




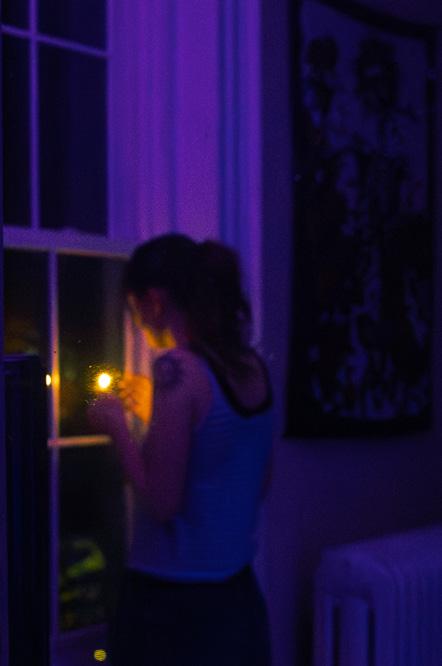











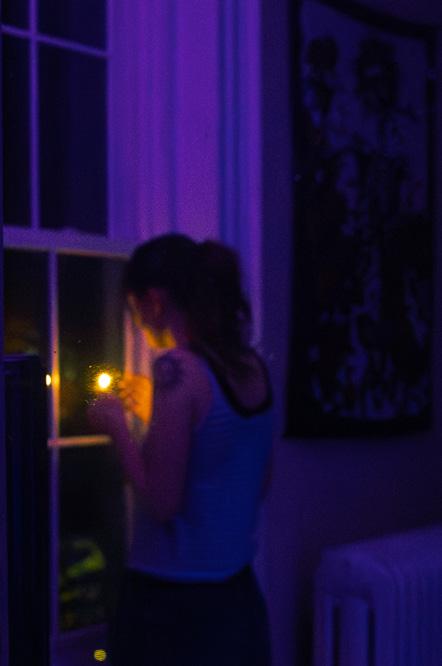












Dear reader,

Welcome back to the glossy pages of another Cynic special issue. This one’s about drugs. ‘Tis the season after all.
This semester, we set out to capture the current conversation surrounding drug use and culture in and around campus, offering a snapshot of young adults in 2026: what, where, how and why they’re using.
We’re not claiming this is entirely comprehensive. If it were, it would be a lot longer and significantly more concerning. If you think we missed something, take it up with us next year. Or better yet, write something yourself.
Whether you read every issue or just the special issues to hang them up on your dorm wall, we hope you enjoy. Roll one up, sit somewhere the cops can’t see you and take in the 18 pages we have to offer. But please, don’t smoke the pages. We worked too hard on them and honestly, the ink’s probably toxic.
In whatever state of being you find yourself right now, please indulge in this once in a semester treat responsibly. And as the last issue we’re sending to the printing press in our time here at the Cynic, we want to leave a little note of gratitude.
To every writer, photographer, illustrator, podcaster, copy editor and Instagram follower, you made our experience here one we can never and will never forget. We cannot express in words how special this publication is to us.
Thank you, Cynics.

Editor-in-Chief
Liliana Mefford Managing Editor


Erika
Josh






BY ANNA BOUCHARD
Idyllic countrysides dotted with red barns, small villages and beautiful views make up the Vermont many imagine.
What goes unseen, however, is how this rural environment can isolate those struggling with substance misuse from treatment programs and resources.
66.1% of Vermont’s population is estimated to live in a rural area, making it the most rural of the 50 states. Vermont also has higher rates of alcohol, marijuana and other illicit drug use than the national average among people aged 12 or older.
“Over the past couple of decades, some of the highest numbers [of overdose deaths] really come out of New England, and some of the highest actually come out of Vermont,” said Devika Singh, an associate professor at the Larner College of Medicine.
Singh is the principal investigator in a five-year study focused on understanding drug use trends and access to substance use treatment and safe syringe sites throughout New England.
Despite Vermont’s high overdose rates, the majority of New England-based studies have focused on urban settings, leaving the unique challenges to rural substance use treatment largely unexplored, Singh said.
“We don’t understand terribly well what the unique challenges are to rural populations, and this is our opportunity to learn,” she said.
As an R1 institution with Vermont’s only
Level 1 Trauma Center, UVM is in a unique position to have a substantial impact on understanding the challenges to substance use treatment in rural Vermont.
“It’s really, to some extent, our responsibility to be involved in this [research],” Singh said.
The study will be an opportunity for UVM to bridge academic research with community allies, Singh said.
“At UVM, we really want to know how to build better bridges and bolster existing ones with folks in downtown Chittenden County and other parts of the state,” Singh said.
For young adults and teens, experimenting with substances can be a common risk-taking behavior, said Christopher Smith, Chief Clinical Officer at Spectrum Youth and Family Services.
What substance use looks like for each person varies, but it becomes problematic when it interferes with the user’s participation in their typical daily activities. This could look like missing classes or no longer participating in hobbies, Smith said.
“People in their late teens and early twenties are looking to forge an identity that is separate and distinct from their families or communities of origin, and their relation to substances is not different,” Smith said.
For 20-year-old Vermont native Sierra Wedge, this exploration started when she was 12. After losing her father, she began to smoke marijuana and vape with friends.
“It was my way of coping. I was getting it from anybody I could, didn’t know if it was even safe. I was just putting my life at risk to be able to cope with that,” Wedge said.
Wedge’s marijuana use continued to increase throughout high school. She began smoking before, during and after school. Eventually, she dropped out.
“I was under a lot of stress,” Wedge said. “So I just resorted to that, and that’s how I spent my days. I dropped out of school because things had gotten so bad, and so I spent my whole day sitting in my bedroom smoking weed.”
While risk-taking behaviors among teens are not unique to Vermont, its significant rural population poses barriers to providing treatment for substance misuse.
“What we see in more rural parts of the state is that it’s harder to get treatment. It’s harder to participate in peer support groups like AA or other recovery activities,” Smith said.
This difficulty is often due to a lack of accessibility to the available services. Those in rural areas may be unable to reach medical and substance use treatment facilities due to a lack of public transportation.
“About four years ago, as an organization, we recognized that people in the young adult and adolescent range were struggling to get vast or immediate access to appropriate mental health and substance use treatment,” Smith said.
To address this, Spectrum increased the volume of its counselors, launched a cen-

