

Daniel’s Dream Takes Flight
WINTER 2026
A Dream Takes Flight
Tulane Sickle Cell Center provides patients with everything they need to navigate their disease from childhood to adulthood. For some, like Daniel Cressy, they also help to put dreams within reach.


In Search of Relief
When Stephanie Joy Brady sought answers for her son Jaylon’s painful skin condition, she found the only place that gave her hope.

TRANSPLANT INSTITUTE
A New Era of Growth
In just over a year, Tulane’s transplant team has completed more than 250 abdominal transplants.
Addy Jensen beats the odds with CAR T-cell therapy from Tulane’s Pediatric Stem Cell Transplant and Cell Therapy Program.
A Message from Tulane’s Associate Dean for Surgical Services
Tulane Doctors are in a remarkable period of growth, and not just in the procedures we perform or the technology we employ, but in how we care for each patient who walks through our doors. In this issue of Wellness Wire, you’ll meet Tulane Doctors and scientists who have dedicated their careers to providing patient-centered, personalized care. You’ll also hear from some of the patients whose lives were transformed by Tulane Doctors. Their stories reflect what drives us: the privilege of restoring health, providing hope and partnering with patients throughout their care journey.
Our recent milestones are just a glimpse of the groundbreaking work happening across our institution. Tulane is the only center in our region offering novel sickle cell gene therapy treatment. We’ve performed four heart transplants and more than 250 abdominal transplants in a little over a year. From robotic surgery to preventive genomics, our physicians are using cutting-edge technology and research to improve patient care across every specialty.
Tulane Doctors combine world-class research with compassionate, personalized care. Backed by Tulane University School of Medicine, our faculty members are part of the same teams conducting groundbreaking studies that shape the future of medicine. This means our patients benefit from the very latest advancements in treatment, access to clinical trials, and a coordinated approach to care that brings together experts from across Tulane.
Technology continues to reshape what’s possible. Minimally invasive surgery is now the standard for many surgical procedures, with smaller incisions and shorter recovery times resulting in better outcomes. Additionally, we’re utilizing genetics and lifestyle data to predict health risks and prevent diseases before they occur.
What truly defines Tulane Doctors is our patient-centered care. Whether helping someone navigate a new diagnosis, supporting them through treatment or partnering with them to maintain long-term health, we provide continuous, individualized support every step of the way.
As Tulane Doctors, we are honored to serve as your partners. Thank you for trusting us with your care.
Warm regards,

Gabriella Pridjian, MD, MBA, FACOG, FACMG Associate Dean for Surgical Services Chair of Obstetrics & Gynecology
Tulane University School
of Medicine




F Daniel Cressy represents Privileged Pilots at The Organization of Black Aerospace’s 49th Annual Conference in August 2025.
G Daniel, center, with his Tulane care team (left to right) Dr. Maria Español, nurse practitioner Amy Kinzie, nurse manager Rihana Galloway-Dawkins, Dr. Benjamin Watkins, pediatric nurse Trenese McDonald, and Dr. Justin Farge. Photo by James Cullen.
A Dream Takes Flight
When Ernest DeJean Jr. first met Daniel Cressy, he was a social worker at the Tulane Sickle Cell Center. Daniel was just ten days old — and newly diagnosed with sickle cell anemia.
His parents were understandably upset. But the minute they walked into Tulane Sickle Cell Center, they knew they had found the lifeline they were looking for. As one of the leading centers of its kind in the state, DeJean, now the administrative director, is proud of the extraordinary community Tulane Sickle Cell Center has built for both patients and their families. In addition to offering expert personalized medical care, the center also provides much-needed emotional and resource support to enable patients to manage life with sickle cell.
“Education and communication are at the core of everything we do. We are asking people to put their faith in us. Our clinical expertise when it comes to sickle cell is important, but we have to make sure we give people the information they need in a timely and understandable way. It makes a huge difference in helping them through the process,” explains DeJean.
While the center stays abreast of the latest treatments and research in sickle cell disease, often participating in national studies so they can provide the most scientifically advanced treatments for sickle cell patients, the caregivers at Tulane know there is so much more to helping people feel well physically.

That’s why they are strong advocates for providing consistent, cohesive medical and non-medical care that will give their patients everything they need to navigate their disease.
“We treat the entire person because feeling healthy is about more than just treatments and tests. It’s about knowing you have someone in your corner. We build strong relationships with our patients. They trust us. They often look to us for help with what I like to call ‘life stuff’ and we are more than happy to assist however we can. It’s not always about sickle cell,” shares DeJean.
In addition, the center provides an unparalleled “lifespan” program to help patients transition from treatment as a child or teen to adulthood.
“The center works hard to remind patients to focus on living, and that they are more than their diagnosis.”
— ERNEST DEJEAN JR.
According to DeJean, “We encourage patients to make plans and think about the future. Sometimes that’s hard when you know the odds tell a different story or when some treatments aren’t available to you. Daniel is the perfect example of what we strive for.”

The reality is that without a bone marrow transplant most sickle cell patients won’t live beyond their 40s. For many, finding that perfect match can be difficult, even among family members. Daniel was one of those patients. But he refused to let that small detail get in the way of his dreams.
Although Daniel has been living with his disease since he was an infant, with Tulane’s help he never let it get in the way of living his life. The disease often meant monthly hospital visits throughout his childhood and took away the opportunity to play team sports, but Daniel still found ways to simply be an active kid, doing the things that most kids do.
“Sickle cell was always part of my life, so it all just seemed normal to me. I never felt like I was missing out on anything,” says the 22-year-old.
“No matter what I wanted to do or try, Tulane always had my back. They were there to talk things through and provide information so I could make informed decisions.”
— DANIEL CRESSY
Recently Daniel came up against something that for many would be considered a showstopper. Once again, Tulane was there for him.
After graduating high school and taking some college classes, he realized his chosen career paths of dental hygienist — and then finance — really didn’t excite him. And he didn’t want to be in an office all day long. Inspired by his brother, he secured his Commercial Driver's License at 19 years old.
He loved operating the powerful 18-wheelers, but soon decided he needed more of a challenge. That’s when a TikTok video of a kid “just like me” flying a plane set Daniel’s future in motion. He was hooked.
His mom connected him with someone she knew at a local flight school and Daniel was soon soaring
above the clouds. He knew this was what he was meant to do.
But his sickle cell threatened to take his dream of becoming a commercial pilot away from him. As challenging as it was to deal with a chronic illness, it was the first time in Daniel’s life his disease became an obstacle to something he really wanted to do.
The Federal Aviation Administration has strict medical standards. People with sickle cell anemia run the risk of high altitudes impacting their cells, causing intense pain if there isn’t enough oxygen. The FAA refused to give him his medical certification, even after several appeals.
Daniel was undeterred.
When Daniel was unsuccessful in finding a bone marrow match, he didn’t want to put his plans on hold. He knew it could take years to find someone to meet the very specific criteria — if ever.
In 2024, a friend of his in Georgia who he met through the sickle cell community and who also wanted to be a pilot had undergone a newly available gene therapy. The success of the treatment opened the door to his friend getting his pilot’s license.
Daniel discussed gene therapy with his doctors, who listened with open ears. “It was so new, they just wanted to make sure it was the right path for me, but they were 100% in my corner and did everything necessary to make it possible.”
As a result, in addition to providing Daniel with the medical treatment he’s needed over the years, Tulane is now carefully coordinating with its partner, Manning Family Children’s, on the groundbreaking and life-changing gene therapy care treatment. Daniel is the first patient in Louisiana to receive this cutting-edge care which promises him a cure — and the chance to fulfill his dream.
In July 2025 he underwent the first of at least two cell collection procedures, the initial step in a process that will see his cells sent overseas for editing and then returned sometime in March 2026 to be infused
back into his body, which will require a month-long hospital stay, and then three months of isolation as his immune system resets.
“It’s a lot to go through,” says Daniel. “To be honest, I’d been managing my sickle cell really well. If this wasn’t the only way for me to be a pilot, I might not have even considered it. But I am more than grateful to be surrounded by healthcare professionals who listen to their patients and are always pushing the envelope to provide the best for them. They have been with me every step of the way for 22 years.”
While becoming a pilot was Daniel’s primary motivation for undergoing this medical journey, his experience also fostered a new mission, the launch of a non-profit to inspire other sickle cell patients to reach for their dreams. According to its website, Privileged Pilots (privilegedpilots.shop) was created to “inspire hope & change in the community & prove that YOU can do ANYTHING! With a little faith, & A LOT of perseverance: NOTHING is IMPOSSIBLE.”
Through his organization, Daniel and his partner — that same friend from Georgia — strive to bring awareness to sickle cell and to act as advocates and
inspiration for those who may be suffering or have loved ones suffering from the disease. Daniel is excited about his future and credits a little divine intervention for getting him on his way. “I know for some people, not finding a bone marrow match is a disappointment. But my faith tells me this was meant to be my path. Not only to help myself, but to help others.”
“Between God, Tulane and Manning, I know I’ll soon be on my way to flying people all over the world and hopefully continuing to help others ‘fly’ in their own way, too.”
— DANIEL CRESSY
For DeJean, who still remembers the tiny baby he met 22 years ago, watching Daniel come full circle from being guided by Tulane and needing their support to now providing guidance and support through his nonprofit has been very gratifying. “It’s the reason we do what we do,” he says.


Scan this code to support the Sickle Cell Center of Southern Louisiana.
F In December 2025, Daniel participated in the Manning Family Children’s annual radiothon where he discussed his experience navigating sickle cell disease and gene therapy treatment.
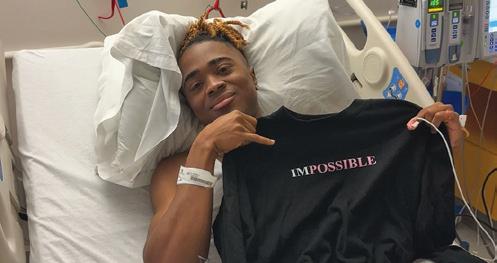
G Daniel holds up a Privileged Pilots “ IM POSSIBLE” shirt while undergoing sickle cell treatment at Manning Family Children’s in May 2025.
Rewriting the Sickle Cell Story
For decades, a diagnosis of sickle cell disease guaranteed a shortened lifespan and relentless pain. At the Tulane Sickle Cell Center of Southern Louisiana, that story is being rewritten. Innovative treatments and compassionate care are giving patients something thought impossible only years ago — the chance to live full, healthy lives. “We are with our patients side by side at every step,” said Dr. Maria Español , the center’s medical director. “We want them to know they don’t have to face this disease alone.”
Tulane’s center will soon make history as the first site in Louisiana to perform a revolutionary gene therapy procedure designed to cure sickle cell disease. The procedure is groundbreaking, having only been approved by the U.S. Food and Drug Administration in December 2023.
The breakthrough is life-changing, but many sickle cell patients are not candidates for gene therapy or the other current cure, a bone marrow transplant. For most, the path forward depends on managing the disease, something the center’s comprehensive approach makes possible. “We offer a multidisciplinary team with nurses, social workers and physicians, and every time patients come in, we see them as a team,” Español said.

“We are with our patients side by side at every step. We want them to know they don’t have to face this disease alone.”
— DR. MARIA ESPAÑOL
“Patients used to live with a lot of comorbidities and a low quality of life,” Español said. “Now, even without a bone marrow transplant or gene therapy, life expectancy has increased. And now it can be cured. However, to truly make a lasting difference, it’s crucial that we support the community through ongoing research and improved access to care. This ensures that all patients, regardless of their circumstances, can benefit from the latest advancements and receive the care they need.”
Sickle Cell profile need headshot
Because Tulane is an academic medical center, patients also have access to cutting-edge research opportunities that may open the door to future advances in care. The center’s transition program further helps adolescents and young adults move seamlessly from pediatric to adult treatment, ensuring consistent support during a critical stage of life.
As the center prepares its first gene therapy patient for treatment, the moment carries profound meaning. “The disease deserved this moment,” Español said. “Now, through research, we are not only gaining a better understanding of the pathophysiology of sickle cell disease, but also unlocking more treatment options for patients.”
With every new treatment and every patient cared for, Tulane is changing the story of sickle cell disease — for good.
FACING

Tulane Sickle Cell Center of Southern Louisiana offers comprehensive care from birth through adulthood. We provide education and scientifically advanced treatments customized to each person’s symptoms, with the goal of preventing complications and improving overall quality of life. METAIRIE Tulane

J Medications
J Gene Therapy
J Blood transfusions
J Pain management
J Hydration
J Bone marrow transplant

NEW ORLEANS
Sickle Cell Community Events
STOPPING HEART DISEASE BEFORE IT STARTS Tulane Heart & Vascular Institute
Using advanced imaging and research, the Tulane Heart & Vascular Institute is attempting to identify and interrupt the aging process in the heart, to prevent arrhythmias instead of just treating them.

