MASTHEAD CLEAR SPACE


The stand-out performance patients need. The name professionals recommend.
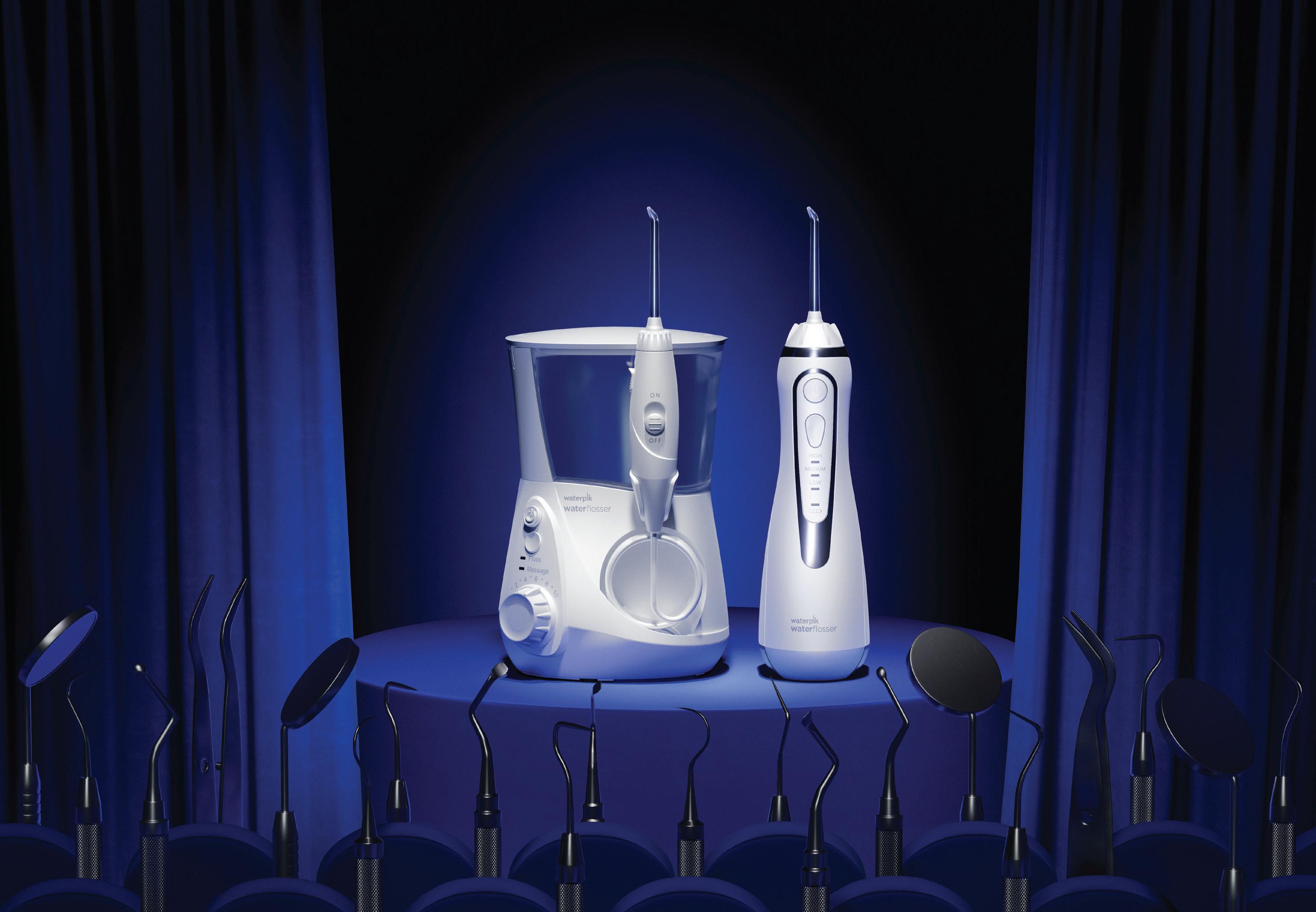

Not all water flossers are equal. Recommend by name.



















The stand-out performance patients need. The name professionals recommend.


Not all water flossers are equal. Recommend by name.




















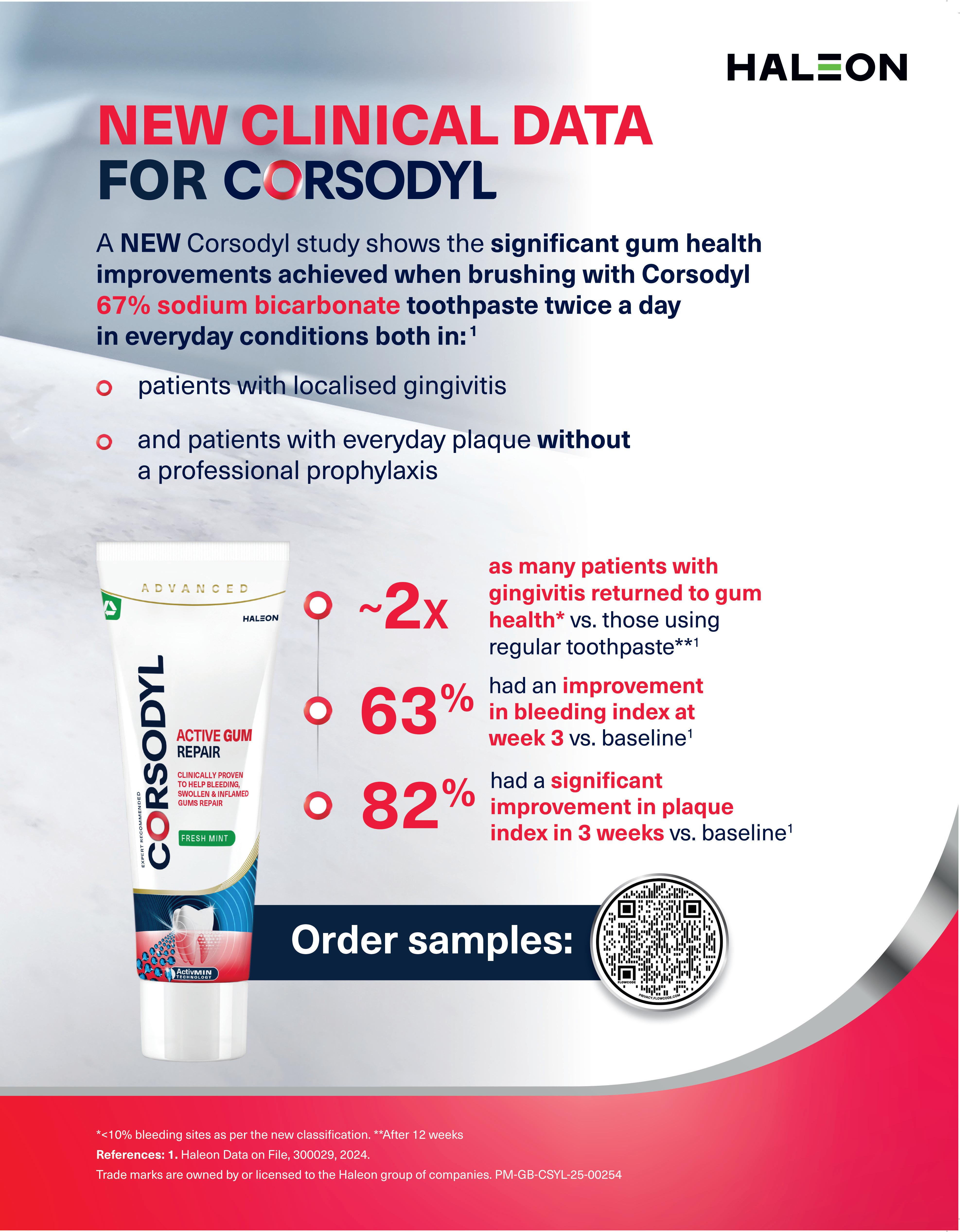
The Department of Health and Social Care and Minister of State for Care Stephen Kinnock MP have revealed a set of reforms for NHS dentistry that it is hoped will provide a major boost for millions of NHS dental patients. The changes are designed to enable patients to access urgent care more efficiently.

What is described as an overhaul of NHS dentistry will see patients with most urgent dental needs and those requiring complex treatments prioritised. There are also new incentives for those under the NHS dental contract to offer longer-term treatments for major issues, such as gum disease and tooth decay, through the NHS.
The government states that deep-rooted reforms are fundamental to its wider rescue plan for dentistry, including the rolling out of urgent and emergency care appointments, supervised toothbrushing for 3-to-5-year-olds, and water fluoridation schemes to reduce decay.
Minister for Care Stephen Kinnock said: “We inherited a broken NHS dental system and have worked at pace to start fixing it – rolling out urgent and emergency appointments and bringing in supervised toothbrushing for young children in the most deprived areas. Now we are tackling the deep-rooted problems so patients can have faith in NHS dentistry – these changes will make it easier for anyone with urgent dental needs to get NHS treatment, preventing painful conditions from spiralling into avoidable hospital admissions.
“This is about putting patients first and supporting those with the greatest need, while backing our NHS dentists, making the contract more attractive, and giving them the resources to deliver more. This marks the first step towards a new era for NHS dentistry after a decade of decline, one that delivers for patients and our dedicated dental professionals.”
Jason Wong, Chief Dental Officer for England, said: “Dentists have been working tirelessly to care for patients, and I want to thank them for their dedication. We listened closely to the profession, and these reforms are centred on improving patients’ experience, from getting urgent care more easily to supporting longer-term and preventative treatment, especially for children.
“By recognising the work of the wide range of professionals in dental teams and making better use of their skills, the NHS can help ensure patients see clear benefits from the changes being made.”
The government will proceed with what is being hailed as ‘the most significant modernisation of the NHS dental contract in years’, following a consultation with the sector and the public. A government response to the NHS dentistry contract: quality and payment reforms consultation has also been published.
Additionally, to help boost for children’s dental health, dental nurses are to be encouraged to apply fluoride varnish to children’s teeth. Dental staff will also reportedly receive a fairer payment for applying fissure sealants to protect children’s teeth from decay as NHS dentistry shifts towards prevention first and foremost.
Dr Oosh Devalia, President, British Society of Paediatric Dentistry (BSPD), said: “BSPD welcomes today’s announcement on NHS dental contract reform as a positive step and we look forward to seeing what this means for children and
young people. Having a contract with prevention at its heart must be the way forward, and the recommendations we submitted during the consultation period are focused on ensuring that the children most in need are prioritised to receive the dental services they deserve.
“A prevention approach will have the biggest impact when it is designed to target the most vulnerable children in our communities. As ever, BSPD looks forward to working with policymakers to establish the details to ensure that the dental contract really delivers for children.”
To improve staff retention, NHS dental teams will receive more support through annual reviews, and learning and development opportunities, in addition to government funding to support sick leave and guidance on NHS contractual terms and benefits.
Dr Nigel Carter OBE, Chief Executive of the Oral Health Foundation, said: “The proposed reforms acknowledge some of the pressures within NHS dentistry, particularly for patients with complex needs, but they stop short of the fundamental change the system requires. Adjusting contractual mechanisms may improve continuity of care for a small cohort of patients, but it does not resolve the structural problems that limit access or drive dentists away from NHS provision. Without sustained investment in prevention, early intervention and population-level public health measures, demand will continue to exceed capacity. A model that remains weighted towards managing disease rather than preventing it risks perpetuating the very pressures these reforms are meant to address.”
The British Dental Association (BDA) has stated its hope that ‘interim changes to the discredited NHS dental contract will offer a boost for patients and practitioners’ but stressed ‘this is not the wholesale change required to save the struggling service’. n




WJames Cooke T: 01732 371 581 E: james.cooke@purplems.com http://www.smile-ohm.co.uk/
elcome to the first issue of Smile Oral Health Matters for 2026! I hope the year is off to a great start for each of you.
Managing Editor James Cooke james cooke @purplems.com Tel: 01732 371 581
Commercial Director Gary Henson gary.henson@purplems.com Tel: 07803 505208
Rates: UK £39.95 per year; Overseas £83 - all cheques in sterling drawn on a UK bank made payable to ‘Smile’. 8 issues including 16 hrs CPD £39.95

Published by Purple Media Solutions
The Old School House, St Stephen’s Street Tonbridge, Kent TN9 2AD Tel: 01732 371 570

Kicking off 2026, I’ve had the privilege of serving as guest host for an episode of the British Society of Dental Hygiene and Therapy’s new podcast: Dental Health Matters. In the episode, titled Future-Ready: What 2025 Taught Us and the Opportunities and Challenges Ahead in 2026, I spoke with BSDHT President Elect Simone Ruzario and President Rhiannon Jones as they reflected on 2025 and looked ahead to what the year ahead has in store for the profession.
Production and Designer 1 Lorna Reekie lorna reekie @purplems.com Tel: 01732 371 584
Production and Designer 2 Rob Tremain rob.tremain@purplems.com

Divisional Administrator Francesca Smith francesca.smith@purplems.com Tel: 01732 371 570







You can read more on page 10, as Rhiannon provides a full introduction to the new show. And for more information, you can visit bsdht.org.uk/podcast
For more dental-related chatter, check out our own podcast in conjunction with sister magazine The Probe at the-probe.co.uk/podcasts
Enjoy the magazine!


in association with:

of Purple Media Solutions
Editorial Advisory Board: Dr Barry Oulton, B.Ch.D. DPDS MNLP; Dr Graham Barnby, BDS, DGDP RCS; Dr Ewa Rozwadowska, BDS; Dr Yogi Savania BChD, MFGDP; Dr Ashok Sethi, BDS, DGDP (UK), MGDS RCS; Dr Paroo Mistry BDS MFDS MSc MOrth FDS (orth); Dr Tim Sunnucks, BDS DRDP; Dr Jason Burns, BDS, LDS, DGDP (UK), DFO, MSc; Prof Phillip Dowell, BDS, MScD, DGDP RCS, FICD; Dr Nigel Taylor MDSc, BDS, FDS RCS(Eng), M’Orth RCS(Eng), D’Orth RCS(Eng); Mark Wright BDS(Lon), DGDP RCS(UK), Dip Imp Dent.RCS (Eng) Adv. Cert, FICD; Dr Yasminder Virdee, BDS.

Other titles include:
Circulation Manager Andy Kirk
Managing Director Ed Hunt ed.hunt@purplems.com Tel: 01732 371 577





The Oral Health Foundation has welcomed a new government announcement confirming that young people leaving care will be entitled to free NHS dental care, prescriptions and eye tests up to their 25th birthday. The new measures aim to reduce health inequalities faced by care leavers, who are more likely to experience poor oral health and face barriers to accessing dental services once statutory support ends at 18. The policy is part of a wider package designed to improve health outcomes and life chances for young people transitioning out of care.
Access to dental care remains a significant challenge for many care leavers, with cost, uncertainty around entitlement and difficulty registering with a dentist often leading to untreated dental problems and avoidable pain. Extending free dental care is intended to remove one of the key obstacles to early intervention.
Dr Nigel Carter, chief executive of the Oral Health Foundation, says: “This is about dignity as much as dentistry. Extending free dental care to 25 is a hugely positive step for young people leaving care, many of whom have grown up facing real barriers to accessing dental services
at a critical time in their lives. It removes a barrier that never should have existed and recognises the heightened risk of poor oral health among care leavers.
“The priority now is making sure this commitment translates into real access on the ground, so every eligible young person can actually secure the care they need as they build independent lives.”
The charity has stressed that successful delivery will depend on clear communication, consistent local implementation and sufficient NHS dental capacity, so that care leavers can access appointments in practice as well as in policy. n
The British Dental Association has said new guidance explaining how local authorities should provide specialist public health advice to Integrated Care Boards (ICBs) risks being undermined given the huge question marks hanging over the dental public health workforce in England.
This guidance, developed by the Faculty of Public Health and the Association of Directors of Public Health for government, aims to ensure that expert public health input should be embedded into ICB commissioning processes. However, the grave uncertainty facing the dental public health workforce in light of the abolition of NHS England is set to undermine aspirations to ensure that

local decisions are informed by population health needs and evidence-based approaches.
Deep oral health inequalities look set to widen. The recent Adult Oral Health Survey revealed decay rates among adults have surged to levels not seen since the 1990s, with decades of oral health gains wiped out. The full guidance is available here.
BDA Chair Eddie Crouch said: “This guidance sets out very worthy aspirations, but local authorities will not meet the challenge of widening inequality without boots on the ground armed with unique expertise. The abolition of NHS England has left dental public health staff flying blind. They deserve real clarity on the future of their vital roles.” n
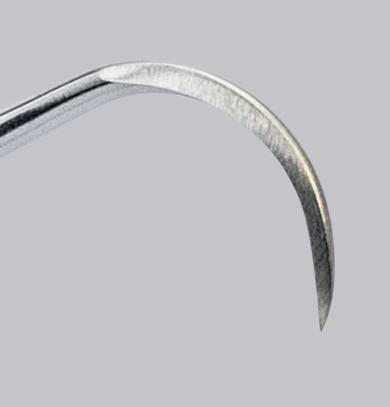


200-300% More Contact than Leading Competitors
Greater adaptation means less scaling strokes. Better for you, better for your patients.




Less Sharpening


PDT blades are thinner, sharper, and heat-treated for durability, lasting up to seven times longer.



























Ultra-lightweight Design
Solid resin handle reduces fatigue and muscle strain during prolonged use.








Superior Tactile Sensitivity
Knurled grip provides superior tactile sensitivity for precise control during procedures.


Expertly crafted to provide maximum comfort and tactile sensitivity


The dental community is joining together in 2026 to take part in a BIG 100km charity challenge – and now is your chance to sign up and be part of it.
Dental groups, suppliers, clinicians and energetic fundraisers are being invited to test their limits and raise money to support Dentaid The Dental Charity in its 30th anniversary year as part of Dentistry’s BIG Community Challenge.

