







































GERALD M. MARLIN, DMD, MSD
At Elite Prosthetic Dentistry, our “dream team” delivers an extraordinary blend of clinical precision and genuine care. Led by Gerald M. Marlin, D.M.D., M.S.D., a renowned specialist with over 3,700 successful implant procedures and a history of crafting crowns that last over 35 years, we are the trusted choice for adults seeking implant, cosmetic, and reconstructive dentistry in the Washington, DC metropolitan area. Why Choose Elite Prosthetic Dentistry?
• Expertise in saving teeth, problem-solving failing restorations, and addressing TMJ issues. Proven success in implant therapy, offering long-term results with minimal bone loss.
• Comprehensive care, including surgical implant placement, bone grafting, and custom restorations—all performed in our state-of-the-art office.
• An in-house laboratory ensuring efficiency and precision for veneers, crowns, and implant restorations.
• A warm, caring environment supported by a highly skilled team with an average tenure with us of 14+ years, complemented by oral and IV sedation protocols. With a commitment to advanced digital technology and artistry, Dr. Marlin works closely with each patient to deliver “simply radiant, simply natural” results. Our crowns last more than three times the national average, and our implants boast a >97% success rate over 20 years. Your journey to a revitalized smile begins here. Contact us today to schedule your consultation and experience the difference of truly exceptional dental care.
SPECIALIZATION
Prosthodontist specializing in cosmetic, implant, and reconstructive dentistry, including crowns, veneers, and dentures.
DESIGNATIONS, AFFILIATIONS, and AWARDS
Invented and Patented an Implant Restoration System, Academy of Osseointegration, American College of Prosthodontics, American Academy of Periodontology, American Dental Association, DC Dental Society, Bethesda Magazine Top Dentist, Washingtonian Top Dentist for 22 years
4400 Jenifer Street, NW, Suite 220 Washington, DC 20015
202.244.2101
Concierge@eliteprostheticdentistry.com
EliteProstheticDentistry.com

By Farzin Ghanavati , DDS Burke Dental
As the days grow longer and the flowers begin to bloom, March naturally inspires a fresh start. Many of us think about spring cleaning our homes, organizing our schedules, and refocusing on our health. But one area that is often overlooked is our smile.
At our Burke Dental, we believe spring is the perfect time for a dental reset — a chance to renew, refresh, and restore your oral health for the months ahead.
Winter habits, such as increased sugar intake, missed routines during the holidays, and postponed dental visits, can take a toll on your teeth and gums. A comprehensive dental exam and professional cleaning in early spring can help identify small concerns before they become larger, more costly problems. Preventive care not only protects your smile, but it also supports your overall wellness.
As a holistic dentist serving Burke and the surrounding community, I take a whole-body approach to dental

care. Oral health is closely connected to systemic health, and what we place in our mouths matters.
One important topic I often discuss with patients is the replacement of old silver (amalgam) fillings. Traditional silver fillings contain a mixture of metals, including mercury. While they have been used in dentistry for many decades, many patients today are choosing to have them safely removed and replaced with modern, tooth-colored composite materials.
Composite restorations are not

only more aesthetically pleasing, blending naturally with your smile, but they also allow us to preserve more healthy tooth structure. For patients who are concerned about long-term wellness and reducing metal exposure, replacing old amalgam fillings can be an important part of their dental reset. In our office, we follow strict safety protocols when removing old silver fillings to ensure the process is done carefully and responsibly. Patient safety and comfort are always our top priorities.
Spring is also an excellent time to:
• Schedule overdue cleanings
• Address bleeding gums or gum inflammation
At Burke Dental, we believe great dentistry goes beyond healthy teeth — it’s about trust, comfort, and confidence in your care. Here’s why families across Burke, Fairfax, and Springfield, VA choose Dr. Farzin Ghanavati and his team for their dental needs:
Top-Rated Dentist in Burke, VA – Hundreds of 5-star reviews from happy patients reflect our commitment to excellence, honesty, and gentle care.
26+ Years of Advanced Experience – Dr. Ghanavati brings decades of skill in cosmetic, implant, and restorative dentistry — with proven results you can trust.
State-of-the-Art Technology – From 3D digital imaging to laser and Invisalign® systems, we deliver precision, safety, and comfort at every visit.
Personalized, Honest Care – No pressure, no upselling — just clear communication, customized treatment, and genuine concern for your oral health.
Comfortable, Modern Environment – Relax in our clean, high-tech office designed for your comfort and peace of mind.

• Repair worn or cracked teeth
• Brighten your smile with professional whitening
• Discuss smile enhancement options before wedding and graduation season
Your smile plays a powerful role in your confidence, your health, and how you connect with others. As your Burke neighborhood dentist, my goal is to provide personalized, comprehensive care in a welcoming and supportive environment. Many of my patients are neighbors and families who have trusted our office for years, and I am honored to serve this wonderful community.
If you have been waiting for the “right time” to prioritize your oral health, consider this your sign. March is the perfect opportunity to refresh your smile and step into spring feeling confident and healthy.
A healthier smile begins with a simple conversation. We look forward to helping you achieve it.

By Marc P. Stanard, DDS, PC
Periodontal disease is one of the most common chronic inflammatory conditions affecting adults, yet it frequently advances without obvious symptoms. Unlike dental caries, which often cause pain or sensitivity early on, periodontal disease can progress quietly—sometimes for years— before patients realize significant damage has occurred.
The disease begins with bac-
terial plaque accumulation along and beneath the gumline. If not adequately removed, these bacteria trigger an immune response that leads to inflammation of the gingival tissues. Over time, this inflammatory process causes the breakdown of connective tissue attachment and resorption of alveolar bone. As bone support is lost, periodontal pockets deepen, teeth loosen, and gums recede, allowing further bacterial colonization and accelerating disease progression.
One of the most challenging aspects of periodontal disease is that patients often adapt to early warning signs. Mild bleeding during brushing, occasional gum tenderness, or chronic bad breath are commonly dismissed as minor issues rather than indicators of active infection. By the time tooth mobility or gum recession

becomes noticeable, significant structural damage may already be present.
Systemic health factors can further influence disease severity. Conditions such as diabetes, cardiovascular disease, and autoimmune disorders are associated with heightened inflammatory responses, increasing susceptibility to periodontal breakdown. Smoking, smokeless tobacco, vaping and chronic stress also impair immune regulation and tissue healing, compounding risk. Early diagnosis is critical. Comprehensive periodontal examinations—including probing depths, bleeding indices, gingival recession, teeth mobility, radiographic evaluation, and assessment of risk factors—allow clinicians to identify disease at stages where intervention is more predictable and less invasive.
Modern periodontal therapy focuses not only on bacterial reduction but also on long-term inflammation control and tissue stability.
When detected early, periodontal disease can often be managed with non-surgical therapy and structured maintenance programs. In more advanced cases, surgical and regenerative techniques may be required to restore lost support and preserve remaining dentition. The goal in all cases is disease control—not merely symptom relief.
Periodontal health is foundational to oral function, comfort, and long-term tooth retention. Regular evaluations and timely intervention remain the most effective strategy for preventing irreversible damage and maintaining oral health over a lifetime.
Maintaining good dental hygiene is crucial, and Dr. Marc Stanard, a periodontist and specialist in surgical implant dentistry, can help you achieve healthy teeth comfortably. We offer a wide range of specialized procedures and services to cater to your periodontal needs, such as bone surgery, scaling, and root planing, gum grafts, crown lengthenings, and sinus lifts.
P. Stanard, DDS
• We provide advanced, affordable dental care tailored to meet your unique needs.
• Our team offers oral hygiene instruction and education on gum disease, bone loss, and other dental health conditions.
• Dr. Marc Stanard has decades of experience and a passion for his work, and he’s earned numerous designations, affiliations, and awards, including Top DDS by Washingtonian and high ratings on Google and Yelp.
• Our office is friendly and welcoming, making it the perfect place to receive top-quality dental care.


Your Health Magazine is on a mission. There are far too many people, insured or not, who do not go to the doctor when they should, and in millions of cases, don’t know who they should go to, or why.
People are encouraged to buy a new house, car, cell phone or big screen TV, and those companies make themselves very visible and their products easily attainable.
Information about, and from, local healthcare providers is not easy to find, and many times those services are difficult to access.
Information and encouragement always lowers fear and trepidation about anything, and this is especially true in healthcare. While general information is available on web-sites, specific information from local providers is almost impossible for people to find. This is one of the key reasons chronic and episodic conditions are not cared for. It is our mission to:
Make A Difference By Empowering and Encouraging People To Live Healthier By Going To the Doctor When They Should.
There is a lot of evidence that the health professionals who participate in Your Health Magazine have helped many people over the years. We at Your Health Magazine salute you!
G. Scott Hunter, Editor-in-Chief
If you would like to find out how you can participate in one of our upcoming editions, please contact the office nearest you.
MARYLAND & WASHINGTON, DC OFFICE One Town Center 4201 Northview Drive, Suite 102 Bowie, MD 20716 Office (301) 805-6805 • Fax (301) 805-6808 info@yourhealthmagazine.net
VIRGINIA OFFICE Office (301) 805-6805 info@yourhealthmagazine.net
© Your Health Magazine, 2026. The magazine and all of its contents are protected by copyright. For permission to reproduce any materials in this magazine, contact info@yourhealthmagazine.net
The content in Your Health Magazine and provided on yourhealthmagazine. net is for informational and educational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always consult with a qualified healthcare provider before starting any exercise program, making changes to your health routine, or acting on any health-related information found on the Internet, or anywhere else.

Foot & Ankle Specialist’s Board Certified doctors have been providing expert care to Northern Virginia families. From sports injuries and diabetic care to surgery and custom orthotics, we’re here to keep you moving—pain-free and confident every step of the way.

Ian Beiser, DPM
Dr. Ian Beiser has practiced podiatric medicine in Washington, DC since 1990. A leader in his field, he specializes in sports medicine and reconstructive foot surgery. He serves on multiple medical staffs, teaches at George Washington University, and holds several regional and national leadership positions.

David Vieweger, DPM
Dr. Vieweger, valedictorian of the Scholl College of Podiatric Medicine, completed his Surgical Residency at MedStar Washington Hospital Center. He specializes in conservative and surgical foot and ankle care, with expertise in trauma, limb salvage, and reconstruction. An avid runner, he lives in Maryland with his family.


Jennifer Gerres, DPM
Dr. Jennifer Gerres, DPM, is a graduate of Des Moines University and completed her Residency at the Cleveland Clinic. A published researcher and educator, she provides compassionate, evidence-based care in podiatric medicine and surgery, combining clinical expertise with a personalized, patient-focused approach.

Haseeb Ahmad, DPM
Dr. Haseeb Ahmad, originally from Philadelphia, earned his Doctor of Podiatric Medicine from Temple University and completed his Surgical Residency at the VA New Jersey Healthcare System. Board Certified in Podiatric Medicine, he specializes in sports medicine, orthopedics, and trauma, and consults for Georgetown University athletics.
Dr. Howard Osterman, a Board-Certified Foot and Ankle Surgeon, serves as Team Podiatrist for the Washington Wizards and Washington Mystics. Recognized by Washingtonian Magazine as a top podiatrist, he is also President of the DC Podiatric Medicine Association and a leader in podiatric sports medicine.


