




































Your smile is more than just teeth — it’s how you greet the world. Whether you’re tired of covering your mouth in photos, hiding stained or crooked teeth, or feeling discomfort when you chew, Smiles International can help you take back your confidence and restore a radiant, youthful smile.
From routine care to advanced cosmetic dentistry, our experienced team delivers natural-looking results in a modern, comfortable environment.
• Invisalign® clear aligners for discreet straightening
• Teeth Whitening for a brighter, more youthful smile
• Veneers and smile makeovers to fix chips, gaps, and discoloration
• Complete family dental care — all in one place






By Elizabeth Shin, DDS
Bethesda Chevy Chase Pediatric Dentistry
When people hear about fluoride and IQ, most are not thinking about research papers or chemical names. They are thinking about the fluoride their children use every day, brushing their teeth, rinsing, or getting fluoride treatments at the dental office. That makes sense. But the studies that raised this question are not about fluoride that touches the teeth and gets spit out. They focus on fluoride that is swallowed, the kind that goes through the body in drinking water, baby formula mixed with tap water, and foods or beverages made with fluoridated water. To understand the science, it helps to separate topical fluoride, which works on the surface of the tooth, from systemic fluoride, which travels through the bloodstream. Both play a role in oral health, but only the systemic kind is being studied for possible effects on the brain and body.
The Study That Reignited the Discussion
In early 2025, JAMA Pediatrics published a review combining 74 studies on fluoride exposure and children’s IQ. The researchers found that, overall, children with higher fluoride levels in their bodies had slightly lower IQ scores. They did not claim fluoride directly causes lower IQ, but the link appeared stronger in studies that measured fluoride inside the body, such as urinary levels, rather than simply using city water data. Their message was straightforward. The pattern is strong enough to warrant a fresh look at how much fluoride children are receiving from all sources combined.
Differing Scientific Opinions
Some academics have questioned the review, noting that many of the studies it included came from countries with higher natural fluoride levels or from communities with co-exposures such as arsenic or poor nutrition. Others have argued that the review’s methods may have combined studies of unequal quality. However, even among critics, there is general agreement that the findings raise valid questions and that more well-controlled research at U.S. exposure levels is urgently needed.
This Was Not the First
A pediatric dentist’s evidence-based look at what new studies are showing and how families can stay both cavity-free and safe.
Time Scientists Saw This
The JAMA study confirmed what earlier research had already noticed. In Canada (2019) pregnant women with higher urinary fluoride had children with slightly lower IQ scores, especially boys. In Mexico (2017–2018) two separate studies linked prenatal fluoride exposure with lower cognitive and attention scores. In Canada (2020) babies fed formula mixed with fluoridated tap water scored lower on non-verbal IQ tests than breastfed babies. Earlier reviews (2012–2018) also showed an inverse relationship between fluoride exposure and IQ, though quality varied. In New Zealand (2015) one study found no difference, but it used residence rather than biomarkers to estimate exposure. Taken together, this growing body of evidence suggests a consistent pattern that deserves attention, especially for developing brains.
Beyond
Health Clues
Even if we set aside brain development, fluoride that is swallowed leaves unmistakable signs inside the body. The most visible sign is dental fluorosis, faint white lines, cloudy patches, or brownish streaks that appear on teeth as they form. Many professionals call it a cosmetic issue, but that view misses the deeper biological meaning.
Fluorosis as a Warning Sign
Fluorosis is not merely a surface change; it is a biological warning sign of overexposure. It tells us that, during tooth development, the body absorbed more fluoride than it could safely manage. At that point, the safe threshold for cellular balance has already been surpassed. Because fluoride is strongly attracted to calcium, it tends to settle in tissues rich in calcium, including teeth, bones, the pineal gland, and even developing regions of the brain. The enamel changes we can see are simply the visible tip of a deeper metabolic shift.
Systemic Effects Beyond the Teeth
The same chemical interactions that create white streaks in enamel may also be occurring silently in the thyroid, kidneys, and nervous system, where we cannot see them with the naked eye. Fluorosis, therefore, should not be dismissed as cosmetic. It is the body’s way of signaling that fluoride exposure has reached a level capable of altering normal cellular activity. The teeth are the dashboard light, and once they show a warning, the rest of the system deserves inspection.
Topical Fluoride:
Still a Trusted Ally
Fluoride that stays on the tooth surface remains one of dentistry’s most effective tools. Toothpaste, varnish, and sealants all work topically to harden enamel and prevent decay. The question today is not whether fluoride works, but how much and how it is delivered. In the 1950s, when toothpaste was rare, water fluoridation helped communities reduce cavities. Now, with widespread fluoride toothpaste, professional varnish, and better nutrition, mass ingestion may no longer add much benefit and could increase total exposure unnecessarily. Modern prevention should be targeted rather than universal ingestion.
Practical Questions People Are Asking About Fluoride
1. If fluoride helps teeth, why are people suddenly worried about it? Because scientists are now examining how swallowed fluoride affects other organs besides teeth. Fluoride is beneficial in small amounts, but it can accumulate in bones and tissues. Researchers are exploring its possible influence on the brain, thyroid, and kidneys. The goal is balance, not elimination.
2. How can parents protect their children without overdoing fluoride? Use toothpaste properly: rice-sized for toddlers, pea-sized for preschoolers, and teach them to spit, not swallow. Professional fluoride varnish and sealants are safe and stay on the teeth. When preparing baby formula, alternate between fluoridated and low-fluoride bottled or filtered water. Good brushing and diet remain the best cavity prevention.
3. Is fluoridated water safe during pregnancy? Pregnancy is a sensitive time for brain and organ development. Expectant mothers can use reverseosmosis or carbon filters for drinking water, mix bottled and filtered water to reduce total intake, and maintain gum health since inflammation during pregnancy can affect the baby. Lowering ingestion is a reasonable precaution, not an alarm.
4. What about adults with kidney or thyroid conditions? People with reduced kidney function clear fluoride more slowly, so it can accumulate. Those with thyroid disorders may also be more sensitive. Choose filtered or non-fluoridated water when possible. Continue using fluoride toothpaste since it acts topically. Inform your doctor about local water fluoridation to help interpret labs. Fluoride is not automatically harmful, but those with chronic illness should manage intake carefully.
5. Are fluoride-removing filters expensive? Not really. Reverse-osmosis systems cost about $150–300 with annual filter changes, and smaller countertop models start near $50. For families with infants or chronic illness, it is a practical safeguard.
6. How can I find out if my water has fluoride? Check your city’s annual water report or the CDC’s “My Water’s Fluoride” website. If you use a private well, have it tested, since natural levels vary widely.
7. Does bottled water contain fluoride? Some brands do and others do not. Always read the label. For baby formula, most pediatricians suggest non-fluoridated bottled or filtered water.
8. What is the safest overall approach? Keep topical fluoride such as toothpaste, varnish, and sealants. Reevaluate systemic exposure during pregnancy, infancy, or chronic illness. Support new U.S.-based studies that measure real fluoride levels instead of relying on decades-old data. Fluoride’s value remains, but dose and delivery are what truly determine safety.
So, Does Fluoride Lower IQ?
The fair answer is that higher systemic fluoride exposure is associated with slightly lower IQ in many studies. At typical U.S. fluoridation levels, the data are still limited. Topical fluoride remains safe and effective. In short, keep fluoride on the teeth, not in the bloodstream.
A Final Word
Community water fluoridation was one of the great health achievements of the twentieth century. Yet children today already receive fluoride from toothpaste, varnish, and food. We can preserve its benefits while reducing unnecessary ingestion. Re-examining systemic fluoride is not anti-science; it is good science. Our responsibility is to use fluoride wisely, to protect both smiles and developing minds. If you have questions about fluoride or your child’s oral health, you are welcome to email me at smile@ bccpediatricdentistry.com. I am always happy to help families make informed, confident choices.
Read the full article, including references, online: yhm.news/FluorideIQ
For more information, contact Dr. Shin at 301-941-7374 or visit the website at BCCPediatricDentistry.com

By Marc P. Stanard, DDS, PC
Periodontal disease is more than a localized oral infection – it is a chronic inflammatory condition with measurable effects on systemic health. For patients with diabetes and cardiovascular disease, this connection is particularly important.
Periodontal disease develops when pathogenic bacteria accumulate below the gumline, triggering a sustained inflammatory response. Over time, this inflammation destroys the supporting gum tissue and alveolar bone. Unlike acute infections, periodontal disease often progresses silently, with minimal pain, allowing inflammation to persist for years if untreated.
In patients with diabetes, this chronic inflammation has a well-
Periodontal disease is more than a localized oral infection – it is a chronic inflammatory condition with measurable effects on systemic health.
documented bidirectional relationship. Elevated blood glucose levels impair immune function and wound healing, increasing susceptibility to periodontal infection. At the same time, periodontal inflammation increases systemic inflammatory markers, which can worsen insulin resistance and make glycemic control more difficult. Studies consistently show that patients with uncontrolled diabetes experience more severe periodontal disease and faster progression.
Cardiovascular health is also affected. Periodontal pathogens and inflammatory mediators can enter the bloodstream, contributing to endothelial dysfunction, arterial inflammation, and atherosclerotic changes. While periodontal disease is not considered a

direct cause of heart disease, it is recognized as a significant contributing risk factor, particularly in patients with existing cardiovascular conditions.
Tooth loss, a common outcome of advanced periodontal disease, carries additional consequences. Missing teeth can compromise proper chewing, leading to dietary limitations that may negatively impact blood sugar and cholesterol management. Bone loss in the jaw also alters oral structure and function, further complicating restorative care if intervention is delayed.
The encouraging news is that periodontal treatment can reduce inflammatory burden. Non-surgical therapy, ongoing periodontal maintenance, and – when necessary – advanced
surgical or regenerative procedures help control infection and stabilize the disease process. In diabetic patients, improved periodontal health has been associated with modest but meaningful improvements in glycemic control.
For patients managing diabetes or cardiovascular disease, periodontal evaluations should be considered part of a comprehensive healthcare strategy. The mouth is not separate from the body; chronic oral inflammation can influence systemic conditions that affect long-term health outcomes. Addressing periodontal disease early is not only about preserving teeth – it is about reducing inflammation and supporting overall metabolic and cardiovascular health.
Maintaining good dental hygiene is crucial, and Dr. Marc Stanard, a periodontist and specialist in surgical implant dentistry, can help you achieve healthy teeth comfortably. We offer a wide range of specialized procedures and services to cater to your periodontal needs, such as bone surgery, scaling, and root planing, gum grafts, crown lengthenings, and sinus lifts.
• We provide advanced, affordable dental care tailored to meet your unique needs.
• Our team offers oral hygiene instruction and education on gum disease, bone loss, and other dental health conditions.
• Dr. Marc Stanard has decades of experience and a passion for his work, and he’s earned numerous designations, affiliations, and awards, including Top DDS by Washingtonian and high ratings on Google and Yelp.
• Our office is friendly and welcoming, making it the perfect place to receive top-quality dental care.



