Ergonomics in Dentistry
Inside: 2025 SDDS Annual Report

Inside: 2025 SDDS Annual Report


March 5, 2026
Sacramento Kings Game
Thursday • 7:00pm
March 10, 2026
General CE Meeting
Tuesday • 5:45– 9:00pm • Social/Exhibits, Dinner and Program
Hilton Sacramento Arden West • 3 CEU, Core
Member Price: $89 early (ends 2/24) / $99 regular (ends 3/7)
$109 late (begins 3/8)
Non-Member Price: $218
Leading with Trust: Tools to Inspire Teams, Prevent Burnout, and Build Wellness
Eric Johnson, DDS
Sponsored by Alpha & Delgadillo OMS
March 26-27, 2026
45th Annual MidWinter Convention & Expo
Toothstock: Peace, Love & CE
SAFE Credit Union Convention Center, Sacramento, California Register online at www.sdds.org
April 7, 2026
Continuing Education Webinar*
Tuesday • 12:00–1:00pm • 1 CEU, Core • Webinar • $45
Member Price: $45 early (ends 3/17) / $70 regular (begins 3/18)
Non-Member Price: $140
HIPAA Without the Headache: What Dental Offices Get Wrong (and How to Fix It)
Dennis Krohn and Sara Baker, MBA; SD Dental Solutions (SDDS Vendor Member)
April 8, 2026
Dentists Do Broadway - MJ (Michael Jackson)
Wednesday • 7:30pm show
April 14, 2026
General CE Meeting
Tuesday • 5:45–9:00pm • Social/Exhibits, Dinner and Program
Hilton Sacramento Arden West • 3 CEU, Core
Member Price: $89 early (ends 3/31) / $99 regular (ends 4/11)
$109 late (begins 4/12)
Non-Member Price: $218
GM: Non-Odontogenic Tooth Pain
Mohd Khalaf, DDS
* Does not qualify for AGD credit

View all CE Courses & Events online with this QR code.
April 18, 2026
CPR–AHA BLS Blended Learning–
Online and Skills Testing, 3 Time Sessions
Saturday • 8:00–8:45am; 9:00–9:45am; 10:00–10:45am
Member Price: $98 total; $37 to AHA / $61 to SDDS (ends 3/28)
$118 total; $37 to AHA/$81 to SDDS (begins 3/29)
Non-Member Price: $199 total; $37 to AHA / $162 to SDDS
Skills Testing, 3 Time Sessions (3 CEU, Core)
SDDS Instructors
April 22, 2026
Licensure Renewal Webinar*
Wednesday • 5:30–7:30pm • 2 CEU, Core • Webinar
Member Price: $75 early (ends 4/1) / $95 regular (begins 4/2)
Non-Member Price: $190
California Dental Practice Act
Joy Brack, RDA
April 28, 2026
Licensure Renewal Webinar*
Tuesday • 5:30–7:30pm • 2 CEU, Core • Webinar
Member Price: $75 early (ends 4/7) / $95 regular (begins 4/8)
Non-Member Price: $190
Infection Control
Joy Brack, RDA
May 1, 2026
Continuing Education Hands-On Friday • SDDS Classroom
Lecture only: 8:30–11:30am • 3 CEU, Core
Lecture and Hands-on: 8:30am–2:30pm • 6 CEU, Core
Lecture only Member Price: $159 early (ends 4/10) / $184 (begins 4/11) Non-Member Price: $368
Lecture and Hands-on Member Price: $395 early (ends 4/10) / $420 (begins 4/11) Non-Member Price: $840
Mimicking Nature: Navigating the Complex Root Canal System
Peter Ham, DDS, MSD
Sponsored by Henry Schein Dental and EdgeEndo
May 8, 2026
Swing For Smile Golf Tournament
Friday • 7:00pm check-in • Teal Bend Golf Course
May 12, 2026
General CE Meeting
Tuesday • 5:45– 9:00pm • Social/Exhibits, Dinner and Program
Hilton Sacramento Arden West • 3 CEU, Core
Member Price: $89 early (ends 4/28) / $99 regular (ends 5/9)
$109 late (begins 5/10)
Non-Member Price: $218
Drugs, Bugs and Dental Products, What to Prescribe!
Peter Jacobsen, DDS
Sponsored by Capitol Periodontal Group
Bryan Judd, DDS; Editor-in-Chief
Ranna Alrabadi, DMD • Nicholas Scordakis, DDS
Ramsen Warda, DDS • Peter Yanni, DMD, MS Idean Rezaei, Student Rep
James Musser, DDS
William Parker, DMD, MS, PhD Bevan Richardson, DDS
Provided by the American Dental Association 12 14 16 18 21
Trapezius Myalgia: Making Dentistry a Pain in the Neck—or Head
Bethany Valachi, PT, DPT, MS,
Understanding Ergonomics: Best Practices, Benefits, and Your Responsibilities as a Dentist
Karen Schaffner; TDIC
The Rise of Ergonomic Loupes: A Smarter Approach to Clinical Precision and Practitioner Health
Jalen Blackman & Tessa Crosby; LumaDent
Getting a Better Grasp: Preventing Hand and Wrist Injuries in Dental Professionals
Noëlle M. Santucci, DDS, MA, RDH, FACD & Justin Jellin, DPT, ART
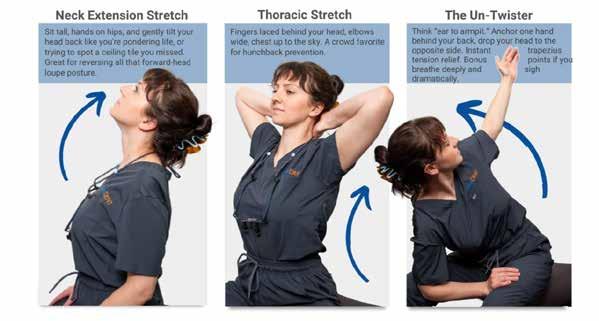
ADA Ergonomic Stretch Guide




I am proud to say we have several early career dentists already volunteering in our committees.




