Requirements
January 2026

Authors: Isabella Belleza, Shamik Bhat Elena Conde, Mera Cronbaugh, Faith Gay, Julia Heinzel, Teddy Knox, Maya Pontón Aronoff, Matteo Treviño, Joshua Varcie
Project Advisors: Heather Howard, J.D., and Daniel Meuse, M.B.A.
Publication Date: March 6, 2026.
Photos courtesy of Moss and Fog.
Data Graphics by Mera Cronbaugh, Joshua Varcie.
Geographic Data Visualization by Isabelle Belleza, Joshua Varcie.
Executive Summary
The “One Big Beautiful Bill Act,” or H.R. 1, will significantly impact how and whether people receive health insurance in Oregon and will likely have major ramifications for health outcomes and healthcare providers in Oregon. The health provisions in H.R. 1 are projected to increase the number of uninsured people in Oregon by over 200,000.1 Furthermore, H.R. 1’s Medicaid and Supplemental Nutrition Assistance Program (SNAP) cuts will reduce annual state and local tax revenue in Oregon by about $240 million while introducing sizable administrative burdens on the state, causing the state to have to do more with less.2 Ultimately, H.R. 1 will not only impact residents’ health, but the entire healthcare system, including hospitals, managed care organizations, providers, and healthcare workers across medical and non-medical jobs.
H.R. 1 is the first federal mandate in history to impose work requirements on Medicaid members.3 In Oregon, this means that members of Oregon’s Medicaid program, known as the Oregon Health Plan (OHP), will have to comply with or claim exemption from the work requirements to keep their OHP coverage.4 Work requirements are projected to reduce federal funding for OHP by $1.4 billion per year after they begin on January 1, 2027, totaling $16 billion over 10 years.5 Moreover, administering work requirements can be very expensive. For instance, since Georgia began implementing work requirements in 2021, its state Medicaid agency has spent twice as much on administration as on healthcare costs.6
This report offers recommendations for how to implement work requirements to ensure that all who are eligible for OHP can get or maintain their healthcare coverage. Oregon has the opportunity to mitigate many of the negative impacts of work requirements via its implementation decisions, which we group into three categories:
• Policy: Although many elements of H.R. 1 are fixed by statute, there is still some flexibility around how Oregon can define terms in the law and take advantage of optional exemptions from work requirements. Oregon can define its state-level policy in ways that ensure eligible individuals maintain access to the care they need, subject to the text of H.R. 1 and current or forthcoming guidance from the federal government.
• Data: Oregon collects data on potential OHP applicants and members that can be used to automatically verify that they are exempt from or compliant with work requirements. Oregon can build on existing data infrastructure, namely the ONE Eligibility system, and stand up new connections to other data systems—such as those maintained by state agencies, healthcare organizations, and other partners—to compile the information it needs. The more effectively Oregon can use these data for verification, the fewer eligible residents will lose coverage.
• Communications: Oregon will need to communicate clearly with potential OHP applicants and members to help them understand what they need to do to have health coverage under work requirements. Even with highly effective data-driven verification processes, some people will still not achieve automatic verification. Oregon can use a range of communications strategies to inform these residents of the forthcoming policy changes and help them supply the information necessary to get or keep coverage.
Implementing work requirements is an immense undertaking that will require the collaboration of many agencies, nonprofit and community-based partners, healthcare organizations, healthcare providers, and more. This will be true for collaborating across data systems, communications, and policy building. Early and consistent coordination and communication with these populations from the Oregon Health Authority (OHA) will be instrumental in this effort.
This report includes four sections, summarized below:
• Introduction: Offers an overview of OHP, how applicants apply, and the estimated impacts of H.R. 1.
• Exemptions and compliance policy: Reviews exemption and compliance policy definitions in H.R. 1. Offers recommendations for defining state-level policy.
• Data: Reviews how Oregon can use data to automatically verify exemption or compliance, both at application and renewal.
• Communications: Details how Oregon should communicate with residents to ensure they know how to prepare for and comply with the work requirements. Provides general and population-specific recommendations.
Acknowledgements
This report was written by Master in Public Affairs (MPA) students at the Princeton University School of Public and International Affairs (SPIA). It is the culmination of extensive research, data analysis, and interviews. This report fulfills Princeton SPIA’s graduation requirements, which stipulate that all students conduct research and produce a policy report for a client. Our project was led by our exceptional advisors Heather Howard and Dan Meuse, who offered course planning, technical expertise, and content advising that enhanced the quality of this work. We thank them for their commitment to our learning and their investment in this report.
We also extend our gratitude to the Oregon Health Authority (OHA) for providing us the opportunity to work on this project. We especially appreciate OHA staff’s patience and timeliness in responding to our many inquiries about the Oregon Health Plan.
Finally, we thank the following partners in Oregon who generously shared their perspectives, which were instrumental in shaping this report and our recommendations:
• Meghan Bours Slotemaker, Hospital Association of Oregon
• Valdez Bravo, Healthcare for All Oregon
• Marty Carty, Oregon Primary Care Association
• Sheeref Elnahal, Oregon Health and Science University
• Amy Fellows, We Can Do Better
• Dani Gehrke, Oregon Primary Care Association
• Robert Gordon, Recoding America Fund and Georgetown University
• Jennifer Griffith, One Community Health
• Becky Hultberg, Hospital Association of Oregon
• Sean Jessup, Eastern Oregon
• Sean Johnson, Center for Civic Design
• Natalie Kean, Justice in Aging
• Sean Kolmer, Hospital Association of Oregon
• Nora Leibowitz, CareOregon
• Vivian Levy, Oregon Health Authority
• Angela Me, One Community Health
• Andy Mendenhall, Central City Concern
• Robert Nosse, Oregon House of Representatives
• Whitney Quesenbery, Center for Civic Design
• Emma Sandoe, Oregon Health Authority
• Gelila Selassie, Justice in Aging
• Mindy Stadtlander, Health Share
• Claire Tranchese, Oregon Primary Care Association
• Robert Uhlenkott, Oregon Employment Department
• Erin Woods, Oregon Primary Care Association
Project Scope
This report aims to inform the Oregon Health Authority about best practices to support the development of technical specifications for implementing Medicaid work requirements. The primary goal is to maximize coverage for state residents who remain eligible for the Oregon Health Plan (OHP) while reducing coverage loss that could result from increased administrative burden for applicants and members. The research is centered around three objectives:
• Prioritize state-level policy options to identify exemptions for those populations without active data sources for ex parte processing, including for initial applicants that may not have previous accounts and claims.
• Identify data sources and ideal data use agreement structures to support automatic, manual, or ex parte exemption and compliance verification.
• Design sample language and identify channels for communications (both official notices and general outreach) to applicants and members to support exemption or compliance.
Introduction
On July 4, 2025, President Trump signed into law the One Big Beautiful Bill Act (H.R. 1).7 Among the most significant changes in H.R. 1 is the imposition of community engagement requirements—also known as work requirements—for Medicaid members who are receiving coverage through the Affordable Care Act (ACA)’s Medicaid expansion. These new requirements are complex, requiring the state to understand which statutory groups are exempt from the work requirements, use data to automatically determine compliance or exemptions, and develop communication strategies to inform Medicaid members of the program changes. The requirements go into effect January 1, 2027.
The Oregon Health Plan
The Oregon Health Plan (OHP) is a joint federal-state program that provides health insurance coverage to certain low-income and medically needy populations in Oregon. About 1.4 million people (32 percent of the population) receive health insurance through OHP, which is administered by the Oregon Health Authority (OHA).8 That share grew significantly after the state expanded OHP after passage of the ACA in 2014. Since 2011, Oregon has seen the number of uninsured people in the state decline by about 400,000, in large part due to the expansion.9 During this time period, Oregon’s efforts to improve access to care have also significantly reduced disparities in insurance rates by demographic group.10
Eligibility for the Oregon Health Plan
Eligibility for OHP can be established if an applicant’s income falls below a certain level or they have certain medical needs. In general, eligible individuals qualify for OHP by having income below 138 percent of the federal poverty level (FPL). Certain statutory groups can also qualify for Medicaid with incomes above 138 percent of the FPL if they meet conditions specified in the Section 1902 of the Social Security Act.11
ACA significantly expanded OHP eligibility based on income. On January 1, 2014, Oregon implemented its Medicaid expansion to allow all adults with income below 138 percent of the FPL to enroll in Medicaid. This newly eligible population is commonly known as the Modified Adjusted Gross Income (MAGI) population; it is for this population that work requirements apply. Prior to the Medicaid expansion, OHP eligibility was limited to certain groups, such as pregnant women and people with
children. Oregon’s Medicaid expansion increased OHP enrollment from about 614,000 members in December 2013 to 1,446,000 in October 2025.1213 Now, individuals eligible through the MAGI adult pathway make up about 40 percent of all OHP members.14
The “medically needy” pathway allows individuals to receive Medicaid if they can demonstrate they have a functional limitation resulting from a disability. To qualify, applicants must also generally demonstrate that their income and assets fall below certain thresholds. Many recipients of Medicaid through this pathway are recipients of long-term services and support. Work requirements do not apply to these OHP members.
There are other qualifications that all applicants must meet to enroll in OHP. For example, OHP members must be U.S. citizens or lawful permanent residents. They must also be residents of the state of Oregon. Individuals residing in Oregon who are not lawfully present may be eligible for coverage under Healthier Oregon, a program that offers Medicaid-like benefits and eligibility rules but is funded entirely through state resources.15
Enrolling in the Oregon Health Plan
To receive health insurance coverage through OHP, applicants must apply and be determined eligible for benefits. There are several ways that new applicants may apply for OHP, including online or via a paper application. New applicants may also receive assistance with the application from a navigator when visiting a healthcare provider, such as a Federally Qualified Health Center (FQHC) or a hospital.
95 percent of applicants to OHP sign up for coverage through the state’s ONE Eligibility system.16 Application and renewal processing also occurs through the state’s ONE Eligibility system. The ONE Eligibility system is housed in the Oregon Department of Human Services (ODHS) and is an integrated eligibility system, meaning that it processes applications for Medicaid alongside other programs like Temporary Assistance for Needy Families (TANF) and the Supplemental Nutrition Assistance Program (SNAP). Integrated systems are beneficial because, on the user side, they streamline the application process for public benefits. On the state’s side, they centralize data collection on compliance and exemptions for various programs, which facilitates data sharing across programs. Oregon’s integrated system has been determined by state audit to be effective at correctly determining eligibility automatically.17
Furthermore, after redetermination in 2023, Oregon had a higher-than-average ex parte renewal rate (69 percent, eight percentage points higher than the nation’s average ex parte renewal rate of 61 percent).18
Eligibility and renewal determinations rely on three forms of verification: automatic verification, manual verification, and ex parte verification. Automatic verification relies on the applicant indicating they meet compliance or exemption standards and the state providing automatic checks using data sources. Manual verification relies on the applicant taking more substantive action, such as submitting documentation, consenting to third-party data verification, or attesting to an eligibility parameter on the Medicaid application. When manual verification is needed, the applicant may work with a caseworker from ODHS, who can help the applicant understand what documentation to submit and how to submit it. Ex parte verification relies on using a combination of state-based or third-party data sources to verify an applicant’s eligibility without requiring any action from the applicant. Ex parte verification occurs during the renewal process and prevents the member from having to take action at the time of renewal.
Once enrolled in benefits, OHP members typically receive care through a coordinated care organization (CCO). Launched in 2012 as part of Oregon’s 1115 Medicaid waiver, CCOs are community-based organizations that deliver care to OHP members through a coordinated care model. CCOs adapt the traditional Medicaid Managed Care Organization (MCO) model by working at the community level, paying providers based on global budgets, and leveraging flexibility in how they spend federal dollars.19 CCOs allow members to visit a range of providers within the CCO’s network. They also serve distinct regions of the state, allowing them to tailor their approaches to both Oregon’s highly rural and urban geographies. Finally, CCOs work to address social determinants of health, taking a more integrative approach to healthcare beyond the typical MCO.
Overview of Medicaid Work Requirements in H.R. 1
H.R. 1 includes provisions affecting health care, taxes, and other policies. This report focuses on one component of H.R. 1: the implementation of work requirements in the Medicaid program. In total, H.R. 1’s health provisions are estimated to lead to up to 200,000 OHP members losing coverage.20 The loss of key financing tools, such as statedirected payments and provider taxes, will limit Oregon’s ability to sustain its health infrastructure for populations with low incomes.
The implementation of work requirements for Medicaid under H.R. 1 is the first time in history that Medicaid enrollment has been explicitly tied to an individual’s employment status. As a result, OHA will need to navigate a new and complex process that will be filled with challenges. OHA will need to verify that members and applicants are working or volunteering for at least 80 hours per month or are enrolled in school at least half-time. Some individuals will fall under exemptions to these requirements, allowing them to maintain insurance coverage without needing to prove their work, volunteer, or student status.
Another component of H.R. 1 that will increase burdens is the increased frequency with which the state will have to verify a member’s compliance or exemption from work requirements. Under H.R. 1, members will need to certify that they remain eligible for OHP and are in compliance with work requirements every six months, a process known as renewal. This is a significant change from the current process, which was not required to occur during the COVID-19 pandemic and now occurs every 24 months in Oregon.21 This change introduces significant administrative burden for both the state and members, in turn increasing the likelihood of churn and eligible individuals losing coverage.
How Work Requirements Will Affect the OHP Population
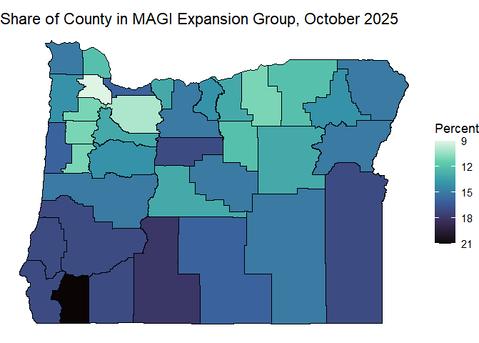
As noted above, estimates suggest that as many as 200,000 members will lose OHP coverage due to the implementation of work requirements.22 About 600,000 current OHP members will be subject to work requirements (40 percent of the total Medicaid population, or those eligible for Medicaid under the MAGI pathway as of October 2025).23 Counties with a high share of MAGI population OHP members, as shown in Figure 1, would be expected to be most affected by the implementation of work requirements.
Administrative Burden
A large portion of the reduction in OHP enrollment from work requirements will result from increased administrative burden. Administrative burdens are the frictions people face in their interactions with public services. These burdens can have costly effects by delaying or preventing people from accessing benefits they are otherwise eligible for. They are “the gap between people’s needs and the policies that are supposed to provide for them.”24 Burdens often disproportionately affect those who are already disadvantaged. As a result, the impacts of administrative burden are particularly onerous for marginalized communities.25
Administrative burdens impose three primary costs: (1) learning costs, or the time and effort required to learn about what government resources are available and whether they apply to an individual’s circumstances; (2) psychological costs, or the stigma associated with accessing certain services along with the stress and emotional toll of applying for them; and (3) compliance costs, or the time and effort required to go through the process of filling out forms, attending interviews, and/or supplying paperwork to comply with program requirements.26
Supporters of H.R. 1’s Medicaid work requirements often suggest that the coverage loss from the new requirements will reflect reductions in “waste, fraud, and abuse.”27 However, many working people will likely also lose access to coverage for which they are legally eligible because of the increased complexity of applying for benefits.28 Furthermore, the administrative burden of proving compliance or exemption every six months to Medicaid’s work requirements will also particularly impact people who most need Medicaid, like members experiencing houselessness or with chronic conditions. Ultimately, there is little evidence that work requirements lead to increased employment or earnings.29
This report’s underlying perspective is that increased administrative burden—rather than non-compliance with the Medicaid work requirements—will be the main factor causing OHP members to lose coverage. Initial estimates from researchers have found that only 6 percent of nonexempt people on Medicaid nationwide are unemployed. Of that 6 percent, one-third are retired but not yet old enough to qualify for Medicare.30
By recognizing work requirements as an administrative burden, this report recommends that OHA approach
implementation with a lens of shifting the burden from the individual to the state 31 There are promising ways of communicating with applicants and members to alleviate psychological and learning costs. Well-designed digital infrastructure will also alleviate compliance costs.
Framework For Recommendations
Our recommendations follow a funnel framework for implementing work requirements in a way that reduces coverage loss among eligible residents (see Figure 2). The funnel’s three stages, Policy, Data, and Communications, correspond to the sections of this report.
The first stage involves making policy decisions where state flexibility exists. This stage considers how OHA can define terms in the law and take advantage of optional hardship exemptions to work requirements to ensure OHP members retain access to care. It is important to consider this stage first because decisions made in this stage have downstream consequences for other considerations. We provide recommendations for policy decisions in the “Policy Considerations” section of this report.
The second stage involves using data to minimize administrative burden for applicants and members. This stage involves making decisions about how to use automatic, manual, and ex parte verification to streamline the enrollment process for applicants and the renewal process for members. The “Data” section of this report puts forward recommendations showcasing the viability of several approaches to data-driven verification of exemptions and compliance and discusses the data systems that can support collaboration when implementing work requirements.
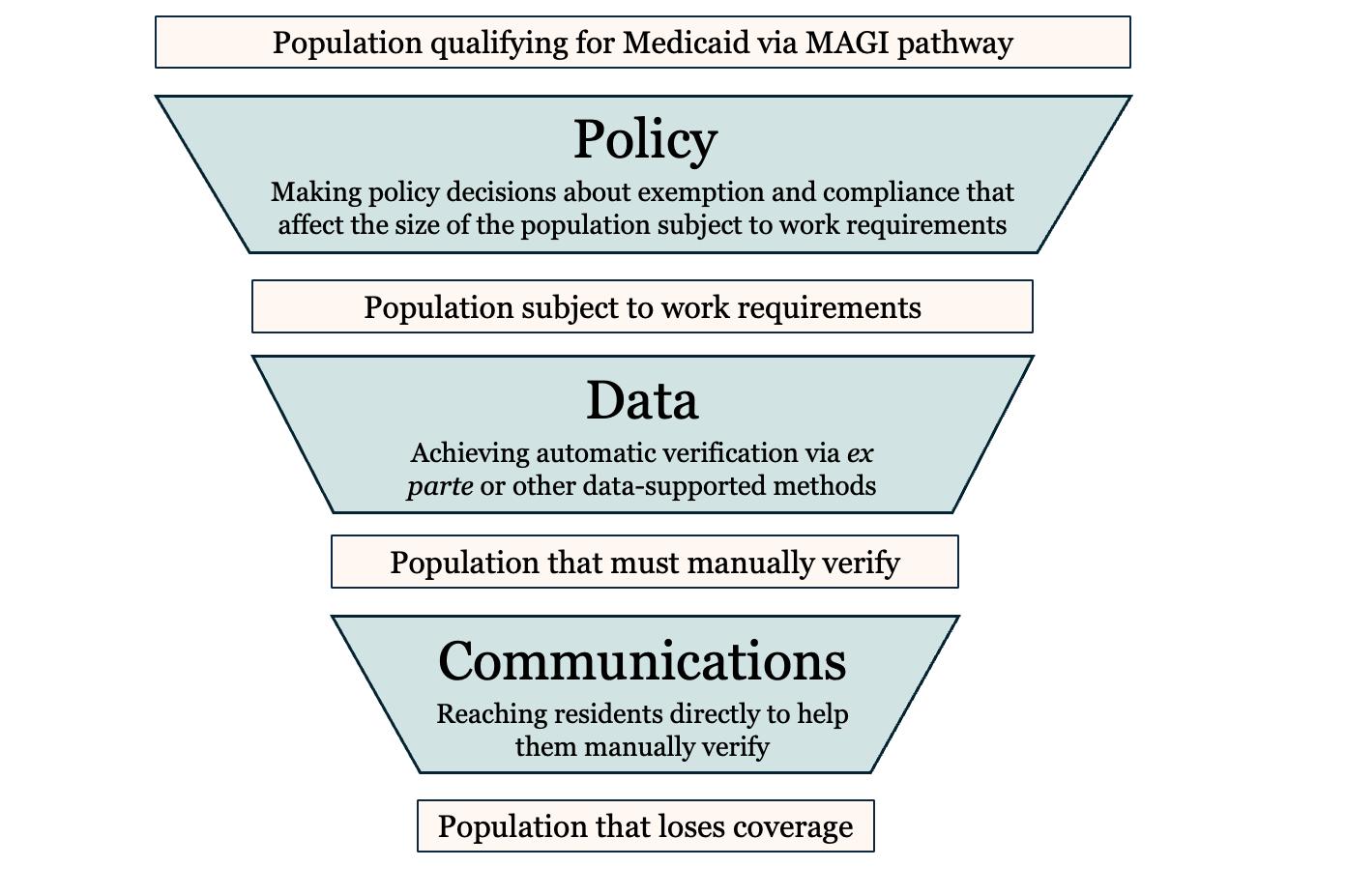
The final stage of this approach is communication with applicants, members, and community partners. Communications are important for those populations where enrollment or renewals are unlikely to be verified with data. We view communications as the final step in the funnel because the communications strategies employed depend on whether the population in question is likely to be successfully verified with data. The “Communications” section of this report proposes general best practices for communications and strategies for outreach to these hardto-reach populations. Specifically, the section offers tailored approaches for groups who may require additional support because they cannot be verified with data, have unique communication needs, or are historically underserved.
Research Team and Process
This report was produced by Masters of Public Affairs students at the Princeton School of Public and International Affairs program as part of the program’s
policy workshop requirement. The research was conducted under the supervision of Professor Heather Howard and Professor Dan Meuse based on guidelines provided by OHA. Research was conducted over the course of seven weeks and included data analysis and desk research informed by learnings from interviews with local government officials, CCOs, an FQHC, national experts in government data capacity and communications, associations representing key Oregon healthcare organizations, and advocates.
This report is not without limitations, and we strive to voice those limitations alongside our recommendations. Furthermore, while our research consulted a wide variety of partners throughout Oregon, our outreach efforts were constrained by the timeline of our research. For this reason, we strongly recommend OHA continue engaging with relevant state agencies, experts, and community leaders to establish strong partnerships that will be required for successful implementation. We present a roadmap for such engagement in a call-out box in Communications.
Policy
H.R. 1 implements new work requirements for individuals aged 19–64 who are eligible for Medicaid through the Affordable Care Act’s Medicaid expansion. Certain groups are exempted from upcoming work requirements. Many of these exemption categories build on familiar program definitions that states already use in Medicaid, SNAP, or TANF. However, H.R. 1 also introduces new classifications and narrower interpretations that may be unfamiliar to implementers. These uncertain terms create uncertainty for applicants, members, and OHA itself. This section outlines the key definitions and policy flexibilities embedded in the statute, focusing on both where H.R. 1 provides clear exemptions and areas where the law contemplates policy flexibility. Given that Oregon is most familiar with its communities, challenges, and local health conditions on the ground, maintaining flexibility in interpreting and applying these provisions is critical to minimizing disruptions in coverage. By clarifying these nuances, OHA can better assess who must comply with work requirements, who may be categorically exempt, and where administrative flexibility may mitigate coverage losses.