tralized intake procedure and began providing mental health counseling through its drop-in centers, Smith said.
While treatment opportunities have increased, there are still significant barriers to accessing them.
“There’s a lot of good things out there, but the waiting lists are long, and there’s a lot of staff turnover at a lot of these really cool programs, and that limits the services that people are able to get,” said Martha, a mother of two teenagers who struggled with substance use, who is using a pseudonym for confidentiality.
Sam, Martha’s 16-yearold daughter, also using a pseudonym for confidentiality, began using nicotine products at age 11 and marijuana and alcohol around age 13. Throughout her teen years, she continued her use and added in a variety of illicit drugs.
family and her son.
“I feel like if we’d been able to get help the year before that, maybe it would have prevented a lot of this really hard, stressful stuff from happening,” Martha said.
Sam was eventually referred to Northwestern Counseling & Support Services by her physician. There, she participated in weekly therapy focused on developing healthy coping mechanisms and finding ways to step away from substance use.
Initially, Sam was hesitant about the treatment plan.
“I was a little bit rebellious. I didn’t want to [participate] and thought it was probably dumb,” Sam said.
With encouragement from her counselor, family and partner, Sam has reduced her
ment throughout Vermont will be connecting existing treatment programs with academics and advocates. In doing so, best practices for treatment can be learned and shared, Singh said.
This involves finding ways to reach those hesitant to find outside support. Like Sam, who was hesitant about participating in treatment through NCSS, Wedge was originally uninterested in participating in a treatment program.
“I didn’t think any programs would have helped me,” Wedge said. “I was a very to myself type of person, so I didn’t want help from anyone.”
When reflecting on her substance use, Wedge said that she was isolated from any support systems.

“[My friends and I] were using substances almost every day,” Sam said. “I definitely chose the wrong people to be around. I stopped talking to my family for a lot of [this time].”
Martha said that she felt her control slipping as Sam began high school and her drug use increased. Around the same time, Martha’s son began using substances as well.
“I had two teenagers spiraling, and I felt like I was not well equipped to handle it,” Martha said. “The only help I got was [the Department and Families] telling me very firmly that I needed to get control of this situation.”
For Martha’s son, the long waitlists for available programs meant that by the time he made it to the top of the list, he had been removed from her custody due to behavioral problems exacerbated by substance use. This put a significant strain on Martha’s
substance use to nicotine and occasionally marijuana.
“I’m glad I had NCSS there and that I had a counselor,” Sam said. “I’ve come so far.”
Martha said that getting her daughter treatment involved pushing aside the shame that can be associated with seeking out treatment programs.
“The instinct can be to hide and not let anybody know,” Martha said. “Reaching out for the help that is out there, and being open to advice, that can be really humbling.”
For those seeking programs for substance use, there can be significant variations in the quality of help.
“We’ve got places that are very strong, and places that could use a lot more of that similar kind of strength and energy,” Singh said.
Part of improving substance use treat-
“[Using substances] ruins your life, and it ruins your family dynamic and it makes people not want to be around you because of it,” Wedge said. It wasn’t until she left a toxic relationship that she opened herself up to the support of her mother and now best friend. With their help, she has been completely sober for four months. In addition to promoting social isolation, using substances at a young age increases the likelihood of lifelong substance use dependence. This makes having substance use treatment programs accessible to young adults particularly vital, Smith said.
For those struggling with substance use, Sam said that while finding available resources is hard, doing so is worth it.
“These programs are there to help you, not to be against you,” Sam said. “Don’t be afraid to reach out to them, because I’m glad that I did.”

