

2
Dr. Sheahan on "the shadow curriculum."

10 News From SVS
Be sure to get your tickets now for the special gala at the Vascular Annual Meeting.



2
Dr. Sheahan on "the shadow curriculum."

Be sure to get your tickets now for the special gala at the Vascular Annual Meeting.
BY MARK S. LESNEY
MDEDGE NEWS FROM THE JOURNAL OF THORACIC AND CARDIOVASCULAR SURGERY
Anew study finds that patients taking fluoroquinolone antibiotics may be at higher risk of aortopathy in part because of human aortic myofibroblast–mediated extracellular matrix (ECM) dysregulation.
“Emerging evidence supports pharmacologic-associated aortopathy in patients receiving fluoroquinolone [FQ] antibiotics,” said first author David G. Guzzardi, PhD, and his colleagues, citing previous research showing that, “compared with patients receiving amoxicillin antibiotics, those receiving FQ have a 66% higher risk of aneurysm or dissection within a 2-month period after commencing FQ use.”

16
Three HIPAA violation cases to learn from.


BY BRUCE JANCIN MDEDGE NEWS
CHICAGO – A closer look at the landmark ATTRACT trial of pharmacomechanical catheter-directed thrombolysis for acute deep vein thrombosis (DVT) shows multiple benefits for the intervention versus standard anticoagulation alone in the subset of participants with iliofemoral DVT, Kush R. Desai, MD, said at a symposium on vascular surgery sponsored by Northwestern University.
ATTRACT, a National Institutes of Health–sponsored,
phase 3, multicenter, open-label, assessor-blinded study, was the first-ever randomized trial of pharmacomechanical catheter-directed thrombolysis (PCDT) for acute DVT. The results caused a major stir because, despite a sound therapeutic rationale for the procedure, the incidence of chronic postthrombotic syndrome (PTS) at 24 months of follow-up was 47% in the PCDT plus anticoagulation group and 48% in controls on anticoagulation alone (N Engl J Med. 2017 Dec 7;377[23]:2240-52). Since then, that overall negative trial has been one
Society for Vascular Surgery Relocates
The new SVS headquarters is located at 9400 W. Higgins Road, Rosemont, Ill. The new building is only 10 minutes from the Chicago’s O’Hare International Airport and will allow members to easily drop in and work with staff or hold council and committee meetings.
BY MALACHI G. SHEAHAN III, MD MEDICAL EDITOR, VASCULAR SPECIALIST
Spend a morning in my clinic and it becomes clear that many U.S. medical schools have no formal training in vascular disease. Certainly the symptoms of PAD are never taught; otherwise, why am I being referred so many patients with spinal stenosis? Some days I would have more use for an MRI than for my vascular lab. Then again, reviewing the aftermath of patients “treated” by other specialties, maybe some are better off going undiagnosed.
What I believe is needed is a longitudinal medical school curriculum in peripheral vascular disease. From the basic sciences to the clinical clerkships, a comprehensive education is essential. Undoubtedly vascular surgeons can provide this, but first we must understand the roadblocks to curriculum change, and they are significant.
In the early 1900s, Abraham Flexner was commissioned by the Carnegie Foundation to survey the quality of North American medical schools. During his travels, Flexner visited 155 schools and found that many had little staffing, no research, and poor or absent clinical facilities. A number of schools were simply money-making enterprises with dubious educational content. Flexner pulled few punches in his descriptions, calling some institutions “indescribably foul” and “the plague spot of the nation.” He published his findings in the Flexner Reports of 1910 and 1912.
These documents shaped modern medical education in the U.S. Flexner urged schools to adopt new standards of curriculum, including a model dividing the 4 years of school into 2 years of basic

Dr. Sheahan is the Claude C. Craighead Jr., Professor and Chair, Division of Vascular and Endovascular Surgery, Louisiana State University Health Sciences Center, New Orleans
science and 2 years of clinical experience.
In the wake of the Flexner Reports, half of U.S. medical schools were forced to merge or close. Still, a standardized system for accreditation was lacking. In 1942, the American Medical Association (AMA) and the Association of American Medical Colleges (AAMC) established the Liaison Commission for Medical Education (LCME) to meet this goal. Today the LCME provides accreditation for U.S. medical schools through an 8-year review cycle.
The LCME defines core curriculum as “the required components of a medical curriculum, including all required courses/modules and clinical clerkships/rotations.”1 Reviewing the LCME documents, one finds the specifications for curricular content are amazingly vague and astonishingly brief. Terms like “biochemistry,” “anatomy,” or even “surgery” are not mentioned.
Per LCME standards, it is the faculty of a medical school who define the competencies to be achieved by the students. The curriculum is then essentially reverse engineered to achieve these competencies. So while the SVS could attempt to open a discussion with the LCME regarding vas-
cular education, it appears change must happen at the individual school level.
The good news is that US medical school curricula are now exceptionally fluid. According to the 2017-2018 AAMC survey,2 85% of schools report a significant curriculum transformation within the past 3 years. Flipped classrooms, longitudinal courses, standardized patients, and team-based learning have become standard methods of medical teaching. The most common change reported is the enhanced integration of basic science content into organ system/case-based curriculum (97/147 schools). Pass/fail grading standards in basic science courses have also been widely adopted to encourage team learning. Those of us who review student applications to residency programs can vouch for the prevalence and extent of these changes. Many dean’s letters now border on the absurd:
Dear Program Director,
At the Medical College of the Everglades, we feel our students achieve a broad range of outcomes. Therefore we assign grades on an unintelligible scale of color hues. In that light, we are pleased to recommend Josh Atkins, MD, as a LEMON DROP YELLOW candidate for your residency.
Plainly we are evolving from the Flexner system which required 2 years of basic science classwork. This traditional medical education forced a divide between the basic sciences and their clinical relevance. Students were asked to memorize facts out of context as passive learners. Then, in the clerkships, would the truths of the Kreb’s cycle magically appear through the wonders of ENT clinic? Not likely. Recently I opened my biochemistry textbook for the first time since medical school (honestly,
VASCULAR SPECIALIST Medical Editor Malachi Sheahan III, MD
Associate Medical Editors Bernadette Aulivola, MD, O. William Brown, MD, Elliot L. Chaikof, MD, PhD, Carlo Dall’Olmo, MD, Alan M. Dietzek, MD, RPVI, FACS, Professor Hans-Henning Eckstein, MD, John F. Eidt, MD, Robert Fitridge, MD, Dennis R. Gable, MD, Linda Harris, MD, Krishna Jain, MD, Larry Kraiss, MD, Joann Lohr, MD, James McKinsey, MD, Joseph Mills, MD, Erica L. Mitchell, MD, MEd, FACS, Leila Mureebe, MD, Frank Pomposelli, MD, David Rigberg, MD, Clifford Sales, MD, Bhagwan Satiani, MD., Larry Scher, MD, Marc Schermerhorn, MD, Murray L. Shames, MD, Niten Singh, MD, Frank J. Veith, MD, Robert Eugene Zierler, MD
Resident/Fellow Editor Laura Drudi, MD.
Executive Director SVS Kenneth M. Slaw, PhD. Interim Director of Membership, Marketing and Communications
Angela Taylor
Managing Editor SVS Beth Bales
Vascular Specialist is the official newspaper of the Society for Vascular Surgery and provides the vascular specialist with timely and relevant news and commentary about clinical developments and about the impact of health care policy. Content for Vascular Specialist is provided by Frontline Medical Communications Inc. Content for the News From the Society is provided by the Society for Vascular Surgery.
The ideas and opinions expressed in Vascular Specialist do not necessarily reflect those of the Society or the Publisher. The Society for Vascular Surgery and Frontline Medical Communications Inc. will not assume responsibility for damages, loss, or claims of any kind arising from or related to the information contained in this publication, including any claims related to the products, drugs, or services mentioned herein.
POSTMASTER Send changes of address (with old mailing label) to Vascular Specialist, Subscription Services, 10255 W Higgins Road, Suite 280, Rosemont, IL 60018-9914.
RECIPIENT: To change your address, contact Subscription Services at 1-800-430-5450. For paid subscriptions, single issue purchases, and missing issue claims, call Customer Service at 1-833-836-2705 or e-mail custsvc.vasc@fulcoinc.com.
The Society for Vascular Surgery headquarters is located at 9400 W. Higgins Road, Suite 315, Rosemont, IL 60018. Vascular Specialist (ISSN 1558-0148) is published monthly for the Society for Vascular Surgery by Frontline Medical Communications Inc., 7 Century Drive, Suite 302, Parsippany, NJ 07054-4609. Phone 973-206-3434, fax 973-206-9378
Subscription price is $230.00 per year.
National Account Manager Valerie Bednarz, 973-206-8954, cell 973-907-0230, vbednarz@mdedge.com
Digital Account Manager Amanda Smith, (973) 206-2321, asmith@mdedge.com
Classified Sales Representative Drew Endy, 215-657-2319, cell 267-481-0133, dendy@mdedge.com
Senior Director of Classified Sales Tim LePella, 484-921-5001, cell 610-506-3474, tlapella@mdedge.com
Advertising Offices 7 Century Drive, Suite 302, Parsippany, NJ 07054-4609 973-206-3434, fax 973-206-9378
©Copyright 2019, by the Society for Vascular Surgery


