JULES STEIN EYE INSTITUTE



July 1, 2024–June 30, 2025
DIRECTOR
Anne L. Coleman, MD, PhD
MANAGING EDITOR
Tina-Marie Gauthier
c/o Jules Stein Eye Institute
100 Stein Plaza, UCLA Los Angeles, California 90095–7000 Tina@EyeCiteEditing.com
PUBLICATION COMMITTEE
Anthony Aldave, MD
Susan Lee DeRemer, CFRE
Deborah Ferrington, PhD
JoAnn Giaconi, MD
Marissa Goldberg
Kevin Miller, MD
Peter Quiros, MD
Roxana Radu, MD
Alfredo Sadun, MD, PhD
CONTRIBUTING EDITORS
Rubi Arias
Leiloni Breidert
Margarita Gonzalez
Chris Laybourn
Peter López Angel Padilla
Mario Schunimann
PHOTOGRAPHY
Reed Hutchinson
Rich Schmitt
Robin Weisz
DESIGN
Robin Weisz/Graphic Design
To view the Annual Report online, visit: www.uclahealth.org/Eye/annual-report
For more information about the UCLA Department of Ophthalmology, see: www.uclahealth.org/eye/
by the Regents of the University of California.


Dear Friends,
I am pleased to share with you the 2024–25 Jules Stein Eye Institute Annual Report, showcasing the remarkable work of our clinicians and vision-scientists this fiscal year as we continue our singular passion: preserving sight and restoring vision.
The work we do today at the Institute and worldwide is made possible by two individuals of incredible foresight: Dr. Bradley Straatsma and Dr. Jules Stein. Together these visionaries saw an opportunity to transform UCLA into a global leader in eye care, research, and education through their creation of the Jules Stein Eye Institute, which has grown to become a vision-science campus at UCLA. The documentary A Celebration of Our Founders was created this year, bringing to life the pivotal moments that shaped the Institute and offering both a personal and historical lens on its enduring impact.
Building on this legacy, the UCLA Department of Ophthalmology marked many noteworthy events, including:
f Dr. SriniVas Sadda serving as president of the 2025 Association for Research in Vision and Ophthalmology (ARVO) annual meeting. Our leadership at ARVO will continue, with Dr. Sophie Deng as 2026 ARVO president and Dr. Joseph Demer as 2026 ARVO vice president.
f The opening of the new Doheny Eye Center UCLA–Pasadena, bringing state-of-the-art clinical care to the Doheny Eye Institute campus— continuing our commitment to excellence.
f The 10th anniversary of the UCLA Stein Eye Surgery Center, marking a decade of providing essential ophthalmic services at the Jules Stein Eye Institute vision-science campus.
f Welcoming eight new faculty members, bringing specialized expertise in clinical practice and vision science.
f Department vision scientists securing 60 R01 and other major competitive vision-science research grants, totaling $14,378,000 in support of cutting-edge investigations.
As we reflect on these milestones, we renew our commitment to eliminating preventable blindness. The unwavering dedication of our community to advancing research and education underscores our shared vision of improving global eye health. Through innovation, collaboration, and a continued pursuit of knowledge, we are working toward a future where the gift of sight is accessible to all.
Sincerely,

Anne L. Coleman, MD, PhD
Bradley R. Straatsma, MD, Endowed Chair in Ophthalmology
Chair, UCLA Department of Ophthalmology
Director, Jules Stein Eye Institute
Affiliation Chair, Doheny Eye Institute
The Jules Stein Eye Institute was born from a powerful partnership between Dr. Jules Stein (left) and Dr. Bradley Straatsma (right). United by purpose, they transformed a bold idea into a world-renowned Institute at UCLA.

On June 25, 2025, the Jules Stein Eye Institute hosted a screening of Jules Stein Eye Institute: A Celebration of Our Founders, a documentary honoring Jules Stein, MD, a former ophthalmologist turned powerful entertainment executive and founder of MCA, and Bradley R. Straatsma, MD, JD, the founding chair of the UCLA Department of Ophthalmology and the Jules Stein Eye Institute’s founding director.
Anne L. Coleman, MD, PhD, chair of the Department of Ophthalmology, director of the Jules Stein Eye Institute, and affiliation chair of Doheny Eye Institute, described the film as a tribute that captures the spirit and legacy of the Institute through the voice of one of its most influential figures—Dr. Straatsma, who through personal stories, preserves the Institute’s rich history.
The event also paid tribute to Lew Wasserman, a philanthropist and former president of MCA, who was instrumental in supporting the Institute’s growth. His grandson, Casey Wasserman, continues to carry forward that legacy alongside the Institute’s Board of Trustees.
Stein:
In the late 1950s, ophthalmology at UCLA existed only as a division within the Department of Surgery. With training from esteemed universities including Yale, Columbia, and Johns Hopkins, as well as the Armed Forces Institute of Pathology, Dr. Straatsma quickly recognized UCLA’s potential to develop a world-class eye program that could rival any in the nation.

Shortly after his arrival at UCLA, Dr. Straatsma learned of a donation from Dr. Stein and requested a meeting, which Dr. Stein declined. Undeterred, Dr. Straatsma persisted and ultimately presented Dr. Stein with a written proposal for an integrated eye institute—combining research, education, and patient care— along with a conceptual sketch of the facility on UCLA’s campus. The idea captured Dr. Stein’s imagination, and their resulting collaboration proved pivotal in shaping the future of ophthalmology at UCLA.
Leadership at the Helm:
UCLA’s Role in Building a World-Class Eye Institute
From its earliest days, the Institute benefited from the support of an exceptional University environment—not merely as an institution, but as a collective of forward-thinking individuals. Key were UCLA’s chancellors, including Vern Knudsen, Franklin Murphy, and Richard Young , whose administrative foresight helped shape a fertile ground for medical innovation.
Founding Dean of the Medical School Stafford Warren, followed by Sherman Mellinkoff, and subsequent deans, played a foundational role in integrating the Institute’s mission with UCLA’s broader medical education and research goals. Their guidance helped secure vital resources, attract top-tier faculty, and ensured the Jules Stein Eye Institute would not only thrive within the University but also influence ophthalmology worldwide.
Under the visionary direction of Dr. Straatsma, the contributions of Drs. Leonard Apt , Dean Bok , Robert Christensen, Robert Foos, Michael Hall, S. Rodman Irvine, and Thomas Pettit were instrumental in shaping the Jules Stein Eye Institute into a driving force of excellence, innovation, and influence within academic medicine. Their impact on the field—and on the Institute’s legacy—cannot be overstated.
The 1966 dedication of the Jules Stein Eye Institute spanned several days, drawing global ophthalmology leaders, donors, UCLA faculty, and members of the Hollywood community. At a gala banquet, guests were blindfolded—offering a powerful, wordless reminder of the vital sense the Institute was committed to preserving: vision.

Concluding his remarks, Dr. Stein declared, “The history of the Institute begins with this dedication. I am confident it will be a proud history.” At that moment, Doris Stein stepped forward to cut the ribbon draped across the entrance—symbolically opening the Institute and ushering in a new era in vision science and care.
Dr. Straatsma held deep admiration for Dr. Stein’s intellect, business acumen, and unwavering commitment to excellence. “I can’t afford to do something unless I do it very well,” Dr. Stein said—an ethos that defined their partnership. Dr. Straatsma’s respect was met with Dr. Stein’s trust, forming a relationship grounded in shared purpose and ambition.
And the personal bond between the two men evolved into a unique partnership that bridged medicine and entertainment. Welcomed into the Steins’ social circle—which included figures like Walt Disney and Alfred Hitchcock, along with the leading movie stars of the day—Dr. Straatsma gained access to influential connections that led to meaningful support for the Institute. Key benefactors emerged from these relationships, while events hosted at the Stein residence and the Institute raised critical funds and awareness, fostering a rare and enduring alliance between Hollywood and academic medicine.
Dr. Straatsma’s commitment to ophthalmology didn’t stop at UCLA’s doorstep; community engagement was equally crucial. Through the UCLA Mobile Eye Clinic and partnerships with regional hospitals, the Institute serves a broad and diverse population. And Institute physicians, international fellows, and alumni advance the Institute’s mission by working tirelessly to eradicate blindness worldwide.
Today, Dr. Straatsma expresses pride in what the Institute has become—a global leader in ophthalmology research, patient care, and education. Yet he remains focused on the future. He credits ongoing leadership, Dr. Bartly J. Mondino and Dr. Anne Coleman, with carrying forward the Institute’s legacy. “The challenge for us at UCLA,” he says, “is to use the opportunities that will emerge for the advance of science, the care of patients, and the education of the students who will arrive from all over the world. That’s the next step in the future of the Jules Stein Eye Institute.”


Our exemplary leaders who have served as chair of the UCLA Department of Ophthalmology and director of the Jules Stein Eye Institute: Dr. Bartly Mondino (1994–2022), Dr. Anne Coleman (2022–present), and Dr. Bradley Straatsma (1964–1994).
Congratulations to our faculty who were honored at the American Academy of Ophthalmology (AAO) annual meeting in Chicago, Illinois. Drs. Federico G. Velez and Stacy L. Pineles received Senior Achievement Awards. Dr. Simon K. Law was a Secretariat Awardee, and Dr. Robert Alan Goldberg was the Wendell L. Hughes Lecturer.
UCLA Department of Ophthalmology faculty presented over 100 educational events over the four-day meeting.
Anthony J. Aldave, MD, Bartly J. Mondino, MD, Endowed Chair in Ophthalmology, achieved a departmental first by receiving both Orphan Drug and Rare Pediatric Disease Designation from the FDA for his gene therapy program targeting congenital hereditary endothelial dystrophy (CHED). Dr. Aldave leads the Jules Stein Eye Institute Cornea Genetics Laboratory, which is part of the NIH’s Bespoke Gene Therapy consortium. His lab also received funding from the California Institute for Regenerative Medicine to further this work. These milestones bring the gene therapy closer to human clinical trials and potential treatment for children affected by CHED-related blindness.
Michael D. Ip, MD, Gavin S. Herbert Endowed Chair for Macular Degeneration, has been elected to the American Ophthalmological Society (AOS), one of the most prestigious honors in the field. Founded in 1864, the AOS limits its membership to 225 board-certified ophthalmologists who demonstrate excellence in clinical care, research, education, or public service. Dr. Ip presented his thesis on imaging and treatment outcomes after anti-VEGF therapy for macular edema due to retinal vein occlusion.
UCLA AOS members include: Drs. Anthony C. Arnold , Joseph Caprioli, Anne L. Coleman, Robert Alan Goldberg, Gary N. Holland, Allan E. Kreiger (deceased), Colin A. McCannel, Kouros Nouri-Mahdavi, SriniVas R. Sadda, Alfredo A. Sadun, David Sarraf, Bradley R. Straatsma, and Michael D. Ip
The Doheny and Jules Stein Eye Institutes had a major presence at the Association for Research in Vision and Ophthalmology (ARVO) annual meeting, held May 4–8, 2025, in Salt Lake City. With nearly 11,000 attendees from 74 countries, this year’s event was especially notable as UCLA’s Dr. SriniVas Sadda served as ARVO president, delivered the opening keynote, and shaped the conference theme: “i3: Imagining Innovation and Intelligence in Vision Science.”

Dr. SriniVas Sadda was recently appointed A. Ray Irvine, Jr, MD, Endowed Chair in Clinical Ophthalmology in support of his vision research. He is recognized internationally for his leadership and expertise.
UCLA faculty and trainees contributed across the educational program, and over 1,500 attendees visited the shared Stein/Doheny Expo booth to learn about the Department’s latest research.
The annual Doheny–UCLA Breakfast Forum focused on “Oculomics,” exploring how retinal imaging can help detect systemic disease early. Esteemed speakers included Drs. Amani Fawzi, Yali Jia, and Jianhua Wang. Drs. Deborah Ferrington, Yuhua Zhang , and Giulia Corradetti led the session.
More than 150 Doheny and Jules Stein Eye Institute alumni, faculty, and friends attended the ARVO Alumni Reception on May 5, with notable guests from leading institutions.
The tradition of leadership continues at ARVO next year, with Dr. Sophie X. Deng serving as 2026 ARVO President and Dr. Joseph L. Demer as 2026 ARVO Vice President.
Members of the UCLA Department of Ophthalmology were active participants at the 2025 Association of University Professors of Ophthalmology (AUPO) annual meeting held January 29 to February 1 in Fort Lauderdale, Florida. The event brought together academic leaders in ophthalmology to discuss key challenges and innovations in the field.
Topics included future training pathways in subspecialties such as neuro-ophthalmology, pediatric ophthalmology, and uveitis; the shift between virtual and in-person residency interviews; and leadership development in academic medicine. UCLA faculty contributed valuable insights through presentations that helped shape ongoing conversations in academic ophthalmology.
On March 4, 2025, Doheny Eye Institute celebrated a major milestone with the ribbon-cutting of the new clinic in Pasadena. Now located on the first floor of 150 N. Orange Grove Blvd., the Doheny Eye Center UCLA–Pasadena brings together operations previously spread across multiple suites at Huntington Pavilion. Situated on the scenic Doheny Eye Institute campus, the modern, centralized facility is designed to elevate patient care, encourage collaboration, and usher in a new chapter in the long- standing partnership between Doheny and UCLA’s Jules Stein Eye Institute in advancing excellence in ophthalmology.
Dr. Debora Farber

On April 7, 2025, the Jules Stein Eye Institute honored Debora B. Farber, PhD, with a symposium celebrating her groundbreaking contributions to vision science and advocacy for women in research. A pioneer in retinal degeneration studies, Dr. Farber joined the Institute in 1976 and became one of its first female faculty members. Her research uncovered key genetic causes of inherited eye diseases, earning her major accolades including the ARVO Proctor Medal and an NIH MERIT Award. Beyond her science, she served in key leadership roles at UCLA and ARVO, leaving a lasting legacy in vision research and mentorship.
Since opening in 2015, the UCLA Stein Eye Surgery Center at the Edie & Lew Wasserman Building has performed nearly 80,000 procedures, becoming a cornerstone of ophthalmic care at the Jules Stein Eye Institute. With state-of-the-art technology and subspecialty-trained surgeons, the Center has increased its surgical volume by 45% in a decade, reflecting rising demand and patient trust. Beyond the numbers, its greatest impact lies in lives transformed through expert, compassionate care. As it enters its second decade, the Center remains dedicated to advancing safe, efficient, and patient-centered surgery. Thank you for 10 years of partnership and progress.

Congratulations to Emile Vieta, MD, on completing the competitive two-year board certification program in medical genetics through the UCLA Intercampus Medical Genetics Training Program. This demanding program requires in-depth expertise in genetics, internal medicine, and pediatrics. Dr. Vieta earned high praise for his clinical performance and is now among a select group of physicians board certified in both medical genetics and ophthalmology. His dual specialization positions him to significantly advance the diagnosis and treatment of inherited eye disorders, strengthening the Jules Stein Eye Institute’s commitment to providing expert, personalized care for patients with genetic vision conditions.

Dr. Bronwyn Bateman (left), who gave a $10 million gift to establish the UCLA Bronwyn Bateman Center for Ocular Genetics, and Dr. Michael Gorin (right), retinal disorders and ophthalmic genetics faculty, congratulate Dr. Emile Vieta on completing the Medical Genetics Training Program, part of the EyeGenetics Medical Genetics track.
On September 4, 2024, the Jules Stein Eye Institute held a memorial honoring Dr. Allan “Buzz” Kreiger, the founding chief of the Retina Division and its first faculty member. Family, friends, alumni, and colleagues gathered to reflect on his remarkable legacy in ophthalmology and his lasting influence as a mentor and friend. Speakers, including Drs. Anne L. Coleman, Gary N. Holland, Colin A. McCannel, Bartly J. Mondino, Pradeep S. Prasad, and Steven D. Schwartz, along with video tributes, shared heartfelt memories that evoked both laughter and tears, celebrating the enduring spirit of a beloved leader and pioneer.








Dr. Joseph Horwitz, a pioneering vision scientist and longtime member of the UCLA Department of Ophthalmology, passed away on October 23, 2024, at age 88. A UCLA alumnus, he joined the faculty in 1971 and served as associate director of research and founding co-chief of the Vision Science Division. His groundbreaking work on alpha-crystallin significantly advanced understanding of lens proteins and cataract formation. Honored with the Proctor Medal, NIH MERIT Award, and more, he published 174 papers and mentored countless colleagues. Remembered for his brilliance, humor, and generosity, Dr. Horwitz leaves a lasting legacy in science and in the lives he touched.

Mona Fayad, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Alexander S. Fein, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Michael J. Gilhooley, MD, PhD
Assistant Professor of Ophthalmology
Emma M. Lessieur, MD, PhD
Assistant Professor of Ophthalmology
Boris E. Malyugin, MD, PhD
Joan and Jerome Snyder Chair in Cornea Diseases (pending) Professor of Ophthalmology
Vivian Qin, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Daniel Sand, MD
James and Catherine Shuler Endowed Chair in Comprehensive Ophthalmology
Health Sciences Associate Clinical Professor of Ophthalmology
Chief, Comprehensive Ophthalmology Division
Joel Zylberberg, PhD
Associate Professor of Ophthalmology

Advancing knowledge is central to our mission to protect sight and end blindness. Major research grants play a critical role in fueling this progress. This year, investigators from the Jules Stein Eye Institute and Doheny Eye Institute secured highly competitive Research Project Grants (R01) from the National Institutes of Health (NIH), the National Eye Institute (NEI), and other significant funding sources in support of pioneering vision research.
We proudly recognize and congratulate these distinguished recipients whose work is shaping the future of ophthalmology:
Joseph L. Demer, MD, PhD , Arthur L. Rosenbaum, MD, Chair in Pediatric Ophthalmology, received a five-year NEI R01 grant of $3,353,271 for his project, “Biomechanical Analysis in Strabismus Surgery,” which has been continuously funded for 38 years.
Congratulations to Drs. Anne L. Coleman , Michael S. Ip , SriniVas R. Sadda, and Alfredo A. Sadun of UCLA’s Department of Ophthalmology for being recognized among the Los Angeles Business Journal ’s Top Doctors of 2025. This honor reflects their exceptional contributions to vision science and patient care. Their dedication advances the field of ophthalmology and positively impacts the Los Angeles community.
Yi-Rong Peng, PhD, assistant professor of ophthalmology and neurobiology, secured two prestigious research grants this academic year. The first, is a fiveyear NEI R01 grant of $1,986,646, which will fund her project to elucidate control of neuronal position and connection in the retina.
Dr. Peng also received a one-year competitive seed grant of $80,000 from the Brain Research Foundation, which will fund her project to generate comprehensive measurements of the membrane proteins that construct the retinal circuit and those that change during retinal degeneration. The total amount of these two awards is $2,048,646.
Alapakkam P. Sampath, PhD, Grace and Walter Lantz Endowed Chair in Ophthalmology, received a four-year, NIH R01 grant of $2,257,565 for his project, “Physiology of Retinal Degeneration.”
Dr. Sampath also received a four-year, multi-principal investigator R01 grant of $513,136 with Kirill Martemyanov, PhD, from the Scripps Institute, University of Florida, to uncover the molecular mechanisms allowing photoreceptors to organize their synaptic contacts with downstream retinal neurons. The total amount of these two awards is $2,770,701.
Yuhua Zhang, PhD, professor of ophthalmology, is among a multidisciplinary group of scientists to receive a $4.7M annual three-year award from the NIH Common Fund Venture Program Oculomics Initiative.
Anthony J. Aldave, MD, Bartly J. Mondino, MD, Endowed Chair in Ophthalmology, the principal investigator of a gene therapy program for congenital hereditary endothelial dystrophy (CHED), was granted both Orphan Drug Designation and Rare Pediatric Disease Designation status by the U.S. Food and Drug Administration (FDA), firsts for an investigator in the UCLA Department of Ophthalmology.
Steven A. Barnes, PhD, professor of ophthalmology and neurobiology, received a Glaucoma Research Foundation Shaffer Research Grant that provides $55,000 in seed money for collaborative glaucoma projects that target one or more of the Foundation’s strategic research goals.
Aya Barzelay Wollman, MD, PhD , assistant professor of ophthalmology, was awarded a prestigious ARPA-H (Advanced Research Projects Agency for Health) grant as the UCLA principal investigator for Project VISION. Viability, Imaging, Surgical, Immunomodulation, Ocular preservation, and Neuroregeneration (VISION) Strategies for whole eye transplant, aims to make whole eye transplantation a clinical reality and has the potential to revolutionize vision restoration.

Joseph Caprioli, MD, David May II Chair in Ophthalmology, presented the keynote lecture, “Evolving Toolkit for a Glaucoma Surgeon,” at the Curso Inaugural LXVIII Curso de Formación y Perfeccionamiento de Oftalmólogos on May 22, 2025, in Santiago, Chile.
Dr. Caprioli also gave the Steven Podos Lecture, “Retinal Ganglion Cell Recovery in Glaucoma,” at the Icahn School of Medicine at Mount Sinai, on June 5, 2025, in New York.
Anne L. Coleman, MD, PhD, Bradley R. Straatsma, MD, Endowed Chair in Ophthalmology, chair and executive medical director, Department of Ophthalmology, director, Jules Stein Eye Institute, and affiliation chair, Doheny Eye Institute, presented the Mansour Armaly Lecture “Has Risk Profiling Improved?” on March 21, 2025, at the University of Iowa Glaucoma Clinical Conference in Iowa City, Iowa.
Dr. Coleman also gave the Bascom Palmer Eye Institute Chair’s Lecture, “Neovascular Glaucoma,” on April 10, 2025, at the Bascom Palmer Eye Institute in Miami, Florida.
Joseph L. Demer, MD, PhD , Arthur L. Rosenbaum, MD, Chair in Pediatric Ophthalmology, was the keynote speaker during the Brazilian Society of Pediatric Ophthalmology and Brazilian Strabismus Center Symposium at the University of São Paulo, Brazil, December 3–7, 2024.
Dr. Demer also presented the inaugural Gary L. Rogers and Don L. Bremer Lectureship in Ophthalmology, “Treating Strabismus Caused by Pathology of the Orbital Pulley System,” on April 10, 2025, at Ohio State University in Columbus, Ohio.
Deborah A. Ferrington, PhD , The Stephen J. Ryan–Arnold and Mabel Beckman Foundation Endowed Presidential Chair, was named Nonprofit Executive of the Year at the 2025 Los Angeles Business Journal Nonprofit and Corporate Citizenship Awards. The honor celebrates outstanding leadership and impact in the region.
Dr. Ferrington, chief scientific officer at Doheny Eye Institute, was also appointed president of the Research Directors Council, part of the Association of University Professors of Ophthalmology, for a one-year term, effective April 2025.
Brian A. Francis, MD, MS, The Rupert and Gertrude I. Steiger Vision Research Chair, and John A. Irvine, MD, health sciences clinical professor, were selected by unanimous vote of the DEC-UCLA faculty as Doheny Eye Center UCLA Co-Medical Directors, effective January 2, 2025.
Kaustabh Ghosh, PhD, associate professor of ophthalmology, was appointed as the holder of the Mary D. Allen Endowed Chair in Vision Research, previously held by Deming Sun, MD, now professor emeritus. Dr. Ghosh is a highly respected researcher and is the recipient of many honors and awards, including the competitive Catalyst Award for Innovative Research Approaches for age-related macular degeneration from Research to Prevent Blindness.
Michael James Gilhooley, MB, PhD, FRCOphth , received the Thomas and Susan Carlow Young Investigator Award from the North American Neuro-Ophthalmology Society. He was the 2025 recipient of the year for his work, “Features and surgical management of acquired esotropia associated with high myopia.”
Michael Kapamajian, MD, was named chief of ophthalmology at Harbor-UCLA Medical Center. As chief, Dr. Kapamajian is responsible for the daily operations of the eye clinic at Harbor-UCLA, clinic staffing, staffing in the OR, and all administrative responsibilities associated with Harbor-UCLA. In addition, Dr. Kapamajian works closely with residents during their rotations at Harbor-UCLA, playing an integral part in their training.
Colin A. McCannel, MD, was named as the new chief of the Retina Division of the Jules Stein Eye Institute. Nationally recognized for his work, Dr. McCannel is dedicated to advancing patient care, fostering collaborative research, and providing unparalleled retinal education to fellows and residents.
In addition, Dr. McCannel was appointed as the Ahmanson Chair in Ophthalmology. This administrative chair is for the Retina Division chief to further research, education, and clinical care programs.
Kevin M. Miller, MD, Kolokotrones Chair in Ophthalmology, was chosen as vice president/president-elect of the American Society of Cataract and Refractive Surgery for 2025–26.
Bartly J. Mondino, MD, distinguished professor of ophthalmology, was awarded the S. Rodman Irvine Prize at the UCLA Department of Ophthalmology Annual Seminar on May 30, 2025. The Irvine Prize recognizes excellence in a Department of Ophthalmology faculty member whose relationships with patients and students are exemplary; whose professional actions illustrate the finest traditions of the medical profession and the vision-science community, and whose teaching demonstrates a dedication to transmission of knowledge to future generations.

Kouros Nouri-Mahdavi, MD, MSc , Kay K. Pick Endowed Chair in Glaucoma Research, presented the KapetanskyAllergan lecture at the 46th annual meeting of the Midwest Glaucoma Society on November 9, 2024, in Louisville, Kentucky.
Pradeep S. Prasad, MD, MBA , health sciences associate clinical professor of ophthalmology, was inducted into the Retina Society on September 14, 2024, in Lisbon, Portugal.
Peter A. Quiros, MD , health sciences clinical professor of ophthalmology, was named assistant division chief of the Neuro-Ophthalmology Division, effective July 1, 2024.
SriniVas R. Sadda, MD , professor of ophthalmology, was named A. Ray Irvine, Jr., MD, Endowed Chair in Clinical Ophthalmology, effective August 7, 2024.
Dr. Sadda also delivered the John H. Dunnington Lecture, “AI in Clinical Practice: Opportunities and Challenges,” at Columbia University on March 6, 2025, in New York.
Alfredo A. Sadun, MD, PhD , Flora L. Thornton Endowed Chair in Vision Research, presented the Daniel M. Jacobson Memorial Lecture, “From Castro to Quantum Mechanics: A Tunnel of Love” on March 19, 2025, at the North American Neuro-Ophthalmology Society (NANOS) annual meeting in Salt Lake City, Utah. The award is given by NANOS to one person each year for their lifetime of research.
David Sarraf, MD, health sciences clinical professor of ophthalmology, presented the Robert Machemer Lecture “PED and RPE Tears: How Can We Reduce Risk?” on March 26, 2025, in Snowmass, Colorado.
Dr. Sarraf also delivered the Neil Della Memorial Lecture “PAMM Detection Can Prevent Blindness and Death” at the Australian and New Zealand Society of Retinal Specialists on June 14, 2025, in Melbourne, Australia.
And Dr. Sarraf gave the keynote lecture, “Type 4 MNV: A New Addition to the Classification of Neovascular AMD” on June 29, 2025, at Maculart in Paris, France.
Gabriel H. Travis, MD , Charles Kenneth Feldman Chair in Ophthalmology, received the Endre A. Balazs Prize on October 21 at the 2024 Biennial Meeting of the International Society for Eye Research (ISER) in Buenos Aires, Argentina, and he delivered the plenary lecture, “Photic mechanisms of visual pigment regeneration in vertebrates.” The award recognizes Dr. Travis’ outstanding contributions in the field of experimental eye research.
Victoria L. Tseng, MD, PhD, Jerome and Joan Snyder Chair in Ophthalmology, was appointed to the American Academy of Ophthalmology (AAO) Council. Dr. Tseng will serve as a liaison between the AAO and the California Academy of Eye Physicians and Surgeons (CAEPS), coordinating the implementation of joint activities and helping to develop council advisory recommendations in conjunction with the leaders of CAEPS.
Edmund Tsui, MD, MS, assistant professor of ophthalmology, was selected for the American Academy of Ophthalmology Leadership Development Program (LDP) Class of 2026.
The LDP is an extremely competitive program providing both orientation and skill development to future leaders of state, subspecialty, and specialized interest societies. Dr. Tsui was nominated by the Association for Research in Vision and Ophthalmology.
Federico G. Velez, MD , Leonard Apt Endowed Chair in Pediatric Ophthalmology, was the Pediatric Ophthalmology and Strabismus Network (POSN) Keynote Lecturer in Strabismus at the POSN meeting in Bengaluru, India, on September 21, 2024.
Dr. Velez presented the Emilio Campos Inaugural Lecture on September 28, 2024, during the Italian Association of Strabismus meeting in Udine, Italy.
Dr. Velez gave the American Association for Pediatric Ophthalmology and Strabismus (AAPOS) 10th Kushner Lecture on Duane syndrome on February 8, 2025 (virtually).
At the AAPOS March 5–9, 2025, annual meeting in Salt Lake City, Utah, Dr. Velez was a Senior Honor Award recipient.
Dr. Velez was also the recipient of the Jules Stein Eye Institute’s annual Golden Eye Award, which is an honor bestowed on the surgeon by the operating room staff for being helpful, kind, and patient.
David S. Williams, PhD, Karl Kirchgessner Foundation Chair in Vision Science, received the Spring 2025 Research to Prevent Blindness (RPB) International Collaborators Award in support of his proposal, “Establishing better models for studying retinal degeneration and developing therapies for Usher syndrome type 1B.” Dr. Williams will be working on the project with collaborators from Germany.
Joel Zylberberg, PhD, associate professor of ophthalmology, was appointed as Fellow of Learning in Machines and Brains at the Canadian Institute for Advanced Research (CIFAR).

The UCLA Department of Ophthalmology held its prestigious clinical and research seminar May 30, 2025, at the UCLA Jules Stein Eye Institute. The event was highlighted by the following keynote lectures:
55th Jules Stein Lecturer
Joan W. Miller, MD
“Developing treatments for age-related macular degeneration: The road we travelled and the road ahead”
55th Doheny Memorial Lecturer
Jane C. Edmond, MD
“Discs in disguise: Unmasking buried optic disc drusen from papilledema”
22nd Bradley R. Straatsma Lecturer
M. Roy Wilson, MD, MS
“Rethinking race in biomedical research: View from the national academies and personal reflections”
22nd Thomas H. Pettit Lecturer
Reza Dana, MD, MSc, MPH
“New ways of doing old things: Translational investigations in management of common corneal and ocular surface disorders”
The 2025 Excellence in Research Awards were also presented at the Seminar. Congratulations to Resident Angela Chen, MD, Clinical Fellow Blake Fortes, MD, International Research Fellow Alessandro Feo, MD, and Postdoctoral Fellow Junqiang Wang, PhD, on receiving this award for their exceptional research projects.
Bartly J. Mondino, MD, distinguished professor of ophthalmology, received the S. Rodman Irvine Prize, an award recognizing outstanding achievement by a faculty member in the UCLA Department of Ophthalmology.



The Aesthetic Eyelid and Facial Rejuvenation Course was held at the Jules Stein Eye Institute July 12–13, 2024. Course directors were Drs. Daniel B. Rootman and Jonathan A. Hoenig.
The 2nd UCLA/American Uveitis Society International Workshop on Objective Measures of Intraocular Inflammation for Use in Clinical Trials was held at the Jules Stein Eye Institute on September 27–28, 2024. The workshop was co-organized by Drs. Gary N. Holland, SriniVas R. Sadda, and Edmund Tsui, and co-sponsored by the American Uveitis Society.
The 6th annual Doheny-UCLA International Glaucoma Symposium was held Saturday, September 28, 2025. The symposium was organized by Drs. Vikas Chopra and Brian Francis
The workshop, Embracing and Exploiting Artificial Intelligence for Neuroscience , was held at Stanford University on October 12–13, 2024. The event was organized by Dr. Greg D. Field (Jules Stein Eye Institute) and Dr. E.J. Chichilnisky (Stanford), and was led by Allison Duettmann, CEO of the Foresight Institute.
The annual Cataract Surgery Essentials Course , in conjunction with Bausch & Lomb, was held on November 2, 2024, in Newport Beach, California. It was led by Course Director Dr. Kevin M. Miller
Doheny Eye Institute hosted its inaugural Oculomics Symposium on November 23, 2024. The event was organized by Dr. Yuhua Zhang
The 3rd annual Doheny-UCLA International Retina Symposium was held on February 1, 2025, at Doheny Eye Institute. Course organizers were Drs. Kirk Hou and Michael Ip

Drs. SriniVas Sadda, Anita Agarwal, David Sarraf, Jacque Duncan (Alexander R. Irvine Award Lecture), and Mike Jumper at the combined IntRIS and Pacific Retina Club meeting.
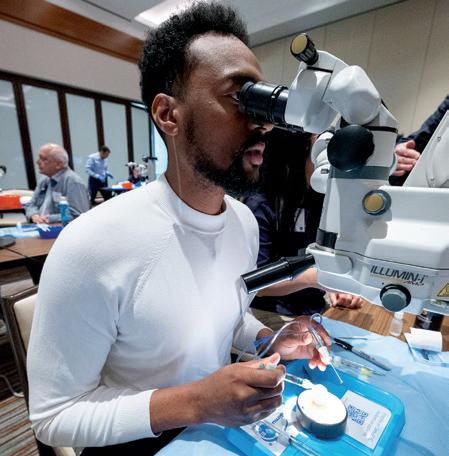
Attendees of the Alcon Advanced Cataract Surgery Course gain hands-on experience under the guidance of expert faculty.
The 2025 Doheny Distinguished Lecture Series began on February 7 with a presentation by Rajendra Apte, MD, PhD, a former fellow of SriniVas R. Sadda, MD; continued on March 25 with a presentation by Robert Mullins, MS, PhD; and concluded on April 25, with a presentation by Julia Busik, PhD, FARVO
The International Master’s Symposium on Thyroid Eye Disease was held at the UCLA Jules Stein Eye Institute on February 21–22, 2025. It was directed by Dr. Daniel B. Rootman
A two-day Ophthalmic Knowledge Assessment Program (OKAP) Review Course for residents was held on February 21–22, 2025, at UCLA’s Jules Stein Eye Institute and USC. The course was organized by Drs. Amanda Lu and Mitra Nejad (UCLA), along with Dr. Annie Nguyen (USC).
The 15th annual Ryan Initiative for Macular Research (RIMR) Conference was held March 26–28, 2025, at the Beckman Center in Irvine, California. This year’s Gerald Lutty Memorial Lecture was delivered by Vinit Mahajan, MD, PhD, a Jules Stein Eye Institute alumnus.
The Alcon Vision Advanced Cataract Surgery Course was held April 5, 2025, in Irvine, California. It was led by Course Director Dr. Kevin M. Miller
The Jules Stein Eye Institute Distinguished Lecture Series hosted two presentations in May 2025: the first by Justin Kumar, PhD, hosted by Alapakkam Sampath, PhD , and the second by Michael Do, PhD, hosted by Greg Field, PhD Dr. Roxana Radu serves as the faculty organizer and coordinator of this series.
The MedTech Innovation Seminar: Advancing Medical Technology was held at the RPB Auditorium in the Jules Stein Eye Institute on May 21, 2025.
The International Retinal Imaging Society (IntRIS) held a combined meeting with the Pacific Retina Club June 5–7, 2025, at the UCLA Meyer & Renee Luskin Conference Center. Course organizers were Drs. David Sarraf, Amani Fawzi, J., Michael Jumper, H. Richard McDonald, Phil Rosenfeld, and SriniVas Sadda

Residents, fellows, and faculty were honored for excellence at the UCLA Department of Ophthalmology graduation ceremony on June 24, 2025, at UCLA’s Luskin Conference Center.
TEACHING
Teaching Award
Mark Volpicelli, MD
Fellowship Faculty Teaching Award
Hamid Hosseini, MD
Resident Teaching Award
Angela Chen, MD
Resident Teaching Award
Alan Kong, MD
Fellow Teaching Award
Bryan Zarrin, MD


The 2024 Visiting Medical Student Scholarship in Ophthalmology was awarded to Chioma Amuzie. Chioma came to UCLA for three weeks in fall 2024 to complete her rotation in ophthalmology as part of the Visiting Student Learning Opportunity. During her time at UCLA, Chioma—a fourth-year medical student at the Miller School of Medicine at the University of Miami—explored how to best serve people whose access to ophthalmic services is limited.
The Vision Science Undergraduate 2024 Summer Research Program hosted four exceptional undergraduate students at Jules Stein Eye Institute research laboratories. Brianna Burns, a junior at the University of Alabama, joined Dr. Anthony J. Aldave’s laboratory. Kiara Abhayaratne, a junior at University of California, Berkeley, elected to conduct investigations in Dr. Greg D. Field’s laboratory. Dragui Salazar, a junior at the Utah Valley University, worked with Dr. Sophie Deng’s team, and Baani Sabharwal, a junior at the University of California, Berkeley, conducted research in Dr. Roxana Radu’s laboratory. The students’ research was presented at the end of the program during the UCLA Sponsored Projects for Undergraduate Research Showcase.
Dr. Clémence Bonnet Awarded JAM Fellowship
Clémence Bonnet, MD, PhD , health sciences assistant clinical professor, was the recipient of a one-year “JAM” fellowship from the David Geffen School of Medicine at UCLA. The JAM fellowship was developed for faculty at the assistant professor level who demonstrate potential for careers in academic medicine and health leadership.

The JAM Fellowship provides comprehensive mentoring training, including extensive coaching, networking, and mentoring opportunities, with the goal of advancing the professional development and retention of faculty in academic medicine. Previous Department of Ophthalmology recipients of the JAM fellowship are Drs. Simon Fung and Edmund Tsui

Alumni Shine at APSOPRS 2024
The Jules Stein Eye Institute family played a major role in the success of the Asia Pacific Society of Ophthalmic Plastic and Reconstructive Surgery (APSOPRS) meeting held November 29–30, 2024, in Seoul, Korea.
Highlights included Robert Alan Goldberg, MD, Bert O. Levy Endowed Chair in Orbital and Ophthalmic Plastic Surgery, delivering the Keynote Lecture; fellow alumni Helen Lew, MD (’09), and Yoon-Duck Kim, MD, PhD (’94), serving as program chairs and local hosts; and international fellowship alumni Kam- Lung “Kelvin” Chong, MD (’10), Chee-Chew Yip, MD (’03), Milind Naik, MD (’07), Alice Goh, MD (’13), Bird Putthirangsiwong , MD, (’19), and Tomoyuki Kashima, MD (’16) presenting papers in the scientific session. Four fellow alumni were nominated to executive positions of APSOPRS, including incoming president Dr. Kelvin Chong
Bronwyn Bateman Receives Gradle Medal
J. Bronwyn Bateman, MD, Department of Ophthalmology alumna, was honored with the 2025 Gradle Medal for Good Teaching from the Executive Committee of the Pan-American Association of Ophthalmology (PAAO). Dr. Bateman was recognized at the Opening Ceremony of the PAAO in Bogota, Colombia, on May 30, 2025.
The Harry S. Gradle Medal is one of the highest awards conferred by the PAAO and recognizes excellence in teaching and education in the field of ophthalmology.

The UCLA Department of Ophthalmology Association held its annual Jules Stein Eye Institute and Doheny Eye Institute reception on October 20, 2024, during the American Academy of Ophthalmology meeting in Chicago, Illinois.







