

ISSUE 2: THE BODY ISSUE APRIL 14 2026




ISSUE 2: THE BODY ISSUE APRIL 14 2026

ARTIST: VERONICA GRIGNANO
Bachelor of Health Sciences (Honours), Class of 2027, McMaster University
Healthy skin with no injury. Blood flow and tissue function are intact, allowing for typical sensation and appearance.
A mild, reversible cold injury with no permanent tissue damage. Skin appears pale or erythematous with a transient numbness or tingling sensation.3
A partial-thickness injury impacting superficial skin tissue. Affected areas may appear waxy or white initially, followed by clear or milky blister formation and edema after rewarming.3

Frostbite is a thermal injury resulting from prolonged exposure to cold temperatures, ranging from superficial injury to deep injury involving necrosis of the skin and underlying tissues.1 Any portion of exposed skin is prone to frostbite, however, frostbite most commonly occurs in peripheral areas such as the fingers, toes, ears, and nose. When tissue temperature drops below freezing, vasoconstriction reduces blood flow to peripheral tissues, resulting in ice crystal formation and cellular damage.2 Further injury can occur during rewarming, as restored blood flow triggers inflammation, vessel damage, clot formation, and fluid leakage into surrounding tissues.2 Timely rewarming is necessary to minimize injury, though severe cases may require amputation.2
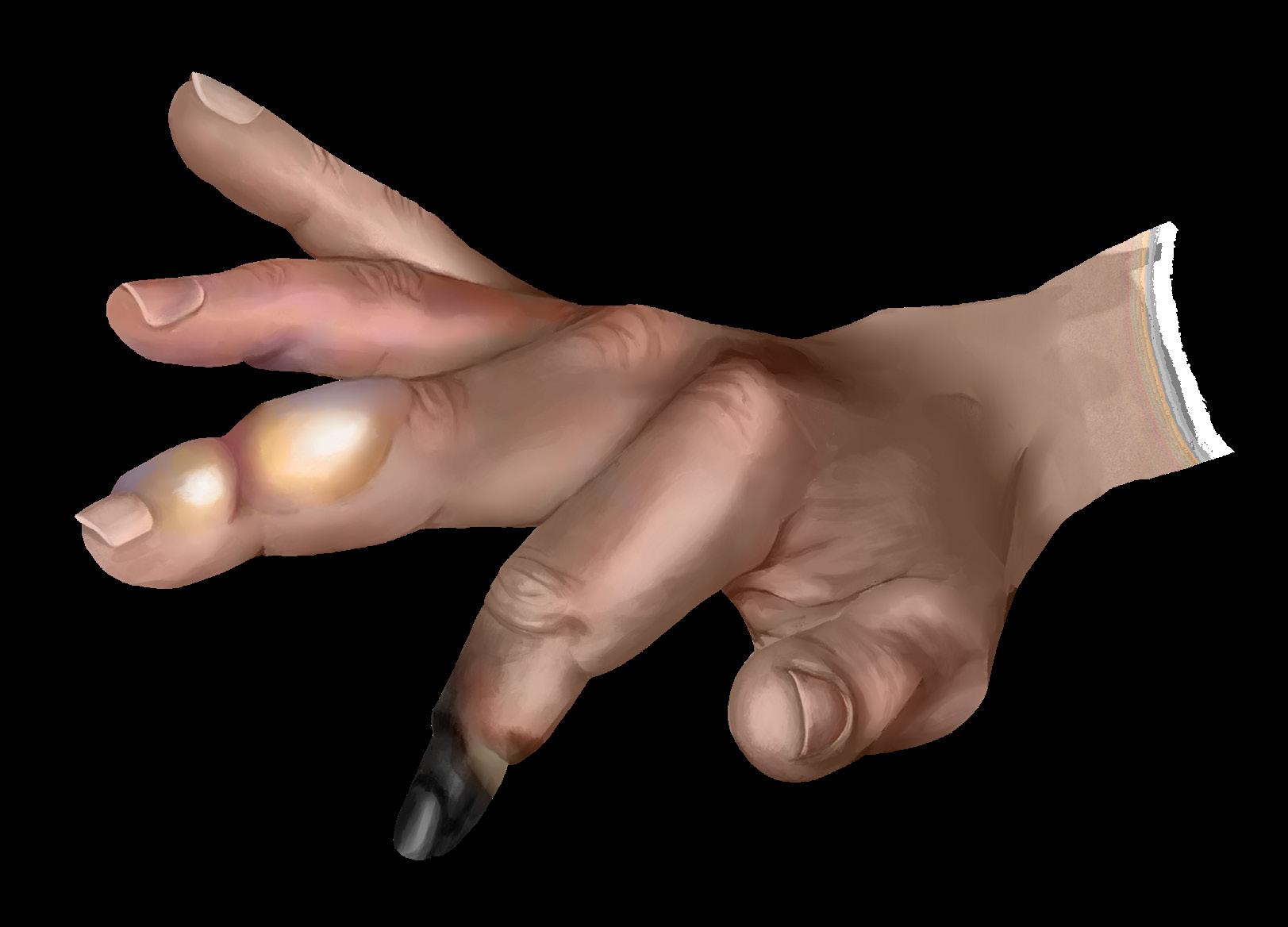
A full-thickness injury extending into muscle, tendon, and bone, resulting in permanent damage. The affected region loses function and sensation, and surrounding tissues become blackened and hardened as a result of tissue death.3

Frostbite disproportionately affects socially and structurally vulnerable populations. Evidence from Canadian emergency department data indicates that individuals experiencing homelessness are overrepresented among cases of deep frostbite compared with superficial injuries.1 Housing insecurity, inadequate shelter capacity, and barriers to timely medical care increase both the likelihood of injury and the risk of delayed presentation, resulting in more severe tissue damage at diagnosis. Mental health disorders and substance use are also prevalent among patients with severe frostbite, as these conditions can impair judgment, reduce awareness of early symptoms, and limit the ability to seek warmth or medical attention.4 Additional risk is observed among individuals living in rural or remote regions, where colder climates, longer emergency response times, and reduced access to specialized care contribute to worse outcomes.5
ARTIST: ELAINE WANG1
1Bachelors of Health Sciences (Honours), Class of 2026, McMaster University
REVIEWED BY: VICKY LIN2
2Masters of Sciences in Biomedical Communication (Honours), Class of 2026, University of Toronto
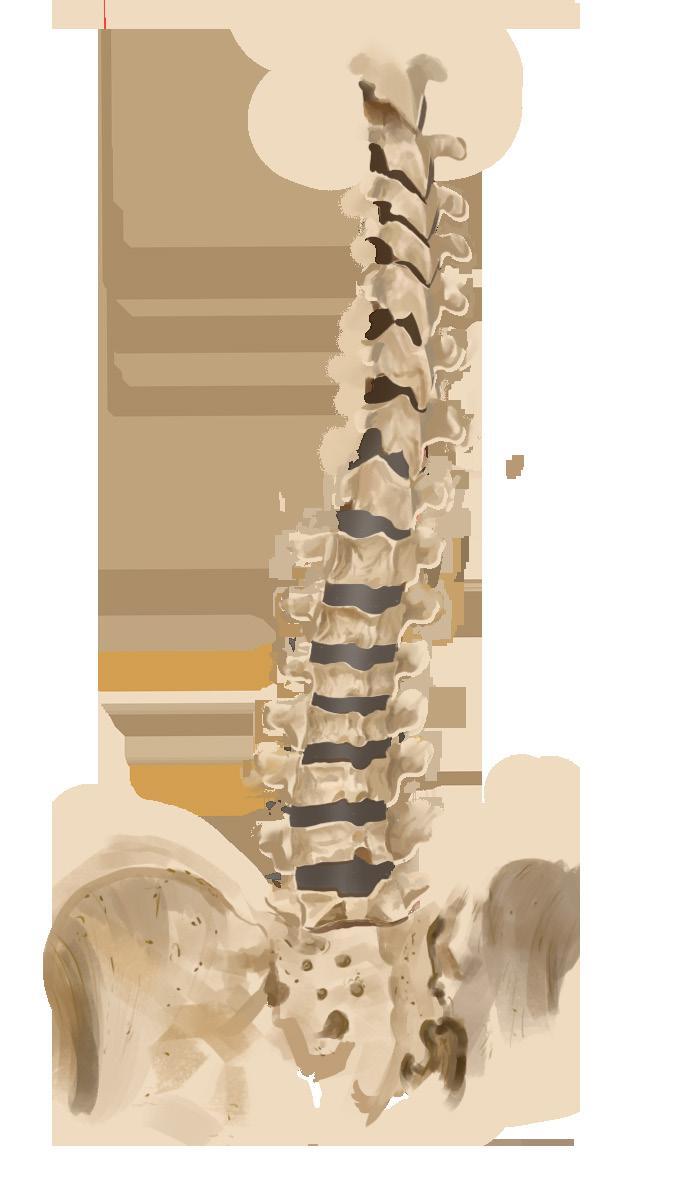
Osteoporosis is a bone disease in which bones gradually lose mass and their internal structure begins to break down, making them weaker and more likely to fracture.