A team with participants from across the profession is entering the ‘original’ 100km London 2 Brighton Ultra Challenge on Saturday 23rd and Sunday 24th May 2026.
For those seeking a shorter route, two oneday challenges are available on the Sunday with
a marathon-distance 42km route and a 25km looped walk from Brighton Racecourse. There will be also be a Walk in a Box option for anyone unable to join the main event.
Event registration is now open and professionals from across the industry are being invited to get their best foot forward and sign up.
The challenge is the brainchild of Mark Allan, MD of Bupa Dental Care and Joe Lovett , owner of Catalyst Sales and Marketing, who wanted to bring teams from across the dental sector together with a shared goal.
Mark Allan said: “Over the last two years I’ve done walking marathons between dental practices, got a few people involved and raised some money for charity.
“However I couldn’t help feeling that this could be done on a much bigger scale – connecting the brilliant dental industry through a walk that could raise significantly more for a fantastic charity like Dentaid is the perfect solution.
“I can’t wait to see everyone getting involved.”
Joe Lovett said: ‘Having worked in the industry for almost 20 years, I know what a strong sense of community there is in dentistry. I am so proud to work on this project alongside Dentaid and am confident we can bring lots of people together to collectively raise a huge amount of money for this incredible cause.”
Participants will get lots of support with regular stations for food and drink, medical
back-up, parking and shuttle transfers and camping options.
There will also be medals, T-shirts and a team cheering on the Dentistry’s BIG Community Challengers who will also be invited to a postevent celebration after they cross the finish line.
The money raised will go towards Dentaid’s work to deliver dental care to vulnerable people across the UK. Dentaid operates 11 outreach mobile dental clinics which offer treatments and oral health advice to people experiencing homelessness, harm, poverty and abuse.
Andy Evans, CEO of Dentaid The Dental Charity, said: “We are honoured to be chosen as the partner charity for the first ever Dentistry’s BIG Community Challenge. It’s a great opportunity to meet up with colleagues from across the industry. Along the way, the dental community will be helping us to change the lives of the most vulnerable people through dental care. The sense of achievement and pride on crossing that finishing line will be incredible and I’m sure it will be an experience no-one involved will ever forget.”
Registration costs £189 for the full challenge, £132 for the marathon challenge and £84 for the 25k challenge. Participants are required to raise at least £500 in sponsorship for Dentaid (£300 if taking part in the 25k event).
To sign up for the event please visit: https://www. ultrachallenge.com/london-2-brighton-challenge/ dentistrys-big-community-challenge/ n






































Rhiannon Jones reflects on the launch of Dental Health Matters, a new podcast from the BSDHT giving space to the conversations that matter most to dental hygienists and dental therapists

There has never been a more important time to listen to the voices of dental hygienists and dental therapists. As prevention takes centre stage, pressures on the workforce continue to grow and expectations of our profession evolve, the need for connection, shared learning and practical support has never been clearer. That is why, earlier this month, the BSDHT was proud to launch Dental Health Matters, a brand-new podcast created for the profession, by the profession.
Dental Health Matters is a space to pause, reflect and feel supported. It is a place where real conversations happen about the realities of practice, the science that underpins prevention, and the people who make oral healthcare what it is.
Why a podcast and why now?
Dental hygienists and dental therapists are busier than ever. Clinical schedules are full, patient needs are increasingly complex, and the emotional demands of care are often underestimated. At the same time, the profession is stepping into a more visible, influential role in prevention, early detection and patient education. That combination creates both opportunity and pressure.
Podcasts offer something uniquely suited to this moment. They fit into real life. You can listen on the commute, between patients or while winding down at the end of the day. Dental Health Matters has been designed with that in mind. Episodes are concise but meaningful, accessible without being superficial, and grounded in evidence as well as lived experience.
The aim is to explore what is happening across the profession, share insights you can apply in practice and remind you that you are not navigating these challenges alone.
What listeners can expect
Dental Health Matters brings together trusted voices from across dentistry, general healthcare
and professional wellbeing. Hosted by the BSDHT, with guests joining throughout the series, the podcast blends clinical relevance with honest discussion and practical takeaways.
The first three episodes, released together at launch, set the tone for what is to come. The series is supported by the Society’s Corporate Friends, EMS, Oral-B and TePe, whose involvement reflects a shared focus on prevention and education and helps ensure the podcast remains freely accessible to the profession.
The opening episode, Beating Burnout: Sustainable Wellbeing Strategies for Dental Professionals , features Dr Mahrukh Khwaja, founder of Mind Ninja. This conversation focuses on mental wellbeing through a preventive lens. Drawing on evidence-informed approaches from psychology, Dr Khwaja explores how dental professionals can recognise early signs of burnout, build resilience and create habits that support long-term wellbeing. It is practical, compassionate and rooted in the realities of dental practice.
The second episode, Early Detection Saves Lives , brings together Jocelyn Harding and Professor Mike Lewis to explore the critical role dental hygienists and dental therapists play in identifying mouth cancer. This conversation highlights why prevention and early detection are central to our professional identity and how confident, clear communication with patients can make a life-changing difference.
The third episode, Future-Ready: What 2025 Taught Us and the Opportunities and Challenges Ahead in 2026 , is hosted by James Cooke and brings together BSDHT President Elect, Simone Ruzario, and myself. This episode reflects on the past year and looks ahead to what is coming next for the profession. It considers policy, education, collaboration and scope of practice, as well as the skills and confidence needed to thrive in a changing landscape.
Together, these opening episodes reflect the breadth of what Dental Health Matters is about: wellbeing, prevention, professional identity and future-focused thinking.
A platform that will grow with the profession
Dental Health Matters is not a one-off project. It is designed to evolve alongside the profession, responding to emerging challenges, celebrating progress and amplifying the voices of dental hygienists and dental therapists across the UK. Future episodes will continue to explore prevention, professional development, leadership, education and the everyday realities of clinical life. Members will also have the opportunity to suggest topics and guests, ensuring the podcast remains relevant, inclusive and grounded in practice.
Listen and join the conversation
Dental Health Matters launched just a few days ago and is available in both audio and video format across all major podcast platforms. Whether you are looking for practical insight, professional reassurance or simply a reminder of why your role matters so deeply, this podcast has been created with you in mind.
To listen, subscribe and find out more, visit bsdht.org.uk/podcast. n
RHIANNON JONES

Rhiannon is the President of the British Society of Dental Hygiene & Therapy.





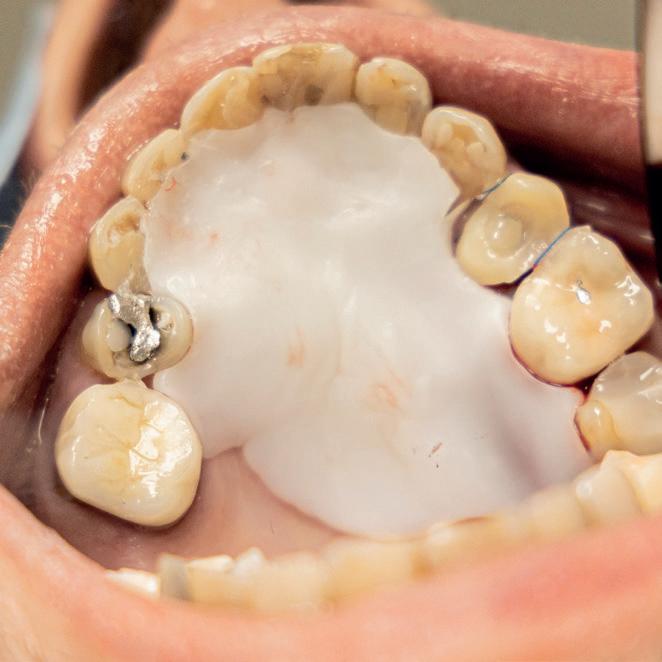
Minimise Complications and Improve Healing Conditions In Mucogingival and Implant Surgery


Leveraging the antibacterial and wound-healing properties of zinc ions, Elemental can be used post-operatively with or without a membrane.


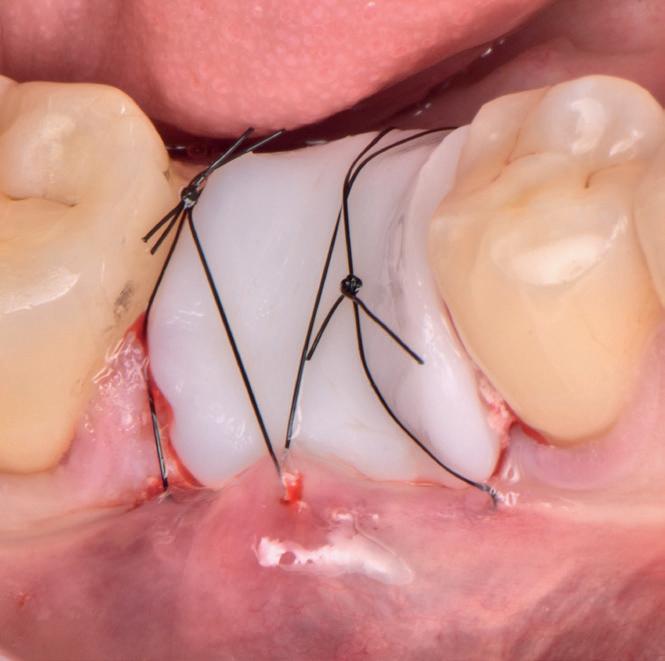
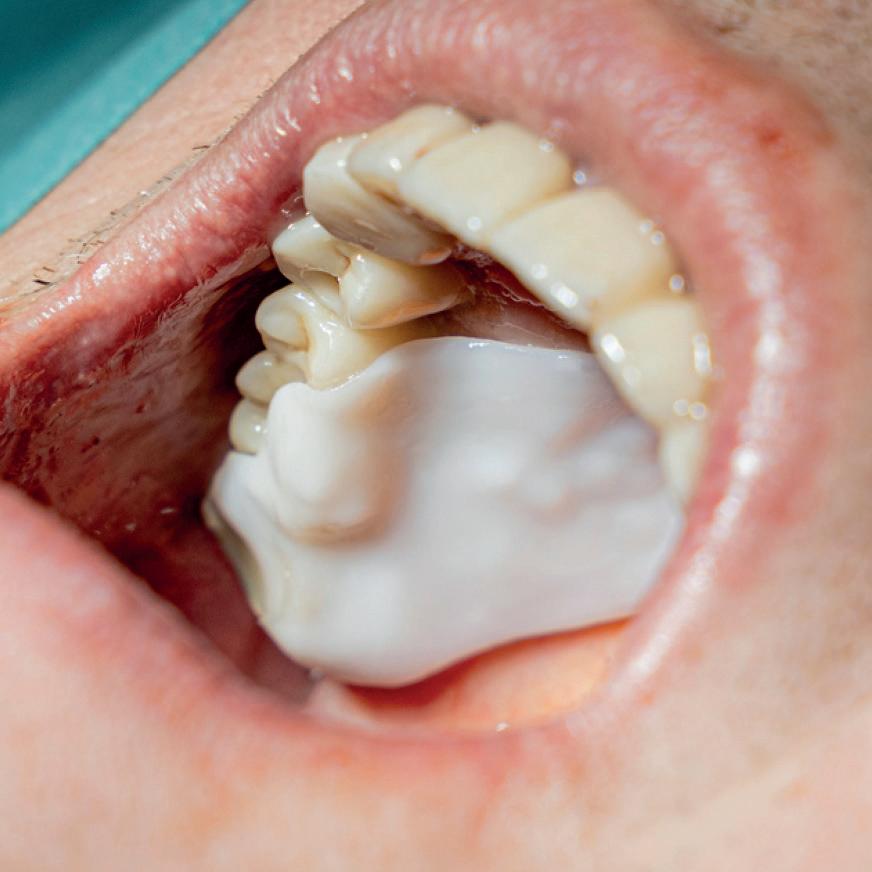
Elemental activates when in contact with boiling water, and the resulting material, which sets rigid and stable, can be quickly and easily moulded and shaped according to the needs of the patient.


























As one of the leading causes of nonodontogenic orofacial pain, temporomandibular joint disorder (TMD) is a major disruptor to everyday life.i Whether effecting mastication and limiting the choice of foods or causing consistent pain that makes it difficult to concentrate at work, the impact of TMD is widespread.
By identifying the aggravating risk factors for TMD, dental practitioners can better help their afflicted patients with managing the condition. Part of this includes learning more about sleep bruxism and being able to understand its correlation with TMD – a contentious link that can often provide contradictory results.

Correlation – but is there causation?
TMD easily progresses from acute to chronic pain; the temporomandibular joint (TMJ) is used throughout the day for talking and eating, whilst parafunctional habits like clenching also mobilise it. Similarly, bruxism is characterised as repetitive jaw-muscle activity, such as the bracing or thrusting of the mandible and grinding, and is self-reported among 12% of the population.i
Research on the association between sleep bruxism and TMD is divisive. One study, assessing an array of literature on the subject, determined that the methodologies used heavily influenced each study’s findings. Effectively, the studies based on a self-reported or questionnaire-based approach to bruxism found an association with TMD.ii This highlights the need for more specific categorisations of both conditions, helping to avoid the conflation of the two.
For sleep bruxism, the Internal Classification of Sleep Disorders has an established criteria, noting the presence of regular or frequent tooth grinding during sleep, morning jaw-muscle pain or fatigue, jaw locking upon awakening, and/or temporal headaches.iii Almost 40% of patients with TMD pain are told by their dentist that they have sleep bruxism, highlighting the overlapping association between the two conditions.iii These patients are expected to exhibit more severe clinical manifestations and report a higher pain intensity.
One of the challenges with defining the association between sleep bruxism and TMD is how the two are often locked in a vicious cycle, raising the question as to which came first. Peak incidence of sleep bruxism is among adults aged 20-40. This is the age for raising a family, finding jobs, owning property and juggling busy social lives. It is unsurprising then that sleep bruxism is linked to elevated levels of stress, anxiety and depression; there’s a lot to manage as an adult. As 90% of TMD patients experience sleep problems (not exclusively sleep bruxism), this increases tiredness the following day, limiting productivity and impacting mood. This decline can further increase stress – the stress hormone cortisol is a significant predictor of sleep bruxism in TMD patients.i

Whilst those with higher levels of cortisol are likelier to grind their teeth, not every sleep bruxer will fall into the cycle of disrupted sleep, impacted mood and TMJ pain. Some studies posit that bruxism itself is a mechanism for stress relief, and is not an exacerbating aetiological factor of it.

For dental professionals, identifying patients who have a higher risk of developing TMD or are showing signs of sleep bruxism (an unawareness they are grinding their teeth or a partner has reported hearing it) is vital to protect their teeth and TMJ. The leading predictors for both conditions are:
• Patient age (20-40)
• Sleep deterioration
• Psychological distress
• Elevated cortisol levels
With these in mind, dental professionals can guide patients towards suitable management strategies. Whilst the discourse around sleep bruxism demonstrates that it may not be a direct cause of TMD, the correlation between the two makes them excellent indicators for the other. If a patient has one, there is a strong chance they have the other due to the shared risk factors, especially around their mental state.
To help patients alleviate the symptoms of TMD and restore strength and function to the jaw, recommend the OraStretch ® Press Rehab System from Total TMJ. A reliable device for at-home rehabilitation, it stretches the orofacial tissues to promote mobility. Diligent use of the OraStretch ® Press, as directed by a clinician, can lead to an improved quality of life, one where jaw pain is no longer a major disruptor to everyday activities – especially sleep.
Whilst easy to look at the overlapping risk factors between TMD and sleep bruxism, the actual cause and effect between the two continues to be controversial. Dental practitioners can help by assessing at-risk patients and highlighting the best ways to limit sleep bruxism and manage TMD for a better night’s sleep and an improved quality of life.
For more details about Total TMJ and the products available, please email info@totaltmj.co.uk n
References available upon request
KAREN HARNOTT

Interdental cleaning is essential for maintaining optimal oral health, as traditional brushing alone cannot reach the spaces between teeth where plaque and bacteria accumulate. Discover TePe’s comprehensive range of interdental cleaning solutions designed to meet the diverse needs of patients.
TePe® Interdental Brush Original
Available in nine sizes, Interdental brushes are the most effective way to remove plaque between the teeth.
TePe Angle™
The long handle and angled head allows easier access to the back teeth from the inside and the outside.


























TePe® Interdental Brush Extra Soft Extra soft filaments for a gentle and safe cleaning around natural teeth and implants.
















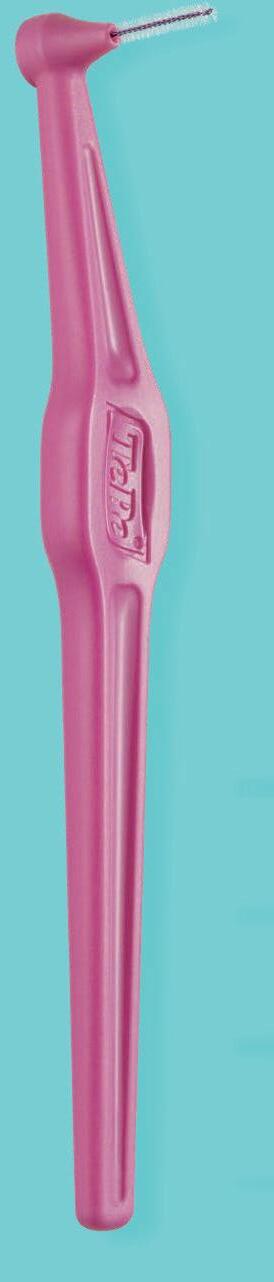







TePe EasyPick™ EasyPicks come in three conical sizes to suit all interdental spaces.
Scan the QR code to view TePe’s products suitable for interdental cleaning.

Pain throughout the gingival tissue is a common symptom of periodontal disease, often accompanied by bleeding during eating or oral hygiene routines, and as well as inflammation.i This discomfort can significantly impact daily life, with patients changing dietary choices or avoiding thorough interdental cleaning due to the soreness it induces.
The latter element can be particularly concerning. Pain throughout the periodontal tissue can be brought on by additional factors such as heavily abrasive brushing – a problem faced by even the most well-intentioned patient. However, avoidance of these effective oral hygiene practices can give way to an increased risk of infection and oral disease, exacerbating the very causes of gingival pain.
Clinicians should be prepared to recognise the causes of gingival sensitivity in any presenting patients. It’s also important to understand how it affects their day-to-day life, and professionals should be able to recommend immediate implementable changes that can improve periodontal health over time.
Traditional oral hygiene routines can cause trauma to the soft tissue, creating gingival abrasions that can cause pain and encourage recession of the tissue. The literature reports that a medium-hard toothbrush is twice as likely to cause tissue damage as a soft toothbrush.ii In the same vein, a medium toothbrush can remove more damaging biofilm than soft toothbrushes.iii To minimise harm whilst maximising the ability to remove plaque and biofilm, patients need to use adopt a more careful technique; gentle, circular brushing that focuses on each tooth surface, and takes care around the gingival margin is key. Proper interdental cleaning should support this, with a variety of solutions available, such as traditional floss or oral irrigators.

