

THE stress less ISSUE




LETTER PRESIDENT FROM THE
Dear Neighbor,
As we approach our 24th year of serving Northeast Florida, I remain deeply humbled by the privilege of being entrusted with your health. While I’m proud to share some of our recent ‘firsts,’ none compares to the pride we feel in being your trusted providers in cardiovascular care, wound healing, pulmonary medicine, and sleep health.
This year, we are thrilled to introduce another major milestone: the launch of the region’s first and only outpatient dedicated cardiovascular surgical center. When my father needed a pacemaker defibrillator 20 years ago, the only option was a hospital procedure followed by an overnight stay. Thanks to today’s medical advancements, the same procedure can now be performed in a more comfortable, cost-effective outpatient setting. My father, special as he is to me, is just one of tens of thousands of patients we’ve served at FCCI, many of whom have asked for greater convenience, comfort, and affordability. We listened. After two years of planning, working with architects, physicians, nurses, and government agencies, we’re proud to be on the brink of opening this groundbreaking facility.
We are fortunate in Northeast Florida to have access to outstanding hospitals with stateof-the-art equipment. In fact, more than 50% of the procedures we perform will continue to be done in hospital settings due to patient preference, procedural complexity, and other factors.
A couple of years ago, I had the honor of working with a dozen cardiovascular physician leaders (out of over 60,000 cardiologists in the US, Canada, and the UK) to create clinical guidelines identifying which procedures and patients are best suited for outpatient care. These guidelines ensure we incorporate the most up-to-date evidence in every patient decision we make.
Another exciting development is our merger with Clearwater Cardiovascular Consultants (CCC), a premier practice in Clearwater, Florida. Our two groups have enjoyed a decade-long friendship, frequently collaborating and sharing best practices to better serve our communities. Now, as one unified group, we deepen that collaboration while preserving the local feel, names, and teams you know and trust. This merger strengthens our infrastructure, helps us stay ahead of inflation and industry challenges, and enhances our ability to recruit top-tier physicians and staff.
We’re also proud to announce our first Interventional Cardiology Fellowship Program at HCA Orange Park. For almost a decade, FCCI has trained outstanding future cardiologists. This new program builds on that tradition by preparing fellows to specialize in life-saving procedures—treating heart attacks and repairing valves, blockages, and aneurysms through minimally invasive techniques like stents and balloon angioplasty. We are honored to share this educational responsibility with only one other institution in our region: the University of Florida.
The future is bright. While economic uncertainty and physician shortages are real concerns, FCCI is rising to the challenge. We are investing in talent, innovation, and education— creating a stronger future for cardiovascular care in Florida and South Georgia.
With gratitude and optimism,
Dr. Yazan Khatib President
First Coast Cardiovascular Institute
First Coast Cardiovascular Institute leads cardiovascular innovation and care at HCA Florida
Orange Park Hospital to best serve you.









Getting an Echocardiogram: What
You Need to Know
Understanding this essential heart test can ease your mind and support your health
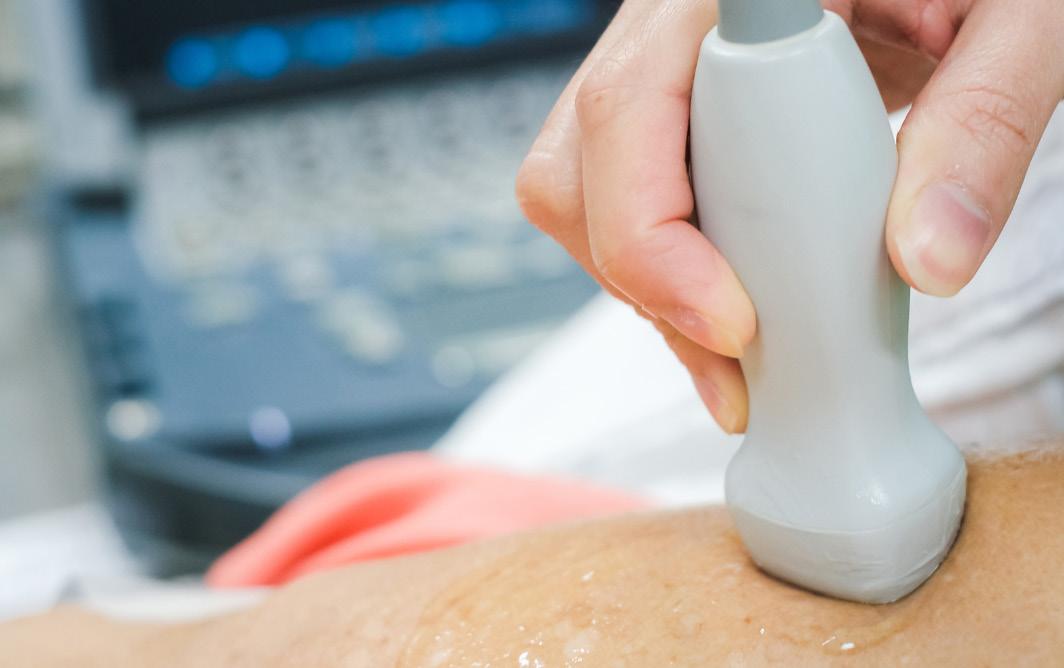
An echocardiogram is a safe, non-invasive test that uses sound waves to create detailed images of the heart. It’s one of the most used tools for diagnosing and monitoring heart conditions—offering valuable insights into your heart’s structure and function. Here’s what you can expect:
Before the Test
• Preparation: Most patients don’t need to do anything special. Eat, drink, and take medications as usual unless your doctor advises you otherwise.
• What to Wear: You may be asked to wear a gown or remove clothing from the waist up for easy access to your chest.
During the Test
• Getting Set Up: You’ll lie on an exam table while a technician places electrodes on your chest to monitor your heart’s electrical activity.
• Gel Application: A small amount of gel is applied to your chest to help the sound waves travel from the transducer (the imaging device) to your heart.
• Image Capture: The technician will gently move the transducer across your chest to record images. You may be asked to change positions or briefly hold your breath to get the clearest views.
• Time: The entire procedure can take up to 40 minutes. It’s painless, though you may feel mild pressure from the device.
After the Test
• Wrap-Up: The gel is wiped off, and you can dress and resume normal activities immediately.
• Quality Matters: For the most accurate results, echocardiograms should be performed by trained technicians in accredited facilities and interpreted by board-certified cardiologists.
• Getting Results: A cardiologist will review the images and explain the findings. If needed, they may recommend further testing or treatment.
What It Shows
An echocardiogram provides detailed information about:
• Heart Chambers: Their size and how well they’re working
• Heart Valves: Whether they’re opening and closing properly
• Heart Muscle: Thickness and motion, which can indicate damage or disease
• Blood Flow: Direction and speed through the heart and major vessels
• Pericardium: The protective sac around the heart and the major vessels like the aorta
This test helps diagnose conditions like heart failure, valve disease, congenital heart defects, and more. It plays a key role in creating a personalized plan to protect and improve your heart health.
If you have questions or concerns about your upcoming echocardiogram, talk to your healthcare provider. Knowing what to expect can help reduce anxiety and make the experience more comfortable.
Source: FirstCoastCardio.com
HOW DOES STRESS AFFECT YOUR HEART?
The Connection Between Stress and Heart Health
A little stress from time to time can actually be helpful. It keeps us alert, focused, and ready to rise to challenges. The balance shifts when stress becomes constant or overwhelming. At that point, it is not only the presence of stress that matters, but how our bodies and minds respond to it. That response plays a powerful role in overall health, especially when it comes to the heart.
Growing research continues to show that unmanaged stress can quietly take a toll on the cardiovascular system, increasing the risk for long-term heart problems. Here is how stress affects heart health in some of the most significant ways.
Increased Heart Rate and Blood Pressure
When stress strikes, the body releases hormones such as adrenaline and cortisol, triggering the familiar “fight or flight” response. Heart rate and blood pressure rise to help the body react quickly. While this response is useful in short bursts, chronic stress keeps these systems switched on longer than necessary. Over time, this ongoing strain can damage blood vessels, raise blood pressure, and increase the risk of heart disease. The American Heart Association notes that sustained stress can contribute to lasting injury to artery walls.
Inflammation
Stress can also fuel inflammation throughout the body, a key contributor to cardiovascular disease. Chronic inflammation is closely linked to the buildup of plaque in the arteries, known as atherosclerosis, which increases the risk of heart attacks and strokes. According to Harvard Health, ongoing emotional stress may disrupt immune function and intensify inflammatory responses, creating another pathway to heart disease.
Elevated Blood Sugar Levels
Cortisol, one of the body’s primary stress hormones, stimulates the liver to release glucose into the bloodstream. This surge is helpful during short-term stress, but persistent stress can cause blood sugar levels to remain elevated. Over time, this may lead to insulin resistance and raise the risk of developing diabetes, a major risk factor for heart disease.
Lifestyle Choices
Stress often influences the choices we make day to day. Many people cope by smoking, overeating, drinking alcohol, or skipping physical activity. While these behaviors may feel comforting in the moment, they place additional strain on the heart and increase the likelihood of chronic illness.

