WINTER 2026 EDITION ROYAL COLUMBIAN HOSPITAL FOUNDATION


WINTER 2026 EDITION ROYAL COLUMBIAN HOSPITAL FOUNDATION
IN THIS ISSUE
The extraordinary work behind opening the Jim Pattison Acute Care Tower
34 MINUTES
Advanced stroke care and rapid response at Royal Columbian Hospital help a Coquitlam woman recover
PREPARING FOR THE UNIMAGINABLE
Inside a Code Orange at Royal Columbian Hospital
LISTENING TO INSTINCT
Early warning signs, advanced care, and family bonding in the NICU


Cameron Belsher

Chair, Royal Columbian Hospital Foundation


President & CEO, Royal Columbian Hospital Foundation
s we share this edition of Your Health Matters, there is a growing sense of anticipation across Royal Columbian Hospital. After years of planning, construction, and preparation, the opening of the Jim Pattison Acute Care Tower is drawing closer. Teams throughout the hospital are preparing for a moment that will mark a significant new chapter in care for patients and families across our region.
The stories in this issue offer a meaningful preview of what is to come. From advanced stroke treatment and critical care to cardiac surgery, neurosurgery, and neonatal intensive care, many of the programs featured here will soon be delivered in purpose-built spaces within the new tower. These patient journeys reflect not only clinical excellence, but also the teamwork, compassion, and precision that
define care at Royal Columbian Hospital today and will be further strengthened in the new building.
As you read these stories, we hope you see how the tower brings together people, expertise, and technology to support some of the most complex and time-sensitive care in British Columbia. It is a place designed to help caregivers do more, respond faster, and support patients through life-changing moments with dignity and respect.
None of this would be possible without you. Your generosity, led by Jim Pattison’s transformational $30 million gift, has helped build the spaces, equip the teams, and advance the care described in these pages. As we look ahead to welcoming the first patients into the Jim Pattison Acute Care Tower, please accept our sincere thanks for being part of this remarkable journey. •
ROYAL COLUMBIAN HOSPITAL FOUNDATION
EXECUTIVE EDITOR
Jeff Norris
EDITOR/WRITER
Jason Howe
CONTRIBUTING WRITER
Jason Manaois
CONTRIBUTING PHOTOGRAPHER
Joshua Klaassen
Jason Manaois
Jerald Walliser
DESIGN + PRODUCTION
Tracy Trydal
COVER
Paula Heal
PUBLISHED BY Lodestar Media
ROYAL COLUMBIAN HOSPITAL FOUNDATION BOARD OF DIRECTORS
Chair Cameron Belsher
Vice Chair
Norm Taylor
Treasurer
Han Shu
Secretary Hayley Woodin Hastings
President and CEO
Jeff Norris
Directors
Hema Bhatt, John Clinton, Aleem Jinnah, Jim McGuigan, Diana Miles, Diane Ormiston, Lynn Radbourne, Puneet Sandhar, Dr. Carolyn Shiau, Fred Withers, Dr. Brian Yang

and Foundation President and CEO Jeff Norris
Inspired giving
Behind-the-scenes of the June 17, 2025 unveiling of the Jim Pattison Acute Care Tower’s external signage.
Listening to instinct
We welcome your comments on Your Health Matters magazine. Please email info@rchfoundation.com or write to us c/o Royal Columbian Hospital Foundation, 330 East Columbia St, New Westminster, BC V3L 3W7.
Established in 1978, Royal Columbian Hospital Foundation raises millions of dollars annually to purchase medical equipment, fund innovative programs, and support training and research. To donate, please visit www.rchfoundation.com or call 604-520-4438
Early warning signs, advanced care, and family bonding in the NICU Preparing for the unimaginable Inside a Code Orange at Royal Columbian Hospital
Hospital on the move
The Extraordinary Work Behind Opening the Jim Pattison Acute Care Tower
Time to recover
How critical care and advanced life support give patients the chance to heal
A mother and daughter’s story of survival, courage, and cardiac care at Royal Columbian Hospital
34 minutes
A rapid response and advanced stroke care at Royal Columbian Hospital help woman recover
Finding room for life
Navigating a brain tumour diagnosis alongside life’s milestones
Anesthesia meets space
Q&A with Royal Columbian Hospital anesthesiologist Dr. Matthew Turnock
On June 17, 2025, Royal Columbian Hospital reached an important milestone in the journey toward opening a transformative new facility with the official unveiling of the external signage for the Jim Pattison Acute Care Tower. The event brought together leaders and partners from the Jim Pattison Foundation, Royal Columbian Hospital Foundation, Royal Columbian Hospital, Fraser Health, and EllisDon to mark a moment that symbolized both progress and gratitude. The signage honours Jim Pattison’s transformational $30 million gift, announced in 2022, which played a pivotal role in advancing the new tower and strengthening critical care services for patients across the region and beyond.