To support the work of Dr. Marrouche and Tulane Heart & Vascular Institute, scan this code or visit giving.tulane.edu/triad
Dr. Nassir Marrouche , director of Tulane University Heart & Vascular Institute (TUHVI), and his collaborators are asking a question: What if we could prevent heart failure and arrhythmias from developing?
To answer that, Marrouche is partnering with Dr. Victor Thannickal and his team to study the fundamental process of cardiac aging. Over time, factors such as high blood pressure, poor diet, genetics, infections and even COVID can cause the heart muscle to scar. This “aging” of the heart tissue is a major driver of AFib and heart failure. Using advanced imaging, along with basic science research, the team is working to identify and interrupt the aging process before irreversible damage occurs.
A major focus at Tulane is harnessing artificial intelligence to detect heart irregularities before symptoms ever arise. “Eighty percent of our work is AI-based,” said Marrouche.
Already, TUHVI is tracking 1,000 patients wearing smart devices that could help predict, identify and understand cardiovascular diseases and comorbidities. TUHVI, in collaboration with Samsung Research America, is testing the relationship between biological signals collected on a Samsung Galaxy Smartwatch and heart-related health problems.
In the lab, scientists are studying how heart cells age. At the same time, that wearable technology and imaging are working to identify people at higher risk long before symptoms appear. “We can now screen, detect and manage heart disease before it causes harm. Early detection and prevention of arrhythmias is the key to saving lives,” Marrouche said.
While Marrouche’s research shapes the future of cardiovascular care globally, the patients in his clinic — the lives he’s saved right here in the New Orleans area — also tell a powerful story.
G Dr. Nassir Marrouche, director of Tulane University Heart & Vascular Institute
“We can now screen, detect and manage heart disease before it causes harm. Early detection and prevention of arrhythmias is the key to saving lives.”
— DR. NASSIR MARROUCHE
One patient credits Marrouche’s innovative earlydetection approach with saving his life. That gratitude inspired a $6 million gift to support Marrouche’s work — the largest donation ever made by a grateful patient at Tulane.
Continued philanthropic investment will be critical to expanding this work. Increased support would allow Marrouche and his team to accelerate clinical trials, recruit additional researchers and trainees, expand advanced imaging and AI capabilities and bring earlydetection tools to more patients across the region. Philanthropy helps move discoveries from the lab to the clinic faster, so that innovations developed at
Tulane translate into lifesaving care for patients in Louisiana and beyond.
The mission remains urgent: use science to save lives and make New Orleans a place known for world-class heart care. With major trials underway, global collaborations and emerging technologies, Tulane stands at the forefront of the next evolution in cardiology. “We’re not just following guidelines, we’re writing them,” said Marrouche.
For Marrouche and his team, the work is far from finished. The future of heart care is being shaped right now, and Tulane is where the next chapter is being written.

G (Left to right) Han Feng, PhD; Mohammad Montaser Atasi, MD; Joe Abi-Rached; Kristie Sanders; Mayana Bsoul, MD; Monique Young, NP; Michel Abou Khalil, MD; Eleanor Christianson; Ghassan Bidaoui, MD; Nassir Marrouche, MD; Hadi Younes, MD; Eli Tsakiris; Christian Massad, MD; Yingshuo Liu; Mario Mekhael, MD
Setting a New Standard of Care
Dr. Nassir Marrouche has helped define how atrial fibrillation, or AFib, is treated around the world. His research reshaped the guidelines for AFib care, changing how physicians approach one of the most dangerous and common cardiac conditions. At Tulane, he is now leading discoveries that could establish new standards of care for the highest-risk heart patients.
Marrouche came to Tulane and New Orleans in 2019 because he realized the need: Louisiana has one of the highest rates of cardiovascular disease in the nation, with heart disease mortality significantly exceeding the national average.
By taking on the role of director of the Tulane University Heart & Vascular Institute (TUHVI), Marrouche would have an opportunity to save lives on a huge scale. “I was drawn to Tulane by the urgent need to combat the cardiovascular disease crisis in Louisiana,” said Dr. Marrouche.
“We are building more than just an institute; we are creating a movement to bring groundbreaking care and renewed hope to this entire region.”
— DR. NASSIR MARROUCHE
Marrouche’s impact on heart care cannot be overstated. When he arrived, specialized cardiology programs barely existed at Tulane. Today, his vision has transformed the cardiac landscape at Tulane, building a comprehensive team of expert health professionals.

Before Tulane, Marrouche was at the University of Utah where he led a landmark clinical trial, proving that catheter ablation significantly reduced heart failure death and hospitalization compared to medication. “Never before had a study shown that the procedure could reduce mortality,” Marrouche said. “The way your AFib is treated today at NYU or Cleveland Clinic or Stanford is mandated by our scientists.” The establishment of a cardiac imaging program, a field that didn’t exist at Tulane prior to Marrouche’s arrival, is now pioneering cardiac imaging capabilities. “That’s why I came here — to use my experience, use my history — to build something unique for the future.”
Marrouche has started a $29 million multicenter trial worldwide to study using catheter ablation for AFib patients whose hearts don’t relax and fill properly with blood between beats, he said. By collaborating with 52 universities across Europe and the United States, his team is building the evidence that could again shift global guidelines.
Born of his own curiosity in the labs of Heidelberg, Germany, and honed through years of innovation, his work reflects a lifelong commitment to turning discovery into lifesaving practice. “In 1993, I was in the lab researching arrhythmias. Fast forward 32 years later, and I can save your life with screening and early detection. So I encourage you to use all the tools we have today to screen yourself and manage your heart health.”
JOIN THE HEARTBEAT RESEARCH STUDY
What is the HEARTBEAT research study?
This research study will test a relationship between biological signals collected on a smartwatch and heart health issues.
What will you need to do during the study?
We will assign you a loaner Samsung Galaxy smartwatch. We ask you to wear the smartwatch at least 18 hours per day for one year. You will have to complete a daily task on the smartwatch (it will take about 1 minute per day).
Using an app on your smartphone, you will have to complete several questionnaires (once in a few months).
Participating in the study is completely voluntary. You may be able to join if: You are at least 18 years of age, You have heart health problems(s): heart failure, cardiac arrhythmia(s), chronic kidney disease, coronary artery disease, history of stroke / transient ischemic attack, or diabetes mellitus. If you don't have any of these conditions, you can be part of the study’s healthy controls group.

PRINCIPAL INVESTIGATOR: Nasir Marrouche, MD Director of TRIAD, professor of medicine, and Vice Chair of Innovation and Entrepreneurship at Tulane University School
Medicine.

of in search RELIEF

When Stephanie Joy Brady sought answers for her son’s excruciatingly painful skin condition, she never imagined moving hundreds of miles from home to seek treatment from the only place that gave her hope.
Miraculous words to a mom desperately trying to find relief for her child — “I can help your son.” Even though I’d been a nurse for 25 years at the time of my son Jaylon’s diagnosis, I’d never heard of hidradenitis suppurativa (HS), a chronic inflammatory skin condition that results in painful, pus-filled lumps and abscesses.
Watching my son suffer daily was absolutely awful. As both a mom and a health professional, I felt helpless for years. Until Tulane changed everything.
Jaylon has always been my pride and joy. Whether doing a complicated math problem in his head, playing the piano better than I ever have, learning how to fly a plane, or graduating from high school with an associate’s degree, he has never ceased to amaze me with his joy of learning. But in a few short years, HS slowly robbed him of the things he loved to do and threatened his dream of becoming an aviation lawyer. I was worried and heartbroken.



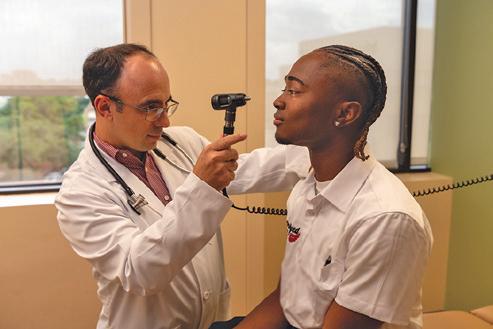
E Jaylon Brady with Dr. Abigail Chaffin and Stephanie Joy Brady.

“Tulane and Dr. Chaffin and all the hardworking, talented people who have been involved in Jaylon’s care have given him the chance at a life that a few years ago we didn’t think was possible.”
I set out to find out everything I could about his condition and what could be done to help him. His dermatologist was amazing and supportive, but even she was unsure how to proceed beyond various medications, especially as his condition worsened.
She recommended a surgeon who had more familiarity with HS. For a minute I was hopeful, but he said there was nothing he could do. He referred us to a second surgeon who was using alternative medicine. I was ready to try anything, but even he didn’t think he could help Jaylon.
I refused to give up.
My “mom and nurse” research led me to a support group on Facebook. I pleaded for anyone to give me some advice on what to do next. Time after time one name kept popping up: Dr. Abigail Chaffin, plastic surgery chief at Tulane. I couldn’t dial her number fast enough.
We traveled from our home in Georgia to New Orleans to meet Dr. Chaffin and her team. From the moment she stepped into the room, I knew we were in the right place. The first thing she did was introduce the other specialists who joined us and made sure Jaylon and I were comfortable with their presence.
Then she got to know my son. Not his disease or his symptoms. Just
Jaylon. She asked him questions about what he liked to do, what he wanted to be. I have worked in many places and dealt with many doctors, and I have never been more impressed. I could see Jaylon relax in her presence.
After 45 minutes, she said the words he and I prayed we would hear: “I can help.” Jaylon simply cried. After years of feeling hopeless, she offered Jaylon a way back to himself. Can you imagine what that felt like?
Dr. Chaffin told us the journey wasn’t going to be easy. We needed to move to New Orleans for at least a year so Jaylon could be carefully monitored after each of four surgeries and the challenging recoveries that would follow.
We were ready to do whatever it took. Dr. Chaffin and her team helped us find housing, referred us to a local primary care physician (her husband’s personal doctor), and supported us in ways I can’t even begin to list, always going above and beyond.
As we went through each surgery, everyone I came across at Tulane was incredibly caring and highly competent. But I always refer to Dr. Chaffin as the G.O.A.T. She has been absolutely worldclass every step of the way.
She treated “mom Stephanie” with patience and compassion. She treated “nurse Stephanie” like part of Jaylon’s medical team,
always appreciating my questions and input. I could not have asked for a better experience.
Because of the expertise of Dr. Chaffin and her team, each of the first three surgeries has been a success. As we await surgery number four, we see a light at the end of what has been a very long and painful tunnel.
Recently Dr. Chaffin asked Jaylon, “Are you ready to go to law school?” His smile lit up the room. Even knowing this last surgery will have the most extensive recovery, Dr. Chaffin wants Jaylon to know his dream is now within reach.
Tulane and Dr. Chaffin and all the hard-working and talented people who have been involved in Jaylon’s care have given the chance at a life that a few years ago we didn’t think was possible.
I would have traveled to the ends of the earth to help my son, but I am grateful every single day he wound up at Tulane. I have always said I would never work at a hospital where I wouldn’t want myself or a family member to be a patient. Well, I would work at Tulane in a heartbeat. And even though Jaylon has already been accepted to a law school close to home, I am secretly hoping Tulane Law might be in his future.
What a full circle moment that would be.