Source: Yale Medicine
The Importance of Managing Stress for Heart Health
The encouraging news is that you have more influence over your heart health than you might think. It’s not just about eliminating stress, but about reshaping how you relate to it. A positive outlook—rooted in gratitude, acceptance, and mindfulness—can make a real difference. Studies have shown that individuals who maintain a hopeful attitude tend to have lower blood pressure, reduced risk of heart disease, and better overall health outcomes.
We hope you’ll find inspiration throughout this edition of The Heart of Jacksonville to empower you to manage stress in a healthier way.

"The greatest weapon against stress is our ability to choose one thought over another."
~ William James, Philosopher, Psychologist, and Harvard Professor
To get you started, we offer:
Ten Ideas to Quickly
Combat Stress Right Now
• Practice acceptance and focus on what you can control
• Take a walk
• Get outside
• Pet your cat or dog
• Have a laugh
• Think of something that makes you smile (a grandchild, a favorite vacation, a funny movie)
• Listen to music
• Deep breathing
• Pray and meditate
• Focus on what you are grateful for
Sources: American Heart Association, Harvard Health Publishing, Yale Medicine

Easy, Delicious, and Comforting: Minestrone Soup
Minestrone is a classic comfort food dish. A couple of editions ago, we featured a light minestrone recipe for Springtime. This version is a bit different with more of a tomato base for a rich and warm eating experience.
Nourishing for the body and spirit, try this easy to make recipe any day of the week. It makes great leftovers the next day. Pair up with a healthy salad of your choice.

PREP 25 MIN
COOK 40 MIN 11 SERVINGS
Instructions
1. In a large saucepan, sauté carrots, celery and onion in oil and butter until tender. Add garlic; cook 1 minute longer.
2. Stir in broth, tomato sauce, kidney beans, chickpeas, tomatoes, cabbage, basil, parsley, oregano and pepper. Bring to a boil. Reduce heat; cover and simmer for 15 minutes. Add macaroni; cook, uncovered, 6-8 minutes or until macaroni and vegetables are tender.
3. Ladle soup into bowls. Sprinkle with cheese. Enjoy!
Ingredients
• 2 large carrots, diced
• 2 celery ribs, chopped
• 1 medium onion, chopped
• 1 tablespoon olive oil
• 1 tablespoon butter
• 2 garlic cloves, minced
• 2 cans (14-1/2 ounces each) reduced-sodium chicken broth (or better yet, make your own broth)
• 2 cans (8 ounces each) no-salt-added tomato sauce
• 1 can (16 ounces) kidney beans, rinsed and drained (or better yet, boil your own dried beans)
• 1 can (15 ounces) chickpeas, rinsed and drained (or better yet, boil your own dried chickpeas)
• 1 can (14-1/2 ounces) diced tomatoes, undrained
• 1-1/2 cups shredded cabbage
• 1 tablespoon dried basil
• 1-1/2 teaspoons dried parsley flakes
• 1 teaspoon dried oregano
• 1/2 teaspoon pepper
• 1 cup uncooked whole wheat elbow macaroni
• 11 teaspoons grated Parmesan cheese
Source: Taste of Home
Every Step Matters:


David Swain, DPM, CWSP
Dr. David Swain specializes in limb salvage and lower extremity wound care, helping patients heal and prevent amputations. Inspired by his grandfather’s experience with diabetic ulcers, he focuses on proactive, patient-centered treatments.
He earned his BS in Biology, magna cum laude, from Georgia Southern University, and his Doctor of Podiatric Medicine from Scholl College of Podiatric Medicine. Following a surgical residency focused on diabetic limb salvage, Dr. Swain became board certified in Podiatric Medicine, Wound Management, Limb Preservation and Salvage, and Podiatric Surgery. He serves as a community educator on limb preservation and, along with Donna Geiger, participates in clinical trials for diabetic and venous ulcers. Outside work, he enjoys family time, golfing, music, and the beach.
Donna Geiger, MSN, FNP-BC, CWON
With over 44 years of nursing experience, Donna Geiger has served Jacksonville’s acute care community and has been a vital part of FCCI’s wound care team for the past 7.5 years.
She earned her BSN from Armstrong Atlantic State University, her Wound, Ostomy, and Continence Nursing certification from Emory University, and her MSN as a Family Nurse Practitioner from Chamberlain College of Nursing. Donna is active in professional nursing organizations, has presented research on pressure injury prevention at national and international conferences, and works with Dr. Swain on clinical trials for diabetic and venous ulcers.
Donna’s dedication to quality patient care addresses amputation prevention and all types of wounds, including pressure injuries, trauma, and surgical sites, taking a holistic approach to treat the patient as a whole. Outside work, she enjoys painting, biking, going to the beach, and spending time with family.
Learn more about FCCI’s wound care and amputation prevention services at www.noamputation.com

Know Your Metrics: Understanding Your Resting and Target Heart Rate
Your heart is more than a muscle—it’s a vital indicator of your overall health and fitness. Two key numbers can help you tune in to your cardiovascular wellness: your resting and target heart rates. Knowing both can guide your workouts, monitor your progress, and alert you to potential health issues.
What is your Resting Heart Rate?
Your resting heart rate is the number of times your heart beats per minute (bpm) when you’re completely at rest. The best time to measure it is right after waking up, before getting out of bed. For most adults, a healthy resting heart rate falls between 60 and 100 bpm
Several factors can influence this number— stress, hormones, medications, and fitness level, among them. In general, a lower resting heart rate means a stronger, more efficient heart. However, if your resting rate dips below 40–50 bpm and you’re not an endurance athlete, it’s worth checking in with a healthcare provider.

