










One in seven WA school students aged 12 to 17 have tried vaping.
Andrea Downey | Managing Editor
YOU ASKED, WE DELIVERED: WE ARE NOW CPD VERIFIED


Complete the self-reflection and claim your CPD time, please scan here
Australia has some of the strictest vaping laws in the world, but it doesn’t always seem that way.
One year ago, the federal government introduced worldleading reforms to curb vaping, prohibiting the sale of vapes unless via a pharmacist for those aged 18 and over.
It means any other shop selling vapes is doing so illegally, but it doesn’t seem to be the deterrent the government had hoped.
In the latest annual National Tobacco Scorecard WA was sent home with a ‘D’ on its report card.
One of the main reasons for this was the rise in vaping and nicotine pouches and their popularity among young people. One in seven WA school students aged 12 to 17 have tried vaping.
Illegal tobacco sales in WA are not just impacting the state’s health, since January 2024, WA authorities had carried out 1600 inspections and seized more than 190,000 vapes worth about $5.8 million.
When the vaping reforms came into play 12 months ago, we knew we would have to wait and see whether they were effective. Given that WA’s once enviable reputation for smoking cessation now seems to be going up in a cloud of bubble-gum flavoured smoke, perhaps the reforms have not been as impactful as hoped.
In this edition we look at why WA received such a bad report card and how GPs can help tackle the rise in vaping.
SYNDICATION AND REPRODUCTION Contributors should be aware the publisher asserts the right to syndicate material appearing in Medical Forum on the mforum.com.au website. Contributors who wish to reproduce any material as it appears in Medical Forum must contact the publisher for copyright permission.
DISCLAIMER Medical Forum is published by Medforum Pty Ltd (Publisher) as an independent publication for health professionals in Western Australia. Neither the Publisher nor its personnel are medical practitioners, and do not give medical advice, treatment, cures or diagnoses. Nothing in Medical Forum is intended to be medical advice or a substitute for consulting a medical practitioner. You should seek immediate medical attention if you believe you may be suffering from a medical condition. The support of all advertisers, sponsors and contributors is welcome. To the maximum extent permitted by law, neither the Publisher nor any of its personnel will have any liability for the information or advice contained in Medical Forum. The statements or opinions expressed in the magazine reflect the views of the authors and do not represent the opinions, views or policies of Medical Forum or the Publisher. Readers should independently verify information or advice. Publication of an advertisement or clinical column does not imply endorsement by the Publisher or its contributors for the promoted product, service or treatment.
Advertisers are responsible for ensuring that advertisements comply with Commonwealth, State and Territory laws. It is the responsibility of the advertiser to ensure that advertisements comply with the Competition and Consumer Act 2010 (Cth) as amended. All advertisements are accepted for publication on the condition that the advertiser indemnifies the Publisher and its personnel against all actions, suits, claims, loss or damages resulting from anything published on behalf of the advertiser.
EDITORIAL POLICY This publication protects and maintains its editorial independence from all sponsors or advertisers. Medical Forum has no professional involvement with advertisers other than as publisher of promotional material. Medical Forum cannot and does not endorse any products.




Our competitions continue this month with a selection that suits everyone.
We have three signed copies of a murder mystery with a medical twist written by Perth author Karen Herbert to giveaway.
See page 44 for the scoop on the new book.
We’ve also got film tickets to give away if watching a story unfold is more your style.
And our round of delicious WA wine giveaways continues with a crate of vino from 3drops in the Great Southern up for grabs this month.
See our lifestyle section for this months wine review and more details on our competitions.
PUBLISHERS
Alice Miles – Director Fonda Grapsas – Director Tony Jones – Director tonyj@mforum.com.au
EDITORIAL TEAM
Managing Editor
Andrea Downey 0437 909 904 andrea@mforum.com.au
Clinical Editor
Dr Joe Kosterich 0417 998 697 joe@mforum.com.au
Graphic Design
Ryan Minchin ryan@mforum.com.au
ADVERTISING
Advertising Manager
Bryan Pettit 0439 866 336 bryan@mforum.com.au
Advertising Account Manager
Rita Murphy 08 9203 5222 rita@mforum.com.au
Clinical Services Directory
Alice Miles 08 9203 5222 alice@mforum.com.au
CONTACT MEDICAL FORUM
Suite 3/8 Howlett Street, North Perth WA 6006
Phone: 08 9203 5222 Fax: 08 6154 6488
Email: info@mforum.com.au www.mforum.com.au


















Landmark legislation to increase access to assisted reproductive technology (ART) and surrogacy is being considered in WA.
The Assisted Reproductive Technology and Surrogacy Bill 2025, introduced to Parliament in August, will remove long-standing barriers to access, enabling same-sex couples, single people, transgender and intersex West Australians to access ART and surrogacy.
It aims to ensure the best interests of children born through ART and surrogacy are paramount and maintains safety and quality assurances through the licensing of fertility clinics by the Department of Health.
It will also extend the rights of donor-conceived people, where records are available, to access important information about their genetic heritage, regardless of when they were conceived, to help them make better informed decisions about family planning and healthcare decisions.
The changes will bring WA in line with much of the rest of the country.
WA fertility specialists have welcomed the move.
Concept Fertility Centre’s Medical Director Dr Sebastian Leathersich said that while WA was one of the first jurisdictions in the world to regulate ART and IVF in 1991, those laws were now outdated.
“These long overdue reforms reflect contemporary societal values and, if passed, will make it easier for West Australians to access ART without needing to travel interstate or overseas,” he said.
GPs will have to split the federal government’s bulk billing incentive equally across practices, in a move labelled disappointing by the RACGP.
Under the Bulk Billing Practice Incentive Program – part of it’s $8.5 billion Medicare package to deliver more bulk billed appointments – participating practices would receive an additional 12.5% incentive payment on every $1 of MBS benefit earned from eligible services.
Federal Minister for Health Mark Butler has confirmed the incentive would be split equally between GPs and practices.
RACGP President Dr Michael Wright said GPs were disappointed by the decision.
“In polling our members, we found fewer than one in 10 want the payment to be split evenly,” he said.

“The proposed legislation will also remove other barriers to fertility treatment such as the need to ‘prove’ infertility before offering IVF, as well as some of the restrictions on pre-implantation genetic testing, giving patients and clinicians the autonomy to choose the best path to parenthood for their specific situation.”
Monash IVF West Medical Director Dr Tamara Hunter also welcomed the legislation.
“We must do more to support those who require fertility treatment to start their families, regardless of their circumstances,” she said.
“This legislation is a step in the right direction and we look forward to seeing meaningful change in the near future.”
But Dr Kiran Puttappa, founder of GP West, said the decision was a “fair call” from the government.
Dr Puttappa, who oversees 20 GP clinics across Perth, said from a practice owner’s perspective 100% of the incentive going to GPs would make running a clinic even more expensive.
“At the end of the day you still have to run a quality medical centre and still keep up all of your accessibility, pay the staff, pay increasing rent.
“If you don’t keep up with all of those services then the GP cannot see the patients in the practice.”
Whether the government will meet its target of nine in 10 GP visits being bulk billed by 2030 is in doubt after Department of Health documents revealed that some patients will still face out-ofpocket costs.
The document estimates that
23% of clinics are unlikely to join the program based on financial incentives.
The RACGP wants to see access to supplements containing certain levels of vitamin B6 restricted.
In a submission to the TGA as part of consultation on its proposal to make products containing 50–200mg of vitamin B6 pharmacistonly medicines, the college said it was a positive step towards reducing the risk of harm.
High doses and/or prolonged use of vitamin B6 has been linked with peripheral neuropathy.
In late June the TGA decided to amend the scheduling of vitamin B6 in the future to restrict the access to medicines providing more than 50mg per recommended
daily dose by classifying these as pharmacist-only medicines.
The RACGP noted that scheduling changes alone would not address the multiple sources through which individuals may be exposed to vitamin B6, including diet, fortified foods, and supplements.
It warned many people were unaware these combined sources could lead to excessive cumulative intake and potential health risks.
The submission stated clinical deficiency of vitamin B6 was rare, and there was limited evidence supporting supplementation benefits in individuals who were not deficient.
The interim measures are set to be in place for 18 months as of February 2027.
New resources to encourage the use of spacers with pressurised metered dose inhalers (pMDIs) are now available.
Developed by the National Asthma Council Australia (NAC), the resources include a new spacer chart and information sheet for health professionals and an accompanying how-to-video.
Clinical Executive Lead at NAC Professor Debbie Rigby said the clinical effectiveness of pMDIs can be significantly improved by using a spacer.
“Only about one in 10 patients can correctly perform all the steps in using a pMDI and three-quarters of patients using a pMDI make at least one error when using their inhaler.
“The spacer helps the medication reach the small airways where it is most needed and this is important for both adults and children.
“The use of a pMDI with a spacer is at least as effective and safe as use of a nebuliser and spacers should be selected individually to fit the pMDI.”
All spacer resources can be downloaded directly from the NAC website.
For more news visit mforum.com.au and hit the ‘news’ tab
Two West Australian doctors have been recognised for their dedication to medicine and community health at this year’s AMA National Conference.
Dr Rajeshwary (Raji) Krishnan’s understanding of and willingness to help overcome barriers to accessing care saw her receive the AMA’s President’s award.
While former state and national AMA President Dr Omar Khorshid was the joint winner of the 2025 AMA Gold Medal alongside Dr Tony Bartone.
Dr Krishnan was recognised for her dedication to improving health outcomes for multiple generations of First Nations families.


Dr Krishnan has worked in Aboriginal healthcare for 45 years and heads the multidisciplinary team at Pramana Medical Centre in Gosnells.
Dr Krishnan said she was humbled by the award, adding: “I acknowledge the immense support I have received from my dedicated practice team, including my daughter and fellow GP Dr Priya Krishnan, co-director, the dynamic Ms Kate Fulford, and lifelong strength and encouragement from my husband,” she said.
“Most importantly, I thank my patients, who continue to share their stories openly and courageously with me, who never cease to motivate me in this tireless journey of service. They have taught me more than I have taught them.”
Dr Khorshid, an orthopaedic surgeon, was elected in August 2020 and played a pivotal role in guiding the COVID vaccine rollout and ensuring GPs played a central role.
In 2022, Dr Khorshid launched the AMA’s Clear the Hospital Logjam, Sickly Sweet and Modernise Medicare campaigns. His advocacy helped secure the $970m investment in Medicare and general practice promised by Labor in the 2022 federal election.
Professor Helen Wilcox has been appointed Dean of the Medical School of UWA. She is the first GP to be appointed to the role.
Parkinson’s WA chief executive Yasmin Naglazas has been appointed to the Board Finance Committee of the National Parkinson’s Alliance (NPA).
Professor David Blacker has also been appointed at Honorary Medical Director at Parkinson’s WA.



What if they told you
The Photon Counting CT machine at ChestRad requires ten times less radiation dose for lung cancer screening
All lung cancer screening bulk billed
1 Heismann, B Photon counting CT versus energy-integrating CT: A comparative evaluation Med Physics Dec 2024
Finding - Siemens Naeotom Alpha PCCT ten times more dose efficient for LCS than Siemens Definition Force
2. American Association of Physicists in Medicine Lung Cancer Screening CT Protocols V 6 0 November 2023
Finding - Siemens Definition Force four times more dose efficient for LCS than the next best CT machine


WA has an enviable reputation when it comes to combatting one of the biggest health scourges of modern time – smoking. But has it lost its edge?
By Cathy
O’Leary
Western Australia has long been recognised as a world-leader in tobacco control, adding its own weight to efforts at a national level to stub out smoking.
Its playlist has included graphic public education campaigns showing surgical removal of a smoker’s larynx, backed up by law reforms that have progressively restricted how cigarettes can be advertised, sold and used.
WA doctors have played a critical role in anti-smoking advocacy from the 1970s, when some risked criminal charges by defacing cigarette advertising on billboards under the cover of night.
In the early 2000s, a Perth cardiothoracic surgeon was filmed removing a lung cancer tumour, to be later used in television advertisements.
As a result of sustained efforts, rates of smoking in WA have been on a steady downward trend since the 1980s when about one in three adults smoked, to 2025 when rates hover around 10%.
But there are concerns that the state is not keeping up with crackdowns on rapid new markets of addiction such as e-cigarettes and nicotine pouches, which are targeting teenagers and young adults.
In a move that surprised many, the latest annual National Tobacco Scorecard by the lobby group Australian Council on Smoking and Health (ACOSH), which names and shames the states falling behind on tobacco and vape reform, gave WA a grade of ‘D’ – second only to the Northern Territory as the worst performer.
It has prompted calls for more action so that the progress made since the 1970s does not start to unravel.
When public health stalwart
Professor Charles Watson wrote the introduction to a 2008 publication on the history of tobacco control in WA, few people had even heard of vaping.
Many thought the battle to eliminate smoking, one of the leading causes of cardiovascular disease and lung cancer, had been largely won.
But Prof Watson, then chair of Cancer Council WA’s medical and scientific committee, voiced what would turn out to be a prophetic note of caution.
“In reflecting on progress in tobacco control in WA we can rejoice in the lives it has saved and the health it has given back to ex-smokers, but much remains to be done,” he wrote.
“There is still a need for concerted action, regular review of achievements, and the invention of new tactics.
“The simple fact is, tobacco is still a major killer despite the gains made over the past four decades.”
In 2025, the health system is still dealing with the legacy of decades of high rates of smoking and the demand for medical services is expected to rise with the launch of the National Lung Cancer Screening Program using low-dose CT scans to look for cancer in high-risk asymptomatic current and former smokers.
But now there are new kids on the block – nicotine products that can be legitimately used as second or third-line treatments to help people quit smoking, but have also developed into a lucrative new target for teenagers and young adults, many of whom have never smoked.
Only introduced to the American market in 2006, e-cigarettes were at the time hailed as a smoking cessation tool and safer alternative. Similarly, nicotine pouches – small bags containing nicotine, sweeteners and flavours which are placed between the lip and gum – were first registered in the early 2000s as a medicinal nicotine replacement tool by a company later bought out by RJ Reynolds (now British American Tobacco).
However, vapes and nicotine
pouches have now become the domain of the young. Illegal to sell over the counter in shops but regularly sold to children, nevertheless.
The downside of reducing smoking rates so much has been that tobacco companies and other industry players have been pushed to look to new products to make money.
As a result, there has been a significant rise in people who use vapes, particularly among teenagers and young adults. One in seven WA school students aged 12 to 17 have tried vaping.
The ‘gateway effect’ to tobacco is now firmly established, with young people who vape three times more likely to take up smoking cigarettes.
ACOSH Chief Executive Laura Hunter said that almost a year on from the Federal Government introducing world leading reforms, the results from the National Tobacco Scorecard showed a stark divide, with some states leading the charge and others lagging.
was capturing was that the Federal Government’s reforms that we saw passed by Parliament last year were world-leading,” she said.
“But without the legislation being updated in every state and territory, there’s a disconnect between the federal laws and the ability of the states to enforce them.
“There are some states yet to update their legislation and, because of that, it’s hamstrung all the compliance and enforcement teams within those states.”
Ms Hunter said states were judged on whether they could crack down on illegal sales and enforce state laws, and a critical area where WA lost marks was in enforcement and compliance on products such as vapes and nicotine pouches.
Under federal and state laws, vapes can only legally be sold with a prescription at a pharmacy. It is illegal to sell, buy or commercially advertise nicotine pouches.