Jaylon has completed three stages of surgery between May and September 2025. He and his mother have moved back home to Atlanta and have connected with Tulane graduate Dr. Vironka Davis at her General Surgery and Wound Care practice in Atlanta. Jaylon is expected to heal completely.
E Jaylon (center right) stands with his brother Matthew, uncle Clarence, and father Maverick.
It Takes a Village to Tackle the Toughest of Cases
Dr. Abigail Chaffin has dedicated her career to treating patients with some of the most challenging and often overlooked medical conditions.
Chaffin is board-certified in general surgery and plastic and reconstructive surgery, and she is a wound-specialist physician. Chaffin has become a beacon of hope for patients suffering from complex conditions like hidradenitis suppurativa (HS), a painful inflammatory skin disorder that often leaves patients feeling isolated and misunderstood.
“It’s a disease that hides in the shadows,” Chaffin said. “Patients with really advanced disease struggle to find someone who will take care of them. It requires a village — a lot of people and significant resources. Many surgeons won’t take this on, because their offices and networks don’t have the bandwidth.”
To change that reality, Chaffin collaborated with colleagues across specialties to build a comprehensive inpatient and outpatient wound team at Tulane.
“We’ve built a kind of ‘super team’ of Tulane Doctors,” she said, bringing together experts from urology, gynecology, dermatology and infectious diseases. She is also medical director of the MedCentris Wound Healing Institute in Metairie, which handles outpatient wound care.
Chaffin is a national leader in her field, serving on the boards of the American Society of Plastic
Surgeons and the Southeastern Society of Plastic and Reconstructive Surgeons. She is also an academic leader, serving as chief of the Tulane School of Medicine Division of Plastic Surgery and program director for the Tulane/Ochsner plastic surgery residency, authoring numerous research papers on HS and presenting her work at national conferences.
Chaffin is gratified when she sees her patients heal — and when she witnesses how that healing transforms them.
“People with HS have been shamed for years,” she said. “They’ve been told it’s about hygiene or that

it’s their fault, but it’s not. It’s an inflammatory disorder. It’s genetic.”
The change after surgery is remarkable. Before, many of her patients wear black because it doesn’t show stains, choosing long garments to hide drainage or dressings. “Then when they come back and they’re healed, the women start to wear nicer, fitted, brighter things. The men wear dressier clothes.”
For Chaffin, those moments say everything. “That’s what makes me happy,” she said. “Seeing them walk in wearing something colorful — it’s like they’re finally free.”

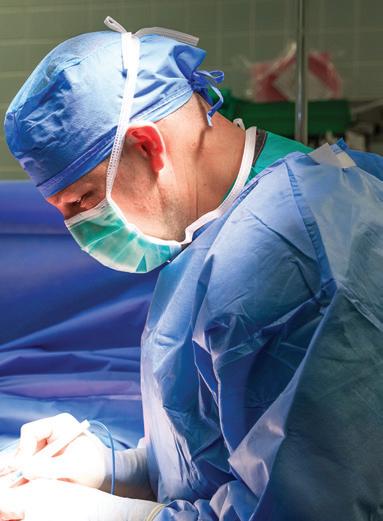

“HS is a disease that hides in the shadows. Patients with really advanced disease struggle to find someone who will take care of them. It requires a village — a lot of people and significant resources. Many surgeons won’t take this on, because their offices and networks don’t have the bandwidth.”
— DR. ABIGAIL CHAFFIN
To support the work of Dr. Chaffin and Plastic Surgery Wound Care, scan this code or visit giving.tulane.edu/ gratefulgiving25, choose “other” and select “Dr. Chaffin – Plastic Surgery.”
H Dr. Chaffin operates on a patient with Dr. Dustin Eck.
A NEW ERA OF GROWTH AND INNOVATION Tulane Transplant Institute
The Tulane Transplant Institute is entering an extraordinary period of growth as a multi-organ transplant center, having achieved major milestones in recent months.
The institute now offers kidney, liver, and pancreas transplants, with heart transplant services newly revived and a lung transplant program on the horizon.
Since relocating to East Jefferson General Hospital in 2024, Tulane’s transplant team has completed more than 370 abdominal transplants. This remarkable achievement highlights both the institute’s expertise and its commitment to expanding access to lifesaving care.
Dr. Anil Paramesh , chief of abdominal transplant and professor of surgery, urology, and pediatrics at Tulane School of Medicine, has been at Tulane for more than 20 years and is key to the institute’s extraordinary growth.
In another milestone for the university, heart transplants have returned to Tulane, with four procedures successfully completed as of press time, a testament to the leadership of Dr. Jamil Borgi , chief of cardiothoracic surgery. Recruited
F (Front row, left to right) Dr. Bonnie Chow, Dr. Brian Borg, Dr. Moh’d Sharshir, Dr. Lee Cummings, Dr. Anil Paramesh, Dr. Giuseppe Morelli, Dr. Matt Pittappilly, Dr. Diala Khirfan, Dr. Arnold “Brent” Alper
F (Back row, left to right) Our dedicated Tulane LCMC Transplant Clinic Nurse Navigators, Dr. Fred Regenstein, Dr. Kiara Tulla, Jennifer Forstall, NP

“At Tulane, we’re committed to the whole person. We approach it from a multidisciplinary perspective in every phase of care.”
– DR. MARY KILLACKEY

from Montefiore Medical Center in New York in 2024, Borgi has rebuilt Tulane’s heart transplant program.
The Tulane Transplant Institute serves a uniquely high-need population in a region with high rates of diabetes, hypertension and organ failure. Patients receive comprehensive, coordinated treatment that spans the full transplant journey, from pre-transplant evaluation through long-term recovery.
“At Tulane, we’re committed to the whole person,” said Dr. Mary Killackey , chair of the Department of Surgery. “We approach it from a multidisciplinary perspective in every phase of care.”
With each milestone, the Tulane Transplant Institute strengthens its legacy as a leader in organ transplantation — and as a beacon of hope for patients across the Gulf South.





of making the most SECOND

Amber Brown’s Tulane story began with something many of us do every year — her annual physical. As a healthy 26-year-old she didn’t think twice about the results of the usual tests her doctor performed. When she received a call that there was an abnormally high amount of protein in her urine, she wasn’t overly concerned.

to take bubble baths (because of her catheter) and having to put her dream of nursing school on hold.



Follow-up testing, including a kidney biopsy, revealed a surprising diagnosis: FSGS — a condition which damages the kidney’s filtration function.
“I felt fine and didn’t have any of the typical symptoms,” explains Amber. “I started on steroids and all seemed to be well. I went about my life.”
Until one day while sitting at her desk at work, she couldn’t feel her legs. They had become so swollen she couldn’t walk. Amber said, “I was shocked to find out my kidney function was at 13 percent! It seemed to come on so suddenly.”


Amber was told she would need a new kidney, but finding a donor could take years. She went on dialysis while she waited and kept her life as normal as possible. Her faith and her family kept her going. Amber’s two biggest complaints? Not being able
“I was able to do my dialysis at home overnight so usually I was able to have a fairly normal day. But nursing school is really hard, and I knew I wasn’t up to it.”
Amber made the best of things, but her mom Nija could tell it was taking a toll on her daughter emotionally and physically. Even though she’d been told it was highly unlikely she’d be a suitable donor, she decided to get tested anyway. She was a match!
And that’s when Tulane came into Amber’s life.
Since the 1960s, Tulane has played an important role in the development of organ transplantations, constantly striving to provide the most advanced care for their patients. For Amber, they not only offered decades of expertise, they also offered the cutting-edge technology of the future. She had the opportunity to be the state’s first kidney transplant using a robotic surgical system.


“I was nervous, but I trusted my Tulane transplant team completely,” shared Amber. I knew using the robot meant a more precise and minimally invasive







CHANCES
procedure with less pain and a faster recovery. Tulane has a highly regarded transplant program, and I felt honored to be chosen for this first-of-itskind option.”


“It’s the exact reason people go to Tulane – they are always investing in the technology that will give their patients better outcomes.”
Amber was equally impressed with her medical team. “The nurses were amazing and my doctors called frequently to check on me personally. That was something! They really made me feel like family.”
It’s been almost three years since her transplant, and both Amber and her mom feel great. In fact, after that well-deserved bubble bath, Amber enrolled in nursing school — and her mom joined her. Both graduated in April 2025 with their RN degrees.


“I’m usually a very private person but I realized this isn’t just my story. I had to release it because I knew it would help others. Sometimes life throws us a medical curve ball and having a place like Tulane, where their team is your team, to get you through is


so important. People need to know that. I couldn’t be more grateful for everything they did for us.”


In addition to her nursing career, Amber has big plans for a bright future. She dreams of starting an organization and website to help dialysis patients, providing encouragement, support and resources. She says, “I was inspired by the wonderful care I received at Tulane, and I want to pay it forward however I can. My mom — and Tulane — gave me a second chance at life and I don’t want to waste a second of it.”

E Amber and her mother Nija prepare for transplant surgery.
Creating a Culture of Caring Through Organ Transplantation

For Dr. Anil Paramesh, the most rewarding part of his work will always be living organ donation, what he calls the purest expression of compassion. These transplants often occur between family members, but sometimes between friends, co-workers or strangers.
Dr. Anil Paramesh was in medical school when he first witnessed a living organ donation, an experience so profound it set the course for his career.
“There’s nothing else in medicine where a healthy person who doesn’t need to put themselves at risk, risks their life to save somebody else,” said Paramesh, director of the Tulane Transplant Institute at East Jefferson General Hospital, and professor of surgery, urology and pediatrics at Tulane School of Medicine.
In a living donation, a healthy person voluntarily gives one of their organs — most often a kidney, or a portion of their liver — to someone in need of a transplant. The act not only saves a life but also forges an unbreakable bond between donor and recipient.
“It’s just so powerful,” Paramesh said, recounting the emotion when the two meet after surgery: the tears of joy, the hugs, the indescribable gratitude. “This is true human nobility and kindness.”
That defining moment ignited a lifelong passion for transplant surgery. Paramesh started at Tulane School of Medicine in 2006, drawn to help rebuild the city’s medical infrastructure after Hurricane Katrina. Today, as Tulane’s chief of abdominal transplants, Dr. Paramesh leads a rapidly expanding program that has already completed more than 250 transplants since mid-2024, providing lifesaving care to patients across the region.
Tulane has built what Paramesh describes as a “culture of caring.” Over nearly two decades at the university, he’s seen the same philosophy in action
every day: treating patients as partners, maintaining close contact with them long after surgery and building relationships with referring physicians.
“Nobody gets lost in a huge corporate system where you’re just a number,” he said. “At Tulane, we treat our patients as individuals and stay in touch with them throughout their lives. It’s a satisfying experience — both for the doctors and for the patients as well.”
As an academic medical center, Tulane is a place where tomorrow’s transplant surgeons learn from today’s experts — and where research fuels progress for patients everywhere.
“When we’re actively engaged in both clinical and basic science research, we’re helping to make organ transplantation better for everybody,” Paramesh said.
Tulane’s faculty participate in numerous national clinical trials, ensuring patients have access to the newest medicines and therapies.
“Our Institute has grown considerably since our move to East Jefferson General Hospital last year. We have been given more resources to grow our team and program. The heart transplant program has had an amazing start. We have been able to hire new doctors to help the liver transplant program grow considerably. And our pediatric transplant program at Manning Family Children’s has made us one of the busiest transplant programs in the region. We have a lot to be proud about.”
Tulane’s abdominal transplant program has also been lauded for its innovative and inclusive approach to patient care. The team has pioneered a groundbreaking bariatric initiative for obese patients who have been turned away from other transplant centers.
Through close collaboration with bariatric surgeons, Tulane’s transplant team helps patients lose weight,
manage comorbidities and ultimately become eligible for transplantation.
“If you just tell somebody they’re too large to get a transplant and never give them the opportunity to lose the weight, you’re putting them in purgatory,” Paramesh said.
For Paramesh, the most rewarding part of his work will always be living organ donation, what he calls the purest expression of compassion. These transplants often occur between family members, but sometimes between friends, co-workers or even strangers.
The Tulane Transplant Institute was the first in Louisiana to perform living donor kidney-swap operations and has currently paired with a national organization to help grow this further. A kidneyswap is a system that helps patients who need kidney transplants and have a willing donor who isn’t a medical match for them. Swapping donors can make more matches happen.
“Organ transplantation is one of the most complex, unique systems in medicine today,” said Paramesh. “There are just so many moving pieces that must fit together on a local, regional, and national framework to make even one transplant happen. In addition, there is so much new technology that is helping us make more organs usable and allowing more people to get an organ. It’s an exciting time in the world of transplant! But the one thing that will not change for us is our culture of caring for the patient first.”
To support the work of Dr. Paramesh and the Tulane Transplant Institute, scan this code or visit giving.tulane.edu/transplant.
TULANE
cracking WHIPthe
Ijust kept thinking, ‘Something’s off…this isn’t normal,’” recalled 78-year-old Metairie resident Robert Mahl.
In May of 2025, Robert began noticing unexpected changes in his bowel habits, which steadily progressed over several weeks and started interfering with daily life. Soon after, he began losing weight rapidly, nearly 20 pounds in a short period. He initially assumed the issue was temporary, but when things did not improve with help from his primary care provider, Robert and his wife, Debbie, knew it was time to look deeper.
A colonoscopy did not reveal anything concerning. However, an MRI uncovered a cyst in the head of Robert’s pancreas. When a biopsy showed atypical cells, his gastroenterologist, Dr. Brett Hymel, immediately referred him to Dr. Lee Cummings, associate professor of surgery at Tulane School of Medicine and surgical director of liver transplantation with the Tulane Transplant Institute at East Jefferson General Hospital (EJGH).
From their first meeting, the Mahls felt a deep sense of trust. “He explained everything clearly,” Debbie said. You could tell he knew exactly what he was doing. After our first meeting, we never second-guessed our decision about choosing him to treat Robert.”