Improving Your Resting Heart Rate
The most effective way to improve your resting heart rate? Exercise. Consistent physical activity helps strengthen the heart, allowing it to pump more efficiently and beat fewer times per minute.
But before you lace up your sneakers, it’s essential to understand your target heart rate—the zone where your heart is working at an optimal level during exercise.

Sources: American Heart Association, John Hopkins Medicine, Cleveland Clinic
Importance of Knowing Your Target Heart Rate
Knowing your target heart rate ensures you’re exercising at the right intensity. It helps you burn calories efficiently, boost endurance, and avoid overexertion. It also provides a benchmark to track progress over time.
Calculating Your Target Heart Rate
1. Maximum Heart Rate (MHR): Subtract your age from 220. For example, if you’re 40, your MHR is 180 beats per minute (bpm).
2. Target Heart Rate Zone: Aim for 50-85% of your MHR. For a 40-year-old, this is 90-153 bpm.
• 50–70% of MHR: Light to moderate intensity—great for beginners or warmups
• 70–85% of MHR: Vigorous intensity—for improving cardiovascular fitness
How Do I Find My Pulse or Heart Rate?
Finding your pulse is easy and takes less than a minute:
1. Place your index and middle fingers on the inside of your wrist, just above the thumb.
2. Press lightly until you feel your heartbeat.
3. Count the beats for 30 seconds and multiply by two.
If your heart rate is above your target zone, that is your cue to slow down. If it's low, you can pick up the pace. Either way, you're gaining valuable insight into how your body responds to movement.

Final Thoughts
Your heart rate tells a story—one that can guide your fitness goals, highlight your progress, and help you stay safe while exercising. Make a habit of checking in with your numbers, and always consult a healthcare provider before starting a new workout program (especially if you have any risk factors for heart disease).
FAST FACTS
Dr. Alan Schimmel is a boardcertified cardiologist with over 30 years of experience in clinical, diagnostic, and interventional cardiology in Jacksonville, FL. A graduate of the prestigious Massachusetts Institute of Technology, he joined First Coast Cardiovascular Institute in 2015 and enjoys spending time with his wife and two sons, along with staying active in the MIT alumni community.

Alan Schimmel, MD
Each minute, your heart pumps nearly 1.5 gallons (5.7 liters) of blood. That’s a pump flow rate that could fill an Olympic-sized swimming pool in less than a year. Talk about a gold medal effort!
Source: Cleveland Clinic
FALL-PROOF YOUR LIFE: EASY EXERCISES FOR BETTER BALANCE
As we age, muscle strength, joint flexibility, and proprioception (awareness of body position) naturally decline, increasing the risk of falls. Engaging in targeted balance exercises helps counteract these changes, maintaining mobility and independence.


Resources: The Mayo Clinic, National Institute on Aging
1

Here are some exercise ideas to keep you upright, steady, and strong:
1. Take a walk. Walking keeps you on your feet and also provides the additional benefits of fresh air, improved mood, and cardiovascular exercise.
2. Stand on one leg. Practice standing on one foot for 10 seconds, then switch to the other foot. You can do this while brushing your teeth, talking on the phone, or watching TV (a fun challenge is to do this every time a commercial comes on).
3. Weighted High Knees. March in place while lifting your knees to hip level. This is another exercise you can do while watching TV.
4. Dance. Get up and dance with a partner or simply turn on some music and move around. It doesn’t matter what type of dance it is. Dancing improves balance, coordination, and cardiovascular health. It also happens to be a lot of fun!
THREE KEYS TO SUCCESS
2 Start slowly
3 Consult your healthcare provider before starting any new exercise program.
Consistency is key: Engage in balance exercises at least two to three times per week for optimal benefits.
“One good thing about music, when it hits you, you feel no pain.”
~ Bob Marley

CAN MUSIC HEAL YOUR HEART?
The Healing Power of Music: A Symphony for the Heart
Music has long been celebrated for its ability to evoke emotions, tell stories, and bring people together. But did you know that it can also play a vital role in healing the heart? Research shows that music has profound effects on both emotional wellbeing and physical health, making it a powerful tool in the fight against heart disease and stress.
The Science Behind Music and Heart Health
Listening to music has been found to reduce stress and anxiety, lower blood pressure, improve recovery from strokes, and improve heart rate variability. These benefits are crucial because chronic stress and high blood pressure are significant risk factors for cardiovascular disease. When we listen to music we love, our brains release endorphins and dopamine, the body’s natural feel-good chemicals. These substances not only enhance our mood but also promote relaxation and reduce the levels of stress hormones like cortisol.
“Music is the divine way to tell beautiful, poetic things to the heart.” – Pablo Casals
A study published in the journal Heart found that patients who listened to music for 30 minutes a day experienced significant reductions in blood pressure and heart rate. Similarly, a report in the Journal of the American College of Cardiology revealed that patients recovering from heart surgery who listened to soothing music experienced less anxiety and, in some cases, required less pain medications and sedatives.


Music as a Stress Reliever
Stress is a common part of modern life, and its effects can be particularly harmful to the heart. Chronic stress contributes to hypertension, arrhythmias, and other cardiovascular issues. Music therapy offers a natural and enjoyable way to combat stress. Gentle, rhythmic music can slow down the heart rate, lower blood pressure, and decrease levels of stress hormones.
Different genres of music can have varied effects on our emotions and physiology. Classical music, for example, is often used in therapeutic settings due to its calming and soothing properties. On the other hand, upbeat music can boost energy and motivation, helping to counteract feelings of fatigue and depression.
Music and Emotional Well-Being
Beyond its physiological benefits, music also plays a crucial role in emotional healing. It provides an outlet for expression, allowing individuals to process and release their emotions. Listening to music can also trigger fond memories from a simpler and happier time. For those dealing with heart disease, music can offer comfort and a sense of connection. Singing, playing an instrument, or simply listening to favorite tunes can improve mood and foster a positive outlook on life.


Incorporating Music into Daily Life
Incorporating music into your daily routine can be simple and highly beneficial. Here are some tips to harness the healing power of music:
1. Create Playlists: Curate playlists of your favorite songs to play during different activities, such as working, exercising, or relaxing.
2. Music Breaks: Take short music breaks throughout the day to relax and re-center your mind. Listening to calming music for just a few minutes can help reduce stress levels.
3. Learn an Instrument: Learning to play an instrument can be a rewarding and therapeutic hobby. It not only engages the mind but also provides a sense of accomplishment.
4. Attend Live Music Events: Experiencing live music can be uplifting and energizing. Concerts, musical theater, and community events are great ways to enjoy music socially.
Sources: Harvard Health, Scientific American, American Heart Association
Breathe Easy: Managing Stress with Simple Breathing Techniques
“Breathing in, I calm body and mind. Breathing out, I smile. Dwelling in the present moment I know this is the only moment” — Thích Nhat Hanh