As we look back on the past year at the Jules Stein Eye Institute, we are deeply thankful for your partnership. Your support has helped advance eye research, enhance patient care, train future specialists, and connect with our community. You have played a vital role in our mission to protect and preserve vision—thank you.
Donations July 1, 2024–June 30, 2025
Major Gifts $25,000 and Above:
Aliza and Marc Guren
Barbara Mack and Norman Levine
BlueStar
Brian N. Lasky
Bruce Ford and Anne Smith Bundy Foundation
Constance M. Calogeris
Corie and Michael Koss
Diane Mellen
Dina Goldstein
Estate of Ralph E. Johnson
Fox Family Foundation
Gerald Oppenheimer Family Foundation
Glenn and Ruthanne Wever
J & P Caballero Trust
John R. Heckenlively, MD
Maralea and Joseph Binz
Memorium for Virginia Fimbres Gomez Research to Prevent Blindness, Inc.
Sally Mishkind
Schepens Eye Research Institute
The Arthur & Patricia Price Foundation
The Louis & Harold Price Foundation
The Douglas Foundation
The Yardi Foundation
Wendy and Theo Kolokotrones
Wendy Ruby
Wilbur May Foundation
Individuals Recognized with a Tribute Gift
IN HONOR OF:
Anne L. Coleman, MD, PhD
Aya Barzelay-Wollman, MD, PhD
Bartly J. Mondino, MD
Bradley R. Straatsma, MD, JD
Cindy Beatty
David Sarraf, MD
Federico G. Velez, MD
Gary N. Holland, MD
Irene E. Jones
Joseph Caprioli, MD
Joseph L. Demer, MD, PhD
Kevin M. Miller, MD
Marissa Hirt
Priscilla Lam
Robert A. Goldberg, MD
Scott M. Whitcup, MD
Sydney Kraft
Tara A. McCannel, MD, PhD
Vikas Chopra, MD
Wendy Shackelly
IN MEMORY OF:
Allan E. Kreiger, MD
George P. Fallon, PhD
Herbert J. Grossman, MD
Irene E. Jones
Jean Stein
Jerrold C. Bocci, MD
Maggi Kelly
Neil Mellen
Ralph J. Shapiro, Esq.
Roger P. Gray and Katherine L. Gray
Jules Stein Eye Institute
Endowed Chairs
Supporting Department of Ophthalmology Faculty
Receiving an endowed chair is one of the highest honors a faculty member can achieve. It reflects UCLA’s deep respect for their leadership and provides crucial financial support. These positions help attract and retain top talent, ensuring the UCLA Department of Ophthalmology remains a leader in its field.
Arthur L. Rosenbaum, MD, Chair in Pediatric Ophthalmology
Established in 2007 by Mr. and Mrs. Gottlieb as an administrative chair for the Division of Pediatric Ophthalmology and Strabismus in honor of the late Dr. Arthur L. Rosenbaum. The chair was originally named the Brindell and Milton Gottlieb Chair in Pediatric Ophthalmology.
Arthur L. Rosenbaum, MD 2008–June 2010
Joseph L. Demer, MD, PhD 2015–Present
Bartly J. Mondino, MD, Endowed Chair in Ophthalmology
Established in 2022 as an administrative chair to support the position of Vice Chair of Academic Affairs in the UCLA Department of Ophthalmology and UCLA Jules Stein Eye Institute.
Anthony J. Aldave, MD 2023–Present
Bert O. Levy Endowed Chair in Orbital and Ophthalmic Plastic Surgery
Established in 2019 as a permanentappointment chair by Mr. Bert Levy to support the teaching and research activities of an outstanding, academic orbital and ophthalmic plastic surgeon.
Robert Alan Goldberg, MD 2019–Present
Bradley R. Straatsma, MD, Endowed Chair in Ophthalmology
Established in 1994 to honor founding director of the Jules Stein Eye Institute, Bradley R. Straatsma, MD, JD.
Bartly J. Mondino, MD 2000–2022
Anne L. Coleman, MD, PhD 2022–Present
Charles Kenneth Feldman Chair in Ophthalmology
Established in 1982 by various donors in memory of Charles Kenneth Feldman, an entertainment industry executive.
Robert D. Yee, MD Professor 1984–1987
Hilel Lewis, MD Scholar 1989–1993
Gabriel H. Travis, MD 2001–Present
David May II Chair in Ophthalmology
Established in 1998 as a termappointment chair by the family of Mr. David May II, a founding member of the Institute’s Board of Trustees, to perpetuate, in memoriam, Mr. May’s association with the Jules Stein Eye Institute; after an additional pledge from the Wilbur May Foundation, it was converted to a permanentappointment chair in 2009.
Gary N. Holland, MD 1999–2004
Joseph Caprioli, MD 2004–Present
Dolly Green Chair of Ophthalmology
Established in 1980 by Ms. Dorothy (Dolly) Green.
Dean Bok, PhD 1984–2013
Dolly Green Chair in Clinical Research
Established in 2021 to support an endowed chair in clinical research.
Dolly Green Chair in Vision Science
Established in 2021 to support an endowed chair in vision science.
Ernest G. Herman Chair in Ophthalmology
Established in 2008 by Mr. Ernest G. Herman to support a vision scientist or a clinician-investigator.
Xian-Jie Yang, PhD 2012–2021
Kouros Nouri-Mahdavi, MD, MSc 2021–2023
Grace and Walter Lantz Endowed Chair in Ophthalmology
Established in 1991 as a termappointment chair by Mr. and Mrs. Lantz and, with an additional pledge, it was converted to a permanentappointment chair in 2010.
J. Bronwyn Bateman, MD
Grace and Walter Lantz Scholar 1993–1995
Sherwin J. Isenberg, MD
Grace and Walter Lantz Scholar 1993–1995 Professor 1996–2004
Joseph L. Demer, MD, PhD Professor 2004–2005
Alapakkam P. Sampath, PhD 2021–Present
Harold and Pauline Price Chair in Ophthalmology
Established in 2000 by the Louis and Harold Price Foundation and, with an additional pledge, it was converted to a permanent-appointment chair in 2006.
Michael B. Gorin, MD, PhD 2006–Present
Hilel Lewis Family Chair in Ophthalmology
Established at UCLA in 2020 in collaboration with Dr. Hilel Lewis via Columbia University to support an outstanding clinician-investigator in retina.
Jack H. Skirball Chair in Ocular Inflammatory Diseases
Initiated in 2008 by The Skirball Foundation in honor of Mr. Jack H. Skirball’s long-standing friendship with Dr. Jules Stein and Mr. Lew Wasserman.
Gary N. Holland, MD 2009–Present
Jerome and Joan Snyder Chair in Ophthalmology
Established in 2008 by Mr. and Mrs. Snyder to support the activities of a distinguished faculty member who directs the ophthalmology residency program, ensuring that UCLA’s accredited program continues to offer rigorous and comprehensive instruction for individuals of the highest caliber.
Anthony C. Arnold, MD 2008–2017
Stacy L. Pineles, MD 2017–2023
Victoria L. Tseng, MD, PhD 2023–Present
Joan and Jerome Snyder Chair in Cornea Diseases
Established in 2013 by Mr. and Mrs. Snyder to support the activities of a distinguished faculty member in the area of corneal diseases and research.
Sophie X. Deng, MD, PhD 2019–2023
Boris Malyugin, MD (pending) 2024–Present
Joan and Jerome Snyder Chair in Vision Science
Established in 2018 by Mr. and Mrs. Snyder, this term chair will support the teaching and research activities of an excellent scientist and faculty member in the Vision-Science Division.
Greg D. Field, PhD 2023–Present
Jules Stein Chair in Ophthalmology
Established in 1982 as a memorial tribute to Dr. Jules Stein by his many friends, with the leadership of Mr. Samuel Goldwyn, Jr.
Wayne L. Hubbell, PhD 1983–Present
Karen and Frank Dabby Endowed Chair in Ophthalmology
Established in 2007 by Dr. and Mrs. Dabby as a term chair to support the activities of a distinguished faculty member in the area of orbital disease.
Robert Alan Goldberg, MD 2008–2018
Daniel B. Rootman, MD, MS 2019–Present
Karl Kirchgessner Foundation Chair in Vision Science
Established in 2001 as a termappointment chair by a colleague of Dr. Jules Stein to promote basicscience research initiatives.
Debora B. Farber, PhD, DPhhc 2001–2018
David S. Williams, PhD 2019–Present
Kay K. Pick Endowed Chair in Glaucoma Research
Established in 2023 as a permanentappointment chair for a faculty member with an expertise in glaucoma research.
Kouros Nouri-Mahdavi, MD, MSc (pending) 2023–Present
Kolokotrones Chair in Ophthalmology
Established in 2004 by Wendy and Theo Kolokotrones to support the teaching and research of a cataract surgeon and scientist.
Kevin M. Miller, MD 2005–Present
Laraine and David Gerber Chair in Ophthalmology
Established in 1998 as a termappointment chair by Mr. and Mrs. Gerber and, with an additional pledge, converted to a permanentappointment chair in 2009.
Joseph L. Demer, MD, PhD 2000–2004
Sherwin J. Isenberg, MD 2004–2019
Leonard Apt Endowed Chair in Pediatric Ophthalmology
Established in 2004 by Professor Emeritus of Ophthalmology and Founding Director of the Division of Pediatric Ophthalmology and Strabismus, Dr. Leonard Apt, with a gift from the trust of Frederic G. Rappaport, Dr. Apt’s nephew.
Joseph L. Demer, MD, PhD 2005–2015
Federico G. Velez, MD 2021–Present
Mary Oakley Foundation Chair in Neurodegenerative Diseases
Established in 2013 by The Mary Oakley Foundation to support neurodegenerative diseases.
Anthony C. Arnold, MD 2017–Present
Olive Bateman and Anga Lundgren Endowed Chair
Established in 2020 by faculty alumna Dr. J. Bronwyn Bateman in the memory of her mother, Olive Anga Lundgren, MD, and grandmother, Anga Lundgren. This administrative chair supports the Director of Consultations overseeing inpatient and emergency care.
Laura Bonelli, MD 2022–Present
Oppenheimer Brothers Chair
Established in 2002 as a term chair by the Oppenheimer Brothers Foundation.
Joseph Horwitz, PhD 2003–2017
Suraj P. Bhat, PhD 2019–Present
Rory Smith, MD, Endowed Chair
Established in 2019 by faculty alumna Dr. J. Bronwyn Bateman in honor of her late husband, Dr. Roderick “Rory” Smith, this administrative chair will be held by the director of the UCLA J. Bronwyn Bateman Center for Ocular Genetics.
James and Catherine Shuler
Endowed Chair in Comprehensive Ophthalmology
Established in 2020 by Dr. and Mrs. James D. Shuler as an administrative chair for the Comprehensive Ophthalmology Division Chief to further research, education, and clinical care programs.
Daniel Sand, MD 2024–Present
Smotrich Family Optometric Clinician-Scientist Chair
Established in 2016 to support an optometric clinician-scientist at the UCLA Jules Stein Eye Institute and will fund the appointee’s education and research programs.
Ava K. Bittner, OD, PhD 2019–Present
The Ahmanson Chair in Ophthalmology
Established in 2006 by The Ahmanson Foundation as an administrative chair for the Retina Division Chief to further research, education, and clinical care programs.
Steven D. Schwartz, MD 2007–2024
Colin A. McCannel, MD 2025–Present
The Fran and Ray Stark Foundation Chair in Ophthalmology
Established in 1992 as a termappointment chair by the Fran and Ray Stark Foundation, and with an additional commitment, it was converted to a permanentappointment chair in 2009.
Joseph Caprioli, MD 1997–2004
Anne L. Coleman, MD, PhD 2004–2022
The Wasserman Professor of Ophthalmology
Established in 1977 by Edie and Lew Wasserman to honor Dr. Jules Stein.
Manfred Spitznas, MD 1979–1981
Bartly J. Mondino, MD Scholar 1984–1988 Professor 1988–2000
Ben J. Glasgow, MD 2003–Present
Vernon O. Underwood Family Chair in Ophthalmology
Established in 1995 as a termappointment chair by Mrs. Adrienne Underwood Pingree in memory of her late husband, Mr. Vernon O. Underwood.
John R. Heckenlively, MD 1997–2004
Gary N. Holland, MD 2004–2009
Lynn K. Gordon, MD, PhD 2012–2020
Roxana A. Radu, MD 2021–Present
Walton Li Chair in Cornea and Uveitis
Established in 2013 by Walton W. Li, MD, as an administrative chair for the Cornea and Uveitis Division to further research and teaching activities.
Anthony J. Aldave, MD 2014–2023
Sophie X. Deng, MD, PhD 2023–Present
Doheny Eye Institute Endowed Chairs Supporting Department of Ophthalmology Faculty
A. Ray Irvine, Jr., MD, Endowed Chair in Clinical Ophthalmology
John A. Irvine, MD 2014–2024
SriniVas R. Sadda, MD 2024–Present
Flora L. Thornton Endowed Chair in Vision Research
Alfredo A. Sadun, MD, PhD 2014–Present
Gavin S. Herbert Endowed Chair for Macular Degeneration
Michael S. Ip, MD 2019–Present
Mary D. Allen Chair in Vision Research
Deming Sun, MD 2015–2024
Kaustabh Ghosh, PhD 2025–Present
The Charles Stewart Warren and Hildegard Warren Endowed Research Chair
Vikas Chopra, MD 2017–Present
The Rupert and Gertrude I. Steiger Vision Research Endowed Chair
Brian A. Francis, MD, MS 2015–Present
The Stephen J. Ryan—Arnold and Mabel Beckman Foundation Endowed Presidential Chair
SriniVas R. Sadda, MD 2015–2020
Deborah A. Ferrington, PhD 2022–Present
Jules Stein Eye Institute Fellowship Funds and Endowments
Abe Meyer Memorial Fellowship Fund
Established in 1969 by various donors to support clinical fellows at the Institute.
Adelaide Stein Miller Research Fellowship
Established in 1977 by Mr. Charles Miller as a tribute to his wife, Adelaide Stein Miller, Dr. Jules Stein’s sister.
Audrey and Jack Skirball Ocular Inflammatory Disease Fellowship
Established in 2011 by The Skirball Foundation to support the training of fellows specializing in ocular inflammatory disease.
Christian Bardan, MD 2024–2025
Bert Levy Research Fellowship Fund
Established in 1995 by Mr. Bert Levy to enhance the educational opportunities of vision-science scholars and advance research in neuro-ophthalmology.
Thanh-Liem Huynh-Tran, MD 2024–2025
Cooperman Fellowship Fund
Established in 1988 by the Coopermans to support eye research and education, with emphasis on clinical ophthalmology.
Marko M. Popovic, MD, MPH 2024–2025
David and Randi Fett Orbital and Ophthalmic Plastic Surgery Fellowship
Established in 2013 by Dr. David R. Fett and Ms. Randi Levine to support fellows in the Orbital and Ophthalmic Plastic Surgery Division.
Katherine M. Lucarelli, MD 2024–2025
David May II Fellowship Fund
Established in 1992 by the family of Mr. David May II to support advanced study and research in ophthalmology and vision science.
Dr. Jack Rubin Memorial Fellowship
Established in 1987 by the family of Dr. Jack Rubin to support postdoctoral fellows.
Cherilyn Palochak, MD 2024–2025
Elsa and Louis Kelton Fellowship
Endowed by the Keltons in 1982 to support postdoctoral research and training.
Frances Howard Goldwyn Fellowship
Established in 1977 by Mr. Samuel Goldwyn, Jr., with gifts from Mrs. Goldwyn’s estate and Dr. and Mrs. Jules Stein.
Prashant Tailor, MD 2024–2025
Frederic G. Rappaport Endowed Fellowship in Retina/Oncology
Established in 2004 by Mrs. Jeanne A. Rappaport as a memorial to her son Frederic.
Adrian C. Au, MD, PhD 2024–2025
Jerome Comet Klein, MD, Fellowship and Lecture Fund
Established in 2007 by the Irving and Estelle Levy Foundation to provide fellowship and lecture support in the areas of orbital and ophthalmic plastic surgery.
John and Theiline McCone Fellowship
Established in 1989 by the McCones to support and enhance education programs and fellowship training in macular disease.
Jules Stein Research Fellowship
Established in 1982 by various donors to honor the memory of Charles Kenneth Feldman.
Blake H. Fortes, MD 2024–2025
Klara Spinks Fleming Fellowship Fund
Established in 1985 by Klara Spinks Fleming to support cataract research.
Leonard Apt Endowed Fellowship in Pediatric Ophthalmology
Established in 2002 by founding chief of the Pediatric Ophthalmology and Strabismus Division, Leonard Apt, MD, to support outstanding clinical fellows in the field of pediatric ophthalmology and strabismus.
Leonard Apt, MD, Pediatric Fellowship Fund
Established in 2015 by the trust of Leonard Apt, MD, founding chief of the Pediatric Ophthalmology and Strabismus Division, to support pediatric ophthalmology fellowships.
Rosalind W. Alcott Fellowship
Established in 1978 by the Rosalind W. Alcott Charitable Remainder Trust for the training of outstanding postdoctoral fellows.
Sanford and Erna Schulhofer Fellowship Fund
Established in 1986 by Mr. Sanford Schulhofer to support postdoctoral research and training in vision science.
Bryan J. Zarrin, MD 2024–2025
The Harold and Pauline Price Fellowship
Established in 1987 by the Louis and Harold Price Foundation to support research and education in ophthalmology and vision care.
Alejandro Itzam Marin, MD 2024–2025
Thelma and William Brand Director’s Fund
Established in 2004 with a trust from Mr. William F. Brand to benefit worthy students at the Jules Stein Eye Institute.
The Mae and Lee Sherman Fellowship Fund
Established in 1981 by the Sherman family to support postdoctoral fellows.
Angela J. Oh, MD 2024–2025
Wilbur D. May Fellowship
Established in 2013 by the May family as a tribute to Mr. Wilbur D. May, the beloved uncle of Mr. David May II.
Robert C. Gunzenhauser, MD 2024–2025
Albert Sarnoff Endowed Cataract Fund
Allan E. Kreiger, MD, and Jerome T. Pearlman, MD, Endowed Lectureship
Amalia Simon Roth and Victor and Edith Roth Endowment
Anne H. West Estate Fund
Annenberg Foundation—Safety Net Children’s Program
Annenberg Foundation—Safety Net Families Program
Annenberg Foundation—Pediatric Contact Lens Fund
Anthony Eannelli Endowment for Retina Research
Arna Saphier Macular Degeneration Fund
Arthur Spitzer Fund
Audrey Hayden-Gradle Trust
Barbara P. Taylor Fund
Bateman Endowment
Bert O. Levy Cornea and Uveitis Quasi-Endowment Fund
Bradley R. Straatsma Research Fund
Chesley Jack Mills Trust
Daniel B. Whipple Fund
Dr. William F. Stein and Ester Elizabeth Stein Memorial Fund
Edward and Hannah Carter Fund
Elsie B. Ballantyne Regents Fund
Elsie B. Ballantyne UCLA Foundation Fund
Emilia B. Gillespie Jules Stein Eye Institute Fund
Emily G. Plumb Estate and Trust
Endowment for Children with Uveitis
Esther Shandler Research Fund
Gerald Oppenheimer Family Foundation Center for the Prevention of Eye Disease Endowment Fund
Harry J. Heitzer Fund
Henry I. Baylis, MD, Endowed Fund in Orbital and Ophthalmic Plastic Surgery
Herb Ritts, Jr., Memorial Vision Fund
Herman King Research Fund
Hintze Glaucoma Research Fund
J. Richard Armstrong and Ardis Armstrong Fund
Jerome T. Pearlman, MD, Fund
John and Theiline McCone Macular Disease Research Fund
Jules Stein Eye Institute Maintenance Fund
Katherine L. Gardner Research Fund
Kay K. Pick Glaucoma Research Fund
Kreiger Retinal Support of Medically Underserved Populations
Levin Family Contact Lens Endowment Fund
Lila Hartman Jules Stein Eye Institute Fund
Maggi Kelly Vision Fund
Marie and Jerry Hornstein Family Endowed Macular Degeneration Research Fund
Michael Huffington Ophthalmology Scholarship Fund
Nancy Chen Endowed Research Fund
Pat and Joe Yzurdiaga Endowed Cataract Fund
Patricia and Joseph Yzurdiaga Endowed Vision Science Research Fund
Patricia Pearl Morrison Research Fund
Paul J. Vicari Endowed Cataract Research Fund
Raymond and Ruth Stotter Vision Science Research Fund
Richard B. Shapiro Vision Fund
Sara Kolb Memorial Fund
Stella F. Joseph Fund
The Card Family Research Fund
The Karl Kirchgessner Foundation Ophthalmology Endowment Fund
The Leonard Apt, MD, Pediatric EyeSTAR Residency Training Fund
The Leonard Apt, MD, Pediatric Ophthalmology Fund
The Skirball Foundation Fund
UCLA Center for Eye Epidemiology
Uncle Claude Fund
Virginia Burns Oppenheimer Endowment Fund
William, Richard, and Roger Meyer Fund


Committed to advancing eye health, UCLA Department of Ophthalmology boardcertified faculty provide services ranging from routine eye examinations to complex sight-saving procedures.
Designated as a tertiary referral center, doctors and hospitals throughout the United States, as well as Mexico, direct patients with the most challenging ophthalmic issues to the UCLA Jules Stein Eye Institute.
The Jules Stein Eye Institute and its affiliation partner, Doheny Eye Institute, are ranked among the top in the nation for ophthalmology. Patients and referring physicians alike trust UCLA Department of Ophthalmology faculty to provide the highest level of care across every subspecialty. Premier services are available at the UCLA Jules Stein Eye Institute vision-science campus in Westwood, as well as at the Stein Eye Center locations in Calabasas and Santa Monica and Doheny Eye Center UCLA locations in Arcadia, Orange County, and Pasadena.











The UCLA Jules Stein Eye Institute vision-science campus in Westwood is home to clinics and laboratories, as well as the UCLA Stein Eye Surgery Center, which has set new standards in surgical excellence.
Direct consultation and treatment, including emerging therapies, is available through the Ophthalmology Faculty Consultation Service . Faculty members have extensive and advanced training in ophthalmic subspecialties and are a valuable resource for referring physicians and patients with complex eye problems. In addition, wide-ranging and subspecialty eye care in all medical and surgical areas of ophthalmology is offered through the Comprehensive Ophthalmology Division, which is staffed by UCLA Department of Ophthalmology faculty, members of the UCLA Medical Group, and subspecialty ophthalmology fellows.
The UCLA Stein Eye Surgery Center, housed in the award-winning Edie & Lew Wasserman Building, is equipped with advanced tools for precision surgery and sets the standard for excellence in patient care and medical progress. Ophthalmic surgery of every kind—from cataract extraction and laser vision-correction surgeries to removal of ocular tumors—is performed. Faculty members and skilled medical specialists, including subspecialty fellows, medical residents, anesthesiologists, nurses, and technicians, ensure that each patient receives the highest quality preoperative, intraoperative, and postoperative care possible.
The Ophthalmology Inpatient Consultation Service, operating 24 hours a day through the Ronald Reagan UCLA Medical Center and UCLA Medical Center Santa Monica, provides ophthalmic consultation and treatment to pediatric and adult patients who are admitted to the medical centers for inpatient care. The consultation team consists of physician-residents at the UCLA Jules Stein Eye Institute, with subspecialty coverage provided by UCLA Department of Ophthalmology faculty. The Director of the Service is Laura Bonelli, MD, Olive Bateman and Anga Lundgren Endowed Chair.
100 Stein Plaza, UCLA
Los Angeles, CA 90095
Referral Service: (310) 825-5000
Emergency Service: (310) 825-3090
After-Hours Emergency Service: (310) 825-2111
UCLA Stein Eye Center
Locations in Calabasas and Santa Monica
The Stein Eye Center–Calabasas and Stein Eye Center–Santa Monica provide excellence in clinical care combined with neighborhood convenience. At each location, UCLA Department of Ophthalmology faculty provide subspecialty care, surgical services, and diagnostic testing.
Stein Eye Center–Calabasas
The Stein Eye Center–Calabasas provides patients in the San Fernando Valley and nearby communities with subspecialty care, including cataract and LASIK surgery, diabetic retinopathy, glaucoma, macular degeneration, and functional and cosmetic oculoplastics. Visual field testing, corneal mapping (corneal topography), intraocular lens measurement, fluorescein angiography, spectral domain optical coherence tomography, and additional diagnostic retinal imaging techniques are available.
The Stein Eye Center– Calabasas has free on-site parking and is located in the UCLA Health Building immediately adjacent to the 101 Freeway, between the Las Virgenes Road and Lost Hills Road exits.
26585 W. Agoura Rd., Suite 270 Calabasas, CA 91302 (818) 431-4414
The Stein Eye Center–Santa Monica offers the comprehensive and subspecialty eye care of the UCLA Jules Stein Eye Institute in Westwood at an easily accessible Westside locale. UCLA faculty provide evaluation and treatment for a range of subspecialties, including eyelid and other oculoplastic surgery, pediatric eye care, and neuroophthalmology. A wide range of ocular assessment is available, including visual field testing, corneal mapping (corneal topography), intraocular lens measurement, fluorescein angiography, spectral domain optical coherence tomography, and other diagnostic retinal imaging techniques.
In addition to on-site parking, the Stein Eye Center–Santa Monica has an in-house optical shop with a comprehensive selection of eyeglasses and contact lenses.
1807 Wilshire Blvd., Suite 203 Santa Monica, CA 90403 (310) 829-0160
The Doheny Eye Centers UCLA support neighborhoods northeast of downtown Los Angeles and south to Orange County. UCLA Department of Ophthalmology faculty provide the finest clinical care, surgical services, diagnostic testing, and treatment available.
The Doheny Eye Center UCLA–Arcadia expands the Department’s reach by caring for patients in the San Gabriel Valley. The renovated office includes 12 exam rooms, dedicated diagnostic equipment, and attractive patient areas. The Center provides comprehensive ophthalmology, and a broad range of subspecialty services, including complex cataracts and secondary intraocular lenses, cornea and external diseases, glaucoma, neuro-ophthalmic disorders, pediatric eye disease, as well as vitreoretinal diseases and disorders. Situated just south of the 210 freeway and north of the 10 freeway, the Doheny Eye Center–Arcadia is easily accessible from the two freeways and provides free, on-site parking.
622 W. Duarte Rd., Suite 101 Arcadia, CA 91007 (626) 254-9010
The Doheny Eye Center UCLA–Orange County broadens the scope of the UCLA Department of Ophthalmology south to Orange County. The Center is located in the Orange Coast Memorial Medical Center, and it offers comprehensive ophthalmology and extensive subspecialty services, including complex cataracts and secondary intraocular lenses, cornea and external diseases, glaucoma, neuro-ophthalmic disorders, pediatric eye disease, as well as vitreoretinal diseases and disorders. Centrally located and accessible to all of Orange County, the Doheny Eye Center UCLA–Orange County includes 12 exam rooms and dedicated diagnostic equipment.
Orange Coast Memorial Medical Center 18111 Brookhurst St., Suite 6400 Fountain Valley, CA 92708 (714) 963-1444
Doheny Eye Center
UCLA–Pasadena
The Doheny Eye Center UCLA–Pasadena is the primary hub of the Doheny Eye Centers UCLA. Appointed with state-of-the-art equipment and imaging systems, the clinic occupies nearly 17,000 square feet on the Doheny Eye Institute campus and is home to UCLA Department of Ophthalmology faculty physicians and staff members who serve patients in Pasadena and the greater communities.
Offering the highest quality vision care, the clinic’s services include detection, diagnosis, and treatment of all ocular diseases. The three suites offer world-class ophthalmology and specialty eye care, with one suite focusing on cornea, glaucoma, neuro-ophthalmology, and retina treatment, another suite specializing on ocular plastics, cataract, and refractive care, and the third suite dedicated to pediatric patients.
The clinic includes 36 exam rooms and an imaging center housing 20 diagnostic and imaging devices, as well as private spaces for patient-doctor consultations, members of the support team, and administrative offices.
The space also supports academic medicine activities, including teaching rounds and clinical research. Additionally, having the clinic on the Doheny campus brings both clinicians and researchers together under the same roof, facilitating interactions that encourage collaborative research and medicine.
Doheny Eye Institute 150 N. Orange Grove Blvd. Suites 1200, 1300, and 1400 Pasadena, CA 91103 (626) 817-4747
Taught by world-class faculty and experts in their field, residents in the UCLA Department of Ophthalmology gain hands-on clinical and surgical experience caring for patients in UCLA-affiliated teaching hospitals. Together with attending physicians, UCLA residents provide vital eye care services to large and diverse patient populations.
Harbor-UCLA Medical Center 1000 W. Carson St. Torrance, CA 90502
Chief: Michael Kapamajian, MD
Olive View-UCLA Medical Center 14445 Olive View Dr. Sylmar, CA 91342
Chief: Jay Sridhar, MD
Veterans Affairs Greater Los Angeles Healthcare System Sepulveda 16111 Plummer St. Sepulveda, CA 91343
Chief: JoAnn Giaconi, MD
Veterans Affairs Greater Los Angeles Healthcare System West Los Angeles 11301 Wilshire Blvd. Los Angeles, CA 90073
Chief: JoAnn Giaconi, MD
The UCLA Department of Ophthalmology has established formal partnerships that advance patient care, the education of ophthalmologists, and research discovery.
Doheny Eye Institute
Doheny Eye Institute began its historic affiliation with the UCLA Department of Ophthalmology in 2014. With that action, UCLA became the only university with two eye institutes: the UCLA Jules Stein Eye Institute and Doheny Eye Institute. Doheny Eye Institute, a top-ranked nonprofit organization, opened its 115,895-square-foot headquarters in Pasadena in 2022. The vision-science campus enhances Doheny’s capabilities for fundamental discoveries that fuel ideas for clinical trials, new treatments, and cures. Its laboratories are equipped to accelerate research and discovery in key areas, including artificial intelligence, regenerative medicine, gene-based therapies, and imaging diagnostics. Educational programs housed in a state-of-the-art conference center enable remote collaborations to meet current demands and evolving opportunities to advance vision research and teaching.
Doheny Eye Institute
150 N. Orange Grove Blvd. Pasadena, CA 91103
Doheny Eye Institute’s headquarters in Pasadena

The Research and Treatment Centers provide subspecialty care from faculty physicians who are actively involved in related research, enabling emerging and experimental treatment options to be developed for a gamut of eye disorders. In addition to comprehensive treatment, the centers provide both patients and physicians with expert diagnostic and consultation services for diseases that are difficult to identify and treat. Ophthalmology faculty work closely with other specialists, both within the UCLA Jules Stein Eye Institute and in other UCLA clinical departments, to create a multidisciplinary team customized for each patient’s unique medical needs.
f Aesthetic Center
f Center for Community Outreach and Policy
UCLA Center for Eye Epidemiology
UCLA Mobile Eye Clinic
f Center to Prevent Childhood Blindness
f Center for Regenerative Medicine in Ophthalmology
f Clinical Research Center
f Contact Lens Center
f Diabetic Eye Disease and Retinal Vascular Center
f Eye Trauma and Emergency Center
f Gerald Oppenheimer Family Foundation Center for the Prevention of Eye Disease
f Glaucoma Center for Excellence in Care and Research
f Macular Disease Center
f Ocular Inflammatory Disease Center
f Ophthalmic Oncology Center
f Optic Neuropathy Center
f Orbital Disease Center
f UCLA Laser Refractive Center
f Vision Genetics Center
f Vision Proteomics Center
f Vision Rehabilitation Center
Ophthalmology diagnostic services provide testing that offers precise measurements, photographs, and quantitative studies of the eye and the visual system. Diagnostic testing increases the accuracy of diagnosis and further augments the effectiveness of disease management. Our diagnostic services are available to eye care physicians in the community.
f Anterior Segment Diagnostic Laboratory
f Corneal Diagnostics
f Glaucoma Imaging Laboratory
f Medical Photography/Ultrasound
f Ocular Motility Clinical and Basic Science Laboratory
f Visual Field Laboratory
f Visual Physiology Diagnostic Laboratory
The Jules Stein Eye Institute has specially equipped laboratories to support vision-science investigations. Laboratory-based research, also referred to as basic vision-science research, forms the foundation for the clinical research, education, and patient care that are the visible hallmarks of the Jules Stein Eye Institute. Organized around the interests of the research faculty, these distinct laboratories offer unique opportunities for students, physicians, and fellows to become involved in nationally and internationally renowned scientific study.
f Computational Visual Neuroscience Laboratory
Dr. Joel Zylberberg
f Corneal Biology Laboratory
Dr. Sophie Deng
f Corneal Genetics Laboratory
Dr. Anthony Aldave
f Developmental Neurobiology Laboratory
Dr. Xian-Jie Yang
f Glaucoma Imaging and Artificial Intelligence Laboratory
Dr. Kouros Nouri-Mahdavi
f Molecular Biology of Retinal Ganglion Cells Laboratory
Dr. Natik Piri
f Molecular Mechanisms of Tear Film Formation Laboratory
Dr. Ben Glasgow
f Ocular Motility Laboratory
Dr. Joseph Demer
f Ocular Neurobiology and Genomics Laboratory
Dr. Michael Gorin
f Ophthalmic Biophysical Chemistry Laboratory
Dr. Wayne Hubbell
f Photoreceptor Biochemistry Laboratory
Dr. Gabriel Travis
f Receptor Signaling and Chemical Targeting Laboratory
Dr. Hui Sun
f Retinal Biochemistry and Clinical Disease Modeling Laboratory
Dr. Roxana Radu
f Retinal Cell Biology Laboratory
Dr. David Williams
f Retinal Circuits and Visual Processing Laboratory
Dr. Greg Field
f Retinal Function and Dysfunction Laboratory
Dr. Yi-Rong Peng
f Retinal Neurophysiology Laboratory
Dr. Alapakkam Sampath
f Retinal Pathophysiology Laboratory
Dr. Nicholas Brecha
f Therapeutic Development in Ophthalmology Laboratory
Dr. Jie Zheng
f Vision Molecular Biology Laboratory
Dr. Suraj Bhat
Find out more about our RESEARCH LABORATORIES
www.uclahealth.org/eye/ research-laboratories.
The UCLA Department of Ophthalmology provides comprehensive training in ophthalmology and vision science to medical students and residents, as well as to clinical and research fellows. Training programs encompass the gamut of ophthalmic and vision-science education, incorporating a full range of subjects in the study of the eye. Residents and clinical fellows serve a large patient population with diverse vision problems that offer innumerable training opportunities. In addition, a wide range of research laboratories ensures a broad choice of vision-science projects for all trainees. Predoctoral and postdoctoral research fellows benefit from the wealth of new and unfolding research generated by UCLA Department of Ophthalmology vision scientists.
The UCLA Department of Ophthalmology extends instruction to UCLA medical students in their second, third, and fourth years of instruction through the UCLA Medical Student Program. With lectures, small group discussions, and clinical experience, all students have numerous training sessions from which to gain knowledge about the eye and eye diseases, and they are taught eye examination skills that should be known by all physicians, regardless of their specialties. Students who are interested in ophthalmology as a career have additional learning opportunities in elective courses.
The UCLA Medical Student Research Program provides select medical students with a year-long opportunity to participate in laboratory or clinical research in the field of ophthalmology. The goal of the program is to encourage medical students to pursue careers in academic ophthalmology.
The UCLA Department of Ophthalmology Residency Program is ranked one of the top in the country and covers the full breadth of ophthalmology training from general ophthalmology to ophthalmic subspecialties. The accredited three-year residency program trains 24 residents with eight new residents beginning the program each July.
Training incorporates the resources of the UCLA Jules Stein Eye Institute, Harbor-UCLA Medical Center, Olive View-UCLA Medical Center, and the Veterans Affairs Greater Los Angeles Healthcare System at West Los Angeles and Sepulveda. Through their clinical rotations, every resident has exposure to each medical center and gains clinical experience with a broad range of ophthalmic problems and patient populations. Certification by the American Board of Ophthalmology is a natural objective of the program.
In addition to their clinical rotations, a night float system was implemented for ophthalmology residents at the Ronald Reagan UCLA Medical Center starting in July 2022. In this system, a PGY2 resident spends a six-week rotation working night shifts in the emergency department and inpatient floors seeing ophthalmology consults from 5 pm to 8 am during the work week. This provides the opportunity to free other PGY2 residents from night call to improve resident education and wellness. The system has been favorably received by multiple classes of ophthalmology residents at UCLA.
PGY2–PGY4 residents also have access to an Area of Focus curriculum that provides two dedicated weeks per academic year to undertake scholarly pursuits. Under the mentorship of a UCLA faculty member, residents have the option to pursue initiatives in research, education, quality improvement, or advocacy and community outreach. Residents who choose to participate in the curriculum present their scholarly work at the annual resident retreat. Examples of initiatives that have
been pursued include research studies leading to manuscript publication, development of specialized order sets for the electronic medical record system at UCLA, and investigation of telemedicine strategies in ophthalmology.
The Department of Ophthalmology Residency Director is Victoria L. Tseng, MD, PhD
For physicians interested in academic careers and professional leadership as clinician-scientists, the UCLA Jules Stein Eye Institute offers the Ophthalmology Specialty Training and Advanced Research Program, referred to as EyeSTAR, which offers visionscience training combined with an ophthalmology residency. Appointees complete a residency program leading to certification in ophthalmology, as well as laboratory research experience leading to a doctorate, or postdoctoral training in the event that the trainee already has a doctorate. EyeSTAR trainees work under the guidance of a faculty advisory panel representing the clinical and research interests of each trainee.
In 2021, the UCLA Department of Ophthalmology introduced a new EyeSTAR track combining ophthalmology residency training with medical genetics certification . This opportunity provides ophthalmology residency training in tandem with training by the UCLA Intercampus Medical Genetics Training Program and leads to Clinical Genetics and Genomics Certification by the American Board of Medical Genetics and Genomics.
EyeSTAR is recognized by the National Eye Institute and the Association of University Professors of Ophthalmology as a model training program for clinician-scientists in ophthalmology.
The UCLA Department of Ophthalmology offers well-qualified persons the opportunity to receive fellowship training in vision-science research or specific areas of clinical ophthalmology.
Vision science fellowship training is laboratory based and offers both predoctoral and postdoctoral opportunities to trainees in specific areas of vision science that encompass a wide range of topics. Trainees work under the supervision of UCLA Department of Ophthalmology faculty members who are engaged in basic-science research and have active laboratories. The predoctoral or postdoctoral trainee and his/her faculty mentor develop the scope and nature of the training program.
An integrated program is also offered under the auspices of a National Eye Institute Vision Science Training Grant for predoctoral and postdoctoral fellows. The grant provides trainees with coordinated and organized exposure to a wide range of techniques, giving each fellow the broadest possible background in ophthalmology and the basic sciences.
Following successful completion of the residency program, clinical fellowship training combines outpatient, inpatient, and surgical experience in an ophthalmic subspecialty. The fellow assumes increasing responsibility for patient care under the supervision of faculty members responsible for the program. In addition to receiving training from faculty, the fellow instructs medical students and residents. Research is an important aspect of specialty training and a major prerequisite for assimilating future developments in ophthalmology. Fellows are expected to undertake independent investigation or to participate in ongoing research projects in a field related to their specialty.
The UCLA Department of Ophthalmology offers clinical fellowships in the following subspecialty areas:
f Cornea and External Ocular Diseases and Refractive Surgery
f Cornea and External Ocular Diseases
f Glaucoma
f Medical Retina
f Neuro-Ophthalmology
f Ophthalmic Pathology
f Orbital and Ophthalmic Plastic Surgery
f Pediatric Ophthalmology and Strabismus
f Uveitis and Inflammatory Eye Disease
f Vitreoretinal Diseases and Surgery
International Fellowship Training
To promote and encourage research and education interaction with ophthalmology institutions throughout the world, the Jules Stein Eye Institute offers an International Ophthalmology Fellowship and Exchange Program consisting of one-year to two-year fellowships under the supervision of specific Institute faculty. Candidates for these fellowships are nominated by prestigious institutions outside the United States and often hold academic positions within their own countries. Fellows participate in the clinical and research activities of ophthalmic subspecialties according to their training needs.
Find detailed information about our TRAINING PROGRAMS at:
https://www.uclahealth.org/ eye/training-programs.
The Jules Stein Eye Institute excels as an Organized Research Unit (ORU). ORUs are entities established by the University of California Regents that are interdisciplinary in scope and advance the University’s research, teaching, and public service missions.
As a UCLA Organized Research Unit, the Jules Stein Eye Institute undergoes a formal review every five years to evaluate its research, education, and community engagement programs. The Institute has been commended for its successful recruitment of faculty in emerging and innovative fields, with recognition that these strategic appointments have strengthened its capacity to integrate basic science discoveries with clinical application.
The Institute’s renovated facilities and advanced core resources have been acknowledged as key assets for promoting collaboration across the UCLA research community. In addition, the Jules Stein Eye Institute’s Clinical Research Center is cited as an important platform for National Institutes of Health and industry-sponsored clinical trials, and the UCLA Mobile Eye Clinic is recognized for its continued role in expanding the Institute’s community impact throughout Los Angeles.
Importantly, the ORU provides essential funding that supports all of the Jules Stein Eye Institute’s education, research, and community outreach activities—ensuring the Institute’s continued growth and impact.

Academic Divisions at UCLA Jules Stein Eye Institute (JSEI) and Doheny Eye Centers UCLA (DEC)
CATARACT AND REFRACTIVE SURGERY
John D. Bartlett, MD
Shawn Lin, MD
Kenneth L. Lu, MD
Kevin M. Miller, MD, Chief JSEI
Mitra Nejad, MD
Optometrists
Tony Chan, OD
Lorraine Cheng, OD
Carolyn Duong, OD
Amanda Havens, OD
Linda Hwang, OD
Roxana Khorrami, OD
Melody Kordnaij, OD
Mark Landig, OD
COMPREHENSIVE OPHTHALMOLOGY
Gavin G. Bahadur, MD
Rachel Feit-Leichman, MD
Amanda Lu, MD
Tania Onclinx, MD
Vivian Qin, MD
Susan S. Ransome, MD
Daniel Sand, MD, Chief JSEI
Meryl L. Shapiro-Tuchin, MD
Ronald J. Smith, MD
CORNEA AND UVEITIS
Anthony J. Aldave, MD, Co-Chief JSEI
Saba Al-Hashimi, MD
Benjamin B. Bert, MD
Clémence Bonnet, MD, PhD
Sophie X. Deng, MD, PhD, Co-Chief JSEI
Gary N. Holland, MD
Hugo Y. Hsu, MD, Chief DEC
John A. Irvine, MD
Batool Jafri, MD
Boris E. Malyugin, MD, PhD
Bartly J. Mondino, MD
Edmund Tsui, MD, MS
Victoria H. Yom, MD
Optometrist
Vivian Shibayama, OD
Find out more about our ACADEMIC DIVISIONS and FACULTY at: www.uclahealth.org/eye/ academic-divisions.
Reza Alizadeh, MD
Joseph Caprioli, MD
Vikas Chopra, MD
Anne L. Coleman, MD, PhD, Department Chair
Brian A. Francis, MD, Chief DEC
JoAnn A. Giaconi, MD
Simon K. Law, MD, PharmD
Kouros Nouri-Mahdavi, MD, Chief JSEI
Victoria L. Tseng, MD, PhD
Optometrist
Saluemeh Abadi, OD
NEURO-OPHTHALMOLOGY
Anthony C. Arnold, MD, Chief JSEI
Laura Bonelli, MD
Jane W. Chan, MD
Alexander Fein, MD
Michael J. Gilhooley, MD, PhD
Lynn K. Gordon, MD, PhD
Stacy L. Pineles, MD
Peter A. Quiros, MD, Chief DEC
Alfredo A. Sadun, MD, PhD
OPHTHALMIC ONCOLOGY
Tara A. McCannel, MD, PhD
OPHTHALMIC PATHOLOGY
Ben J. Glasgow, MD, Chief JSEI
ORBITAL AND OPHTHALMIC
PLASTIC SURGERY
Cynthia A. Boxrud, MD
Robert Alan Goldberg, MD, Chief JSEI
Justin Karlin, MD, MS
Daniel B. Rootman, MD, MS
PEDIATRIC OPHTHALMOLOGY AND STRABISMUS
Joseph L. Demer, MD, PhD, Chief JSEI
Mona Fayad, MD
Monica R. Khitri, MD
Stacy L. Pineles, MD
Soh Youn Suh, MD
Laura Syniuta, MD
Federico G. Velez, MD
Optometrist
Laura Robbins, OD
RETINA
Aya Barzelay-Wollman, MD, PhD
Michael B. Gorin, MD, PhD
Gad Heilweil, MD
Hamid Hosseini, MD
Michael S. Ip, MD, Chief DEC
Phillip Le, MD, PhD
David Lozano Giral, MD
Colin A. McCannel, MD, Chief JSEI
Tara A. McCannel, MD, PhD
Steven Nusinowitz, PhD
Moritz Pettenkofer, MD
Pradeep S. Prasad, MD, MBA
SriniVas R. Sadda, MD
David Sarraf, MD
Irena Tsui, MD
Optometrists
Ava K. Bittner, OD, PhD, Chief Optometric Services
Jennie Kageyama, OD
VISION SCIENCE
Steven A. Barnes, PhD
Suraj P. Bhat, PhD
Nicholas C. Brecha, PhD
Gordon L. Fain, PhD
Deborah Ferrington, PhD, Chief Scientific Officer, DEI
Greg D. Field, PhD, Assistant Director, JSEI
Kaustabh Ghosh, PhD
Ben J. Glasgow, MD
Wayne L. Hubbell, PhD
Alexander Huk, PhD
Emma M. Lessieur, MD, PhD
Steven Nusinowitz, PhD
Yi-Rong Peng, PhD
Natik Piri, PhD
Roxana A. Radu, MD
Alapakkam P. Sampath, PhD, Associate Director, JSEI
Deming Sun, MD
Hui Sun, PhD
Gabriel H. Travis, MD
David S. Williams, PhD
Xian-Jie Yang, PhD
Yuhua Zhang, PhD
Jie Zheng, PhD
Joel Zylberberg, PhD