Saylee Tulpule, DPM
Dr. Saylee Tulpule, a graduate of the California School of Podiatric Medicine, completed her Surgical Residency at Long Beach Memorial, where she served as Chief Resident. Practicing since 2010, she specializes in podiatric medicine, sports medicine, biomechanics, and elective forefoot surgery with a patient-focused approach.

Lee Firestone, DPM
Dr. Firestone, Board Certified in Foot Surgery and Sports Medicine, specializes in surgical and non-surgical foot and ankle care. An accomplished marathoner and RRCA-certified coach, he’s been recognized among Washington’s top podiatrists and sports medicine providers, serving the DC area since 1994.
Dr. Erika Schwartz, Board Certified in Foot Surgery, serves on the Maryland Podiatric Medical Association Board and teaches at MedStar Washington Hospital Center. A past president of the American Association for Women Podiatrists, she’s been recognized by Washingtonian Magazine and featured in major national media outlets.
By Kari Bailey, MD Anne Arundel Urology
Urologic malignancies encompass a range of cancers that affect the urinary system, including the kidneys, bladder, ureters, prostate, and testicles. These cancers present unique challenges in diagnosis, treatment, and management, making awareness and education essential for both patients and healthcare providers.
Types Of Urologic Malignancies
Kidney Cancer: Renal cell carcinoma (RCC) is the most common type of kidney cancer. Risk factors include smoking, obesity, and hypertension. Symptoms may include blood in urine, persistent back pain, and unexplained weight loss. Early detection is crucial, often achieved through imaging studies such as ultrasound or CT scans.
Bladder Cancer: This is characterized by malignant growths in the bladder lining. The most common symptom is hematuria (blood in urine). Risk factors include smoking,
exposure to certain chemicals, and chronic bladder infections. Diagnosis often involves cystoscopy and biopsy, while treatment may include surgery, chemotherapy, or immunotherapy.
Prostate Cancer: One of the most prevalent cancers among men, prostate cancer typically grows slowly and may not present symptoms in early stages. Risk factors include age, family history, and race. Screening methods like PSA (prostate-specific antigen) tests are vital for early detection. Treatments vary from active surveillance to surgery and radiation therapy.



Testicular Cancer : Although rare, testicular cancer is the most common cancer in young men aged 15 to 35. Symptoms might include a lump in the testicle, swelling, or discomfort. Self-examinations are encouraged for early detection as early stage cancers have cure rates above 90%. Treatment usually involves surgery, and may involve chemotherapy and radiation.
Ureteral Cancer : This malignancy affects the ureters, the tubes connecting kidneys to the bladder. Symptoms can be similar to those of kidney or bladder cancer. Diagnosis often requires imaging and biopsy. Treatment options depend on the stage and location of the cancer.
Risk
Understanding risk factors is crucial for prevention and early detection. Modifiable factors include lifestyle choices such as smoking cessation, maintaining a healthy weight, and regular exercise. Additionally, awareness of family history can guide individuals in discussing screening options with their healthcare providers.
Diagnosis of urologic malignancies typically involves a combination of physical exams, imaging tests, and laboratory tests. Biopsies are often necessary to confirm the presence of cancer. Once diagnosed, treatment plans are tailored to the individual’s needs and may involve surgery, radiation therapy, chemotherapy, or targeted therapies.
Early detection significantly improves the prognosis for patients with all types of cancer, including urologic malignancies. Regular check-ups and discussions about risk factors and symptoms with healthcare professionals based on your individual lifestyle and habits. For instance, men over 50 or those with a family history of prostate cancer should consider regular screenings with PSA and/or DRE.


By Rashmi K. Parmar, DMD, D-ABDSM and Neelima K. Yerra, DDS – Sleep Better Maryland
Sleep apnea is a serious and often underdiagnosed sleep disorder that affects people of all ages and genders. Marked by repeated pauses in breathing during sleep, it disrupts normal rest and lowers oxygen levels, placing significant strain on the body. Although sleep apnea is commonly associated with men, growing evidence shows it is frequently overlooked in women, leading to delayed diagnosis and avoidable health risks.
Obstructive sleep apnea (OSA), the most common form, occurs when the airway collapses or becomes blocked during sleep. Classic symptoms include loud snoring, gasping for air, and excessive daytime sleepiness. However, women often experience subtler symptoms that are easier to miss. Instead of loud snoring, many women report chronic fatigue, insomnia, morning headaches, anxiety, depression, difficulty concentrating, or unexplained weight gain. These symptoms are frequently attributed to stress, aging, or hormonal changes, which can delay proper evaluation and treatment.
Hormonal changes play an important role in women’s risk for sleep apnea. Pregnancy, perimenopause, and menopause can all increase vulnerability to airway obstruction during sleep. Declining estrogen and progesterone levels may affect muscle tone and breathing regulation. After menopause, a woman’s risk of sleep apnea rises significantly and can approach that of men, yet many women remain undiagnosed and untreated.
Untreated sleep apnea can have serious consequences for both women and men. It has been linked to high blood pressure, heart disease, stroke, type 2 diabetes, and metabolic disorders. For women in particular, sleep apnea may worsen hormonal imbalance, contribute to mood disorders, and increase cardiovascular risk – the leading cause of death among women. During pregnancy, untreated sleep apnea has also been associated with complications such as gestational diabetes and preeclampsia.
Diagnosis is a critical step toward better health. Sleep apnea is typically
identified through a sleep study, conducted either in a sleep laboratory or at home, depending on individual needs. Once diagnosed, effective treatment options are available. While Continuous Positive Airway Pressure (CPAP) therapy remains the most well-known
treatment, many patients struggle with comfort or compliance. For these individuals, custom oral appliance therapy can offer a comfortable, discreet alternative, especially for those with mild to moderate sleep apnea or CPAP intolerance.
Treating sleep apnea can greatly improve quality of life. Many patients experience better energy,
improved mood, sharper focus, and more restorative sleep. For women, effective treatment may also support improved cardiovascular health, weight management, and overall well-being. Sleep apnea is not just a men’s health issue – it is a widespread condition that deserves awareness, timely diagnosis, and treatment for everyone.

We are pleased to announce that Dr. Parmar and Dr. Yerra are now partners, united by a shared commitment to providing high-quality, patient-centered care to our community. Together, they bring experience, compassion, and a dedication to helping patients achieve better health and lasting wellness.

Rashmi K. Parmar, DMD, D-ABDSM
Dr. Rashmi Parmar is Diplomate of the American Board of Dental Sleep Medicine. She received her professional degree from University of Pennsylvania School of Dental Medicine. She completed the comprehensive general practice Residency at Carolinas Medical Center in Charlotte, NC and has been in practice in the Columbia Clarksville area since 1991.

Neelima K. Yerra, DDS
Dr. Neelima K. Yerra is an American Academy of Dental Sleep Medicine- Qualified Dentist. She has extensive expertise in the diagnosis and management of Obstructive Sleep Apnea. Dr. Yerra received her professional degree, Doctor of Dental Surgery from New York University College of Dentistry in 2015.
We are honored to continue serving the community together and look forward to welcoming new and returning patients.



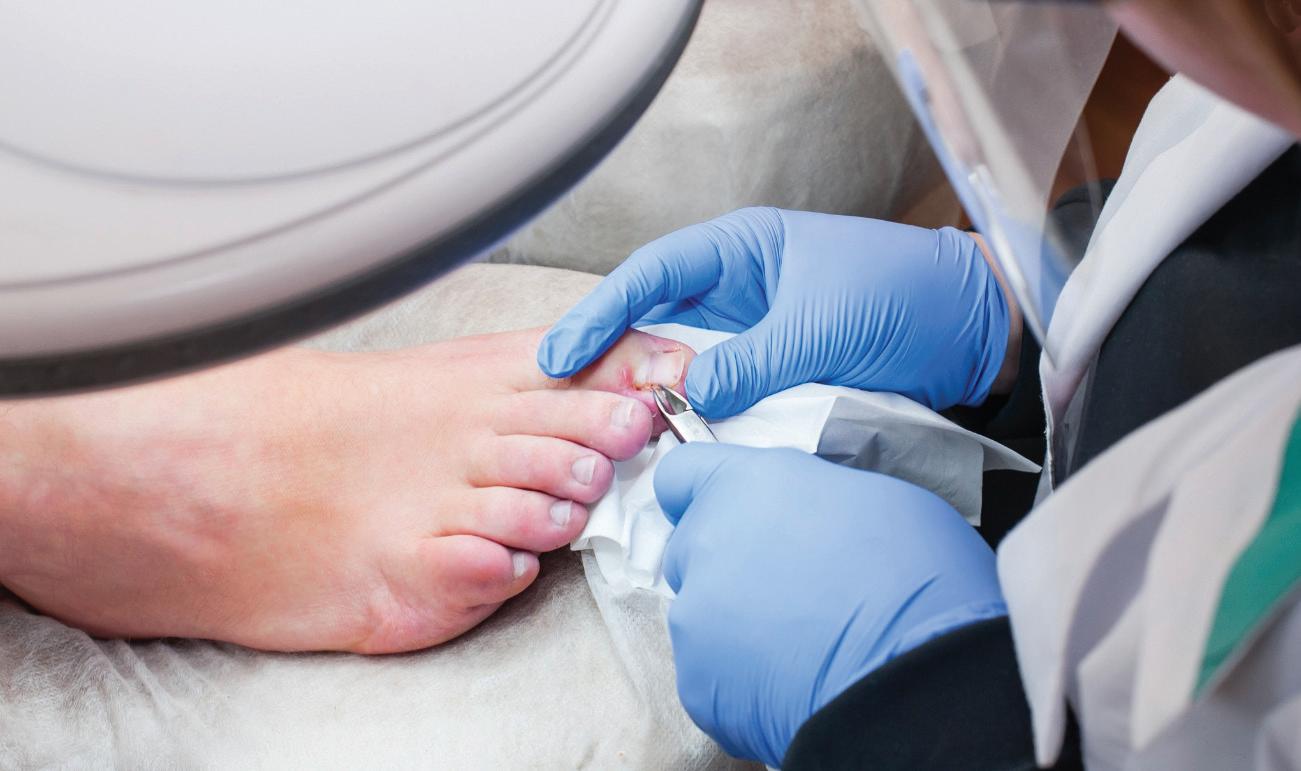
By Mikel Daniels, DPM
We Treat Feet Podiatry and ankles!
Your feet quietly run your life. If they hurt, everything gets harder. Work, exercise, sleep, even walking from the couch to the kitchen can feel like a chore. Most people don’t think about their feet until something goes wrong, and in my office at WeTreatFeet Podiatry, many patients arrive already in crisis. I see ulcers, fractures, infections, and severe arthritis every day. Much of this is preventable – and a surprising amount of it starts not with your shoes, but with what’s on your plate.
When people think about foot health, they expect me to talk about arch supports or fancy sneakers. They’re usually surprised when I start with breakfast. Your feet are made of bone, muscle, fascia (that fibrous tissue under the skin), nerves, blood vessels, and skin. These are living tissues, and they need fuel. Food provides the building blocks that keep them strong and resilient.
Structurally, your feet depend on strong bones. That means adequate calcium, vitamin D, magnesium, and protein to maintain density and resist stress fractures and deformity. Joints and cartilage rely on collagen, vitamin C, and healthy fats to stay smooth and pain-free. Muscles and tendons need protein and minerals to generate power and absorb shock. Skin and soft tissue depend on protein, zinc, vitamins C and E, and healthy fats to resist cracking, ulcers, and infection.
I’ve lost count of how many times I’ve seen “mystery” foot pain in people living on processed food and sugary drinks. When we check labs, vitamin D deficiency is common. When diet improves – more whole foods, better hydration, fewer inflammatory foods – patients often feel better. Sometimes their entire pain profile changes. That isn’t magic; it’s basic physiology.
If you remember one thing from this article, let it be this: circulation and nerves will make or break your feet over your lifetime. Healthy feet need blood flow – oxygen in, waste out. When arteries narrow due to
cholesterol buildup, diabetes, smoking, or high blood pressure, toes and heels suffer first. Reduced blood flow means slower healing, pain with walking, and a dramatically higher risk of ulcers and amputation.
Certain foods protect blood vessels. Leafy greens and beets are rich in nitrates that boost nitric oxide and relax vessels. Fatty fish like salmon, mackerel, and sardines provide omega-3s that reduce vascular inflammation. Olive oil, nuts, and seeds support healthy cholesterol and vessel flexibility. Colorful fruits and vegetables supply antioxidants that protect the vessel lining.
The opposite is also true. Diets high in trans fats, fried foods, and ultra-processed snacks accelerate plaque buildup and damage blood vessels. I’ve seen this play out repeatedly – in angiography suites with my vascular colleagues and in wound care centers. Different patient, same story.
Nerves in your feet act as your early warning system. They tell you when a shoe is rubbing or when a surface is too hot. In diabetes, chronically high blood sugar damages nerves and blood vessels, leading to neuropathy – numbness, tingling, burning, or complete loss of sensation. Tight glucose
control, B vitamins, antioxidants, and a low-glycemic, anti-inflammatory eating pattern can slow damage and help preserve remaining nerve function.
I see patients daily who walk in with what they think is a “small sore.” One man in his 60s couldn’t feel a wound on his toe at all. That small sore turned out to be a deep ulcer tracking to bone. We saved the toe, but it took months of care. Better sensation and circulation could have prevented it.
Poor nutrition may not shorten your life outright – but it can make the later years far more difficult for you and your family.