Women who are underweight and entering menopause are at a particularly high risk of developing the condition, since both factors speed up the process of bone loss. This is because hormones play a key role in keeping bones healthy. Estrogen, in particular, helps regulate the balance between bone formation, where new bone tissue is built, and bone resorption, where old bone is broken down. When estrogen levels drop during menopause, this balance is disrupted and bone breaks down faster than it can be replaced. Over time, both the dense outer layer and the spongy inner layer of bone become thinner and weaker, making fractures more likely even from relatively minor falls or impacts.
The scale of this disease is significant. The Public Health Agency of Canada estimates that 80% of those living with osteoporosis are women.1 Osteoporosis is dangerous for older adults because
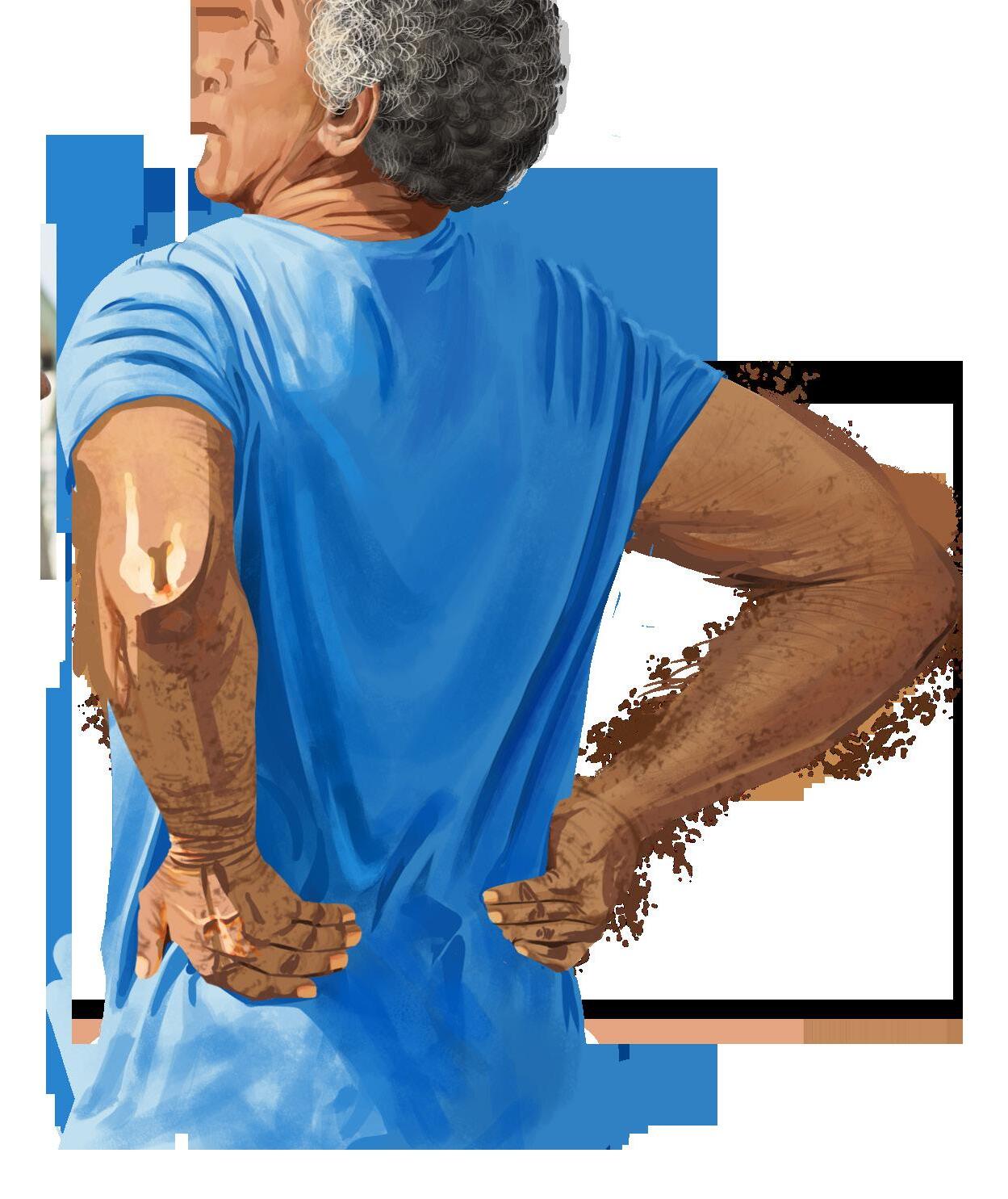
it increases people's risk for hip fractures, which are among the most serious injuries an older aduvvlt can experience. Women account for 75 to 80 percent of all hip fractures in Canada (figure 1).2 A hip fracture often marks the point at which a person can no longer live independently, and frequently leads to admission into a long-term care facility. Because of this, osteoporosis threatens not only a woman's physical health, but also her ability to maintain independence as she ages.3
Preventing and managing osteoporosis requires a comprehensive approach that combines lifestyle changes with medical treatment. Weight-bearing exercises like walking and strength training help slow bone loss, while getting enough Calcium and Vitamin D through food or supplements supports bone density.4 Adjusting the home environment to reduce fall risks is also a routine part of care. When medication is necessary, bisphosphonates are the most commonly prescribed and are considered the first-line treatment. They work by attaching to bone tissue and slowing down the cells that break bone down, which helps preserve bone strength over time.4 Used together, these treatments aim to protect skeletal health and help patients maintain their functional independence for as long as possible.
1,400 1,200 1,000 800 600 400 200 figure 1. Annual Rate of Hip Fractures in Canada Rate (per 100, 000)
1. Osteoporosis and related fractures in Canada, 2023 [Internet]. Government of Canada. 2016. Available from: https://www.canada.ca/en/public-health/services/publications/diseases-conditions/osteoporosis-related-fractures-canada-2021.html
2. Public Health Agency of Canada. Osteoporosis and related fractures in Canada: Report from the Canadian Chronic Disease Surveillance System 2020 [Internet]. www.canada.ca. 2020. Available from: https://www.canada.ca/en/public-health/services/publications/diseases-conditions/osteoporosis-related-fractures-2020.html
3. Osteoporosis Risk Factors [Internet]. UC San Diego Health. Available from: https://health.ucsd.

Age

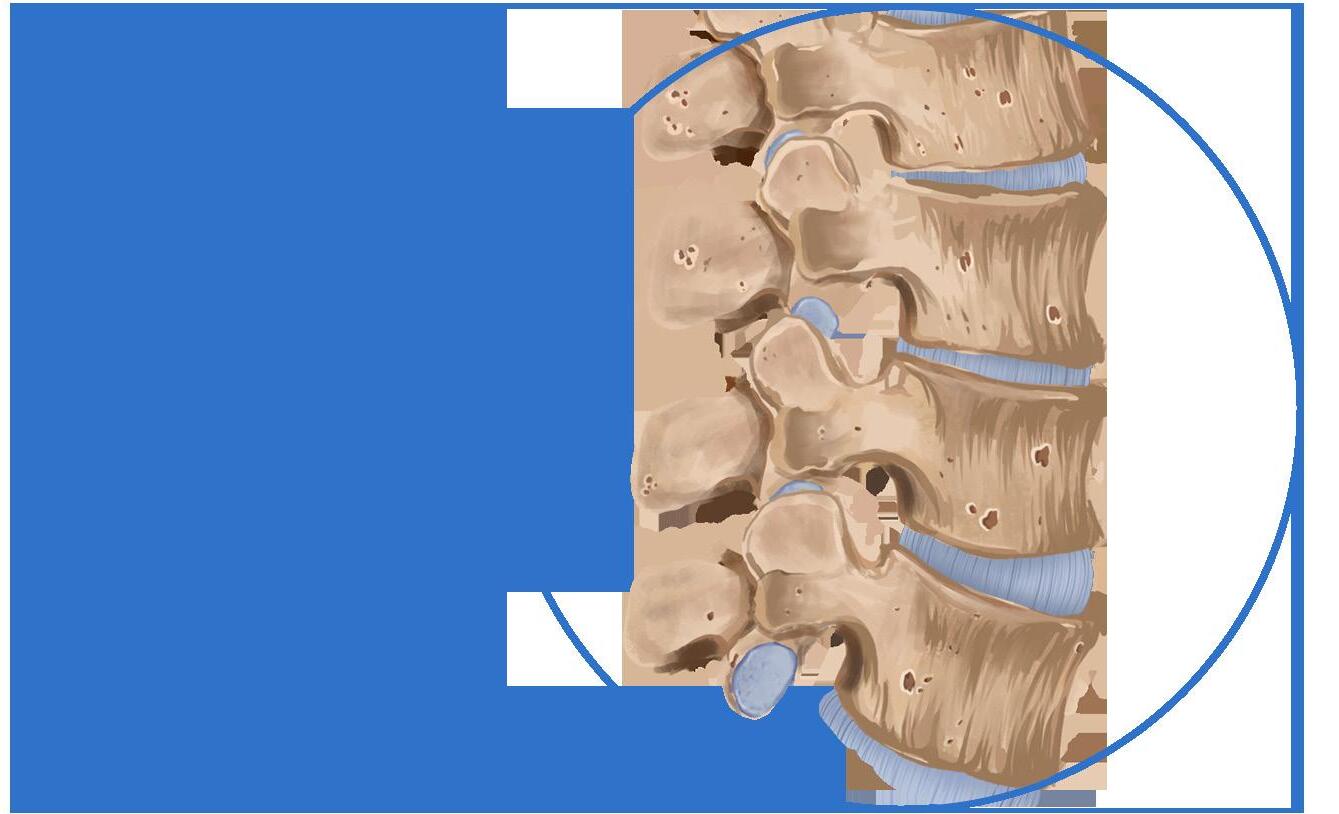
Healthy Trabecular Bone low porosity
Osteoporotic Trabecular Bone high, visible cavitation
edu/care/endocrinology-diabetes/osteoporosis/risk-factors/#women-and-osteoporosis
4. Qaseem A, Hicks LA, Etxeandia-Ikobaltzeta I, Shamliyan T, Cooney TG. Pharmacologic Treatment of Primary Osteoporosis or Low Bone Mass to Prevent Fractures in Adults: A Living Clinical Guideline From the American College of Physicians. Annals of Internal Medicine. 2023 Jan 3;176(2).