Jeff Norris, President and CEO of Royal Columbian Hospital Foundation, addresses guests during the June 17, 2025 unveiling of the Jim Pattison Acute Care Tower external signage, with Jim Pattison and partners in attendance for the milestone moment.

Jim Pattison stands beneath the newly unveiled external signage for the Jim Pattison Acute Care Tower, marking the occasion that honours his transformational support and brings the hospital one step closer to welcoming its first patients in 2026.

As part of the ceremony, Jim Pattison places an original brick from the hospital’s 1912 building, symbolizing the connection between Royal Columbian Hospital’s long history and its future as a leading centre for advanced critical care in British Columbia.

Jim Pattison smiles inside the main lobby of the Jim Pattison Acute Care Tower during the June 17, 2025 signage unveiling, a moment that reflects both gratitude and the promise of care to come.

As Lauren Phillips woke up 25 weeks into her pregnancy, she could not ignore the feeling that something was off. Trusting her instincts, the 31-year-old Port Moody resident and her husband went to Royal Columbian Hospital to make sure everything was okay. Instead, they began a four-month journey that included an emergency C-section and a prolonged stay in the neonatal intensive care unit following the birth of their son, Wesley.
“He kicked me all the time,” says Lauren, recalling a joyful but otherwise uneventful first two trimesters. “I’d wake up every night between two and four, and I knew he was there. But he just didn’t kick me in those hours that day, and he had every night since he could.”
Although Lauren was not in labour, monitoring revealed subtle changes in Wesley’s heart rate. “His heart rate, they noticed, would just dip ever so slightly every now and then,” she says. “So they checked me in overnight.”
When his heart rate dropped further, the decision was made to deliver immediately. Born weighing just 720 grams, Wesley was rushed to the NICU as Lauren went into recovery.
“Once the baby is born, we place them on a warmer and cover the body with the plastic bag to retain the heat,” explains neonatologist Dr. Miroslav Stavel. “Then you need to make sure that the airway is secure, the baby is breathing, and that the circulation is working.”
Wesley required mechanical breathing support and was placed on a jet ventilator. With careful coordination, the neonatal team helped Lauren hold her son for the first time six days later.
Lauren admits she was scared, but grateful. “The bond that we built over those months, I think, is a big reason why he’s been successful,” she says.
The NICU Lauren came to know so well will soon be transformed in the Jim Pattison Acute Care Tower. The current open-concept unit will be replaced by 24 single-family rooms, designed to offer greater privacy, natural light, and space for parents to remain close to their babies. In addition, a new obstetrics unit will open with two dedicated operating rooms for emergency and planned C-sections.
After more than 125 days, Wesley finally went home.
“I would like other families to know that the experience is not easy,” Lauren says. “But you have the most amazing team to get you through those bumps.” •


At Royal Columbian Hospital, a dedicated group of physicians, nurses and operational leaders spend countless hours preparing for something that feels almost unthinkable: a sudden mass-casualty situation where a large number of patients arrive at once. These teams plan, rehearse and refine processes to ensure the hospital can continue to provide exceptional care even under the most challenging circumstances. A major earthquake, for example, could send many injured people to hospital within a very short period of time.
A Code Orange is the emergency designation used when the number and severity of incoming patients exceed the hospital’s immediate capacity. As Dr. Kenneth Chan, Head of the Emergency Department, explains, “Code Orange is usually in situations where the number of patients will overwhelm our resources. We need to mobilize our forces, gather all our resources and systematically prepare and triage patients appropriately so they go to the right places.”
A small, unexpected surge of critically injured patients can often be managed by calling in additional staff. But when hospital leaders anticipate a much larger influx, they must consider whether regular operations can safely continue.
“We look at our current status and ask, ‘Can we handle this situation on top of everything else happening in the hospital right now?’” says Dr. Chan. “If the answer is no, then we would call a Code Orange.”
In mass-casualty scenarios, experience shows that approximately 20 percent of patients require immediate life-saving care. About 30 percent have serious but stable injuries, and roughly 50 percent