The truth about untreated foot issues – and how We Treat Feet can help you get back to living pain-free.
Every step you take should bring you forward – not closer to chronic pain, mobility loss, or costly surgery. At We Treat Feet Podiatry, we don’t just treat symptoms – we solve the problem at its root, using the latest techniques in foot and ankle care.
Whether you’re battling bunions, heel pain, diabetic wounds, or sports injuries, we help you walk, run, and move with confidence again.
Why Washingtonians Trusted Us:
• Expert care from board-certified foot & ankle specialists
• 12+ locations for your convenience
• Advanced diagnostics & same-day appointments available
• Custom orthotics, surgical options & diabetic foot programs
• We’re the Official Podiatry Partner of the Baltimore Orioles




By Michael Rogers, DDS Fairlington Dental
Temporomandibular joint disorders, often called TMJ or TMD, can affect much more than your jaw. Many people do not realize that TMJ dysfunction can contribute to persistent headaches, neck discomfort, and even back pain. At Fairlington Dental, we focus on identifying and treating TMJ related pain so you can enjoy daily life without chronic discomfort.
What
The temporomandibular joints connect your lower jaw to your skull and
allow you to chew, speak, and yawn. When their function is disrupted by muscle tension, misalignment, grinding, or stress, symptoms can extend far beyond the jaw. Headaches, neck strain, and referred discomfort throughout the upper body are common.
Headaches and TMJ
The jaw joints and chewing muscles are closely connected to the muscles and nerves of the head. When the TMJ is irritated or overworked, surrounding muscles tighten, often leading to headaches felt at the temples, around the eyes, or at the base of the skull. Many patients with frequent tension type headaches are unknowingly clenching or grinding their teeth, placing additional strain on these muscles.
Neckaches and TMJ
The jaw, neck, and upper spine function as a connected system. When jaw muscles are overactive due to clenching or bite imbalance, neck muscles often compensate, resulting in tightness and discomfort. Poor posture can intensify this strain. Over
time, TMJ tension can contribute to persistent neck pain and stiffness.
Backaches and TMJ
Although less obvious, TMJ dysfunction can also influence the upper back. Muscle imbalance in the jaw affects posture and head position. When the neck and shoulders remain tense, the upper back muscles compensate, which can lead to ongoing aching and fatigue.
TMJ dysfunction does not always present as severe jaw pain. Other symptoms may include:
• Pain or tenderness in the jaw joint
• Clicking or popping when opening or closing the mouth
• Difficulty chewing or changes in bite
• Ear pain, pressure, or ringing
• Frequent headaches or migraines
• Neck tension or stiffness
• Discomfort extending into the shoulders or upper back Many patients are surprised to learn their symptoms trace back to
the jaw, which is why a thorough TMJ assessment is an important step toward lasting relief.
What You Can Do
If you regularly experience headaches, neck tension, or back discomfort that seems connected to jaw movement or clenching, you should consult your dentist. Identifying whether TMJ dysfunction contributes to these symptoms is the first step toward meaningful relief. A comprehensive evaluation can reveal bite imbalance, muscle strain, or joint dysfunction that may be driving your pain.
Your local dentist will take an integrative approach to TMJ care that considers both oral health and overall well being. Treatment may include custom oral appliances designed to support proper jaw alignment and reduce strain on surrounding muscles. When the jaw functions in balance, it can help restore comfort not only in your smile but throughout your head, neck, and upper body.


At Fairlington Dental, we understand the connection between a healthy smile and a healthy body. As a result, we look at the whole person to discover the reasons a patient may have gum disease or a bad bite. A number of studies link heart disease and other serious conditions to the presence of periodontal (gum) disease. This research makes it vital that we take a Complete Health approach to your dental care. Dr. Rogers will listen to you, conduct a careful assessment, and carefully explain your proposed customized wellness plan. He will then take the time to answer all of your questions. You become a partner in your oral health goals!
Our team has mastered the techniques of gentle dentistry and is skilled at helping patients with any level of apprehension relax and grow comfortable with visiting the dentist. Anxiety and tension have a variety of sources, so it’s important for us to listen to your concerns as well as your goals and history. Then we address your anxieties and proceed with gentle treatment only when you’re ready. We deliver all of this in an office that is environmentally aware, while you enjoy a variety of spa-like amenities during your visit.
One of our greatest joys is helping patients smile again, especially those who may not have seen a dentist in a while. You’ll be amazed at how the quality of life can change! We strive to create a partnership with you that starts the moment you walk through our door.

By Lubrina Bryant, DPM District Podiatry, PLLC
Foot pain can stem from various conditions, including plantar fasciitis, bunions, flat feet, arthritis, or injuries like sprains and fractures. Even seemingly minor discomfort can significantly impact daily activities, affecting mobility, balance, and overall quality of life. Chronic foot pain may also lead to compensation issues, causing pain in the knees, hips, or back. Ignoring persistent pain can worsen underlying conditions, making treatment more complex.
Addressing foot pain begins with identifying the cause. Rest, proper footwear, and targeted stretching exercises can help in mild cases. Custom orthotics or surgical intervention may be necessary for persistent or severe pain. Early intervention is key to preventing long-term complications. If foot pain disrupts your routine, it is suggested that you consult a podiatrist for an accurate diagnosis and an effective treatment plan tailored to your needs.
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Dr. Lubrina Bryant from District Podiatry, PLLC. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
• Bunions
• Hammertoes
• Plantar Fasciitis
• Bone Spurs
• Corns
• Tarsal Tunnel Syndrome
• Ingrown Toenails
• Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
• Flat Feet
• Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
• And more
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events
will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.


By Jeffrey L. Brown, DDS Sleep & TMJ Therapy
Obstructive Sleep Apnea (OSA), and Temporomandibular Disorder (TMD) are conditions that can severely disrupt daily life. OSA occurs when the airway is blocked during sleep, leading to pauses in breathing. This not only disrupts sleep but also poses significant health risks, such as cardiovascular issues, diabetes, and even cancer.
Temporomandibular Disorder –TMD – affects the jaw joint and the muscles controlling jaw movement. Symptoms often include jaw pain, difficulty chewing, and a clicking or locking of the jaw. These symptoms can vary in intensity and may sometimes lead to chronic discomfort.
Both Sleep Apnea and TMD are often overlooked or misdiagnosed, making awareness crucial for effective management. People experiencing symptoms of either condition should



seek medical evaluation to prevent long-term complications. Understanding the underlying mechanisms of these conditions can help in recognizing the need for timely and appropriate treatment.

Effective diagnosis usually involves a combination of medical history, physical examination, and advanced diagnostic tools. In the case of Sleep Apnea, sleep studies are commonly used to measure breathing patterns, while TMD diagnosis may involve imaging techniques like X-rays or MRIs to examine the jaw joint and surrounding tissues. Recognizing the signs and seeking professional help are key steps in managing these disorders. If you look for studies, there are clear links between OSA and TMD.
Both Sleep Apnea and TMD share several risk factors that can exacerbate symptoms. If the discs in the jaw joints are displaced, this will greatly contribute to TMD as well as OSA. Oftentimes, genetics are involved – a family history of OSA and/or TMD is common.
Another important factor is age; the likelihood of developing Sleep Apnea and TMD increases as one gets older. Being overweight is another significant risk factor for Sleep Apnea, as excess fat can obstruct the airway. This excess weight can also put additional stress on the jaw muscles, contributing to TMD symptoms.
Dr. Jeffrey Brown has limited his practice to focus only on TMJ Disorders, Craniofacial Pain Management and Sleep Apnea. By fixing slipped discs in the jaw joints, Dr. Brown can significantly reduce the pain patients experience in the head/neck region and other symptoms associated with jaw joint problems. Sleep & TMJ Therapy may be able to improve the quality of life for you or a loved one – we encourage you to contact us with any questions or concerns.
“Dr. Brown and his staff are absolutely wonderful. I was diagnosed with Dystonia. I could not turn my head and had a ton of pain. My doctors offered no help and no advice besides Meds and Botox. Since having the appliance I have NO pain and I can turn my head. I would highly recommend them to anyone. I feel Dr. Brown and his staff really care about their patients and helping them to get better. They do not just numb the symptoms but fix the problem. Thank you from the bottom of my heart. I feel like the old me again!”
- D. Thomas
“My daughter has been treated by Dr. Stack and Dr. Brown for the last 2 1/2 years, and we are very fortunate to have found them. Prior to that she was being treated by a neurologist at a Children’s hospital. She was on medications for tics and associated muscle pain, OCD/repetitive thoughts, sleeplessness and more (all possibly associated with Tourettes). Drs. Stack and Brown installed spacers to alleviate pressure on nerve bundles in the jaw, and subsequently braces to complete the process. Her symptoms have diminished significantly. She is off medication, her tics have all but disappeared, she can concentrate better in school, and she is once again cheerful and relaxed.” - Susan
Technological advancements are making significant strides in the diagnosis and treatment of both OSA and TMD. For Obstructive Sleep Apnea, the use of devices like Continuous Positive Airway Pressure (CPAP) machines has been revolutionary. These machines ensure that airways remain open during sleep by providing a constant flow of air through a mask. A custom fitted dental appliance is made for those who cannot tolerate CPAP.
On the TMD front, laser therapy is being increasingly utilized to treat jaw pain and inflammation. Laser treatments can reduce pain and promote healing by stimulating blood flow and tissue repair. Additionally, advancements in imaging techniques, such as digital X-rays and MRIs, provide detailed views of the jaw joint and surrounding structures. This allows healthcare providers to make more accurate diagnoses and tailor treatments to individual needs. Appliance therapy like the Gelb orthotic and the amazing ALF have come to the forefront in TMD treatment, and coincidentally helps with OSA.
Be sure to talk to a well educated healthcare professional who understands your needs and can analyze the situation correctly.