Infections linked to periodontal pain are manifold. The most prominent link is periodontal disease; almost a fifth (19%) of adults in the UK have been told they have gum disease.iv Gingivitis will typically present with inflammation and bleeding upon brushing or flossing, as well as dull pain, but progression to periodontitis may create a tender feeling simply upon being touched, which can be troubling for many patients.v,vi As oral hygiene routines improve, and plaque and bacteria is kept away from the gingival margin, patients can expect inflammation to subside over time, and discomfort to fade with it. Discomfort can also be the result of gingival and periodontal abscesses, necrotising periodontal diseases, injuries related to traumas such as piercings, gingival recession, and more.vi Gingival
recession is likely the most prevalent condition of these, and can be caused by aggressive brushing, poor oral hygiene and frequent tobacco use. The reduced width of keratinised connective tissue can once again cause inflammation, which may also increase dentine hypersensitivity.vi
Sensitivity and pain throughout the periodontal tissue can place a significant strain on everyday life. Patients may find certain foods being uncomfortable to eat or meals being interrupted entirely.vii If a patient avoids certain types of food because of this, they could encounter various issues. Harder fruits and vegetables, such as apples and carrots, often contain vital nutrients, and replacing these with unhealthy alternatives can be detrimental.
Inadequate oral hygiene routines and, in particular, interdental cleaning approaches, can be extremely detrimental to gingival health, with evidence of abrasion and physical injury in some cases.viii Whilst patients may be motivated to look after their oral health, and take on new routines such as conventional flossing as a result, the pain caused by this may lead to them ceasing such a behaviour. The benefits of flossing outweigh the risk of damage,viii but an interdental cleaning alternative that reduces any aggravation of pain would be ideal.
Conventional flossing is technique sensitive, and so alternative interdental cleaning solutions may be helpful in order to improve oral hygiene whilst managing pain.ix Patients rely on their dental professionals to provide effective recommendations. ix An oral irrigator could be an ideal solution for individuals with gingival pain, with studies showing a statistically significant reduction in bleeding on probing in just four weeks.ix
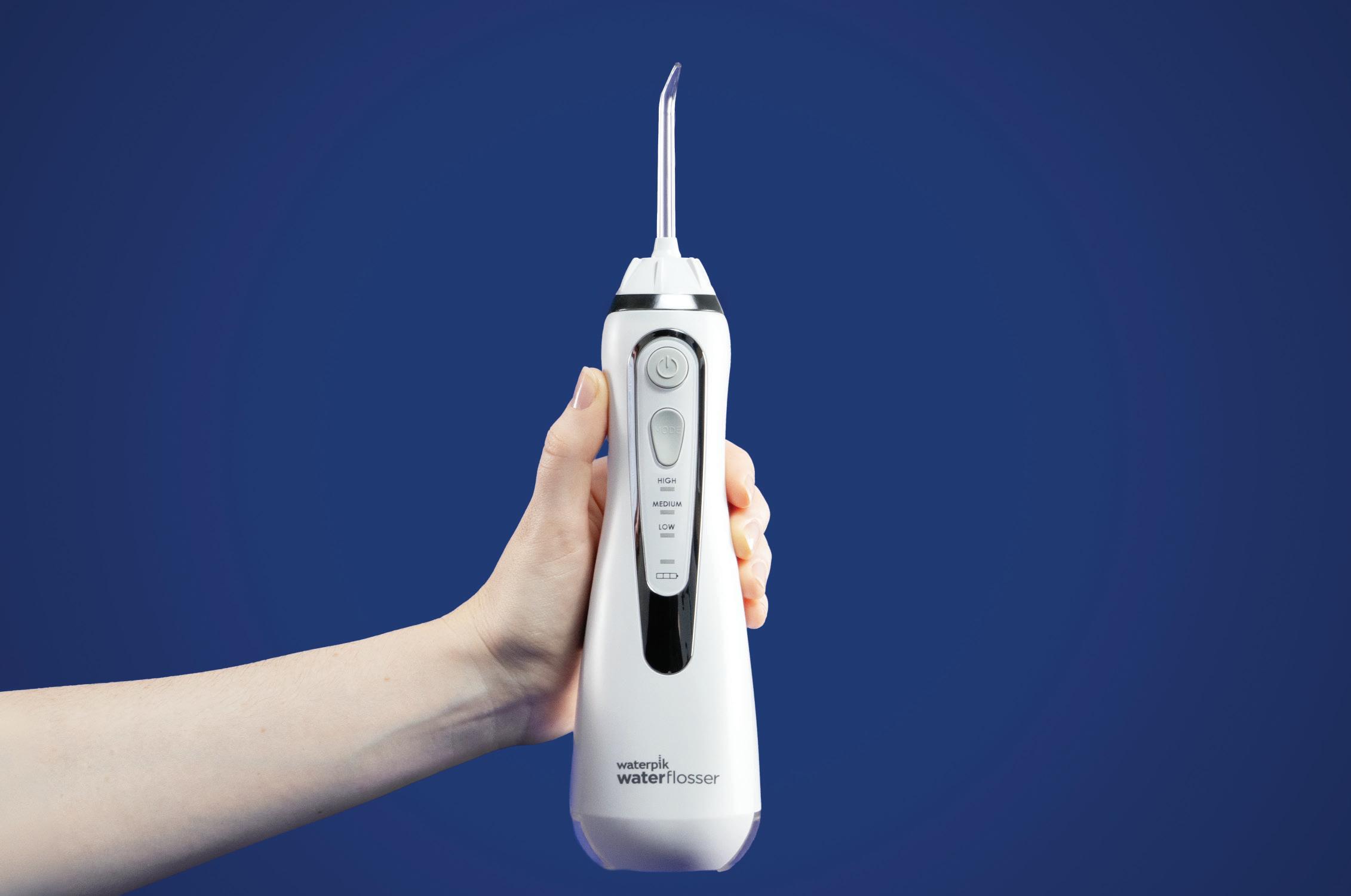
A solution such as the Cordless Advanced water flosser from Waterpik™ can aid patients with up to 99.9% of plaque and bacteria removed with just a three second application,x reaching below the gingival margin and in the interdental spaces, where brushing alone cannot access. Patients with sensitive gums can choose between three pressure settings, for an effective clean without compromising on comfort.

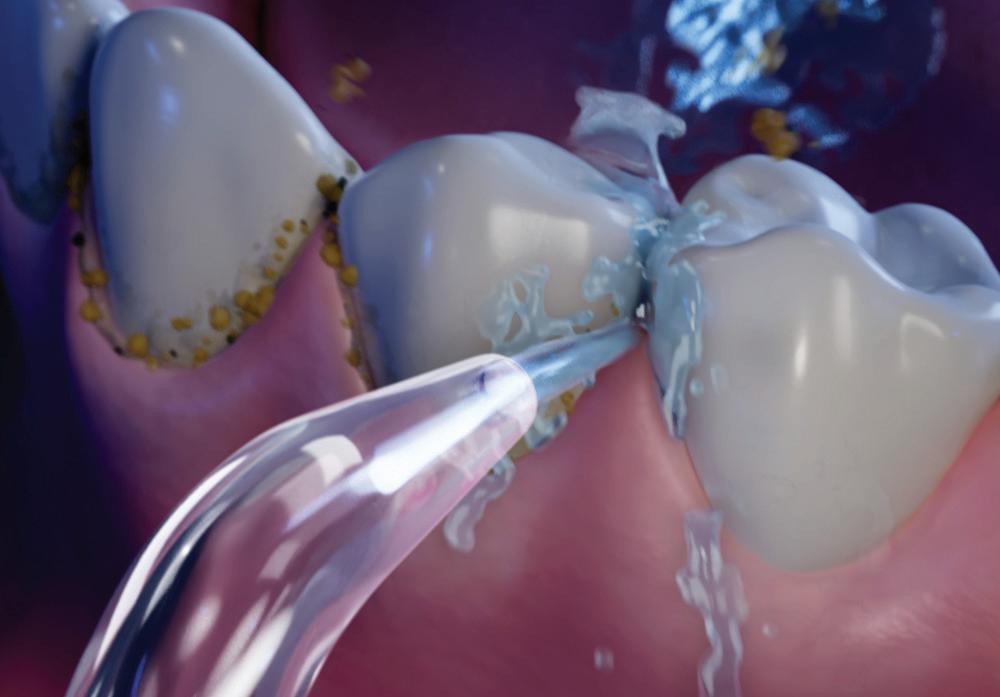
Waterpik™ is the #1 water flosser brand recommended by dental professionals, xi and is the only water flosser brand to be approved by the Oral Health Foundation – ensure you recommend by name.
Pain and discomfort throughout the gingival tissue can be caused by a number of issues, but ensuring gentle and effective oral hygiene routines are in place will minimise risk in a number of ways. This can help patients return to smiling and living in comfort, every day.
For more information on WaterpikTM water flosser products visit www.waterpik.co.uk. WaterpikTM products are available from Amazon, Costco UK, Argos, Boots and Tesco online and in stores across the UK and Ireland. n
References available upon request
RACHEL BENNETT

Oral hygiene needs differ between every patient. Individuals undergoing orthodontic care need to be mindful of irritating brackets and wires, whilst those with implants and crowns will endeavour to maximise the lifespan of their restoration.
Expert assistance is offered by clinicians, who can develop patient’s knowledge and provide them with access to effective solutions through the Waterpik™ Advocacy Programme. Designed to help individuals find effective interdental cleaning aids that can transform their oral hygiene routines, the Advocacy Programme equips practices with everything needed throughout the treatment journey.
It’s important to first understand how Waterpik™ water flossers can support your patients, no matter their needs. Then clinicians can bring the benefits of the Advocacy Programme to their patients, with informed knowledge of the opportunities available for improved oral health outcomes.
Versatility for your patients
Effective oral hygiene routines don’t just stop at twice daily brushing. Interdental cleaning is an essential element that can be forgotten by some individuals. Removing plaque and bacteria that rests in the interproximal spaces and below the gumline minimises the risk of developing caries, bad breath, and periodontal disease. For patients with fixed orthodontic appliances, removing plaque and debris from these areas can be especially difficult. The Cordless Advanced water flosser from Waterpik™ is readily equipped to provide support, thanks to the unique Orthodontic Tip. With this attached, the Cordless Advanced is up to three times as effective as string floss for removing plaque around braces.
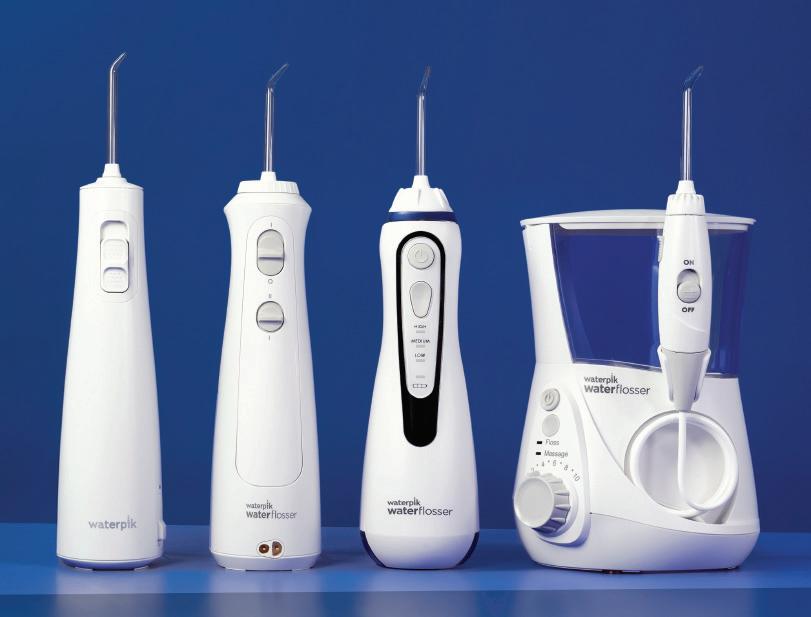
Individuals can use the Orthodontic Tip, which features a tapered brush head to remove plaque and debris in hard-to-reach areas, for a gentle yet effective clean. Together, the Cordless Advanced water flosser and the Orthodontic Tip work quickly – true of any Waterpik™ pairing – with 99.9% of bacteria removed from targeted areas with just a three second application.ii
If an individual needs to debride plaque and bacteria from sensitive areas surrounding restorations, such as an implant or crown, they can opt for the Plaque Seeker™ tip, available with the Ultra Professional countertop water flosser. Bristles connected to the tip help to remove plaque from hard-to-reach areas, whilst flushing out bacteria with gentle water pressure. When used with a Waterpik™ water flosser, the solution is more than two times as effective as string floss for improving gingival health around implants, with research showing a reduction in bleeding.iii

With a greater understanding of the capabilities of the Waterpik™ water flosser, clinicians can better support patients with advanced oral hygiene needs. The Advocacy Programme is designed to help both dental professionals and patients recognise the solutions available to them.
Clinicians that sign up receive a bespoke welcome kit, containing access to a free CPD module with the Health Professional Academy, designed and created in collaboration with Waterpik™. The module called “Should water flossing become an integral part of oral hygiene?”, develops knowledge of why and how to use water flossers, especially for those that face increased difficulties with a standard oral hygiene routine.
Free patient brochures, provided to members of the Advocacy Programme, enable patients to take away key information from every appointment. This means they can spend time considering the Waterpik™ water flossers that meet their needs, and return to the practice prepared with any questions that they may have.
Practitioners also receive unique discount codes that can be used by patients, giving them even better access to industry-leading water flossers that make a difference in their oral hygiene routines.
Want to learn more about the Advocacy Programme, and find out how you and your patients can receive all-new benefits? Visit the Waterpik™ website today.
For more information on WaterpikTM water flosser products visit www.waterpik.co.uk. WaterpikTM products are available from Amazon, Costco UK, Argos, Boots and Tesco online and in stores across the UK and Ireland.
References available upon request








Harry Morris explores why prevention is moving from aspiration to expectation in modern dental practice, and how structured biofilm management is helping teams deliver this shift with confidence.
The aim of this article is to explore why prevention-led dentistry is gaining momentum in 2026 and how Guided Biofilm Therapy can support this approach in clinical practice.
On completing this Enhanced CPD session, the reader will:
• Recognise the key drivers behind the shift towards prevention-led dentistry in 2026
• Appreciate the relationship between oral health, systemic health and long-term disease prevention
• Appreciate the principles of structured biofilm management within preventive dental care
• Identify the key components of the Guided Biofilm Therapy protocol and its clinical applications
• Understand how prevention-led approaches, including Guided Biofilm Therapy, can support patient-centred care and long-term oral health outcomes.
Learning Outcomes: C,D
Dentistry enters 2026 at a point of clear transition. For years, prevention has been championed in policy documents and professional guidance, yet delivery at scale has remained inconsistent. What makes this year different is the convergence of clinical evidence, system reform and patient expectation, shifting prevention from aspiration into everyday practice.
Rising oral disease burden, a growing evidence base linking oral and systemic health, increasing patient expectations and renewed emphasis on prevention within the national healthcare strategy are reshaping how care is planned, delivered and evaluated.
In the UK, oral health inequalities persist, with caries and periodontal disease continuing to affect large sections of the population despite decades of clinical advancement. At the same time, clinicians are seeing more complex patient presentations. Ageing populations, increasing prevalence of long-term conditions, polypharmacy and implantsupported restorations all raise the stakes for ongoing preventive care.
Alongside this clinical reality sits a broader shift in how health is viewed. Patients are increasingly informed, digitally engaged and motivated by long-term wellbeing rather than sporadic intervention. Preventive healthcare, once positioned as a future ambition, is now a consumer expectation, and dentistry is not immune to this change.
Against this backdrop, many practices are re-evaluating traditional models of hygiene and maintenance care. Rather than responding to disease progression, there is growing momentum behind structured, prevention-led approaches that prioritise early detection, patient education and minimally invasive biofilm management.
Oral health, systemic links and prevention
The link between oral health and systemic health is now well established, with periodontal disease associated with conditions including diabetes, cardiovascular disease and adverse pregnancy outcomes. This understanding has practical implications for dental teams, positioning prevention not simply as tooth and gum care, but as part of wider health maintenance.

This shift is also reflected in policy direction. The NHS Long Term Plan and subsequent reform measures have reinforced prevention, early intervention and personalised care as priorities, with recent dental recovery initiatives signalling a move towards prevention being designed into care delivery, rather than positioned as an adjunct to treatment.
Central to this approach is greater utilisation of skill mix, with dental hygienists and dental therapists playing an expanded role in delivering preventive care, periodontal maintenance and patient education. This reflects recognition that prevention-led dentistry cannot be delivered by dentists alone, and that enabling the wider team to work to full scope is essential to embedding prevention consistently across patient pathways.
For practices, this creates both opportunity and responsibility. Skill mix offers a practical route to scaling prevention, but consistent delivery depends on clear approaches to diagnosis and delegation, supported by structured systems and protocols that align assessment, treatment and maintenance. Central to this shift is greater emphasis on risk-based maintenance and recall, allowing preventive care to be tailored to individual disease susceptibility rather than delivered as a one-size-fits-all intervention.
One of the most visible changes within prevention-led dentistry is the reframing of the hygiene visit. Traditionally perceived by patients as a routine scale and polish, the modern hygiene appointment is increasingly positioned as the foundation of preventive care.
This evolution reflects a deeper understanding of biofilm as the primary aetiological factor in caries and periodontal disease. Biofilm is invisible, persistent and patient-specific. Managing it effectively requires assessment, disclosure, motivation and targeted removal, rather than forceful instrumentation alone. Clinical research over several decades has demonstrated the impact of consistent plaque control and professional maintenance on long-term oral health outcomes. Landmark longitudinal studies by Axelsson, Lindhe and colleagues showed that structured preventive programmes could significantly reduce caries, periodontal disease and tooth loss over periods of 15 to 30 years.1-4 These findings underpin much of modern preventive dentistry and remain highly relevant today.
More recent research has explored how advances in air polishing, plaque disclosure and minimally invasive technologies can enhance both clinical outcomes and patient experience. Systematic reviews and randomised controlled trials have shown that air polishing with low-abrasive powders can effectively remove supra- and subgingival biofilm, support periodontal maintenance and improve comfort compared with traditional approaches.5-7 For busy practices, the challenge lies in translating this evidence into workflows that are repeatable, efficient and aligned with patient expectations. This is where structured protocols have gained traction.
Guided Biofilm Therapy (GBT), developed by EMS in collaboration with the Swiss Dental Academy (SDA), offers a structured, evidence-based approach to preventive and maintenance care. Rather than a single technology or product, GBT is a clinical protocol designed to support systematic biofilm management across a wide range of indications. At its core, GBT is built around eight sequential steps: assessment, disclosure, motivation, targeted biofilm removal, calculus removal only where necessary, and recall planning. Each stage is supported by clinical evidence and designed to promote minimal intervention with maximum effect.6,7
The emphasis on disclosure and patient education is particularly significant. Making biofilm visible transforms the hygiene visit into a shared experience, where patients can see, understand and engage with their own risk factors. Studies have shown that visualisation techniques improve oral hygiene behaviours and enhance patient motivation, reinforcing the role of education within preventive care.8
From a clinical perspective, the use of air polishing with low-abrasive powders allows biofilm to be removed efficiently from teeth, restorations and implants. This supports comfort, reduces chair time in many cases, and aligns with a minimally invasive philosophy.
GBT is indication-oriented, so that treatment is tailored to individual diagnosis and risk. This flexibility is particularly relevant in practices managing diverse patient groups, from children and anxious patients to those with periodontal disease or dental implants.
Patient acceptance plays a critical role in the sustainability of preventive care. Such protocols are only effective if patients attend regularly, engage with advice and feel positive about their experience.
Large-scale patient surveys referenced within EMS clinical literature have consistently reported high levels of satisfaction with GBT-based care, including a strong preference compared with conventional prophylaxis. Patients commonly cite comfort, reduced pain and a clearer understanding of their oral health as key factors influencing their preference.9
These findings reflect broader trends within healthcare, where patient experience, shared decision-making and perceived value increasingly influence compliance and loyalty. For dental teams, a preventive approach that patients actively prefer supports long-term engagement and recall adherence.
As dentistry moves further into 2026, preventionfirst models are becoming a defining feature of progressive practices. This shift is not limited to private dentistry. Across mixed and NHS settings, clinicians are seeking ways to deliver prevention more effectively within existing constraints. Several factors are accelerating this change, including ongoing workforce pressures that require practices to adopt more efficient and predictable