Your Health Magazine is on a mission. There are far too many people, insured or not, who do not go to the doctor when they should, and in millions of cases, don’t know who they should go to, or why.
People are encouraged to buy a new house, car, cell phone or big screen TV, and those companies make themselves very visible and their products easily attainable.
Information about, and from, local healthcare providers is not easy to find, and many times those services are difficult to access.
Information and encouragement always lowers fear and trepidation about anything, and this is especially true in healthcare. While general information is available on web-sites, specific information from local providers is almost impossible for people to find. This is one of the key reasons chronic and episodic conditions are not cared for. It is our mission to:
Make A Difference By Empowering and Encouraging People To Live Healthier By Going To the Doctor When They Should.
There is a lot of evidence that the health professionals who participate in Your Health Magazine have helped many people over the years. We at Your Health Magazine salute you!
G. Scott Hunter, Editor-in-Chief
If you would like to find out how you can participate in one of our upcoming editions, please contact the office nearest you.
One Town Center 4201 Northview Drive, Suite 102 Bowie, MD 20716 Office (301) 805-6805 • Fax (301) 805-6808 info@yourhealthmagazine.net
VIRGINIA OFFICE Office (301) 805-6805 info@yourhealthmagazine.net
© Your Health Magazine, 2026. The magazine and all of its contents are protected by copyright. For permission to reproduce any materials in this magazine, contact info@yourhealthmagazine.net
The content in Your Health Magazine and provided on yourhealthmagazine. net is for informational and educational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always consult with a qualified healthcare provider before starting any exercise program, making changes to your health routine, or acting on any health-related information found on the Internet, or anywhere else.

Foot & Ankle Specialist’s Board Certified doctors have been providing expert care to Northern Virginia families. From sports injuries and diabetic care to surgery and custom orthotics, we’re here to keep you moving—pain-free and confident every step of the way.

Ian Beiser, DPM
Dr. Ian Beiser has practiced podiatric medicine in Washington, DC since 1990. A leader in his field, he specializes in sports medicine and reconstructive foot surgery. He serves on multiple medical staffs, teaches at George Washington University, and holds several regional and national leadership positions.

David Vieweger, DPM
Dr. Vieweger, valedictorian of the Scholl College of Podiatric Medicine, completed his Surgical Residency at MedStar Washington Hospital Center. He specializes in conservative and surgical foot and ankle care, with expertise in trauma, limb salvage, and reconstruction. An avid runner, he lives in Maryland with his family.


Jennifer Gerres, DPM
Dr. Jennifer Gerres, DPM, is a graduate of Des Moines University and completed her Residency at the Cleveland Clinic. A published researcher and educator, she provides compassionate, evidence-based care in podiatric medicine and surgery, combining clinical expertise with a personalized, patient-focused approach.

Dr. Haseeb Ahmad, originally from Philadelphia, earned his Doctor of Podiatric Medicine from Temple University and completed his Surgical Residency at the VA New Jersey Healthcare System. Board Certified in Podiatric Medicine, he specializes in sports medicine, orthopedics, and trauma, and consults for Georgetown University athletics.
Dr. Howard Osterman, a Board-Certified Foot and Ankle Surgeon, serves as Team Podiatrist for the Washington Wizards and Washington Mystics. Recognized by Washingtonian Magazine as a top podiatrist, he is also President of the DC Podiatric Medicine Association and a leader in podiatric sports medicine.


Saylee Tulpule, DPM
Dr. Saylee Tulpule, a graduate of the California School of Podiatric Medicine, completed her Surgical Residency at Long Beach Memorial, where she served as Chief Resident. Practicing since 2010, she specializes in podiatric medicine, sports medicine, biomechanics, and elective forefoot surgery with a patient-focused approach.

Lee Firestone, DPM
Dr. Firestone, Board Certified in Foot Surgery and Sports Medicine, specializes in surgical and non-surgical foot and ankle care. An accomplished marathoner and RRCA-certified coach, he’s been recognized among Washington’s top podiatrists and sports medicine providers, serving the DC area since 1994.
Dr. Erika Schwartz, Board Certified in Foot Surgery, serves on the Maryland Podiatric Medical Association Board and teaches at MedStar Washington Hospital Center. A past president of the American Association for Women Podiatrists, she’s been recognized by Washingtonian Magazine and featured in major national media outlets.
By Troy Sukhu, MD Anne Arundel Urology
What is BPH?
Benign Prostatic Hyperplasia (BPH), commonly known as an enlarged prostate, is a condition that affects millions of men, particularly as they age. The prostate gland, located just below the bladder, tends to grow larger over time, which can lead to uncomfortable urinary
symptoms.
• Frequent or urgent need to urinate
• Increased frequency of urination at night (nocturia)
• Difficulty starting urination
• Weak urine stream or a stream that stops and starts
• Dribbling at the end of urination
• Inability to completely empty the bladder
Living with BPH can significantly impact your quality of life. The symptoms can interfere with daily activities, disrupt sleep, and lead to complications such as urinary tract infections or bladder damage. Seeking treatment can help alleviate these symptoms and improve your overall well-being.
Treatment Options: There are



various treatment options available for BPH, ranging from medications to minimally invasive procedures and surgery. Some of the most effective treatments include:
• Medications: Alpha blockers and 5-alpha reductase inhibitors can help relax the prostate muscles and reduce its size.
• Minimally Invasive Procedures: Techniques like Urolift, Rezum, and the Optilume BPH Catheter System offer relief with fewer side effects and quicker recovery times.
• Surgery: For more severe cases, surgical options such as Transurethral Resection of the Prostate (TURP) can provide significant symptom relief. Patient Testimonials: Many men have found relief from BPH symptoms through various treatments. Here are some experiences:
• John’s TURP Experience: “After struggling with BPH symptoms for years, TURP provided me with the relief I needed. The recovery was smooth, and I can finally sleep through the night without frequent trips to the bathroom”.
• Mike’s Aquablation Journey: “Aquablation was a game-changer for me. The minimally invasive procedure was quick, and I experienced minimal discomfort. My urinary symptoms have improved dramatically”. Take Control Of Your Health Don’t let BPH control your life. Consult with your healthcare provider to explore the best treatment options for you. With the right approach, you can manage your symptoms and enjoy a better quality of life.

By James Lynch, MD
A landmark study published last month in the Journal of Psychotherapy and Psychosomatics demonstrates a novel combination therapy that greatly improved symptoms of posttraumatic stress disorder (PTSD).
This study adds to the broader body of work over the past 15 years on a medical procedure called stellate ganglion block (SGB) used to treat anxiety and PTSD. In this randomized controlled trial (RCT), we examined whether adding SGB to cognitive processing therapy (CPT)—a wellestablished talk therapy—improved PTSD symptoms. We tested whether giving SGB before CPT works better than giving CPT alone, and whether SGB can help people who still have symptoms after therapy.
SGB is an injection of local an-

By Mikel D. Daniels, DPM, MBA President and Chief Medical Officer
WeTreatFeet Podiatry
Living with diabetes means your feet need extra attention. Not because something is wrong right now, but because the smallest change, something like a new callus, a temperature difference, or rubbing of a shoe, can quietly snowball into a serious problem. This is exactly why practices like WeTreatFeet Podiatry focus so heavily on prevention and why they work with advanced limb preservation programs to reduce amputations before they ever become a conversation. WeTreatFeet Podiatry is at the forefront of diabetic foot amputation prevention and is the only podiatry practice in Washington, DC, and the first in the region, to participate in ArcheHealthcare’s
esthetic along a nerve in the side of the neck that helps reset the body’s “fight-or-flight” system. It has been used safely for 100 years to treat pain and over the past 15 years has also been used to reduce anxiety and PTSD symptoms.
Eighty-six people with PTSD took part. One group received SGB before starting two weeks of daily CPT sessions. The other group completed CPT first and received SGB three months later if they were still struggling.
What we found:
• Everyone improved, but people who got SGB before CPT improved much faster.
• Those who received SGB first had quicker and greater reductions in PTSD symptoms, as well as depression, anxiety, and physical (body-related) symptoms—reducing scores by roughly 50% on PCL-5, GAD-7, PHQ-9, and PHQ15 symptom checklists.
• By week 8, 48% of SGB-before-
CPT participants reached good end-state functioning, compared to 16% in the SGB-afterCPT group.
• For people who did not improve enough with CPT alone, receiving SGB afterward led to significant symptom relief, showing it can help even when therapy by itself is not enough.

Faster symptom relief may help people better engage in therapy, feel less overwhelmed, and return to daily functioning sooner.
• By week 52, 81% of SGB-beforeCPT participants showed reliable improvement in PCL-5 scores, while 62% of SGB-after-CPT participants did.
• This study adds evidence that SGB can be both an effective symptomreducing procedure on its own and a valuable adjunct that enhances the impact of proven therapies like CPT.
Bottom Line
SGB is a helpful add-on to PTSD therapy. Getting SGB before intensive therapy leads to faster improvement, and getting it afterward can still help those who need more support.
Reference: Effectiveness of combined cognitive processing therapy with stellate ganglion block: an open-label randomized wait-list clinical trial
LEAP, (Lower Extremity Amputation Prevention) collaborative, a nationally recognized system designed to identify risk early and protect your limbs.
Diabetes can damage both the nerves and the blood vessels in your feet. That combination is dangerous because you can injure your foot and not even know. A small wound may not get enough blood flow to heal, and infections can spread quickly. In the
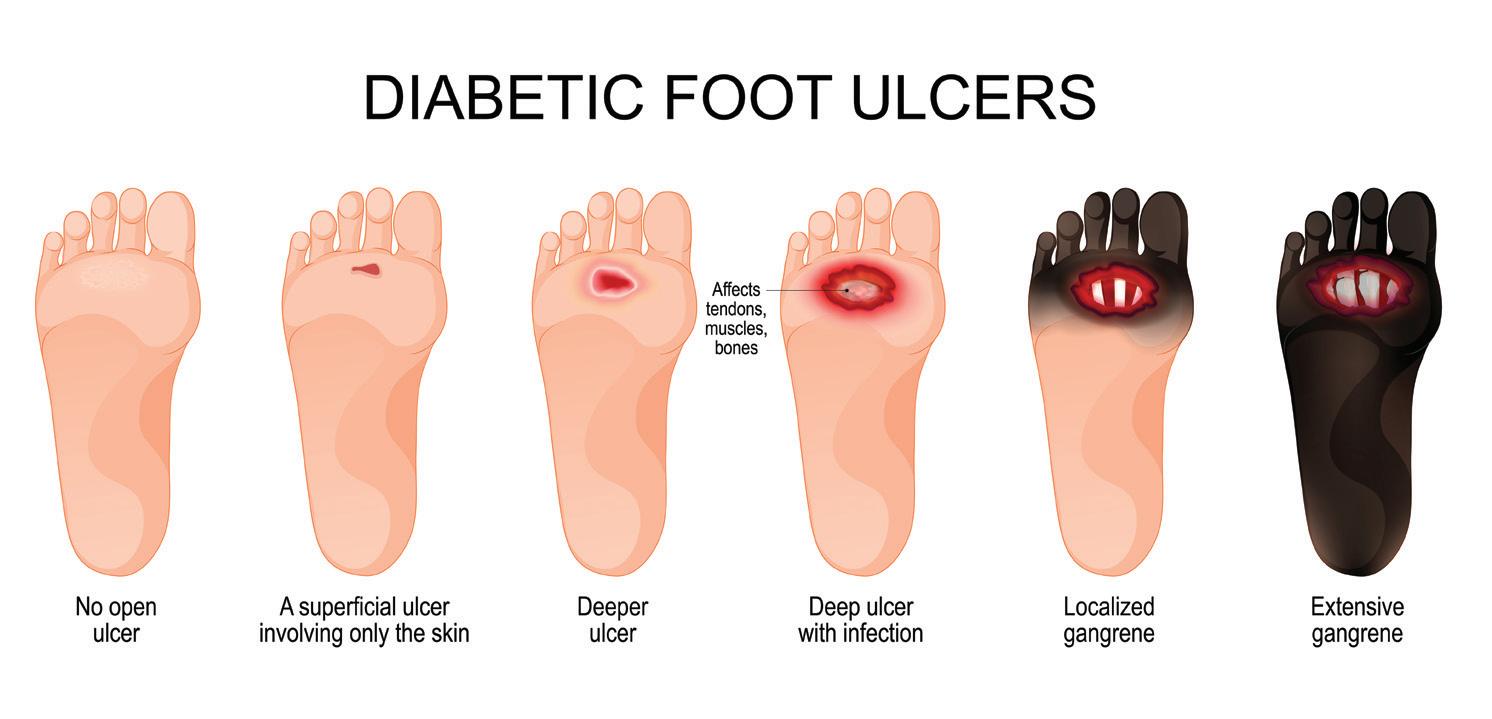
worst cases, this can lead to amputation.
One subtle sign of circulation trouble is a temperature difference between your feet, for example if one foot feels noticeably cooler than the other. That is not something to brush off. It is one of the things a comprehensive diabetic foot exam is designed
to pick up. When a podiatrist notices changes like this, we often order tests such as an arterial ultrasound and coordinate with a vascular specialist. The goal is not to scare you, but to catch problems early enough to treat them or slow them down.
Hammer toes and calluses may sound minor, but in a diabetic foot they
can be the quiet beginning of a serious ulcer. Hammer toes bend the toes so that certain parts of the toes or the ball of the foot press harder into your shoe. That extra pressure causes rubbing and callus buildup. Under a thick callus, the skin can break down without you
Please see “Foot Care,” page 34