Choose Adventist Medical Group Primary Care in Fort Washington, Maryland, to provide a full range of primary care services for adults.
Learn to better manage your health and prevent illnesses with personalized care from our experienced, primary care providers. Our specialists in family medicine and internal medicine work as a team to deliver expert care when you need:
• Same-day Sick Visits
• Women’s and Men’s Health and Wellness Exams
• Health Physicals, Health Maintenance and Preventive Care
• Geriatric (Senior) Wellness Exams
• Vaccinations and Immunizations, including Flu Shots
• Health Management for:
• Asthma and Allergies
• High Blood Pressure
• High Cholesterol
• Diabetes
• Heart Disease
You also benefit from coordinated care that helps you effectively handle all aspects of your health—from preventive medicine and preoperative appointments to management of chronic health conditions.
To schedule an appointment, please call 240-724-6018 10709 Indian Head Highway, Suite D1 Fort Washington, Maryland 20744 AdventistMedicalGroup.org

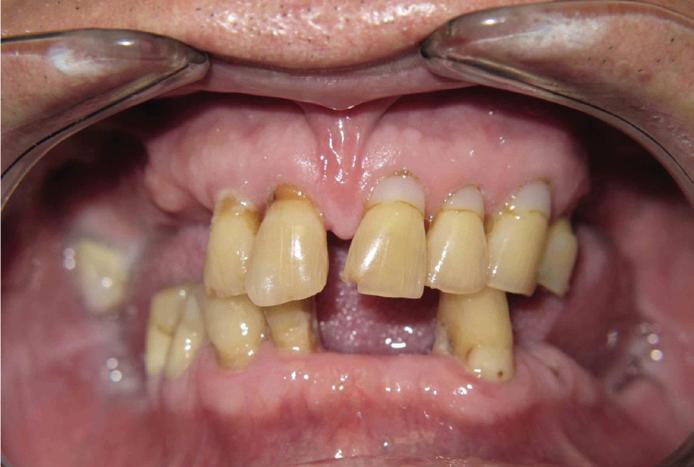
Submitted By Sivakumar Sreenivasan, DMD, MDS Dental Implant Center of Rockville
Can just four implants replace all of the teeth on the top or the bottom of your mouth? Thanks to advances in dental implant technology, that answer is a resounding yes.
Believe it or not, tooth loss is extremely common among adults, especially as we age. In fact, more than 35 million people in America are missing all of their upper and/or lower teeth. Rather than living with the discomfort and hassles of dentures, many people are opting for what is called “all-onfour” dental implant restoration.
All-On-Four: One Full Arch Of Teeth, Four Dental Implants
To fully understand this remark-
able technique for replacing teeth, you should first understand what a dental implant is. An implant is a small titanium screw that fits inside your jawbone and replaces the root-part of a missing tooth. Minor surgery is required to insert the implants. Once the implant is in place, a crown is attached to give you a highly realistic-looking and functional prosthetic tooth.
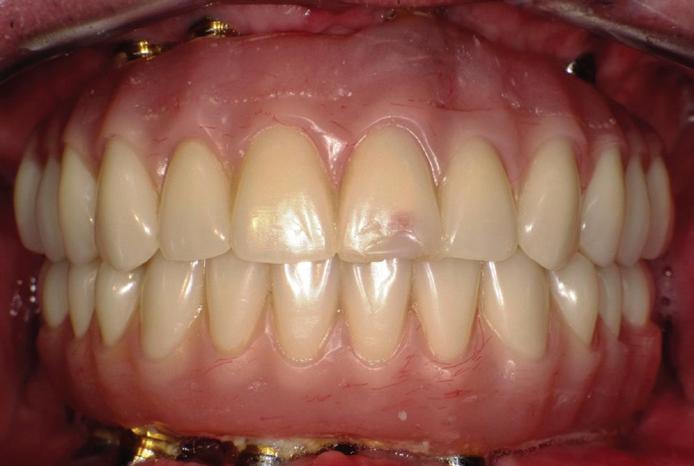
Here’s where it gets really interesting: You do not need a dental implant for each and every one of your missing teeth. All you need is four precisely placed implants on the top of your mouth, and four on the bottom, to restore your full smile. That’s the beauty of the all-on-four. And because the implant is made of titanium, it has the unique ability to fuse to living bone and function as part of it. So eventually, the dental implant becomes part of the jawbone and serves as a strong, long-lasting foundation for your new teeth.
Besides ensuring that your implants are permanently fixed in place,

this bone fusion has another important benefit: it prevents future bone loss in the jaw. This helps to maintain a more youthful facial structure – and better oral health. But perhaps the biggest surprise about the all-on-four is how quickly it can transform your life.
What’s The All-On-Four Dental Implant Procedure Like?
It can be scary to get implants for the first time. Most of that fear is probably due to the uncertainty, so here is the step-by-step process for getting an All-On-Four dental implant.
First, your dentist will want to make sure your comfortable, so either local or general anesthesia will be administered.
Second, the dentist or surgeon will prepare your mouth for the implants, which involves removing your remaining teeth that are failing. They will then remove any diseased or infected tissue from your jaw and gums.
After the implants have been placed, they will thoroughly clean the surgical sites and suturing all the incisions. Then you’ll be taken to a recovery room where you can relax and take time to wake up from the anesthesia.
Do
If The All-On-Four Procedure Is The Right Option For You?
At your All-On-Four consultation, you’ll receive a 3D CT Scan. This scan will help determine if you need implants and assist your doctors in creating your treatment plan. So if you want to learn more about dental implants, simply schedule a consultation with an All-On-Four provider. It’s the best way to find out how dental implants can change your life.
Next, they will begin the implantation process. This means they will insert the titanium screws into your jawbone. Most likely, they will place two implants toward the front of your mouth and two towards the back of your mouth so the “anchors” can evenly bare the force of the denture.


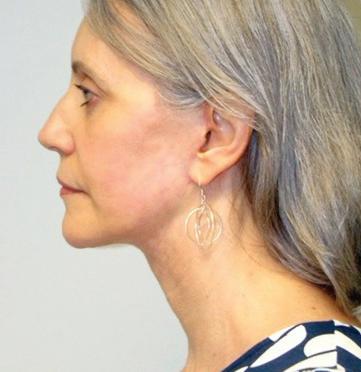
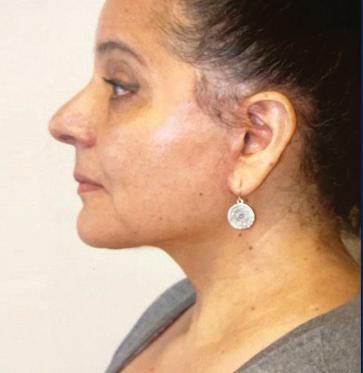
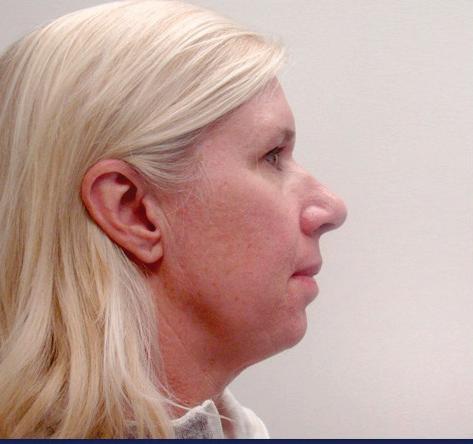
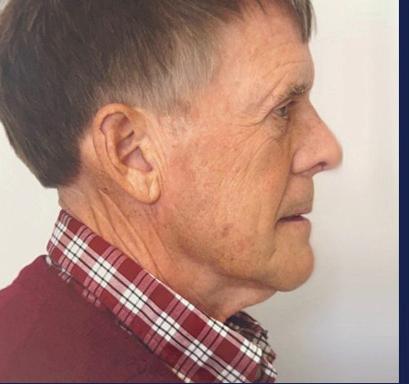
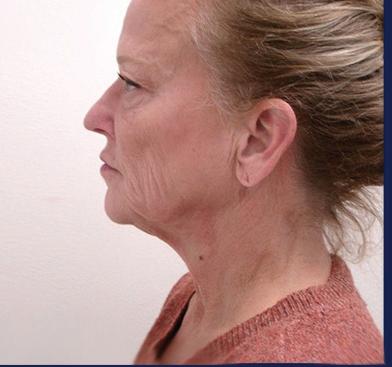
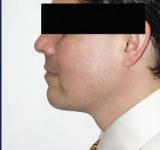
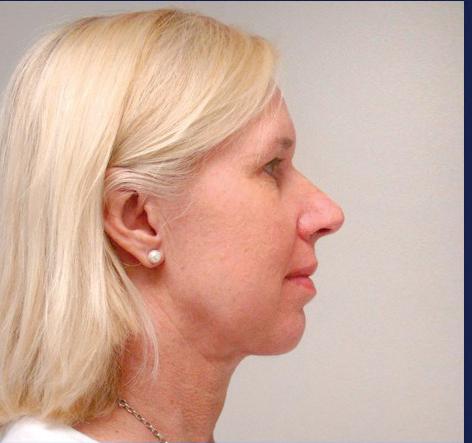
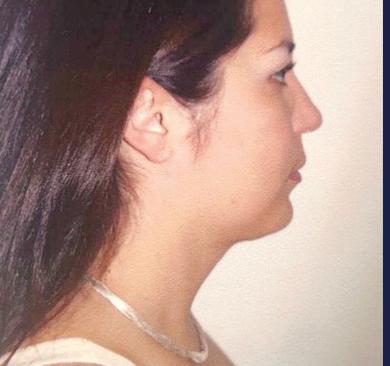
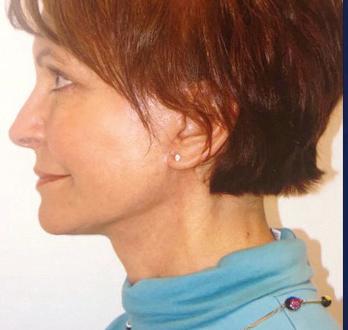
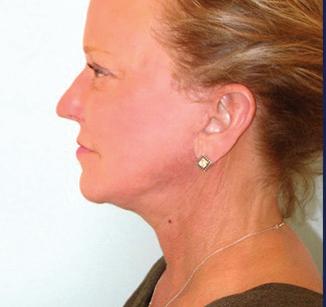
A neck lift can be performed for men and women of varying ages who are often frustrated by changes of the appearance of their neck and jawline. Depending on your age, a neck lift can be a short one-hour procedure to remove fat or a 3-hour procedure to remove fat, visible neck bands, and excess skin.
Remove Excess Skin (Cervicoplasty) • Liposuction to Remove Excess Fat
Remove or Alter Neck Muscles (Platysmaplasty)
Liposuction can be performed alone or with surgical removal of the fat under the chin through a small incision under the chin.
In patients with vertical bands in the neck, a platysmaplasty can be performed to reduce the appearance of the bands.
Sometimes a chin implant is recommended to improve the overall contour and help with excess skin.



