have less urgent conditions. This mix helps teams estimate how many physicians, nurses, beds and operating rooms may be needed within minutes.
A Code Orange changes the operations of the entire hospital. Dr. Chan notes, “It really is an all-hands-on-deck situation.” The Emergency Operations Centre is activated, bringing together clinical leaders, logistics experts, communications staff and others responsible for coordinating the response.
To make space for incoming patients, existing emergency patients are rapidly moved to inpatient units or other designated areas. Staff begin “decanting” beds, accelerating discharges when safe to do so and relocating stable patients out of high-acuity zones.
Outside, triage often moves to the ambulance bay or a large open area where teams can quickly assess patients and direct them to the most appropriate clinical space.
Inside, areas are reconfigured so patients with the most urgent needs can be assessed and treated promptly, while those with less severe injuries are

managed in separate dedicated areas. Operating rooms, imaging departments and critical care teams shift into emergency-only mode. Elective surgeries are paused. It becomes a coordinated hospital-wide effort.
As a Level 1 trauma centre, Royal Columbian is uniquely positioned to care for the most complex emergency cases. “We do a lot of things here,” Dr. Chan says. “In a Code Orange we have to reprioritize our operations to take care
of the sickest as urgently as possible.”
The opening of the Jim Pattison Acute Care Tower will significantly strengthen Royal Columbian Hospital’s ability to respond to a Code Orange. The new Emergency Department is substantially larger than the current space, with modern layouts designed to improve patient flow and coordination during both everyday operations and large-scale emergencies.
The new Emergency Department also
