April 25, 2026 | 8 AM-12 PM
Join us in celebrating the high-caliber research conducted by our medical students, residents, and fellows. Learners will present their research and Christopher Hess, MD, PhD will deliver the keynote presentation. Visit the webpage to learn more.
August 10 & 11, 2026
CT-POW is an interdisciplinary, hands-on conference dedicated to enhancing CT protocols and workflows. This event provides a unique opportunity to collaborate, learn, and implement practical solutions to optimize CT imaging practices. View the agenda online
This multi-day educational event offers opportunities to learn, connect, and ski the beautiful mountains in Park City, Utah. The date for the 2027 Summit will be announced on the webpage.
The Department will celebrate our Centennial Anniversary in 2027!
To mark this monumental moment in our history, we will be hosting various events throughout 2027 and encourage alumni to join us in our celebrations. More details to come as this milestone draws near.
While the chill of winter still clings to the air, there’s always a spring in our step!
This newsletter is filled with the exciting work that energizes us even on the coldest days. If you watch the news, you may already know about some! Our participation in the national trial of AI use in breast cancer screening generated national media coverage and our faculty were interviewed by multiple Wisconsin outlets. We were also featured in news about theranostics, testing AI models, and breast cancer occurrence in men.
In addition to making headlines, we’re creating new treatment options including thyroid artery embolization. We’re one of the few institutions in the Midwest offering this minimally invasive alternative. And while not new, we continue to provide patients with the option of CT colonography to screen for colon cancer, based on 20 years of research on the benefits of this alternative to optical colonoscopy and emerging multitarget stool DNA-based testing.
We’re also making a difference in our field through summer programs for medical students, innovations in curriculum development, CT protocol education, and winning awards at RSNA – including a gold medal!
What energizes us today, fuels tomorrow’s discoveries. I am inspired by the passion of our physicians, trainees, and researchers every day. Together we are ensuring a brighter tomorrow.
“What energizes us today, fuels tomorrow’s discoveries.”
On Wisconsin!
Scott B. Reeder, MD, PhD

Scott Reeder, MD, PhD
For patients suffering from thyroid goiters, undergoing surgery can be a daunting treatment. However, for many patients, it’s not the only option. UW Department of Radiology interventional radiologists Sean Golden, MD and Matthew Niemeyer, MD offer thyroid artery embolization (TAE) as a minimally invasive alternative.
TAE can be a good fit for patients who are hesitant to undergo surgery or have medical conditions that prevent them from doing so. Dr. Golden and Dr. Niemeyer guide a catheter inserted into a small puncture in the patient’s wrist or thigh through the complex network of arteries within the body to those that supply blood flow to the thyroid gland.
To help them navigate, the interventional radiologists use fluoroscopy, a specialized live x-ray that shows the catheter moving through the body; similar to how a person can watch their car navigate in real-time on a GPS.
Once they reach the thyroid artery, they inject small particles through the hollow catheter. These particles build up a barricade that blocks the flow of blood, and the restriction of blood flow causes the goiter to reduce in size. Recent cases are showing a 60% reduction in goiter size.
The entire process takes around two hours, and patients can return home the same day they undergo TAE. They may experience mild neck soreness for up to two weeks afterward and should avoid vigorous activities like running for the first week; but are otherwise able to resume their normal daily activities the day following the procedure.
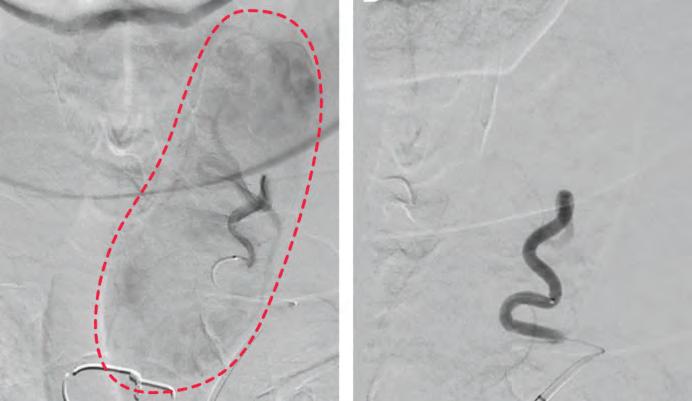
Intra-procedure angiograms depicting the left thyroid gland pre-embolization (left) and post-embolization (right). Pre-embolization shows an area of blush, indicating the blood supply. Post-embolization shows the absence of blood supply as the supply is blocked during the procedure.
To lay the groundwork for incorporating TAE as a treatment option, Drs. Golden and Niemeyer spoke with interventional radiologists across the nation. Once they’d gained a thorough understanding of the procedure, they connected with endocrine surgery specialist Alex Chiu, MD. A phenomenal collaborator, Dr. Chiu refers patients who are good candidates for TAE. Now that the embolization clinic is up and running, colleagues throughout the institution are referring candidates.
Ensuring the best possible care for patients is a collaborative effort. A multidisciplinary team consisting of surgeons, endocrinologists, and diagnostic neuroradiologists each play a part in the patient’s care journey, from the initial diagnosis and consult through to treatment and post-procedure follow-up.
UW Health is one of the few institutions in the Midwest offering TAE. “One of the great things about UW is that we have access to an amazing hybrid CT angiography room. This allows us to perform a diagnostic CTA prior to embolization so we can confirm blood supply to the thyroid and look for non-target embolization” Dr. Golden explained.
“Most other practices use cone beam CT, which provides less detailed imaging. We are researching whether contrast deposition in the thyroid gland on our post-procedure CT predicts the degree of thyroid shrinkage after embolization. We are also researching how long it takes for the thyroid to shrink and alterations in thyroid and parathyroid hormone levels after embolization.”
This November, nationally recognized experts in computed tomography (CT) gathered virtually for the University of Wisconsin Department of Radiology CT Medical Advisory Board meeting. Held biennially and hosted by the department through the CT Education and Collaboration Collective (C-TECC), the meeting ensures that the CT Protocols developed at UW–Madison are up to date, leverage the latest technological advances, and incorporate novel research.
The week long meeting included multiple sessions on subspecialties as well as numerous breakout sessions. There was a strong focus on photon counting CT across sessions, citing the exciting potential that this new technology has and how it could make a difference in
clinical settings. Experts also discussed potential updates to existing protocols, evaluating the benefits to removing oral contrast for Emergency Department imaging; creating a new protocol for emergent scans of the aorta in the emergency room, and implementing a whole body bone marrow scan protocol to screen for multiple myeloma; among others.
Additionally, the advisory board set goals related to usability and workflow improvements; like condensing the amount of abdominal protocols to reduce technologist confusion and implementing specific protocols into Healthlink at the exam ordering level to reduce back-and-forth between technologists and providers.