Scan this QR Code to visit vascularspecialistonline.com
FRONTLINE MEDICAL COMMUNICATIONS SOCIETY PARTNERS
Director, FMC Society Partners Mark Branca
Editor in Chief Mary Jo M. Dales
Executive Editors Denise Fulton, Kathy Scarbeck
Managing Editor Mark S. Lesney
Creative Director Louise A. Koenig
Director, Production/Manufacturing Rebecca Slebodnik
Letters to the Editor: VascularSpecialist@vascularsociety.org
Editorial Offices: 2275 Research Blvd, Suite 400, Rockville, MD 20850, 240221-2400, fax 240-221-2548
Corporate
President/CEO Alan J. Imhoff
CFO Douglas E. Grose
SVP, Finance Steven J. Resnick
VP, Operations Jim Chicca
VP, Sales Mike Guire
VP, Society Partners Mark Branca
VP, Editor in Chief Mary Jo M. Dales
VP, Editorial Director, Clinical Content Karen Clemments
Chief Digital Officer Lee Schweizer
VP, Digital Content & Strategy Amy Pfeiffer
President, Custom Solutions JoAnn Wahl
VP, Custom Solutions Wendy Raupers
VP, Marketing & Customer Advocacy Jim McDonough
VP, Human Resources & Facility Operations
Carolyn Caccavelli
Data Management Director Mike Fritz
Circulation Director Jared Sonners
Corporate Director, Research & Comms. Lori Raskin
Director, Custom Programs Patrick Finnegan
In affiliation with Global Academy for Medical Education, LLC
President David J. Small, MBA
I don’t think I opened it too many times there). I thumbed through the prelude, which distressingly discusses the new (!) technology of recombinant DNA (I’m old – sigh.).
The rest of the text is hundreds of pages of biomolecules and glycolysis, but no mention of disease or any clinical application. AAMC surveys show that students report biochemistry and histology as the most deficient courses in terms of preparing them for clinical duties. Neurology and OB/ Gyn receive the lowest scores of the required clinical clerkships.
Think of how much time you spent in medical school learning the signs, symptoms, and treatments of endocrine disorders such as Cushing’s syndrome, Graves’ disease, and primary hypoparathyroidism. Together they are found in less than 500,000 Americans annually. PAD affects over 10 million. If we are graduating students with a poor understanding of vascular disease, change is needed. Shoehorning vascular education into the surgical clerkship is a weak solution.
According to the AAMC, the average number of required weeks on surgery is less than 8. Only about onethird of schools mandate a rotation on surgical specialties. There is time available for a longitudinal integrated curriculum in vascular disease, but not in the clinical years. Medical schools report an average of 12 elective weeks in each of the first 2 years. Here is where we can establish our course. There is, however, one more barrier to change — the “shadow curriculum” of the U.S. medical schools.
As medical students strive to earn positions in competitive residencies,
Continued from page 1
Upcoming Meetings
Advanced Practice Course for Vascular Surgeons on Venous Interventions
The Midwestern Vascular Surgical Society will host the new course in Indianapolis Apr. 19-20, 2019. It will feature a comprehensive program delivered by venous experts. The course will target 20 Vascular Surgeons/Senior Fellows; intentional limited attendance promotes one to one interaction between attendees and faculty. Program highlights for the 2019 course will include: Thermal and non-thermal options for the treatment of super-
they must differentiate themselves. But, as I have previously pointed out, more schools are adopting pass/fail grading systems rendering their class rank structures nebulous. What will make a residency application stand out? Personal statements are subjective at best. Faculty letters of recommendation? Unfortunately, these are often wild collages of impossible math, broad generalizations, and ambiguous superlatives.
“Kyle definitively rotated with us.”
“Top 5.8% of students I’ve worked with!”
“The residents seemed to like him.”
“Would do well in YOUR program.”
While “great,” “excellent,” and “outstanding” are synonyms in Webster’s Dictionary, for many surgeons they are proxies for “imbecile,” “meh?”, and “somewhat good.” With few objective measures of academic performance to select candidates for interviews, most residencies are turning to the USMLE scores as a barometer. Medical students have noticed.
The USMLE is a joint program of the Federation of State Medical Boards and the National Board of Medical Examiners (NBME). The exam was implemented in 1992 with the stated goal to provide medical licensing authorities with meaningful information regarding the ability of physicians to provide safe and effective patient care.
I was a first-year medical student when the process began. Medical schools at the time had a general consistency in the basic science topics taught, but wide variations in the
depths to which these subjects were covered. So while my pathology course lasted 4 weeks and gross anatomy a full year, on the USMLE Step 1 exam, this emphasis was essentially reversed. Pathology accounted for nearly half of the material, while anatomy was less than 10% of the test. Medical schools bristled against the idea of “teaching to the exam.”
Little if any USMLE prep books were available, so the goal was merely to achieve a passing score. Today, as the preclinical courses move to
perts in the diagnosis and treatment of peripheral vascular disease at the medical school level. Existential threats to our specialty abound. A poll of recent medical student graduates revealed that more would consult interventional radiology (56%) than vascular surgery (39%) for the performance of a peripheral angiogram. There is a void in medical education that we must fill. Recently the Chairs of the Peripheral Vascular Disease section of the American College of Cardiology and the Pe-
A poll of recent med student graduates showed more would consult interventional radiology than vascular surgery for a peripheral angiogram.
lower stakes pass/fail grading, students are abandoning their school curriculum and focusing their efforts on the Step 1 exam. Even as schools try to deemphasize subjects like biochemistry and histology, these topics still account for about one-third of the Step 1 content.
The USMLE subject matter has become the de facto curriculum of U.S. medical schools. The traditional “2 weeks, 2 days, 2 pencils” algorithm for preparing for Steps 1-3 has been abandoned. Many students now spend months studying for the pivotal Step 1 exam. As evidence, scores have been steadily rising as students seek to increase the competitiveness of their residency applications.
ripheral Vascular Disease Council of the American Heart Association cowrote an editorial4 claiming “the lack of an American Board of Internal Medicine-certified specialty focused on patients with PAD has undermined their medical care.”
While we know time spent on vascular surgery rotations increases knowledge and interest, many specialties are competing for this time. A longitudinal curriculum could be established during the available elective blocks in the first 2 years of medical school. Unfortunately, due to the reliance of the LCME on individual schools to set up their curricula, this effort will require a national grassroots campaign.
ficial venous disease, deep venous interventions, contemporary indications for open venous surgery, proprietary foam therapy, new mechanical thrombectomy options for venous thromboembolism, and techniques for difficult IVC filter retrieval.
The Congress is being held at the Lowes Miami Beach hotel, Miami Beach, Fla., on Apr. 25-27, 2019. This CME event covers the treatment of superficial and deep venous disease, including topics from sclerotherapy optimization to managing thrombophilias and discussing clot bursting strategies.
A recent commentary in Academic Medicine3 makes a compelling argument for ending the use of Step 1 scores when selecting residency applicants. The authors compare this practice to the use of an off-label drug for an untested purpose. They also note the exam’s restraining effect on curriculum change, the inordinate amount of time and money students spend preparing, as well as unintended consequences such as discouraging students with average scores from pursuing competitive residencies.
They even note that the stress of the exam likely contributes to student burnout. The remarkable thing about this commentary is that its senior author is the president and CEO of the NBME, which sponsors the USMLE. Of course, the USMLE could end all of this tomorrow by publicly reporting only pass/ fail scores. Unfortunately, they have openly stated they have no intention to do so.
It is imperative that vascular surgeons establish themselves as the ex-
There are many LCME standards that can be referenced to make our case. ED-33 requires schools to monitor the content in each discipline “including the identification of omissions.” IS-16 notes the importance of meeting the health care needs of “medically underserved populations”, groups which have a disproportionate prevalence of PAD. The SVS, in collaboration with the other major regional and national societies, has the opportunity to lead this campaign to improve the care of vascular patients and solidify the future of our specialty.
References
1. https://med.virginia.edu/ume-curriculum/wp-content/uploads/ sites/216/2016/07/2017-18_Functions-and-Structure_2016-03-24.pdf.
2. https://www.aamc.org/download/490454/data/2018gqallschoolssummaryreport.pdf.
3. Acad Med. 2016 Jan;91(1):12-5. doi: 10.1097/ACM.0000000000000855.
4. Circulation. 2016 Aug 9;134(6):438-40.
5. J Vasc Surg. 2010 Jan;51(1):252-8.
BY FRANK J. VEITH, MD
Bias can be defined as a prejudice or a preformed inclination. Bias is reflective of one’s inherent mind set about any thing, concept, ideology, claim, product, person, or group of people. Since biases are well known to be inherent in human nature, one can fairly ask how important and how widespread are they and what are their effects?
Bias affects many fields including medicine. One example is the statin controversy. Some experts interpret existing data, which include randomized controlled trials, to make a strong case that statins are harmful and do little good. In contrast, other qualified experts interpret precisely the same data to conclude that statins are miracle drugs that sharply diminish the mortality and morbidity from atherosclerosis. Again bias rules and leads to disagreement, controversy, and damaging public uncertainty.
A second example in medicine – and there are many – is the current controversy over what constitutes the optimal treatment for patients with asymptomatic carotid stenosis. Some authorities believe no such patients should be treated invasively, while others hold the position that many should be. Still other experts opine that only a

Dr. Veith is professor of surgery at New York University Langone Medical Center and Case Western Reserve University, Cleveland, as well as the William J. von Liebig Chair in Vascular Surgery at the Cleveland Clinic Foundation.
rare asymptomatic patient should undergo invasive treatment. All three groups use the same existing factual data to support their differing and sometimes totally opposite opinions. These contrasting views are reflected in articles in leading journals and differences among various guidelines from prestigious learned groups. The only explanation for their differing conclusions appears to be the fact that they are largely based on the bias of the authors of the articles or guidelines. Again, bias rules.
So these and many other examples exist in every phase of human endeavor. Biases are omnipresent and critically important in everything people do. They control our thinking, our opinions, our reasoning, our behavior, and most importantly, our
BY GREGORY TWACHTMAN MDEDGE NEWS FROM JAMIA
Physicians who experience stress related to the use of health information technology (HIT) are twice as likely to experience burnout.
Rebekah Gardner, MD, of Brown University in Providence, R.I., and her colleagues surveyed all 4,197 Rhode Island physicians in 2017 to learn how the use of electronic health records affected their practices and their job satisfaction.
Just over a quarter (25.0%) of 1,792 respondents reported burnout. Among electronic health record users (91% of respondents), 70% reported health IT-related stress (J Am Med Inform Assoc. doi: 10.1093/jamia/ ocy145).
“After adjustment, physicians reporting poor/marginal time for documentation had 2.8 times the odds of burnout (95% confidence interval, 2.0-4.1; P less than .0001) compared to those reporting sufficient time,” according to the researchers.
The team looked at three stress-related variables: whether the EHR adds to the frustration of one’s day; whether physicians felt they had sufficient time for documentation; and the amount of time spent on the EHR at home. Variables were measured on a four- or five-point scale depending on the question related to the specific stress variable.
Almost two-thirds (64.2%) of respondents “agreed” or “strongly agreed” that EHRs add to the frustration of their day.
“It was the most commonly cited HIT-related stress measure in almost every specialty, with the highest prevalence among emergency physicians (77.6%),” the investigators wrote.
More than a third of physicians (37.7%) reported “moderately high” or “excessive” time spent on EHRs at home; this metric was the most commonly cited stress measure among pediatricians (63.6%).
Nearly half (46.4%) of physicians reported “poor” or “marginal” sufficiency of time for documentation.
decisions. They override most other forces that influence how we humans behave.
What can be done about this dominance of bias? The main safeguard against it is to recognize its controlling importance in all human thinking. Such recognition will help to offset the harmful effects of bias and encourage other, more laudable forces to influence behavior and actions. Logic is one such force. Even more important is objective interpretation of facts and a clear assessment of their validity. Such objectivity may be difficult currently because of the overt bias expressed in our media and publications. If one doubts the influence of such bias, watch reports of the same event on CNN and Fox News. It is hard to believe the two sources are describing the same event. The same can be true of news reports in the New York Times and the Wall Street Journal. Bias often overrides objective reporting.
Somewhat surprisingly, even articles in our highly rated scientific journals are subject to the influences of bias. As in the lay press, scientific authors, reviewers, and editors all function under its spell. By recognizing the importance, the dominance, and the universality of bias, individuals and groups can move toward neutralizing its divisive, damaging, and overall negative effects. Such recognition of bias will not eliminate it, but it would help to make the world a better place.

“Presence of any 1 of the HIT-related stress measures was associated with approximately twice the odds of burnout among physician respondents,” Dr. Gardner and her colleagues noted, adding that “measuring and addressing HIT-related stress is an important step in reducing workforce burden and improving the care of our patients.”
To alleviate burnout, the authors recommended increased use of scribes, use of medical assistants
to help create a more team-based documentation function, improved EHR training, provided more time during the day for documentation, and streamlined documentation expectations, with certain culture shifts needed in some cases (i.e., banning work-related email and clinical tasks for vacationing physicians).
gtwachtman@mdedge.com
SOURCE: Gardner R et al. J Am Med Inform Assoc. doi: 10.1093/jamia/ocy145.