Proud to be in network with PPO plans: Delta Dental, MetLife, United Concordia, United Healthcare, Aetna, GEHA, CIGNA, Anthem, BlueCross BlueShield, United Healthcare, Guardian, Principal Ameritas, DentaQuest, Dominion Dental, Connection Dental, Himan, Assurant/Dental Health Alliances, Smiles for Children. Dr. Afreen Sayeed Services provided include: Implants, Implant Crowns, Invisalign, CEREC, Crowns, Root Canals, Cosmetic Dentistry, iTero Digital Scanner, Tooth-Colored Fillings and Extractions. Schedule an appointment for you and your family today!



Dr. Brown’s practice focuses on TMJ, sleep apnea and orthodontics. This allows Dr. Brown and his team to provide individualized, focused care for patients dealing with these specific issues. Every day, his practice helps patients of all ages with facial development, sleep issues, chronic headaches, migraines, neck pain, movement disorders, and much more. His training also includes multiple disciplines involving the cranial bones in the skull, and the discs in the jaw joints. Through treatment, Dr. Brown is able to reduce these symptoms, align cranial bones, avoid extractions, and greatly reduce the need for traditional braces. His expertise allows him to identify issues early on which promotes proper facial development using dental appliances. If there is an internal imbalance, whether an adult or child, the body does not develop or function properly. When the cranial bones are lined up correctly, patients are able to function, sleep and generally live better.
With that in mind, the team at Sleep & TMJ Therapy takes a whole-body approach when treatment planning. They work hand in hand with physical therapists and osteopathic doctors for a better success rate. Dr. Brown is devoted to helping patients of all ages live a symptom free life.
Degrees & Certifications
Dr. Brown earned his degree from Georgetown Dental School and completed residencies with Emory University Hospital for Dental Sleep Medicine and the ALF Appliance Therapy Institute.
Outside the Office
When not seeing patients, Dr. Brown is a sought-after speaker. He has lectured all over the world, including D.C., Dubai, Seoul, London, Norway and Toronto. He has also been featured on Channel 9’s Good Morning Washington, several podcasts, and numerous magazines and journals.
Professional Affiliations
Dr. Brown is a diplomate of the American Academy of Craniofacial Pain, a member of the American Academy of Dental Sleep Medicine, American Academy of Gnathological Orthopedic, Academy of Integrative Pain Management American Dental Association, a Fellow of the American Academy of Craniofacial Pain, and Legacy Provider for the ALF Interface Academy.
Do you have TMD or Sleep Apnea?
TMD Symptoms: Noise in the jaw joints when opening and closing your mouth, difficulty chewing, limited opening, tender facial muscles, ear ringing, uncomfortable bite, jaw locking, headaches, migraines, dizziness, vision issues as well as pain in the jaw area which can radiate to the ears, head, neck, shoulders, and back.

Sleep Apnea Symptoms: Snoring, waking up gasping for air, feeling tired and irritable in the morning, difficulty controlling weight, concentration problems, morning headaches, episodes of not breathing, waking with a sore throat, forgetfulness and mood changes. If you believe you may be suffering from TMD or Sleep Apnea, don't wait... Call today to schedule a consultation with Dr. Brown: 703-821-1103. Germantown Square Shopping Center, Lower Level
Wisteria Drive, Suites C & D

I knew I wanted to be a veterinarian at age five and started working in clinics at 14. I earned my DVM from Ohio State University in 1977 and spent a decade in clinical practice before discovering holistic medicine. When seeking alternative ways to improve pet health, I became certified in veterinary acupuncture, natural health, and homeopathy, training with Dr. Richard Pitcairn. My passion is Traditional Chinese Medicine (TCM) which includes Acupuncture, Aquapuncture, Food Therapy, and Chinese Herbal Medicine. I am also certified in Medical Ozone Therapy for Animals and am a Certified Fear Free Practitioner. Our complete Integrative approach to medicine enhances our patients’ longevity and quality of life. In 1993, I sold my practice in Germantown, MD and moved to Sedona, AZ, embarking on a spiritual journey. I was a Tibetan Buddhist nun from 2002 to 2023, dedicating myself to relieving suffering. I also studied energy healing and volunteered in disaster relief efforts, including Katrina Relief and Tara’s Babies Animal Sanctuary.
Returning to Maryland in 2006, I worked at Veterinary Holistic Care before co-founding Holistic Veterinary Healing in 2013 with Dr. Kitty Raichura.
In 2009, I received a Master’s in Human Acupuncture and practiced on both humans and animals until Dr. Raichura’s passing in 2016. Now, I focus solely on treating animal patients.
I live in Germantown with my dogs, Bodhi and Jack. In my free time, I enjoy meditating, watching movies, and taking my dogs for walks.

Growing up with a background in Traditional Chinese Medicine, I discovered my passion for integrative veterinary medicine early on. My father introduced me to Gua Sha and acupressure massage, sparking my fascination with healing modalities. Initially pursuing human medicine, I worked in acupuncture clinics, volunteered at Walter Reed, and conducted research at UMD and FDA.
In 2015, I encountered Traditional Chinese Veterinary Medicine (TCVM) through Dr. Allison Marshall, a veterinarian certified in acupuncture. Inspired, I pursued veterinary medicine, earning a Bachelor’s in Biomedical Engineering at VCU in 2017 and completing my DVM at Virginia-Maryland College of Veterinary Medicine in 2021.
I specialize in integrative medicine, blending holistic and conventional approaches to provide optimal care. Certified in veterinary acupuncture (CVA) through Chi University, I also have experience in pathology, surgery, and exotics.
In my free time, I enjoy lion dancing, spending time with family, and exploring new foods.


Dr. Mikel Daniels is a highly skilled podiatrist dedicated to delivering exceptional, patient-centered care. With decades of experience and a deep commitment to improving foot and ankle health, he blends medical expertise with compassionate service to help patients achieve lasting wellness and mobility.
Dr. Daniels earned his Bachelor of Science in Biology with a minor in Economics from Muhlenberg College in 1996, followed by his Doctor of Podiatric Medicine (DPM) degree from Temple University School of Podiatric Medicine in 2000. He completed his Podiatric Surgical Residency at the University of Maryland, Mercy Medical Center, where he gained extensive clinical and surgical experience. In addition, Dr. Daniels holds an MBA with a concentration in Healthcare Management from Western Governors University, earned in 2014— giving him a unique combination of medical and business education that informs his approach to both patient care and practice management.
Dr. Daniels has been named one of Baltimore’s Top Doctors in 2023, 2024, and 2025, a reflection of his outstanding reputation among peers and patients alike. He is a frequent podcast guest and has been featured as an expert in foot and ankle care by major media outlets including CNN and Parade. Locally, he has also appeared on television to discuss common foot and ankle issues, offering practical tips for maintaining mobility and preventing injury.
Dr. Daniels’ special areas of interest include diabetic wound care, medical and practice economics, and advancing equity within healthcare. His mission is to ensure every patient receives comprehensive, evidence-based treatment tailored to their individual needs—helping them stay active, comfortable, and confident on their feet.

Dr. Janet V. Johnson was born in Brooklyn, NY. She received her undergraduate degree in Biology at Hunter College in Manhattan, NY. She pursued a career in research medicine as a research assistant at Downstate Medical School in the Department of Gastroenterology. Obtaining her masters degree in Physiology at Long Island University in Brooklyn, NY. Dr. Johnson received her medical degree from State University of New York at Buffalo School of Medicine in 1991. She completed her Internship and Residency at Howard University/ DC General Hospital in 1994.
After becoming Board Certified by the American Board of Pediatrics, Dr. Johnson worked as an Emergency Room Pediatric Physician at DC General Hospital and for a local pediatrician before she began her practice: Loving Care Pediatrics in Hyattsville, MD in 1998. She is continuing to pursue CME credits to maintain board certification. Concurrently, she serves as a Clinical Instructor to nursing students at Howard University Family Nurse Practitioner (FNP) Program; John Hopkins Family Nurse Practitioner (FNP) Program; Marymount Family Nurse Practitioner (FNP) Program; and University of Maryland Baltimore Family Nurse Practitioner (FNP) Program. She also serves as a Clinical Instructor for medical assistant students at Stratford University; Fortis College, Brightwood College and Career Technical Institute. She is a Fellow of the American Academy of Pediatrics (FAAP). Dr. Johnson is also a member of the Prince George’s Community Advisory Group (CAG), Washington Adventist Health Ministry Network and the Medical Advisory Committee for Amerigroup Insurance. Dr. Johnson has given lectures on Teen Suicide and Teen awareness on HIV/AIDS to youth groups in Washington, DC and continues to publish articles in Washington Woman’s Journal and Your Health Magazine in Prince George’s County. She served as Medical Director of the Mid-Maryland Mission of Mercy and Health Equity Festival, which provides free dental care. She annually gives talks “Suicide Is Not an Option” and “Teen HIV/AIDS Awareness” to a group for youth summer program in Washington, DC. She integrates Christian prayer into her practice when appropriate and regularly incorporates social justice topics into her magazine articles.
With offices in Charlotte Hall, and La Plata, we are conveniently located to help with all of your chiropractic needs. Since serving the community since 2003, we offer many services such as chiropractic adjustments, physical therapy, exercise therapy, children’s therapy, DOT/CDL Physicals, and more. Winters Chiropractic and Physical Therapy is a full service care office. We focus on our patients comfort while providing the latest techniques to relieve persistent pain.