1. What is recognised as the primary aetiological factor in caries and periodontal disease?
a) Calculus accumulation
b) Poor brushing technique
c) Biofilm
d) Dietary sugar
2. How is Guided Biofilm Therapy defined in relation to preventive and maintenance care?
a) A single air-polishing technique
b) A structured, evidence-based approach to preventive and maintenance care
c) A product-based hygiene system
d) A replacement for periodontal therapy
3. How many sequential steps form the Guided Biofilm Therapy protocol?
a) Six
b) Seven
c) Eight
d) Ten
4. Which approach underpins prevention-led dentistry in contemporary clinical practice?
a) Minimally invasive management of disease risk
b) Reactive treatment planning
c) Symptom-led intervention
d) Forceful debridement
5. Which practice model is increasingly being adopted in response to clinical, patient and system pressures?
a) Treatment-focused practice
b) High-volume practice
c) Technology-led practice
d) Prevention-first practice
workflows, rising patient expectations for clear communication and evidence-based care, and continued emphasis from regulators and commissioners on prevention and risk management. At the same time, clinicians increasingly value approaches that support professional satisfaction and align with ethical, prevention-focused care. Structured preventive protocols offer a way to meet these demands. By standardising assessment, disclosure and treatment planning, teams can deliver consistent care while retaining clinical autonomy. Education becomes embedded within the appointment rather than an optional extra, while recall intervals can be tailored based on risk rather than routine.
Prevention in dentistry has moved from ambition to necessity. Clinical evidence, understanding of systemic health, patient expectations and healthcare policy are now converging, making 2026 not simply a moment of change, but a point at which preventionfirst practice becomes the expected standard of care. For dental teams, embracing prevention-first care is not about adopting a single technique or technology. It is about committing to a philosophy that prioritises early intervention, patient education and minimally invasive management of disease risk.
GBT provides one framework through which this philosophy can be delivered in daily practice. By combining decades of preventive research with modern technology and structured protocols, it supports clinicians in translating prevention from principle into practice.
As the profession continues to evolve, the practices that thrive will be those that place prevention at the centre of care; not as an add-on, but as the foundation of everything they do. n
References available upon request

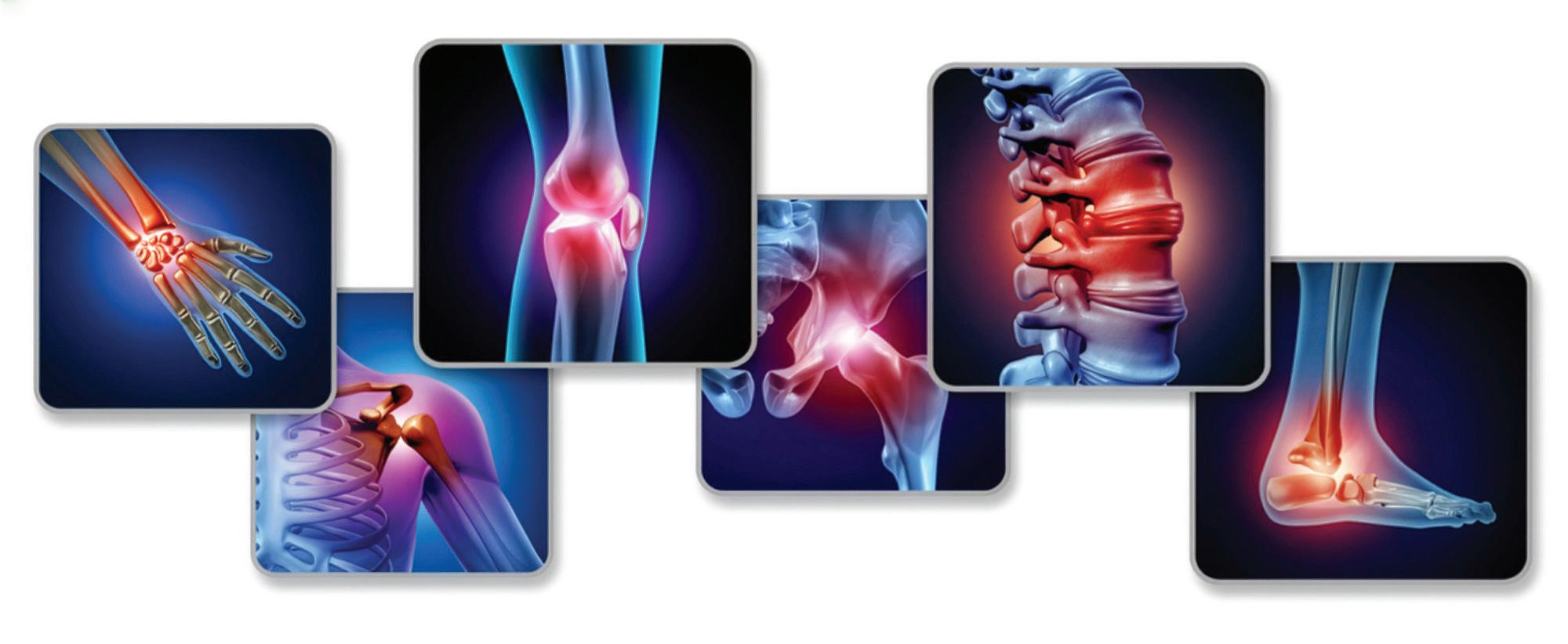
Rheumatoid arthritis (RA) is a chronic autoimmune disease in which a person’s synovial linings are attacked by their immune system throughout the body. RA causes joint inflammation, which, in extreme cases, can progress to permanent joint damage and disability. i
Affecting at least 1 in every 200 adults worldwide, rheumatoid arthritis has long been categorised as a disease of the musculoskeletal system.ii However, research also indicates that RA extends beyond joints, with oral health – particularly periodontitis – being regarded as a factor in the onset and progression of the disease. Research surrounding the connection between oral conditions and inflammatory arthritis dates back centuries, with Hippocrates suggesting that tooth removal could cure arthritis.iii
Shared inflammatory responses
Rheumatoid arthritis and periodontitis share the same processes of chronic inflammation – the suffix of “-itis” itself quite literally connotes inflammation.iv In RA, the joint linings’ destruction causes stiffness, extreme swelling, and ultimately, complete joint deterioration.
Similarly, in periodontitis, microbial plaque builds up along the gingival margin, instigating an intense immune response. This eventually provokes an exaggerated reaction, resulting in the disintegration of periodontal tissue and the alveolar bone.v
The interchange between these inflammatory mechanisms has led to evidence surrounding the bidirectionality of the relationship. There is a high correlation between patients suffering with RA and their rate of periodontitis compared to the general population. Furthermore, severe periodontitis can intensify systemic inflammation and exacerbate the symptoms of RA further.
Rheumatoid arthritis and xerostomia
Dependent upon the severity of the condition, RA is treated through various methods. This ranges from over-the-counter analgesics, anti-inflammatory medication, disease-modifying antirheumatic drugs, and in some cases, surgery.vi Unfortunately, a side effect of many of these medications is decreased salivary flow.
RA is strongly associated with xerostomia symptoms indicative of reduced salivary flow even in patients who are not taking xerogenic medications – affecting more than 50% of RA patients.vii Furthermore, RA is linked to conditions such as Sjögren’s
syndrome (SS), which is also associated with xerostomia.viii Due to this connection, patients with RA are more likely to experience periodontitis as a result of xerostomia reducing the oral clearance effect of the saliva.
Joints and dexterity
RA can directly impact the temporomandibular joint (TMJ), causing severe pain in the entire orofacial region.ix Due to the inflammation in the TMJ, the cartilage and other structures become damaged, causing stiffness and restricted movement, particularly in opening the mouth.
The relationship between RA and oral health is far from restricted to biology – there is also a functional element of bidirectionality. RA is renowned for compromising dexterity and grip strength, which further impairs patients’ ability to perform effective oral hygiene procedures and routines. Consequently, more plaque accumulates, instigating greater susceptibility to gingival inflammation. This vicious cycle is sustained by the individual’s inability to efficiently manage their oral health – an issue that is exacerbated by RA to begin with.
The systemic and practical challenges that RA patients face must be considered by dental professionals, with considerate oral health interventions tailored to each individual’s capability.
Prevention and management

The right strategies and support can alleviate the symptoms of both RA and periodontitis. Oral health can be proactively managed with twicedaily toothbrushing, daily plaque control, the use of fluoride products, and effective interdental cleaning.
Even without the dexterity difficulties associated with toothbrushing, it is commonly understood that using toothbrushes alone is inadequate in removing dental plaque, with evidence suggesting that 40% of dental plaque remains.x This means that combined with limited dexterity, the effectiveness of toothbrushing alone is insufficient.
The role of interdental cleaning
Interdental areas are extremely susceptible to gingival inflammation which makes thoroughly cleaning them vital to reduce the risk of periodontal disease, which may in turn reduce the risk of developing RA. For individuals living with RA, interdental cleaning often presents a challenge. Regular floss is difficult to operate due to patients’ minimal hand
function. This is evident through the anatomical and neuromuscular changes, the muscle, grip, and pinch strength loss, and diminishment of sensory management and coordination experienced by those with RA.xi Due to this, the success of conventional dental flossing is limited for RA patients. Interdental brushes, however, provide a practical and effective alternative.
High quality tools like the FLEXI interdental brushes from TANDEX promote healthy gingivae by reducing the amount of plaque build-up. FLEXI brushes are available in 11 different sizes, delivering tailored care to each individual circumstance –accommodating anatomical variation for all stages of RA. The ergonomic design of the brushes improves ease of use for those with joint stiffness and minimal dexterity, offering them an alternative against their physical limitations. Combining the brushes with the TANDEX PREVENT Gel allows patients to take full control of their oral health. Containing 0.12% chlorhexidine and 900 ppm fluoride, the gel delivers anti-caries and anti-inflammatory advantages which is ideal for minimising periodontitis in RA patients.
support against inflammation
The research connecting rheumatoid arthritis and oral health continues to evidence that the successful management of periodontal disease extends beyond the oral cavity, but can positively impact more systemic health and wellbeing too. Supporting patients with tailored, accessible, and effective advice and tools allows dental professionals to provide more considerate and holistic inflammation control.
For more information on Tandex’s range of products, visit https://tandex.dk/
Our products are also available from DHB Oral Healthcare https://dhb.co.uk/ n
References available upon request
JACOB














As the pressure of practice grows, your wellbeing matters too. With confidential counselling and wellbeing support available at no extra cost, Dental Protection is by your side every step of the way. It’s time to put yourself first, with the support you deserve.












In dentistry, pain – particularly toothache –remains one of the most common reasons for patients seeking treatment, but is often more than a simple, short-term issue. The oral cavity and teeth are heavily innervated by the trigeminal nerve, one of the largest cranial nerves. Due to this, oral pain is more than an isolated issue and presents in various intensities – bringing great discomfort to most, and can even be debilitating for some.
Toothache can arise suddenly and affect every day wellbeing like sleeping, working, mood, and confidence. Dental professionals have both the duty to identify the clinical cause of toothache and to guide patients through safe and effective methods of management until clinical treatment is completed, if necessary.
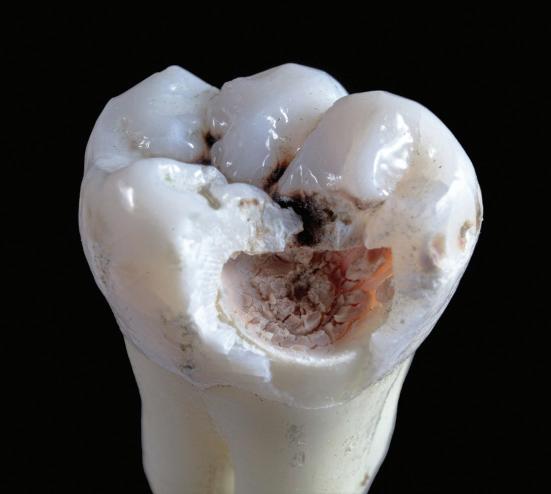
The nature of toothache
Toothache presents in several ways, from transient or intermittent pain, to more acute or persistent pain. The underlying causes are just as varied: reversible pulpitis, for example, can produce rapid, sharp twinges of localised pain when exposed to thermal stimuli – this fast pain conduction is due to the nerve pathway of myelinated A-delta fibres (A∂ fibres). Conversely, unmyelinated C-fibres are responsible for slower pain conduction which is difficult to localise – their pain activation signifies that the pulp damage could be irreversible.
Caries-related irreversible pulpitis is caused by the progression of bacterial infection and inflammation that decays into the dental pulp which can lead to the eventual need for root canal treatment. Other causes of toothache include cracked teeth, occlusal trauma, exposed dentine, and more.
Starting with emotional support
Dental professionals deal with a plethora of intense cases daily. However, regardless of the extremity of a case, something that may seem slightly minor in contrast, like toothache, can feel colossal to a patient – particularly when it is evidenced to interfere with eating or socialising.


Anxiety and fear can exacerbate the sensation of pain and many patients often fear that oral pain can mean something serious that will worsen whilst anxiously awaiting a dental appointment. For professionals, treating this unease is as important as clinical treatment –particularly in preventing patients from assuaging these feelings and sourcing their own relief with remedies that could do more harm than good.
Guiding efficient self-care
There are many “home remedies” that patients might attempt to find relief. These are often unverified methods, and can actually inhibit or exacerbate the initial problem such as alcohol-based mouth washes or hot compresses. Moreover, though “home remedies” might seem to ease anxieties and mildly diminish discomfort, a recent study evidenced that only 26% of individuals found that they helped “a lot”, with 10.6% declaring them “not at all” effective.
As such, dental professionals should intervene, with safe, pharmacy-available options being recommended until appointments and treatments are available. In discussing self-care, each minor detail has an impact on the reception and fulfilment of such – small details matter. Patients that understand their pain, and available relief options, are more likely to progress confidently and compliantly in their path to recovery.
Long-term toothache solutions begin with addressing the cause – from caries removal or endodontic therapy to full extraction or occlusal adjustment. Yet, to bridge the gap between presentation and treatment, evidence-based selfmanagement strategies are most useful, especially as alternatives to hindering “home remedies”. Primarily, systemic analgesics are both accessible and effective methods of pain relief – which should be recommended with appropriate advice. Alongside systemic medication, topical treatments can offer a huge consolation. The targeted nature of the medication makes relief more localised and source-specific. As such, offering patients a method of self-managing their discomfort can assist them both physically and psychologically – allowing them to regain control over their pain and recovery. Practitioners should explain how topical gels work, the recommended frequency of use, and when to seek professional intervention.
Orajel® has paved the way of dependable and effective oral pain management for decades. Within its range, Orajel® Dental Gel is the ideal solution for toothache pains. Offering rapid toothache relief where and when you need it most – delivering localised treatment in under 2 minutes. The gel contains 10% w/w benzocaine, a local anaesthetic that temporarily blocks the pain signal pathways along the nerves – numbing the area for up to 2 hours of relief. Orajel® also offer an Extra Strength option, containing 20% w/w benzocaine, for those seeking a stronger solution to their discomfort. The Orajel® Extra Strength Gel can be found at the pharmacy and should not be used consistently.
Toothache extends far beyond solely the oral pain, but can impact major aspects of a patient’s wellbeing – from eating and sleeping, to socialisation, and more. Dental teams can best assist their toothache patients firstly by offering empathy-driven understanding into the pain and anxieties associated with their suffering.
Furthermore, self-management advice is critical in ensuring the avoidance of detrimental ”home remedies”, guaranteeing that patients are sourcing evidence-based solutions whilst awaiting professional treatment.
Visit www.orajelhcp.co.uk to explore the full Orajel range. n
References available upon request
SUMERA BASHIR

Dental pain can have a huge impact on patients’ lives – affecting their work, sleep, and ability to eat the foods they love. Because of this, it’s important that the dental team can help to assist patients in their pain management, even before they visit the practice.
Toothache causes, management, and relief
When the dental pulp is exposed, irritated, or inflamed, patients experience toothache. There are a number of causes for this to happen, including dental decay, dental fracture, receding gums, or dental treatment complications – like a loose filling, for example.
There are a number of triggers which may cause the pain to worsen, and it can be helpful to make patients aware of these to help them avoid pain whilst they wait for a dental appointment. These triggers include:
• Cold food or drinks
• Sweet foods
• Biting down whilst eating, for example
• Pressure, such as from orthodontic treatment
Orajel® Dental Gel is ideal for patients with toothache. It contains 10% benzocaine, a powerful local anaesthetic, which reduces pain associated with a broken tooth or a tooth that may require a filling. Patients are able to apply the gel directly to the painful area, giving them control over the product, allowing it to provide targeted relief. Unlike traditional pain relief methods, including painkiller drugs and hot and cold compresses, Orajel® Dental Gel works almost instantly, reaching its full effect in under two minutes.
For patients experiencing more acute toothache, Orajel® Extra Strength is an excellent solution. It
delivers rapid pain relief as its formula features the maximum level of benzocaine available without a prescription (20%) – with individuals able to purchase it at the pharmacy. In the same way as Orajel® Dental Gel, Orajel® Extra Strength can be applied directly to the affected tooth, for effective and targeted relief, quickly.
Mouth ulcers and denture pain
Of course, toothache is not the only reason a patient might contact their dental practice reporting pain in their mouth. Mouth ulcers can be incredibly uncomfortable, sometimes leading people to contact their dentist and ask for advice. Usually they are minor, caused by trauma to the mouth – for example, biting the cheek or injury during brushing, and heal without medication.
Whilst they usually heal on their own, mouth ulcers can be painful. As such, it’s important to offer patients appropriate advice to help them manage their pain whilst they heal. This might include avoiding triggers:
• Lowering stress, as fatigue and emotional stress are associated with mouth ulcers, ensuring patients aim to increase rest and relaxation


• Chewing carefully to avoid further or worsening mouth injuries
• Avoiding hot, spicy, and acidic foods to prevent mouth ulcers from becoming more painful
In terms of actively reducing pain, Orajel® Mouth Gel is a fantastic choice. The gel contains 10% benzocaine, and provides temporary relief of pain from mouth ulcers and from wearing dentures. By managing their pain at home whilst they heal, patients are able to maintain their quality of life, keep their teeth clean, and eat a balanced diet.
Dental pain is a very common issue, with an Orajel® 2025 Survey revealing that 50.8% of dental professionals are contacted by a patient in dental pain every day. In order to meet this demand, 74.2% of respondents reported that they usually offer an emergency appointment on the same day, with a further 18.2% offering emergency appointments the next day. As such, it is sometimes necessary to offer advice for at home management of pain, particularly if patients are waiting hours or days to be seen by a clinician.
Pain relief gel is an excellent option for patients who require immediate relief from dental and mouth pain. Orajel® contains benzocaine, which enables patients to apply the local anaesthetic to the painful area, making it incredibly easy to use, and ensuring very fast results, perfect for those awaiting emergency dental appointments.
For essential information, and to see the full range of Orajel products, please visit https:// www.orajelhcp.co.uk/