EXPERIENCE THE DIFFERENCE IN
























Choose the distinctive performance of our balloon dilatation catheters

Engineered to provide best-in-class PUSHABILITY* with a small profile for accessing target lesions1
Complete support for complex BTK cases
PINNACLE® DESTINATION®

Guiding Sheath NAVICROSS® Support Catheters



Demonstrated excellence in CROSSABILITY with a low deflation time1

ADVANTAGE® Peripheral Guidewires
GOLD Hydrophilic Coated Guidewire
*Tested against select leading competitors When RX tested against Boston Scientific Sterling™ Monorail™ and OTW tested against Bard Ultraverse® 0.018"


The Midwestern Vascular Surgical Society continues to prioritize educational and recruitment efforts for our regional membership. We are excited to report the following updates from our 2018 Annual Meeting:
The Midwestern Vascular Surgical Society (MVSS) Educational Committee hosted the 7th Annual Mock Oral Examination and 5th Annual Simulation and Technical Skills Assessment Program at our 2018 Annual Meeting in St Louis. The program was generously supported, in part, by a grant from W.L. Gore. The Simulation and Surgical Skills Assessment Program included facultyobserved clinical simulation stations encompassing advanced open surgical and endovascular models. Mock oral examinations provide feedback to both trainee and program directors in order to identify strengths and weaknesses prior to Certifying Examination. In total, 20 senior integrated vascular residents and fellows from across the Midwest participated, proctored by 29 vascular surgery faculty. Concurrently, the 4th Annual MVSS Medical
Antibiotic from page 1
Based upon such data, the Food and Drug Administration issued a December 2018 warning about the increased risk of ruptures or tears in the aorta with fluoroquinolone antibiotics in certain patients, updating their May 2017 warning regarding “disabling and potentially permanent side effects of the tendons, muscles, joints, nerves, and central nervous system that can occur together in the same patient,” upon exposure to this class of antibiotics. Earlier in 2018, the FDA had reinforced their safety information about serious and potentially fatal low blood sugar levels and mental health side effects with fluoroquinolone antibiotics.
Dr. Guzzardi and his colleagues at the University of Calgary (Alta.) isolated human aortic myofibroblasts from nine patients with aortopathy who were undergoing elective ascending aortic resection. Following exposure of cells to FQ, the researchers assessed secreted matrix metalloproteinases relative to tissue inhibitors of matrix metalloproteinases (TIMPs). In addition, they examined ECM degradation by using a three-dimensional gelatin-fluorescein isothiocyanate fluorescence microgel assay. Aortic cellular collagen type I expression following FQ exposure was determined by immunoblotting and immunofluorescent staining. Dr. Guzzardi and his colleagues also

students from 10 Midwest medical schools. The students received travel scholarships and free conference registration. The program was generously supported by a grant from the Association of Program Directors in Vascular Surgery.
Considering 18 highly competitive candidates from the 2018 MVSS Scientific Session, The D. Emerick Szilagyi Award was presented to Donald Harris, MD (mentored by Paul Dimusto, MD) from the University of Wisconsin for his work entitled: “Frailty Based Risk Score Predicts Morbidity and Mortality After Elective Endovascular Thoracic Aortic Aneurysm Repair.”
Student Education and Participation Program “Introducing Vascular Surgery as a Career Choice” offered medical students in the Midwest region an introduction to the specialty of vascular surgery as a career choice, provided basic skills training (photo) and important mentorship opportunities. The program grew this year to support 30 medical
looked at cell apoptosis, necrosis, and metabolic viability using two versions of vital staining.
They found that FQ exposure significantly decreased aortic cell TIMP1 (P less than .004) and TIMP-2 (P less than .0004) protein expression, compared with controls, and the ratio of matrix metalloproteinase 9/ TIMP-2 was increased (P less than .01). This suggests an increased capacity for ECM degradation after FQ exposure, according to the researchers. In addition, FQ exposure attenuated collagen type I expression (P less than .002).
“FQ induces human aortic myofibroblast–mediated ECM dysregulation by decreasing TIMP expression and preventing compensatory collagen deposition. These data provide novel insights into the mechanisms that may underlie the clinical association of FQ exposure and increased risk of acute aortic events in the community. Our data suggest cautious use of FQ in selected patient populations with preexistent aortopathy and connective tissue disorders,” the researchers concluded.
In an accompanying editorial, while warning that these are preliminary observations, Ari A. Mennander, MD, PhD, of Tampere (Finland) University, wrote that, “for the first time, the wild theory of fluoroquino-
The 2018 Best Poster Winner was Martina S. Draxler, MD, PhD (mentored by Alexander D. Shepard, MD) from the Henry Ford Health System in Detroit, MI for her work entitled “Thirty-days and One-year Outcomes of Patients Treated for Acute Limb Ischemia – A Single Center Analysis.” – Dawn Coleman, MD
PERSPECTIVE by Dr. Russell H. Samson
The issue of fluoroquinolones is certainly of concern. I wonder how many of my patients who have suffered a ruptured aneurysm were on one of these drugs? In the last few years, Cipro (ciprofloxacin) and Levaquin (levofloxacin) were commonly used by our family practice and internal medicine colleagues for almost all outpatient infections. It was so common that even my wife, who is not a physician, would request Cipro whenever she had a sneeze. We would also bring large bottles of Cipro every time we went traveling to some exotic destination, reassuring ourselves that the only “runs”

Russell H. Samson, MD, FACS, DFSVS, is a clinical professor of surgery at Florida State University, Sarasota, a senior surgeon at Sarasota Vascular Specialists, and President of the Mote Vascular Foundation.
we would have would be in the airport trying to catch a flight. A cousin of mine, prescribed Levaquin by a well-meaning physician while he was cruising the Nile River, ruptured his Achilles tendon. Clearly, these medications do bad things to collagen, and we should avoid them in all patients who are at risk for aneurysmal development. I am unsure about the medicolegal responsibility for informing outpatients; however, our practice has put out an email blast to all patients who have aneurysms or are at risk for an aneurysm, informing them of the dangers of these drugs.
lone-associated aortopathy has a molecular hint that is based on collagen degeneration and progression of aortic disease. ... The enigmatic puzzle of the progression of some aortic events may alarmingly be iatrogenic, and the clinician may wisely consider a prudent use of fluoroquinolones in
patients with aortic dilatation.” The authors and commentators reported that they had no commercial conflicts to disclose.
mlesney@mdedge.com
SOURCE: Guzzardi DG et al. J Thorac Cardiovasc Surg. 2019;157:109-19.
BY MARK S. LESNEY MDEDGE NEWS FROM THE JOURNAL OF SURGICAL RESEARCH
An increased peripheral arterial stiffness index was associated with an increased rate of major adverse cardiac events (MACEs), independent of age, coronary artery disease, and Rutherford category, according to the results of a study of patients with peripheral arterial disease (PAD) presenting to the vascular surgery outpatient clinic at the San Francisco Veterans Affairs Medical Center.
Seventy-two patients with PAD were recruited during 2011-2016 and each had baseline radial artery applanation tonometry performed at a baseline visit. Their central radial
artery augmentation index (AIX), normalized to 75 beats/min, and the peripheral AIX were calculated using pulse wave analysis. Subsequent MACEs were identified by chart review in the Journal of Surgical Research.
The cohort was predominately male (96%) and white (69%), with an average age of 69.4 years.
During a median follow-up period of 34 months, 14 patients experienced a MACE (19%). These events included eight myocardial infarctions or coronary revascularizations, four deaths from a cardiac cause, one stroke, and one transient ischemic attack. Unadjusted Cox proportional hazards models identified a significant association between the peripheral AIX and rate of MACE (hazard ratio, 1.54; 95% confidence
interval, 1.06-2.22; P less than .02).
“These findings suggest that increased stiffness of the peripheral arteries may play a predictive role in patients with PAD. Furthermore, these findings inform future studies and suggest that the peripheral AIX may be used to risk stratify patients with PAD,” the researchers concluded.
The study was funded by public
institutions including the National Institutes of Heath, the University of California, San Francisco, and a Society for Vascular Surgery Seed Grant and Career Development Award. The authors reported that they had no disclosures.
mlesney@mdedge.com
SOURCE: Ramirez JL et al. J Surg Res. 2019;235:250-7.
BY ERIK GREB MDEDGE NEWS REPORTING FROM ISC
HONOLULU – A combination of cilostazol and aspirin or clopidogrel reduces the risk of recurrent ischemic stroke, compared with aspirin or clopidogrel alone, among patients at high risk for recurrent stroke. The combination also entails a similar risk of major bleeding, compared with aspirin and clopidogrel alone, according to results from the Cilostazol Stroke Prevention Study for Antiplatelet Combination (CSPS.com).
Dual-antiplatelet therapy with aspirin and clopidogrel reduced the rate of recurrent stroke in previous studies. The benefit of this drug combination is relatively short lived, however, and long-term concomitant use of aspirin and clopidogrel entails a risk of major bleeding. Other data have indicated that cilostazol, which is approved by the Food and Drug Administration to alleviate intermittent claudication in patients with peripheral vascular disease, prevents stroke recur-
rence without increasing the incidence of serious bleeding, compared with aspirin, said Kazunori Toyoda, MD, PhD, who presented the results of the CSPS.com trial at the International Stroke Conference sponsored by the American Heart Association.