Cummings recommended moving forward with surgery rather than waiting, explaining that the cyst had the potential to be malignant. Waiting, he warned gently, could significantly change the course of treatment. He recommended a robotic Whipple, a technically complex operation traditionally performed through a large open incision.
For decades, the Whipple has been considered one of the most demanding abdominal procedures in medicine. Cummings, who spent years performing open Whipple operations before transitioning to robotic approaches, describes it as the same operation performed through a very different lens, literally. Robotic surgery provides magnified 3D visualization and allows the surgeon to “see around corners,” navigating spaces impossible to view through an open incision. Patients benefit from smaller incisions, less pain, less blood loss, and faster recovery, even though the operation itself can take longer.
Robert underwent the robotic Whipple at EJGH on September 23, 2025. The pathology would confirm a rare colloid carcinoma arising from an intraductal papillary mucinous neoplasm (IPMN), a form of early-stage pancreatic cancer that Cummings was able to remove completely with clear margins and 24 negative lymph nodes.

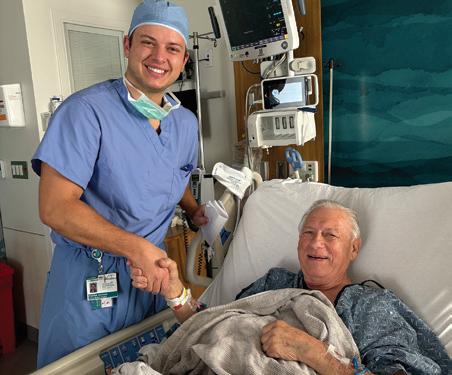
Robert remembers little of the first two days following surgery, but by day three, he stood up and walked the hallway with the physical therapy team. “I was surprised,” he recalled. “I thought it would hurt, but it really didn’t.”
He was also eating full meals by day three: eggs, bacon, and even a pork chop for dinner. Debbie laughed, recounting it. “He hadn’t eaten in days, and there he was, finishing everything they brought. It amazed us.”
His symptoms began to improve immediately. The unpredictable bowel movements that had kept him close to home for months disappeared. Even the change in the odor of Robert’s breath, something Debbie hadn’t connected to his illness, resolved after surgery, a subtle but telling sign of how much his pancreatic function had been affected.
After eight days in the Transplant ICU and surgical unit, Robert returned home and soon was walking outside on his own. “I feel like I didn’t even have major surgery,” he said. “It’s amazing.”
For Debbie, the ability to receive this level of care without leaving Louisiana was one of the greatest gifts. “We have friends who had to spend months

in Houston for cancer treatment,” she said. “We were blessed to have this here at home.”
At Robert’s postoperative visit, EJGH medical oncologist Dr. Rachel Caldwell delivered the news they had been praying for: no chemotherapy would be necessary. Instead, Robert would get scans and bloodwork every three months. “It felt like a weight was lifted off my shoulders,” he said.
Stories like Robert’s reflect the momentum building within Tulane’s robotic HPB and complex GI surgery program. Robotic Whipple procedures remain uncommon, but with the expertise of Tulane surgeons like Cummings, the capability is expanding. “This is exactly the kind of care our patients deserve,” Cummings said. “We’re providing world-class, minimally invasive surgery right here in our community.”
For Robert and Debbie, the experience comes down to deep gratitude for the technology, for the care team, and for the surgeon they felt they were incredibly fortunate to find. “Dr. Cummings really was our angel,” Debbie said, and Robert agrees. “I can’t thank Dr. Cummings enough. I’m here today because he knew what needed to be done, and because we didn’t wait.”
E Dr. Lee Cummings, surgical director of liver transplantation, Tulane Transplant Institute
F Robert shakes hands with Tulane medical student Patrick Burnam
Redefining Cardiac Care Across the Gulf South
Dr. Jamil Borgi came to Tulane because he saw a great need — a gap in high-complexity heart care in a city with some of the nation’s highest rates of heart disease. At the time, Tulane School of Medicine had no division of cardiothoracic surgery, and patients with advanced heart conditions often had to travel elsewhere for lifesaving treatment.
“I felt there was a good opportunity to make a difference,” said Borgi.
The need was clear. In years past, about 90 to 100 heart transplants were performed annually in New Orleans. In recent years, that number had fallen to roughly 20 — even as national transplant rates rose by nearly 50 percent. “It’s not because people here suddenly got healthier,” Borgi said. “It’s because access to care became harder.”
He estimates that Louisiana should see between 100 and 150 heart transplant patients each year, but many of those cases have gone untreated or were sent to centers in other states. “Too many patients were simply managed medically and died prematurely,” he said. “That’s one of the reasons I decided to come here — to make sure those patients have a chance.”
And so he has. In just 18 months as chief of cardiothoracic surgery, Borgi built Tulane’s heart program from the ground up, bringing worldclass expertise and innovative procedures that are redefining cardiac care across the Gulf South.

“I come from three generations of physicians, and I always knew I wanted to be a surgeon. Cardiac surgery is the most dynamic, technically demanding surgery, and I knew this was where I could make the greatest difference in people’s lives.”
— DR. JAMIL BORGI
What began with Borgi alone has expanded into a team of six surgeons, including three new physicians and two existing colleagues from East Jefferson General Hospital. One of the new doctors is advanced heart failure specialist Dr. Sasha Vukelic .
Both Borgi and Vukelic came to Tulane from Montefiore Medical Center in New York, where Borgi was part of a nationally recognized team known for outstanding outcomes: at Montefiore,
his program achieved the highest one-year survival rates for heart transplants in the country.
“We had extraordinary results at Montefiore, and now we have the same team here,” Borgi said. “We’ve built a program at Tulane that’s thriving.”
Under Borgi’s leadership, the program earned approval for heart transplants in December 2024 and is now pursuing certification to launch a lung transplant program — another leap forward in Tulane’s mission to provide advanced care close to home.
The program’s accomplishments speak for themselves. Since December 2025, Borgi’s team has completed 11 heart transplants. They have also performed 26 left ventricular assist device (LVAD) procedures, providing lifesaving support for patients with end-stage heart failure.
Tulane has also established a robust aortic program, drawing highly complex and emergency
cases from across Louisiana and Mississippi and positioning the university as a regional leader in advanced aortic care.
Borgi brings both exceptional skill and a deep sense of purpose. He said, “I come from three generations of physicians, and I always knew I wanted to be a surgeon. I felt that cardiac surgery is the most dynamic, technically demanding surgery, and I knew this was where I could make the greatest difference in people’s lives.”
And that is what he’s already doing at Tulane. By restoring access to world-class cardiac care, he’s giving hope to patients with the most complex heart conditions — right here at home.
To support the work of Dr. Borgi and the Tulane Transplant Institute, scan this code or visit giving.tulane.edu/transplant.

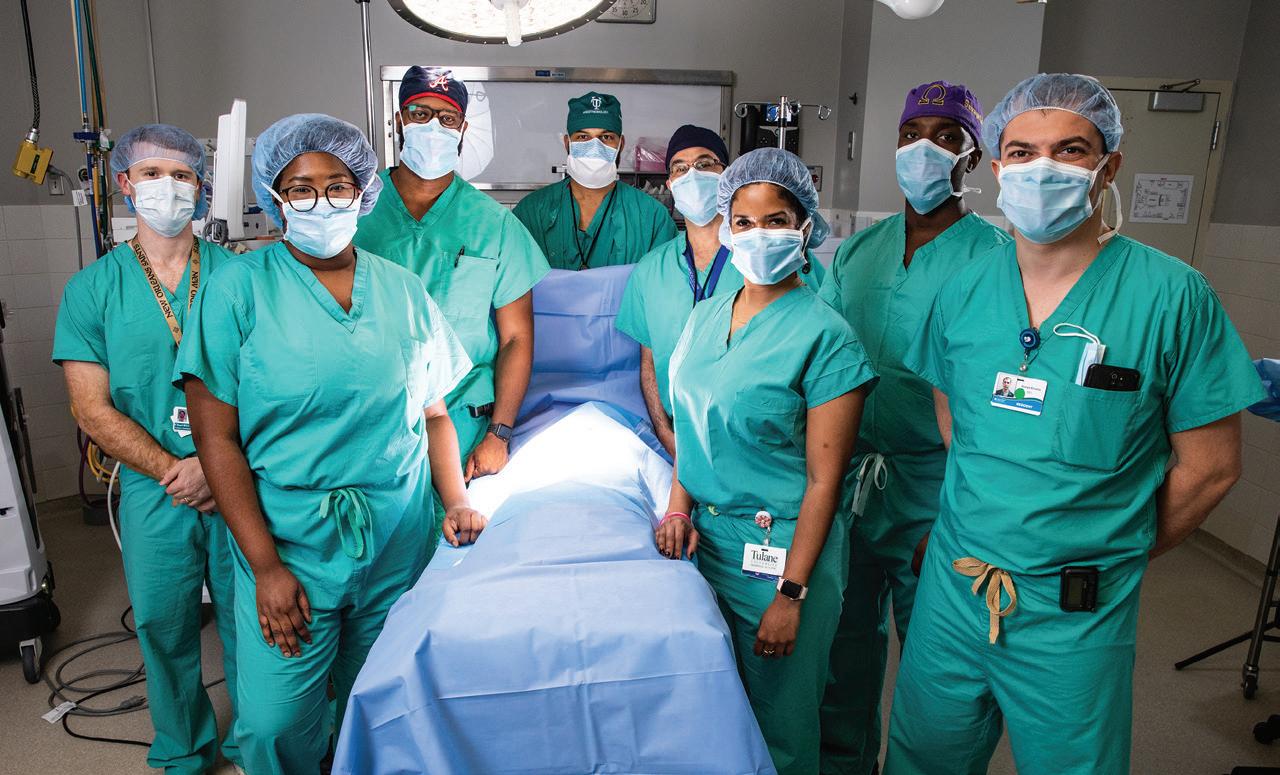
H (From left) Dr. Aabha Divya, Dr. Harry Roach, Anna Grace Koepp, Tavarius Walker, Matthew Boles, Dr. Jamil Borgi, Amaris Hollins, Beth Evers, and Amanda Walker.
PULLED the brink from W
When Tulane Doctors were faced with one of the most complex cardiac cases they ever saw, a team of three dozen medical professionals worked tirelessly to pull their patient back from the edge.

hen Benny Nunez suffered a sudden heart attack, his heart stopped not once, but several times. Each time, Tulane Doctors shocked him back to life. His condition was critical, and survival meant months in the hospital, advanced life support, and ultimately, a heart transplant. Yet through expert care, his deep faith, and the unwavering support of his family, Benny began an extraordinary journey from the brink of death to a second chance at life.
Looking back on his care, Benny speaks with deep gratitude for the doctors who saved his life. “I couldn’t have landed in a better spot. They’re the best people I ever met in my life — the whole staff.”
Benny was doing yard work at his Mississippi home in May 2025 when he felt unwell and was rushed to the hospital in Slidell.
When his family arrived at the hospital, there was confusion and urgency, according to son Benny Nunez Jr. “The doctors really didn’t understand what was going on with him. They were thinking more of like a brain aneurysm… but they did a CT of his chest and realized that he had a massive heart attack.”