SLS-free and non-foaming –gentle on dry and sensitive mouths 1450ppm fluoride and xylitol to help protect teeth


Designed specially for individuals experiencing dry mouth, taste sensitivity, or aversions to strong flavours. No added flavours















The design of a dental practice has an impact on many aspects of the business. Everything from the patient experience to the professional workflow, and the health and safety of all on the premises, will be influenced by the layout of the practice. For principals, whether starting from scratch or refreshing an existing business, it is crucial to integrate intentional design elements that will add value to patients, the professional team and the business.
Dental practice design can have an emotional and psychological impact on patients from the moment they walk through the doors. Research has found that design features such as ambient lighting, indoor plants, and seating options can help to reduce stress levels among patients. Colour psychology – with a focus on blues, pinks, greens, and yellows – can also be implemented within the décor to lower patient anxiety. A clutter-free reception and waiting area contributes to reduced tension and a more calming atmosphere as well.
Boosting productivity
The research also demonstrates the benefits of ergonomic practice design for the wellbeing of professionals. When ergonomic principles are applied – such as dental chairs or stools that improve posture – professional health is protected and the risk of musculoskeletal disorders is reduced. Improved ergonomics have several other benefits for the business, including increased productivity. This is achieved not only by minimising the risk of professional injuries and staff absence, but also has positive implications for daily workflows across the practice, which can lead to improved patient satisfaction. Spatial design has been shown to increase the efficiency of the healthcare team, allowing faster patient care with no compromise on the quality of care delivered.
One of the most important benefits of effective dental practice design is the enhanced health and safety standards it facilitates for patients and
staff alike. The decontamination workflow requires significant attention in order to ensure practice compliance, streamline processes, and maintain reliability for complete peace of mind.
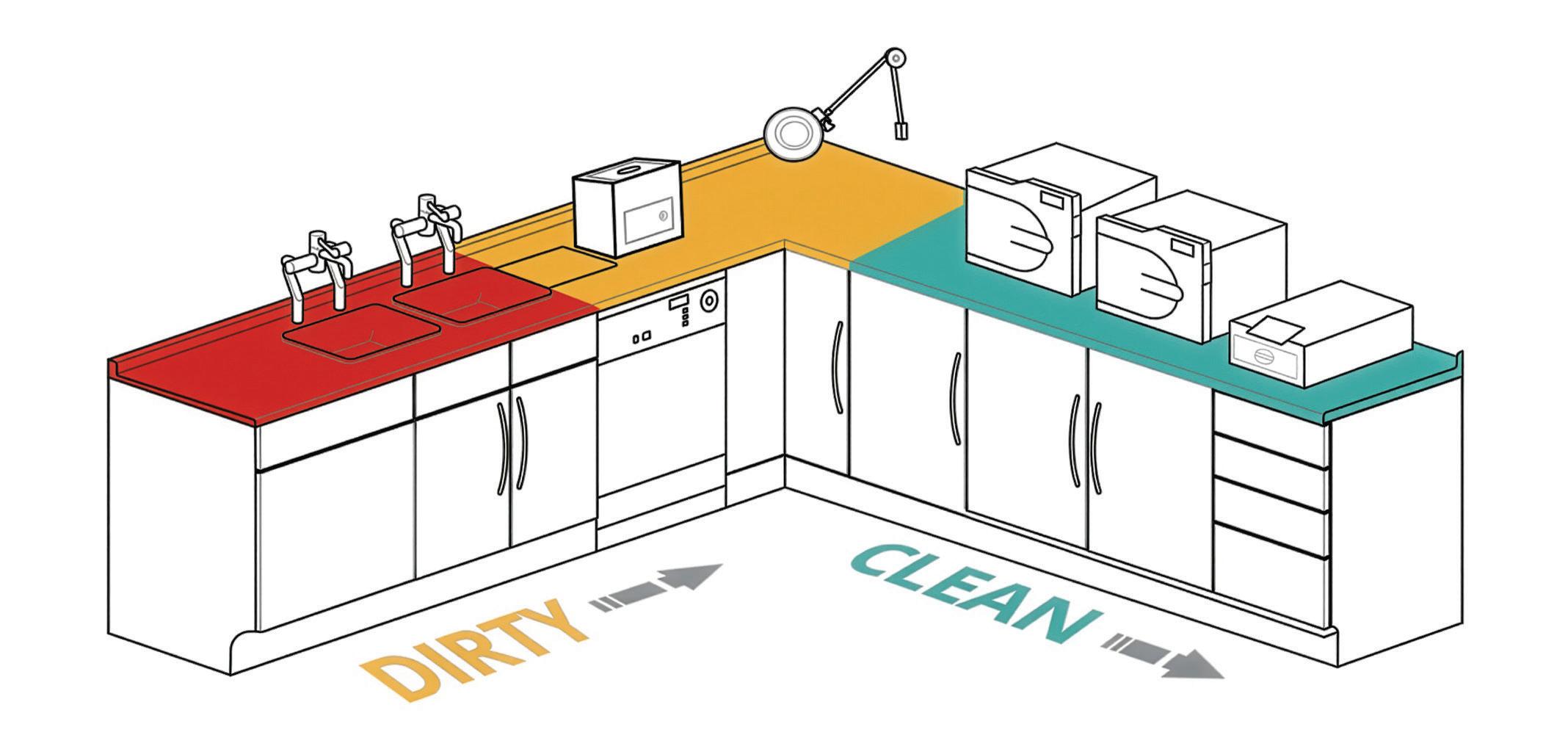
A dirty-to-clean workflow should be implemented for the cleaning, disinfection and sterilisation of reusable instruments. Best practice guidelines encourage practices to assign a separate room. As such, the physical layout of the space should ensure that dirty and clean items are kept apart. The objective is to minimise the risk of contaminating clean instruments via inadvertent contact with dirty items.
For practices without the space for a dedicated decontamination room, the instrument reprocessing area must be located as far from the dental chair as possible. Measures are also required to reduce the risk of exposure to bacterial aerosol, such as not manually washing instruments or using an ultrasonic cleaner without a lid when a patient is in the room.
Achieving this dirty-to-clean workflow relies on a carefully designed physical environment. Firstly, the space should be uncluttered, with places for all equipment and instruments to be kept tidy. The ‘dirty’ area or room should be set up to receive used instruments. Initial cleaning and disinfection should occur adjacent to the dirty area. Manual cleaning is possible at this point, although a washer disinfector affords several advantages over manual processes by automating and validating this step in the workflow.
After visual inspection of the instruments, they are then due for sterilisation in the autoclave, which should be situated in the clean area as far from the dirty receiving area as possible. Figure 1 offers an example of how the decontamination room could be designed and where each piece of equipment may be situated in relation to others.
Whether you are updating your existing practice design, expanding your surgeries or setting up a new squat practice, meticulously planning the
layout is crucial for success. From your entrance area to reception and the waiting room, the surgery and the bathrooms, your patients will expect a modern, comfortable, and safe space.
To achieve all this while managing budgets and future-proofing the practice, it can be invaluable to seek the advice of specialists in their respective fields. For example, Eschmann is the expert in instrument decontamination, and the team is more than happy to provide guidance and support on the design of your infection control area(s). With years of experience and extensive market knowledge, Eschmann offers bespoke advice, industry-leading equipment and ongoing support that will help you elevate your safety standards no end.
Thoughtful practice design will impact the team and patients in a number of ways. The right layout can improve the patient experience by promoting positive emotions and increasing efficiency of their care. Professionals also benefit from improved ergonomics and productivity. The design of the decontamination area is particularly important for the health and safety of all.
For more information on the highly effective and affordable range of decontamination solutions available from Eschmann, please visit www.eschmann.co.uk or call 01903 753322 n
References available upon request
NICKY VARNEY,


For little ones, losing a tooth is more than just that… it’s a magical dental milestone. It’s a moment driven by excitement, wonder, and the dream of being visited by the tooth fairy. Now, imagine a combination of using that bright, imaginative moment to simultaneously educate children on lifelong oral health. Curaprox realises this possibility with its Tooth Fairy Gift Set, a wonderfully packaged collection designed to celebrate children’s priceless moments whilst subtly introducing them to correct and effective brushing habits, keeping it fun and augmenting the entire experience.
From magical milestones to healthy habits
The tooth fairy has long been a welcome part of a child’s upbringing , but beyond the handwritten letters exchanged for token gifts and coins, this moment can also be reutilised. Imagination is the perfect tool for parents/guardians to educate their children, and good oral hygiene habits being taught early on will last a lifetime.
Curaprox upholds the fantastic balance between playfulness and truly effective oral care, revolutionising the field with this enchanting gift set. It includes a high-quality, super soft Curaprox children’s toothbrush, specially adapted for little hands and developing gingiva. With ultra-soft Curen® filaments, it is gentle on the hard and soft tissues, whilst offering a thorough clean with the efficient easy-grip and hexagonal shaping.

All this comes packaged with a little fairy magic – offering an enchanting tooth pouch to safely store the teeth and handy ‘Tooth Receipts’ to assist parent/guardians in maintaining excitement after the departure of the tooth fairy.
Perfect for dental practices, perfect for home
For parents/guardians, the Tooth Fairy Gift Set is more than merely another exciting product for their children, but a reliable, approved tool that offers fun and lifelong oral health support.
The Tooth Fairy Gift Set isn’t just for home use. It’s a handy addition to any dental practice wanting to reduce paediatric patients’ anxieties and enhance their experience, making it – and your practice – memorable for all the right reasons. Proposing the purchase of the gift set after a check-up or treatment creates a lasting impression, helping to create positive associations with visits to the dentist.
fun into learning
The holistic experience of combining amusement, education, and health, make for the perfect learning environment, proven to enhance more longstanding habits.i The addition of a five-step guide to teeth cleaning, which is bright and aesthetic, pushes learning even further. Additionally, the fairy door hangar, educational activity packs, and a tooth chart to further anatomical understanding, each help to make oral hygiene a pleasure and not a chore, encouraging knowledge retention.


The magic continues through the flavour of the Curaprox Kids toothpaste – a juicy watermelon delight in a vibrant pink colour. With a fluoride content of 1,450ppm, this toothpaste provides deciduous teeth with effective caries protection as well as helping to defend against acid attacks from food and drinks. The Curaprox Kids toothpaste has an SLS free formula and is free from microplastics. Designed to work in harmony with children’s mouths, no harmful ingredients are incorporated within the product, and the low abrasion formula also contains xylitol and enzymes for additional protection and a healthier mouth for kids.
With evidence supporting the sentiment that children prefer toothpaste flavour options other than mint,ii this product personalises their experience even further by reinventing a once-monotonous chore.
Tooth fairy visits have always been an enlivening tradition, but by adding the extra layer of Curaprox’s Tooth Fairy Gift Set, they can be revolutionised. They offer a simple and effective chance to support the building of positive habits, reduce dental anxiety, and establish healthy oral care well into the future. Learn more about the magical combination of fun and learning with Curaprox’s Tooth Fairy Gift Set. To arrange a Practice Educational Meeting with your Curaden Development Manager please email us on sales@curaden.co.uk
For more information, please visit www.curaprox. co.uk and www.curaden.co.uk n
References available upon request
The seamless Sensei Cloud from Carestream Dental Agility, and connection. Sensei Cloud from Sensei, the practice and patient management brand of Carestream Dental, offers all this plus peace of mind, so dental professionals can focus on what’s important – delivering remarkable patient care.
Modern dental practices require modern workflows with minimal risk and resilience to change. The cloudbased platform offers this flexibility, whilst eliminating the need to update systems or worry about backups. Your data is stored and protected in Microsoftmanaged data centres, enhancing its uninterrupted performance and reliability.
On the note of seamless operation is the streamlined transition to Sensei software. Carestream Dental ensures undisrupted migration with additional
Whether you are looking for a permanent or locum role, Dental Elite offers a comprehensive recruitment service that can quickly match to you your ideal position.
The now reunited Dental Elite locum recruitment dream team – Luke Arnold and Lisa McCusker – are back together and helping practices across the UK source Locum Dentists and Dental Hygienists. They have had so much success recently that they have broken their own record for the largest number of locum shifts allocated in one month! A figure they look to break again this month…
For support you can rely on, whether you’re looking for permanent or locum roles, contact
Effective, natural protection
A new, effective chlorhexidine-free mouthwash –introducing the Perio plus Zero from Curaprox. Featuring a next generation formula to support oral prophylaxis, the Perio plus Zero offers powerful protection against harmful bacteria. Without chlorhexidine, it better maintains the natural balance of the oral microbiome and can specifically target the pathogens responsible for caries and gum disease.
The advanced formula uses a biohacking method: it disrupts bacterial communication and inhibits the formation of harmful colonies. This reduces the build-up of plaque and the risk of oral diseases.
Ideal for treating halitosis, xerostomia, gingival diseases and orthodontic patients, Perio plus is
guidance and support for future upgrades too.
The innovative, userfriendly platform makes it the perfect addition to any modern practice, empowering you to optimise patient care and accelerate growth.
Find out more about future-proofing your practice with the Sensei Cloud today!
For more information on Sensei Cloud visit the website below.
For the latest news and updates, follow us on Facebook and Instagram @carestreamdental.uk
gosensei.co.uk

Dental Elite today to find out more.
For more information on Dental Elite visit www.dentalelite.co.uk, email info@dentalelite.co.uk or call 01788 545 900
dentalelite.co.uk
suitable and effective for both short and long-term use.
An excellent synthesis of ground-breaking science and prophylactic power, recommend Perio plus Zero from Curaprox today.
To arrange a Practice Educational Meeting with your Curaden Development Manager please email us on sales@curaden.co.uk.

For more information, please visit www.curaprox.co.uk and www.curaden.co.uk.
curaprox.co.uk
The WaterpikTM Cordless Advanced offers convenient oral care, without compromising on quality.
The device is perfect for travel being compact yet powerful. It is rechargeable, waterproof, and portable, which combined with its ergonomic design make it ideal for patients requiring a practical solution for on-the-go oral care.
Better yet, the four-hour rapid charge, lightweight design, and compatibility with global voltage make it the perfect travel companion. The tip storage case and travel plug prevent leakage during transportation, paired with the handy travel bag to enhance your mobile oral care further.
With three pressure settings and a 45-second water capacity, the Cordless Advanced establishes
a great addition to oral hygiene routines in a fast and comfortable approach.
Learn more about enhancing your oral care routine, on-the-go! Recommend by brand.
For more information on Waterpik™ water flosser products visit www.waterpik.co.uk. Waterpik™ products are available from Amazon, Costco UK, Argos, Boots and Tesco online and in stores across the UK and Ireland.
waterpik.co.uk
Dr Charlie Evans, a member of the Clinical Team at Clyde Munro Dental, offers comprehensive clinical support to clinicians across the group. He says:

“Clinical support is critical for clinicians as they develop their skills and advance in their careers. At Clyde Munro, we provide dedicated support programmes for dentists fresh out of their VT year and those within 5 years of qualification. We also have a team of regional Clinical Advisors who help clinicians tackle complex cases or overcome any other challenges in practice.
“In addition, Clyde Munro has a dedicated Advanced Dentistry & Clinical Skills Centre with nine phantom head stations and a suite of the latest equipment, which provides training courses and trips to help clinicians engage with the wider industry, meet suppliers and discover new innovations as part of their career progression.”
The Advanced Dentistry & Clinical Skills Centre features state-of-the-art surgeries with comprehensive audio and visual facilities to allow live demonstrations, as well as cuttingedge latest digital imaging and manufacturing equipment to ensure an exceptional hands-on learning experience.
Discover this and more with Clyde Munro today.
careers.clydemunrodental.com
The new Miele PWD 8682 underbench washer disinfector from Eschmann allows dental teams to work smarter, not harder.

It provides an automated and validated method of heavyduty cleaning and disinfection for reusable instruments, prior to sterilisation. Cycles are completed in under an hour for up to 360 instruments, elevating productivity and workflow efficiency for staff. These benefits are compounded by features like intuitive user controls and fast-touch operation.
The equipment can also be protected with the Eschmann Care & Cover servicing package, which offers expert testing, maintenance and annual validation. Not only does this support practice compliance, but it also helps optimise product life and minimise the risk of equipment downtime. Care & Cover also includes annual Enhanced CPD staff training for maximum return on your investment.
For more information on the highly effective and affordable range of decontamination solutions available from Eschmann, please visit www.eschmann.co.uk or call 01903 753322
eschmann.co.uk
It’s the end of the first year of the amalgam phase-down across the EU, but it’s clear that safe waste management solutions like the PureGuard™ Dental Container Range from Initial Medical are as important as ever before.
The PureGuard™ Dental Container Range features a specialised suppressant, which absorbs mercury vapours, protecting your team and providing a safe storage solution for amalgam contaminated waste streams. Containers are collected by the Initial Medical team to be fully recycled at their ISO 14001:2015 (environment) certified dental recycling facility.
Clinicians are provided with recycled containers to ensure their practice faces no down time, and
Have you discovered the oral health duo redefining interdental maintenance?
The TANDEX WOODI is an expertly designed premium product meeting the widest range of oral needs.
Did you know the TANDEX WOODI is available in six different sizes, providing interdental maintenance for gaps of all shapes and sizes?
It is also designed with sustainability in mind, made from responsibly sourced birchwood and supplied in a recyclable cardboard box.
The TANDEX PREVENT GEL is an excellent pairing with the WOODI, providing enamel strengthening and antibacterial properties working to remineralise the teeth and fight

the cycle of green amalgam waste collection continues. Find out more about dental waste solutions from Initial Medical by contacting the team today.
To find out more, get in touch at 0808 304 7411 or visit the website today.
The best introduction to water flossing for your patients is the Cordless Pulse water flosser from Waterpik™, a versatile, effective solution that fits into any oral hygiene routine.