• Lakshmi Ananthakrishnan, MD, Medical Director of CT, UT Southwestern Medical Center
• Francis Baffour, MD, Associate Medical Director, CT Clinical Innovation Center, Mayo Clinic
• Amit Gupta, MD, MRMD, CIIP, Division Chief of Cardiothoracic Imaging, Modality Director of Diagnostic Radiology, University Hospitals Cleveland Medical Center
• David Haynor, MD, PhD, Harborview Medical Center, Seattle WA
• Alan Ropp, MD, Modality Director, Thoracic & MR Imaging, Co-Director, Cardiothoracic Imaging Fellowship, Director B Reading Program for Occupational Lung Disease, University of Virginia Health
• Ramandeep Singh, MD, MBBS, Medical Director of CT, Associate Chief Health Information Officer, Director of Imaging Informatics, Peer Learning Leader, University of Iowa
• Naveen Subhas, MD, MPH, Director of Operation Efficiency & Strategy, Director of MSK Imaging Fellowship, Cleveland Clinic
Despite being preventable, colorectal cancer (CRC) is one of the leading causes of cancer deaths in the United States. Colonoscopy has been the predominant option for screening and identifying precancerous polyps, but multitarget stool DNA (mt-sDNA) has gained popularity in recent years due to its non-invasive nature. At UW Health, another non-invasive option, CT Colonography (CTC), is available; and according to data from a 20-year-long program led by Perry Pickhardt, MD and David Kim, MD, it may be the best option for many patients.
Unlike colonoscopy, there’s no risk of bleeding or perforating the colon associated with CTC. Instead of a scope, computed tomography scans are used to create 3D images of a patient’s colon from different angles. Patients are able to resume normal activities and even drive themselves home following the procedure. If polyps are detected, same-day GI Clinic services are available for polypectomies.
While stool testing is also a non-invasive screening method, CTC outperforms it in a crucial area: detecting precancerous polyps. By identifying and removing these types of polyps, patients can effectively prevent cancer that they may have developed later in life.
Key findings from the study include:
• A polyp ≥ 6 mm was detected in 15.9% of examinations, and polyp detection had a positive predictive value of 91.6%.
• 0.2% of examinations detected histologically confirmed adenocarcinoma, yet 4% detected histologically confirmed advanced adenoma, which is considered a CRC precursor
• Additionally, CTC detected in this group unsuspected extracolonic malignancies in 0.4% of examinations and abdominal aortic aneurysm in 0.3% of examinations.
• No major complications occurred after any examination
The CTC screening program was established in 2004 and has completed over 15,000 CTC exams, including over 9,000 primary asymptomatic screening exams, in nearly 12,000 patients. Notably, it is the largest and longest running CTC data set in the country.
This summer, Drs. Pickhardt and Kim published “CT Colonography for Colorectal Cancer Screening and Prevention: 20-Year Programmatic Experience at a U.S. Academic Medical Center” in the American Journal of Roentgenology (AJR). Insights support CTC as a safe, noninvasive way to detect and prevent CRC. Dr. Pickhardt discussed the study with AJR Editor in Chief Andrew Rosenkrantz, MD.
The department has seen success with the CTC screening program; however, the study shows that there’s been a decrease in the number of scans performed in recent years. Despite widespread insurance coverage, including Medicare coverage, CTC has been slow to gain traction as a screening option nationwide.
In the AJR Conversations podcast episode “CT Colonography for Colorectal Cancer Screening”
Dr. Kim discussed some of the barriers for clinical implementation of CTC with AJR Gastrointestinal Imaging Section Editor Federica Vernuccio, MD, PhD He noted that acceptance from primary care providers, hesitancy among radiologists, and the need for quality training as key factors to overcome.
Dr. Kim acknowledged that while hesitancy to incorporate a new exam into a practice is understandable, there is a robust body of literature supporting CTC as a safe and effective screening method that excels at detecting and preventing CRC. He highlighted that now that coverage is widespread, it’s up to radiologists to advocate for CTC screening.
“We need radiologists to champion CTC use. If radiologists don’t accept it in general throughout the world, then it will never get into widespread use. You need to get down into the local level, talk to your primary
care physicians, and explain the test; what it can do and engage your primary care physicians. Otherwise, that referral will never happen.”
In the same conversation, Dr. Kim emphasized that regardless of method, screening levels for CRC remain low. An acceptable screening level is considered to be about 80% adherence rate for a given population, and many institutions are within a range of high 60s to low 70s. Widespread implementation of CTC could help close this screening gap and reduce the overall rate of CRC occurrence.
Comparisons can be drawn and advantages weighed between the various CRC screening methods, but opportunistic screening is a benefit gained from CTC which neither colonoscopy nor stool screening can offer. It’s the practice of reviewing medical images taken for one concern and evaluating them to potentially identify other health conditions.
CT scans taken for CRC screening can show characteristics like bone mineral density, skeletal muscle, liver fat, and aortic plaque; which can be used to evaluate the patient’s overall health and wellness. In his interview with AJR discussing the 20-year CTC program, Dr. Pickhardt acknowledged that opportunistic screening does take additional time. However, he noted that artificial intelligence (AI) tools can aid radiologists in reading opportunistic screening studies.
“I think the opportunistic CT screening revolution is just getting started. Screening for things like colorectal cancer and lung cancer fit in perfectly with this approach. I think as all radiologists are by now aware, body CT scans contain very rich cardiometabolic health information and that using these explainable AI algorithms, we can now efficiently and objectively assess these.”
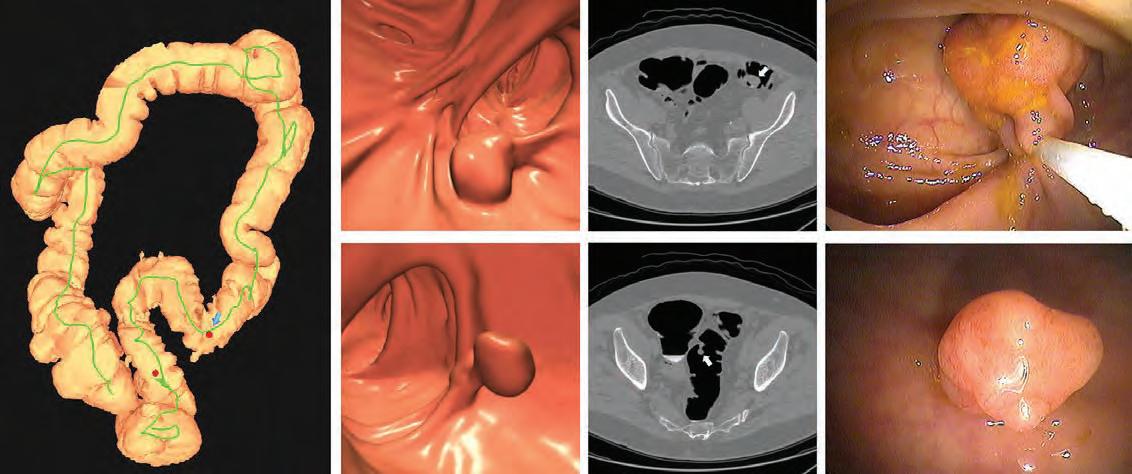
Images of positive CT colonography (CTC) screening examination result in an asymptomatic patient. Colon map from CTC (left image) shows the location of two sigmoid polyps that were detected (red dots). Three-dimensional endoluminal and confirmatory two-dimensional transverse CTC images show a large 1.6-cm pedunculated polyp on top row (arrow) and a 9-mm pedunculated polyp in the distal sigmoid on the bottom row (arrow). Both polyps were confirmed and resected at optical colonoscopy performed the same day (right images), avoiding the need for a second bowel preparation. The larger polyp proved to be a tubulovillous adenoma (large advanced adenoma), whereas the smaller polyp was a nonadvanced tubular adenoma.

Elizabeth Burnside, MD, MPH received a 5-year $4M grant renewal for the UW BIRCWH Scholars Program from the NIH/NIAMS.

Christoph Lee, MD, MS, MBA received:
• 1-year $1.4M grant for “PopulationBased Evaluation of Artificial Intelligence for Mammography Prior to Widespread Clinical Translation” from the NIH/ NCI.
• 5-year $1.2M grant for “Comparing Screening Mammography With and Without Assistance from Artificial Intelligence for Breast Cancer Detection and Recall Rates” from PCORI.
• 1 year $675K grant for “Improving Outcomes in the Breast Cancer Screening and Diagnostic Continuum” from the NIH/NCI.

Tim Szczykutowicz, PhD received a 1-year $220K grant for “Collaboration on Photon Counting CT Development” from GE HealthCare.

Sarv Priya, MD, MBBS received a 1-year $50K grant for “10-Minute Cardiac MRI: Comprehensive Cine, Flow, and Angiography in a Single Exam” from the Congenital Heart Defect Coalition.

James Pipe, PhD received a 4-year $2.2M grant for “MRI Technology for “Greater Efficiency and Improved Value” from the NIH/NIBIB.

Pallavi Tiwari, PhD received a 3-year $1.1M grant for “Image informatics tools for curation and prognostic modeling in pediatric brain tumors” from the NIH/NCI.

Timothy Ziemlewicz, MD received a 5-year $353K grant for “Ultrasound Device Evaluation” from GE HealthCare.

John Garrett, PhD received a 1-year $302K grant for “Foundation Models for Medical Imaging Analysis and Interpretation” from GE HealthCare.