Dr. Toyoda of the National Cerebral and Cardiovascular Center in Osaka, Japan, and his colleagues randomized 1,879 high-risk patients at 8-180 days after the onset of noncardioembolic ischemic stroke identified on MRI to receive 81 or 100 mg aspirin or 50 or 75 mg clopidogrel alone, or a combination of cilostazol 100 mg twice daily with aspirin or clopidogrel. They conducted their open-label, parallel-group trial at 292 sites in Japan from December 2013 through March 2017. To be considered at high risk, participants had to meet one or more of the following criteria: 50% or greater stenosis of a major intracranial artery, 50% or greater stenosis of an extracranial artery, and two or more vascular risk factors. The trial’s primary efficacy outcome was the first recurrence of ischemic stroke. Safety out-
comes included severe or life-threatening bleeding. The investigators ended the trial early because of a delay in recruiting patients. They enrolled 1,884 and randomized 1,879 of an anticipated 4,000 patients. At randomization, 41% in the dualtherapy group received aspirin and 59% clopidogrel, and in the monotherapy group, 40% received aspirin and 60% clopidogrel. Baseline characteristics were similar between the treatment groups. The population’s mean age was 70. Approximately 30% of patients were women.
During a median follow-up period of 17 months, ischemic stroke recurred in 29 of 932 patients receiving dual therapy including cilostazol for an annual rate of 2.2% and in 64 of 947 patients receiving monotherapy for an annual rate of 4.5% (hazard ratio, 0.49; 95% confidence interval, 0.31-0.76; P = .001). Severe or life-threatening bleeding occurred in 8 patients (0.6% per year) receiving dual therapy and 13 patients (0.9% per year) receiving monotherapy (HR, 0.66; 95% CI, 0.27-1.60; P = .354).
The study was funded by Otsuka Pharmaceutical, which manufactures cilostazol. Dr. Toyoda reported receiving support from Bayer Yakuhin, Daiichi Sankyo, Bristol-Myers Squibb, and Nippon Boehringer Ingelheim.
egreb@mdedge.com
SOURCE: Toyoda K et al. ISC 2019, Abstract LB3.
ATTRACT from page 1
of the hottest topics in DVT.
“This is the first thing your educated patients who come to the emergency department with DVT will ask about. It’s the first thing they’ll see when they go online and type in ‘thrombolysis DVT,’ ” noted Dr. Desai, an interventional radiologist at Northwestern University, Chicago.
But the trial has several major flaws, he cautioned. And contrary to popular opinion, ATTRACT is not the death knell for PCDT. Far from it.
“I don’t think the story stops with ATTRACT. This isn’t the end for PCDT in patients with iliofemoral DVT,” he asserted.
That’s in part because 301 of the 692 participants in ATTRACT had DVT of the femoropopliteal segment. That’s a population in which Dr. Desai and other interventionalists wouldn’t have anticipated seeing a benefit for PCDT, because their risk of PTS is so low.
“We know through historical data that patients with iliofemoral DVT are much more likely to develop PTS and to have recurrent DVT, so this is probably one of the major shortcomings of the trial,” he explained. “It’s through no fault of the trial investigators, because the study was planned years ago when we just didn’t know as much about PTS as we do now.
“The way I look at it is, I don’t practice in the way that ATTRACT was designed,” Dr. Desai said. “I don’t typically lyse or get referrals for lysis or thrombectomy in patients who have isolated femoropopliteal DVT. It has to involve at least the common femoral vein and frequently goes up to the iliac vein.”
The ATTRACT investigators’ recent subanalysis of the 391 participants with iliofemoral DVT showed that, although there was no difference between the two study arms in the occurrence of PTS through the first 24 months of follow-up, PCDT led to a 35% reduction in the incidence of moderate or severe PTS – by a margin of 18% versus 28% in controls.
Patients in the PCDT arm also experienced significantly greater improvement in venous disease-specific quality of life through 24 months, and a greater reduction in leg pain and swelling at 10 and 30 days (Circulation. 2018 Dec 4. doi:
10.1161/CIRCULATIONAHA.118.037425).
And moderate to severe PTS is a key outcome, Dr. Desai continued. Multiple studies have shown that patients with PTS have a worse quality of life than those with chronic lung disease, arthritis, or diabetes. Moreover, the 5%-10% of patients with symptomatic DVT who develop the most-severe form of PTS – characterized by severe pain, chronic ulcerations, stasis dermatitis, venous claudication, and intractable edema – have a quality of life com-
catheter to infuse a fibrinolytic drug directly to the thrombus to dissolve it rapidly.
But that form of catheter-directed thrombolysis has major disadvantages, Dr. Desai explained: It’s a multiday procedure requiring ICU-level care and prolonged exposure to powerful lytic agents.
“This is where things have changed with PCDT,” he said. “We can now, with on-label devices, accelerate the thrombolysis time, reduce lytic exposure, and I think also reduce the bleeding risk, although that hasn’t been shown in a trial yet. PCDT also reduces the necessity for ICU-level care and prolonged hospitalization.”
Dr. Desai no longer performs multiday lytic procedures. “In fact, with the introduction of the newer on-label devices, I haven’t done a multiday unilateral limb lytic procedure in a couple years. I think we’ve gotten to the point where we don’t need to do that anymore.”
Patients who develop the most-severe form of PTS – characterized by severe pain, chronic ulcerations, stasis dermatitis, venous claudication, and intractable edema – have a quality of life comparable with patients with cancer or heart failure.
parable with patients with cancer or heart failure.
The 1.5% incidence of major bleeding within 10 days in the PCDT group was 200% higher than in controls, but none of it was life threatening.
“This is reassuring: Nobody had intracranial hemorrhage; nobody had a GUSTO 5 bleed,” Dr. Desai said.
Another limitation of the ATTRACT trial is that all but one of the devices utilized for PCDT were used off label. They weren’t designed for venous application. Several on-label rheolytic, rotational thrombectomy, or clot aspiration devices have been approved since enrollment in ATTRACT was closed. Future randomized trials will utilize on-label devices in patients with acute iliofemoral DVT to clarify the role of PCDT.
It’s noteworthy that nearly half of ATTRACT participants developed PTS within 24 months of their DVT despite being on optimal anticoagulation. It’s a finding that underscores the need for improved therapies. That was the impetus for development of first-generation catheter-directed thrombolysis utilizing a percutaneously inserted
Indeed, PCDT makes recanalization possible as a single-day, single-session procedure.
Dr. Desai views the recent ATTRACT subanalysis as hypothesis generating.
“Should PCDT be the first-line treatment in all proximal DVT patients? No it should not – and that’s not what I would have advocated even before ATTRACT came out,” he explained. “It’s sort of a salvage procedure for patients with iliofemoral DVT and moderate to severe symptoms. And there are a significant number of such patients.”
Current understanding of the pathophysiology of PTS is that a nondissolved thrombus at the valve leaflets becomes inflammatory, with resultant valvular dysfunction leading to venous reflux and venous hypertension. PCDT is consistent with the open-vein hypothesis, which posits that, by eliminating thrombus much faster than achievable via anticoagulation, valve integrity is maintained and PTS is prevented.
Dr. Desai reported receiving consulting fees from AngioDynamics, Boston Scientific, Cook Medical, and Spectranetics.
bjancin@mdedge.com
BY BRUCE JANCIN
MDEDGE NEWS
EXPERT ANALYSIS FROM THE NORTHWESTERN VASCULAR SYMPOSIUM
CHICAGO – Clinically significant aortic neck dilation occurs in one-quarter of patients after endovascular abdominal aortic aneurysm repair and is associated with sharply increased risk for type Ia endoleak, stent migration at the proximal seal zone, continued aneurysmal sack
enlargement, and even aneurysm rupture, Jason T. Lee, MD, said at a symposium on vascular surgery sponsored by Northwestern University, Chicago.
He cited what he considers to be the best-quality systematic review of the literature regarding proximal neck dilation after endovascular aneurysm repair (EVAR), which was conducted by investigators at Paracelsus Medical University in Nuremberg, Germany. The data, he said, speak to the importance of trying to minimize the chances of aortic neck dilation (AND).
The review, which included 26 published studies through 2015 and nearly 10,000 EVAR patients, concluded that AND occurred in 24.6% of these patients. The investigators defined AND as more than 3 mm of dilation, which with an average neck diameter of about 30 mm in all comers, would represent a 10% aortic neck–diameter expansion. The incidence of the composite adverse outcome of type I endoleak, stent migration, and reintervention during a maximum of 9 years of follow-up was 29-fold
greater in the AND group than in AND-free patients (J Endovasc Ther. 2017;24[1]:59-67).
Continuing controversy exists regarding the extent to which postEVAR AND is a manifestation of the underlying aneurysmal process as opposed to an adverse effect caused by the outward radial force applied by the stent. That being said, there are several factors related to AND that are potentially within the vascular interventionalist’s control. Topping
Dilation continued on following page
continued from previous page
the list is aggressive oversizing of self-expanding stent grafts in an effort to obtain an excellent seal, according to Dr. Lee, a professor of surgery at Stanford (Calif.) University.
“The data from multiple series definitely suggests that more than 20% oversizing is correlated with a higher incidence of AND. So maybe the answer is oversizing by more like 10%-15%,” the vascular surgeon said.
Another factor contributing to AND is the overwhelming popularity of self-expanding aortic stent grafts, now utilized in 95% of all EVARS done in the United States.

Balloon-expandable stent grafts require much less oversizing – less than 5% – to maintain their diameter post deployment, but they are rarely used. Indeed, the only commercially available balloon-expandable device in the United States is the TriVascular Ovation stent system, which seals the stent graft to the wall of the aorta via polyethylene glycol rather than by radial force.
Intriguingly, Italian investigators have reported that, in a multicenter series of 161 patients who under-
A factor contributing to AND is the overwhelming popularity of selfexpanding stent grafts, used in 95% of EVARS in the U.S.
went EVAR with the Ovation endograft, no AND occurred at CT scanning done after a minimum of 24 months of follow-up (J Vasc Surg. 2016;63[1]:8-15).
Previous studies of the implications of AND after EVAR have been limited to comparisons of early-generation devices, so Dr. Lee and his coinvestigators conducted a retrospective review of a prospective Stanford database that included 86 patients who underwent elective, uncomplicated infrarenal endovascular abdominal aortic aneurysm repairs using a variety of
contemporary stent grafts. Eightysix percent of patients experienced AND during a median radiologic follow-up of 21.9 months, with a mean 1.3-mm increase at 30 days and 3.3 mm at most recent follow-up. The degree of AND correlated with the amount of oversizing. However, AND didn’t vary
significantly by device type, which included the Cook Zenith, Gore Excluder, Medtronic Endurant, and Endologix Powerlink self-expanding stent grafts (Ann Vasc Surg. 2017;43:115-20).
Aortic anatomy also plays a role in AND. Shorter necks with severe angulation have been found to pose
a higher risk. Open repair, which entails much less AND than does EVAR, may make more sense in that challenging anatomic situation, according to Dr. Lee.
He reported current research funding from Cook, Gore, and Medtronic.
bjancin@mdedge.com
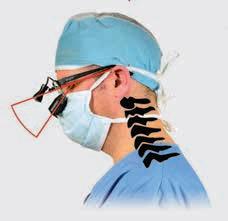

• Magnification: SurgiTel offers the most magnification options (2.5x - 8.0x) with our patented lightweight optics
• Depth-of-Field: Long depths-of-field for easier, faster work, and better outcomes
• Field-of-View: Maximized field-of-view utilizing both oculars for a binocular effect
• Comfort: Patented designs minimize ocular weight, reduce strain on the face
Pictured right: the same scene, equally magnified,binocularviewvs.monocularview




The early response has been “spectacular.”
That’s as in “Vascular Spectacular,” the gala that will be a central festivity of the 2019 Vascular Annual Meeting.
The glitzy, fun-filled evening will include live and silent auctions, cocktails and dinner, headliner entertainment and dancing to a DJ. All proceeds benefit the work of the SVS Foundation.
Within the first week, members and friends donated, among other attractions, a one-week Caribbean sailboat cruise, art, fine wine and hotel stays in Toronto and Chicago, as well as many and varied entertainment offerings, including two tickets to any production at the renowned Ore-
gon Shakespeare Festival in Ashland, Ore.
Member Enrico Ascher, MD, was first out of the box on ticket sales, purchasing a table for 10 almost as soon as the ticket website opened. Seating is limited for the event.
SVS President Michel Makaroun, MD, suggested hosting the gala instead of the President’s Reception. His goal is to celebrate the specialty and bring everyone together while also benefitting the SVS Foundation and continuing its work. He has asked those who typically hold alumni receptions to gather at the gala, instead.

What: Vascular Spectacular
When: 6:30 p.m. Friday, June 14
Where: Riverview Ballroom, Gaylord National Resort & Convention Center, National Harbor, Md.
Tickets: $250 each, $150 of which is considered a tax-deductible donation to the SVS Foundation
Cynthia Shortell, MD, and Benjamin Starnes, MD, were quick to volunteer both ideas and time for the gala and are co-chairing the planning committee. “I love what Dr. Makaroun is trying to achieve: convergence, rather than divergence,” said Dr. Starnes. “For years, many of our academic institutions held alumni receptions at the Vascular Annual Meeting and, while they have been wonderful, they’ve also been somewhat insular.
Buy tickets; donate auction items: vam19gala.givesmart.com
“This year, we’re trying to redirect some of those people, as well as the President’s Reception, into one large, fun gathering,” said Dr. Starnes. “We’re bringing people together for a very worthy cause.
“It’s going to be one great party.”
Everyone, whether attending VAM or not and wherever they are on June 14, can participate in the Vascular Spectacular gala, including donating items to both the Live and Silent auctions, and bidding on Silent Auction items.
SVS has created a special ticket and auction website, VAM19gala.givesmart.com. There, people may purchase tickets at $250 apiece or a table for 10 at $2,500. Already more than 150 tickets have been sold, many in tables of 10.
Seating will be limited.
Members, family and friends go to the same site to donate auction items and (in late May) begin to bid on those and additional offerings. The process of how to handle the submission process (photos are requested) is straightforward, and the bidding process will be equally so.
Silent Auction bidders even will know just who they’re bidding against, said Co-Chair Dr. Cynthia Shortell. “I think that both the silent and live auctions will bring out our competitive sides in a fun and playful way, which will hopefully increase participation.”
Vascular calcification affects the vascular health of millions of patients. No current therapies exist to prevent or reverse it, and the problem has confounded researchers and physicians for decades.
The development of innovative treatment strategies requires both a better fundamental understanding of the problem and collaboration between vascular surgeons and vascular biologists/biomedical engineers. This year’s Vascular Research Initiatives Conference (VRIC) will bring these audiences together and provide insight from key investigators in this field.
VRIC, which focuses broadly on emerging vascular science and translational research relevant to vascular patients, will be Monday, May 13, in Boston, one day prior to the American Heart Association’s Vascular Discovery Conference. More than 200 abstracts were submitted for presentation, and as such, organizers
have expanded the scientific program. Visit vsweb.org/VRIC19 to view the preliminary program and to register.
Cecelia Giachelli, PhD, is the W. Hunter and Dorothy Simpson Professor and Endowed Chair of Bioengineering at the University of
Panel members are fellow vascular calcification experts Elena Aikawa MD, PhD (director of the Vascular Biology Program at Brigham and Women’s Hospital/Harvard Medical School); Dwight Towler, MD, PhD (J.D. and Maggie E. Wilson Distinguished Chair in Biomedical