With two pressure settings and two unique flossing tips (including a Tongue Cleaner for a fresher breath), your patients can choose the set up that meets their needs. This allows them to not only optimise for comfort, but take charge of their oral hygiene routine, and effectively combat plaque around the mouth.
caries.
To discover this dynamic duo and to see how TANDEX is redefining interdental cleaning, visit the website today.
For more information on Tandex’s range of products, visit https://tandex.dk/ Our products are also available from DHB Oral Healthcare https://dhb.co.uk/

For patients seeking the highest standard in oral care, they should look no further than the Ultra Professional water flosser from WaterpikTM. Specialist care from the comfort of one’s home and the #1 water flosser brand recommended by dental professionals, this device has it all. 10 pressure settings and 5 flossing tips offer the user a comprehensive clean – up to 2X as effective as string floss for improving gum health. The option of 5 flossing tips makes it the perfect device for all: including implants and all advanced gum care requirements.
The Hydro-Pulse Massage Mode provides gentle gum stimulation which increases blood circulation in gingival tissues and offers an easy, comfortable alternative to flossing with sensitive
gums.
Take oral care routines to the highest level – find out more today! Recommend by brand.
tandex.dk

For more information on Waterpik™ water flosser products visit www.waterpik.co.uk. Waterpik™ products are available from Amazon, Costco UK, Argos, Boots and Tesco online and in stores across the UK and Ireland.
waterpik.co.uk
The beauty of a career in dentistry is that learning and personal progression is limitless. The Best Foot Forward programme from Clyde Munro is tailored to support those participating in the Vocational Trainee (VT) Programme during their transition into independent practice.
The sessions include the in-depth learning of topics including brand creation, digital dentistry, and establishing partnerships. The programme also incorporates one-to-one support for schedule management and the benefit of a strong network of peers.
The Best Foot Forward programme represents the foundations as a launchpad into the Flying Start programme, which ensures that after the VT year, associates can continue their professional growth with
structured support and continuous learning opportunities.

Build upon your foundations of knowledge and become a more well-rounded professional with the Best Foot Forward Programme at Clyde Munro today!
To find out more about the career development opportunities available at Clyde Munro, please visit https://careers.clydemunrodental.com/.
careers.clydemunrodental.com
The Cordless Pulse removes up to 99.9% of plaque from treated areas in just 3 seconds, giving patients confidence in their ability to debride bacteria between dental appointments.
As a cordless solution, the water flosser can be used at home, but also taken away in a compact wash bag.
You can learn more by contacting the Waterpik™ team today.
For more information on Waterpik™ water flosser products visit www.waterpik.co.uk. WaterpikTM products are available from Amazon, Costco UK, Argos, Boots and Tesco online and in stores across the UK and Ireland.
waterpik.co.uk
Toothache can be debilitating, making day-to-day life for sufferers uncomfortable. As such, its essential for clinicians to recommend fast acting solutions for the rapid relief of toothache.

Orajel™ Dental Gel absorbs swiftly through the oral mucosa, acting quickly to target the source of dental pain directly, ensuring immediate comfort by effectively numbing the area. It contains 10% benzocaine, a powerful local anaesthetic, applied directly to the painful site. It delivers toothache relief in 2 minutes or less, providing up to 2 hours of relief.
For more acute pain, recommend Orajel™ Extra Strength, which contains 20% benzocaine to block pain signals along the nerves.
For more information, please visit the website.
For essential information, and to see the full range of Orajel products, please visit: https://www.orajelhcp.co.uk/.
orajelhcp.co.uk

2025’s Dental Therapist of the Year, Emily Banks, on how communication is key, mental health, and skill-mix
Your clinical work is centred on a challenging paediatric demographic, often involving patients with phobias or additional needs. How has your focus on communication affected your career and are there any examples you could share of how communication skills have played a significant role in providing patient care?
I think that communication with paediatric patients succeeds when delivered with confidence. I think every dental professional out there will have their own strength in communication to lean into with paediatric patients, whether that’s empathy in delivery, distraction, positive reinforcement or asking questions. Personally, I lean into being a bit silly as it creates a good distraction and builds rapport. There is also an evidence base behind medical clowning that shows decreased stress levels in paediatric patients.
For professionals who want to grow more confidence with paediatrics, I would recommend shadowing a clinician who is confident with treating paediatrics – there is likely a nurse in practice, who has a secret skill of child taming, who could teach you a few tips and tricks to get started. Managing paediatric patients is a skill that needs to be developed over time, and this can be done by anyone as long as they are committed to enhancing their skills.

Your research focusing on postgraduate training opportunities for dental therapists is set for publication in the European Journal of Dental Education. As a champion of the dental therapist role, what is the most critical conversation you want this research to spark regarding the empowerment and maximisation of the therapist’s skill set, both in the UK and on an international level?
I chose this research path based on my own ambition to gain additional skills. I wanted to see opportunities grow for dental therapists in the postgraduate field, and this got the ball rolling. The conversation I want to spark is related to upskilling an already very dedicated work force. Important discussions around vacancies and future planning of dental provisions are happening at national level,

and education should always be the basis of this. Dental Schools Council has released a statement outlining the need for increased undergraduate provision. What would be sensible is to start looking at upskilling the current workforce, so we don’t end up with a plateau of skill sets in dental practice and academia. I understand it is a brave move in a volatile environment such as postgraduate delivery, but conversations need to be had. At an international level, the UK would be set to make an example of good practice in further training for dental auxiliary staff.
As a Lecturer in Dental Therapy at Cardiff University, you are dedicated to equipping future clinicians in paediatric management. Your local audits have demonstrated the efficacy of dental therapists in the hospital paediatric environment. What key operational or educational changes would you like to see implemented across the wider UK dental workforce to fully embrace this model of skill-mix?
Obviously, there are external factors related to care provision and NHS commissioning that dictate the dental workforce and its future success, and it would be fabulous to have a crystal ball to see how dental therapists will be used in the next 3-5 years, but alas, I just have to wait. Luckily, the dental therapy community has advocates in the form of its professional societies, BADT and BSDHT, who do extraordinary work with developing the profession, exemplified in the recent Human Medicines Regulations amendments. Understanding of varying scopes of practice will be essential in the next few years in order to facilitate a skill-mix model that works. This is being nurtured at undergraduate institutions and benefits will be seen in a workforce that can play to each other’s strengths and scopes. Dental care providers should be leaning into this efficient way of working and, if they need guidance and help, training is available to support this in the UK. The orthodontic sector has demonstrated this well with the use of orthodontic therapists being utilised to their full abilities. The rest of the dental sector should be catching up, and there are multiple practices and dental settings providing evidence of good practice that should be shared and celebrated!
You have openly shared your personal experiences with mental health conditions, writing articles and delivering talks that prompt clinicians to think about their own wellbeing and occupational risks. What is the single most important step the dental profession, as an industry, needs to take right now to better support the mental health and longevity of its professionals?
Compassion within management. I aim to embed compassion into my educational approach with students and clinical delivery of care. However, this is with active effort and



participation in self-reflective practice. Reflection is a huge part of my own management of my mental illness.
In my previous talks, I have focussed on participating in reflection and this leading to advocation of one’s needs. This seems like a simple thing to do, but so many people overlook it and focus on what their patients need, what their employers need, what their family or partner need, but neglect their own needs. Once someone has had that realisation of ‘I need help’, the compassion (or lack thereof) upon talking to management, will set the course of mental and wellbeing improvements.
Your day-to-day management of patients actively aims to counteract the negative impact of social determinants of health through family-wide goal setting and adaptive routines. For a widespread public health challenge like this, what are the core, non-negotiable principles that underpin your adaptive behaviour management strategy to ensure sustainable oral health improvements for the most vulnerable families?
That makes it sound like I’m doing something incredibly fancy, but really it is just using common sense to apply routine and structure to a day to increase health benefits. I have a lot of experience in childcare, and understanding the power of family dynamics, role modelling and rules contribute to a lot of the changes I recommend to families.
We know that dental caries incidence is heightened if a sibling has active caries – so although the patient in the chair is my patient, addressing a whole family in one foul swoop is more my approach. If you ban one child from squash but mum, dad and big brother are still having it, the overall success if hindered by cries of “it’s not fair!”, so applying a no squash rule to the house or a dinner table only rule works. This is just one example of family wide goal setting, and it does take confidence and creativity in your approach as a healthcare provider.
How did it feel to be named Dental Therapist of the Year?
It was all a bit crazy really! I felt very awkward being on a video call with fellow shortlisted applicants, so much so that I practiced my disappointed face and shocked face, just as stars at the Oscars do – but that was all for nothing and excitement came over me when I was told the news. I rarely grin that widely, normally reserved for music concerts and seeing kittens. I was very grateful to go to the awards celebration and meet some of the judges, fellow award winners, and the organisers from The Probe I took my mum along to the day and it was lovely to have her to celebrate with me – *insert typical “I couldn’t have done it without her” quote here*.
It feels fantastic to be Dental Therapist of the Year, something I never thought I would be able to say!















Ramadan is a significant religious period that involves daily fasting from dawn (suhoor) until sunset (iftar) for approximately one lunar month. During this time, individuals refrain from eating food and drinks between these times.
As dental professionals, an understanding of the physiological and metabolic effects of fasting, particularly on blood glucose regulation, energy metabolism, and hydration, is essential to providing safe, effective, and culturally acceptable care. Those who are pregnant or medically compromised, or unwell, are exempt from fasting. Fasting alters normal daily routines, which can have both systemic and oral health implications relevant to dental treatment.
While Ramadan offers numerous spiritual and health benefits, such as improved blood sugar regulation and cholesterol levels, it also presents challenges for maintaining oral health. Essential oral care is crucial during fasting to prevent issues, such as halitosis, xerostomia, periodontal disease, and dehydration. Fasting affects the body primarily through metabolic changes. During fasting, the body uses stored energy sources, such as glycogen and fat, to sustain itself. This can aid in improving cholesterol levels and enhancing insulin sensitivity.
Ramadan not only fulfils a spiritual purpose but also instils a disciplined fasting habit, very similar to intermittent fasting, which can help to regulate weight and blood sugar.
Dehydration is a common physical effect felt whilst fasting due to the lack of water intake during fasting hours, which can, in turn, affect energy levels, concentration, and bodily functions. The changes in energy levels may fluctuate as the body adapts to using fat reserves for fuel. Fatigue and weakness can occur initially as the body adjusts, but many people report feeling more alert and focused over time.
The metabolic effects of fasting
Under normal conditions, blood glucose levels are maintained by dietary intake of carbohydrates and glucose production within the body. When fasting, the body goes through a period of change. It first uses up glucose for energy, then switches to burning stored fats and then can also break down proteins if the fasting period is long.
Energy levels and fatigue
Reduced daytime caloric intake and altered sleep patterns can lead to transient fatigue,
reduced alertness, and mild dehydration, particularly in the first 1–2 weeks of Ramadan as the body adapts. From a dental perspective, this may affect:
• Patient tolerance of lengthy procedures
• Stress responses during treatment
• Postural hypotension when moving from supine to upright positions
Dental teams should remain attentive to signs of hypoglycaemia, such as dizziness, sweating, confusion, or tremor, especially in diabetic patients.
These things do not break your fast
• Brushing your teeth with toothpaste or a miswak stick
• Cleaning teeth with a toothbrush and toothpaste, and in between the teeth
• Visiting a dentist, dental hygienist, and dental therapist for checkups or treatments, provided water is not swallowed. Treatment under rubber dam, if applicable, is ideal
• Lightly rinsing your mouth during ablution (cleansing before prayer)
The benefit of using an electric toothbrush
I personally use the Philips Sonicare toothbrush and recommend it to my patients. The Sonicare technology uses sonic vibration to create a dynamic fluid action, moving water and toothpaste between teeth to move food particles and plaque biofilm. This helps to move more plaque bacteria and offers gum protection through a thorough cleaning. This toothbrush can help maintain a fresh breath feeling to combat halitosis during fasting hours. Combining a Sonicare toothbrush with the Philips Cordless Power Flosser will help to remove plaque effectively between the teeth. It also uses a mixture of water droplets and bursts of air to disrupt the plaque and bacteria. It’s quick and easy and can be particularly useful when time is pushed.
Oral hygiene tips during Ramadan
• Maintain a consistent oral care routine as normal:
- Brush twice daily with fluoride toothpaste – once after iftar (breaking fast) and again before suhoor (in the morning)
- Wait 30 minutes after eating to brush to avoid enamel erosion
• Use interdental brushes and/or floss:
- Clean between teeth to prevent plaque biofilm buildup/remove food debris, to maintain gum health. Alcohol-free mouthwash as an adjunct
• Hydrate between fasts:
- Drink water between iftar and suhoor to keep your body and mouth hydrated
• Combat bad breath:
- Use a tongue scraper to reduce bacteria on the tongue
- Chew sugar-free gum (with Xylitol) after evening meals to stimulate saliva and fight bacteria
• Choose friendly foods:
- Eat Vitamin C-rich fruits like berries, guavas, and oranges
- Avoid sugary and acidic foods that can contribute to tooth decay
- Include low glycemic index (GI) foods, such as porridge, lentils or whole grains, yoghurt, protein eggs, and dates for sustained energy and oral health benefits
• Avoid caffeine and excessive salt:
- These can increase dehydration, exacerbating dry mouth and gum sensitivity
Ramadan in practice
Whilst this article is patient-focused, many colleagues in the dental team will also be balancing their professional responsibilities of patient care with spiritual commitments during Ramadan. Ensure that the surgery is wellventilated and regular rest periods are taken to maintain focus and energy levels.
Ramadan Kareem from Sakina.
SAKINA
SYED

Dental Hygienist & Dental Therapist Sakina Syed works in private practice at Bupa Dental Care, London Bank and Serene by Dr Safa, Knightsbridge, London. She is a key opinion leader for Philips, and an ambassador for EMS and The British Society of Dental Hygiene and Therapy (BSDHT) London Regional chair. @bank_dentalhygienist (Instagram)

Clyde Munro Dental Group was thrilled to bring together more than 200 clinicians and practice team members at their hugely successful Clinical Conference 2025 in Glasgow.
The day offered a complimentary educational programme with inspirational guest speakers sharing expert insights, advice and motivation to help individuals progress their careers. Various CPD-accredited sessions also enabled attendees to develop their knowledge and skills in partnership with the group’s Advanced Dentistry & Clinical Skills Centre. Sessions covered a broad range of clinical and nonclinical topics to ensure a diverse and enriched learning experience for all in attendance.
An educational journey
Exploring a particularly pertinent subject right now, Sarah Morgan and Heather MacMillan from Denplan discussed how to expand services in private dentistry. Sharing several decades of experience in the profession, the dynamic duo explored the different routes clinicians and businesses can take as they build up their private dental offerings, while

maintaining NHS services. Practical, financial and cultural aspects were discussed, highlighting the value of introducing elements like Denplan.
Dr Barry Oulton kept spirits high with an inspiring session designed to help dental professionals break free from the conventional constraints of practice life. Drawing on his success as a practising dentist, coach and founder of The Confident Dentist Academy, he demonstrated how he transformed his own practice from £250,000 to over £1 million in turnover – providing routine dentistry just three and a half days per week and without any marketing spend!
Roy McGillivray and Ben McGillivray also shared their stories by outlining the strategic evolution of Swift Dental Laboratory – one of the UK’s largest and most innovative full-service dental labs –over the past four decades. The session explored the importance of digital workflows and how these can strengthen the collaboration between practice and lab for partnerships that last.
With a more clinical focus, by Dr Duncan Black – a pioneering clinician in the field of digital dentistry – presented a session supported by Dentsply. He reflected on just how much digital solutions have revolutionised the planning and restorative phase of dental treatment, discussing the opportunities and limitations of technology available today.
Dr Niall McGoldrick, Specialist in Dental Public Health, brought the essential topic of mouth cancer to the fore. He examined the epidemiology, clinical presentation and referral pathways for oral cancer, providing practical guidance on chairside strategies for addressing smoking and alcohol-related risks. The Q&A gave delegates an opportunity to explore key aspects further with an experienced public health specialist.
Taking delegates in a completely different direction and offering rare insights into a unique and fascinating field of dentistry was Dr Douglas Sheasby – a forensic odontologist. He shared with delegates the complexities of bite mark evidence, the impact of skin distortion on interpretation and the importance of applying scientific rigor to
forensic investigations. It was a unique opportunity to understand both the potential and the pitfalls of dental evidence in legal contexts.
A lively Q&A panel provided further opportunity for discussion, with attendees keen to engage with speakers for further insights and information.
After a busy day of building knowledge, connecting with experts and engaging with colleagues, attendees enjoyed drinks and dinner with live entertainment.
Many thanks go to all the speakers, trade partners and sponsors who helped deliver the diverse learning and networking opportunities available on the day, including Dr Barry Oulton, Lupin Dental, Dentsply Sirona, Wrights, Denplan and Swift Dental, as well as the 20+ exhibitors who supported attendees throughout the event! This was a fantastic opportunity for individuals to see products, materials and technologies first-hand, and to explore how the latest innovations could elevate their own dentistry.
The Advanced Dentistry & Clinical Skills Centre is a purpose-built educational facility that features cutting-edge technologies to support professional learning. While access to the Centre is one of many advantages available to Clyde Munro professionals, there are opportunities for external professionals to benefit from it also. Various independently run training courses are hosted throughout the year by industry-leading experts and brands. The Centre also has a dedicated entrance, separate branding and its own operational team, helping all dental professionals advance their knowledge and skills with confidence.
To find out more about the career development opportunities available at Clyde Munro, please visit https://careers.clydemunrodental.com/.
To browse all the courses available through the Advanced Dentistry & Clinical Skills Centre, please visit https://education. clydemunrodental.com/events n
Nina Frketin introduces a topic that sits quietly in the minds of dental professionals everywhere – even though few ever say it out loud: imposter syndrome
Imposter syndrome is that quiet voice insisting you are not as good as people think you are, even when your work says otherwise. It shows up as hesitation, overthinking, comparison and the sense that someone else would have done it better.
Many dental professionals carry these feelings silently, yet imposter syndrome is far more common than most realise. It is estimated to affect most of us at some point, including two-thirds of women at work, according to the National Institute for Health and Care Research (NIHR).
For Nina, the realisation came through conversations with dental technicians across the profession. “No matter the role or experience, the same little voice kept coming up,” she says. What struck her most was how many people admitted to feeling this way only after someone else voiced it first. “It clicked for me that this wasn’t a private battle. It was a quiet epidemic.”
The anatomy of self-doubt
Why does imposter syndrome take such a strong hold in dental technology? Nina sees several forces at play. The profession demands precision,
Nina Frketin is a dental technician at Queensway Dental Laboratory and the founder of Nightshift, a community initiative that champions visibility and support for women in dental technology. She is a published author, international speaker and educator, as well as an ambassador for the charity Den-Tech. Nina is committed to shaping the future of dentistry and inspiring the next generation of dental technicians through education, advocacy and community leadership.
scrutiny and meticulous care. Every case carries an expectation of near-flawless output, and when perfection feels like the baseline, the natural fluctuations of skill, confidence and human fallibility can be misread as falling short.
“We’re artists with microscopes pointed at us,” she says. “And sometimes, that can be brutal.”
For many women in dental technology, the internal pressure is amplified further. Nina describes an “unspoken expectation to prove yourself twice to be taken seriously once,” an exhausting dynamic that reinforces the belief that anything short of perfection is insufficient.
When combined with an already critical internal voice, this creates a psychological load far heavier than most people acknowledge.
Nina is open about how imposter syndrome has affected her career. It has appeared as overthinking, procrastination driven by a fear of making mistakes, comparison with peers, and craving external validation. Naming these patterns