By Caroll Badgley SDDS Executive Director
Through conversations at Society events, I’ve had the chance to really listen and better understand the realities you face in practice today. You’ve shared that your focus is on running healthy practices, managing growing administrative demands, finding continuing education that truly adds value, and staying connected with colleagues who understand what practicing dentistry is really like. At the same time, there’s a shared concern about the future of the profession and a desire to support the next generation of dentists.
That desire is at the heart of much of what we do at the Sacramento District Dental Society (SDDS). Supporting students and young dentists is one of the most meaningful ways we can strengthen the future of dentistry, and we are intentional about creating opportunities for connection, mentorship, and community early in their careers.
Through our CSUS Pre-Dental Committee, members share real-world insight that goes far beyond the classroom, helping students better understand the profession they hope to enter. The SDDS Foundation also proudly administers the Dr. Herbert and Inez Yee Family Scholarship, established by the Yee Family, providing annual financial support to CSUS pre-dental students every year.
We believe it’s important for students to have a voice, which is why SDDS includes two non-voting student representatives on our Board of Directors, one from California Northstate University and one from the University of the Pacific. Their perspectives help inform our discussions and keep us connected to those entering the profession.
Mentorship continues at our General Meetings, where dentist members sponsor students to attend, connect, ask questions, and build relationships that often extend well beyond a single evening. These experiences reinforce that organized dentistry is more than an organization, it’s a community.
Students and members also come together through service, volunteering side by side at events like Smiles for Kids Day, local school screenings, and the MidWinter Convention. And sometimes, connection is simply about coming together socially, as we saw with strong student attendance from CNU and UOP at last summer’s Ice Cream Social.
All of this reflects a simple truth: organized dentistry is strongest when we stay connected across generations. By investing in students today, we help ensure a strong, engaged, and prepared dental community for tomorrow.
Thank you for being part of this shared effort. I look forward to seeing you at an upcoming event and continuing these important conversations together.
Warm regards,
President: Jeffrey Sue, DDS
President-Elect/Treasurer: Craig Alpha, DDS
Secretary: Chirag Vaid, DDS
SDDS BCR Rep: Bryan Judd, DDS
Editor-in-Chief: Bryan Judd, DDS
Executive Director: Caroll Badgley
Andrea Cervantes, DDS
Diana Fat, DDS
Eric Grove, DDS
Kart Raghuraman, DDS, MPH
Cherag Sarkari, DDS
Joel Whiteman, DDS
Rosemary Wu, DMD, MS
Guest of the Board: Sarmad Paydar, DDS, MS
CNU Student Rep: Christopher Brandon Azali
UOP Student Rep: Resha Shah
CPR: Margaret Delmore, MD, DDS/ Brad Archibald, DDS
Membership/Engagement:
Shahrzad Paydar Hogan, FAADOM
Nominating/Leadership Development:
Nima Aflatooni, DDS
Budget & Finance Advisory: Craig Alpha, DDS
Bylaws Advisory: Nima Aflatooni, DDS
CE Advisory: Arryan V. Emamian, DDS
CSUS Pre-Dental:
Brian Orcutt, DDS/Shannon Chris, DDS
Social Media Advisory: Jasraj Sandhu, DMD
Strategic Planning Advisory: Chirag Vaid, DDS/Craig Alpha, DDS
Foundation President: Carl Hillendahl, DDS
Caroll Badgley | Executive Director
Della Yee | Director of Operations
Sofia Gutierrez | Foundation Projects/CPR
Jessica Luther | Graphic Designer
Jen Jackson | Member Liaison
Katie Carrillo | Administrative Assistant
(916) 446-1211. Acceptance of advertising in The Nugget in no way constitutes approval or endorsement by Sacramento District Dental Society of products or services advertised. SDDS reserves the right to reject any advertisement.
Postmaster: Send address changes to SDDS, 2035 Hurley Way, Ste 200, Sacramento, CA 95825.
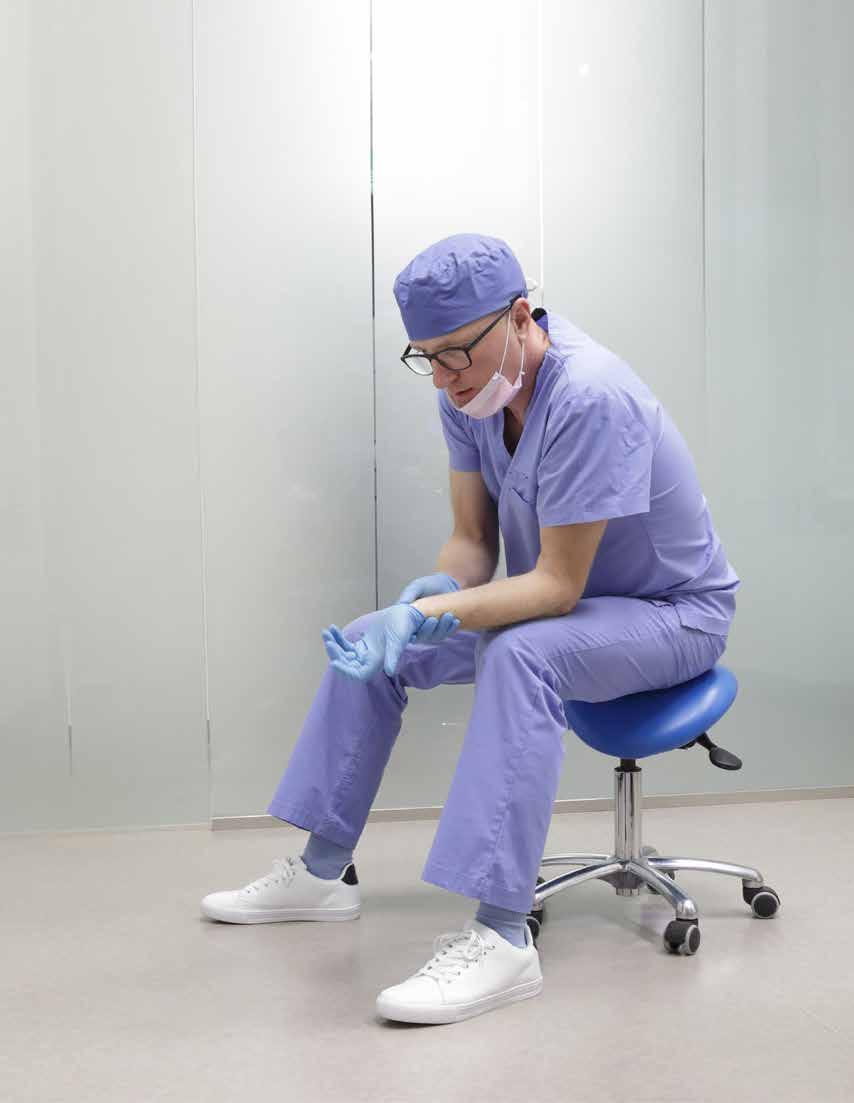
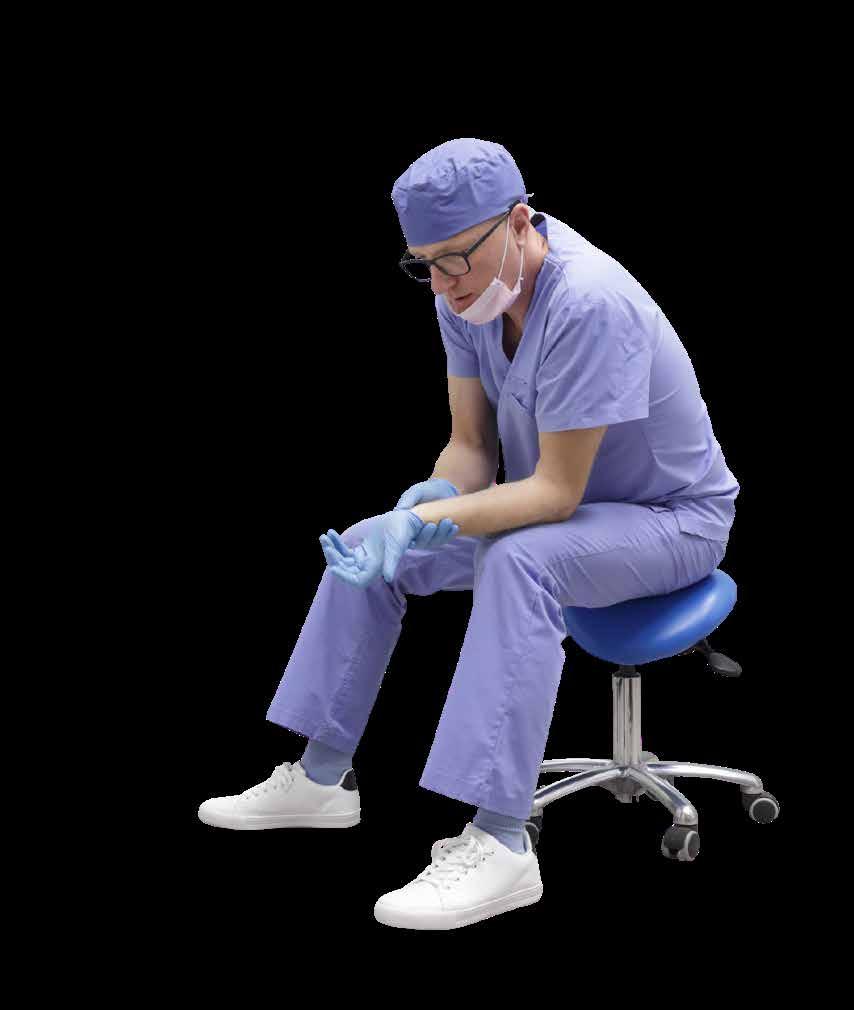
Bringing awareness and education to the impacts of ergonomics while applying evidence-based techniques for a healthier and long-lasting dental career.
It is well known that dentists have long been associated with having back, neck, and wrist pain. Photography, going back to the 1800s show dentists hunched over and in awkward positions delivering dental care to their patients. It is this portrayal that was in newspapers, movies, and now in social media that is embedded in the minds of many generations.
Unfortunately for dentists, the struggle is not just a theatrical depiction in cinema or a social media post, but it is a reality.
According to the United States Bureau of Labor Statistics, 30% of work-related injuries are caused by musculoskeletal disorders (MSDs). Even more alarming, many dentists are forced into early retirement due to suffering from MSDs.
As dentists and specialists in the dental field, we are expected to deliver high quality dentistry with efficiency, precision, and quickly adapt to challenging situations.
Many of these challenges require dentists to work in a non-ergonomic form. This is familiar territory among dentists and can be influenced by a myriad of situations, including patients with limited jaw opening, operating on surfaces and teeth with limited accessibility, such as third molars, or patients who present with a medical condition that prevents them from being reclined in the dental chair, or a combination of all three.
These are just some of the many situations that dentists face on a daily basis that impact our ability to have proper ergonomic form.
To achieve high levels of expectations, and in keeping with our calling and duty as dental practitioners, patients are put first at all times.
Yet this brings up an important question: how can we as dentists continue to provide the best care for our patients?
This reminds me of a common saying, “you can’t take care of others if you don’t take care of yourself.”
I encourage readers to ask themselves, “When was the last time I checked on my ergonomic form?”
This is a similar approach to how I work with patients who clench their teeth during the daytime. The first step to prevention is bringing awareness to the situation.
Many dentists may not even realize the toll their daily habits are taking on their physical health until it’s too late.
This issue of The Nugget features a collection of experts sharing their perspectives on ergonomics in dentistry.
Dr. Bethany Valachi, a world-renowned physical therapist, author, and clinical instructor of ergonomics at OHSU School of Dentistry, discusses Trapezius Myalgia — a common condition that many dental professionals suffer from — and provides evidence-based strategies to improve the health and well-being of dental professionals.
TDIC Workers’ Compensation Claims Manager, Karen Schaffner, illustrates cases

By Ranna Alrabadi, DMD Associate Editor
of ergonomic injuries sustained by dental staff and actions dentists can take to mitigate liability.
LumaDent Marketing Coordinator, Tessa Crosby, and Lead Clientele Advocate and head of LumaDent’s VIP program, Jalen Blackman, discuss the emergence, efficiency, and popularity of ergo loupes.
Lastly, co-founders of Ergonomic Dental Consultants, Dr. Noëlle Santucci, a dentist and associate professor in the Department of Preventive and Restorative Dentistry at UOP, and Dr. Justin Jellin, a distinguished physical therapist and faculty member at the UOP Dugoni School of Dentistry and UCSF, discuss the prevention of hand and wrist injuries in a co-authored article.
Pain and early retirement does not have to be inevitable. Advancements in dental loupes, techniques, education, and bringing awareness to ergonomics have drastically shifted the paradigm of practicing dentistry. Ergonomics in dentistry is more than taking a five-minute break in between patients or just sitting up straight. Rather, it is a way of practicing dentistry to prolong our careers and to live a healthier lifestyle. This will support our mission as dentists to deliver the best patient care possible as we redefine the image and reality of practicing dentistry.
Are You Signed Up to Play on Friday, May 8, 2026? Golf Tournament Proceeds Bene t the SDDS Foundation | Register Today!

As I reflect on my year serving as President of SDDS, I do so with a deep sense of gratitude and pride. It was a year marked by both success and change, yet, all grounded in our shared commitment to serving Sacramento’s dental community.
We continued to see strong momentum in the areas that matter most to our members. Our continuing education programs remained robust and well attended, reinforcing SDDS’s role as a trusted source of high-quality, relevant continuing education. This was perhaps most evident at our MidWinter Convention, which reached record attendance with 809 registrants.
With a market share of 78.2% and an engagement rate of 80%, the trust, relevance, and value our members place in SDDS is evident and continues to hold strong.
Community and philanthropy were also front and center this year. Our SDDS Holiday Party was not only a wonderful opportunity to connect as colleagues, but it also raised an impressive $25,000 for the Sacramento District Dental Foundation. That generosity directly supports the
important work of caring for our community through SDDF’s Smiles for Kids and Smiles for Big Kids programs and reminds us of the impact we can have when we come together. SDDF is truly the heart of SDDS.
This year also brought significant leadership transition. We bid a fond and heartfelt farewell to Cathy Levering, who served as Executive Director of SDDS for 24 years. Cathy’s leadership helped shape the direction, culture, and stability of this organization, and her influence will be felt for many years to come. At the same time, we were pleased to welcome Caroll Badgley as our new Executive Director. Caroll has stepped into this role with purpose, conviction, and a clear commitment to advancing SDDS’s mission into the future. The foundation Cathy built has allowed Caroll to lead with momentum, vision, and confidence.
None of this would be possible without the tireless work of our SDDS staff, they truly are the heart and soul of the organization. They work behind the scenes to put on our events and make sure our members’ needs are met.

By Nima Aflatooni, DDS 2025 SDDS President
That sense of dedication continues with our Board of Directors, committee members, and committee chairs. Their commitment ensured that the needs of Sacramento dentists were served and that our profession was represented thoughtfully and effectively at both the local and state levels.
It has been an honor to serve as your President. SDDS remains in great hands under the incomparable Dr. Jeff Sue, and I know he will continue to build on the success of this organization. I remain optimistic about the future of SDDS and grateful to be part of an organization that continues to evolve, lead, and support its members with intention and excellence.

Respectfully,
Nima Aflatooni, DDS

MEMBERS DHP (Dental Health Professionals): 57

365 Dental Studio
Adams Dental Consulting
Align Technologies, Inc.
Alltion/Verex Dental
Analgesic Services, Inc.
Andau Medical
Arklign
Asesso Health
Aspen Dental
Bank of America Practice Solutions
BMO Bank - Practice Finance
BPE Law Group
Brasseler USA
Business PC Support, Inc.
California Northstate University, College of Dental Medicine
CareCredit
Carestream Dental
CariFree (Oral BioTech)
Columbia Bank Healthcare
Corvia Real Estate
Dandy
DDSmatch
Dental & Medical Counsel, PC
Dental Intelligence
DentaQuest -
a Sun Life company
Dentsply Sirona - Consumables
Dentsply Sirona - Implants
Dentsply Sirona - Technology
Desco Dental
DIO Implant
Earned
Elevate Oral Care
Fotona
Gargle
GC America
Haleon
Health Net Dental
Henry Schein Dental
Henry Schein Dental Practice Transitions
HR for Health
Huntington National Bank
Impladent LTD
Implant Direct
Integrity Practice Sales
J Productions Dental
Seminars, Inc.
Kettenbach LP
Kids Care Dental and Orthodontics
Kuraray America, Inc./Noritake
Laguna Dental Arts
LIBERTY Dental Plan
Lovely32
LumaDent, Inc.
Lumina HealthCare
Medi-Cal Dental
Meds 2U Pharmacy Supply
Melinda Heryford, Inc.
MME Consulting Inc.
MUN CPAs, LLC
Murphy Dental Sales
NEO Dental Lab
Nextsum Dental
NSK America
NW Staffing Resources
Olson Construction, Inc.
Omni Practice Group
Osborne Group (The), Gallelli
Real Estate
Patterson Dental
PepCreative Architecture + Interior Design
Philips Sonicare and Zoom Whitening
Professional Practice Sales
Provide, Inc.
Q-Optics
Sacramento Safety & Training
SD Dental Solutions
SDI (North America) Inc.
Shofu Dental Corporation
Snap On Optics
Solventum
Spin Doctor Handpiece Repair
Star Refining Inc.
Straumann USA
Supply Doc
TDIC Insurance Solutions
Tokuyama, Preventech, Cranberry, Cetylite uLab Systems
Ultradent Products, Inc.
Ultralight Optics Inc.
US Air Force Health Professions
US Bank
Vionex Med Tech LLC
VOCO America, Inc.
Weave
Western Practice Sales
Woods Technologies, Inc.
Yaeger Dental Supply, Inc.
(confirmed exhibitors as of 2/17/2026)