“If this were an exam result, you’d have to say some states and territories are struggling,” Ms Hunter said.
“The results show that while South Australia and Queensland are leading the charge, jurisdictions like the NT and WA are falling behind — and are needing to prioritise urgent updates to state tobacco laws.
“In WA, we’ve seen regulations introducing the prescription-model for vaping products, a very welcome direction but the state tobacco laws haven’t been updated in seven years. Bringing these up to date will play a critical role in giving authorities the power to shut down illegal vape shops and introduce tougher penalties that deter offenders.”
Ms Hunter told Medical Forum that many people were shocked to see the report card for WA and she had received a lot of calls, including from Members of Parliament asking what was going on.
“As West Australians it was quite upsetting to people to see WA fall behind, but what this score card
In June WA’s state budget estimates was told that since January 2024, WA authorities had carried out 1600 inspections and seized more than 190,000 vapes worth about $5.8 million.
But no on-the-spot fines had been issued for illegally selling vapes because the WA Health Department did not have the powers, although some prosecutions were going through.
In contrast, Ms Hunter said that in South Australia there have been more than 500 inspections conducted with closures of retailers who did the wrong thing and huge resourcing and investment into government taskforces that were seizing millions of dollars’ worth of illicit cigarettes and vapes.
Significant penalties had been introduced in Queensland, with large-scale seizures and stronger enforcement.
“You can pump as many resources as you like into compliance and enforcement, but at the end of the day if their hands are tied they can’t shut down retailers who are doing the wrong thing,” she said.
“Some states, like South Australia and Queensland, are doing a lot, they’ve updated their legislation, but
continued on Page 10
continued from Page 9
others like the Northern Territory and WA are lagging.
Shonky retailers
“With WA being the only state that hasn’t updated its tobacco laws, it means that if you have someone who reports a vape shop for selling illegal vapes to kids in school uniform, it goes to the compliance team in the WA Health Department,” she said.
“They would have to go out and witness it in person, then they would have to go to a JP for a warrant, issue it to the store, and meanwhile the shop owner, who’s not stupid, has cottoned on quickly and the stock magically disappears.
“I’ve even seen retailers put all the stock into the boot of their car, and some retailers have secret knocks, whereby they get the stock and leave it in a certain spot and kids in school uniform walk out the store with vapes in between two packets of crisps. The retailers do it because they can get away with it.”
In South Australia, enforcement teams could shut down stores immediately and the penalties were “eye-watering”.
“This is really a scorecard on political will, and if politicians have a real fire in their belly and see the insidious tactics by the industry, they prioritise the necessary changes in the law,” Ms Hunter said.
“It’s like a game of Whack-a-Mole, where you deal with cigarettes and you get the lowest use in history, then the industry moves on and creates things like nicotine pouches.
“I went into a Subiaco convenience store and purchased a packet of nicotine pouches, even though they’re illegal, but for $25 they had all the flavours.
“I’m not a policy expert, and I appreciate that compliance enforcement is complex and they would need to work out the necessary laws from a WA context, but it can be done if politicians are serious about protecting the public, particularly kids.
“Vapes are not harm-free. There is now good evidence that if someone picks up a vape and they’ve never vaped or smoked before, they’re

“Of all the things that will confuse historians in the next century, certainly the idea of a lethal product, a product of illness and despair, peddled to youngsters for the profit of the peddler, will be the most confusing.”
–
William Foege, Proceedings of the 8th World Conference on Tobacco
or Health (1992)
five times more likely to go onto cigarettes. From the tobacco industry’s angle, that’s a genius business model.”
WA’s Police Commissioner Col Blanch has recently spoken out about the issue of illegal tobacco sales in WA, saying the penalties that could be imposed were too low.
Speaking to ABC Radio Perth he said he wanted the state to follow in South Australia’s footsteps to allow authorities to issue interim closures.
GPs have a role
Ms Hunter said there was still some scepticism or under-appreciation about the dangers of vapes, even among doctors.
“GPs would be seeing vaping a lot now, it’s an addiction, and it’s not like a fast-food drive-through habit to get burgers, this is a chemical addiction. One vape can contain the same amount of nicotine as you would get in nine packets of cigarettes, so it’s really potent doses,” she said.
“Australia has always taken a very cautionary approach around vapes but globally some countries have adopted a different model and allowed vapes to be sold alongside cigarettes. And as soon as you have an open retail market, the prevalence and use among teenagers skyrockets.”
Ms Hunter said Australia had come to a middle point where it had a pharmaceutical model for vapes, but it was a second or third-line treatment option.
They were safer because they were limited to three ingredients and two flavours, and were in pharmaceutical-style packaging.
“I would be encouraging GPs to look at the evidence around combination nicotine replacement therapy first and foremost, even for giving up vapes,” she said.
“The RACGP has published some incredible guidelines around nicotine dependency that incorporates all of that. GPs have a huge opportunity to use evidence-based methods
when they’re helping people get off cigarettes and vapes.
“GPs are going to be really important as we move forward and start cracking down on illicit use.”
The RACGP guidelines on nicotine vaping products urge doctors to minimise risk.
“The recommended first-line smoking cessation support includes TGA-approved pharmacotherapies and behavioural support. Nicotine vaping products (NVPs) are not first-line treatments for smoking cessation,” the guidelines state.
“NVPs may be considered with ongoing behavioural support for people who have tried to achieve smoking cessation with TGAapproved pharmacotherapies combined with behavioural intervention but failed and are still motivated to quit smoking.”
Ms Hunter said vapes had been painted as the holy grail for quitting smoking, but the real market was to addict a new generation of people to dangerous products.
“I struggle to find a 50 or 60-yearold smoker who’s been trying to give up cigarettes and then reaches for a unicorn milk flavoured vape – that’s not the market for vapes,” she said.
Upping the ante
Cancer Council WA (CCWA), which runs the Government-supported Make Smoking History program, said there had been some solid wins but more needed to be done.
Cancer Prevention and Research Director Melissa Ledger said important amendments had been made to the state’s tobacco laws in 2018 to ban the sale of flavoured cigarettes and splitable packs, and the sale of cigarettes to children.
Amendments to state legislation could have been delayed in anticipation of national vaping reforms, which came into effect in July last year and had brought big benefits to WA without duplication of efforts.
But CCWA wanted to see significantly increased resourcing for compliance and enforcement in

relation to the illicit trade of tobacco, and to prevent the sale of cigarettes to children.
“We do wish to see some amendments made to state legislation to strengthen some areas, to prohibit the sale and supply of e-cigarette products that are not prescribed or otherwise legally authorised, and strengthen legislative enforcement measures and penalties to effectively deter the unlawful sale of e-cigarettes and illicit tobacco,” Ms Ledger said.
When Medical Forum contacted the WA Health Department about WA’s poor grade in the National Tobacco Scorecard, it said some other states have recently updated their legislation, which has resulted in ACOSH recognising their progress.
A spokesperson said WA had benefitted from federal tobacco and vaping reforms, while WA laws had also been amended to require nicotine vapes be supplied only on prescription.
“The State Government is committed to complementing national tobacco and vaping reforms and is considering appropriate amendments to the Tobacco Products Control Act 2006,” the spokesperson said.
“This includes ensuring WA legislation is in lock step with the Commonwealth’s tough stance on vapes and on tobacco control.
“The department continues to conduct compliance activities in relation to the sale and use of tobacco products and the illegal supply of nicotine vaping products in both metropolitan and regional

In the past two years, it had inspected more than 3000 tobacconists across WA and seized more than 550,000 vapes, worth an estimated $21 million.
Ms Hunter said ACOSH would revise the scorecard next year.
“Across the board lots of people are concerned about smoking and vaping, and while we’re hearing about priority being given to the necessary reforms, our argument is let’s not delay it anymore, because we can’t afford to miss the boat.”
Amid a concerning rise in respiratory disease among Aboriginal and Torres Strait Islands people, how can we provide more accessible, culturally safe care to close the gap?
By Suzanne Harrison

For 30 years Trish Bushby has been working with First Nations people in the health support sector. During that time, she has seen huge change.
Now an Aboriginal Health Manager with Arche Health in Bentley – which partners with Respiratory Care WA – Ms Bushby said when she first started out, there were only two Aboriginal health workers in the sector.

with a recent rise in respiratory disease – it’s the fourth leading cause of death among Indigenous Australians, according to the National Indigenous Australians Agency in 2024.
pulmonary disease (COPD) and 1.6 times more likely to report asthma, compared to the non-Indigenous population.
In 2021/22, more than 5400 asthmarelated emergency department visits were recorded among First Nations people.
“We still have a long way to go, but there are a lot more self-led programs and more community programs,” she said.
“We’ve got Aboriginal staff who get to have input in developing services and programs. It’s very exciting to see that.”
But despite positive steps, there is still a significant gap when it comes to culturally safe, easily accessible medical care, particularly now
“Our team delivers support programs to Aboriginal and Torres Strait Islander clients who are living with a variety of chronic conditions,” Ms Bushby adds.
“A large portion of our clients have respiratory conditions that require different levels of education, review, and support to manage their respiratory health.”
Her comments are reflected in the statistics. According to the Australian Institute of Health and Welfare (2023), First Nations people are 2.2 times more likely to report having chronic obstructive
According to the latest Aboriginal and Torres Strait Islander Health Performance Framework (HPF) reports, respiratory diseases among Indigenous Australians accounted for 10% of all deaths between 2015 and 2019.
Rates of death due to COPD are 2.8 times higher than the nonIndigenous rate, and asthma-related deaths about 2.5 times higher. There has also been a 32% increase in hospitalisations for respiratory diseases among Indigenous Australians over the last decade. According to Dr Jeanita Wong, Acting Medical Director of the
integrated Derbarl Yerrigan Health Service (DYHS), common contributors to respiratory disease –and in fact, all diseases – are barriers including poor housing, awareness, education, and stigma of seeking help from a medical professional.
“It’s ongoing. It comes back to a lot of social determinants, which require a multi-sector responsibility such as safe, reliable housing and people with jobs to pay for their medications,” she told Medical Forum
Other factors are also at play. The HPF notes that nearly half (47%) of the respiratory disease burden is attributed to smoking.
However, Dr Wong says the DYHS Tackling Indigenous Smoking (TIS) program – a government initiative aimed at reducing smoking rates among Aboriginal and Torres Strait Islander people – has already delivered.
The program has helped more than 100 families create a smoke and vape-free home.
“I would say that smoking rates have improved, which has a lot to do with health promotion. Our TIS team has recently ranked second in the nation for its program.”
Kate Fulford, Associate Director, Strategy and Clinical Innovation at Pramana Medical Centre in Gosnells, said that chronic respiratory conditions are often caused, or significantly worsened by exposure to dust, mould, and chemicals, which are common in overcrowded or substandard housing.
“These exposures make it harder to avoid triggers, leading to chronic inflammation and persistent respiratory issues. Higher rates of smoking and exposure to secondhand smoke also contribute,” she said.
“While smoking rates are thankfully decreasing over time, there’s still more work to be done.”
A focus on the importance of community-based, culturally relevant initiatives are at the heart of Respiratory Care WA (RCWA).
It has stressed that to bridge the gap in care there is a need to provide greater access to more culturally safe spaces for education, support, and care that respects and reflects First Nations cultures and identities.
RCWA Acting Chief Executive Rael Rivers told Medical Forum that more people are seeking their services and that partnerships with Aboriginal-led organisations were vital.

“These partnerships enable us to deliver free lung health diagnostics, education, and support in settings that are culturally safe, trusted, and accessible,” she said.
“However, demand is growing, and many First Nations people – particularly those in remote communities – still face barriers to accessing lung health care.
“While we and our partners are working hard to reduce this inequity, without greater government and corporate investment, our ability to make meaningful progress remains limited.”
Through its partnerships with Aboriginal-led organisations RCWA reaches more than 1100 First Nations people in WA each year.
These sessions are held in culturally safe, familiar settings where community members feel respected, supported, and empowered to ask questions freely.
RCWA Community Outreach Coordinator Melanie Preen said culturally safe care involves being in a space that feels familiar and acknowledges Country and connection to culture.
“These trusted settings help build relationships and encourage patients to open up about their respiratory health and the challenges they’re facing,” she said.
be there for my family and help the grandkids with their asthma too.”
There are many Aboriginal Health Services in WA, including communitycontrolled and mainstream services, all working toward trauma-informed, accessible, and culturally safe care.
“Culturally safe care shouldn’t be limited to specific services,” Ms Fulford said.
“It should be embedded across all health and social services, so that every patient can receive equitable care, no matter their background.”
Sending this message to the community is a positive step towards closing the health gap, but how can GPs prepare themselves to offer culturally safe care, or refer patients to those who are the best fit for their needs?
“One key area is better understanding and addressing the social determinants of health — particularly housing — alongside medical treatment,” Ms Fulford said.
“A puffer alone won’t be effective if a patient is living with constant environmental triggers.
“It’s also essential to ensure correct diagnosis through tools like spirometry or full lung function tests to avoid misdiagnosis or overdiagnosis of asthma, which is common due to fragmented care or old, inaccurate medical records.”

She adds that at Pramana Medical Centre they find lung function testing invaluable, not just for diagnosis, but also as an opportunity for patient education.
“It helps explain how and why to use inhalers properly, and why preventers are essential, not just relievers,” she said.
“It encourages openness, builds trust, and helps people engage in meaningful learning.”
During yarning circles held in 2024 and 2025, RCWA said participants shared powerful stories about their experiences with respiratory illness.
One elder reflected: “For the first time, I felt comfortable talking about my asthma and learned how to manage it better so that I can
“We’re fortunate to have Respiratory Care WA visit our clinic monthly to conduct these tests and deliver patient education. We've observed a strong correlation between this education and improved inhaler technique and medication adherence.” continued on Page 15
THE QUICK AND EASY WAY FOR GPs TO DIAGNOSE HEART RHYTHM ISSUES

D E V I C E
F I T T I N G
R E P O R T S
C O S T S
G P S U P P O R T

O l d , b u l k y H o l t e r m o n i t o r s a r e d i f f i c u l t t o
u s e a n d u n c o m f o r t a b l e f o r p a t i e n t s t o w e a r
P a t i e n t i s r e f e r r e d o f f - s i t e , h a v i n g t o b o o k a n d
t r a v e l f o r f i t t i n g w h i c h c a u s e s d e l a y s i n t e s t i n g
T y p i c a l l y r e p o r t e d b y g e n e r a l c a r d i o l o g i s t s , o f t e n
l a c k c l i n i c a l d e t a i l a n d r e t u r n e d i n d a y s o r w e e k s
O f t e n r e q u i r e s p a t i e n t s t o p a y o u t o f p o c k e t e x p e n s e s l e a d i n g t h e m t o s k i p t e s t i n g
O n l y r e p o r t s H o l t e r , n o f u r t h e r s u p p o r t i s p r o v i d e d t o r e f e r r i n g G P s t o a s s i s t i n p a t i e n t c a r e

S m a l l l i g h t c u t t i n g e d g e H o l t e r m o n i t o r Q u i c k
a n d e a s y t o u s e , c o m f o r t a b l e f o r p a t i e n t s t o w e a r
P a t i e n t s a r e c o n v e n i e n t l y f i t t e d a t y o u r p r a c t i c e , a v o i d i n g t r a v e l a n d d e l a y s
D e t a i l e d c l i n i c a l r e p o r t s p r e p a r e d b y o u r t e a m o f
c a r d i a c e l e c t r o p h y s i o l o g i s t s r e t u r n e d i n h o u r s
1 0 0 % b u l k b i l l e d t e s t i n g w i t h o u t a n y a d d i t i o n a l
c o s t s f o r p r a c t i c e o r p a t i e n t s
C o m p r e h e n s i v e s u p p o r t p r o t o c o l s t o h e l p G P s
c o n f i d e n t l y a n d e f f i c i e n t l y m a n a g e p a t i e n t c a r e
w w w . C l o u d H o l t e r . c o m . a u