Richard Bruce, MD received a 1-year $54K grant for “Intelligent Protocoling Integration and Write-Back” from GE HealthCare.

Sanna Herwald, MD, PhD received a 1-year $28K grant for “Prediction of Clinical Abscess Drainage Outcomes and the Efficacy of Potential Viscosity Modifying Biochemical Treatments by Measuring Quantitative Abscess Fluid Viscosity” from RSNA.

Nicholas Burris, MD received a 3-year $1.5M grant for “Non-invasive hemodynamic and biomechanic imaging methods for early risk prediction in aortic dissection” from the NIH/NHLBI.


Orhan Unal, PhD and Pallavi Tiwari, PhD received a 1-year $380K grant for “Imaging Fabric POC License & Development SOW –Imaging Visualization, Annotation, and Segmentation” from GE HealthCare.

Alan McMillan, PhD received a 2-year $250K grant for “Ultra-high sensitivity, high spatial resolution single photon emission tomography using mechanical flux manipulation” from the NIH.

Vivek Prabhakaran, MD, PhD received a 1-year $200K grant for “Establishing Concordance, Reproducibility and Multimodal Cross-Validation of Water Exchange MRI Technique for Glymphatic Function Across the Alzheimer’s Disease Continuum” from ARPA-H/GE.

Giuseppe Toia, MD received a 3-month $18K grant for “PROView DL Feasibility Study: Algorithm Usability and Performance” from GE HealthCare.
The University of Wisconsin–Madison and UW Health will assess whether artificial intelligence (AI) can effectively assist radiologists in the interpretation of mammograms as part of a national clinical trial. Wisconsin media outlets interviewed Christoph Lee, MD, MS, MBA; Mai Elezaby, MD; and Ryan Woods, MD, MPH about the exciting potential of improving cancer detection and reducing unnecessary callbacks and anxiety for patients.
Funded by a $16 million grant from the Patient Centered Outcomes Research Institute (PCORI) and co-led by UCLA and UC Davis, the PRISM Trial (Pragmatic Randomized Trial of Artificial Intelligence for Screening Mammography) will comprise of 400,000 patients at seven sites across the United States, including an estimated 50,000 in Wisconsin, over the next two years.
Christoph Lee’s Interview with WMTV 15 News
During a WMTV 15 News segment, Dr. Lee discussed the trial with reporter Ashley Weil and how it differs from previous studies of AI use for reading mammograms.
“Even with expert interpreters and improved technologies, we still miss about one in eight breast cancers,” said Dr. Lee. “These cancers could be very small, maybe imperceptible to the human eye, or hidden behind dense breast tissue. So these deep learning algorithms that could see texture features and possibly different patterns in the images that humans can’t, could lead to earlier cancer detection.”
While a radiologist will read every mammogram, the AI tool will be turned on for half and generate information that may or may not help the radiologist make the final diagnosis.
In addition to Dr. Lee, who serves as the national co-principal investigator, four other UW Department of Radiology faculty members will help lead this pivotal trial. That includes Drs. Elezaby and Woods as co-site PIs, as well as Richard Bruce, MD and John Garrett, PhD as co-investigators.
Through TV news segments, radio interviews, podcasts, and articles in October 2025, Drs. Lee, Elezaby and Woods provided information about the trial and their hopes for AI use in breast cancer screening.
Ryan Woods’s Interview with WBAY Action 2 News WBAY Action 2 News Host Chris Roth interviewed Dr. Woods and discussed the skepticism of AI usage. Dr. Woods emphasized that the AI tool would only be used to support the radiologist.
Ryan Woods’s Interview with Wisconsin’s Midday News
Dr. Woods sat down with hosts Greg Matzek and Jessica Tighe for the 620 TMJ Radio show, Wisconsin’s Midday News. He explained how UW–Madison became the only trial site in the Midwest and shared his hopes for how an AI tool could help rural communities.
“In rural practices you may have radiologists who don’t have specific fellowship training in breast imaging,” Dr. Woods explained. “A tool like this can really improve their confidence and accuracy and ability to identify cancers and also decrease those false positives.”
Mai Elezaby and Christoph Lee’s Interview with Milwaukee Journal Sentinel
Drs. Elezaby and Lee emphasized the importance of balancing the excitement for the tool’s potential and the need to truly evaluate its effectiveness.
“With every technological advancement, there’s the enthusiasm for it, but I think the important thing is the caution,” Dr. Elezaby stated. She also noted that the trial will only use AI as an aid for the radiologist. “It’s almost like having a partner that is giving you some feedback,” she said.

Vivek Prabhakaran, MD, PhD contributes his expertise in neuroradiology to a new study examining why Native Americans in Wisconsin face disproportionately high rates of stroke.
The project, led by UW Department of Neurological Surgery Chair Robert Dempsey, MD, brings together citizens of the Oneida Nation and a team of researchers from the UW School of Medicine and Public Health.
The study aims to measure health factors in Native Americans. Ultrasound scans will check for plaque in the carotid arteries, which supply blood to the brain. In addition, MRI scans will track brain changes that may show signs of increased stroke risk.
“We hope that understanding the root causes of stroke risk disparity in this community will lead to more biomarkers to target in terms of future stroke preventive measures,” said Dr. Prabhakaran.
The research builds on an earlier study the Oneida Nation and university partnered on, which found about 80% of individuals age 54 or older had atherosclerotic plaque, and more than 40% had diabetes. The participants in this study also showed high levels of inflammatory proteins that can damage blood vessels and accelerate atherosclerosis.
Native Americans face the highest stroke risk of any racial group in the United States. The study conducted by the Oneida Nation and University of Wisconsin-Madison will explore how stress, historical loss and food sovereignty contribute to the onset of stroke risk factors.
“This partnership represents an important step forward in understanding and addressing the unique health challenges faced by Oneida people. By participating in research grounded in respect for our culture, we can better identify the factors driving stroke risk and work toward long-term prevention. The knowledge gained through this program not only benefits the Oneida Nation today but strengthens the health and well-being of future generations,” said Debra Danforth, Oneida Comprehensive Health Division Director.
Though focused on a small population, the project will provide preliminary data for a planned larger study which could benefit all Native American populations. The goal is to shape culturally sensitive approaches to reduce stroke risk in Native Americans and to gain knowledge about stroke prevention therapies.
“It’s a population that is unique in Wisconsin,” said Dr. Prabhakaran. “We need to be respectful of the Indigenous community’s system of beliefs and practices while conducting the study.”