You should never send your credit card number by email. Email is not a secure method of transmitting sensitive financial information; messages can be intercepted, forwarded, stored on multiple servers, or accessed if an account is compromised. Even when sent with good intentions, email exposes both you and the recipient to unnecessary risk of fraud and identity theft.
Following PCI compliance requirements, we want to remind you to never submit your full credit card details via email. Please be sure to use only approved, secure payment methods when providing payment information.
By Olivia Anderson, ADA News
ADVOCACY MILESTONES
• The ADA pushed for the extension of crucial small business tax provisions in the budget reconciliation bill. Due to ADA advocacy:
• The pass-through entity tax deduction was restored, guaranteeing tax parity for small business dental practices and protecting dentists from a 1.5%-5% tax hike.
• The bill includes a permanent 20% small business income deduction, restoration of 100% bonus depreciation, new domestic research tax incentives, the preservation of a 21% corporate tax rate, and a $40,000 individual state and local tax deduction.
• The ADA defended critical oral health funding for the CDC, HRSA, NIDCR and IHS to pass a bill with strong investments in programs essential to dentistry, funding for dental research and oral health efforts.
• Congress passed the National Defense Authorization Act, which included an ADAsupported provision, sponsored by Rep. Brian Babin, D.D.S., R-Texas, to strengthen accreditation standards for military dental treatment facilities to help ensure the highest standard of care for service members
DENTAL INSURANCE REFORMS
• The ADA has successfully encouraged 93 co-sponsors of H.R. 1521, or the Dental and Optometric Care Access Act of 2025.
• With ADA support, both strategic and financial, state dental societies were successful in 40 dental insurance reform campaigns in 2025. Thirty-nine new laws passed and one legislative effort was successful in preventing the loss of an important, long-standing claim payment statutory protection.
• The National Council of Insurance Legislators made two ADA-supported changes to the Transparency in Dental Benefits Contracting Model Act, first adopted in 2020. Should the new language be adopted in a state, the insurer must first get dentists’ express permission prior to using virtual credit card payment methods that require dentists to pay a fee to collect claim payment. Second, dentists’ election on payment methods remains active until the dentist changes it or a new contract is executed.
To view the rest of the highlights, visit: https://adanews.ada.org/media/nz2b2cu1/ada2025-advocacy-highlights.pdf
The 2026 salary survey is soon to be underway. You will receive an email from Survey Monkey and it will be titled “SDDS 2026 Salary and Benefits Survey.” It will come April 7, detailing how you can participate in the survey and get the findings at a discounted rate. Please be sure to check your emails and be sure to take the survey. Your input is invaluable, the more responses we receive, the more accurate and comprehensive the salary data will be, enabling you to make informed decisions that benefit your entire team.
We would like to invite you to consider mentoring or sponsoring a UOP or CNU student at an upcoming General Meeting. Students receive a discounted rate to attend GMs, and sponsorship is a great way to welcome them into our community and support their professional growth. If you are interested in sponsoring a dental student at any future General Meeting, please call (916) 446-1227 or email sdds@sdds.org - we’d be glad to help make the connection.
CDA’s new Future of Dentistry workgroup will address the issues shaping the profession, including dental plan reform and what meaningful coverage could look like for both providers and patients.
Opportunities to get involved will include town hall meetings, focus groups and surveys. Dentists who are interested in participating can complete this interest form. Stay connected to updates in CDA communications and our Dental Plan Action Center. https://www.cda. org/practice/practice-support/dental-benefitplans/dental-plan-action-center/

By Bethany Valachi, PT, DPT, MS, CEAS
Dr. Bethany Valachi is author of the book, “Practice Dentistry Pain-Free”, clinical instructor of ergonomics at OHSU School of Dentistry in Portland, OR and is recognized internationally as an expert in dental ergonomics. Bethany is founder and CEO of Posturedontics®, a company that provides research-based dental ergonomic education. For over 20 years, Dr. Valachi has helped thousands of dental professionals prevent pain and extend their careers with her ground-breaking dental ergonomic education. She has published more than 80 articles in dental journals and offers online dental ergonomic CE courses at www.posturedontics.com.
By midmorning, it starts ... again; the all-toofamiliar “tension headache” that soon evolves into a headache behind the dentist’s right eye and pain in the right temple. In an adjacent operatory, the hygienist experiences burning pain on the left side of the neck. Why does this happen? Both clinicians recently embarked upon diligent exercise programs with their personal trainers in an effort to improve their musculoskeletal health and avoid such painful episodes.
Does this sound familiar? If so, you’re in good company—the incidence of neck pain among dentists and hygienists has been reported as high as 71% and 82%, respectively. The causes of headaches and neck pain are multifactorial; however, in dentistry, the upper trapezius muscle is the culprit in a myriad of head and neck pain syndromes.
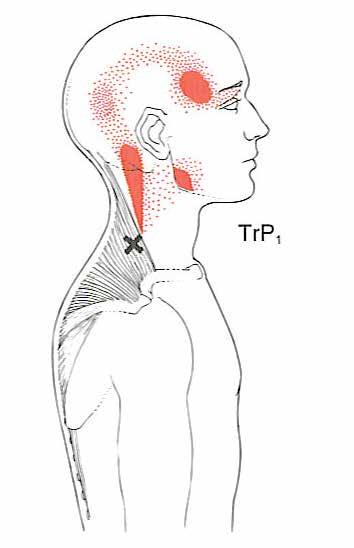
The delivery of dental care places high demands on this muscle and can result in a painful condition called trapezius myalgia. Symptoms include pain, spasms, or tenderness in the upper trapezius muscle, often on the side of the mirror, or retracting arm (figure 1). Trigger points in this muscle result in headaches behind the eye, into the temple, and in the back of the neck.
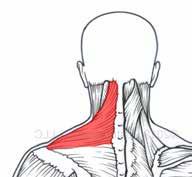
The upper trapezius muscles are responsible for elevating the shoulders and rotating the neck. In a rounded shoulder posture, the upper trapezius and neck muscles largely support the arm’s weight, increasing muscular strain on the neck and shoulder. In dentistry, trapezius myalgia is caused by static, prolonged elevation
of the shoulders, mental stress, infrequent breaks, and poor head posture.
CAUSES OF TRAPEZIUS MYALGIA
Positioning the patient too high. When the patient is positioned too high (Fig 1), the operator is forced to assume one of two postures—working with the shoulders elevated (which leads to trapezius myalgia) or shoulder abduction (which leads to rotator cuff impingement). Patients should be positioned so the oral cavity is at elbow level or 4 cm above elbow level. When the patient is higher than this, arm abduction or shoulder elevation typically occurs, especially when working between the 8 o’clock and 10 o’clock positions. Working in the correct clock position for a specific tooth surface & quadrant, while preserving your optimal posture AND patient comfort, is critical for preventing upper trapezius pain.
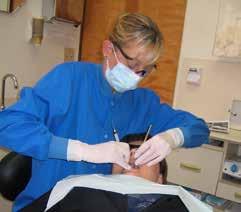
Non-ergonomic magnification. Poor head posture is commonly observed in the operatory and strains the upper trapezius muscles. Loupes with poor declination angles are one of the biggest culprits I’ve seen that can cause or worsen trapezius myalgia. About 70% of the loupes on the market today don’t offer a steep enough declination angle to prevent trapezius myalgia. No armrests/Improper height. Supporting the arm weight is especially important for
trapezius myalgia sufferers. Clinicians should make sure their armrest height is adjusted properly. Adjusting the armrests too high can cause neck stiffness and pain at the crook of the neck and shoulder, adjusting them too low can also lead to neck pain.
Dental professionals are prone to a unique muscle imbalance that causes and worsens trapezius myalgia. Team members should target this imbalance with shoulder stabilization exercises.
Infrequent breaks/tightness. One EMG study of the neck, shoulders, and arms showed that the highest muscular activity during dental work occurs in the trapezius muscles. Sustained low-level contraction of these muscles with few breaks greatly increases susceptibility to pain. With insufficient rest periods or dynamic movement (i.e., chairside stretching), tension can accumulate in these muscles, and by the end of the day, you may be wearing your shoulders as “earrings” without realizing it. Chairside stretching every 45 minutes is important to prevent trapezius myalgia.
Stress. Common clichés such as “pain in the neck” allude to stress as a cause of pain. This association is actually quite true. High levels of emotional stress and working at complex tasks can elicit muscular contraction in the upper trapezius muscle. This subconscious muscular contraction in response to stress is called neuromuscular hypertension. If the stress response is not followed by dynamic muscular activity, the blood pressure has no outlet and continues to rise. The statically contracted muscle becomes ischemic and painful while the
blood pressure remains high. Therefore, stress management strategies that specifically target muscular-type pain are helpful in prevention.
Improper exercises. Training the upper trapezius muscle with heavy weight resistance is one of the most common exercise mistakes dental professionals make. Fig. 3.

3 Certain exercises ( that aren’t a problem for the general public) can throw dental professionals into the ‘vicious pain cycle’, causing trapezius myalgia.
This can worsen the unique muscle imbalance to which they are already prone, create trigger points, and worsen neck pain. Dental professionals are prone to a unique muscle imbalance that causes and worsens trapezius myalgia. Team members should target this imbalance with shoulder stabilization exercises. Wardrobe risk factors. Narrow bra straps can compress the upper trapezius muscles, worsen neck pain, and create headaches, especially among female dental professionals with large chests. Racer-back sports bras have wider straps and are a better choice. A purse slung over one shoulder can also perpetuate muscle imbalances to which female dental professionals are prone, since the trapezius muscle must contract unilaterally to support the weight.
Trigger points. Trigger points in the upper trapezius muscles can refer pain to the temple, cause a “headache behind the eye”, or cause pain in the back of the neck. (Fig 4) Once the diagnosis is determined to be myofascial or muscular in nature, consider self-treating your own trigger points. An effective combination is moist heat, then trigger point self-treatment, followed by a sustained stretch of the affected muscle.