By Lubrina Bryant, DPM District Podiatry, PLLC
signed to reduce pressure points and improve stability.
Diabetes affects millions of Americans and can have serious consequences throughout the body if not carefully managed. One of the most commonly overlooked — yet critically important — areas impacted by diabetes is the feet. Proper foot care is essential for people with diabetes, as nerve damage and poor circulation can turn small problems into serious, even limb-threatening complications.
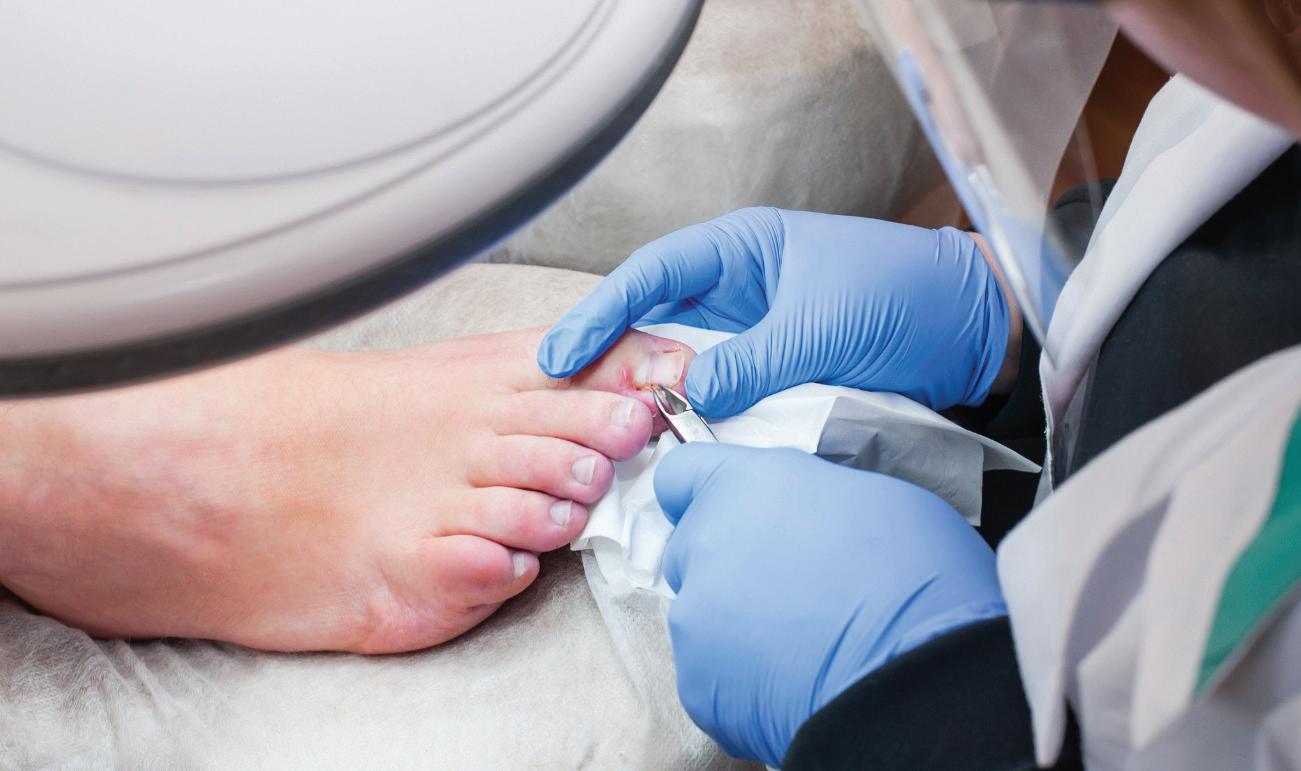
People with diabetes are at increased risk for peripheral neuropathy, a condition that reduces sensation in the feet. When feeling is diminished, cuts, blisters, pressure points, or ingrown toenails may go unnoticed. At the same time, diabetes can impair blood flow, slowing the body’s ability to heal wounds and fight infection. Together, these factors create the perfect environment for ulcers, infections, and, in severe cases, amputation.
Daily foot care is one of the most effective ways to prevent complications. Individuals with diabetes should inspect their feet every day, checking for redness, swelling, cracks, sores, or changes in skin color or temperature. Even minor issues should be taken seriously. Using a mirror or asking for help can ensure the bottoms of the feet are not overlooked.
Good hygiene is also essential. Feet should be washed daily with lukewarm water and mild soap, then dried thoroughly, especially between the toes. Moisturizing lotion can help prevent dry, cracked skin, but should not be applied between the toes, where excess moisture can lead to fungal infections. Toenails should be trimmed straight across and filed carefully to avoid injury.
Proper footwear plays a significant role in diabetic foot health. Shoes should fit well, provide adequate support, and protect the feet from friction and pressure. Tight shoes, high heels, or footwear with narrow toe boxes can cause blisters or calluses that may worsen over time. Many people with diabetes benefit from professionally fitted shoes or custom orthotics de-
Regular medical foot exams are equally important. Healthcare providers can identify early signs of nerve damage, circulation issues, or structural problems that increase the risk of injury. Podiatrists are specially trained to manage diabetic foot concerns, including callus care, nail treatment, and ulcer prevention. Early intervention often prevents more
serious outcomes.
Lifestyle choices also influence foot health. Maintaining healthy blood sugar levels helps protect nerves and blood vessels, reducing the risk of complications. Staying physically active, eating a balanced diet, quitting smoking, and managing blood pressure all contribute to better circulation and healing.
Diabetic foot problems are com-
mon, but they are not inevitable. With daily attention, proper footwear, routine medical care, and good diabetes management, most serious foot complications can be prevented. Paying close attention to foot health is not just about comfort — it is about preserving mobility, independence, and overall quality of life. If you have diabetes, caring for your feet should be an essential part of your daily health routine.


By Jeffrey L. Brown, DDS Sleep & TMJ Therapy
It may be hard to believe, but when you have a TMJ disorder (otherwise called TMD), this can correlate to sleep-disordered breathing (SDB). The way this works is that when the jaw joint discs are displaced – just like a kneecap can slip out of place – you get pain. Pain and inflammation are quite common with a displaced jaw disc. When you are hurting, you just cannot
sleep all that well. Also, the quality of sleep is compromised because it is now harder to get the good, deep, non-REM sleep that helps our body to heal.
It is unfortunate that TMD is so poorly understood because so many people really do need help in this area. It is actually fairly easy to get a handle on this disorder, however. One of the first signs of TMD is that you have clicking and/or popping in the jaw joints. This is often a clear sign that



the articular discs (jaw joint discs) are displaced and causing an inflammatory reaction.
Another very clear sign of TMD is that you cannot open your jaw widely. The “normal” range of motion is generally considered to be around 50 mm. This means measuring from the tip of the upper front teeth to the tip of the lower front teeth when opening wide, you should get around 50 mm.

Some practitioners say that 35mm is around normal, but in general most agree that 50mm is a healthier way to be. This measurement can readily be done when you see your dentist or hygienist but most of the time it is not done.
So, now let’s get back to the link to sleep problems. If and when the articular discs in the jaw joints are displaced, they are going to rub around in the jaw sockets and will quite literally pinch or rub against nerves and blood vessels in the joint. Diagnosis: It just plain hurts. In the human body when a bone rubs against bone or other vessels, it just hurts, simple as that. This in turn begins an inflammatory reaction in which the body releases the mediators of inflammation called “cytokines”. Now these cytokines are floating around inside your body causing a chronic irritation. It’s kind of like being chronically sick all the time.
Dr. Jeffrey Brown has limited his practice to focus only on TMJ Disorders, Craniofacial Pain Management and Sleep Apnea. By fixing slipped discs in the jaw joints, Dr. Brown can significantly reduce the pain patients experience in the head/neck region and other symptoms associated with jaw joint problems. Sleep & TMJ Therapy may be able to improve the quality of life for you or a loved one – we encourage you to contact us with any questions or concerns.
“Dr. Brown and his staff are absolutely wonderful. I was diagnosed with Dystonia. I could not turn my head and had a ton of pain. My doctors offered no help and no advice besides Meds and Botox. Since having the appliance I have NO pain and I can turn my head. I would highly recommend them to anyone. I feel Dr. Brown and his staff really care about their patients and helping them to get better. They do not just numb the symptoms but fix the problem. Thank you from the bottom of my heart. I feel like the old me again!”
- D. Thomas
“My daughter has been treated by Dr. Stack and Dr. Brown for the last 2 1/2 years, and we are very fortunate to have found them. Prior to that she was being treated by a neurologist at a Children’s hospital. She was on medications for tics and associated muscle pain, OCD/repetitive thoughts, sleeplessness and more (all possibly associated with Tourettes). Drs. Stack and Brown installed spacers to alleviate pressure on nerve bundles in the jaw, and subsequently braces to complete the process. Her symptoms have diminished significantly. She is off medication, her tics have all but disappeared, she can concentrate better in school, and she is once again cheerful and relaxed.”
- Susan
When the body is running in inflammation mode, it hurts, and this leads to sleep difficulties. What happens in so many people are the jaw joints ache, which in turn leads to the neck being irritated, and then it travels down the back as well. This makes the deep sleep – called non-REM III – unable to happen the way it should. Now you are sleep deprived and not able to heal the body like your body intended. This cycle just gets worse and worse over time. In so many people, this will lead to OSA – obstructive sleep apnea. So be safe, be smart, learn about TMD and how to treat it for a good night sleep.