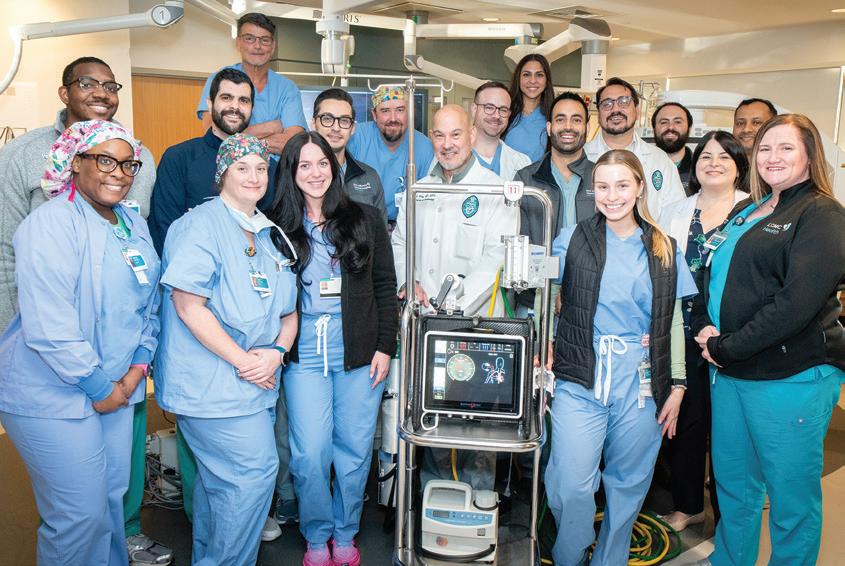
E (Top row, from left) Jay Culbertson, Jason Graham, Dr. Adam Lick, Hannah Cantrelle, Dr. Sasha Vukelic, Dr. Paterson Graham, and Dr. Abhinav Saxena.
(Middle row, from left) Dr. Benjamin Pickard, Dr. Samer Zakhour, Dr. Ali Ayoub, Dr. Jose Wiley, Dr. Ala Mohsen, and Nicole Jones.
(Bottom row, from left) Tarriana Betha, Lauren LeBlanc, Madison Connely, Katie Champagne, and Brandi Richardson.
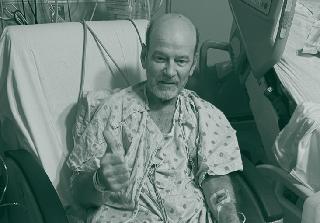
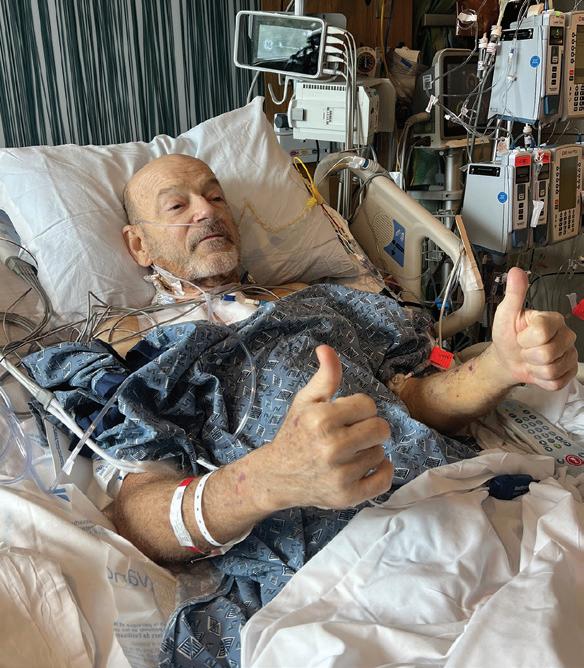
H Benny Nunez gives two thumbs up to the care he received from Tulane Doctors and staff.
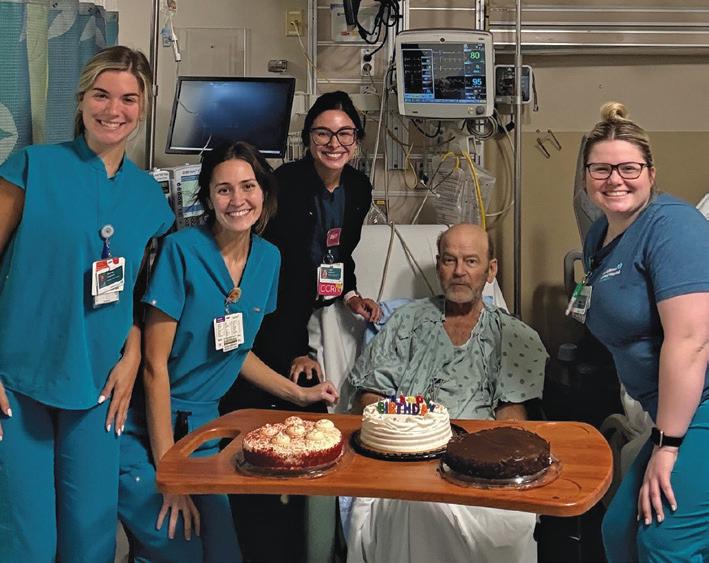
His father coded multiple times. “When the doctor came out, it was pretty grim,” Benny Jr. recalled. “They said, ‘Your dad’s very sick.’ His chances of survival were slim to none.”
Benny went to the hospital in Slidell in the afternoon, but by the evening, the doctors there called the Tulane interventional cardiology team at East Jefferson General Hospital because it was clear he needed advanced care.
The transfer to East Jefferson carried its own dangers — there was no guarantee Benny would survive the trip. But without it, he had no chance at all. The damage to his heart from the heart attack was so severe, his kidneys and liver had stopped working. As his systems began to shut down, he grew extremely weak and winded and ultimately required dialysis.
That critical night was also when his family first met Dr. Sasha Vukelic , Tulane associate professor of medicine, vice chief of the section of cardiology, director of advanced heart failure and transport cardiology and director of mechanical circulatory support. He said Benny’s case was one of the most complex cases he ever saw; a team of three dozen medical professionals worked on him tirelessly.
At East Jefferson, Vukelic and his team quickly performed several life-saving interventions to stabilize Benny, opening blocked arteries and placing him on ECMO, a form of advanced life support that temporarily takes over the work of the heart and lungs to give the body a chance to recover.
Benny’s son, Adam Nunez, recalls meeting Vukelic in the earliest hours after the transfer.
F Benny celebrates his birthday in August 2025 with members of the nursing staff at East Jefferson General Hospital.
“By the time everything got settled, it was probably one or two o’clock in the morning. But immediately, Dr. Sasha came out and talked to me and my brother and explained everything that was going on. You could tell they were working tirelessly back there — they looked wiped out themselves by the time we saw them.”
That late-night conversation was just the beginning. “After that, we saw him so much,” Adam said. “He was always there and always willing to sit with us and explain everything that was going on.”
Even with expert care, the road was still uncertain. “We actually lost him several times throughout the first couple of weeks,” Adam shared. “I didn’t think he was going to make it out of there. As a matter of fact, we got quotes on his funeral.”
Vukelic was impressed with Benny’s fortitude, telling WWLTV: “His heart stopped multiple, multiple times. He was shocked multiple, multiple times. That’s a lot of pain and suffering. … This is like PTSD, like you’ve been in a war.”
“He was in a coma for three weeks,” Adam said. “They didn’t really understand if he was going to have any brain activity left because of the amount of time he went without oxygen.” Still, Adam remembers that the doctors never gave up on his father, and that gave the family hope too.
Over time, with close monitoring and continuous care, he began to stabilize. But Benny still wasn’t strong enough to leave the hospital. His heart was failing so severely that he would get winded just walking a few steps, even to the end of his hospital bed. The medical team discussed two options. One was the use of an LVAD, a left ventricular assist device that helps the heart pump blood through the body. However, the LVAD requires a wire connecting the device to
a power source outside the body, meaning Benny would remain hooked up to it, and there was a concern that he might not be strong enough to tolerate it.
The other option was a heart transplant. Fortunately for Benny, Tulane had just resumed its heart transplant program under the leadership of Dr. Jamil Borgi , Tulane School of Medicine associate professor of surgery and chief of cardiothoracic surgery.
On October 4, Benny received the gift of a new heart. He had deep confidence in his doctors going into the complex procedure. “They made you feel comfortable with what they were getting ready to do,” he said. “And like I told them — win or lose — at least y’all tried.”
But win they did. And the improvement to Benny’s quality of life was immediate. “As soon as I woke up, I could breathe again. That was unbelievable,” he recalled.
Benny Jr. remembers the quiet reassurance that came from Borgi’s steady presence. “He was there almost every day, giving us updates,” he said. “When I saw him work, I thought — this guy really knows what he’s doing. He felt like a superhero to me.”
And the family felt the same about the nurses. They saw strength and compassion in every shift change and bedside conversation, calling the nurses heroes, who encouraged their father.
“Some days he wanted to give up, and [the nurses] would point him back in the right direction… constantly changing out IV bags and cleaning wounds. They treated my dad like family.”
— ADAM NUNEZ
Even small gestures meant everything to Benny. “A nurse gave me three cakes,” he said, smiling as he recalled celebrating his sixty-second birthday from his hospital bed in August 2025.
Benny Jr. felt grateful that his father’s care allowed them more time together.
“With all of this going on, I spent a lot more time with my dad than I normally would. I visited every single day, and I probably had more conversations with him in the last six months than I’ve ever had. I learned a lot more about him.”
— BENNY NUNEZ JR.
That time brought a different kind of closeness. “Normally when you see your dad, it’s just like, ‘Hey, how’s it going?’” he said. “But when you spend time with him like this, you really get to see inside. Stories he never shared before — now he’s sharing them.”
While recovering, Benny said he reflected on personal loss, including his first wife who died in an accident and a son who passed away as an infant nearly 40 years ago. He also said he experienced powerful spiritual moments while healing.
During the time when he had coded shortly after the heart attack, he said, “I believe Jesus was talking to me. He was telling me different things, telling me to keep going.” Benny was shown three Bible passages, and when doctors removed a piece of equipment
from his head, he recalls seeing three crosses marked on his forehead. It was a moment that strengthened his resolve to heal and return to the life waiting for him.
That determination is rooted in love for his wife of 26 years, Mary, whom he had cared for since she suffered a stroke and lost most of her ability to speak. He is the only family member who can understand her, and while he was hospitalized, she had to be moved to a nursing home. Now he is focused on regaining enough strength to bring her home.
He hasn’t seen her since the heart attack and has lost 40 pounds in the past several months, dropping from 190 to 150. “I’ll walk through that door a skinny old man. She’s barely going to recognize me.”
In the meantime, Benny has been staying with his son Adam, who takes him to doctors’ appointments, sometimes several in a single day. Adam said he is especially grateful that Tulane now has specialists like Vukelic and Borgi, who both came from Montefiore Medical Center in New York, where they previously practiced and built their expertise in advanced heart care.
“It’s wonderful to know that they have people of that caliber down here in South Louisiana,” Adam said.
Now, as Benny grows stronger each day and prepares to return home to his wife, he does so with deep gratitude for the Tulane team whose expertise made his recovery possible. His story is a testament to what access to advanced heart care can do. At Tulane, those second chances are just beginning.
Honor compassionate care. Support Tulane Doctors.
Tulane Doctors are defined by their dedication, their expertise and their extraordinary care for their patients. By making a gift of $2,500 or more , you can directly strengthen our partner clinics and physician-led research that Tulane Doctors are known for.
Members of the 1834 Society are some of our most committed partners, empowering Tulane Doctors to pursue the groundbreaking research and innovative care that transforms lives.
Expand access. Improve treatments. Accelerate discovery.
Contact Ally Bradley, Director, School of Medicine Annual Giving, at 504-247-1833 or 1834society@tulane.edu for more information.
Annual gifts of $2,500 or more to the Tulane University School of Medicine enroll you as a member of the 1834 Society. Members receive invitations to exclusive School of Medicine events and special access to Tulane Associates programs throughout the year.
Join the 1834 Society by making a gift of $2,500 or more today. Scan the code or visit tmaa.tulane.edu/1834 to learn more.
Stroke Awareness Event is a Lifesaver
As the housing intake coordinator for A New Way of Life – New Orleans and the executive director of Operation Inclusion Center for Women, Denise Williams supports formerly incarcerated women as they rebuild their lives and navigate multiple health challenges. On May 20, 2025, she attended the “Towards a Healthier Us” Stroke Awareness event, held at Voice of the Experienced (VOTE) and supported by The Fit Clinic NOLA. The event featured a presentation by Tulane neurosurgeon Dr. Kendrick Johnson, director of the Tulane Stroke Outreach Program.
Williams said she found the session enlightening, particularly given her own family history of stroke and her age group’s increased risk. She had no idea how quickly that information would become vital.
The session taught Williams about the main signs of stroke and what to do if you see someone exhibiting symptoms.
Just remember the acronym F.A.S.T.
Face: Does one side of the face droop when smiling?
Arms: Does one arm drift downward when raised?
Speech: Is speech slurred or hard to understand?
Time: If you notice any of these signs, call 911!
“Just a few days later, I was at church when I noticed a friend showing some subtle, strange signs, his fingers were twitching, his arm was moving oddly, and his speech was slurred,” Williams recalled. “Because of what I had just learned, I immediately recognized he was likely having a stroke and called 911.”
Her friend was rushed to the hospital, where he was treated in time to avoid lasting damage. He is now recovering and recently sent Williams a photo from his hospital bed with a big smile and heartfelt thanks. “I never imagined how quickly that knowledge would become essential,” said Williams. “This experience reminded me how crucial these kinds of educational events are — not just for those we serve, but for our own lives and loved ones.”