By Karen Schaffner TDIC
Karen
A busy day in the dental practice is a marathon, not a sprint. And much like marathon runners, each member of the practice team needs training to condition their body for enduring the day-to-day demands and understand proper form for safety and efficiency.
Proactively addressing ergonomics in both clinical and administrative areas supports endurance and proper form, protects musculoskeletal health, reduces fatigue, and improves clinical efficiency. Appropriate posture, equipment setup, and workflow design can significantly reduce the risk of work-related injuries and promote overall well-being.
Between 60% and 80% of dental professionals experience some form of musculoskeletal pain during their careers, according to data from the American Dental Association and the National Institute for Occupational Safety and Health. Continuous trauma is the primary driver of musculoskeletal disorders and the second most common type of workers’ compensation claim for dental practices. The Dentists Insurance Company notes that its policyholders have filed more than 600 claims of this type since 2020.
Continuous trauma, often called cumulative trauma, is an injury caused by repetitive motion or overextension over a protracted period of time. In the dental office, they almost exclusively show up as tendon and nerve disorders, such as tendonitis and carpal tunnel syndrome.
Most ergonomic injuries are both foreseeable and preventable, making them an area of liability exposure that practice leaders can take steps to reduce. If a staff member alleges that a workplace injury occurred due to unsafe or poorly designed working conditions, the practice could face costly liability exposure in addition to workers’ compensation claims.
Just as importantly, a culture that values ergonomics signals to team members that their long-term well-being matters, fostering higher
levels of job satisfaction, performance, loyalty, and retention.
The Dentists Insurance Company shared two examples that illustrate practice roles and responsibilities.
In the first, a front-office receptionist reported pain and numbness in her wrist and fingers that she attributed to her workstation. The practice owner recommended she take breaks from typing and stretch as needed, but the symptoms persisted for several weeks. The employee began to call out of work due to ongoing discomfort, prompting the dentist to contact TDIC’s Risk Management Advice Line.
The Advice Line analyst recommended that the practice owner file a workers’ compensation claim so the employee could be evaluated by an occupational health provider. An ergonomic evaluation of the employee’s workstation revealed several issues, and adjustments were made to correct them. Within days of the adjustments, the employee reported her symptoms were improving. She was discharged from care at her follow-up visit, and the claim was closed without the need for additional intervention.
In another instance, a practice owner called TDIC’s Risk Management Advice Line as soon as a hygienist reported she was suffering neck pain toward the end of each shift. The risk management analyst warned that using dull instruments requires additional physical force and repetitive motion. Along with this reminder, the analyst advised the dentist to discuss ergonomics best practices with the hygienist and to inform her of her rights to file a workers’ compensation claim.
Ergonomics in Practice
Injury prevention begins with identifying the most common ergonomic hazards in the operatory and front office, then addressing them through thoughtful design, proper
equipment selection, and consistent training. TDIC’s risk management analysts recommend the following best practices.
For clinical staff working in the operatory:
• Use neutral hand and body postures whenever possible.
• Use sharp, lightweight instruments to reduce the required force and number of repetitions.
• Use properly fitted gloves, preferably left- and right-handed gloves.
• Spread out appointments that include heavy scaling work to allow muscles to rest.
• Lift heavy boxes or equipment with leg muscles and keep the back straight.
• Avoid lifting below the knee and above shoulder height.
For front office staff, office managers, and those working primarily on computers:
• The computer monitor and keyboard should be directly in front of the user.
• The wrists should be kept in a neutral (straight) position.
• The elbows and knees should be bent at an approximately 90-degree angle.
• The top of the monitor should be at eye level or slightly below.
• Feet should be flat on the floor or on a footrest.
• Chairs and desks should be adjustable to the employee’s needs.
A certified ergonomist can look for specific actions, processes, or operations that may contribute to repetitive motion injuries and inform your ergonomics plan. A comprehensive plan includes employee training on the risks and exposure associated with repetitive motion injuries, the symptoms and consequences of those injuries, the necessity of reporting injuries, and the reporting procedure.
If any team member complains of ongoing pain or reports an acute injury related to their work, practice leaders must follow required protocols, similar to reporting needlestick injuries.
• Notify your workers’ compensation carrier of the injury immediately to determine where you can send the employee for medical care.
• Provide the applicable workers’ compensation claim forms to the employee within the required time-frame (typically, one working day after being made aware of the injury).
• Remain in contact with the employee throughout the life of their workers’ compensation claim and obtain work status reports from the employee.
• Discuss the options for accommodation with the employee, if applicable.
• Document all discussions regarding workplace accommodations in the employee’s workers’ compensation file.
Ergonomic safety should be integrated into dental practice culture, not treated as an afterthought. Leaders can set the tone by prioritizing team wellness, investing in ergonomic equipment, and providing regular training. Ultimately, protecting against ergonomic injury is about more than preserving productivity; it’s part of a holistic wellness approach to long, healthy careers.



By Jalen Blackman & Tessa Crosby LumaDent
Jalen Blackman is a first-generation college graduate with a Bachelor’s degree in Marketing from Western Michigan University. In addition to working closely with customers and VIP members, Jalen coordinates LumaDent events and develops a wide range of marketing materials, including flyers, reels, social media content, newsletters, and sales rep resources. Jalen also collaborates directly with management to oversee student ambassadors, manage influencer relationships, and support multiple dentistry-focused Facebook groups. Outside of work, Jalen is an avid movie enthusiast and has recently developed a passion for hiking since moving out west.
Originally from the south of France, Tessa Crosby moved to the United States for college and earned a degree in Digital Media from UC Berkeley. She currently works as the Marketing Coordinator at LumaDent, where she supports events and sales while creating engaging marketing content such as social media reels, flyers, and email campaigns. When she’s not working, Tessa enjoys baking, thrifting, and spending time at the beach.
A career in dentistry demands precision, focus, and endurance. The physical strain on the neck, shoulders, and back has long been normalized as part of the job, at times, even cutting the career short. However in recent years , ergonomic innovations have begun to change that narrative. The introduction of ergonomic loupes not only improve vision, but protect the dental professional’s body long term.
When Ergo Loupes Were Introduced Traditional loupes have been used in dentistry for many years to enhance magnification and accuracy. However, this design requires clinicians to tilt their heads downward for extended periods, leading to poor posture and health issues. With greater awareness of musculoskeletal strain in dentistry, ergonomic loupes emerged as a solution.

Dentists choose ergonomic loupes for a simple reason. They allow you to see clearly without compromising posture. By looking forward rather than down, ergo loupes reduce the need to hunch over the patient, making it a more comfortable experience. This upright posture helps dentists focus and maintain an ergonomic position throughout long procedures and busy days. These loupe magnifications range from 3.0x to 10.0x allowing the clinician to see the appropriate level of detail needed for
their specialty and workflow. Investing in ergonomic loupes is an investment in your long term health, reducing time spent seeking chiropractic care.
Ergonomic loupes use internal prisms to bend light and project the image back to the user’s eyes in a natural line of sight, allowing dentists to look straight ahead rather than tilt the head downward as with traditional loupes. In ergonomic designs, the declination angle is optimized to support clear vision while keeping the head upright minimizing unnecessary movements. This neutral head position helps maintain proper spinal alignment, reducing muscle strain that contributes to physical stress over time. While there is a learning curve, the long-term benefits include reduced back and neck pain and the ability to extend your career for years to come. Additional design considerations using lightweight materials such as anodized aluminum or titanium. Additional design features, such as balanced
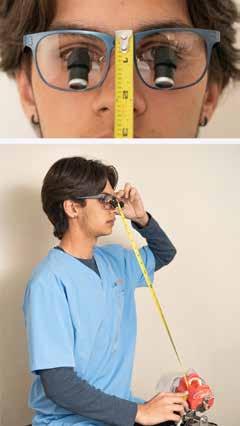
weight distribution, a wide field of view and lightweight materials like anodized aluminum or titanium help reduce eye strain and neck and head discomfort
Studies show that dental practitioners can lose up to 33% of potential career earnings due to early retirement because of neck and back pains or Musculoskeletal disorders. Ergo loupes help these issues by: preventing continuous neck strain and shoulder tension, supporting a neutral spinal posture, and minimizing fatigue during long procedures. Although no single tool removes all physical strain, ergonomic loupes play a key preventive role, particularly when used alongside ergonomic seating such as a saddle chair.
Ergonomic loupes move society toward healthier dental practices. When dentists invest in tools that support the body as well as the eyes, they improve endurance, reduce pain, and extend career longevity. For dentists in Sacramento and beyond, ergonomic loupes represent a shift toward working smarter not harder while protecting long term health.



CAMERON PARK/PLACERVILLE: GP, 4 Ops+RE, 4 Hyg days/wk Dentrix PMS, No Delta Premier 2024 GR $755K #CA4702
CARMICHAEL/FAIR OAKS AREA: 4 Ops, 19+ Yrs Goodwill, 1,310 Sq Ft , Open Dental PMS, Paperless, Digital, 55% Delta Premier. 2024 GR $516K #CA4300
EL DORADO HILLS/FOLSOM/GRANITE BAY AREA: Highly Desirable GP Practice & RE in a highly desirable city/community 6 Ops, 8 Hyg/days and $1 1M Collections! #CA4628
ELK GROVE AREA: High-end North Sacramento Area GP with beautiful RE 5 Ops, 8 Hyg/days and collected $1.37M in 2024! #CA4588
ELK GROVE/SOUTH SACRAMENTO AREA: New Listing! Amazing 6 Op GP Practice, Eaglesoft PMS, New 3D Conebeam, Pano, 5 Hyg days/wk 2025 GR $370K #CA4731
GREATER MODESTO AREA: 7 Ops+RE, GP, 16+ Yrs Goodwill, Dentrix PMS, Digital GR $469K #CA2795
GREATER STOCKTON METRO & SURROUNDING AREA: 6 Ops, GP, 55+ Yrs Goodwill, FFS, 8 days/wk Hygiene, 1,880 sq ft 2024 GR $1 4M #CA4533
REDDING/RED BLUFF/SHASTA COUNTY AREA: 6 Ops+RE, GP, 41+ Yrs. Goodwill, 3,000 Sq. Ft., Dentrix PMS, CEREC, 3D Conebeam, Hi Tech! GR $1 73M #CA3790
SOLANO COUNTY AREA: 8 Ops, GP, 45+ Yrs Goodwill, 3,800 sq ft Paperless, Dentrix PMS, Digital 2024 GR $1 535M #CA3586



By Noëlle M. Santucci, DDS, MA, RDH, FACD & Justin Jellin, DPT, ART
Dr. Santucci received her dental degree, her Advanced Education in General Dentistry Certification, and her Masters Degree in Educational Psychology and Counseling from the University of the Pacific and her Degree in Dental Hygiene from Marquette University.
She is co-founder of Ergonomic Dental Consultants, with her business partner, Dr. Justin Jellin, delivering inter-disciplinary continuing education on dental ergonomics and streamlining it into practical and clinical pearls. She has been private practice for over 30 years with her husband, Eugene Santucci, in Atherton, CA.
Dr. Jellin earned his Doctor of Physical Therapy degree from the University of the Pacific and has an undergraduate degree in Sports Sciences. He is the co-founder of Ergonomic Dental Consultants with his business partner Dr. Noëlle Santucci, delivering continuing education on the latest research in dental ergonomics and streamlining it into practical clinical pearls.
Musculoskeletal disorders (MSDs) are very common disorders among dental professionals with prevalence among dentists and hygienists reaching as high as 94%.1,2 It is also one of the leading causes of early retirement among dentists.
One of the most commonly affected parts of the body are the dental operator’s wrist and hands. Studies indicate that up to 66% of dentists and 69% of dental hygienists suffer from MSDs in this area.3
Using incorrect grasps of the dental instruments and handpieces can result in practitioners developing MSDs of the hands and wrists. This can lead to pain, tactile disturbances, reduced grip strength, shorter range of motion, and loss of coordination.4,⁵
Despite the formal training dental professionals receive on how to correctly hold dental instruments, many clinicians develop maladaptive grasping patterns over time, often unconsciously. This can be in response to fatigue, stress, poorly designed instruments, or poor ergonomics. Unfortunately, with time, these modifications are incorporated more permanently, leading to the development of detrimental grasping habits.
As we delve into MSDs of the hands, we begin by analyzing how humans grip pens or pencils. As we first learn to grasp writing instruments, there are a couple of stages young children go through in the development of this skill.6 Initially, children go through an immature phase, where several permutations of pencil grips are used. As they get older, their grasp changes into what is called the mature phase.
One form of the mature pen grasp is known as the Dynamic Tripod Pencil grasp (Figure 1). In dentistry, this grasp is modified into the Modified Pen Grasp (Figure 2), where the middle finger is moved from below the pencil to the side of the shank of the dental instrument. This tripod effect serves to:6
Facilitate holding and manipulating the handpiece or dental instrument.
1. Balance a dental instrument in the clinician’s hand to provide stability.
2. Facilitate rolling the instrument between the 3 digits with more ease and control.
3. Prevent finger fatigue.
4. Increase tactile sensitivity.
Detrimental Grasping Habits and Their Consequences
Common detrimental grasping habits include:
1. Finger and thumb hyperextension rather than maintaining gentle flexion. (Figure 3)
2. Incorrect finger placement, increasing intrinsic muscle strain, such as when holding instruments with fingers too wide apart. (Figure 4)
3. Thumb abduction (hitchhiker’s thumb) increases stress at the carpometacarpal (CMC) joint. (Figure 5)
The wrist is another area that is affected by poor ergonomics. It results from overextending, flexing, or deviating the wrist from its neutral position (Figure 6). Ideally, the shoulders should remain parallel to the floor, the elbows bent to 90 degrees, all while keeping the wrist neutral throughout the treatment of a patient (Figure 7). This can help minimize the development of carpal tunnel syndrome. It also helps to prevent injuries of repetitive stress, of overuse, and compression in the carpal tunnel, which includes the wrist flexor tendons and the median nerve.
Common Hand and Wrist MSDs in Dental Professionals
Improper grasp and wrist posture contribute to the development of several clinically significant conditions.
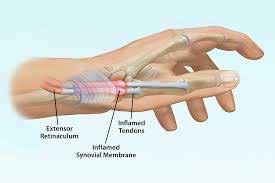
1. Tendinitis and Tenosynovitis
Inflammation of the flexor or extensor tendons due to repetitive motion and forceful gripping. Symptoms include pain, swelling, and reduced grip endurance.
2. De Quervain’s Tenosynovitis
A specific form of tenosynovitis affecting the abductor pollicis longus and extensor pollicis brevis tendons at the radial wrist. Strongly associated with repetitive thumb abduction (“hitchhiker’s thumb”) and sustained pinch force. (Figure 8)
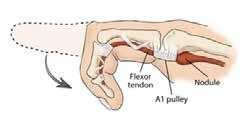
3. Trigger Finger (Stenosing Tenosynovitis)
Caused by thickening of the flexor tendon sheath, resulting in finger locking or catching during extension due to repetitive gripping or forceful hand use (Figure 9).
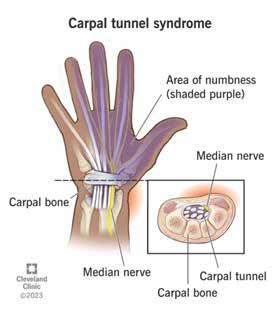
4. Carpal Tunnel Syndrome
Compression of the median nerve due to prolonged wrist flexion, extension, or deviation, compounded by increased intracarpal pressure from sustained gripping (Figure 10).
commonly referred to as basal thumb arthritis. It presents as chronic pain at the base of the thumb, commonly caused by hyperextension of a joint or over-gripping (Figure 11).