This summer, seven dedicated medical students explored research opportunities with the UW Department of Radiology through the Shapiro Summer Research Program and the Radiology Equity Program. The Shapiro Program is part of a broader research initiative from the UW School of Medicine and Public Health, while the Radiology Equity Program is unique to the department. Both programs follow a similar structure: students work closely with a radiology faculty mentor, participate in clinical shadowing opportunities, and attend seminars that offer insight into the day-to-day life as a radiologist.
Meghan Lubner, MD has participated as a Shapiro mentor nearly every summer for the past decade. “It’s a nice way to expose students to radiology outside of the reading room” she explained. “When they’re on rotation, it can be difficult to showcase the field in all its glory. By conducting research, they can think more clinically, see the tools, and understand the data that we can extract beyond what we’re looking for to make a diagnosis in the reading room.”
Tai Le worked with Dr. Lubner and Perry Pickhardt, MD on a project focusing on opportunistic screening using body composition biomarkers extracted from abdominal CT scans by AI-tools. Specifically, he compared a Kenyan patient cohort and matched US African American and white American cohorts to understand how body composition biomarkers vary with race and geographic location.
Le echoed Dr. Lubner’s sentiments on the program’s benefits. “The clinical shadowing sessions dispelled a lot of the myths about the specialty for me. A common misperception is radiologists grind cases in a dark room all day without any human interactions. On ultrasound, I saw a mix of cool procedures like ultrasound-guided biopsy and paracentesis. And yes, bedside manners are still important to help patients feel comfortable during the procedures.” He noted that his experience with the program enhanced his understanding of the field and sparked interest in radiology as a potential career path.
Le also highlighted the positive atmosphere created within the department. “In the reading room, there was a lot of camaraderie between the residents and faculty radiologists. They worked as a team to manage the reading list and shared interesting cases with each other.”
• Kiara Didriksen, Mentor: Anand Narayan, MD, PhD
• Adam Ghouse, Mentor: Erica Knavel Koepsel, MD
• Muhaison Ibrahim, Mentor: Aaron Eifler, MD
• Tai Le, Mentors: Meghan Lubner, MD and Perry Pickhardt, MD
• Zamzam Nur, Mentor: Pallavi Tiwari, PhD
• Brent Robley, Mentor: Ryan Woods, MD, MPH
• Joey Yang, Mentor: Pallavi Tiwari, PhD
Lonie Salkowski, MD, PhD brings three qualities to the world of radiology education: passion, creativity and a spirit of intellectual generosity. Through her innovative approaches to curriculum development, she is deeply committed to refining the best practices for teaching students and sharing her insights with fellow educators, fostering a culture of collaboration and continuous improvement.
Dr. Salkowski began her educational path in science earning a bachelor’s degree in biology and chemistry from Mount Mary College in 1986. She earned her medical degree at the Medical College of Wisconsin in 1991, where she later completed a breast imaging fellowship in 1998. While studying radiology, she saw how steep the learning curve could be.
“The first time you’re looking at medical images, it’s a huge jump to take what you learned in anatomy and apply it to the X-ray,” she said.
Dr. Salkowski joined the University of Wisconsin Department of Radiology as a faculty member in 2005. She enrolled in the UW School of Education soon after and earned her master of science in Educational Leadership and Policy Analysis in 2013 and then her doctorate in Curriculum and Instruction in 2017. Dr. Salkowski traces her interest in learning and education during her time as a medical student.
“I realized that everybody learned differently,” Dr. Salkowski recalled. “Some caught on really fast, and some took a little bit longer. I started thinking, ‘why did that person do it so efficiently, and why is that person struggling?’”
After earning her master’s and doctorate, Dr. Salkowski explored new ways to teach to help those who struggled with learning, including through games. She co-designed Anatomy Pro-Am, a Facebook game that taught anatomy, biomedical imaging and cancer treatment, while also helping medical professionals improve treatment strategies for patients.
She collaborated with colleagues from across the university, including R. Benjamin Shapiro of the

Wisconsin Institutes for Discovery; Kurt D Squire, a former digital media professor; and Rock Mackie, a professor of medical physics. Together, they tackled a common challenge: students struggling to connect twodimensional diagrams with three-dimensional anatomy. Their efforts expanded into several projects, including a simulation lab funded by a grant from the Radiological Society of North America’s Research & Education (RSNA) Foundation.
The original version of the lab allowed users to guide a CT scan of the human torso with a handheld probe and view real-time images on an iPad. Dr. Salkowski utilized the lab in a study researching how novices and experts interpret radiology images. The goal of the project was
to find ways to improve how students achieve expertise in the field of radiology.
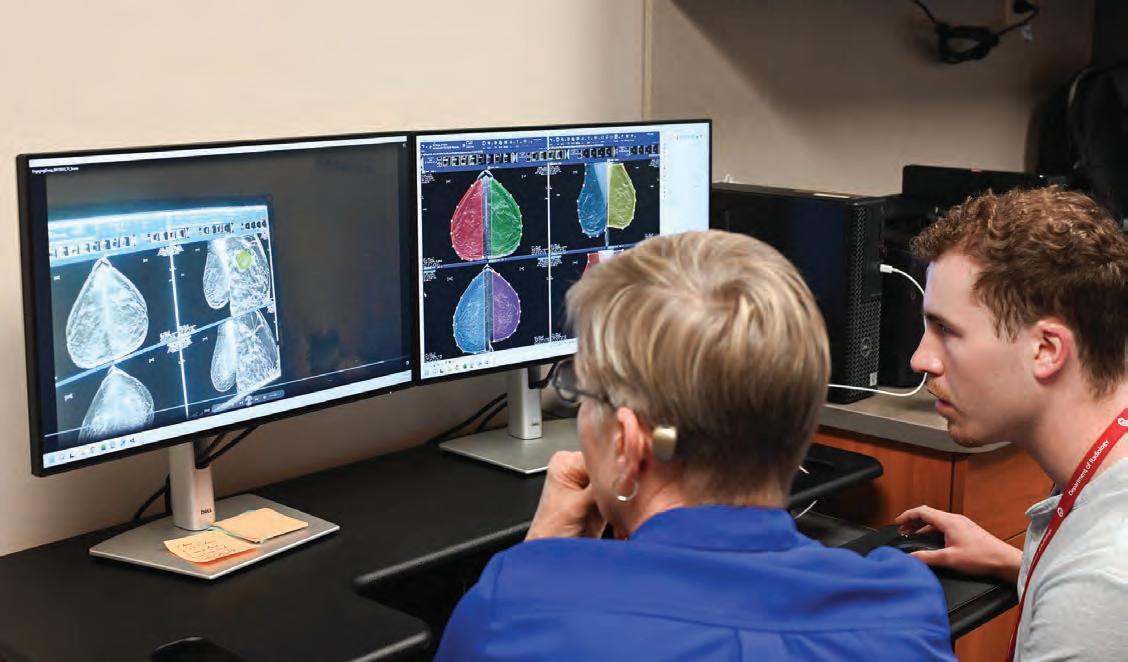
As technology evolved, the simulation lab has also undergone changes. Today, the torso is gone and has been replaced with several computer stations and a pair of special glasses that can track the user’s eye movements while they review cases. This allows the system to follow exactly how the learner examines images of breast scans.
“In real time, the work we’re doing is giving us some idea of how residents are processing mammograms,” Dr. Salkowski explained. “We can turn that knowledge back into improving how we teach them.”
In addition to scientific research, Dr. Salkowski has also shared her expertise through textbooks. She co-authored several editions of Weir & Abrahams’
Imaging Atlas of Human Anatomy, even reaching international audiences with translations in French, Spanish, Italian, Portuguese, Japanese, Chinese, and Korean.
Her contributions to the textbook have earned recognition from The British Medical Association, including the honor of Highly Commended Title in the Basic and Clinical Science category for the fifth edition of Weir & Abrahams’ Imaging Atlas of Human Anatomy. In 2021, Dr. Salkowski received the Medical Book Award in the same category for the sixth edition of the textbook.
For Dr. Salkowski, her work in research and education is both a profession and a passion, that keeps evolving.
“You can’t stay in an old format just because you want to,” Dr. Salkowski said. “You have to adapt, and I like using technology to make that possible.”

This year, over 50 faculty members, trainees, and medical students shared their expertise through presentations, posters, and workshops at the Radiological Society of North America (RSNA) 2025 Annual Meeting.
Thomas Grist, MD received the RSNA Gold Medal, the highest honor awarded by the society, in recognition of his remarkable service to the science of radiology. This marks the second RSNA Gold Medal for a faculty member, with Elizabeth Burnside, MD, MPH receiving one at the 2024 meeting.
Mark Schiebler, MD received an Honored Educator award, and Christopher Brace, PhD; Paul Laeseke, MD, PhD: and James Pipe, PhD were inducted into the Council of Distinguished Investigators Class of 2025 by the Academy for Radiology & Biomedical Imaging Research.
Faculty, trainees, and students also received the following accolades:
• Giuseppe Toia, MD, MS; Prashant Nagpal, MD; and Nicholas Laucis, MD were featured speakers at GE HealthCare’s CT Innovation Night.
• Matthew Lee, MD; John Garrett, PhD; Joshua Warner, MD, PhD; and Perry Pickhardt, MD received a Certificate of Merit for their education exhibit “Untapped Potential: Adding Value Through Image-Based Opportunistic Screening.”
• Dania Daye, MD, PhD and Perry Pickhardt, MD received a Certificate of Merit at for “Transforming Patient Care: Radiologist-Driven Consultations with Opportunistic CT Screening.”
• Cardiothoracic Imaging Fellow Andrew Moore, MD received a Certificate of Merit for the education exhibit “A Fundamental Approach to Smoking Related Interstitial Lung Disease.”
• Nuclear Medicine Resident Anna Giarratana, MD, PhD was selected for the RSNA Introduction to Academic Radiology (ITAR) program.