Nina Frketin will be speaking at Dental Technology Showcase (DTS) which takes place on the 15th -16th May 2026 at NEC Birmingham and runs alongside the British Dental Conference & Dentistry Show (BDCDS). She will explore imposter syndrome with candour, humour and practical insight. If you have ever second-guessed your worth, this is a conversation that could change the way you see yourself and your work. For further information, visit the-dts.co.uk and birmingham.dentistryshow.co.uk.
helped her interrupt them, and speaking honestly about them helped others feel seen.
Her work with Nightshift reinforced this (nightshiftdentaltech.com). Within the community, she saw technicians share not only their successes but also the late-night panic, the perfection fatigue and the frustration of not feeling enough. In return, she saw genuine empathy. “It reflected both our struggles and our strengths,” she says. “That shaped everything about how I approach this issue.”
While personal growth plays a role, Nina believes the profession itself must evolve. Confidence cannot thrive in environments structured around fear. Psychological safety must be cultivated intentionally. She calls for feedback that builds rather than breaks; for recognition of progress, not just perfection; and for conversations that move beyond materials and techniques to the human experience of the technician. “When techs feel seen and supported everything else improves naturally.”
With all this in mind, Nina will be presenting on the topic of imposter syndrome at the Dental Technology Showcase (DTS) in May, mixing honesty, self-reflection and humour. As she puts it: “If you can laugh at that inner critic, you’ve already won half the battle.” She also wants delegates to feel “seen, relieved and maybe slightly called out in a good way.”
Most of all, Nina wants to leave her audience with a new internal narrative. One that sounds less like self-criticism and more like self-recognition. If they can walk away with even a fraction of that shift, she believes the session will have done its job.
“For anyone who has ever felt like they’re faking it or falling behind, this talk is for you,” she says. “You’ll walk out feeling lighter and a little more equipped to quiet that ridiculous inner voice that’s been holding you back.
“Imposter syndrome is heavy enough. The conversation doesn’t have to be.” n
Set to deliver new learning, innovation and inspiration for the whole dental team
The British Dental Conference & Dentistry Show (BDCDS) – the UK’s leading dental event – is set to return to NEC Birmingham on 15-16 May 2026, promising two days of world-class education, cutting-edge innovation, and unrivalled networking for the entire dental profession.
Free for all delegates, BDCDS 2026 will once again bring together thousands of dental professionals from across the UK for an unmissable showcase of clinical excellence, business insights, and the latest product and technology developments transforming modern dentistry. Register your interest today and mark the date in your calendar!
New for 2026: The ADI Implant Theatre
Among the exciting additions for next year’s show is the brand-new ADI Implant Theatre, supported by the Association of Dental Implantology (ADI).
Designed to provide a focused platform for all levels of implant dentistry experience – from those already passionate about the field to practitioners looking to get started – the ADI Implant Theatre will offer practical, real-world learning that delegates can take straight back to practice.
Sessions will spotlight cutting-edge techniques, advanced surgical workflows, and the latest developments in digital planning and full-arch

rehabilitation, all led by some of the UK’s most experienced implantologists. With a focus on evidence-based outcomes and sustainable success, the programme aims to support improved clinical outcomes and long-term patient care.
“The introduction of the ADI Implant Theatre reflects the ongoing evolution of BDCDS and our commitment to delivering content that meets the real educational needs of today’s dental professionals,” said Stewart Turner, Senior Show Manager. “Whether you’re refining your implant workflow or exploring new treatment possibilities, this theatre offers the tools, insights and inspiration to elevate your practice.”
A must-attend event for every member of the dental team
Following on from the footsteps of the phenomenal Dentistry Show London (DSL) in October 2025, the event promises to be bigger and better than ever –
providing an unparalleled exploration of the latest innovations in dental technology and practice, as well as the best treatments available for patients.
More than 400 exhibitors are expected, showcasing the very latest in dental technology, materials and services, while a host of internationally renowned speakers will take to the stage to deliver ground-breaking and inspirational talks on a wide range of topics, including clinical updates, business strategies and the latest in aesthetic and digital dentistry.
In addition to the new implant-dedicated theatre, BDCDS 2026 will feature over 150 free eCPD hours, multiple conference streams tailored for different team roles, and exceptional networking opportunities. With a strong reputation for bringing the dental community together for personal and professional growth, this is one event not to be missed.
Stewart adds: “BDCDS remains the definitive annual meeting place for learning, collaboration and professional growth and we can’t wait to open our doors again next year. Make sure you block out the 15-16 May 2026 in your calendar, sign up and stay tuned for more exciting developments in early 2026.”
For more information and to register your interest, visit birmingham.dentistryshow.co.uk as well as following @dentistryshowCS on Instagram to receive n
The British Dental Conference & Dentistry Show is the event where over 10,000 dental professionals meet to shape the future of dentistry. With 400+ exhibitors, 11 theatres, 200+ expert speakers and 150+ hours of free Enhanced CPD, this is the place to unite with your dental community. Embrace new ideas, explore the innovations of tomorrow and take your practice to the next level.





Finding a new job is more than just moving practices, it is an investment in your future. That’s why it’s so important to make your decision carefully and to find a role that will allow you to both develop and flourish. It is important to take a strategic approach to each position you take on. This means setting yourself some goals and driving your career development in a way that will help you to achieve your ambitions.
Just as the SMART principles are applied to marketing and other business targets, they offer a useful tool for professional development. By following the concept, you will create career objectives that are Specific, Measurable, Achievable, Relevant and Time-bound. This ensures that aspirations are tailored to you and your interests, and that they can be monitored so that you know you’re on track. The framework also ensures that goals are realistic and that there is a deadline to reach each milestone.
Some career objectives that follow these guidelines may be to start delivering fixed orthodontics to patients within the next two years, or to increase the number of implants placed to 25 in a year. Other examples may be to establish and host a monthly study club dedicated to endodontics in 6 months, or to buy your own practice in 5 years.
Whatever your ambitions, clearly defining them will be key to driving your personal and professional growth. Your objectives will also be critical to any decisions around new job roles.
In fact, your career goals may be the reason that you look for a job vacancy in the first place. If your current practice doesn’t have the capacity or opportunity to accommodate your aspirations and allow you to grow in the area you wish, then finding somewhere that will facilitate this will be a priority. Your targets will also influence your choice of new practice – if hoping to develop within dental implantology, you’ll need to join a practice that can offer the appropriate clinical mentorship and support specifically in the field. Should your interests lie in facial aesthetics, it might be more advantageous to find a practice that doesn’t currently provide the service at all, reducing the competition you would face and creating exciting opportunities for you and the business to grow.

When preparing for the next step in your professional journey, it is important to understand the broader market. A little research into average UDA rates for the area you’re looking to stay in or move to, average pay for associates in different disciplines or with various years of experience, and even general patient need for the area will offer insight into the jobs available.
Your CV and professional portfolio should then be tailored according to your research. It should present the very best of you while highlighting the value that you will bring to the practice you join.

Where you can include previous achievements such as an increase in new patients, communitybased projects you ran or income you have generated for previous businesses, this offers tangible evidence of your worth.
From here, attention will turn to the interview process. This is no longer just your opportunity to impress a potential new employer, but rather, it should be a two-way conversation with both parties selling themselves. As such, you are assessing the practice as much as the manager or principal in front of you is evaluating you. Be prepared to engage, to ask questions, and to really get a feel for what working in the practice would be like. Think beyond pay too – consider the clinical support, mentorship, autonomy, flexibility, education and training available to you.
For anyone looking for a new job right now, it is a candidate’s market. The recruitment challenges experienced by practices nationwide mean that most are offering highly competitive opportunities for the right clinician. Be sure to use this to your advantage by discussing any additional value a potential new practice is willing and able to offer to the right candidate. You will be able to utilise your experience, your skills, and your value to the business to leverage the most mutually-beneficial contract. Of course, while candidates are wellpositioned to find a great role in today’s market, it is still crucial to sell yourself to secure the job you want in the best possible practice for you.
For bespoke support in finding the most appropriate vacancies and presenting yourself in the

strongest way, work with the recruitment experts from Dental Elite. They have years of experience helping dental professionals accelerate their career progression with new roles that unlock exciting opportunities to grow. Whether you’re seeking fulltime, locum or other work, give us a call today!
A career in dentistry can take various different paths, each as rewarding and fulfilling as the other. Which direction you take will depend on your personal interests and clinical strengths, but strategically guiding your career towards identified goals will help you achieve your objectives faster and more effectively. This will often coincide with finding a new role, which can be done very successfully with a little planning and support.
For more information on Dental Elite visit www. dentalelite.co.uk, email info@dentalelite.co.uk or call 01788 545 900 n
ADAM NEEVES


Learning objectives
• To understand some of the factors influencing the oral microbiome
• To appreciate key factors contributing to dysbiosis of the gut microbiome
• To better understand the links between oral and gut health, and the impact of oral hygiene on both
GDC Development Outcome: C
The mouth is often referred to as ‘the gateway to the body’, with oral health issues frequently associated with concerns elsewhere. One of the better understood connections is that between the oral cavity and the gut, with one having a direct impact on the other. This is relevant for patients of all ages, backgrounds, and oral health needs, making it crucial for dental professionals to understand their role in reducing the risks and preventing disease.
The oral microbiome consists of a diverse range of microorganisms, which include bacteria, fungi and viruses. When balanced, it forms a protective biofilm that prevents the pathogenic infiltration that can lead to caries or periodontal disease.
There are several factors that can affect the oral microbiome. The first is important for everyone to understand: diet. A person’s nutritional intake significantly affects their mouth, as consuming a higher amount of sugar and carbohydrates leads to an increase in Streptococcus mutans – the primary bacteria implicated in dental caries.i Excessive protein and simple carbohydrates have also been shown to create an acidic oral environment that favours inflammation and increases the risk of periodontal disease. ii The Mediterranean diet – rich in antiinflammatory and antioxidant compounds – is widely recognised as one of the most supportive for oral and general health.iii A number of lifestyle factors also influence the oral microbiome, including smoking and alcohol consumption. The former presents a multifaceted problem that leads to altered salivary pH and compromised immune

responses, with nicotine found to raise the virulence of oral microorganisms. Tobacco smoke also reduces oxygen levels, which encourages anaerobic bacterial growth. When it comes to alcohol, prolonged excessive consumption disrupts the oral mucosa, salivary glands and saliva composition. Neutrophil function is impaired too, paving the way for accelerated bacterial growth. In addition, ethanol promotes bone resorption and suppresses bone formation, causing further issues for the teeth and supporting bony infrastructure.iv
Finally, as would be expected, oral hygiene is a critical factor in the protection of a balanced oral microbiome. Where plaque is allowed to accumulate and form its own biofilm, the chance of developing various oral diseases such as dental caries and periodontitis increases substantially.v Regular and effective mechanical removal of plaque
is, therefore, crucial for the long-term maintenance of a healthy oral microbiome.
Managing gut health
Many of these same factors have an influence on gut health too. This microbiome is equally as complex with a dense colony of microbes that facilitate, or hinder, metabolism and immune response. A healthy gut relies on sufficient bacterial diversity, composition, and functionality; natural pH levels; the absence of inflammatory markers; and more.vi Imbalance of the microbiome in favour of pathogenic bacteria is closely linked with systemic health concerns, including inflammatory bowel disease (IBD) – although it is not yet known whether the dysbiosis or disease comes first.vii
For obvious reasons, diet is a major contributor to gastrointestinal wellbeing. To
aid digestion, whole-foods like fruit and vegetables are preferred over processed alternatives with added sugar or salt. Fermentable fibres (known as microbiotaaccessible carbohydrates or MACs) are particularly important in this respect, as they support microbiota composition, diversity and health.viii The Mediterranean diet, once again, comes out on top for gut health, along with plant-based diets. ix Official recommendations regarding the consumption of food types and amounts are consistent around the world, and are supported by high-quality research.x
Smoking and chronic alcohol consumption also negatively affect the gut microbiome, with the literature reporting alterations to the microbiota composite that induce dysbiosis.xi,xii Antibiotic use is another important consideration, with initial studies pointing to a reduction in microbiota richness and diversity, including a decreased volume of beneficial bacteria.xiii
An emerging area of research is focusing on the impact of microplastics on gut microbiome health. Exposure to microplastics through aerosol inhalation or food consumption, as well as other sources, has led to the accumulation of microplastics in the lungs, placenta, faeces and blood, with links found to various gastrointestinal conditions like IBD due to gut dysbiosis.xiv Greater understanding is needed to fully appreciate the size of the problem, but it’s an interesting, yet still somewhat novel, topic that we should all remain aware of as it develops.
Making the connection
The links between oral and gut health go beyond common risk factors. The literature demonstrates a direct correlation between oral bacteria and the oral-gut axis. In fact, a potential bi-directional relationship has
been proposed, with periodontopathic bacteria capable of inducing gut dysbiosis, and disruption of the gut microbiota increasing the pathogenesis of periodontal disease.xv The risks appear to be greater among patients with obesity, highlighting the links with other systemic health conditions too. Various mechanisms have been put forward, including the action of bacterial components and inflammatory mediators, and even gastrointestinal transmission which involves ingestion of periodontopathic bacteria from the oral cavity.
Other research suggests the potential for periodontitis to play a role in the carcinogenesis of the gastrointestinal tract. The dysbiosis of the various microbiomes and consequential chronic inflammation are once again considered responsible.xvi
This is yet another reason why effective oral hygiene is so important for all patients.
As mentioned, the physical removal of plaque biofilms from the mouth is an essential step in reducing the opportunity for pathogens to accumulate in the mouth and/ or be ingested. The most effective and wellestablished method for achieving this is by brushing the teeth twice a day and cleaning interdentally once a day. Patients need to be educated on the appropriate techniques required for each step and be supported by a dental professional to establish a comprehensive daily routine.
As part of this patient-practitioner interaction, information should be exchanged on recommended products for at-home use. The FLEXI interdental brush and PREVENT Gel from TANDEX are the perfect duo to suggest, offering reliable interdental cleaning that’s gentle on the gingivae, with an antibacterial boost to protect against caries. The brushes are available in different sizes,

colour-coded for convenience, to ensure a solution to suit each patient.
A growing body of research has evidenced the connections between oral and systemic health for many years now. The link between oral and gut bacteria is of growing interest and provides yet another motivation for patients to maintain exceptional oral hygiene.
For more information on TANDEX's range of products, visit https://tandex.dk/
Our products are also available from DHB Oral Healthcare https://dhb.co.uk/
i. Moye ZD, Zeng L, Burne RA. Fueling the caries process: carbohydrate metabolism and gene regulation by Streptococcus mutans. J Oral Microbiol. 2014 Sep 5;6. doi: 10.3402/ jom.v6.24878. PMID: 25317251; PMCID: PMC4157138.
ii. Santonocito S, Giudice A, Polizzi A, Troiano G, Merlo EM, Sclafani R, Grosso G, Isola G. A CrossTalk between Diet and the Oral Microbiome: Balance of Nutrition on Inflammation and Immune System's Response during Periodontitis. Nutrients. 2022 Jun 11;14(12):2426. doi: 10.3390/nu14122426. PMID: 35745156; PMCID: PMC9227938.
iii. Augimeri G, Caparello G, Caputo I, Reda R, Testarelli L, Bonofiglio D. Mediterranean diet: a potential player in the link between oral microbiome and oral diseases. J Oral Microbiol.
2024 Mar 19;16(1):2329474. doi: 10.1080/20002297.2024.2329474. PMID: 38510981; PMCID: PMC10953787.
iv. Rajasekaran JJ, Krishnamurthy HK, Bosco J, Jayaraman V, Krishna K, Wang T, Bei K. Oral Microbiome: A Review of Its Impact on Oral and Systemic Health. Microorganisms. 2024 Aug 29;12(9):1797. doi: 10.3390/microorganisms12091797. PMID: 39338471; PMCID: PMC11434369.
v. Gm A. Oral Biofilm and Its Impact on Oral Health, Psychological and Social Interaction. Int. J. Oral Dent. Health. 2021;7:127. doi: 10.23937/24695734/1510127
vi. Van Hul M, Cani PD, Petitfils C, et al. What defines a healthy gut microbiome? Gut 2024;73:1893-1908.
vii. Aldars-García L, Chaparro M, Gisbert JP. Systematic Review: The Gut Microbiome and Its Potential Clinical Application in Inflammatory Bowel Disease. Microorganisms. 2021 Apr 30;9(5):977. doi: 10.3390/ microorganisms9050977. PMID: 33946482; PMCID: PMC8147118.
viii. Sonnenburg ED, Sonnenburg JL. Starving our microbial self: the deleterious consequences of a diet deficient in microbiota-accessible carbohydrates. Cell Metab., 20 (2014), pp. 779-786, 10.1016/j. cmet.2014.07.003
ix. Duncanson K, Williams G, Hoedt EC, Collins CE, Keely S, Talley
NJ. Diet-microbiota associations in gastrointestinal research: a systematic review. Gut Microbes. 2024 Jan-Dec;16(1):2350785. doi: 10.1080/19490976.2024.2350785. Epub 2024 May 9. PMID: 38725230; PMCID: PMC11093048.
x. Armet AM, Deehan EC, O'Sullivan AF, Mota JF, Field CJ, Prado CM, Lucey AJ, Walter J. Rethinking healthy eating in light of the gut microbiome. Cell Host Microbe. 2022 Jun 8;30(6):764-785. doi: 10.1016/j. chom.2022.04.016. PMID: 35679823.
xi. Antinozzi M, Giffi M, Sini N, Gallè F, Valeriani F, De Vito C, Liguori G, Romano Spica V, Cattaruzza MS. Cigarette Smoking and Human Gut Microbiota in Healthy Adults: A Systematic Review. Biomedicines. 2022 Feb 21;10(2):510. doi: 10.3390/ biomedicines10020510. PMID: 35203720; PMCID: PMC8962244.
xii. Grodin EN, Burnette EM, Rodriguez C, Fulcher JA, Ray LA. The gut microbiome in alcohol use disorder and alcohol-associated liver disease: A systematic review of clinical studies. Alcohol Clin Exp Res (Hoboken). 2024 Jul;48(7):1221-1242. doi: 10.1111/ acer.15338. Epub 2024 May 8. PMID: 38719790; PMCID: PMC11827555.
xiii. McDonnell L, Gilkes A, Ashworth M, Rowland V, Harries TH, Armstrong D, White P. Association between antibiotics and gut microbiome dysbiosis in children: systematic review and meta-analysis. Gut
To answer the questions below, visit cpd.the-probe.co.uk and register/log in.
Click on ‘Courses’. Search for the course with the same headline as the corresponding article.
1. Which general diet is considered one of the best to support a healthy oral microbiome?
a) A diet high in sugar
b) Mediterranean diet
c) A diet low in protein
d) None of the above
2. How does smoking impact the oral microbiome?
a) Alters salivary pH
b) Compromises the immune system
c) Raises virulence of oral microorganisms
d) All of the above
3. How can antibiotic use affect the gut microbiome?
a) Induces dysbiosis
b) Improves gut pH
c) Manages digestion of proteins
d) None of the above
Microbes. 2021 Jan-Dec;13(1):1-18. doi: 10.1080/19490976. 2020.1870402. PMID: 33651651; PMCID: PMC7928022.
xiv. Thin ZS, Chew J, Ong TYY, Raja Ali RA, Gew LT. Impact of microplastics on the human gut microbiome: a systematic review of microbial composition, diversity, and metabolic disruptions. BMC Gastroenterol. 2025 Aug 13;25(1):583. doi: 10.1186/ s12876-025-04140-2. PMID: 40804621; PMCID: PMC12351775.
xv. Yamazaki K. Oral-gut axis as a novel biological mechanism linking periodontal disease and systemic diseases: A review. Jpn Dent Sci Rev. 2023 Dec;59:273-280. doi: 10.1016/j. jdsr.2023.08.003. Epub 2023 Aug 28. PMID: 37674899; PMCID: PMC10477752.
xvi. Baima G, Ribaldone DG, Romano F, Aimetti M, Romandini M. The GumGut Axis: Periodontitis and the Risk of Gastrointestinal Cancers. Cancers (Basel). 2023 Sep 15;15(18):4594. doi: 10.3390/cancers15184594. PMID: 37760563; PMCID: PMC10526746. n
About the author
Jacob Watwood on behalf of Tandex.