There are several dental modifications that can be made to prevent MSDs of the hands and wrists. These include:
1. Adjusting your operator chair so you are properly aligned. Feet flat on the floor, knees slightly lower than the hips, trunk in neutral and upright position, forward proclination as needed up to 5 degrees, head over shoulders, neck flexion as needed up to 5 degrees, elbows at 90 degrees close to your side, and wrists neutral.
2. Adjust the patient’s chair so their head is opposite your navel.
3. Make sure that the handpiece swivels at the junction of the handpiece and its attachment to the cord.
4. Use wide-diameter instruments, as opposed to thin instruments, that are serrated in texture and not smooth. This will decrease the pinch force in your hands while holding the instrument.
5. For hygienists, be sure to sharpen your instruments for each patient. This makes your scaling stroke effective and decreases the repetitions required with dull instruments.
6. Move around the patient in different clock positions and turn the patient’s head to facilitate keeping your spine and body in its neutral position.





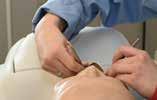
5. Osteoarthritis
Degenerative joint changes, particularly at the first carpometacarpal (CMC) joint, are
7. Using off-angle instruments can help keep the wrists from overextending, flexing, or deviating.
Continued on page 20
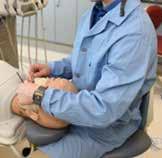
The focus of this article was to highlight common musculoskeletal disorders affecting the hands and wrists of dental practitioners. It is important to recognize that effective prevention of MSDs begins with proper ergonomics and equipment selection that set the clinician up for long-term success. This includes investing in an appropriate operator chair with at least four independent adjustments: seat height, seat pan tilt, vertical backrest adjustment, and independent horizontal backrest positioning. A high-quality saddle seat may also be an excellent alternative for some clinicians.
Equally important is the adjustability of the patient chair, which should accommodate clinicians of varying stature and allow the patient’s head to be positioned opposite the clinician’s navel in order to maintain approximately 90 degrees of elbow flexion during treatment. Properly measured and fitted ergonomic loupes further support neutral spinal alignment and reduce postural strain. Clinicians
should also remain mindful of fundamental principles taught during dental training, including appropriate clock positioning, the use of handpieces with swiveling connections, and selecting instruments with optimal handle diameters. Finally, preventive strategies such as regular stretching and strengthening exercises play a critical role in sustaining a long, pain-free clinical career.
1. Hayes M, Cockrell D, Smith DR. A systematic review of musculoskeletal disorders among dental professionals. Int J Dent Hyg. 2009 Aug;7(3):159-65.
2. Hayes MJ, Smith DR, Taylor JA. Musculoskeletal disorders and symptom severity among Australian dental hygienists. BMC Res Notes. 2013 Jul 4;6:250. doi: 10.1186/1756-0500-6-250. PMID: 23822098; PMCID: PMC3704656.
3. Haas Y et al. Prevalence of self-reported musculoskeletal disorders of the hand and associated conducted therapy approaches among dentists and dental assistants in Germany. PLoS One. 2020; 15(11):e0241564.
4. Int. J. Environ. Res. Public Health 2020, 17, 3482
5. AlSahiem J, Musculoskeletal disorders among dental students: a survey from Saudi Arabia. BMC Oral Health. 2023; 23: 795.
6. https://www.griffinot.com/what-does-goodpencil-grasp-look-like
7. Canakci V, Orbak R, Tezel A, Fatih C, Canakci CF. Influence of different periodontal curette grips on the outcome of mechanical non-surgical therapy. Int Dent J 2003 Jun;53(3):153-8.
8. Haas Y, Naser A, Haenel J, Fraeulin L, Holzgreve F, Erbe C, Betz W, Wanke EM, Brueggmann D, Nienhaus A, Groneberg DA, Ohlendorf D. Prevalence of self-reported musculoskeletal disorders of the hand and associated conducted therapy approaches among dentists and dental assistants in Germany. PLoS One. 2020 Nov 6;15(11):e0241564. doi: 10.1371/journal. pone.0241564. PMID: 33156851; PMCID: PMC7647093.

Taking regular breaks to stretch throughout the day can help prevent work-related pain and injuries.
Get more in-depth resources to help you practice at your best at ADA.org/wellness .
The SDDS Continuing Education (CE) Advisory Committee plays a key role in advancing the professional development of our members by helping shape the educational programming offered throughout the year. From large-scale conventions to focused CE courses and business forums, the committee is committed to delivering timely, relevant, and high-quality educational opportunities that support both clinical excellence and practice success.
The primary purpose of the CE Advisory Committee is to identify, propose, and select speakers and topics for future events, such as the MidWinter Convention, general meetings, and continuing education courses. In addition, the committee provides speaker and topic recommendations, planning up to three years in advance. A core expectation of this work is that all presentations remain educational and non-commercial in nature for the benefit of our profession.
During our most recent meeting, the committee reviewed the 2025 MidWinter Convention recap and discussed registration numbers and sponsorships to date for the 2026 MidWinter Convention. These discussions help guide future planning efforts with
improvements and ensure that educational offerings continue to meet member needs and interests, as well as attendance.
The committee devoted significant time to suggesting speakers and topics across multiple formats. Proposed General Meeting topics included: occlusion; TMJ and radiology with a dual-presenter approach; implant complications; minimally invasive dentistry; gum recession treatment options; and advancements in 3D printing. Business Forum suggestions focused on practical topics such as key performance indicators, transitioning into practice ownership, fee-for-service models, managing complicated patients, and buying or selling a dental practice.
For the MidWinter Convention, suggested topics spanned clinical, leadership, and practice management areas, including: composite restoration techniques, CEREC, restorative dentistry, communication, conflict resolution, marketing and branding, periodontics, and emerging technologies such as exocad and 3D printing.
An exciting focus for the coming year is the expansion of hands-on CE courses. Based on prior attendance trends and member feedback, the committee discussed offering

By Arryan Emamian, DDS Chair; CE Advisory Committee
hands-on courses in the potential future to improve accessibility and participation. These sessions aim to provide practical, skill-based learning that participants can immediately apply in their practices locally.
The CE Advisory Committee encourages all members to take advantage of upcoming CE opportunities offered throughout the year. These programs are designed to support professional growth, enhance practice management skills, and keep members informed about advances in dentistry. Members interested in contributing to the future of SDDS education are also encouraged to consider joining the CE Advisory Committee next year. Serving on the committee offers a valuable opportunity to collaborate with colleagues, share ideas, and help shape meaningful educational experiences for the membership.
Through collaboration and strategic planning, the CE Advisory Committee continues to strengthen SDDS educational offerings and support lifelong learning for our members. We look forward to building on this momentum and invite members to participate in upcoming programs or contribute by serving on the committee in the year ahead.
Wednesday, April 7, 2026 • 1 CEU, Core • Webinar
Member Price: $45 early (ends 3/17) / $70 regular (begins 3/18) / Non-Member Price: $140


Speakers: Sara Baker, MBA; CEO & Founder and Dennis Krohn, President & Founder; SD Dental Solutions (SDDS Vendor Member)
HIPAA compliance isn’t just about policies in a dusty binder: it’s about real-world risks, real penalties, and real patients trusting your practice every day.
In this no-fluff, straight-talk webinar, Sara Baker and Dennis Krohn Jr. pull back the curtain on what HIPAA actually means for dental offices today. From everyday compliance blind spots to cybersecurity mistakes that trigger Office for Civil Rights investigations, this course breaks down what dental practices get wrong… and how to fix it before it becomes a problem.
Whether you’re a practice owner, office manager, or part of the dental support team, this webinar will help you reduce risk, protect patient data, and build a culture of compliance that actually works in the real world.
Learning Objectives:
• Identify the most common HIPAA compliance and cybersecurity failures in dental offices and understand why they lead to investigations, breaches, and penalties.
• Evaluate how everyday technology use, staff behavior, and workflows impact HIPAA compliance, revealing hidden risks most practices overlook.
• Apply practical, real-world strategies to reduce risk, strengthen security, and build a sustainable culture of HIPAA compliance within dental practice.

Register online today with this QR code.
PPS pioneered the business of selling dental practices in 1966. Our understanding of this activity is unmatched. We do not outsource appraisals to parties who will never set foot in your office. We do not subscribe to industry multiples regarding valuations as each practice is unique. We are not a listing factory where opportunities get stale and little attention. We provide realistic expectations in a fast-changing marketplace. We employ strong risk-management applications. Tailored staging is our hallmark. Detailed toolboxes are assembled allowing us to immediately respond to interested parties, their advisors and lenders. We never want the rhythm of a sale to slow down because we were not prepared. We manage each engagement from start-to-finish.
As you approach this change, talk to us. These initial conversations have paved the way to successful outcomes in the Sacramento District Dental Society the last 6+ Decades.
Citrus Heights
Collected $1.3M+. Included Building
Elk Grove
Collected $900K. Included Condo.
Sale in Progress
Arden Arcade
Collects $750K. Includes building.
New Listing
Carmichael
Collects $645K. 7-days of Hygiene.
Smiles for Kids Day was a tremendous success thanks to the generosity of our volunteer dental community. Across eight host sites, more than 100 volunteers, including SDDS Dentist Members, DHPs, interpreters, and community members, came together to provide care for 144 children. The total value of treatment delivered exceeded $100,000.
This incredible day highlights the power of collaboration and our shared commitment to improving children’s oral health. We extend our sincere thanks to every volunteer and host site that helped make this event possible.
you...
to our SFK Day Sites, Dentists and to our many volunteers!