This fall, radiology residents and medical students took part in Communities Crushing Cancer, a national patient outreach effort. They spoke with patients at UW Health to explain image-based screening options and distribute educational graphics that they helped create.


Mai Elezaby, MD and Anand Narayan, MD, PhD spoke at the state assembly, advocating for Gail’s Law, a bill that would require health insurance to cover diagnostic and supplemental breast screenings for individuals at increased risk of breast cancer.


Faculty members have been busy connecting with medical students! Activities have included small group mentoring sessions, radiology jeopardy, hands-on interventional radiology demonstration sessions, and more!

This fall, Perry Pickhardt, MD spent two weeks touring China, building interdisciplinary relationships and delivering talks on the use of artificial intelligence (AI) in radiology. The tour was part of Dr. Pickhardt’s Distinguished Scientist, President’s International Fellowship Initiative (PIFI) award that he received from the Chinese Academy of Science (CAS).
Open to scientific research personnel worldwide, PIFI encourages scientific cooperation and promotes research communication globally. Xin Gao, PhD, an expert on AI and imaging technology research at the Suzhou Institute of Biomedical Engineering and Technology, nominated Dr. Pickhardt for the Distinguished Scientist award. Drs. Pickhardt and Gao have previously collaborated on a multicenter research project to develop and evaluate a deep learning model to diagnose rectal cancer.
Dr. Pickhardt spoke at several institutions throughout China. In his lectures, he focused on how AI can be leveraged in radiology; highlighting his work on opportunistic screening and estimating biological age using CT biomarkers.
Both topics utilize AI-based tools to analyze characteristics of a patient’s CT scan that would otherwise be time consuming in a clinical setting. Typically, a patient undergoes a CT scan to determine a diagnosis, like the cause of acute abdominal pain. Opportunistic screening goes a step further by looking at the additional metrics such as bone mineral density, skeletal muscle, and liver fat; which can be used to evaluate the patient’s overall health and wellness.
In a related sense, biological age estimations use metrics from CT scans to form a predictive model that appears to outperform other metrics like chronological age and epigenetic data. In clinical settings, this could help health care professionals better understand the characteristics that may be causing a higher biological age in a patient and tailor medical and lifestyle changes to lower the advanced biological age.
In addition to his lectures, Dr. Pickhardt engaged in the culture such as visiting the famed Terracotta Army and other UNESCO World Heritage Sites.

Physician. Teacher, Inventor. These are just a few of many roles that Fred Lee Jr., MD has embraced throughout his career with the University of Wisconsin Department of Radiology. He is widely recognized as a passionate advocate for advancing the field, whether it’s through improving patient care, mentoring the next generation of radiologists, or translating groundbreaking research.
This spirit of excellence embodies the newly established Fred Lee, Jr., MD Professorship of Abdominal Imaging and Intervention. Made possible by a generous gift from Dr. Lee, the endowed professorship will support the research of a faculty member in the Section of Abdominal Imaging and Intervention. Dr. Lee has been steadfast in his belief that UW Radiology is one of the best and brightest departments, and the professorship will ensure that it continues to be a driving force for innovation.
In part, Dr. Lee was inspired to donate funds to create the professorship to help support others who have novel ideas. He often cites that his success is due to the support he received throughout his career.
“All of our chairs have been huge supporters, from Joe Sackett who helped purchase our first ablation equipment, Pat Turski who didn’t fire me when I lost a rat in the CT scanner and gave me my first leadership position as abdomen section chief, Tom Grist who encouraged the translation of our ideas into products that have changed the world, and now Scott Reeder
who is pushing us to get histotripsy into widespread clinical use. This is a special place, and we shouldn’t take it for granted.”
There is no doubt that Dr. Lee has made a lasting impact on both the department and the field of radiology itself. With the establishment of the Fred Lee Jr., MD Professorship of Abdominal Imaging and Intervention; the department looks forward to the next generation of novel ideas that Dr. Lee’s legacy will inspire.
Several of Dr. Lee’s colleagues and collaborators shared their insight into how he has helped shape the department and make a difference in the lives of patients worldwide.
Thomas Grist, MD, former department chair:
“Dr. Fred Lee combines his clinical acumen, creativity, and transformative leadership to improve the health of his patients and raise the level of health care provided by his colleagues near and far. As section chief, he transformed the Abdominal Imaging and Intervention section into one of the world’s most recognized team of leaders in the field.
As vice chair for clinical operations for UW Radiology, he helped the department become a clinical leader within UW Health and applied his creative energy in areas well beyond his immediate clinical interests. Finally, as an inventor and entrepreneur, Dr. Lee successfully navigated the complex world of technology development and commercialization to disseminate his research for the benefit of countless cancer patients throughout the world.
As his professional colleague for the past three decades, I can think of few others who demonstrated such a transformative impact on our field. Fred truly embodies the Wisconsin Idea in action.”
Michael Tuite, MD, longtime colleague of Dr. Lee:
“Fred Lee was a year ahead of me as a resident at the University of Rochester, New York. Even then Fred was super smart and ambitious, so I knew he was destined to be one of the top abdominal radiologists when he joined
UW–Madison. Fred’s enthusiasm for UW Radiology got me excited to join a year later, and in those early years when Fred, Tom Grist and I would be on a fishing trip sitting around the campfire he would always proclaim in his understated way that ‘We’re making UW the best radiology department in the country.’ Fred truly made the Abdominal section the best in the country!”
Erica Knavel Koepsel, MD, current chief of the Section of Interventional Radiology and former mentee of Dr. Lee:
“Fred is a force. He is brilliant, contagiously inspiring, and operates on a level we can only hope to reach. Fred took a chance on me as a medical student and changed my career trajectory. It was his strong mentorship that set the tone, fair and tough but always having fun. Fred is the greatest advocate and sponsor, not just for me, but for those who have the opportunity to work with him. We stand on his shoulders of greatness; and I am honored to be his mentee, colleague and friend.”
Daniel Van Der Weide, PhD, professor of engineering and longtime collaborator of Dr. Lee:
“I first met Fred through our kids and being in the same Nakoma neighborhood of Madison. We soon found a shared interest in solving immediate clinical problems with rigorous engineering. Fred would identify these needs, and I would propose solutions borne out of naïveté that once in a while showed some promise. Fred had an unusually clear way of articulating unmet clinical needs, not in abstract terms, but grounded in
what actually happens in procedures. Furthermore, his enthusiasm and care for patients is infectious, in the best way possible.
What many people do not see behind the scenes is how deeply Fred would engage in the problem-solving process, which is the essence of engineering. With both NeuWave and Elucent, he was not just a clinical advisor but a true co-inventor. He challenged assumptions, pushed for simplicity and reliability, and constantly asked how a technology would behave in the hands of a busy clinician. Those conversations fundamentally shaped the designs and helped ensure that the systems we built were not just technically elegant, but clinically relevant. His willingness to take the long view and not the short-term easy way out was what kept us going in the early days.
Some of my favorite memories working with Fred are working in the animal lab, especially when we tried low-cost but somewhat less polished microwave power generation techniques that would generate sparks, burnishing my mad-scientist bona fides in his eyes. We held many candid discussions where medicine, engineering and management of a startup all got balanced attention. He has brought humility, curiosity, and an unwavering focus on patient outcomes to every interaction. Fred had a rare ability to bridge disciplines and people, and that is a big part of why both NeuWave and Elucent succeeded in moving from ideas to technologies that have helped tens of thousands of patients.”

Anu Brixey, MD joined the Section of Thoracic Imaging as an associate professor. Dr. Brixey was previously a faculty member at Oregon Health & Science University (OHSU) and subsequently the Portland VA where she served as chief of cardiac imaging and chief of ultrasound. Her professional interests include interstitial lung disease, pulmonary embolism, and trainee education.

Nancy Ann Little, MD joined the Division of Community Radiology as a clinical assistant professor. Dr. Lit tle served as chief resident during her diagnostic radiology residency with the UW Hospitals and Clinics. After residency, she trained in interventional radiology at the University of Alabama Birmingham. Her professional interests include pelvic, deep venous and oncologic interventions.

