NEWS eyes
Endocrinologists and Scientists



03 From your EYES Co-Chairs, plus Celebrating 20 years of ESE
04 Amazing careers: Maria Yavropoulou
09 The EYES community at ECE 2026, plus Belgrade calls you to the EYES Annual Meeting
10 Get ready for Summer School, plus Introducing #ThisIsEndocrinology and Are you making use of EndoCompass?
11 Apply for your Observership now, plus Get involved in World Hormone Day 2026
05 Advanced prostate cancer and the gut microbiota
06 The gut microbiota and weight loss
07 Healing the heart through the gut
07 The gut microbiome and oestrogens
08 Thyroid autoimmunity and the gut microbiota
08 The gut microbiota in type 1 diabetes
12 Meet the Czech Young Endocrinologists







It is an honour and a responsibility to step into the role of Editor of EYES News. I do so with excitement and appreciation, following Juan, whose work shaped this magazine and reminded us that true clinical progress begins with strong basic science.
I am fortunate to work with an extraordinary EYES News Editorial Board, as well as a brilliant Sub-editor and Designer. Their dedication, creativity and constant support turn challenges into shared achievements, and the joy we feel after every successful issue is, for me, the greatest reward.
Editor: Dorota Filipowicz, Poland
Deputy Editor: Shamini Ramkumar Thirumalasetty, Germany
Editorial Board: Mirjana Đukić, Croatia
Juan Manuel Jiménez Vacas, UK
Lorenzo Marinelli, Italy
Petros Papalexis, Greece
Victoria Withy, UK
Sub-editor: Caroline Brewser
Design: Qube Design Associates
Website: www.ese-hormones.org
©2026 European Society of Endocrinology
The views expressed by the contributors are not necessarily those of ESE
EYEScientists fb.com/groups/eyes.endo
ESE Young Endocrinologists and Scientists eyescientists ese-eyes
We welcome contributions and suggestions for articles. Please contact EYES News at eyesnewsletter@gmail.com
The addresses used to email this issue of EYES News were supplied by the members of ESE. If you do not wish to receive further mailings, you can update your mailing preferences by going to My ESE area EXTERNAL-LINK-ALT or emailing info@ese-hormones.org
Cover image: Depiction of the human intestinal microbiome ©iStock/nopparit
This issue is the first of 2026, and I wish you health, curiosity and renewed energy for the year ahead. May it bring inspiration, meaningful connections, and exciting discoveries for our entire EYES community.
Read on, as we open the door to a hidden universe that lives within us: the world of bacteria EXTERNAL-LINK-ALT. The microbiome has rapidly become known as an important player in medicine and endocrinology. In these pages, you will explore its links with prostate cancer, obesity, menopause, type 1 and type 2 diabetes, and thyroid autoimmunity − revealing how microscopic ecosystems may influence systemic health in ways we are only beginning to understand.
Our Amazing Careers interview with Maria Yavropoulou EXTERNAL-LINK-ALT is another highlight of the issue. Also, be sure to register for ECE 2026 EXTERNAL-LINK-ALT, where we invite you to the EYES pituitary session and the announcement of the new EYES Observership Programme awardees. And don’t miss the 13th EYES Annual Meeting EXTERNAL-LINK-ALT in Belgrade, Serbia, or the ESE Summer School EXTERNAL-LINK-ALT in Innsbruck, Austria. We round off the issue with a chance to meet the young endocrinologists from the Czech Republic EXTERNAL-LINK-ALT who will host us in Prague this May.
Finally, I am thrilled to announce that Shamini has stepped into the role of Deputy Editor, while Mirjana and Lorenzo have become Social Media and Scientific Articles Co-ordinators, helping make our content even stronger and more visible.
Dive in!
Dorota Filipowicz Editor EYES News
In 2026, we will celebrate the 20th anniversary of ESE! You can be sure that the EYES community has started the year with renewed energy for our many different endeavours.
We are pleased to share that preparations are well underway for ECE 2026 (see page 9), which you will be able to enjoy in Prague, Czech Republic, on 9–12 May. From an early-career perspective, we can promise an outstanding EYES Symposium, focused on exciting and innovative pituitary research, presented by brilliant early-career scientists from across Europe. We warmly invite you to join us for lively scientific discussions in a vibrant atmosphere.
In addition, we have planned an engaging EYES social event, designed to offer plenty of opportunities to network, connect and get to know one another, always with a fun and relaxed vibe. Find out more about ECE 2026 and book your place EXTERNAL-LINK-ALT
Of course, the excitement does not stop in Prague. It’s only a few months until our EYES Annual Meeting. This year, we head to Belgrade, Serbia, a dynamic city where history, culture and nightlife meet. Join your colleagues on 4−6 September, when we come together for cutting-edge science, meaningful networking, career-boosting opportunities and unforgettable social events. You can read more on page 9
Many other activities are coming up, including your chance to benefit from the ESE Observership Programme (see page 11). The Observership Programme gives early-career clinicians and scientists the chance to grow and learn during short stays at leading endocrine centres across Europe. This year offers more centres and opportunities than ever before, so don’t miss out! Find out more and apply EXTERNAL-LINK-ALT.
You can also take part in the ESE Summer School, on 5−8 July in Innsbruck, Austria (page 10). This unique event combines outstanding scientific training with an extensive social programme. Beyond professional development, it offers the chance to build lasting connections across Europe through networking activities, sports and more. Registration is now open, and travel and attendance grants are available. Find out more EXTERNAL-LINK-ALT

This will be the last time Juan writes in his role as EYES Co-Chair, but EYES will still be in excellent hands. Under the continuing leadership of Kristina, with a highly motivated and dedicated EYES Committee, the team is already working towards the future, creating new opportunities, expanding benefits for early-career members, and ensuring that your voices continue to be heard and represented within ESE.
We look forward to seeing you very soon.
Juan Manuel Jiménez Vacas, UK Kristina Saravinovska, Serbia

2026 marks ESE’s two eventful and productive decades as the voice for endocrinology.
Since 2006, your Society has grown from just 375 individual members to 4810 individual members at the time of the 2025 AGM, last May.
To mark the anniversary, a celebratory digital booklet entitled ‘ESE: the first 20 years’ will recall key events in ESE’s development and also look to the future, with plenty of photographs and fascinating facts.
You will learn how the roots of ESE can be traced back to a collaboration between national societies as long ago as the 1940s, how the journal they founded (Acta Endocrinologica) developed to become European Journal of Endocrinology, and how its growth supported the Society which, in turn, supports you!