Get ready to tee off for a day of fun at this year’s annual SDDS’ golf tournament at Teal Bend Golf Course! We are excited to welcome back our returning players as well as welcoming new participants for a memorable day on the course.
We’d love to have you play, invite your friends (dentists and non-dentists) for a day of golf, fun and games, and camaraderie - all to support the Foundation! Here are ways to participate in this year’s golf tournament:
• Put a foursome together – invite your dentist and/or non-dentist friends to introduce them to our Foundation
• Sign up as a single player – we’ll pair you with a fun foursome
• Sponsor a tee and be front and center as players tee off, please consider being a green sponsor – if you aren’t able to attend in person
• Donate a raffle prize
• Be a major sponsor - lots of great sponsorship opportunities still available The golf tournament includes breakfast and lunch, snacks and libations from the sponsors on the course and loads of fun.
Please sign up for this awesome event (the signup form is included as an insert in this issue). It’s sure to be a great time and, best of all, it supports our wonderful Foundation and all the great projects it supports for our community!








By Stanislav Samokysh SDDS DHP Member
Stanislav Samokysh, a dentist from Ukraine now based in California, works as Dental Dispensary Staff at CNU. He’s passionate about dentistry and eager to grow within the U.S. dental community.
I’ve always believed that change is for the better—well, maybe not always, but at least most of the time (let’s keep it honest). We recently witnessed one of the biggest changes yet at California Northstate University’s College of Dental Medicine (CNU). After years of planning, effort, and anticipation, the clinical program has finally completed its move from Elk Grove to a brand-new facility in the heart of Sacramento, 22nd Street and Broadway.
Even though CNU is still a young dental school, only graduating our first group of students in June 2025, we are proud that they are carrying the name of their alma mater into the profession. While they move forward in their careers, the university itself took a huge leap into its next stage of growth in July 2025 as it moved its clinical operations from Elk Grove to downtown Sacramento, just off Broadway.
We didn’t just pack up and change ZIP codes. This move expanded the clinical operation—from 23 operatories at the Elk Grove/Maritime Clinic to 34 operatories at the downtown Sacramento/Broadway Clinic. The Broadway clinic is spacious, bright, and full of possibilities. It sets an exciting stage for what comes next, especially as other parts of the clinic continue to be under construction to allow operations to further double in size.
This is not just about new chairs and shiny floors. Rather, it’s about what happens when you bring people, ideas, and systems together into a single, unified campus. Students will now be able to attend lectures, provide clinical care, participate in grand rounds, meetings, and classes all under one roof. No more bouncing across town to make it from one building to the next.
For the faculty and staff, the layout makes daily life easier. We’ve got more room, better flow, and a setup that improves clinic efficiency and better accommodates the teaching aspects of our clinical care. A lot of decisions were made based on our lived
experience back in Elk Grove. That’s the thing about change; you don’t always need to reinvent everything. Sometimes you just need to build on what worked and tweak what did not work.
The sterilization room? It deserves its own paragraph. It’s huge and beautiful. We’re talking about high-end industrial machines, smart zoning, and a conveyor-style process that moves instruments from used to clean to sterile without crossing paths. It is built to minimize cross-contamination and maximize efficiency. Honestly, it’s one of the highlights of the whole clinical operation –and one that patients can see in action.
Personally, this move has been a milestone for me. Coming to California from Ukraine not long ago, one of my biggest hopes was to experience real American dentistry up close, not just the treatment, but the environment, the teamwork, the protocols, and the systems behind it all. What I’ve been lucky enough to experience at CNU has exceeded all expectations.
Over the past few months, I’ve helped assemble furniture, organize materials, set up the dispensary room, and make small but meaningful choices about how we’ll work going forward. Every drawer we filled, every light we tested felt like a small win. Now, if only I could figure out where we put the extra gloves.
But truly, this moment isn’t just about convenience or space. It reflects how dental education is evolving in America. Because before we can teach complex treatment planning and clinical judgment, we need to start with the basics: comfort, access, and thoughtful design. Once that foundation is solid, everything else can grow on top of it: mentorship, knowledge, and experience. And in the end, we get confident, wellprepared dentists who not only know what to do but why they’re doing it.
I’m just one piece of the puzzle, but I’m proud to help it come together


The OsteoGen® Bone Grafting Strip is a collagen sheet infused with the same crystal technology used in the OsteoGen® Bone Grafting Plug – OsteoGen® bone graft crystals that provide a cohesive delivery system that maintains graft containment. The bioactive particles assist to control the migration of connective tissue.1-4
The OsteoGen® Strip offers a reliable and straightforward solution for sinus lift procedures, and grafting gaps between the implant and the extraction socket wall.


The SDDS Board of Directors met on January 6, 2026, to begin the new year with a focus on member engagement, governance, advocacy, and upcoming programs. Dr. Jeff Sue called the meeting to order and welcomed the Board to the first meeting of 2026.
Dr. Sue emphasized the importance of Board participation in SDDS activities, particularly attendance at General Membership Meetings, assigned committee meetings, and full participation in the 2026 CDA House of Delegates.
Consent items, including the November 2025 meeting minutes and 2026 planning documents, were reviewed and approved. Board members also completed annual conflict-of-interest disclosures.
Dr. Chirag Vaid reported on year-end membership and engagement, noting continued growth and strong member participation across the Society.
• 2025 Total Membership – 2,077
• New Members in 2025 – 122
• Market Share 78.2%
• Engagement 80%
Executive Director Caroll Badgley reviewed key governance and operational items, including bylaws, policies, the 2026 calendar of events, committee structure, and Board liaison responsibilities. Committee liaison assignments for 2026 were confirmed. Delegates for the 2026 CDA House of Delegates were confirmed, with Drs. Jeff
Sue, Craig Alpha, Chirag Vaid, Bryan Judd, Eric Grove, Cherag Sarkari, Kart Raghuraman, Nima Aflatooni. Additional Delegates and Alternates will be added after the Leadership Development meeting. The House of Delegates will be held in Los Angeles on November 13–14, 2026.
Dr. Bryan Judd provided an update on BCR, highlighting its role as the collective voice of local dental components and outlining a goal for 2026 to establish clear SDDS priorities for regional advocacy. Dr. Judd also announced that Executive Director Caroll Badgley was selected by California’s components to serve as a non-voting member of BCR in 2026.
Dr. Cherag Sarkari presented an educational overview of Proposition 56 and its impact on Medi-Cal dental reimbursement. The discussion focused on anticipated changes beginning in mid-2026, potential accessto-care challenges, and the importance of

member education, communication, and coordination with CDA advocacy efforts. Dr. Sarkari agreed to write an article for the March/April issue of the Nugget
Dr. Rosemary Wu shared details on the upcoming Asian Dental Recognition Dinner, scheduled for March 12, 2026, at Fuji Restaurant on Broadway in Sacramento, with early registration available through February 12.
Caroll Badgley concluded with an overview of recent and upcoming SDDS events, including the successful Holiday Party and Installation of Officers, ongoing registration for the MidWinter Meeting, and future convention planning. Operational updates and staff transitions were also shared.
The meeting concluded with a group photo.
The next SDDS Board of Directors meeting is scheduled for March 3, 2026.











By the HR Hotline Advisors; California Employers
One complicated issue that comes up for many employers is when an employee has exhausted all protected leave but then requests an extension of leave as a reasonable accommodation for a disability or medical condition. Particularly in situations when employees request multiple extensions, employers often wonder:
• Whether they have to continue “holding the position.”
• Whether they must continue health care coverage.
• At what point is it reasonable to terminate?
Holding the Position
PDL/CFRA/FMLA
First, if the employee is on a protected leave such as Pregnancy Disability Leave (PDL), California Family Rights Act Leave (CFRA), and/or Family and Medical Leave (FMLA), they have a formal “right to reinstatement” to an equivalent position upon return. This means the employer is obligated to “hold the position” under almost all circumstances.
If the employee is not eligible for these leaves or has exhausted these leave entitlements, it becomes a bit more complicated. Remember, even if your employee does not qualify for these protected leaves, you must still consider providing them an unpaid leave of absence as a reasonable accommodation under the federal Americans with Disabilities Act (ADA— applies if you have 15 or more employees) and/ or California’s Fair Employment and Housing Act (FEHA—applies if you have 5 or more employees).
When an employee is on an ADA/FEHArelated leave only, you must generally hold the position, but there may be circumstances when the employer is not required to do so.
For example, if the employer can show that holding the position creates an undue hardship and they need to fill it, the employer may do so, but then must offer the employee any vacant position for which they are qualified, as follows:
• The employer must first offer any available positions equivalent in pay and seniority.
• The employer may only offer positions that result in less pay or status if that is all that is available.
• The employer is not obligated to create a new position for the employee that does not exist.
If the employee is on PDL, CFRA, and/ or FMLA, their health care benefits must continue as if they were currently working for you, for the entire duration of those leaves. You may require the employee to still pay their share of the premiums. Be sure to arrange in advance how the employee will cover their premiums when you aren’t able to make payroll deductions (e.g., cut you a separate check each month, pay upon return, etc.)
If the employee is on an ADA/FEHA-related leave only, then whether you must continue health care benefits depends on your specific policies—be sure to check with your benefits carrier. Also, if you continue health care
benefits for employees in a similar leave status (for example, during unpaid personal leaves of absence), then you may be required to continue health care coverage during ADA/FEHA leaves as well.
Employers should not take it lightly when considering ending the employment relationship instead of granting an extended leave request, as this often carries significant legal risk. While courts have held that employers are not required to accommodate an “indefinite” leave, there is no bright-line rule on how long an employer must hold a position after protected leave entitlements are exhausted. There is at least one unpublished case in California where the court found the employer satisfied their reasonable accommodation requirements, where leave was granted for “about a year.”
For this reason, employers should not implement “maximum leave policies” resulting in automatic termination after a set period of time. Instead, employers should evaluate on a case-by-case basis whether they can reasonably accommodate the employee or whether the extended leave request would cause an “undue hardship.”
Because the “undue hardship” standard is often difficult for employers to satisfy, it is recommended to get guidance before deciding to terminate. The Job Accommodation Network (www. https://askjan.org/) has helpful resources for employers on reasonable accommodation obligations.


By Santiago Mendoza CNU Dental Student (D1)
Originally from Tijuana, Santiago received his bachelor degree in neurobiology from UC Davis and his master’s in biology from Point Loma Nazarene University. He is now in his third year of dental school where he serves as president of his class. He is also planning on pursuing an oral surgery specialty upon graduation. Outside of dentistry, his hobbies include plants and running.
Dental school is demanding by design. Between lectures, preclinical labs, examinations, and clinical preparation, students are constantly challenged to adapt and perform at a high level. An additional layer of complexity is added by my role as class president. This responsibility is further shaped by the fact that my class is only the third cohort to matriculate at California Northstate University College of Dental Medicine. Because this is a new dental program, change is constant, and I have taken on the responsibility of helping guide these transitions by centralizing and communicating feedback from my classmates to faculty.
Being part of a developing program has meant navigating frequent adjustments over the past three years. These have included changes in physical locations, revised schedules, and the introduction of multiple systems used to track both didactic and clinical progress. While adapting individually can be challenging enough, serving as class president requires that I also help guide my classmates through these changes while addressing concerns as they arise. Although these situations can be unpredictable and demanding, I view this role as an extension of my dental education, almost like an elective course in leadership. As a future dentist, I know I will one day lead a team and manage a practice, and these experiences provide valuable early exposure to that responsibility.
I have learned that effective leadership often comes down to ensuring people feel heard and acknowledged, especially during moments of frustration or uncertainty. One of the most important lessons I learned early on was understanding what is within my control as a student leader and what is not. Communicating
this distinction to my classmates without making anyone feel dismissed is a delicate balance and one of the most challenging aspects of leadership. Similarly, relaying class concerns to faculty in a respectful and constructive manner requires careful communication. I learned to avoid speaking in the first person and instead frame discussions around the collective perspectives of students and faculty to foster productive dialogue and minimize conflict.
Now in my third year and beginning clinic, I am seeing how these leadership skills directly translate to patient care. Acknowledging patients’ feelings about their oral health has proven essential in building trust and rapport. While clinicians often focus on education and treatment planning, many patients feel powerless due to financial limitations or perceived predispositions to poor oral health. Regardless of whether these concerns are clinically accurate, allowing patients to express how they feel is critical to addressing their needs in a way that is meaningful and effective for them.
When I first accepted the role of class president, I questioned whether I could successfully balance it alongside the demands of dental school. There were many moments that tested my confidence unexpectedly. Looking back now, I see those challenges no differently than a difficult didactic course or complex clinical case experiences from which I have learned the most. Ultimately, serving as class president has strengthened my confidence, reinforced my resilience, and shaped me not only as a dental student, but as a future professional.
MAY 1

Presented by Peter Ham, DDS, MSD
Sponsored by Henry Schein Dental and EdgeEndo
The root canal system is inherently complex, often presenting significant challenges in achieving efficient negotiation and instrumentation. With the proper armamentarium, clinicians can streamline their approach, improve consistency, and enhance predictability in clinical outcomes. Join Dr. Ham as he shares his strategies for managing anatomical complexities.
By the end of this session, participants will be able to:
• Identify common anatomical challenges within the root canal system and understand how they influence negotiation and instrumentation strategies.
• Implement step-by-step instrumentation techniques demonstrated by Dr. Ham to improve efficiency and predictability in complex cases.
• Apply strategies to minimize file separation risk and enhance overall procedural consistency across varied canal anatomies.
• Integrate optimized rotary workflows that support smoother clinical performance and improved patient outcomes.