Current Enrollment Process and Potential Changes
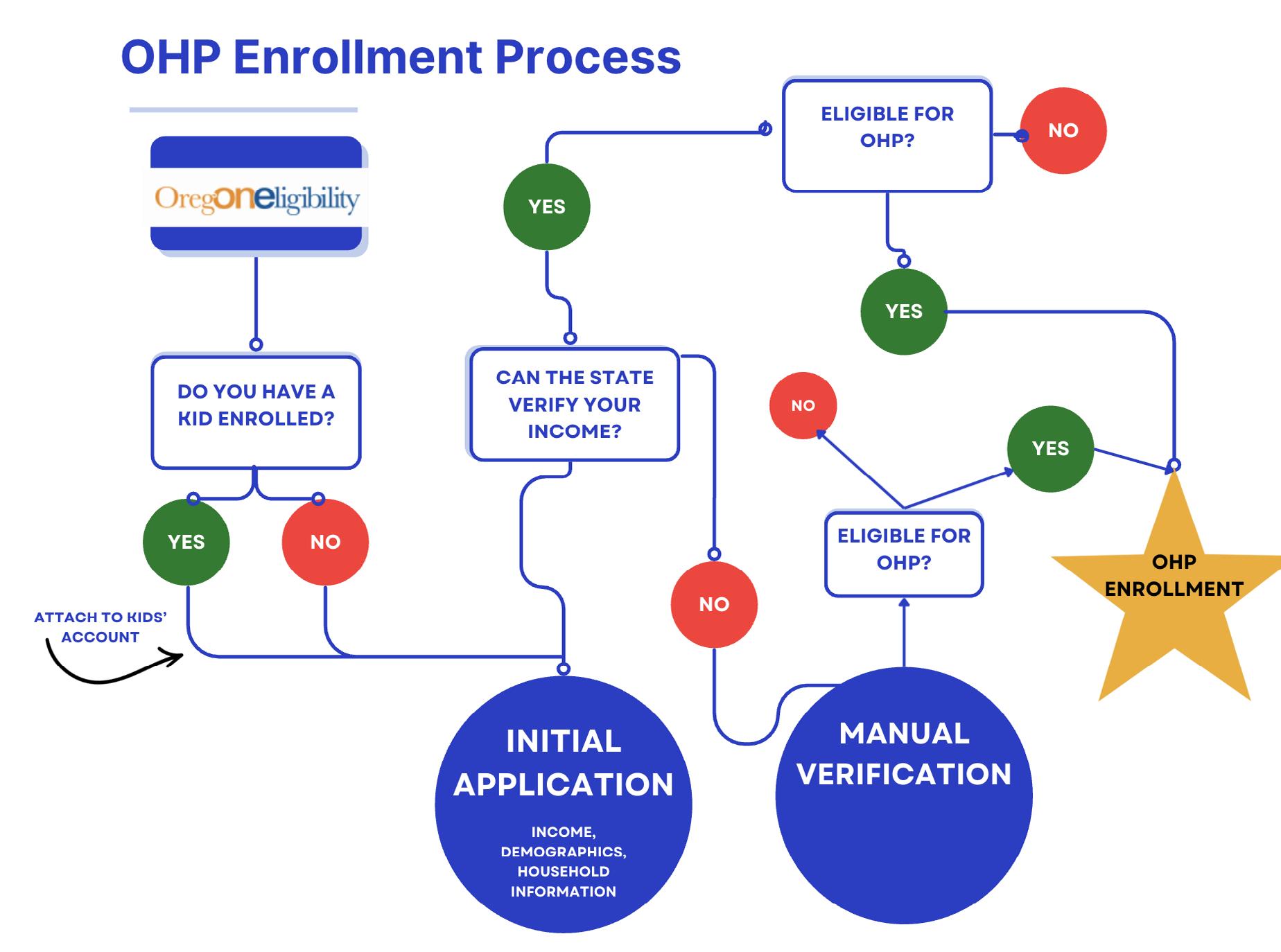
The changes to Medicaid eligibility and verification in H.R. 1 are significant. When considering additions to the OHP application and communications with members, it is important to first detail the current enrollment process and its potential burdens, as outlined in Figure 3.To enroll in OHP, new applicants go through the following process:
Step 1: Initial application. Applicants fill out the OHP application for their household.32 They must provide information on identification (name, birth date, and Social Security Number), address, income, citizenship, immigration status, tribal status, and disability. They also have the option to provide additional demographic information.
• If applicants have children on OHP, they will attach their application to their children in the ONE eligibility system. If applicants do not have children on OHP, they will start a new application in the ONE eligibility system.
• Applicants can apply online, via paper, or in the app. They can receive assistance with the application from a navigator when visiting a provider, such as a Federally
Qualified Health Center (FQHC), a hospital, or mobile clinic.
Step 2: Income verification. The state tries to verify the income information in the application.
• If income can be verified and the applicant is eligible, the applicant is enrolled in OHP.
• If income renders the applicant ineligible, they are encouraged to apply to Oregon’s Marketplace.
• If income cannot be verified, OHA contacts the member for additional verification (e.g., self-employed income). Nearly half of applicants are contacted for additional verification.
As OHA implements changes required in H.R. 1, it may choose from two options. First, OHA may add additional questions to the initial OHP application, such as questions that ask for self-reporting of data for exemptions. OHA may also choose to minimize changes to the initial OHP application and add questions during the manual verification stage (that is, if eligibility is not automatically determined). Adding questions to the initial OHP application risks greater burden for applicants when filling out the application. However, given the numerous exemptions to work requirements present in H.R. 1, it is crucial that OHA collect self-reported exemption data efficiently, and adding questions to the initial application makes this possible. Reserving these questions for the manual verification stage avoids adding greater burden to OHP applicants, but risks greater challenges for hardto-verify populations: manual, mail-based verification is prone to attrition, confusion, and time delays. OHA should lean on both its community partners and internal experience to determine which approach is more likely to maintain coverage for eligible members.
RECOMMENDATION
Determine whether initial queries or secondary, manual queries are more efficient in minimizing coverage loss.
Timeline for Compliance Verification
H.R. 1 requires individuals or the state to verify compliance with work requirements based on a “lookback” period prior to application or renewal. At application, states can choose to verify compliance for up to three consecutive months. At renewal, states can opt for a lookback period
of up to six months, asking members to demonstrate compliance for a single month or more. Proving even a single month is challenging for applicants and members; in Georgia, proving that an applicant met the work requirements proved to be a key hurdle. Over 40 percent of people who expressed interest in Georgia’s expanded Medicaid program did not complete their application because they could not complete a report showing their qualifying hours.33
RECOMMENDATION
Require individuals to demonstrate only a single month of compliance at application. At renewal, use the maximum six-month lookback period and verify a single month.
Exemptions
H.R. 1 defines specific populations that are exempt from work requirements and can access Medicaid without needing to prove they meet work requirements. Although H.R. 1 applies work requirements to a broad swath of the Medicaid expansion population, the law also identifies several well-defined categories of individuals who are excluded or excepted, referred to in this report as
exemptions.34 These exemptions are exact, technical, or well-established in federal Medicaid policy, leaving little discretion to states.
To determine exemption status, OHA can and should rely on self-reported data at the time of application. Where possible and relevant, OHA should ex parte verification to automatically re-verify exemption status without contacting members. If ex parte verification fails, OHA should then contact members to collect updated, accurate exemption status via manual verification. Some exemptions, such as demographic or disability status mechanisms, are immutable; it is impractical to reverify every six months. To minimize administrative burden, we recommend that such exemptions are not reverified at renewal and that these members should be considered permanently exempt from work requirements.
To accurately self-report exemption status at application, applicants must first recognize that an exemption applies to them. Whether an applicant recognizes that they fall within an exemption depends on how clear, intuitive, and welldefined that category is to the community it affects and on the application itself, as well as what type of information must be provided by the applicant. Accordingly, in addition to explaining definitions and clarifying flexibilities, this section highlights nuances in definitions that OHA may need to emphasize in the application or renewal process.
RECOMMENDATION
Ensure that the Medicaid application clearly defines exemptions. Accept self-reported data for exemptions and use ex parte verification to verify mutable exemptions at renewal.
Former Foster Youth
Former foster youth under the age of 26 who aged out of the foster care system and were enrolled in Medicaid at the time they turned 18 are exempt from work requirements. (Note that foster youth who did not age out of the system because they were adopted are not exempt).
In exempting former foster youth under the age of 26, H.R. 1 preserves a protection for foster youth established by the Affordable Care Act (ACA). One of the ACA’s widelysupported provisions allowed young adults to remain on a parent’s health insurance plan until age 26. Recognizing that youth aging out of foster care do not have that option, the ACA created a parallel pathway that enables eligible young adults who were in foster care at age 18 to remain enrolled in Medicaid until age 26. Because an individual’s “former foster youth” status is an existing pathway to Medicaid coverage, it is relatively straightforward for individuals who meet this exemption to identify they qualify for the exemption.
American Indians
American Indians, Alaska Natives, and California Indians are exempt from work requirements in H.R. 1. “American Indians” are defined in H.R. 1 as members of federally recognized tribes and anyone eligible for services from an Indian health care provider. This includes persons of “Indian descent” who are not enrolled members of their tribe, spouses of tribal members (if the tribe has passed a resolution allowing them to receive services), children adopted by tribal members, and non-Indian women who are pregnant with the child of an eligible “American Indian.” It does not include members of state-recognized tribes. This definition is the same as the definition already used and explained on Medicaid application forms, and to determine eligibility for Oregon waiver programs like coverage of traditional health practices. The state does not have any policy flexibility in defining this exemption.
Parent, Guardian, Caregiver Of A Dependent Child 13 Or Younger Or A Disabled Individual
Parents and guardians are well-defined terms, but caregiver merits additional consideration. H.R. 1 refers
to the definition of family caregiver used in the RAISE Family Caregivers Act, which defines the term as “an adult family member or other individual who has a significant relationship with, and who provides a broad range of assistance to, an individual with a chronic or other health condition, disability, or functional limitation.” The RAISE Family Caregivers Act definition is broader than the term “family caregiver” in H.R. 1 may immediately imply; it does not require that the caregiver be a blood relative or that the caregiver and receiver live together.
While some individuals (such as parents of a child 13 or younger) will be determined exempt via ex parte verification at renewal, exempting caregivers will be more challenging. Many individuals providing caregiving tasks do not self-identify as caregivers; therefore, the application itself will require clear guidance to ensure this population is correctly captured.35
There is also legal ambiguity in who exactly is eligible for the caregiver exemption. Recent recommendations developed by Justice in Aging, the National Health Law Program, and the Bazelon Center for Mental Health Law argue that caregiving for any individual with a “chronic or other health condition, disability, or functional limitation,” as defined by the RAISE Caregiver Act, renders the caregiver exempt.36 This would likely also include adults with “elderly parents in their care” as exempt.37 Other experts, however, highlight that the language in H.R. 1 limits caregiving recipients to “[children] 13 or younger or disabled individual[s].”
Ultimately, OHA should seek further legal advice on this exemption. If OHA chooses to implement the latter definition, it should consider someone a caregiver of a disabled individual according to the state’s statutory definition of “disabled individual,” which defines the term to include “any person who a) has a physical or mental impairment which substantially limits one or more major life activities; b) has a record of such an impairment; or c) is regarded as having such an impairment.”38
RECOMMENDATION
Consult with legal experts to determine the precise definition of “disabled individual” and “caregiver” and communicate these definitions clearly to new and renewing members.
Veteran With A Total Disability Rating
This exemption applies to veterans who have been assigned a 100 percent disability rating, as specified in Section 1155 of Title 38 of the United States Code. This rating is determined by the Veterans Affairs (VA) following a claim for a service-connected condition. A condition is service-
connected if it was incurred or aggravated during the veteran’s active military service. The VA assigns a rating from 0 percent to 100 percent to reflect the severity of this condition and establish the level of monthly compensation. Because their rating is highly salient to them and influences the level of treatment they receive, veterans will know their own status and can easily document this rating using a notification letter from the VA.39
Supplemental Nutrition Assistance Program
H.R. 1 exempts from Medicaid work requirements individuals in households receiving SNAP benefits and subject to SNAP work requirements. Unlike the new Medicaid work requirements, individuals applying for SNAP do not need to meet the work requirements at application. Instead, individuals who do not meet work requirements receive SNAP for three months before being disenrolled from SNAP and losing those benefits.40
SNAP has required many of its participants to meet work requirements for decades, though SNAP work requirements differ slightly from the Medicaid work requirements imposed in HR 1.41 For example, unhoused people are excused from SNAP requirements, while they are not automatically exempt from Medicaid work requirements.42 The SNAP exemption in H.R. 1 prevents the creation of parallel or conflicting compliance regimes across the two programs and allows states to rely on determinations already made by SNAP administrators or eligibility systems (e.g., ONE Eligibility).
Pregnant And Postpartum
Individuals who are pregnant or entitled to postpartum medical assistance are exempt from work requirements. Individuals are entitled to postpartum care for 60 days after delivery at a minimum, and OHP extends that coverage to 12 full months after pregnancy end-date. For example, if an individual’s pregnancy ends 5/3/2022, the post-partum period continues until 5/31/2023.43
RECOMMENDATION
Clarify in implementing documents that postpartum individuals are exempt from work requirements for the full 12 months following childbirth. Highlight this clarification in communications materials with new parents.
Drug Rehabilitation Program
H. R. 1 exempts individuals participating in a drug addiction or alcoholic treatment and rehabilitation program as defined in the Food and Nutrition Act of 2008.44 That definition specifies programs conducted by a private nonprofit organization or institution, or a publicly operated community mental health center, that provide rehabilitative treatment of individuals with drug or alcohol use disorder. Rehabilitation programs likely file claims for Medicaid enrollees they treat; OHA should use this claims data to form a public list of relevant treatment programs.
RECOMMENDATION
Consider posting a list of relevant public and private rehabilitative treatment programs to clarify exemption status for individuals.
Former Inmates Of Public Institutions
A “public institution” is an institution that is the responsibility of a governmental unit or over which a governmental unit exercises administrative control.45 Generally, an individual detained in a local jail, state or federal prison, or detention facility is considered an inmate of a public institution.46 By federal law, incarcerated individuals are generally not allowed to be enrolled in OHP; instead, they receive healthcare services from the facility where they are incarcerated. However, upon release, individuals are exempt from work requirements for the following three months. Notably, individuals on probation or parole, under home confinement, or residing in halfway houses are not considered inmates and therefore would not qualify for this exemption, unless they are in the threemonth window before release.47, 48
Medical Frailty
H.R. 1 explicitly exempts medically frail individuals from work requirements. “Medically frail” is a broad category, including people who are blind or disabled; have a substance-use disorder or a disabling mental illness; have a physical, intellectual, or developmental disability that limits at least one activity of daily living; or have a serious or complex medical condition. States have discretion to define medical frailty, potentially providing OHA greater flexibility to develop processes for identifying medically frail individuals. CMS guidance, which is due by June 1, 2026, may impose constraints on how states can define medical frailty.49
Disability and medical frailty
When OHA defines medical frailty, it must consider the complex pathways through which people with disabilities access Medicaid. 70 percent of people with disabilities on Medicaid in Oregon are not receiving Supplemental Security Income (SSI) or Social Security Disability Insurance (SSDI). These individuals qualify through income or other nondisability-based pathways due to the restrictive and challenging nature of applying for federal disability programs (e.g., high denial rates, low asset limits).78
While people qualified through SSI, SSDI, or similar disability categories may be automatically verified, the remaining 70 percent face significant risk of losing coverage. They may be subjected to work requirements or need clear communication to understand their new eligibility under medical frailty. A lapse in coverage for this vulnerable group, particularly those with chronic conditions like diabetes or those receiving home-care services, carries severe, potentially life-threatening consequences. Given these concerns, OHA’s definition of medical frailty should pay close attention to those with disabilities, ensuring that examples and communications include the diverse experiences of disabled Oregonians.
Defining Medical Frailty
Several states have defined medical frailty for the purposes of Alternative Benefit Plans (ABP)—customized Medicaid benefit packages that states can offer to certain adult populations—or work requirement waivers for their adult Medicaid expansion population.50 The following are examples of state medical frailty definitions:
Arkansas (ABP and work requirement waiver): Defines a medically frail individual as a person who has a physical or behavioral health condition that limits what he or she is able to do (bathing, dressing, daily chores, etc.), a person who lives in a medical facility or nursing home, a person who has a serious mental illness, a person who has a long-term problem with drugs or alcohol, a person with intellectual or developmental disabilities, or a person with some other serious health condition.51
Kentucky (work requirement waiver): Refers to the federal definition of medical frailty, then provides examples of medically frail conditions, including but not limited to: active cancer, aplastic anemia, blood clotting disorders, chronic alcohol or substance abuse, and mental illness, including major depression or bipolar disorder.52 In addition, individuals otherwise eligible for Kentucky HEALTH who are either receiving hospice care, diagnosed with HIV/AIDs, or eligible for Social Security Disability Insurance (SSDI) will automatically be determined medically frail upon verification of the qualifying condition.53
Arkansas and Kentucky represent two approaches to defining medical frailty. The Arkansas definition focuses on functional needs (for example, difficulty performing daily activities such as bathing or dressing) while the Kentucky definition focuses on specific diagnoses. However, even with a definition, it can still be challenging to consistently identify all individuals who qualify as medically frail, and
care should be taken to ensure that definitions are not restrictive of individuals who may qualify as medically frail. A definition that focuses on functional needs instead of specific diagnoses, or vice versa, may increase the risk that segments of the medically frail population will be excluded.
RECOMMENDATION
Develop a definition of medical frailty that encompasses both functional need and medical diagnoses in order to reflect the population’s diverse needs.
Identifying Medical Frailty
After defining medical frailty, states must also identify medically frail individuals. While H.R. 1 likely accepts self-reported status for initial exemption processing, ex parte verification of exemptions at renewal is critical in maintaining coverage retention for the medically frail. Notably, Michigan developed a medically frail identification process applicable for specific ABP exemptions in preparation for work requirements that had been mandated to take effect January 1, 2020 but were invalidated in court before implementation.54, 55 Their identification process thus offers a model for OHA to consider.
Self-reporting: Michigan developed questions for individuals to self-report their medical frailty at the time of application. Answering “yes” to either of these questions allowed an individual to be designated as medical frail:
1) Does the applicant “have a physical, mental, or emotional health condition that causes limitations in activities (like bathing, dressing, daily chores, etc.) or live in a medical facility or nursing home?” (Paper Application)
2) Does the applicant: a) “have a physical disability or mental health condition that limits their ability to work, attend school, or take care of their daily needs?” or b) “need help with activities of daily living (like bathing, dressing, and using the bathroom), or live in a medical facility or nursing home?” (Online Application)
Claims data: Michigan developed a set of over 500 ICD-10 diagnostic codes. The Michigan Department of Health and Human Services then used these codes to review health care claims data from the preceding 12 months, identifying conditions that qualify an individual as medically frail.56 Additional detail on the use of claims data in ex parte verification is located in the Data section of this report.
Medical provider verification: Michigan also allowed providers to recommend an individual be considered medically frail via a Medical Exemption Request form, which the state would accept at any time as verification.
Following this precedent, OHA should develop a similar multi-pronged approach to identify and verify medically frail individuals for exemption. Utilizing three distinct avenues—claims data review, provider verification, and self-reporting—ensures that medically frail individuals are not blocked from eligible exemption due to challenges seeking care or low medical literacy. Self-reporting is especially critical as it removes administrative barriers; OHA can and should accept self-reported data to qualify an applicant or member for an exemption. It is important that questionnaires include both diagnoses and measures of functional needs and challenges—this helps identify individuals who may not realize they qualify as “medically frail.” At renewal, claims data and provider verification serve as crucial sources of ex parte verification data.
RECOMMENDATION
Allow identification of medical frailty through multiple channels, including self-reported and ex parte verification through claims data, health provider information, and other sources of medical data (see Data).
Explicitly Mentioned Qualifying Conditions
The following medical frailty categories are specifically mentioned in H.R. 1 and are currently incorporated into Oregon social services and health programs; OHA can likely continue using these definitions to verify medical exemptions.
Blindness
Medical blindness is well-defined in federal regulations as having either a central visual acuity of 20/200 or worse in
the better eye with corrective lenses, or a visual field of 20 degrees or less.57
RECOMMENDATION
Follow the federal definition of blindness in processing medical exemptions ex parte
Substance use disorder (SUD)
“Substance use disorder” is defined in Oregon Administrative Rule 415-050-0105, which lists disorders related to the taking of a drug of abuse including alcohol, to the side effects of a medication, or a toxin exposure. Notably, the definition also includes substance-related delirium, neuro-cognitive disorders, and substanceinduced psychotic disorders.58
RECOMMENDATION
Follow state definitions of substance use disorder in processing medical exemptions ex parte
Disabling Mental Disorder
Under Administrative Rule 436-035-0400, “mental disorders resulting in an impairment” must be diagnosed by a psychiatrist or other mental health professional.59 Note that this is a source of conflict, since H.R. 1 generally allows for the use of self-reported data in determining exemptions. If OHA uses the Oregon Administrative Rule’s definition, it may limit the exemption to individuals with formal diagnoses. This would potentially restrict many eligible disabled individuals from exemption. However, if this definition in state law poses a challenge to accepting self-reported disabling mental disorder status, OHA may also exempt individuals under the “serious or complex medical condition” exemption (detailed below). Individuals with disabling mental disorders often also have comorbid physical illnesses, likely making them eligible for either exemption pathway.60 It is also important to note that a “mental disorder resulting in an impairment” and “disabling mental disorder” are not identical terms.
RECOMMENDATION
Accept self-reported mental health information for either the “disabling mental disorder” or “serious or complex medical condition” exemption pathways. Rely on sources of medical data (see Data) for ex parte verification of mental disorders at renewal.
Physical, Intellectual, or Developmental Disability
Individuals with a physical, intellectual or developmental disability that significantly impairs their ability to perform one or more activities of daily living explicitly qualify for an exemption under H.R. 1’s medically frail category. Definitions of developmental and intellectual disability can be found in Oregon Administrative Rule 411-3200020.61 OHA should pay close attention to individuals with chronic, permanent, and/or degenerative disabilities; ex parte verification or permanent exemption status is crucial in ensuring these individuals do not have to manually verify their disability at renewal every six months.
RECOMMENDATIONS
Utilize sources of medical data to ensure individuals with physical, intellectual, or developmental disabilities receive ex parte verification.
Ensure ex parte or permanent exemption status for individuals with chronic, permanent and/or degenerative disorders.
Serious or Complex Medical Condition
H.R. 1 does not define “serious or complex” medical conditions, providing states with discretion to define qualifying conditions of this nature. This is consistent with past practices and allows states to use their more nuanced understanding of local health conditions and challenges. A “serious health condition” is defined in Oregon Administrative Rule 471-070-1000 for the Paid Leave Oregon program (see Appendix).62 OHA should consider using this Administrative Rule definition to identify individuals with serious or complex medical conditions, for the following reasons:
Comprehensive definition: This definition not only includes conditions that involve long-term incapacity such as severe strokes and terminal illnesses, but also includes chronic conditions that require periodic treatments over an extended period of time and cause episodic periods of incapacity. Examples of these conditions include asthma or diabetes, both of which are associated with a decrease in the likelihood of employment or an increase in work missed due to illness.63 Using the state’s paid leave definition would ensure that medical exemptions reflect the diverse experiences and clinical presentations of disabled individuals, and that OHA maximizes retention of eligible individuals in OHP. OHA could consider expanding this definition to highlight clinical conditions that see significant increases in mortality due to lapses in coverage. The agency should also consider the compounding effects of multiple comorbidities; for example, asthma and hypertension can compound to create a challenging, complex clinical picture.