BY ERIKA TALLY
During an advertisement featured in Super Bowl LX, 125.6 million viewers watched as a fit and toned Serena Williams cheerfully injected herself with a GLP-1 medication.
Graphics behind Williams touted her 34-pound weight loss, which she attributes to the company Ro, a direct-to-patient telehealth company — specifically its GLP-1-focused weight-loss program.
GLP-1 receptor agonists are a class of medications that imitate the naturally occurring GLP-1 hormone made by the small intestine, which regulates hunger, blood sugar levels and slows digestion.
These medications are marketed under recognizable brand names, such as Ozempic, Wegovy and Zepbound.
Williams’ endorsement comes at a decisive moment for the acceptance of these drugs in broader society.
Researchers at the University of Michigan found there was a 594% increase in the monthly number of adolescents and young adults using GLP-1s between 2020 and 2023.
With their rapid rise in popularity, GLP-1s are a new development in the cultural landscape of weight loss, but their controversial reputation and social stigma can overshadow the lived experiences of real patients.
In 2005, the FDA approved the first GLP-1 agonist, exenatide, for the treatment of type 2 diabetes. However, in recent years, the administration has approved several new GLP-1 medications to treat a different disease: obesity.
Taken either orally or via injection, GLP1s are effective for weight loss because they slow stomach emptying, making patients feel fuller for longer. They also send signals to the brain that increase feelings of satiety, which decreases food intake and appetite.
These drugs have entered the market at a crucial time in public health. According to the CDC’s National Health and Nutrition Examination, the prevalence of obesity among adults in the United States was 40.3% between 2021 and 2023.
Dr. Kaitlyn Vennard Barrett works as an assistant professor in the UVM Department of Medicine, specifically in the Division of Endocrinology and Diabetes. She describes GLP-1s as an important medical breakthrough for the treatment of obesity.
“These medications have totally changed the landscape of how we treat diabetes and obesity,” Barrett said. “We have clinical studies and a lot of anecdotal and real-life evidence to show us that on average, patients are losing 10% to 15% of their body weight, but a lot of times it’s a lot more than that.”
Medical professionals like Barrett stress the importance of having proper physician oversight during GLP-1 treatment to ensure that weight is lost safely. However, this advice has been largely ignored as GLP-1 drugs permeate the cultural zeitgeist, feeding into the media and society’s obsession with thinness.
This familiar preoccupation with body image has only intensified with the expansion of the GLP-1 market. Celebrities like Meghan Trainor and Sharon Osbourne confirmed that they used GLP-1s for weight loss, with Osbourne becoming the poster child for ‘Ozempic Face.’
Other stars have faced criticism for their drastic transformations, such as Ariana Grande and Cynthia Erivo, who were
accused of promoting unhealthy thinness during media tours for their movie “Wicked: For Good.”
Though the pair never confirmed the cause of their weight loss, the rapid change in their appearances sparked debate about how to talk about weight in the age of GLP-1s.
Celebrities are not the only ones swept up in the discourse. As awareness about GLP1s spreads, non-famous people on the drugs are facing mounting social disapproval surrounding their usage.
Dr. Barrett refuted this negative public perception, highlighting that the taboo surrounding obesity and weight loss is often to blame for pushback against these medications.
“I think, in general, being overweight and struggling with obesity is stigmatized. I think in mainstream media and popular culture, that sometimes medication can be looked at as a scapegoat or an easy way out,” said Barrett.
However, for patients like UVM sophomore Madeline Wick, taking these drugs was anything but easy. Wick started taking Zepbound during her senior year of high school, citing issues with weight loss and binge eating as her motivation.
“THESE MEDICATIONS HAVE TOTALLY CHANGED THE LANDSCAPE OF HOW WE TREAT DIABETES AND OBESITY.”
While taking the medication, Wick experienced uncomfortable side effects attributed to GLP-1 usage, such as nausea and vomiting.
“There were days where I would wake up, throw up and go to class. It could be really bad. And there are some days where you really just don’t want to eat and foods will kind of ick you out,” Wick said.
Despite the side effects, Wick continued with her treatment, recently reaching a point where she feels ready to taper off the drugs. Wick dispels rumors that GLP-1s are a shortcut for weight loss, emphasizing the work she had to put in to achieve the results she wanted.
“If someone were to ask me, say, like someone from high school, they’d be like, oh my God, you were totally on a GLP-1. I’d be like, yeah, sure. But also diet and exercise. That was really kind of the starting point to really get me somewhere where I could keep going with it,” said Wick.
Regardless of the negative media attention, the perception of GLP-1s as a trick to
‘get skinny quick’ has fueled their popularity.
Jack, a UVM junior who requested to go by a pseudonym, began taking Zepbound for weight loss during his senior year of high school. Despite being a varsity athlete and following a healthy diet, Jack continued to struggle reaching his personal goals.
Jack described how the popularized exploitation of the drugs has spread misinformation about their purpose, and tied the usage of GLP-1s solely to changing physical appearance rather than improving overall health.
“It’s [misuse is] ridiculous, and it’s expanding this negative body image that like, oh yeah, fat people can’t be happy in their own bodies. I don’t think that’s really what it’s supposed to be for,” said Jack.
Since beginning treatment, Jack has lost over 100 pounds. Like Wick, he emphasized that his success was not all due to his GLP1 medication, but also changes to his lifestyle that improved his mental and physical health.
Despite conflicting public opinions on their usage, it seems GLP-1s are here to stay.
A Gallup survey published in 2025 revealed that 12.4% of adults surveyed were taking a GLP-1 for weight loss, up 6.6% from 2024.
The same survey determined a possible connection between a slight decrease in the U.S obesity rate and a rise in the prescription rates of GLP-1 medications. Those in the public health sphere champion the use of GLP-1 medications in the fight against obesity.
“Obesity is a chronic disease, and it’s finally kind of being recognized as such, and it’s really wonderful in our world of endocrinology to finally have a tool that has pretty limited side effects compared to kind of older obesity medications and works so well,” Barrett said.
As society continues to determine where these drugs fit into the public health sphere, including more nuance in the discussion could paint a clearer picture of GLP-1s, not as a cheat, but as a pathway to improved well-being.


BY JOSH PARK
a truly nightmarish time in my life, the final trial before I could escape the horror that is the American public school system. The only thing that kept me chugging was the love of my life: Mary Jane.
With Mary, every day was a new adventure. She brought out the best in me in the worst of times. I believe Mary saved my life; she fought off the bad vibrations that rattled the walls of my hillbilly high school.
Mary motivated me to be more social. I actually reached out to others first and began participating in class far more than usual.
She gave me creative inspiration, and I penned some of my best writing while under her influence.
My girl aided me in improving myself, both physically and emotionally; I found the motivation to exercise more and eat better.
Most importantly, Mary Jane lulled me to sleep every night with her sultry tones. I slept like a baby and awoke refreshed and rejuvenated every morning.
require serious focus and dedication, and Mary Jane would just be a distraction in this kind of environment.
Yet, relaxation would pose a challenge in these circumstances. I had to stay on top of my game and keep up on my work; even the slightest distraction could lead me astray.
I tried to bargain with myself — maybe I would just smoke on weekends. And maybe include Friday nights. Or every night before bed … just for sleep, I promise.
And so, I sat depressed in my bedroom the day before I left for college, sad to leave my home and family behind.