32% increase in hospitalisations over the last decade

Rosedie Milne, Specialist and Allied Health Coordinator at DYHS said:
“While we offer transport for elderly patients, there’s little support for younger people aged 20–40.”
To help address this, DYHS has partnered with RCWA to deliver integrated respiratory assessments, combining specialist consultations and lung function testing in a single visit.
around maintaining good respiratory health.
“Breaking down information shared in client consults and delivering it in culturally appropriate ways – particularly with medication reviews to check if the client has the right medications and is using them correctly – has led to a vast improvement in many of our clients’ respiratory health and understanding of their conditions.”
Ms Bushby told Medical Forum that Arche has a good relationship with funding representatives, but with costs for equipment and demand increasing, more reliable funding is imperative.
For example, education in the community about sleep apnoea has improved greatly, resulting in an increase in diagnoses, but that means more Continuous Positive Airway Pressure (CPAC) equipment is required.
“It would also be great for more people to be on the ground to bring more services to the community; not just at the top level. It needs to hit the grass roots,” Ms Bushby adds.
Ms Fulford concludes: “It’s critical that First Nations people have real choice in where they access care, not just from designated services in specific locations.
“Siloing healthcare doesn't improve outcomes. We all need to work collaboratively and ensure more integrated and inclusive access to care, rather than selective or restricted access.”
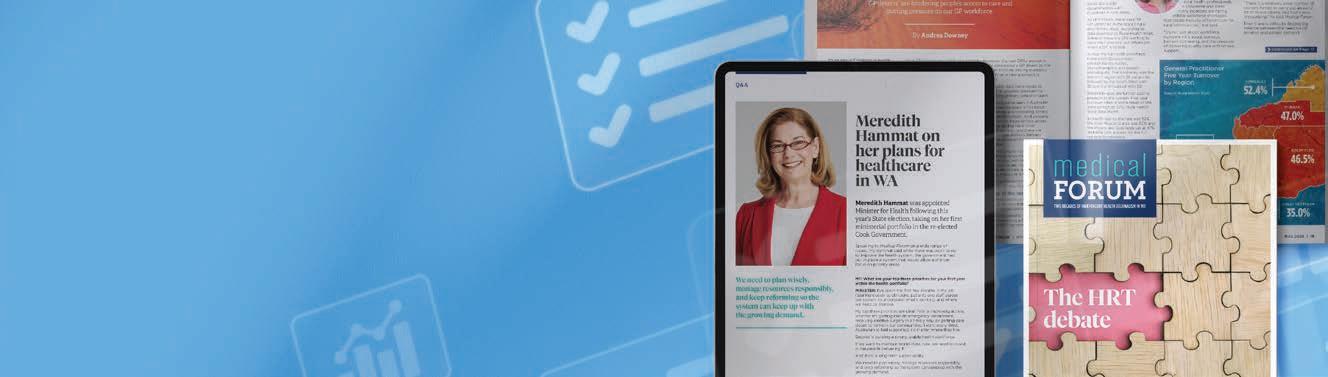
Thank you to everyone who took part in our readership survey*.
It was good to know our clinical updates, guest columns and WA-led news were important to our readers.
Going forward we will expand our offering of CPD verified content, clinical education and local health news to continue delivering more of what you want.
*n= 241 respondents unaudited
94% of respondents say they read Medical Forum to keep
with WA health news
Over 84% find Medical Forum clinical updates keep them abreast of changes to clinical practice
I find the clinical updates useful to stay abreast of changes to clinical practice
How often do you read Medical Forum magazine?
“More medical business articles”
“More opinion pieces, interactive clinical quizzes”
“More CPD opportunities”
“Clinical cases with answers next edition”
“It’s great as it is”


Plans to further expand WA pharmacists’ scope of practice has sparked concern over increased risk of misdiagnoses and fragmented care.
The State Government has confirmed pharmacists will be able to diagnose and treat a further 17 conditions including asthma, acne, ear infections, hormonal contraception and obesity management, under its Enhanced Access Community Pharmacy Pilot.
Training will begin in September for the first cohort of pharmacists through accredited Graduate Certificate programs at Western Australian universities.
Health Minister Meredith Hammat said the move will reduce pressure on hospitals and GPs while giving patients safe care options closer to home.
But the move has been criticised by RACGP Vice President and WA Chair Dr Ramya Raman, who said chronic conditions like asthma, respiratory conditions and obesity management do not belong in the retail space. She said this was not a turf war, but about patient safety.
“First and foremost, I want to say in terms of pharmacists and the work they do, they play a really important role in the community,” she told Medical Forum
“But the considerations we have to take on board is ensuring quality of care for patients and that the outcomes for patients are not compromised.
“Studies have shown that patients who see the same GP are healthier, they live longer, they’re much more satisfied with their care.”
Dr Raman said similar pharmacy pilots in Queensland had not resulted in less pressure on GPs and that workforce issues within the pharmacy sector would also

likely lead to increased pressure if prescribing powers were expanded.
“There is an increased risk of things falling through the cracks and, while the patient may think it is adequate, there is an increased risk of delayed diagnosis,” she added.
It comes as the Pharmacy Guild of Australia published its 10-year plan Towards 2035, which aims to make community pharmacists the “first
port of call for primary healthcare services through the adoption of full scope of practice”.
It outlines a goal to have 80% of community pharmacists across Australia qualified as prescribing pharmacists by 2035. Under the plan pharmacists would be able to diagnose and treat more than 22 common acute and chronic health conditions.
The full list of conditions WA pharmacists will be able to prescribe for includes:
Asthma
Smoking cessation
Shingles
Impetigo
Allergic and nonallergic rhinitis
Mild to moderate acne
Mild to moderate atopic dermatitis
Gastro-oesophageal reflux and Gastro-oesophageal reflux disease
Oral health risk assessment and fluoride application
Acute otitis externa
Acute otitis media
Acute nausea and vomiting
Acute minor wound management
Mild, acute musculoskeletal pain
Hormonal contraception
Mild psoriasis
Weight loss and management of obesity

Stepping up as President felt like the right way to push for real change. I believe this role has the power to hold the system to account and help shape a future where our patients and our profession get the support they need and deserve.
Dr Kyle Hoath took up the role of AMA (WA) President in July. He told Medical Forum his plans for the role and the issues he has already raised with the Health Minister in his first weeks as head of the association.
MF: Why did you put your hand up for the role of AMA (WA) President?
DR HOATH: I’ve always been driven by community service through advocacy. I joined the AMA (WA) as a medical student because I wanted to speak up for medical students and doctors, and patients who deserve better.
Over the years on the AMA (WA) Council, including as Vice President, I’ve seen just how much work still needs to be done to strengthen our system, especially in mental health. As a psychiatrist who has worked across public and private practice, I see daily the barriers that stand in people’s way when they need care the most.
Stepping up as President felt like the right way to push for real change. I believe this role has the power to hold the system to account and help shape a future where our patients and our profession get the support they need and deserve.
MF: What are your long-term priorities in this role?
DR HOATH: My vision rests on three foundations. First, we need to make sure every West Australian can get care when they need it, regardless of where they live. That means tackling ramping, boosting hospital capacity, and making mental health support accessible.
Second, we have to strengthen and keep our medical workforce. More training places, better working conditions for junior doctors, fair pay, and opportunities to build a career here in WA, not interstate.
Third, we must invest properly in prevention. That means getting serious about tackling issues like obesity, smoking, alcohol harm, and the mental health crisis at their roots. It’s smarter, more cost-effective, and most importantly keeps people healthier for longer.
MF: Have you met with the Health Minister since taking up the role and what are three issues you raised?
DR HOATH: Yes, I’ve already had the chance to sit down with Health and Mental Health Minister Meredith Hammat and we had a really constructive conversation.
The first issue I raised was the urgent need to increase capacity and reduce pressure on our hospitals, which means more beds, more doctors, nurses and allied health, and more community-based services.
Secondly, we talked about workforce shortages, particularly outside the metropolitan area. We need real investment to attract and keep rural doctors including GPs, generalists, and other specialists, so people don’t have to travel for hours just to see a doctor.
Thirdly, I emphasised the need for a stronger focus on prevention and mental health. We have a Minister for Preventative Health now and I think that’s a huge opportunity. I want to see us move beyond bandaid solutions and invest in keeping people well before they reach crisis point.
All of this is about working with government but not shying away from highlighting what’s missing.
MF: How has the medical community found the sharing of health responsibilities between multiple State Government ministers since the election?
DR HOATH: There’s been cautious optimism about the team approach. Having multiple ministers acknowledges that health is massive, and that mental health and prevention deserve dedicated focus.
Many doctors have said it could bring fresh energy to areas that have struggled for too long. Of course,
Smoking, vaping, alcohol harm and poor mental health drive too many of our health problems. WA can and should lead the nation in smart public health – but it takes real investment and follow-through, not just words.
this only works if there’s clear coordination.
As President, I’ll be keeping a close eye on how the ministers work together so gaps don’t open between portfolios. We will continue to support good collaboration, but we’ll speak up if things fall through the cracks.
MF: Where do you think WA needs to improve most in terms of preventative health?
DR HOATH: Prevention is a huge part of why I wanted this role. We spend so much money treating preventable illness when we should be tackling it at the source.
Smoking, vaping, alcohol harm and poor mental health drive too many of our health problems. WA can and should lead the nation in smart public health – but it takes real investment and follow-through, not just words.
I’m keen to sit down with Education, Early Childhood and Preventative Health Minister Sabine Winton. I want us to build practical programs that reach people early in schools, families, and communities. That’s where we get the biggest health gains and the best value for taxpayers too.
MF: Your predecessor repeatedly spoke about a shortage of hospital beds in WA. How many more do we need?
DR HOATH: The numbers can vary but the bottom line is clear: WA has the lowest ratio of public hospital beds per capita in the country, and it shows. We’re at least 600 beds short just to match the national average and that’s before you factor in the growing population and extra demands on mental health and aged care.
So realistically, we need hundreds more beds plus the doctors, nurses and allied health staff to run them properly. Our private hospitals do a
great job, but they can’t plug that gap alone.
If we want to end ramping and waitlists, we need to stop pretending we can do more with less. We need to plan now and get building.
MF: What more can be done to ensure the private health system remains viable?
DR HOATH: Our private hospitals and practices take huge pressure off the public system, especially for elective surgery and specialist care, but they need to stay viable.
That means fair funding and better collaboration between government, private providers and insurers. We need policies that help specialists stay in private practice without being buried in red tape and costs.
It’s also about making sure patients can afford to use their private cover when they want to. I want us to work with the private sector as genuine partners, because when private and public work well together, the whole community benefits.
MF: Are you comfortable with how the Expedited Specialist Pathway has been operating to serve WA?
DR HOATH: In principle, yes. Bringing more qualified overseas specialists to WA is a good step, especially in fields like psychiatry, anaesthesia and obstetrics where we have clear shortages.
It’s early days but I want to make sure those doctors feel supported once they arrive and that they take up positions where they’re needed most, including in our regions. This is one part of fixing workforce gaps, but it needs to be backed up by local training and retention too.
continued on Page 21
Advert removed in compliance with Medicines Australia's Code of Conduct and the Therapeutic Goods Administration's Therapeutic Goods Act.
https://medicinesaustralia.com.au/code-of-conduct/about-the-code/ https://www.tga.gov.au/legislation-legislative-instruments
continued from Page 19
MF: What steps should the state and federal governments be taking to meet the shortfall of GPs in WA?
DR HOATH: It’s no secret WA needs more GPs, we can’t keep expecting rural councils to pay huge subsidies to get just one doctor to town. Both the state and federal governments should share that responsibility by providing practical incentives like housing support, relocation help and fair remuneration.
We also need to expand GP training places and make it easier for registrars to do placements in regional and remote WA and stay there. We should respect general practice as a specialty and pay GPs fairly for the complex work they do.
At the end of the day, strong primary care keeps people out of hospital and that benefits everyone.
MF: With the Federal Government funding health and the state delivering it, what could work better?
DR HOATH: Everyone knows the split can be messy. Funding and delivery don’t always line up, and the cracks show up in long waiting lists and clunky hand-offs.
We need better integration. That means the state and commonwealth working together on funding models that reward keeping people healthy, not just treating them when they’re sick.
We also need to invest in good data systems that let GPs and hospitals share information quickly and safely. And we should have regular forums

that bring clinicians to the table, so the people doing the work can shape the solutions.
MF: How is work with the State Government on the GP ASK program going?
DR HOATH: The GP ASK pilot is a great example of the system trying to join the dots. It’s early days but so far, it’s promising.
Giving GPs fast access to specialist advice helps them manage patients in the community and can stop people ending up in hospital unnecessarily.
Our system is functional but fragile. It’s held up by the dedication of our workforce, but that’s not enough on its own. If we want a health system that’s genuinely world class and sustainable, we can’t keep patching holes and hoping for the best.
We’ll keep working with the State Government to make sure the program stays practical and easy to use. If it works, we’d love to see it expand to more specialties and regions so that every GP has a realtime safety net when they need it.
MF: How would you rate the WA health system as it is today?
DR HOATH: I’d say our system is functional but fragile. It’s held up by the dedication of our workforce, but that’s not enough on its own. If we want a health system that’s genuinely world class and sustainable, we can’t keep patching holes and hoping for the best.
We need real planning, proper capacity and investment, and we need to fix the root causes so that every West Australian can get care when they need it.








Writing a script is rarely just a five-minute job, it requires established relationships and a knowledge of patient history, writes Dr Ramya Raman
From the outside, a repeat prescription can look like a fiveminute administrative task: patient comes in, a few clicks, a signature, job done.
Inside the consulting room, it’s something else entirely. Safe prescribing draws on years of training, a deep knowledge of a person’s history and risks and, most importantly, the trust and rapport built over time with their GP and family.
That diagnostic triad represents the quiet engine room of our health system.
Western Australia is moving to test how far the definition of that engine room can be stretched. Under the Enhanced Access Community Pharmacy Pilot, pharmacists will be trained to identify and treat more than 17 conditions, including asthma, ear infections, acne, shingles, reflux, hormonal contraception and weight management.
The intent is understandable: make care faster and closer to home. But the question isn’t who is ‘allowed’ to treat what, but instead what model actually delivers safer care, fewer adverse events and genuine system relief?
Continuity of care is the lever most likely to achieve those goals. The OECD’s Patient-Reported Indicator Survey (PaRIS) survey, Australia’s first national, patient-reported snapshot of chronic-condition care, shows how strongly outcomes track with therapeutic relationships.
Some 94% of Australians with chronic conditions reported positive experiences at their GP practice, above the OECD average. Among people who had the same GP for three to five years, 97% rated their care positively, compared with 79% among those without a regular GP.

Some 94% of Australians with chronic conditions reported positive experiences at their GP practice. Among people who had the same GP for three to five years, 97% rated their care positively, compared with 79% among those without a regular GP.
Better coordination and trust followed the same pattern – the longer and steadier the therapeutic relationship, the better the experience and outcomes. In policy terms, this is not soft evidence.
General practice remains the most cost-effective way to uphold the health system, not because it is cheaper in isolation, but because it prevents expensive problems downstream.
The OECD’s analysis of PaRIS data is blunt – doing more for people with chronic conditions “does not necessarily mean spending more”.
The features that matter are person-centred, coordinated primary care delivered by a workforce patients know and trust. That is precisely what highfunctioning general practice offers when it is supported well.
This is where WA has a choice. We can extend roles in ways that fragment care, have multiple entry points, variable records, and no guaranteed feedback to the usual GP.
Or we can aim for continuity, strive for same-day communication with the patient’s nominated GP and upload to My Health Record, establish clear escalation thresholds, and mandate time-
limited prescribing linked to follow-up.
It also means measuring the right things; not just service counts and satisfaction, but adverse events, antibiotic stewardship, confirmed follow-up with the usual GP, and changes in ED presentations for those specific conditions, reported independently and transparently.
It also means investing in access inside general practice funding for same-day or next-day acute appointments and after-hours cooperatives, so patients don’t have to choose between timeliness and continuity.
Pharmacists, nurses, allied health professionals and GPs already work side-by-side every day. The task ahead is not to pit us against each other, it’s to knit our contributions together around a patient’s medical care.
The five-minute script is rarely just a script, it’s the product of a relationship that prevents harm, reduces duplication and quietly keeps hospital doors a little less busy.
ED: Dr Raman is the RACGP Vice President and WA Chair.