Flexible verification: In the case that ex parte verification fails and members are asked to verify exemption status manually, Oregon Paid Leave’s “Verification of Serious Health Condition Form” could be a model for OHA, as the form reduces burdens for eligible, disabled individuals. For example, the definition of health care provider includes a “regulated social worker,” benefitting individuals who have limited access to clinical providers but regularly engage with social workers.
RECOMMENDATION
If ex parte verification of medical exmptions fails at renewal, consider adopting the Oregon Paid Leave definition of a “serious or complex medical condition” in manual verification processes.
Short-Term Hardship Exemptions
H.R. 1 allows states to offer optional exemptions from work requirements if an individual experiences a short-term hardship event during the month. These exemptions are not mandated by the federal government and the state can choose whether to offer them. These exemptions present important opportunities to protect vulnerable groups, and we recommend OHA offer them. OHA should consider accepting self-reported data at the time of application and rely on ex parte verification at renewal to the extent feasible. The four short-term hardship exemptions are listed and analyzed below.
Inpatient Care
The state may waive work requirements for an individual if, during a month that they were subject to work requirements, that individual received inpatient hospital services, nursing facility services, services in an intermediate care facility for individuals with intellectual disabilities, inpatient psychiatric hospital services, or other services of similar acuity.
RECOMMENDATIONS
Offer the inpatient care exemption and conduct ex parte verification of inpatient care at renewal using the PointClickCare system (see Data).
Emergency Declaration
The state may waive work requirements for an individual if, during a month that they were subject to work requirements, that individual resided in a county in
Tier
Tier
Tier 1
Tier 2
Tier 3
Primary Care, Primary Care Dentistry, Mental Health, Pharmacy, SUD Treatment
Cardiology, Durable Medical Equipment, Hospital, Methadone Clinic, Neurology, Obstetrics and Gynecology, Occupational Therapy, Medical Oncology, Radiation Oncology, Ophthalmology, Optometry, Physical Therapy, Podiatry, Psychiatry, Speech Language Pathology
Allergy & Immunology, Dermatology, Endocrinology, Gastroenterology, Hematology, Nephrology, Otolaryngology, Pulmonology, Rheumatology, Skilled Nursing Facility, Urology
Figure 4. CCO Network Adequacy Standards across areas and tiers
which there was an emergency or disaster declared by the President.
RECOMMENDATION
Offer the emergency declaration exemption.
Unemployment Rate
The state may waive work requirements for an individual if, during a month that they were subject to work requirements, that individual resided in a county or local jurisdiction that has an unemployment rate of 8 percent or 1.5 times the national unemployment rate (whichever is lower). As of August 2025, while no Oregon counties had an unemployment rate of 8 percent, Douglas, Coos, Curry, Josephine, and Klamath counties had an unemployment rate greater than 6.45 percent, which is 1.5 times the national unemployment rate of 4.3 percent. Given the variability of national and county-level unemployment, regular monitoring will be necessary to minimize coverage loss.
RECOMMENDATION
Offer the unemployment rate exemption and track the unemployment rate in all counties every month.
Travel for Care
The state may waive work requirements for an individual if, during a month that they were subject to work requirements, that individual or their dependent had to travel outside of their community for an extended period of time to receive medical services to treat a
serious or complex medical condition. “Travel outside of a community” is not defined at the federal or state level, giving OHA the discretion to develop definitions for this exemption. This exemption is particularly salient for OHA to consider, given the state’s diversity of geography and disparities in healthcare access across urban, rural, and frontier areas. Areas where OHA has flexibility to determine criteria and definitions include:
“Community”
There are two existing frameworks OHA could consider adapting in its definition of “community” when considering the travel for care exemption. These frameworks are not exhaustive, but serve as potential resources to inform policy development.
Office of Rural Health Primary Care Service Areas (PCSAs): PCSAs consist of 128 pre-defined, sub-county regions of contiguous ZIP codes. Each PCSA serves as a “rational” medical market area, containing at least 800 to 1,000 residents. Access to care within these areas is generally high, with resources available within 30 to 40 minutes of travel. The average drive time to a Patient Centered Primary Care Home (PCPCH) varies by region: 14 minutes across all 128 areas, 23 minutes in remote counties, and 28 minutes for the 27 rural or remote areas that currently do not have a PCPCH.
PCSAs are already used to calculate areas of unmet healthcare needs and account for local factors that affect travel times, such as topography and travel patterns. The service areas are smaller than counties; given the large size of some Oregon counties, PCSAs are likely a more accurate and inclusive method of determining travel distance exemptions. While most service areas have PCPCHs, OHP members may travel to other service areas for care. OHA should render the travel exemption relevant in these cases, ensuring that ex parte medical sources are fully used to
automatically determine whether patient care occurred in a non-home PCSA (see Data).
Coordinated Care Organization (CCO) Network
Adequacy Standards: The network adequacy standards outlined by the State of Oregon require CCOs to ensure that members have access to providers within acceptable travel time or distance. OHA has four area types: County with Extreme Access Considerations, Rural, Urban, and Large Urban Areas (see Appendix). There are tiers of providers, with higher time and distance standards for Tier 1 providers (primary care providers) than for Tier 2 or Tier 3 providers (specialty providers).64
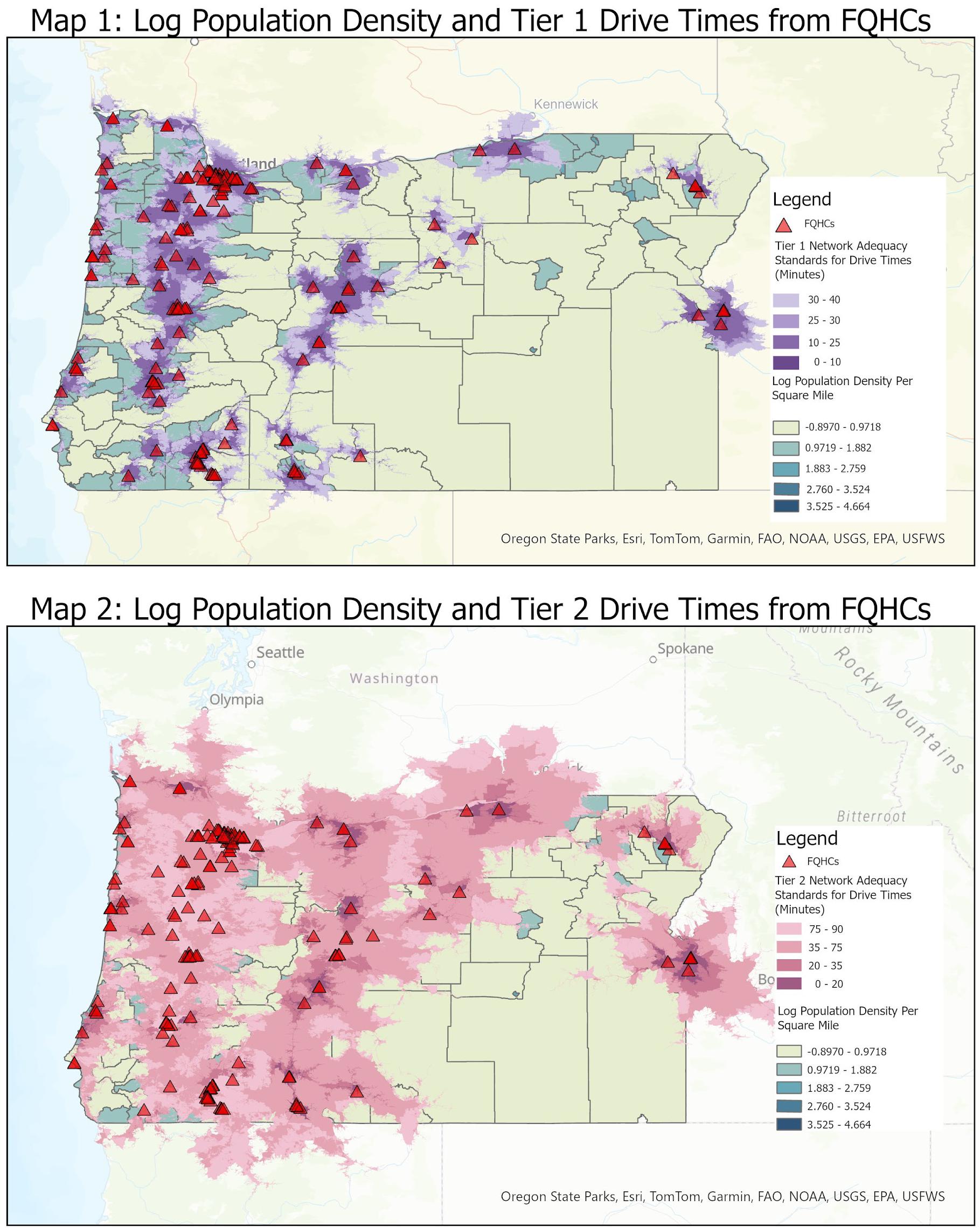
Given the existence of pre-existing distance standards, OHA should consider adapting them for the travel for care exemption. Tiered providers is an important consideration: rural and frontier members in particular likely travel farther for specialized care than for primary care, often traveling to urban areas. Using ACS data, Geographic information system (GIS) analysis of travel times fromFQHCs according to Tier 1 and Tier 2 standards has demonstrated that significant parts of the state are in Tier 2 (see Maps 1 and 2). In contrast, there are some populated census tracts that fall outside of the Tier 1 travel times, meaning that these communities must travel far distances to reach FQHCs.65To maximize retention of eligible individuals and minimize disenrollment due to distance from care, OHA should consider defining “community” as Tier 1 distances to providers.
“Extended period of time”
OHA should also interpret H.R. 1’s definition of “extended period of time” to determine eligibility for the travel for care exemption, recognizing that the required length and frequency of medical visits can vary widely based on individual needs. To establish clear thresholds, OHA should consider both existing federal and state benchmarks, such as the CMS criterion of a 25-day average inpatient stay for long-term care hospitals66 and OHA’s goal of a 30-day average length of stay for residential treatment.67 Listed below are definitions OHA should consider in implementation of the travel for care exemption. To add clarity to this exemption, OHA should also confer with clinicians to identify specific numerical threshold or minimum number of multiple medical visits (if applicable) required to address episodic or chronic conditions.
Defined number of days spent in treatment or care (e.g., a member received medical care for X days or more): This definition would include conditions that require prolonged treatment in residential or longer-term inpatient care, during which they would not be able to fulfill work requirements. Examples of treatments that may require a period of consecutive days spent in medical care include
prolonged oncology, extended inpatient behavioral health, and prenatal treatment.
Minimum number of multiple visits within a defined time period (e.g., member must make X number of visits to see a medical provider within a X day period): This definition would include conditions that require periodic treatment over an extended period of time that may cause episodic rather than continuing periods of incapacity. Examples of treatments include chemotherapy or radiation, dialysis, or physical therapy.
Separate definition specifically for rural and frontier residents (e.g., a member in a rural or frontier county with an overnight stay outside their community): This definition would include individuals for whom an overnight stay for a serious or complex medical condition is unavoidable, given long travel distances and lack of access to care in home communities. Examples of conditions include surgery, post-operative care, or oncology imaging.
RECOMMENDATIONS
Offer the travel outside community for care exemption. Carefully define “community” and “extended period of care,” ensuring that both reflect the diverse medical needs of OHP members and varying travel times for rural and frontier county residents.
Compliance
For individuals not exempted from Medicaid work requirements, the law provides individuals several options to comply, including work, community service, and education.
Work
Members can demonstrate compliance with the work requirement by working 80 hours in a given month. Alternatively, individuals can demonstrate a monthly income of at least eighty hours at federal minimum wage ($580 per month). Oregon’s relatively high minimum wage—currently $15.45 per hour in the Portland metro area, $14.20 per hour in standard counties, and $13.20 per hour in non-urban areas—is nearly twice the federal rate, allowing many residents to reach the monthly income level more readily.68 The required hours will continue to decline as Oregon’s minimum increases annually according to calculations by Oregon’s Bureau of Labor Statistics.69 Finally, seasonal workers can demonstrate an average monthly income over six months equivalent to 80 hours at federal minimum wage to be in compliance with work requirements.
Community Service
OHP members can also demonstrate compliance with 80 hours of volunteering or community service in one month. H.R. 1 does not define community service, so OHA retains flexibility in implementing this compliance mechanism. Oregon currently does not have a statutory definition of community service, often used in probation or parole. Traditionally, judges ordering community service in that context may recommend a non-profit, food bank or church, or refer individuals to parole and probation offices, which may have additional community service suggestions.
OHA could adapt the definition of community service used in TANF. Generally, TANF defines community service to be structured programs and activities where individuals perform work directly benefiting the community under the auspices of a public or non-profit organization. This work must serve a useful community purpose in areas like health, education, social services, and public safety.70 This federal criteria offers a thorough baseline for OHA to use. OHA should keep in mind, however, that significant community service also occurs outside of incorporated organizations. Communications and verification methods, whether electronic, ex parte, or manual, should account for this variability.
RECOMMENDATIONS
Build on the TANF community service definition in reporting forms and communications, allowing for nonorganizational volunteering.
Education
H.R. 1 allows individuals to fulfill work requirements by enrolling in educational programs at least half-time. The law states that the term “educational program” includes (i) an institution of higher education (as defined in section 101 of the Higher Education Act of 196571) and (ii) a program of career and technical education (as defined in section 3 of the Carl D. Perkins Career and Technical Education Act of 2006).72 While “half-time enrollment” is a common term, OHA should be intentional in defining what counts as half-time enrollment within the state and what educational programs are eligible.
There is no strict federal definition for half time enrollment—individual schools set their own policies.73 Higher education institutions commonly define enrollment status by the number of credits a student is enrolled in as of a given date on the academic calendar, often called a census date.74 Educational programs use enrollment status for two key activities: tuition billing and federal financial aid. The University of Oregon, for example, defines parttime enrollment for undergraduate students as fewer than 12 credits per term and part-time enrollment for graduate students as less than 9 credits per term.75 For tuition purposes, all classes count towards enrollment. For federal financial aid purposes, however, audit credits, independent study, non-credit courses, and credit-by-exam courses do not count towards enrollment.
Summer enrollment also presents challenges for students maintaining OHP coverage, as they might not be able to demonstrate that they were enrolled in school part time in the prior month. However, those students may be able to demonstrate compliance through other pathways: 80 percent of prime-age adults who are enrolled in postsecondary education are working.76 Those who are not working may be among the 18 percent of postsecondary students who are parents of dependent children.77
Finally, thousands of students pursue short-term, noncredit programs from community colleges that provide skills training in response to regional occupational needs. In Oregon, these types of programs include certified nursing assistants, phlebotomists, and pharmacy techs. Oregon’s Higher Education Coordinating Commission (HECC) regularly assigns students part-time or full-time enrollment status in those programs based on a calculation of clock hours. That same application of clock hours could be applied to private trade schools, as well, including trucking schools or cosmetology programs.
RECOMMENDATION
Define half-time enrollment for work requirement compliance to include all coursework, including audited courses and independent study. Publish a definition of half-time enrollment based on clock hours, so that current students can understand whether their own program will qualify.
Table 1. Recommendations
Domain Recommendation
Enrollment process
Timeline for compliance
Exemptions under H.R. 1
Caregivers
Postpartum
Drug rehabilitation programs
Determine whether initial queries or secondary, manual queries are more efficient in minimizing coverage loss.
Require individuals to demonstrate only a single month of compliance at application. At renewal, use the maximum six-month lookback period and verify a single month.
Ensure that the Medicaid application clearly defines exemptions. Accept self-reported data for exemptions and use ex parte mechanisms to verify mutable exemptions at renewal.
Consult with legal experts to determine the precise definition of “disabled individual” and “caregiver” and communicate these definitions clearly to new and renewing members.
Clarify in their implementing documents that postpartum individuals are exempt from work requirements for the 12 months following childbirth. Highlight this clarification in communications materials with new parents.
Consider posting a list of relevant public and private rehabilitative treatment programs to clarify exemption status for individuals.
Develop a definition of medical frailty that encompasses both functional need and medical diagnoses in order to reflect the population’s diverse needs.
Allow identification of medical frailty through multiple channels, including self-reported and ex parte verification through claims data, health provider information, and other sources of medical data.
Follow the federal definition of blindness in processing medical exemptions ex parte.
Follow state definitions of substance use disorder in processing medical exemptions ex parte.
Medical frailty
Inpatient care
Emergency declaration
Unemployment rate
Accept self-reported mental health information for either the “disabling mental disorder” or “serious or complex medical condition” exemption pathways.
Rely on sources of medical data (see Data) for ex parte verification of mental disorders at renewal.
Utilize sources of medical data to ensure individuals with physical, intellectual, or developmental disabilities receive ex parte verification. Ensure ex parte or permanent exemption status for individuals with chronic, permanent and/or degenerative disorders.
If ex parte verification of medical exemptions fails at renewal, consider adopting the Oregon Paid Leave definition of a “serious or complex medical condition” in manual verification processes.
Offer the inpatient care exemption.
Conduct ex parte verification of inpatient care using claims data, medical providers, or other sources.
Offer the emergency declaration exemption.
Offer the unemployment rate exemption.
Track the unemployment rate in all counties every month.
Offer the travel outside community for care exemption.
Travel for care
Community service
Education
Carefully define “community” and “extended period of care,” ensuring that both reflect the diverse medical needs of OHP members and varying travel times for rural and frontier county residents.
Build on the TANF community service definition in reporting forms and communications, allowing for non-organizational volunteering.
Define half-time enrollment for work requirement compliance to include all coursework, including audited courses and independent study.
Publish a definition of half-time enrollment based on clock hours, so that current students can understand whether their own program will qualify.
Data
This section provides recommendations for how the OHA can use data to verify compliance or exemption from Medicaid work requirements at application and renewal. These recommendations are intended to maintain access to care for OHP members and applicants and decrease administrative burdens on both residents and the state. In the funnel framework (see Introduction), the Data section follows Exemptions Policy—as automatic and ex parte verification depend on those definitions—and precedes Communications, which covers strategies for reaching individuals who do not receive automatic or ex parte verification.
Achieving automatic or ex parte verification is preferable to manual methods because it decreases burdens on both individuals and the state. For new applications, automatic verification of compliance can ease applicants’ and case workers’ burdens by reducing the amount of documents they must review. For renewals, ex parte verification allows OHA to avoid a touchpoint with the member entirely, which significantly reduces churn risk and eliminates burden on the member.79 Note that automatic and ex parte verification mechanisms are similar, as they both rely on OHA using a variety of data sources to verify exemptions or compliance with work requirements without action on the applicant or member’s behalf. Automatic verification is the use of data sources to automatically verify exemption
or compliance status at the time of application, once the applicant submits preliminary information. Ex parte verification, on the other hand, takes place without the member sending or receiving any information, and thus, generally refers to verifications of both exemptions and compliance at renewal.
Recommendations are divided into three categories: updating existing systems, integrating additional data sources, and using data-supported manual verification methods. Each recommendation is scored and prioritized based on the estimated cost of implementing it and the scale of its impact in terms of the number of individuals who would achieve verification. A full analysis of cost and scale, as well as recommended prioritization, is available in the “Prioritized Recommendations” section. In addition to recommendations, we highlight some “considerations”; actions that OHA can take to enable effective implementation of the recommendations.
Verifying Medicaid Eligibility in Oregon
OHA works with the Oregon Department of Human Services (ODHS) to verify an applicant’s OHP eligibility. The Oregon Eligibility Partnership (OEP) within ODHS runs the ONE Eligibility system, which processes the
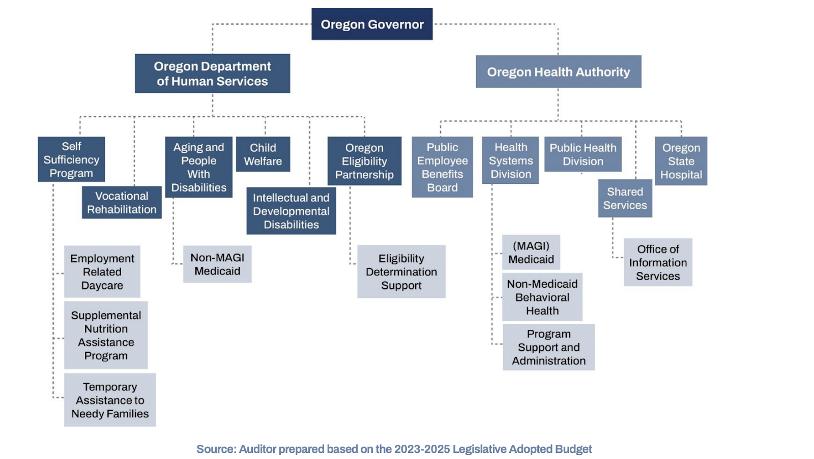
state’s OHP verification process. ONE Eligibility also allows residents to apply for the Supplemental Nutrition Assistance Program (SNAP) and Temporary Assistance for Needy Families (TANF) in addition to OHP membership.
OEP was established in 2023 to consolidate eligibility functions and staff through ODHS. The OEP runs with a two-year budget of $800 million (FY 2023-25), which includes funding for 2,599 full-time staff positions.80 The relationship between OHA and ODHS is illustrated in the diagram below.
OHA currently uses a variety of methods to verify eligibility for OHP, many of which involve ex parte verification. As discussed in the introduction, ex parte is a uniquely critical tool in eligibility verification, as it allows the state to verify without needing to ask members for additional information, saving members time and effort and preventing members who are eligible for OHP from otherwise losing their enrollment status due to paperwork burden or clerical error. Ex parte verification also reduces paperwork filing and verification effort for eligibility case workers.81 After the redetermination of Medicaid’s continuous enrollment in 2023, Oregon had a 69 percent ex parte renewal rate (eight percentage points higher than the nation’s average ex parte renewal rate of 61 percent).82 That same year, Oregon’s ONE Eligibility system was also determined by state audit to be effective at correctly determining eligibility automatically.83
Implementers should note that ex parte verification generally takes place two months before a member’s eligibility period ends, to ensure that the member does not have a lapse in coverage due to verification delays. The downside of this approach, however, is that mechanisms of exemption or compliance that occur within two months of the eligibility period ending are at higher risk of being missed by ex parte data checks. In cases where ex parte verification fails, manual verification by the member is then necessary.
Estimating the Population Size of Those Subject to Work Requirements
To understand how to allocate the state’s limited resources for ex parte verification of exemptions or compliance with Medicaid work requirements, it is crucial to understand the relative sizes of each statutory group defined in H.R. 1. Below, we estimate the sizes of these groups based on data from the American Community Survey (ACS), a nationwide, yearly survey that collects demographic, social, and economic data on millions of households. In cases where ACS data are insufficient, we supplement our results with additional data sources. The estimates are subject to significant uncertainty due to data limitations, a lack of clear definitions for certain statutory groups in H.R. 1, and the flexibilities the state has in defining exemptions for statutory groups (see Policy Considerations). Nonetheless, understanding the size of populations affected by the new requirements can help the state prioritize effective automatic, ex parte, and manual verification plans. A detailed description of the methodology underlying these estimates is available in the Appendix.