Washington and a world-renowned expert in vascular calcification. She will present the Third Annual Alexander W. Clowes Distinguished Lecture on “New Concepts in Regulation and Bioengineered Therapies for Vascular and Valvular Calcification.” The interactive Translational Panel will follow, discussing calcific arteriosclerosis, or hardening of the artery.
Research and the Louis V. Avioli Professorship in Mineral Metabolism Research and vice chair, research, Internal Medicine at UT-Southwestern); and Raul Guzman, MD (vascular surgeon, Beth Israel Deaconess/ Joslin Diabetes Center and chair of the SVS Clinical Research Committee).
“Since calcium turns normally
compliant and energy-efficient arteries into hard pipes, vascular surgeons are commonly frustrated by this disease,” said Luke Brewster, MD, PhD, chair of the SVS Research and Education Committee, which organizes the VRIC program. “Medical therapies for this are lacking, in contrast to atherosclerosis. This is a field where vascular surgeons bring much needed value to translational science in vascular calcification.”
Given the increased incidence and survival of patients with diabetes and/or end-stage renal disease, calcific arteriosclerosis will only become more of a clinical problem in the future, he said.
As with any complicated process, a broad group of investigators is needed to solve this terrible problem, said Dr. Brewster. And when the problem IS solved, he said with a laugh, someone “will win a Nobel Prize or own a winery!”
Registration and housing have opened for the 2019 Vascular Annual Meeting. This year’s premier educational event for vascular professionals will be June 12 to 15 at the Gaylord National Resort & Convention Center in National Harbor, Md., outside of Washington, D.C.
Wednesday, June 12, will include postgraduate courses, abstract-based sessions with the Vascular and Endovascular Surgery Society and a host of international events. Scientific sessions are June 13 to 15 and the Exhibit Hall will be open June 13 to 14. See the “Schedule at a Glance” of VAM events at vsweb.org/VAM19
This year’s meeting will feature a gala (see stories on p. 10) for the first time in more than a decade. The “Vascular Spectacular” on Friday,
June 14, will benefit the SVS Foundation and its activities.
Also of note are:
Dedicated programming for vascular trainees and fellows to help them make the transition from training to practice, and to explore leadership development. Topics include billing and coding, contract negotiation, tips for a successful career and what vascular societies have to offer. Representatives of several associations and regional vascular societies will be on hand.
“The focus of the Fellows program is business, because we feel this is missing from residency programs. And it also isn’t covered by regional societies, which already include excellent fellows programming,” said Matthew Eagleton, MD. He chairs the Program Committee, which oversees VAM programming. “We’re

also including industry representatives in the Fellows dinner, to focus on what’s in the pipeline in terms of industry, and what’s coming down the road.”
Programming for those involved in outpatient-based facilities, requested by members in the SVS’ newest membership section, the Section for Outpatient and Office Vascular Care. This includes a breakfast session co-sponsored with the Outpatient Endovascular and Interventional Society. Two new programs for international participants, the Young Surgeon Competition and International Poster Competition, both on Wednesday.
Additional Ask the Expert sessions, which proved enormously popular in 2018. Topics for these small groups include infected grafts, IVC filter complications, open aorta,
As of this Specialist deadline date in late February, the SVS staff was still settling in, unpacking boxes, creating new work spaces and – a very important task! – locating the coffeemaker.
The Society for Vascular Surgery is open for business in its new headquarters office at 9400 W. Higgins Road in Rosemont, Ill., just minutes from O’Hare International Airport. Its new digs are, in the words of President Dr. Michel S. Makaroun, “a home for vascular surgeons from all over the country and around the world.”
At 12,000 square feet, SVS’ new space is nearly twice the size of the Chicago office and has room for growth in programming, initiatives, member benefits, and for staff to support those priorities.
Personnel that interact frequently are located near each other, to make collaboration simpler. The new HQ features a 4,000-square-foot meeting center that can seat up to 40 for a large meeting or training session, and has moveable airwalls to configure the space into one, two or three meeting rooms; up to three councils, committees, sections or task forces can meeting simultaneously. All meeting rooms are equipped with state-of-the-art technology to accommodate webinars and web conference calls. Day-to-day, the meeting center can accommodate the entire staff for meetings. “It will be a pleasure to convene the staff and not have colleagues forced to stand or sit along the perimeter of the room,” noted Executive Director Kenneth M. Slaw, PhD.
mesenteric/hybrid, open tibial exposures, Thoracic Outlet Syndrome and spine exposure.
Workshops moved from Wednesday to Thursday and Friday. Topics include transcarotid artery revascularization, fenestrated EVAR (ZFEN) and below-the-knee access and intervention.
An “Aortic Summit” Saturday afternoon, co-sponsored by SVS and The Society of Thoracic Surgeons.
“We are really focused on presenting a great program with content specific to many career needs,” Dr. Eagleton said. “We want to showcase the best abstracts representative of critical research, and we’re adding programming for targeted audiences. We have something for everyone.”
Register and book hotel rooms today. Visit vsweb.org/VAM19.


Your SVS team in their new surroundings
The new SVS office also offers:
» A convenient location near O’Hare, eliminating the need to rent meeting space several times a year
» Access
• To additional educational space in the building
• To a state-of-the-art surgical simulation training facility
• For members to staff
» Double-duty spaces, such as the lunchroom/coffee room that in other hours can become a large space for collaboration.

We’re open for business. And the next chapter in the history of the SVS has begun. Next time you swing through O’Hare and have a few minutes, come visit us!
Address, Phone Information
9400 W. Higgins Road, Suite 315
Rosemont, IL 60018
Phone: 312-334-2300 or 1-800-257-8188
Fax: 312-334-2320
019 is in full swing, with work continuing on a wide array of SVS objectives, events and priorities.
But before shutting the door completely on 2018, SVS members will be interested to see the lengthy list of achievements for the year.
Executive Director Kenneth M. Slaw, PhD, reviewed 2018 activities and their impact for the coming year for the Strategic Board of Directors at its retreat in early January:
• A new Branding Initiative Task Force, led by Joe Mills, MD, made substantial progress in 2018 researching and exploring new messaging, imaging and taglines that optimally position the vascular surgeon and SVS for the future. SVS members will hear more at VAM 2019! Another major focus: outreach and collaborative education with referral physicians.
• SVS now has two thriving membership “sections,” one for vascular physician assistants (145 members) and the new Section on Outpatient
and Office Vascular Care (155 members), approved in late December.
• SVS established and announced availability of the new Fellow (FSVS) and Distinguished Fellow (DFSVS) designations.
• The Document Oversight Committee produced three published guidelines, has six in the pipeline and is working with the Quality Council to explore a process for adding appropriate use criteria.
• The SVS Wellness Task Force has completed a comprehensive study with Mayo Clinic. Data presentations have been submitted for the 2019 Vascular Annual Meeting.
• The SVS Foundation created and awarded three Community Awareness Prevention Project Grants; SVS also is linking the Community Practice Committee to the Resident/ Student and Young Surgeons committees plus the Vascular and Endovascular Surgery Society to address community-based mentoring.
• In June, the Society created the
Quality Council, headed by Dr. Larry Krais
• The SVS/ACS Vascular Center Verification and Quality Improvement Program was created; standards are 90 percent written. A pilot program is planned for 2019.

Other achievements in 2018, and plans for 2019 include:
• Seeing the Vascular Quality Initiative and Patient Safety Organization hit milestones of more than 500,000 procedures registered and more than 500 centers participating; piloting a method to track guideline adherence (AAA); creating new dashboards; leading collaboration with other agencies, including the Food and Drug Administration; tracking 30-day follow-up information; adding registries and updating others; and holding 17 educational webinars.
• Developing a new comprehensive education plan for early-career vascular surgeons
• Creating a Fellows Program of educational programming for the 2019 Vascular Annual Meeting.
• Holding a successful 2018 Vascular Research Initiatives Conference, with good fundraising support
• Working with the Journal of Vascular Surgery to create a basic science journal, with a likely 2019 launch.
• The Coding Committee developing templated coverage documents by procedure.
• Advocacy staff and committee members convincing the CMS to hold the line on Medicare payments and reimbursements on many fronts.
• Providing comments on the episode-based measure for Revascularization for Lower Extremity Chronic Critical Limb Ischemia.
• Providing education, including monthly columns in JVS and JVS-VL and webinars, to SVS members on the Quality Payment Program, and writing comments to CMS on Year 3 QPP Proposed Rule.
• Launching SVSConnect, the new member interaction and networking online platform for SVS members.








• Seeing the Alternative Payment Models Task Force near completion of its analysis and a potential vascular APM model for presentation to the Centers for Medicare & Medicaid Services.
• Submitting re-accreditation materials to the Accreditation Council for Continuing Medical Education, with an interview set for March.
• Choosing a vendor for the Learning Management System (LMS) to store/ organize online learning materials
• Beginning the process of building the new SVS Headquarters in Rosemont, Ill., with the move accomplished in late February. (See story and pictures on page 11.)
“The SVS is a vibrant, thriving medical society thanks to its dedicated members and leaders,” noted Dr. Slaw. “It is an honor and privilege to serve our members, and our mission.”

The April Journal of Vascular Surgery takes a look at the “adequate” proximal seal for complicated type B aortic dissections. Failure to achieve any intramural hematoma-free proximal seal zone during such surgeries may be associated with higher degrees of retrograde type A dissection. The article is available open source through May 31 at vsweb.org/ JVS-Proximal
BY DANIEL MCDEVITT, MD
On behalf of the Leadership Development and Diversity Committee
Barry Posner and James M. Kouzes’ “The Truth About Leadership” describes 10 critical “truths.” In this latest column highlighting the evidence-based behaviors and attributes that define great leadership, we focus on “you either lead by example or you don’t lead at all.”
Q: Everyone’s leadership journey begins somewhere. What was it that inspired you to want to lead?
A: I started my practice in 1987. The chairman of surgery at the time was a great leader. While working with him, I had the opportunity to see how he interacted with physicians and administrators. I admired the way he handled himself. Academically, I was lucky to work and train with surgeons who were great leaders, some of them inspirational leaders. I tried to model the way I interacted with residents, medical students and fellow faculty in the same way. There is a practical side as well. If you’re not leading, then someone else is going to be doing it. In a lot of hospitals, if you’re busy and outspoken about your concerns, which I certainly always was, they recruit you to help solve the problems.
Q: You mentioned that you worked with Frank LoGerfo. Is there a pearl of wisdom from him that you would like to pass along?
A: I think the most important piece of wisdom that Frank gave me, that I always adhered to, was that it’s very important to know who you are and be that person. I’m sure you’ve seen where people are in leadership and you get the sense they are almost acting the role. I think people can tell when leaders are real or phonies.
Q: What leadership skills do you rely on for day-to-day success and where did you learn these skills?
A: I never had any formal leadership training. I saw qualities I liked in people who led me and I tried to emulate those. Leaders fall into three broad categories. Bad leaders lead by fear and intimidation. Good leaders are persuasive. Truly great leaders lead by inspiration.
The first part of inspirational leadership is leading by example. Great leaders don’t ask people to do things they wouldn’t do themselves. I’ve
tried to be that kind of leader. When I first started in my current position, I was the only vascular surgeon, which was a tremendous change from being part of a big vascular surgery program. I did a lot of operating. People could say, “This guy’s the real deal. He’s not some guy sitting in an office working on his computer all day. He’s a real surgeon.” To be a surgical leader you first have to be a surgeon. You also need to interact well with people. I treat everybody the same whether it’s the guy sweeping the floors or the hospital president. Treat people the way you want to be treated. Have a little humility no matter how high up the ranks you go. Be prepared when you go to meetings and know what you’re talking about. Be honest. If you don’t like something, say you don’t like it. I think being memorable to people is also important. You remember what good leaders tell you and the lessons that they taught you. Being more of an inspiration to people than just the boss is how I try to do it.
a better listener was something I wish someone had told me early on.
Q: What do you regard as your best leadership success to date?