Her story reflects exactly the kind of impact that Johnson, an assistant professor of neurosurgery at Tulane University School of Medicine, hopes to make through his outreach and education efforts.
Stroke is a national emergency that can affect anyone, regardless of age or background.
Johnson is on a mission to raise awareness about stroke prevention and treatment. He knows firsthand how geography and socioeconomic status can dramatically impact healthcare access. Growing up in St. Joseph, Louisiana, a town of just 1,000 residents, he understands the challenges facing rural communities when it comes to critical medical care.
Johnson said that when he compares maps showing poverty rates and stroke cases, a pattern emerges: strokes are more common in areas with fewer
resources. Because most advanced stroke centers are located in cities, people in rural communities face much higher risks.
“Time is brain,” he said, highlighting the importance of immediate medical attention. A few crucial minutes can mean the difference between recovery and permanent disability. Johnson advocates for improved healthcare systems, better access to stroke care and increased public education about this serious health threat.
For Denise Williams and her friend, Johnson’s work has already made a life-changing difference — proof that education, awareness and quick action can truly save lives.
E Dr. Kendrick Johnson, director of the Tulane Stroke Outreach Program
H Stroke awareness event attendee and lifesaver Denise Williams
by sidelined SPINE A
When Jeanette Weiland began experiencing lower back pain, she chalked it up to her workout routine. After being diagnosed with a slipped disc, she knew she needed spine surgery, and she knew just where to go.
s a high school softball player, I spent a lot of time working out and pushing my body to its limits. Many years later, staying physically active is still an important part of my life. So, when the periodic lower back pain I had experienced for decades turned into something more serious, I wondered if my gym days were a thing of the past.
It all began two years ago when I felt a sharp pain in my glute. I’d recently started weightlifting more than spinning, and assumed I’d just strained something. When the pain moved down my left leg, it became debilitating to a degree that I never knew possible. I saw a local orthopedic surgeon who diagnosed me with a slipped disc pressing against my spinal nerve.
I tried everything I could to avoid surgery: cupping, physical therapy, acupuncture, and more. After six months with no relief, it was clear nothing would help.
Given the extremely delicate nature of the procedure I would need, a friend recommended Dr. Christopher Maulucci, a Tulane spinal neurosurgeon and director of their Neurosurgery Spine Program.
PAIN
Just thinking about having spine surgery terrified me. I have two young children. There were so many “what ifs” floating around in my head. However, as soon as I met Dr. Maulucci, I knew I was in the best of hands.
In addition to clearly being an expert in his field, his bedside manner was calming and reassuring. I felt seen and heard, and all my questions were patiently answered in language I could understand. A bonus is that Dr. Maulucci has a wonderful sense of humor, which is extra helpful when you’re facing the prospect of someone operating on your spine!
I am usually the kind of person who gets multiple opinions about anything medical, but given the comfort and confidence I felt with Dr. Maulucci, I didn’t feel the need. Having skillfully performed thousands of complex surgeries like mine (because you know I asked!), it’s no surprise the discectomy he performed on my spine was a complete success.
During follow-up visits, I felt cared for and supported. And although it was scary, with Dr. Maulucci’s

encouragement, I slowly got back to my weightlifting routine and joined a moms’ softball team. There were days I questioned if I’d ever get back to normal, but Dr. Maulucci had no doubt. His whole demeanor was so uplifting.
Coincidentally, about two weeks after my surgery, I started working at Tulane University. The time I spend interacting with the amazing medical professionals at Tulane has only reinforced my appreciation for the importance of academic medicine, which helps ensure that Dr. Maulucci, his team, and all the healthcare providers at Tulane have the most advanced resources and treatments.
The kind of treatments and resources that made a life-changing difference for me. I am beyond grateful to Dr. Maulucci and Tulane for giving me back my active lifestyle.
A Little Patience Eases Patient
As a high school student, Thomas Barbera was a three-sport athlete. While he was accomplished in both swimming and soccer, Tom’s passion was hockey, and he went on to play in college as well.
Even as he neared retirement, Tom jogged five miles a day. After practicing law for 40 years, it was a great way to clear his mind. His back started to bother him occasionally, but he chalked it up to getting older. But when he took a slight fall and was unable to get up, Tom suspected there was more going on than aging.
Unable to help him off the floor, his wife Carol called for help, and soon Tom found himself on the way to the hospital in a firetruck. He wouldn’t return home for almost four months.
“As soon as I got to the hospital, they did an MRI and an angiogram. I barely had time to process what was going on when they told me I needed back surgery that day,” explains Tom. That’s when he met board-certified neurosurgeon Dr. Christopher Maulucci.
As an attorney, Tom questions people for a living. So even with limited time to prepare before surgery, he had a list of questions ready. “When someone is going to be operating on my spine, you can bet I want to get as much information as possible.” But Tom’s list sat unused.
“Dr.
Maulucci went over everything so clearly and patiently that he answered every single one of my questions before I had a chance to ask. It was obvious to me he knew his stuff, and I was in the best of hands.”
After a successful surgery, Tom went from not being able to do anything for himself to walking unassisted and pain free. Although he worked hard to regain all he lost, Tom was impressed with how the Tulane team supported him every step of the way — both literally and figuratively.
“When you first wake up after surgery, you wonder if things will ever return to normal. Dr. Maulucci and his team were nothing but encouraging. They made me see the light at the end of the tunnel. I couldn’t have asked them for anything more.”


Precision, Progress and Patient Focus
At Tulane, the future of spine surgery is already here. Under the leadership of Dr. Christopher Maulucci , director of the Neurosurgery Spine Program, Tulane has become a pioneer in roboticassisted spine surgery — an advancement that’s redefining precision, safety and patient outcomes.
“It’s helped us do procedures and place implants more accurately and consistently,” Maulucci said. “It’s still a hands-on procedure, but the robot adds that unwavering third arm to hold an instrument still and in a perfect trajectory every time.”
Robotic surgery has also made procedures safer for patients and operating room staff as well. Traditional spine surgeries require multiple X-rays throughout the procedure. The improved imaging of the new system greatly reduces that need and greatly reduces the amount of radiation exposure endured by patients and staff.
“In addition to the decreased radiation exposure,” Maulucci said, “robotics diminishes surgical time. Furthermore it aids in the planning process prior to surgery so as to execute an ideal plan in an effort to prevent subsequent surgeries.”
Tulane was an early leader in robotic spine surgery. “We were the sixth site in the world to use the technology,” Maulucci said. “We were very eager to adopt new technology and try something new for the betterment of our patients.”
That willingness to innovate defines Tulane’s culture. “Tulane has been really willing to let us invest in newer technologies and take a risk,” he said. “That open-mindedness has been incredibly

“We were the sixth site in the world to use [robotic spine surgery]. We were very eager to adopt new technology and try something new for the betterment of our patients.”
— DR. CHRISTOPHER MAULUCCI
To support the work of Dr. Maulucci and the Tulane Center for Clinical Neurosciences, scan this code or visit giving.tulane.edu/neurosciences.
welcome, letting us try new things, thrive with them, and continue to push the envelope.”
Equally important, Maulucci added, is the program’s unwavering focus on the patient. “There’s a real thoughtfulness that goes into the care of each person,” he said. “Tulane Doctors really listen, synthesize the data given to them about that particular person, then put together a plan for that individual. We strive to find the right balance so every patient gets the best and safest path to recovery.”
A RESEARCH RACE AGAINST TIME Tulane Cancer Center
Through the combined efforts of Tulane’s clinicians and scientists, one patient’s surgery has opened the door to discoveries that could reshape understanding of a rare cancer — and potentially many others.
When scans revealed multiple tumors in a patient’s abdomen, Tulane physicians quickly realized they were dealing with something almost unprecedented — a rare metastatic meningioma, a type of tumor that almost never spreads outside the brain. Recognizing the opportunity to advance science, the patient’s oncologist and surgeon worked side by side. The team carefully removed the tumor tissue in surgery, and, racing against time, delivered it to Tulane researchers, who began preparing it for study — an effort that could help shed new light on how this rare cancer behaves.
Efforts like this are made possible through the close collaboration between Tulane’s physicians and scientists, ensuring that discoveries made in patient care can be rapidly translated into research models to understand drivers of cancer spread and drug resistance.