Table 2 presents the results of our findings. Importantly, this table indicates that three exemptions will capture the most individuals via electronic or ex parte verification: the exemption for SNAP household members, the exemption for parents caring for a child 13 years of age or younger, and the exemptions for medical frailty (including exemptions for disability, substance use disorder, and mental health disorders). Our estimates also show that nearly two in three individuals potentially subject to work requirements are already working at least 80 hours per month.
Statutory Group
Exemptions
Table 2. Estimates of the Population Subject to Exemptions or Compliance with H.R. 1
Member of a household receiving SNAP and is not exempt from SNAP work requirements 16%-43%*
Parent, guardian, caretaker relative, or family caregiver of a dependent child age 13 and under 21%
Medically frail—have a significant physical, intellectual, or developmental disability that interferes with one or more activities of daily living 19%
Medically frail— have substance-use disorder 10%-21%**
Medically frail—have disabling mental disorder 9%-17%***
Parent, guardian, caretaker relative, or family caregiver of a disabled individual 6%
American Indian or Alaska Native (AI/AN) 5%
Meeting TANF work requirements
Former foster youth under age 26
Living in a county with high unemployment rate
Inmate of a public institution
Recently released from incarceration within the past 90 days
Medically frail — Blind 1%
Participating in a drug or alcohol addiction treatment program 1%
Veteran with disability rated as total
Living in a county impacted by a federally declared emergency or disaster 0%
Receiving inpatient hospital care, nursing facility services in an intermediate care facility for individuals with intellectual disabilities, inpatient psychiatric hospital services, or such other services of similar acuity
Traveling for an extended period to access medically necessary care for a serious or complex medical condition that is not available in the individual’s community for either themselves or their dependent(s)
Medically frail—have a serious or complex medical condition
Compliance
Not Estimable
Not Estimable
Not Estimable
Note: This table calculates the share of the work requirement population that will qualify for an exemption for a given statutory group or be determined to be compliant under a compliance pathway. Individuals may qualify for multiple exemptions or may comply with; therefore, the totals in the table will be greater than 100%.
Statutory Group
Income of at least $580/month (as of 2025), equivalent to working at least 41 hours per month in Oregon
Average monthly income of at least $580/month for seasonal worker over six month period
80 hours of work program
80 hours of community service
At least half-time enrollment in educational program
80 hours combination of work, work program or school
Notable subsegments for compliance
estimable
*The lower bound estimate includes individuals who self-report receiving SNAP and have usual hours per work greater than 20 hours per week, and the upper bound estimate includes any individual who self-reports having SNAP.
**The lower bound only includes people with severe substance use disorder, while the upper bound includes people with any substance use disorder.
***The lower bound includes people with serious mental illness only, while the upper bound includes people with serious or moderate mental illness.
Note: This table calculates the share of the work requirement population that will qualify for an exemption for a given statutory group or be determined to be compliant under a compliance pathway. Individuals may qualify for multiple exemptions or may comply with; therefore, the totals in the table will be greater than 100%.
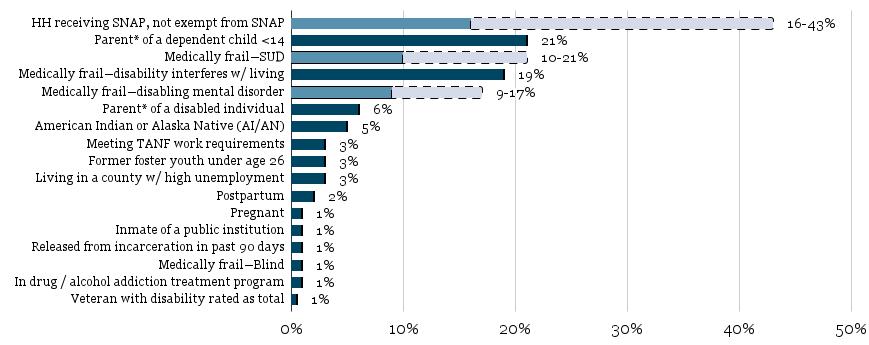
6. Estimates of the Population Subject to Exemptions
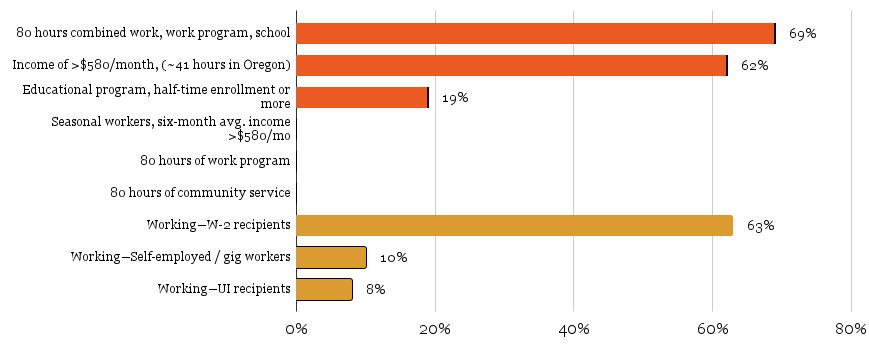
7. Estimates of the Population Subject to Compliance
Strategies to Improve Automatic Verification
Using Existing Systems for Automatic Verification
Oregon’s ONE system currently uses numerous sources of data to verify OHP eligibility; there are specific statutory exemptions and methods of compliance that these data sources can be used, either as currently used or with minor tweaks, to verify.
Exemptions
Parents or caregivers of children 13 years or younger
The ONE Eligibility process currently includes selfreporting to determine household composition for OHP and the Children’s Health Insurance Program (CHIP); where possible, these data are verified with data the state may have on the household, including the Office of Child Support Enforcement or other ongoing state benefits.84 This system of verification, including its use of self-reported information, can be used to assign automatic exemptions to parents or caregivers of children 13 years or younger. ONE currently likely uses household composition to determine its OHP eligibility pathway. System implementers can simply ensure that collected information now triggers an exemption if individuals have children 13 years or younger.
RECOMMENDATION
Ensure that children’s ages are collected in ONE and enable automatic exemption for parents with children 13 years or younger.
Low cost, medium scale; prioritize.
Individuals complying with TANF work requirements
The ONE Eligibility system currently manages TANF work requirement compliance using data sources that may include The Work Number, quarterly wage data from the Oregon Employment Department, and manual verification by case workers. If an OHP applicant is receiving TANF benefits and is in compliance with its work requirements, the individual can be swiftly rendered exempt from Medicaid work requirements with no additional steps.
RECOMMENDATION
Enable automatic exemption for individuals in compliance with TANF work requirements.
Low cost, large scale; prioritize.
Individuals in households receiving SNAP benefits and subject to SNAP work requirements
As with TANF work requirements above, the ONE Eligibility system currently determines compliance with SNAP and collects aforementioned household composition data. Administrators and case workers can ensure that SNAP applicants’ household members are identified. Their exemption status for SNAP work requirements is currently determined through ONE; if they are not exempt from (i.e., they are subject to) SNAP work requirements, household members are then exempt from upcoming Medicaid work requirements.
RECOMMENDATION
Identify and automatically exempt individuals in households receiving SNAP benefits.
Low cost, large scale; prioritize.
Pregnant individuals or those receiving postpartum coverage
The ONE Eligibility system collects information on pregnancy status to determine Modified Adjusted Gross Income (MAGI) pathway eligibility for OHP. Self-reporting is currently accepted, and additional documentation is requested for “questionable” reporting. In cases where no additional documentation can be provided, self-reported status is accepted. Accurate pregnancy status from new and renewing applicants is crucial; OHA can inquire how often ONE collects pregnancy data and suggest collection every six months to align with H.R. 1 requirements on eligibility determination frequency. If pregnancy status is collected accurately in ONE, automatic exemptions from Medicaid work requirements can apply.
RECOMMENDATION
Collect frequent and accurate pregnancy data and automatically exempt pregnant individuals.
Low cost, small scale; implement if spare capacity.
Indians and California Indians
The ONE Eligibility system currently collects these demographic data at the time of application, and we expect no major changes will be required in data collection to process automatic exemptions for American Indians.
This self-reporting of race and ethnicity, along with other demographic data, is likely sufficient for processing this exemption automatically within ONE at the time of application. As Indian identification is immutable, this exemption should not be verified every six months and should instead be considered permanent; this will avoid needless and burdensome verification steps.
RECOMMENDATION
Accept self-reported American Indian identification and continuously exempt Indian individuals.
Low cost, small scale; implement if spare capacity.
Compliance
Individuals with monthly income equivalent to at least 80 hours at federal minimum wage ($580) or W-2 employees working at least 80 hours in one month
Some employed individuals, such as those receiving W-2 forms from their employers, can have their income or work hours verified using current ONE Eligibility system practices. Currently, to verify income for OHP applicants, ONE largely uses the Verify Current Income (VCI) function from the Federal Data Services Hub (FDSH). The FDSH includes federal income data from the Internal Revenue Service, Social Security retirement and Social Security Disability Insurance, and Supplemental Security Income.85 While VCI can draw information from Equifax’s The Work Number service, ONE largely uses The Work Number for verifying SNAP eligibility, while preferring VCI and its sources for OHP income eligibility. Quarterly wage data are currently not used heavily, due to inherent delays and lack of precision. Note that this is our current understanding of income verification based on initial conversations; OHA should obtain further details from the ONE Eligibility team.
OHA can use and expand this framework of income verification for W-2 recipients, which we estimate comprise nearly two-thirds of the population work requirements apply to. ONE can continue pinging the FDSH for updated federal documentation of earned and unearned income, and can consider additionally referencing quarterly wage data and The Work Number. Quarterly wage data, while often delayed by one or more quarters, likely cover a larger portion of W-2 employees than The Work Number and are much more cost effective. While quarterly wage data’s delay likely renders it ineffective for verifying income-based compliance for new applicants (where we recommend OHA use a one-month lookback), it can likely be used for renewing applications (where we recommend OHA
use the maximum six-month lookback). Administrative guidance from the Centers for Medicare and Medicaid Services (CMS) is expected to be released in 2026; if guidance allows for use of quarterly wage data for income verification, no further action would be needed. If guidance precludes the use of quarterly wage data, OHA can pursue additional sources of income data.
W-2 employee income can also be verified using Equifax’s The Work Number, which contains weekly or bi-weekly payroll information. Income and employment hours would thus be available to OHA much quicker, but at significant cost: Equifax charges a high marginal cost on each look-up, and these costs are expected to rise drastically in coming years.86 The Work Number’s more recent data makes it an important, additional resource OHA can use in addition to quarterly wage data; it will be particularly useful for verifying income data automatically in the one-month lookback period for new applicants. Information on work hours in particular is important for individuals who meet the 80-hour requirement through a combination of employment, community service, and/or educational enrollment; for these applicants, The Work Number will be a crucial, updated source of employment data. While The Work Number is the only source of work hours in many states, Oregon’s quarterly wage data does also include hours worked. Note that verifying hours worked in one month may be challenging if hours span across two different months (e.g., if hours span the last week of April and first week of May); however, given Oregon’s high minimum wage, we expect most such individuals will be meeting income-related compliance guidelines regardless.
Individuals receiving unemployment insurance (UI) or compensation may also be compliant with Medicaid work requirements if they are receiving at least $580 in any given month. Oregon’s unemployment insurance minimums were increased in 2025 to $204 per week ($816 per month), implying that all individuals receiving unemployment insurance for at least three weeks out of any four-week period are compliant with Medicaid work requirements.87 The ONE Eligibility system currently includes integration with the Employment Department to verify unemployment compensation, but only does so for program renewal or post-enrollment. We recommend expanding this integration to include income verification at time of application; this will ensure that new applicants’ unemployment compensation is included in monthly income calculations when determining automatic compliance with Medicaid work requirements. Oregon’s FRANCES data system that houses these data can report UI payouts in real time, making it a valuable source of income compliance verification for both new and renewing applications.
RECOMMENDATIONS
Expand ONE Eligibility income verification to include The Work Number (applicants and members), quarterly wage data (members), and unemployment insurance (applicants and members).
Medium cost, large scale; prioritize for implementation.
Self-employed or gig workers, comprising roughly 10 percent of the Medicaid work requirements population, are unlikely to receive ex parte income verification through quarterly wage data or The Work Number. However, they may have relevant income data already stored in the FRANCES system if they participate in Paid Leave Oregon, Oregon’s family leave program that began accepting contributions in 2023.88 Uptake in this system is currently low—our interviews suggest approximately 10 percent of self-employed workers pay into the system—but may increase over time. There is a three-to-six month lag on Paid Leave Oregon queries, meaning that these data would be useful for most renewals but not for first-time applications.
RECOMMENDATION
Expand ONE Eligibility income verification to include data on contributions to Paid Leave Oregon.
Medium cost, medium scale; implement if spare capacity.
Integrating Additional Data Sources for Automatic and Ex Parte Verification
There are data sources ONE Eligibility currently does not include in its automatic or ex parte verification processes but could include in coordination with other state data sources. Given the various statutory groups and exemptions in H.R. 1, these integrations could significantly improve rates of both automatic and ex parte verification if pursued.
Medical Exemptions
Many applicants and members will be exempt from work requirements because they have a medical condition. These exemptions encompass those who are medically frail or have a special medical need as discussed in the policy section of the report. We also consider medical exemptions to include. For the purposes of this section, we also consider the short-term inpatient care exemption to be a medical exemption.
OHA should consider how to determine whether an individual has a medical exemption at two stages in the process: application and redetermination. At application,
OHA should update its OHP application to include additional questions to allow applicants to self-report a medical exemption to support automatic verification. Many of these questions are already asked in the application, including questions about blindness and disability, activities of daily living, and pregnancy. Questions will need to be added to the application about whether an applicant has a substance use or mental health disorder, a serious or complex medical condition, is postpartum up to 12 months, has received inpatient care in the last month, or is participating in a drug or alcohol treatment program.
RECOMMENDATION
Add questions to the OHP application about whether the applicant has a substance use or mental health disorder, a serious or complex medical condition, is postpartum up to 12 months, or has received inpatient care in the last month, and participation in a drug or alcohol treatment program.
Low cost, large scale; prioritize.
At renewal, OHA should build capacity to verify a member meets a medical exemption through ex parte verification. Ex parte verification is preferable to other forms of verification of a medical exemption, such as self-reporting, because a member does not need to submit any documentation or make any judgment calls about whether they are eligible to receive an exemption. These actions would be onerous for a member and would create administrative burdens for both the member and OHA. OHA has existing data capacities that can help to minimize these burdens through ex parte verification.
To conduct ex parte verification of a medical exemption, OHA would need to analyze existing data sources containing information on a member’s medical claims. Several data sources exist for analyzing medical claims, but those data sources are not yet integrated into the ONE Eligibility system. For example, medical claims data are accessible through the state’s Medicaid Management Information System (MMIS), as well as its All Payer All Claims database (APAC). Additional data could also be extracted from the state’s Prescription Drug Monitoring Program (PDMP), disease registries (such as cancer registries), and hospital and emergency department discharge data.
The process for ex parte identification of a medical exemption for an OHP member involves the following steps.
1. Develop a list of medical conditions that qualify for each medical exemption.
OHA should first establish a list of medical conditions that would qualify for each medical exemption. The
“Policy Considerations” section of this report discusses considerations for defining specific medical exemptions in detail.
When designing these definitions, OHA should be aware that certain diagnoses may be underreported. For example, research indicates that using ICD-10 codes to detect substance use disorders leads to an undercount of those disorders.89 Underreporting of disorders threatens the ex parte verification process because it systematically excludes certain individuals from the ex parte process, creating administrative burden for those individuals and the state. A robust manual verification system may help, and will likely be necessary for some of these cases, but the state can also consider unique ways to identify populations with underreported diagnoses without using standard diagnosis codes. For example, the state could consider identifying individuals with substance use disorder by using data from prescription drug monitoring programs to identify individuals undergoing treatment for opioid use disorder. Similarly, OHA can also rely on prescription drug claims data to exempt people prescribed medications that treat mental health disorders.
Additionally, some diagnoses might qualify an individual for a medical exemption only if the diagnosis is recent. For example, an individual who fractures their leg might be considered temporarily disabled, but would not receive a medical exemption once the bone is healed. In these cases, OHA should determine the maximum number of days a diagnosis qualifies an individual for a medical exemption and include that information in communications with relevant parties.
The final product from these efforts should be a machinereadable data file containing the possible medical conditions that would qualify for an exemption tied to common claims identifiers. The most common identifier would be an ICD-10 code. However, additional codes, such as CPT codes, ICD-9 codes, DRG codes (for hospital inpatient stays), and NDC codes (for prescription drug use) can also be considered. The data should be created in a tidy data format so that it is easy to query. An example product for the case of sickle cell disorder is shown in the Appendix.
CONSIDERATION
Develop a list of medical conditions for each medical exemption, keeping in mind that some diagnoses are commonly underreported.
2. When a member becomes eligible for renewal, query existing databases to determine whether the member meets any of the conditions.
OHA can develop a process to query existing medical claims databases to determine if a member meets a medical exemption by having one or more of the identified codes attached to their medical claim. OHA can first prioritize querying its MMIS data, followed by its APAC data. Several other data sources, including the state’s prescription drug monitoring program (PDMP) data, the Oregon State Cancer Registry, and PointClickCare platform can provide further sources of data for specific statutory groups. Since OHA manages or contracts out the development and management of these databases, the agency likely has access to all the recommended data sources. However, the ease of integrating these data sources into eligibility determinations will vary.
Several considerations are relevant to the querying process. First, OHA must decide whether to run queries on all members subejct renewal or only on members who have previously indicated they qualify for a medical exemption on their OHP application. Querying all members would expand the universe of people who might be eligible for a medical exemption, but it would also place additional burdens on state agencies conducting queries. Similarly, the frequency with which to conduct queries must be considered; higher frequency could lead to faster renewal approval times but could create additional administrative burdens. Based on conversations with experts, we expect administrative burden of these queries to generally be minimal.
CONSIDERATION
Conduct frequent (at least twice per month) data queries to examine whether any member subject to redetermination is eligible for a medical exemption.
Finally, OHA must consider that, even with a robust ex parte verification system, certain members eligible for medical exemptions will not be captured by an ex parte verification process. One such example comes from recently enrolled members who were uninsured before enrolling in OHP, since the care those members received while uninsured likely was not recorded in a medical claim. Similarly, members who recently received a diagnosis might not yet have their data appear in a medical claims database due to processing delays. For these reasons, the state will still have to develop processes to manually verify these conditions. A more detailed discussion of best practices for manual verification is discussed in further sections (see Data-supported alternatives to ex parte verification).
CONSIDERATION
Supplement ex parte data pulls with a robust selfreporting mechanism for medical exemptions.
Medicaid Management Information System (MMIS)
There are several medical claims databases that would provide OHA with the data needed to verify medical exemptions ex parte. The most robust of these datasets is the Medicaid Management Information System (MMIS). MMIS data contain medical claims for nearly all OHP members dating back to at least 2008. These data include personally identifiable information (such as name and Social Security number) as well as ICD-10 diagnosis codes and prescription drug NDC codes. As a result, MMIS data can be queried to return an indicator for whether a member would be eligible for a medical exemption using rich data on their medical history.
A few considerations should be top-of-mind when using these data. First, given the length of time covered in these data, older diagnosis codes may differ from the most upto-date codes. For example, CMS transitioned from using ICD-9 to ICD-10 codes in the early 2010s.90 Appropriate crosswalks can be developed so that ICD-9 and ICD-10 diagnoses are accurately matched in queries.
RECOMMENDATION
Query the MMIS database to determine whether members are eligible for a medical exemption, looking for matches based on both ICD-9 and ICD-10 codes.
Medium cost, large scale; prioritize.
Second, implementers should be aware that some MMIS diagnosis codes may not accurately reflect a patient’s diagnosis. In MMIS, all medical claims for an OHP member must have a diagnosis code. This includes claims that occur at the very early stages of treatment, when a formal diagnosis may not yet have been reached. For example, an EMT might need to include a diagnosis code on a claim for ambulance services despite the fact that the member has not yet been evaluated by a physician. As a result, some diagnosis codes are based on incomplete information and may not provide an accurate reflection of a member’s true medical condition. For this reason, implementers might consider categorically removing certain types of providers from their claims analysis.
CONSIDERATION
Limit MMIS queries to certain types of providers to avoid conclusions based on inaccurate diagnoses.
Finally, there are notable limitations of MMIS data. Most notably, MMIS only includes claims from periods of time when a member was enrolled in the Oregon Health Plan (OHP). As a result, MMIS data may miss diagnoses that occurred when a member was not enrolled in OHP, such as if the member had another form of insurance, was uninsured, or lived outside of Oregon. For those who previously lived outside of Oregon, OHA might be able to query national Medicaid claims data (T-MSIS), but this would require negotiating data use agreements (DUAs) with CMS.91 MMIS data may also have some small time delays due to claims processing, so some diagnoses might not be immediately viewable in the MMIS data.
All Payer All Claims (APAC) database
Another database with which OHA can verify medical claims is its APAC database. Oregon’s APAC database contains medical claims submitted from insurance companies, third party administrators, and pharmacy benefits managers to the OHA. Like MMIS, the database contains diagnostic codes and can link individuals to medical records using personally identifiable information. The data have been collected since 2009, and the database currently includes data for about 92 percent of state residents.92 Given its wide coverage across individuals and time, the APAC database is a valuable source of medical claims data that OHA can use to verify medical exemptions ex parte. The data in the APAC are a particularly valuable source of data for recently enrolled members who may have a medical condition that qualifies them for an exemption but have not yet received treatment for that condition under the Medicaid program.
CONSIDERATION
Query the APAC database to determine whether members are eligible for a medical exemption.
Medium cost, medium scale; implement if spare capacity.
Several features of the APAC database are notable. For example, similar concerns to the MMIS data may be present regarding different diagnostic code formats and inaccurate diagnoses in the APAC database. Furthermore, based on conversations with experts, querying the APAC database and establishing data pipelines with the ONE Eligibility system may be more challenging than with the MMIS data. State officials can consider allocating additional resources to Oregon’s Office of Health Analytics to implement these changes.
CONSIDERATION
Increase staffing capacity for the APAC database to improve the ability to conduct timely queries.