5. Kado DM, Huang MH, Barrett-Connor E, Greendale GA. Hyperkyphotic posture and poor physical functional ability in older community-dwelling men and women: the Rancho Bernardo Study. J Gerontol A Biol Sci Med Sci. 2005;60(5):633–7
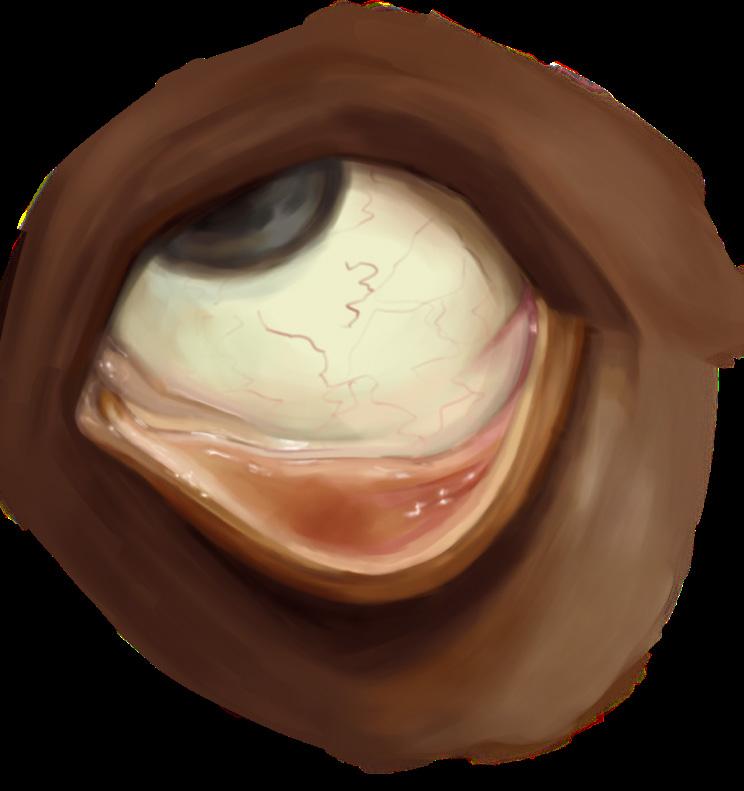
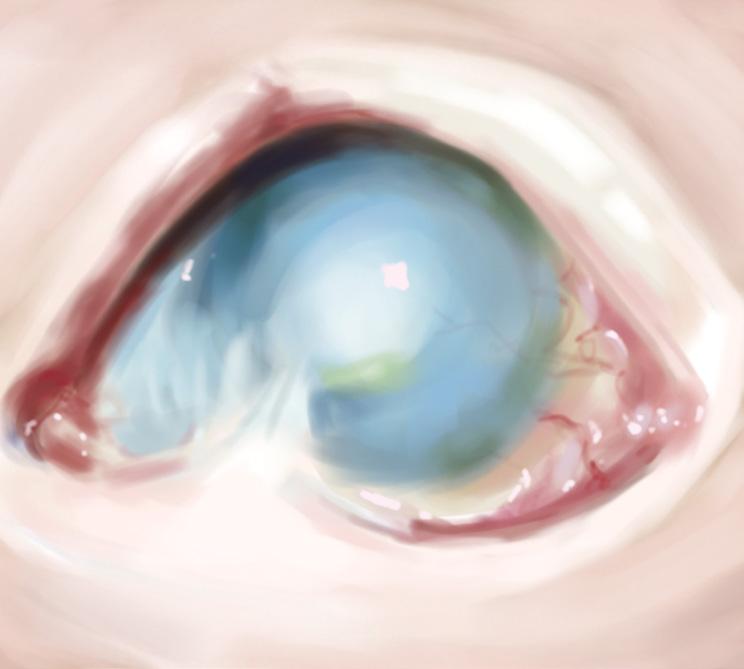
Ocular cicatricial pemphigoid (OCP) is a rare, chronic autoimmune disease with a 0.015% incidence rate, though due to underdiagnosis, prevalence is expected to be higher.1 This disease is a subset of Mucous Membrane Pemphigoid that targets the eye. Onset occurs approximately at 60 years and predominantly found in women than men with a 2 to 1 ratio.1,2 The primary place of inflammation is the eye’s conjunctiva, the thin mucous membrane lining the eyelid, a vulnerable area that increases in risk with age.3,4 As the disease progresses, serious complications develop including scarring of the eye tissues, clouding of the cornea, abnormal growth of eye tissue, and compromisation of the eyelid.3 This creates significant implications for the individual’s quality of life. OCP’s morphological damage may result in visual impairment, visual loss, or blindness.1 The disease symptoms differ in the extent of its severity and progression across patients.1,3 Initial symptoms often mimic chronic, non-specific eye irritation that frequently get misdiagnosed as allergies or chronic conjunctivitis.1 Early diagnosis and treatment are decisive to disease management and progression.
Older women are established to have a stronger association with developing OCP, in particular, postmenopausal women.5 However, there is a notable lack of research directed at this gender difference despite the large disparity.6 The present theories addressing the demographic disparity appoint a variety of factors including biological, societal, cultural, and behavioural.6 Research has mainly been aimed at investigating the physiological and pathological differences of the individual’s biological sex.6,7 The body’s ocular tissues have systems that directly respond to sex steroid hormones of the reproductive system.8 Understanding the mechanisms contributing to disease incidence, can aid health providers and researchers to better help those impacted.
Progression of OCP can be evaluated through a clinical scale or depth of the inferior fronix.1 Inferior fornix depth loss varies in individuals and refers to: 0-25%, 25-50%, 50-75%, 75-100%.1,9 The modified grading scale is as follows:9,10
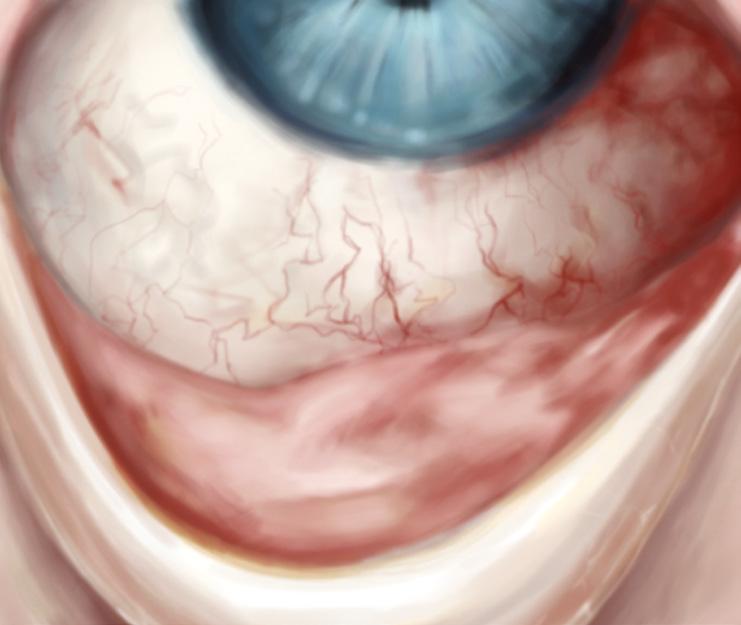
STAGE 1: SUBEPITHELIAL FIBROSIS
• Chronic inflammation, early scarring, no structural distortion
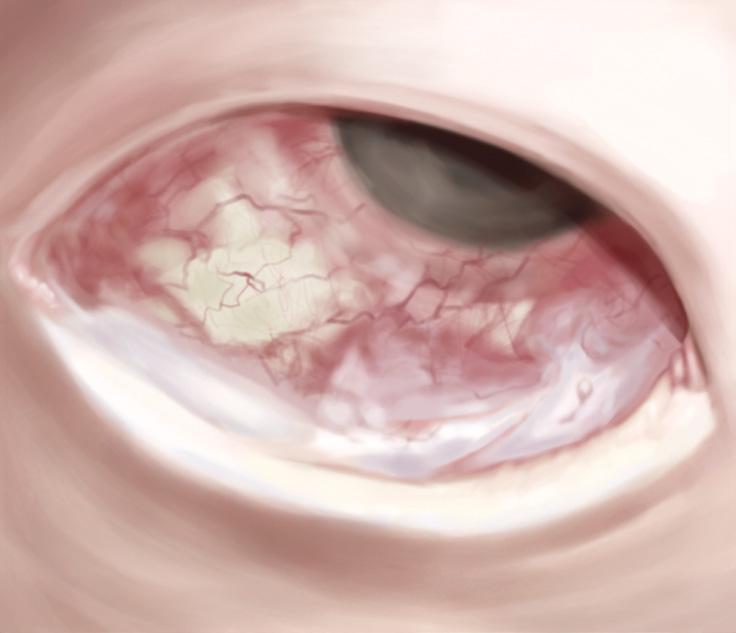
STAGE 2: INFERIOR FORNICEAL SHORTENING
• Tightening of lower fornix due to scarring, measured depth loss
STAGE 3: SYMBLEPHARON FORMATION
• Adhesion of conjunctiva to the retinal globe in one or more areas
• Restricted, painful eye movement and measured lower fornix depth loss
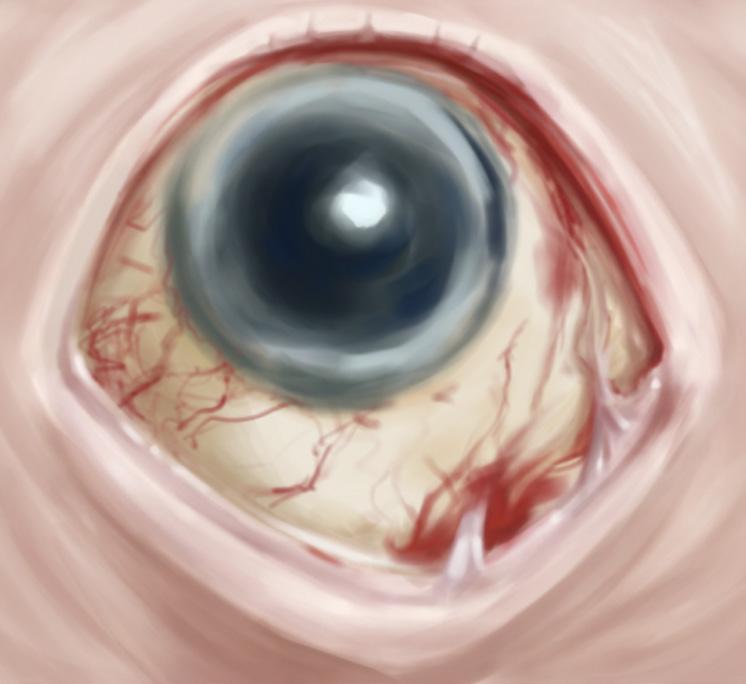