Degrees, Training, and Certifications: Doctor of Chiropractic, Northwestern College of Chiropractic; Bachelor of Science, North Dakota State University; Certified Medical Examiner, FMCSA (Federal Motor Carrier Safety Administration). Doctor of Chiropractic w/Physical Therapy Privileges, FMCSA DOT/CDL Certified Medical Examiner.
Professional Memberships/Associations: Maryland Chiropractic Association, Maryland Board of Chiropractic & Massage Therapy Examiners.
Techniques: Diversified, Thompson, SOT, Active Release Technique, Passive Release Technique, Trigger Point Therapy
Expertise: Personal/Work/Sports Injuries, DOT/CDL Medical Certifications, Musculoskeletal Disorders, Nutrition.
Personal Interests: Family and Vacationing, Motorcycling (Harley Davidson), Snowmobiling, Target Shooting, Computers
Degrees, Training, and Certifications: Doctor of Chiropractic, Northwestern College of Chiropractic; Bachelor of Science, Human Biology Minnesota State University. AMA Guides to Evaluating Permanent Impairment, Certified Disability Examiner, Manipulation Under Anesthesia Certified.
Professional Memberships/Associations: Maryland Chiropractic Association
Techniques: Diversified, Thompson, SOT, ART/PRT, TPT, MUA
Expertise: Personal, Work and Sports Injuries, Spinal and Extremity Conditions, Musculoskeletal Disorders and Nutrition
Personal Interests: Family, Home, The Great Outdoors, Motorcycles, Snowmobiles

Dr. Mary Alexander, periodontist, obtained a Bachelor of Science degree in Biology from the University of South Carolina and continued her education in dentistry at the University of Maryland School of Dental Surgery where she received her DDS degree. Prior to and during her dental studies, Dr. Alexander received funding and support from the National Institutes of Dental Research for her involvement in the periodontal research. After obtaining her DDS degree Dr. Alexander spent one year at the Veteran’s Administration Hospital, in general practice residency focusing her training in the area of anxiety patient management. She then attended Harvard University and earned her clinical specialty in periodontics and a doctorate in medical science. Her doctoral research was focused in the study of bone function and metabolic disease of the bone.
Dr. Alexander received extensive training in dental implantology, periodontal plastic surgery, bone regenerative procedures and sedation dentistry. All aspects of Dr. Alexander’s training are incorporated in her periodontal practice assuring patient’s thorough and comprehensive periodontal treatment.




dental school again at Boston University and Oral and Maxillofacial Surgery residency at University of Medicine and Dentistry of New Jersey.
As an Oral and Maxillofacial Surgeon, Dr. Sreeni manages a wide variety of problems relating to the Mouth, Teeth and Facial Regions. He practices a full scope of Oral and Maxillofacial Surgery with expertise ranging from Corrective Jaw Surgery to Wisdom Teeth Removal. His passion is in implant surgery and he is well known for same day placement of implants following teeth removal be it for single teeth or a complete “makeover” (Smile in a day). He can also diagnose and treat Facial Pain, Facial Injuries and TMJ disorders and perform Bone Grafting and Sinus lift procedures.
Dr. Sreeni completed a residency in Anesthesiology at Mount Sinai Hospital, New York in 1994 and has worked as an Attending providing anesthesia services for children and adults in the ambulatory outpatient center of the hospital.
Dr. Sreeni is an Advanced Cardiac Life Support instructor with the Adventist group. He is also certified in Pediatric advanced life support and is very capable of handling emergencies that could possibly arise in the office. Dr. Sreeni’s staff are trained in assisting with IV Sedation/ General Anesthesia within our state of the art office setting. Patients are continuously monitored during and after surgery. The goal of our office is to provide professional service with compassion and an understanding of the patients’ perspective.


Dr. Lynese Lawson is the founder and medical director of Proactive Wellness Centers, PLC, an integrative and functional medicine practice in Tysons Corner, Virginia. Since opening in 2006, the center has become a leading destination for patients across the DC metropolitan area and beyond.
A Doctor of Osteopathic Medicine, Dr. Lawson spent 20 years in traditional medicine before establishing her practice to focus on bioidentical hormone replacement, weight management, CIRS/ Mold illness, Lyme disease, parasitic infections, and chronic disease prevention. She is Board Certified in Anti-Aging/Regenerative Medicine (ABAARM), an Institute for Functional Medicine Certified Practitioner, and one of the select Bredesen Certified practitioners in the ReCode 2.0 protocol for treating early Alzheimer’s and cognitive decline.
Dr. Lawson also trained at the BaleDoneen Institute in advanced prevention of heart attacks, strokes, and type 2 diabetes. She is Shoemaker-Certified in diagnosing and treating CIRS/Mold illness, an emerging epidemic often linked to water-damaged buildings. Her expertise integrates scientific research with personalized care, especially for patients facing complex, overlapping conditions. Through her dedication to functional medicine, advanced training, and ongoing research, Dr. Lawson helps patients achieve better health, restore vitality, and improve quality of life.
Wellness-Peptides-BHRT-Lyme Disease-Mold/CIRS
aaybar@kidsgastro.com

Every patient and their parents are given the time they need during a consultation at Annapolis Pediatric Gastroenterology and Nutrition to fully understand what’s happening and ask any questions they may have. If your child needs to undergo any procedures, Dr. Aybar performs them at the Anne Arundel Medical Center in Annapolis, Maryland.
A board-certified pediatrician who specializes in pediatric gastroenterology after finishing his fellowship at University of Maryland. Dr. Aybar was born in Turkiye, and received his medical degree from the University of Istanbul. He completed an internship in pediatrics and adolescent medicine at the Cleveland Clinic Foundation Children’s Hospital and a residency in pediatrics at Sinai Hospital in Baltimore, Maryland, where he served as chief resident. Dr. Aybar gained valuable experience working in several Baltimore Metropolitan Area hospitals as a pediatrician in the emergency department and as a pediatric hospitalist.

Call

After completing his fellowship in Colon and Rectal Surgery at Robert Wood Johnson University Hospital-Rutgers University, Rami Makhoul, MD, joined Holy Cross Health Hospital in 2014 to serve patients of the DMV area.
Upon graduating from medical school, Dr. Makhoul first completed his internship in General Surgery at the University of Massachusetts Medical School. He, then, completed his residency training in General Surgery at the George Washington University Hospital in Washington, DC.
During his residency training at GW, he spent a year in clinical research where he published some of his work on colon and rectal cancer, and the use of Robotic Surgery in various abdominal procedures performed in the Colon and Rectal Surgery field. He continued with his passion for research and published peer-reviewed articles during his fellowship training. Several of his work, was presented at national conferences including the American Society of Colon and Rectal Surgery, and the Society of American and Gastrointestinal and Endoscopic Surgeons annual conferences.
Dr. Makhoul diagnoses and treats various diseases of the colon, rectum, anus, and other parts of the GI tract using national standards and guidelines. He has a special interest in treating colon and rectal cancer using advanced surgical minimally invasive techniques including robotic, laparoscopic, and transanal minimally invasive surgery. Dr. Makhoul is Board Certified in both General Surgery and Colon and Rectal Surgery and is an active member of the American Society of Colon and Rectal Surgeons education committee.
As part of his commitment to surgical training and education, Dr. Makhoul serves as a Clinical Instructor of Surgery at the George Washington University. Dr. Makhoul is currently the chairman of the Department of Surgery at Holy Cross Hospital in Silver Spring. He also holds the position of Cancer Liaison Physician for Holy Cross Health, where he manages and overlooks clinically related cancer activities in collaboration with the Commission on Cancer and American Cancer Society. When he is away from the office, Dr. Makhoul may be found spending time with his family. Dr. Makhoul enjoys skiing, cycling, scuba diving, tennis, and traveling.


Dr. Matthew Skancke is a colon and rectal surgeon serving Maryland, Virginia and Washington, DC. Dr. Skancke grew up in Great Falls, VA earning his undergraduate degree in electrical and biomedical engineering at the University of Virginia’s engineering school. After engineering school he spent three years working for a Swiss based GPS company U-blox America while going to night school to finish his premedical degree. He then attended medical school at the University of North Carolina at Chapel Hill where he did basic science research of mesenchymal stem cells to progress the field of regenerative medicine. Dr. Skancke continued his General Surgery training at the George Washington University Hospital and subsequently did his Colon and Rectal Surgery Fellowship at the Cleveland Clinic.
During his training, Dr. Skancke has published over 24 peer reviewed publications, authored three book chapters, and presented over 45 times at national conferences in medicine and surgery. He has participated in clinical trials of bench top and mechanical sciences and is a member of the American College of Surgeons and the American Society of Colon and Rectal Surgeons. Dr. Skancke is Coard Certified in General Surgery and Colon and Rectal Surgery and is an active member of the American Society of Colon and Rectal Surgeons Quality and Safety National committee.
Outside of work, Dr. Skancke has found a new love for French cooking and North Carolina barbeque. To offset these vices, Dr. Skancke also enjoys running and powerlifting in his free time.







If you are struggling with acute and chronic pain, post-radiation/post-chemotherapy-induced dry mouth, neuropathy, headaches, or stress-related conditions (anxiety, depression, PTSD), Rapid Acupuncture offers targeted, evidence-based treatment designed to activate your body’s natural healing response – often with noticeable improvement after the first session.
You probably know family and friends whose lives were cut short by heart disease or cancer. Then you ask yourself “Is there any way to keep that from happening to me?” The answer is “yes.” Today there is a simple non-invasive test that can often identify these illnesses in their earliest stages, when they can most effectively be treated and cured.
It’s called the Virtual Physical. The Virtual Physical takes less than twenty minutes and is a safe, painless, high-speed full Body, Heart and Colon scan. It has already saved many lives by uncovering many illnesses like cancer, heart disease, aneurysms, and tumors.
The Virtual Physical is a test that gives you the advantage in finding diseases and abnormalities at their early stages, long before symptoms occur. Make the choice that could save your Life.
Dr. Songxuan (Song) Zhou-Niemtzow received her medical degree and acupuncture training at Yunnan University of Traditional Chinese Medicine in Kunming, China. She subsequently trained with several renowned acupuncture masters in the Yunnan and Sichuan provinces, as well as in Beijing, before establishing a thriving private practice in Beijing’s Embassy District. There, she provided care for an international clientele, including patients from the U.S., French, and Japanese embassies. She also worked for many years in U.S. military hospitals, including Malcolm Grow Medical Clinics and Surgery Center at Joint Base Andrews (formerly Andrews Air Force Base), where she provided integrative acupuncture and integrative medicine to service members and their families.
Sciatica
TMJ Dysfunction • Frozen Shoulder • Plantar Fasciitis • Carpal Tunnel
Fibromyalgia • Migraine & Headaches • Trigeminal Neuralgia
• Peripheral Neuropathy
• Post-Stroke Recovery
• Essential Tremor
• Parkinson’s Disease
• Chronic Pelvic Pain
• Female Infertility
• Menopause Symptoms
• Insomnia
• PTSD
• PMS & Menstrual Disorders • Anxiety/Depression
• Radiation-Induced Dry Mouth
• Tinnitus
• Macular Degeneration (Stable Dry Type)
• Smoking Cessation
10111 Martin Luther King Jr. Highway, Suite #102 Bowie, MD
6196 Oxon Hill Road Suite #240, Oxon Hill, MD

Dr. Trent has a passion for helping people. She has practiced Audiology since 1984, in a number of clinical settings. Her diverse career has included 16 years of teaching and clinical supervision at Howard University, Washington, DC and Temple University, Philadelphia, PA. Dr. Trent has also worked as a clinical audiologist in hospital settings and private ENT practices. Education:
Clinical Doctoral Degree – Audiology-University of Florida, Gainesville, FL
Master of Education – Audiology- Northeastern University, Boston, MA
Bachelor of Science – Communication Sciences and Disorders – Hampton University, Hampton, VA
Dr. Trent holds her Maryland State Licensure in Audiology. She is a Certified Clinical Audiologist (CCC-A) through the American Speech-Language-Hearing Association (ASHA). Presently, she serves on the Board of Directors for ASHA as Vice President for Audiology Practice.