Find out how travel to ECE 2010 was nearly grounded by a volcano, how the Executive Committee had a police escort to the Congress dinner at ECE 2007, and read about the many developments that make ESE the strong, collaborative and diverse organisation that it is today.
An exciting range of activities is planned at ECE 2026, including a special celebration during our ECE Welcome Reception and a fascinating symposium centred around endocrinology over the past 20 years. There will be other activities that you can take part in, and you will receive a special 20th anniversary pin badge.
A dedicated ‘History of ESE’ web page will evolve throughout the year. Make sure you visit it regularly EXTERNAL-LINK-ALT 2026 also sees the end of ESE’s current five-year transformation strategy, so the Executive Committee and leadership team, led by ESE President Wiebke Arlt and CEO Helen Gregson, will develop the next five-year strategy for 2027−2031.
This will be the next exciting chapter in the ongoing development of ESE as the voice for endocrinology.
Maria Yavropoulou is a Consultant Endocrinologist in the 1st Department of Propaedeutic and Internal Medicine at the Medical School of the National and Kapodistrian University of Athens, Greece, and Deputy Director of the National Center of Expertise in Rare Endocrine Diseases. In 2020, she received the Jens Sandahl Christiansen Award in Basic Science from ESE. EYES News Editorial Board Member Petros Papalexis interviewed Maria about her amazing career to date.

What motivated you to pursue a career in endocrinology?
From very early in my medical studies I was fascinated by how hormones − such tiny molecules − can orchestrate such complex biological processes. Endocrinology felt like the specialty that combined detective work, physiology and long-term patient relationships.
In the beginning, I actually believed I would become an oncologist: I admired the field deeply. But, as I progressed in my training, I realised that I did not want a career where I would often have to deliver bad news to patients and their families.
At around that time, Professor John Yovos, who later became one of my mentors during my early steps at the Aristotle University of Thessaloniki, gave a truly fascinating lecture on how hormones regulate general homeostasis. I still remember sitting there, completely captivated, and imagining myself many years later working with these beautifully interconnected systems. That moment changed my direction and led me to endocrinology.
What are you currently working on?
At the moment, my work has two main strands. First, clinically, I am heavily engaged in the management of rare bone diseases and disorders of calcium and phosphate metabolism through the Center of Expertise in Rare Endocrine Diseases at Laiko Hospital. This is precisely the field in which I trained at Leiden University Medical Center in The Netherlands, under Dr Neveen Hamdy and Professor Socrates Papapoulos, so it is especially meaningful for me to apply that knowledge directly to patient care every day.
Secondly, scientifically, we have a special focus on hypoparathyroidism, particularly on skeletal fragility and the broader disease burden in this population. In parallel, we are running multicentre studies on the long-term and sequential management of osteoporosis.
What work led to your award from ESE?
The research focused on the role of microRNAs in predicting fractures in patients with osteoporosis. We examined how specific microRNAs change with treatment, and how these changes mirror the complex molecular mechanisms of bone remodelling at the cellular level. What was particularly exciting was the ability to connect these molecular signatures with real clinical outcomes, offering the potential for microRNAs to serve as biomarkers for fracture risk and therapeutic response.
Since then, however, technology has advanced rapidly, especially with the evolution of various omics platforms. For a clinician-scientist, it has been challenging to keep pace with such a highly sophisticated and rapidly expanding field, so I decided to change focus away from microRNAs.
What has been most challenging: laboratory research, hospital work or guideline development?
Each has its own challenges. The most demanding aspect has been balancing all of them simultaneously. Laboratory work requires patience and precision, hospital work demands emotional resilience and rapid decision making, and guideline development requires consensus building and responsibility towards the wider medical community.
What has been your biggest achievement?
If I had to choose one, it would be contributing to the clinical care and improved quality of life of patients living with rare metabolic bone diseases. Research awards and academic milestones are important, but seeing patients benefit from our scientific progress is the true accomplishment.
What is the biggest challenge for early-career endocrinologists?
This will be the rapidly evolving landscape of medical knowledge. New technologies, from omics to artificial intelligence, are transforming how we diagnose and treat endocrine diseases.
Not only must young endocrinologists master classical endocrinology, they must also integrate these new tools thoughtfully and ethically into practice. Maintaining compassion and clinical intuition while navigating technological change will be essential.
What advice would you give young people?
Be curious. Be persistent. And never be afraid to ask questions − even the ones that seem simple. Seek mentors who inspire you, collaborate generously, and remember that science advances through collective effort, not competition. Most importantly, stay connected to the reason you entered medicine in the first place: to help people.
Who have been your role models?
I have been fortunate to be surrounded by inspiring mentors throughout my career. I have already mentioned Neveen Hamdy, John Yovos and, of course, Socrates Papapoulos. I should also add Stavros Manolagas and Maria Almeida from the University of Arkansas for Medical Sciences in Little Rock, USA, both of whom shaped my scientific thinking in profound ways.
As I grow older and, hopefully, a bit wiser, I have come to believe that academic mentality is not just about being hard-working or scientifically productive. What truly matters is the ability to inspire young people, to make them want to stay, learn and work with you.
Please share a significant moment from your career
One of the most meaningful moments was diagnosing a rare metabolic bone disorder in a young patient who had gone years without answers.
Seeing the impact that a correct diagnosis and targeted treatment had on her life reaffirmed why rare disease expertise matters so much. It reminded me that, at the end of the day, every hour spent in the lab and every page of research read serves someone who desperately needs answers.
Our bacterial companions have a big say in our health − not least of all in regulating our hormones.
Prostate cancer is the most frequently diagnosed cancer among men in developed countries. How might microbes play a part in its pathogenesis?
When detected at an early stage, prostate cancer is highly treatable, with excellent survival rates. However, it becomes a major clinical challenge when it progresses to an advanced stage, once it spreads to distant organs or if it relapses after initial therapy. In these cases, the disease frequently evolves into a lethal form, despite modern therapeutic advances.1
The cornerstone of treatment for advanced prostate cancer remains the inhibition of the androgen receptor signalling pathway. Prostate cancer cells are highly dependent on androgens for growth and survival. For this reason, standard therapies aim either to reduce circulating androgen levels (a strategy known as androgen deprivation therapy) or to block the androgen receptor directly using specific inhibitors. While these approaches are initially effective in most patients, the majority eventually develop castration-resistant prostate cancer (CRPC), a stage during which tumours continue to grow, despite very low levels of circulating androgens.