I’ve always had sleep issues, since I was a wee lad suffering from night terrors. When Mary Jane came into my life, things started looking up.
As college approached, though, I quickly came to the realization that all good things must come to an end. I had to “lock in,” as the kids say, and focus on the upcoming workload.
When I came to UVM this spring and decided to study biochemistry, I knew I was
Some may be asking why I would choose biochem if I wanted to relax. The answer is because I am insane, in a mad scientist kind of way.
Maybe if I got my PhD, I could introduce Mary Jane to my contacts in the pharmaceutical industry and work towards normalizing her presence. Or maybe I could invent a new weight loss drug and retire, spending my millions on new accessories for Mary.
Just my love-induced daydreaming. But
To take my mind off things, I began staring at my beautiful cart collection. All of a sudden a question shot to the forefront of my mind: should I take all of them with me to school? Should I just take one?
These questions were racing around in my brain, my soul torn apart by this vile dilemma.
Goddamn you, STEM. I placed my carts back in the bottom nightstand drawer where they made their quiet home. In that drawer they stay, wallowing in the darkness, crying out for me.
Thus, my first true tolerance break began. I waved goodbye to Mary Jane, who stared sadly in the rearview mirror of my parents’ car as we drove off to the snowy north.
As the scenery passed me by, I knew I wouldn’t be reunited with Mary until spring break. Tears rolled down my face as I contemplated the horror I was about to experience. All alone in a foreign land … and with no zaza.
Now I sit here typing this piece, a little over a month into my first real tolerance break. I had tried t-breaks in the past, but I

usually cracked after a week.
This experience has been the greatest test of my stoner discipline. I have made the choice to choose academics over the joy of Mary Jane.
I have noticed a personality change since I’ve stopped smoking weed. I seem more rigid now — less fun and interesting. I am quieter, more closed off to the outside world.
I’ve always been very shy, and Mary Jane gave me the confidence to break out of my shell.
For the first few weeks after stopping, I began to enjoy things less.
I was even depressed. When I smoked weed, I was able to focus on a book for hours at a time; Reading Pynchon and Gaddis while high was some of the most fun I have ever had. Weed enhanced the “theater of the mind,” as Harlan Ellison once described imagination.
I used to love every second of every little thing I did, both stoned and sober. But when I stopped smoking, things I used to enjoy became boring.
This has to do with how weed changes your brain. Some chemistry for you all: When you smoke weed daily as I did, you develop marijuana withdrawal when you stop.
Daily THC use causes heightened serotonin and dopamine levels, which puts the brain in a deficit after stopping. This can lead to the aforementioned symptoms of weed withdrawal.
Now that Mary Jane is gone, I am locked into the sober mindset. That is to say, I am constantly upset and worried, not to mention the sleep issues. Dear God, the sleep issues.
The title of this piece is only a slight hyperbole. As I said previously, I’ve always had sleep issues, and I’m a very light sleeper. The slightest noise will send me leaping out of bed in a drowsy rage.
When I was using weed daily, though, this problem simply disappeared. I had never slept better in my entire life.
Every single night, I would gas myself into a deep coma, sometimes dreamless and sometimes dreamy. I would awake to the sun’s rays alighting upon my face, feeling fresh and ready to go.
People underestimate just how much bad sleep can screw you up. Sleep deprivation can cause increased risk of cancer, diabetes and heart disease, according to John Hopkins,
With Mary Jane at my side, I slept better, felt better and I think I was a better person overall. Weed made me nicer and more understanding of others; it made me feel more connected.
I don’t mean to glamorize drug use; being sober is a perfectly good decision, but I prefer to give in to MJ’s sweet embrace.
Some may call me an addict, but the beauty of marijuana is that I quit cold turkey and was fine. I did not die, I was not in severe pain and after a while, I did not even crave the feeling of being high.
It was not like that freaky baby scene in “Trainspotting” whatsoever. I was just slightly disappointed for a few weeks.
But from now on, weed will be a special treat, not a daily occurrence. I deeply love Mary Jane, but we had to take some time apart.
Let this be a lesson to all stoners — everything in moderation.
And just remember that this is all my opinion, weed has different effects on different people, and my experience is in no way reflective of anyone else’s.
And so, the t-break marches on. I look forward to summer break, when I can return and make sweet love to Mary Jane. While our relationship won’t be as committed, I still plan to maintain it so I can finally get a good night’s rest again. And in the words of Rick James:
“I’m in love with Mary Jane. She’s my main thing. She makes me feel alright. She makes my heart sing. And when I’m feeling low, She comes as no surprise. Turns me on with her love. Takes me to paradise.”
BY MACKENZIE BENDER


From weed to ketamine, many different drugs make their way through the UVM campus. These drugs might just have their own personalities.
Ever wonder what your personality says about what drug you would be? Take this quiz and find out!
Question 1
What is your ideal Thursday night?
a) Going to the bars with friends
b) Craft night with fun drinks
c) Movies and munchies
d) Going to a rave
Question 2
What was your favorite 2010s teen drama?
a) Gossip Girl
b) Glee
c) Teen Wolf
d) Skins
Question 3
What is your go-to drink?
a) Vodka Redbull
b) Strawberry margarita
c) Hard seltzers
d) Shots
Question 4
What is your least favorite genre of music?
a) EDM
b) Pop music
c) Country
d) Indie sad girl music
Question 5
What is your favorite summer activity?
a) Going to the beach
b) Hikes
c) Burlington Vintage Market
d) Music festivals