Choose Adventist Medical Group Primary Care in Fort Washington, Maryland, to provide a full range of primary care services for adults.
Learn to better manage your health and prevent illnesses with personalized care from our experienced, primary care providers. Our specialists in family medicine and internal medicine work as a team to deliver expert care when you need:
• Same-day Sick Visits
• Women’s and Men’s Health and Wellness Exams
• Health Physicals, Health Maintenance and Preventive Care
• Geriatric (Senior) Wellness Exams
• Vaccinations and Immunizations, including Flu Shots
• Health Management for:
• Asthma and Allergies
• High Blood Pressure
• High Cholesterol
• Diabetes
• Heart Disease
You also benefit from coordinated care that helps you effectively handle all aspects of your health—from preventive medicine and preoperative appointments to management of chronic health conditions.
To schedule an appointment, please call 240-724-6018
10709 Indian Head Highway, Suite D1 Fort Washington, Maryland 20744 AdventistMedicalGroup.org

Submitted By Sivakumar Sreenivasan, DMD, MDS Dental Implant Center of Rockville
Can just four implants replace all of the teeth on the top or the bottom of your mouth? Thanks to advances in dental implant technology, that answer is a resounding yes.
Believe it or not, tooth loss is extremely common among adults, especially as we age. In fact, more than 35 million people in America are missing all of their upper and/or lower teeth. Rather than living with the discomfort and hassles of dentures, many people are opting for what is called “all-onfour” dental implant restoration.
All-On-Four: One Full Arch Of Teeth, Four Dental Implants
To fully understand this remark-
able technique for replacing teeth, you should first understand what a dental implant is. An implant is a small titanium screw that fits inside your jawbone and replaces the root-part of a missing tooth. Minor surgery is required to insert the implants. Once the implant is in place, a crown is attached to give you a highly realistic-looking and functional prosthetic tooth.
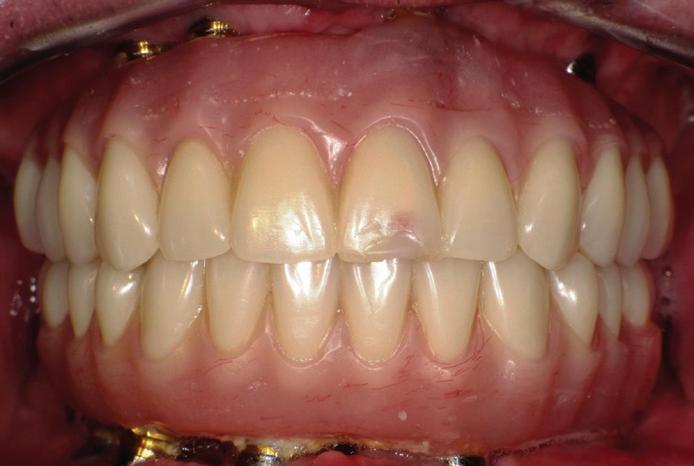
Here’s where it gets really interesting: You do not need a dental implant for each and every one of your missing teeth. All you need is four precisely placed implants on the top of your mouth, and four on the bottom, to restore your full smile. That’s the beauty of the all-on-four. And because the implant is made of titanium, it has the unique ability to fuse to living bone and function as part of it. So eventually, the dental implant becomes part of the jawbone and serves as a strong, long-lasting foundation for your new teeth.
Besides ensuring that your implants are permanently fixed in place,
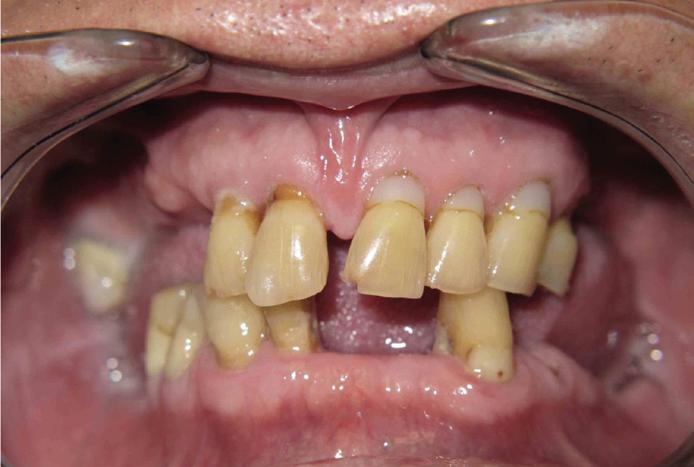

this bone fusion has another important benefit: it prevents future bone loss in the jaw. This helps to maintain a more youthful facial structure – and better oral health. But perhaps the biggest surprise about the all-on-four is how quickly it can transform your life.
What’s The All-On-Four Dental Implant Procedure Like?
It can be scary to get implants for the first time. Most of that fear is probably due to the uncertainty, so here is the step-by-step process for getting an All-On-Four dental implant.
First, your dentist will want to make sure your comfortable, so either local or general anesthesia will be administered.
Second, the dentist or surgeon will prepare your mouth for the implants, which involves removing your remaining teeth that are failing. They will then remove any diseased or infected tissue from your jaw and gums.
After the implants have been placed, they will thoroughly clean the surgical sites and suturing all the incisions. Then you’ll be taken to a recovery room where you can relax and take time to wake up from the anesthesia.
Do
If The All-On-Four Procedure Is The Right Option For You?
At your All-On-Four consultation, you’ll receive a 3D CT Scan. This scan will help determine if you need implants and assist your doctors in creating your treatment plan. So if you want to learn more about dental implants, simply schedule a consultation with an All-On-Four provider. It’s the best way to find out how dental implants can change your life.
Next, they will begin the implantation process. This means they will insert the titanium screws into your jawbone. Most likely, they will place two implants toward the front of your mouth and two towards the back of your mouth so the “anchors” can evenly bare the force of the denture.




By Rashmi K. Parmar, DMD, D-ABDSM and Neelima K. Yerra, DDS – Sleep Better Maryland
Sleep apnea is a very serious condition, yet more than 80% of people who have it are undiagnosed. This means out of the 24 million plus people that have it, approximately 19.2 million don’t even know they have it.
This is tragic in many cases as they develop life-threatening health issues. They don’t even know that their health problems are tied directly to their lack of sleep due to sleep apnea.
Your body needs sleep in order to reboot and repair itself. Lack of sleep causes oxygen levels to decrease and carbon dioxide levels to increase. Your brain signals your body to wake up and start breathing again.
These micro-awakenings have a severe impact on your quality of sleep and overall health.
Who Is At Risk For Developing Sleep Apnea?
There is no one that is immune to sleep apnea. However, there are some who are at risk more than others. Here is a list of factors and a brief explanation:
• Excess weight. Most but not all people with obstructive sleep apnea are overweight. Fat deposits around the upper airway may obstruct breathing. Medical conditions that are associated with obesity, such as hypothyroidism and polycystic ovary syndrome, also can cause obstructive sleep apnea. However, not everyone with obstructive sleep apnea is overweight and vice versa. Thin people can develop the disorder, too.
• Narrowed airway. You may inherit naturally narrow airways. Or your tonsils or adenoids may enlarge, which can block your airway.
• High blood pressure (hypertension). Obstructive sleep apnea is relatively common in people with hypertension.
• Chronic nasal congestion. Obstructive sleep apnea occurs twice as often in those with consistent nasal congestion at night, regardless of the cause. This may be due to narrowed airways.
• Smoking. People who smoke are more likely to have obstructive sleep apnea.
• Diabetes. Obstructive sleep apnea
may be more common in people with diabetes.
• Sex. In general, men are twice as likely as premenopausal women to have obstructive sleep apnea. The frequency of obstructive sleep apnea increases in women after menopause.
• A family history of sleep apnea.
If you have family members with obstructive sleep apnea, you may be at increased risk.
• Asthma. Research has found an association between asthma and the risk of obstructive sleep apnea.
How Do You Know If You Might Have Sleep Apnea?
There are several signals you might have sleep apnea, but two of
them are prominent. One is daytime sleepiness. You don’t sleep at night so you are tired and fatigued all day. The other is snoring. It is a sign that your airway is obstructed.
The way to know for sure is to have a sleep study. This will tell you whether or not you have it and how severe it is. Call a sleep apnea specialist today and be on your way to a better night’s rest and better health.

We are pleased to announce that Dr. Parmar and Dr. Yerra are now partners, united by a shared commitment to providing high-quality, patient-centered care to our community. Together, they bring experience, compassion, and a dedication to helping patients achieve better health and lasting wellness.

Rashmi K. Parmar, DMD, D-ABDSM
Dr. Rashmi Parmar is Diplomate of the American Board of Dental Sleep Medicine. She received her professional degree from University of Pennsylvania School of Dental Medicine. She completed the comprehensive general practice Residency at Carolinas Medical Center in Charlotte, NC and has been in practice in the Columbia Clarksville area since 1991.

Neelima K. Yerra, DDS
Dr. Neelima K. Yerra is an American Academy of Dental Sleep Medicine- Qualified Dentist. She has extensive expertise in the diagnosis and management of Obstructive Sleep Apnea. Dr. Yerra received her professional degree, Doctor of Dental Surgery from New York University College of Dentistry in 2015.


By Dr. Tiffany Daniel Live To Day Wellness
The month of February has been nominated Healthy Heart Month.
Why February? Could it be because it’s the month of Valentine’s Day, where the symbol is the red heart? Or could it have something to do with romance, chocolates and wine? Ironically, romance, chocolates and wine are good for the heart too for various reasons, so why don’t we celebrate Valentine’s Day all month instead of heart disease? And why is it that heart disease plagues women more so than men?
The American Heart Association created the Go Red for Women Campaign in 2003 to help increase the awareness of women’s heart disease and studies. The month of February has been designated Healthy Heart month to focus on heart studies, check-ups and tests to learn more on preventing heart disease and heart attacks. However, the most common cause of death in women is still heart disease.
So let’s talk about some of the

We believe total well-being starts with balance—of body, mind, and spirit.
Our mission is to empower women, veterans, and families through movement, mindfulness, and nutrition. Join our workshops and wellness programs featuring: Mindful Movement & Breathwork – Therapeutic Horticulture Yoga for Trauma & Stress Relief – Nutrition and Wellness Coaching Whether you’re healing from life’s challenges or simply ready to grow stronger inside and out—there’s a place for you here.

things that can be done to help prevent heart disease in both men and women. This list is called the “Simple Seven” and it is very simple to maintain for your heart’s sake.
Because the heart is a muscle, if these conditions are detected in time, they can possibly be prevented with daily physical activity, which increases your length and quality of life.
If you get at least 30 minutes of moderate physical activity each day, five times per week, you can almost guarantee an improvement.
Learn to control your cholesterol and give your arteries a break by allowing them to stay clear of plague build up.
Choose healthy foods that are fueled with vitamins and minerals that our bodies use to make new cells and create the energy we need to thrive and fight diseases.
The month of February has been nominated Healthy
Manage your blood pressure and keep it within healthy ranges so you can reduce the strain on your heart, arteries, and kidneys, which keeps you healthier longer.
If you’re overweight, you can reduce your risk for heart disease by successfully losing weight and keeping it off; especially if it is in your mid-section as this is the danger zone for auto-immune diseases.
Diabetes appears when your body is unable to create insulin to carry your food energy into your cells. This is a good indication that your blood sugar levels are too high and need to be managed.
And last but not least, smoking damages your entire circulatory system, and increases your risk for coronary heart disease, hardened arteries, aneurysm and blood clots.
Don’t ignore the signs as they can be different in men and women. Get your check-up. Eat healthy and stay active.