Declining rates of spirometry testing is posing a problem for COPD diagnosis and management, writes Rael Rivers, acting chief executive of Respiratory Care WA and Dr Li Ping Chung, Respiratory Consultant at Fiona Stanley Hospital.
We’re seeing fewer spirometry tests being done – and that’s a problem.
In 2024, Australia introduced the first Chronic Obstructive Pulmonary Disease (COPD) Clinical Care Standard which sets out best practice care for patients. A key component is the emphasis on spirometry as an essential diagnostic tool for assessing symptoms, disease severity and comorbidities.
Without spirometry, too many people are missing out on an accurate COPD diagnosis and the chance for early treatment that can significantly improve outcomes.
The reasons behind the decline are complex, but the way forward is clear: keep spirometry front and centre, equip GPs with the tools and pathways they need, and invest in proven models of care, such as Respiratory Care WA’s Respiratory Hubs.
Earlier this year, the Atlas Focus Report: COPD by the Australian Commission on Safety and Quality in Health Care, highlighted a troubling trend – a 31% drop in spirometry testing across Australia between 2015/16 and 2022/23. In WA the decline was sharper at 39%.
This decline is particularly concerning given that spirometry remains the only reliable way to definitively diagnose COPD. Without this essential test, patients face delayed or incorrect diagnosis, leading to worse health outcomes and reduced quality of life.
It is likely that several factors have contributed to the decline including:
• High equipment and maintenance costs for clinics

• Spirometry being resource intensive and time consuming
• Reduced prioritisation or awareness of spirometry in COPD diagnosis
• Limited access to trained and experienced clinicians and scientists capable of interpreting tests.
Interpreting spirometry results and developing tailored treatment plans demand years of experience and specialised training.
This expertise is crucial to ensuring accurate diagnosis and
effective, personalised care plans. Shortcutting this process risks misdiagnosis, unnecessary patient harm and further delays in receiving appropriate treatment.
While the health system, including general practice, is already under immense pressure, there are ways GPs can help ensure their patients with respiratory conditions such as COPD are on the right path. These include:
• Keep spirometry front-of-mind when assessing patients with persistent cough, breathlessness,
The Atlas Focus Report: COPD by the Australian Commission on Safety and Quality in Health Care, highlighted a troubling trend – a 31% drop in spirometry testing across Australia between 2015/16 and 2022/23. In WA the decline was sharper at 39%.

Restoring spirometry as a routine step in diagnosing at-risk patients will enable earlier intervention, improving quality of life, slowing disease progression, and reducing hospital admissions.
or smoking history
• Refer patients to accredited lung testing laboratories in the communities or specialised services that provide expert interpretation and access to high quality spirometry testing
• Engage in ongoing education on COPD diagnostic best practices and collaborate with organisations such as Respiratory Care WA or Lung Foundation Australia for advice and referrals
• Incorporate spirometry into annual health checks for high-risk groups including those with a history of smoking and exposure to air pollutants.
Early diagnosis is key
The decline in spirometry testing is leading to later stage COPD diagnosis, when the disease is
harder to manage, and quality of life is significantly impaired.
Restoring spirometry as a routine step in diagnosing at-risk patients will enable earlier intervention, improving quality of life, slowing disease progression, and reducing hospital admissions.
It will also prevent inappropriate use of inhalers for those without COPD or other airways disease. Unnecessary inhaler use not only poses health risks for patients but also contributes to environmental harm through increased greenhouse gas emissions.
To address the decline in spirometry testing and improve COPD outcomes, sustained and increased funding is critical along with policy change by government policy makers and leadership.
This should include targeted GP engagement and education campaigns; subsidised testing for patients who cannot afford it; and an expansion of mobile and outreach testing services to reach underserved areas.
The decline in spirometry testing poses a significant challenge to COPD diagnosis and management in Australia, but the solution is within reach.
By supporting GPs, backing proven service models and outreach programs, ensuring sustainable funding, and prioritising spirometry – ideally by advocating to government policymakers and leaders to make it mandatory –we can turn the tide and improve health outcomes for thousands of Australians living with COPD.
ED: Respiratory Care WA’s Respiratory Hubs are integrated hubs that combine lung function testing, specialist review and reporting, and education. They operate in Perth and the South West.
The rise of social media and blogs has resulted in some patients refusing conventional cancer treatments, raising new challenges for clinicians, writes Associate Professor Moira O’Connor from the Curtin School of Population Health.
In some cases, against medical advice, a person with cancer decides not to undergo conventional treatments such as chemotherapy, radiation therapy, hormone therapy, and others.
While estimates vary and do not account for silent withdrawals, up to a quarter of patients may decline treatment. Refusing evidencebased, conventional cancer treatments can pose significant risk to patients and is linked to rapid deterioration, poor prognosis, lower quality of life, and a substantially higher risk of premature death.
Treatment refusal also has implications for clinicians, due to the demands on time and resources needed to engage hesitant patients.
People refusing conventional treatments not only choose to overlook options for effective cancer care and management but may also opt to use non-evidencebased treatments, commonly referred to as ‘alternative therapies’, that have limited or no demonstrated benefits for managing cancer.
While the internet can be a tool to access valuable information when given a cancer diagnosis, it can also promote misinformation.
Alternative therapies represent a multibillion-dollar industry, and their products are aggressively promoted via the internet and without regulation.
Social media and blogs allow users to join groups of other people who share similar beliefs, resulting in the reinforcement of anti-science views.
Developing an understanding of the relationship between health


professionals and patients, where a therapeutic alliance is established, is seen as a key first step to creating new and effective approaches to increase conventional treatment uptake.
A recent survey aimed to explore oncology health professionals’ experiences and views on why patients refuse standard cancer treatments.
Four main themes were identified as follows:
1. I want to do it my way
2. Keeping the door open
3. It can be draining
4. Where to from here?
Exploring oncologists’ experiences of people refusing standard conventional treatments for cancer revealed multiple, complex motives.
These ranged from mistrust in medical authority, cultural beliefs, and the fear of toxicity from standard treatments. Decisions by patients appeared to be influenced by the lived experiences of others’ negative experiences.
Participants highlighted that it was essential to keep lines of communication open between clinicians and the patient, and that generally, but not always, a key focus was to keep the doors open to patients, including those who sought non-evidence-based treatments.
Even though participants reported that numbers were small, they recalled patients refusing treatment in great detail.
They reported experiencing an emotional and professional burden
Developing an understanding of the relationship between health professionals and patients, where a therapeutic alliance is established, is seen as a key first step to creating new and effective approaches to increase conventional treatment uptake.
Treatment refusal is not common, but it is deeply challenging. Treatment refusal after a cancer diagnosis creates a burden for people diagnosed including increased morbidity, premature death and, importantly, lower quality of life.
when patients refused conventional treatments, and mentioned time and effort taken to work with patients who were refusing or not adhering to prescribed standard treatments.
They also reported professional tensions, ethical considerations, and trying to accommodate patients’ wishes.
The final theme of the survey addressed the way forward. Recommendations included patient education on credible data, clinician training in engagement communication, and
targeted campaigns to counter misinformation.
Social media was mentioned and a quote from the study sums up the value of meeting people where they are.
“You need to meet the audience where they are and use some of the same hooks that get them in. Journal articles don’t get read but summarising systematic reviews and turning them into reels, which are the latest thing on Instagram that get a lot of eyes on them, it’s like a quick slideshow of four or five tiles that just say did you ever wonder about this?”
Advanced Oncoplastic Breast Surgery Thyroid Surgery
Cutting-Edge Breast Cancer Surgery Minimally Invasive Hernia Repair
Mr Saud Hamza
Specialising in:
Oncoplastic Breast Surgery including breast reconstruction and rotation flaps
Breast reduction and mastopexy (nipple lifting)

Removal of breast implants and mastopexy
Thyroid Surgery.
Practicing Location: Mandurah & Murdoch
Operating Locations:
St John of God Murdoch, Murdoch Peel Health Campus, Mandurah
Hollywood Private Hospital, Nedlands
The Mount Hospital, Perth
Email: info@saudhamza.com.au
Healthlink EDI: mrhamzas

Dr Wei Ling Ooi
Specialising in:
Oncoplastic Breast Surgery including breast reconstruction and rotation flaps
Breast reduction and mastopexy (nipple lifting)

Removal of breast implants and mastopexy.
Practicing Location: Murdoch
Operating Locations: St John of God Subiaco, Subiaco
Email: secretarydrooi@gmail.com
Healthlink EDI: wlingooi
Health professionals also face a burden of care. Equipping clinicians with practical skills to manage difficult conversations - and reaching patients with accurate information where they already seek advice can bridge the gap between evidence and choice.
ED: The author was involved in the study mentioned, alongside:
• Darren Haywood, Postdoctoral Research Fellow (Cancer Survivorship), UTS
• Nicolas Hart, Senior Researcher at UTS
• Tracey Williams, School of Population Health, Curtin University
• Jordan Joseph, School of Population Health, Curtin University
Dr Kai Hellberg
Specialising in:
Gallbladder Surgery
Hernia Surgery
Endoscopic Services with Gastroscopy & Colonoscopy

Haemorrhoid treatments and other benign procto-rectal conditions
Ingrown Nail Surgery
All Skin and Soft Tissue Procedures.
Practicing Location: Mandurah & Murdoch
Operating Locations:
St John of God Murdoch, Murdoch Peel Health Campus, Mandurah
Email: murdochrooms44@gmail.com
Healthlink EDI: hellberg
Postal Address | Suite 44, Level 2, Murdoch Clinic, 100 Murdoch Drive, Murdoch WA 6150 Appointment Bookings | Phone: (08) 6148 0540 Fax: 9332 9425
www.perthsurgeons.com.au
An advocate for men’s health, Dr Tom Shannon likes to set a good example for his patients and encourage self-care for the prevention of illness.
Urologist and prostate cancer surgeon Dr Tom Shannon aims to be in his patient’s lives for the shortest time possible.
“I love the fact that I can be important to a patient for a very short period of time. The goal is not to need me and to get on with their lives, free of cancer, which is such a privilege to be part of. Our team makes a difference,” he says.
Tom has been a urologist for more than 25 years, specialising in prostate cancer diagnosis and treatment. He still loves his profession as much today, if not more than when he started.
From a young age Tom knew he wanted to be a doctor, even though it wasn’t something that was in his family. Fascinated with the human body, he was drawn to books about how the body worked.
Tom was also very clear he was going to be a physician during medical school, but exposure to some great surgical bosses in early years changed his view. As a young intern at Hollywood Hospital he had his own theatre list, developing a love for surgery.
“Hollywood was a great place to be a junior doctor. I had a great boss who gave true one-on-one mentoring. I learnt so much. When I finished my internship, I just started studying for surgery. I was really interested in cardiothoracics but after a year realised it wasn’t for
A/Prof Shannon is a graduate of the University of WA. He completed his Fellowship in Urology in 1999 and completed post-fellowship training in the UK and the US focusing on minimally invasive surgery and prostate brachytherapy. He was a pioneer of minimally invasive urological surgery in WA and is a leader in the development of prostate MRI. He is a strong advocate for men’s health and has been a board member of the Prostate Cancer Foundation of Australia (WA) for over 10 years.
me. I was sent to do urology for a rotation and remember complaining loudly. I was given great advice –the only way to know if I liked it was to approach it like I would be doing that job every day for the rest of my career.
Among other accomplishments, in 2004 Tom operated in WA with the pioneering French surgeon Professor Claude Abbou for the first demonstration of a laparoscopic radical prostatectomy. To date, the urologist has cared for more than 10,000 men and performed more than 3,000 open, laparoscopic and robotic surgeries.
A big advocate of self-care and the prevention of illness, Tom actively advocates for men’s health and prostate cancer. He has been involved with the Prostate Cancer Foundation of Australia since inception and holds an adjunct associate professor role with Edith Cowan University in exercise medicine.
With around 26,400 cases diagnosed in 2024, prostate cancer is estimated to account for 28% of the cancers to be diagnosed in
males for the year. Because prostate cancer survival rates are high, Tom says it’s a rewarding field to be working in.
He says there’s still work to do to bring equality to early detection. There’s excellent data showing the benefits of Prostate-Specific Antigen (PSA) testing and new Australian guidelines advocate men start testing at 40 and at regular intervals after, depending on personal risk. Tom argues that we could achieve significant gains with simple, but uniform changes.
“The goal is to find significant cancers early and cure them. Cures are achieved by complete surgical resection, which is a challenge, because you get one chance to do it really well. There are minimal margins for the cancer. To cure and retain continence and sexual function, you must be precise. The trifecta is the goal. Cure avoids needing testosterone suppression, which can be devastating.”

The inherent assumption is that all presentations are the same, but they are not. Medicine has nuance and complexity and requires judgement. What matters is patient outcomes.
What can be measured will be measured, but that doesn’t make it useful. Ambulance ramping always makes headlines, especially in winter when another record is reached.
On July 31 ramping at WA hospitals reached 7009 hours.
St John WA describes ramping as: “Hospitals aim to receive all patients within 30 minutes of our arrival at the ED. If it takes longer than 30 minutes, this is referred to as ramping.”
On August 19 some 80 category two and category three elective surgeries were postponed across public hospitals in Perth due to unprecedented pressure on emergency departments. The AMA (WA) said the state’s public health system was facing a “full-blown emergency”.
As the party of government changes, so too does their view on ramping. When in opposition it is a crisis, as 1000 hours was described by then Shadow Minister for Health Roger Cook in 2016. Now in Government, the attitude seems to have changed.
Is tracking ramping a useful measure? Probably not.
Why is there a focus on 30 minutes, why not 15 or 60? Similarly, why does everyone arriving in an ED need to be seen in four hours? Some need immediate care while others could wait many hours with no ill effects. Some, arguably, don’t belong in an ED.
One-size-fits-all models are beloved by bureaucrats because they require no nuance and are easy to measure.
The inherent assumption is that all presentations are the same, but they are not. Medicine has nuance and complexity and requires judgement.
What matters is patient outcomes, but these have multiple inputs with some uncontrollable and not easily measured.
We can expect the same noises when the next record of 7500 hours is reached, but will this data change the system? Perhaps it’s time we change the measurements.