“The whole idea is bench-to-bedside and bedside-to-bench,” said Dr. Mark Sides , director of Tulane’s Thoracic Oncology Program and the patient’s doctor. “I recognized that this was a rare opportunity, so I connected the surgeon performing the operation with the basic science researcher who had the tools to study it.”
He explained that the research could have global impact because scientists created a tumor model — a living sample of cancer cells that can be grown and studied for future research — from the patient’s tissue. “Now we have a cell line created for this extremely rare cancer, and looking at the differences in this cancer versus the standard version of this cancer can help us better understand cancer biology that may lead to advances beyond just meningiomas. This could possibly give us insight into a more global picture of cancer biology.”
Sides noted that, to his knowledge, there were no existing cell lines for metastatic meningioma.
G Medical research technician Sophie Dietrich monitors and images live cells in Dr. Burow’s lab.
Tulane cancer researcher Matthew Burow, PhD , said that when Sides contacted him and told him about the rare tissue, he immediately understood the value of the collaboration.
“Meningiomas are usually confined to the brain’s lining and are typically benign. This case was rare because the tumor had spread to the patient’s gastrointestinal tract and peritoneum,” explained Burow, associate professor of medicine and associate chair of research in the John W. Deming Department of Medicine, who also serves as associate director for translational research at the Tulane Cancer Center (TCC). “We knew that if we created this model, it would be a benefit in the future for research in meningioma for other scientists around the country.”
Dr. Kristen Limbach , assistant professor of surgery and a Tulane surgical oncologist who specializes in rare cancers, performed the complex operation to remove the patient’s tumors and ensure the tissue could be preserved for research. After the tissue had been given to pathologists, she finished up in the operating room while a team from the Louisiana Cancer Research Center (LCRC) Biobank transported the tissue to keep it viable for study. It was, quite literally, a race against time.
“Dr. Sides reached out about this rare case, and it really became a collaborative effort,” Limbach said. “It’s a story of exceptional collaboration for all these different players working together to get this tissue over to Burow’s lab in an appropriately processed way.”
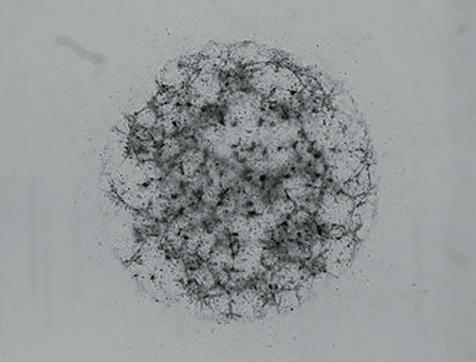
Inside Burow’s lab, the team worked quickly to implant the tissue into mice and culture the organoids — tiny, threedimensional clusters of cells that mimic how tumors behave inside the body. The tissue is being studied through both patient-derived xenograft (PDX) and organoid models.
“ It really became a collaborative effort. It’s a story of just exceptional collaboration for all these different players working together.”
— DR. KRISTEN LIMBACH
E View of meningioma organoid in culture
This work is supported through TCC’s Organoid Core, a special lab where scientists grow tiny models of tumors from patient cells.
“These donor tissue-derived systems would more accurately mimic clinical features of the tumors than traditional cell cultures,” according to Van Barnes, PhD , assistant director of the TCC Organoid Core and a School of Medicine research faculty member. “Among the benefits, this work would enable evaluation of drugs that may guide treatment decisions and drive the development of novel therapeutic strategies to benefit patients.”
Delia Carlino , a medical research specialist in the TCC Organoid Core, was on hand on the day of the surgery. She explained the urgency everyone felt. “It ends up being a long day for the team — while the surgery is happening, we’re setting up and preparing everything in the lab to keep the tissue viable.”
Sophie Dietrich , a medical research technician in Burow’s lab explained the race against time. “It was critical to keep the tissue alive,” Dietrich said. “Once removed from the body, tumor cells begin to deteriorate quickly. To study them, researchers must act fast, processing and preserving the sample within hours so they can continue to grow and function in the lab. Implanting the samples in mice enables more indepth analysis to understand tumor growth and spread in a whole system rather than isolated on a dish.”
Behind every step of the process — from surgery to research — was a network of Tulane colleagues who know each other well and share a common purpose. Sides said he has known Burow for nearly two decades, since their early days at Tulane. “I’ve worked with Matt since I was a graduate student and postdoc, back when he was a junior investigator,” Sides said with a smile. “We were in labs just a floor apart, and we talked often.”
Limbach agrees that the real story is one of interdisciplinary collaboration. She says, “It was truly a team effort — all of us working together to get the tissue where it needed to go, quickly and correctly,” she said. “Because we know each other and have built those relationships, we can move fast when unique opportunities like this arise.”
“When you go to Tulane doctors from the TCC, there’s a high degree of collaboration between us. We’ve worked together closely for years, and patients benefit from that multidisciplinary team that listens, shares ideas, and explores every option across the spectrum of cancer care.”
— DR. KRISTEN LIMBACH
Limbach added that this kind of seamless coordination reflects what sets Tulane apart. Through the combined efforts of Tulane’s clinicians and scientists, one patient’s surgery has opened the door to discoveries that could reshape understanding of this rare cancer — and potentially many others.
Carlino said, “Because it’s so rare, we want to see how it reacts in organoid form, how it responds to different treatments, and what kinds of proteins it expresses.”
To support cancer research at Tulane Cancer Center, scan this code or visit medicine.tulane.edu/giveTCC


H Medical research specialist Delia
under sterile conditions.
E (From left) Dr. Matthew Burow, Sophie Dietrich, Dr. Van Barnes, Dr. Kristen Limbach, and Dr. Mark Sides
Carlino cultures patient-derived breast organoids
kicking leukemia!

H Addy received treatment for leukemia at Manning Family Children’s in 2024.
E A year later, Addy was back in school.
Summer had just begun for 11-year-old Adalyn Jensen, known to her family and friends as “Addy.” She should have been swimming, going to sleepovers and counting down the days until her family’s annual trip to Florida. Instead, she and her family found themselves living inside the sterile halls of Manning Family Children’s pediatric oncology unit.
There, she would rely on both cutting-edge treatment and exceptional, hands-on care to survive.
In June 2024, during a Father’s Day dinner, Addy told her mom, Stacey, that she didn’t feel well. Minutes later, she was vomiting what looked like blood.
At first, they thought it was a stomach bug. Over the next several weeks, Addy went to urgent care and the ER repeatedly, complaining about back and leg pain, and then she’d bounce back before the exhaustion, vomiting and pallor continued.
On July 3, after being urged to go to Manning Family Children’s, Addy was then diagnosed with B-cell acute lymphoblastic leukemia.
Treatment began immediately, and so did the side effects. Infections, high blood sugar and neuropathy left Addy unable to eat or walk for stretches at a time.
Dr. Justin Farge, Addy’s oncologist, quickly became a trusted confidant. “He was amazing,” said Stacey Jensen, Addy’s mother. “If I ever had a concern or something that was bothering me, he would take the time out of his day to physically sit in the room with us and talk it over, hash it out, go over options.”
Despite months of chemotherapy, Addy still had residual cancer. Her body was exhausted. It was time for a new path.
Farge, assistant professor of pediatrics at Tulane, called in Dr. Ben Watkins, director of the Pediatric Stem Cell Transplant and Cell Therapy Program at
Tulane University and Manning Family Children’s. Her best option: CAR T-cell therapy, an advanced treatment in which a patient’s own immune cells are collected, genetically reprogrammed to attack cancer, and infused back into the body. And Addy was at the only pediatric center in Louisiana offering it.
“When we first heard about CAR T therapy, I was honestly very nervous. The idea of having your child’s cells taken out and modified in a lab was incredibly scary. But after meetings with Dr. Watkins and his team, we were put completely at ease. There was no need to go anywhere else.”
— STACEY JENSEN
Stacey vividly remembers the uncertainty and fear that accompanied their initial suggestion. “When we first heard about CAR T therapy, I was honestly very nervous,” she recalled. “The idea of having your child’s cells taken out and modified in a lab was incredibly scary. But after meetings with Dr. Watkins and his team, we were put completely at ease. There was no need to go anywhere else.”
Their medical odyssey spanned an incredible 115 days of inpatient treatment, during which Stacey became intimately familiar with every nuance of Addy’s care. “I was the main caretaker,” she explained. “My husband would stay a night or two to give me a break, but I never wanted to leave her alone.”
She said that looking over the medical notes revealed just how dire the situation was. “Looking back at her clinical notes,” Stacey said, her voice catching, “I was taken aback to find a note stating that if she wouldn’t have done CAR T, she wouldn’t have survived. I never knew just how serious her complications were.”
The Tulane medical team’s approach transcended traditional patient care. Stacey describes how they made complex medical information accessible: “They would always do their best to help me understand. I’ve been in this for over a year now, and I almost feel like I could be a doctor because of all the knowledge I’ve gained.”
Dr. Watkins and Dr. Farge emerged as trusted allies, she said.
“[Dr. Watkins and Dr. Farge] are down to earth, knowledgeable, with amazing bedside manner. They never made me feel like my concerns weren’t valid. I consider the doctors and nurses like family.”
— STACEY JENSEN
Today, Addy is back in school, though not without challenges. Side effects from her prolonged hospital stay include bone demineralization, making her prone to fractures. “She broke her toe a few months ago, and then she tripped and broke her leg,” Stacey said. “But she’s resilient, always counting down the days until her next milestone.”
Eight months post-infusion, Addy has already undergone seven bone marrow biopsies. Each positive result brings hope and a renewed appreciation for the medical team that saved her life.
When asked what she would say to the doctors and nurses who cared for Addy, Stacey’s response is simple yet profound: “I couldn’t be any more grateful for what they did. They saved her life.”


E Addy (seated) having fun with her mom Stacey, brother Joey, and dad Jon on her dream trip to New York City in October 2025.
F Addy and her mom in NYC

Advancing Pediatric Cancer Care Locally and Globally
Dr. Benjamin Watkins was raised in a log cabin on a blueberry farm in the Ozark Mountains of rural Arkansas. The closest stoplight was an hour away, and adequate medical care was even farther. “I grew up witnessing what the lack of access to medical care could do to a community.”
Today, as director of the Pediatric Stem Cell Transplant and Cell Therapy Program at Tulane University and Manning Family Children’s, he has dedicated his career to ensuring that all children have access to the advanced treatments and compassionate care they deserve.
Watkins came to New Orleans from Emory University in 2023 after seeing the great need in the region. “Coming here felt like an opportunity to bring new therapies, expand what we can offer, and help address some of the health disparities that exist in this state.”
An associate professor of pediatrics at Tulane School of Medicine, Watkins is glad to be part of an academic medical center like Tulane, where discovery and care go hand in hand. “Academic institutions are where innovation occurs,” Watkins said. “Centers like Tulane are pushing the field forward. That’s where the research is being done, the clinical trials are taking place, and the latest therapies are being developed.”
For many of his young patients, a stem cell transplant represents a second chance at life. “Stem cell transplant is often the last hope for a cure,” Watkins said. “It’s like a rebirth, a chance to start over with a brand-new immune system, a
brand-new blood system, and hopefully a life free of the disease that brought them here.”
Watkins’ groundbreaking research has focused on graft-versus-host disease, one of the leading causes of death after a stem cell transplant. One of the greatest challenges in transplantation, he explained, is finding a donor whose immune system closely matches the patient’s. For Black, Indigenous, and other communities of color, compatible donors are far less common, increasing the risk of severe complications such as graft-versus-host disease. These disparities in donor matching contribute to lower survival rates and deepen existing inequities in health outcomes.
To address that problem, Watkins helped lead the clinical trial evaluating the drug abatacept in the prevention of graft-versus-host disease. The addition of abatacept resulted in a dramatic reduction in the disease — from about 30 percent to just 2 percent. Thanks to his work, abatacept became the first FDA-approved drug for preventing this life-threatening condition.
“Our survival rates were better; our outcomes were much improved,” Watkins said. “The goal was to level the playing field and reduce some of the health disparities that exist and this drug helped do just that.”
Today, Watkins is building on that success. He’s leading research to test abatacept for use in other diseases and directing an early-phase clinical trial of a drug aimed at preventing post-transplant leukemia relapse, which could improve survival
rates for children undergoing stem cell transplants. In addition, Watkins is leading new efforts in gene therapy for sickle cell disease and thalassemia, which he believes will dramatically change the treatment landscape for numerous diseases.
A pediatric hematologist/oncologist, Watkins focuses on building trust and forming deep connections with patients and their families facing life-altering diagnoses. In Cambodia, where he directs a pediatric oncology program, he has helped transform childhood cancer care.
“When we started working in Cambodia in 2013, there was no treatment for pediatric cancer in the entire country,” Watkins said. “Children were diagnosed, but they weren’t receiving care. They were dying of curable diseases due to lack of access. There was zero opportunity to be treated.”
To address that need, Watkins, colleagues from the American Society of Hematology and Health Volunteers Overseas, and other U.S. healthcare providers worked at a children’s hospital in Siem Reap where they trained local physicians, established treatment protocols, and provided resources so they could care for young patients. The results have been remarkable. Today, 70 to 80 percent of children with cancer in Cambodia are being treated, and survival rates for leukemia have risen from zero to more than 50 percent for some diseases.
Watkins’ mission of improving access to health care reflects Tulane’s enduring commitment to improving health — for all.