Bradley R. Straatsma, MD, Endowed Chair in Ophthalmology
Chair and Executive Medical Director, UCLA Department of Ophthalmology
Director, Jules Stein Eye Institute
Affiliation Chair, Doheny Eye Institute
Professor of Epidemiology, UCLA Jonathan and Karin Fielding School of Public Health
Dr. Coleman was appointed director of the Jules Stein Eye Institute, chair of the UCLA Department of Ophthalmology, and affiliation chair of the Doheny Eye Institute in 2022, having served as a national leader in ophthalmology, including as president of the American Academy of Ophthalmology (AAO), chair of the National Eye Institute’s National Eye Health Educational Program, president of Women in Ophthalmology, president of the Council for the American Ophthalmological Society, and as associate editor of the American Journal of Ophthalmology. In recognition of her contributions to the field, Dr. Coleman has received numerous honors, including the AAO Life Achievement Award and Secretariat Award and being elected to the National Academy of Medicine.
Dr. Coleman has a passion for patient care, particularly for those traditionally underserved by mainstream medical systems. As director of the Jules Stein Eye Institute Center for Community Outreach and Policy and the UCLA Mobile Eye Clinic, Dr. Coleman has overseen outreach efforts to screen and treat over 180,000 medically underserved children and adults of Southern California.
An accomplished researcher, Dr. Coleman focuses on the diagnosis, treatment, risk factors, geneenvironment interactions, and the societal impact of glaucoma, cataracts, myopia, and age-related macular degeneration. In the surgical arena, Dr. Coleman pioneered the use of the Ahmed glaucoma valve—the world’s leading glaucoma drainage device—and published the first peer-reviewed article describing its safety and efficacy. She has more than 282 peer-reviewed publications and has currently received over 20 million dollars in federal/private funding.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Anthony J. Aldave, MD
Bartly J. Mondino, MD, Endowed Chair in Ophthalmology
Professor of Ophthalmology
Vice Chair of Academics
Co-Chief of the Cornea and Uveitis Division
Director of the Corneal Genetics Laboratory
Discovering the Genetic Basis of the Corneal Dystrophies
Dr. Aldave’s clinical specialties are cornea and external disease. His laboratory research focuses on the molecular genetics of the corneal dystrophies, a group of inherited disorders that affect corneal clarity and constitute one of the primary indications for corneal transplantation.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Saba Al-Hashimi, MD
Health Sciences Associate Clinical Professor of Ophthalmology
Cornea, External Disease, and Refractive Surgery Specialist
Dr. Al-Hashimi is a clinician with a research interest in keratoconus and corneal crosslinking. His research focus involves halting the progression of corneal disease by using light and chemicals to strengthen the cornea. He also participates in training fellows and residents at Harbor-UCLA Medical Center.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood
Stein Eye Center–Calabasas
Reza Alizadeh, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Glaucoma and Refractive Cataract Surgery
Dr. Alizadeh specializes in the medical and surgical treatment of glaucoma and refractive cataract surgery.
Dr. Alizadeh was a board-certified ophthalmologist in his home country of Iran before completing a two-year glaucoma research fellowship at the UCLA Jules Stein Eye institute. He then completed his ophthalmology residency at the University of Arizona, where he served as chief resident and went on medical missions to rural Mexico. He completed his fellowship at the Havener Eye Institute at Ohio State University, receiving advanced training in glaucoma surgery, including laser and minimally invasive glaucoma surgery.
Dr. Alizadeh is an avid supporter of scientific advancements in improving outcomes, and he is excited to share his expertise with his patients. He has authored dozens of peer-reviewed articles and has presented his work at scientific meetings. He is an active member of the American Academy of Ophthalmology and the American Glaucoma Society.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood
Stein Eye Center–Calabasas
Stein Eye Center–Santa Monica
Anthony C. Arnold, MD
Mary Oakley Foundation Chair in Neurodegenerative Diseases
Professor of Clinical Ophthalmology
Vice Chair of Education
Chief of the Neuro-Ophthalmology
Division, UCLA Jules Stein Eye Institute
Director of the UCLA Optic Neuropathy Center
Ischemic and Inflammatory Diseases of the Optic Nerve
Dr. Arnold’s clinical expertise is in neuroophthalmology, with a special emphasis on ischemic and inflammatory optic neuropathies and manifestations of tumors, stroke, and inflammation of the central nervous system. His research has focused on advanced imaging techniques to identify optic nerve circulatory diseases and to investigate their causes.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Gavin G. Bahadur, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Associate Medical Director, Stein Eye Center–Santa Monica
Cataract Surgery Outcomes and Glaucoma Detection
Dr. Bahadur’s clinical specialties are comprehensive ophthalmology including cataract, pterygium, and glaucoma. His research activities include machinelearning algorithms for cataract surgery outcomes and glaucoma detection. He also performs manual small incision cataract surgery (MSICS) with Surgical Eye Expeditions International.
LOCATION:
Stein Eye Center–Santa Monica
Steven A. Barnes, PhD
Professor of Ophthalmology and Neurobiology
Ion Channel Function in Retinal Neurons
Dr. Barnes’ research is focused on the biophysical impact of healthy and bioenergetically stressed conditions on the cellular ion channels that mediate signaling within and between retinal neurons. The activity of ion channel proteins in retinal neurons governs how the retinal network processes and optimizes image processing, as well as transmitting these signals to the brain. Dr. Barnes seeks to define ion channel targets that could aid interventions via early detection and slow or prevent vision loss in diseases such as glaucoma and macular degeneration.
Investigations concern the limits that the bioenergetic environment imposes on photoreceptor and ganglion cell sensitivity and signaling, as well as how early stages of bioenergetic dysfunction are manifested and, in some cases mitigated, by self-regulated ion channel modulation.
LOCATION:
Doheny Eye Institute, Pasadena
Health Sciences Associate Clinical Professor of Ophthalmology
Chief of the Comprehensive Ophthalmology Division
Cataract and Refractive Surgery, Clinical Informatics
Dr. Bartlett’s clinical interest is cataract and refractive cataract surgery, with the goal to improve the focus of the eyes, reduce dependence on glasses, and restore vision potential. He teaches Jules Stein Eye Institute residents, training the next generation of eye surgeons to deal with challenging cases.
Dr. Bartlett is a UCLA physician informaticist and is involved in the implementation and optimization of electronic health records (EHRs) to promote effective organization, analysis, management, and use of clinical information. He is interested in using EHRs to enhance patient care, improve population health, and decrease health care costs.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Aya Barzelay-Wollman, MD, PhD
Assistant Professor of Ophthalmology
Retinal and Vitreoretinal Diseases and Surgery
Dr. Barzelay-Wollman specializes in the treatment of retinal and vitreoretinal diseases. Her research focuses on developing stem cell-based therapies for retinal degeneration and blindness, as well as advanced robotic-assisted retinal surgery. She is a key investigator in multiple funded projects from the California Institute for Regenerative Medicine, National Institutes of Health, and the National Eye Institute.
She completed her internship at Tel Aviv Sourasky Medical Center, followed by her residency in the Institute’s Department of Ophthalmology. She specialized in surgical retina during her fellowship at Sheba Medical Center in Israel and completed an international fellowship in the Retina Division at the UCLA Jules Stein Eye Institute.
Dr. Barzelay has received numerous awards, including the Eli and Edythe Broad Center of Regenerative Medicine and Stem Cell Research Scholarship and the Elrov Scholarship for Excellent Physicians. She serves on PhD committees, is a review editor for prominent journals, and is a member of professional ophthalmologic societies.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Benjamin B. Bert, MD
Health Sciences Associate Clinical Professor of Ophthalmology
Medical Director, Doheny Eye Center UCLA–Orange County
Cornea-External Ocular Disease and Refractive Surgery
Dr. Bert provides comprehensive ophthalmic care and is a subspecialist in cornea/external disease. His areas of expertise include: dry eye/ blepharitis, conjunctivitis, uveitis, acute corneal injury, and genetic corneal disorders, as well as cataract surgery with advanced intraocular lenses and refractive surgery.
LOCATIONS:
Doheny Eye Center UCLA offices in Orange County and Pasadena
Suraj P. Bhat, PhD
Oppenheimer Brothers Chair Professor of Ophthalmology
Director of the Vision Molecular Biology Laboratory
Member of the Molecular Biology Institute
Molecular Biology of Vision
Dr. Suraj Bhat’s research impacts two important areas of vision: the ocular lens in the anterior eye and the retinal pigment epithelium (RPE) in the posterior eye. His laboratory, the Vision Molecular Biology Laboratory (VMBL), investigates gene activity that generates transparency within the ocular lens and gene activity that maintains the physiological health of the RPE, which in turn sustains the neural activity in the retina that makes vision possible. VMBL is investigating single cells in an effort to delineate very early events (at the genetic and molecular level) that culminate in cataractogenesis in the ocular lens and age-related macular degeneration in the RPE.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Ava K. Bittner, OD, PhD
Smotrich Family Optometric Clinician-Scientist Chair
Director of the Vision Rehabilitation Center
Chief of Optometric Services
Professor of Ophthalmology
Low Vision Rehabilitation
Dr. Bittner’s specialty is low vision rehabilitation. Her research activities include clinical trials to assess the use of novel approaches and technologies to improve access to low-vision rehabilitation care and reading ability with visual assistive aids. Specifically, she is evaluating telerehabilitation, Bluetooth low energy beacon sensors, socially assistive robots, and visual assistive mobile apps for low vision.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Laura Bonelli, MD
Olive Bateman and Anga Lundgren Endowed Chair
Health Sciences Assistant Clinical Professor of Ophthalmology
Neuro-Ophthalmology
Dr. Bonelli completed her residency in ophthalmology, as well as fellowships in neuro-ophthalmology and oculoplastics, at the Hospital de Clínicas, University of Buenos Aires, Argentina.
Joining the UCLA Department of Ophthalmology in 2008, Dr. Bonelli specializes in comprehensive ophthalmology and neuro-ophthalmology.
A committed educator, Dr. Bonelli teaches medical student courses at the David Geffen School of Medicine, regularly lectures at educational conferences, and instructs residents and neuroophthalmology fellows in the Department. She is the director of inpatient consultation services for the Ronald Reagan UCLA Medical Center and UCLA Medical Center, Santa Monica, where she oversaw a broad reorganization to improve services and to provide more efficient patient care. In recognition of her work with ophthalmology residents on the consultation services, Dr. Bonelli received the Jules Stein Eye Institute Faculty Teaching Award in 2014.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood Stein Eye Center–Santa Monica
Clémence Bonnet, MD, PhD
Health Sciences Assistant Clinical Professor of Ophthalmology
Cornea, External Disease, and Refractive Surgery
Dr. Bonnet joins the faculty of the Cornea Division as assistant clinical professor where she specializes in the clinical and surgical treatment of corneal diseases and conducts research on limbal stem cell deficiency, ocular surface diseases, and corneal imaging.
Dr. Bonnet obtained her MD at Paris Descartes University in 2015. She obtained her master’s degree in surgical sciences from Université Paris Creteil in 2018. She graduated with a research international fellowship degree in cornea diseases and surgery at the UCLA Jules Stein Eye Institute in 2019. She obtained her PhD in cell biology from Paris Cité Université and UCLA in 2022 summa cum laude, publishing several papers advancing the understanding of limbal stem cell biology in major peerreviewed journals.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood UCLA Santa Monica Medical Center
Nicholas C. Brecha, PhD
Distinguished Professor of Neurobiology, Ophthalmology, and Medicine
Director of the Retinal Pathophysiology Laboratory
Member of the Brain Research Institute
Member of CURE: Center for Digestive Diseases
Member of the California NanoSystems Institute
Functional and Structural
Organization of the Mammalian Retina
Dr. Brecha is a visual system neuroscientist whose expertise includes retinal neurochemistry, transmitters, synaptic and cellular structure, and neuronal circuitry regulating visual function.
His current research studies are furthering the understanding of 1) fundamental synaptic inhibitory processes mediating early vision in the outer retina and 2) neuronal cell structure and function mediating visual processing in the inner retina.
His studies are a prerequisite for understanding normal retinal function, and the impact on the development of therapeutic approaches and diagnostic tools essential for the treatment, prevention, and restoration of vision loss due to retinal injury and disease.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood

Judy L. Chen, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Uveitis and Glaucoma
Dr. Chen specializes in the evaluation and treatment of uveitis and glaucoma. She received her MD from UCLA and completed her ophthalmology residency at the Illinois Eye and Ear Infirmary in Chicago. She pursued clinical fellowships in uveitis and inflammatory eye diseases at UCLA and a glaucoma fellowship at UC Davis. Dr. Chen is developing clinical and research programs focused on glaucoma as a complication of uveitis, with an emphasis on long-term outcomes of uveitic glaucoma among children with chronic anterior uveitis related to juvenile idiopathic arthritis.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood
Doheny Eye Center UCLA offices in Arcadia and Pasadena
The Charles Stewart Warren and Hildegard Warren
Endowed Research Chair
Health Sciences Clinical Professor of Ophthalmology
Medical Director, Doheny Eye Center UCLA–Pasadena Glaucoma
Dr. Chopra has more than 20 years of expertise in glaucoma clinical care, ophthalmic research, and medical education. He delivers evidence-based care utilizing the latest technologies including SLT, LPI, trabeculectomy, aqueous tube shunts, and the newest minimally invasive glaucoma surgeries (MIGS).
Dr. Chopra’s research activities include advanced optic nerve and retinal nerve fiber layer imaging for early glaucoma detection, as well as development and validation of novel parameters for use in anterior segment optical coherence tomography devices as principal investigator at the Doheny Image Reading Center. To date, Dr. Chopra has authored more than 90 peer-reviewed publications in leading journals.
Dr. Chopra holds leadership positions at the American Board of Ophthalmology, American Glaucoma Society, and the American Academy of Ophthalmology. Furthermore, Dr. Chopra teaches surgical courses at the American Academy of Ophthalmology for residents, fellows, and practicing physicians, as well as at the annual Harvard Surgical Course for ophthalmology residents.
LOCATIONS:
Doheny Eye Center UCLA offices in Arcadia and Pasadena
Joseph L. Demer, MD, PhD
Arthur L. Rosenbaum, MD, Chair in Pediatric Ophthalmology
Distinguished Professor of Ophthalmology and Neurology
Chief of the Pediatric Ophthalmology and Strabismus Division
Director, Fellowship in Pediatric Ophthalmology and Strabismus
Director of the Ocular Motility Laboratory
Chair, EyeSTAR Residency PhD/ PostDoc Program in Ophthalmology and Visual Science
Motility and Vision
Dr. Demer’s clinical specialties include pediatric ophthalmology, adult strabismus, and other ocular motility disorders. He is a biomedical engineer whose research includes anatomy and imaging of the eye muscles, and the biomechanics of eye movements and optic nerve disorders. Dr. Demer employs modern scientific and engineering techniques to understand the basis and consequences of disorders of ocular motility in order to save ocular function and promote normal binocular vision. He has developed basic science and clinical imaging methods that have clarified fundamental mechanisms of eye movements and their clinical implications for diagnosis and surgery.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Sophie X. Deng, MD, PhD
Walton Li Chair in Cornea and Uveitis
Co-Chief of the Cornea and Uveitis Division
Professor of Ophthalmology
Vice Chair of Inspiring Physician Excellence
Director of the Corneal Biology Laboratory
Member of the UCLA Jonsson Comprehensive Cancer Center
Member of the UCLA Broad Stem Cell Research Center
Co-Director of Center of Regenerative Medicine in Ophthalmology
Stem Cell-Based Therapies for Corneal Diseases
Dr. Deng specializes in corneal and external ocular diseases, and cataracts. Her surgical areas include endothelial keratoplasty (DSEK and DMEK), deep anterior lamellar keratoplasty (DALK), penetrating keratoplasty, limbal stem cell transplantation, artificial cornea, and cataract.
Dr. Deng is the director of the Cornea Biology Laboratory at the Jules Stein Eye Institute. Her research focuses on corneal epithelial stem cell regulation, deficiency, and regeneration. She aims to improve the current treatment for patients with limbal stem cell deficiency and corneal scars by using stem cellbased therapy to restore vision. Dr. Deng also conducts clinical studies to develop new diagnostic tests using live imaging techniques.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Mona Fayad, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Pediatric Ophthalmology and Strabismus
Dr. Mona Fayad is a pediatric ophthalmologist and strabismus specialist. She completed her medical residency at New York Eye and Ear Infirmary of Mount Sinai followed by a pediatric ophthalmology and adult strabismus fellowship at the UCLA Jules Stein Eye Institute. She specializes in the evaluation and management of strabismus and ocular muscle disorders, amblyopia (“lazy eye”), pediatric cataracts, pediatric glaucoma, lacrimal disorders, and more. Dr. Fayad is also the chief of the Pediatric Ophthalmology Service at Harbor-UCLA Medical Center, where she teaches medical students, ophthalmology residents, and fellows. Her academic interests include surgical outcomes in strabismus surgery and disparities in access to pediatric eye care.
LOCATIONS:
Doheny Eye Center UCLA–Orange County
UCLA Jules Stein Eye Institute, Westwood Harbor-UCLA Medical Center, Torrance
Alexander S. Fein, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Neuro-Ophthalmology
Dr. Fein is a neurology-trained neuroophthalmologist who sees patients with a breadth of neuro-ophthalmic disorders. Dr. Fein has a particular interest in optic neuritis, idiopathic intracranial hypertension, neuro-inflammatory conditions, autoimmune and paraneoplastic disorders. He is a member of the North American Neuro-Ophthalmology Society and serves on multiple professional committees. With a background as a science educator and with a passion for medical education, Dr. Fein enjoys teaching medical students, residents, and fellows.
Dr. Fein earned his MD from SUNY Upstate Medical University. He completed his residency and fellowship training at New York University.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood Doheny Eye Center UCLA–Pasadena

Deborah A. Ferrington, PhD
The Stephen J. Ryan-Arnold and Mabel Beckman Foundation Endowed
Presidential Chair
Professor of Ophthalmology
Chief Scientific Officer, Doheny Eye Institute
Examining a “Personalized Medicine” Approach for Treating AMD
Dr. Ferrington’s research is focused on investigating the molecular changes that occur with age-related macular degeneration (AMD), the leading cause of blindness among the elderly in the developed world. Using human donor tissue graded for the presence and severity of AMD, Dr. Ferrington’s laboratory discovered that AMD has a negative impact on the energy-producing mitochondria in the retinal pigment epithelium (RPE). Notably, damaged mitochondria are present at an early stage of AMD, which provides an opportunity for early intervention. Her work is now focused on identifying and testing drugs that promote mitochondrial function using cultured primary human RPE cells and RPE differentiated from induced pluripotent stem cells (iPSC) obtained from AMD patients. The goal is to use patient-specific iPSC-RPE to develop a “personalized medicine” approach for treating AMD.
LOCATION:
Doheny Eye Institute, Pasadena
Joan and Jerome Snyder Chair in Vision Science
Associate Professor of Ophthalmology
Assistant Director of Research, Jules Stein Eye Institute
Director of the Retinal Circuits and Visual Processing Laboratory
Investigating the Retina
Dr. Field’s laboratory is developing new technologies for understanding how the retina works, and how diseases of the retina can be treated and prevented. His laboratory research uncovers how the retina transforms light into electrical signals that are sent to the rest of the brain, and how the retina works both in healthy states and with diseases such as glaucoma and retinitis pigmentosa.
Dr. Field majored in physics at the University of Puget Sound in Tacoma, Washington, before receiving his PhD in physiology and biophysics from the University of Washington. He conducted his postdoctoral research at the Salk Institute for Biological Studies in La Jolla, California. He started his first laboratory at the University of Southern California in 2012, before moving to Duke University in Durham, North Carolina, in 2015.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Brian A. Francis, MD, MS
The Rupert and Gertrude I. Steiger
Vision Research Endowed Chair
Health Sciences Clinical Professor of Ophthalmology
Co-Medical Director, Doheny Eye Centers UCLA
Chief of Service, Glaucoma, Doheny Eye Centers UCLA Glaucoma
Dr. Francis’ clinical specialties are glaucoma and complex cataract. His research activities include innovative glaucoma surgeries, minimally invasive glaucoma surgery, novel visual field techniques, glaucoma diagnostic and functional imaging, anterior segment imaging (ultrasound biomicroscopy and Fourier domain optical coherence tomography), and glaucoma laser surgery.
LOCATIONS:
Doheny Eye Center UCLA offices in Arcadia, Orange County, and Pasadena
Kaustabh Ghosh, PhD
Mary D. Allen Endowed Chair in Vision Research
Associate Professor of Ophthalmology
Vascular Inflammation, Mechanobiology, Bioengineering, and Nanomedicine
Dr. Ghosh is an interdisciplinary researcher with expertise in vascular inflammation, mechanobiology, bioengineering, and nanomedicine.
He obtained his undergraduate degree in chemical engineering from the National Institute of Technology, India; his PhD in biomedical engineering from Stony Brook University, New York; and conducted his postdoctoral fellowship in the Vascular Biology Program at Boston Children’s Hospital and Harvard Medical School.
Dr. Ghosh was associate professor of bioengineering at the University of California, Riverside (UCR), and participating faculty in the UCR Division of Biomedical Sciences, Stem Cell Center, and the Program in Cell, Molecular and Developmental Biology. The Ghosh Research Group at UCR focused on leveraging the principles of mechanobiology to examine and treat inflammation-mediated vascular degeneration associated with diabetic retinopathy and age-related macular degeneration.
Dr. Ghosh has active R01 grants from the National Eye Institute and was recently honored as Featured Scientist by the BrightFocus Foundation.
LOCATION:
Doheny Eye Institute, Pasadena
JoAnn A. Giaconi, MD
Professor of Clinical Ophthalmology
Vice Chair of Affiliated Hospitals
Chief of the Ophthalmology Section at the Greater Los Angeles
VA Healthcare System
Co-Director of Medical Student Education at the David Geffen School of Medicine, UCLA
Adult and Pediatric Glaucoma
Dr. Giaconi’s areas of clinical specialty are adult and pediatric glaucoma and cataract surgery. Her research interests are in the outcomes of glaucoma surgery. She also has a strong interest in medical education.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood
Veterans Administration Eye Clinic, West Los Angeles campus
Michael J. Gilhooley, MD, PhD
Assistant Professor of Ophthalmology
Strabismus and Neuro-Ophthalmology
Dr. Gilhooley is a surgeon-scientist with clinical expertise in adult strabismus and neuro-ophthalmology. His research focuses on genetics with a particular interest in inherited optic neuropathies.
Originally from Scotland, Dr. Gilhooley completed his medical degree at the University of Cambridge and earned a PhD from the University of Oxford. He completed his ophthalmology residency and a fellowship in adult strabismus at Moorfields Eye Hospital in London, United Kingdom. He later undertook further subspecialty training in neuroophthalmology, with a fellowship at the University of Colorado.
Dr. Gilhooley’s research has been published in leading peer-reviewed journals. He is a recipient of the NANOS Carlow Young Investigator Award and actively contributes to the field through roles on several professional committees and journal editorial boards.
In clinical practice, Dr. Gilhooley focuses on the evaluation and management of the full spectrum of neuroophthalmic disorders, as well as complex strabismus and other oculomotor disturbances.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood Doheny Eye Center UCLA–Pasadena
Ben J. Glasgow, MD
The Wasserman Professor of Ophthalmology
Professor of Pathology and Laboratory Medicine
Chief of the Ophthalmic Pathology Division
Director of the Molecular Mechanisms of Tear Film Formation Laboratory
Ophthalmic Pathology
Dr. Glasgow specializes in ophthalmic pathology, and his research focus is the role of human lacrimal gland proteins in the protection and maintenance of the eye. His laboratory is investigating the structure-function relationship of tear lipocalin. By studying the molecular mechanisms of tear proteins, Dr. Glasgow is seeking to learn the normal functions of tear lipocalin and its role in maintaining the health of the ocular surface and in the prevention of dry eye diseases. Ideally this research will lead to new treatments for dry eye and have broad application to numerous other members of this protein family that transport small, insoluble molecules through the body.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood

Robert
Alan Goldberg, MD
Bert O. Levy Endowed Chair in Orbital and Ophthalmic Plastic Surgery
Professor of Ophthalmology
Chief of the Orbital and Ophthalmic Plastic Surgery Division
Director of the UCLA Orbital Disease Center
Co-Director of the UCLA Aesthetic Center
Diseases and Therapy of the Eyelid and Orbit
Dr. Goldberg is an internationally recognized surgeon, researcher, and teacher. He has developed surgical procedures that are now globally taught and practiced, including less invasive treatments for eye and orbit cancers, new surgeries for thyroid eye disease, and innovative surgical techniques for tearing problems. His research into orbital and eyelid anatomy is resulting in improved techniques and approaches to deep orbital disease. He has had leadership and executive positions in the American Society of Ophthalmic Plastic and Reconstructive Surgery, the American Academy of Cosmetic Surgery, and the American College of Surgeons.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Michael B. Gorin, MD, PhD
Harold and Pauline Price Chair in Ophthalmology
Professor of Ophthalmology
Professor of Human Genetics
Director of the Ocular Neurobiology and Genomics Laboratory
Hereditable Eye Disorders and Molecular Genetics of Age-Related Maculopathy
Dr. Gorin’s clinical expertise is in medical retina and ophthalmic genetic disorders. He has both a basic and translation research program that address the genetics of inherited retinal dystrophies and age-related macular degeneration, the biological basis of pain caused by light exposure, the study of von Hippel Lindau disease, etiology of central serous chorioretinopathy, drug and autoimmune-related retinopathies, genetics-based therapies for disease, and late-life morbidities associated with retinopathy of prematurity.
Dr. Gorin was among the first UCLA physicians to be boarded in Clinical Informatics, and he is exploring the use and analysis of clinical datasets to better understand disease and clinical outcomes.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Gad Heilweil, MD
Health Sciences Associate Clinical Professor of Ophthalmology
Degenerative Retinal Disease
Dr. Heilweil’s research activities include stem-cell therapy for degenerative retinal disease; retinal and uveal drug toxicity; and pharmacokinetics of intravitreal drugs.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood
Stein Eye Center–Calabasas
Doheny Eye Center UCLA offices in Arcadia, Orange County, and Pasadena
Gary N. Holland, MD
Jack H. Skirball Chair in Ocular Inflammatory Diseases
Distinguished Professor of Ophthalmology
Vice Chair of Patient-Based Research Director of the Ocular Inflammatory Disease Center, UCLA Jules Stein Eye Institute
Director of the UCLA Department of Ophthalmology Clinical Research Center
Uveitis and Cornea-External Ocular Diseases
Dr. Holland specializes in uveitis and other inflammatory diseases of the eye. His research activities focus on the evaluation and management of infectious and inflammatory diseases, including ocular toxoplasmosis, cytomegalovirus retinitis and other HIV-related eye disorders, and various non-infectious forms of uveitis, such as chronic anterior uveitis in children and the autoimmune disease birdshot chorioretinitis. Among current studies are those investigating risk factors, disease mechanisms, and response to treatment. Many of these studies are conducted in multicenter clinical trials. In addition to his clinical and research work, Dr. Holland is associate editor of the American Journal of Ophthalmology
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Kirk Hou, MD, PhD
Assistant Professor of Ophthalmology
Vitreoretinal Diseases
Dr. Hou specializes in the evaluation and treatment of vitreoretinal diseases, including diabetic retinopathy, macular degeneration, and complex retinal detachment. He obtained his medical degree from Washington University School of Medicine in St. Louis, Missouri, during which time he also completed a PhD in computational and molecular biophysics. He conducted both his ophthalmology residency and fellowship in vitreoretinal surgery at the UCLA Jules Stein Eye Institute. He is an interdisciplinary researcher with expertise in nanomedicine and drug delivery. He holds patents for his work developing nanoparticles for the delivery of therapeutic nucleic acids. Dr. Hou also teaches residents at Olive View-UCLA Medical Center.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood
Doheny Eye Center UCLA–Pasadena
Hugo Y. Hsu, MD
Health Sciences Clinical Professor of Ophthalmology
Chief of Service, Cornea, Doheny Eye Centers UCLA
Cornea and External Diseases
Dr. Hsu specializes in corneal infection and inflammation, corneal transplantation, anterior segment reconstruction, and cataract surgery. His research interests include corneal and ocular infections and ophthalmic antibiotics.
LOCATIONS:
Doheny Eye Center UCLA offices in Arcadia, Orange County, and Pasadena
Alexander Huk, PhD
Professor of Ophthalmology
Professor, Department of Psychiatry and Biobehavioral Science
Vision and Visually Guided Cognition
Dr. Huk focuses on studying vision and visually guided cognition in increasingly naturalistic conditions. He was the Raymond Dickson Centennial Professor and director of the Center for Perceptual Systems at the University of Texas at Austin before coming to UCLA in 2022. He received his PhD from Stanford University and conducted behavioral and cortical studies of the human visual system there with Drs. David J. Heeger and Brian A. Wandell. His postdoctoral research was at the University of Washington in Seattle. Dr. Huk received the Young Investigator Award from the Vision Sciences Society in 2011, and he is a permanent member of a National Eye Institute focused study section.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Michael S. Ip, MD
Gavin S. Herbert Endowed Chair for Macular Degeneration
Professor of Ophthalmology
Chief of Service, Retina, Doheny Eye Centers UCLA Medical Director, Doheny Image Reading Center
Vitreoretinal Disease
Dr. Ip is the chief of the Vitreoretinal Surgery Service at the Doheny Eye Centers UCLA. His practice concentrates on the surgical management of complex retinal detachment, complications of diabetic retinopathy, macular holes, epiretinal membranes, and other vitreoretinal diseases amenable to surgical intervention. Dr. Ip’s research focuses on the design and conduct of clinical trials investigating treatments for diabetic retinopathy, age-related macular degeneration, and retinal venous occlusive disease. As medical director for the Doheny Image Reading Center, endpoint analysis for clinical trials is an additional area of research focus. In addition, Dr. Ip has served as the national director for numerous NIH-funded ophthalmic clinical trials.
LOCATIONS:
Doheny Eye Institute, Pasadena Doheny Eye Center UCLA–Arcadia

Monica R. Khitri, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Pediatric Ophthalmic Diseases and Strabismus
Dr. Khitri specializes in the evaluation and treatment of pediatric ophthalmic diseases, including pediatric cataracts, nasolacrimal duct obstructions, amblyopia, and retinopathy of prematurity. She also treats and operates on strabismus in both children and adults.
She received her medical degree from the David Geffen School of Medicine at UCLA and completed her residency in ophthalmology at the Jules Stein Eye Institute, followed by a fellowship in pediatric ophthalmology and strabismus at the Children’s Hospital of Philadelphia.
Dr. Khitri is also a medical educator, researcher, and winner of over two dozen academic and professional awards, including the 2018 Faculty Teaching Award for the Jules Stein Eye Institute ophthalmology residency program. She teaches residents and fellows at HarborUCLA Medical Center, where she is chief of the Pediatric Ophthalmology Service.
LOCATIONS:
Doheny Eye Center UCLA offices in Arcadia, Orange County, and Pasadena
Simon K. Law, MD, PharmD
Health Sciences Clinical Professor of Ophthalmology
Optic Disc Evaluation
Dr. Law’s clinical specialties are glaucoma and cataract. His research activities include evaluation of the optic nerve in different racial groups and ocular pathologies, different patterns of glaucomatous visual function decline, outcomes of different glaucoma surgical procedures and medications in eye pressure control and vision restoration, and alternative therapy in glaucoma care.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Emma M. Lessieur, MD, PhD
Assistant Professor of Ophthalmology
Causes and Prevention of Diabetic Retinopathy
Dr. Lessieur is a scientist who studies what causes retinopathy in diabetes, and how it can be prevented. Efforts in her lab are focused on understanding the cellular and molecular mechanism that led to the disease and the development of novel unconventional therapies to halt the progression of the retinopathy.
Dr. Lessieur earned her medical degree from the Universidad Autónoma de Tamaulipas in México and completed her PhD in Molecular Medicine at the Cleveland Clinic Lerner College of Medicine of Case Western Reserve University in Cleveland, Ohio. During her postdoctoral training at the University of California, Irvine, under Professor Timothy Kern, she investigated how extracellular vesicles mediate immune signaling in the early stages of diabetic retinopathy. Her innovative work is supported by a prestigious K99/R00 MOSAIC Career Transition Award from the National Eye Institute.
LOCATION:
Doheny Eye Institute, Pasadena
Shawn R. Lin, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Medical Director, Stein Eye Center–Calabasas
Associate Residency Director, Department of Ophthalmology
Cataract and Refractive Surgery
Specializing in cataract and refractive surgery, Dr. Lin obtained his MD and MBA from Stanford University. He conducted his ophthalmology residency at the UCLA Jules Stein Eye Institute, and he completed a Heed Cornea and Refractive Surgery Fellowship at the Massachusetts Eye and Ear Infirmary at Harvard University.
Dr. Lin’s research is focused on combining human and artificial intelligence to deliver exceptional surgical results. He has authored more than a dozen peerreviewed publications in leading ophthalmology journals, has written chapters on ophthalmology and cornea for textbooks, and has delivered keynote presentations at international scientific meetings.
Dr. Lin founded EyeGuru, an online educational platform visited more than one million times a year by ophthalmologists from 125 countries. In this role, Dr. Lin helps to advance knowledge in the field and train the next generation of ophthalmologists.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood
Stein Eye Center–Calabasas
David Lozano Giral, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Director, Ocular Trauma Service
Retina and Vitreous Diseases
Dr. Lozano Giral specializes in the clinical and surgical treatment of retina and vitreous diseases, and also serves as ocular trauma faculty.
He received his medical degree in 2014 and a master’s degree in medical science in 2016, both at Universidad Anahuac in Mexico City. He joined the Genetics Research Department at the Instituto de Oftalmología Conde de Valenciana in Mexico City, publishing peer-reviewed papers on genetic polymorphisms and mutations related to ophthalmologic pathologies. He conducted his residency at the Instituto de Oftalmología Conde de Valenciana in 2020 and was an international retinal fellow at the Jules Stein Eye Institute in 2023. He has been involved in development of new platforms for surgical robotics, and his work has been published in journals and in chapters of national and international medical books.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood Ronald Reagan UCLA Medical Center
Amanda Lu, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Comprehensive Ophthalmology
Dr. Lu sees patients in the Comprehensive Ophthalmology Division where she provides primary ophthalmic and surgical care. Dr. Lu, who was born and raised in Dallas, Texas, graduated from Harvard University with a BA in organismic and evolutionary biology and with a minor in global health. She was awarded the prestigious Trustman Fellowship to study ethnobotany in Peru, following her passion for environmental interactions and health.
Dr. Lu earned her MD at Yale School of Medicine and her MBA from Quantic School of Business and Technology. She completed her medical internship at Manchester Memorial Hospital, and she received her ophthalmology residency training at the UCLA Jules Stein Eye Institute. Dr. Lu’s academic interests include studying perioperative cataract outcomes and factors driving healthcare costs, and her research has been featured in national presentations and peer-reviewed publications.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Kenneth L. Lu, MD
Health Sciences Associate Clinical Professor of Ophthalmology
Medical Director, Doheny Eye Center UCLA–Arcadia Cataract and Refractive Surgery
Dr. Lu specializes in cataract and refractive surgery, and his research activities are focused in the same areas.
LOCATION:
Doheny Eye Center UCLA–Arcadia
Boris E. Malyugin, MD, PhD
Joan and Jerome Snyder Chair in Cornea Diseases (pending) Professor of Clinical Ophthalmology Cataract Surgery and the Treatment of Corneal Diseases
Dr. Boris Malyugin joins the Cornea and Uveitis Division where he specializes in cataract surgery and the treatment of corneal diseases.
Born in Moscow, he was trained and worked at the Fyodorov Eye Microsurgery—the leading eye care provider in Russia. Dr. Malyugin has developed innovative surgical techniques and devices, including the “Malyugin Ring,” a device which is used to temporarily stretch and expand the pupil during cataract surgery. He is highly regarded for development of complex cataract surgery techniques, secondary intraocular lens implantation, keratoplasty techniques (both lamellar and full thickness), and ocular surface reconstruction.
Dr. Malyugin’s research has been featured in peer-reviewed journals, and he has also contributed to many ophthalmic surgery textbooks and atlases. He is an active member of leading ophthalmic organizations and serves on the editorial boards of several ophthalmology journals.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood
Stein Eye Center–Santa Monica
Colin A. McCannel, MD
The Ahmanson Chair in Ophthalmology
Chief of the Retina Division
Professor of Clinical Ophthalmology
Medical Director, Stein Eye Center–Santa Monica
Vitreoretinal Surgery
Dr. McCannel has a longstanding interest in the management of vitreoretinal conditions, particularly complex retinal detachments, complications of diabetic retinopathy, macular holes and epimacular membranes, and age-related macular degeneration. His clinical research efforts are directed at the improvement of vitreoretinal surgical techniques and outcomes, including the prevention of endophthalmitis following intravitreal injections.
Dr. McCannel devotes time to educational research as well. Currently, he is investigating the utility of virtual reality surgery simulation in teaching ophthalmic surgery. He has several ongoing protocols that assess ophthalmic surgical simulation in surgical teaching.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood
Stein Eye Center–Santa Monica
Tara A. McCannel, MD, PhD
Health Sciences Clinical Professor of Ophthalmology
Director of the Ophthalmic Oncology Center
Metastatic Ocular Melanoma and Diseases of the Retina and Vitreous
Dr. McCannel is an ophthalmic oncologist, as well as a vitreoretinal surgeon. Dr. McCannel’s Ophthalmic Oncology Laboratory is studying molecular markers in ocular melanoma to provide prognostic information to patients and advance understanding of metastatic disease. Discovery of candidate genes from tissue of patients undergoing surgical treatment for ocular melanoma is being explored. This information will be important to establish a better understanding of the biology of metastatic ocular melanoma and help develop better treatments for this cancer. New modalities are being investigated to predict, detect, and ultimately treat choroidal melanoma metastasis.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood

Kevin M. Miller, MD
Kolokotrones Chair in Ophthalmology
Professor of Clinical Ophthalmology
Chief of the Cataract and Refractive Surgery Division
Director of the Anterior Segment Diagnostic Laboratory
Cataract and Refractive Surgery
Dr. Miller is chief of the Cataract and Refractive Surgery Division and director of the Anterior Segment Diagnostic Laboratory. He also manages the UCLA Laser Refractive Center. His research interests include devices and implants used in cataract and refractive surgery, outcomes of surgical procedures, astigmatism management, and artificial iris implantation.
He specializes in refractive cataract surgery including femtosecond laser assistance, intraoperative refractive guidance, and postoperative refractive enhancement. He performs refractive procedures such as LASIK, PRK, SMILE, ICL implantation, and clear lens extraction. He also performs complex anterior segment surgery including artificial iris implantation.
He is an executive editor for the American Journal of Ophthalmology and a member of the EyeWorld editorial board. Dr. Miller is president-elect of the American Society of Cataract and Refractive Surgery and serves in leadership roles at the American Academy of Ophthalmology and as a consultant for industry.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Mitra Nejad, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Associate Residency Director, Department of Ophthalmology
Cataract and Refractive Surgery
Dr. Nejad is an assistant clinical professor in the Cataract and Refractive Division. She graduated summa cum laude from UCLA and earned her MD from the David Geffen School of Medicine (DGSOM) at UCLA. Dr. Nejad conducted her internship at Harbor-UCLA Medical Center and her ophthalmology residency at the Jules Stein Eye Institute, where she remained on staff. She recently completed the DGSOM Medical Education Fellowship and serves as a residency assistant program director and co- director of Medical Student Education. Dr. Nejad has contributed to the cataract surgery curriculum and microsurgery wet lab curriculum, and she attends resident cataract surgery at both the Jules Stein Eye Institute and Harbor-UCLA. She is a certified proctor in laser refractive surgery and supervises Jules Stein Eye Institute residents’ refractive surgery cases. She also serves on the residency program evaluation and selection committees.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Kouros Nouri-Mahdavi, MD, MSc
Kay K. Pick Endowed Chair in Glaucoma Research (pending)
Chief of the Glaucoma Division
Director of the Glaucoma Imaging and Artificial Intelligence Laboratory
Structural and Functional Measurements for Detection of Glaucoma and its Progression, Surgical Outcomes, and Artificial Intelligence in Glaucoma Diagnostics
Dr. Nouri-Mahdavi’s areas of clinical focus are management of adult glaucoma and advanced and complex cataract surgery. His research activities currently focus on optimizing the role of structural and functional measurements for detection of glaucoma progression with an emphasis on advanced disease and macular optical coherence tomography imaging. More recently, his research laboratory has been exploring the use of artificial intelligence and digital phenotyping in glaucoma diagnostics.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood Stein Eye Center–Calabasas
Yi-Rong Peng, PhD
Assistant Professor of Ophthalmology and Neurobiology
Director of the Retinal Function and Dysfunction Laboratory
Pathogenesis of Retinal Diseases
Dr. Peng is a neuroscientist whose research focuses on large-scale transcriptomic profiling of retinal cells in healthy and pathological conditions to understand human vision and provide insights for the study of ocular diseases.
Dr. Peng received her PhD in neurobiology from the Institute of Neuroscience, Chinese Academy of Sciences, Shanghai, China. Her doctoral research examined the role of functional interactions between inhibitory and excitatory synapses that maintain the stability of neural networks. Dr. Peng then joined the laboratory of Dr. Joshua Sanes at Harvard University as a postdoctoral fellow, where she leveraged high throughput single-cell transcriptomic methods to uncover key transcriptional factors that control the specification of retinal cell types.
At the Jules Stein Eye Institute, Dr. Peng is continuing her development of state-of-the-art transcriptomic and genomic tools to reveal the molecular underpinnings of the formation of retinal circuits and the pathogenesis of retinal diseases.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood

Moritz S. Pettenkofer, MD
Health Sciences Clinical Assistant Professor of Ophthalmology
Macular Diseases
Dr. Pettenkofer obtained his medical degree at the University of Göttingen in Germany and completed his residency training in ophthalmology at the Technical University of Munich in Germany. He then completed an international fellowship in vitreoretinal diseases at the UCLA Jules Stein Eye Institute.
Dr. Pettenkofer joined the faculty in 2022 and specializes in macular diseases with a particular focus on agerelated macular degeneration, diabetic retinopathy, and retinal vein occlusions. He has contributed to more than a dozen peer-reviewed publications in the field of retina, and his research focuses on imaging, evaluation, and treatment of macular diseases, notably dry macular degeneration. His in-office procedures include retinal laser and intravitreal injections.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood Stein Eye Center–Calabasas
Professor of Ophthalmology
Pediatric Neuro-Ophthalmology, Amblyopia, and Neurologic Causes of Strabismus
Dr. Pineles’ research interests include evaluating the surgical outcomes of strabismus surgery and studying pediatric optic nerve diseases. With her dual training in pediatric ophthalmology and neuro-ophthalmology, she has a special interest in pediatric neuro-ophthalmic diseases, as well as adult patients with amblyopia and neurologic causes of strabismus.
Dr. Pineles is the chair of a national research network, the Pediatric Eye Disease Investigator Group (PEDIG) sponsored by the National Institutes of Health.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Natik Piri, PhD
Professor of Ophthalmology
Director of the Molecular Biology of Retinal Ganglion Cells Laboratory Retinal Ganglion Cell Biology, Glaucomatous Neurodegeneration, and Neuroprotection
Dr. Piri’s primary research is defining the mechanisms leading to retinal ganglion cell (RGC) degeneration in glaucomatous neuropathy; developing strategies for preserving RGCs against neurodegeneration; and identifying and characterizing the genes critical for RGC function and integrity. Characterization of RGC- expressed genes is fundamental to a better understanding of normal RGC physiology and pathophysiology. Dr. Piri also focuses on understanding the degeneration of RGCs and their axons, which is a hallmark of glaucoma. He is also studying the involvement of oxidative stress and proteins of the thioredoxin system, particularly in RGC degeneration in the glaucoma model, and the neuroprotective effects of these proteins against glaucomatous RGC death.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Pradeep S. Prasad, MD, MBA
Health Sciences Associate Clinical Professor of Ophthalmology
Assistant Chief of Clinical Affairs, Retina Division
Vitreoretinal Surgery and Disease Management
Dr. Prasad specializes in the medical and surgical management of diseases of the retina and vitreous. His research is focused on teleretinal screening for diabetic retinopathy, applications of widefield fundus photography for retinal vascular disease, and health care delivery for low-income populations.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Health Sciences Assistant Clinical Professor of Ophthalmology
Glaucoma Care
Dr. Qin was raised in New Jersey, where she graduated from Princeton University summa cum laude with a degree in molecular biology and a certificate in global health and health policy. She earned her MD at Case Western Reserve University School of Medicine in Cleveland, Ohio, and graduated with AOA medical society honors. She spent her medical intern year at Lankenau Hospital in Philadelphia and conducted her ophthalmology residency at Scheie Eye Institute at the University of Pennsylvania. Dr. Qin completed a fellowship in glaucoma at University of California, San Francisco and is excited to be bringing her passion for glaucoma care and medical education to UCLA.
LOCATIONS:
Doheny Eye Center UCLA locations in Pasadena and Arcadia
Peter A. Quiros, MD
Professor of Clinical Ophthalmology
Assistant Division Chief of the Neuro-Ophthalmology Division
Chief of Service, Neuro-Ophthalmology, Doheny Eye Centers UCLA
Neuro-Ophthalmology
A neuro-ophthalmologist, Dr. Quiros specializes in optic nerve disease, including optic neuritis and ischemic optic neuropathy; double vision and adult strabismus; idiopathic intracranial hypertension; thyroid eye disease; orbital inflammatory syndromes; and stroke. Research includes idiopathic intracranial hypertension, headache, ocular myasthenia gravis, and ischemic optic neuropathy. He was the principal investigator for the idiopathic intracranial hypertension treatment trial. He is currently president-elect of the North-American Neuro-Ophthalmology Society and a member of the Neuro-Ophthalmology Researchers and Disease Investigators Consortium (NORDIC).
Dr. Quiros obtained his MD from the Yale University School of Medicine. He completed his residency training at LAC/ USC Medical Center and his fellowship training at Doheny Eye Institute.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood Doheny Eye Center UCLA–Pasadena
Roxana A. Radu, MD
Vernon O. Underwood Family Chair in Ophthalmology
Associate Professor of Ophthalmology
Director of the Retinal Biochemistry and Clinical Disease Modeling Laboratory
Retina Biochemistry and Clinical Disease Modeling Laboratory
Dr. Radu’s scientific interest is to understand the mechanism of photoreceptor cell degeneration by integrating genetic, biochemical, cellular, and molecular approaches. Dr. Radu’s research focuses on the formation and pathogenic role of bisretinoids in retinopathies such as recessive Stargardt disease and age-dependent macular degeneration. Her group has developed both mouse and human disease cell-based models to identify fundamental biological processes at the intersection between the complement system, retinoid- lipid metabolism, mitochondria, and endolysosomal pathways in normal and immunecompromised retinal pigment epithelium cells. Her studies are supported by the NIH grants, sponsor- initiated research programs, and philanthropic funds. Dr. Radu is also actively involved in training and teaching undergraduates, pre-/ post-graduate fellows, and medical students.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood

Daniel B. Rootman, MD, MS
Karen and Frank Dabby Endowed Chair in Ophthalmology
Associate Professor of Ophthalmology
Orbit and Ophthalmic Plastic Surgery
Dr. Rootman is an orbit and ophthalmic plastic surgery specialist with expertise in Graves disease, orbital surgery, orbital tumors, ptosis, lacrimal disorders, blepharoplasty, blepharospasm, Botox®, cosmetic dermal fillers, endoscopic eyebrow lift, eyelid surgery, eyelid tumors, and trauma. His research is developing and refining patient-centered outcome measures for surgical care; randomized clinical trials in surgery, including ptosis, Graves orbitopathy and lacrimal disease; health economics of eyelid and facial surgery; sociodemographics of facial trauma; physiology and pathobiology of ptosis; new approaches to surgery; and measurement and assessment in medical education.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood
Doheny Eye Center UCLA offices in Orange County and Pasadena
SriniVas R. Sadda, MD
A. Ray Irvine, Jr., MD, Endowed Chair in Clinical Ophthalmology
Professor of Ophthalmology
Retinal and Macular Diseases
Dr. Sadda received his MD from Johns Hopkins University, where he also completed his ophthalmology residency and neuro-ophthalmology and medical retina fellowships. His clinical interests are macular degeneration and diabetic retinopathy, and his research includes automated retinal image analysis and advanced retinal imaging technologies. He has more than 800 peer-reviewed publications and 20 book chapters, and he has given over 500 presentations worldwide. He also serves as an editorial board member of Ophthalmic Surgery, Lasers & Imaging, Retina, Ophthalmology Retina, Ophthalmology, and is editor-inchief of Graefe’s. He is also the editorin-chief of the 7th edition of the Ryan’s Retina textbook.
LOCATIONS:
Doheny Eye Center UCLA offices in Arcadia and Pasadena
Alfredo A. Sadun, MD, PhD
Flora L. Thornton Endowed Chair in Vision Research
Professor of Ophthalmology
Vice Chair of Doheny Eye Centers UCLA
Neuro-Ophthalmology
Dr. Sadun conducted his ophthalmology residency and fellowship in neuroophthalmology at Massachusetts Eye and Ear, Harvard Medical School. His clinical interests are diseases of the optic nerve, and more particularly, Leber hereditary optic neuropathy, toxic and nutritional optic neuropathies, and anterior and posterior ischemic optic neuropathies. He conducts research in these areas, as well as the assessment of the retina and optic nerve in Alzheimer disease and other neuro-degenerations.
Dr. Sadun has authored approximately 400 peer-reviewed publications and 75 book chapters. His research activities focus on human visual neuro-anatomy; retinal ganglion cell degeneration and regeneration; and axon populations in the human optic nerve in development, aging, and disease. He has six clinical trials involving treatment of optic nerve diseases, and most particularly, mitochondrial impairments as a cause of optic nerve disease.
LOCATION:
Doheny Eye Center UCLA–Pasadena
Alapakkam P. Sampath, PhD
Grace and Walter Lantz Endowed Chair in Ophthalmology
Professor of Ophthalmology and Neurobiology
Associate Director of Research Chief, Vision Science Division
Director of the Retinal Neurophysiology Laboratory
Molecular Mechanisms Underlying Early Visual Processing
The Sampath laboratory is interested in understanding the molecular mechanisms underlying early visual processing. In particular, the focus of laboratory researchers has been on elucidating mechanisms that set the sensitivity of night vision. Night blindness, or nyctalopia, is a condition that results from abnormal signaling by the rod photoreceptors, or the retinal circuits that process roddriven signals. Using physiological and genetic methods, the laboratory studies signal transmission in these retinal rod pathways to identify how these processes are optimized to allow our exquisite visual sensitivity.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Daniel Sand, MD
James and Catherine Shuler Endowed Chair in Comprehensive Ophthalmology (pending)
Health Sciences Associate Clinical Professor of Ophthalmology
Chief, Comprehensive Ophthalmology Division
Comprehensive Ophthalmic Care
Dr. Sand is the new chief of the Comprehensive Ophthalmology Division. He practices a full scope of comprehensive ophthalmology and cornea/refractive surgery.
Dr. Sand attended medical school at Case Western Reserve University in Ohio, where he was elected into the Alpha Omega Alpha Honor Medical Society. He completed his internship at Olive View-UCLA Medical Center and his residency at Doheny Eye Institute/University of Southern California. He did his cornea, external disease and refractive surgery training as a Heed Ophthalmic Foundation Fellow at the University of Michigan, Kellogg Eye Center. There he also completed an eye banking fellowship as the inaugural Eversight Eye Bank Fellow. He is continuing his involvement with the Eye Bank Association of America as a member of multiple national committees. He most recently was in private practice and taught USC residents in surgery and clinic.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
David Sarraf, MD
Health Sciences Clinical Professor of Ophthalmology
Age-Related Macular Degeneration and Retinal Imaging
Dr. David Sarraf is clinical professor of ophthalmology at the UCLA Jules Stein Eye Institute and member of the Retinal Disorders and Ophthalmic Genetics Division. He has published close to 300 peer-reviewed research papers, case reports, and reviews and has authored 22 book chapters. He is co-author for the second edition of the Retina Atlas and will be section editor for the 7th edition of Ryan Retina. Dr. Sarraf is a world leader in the field of advanced retinal imaging and has delivered over 300 invited lectures at various meetings worldwide, including close to a dozen endowed and keynote lectures.
Dr. Sarraf is associate editor for the British Journal of Ophthalmology and Ophthalmology Science, and he is section editor of the Ocular Imaging Section for the Canadian Journal of Ophthalmology. He is also associate editor for the journal Retinal Cases and Brief Reports and editorial board member of the journals Retina and OSLI Retina
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Health Sciences Clinical Assistant Professor of Ophthalmology
Chief, Pediatric Ophthalmology and Strabismus Division, Olive View-UCLA Medical Center
Pediatric Ophthalmology and Adult Strabismus
Dr. Suh is a pediatric ophthalmologist specializing in pediatric ophthalmic diseases including amblyopia, strabismus, nasolacrimal duct obstruction and congenital optic nerve anomalies. She is also a strabismus specialist and performs strabismus surgery in both children and adults.
Dr. Suh’s clinical research focuses on surgical dosing in strabismus surgery and myopia control in pediatric patients.
Dr. Suh serves as both a course director for medical students and the chief of the Pediatric Ophthalmology and Strabismus Division at Olive View-UCLA Medical Center.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood Olive View-UCLA Medical Center
Professor of Physiology and Ophthalmology
Director of the Receptor Signaling and Chemical Targeting Laboratory
Member of Jonsson Comprehensive Cancer Center
Molecular Mechanism of Vitamin A Transport for Vision; Identification of New Therapeutic Targets for Blinding Diseases
Dr. Sun’s laboratory aims to identify new therapeutic targets to treat still incurable human diseases, to study their molecular mechanisms, and to develop novel therapies based on the mechanisms. Through many years of research efforts, his laboratory has identified the cell-surface receptors for the most potent endogenous inhibitor of angiogenesis, developed novel techniques to screen for drugs that target these receptors, and developed the first small molecule drug candidates that specifically suppress pathogenic angiogenesis in diverse vision diseases and in cancer. These molecules have achieved therapeutic effects that no existing drugs can achieve and are being prepared for clinical trials.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood

Gabriel H. Travis, MD
Charles Kenneth Feldman Chair in Ophthalmology
Professor of Ophthalmology
Director of the Photoreceptor
Biochemistry Laboratory
Biochemistry of Vertebrate Photoreceptors and Mechanisms of Retinal Degeneration
Dr. Travis’ laboratory uses biochemical and genetic approaches to study the visual cycle and its role in retinal and macular degenerations. Vision in vertebrates is mediated by two types of light-sensitive cells: rods and cones. These cells contain light-detecting molecules called opsin pigments. Detection of a single light particle bleaches the opsin pigment. Restoring light sensitivity to a bleached opsin involves an enzymatic pathway called the visual cycle. Mutations in the genes for many proteins of the visual cycle cause inherited blinding diseases.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Victoria L. Tseng, MD, PhD
Jerome and Joan Snyder Chair in Ophthalmology
Assistant Professor of Ophthalmology
Residency Director, Department of Ophthalmology
Glaucoma and Cataract
Dr. Tseng specializes in the treatment of glaucoma and cataracts in the UCLA Department of Ophthalmology. Committed to the education of future ophthalmologists, she teaches ophthalmology residents at Olive View-UCLA Medical Center and is the director of the UCLA Department of Ophthalmology Residency Program.
Dr. Tseng’s research focuses on the intersection of epidemiology, disparities, and population health within ophthalmology. She is a recipient of multiple research grants and honors including the Research to Prevent Blindness Career Development Award, the Research to Prevent Blindness and American Academy of Ophthalmology (AAO) Award for IRIS Registry Research, and the American Glaucoma Society Mentoring for the Advancement of Physician Scientists Research Grant.
Dr. Tseng is involved with national ophthalmology organizations and is a regional representative for AAO State Affairs.
LOCATION:
Doheny Eye Center UCLA, Pasadena
Edmund Tsui, MD, MS
Associate Professor of Ophthalmology Uveitis and Ocular Inflammatory Diseases
Dr. Tsui specializes in the management of uveitis and ocular inflammatory diseases. He completed his medical training at Dartmouth Medical School followed by an ophthalmology residency at the New York University School of Medicine. He completed his fellowship in uveitis and ocular inflammatory disease at the Francis I. Proctor Foundation at the University of California, San Francisco.
Dr. Tsui’s National Institutes of Healthfunded research focuses on the evaluation of imaging biomarkers to measure and quantify intraocular inflammation with optical coherence tomography and laser flare photometry. Dr. Tsui is also the site principal investigator for clinical trials investigating novel therapeutics for uveitis. He serves on the Executive Committee of the American Uveitis Society and is the chair of the Association for Research in Vision and Ophthalmology Professional Development and Education Committee. He is also the senior social media editor for the journals Ophthalmology, Ophthalmology Retina, and Ophthalmology Glaucoma
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Irena Tsui, MD
Associate Professor of Ophthalmology Assistant Chief of Research, Retina Division
Clinical Vitreoretinal Research
Dr. Tsui’s clinical activities include adult and pediatric vitreoretinal diseases. Her research interests focus on retinopathy of prematurity and Zika virus eye abnormalities. Dr. Tsui teaches ophthalmology trainees and serves veterans at the Greater Los Angeles VA Healthcare System.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood
Doheny Eye Center UCLA–Arcadia
Federico G. Velez, MD
Leonard Apt Endowed Chair in Pediatric Ophthalmology
Professor of Clinical Ophthalmology
Strabismus and Childhood Eye Disorders
Dr. Velez is a pediatric ophthalmology specialist who studies the mechanisms of congenital and acquired forms of strabismus. In addition, Dr. Velez conducts research on artificial muscle stimulation and management of orbital fibrosis, amblyopia therapy, and medical management of thyroid eye disease. He has participated in development of guidelines for preoperative assessment and surgical approaches to patients with convergent (esotropia), divergent (exotropia), and vertical forms of strabismus, and he has advanced techniques to treat pediatric patients with eyelid abnormalities and cataracts.
LOCATIONS:
UCLA Jules Stein Eye Institute, Westwood
Stein Eye Center–Calabasas
Doheny Eye Center UCLA–Orange County
S. Williams, PhD
Karl Kirchgessner Foundation Chair in Vision Science
Professor of Ophthalmology and Neurobiology
Director of the Retinal Cell Biology Laboratory
Cell Biology of the Retina and Inherited Retinal Disease
Dr. Williams’ laboratory focuses on the cell biology of photoreceptor and retinal pigment epithelium cells. His group is especially interested in proteins that function in transport and compartmentalization within these cells. These proteins include those that underlie Usher syndrome and macular degeneration. Translational areas of his research involve gene therapy experiments aimed at preventing the blindness that ensues from Usher syndrome type 1B and studies on stem cell-derived RPE cells, which may be transplanted into retinas afflicted by macular degeneration.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Xian-Jie Yang, PhD
Professor of Ophthalmology
Director of the Developmental Neurobiology Laboratory
Member of the Molecular Biology Institute
Member of the Brain Research Institute
Member of the UCLA Broad Stem Cell Research Center
Director of the Gene and Cell Delivery Core for Vision Research
Development and Repair of the Retina
Dr. Yang obtained her PhD at Cornell University and received postdoctoral training at Harvard University and Harvard Medical School before joining UCLA Jules Stein Eye Institute as a faculty member. Dr. Yang’s research is focused on molecular and cellular mechanisms underlying retina development and repair. Her research includes using genetically engineered retinal degeneration models and recombinant virus-mediated gene delivery to study neuroprotection mechanisms. In addition, her research team has established stem cell based retinal organoid models to derive human retinal neurons, simulate retinal diseases, and develop gene editing and replacement therapies.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Victoria H. Yom, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Cornea and External Diseases
Dr. Yom specializes in corneal and external diseases. Her expertise includes surgical and medical management of complex ocular inflammatory conditions and anterior uveitis. Procedures performed include corneal transplant surgery and cataract surgery.
Dr. Yom received her MD and Master of Science in Clinical Investigation from Washington University School of Medicine in St. Louis, where she also completed her residency. She obtained a fellowship in cornea and external diseases at the Doheny Eye Centers UCLA and has been a member of the UCLA Department of Ophthalmology since 2017. Dr. Yom enjoys introducing medical students to the field of ophthalmology during their preclinical clerkships, and she regularly lectures at educational conferences and is an active member of the American Academy of Ophthalmology.
LOCATIONS:
Doheny Eye Center UCLA offices in Arcadia and Pasadena

Yuhua Zhang, PhD
Professor of Ophthalmology
Retinal Imaging
Dr. Zhang is a professor whose research focuses on developing state-of-the-art imaging tools to study blinding eye disorders and small-vessel diseases related to systemic conditions and central nervous systems. His work includes 3-D imaging technologies for viewing the retina at the cellular level in patients with age-related macular degeneration, diabetic retinopathy, hypertensive retinopathy, and small-vessel diseases.
His advanced imaging systems integrate adaptive optics, scanning laser ophthalmoscopy, optical coherence tomography, and fluorescence lifetime imaging to study vision-producing cells, retinal blood vessels, and individual red and white blood cells within the eye. Understanding their interactions will help answer fundamental questions about the causes of vision loss and systemic diseases, improve prognoses for patients, and lead to targeted treatments to slow or prevent vision loss.
LOCATION:
Doheny Eye Institute, Pasadena
Jie J. Zheng, PhD
Professor of Ophthalmology
Director of the Therapeutic Development in Ophthalmology Laboratory
Member of the Molecular Biology Institute
Member of the Jonsson Comprehensive Cancer Center
Member of the Brain Research Institute
Member of the California NanoSystems Institute
Therapeutic Development in Ophthalmology
Dr. Zheng’s research is at the interface of biochemistry, computational biology, systems pharmacology, and drug discovery with an emphasis on therapeutic development in ophthalmology. His laboratory is currently developing proteins and small molecules that can modulate signal transduction pathways, such as Wnt, Hedgehog, BMP, and Hippo pathways, in an effort to better understand the biological functions of these signaling pathways and to explore the therapeutic potential of these compounds and proteins. Aiming to establish new translational research within the scientific community at UCLA, Dr. Zheng’s goal is to develop novel therapies for retinal degenerative diseases, glaucoma, and corneal disorders.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Joel Zylberberg, PhD
Associate Professor of Ophthalmology
Director of the Computational Visual Neuroscience Laboratory
Computational Visual Neuroscience and Artificial Intelligence
Dr. Zylberberg is a neuroscientist who studies the transmission of visual information along the optic nerve. His laboratory specializes in developing new computational frameworks—typically using machine learning and artificial intelligence—to integrate information from many different experiments.
Dr. Zylberberg completed his PhD in Physics at UC Berkeley and then underwent postdoctoral training at the University of Washington where he worked with retinal neuroscientist Fred Rieke and applied mathematician Eric Shea-Brown. He started his own laboratory and held his first faculty position at the University of Colorado School of Medicine before moving to York University in Toronto, where he served as Canada Research Chair in Computational Neuroscience. Dr. Zylberberg’s work has received funding from Google, the Sloan Foundation, National Institutes of Health, Canadian Institute for Advanced Research, and Canada’s Natural Sciences and Engineering Research Council. He joined UCLA in January 2025.
LOCATION:
UCLA Jules Stein Eye Institute, Westwood
Bruce Becker, MD
Health Sciences Clinical Professor of Ophthalmology
Olive View-UCLA Medical Center
Clinical Oculoplastics
Ekjyot Gill, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Olive View-UCLA Medical Center
Cornea
Hamid Hosseini, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Harbor-UCLA Medical Center
Retinal and Macular Conditions
Dr. Hosseini specializes in retinal and macular conditions, such as macular degeneration, diabetic retinopathy, and retinal detachment.
Dr. Hosseini completed two fellowships at the UCLA Jules Stein Eye Institute, the first in glaucoma and the second in retina.
Michael Kapamajian, MD
Associate Clinical Professor of Ophthalmology
Chief of Ophthalmology, Harbor-UCLA Medical Center
Uveitis/Glaucoma
Julie Kwon, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Olive View-UCLA Medical Center
Medical Retina/Ophthalmic Genetics
Ronald J. Smith, MD
Associate Physician Diplomate Veterans Affairs Greater Los Angeles Healthcare System
Objective Assessment of Surgical Technique and Training
Dr. Smith’s research interest is the objective assessment of surgical technique and development of evidence-based surgical training for residents to improve patient care. In addition to teaching residents at the Veterans Affairs Greater Los Angeles Healthcare System and in the UCLA Microsurgery Laboratory, Dr. Smith provides cornea and comprehensive eye care to patients at the Stein Eye Center–Santa Monica.
Jayanth Sridhar, MD
Associate Clinical Professor of Ophthalmology
Chief of Ophthalmology, Olive View-UCLA Medical Center
Medical and Surgical Treatment of Vitreoretinal Disease
A member of the Retina Division specializing in the medical and surgical treatment of vitreoretinal diseases, Dr. Sridhar is chief of ophthalmology at Olive View-UCLA Medical Center, where he supervises and teaches residents and surgical fellows. Dr. Sridhar completed his residency at the Bascom Palmer Eye Institute, University of Miami, and fellowship at Wills Eye Hospital, where he was named “Fellow of the Year.” He served on the faculty at Bascom Palmer for seven years, earning “Faculty of the Year” honors before transitioning to the UCLA Jules Stein Eye Institute. He has over 240 peer-reviewed publications and has earned several international commendations, including the American Academy of Ophthalmology Secretariat Award, the American Society of Retina Specialists Presidential Award, and induction into the prestigious Retina and Macular Societies.
Homayoun Tabandeh, MD
Health Sciences Associate Clinical Professor of Ophthalmology
Harbor-UCLA Medical Center
Retina
Mark Volpicelli, MD
Health Sciences Assistant Clinical Professor of Ophthalmology
Harbor-UCLA Medical Center
Cornea
UCLA Jules Stein Eye Institute Members Based at Other Sites
James W. Bisley, PhD
Ethel Scheibel Chair in Neuroscience Professor of Neurobiology and Psychology Member of the Brain Research Institute
Cognitive Processing of Visual Information
Dr. Bisley’s research revolves around understanding the neural mechanisms underlying the cognitive processing of visual information. These cognitive processes include visual perception, visual memory, visual attention, and the visual guidance of eye movements. Recent work has focused on how the responses of neurons in the posterior parietal cortex and prefrontal cortex are involved in the allocation of visual attention and how they guide eye movements in goaldirected visual search.
Aaron Savar, MD
Health Sciences Associate Clinical Professor of Ophthalmology
Veterans Affairs Greater Los Angeles Healthcare System
Oculoplastics
Patrick T. Dowling, MD, MPH
Chair, UCLA Department of Family Medicine
The Kaiser Endowed Professor of Community Medicine
Health Care Policy and Access for Underserved Populations
For 20 years, Dr. Dowling has received funding to link medical education to underserved neighborhoods. For a decade, several departments from UCLA have volunteered in the yearly event known as “Care Harbor,” providing 3,500 individuals with free medical, dental, and eye care. The UCLA Mobile Eye Clinic, led by Dr. Anne Coleman, provides free eyeglasses made onsite to low-income families and the homeless in LA County.
Professor of Medicine, Surgery, and Molecular and Medical Pharmacology
Malignant Melanoma
Dr. Ribas is a physician-scientist conducting laboratory and clinical translational research in how melanoma responds to or resists cancer immunotherapies, and developing gene engineered adoptive cell transfer therapies. He has been instrumental in the clinical development of several agents approved by the FDA, including the first anti-PD-1 pembrolizumab (Keytruda), the anti-CTLA-4 tremelimumab (Imjudo), and two combinations of BRAF and MEK inhibitors, vemurafenib (Zelboraf) and cobimetinib (Cotellic), and dabrafenib (Tafinlar) and trametinib (Mekinist).
Dario L. Ringach, PhD
Professor of Neurobiology and Psychology, Biomedical Engineering Program
Visual Perception and Neurophysiology
Dr. Ringach’s research focuses on the relationship between eye movements and visual perception, as well as how motor planning and execution, such as reaching, grasping, navigating, and adjusting body posture, is influenced by visual information and impaired vision. In collaboration with a team of neurosurgeons at UCLA, Dr. Ringach’s laboratory is also recording the brain activity of patients with epilepsy who are undergoing clinical evaluation for surgical treatment, shedding new light into the processes involved in object recognition and perception.
Christian Altenbach, PhD
Research Ophthalmologist (Recall)
Structure and Function of Rhodopsin
The membrane protein rhodopsin is a critical first step in visual transduction, converting light energy into a chemical form in the photoreceptor cell of the eye. To understand this process on a detailed molecular level, Dr. Altenbach is using site-directed spin labeling and electron paramagnetic resonance spectroscopy to study the structure of rhodopsin in the absence of light, as well as the changes in structure caused by light.
Michael Bridges, PhD
Assistant Project Scientist
Paramagnetic Resonance Methodologies
Dr. Bridges’ research in the laboratory of Dr. Wayne Hubbell is centered on the development and application of new pulsed electron paramagnetic resonance methodologies. Protein conformational dynamics and structural relaxation are his central focus with the goal of characterizing the timescales and motional amplitudes of functional activation.
Barry L. Burgess, BS
Research Specialist (Recall)
Degenerative Retinal Disease Research
Mr. Burgess provides research support for the Photoreceptor/RPE Cell Biology Laboratory of Dr. David Williams. Research interests include production of differentiated RPE cells from human stem cell precursors and developing in vitro models of oxidative stress involved in degenerative retinal disease progression.
Doug Chung, PhD
Assistant Project Scientist
Corneal Endothelial Biology and Disease
Dr. Chung’s research focus includes investigating the biology of the corneal endothelium, determining the utility of ex vivo expansion of human corneal endothelial cells for transplantation, and elucidating the mechanisms involved in the pathogenesis of inherited corneal endothelial dystrophies in an effort to develop novel therapeutic approaches.
Assistant Project Scientist
Photoreceptor and RPE Cell Biology
Dr. Paniagua’s research is primarily focused in studying the molecular mechanisms of the photoreceptor outer segment (POS) renewal. This key organelle for vision is formed as evaginations of the photoreceptor ciliary membrane and recycled in the daily ingestion of POS phagosomes by the retinal pigment epithelium. Both processes represent intrincated mechanisms affected in many types of retinal degeneration.
Rikard Frederiksen, PhD
Assistant Research Ophthalmologist
Adaptation
Dr. Frederiksen’s main research interest is adaptation, specifically how the rods and cones in the retina adapt to different light intensities.
Sheyla Gonzalez Garrido, PhD
Associate Project Scientist
Limbal Stem Cells
Dr. Garrido’s research aims to improve the ex vivo expansion of limbal epithelial stem cells (LSCs) by modulating Notch signaling in individuals suffering from limbal stem cell deficiency. The identification of niche factors could help to improve the in vitro production of LSCs for transplantation.
Somaye Jafari, PhD
Assistant Project Scientist
Yuekan Jiao, PhD
Research Specialist
Microscopy Specialist
Dr. Jiao’s work includes running and supporting the electron microscope and helping with image processing on the images from all the imaging platforms in the microscopy core. He also conducts eye research in collaboration with research labs at the Institute.
Joanna J. Kaylor, PhD
Associate Project Scientist
Visual Chromophore Regeneration in the Retina of the Eye
Dr. Kaylor’s research focuses on identification of biochemical pathways essential for visual chromophore production in the retina. She previously discovered an enzymatic complex that generates visual chromophore precursor, which sustains vision in bright light. She also revealed the presence of a non- enzymatic process that occurs in photoreceptor membranes that aids in chromophore regeneration. Dr. Kaylor is currently studying an enzyme she identified that is responsible for a unique visual chromophore processing activity present in cone photoreceptors.
Joseph Wekselblatt, PhD
Assistant Researcher
Cynthia A. Boxrud, MD
Associate Physician Diplomate
Orbital and Ophthalmic Plastic Surgery
Dr. Boxrud is a board-certified surgeon who specializes in oculofacial and reconstructive surgery, as well as orbital and ophthalmic oncology. She sees patients at the Stein Eye Center–Santa Monica.
Jane W. Chan, MD
Associate Physician Diplomate Doheny Eye Centers UCLA Neuro-Ophthalmology
As a physician-scientist at UCLA, Dr. Chan’s expertise in diagnosing and managing optic nerve disorders is widely recognized. Her acclaimed textbook, “Optic Nerve Disorders,” has become an indispensable reference, solidifying her reputation in the field. Dr. Chan’s cutting-edge research leverages multimodal retinal imaging techniques to explore biomarkers at the cellular and molecular levels in pre-Alzheimer’s disease. She sees patients at the Doheny Eye Center UCLA locations in Orange County and Pasadena.
Juliet Chung, MD
Associate Physician Diplomate
After ten years in private practice, Dr. Chung is returning to UCLA, her alma mater. She studied at UCLA for her undergraduate studies and also for her glaucoma fellowship. She is currently at the Stein Eye Center–Santa Monica.
Rachel Feit-Leichman, MD
Associate Physician Diplomate Cataract Surgery
Dr. Feit-Leichman divides her time between supervising residents and providing patient care at the Jules Stein Eye Institute’s Urgent Care Clinic, and teaching cataract surgery and overseeing residents at the ophthalmology clinic of the Harbor-UCLA Medical Center. Dr. Feit-Leichman is also active in striving to improve patient access to eye care in the greater Los Angeles County Healthcare System.
Reza Ghaffari, MD
Associate Physician Diplomate
Cornea and External Ocular Disease
Dr. Ghaffari’s clinical focus is cornea and external ocular disease, including corneal transplantation (full thickness and lamellar), artificial cornea, keratoconus, and management of ocular surface disease. Dr. Ghaffari has contributed to peer-reviewed publications in fields such as corneal imaging, outcomes of Boston keratoprosthesis implantation, and complications of cosmetic iris implants. Dr. Ghaffari’s research interests include outcomes of keratoprosthesis implantation and corneal transplantation.
Batool Jafri, MD
Associate Physician Diplomate Cornea/External Disease/ Refractive Surgery
Dr. Jafri’s practice interests are cataract surgery, LASIK, keratoconus, glaucoma, diabetic retinopathy, dry eye, and allergic conjunctivitis. She offers subspecialized surgical care including LASIK, refractive cataract surgery, pterygium excision, ocular surface disease management, treatment of ocular surface malignancies, implantable contact lens, corneal transplantation, and corneal collagen crosslinking for keratoconus. She offers personalized, world-class care to all of her patients. Dr. Jafri sees patients at the Stein Eye Center in Santa Monica.
Justin Karlin, MD, MS
Health Sciences Assistant Clinical Professor of Ophthalmology
Orbital, Lacrimal, and Ophthalmic Plastic Surgery
Dr. Karlin specializes in orbital, lacrimal, and oculofacial plastic surgery. He has developed artificial intelligence diagnostic tools, cartilage grafts for use in eyelid reconstruction, and novel approaches to the production of autologous plasma eye drops.
He graduated from the rigorous ASOPRS fellowship at the UCLA Jules Stein Eye and Doheny Eye Institutes in 2020.
As a resident, he was awarded the University of Virginia “All University” Teaching Award and was honored with the UCLA Jules Stein Eye Institute Fellow Teaching Award in 2019. He continues to participate actively in mentoring and teaching activities for undergraduates, medical students, residents, and fellows.
Phillip Le, MD, PhD
Associate Physician Diplomate Retinal and Macular Diseases
Dr. Le is a comprehensive ophthalmologist who specializes in retinal and macular diseases. He sees patients at the Doheny Eye Center UCLA–Pasadena.
Nariman Nassiri, MD
Associate Physician Diplomate Diagnosis and Treatment of Glaucoma
Dr. Nassiri’s research focuses on two areas: The first is drug delivery systems in ocular diseases, which includes developing biodegradable implants, adhesive patches, and microneedles, with the aim of enhancing treatment efficacy. The second is to gain better understanding of the pathogenesis of glaucoma.
Christine V. Nguyen, MD
Associate Physician Diplomate Doheny Eye Centers UCLA
Tania Onclinx, MD
Associate Physician Diplomate Urgent Care and Clinical Supervision
Dr. Onclinx attends at the Urgent Care Walk-In service at the Jules Stein Eye Institute, and she teaches resident physicians and medical students at the Jules Stein Eye Institute during their subspecialty clinical rotation. She also provides clinical supervision to resident physicians at Ronald Reagan UCLA Medical Center and UCLA Medical Center, Santa Monica.
Susan S. Ransome, MD
Associate Physician Diplomate HIV and Diabetic Retinopathy
Dr. Ransome is participating in a clinical research study involving HIV- infected patients who have diabetes to see whether there is increased risk of development or progression of diabetic retinopathy when subjects are treated for abdominal lipodystrophy with Egrifta (tesamorelin).
Meryl L. Shapiro-Tuchin, MD
Associate Physician Diplomate Co-Director of the Ophthalmology Inpatient Consultation Service
Comprehensive Ophthalmology
Dr. Shapiro-Tuchin provides clinical supervision to resident physicians. She functions as co-director of the Ophthalmology Inpatient Consultation Service, assisting resident physicians in their evaluation of inpatients admitted to the Ronald Reagan UCLA Medical Center and the UCLA Medical Center, Santa Monica.
Ronald J. Smith, MD
Associate Physician Diplomate
Objective Assessment of Surgical Technique and Training
Dr. Smith’s research interest is the objective assessment of surgical technique and development of evidence-based surgical training for residents to improve patient care. In addition to teaching residents at the Veterans Affairs Greater Los Angeles Healthcare System and in the UCLA Microsurgery Laboratory, Dr. Smith provides cornea and comprehensive eye care to patients at the Stein Eye Center–Santa Monica.
Laura A. Syniuta, MD
Associate Physician Diplomate
Pediatric Ophthalmology and Strabismus
Dr. Syniuta completed her fellowship training in pediatric ophthalmology and strabismus at the Jules Stein Eye Institute in 1999. With children’s eye and learning disorders being her passion, she sees patients at the Stein Eye Center–Santa Monica and has staffed the UCLA Mobile Eye Clinic since 2011.
Associate Physician Diplomate
UCLA Mobile Eye Clinic
Dr. Young is a glaucoma specialist and provides comprehensive ophthalmic care. He has staffed the UCLA Mobile Eye Clinic since 2008. His research interests include pediatric vision epidemiology and eye health screenings in community-based settings.
Dean Bok, PhD
Dolly Green Chair of Ophthalmology
Professor of Ophthalmology Emeritus
Distinguished Research Professor of Neurobiology
Member of the Brain Research Institute
Joseph Caprioli, MD
David May II Chair in Ophthalmology
Distinguished Professor of Ophthalmology Emeritus (Active Recall)
Vice Chair of Quality Past Chief of the Glaucoma Division
Richard Casey, MD
Health Sciences Clinical Professor of Ophthalmology Emeritus
Gordon L. Fain, PhD
Distinguished Professor of the Departments of Integrative Biology/ Physiology Emeritus
Professor of Ophthalmology Emeritus (Active Recall)
Debora B. Farber, PhD, DPhhc
Distinguished Professor of Ophthalmology Emeritus
Doctor honoris causa
Member of the Brain Research Institute
Member of the Molecular Biology Institute
Lynn K. Gordon, MD, PhD
Professor of Ophthalmology Emeritus (Active Recall)
Emeritus Senior Associate Dean for Equity and Diversity Inclusion
Michael O. Hall, PhD
Professor of Ophthalmology Emeritus
Founding Member of the Jules Stein Eye Institute
Robert S. Hepler, MD
Professor of Ophthalmology Emeritus
Founding Chief, Neuro-Ophthalmology Division
Joseph Horwitz, PhD
(died October 23, 2024)
Distinguished Professor of Ophthalmology Emeritus
Wayne L. Hubbell, PhD
Jules Stein Chair in Ophthalmology
Distinguished Professor of Ophthalmology Emeritus (Active Recall)
Distinguished Professor of Chemistry and Biochemistry Emeritus Director of the Ophthalmic Biophysical Chemistry Laboratory
John A. Irvine, MD
Health Sciences Clinical Professor of Ophthalmology (Active Recall)
Co-Medical Director, Doheny Eye Centers UCLA
Sherwin J. Isenberg, MD
Distinguished Professor of Ophthalmology and Pediatrics Emeritus
Ralph D. Levinson, MD
Health Sciences Clinical Professor of Ophthalmology Emeritus
Bartly J. Mondino, MD
Distinguished Professor of Ophthalmology Emeritus (Active Recall)
Director Emeritus, Jules Stein Eye Institute
Chair Emeritus, UCLA Department of Ophthalmology
Affiliation Chair Emeritus, Doheny Eye Institute
President, Jules and Doris Stein UCLA
Support Group
Member, UCLA Brain Research Institute
Steven Nusinowitz, PhD
Professor of Ophthalmology Emeritus (Active Recall)
Co-Director of the Visual Physiology Laboratory
Bradley R. Straatsma, MD, JD
Professor of Ophthalmology Emeritus
Founding Chair, Department of Ophthalmology
Founding Director, Jules Stein Eye Institute
Deming Sun, MD
Professor of Ophthalmology Emeritus
Barry A. Weissman, OD, PhD
Professor of Ophthalmology Emeritus
Marc O. Yoshizumi, MD
Professor of Ophthalmology Emeritus
RESIDENTS AND FELLOWS
Residents
THIRD-YEAR RESIDENTS
2022–2025
Angela Chen, MD
Erika Ellis, MD, PhD
Elise Ma, MD
Lukas Mees, MD
Yaqoob Qaseem, MD
Sagar Rambhia, MD (EyeMBA)
Junru Yan, MD
Kelly Yom, MD
SECOND-YEAR RESIDENTS 2023–2026
John Cheng, MD
Leila Chew, MD
Bradley Gundlach, MD
Ken Kitayama, MD, PhD (EyeSTAR)
Alan Kong, MD
David Peprah, MD
Weilin Song, MD
Sydney Wendt, MD
FIRST-YEAR RESIDENTS 2024–2027
Sara Emami, MD, MSc
David Hsu, MD
Matthew Miller, MD
Erin Napier, MD
Ethan Osias, MD
Jason Strawbridge, MD
Jessica Tran, MD, MSCR
Maria Villalba, MD, MS
EyeSTAR Trainees
Ken Kitayama, MD, PhD
Elise Ma, MD
EyeMBA Trainee
Sagar H. Rambhia, MD
EyeSTAR Genetics Trainee
Emile Vieta, MD (EyeSTAR Genetics)
Cornea/External Ocular Diseases and Refractive Surgery
Roxana Godiwalla, MD (Doheny Eye Centers UCLA)
Christian Bardan, MD
Bryan Zarrin, MD
Glaucoma
Adam Tanaka, MD, MPH (Doheny Eye Centers UCLA)
Robert Gunzenhauser, MD
Alexandra Schulte, MD
Medical Retina and Ophthalmic Genetics
Marko Popovic, MD
Neuro-Ophthalmology
Thanh-Liem Huynh-Tran, MD
Orbital and Ophthalmic Plastic Surgery
Katherine Lucarelli, MD
Angela Oh, MD
Pathology (Eye)
None
Pediatric Ophthalmology and Strabismus
Mona Fayad, MD
Uveitis and Inflammatory Eye Disease
None
Vitreoretinal Diseases and Surgery
Adrian Au, MD, PhD
Blake Fortes, MD
A. Itzam Marin, MD
Cherilyn Palochak, MD
Prashant Tailor, MD
Cornea Research
Faycal Moujane, MD Belgium
Comprehensive Ophthalmology/ Cataract
None
Glaucoma
Kwanghyun Lee, MD South Korea
Abbas Habibi, MD Iran
Sajad Besharati, MD Iran
Maryam Ashrafkhorasani, MD Iran
Medical Retina and Ophthalmic Genetics
Ahmad Santina, MD Lebanon
Alessandro Feo, MD Italy
Shahin Faghihi Habibabadi, MD Iran
Tal Eshkoly Lior, MD Israel
Neuro-Ophthalmology
Maryam Golmohommadi, MD Iran
Orbital and Ophthalmic Plastic Surgery
Maria Paula Quintero Mutis, MD Colombia
Pediatric Ophthalmology
Veronika Yehezkeli, MD Israel
Qing-Yu Meng, MD China
Uveitis
none
Visual Physiology
None
Vitreoretinal Diseases and Surgery
Hyunduck Kwak, MD
China
Yu-Chien Chung, MD
Taiwan
Rouzbeh Abbasgholizadeh, MD
Turkey
Ceren Soylu, MD
Turkey
Mostafa Mafi, MD
Iran
Kangyeun Pak, MD
South Korea
Predoctoral Research Fellows
Marissa Balagtas
Bita Behziz
Martina Cavallini
Mengzhen Chen
Tierney Daw
Niloufar Ghazavi
Peipei Melody Huang
Kyle Kim
Ravi Komirisetty
Christopher Meredith
Manuel Mora
Karla Murillo
Atharva Shetye
Nathan Siu
Alejandro Torres
Postdoctoral Research Fellows
Mahesh Agarwal, PhD
Sathish Baggam, PhD
Paul Bonezzi, PhD
Priyanka Boro, PhD
Mengzhen Chen, PhD
Arpita Dave, PhD
Lei Fu, PhD
Alejandro Gallego-Ortega, PhD
Juanzi Gao, PhD
Mihir Ghosh, PhD
Rajesh Goit, PhD
Roni Hazim, PhD
Nan Hultgren, PhD
Menglin Li, PhD
Declan Rowley, PhD
Maxime Ruiz, PhD
Saki Sakakura, PhD
Chao Sui, PhD
Jhuwala Venkatakrishnan, PhD
Junqiang Wang, PhD
Xiaoyu Wang, PhD