Most of us react to stress with shallow chest breathing. We are programmed to respond to a perceived threat with a fight or flight response which includes rapid breathing to gear our bodies up to flee from danger. In modern daily life, however, there is usually not an actual threat to our safety. Instead, we experience ongoing tension due to an abundance of emails, media exposure, traffic, too many obigations on our calendars, etc.
Breathing exercises can help calm the mind and body. By focusing on your breath, you can activate the body’s relaxation response, lowering your heart rate and blood pressure, and reducing the production of stress hormones.
“I love breathwork because it’s easy, it can be done anywhere and it has a potent effect on your physiology,” Cleveland Clinic Integrative Medicine Specialist Melissa Young, MD says. “It’s really very powerful.”
Here are a few simple techniques to try:
Diaphragmatic (Belly) Breathing
Instructions:
• Sit or lie down in a comfortable position.
• Place one hand on your chest and the other on your abdomen.
• Take a deep breath in through your nose, allowing your abdomen to rise while keeping your chest relatively still.
• Exhale slowly through your mouth, feeling your abdomen fall.
• A good pace is one where the “inhaleexhale” cycle above takes up to 10 seconds.
• Repeat for 5-10 minutes, focusing on the rise and fall of your abdomen.
4-7-8
Breathing
Instructions:
• Sit or lie down in a comfortable position.
• Close your eyes and take a deep breath in through your nose for a count of 4.
• Hold your breath for a count of 7.
• Exhale completely through your mouth for a count of 8.
• Repeat the cycle 4-8 times, gradually increasing as you become more comfortable.
Box Breathing (also known as 4-4-4-4 or Square Breathing)
Instructions:
• Sit in a comfortable position with your back straight and feet flat on the floor.
• Close your eyes and inhale slowly through your nose for a count of 4.
• Hold your breath for a count of 4.
• Exhale slowly through your mouth for a count of 4.
• Hold your breath again for a count of 4.
• Repeat the cycle several times, maintaining a steady rhythm.
Alternate Nostril Breathing
Instructions:
• Sit in a comfortable position with your back straight.
• Use your right thumb to close your right nostril.
• Inhale deeply through your left nostril.
• Close your left nostril with your right ring finger, releasing your right nostril.
• Exhale through your right nostril.
• Inhale through your right nostril.
• Close your right nostril with your right thumb and release your left nostril.
• Exhale through your left nostril.
• Continue alternating for several cycles.

Working Breathing Exercises into Your Daily Routine
Incorporating these breathing exercises into your daily routine can have profound effects on your stress levels and heart health. Here are a few tips to help you get started:
• Set Aside Time: Dedicate 5-10 minutes each day to practicing your chosen breathing technique.
• Find a Quiet Space: Choose a calm environment where you won’t be disturbed.
• Be Consistent: Regular practice is key to reaping the benefits of these exercises.
• Combine with Other Techniques: Pair breathing exercises with mindfulness, meditation, or yoga.
• Our doctors also suggest a shorter and more frequent routine of 1-2 minutes every 2 to 3 hours.
Sources: Harvard Health and Cleveland Clinic
The Connection Between Good Oral Hygiene and Cardiovascular Health
Scientists have been studying the link between oral health and heart health for years, and recent findings make the case even stronger:
• Flossing and Stroke Prevention: A study presented at the American Stroke Association conference found that flossing just once a week could lower the risk of ischemic stroke by 22%. That’s a pretty big payoff for such a small habit!
• Tooth Loss and Heart Disease: Researchers at Case Western Reserve University discovered a strong link between losing teeth and a higher risk of fatal heart disease. Losing teeth isn’t just a cosmetic issue—it could be a warning sign of deeper health problems.
• Dental Check-Ups Matter: A study published in Scientific Reports showed that people who get regular dental care have a lower risk of cardiovascular disease and other health complications. Preventive care isn’t just good for your teeth—it’s good for your whole body.

How Poor Oral Health Affects Your Heart
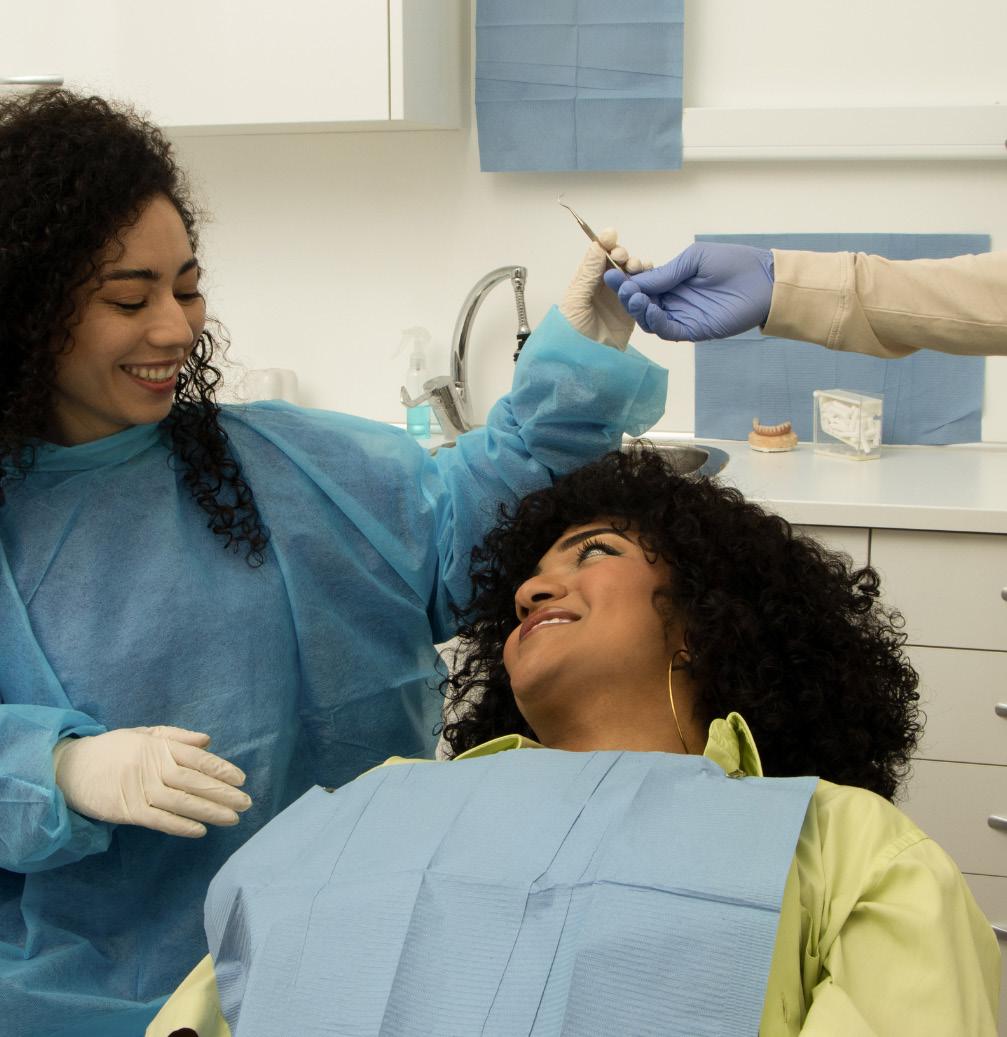
So, how exactly does skipping the floss or ignoring that bleeding gumline impact your heart? Here are a few ways:
1. Bacteria in the Bloodstream – Infected gums can allow harmful bacteria to enter the bloodstream, traveling to the heart and potentially causing infection in the valves.
2. Chronic Inflammation – Gum disease increases overall inflammation in the body, which can contribute to high blood pressure, arterial plaque buildup, and other heart problems.
3. Impaired Blood Vessels – Some research suggests that the bacteria from gum disease can damage the lining of blood vessels, making it harder for them to function properly.
What You Can Do
The good news? Taking care of your mouth is one of the simplest ways to support your heart health. Here’s how:
• Brush and Floss Daily – Brush your teeth twice a day for at least two minutes and floss at least once a day (or at least once a week—every little bit helps!).
• See Your Dentist Regularly – Don’t wait until something hurts. Regular check-ups and cleanings help prevent problems before they start.
• Eat a Heart-Healthy Diet – A diet rich in fresh fruits, vegetables, lean proteins, and whole grains helps both your teeth and your heart.
• Quit Smoking – Tobacco use is a major risk factor for both gum disease and heart disease. If you smoke, quitting is one of the best things you can do for your health.
• Manage Health Conditions – If you have diabetes or high blood pressure, keeping them under control will help reduce your risk of gum disease and heart problems.