Friday, May 1, 2026
Lecture only 8:30–11:30am • 3 CEU, Core
Member Price: $159 early (ends 4/10), $184 regular (begins 4/11)
Non-Member Price: $368
Lecture and Hands-on: 8:30am–2:30pm • 6 CEU, Core
Member Price: $395 early (ends 4/10), $420 regular (begins 4/11)
Non-Member Price: $840
SDDS Classroom Register online today with this QR code.





Rock Rd
El Dorado Hills, CA 95762




By Cherag Sarkari, DDS (SDDS Member)
For nearly a decade, Proposition 56 has been a cornerstone of the Medi-Cal Dental Program, strengthening a system that had long struggled under the weight of inadequate reimbursement rates. Approved by voters in 2016, Prop 56 increased tobacco taxes and directed revenue to support Medi-Cal health programs, including supplemental payments to dental providers. These payments have been essential in stabilizing provider participation, improving practice sustainability, and expanding access to care statewide.
Before Prop 56, California had some of the lowest Medicaid dental reimbursement rates in the country. Many dentists faced financial losses for every Medi-Cal Dental patient they treated, leading some to reduce participation or withdraw entirely. As a result, patients in many communities—particularly rural and low-income areas—faced long wait times for even routine dental care. Prop 56 helped reverse this trend by supporting provider expansion, reducing wait times, and improving availability in historically underserved regions.
The Department of Health Care Services (DHCS) confirmed in All Plan Letter APL 25-011 Discontinuation of Prop 56 that Proposition 56 supplemental payments will end for all dates of service on or after July 1, 2026. This decision follows legislative actions that preserved Prop 56 funding only through the 2025–26 fiscal year, despite significant advocacy efforts from the dental community. California’s 2025–26 May Revision proposed major reductions to Medi-Cal, driven by declining state revenues and rising program expenditures. While advocacy from organizations such as the California Dental Association (CDA)
prevented immediate cuts, the scheduled elimination remains.
The loss of Prop 56 will have far-reaching consequences for dental providers. Many practices depend on supplemental payments to offset Medi-Cal Dental’s historically low reimbursement rates. Without Prop 56 supplemental reimbursement, practices may be forced to reduce the number of Medi-Cal Dental patients they serve or withdraw from the program completely. This would widen access gaps, raise operational pressures, and exacerbate health disparities—particularly in Sacramento, where Medi-Cal Dental enrollment is high.
But the burden on dentists goes beyond reimbursement. Many providers have built their care models, staffing plans, scheduling templates, and operational workflows around the stability Prop 56 created. Its elimination disrupts not only the financial picture but the clinical one as well. Dentists may face difficult
decisions about reducing hours, restructuring teams, or scaling back preventive programs that have been successfully implemented over the last decade. For early career dentists or those operating small practices, this uncertainty becomes especially destabilizing and may influence long-term decisions about staying in the Medi-Cal Dental program or even remaining in private practice. Patients will experience the most severe consequences. Reduced dentists’ participation will lengthen wait times and make it harder for families to find dentists willing to accept Medi-Cal Dental patients. Delays in preventive and restorative care increase the likelihood of worsening oral disease, higher emergency room utilization, and broader impacts on systemic health.
Vulnerable groups—including children, seniors, people with disabilities, and undocumented adults—are at particular risk of losing consistent access to essential dental services.
The broader Medi-Cal environment compounds these concerns. Policy changes scheduled for 2026, including enrollment freezes for undocumented adults, will further restrict access. Combined with the loss of Prop 56 supplemental payments, these shifts threaten to undermine nearly a decade of progress toward equitable oral healthcare in California.
CDA continues to lead statewide advocacy efforts to preserve Medi-Cal Dental funding. Dentists can learn more, participate in campaigns, and join the coalition through the CDA Advocacy & Coalition Hub: https://www.cda.org/advocacy/advocacyinitiatives/ - Strong engagement is essential. During prior budget debates, thousands of dental professionals mobilized to protect Prop 56 funding, demonstrating the power of unified grassroots advocacy.
As the state capital, Sacramento has an especially critical role to play. Our lawmakers see firsthand how gaps in dental access affect families, schools, and community health systems. SDDS members are uniquely positioned to amplify the importance of preserving Prop 56 by sharing patient stories, meeting with legislators, engaging through the CDA Action Center, and partnering with local organizations.
To build visibility around this opposition, SDDS, in conjunction with CDA, will begin coordinating structured outreach efforts—such as letter-writing campaigns, local advocacy, social media messaging, and targeted meetings with local legislators.
Members can help by hosting visits at their offices, joining community events where Medi-Cal Dental access is discussed, and encouraging patients who are willing to share their stories. Collective storytelling is often the most persuasive advocacy tool we have.
SDDS stands ready to support its members through these challenging times. Whether you need help connecting with policymakers, coordinating advocacy efforts, or accessing educational resources, the Society is here to help. Members wishing to participate in advocacy activities or learn more about how they can support Medi-Cal Dental should contact SDDS@SDDS.org or (916) 4461227.
The future of Medi-Cal Dental—and the oral health of millions of Californians—depends on what we do next. Together, we must raise our voices, strengthen our advocacy, and reaffirm our commitment to health equity. Now is the time for Sacramento to lead.

Visit CDA’s Share Your Story site (with QR code) to download flyers to place in offices and other patientaccessible sites. (Available in English and Spanish) Each flyer includes a QR code that will refer individuals to the CDA share your story collection site.
Ways to volunteer and support the SDDS Foundation:
Become a member of the Foundation –it’s only $75 per year
Donate to the programs of the Foundation –donations help provide screening supplies, toothbrushes and fund the puppet shows
Smiles for Kids Day – 2026 was a success! Now we need DDS volunteers to adopt a child post SFK Day to complete any treatment not completed on SFK Day.
To volunteer, Contact: SDDS office by March 16. 916.446.1227 • smilesforkids@sdds.org
Smiles for Big Kids is ongoing all year long –we need volunteers to adopt the BIG kids too (especially vets and the elderly)
Volunteers Needed: Dentists willing to “adopt” patients for immediate/emergency needs in their office.
To volunteer, Contact: SDDS office 916.446.1227 • sdds@sdds.org
Willow Dental Clinic
One Saturday every other month Contact dental@willowclinic.org for more information. You can check out their website here: www.willowclinic.org/services/dental
CCMP (Coalition for Concerned Medical Professionals) Volunteers needed: General Dentists, Specialists, Dental Assistants and Hygienists.
To volunteer, Contact: 916.925.9379 • ccmp.pa@juno.com
SDDS has dozens of dental industry Vendor Members who are here to serve you. Many vendor members have special offers for SDDS members. These vendors often attend General Meetings and would love to talk to you about ways they can help your practice. The SDDS Vendor Members are an invaluable source of knowledge, expertise and support. You can see all the current Vendor Members on page 39-41 of this Nugget or online using the QR code below.
Everyone for Veterans
To volunteer, Contact: SDDS office 916.446.1227 • sdds@sdds.org everyoneforveterans.org/for-dentists.html
(as of 2/4/2026) 2,084
Gabriel Casias, DDS
General Practice
• Graduated from University of Colorado in 2020.
Sarfraz Momin, DDS
General Practice
• Graduated from Mexico- Universidad De La Salle in 2025.
ENGAGEMENT RATE:
79% active
MARKET SHARE: 78% RETENTION RATE: 99.5%
59% retired Mar/Apr
Mara Kamila Estoesta, DDS
General Practice
• Graduated from Midwestern University in 2023.
Billy Holguin, DDS
General Practice
• Graduated from UCSF School of Dentistry in 2023.
Jennifer Hom, DMD
General Practice
• Graduated from Temple University School of Dentistry in 2014.
Carol Lee, DMD
TOTAL ACTIVE MEMBERS: 1,383
TOTAL RETIRED MEMBERS: 382
TOTAL DUAL MEMBERS: 10
TOTAL AFFILIATE MEMBERS: 1
TOTAL STUDENT MEMBERS: 229
TOTAL CURRENT APPLICANTS: 0
TOTAL DHP MEMBERS: 59
TOTAL NEW MEMBERS FOR 2026: 11
General Practice
• Graduated from Roseman University in 2024.
Hansel Poerwanto, DDS
General Practice
• Graduated from UCSF School of Dentistry in 2016.
Congratulations to Our New Retired Members!
John Adams, DDS
Steven Brazis, DDS
Oscar Chen, DDS
Lindsay Grady, DDS
Gregory Heise, DDS
William Huiras, DDS
Thomas Jarrett, DDS
Keven Keating, DDS, MS
Michael Phelps, DDS
Dr. Vincenzo Castaldo passed away on January 26, 2026. He was an active member for over 50 years. He graduated from dental school in 1967 from Tufts University School of Dentistry. He then went on to earn his Oral and Maxillofacial Surgery specialty from VA Medical Center in Long Beach in 1971.