Prostate cancer cells can escape androgen receptor inhibition through multiple mechanisms. One common strategy is hypersensitisation of the androgen receptor, whereby mutations or gene amplification lead to increased receptor expression or activity, allowing these cancer cells to respond to minimal hormone levels. Another mechanism involves the production of androgen receptor splice variants that lack the ligand-binding domain, the region of the protein targeted by current inhibitors; these truncated receptors remain constitutively active, even in the absence of androgens. In addition, prostate cancer cells may bypass androgen receptor signalling altogether by activating alternative growth pathways, such as PI3K/AKT or MAPK signalling. Less frequently, prostate tumours can undergo treatment-derived neuroendocrine transdifferentiation, losing androgen receptor expression or activity and adopting a highly proliferative and aggressive state.1
Given the absence of curative treatments for CRPC, unveiling novel mechanisms driving castration resistance is a major priority in prostate cancer research. In recent years, an unexpected player has emerged: the microbiota.
The human body is home to trillions of micro-organisms that collectively form the microbiota. Far from being passive passengers, these microbes play essential roles in digestion, immune regulation, metabolism, and even hormone homeostasis. Alterations in the microbiota have been linked to a wide range of diseases, including inflammatory bowel disease, obesity, diabetes and, increasingly, cancer. In oncology, the microbiota has been shown to influence tumour development, the response to immunotherapy, and the efficacy of anti-cancer drugs.2
Until recently, however, the potential contribution of the gut microbiota to CRPC had not been explored. A study has now shown that androgen deprivation therapy can alter the intestinal microbiota and promote the emergence of castration resistance. In both mouse models and patients, the gut microbiota of individuals with CRPC was found to be enriched in species capable of converting androgen precursors into active androgens. Remarkably, depletion of the gut microbiota using antibiotics delayed the onset of castration resistance.
To directly assess causality, researchers employed faecal microbiota transplantation (FMT), a procedure in which micro-organisms from a donor are transferred to a recipient. FMT has gained prominence in recent years as a tool for studying and manipulating the microbiota, and it is already used clinically to treat recurrent Clostridioides difficile infections. When FMT from patients with CRPC or CRPC mouse donors was administered to mice bearing prostate tumours, the tumours rapidly became resistant to castration. In contrast, FMT from patients with
hormone-sensitive prostate cancer was able to restrain tumour growth. Among the bacterial species associated with this protective or antitumour effect, Prevotella stercorea, a common gut commensal involved in carbohydrate metabolism, stood out.3
Together, these findings suggest a previously unrecognised mechanism of endocrine resistance in prostate cancer. The gut microbiota can act as an alternative source of androgens, fuelling tumour growth when systemic androgen levels are low. Beyond the mechanistic insight, these results open exciting therapeutic possibilities. Modulating the microbiota through diet, probiotics, antibiotics or targeted microbial interventions may, in the future, complement existing treatments for advanced prostate cancer.
These discoveries highlight the fact that tumours do not act in isolation. They are embedded within a complex biological ecosystem that includes not only host cells but also the microbial communities we carry with us. In the fight against cancer, the gut microbiota may prove to be an unexpected ally ... or a silent adversary.
Juan Manuel Jiménez Vacas UK
REFERENCES
1. Westaby et al. 2022 Annual Review of Pharmacology & Toxicology https://doi.org/10.1146/annurev-pharmtox-052220-015912
2. Hou et al. 2022 Signal Transduction & Targeted Therapy https://doi.org/10.1038/s41392-022-00974-4
3. Pernigoni et al. 2021 Science https://doi.org/10.1126/science.abf8403
What importance does the gut microbiota have for the effectiveness of weight loss – and how might glucocorticoids be involved?
Modern lifestyles, characterised by highcalorie diets and physical inactivity, contribute significantly to the global rise in obesity and related metabolic disorders, such as type 2 diabetes, metabolic dysfunctionassociated steatotic liver disease (MASLD) and cardiovascular disease. Obesity also negatively affects bone health and reproductive function, and increases the risk of certain cancers. According to the World Health Organization, in 2022, approximately 1 in 8 people worldwide were living with obesity. This included over 390 million children and adolescents (aged 5–19 years) who were overweight, of whom 160 million had obesity. The increasing prevalence of obesity places a significant burden on healthcare systems, with obesity-related conditions accounting for an estimated 8.4% of total health expenditure across OECD countries.
The role of the microbiota
There is now considerable evidence that disruption of the composition of the gut microbiota, or dysbiosis, plays a role in several diseases, including obesity, inflammatory bowel disease and type 2 diabetes.1 Modulating the gut microbiota has emerged as a promising strategy for improving obesity and related metabolic disorders.
Our recent study found that gut microbiota composition correlates with weight loss in children with obesity who are undergoing dietary treatment. Specifically, a higher abundance of Lachnospiraceae family members correlated with greater weight loss, while a higher abundance of Erysipelotrichaceae and Enterobacteriaceae was negatively associated with weight loss efficacy.2
Although many animal studies suggest that probiotic strains, particularly Lactobacillus spp. and Bifidobacterium spp., can enhance gut barrier integrity, reduce inflammation, exhibit anti-diabetic properties and positively influence liver function in MASLD, the probiotics that are currently used have only marginal effects on reducing body weight. This may be due to the use of bacterial taxa that are not directly linked to weight gain or loss in humans, and are not involved in the main mechanisms of obesity development.
Understanding the mechanism
Gut bacteria metabolise various substrates, including dietary proteins, fibre, sterols, bile acids, short-chain fatty acids and steroid hormones. Among steroid hormones, glucocorticoids are important endocrine mediators implicated in the development of obesity and metabolic diseases, acting through the regulation and modulation of metabolic, inflammatory and behavioural processes in different tissues.3 However, considerable controversy remains regarding their role in either aggravating or reducing obesity, and whether glucocorticoids are a cause or a cure for this condition.