Question 6
What is your favorite form of caffeine?
a) Black coffee
b) Yerba Mate
c) Iced latte
d) Monster
Question 7
Which interest did you have as a kid?
a) Collecting rocks
b) Bugs and worms
c) Harry Potter
d) Horses
Question 8
How do you listen to music?
a) Airpods
b) Wired earbuds
c) In the car
d) Speakers
Question 9
What is your ideal skirt length?
a) Mid-thigh
b) Maxi skirt
c) Above knee
d) The size of a belt
Question 10
Which horse idiom do you like the most?
a) “Save a horse, ride a cowboy”
b) “That’s a horse of a different color”
c) “No point in beating a dead horse”
d) “Don’t look a gift horse in the mouth”


Results
Mostly A: Cocaine
You care a lot about what people think of you. Sometimes it comes off the way you think, but other times it doesn’t. You have a good time with most people, whether that’s going out to bars or just hanging out with friends.
Mostly B: LSD
You are definitely chronically online and full of whimsy. Your humor is not for everyone, but you entertain yourself consistently. You love a craft night, or a nature walk and hanging out with small groups of friends.
Mostly C: Weed
You are a little basic and boring, but you know what you enjoy and are content with it. You don’t try new things very often, but you can have fun with a weekend in. You often remain with a consistent schedule.
Mostly D: Ketamine
You always love a party, no matter the day of the week. You can stay up until the sun starts rising in the morning and crash as soon as you make it back in bed. Maybe a little too crazy, but you know how to have fun.


BY
Between housing, food, transportation and entertainment, the average college student spends $3,016 a month on living expenses.
Even in the face of these high costs, UVM students have decided to factor something else into their limited budgets: marijuana.
Despite cannabis prices remaining high after legalization, cannabis usage has been on an incline, with more people reporting daily cannabis use than alcohol in 2022.
Marijuana has often been at the forefront of UVM’s social scene. In a 2024 survey conducted by the Cynic, 95% of 521 students said that they would consider UVM a “stoner school.”
In a recent survey of UVM students conducted by the Cynic this semester, 43.4% of respondents reported smoking weed every day.
Weekly spending on cannabis ranged up to $100 weekly for those who reported using marijuana multiple times daily.
68.2% of students surveyed said they purchase their weed from dispensaries, with the rest sourcing their product from independent sellers or by home growing.
The nationwide price of cannabis
has begun to equalize since legalization as consumers are driven away from underground sources, making dispensaries the preferred source of supply, according to a 2021 article published by NPR.
After legalization, most states saw an increase in cannabis pricing that has remained steady since. In Vermont, the average price for an ounce of flower is $346, according to the Oxford Treatment Center.
Float On, a local dispensary on Church Street, has prices that range from $20 to $48 for 3.5 grams of weed. An employee, who wished to remain anonymous, said that price options were often a key factor in buyers’ purchases.
“Like 60% of people really do care about the price. So the majority, for sure, go towards the lower end,” they said.
However, 63.6% of student respondents said the price of weed wasn’t likely to affect their usage.
The employee described the consumer age demographic as ranging from 21 to roughly 90 years old. Though given their location on Church Street, the employee also said that they do see many student consumers.

“Because we have the bars right by us, we have a lot of you know, partiers or like 21 to like 23 [year olds], especially when the colleges are in session. We can tell,” they said.
Although the price of weed has not changed much since weed’s legalization, students are still getting creative in the ways of budgeting their bud. Sophomore Theo, who preferred not to give his last name, has found a way around dispensary pricing: growing his own weed.
“If you look up seeds on the internet they are very, very cheap compared to buying any amount of weed,” he said.
By growing his own weed, Theo has eliminated his need for a dispensary, but by doing so avoids the regulations and quality assurance that dispensaries provide.
Despite not smoking much himself, Theo started home growing weed as a fun summer project, but now gets to share the flowers of his labor with friends.
“It’s funny… I think it’s technically the cheapest way to get high,” he said.
“Students are still getting Creative in the wayS of budgeting their bud . ”
BY ASHLEY GOLDEN
My hands melted into her skin.
Everyone has heard some version of that sentence as a metaphor for intimacy. Whether that be melting into a hug, a kiss or the cliché of two bodies becoming one during sex: this is a well-known sentiment.
But for those who have taken hallucinogenic drugs, this — frankly tiresome — metaphor can very much become reality.
Hallucinogens are a broad category of psychoactive substances that include psychedelics, empathogens and dissociatives like LSD, Ecstasy, Ketamine and Magic Mushrooms, according to a Dec. 2001 Journal of Dialogues in Clinical Neuroscience article.
These drugs interact with a variety of receptors in the brain, like serotonin, dopamine and glutamate, to produce an altered state of consciousness. This state includes changes in perception, mood, senses, cognition, empathic capabilities and self-experience, according to an Aug. 2025 Journal of Neuroscience & Biobehavioral Reviews article.
This is all one long way of saying that hallucinogenic drugs temporarily change one’s reality. You can feel sounds, taste colors; soft textures like fur and hair can feel like heaven; feelings like love, desire, empathy and care are more intense than ever.

All emotions are heightened, and you may come face-to-face with a level of gratitude that you’ve never come close to before.
Once, after taking a dose of MDMA, all that I wanted to do in between moments of somewhat embarrassing dancing at Higher Ground was tell my best friend how much I loved and was thankful for her.
The prosocial aspect of hallucinogens is nothing new. For thousands upon thousands of years, humans have ingested natural hallucinogenic compounds like psilocybin, the active chemical in magic mushrooms, for spiritual and medicinal purposes and for social connection, according to a Jan. 2020 PNAS article. But one of the most famous and powerful aspects of the connection between interpersonal relationships and hallucinogens is, of course, sex. MDMA, or ecstasy, also referred to as the “Love Drug,” is one of the most commonly used substances for enhancing sex, with users citing it as increasing emotionality and intimacy.