Monique Mogensen, MD joined the Section of Neuroradiology as an associate professor. While she was at the University of Washington School of Medicine, Dr. Mogensen served as director for the neuroradiology fellowship program. Her professional interests include general neuroradiology, CT applications in neuroradiology, and training and education.

Jennifer Pitts, MD has joined the Section of Emergency Radiology as a clinical assistant professor. Dr. Pit ts completed her Diagnostic Radiology residency at the UW Hospitals and Clinics where she served as chief resident. After training, Dr. Pitts practiced at the Virtual Radiologic Corporation where she read primarily emergent studies from facilities in 11 states.

Nathan Skinner, MD, PhD joined the Section of Abdominal Imaging and Intervention as an assistant professor. He earned his medical degree and doctorate in biophysics at the Medical College of Wisconsin. He attended the Mallinckrodt Institute of Radiology in St. Louis for his residency and advanced abdominal imaging fellowship. His professional interests include education and magnetic resonance imaging.

Alexandra Christensen, PhD joined the Section of Clinical Imaging Physics as an assistant professor (CHS). While earning her master’s degree and doctorate in medical physics at UW, Dr. Christensen worked in the Quantitative Ultrasound Lab. Her professional interests include using quantitative ultrasound techniques to explore tissue microstructure.

Kevin McDonald, MD has joined the Sections of Cardiovascular Imaging and Thoracic Imaging as an assistant professor. Dr. McDonald completed his intern year, residency, and cardiothoracic imaging fellowship at the University of Wisconsin Hospitals and Clinics. During his residency, he was awarded the Medical Student Award for Outstanding Teaching by a Resident.

Katharine Molinarolo, MD joined the Division of Community Radiology as a clinical assistant professor. Dr. Molinarolo completed her bachelor’s and medical degrees at UW–Madison as well as her abdominal imaging and intervention fellowship. Most recently, she practiced at Radiology Associates in Appleton, WI. Her professional interests include collaborative learning and community engagement.

Leonardo Rivera-Rivera, PhD has joined the Section of Imaging Sciences as an assistant professor. He obtained his PhD in physics and completed his postgraduate studies in MRI neuroimaging at UW–Madison. Most recently, he worked in the Department of Medicine as an associate scientist and will continue to serve as co-leader and MRI service leader of the Wisconsin Alzheimer’s Disease Research Center Imaging Core.

Troy Tenbrunsel, MD joined the Division of Community Radiology as a clinical assistant professor. Dr. Tenbrunsel joined the University of Wisconsin Hospitals and Clinics for his residency and abdominal imaging and intervention fellowship. His professional interests include medical education, abdominal MRI, and ultrasound-guided intervention.

Justin Brucker, MD and Susan Rebsamen, MD featured in


Anu Brixey, MD interviewed by
Justin Brucker, MD and Susan Rebsamen, MD had their case report “Sturge-Weber Syndrome Without Cutaneous Stigmata Versus Encephalocraniocutaneous Lipomatosis Without Craniocutaneous Lipomatosis” featured in the latest issue of the Wisconsin Medical Journal Read the case report here.
Anu Brixey, MD was featured in the Modern Healthcare article “The new side gig for doctors - testing AI models for developers.” Read the article here.

Christoph Lee, MD, MS, MBA featured by


Jamey Weichert, PhD interviewed by


Woods, MD, MPH

Christoph Lee, MD, MS, MBA was featured in an article from the UW School of Medicine and Public Health for World Breast Cancer Research Day. The article highlighted Dr. Lee’s work on an NIH funded study evaluating four different FDA-approved algorithms for mammography interpretation. Read the article here.
Jamey Weichert, PhD was interviewed for the Medscape article “How ‘Theranostic’ Drugs Diagnose and Treat at the Same Time.” He explained how theranostic drugs target tumors directly. “Theranostics uses a tumor-selective molecule that’s injected intravenously and finds all the tumors in the body.” Read the article here.
In an October 22, 2025, News 3 Now segment, Ryan Woods, MD, MPH helped raise awareness of breast cancer occurrence in men and what symptoms to look out for. Watch the segment here.
The second annual University of Wisconsin Radiology Summit gathered together new and familiar faces from across the country for a week of learning, connecting and skiing the majestic mountains in Park City, Utah. Hosted by the UW Department of Radiology, the Summit grew in attendance while continuing to provide a relaxed atmosphere ideal for the educational event.
“In addition to alumni and UW colleagues, we were happy to welcome radiologists who heard about the Summit by word-of-mouth and the internet,” said Summit Co-Director Tabby Kennedy, MD. “This demonstrated a need for in-person, informal events where radiologists can earn CME credits while building a wider network of colleagues.”
Planned by Co-Directors Dr. Kennedy and Roberta Strigel, MD, MS, the program ran from Monday, January 19 through Thursday, January 22, 2026, and featured 24 sessions led by 11 faculty members. Participants learned about fetal anomalies, contrast agents, mammographic
• Hailey Allen, MD
• Gregory Avey, MD
• Jeffrey Kanne, MD
• Tabassum (Tabby) Kennedy, MD
• Thomas (Tommy) LoDuca, MD
• Alan McMillan, PhD
• Ali Pirasteh, MD
• Scott Reeder, MD, PhD
• Jessica Robbins, MD
• Roberta Strigel, MD, MS
• John Symanski, MD
Trainee Exhibitors:
• Bhoomi Davé, MD
• Sean Duminie, MD
• Jessica Perry, MD
• Erik Winterholler, MD
asymmetries and even ski injuries. They also received an AI starter kit tailored for radiologists.
Joining the faculty presenters, trainees had the opportunity to share their research as electronic exhibits.
“Including residents and fellows was always a priority when planning the Summit,” Dr. Strigel explained. “We’re fostering connections that will span careers so it’s never too early to participate!”
The welcome reception at the start of the week gave people a chance to introduce themselves – and find a partner to ski the slopes with!
Park City boasts 7,300 acres of skiable terrain including paths into the historic downtown – the perfect way to slide into a leisurely lunch or gourmet dinner! And if a day of learning and outdoor activities require a more low-key evening, the Grand Summit Hotel offered an expansive heated pool and hot tubs.


To confirm that the department has updated contact information, people can send an email to radnews@uwhealth.org or contact the co-directors directly. Next year’s dates will be announced on the UW Radiology Summit webpage

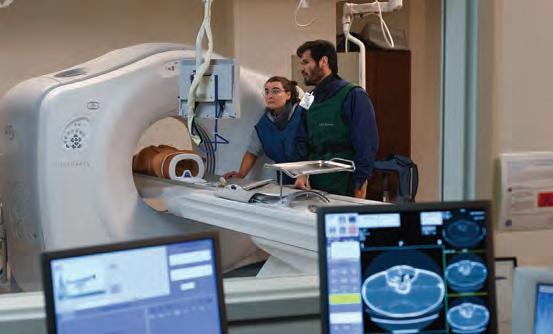
This summer, the department hosted our first Computed Tomography Protocol Optimization Workshop (CT-POW).
CT-POW is an interdisciplinary, hands-on conference dedicated to enhancing CT protocols and workflows. This event provides a unique opportunity to collaborate, learn, and implement practical solutions to optimize CT imaging practices.
Join us this August for the next session! In addition to the immersive lab sessions, participants will gain skills to help with problem solving everyday CT protocol challenges and actionable takeaways that can be immediately implemented into practice.
The workshop is recommended for professionals in CT imaging, including:
• Radiologists - Learn how protocol optimization impacts diagnostic accuracy and patient outcomes.
• CT Technologists - Gain insight into advanced scanning techniques and workflow improvements.
• Medical Physicists - Explore strategies to minimize radiation dose while maintaining image quality.
• Imaging Informaticists - Discover best practices for integrating protocols into clinical systems.
Learn more and sign up online



Matthew Larson, MD, PhD became the faculty leader of the Clinical Research Imaging Core (CRIC).
Scott Perlman, MD is serving as interim chief of the Section of Nuclear Medicine & Molecular Imaging and interim program director of the Nuclear Medicine Residency Program. The role was previously held by Steve Cho, MD.