ADMINISTERED BY THE STEIN EYE INSTITUTE
Faculty
Anthony J. Aldave, MD
AAV Gene Therapy for Treating Biallelic SLC4A11 Mutations
Associated Congenital Hereditary Endothelial Dystrophy
California Institute for Regenerative Medicine (CIRM)
Duration: 8/1/23–1/31/26
$970,000
Ava K. Bittner, OD, PhD
Scanning and Detection at Intersections Schepens Eye Research Institute, The (AFF. w/ Harvard Univ.)
Duration: 9/1/22–8/31/25
$19,233
Beacon Sensors and Telerehabilitation to Assess and Improve Use of Devices for Visual Functioning (BeST-AID)
NIH-National Eye Institute
Duration: 9/30/23–6/30/28
$359,984
Anne L. Coleman, MD, PhD
Impact of Routine Eye Care Coverage on Access to Eye Care and Fall-Related Outcomes Among Low-Income Medicare Enrollees
UCI/NIH-National Eye Institute
Duration: 2/1/23–5/31/26
$65,096
Impact of Routine Eye Care Coverage on Access to Eye Care and Fall-Related Outcomes Among Low-Income Medicare Enrollees
San Diego State University
Research Foundation
Duration: 6/1/22–9/30/26
$22,842
RPB Unrestricted Grant
Research to Prevent Blindness, Inc.
1/1/12–12/31/26
$150,000
Karla Murillo
(Dr. Anne Coleman, mentor)
Examining Mobile Health and Telehealth Applications to Extend Access to Ophthalmic Care to Underserved Rural Communities
Research to Prevent Blindness, Inc.
Duration: 7/1/23–6/1/25
$30,000
Protecting Vision Through Occupational Eye Clinics for Day Laborers
California Healthcare Foundation
Duration: 8/1/23–10/15/25
$50,000
UCLA Mobile Eye Clinic Program (UMEC)
Fox Family Foundation
Duration: 10/1/22–10/1/25
$100,000
Joseph L. Demer, MD, PhD
Biomechanical Analysis in Strabismus Surgery
NIH-National Eye Institute
Duration: 6/1/24–5/31/29
$668,209
Sophie X. Deng, MD, PhD
Safety and Feasibility of Cultivated Autologous Limbal Stem Cells for Limbal Stem Cell Deficiency
California Institute for Regenerative Medicine (CIRM)
Duration: 12/1/19–4/30/27
$2,350,000
Extracellular Vesicle-based Therapy for Corneal Scars
California Institute for Regenerative Medicine (CIRM)
Duration: 8/1/23–1/31/26
$646,710
Gordon L. Fain, PhD
Physiology of Photoreceptors
NIH-National Eye Institute
Duration: 1/1/22–12/31/26
$351,000
Greg D. Field, PhD
Visual Signaling from Retina to Superior Colliculus
NIH-NEI National Eye Institute
Duration: 5/1/23–4/30/29
$524,104
Molecular and Cellular Requirements for Crb1 Gene Function in the Onset and Therapeutic Rescue of an Inherited Retinal Degeneration
NIH-National Eye Institute
Sub-award from Duke University
Duration: 2/1/24–11/30/28
$71,544
High-Resolution Measurement of Natural Stimuli and Ethologically Relevant Behavior as Platform for Understanding the Nervous System
NIH-National Institutes of Drug Abuse
Sub-award from Duke University
Duration: 2/25/24–1/31/26
$32,441
Plasticity and Function of the Rod/Cone Gap Junction
Sub-award from University of Houston
NIH-National Eye Institute
Duration: 5/1/23–4/30/27
$68,381
Dynamic Coding in Retinal Dynamics
Sub-award from the University of Washington
NIH-National Eye Institute
Duration: 9/1/2024–5/31/2029
$320,380
Alex Huk, PhD
Mechanisms of Persistent
Neural Activity
NEI-National Eye Institute
Duration: 5/1/2023–4/30/2027
$2,092,080
Michael Ip, MD
A Randomized Trial Evaluating Fenofibrate for Prevention of Diabetic Retinopathy Worsening
NIH-National Eye Institute
Sub-contract from Jaeb Center for Health Research
Duration: 4/11/25–12/31/28
$174,959
Kouros Nouri-Mahdavi, MD
Detection of Disease Progression in Advanced Glaucoma
National Eye Institute
Duration: 3/1/20–2/28/26
$387,500
Yi-Rong Peng, PhD
Deciphering the Molecular Underpinnings of Foveal Formation Research to Prevent Blindness, Inc.
Career Development Award
Duration: 1/1/22–12/31/26
$100,000
Transcriptional Control of Neuronal Position and Connection in the Retina
NIH-National Eye Institute
Duration: 6/1/24–5/31/29
$393,646
Decoding the Formation of Degeneration of Neural Circuits via Cell-Type-Specific Surface Proteomics
Brain Research Foundation
Duration: 6/1/24–5/31/26
$80,000
Stacy L. Pineles, MD
Pediatric Eye Disease
Investigator Group (PEDIG) and Jaeb Center for Health Research
Duration: 1/1/19–12/31/28
$231,200
Randomized Trial of Dichoptic Treatment for Amblyopia in Children 4 to 7 Years of Age
Pediatric Eye Disease Investigator Group (PEDIG) and Jaeb Center for Health Research
Duration: 10/28/24–12/31/28
$6,900
Alapakkam P. Sampath, PhD
Vision Science Training Program
National Eye Institute
Duration: 9/1/22–8/31/27
$172,794
Instrumentation Grant for Stein Eye Investigators
Bruce Ford and Anne Smith Bundy Foundation
Duration: 8/16/24–8/15/25
$100,000
Molecular Basis of Photoreceptor Wiring
National Eye Institute
Sub-award from University of Florida
Duration: 5/1/24–4/30/28
$128,233
Physiology of Retinal Degeneration
NIH-National Eye Institute
Duration: 5/1/25–4/30/29
$449,920
David Sarraf, MD
In Vivo Ultrastructure of Chorioretinal Disease
NIH-National Eye Institute
Sub-award from Doheny Eye Institute
Duration: 9/30/21–8/31/24
$21,146
In Vivo Characterization of Retinal Hemodynamics
NIH-NEI National Eye Institute
Sub-award from Doheny Eye Institute
Duration: 9/30/22–7/31/26
$73,975
Gabriel H. Travis, MD
Mechanisms for Light-Driven Chromophore Synthesis by Müller Cells to Regenerate Cone Opsin and Maintain Cone Sensitivity
NIH-National Eye Institute
Duration: 1/1/20–12/31/25
$430,727
Functional Characterization of the ABCA4 Transporter in Photoreceptors from a Zebrafish Model of Recessive Stargardt Disease
Research to Prevent Blindness, Inc.
Duration: 7/1/2021–3/31/2025
$300,000
Victoria L. Tseng, MD, PhD
Neovascular Glaucoma: Individual and Neighborhood-Level Associations with Incidence and Outcomes in the California Medicare Population Research to Prevent Blindness, Inc.
1/1/23–12/31/27
$150,000
Edmund Tsui, MD, MS
Objective Measures of Intraocular Inflammation in Pediatric Anterior Uveitis
NIH-National Eye Institute
Duration: 9/1/21–7/31/26
$246,583
Objective Quantification of Vitreous Inflammation Using Optical Coherence Tomography
NIH-National Eye Institute
Duration: 2/1/23–1/31/26
$249,988
Adalimumab Levels in Induction Control for Chronic Anterior Uveitis
Sub-award from Children’s Hospital of Philadelphia
Childhood Arthritis and Rheumatology Research Alliance (CARRA)
Duration: 7/1/2024–4/14/2026
$2,156
Irena Tsui, MD
Neonatal Optical Coherence
Tomography Angiography to Assess the Effects of Postnatal Exposures on Retinal Development and Predict Neurodevelopmental Outcomes
NIH-National Eye Institute
Duration: 7/1/23–6/30/27
$406,750
David S. Williams, PhD
Vision Research Core at UCLA
National Eye Institute
Duration: 9/1/20–6/30/25
$779,998
Cellular Mechanisms of Photoreceptor Disk Morphogenesis
NIH-NEI National Eye Institute
Duration: 5/1/22–3/31/26
$458,936
Outer Segment Tip Ingestion by the RPE
NIH-National Eye Institute
Duration: 1/1/25–12/31/29
$301,868
Roni Hazim, PhD
(Dr. David Williams, mentor)
In-Depth Molecular Studies of Dynein Transport in the RPE
NIH-National Eye Institute
Duration: 6/1/23–5/31/25
$208,798
Nan Hultgren, PhD
(Dr. David Williams, mentor)
Understanding How Mitochondrial Interaction with Other Organelles in the Retinal Pigment Epithelium (RPE)
Affect Its Function in the Outer Retina
NIH-National Eye Institute
Duration: 1/1/24–12/31/25
$229,650
Xian-Jie Yang, PhD
Metabolism and Neuronal Viability of the Retina
NIH-NEI National Eye Institute
Duration: 9/30/22–7/31/26
$390,000
Yuhua Zhang, PhD
In Vivo Characterization of Metabolic Function of Photoreceptors and Retinal Pigment Epithelium Cells in Age-Related Macular Degeneration Research to Prevent Blindness, Inc.
Duration: 1/1/22–12/31/27
$150,000
In Vivo Imaging of the Human Retina at the Molecular Level
NIH-National Eye Institute and Doheny Eye Institute
Duration: 3/1/24–2/28/28
$105,142
Joel Zylberberg, PhD
Dynamic Coding in Retinal Dynamics
Sub-award from the University of Washington
NIH-National Eye Institute
Duration: 9/1/2024–5/31/2029
$145,479
CIFAR Fellow Award for Learning in Machines and Brains
Canadian Institute for Advanced Research (CIFAR)
Duration: 4/1/2025–3/31/2026
$20,721
ADMINISTERED BY THE DOHENY
Steven Barnes, PhD
Visual Processing by GABA-pH Hybrid Feedback at the Photoreceptor Synapse
The Plum Foundation
Duration: 7/22/20–9/30/25
$110,000
Retinal Ganglion Cell Signaling Regulated by Intrinsic Oxygen Species
National Eye Institute
Duration: 8/1/23–3/31/28
$250,000
[Physiology] Intrinsic Ion Channels Reduce Excitability During Energy Stress
Glaucoma Research Foundation
Duration: 3/1/25–2/28/26
$27,500
Deborah Ferrington, PhD
Role of Immunoproteasome in Airway Viral Infection
National Jewish Health
Sub-award on NIAID Grant AI50082
Duration: 5/1/22–4/30/25
$83,999
Deciphering Mechanisms Associated with High-Risk AMD Genotypes for ARMS/HTRA1 and Complement Factor H
National Eye Institute
Duration: 9/30/22–8/31/25
$282,116
Mitochondrial Defects in the Retinal Pigment Epithelium and the CFH Risk Allele for Age-Related Macular Degeneration
National Eye Institute
Duration: 9/30/22–6/30/26
$500,306
Ram Kannan, PhD
Novel Mechanism of Subretinal Fibrosis in Age-Related Macular Degeneration
National Eye Institute
Duration: 5/1/20–4/30/25
$309,041
Therapeutic Strategies for Mitochondrial-Based Optic Diseases via Upregulation of OPA1 Expression and Mitochondrial Function in RPE Using Antisense Oligonucleotides, Part 2
Stoke Therapeutics, Inc.
Duration: 12/8/23–7/31/25
$147,912
Therapeutic Strategies for Mitochondrial-based Optic Diseases via Upregulation of OPA1 Expression and Mitochondrial Function in RPE Cells Using Antisense Oligonucleotides, Part 3
Stoke Therapeutics, Inc.
Duration: 2/20/25–2/20/26
$179,239
SriniVas R. Sadda, MD
Functionally Validated Structural Endpoints for Early AMD University of Alabama at Birmingham
Sub-award on NEI Grant EY029595
Duration: 5/1/19–2/28/25
$158,464
Epidemiology of Biomarkers of AMD Progression
National Eye Institute
Duration: 9/30/21–8/31/27
$481,737
iSafe/VCCM
NASA/KBR Wyle
Sub-award on NASA Prime Duration: 10/1/19–9/30/26
$18,187
NASA SANSA
NASA
Sub-award from University of California, San Diego
Duration: 8/22/22–8/21/25
$27,582
In vivo Imaging of the Human Retina at the Molecular Level
National Eye Institute
Duration: 3/1/24–2/29/28
$413,020
Alfredo Sadun, MD, PhD
National Institute on Aging
Sub-award on Cedars-Sinai Prime Duration: 9/30/23–6/30/28
$15,000
Deming Sun, MD
Role of IL-17+ Autoreactive T Cells in Experimental Autoimmune Uveitis (EAU)
National Eye Institute
Duration: 1/1/20–12/31/24
$270,547
Yuhua Zhang, PhD
In Vivo Ultrastructure of Chorioretinal Disease
National Eye Institute
Duration: 1/1/15–8/31/25
$258,566
In Vivo Characterizations of Retinal Hemodynamics
National Eye Institute
Duration: 9/30/22–7/31/26
$270,721
Novel Retinal Higher-Order Capillary Hemodynamics Imaging for Detecting Cerebral Small Vessel Disease
National Institute of Health
Sub-award on University of Miami Prime
Duration: 9/15/24–9/14/25
$250,000
ADMINISTERED BY UCLA
Anthony J. Aldave, MD
A Phase IIa, Randomized, Double-Masked, Placebo-Controlled, Parallel-Group, Multicenter Study
Assessing the Efficacy and Safety of STN1010904 Ophthalmic Suspension
0.03% and 0.1% Compared with Vehicle in Subjects with Fuchs Endothelial Corneal Dystrophy (FECD)
PHANTOM Study
Duration: 2/3/23–2/2/27
$144,089
A Phase 2, Multicenter, Randomized, Controlled, Double-Masked, Clinical Trial to Evaluate the Efficacy and Safety of OC-01 (Varenicline) Nasal Spray in Subjects with Neurotrophic Keratopathy (the Olympia Study) (Protocol# OPP-102)
Oyster Point Pharma, Inc.
Duration: 8/11/21–8/10/25
$53,936
A Phase 2, Randomized, Prospective, Double-Masked, Vehicle-Controlled Study to Assess the Efficacy and Safety of Nexagon® (NEXAGON) Applied Topically in Subjects with Corneal Persistent Epithelial Defects (PED) Resulting from Severe Ocular Chemical and Orthermal Injuries
(Protocol# NEX-PED-005)
OcuNexus Therapeutics, Inc.
Duration: 3/8/22–3/7/26
$45,775
A Study to Evaluate the Safety and Efficacy of KPI-012 Ophthalmic Solution in Participants with Persistent Corneal Epithelial Defect (PCED) (Protocol # KPI-012-C-001) Combangio, Inc.
Duration: 3/26/24–3/25/28
$121,887
Diabetes Endothelial Keratoplasty Study (DEKS): Impact of Diabetes on Corneal Transplant Success and Endothelial Cell Loss
JAEB Center for Health Research
Duration: 1/27/22–4/30/26
$15,000
Benjamin B. Bert, MD
Observational Study of Conjunctivitis of Dupixent Treatment for Atopic Dermatitis
Regeneron Pharmaeuticals
Duration: 3/11/21–3/10/26
$163,828
Clémence Bonnet, MD, PhD
Structural and Functional Changes of Corneal Innervation After Treatment with Cenegermin
Dompé S.p.A. (20-000833)
Duration: 3/12/20–5/31/26
$287,946
Sophie X. Deng, MD, PhD
A Multi-Center, Randomized, Double-Masked, Vehicle-Controlled, Parallel-Group, Study to Evaluate the Safety and Efficacy of CSB-001 Ophthalmic Solution 0.1% in Stage 2 and 3 Neurotrophic Keratitis Subjects
Claris Biotherapeutics, Inc.
Duration: 9/9/21–9/8/25
$95,196
ST266-PED-202
Noveome Biotherapeutics, Inc.
Duration: 2/8/22–2/7/26
$202,440
Brian A. Francis, MD, MS
A Prospective, Multicenter Clinical Study to Evaluate the Safety and Effectiveness of Ab Externo Implantation of Glaucoma Gel Stent
AbbVie, Inc.
Duration: 5/9/23–12/31/25
$181,974
Michael B. Gorin, MD, PhD
ALK-001 (16-0116)
Alkeus Pharmaceuticals
Duration: 5/23/16–11/20/25
$57,395
SOLSTICE (20-000696)
NightstaRX
Duration: 11/17/20–11/16/25
$377,557
Michael Ip, MD
ADV-022-11 (22-1082)
Adverum Biotechnologies
Duration: 10/26/22–10/25/26
$210,189
ALXN2040-GA-201 (21-1957)
Alexion Pharmaceuticals, Inc.
Duration: 11/21/22–11/20/26
$297,870
ISEE2008
IVERIC Bio, Inc.
Duration: 7/1/20–7/1/25
$232,530
ISEE2009 (23-5018)
IVERIC Bio, Inc.
Duration: 6/9/23–6/8/27
$104,643
OTT166-201 (22-1019)
OcuTerra Therapeutics, Inc.
Duration: 12/20/22–12/19/26
$221,534
OTX-TKI-2023-AMD-301 (24-5013)
Ocular Therpautix, Inc.
Duration: 7/10/24–7/9/28
$388,321
RGX-314-2104 (21-1374)
REGENXBIO, Inc.
Duration: 12/2/21–12/1/25
$395,430
RGX-314-5101
REGENCXBIO, Inc.
Duration: 12/20/24–12/19/28
$141,921
KS301P103 (21-0073)
Kodiak Sciences, Inc.
Duration: 9/22/21–9/21/25
$162,638
KS301P105
Kodiak Sciences, Inc.
Duration: 9/23/21–9/23/25
$80,068
APL2-GA-305 (21-0534)
Apellis Pharmaceuticals
Duration: 11/4/21–11/3/25
$364,425
Colin A. McCannel, MD
GR40549
Genentech, Inc.
Duration: 11/26/18–4/10/25
$571,210
Tara A. McCannel, MD, PhD
AU-011-202
Aura Biosciences, Inc.
Duration: 4/16/21–4/15/25
$268,788
AU-011-301
Aura Biosciences, Inc.
Duration: 8/11/25–8/10/29
$237,997
Daniel B. Rootman, MD, MS
VGN-TED-301 (22-0271)
Sling Therapeutics
Duration: 12/16/22–12/15/26
$150, 932
VGN-TED-302 (24-5105)
Sling Therapeutics
Duration: 3/27/24–5/6/28
$199,594
SriniVas R. Sadda, MD
Belite Bio
Phase 3, Multicenter, Randomized, Double-masked Placebo-Controlled Study of Tinlarebant to Explore Safety and Efficacy in the Treatment of Geographic Atrophy (the PHOENIX Study)
Duration: 11/29/23–11/28/27
$205,628
Boehringer-Ingelheim
Diabetic Muscular Ischemia in Patients with Diabetic Retinopathy Treated with Panrental Photocoagulation
Duration: 2/9/2021–10/27/2025
$136,027
Alfredo A. Sadun, MD, PhD
GS-LHON-CLIN-05
GenSight Biologics
Duration: 8/23/18–7/28/25
$0
Edmund Tsui, MD, MS
ADalimumab Versus Conventional ImmunoSupprEssion for Uveitis (ADVISE) Trial
National Eye Institute
Sub-award from Johns Hopkins University
Duration: 9/30/18–8/31/25
$30,000
Kowa FM-700
Kowa Research Institute, Inc.
Duration: 2/1/20–4/25/25
$0
21103
Acelyrin, Inc.
Duration: 9/27/22–9/26/26
$251,971
The LEOPARD Study: Efficacy and Safety of Dexamethasone
Ophthalmic Suspension Eye Drops in Uveitic and Postsurgical Macular Edema
Global Ophthalmic Research Center
Duration: 5/20/23–5/19/25
$472,634
GR44277
Genentech, Inc.
Duration: 2/22/23–2/22/27
$435,299
PVT-2201-201
Priovant Therapeutics, Inc.
Duration: 2/14/23–2/13/27
$92,378
PVT-2201-303
Priovant Therapeutics, Inc.
Duration: 10/23/24–10/23/28
$280,931
Imaging Biomarkers in Juvenile Idiopathic Arthritis-Associated Uveitis
Pfizer Health Solutions Inc.
Duration: 6/16/21–6/30/24
$150,000
Comparison of Biometry Measurements Using Cylite HP-OCT and Argos SS-OCT in Dense Cataracts
Cylite Pty Ltd.
Duration: 1/18/21–1/17/26
$25,573
RECRUITING IN FISCAL YEAR 2025
ATS23 Amblyopia (24-5245)
Amblyopia Treatment Study 23 is a randomized trial of dichoptic treatment for amblyopia in children 4 to 7 years of age. Investigator: Stacy Pineles, MD.
AU-011
AU-011 is a phase 3 trial of belzupacap sarotalocan (AU-011) treatment versus sham in subjects with primary indeterminate lesions or small choroidal melanoma. Investigator: Tara McCannel, MD.
CHOP-ADA Level Uveitis (24-5326)
CHOP-ADA Level Uveitis is a study evaluating Adalimubab levels in induction control for chronic anterior uveitis. Investigators: Edmund Tsui, MD, and Judy Chen, MD.
Gene Therapy Study for GA
Secondary to AMD (22-5125)
A phase 2b, randomized, doublemasked, multicenter, dose-ranging, sham-controlled clinical trial to evaluate intravitreal JNJ-81201887 (AAVCAGsCD59) compared to sham procedure for the treatment of geographic atrophy (GA) secondary to age-related macular degeneration (AMD). Investigators: Prasad Pradeep, MD, Adrian Au, MD, Aya Barzelay Wollman, MD, Blake Fortes, MD, Hamid Hosseinin, MD, David Lozano, MD, Moritz Pettenkofer, MD, Melanie Schmitz, NP, Jiwei Sheng, MD, and Stefanie Uechi, NP.
IDE196-009 Ocular Melanoma (23-001460)
Neoadjuvant IDE196 (Darovasertib) in patients with localized ocular melanoma (IDE196-009). Investigators: Tara McCannel, MD, Adrian Au, MD, Bartosz Chmielowski, MD, Meetal Dharia, MD, John Glaspy, MD, Alejandro Marin, Cherilyn Palochak, MD, Antoni Ribas, MD, Prashant Tailor, MD, and Deborah Wong, MD.
ISEE2009 Macular Degeneration (23-5018)
An open-label extension (OLE) phase 3 trial to assess the safety of intravitreal administration of Avacincaptad Pegol (complement C5 inhibitor) in patients with geographic atrophy who previously completed phase 3 study ISEE2008 (GATHER2). Investigators: Michael Ip, MD, Adrian Au, MD, Hamid Hosseini, MD, Moritz Pettenkofer, MD, and Pradeep Prasad, MD, MBA.
Jaeb Protocol AF Non-proliferative Diabetic Retinopathy (24-5762)
A randomized clinical trial evaluating fenofibrate for prevention of diabetic retinopathy worsening (Protocol AF). Investigators: Michael Ip, MD, Kirk Hou, MD, and Gad Heilweil, MD.
K-321-301 (23-5047)
A double-masked, randomized, placebo-controlled, parallel-group, 12-week administration with twoweek gradual dose taper phase and 38-week follow-up phase, phase 3 study to investigate the safety and efficacy of ripasudil (K-321) eye drops after descemetorhexis in subjects with Fuchs endothelial corneal dystrophy. Investigators: Sophie X. Deng, MD, PhD, and Anthony J. Aldave, MD.
KPI-012 Ophthalmic Solution (23-5170)
A study to evaluate the safety and efficacy of KPI-012 ophthalmic solution in participants with persistent corneal epithelial defect (PCED). Investigators: Anthony J. Aldave, MD, Seyed Reza Ghaffari, MD, Melanie Schmtz, NP, and Stefanie Uechi, NP.
MEERKAT Study (Genentech) (22-5108)
A phase III, multicenter, randomized, double - masked, sham - controlled study to investigate the efficacy, safety, pharmacokinetics, and pharmacodynamics of RO7200220 administered intravitreally in patients with uveitic macular edema. Investigators: Edmund Tsui, MD, Adrian Au, MD, Judy Chen, MD, Blake Fortes, MD, Moritz Petenkofer, MD, Pradeep Prasad, MD, and Irena Tsui, MD.
OTX-TKI-2023-AMD-301 (24-5013)
A phase 3, multicenter, doublemasked, randomized, parallel-group study to evaluate the efficacy and safety of intravitreal OTX-TKI (axitinib implant) in subjects with neovascular age-related macular degeneration/ OTX-TKI-2023-AMD-301. Investigators: Michael S. Ip, MD, and Gad Heilweil, MD.
Priovant PVT-2201-303 Uveitis (24-5274)
A phase 3 randomized, doublemasked, placebo-controlled study to investigate the safety and efficacy of oral brepocitinib in adults with active, non-infectious intermediate-, posterior-, and panuveitis. Investigators: Edmund Tsui, MD, Adrian Au, MD, Judy Chen, MD, Alejandro Marin, MD, Cherilyn Palochak, MD, and Prashant Tailor, MD.
RGX-314-2104 (21-1374)
A randomized, partially masked, controlled, phase 2b/3 clinical study to evaluate the efficacy and safety of RGX-314 gene therapy in participants with wet AMD (ATMOSPHERE). Investigators: Michael S. Ip, MD, Irena Tsui, MD, and Gad Heilweil, MD.
RGX-314-5101 nAMD (23-5267)
A long-term follow-up study to evaluate the safety and efficacy of RGX-314 following subretinal administration in participants with neovascular agerelated macular degeneration and fellow eye treatment substudy. Investigator: Michael Ip, MD.
Safety and Feasibility of Cultivated Autologous Limbal Stem Cells (LSCs) for Limbal Stem Cell Deficiency (19-1056)
Cell therapy using cultivated autologous LSCs has been developed as a potentially better alternative to various direct transplantation methods of limbal tissues, as it greatly lowers the risk of damage to the donor eye by decreasing the amount of tissues that need to be harvested from the donor. Investigators: Sophie X. Deng, MD, Anthony J. Aldave, MD, and Vivian Shibayama, OD.
VGN-TED-302 (24-5105)
A multicenter, extension study to evaluate the efficacy, safety, pharmacokinetics, and pharmacodynamics of two doses of linsitinib in subjects with active, moderate-to-severe thyroid eye disease (TED). Investigator: Daniel B. Rootman, MD, MS.
Xiidra Study (19-000843)
This is a prospective study evaluating the benefit of Xiidra in treating patients currently using one or more topical glaucoma antihypertensives and who self-describe symptoms of ocular surface irritation. Investigators: Benjamin B. Bert, MD, and Brian A. Francis, MD, MS.
ABP 938 (20-0448)
A randomized, double-masked, phase 3 study of ABP 938 efficacy and safety compared to aflibercept (Eylea®) in subjects with neovascular age-related macular degeneration. Investigators: David Sarraf, MD, Michael B. Gorin, MD, PhD, and Colin A. McCannel, MD.
Acelyrin Non-infectious Intermediate Uveitis, Posterior Uveitis or Panuveitis
Phase 2 Study of Izokibep (22-0504)
A phase 2 dose-finding study to evaluate the efficacy, safety, and immunogenicity of izokibep in subjects with noninfectious intermediate uveitis, posterior uveitis or panuveitis. Investigators: Edmund Tsui, MD, MS, Gary N. Holland, MD, and Judy L. Chen, MD.
APL2-GA-305 (21-0534)
A phase 3, open-label, multicenter, extension study to evaluate the longterm safety and efficacy of pegcetacoplan in subjects with geographic atrophy secondary to age-related macular degeneration. Investigator: Michael S. Ip, MD.
ASP7317 (17-000835)
A phase 1b, multicenter, dose escalation, evaluation of safety and tolerability of ASP7317 for geographic atrophy secondary to age-related macular degeneration. Investigators: Pradeep Prasad, MD, Adrian Au, MD, Aya Barzelay, MD, Jennifer Grossman, MD, Hamid Hosseini, MD, Kirk Hou, MD, David Lozano, MD, Alejandro Marin, MD, Colin McCannel, MD, Maureen Mcmahon, MD, Cherilyn Palochak, MD, Moritz Pettenkofer, MD, Prashant Tailor, MD, and Irena Tsui, MD.
Corneal Nerves After Cenegermin— Dompe (20-0833)
This study is to determine the structural and functional effects of cenegermin on the cornea, using noninvasive technologies, including the Ocular Surface Disease Index, corneal sensitivity testing, tear film testing, imaging, and confocal microscopy. Investigators: Clemence Bonnet, MD, Anthony J. Aldave, MD, Saba Al-Hashimi, MD, and Sophie X. Deng, MD, PhD.
Corticosteroids for Uveitic Macular Edema (ADVISE) (19-0668)
This research study compares three treatments for macular edema in patients who have uveitis. Macular edema is swelling of the retina at the back of the eye, and it can cause vision loss. The standard treatment is to inject corticosteroid drugs next to the eye or directly into the eye. Investigators: Edmund Tsui, MD, MS, Gary N. Holland, MD, and Colin A. McCannel, MD.
ESK-001-014 OPTYK 1 Panuveitis (23-5169)
A proof-of-concept, randomized, double-masked study to evaluate the efficacy and safety of ESK-001 in patients with active noninfectious intermediate, posterior, or panuveitis (OPTYK-1). Investigators: Edmund Tsui, MD, and Judy Chen, MD.
Evaluation of a New Drug for Alkeus Stargardt Disease (16-0116)
The study purpose is to find out whether a new drug for Stargardt disease is safe and effective. There are currently no proven treatments for Stargardt disease, a disease that leads to blindness in almost all cases. Investigators: Michael B. Gorin, MD, PhD, and Steven Nusinowitz, PhD.
Multicenter, Open-Label Extension Study to Evaluate the Long-Term Safety and Tolerability of the Port Delivery System with Ranibizumab in Patients with Neovascular Age-Related Macular Degeneration (PORTAL) (18-1405)
Continuous delivery of ranibizumab from the implant, with a prolonged fixed period between refills, is a novel approach that may result in lessfrequent need for retreatment than monthly dosing and patient monitoring. Investigators: Colin A. McCannel, MD, Pradeep S. Prasad, MD, MBA, and David Sarraf, MD.
Phantom Trial FECD (22-0912)
A phase IIa, randomized, doublemasked, placebo-controlled, parallelgroup, multicenter study assessing the efficacy and safety of STN1010904 ophthalmic suspension 0.03% and 0.1% compared with vehicle in subjects with Fuchs endothelial corneal dystrophy (FECD). Investigators: Anthony J. Aldave, MD, Saba Al - Hashimi, MD, Sophie X. Deng, MD, PhD, Simon Fung, MD, MA, and Reza Ghaffari, MD.
Priovant NEPTUNE Study (22-5103)
A phase 2 randomized, doublemasked, dose-ranging study to investigate the safety and efficacy of oral brepocitinib in adults with active noninfectious intermediate-, posterior-, and pan-uveitis. Investigators: Edmund Tsui, MD, MS, and Judy L. Chen, MD.
VGN-TED-301 (22-0271)
A phase 2b, randomized, double-mask, placebo-controlled, study to evaluate the safety, pharmacokinetics, and efficacy of linsitinib in subjects with active, moderate-to-severe thyroid eye disease (TED). Investigator: Daniel B. Rootman, MD, MS.
XEN45 AbbVie Study (22-5039)
A prospective, multicenter clinical study to evaluate the safety and effectiveness of ab externo implantation of glaucoma gel stent. Investigators: Brian A. Francis, MD, MS, and Victoria L. Tseng, MD, PhD.
Zoster Eye Disease Study (ZEDS) (17-0982)
The purpose of this study is to find out whether one year of a low dose of valacyclovir reduces complications of shingles affecting the eye. The study will involve two groups of participants who have eye problems due to shingles. One group will receive daily valacyclovir medication and the other group will receive a placebo. Investigators: Gary N. Holland, MD, Anthony J. Aldave, MD, Sophie X. Deng, MD, PhD, and John A. Irvine, MD.
AI Imaging Analysis (25-0614)
This study is to assess whether vascular pathology features quantified using Emagix algorithms are comparable to expert diagnoses based on manual image inspection. Additionally, the study aims to examine the capability of AI-measured vascular pathology features to predict disease progression and patient response to treatment, thereby evaluating the potential of these algorithms to support clinical decision-making and improve patient outcomes. Investigator: Edmund Tsui, MD, MS.
AMD Ryan Initiative Study–
Longitudinal Study of Early AMD and Reticular Pseudodrusen
The primary objectives of the study are to enroll participants with early AMD to assess rate of change in drusen volume and progression rates to large drusen and associate these morphologic changes with psychophysical changes, including visual acuity and dark adaptation. Investigators: Michael B. Gorin, MD, PhD, and SriniVas R. Sadda, MD.
Analysis of the Corneal and Limbal Epithelial Changes in Limbal Stem Cell Deficiency Using In Vivo Confocal Microscopy
Investigators are working to establish a system for diagnosing limbal stem cell deficiency at a cellular level by correlating the information from impression cytology tests, confocal microscopy pictures, and medical records. Investigators: Anthony J. Aldave, MD, and Sophie X. Deng, MD, PhD.
SS-OCT (22-1545)
Swept source optical coherence tomography (SS-OCT) will be used to capture detailed images of patients with various eye conditions, including cataracts, corneal and macular diseases, optic nerve disorders, iris abnormalities, and uveitis. The highresolution images obtained from SS - OCT will be compared to those taken with standard imaging devices, such as the FDA-approved Optovue OCT, to evaluate differences and potential advantages of this newer technology. Investigators: Edmund Tsui, MD, MS, Gary N. Holland, MD, and Judy L. Chen, MD.
Anterior Chamber Flare Measurements (19-1602)
The evaluation and detection of inflammation is critical in management of uveitis. Flare, which is one of the commonly assessed ocular inflammation parameters, is the appearance of light reflected from solutes in the anterior chamber. This study seeks to compare two platforms of laser flare photometry and to evaluate the reproducibility of these measurements. Investigators: Edmund Tsui, MD, MS, and Gary N. Holland, MD.
Anterior Imaging of Ocular Muscles
Presbyopia is poorly understood and may be due to the lens in the eye becoming harder or the muscles that help focus vision for reading becoming weaker with age. The aim of this study is to utilize OCT imaging technology to better understand and develop therapies to combat presbyopia. Investigator: Alex A. Huang, MD, PhD.
Arm-Mounted Heidelberg OCT-A for Noninvasive Vascular Zone
Imaging in Infants with Retinopathy of Prematurity (ROP)
This study evaluates OCT-A imaging data on preterm infants who are screened and/or treated for ROP, especially evaluating the potentially beneficial effects of anti-VEGF treatment on foveal development and visual outcomes. Investigators: Alex A. Huang, MD, PhD, and Irena Tsui, MD.
Beacon Sensors and Telerehabilitation
The primary goal of this project is to refine the methods and procedures for implementing innovative technologies for low-vision rehabilitation in order to develop future protocols for randomized controlled trials. Investigators: Ava K. Bittner, OD, PhD, Melissa Chun, OD, and Jennie Kageyama, OD.
Biomechanical Analysis in Strabismus Surgery
This study aims to develop new diagnostic tests and computer models that will lead to improvements in strabismus surgery. Tests of binocular alignment and eye movements, as well as magnetic resonance imaging of the extraocular muscles, are being performed in the Institute’s Clinical and Basic Science Ocular Motility Laboratory before and after strabismus surgery. To date, this research has fundamentally contributed to the knowledge of the functional anatomy of the extraocular muscles and connective tissues and allowed discovery of causes of common strabismus and development of new types of surgeries. Investigator: Joseph L. Demer, MD, PhD.
CAPRICORN (23-5071)
This study will collect and analyze genetic material from patients with corneal ulcers across multiple sites, enrolling a total of 1,200 participants including 100 at UCLA. Each patient will be evaluated over two visits spaced one month apart, during which up to three ocular surface swabs will be collected. These samples will be sent to the University of California, San Francisco, for advanced DNA testing aimed at identifying the pathogens responsible for infection. Investigators: Edmund Tsui, MD, MS, and Amanda Lu, MD.
Characteristics of the Brow-Eyelid Margin Relationship
The study purpose is to determine if changing the effect of gravity has an effect on eyelid position. Investigators: Robert Alan Goldberg, MD, and Daniel B. Rootman, MD, MS.
Choroideremia Health Outcomes
The purpose of this observational study is to gather information on patient and caregiver experience with choroideremia. Investigator: Michael Gorin, MD, PhD.
Clinical Measurements of the Optic Nerve in Glaucoma
The goal of this study is to develop novel structural measures of the optic nerve and nerve fiber layer, which are sensitive and specific for early and progressive glaucomatous optic nerve damage. Investigators: Joseph Caprioli, MD, Anne L. Coleman, MD, PhD, and Simon K. Law, MD, PharmD.
This study will test a new MHz OCT system developed by engineering collaborators and compare the performance of this new OCT system to a standard clinical OCT device. The newly designed OCT system will be five to 10 times faster, leading to a marked improvement in resolution and significant reduction of artifacts. Investigator: Kouros Nouri-Mahdavi, MD.
Development of a Behavioral Intervention with Socially Assistive Robots to Enhance Magnification Device Use for Reading
The primary goals of this research are to perform the initial development and preliminary evaluation of a prototype socially assistive robot specifically for low vision rehabilitation involving reading with magnifiers, in order to develop future protocols for larger scale clinical trials. Investigators: Ava K. Bittner, OD, PhD, Melissa Chun, OD, and Jennie Kageyama, OD.
Effect of External Eyelid Weighting on Lid Position in Normal and Ptosis Patients
This investigation compares the ability of normal and ptotic patients to maintain eyelid position by adapting to acute and dramatic changes in protracting forces by using eyelid weights. This project will help elucidate the physiology of the eyelid position maintenance system and provide insight into its ability to respond to changes in disease. Investigator: Daniel B. Rootman, MD, MS.
Effect of Glaucoma Drainage Devices on the Cornea in Comparison to Filtering Surgery with Antimetabolites in Cases of Glaucoma
This study aims to evaluate the endothelial cell number in patients undergoing glaucoma drainage device implantation as part of their regular eye care in comparison to the endothelial cell number in patients having filtering surgery with antimetabolites or medical treatment. Investigators: JoAnn A. Giaconi, MD, Joseph Caprioli, MD, Anne L. Coleman, MD, PhD, Simon K. Law, MD, PharmD, and Kouros Nouri - Mahdavi, MD.
Effect of Yoga on Glaucoma
The purpose of this study is to examine the practice of yoga and its ability to improve a patient’s vision by relieving stress and reducing eye pressure. Investigator: Anne L. Coleman, MD, PhD.
Evaluating a Microshunt for the Treatment of Glaucoma
This study is to assess the safety and efficacy of a microshunt when used to lower intraocular pressure (IOP) in subjects with primary open angle glaucoma whose IOP is not controlled when using maximum-tolerated glaucoma medications. Investigators: Joseph Caprioli, MD, Anne L. Coleman, MD, PhD, JoAnn A. Giaconi, MD, Simon K. Law, MD, PharmD, and Brian A. Francis, MD, MS.
Extended-Use Program of Elamipretide Topical Ophthalmic Solution for Patients with Leber Hereditary Optic Neuropathy (LHON)
This extended-use program is to provide elamipretide to patients with LHON previously enrolled in the SPILH -201 clinical trial who are still benefitting from treatment per the discretion of the treating physician. Investigators: Alfredo A. Sadun, MD, and Rustum Karanjia, MD.
DMI
This epidemiological study evaluates the prevalence and progression of diabetic macular ischemia in patients with diabetic retinopathy treated with panretinal photocoagulation. Investigator: David Sarraf, MD.
Eye Health Imaging Study
The purpose of this study is to expand the normative database for the Heidelberg Spectralis OCT by collecting ophthalmic data from healthy eyes of people of Hispanic/Latino, Asian, and African American descent. Investigators: Kouros Nouri-Mahdavi, MD, and Joseph Caprioli, MD.
Field Test of Glaucoma Outcomes Survey (GOS)
The American Glaucoma Society is interested to learn how quality of life improves for patients after minimally invasive glaucoma surgery combined with cataract surgery. They have designed a questionnaire and are conducting research to find out how reliable the questionnaire is as a tool for measuring patient quality of life after surgery. Investigator: Brian A. Francis, MD.
Genetic and Anatomic Studies of Eye Movement Disorders
This study is conducting magnetic resonance imaging of the extraocular muscles. This procedure clarifies the phenotypes and mechanisms of congenital cranial dysinnervation syndromes whose hereditary properties have been characterized using modern molecular genetics. Patients with these syndromes have severe forms of strabismus. Investigator: Joseph L. Demer, MD, PhD.
Glaucoma Imaging Study
This study is evaluating different imaging techniques and their use in improving open-angle glaucoma detection.
Investigators: Kouros Nouri-Mahdavi, MD, and Joseph Caprioli, MD.
Hyaluronic Acid Gels for Upper Lid Retraction in Active State Thyroid Eye Disease
This study is to determine if hyaluronic acid gel (HAG) can be used to correct upper eyelid retraction, improve dry eye related symptoms, aesthetic appearance, and quality of life in active-stage thyroid eye disease (TED). The study also aims to determine the long-term outcome of TED and how long the effects of HAG can last. Investigator: Daniel B. Rootman, MD, MS.
Identifying Novel Genes for Fuchs Corneal Endothelial Dystrophy
Investigators are working to identify the gene(s) responsible for Fuchs corneal endothelial dystrophy, an inherited disorder that may result in irreversible corneal swelling and loss of vision. Investigators: Anthony J. Aldave, MD, Gary N. Holland, MD, and Bartly J. Mondino, MD.
Imaging of Intraocular Inflammation (19-1732)
Uveitis, a major cause of blindness, can lead to severe complications, making accurate inflammation assessment essential. This study will use advanced imaging (OCT, OCT angiography, laser flare photometry) to obtain objective, reproducible measurements in patients with infectious or noninfectious uveitis, compare them with SUN criteria, and evaluate their correlation with complications and treatment response. Investigators: Edmund Tsui, MD, MS, Gary N. Holland, MD, and Judy L. Chen, MD.
Imaging of Vitreous Inflammation (24-1043)
The study will utilize multiple imaging instruments to quantitatively assess intraocular inflammation in patients diagnosed with either infectious or noninfectious uveitis. Imaging-based inflammation measurements will be systematically compared with the SUN Working Group criteria to evaluate their concordance and reliability. The study will investigate how changes in these imaging and clinical outcome measures correlate with the development of uveitis-related complications and patient responses to treatment over time, thereby enhancing understanding of disease progression and management effectiveness. Investigators: Edmund Tsui, MD, MS, Gary N. Holland, MD, and Judy L. Chen, MD.
In-Vivo Ultrastructure of Chorioretinal Diseases
The study will utilize a novel adaptive optics (AO) imaging instrument that integrates scanning laser ophthalmoscopy and optical coherence tomography (AO-SLO-OCT), allowing for in -vivo ultrastructure assessment of RPD and individual photoreceptors in both en face and cross-sectional planes. The study will use the AO imaging to monitor the progression of the RPD and their impact on overlying photoreceptors. Investigators: David Sarraf, MD, and Yuhua Zhang, PhD.
Long-term Follow-up of ND4 LHON
Subjects Treated with GS010
Ocular Gene Therapy in the RESCUE or REVERSE
This study is to assess the long-term safety of intravitreal GS010 administration up to five years post treatment in subjects who were treated in the RESCUE or REVERSE studies. Investigators: Alfredo A. Sadun, MD, and Rustum Karanjia, MD.
Lotus (24-5309)
To improve the diagnosis and understanding of uveitis by employing multimodal molecular techniques to characterize pathogens, host transcriptomes, proteomic, and metabolite signatures. This will be achieved by collecting and analyzing intraocular samples, tears, and conjunctival swabs from patients with suspected infectious and noninfectious uveitis, as well as controls, using standard-of-care procedures and advanced molecular analyses at UCSF and Stanford. The study aims to contribute to global infectious uveitis surveillance, pathogen discovery, biomarker identification, and enhanced understanding of host responses, ultimately advancing uveitis diagnosis and treatment to reduce ocular morbidity and vision loss. Investigators: Edmund Tsui, MD, MS, and Judy L. Chen, MD.
This prospective longitudinal study aims to evaluate low vision patients’ reading performance and level of difficulty when using additional preferred lighting for near reading as provided by a commercially available desk lamp or a bulb placed in a generic gooseneck desk lamp specified according to the patient’s preferred settings with a lighting assessment tool. Investigators: Ava K. Bittner, OD, PhD, Melissa Chun, OD, and Jennie Kageyama, OD.
This research is to study ocular melanoma tumor tissue and to identify key molecular and genetic features that could help predict those patients who may be at high risk for metastasis. Investigators: Lynn K. Gordon, MD, PhD, Tara A. McCannel, MD, PhD, and Bradley R. Straatsma, MD, JD.