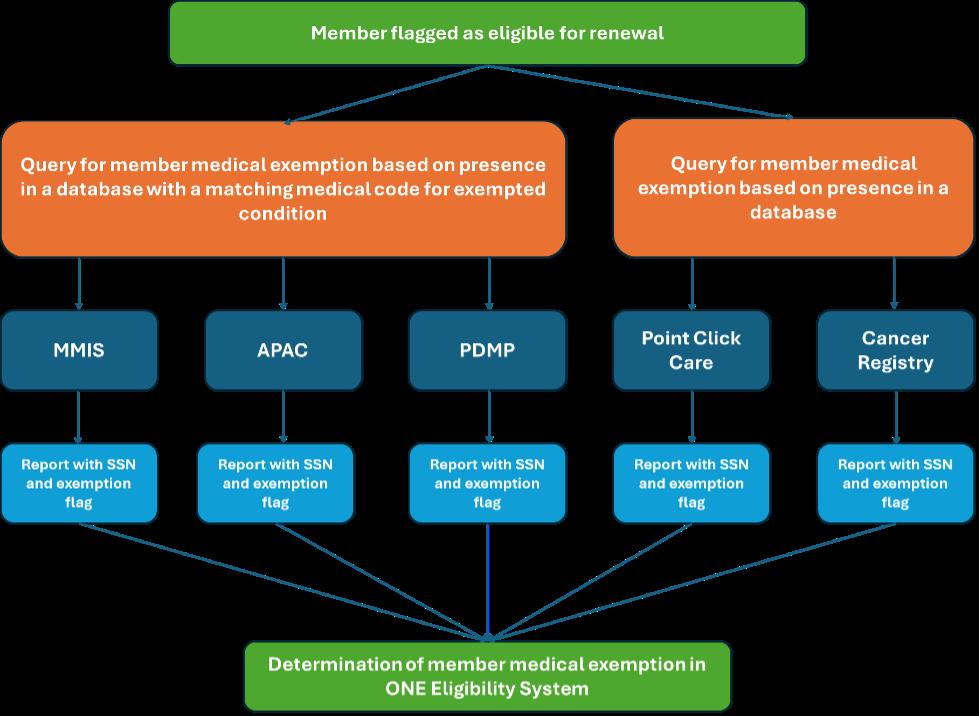
Figure 8. Overview of automatic verification of medical exemptions and necessary data sources.
There are notable limitations of the APAC database. While the database covers a large share of state residents, it only covers individuals who receive care through an insurer. Most notably, this means that claims from uninsured individuals are not included in the data, at least for care received during the period of uninsurance. Furthermore, information in the APAC database is only submitted quarterly and can be subject to significant reporting lags. For this reason, in cases where data from the APAC database duplicate other data sources (as is the case with MMIS), we recommend that OHA rely on those data sources before querying the APAC database.
CONSIDERATION
Prioritize building capability to conduct MMIS queries before conducting APAC queries.
Other data sources
Several other data sources may be useful for identifying members who are exempt from work requirements because they have a medical condition. These data sources include
data from Oregon’s PDMP, the Oregon State Cancer Registry, and data from the PointClickCare system. While these data sources can provide information on members who may be difficult to identify through other data sources, these data are likely to apply to fewer members. Therefore, OHA could consider consulting these data sources only after consulting the MMIS and APAC data, or if the state has a particular interest in identifying medical exemptions for a certain population.
Oregon’s prescription drug monitoring program (PDMP)
Oregon’s PDMP collects data from pharmacies on prescriptions for all Schedule II, III and IV controlled substances, as well as gabapentin and naloxone.93 The data have identifying information for individuals prescribed these drugs. The data could be queried by NDC to identify members using drugs that treat substance use disorders. These data are particularly valuable for members who are receiving treatment for a condition but do not have a formal diagnosis from a medical provider. Since data in PDMPs are reported by pharmacies when a prescription is filled, they are generally subject to minimal time delays.
RECOMMENDATION
Develop capability to query PDMP data
Medium cost, small scale; deprioritize
Oregon State Cancer Registry
The Oregon State Cancer Registry collects statewide data on cancer cases occurring in Oregon.94 The data contain identifying information on patients, as well as diagnosis codes.95 The data can be queried to exempt any members with cancer (which would likely qualify under the serious or complex medical condition exemption) or by ICD-10 code or cancer stage to exempt members with certain cancers. Data must be reported to the registry within 180 days of receiving the first diagnosis or treatment for cancer at a facility.96 Because of this timeline, the first renewal after a cancer diagnosis may not be captured ex parte, but subsequent renewals will likely be captured.
RECOMMENDATION
Develop capability to query Oregon State Cancer Registry data
Medium cost, small scale; deprioritize
PointClickCare Platform
OHA receives real-time emergency department, inpatient, and post-acute care Admit, Discharge, and Transfer (ADT) data from the PointClickCare system.97 Since these data are updated in real-time, they could be useful in identifying members eligible to receive a temporary exemption for an inpatient hospital stay in a given month.98
RECOMMENDATION
Develop capability to query Oregon State Cancer Registry data
Medium cost, small scale; deprioritize
3. Send a report to the ONE Eligibility system indicating which members meet a medical exemption.
Once the data are queried, each state agency responsible for the query will need to generate a report on the queried members and send it to the ONE Eligibility system. Those reports should include, at minimum, an identifier for the member (such as a name and date of birth or Social Security number), along with a binary variable for each member indicating whether the member meets a medical exemption. To the extent that OHA decides to permanently exempt members based on certain medical diagnoses, an additional binary variable should also be included
for whether the exemption is permanent or temporary. Reports should also follow a standardized process across different databases that are queried. See the Appendix for an example report.
CONSIDERATION
Produce a standardized report from each medical exemption query including, at minimum, a member identifier, a binary variable indicating whether the member meets a medical exemption, and a binary variable indicating whether the exemption is temporary or permanent.
Once the report is created, the agency will need to send the report to the ONE Eligibility system so the exemptions can be integrated into the system. In the short-term, agencies could share the results of those queries through secure file transfer protocols. In the long-term, however, OHA would benefit from integrating their data sources into the ONE Eligibility system. Such integration would allow for the verification process to be automated and would better protect the sensitive personally identifiable information (PII) data being transmitted.
Integrating these data sources into the ONE Eligibility system would have benefits and costs. Automation and integration of the ONE Eligibility system would create a standardized process that could increase application processing speed, avoid the transfer of secure data, and save resources in the long-term. However, this process would involve significant up-front development costs. Those costs include agreements with Oregon’s private contractor as well potential legal costs to create data-use agreements. Consultations with experts in OEP and OHA have made clear that OHA must develop short-term protocols for transferring data between agencies without integrating data into the ONE system. However, a long-term plan can still be developed to integrate data sources into the ONE system in the long-term, with MMIS integration being the highest priority.
CONSIDERATION
In the short-term, transfer reports on medical exemptions to the ONE Eligibility system via a secure file transfer protocol. In the long-term, build capacity to integrate data sources verifying medical exemptions into the ONE Eligibility system.
Legal Considerations
The data sources explored in this section are either maintained directly by OHA or through contracts on behalf of OHA. Therefore, existing DUAs are likely already in place to allow OHA to explore and conduct queries on
these data. However, OHA may need to modify existing DUAs to explicitly permit the use of the data to verify Medicaid work requirement exemptions in accordance with the Health Insurance Portability and Accountability Act (HIPAA). OHA can follow best practices outlined later in this section to update those DUAs.
CONSIDERATION
Update existing DUAs to permit the explicit use case of verifying Medicaid work requirement exemptions.
Additional legal processes are likely necessary for longterm integration of these data sources into the ONE Eligibility system. Since the ONE Eligibility system is housed within the Department of Human Services, it likely does not have the same existing legal data privileges as OHA in terms of using personally-identifiable health data under HIPAA. As a result, the ONE Eligibility system will likely have to create new DUAs with OHA to permit the integration of data sources. Even with DUAs, the ONE Eligibility system may be constrained in the information it is allowed to integrate because of HIPAA. However, even with such limitations, OHA would likely still be able to automate certain processes, such as the sharing of aggregated reports with the ONE Eligibility system.
CONSIDERATION
Consult with legal experts to determine the extent to which health data can be integrated into the ONE Eligibility system and adjust long-term integration strategy accordingly.
Education
One method of compliance with Medicaid work requirements is at least half-term enrollment in an educational program. More than 200,000 students are enrolled in colleges and universities across Oregon, comprising 19 percent of the population subject to Medicaid work requirements Automatic verification of enrollment in educational programs, including public and private universities, community colleges, trade schools, and work programs, will ensure that students in such programs can access Medicaid coverage without costly manual verification. OHA can consider two approaches to automatic verification: pinging the Higher Education Coordinating Commission (HECC) and direct ONE Eligibility integration with educational institutions.
Higher Education Coordinating Commission
HECC receives data from nearly all post-secondary education institutions, including trade schools, work programs, and community colleges, the latter of which
also include non-credit career training, for-credit technical training, and for-credit lower division courses. The detail and recency of data transmitted to HECC varies by institution, however, limiting its effectiveness to specific use cases.
The granularity and content institutions transmit to HECC varies by type (e.g., public university vs. trade college), as does the delay present between an academic term ending and data being transmitted. All Oregon institutions use quarters rather than semesters, and data is transmitted to HECC after each quarter. Public universities generally transmit the most thorough data, including individual student identifiers and information on credit hour enrollment, and the data is submitted at the completion of the academic quarter with a one or two month delay. Community colleges send draft data to HECC with the same one or two month delay, then transmit final data the following fall after an academic term (e.g., data transmitted in November 2025 contains enrollment information from summer 2024 through spring 2025 terms). Draft data contains individual student enrollment data and is thus usable for data-supported compliance verification; it simply lacks additional checks for details such as students enrolled at multiple institutions. HECC has a standardized method of determining half-time and full-time enrollment, ensuring that school variation in enrollment definitions of half-time do not contribute to verification complexity. Trade schools and small career/technical training programs submit less data to HECC, likely due to technical limitations; they send more rudimentary data that simply verifies if a student was enrolled in the last term, without details on credit hours (necessary to determine at least half-time status). Credit hour details are important for verification: any combination of half-time enrollment, work program enrollment, and work or community service totaling to 80 hours satisfies the work requirement.
These data makes HECC an invaluable resource as OHA looks to verify compliance for members enrolled in educational programs. H.R. 1 instructs states to check for work requirement compliance for one to three consecutive preceding months for OHP applicants and one to six nonconsecutive or consecutive preceding months for members at renewal. Because we recommend OHA verify enrollment for only the month directly preceding the application, HECC will not yet have updated academic term data, limiting the usefulness of HECC data for automatic verification at application. For example, if a student applies for OHP coverage in February, OHA will look to verify enrollment in HECC for the month of January. These data will not be transmitted to HECC until the end of the quarter (plus an additional one or two months), which may be as late as May. For renewing members, however, HECC data is quite useful: If a member is eligible for renewal in June 2025, for example, OHA can query HECC in April or May 2025 (accounting for ex
parte checks occurring two months before eligibility ends) to check for student enrollment in the last six months, going back to October 2024. Despite ex parte processing occurring months before eligibility ends, HECC will likely contain data from at least some of this period, making it a valuable data source in ex parte verification of compliance. Trade schools remain a weakness in HECC data for both application and renewal.
HECC integration may prove complex. The Family Educational Rights and Privacy Act (FERPA) limits schools’ ability to share student-level data: schools may only share student-level data for educational purposes or audits. Compliance verification for Medicaid work requirements may fit within the audit designation, but further legal exploration is necessary. There are also logistical concerns: OHA queries to HECC may impose significant costs on HECC, which may require additional labor, financial, or logistical support to handle the additional data manipulation and management required.
RECOMMENDATION
Build data-sharing between HECC database and OHA for ex parte verification, pending legal feasibility.
Medium cost, large scale; prioritize for implementation.
Direct ONE Eligibility integration with educational institutions
Given limitations inherent in HECC data, direct studentlevel data integration between post-secondary institutions and the ONE Eligibility system may be useful in the long term. ONE could then directly check applicants’ or members’ information in a database receiving standardized, timely transmission of enrollment data from all Oregon educational institutions. This would likely reduce burden on OHA itself, as automatic or ex parte verification would occur through ONE itself. There would be logistical constraints involved in establishing communication with a new database; this work is likely manageable for most universities, while trade schools may likely need additional support to send regular data. Estimates for implementation in our interviews ranged from one or two months for large universities to 12 months for schools with fewer resources. Given that work requirements must be implemented on January 1, 2027, there may be sufficient time for direct integration between institutions and ONE to build on the data HECC provides.
RECOMMENDATION
Develop a standardized database of educational enrollment to integrate with the ONE Eligibility system.
High cost, large scale; consider for long-term.
Incarceration
Inmates of a public institution (both jails and prisons) and those who have been recently released from incarceration within the past 90 days are exempt from Medicaid work requirements. OHP coverage is suspended for inmates in all Oregon prisons or jails, which adds an additional level of complexity to a challenging verification process.99 Given these complications, a direct data-sharing pathway between OHA and the Department of Corrections would allow for automatic verification of inmates based on correctional data.
The Department of Corrections maintains data on all individuals under its supervision, including those who are incarcerated or in the community (e.g., on parole, probation, or post-prison supervision). As of 2025, there are approximately 12,000 inmates and over 19,000 individuals in the community under Department of Corrections supervision.100101 There are also several thousand inmates in local and county jails. While this population may seem nominally large, the relevant population for verification are those inmates within 90 days of release; this population, we estimate, is about 1 percent of the total population subject to work requirements. There are two sources of data OHA could look to integrate with the ONE Eligibility system for verification, detailed below.
The Prisoner Update Processing System
The federal Prisoner Update Processing System (PUPS), managed by the Social Security Administration, tracks incarcerated individuals who may be recipients of Social Security benefits. The PUPS collects data from correctional facilities, manages records, and helps the SSA verify the identity and confinement status of the recipients. Correctional facilities send data on inmates (e.g., names, Social Security numbers, and dates of incarceration) to the SSA; PUPS then houses a record for each inmate to be verified, allowing the system to keep records of members, benefit suspensions, and reinstatements. PUPS data could be used for data-supported exemption verification.102 It is unclear how up-to-date PUPS data is in Oregon; given that the exemption applies to individuals 90 days from their release, additional information on update frequency will be important in determining whether PUPS data can be used.
To link the PUPS with the ONE Eligibility system, OHA and/or ODHS would need to develop data-use agreements with the Social Security Administration; it is unclear how much time this process would require. These data are not
publicly available, and developing data use agreements may limit OHA staff’s ability to pursue other data integrations for larger statutory groups. Additionally, a major limitation of these data is that it only includes detailed information for recipients of Social Security benefits, likely leaving significant gaps in its coverage of the incarcerated population.103
Institutional-level data from the Department of Corrections
Given the Department of Correction collects data on all individuals under its supervision, OHA can consider direct integration with Department of Corrections databases. However, the data use agreements required for such a partnership, and the amount of people contained in the relevant exemption, would likely render the effort high-cost and low-scale. Similar to the PUPS–ONE linkage proposed above, data from correctional institutions would have to be recent and up-to-date to allow for automatic verification.
Additionally, data sharing across county jails has proved to be a recurring problem, due to the different data tracking measures across various institutions. While the governor signed a bill in 2019 to improve data sharing across county carceral facilities, at the time of passage there existed no statewide unified computer system for jails, making data collection a challenge and data sharing nearly impossible.104 An independent oversight report published in 2025 found that the correctional healthcare system still lacked a unified records system and was heavily paper-based, making coordination across facilities difficult.105
RECOMMENDATION
Streamline the automatic verification process for inmates by partnering with SSA’s PUPS database or state institutions.
High cost, small scale; deprioritize.
Data-Supported Alternatives to Automatic or Ex Parte Verification
Using Data-Supported Verification Where Automatic or Ex Parte Is Not Possible
Some individuals applying for or renewing OHP coverage may find that automatic or ex parte verification
of compliance is not possible and self-reporting is burdensome. OHA can increase the verification rate and reduce burdens on these individuals by implementing other data-supported verification methods, including consent-based verification, commercial third-party queries, and data-sharing partnerships with employers or other data owners.
Several statutory groups are likely to be in this population, particularly self-employed workers, including independent contractors and gig workers (10% of the work requirements population), students (19%), seasonal workers (<1%), and individuals participating in work programs or community service (<1%).106 Additionally, in the case that quarterly wage data are deemed unusable for ex parte verification by CMS guidance, W-2 employees will be a large (63%) group that will benefit from data-supported verification.
Volunteer Activity
Ex parte verification of volunteering hours is challenging. While community-based organizations (CBOs) may have individualized tracking methods for volunteering hours, there is no centralized process or database for tracking participation. A forthcoming interim rule from the Department of Health and Human Services (HHS) is expected to provide criteria for verifying compliance with qualifying community service activities. However, this rule is not expected to be released until June 2026, giving OHA limited time to develop or change implementation plans.107 Therefore, OHA will likely need to make a decision on how to streamline these processes before additional clarification comes from HHS. Given the data limitations and forthcoming guidance from HHS, OHA should accept manual reporting for compliance from volunteering until data systems are in place that will allow for a more automatic system.
There are alternate options that OHA could pursue to increase data collection on volunteer hours. First, OHA could explore the development of a database within ONE Eligibility portal to house all volunteer/service organization information and hours. CBOs could report volunteer membership and hours within this portal, allowing ONE or OHA to quickly verify volunteer hours for new applicants or renewing members. A volunteering database could be useful for other programs as well, as volunteer activity can also be used to comply with work requirements for SNAP.108
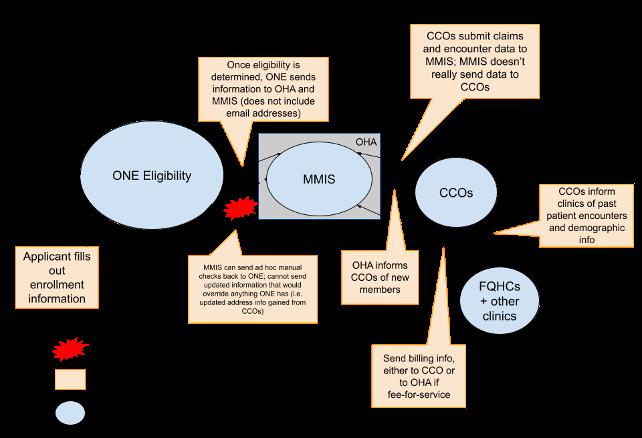
RECOMMENDATION
Implement a database within the ONE Eligibility system to house volunteer information reported by organizations and hours in one centralized location.
Medium cost, small scale; deprioritize.
OHA could also work directly with CBOs to verify compliance, prioritizing building data-sharing partnerships with organizations that work with a large number of individuals subject to work requirements. CBOs may struggle to incorporate reporting requirements given budget and staffing constraints; as a result, OHA may struggle to receive data from small organizations with few permanent employees.
RECOMMENDATION
Partner with large CBOs directly to verify compliance.
High cost, small scale; deprioritize.
Lastly, OHA could allow individuals to self-report their volunteer hours in the ONE Eligibility portal at time of application or renewal. This places additional burden on applicants, but may be the most efficient way to obtain volunteering participation data. Upcoming CMS guidance may preclude self-reporting of compliance mechanisms (including volunteering); in this case, OHA should further prioritize organization-level data collection methods listed above. If pursuing this recommendation, OHA could
accept manual reporting for volunteer hours until capacity is built for a more systematic, data-driven process to be used.
RECOMMENDATION
Accept self-reported volunteer hours at application and renewal.
Low cost, small scale; implement if spare capacity.
Data-supported employment verification
Consent-based verification
Consent-based verification (CBV) allows applicants and members to give consent to payroll providers, gig work platforms, bank accounts, and other sources to share relevant data with the state directly. Implementing CBV requires procuring a commercial vendor but tends to have lower cost-per-verification than commercial third-party queries. The ONE Eligibility system is currently running a pilot program for CBV to verify income for some gig workers; if implemented at a greater scale, CBV could be the lowest-cost way to verify compliance for self-employed workers and those W-2 employees who cannot achieve automatic or ex parte verification via aforementioned data sources (e.g., VCI).
Beginning conversations with vendors early can help ensure that Oregon has a scalable CBV solution in time for Medicaid work requirements and can help plan the rest
of the income verification waterfall (see below). Leading private sector vendors include Steady IQ, Truv, truework, and Plaid.109 CMS is piloting a CBV platform in Louisiana and Arizona, but some experts have expressed concerns that an effective product will not be ready for all states in time for the rollout of work requirements.110
RECOMMENDATION
Scale up consent-based verification.
Medium cost, large scale; prioritize.
Commercial third-party queries
States, including Oregon, supplement their ex parte quarterly wage data queries with queries to commercial databases such as Equifax’s The Work Number or Experian Verify. These queries tend to have high marginal cost relative to other options, ranging up to $15 per match for some leading platforms.111
Data-sharing partnerships with non-state entities
OHA can partner with employers, schools, work program administrators, and other entities that keep relevant data to share data for verifications. This approach will likely involve larger fixed costs of setting up data-sharing infrastructure and agreements, but could be worthwhile to pursue with institutions that employ or educate large numbers of residents.112
CONSIDERATION
Create data-sharing partnerships with non-state entities.
The income verification waterfall
Combining multiple verification methods into an “income verification waterfall” is the best way for OHA to maximize the number of successful verifications while minimizing marginal costs. The Center on Budget and Policy Priorities’s “Guide to Reducing Coverage Losses” describes the waterfall approach as follows: “first attempt to verify income through lower-cost sources, only check more expensive data sources if necessary, and only request documents from individuals as a last resort.”113 OHA can collaborate with the administrators of the ONE Eligibility system to design an OHP income verification waterfall that models the costs of each potential member journey and includes contingencies for potential scenarios—for example, models may include whether CBV is possible for various groups, or alternative data sources if CMS guidance rules out VCI verification.
In Oregon’s case, a simple baseline version of the Medicaid waterfall could look like:
1. Query VCI via FDSH for earned income (ex parte verification)
2. Query SSA for unearned income (ex parte verification)
3. Send CBV (data-supported verification)
4. Query commercial data sources (ex parte verification, but high marginal cost)
5. Reach out to applicant directly to request documents (manual verification)
CONSIDERATION
Design an income verification waterfall.
Collaborative Data Systems
OHA can work with its Coordinated Care Organization (CCO) partners and ODHS to create a streamlined data structure that will promote collaboration, which is especially important in cases where ex parte verification is not possible but data can point to methods of effective outreach via communications channels.
One potential data hazard is MMIS’s inability to update demographic or contact information held in the ONE Eligibility system. This has significant implications for outreach efforts: Federally Qualified Health Centers (FQHCs) and CCOs are often the first to receive accurate updates from OHP members but are unable to update member information centrally held in the ONE Eligibility system. ONE should include the ability for MMIS to update contact information within its database. This capability would also improve SNAP and TANF information accuracy; if a CCO or FQHC receives and transmits a change in contact information to ONE, SNAP, TANF, and Medicaid would all have access to the new, accurate member information.
To facilitate coordinated outreach, we recommend updating the OHA data portal, which is used by CCOs and FQHCs for tracking patient claims, to include detailed enrollment status information. This status should specify a member’s next renewal timeline and their last eligibility determination method (e.g., exemption or income). Crucially, the portal must also include a field allowing CCOs and FQHCs to enter updated contact information, which can then be transferred via MMIS to the ONE system to ensure member data remains current.
RECOMMENDATION
Update existing data flow infrastructure to efficiently coordinate outreach to members when ex parte verification is not feasible.
Medium cost, large scale; prioritize.