includes a dedicated mass casualty hallway, a wide and purpose-built space that allows for rapid assessment and movement of patients during a surge. The expanded ambulance bay provides more room for offloading and triage, helping teams work efficiently even in high-volume situations.
These modernized spaces, combined with the expertise of Royal Columbian’s emergency, surgical, imaging and critical care teams, will help ensure that if the unimaginable ever occurs, the hospital is as prepared as possible to respond. •
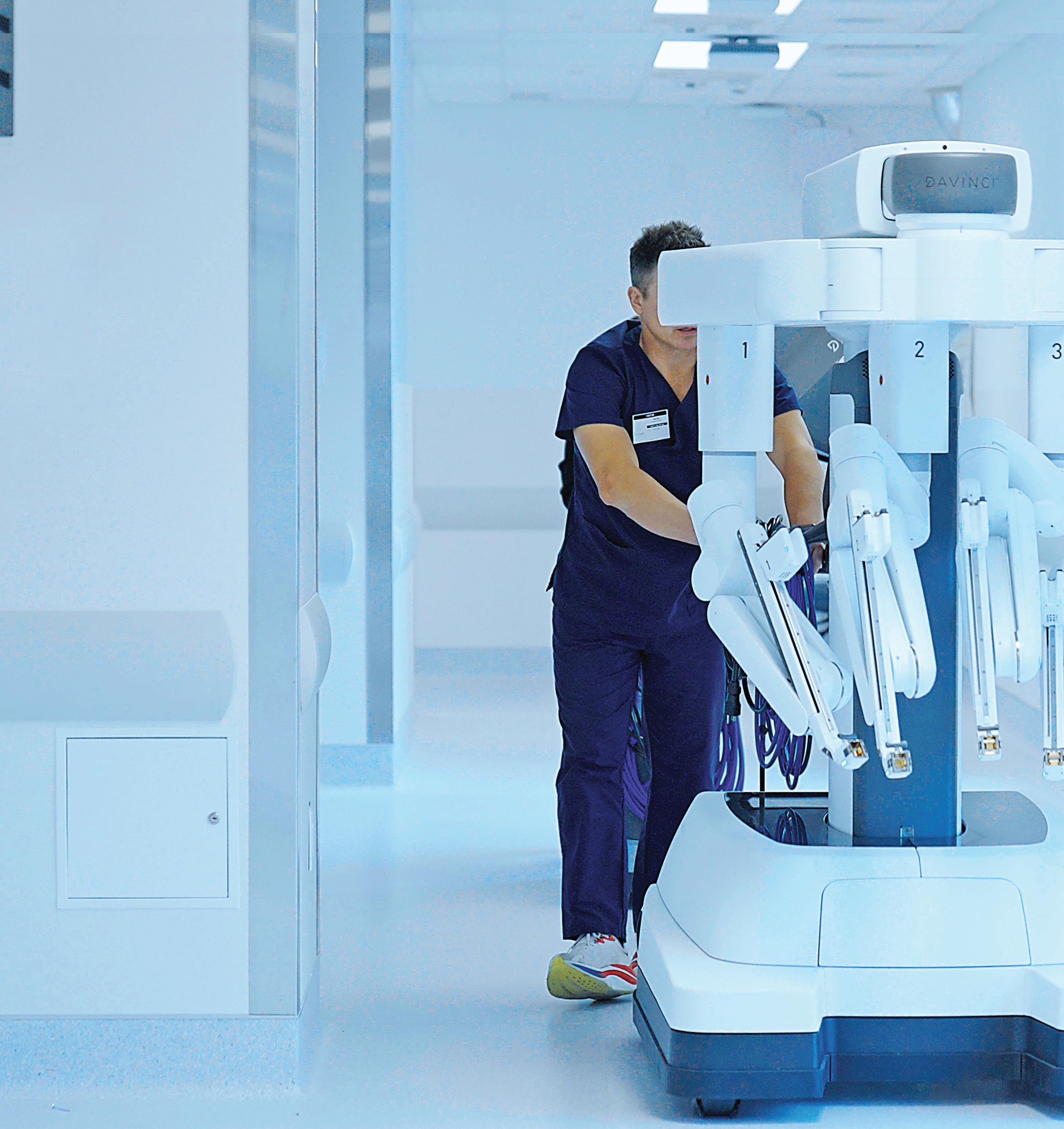
Behind the scenes at Royal Columbian Hospital, an extraordinary effort has been unfolding. As the Jim Pattison Acute Care Tower edges toward its 2026 opening, teams across the hospital are deep into one of the most complex transitions in Royal Columbian’s history. Equipment is being installed and tested, workflows are being redesigned, and hundreds of staff are preparing to move people, programs, and technology into an entirely new centrepiece for acute and critical care in British Columbia.
Few know the scale of this better than Ramona Fonseka, Chief Clinical Planner for Redevelopment at Royal Columbian Hospital. “There are thousands of items, everything from medical instruments to the amount of PPE a hospital needs,” she explains. “Anything and everything required to run a hospital has to be in place for first patient day.”
Her team, together with activators and superusers from across the hospital, is working floor by floor to ensure every piece is installed, tested, and ready before opening day.
Those activators, experienced clinicians and operational experts, are validating room layouts, confirming equipment placement, and ensuring the full inventory of supplies is exactly where care teams will expect it.
Superusers, meanwhile, are preparing to be the first wave of staff trained on new equipment, new technologies, and new workflows unique to the Tower. These champions will guide colleagues through orientation, troubleshooting, and readiness activities in the months and weeks before opening.
“What staff need most is orientation