301-805-4664
12200 Annapolis Road Suite #116 Glenn Dale, MD 20769
EnvisionEyeandLaser.com

Board Certified, Ophthalmology by the American Board of Ophthalmology
Degrees, Training and Certificates: UCLA Medical School; Yale University Hospital for Residency; Louisiana State University for Cornea and Refractive Fellowship
Professional Memberships/Associations: American Academy of Ophthalmology; American Society of Cataract and Refractive Surgery; International Society of Refractive Surgery
Areas of Interest: All laser custom LASIK; Cataract Surgery; Botox; Dermal Fillers; Cornea Comprehensive Ophthalmology
Practice Philosophy: Envision Eye and Laser is committed to delivering superior ophthalmic care with state-of-the-art technology and patient education in a caring, compassionate environment. We cater to a diverse population of adults and work with your primary care physician to improve the quality of your overall health and life. Your best vision is our focus.




By Dr. Tiffany Daniel Live To Day Wellness
The majority of our clients suffer from chronic pain or trauma which inhibits them from conducting their daily living activities or reaching their goals of being pain and stress free.
Mindfulness and movement can be combined together to complement the primary care provider’s prescribed treatment. So many clients are living with chronic pain, trauma, and disease that it has become a common household topic.
Today some of the most popular practices for well-being are through equine training, therapeutic horticulture, meditation and yoga. All the above can provide forms of mindful movement.
Mindfulness is a mental state achieved by focusing one’s awareness on the present moment, while calmly acknowledging and accepting one’s feelings, thoughts, and bodily sensations, used as a therapeutic technique.
Mindful movement can be described as any movement activity that is practiced mindfully, by giving attention, presence, and intention to whatever the form of movement may be. It can be accomplished through activities such as equine therapy, gardening, walking, yoga, etc,. to name a few.
We implement programs geared toward individual needs to glean from the incentives gathered from the practice of mindfulness.
Mindful Resilience (MR), or therapeutic yoga is a program that was developed by Dr. Dan Libby of the Veteran Yoga Project (VYP) which includes practices that have been chosen based on the feedback of hundreds of veterans and active service members who suffer from the aftereffects of combat or other trauma. MR programs report improvements in mood, impulse behavior, irritability, concentration, and sleep.
There are five parts to Mindful Resilience training:
• Breathing – Techniques that can help relieve anxiety and can be used anywhere and anytime.
• Meditation – Enhances focus and concentration, settles the mind, and promotes a sense of wellbeing.
• Mindful Movement – Postures that
bring the body through its natural range of motion to enhance strength and flexibility and reinforce the connection between mind and body.
• Guided Rest – Guided exercises can lead to deep and profound relaxation.
• Gratitude – Simple practices that promote a positive outlook.
Equine Facilitated Therapy, used for personal development and learning can be used effectively for both adults and youth where they are offered social activities based on their horse experience. This type of training provides positive results to
improve cognitive functions including strategies for organized behavior and self-awareness with mindfulness skills as a recovery tool for individuals under enormous amounts of stress.
This therapy is also known to be beneficial in improving motor skills for those seeking treatment for cerebral palsy, Downs syndrome, autism, and sensory integration disorder. When this type of therapy is offered, we partner with equine and physical therapist.
Therapeutic Horticulture, uses plants and outdoor environments to achieve the mindfulness health
goals. The American Horticulture Therapy Association (AHTA) defines therapeutic horticulture as “the process through which participants enhance their well-being through active or passive involvement in plantrelated activities. Nonetheless, there have been breakthroughs reported for eating disorders, PTSD, depression, anxiety, developmental disabilities, dementia, brain injury, cancer, and physical disabilities.
And lastly rest, walking and water, will never steer you wrong. So let’s relax and let it go.

We believe total well-being starts with balance—of body, mind, and spirit. Our mission is to empower women, veterans, and families through movement, mindfulness, and nutrition. Join
and wellness programs featuring: Mindful Movement & Breathwork – Therapeutic Horticulture Yoga for Trauma & Stress Relief – Nutrition and Wellness Coaching Whether you’re healing from life’s challenges or simply ready to grow stronger inside and out—there’s a place for you here.


By Quansheng Lu, CMD, PhD, LAc Wholelife Chinese Medicine & Acupuncture Center

Chinese acupuncture has a rich history spanning over 3,000 years, forming an integral part of traditional Chinese medicine (TCM). Acupuncture entails the delicate insertion of fine needles into specific points on the skin, aiming to induce therapeutic benefits.
The Mechanism Behind Acupuncture
Within the framework of Chinese medicine, acupuncture is rooted in the belief that it acts by clearing the blockages in the flow of energy along pathways known as “meridians.” The
Quansheng Lu, CMD, PhD, L.Ac www.wholelifeherb.com • luquansheng@gmail.com 301-340-1066 • fax: 301-340-1090
Guest professor, Henan University of Traditional Chinese Medicine (TCM) Chief TCM Physician, WFCMS; M.S. in TCM, Beijing University of TCM PhD in integrated medicine, China Academy of Chinese Medical Sciences Fellowship, Georgetown University & Children’s National Medical Center 3 patents, 8 books of TCM, 30 papers, 30+ years of experience in TCM
Low back pain • eczema • arthritis • allergies
cough
insomnia
paralysis obesity • nephritis • hepatitis
infertility • PMS • side effects of cancer treatment 416 Hungerford Drive, #300 Rockville, MD 20850 5022 Dorsey Hall Drive, #101 Ellicott City, MD 21042



underlying theory suggests that when these energy channels are obstructed, discomfort ensues.
The primary causes of neck pain often stem from extended periods of maintaining a fixed posture, leading to increased neck tension. Injuries can also trigger neck pain. Among adults, cervical spinal stenosis, which involves the narrowing of the spinal canal in the neck, is a prevalent factor. In the context of Chinese medicine, it is believed that external factors like wind, cold, injuries, or excessive physical activities can disrupt the flow of qi and blood in the neck, ultimately resulting in neck pain.
Common symptoms associated with neck pain include the presence of knots, stiffness, or sharp pain in the neck region. This discomfort may radiate to the shoulders, upper back, or arms. In some cases, individuals might also experience headaches, difficulty in head and neck movement, as well as sensations of numbness, tingling, or weakness in the arms.
Acupuncture serves as a widely recognized approach for addressing neck pain and various musculoskeletal issues, with some compelling evidence to support its efficacy in both short-term and long-term pain relief. An Australian randomized controlled trial sought to compare the effectiveness of acupuncture with simulated acupuncture in individuals dealing with sub-acute and chronic whiplash-related disorders. The study involved a series of 12 acupuncture sessions over a six-week period, with follow-up assessments at three and six months. The results revealed that those who received genuine electroacupuncture treatment experienced significantly greater reductions in pain intensity at three and six months, as compared to the sham electro-acupuncture group (Spine, April 2011).
Incorporating Traditional Chinese Medicine
Traditional Chinese medicine encompasses a diverse array of practices, including Chinese herbal medicine and acupuncture/moxibustion, among others. The use of Chinese medicine therapies, such as herbal remedies and acupuncture, for managing neck pain,
Please see “Neck Pain,” next page

By Janet V. Johnson, MD Loving Care Pediatrics
Teen Suicide Awareness and Prevention
Teen suicide is a concerning issue that ranks as the third leading cause of death among teenagers. Every 17 minutes, a teenager tragically succeeds in taking their own life. These statistics underscore the gravity of the problem and emphasize the importance of understanding who may be at risk and how to offer assistance.
Teenagers often grapple with thoughts of death, making it crucial to take suicide attempts seriously. The National Institute of Mental Health
estimates that for every completed suicide, there may be as many as 25 suicide attempts that go unreported. Recognizing that a teen’s suicide attempt is a plea for help is vital in preventing future, potentially fatal attempts.
Several strong risk factors contribute to teenage suicide, including aggressive or disruptive behavior, substance abuse, and depression. These factors often intensify the turbulent emotions experienced during adolescence, fostering a sense of hopelessness and despair. Acknowledging these feelings as legitimate and offering support is critical in the battle against teen suicide.
Access to firearms is another risk factor to consider, given that they are involved in over half of teen suicides. Limiting access to firearms and ammunition for teenagers expressing suicidal thoughts is an essential safety measure. Understanding warning signs is paramount, as studies indicate that four out of five teen suicide attempts are preceded by clear indicators. These warning signs encompass neglect of personal hygiene, physical complaints arising from emotional distress, de-
has not only been widespread but also highly effective, extending its reach not just within China but also across Europe. Navigating Acupuncture Safety
While acupuncture is generally acknowledged as a safe therapeutic method, potential side effects may include dizziness, localized internal
clining academic performance, loss of interest in school and extracurricular activities, risky behavior, boredom, and more. Recognizing these signs can be a life-saving intervention.
Preventing teen suicide requires unwavering vigilance and support. It is imperative for guardians to convey love

From Page 30
bleeding, dermatitis, nerve damage, or occasionally heightened pain—especially when administered by less experienced practitioners. Therefore, the role of a well-trained and seasoned acupuncturist is paramount in ensuring both safety and effectiveness.
From Page 30
and support to teenagers, letting them know they are not alone in their struggles. Additionally, educating oneself about the signs of suicidal thoughts and feelings is crucial, as is seeking professional help when needed. Together, we can work towards reducing the devastating impact of teen suicide on our youth.