Legal and Data Use Agreement Considerations
Data sharing requires clear frameworks for accessing, sharing, and using data across agencies while maintaining privacy and minimizing costs. Data use agreements (DUAs) or data sharing agreements are critical tools to ensure secure and responsible sharing of information between state agencies. They establish clear terms for protecting privacy, ensuring compliance with regulations, and creating a concrete understanding of the scope and nature of any data partnership. Ideally, DUAs not only foster streamlined and protected data sharing but also promote collaboration across agencies.114
In addition to DUAs, designated data management bodies, responsible for storing and sharing data as requested, can streamline the processes of frequent data sharing among many agencies. Oregon does not currently operate with a designated data management body. However, it does have an open data portal, created by legislation in 2017.115 The same law also requires the Chief Data Officer to create an enterprise Memorandum of Understanding (MOU) that helps facilitate data sharing.116 However, MOUs are limited in that they are not legally binding, while legislating data sharing or drafting data use agreements are.
Ohio’s InnovateOhio platform can serve as an example of a data management body. Ohio’s governor signed an executive order in 2019 creating the InnovateOhio platform, which consolidates data systems across the state. The executive order created a presumption of data sharing between state agencies, except where a specific legal prohibition is identified in writing. Ohio’s initiative has been successful—it is now considered a leading example in data-sharing policies, and nearly 1,600 information systems have been incorporated into the state’s cloud environment.117
In the absence of more explicitly legislated data sharing, the ONE Eligibility system should create template DUAs,
ideally based on existing protocols. These templates would streamline system-wide data sharing with the sources described in this report. Establishing DUAs formalizes critical aspects: the scope of the data, agency responsibilities, the expected output, and allowed uses by analysts, thereby ensuring a common understanding among all parties.118
A template data use agreement should include the following elements: (1) purpose statement, (2) definitions, (3) justification for access, (4) any state requirements to consider, (5) benefits to sending agency, (6) benefits to receiving agency, (7) mutual benefits, (8) description of data, (9) method of data transfer or access, (10) plan for regulatory compliance (i.e., for data protected under HIPAA), (11) location of matched data, (12) declaration of custodial responsibility, (13) timeline for agreement, (14) any relevant exclusions, (15) methods for amending, (16) liaison officials from each agency.119
Recommendations
:
• MMIS: The ONE Eligibility system shares eligibility information on applicants to the MMIS. However, MMIS does not currently share data back to the ONE Eligibility system, except through ad-hoc queries. We recommend developing a data use agreement between MMIS and ONE that allows MMIS to more systematically share back (1) claims and diagnostic data for Medicaid eligibility verification and (2) updated addresses, phone numbers, or other crucial contact information.
• APAC: The APAC database currently faces capacity constraints in managing ad-hoc queries. Developing a systematic plan for querying claims data through a data use agreement, along with additional staffing resources, could significantly mitigate these challenges.
• HECC: Similar to APAC, HECC is expected to face significant constraints when responding to queries from ONE. To systematize this process before implementation begins, HECC should establish a data use agreement and receive the necessary staffing and financial support to identify and mitigate anticipated data-sharing challenges.
Prioritized Recommendations
The Cost-Scale Framework
OHA has many options for increasing the number of people deemed exempt or compliant with work requirements via automatic and ex parte verification. However, given resource and timeline constraints, it will not be possible to implement every recommendation. To help OHA prioritize among recommendations, we introduce a “cost-scale framework,” which can help ensure the greatest impact and retention of coverage for eligible OHP members.
Scale is measured, for each recommendation, as the increase in the number of people who receive verification as a result of implementing it. Scale is the product of two components:
• Base, the size of the work requirements population that would be affected. Bases are sourced from our analysis in the section “Estimating the population size of those subject to work requirements.”
• Lift, the expected increase in verification rate due to implementing the recommendation. Lifts are approximated by qualitative analysis of the recommendation’s likely impact if implemented successfully.
For example, a recommendation that affects a group comprising 30 percent of the work requirements population and is expected to increase the rate of automatic verification from 25 to 35 percent would have a total scale of 30% × (35% - 25%) = 3 percentage points. To accommodate uncertainty in the lift estimates, we group scale into three categories: “large” (greater than 5 percentage point increase to total verifications), “medium” (1 to 5 percentage points), and “small” (less than 1 percentage point).
Cost is multifaceted, including the dimensions of the time cost, fiscal cost, and administrative burden associated with implementing the recommendation. Fixed costs (initial setup costs) and variable costs (any costs associated with each marginal verification) are both considered. To represent cost in a way that captures its multifaceted nature but is still useful for prioritization, recommendations are
divided into three cost scores of “high,” “medium,” and “low.”
There are other considerations that may be relevant to prioritization that are not included in this simple framework. Particularly, it is important to keep in mind that this method considers each person who receives automatic, data-supported verification to be equal in terms of scale measurement; however, there are many reasons why some individuals or groups could be prioritized for automatic verification over others. First, a recommendation may be more desirable if (all else equal) it increases automatic verification for a group that is more difficult to reach via direct channels, or for a group that will struggle more with manual verification, as verifying those groups manually is more costly. Second, in accordance with Oregon’s health equity principles, OHA may want to prioritize a recommendation more if it contributes to “recognizing, reconciling, and rectifying historical and contemporary injustices.”120 Note that in many cases this consideration will be aligned with the former. Finally, some pairs of recommendations will affect overlapping groups, and thus implementing them both would have a lower scale than just adding together the scale scores of each would suggest. We highlight these overlaps qualitatively where we expect them to be consequential.
High-Priority Recommendations
Table 3 highlights how we determined which recommendations to prioritize for automatic or ex parte verification according to the cost-scale framework described above. Table 4 shows recommendations for whether to implement each action based on its cost-scale score.
The actions that we recommend prioritizing correspond to the green boxes in Table 3, and are listed here:
Low cost, large scale; prioritize.
• Ensure that children’s ages are collected in ONE and enable automatic exemption for parents with children 13 years or younger.
• Identify and automatically exempt individuals in households receiving SNAP benefits.
• Add questions to the OHP application pertaining to medical exemptions
Medium cost, large scale; prioritize.
• Expand ONE Eligibility income verification to include The Work Number (new and returning applicants), quarterly wage data (returning applicants), and unemployment insurance (new and returning applicants).
• Query the MMIS database to determine whether members are eligible for a medical exemption
• Build data-sharing between HECC and OHA to verify members’ educational enrollment
• Scale up consent-based verification
• Update existing data infrastructure to coordinate outreach to members when ex parte is not feasible
Low cost, medium scale; prioritize.
• Accept self-reported American Indian identification and continuously exempt Indian individual
Table 4. Recommendations and cost-scale estimates for Data section
Recommendation
Using existing systems
Ensure children’s ages are collected in ONE; enable automatic exemption for parents with young children
Enable automatic exemption for individuals in compliance with TANF work requirements
Identify and automatically exempt individuals in households receiving SNAP benefits
Collect frequent and accurate pregnancy data and automatically exempt pregnant individuals
Accept self-reported American Indian identification and continuously exempt Indian individuals
Expand ONE income verification to include The Work Number (applicants and members), quarterly wage data (members), and UI (applicants and members)
Expand ONE Eligibility income verification to include data on contributions to Paid Leave Oregon.
Further integration of existing data sources
Add questions to the OHP application pertaining to medical exemptions (see full text in body)
Query the MMIS database to determine whether members are eligible for a medical exemption
Query the APAC database
Develop capability to query Presc. Drug Monitoring Program
Develop capability to query Oregon State Cancer Registry
Develop
to query PointClickCare platform
Build data-sharing between HECC and OHA to verify members’ educational enrollment
Develop a standardized database of educational enrollment to integrate with the ONE Eligibility system
Streamline the automatic verification process for inmates by partnering with SSA’s PUPS database or state institutions
of children 13 years or younger
with TANF work requirements
recipients NOT exempt from SNAP WRs
individuals and those receiving postpartum coverage
California Indians
Note: Color codes in rightmost columns refer to recommended prioritization (see Table 3).
Non-ex parte, data-supported
Implement a database within ONE to house all volunteer information and hours in one centralized location
Partner with large CBOs directly to verify compliance
Accept self-reported volunteer hours
Update existing data infrastructure to coordinate outreach to members when ex parte is not feasible
Note: Color codes in rightmost columns refer to recommended prioritization (see Table 3).
Communications
The disruption stemming from the imposition of new work requirements cannot be overstated; indeed, lessons from the two states that have already instituted work requirements demonstrate that significant coverage losses are likely.122 Even after OHA makes clear policy decisions and establishes a robust ex parte data verification system, many potential OHP members will still require additional information from OHA to enroll successfully in OHP and fulfill renewal requirements. Some of this information will need to be communicated to all potential OHP applicants and members, and some information will need to be targeted to address the needs of specific populations.
In this section, we offer recommendations centered around four pillars:
• General best practices for design and delivery of messages to the entire population across all channels;
• Channel-specific best practices for design and delivery of messages through various channels, including mail, websites, text messaging, or radio;
• Engaging partners to amplify and deliver information and co-create the communications, data, and policy strategies to address work requirements; and
• Population-specific strategies that explore channelspecific best practices and reliable partners for hard-toreach populations.
The goal of this section is to provide considerations for OHA’s communication with OHP applicants and members to ensure that all individuals eligible for OHP can retain their Medicaid coverage. First, we review the general best practices for the design and delivery of messages to the population of interest. These strategies include adopting best practices around language, framing, timing, and delivery. The following section recommends solutions to the unique design and delivery challenges present for certain channels, including mailers, flyers, ONE Eligibility system push notifications, text messages, websites, phone calls, radio, and in-person outreach. The third section recommends a framework for OHA’s partnerships with other institutions and organizations, including 1) cocreation of its strategy around work requirements, similar to its process during redetermination, and 2) working with partners to strengthen and distribute information. Fourth, we discuss population-specific strategies for certain hardto-reach populations, such as people living in rural areas, houseless people, former foster youth, and people of color. These populations may warrant additional attention as they
may have different communications needs or are underserved.
General Best Practices For Communication
OHA can integrate general best practices for communication into its communications strategies with OHP applicants and members. These best practices are applicable to all populations and regardless of the channel or partners through which the communication occurs. This section considers two steps of the communications process that are essential for effective communications: design and delivery. By adopting these strategies across all communications with OHP applicants and members, OHA can provide accurate, timely, and easy-to-understand communications, which will increase the number of eligible people who enroll in OHP and reduce the number of eligible people who lose OHP coverage due to the information challenges associated with work requirements.
Design
An effective communication strategy makes its intended action clear, direct, and achievable. Designing communications that use language effectively maximizes the likelihood that an OHP applicant or member takes the action desired by OHA. Best practices include using plain language, framing the message, and employing humancentered design.
Use plain language
Plain language is language that is clear and easy to understand for the target audience. Plain language is the gold standard for public information and the federal standard under the 2010 Plain Writing Act.123
Plain language communications are structured and conversational. Conversational language involves employing words that a general audience confidently knows, as part of broader messaging it can quickly understand, even without professional expertise. In practice, this means using a fourth-grade reading level.124,125
Plain language should also pay close attention to voice and tone. Successful plain language campaigns write directly to the reader in active, positive sentences that tell them what they need to know and what they have to do.
Finally, plain language avoids conditional statements that could confuse people, like “You may be automatically renewed,” or “Most people must complete a form, but some will not.”
Additional effective practices for using plain language in communications include the following:
• Keep sentences short;
• Present important information first, section by section;
• Include relevant details that help audiences complete tasks;
• Standardize titles, lists, headers, and other forms of design; and
• Connect varying elements through transitions.126
Applicants and members may not be familiar with certain words or terms. For one thing, many OHP members may not know that they are on Medicaid because their insurance is not branded as Medicaid. For example, members may think that their plan is actually a private plan or state-sponsored, or they may not understand that OHP and Medicaid are the same program.127 In this case, using plain language means helping people to understand that they may know their Medicaid coverage by a different name, such as the Oregon Health Plan or the name of their Coordinated Care Organization (CCO). Acronyms and jargon may also be unfamiliar, like “OHP” for the Oregon Health Plan or “Medicaid expansion population.” When drafting communications, OHA should avoid using these terms.
OHA can rely on several existing tools and processes to understand whether its communications meet plain language standards. For example, online tools such as the Hemingway Editor allow policymakers to test the grade level at which their forms are written. OHA can test communications prototypes with members using the Medicaid Beneficiary Advisory Council for plain language, as discussed below. Additional resources that can provide guidance on implementing plain language best practices include Federal Plain Language guidance, a field guide to designing government forms from The Lab @ DC, and plain language review best practices from Massachusetts.128, 129, 130
RECOMMENDATIONS
Adopt best practices for plain language use in communications with OHP applicants and members:
• Identify a target audience and purpose for content.
• Write content in plain language and avoid jargon.
• Test prototypes internally with online readability assessment tools and externally with target user groups.
Frame the message
Message framing considers how the way information is presented influences whether people are motivated to take the action desired by a messenger. Calls-to-action can encourage applicants and members to enroll in OHP or submit renewals.
A call-to-action is a clear, simple instruction that tells an applicant or member what specific step(s) to take, how to take them, and how taking those steps will help the applicant or member gain or retain access to coverage. Calls-to-action provide an easy, concrete next step— such as updating contact information, completing a renewal form, submitting documentation, or attending an appointment—so the member knows exactly what to do to stay covered and avoid losing benefits.
Research from redetermination shows that two message frames are particularly effective when encouraging Medicaid members to take action to renew their eligibility for Medicaid:131
1. The “Keep Your Benefits” Frame: “If you want to keep your Medicaid, it’s important to complete your renewal when you get your notice. Respond right away to keep your benefits.”
2. The “Access to Care” Frame: “To keep your health coverage for doctor visits, prescriptions, and more, you must complete your Medicaid renewal. Respond right away to make sure you can continue to get the care you need.”
These frames outperformed two other frames, which focused on the hassle of reapplying for benefits and the threat of losing coverage. The results also varied by population segment; while most segments found the “Keep Your Benefits” to be most effective, young adults and people without children found the “Access to Care” frame more motivating. OHA can use these frames as a starting point and engage in user testing to understand how the frames might be interpreted by various population segments.
RECOMMENDATIONS
Use calls-to-action to frame messages in a way that will encourage OHP applicants and members to take action. Center calls-to-action around how taking action will help applicants and members keep their benefits or continue to have access to care.
Employ human-centered design
OHA can bridge the gap between the human and technical needs of service delivery by continuing to
use human-centered design (HCD) while creating its work requirements communications strategy. HCD is a method that places the emphasis on designing for the needs of humans, not systems. The method comprises four phases: discovery, design, deliver, and measure. In practice, this looks like researching user needs (discovery), developing and testing prototypes (design), publishing the best iteration of the product (deliver), measuring its effectiveness (measure), and then continuing to iterate on the design.
The Center for Civic Design’s best practices for the “design” phase include testing communications prototypes by soliciting direct feedback in conversations with members of the public.132 In these conversations, the goal is to identify how well members of the public can understand the processes outlined in the communications and the ways in which the intended message might be misinterpreted. The feedback provided should then be used to revise the prototypes. OHA’s Medicaid Beneficiary Advisory Council, created to elevate the voice of people with lived experience in the Oregon Health Plan, can serve as a representative sample of OHP beneficiaries.
Rich human-design conversations are fueled by unbiased, open-ended, and probing questions.
Potential questions for a conversation about a prototype mailer that informs an OHP member that they may be subject to work requirements beginning January 1, 2027, include:
• Why do you think OHA is sending this notice to OHP members?
• After reading this notice, what do you think is going to change for OHP members starting January 1, 2027? Does that depend on whether the member is working?
• What do you think “work requirements” means in the context of this notice?
• Can you walk me through the actions you would need to take to be compliant with work requirements?
RECOMMENDATION
Apply human-centered design principles to communications design, with a focus on testing prototypes with users.
Delivery
Even with effective design, communications will only be effective if they reach the member. This section considers general best practices for delivering communications regarding changes resulting from H.R. 1, with a focus
on ensuring that messages reach members and are internalized. We offer three recommendations to ensure effective delivery of communications: use repeated messages across multiple channels, time messages, and work with partners.
Use repeated messages across multiple channels of communication
H.R. 1 requires OHA to send information via mail and use at least one additional channel of communication when communicating changes to OHP members. Additional channels of communication may include push app notifications from the ONE Eligibility app, mailers, flyers, text messages, phone calls, websites, and social media posts.
Marketing research suggests that individuals need to “be exposed to messaging 10 to 13 times across multiple channels” for a message to stick and that messages should be consistent across platforms.133 For OHA’s purposes, this includes adopting consistent language, logos, color schemes, message frames, and calls-to-action across all communications about work requirements.
Using multiple channels of communication may motivate an OHP applicant or member to take action for several reasons. First, existing research shows that repeating key messages across multiple channels increases the likelihood of a member taking the desired action of the messenger.134 Furthermore, members may expect to receive communications via mail, text, and email, among other forms of outreach.135 Using multiple channels of communications allows members to use the medium with which they are most comfortable. Finally, using multiple channels of communication ensures that a member can receive important information even if there are barriers to using certain channels. For example, a member who lacks a reliable mailing address may still be able to view a social media post, while a member without broadband access may still receive phone calls.
RECOMMENDATIONS
Communicate with applicants and members through consistent, repeated messages across as many channels as possible.
Time messages
States are required to begin conducting outreach to members between June 30, 2026 and August 31, 2026, to inform them about upcoming changes to Medicaid resulting from H.R. 1. Once work requirements go into effect on January 1, 2027, states will have to verify members comply or are exempt from work requirements at least
once every six months. States also must verify compliance or exemption for at least one month prior to application. This staggered timing means that OHA will have to send messages at different times to certain groups.
To account for the staggered timing of various deadlines, OHA will need to develop a strategy so that messages land at the appropriate time in a highly congested media environment. While the development of a detailed communications timeline is out-of-scope, following general message timing considerations apply across populations and timelines.
• Send communications far enough in advance so that affected individuals have sufficient time to act: OHA should consider the amount of time it will take members to understand requirements and gather and submit documentation and send notices to allow sufficient time to do so.
• Create a sense of urgency by sending notifications at key intervals: OHA should send strategically timed reminders in the final weeks and days before a deadline, which can note the deadline to create urgency.
• Stagger communications to avoid overwhelming customer service channels: OHA should sequence messages across member groups and deadlines so that the workload of call centers and caseworkers is evenly distributed over time.
RECOMMENDATION
Ensure communications are sent in advance, send notifications at key intervals, and stagger communications.
Channel-Specific Best Practices For Communication
Alongside the general best practices for communications outlined above, there are channel-specific factors to consider when designing an effective communications strategy. This section outlines the best practices for channel-specific communications, including mailers, flyers, ONE Eligibility system push notifications, text messages, websites, phone calls, radio, and in-person outreach.
Mailers
Mailers are often the default mode of communication for government agencies and for good reason: Sending mail is the most straightforward way to reach every address that
OHA has on file. Mail is also more effective for populations who are uncomfortable using digital services, like older people, or populations in rural areas, who may lack dense community spaces where people may see information about work requirements.
Unfortunately, most government mailers suffer from unclear, convoluted writing that does more to confuse people than enlighten them.136 Many of these shortcomings arise from challenges that are unique to mailers. For example, since mailers must be contained on paper—rather than a computer screen—they are limited to one-way communication. This challenge prevents certain actions, like the use of conditional logic, where a dynamic prompt appears based on a user’s previous response. Second, taking action by mail can be a slow and complicated process for many users. For example, some younger people might not know how to address an envelope. Finally, applicants or members may discard unfamiliar envelopes.
An additional consideration when using mailers is that mailers are typically effective only when they reach their recipient, which is increasingly rare. When Arkansas tried work requirements, one health provider attempting to notify their patients about the new requirements found that only about 10 to 15 percent of the mail sent to beneficiaries reached its intended recipient.137
To address these challenges, we offer four mailer-specific recommendations to address these challenges, adapted from recommendations from the Center for Civic Design:
• Make it trustworthy. Help the recipients identify the office it came from with a few universally recognizable elements on the outside of the envelope: the name of the office, contact information, and an official seal, if possible. OHA can also include basic information on the outside of the envelope, so that anyone can read crucial information that their benefits are at risk.
• Be specific about the problem. Tell each person why they are getting this letter and show them what information it is based on. Create separate letters for different problems, so everyone gets the details they need without relying on conditional logic.
• Tell them how to take action successfully. If applicants or members have to return a form, tell them why and how. Additionally, if there is an online version or more information on the web, give them a link (and a QR code for a web page). Finally, make the requirements for success clear: Do they have to sign the form? Is there other required information? What is the deadline?138
Designing with these principles yields a much friendlier, more effective mailer.
RECOMMENDATION
OHA should design mailers that are designed to be trustworthy, are specific about the problem, and tell recipients how to take actions successfully.
Flyers
Flyers can be helpful for reaching members or applicants who are not reached by direct mailers or internet outreach. This is especially true if they are posted in strategic places likely to reach potential OHP applicants or members, such as health care providers and clinics; state or local health departments; offices that administer social services such as SNAP, WIC, housing, or disability benefits; and community spaces like schools or places of worship.139 CMS offers channel-specific communications toolkits with guidance and example materials for several types of locations, including schools and childcare settings, places of worship, and clinical offices and health care settings.140
Flyers present two unique communications challenges. First, like mailers, flyers involve one-way communication. Second, flyers must catch a member’s eye, often on crowded pinboard spaces.
We offer a few key recommendations for how to deal with these challenges unique to flyers in accordance with guidance from CMS:141
• Make key messages large and striking on the page
• Include specific dates and timeframes wherever possible
• Include specific, relevant information so that viewers will not need to fill in missing gaps or guess where they fit in
• Provide clear guidance on how to take the desired action
See the Appendix for a discussion of flyer design with three example flyers.
RECOMMENDATION
OHA should work with partners to post flyers that highlight a large key message and include specific dates and instructions in clinics, schools, social service offices, faith institutions, community centers, and other public spaces.
One Eligibility Push Notifications & Text Messages
States have embraced text messaging as a way of communicating with Medicaid applicants and enrollees since the Federal Communications Commission (FCC) began allowing it in 2023.142 Some have used text messaging to great success: Oklahoma, for example, found that texts sent during open enrollment increased the daily enrollments per day from 6,000 to 14,000 and helped the state surpass its enrollment goal by 200 percent.143
Research shows that text messaging is effective: Members are more likely to respond to requests to update their contact information if they receive the request via text message as opposed to mail or email.144 However, text messages have their limits. The City of Norfolk, Virginia, has found that some Medicaid members either do not trust text messages or do not read them.145 Similarly, push notifications must compete with several other notifications that people receive daily and may be ignored. Finally, FCC guidance from 2023 suggests that Medicaid agencies send no more than eight text messages to any single person per calendar year.146
Several strategies can overcome the challenges associated with push notifications and text messages, adopted from best practices developed by State Health and Value Strategies (SHVS).147
• Establish credibility: Send a “credibility” text message (a message that identifies the sender and states OHA will never ask for personal information over text). Making a follow-up phone call afterwards will improve response rates further. The city of Norfolk is currently conducting an evaluation to understand the effectiveness of this intervention.148
• Keep it short. Limit messages to 160 characters to ensure deliverability.
Sample Text Message
This is the Oregon Health Authority reminding you to update your mailing address. It’s important that we can contact you about your health insurance. Visit [SHORT URL] or call 800-273-0557 to update your contact info today.
Adapted from State
• Don’t send too frequently. Limit messages to two to four per month. Prioritize critical messages, deadlines, and alerts to take action.
• Share a clear call to action: Give members the information they need to act quickly, such as how and where they can comply with work requirements.