Dr. Jeff Kwong (L) on being installed as President of the California Association of Orthodontists (2).
Dr. Dean Ahmad who is a graduate of the Executive Leadership Program at Stanford Graduate School of Business (1).
Caroll Badgley for volunteering her time in Thailand in late December assisting another artist with a mural. The mural was painted at the Elephant Nature Park, Sanctuary in Chiang Mai - Northern Thailand (3)
Dr. Maya Giannetti on the birth of her son and Dr. Kelly Giannetti on becoming a grandma. Annon Luke Bradley Giannetti was born January 5, 2026 to Dr. Maya Giannetti and Mr. Conner Bradley (4)

2
Send us your news to sdds@sdds.org to let everyone know about the great things that are happening!




Olson Construction, Inc. is a design/build construction firm who will take your office from design to finish. They have proven themselves to be the go-to company when you want your dental office done on time and within budget.
ph: (209) 366-2486 | olsonconstructioninc.com
David Olson dave@olsonconstructioninc.com

U.S. Bank is a subsidiary of U.S. Bancorp (NYSE: USB), the fifth largest commercial bank in the United States. U.S. Bank operates 52 banking offices in the Sacramento Region and provides a comprehensive line of banking, investment, mortgage, trust and payment services products to consumers and businesses in the local market. Visit us on the web at www.usbank.com.
ph: (916) 932-6360 | usbank.com
Dave Nelson dave.nelson@usbank.com
Danny Smith danny.smith7@usbank.com
of The Great West
Professional Practice Sales has been faithfully serving members of the Sacramento District Dental Society since 1966.
Benefits, Services, Special Pricing and/or Discounts Extended to SDDS Members: PPS shall perform a thorough scrub on the practice prior to our having a meaningful discussion with the Owner as they contemplate this event. The Owner shall receive the candid feed-back they need regarding their practice, so they can then make the proper decisions. The Owner shall be properly prepared for this unique journey, with their understanding their role in the process.
ph: (415) 899-8580 | PPSsellsDDS.com
Ray Irving
Ray@PPSsellsDDS.com
Edna Irving
Edna@PPSsellsDDS.com

Laguna Dental Arts: Where Digital Precision & Custom Artistry Meet. At Laguna Dental Arts, we take pride in our personalized service, complimented by a full catalog of dental restorative options. With roots in Northern California for nearly 30 years, we have helped local and distant doctors achieve the best dentistry for their patients through detailed collaboration and communication.
ph: (916) 688-1333 | lagunadentalarts.com/
Jeton Zajmi
jzajmi@lagunadentalarts.com

California Northstate University (CNU) is an educational institution dedicated to educating, developing, and training individuals to provide competent, patient-centered care. The University offers bachelor's (BS) and graduate degrees (MS, MHA, MA) as well as terminal professional degrees (MD, DMD, PsyD, PharmD) all focused in various areas related to practice and management of healthcare.
ph: (916) 686-7300 | cnsu.edu
Pinelopi Xenoudi, DDS, MS (Interim Dean) Shagufta Ali shagufta.ali@cnsu.edu
California Employers Association TM
CEA’s services are dedicated to those business professionals who demand accurate, immediate and cost-effective solutions to human resource and labor relations issues.
HR Hotline: 1-888-784-4031
ph: (916) 921-1312 | employers.org
Kim Gusman, President/CEO ceainfo@employers.org

NW Staffing Resource provides comprehensive staffing services to premier companies along the West Coast. From our establishment in 1985, we have been committed to a high level of professionalism, the best customer service and sustainability.
Benefits, Services, Special Pricing and/or Discounts Extended to SDDS Members: 5% discount for SDDS members who place a Direct Hire order.
ph: (916) 993-4182 www.resourcestaff.com/employers/dental
our Vendor Members! learn more about these Vendor Members!
Wendie Richards, Dental Staffing Consultant wrichards@resourcestaff.com

At TDIC, protecting dentists is all we do. Since 1980, when we were founded by a bold group of dentists, this has been our singular focus.
Benefits, Services, Special Pricing and/or Discounts Extended to SDDS Members: Generous discounts are available for new graduates, multipolicy coverage and participation in a risk management seminar.
ph: (888) 627-3318 | www.tdicinsurance.com
Bryan Johnson, Account Manager Advisor ph: (888) 654-2374 | bryan.johnson@tdicins.com
Analgesic Services, Inc.
Jeff Hardin, Vice President
916.928.1068
asimedical.com

Impladent
Steven Weinreich 916.805.1805
impladentltd.com/

Amin Amirkhizi, Founder & CEO 877.311.7373 supplydoc.com

Roy
916.918.5752 ddsmatch.com

Dr. Brigid
916.678.3565 kidscaredental.com

Benco
Peter Joy, Regional Manager 530.828.1723 benco.com

Meds 2U Pharmacy: Emergency Dental Kit
William Huynh, Pharm D 916.221.7789 www.meds2urx.com/emergency-dental-kit
Tony
916.508.9218 straumanngroup.us

Tim Yaeger 650.593.5100 yaeger.dentist

Brian
Jay Harter 916.812.0500 henryscheindpt.com


Frank





Wendie
916.993.4182
nwstaffing.com


CJ
614.560.5417
Forrest Wiederman
949.910.3343 bofa.com/practicesolutions





Clint Bedolido, CPA, Partner 916.774.4208 muncpas.com



Ashlee Adams
866.232.7640
adamsdentalconsulting.com





Dental
The SDDS Job Bank is a service offered only to SDDS Members. It is for job seekers to reach other Society members who are looking for dentists to round out their practice, and vice versa. If you are a job seeker or associate seeker contact SDDS at (916) 446-1227 or by email at sdds@sdds.org, we can also provide contact information for the members listed below.
Cindy Weideman, DDS • Citrus Heights/Rocklin • PT • Ortho
Matthew Comfort, DDS • Roseville • PT • GP
Sukhjeet Kaur, DDS • Jackson • FT/PT • GP
Dan Gustavson, DDS • Auburn • PT • GP
Gautam Dogra, DDS • Sacramento • PT/FT • GP
Harkeet Sappal, DDS • Sacramento • PT • Endo
Mugunth Nandagopal, DDS • Sacramento • FT/PT • GP
Sean Roth, DDS • Folsom • FT • GP
Peter Kim, DDS • Sacramento • PT • GP
Hossein Kazemi, DDS • Roseville • PT/FT • GP/Perio
Arash Aghakhani, DDS • Sacramento • FT/PT • GP
Darryl Azouz, DDS • Lake Tahoe • FT/PT • GP
Oleg Oliferuk, DDS • Folsom • PT • GP
Siamak Okhovat, DDS • Roseville • PT/FT • GP
Monica Tavallaei, DDS • Sacramento • PT/FT • GP/PEDO
Sabrina Jang, DDS • Sacramento • PT/FT • GP
Albert Lee, DDS • Sacramento • PT • GP
Amandeep Behniwal, DDS • Roseville • PT/FT • GP
Elizabeth Johnson, DDS • Wellspace - various locations • FT/PT/Fill-In • GP
Amy Woo, DDS • Sacramento • PT 1 Day • Endo
David Park, DDS • several/multiple positions • FT/PT • GP
Gassan Hawari, DDS • PT/ Tue-Thur • GP
Navneet Sehgal, DDS • FT • GP
Gaetan Tchamba, DDS • PT/locum tenans • GP
Join Make a Smile Dental! We’re hiring Dental Assistants, Hygienists, and Dentists across specialties. Enjoy competitive pay and a supportive team. Apply today: makeasmile.com/ careers 11-12/24
ENDODONTIST: Seeking a Endodontist to join our professional dental team. We have been serving Sacramento for over 25 years and Voted Top Dentist by Sacramento Magazine. If you like to experience the many facets of dentistry, our practice consists of general, periodontist, endodontist, and orthodontist this practice is for you. For more information about us, please visit DrAmyWoo.com. 1-2/24
Kids Care Dental & Orthodontics seeks doctors to join our teams in the greater Sacramento and greater Stockton areas. We believe when kids grow up enjoying the dentist, healthy teeth and gums will follow. As the key drivers of our mission—to give every kid a healthy smile— our dentists, orthodontists and oral surgeons exhibit a genuine love of children and teeth. A good fit for our culture means you are also honest, playful, lighthearted, approachable, hardworking, and compassionate. Patients love us... come find out why! Send your CV to drtalent@kidscaredental.com. 6-7/17
WELLSPACE HEALTH ORGANIZATION (an FQHC) is taking applications for fill-in/part-time/ full-time dentists. Send your resume/CV to eljohnson@wellspacehealth.org. 1/15
Kids Care Dental & Orthodontics seeks orthodontists to join our teams in the greater Sacramento and greater Stockton areas. We believe when kids grow up enjoying the dentist, healthy teeth and gums will follow. As the key drivers of our mission—to give every kid a healthy smile—our dentists, orthodontists and oral surgeons exhibit a genuine love of children and teeth. A good fit for our culture means you are also honest, playful, lighthearted, approachable, hardworking, and compassionate. Patients love us... come find out why! Send your CV to drtalent@kidscaredental.com. 6-7/17
Dental Office Condo for sale or lease. One story prime location corner opposite Kaiser Hospital. 2,743 square feet of NRA located at 1603 Eureka Rd., Roseville. Six operatories with equipment. Call (916) 797-7436 for details. 1-2/26
Roseville New Construction/Sacramento Dental Building Orthodontic Office/Dental Offices for Lease/Sale; Ranga Pathak, Broker Associate, RE/ MAX Gold, DRE01364897; Tel: (916) 201-9247; Email: ranga.pathak@norcalgold.com. 8-9/21
SACRAMENTO DENTAL COMPLEX has one 3 unit suite which is equipped for immediate occupancy. Two other suites total 1630 sq. ft which can be remodeled to your personal office design with generous tenant improvements. 2525 K Street. Please call for details: (916) 539-1516. 10/11
SDDS’ weekly “This Week at SDDS” eblast reaches our entire membership every Sunday at 8:00am, with a circulation of 2,200 and an impressive open rate of 67% – contract due by noon on the Wednesday prior to the Sunday e-blast.
Guidelines for Online Classified Advertising:
• Members must place and pay for the ad themselves
• Non-Vendor Member companies and representatives cannot be listed in the ad
• Contact info in the ad must be direct to member/member’s office, non-member emails and phone numbers are prohibited
Visit www.sdds.org/publications-media/advertise/ to advertise NEW Online “This Week” Classified Advertising for SDDS
Selling your practice? Need an associate? Have office space to lease? SDDS member dentists get one complimentary, professionally related classified ad per year (30 word maximum). For more information on placing a classified ad, please call the SDDS office at 916.446.1227 or visit www.sdds.org/publications-media/advertise/
2035 Hurley Way, Suite 200 • Sacramento, CA 95825
916.446.1211 • www.sdds.org
ADDRESS SERVICE REQUESTED
5 Sacramento Kings Game
Thursday • 7:00pm
10 GM: Leading with Trust: Tools to Inspire Teams, Prevent Burnout, and Build Wellness
Eric Johnson, DDS
Sponsored by Alpha & Delgadillo OMS
Tuesday • 5:45–9:00pm
26
MidWinter Convention Day 1
SAFE Credit Union Convention Center
27 MidWinter Convention Day 2
SAFE Credit Union Convention Center
For full details and to sign up for courses online, visit: www.sdds.org
7 HIPAA Without the Headache: What Dental Offices Get Wrong (and How to Fix It)
Dennis Krohn and Sara Baker, MBA; SD Dental Solutions (SDDS Vendor Members)
Tuesday • 12:00–1pm
1 CEU, Core • Webinar
8 Dentists Do Broadway
MJ (Michael Jackson)
Wednesday • 7:30pm show
14 GM: Non-Odontogenic Tooth Pain Mohd Khalaf, DDS
Tuesday • 5:45–9:00pm
18 CPR-AHA BLS Blended Learning –Online and Skills Testing, 3 Time Sessions SDDS Instructors
Saturday • 8:00–8:45am; 9:00–9:45am; 10:00–10:45am
3 CEU, Core • SDDS Classroom
22 California Dental Practice Act Joy Brack, RDA
Wednesday • 5:30–7:30pm
2 CEU, Core • Webinar
28 Infection Control Joy Brack, RDA
Tuesday • 5:30–7:30pm
2 CEU, Core • Webinar
Come support the Foundation at the annual Golf Tournament on May 8 at Teal Bend Golf Club!
10
Tuesday • 3 CEU, Core • $89 early price thru 2/24
Presented by Eric Johnson, DDS
Sponsored by Alpha & Delgadillo OMS
This session explores how trust-centered leadership transforms dental teams by strengthening relationships, reducing stress, and promoting resilience. Participants will gain evidence-based strategies to address burnout, foster team wellness, and create a culture of purpose and engagement that sustains both professional success and personal fulfillment.
14
Tuesday • 3 CEU, Core • $89 early price thru 3/31
Presented by Mohd Khalaf, DDS
The primary cause of tooth pain is a dental disease that ends up sometimes needing restorative work, root canal treatment or even extraction. What if the pain persists beyond the dental treatment? Would this be a medical condition related to jaw or head and neck issues? This lecture will discuss how to recognize, differentiate and manage dental pain due to medical (Non-odontogenic) conditions and how to collaborate with an orofacial pain specialist on management.
5:45–9:00pm: Hilton Sacramento Arden West (2200 Harvard Street, Sac)