STAGE 4: END-STAGE CICATRICIAL DISEASE
• Complete lower fornix loss (100%; no lower pocket; sight-threatening)
• Eye to lid fusion and severe opening restriction
• Corneal keratinization: opaque, rough, painful cornea & vision loss
REVIEWED BY: JOSIP PETRUSA2
2Masters of Sciences in Biomedical Communication (Honours), Class of 2026, University of Toronto References can be found on our webstie: www.themeducator.org
1Bachelors
ARTIST: NICOLE KIM1
1Bachelors of Health Sciences (Honours), Class of 2026, McMaster University
REVIEWED BY: CATHY
ZHOU2
2Masters of Sciences in Biomedical Communication (Honours), Class of 2026, University of Toronto
Jaundice is a condition in which there is too much bilirubin in the blood.1 This occurs in 60% of term babies and up to 80% of preterm babies, when it is called neonatal jaundice.1,2 Although neonatal jaundice typically resolves within two weeks, 1 in 20 babies require early diagnosis and treatment or else risk kernicterus (a form of brain damage resulting from excess bilirubin in newborns).1
Because bilirubin is a yellow substance, jaundiced neonates typically present with slightly yellow skin.1 There is a great reliance on such visual signs to identify neonatal jaundice during newborn examinations.1 Babies with brown or black skin, in whom yellowing is less noticeable, are more likely
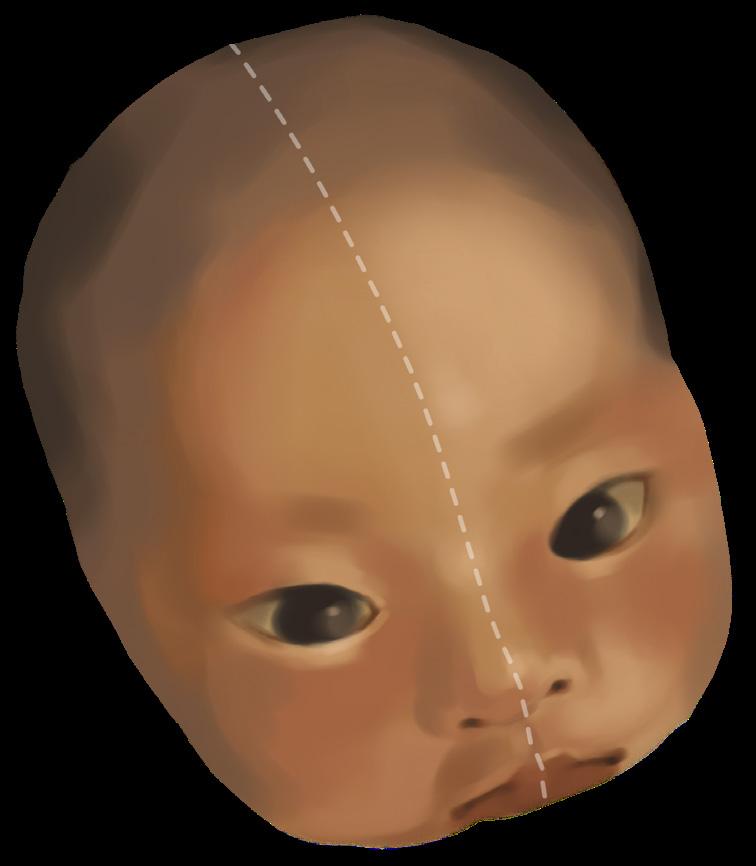
Fig. 1. Comparison of jaundiced state (left) versus healthy state (right) in an East Asian baby. Neonatal jaundice has a higher incidence in East Asian and Native American babies than other racial groups, which stresses the importance of such babies to be accurately assessed and diagnosed in a timely manner.7
to face delayed diagnosis of neonatal jaundice as the lack of clear visual signs can lead clinicians to overlook high bilirubin levels on blood tests.3 Unsurprisingly, kernicterus disproportionately affects babies from ethnic minorities.2
While it is widely known that diagnosing neonatal jaundice in darker skin tones poses a challenge, there has not been adequate direction from clinical guidelines to address this issue.1 Minimal evidence exists to inform how jaundice is identified and managed across skin tones,2 and textbooks and training are repeatedly modelled on white skin.4
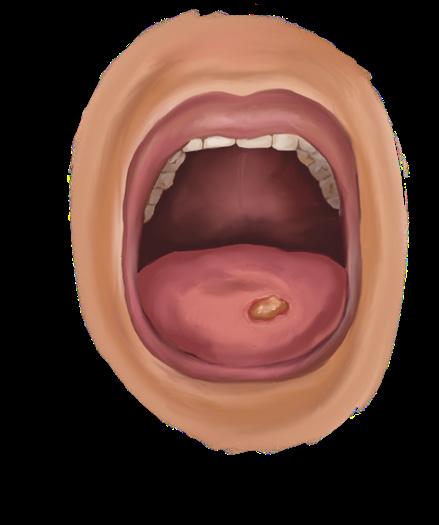
Jaundiced skin may appear normal and healthy on darker skin tones, such as found on Black, Asian, and other ethnic minority babies.5 In such babies, it is recommended to instead look for yellowing in the sclerae of the eyes (figure 1), inside of the mouth, palms of the hands, soles of the feet, and on “blanched” skin (skin that is made lighter by pressing down on it as shown in figure 2).3,6 Additional signs of neonatal jaundice are dark urine, pale stools, fatigue, and/or abdominal pain.5
Blanched nose revealing a yellow tinge
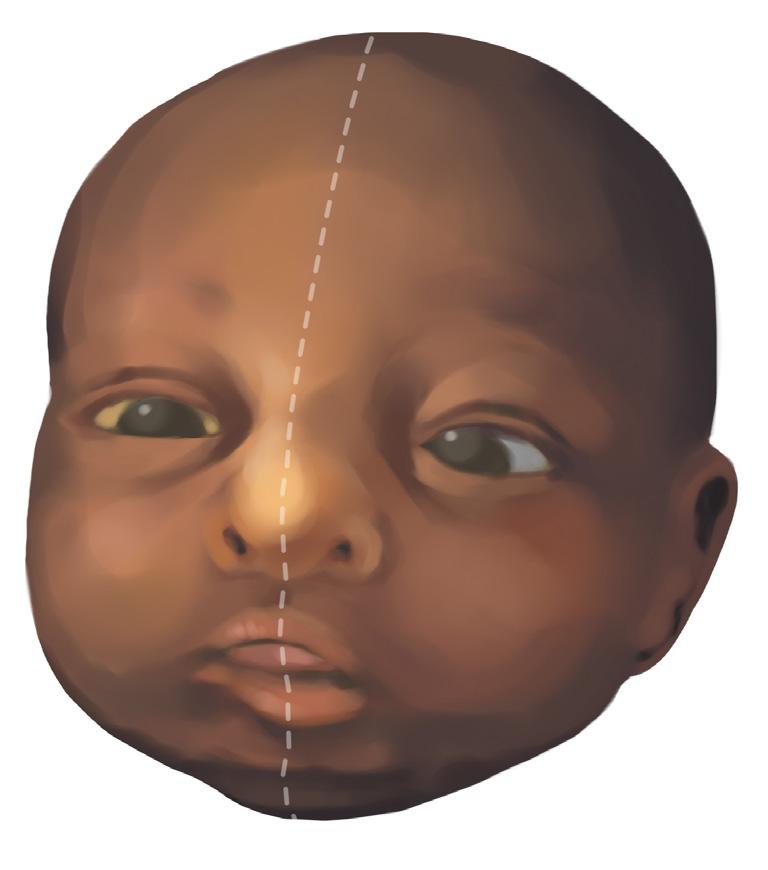
Fig. 2. Comparison of jaundiced state (left) versus healthy state (right) in a Black baby.