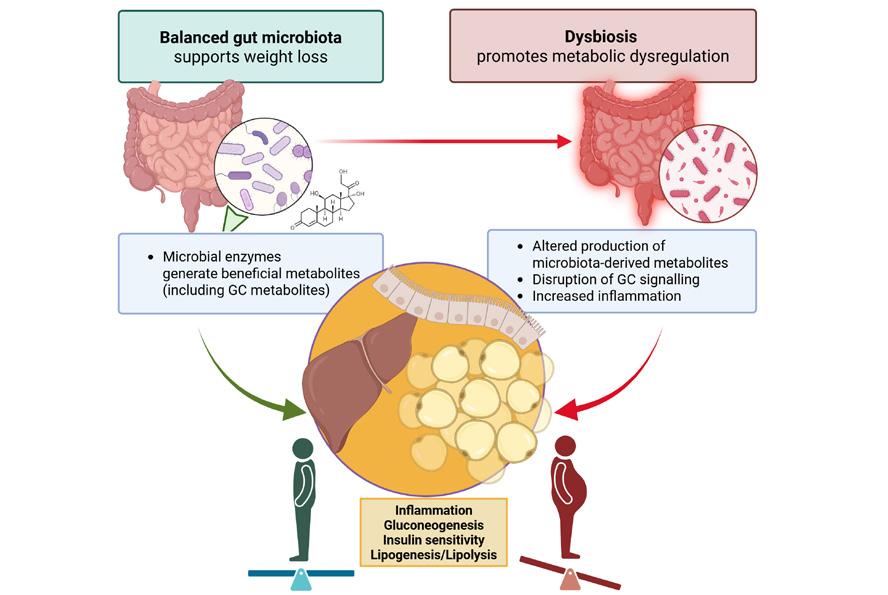
Chronic glucocorticoid treatment typically results in weight gain, increased visceral obesity and hypertension, while acute treatment usually causes weight loss, particularly through lipolysis in adipose tissue. Research has focused on the dysregulation of tissue-specific glucocorticoid metabolism and the role of peripheral glucocorticoid metabolites in obesity, revealing significant differences in glucocorticoid signatures among patients with obesity. Although glucocorticoids are involved in the regulation of diet-induced weight loss, the role of microbiota-derived intestinal glucocorticoids and their metabolites in obesity remains unclear.
Microbial glucocorticoid metabolism
Emerging evidence indicates a bidirectional relationship between gut microbiota and glucocorticoid metabolism that contributes to obesity. As previously mentioned, certain intestinal bacteria can metabolise hostproduced glucocorticoids, thereby regulating intestinal glucocorticoid synthesis. Steroid transformations by gut bacteria include side chain cleavage (desmolase activity), dehydroxylation of the 21-hydroxyl group, formation of 11-oxy-androgens (20α-hydroxysteroid dehydrogenase (20αHSD) activity) and reduction of the A ring (5βand 5α-reductase activity), all resulting in glucocorticoid metabolites with markedly different physicochemical properties from their precursors.4
These metabolites act both locally (affecting the intestinal glucocorticoid pathway, regulating local immune responses and altering epithelial barrier integrity) and systemically, as they are absorbed into the portal circulation to act in other organs, such as the liver and adipose tissue, before being excreted in urine. Some of these metabolites, such as 3,5-tetrahydrocorticosterone and 11-hydroxyprogesterone, strongly inhibit both 11βHSD1 and 11βHSD2 (the enzymes responsible for glucocorticoid prereceptor metabolism), while the microbial metabolite 21-desoxycortisol potently inhibits only
GC, glucocorticoid Created using BioRender.com
11βHSD2. Thus, gut microbiota can influence systemic glucocorticoid signalling not only by producing metabolites, but also by modulating glucocorticoid prereceptor metabolism.5
Disruption of the glucocorticoid pathway in intestinal epithelial cells due to dysbiosis, a feature of obesity, may lead to increased inflammatory responses and greater tissue damage. Dysbiosis associated with obesity often results in altered production of microbiotaderived metabolites, including short-chain fatty acids, bile acids and tryptophan derivatives, which can modulate glucocorticoid receptor signalling and adipose tissue glucocorticoid activity. This interaction promotes visceral fat accumulation, low-grade inflammation and insulin resistance, creating a vicious cycle in which dysbiosis worsens glucocorticoidmediated metabolic dysfunction and further drives obesity.
Identifying gut bacteria that can restore local glucocorticoid synthesis and enhance beneficial glucocorticoid-mediated effects in the intestine may help explain how the microbiota contributes to inconsistent outcomes in weight-loss interventions. Further studies demonstrating the causal relationship between glucocorticoid-metabolising bacteria and weight loss, as well as investigating the underlying molecular mechanisms, could enable an effective microbiota-based approach to obesity prevention or treatment, and serve as the basis for developing ‘tailor-made’ nextgeneration probiotics.
REFERENCES
1. Guarner & Malagelada 2003 Lancet https://doi.org/10.1016/S0140-6736(03)12489-0
2. Kovačević et al. 2025 Journal of Endocrinological Investigation https://doi.org/10.1007/s40618-025-02672-8
3. Morris & Brem 2019 Physiological Genomics https://doi.org/10.1152/physiolgenomics.00115.2018
4. Ly et al. 2021 Molecular & Cellular Endocrinology https://doi.org/10.1016/j.mce.2021.111174
5. Tomlinson et al. 2004 Journal of Clinical Endocrinology & Metabolism https://doi.org/10.1210/jc.2003-031376
How can diet and the microbiota help prevent, or reverse, diabetes in patients with coronary heart disease?
In recent years, research has revealed that the gut plays a central role in regulating cardiometabolic health. Evidence from the CORDIOPREV study (a long-term nutritional intervention in patients with coronary heart disease) indicates that changes in the gut microbiota can precede and predict the development of type 2 diabetes (T2DM).
A characteristic intestinal microbiota profile has been identified in individuals at risk of developing T2DM.1 This ‘diabetic microbiota’ is characterised by a lower abundance of butyrate-producing bacteria, such as Faecalibacterium prausnitzii and Roseburia spp., along with an increase in pro-inflammatory genera such as Ruminococcus, Collinsella and Dorea. This dysbiosis promotes increased intestinal permeability, low-grade endotoxaemia and insulin resistance, even years before the clinical onset of the disease. Integrating microbiome data with traditional clinical factors significantly improved predictive ability, suggesting that gut bacteria could act as early biomarkers of metabolic risk.1 This microbiota, however, differs significantly between men and women, making sex one of the key factors in microbiota research, according to the latest studies.2
Women without T2DM have lower plasma concentrations of lipopolysaccharides (LPS) and trimethylamine oxide (TMAO), metabolites derived from the gut microbiota associated with inflammation and atherosclerosis. However, this traditional advantage disappears once T2DM develops, indicating that T2DM alters intestinal integrity and eliminates sex-related cardiovascular protection.