BEYOND THE WHITE COAT: FIRAS EL SABBAGH, MD, FHRS
Director of Electrophysiology, FCCI
Dr. Firas El Sabbagh joined First Coast Cardiovascular Institute in 2019 as Director of Electrophysiology and also serves in the same role at HCA Orange Park Medical Center. Boardcertified in cardiac electrophysiology, cardiovascular disease, and echocardiography, he is a member of both the American College of Cardiology and the Heart Rhythm Society.
A graduate of the American University of Beirut, Dr. El Sabbagh completed his internal medicine residency at the prestigious Cleveland Clinic, followed by a cardiology fellowship at the University of Missouri and advanced training in cardiac electrophysiology at University Hospitals Case Medical Center.
Since beginning his practice in 2012, Dr. El Sabbagh has specialized in device-based therapies such as pacemakers, ICDs, and CRT for heart failure. He is also highly skilled in left atrial appendage occlusion (Watchman and Amulet) and catheter ablation for atrial and ventricular arrhythmias, utilizing both radiofrequency and cryoballoon techniques.
Recognized nationally for his expertise, he proctors and mentors junior cardiologists across the country on how to perform new procedures safely.
Passionate about innovation and patient care, Dr. El Sabbagh says, “The field challenges you to stay up to date and use these advancements in the best interest of our patients.”
Outside of work, he enjoys traveling and spending quality time with his wife and two daughters.

Quality Care for All: Addressing the Unique Needs of Rural Communities
Healthcare is a fundamental need for all, yet access to quality healthcare services remains a significant challenge in many rural communities across the United States. According to the U.S. Government Accountability Office (GAO), more than 60 million Americans – about 20 percent of the U.S. Population live in rural areas. However, only 1/10 of physicians practice in these areas. More than 100 (or 4%) of rural hospitals closed between 2013 to 2020.
Rural communities face various healthcare challenges that are often less prevalent in urban areas. These include:
• Limited Access to Healthcare Providers: Rural areas often have fewer healthcare providers, and hospitals are closing, making it difficult for residents to receive timely and adequate care.
• Long Travel Distances: Patients in rural areas may need to travel long distances to reach the nearest healthcare facility, which can be a significant barrier to accessing care.
• Economic Challenges: Rural populations often have lower incomes and higher rates of uninsured individuals, making healthcare affordability a major concern. Rural and lowincome areas also often have less broadband internet access which limits health information to residents, resulting in lower health literacy.
• At Higher Risk: Rural populations tend to be older, have higher rates of cigarette smoking and obesity.
• Higher Prevalence of Chronic Conditions: Rural residents may be at higher risk for heart disease, diabetes, hypertension, stroke, chronic lung disease, and suicide risk.