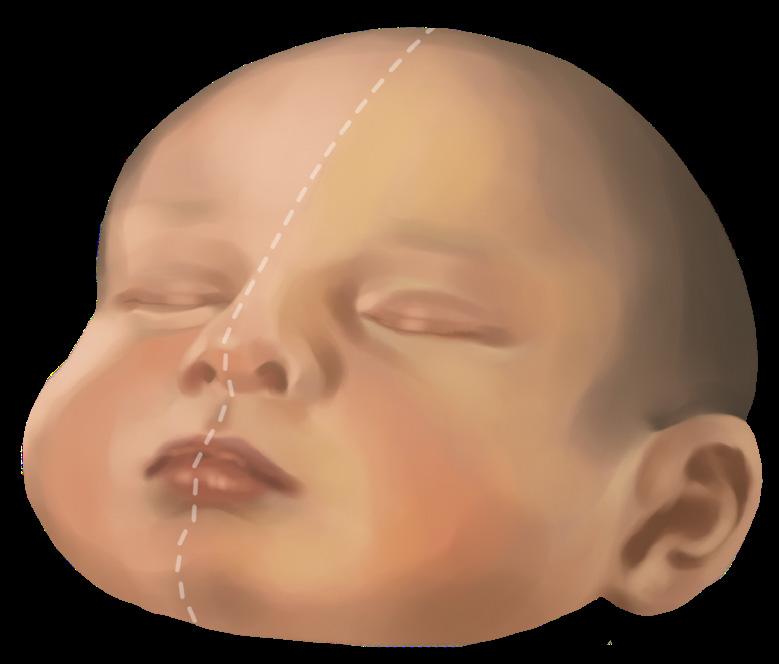
Fig. 3. Comparison of jaundiced state (right) versus healthy state (left) in a White baby. Note that the degree of visible yellowing is more striking than in Fig. 1 and 2.
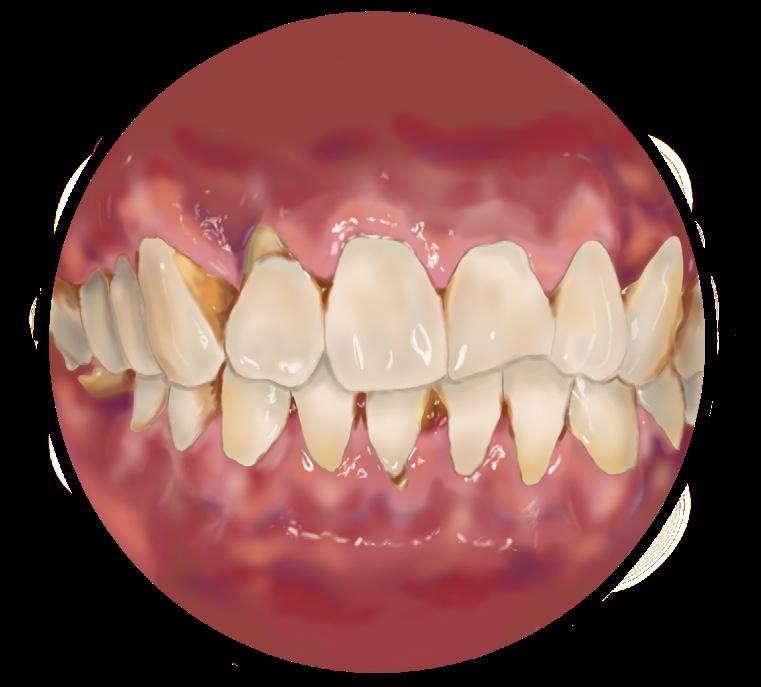
Gums appear swollen, red or darker than usual, are tender, and bleed easily. Patient experiences bad breath due to plaque buildup. Symptoms are reversible at this stage.3
ARTIST: RUCHI TILVA1
1Bachelors of Health Sciences (Honours Biochemistry), Class of 2028, McMaster University
REVIEWED BY: CATHY ZHOU2
2Masters of Sciences in Biomedical Communication (Honours), Class of 2026, University of Toronto
Periodontitis, or gum disease, is the inflammation of the gums due to the buildup of plaque and tartar, and the collection of bacteria.1 This disease progresses in three stages: gingivitis, mild/moderate, and advanced (figure 1). While some people are more prone to getting this infection, it is most often caused by poor oral hygiene.
Globally, severe periodontitis is projected to affect over 1.5 billion people by 2050.2 However this disease has the highest prevalence in Asian countries, specifically Indonesia, Vietnam, India, and the Philippines.2 The lack of accessibility to dental care and lack of literacy surrounding oral health coupled with high sugar consumption exacerbates this issue.2 The socioeconomic factors that are associated with healthcare mean that low-income communities arem most likely to not receive treatment. Ultimately, mitigating the effects of periodontitis requires developing health policies that prioritize oral health literacy and ensure equitable dental access to marginalized communities.
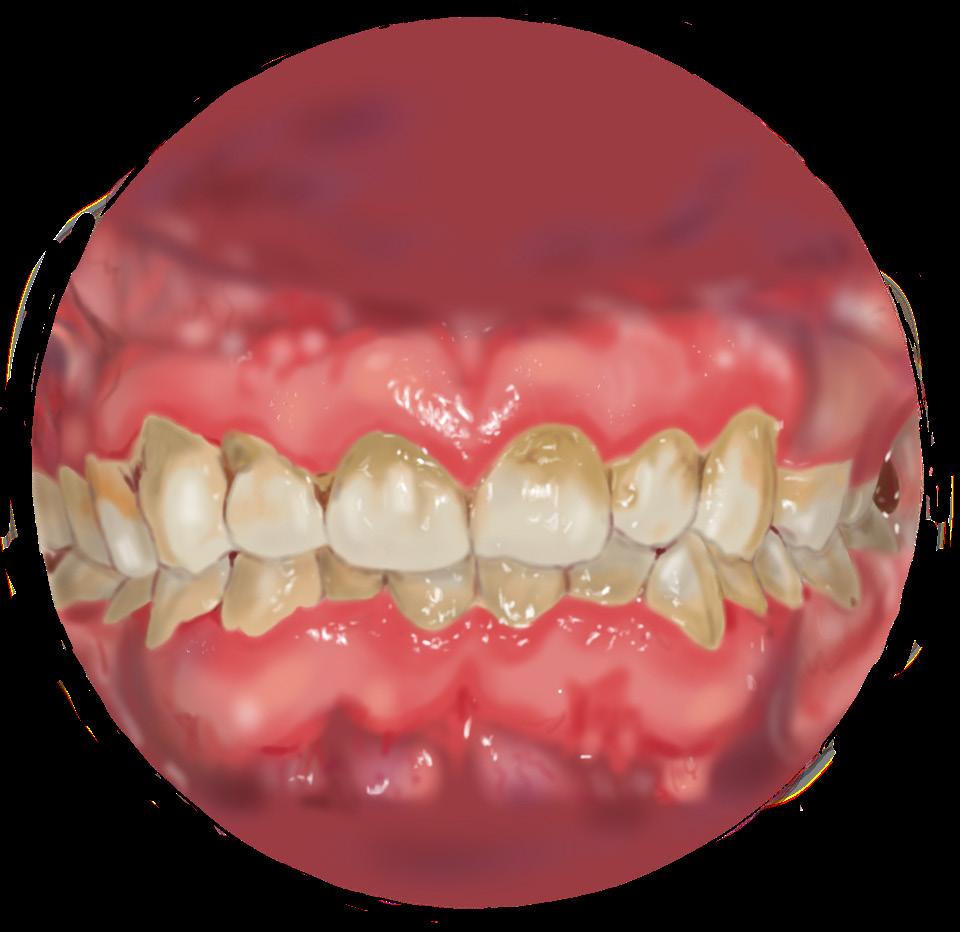
Gums retract from teeth to form pockets. Plaque accumulates and bacteria roots itself deeper while affecting bone. Aggressive scaling and root planing required to treat, as well as antibiotics.3
1. Mayo Clinic. Gingivitis - Diagnosis and treatment - Mayo Clinic [Internet]. Mayoclinic.org. 2017. Available from: https://www.mayoclinic.org/diseases-conditions/gingivitis/diagnosis-treatment/ drc-20354 459
2. Chapple I, Rudiktyo E, Sulijaya B, Marlina E, Oktawati S, Tahapary D, et al. The burden of periodontal disease in Southeast Asia (Indonesia and Vietnam): A call to action. Journal of
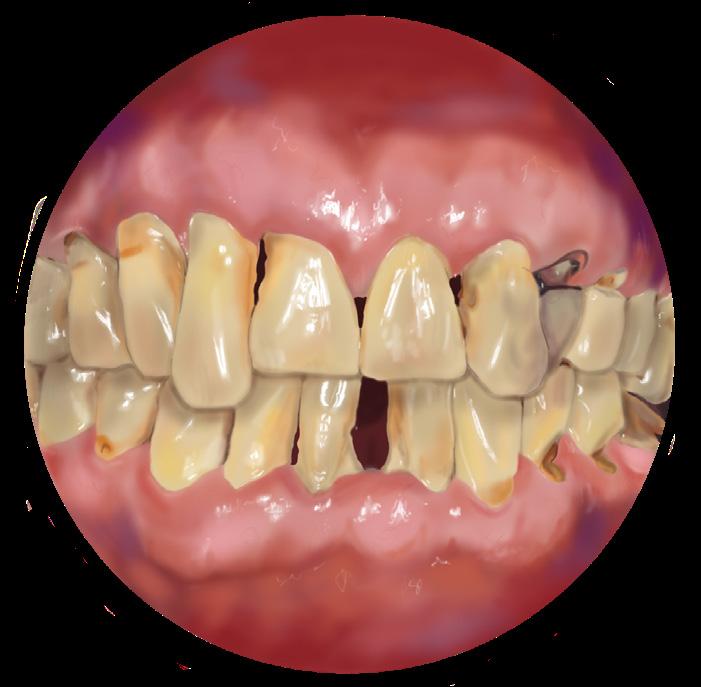
Gums continue to recede causing more bone loss. Teeth may become loose and fall out. Treatment involves pocket reduction surgery to remove deep tartar and plaque. Bone grafts may be used to replace bone.3
Dentistry [Internet]. 2025 Oct 8;163:106160. Available from: https://www.sciencedirect.com/ science/article/pii/S0300571225006062
3. Cleveland clinic . Gum (Periodontal) Disease: Causes, Symptoms, Treatment & Prevention [Internet]. Cleveland Clinic. 2023. Available from: https://my.clevelandclinic.org/health/ diseases/21482-gum-periodontal-disease
Fig. 1. An older female patient experiencing chest discomfort, characteristic of cardiac distress.