Jakub Siembida, MD is now an associate program director of the MRI fellowship.
Giuseppe Toia, MD, MS is now the modality chief of computed tomography. The role was previously held by Meghan Lubner, MD.
Diego Hernando, PhD and Oliver Wieben, PhD each received a Vilas Faculty Mid-Career Investigator Award in recognition of research and teaching excellence.
Meghan Lubner, MD was a guest on the Science Fare podcast episode “Careers in Cancer Care, How Oncologists and Radiologists Can Best Communicate, and How AI is Helping in Cancer Diagnosis and Treatment.”
Pamela Propeck, MD has been selected for a third term as a trustee for the American Board of Radiology (ABR) and will serve in this position through October 2028.
Wenhui Zhou, MD, PhD has been appointed to the UW Building Interdisciplinary Research Careers in Women’s Health (BIRCWH) program’s 202527 cohort of scholars and will receive mentoring, curricular, and research support to advance their careers in women’s health.

Alan McMillan, PhD became the new section chief for the Section of Imaging Sciences in January 2026 after Frank Korosec, PhD stepped down from the role after 15 years.

Scott Reeder, MD, PhD has been elected to serve as Clinical Department Chair Director on the UWMF Board of Directors. He will serve a three-year term.

Teresa Sommerfeld became the interventional radiology manager. She will have oversight of UH, AFCH, and EMC operations and will continue to work closely with physicians, technologists, and the nursing team to streamline operations.
Elizabeth Burnside, MD, MPH and Weibo Cai, PhD were honored at a reception hosted by Chancellor Jennifer Mnookin, highlighting Dr. Burnside’s RSNA Gold Medal and Dr. Cai’s American Association for the Advancement of Science fellowship.
Due in part to Robert Bour, MD’s leadership and Greg Avey, MD’s subspecialty expertise, the National Government Services has officially added coverage for MRA head and neck for stroke symptoms. This has been a multi-year priority for the Wisconsin Radiological Society and the American College of Radiology.
Alisa Walz-Flannigan, PhD and Frank Ranallo, PhD were invited to serve on the Wisconsin Department of Health Services’ DHS 157 Advisory Committee.
Shawn Drulia, PA was nominated for the Excellence in Clinical Practice Award by UW Health for their celebrations during Advanced Practice Provider week.
Elizabeth Sadowski, MD has been appointed as the next chair of the American College of Radiology (ACR)’s O-Rads Committee.
Perry Pickhardt, MD has been interviewed by the American Journal of Roentgenology (AJR), RSNA, and AuntMinnie.com about the recently published paper “CT Colonography for Colorectal Cancer Screening and Prevention: 20-Year Programmatic Experience at a U.S. Academic Medical Center. Max Golden, MD and David Kim, MD co-authored the paper.
Laura Eisenmenger, MD was featured by the National Center for Advancing Translational Sciences (NCATS) at the CTSA program update for her research on vessel wall imaging and continued research on imaging development.
David Bluemke, MD, MSD, PhD’s study “Use of CT-derived non-cardiovascular calcification marker for predicting cardiovascular events among diabetic older adults: the multi-ethnic study of atherosclerosis” was featured in The Imaging Wire.
Weibo Cai, PhD was quoted in an Imaging Technology News article on a new PET tracer for same-day imaging of triple-negative breast and urothelial bladder cancers.
Matthew Lee, MD; Perry Pickhardt, MD; Giuseppe Toia, MD; Meghan Lubner, MD and David Kim, MD’s publication “Acute Mesenteric Ischemia: Pathophysiology-based Approach to Imaging Findings and Diagnosis” was featured in RSNA’s Highlights newsletter.
Resident Christian Cuevas, MD received a Cum Laude Award at SABI for “AI-derived visceral fat attenuation is a better predictor of all-cause mortality than visceral fat area and BMI.”
Alejandro Roldán-Alzate, PhD received the Ser Saber and Servir Award from Universidad EIA. The award celebrates the important contributions and impact that the university’s alumni have made.
Ali Pirasteh, MD was inducted as a society fellow at the Society for Advanced Imaging (SABI) annual meeting.
Matthew Lee, MD received the Foundation Award at the SABI meeting for “AI-derived CT muscle attenuation is a stronger predictor of mortality risk than muscle area in a large adult population with age and sex specific variation.”
Ryan Woods, MD, MPH will be inducted as a Fellow of the American Medical Informatics Association (AMIA) during their 2026 conference.
Anand Narayan, MD, PhD received a Silver Medal for Exceptional Manuscript Review from the Journal of the American College of Radiology.
Jessica Robbins, MD has been elected as senior deputy editor for Academic Radiology and as a member of the editorial executive committee. Allison Grayev, MD has been elected as a deputy editor; Teresa Chapman, MD and Dania Daye, MD, PhD have been elected as associate editors.
Giuseppe Toia, MD, MS was featured in the DOTmed HealthCareBusiness News article, “GE HealthCare unveils its first photon-counting CT system ahead of RSNA.”
Christoph Lee, MD, MS, MBA was interviewed by Diagnostic Imaging about multi-stage AI-driven workflow for breast cancer detection for the article “Mammography Study: Multi-Stage Use of AI for DBT Exams Yields Over 21 Percent Increase in Breast Cancer Detection.”
B. Dustin Pooler, MD; John Garrett, PhD; Matthew Lee, MD; and Perry Pickhardt, MD’s paper “CT-Based Body Composition Measures and Systemic Disease: A Population-Level Analysis Using Artificial Intelligence Tools in Over 100,000 Patients” received the Best of AJR award in the Multispecialty Imaging section for 2025.
Perry Pickhardt, MD was interviewed by RSNA for their article “Knowing When to Respond to Incidental Findings.“
Jade Anderson, MD has been selected by the Wisconsin Medial Society Foundation as the 2026 recipient for the Kenneth M. Viste, Jr., MD Young Physician Leadership Award.
John Swietlik, MD and Erica Knavel Koepsel, MD have opened the BOOMBOX clinical trial for histotripsy of liver tumors, and accrued their first two patients.
Christopher Brace, PhD; Paul Laeseke, MD, PhD; and James Pipe, PhD were inducted into the Council of Distinguished Investigators Class of 2025 by the Academy for Radiology & Biomedical Imaging Research at RSNA 2025.
Abdominal fellow Ben Prout, MD won first place in the Kalender Competition Early Career Investigators Award for Recognizing Outstanding Scientific Research at the International Society of Computed Tomography (ISCT).
Prashant Nagpal, MD has been appointed chair of the Society of Cardiovascular CT’s Cardiac CT Board.
Wenhui Zhou, MD, PhD has been selected to participate in the 2025-26 RSNA Advanced Course in Grant Writing.
Alan McMillan, PhD has been selected as a deputy editor for Radiology and will take lead for AI-related submissions.
Michael Hartung, MD was featured in the Class Notes of Quarterly for collaborating and launching the Abdominal CT Essentials continuing medical education course with Radiopaedia.
Thekla Oechtering, MD, PD Dr med was named junior fellow of the Society for Magnetic Resonance Angiography (SMRA).
Matthew Lee, MD was interviewed for the RSNA News article “Imaging Plays a Pivotal Role in Diagnosing Acute Mesenteric Ischemia.”
Zahra Alyani Nezhad, a PhD student advised by Tim Szczykutowicz, PhD, won a Blue Ribbon Poster award for “Quantitative Analysis of Three Strategies for CTPA Scan Timing Optimization” at the annual American Association of Physicists in Medicine meeting.
PET Instrumentation Technologist Trish Tolan received the SNMMI-Technologist Section Career Advancement Grant, which supports nuclear medicine technologists wishing to pursue additional educational opportunities to advance their professional career.
Sean Golden, MD and Matthew Niemeyer, MD were featured in the Class Notes of Quarterly for performing the first known thyroid artery embolization for thyroid goiter in Wisconsin.
Anand Narayan, MD, PhD received the 20242025 Editor’s Distinguished Reviewer award from the Journal of Breast Imaging (JBI).
Sanna Herwald, MD, PhD has been selected to participate in RSNA’s 2026 Clinical Trials Methodology Workshop.
Amy Fowler, MD, PhD has been elected to serve as assistant editor, breast imaging for RSNA’s RadioGraphics editorial board.
Andrew Ross, MD, MPH was named as one of AJR’s Distinguished reviewers for 2025.
Bracco Fellow Julius Heidenreich, MD received the Moncada Award at SABI for “Pulmonary MR angiography with gadopiclenol can reduce gadolinium exposure while maintaining signal enhancement.”