Natural History Study of Leber Hereditary Optic Neuropathy
Leber hereditary optic neuropathy (LHON) is one of the diseases where the mitochondria of the retina cells are not functioning correctly, which can lead to loss of vision. This study is to obtain electroretinography (ERG) data and optical coherence tomography (OCT) data from patients who carry the Leber hereditary optic neuropathy gene. Investigator: Alfredo A. Sadun, MD, PhD.
Natural History Study of Macular Telangiectasia
The primary study objective is to develop a registry of participants with MacTel Type 2 (as confirmed by the Reading Center) who may agree to be contacted for inclusion in future clinical trials. Investigators: Hamid Hosseini, MD, Tara A. McCannel, MD, PhD, Pradeep S. Prasad, MD, MBA, and Irena Tsui, MD.
Natural History of the Progression of Choroideremia
This study characterizes the visual function and retinal structural changes associated with X-linked choroideremia with the intention of determining the best means of measuring disease progression and the rate of natural progression for this condition. Investigators: Michael B. Gorin, MD, PhD, and Steven Nusinowitz, PhD.
Natural History of the Progression of X-Linked Retinitis Pigmentosa
This study is to characterize the visual function and retinal structural changes associated with X-linked retinitis pigmentosa to determine the best means of measuring disease progression and the rate of natural progression for this condition. Investigator: Michael B. Gorin, MD, PhD.
Neuroendocrine Tumor Metastases in the Eye and Orbit
The purpose of this study is to understand the diversity in presentation of carcinoid tumors of the orbit, as well as to identify, stage, and grade related factors that may affect prognosis and thus treatment decisions. Also considered will be if there are features of carcinoid tumor presentations in the orbit that can predict outcome and thus guide therapeutic decision- making. Investigator: Daniel B. Rootman, MD, MS.
NGS Based Metagenomic Screening of Ocular Infections (24-5434)
The purpose of this study is to characterize the ocular microbiome and identify potential pathogens in presumed infectious eye conditions by collecting samples from patients undergoing standard-of-care eye surgeries or procedures. The study will compare traditional molecular diagnostic methods, such as cultures and PCR, with advanced techniques like Next Generation Sequencing (NGS) to improve pathogen detection. Ultimately, the goal is to discover previously unidentified infectious agents to inform treatment approaches and improve outcomes for patients with eye infections and related diseases. Investigator: Edmund Tsui, MD, MS.
Nonexudative Age-Related Macular Degeneration Imaged with Swept Source OCT
OCT imaging with SS-OCTA will be utilized to study the natural history of disease. Investigator: SriniVas R. Sadda, MD.
Noninvasive Methods for Early Detection of Alzheimer Disease
The purpose of this study is to obtain electroretinography data and optical coherence tomography data from patients with Alzheimer disease, with the aim of permitting earlier intervention and improved disease monitoring. Investigator: Alfredo A. Sadun, MD, PhD.
Observational Study of Conjunctivitis in the Setting of Dupixent Treatment
The primary objective of the study is to characterize the clinical phenotype(s) of DUPIXENT®-associated conjunctivitis events. Investigator: Benjamin B. Bert, MD.
Observational Study of Patients Diagnosed with Idiopathic Bilateral Cataracts
The purpose of this study is to understand better how many people who have been diagnosed with early-onset idiopathic bilateral cataracts may have a rare but treatable disease called cerebrotendinous xanthomatosis (CTX). Often one of the first signs of CTX is cataract from an unknown cause at an early age. Investigators: Federico G. Velez, MD, Stacy L. Pineles, MD, and Joseph L. Demer, MD, PhD.
OCT-A and Visual Acuity in Human Immunodeficiency Virus Associated Neuroretinal Disorder
This study aims to characterize the microvascular abnormalities in patients with HIV via OCT-A and investigate the relationships between capillary density, nerve fiber layer thickness, and other measures of visual function (visual acuity, contrast sensitivity, color vision, visual fields). In addition, to compare the OCT-A data in HIV-positive patients versus controls to evaluate the hypothesis that HIV-positive patients have significant differences in microvascular flow compared to normal eyes. Investigators: Gary N. Holland, MD, and David Sarraf, MD.
Ocular Biometric Measurements in Angle-Closure Glaucoma
The purpose of this study is to determine the potential contributing factors in angle-closure patients of different ethnicities and to determine predictive factors for this type of glaucoma.
Investigators: Joseph Caprioli, MD, Anne L. Coleman, MD, PhD, Simon K. Law, MD, PharmD, and Kouros Nouri-Mahdavi, MD.
Ocular Hypertension Treatment Study
Since topical hypotensive medications are safe and effective in delaying or preventing primary open angle glaucoma, this study is examining whether other forms of treatment can be deferred with little or no penalty. Investigator: Anne L. Coleman, MD, PhD.
Ocular Imaging Study
This study is about improving existing anterior and posterior segment imaging using optical coherence tomography (OCT) instruments and/or other imaging devices. Investigators would like to know if different imaging devices can improve the quality of images and visualization of imaged tissues.
Investigators: SriniVas R. Sadda, MD, Anthony C. Arnold, MD, Vikas Chopra, MD, Brian A. Francis, MD, MS, Gad Heilweil, MD, Hugo Y. Hsu, MD, Michael S. Ip, MD, John A. Irvine, MD, Phillip Le, MD, Alfredo A. Sadun, MD, PhD, David Sarraf, MD, James C. Tan, MD, PhD, and Irena Tsui, MD.
Ocular Protrusion in Sitting and Supine Positions
The aim of this study is to compare the degree of ocular protrusion in normal individuals and patients with thyroid eye disease between sitting and lying (supine) positions. Investigators: Robert Alan Goldberg, MD, and Daniel B. Rootman, MD, MS.
Ocular Surface Microbiome Study
This study aims to investigate and understand the normal ecosystem of microbes that live on the eye’s surface and how their ecological system changes and responds to routine eye care and treatments. Investigators: Hugo Hsu, MD, Vikas Chopra, MD, and Gad Heilweil, MD.
Oculoplastic Registry
Many orbital and ophthalmic plastic surgical diseases are not well studied in the medical literature. The purpose of this study is to contribute to a large database of electronic measurements from medical records that allow us to study diseases in a way that was difficult or impossible before. Investigators: Robert Alan Goldberg, MD, and Daniel B. Rootman, MD, MS.
Optic Nerve Appearance in Age-Related Macular Degeneration
In order to evaluate the relationship between macular degeneration and optic nerve change, digital imaging technology and photography are being used to assess the structural appearance of the optic nerve in patients with age-related macular degeneration. Investigator: Simon K. Law, MD, PharmD.
Optical Coherence Tomography
Angiography Images of Pregnant Women
This study aims to identify changes that occur in the retina as a result of gestational associated diseases (eg, gestational diabetes, high blood pressure, increased myopia) and unknown changes that may affect the eyes during gestation and in the two to three months following birth. Investigator: Irena Tsui, MD.
Optical Coherence Tomography
Angiography of Foveal Avascular Zone in Premature Children
This prospective study evaluates blood vessel development in children and adults who are born early and compares them with children and adults who were not born early, by getting optical coherence tomography (OCT), OCT-angiography, color pictures, refraction, and axial length on subjects with retinopathy of prematurity and without retinopathy of prematurity. Investigators: Irena Tsui, MD, Stacy L. Pineles, MD, and Federico G. Velez, MD.
Amblyopia is a major cause of childhood visual loss. This study uses high resolution, surface-coil magnetic resonance imaging to study optic nerve size in amblyopia. It tests the theory that the optic nerve is smaller than normal in amblyopia and that optic nerve size may be a limiting factor in restoration of vision by amblyopia treatment. Investigator: Joseph L. Demer, MD, PhD.
Outcomes of Ocular Inflammatory Diseases (22-0678)
The study aim is to collect core clinical data on children and teens undergoing surgery for cataracts in order to conduct analyses and generate hypotheses. Investigators: Edmund Tsui, MD, MS, and Irena Tsui, MD.
Pediatric Cataract Surgery Outcomes Registry
This study is to evaluate the underlying risk factors and treatment outcomes of ocular inflammatory diseases, utilizing advanced imaging technology with the Anterion camera to obtain highresolution anterior segment images. This approach aims to enhance the characterization of disease patterns and to assess the effectiveness of current therapeutic interventions to inform and improve future management strategies. Investigators: Edmund Tsui, MD, MS, and Irena Tsui, MD.
Pediatric Cornea and Anterior Segment Diseases Registry
Pediatric cornea and anterior segment diseases are rarely encountered by ophthalmologists. As such, details on the causes, features, and optimal treatment for these conditions are inadequately described. The information on this registry would allow us to study these diseases. Investigator: Simon Fung, MD.
Pediatric Optic Neuritis Prospective Outcomes Study (PON1)
Optic neuritis is an acute inflammatory disease of the optic nerve. The purpose of this study is to collect information about children who have optic neuritis and what happens to their eyesight. Investigator: Stacy L. Pineles, MD.
PET/CT Imaging for Early Detection of Ocular Melanoma
This research involves the use of combined positron emission tomography (PET)/computed tomography (CT) scans in subjects with ocular melanoma to ideally develop better ways of monitoring for tumor spread and allow for early treatment if metastasis is found. Investigators: Tara A. McCannel, MD, PhD, and Bradley R. Straatsma, MD, JD.
Predicting Eye Disease in Childhood Arthritis-Uveitis Study (PEDIA-U)
The purpose of this study is to further the understanding of juvenile idiopathic arthritis and uveitis (JIA-U). Investigators: Gary N. Holland, MD, and Edmund Tsui, MD, MS.
Pro-Inflammatory Cytokines, Dry Eye, and Thyroid Eye Disease
This study is to determine whether there are specific inflammatory proteins in tears of patients with active-stage thyroid eye disease (TED). If these inflammatory proteins exist, the study aims to determine whether they can be used to predict dry eye symptomatology and TED activity. Investigators: Robert Alan Goldberg, MD, and Daniel B. Rootman, MD, MS.
Prospective Study Examining Pentosan Retinal Toxicity
Patients will be evaluated for the dose and treatment duration of Pentosan. The goal is to determine the risk and toxic profile of Pentosan, as well as the incidence of interstitial cystitis, in an effort to establish clinical guidelines for retinal toxicity screening. Investigator: David Sarraf, MD.
Ptosis Surgery Outcomes Scale
This investigation is to define and validate a universal measure for ptosis outcomes that can be used in defining both value and efficacy in ptosis surgery. Investigator: Daniel B. Rootman, MD, MS.
Research to Evaluate Latest Improvements with Electronic Visual Enhancement Devices (RELIEVED)
This prospective study aims to evaluate patient preferences for wearable electronic visual aids for low vision rehabilitation and changes in visual functioning with these devices. Investigators: Ava K. Bittner, OD, PhD, Melissa Chun, OD, and Jennie Kageyama, OD.
Role of Pattern Electroretinogram (PERG) in Glaucoma
This study is researching the electrophysiological test, pattern electroretinogram (PERG) to determine the role of PERG in estimating the risk of future glaucoma progression and the reversibility of glaucomatous damage after treatment. The latter could help clinicians better determine to what extent eye pressure needs to be lowered to prevent disease progression. Investigators: Joseph Caprioli, MD, Anne L. Coleman, MD, PhD, JoAnn A. Giaconi, MD, Simon K. Law, MD, PharmD, and Kouros Nouri-Mahdavi, MD.
To assess the diagnostic accuracy and clinical utility for identifying specific pathogens in patients presenting with inflammation or infection of the ocular surface. This will be accomplished by collecting nasal and conjunctival swab samples during routine clinical visits and analyzing the results to determine the test’s effectiveness in detecting and differentiating various infectious agents. Investigators: Edmund Tsui, MD, MS, and Amanda Lu, MD.
Studies on Tissue in Autoimmune Diseases
This study aims to determine the cause of eye problems in Graves disease and other autoimmune diseases. Examination is being done of material removed from orbits during surgical therapy for Graves disease or other problems requiring surgery on the tissue surrounding the eyes, of thyroid tissue removed during the course of surgical therapy, or of blood drawn for laboratory tests. Investigator: Robert Alan Goldberg, MD.
Study of Macular Disease Using Spectral Domain Optical Coherence Tomography Angiography (SD-OCTA)
The RTVue XR 100 Avanti with SSADA will be used to screen patients with macular disease as detected with clinical examination or ancillary testing, such as with standard OCT, color fundus photography, fluorescein angiography, or fundus autofluorescence. Investigators: Michael B. Gorin, MD, PhD, Colin A. McCannel, MD, and David Sarraf, MD.
Tear Collections for Patients with Limbal Stem Cell Deficiency
The purpose of this study is to find markers specific to limbal stem cell deficiency not present in normal or dry eye diseased eyes. These markers could become additional diagnostic markers to confirm the disease and possibly targets for drug development. Investigator: Sophie X. Deng, MD, PhD.
Temporal Fossa in Different Ethnicities
The aim of this study is to investigate differences in anatomy of temporal fossa between different ethnicities using three-dimensional CT scan images. Better knowledge of these differences is important for cosmetic procedures to achieve better results and fewer complications. Investigators: Robert Alan Goldberg, MD, and Catherine J. Hwang, MD.
This study searches for the gene(s) responsible for inherited disorders that are either specific to the eye or are part of the medical condition. The study provides for the clinical characterization of affected individuals and at-risk family members, in conjunction with molecular genetic testing, to identify the causative genes and mutations. Investigators: Anthony J. Aldave, MD, and Michael B. Gorin, MD, PhD.
This study is designed to evaluate how quality of life is impacted by glaucoma in relation to eye dominance. It aims to determine whether quality of life is affected more by glaucoma if it primarily affects the dominant eye. Investigators: Joseph Caprioli, MD, Anne L. Coleman, MD, PhD, JoAnn A. Giaconi, MD, and Simon K. Law, MD, PharmD.
Books, book chapters, and articles published in peer-reviewed journals play a vital role in academic excellence. Through rigorous expert evaluation, faculty research contributes meaningfully to the advancement of our knowledge in vision science. The following highlights works published this academic year by our full-time faculty.
JULY 2024
Aguirre B, Lin MC, Araujo E, Lu CH, Casero D, Sun M, Nusinowitz S , Hanson J, Calkins K, Gordon L , Wadehra M, Chu A. Epithelial Membrane Protein 2 (EMP2) Blockade Attenuates Pathological Neovascularization in Murine Oxygen-Induced Retinopathy. Invest Ophthalmol Vis Sci. 2024 Jul 1;65(8):10. doi: 10.1167/iovs.65.8.10. PMID: 38958972; PMCID: PMC11223617.
Baek J, He Y, Emamverdi M, Mahmoudi A, Nittala MG, Corradetti G, Ip M , Sadda SR . Prediction of Long-Term Treatment Outcomes for Diabetic Macular Edema Using a Generative Adversarial Network. Transl Vis Sci Technol. 2024 Jul 1;13(7):4. doi: 10.1167/ tvst.13.7.4. PMID: 38958946; PMCID: PMC11223618.
Feo A, Sarraf D. Schlaegel Lines 360 Degrees in Punctate Inner Choroidopathy. Ophthalmol Retina. 2025 Jan;9(1):e2. doi: 10.1016/j.oret. 2024.05.015. PMID: 38958617. Epub 2024 Jul 1.
Kar D, Amjad M, Corradetti G, Swain TA, Clark ME, McGwin G Jr, Sloan KR, Owsley C, Sadda SR , Curcio CA. Choriocapillaris Impairment, Visual Function, and Distance to Fovea in Aging and Age-Related Macular Degeneration: ALSTAR2 Baseline. Invest Ophthalmol Vis Sci. 2024 Jul 1;65(8):40. doi: 10.1167/iovs. 65.8.40. PMID: 39042400; PMCID: PMC11268449.
Lee B, Josic K, Nittala MG, Velaga SB, Karamat A, Srinivas S , Corvi F, Singh G, Sadda S , Sun JK, Ip M ; DRCR Retina Network. Long-Term Effects of Intravitreal Ranibizumab Compared with Panretinal Photocoagulation on Optical Coherence Tomography Measured Choroidal Thickness and Vascularity. Transl Vis Sci Technol. 2024 Jul 1;13(7):19. doi: 10.1167/tvst. 13.7.19. PMID: 39058503; PMCID: PMC11282891.
Wang X, Hoshi S, Liu R, Zhang Y Modeling Human Macular Cone Photoreceptor Spatial Distribution. Invest Ophthalmol Vis Sci. 2024 Jul 1; 65(8):14. doi: 10.1167/iovs.65.8.14. PMID: 38975943; PMCID: PMC11232901.
Kaylor JJ, Frederiksen R, Bedrosian CK, Huang M, Stennis-Weatherspoon D, Huynh T, Ngan T, Mulamreddy V, Sampath AP, Fain GL , Travis GH RDH12 allows cone photoreceptors to regenerate opsin visual pigments from a chromophore precursor to escape competition with rods. Curr Biol. 2024 Aug 5;34(15):3342-3353.e6. doi: 10.1016/j.cub.2024.06.031. Epub 2024 Jul 8.
Tang D, Zylberberg J, Jia X, Choi H. Stimulus type shapes the topology of cellular functional networks in mouse visual cortex. Nat Commun. 2024 Jul 9; 15(1):5753. doi: 10.1038/s41467-02449704-0. PMID: 38982078; PMCID: PMC11233648.
Wu EG, Rudzite AM, Bohlen MO, Li PH, Kling A, Cooler S, Rhoades C, Brackbill N, Gogliettino AR, Shah NP, Madugula SS, Sher A, Litke AM, Field GD, Chichilnisky EJ. (2025) Decomposition of retinal ganglion cell electrical images for cell type and functional inference. J Neural Eng. 2025 Jul 9;22(4). Doi: 10.1088/1741-2552/ade344. PMID: 40494387.
Aleman AI, Kiryakoza L, Sridhar J, Sengillo J. Management of vitreous floaters: a review. Curr Opin Ophthalmol. 2024 Sep 1;35(5):365-368. doi: 10.1097/ICU.0000000000001075. Epub 2024 Jul 11. PMID: 39046174.
Behera UC, Brar AS, Kelgaonkar A, Sahoo J, Narayanan R, Sadda SR Efficacy of dexamethasone implant in the management of chronic central serous chorioretinopathy without choroidal neovascularization. Indian J Ophthalmol. 2025 Jan 1;73(Suppl 1): S100-S106. doi: 10.4103/IJO. IJO_626_24. Epub 2024 Jul 11. PMID: 38990618.
Shah S, Chou B, Patel M, Watane A, Shah L, Yannuzzi N, Sridhar J. Review and analysis of history and utilization of panretinal photocoagulation and ranibizumab after publication of protocol S. Curr Opin Ophthalmol. 2024 Sep 1;35(5):369-375. doi: 10.1097/ ICU.0000000000001076. Epub 2024 Jul 12. PMID: 39115058.
Fragiotta S, Parravano M, Corradetti G, Bousquet E, Polito MS, Sacconi R, Capuano V, Costanzo E, Tombolini B, Souied EH, Bandello F, Sadda SR , Sarraf D, Querques G. Vitelliform Lesions Associated with Leptochoroid and Pseudodrusen. Ophthalmol Retina. 2024 Dec;8(12):1151-1162. doi: 10.1016/ j.oret.2024.07.003. Epub 2024 Jul 14. PMID: 39004281.
Rojas-Carabali W, Cifuentes-González C, Gutierrez-Sinisterra L, Heng LY, Tsui E , Gangaputra S, Sadda S , Nguyen QD, Kempen JH, Pavesio CE, Gupta V, Raman R, Miao C, Lee B, de-la-Torre A, Agrawal R. Managing a patient with uveitis in the era of artificial intelligence: Current approaches, emerging trends, and future perspectives. Asia Pac J Ophthalmol (Phila). 2024 Jul-Aug;13(4):100082. doi: 10.1016/j. apjo.2024.100082. Epub 2024 Jul 15. PMID: 39019261.
Skorodumova LO, Grafskaia EN, Kharlampieva DD, Maltsev DI, Petrova TV, Kanygina AV, Fedoseeva EV, Makarov PV, Malyugin BE . TACSTD2 in gelatinous drop-like corneal dystrophy: variant functional analysis and expression in the cornea after limbal stem cell transplantation. Hum Genome Var. 2024 Jul 16;11(1):26. doi: 10.1038/ s41439-024-00284-x. PMID: 39013858; PMCID: PMC11252363.
Ersoz MG, Demirel S, Iovino C, Chhablani J, Sarraf D. Is Pachychoroid Serous Retinopathy a Better Name to Describe the Features of Central Serous Chorioretinopathy? Retina. 2024 Sep 1;44(9):1475-1477. doi: 10.1097/IAE.0000000000004215. PMID: 39024659. Epub 2024 Jul 16.
Cheng JY, Santina A, Margines JB, Voichanski S, Ramtohul P, Bousquet E, Bijon J, Freund KB, Yannuzzi L, Sarraf D. Acute posterior multifocal placoid pigment epitheliopathy and placoid variant diseases masquerading as agerelated macular degeneration in the elderly: A Case Series. Retina. 2024 Oct 1;44(10):1666-1678. doi: 10.1097/ IAE.0000000000004191. PMID: 39027974. Epub 2024 Jul 17.
Topouzis N, Kitayama K, Puran A, Yu F, Tseng VL , Coleman AL . Association of Open-Angle Glaucoma with Dementia in California Medicare Beneficiaries. Am J Ophthalmol. 2024 Dec;268:165173. doi: 10.1016/j.ajo.2024.07.009. Epub 2024 Jul 18. PMID: 39029771.
Khanani AM, Sadda SR , Sarraf D, Tadayoni R, Wong DT, Kempf AS, Saffar I, Gedif K, Chang A. Effect of Brolucizumab and Aflibercept on the Maximum Thickness of Pigment Epithelial Detachments and SubRetinal Pigment Epithelium Fluid in HAWK and HARRIER. Ophthalmol Retina. 2025 Jan;9(1):13-21. doi: 10.1016/ j.oret.2024.07.012. Epub 2024 Jul 19. PMID: 39033924.
Oquendo PL, Sodhi GS, Naidu SC, Martins Melo I, Pecaku A, Demian S, Belin PJ, Lee WW, Christakis PG, Hamli H, Bansal A, Andreoli MT, Tsui E , Muni RH. Optical Coherence Tomography Features in Fovea-Off Exudative vs Rhegmatogenous Retinal Detachment. Am J Ophthalmol. 2024 Dec;268:212221. doi: 10.1016/j.ajo.2024.07.003. Epub 2024 Jul 19. PMID: 39033833.
Tseng VL , Pan D, Kitayama K, Yu F, Coleman AL . Racial and Ethnic Differences in the Prevalence and Treatment Patterns for Neovascular Glaucoma in the American Academy of Ophthalmology IRIS® Registry. Ophthalmol Glaucoma. 2024 NovDec;7(6):615-623. doi: 10.1016/j. ogla.2024.07.006. Epub 2024 Jul 19. PMID: 39032697.
Ghosh S, Sharma R, Bammidi S, Koontz V, Nemani M, Yazdankhah M, Kedziora KM, Stolz DB, Wallace CT, Yu-Wei C, Franks J, Bose D, Shang P, Ambrosino HM, Dutton JR, Geng Z, Montford J, Ryu J, Rajasundaram D, Hose S, Sahel JA, Puertollano R, Finkel T, Zigler JS Jr, Sergeev Y, Watkins SC, Goetzman ES, Ferrington DA , Flores-Bellver M, Kaarniranta K, Sodhi A, Bharti K, Handa JT, Sinha D. The AKT2/SIRT5/TFEB pathway as a potential therapeutic target in non-neovascular AMD. Nat Commun. 2024 Jul 21;15(1):6150. doi: 10.1038/s41467-024-50500-z.PMID: 39034314.
Khanani AM, Sadda SR , Sarraf D, Tadayoni R, Wong DT, Kempf AS, Saffar I, Gedif K, Chang A. Effect of Brolucizumab and Aflibercept on the Maximum Thickness of Pigment Epithelial Detachments and Sub-Retinal Pigment Epithelium Fluid in HAWK and HARRIER. Ophthalmol Retina. 2025 Jan;9(1):13-21. doi: 10.1016/j.oret. 2024.07.012. PMID: 39033924. Epub 2024 Jul 19.
Tseng VL, Kitayama K, Yu F, Coleman AL . Racial and ethnic differences in the prevalence and treatment patterns for neovascular glaucoma in the American Academy of Ophthalmology Intelligent Research in Sight Registry. Ophthalmol Glaucoma. 2024 Nov-Dec;7(6):615-623. doi: 10.1016/j.ogla.2024.07.006. Epub 2024 Jul 19. PMID: 39032697.
Feo A, Tojjar J, Sarraf D. Polyp with large aneurysmal ring. Can J Ophthalmol. 2024 Dec;59(6): e842-e843. doi: 10.1016/j.jcjo.2024. 06.002. PMID: 39043255. Epub 2024 Jul 20.
Fu C, Yang N, Chuang JZ, Nakajima N, Iraha S, Roy N, Wu Z, Jiang Z, Otsu W, Radu RA , Yang HH, Lee MP, Worgall TS, Xiong WC, Sung CH. Mutant mice with rod-specific VPS35 deletion exhibit retinal α-synuclein pathologyassociated degeneration. Nat Commun. 2024 Jul 23;15(1):5970. doi: 10.1038/s41467-024-50189-0. PMID: 39043666; PMCID: PMC11266608.
Mohammadzadeh V, Wu S, Davis T, Vepa A, Morales E, Besharati S, Edalati K, Martinyan J, Rafiee M, Martynian A, Scalzo F, Caprioli J, Nouri-Mahdavi K Prediction of visual field progression with serial optic disc photographs using deep learning. Br J Ophthalmol. 2024 Jul 23;108(8):1107-1113. doi: 10.1136/bjo2023-324277. PMID: 37833037; PMCID: PMC11014894.
Ueda-Consolvo T, Ishida M, Nakamura T, Yanagisawa S, Tsuboi K, Wakabayashi T, Hayashi A, Sharma A; International Retina Biosimilar Study Group (Inter BIOS Group) (Sridhar J ). Biosimilar ranibizumab (BS1) - early experience from Japan (BRIJ study). Eye (Lond). 2024 Nov;38(16):3193-3196. doi: 10.1038/s41433-024-03220-z. Epub 2024 Jul 23. PMID: 39043816; PMCID: PMC11543661.
Falavarjani KG, Sarraf D. Improvement of Tamoxifen Induced Foveal Cavitation with Topical Dorzolamide Therapy. Retin Cases Brief Rep. 2024 Jul 29. doi: 10.1097/ICB.0000000000001645. PMID: 39079100. Epub 2024 Jul 29.
Bittner AK , Yoshinaga PD, Kaminski JE. Transitioning vision rehabilitation patients from over-the- counter magnifiers to prescribed aids. Disabil Rehabil Assist Technol. 2025 Feb;20(2):298303. doi: 10.1080/ 17483107. 2024. 2384512. Epub 2024 Jul 31. PMID: 39083649; PMCID: PMC12118344.
Lee SY, Paul ME, Coleman AL , Kitayama K, Yu F, Pan D, Tseng VL. Associations between statin use and glaucoma in the All of Us Research Program. Ophthalmol Glaucoma. 2024 Nov-Dec;7(6):563-571. doi: 10.1016/j. ogla.2024.07.008. Epub 2024 Jul 31. PMID: 39094953.
AUGUST 2024
Cohen SA, Sridhar J, Tseng VL Geographic Trends in Ophthalmology
Resident Physician Compensation and Cost-of-Living Expenses. JAMA Ophthalmol. 2024 Aug 1;142(8):761767. doi: 10.1001/jamaophthalmol. 2024. 2408. PMID: 38990549; PMCID: PMC11240227.
Javaheri M, Oh AJ, Prasad PS Macular Hole Self Closure While Awaiting Pre-operative Clearance. Ophthalmic Surg Lasers Imaging Retina. 2025 Jan;56(1):54-56. doi: 10.3928/23258160-20240729-01. Epub 2024 Aug 1. PMID: 39231107.
Borrelli E, Boscia G, Gelormini F, Ricardi F, Ghilardi A, Marolo P, Parisi G, Fallico M, Lupidi M, Mariotti C, Bandello F, Sadda S , Reibaldi M. Macular thickness and visual acuity are characterized by a quadratic nonlinear relation in previously treated neovascular AMD eyes. Eur J Ophthalmol. 2025 Mar;35(2):650659. doi: 10.1177/11206721241265998. Epub 2024 Aug 2. PMID: 39094557.
Mohammadi M, Su E, Mohammadzadeh V, Besharati S, Martinyan A, Coleman AL , Law SK , Caprioli J, Weiss RE, Nouri-Mahdavi K . Comparison of Retinal Nerve Fiber Layer and Ganglion Cell Complex Rates of Change in Patients with Moderate to Advanced Glaucoma. Am J Ophthalmol. 2024 Dec;268:190-198. doi: 10.1016/j.ajo. 2024.07.025. Epub 2024 Aug 5. PMID: 39111519.
Alsalloum A, Mosin I, Shefer K, Mingaleva N, Kim A, Feoktistova S, Malyugin B, Boiko E, Sultanov S, Mityaeva O, Volchkov P. Novel and Previously Known Mutations of the KCNV2 Gene Cause Various Variants of the Clinical Course of Cone Dystrophy with Supernormal Rod Response in Children. J Clin Med. 2024 Aug 6;13(16):4592. doi: 10.3390/ jcm13164592. PMID: 39200733; PMCID: PMC11354624.
Ashrafkhorasani M, Habibi A, Nittala MG, Yaseri M, Emamverdi M, Velaga SB, Wykoff CC, Ciulla TA, Ip M , Sadda SR . Spectral-domain OCT characteristics of intraretinal hyper-reflective foci associated with age-related macular degeneration and diabetic retinopathy. Can J Ophthalmol. 2025 Apr;60(2):9199. doi: 10.1016/j.jcjo.2024.07.017. Epub 2024 Aug 8. PMID: 39128832.
Finn AP, Sridhar J. Challenges and controversies in ophthalmology in 2024. Curr Opin Ophthalmol. 2024 Sep 1;35(5):351-352. doi: 10.1097/ICU. 0000000000001073. Epub 2024 Aug 8. PMID: 39115057.
Gedde SJ, Vinod K, Bowden EC, Kolomeyer NN, Chopra V, Challa P, Budenz DL, Repka MX, Lum F. Special Commentary: Reporting Clinical Endpoints in Studies of Minimally Invasive Glaucoma Surgery. Ophthalmology. 2025 Feb;132(2):141153. doi: 10.1016/j.ophtha.2024.07.030. Epub 2024 Aug 8. PMID: 39127407.
Park J, Lee I, Jafari S, Demer JL Tensile properties of glaucomatous human sclera, optic nerve, and optic nerve sheath. Biomech Model Mechanobiol. 2024 Dec;23(6):18511862. doi: 10.1007/s10237-024-01872-0. Epub 2024 Aug 8. PMID: 39112729.
Feo A, Fossataro C, Abraham N, Voichanski S, Lemon JD, Sarraf D Long Term Follow Up of a Family with A3243G Mitochondrial Syndrome. Retin Cases Brief Rep. 2024 Aug 14. doi: 10.1097/ICB.0000000000001647. PMID: 39151174.
Sivaprasad S, Chandra S, Sadda S , Teo KYC, Thottarath S, de Cock E, Empeslidis T, Esmaeelpour M. Predict and Protect: Evaluating the DoubleLayer Sign in Age-Related Macular Degeneration. Ophthalmol Ther. 2024 Oct;13(10):2511-2541. doi: 10.1007/ s40123-024-01012-y. Epub 2024 Aug 16. PMID: 39150604; PMCID: PMC11408448.
Bonnet C , Han CS, Deng SX , Zheng JJ. Positive cooperativity in synergistic activation of Wnt proteins. Mol Biol Rep. 2024 Aug 18;51(1):914. doi: 10.1007/ s11033-024-09831-9. PMID: 39154310; PMCID: PMC11330945.
Lai WY, Demer JL . Laterality Targeting in Graded Inferior Rectus Tenotomy Corrects Lateral Incomitance of Hypertropia in Sagging Eye Syndrome. Am J Ophthalmol. 2025 Jan;269:7883. doi: 10.1016/j.ajo.2024.08.012. Epub 2024 Aug 22. PMID: 39179127.
Zhuang I, Ashrafkhorasani M, Mohammadzadeh V, Nouri-Mahdavi K . Sources of Discrepancy between Retinal Nerve Fiber Layer and Bruch’s Membrane Opening-Minimum Rim Width Thickness in Eyes with Glaucoma. Ophthalmol Sci. 2024 Aug 22;5(1):100601. doi: 10.1016/j.xops. 2024.100601. PMID: 39411541; PMCID: PMC11474368.
Sharma A, Kaiser PK, Tadayoni R, Holz FG, Nicholson L, Vazquez-Alfageme C, Sivaprasad S, Wakabayashi T, Woo SJ, Sarraf D, Kumar N, Parachuri N, Regillo CD, Rezaei KA, Khanani AM, Bandello F, Shanamugam M, Verma L, Dogra MR, Ns M, Agarwal M, Loewenstein A, Kuppermann BD; International Retina Biosimilar Study Group (Inter BIOS Group) (Sridhar J ). Anti-VEGF Biosimilars for Retinal Diseases Survey 2023- India (Bio-INDAS) by the International Retina Biosimilar Study Group (Inter-BIOS Group) in collaboration with the Vitreo-Retinal Society of India (VRSI). Eye (Lond). 2024 Dec;38(17):3392-3395. doi: 10.1038/ s41433-024-03284-x. Epub 2024 Aug 26. PMID: 39187656; PMCID: PMC11584715.
Song D, Ginsberg C, Nudleman E, Borooah S, King A, Bousquet E, Sarraf D, Goldbaum M. Catastrophic retinal vascular occlusion and vision loss due to crystal deposition in end-stage kidney disease treated with peritoneal dialysis. Am J Ophthalmol Case Rep. 2024 Aug 26;36:102153. doi: 10.1016/j. ajoc.2024.102153. PMID: 39282596.
Bakhoum CY, Au A , Bousquet E, Matesva M, Singer MB, Jayaraj C, Romero-Morales VA, Somisetty S, Santina A, Bajar B, DeMaria AN, Goldbaum MH, Meadows J, Spatz ES, Sarraf D, Bakhoum MF. Retinal Ischemic Perivascular Lesions Are Associated with Stroke in Individuals with Atrial Fibrillation. J Am Heart Assoc. 2024 Sep 3;13(17):e035079. doi: 10.1161/JAHA.123.035079. Epub 2024 Aug 27. PMID: 39190603.
SEPTEMBER 2024
Chawla K, Tailor PD, Sridhar J Evaluating the necessity of topical and subconjunctival antibiotic prophylaxis in ocular surgery. Curr Opin Ophthalmol. 2025 Sep 1;36(5):389-400. doi: 10.1097/ICU.0000000000001136. Epub 2025 Mar 27. PMID: 40145558.
Govetto A, Lucchini S, Sebag J, Gianfrate F, Ranno S, Carini E, Virgili G, Romano MR, Sarraf D, Radice P. En face optical coherence tomography morphology of macular pucker correlates with metamorphopsia. Retina. 2024 Sep 1;44(9):1513-1520. doi: 10.1097/ IAE.0000000000004160. PMID: 39167572.
Rohowetz LJ, Shaheen A, Magraner M, Flynn HW Jr, Williams BK Jr, Smiddy WE, Sridhar J, Russell JF, Townsend JH, Berrocal AM, Albini T, Yannuzzi NA. Surgical outcomes in concurrent sickle cell and diabetic retinopathy. Retina. 2024 Sep 1;44(9):1560-1564. doi: 10.1097/IAE.0000000000004156. PMID: 39167577.
Jin SW, Bouris E, Morales E, Caprioli J Long-Term Rate of Optic Disc Rim Loss in Glaucoma Patients Measured from Optic Disc Photographs with a Deep Neural Network. Transl Vis Sci Technol. 2024 Sep 3;13(9):9. doi: 10.1167/tvst. 13.9.9. PMID: 39235397; PMCID: PMC11379101.
Song W, Randhawa S, Johnson MW, Bohn M, Agarwal A, Rahimy E, Taubenslag KJ, Charbel Issa P, Mahroo OA, Bijon J, McDonald HR, Walter SD, Yonekawa Y, Sadda S , Freund KB, Sarraf D. Multifocal Vitelliform Paravascular Retinopathy (MVPR): A New Disorder in the Vitelliform Spectrum. Am J Ophthalmol. 2025 Jan; 269:362-372. doi: 10.1016/j.ajo.2024. 08.028. Epub 2024 Sep 4. PMID: 39237051.
Saffari PS, Glasgow BJ, Lucarelli KM, Roelofs KA. Periorbital Intravenous Lobular Pyogenic Granulomas: A Case Report and Literature Review of This Peculiar Pathology. Ophthalmic Plast Reconstr Surg. 2025 Jan-Feb 01;41(1):e15-e18. doi: 10.1097/IOP. 0000000000002778. Epub 2024 Sep 10. PMID: 39254957 Review.
Nanegrungsunk O, Corradetti G, Phinyo P, Choovuthayakorn J, Sadda SR . Relationship between hypertransmission defect size and progression in eyes with intermediate age-related macular degeneration. Eye (Lond). 2024 Dec;38(18):3488-3494. doi: 10.1038/s41433-024-03338-0. Epub 2024 Sep 15. PMID: 39279009; PMCID: PMC11621391.
Kim JJ, Law MX, Buckley EG, Pineles SL , Prieto-Díaz F, Gamio S, Go M, Velez FG. Anterior Nasal Superior Oblique Tendon Syndrome: A Case Series. Am J Ophthalmol. 2024 Dec;268:329-339. doi: 10.1016/j.ajo.2024.09.013. Epub 2024 Sep 16. PMID: 39293569.
Pilotte J, Khoury S, Tafreshi A, Mandel ZT, Sharma SV, Vanderklish P, Sarraf ST, Sadun AA , Weinreb RN, Huang AS. Identification of Retinal AmyloidBeta in Ex-Vivo Human Glaucoma Eyes Using a Novel Ocular Tracer. J Glaucoma. 2024 Sep 17. doi: 10.1097/ IJG.0000000000002496. PMID: 39283690.
Yadlapalli N, Hollinger R, Berzack S, Spies D, Patel A, Sridhar J. Potential Gaps in Eye Care Based on Evaluation of Federally Qualified Health Centers. JAMA Ophthalmol. 2024 Sep 19;142(11): 1018–26. doi: 10.1001/ jamaophthalmol. 2024.3569. PMID: 39298148; PMCID: PMC11413758.
Petrovic M, Fischer JL, Goldberg RA , Suh JD. Rapid Vision Loss After Root Canal Treatment Due to Invasive Fungal Sinusitis. Ear Nose Throat J. 2024 Sep;103(2_suppl):7S-11S. doi: 10.1177/01455613241281861. Epub 2024 Sep 20. PMID: 39305069.
Cohen SA, Tseng VL , Sridhar J, Coleman AL . A New Era of Ophthalmology Leadership? A Descriptive and Comparative Analysis of Ophthalmology Department Chairs in 2024. Am J Ophthalmol. 2025 Jan;269:373-380. doi: 10.1016/j.ajo.2024.09.020. Epub 2024 Sep 21. PMID: 39313085.
Davis MR, Robinson E, Koronyo Y, Salobrar-Garcia E, Rentsendorj A, Gaire BP, Mirzaei N, Kayed R, Sadun AA , Ljubimov AV, Schneider LS, Hawes D, Black KL, Fuchs DT, Koronyo - Hamaoui M. Retinal ganglion cell vulnerability to pathogenic tau in Alzheimer’s disease. bioRxiv [Preprint]. 2024 Sep 21:2024.09.17.613293. doi: 10.1101/2024.09.17.613293.
Ferro Desideri L, Sim PY, Bernardi E, Paschon K, Roth J, Fung AT, Wu XN, Chou HD, Henderson R, Tsui E , Berrocal M, Chhablani J, Wykoff CC, Cheung CMG, Querques G, Melo GB, Subhi Y, Loewenstein A, Kiilgaard JF, Zinkernagel M, Anguita R. Evidencebased guidelines for drug dosing in intravitreal injections in silicone oilfilled eyes: Pharmacokinetics, safety, and optimal dosage. Surv Ophthalmol. 2025 Jan-Feb;70(1):96-105. doi: 10.1016/j.survophthal.2024.09.006. Epub 2024 Sep 27. PMID: 39343316.
Lescrauwaet B, Vansteelandt S, Jackson TL, Sadda SR , Duchateau L. A Causal Inference Approach to Mediation Analysis in Vitreomacular Traction: How Much Does Traction Resolution Mediate Functional Outcomes? J Mark Access Health Policy. 2024 Sep 30;12(4):280-293. doi: 10.3390/jmahp12040022. PMID: 39464178; PMCID: PMC11503358.
Rahn U, Rahn CD, Arora S, Ng E, Kozak I, Chhablani J; Subthreshold Laser Planning Group ( Prasad P ). Variability of thermal subthreshold retinal laser treatment plans. Sci Rep. 2024 Sep 30; 14(1):22723. doi: 10.1038/s41598-02473763-4. PMID: 39349668; PMCID: PMC11442868.
Zhu E, Li Y-R, Margolis S, Wang J, Wang K, Zhang Y, Wang S, Park J, Zheng C, Yang L, Chu A, Zhang Y, Gao L, Hsiai TK. Frontiers in artificial intelligencedirected light-sheet microscopy for uncovering biological phenomena and multiorgan imaging. VIEW. Vol. 5, Issue 5. Oct 2024. 20230087. https://doi. org/10.1002/VIW.20230087.
Avram O, Durmus B, Rakocz N, Corradetti G, An U, Nittala MG, Terway P, Rudas A, Chen ZJ, Wakatsuki Y, Hirabayashi K, Velaga S, Tiosano L, Corvi F, Verma A, Karamat A, Lindenberg S, Oncel D, Almidani L, Hull V, Fasih-Ahmad S, Esmaeilkhanian H, Cannesson M, Wykoff CC, Rahmani E, Arnold CW, Zhou B, Zaitlen N, Gronau I, Sankararaman S, Chiang JN, Sadda SR , Halperin E. Accurate prediction of disease-risk factors from volumetric medical scans by a deep vision model pre-trained with 2D scans. Nat Biomed Eng. 2025 Apr;9(4):507-520. doi: 10.1038/s41551-024-01257-9. Epub 2024 Oct 1. PMID: 39354052.
Tong N, Fan W, Su L, Ebraheem A, Uji A, Marion K, Sadda S . Relationship between optical coherence tomography biomarkers and number of intravitreal ranibizumab injections in eyes with neovascular age-related macular degeneration in the harbor study. Retina. 2024 Oct 1;44(10):1696-1703. doi: 10.1097/IAE.0000000000004171. PMID: 39287532.
Badalà F, Bona E, Devincenzi G, Nouri-Mahdavi K . Long Term Visual Outcomes of an Extended Macular Vision IOL in Eyes with Macular Disease and Visually Insignificant Cataract. Clin Ophthalmol. 2024 Oct 4;18:2765-2775. doi: 10.2147/OPTH. S481570. PMID: 39386174; PMCID: PMC11461591.
Bowe T, Richards CJ, Mansour HA, Ali FS, Sridhar J, Williams JBK, Yonekawa Y, Cohen MN, Xu D, Deaner JD, Sivalingam M, Orlin A, Patel S, Kuriyan AE. Disparities Between Clinical Trial Recruitment and Real-World Demographics in Macular Edema Secondary to Retinal Vein Occlusion. Am J Ophthalmol. 2025 Jan;269:429434. doi: 10.1016/j.ajo.2024.09.031. Epub 2024 Oct 4. Erratum in: Am J Ophthalmol. 2025 Aug;276:416. doi: 10.1016/j.ajo.2025.04.015. PMID: 39369931.
Lai WY, Demer JL . Cutaneous Lower Eyelid Retractor Release Averts Lower Lid Malposition After Inferior Rectus Muscle Recession. Am J Ophthalmol. 2025 Jan;269:466-470. doi: 10.1016/j. ajo.2024.09.030. Epub 2024 Oct 10. PMID: 39393423.
Margines JB, Huang C, Young A, Yu F, Coleman AL . Epidemiological Characteristics Associated with Astigmatism in a Population of 3- to 5-Year-Old Children in Los Angeles, CA. Ophthalmic Epidemiol. 2024 Oct 10:1-6. doi: 10.1080/09286586. 2024.2410302.
Bousquet E, Abraham N, Estawro R, Khadka S, Voichanski S, Mafi M, Au A , Santina A, Sadda S , Sarraf D Subretinal pigment epithelium hyporeflective spaces preceding large drusen collapse. Retina. 2024 Dec 1;44(12):2041-2048. doi: 10.1097/ IAE.0000000000004233. PMID: 39116541. Epub 2024 Oct 12.
Yu S, Jones IL, Maunz A, Bachmeier I, Albrecht T, Ebneter A, Gliem M, Staurenghi G, Sadda SR , Chakravarty U, Fauser S. Artificial intelligencebased analysis of retinal fluid volume dynamics in neovascular age-related macular degeneration and association with vision and atrophy. Eye (Lond). 2025 Jan;39(1):154-161. doi: 10.1038/ s41433-024-03399-1. Epub 2024 Oct 15. PMID: 39406933; PMCID: PMC11732971.
Chatterjee SK, Talebi R, Kitayama K, Young AG, Yu F, Tseng VL, Coleman AL . The association between glaucoma severity and hip fractures in California Medicare beneficiaries. Ophthalmol Glaucoma. 2025 Mar-Apr;8(2):167-174. doi: 10.1016/j.ogla.2024.10.002. Epub 2024 Oct 16. PMID: 39419201.
Duan E, Robinson M, Davis C, Pruthi S, Shin C, Lewis M, Martinez-Agosto JA, Gorin MB, Shuch BM, Friedman DL, Chang VY. Pediatric patients with von Hippel-Lindau and hemangioblastomas treated successfully with belzutifan. Pediatr Blood Cancer. 2025 Jan;72(1):e31371. doi: 10.1002/pbc.31371. Epub 2024 Oct 16. PMID: 39415342.
Edmonds B, Ngo JP, Groves A, Reyes B, Gott RA, Chia DJ, Mirbaha H, Magaki S, Khanlou N, Pineles SL , Salamon N, Thompson RM, Newman M, Rajaraman RR, Hussain SA, Fallah A, Russell B, Nariai H. Multidisciplinary team approach for pediatric hemimegalencephaly: Insights from a single institutional case series. Epilepsia Open. 2024 Dec;9(6):2510-2517. doi: 10.1002/ epi4.13079. Epub 2024 Oct 23. PMID: 39442533; PMCID: PMC11633684.
Gobeille M, Bittner AK , Malkin AG, Ho J, Idman-Rait C, Estabrook M, Ross NC; CARE Study Team. Rasch analysis of the new general self efficacy scale: an evaluation of its psychometric properties in older adults with low vision. Health Qual Life Outcomes. 2024 Oct 23;22(1):90. doi: 10.1186/s12955-02402306-2. PMID: 39443965; PMCID: PMC11515722.
Salvi A, Cluceru J, Gao SS, Rabe C, Schiffman C, Yang Q, Lee AY, Keane PA, Sadda SR , Holz FG, Ferrara D, Anegondi N. Deep Learning to Predict the Future Growth of Geographic Atrophy from Fundus Autofluorescence. Ophthalmol Sci. 2024 Oct 23;5(2):100635. doi: 10.1016/j. xops.2024.100635. PMID: 39758130; PMCID: PMC11699103.
Rosenblatt TR, Ghoraba HH, Ji MH, Baumal CR, Berrocal AM, Besirli CG, Drenser KA, Ells AL, Harper CA 3rd, Hubbard GB 3rd, Nudleman ED, Quiram PA, Tsui I , Yonekawa Y, Wood EH, Kumm J, Moshfeghi DM. Longitudinal Assessment of Retinopathy of Prematurity (LONGROP) Study: Impacts of Viewing Time and Ability to Compare on Detection of Change. Am J Ophthalmol. 2025 Mar;271:31-37. doi: 10.1016/j.ajo. 2024.10.015. Epub 2024 Oct 24. PMID: 39461403.
Faes L, Feo A, Sheng J, Ramtohul P, Gundlach BS, Jumper JM, Sarraf D, Freund KB. Features of ValsalvaInduced Choroidal Hemorrhage in High Myopia. Ophthalmol Retina. 2025 Feb;9(2):194-196. doi: 10.1016/j. oret.2024.10.021. Epub 2024 Oct 29. PMID: 39477208.
Qaseem Y, Hou KK , Pettenkofer MS
Outcomes After Switching to Faricimab for Refractive Macular Edema in Treatment-Experienced Eyes with Neovascular Age-Related Macular Degeneration. Clin Ophthalmol. 2024 Oct 29:18:3097-3102. Doi: 10.2147/ OPTH.S483563.
Su BE, Weiss RE, Nouri-Mahdavi K , Holbrook AJ. A spatially varying hierarchical random effects model for longitudinal macular structural data in glaucoma patients. Ann Appl Stat. 2024 Dec;18(4):3444-3466. doi: 10.1214/24aoas1944. Epub 2024 Oct 31. PMID: 40017564; PMCID: PMC11864210.
NOVEMBER 2024
Hou KK , Aldave AJ, Kreiger AE
Chronic hypotony and uveitis managed with pars plana vitrectomy, silicone oil tamponade, and permanent keratoprosthesis. Retin Cases Brief Rep. 2024 Nov 1;18(6):671-674. doi: 10.1097/ ICB.0000000000001475. PMID: 37603441.
Schildroth KR, Peterson KD, Altaweel MM, Channa R, Chang JS, Gottlieb JL, Ip MS , Nork TM. Supplemental dextrose in the infusion fluid during diabetic vitrectomy. Retina. 2024 Nov 1;44(11):1931-1936. doi: 10.1097/ IAE.0000000000004203. PMID: 39437216; PMCID: PMC11884518.
Strawbridge J, Cheng JY, Gundlach BS, Gillespie T, Karmouta R, Khitri M , Chu A, Tsui I . Short-term reactivation of retinopathy of prematurity after primary ranibizumab treatment. Retina. 2024 Nov 1;44(11):1945-1951. doi: 10.1097/ IAE.0000000000004206. PMID: 39024625.
Shang P, Ambrosino H, Hoang J, Geng Z, Zhu X, Shen S, Eminhizer M, Hong E, Zhang M, Qu J, Du J, Montezuma SR, Dutton JR, Ferrington DA The Complement Factor H (Y402H) risk polymorphism for age-related macular degeneration affects metabolism and response to oxidative stress in the retinal pigment epithelium. Free Radic Biol Med. 2024 Nov 20;225:833-845. doi: 10.1016/j.freeradbiomed.2024.10.307. Epub 2024 Nov 2. PMID: 39491736.
Gedde SJ, Vinod K, Bowden EC, Kolomeyer NN, Chopra V, Challa P, Budenz DL, Repka MX, Lum F. Reply. Ophthalmology. 2025 Feb;132(2):e22. doi: 10.1016/j.ophtha.2024.10.003. Epub 2024 Nov 4. PMID: 39503662.
Rabiolo A, Montesano G, Gazzard G, Caprioli J, De Cillà S. Re: Gedde et al: Special Commentary: Reporting clinical endpoints in studies of minimally invasive glaucoma surgery (Ophthalmology. 2025;132:141-153). Ophthalmology. 2025 Feb;132(2):e20-e22. doi: 10.1016/j. ophtha.2024.10.002. Epub 2024 Nov 4. PMID: 39503658.
Cavanaugh BL, Milstein ML, Boucher RC, Tan SX, Hanna MW, Seidel A, Frederiksen R, Saunders TL, Sampath AP, Mitton KP, Zhang DQ, Goldberg AFX. A new mouse model for PRPH2 pattern dystrophy exhibits functional compensation prior and subsequent to retinal degeneration. Hum Mol Genet. 2024 Nov 5;33(21):1916-1928. doi: 10.1093/hmg/ddae128. PMID: 39231530.
Hanson J, Hui M, Strawbridge JC, Chatterjee S, Goodyear K, Giaconi JA , Tsui I . High Rates of Eye Surgery Cancellation in Veterans Related to Mental Health. Mil Med 2024 Nov 5; 189(11-12):e2588-e2593. PMID 38687601.
Cavuoto KM, Trivedi RH, Prakalapakorn SG, Oatts JT, Nallasamy S, Morrison DG, Pineles SL , Chang MY. Multifocal Soft Contact Lenses for the Treatment of Myopia Progression in Children: A Report by the American Academy of Ophthalmology. Ophthalmology. 2025 Apr;132(4):495-503. doi: 10.1016/ j.ophtha.2024.09.031. Epub 2024 Nov 7. PMID: 39503665; PMCID: PMC11930616.
Good SD, Adamus G, Gorin MB, Jacquez J, Grossman J, Matsuura I, Hasan A, Skaggs B, McMahon M. Anti-retinal Autoantibodies in Hydroxychloroquine Eye Toxicity. ACR Open Rheumatol. 2025 Jan;7(1):e11743. doi: 10.1002/acr2.11743. Epub 2024 Nov 7. PMID: 39511790; PMCID: PMC11694172.
Ashrafkhorasani M, Besharati S, Mohammadzadeh V, Zou J, Figueroa J, Mohammadi M, Nouri-Mahdavi K Enhancing Detection of Glaucoma Progression: Utility of 24-2 Visual Field Central Points vs. 10-2 Visual Fields. Ophthalmol Glaucoma. 2025 Mar-Apr;8(2):117-125. doi: 10.1016/j. ogla.2024.11.004. Epub 2024 Nov 12. PMID: 39542212.
Fabiani C, Shantha J, Gangaputra S, Vitale A, Thorne JE, Jabs DA, Fawzi A, Smith JR, Accorinti M, Smet MD, Agrawal R, Munk MR, Agarwal A, Pichi F, Carreño E, Invernizzi A, Chee SP, Davis JL, Sarraf D, Gupta V. Is it Time to Adopt a New Nomenclature and Classification for White Dot Syndromes Using Multimodal Imaging Techniques? Ocul Immunol Inflamm. 2025 May;33(4):561-569. doi: 10.1080/09273948.2024.2423870. Epub 2024 Nov 13. PMID: 39535406.
Corradetti G, Karamat A, Srinivas S , Lindenberg S, Velaga SB, Corvi F, Attiku Y, Nittala MG, Desai D, Zhu L, Abulon D, Sadda SR . Progression to complete retinal pigment epithelium and outer retinal atrophy (cRORA): post hoc analysis of the GATHER1 trial. Graefes Arch Clin Exp Ophthalmol. 2025 Mar;263(3):669-677. doi: 10.1007/ s00417-024-06676-7. Epub 2024 Nov 14. PMID: 39538001; PMCID: PMC11953152.
Hubschman S, Sojitra B, Ghiam S, Sears C, Hwangbo N, Goldberg RA , Rootman DB. Teprotumumab and Orbital Decompression for the Management of Proptosis in Patients with Thyroid Eye Disease. Ophthalmic Plast Reconstr Surg. 2024 May-Jun 01;40(3):270-275. doi: 10.1097/IOP. 0000000000002563. Epub 2023 Nov 16. PMID: 37972968.
Heyman A, Zylberberg J. Fine Granularity Is Critical for Intelligent Neural Network Pruning. Neural Comput. 2024 Nov 19;36(12):26772709. doi: 10.1162/neco_a_01717. PMID: 39383032.