ARTIST: DANIELA KLOBUCAR1
1Bachelors of Sciences (Life Sciences Co-Op ), Class of 2026, McMaster University
REVIEWED BY: JOSIP PETRUSA2
2Masters of Sciences in Biomedical Communication (Honours), Class of 2026, University of Toronto
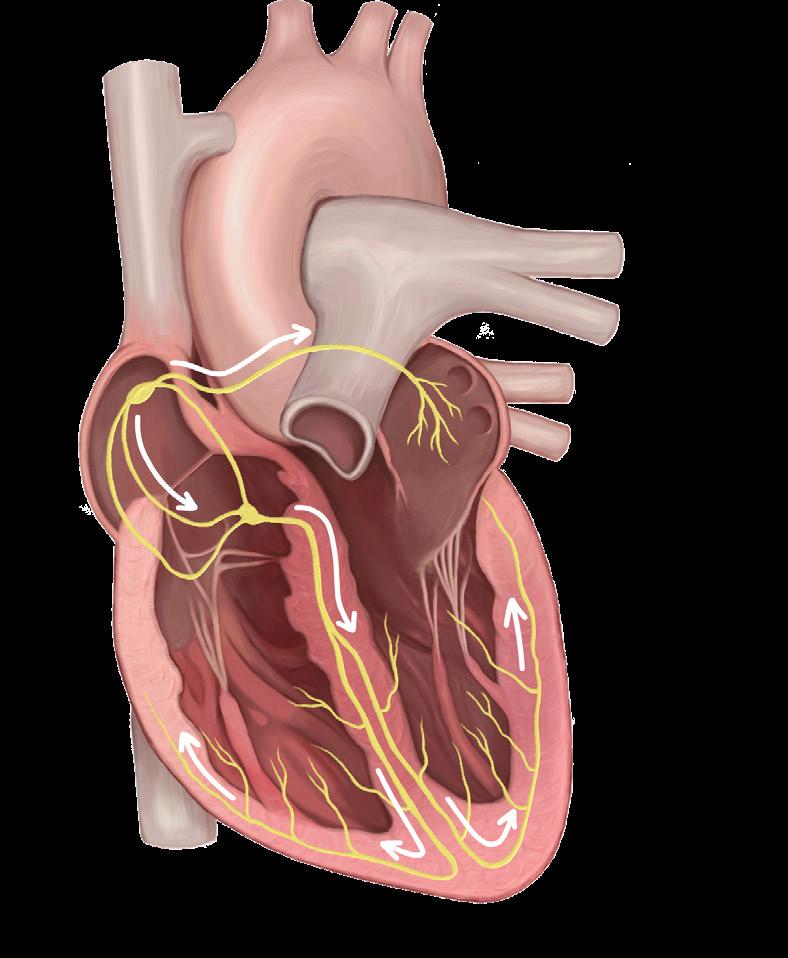
Cardiac arrhythmia is a disorder in which the heartbeat is abnormal, characterized by a fast, slow or irregular heartbeat that can impair the heart’s ability to pump sufficient blood to the rest of the body.1 Atrial fibrillation (AF), the most common cardiac arrhythmia, is marked by irregular contractions of the upper chambers, the atria, of the heart.t Under normal conditions, electrical signals originating in the sinoatrial node stimulate coordinated contraction of the right and left atria, allowing blood to flow efficiently into the lower chambers, the ventricles, of the heart.3

During AF, irregular, chaotic electrical signals disrupt this normal signalling, leading to irregular atrial contractions and impaired blood flow (figure 2). As a result, blood may pool in the atria due to the loss of synchronized atrial and ventricular beating. When blood sits still, it tends to clot. If one of these clots is pumped out of the heart and travels to the brain, it blocks oxygen and significantly increases the risk of stroke.2 Symptoms of cardiac arrhythmia can vary but often manifest as chest pain, paleness, sweating, light-headedness or dizziness, fainting and/or shortness of breath.1

The global prevalence of AF reached 59.7 million cases in 2019 and is expected to increase due to the aging population of multiple countries.4 AF affects about 350,000 Canadians and is particularly prevalent among older adults.5 Aging leads to substantial structural and electrical remodeling of the cardiac tissue. Often, this involves scarring or stiffening of the heart walls. This is joined by increased oxidative stress, along with other age-related challenges such as frailty and the present of multiple comorbidities.8 Elderly women face a disproportionately high risk of AF and its complications, yet they remain underrepresented in cardiovascular research and clinical trials. Emerging research shows that women aged 75 and older with AF have a significantly higher risk of stroke than men, despite similar adherence to anticoagulant therapy.6 This suggests that standard treatments may be less effective in women, possibly due to sex-specific differences in vascular health and therapeutic response. Important cardiovascular differences exist between males and females, including variations in electrocardiographic and
electrophysiological characteristics influenced by sex hormones and autonomic function.7
Historically, women have been underrepresented in cardiovascular studies, resulting in critical gaps in evidence that limit the optimization of care for female patients. Women in developed countries face disadvantages due to limited sex-specific data on medication effectiveness, while women in disadvantaged socioeconomic settings encounter additional barriers such as reduced healthcare access and limited health literacy, further delaying diagnosis and treatment.6 With the global population of individuals over 80 years projected to triple by 2050 from the current 137 million, the need for targeted research and effective management strategies, including improved anticoagulation approaches for elderly women, is increasingly urgent.5 Greater inclusion of older women in heart disease research is essential to develop equitable, evidence-based strategies for managing arrhythmias and reducing stroke risk in this growing and vulnerable population.