Ecstasy also prolongs the time it takes to reach climax and increases the intensity of orgasm, according to a Feb 2022 Psychedelic Health article.
Though that delay may just be due to the fact that MDMA can cause temporary impotence in around 40% of males, according to the same source.
The famous 1967 summer of love was also the summer of LSD. Sex with strangers was practically seen as an act of generosity, according to a June 2012 Vanity Fair article.
Around the same time, renowned philosopher Michel Foucault became known as the “last man” to take LSD. Foucault admitted his experience with the drug caused him to massively rewrite the entire first volume of his renowned work “The History of Sexuality,” according to a March 2021 Salon article.
Studies have also found that users of hallucinogens report increased sexual satisfaction for months after ingestion, according to a Feb. 2024 study from the Imperial College of London.
My own experiences with these substances and physical intimacy have been everything from mundane to heart-wrenching to orgasmic.
While the more explicit of these experiences belong not in a newspaper but on the pages of my diary, or at most in a letter to Penthouse, some are actually sweet.

Her soft skin, my skin, soft skin; it felt like nothing I’d felt before
One night, high on ketamine after a party, the foul metallic taste of the powder coating the walls of my throat and the beautiful lights in my apartment shifting between blues and purples and reds much more vibrantly through my eyes than they were really shining, I held a beautiful girl in my arms.
This was not the first time I had held her, and yet it felt like a completely new experience — something I’d never even imagined before.
Ketamine, a dissociative, can have a profound impact on your sense of touch and especially so on your ability to distinguish between touch produced by yourself and touch produced by another, according to a June 2024 Journal of Neuropsychopharmacology article.
To put it more simply, it can become a lot harder to tell where your body ends and
another person begins.
When I held this beautiful woman, it truly felt like I was melting into her. Her soft skin, my skin, soft skin; it felt like nothing I’d felt before.
And as I felt her heartbeat under my head, the rhythm reverberating through my skull like music, I felt a level of lightness in my mind and body that I’d never imagined. Every feeling floated to the surface like feathers on water.
There is no denying that all drug use carries some degree of risk.
What comes up must come down, and with every high there is often a low. Hallucinogenic drugs, upon wearing off, can famously cause an onslaught of intense negative feelings and sensations like exhaustion and depression called the “come down,” according to a Nov. 2025 Verywell Mind article.
This negative state is temporary and is rarely dangerous, according to the same source.
It would also be irresponsible to write this piece without acknowledging the incredibly complex relation between drug use and consensual sex or any type of physical intimacy.
It is of vital importance to have an open, clear and incredibly intentional conversation regarding boundaries, expectations and consent prior to engaging in any sexual activity while under the use of drugs and before the ingestion of those drugs.
With chemicals as powerful as hallucinogens, someone can reach a state of mind in which they are no longer able to give consent. Consistent and enthusiastic consent is paramount.
But for those who wish to have an intimate experience on hallucinogens and do so responsibly, of course, they will feel sensations that people couldn’t even imagine. You truly can feel like you’ve become one with your partner, the boundary between your two bodies blurring into non-existence.
Touch becomes electric. Their hair is the most beautiful thing you have ever felt in your life. Their eyes become literal stars. My hands melted into her skin.