to the space, how to function and work within it, how to react, how to go and find the Code Blue button, where the crash cart is,” says Fonseka. “Then there’s training on new and different equipment that we don’t have access to in our current space.”
Supporting all of this is Health Care Relocations (HCR), a global leader in hospital moves. For HCR Senior Project Manager Cameron Goes, this is a signature project.
“We’ve done a lot of projects all over the world,” he says. “This will certainly be the biggest in BC’s history.”
HCR’s role is both meticulous and
mission-critical. The team plans how departments will ramp down in their current spaces, sequences the move of equipment carefully, and orchestrates a single-day transfer of more than 300 patients into the new Tower.
“You can’t snap your fingers and have all your people and equipment over there,” Goes explains. “We bring a phased approach to department moves so that services can ramp down and ramp back up to the levels needed for the public.”
On patient-transfer day, dozens of teams, including Registration, Clean Team, Security, transport teams, and unit-based clinical staff, will work in tightly choreographed cycles.


“We implement a very efficient patient transfer process where all the patients move in essentially one day,” says Goes. Every team member will wear colourcoded T-shirts identifying their role, an approach honed through years of experience. “Everyone stays in their role, and we get the job done.”
Before that day arrives, the hospital will run a full patient-transfer rehearsal. This is an essential test of routes, timing, communication processes, elevator access, and staffing.
“We do it to gain that experience perspective,” Goes says. “We want to actually test it with equipment and a bed. Something can look good on paper, but in real time it may look a little different.”
Across the hospital, anticipation is building, not only for the building’s
advanced technology, expanded capacity, and single-patient rooms, but for the sense of calm and dignity the new environment will offer.
“With the Jim Pattison Acute Care Tower, one of the pieces people will sense right away is how spacious and inviting the main entrance is,” says Fonseka. “Access to natural light, beautiful single rooms, alcoves for families, we finally have a hospital that will match the exceptional care that is provided here.”
The move into the Jim Pattison Acute Care Tower is far more than a logistical event. It reflects the precision, care, and dedication that define Royal Columbian’s provincial role. When the doors open, patients and families will step into a modern, thoughtful, purpose-built environment, one shaped by thousands of hours of preparation and a shared commitment to exceptional care. •

Russ Moore first noticed a slight shortness of breath that would come and go. The episodes were so brief that he dismissed them. But when the sensation returned one morning in late July 2025, while he was alone at his mother’s home in North Delta, he trusted his instincts and reached for his phone. His next memory was waking up bleeding from his head.
“I called 911 and then made my way down the stairs,” Russ recalls. “I was just sitting there. I didn’t think I could stand up.”
Paramedics transported Russ to Surrey, where tests revealed a large blood clot in his lungs. He was immediately transferred to Royal Columbian Hospital.
“A pulmonary embolism is a blood clot
that moves through the heart and into the pulmonary arteries where it blocks up a pulmonary artery,” explains Dr. Derek Gunning, a critical care physician at Royal Columbian Hospital.
As an interventional radiology team worked to remove the clot, Russ went into cardiac arrest. He was soon connected to ECMO, or extracorporeal membrane oxygenation, a specialized machine that temporarily takes over the function of the heart and lungs to give the body time to recover.
“After we stabilize people (on ECMO), we next have to determine if they have had a brain injury, are they going to be able to wake up, and are they going to be able to return to a normal functional life,” says Dr. Gunning. “And, unfortunately, on day one, we never know.”
As Royal Columbian Hospital cares for a high volume of critically ill patients, this level of care is expanding in the Jim Pattison Acute Care Tower. Level four of the new building is dedicated entirely to intensive care, with 47 ICU beds, 20 Cardiac Surgery beds, and 17 Cardiac Intensive Care beds, bringing advanced technology and specialized teams together to support patients at their most vulnerable.
Despite his grave condition, Russ responded remarkably well and was removed from ECMO before the end of the third day. He was discharged within a couple of weeks.
“All the doctors and nurses were astounded at how fast I recovered,” he says. “I didn’t realize just how sick I was.” •
When Robin Shingler collapsed in her yard, she faced one of the most life-threatening cardiac emergencies, a ruptured aortic aneurysm. She was rushed to Royal Columbian Hospital, where an emergency operation saved her life.
Robin’s medical emergency would soon have a profound impact on her daughter.
Annalise Schatz, an environmental educator, had already been diagnosed with an aortic aneurysm. Until her mother’s sudden collapse, however, she had struggled with whether to proceed with surgery herself.
“I had no signs, no warnings. If it wasn’t for my mom’s experience, I never would have gone ahead with my surgery,” Annalise says.
Unlike her mother’s crisis, Annalise had the rare opportunity to undergo a planned operation to repair her aorta before it became life-threatening. The decision was not easy, but with the guidance of the cardiac team at Royal Columbian Hospital, she chose to move forward.
Throughout her journey, Annalise wore a heart-shaped necklace made from a stone she found on Vancouver Island. It became a quiet source of reassurance during surgery and remains a symbol of resilience and hope.
Care for patients like Robin and Annalise will be further strengthened as the Jim Pattison Acute Care Tower comes into use. The superfloor on the second level of the new building will expand Royal Columbian Hospital’s operating rooms from 12 to 17, including three dedicated cardiac operating rooms designed for complex and time-sensitive
heart surgery. Interventional cardiology and interventional radiology suites will also be located on the same floor, bringing related services together in one integrated space.
Today, both mother and daughter are grateful for the care they received and the second chance they’ve been given.
“We’ve kind of won the life lottery twice,” Annalise reflects. “And it just fills us with a huge sense of gratitude going forward.”
Robin shares that perspective. “I think we’re all strong. We all have this inside us. Unfortunately, it takes something like this to happen before you know what you’re made of.”. •
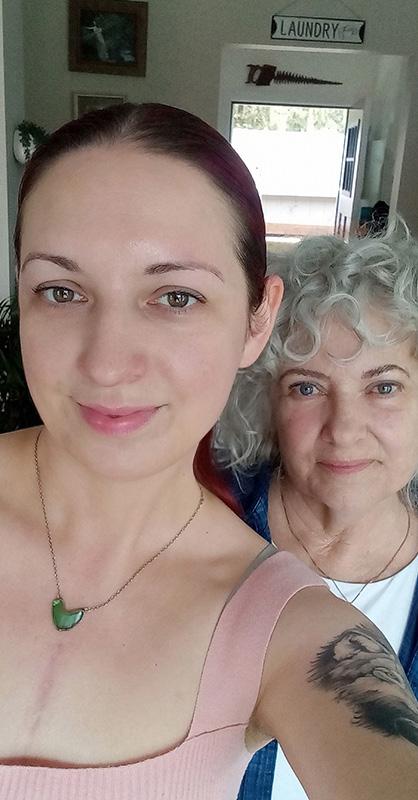