“Improving access is at the heart of everything I do. I’ve seen firsthand how the lack of access can devastate communities, and that experience continues to drive my work. We have to do better — locally, regionally, nationally, and globally — because lives depend on it.”
— DR. BENJAMIN WATKINS
To support the work of Dr. Watkins and Tulane Cancer Center, scan this code or visit giving.tulane.edu/ pediatric_hematology_oncology.
SUPPORTING RESEARCH AT EVERY STAGE Tulane Center for Clinical Research
Before a new drug ever reaches a pharmacy shelf or a new procedure becomes standard of care, it must first be thoroughly tested with patients. That’s clinical research, and it’s happening every day through the Tulane Center for Clinical Research.
“The Tulane Center for Clinical Research was set up to provide comprehensive and centralized research infrastructure to our physicians and other investigators,” said Eva Lustigova , senior director of the center. “We support our physicians throughout the entire process.
That means helping with every step of the way — from developing a research proposal or clinical trial protocol, to securing approvals, recruiting participants, managing data, ensuring regulatory compliance, and finally, assisting with study closeout. The goal, Lustigova said, is to make it as seamless as possible for Tulane researchers to move from an idea to a discovery that can ultimately change lives.
Advancing research initiatives
The center supports research studies across a wide range of School of Medicine specialties such as endocrinology, cardiology, nephrology, pulmonary medicine, infectious diseases, and orthopedics — and also partners with the School of Science and Engineering and the Celia Scott Weatherhead School of Public Health and Tropical Medicine to advance their research initiatives. More than 200 studies have been supported by the center over the past ten years.
When science and research touch lives, it becomes something greater. “Patients can get access to novel therapies that may not be available on the market,” Lustigova said. “For patients who have conditions where they’ve run out of treatment options, a clinical trial may provide a new possibility.”
Participants in Tulane studies often experience benefits beyond access to new treatments. “You get more frequent touchpoints with the research team and healthcare providers, offering almost personalized care,” Lustigova said. “There’s also an altruistic benefit — potentially helping others down the road get access to better treatments. Patients who decide
G Eva Lustigova, senior director, Tulane Center for Clinical Research (center, red boa) and Sarah Bigelow, executive director, Clinical Trials at the Tulane Cancer Center (center, green boa) surrounded by staff and medical students pose for a photo at Clinical Trials Day in May 2025.
to volunteer in clinical trials are the true heroes who help move medicine forward.”
During the COVID-19 pandemic, the center played a pivotal role in vaccine and treatment trials, showcasing its flexibility and commitment to urgent global health needs.
More than drug development
While many projects focus on pharmaceutical trials, the center’s work extends beyond drug development. One example is an investigator-initiated study that will explore continuous glucose monitoring for patients with type 2 diabetes — research that could demonstrate how this technology improves long-term outcomes.
The center is just one part of Tulane’s expansive research enterprise, where discoveries made in the lab or at the bedside are advancing science, improving human health, and shaping a healthier future for all.
“The goal of the center is to make it as seamless as possible for researchers to move from an idea to a discovery that can ultimately change lives.”
– EVA LUSTIGOVA
To support the Tulane Center for Clinical Research, scan this code or visit giving.tulane.edu/ gratefulgiving25. Under “Designations” select “Dean’s Discovery Fund - Medical Research.”



ADVANCING WOMEN’S HEALTH
Tulane Obstetrics & Gynecology
Tulane’s Department of Obstetrics and Gynecology is leading the way in women’s health care, addressing every stage of a woman’s life.
Read on to learn how physicians in the Department of Obstetrics and Gynecology are collaborating across Tulane and pioneering new frontiers in women’s health.

From groundbreaking research in preeclampsia and menopause to innovative, minimally invasive treatments and cancer prevention, Tulane Doctors are advancing care and improving outcomes for women across generations.
“We deliver patient-centered care with the strength of Tulane School of Medicine and Tulane’s clinical and basic research and innovation at our side,” said Dr. Gabriella Pridjian , chair of obstetrics and gynecology and associate dean for surgical services at Tulane School of Medicine.
Through interprofessional collaboration with clinical specialists across Tulane, the department provides access to cutting-edge clinical trials and personalized medicine that drive better outcomes for every patient.
The breadth of expertise at Tulane sets the department apart, meeting women where they are at any stage of life. For example, Dr. Cecilia Gabala and the maternal fetal medicine team offer integrated genetics, ultrasound and high-risk pregnancy care. Dr. Amber Naresh brings exceptional expertise in pre-cancer cervical lesions, while Dr. Jessica Shank leads the innovative gynecological oncology program.
While having a baby remains a joyful milestone, complications can arise unexpectedly. For example, preeclampsia — a dangerous high blood pressure condition — can develop rapidly during otherwise normal pregnancies. Tulane faculty have made the prediction and treatment of preeclampsia a research priority, directly improving how this life-threatening condition is managed.
That same commitment extends to menopause management, where the landscape is shifting dramatically. For years, women endured menopausal symptoms without access to estrogen replacement therapy. Now, recent studies from Tulane and peer institutions reveal that carefully selected patients can benefit significantly from hormone replacement
G (From left) Tulane Obstetrics & Gynecology Doctors Amy Vaughan, Gabriella Pridjian, Amy Grace and Elizabeth Kelly stand in front of Tulane Lakeside Hospital.
“Caring for women is a continuum with different needs along the way. As Tulane Doctors, we are honored to help you throughout this journey.”
— DR. GABRIELLA PRIDJIAN
therapy, experiencing relief from menopausal symptoms, decreased osteoporosis risk, cardiovascular protection and potentially improved cognitive function.
“Every woman is different… and that is where individual evaluation and treatment are paramount,” Pridjian said.
Noninvasive or minimally invasive techniques are now the standard of care for most women who need gynecologic surgery. These innovative new procedures offer patients smaller incisions, enhanced precision and shorter recovery times. In addition, Tulane offers many procedures on an outpatient basis, allowing women to return home the same day.
Tulane is pioneering new frontiers in cancer risk reduction. By integrating genetics, lifestyle data and other predictive factors, Tulane Doctors help women prevent disease before it starts. The Papanicolaou (PAP) smear screening test for cervical cancer has evolved significantly, and HPV testing combined with vaccination may eventually eliminate cervical cancer entirely. For women with hereditary risk factors, genetic testing enables personalized screening protocols with more sensitive detection methods and the option for riskreducing surgery.
“Caring for women is a continuum with different needs along the way,” said Pridjian.
“As Tulane Doctors, we are honored to help you throughout this journey.”

To support the work of Dr. Pridjian and Women’s Health, scan this code and select “OBGYN/ Women’s Health Support Fund.”
Compassionate Care Across Women’s Life Stages
Dr. Amber Naresh is there for her patients through every stage of life — from a teenager’s first gynecological visit, to the excitement and challenges of pregnancy, to the changes that come with menopause. For Naresh, that continuity of care is at the heart of why she chose obstetrics and gynecology as her specialty. “I enjoy getting to know people over time and being able to help them through different health challenges,” Naresh said.
Knowing her patients across decades also means Naresh understands what matters most when they need surgery: effective treatment with the fastest possible recovery time. That’s why she’s embraced minimally invasive robotic surgery.
“We’re able to perform much more complex procedures using minimally invasive techniques than ever before,” Naresh said. “That’s true for me individually, but also for us as a department and as a specialty — we can do so much more with fewer and smaller incisions.”
Beyond the operating room, Naresh is helping shape the future of cancer prevention and treatment through research. She manages an HPV registry at Tulane, gathering data that could transform how physicians approach cervical cancer screening and treatment. “The information could be used to answer a wide array of questions about cancer prevention,” Naresh said. “We can evaluate current techniques for managing precancerous conditions, assess emerging approaches, and identify patterns that help us prevent cancer more effectively.”

“I enjoy getting to know people over time and being able to help them through different health challenges.”
— DR. AMBER NARESH
Throughout all her work, whether in surgery, research or the exam room, Naresh maintains a collaborative approach to patient care.
“I really view myself as a consultant, not someone dictating care,” she said. “I’m here to provide accurate, up-to-date information and help guide patients.” She believes patients should be fully informed partners in their own healthcare decisions, equipped with knowledge to choose what’s right for their lives.
This blend of advanced surgical expertise, groundbreaking research and patient partnership defines Naresh’s approach to women’s health, which is comprehensive, compassionate and designed to empower every patient she treats.
Ask a Tulane Doctor
Have a health or wellness question you’ve always wondered about? Tulane experts are here to help.
With Wave Advice, Wellness Wire connects your everyday questions with Tulane doctors and health professionals. Share what’s on your mind, and our team will route your questions to the right Tulane expert for general guidance.
• Ask about everyday health and wellness (sleep, movement, heart and brain health, kids’ health, stress, aging, and more).
• No question is too basic or too “awkward,” as long as it’s not an emergency or a substitute for a medical visit.
We’ll publish a selection of questions and answers on our website and feature highlights in future issues of Wellness Wire , so you can learn from what others are asking too.


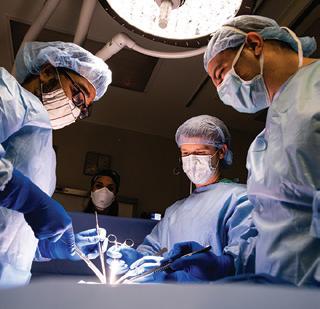
We Heal Communities
At Tulane, we understand that medical care — whether routine or life-changing — often comes during one of the most challenging moments in a patient’s life. That is why we are committed to providing compassionate, world-class care to every patient we serve and to the families who walk alongside them.
When we care for an individual, we are entrusted with more than a medical outcome. We are entrusted with the well-being of families, friends, and communities. This belief is central to our mission and reflected in our guiding principle: We Heal Communities.
Your philanthropic support plays a vital role in this mission. Gifts help advance innovative treatments, fuel physician-led research into complex diseases, and train the next generation of caregivers. Together, we can ensure that exceptional care reaches more patients and builds healthier communities — today and for generations to come.
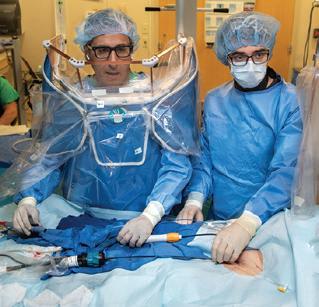


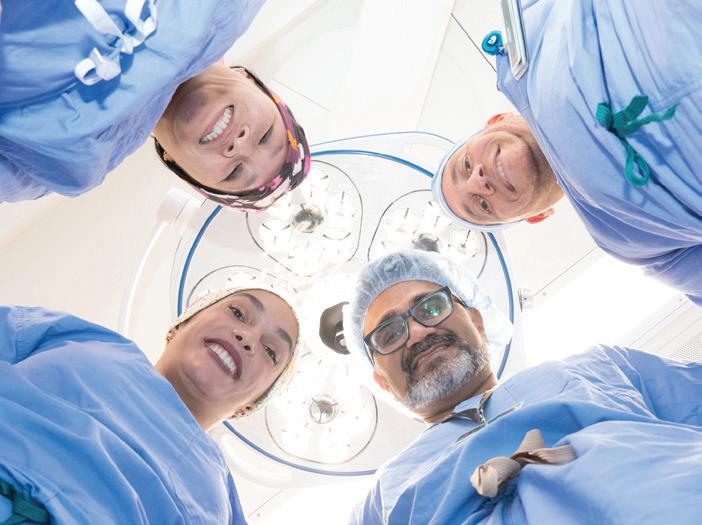
Join Us in Making a Lasting Impact
• Make a gift in honor or memory of a loved one
• Make a gift in honor of a caregiver
• Support medical research that is important to you
Continue the Conversation
• Share your story about a special caregiver who has made a difference in your life
• Include Tulane School of Medicine in your estate plan
At Tulane, we understand that philanthropy is deeply personal. Many choose to give in gratitude for care that touched their lives or the lives of those they love. We are committed to honoring those motivations with meaningful, lasting impact.
From recognizing a specific caregiver to advancing patient care and medical research, we work with donors to ensure their generosity supports what matters most to them.
If you would like more information about patient care initiatives, clinical innovation, or physician-led research at Tulane Doctors and the Tulane School of Medicine, we welcome the opportunity to connect.
Contact:
Krystal Oliveira Springgate, CFRE Executive Director, Health Systems Office of Advancement koliveira@tulane.edu
Cell: 504-224-1715
Michael Richmond, CFRE Director of Annual Giving, Health Systems mrichmond@tulane.edu
Cell: 702-813-5713

WELLNESS WIRE
Writing and Editorial Contributors
Krystal Oliveira Springgate, Michael Richmond, Mary Sparacello, Stephanie Hoina, Studio Mundi, Inc.
Design Studio Mundi, Inc.

Thank you for entrusting Tulane to be your healthcare provider.
Our Tulane Doctors work tirelessly to provide exceptional care, lead groundbreaking research and train the next generation of medical professionals through our network of clinics and centers. They are the heart of Tulane’s mission to move medicine forward.
Together, we can ensure our doctors continue to deliver the high-quality care and innovative treatments that define Tulane’s legacy. By making a gift at gratefulgiving.tulane.edu, you help to enhance care and spark medical breakthroughs. Your generosity is more than a donation — it is a testament to your profound trust and appreciation for Tulane Doctors.