Erin Bravo, MD completed her residency and Breast Imaging and Intervention fellowship at University of Wisconsin Hospital and Clinics in 2017. Currently, Dr. Bravo works as the medical director at Solis Mammography in Phoenix, Arizona; a breast-only outpatient imaging center. Learn more about Dr. Bravo, and her time at UW–Madison below!
What’s your favorite aspect of being a radiologist?
I am a big true crime fan! In radiology, I feel we get to be detectives, as we play a large role in putting together the pieces in order to “solve” the case and make the diagnosis for our clinical colleagues.
As a breast radiologist, I love how my time is split between doing procedures, discussing diagnostic results with patients, and reading screening mammograms in my quiet reading room (often while listening to true crime podcasts).
What career milestones have you achieved since your time at UW–Madison?
Due to the outstanding training I received at UW–Madison, I have become a well-respected breast radiologist in the Phoenix community. Many of the breast surgeons have me on speed-dial and often look to me for my opinion on breast radiology cases. Also, my time at UW provided me with the tools to be the Medical Director for the Solis Mammography Centers in the greater Phoenix area.
How would you say your training at UW–Madison has helped you in your career?
The radiology training at UW is top notch. Being able to train under radiologists who are world-renowned experts allowed me to be a successful radiologist in my community. The attendings at UW made resident and fellow education a priority, and I felt more than prepared to practice on my own upon completion of training. Reading exams independently while on call, regular didactic lectures and case conferences, extensive board review lectures, and staffing-out with attendings during the day all have contributed to my career success.
What’s your favorite memory from your time at UW–Madison?
The camaraderie and friendships you develop during training will last a lifetime! I have so many good memories of us hanging out in the resident room after morning and noon conferences; to the dismay of some attendings because we were a little late getting back to our assigned reading rooms. We developed friendships that have lasted to this day.
What advice would you share with prospective and current trainees at UW–Madison?
Enjoy your time and try to enjoy the training process as much as you can. The more you get out of residency, the easier your career will feel.
Also, try to enjoy Madison as much as you are able. Madison has so much to offer and is a great place to live, so take advantage while you can!

Although Joseph Sackett, MD stepped down as chair of the University of Wisconsin Department of Radiology 30 years ago, his impact continues to be felt throughout the field. From advancing spine imaging to transforming the department’s structure and policy, Dr. Sackett’s research and leadership helped shape modern radiology in Wisconsin and beyond.
Dr. Sackett graduated from Tulane University School of Medicine in 1966 and joined the department in 1974. He was the first radiologist in North America to publish a pivotal study demonstrating the safety and efficacy of metrizamide as a contrast agent for spine imaging in 1977. His research marked a significant improvement over oil-based agents, and today’s metrizamide techniques are still informed by his findings.
In the 1970s, Dr. Sackett assisted colleague Charles Mistretta, PhD in developing digital subtraction angiography (DSA), even volunteering himself as a test subject. The procedure went smoothly, aside from the contrast solution giving Dr. Sackett hives, which he shrugged off when recalling the incident.
“It was not a major reaction,” he said.
Despite the minor allergic episode, their work paid off. Today, DSA remains a vital medical imaging technique for visualizing blood vessels. A 2019 article from the journal Stroke hailed the procedure as the “current gold standard for confirming aneurysmal obliteration.”
Dr. Sackett’s collaborative leadership emerged early. He served as vice chair under Francis Ruzicka, MD who led the institution from 1976 to 1981. That partnership prepared Dr. Sackett to succeed Dr. Ruzicka as department chair.
“I worked closely with him,” Dr. Sackett said. “There weren’t any major secrets.”
Dr. Sackett also served as a mentor to Patrick Turski, MD who completed his internship and residency at UW–Madison. Dr. Sackett introduced Dr. Turski to the field of radiology and convinced him to pursue it as a career. In

1981, Dr. Turski joined the faculty, becoming chief of MRI in 1986, chief of the Section of Neuroradiology in 1993 and eventually replacing Dr. Sackett as the department chair in 1995, a full-circle moment.
“He’s an outstanding individual,” Dr. Sackett reflected on his successor. “I’m pleased he was willing to step in as chair when I retired.”
During Dr. Sackett’s career, more women were slowly joining the field of radiology. According to an American College of Radiology article, only 5.3% of radiologists were women in 1970, gradually increasing to 14% in 1995 when Dr. Sackett stepped down from his leadership role. The rise in female radiologists and trainees inspired many institutions to develop more inclusive cultures.
Shortly after his appointment as chair, a high-performing female resident approached Dr. Sackett, requesting time off to manage morning sickness and stress during her pregnancy. At the time, the residency program lacked a pregnancy policy, adhering to the Board of Radiology’s 6-week annual leave limit. Recognizing the gap, Dr. Sackett and faculty members established the first departmental pregnancy policy, granting up to four weeks of paid maternity leave for residents.
Soon after, male residents and staff requested leave to support their partners during childbirth. Dr. Sackett recommended one week of paid paternity leave, provided the service chief resident cleared it. These early policy changes reflected Dr. Sackett’s philosophy of supporting trainees as they pursued their personal and career goals, even if they went against contemporary recommendations.
“These policies do not deal with the broader issue of how a resident-in-training or a junior faculty member can be a mother and spouse, do justice to the training program and remain academically productive,” Dr. Sackett wrote in a 1987 Investigative Radiology article. “I know this opposes the position of some national organizations in radiology, but I believe we must be flexible in dealing with individual trainees and junior faculty.”
In the same article, he described an innovative part-time training arrangement for a female resident balancing child care while completing the residency program. Though the position extended the resident’s training, she wouldn’t have to sacrifice her career for motherhood.
Alongside policy changes, Dr. Sackett recognized the need to modernize the department’s technological capabilities. Though MRI technology was in its infancy when he became chair, he quickly positioned the institution to lead in this emerging field.
In 1984, the department began a collaborative research program with General Electric Medical Systems (now GE HealthCare) and installed the first MRI machine on campus. Previously, researchers traveled to GE’s facility in Waukesha, Wisconsin to access equipment.
Today, the department has access to over 20 MRI scanners for research, and its longstanding relationship with GE HealthCare has generated over 100 patents. In November 2023, GE HealthCare and UW–Madison announced a 10-year strategic collaboration to continue to advance medical imaging and improve patient care.
In 1981, the department comprised five subdivisions: radiotherapy, medical physics, nuclear medicine, radiobiology and diagnosis. During his tenure, radiotherapy joined the Department of Human Oncology, medical physics became a separate department and radiobiology shifted to the Clinical
Cancer Center (now UW Carbone Cancer Center). During this time, the advances in medical imaging technology necessitated additional subspecialties. By 1995, the department expanded to ten major sections, including skeletal, angio/interventional, neuroradiology, pediatrics, mammography, chest, VA radiology, nuclear medicine, MRI and body imaging.
Today’s 14 sections include most of those created in the Sackett era, with some renamed to accommodate changes in medical terminology or additional subspecialties. Recent additions include the Section of Emergency Radiology and Clinical Imaging Physics. Current Chair Scott Reeder, MD, PhD noted the latter “demonstrates the continued legacy and commitment of UW–Madison to the high standards in medical imaging required to provide optimal patient care.”
Dr. Sackett’s incredible work as a faculty member and chair lives on through the department’s legacy while his personal legacy is most visible in the Joseph F. Sackett Professorship in Radiology created in his honor to support the Section of Neuroradiology chief. Recipients of the professorship include inaugural honoree Howard Rowley, MD and the current holder, Tabassum (Tabby) Kennedy, MD
As the department approaches its centennial in 2027, Dr. Sackett’s words to present and future members remain simple.
“Just carry on and do as well as they have.”