Avisit to the gym in Coquitlam was part of Margaret Swanson’s active lifestyle, until a sudden shift in her vision one day in August 2025 signalled something was wrong. What began as a familiar workout quickly turned life-threatening when everything in front of her appeared “sparkly” and she collapsed. At 69 years old, Margaret was experiencing a major
stroke. “The next thing I knew, I was on the floor,” Margaret recalls. “I could not speak, and I could not move properly. I was confused more than anything.”
Paramedics arrived quickly and rushed her to Royal Columbian Hospital. Inside the ambulance, Margaret remembers an unusual calm. “It was very quiet,” she says. “I knew something was not right.”
When Margaret arrived at Royal
Columbian Hospital, the stroke team was already waiting. Dr. Zameer Hirji, interventional radiologist, had been alerted by Royal Columbian Hospital stroke neurologist Dr. Hassanain Toma before she reached the hospital. “I received the call at 1:06 p.m. that a patient with a high likelihood of a largevessel stroke was on the way,” says Dr. Hirji. “From that moment, everything
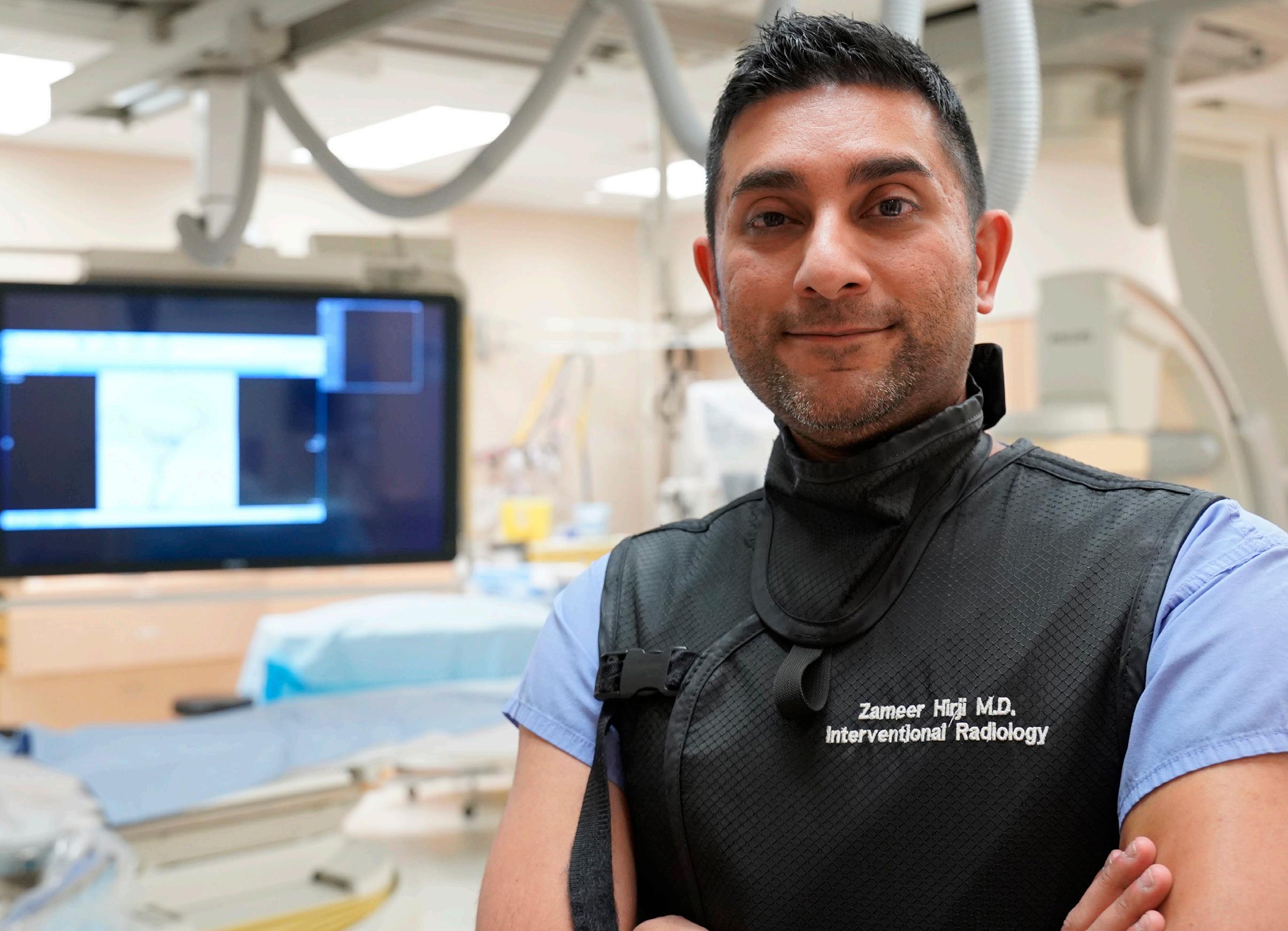
moved very quickly. Mrs. Swanson arrived in our ER at 1:08pm and by 1:42 p.m., we had removed the clot and fully restored blood flow to her brain.”
“Removing a clot from someone’s brain within 34 minutes of them entering the RCH doors is remarkable,” Dr. Hirji adds.
“When they told me how fast it all happened, I was amazed,” Margaret says. “I did not even realize things like that were possible.”
The procedure, known as a mechanical thrombectomy, involves accessing a blood vessel through the groin and navigating a catheter or “thin tube” using imaging guidance to the brain to remove the clot. At the time, Margaret had no idea how it was done. “I was fascinated when they explained it to me,” she says. “The technology is unbelievable.”
When the Jim Pattison Acute Care Tower opens, treatments like Margaret’s will take place on the second level’s interventional superfloor, which brings interventional radiology, interventional cardiology, and operating rooms together. Following procedures, patients requiring specialized neurological care will recover on the ninth-floor Neurosciences inpatient unit. Margaret spent about a week in hospital before returning home. Nurses and staff ensured she was ready to leave safely, checking her strength, balance, and recovery every step of the way. “The nurses were incredible,” Margaret says. “They explained everything, made sure I was okay, and helped me feel confident going home.”