By Linda Penkala, Author, LMT Optimum Health For Life
What is the #1 killer of women that less than half of us even know exists? That would be heart disease, and it claims more lives than all the cancer deaths combined, according to the American Heart Association’s Go Red for Women. One unknown fact that many don’t know is that CVD is the #1 killer of new moms. But when I read that the number of casualties among younger women (30-50s) is rising, with unique factors affecting their hearts, it becomes clear that more needs to be done.
One silent player in the CVD realm is chronic stress. For decades, it was not even mentioned in discussions of heart health. Stress has its physiological manifestations in the mind/body continuum, by way of anxiety, depression, fear, pain, and impaired mental health. The body’s “pre-wired” 911 call for help via the sympathetic nervous system triggers the fight-orflight response, along with chemical changes. Unfortunately, it may get stuck sounding the bell constantly with that steady surge of cortisol, adrenaline, or norepinephrine, setting the stage for inflammation that impacts every organ.
Having a roadmap for heart health comes down to understanding your medical results from a physical, being aware of your stress levels, and incorporating movement daily. Lifestyle choices such as not smoking, eating, and drinking red (hibiscus tea, red fruits/veggies), and taking time for relaxation are fundamental solutions that add quality and overall health for years. Friendships offer a myriad of wellness benefits, from laughing to lessen stress and cortisol, to going outside to be in nature, walking, and talking together. One important choice that impacts CVD is regular dental visits for cleaning to be sure gum disease is not present.
From my book, The Pause to Relax, A Woman’s Guide to Robust Heart Health on Amazon, comes these heart healthy lifestyle choices to address and lessen the impact of stress:
Breathwork: Box breathing taught in the Navy Seals training for focus, and clarity: inhale 4 counts, pause 4 counts, exhale 4 counts, pause 4 counts. Or 3-5-8 breathing, inhaling, holding, then exhaling for a state of calm.
Aromatherapy: The oldest form of medicine, with clinical aromatherapy using essential oils, currently a worldwide alternative modality. Cardioprotective oils can be orange, cypress, ylang ylang, marjoram, and lavender.
Prayer: If you are a faith-filled person, praying to God is a grounding, meaningful moment in the day, with solid research that this impacts health: https://newsroom.heart.org/news/reli-
giousness-spirituality-linked-to-betterheart-health-among-african-americans.
Receiving a Massage: Relaxation promotes cellular and mental balance besides lessening pain.
Find Your Friends : Choose to schedule gal time for fun, and laughter.
Volunteer For a Cause: Super research is showing the steep decline in stress when partnering with other likeminded volunteers for a passionate cause.

Linda Penkala, Author, LMT, Holistic Healthcare Presenter, and Wellness Catalyst shares her passion and heart for holistic lifestyle choices through: • Keynote Presentations • Massage Therapy • Aromatherapy • Book Signings • Breathwork for Healing
• Her book, The Pause to




CORPORATE OR COMMUNITY PRESENTATIONS:
• Wise Self Care for Life
• Nine Pillars to Prevent Heart Disease
• Wise Heart Health for Women
• Navigating New Waters of Wellness
• Tapping with Essential Oils for Health
LIVE ZOOM PRESENTATIONS
• Mindful Meditation Massage (at night, pre-sleep)
• Mindful Massage and Stretching (at desk)
• Aromatherapy 101
• Essential Oils and Your Pet
• Wise Self Care for Life
• Wise Heart Health for Women





Dr. Brown’s practice focuses on TMJ, sleep apnea and orthodontics. This allows Dr. Brown and his team to provide individualized, focused care for patients dealing with these specific issues. Every day, his practice helps patients of all ages with facial development, sleep issues, chronic headaches, migraines, neck pain, movement disorders, and much more. His training also includes multiple disciplines involving the cranial bones in the skull, and the discs in the jaw joints. Through treatment, Dr. Brown is able to reduce these symptoms, align cranial bones, avoid extractions, and greatly reduce the need for traditional braces. His expertise allows him to identify issues early on which promotes proper facial development using dental appliances. If there is an internal imbalance, whether an adult or child, the body does not develop or function properly. When the cranial bones are lined up correctly, patients are able to function, sleep and generally live better.
With that in mind, the team at Sleep & TMJ Therapy takes a whole-body approach when treatment planning. They work hand in hand with physical therapists and osteopathic doctors for a better success rate. Dr. Brown is devoted to helping patients of all ages live a symptom free life.
Degrees & Certifications
Dr. Brown earned his degree from Georgetown Dental School and completed residencies with Emory University Hospital for Dental Sleep Medicine and the ALF Appliance Therapy Institute.
Outside the Office
When not seeing patients, Dr. Brown is a sought-after speaker. He has lectured all over the world, including D.C., Dubai, Seoul, London, Norway and Toronto. He has also been featured on Channel 9’s Good Morning Washington, several podcasts, and numerous magazines and journals.
Professional Affiliations
Dr. Brown is a diplomate of the American Academy of Craniofacial Pain, a member of the American Academy of Dental Sleep Medicine, American Academy of Gnathological Orthopedic, Academy of Integrative Pain Management American Dental Association, a Fellow of the American Academy of Craniofacial Pain, and Legacy Provider for the ALF Interface Academy.
Do you have TMD or Sleep Apnea?
TMD Symptoms: Noise in the jaw joints when opening and closing your mouth, difficulty chewing, limited opening, tender facial muscles, ear ringing, uncomfortable bite, jaw locking, headaches, migraines, dizziness, vision issues as well as pain in the jaw area which can radiate to the ears, head, neck, shoulders, and back.
Sleep Apnea Symptoms: Snoring, waking up gasping for air, feeling tired and irritable in the morning, difficulty controlling weight, concentration problems, morning headaches, episodes of not breathing, waking with a sore throat, forgetfulness and mood changes. If you believe you may be suffering from TMD or Sleep Apnea, don't wait... Call today to schedule a consultation with Dr. Brown: 703-821-1103.
Varnum

Foot doctor Lubrina Bryant, DPM is dedicated to getting to the root of your foot or ankle problem.
District Podiatry, PLLC specializes in general foot, ankle and leg care. Having chronic foot and ankle pain can affect the quality of your life and finding the right foot and ankle specialist can be just as difficult. We know how hectic life can be and we are committed to making our practice and care convenient and accessible.
From routine checkups to minor foot surgery, Lubrina Bryant, DPM is a podiatrist who is equipped to handle all your foot and ankle needs.
Services Include: Routine Foot Care, Diabetic Foot Care, Wart Removal, Ingrown Toenails, Foot, Ankle or Heel Pain, Toenail Fungus, and Bunions.



Dr. Mikel Daniels is a highly skilled podiatrist dedicated to delivering exceptional, patient-centered care. With decades of experience and a deep commitment to improving foot and ankle health, he blends medical expertise with compassionate service to help patients achieve lasting wellness and mobility.
Dr. Daniels earned his Bachelor of Science in Biology with a minor in Economics from Muhlenberg College in 1996, followed by his Doctor of Podiatric Medicine (DPM) degree from Temple University School of Podiatric Medicine in 2000. He completed his Podiatric Surgical Residency at the University of Maryland, Mercy Medical Center, where he gained extensive clinical and surgical experience. In addition, Dr. Daniels holds an MBA with a concentration in Healthcare Management from Western Governors University, earned in 2014— giving him a unique combination of medical and business education that informs his approach to both patient care and practice management.
Dr. Daniels has been named one of Baltimore’s Top Doctors in 2023, 2024, and 2025, a reflection of his outstanding reputation among peers and patients alike. He is a frequent podcast guest and has been featured as an expert in foot and ankle care by major media outlets including CNN and Parade. Locally, he has also appeared on television to discuss common foot and ankle issues, offering practical tips for maintaining mobility and preventing injury.
Dr. Daniels’ special areas of interest include diabetic wound care, medical and practice economics, and advancing equity within healthcare. His mission is to ensure every patient receives comprehensive, evidence-based treatment tailored to their individual needs—helping them stay active, comfortable, and confident on their feet.



Board Certified, Ophthalmology by the American Board of Ophthalmology
Degrees, Training and Certificates: UCLA Medical School; Yale University Hospital for Residency; Louisiana State University for Cornea and Refractive Fellowship
Professional Memberships/Associations: American
Academy of Ophthalmology; American Society of Cataract and Refractive Surgery; International Society of Refractive Surgery
Areas of Interest: All laser custom LASIK; Cataract Surgery; Botox; Dermal Fillers; Cornea Comprehensive Ophthalmology
Practice Philosophy: Envision Eye and Laser is committed to delivering superior ophthalmic care with state-of-the-art technology and patient education in a caring, compassionate environment. We cater to a diverse population of adults and work with your primary care physician to improve the quality of your overall health and life. Your best vision is our focus.

Interal Medicine / Diabetes Management
in Accokeek, MD

Rejuve Medical Group is a family-owned interal medicine practice committed to your total well-being. The Group is a blend of RejuVe Health and Medispa/SpinaTherapeutics. We hope to inspire you to feel, look, and live your best life!
We offer medically guided services designed to support blood sugar control, metabolic health, and long-term mobility:
• Semaglutide (GLP-1 therapy) – A clinically proven option that helps regulate appetite, improve insulin sensitivity, support weight loss, and reduce cardiometabolic risk when medically appropriate.
• Private, Customized Workouts – Individually designed exercise programs that help improve glucose utilization, increase insulin sensitivity, and support safe, sustainable physical activity for patients with diabetes or prediabetes.
• Emsculpt Neo – Builds lean muscle while reducing fat, helping improve metabolic rate and glucose control. Increased muscle mass plays a key role in better blood sugar regulation.
• Emsella – Strengthens pelvic floor muscles, which can be especially beneficial for patients experiencing urinary changes related to aging, diabetes, or childbirth.
• Emtone – Helps tighten loose skin that can occur after significant weight loss, supporting comfort and confidence during body-composition changes.
• Robard Meal Replacement Program – A medically supervised, evidence-based nutrition program developed from extensive academic research, designed to support weight management, glycemic control, and long-term lifestyle change.

Dr. Mary Alexander, periodontist, obtained a Bachelor of Science degree in Biology from the University of South Carolina and continued her education in dentistry at the University of Maryland School of Dental Surgery where she received her DDS degree. Prior to and during her dental studies, Dr. Alexander received funding and support from the National Institutes of Dental Research for her involvement in the periodontal research. After obtaining her DDS degree Dr. Alexander spent one year at the Veteran’s Administration Hospital, in general practice residency focusing her training in the area of anxiety patient management. She then attended Harvard University and earned her clinical specialty in periodontics and a doctorate in medical science. Her doctoral research was focused in the study of bone function and metabolic disease of the bone.
Dr. Alexander received extensive training in dental implantology, periodontal plastic surgery, bone regenerative procedures and sedation dentistry. All aspects of Dr. Alexander’s training are incorporated in her periodontal practice assuring patient’s thorough and comprehensive periodontal treatment.




dental school again at Boston University and Oral and Maxillofacial Surgery residency at University of Medicine and Dentistry of New Jersey.
As an Oral and Maxillofacial Surgeon, Dr. Sreeni manages a wide variety of problems relating to the Mouth, Teeth and Facial Regions. He practices a full scope of Oral and Maxillofacial Surgery with expertise ranging from Corrective Jaw Surgery to Wisdom Teeth Removal. His passion is in implant surgery and he is well known for same day placement of implants following teeth removal be it for single teeth or a complete “makeover” (Smile in a day). He can also diagnose and treat Facial Pain, Facial Injuries and TMJ disorders and perform Bone Grafting and Sinus lift procedures.
Dr. Sreeni completed a residency in Anesthesiology at Mount Sinai Hospital, New York in 1994 and has worked as an Attending providing anesthesia services for children and adults in the ambulatory outpatient center of the hospital.
Dr. Sreeni is an Advanced Cardiac Life Support instructor with the Adventist group. He is also certified in Pediatric advanced life support and is very capable of handling emergencies that could possibly arise in the office. Dr. Sreeni’s staff are trained in assisting with IV Sedation/ General Anesthesia within our state of the art office setting. Patients are continuously monitored during and after surgery. The goal of our office is to provide professional service with compassion and an understanding of the patients’ perspective.