At FCCI, we believe that everyone deserves access to high-quality healthcare, regardless of their location. By setting up clinics in rural areas like Palatka, FL, and Waycross, GA, we bring healthcare services closer to those who need them most. These clinics offer a range of cardiovascular services, ensuring that patients have access to specialized care without having to travel long distances.
To learn more about our locations and services, www.firstcoastcardio.com
Protecting Your Kidney Health:
From Prevention to Dialysis and Innovative Access Solutions
Kidney disease often progresses in silence. Many people with chronic kidney disease (CKD) have no symptoms until more than 70% of their kidney function is already lost. In fact, countless patients only discover they have advanced kidney disease when they’re on the brink of needing dialysis.
Why Kidneys Fail
While kidney failure can result from infections or autoimmune disorders, the most common causes are uncontrolled diabetes and high blood pressure—the same culprits that increase the risk of heart disease. Over time, these conditions damage the kidneys’ tiny filtering units, called glomeruli, reducing their ability to remove waste and excess fluid from the body. This function is measured using the glomerular filtration rate (GFR).
Because the decline in kidney function is often symptomless, early injury may go unnoticed unless caught through routine blood and urine tests. Smoking can also contribute to kidney damage by reducing blood flow to the kidneys, compounding the effects of chronic conditions.
The Stages of CKD
CKD is classified into five stages, based on GFR levels and the rate of progression. The earlier it’s detected, the more effectively it can be managed. In many cases, controlling blood sugar and blood pressure, along with healthy lifestyle changes, can slow or even stop the progression of kidney disease.
The good news: the body can often function well with as little as 30% of original kidney function. With early intervention and proper management, many patients can avoid dialysis for years—or altogether.
The Heart-Kidney Connection
The kidneys and the heart are closely linked. That’s why managing CKD is a team effort, often involving your primary care doctor, nephrologist, and cardiologist. Certain medications can protect kidney function while also improving heart health and managing diabetes.
At First Coast Cardiovascular Institute (FCCI), we emphasize a collaborative approach to care. Our team helps patients reduce risk factors and avoid common pitfalls such as:
• Avoiding blood draws and IV lines at the elbow: These veins may be needed later for dialysis access.
• Minimizing contrast exposure during imaging: FCCI prioritizes kidney-friendly alternatives such as ultrasound and CO2 imaging to reduce the risk of contrastinduced kidney injury.
When Dialysis Becomes Necessary
Despite the best efforts, some patients reach a point where dialysis is essential. At that stage, having a well-planned dialysis access site is critical. The safest and most effective method is through an arteriovenous fistula (AVF) connection between an artery and vein, typically in the arm.
However, many patients still receive dialysis through a catheter placed in the upper chest, which carries higher risks of infection, blood clots, and long-term complications. At FCCI, we’ve long championed the effort to move patients away from catheters and toward safer, more reliable options.
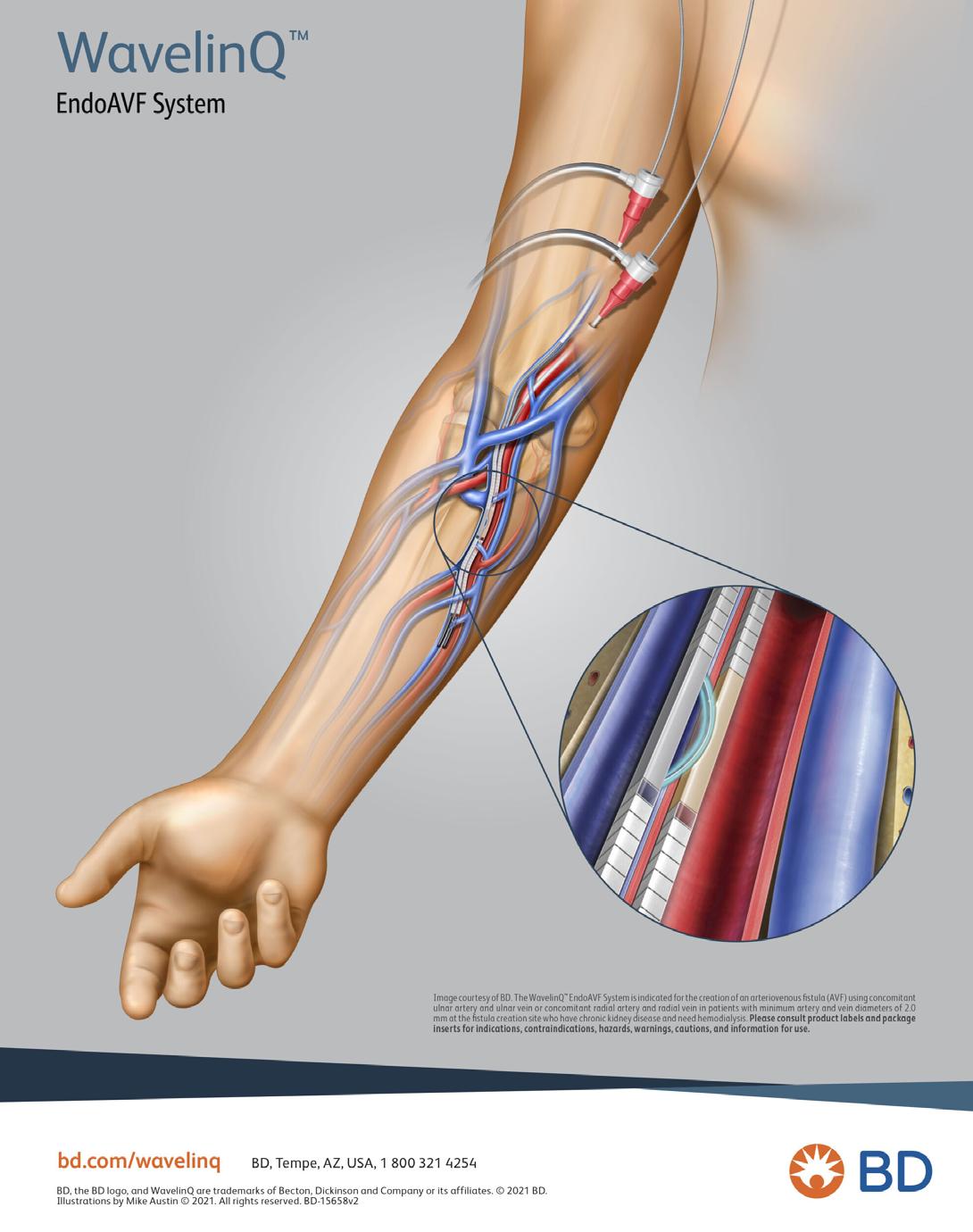
Historically, fistulas could only be created through open surgery. But new advances in vascular medicine have changed that. Today, patients have access to less invasive options like the WavelinQ™ EndoAVF System which FCCI is proud to offer.
What Is the WavelinQ System?
WavelinQ is a catheter-based procedure that creates a fistula using two small incisions and radiofrequency energy to form a connection between a vein and an artery without the need for open surgery.
Benefits of WavelinQ:
• Minimally invasive and with no surgical wound there is less trauma and a faster recovery
• Lower complication risk: Markedly reduced chances of infection or scarring
• Comfortable for patients: Less discomfort and quicker return to daily activities
• Improves dialysis outcomes: Creates reliable access for long-term treatment
At FCCI, our vascular specialists are leaders in these cutting-edge approaches. We are committed to eliminating the use of dialysis catheters whenever possible, improving both safety and quality of life for our patients.
The Importance of Planning Ahead
National guidelines now recommend that patients begin preparing for dialysis when they reach stage IV CKD, even if dialysis isn’t immediately needed. Creating a fistula early can
help ensure smoother treatment and prevent emergency catheter placement.
Our team at FCCI works closely with each patient and their nephrologist to plan and prioritize the patient’s comfort, safety, and to reduce complications down the line.
The Takeaway:
Your kidneys and your heart are partners in health.
Managing chronic conditions, staying proactive with screenings, and taking advantage of innovative options like WavelinQ can help you navigate kidney disease with more confidence and control.
At First Coast Cardiovascular Institute, we’re proud to offer state-of-the-art care for both heart and kidney health. If you or a loved one is facing CKD, we’re here to guide you every step of the way.
Learn more about the WavelinQ™ system at wavelinq.bd.com.

A New Era of Heart Care: FCCI’s Cardiovascular Ambulatory Surgical Center
In yet another first, First Coast Cardiovascular Institute brings Northeast Florida the first and currently only surgical center dedicated exclusively to cardiovascular care.
First Coast Cardiovascular Institute (FCCI) is proud to announce the upcoming opening of its Cardiovascular Ambulatory Surgical Center (ASC), a state-of-the-art facility designed to make advanced heart and vascular care more accessible than ever.
Unlike traditional hospitals, an ASC provides specialized outpatient procedures that do not require an overnight stay. This allows patients to receive the cardiovascular care they need in a comfortable, patient-focused environment and return home the very same day.
Why we built it: The healthcare landscape is rapidly shifting, with more procedures moving from hospitals to outpatient settings. FCCI built its ASC to meet this challenge head-on by expanding access to care, lowering costs, and maintaining the high-quality cardiovascular services our community has come to expect.


Who it serves: The Cardiovascular ASC is designed for patients who require minimally invasive, same-day procedures. By focusing on appropriate low- to moderate-risk cases, the center enhances patient convenience and safety while supporting physician practices, insurers, and the broader community with a cost-effective alternative to hospital-based care.

Patient benefits: For patients, the advantages are clear: shorter recovery times, reduced costs, and a more personalized, comfortable care experience without compromising quality or safety. The ASC also strengthens care coordination, ensuring patients remain closely connected with their FCCI physicians throughout every stage of treatment.
“Our Cardiovascular Ambulatory Surgical Center delivers safe, high-quality heart and vascular care that is affordable, convenient, and designed
to get patients home the same day they receive their procedure.”

- Walid Abdalla, MHA, FACHE, FACHDM, Vice President & ASC Administrator
The FCCI Cardiovascular ASC reflects our ongoing mission of bringing world-class, patient-centered cardiovascular care closer to home. While the official opening date and operating hours will be announced soon, one thing is certain: patients can look forward to a new era of heart and vascular care that is safe, efficient, and truly centered on their wellbeing.
To learn more, visit fccsurgicalcenter.com
The FCCI Family is Growing

Welcome
Dr. Deepak Kumar Pasupula, MD, MPH
We are pleased to welcome Dr. Deepak Kumar Pasupula to FCCI’s cardiac electrophysiology practice. Board-certified in cardiovascular disease, echocardiography, and nuclear cardiology, he trained in India and completed fellowships at MercyOne North Iowa and the Mayo Clinic in Jacksonville. A Harvard-trained public health scholar with over 45 publications, he is skilled in advanced ablation techniques, conduction system pacing, cardiac device procedures, and lead extraction. He specializes in treating arrhythmias and device infections, collaborates on research with the Mayo Clinic, and is known for his compassionate, patient-first care. Outside of medicine, he enjoys swimming, cooking, and time with his wife and two children.
Welcome
Dr. Rabih Tabet, MD
Dr. Rabih Tabet, an interventional and vascular cardiologist, is now seeing patients at First Coast Cardiovascular Institute. Triple board-certified in Interventional Cardiology, Cardiovascular Disease, and Internal Medicine, he trained at Lenox Hill Hospital and Yale New Haven Hospital. He specializes in limb preservation, carotid and renal artery interventions, and comprehensive cardiac care.
Fluent in English, French, and Arabic, Dr. Tabet is recognized for his compassionate bedside manner and commitment to patient care and research. Outside of medicine, he enjoys time with his family, bonsai trees, stargazing, and music.