A: That is a hard question to answer. I’d say the thing I was most proud of was becoming chief of vascular surgery at Beth Israel Deaconess. That was an aspirational goal along with becoming professor of surgery. On a practical side, there are two other things. One is that I pushed forward into the endovascular era at a time when there was a lot of resistance to it. That proved to be transformational both in my own practice and for our division at the time. My other great leadership accomplishment is when I run into former fellows and they tell me how the lessons I taught them were so important and how they remember
them and how much they appreciate them. When fellows come up in meetings and say, “You taught me so much! I’m so appreciative of what I learned from you,” then that’s the pinnacle as well. When those who have achieved more academic and clinical success than I have tell me these things, it makes me feel like I must have done a few things right along the way.
Q: When you think of the SVS, what do you think its role might be in creating vascular leaders?
A: We have a mentorship program for young people, medical students, general surgery residents, vascular fellows, but we probably need a mentorship program for people who are entering their midcareer and start assuming leadership roles. They have the E.J. Wiley Traveling Fellowship where people travel around and see what’s going on in other places. Maybe we could create something similar where people could come and spend time with people, not so much in their role as a vascular surgeon, but in their role as a leader, mentor and role model.
Q: For those who are just starting out, what skills do you think are critical to successful leadership and are there personality traits or behaviors that are more conducive to success?
A: For the young surgeon just starting out in practice, I think the first thing they need to do is concentrate on developing their practice, developing their academic career, and so forth. Some of the things all great leaders share is they have to be good communicators, be personable and become risk-takers. Leaders are not afraid to take a risk and, at the same time, be one of the first ones to admit when they make a mistake.
Q: What do you wish somebody had told you early on in your leadership development that would have been very valuable?
A: The most important thing someone could have told me personally is: shut up, say less and listen more. I am direct and outspoken and there’s no question that, over the years, I made some colossal mistakes as a result. Learning to be

In response to member requests, the Vascular Quality Initiative now includes 30-day follow-up forms in most of its 12 registries.
The addition of the form — there already is a mandatory Long-term Follow-up Form — permits VQI participants to collect 30-day re-admission data. Surgeons and hospital administrators find this information important as the Centers for Medicare and Medicaid Services has focused on readmissions as part of the reimbursement process.
This 30-day information is not currently being captured on the long-term forms, and the long-term form isn’t timely enough for 30-day purposes, said Jens Eldrup-Jorgensen,
MD, SVS PSO medical director.
“Now users will be able to collect 30-day re-admission data in addition to other important short-term outcomes, such as acute myocardial

infarction, heart failure and pneumonia,” he said. “CMS defines many of those outcomes and is interested in when, where and how they occur.”
The 30-day form is a big departure for VQI registry collection data, he/ she said. “It’s always been thought
that it’s more important to look at vascular patients long-term; that’s why we have the one-year follow-up,” Dr. Eldrup-Jorgensen said. Other registries typically do only 30-day follow-up and don’t track long-term disease progression, as VQI does.
“But because of the government focus on 30-day re-admissions, it was important for us to add this data point where we can,” said Dr. Eldrup-Jorgensen. “Members have really been eager to have this information to help their focus on quality improvement efforts.”
The new forms can be used with the registries for carotid artery stent, carotid endarterectomy, endovas-
Your online community, SVSConnect, is now on the go.
The SVSConnect mobile app — for cell phones and tablets — brings easy access to collaboration, engagement and communication with your SVS member colleagues and thought leaders. It only takes a few minutes to get set up – just follow the below steps.
1. Search for “MemberCentric” in either the App Store or Google Play.
2. Download the “MemberCentric (HUG)” app.
3. Once installed, search for “SVS” on the welcome screen.
4. Login with your SVS account credentials.
5. Hit ‘OK’ when you receive a notification prompt about the app icon change.
6. Join a discussion, search for fellow members and share resources right from your phone.
Within the app you can do everything you’re able to do on your desktop computer, but more easily. Continue discussing topics such as outpatient treatment centers, popliteal artery access
cular AAA repair, open AAA repair, infra-inguinal bypass, supra-inguinal bypass, lower extremity amputation, peripheral vascular intervention, and thoracic and complex EVAR. The forms are not available for the hemodialysis access, inferior vena cava filter and varicose veins registries.
VQI presented a webinar on the 30-day form at the end of 2018. VQI members may view the webinar at vsweb.org/30DayWebinar
The VQI is a collaborative of regional quality groups that collects and analyzes data in an effort to improve patient care. It is governed by the SVS Patient Safety Organization. For more, visit vqi.org.
and carotid surveillance imaging. Follow our newly launched bi-weekly “Tip Tuesday” that we share to enhance both your community experience and your SVS membership experience. Coming soon, we’ll have smaller communities

where committees, affiliate members or interest groups can communicate and collaborate privately.
Get started today to join the discussion, expand your network and build your community.
BY LARRY A. SCHER, MD
Hemodynamic complications of arteriovenous (AV) access are uncommon but can be potentially life threatening. Fistulas and grafts can cause a decrease in systemic vascular resistance and secondary increase in cardiac output in patients who may already have myocardial dysfunction secondary to their end-stage renal disease.1 This increased cardiac output is usually insignificant but in rare cases can result in clinically significant cardiac failure. Patients with high-output fistulas with volume flow greater than 2 L/ min may be at increased risk of heart failure but volume flow less than 2 L/min does not preclude this complication.2
In patients with AV access–related heart failure, optimal medical management and reduction of fistula flow or ligation of the dialysis access should be considered. If continued hemodialysis is necessary, loss of a functioning dialysis access is problematic and difficult management decisions must be made. Following successful renal trans-

Dr. Scher, is a vascular surgeon at the Montefiore Greene Medical Arts Pavilion, New York, and an associate medical editor for Vascular Specialist.
plantation, ligation of vascular access in the presence of symptomatic heart failure may represent a straightforward decision. Nonetheless, there is no clear consensus of how to manage patent fistulas or grafts in patients following renal transplantation in the absence of significant cardiac symptoms with particular concern to the important issues of transplant survival and long-term cardiac prognosis. Yaffe and Greenstein3 recommend preservation of almost all fistulas after transplantation in the absence of significant complications such as ve-
nous hypertension, pseudoaneurysm, significant high-output cardiac failure or hand ischemia. They recommend taking into account the 10-year adjusted renal transplantation graft survival rates and the relative paucity of donors, recognizing the possibility that the patient may have to return to dialysis at some point in the future. They also reference the lack of information regarding the beneficial impact of fistula ligation on cardiac morphology and function as a rationale for access preservation.
A recent presentation at the American Heart Association Scientific Sessions by Michael B. Stokes, MD,4 from the department of cardiology at Royal Adelaide Hospital in Australia, suggests that cardiovascular disease is responsible for 40% of deaths among kidney transplant recipients and that left ventricular (LV) mass is strongly associated with cardiovascular mortality.
He states that, although there is no guideline consensus on the management of an AV fistula following successful renal transplantation, the fistula continues to contribute adversely to cardiac
continued on following page
BY MARK S. LESNEY
MDEDGE NEWS FROM THE JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY
Mortality after the use of drug-coated balloons (DCB) for femoropopliteal peripheral arterial disease (PAD) was not correlated with paclitaxel exposure, according to the results of a meta-analysis of 5-year outcomes, according to a report published online.
“Paclitaxel DCBs are safe and effective to treat the symptoms of [Rutherford classification categories] 2-4 femoropopliteal PAD,” according to Peter A. Schneider, MD, of Hawaii Permanente Medical Group, Kaiser Foundation Hospital, Honolulu, and his coauthors.
Their study analyzed data pooled from five clinical trials NCT01175850, NCT01566461, NCT01947478, NCT02118532, and NCT01609296, comprising 1,980 patients from a variety of ethnic populations with Rutherford classification 2-4 disease.
Among these patients, 1,837 received DCB and 143 received uncoated percutaneous transluminal angioplasty (PTA). The mean age of the overall cohort was 68.5 years; 68.4% of patients were men. Baseline characteristics were similar between groups. However, patients treated with a DCB were more likely to have critical limb ischemia,
continued from previous page
remodeling and function. The lack of previous randomized controlled trials in this area led Dr. Stokes and his colleagues to randomly assign 64 patients at least 1 year following successful kidney transplantation with stable renal function and a functioning AV fistula to either fistula ligation or no intervention. All patients underwent cardiac MRI at baseline and 6 months.
The primary endpoint of decrease in LV mass at 6 months was significant in the ligation group but not in the control group. The ligation group also had significant decrease in LV end diastolic volume, LV end systolic volume, and multiple other parameters. In addition, NT-proBNP levels and left atrial volume were significantly reduced in the ligation group when compared with the control group. Complications in the ligation group included six patients with thrombosis of their fistula vein and two infections, all of which resolved with outpatient anti-inflammatory or antimicrobial therapy.
Dr. Stokes believes that control patients in his study face “persisting and substantial deleterious cardiac remodeling” and that “further investigation would clarify the impact of AV fistula ligation on clinical outcomes following kidney transplantation.”
I believe this is important information and represents the first randomized controlled data regarding the long-term adverse cardiac effects of a patent fistula after renal transplantation. Unfortunately, information regarding baseline fistula volume flow is not provided in this abstract. As
compared with PTA. DCB subjects were less likely to have hyperlipidemia, coronary artery disease, and diabetes mellitus than were those treated with uncoated PTA. In addition, PTA patients who died were more likely to be active smokers than were DCB patients that died.
There was no statistically significant difference in all-cause mortality between DCB and PTA through 5 years (9.3% vs 11.2%, respectively, P = .399).

A Kaplan-Meier survival analysis stratified paclitaxel dosage into three groups: low-dose, mid-dose, and upper-dose groups. Mean dosages for the three groups were 5,019, 10,008, and 19,978 mcg, respectively. The analysis showed no significant difference in mortality between groups, “demonstrating no direct impact of levels of nominal paclitaxel dose exposure at the index procedure and survival status in the DCB patients through 5 years (P = .700),” according to the authors.
Limitations of the study reported by the authors include the fact that pooling data from distinct trials has shortcomings. Some of data included had not yet undergone peer review, and PTA patients
were included in only two randomized trials in a 2:1 ratio.
“The small numbers of PTA control patients (less than 10%) may not be representative of PTA patients in general and limits the strength of this analysis of mortality.” In addition, only patients with Rutherford classification 2-4 were included in these studies.
“Results from this independent patient-level metaanalysis show no difference in mortality between DCB and PTA at 5 years and no correlation between varying levels of paclitaxel exposure and mortality. ... Data transparency and additional analyses are needed to better understand how other factors influence long-term outcomes in this complex patient population,” the researchers concluded. The study was funded by Medtronic, which provided the data for independent analysis to the Baim Institute for Clinical Research. Dr. Schneider is a member of the advisory board for Medtronic, Abbott, and Boston Scientific and is a consultant for Medtronic and other device companies. Coauthors had consulting, advisory board, or honoraria relationships with Medtronic and other device companies.
mlesney@mdedge.com
SOURCE: Schneider PA et al. JACC. 2019 Jan 25. doi: 10.1016/j.jacc.2019.01.013.
The AV Fistula Ligation Study showed that ligation of the hemodialysis arteriovenous fistula (AVF) in stable post–renal transplant patients improves left ventricular (LV) remodeling, according to a presentation by Michael B. Stokes, MD, at the American Heart Association Annual Scientific Sessions in Chicago in November last year. In addition, significant improvements were noted in N-terminal pro–B-type natriuretic peptide (NT-proBNP), LV end-diastolic volume, LV end-systolic volume, and left and right atrial area in the AV fistula ligation arm, but not in the control arm, according to the summary published online at the American College of Cardiology website.
The study was an open-label, multicenter, two-group, parallel-design, randomized controlled trial. Australian and New Zealand clinical trials registry ACTRN12613001302741.
The primary outcome of LV mass reduction at 6 months, for AV fistula ligation vs. control, was –22.1 g vs. 1.2 g (P less than .001).
Cardiac output at 6 months also improved in the ligation vs. the nonligated patients at 6.8 vs. 4.8 L/min, respectively (P less than .05).
The study was funded by the Royal Adelaide Hospital Research Foundation, and the authors reported no disclosures.
discussed earlier, patients with high-flow fistulas may be at increased risk of heart failure and hemodynamic data can be critical in establishing an algorithm for managing these challenging patients. Ligation of a functioning and asymptomatic access in a patient with a successful renal transplant should be recommended only after informed discussion with the patient weighing the ongoing potential negative effects on cardiac function of continued access patency versus the potential need for future hemodialysis. Dr. Stokes presents interesting data that must be considered in this controversy. I believe that, in the absence of a universally applicable algorithm, the clinical
decision to recommend AV fistula ligation after successful kidney transplantation should be individualized and based on ongoing assessment of cardiac and renal function and fistula complications and hemodynamics.
References
1. Eur Heart J. 2017;38:1913-23.
2. Nephrol Dial Transplant. 2008;23:282-7.
3. J Vasc Access. 2012;13:405-8.
4. Stokes MB, et al. LBS.05 – Late Breaking Clinical Trial: Hot News in HF. Presented at American Heart Association Scientific Sessions. 2018 Nov 1012. Chicago.
BY ALICIA GALLEGOS MDEDGE NEWS
Data security experts say three HIPAA violations that resulted in significant fines by the Office for Civil Rights (OCR) in 2018 hold important lessons for health professionals about safeguarding records and training staff in HIPAA compliance.
Read on to learn how the cases unfolded and what knowledge practices can gain from the common HIPAA mistakes.
to defend themselves if they are being accused by a patient,” she said. “However, under the HIPAA rules, health care providers have to understand that they are prohibited from making such public statements about any patient.”