Before her stroke, Margaret lived a very active life. She was a dragon boat paddler, a volunteer, and a gardener who loved
being outdoors. While she continues to recover, she remains deeply grateful for the care she received. “I think about it now and I realize how lucky I was,” she says. “If that technology and that team had not been there, I might not be here.”
For Dr. Hirji, stories like Margaret’s are the reason he does this work. “You do not think about the bigger picture in the moment,” he says. “You are focused on getting from the groin to the brain safely and quickly. But when you see that person later, talking, walking, living their life again, that is when it really hits you why this work matters.”
Margaret looks back with gratitude for the quick-thinking gym staff, the paramedics, and the Royal Columbian Hospital team that acted without hesitation. “I am just so thankful,” she says. “It is amazing what they can do. Truly amazing.” •
The seizure came without warning, in the middle of the night, and instantly reframed everything Jasmine Martin thought she knew about her health.
“I had been feeling off for a few weeks but brushed it off as something minor,” Jasmine recalls. “It wasn’t until I had a Grand Mal seizure in my sleep that I realized something was seriously wrong.”
The diagnosis of a brain tumour was shocking, but Jasmine was grateful for the swift and thorough care she received at Royal Columbian Hospital. “It was good to know what I was dealing with right away,” she says.
At the hospital, Jasmine met neurosurgeon Dr. Zurab Ivanishvili, whose direct and compassionate approach immediately stood out. “Dr. Ivanishvili had the best bedside manner,” she says. “He didn’t sugarcoat anything but gave us all the details we needed. For me, the more information, the better.”
Dr. Ivanishvili recalls being struck not only by the size of the tumour, but by Jasmine herself. “On one hand, she was facing a huge challenge with such a large tumour,” he says. “But on the other, she had the personality that made me think, if anyone can fight this, it would be her.”
Throughout her care, he remained closely involved, ensuring Jasmine understood both her diagnosis and the options ahead.
Nurses and staff also left a lasting impression, particularly as Jasmine’s treatment coincided with her wedding plans. Rather than postponing, her care team worked around important milestones. “I had not one but two small weddings,” she says. “Dr. Ivanishvili even encouraged me to enjoy a dance and a bit of champagne at the reception. Those moments were some of the happiest of my life.”
Today, Jasmine reflects with gratitude and purpose. “This has taught me how