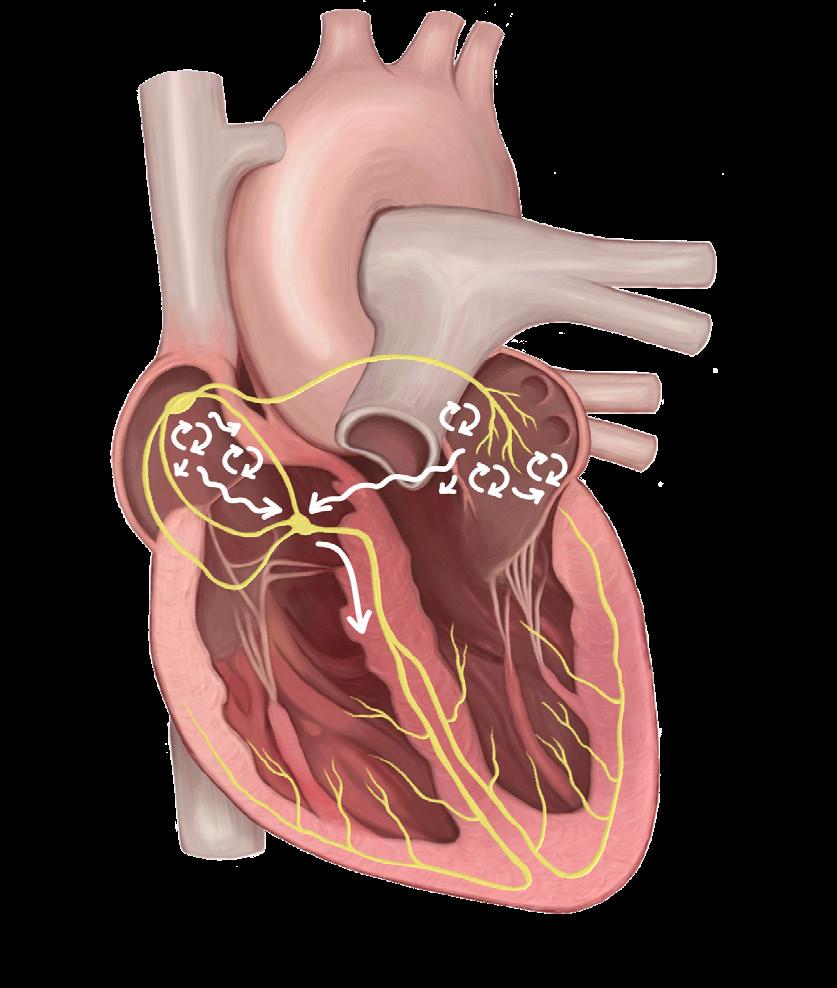
Irregular electrical activity
Fig. 2. Comparison of electrical conduction in a normal heartbeat vs. atrial fibrillation
1. Cox N. Arrhythmia. Melbourne Cardiology. Accessed March 22, 2026. https://www.melbournecardiology.com.au/arrhythmia-interventional-cardiologist-glen-waverley-vic.html
2. American Heart Association. What is Atrial Fibrillation? American Heart Association. March 26, 2025. Accessed March 22, 2026. https://www.heart.org/en/health-topics/atrial-fibrillation/whatis-atrial-fibrillation-afib-or-af
3. National Heart, Lung and Blood Institute. Atrial Fibrillation - Causes and Risk Factors. National Heart, Lung and Blood Institute. November 30, 2022. Accessed March 22, 2026. https://www. nhlbi.nih.gov/health/atrial-fibrillation/causes
4. Robert J. Elderly women with irregular heartbeat at higher risk for stroke. McGill Newsroom Institutional Communications. May 9, 2012. Accessed March 22, 2026. https://www.mcgill.ca/ newsroom/channels/news/elderly-women-irregular-heartbeat-higher-risk-stroke-216318
5. Siyuan Cheng, JinZheng He, Yuchen Han, Shaojie Han, Panpan Li, Huanyan Liao, Jun Guo,
Global burden of atrial fibrillation/atrial flutter and its attributable risk factors from 1990 to 2021, EP Europace, Volume 26, Issue 7, July 2024, euae195, https://doi.org/10.1093/europace/ euae195
6. Tsadok MA, Jackevicius CA, Rahme E, Humphries KH, Behlouli H, Pilote L. Sex Differences in Stroke Risk Among Older Patients With Recently Diagnosed Atrial Fibrillation. JAMA. 2012;307(18):1952. doi:10.1001/jama.2012.3490
7. Zeitler EP, Poole JE, Albert CM, et al. Arrhythmias in Female Patients: Incidence, Presentation and Management. Circulation Research. 2022;130(4):474-495. doi:10.1161/CIRCRESAHA.121.3198
8. Curtis AB, Karki R, Hattoum A, Sharma UC. Arrhythmias in Patients ≥80 Years of Age. J Am Coll Cardiol. 2018;71(18):2041-2057. doi:10.1016/j.jacc.2018.03.019
1Bachelors of Biochemistry (Honours), Class of 2028, McMaster University
REVIEWED BY: ELLA EBERHARDT2
2Masters of Sciences in Biomedical Communication (Honours), Class of 2026, University of Toronto
Syphilis is a bacterial sexually transmitted infection (STI) caused by Treponema pallidum as shown in figures 1 and 2.1 Transmission occurs primarily through direct sexual contact (infectious syphilis) or vertical transmission from mother to fetus during pregnancy (congenital syphilis).1 While highly curable with penicillin, untreated cases progresses through primary, secondary, latent, and tertiary stages that lead to severe neurological
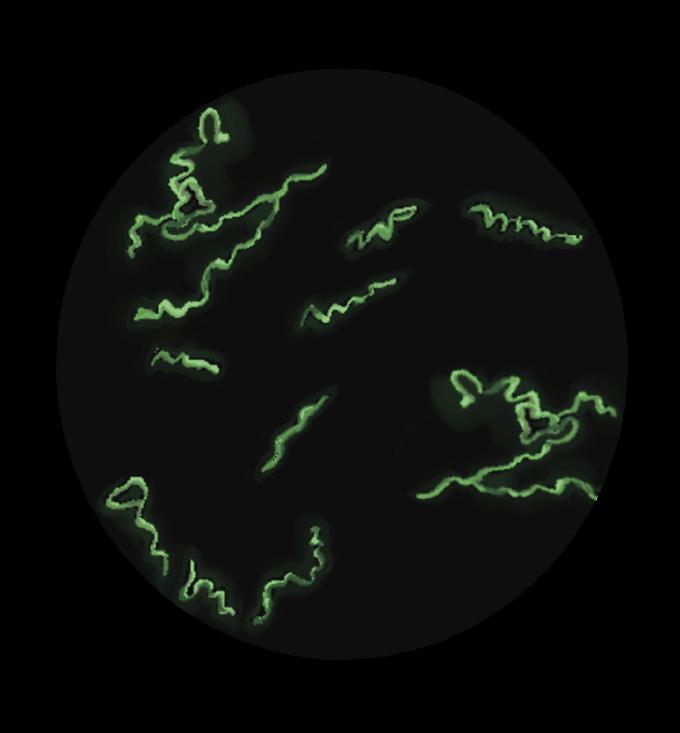
, the causative agent of syphilis.
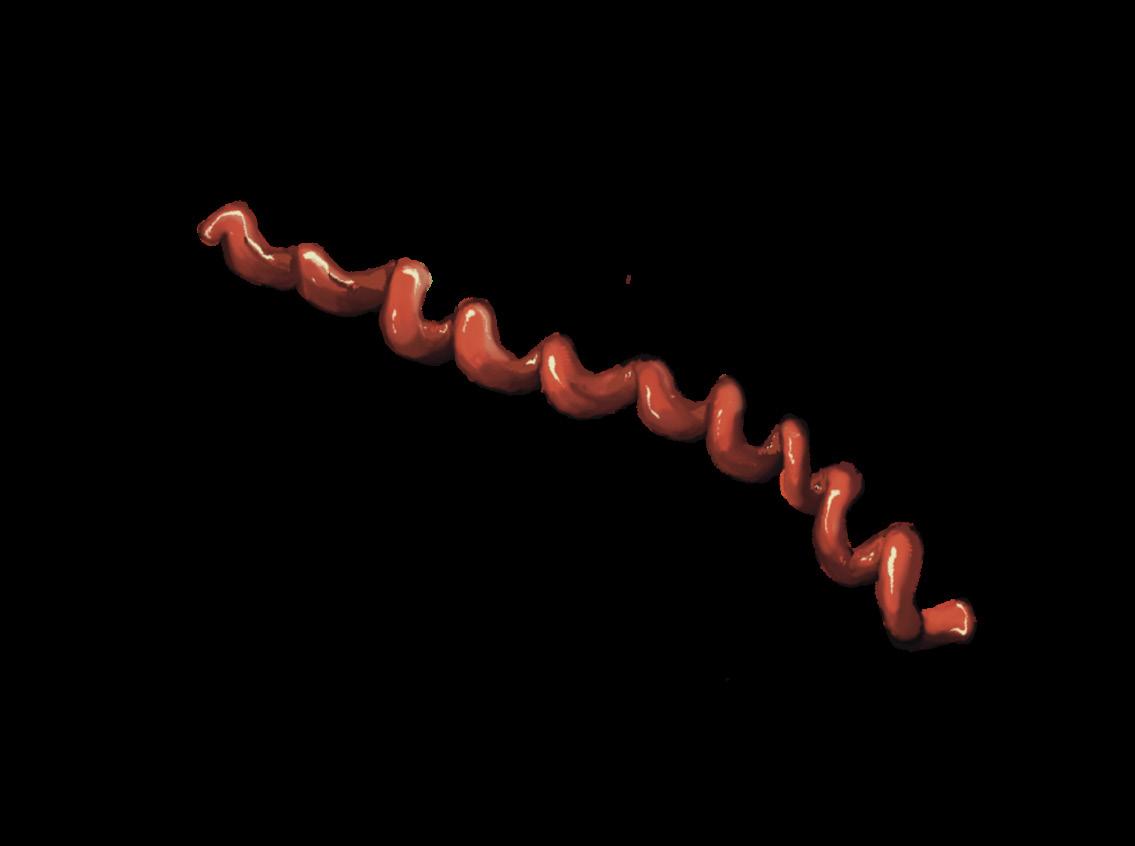
pallidum
1. Canada,. Key Messages from the CIHR Mid-Term Knowledge Mobilization Virtual Event: Addressing Infectious and Congenital Syphilis in Canada - CIHR [Internet]. Cihr-irsc.gc.ca. 2017. Available from: https://cihr-irsc.gc.ca/e/54356.html
2. Canada PHA of. Infectious Syphilis and Congenital Syphilis in Canada, 2022 [Internet]. www. canada.ca. 2023. Available from: https://www.canada.ca/en/public-health/services/reports-publications/canada-communicable-disease-report-ccdr/monthly-issue/2023-49/issue-10-october-2023/infectious-congenital-syphilis-canada-2022.html
3. Healthwise I. Stages of Syphilis [Internet]. myhealth.alberta.ca. 2025. Available from: https:// myhealth.alberta.ca/Health/Pages/conditions.aspx?hwid=tm6404
4. CDC. Syphilis Images [Internet]. Syphilis. 2024. Available from: https://www.cdc.gov/syphilis/ hcp/images/index.html
5. Aryal S. Laboratory Diagnosis of Syphilis Caused by Treponema Pallidum [Internet]. Online Microbiology Notes. 2017. Available from: https://microbenotes.com/laboratory-diagnosis-of-syphilis-caused-by-treponema-pallidum/
Painless sore (chancre) at the site of infection. The chancre typically heals without intervention, but the patient remains infectious.3
Systemic response, where symptoms may resolve, but bacteria remains active:3
• Maculopapular rash (frequently on the palms and soles)
• Neurosyphilis
• Ocular syphilitic manifestations,
• Genito-inguinal rashes
• Internal organ manifestations.