Dietary interventions modify the intestinal microbiota of the patient.2 The Mediterranean diet, rich in fibre, polyphenols and healthy fats, also reduces inflammatory markers and promotes remission of T2DM, compared to a low-fat diet.3 At the same time, maintaining healthy eating patterns helps preserve telomere length, delaying biological ageing,4 while certain circulating microRNAs (miR-15a, miR-223, miR-150) respond to nutritional therapy and act as molecular signatures of metabolic improvement and T2DM improvement.5
Taken together, these pioneering findings from the Spanish CORDIOPREV study highlight the powerful interaction between the Mediterranean diet, gut microbiota health and its implications for metabolic and cardiovascular health. Personalised nutrition aimed at restoring microbiome balance and shaping an optimal ‘anti-diabetes’ profile could become a key tool in preventing and even reversing T2DM, as these studies demonstrate.
Helena García-Fernández Spain
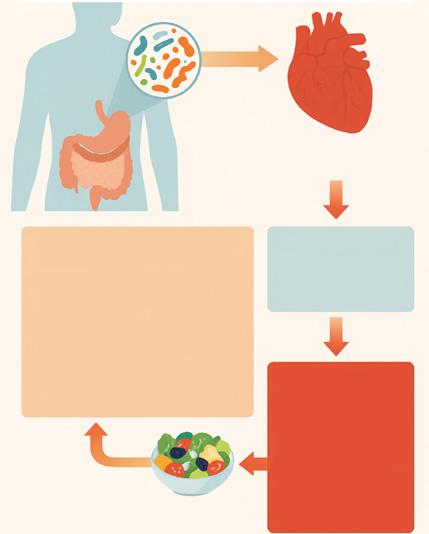
Gut microbiota
Coronary heart disease
Sex differences
Characteristic intestinal microbiota profile in T2DM
- ↓ butyrate-producing bacteria
- ↑ proinflammatory genera
- intestinal permeability
- low-grade endotoxaemia
- insulin resistance
In non-T2DM women
↓ LPS and TMAO
Dietary intervention (CORDIOPREV)
- ↓ inflammatory markers
- T2DM remission
- preserved telomere length
- circulating microRNAs Mediterranean diet
The gut microbiota-T2DM-coronary heart disease axis
REFERENCES
1. Vals-Delgado et al. 2021 Clinical & Translational Medicine https://doi.org/10.1002/ctm2.326
2. García-Fernández et al. 2025 Frontiers in Cardiovascular Medicine https://doi.org/10.3389/fcvm.2025.1527406
3. Boughanem et al. 2025 Nutrition & Diabetes https://doi.org/10.1038/s41387-025-00360-3
4. Ojeda-Rodriguez et al. 2024 Cardiovascular Diabetology https://doi.org/10.1186/s12933-024-02175-5
5. Alcala-Diaz et al. 2025 Nutrition & Diabetes https://doi.org/10.1038/s41387-025-00362-1.
What are the implications of the gut microbiome for premature ovarian insufficiency (POI) and postmenopause?
The gut microbiome is increasingly recognised as a modulator of women’s hormonal health. Beyond its metabolic and immune roles, it potentially affects oestrogen metabolism through the oestrobolome, a collection of bacterial genes capable of modulating systemic oestrogen levels.1 Specifically, oestrogenic compounds undergo glucuronidation in the liver and are mainly excreted through urine and faeces. However, bacteria producing β-glucuronidase can deconjugate these metabolites in the gut, leading to their reabsorption, thus increasing circulating oestradiol levels.2
Indeed, a recent study combining liquid chromatography−tandem mass spectrometry and meta-genomic shotgun sequencing showed that the gene copy number for oestrogendeconjugating enzymes (β-glucuronidase and arylsulfatase) was significantly higher in premenopausal than in postmenopausal women. Moreover, the abundance of these genes was associated with individual plasma oestrogen metabolites in premenopausal women.3 These findings support the concept that gut microbial β-glucuronidase and arylsulfatase activity influence the deconjugation of gut oestrogens and, as a result, oestrogen homeostasis.
Several studies investigated the gut microbiome in hypo-oestrogenic states, including POI and postmenopause. POI (defined as loss of ovarian function before the age of 40) and menopause (typically occurring between 45 and 55 years of age) share a state of ‘hypergonadotrophic hypogonadism’, characterised by high follicle-stimulating hormone and low oestradiol levels.4,5 Beyond reproductive implications, these women face increased risks of cardiovascular disease, osteoporosis, metabolic syndrome, premalignant and malignant diseases, and cognitive decline.
Recent evidence links gut dysbiosis to these conditions. Women with POI have increased abundance of Eggerthella species in faecal samples, which normalises after sequential oestro-progestagen therapy. In vivo studies showed that Eggerthella inoculation in mice induced ovarian fibrosis and inflammation − changes that were reversed by oestradiol, indicating the bidirectional relationship between oestrogen and gut microbiome alterations.6 Additionally, reduced gut microbiome diversity has been observed both in women with POI6 and in postmenopausal women, associated with greater faecal oestrogen loss and diminished oestrogen recycling.7 Furthermore, the postmenopausal microbiome more closely resembles those of men than those of premenopausal women,8 highlighting the role of oestrogen in shaping the microbial environment.
However, a recent meta-analysis found no differences in gut microbiome composition between postmenopausal and premenopausal women, nor between women with POI and premenopausal controls. These results should be interpreted with caution, as the studies included were heterogeneous in terms of populations, methods and confounding factors.9
Future research should prioritise well-defined, homogeneous populations and exclude known gut microbiome disruptors. Understanding the gut−oestrogen axis could guide targeted treatments and interventions that could improve the management and outcomes of oestrogendependent states.
Kristina Saravinovska, Serbia
REFERENCES
1. Ervin et al. 2019 Journal of Biological Chemistry https://doi.org/10.1074/jbc.RA119.010950
2. Plottel & Blaser 2011 Cell Host & Microbe https://doi.org/10.1016/j.chom.2011.10.003
3. Li VW et al. 2025 Molecular & Cellular Endocrinology https://doi.org/10.1016/j.mce.2025.112534
4. Vujovic et al. 2010 Maturitas https://doi.org/10.1016/j.maturitas.2010.04.011
5. Randolph et al. 2004 Journal of Clinical Endocrinology & Metabolism https://doi.org/10.1210/jc.2003-031183
6. Jiang et al. 2021 Frontiers in Endocrinology https://doi.org/10.3389/fendo.2021.794496.
7. Flores et al. 2012 Journal of Translational Medicine https://doi.org/10.1186/1479-5876-10-253
8. Peters et al. 2022 mSystems https://doi.org/10.1128/msystems.00273-22
9. Saravinovska et al. 2025 Endocrine Abstracts https://doi.org/10.1530/endoabs.110.P1058
What mechanisms might underlie interactions between the gut microbiota and the thyroid system?