Who? Allergy Associates of Hartford, Conn. What happened? A patient contacted a local television station to complain about a dispute between herself and a physician at Allergy Associates. The disagreement stemmed from the office turning away the patient because she allegedly brought her service animal, according to a Nov. 26, 2018, announcement by the Department of Health & Human Services. The reporter contacted the doctor in question for a news story, and in responding, the physician disclosed protected patient information to the reporter. What else? An OCR investigation determined that a privacy officer with Allergy Associates had instructed the physician not to respond to the media about the complaint or to respond with “no comment”; that advice was disregarded. The practice then failed to discipline the physician or take any corrective action following the disclosure, according to the OCR. How much? The OCR imposed a $125,000 fine on the practice and a corrective action plan that includes 2 years of OCR monitoring.
Lessons learned: Had the practice disciplined the physician or taken corrective action after the disclosure, the OCR may not have penalized the group so severely, according to Jennifer Mitchell, a Cincinnati-based health law attorney and vice chair of the American Bar Association eHealth, Privacy, & Security Interest Group.
“In my opinion, the government levied these penalties because the provider did not sanction the doctor,” Ms. Mitchell said in an interview. “Health care entities need to take proper steps to remediate and, at a minimum, hold their workforce responsible for their behavior and ensure that it won’t happen again.”
The case emphasizes the need to train team members on media protocols and to ensure that protected health information is not mistakenly released. In addition to implementing policies and procedures, practices must also be willing to discipline health professionals when violations occur.
“A health care provider’s natural inclination is
Who? Advanced Care Hospitalists of Lakeland, Fla. What happened? Advanced Care Hospitalists (ACH) received billing services from an individual who represented himself to be affiliated with a Florida-based company named Doctor’s First Choice Billing. A local hospital later notified ACH that patient information, including names and Social Security numbers, were viewable on the First Choice website. ACH identified at least 400 patients affected by the breach and reported the breach to the OCR. However, ACH later determined that an additional 8,855 patients may have been affected and revised its OCR notification. What else? During its investigation, the OCR found that the hospitalist group had never entered into a business associate agreement for billing services with First Choice, as required by HIPAA, and that the practice also failed to adopt any policies regarding business associate agreements until 2014, according to a Dec. 4, 2018, announcement from HHS. How much? The OCR fined the practice $500,000 and also imposed a robust corrective action plan that includes an enterprise-wide risk analysis and the adoption of business associate agreements. Roger Severino, OCR director, called the case especially troubling because “the practice allowed the names and Social Security numbers of thousands of patients to be exposed on the Internet after it failed to follow basic security requirements under HIPAA.” Lessons learned: The case illustrates the importance of having a business associate agreement in place for all third parties that may have access to protected health information, said Clinton Mikel, a Farmington Hills, Mich., health law attorney specializing in HIPAA compliance.
Under HIPAA, a business associate is defined as a person or entity, other than a member of the workforce of a covered entity, who “performs functions or activities on behalf of, or provides certain services to, a covered entity that involve access by the business associate to protected health information.”
HIPAA requires that covered entities enter into contracts with business associates to ensure appropriate safeguarding of protected health information.
“If your business associate has a breach, your practice must report the breach to OCR and your patients,” Mr. Mikel said in an interview. “The OCR will then investigate your practice and your relationship with the business associate. Just because the breach and fault clearly happened elsewhere, you will still be investigated, and could face a penalty if HIPAA requirements weren’t met.”
Who? Filefax of Northbrook, Ill.
What happened? The OCR opened an investigation after receiving an anonymous complaint that medical records obtained from Filefax, a company that provided storage, maintenance,
and delivery of medical records for health professionals, were left unmonitored at a shredding and recycling facility. OCR’s investigation revealed that a person left the records of 2,150 patients at the recycling plant and that the records contained protected health information, according to an HHS announcement. It is unclear if the person worked for Filefax.
What else? The OCR discovered that, in a related incident, an individual who obtained medical records from Filefax left them unattended in an unlocked truck in the Filefax parking lot.
How much? The OCR imposed a $100,000 fine on Filefax. The company is no longer in business; however, a court-appointed liquidator has agreed
HIPAA violations that resulted in significant fines by the Office for Civil Rights in 2018 hold important lessons for health professionals about safeguarding records and training staff.
to properly store and dispose of the remaining records.
Lessons learned: Although the case did not involve a health provider, the circumstances are applicable to physicians, particularly when practices move or close, Mr. Mikel said. In some cases, a former patient may contact a shuttered practice only to learn their record cannot be located, or worse, that a breach has occurred.
“[Such a case is] ripe for a patient to complain to OCR,” he said. “OCR doesn’t care if you’re closed or retired, they’re going to look.”
HIPAA requires that covered entities apply appropriate administrative, technical, and physical safeguards to ensure the privacy of protected health information in any form when moving or closing. The safeguards must prevent prohibited uses and disclosures of protected health information in connection with the disposal of such information, according to the rule. The HHS provides guidance for the disposing of medical records; further, the American Academy of Family Physicians has created a checklist on closing a practice that addresses the transferring of medical records.
Without taking the correct measures, doctors may end up drawing scrutiny from OCR and face a potential fine if violations are found, experts said.
“Covered entities and business associates need to be aware that OCR is committed to enforcing HIPAA regardless of whether a covered entity is opening its doors or closing them,” Mr. Severino of the OCR said in a statement. “HIPAA still applies.”
BY SHARON WORCESTER MDEDGE NEWS REPORTING FROM THE ACR ANNUAL MEETING
CHICAGO – Nonwhite ethnicity and limb infection at diagnosis predict vascular events in patients with thromboangiitis obliterans (TAO), and the latter also predicts amputation, which occurs within 10 years of diagnosis in nearly a third of patients, according to findings from a large retrospective French cohort study.
After a mean follow-up of 5.7 years, 58.9% of 224 patients with TAO – also known as Buerger’s disease – experienced a vascular event, 21.4% experienced at least one amputation, and 1.3% died, Alexandre Le Joncour, MD, reported at the annual meeting of the American College of Rheumatology.
The 5- and 15-year vascular eventfree survival rates were 45% and 28%, respectively, and the 10- and 15year amputation-free survival rates were 74%, and 66%, respectively, said Dr. Le Joncour of Sorbonne University, Paris.
Of note, no significant difference was seen in the vascular event-free survival rates based on tobacco use
The 5- and 15-year vascular eventfree survival rates, were 45% and 28%, respectively.
levels (more than 22 pack-years vs. 22 or fewer pack-years; hazard ratio, 1.2), he said.
Patient characteristics and clinical factors found to independently predict vascular events included nonwhite ethnicity (HR, 2.35; P = .005) and limb infection at diagnosis (HR, 3.29; P = .045). Limb infection at diagnosis also independently predicted amputation (HR, 12.1; P less than .001), he said.
“But there was no significant [association with amputation] in patients who had claudication, critical ischemia, or ischemic ulcers/necrosis,” he noted, adding that a comparison of white and nonwhite patients showed that the groups were sim-
ilar with respect to epidemiologic and cardiovascular factors, clinical symptom distribution, and rates of
addiction to tobacco, alcohol, and illicit drugs. It was also clear that patients who
quit using tobacco had a significantly lower risk of amputation than did Prognostic continued on page 19
BY MARK S. LESNEY MDEDGE NEWS FROM THE ANNALS OF VASCULAR SURGERY
Adeveloping feature of modern health care is the formation of eHealth communities based upon particular disease conditions. An analysis of one such forum dedicated to peripheral arterial disease indicated that this form of communications outlet can provide “a rich source of information related to the experiences of patients with PAD, their treatment preferences, questions they consider important, and terminology that they use,” according to a study published in Annals of Vascular Surgery.
The researchers collected 103 posts from an online open-access PAD Medical Support Community forum (MedHelp) based in the United States. Posts were selected from PAD-specific threads and were analyzed for thematic content, common vernacular, and self-reported characteristics of the participants using a qualitative analysis software pro-