Jafari S, Hollister J, Kavehpour P, Demer JL . Shear viscoelastic properties of human orbital fat. J Biomech. 2024 Dec;177:112416. doi: 10.1016/j. jbiomech.2024.112416. Epub 2024 Nov 19. PMID: 39579590.
Sacconi R, Forte P, Corradetti G, Costanzo E, Capuano V, Bousquet E, Beretta F, Iannuzzi S, Polito MS, Nicolò M, Parravano M, Souied E, Sarraf D, Sadda S , Bandello F, Querques G. Type 3 Macular Neovascularization in Age-related Macular Degeneration: Baseline Predictors of 3-Year Macular Atrophy Development. Ophthalmol Retina. 2025 Jun;9(6):546-555. doi: 10.1016/j.oret.2024.11.011. Epub 2024 Nov 19. PMID: 39566885.
Nanji K, Phillips M, Thabane L, Tham YC, Wong TY, Steel DH, Munk MR, Wykoff CC, Chaudhary V; Retina Evidence and Trials INternational Alliance (R.E.T.I.N.A.) Study Group (Sarraf D). Pilot and feasibility studies in ophthalmology: fundamental keys to success. Eye (Lond). 2025 Jan;39(1): 4-6. doi: 10.1038/s41433-024-03413-6. Epub 2024 Nov 21. PMID: 39572846.
Anegondi N, Steffen V, Sadda SR , Schmitz-Valckenberg S, Tufail A, Csaky K, Lad EM, Kaiser PK, Ferrara D, Chakravarthy U. Visual Loss in Geographic Atrophy: Learnings from the Lampalizumab Trials. Ophthalmology. 2025 Apr;132(4):420430. doi: 10.1016/j.ophtha.2024.11.017. Epub 2024 Nov 23. PMID: 39581330.
Szeto SK, Lai TY, Vujosevic S, Suns JK, Sadda SR , Tan G, Sivaprasad S, Wong TY, Cheung CY. Corrigendum to “Optical coherence tomography in the management of diabetic macular oedema” [Prog. Retin. Eye Res. 98 (2024) 101220]. Prog Retin Eye Res. 2025 Jan;104:101319. doi: 10.1016/j. preteyeres.2024.101319. Epub 2024 Nov 30. Erratum for: Prog Retin Eye Res. 2024 Jan;98:101220. doi: 10.1016/ j.preteyeres.2023.101220. PMID: 39616093.
DECEMBER 2024
Feo A, Sarraf D. Fluid Pathways in Age-Related Macular Degeneration Elucidated with Advanced Retinal Imaging. Ophthalmol Retina. 2024 Dec;8(12):1115-1117. doi: 10.1016/j.oret. 2024.08.019. PMID: 39632019.
Mohammadi M, Su E, Mohammadzadeh V, Besharati S, Martinyan A, Coleman AL , Law SK , Caprioli J, Weiss RE, Nouri-Mahdavi K . Comparison of Retinal Nerve Fiber Layer and Ganglion Cell Complex Rates of Change in Patients with Moderate to Advanced Glaucoma. Am J Ophthalmol. 2024 Dec;268:190-198. doi: 10.1016/j.ajo. 2024.07.025. PMID: 39111519.
Cheng JY, Margines JB, Abraham N, Tsui I , Sarraf D. Blue Rubber Bleb Nevus Syndrome and Retinal Cavernous Hemangioma. Retina. 2024 Dec 1;44(12):e78-e80. doi: 10.1097/ IAE.0000000000004199. PMID: 39187262.
Huang RS, Naidu SC, Mihalache A, Popovic MM, Kertes PJ, Sarraf D, Sadda SR , Muni RH, Kohly RP. Loss to Follow-Up in Patients with Proliferative Diabetic Retinopathy or Diabetic Macular Edema. JAMA Netw Open. 2024 Dec 2;7(12):e2450942. doi: 10.1001/jamanetworkopen.2024.50942. PMID: 39671194; PMCID: PMC11645645.
Akpek EK, Aldave AJ, Amescua G, Colby KA, Cortina MS, de la Cruz J, Parel JA, Foster JW. Prognostic significance of biointegration at the optic-cornea joint in keratoprosthesis implantation. Cornea. 2024 Dec 3; 44(5):628-636.
Hultgren NW, Petcherski A, Torriano S, Komirisetty R, Sharma M, Zhou T, Burgess BL, Ngo J, Osto C, Shabane B, Shirihai OS, Kelesidis T, Williams DS Productive infection of the retinal pigment epithelium by SARS-CoV-2: Initial effects and consideration of long-term consequences. PNAS Nexus. 2024 Dec 3;3(12):page500. doi: 10.1093/ pnasnexus/pgae500. PMID: 39712068; PMCID: PMC11660945.
Tan C, Puran AI, Santina A, Yu F, Kitayama K, Tseng VL , Coleman AL Social determinants of health as risk factors for keratoconus in the All of Us database. J Ophthalmol. 2024 Dec 10:bjo-2024-326229. doi: 10.1136/bjo2024-326229. PMID: 39658142.
Aziz AA, Khanani AM, Khan H, Lauer E, Khanani I, Mojumder O, Khanani ZA, Khan H, Gahn GM, Graff JT, Abbey AM, Almeida DRP, Barakat MR, Corradetti G, Graff JM, Haug SJ, Nielsen JS, Sheth VS, Sadda SR , Hadas I, Benyamini G, Nahen K, Mohan N. Retinal fluid quantification using a novel deep learning algorithm in patients treated with faricimab in the TRUCKEE study. Eye (Lond). 2025 Apr;39(6):1099-1106. doi: 10.1038/s41433-024-03532-0. Epub 2024 Dec 11. PMID: 39663398; PMCID: PMC11978878.
Santina A, Feo A, Bousquet E, Velaga SB, Abraham N, Fogel-Levin M, Romero-Morales V, Somisetty S, Wong A, Lu A, Nittala M, Chhablani J, Voichanski S, Au A , Sadda S , Sarraf D Pentosan polysulfate sodium maculopathy: Final analysis of a prospective cohort, updated review, and association with inflammatory bowel disease. Surv Ophthalmol. 2025 MayJun;70(3):583-592. doi: 10.1016/j. survophthal. 2024.12.002. Epub 2024 Dec 12. PMID: 39674406.
Bousquet E, Santina A, Somisetty S, Morales VR, Holland GN , Sarraf D Hydroxychloroquine retinopathy in a 23-year-old male. Retin Cases Brief Rep. 2024 Dec 13. doi: 10.1097/ ICB.0000000000001704. PMID: 39689289.
Darzi AJ, Busse JW, Torabiardakani K, Phillips M, Thabane L, Bhandari M, Borrelli E, Steel DH, Wykoff CC, Chaudhary V; Retina Evidence and Trials INternational Alliance (R.E.T.I.N.A.) Study Group (Sarraf D). Risk assessment models: considerations prior to use in clinical practice. Eye (Lond). 2025 Mar;39(4):617-619. doi: 10.1038/s41433-024-03557-5. Epub 2024 Dec 18. PMID: 39695254.
Diep BL, Glasgow BJ, Bert BB Remission of Ocular Surface Squamous Neoplasia. Ophthalmology. 2024 Dec;131(12):1475. doi: 10.1016/j.ophtha. 2023.11.010. Epub 2023 Dec 18. PMID: 38108681.
Forte P, Feo A, Sarraf D, Romano MR, Nicolò M. Current insights and challenges in the management of perifoveal vascular anomalous complex (PVAC): a systematic review of multimodal imaging features and treatment strategies. Eye (Lond). 2025 Feb;39(3):449-459. doi: 10.1038/ s41433- 024-03544-w. Epub 2024 Dec 19. PMID: 39702788.
Yu-Wai-Man P, Newman NJ, Biousse V, Carelli V, Moster ML, Vignal-Clermont C, Klopstock T, Sadun AA , Sergott RC, Hage R, Degli Esposti S, La Morgia C, Priglinger C, Karanja R, Taiel M, Sahel JA; LHON Study Group. FiveYear Outcomes of Lenadogene Nolparvovec Gene Therapy in Leber Hereditary Optic Neuropathy. JAMA Ophthalmol. 2024 Dec 19. doi: 10.1001/ jamaophthalmol.2024.5375. PMID: 39699886.
Tsui E , Jackson NJ, Chen JL , Holland GN . Establishment of a Standard Technique for Determining Laser Flare Photometry Values during Assessment of Intraocular Inflammation. Ophthalmol Sci. 2024 Dec 20;5(3):100690. doi: 10.1016/j.xops.2024.100690. PMID: 40114710; PMCID: PMC11925576.
Chaudhary V, Mar F, Amador MJ, Chang A, Gibson K, Joussen AM, Kim JE, Lee J, Margaron P, Saffar I, Wong D, Wykoff C, Sadda S . Emerging clinical evidence of a dual role for Ang-2 and VEGF-A blockade with faricimab in retinal diseases. Graefes Arch Clin Exp Ophthalmol. 2025 May;263(5):12391247. doi: 10.1007/s00417-024-06695-4. Epub 2024 Dec 21. PMID: 39708087; PMCID: PMC12148975.
Lakkaraju A, Boya P, Csete M, Ferrington DA , Hurley JB, Sadun AA , Shang P, Sharma R, Sinha D, Ueffing M, Brockerhoff SE. How crosstalk between mitochondria, lysosomes, and other organelles can prevent or promote dry age-related macular degeneration. Exp Eye Res. 2025 Feb;251:110219. doi: 10.1016/j.exer.2024.110219. Epub 2024 Dec 22. PMID: 39716681 Review.
Kianian R, Sun D, Rojas-Carabali W, Agrawal R, Tsui E . Large Language Models May Help Patients Understand Peer-Reviewed Scientific Articles About Ophthalmology: Development and Usability Study. J Med Internet Res. 2024 Dec 24;26:e59843. doi: 10.2196/59843. PMID: 39719077; PMCID: PMC11707445.
Wang J, Zhang L, Cavallini M, Pahlevan A, Sun J, Morshedian A, Fain GL , Sampath AP, Peng YR . Molecular characterization of the sea lamprey retina illuminates the evolutionary origin of retinal cell types. Nat Commun. 2024 Dec 30;15(1):10761. doi: 10.1038/s41467024-55019-x. PMID: 39737973; PMCID: PMC11685597.
Field, GD. (2025). Information processing: Ganglion cells. In P. A. D’Amore (Ed.), Encyclopedia of the Eye (Vol. 3, pp. 224–233). Elsevier, Academic Press.
Field, GD. (2025). Information processing in the retina. In P. A. D’Amore (Ed.), Encyclopedia of the Eye (Vol. 3, pp. 246–254). Elsevier, Academic Press.
Cohen SA, Tseng VL , Sridhar J, Coleman AL . A New Era of Ophthalmology Leadership? A Descriptive and Comparative Analysis of Ophthalmology Department Chairs in 2024. Am J Ophthalmol. 2025 Jan;269:373-380. doi: 10.1016/j.ajo.2024.09.020. PMID: 39313085.
Hazim RA, Williams DS . The Importance of Differentiated RPE Cultures for Studying Cell Biological Processes. Adv Exp Med Biol. 2025; 1468:351-355. doi: 10.1007/978-3-03176550-6_58. PMID: 39930221.
Paniagua AE, Chang A, Williams DS Mechanism of Photoreceptor Outer Segment Tip Ingestion: Evidence of Trogocytosis. Adv Exp Med Biol. 2025;1468:309-311. doi: 10.1007/978-3031-76550-6_51. PMID: 39930214.
Feo A, Sarraf D. Outer Retinal Holes in Degenerative Retinoschisis. Retina. 2025 Jan 1;45(1):e1-e2. doi: 10.1097/ IAE.0000000000004241. PMID: 39121501. No abstract available.
Demer JL , Clark RA, Suh SY, Giaconi JA , Nouri-Mahdavi K , Law SK , Bonelli L , Arnold AC , Quiros P, Coleman AL , Caprioli J. Eye Movements and the Intraorbital Subarachnoid Space: Potential Contribution of Altered Cerebrospinal Fluid Pumping in Optic Neuropathies. Invest Ophthalmol Vis Sci. 2025 Jan 2;66(1):53. doi: 10.1167/ iovs.66.1.53. PMID: 39847366; PMCID: PMC11758931.
Moujane F, Zhang C, Knight R, Lee JY, Deng SX , Zheng JJ. Corneal Stromal Stem Cell-Derived Extracellular Vesicles Attenuate ANGPTL7 Expression in the Human Trabecular Meshwork. Transl Vis Sci Technol. 2025 Jan 2;14(1):21. doi: 10.1167/tvst. 14.1.21. PMID: 39847376; PMCID: PMC11759583.
Figueroa J, Su E, Mohammadzadeh V, Besharati S, Mohammadi M, Ashrafkhorasani M, Law SK , Coleman AL , Caprioli J, Weiss RE, Nouri - Mahdavi K . Association of Blood Pressure and Retinal Nerve Fiber Layer Rates of Thinning in Patients with Moderate to Advanced Glaucoma Ophthalmol Glaucoma. 2025 Jan 3:S2589-4196(24)00225-4. doi: 10.1016/j.ogla.2024.12.009. PMID: 39756794.
Frederiksen R, Peng YR , Sampath AP, Fain GL . Evolution of rod bipolar cells and rod vision. J Physiol. 2025 Jan 7. doi: 10.1113/JP287652. PMID: 39775947. Review.
Rabiolo A, Triolo G, Khaliliyeh D, Jin SW, Morales E, Ghirardi A, Anand N, Montesano G, Virgili G, Caprioli J, De Cillà S. Hypotony Failure Criteria in Glaucoma Surgical Studies and Their Influence on Surgery Success. Ophthalmology. 2024 Jul;131(7):803814. doi: 10.1016/j.ophtha.2024.01.008. Epub 2024 Jan 8. PMID: 38199527.
Pillar S, Kadomoto S, Chen K, Gonzalez SS, Cherian N, Privratsky JK, Zargari N, Jackson NJ, Corradetti G, Chen JL , Sadda SR , Holland GN , Tsui E
Automated quantification of anterior chamber cells using swept-source anterior segment optical coherence tomography. J Ophthalmic Inflamm Infect. 2025 Jan 9;15(1):3. doi: 10.1186/s12348- 025-00456-y. PMID: 39786628; PMCID: PMC11717729.
Tailor PD, Au AC, Pineles S . Ocular Type 1 Sialidosis. Ophthalmol Retina. 2025 Jan 10:S2468-6530(24)00585-2. doi: 10.1016/j.oret.2024.12.009. PMID: 39797873.
Ruamviboonsuk P, Ng DSC, Chaikitmongkol V, Chang A, Chen SJ, Chen Y, Cheung CMG, Gomi F, Guymer R, Kim JE, Koh A, Kokame GT, Lai CC, Lai TYY, Lee WK, Ogura Y, Sadda S , Teo KYC, Wong TY, Yanagi Y, Lam DSC. Consensus and guidelines on diagnosis and management of poly poidal choroidal vasculopathy (PCV) from the Asia-Pacific Vitreo-retina Society (APVRS). Asia Pac J Ophthalmol (Phila). 2025 Jan-Feb;14(1):100144. doi: 10.1016/ j.apjo.2025.100144. Epub 2025 Jan 15. PMID: 39824255.
Manta AI, Demer J, Goldberg R
Magnetic Resonance Imaging
Demonstrates Differences in Brow and Upper Eyelid Fat and Muscle Layers Between East Asians and Caucasians. Ophthalmic Plast Reconstr Surg. 2025 Jan 16. doi: 10.1097/ IOP.0000000000002904.
Pohl KA, Zhang X, Ji JJ, Stiles L, Sadun AA , Yang XJ. Derivation and Characterization of Isogenic OPA1 Mutant and Control Human Pluripotent Stem Cell Lines. Cells. 2025 Jan 17; 14(2):137. doi: 10.3390/cells14020137. PMID: 39851566; PMCID: PMC11764107.
Peshkar-Kulkarni S, Chung DD, Aldave AJ. Antioxidant MitoQ increases viability of human corneal endothelial cells with congenital hereditary endothelial dystrophy- associated SLC4A11 mutations. Ophthalmic Genet. 2025 Apr;46(2):166-173. doi: 10.1080/13816810.2025.2450455. Epub 2025 Jan 20.
Kashani AH, Koronyo-Hamaoui M, Koronyo Y, Shi H, Alluwimi M, Singer M, Sagare A, Hawes D, Tang A, Jiang X, Collazo Martinez A, Ross-Cisneros FN, Sadun AA , Ringman JM. Retinal and Optic Nerve Lesions Correspond to Amyloid in Autosomal Dominant Alzheimer’s Disease. medRxiv. 2025 Jan 22:2025.01.21.25319904. doi: 10.1101/2025.01.21.25319904. PMID: 39974084.
Bartzoulianou RC, Coleman AL , Wilson MR, Harris A, Bougioukas KI, Pappas T, Giannoulis DA, Yu F, Raptou A, Tzoanou G, Topouzis F. Factors Associated with Corneal Hysteresis in an Elderly White Population: The Thessaloniki Eye Study. J Glaucoma. 2025 Jan 23. doi: 10.1097/IJG.0000000000002541. PMID: 39841091.
Iwundu CN, Chen Y, Coleman AL , Hansen J, Kwon J, Heck JE. Occupational Exposures and Age-related Cataract: A Review. Arch Environ Occup Health. 2025 Jan 24:1-10. doi.org/ 10.1080/19338244.2025.2451907. PMID: 39850981.
Munk MR, Turgut F, Faes L, Jaggi D, Freund KB, Sadda SR , Peto T, Wang RK, Pircher M, Curcio CA, Sun J, Kashani AH; International Retinal Imaging Society Research Group. Standardization of OCT Angiography Nomenclature in Retinal Vascular Diseases: Consensus-Based Recommendations. Ophthalmol Retina. 2025 Jul;9(7):645-654. doi: 10.1016/j. oret. 2025.01.015. Epub 2025 Jan 31. PMID: 39894444.
Yehezkeli V, Pineles SL , Demer JL , Meng Q, Velez FG. Strabismus Surgery in Patients Aged Over 80 Years: Indications, Safety, and Outcomes. Am J Ophthalmol. 2025 Apr;272:145-149. doi: 10.1016/j.ajo.2025.01.021. Epub 2025 Jan 31. PMID: 39894427.
FEBRUARY 2025
Choi H, Corradetti G, Lindenberg S, Karamat AN, Oncel D, Liu H, Gnanaraj R, Fasih-Ahmad S, Marion KM, Baker KL, Gulati S, Foster B, Lam A, Sadda SR , Lally DR. Incomplete RPE and Outer Retinal Atrophy (iRORA) Development in Eyes with Felloweye Neovascular Age-related Macular Degeneration. Ophthalmic Surg Lasers Imaging Retina. 2025 May;56(5): 274-279. doi: 10.3928/2325816020250108-01. Epub 2025 Feb 1. PMID: 39960315.
Qaseem Y, Ben Margines J, Song W, Au A , Gupta OP, Sridhar J. Scleral Fixation of an Intraocular Lens with Gore-Tex ® Suture from a Temporal Approach. Ophthalmic Surg Lasers Imaging Retina. 2025 Mar;56(3):136138. doi: 10.3928/23258160-2024120401. Epub 2025 Feb 1. PMID: 39960302.
Yu-Wai-Man P, Newman NJ, Biousse V, Carelli V, Moster ML, Vignal-Clermont C, Klopstock T, Sadun AA , Sergott RC, Hage R, Degli Esposti S, La Morgia C, Priglinger C, Karanja R, Taiel M, Sahel JA; LHON Study Group ( Tsui I ). Five-Year Outcomes of Lenadogene Nolparvovec Gene Therapy in Leber Hereditary Optic Neuropathy. JAMA Ophthalmol. 2025 Feb 1;143(2):99108. doi: 10.1001/jamaophthalmol. 2024.5375. PMID: 39699886; PMCID: PMC11843360.
Yamamoto MH, Marin AI, Tsui I Management of traumatic macular hole and retinal detachment using amniotic membrane transplantation: A case report. Am J Ophthalmol Case Rep. 2025 Feb 2;37:102267. doi: 10.1016/j. ajoc.2025.102267. PMID: 40104278; PMCID: PMC11916789.
He Y, Heumann P, Weilin Song M, Kadomoto S, Sadda SR , Pluym ID, Tsui I . Changes in Optical Coherence Tomography Angiography Precede Clinical Onset of Placental Insufficiency. Invest Ophthalmol Vis Sci. 2025 Feb 3;66(2):36. doi: 10.1167/ iovs.66.2.36. PMID: 39937495; PMCID: PMC11827859.
Mukherjee S, Arunachalam T, Duic C, Abraham M, Orndahl C, Menezes S, Agrón E, Pfau M, de Silva T, Bailey C, Thavikulwat AT, Bellur S, Sadda SR , Chew EY, Jeffrey BG, Wong WT, Keenan TDL. Structure-Function
Relationships in Geographic Atrophy Based on Mesopic Microperimetry, Fundus Autofluorescence, and Optical Coherence Tomography. Transl Vis Sci Technol. 2025 Feb 3;14(2):7. doi: 10.1167/tvst.14.2.7. PMID: 39908134; PMCID: PMC11806430.
Okawa H, Sampath AP. Temporal Transformation of the Rod SinglePhoton Response in the Retinal Circuitry. Invest Ophthalmol Vis Sci. 2025 Feb 3;66(2):52. doi: 10.1167/ iovs.66.2.52. PMID: 39976956.
Savastano MC, Fossataro C, Carlà MM, Cestrone V, Biagini I, Rizzo C, Kilian R, Zweifel SA, Muth DR, Faraldi F, Rizzo S, Sarraf D. OCT Angiography of Type 1 Macular Neovascularization in AMD: A Morphometric Evaluation. Transl Vis Sci Technol. 2025 Feb 3;14(2):23. doi: 10.1167/tvst.14.2.23. PMID: 39992662.
Wang X, Hoshi S, Liu R, Corradetti G, Ip M , Sarraf D, Sadda SR , Zhang Y
Photoreceptor Function and Structure in Retinal Areas with Intraretinal Hyperreflective Foci in Age- Related Macular Degeneration. Invest
Ophthalmol Vis Sci. 2025 Feb 3; 66(2):27. doi: 10.1167/iovs.66.2.27. PMID: 39928312; PMCID: PMC11812613.
Yoshida K, Anegondi N, Pely A, Zhang M, Debraine F, Ramesh K, Steffen V, Gao SS, Cukras C, Rabe C, Ferrara D, Spaide RF, Sadda SR , Holz FG, Yang Q. Deep Learning Approaches to Predict Geographic Atrophy Progression Using Three-Dimensional OCT Imaging.
Transl Vis Sci Technol. 2025 Feb 3; 14(2):11. doi: 10.1167/tvst.14.2.11. PMID: 39913124; PMCID: PMC11806428.
Hanson J, Khorrami R, Kanamoto K, Strawbridge J, Miller KM , Lin SR
Evaluating the Protective Effects of a Dispersive Ophthalmic Viscosurgical Device Versus Balanced Salt Solution on the Cornea During Cataract Surgery. Eye Contact Lens. 2025 Apr 1;51(4):165-170. doi: 10.1097/ICL. 0000000000001161. Epub 2025 Feb 4. PMID: 39901353.
Feo A, Govetto A, Ramtohul P, Abraham N, Cabral D, Chang PY, Chaudhry N, Chen FK, Eliott D, Faes L, Heath Jeffery RC, Mrejen S, Popovic MM, Tieger MG, Zatreanu L, Sadda SR , Freund KB, Romano MR, Sarraf D Stellate Nonhereditary Idiopathic Foveomacular Retinoschisis and Central Anomalous Retinoschisis with mid-Peripheral Traction (CARPET). Ophthalmol Retina. 2025 Feb 6:S24686530(25)00051-X. doi: 10.1016/j.oret. 2025.01.019. PMID: 39922381.
Yehezkeli V, Demer JL . Common Forms of Adult Esotropia Require Augmented Surgical Dosing. Am J Ophthalmol. 2025 May;273:74-81. doi: 10.1016/j.ajo.2025.02.007. Epub 2025 Feb 11. PMID: 39947270
Kalavar M, Sridhar J. Clinical trials and real-world studies examining faricimab and high-dose aflibercept for wet agerelated macular degeneration and diabetic macular edema. Curr Opin Ophthalmol. 2025 May 1;36(3):189-198. doi: 10.1097/ICU.0000000000001129. Epub 2025 Feb 12. PMID: 39937692.
Gijs M, van de Sande N, Bonnet C , Schmeetz J, Fernandes R, Travé - Huarte S, Huertas-Bello M, Bo Chiang JC, Boychev N, Sharma S; Tear Research Network Scoping Review taskforce. A comprehensive scoping review of methodological approaches and clinical applications of tear fluid biomarkers. Prog Retin Eye Res. 2025 May;106:101338. doi: 10.1016/j.preteyeres.2025.101338. Epub 2025 Feb 13. PMID: 39954936.
Davis MR, Robinson E, Koronyo Y, Salobrar-Garcia E, Rentsendorj A, Gaire BP, Mirzaei N, Kayed R, Sadun AA , Ljubimov AV, Schneider LS, Hawes D, Black KL, Fuchs DT, Koronyo-Hamaoui M. Retinal ganglion cell vulnerability to pathogenic tau in Alzheimer’s disease. Acta Neuropathol Commun. 2025 Feb 15;13(1):31. doi: 10.1186/s40478-02501935-y. PMID: 39955563.
Sakuno G, Sarraf D, Sadda SR , Preti RC, Oliveira BPM, Damico FM. Coronary artery and retinal vascularization by optical coherence tomography angiography: are eyes the window to the heart? Graefes Arch Clin Exp Ophthalmol. 2025 Jun;263(6):15031513. doi: 10.1007/s00417-025-06769-x. Epub 2025 Feb 15. PMID: 39954049.
Gunawardene AN, Suraneni S, Rohowetz LJ, Sridhar J. Characteristics and Medical Accuracy of Online Discussions of Retinal Conditions on a Social Media Platform. J Vitreoretin Dis. 2025 Feb 19:24741264251315139. doi: 10.1177/24741264251315139. PMID: 39991040; PMCID: PMC11840817.
Miller JML, Thompson BR, Handa JT, Luthert P, Chakravarthy U, Csaky KG, Bird A, Young BK, Iyengar SK, Baek J, Zouache MA, Richards BT, Hageman GS, Rodrigues G, Bharti K, Flannery JG, Gorin MB, Bowes Rickman C. Dissecting the biological complexity of age-related macular degeneration: Is it one disease, multiple separate diseases, or a spectrum? Exp Eye Res. 2025 May;254:110304. doi: 10.1016/j.exer.2025.110304. Epub 2025 Feb 19. PMID: 39983974; PMCID: PMC12066171.
Malyugin B, Kalinnikova S, Nefedova O, Gerasimov M, Müller F, Bernau W. Autologous Glueless Simple Limbal Epithelial Transplantation for Unilateral Stem Cell Deficiency Using Femtosecond Laser-Assisted Limbal Stem Cell Harvesting: The Report of the First 3 Clinical Cases. Cornea. 2025 Feb 21;44(8):1058-1069. doi: 10.1097/ ICO.0000000000003838. PMID: 40591740.
Meng Q, Yehezkeli V, Demer JL Surgical Management of Masquerading Superior Oblique Palsy. Am J Ophthalmol. 2025 May;273:240-247. doi: 10.1016/j.ajo. 2025.02.015. Epub 2025 Feb 21. PMID: 39986638.
Sharma A, Holz FG, Kumar N, Sarraf D, Ayachit S, Mishra C, Tufail A, Chakraborty D, Rachitskaya A, Eichenbaum D, Banker A, Parachuri N, Kumar A, Loewenstein A, Bandello F, Wakabayashi T, Woo SJ, Kuppermann BD. Biosimilar ranibizumab (Ranieyes) safety and efficacy in the real world: BRESER Study. J Vitreoretin Dis. 2025 Feb 27. doi:10.1177/24741264251322213. PMID: 40028177.
MARCH 2025
Engelmann AR, Pargalava N, Sadun AA . Blindness following hydrogen peroxide ingestion and recovery with hyperbaric oxygen therapy. Toxicol Rep. 2025 Mar 1;14:101985. doi: 10.1016/ j.toxrep.2025.101985. eCollection 2025 Jun.
Sadda SR . Photobiomodulation for Age-Related Macular Degeneration. JAMA Ophthalmol. 2025 Mar 1;143(3): 195-196. doi: 10.1001/jamaophthalmol. 2025.0077. PMID: 39854014.
Mohammadzadeh V, Su E, Zhuang I, Besharati S, Park J, Yonge A, Shi L, Caprioli J, Weiss RE, Nouri-Mahdavi K Retinal Nerve Fiber Layer Rates of Change: Comparison of 2 OCT Devices. Ophthalmol Glaucoma. 2025 Mar 4:S2589-4196(25)00033-X. doi: 10.1016/j.ogla.2025.02.005. PMID: 40049324.
Oh AJ, Bouris E, Leyva BK, Malik M, Caprioli J. Telemedicine in Glaucoma Management: Patient Perspectives. J Glaucoma. 2025 May 1;34(5):365-370. doi: 10.1097/IJG.0000000000002558. Epub 2025 Mar 4. PMID: 40029196.
Feo A, Ramtohul P, Govetto A, Borrelli E, Sacconi R, Corradetti G, Querques G, Romano MR, Rosenfeld PJ, Spaide RF, Freund KB, Sadda S , Sarraf D. En face OCT: breakthroughs in understanding the pathoanatomy of retinal disease and clinical applications. Prog Retin Eye Res. 2025 May;106: 101351. Epub 2025 Mar 5. doi:10.1016/ j.preteyeres. 2025.101351. PMID: 40054600.
Lee SY, Paul ME, Coleman AL , Kitayama K, Yu F, Pan D, Tseng VL. Author Reply to Shah et al. Ophthalmol Glaucoma. 2025 May-Jun;8(3):e5-e6. doi: 10.1016/j.ogla.2025.01.004. Epub 2025 Mar 7. PMID: 40057903.
Moussa K, Virk JS, Paciotti B, DurbinJohnson BP, Shantha JG, Tsui E , Sun CQ, Baxter SL, Gore C, Yiu GY. Adherence to Hydroxychloroquine Dosing Guidelines at the University of California. Ophthalmol Retina. 2025 Mar 10:S2468-6530(25)00100-9. doi: 10.1016/j.oret.2025.03.003. PMID: 40074061.
Tseng VL, Kitayama K, Yu F, Coleman AL . Associations between socioeconomic factors and neovascular glaucoma in a United States Medicare population. J Glaucoma. 2025 Mar 10. doi: 10.1097/IJG.0000000000002561. PMID: 40052874.
Ku PI, Sreeja JS, Chadha A, Williams DS , Engelke MF, Subramanian R. Collaborative role of two distinct ciliumspecific cytoskeletal systems in driving Hedgehog-responsive transcription factor trafficking. Sci Adv. 2025 Mar 14; 11(11):eadt5439. doi: 10.1126/sciadv. adt5439. Epub 2025 Mar 12. PMID: 40073114; PMCID: PMC11900865.
Rodrigues-Braz D, Bonnet C , Zhu L, Yesilirmak N, Gélizé E, Jonet L, Jaisser F, Bourges JL, Behar-Cohen F, Zhao M. Mineralocorticoid receptor antagonism improves corneal integrity in a rat model of limbal stem cell deficiency. Biomed Pharmacother. 2025 Apr;185:117979. doi: 10.1016/j.biopha. 2025.117979. Epub 2025 Mar 12. PMID: 40080998.
Gim N, Ferguson A, Blazes M, Soundarajan S, Gasimova A, Jiang Y, Sánchez CI, Zalunardo L, Corradetti G, Elze T, Honda N, Waheed NK, Cairns AM, Canto-Soler MV, Domalpally A, Durbin M, Ferrara D, Hu J, Nair P, Lee AY, Sadda SR , Keenan TDL, Patel B, Lee CS; Ryan Initiative for Macular Research (RIMR) Consortium. Publicly available imaging datasets for age-related macular degeneration: Evaluation according to the Findable, Accessible, Interoperable, Reusable (FAIR) principles. Exp Eye Res. 2025 Jun;255:110342. doi: 10.1016/ j.exer. 2025.110342. Epub 2025 Mar 13. PMID: 40089134; PMCID: PMC12058379.
Gim N, Blazes M, Sánchez CI, Zalunardo L, Corradetti G, Elze T, Honda N, Waheed NK, Cairns AM, Canto-Soler MV, Domalpally A, Durbin M, Ferrara D, Hu J, Nair P, Sadda SR , Keenan TDL, Lee CS; RIMR Consortium. Retinal imaging in an era of open science and privacy protection. Exp Eye Res. 2025 Jun;255:110341. doi: 10.1016/ j.exer. 2025.110341. Epub 2025 Mar 14. PMID: 40090567; PMCID: PMC12059805.
Guymer RH, Rosenfeld PJ, Ehlers JP, Attar M, Chen H, Ferris F, Fujimoto JG, Ip M , Pfau M, Saßmannshausen M, Shen J, Zacks DN, van Zyl T, Wu Z, Jaffe GJ. Designing the next generation of clinical trials in intermediate AMD—a consensus driven, pragmatic, proof of concept early intervention study. Exp Eye Res. 2025 Jun; 255:110340. doi: 10.1016/j.exer. 2025. 110340. Epub 2025 Mar 14. PMID: 40090569.
Idrees S, Manookin MB, Rieke F, Field GD, Zylberberg J. Biophysical neural adaptation mechanisms enable artificial neural networks to capture dynamic retinal computation. Nat Commun. 2024 Jul 16;15(1):5957. doi: 10.1038/ s41467-024-50114-5. Erratum in: Nat Commun. 2025 Mar 14;16(1):2537. doi: 10.1038/s41467-025-57762-1. PMID: 39009568; PMCID: PMC11251147.
Boychev N, Sethu S, de Laak RO; Tear Research Network Survey Taskforce ( Bonnet C ); Gijs M. Global practices of tear fluid collection, storage, and molecular analysis—A questionnaire by the Tear Research Network. Cont Lens Anterior Eye. 2025 Jul;48(4):102388. doi: 10.1016/j.clae.2025.102388. Epub 2025 Mar 17. PMID: 40102139.
Feo A, Omidtabrizi A, Sarraf D
Ultrawidefield imaging of choroidal abnormalities in Neurofibromatosis Type 1. Ophthalmology. 2025 Mar 17. doi:10.1016/j.ophtha.2025.01.009. PMID: 40100194.
Saffari PS, Strawbridge JC, Roelofs KA, Rootman DB, Goldberg RA , Karlin JN. Facial Aging in Thyroid Eye Disease: Quantification by Artificial Intelligence. J Craniofac Surg. 2025 Mar 17. doi: 10.1097/SCS.0000000000011224. PMID: 40096588.
Yan D, Prajna NV, Lalitha P, Sansanayudh W, Satitpitakul V, Laovirojjanakul W, Chaudhary M, Bountogo M, Sie A, Coulibaly B, Amza A, Nassirou B, Almou I, Tran H, Tran Y, Tsui E , Onclinx T, Sella R, Goren L, McClean E, Tham V, Chen C, Ouimette K, Zhong L, Liu Y, Yu D, Abraham T, Lebas E, Arnold BF, McLeod SD, Deiner MS, Porco TC, Seitzman GD, Lietman TM, Shantha J, Hinterwirth A, Doan T. Association of Weather Variables with Pathogens Contributing to Conjunctivitis Worldwide. Clin Infect Dis. 2025 Mar 17;80(3):551-561. doi: 10.1093/cid/ciae417. PMID: 39158989; PMCID: PMC11912971.
Lubeck D, Woodard L, Hsiao C, Pan SM, Son D, Zhou A, Miller KM Costs of Treating Cataract Surgery Complications from a US Provider Perspective: A Micro-costing Approach for Health Economic Analyses. Expert Rev Ophthalmol 2025 Mar 19; 20(2):67-78.
Wu Z, Sadda SR , Ach T, Blodi BA, Bottoni F, Chakravarthy U, Chew EY, Curcio CA, Ferris FL 3rd, Fleckenstein M, Freund KB, Grunwald JE, Holz FG, Jaffe GJ, Liakopoulos S, Lim TH, Monés JM, Pagliarini S, Pauleikhoff D, Pfau M, Rosenfeld PJ, Sarraf D, SchmitzValckenberg S, Spaide RF, Sparrow JR, Staurenghi G, Tufail A, Viola F, Guymer RH. Onset of end-stage atrophic age-related macular degeneration as an endpoint—a Delphi Study: Classification of Atrophy Meetings Report 7. Ophthalmol Sci. 2025 Mar 28;5(5):100777. Epub 2025 Mar 20. doi:10.1016/j.xops.2025.100777. PMID: 40469898.
Chew EY, Cukras C, Duncan JL, Dysli C, He Y, Henry E, Holz F, Moult E, Owsley C, Roorda A, Sarraf D, Schwartz R, Spaide R, Taylor L, Teussink M, Zhang Y, Staurenghi G. Assessing structure-function relationships in non-neovascular agerelated macular degeneration. Exp Eye Res. 2025 Jun;255:110349. Epub 2025 Mar 22. doi:10.1016/j.exer. 2025. 110349. PMID: 40127748. PMCID: PMC12058413.
Dagi Glass LR, Aakalu VK, Foster JA, Grob SR, McCulley TJ, Tao J, Vagefi MR, Yoon M, Pineles SL , Wladis EJ. Patch Testing for Eyelid Dermatitis: A Report by the American Academy of Ophthalmology. Ophthalmology. 2025 Jul;132(7):842-847. doi: 10.1016/j.ophtha. 2025.01.019. Epub 2025 Mar 22. PMID: 40119863.
Racioppo P, Alhasany A, Pham NV, Wang Z, Corradetti G, Mikaelian G, Paulus YM, Sadda SR , Hu Z. Automated Foveal Avascular Zone Segmentation in Optical Coherence Tomography Angiography Across Multiple Eye Diseases Using Knowledge Distillation. Bioengineering (Basel). 2025 Mar 23;12(4):334. doi: 10.3390/ bioengineering12040334. PMID: 40281694; PMCID: PMC12025180.
Zhong L, Ip M , Hou KK . Epstein-Barr Virus Lymphoproliferative Disorder in a Patient with Acute Lymphoblastic Leukemia. Ophthalmol Retina. 2025 Mar 25:S2468-6530(25)00096-X. doi: 10.1016/j.oret.2025.02.026.
Csete M, Ferris FL 3rd, Sadda SR Introduction to the RIMR 2024 special issue. Exp Eye Res. 2025 Jun; 255:110354. doi: 10.1016/j.exer. 2025. 110354. Epub 2025 Mar 27. PMID: 40157628.
Gupta AS, Linaburg TJ, Iacobucci E, Augello PA, Qin VL , Ying GS, Bunya VY, Massaro M. Varenicline Solution
Nasal Spray for the Treatment of Dry Eye Disease in Sjogren’s Disease: A Pilot Study. Clinical Ophthalmology. 2025 March 27; 19:1073-1086. PMID: 40166690.
Sridhar J, Kuriyan AE. The everchanging world of medical and surgical retina: a 2025 snapshot. Curr Opin Ophthalmol. 2025 May 1;36(3):159-160. doi: 10.1097/ICU.0000000000001132. Epub 2025 Mar 27. PMID: 40145316.
Zaidi H, Sridhar J. Optical Coherence Tomography in Retinal Detachment: Prognostic Biomarkers, Surgical Planning, and Postoperative Monitoring. Diagnostics (Basel). 2025 Mar 28;15(7):871. doi: 10.3390/diagnostics15070871. PMID: 40218221; PMCID: PMC11988441.
Cohen EJ, Troxel AB, Liu M, Hochman JS, Baratz KH, Mian SI, Choulakian MY, Warner DB, Lu Y, Twi-Yeboah A, Lee TF, Kim J, Lopez-Jimenez C, Laury SC, Jeng BH; ZEDS Trial Research Group ( Holland GN ). Low-Dose Valacyclovir in Herpes Zoster Ophthalmicus: The Zoster Eye Disease Randomized Clinical Trial. JAMA Ophthalmol. 2025 Apr 1;143(4):269-276. doi: 10.1001/ jamaophthalmol.2024.6114. PMID: 40048183; PMCID: PMC11886868.
Kittipibul T, Bonnet C , Patarajierapun P, Deng SX . Use of automated epithelial thickness measurements by anterior segment optical coherence tomography in the diagnosis of limbal stem cell deficiency. Cornea. 2025 Apr 1;44(4):422-426.
Modjtahedi BS, Palestine AG, Jampol LM, Sarraf D, Sen HN, Sobrin L, Chen JJ, Yang P, Adamus G, Fong DS, Qian CX, Lum F. Guidelines for the diagnosis, management, and study of autoimmune retinopathy from the American Academy of Ophthalmology’s Task Force. Ophthalmol Retina. 2025 Apr 1. doi:10.1016/j.oret.2025.03.024. PMID: 40180315.
Warner DB, Jeng BH, Kim J, Liu M, Troxel AB, Hochman JS, Baratz KH, Mian SI, Choulakian MY, Meyer JJ, Lu Y, Twi Yeboah A, Lee TF, Lopez-Jimenez C, Laury SC, Cohen EJ; ZEDS Trial Research Group ( Holland GN ). LowDose Valacyclovir for Postherpetic Neuralgia in the Zoster Eye Disease Study: A Randomized Clinical Trial. JAMA Ophthalmol. 2025 Apr 1;143(4): 277-285. doi: 10.1001/jamaophthalmol. 2024.6113. PMID: 40048191; PMCID: PMC11886865.
Tsedilina TR, Sharova EI, Kanygina AV, Malyugin BE , Antonova OP, Belodedova AV, Tkachenko IS, Gelyastanov AM, Zolotarev AV, Klokov AV, Murashev AO, Fedyushkina IV, Generozov EV, Skorodumova LO. From Genes to Disease: Reassessing LOXHD1 and AGBL1’s Contribution to Fuchs’ Dystrophy. Int J Mol Sci. 2025 Apr 3;26(7):3343. doi: 10.3390/ ijms26073343. PMID: 40244234; PMCID: PMC11989410.
Chang EL, Liu R, Keyhanian K, Huynh K, Berkenstock M, Bhatti MT, Chen JJ, Chodosh J, Costello F, Dalvin LA, DeLott LB, Dinkin M, Egan RA, Fraser CL, Freitag SK, Gangaputra S, Gordon LK , Guidon AC, Johnson DB, Kombo N, Kramer M, Lee AG, Levy M, Lobo-Chan AM, Mantopoulos D, Papaliodis G, Pless M, Pimkina J, Rubin KM, Sen HN, Shariff A, Subramanian PS, Tsui E , Yoon MK, McDunn J, Rine J, Reynolds KL, Sobrin L, Chwalisz BK. Consensus disease definitions for ophthalmic immune-related adverse events of immune checkpoint inhibitors. J Immunother Cancer. 2025 Apr 8;13(4):e011049. doi: 10.1136/jitc-2024011049. PMID: 40199607; PMCID: PMC11979595.
Feo A, Bousquet E, Faes L, Ramtohul P, Sacconi R, Rissotto F, Boscia G, Abraham N, Lior TE, Faghihi S, Popovic MM, Chan HH, Cheung CMG, Fouad Y, Cabral D, Govetto A, Romano MR, Querques G, Farvo SRS, Freund KB, Sarraf D. Vitelliform lesions associated with angioid streaks: long-term follow-up of a rarely described phenotype. Retina. 2025 Apr 11. doi:10.1097/ IAE.0000000000004485. PMID: 40239167.
Carpentiero E, Hughes S, Rodgers J, Xhaferri N, Biswas S, Gilhooley MJ, Hankins MW, Lindner M. Interaction between native and prosthetic visual responses in optogenetic visual restoration. JCI Insight. 2025 Apr 15;10(11):e190785. doi: 10.1172/ jci.insight.190785. PMID: 40232851; PMCID: PMC12220941.
Gangaputra SS, Newcomb CW, Ying GS, Dreger KA, Fitzgerald T, Artornsombudh P, Kothari S, Liesegang TL, Rosenbaum JT, Sen HN, Suhler EB, Thorne JE, Bhatt NP, Foster CS, Jabs DA, LevyClarke GA, Lowder CY, Goldstein DA, Holland GN , Jaffe GJ, Davis JL, Acharya NR, Latkany PA, Read RW, Garg SJ, Liederman YI, Buchanich JM, Kempen JH, For The Systemic Imunosuppressive Therapy for Eye Diseases Site Cohort Study Research Group. Effectiveness of Frequently Used TNF Inhibitors vs.Conventional Immunosuppressive Therapies for Noninfectious Uveitis. Ocul Immunol Inflamm. 2025 Aug;33(6):948-956. doi: 10.1080/09273948.2025.2479802. Epub 2025 Apr 15. PMID: 40233243; PMCID: PMC12286736.
Saks AA, Saks C, Bert B. Visual rehabilitation in keratoconus by altering corneal shape using the corneal crosslinking pen: initial results. Graefes Arch Clin Exp Ophthalmol. 2025 Apr 17. doi: 10.1007/s00417-025-06825-6. PMID: 40240685.
Schmidt RE, Pohodich AE, Birch D, Jones K, Lam BL, Jung EH, Jain N, Georgiou M, Mahroo OA, Webster AR, Michaelides M, Bakall B, Iannaccone A, Vincent A, Parameswarappa DC, Heon E, Scholl HPN, Janeschitz-Kriegl L, Traboulsi EI, Zein W, Brooks BP, Cukras C, Hufnagel R, Aleman TS, Sylla MM, Tsang SH, Alabek M, Sahel J, Gorin MB, van Genderen MM, Stingl K, Reith M, Kohl S, Amaral RAS, Sallum JMF, Vincent AL, Hull S, Duncan JL, Hanson JVM, Tedeus M, Maggi J, Graf U, Koller S, Berger W, Gerth-Kahlert C, Marra M, Everett LA, Yang P, Pennesi ME. Variants in CFAP410 cause a range of retinal and skeletal phenotypes. NPJ Genom Med. 2025 Apr 17;10(1):32. doi: 10.1038/s41525-025-00489-1. PMID: 40246852; PMCID: PMC12006490.
Yan J, Fung SSM , Tsui E . SweptSource Anterior-Segment OCT of Lens Subluxation in Marfan Syndrome. JAMA Ophthalmol. 2025 Apr 1;143(4): e250215. doi: 10.1001/jamaophthalmol. 2025.0215. Epub 2025 Apr 17. PMID: 40244626.
Govetto A, Lucchini S, Sebag J, Gianfrate F, Ranno S, Carini E, Virgili G, Romano MR, Sarraf D, Radice P. En face OCT morphology of macular pucker correlates with metamorphopsia: possible role of the Henle fiber layer: Erratum. Retina. 2025 May; 45(5):e41. Epub 2025 Apr 20. doi: 10.1097/IAE.0000000000004432. PMID: 40262069.
Gundlach BS, Tsui I , Tsui E Visualization of the Suprachoroidal Space with Swept-Source Anterior Segment OCT before and after Suprachoroidal Triamcinolone Acetonide Injection. Ophthalmol Retina. 2025 Apr 21:S2468-6530(25)00106-X. doi: 10.1016/j.oret.2025.03.007. PMID: 40261231.
Song W, Au A , Sarraf D, Prasad P, Tsui E . Bilateral acute multifocal retinitis and retinal vasculitis secondary to Rickettsia typhi infection. J Ophthalmic Inflamm Infect. 2025 Apr 21;15(1):38. doi: 10.1186/s12348-025-00496-4. PMID: 40259155; PMCID: PMC12011691.
Olawoye O, Young BP, Nyunt AW, Fafowora OF, Ajani M, Sarimiye T, Creemer BA, Roos BR, Coleman AL , Gorin MB, Hauser MA, Scheetz TE, Ashaye A, Fingert JH. Prevalence of Myocilin Mutations in a Cohort of Patients with Juvenile Open-Angle Glaucoma from sub-Saharan Africa. Ophthalmol Glaucoma. 2025 Apr 23:S2589-4196(25)00078-X. doi: 10.1016/j.ogla.2025.04.010. PMID: 40280414.
Kevin MF, Querques G, Sacconi R, Miller JML, Johnson MW, Miere A, Souied E, Kunkler A, Yannuzzi NA, Fung AT, Freund KB, Bacci T, Ramtohul P, Yannuzzi L, Sadda SR , Baumal CR, Christakis P, Gupta RR, Ip M , Santina A, Au A , Sarraf D. Central bouquet hemorrhage with Henle fiber layer extension in myopic eyes. Can J Ophthalmol. 2025 Apr 24:S0008-4182(25)00145-0. doi: 10.1016/j.jcjo.2025.03.019. PMID: 40288421.
Gangaputra S, Agarwal A, Norel JO, Tsui E , Thorne JE, de-la-Torre A, Altaweel M, Biswas J, Sadda S , Invernizzi A, Agrawal R, Shantha JG, Accorinti M, Fawzi A, Jabs DA, Sarraf D, Gupta V; MUV Taskforce. Evidence and consensus-based imaging guidelines in multifocal choroiditis with panuveitis and punctate inner choroiditis—MUV Taskforce Report 5. Am J Ophthalmol. 2025 Aug;276:272285. Epub 2025 Apr 25. doi:10.1016/j. ajo.2025.04.018. PMID: 40288596.
Rojas-Carabali W, Chan K, CifuentesGonzalez C, Agarwal M, Sen A, Biswas J, Kharel Sitaula R, La Distia Nora R, Utami A, Khatri A, Mahendradas P, Schlaen A, Mishra C, Guex-Crosier Y, Tsui E , Ayachit A, Gangaputra S, Kempen JH, Gupta V, de-la-Torre A, Lee B, Agrawal R; OASIS 1 and OASIS 2 study groups. Programme for ocular inflammation & infection translational research (PROTON) registry: Crosssectional analysis of baseline patient characteristics. Asia Pac J Ophthalmol (Phila). 2025 May-Jun;14(3):100199. doi: 10.1016/j.apjo.2025.100199. Epub 2025 Apr 25. PMID: 40288758.
Talebi R, Fortes BH, Yu F, Coleman AL , Tsui I . Real-world Associations Between GLP-1 Receptor Agonist Use and Diabetic Retinopathy Accounting for Longitudinal Glycemic Control. Retina. 2025 Apr 30. doi: 10.1097/ IAE.0000000000004507. PMID: 40334190.
Cascavita C, Santina A, Kitayama K, Yu F, Tseng VL, Coleman AL . The association between sensory impairment and adherence to COVID-19 prevention measures in the adult California Health Interview Survey population. Vision (Basel). 2025 May 2;9(2):40. doi: 10.3390/vision9020040. PMID: 40407622.
Avadzadeh S, Sharma A, Parvaresh MM, Ghasemi Falavarjani K; International Retina Biosimilar Study Group (Inter BIOS Group) (Sridhar J ). Aflibercept 2 mg biosimilar (Tyalia)real-world experience from IRAN (ATRIA study). Eye (Lond). 2025 Aug;39(11):2159-2163. doi: 10.1038/ s41433-025-03813-2. Epub 2025 May 3. PMID: 40319174; PMCID: PMC12274603.
Boghosian T, Patarajierapun P, Glasgow BJ, Berkowitz CB, Bonnet C , McCannel TA , Barrows BD, Fung SSM Spontaneously resolved invasive conjunctival squamous cell carcinoma with anterior chamber invasion in low-grade lymphoma patient. Am J Ophthalmol Case Rep. 2025 May 3;38:102348. doi: 10.1016/j.ajoc.2025.102348. PMID: 40475126; PMCID: PMC12139222.
Rämö JT, Gorman BR, Weng LC, Jurgens SJ, Singhanetr P, Tieger MG, van Dijk EH, Halladay CW, Wang X, Hauser BM, Kim SH, Brinks J, Choi SH, Luo Y; FinnGen; VA Million Veteran Program; Pyarajan S, Nealon CL, Gorin MB, Wu WC, Anthony SA, Roncone DP, Sobrin L, Kaarniranta K, Yzer S, Palotie A, Peachey NS, Turunen JA, Boon CJ, Ellinor PT, Iyengar SK, Daly MJ, Rossin EJ. Rare genetic variation in PTPRB is associated with central serous chorioretinopathy, varicose veins and glaucoma. Nat Commun. 2025 May 3;16(1):4127. doi: 10.1038/s41467-02558686-6. PMID: 40319023; PMCID: PMC12049426.
Yoon MK, Aakalu VK, Dagi Glass LR, Grob SR, McCulley TJ, Vagefi MR, Pineles SL , Wladis EJ. Orbital PatientSpecific (Customized) Implants: A Report by the American Academy of Ophthalmology. Ophthalmology. 2025 May 3:S0161-6420(25)00168-X. doi: 10.1016/j.ophtha.2025.03.006. PMID: 40317276.
Yun JS, Santina A, Tseng VL. Medical and surgical management of neovascular glaucoma. Curr Opin Ophthalmol. 2025 May 5. doi: 10.1097/ ICU.0000000000001151. PMID: 40314467.
Liu D, Oh A, Shirriff A, Rapola EW, Singh P, Gout T, Goldberg RA . Intralesional Bleomycin Palliation: An Option for Nonoperative Sebaceous Cell Carcinoma of the Eyelid. Ophthalmic Plast Reconstr Surg. 2025 May 6. doi: 10.1097/IOP.0000000000002949. PMID: 40326578.
Lakhani M, Kwan ATH, Mihalache A, Popovic MM, Nanji K, Xie JS, Feo A, Rabinovitch D, Shor R, Sadda S , Sarraf D, Hurley B, Margolin EA, Kertes PJ, Chaudhary V, Muni RH. Association of glucagon-like peptide-1 receptor agonists with optic nerve and retinal adverse events: a population-based observational study across 180 countries. Am J Ophthalmol. 2025 May 16; 277:148-168. Epub 2025 May 9. doi: 10.1016/j.ajo.2025.05.007. PMID: 40383360.
Boneva SK, Nguyen JH, Mamou J, Yee KM, Hoerig C, Silverman RH, Ketterling JA, Stanga PE, Reinstein DZ, Sadun AA , Sebag J. Clinical Management of Vision Degrading Myodesopsia from Vitreous Floaters— Observation vs. Limited Refractive Vitrectomy. Ophthalmol Retina. 2025 May 15:S2468-6530(25)00221-0. doi: 10.1016/j.oret.2025.05.014.
Phillips MJ, Reid MW, Gaier ED, Gise RA, Heidary G, Beres SJ, Pineles SL , Borchert MS, Chang MY; Pediatric Optic Nerve Investigator Group (PONIG). Agreement and Accuracy of Papilledema and Pseudopapilledema Classification Among Pediatric NeuroOphthalmologists Using Optic Disc Photographs. J Neuroophthalmol. 2025 May 15. doi: 10.1097/WNO. 0000000000002316. PMID: 40378038.
Ko M, Talebi R, Yu F, Tseng VL, Coleman AL , Hosseini H . Socioeconomic disparities in intravitreal injection use and anti-VEGF agent selection: Aflibercept/ranibizumab versus bevacizumab. Clin Ther. 2025 May 17:S0149-2918(25)00129-8. doi: 10.1016/j.clinthera.2025.04.010. PMID: 40383690.
Huang A, Wu Z, Ansari G, Von Der Emde L, Pfau M, Schmitz-Valckenberg S, Fleckenstein M, Keenan TDL, Sadda SR , Guymer RH, Cheung CMG, Chakravarthy U. Geographic atrophy: Understanding the relationship between structure and function. Asia Pac J Ophthalmol (Phila). 2025 May-Jun;14(3):100207. doi: 10.1016/j. apjo.2025.100207. Epub 2025 May 19. PMID: 40398512; PMCID: PMC12235197.
Groth SL, Newcomb CW, Yang W, Payal A, Begum H, Khachatryan N, Kaçmaz RO, Dreger KA, Rosenbaum JT, Sen HN, Suhler EB, Thorne JE, Bhatt NP, Foster CS, Jabs DA, Levy- Clarke GA, Buchanich JM, Ying GS, Kempen JH, Gangaputra S; Systemic Immunosuppressive Therapy for Eye Diseases (SITE) Cohort Study Research Group ( Holland GN ). The Rate of Failure of Trabeculectomy and Tube Shunt Surgery in Eyes with Uveitic Glaucoma and Ocular Hypertension. Ophthalmol Glaucoma. 2025 May 22:S25894196(25)00108-5. doi: 10.1016/j.ogla. 2025.05.004. PMID: 40412807.
Berni A, Foti C, Bandello F, Boscia F, Breazzano MP, Cicinelli MV, Corradetti G, Dolz-Marco R, Feo A, Gallego - Pinazo R, Marolo P, Russo A, Sadda SR , Sarraf D, Soylu C, Viggiano P, Reibaldi M, Borrelli E. Predictors of macular atrophy after serous pigment epithelial detachment collapse in type 3 macular neovascularization and age-related macular degeneration. Ophthalmol Retina. 2025 May 27. doi:10.1016/j.oret.2025.05.028. PMID: 40441379.
Ip M , Modi Y, Fekrat S, Gibson K, Boucher N, Arrisi P, Ishii F, Liu Y, Paris LP, Fenech M, Chi GC. Treatment Patterns and Long-Term Outcomes with Anti-VEGF Therapy for Retinal Vein Occlusion: An Analysis of the Vestrum Database. Ophthalmol Retina. 2025 May 27:S2468-6530(25)00251-9. doi: 10.1016/j.oret.2025.05.025.
Yang A, Reid M, Nguyen AM, Nallasamy S, Velez FG, de Alba Campomanes AG, Chang MY. Quality and Readability of Patient Educational Materials Generated by ChatGPT-4o for Pediatric Ophthalmologic Surgeries. J Pediatr Ophthalmol Strabismus. 2025 May 27:1-7. doi: 10.3928/0191391320250404-01. PMID: 40423504.
Frederiksen R, Bonezzi PJ, Fain GL , Sampath AP. The Role of the Ca2+activated Cl - Conductance in the Membrane Potential and Light Response of Mouse Rods. J Neurosci. 2025 May 28;45(22):e1920242025. doi: 10.1523/JNEUROSCI.1920-24.2025. PMID: 40280711.
Oh AJ, Chen AC, Pirakitikulr N, Rootman DB, Glasgow BJ. Amyloid in the orbital apex and cavernous sinus. Orbit. 2025 May 28:1-5. doi: 10.1080/01676830.2025.2509834. PMID: 40434011.
Arnold RW, Birch E, Bradford G, Collins M, Donahue SP, Gaier ED, Ghasia F, Greninger DA, Hutchinson AK, Jastrzembski B, Kemper AR, O’Neil J, Pineles S , Rotruck J, Wang B, Wygnanski-Jaffe T. Defining and measuring population-level amblyopia treatment outcomes: a proposal by the AAPOS Vision Screening and Research Committees. J AAPOS. 2025 May 29: 104231. doi:10.1016/j.jaapos. 2025. 104231. PMID: 40449829.
Jafari S, Cai S, Demer JL . Finite Element Model of the Effect of Optic Nerve Sheath Anisotropy on Ocular Loading During Horizontal Duction. Bioengineering (Basel). 2025 May 29;12(6):587. doi: 10.3390/ bioengineering12060587.PMID: 40564404.
Agarwal A, Agarwal A, Goldstein DA, Invernizzi A, Janetos TM, Cimino L, Nguyen QD, Jabs DA, Agrawal R, Fawzi A, Sarraf D, Gupta V; MUV Taskforce. Evidence and consensus-based imaging guidelines in serpiginous choroiditis—MUV Taskforce Report 4. Am J Ophthalmol. 2025 Jun 4;278:81-92. Epub 2025 May 28. doi:10.1016/j.ajo. 2025.05.052. PMID: 40480346.
Carreño E, Maghsoudlou P, Fonollosa A, Leal I, Schlaen A, Abraham AR, Dick AD, Agarwal A, Gangaputra S, Invernizzi A, Fawzi A, Miserocchi E, Agrawal R, Jabs DA, Sarraf D, Gupta V; Multimodal Imaging in Uveitis (MUV) Taskforce. Evidence and consensusbased imaging guidelines in acute posterior multifocal placoid pigment epitheliopathy—MUV Taskforce Report 7. Am J Ophthalmol. 2025 Jun 6;278:3851. Epub 2025 May 30. doi:10.1016/j. ajo.2025.06.007. PMID: 40484301.
Popovic MM, Feo A, Sadda SR , Freund KB, Muni RH, Munk MR, Fawzi AA, Rosen RB, Agarwal A, Balaratnasingam C, Dubovy SR, Byeon SH, Fossataro F, Voichanski S, Faes L, Mihalache A, Huang RS, Sarraf D; International Retinal Imaging Society. Large retinal capillary aneurysm: a Delphi consensus study and updated nomenclature for a signature optical coherence tomography lesion. Retina. 2025 May 30. doi: 10.1097/IAE.0000000000004502. PMID: 40456130.
Tan C, Puran AI, Santina A, Yu F, Kitayama K, Tseng VL, Coleman AL Social determinants of health as risk factors for keratoconus in the All of Us database. Br J Ophthalmol. 2025 May 30;109(6):645-651. doi: 10.1136/bjo2024-326229. PMID: 39658142.
Talebi R, Yu F, Tseng VL, Coleman AL The association between food insecurity and chronic eye disease in the National Institutes of Health All of Us Research Program. Ophthalmol Sci. 2024 Dec 30;5(3):100697. doi: 10.1016/ j.xops.2024.100697. eCollection 2025 May-Jun. PMID: 40165908.
Arepalli S, Kopplin L, Tsui E , Brill D, Sobrin L, Papaliodis G, Darwish D, Raiji V, Janardhana P, Emami-Naeini P, Nore L, Parker M, Thomas AS. The heterogeneous presentations of de novo and recurrent ocular inflammation after Covid-19 vaccination: A multicenter report and a review of the literature. Retina. 2025 Jun 1;45(6):1175-1183. doi: 10.1097/IAE.0000000000004413. PMID: 39841907.
Huang RS, Mihalache A, Benour A, Zaman M, Popovic MM, Kertes PJ, Muni RH, Sarraf D, Sadda SR , Kohly RP. Eplerenone and spironolactone for chronic central serous chorioretinopathy: a systematic review and meta-analysis. Am J Ophthalmol. 2025 Jun 11;278:22-37. Epub 2025 Jun 1. doi:10.1016/j.ajo.2025.06.012. PMID: 40513762.
Mafi M, Govetto A, Mahmoudinezhad G, Prasad P, Bousquet E, Voichanski S, Feo A, Sarraf D. Pathogenesis of ectopic inner foveal layers and its impact on visual recovery after epiretinal membrane peeling. Retina. 2025 Jun 1;45(6):1108-1116. Doi: 10.1097/ IAE.0000000000004418. PMID: 39899800.
Akpek EK, Li G, Aldave AJ, Amescua G, Colby KA, Cortina MS, de la Cruz J, Parel JA, Schmiedel T. Artificial intelligence aided analysis of anterior segment optical coherence tomography imaging to monitor the device-cornea joint after synthetic cornea implantation. Transl Vis Sci Technol. 2025 Jun 2;14(6):1.
Feo A, Santina A, Abraham N, Mafi M, Popovic MM, Govetto A, Romano MR, Johnson MW, Sarraf D. En face OCT imaging of epiretinal membranes complicated by internal limiting membrane tears. Ophthalmol Retina. 2025 Jun 2. doi:10.1016/j.oret.2025.05.031. PMID: 40466769.
Fogel Levin M, Querques G, Sacconi R, Miller JML, Johnson MW, Miere A, Souied E, Kunkler A, Yannuzzi NA, Fung AT, Freund KB, Bacci T, Ramtohul P, Yannuzzi L, Sadda SR , Baumal CR, Christakis P, Gupta RR, Ip M , Santina A, Au A , Sarraf D. Central bouquet hemorrhage with Henle fiber layer extension in myopic eyes. Can J Ophthalmol. 2025 Jun 4. doi:10.1016/ j.jcjo.2025.03.019. PMID: 40288421.
Kong AW, Jeon MJ, Lin SR , Bartlett JD, McCannel CA , Hoffer KJ, Savini G, Nejad M . Comparison of IOL formula accuracy for eyes with prior scleral buckle surgery. J Cataract Refract Surg. 2025 Jun 9. doi: 10.1097/j. jcrs.0000000000001715. PMID: 40494275.
Chen C, Han J, Sanchez L, Chen JL , Zheng JJ. Characterizing the expression profile of Dexras1 in human trabecular meshwork cells. Biochem Biophys Rep. 2025 Jun 10;43:102077. doi: 10.1016/j.bbrep.2025.102077. PMID: 40546349; PMCID: PMC12182328.
Huang RS, Mihalache A, Benour A, Zaman M, Popovic MM, Kertes PJ, Muni RH, Sarraf D, Sadda SR , Kohly RP. Eplerenone and Spironolactone for Chronic Central Serous Chorioretinopathy: A Systematic Review and Meta-Analysis. Am J Ophthalmol. 2025 Jun 11;278:22-37. doi: 10.1016/j. ajo.2025.06.012. PMID: 40513762.
Sandoval Gonzalez S, Song W, Privratsky JK, Lemon J, Tsui E
Swept-Source Anterior Segment Optical Coherence Tomography of a Vascularized Syphilitic Iris Lesion. Ocul Immunol Inflamm. 2025 Jun 11:1-3. doi: 10.1080/09273948.2025.2514693. PMID: 40499096.
Fein AS , Grossman SN, Pillai C, Gold DM. Progressive Cranial Neuropathies. J Neuroophthalmol. 2025 Jun 18. doi: 10.1097/WNO.0000000000002375. PMID: 40528293.
Pichi F, Miserocchi E, Grewal DS, Sharma S, Brézin AP, Bodaghi B, Agarwal A, Jabs DA, Fawzi A, Sarraf D, Gupta V; Multimodal Imaging in Uveitis (MUV) Taskforce. Evidence and consensusbased multimodal imaging guidelines in birdshot chorioretinopathy—MUV Taskforce Report 8. Am J Ophthalmol. 2025 Jun 20. doi:10.1016/j. ajo.2025.06.029. PMID: 40545009.
Ramirez M, Kitayama K, Puran AI, Tseng VL, Yu F, Coleman AL . The associations between glaucoma, glaucoma severity and circadian rhythm sleep disorders in California Medicare beneficiaries. Am J Ophthalmol. 2025 Jun 20:S0002-9394(25)00313-7. doi: 10.1016/j.ajo.2025.06.021. PMID: 40545017.
Gupta V, Davis JL, Gangaputra S, Chee SP, Thorne JE, Agrawal R, Invernizzi A, Agarwal A, de Smet MD, Sarraf D, Jabs DA; Multimodal Imaging in Uveitis (MUV) Taskforce. Evidence and consensus-based guidelines for imaging in non-infectious posterior uveitis— Methodology of the MUV Project: Report 2. Am J Ophthalmol. 2025 Jun 21. doi:10.1016/ j.ajo.2025.06.033. PMID: 40550447.
Desideri LF, Anguita R, Sacconi R, Beretta F, Corradetti G, Feo A, Dobovsek D, Parravano M, Capuano V, Souied E, Sarraf D, Zinkernagel M, Querques G. Unilateral reticular pseudodrusen: clinical features and potential protective factors. Retina. 2025 Jun 23. doi:10.1097/ IAE.0000000000004575. PMID: 40591950.
Munk MR, Stillenmunkes R, Tillmann A, Jampol LM, Cicinelli MV, Lin P, Pepple KL, Freund KB, Tugal-Tutkun I, Habot-Wilner Z, Agarwal A, Gangaputra S, Agrawal R, Jabs DA, Sadda S , Sarraf D, Gupta V; Multimodal Imaging in Uveitis (MUV) Taskforce. Evidence and consensus-based imaging classification criteria in multiple evanescent white dot syndrome: Multimodal Imaging in Uveitis (MUV) Taskforce Report 6. Am J Ophthalmol. 2025 Jun 24. doi:10.1016/j.ajo.2025.06.039. PMID: 40571046.
Bonezzi PJ, Frederiksen R, Tran AN, Kim K, Fain GL , Sampath AP Photoreceptor degeneration induces homeostatic rewiring of rod bipolar cells. Curr Biol. 2025 Jul 7;35(13): 3263-3268.e2. doi: 10.1016/j.cub.2025. 05.057. Epub 2025 Jun 25. PMID: 40570846; PMCID: PMC12276929.
Feo A, Eshkoly-Lior T, Sarraf D Multimodal imaging of laser pointer maculopathy. Can J Ophthalmol. 2025 Jun 28. doi:10.1016/j.jcjo.2025.05.009. PMID: 40456281.
Thomas AS, Tsui E , Armbrust KR, Kodati S, Berkenstock MK, Davis EC, Thomas MK, Gangaputra S. Burnout Among US Uveitis Specialists— An Assessment of Prevalence and Contributing Factors. Am J Ophthalmol. 2025 Jun 28:S0002-9394(25)00342-3. doi: 10.1016/j.ajo.2025.06.042. PMID: 40588207.
Ko MY, Glasgow BJ, Ghaffari R . Late onset bilateral annular subepithelial corneal haze after LASIK. Am J Ophthalmol Case Rep. 2025 Jun 28; 39:102371. doi: 10.1016/j.ajoc. 2025. 102371. PMID: 40678733; PMCID: PMC12270613.
Fehilly JD, McCann T, Ruddin G, Kaylor JJ, Grenville H, Ward R, Wynne K, Sánchez AG, Strachan E, Travis GH , Collery RF, Kennedy BN. Germline Disruption of Retinal Pigment Epithelium-Expressed Zebrafish rlbp1b -/- Results in Selective Dim Light Visual Behavior Deficits and Provides a Screening Platform for Evaluating the Pathogenicity of Human RLBP1 Variants. FASEB J. 2025 Jun 30;39(12):e70754. doi: 10.1096/ fj.202500600R. PMID: 40552921.