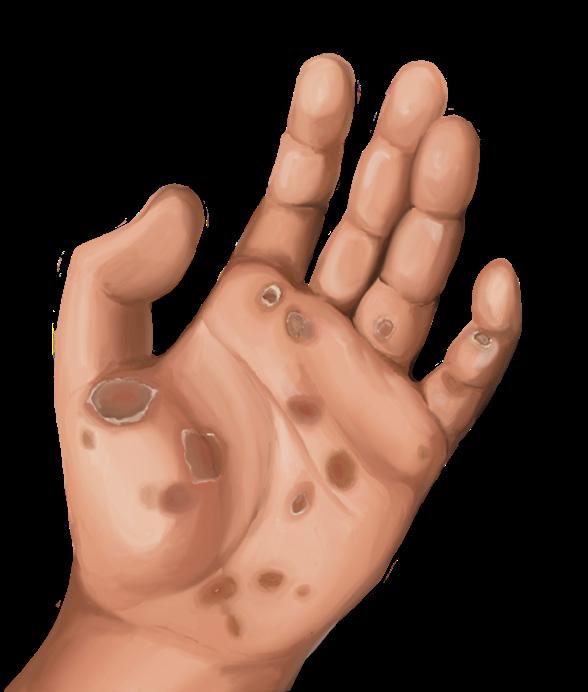
Characteristic maculopapular
Asymptomatic (~20 years), where the patient may not be contagious via sexual contact, but gestational transmission remains a high risk, potentially leading to misacarriage, stillbirth, or neonatal congenital syphilis.3
Develops in about 25-40% of untreated cases, involving multi-organ involvement, such as cardiovascular syphilis, neurosyphilis, gummatous syphilis.3
ARTIST:
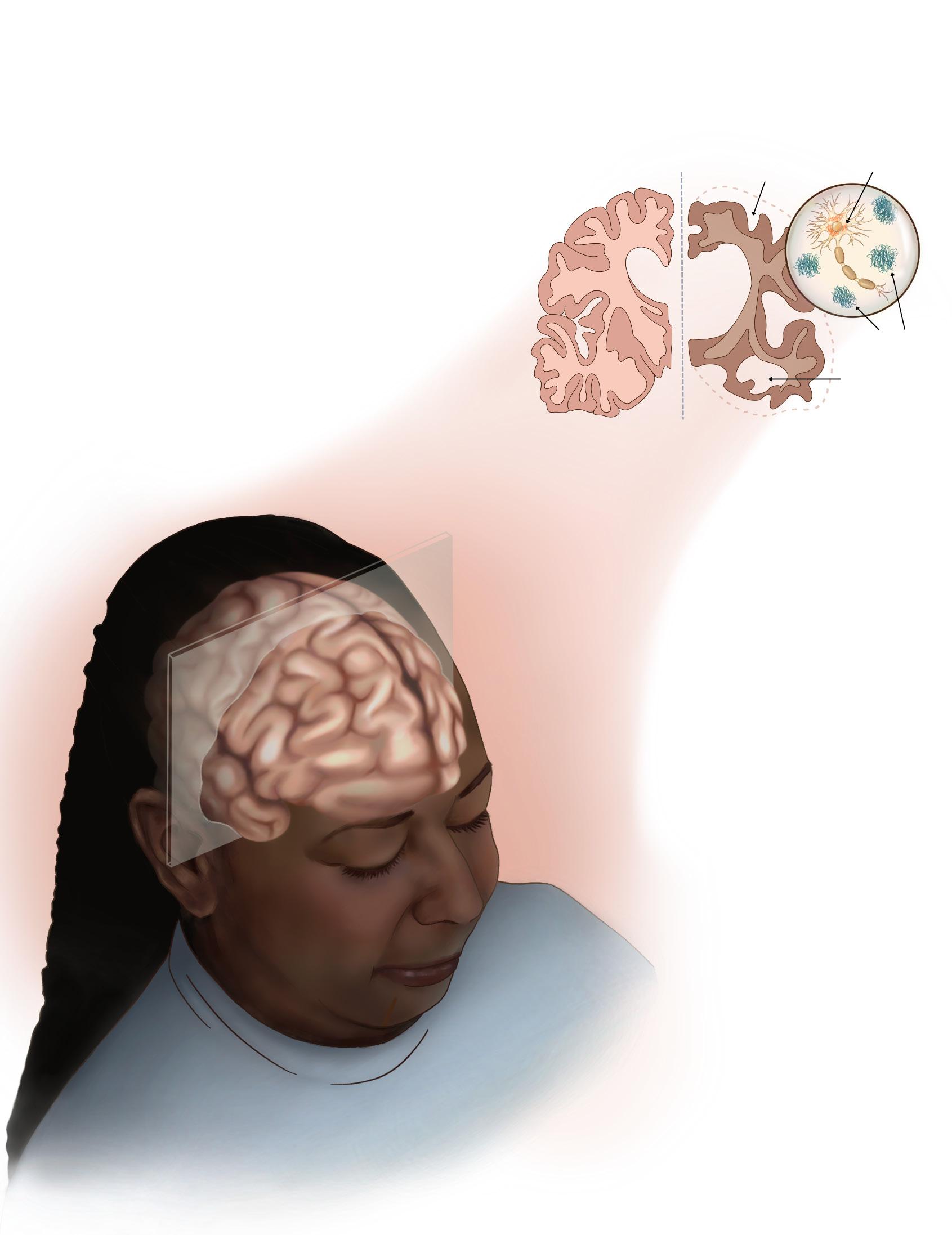
Alzheimer’s disease (AD) is a neurodegenerative disorder that causes the death of cells in the brain and shrinking of the brain size over time.1 The disease is marked by two proteins: amyloid plaques which block messages between brain cells, and tau tangles which stop nutrients from moving inside the cells (figure 1).2 As the disease progresses, people begin to struggle with memory, language, problem solving, and everyday tasks.2 As the seventh leading cause of death, affecting over 57 million people worldwide, Alzheimer’s disease unfortunately has no cure.3 Therefore, early diagnosis of AD is important because it allows patients to access treatments and support sooner, helping to manage symptoms and maintain quality of life for as long as possible.4
REVIEWED BY: VICKY LIN
2Masters of Sciences in Biomedical Communication (Honours), Class of 2026, University of Toronto
1Bachelors of Sciences (Honours Life Sciences), Class of 2026, McMaster University
brain strinkage
tau tangles neurodegeneration
1. Cross-section of the brain showing a healthy side and a side affected by Alzheimer’s disease.
Older age and being female are both risk factors for AD.5 However, Black women face an even greater risk compared to other groups. Research shows that Black individuals are two to three times more likely to develop AD, yet they are often diagnosed later, when symptoms are more severe and harder to treat.5 Black women are especially at risk due to a combination of biological, social, and healthcare factors, including higher rates of chronic stress-related damage and cardiovascular issues.5
Despite being at higher risk, Black individuals are underrepresented in Alzheimer’s research, as they make up only five percent or less of participants in clinical studies and drug trials.6 This lack of representation is a result of historically rooted medical mistrust, limited access to clinical studies, and restrictive study inclusion criteria.6 This combined result of systemic injustices limits our understanding of how the disease affects them and creates racial gaps in care, prevention, and treatment of AD.
1. Lui F, Tsao JW. Alzheimer Disease [Internet]. National Library of Medicine. StatPearls Publishing; 2024. Available from: https://www.ncbi.nlm.nih.gov/books/NBK499922/
2. Breijyeh Z, Karaman R. Comprehensive Review on Alzheimer’s Disease: Causes and Treatment. Molecules (Basel, Switzerland). December 8, 2020;25(24):5789.
3. World Health Organization. Dementia [Internet]. World Health Organization. 2025. Available from: https://www.who.int/news-room/fact-sheets/detail/dementia
4. Rasmussen J, Langerman H. Alzheimer’s Disease – Why We Need Early Diagnosis. Degenerative neurological and neuromuscular disease. December 1, 2019;9:123–30.
5. Findley CA, Cox MF, Lipson AB, Bradley R, Hascup KN, Yuede C, et al. Health disparities in aging: Improving dementia care for Black women. Frontiers in aging neuroscience. February 9, 2023;15:1107372.
6. Stradford J, Heyworth NC, Jackson M, Norman M, Banks SJ, Sundermann EE, et al. Increasing research study engagement in minoritized populations: An example from the Black Women Inflammation and Tau Study. Alzheimer’s & dementia. October 2024;20(10):7403–10.