Welcome
Kelechukwu Okoro, MD
We’re excited to welcome Dr. Kelechukwu Okoro as a fulltime physician at FCCI. Board certified in internal medicine, cardiovascular diseases, and interventional cardiology, he recently completed his endovascular fellowship with us.
Dr. Okoro earned his medical degree from St. Matthew’s University, completed residency at Virginia Tech Carilion, and was Chief Fellow during his fellowships at Marshall University.
Dr. Okoro stood out for his skill, dedication, and compassionate care, and we’re excited to have him continue with us as part of our expert team.


Welcome
Siva Suryadevara, MD, FACC, FSCAI
Dr. Siva Suryadevara is a board-certified interventional cardiologist with more than a decade of experience providing comprehensive cardiovascular care. He earned his medical degree from the University of the West Indies and completed his graduate medical education at the University of Florida College of Medicine–Jacksonville after relocating to Northeast Florida.
Board certified in internal medicine, cardiovascular disease, interventional cardiology, and cardiovascular CT, his clinical interests include complex coronary artery disease, heart failure, peripheral vascular disease, and preventive cardiology. Known for his patient-centered approach, Dr. Suryadevara focuses on clear communication and personalized care to build long-term patient relationships.
First Coast Cardiovascular Institute is pleased to welcome “Dr. Siva” Suryadevara to the practice beginning January 2026.



















Spotlight on Lung Health:
The Critical Importance of Lung Cancer Screening in Smokers
By Irram Hamdani, M.D., Pulmonologist and Sleep Specialist
Each year, lung cancer claims more lives in the United States than breast, prostate, colorectal, and pancreatic cancers combined. Yet despite its devastating impact, lung cancer remains under-screened, often diagnosed in its later, less treatable stages.
As both a pulmonologist and sleep medicine specialist, I regularly see the long-term impact of tobacco use. About 81% of lung cancers are directly related to smoking. This risk increases with the number of packs smoked, the duration of use, and how early someone began smoking. Lung cancer screening, particularly with low-dose CT scans, offers a life-saving opportunity to detect cancer at a stage when it is still curable.
The numbers are sobering. More than 340 people die from lung cancer each day. Overall, the five-year survival rate is just 18% when diagnosed in late stages. For individuals diagnosed at early stages 5 years survival rate climbs to an impressive 92%. This makes early detection not just beneficial. It is critical.

So, who should be screened?
Current and former smokers aged 50 to 74 with a 20-pack-year smoking history, including those who quit within the last 15 years, are prime candidates. The U.S. Preventive Services Task Force recommends annual low-dose CT scans for these individuals.
Lung screening isn’t just about cancer. Smoking is also a leading cause of cardiovascular disease (CVD), contributing to one in four CVD-related deaths in the U.S. Smokers are up to four times more likely to develop heart disease than non-smokers. In both cancer and heart disease prevention,
quitting smoking and routine screening are essential.
It’s time we treat lung screenings the way we do mammograms and colonoscopies. When caught early, lung cancer is treatable. Early screening is the key to changing the course of this disease for our patients, families, and communities.
About Dr. Irram Hamdani
Dr. Irram Hamdani is a board-certified pulmonologist and sleep medicine specialist at First Coast Cardiovascular Institute. With a compassionate approach and years of experience, she is dedicated to improving patients’ lung and sleep health through education, early detection, and expert care.
Learn more about Dr. Hamdani at firstcoastcardio.com

TESTIMONIALS PATIENT
Patient reviews are the heart of our practice. Nothing is more heartwarming than seeing we have made the experience of visiting a doctor’s office just a little bit easier.
“Dr. Fahdi took the time to explain test results and the reasoning behind them. He was very patient and understanding. His professional expertise was appreciated.”
~ Verified Healthgrades Review
“This was my first visit with Dr. Thielemann. Amazing experience. He explained things on my knowledge level and terminology, making sure I understood the process and next steps of treatment. I appreciate his caring attitude and look forward to my next appointment. Sincerely thankful!!”
~ Verified Google Review
“Dr. Lamba is very informative and spent much time with me to answer any questions. He has been my mother’s cardiologist for many years and saved her life.”
~Verified Patient Survey
“Dr. Al Saghir did not rush us at all. He took his time explaining exactly what the diagnosis was. He was very pleasant and answered all questions.”
~ Verified Healthgrades Review
“Dr. Ali and the staff have always made me feel relaxed during visits and at the same time being informative and honest. A smile, small conversation, and honesty goes a long way! Thanks again for caring!”
~ Verified Google Review
“First Coast Cardiovascular Institute –Palatka. They are the best. I would not trust another cardiology group. I love these people.”
~ Verified Google Review
These reviews have been edited for spelling and grammar.
Berry Good for You:
The Health Benefits of Nature’s Superfruit
Berries are not only delicious but also packed with nutrients that offer numerous health benefits. Incorporating berries into your daily diet can improve heart health, enhance brain function, and reduce the risk of chronic diseases.
Nutrient Powerhouses
Berries such as blueberries, strawberries, raspberries, and blackberries are rich in vitamins, minerals, and antioxidants. They provide essential nutrients like vitamin C, vitamin K, fiber, and manganese, all of which contribute to overall health. The high antioxidant content in berries helps combat oxidative stress, reducing inflammation and protecting cells from damage.
Heart Health
Regular consumption of berries has been linked to improved cardiovascular health. A study by Harvard School of Public Health reported that eating berries, such as blueberries, appeared to reduce the risk of heart attack in women by 33%. The anthocyanins in berries help dilate arteries, reduce plaque buildup, and decrease blood pressure, all of which support heart health.
Cognitive Benefits
Berries also play a role in maintaining and improving brain function. Research indicates that the antioxidants in berries may delay brain aging and enhance memory.
A study from the University of Cincinnati found that daily consumption of blueberries improved memory and cognitive performance in older adults.
Cancer Prevention
The high levels of antioxidants, particularly anthocyanins, in berries have been associated with cancer prevention. These compounds help neutralize free radicals, reducing DNA damage that can lead to cancer. Some studies suggest that berries may inhibit the growth of cancer cells and reduce the risk of certain types of cancer.
Blood Sugar Control
Despite their sweetness, berries have a low glycemic index, making them suitable for individuals monitoring their blood sugar levels. Studies have shown that berries can improve insulin sensitivity and reduce blood sugar responses when consumed with highcarb foods.
Digestive Health
The fiber content in berries aids digestion and promotes a healthy gut microbiome. Regular intake can prevent constipation and contribute to overall gastrointestinal health.
The FCCI team encourages mindful eating. Remember, even healthy foods like berries are best in moderation.
Resources: Harvard Health, NIH
Incorporating Berries into Your Diet

Berries are versatile and can be enjoyed in various ways:
• Fresh Snacks: Enjoy them raw as a quick and nutritious snack.
• Smoothies: Blend them into smoothies for a refreshing drink.
• Salads: Add them to salads for a sweet and tangy flavor.
• Breakfast: Top your cereals, oatmeal, or yogurt with berries.
• Desserts: Incorporate them into desserts like parfaits or use them as toppings for cakes and pastries.