BY ELIAS GALLIGAN
In a culture where drinking is expected for college students, the words “I don’t drink” can feel charged.
It can invite confused questions or persistent “you should just have one” offers. Worse, though, is the raging fear of missing out. Because of this, making a conscious effort not to drink in college can feel like an uphill battle.
I remember standing outside a crowded house party, holding a cup of iced tea while others around me were drinking. After dodging questions and using my red Solo cup as a decoy, I decided that alcohol-centric events were more work than they were worth.
At my first college party, I wanted to have fun. Instead, all I could think about was whether it was obvious that my cup held iced tea instead of alcohol.
As someone with an anxiety disorder, I learned that alcohol and anxiety don’t always mix. In fact, many of my preexisting anxiety symptoms were exacerbated by the consumption of alcohol.
The first time I tried drinking, it was a margarita at dinner. For a moment, nothing happened. Then, my heart began to race and my chest felt tight. I felt completely out of control.
I excused myself and spent most of that embarrassing night trying to steady my breathing and wondering why I had that reaction in the first place.
Even small amounts of alcohol would trigger a pounding heartbeat and the overwhelming feeling of a panic attack coming on.
While some people with anxiety disorders enjoy alcohol without issue, research suggests that alcohol consumption can worsen anxiety symptoms for many others, according to a Feb. 2025 American Addiction Centers article.
As a depressant, alcohol can mask acute anxiety symptoms. For those who experience social anxiety, this can serve as an initial appeal.
When alcohol enters your system, it increases the production of dopamine and serotonin, which can create a relaxed feeling, according to an April 2025 Brentwood Behavioral Healthcare article.
This is because alcohol affects the brain’s gamma-aminobutyric acid receptors, the same receptors targeted by anti-anxiety benzodiazepines like Xanax or Ativan, making our brains feel more relaxed, according to an April 2023 Cleveland Clinic article.
However, this feeling only lasts for a limited time.
As the effects start to wear off, the brain increases glutamate to restore chemical balance, making us feel more anxious, according to a Feb. 2023 Alcohol and Drug Foundation article.
In other words, what starts as taking the edge off can turn into a cycle: drinking to relieve anxiety, only for it to return later. As I’ve sobered up in the past, I dissociated, zoned out and felt an overwhelming sense of dread.
In these moments, I was often told to just drink more. It felt strange that the solution people offered to the horrible feeling was to simply keep going.
Beyond these short-term effects, repeated drinking can have longer-term consequences. The more you drink alcohol, the more you build tolerance to it, making it harder to achieve the same calming results, according to an Oct. 2016 University Health Services article.
Because of this, those who rely on alcohol to relax are at a greater risk of alcohol dependence disorders.
Twenty to 40% of people with internalizing disorders, such as anxiety, suffer from
alcohol use disorder, compared to just 5% of the general population, according to a May 2023 University of Minnesota Medical School article.
Even people who previously suffered from depression or anxiety but are now in remission show higher rates of AUD, according to the article.
Learning about the connection between anxiety and alcohol dependence further reinforced why choosing not to drink felt like the right decision for me despite the social pressures.
In many cases, alcohol-centric events or parties can feel inaccessible or exclusionary for those who do not drink, contributing to isolation.
There have been many instances in which I’ve had to turn down invites to parties or get-togethers that I genuinely wanted to go to, because I didn’t want to be the only person not drinking.
Despite these pressures, choosing not to drink can have many benefits for the brain.
One benefit I noticed from not drinking is better sleep. Because alcohol can disrupt sleep cycles, choosing to stay sober can help improve the quality of sleep and reduce anxiety, according to a Dec. 2025 Addiction Center article.
Over time, I began to notice my mood was more stable as well. Research suggests that this may happen because the serotonin levels in the brain stabilize, which can result in less anxiety and a reduction in mood swings, according to the article.
While choosing not to drink can occasionally be uncomfortable in social settings, the mental health benefits have made it worth it for me.
These days, I will gladly drink my iced tea in peace with a balanced and stable mind.
BY AUTUMN ANDERSON
We are lost in our disconnect. Lost from the Earth we walk on, from the people we share a community with, from the truth about what we are capable of.
We have become paralyzed by this lack of connection.
Society has taught us that we exist to work and our worth is decided by our ability to produce, and we face the repercussions in every facet of life.
I used to have nightmares about ending up in a treacherous 9-to-5 job, fantasizing about retirement just to get through the day. I tried to remind myself that this doesn’t need to be my path.
But I fear it’s my friends’ and my only option to survive. And this fear, this crushing weight, is eating away at the people and community I care so much about.
When my peers aren’t drowning in their phones, they complain as a way to bond with others. If their primary form of connection is through expressing their dissatisfaction, they haven’t even scratched the surface of what real connection entails.
To find a way out of this mess we are in, I’ve been searching for a new means of connecting.
Recently, I met a student by the name of Julia Hart, who opened my eyes to therapy involving psychedelics, and over the course of our discussions, we came to call this treatment the “therapy of connection.
Hart, a UVM sophomore, is working to-
ward creating her own major surrounding this topic.
“[I] want to understand the ways in which humans can connect with plants, and the ways that we’ve forgotten how to use plants,” Hart said.
Hart is a research assistant in the Vermont Conversation Lab, where she works on interpersonal grounding concepts through psychedelic-assisted therapy, specifically using psilocybin.
It is important to note that other drugs, such as LSD and MDMA, are also being researched for therapeutic purposes, according to an April 2022 Front Journal article.
Psychedelic therapy, formally referred to as integrational therapy is not an invitation to take these drugs carelessly. This treatment requires supervision and guidance by a trained medical professional.
Risks can be much higher for users ingesting psilocybin if they are also using SSRIs or have a family history of schizophrenia, according to the University of California San Francisco.
Integrational therapy targets what patients learn from the psychedelic experience to incorporate it into their daily lives.
The therapy consists of two prep sessions where participants are given the necessary information needed to give informed consent, including the therapist’s limitations surrounding their role during the trip; after which come the dosing and integration ses-

sions, stated Hart.
“Taking the insights that you have and figuring out how you can change the way you are living your life and the way you are responding to things is the goal,” Hart said.
Western culture is not the first to engage with the healing effects of these drugs. Long before them, various Indigenous cultures used psychedelics to heal physical, spiritual and mental ailments, according to an April 2025 article in the Journal of Anthropology of Consciousness.
Typically, these practices involve a healing shaman or leader who advises members through the experience. That person is someone who has a connection to the spirit of the plant that is healing you and the community, Hart stated.
The classification of targeted symptoms points to how vast the application of integrational therapy can be.
Disorders that involve a lack of brain connectivity, like post-traumatic stress disorder, major depressive disorder, anxiety disorders and OCD, fall into this category, according to Hart.
Psilocybin disrupts the way the brain typically functions, including how information is processed. Hart compares the constantly-filtering nature of the brain, known as the Default Mode Network, to a labyrinth.
While the role of DMN is helpful to avoid being overwhelmed by too much informa-
tion, this maze becomes an obstacle when attempting to see past habitual patterns of thought present in mental illnesses; in other words, to think differently.
Once psilocybin enters your system, DMN function is disrupted, allowing every section of your brain to interact with itself, causing thoughts to travel in ways they’ve never been able to before, according to a March 2023 article in the International Journal of Neuropsychopharmacology.
The pathways opened up in participants’ brains are part of why Hart and I have coined this as a “therapy of connection.”
The intense connectivity lasts 21 days after you ingest the drugs. In these 3 weeks, known as the critical period, you are able to integrate what was learned during your trip to change habits and reactions about the self, according to John Hopkins Medicine. This is possible because of the brain’s neuroplasticity, according to a Nov. 2022 article in the Journal of Neuroscience.
With increased brain plasticity, we are able to access other ways of thinking that were there the whole time, but not accessible from our current pathways. It’s like trying on glasses for the first time.
The other reason we call this the “therapy of connection” is because of its ability to end maladaptive thought patterns.
“You might have one really negative experience that forces you to react in a certain way out of habit … If a stimulus happens,