A possible link between gut microbiota composition and thyroid homeostasis was first suggested about 100 years ago, but only in recent years has knowledge of this topic deepened, leading to the concept of the ‘thyroid−gut axis’.1
A hypothesis of gut microbiota-related induction of autoimmunity in genetically predisposed subjects stems from the microbiota’s impact on both innate and adaptive immunity, as demonstrated in murine models. The intestine hosts approximately 70% of the entire immune system, known as gut-associated lymphoid tissue.1 According to the ‘intestinal barrier hypothesis’, dysbiosis, which represents an imbalance between commensal and pathogenic bacteria, may lead to an increased
translocation of bacterial antigens into the systemic circulation, where their epitopes may trigger auto-aggressive processes, establishing a sort of ‘vicious circle’.2
An additional mechanism may involve indirect mediation by a variation in short-chain fatty acids, metabolites produced by specific strains of bacteria, known to exert anti-inflammatory effects (see Figure).3
For example, in NOD H2h4 mice, bacterial lipopolysaccharide can interact with Toll-like receptor 4 expressed on thyrocytes, triggering thyroiditis. Using animal models established by immunisation with human thyrotrophin receptor, researchers have demonstrated that different gut microbiota can vary the clinical manifestation of both Graves’ disease and
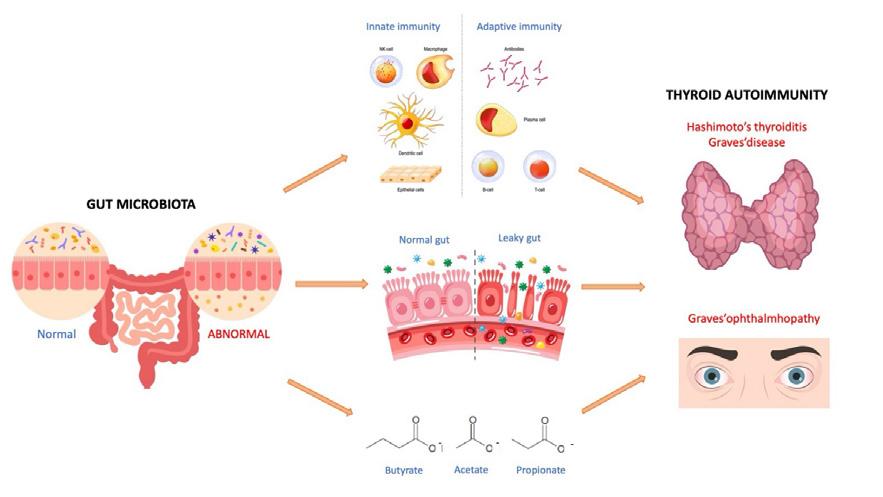
Graves’ ophthalmopathy. Furthermore, animal studies on gut microbiota transplantation confirmed that a dysbiotic state may increase the susceptibility to thyroid autoimmunity.1 Of note, increased direct and indirect markers of gut barrier leakiness have been described in patients with Hashimoto’s thyroiditis and Graves’ disease, with or without ophthalmopathy.1 Several studies have reported a dysbiotic gut microbiota in patients with autoimmune thyroid diseases and, in some cases, a direct correlation has been found between thyroid biomarkers (e.g. thyroid-related autoantibodies) and specific bacterial taxa.4 However, further research is still needed due to geographical variability, small sample sizes and the numerous environmental factors influencing gut microbiota composition that are often not carefully analysed.5
Finally, no studies have yet been published on the effects exerted by the other components of gut microbiota, such as viruses, bacteriophages and protozoa, on thyroid homeostasis. Despite these limitations, microbiota− host interactions may open a new era in the pathophysiological research on thyroid autoimmunity.
Camilla Virili, Italy
REFERENCES
1. Virili et al. 2024 Reviews in Endocrine & Metabolic Disorders https://doi.org/10.1007/s11154-023-09839-9
2. Akdis 2021 Nature Reviews Immunology https://doi.org/10.1038/s41577-021-00538-7
3. Saadh et al. 2025 Seminars in Oncology https://doi.org/10.1016/j.seminoncol.2025.152398
4. Sawicka-Gutaj et al. 2022 International Journal of Molecular Science http://doi.org/10.3390/ijms232113450
5. Ludgate et al. 2024 Nature Reviews Endocrinology https://doi.org/10.1038/s41574-024-01003-w
How can the relative abundance of different bacterial strains affect development of this autoimmune disease?
In type 1 diabetes (T1DM), predisposed people experience autoimmune destruction of pancreatic β cells. Factors that may influence the development and progression of this disease are being investigated. The intestinal microbiota is one such factor, potentially impacting the disease’s course, metabolic control and the risk of developing chronic complications.
The pathomechanism of T1DM development may be related to the reduced occurrence of butyrate-producing strains. This affects the function of enterocytes, peri-intestinal lymphoid tissue and tight junction proteins.1 The proteins claudin-2, occludin and zonulin also have a modulatory effect on the intestinal barrier, and their levels are modified depending on the colonisation of bacterial strains.2 Damage to the intestinal barrier’s components leads to the translocation of bacteria and their metabolites into the bloodstream, potentially triggering the activation of autoimmune processes.
In patients with T1DM, there is a disturbance in the ratio of Gram-positive bacteria (Firmicutes) to Gram-negative bacteria (Bacteroidetes), as well as excessive or reduced
colonisation of some species − an increase in Clostridiales and Dorea and a decrease in Dialister 3 The first significant meta-analyses examined the potential impact of the intestinal microbiota on the risk of developing T1DM. The TEDDY study evaluated the influence of environmental factors on alterations in the intestinal microbiota that may promote the development of T1DM. In addition, differences in the composition of the microbiota were assessed between children who had T1DM and those who did not develop this disease. The microbiome of children without T1DM contained more genes related to the fermentation and biosynthesis of short-chain fatty acids.4,5
A consequence of changes in the ratio of individual species is the activation of Toll-like receptor 4 and an increase in the expression of inflammatory pathways, such as c-Jun N-terminal kinase and nuclear factor-κB. Moreover, an increased concentration of trimethylamine-N-oxide is also observed, which may contribute to the development of atherosclerosis and microangiopathic complications in this patient group.6
A correlation was also found between the colonisation of the intestines by some species and the development of specific complications.7 This study showed that changes in the composition of the intestinal microbiota occurring in people with T1DM may be related to its compensation.
The role of the intestinal microbiota in patients with T1DM remains unclear and requires further investigation.