Sign up to our Wednesday clinical newsletter to get the latest updates from your local specialists.
Head to our website and click the subscribe button or scan the QR code
By Dr Scott Claxton, Respiratory Physician, Joondalup
Respiratory diseases are common and, although they may not seem overtly severe, can still impact the patient’s sleep.
This may be as a part of the disease, for example pulmonary fibrosis and nocturnal hypoxaemia; part of a sleep disorder such as COPD and obstructive sleep apnoea (OSA); or it may be sleeping disturbance as part of a chronic disease and mood disorders.
As part of improving the symptoms for any chronic disease, assessing what might happen at night in sleep can improve feelings of wellbeing and can improve disease outcomes. Assessing sleep in respiratory disease is more than just OSA, there can be many causes.
During sleep several changes take place that can alter respiratory function. Ventilatory drive reduces in sleep, more so in REM sleep compared with non-REM sleep.
Anything that further impacts on ventilation can make things worse. This includes upper and lower respiratory muscle function, which can also be impacted by an increased load (obesity).
The fluid shifts occurring normally when changing from upright to supine also impact on the upper airway size.
This can be more so in comorbid heart failure, which can also contribute to pulmonary congestion and reduced lung compliance.
Changes in airway function and size during sleep as well as changes in ambient air, such as temperature, may contribute to sleep disturbance, for example when asthma is not optimally controlled.
This can mean that anything that impairs breathing – airway narrowing (COPD), lung stiffness (ILD), chest wall compliance (obesity) – can make breathing worse, reducing oxygen and raising carbon dioxide.
Sleep is important for wellbeing, both physical and mental. Poor sleep can have a substantial negative impact on patients with chronic lung disease
In these patients, the impact on sleep may be part of the disease, be related to the treatments or be part of the psychological impact of poor health
Assessment is important and although management may be challenging, it may provide some positive benefits for patients.
As with any chronic disease, sleep can be impacted by poor mood, anxiety and depression. As with other chronic diseases, there are common co-morbidities with chronic respiratory disease.
Concerns regarding the impact of the disease on family, risks of exacerbations and illness, and hospitalisation are major contributors to poorer mood and impaired quality of life, especially in COPD.
The life shortening which results from lung disease such as ILD and COPD are also significant factors in poorer mental health.
Treatment side effects can negatively impact sleep.
Corticosteroid therapy either as short-term high dose or long-term can negatively impact mood and is associated with insomnia.
Long-term steroid therapy leading to osteoporosis and fracture can impact sleep due to pain.
Nocturnal oxygen therapy can lead to nasal symptoms with dryness and epistaxis, as well as discomfort form the delivery system – usually nasal cannula.
PAP therapy, if used thoughtfully and with good patient education, is often beneficial but can impact sleep quality if not properly set up.

Assessing sleep in patients with chronic respiratory disease initially can be done on history – how do they sleep, what issues do they have with sleep.
Disease specific questionnaires have sleep related questions, for example the COPD Assessment Test (CAT) and the Asthma Control Questionnaire (ACQ).
Sleep quality questionnaires, such as Epworth Sleepiness Score and Pittsburgh Sleep Quality Index, are more sleep specific and the DAS (Depression and Anxiety Scale) can be helpful in identifying mood changes in patients.
A sleep study may be beneficial, particularly if there is a consideration of OSA, hypoxaemia or hypoventilation in sleep. Whether a home or a lab sleep study is better may depend on the specific question, but the assessment of the study in the context of the patient is imperative, as is the discussion and supervision of any therapy.
Management of the other causes of poor sleep in this patient group, however, can be more challenging. Pharmacological management of insomnia is ideally only short term.
Psychological and behavioural strategies are better long-term options, but access to therapies like CBT-I can be difficult and cost can be a deterrent.
Medication to improve anxiety, help with sleep and manage pain can all have the potential issues of respiratory depression. Generally, careful supervision and starting with low doses is safe.
Informing the patient and family of what to look out for can avoid significant respiratory depression. Balancing the positive with the negative effects may bring about an acceptable positive response with tolerable side effects.
Author competing interests – nil
By Dr Peter Baumgartner, Anaesthetist, West Leederville
The list of conditions that could benefit from Glucagon-like Peptide 1 Receptor Agonists (GLP-1 RA) grows.
In June the Therapeutic Goods Administration (TGA) approved Tirzepatide as the first medical treatment for obstructive sleep apnoea (OSA). It has GLP-1 and glucose-dependent insulinotropic peptide activity (GIP).
Not surprisingly OSA is improved by weight loss, as 70% of OSA patients are overweight.
The indications for GLP-1 RA include morbid obesity, glycaemic control in Type 2 Diabetes Mellitus (T2DM), reducing cardiovascular events in T2DM, and reduction of renal deterioration in T2DM with chronic kidney disease.
Inclusion criteria suggest a BMI greater than 30, or a BMI of 27 with at least one weight related condition such as hypertension, hypercholesterolaemia or T2DM, and now presumably OSA.
Glucagon was found to increase blood glucose levels and incretins were first discovered in the 1970s. GLP-1, produced in the gut, was discovered in the 1980s. It can increase insulin release and activity.
Later its role in appetite regulation, slowing gastric emptying, and in glucose regulation was shown. When researchers discovered a GLP-1 like peptide, exendin-4 in Gila monster saliva, it led to the development of exenadine being the first drug approved in 2005 by the FDA for T2DM.
Other drugs such as liraglutide and semaglutide followed, with newer medications showing enhanced weight loss effects, eventually leading to the approval for obesity treatment.
GLP-1 receptors are found in multiple tissues including the hypothalamus and brainstem where stimulation leads to reduced food intake. Hepatic glucose production is reduced by activation of hindbrain receptors and autonomic nervous system influences lead to a modest
GLP-1 RA increases the risk of aspiration under anaesthesia and sedation
Ask specifically if the patient is taking a GLP-1 RA. Contact your treating team for a diabetic management plan, with monitoring of glucose levels
Withhold dose for a week and follow a liquid diet for 24 hours before procedure.
reduction in blood pressure and increases in heart rate. Pancreatic action results in increased insulin secretion and decreased glucagon secretion.
Several drugs are now available, mostly once weekly injectables, with oral versions recently approved. Offlabel use is widespread, and patients should be asked directly if they are taking them.
Side effects are common and may improve with time and dose adjustment. Gastrointestinal effects including nausea, vomiting, stomach pain, constipation and diarrhoea, heartburn and reflux are noted, however the absence of these does not guarantee an empty stomach.
The advice about how to manage GLP-1 RA in the preoperative period is not well known.
It could be said that the majority of GPs and surgeons are also in the dark about how best to advise patients when they are booked for a procedure under sedation or general anaesthesia.
The concern is an increased risk of regurgitation and aspiration when airway reflexes are obtunded in the presence of a stomach that does not empty in the usual way.
GLP-1 agonists slow gastric emptying and thus cause reduced hunger and calorie intake. The effect has been seen to last over four weeks, with patients noted to still have significant food and liquid residue at

gastroscopy despite fasting periods of six to eight hours being observed.
Guidelines on the management of GLP-1 RA and surgery have been produced by different organisations, with concerns specific to each specialty and disagreement about the best way to manage these medications.
Many anaesthetists believe that a compromise of withholding the injection for one week has a low risk to patient management while allowing gastric emptying to improve.
The use of a pre-operative 24-hour liquid diet is recommended widely. ANZCA has produced the following guideline relating to GLP-1RAs and GLP-1/GIPRAs in cases requiring sedation or anaesthesia including endoscopy.
“All patients should be asked about the use of GLP-1RAs and GLP-1/ GIPRAs and be involved in discussion and planning regarding aspiration risk.”
Elective pre-procedural cessation of GLP-1RAs and GLP-1/GIPRAs is not recommended. It risks hyperglycaemia in people with diabetes and may compromise weight control in patients who are taking GLP-1RAs and GLP-1/GIPRAs for this indication.
Patients should be asked about the use of other medications and medical conditions which may exacerbate gastrointestinal symptoms and delay gastric emptying, for example bowel dysmotility, gastroparesis, and Parkinson’s disease.
Pre-procedural diet modification with 24-hour clear fluid diet, followed by standard six-hour fasting, should be recommended
Risk mitigation options should be undertaken for those who have not withheld solids for 24 hours. These include detection of residual gastric contents, prokinetic agents, modification of anaesthesia technique, or deferral of procedure.
Author competing interests – nil.
By Prof Desiree Silva , Director of Research, Joondalup
Childhood asthma accounts for 43% of asthma hospitalisations and remains the leading cause of total disease burden in children aged between one and nine years.
An estimated $1.192 billion was spent on the treatment and management of asthma in 2022 and 2023. But what if we could pinpoint the children who are on the genetic pathway to develop asthma, before the wheeze and hospital visits, and intervene early enough to change that trajectory?
This is the ambitious goal of AERIAL, a sub-project within ORIGINS, Australia's largest longitudinal birth cohort study of its kind.
AERIAL is investigating one of the most compelling theories in asthma research: that there are gene signature patterns associated with the development of wheeze and asthma later in childhood.
The hope is to identify these patterns, alert parents that their child is on a pathway to developing asthma, and provide an interventional treatment plan to halt its progression, ultimately reducing asthma diagnoses.


The focus of this study to date has centred around epithelial cells, which line the airways in the nose and lungs. When working correctly, these cells act as a tight, strong, and efficient barrier to protect the lungs from toxins.
However, in children with asthma, epithelial cells cannot form a tight barrier and behave differently to viral
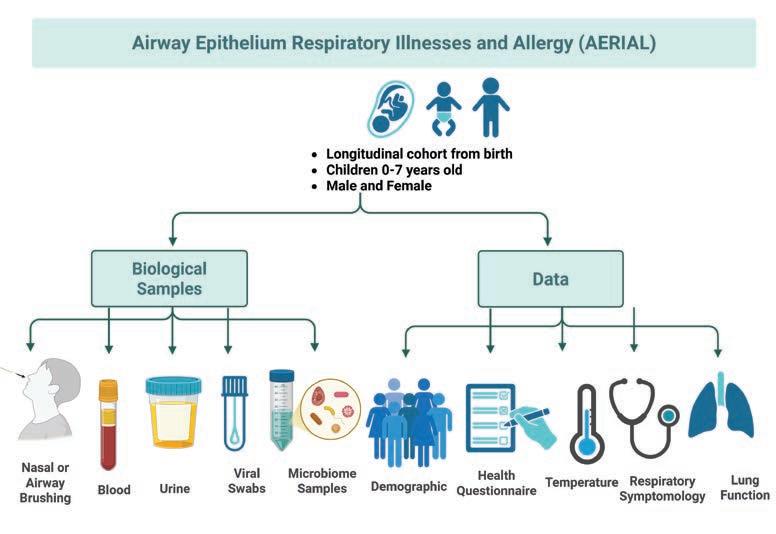
infections, making the lungs more vulnerable.
AERIAL recruited 460 mothers who birthed at Joondalup Health Campus, where a nasal swab was taken from their newborns at birth, alongside other samples like the placenta, meconium and colostrum, which make up over 400,000 samples in the ORIGINS Biobank.
During the first year of life, AERIAL participants were asked to use a mobile app to record their baby’s temperature and symptoms associated with viral infections, like a runny nose or cough.
If required, parents would take a nose swab from their child to identify the type of infection, to determine the number and type of viral infections, and how this may leave a ‘fingerprint’ on the epithelial cell gene signatures.
Alongside continued nasal swabs, children aged three to seven undergo a lung function test using oscillometry rather than spirometry, which typically requires strong forceful breathing alongside specific timing instructions that can be difficult for small children.
Oscillometry is a simple gentle test which asks the child to breathe normally into a mouthpiece for
AERIAL is investigating whether there are gene signature patterns associated with the development of wheeze and asthma later in childhood
There are significant implications for public health and awareness campaigns if asthma’s genesis is in the antenatal period is confirmed
If at-risk children can be identified earlier, we can work to drastically reduce the rate of lung damage in children and improve respiratory health outcomes during their lifetime.
around 30 seconds. It has been shown to be both feasible and effective in detecting poor lung health in children.
By assessing lung health through oscillometry, we can begin to correlate the results with the unique genetic signatures found in their epithelial cells, to see if there are any indicators in the children who have developed, or are on track, to develop asthma.
Our ultimate goal is to develop a simple RAT like swab test that could flag children at higher risk of developing asthma.
With early identification, families could be provided with an interventional action plan outlining proactive steps to reduce asthma risk as the child grows.
This might include staying up to date with vaccinations, limiting exposure to respiratory infections through adapting daycare routines, initiating timely antibiotic treatment, and potentially even using targeted preventative therapies developed for children on the pathway to asthma.
Early identification of at-risk children could reduce the rate of lung damage in children and improve lifelong respiratory health outcomes, as well as lighten the physical, mental and financial strain on families with children living with the condition.
It is hoped that the sub-project can be further expanded to begin analysing participating mother’s amniotic membranes to see if they share the same genetic signature as
their child’s epithelial cells. This would indicate that exposures during pregnancy may have a ‘fingerprint’ that could lead to a child developing asthma in their early years.
If we can confirm asthma’s genesis is in the antenatal period and can pin down the specific exposure risks, the implication for public health campaigning and advice to pregnant women and their partners could be enormously significant.
For the children participating in the AERIAL study, this isn’t just research, this is a potential turning point in their health journey, particularly if they receive an asthma diagnosis.
For researchers, clinicians, and families around the world, it’s a glimpse into a future where asthma could be identified and tackled before it even starts.
Author competing interest - the author is involved with the AERIAL research
ED: ORIGINS is a collaboration between Joondalup Health Campus and The Kids Research Institute Australia. AERIAL is one of 60 sub-projects and is run in collaboration with the Wal-yan Respiratory Research Centre.