4. What novel factor does the article suggest may influence gut microbiome, though more research is needed?
a) Water consumption
b) Microplastics
c) Climate change
d) Clothing materials
5. What type of relationship has been postulated between gut and oral dysbiosis?
a) The gut causes problems in the oral cavity
b) The oral cavity causes problems in the gut
c) A bi-directional relationship
d) No relationship exists
6. What mechanisms may influence the oral-gut axis?
a) Action of bacterial components
b) Inflammatory mediators
c) Gastrointestinal transmission
d) All of the above
Learning objectives
• Explain how hormonal and microbial changes during pregnancy influence gingival health.
• Describe the relationship between periodontal inflammation and adverse pregnancy outcomes.
• Apply preventive care strategies to help pregnant patients maintain optimal oral health.
GDC Development Outcome: C
Pregnancy represents a time of significant physiological and immunological change as many expecting patients experience anticipated changes like cravings, morning sickness, or fatigue.i Some systemic changes are vital for the healthy development and functioning of the foetus. However, due to the fluctuations in hormones – namely oestrogen and progesterone – the oral microbiome alters in composition leading to different responses involving the oral microbiome, blood flow, and inflammatory reactions within the gingivae.ii
Research increasingly explores the intersection between these oral manifestations and systemic inflammation. This is something which can be better understood and managed by patients with the right dental support – offering preventive strategies to protect both the maternal and foetal health and wellbeing.
The influence of pregnancy on oral health
Rising levels of oestrogen and progesterone during pregnancy lead to increased blood vessel dilation and permeability in the gingival tissues.iii The environment it creates is more detrimentally responsive to the tiniest amounts of plaque biofilm, which can consequently instigate intense inflammation. This creates a more reactive environment where even small amounts of plaque biofilm can provoke exaggerated inflammation.iv The resulting pregnancy-associated gingivitis, which demonstrates symptoms like red, swollen gingiva that bleed easily when provoked, is commonly seen, affecting up to 70% of pregnant women.v Regularly, it is noticed in the second month of pregnancy, peaking throughout the second trimester, and subsiding post-birth. The impact it has on oral health is normally reversible, but can be more damaging in the long term combined with poor oral hygiene – making plaque control integral and the dental professional’s role more important than ever.

During pregnancy, the oral microbiome also undergoes change, with higher levels of Prevotella intermedia and Porphyromonas gingivalis – both heavily linked to periodontitis, due to their nature of growth being dependent on oestrogen and progesterone.vi Whilst excellent oral hygiene can help prevent the progression of such, the hormonal attributes are not always avoidable.viii
Oral changes and pregnancy epulis
Pregnant patients will experience a variety of oral changes – some may experience many and some none. It’s always a good idea to prepare these patients in
advance on what to expect, to reduce anxiety surrounding the issues. These different changes include mild xerostomia, increased gag reflex, and enamel erosion derived from morning sickness – due to the contact of gastric acid on the enamel.vii Professionals can recommend post-vomit water rinses or fluoride mouthwashes, and the avoidance of brushing until 30 minutes after to minimise abrasion.viii

Affecting up to 5% of pregnant women is the benign overgrowth pregnancy epulis, also known as pregnancy-associated pyogenic granuloma.ix The growth is a tumour of inflammatory and vascular origin which causes an amplified gingival response to the local irritants under the impact of hormonal alterations. Due to this, gingival tissue becomes much more vulnerable to plaque, calculus, and other irritants, which may then lead to invasive procedures like surgical excision, curettage and electrocautery, and vascular laser.x However, in most cases the pregnancy epulis will resolve post-partum once hormone levels return to normal.
Beyond inflammation as an oral complication throughout pregnancy, there is also research to indicate a connection between periodontal disease and systemic complications such as preterm births and low birth weight.xi
A recent study saw that women with periodontitis were 1.6x more likely to give birth to low-birth-weight infants. Furthermore, a 2024 systematic review of over 2,000 women found that those with periodontitis were twice as likely to give birth prematurely compared to women without periodontitis.xii Periodontal therapy has been deemed safe for women during pregnancy, supporting the significant reduction of periodontitis. However, precautionary and preventive measures should be a priority, starting with greater attention to oral hygiene throughout pregnancy.
In order to effectively support pregnant patients with their oral health, the starting point should always be prevention. Many expecting patients are uninformed of the ‘dos and don'ts’ of oral health and dental appointments throughout pregnancy, with some believing that dental treatment is unsafe throughout. However, these misconceptions can be corrected with the right advice from the right source –dental professionals.
Patients should be advised to attend regular dental appointments, where the progression of issues such as periodontitis can be assessed. Other important advice should involve:xiii,xiv
• Brushing twice daily with a toothpaste containing 1,000-1,500 ppm fluoride
• Using alcohol-free fluoride mouthwash
• Reducing the intake of sugar through a well-balanced diet
• Orally rinsing after vomiting with water or a fluoride mouthwash
• Cleaning a minimum of 30 minutes after vomiting
• Interdental cleaning with soft, flexible brushes
Pregnant patients have a vast amount of systemic and lifestyle changes that can often take precedence over oral hygiene on their list of priorities. This can lead to neglected care routines that continue postnatally with less time or motivation to make dental appointments – which is particularly difficult to maintain with a newborn and new changes.
Furthermore, pregnancy-associated gingivitis and morning sickness often contribute to the difficulties due to the discomfort faced when brushing, which can

discourage patients to clean as thoroughly or as often as they should. Recommending gentle, easy-to-use tools can be particularly helpful, particularly ones that are fast and easy methods of maintaining oral hygiene.
The TANDEX FLEXI offers a perfect solution to consistent and adequate oral care for pregnant patients. In a class of their own, the soft brushes deliver a thorough interdental clean, from between teeth to the niches of sensitive gumlines. The unique non-slip rubber handle, vast range of sizes, and plastic-coated wire make cleaning simple and effective –minimising the risk of abrasive damage and avoiding sensitivity with its ergonomic design. By recommending these efficient preventive tools to pregnant patients, their daily routines and overall wellbeing can be protected.
Expecting mothers have an extensive to-do list, which can often mean that daily habits lose their position of importance within their routine. Pregnancy-associated gingivitis is one of the most common oral conditions that these patients face – yet it is reversible. However, when left unmanaged or without the right recommendations and tools to support recovery, chronic inflammation can cause both oral health detriment and stem to greater systemic issues.
Dental professionals perform an important role in informing patients of the potential issues, recognising the changes and effects, and providing judicious care to individuals suffering – always ensuring safety and benefit. High-quality tools can assist in attaining effective results, supporting ongoing maternal and newborn health. For more information on Tandex’s range of products, visit https://tandex.dk/ Our products are also available from DHB Oral Healthcare https://dhb.co.uk/

Referneces
i. Pownall, M., Hutter, R. R. C., Rockliffe, L., & Conner, M. (2022). Memory and mood changes in pregnancy: a qualitative content analysis of women’s first-hand accounts. Journal of Reproductive and Infant Psychology, 41(5), 516–527. https://doi.org/10.108 0/02646838.2022.2052827
ii. Peruga, M., Piwnik, J., & Lis, J. (2023). The Impact of Progesterone and Estrogen on the Tooth Mobility. Medicina, 59(2), 258. https://doi. org/10.3390/medicina59020258
iii. Anneli Laine, M. (2002) Effect of pregnancy on periodontal and dental health, Acta Odontologica Scandinavica. Available at: https:// medicaljournalssweden.se/ actaodontologica (Accessed: 09 October 2025).
iv. Sachelarie L, Iman AEH, Romina MV, Huniadi A, Hurjui LL. Impact of Hormones and Lifestyle on Oral Health During Pregnancy: A Prospective Observational Regression-Based Study. Medicina (Kaunas). 2024 Oct 30;60(11):1773. doi: 10.3390/ medicina60111773. PMID: 39596958; PMCID: PMC11596282.
v. Anneli Laine, M. (2002) Effect of pregnancy on periodontal and dental health, Acta Odontologica Scandinavica. Available at: https:// medicaljournalssweden.se/
actaodontologica (Accessed: 09 October 2025).
vi. Wu M, Chen SW, Jiang SY. Relationship between gingival inflammation and pregnancy. Mediators Inflamm. 2015;2015:623427. doi: 10.1155/2015/623427. Epub 2015 Mar 22. PMID: 25873767; PMCID: PMC4385665.
vii. Yilmaz, F., Carti Dorterler, O., Eren Halici, S. et al. The effects of pregnancy on oral health, salivary ph and flow rate. BMC Oral Health 24, 1286 (2024). https://doi.org/10.1186/ s12903-024-05057-0
viii. Vt H, T M, T S, Nisha V A, A A. Dental considerations in pregnancy-a critical review on the oral care. J Clin Diagn Res. 2013 May;7(5):948-53. doi: 10.7860/JCDR/2013/5405.2986.
Epub 2013 Mar 21. PMID: 23814753; PMCID: PMC3681080.
ix. Sarfi Dounia, Ben Yahya Ihssane, Extensive pyogenic granuloma in a pregnant woman, Advances in Oral and Maxillofacial Surgery, Volume 20, 2025, 100563, ISSN 2667-1476, (https://www. sciencedirect.com/science/article/pii/ S2667147625000494)
x. Weiss ES, Wood D. Simple, safe, and effective treatment for pyogenic granuloma. Can Fam Physician. 2023 Jul;69(7):479-480. doi: 10.46747/ cfp.6907479. PMID: 37451992; PMCID: PMC10348791.
xi. Xu H, Cai M, Xu H, Shen XJ, Liu J. Role of periodontal treatment in pregnancy gingivitis and adverse outcomes: a systematic review and
To answer the questions below, visit cpd.the-probe.co.uk and register/log in. Click on ‘Courses’. Search for the course with the same headline as the corresponding article.
1. Which two hormones are primarily responsible for increased gingival inflammation during pregnancy?
a) Thyroxine and progesterone
b) Insulin and dopamine
c) Oestrogen and progesterone
d) Dopamine and oestrogen
2. According to the article, when does pregnancy-associated gingivitis peak?
a) First trimester
b) Second trimester
c) Third trimester
d) Post-partum
3. Women with periodontitis were how many times more likely to give birth to low-birth-weight infants?
a) 1.6
b) 2.6
c) 3.5
d) 1.5
meta-analysis. J Matern Fetal Neonatal Med. 2025 Dec;38(1):2416595. doi: 10.1080/14767058.2024.2416595. Epub 2024 Dec 25. PMID: 39721768.
xii. Tsikouras P, Oikonomou E, Nikolettos K, Andreou S, Kyriakou D, Damaskos C, Garmpis N, Monastiridou V, Nalmpanti T, Bothou A, Iatrakis G, Nikolettos N. The Impact of Periodontal Disease on Preterm Birth and Preeclampsia. J Pers Med. 2024 Mar 26;14(4):345. doi: 10.3390/ jpm14040345. PMID: 38672972; PMCID: PMC11051368.
xiii. Adamska, P., Sobczak-Zagalska, H., Gromek, Z., Wojciechowska, B., Doroszkiewicz, P., Chmielewski, M., Cichonska, D., Zedler, A., & Pilloni, A. (2025). The Impact of Oral Health and Dental Care on Pregnancy: A CrossSectional Study Among Women of Reproductive Age. Journal of Clinical Medicine, 14(14), 5153. https://doi. org/10.3390/jcm14145153
xiv. Oral health care during pregnancy and through the lifespan (no date) ACOG. Available at: https://www.acog.org/ clinical/clinical-guidance/committeeopinion/articles/2013/08/oral-healthcare-during-pregnancy-and-through-thelifespan (Accessed: 10 October 2025). n
About the author
Jacob Watwood on behalf of Tandex.

4. According to the article, women with periodontitis were how many times more likely to give birth prematurely?
a) 0.5
b) 2
c) 2.5
d) 3.5
5. A minimum of how many minutes after vomiting should pregnant women be advised to brush?
a) 2 minutes
b) 10 minutes
c) 20 minutes
d) 30 minutes
6. Which oral hygiene aid is particularly suitable for pregnant patients experiencing gingival tenderness?
a) Any type of floss
b) Soft-tipped interdental brushes like TANDEX FLEXI
c) Alcohol-based mouthwash
d) Vigorous cleaning right after morning sickness











For more information visit https://tandex.dk/ To request samples and place orders, please visit
at https://dhb.co.uk/
Arandom meeting in Spring 2024 with Shaenna Loughnane from Bridge2Aid, led to NSK Ikigai Educator, personal coach and dental hygienist Siobhan Kelleher gathering a team of Ikigai hygienists and therapists to help launch a new Bridge2Aid initiative operating in Northern Tanzania, aimed at educating community leaders about the dangers of Infant Oral Mutilation (IOM).
Now, just a few weeks before embarking on a trip to Tanzania with five of their colleagues, Siobhan and fellow educator and dental hygienist, Amanda Harbrow-Harris, explain their aims, aspirations and trepidation, for their forthcoming expedition.
Siobhan explained, “I have been aware of the work of Bridge2Aid for a number of years and have also been involved with oral hygiene instruction in the UK and Ireland, so it seemed like a really good fit and something I was really interested in supporting. I told the group of Ikigai educators about it and was bowled over by their response, so now there’s a group of seven of us, leaving on Jan 24th for a week.”
According to Bridge2Aid the practice of Infant Oral Mutilation (IOM) is carried out on around 2.5 million children under the age of three, each year in East Africa. It is practiced, often by traditional healers, to cure sickness and diarrhoea when children when they are developing their first set of teeth, The ‘treatment’ involves removing the growing canine teeth, without the use of anaesthetic, and usually with unsterilised or improvised implements. This practice is extremely painful, dangerous, and leads to a serious risk of subsequent infection and in some cases can even be fatal.
The role of the educators is to deliver an education programme aimed at creating local community champions, including teachers, health workers, traditional healers and faith leaders. The message is simple; to inform and educate about the dangers of IOM, with the aim of cascading the key messages into communities and schools. It’s estimated that the Ikigai group’s education will reach around 1200 trainers and in turn these people will be able to impact almost 6 million people.
One of the group is Ikigai Educator and Dental Hygienist of the Year 2024, Amanda Harbrow-Harris, who works at Springfield Dental Care in Chelmsford. She is very much looking forward to the upcoming trip, “I’ve always wanted to get involved with a really good cause like this one, but it’s never been quite the right time. I don’t know if I it is now, to be fair, but it is something I’ve always wanted to do, and I’ve always admired other people who’ve done trips like this.”
Like everyone Amanda has raised money to fund the trip and raise much needed funds for Bridge2Aid and her patients have been particularly supportive. “My patients have been



so excited and encouraging and keep saying how interested they are to hear all about the trip when I get back.”
Bridge2Aid has worked with a Tanzania partner – Dr Nila Jackson on the IOM programme and on this trip the launch will be attended by Tanzania’s Health Minister, Education Minister and Chief Dental Officer who will follow the work being done on the ground. In 2024 Bridge2Aid assessed the impact of a trial IOM programme, which recorded some outstanding results, with the number of attendees believing that IOM will stop childhood sickness falling from 77% to 25%, and those who felt confident in sharing messages in their community about the dangers of IOM rising from 33% to 95%.
Amanda elaborated on what awaits the team when they reach Tanzania, “The children who have suffered Infant Oral Mutilation,


don’t just have the dreadful experience itself to deal with – there are all sort of knock-on effects, like sepsis, developmental issues, pain, trauma, and infections, as well how the adult teeth will erupt. But we are also very sensitive to the fact that the education needs to be done in a way that is mindful and respectful of the local culture.”
The whole Ikigai team is excited about the forthcoming trip and although there are some aspects they are nervous about, Siobhan is clear about the need for people to get involved in this type of project. She said “It’s a massive challenge for us, as a team, to come together and do this. We know it’s going to be really hard work, physically but also mentally and emotionally, but I’m very confident that we can make a difference, even if just a small one. I appreciate there’s a lot of work to be done on oral health education here in the UK, but this need is so basic and so fundamental that I believe we can make a real difference, even in the short time we are there.”
The Ikigai Educator team going to Tanzania are Siobhan Kelleher, Amanda Harbrow-Harris, Lauren Long, Gulab Singh, Cat Edney, Anna Peterson and Robbie Stewart
The NSK Ikigai Educators trip to Tanzania takes place 24th Jan 2026. You can follow their progress on the-probe.co.uk and if you would like to donate visit: https://www.justgiving. com/page/siobhan-kelleher-1727613792161
CPD 4 DCPs is a fully veri able ECPD programme that enables each member of the dental team to complete one year’s ECPD requirement in a highly cost-effective manner. Covering all the highly recommended subjects, each volume is specially designed to cover the ECPD needs of up to 10 DCPs.
Providing 10 hours of veri able ECPD, one Volume covers the annual veri able ECPD needs of most practices.

Subjects covered:
• The reality of mouth cancer
• Young patients and consent
• Complaints and how to avoid them
• Regulating X-rays








• Supporting patients through menopause
• Tracking infectious touchpoints
• Managing patient care prior to an emergency appointment
• Trismus and cancer treatment
• Sepsis – knowing the signs, and preventing infection
• Understanding dental risks

Our exclusive TrueFit® Technology analyses your unique facial features and working posture to deliver comfort, perfect visual alignment, and lasting ergonomic support.
Our exclusive TrueFit® Technology analyses your unique facial features and working posture to deliver comfort, perfect visual alignment, and lasting ergonomic support.
CUSTOM MEASURED • CUSTOM FITTED • CUSTOM MADE
CUSTOM MEASURED • CUSTOM FITTED • CUSTOM MADE
CUSTOM MEASURED
CUSTOM FITTED • CUSTOM MADE