then your brain immediately goes to another thought. That’s this connection, this loop that keeps occurring. Bad stimuli, bad reaction,” Hart said.
With increased brain plasticity, this connection between bad stimuli and bad reactions can be disrupted while new connections are made.
These psychedelic experiences can bring up a lot of suppressed negative emotions and feelings.
This phenomenon is often called a “bad trip.”
While these experiences can be quite frightening, Hart believes, under the right circumstances, they can also be beneficial.
Hart uses an analogy in Buddhism, where the Buddha claims that life will inevitably hit you with pain, or “the first arrow.”
What dictates whether life hits you with another arrow depends on the way you react to this pain.
“There’s always going to be pain, but you have the choice in how to react to that pain. If you resist the pain, it becomes suffering because you aren’t allowing the pain to pass through you,” Hart said.
We can see this first arrow as whatever negative experience or emotion you have that has been pushed down over time, that psychedelics bring to the surface.
If one chooses to resist the pain, they are refusing to let the pain properly pass and prohibiting their ability to heal from it,
but if one doesn’t resist, new insight will be brought to light.
This increased connectivity allows a new sense of openness to experience. Taking the power away from the oppressive conditioning of our society and allowing us to find what it means to be truly connected to a community.
Although we may feel isolated in this world, we have never been alone. We will never be alone.
After this “therapy of connection,” random interactions that once may have seemed pointless may now fill you with purpose. Instead of viewing people as judging you, you can see it as lighthearted curiosity.
The childlike lens you used to view the world through may finally open again, bringing along wonder and amazement into a world you once viewed as dull and predictable.
Life is like a “choose your own adventure” novel. The path we take is completely up to us, and psilocybin allows us to see the options that have always been present in the background, but it is still our responsibility to make that choice.
While it may feel like we aren’t able to leave this isolated world, this treatment may be the key to providing the connectivity that we need to feel differently.

BY AYELET KAMINSKI
Every day on my way to Howe Library, I walk past countless blue signs alleging that “UVM is a Tobacco-Free Campus.”

UVM has been “tobacco-free” for over a decade, according to a Sept. 2, 2015 Vermont Cynic article.
However, as I approach the steps, the ever-permeating scent of cigarette smoke fills my nose in stark defiance. Smoking on the steps of Howe Library has become such a favored pastime of UVM students that to mention it borders on cliché.
Given the pervasiveness of signs forbidding tobacco use, I’d find it hard to believe anyone is unaware of the policy.
I would say they’re hard to miss, but I can understand that after a while, they just become part of the scenery on campus. Kind of like the lack of trash cans or a frat bro wearing shorts in January.
It doesn’t help that in all my years at UVM, I’ve never once seen of the policy being enforced, unlike the alcohol and cannabis prohibitions.
Sure, enforcement might be relaxed — or temporarily suspended for campus holidays like 4/20 — but I’ve met enough people who’ve been busted for walking around
drinking from an open container or smoking weed to know to take it semi-seriously.
Meanwhile, when it comes to tobacco, there is absolutely no pretension of upholding the policy; many smoke in broad daylight during passing periods.
The presence of cigarettes on campus is so prolific that the Cynic has published an article investigating the phenomenon twice in the past two years.
“It’s more than a ‘drunk cig:’ cigarettes on UVM’s cam pus,” and “Nicotine’s generational comeback” both ac knowledge the ubiquity of nicotine consumption through vaping and smoking.
Both articles also acknowledge that the trend stretch es beyond the classic “drunk cig” or the occasional social smoke into habitual use.
This tendency isn’t specific to UVM. Instead, it rep resents a broader trend of cigarettes rising in popularity throughout Gen Z in tandem with the resurgence of cigarette imagery and aesthetics in pop culture, according to a Nov. 6, 2025 Bloomberg article.

In a survey of 162 UVM students conducted by the Cynic, over 80% of respondents reported consuming nicotine on a regular basis, according to the aforementioned April 30, 2025 Vermont Cynic article.
Over a third of respondents admitted to trying to quit nicotine and relapsing, according to the same article.
It’s ironic; e-cigarettes were originally marketed as a

tool to aid in smoking cessation, but now I know people who have started smoking cigarettes as a way to stop vaping.
Still, the public health detriments of widespread cigarette smoking, including those of increased exposure to secondhand smoke, cannot be understated.
I know some people will interpret this as a tyrannical call to discipline students, but that’s ignoring why the policy exists in the first place. The decision to become a tobacco-free campus was always intended as a public health measure, not as a punishment.
As spring begins to creep in, I have noticed an increased effort to remind students of the policy through the addition of a new sign outside of Howe. The sign reads:
“There is no smoking allowed on this campus. For the health and safety of all patrons, the Libraries will call Police Services to help us uphold this UVM policy.”
Thus far, I have not heard of Police Services actually being called, as I imagine the librarians may hope the sign itself will act as enough of a deterrent.
I don’t agree with getting the cops involved in most situations, and the University has moved away from punitive measures in response to drug use and towards recovery-focused ones, according to a Cynic news report published in last year’s drug issue.
Michael Schirling, UVM chief of safety and compliance officer, said that the decrease in disciplinary referrals for
drug use may be due to more drug and alcohol referrals being sent to the Vermont Catamount Recovery Center rather than the Center of Student Conduct, according to the same article.
While increasing reminders and enforcing the tobacco-free policy through a recovery-focused approach are steps in the right direction, UVM must also increase its efforts to educate and spread awareness of the harm longterm tobacco use can cause.

As a non-smoker, I want to be mindful that nicotine is an extremely addictive chemical and that quitting is no small task, and the social aspect of nicotine addiction cannot be understated.
To enact real change and improve public health on cam pus, we as a student body must engage in transforming campus culture around smoking. The signs clearly aren’t working.

UVM offers a variety of smoking cessation resourc es, such as the Catamount Recovery Program, behavioral health appointments through the Center for Health and Wellbeing and 802Quits kits available at Living Well.