By Dr Sumit Mehra , Respiratory & Sleep Physician, Dr Alice Culliford, Respiratory Registrar & Dr Mabel Gaastra , Medical Registrar, Joondalup
There is a wide differential for acute eosinophilia in association with respiratory symptoms, most commonly asthma, vasculitis and eosinophilic pneumonias.
However unusual infectious causes, particularly parasites, should be considered, especially where a relevant history of travel is present.
Interestingly, Type 2 inflammation, involving eosinophils and driving conditions such as asthma, eczema, chronic rhinosinusitis, eosinophilic esophagitis and food allergies, originally evolved to combat parasitic worms.
Loeffler’s syndrome
This is a transient respiratory illness characterised by lung inflammation and pulmonary and peripheral eosinophilia.
It results from larval migration through the lungs, where parasite invasion into the alveolar space triggers an eosinophilic response. Ascaris lumbricoides (Ascariasis) and Strongyloides stercoralis (Strongyloidiasis) are common causes.
Ascariasis is more prevalent in areas with poor sanitation and is acquired through ingestion of contaminated food or water. Respiratory symptoms such as cough and wheeze precede gastrointestinal symptoms as the parasites migrate to the gut.
Migratory infiltrates on chest X-ray, marked peripheral eosinophilia, clinical presentation, and exposure history support diagnosis. Larvae may appear in sputum, but eggs are more often detected in stool. Treatment includes albendazole or mebendazole.
Strongyloidiasis is endemic in tropical and subtropical regions, including Australia’s Northern Territory. It typically follows skin contact with contaminated soil, especially in those walking barefoot.
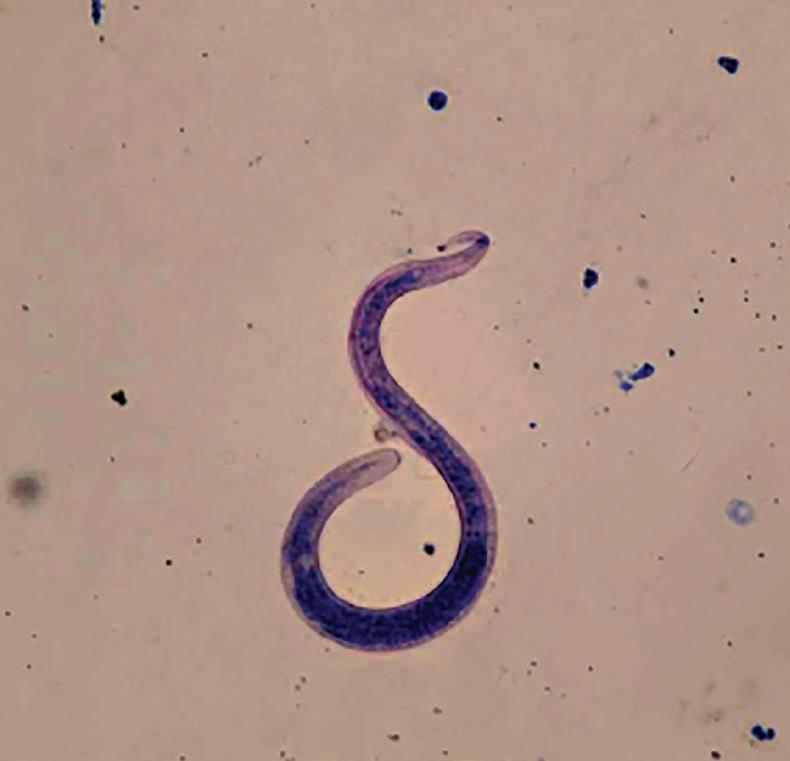
Immunocompromised patients, particularly those on steroids, are at risk of life-threatening hyperinfection.
Clinical signs include GI symptoms, urticarial rash, and respiratory symptoms during larval lung migration. Imaging shows patchy, migratory infiltrates, and eosinophilia is common.
Unlike other helminths, S.stercoralis can complete its life cycle within humans, leading to false-negative stool tests. Ivermectin is the firstline treatment.
Pulmonary visceral larva migrans is a parasitic condition caused
by migrating Toxocara canis or Toxocara cati larvae, typically acquired through ingestion of eggs from soil contaminated with dog or cat faeces.
It primarily affects children and immunocompromised individuals in areas with poor sanitation and pet exposure.
After ingestion, larvae penetrate the intestinal wall and migrate via the bloodstream to visceral organs such as the lungs, liver, and eyes.
As Toxocara invades these organs, it triggers intense eosinophilia and leucocytosis, resulting in a granulomatous response. Patients may develop fever and respiratory
Parasitic infections are important causes of eosinophilic lung disease, particularly in those with relevant travel or exposure history
Symptoms can be non-specific and require prompt targeted treatment to avoid chronic disease, so consideration of specific investigations is worthwhile
ABPA is an important nonparasitic cause seen in asthma.
symptoms like dry cough, wheeze, and dyspnoea.
In children, hepatomegaly and fatigue are common. Marked eosinophilia and elevated IgE result from a T-cell response to a parasitic protein.
Diagnosis is supported by clinical features, positive Toxocara IgG serology, and chest X-ray findings such as ground-glass opacities and patchy infiltrates.
As with Loeffler’s syndrome, treatment targets the parasitic infection, with supportive care as needed for vulnerable groups. Prognosis is excellent with treatment, though chronic infection and inflammation may cause pulmonary fibrosis.
Schistosomiasis
Caused by the trematode Schistosoma, it is endemic to tropical regions such as Japan, the Philippines, China, Indonesia, Africa, and Latin America. The lungs can be affected in both acute and chronic stages.
In acute schistosomiasis (AS), respiratory symptoms like dyspnoea and cough result from immunoallergic reactions to parasite eggs in the lungs, often appearing on CT as nodular lesions.
Eosinophilia occurs in 75% of AS cases within weeks, reflecting the acute immune response.
In chronic schistosomiasis (CS), eggs in the pulmonary vasculature trigger granulomatous inflammation that may progress to fibrosis. While serum eosinophilia is less common in CS, granulomas show high eosinophil concentrations.
Diagnosis is confirmed by
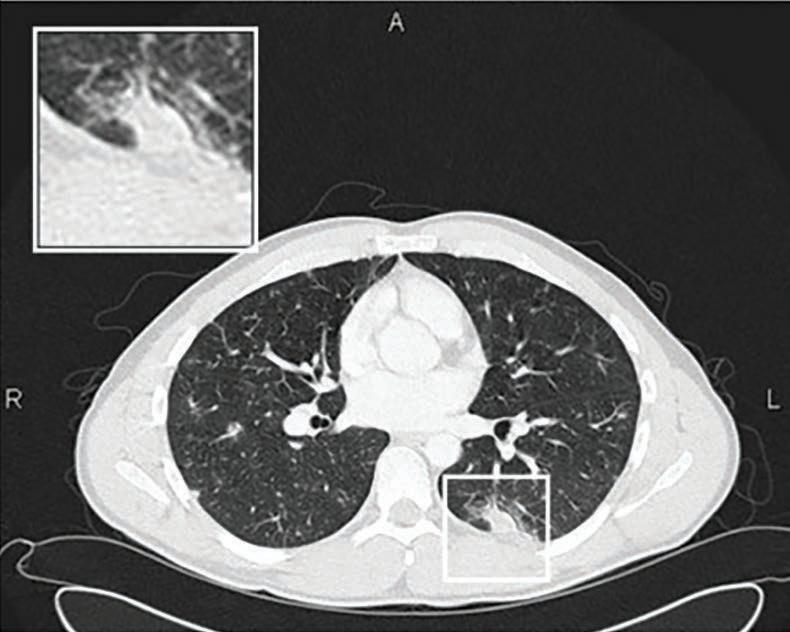
CT Chest showing ground-glass nodules and subpleural consolidation of the left lung consistent with eosinophilic infiltration in acute pulmonary schistosomiasis
microscopic detection of eggs in stool or respiratory samples. If eggs are absent, AS can be diagnosed clinically based on symptoms, eosinophilia, and relevant travel history.
Treatment is a single dose of praziquantel, which usually offers a complete cure.
Allergic Bronchopulmonary Aspergillosis
Aspergillus fumigatus is the primary non-parasitic cause of infectious eosinophilia in the lung.
Allergic Bronchopulmonary
Aspergillosis (ABPA) is a hypersensitivity reaction to airway colonisation by Aspergillus fungus and is nearly exclusively seen in patients with asthma or cystic fibrosis.
Presentation is with recurrent asthma exacerbations, often with mucus expectoration. Blood eosinophilia (>500 cells/uL) is characteristic, in addition to raised total serum IgE level.
Specific IgE and IgG to Aspergillus confirms the diagnosis, and sputum often cultures Aspergillus fungus.
HRCT is the gold standard imaging choice, showing fleeting opacities bronchiectasis (which is usually central and involving upper and middle lobes) plus findings
related to mucus impaction and bronchiolar obstruction.
Other manifestations include centrilobular nodules, ground glass changes, peripheral consolidation and gas trapping.
Acute ABPA is traditionally managed with a tapering course of oral steroids. Azole antifungals may be used as steroid-sparing agents, though relapse after cessation is common.
Emerging smaller studies suggest a possible role for asthma biologics in patients with recurrent ABPA exacerbations or inability to taper off oral glucocorticoids, though long-term studies on efficacy and safety are pending.
Author competing interests – nil
Advert removed in compliance with Medicines Australia's Code of Conduct and the Therapeutic Goods Administration's Therapeutic Goods Act.
https://medicinesaustralia.com.au/code-of-conduct/about-the-code/ https://www.tga.gov.au/legislation-legislative-instruments

By A/Prof Kaushalendra Rathore, Cardiothoracic Surgeon,
Primary lung cancer accounts for 18-20% of cancer-related deaths annually.
Early diagnosis of small tumours, followed by multidisciplinary management, has been shown to improve five-year survival rates.
Tumour size and volume, particularly in solid or sub-solid pulmonary nodules (SSPN) and ground glass opacities (GGO), are key predictors of overall and cancer-free survival at any pathological stage.
The National Lung Cancer Screening Program (NLCSP), which launched in July, was established based on findings from the National Lung Screening Trial (NLST) in the United States. The NLST demonstrated a 20% improvement in cancer related mortality and these findings were further reinforced by other trials.
However, thoracic surgery training in Australia remains integrated with cardiac surgery fellowship programs, leading to a relative shortage of dedicated minimally invasive thoracic surgeons.
The introduction of the NLCSP is expected to increase the volume of surgical and surveillance cases, exacerbating this deficit further.
Firstly, there will be a rise in younger, asymptomatic patients with earlystage (IA, IB) lung cancer. Secondly, there will be an initial increase in newly diagnosed locally advanced (IIB-IIIA) tumours during the initial years of screening.
Both scenarios require highly skilled thoracic surgeons capable of performing lung-sparing surgeries for early-stage cases like complex wedge resections and segmentectomies for SSPN or GGO, and handling intricate locally advanced tumours following neoadjuvant chemo-immunotherapy in a multimodal approach.
Recent studies advocate for lungsparing surgeries in early-stage screening positive tumours (T1aN0, <2 cm diameter, node-negative) due to comparable five-year disease-free
Primary lung cancer accounts for around one in five cancer deaths in Australia
The new Lung Cancer Screening Program has potential to improve this by earlier detection
There remains significant inequity between services in rural and metropolitan areas.
survival rates between sublobar and lobar resections.
Surgical margin and tumour characteristics significantly impact recurrence rates. Studies indicate that a surgical margin of under 10mm and tumour margin distance to solid-component-size ratio below one correlate with higher locoregional recurrence rates, reinforcing the necessity of specialised thoracic surgeons for precise surgical decision-making.
Australia's healthcare distribution is highly uneven, with 29% of the population residing in rural and remote areas where lung cancer outcomes are notably poorer.
Lung adenocarcinoma is more prevalent than squamous cell carcinoma, and 75% of cases are operated on in stages I and II, with most surgeries occurring within a fortnight of referral.
A major barrier to equitable care is the unequal distribution of dedicated thoracic surgeons and specialised

units. Additionally, essential services like radiotherapy, stereotactic ablative body radiotherapy (SABR), and chemotherapy centres must be accessible to all regions.
Delayed lung cancer diagnosis is a significant contributor to poor survival rates, particularly in cases involving larger nodules with high VDT.
Other prognostic factors include histological patterns, molecular features, SSPN type (pure GGO vs heterogeneous nodules), smoking status, previous lung cancer history, and nodule size (>10mm).
Maintaining engagement among high-risk individuals remains challenging due to variable tumour growth rates, which are influenced by age, gender, smoking history, tumour type, stage, histology, remoteness of living and genetic mutations.
The incidence of GGOs in the general population is 1-1.7%, with 29% of pure GGOs progressing to part-solid cancerous nodules.
Long-term lung cancer screening presents challenges such as physical and psychological consequences, cumulative radiation exposure, overdiagnosis, overtreatment, costeffectiveness issues, and incidental findings, such as coronary artery calcification and other malignancies.
Current NLCSP eligibility criteria focus primarily on age and smoking history, potentially overlooking highrisk individuals with occupational exposure such as asbestos, family history, prior cancers, or underlying lung diseases including emphysema and pulmonary fibrosis.
Despite the challenges associated in implementing the NLCSP, ongoing research will refine screening protocols. Incorporating additional variables to improve risk stratification, alongside improved healthcare infrastructure, will ensure optimum patient outcomes.
Author competing interests – nil
By Dr Kriti Sharma, Paediatric Surgical Registrar, & Mr Sanjay Sharma, Cardiothoracic Surgeon
Pulmonary lobectomy has been the mainstay of treatment for early-stage lung cancer, but videoassisted thoroscopic surgery (VATS) has essentially replaced open thoracotomy for smaller tumours.
This is due to lower amounts a pain, a shorter length of stay, lower bleeding/transfusion rates, and less air leak with equivalent oncological outcomes.
Rates of 90% five-year survival can be achieved with early-stage lesions. More recently roboticassisted thoracic surgery (RATS) has been used for lung resection.
With the commencement of the National Lung Cancer Screening Program from July this year, there will be increased requirement for surgical resection.
The hope is to find patients with lower stage lung cancer in highrisk smoking cohorts and to improve survival rates with more surgical intervention. RATS is slowly becoming more available to patients in Perth with increased access to the Da Vinci Robot.

The migration from open surgery to VATS required radical changes in surgeon perceptions, strategies and surgical skills – including loss of precision due to lack of wristed instruments – resulting in a slow adoption of the technique.
In contrast, the learning curve from


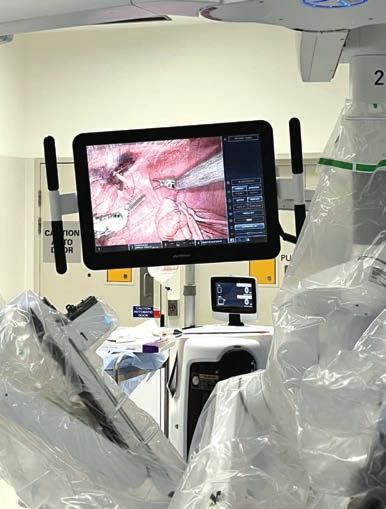
VATS to robotic surgical lobectomy has been exponentially quicker with some studies reporting 2030 procedures being sufficient to achieve proficiency for surgeons who are expert in VATS.
A multitude of retrospective studies demonstrate that robotic techniques result in fewer pulmonary complications, shorter length of hospital stay, shorter chest tube duration and quicker recovery than VATS. Others describe, at the very least, noninferiority of robotic lobectomy when compared with VATS, with no significant difference in operative time, blood loss, or overall complications.
With long-term outcomes only recently maturing, robotic surgery is showing excellent and equivalent cancer survival and recurrence rates when compared to VATS.
Despite the potential advantages of robotic surgery, opponents of this newer surgical approach cite major barriers, namely higher cost, lack of access and lack of high-quality prospective data.
The ability to sit and adjust the robot consul allows for better
With the introduction of the Lung Cancer Screening Program, increased surgical resection will be required
RATS lung resection offers advantages over VATS – including better visualisation, ergonomics, less pain and bleeding, and shorter length of hospital stays.
surgical ergonomics. This has the potential to extend the surgeon’s career.
The surgeon has magnified 3D imaging allowing for extraordinary accuracy and precision. Wristed instruments improve dexterity that leads to greater lymph node harvesting, which improves staging and potentially oncological outcome.
Robotics also allows for sublobar resection leading to lung conserving resection.
No prospective studies have yet been published, however data collection is currently underway for the ‘RAVAL’ trial, the first
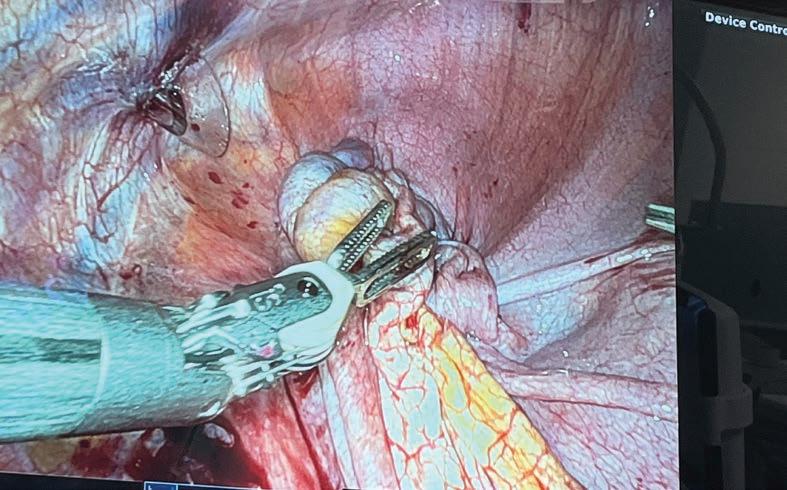
prospective randomised controlled trial comparing VATS and RATS assisted lobectomy for early-stage lung cancer, with research protocol published in 2022.
Overall, RATS offers many surgical advantages over VATS, including superior visualisation, enhanced dexterity, and potentially faster recovery times with equivalent oncological outcomes to VATS.
Further robust prospective research is underway in this exciting field to further characterise the benefits of robotic lobectomy over VATS and its long-term oncological outcomes.
Author competing interests – nil
Dr Guru O is a highly trained Oral Medicine Specialist bringing a wealth of experience from both Australia and overseas. With a career built on compassion, precision, and academic excellence, Dr Guru specialises in: Orofacial Pain Temporo-mandibular Disorders (TMD) Dental management of obstructive sleep apnoea Oral mucosal diseases
Perth Orofacial Pain and TMJ Clinic is a well-known specialist practice focusing on the diagnosis and management of complex oral and facial pain conditions. We work collaboratively with medical, dental and other health care professionals across disciplines to deliver integrated care for patients with persistent pain and jaw dysfunction.
Dr Guru O graduated from the University of Adelaide with a Bachelor of Dental Surgery in 2012. He gained valuable experience in Singapore before completing a Masters in Orofacial Pain at the University of Sydney and his Doctor of