important it is to raise awareness about epilepsy and seizures, which are more common than people realize,” she says. Looking ahead, patients like Jasmine will benefit from continued advances in neurological care. The Jim Pattison Acute Care Tower will include a purpose-built Neurosciences inpatient floor that brings
neurosurgery, neurology, and stroke care together in one integrated environment, designed to support comfort, dignity, and recovery for patients with complex brain and spine conditions.
“You can live a very happy life regardless of what you’re going through,” Jasmine says. •
Over three days in September 2025, Royal Columbian Hospital anesthesiologist Dr. Matthew Turnock fulfilled a childhood dream while helping to advance medical knowledge when he experienced weightlessness. Supported by the European Space Agency, the Canadian Space Agency, and an innovation grant established by Royal Columbian’s anesthesiologists through the Foundation, Dr. Turnock travelled to France with team members Dr. Alex Suen, Dr. Siobhan Wagner, and Adrian Tabari to conduct experiments aboard the Airbus A310 Zero G. His research explored how anesthetic drugs behave in microgravity, a question that could have implications for future space missions and medical care beyond Earth.
Foundation

What was it like to conduct your experiment in microgravity?
It wasn’t until I was sitting in front of the experiment in the air with my medical student, surrounded by the other research teams, that it all became very real. I had heard many accounts of weightlessness before, but nothing quite prepares you for experiencing it yourself. It is an intense experience. Before and after each parabola, the aircraft experiences 1.8 g, so every part of your body feels twice as heavy. Then, virtually instantaneously, you feel no gravity at all, and every limb is suddenly floating in the air.
Foundation
Where did your interest in space develop?
Dr. Turnock
I always wanted to be an astronaut. And when I was in undergrad, I saw a talk by Dr. Dave Williams, who is now a retired physician astronaut. He made it clear that you didn’t have to be an engineer or pilot to become an astronaut. Really what it comes down to is your leadership ability or personality, ability to work with others, your ingenuity and creativeness.
Foundation
What is your experiment?
Dr. Turnock
Here on Earth, we give most general anesthetics through inhaled gases. In space, though, that’s just not an option. If any of that gas leaked into the cabin, you could end up anesthetizing the whole crew. So, people have looked at other ways of providing anesthetics, either injection anesthetics or through spinal anesthesia. For our experiments, we examined how spinal anesthesia behaves when you take away gravity.
Foundation
What did you learn from the initial tests?
Dr. Turnock
Not only did it not spread up to the brain like people predicted, in fact it spread a lot less than it did on Earth. Do we need to increase how much medication we inject? Do we need to inject it faster? Slower? Dilute the medication? These are all questions that we could test on future parabolic flights.
Foundation
Now that you have completed your first experiments, what’s next?
Dr. Turnock
Like all good research, we generated more questions than we answered, and the team is already buzzing with ideas for future research. The thought that we’re going to be doing a surgery in space is far fetched. We’re a long way from doing that. But everything we do now sets the groundwork for 10, 20, 50 years in the future.