• Send during appropriate times. Messages sent midweek during the afternoon have the highest click rates.
• Use short URLs. Easy to follow links direct people to further information.
• Check the Reassigned Number Database. This can reduce the chance of texting the wrong person.
In addition to these best practices, OHA can consider testing different text messaging tactics. For example, OHA can test adopting a conversational tone or adding emojis to messages to see if members respond more positively to them. Testing and tracking what works can enhance the effectiveness of a text message campaign over time.
RECOMMENDATION
OHA should use text messaging in its communication plan. Text messages should be credible, short, infrequent, and timely; include short URLs; and checked using the Reassigned Number Database.
Websites
A well-designed website will allow OHP members to learn about work requirements and exemptions and complete any required tasks. The website should be easy to access, navigate, and understand. Websites offer a number of advantages over traditional communications, including providing opportunities to use conditional logic, organize information, and link to external sites. However, this added content creates additional layers of complexity.
The following recommends can help OHA design effective website content work requirements:
• Use QR codes. Provide QR codes that link to OHA’s homepage about work requirements on all external communication materials.
• Organize text into accordions. Use accordions, or vertically stacked lists of headers that can show or hide content when clicked, to organize text on long pages. Accordions ensure visitors can quickly see the main topics on the page without overloading them with text.
• Provide contact information. Ensure that contact information for OHA is easy to find on all pages throughout the website, including any relevant phone numbers, email address, and mailing address.
• Flag navigation to external sites. Notify users when they are navigating to another website. Testing has shown that people can get confused when they navigate to external websites and can struggle to retrace their steps.
A sample of a website that applies many of these best practices is shown in the Appendix.
RECOMMENDATION
OHA should use well-designed websites to communicate with potential OHP applicants and members. Well-designed websites should use QR codes and accordions, clearly display contact info, and warn users when leaving the site.
Radio
Radio is a key strategic communication channel with a number of strengths, particularly its high reach and low cost. Radio remains one of the most widely used audio platforms in the U.S., and through its passive medium, it can easily be consumed outside of the home during daily routines. Research shows that around 27 percent of individuals report obtaining health information via radio even if not actively seeking it.149
Radio is also portable, low-cost, and inclusive. It requires no broadband, which may be especially beneficial for rural and frontier counties in Oregon. Radio also can reach multilingual audiences through language-specific local stations.
There are certain challenges with using radio. Perhaps the greatest limitation is that radio is not a visual medium, so communicating action-oriented next steps is particularly difficult. Furthermore, radio broadcasts are often localized,
Using OHP’s website to assist with SNAP
Since many OHP members also benefit from SNAP, and SNAP is also changing, OHA might consider including a footer banner with a notice about the upcoming changes to SNAP, such as “Do you have SNAP? Changes are coming to SNAP. Learn how to keep your benefits here,” and a link to the SNAP webpage.
with FM radio signals typically having a range limited to less than 150 miles.150
OHA has several options to address these challenges unique to radio, as adopted from a toolkit Oregon State University (OSU) developed to increase mental health programming in rural Oregon.151
• Keep messages short and action-oriented. In Union County, partners reported that 30-minute radio interviews did not match local needs. Instead, short public service announcements and soundbites offering one specific resource were more effective, allowing nine PSAs to be aired over 900 times across four Eastern Oregon counties. Given that listeners are often listening passively or multi-tasking, messages with one specific next step are more effective than broad guidance.
• Tailor messages to local context. Through the same toolkit, researchers found that county-specific resource guides, reviewed by local partners, were better received. These toolkits included localized references, like local crisis line numbers, county services, or regional examples. Local messages are also bolstered by mentions of local partners, such as county mental health departments and OSU extension offices. Short community testimonials also can help to increase trust.
• Target messages to certain population segments through format radio stations. Radio uniquely allows for specifically tailored messages to audience segments through format radio stations targeted to specific audiences (e.g. agricultural workers, tribal communities, Spanish-language listeners). The study found broader uptake when messages were distributed across stations rather than relying on a single partner. Communicating through multiple channels can also allow for a partnership to be built between radio stations and guests.
RECOMMENDATION
OHA should use radio stations to communicate with potential OHP applicants and members. Messages delivered via radio should keep messages short and action-oriented, be tailored to the local context, and target messages to certain population segments through format radio stations.
Engaging Partners in Communications Strategies
OHA should engage in sustained and coordinated engagement with partners to co-create communications
strategy and/or amplify messages regarding work requirements. OHA’s partners can provide vital insight into the policy, data, and communications strategy. Throughout interviews for this report, CCOs, Federally Qualified Health Centers (FQHCs), and communitybased organizations (CBOs) expressed the desire for strategy sessions similar to those that took place during redetermination.
In this section we review key partners OHA should engage with to amplify their messaging. We begin by offering an overview of the benefits of establishing partnerships with outside organizations. We then review the landscape of partners OHA works with across entire populations and offer key considerations for partnerships. Finally, we suggest a framework that OHA can use when evaluating partnerships to determine the degree of engagement OHA pursues with different organizations.
Benefits of Engaging Partners in Communications Outreach
Engaging partners in communications outreach can help to amplify messaging in several ways, including allowing OHA to rely on existing networks to exponentially increase the reach of its messaging at minimal cost. For example, OHA can spread information to uninsured Oregon residents about enrollment into OHP much more effectively through its network of FQHCs.
Additionally, much of the engagement conducted by partners is likely to be in-person outreach and community engagement via trusted messengers. This type of engagement uniquely allows for a human touch and two-way communications that can drive potential applicants members to take action. Research shows that ideal in-person outreach and community engagement involves using trusted messengers, hosting public events, and physically operating in community “hot spots.” These features can be especially effective in increasing the uptake of information when coupled with other strategies.152 For example, one study found that awareness among respondents increased 7.5 percent among those who received a “second touch” flyer at an in-person community event when compared to those that only received an initial mailer.153 These second-touch strategies include cultivated relationships with providers, appearances at local familyoriented events and celebrations (e.g. health fairs, parades), community forums, and presentations to local community leaders.
Finally, engagement conducted by partners can help to overcome certain barriers experienced by hard-toreach populations. Many CBOs, Tribal organizations, and CCOs already have tailored outreach materials, multilingual capacity, and deep cultural competence. This allows messages from OHA to be adapted into formats
and languages that resonate more directly with these communities. We later provide recommendations for population-specific engagement partners for hard-to-reach populations.
RECOMMENDATION
Engage with relevant partners in communications outreach.
Core Engagement Partners
This section describes the engagement partners for whom OHA could establish partnerships with to help implement work requirements. This section focuses on broad groups of engagement partners, rather than specific partners. However, some specific engagement partners are discussed in the next section, which reviews communications strategies for hard-to-reach populations.
Coordinated Care Organizations (CCOs) are OHA’s primary delivery system partners and maintain ongoing relationships with the OHP members they serve. Because CCOs handle care coordination, member services, and case management, they are often among the most trusted and frequently used access points for members to receive information about coverage. CCOs also have a large network of providers who can reinforce messaging about work requirements, help applicants and members understand whether they qualify for exemptions, and support applicants and members in completing required documentation. In interviews with partners, CCOs expressed a shared interest in minimizing coverage loss from work requirements and a willingness to amplify messages in accordance with guidance from OHA.
Federally Qualified Health Centers (FQHCs) serve large volumes of OHP and uninsured patients across Oregon, making them a critical partner in outreach. Interviews with leaders of FQHCs demonstrated that FQHCs are often intimately involved with an applicant’s OHP enrollment or a member’s renewal application. Because FQHCs already help patients enroll in OHP, their staff are uniquely positioned to help OHP explain work-requirement rules, identify the exemptions an individual might qualify for, and provide hands-on support with verification for renewal. In interviews with partners, FQHCs expressed a shared interest in minimizing coverage loss from work requirements and a willingness to amplify messages in accordance with guidance from OHA.
County Public Health Departments regularly communicate with a county’s residents regarding countywide health care services or disease prevention programs. County health departments can also work closely with other partners within the county to spread information
about health. For this reason, county health departments are a trusted messenger and an effective partner for disseminating information about work requirements. In interviews with partners, county public health departments expressed a shared interest in minimizing coverage loss from work requirements and a willingness to amplify messages in accordance with guidance from OHA.
Hospitals regularly engage with potential OHP applicants and members when those individuals receive care at their facilities. Furthermore, hospitals play a crucial role in helping individuals enroll in OHP, especially through the issuance of presumptive eligibility determinations. Because many OHP members receive care at hospitals and hospitals are usually trusted messengers in the community, hospitals offer a powerful engagement partner for OHA. In interviews with partners, hospitals expressed a willingness to amplify messages in accordance with guidance from OHA.
Community-based organizations play a valuable role in helping OHA spread its messages. OHA’s Office of Community Health and Engagement has a robust network of over 350 organizations and 1,900 community partners to support its work. In interviews with partners, CBOs expressed a shared interest in minimizing coverage loss from work requirements and a willingness to amplify messages in accordance with guidance from OHA.
RECOMMENDATION
Establish partnerships with CCOs, FQHCs, county health departments, hospitals, and community-based organizations to collaborate, inform, and amplify messaging.
Considerations for Engagement With Partners
While establishing partnerships with organizations can help to amplify OHA’s messaging, there are certain coordination challenges that may arise. Below, we offer a few key recommendations to ensure successful engagement with partners:
• Ensure consistent messaging: Employ a top-down approach to communications so that messaging is consistent between OHA and its engagement partners. This approach would involve developing messaging toolkits and guides that can be easily adopted by engagement partners.
• Create opportunities for support: Ensure that resources are dedicated to helping engagement partners understand the new requirements. For example, OHA might set up an engagement partner helpline within
its Office of Community Health and Engagement that specifically answers work requirement questions.
• Develop two-way collaboration opportunities: Rely on the expertise of OHA’s engagement partners to refine communications strategies. One way to do so is to form an advisory working group, as discussed below.
RECOMMENDATION
Ensure consistent messaging between OHA and each engagement partner, create opportunities for the partner to receive support from OHA, and develop two-way collaboration opportunities.
The Ladder of Engagement Framework
When deciding the level of engagement to pursue with partners, we recommend OHA adopt a ladder of engagement framework. The approach groups engagement levels into tiers, which determine the extent of the collaboration between OHA and the organization. Table 5 highlights certain engagement strategies we determined to be most effective; additional strategies and considerations are presented in the Appendix.
The ladder of engagement approach is beneficial for two reasons. First, it allows organizations to choose levels of collaboration based on their own capacity. Second, it also allows OHA to vary its degree of collaboration with outside organizations based on the agency’s capacity, whether it has a history of trusted partnership with an organization, and whether the communication is well-targeted to reaching the population OHA is interested in communicating with.
Table 5. Ladder of Engagement for OHA Communications Partnerships
Collaboration Level Strategy Detail
Step 1: Low Implementing comms strategy
Share a communications toolkit for partners to disseminate, including:
• Fact sheets with basic information on work requirements,
• Brand kit and graphics
• Social media copy
Step 2: Medium Sharing in-depth information, including briefings on what work requirements are and how to comply
Enlist groups to update their communities on work requirements in OHP. Inform organizations how they can help support compliance verification.
Recommended partner types
• All public state and municipal buildings, including public schools
• Grocery stores
• Food pantries
• Community centers
• Universities and community colleges
• Houseless shelters
• Small businesses
• Civil rights organizations
• Libraries
• Public housing authorities
• Healthcare organizations:
• Hospitals
• FQHCs, CCOs, healthcare providers, clinics
• Social service agencies
• Community centers with deep ties to their members—e.g., churches, mosques, synagogues, unions, immigrant justice organizations, civil rights groups, health equity organizations, disability justice groups, and/or unions
Step 3: High Co-create strategy for communications
Some organizations will have unique insight into patients’ needs and questions, and how well the implementation of work requirements is going.
OHA should look to these organizations as a thought partner and collaborator in developing outreach strategies
• CBOs that represent populations with lower rates of insurance coverage, such as Black people, Latinx people, immigrants, Indigenous people, the unhoused population, and former foster youth.
• Healthcare organizations: Hospitals, FQHCs, CCOs, healthcare providers
• Beneficiary Advisory Council
• Tribal Governments
Establishing a working group for successful implementation
Governor Tina Kotek has recently convened an advisory group on Medicaid sustainability. In addition to OHA, members include CCOs, unions, hospital executives and associations, Oregon Health and Science University, and the Department of Consumer and Business Services.226
This advisory group will meet every two weeks until recommendations are provided to the governor in July 2026. While these meetings will provide important insight for the Governor’s plans around Medicaid, we recommend OHA itself seek input from additional organizations to inform policy for the purposes of implementing Medicaid’s work requirements. There are many opportunities for collaborative and creative implementation to ensure the process of implementing Medicaid’s work requirements will be as effective as possible by establishing buy-in for both strategy and implementation.
OHA currently engages with its members through its Beneficiary Advisory Committee and Medicaid Advisory Committee.227 We recommend OHA expand its engagement to develop a working group of work requirement implementers, including key staff members from the ecosystem of Medicaid implementation who can create a collaborative approach to reach Oregon’s Medicaid population through regular meetings.
The most common suggestion we heard from the CCOs, CBOs, and local government officials we interviewed was the desire for multi-way communication with OHA leading up to the implementation of work requirements. During Oregon’s effective approach to the unwinding of the continuous coverage requirement (when the state successfully retained member coverage at a higher rate than the national average228)CCOs and OHA met regularly to troubleshoot and share critical information. OHA should generally look back to its lessons from unwinding.229 Knowing it will need to implement similar systems to unwinding at a much faster pace, it can look to CCOs, community health workers, and community-based organizations as thought and strategy partners. These organizations will have valuable insight into the best strategies for communications, enrollment, and data collection based on their intimate connections with members and experiences with unwinding.
The Center for Health Care Strategies describes several best practices for creating cross-system partnerships when it comes to implementing H.R. 1’s Medicaid work requirements.230 In particular, as OHA sets up a working group, it should prioritize aligning on leadership practices and establishing a cadence of expected engagement with organizations that are part of this group. These practices can lead to an easier exchange of ideas and built-in spaces to troubleshoot arising issues.
We recommend proactively considering the following agencies and organizations for this working group, given either (1) their proximity to implementation and/or (2) connections to OHP members or applicants who may be hard to verify ex parte
• Hospital Associations
• Oregon Primary Care Association (and/or select FQHCs)
• Tribal representatives*
• Higher Education Coordinating Commission
• State Foster Care office
• CCOs
*We note that, based on the OHA Tribal Consultation and Urban Indian Health Program (UIHP) Confer Policy as outlined in OHA’s Strategic Plan, OHA should develop a plan to consult directly with Tribal nation representatives in respecting their sovereignty.231
We provide more specific recommendations for potential relationship-building goals with other agencies or organizations throughout the report’s communications and data sections, which OHA should consider for proactively setting up partnerships for data-sharing and/or communications-strategy purposes.
Population-Specific Strategies
This section contains considerations and recommendations for crafting communications strategies that are specific to population segments. Some of the populations correspond to statutory groups—self-employed and gig workers, medically frail people, Tribal residents, and former foster youth—and the rest cut across statutory groups but still have shared characteristics that will make a differentiated communications approach more effective. For each population we provide:
• An overview describing the population and sharing key facts about it
• An assessment of communication challenges specific to the population
• A list of communication strategies that could be used to reach the population
• Recommendations for which strategies should be prioritized
To prioritize recommendations we follow a cost-scale framework similar to that used in the “Data” section. We score recommendations as “high,” “medium,” or “low” priority based on cost—how much capacity will it take for OHA to pursue the strategy—and scale—how many members of the group would be reached if the recommendation were implemented successfully. See Table 6 in the Prioritized Strategies section for a summarized list of all strategies and recommendations for prioritization.
Importantly, in this section we consider priority, cost, and scale relative to the other recommendations for the same population; these scores should not be compared across populations. For example, a large-scale recommendation for the Rural population impacts more residents than a medium-scale recommendation for the Rural population, but does not necessarily impact more residents than a medium-scale recommendation for any other population.
Rural Residents Population Overview
Medicaid is critical for rural populations, with nearly 1-in4 rural residents nationwide relying on the program.154 Oregon mirrors this pattern: 33 percent of its population lives in rural areas and 2 percent in frontier areas; these communities have higher Medicaid enrollment rates than their urban counterparts. The counties with the highest percentages of Medicaid enrollment include Malheur (54%), Josephine (47%), and Jefferson (47%).155 Given the remote nature of the rural and frontier counties, OHA faces unique communication challenges in reaching these
residents. However, it is important for this population to be aware of the work requirements in case they are eligible for exemption. Certain exemptions such as the “Travel for Care” exemption, may be especially applicable to rural and frontier residents that live far from health care resources.
Communication Challenges
CCO and FQHC leaders reported the following key challenges in communicating with rural residents: limited internet access, limited phone minutes, low technological literacy, and unopened and returned mail. Further, limited health care resources and longer travel times in rural and frontier areas make consistent information-sharing between providers and members more difficult, even though providers are trusted sources of information.156 While community-based organizations have been key partners in redetermination efforts, they may not always reach individuals in remote areas.
Communication Strategies
• Partner with rural CBOs. OHA should hold regular meetings with rural and frontier CBOs to provide implementation information and receive feedback from rural communities. In interviews, CCOs praised CBOs as critical partners for communicating with rural populations during redetermination.
• Engage healthcare providers, particularly FQHCs. Providers and caseworkers at FQHCs can be trusted sources of information and support for rural populations. OHA can distribute information to FQHCs for dissemination to members.
• Distribute communications through CCOs. CCOs noted that rural members are more responsive to correspondence from their CCO than from OHA due to greater familiarity with the name of coverage plans and CCOs.
• Prepare local and regional government offices. Ensure that updated information on Medicaid eligibility and compliance is shared with local social service agencies and public health authorities. Interviews reported that OHA communications with regional government offices are important for distributing official and consistent information.
• Supplement mail communications with text messages and radio broadcasts. Interviews with CCOs noted that mail has limitations in rural areas, citing high return mail rates during redetermination. Text and radio will be effective, broad-reaching supplements to mail; interviewees indicated that rural areas have large radio audiences and that texting can help reach residents that are less likely to receive or open mail.
Recommendations
High-priority strategies:
• Partner with rural CBOs. CBOs already have deep trust, knowledge, and reach in rural communities and were proven vital during redetermination. They can be partners for two-way information sharing by distributing communications to rural residents and helping OHA understand community-specific concerns.
• Engage healthcare providers, particularly FQHCs. Rural providers are highly-trusted messengers for Medicaid information, making them an efficient and reliable channel for reaching rural residents at scale.
Medium-priority strategies:
• Distribute communications through CCOs. CCOs offer a broad-reaching, trusted channel for many rural members, though they will be less effective for reaching non-members.
• Supplement mail communications with text messages and radio broadcasts. Texting and radio can broaden reach and mitigate mail limitations in rural areas.
• Prepare local and regional government offices. These offices can help ensure consistency of information, but may be less direct points of contact for rural residents.
Houseless Residents
Population Overview
Oregon’s houseless population is particularly at risk of losing coverage under work requirements, a concern that was consistently expressed across almost all of our interviews. Houselessness is a growing problem in Oregon, with unsheltered counts reporting a 16 percent increase to 8,403 individuals and sheltered counts seeing a 24 percent increase to 8,842 individuals over the course of 2023.157 Houseless individuals face many barriers to compliance with work requirements and staying enrolled in Medicaid, including challenges with having a reliable residence, having documented or consistent employment, and overcoming administrative burdens. Medicaid is especially important for houseless people because they are at increased risk for infectious and non-infectious diseases and commonly face alcohol and substance use disorder, diabetes, mental illness, and other challenges.158 Depending on their health conditions and co-morbidities, houseless individuals may be eligible for exemptions on the basis of medical frailty.
Communication Challenges
Official notices are often delivered by mail, posing a significant administrative barrier for houseless people. Individuals without reliable residences face challenges in receiving mail, fulfilling mandatory residency checks, storing personal documentation, or losing mail. Personal identification documents can be lost in encampment raids. However, interviewees noted that some individuals can receive mail at shelters and nonprofits. Social media and text messaging are viable communication channels, given that studies have estimated mobile ownership ranging from 44 to 62 percent159 and even up to 94 percent,160 but houseless individuals may lose access to their phones or have limited access to the internet. Houseless individuals may have strong mistrust of the medical system and may prefer to verify health-related information from multiple sources.
Communication Strategies
• Provide messaging through healthcare providers. Houseless individuals prefer receiving health information face-to-face from trusted healthcare providers, which allows individuals to ask questions in private. According to interviewees, houseless individuals commonly receive care at FQHCs, shelters, and mobile health clinics. OHA should ensure that healthcare providers receive consistent messaging and clear information that they can share with houseless patients.
• Partner with CBOs and social service providers OHA should distribute messaging to clinics, shelters, and other social service providers that serve the houseless populations. Interviewees also reported that mobile clinics and related services such as mobile showers were effective in reaching unhoused populations, making them another channel for information sharing.
• Engage local health departments (city and county). Interviewees mentioned that health departments can be another effective communications channel, given that they operate health services (primary, dental, behavioral), mobile clinics, and other community health services that can reach houseless populations.
• Run social media and text campaigns with actionoriented messaging. Research on communications with houseless populations suggests pairing a recommended action with instructions and resources on how to take that action.161 OHA should develop action-oriented messaging specifically for individuals who must comply with work requirements.
Houselessness and Incarceration
Houseless individuals are at increased risk of becoming incarcerated,232 and some may even choose to become incarcerated to access reliable state-provided shelter, food, and healthcare.233 Incarceration has significant implications for Medicaid enrollment: Individuals are disenrolled or have coverage suspended when they enter prison, but can be re-enrolled upon release. Delays in data-processing and re-enrollment can lead to churn and gaps in coverage, leaving vulnerable individuals without access to health care.
Recommendations
High-priority strategies:
• Provide messaging through healthcare providers. Healthcare providers are highly-trusted messengers and come into contact with a large portion of the unhoused population.
• Partner with CBOs and social service providers. CBOs and social service providers can reach unhoused individuals who do not frequently come into contact with healthcare providers.
• Engage local health departments (city and county). Local health departments have deep relationships with their communities and will be able to support engagement with CBOs and social service providers.
Medium-priority strategies:
• Run social media and text campaigns with actionoriented messaging. Social media posts can have wide reach and serve as a medium for individuals to double-check the information they hear from other sources. Text messages can have wide reach if members have regular access to a phone. Sometimes phones are destroyed or lost in encampment raids.
Self-Employed/Gig Workers
Population Overview
Self-employed and gig workers comprise approximately 10 percent of the Medicaid work requirements population and 7 percent of Oregon’s overall labor force (see Data section).162 Of Oregon’s 300,000 “nonemployers,” or individuals receiving at least $1,000 in business income with no employees, most are in professional, scientific, and technical services; real estate and rental and leasing; retail trade; transportation and warehousing, or other services.163 In 2022 there were 12,000–13,000 rideshare drivers in Portland, typically working less than 20 hours a week at $22 per hour.164 In general, residents of Oregon work multiple jobs at higher than the national average.165
Gig workers, self-employed workers, and those working multiple jobs may struggle to verify their compliance with work requirements for the following reasons:
• They are unlikely to have income that is verifiable ex parte. Nationally, only 1 percent of gig workers use online platforms to connect with their work (such as Uber, Lyft or Doordash).166 Most gig workers receive a 1099-NEC form from the companies they work for instead of a W-2, which summarizes annual income, not monthly or hourly.