A native of New Jersey, Dr. Stephen Price attended the University of Connecticut on a football scholarship, and earned his Doctorate of Dental Surgery from Georgetown University School of Dentistry in 1973.
For over 50 years Dr. Stephen Price has been doing procedures such as implant placements, full mouth reconstruction, porcelain crowns, and surgical extractions. He is most proud of all of the smiles that he has created in patients that have completely changed their lives. says Dr. Price and his team set themselves apart in the industry by listening to their patients’ wishes and needs, and understanding their apprehension. They go the extra mile to make them feel comfortable during treatment, and treat their patients like family.
In 2017 Dr. Price, an Elite Invisalign® provider and a Certified Invisalign® instructor, was honored as the best treatment winner at the Invisalign® Summit in Maryland. He is a member of the American Dental Association, the Northern Virginia Dental Society, and the Virginia Dental Society. Start Invisalign®


Stellate Ganglion Block (SGB) provides clinically significant relief of Anxiety and post-traumatic stress disorder (PTSD) symptoms.
• Feeling on edge all the time?
• Angry outbursts? Irritability?
• Nervous, restless, or tense?
• Poor sleep or concentration?
What is SGB? An ultrasound-guided injection of a long-acting anesthetic near the stellate ganglion, a nerve cluster that regulates the body’s “fight or flight” response. This process resets the central autonomic network, offering immediate and long-term improvements in anxiety and hyperarousal symptoms.
Dr. James Lynch is a world expert in SGB , providing relief to thousands of patients since 2011. Dr. Lynch’s patients have traveled to Maryland from 48 US states and 13 different countries to receive his expert care.
His clinic is in Waugh Chapel-Gambrills.
For more information see:

Double Board-Certified Psychiatrist and Addiction Medicine Physician
Affiliated with Sibley Memorial Hospital and Johns Hopkins Medicine, Washington, DC
Licensed in Maryland, Virginia, and Washington, DC
242 Merrimac Court, Suite #9, Prince Frederick, MD 20678
Phone: 410-535-6520
Email: dr.veneramiller@cipmexam.org
Dr. Venera R. Miller offers specialized Psychiatric and Addiction Services and expertise in the following areas:
• Diagnosis and treatment of a wide range of psychiatric and substance use disorders
• Psychiatric evaluations for bariatric, plastic, general, and gender-affirmation surgeries
• Court-ordered psychiatric evaluations and expert witness testimony
• Independent medical opinions, nexus letters, and related evaluations
Dr. Venera R. Miller is a physician with more than 20 years of clinical experience. She earned her medical degree from Bashkir State Medical University in Ufa, Russian Federation, graduating with a Diploma of Excellence, and completed internship and residency training in Internal Medicine. Dr. Miller later completed her Psychiatry Residency at St. Elizabeths Hospital in Washington, DC, where she was nominated Chief Resident and received extensive training in forensic psychiatry. She has over 18 years of experience treating opioid addiction and substance use disorders, and is skilled in advanced therapies including Electroconvulsive Therapy (ECT), Transcranial Magnetic Stimulation (TMS), and ketamine treatment for treatment-resistant depression, supporting a comprehensive, psychosomatic approach to care.



Dr. Beverley Boothe is the President and CEO of Life Enrichment Counseling Center, Inc., founded in 2005 and serving clients throughout Northern Virginia and the DMV. With locations in Gainesville, Alexandria, and Haymarket, the practice provides in-person and telehealth counseling for children, adolescents, adults, and families. A Licensed Clinical Social Worker in Virginia, Dr. Boothe holds a Ph.D. from Regent University, an MSW from Howard University, and undergraduate degrees in Social Work and Psychology from York University. Her experience across private, nonprofit, and government settings informs a holistic, compassionate approach to care, empowering clients to lead meaningful, fulfilling lives.

Nadia Lassic is a Board Certified Psychiatric Mental Health Nurse Practitioner providing compassionate, holistic care. She takes a collaborative, therapy-informed approach that looks beyond symptoms to understand each individual’s experiences and environment. Nadia integrates medication management and lifestyle strategies to support adolescents and adults navigating anxiety, ADHD, mood disorders, and high-functioning stress. She creates a warm, judgment-free space where clients feel seen, supported, and empowered to grow, and is a strong advocate for nervous system regulation and everyday mental wellness.

Elena Acosta is a Virginia licensed clinical social worker with experience across the lifespan. She provides culturally responsive, trauma-informed, client-centered care, specializing in anxiety, life transitions, substance use, and trauma, including sexual assault. Using CBT, psychodynamic, and narrative approaches, Elena supports adolescents and adults in building coping skills, resilience, and confidence. As a Latina therapist, she values authenticity and collaboration, creating a supportive, respectful space that honors each client’s pace, lived experience, and personal goals.




Dr. Zviadi Aburjania is a Board Certified Psychiatrist who works with children, teens, and adults to help them understand themselves more deeply and create lasting change. His approach combines up-to-date medical knowledge with a deep interest in the emotional lives of his patients.
After earning his medical degree from Tbilisi State Medical University in Georgia, Dr. Aburjania spent several years in the United States doing research before completing his psychiatry residency and child psychiatry fellowship at the University of Alabama at Birmingham. He now practices in Virginia and continues advanced psychoanalytic training at the Cincinnati Psychoanalytic Institute. In his work, Dr. Aburjania integrates psychotherapy and medication when needed, believing that true healing comes from both scientific understanding and emotional insight. He treats a wide range of concerns, including depression, anxiety, ADHD, OCD, and personality patterns.
Dr. Aburjania is known for his thoughtful, patient-centered style. He takes time to listen carefully, explore what lies beneath symptoms, and help his patients gain clarity about themselves—the kind of understanding that supports lasting relief, growth, and healing. In his free time he likes to hike, read and learn how to play piano.
Degrees, Training & Certifications: Dr. Cardinal is a Midwest native and finished his undergraduate studies at the University of Minnesota. He pursued his doctoral education at Scholl College of Podiatric Medicine in North Chicago, IL and graduated with a dual degree of Doctor of Podiatric Medicine and Master of Science in Healthcare Administration and Management. Dr. Cardinal went on to complete a 3-year medical and surgical Residency with the VA Maryland Healthcare System with a focus in wound care, general podiatry and surgery. Dr. Cardinal is Board Certified by the American Board of Podiatric Medicine and is a Fellow of the American College of Foot and Ankle Orthopedics.
Special Interests/Services: Podiatrist in Motion is a unique practice whose primary focus is house calls for foot and ankle concerns. Dr. Cardinal will come to you, to your home or office; meaning no waiting rooms, no traffic and no rushed visits. He treats all ages specializing in many general podiatric concerns such as heel pain, medical pedicures, ingrown nails, warts and pediatric podiatry. He performs biomechanical exams and casting for custom orthotics. Dr. Cardinal also offers cutting-edge treatments such as laser therapy for fungal nails and musculoskeletal pain.
Personal Interests & Hobbies: In his free time, Dr. Cardinal enjoys playing tennis, running, spending time with family and friends and playing the guitar.
Practice Philosophy: Podiatrist in Motion’s mission is to bring the foot care clinic to you, in the comfort of your own home, office or wherever you may need care. Private-pay only.


Dr. Horowitz arrived in the Washington metro area in 1986 and established Bowie Foot and Ankle later that year. He quickly joined the staff at the newly opened Bowie Health Center Surgery Center. Dr. Horowitz enjoys the general nature of his practice and sees patients of all ages with a variety of foot problems. He especially enjoys dealing with the orthopedic nature of many podiatric problems, whether they be of recent onset or long standing. He has found that chronic problems affecting the ankle, knee, hip or back, can often be traced to recent symptoms within the foot, or vice versa.
Dr. Horowitz has been practicing in the Bowie area for over 25 years. He graduated from the Illinois College of Podiatric Medicine with a Doctorate of Podiatric Medicine and did his postgraduate training in podiatric medicine and surgery in association with the Podiatry Group of Greater New York and the New York College of Podiatric Medicine. Dr. Horowitz remained in New York for an additional two years to practice with several of his training program’s attending doctors in order to further hone his medical and surgical skills. Dr. Horowitz continues to expand his knowledge in podiatric medicine, in an effort to bring advances in treatment and technology to his patients.
Professional Affiliations: American Podiatric Medical Association, Maryland Podiatric Medical Association and American Academy of Podiatric Sports Medicine
Special Interests: Chronic foot and ankle musculoskeletal issues, Orthopedics, Surgery
Board Certifications: Podiatric Surgery - American Board of Medical Specialties in Podiatry; Podiatric Surgery, Podiatric Orthopedics - American Board of Podiatric Orthopedics and Medicine, Prosthetics, Custom Orthotic / Brace Fabrication and Shoe Modification
Family: Wife: Karin and Children: Aliza and Talia



Since age 5, my passion for veterinary care has guided me. At 14, I embarked on my journey, working in veterinary clinics. Graduating from The Ohio State University with a DVM degree in 1977, I’ve devoted my life to caring for both pets and their families. After a decade in clinical practice, I sought new avenues due to concerns about pets’ health. In 1988, I delved into veterinary acupuncture, earning certification from the International Veterinary Acupuncture Society. This led me into holistic medicine, where I gained certification in homeopathy and underwent training with Dr. Richard Pitcairn. In 1993, I sold my practice in Maryland and pursued spirituality in Sedona, AZ, becoming a Tibetan Buddhist nun until 2023. Embracing the belief in the equality of all life, I dedicated myself to alleviating suffering. Returning to Maryland in 2006, I cofounded Holistic Veterinary Healing in 2013. Recognizing the interconnectedness of human and animal health, I pursued a Master’s degree in Human Acupuncture in 2010. Since 2016, I’ve focused solely on animal patients, certified in Medical Ozone Therapy and as a Fear Free Practitioner. Residing in Germantown with my dogs, I cherish moments with family and friends, and find solace in meditation and loving my dogs.


Dr. Mara Holton grew up in Maryland and has practiced with AA Urology for more than a decade since completing her residency.
Dr. Holton earned her undergraduate degree from The University of Vermont before attending medical school at Temple University in Philadelphia. She then completed her general surgery internship and urologic surgery residency at University of Maryland Medical System. While in residency, Dr. Holton practiced the full breadth of urologic training and surgery. Additionally, while there, she spent a year doing research dedicated to interstitial cystitis / pelvic pain alongside leaders in the field.
In clinical practice, Dr. Holton treats all urologic conditions but has a special interest in female incontinence and pelvic floor dysfunction along with the noninvasive treatment of kidney stones. She is trained in the all of the most current and minimally invasive options to facilitate patients ability to recover from procedures quickly so that they can get back to their lives and families.
As the managing partner of her group, Dr. Holton has overseen the expansion of AA Urology over the past several years and is excited by the growing presence of the group while maintaining the practice ethos of compassionate care in our communities. She is also very involved in the advancement of independent physician practices as a critical resource for patients and participates in advocacy as a board member of national organizations, including the Large Urology Group Practice Association.
In her free time, Dr Holton enjoys traveling, hiking and spending time with her family and dogs.