Clinical Dentistry in Oral Medicine at the University of Western Australia. He has gained experience in multiple hospital departments including pain medicine, immunology, dermatology, rheumatology, and sleep medicine, and continues to publish in peer-reviewed journals and book chapters.
We are delighted to welcome Dr Guru to our clinic at St John of God Hospital, Subiaco. His commitment to education and excellence in delivering evidence-based, patient-centred care makes him a valued member of our team.
St John of God Hospital – Subiaco Clinic Suite 319, 25 McCourt Street Subiaco, WA 6008
Phone: (08) 9382 1200 Fax: (08) 9382 1211 Email: info@orofacialpain.com.au www.orofacialpain.com.au
By Prof Phil Thompson, Respiratory Physician, Nedlands
Airway diseases including asthma, chronic bronchitis, bronchiectasis and rhinosinusitis are complex.
They have a variety of subsets, can co-exist, and are often confused with each other, creating challenges for patients and doctors alike.
This has encouraged a treatment paradigm focussing on treating key pathological features of a patient’s disease. The evolution of monoclonal antibodies targeting specific mediators and impacting cell function have encouraged this.
An increased understanding of biological pathways, thereby informing therapeutic choices, has supported this.
In airway diseases this has led to treatments targeting airway epithelial driven pro-inflammatory pathways that cause proliferation, migration and activation of
Monoclonal antibody therapies are a major step forward in treating severe brittle and/or oral steroid dependent asthma
Clinical features, eosinophil counts, exhaled nitric oxide, together with standard lung function, IgE and allergen testing are useful monitoring and decision-making tools for management
More therapies are on the immediate horizon that will broaden treatment options for severe and difficult asthma.
eosinophils and/or neutrophils.
At the epithelial surface allergic (IgE mediated), non-allergic eosinophilic pathways and non-








allergic neutrophilic pathways can be triggered. These three pathways are activated by alarmins/defensins (TSLP, IL25 & IL33) that sit at the epithelial surface.
These in turn trigger cascades of cell activation and associated cytokine production which includes IL4 and IL13 and downstream IL5. Collectively these cause mast cell activation, mucus production, airway reactivity, nitric oxide (NO) production, enhanced B cell switching to generate IgE and eosinophil proliferation.
Monoclonal antibody treatments
The anti-IgE monoclonal antibody Omalizumab was developed in 1993 gaining FDA registration in 2003. Being an early monoclonal, it was not perfect, with complex dosing schedules, an inability to measure
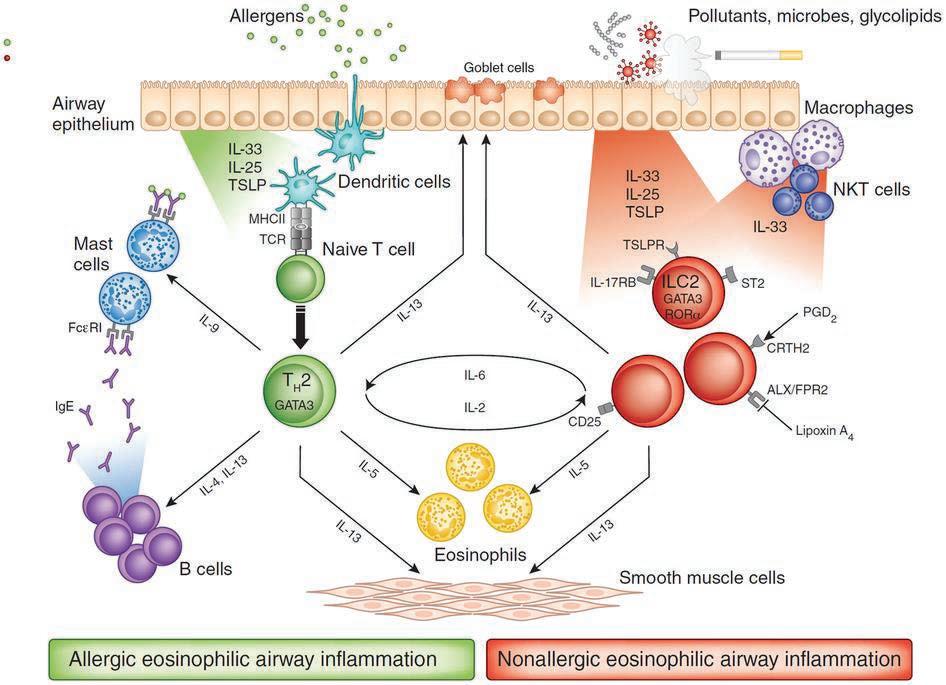

IgE on treatment and periodic drug induced anaphylaxis.
Nevertheless it is used therapeutically for asthma (IgE mediated), chronic rhinosinusitis and polyps, chronic urticaria and food allergy. Increasing evidence suggests limiting mast cell activation underpins its clinical benefit.
A biosimilar was approved in Europe and the USA (2024/25) and its impact on clinical practice and cost is yet to be seen.
Anti-Interleukin 5 (Anti-IL5) (mepolizumab 4 weekly), Anti-IL5 receptor (benralizumab 8 weekly) were approved for Australian use in 2016/17 by the TGA and have significantly impacted on the management of severe asthma, which is often eosinophilic and oral steroid dependent.
Anti-IL5 therapy reduces steroid dependence and improves clinical outcomes. Their side effect profiles are minimal, highlighting the specificity monoclonals provide and the relatively redundant role of eosinophils in human biology.
Eosinophil counts are a predictor of treatment response but not all eosinophilic asthma patients respond effectively to Anti-IL5 therapies. This might reflect patient selection but if persistently elevated exhaled (Ex) NO and symptoms occurs, review is warranted.
Anti IL4/IL13 -Dupilumab can knock out both IL4 & IL13 by targeting a common subunit resulting in many actions, including inhibiting the production of ExNO. As such, ExNO is a useful biomarker for likely response and outcome assessment.
Dupilumab is also extremely effective in treating eczema and rhinosinusitis/nasal polyps as well as asthma. In some patients eosinophil

FeNO patterns post anti-TH2

counts may rise dramatically suggesting deterioration, but the cells are not active.
In patients with significant eczema there is a risk of self-limiting but severe conjunctivitis. Dupilumab is a subcutaneous injection given fortnightly. In patients with mixed disease (asthma & rhinosinusitis and/or eczema) there is an obvious therapeutic appeal.

Prednisolone 7.5mg

Prednisolone 7.5mg



Similarly, patients with high or resistant ExNO production are likely to respond to Dupilumab.
Tezepelumab inhibits TSLP and so inhibits the three key pro-asthma pathways located in the airway epithelium. It can achieve the same outcomes as the other biologics but potentially more so.
It is four weekly dosing and is registered in Australia, but is not currently on the PBS
anti TH2 therapy

FeNO patterns post anti TH2 therapy


Mepolizumab started Dec 2016 98ppb 11ppb


Immediate good control & fall in FeNO
Immediate good control & fall in FeNO
Mrs WK PRN Prednisolone


Mrs WK PRN Prednisolone

Mrs WK PRN Prednisolone

Started Dupilumab May 24



Mr TB Pred 15mg

High FeNo; given Dupilumab, now clinically normal & FeNO has fallen significantly 150ppb 24ppb


Started Dupilumab May 24
High FeNo; given Dupilumab, now clinically normal & FeNO has fallen significantly 150ppb 24ppb


Mr TB Pred 15mg

Started Benra May2020
Inhibiting pathways at, or near, the point of origin is appealing but comes with greater risk of side effects. However, to date this has not been the case.

The above represent a major turning-point in managing severe airways disease. However, the field is not standing still.
Clinical trials (SWIFT & ANCHOR) assessing a six-monthly equivalent of Mepolizumab (Depemokimab) have led to registration applications in Europe and USA.
Early phase trials of an anti IL33 (Itepekimab) have been encouraging, as have assessments of an Ox-40 ligand inhibitor (Amlitelimab) that inhibits immune cell stimulation.
Nanobodies targeting both TSLP & IL13 (Lunsekimig) are at an early
High FeNo; given Dupilumab, now clinically normal & FeNO has fallen significantly 150ppb
Mr TB Pred 15mg
310ppb


310ppb

Started Dupilumab May 24
310ppb
Started Benra May2020 Started May 24

Started Benra May2020


88ppb


88ppb
Started Dupilumab May 24

Rising FeNo with Benralizumzb Some control. Much better on Dupilumab



Rising FeNo with Benralizumzb Some control. Much better on Dupilumab


Rising FeNo with Benralizumzb Some control. Much better on Dupilumab


Figure 2: Nitric oxide measurements on three patients with difficult to control asthma and different outcomes with respect to biologic therapy. Normal ExNO is <25ppb, 25-50ppb limited control without symptoms, >50ppb poor control and symptomatic
phase of clinical assessment. Oral agents targeting IL4/IL3 via STAT 6 degradation are in clinical trials in asthma and eczema.
Studies of a biosimilar for Mepolizumab (Bio-Thera:BAT2606) are underway.
If eosinophils are consistently raised in difficult to control asthma pursue one of the Anti-IL5 therapies. If, despite this, their disease is still brittle and ExNO has not been significantly reduced, trial Dupilumab.
If there are multiple disease manifestations (nasal polyps/ rhinosinusitis and/or eczema) consider Dupilumab or Mepolizumab, depending upon current PBS regulations.
Author competing interests – nil Mepolizumab started Dec 2016 98ppb
By A/Prof George Sim , Paediatric ENT Surgeon, Murdoch
Childhood upper respiratory tract infections (URTIs), especially common over the winter months, include colds, croup, bronchiolitis and pneumonia.
These infections are often viral in origin and self-limiting with supporting measures like analgesia, adequate fluid rehydration and rest. We reduce the spread of respiratory infections by handwashing, covering coughs and sneezes, face masks, limiting contact when sick and vaccinations.
However, some children will develop ENT related infections like ear infections, chronic nasal congestion and sore throats/tonsillitis. Chronic or recurrent ENT infections will affect the health of these children and their quality of life, such as missing time at school, frequent GP visits and antibiotics.
Otitis media (OM) can often arise in children who are frequently sick with upper respiratory issues. OM is one of the most common reasons why younger children present to GPs.
Approximately 75% of children have at least one episode of OM by school age. OM can be acute otitis media (AOM) or otitis media with effusion (OME).
AOM causes pain, fever, irritability and occasionally perforation. Initial management is symptomatic relief with analgesia and an oral antibiotic may be required if symptoms persist.
Symptoms may take one to two weeks to resolve. Recurring middle ear infections of three episodes or more in six months may warrant further assessment.
OME or ‘glue ear’ is accumulation of middle ear fluid. The fluid can be thick, hence the term glue ear. Children with glue ears have less obvious symptoms compared to AOM. Hearing loss, speech delay, learning difficulties at school and imbalance can be associated with the condition.
They may also cause mild earaches that can keep the child awake. Some


younger children will pull or poke at their ears frequently as a result.
Predisposing factors include daycare attendance, frequent URTIs, exposure to cigarette smoke, bottle feeding and use of pacifiers.
Very often the care of a paediatric ear, nose and throat surgeon will be involved in children with recurrent middle ear infections. A hearing test, including an audiology and tympanometry, is usually part of the ENT assessment.
Surgery such as grommet insertion and/or adenoidectomy may be recommended.
Sore throats can be viral or bacterial in origin. Treatment starts with symptomatic relief with analgesia, adequate fluid rehydration and rest.
Sometimes bacteria tonsillitis occurs and needs antibiotic treatment. Symptoms of tonsillitis can include sore throat, difficulty swallowing, halitosis, fever and cervical
Up to 75% of children will have otitis media by school age
Sinusitis is uncommon in children
Obstructive sleep apnoea in children is usually due to enlarged adenoids/tonsils. Surgery is often required.
lymphadenopathy. If a child has recurrent tonsillitis, there are guidelines as to the frequency of tonsillitis to warrant an ENT referral.
There should also be considerations for other factors such as frequency of antibiotics, time off school and time taken off work by parents to look after their child.
Our GPs are generally an expert in ENT issues in children. However, for some children who are chronically unwell or going through frequent cycles of illnesses, a paediatric ENT assessment may be considered in

linings causing rhinitis. This often has an allergy component as well (allergic rhinitis).
Sinusitis is not common in younger children as their sinuses are usually not fully developed. Symptoms of sinusitis may include nasal congestion, discoloured nasal discharge, pyrexia, postnasal drip/ cough and pain in the facial/cheek areas.
Children with allergies and large adenoids may be more prone to sinusitis. Treatment includes analgesia, saline nasal sprays/ flushes, antibiotics and possibly surgery.
Children with enlarged adenoid and/or tonsils can frequently be nasally congested with a runny nose, postnasal drip and cough. These children appear sick all the time and may have associated obstructive sleep symptoms.
Obstructive sleep disorder (OSD) is a range of presenting symptoms from heavy breathing/snoring to sleep apnoea. Symptoms include mouth breathing, sleeping in unusual
positions, nightmares/night terrors, bedwetting, waking up tired and also daytime issues with behaviour or concentration.
Some children can have difficulty with swallowing certain foods. The presenting symptoms vary according to the severity and also age of presentation. OSD symptoms are very often made worse in children with frequent URTIs.
Enlarged tonsils and/or adenoids are usually the main causes of OSD in children.
A comprehensive history to explore symptoms with parents and a detailed examination usually suffices for diagnosis. Treatment for OSD often results in surgical intervention.
Author competing interests – nil
Paediatric ENT considerations
GLP-1 RA and aspiration risk
Unusual infectious causes of pulmonary eosinophilia
Predicting childhood asthma
New treatments for airway disease
Robotic assisted lung surgery
Managing refusal of cancer treatment
Respiratory care gaps
Smoking prevention
Sleep and respiratory disease
Managing childhood leukemia
Aortic Stenosis in low risk patients
Spirometry testing
A patient is looking out of a hospital window where a forensic team are working, word on the ward is it’s the body of a doctor.
Perth author Karen Herbert’s latest book looks at a crime through the eyes of a character with cystic fibrosis.
A conversation with an old friend led author Karen Herbert to explore how to portray a main character with cystic fibrosis.
In her new novel The Ghost Walk, Ruby Rose Gillespie is also a lung transplant recipient whose surgeon is found dead. Dr Gabriel Beaufort and Ruby were secret lovers and she’s determined to find out what happened, digging back into their shared history and starting to wonder if she ever really knew him at all.
The Perth author’s fourth novel crosses genres with elements of a medical drama, suspense and romance. There’s also a fun level of detail of 80s and 90s suburban Australian nostalgia.
What might be most interesting however is that Karen’s childhood friend Jo Giles was the inspiration for Ruby.
Jo is a Perth writer and the 2024 Australian Poetry Slam Champion, who also lives with CF and litany of other issues, which she lists in her winning poem. The pair met in Narrogin when they were kids and have stayed in touch over the years.
“Jo also has an academic interest in the representation of people with disabilities,” said Karen. “She gave me some points to think about and
By Ara Jansen

how a person with CF would do particular things.”
Their conversations led Karen to draw a character who is living with CF and how daily activities, perhaps taken for granted by others, are much harder or need to be done differently. Equally, could living with such restrictions also give Ruby particular insight or an ability to see things differently from other people.
For her previous book, Vertigo, Karen drew on her own experience of Meniere’s disease, a disorder affecting the inner ear which can cause episodes of vertigo, vomiting,
dizziness, hearing loss and tinnitus. Her main character, Frances, has vertigo.
Writing that book helped Karen use her own experiences and in turn, when it came to The Ghost Walk, made her more comfortable drawing on her conversations with Jo and her research to authentically convey Ruby’s journey.
Karen and Jo also talked about self-determination and dignity, ensuring that as an adult Ruby had autonomy over her choices, even when other characters in the book were trying to take over some control.
“I worked in aged care for a long time and one of the big things is dignity of risk,” Karen adds. “If you’re 88 and want to eat donuts every day, you have the right to make that choice.” Separate from whether it might be the best choice.
The Ghost Walk started with a scene where a patient in hospital was looking out over a swamp and could see the forensic team working, while on the ward people were saying it was the body of a doctor. If you’re a local to Perth, you’ll likely recognise the real place Karen drew from.
“I wrote that scene and then kept writing to see what would happen.