Agnieszka Zawada, Poland
REFERENCES
1. Bibbò et al. 2017 Annals of Medicine https://doi.org/10.1080/07853890.2016.1222449
2. Wang et al. 2000 Journal of Cell Science https://doi.org/10.1242/jcs.113.24.4435
3. Del Chierico et al. 2022 International Journal of Molecular Science https://doi.org/10.3390/ijms231810256
4. Vatanen et al. 2018 Nature https://doi.org/10.1038/s41586-018-0620-2
5. Stewart et al. 2018 Nature https://doi.org/10.1038/s41586-018-0617-x
6. Kasselman et al. 2018 Atherosclerosis https://doi.org/10.1016/j.atherosclerosis.2018.02.036
7. van Heck et al. 2022 Diabetes Care https://doi.org/10.2337/dc21-2225
Don’t miss out: book your place at ECE in Prague, Czech Republic, on 9−12 May 2026!
ECE 2026 is fast approaching, and your EYES Committee is determined to leaving nothing to chance. Once again, we will make sure that young endocrinologists have a central role during the most important event of the year. For this reason, we are thrilled to announce our exciting line-up of activities.
The EYES Symposium on 11 May will be an excellent opportunity to encounter high-impact early-career endocrinologists presenting the new cutting-edge developments in pituitary science, providing young clinicians and scientists with valuable insights into the most recent advances in this field. This will also be the chance to learn more about our community, and receive updates on EYES activities, our year-round initiatives and, last but not least, the announcement of the recipients of the current round of Observership Programme funding.

Meeting Grant application deadline: 25 March 2026
Super Early Bird deadline: 31 March 2026
Early Bird deadline: 21 April 2026
www.ese-hormones.org/ece2026
But the experience doesn’t stop there! The best way to fully immerse yourself in the Congress atmosphere will be to join the EYES social event − a fantastic evening designed to offer a relaxed environment − and to engage in high-quality networking with peers from across Europe.
So mark your calendar and register now EXTERNAL-LINK..... You can also take the opportunity to browse the Congress programme EXTERNAL-LINK....
The EYES Committee looks forward to welcoming you to ECE 2026 and to contributing to a meaningful and enriching Congress experience.
Clara Lazzaretti EYES Representative, ECE 2026 Programme

Are you ready for the 13th EYES Annual Meeting on 4−6 September 2026?
Spring always brings a sense of renewal, and this year it arrives with special anticipation, as we are only a few months away from welcoming you to the 13th EYES Annual Meeting in Belgrade, the capital of Serbia. Preparations are already fully underway, and the Local Organising Committee is channelling its shared curiosity and drive into creating a meeting that reflects everything the EYES community stands for: connection, growth and bold ideas.
Expect sessions that spark critical thinking and challenge assumptions, and a programme that is designed to push conversations across borders. The meeting will offer opportunities to present your work, engage with exceptional speakers and peers, and contribute to discussions that shape the future of endocrinology.
Once the sessions are over, Belgrade invites you onto its vibrant stage, for networking. The city’s riverside promenades and
irrepressible energy offer the perfect setting for informal social events, novel collaborations, and a creative spirit that adds to the momentum.
As you plan your journey to Belgrade, make sure to submit your abstract. Bring the work that excites you, the questions that drive you, and the ambition that brought you into this field. We look forward to welcoming you to a meeting that doesn’t just report progress − it creates it.

Watch out for more information EXTERNAL-LINK-ALT
See you in Belgrade.
Antoan Stefan Šojat and Kristina Saravinovska 13th EYES Annual Meeting Local Organising Committee

The 2026 ESE Summer School is an unmissable event for early-career basic scientists and clinical investigators.
In 2025, we had an amazing time in Innsbruck, Austria, at last year’s ESE Summer School. The event offers young researchers, PhD students and early-career scientists from around the world a valuable opportunity to deepen their knowledge and broaden their professional horizons. This inspiring event returns on 5−8 July 2026 at the exceptional TBI-Grillhof, immersed in nature and surrounded by the breathtaking Austrian Alps. Once again it will provide the perfect setting for learning, discussion and connection with one another.
Over four intensive days, you have the chance to attend high-level lectures delivered by

internationally renowned experts in the main areas of endocrinology. They will share insights into the latest scientific advances and their relevance to future applications. You will hear about new directions in endocrine research: from adrenal diseases to diabetes and obesity, from receptor signalling to the emerging role of artificial intelligence in research, and much more. The impact of endocrine-disrupting chemicals across the lifespan will be in the spotlight, as we address one of the most pressing and relevant challenges faced by young endocrinologists today.
Beyond the academic programme, the ESE Summer School is designed to emphasise interaction and networking. Dedicated poster sessions and informal gatherings will encourage dialogue between peers and senior researchers, fostering collaboration, mentorship and the exchange of ideas in a stimulating and inclusive atmosphere.
Learning will not be limited to the lecture halls. The surrounding, majestic mountains are a wonderful backdrop for outdoor activities. Team-based sports, lake swimming and hiking will offer a break from the scientific programme, allowing you to relax while building valuable connections.
The EndoCompass Research Roadmap EXTERNAL-LINK-ALT is set to strengthen endocrine research and improve hormone health.
This major initiative was led by ESE and the European Society for Paediatric Endocrinology, with contributions from over 228 European experts. Its recommendations aim to inform policy and funding decisions at European and national levels by identifying areas where research and investment can have the greatest impact.
You can use the Roadmap as a practical tool in planning research projects, clinical trials and careers. Cite it in your research papers and funding proposals, and let it help you identify how to make the biggest impact in your career (e.g. in emerging areas such as endocrine-disrupting chemicals and artificial intelligence).

Please tell people about the Roadmap!
Share it with colleagues, add it to meeting agendas, and post about it on social media. You can also use the EndoCompass Toolkit EXTERNAL-LINK-ALT, with slides, graphics and other materials, in your presentations and communications.
5−8 July
The ESE Summer School is an unmissable event for any young scientist who is eager to stay at the forefront of endocrinology, while engaging with a global community in one of Europe’s most beautiful alpine settings.
Clara Lazzaretti
EYES Representative, ESE Summer School
Watch out for this new ESE initiative for all endocrine researchers!
#ThisIsEndocrinology is a new campaign from the ESE Science Committee, to communicate the benefits of ESE membership to all scientists working on hormones.
Many scientists working in relevant areas may not consider themselves ‘endocrinologists’. By showcasing the people, science and careers that define modern endocrinology, #ThisIsEndocrinology will raise awareness of our discipline and of ESE, highlighting the breadth of fields that contribute to endocrine discovery. ESE seeks to ensure that basic scientists feel visible, valued and fully represented within the Society, and that they recognise endocrinology – and ESE – as their scientific home.