gram. In addition, the investigators assessed disease-specific comments with regard to their match to contemporary PAD treatment guidelines, according to Peris Castaneda, a medical student, and her colleagues at the University of Michigan, Ann Arbor. They found that, among original posts, the most common themes included PAD diagnosis and differential (25%), epidemiology and pathophysiology (21%), disease symptoms and
effects on activities of daily living (15%), and health care provider recommendations (13%). Negative posts related to experiences with health care providers were identified in 10 of 18 (55.6%), while overall, 15.9% of posts mentioned medical advice that was inconsistent with clinical treatment guidelines.
“This information can be used to understand unmet patient needs, develop educational resources, and improve
Vascular specialists practice in a world where technology changes constantly and evidence often lags behind. As daunting as it may seem to stay abreast of evidence-based practices for physicians, patients seeking additional information about their symptoms, prognosis, or treatment options face an even greater challenge. Most patients lack familiarity with medical terminology and also may have difficulty distinguishing between sources of information that are trustworthy versus not.
Any busy practicing clinician can probably recall multiple examples from a given clinic where they were asked about information that a patient or patient family member obtained from the Internet (often without recollection of the specific site or author).
This study provides the medical community with a survey of eHealth forums about peripheral artery disease (PAD), a common and chronic condition where patients sometimes get multiple opinions from specialist and nonspecialist providers that may not be harmonious. Beyond inconsistencies between user advice and medical evidence identified (15% was medically
inaccurate), the study also provides insight into who is posting and what they are posting about. The most important takeaway, however, may be why the users were there in the first place, and what opportunities the answers to this question provide to improve patient care and education. Posts from some users suggested that they are concerned about leg symptoms but haven’t seen a doctor, and are wondering what to do.
What a great opportunity to rethink our approach to awareness and patient education, since many resources explain PAD rather than thinking upstream to questions about leg symptoms that might be caused by a variety of diagnoses. Other users expressed frustration at barriers to specialist care, providing useful examples for advocacy and policy, underscoring the importance of having a vascular specialist workforce available and appropriately distributed to meet patient needs. A third category of users had seen a doctor (or several) and just wanted more information. This last category would benefit from some direction from the medical community about patient-facing sources of information that are both accurate and free of confusing medical jargon (posts in this study had
"We hope that the results of this analysis can be applied to the development of additional resources targeting unmet patient and family needs and improved communication."
communication,” the authors wrote.
“We hope that the results of this analysis can be applied to the development of additional resources targeting unmet patient and family needs and improved communication,” they concluded. The were no disclosures reported in the article.
mlesney@mdedge.com
SOURCE: Castaneda P et al. Ann Vasc Surg. 2019;54:92-102.
7th-grade reading level). If those don’t exist, then we need to get to work designing better resources. The Internet is a vast source of information juxtaposed with misinformation, and patients aren’t necessarily able to distinguish between the two. The source a user arrives at may depend more upon search engine optimization, advertising dollars, and terminology than medical evidence or accuracy. We should expect patients to seek additional information when they leave our clinics, where we may spend less than 15 minutes with them and it is virtually impossible to cover everything face-to-face. By directing patients to reliable sources rather than hoping they will figure it out on their own, we stand lots to gain. Making patients smarter information shoppers will benefit both patients and physicians, allowing them to spend less of their precious time together focused on misconceptions, unreasonable expectations, or other harms inflicted by unreliable sources.
Matthew A. Corriere, MD, is Frankel Professor of Cardiovascular Surgery and associate professor of surgery, Michigan Medicine, Ann Arbor, Mich.
continued from page 17
those who continued using tobacco (P = .001), he said, explaining that 43 of the 48 patients who experienced amputation were current smokers, and 5 were ex-smokers at the time of amputation.
Dr. Le Joncour and his colleagues included TAO patients diagnosed between 1967 and 2016 at a median age of 36 years at the time of first symptoms, with a median of 12 months from symptom onset until diagnosis. About 76% were men, and about 83% were white. Patients
with diabetes, atherosclerosis, arterial emboli, connective tissue disease, and/or thrombophilia were excluded.
Vascular events in this study were defined as “an acute worsening of the disease course requiring treatment modifications,” and included critical ischemia (35% of cases), ulcers/necrosis (33%), claudication worsening (16%), deep vein thrombosis (3%), superficial phlebitis (7%), limb infection (4%), and “other” events (2%).
Major amputation was defined as “an amputation involving the tibio-tarsian articulation for lower
limbs and the metacarpophalangeal articulation for upper limbs,” he explained.
The median time to amputation was 4 years, and patients who experienced amputation had a median age of 39 years. Half of the 48 patients who experienced amputation had one amputation, nearly a third had two amputations, and 19% had three amputations. About two-thirds had minor amputations and a third had major amputations.
The findings provide important prognostic information regarding TAO, Dr. Le Joncour said, noting that long-term data on outcomes in
MAXIMIZE RADIAL SOLUTIONS TO PERIPHERAL CHALLENGES – RADIAL TO PERIPHERAL (R2P™) by TERUMO
From the leaders in radial access, Radial to Peripheral (R2P™) is the first and only portfolio of longer-length radial devices specifically designed for peripheral procedures, including Above-theKnee (ATK) and PAD/CLI vascular interventions.
With R2P™, TERUMO continues to advance procedural solutions, enabling physicians to utilize a comprehensive radial to peripheral approach to perform more peripheral procedures for more patients:
TAO patients have been lacking.
“We found specific characteristics that identified those at highest risk for subsequent vascular complications, and these factors are not only important predictors of vascular complications or relapse, but may also serve to adjust more aggressive management and close follow-up of these patients,” he concluded.
Dr. Le Joncour reported having no disclosures.
sworcester@mdedge.com
SOURCE: Le Joncour A et al. Arthritis Rheumatol. 2018;70(Suppl 10), Abstract 1885.

• Optimize entry site management with Slender Technology™
• Enable the potential for quicker ambulation, improved patient comfort, and satisfaction
• May increase cath lab efficiencies and decrease overall costs per procedure
The R2P™ portfolio is comprised of:
• GLIDESHEATH SLENDER® Hydrophilic Coated Introducer Sheath
o 7/6 Fr Size
o 10 cm and 16 cm lengths
• R2P™ DESTINATION SLENDER® Guiding Sheath
o 6 Fr Size
o 119 cm and 149 cm lengths
• R2P™ SLENGUIDE® Guiding Catheter
o 7 Fr Size
o 120 cm and 150 cm lengths
• GLIDEWIRE® Hydrophilic Coated Guidewire
o Straight, Angled, 1.5 mm and 3 mm J Tip
o 350 cm, 400 cm, and 450 cm lengths
• GLIDECATH® Hydrophilic Coated Catheter
o 4 Fr Size
o 150 cm length
• NAVICROSS® Support Catheters
o Straight, Angled
o 135 cm and 150 cm lengths
• R2P™ METACROSS® RX PTA Balloon Dilatation Catheter
o 3-8 mm diameter x 20-200 mm length
o 200 cm shaft length
• R2P™ MISAGO® RX Self-expanding Peripheral Stent
o 6-8 mm diameter x 40-150 mm length
o 200 cm shaft length
o Coming soon—contact a TERUMO representative for availability
Indications
The MISAGO® RX Self-expanding Peripheral Stent is indicated to improve luminal diameter in symptom-
atic patients with de novo or restenotic lesions or occlusions of the Superficial Femoral Artery (SFA) and/or proximal popliteal artery with reference vessel diameters ranging from 4 to 7 mm and lesion length up to 150 mm.
Do not use this device in pregnant patients or patients who may be pregnant, patients who exhibit angiographic evidence of severe thrombus in the target vessel or lesion site before/ after undergoing Percutaneous Transluminal Angioplasty (PTA) procedure, patients with contraindication to antiplatelet and/or anticoagulation therapy, patients with known allergy to nickel-titanium alloy, gold or contrast media, vessels in which there may be a residual stenosis of 50% diameter or larger in the target vessel after the planned intervention, a lesion that is within an aneurysm or an aneurysm with a proximal or distal segment to the lesion, a lesion through which a guide wire cannot pass. This device should only be used by a physician who is familiar with, and well trained in, Percutaneous Transluminal Angioplasty (PTA) techniques and stent implantation.
• TR BAND® Radial Compression Device
o Regular 24 cm and Long 29 cm
Discover what’s next in peripheral intervention – learn more at www.terumois.com/r2p
RX ONLY. Refer to the product labels and package insert for complete warnings, precautions, potential complications, and instructions for use.
©2019 Terumo Medical Corporation. All rights reserved. All brand names are trademarks or registered trademarks of Terumo. PM-01504
LESIONS ACROSS THE ELBOW
Thrombosed AV grafts
Complex iliac lesions
In-stent restenosis of the SFA
PTA failures of AV graft lesions
Long SFA lesions
Chronic total SFA occlusions
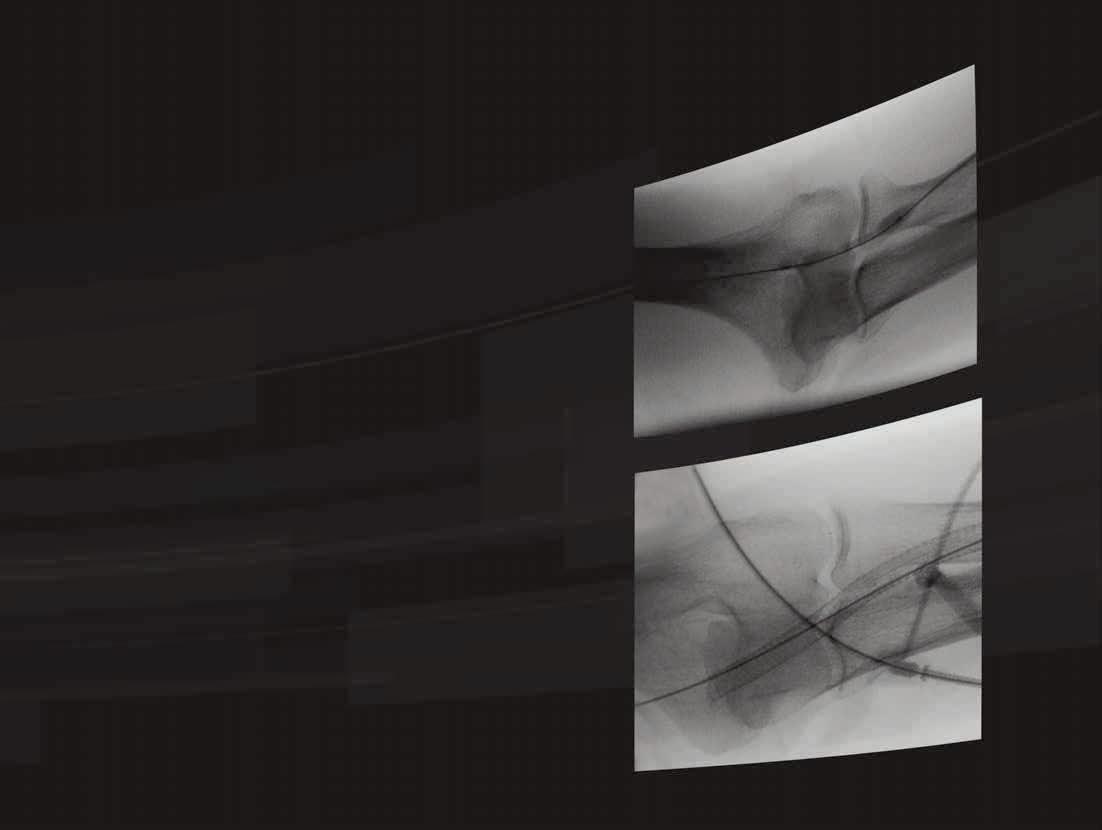






Physicians are achieving durable outcomes across the elbow with fewer reinterventions in rapidly failing AV access circuits. See the NEW case study at goremedical.com/viabahn/elbow
Images courtesy of Minneapolis Vascular Physicians. Used with permission.
INDICATIONS FOR USE IN THE U.S.: The GORE® VIABAHN® Endoprosthesis is indicated for improving blood flow in patients with symptomatic peripheral arterial disease in superficial femoral artery de novo and restenotic lesions up to 270 mm in length with reference vessel diameters ranging from 4.0 –7.5 mm, in superficial femoral artery in-stent restenotic lesions up to 270 mm in length with reference vessel diameters ranging from 4.0 – 6.5 mm, and in iliac artery lesions up to 80 mm in length with reference vessel diameters ranging from 4.0 – 12 mm. The GORE® VIABAHN® Endoprosthesis is also indicated for the treatment of stenosis or thrombotic occlusion at the venous anastomosis of synthetic arteriovenous (AV) access grafts.
CONTRAINDICATIONS: The GORE® VIABAHN® Endoprosthesis with Heparin Bioactive Surface is contraindicated for noncompliant lesions where full expansion of an angioplasty balloon catheter was not achieved during pre-dilatation, or where lesions cannot be dilated sufficiently to allow passage of the delivery system. Do not use the GORE® VIABAHN® Endoprosthesis with Heparin Bioactive Surface in patients with known hypersensitivity to heparin, including those patients who have had a previous incidence of Heparin-Induced Thrombocytopenia (HIT) type II. Refer to Instructions for Use at goremedical.com for a complete description of all warnings, precautions and adverse events. Only
W. L. Gore & Associates, Inc. | Flagstaff, AZ 86004 | goremedical.com
Products listed may not be available in all markets.
GORE®, VIABAHN®, and designs are trademarks of W. L. Gore & Associates. © 2018 W. L. Gore & Associates, Inc. AX1547-EN1 DECEMBER 2018