QWhat is your favorite time of year?
Dr. DeNeen: Autumn (true autumn further up north)
Dr. Khatib: Thanksgiving
QDo you have any pets?
Dr. Khatib: TICO is A cute little Yorkee/ Shitsu hybrid and Fergus and Merida are kittens adopted from the Humane Society.
QWhat is something new you would like to try?
Dr. Khatib: This will sound funny, but in my case, it is “chilling”
Q & A

QWhat scares you, but you do it anyway?
Dr. DeNeen: Letting my daughter drive
Dr. Khatib: Trust/Allow/Enable my growing kids to make more independent life decisions.
QWhat important life lesson did you learn early in life that has stayed with you?
Dr. DeNeen: Be the person people want to work with - not the person they dread working with
Dr. Khatib: All along and I still am working on the “blame yourself for the negatives & credit God for the positives in your life”

Tomorrow’s Heart Care, Here Today
How our research program brings the latest treatments and technology to our patients first.
At First Coast Cardiovascular Institute (FCCI), our Clinical Research Program brings tomorrow’s treatments to patients today.
We partner with leading pharmaceutical and medical device companies to test new medications, procedures, and technologies for conditions like heart failure, peripheral artery disease, diabetic wounds, and coronary artery disease.
Why Consider a Clinical Trial?
• Early access to innovative treatments
• Extra attention and close monitoring from our research and clinical teams
• A chance to help future patients by advancing science
What to Know
Clinical trial patients may have more frequent follow-up visits—which means more personalized care. There’s also a small possibility of side effects not yet recognized. But according to Dr. Khatib, all studies are carefully reviewed by the FDA, and in our 20+ years of research, major unexpected complications have been very rare.
Your safety is always our top priority.
Current Enrolling Studies
We are currently enrolling for studies in several key areas:
Heart Failure
• Testing a new medication combination for patients with preserved ejection fraction.
Peripheral Artery Disease (PAD)
• New devices and treatments to open blocked leg arteries and improve blood flow.
Below-the-Knee PAD
• Innovative balloons and scaffolds designed for hard-to-treat arteries in the lower legs and feet.
Who Can Participate?
Post-Approval Device Studies
• Ongoing monitoring of FDA-approved technologies to ensure long-term safety and effectiveness.
Wound Healing
• New topical therapies for chronic venous ulcers and diabetic foot wounds.
Coronary Artery Disease
• A device using sound wave technology to break up hard calcium deposits in the heart’s arteries.
If you have a cardiovascular condition—or symptoms like leg pain, foot ulcers, or shortness of breath—you may qualify. Eligibility depends on the specific study, but we welcome anyone interested in exploring advanced care options.
What to Expect
• Review of your medical history
• Discussion about eligibility
• Clear answers about risks and benefits
• Support before, during, and after the study
Participation is always voluntary and there is never any pressure to join

Learn More
Visit firstcoastcardio.com/research or email our Research Manager, Vanessa Hernandez, at vhernandez@firstcoastcardio.com for details.
We’re here to help you explore every option for a healthier heart and life.
Transform Your Heart from the Comfort of Home

First Coast Cardiovascular Institute now offers an innovative home-based cardiac rehab program designed to improve your heart health.

Having a heart event or procedure can be a challenging and emotional experience, but you don’t have to go through this alone.
In collaboration with virtual educators at Pritikin Intensive Cardiac Rehab, FCCI’s team of cardiology professionals is ready to provide the support you need as you continue the recovery process and commit to a heart-healthy lifestyle, all from the comfort of home.
Beyond Exercise:
Nutrition Workshops – Learn to read nutrition labels while grocery shopping and make balanced choices when dining out.
Healthy Mind-Set Workshops –Discover how to manage stress and anxiety, improve your communication skills, and set effective goals.
Cooking School Demos – See just how easy it can be to prepare satisfying, heart-healthy meals.
Qualifying Conditions
Your physician can determine if you qualify for home-based cardiac rehab and whether the program will be a good fit for you.
Patients with the following conditions may participate:
z Heart attack
z Coronary artery bypass surgery
z Stenting or angioplasty
z Current stable angina (chest pain)
z Heart or heart-lung transplant
z Heart valve repair or replacement
z Chronic heart failure
What to Expect
After an Initial Evaluation appointment, you will receive an at-home rehab kit with everything you need to participate in the program, including exercise bands and a pulse oximeter.
Each appointment will consist of two components: exercise and education. Our team of cardiac rehab experts will tailor exercise to your current fitness level and create a personalized plan to help you meet your health and wellness goals.
As you continue through the program, the cardiac rehab team will monitor your progress and communicate with your doctor every step of the way.
QUOTES to relax your mind

In the middle of difficulty lies opportunity.
~ Albert Einstein
“There is no trouble so great or grave that cannot be much diminished by a nice cup of tea.”
~ Bernard-Paul Heroux
I have many problems in life. But my lips don’t know that. They always smile.
~ Charlie Chaplin
“Peace is the result of retraining your mind to process life as it is, rather than as you think it should be.”
~ Wayne W. Dyer
“A good way to overcome stress is to help others out of theirs.”
~ Dada J.P. Vaswani
Sources: hope+wellness

Just when the caterpillar thought the world was ending, he turned into a butterfly.
~ Proverb
“Breathe. Let go. And remind yourself that this very moment is the only one you know you have for sure.”
~ Oprah Winfrey

“Don’t believe every worried thought you have. Worried thoughts are notoriously inaccurate.”
~ Renee Jain

Serving the Hearts of the First Coast Since 2002

Cardiovascular
Medicine Interventional Cardiology
Pulmonology
Cardiology
Sleep Medicine Nuclear
Vascular & Endovascular
Medicine
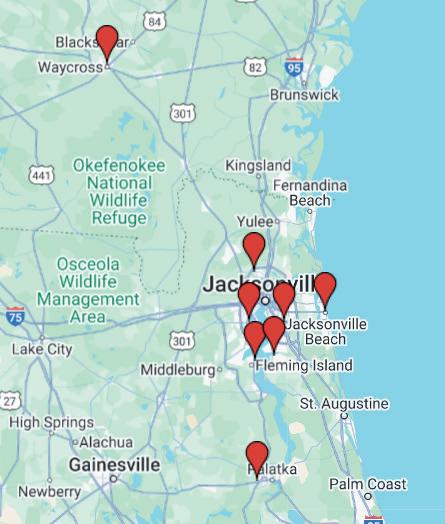
We Are Growing! Offering Multiple Locations to Best Serve YOU

Amputation Prevention Electrophysiology
Varicose and Vein Disease
Cardiac & Vascular Testing
Hemodialysis Access, Creation, and Management Wound Management
SOUTHSIDE OFFICE/OUTPATIENT CATHETERIZATION LAB: 7011 AC Skinner Pkwy, Ste 160
JACKSONVILLE BEACH OFFICE: 905 Beach Blvd
UNIVERSITY BLVD OFFICE: 3627 University Blvd S, Ste. 435
FRUIT COVE OFFICE: 115 Bartram Oaks Walk, Ste. 104
NORTHSIDE OFFICE: 3890 Dunn Ave, Ste. 203
WESTSIDE OFFICE: 5851 Timuquana Rd, Ste 204
ORANGE PARK OFFICE: 1465 Kingsley Ave
PALATKA OFFICE/OUTPATIENT CATHETERIZATION LAB: 205 Zeagler Dr, Ste. 101
WAYCROSS GEORGIA OFFICE: 501 Riverside Drive