Established in 1966, the Jules Stein Eye Institute vision-science campus is the fulfillment of a dream—an ambitious plan developed by Jules Stein, MD, to prevent blindness by transforming the quality of vision research, education, patient care, and community outreach.
The Institute exists because of Dr. Stein, one of the most influential executives in entertainment who returned to his roots as a medical doctor to become a national advocate for vision science; and Bradley R. Straatsma, MD, JD, founding director of the Jules Stein Eye Institute and founding chair of the UCLA Department of Ophthalmology, who created a bold plan for building the scope of ophthalmology in the UCLA School of Medicine. Together Drs. Stein and Straatsma ensured the Institute would take a central role in transforming vision science as a powerful platform for discovery and patient care to eradicate one of the great scourges of human existence: blindness.
Under the leadership of Bartly J. Mondino, MD, director and chair from 1994 to June 30, 2022, the Institute’s core pillars were developed and a broad agenda of program-building and expansion was implemented. Dr. Mondino also forged a historic partnership—a first of its kind—with Doheny Eye Institute in 2013, creating the nation’s preeminent organization for ophthalmic care and vision research under the banner of the UCLA Department of Ophthalmology.
Anne L. Coleman, MD, PhD, assumed leadership of the Jules Stein Eye Institute and UCLA Department of Ophthalmology in July 2022, and brought with her a broad agenda to address the growing challenges for patient care, education, vision-science research, and community outreach.
And today, the original dream for ophthalmology at UCLA has evolved into the Institute’s bold transformation to a vision-science campus—an interconnected community of facilities and people that merge research, training for new ophthalmologists, premier patient care, community outreach programs, and ongoing education for doctors worldwide.
Patients across the Southland have access to the finest vision care at the UCLA Jules Stein Eye Institute in Westwood; Stein Eye Center locations in Calabasas and Santa Monica; Doheny Eye Centers UCLA in Arcadia, Orange County, and Pasadena; and UCLA-affiliated hospitals in Sylmar, Torrance, and West Los Angeles/Sepulveda.
Since its opening on November 3, 1966, the Institute’s original mandate remains paramount: the relentless drive for excellence and the constant search for new possibilities in the treatment of the eye. The Institute’s decades of accomplishments may have even exceeded the original soaring expectations of Dr. Stein who at the dedication ceremony defined his own prophecy for the Institute and the medical field he loved:
“The men and women who will occupy this building and use its resources will share in future achievements that will outstrip any that have been seen; for science today is moving ahead with fantastic speed, and we must be sure that eye research moves with it. The history of this Institute begins with this dedication. I am confident that it will be a proud history.”
“If I am remembered for anything, it will not be for anything I did in show business, but for what I did to prevent blindness.”
DR. JULES STEIN

Doris and Jules Stein
The legacy of Dr. and Mrs. Jules Stein arises from their role in the 20th century as visionaries. Through brilliance and beneficence, they created a multitude of programs aimed specifically at one goal: preserving and restoring eyesight. They approached this task dauntlessly, integrating the worlds of business, medicine, and philanthropy in such a way as to enhance each and leave in trust the promise of limitless accomplishment in the advancement of eye research and treatment. The Jules Stein Eye Institute was established as a result of their philanthropy.
The Board of Trustees was established in 1977 and ensures the Jules Stein Eye Institute’s orderly growth and development. The Board meets regularly during the year, with each trustee providing their unique counsel. Collectively, their invaluable contributions have included fiscal planning for the Institute, adoption of measures to facilitate recruitment of the world’s finest vision scientists, allocation of funds for the purchase of vision research equipment, and recommendations for expansion programs.
Norman Abrams, Esq.
Distinguished Professor of Law Emeritus Acting Chancellor Emeritus UCLA 2015–present
Anne L. Coleman, MD, PhD Chair, UCLA Department of Ophthalmology Director, Jules Stein Eye Institute Affiliation Chair, Doheny Eye Institute 2022–present
Charles T. Foscue
President and Chief Executive Officer HAI Financial, Inc. 2020–present
Ronald L. Olson, Esq. Partner
Munger, Tolles & Olson 1995–present
Katrina vanden Heuvel Publisher and Editor The Nation 1984–present
Casey Wasserman
President and Chief Executive Officer The Wasserman Foundation 1998–present
Bart H. Williams, Esq. Partner Proskauer Rose LLP 2021–Present
Marissa Goldberg OBSERVER
Executive Director and Chief Financial Officer Doheny Eye Institute 2015–present

The Executive Committee of the Jules Stein Eye Institute and UCLA Department of Ophthalmology meets regularly during the year, with each member providing their unique expertise. The Committee ensures the orderly growth and development of the Institute and Department. It is involved in fiscal planning, expansion, recruitment, program development, and resolution of interdivisional issues.
Anne L. Coleman, MD, PhD Chair, UCLA Department of Ophthalmology Director, Jules Stein Eye Institute Affiliation Chair, Doheny Eye Institute
Anthony J. Aldave, MD Vice Chair of Academics
Anthony C. Arnold, MD Vice Chair of Education
Peter A. Quiros, MD
Associate Vice Chair of Education
Joseph Caprioli, MD Vice Chair of Quality
Colin A. McCannel, MD Associate Vice Chair of Quality
Sophie X. Deng, MD, PhD Vice Chair for Inspiring Physician Excellence
Trashon Fearington Chief Administrative Officer, Jules Stein Eye Institute
JoAnn A. Giaconi, MD Vice Chair of Affiliated Hospitals
Marissa Goldberg Executive Director and Chief Financial Officer Doheny Eye Institute
Gary N. Holland, MD Vice Chair of Patient-Based Research
Stacy L. Pineles, MD Irena Tsui, MD Associate Vice Chairs of Patient-Based Research
Alfredo Sadun, MD, PhD Vice Chair of Doheny Eye Centers UCLA
Alapakkam P. Sampath, PhD Associate Director of Research
Greg D. Field, PhD Assistant Director of Research

The Jules Stein Eye Institute is a vision-science campus dedicated to the preservation and restoration of vision through its global programs in innovative research, quality patient care, and multidisciplinary, integrative education, all with community outreach.
IMAGINE a world where the faces of loved ones are blurred or the simple joy of reading is a struggle. For many, this is a daily reality. But with your support, we can continue to change lives through the groundbreaking work at the Jules Stein Eye Institute.
Our mission to preserve and restore sight continues to guide everything we do, from patient care to research, education, and community outreach.
It is only because of your support that we have been rated the #5 Ophthalmology Hospital in the U.S. for more than 30 years. Join us in advancing vision research, providing access to sight-saving patient care, educating tomorrow’s leaders in ophthalmology, and delivering critical community outreach.
There are many ways you can donate to the Jules Stein Eye Institute and give the gift of sight, from traditional cash gifts to those that offer various additional tax benefits.
For information about making a gift or incorporating the Jules Stein Eye Institute into your estate and retirement planning, please contact:
Susan Lee DeRemer, CFRE Director of Development
Jules Stein Eye Institute
100 Stein Plaza, Room 3-138 Los Angeles, CA 90095-7000
Phone: (310) 825-3381
Cell/Text: (424) 325-9076 sderemer@mednet.ucla.edu
See UCLA and the UCLA Foundation’s Disclosure Statements for Prospective Donors at: https://mygiving.ucla.edu/faq#disclosure.

Checks may be made payable to the “UCLA Foundation” and mailed to Susan DeRemer at the address below. To make a donation by credit card, please call: (310) 206-6035.
Recommending a grant from your DAF to the Jules Stein Eye Institute is an efficient and tax-effective way to give.*
Donate cash, securities, or other assets in trust to the Jules Stein Eye Institute, and in return, receive lifetime payments to you and up to one additional person. This may qualify for a partial tax deduction, and the Institute ultimately receives the trust.*
Donating stocks or bonds can potentially offer you more significant tax benefits than a cash gift.*
If you are 70½ years old or older, consider donating from your IRA directly to the Jules Stein Eye Institute. This distribution can also count towards your required minimum distribution (RMD) and is excluded from a donor’s taxable income.*
Leave a lasting legacy by including the Jules Stein Eye Institute in your will or estate plans.
*Consult your tax advisor to determine the best way to support the Institute’s vital work.
UCLA DEPARTMENT OF OPHTHALMOLOGY
DAVID GEFFEN SCHOOL OF MEDICINE AT UCLA