I also didn’t really know what had happened until close to the end, much like my other books. I spend a lot of time getting to know my characters, to the point that they let me know what’s going to happen next.”
Karen says sometimes a character will react in a particular way or reveal an historical detail and she doesn’t really agree. Then she’ll realise that in fact it makes perfect sense and becomes part of the story.
“It’s interesting the way creativity works. Writing these stories is teaching me so much about creativity – I can feel all these new neural networks making connections as I write each book.”
While Karen’s books usually have a crime underpinning them, her angle is different from many other stories. She uses crime as a vehicle to “make observations about bigger things”.
In the case of The Ghost Walk, it’s shining a light on illness and disability while Vertigo looked issues such as homelessness alongside corruption.
The Ghost Walk is available now at all good bookstores.

We have a bumper round of competitions for you this month, from films to books and wine.
We have three signed copies of The Ghost Walk to give away – can Ruby help solve the mystery of Dr Beaufort’s death?
We also have five double passes to the St. ALi Italian Film Festival, running from September 25 to October 22 at Luna Palace Cinemas.
If a hard-earned tipple at the end of a long week is more your style, you can win premium wines from 3drops Wine in Mount Barker. See over the page for entry details.
To enter, use the QR code on this page or go to mforum.com.au and hit the competitions tab.
The Perth Hills are the place to be over the September long weekend. WanderFest celebrates hikers of all abilities and invites you to lace up your boots.
By Ara Jansen

Whether you’re an experienced hiker or a novice, you’ll find a trail which fits you like a pair of wellloved hiking boots during spring’s Perth Hills WanderFest.
Taking place on the long weekend of September 26-29, hikers and walkers can enjoy a tailored hike series in Gidgegannup, Kalamunda, Chidlow, Bedfordale and Jarrahdale. Hikers of all abilities can hit the trails to experience the beauty of the Perth Hills as the weather warms.
Step into landscapes rich in history and overflowing with breathtaking views – spot wildflowers and waterfalls, quendas rustling in the undergrowth and Carnaby’s black cockatoos soaring overhead in a magical afternoon out in nature.
Hikes tailored for beginners, youth, seniors, advanced and those with accessibility needs will be led by award-winning local tour operators
The Hike Collective and Off the Beaten Track WA, who specialise in creating safe, engaging and memorable guided walks.
Destination Perth has teamed up with the Perth Hills Tourism Alliance to deliver the event for the first time. Chief executive Sonja Mitchell is excited about the new initiative and
said September is a perfect time for locals to get out on the trails.
“I think people will be amazed at the variety of what they will see if they head out on a trail,” Sonja said.
“People are quick to think overseas is better, but we have this wonder on our doorstep. Plus, at this time of the year the weather is stunning for getting outdoors.”
With five different levels of hikes, the festival encourages people who have not gone of a walk or a hike before to take to the beginner trail in Gidgegannup, which is an easygoing 3km loop and includes a waterfall lookout.
In contrast the advanced hike is Kitty’s Gorge, a 16km return trail in Serpentine National Park and ready to push your limits. It tackles rugged terrain, steep climbs and long stretches of uninterrupted wilderness, all leading to the breathtaking Serpentine Falls. Your legs will feel the burn, but the views make every step worth it.
“I’m a hiker but I’ve not done all of the hikes, so I am looking forward to trying them. For people on the trails, it’s not just about physical accessibility, but the hikes ask you
to open your senses – smell, see and listen. It’s a chance to take in some deep breaths and enjoy the fresh air,” Sonja adds.
“For me getting out into the bush means ignoring the phone and letting my body relax and my mind expand and not be cluttered. Being away from that constant connection refreshes me and helps me be more creative.
“I encourage people to take photos with their mind and not their phones and let that be your photo library. It’s good to give yourself that time and space.”
WanderFest also encourages you to linger longer in the Perth Hills –rest weary legs with a night or two at a local retreat, fuel up or reward yourself with a pub meal or shop for fresh produce at the local markets and orchards.
A new downloadable guide to ensure visitors can return to safely explore the trails at their leisure will be available from October 1.
Hike tickets are $30. Get all the details at experienceperthhills.com.au/ campaign/wanderfest
3drops winery celebrates everything there is to love about the Great Southern and offers a variety of wine for all drinkers, writes Master of Wine Craig Drummond.
This impressive property is located just off the picturesque St Werburgh’s Road, close to the town of Mount Barker in the heart of the expansive Great Southern wine region. Its name derives from three wonderful and precious liquids – wine, olive oil and water. Both wine and olive oil are produced on the estate and water refers to the wetlands located on the property.
Plantings on Joanne and John Bradbury’s farm began in 1999 with eight hectares making up the property. A further seven hectares followed in 2002 before they expanded to purchase the nearby Patterson’s vineyard in 2007 to add a further six hectares to their land.
These properties together supply a spectrum of varieties including Riesling, Sauvignon Blanc, Chardonnay, Cabernet Sauvignon, Cabernet Franc, Merlot, Pinot Noir, Shiraz and Nebbiolo.
Winemaking since the estates inaugural 2003 vintage has been overseen by Rob Diletti, one of the most celebrated winemakers of the region. This has only added to the good viticultural practices and resulting in wines of profound quality. It is of no surprise to me that 3drops Wine has received many accolades, including a 5-star rating in the 2025 Australian Wine Companion, entry into The Real Review Top Wineries of Australia 2024, and Small Producer of the Year at the 2025 WA Wine Review. Much of my early oenological journey has been in Mount Barker and the wines reviewed certainly depict the varietal expression and cool climate characters that I look for from this sub-region.


3drops 2025 Great Southern Riesling, RRP $29
From the Wragg Rd home vineyard, a classic Great Southern example of Riesling. Aromas are overt, fresh and vibrant. Floral and lemon citrus characters lead to great flavours of grapefruit and lemon zest and background minerality. It is crisp, focused and zesty with palate length and a clean finish. Will reward cellaring up to 10 years.
A nice dry, crisp, refreshing wine with an attractive salmon pink colour. Shows flavours of freshly picked strawberries, but with background Nebbiolo savoury characters. A subtle and vibrant Rosé considering it is made from the dominating Nebbiolo grape known for its firm tannins, high alcohol and high acidity. A good wine to drink now as an aperitif, or accompanying salads and seafoods.
3drops 2023 Great Southern Chardonnay RRP $33
3drops 2024 Great Southern Pinot Noir, RRP $40
From the Patterson’s vineyard, a full bodied Pinot style atypical for the region but very drinkable. Shows a full purple beetroot colour with spicy aromas, herbaceous with a touch of cloves. Palate shows blackcurrant and rhubarb with spice and herbal elements. Tannins are fine and silky, a ‘serious’ Pinot. Drink now and up to five years.
The Great Southern is renowned for its cool climate Shiraz and this is a fine example. Displays white pepper, dark plum and flavours of blackcurrant, blueberry and spices. Peppery on the end palate, good current drinking and will reward for eight to 10 years cellaring.
Difficult to separate from the Riesling, it combines great depth and purity of fruit enhanced by cool climate delicacy and acidity. The nose is inviting with white peach and lifted toasty oak. On the palate it is fresh and fruity, yet complex and integrated. Peach and ripe melon, vanillin oak comes through. Partial malolactic fermentation adds to the mouthfeel. A balanced, intense, complex cool climate Chardonnay. Great current drinking and will go another few years. This wine is a steal at this price.



Our podcasts bring you the latest updates and key insights into new treatment options available.
Join our clinical editor Dr Joe Kosterich in conversation with WA specialists to learn more about developments to improve patient outcomes. Our podcasts are now CPD verified. Look for the CPD logo to complete your self-reflection and claim your time.
Topics covered in this series:
Rethinking radiation oncology with A/Prof Yvonne Zissiadis & Celia Byatt
Management of Childhood Leukemia with Prof Cathy Cole
Difficult-to-treat depression with Dr Kyle Hoath
Advances in lung cancer management with A/Prof Tim Clay
Improving outcomes of Aortic Stenosis with Dr Kevin Chung
Listen on your favourite podcast platform – scan the QR code to follow us!

CONTACT
Sharon:
P: 08 9310 4400
Full-Time General Practitioner
To replace departed Male GP and longestablished GP also reducing hours.
• Private Billing Practice
• Well established small but busy General Practice
• Individual large room available in comfortable and relaxed setting
• Fully Accredited
E: admin@hatherleymedical.com.au
Scan QR code for more details

MOUNT LAWLEY
CONTACT
General Practitioner
Convenient location with adjacent pharmacy and allied health services.
• $200–$300 per hour with 6–7 sessions available
• Modern, well-equipped working environment with excellent facilities
• Skilled nursing staff and onsite nondispensing pharmacist.
Practice Manager Rachael Hadlow:
E: rhadlow@3rdave.com.au www.thirdavenuesurgery.com.au
Scan QR code for more details

COMO
CONTACT
Practice Manager:
P: 08 6165 2444
E: reception@comogp.com.au
Scan QR code for to email

SCARBOROUGH
CONTACT
Practice Manager:
P: 0478 021 910
Opening for VR GP - F/time or P/time Full Private List Available
Unique opportunity to join our family orientated practice in one of Perth’s fastest-growing suburbs.
• FRACGP essential
• Up to 70% private billings
• Enjoy working for a doctor-owned, non-corporate, well support, and accredited practice.

CONTACT
P: 1300 420 272
E: work@dyhs.org.au
Scan QR code for more details

CONTACT
Jasmine Brierty:
P: 0457 905 538
Derbarl Yerrigan Health Service
General Practitioners
(Healthcare & Medical)
• Full Time
• $238k pa (pro rata) + Super & Medicare Incentive
• 12 days of personal leave per year
• Personalized professional development opportunities
• NAIDOC Day holiday
Doctor Opportunity GP to join our growing team
• No Weekends or afterhours work
• Nursing support
• FRACGP qualification
• Vocational Registered
• AHPRA Registration
E: practicemanager@thewoodsmedical.com.au
Scan QR code for more details

PARKWOOD
CONTACT
Practice Manager Folu:
P: 0435 800 320
• Busy mixed billing general practice
• Well established patient base
• Flexible working hours
• Nursing support
• Positive team environment
E: pmanager@parkwoodmc.com.au
Scan QR code for more details
Jindalee Medical Centre
Full or Part-time GP
• Flexible arrangement to suit lifestyle
• Private billing Mon-Fri practice
• On site pathology
• DPA approved location
• 12 consult rooms, treatment & procedure rooms
E: Jasmine.Brierty@ipn.com.au
Scan QR code for more details
FULL OR PART-TIME GP
• Private billing practice
• Fully computerised
• On site Pathology
• RN Support
CONTACT
Call/sms: 0403 016 092
E: managerbmc@gmail.com
Scan QR code for to email

Eastern Perth Metro GP Practice looking for FT or PT GPs
What We Off er:
• Current AHPRA registration and right to work in Australia
• FRACGP (or equivalent), VR General Practitioner. Non-VR on pathway to achieving VR registration are welcome to apply
• Current medical indemnity insurance.
We are looking for an enthusiastic and experienced GP to join our growing team.
What we can off er You:
• DPA location – suitable for doctors under the 10-year moratorium
• Experienced and well-trained staff
• VERY Competitive service fee rates
• Agreed Guarantee period. 70% Tops of Mixed Billing
• Supportive GPs
• Family friendly culture, with great community links
• Reliable clinical software
• Potential Pathway to equity options.
CONTACT
Forward CVs to Practice Manager: E: practice.manager@swanviewfp.com.au
Scan QR code for more details




is seeking expressions of interest from vocationally registered general practitioners
15% service fee
Mixed billing
Free, reserved parking
Full time registered nurse support
Exceptional administrative support team
Best Practice Premier (Spectra)
Flexibility of four to six sessions per week.
Monday to Friday, 8.30am – 4.30pm.
No weekends or after-hours.
Located within the Wellbeing Precinct on the ECU Joondalup Campus, our AGPAL accredited, purpose-built general practice is on the same floor as the free student psychological services, the Living Room (a peer led support and guidance service), with a coffee shop and free reserved GP parking close by.
The ECU Health Service assists students, staff and the university community with their health care needs. The primary function of the service is to provide our students with accessible and affordable health care for the duration of their studies.
Students are charged the rebate fee or bulk billed, and staff and other patients are charged private commercial rates.
Applications are now open from candidates who have either Permanent Residency or Australian citizenship, unrestricted Medical Board of Australia registration and no Provider Number restrictions.
Please contact Laura Harnett – Practice Manager on telephone 0479 188 513 / 08 6304 5618 or email practicemanager@ecu.edu.au.




Development Approved for Medical Centre
Estimated completion August 2026
Excellent street frontage exposure
27 Parking Bays
We are seeking Expressions of Interest from experienced medical operators for:
Medical Centre 495m2
Pharmacy 200m2



at 162 Cambridge St West Leederville (directly opposite SJOG Subiaco).
2 large fully fitted consults rooms (including sink and treatment bed) available and seperate treatment room available.
This exciting site offers plenty of traffic exposure and convenience making it a key location at the northern entry to the growing communities of Anketell, South Wandi and surrounding areas.
Contact exclusive Leasing Agent Kong Wai Wong on 0421 883 338 to secure your next medical business premise


CLAREMONT – CONSULTING ROOMS AVAILABLE FOR SESSIONAL RATE
Level 1, Claremont Medical Centre building
16m2
Full fit out including sink
Please contact Kristy at Health in Mind kristy@healthmind.com.au / (08) 6183 1908 ANKETELL – RARE OPPORTUNITY OF BRAND NEW MEDICAL CENTRE IN
Double French doors onto balcony provide natural light
Onsite parking
GP, Physio and Psychology in same building
Includes use of waiting area, kitchen
$200 half day; $300 full day
Admin support available for additional fee

Each consult room $250 per half day session (includes use of waiting room and kitchen area). Reception/Admin support available for an additional fee.
For further information regarding availability or to arrange inspection please contact: reception@oswa.com.au/ (08) 9332 0066
















Partner with Australia’s largest independent practitioner network and experience freedom over your billings, appointment types, and clinic care.
Explore our WA GP vacancies









At Humphrey Homes, every home we design and build starts with listening. We take the time to understand your vision, your lifestyle and your budget - then translate that insight into thoughtful spaces that are beautifully crafted. By integrating architecture, interior design and construction under one roof, we make the journey to your forever home harmonious, effortless and deeply personal.
Discover how we can bring your vision to life. Visit humphreyhomes.com.au or call Dean on 9284 5444.