Find more information to share EXTERNAL-LINK-ALT and highlight the campaign and the importance of basic endocrine science on your socials and to earlycareer colleagues.
Julia Beck gives an insight into the EYES Advanced Research Observership Programme.
The EYES Observership Programme is one of the most valuable initiatives for early-career endocrinologists and scientists within ESE.
Within this framework, the EYES Advanced Research Observership Programme (AdROP) EXTERNAL-LINK-ALT is specifically designed for experienced early-career basic and translational scientists who wish to develop their academic profile through sustained international research exposure. Applicants are expected to demonstrate prior research experience and a defined scientific interest aligned with the expertise of participating centres, ensuring a productive and mutually beneficial match between awardees and host institutions.
AdROP differs from the shorter, one-month observational visits offered by the other EYES Observership Programmes. AdROP awardees are embedded in host institutions for up to three months, allowing for more active involvement in ongoing basic or translational research projects.
‘The AdROP is designed for experienced early-career scientists who wish to further develop their academic profile.’
This extended duration enables meaningful scientific contribution, close integration within research teams, and in-depth exposure to new experimental approaches and research cultures.
For early-career scientists seeking hands-on research experience rather than short-term observation, AdROP provides a particularly valuable opportunity.
ESE offers funding of up to €3000 per AdROP awardee, to help reduce barriers related to travel and living costs, allowing participants to focus on research activities, skill development and collaboration throughout the Observership.
The value of AdROP can be perfectly illustrated by the experiences of its participants, such as 2025 awardee Rosa Catalano EXTERNAL-LINK-ALT and 2024 recipient Mario Detomas EXTERNAL-LINK-ALT, both of whom describe it as a formative step in their scientific development. Rosa worked in Würzburg in a highly collaborative research environment that encouraged close interaction between clinicians and scientists, strengthening her ability to integrate clinical and biological perspectives. Similarly, Mario Detomas highlighted the programme’s intensive research focus and exposure to new methodologies during his stay in London. Together, their experiences underline a key strength of AdROP: it enables early-career researchers to actively contribute to research while advancing their technical skills and building international collaborations within a broader European network.
As the programme enters its 2026 cycle, AdROP continues to offer early-career scientists a structured opportunity to strengthen their research profile, gain international experience and establish collaborations that support long-term academic development. Apply by the closing date of 12 March 2026.
Julia Beck Switzerland
Find out more about Clinical, Research and Advanced Research Observerships EXTERNAL-LINK.... and apply before 12 March 2026
In 2026, World Hormone Day aims to exceed last year’s reach of over 136 million people across 40 countries.
This year’s campaign also aims to encourage even more conversations about why hormones matter. Engaging with as many people as possible is especially important in 2026, as World Hormone Day will have a stronger publicfacing focus on helping people understand hormones, with new materials designed for the general public.

ESE President, Professor Wiebke Arlt, says: ‘There is still a major gap in public understanding of what hormones are and how people can look after their hormone health. Hormones influence almost every process in the body, yet most people only think about them when something goes wrong. World Hormone Day is a chance to change that, by raising awareness and sharing practical steps that everyone can take towards better hormone health.’
You can join in online by following #BecauseHormonesMatter, or you can get involved in person. Make use of the World Hormone Day information and toolkit from ESE EXTERNAL-LINK-ALT. This includes infographics, posters, videos, social media graphics and more, for anyone who would like to support the campaign. If you want to translate materials, contact ESE for guidance at info@esehormones.org. Translations of last year’s materials are included in the toolkit.
The Young Endocrinologists Section of the Czech Endocrine Society EXTERNAL-LINK-ALT is one of the newest initiatives within the national endocrine community.

This fresh and energetic group is ready to connect, inspire and support the next generation of endocrinologists. Much like similar Sections across Europe, our goal is to bring together early-career clinicians and researchers from all over the Czech Republic, fostering collaboration, education and professional growth in the ever-evolving field of endocrinology.
Aims and vision
Our mission is simple yet ambitious: to strengthen postgraduate education in endocrinology and bring new perspectives to current forms of training. We want to create a vibrant platform where young professionals can bridge the gap between theory and clinical practice, share ideas, discuss challenges and learn from each other’s experiences.
Another key goal is to build a strong community − a network that connects young endocrinologists from different institutions and backgrounds. In a field as dynamic as endocrinology, professional collaboration is essential for staying up to date with advances in diagnostics, treatment and research. The Section aims to serve as a hub for co-operation and shared inspiration, where ideas can turn into joint projects and where both academic and clinical ambitions can thrive. These connections are particularly valuable in smaller countries such as the Czech Republic, where close collaboration can have a truly meaningful impact.
Inclusivity and collaboration
Although the Section primarily brings together endocrinologists under the age of 35, participation is open and flexible. We warmly welcome all colleagues, regardless of age, who wish to contribute, share their expertise, mentor younger members or take part in our activities. Our guiding

principle is inclusivity and intergenerational collaboration. The exchange of knowledge and experience between senior and junior endocrinologists enriches our entire community and strengthens the continuity of our field.
We are planning a range of events focused on education, skill development and community building. From informal case discussions and research presentations to workshops and networking sessions, our activities are designed to be open, friendly and engaging, creating a space where every young endocrinologist feels comfortable to share and learn.
A highlight of our activities will be a dedicated session for earlycareer endocrinologists during the annual Czechoslovak Endocrinology Conference: the largest regional meeting in our field. This platform will offer young professionals a unique opportunity to present their work, connect with leading experts and participate in meaningful clinical and scientific exchanges in a supportive atmosphere.
Representatives of the Young Endocrinologists Section are also invited to attend meetings of the Executive Committee of the Czech Endocrine Society. This ensures that the voices, perspectives and ideas of younger members are heard and reflected in the Society’s future direction. By taking part in these discussions, our members will have a real chance to shape the development of Czech endocrinology for years to come.
The creation of the Young Endocrinologists Section represents an exciting step towards a more connected, dynamic and forward-looking endocrine community. We offer a supportive environment where young specialists can grow professionally, expand their networks and find inspiration in each other’s journeys. We hope that, together, we can build a strong foundation for the future of Czech endocrinology, and to contribute to the field of endocrinology across Europe as well.
Tomáš Brutvan and Jan Drugda on behalf of the Section of Young Endocrinologists of the Czech Endocrine Society