ACUPUNCTURE
Eastern Medical Holistic Healing Center, Angel Wood, 240755-5925. www.acupuncture4wellness.webs.com
ALTERNATIVE HEALTHCARE
Holistic Family Health - Thermal Imaging, Herndon, VA. 703-635-6324 For More information visit www.fhtid.com
BEAUTY/SKIN
A Better You, Dr. ClarkeBennett, 410-672-2742.
BREAST HEALTH
University of Maryland Charles Regional Medical Center. 11340 Pembrooke Square, Suite 202, Waldorf, MD 20603. 240-607-2010. UMCharlesRegional.org
CHINESE MEDICINE & ACUPUNCTURE
Wholelife Chinese Medicine & Acupuncture, 301-526-9898, 416 Hungerford Dr., Rockville www.wholelifeherb.com
DENTAL IMPLANTS
Dental Implants Center of Rockville – Dr. Sreenivasan Sivakumar, DMD, MSD –301-294-8700 – 77 South Washington Street, Suite #205, Rockville, MD 20850 – www.DrSreeni.com.
Karl A Smith, DDS, 2550 N. Van Dorn St., Suite #128, Alexandria, VA. Call 703-894-4867, Visit www.drkarlsmith.com
Richard Hughes, DDS, 703444-1152, 46440 Benedict Dr., Suite #201, Sterling, VA. www. SterlingImplantDentist.com
Marc P. Stanard, DDS – 202887-5441 – 1350 Connecticut Avenue, NW, Suite #305, Washington, DC 20036 – wdcperioimplant.com.
EYE CARE
Visual Eyes, Alexander Nnabue OD, 301-324- 9500.
FERTILITY
Montgomery Women’s Fertility Center – 301-946-6962 – MontgomeryFertilityCenter. com – Rockville, MD.
HOLISTIC WELLNESS COACH
Nutrition Lifestyle Digestion and More – Lisa@LisaThorne.Me – Text 269861-7565.
HYPNOSIS/YOGA
Toni’s Happy Hour Yoga and Holistic Wellness Center • 6504 Old Branch Avenue, Temple Hills, MD 20748 • 301-449-8664.
MEDICAL SPACE
Charles L. Feitel Company, 301-571-9333, www.medicalanddentalspace.com.
MENTAL HEALTH SERVICES
House Calls, LLC. 301-3466732. callingonbeth@gmail. com. www.CallingOnBeth.net.
Nutritional Healing Center, Thomas K. Lo, DC, MA, 240-651-1650, 7310 Grove Road, Suite 107, Frederick, MD 21704. doctorlo.com.
Good Health Nutrition Services,LLC – 1300 Mercantile Lane, Suite 129-37, Largo, MD 20774 – 301-341-4680 –www.ghnutritionservices.com – We accept Insurance.
OPHTHALMOLOGY
NewView Laser Eye Center – Jacqueline D. Griffiths, MD – Reston (703) 834-9777 – Visit us at www.NewViewEye.com.
All Smiles Orthodontics – 9010 Lorton Station Blvd., Suite #260, Lorton, VA 22079 – www. AllSmilesBraces.com – For info call us at 703 337-4414.
To Order: Include you NAME, ADDRESS, PHONE, EMAIL AND WHAT HEADING YOU WISH TO BE LISTED UNDER, AND ANY SPECIAL OFFER OR TEXT TO INCLUDE. We will prepare a proof and email to you for approval.
Email your information to: info@yourhealthmagazine.net or Fax to: (301) 805-6808. Call (301) 805-6805 for assistance.
MARYLAND/WASHINGTON, DC OFFICE
4201 Northview Drive, Suite #102, Bowie, MD 20716 phone: (301) 805-6805 • fax: (301) 805-6808 • email: Info@YourHealthMagazine.net VIRGINIA OFFICE phone: (703) 288-3130 • fax: (703) 288-3174 • email: Publish@YourHealthMagazine.net

Loving Care, Janet Johnson, MD – 301-403-8808.
PHYSICAL THERAPY/ REHABILITATION
Active Physical Therapy. Various Locations across Maryland and Washington, DC. Active-physicaltherapy.com.
Largo Foot and Ankle Health Center, Ade Adetunji, DPM, 301-386-5453.
District Podiatry – Lubrina Bryant, DPM – 202-388-5303 – 1140 Varnum Street, Suite #30, Washington, DC 20017
www.DistrictPodiatry.com.
Chevy Chase Home Care. Help at a time you need it most. Any Ages. Any situations. Any shifts. MD, DC, VA. www.CHCHhomecare. com 202-374-1240.
AA Urology – Odenton, 1106 Annapolis Road, Suite #250, Odenton, MD 21113 – Glen Burnie, 305 Hospital Drive, Suite #303, Glen Burnie, MD 21061 – Bowie, 4201 Northview Drive, Suite #201, Bowie, MD 20716 – West Campus Surgery Center, 7855 Walker Drive, Suite #102, Greenbelt, MD 20770 – Greenbelt , 7855 Walker Drive, Suite #100, Greenbelt, MD 20770.






SUBSCRIBING IS EASY:
1) Call 301-805-6805 with your name, contact info, and credit card payment for $24, or
2) Simply mail this form along with your check for $24:
Your Health Magazine 4201 Northview Dr. Suite 102 Bowie, MD • 20716




Now you can get the latest issues delivered directly to your home!
• Health articles and advice
• Doctors near YOU!
• Maryland, Washington, DC & Virginia editions
• Only $24 for a year’s subscription (12 issues)!


By Angela Akinpelu, PA-C SpinaTherapeutics / Rejuve Medical Group
She sat in front of me with her hands folded tightly in her lap –polite, composed, and exhausted.
Not the “I didn’t sleep well” kind of exhausted.
The deep exhausted. The kind that comes from trying… and trying… and trying – yet feeling like your body is working against you.
Her A1c had climbed. Her weight was up. Her medication list had grown. And the message she’d been hearing for years was this:
“This is progressive. It only gets worse. We’ll just keep adding medications.”
What she didn’t say out loud –but what so many patients feel – is:
“So this is just my life now?”
And that moment is exactly why this conversation matters.
Because for millions of Americans living with prediabetes, type 2 diabetes, and obesity, there is a truth that is often overlooked:
Reversal is possible.
Not in a gimmicky way.
Not by throwing medications away.
Not with shame or starvation.
But in a medically grounded, evidence-supported, metabolismfocused way that restores something many patients have lost: hope.
Many people believe type 2 diabetes is permanent – genetic destiny that can only be “managed.”
That mindset often means:
• more medications
• stricter warnings
• waiting for complications
Neuropathy. Kidney disease. Vision problems. Heart attacks. Strokes.
One of the cruelest parts of this myth is what it does emotionally. It teaches patients to accept decline as inevitable. But type 2 diabetes is not simply high blood sugar. It is a metabolic disease – often driven by insulin resistance – and metabolic states can change.
In clinical practice, I see reversal regularly. Patients who once believed they were destined to worsen begin seeing improvements in A1c, fasting glucose, energy, and medication needs – under careful medical supervision.
This isn’t theory. It’s real life.
Prediabetes Is Not “Almost Diabetes”
Prediabetes is often treated casually. But prediabetes is diabetes already in motion.
Insulin levels are often elevated. Weight gain begins to feel automatic. Many patients are told: “Just watch it.” But watching it is not a plan.
Prediabetes should be treated with urgency – because it is often the stage where reversal is most achievable.
Obesity is not laziness.
And it is not always solved by “eat less and move more.”
If it were, we wouldn’t be facing a national crisis.
Many patients are already doing what they were told:
• smaller portions
• low-fat foods
• calorie counting
• cardio workouts
Yet they feel stuck. Constant hunger. Weight regain. Self-blame.
What’s happening is deeper than discipline.
It’s biology.
The Real Culprit: Insulin Resistance
When the body becomes
resistant to insulin, it produces more and more of it. That creates a metabolic cycle:
• elevated insulin promotes fat storage
• fat storage fuels inflammation
• inflammation worsens insulin resistance
• insulin resistance drives more insulin production
That cycle drives:
• prediabetes
• type 2 diabetes
• stubborn weight gain
• fatigue
• high triglycerides
• fatty liver
The goal isn’t only to lower blood sugar. The deeper goal is to calm the insulin signal and restore metabolic flexibility.
Most conventional care focuses on glucose numbers. And glucose control matters.
But when insulin resistance isn’t addressed, patients often experience a pattern:
• temporary improvement
• rising hunger
• stalled weight loss
• increasing fatigue
• escalating medication
It becomes a treadmill.
And patients blame themselves
– when they were never given the right metabolic strategy.
The Turning Point
When patients finally hear, “This can change,” many don’t believe it.
But once they understand the relationship between carbohydrates, glucose, insulin, hunger, and fat storage, something shifts.
Carbohydrate reduction –including low-carb and ketogenic nutrition – can lower insulin demand.
When insulin demand drops:
• glucose stabilizes
• fat burning increases
• cravings decrease
• appetite becomes manageable
• energy improves
For many, that shift feels like freedom.
What Reversal Actually Looks Like
Reversal doesn’t mean perfection.
It means:
• blood sugar in a non-diabetic range
• significantly lower A1c
• safe medication reduction
• weight normalization
• improved metabolic markers
But the greatest change is often invisible:
Patients stop living in fear of food. They stop feeling powerless. They begin trusting their bodies again.
A Key Safety Point
Nutritional change can alter medication needs quickly. If someone reduces carbohydrates while taking insulin or certain diabetes medications, blood sugar can drop too low.
Reversal should never be done recklessly or unsupervised.
The safest approach includes:
• clinical monitoring
• blood sugar tracking
• medication adjustment protocols
• individualized planning
Reversal is not anti-medication.
It is pro-health.
A Closing Message
If you’ve been told diabetes is forever, hear this:
You are not broken. You are not weak. And you are not destined to decline. Your body is responding to metabolic signals. And those signals can change.
Reversal is possible. And hope belongs in the diabetes conversation.


James Van Der Beek, who died at age 48 from colon cancer, helped bring renewed attention to the rising risk of colorectal cancer in younger adults and the importance of early detection.
Submitted by ScholarsHub.net
For students and working professionals, health concerns are often pushed aside in favor of deadlines, exams, and career demands. Long hours, chronic stress, and irregular routines become the norm, creating a mindset where symptoms are minimized and preventive care is delayed.
Recent public attention following the death of actor James Van Der Beek at age 48 from colon cancer has brought
renewed focus to why this approach can carry serious risks.
Colon cancer has traditionally been viewed as a disease of older adults, yet diagnoses in people under 50 have been rising steadily for decades. One of the most concerning aspects of this trend is how frequently early warning signs go unnoticed— particularly among individuals who are busy, stressed, and otherwise functioning day to day.
Chronic stress affects more than mental well-being. Prolonged exposure to stress hormones can disrupt digestion, alter the gut microbiome, and contribute to systemic inflammation. When combined with sedentary behavior, inconsistent meals, poor sleep, and heavy reliance on ultraprocessed foods, these factors can undermine long-term colon health. While stress alone does not cause cancer, it often contributes to delayed diagnosis by discouraging people from paying attention to persistent symptoms.
Early signs of colon cancer may include changes in bowel habits, abdominal discomfort, rectal bleeding, ongoing diarrhea, or unexplained anemia. For students and professionals, these symptoms are frequently attributed to diet, caffeine, travel, or stress. The tendency to “wait it out” can allow a slow-growing disease to progress undetected.
Colon cancer is often highly treatable when caught early. Current medical guidelines recommend routine screening beginning at age 45
for people at average risk, with earlier evaluation advised for those with family history or concerning symptoms. Screening is not just about diagnosis—it can prevent cancer by identifying and removing precancerous growths before they become dangerous.
From an integrative health standpoint, prevention extends beyond screening alone. Regular physical activity, fiber-rich diets, adequate hydration, stress management, and quality sleep all support digestive health and metabolic balance. These same habits also improve focus, stamina, and resilience—qualities essential for academic success and career longevity.
For younger adults, health is not separate from education or career goals—it supports them. Awareness, early action, and preventive care are informed decisions that protect both personal well-being and longterm potential. Colon cancer awareness is ultimately about education, and informed individuals are better equipped to act before it’s too late.