Dr. Troy Sukhu is originally a Maryland native who is thrilled to have the opportunity to give back to the Maryland community through a patient-centered approach. Dr. Sukhu earned his undergraduate degree from the University of Pennsylvania prior to attending the University of Virginia for medical school. He then completed his Urologic Surgery Residency at The University of North Carolina in Chapel Hill where he had extensive training in open, laparoscopic / robotic, and endoscopic surgeries. Dr. Sukhu is listed as an author on over 30 research papers and abstracts, and has presented at various regional and national conferences.
Dr. Sukhu treats all areas of urology but his main areas of focus are laparoscopic / robotic surgery for kidney and prostate cancer, treatment of benign prostatic hyperplasia (BPH), minimally invasive treatment and prevention of kidney stones, and men’s health including erectile dysfunction and Peyronie’s disease. He strives to utilize cutting-edge technologies to achieve the best outcomes possible for his patients.
Outside of work, he enjoys spending time with his wife and daughter.
Dr. Sukhu is an avid Washington D.C. and Maryland sport fan, enjoys being outdoors, and is always looking forward to trying new restaurants.


By Quansheng Lu, CMD, PhD, LAc
Wholelife Chinese Medicine & Acupuncture Center
Polycystic Ovarian Syndrome (PCOS) is a complex condition where the ovaries produce excessive levels of

male hormones and develop numerous small cysts. While its exact origins remain somewhat elusive, it’s a prevalent gynecological endocrinopathy that affects approximately 6-8% of women in their reproductive years. This condition’s impact on women’s reproductive health is undeniable, as it can lead to an astonishing 75% of anovulatory infertility and is a contributing factor to increased rates of early pregnancy loss. Beyond its gynecological aspect, PCOS brings ad-
Wholelife Acupuncture & Fitness Center
Quansheng Lu, CMD, PhD, L.Ac www.wholelifeherb.com • luquansheng@gmail.com 301-340-1066 • fax: 301-340-1090
Guest professor, Henan University of Traditional Chinese Medicine (TCM) Chief TCM Physician, WFCMS; M.S. in TCM, Beijing University of TCM PhD in integrated medicine, China Academy of Chinese Medical Sciences Fellowship, Georgetown University & Children’s National Medical Center 3 patents, 8 books of TCM, 30 papers, 30+ years of experience in TCM
Low back pain • eczema • arthritis • allergies • cough • insomnia • paralysis obesity • nephritis • hepatitis • infertility • PMS • side effects of cancer treatment 416 Hungerford Drive, #300 Rockville, MD 20850 5022 Dorsey Hall Drive, #101 Ellicott City, MD 21042



ditional metabolic challenges, including insulin resistance (IR), impaired glucose tolerance, and dyslipidemia.
PCOS is not solely a gynecological concern; it extends its influence from puberty to postmenopause, making it a persistent concern throughout a woman’s life.
Therefore, it is crucial not only to address the immediate complaints of PCOS patients but also to prioritize their long-term health, particularly those with obesity and/or IR. Timely and effective interventions are paramount to mitigate the adverse consequences associated with PCOS.
Conventional medical treatments for PCOS encompass prescription medications, surgical options, and lifestyle modifications.
Studies on acupuncture in PCOS, though non-randomized, indicate a low incidence of adverse events, no
heightened risk of multiple pregnancies, and cost-effectiveness.
Acupuncture’s potential impact on beta-endorphin production, which in turn may influence gonadotropinreleasing hormone (GnRH) secretion, suggests a role in ovulation induction and fertility enhancement.
Recent research has highlighted traditional Chinese medicine’s capacity to regulate gonadotropin-releasing hormone, induce ovulation, enhance uterine blood flow, and address menstrual irregularities associated with PCOS. Additionally, it has shown promise in aiding individuals with infertility linked to polycystic ovarian syndrome, as well as those grappling with anxiety, stress, and immunological disorders. However, it is imperative to seek out a well-trained professional acupuncturist to achieve optimal outcomes.

By Janet V. Johnson, MD Loving Care Pediatrics
Parents and caregivers can help their child develop heart healthy habits early in life. They can encourage their children to evaluate their food choices and physical activity habits. Here are some tips to help get you started.
Be a role model. No one is perfect, however if your child sees that you are trying to eat healthy and are exercising, they will notice your efforts and begin to understand that good health is important to the family. Keep things fun and positive. Don’t focus on the restrictions but
offer praise for a job well done. Celebrate successes along with helping children and teens develop a good self-image. Don’t reward with video games, TV, candy or snacks, these habits lead to a sedentary lifestyle, which increase obesity and cardiovascular disease.
Get moving. Plan family time for every member to participate including family pets. Take walks, hikes, bike rides or just play outdoors. Everyone in the family will benefit from the exercise and time together.
Dinnertime should be family time. All members of the family should come together to sit down and eat, there is less opportunity for children eating the wrong foods or snacking too much. Have your children help in meal planning, grocery shopping and cooking the meals. All involved will develop good eating habits and benefit from the quality time with the family.
Make a game of reading labels while shopping and at home preparing your meals. This way the whole family learns what is good for their health
Please see “Heart Habits,” page 34



Services provided include: Implants, Implant Crowns, Invisalign, CEREC, Crowns, Root Canals, Cosmetic Dentistry, iTero Digital Scanner, Tooth-Colored Fillings and Extractions. Schedule an appointment for you and your family today!

Dr. Afreen
Proud to be in network with PPO plans: Delta Dental, MetLife, United Concordia, United Healthcare, Aetna, GEHA, CIGNA, Anthem, BlueCross BlueShield, United Healthcare, Guardian, Principal Ameritas, DentaQuest, Dominion Dental, Connection Dental, Himan, Assurant/Dental Health Alliances, Smiles for Children.


A neck lift can be performed for men and women of varying ages who are often frustrated by changes of the appearance of their neck and jawline. Depending on your age, a neck lift can be a short one-hour procedure to remove fat or a 3-hour procedure to remove fat, visible neck bands, and excess skin.
Remove Excess Skin (Cervicoplasty)
Liposuction to Remove Excess Fat
Remove or Alter Neck Muscles (Platysmaplasty)
Liposuction can be performed alone or with surgical removal of the fat under the chin through a small incision under the chin.
In patients with vertical bands in the neck, a platysmaplasty can be performed to reduce the appearance of the bands.
Sometimes a chin implant is recommended to improve the overall contour and help with excess skin.
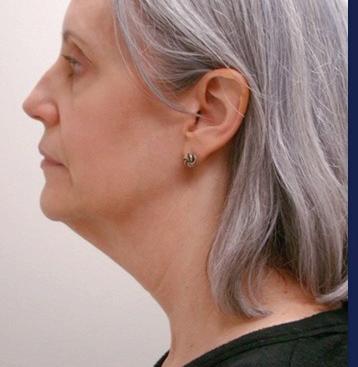
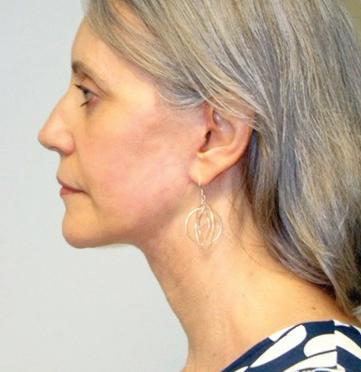

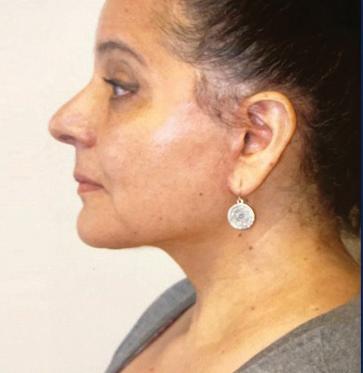



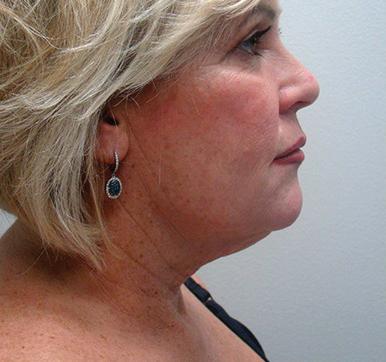



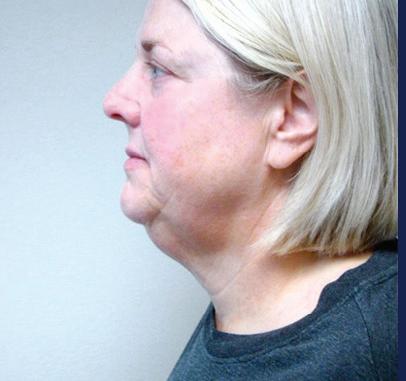
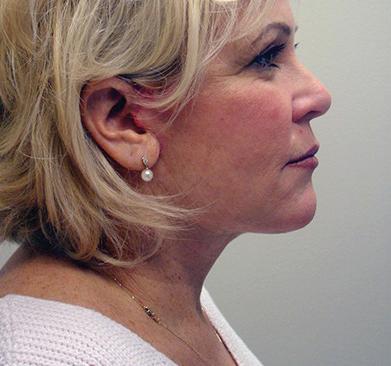
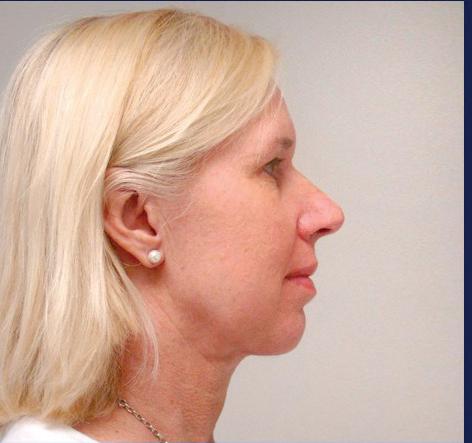
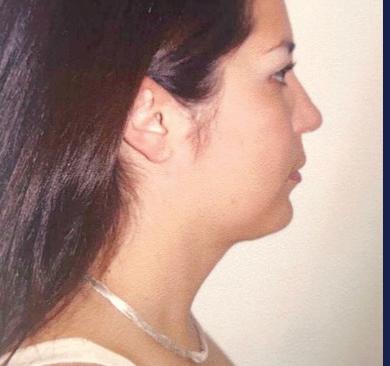


ACUPUNCTURE
Eastern Medical Holistic Healing Center, Angel Wood, 240755-5925. www.acupuncture4wellness.webs.com
ALTERNATIVE HEALTHCARE
Holistic Family Health - Thermal Imaging, Herndon, VA. 703-635-6324 For More information visit www.fhtid.com
BEAUTY/SKIN
A Better You, Dr. ClarkeBennett, 410-672-2742.
BREAST HEALTH
University of Maryland Charles Regional Medical Center. 11340 Pembrooke Square, Suite 202, Waldorf, MD 20603. 240-607-2010. UMCharlesRegional.org
CHINESE MEDICINE & ACUPUNCTURE
Wholelife Chinese Medicine & Acupuncture, 301-526-9898, 416 Hungerford Dr., Rockville www.wholelifeherb.com
DENTAL IMPLANTS
Dental Implants Center of Rockville – Dr. Sreenivasan Sivakumar, DMD, MSD –301-294-8700 – 77 South Washington Street, Suite #205, Rockville, MD 20850 – www.DrSreeni.com.
Karl A Smith, DDS, 2550 N. Van Dorn St., Suite #128, Alexandria, VA. Call 703-894-4867, Visit www.drkarlsmith.com
Richard Hughes, DDS, 703444-1152, 46440 Benedict Dr., Suite #201, Sterling, VA. www. SterlingImplantDentist.com
Marc P. Stanard, DDS – 202887-5441 – 1350 Connecticut Avenue, NW, Suite #305, Washington, DC 20036 – wdcperioimplant.com.
EYE CARE
Visual Eyes, Alexander Nnabue OD, 301-324- 9500.
FERTILITY
Montgomery Women’s Fertility Center – 301-946-6962 – MontgomeryFertilityCenter. com – Rockville, MD.
HOLISTIC WELLNESS COACH
Nutrition Lifestyle Digestion and More – Lisa@LisaThorne.Me – Text 269861-7565.
HYPNOSIS/YOGA
Toni’s Happy Hour Yoga and Holistic Wellness Center • 6504 Old Branch Avenue, Temple Hills, MD 20748 • 301-449-8664.
MEDICAL SPACE
Charles L. Feitel Company, 301-571-9333, www.medicalanddentalspace.com.
MENTAL HEALTH SERVICES
House Calls, LLC. 301-3466732. callingonbeth@gmail. com. www.CallingOnBeth.net.
Nutritional Healing Center, Thomas K. Lo, DC, MA, 240-651-1650, 7310 Grove Road, Suite 107, Frederick, MD 21704. doctorlo.com.
Good Health Nutrition Services,LLC – 1300 Mercantile Lane, Suite 129-37, Largo, MD 20774 – 301-341-4680 –www.ghnutritionservices.com – We accept Insurance.
OPHTHALMOLOGY
NewView Laser Eye Center – Jacqueline D. Griffiths, MD – Reston (703) 834-9777 – Visit us at www.NewViewEye.com.
All Smiles Orthodontics – 9010 Lorton Station Blvd., Suite #260, Lorton, VA 22079 – www. AllSmilesBraces.com – For info call us at 703 337-4414.
To Order: Include you NAME, ADDRESS, PHONE, EMAIL AND WHAT HEADING YOU WISH TO BE LISTED UNDER, AND ANY SPECIAL OFFER OR TEXT TO INCLUDE. We will prepare a proof and email to you for approval.
Email your information to: info@yourhealthmagazine.net or Fax to: (301) 805-6808. Call (301) 805-6805 for assistance.
MARYLAND/WASHINGTON, DC OFFICE
4201 Northview Drive, Suite #102, Bowie, MD 20716 phone: (301) 805-6805 • fax: (301) 805-6808 • email: Info@YourHealthMagazine.net VIRGINIA OFFICE phone: (703) 288-3130 • fax: (703) 288-3174 • email: Publish@YourHealthMagazine.net

Loving Care, Janet Johnson, MD – 301-403-8808.
PHYSICAL THERAPY/ REHABILITATION
Active Physical Therapy. Various Locations across Maryland and Washington, DC. Active-physicaltherapy.com.
Largo Foot and Ankle Health Center, Ade Adetunji, DPM, 301-386-5453.
District Podiatry – Lubrina Bryant, DPM – 202-388-5303 – 1140 Varnum Street, Suite #30, Washington, DC 20017
www.DistrictPodiatry.com.
Chevy Chase Home Care. Help at a time you need it most. Any Ages. Any situations. Any shifts. MD, DC, VA. www.CHCHhomecare. com 202-374-1240.
AA Urology – Odenton, 1106 Annapolis Road, Suite #250, Odenton, MD 21113 – Glen Burnie, 305 Hospital Drive, Suite #303, Glen Burnie, MD 21061 – Bowie, 4201 Northview Drive, Suite #201, Bowie, MD 20716 – West Campus Surgery Center, 7855 Walker Drive, Suite #102, Greenbelt, MD 20770 – Greenbelt , 7855 Walker Drive, Suite #100, Greenbelt, MD 20770.






SUBSCRIBING IS EASY:
1) Call 301-805-6805 with your name, contact info, and credit card payment for $24, or
2) Simply mail this form along with your check for $24:
Your Health Magazine 4201 Northview Dr. Suite 102 Bowie, MD • 20716




Now you can get the latest issues delivered directly to your home!
• Health articles and advice
• Doctors near YOU!
• Maryland, Washington, DC & Virginia editions
• Only $24 for a year’s subscription (12 issues)!








and are more conscious of what they eat. Developing behavioral changes that will bring lifelong benefits.
Eating healthy on a budget can be done. One just has to be creative to stick within the budget to incorporate nutritious foods into the diet. Include in your diet: Bananas, apples (raw with skin), fat-free milk, oranges, pears, lentils, barley, brown rice, oatmeal, beans and a host of other fruits and vegetables. Try to incorporate some of these healthy foods under $1.00 into the weekly menu planning.
It can be challenging cooking for children who refuse to eat some foods. It is also concerning since they miss out on important nutrients found
in foods. Include picky eaters when shopping for and meal planning of foods. Asking them to help with the shopping and cooking gives them investment in the final product and kids are more likely to taste a dish if they helped plan or prepare it.
Start at home, and insist on good food choices in the school for breakfast and lunch, along with healthy choices for vending machines located in the schools and fundraisers. Your children’s healthcare provider will be monitoring cardiovascular indicators like blood pressure, BMI and lipid panels. Make your voice heard, know and understand your child’s numbers.
realizing it, especially if you have neuropathy and do not feel pain even when a deep sore is forming. This is why properly fitted diabetic shoes and custom inserts are so important. They are not just comfortable shoes. They are medical tools that spread pressure evenly across your foot, protect bony areas from rubbing, and lower your risk of ulcers and infections. For people at higher risk, podiatrists usually recommend professional nail and callus care every three to four months. Let your foot specialist handle thick nails and calluses with sterile instruments instead of trying to cut or shave them at home.
small changes are noticed and acted on rather than missed.







Many people with diabetes also develop onychomycosis, a fungal infection that makes the toenails thick, discolored, and crumbly. It is not attractive, and it can catch on socks or shoes, but if your circulation is compromised, aggressively removing the nail can create more danger than benefit. Removing the nail creates an open wound. Poor blood flow means that wound might not heal properly, and any open area becomes a doorway for infection, which can spread quickly in a high-risk foot. Because of that, we may recommend a conservative approach rather than nail surgery. That can include carefully thinning the nail in the office, discussing topical or oral treatments when appropriate, and focusing more on preventing pressure and trauma than on making the nail look normal. It can be frustrating to live with a nail that does not look good, but in the setting of diabetes and vascular disease, the priority is keeping the foot intact, not cosmetic perfection.
A true preventive diabetic foot exam goes far beyond a quick visual check. A thorough visit typically includes a careful skin evaluation to look for cracks, calluses, redness, blisters, or early ulcer changes, an assessment of the nails for thickness, fungal infection, or ingrowing edges, and testing of sensation with tools that check whether you can feel light touch and pressure. Temperature and circulation are assessed by comparing warmth between feet, feeling pulses, and looking at skin color and refill. Structural issues such as hammer toes, bunions, flat feet, or bone spurs can be identified because they change how you walk and where pressure lands. Practices that work within lower extremity amputation prevention programs use these exam findings in a structured way each year, so even
No matter how advanced the clinic or technology, your daily habits are the real frontline of protection. A realistic, high risk foot care plan usually includes daily inspection of the top, bottom, and between the toes on both feet, using a mirror or help from another person if you cannot see well. You look for cuts, blisters, redness, swelling, or color changes. Daily moisturizing of the feet, avoiding the spaces between the toes, helps keep the skin from drying and cracking, which could let infection in. If you have been prescribed compression stockings, especially after a blood clot or when you have chronic swelling, using them as directed can help support the veins and control fluid buildup. Avoid walking barefoot, even at home or for a short distance, because you may not feel something sharp or hot until damage is already done. Do not perform home surgery on your feet. That means no razors on calluses, no digging at ingrown nails, and no over the counter corn removers that can chemically burn the skin.
It is also important to know your red flags and act quickly. You should contact your podiatrist or seek urgent care if you notice a new wound or blister, redness that spreads, swelling that is new or clearly worse, black, blue, or very pale areas on the skin, or a sudden change in temperature or feeling in one foot compared to the other. These signs can mean infection, loss of blood flow, or both, and they are time sensitive problems in a diabetic foot.
All of these pieces, the detailed exams, the vascular testing, the careful shoe fittings, the decision to avoid unnecessary surgery, and the time spent on education, come together with one main goal, keeping you walking on your own feet for as long as possible. That is the heart of lower extremity amputation prevention programs and a major reason it matters that WeTreatFeet Podiatry participates in this type of structured, evidence-based care. It means your visits are guided by a system specifically designed to lower your risk of ulcers and amputations, not just to treat problems once they are severe.
If you live with diabetes and have not had a comprehensive diabetic foot exam in the last year, scheduling that visit is one of the most important steps you can take to protect your mobility and independence.

Submitted by ScholarsHub.net
Burnout is often discussed as a mental or emotional issue, but its effects extend far beyond motivation and mood. For students, job seekers, and working professionals, chronic stress and burnout can have a measurable impact on physical health—particularly on blood sugar regulation. Understanding this connection is critical for long-term health, especially in fast-paced academic and professional environments.
When the body experiences stress, it activates the “fight-orflight” response, releasing hormones such as cortisol and adrenaline. These hormones are designed to provide a quick burst of energy by increasing glucose levels in the bloodstream. In short-term situations, this response is helpful. However, when stress becomes chronic—as it often does with heavy workloads, job insecurity, or academic pressure—the body remains in a constant state of alert.
Elevated cortisol levels interfere with insulin’s ability to move glucose from the bloodstream into cells. Over time, this can lead to insulin resistance, a condition in which the body requires more insulin to keep blood sugar levels stable. Persistent insulin resistance increases the risk of prediabetes and type 2 diabetes, even in individuals who appear otherwise healthy.
Burnout is characterized by emotional exhaustion, reduced performance, and detachment from work or studies. These symptoms often lead to unhealthy coping behaviors such as poor sleep, irregular eating patterns, increased caffeine or sugar intake, and reduced physical activity—all of which further disrupt blood sugar control. Long hours spent sitting, combined with mental fatigue, compound the problem.
Blood sugar dysregulation does not always cause immediate symptoms. Many people feel “fine” while underlying metabolic changes progress silently. Over time, these changes increase the risk of cardiovascular disease, fatigue, impaired concentration, and reduced productivity—directly affecting academic success and career performance.
Breaking the Cycle
Addressing burnout is not just about improving work-life balance; it is a preventive health strategy. Regular physical activity, adequate sleep, structured breaks, and stressmanagement techniques such as mindfulness or deep breathing help lower cortisol levels and support insulin sensitivity. Seeking medical guidance when stress feels unmanageable is also an important step. The Takeaway Burnout is more than a productivity issue—it is a metabolic one. By recognizing the hidden link between stress and blood sugar, students and professionals can take proactive steps to protect both their health and their future performance.