• Hours may be unpredictable week to week, making it difficult to compile the necessary information to verify their eligibility.167
• They often lack the documentation needed for manual verification; even if they have it, assembling documents from multiple sources is burdensome. Nationally only 10 to13 percent of gig workers do gig work full-time, and less than half rely on it for their primary income.168
• Non-benefited worker populations also have “perceived affordability bias,” meaning that they might assume they can’t afford care, even if they can. In 2022, 58 percent of uninsured gig workers said affordability was the reason they were not insured nationally, but 45 percent of insured gig workers paid $0 in premiums.169 Thus some gig workers may give up before even trying to obtain Medicaid.
Communication Challenges
Self-employed and gig workers face additional obstacles to complying with work requirements and greater administrative burdens to verify their compliance. In addition, the lack of identifying data in state data systems makes it difficult for the state to communicate with them. The most effective way to ease these burdens is likely via consent-based verification (see Data section); CBV requires making contact with the worker, and thus necessitates an effective communications strategy.
When applying or renewing OHP, self-employed and gig workers typically get their applications returned so they can provide documentation of their income. Application support personnel (such as state case workers or provider-based benefits navigators) are used to helping
self-employed workers in the application and manual verification process, according to our interviews. However, increased information demands of work requirements and the six-month renewal frequency required by H.R. 1 will strain the capacity of these supporting functions.
Strategies
• Work with organizations that support self-employed or gig workers to share information. OHA will need to inform self-employed workers about the changes coming with H.R. 1, including the nature of work requirements, what documentation will be required to verify compliance, and the six-month renewal frequency. If OHA implements datasupported verification solutions (see Data), it will need to communicate those solutions to self-employed workers.OHA should engage organizations that serve significant populations of self-employed or gig workers, including:
• The National Domestic Workers Alliance (NDWA) Oregon and NDWA Gig Worker Advocates. These organizations advocate for gig workers in home care, childcare, and eldercare.
• Voz Workers’ Rights Education Project in Portland, a worker center for day laborers. This organization includes immigrant and Limited English Proficiency workers, who will benefit from additional communication for multiple reasons.
• Western Farm Workers Association (WFWA), an organization that advocates for seasonal workers. Many seasonal workers in Oregon are enrolled in Medicaid in other states; organizations that work with seasonal workers can help communicate necessary information to them.
• Distribute information via tax preparation services and volunteer income tax assistance (VITA) sites. Gig and self-employed workers interact regularly with tax preparers and free VITA sites, making them ideal settings for sharing relevant information, and verification expectations. Tax preparers are trusted sources for financial guidance and already assist selfemployed workers with compiling 1099s, hours logs, and receipts.
Recommendations
High-priority strategies:
• Work with organizations that support selfemployed or gig workers to share information. These organizations are trusted messengers that can reach the diffuse population of self-employed workers. They are mostly industry-specific and thus will be able
to support the particular needs of their constituent workers.
• Distribute information via tax preparation services and VITA sites. Tax preparers and VITA sites are high-leverage touchpoints because many self-employed workers already rely on them.
People With Medical Frailty
Population Overview
Medically frail people comprise one of the largest segments of the Medicaid work requirements population in Oregon. 19% of Oregon residents in the work requirements population have a “significant physical, intellectual, or developmental disability that interferes with one or more activities of daily living,” 10–21% have substance-use disorder, and 9–17% have a disabling mental disorder.170
Medically frail people are disproportionately vulnerable. Medicaid members with disabilities on average have lower incomes, are less likely to access insurance through employment, experience higher healthcare costs, and are older.171 60% report having two or more health difficulties.172 Communities of color experience higher rates of disability compared to the white population.173 Half of rural residents are over the age of 50, and older adults in rural areas are more likely to reside alone, near or at the poverty level, and suffer from a chronic condition or physical disability.174
The stakes for keeping coverage are high, as medically frail people face more severe health and financial costs from Medicaid disenrollment. For example, the consequences for a diabetic resident forgoing insulin due to even a short lapse in coverage could be deadly. Those who receive home-care based services may face institutionalization if they lose their coverage.175
Communication Challenges
Medically frail people are exempt from work requirements but may be difficult to verify ex parte (see Data section), so many of them will need to self-report to claim their exemption; thus it is particularly important that OHA have an effective strategy for communicating with them.
Over half of Medicaid recipients with disabilities report having cognitive challenges impacting concentration, memory, and understanding.176 This makes it even more difficult to navigate administrative burdens such as completing long and complex forms, calling multiple agencies, and obtaining medical forms from multiple providers. Additionally, the disabled population has diverse access needs, which are unlikely to be met by communications designed for the general population.
Communications Strategies
• Make accessible communications materials. OHA should produce communications materials modified to be accessible for audiences with various disabilities.
• Common accessibility measures include: Using plain language, including alternative text for images on social media and open or closed captions for videos, appropriate color contrast for those with low-vision and colorblindness at a 4:5:1 ratio between background and foreground color, making ASL interpreters for public meetings, providing written materials in Braille and large-font, and providing virtual support from community health outreach workers.
• When designing accessible communications, OHA can consult toolkits such as those from the Northwest ADA Center,177 the National Center on Health, Physical Activity and Disability,178 and the National Association of County and City Health Officials.179
• Involve disability justice organizations. OHA should integrate communication with national and local disability justice organizations into its partner engagement strategy and ensure its planned communications are validated by those experts.
• In Oregon, relevant organizations include We Can Do Better, Disability Rights Oregon, and other groups in the Aging and Disability Resource Connection database; relevant national groups include Justice in Aging, the Arc, and the National Health Law Program.
• Educate CCOs and healthcare providers on the medical frailty exemptions. OHA should work with CCOs and providers to help them understand who qualifies for a medical frailty exemption and what they need to do to claim it; trainings can prepare CCOs and providers to present patients with their options and ensure those who want to receive diagnoses and apply under medical frailty exemptions have access to them.
• OHA can partner with organizations focused on chronic conditions, disability justice, or substance abuse to produce materials for or even facilitate training.
Recommendations
High-priority strategies:
• Make accessible communications materials. Many medically frail people will be reached through channels targeted at the general population; making accessible
materials is a low-cost, high-scale way to make sure that general outreach will be effective for them.
• Educate CCOs and healthcare providers on the medical frailty exemptions. Medically frail individuals are likely to have contact with CCOs and healthcare providers; training them on how to support this population will be a high-leverage way to distribute critical information.
Medium-priority strategies:
• Involve disability justice organizations. Involving disability justice organizations is a low-cost way to improve and validate OHA’s communications strategy for the disabled population. Distributing information through these partners can be more costly but will help with reaching disabled individuals who have less contact or trust with healthcare providers.
People With Limited English Proficiency
Population Overview
15.5 percent of Oregon’s population primarily speak a language other than English, and 5.4 percent of residents speak English “less than very well.” These 220,000 Oregonians with limited English proficiency (LEP) include 44 percent of Oregon’s 403,000 foreign-born residents.180 Among the LEP population, the most common languages spoken at home are Spanish (66% of LEP speakers), Chinese (7%), Vietnamese (5%), Russian (3%), Other Slavic Languages (2%), and Korean (2%).181
The Portland metropolitan area contains the highest language diversity in the state. Residents with LEP are disproportionately lower-income, are 80 percent foreignborn, and include some people who will be losing Medicaid entirely under the new restrictions on non-citizen members.182
Communication Challenges
In one study in Illinois, individuals with LEP were five times more likely to become disenrolled than those who were English proficient; 99 percent of individuals with LEP received a renewal notice in English and 85 percent needed support filling out the form.183 The default communication language for OHA, CCOs, and healthcare providers in Oregon is English; without an intentional strategy, the LEP population will struggle to access critical information.
The LEP population also faces challenges accessing healthcare in general, which can impact their ability to receive information about work requirements from their providers or access diagnoses they will need for exemptions. Only 13 percent of hospitals meet
Culturally and Linguistically Appropriate Services (CLAS) benchmarks due to lack of qualified interpreters, insufficient multilingual materials, lack of clinician awareness, a lack of cultural competence, or technology barriers for remote interpreters.184 About half of adults with LEP say they encountered at least one language barrier in a health care setting in the last three years—including having difficulty filling out forms, communicating with medical office staff, understanding provider instructions, or schedule an appointment.185 LEP residents are at greater risk of being targeted by Immigration and Customs Enforcement and other federal agencies, meaning that they may be afraid to give personal information to the state or even attend doctors appointments.186
Communication Strategies
• Make official documents in multiple languages. All official documents—including application materials, letters, calls, texts/push notifications, and websites— should be available in all seven language options of the ONE eligibility system.
• The ONE Eligibility system should track each applicant’s preferred language and ensure that communications are in that language.
• ODHS offices should have translation available.
• Engage CBOs that serve LEP populations. OHA should share materials in the appropriate language with CBOs that serve LEP populations. CBOs are often the most-trusted messengers for LEP residents and they may have deep knowledge about community hot-spots for information distribution, which will be unique to different localities and immigrant populations.
• Relevant CBOs include: Oregon Latino Health Coalition, Familias en Acción, Latino Network, Oregon Health Justice Recovery Alliance, Latino Community Association of Central Oregon, The Next Door (Hood River), Oregon for All, Portland Immigrant Rights Coalition, Immigrant and Refugee Community Organization (Portland), Russian Oregon Social Services (Portland), and Asian Pacific American Network of Oregon.
• Broadcast on non-English-language Radio stations: OHA should conduct radio outreach via non-English stations.
• Spanish language radio stations include: 93.1 “El Rey” / KRYP-FM (Portland), La Zeta Network (Portland), 97.7 KEQB “La Que Buena” (Eugene), KLCC “Ahora Sí!” (Western / Central Oregon)
• Russian language stations include: KXPD 1040 AM (Portland) and KBSF 100.7 FM “Prime FM” (Portland)
• Share immigrant-relevant information: Communications should include information for how Medicaid eligibility will be impacted by immigration status, particularly in cases where immigration status will require residents to supply additional verification or will cause them to lose their eligibility. This information should be shared on the OHA website and in materials and briefings shared with partners.
Recommendations
High-priority strategies:
• Make official documents in multiple languages. Making all official materials available in residents’ preferred languages significantly improves accessibility and is relatively low-cost.
• Share immigrant-relevant information. Clearly communicating how immigration status affects eligibility and verification supports a population that faces uniquely high information barriers.
• Broadcast on non-English-language Radio stations. Radio is a cost-effective, high-reach channel for LEP residents who speak Oregon’s more common nonEnglish languages.
Medium-priority strategies:
• Engage CBOs that serve LEP populations. CBOs are highly-trusted and knowledgeable community messengers, but coordinating across many localized groups requires more staff effort.
Caregivers
Population Overview
Caregivers are exempt from work requirements under H.R. 1., including caregivers of children 13 and younger and disabled people (see Exemptions Policy section for full definition). 21 percent of the Oregon’s Medicaid work requirements population is a caretaker of a dependent child age 13 and under, and 6 percent is a caretaker of a disabled individual (see Data). Nationally, family caregivers perform an average of 30 hours of unpaid care work per week.187 More than 66 percent of caregivers are women,188 and Hispanic, Black, and Asian survey respondents report higher rates of caregiving than their white counterparts.189
Communication Challenges
Parents of children 13 and younger self-report their children’s ages at time of application and will likely receive high rates of ex parte verification during renewal.
However, other types of caregivers will not be visible in the data or may not realize they qualify for an exemption, meaning it will be especially important to communicate with them directly to realize they can be exempt from work requirements. Caregiving work is often invisible and unpaid in American culture and society;190 as a result, many people providing caregiving tasks do not think of themselves as caregivers.191
Communication Strategies
• Distribute caregiver-focused messaging in pediatric, geriatric, and disability-related healthcare settings. OHA should supply healthcare providers—e.g., pediatric practices, FQHCs, behavioral health clinics, geriatric care providers, and rehabilitation centers— with materials informing caregivers that they may qualify for exemptions.
• Partner with organizations that naturally interact with informal caregivers. OHA should work with senior centers, Area Agencies on Aging (AAAs),192 Aging and Disability Resource Connection (ADRC) sites,193 disability rights organizations (see Medical Frailty section), and family resource centers, to distribute tailored information about the caregiver exemption. These entities routinely interact with people providing unpaid or informal care and can help reach caregivers who don’t identify as such.
• Use school communication channels to reach adult relatives providing child care. Schools should receive materials that explain the caregiver exemption for adults caring for children ages 13 and younger. Many informal caregivers (aunts, grandparents, siblings, neighbors) interact with schools.
Recommendations
High-priority strategies:
• Distribute caregiver-focused messaging in pediatric, geriatric, and disability-related healthcare settings. Caregivers regularly accompany care recipients to appointments, making clinics one of the most reliable places to reach otherwise “invisible” caregivers. OHA already has strong ties to healthcare providers so placing additional messaging there will require smaller start-up costs.
Medium-priority strategies:
• Partner with organizations that naturally interact with informal caregivers. These organizations have strong relationships with caregivers and can effectively share information, but coordination across many diverse partners may require significant capacity.
Low-priority strategies:
• Use school communication channels to reach adult relatives providing child care. Schools can help reach adults providing informal child care, but this is a relatively small population and schools require highlydecentralized outreach.
Tribal Residents
Population Overview
An estimated five percent of the Medicaid work requirements population is American Indian or Alaska Native (see Data). This population is exempt from work requirements in H.R. 1 (see Exemptions Policy section).194 Because this definition is the same as the one currently used in required questions on the OHP application form, the ONE Eligibility system already has information on Tribal status for existing OHP members. However, it will still be important to communicate to Tribal members that they are exempt from work requirements and that they will be subject to the new six-month renewal frequency.
Due to the impacts of colonialism on social determinants of health and access to healthcare, this population faces disproportionate health care needs, costs, and barriers to accessing care. H.R. 1 and federal healthcare cuts in general are expected to critically impact Tribal communities and healthcare centers, meaning that work requirement implementation is taking place in the context of a broader crisis.195, 196
Communication Challenges
Many Tribal families may have mistrust towards the state government, the federal government, and healthcare services due to historic trauma;197 this mistrust may lead to resistance to services or avoiding communication with government officials. As a result, OHA must be very intentional in its communications with Tribal communities and work closely with Tribal partners to inform its approach.
Indigenous people in different parts of the state may also face different communication challenges. Tribal communities on reservations and in rural areas may have less access to cellular, broadband, and healthcare providers (see Policy). Portland, the ninth largest urban Indigenous community in the country, may have a large concentration of indigenous residents who are not connected to a specific Oregon Tribe from which they can receive communications directly.198
Communications Strategies
• Co-create an engagement timeline. OHA should work with Oregon’s nine sovereign Tribal nations to co-create a timeline for government-to-government engagement, following the ODHS-OHA Tribal Consultation and Urban Indian Health Program Confer Policy.199
• The Confer Policy requires OHA and ODHS to maintain intentional engagement with Tribal governments when there is “significant, specific or disproportionate” impact to Tribes, at the earliest point in the process.
• While work requirements alone will not necessarily have a disproportionate impact on Tribes, H.R. 1 as a whole will, and OHA should include cocreation of communications strategies on work requirements in those broader conversations. It is likely that this engagement will not result in a communications strategy specific to work requirements, but rather integrate information about the work requirements exemption into a broader approach to H.R. 1.
• Partner with indigenous healthcare providers. OHA should share communications through healthcare providers that serve indigenous populations, both by distributing materials at provider sites and training provider staff on what messages they will need to share.
• Important providers for indigenous residents include the Portland Area Indian Health Service200 and Oregon’s 10 Rural Tribal Clinics.201
• Health professionals, health clinics, and Tribal health organizations have been found to be the most-trusted messengers to Tribal individuals in healthcare contexts.202
• Engage CBOs in urban areas. OHA should work with trusted CBO partners to reach indigenous residents of urban areas who are not in close contact with a tribe or are not members of a federally-recognized tribe.
• In Portland, Coalition for Communities of Color is home to 28 Portland-area Native organizations that could be hubs for connection and collaboration.203
• Engage directly with indigenous residents, according to best practices.204
• Engage early to establish a relationship and determine what reciprocal partnership should look like.
• Emphasize in-person communication; traveling to and spending time with Indigenous communities
demonstrates commitment. Bringing food to potluck events, accepting invitations when offered, being mindful about the number of government staff at an event, and applying cultural competency and humility are all important to keep in mind when approaching in-person outreach.
• Be transparent about OHA’s goals, and flexible and guided by Tribal communities schedule and pace.
Recommendations
High-priority strategies:
• Co-create an engagement timeline. This approach aligns with mandated government-togovernment consultation, is foundational to all other communication efforts, and ensures that OHA’s outreach reflects Tribal priorities from the start.
Medium-priority strategies:
• Partner with indigenous healthcare providers. Healthcare providers are highly-trusted messengers for Tribal and Indigenous communities, and will provide good leverage for OHA’s capacity.
• Engage directly with indigenous residents, according to best practices. Direct engagement builds trust and cultural alignment that can greatly improve communication effectiveness, though the time and travel required make it more resource-intensive.
Low-priority strategies:
• Engage CBOs in urban areas. While urban CBOs can help reach indigenous residents outside of Tribal settings, this channel is less consistently high-impact and may require more effort to identify and coordinate with the right partners.
People of Color
Population Overview
People of color make up a quarter of Oregon’s population, with 13% of residents identifying sa Latino, 6% as Asian, 3% as American Indian or Alaska Native, and 3% as Black.205 OHA has acknowledged the importance of particularly reaching communities of color—Latino, Asian, AAPI, Native, and Black Oregonians—and defined its strategies for serving them in its 2024 “Strategic Plan to Eliminate Health Inequities.”206 OHA’s attention to people of color should continue in its communications strategy as H. R. 1 is implemented.
People of color have unique needs pertaining to healthcare and Medicaid work requirements. They have higher
uninsured rates than white people in Oregon.207 For instance, Latinx people are uninsured at nearly three times the rates of white people.208 They are more likely to be on Medicaid or uninsured (see Appendix). They tend to have worse health outcomes due to the longstanding impacts of poverty, segregation, and structural racism; for example, “American Indian and Alaska Native people in Oregon have the highest rates of asthma; Black/African American, Pacific Islander, American Indian and Alaska Native people have the highest rates of high blood pressure; and people in Latino/a/x/e and Pacific Islander communities have the highest rates of diabetes.”209 The experience of racism may cause some people of color to have lower trust in healthcare providers and government healthcare entities. Indeed, a 2020 study found that in ten out of eleven focus groups, families of Black and Latino immigrant children with special needs experienced racism in healthcare.210
Communications Challenges
Systemic racism in the healthcare system has generated mistrust among communities of color; Black and Hispanic individuals in particular have reported medical mistrust at higher rates than the general population.211 Experiences of perceived racism are associated with delayed care, decreased disclosure of health concerns, and reduced adherence to medical advice among racial and ethnic minority patients.212 Administrative burden tends to impact people of color more than it does white people, leading to reduced enrollment in public programs.213,214 OHA’s communications strategies must address relational barriers rooted in mistrust by building transparent, culturally competent, and equity-focused outreach and enrollment systems.
Communications Strategies
• Host briefings with trusted community leaders. OHA should host briefings with csrt them in sharing information about work requirements and helping their eligible community members keep enrolled.
• OHA should ask these leaders to verbally share information with their communities and also provide physical information such as flyers and business cards that community members can bring home.
• Community leaders likely to be effective include:
• Faith leaders; especially faith leaders who work with people of color, such as at Black or Latin churches, mosques, temples, or sanghas
• Civil rights organizations such as the Urban League of Portland, Don’t Shoot Portland, the Black Resilience Fund
• Small business owners of color.
• OHA should also use briefings to seek feedback from community leaders, who will have valuable community-specific knowledge and creative ideas about how to reach their local residents.
• Local elected officials and CBOs can help OHA identify the appropriate community leaders to include in briefings.
• Coach providers on culturally competent communications. OHA should work with provider partners to ensure that they are communicating with their patients of color in ways that are culturally responsive.
• OHA should develop short, actionable training sessions that coach providers on acknowledging historical and contemporary sources of mistrust, engaging in active listening, and avoiding assumptions about cultural beliefs or health practices. Coaching should include specific guidance on culturally relevant discussions of Medicaid work requirements.
• Patients who perceive their providers as culturally competent report higher trust, better communication, and greater service utilization,215 whereas communication mismatches lead to reduced adherence, delayed care, and lower engagement.216
Recommendations
High-priority recommendations:
• Host briefings with trusted community leaders. Community leaders are impactful messengers who can both spread information widely and provide culturally grounded feedback to OHA.
Medium-priority recommendations:
• Coach providers on culturally competent communications. Improving provider-patient interactions can help build medical trust, but its impact is indirect and may take a longer applied effort before yielding results.
Former Foster Youth
Population Overview
Foster youth who have aged out of foster care are exempt from Medicaid work requirements until they turn 26 (see Policy); those exempt make up 3 percent of the work requirements population (see Data). Approximately 200 to
600 foster children age out of the system in Oregon each year.217
Former foster youth (“FFY”) are a small but vulnerable population, given their high medical needs. CMS reports that “foster youth frequently experience adverse childhood experiences—such as abuse, neglect, domestic violence, and parental substance abuse—that increase the risk of serious health problems later in life, including severe obesity, diabetes, heart disease, cancer, stroke, chronic obstructive pulmonary disease (COPD), and broken bones.”218 FFY are twice as likely to experience depression compared with the general population, and more likely to suffer from anxiety and attempt suicide. Furthermore, compounding socioeconomic problems worsen health outcomes: Medicaid reports that “43 percent of FFY report experiencing houselessness, often multiple times, by age 21.”219
Young people in general tend to have lower insurance rates,220 and FFY are particularly likely to be uninsured; a 2014-2016 survey found that 90 percent of 19-year-olds in foster care had Medicaid coverage, while only 30 percent of 19-year-olds no longer in foster care had Medicaid coverage.221 Lastly, research shows that youth face greater administrative burdens; young adults struggle more than older adults222 to navigate bureaucracy and are also more likely to move than older adults,223 which could place them at risk of not receiving renewal notifications sent to outdated addresses. In helping FFY claim their exemptions from Medicaid work requirements, OHA may also be able to increase general insurance rates across FFY.
Communications Challenges
Lack of continuity of care poses a significant challenge to communicating with FFY. Across the nation, including in Oregon, state systems that do not ensure continuity of coverage for youth leaving foster care or facilitate streamlined re-enrollment can result in coverage lapses. FFY who have had negative experiences with government services in foster care tend to be distrustful of government.224
Moreover, reaching FFY is difficult, especially because higher rates of houselessness means that may be more difficult to reach by mail and lower insurance rates mean they have fewer touchpoints with healthcare providers. It is for this reason that a foster youth strategy should reach foster youth before they age out of the system and as they are interacting with other social services.
Communications Strategies
Primary Strategy:
• Communicate to child welfare agencies that it is their responsibility to enroll aging-out foster youth. OHA should clearly communicate with child welfare agencies that an essential part of preparing a foster child to age out of the system should be maintaining Medicaid enrollment. The child welfare agency and its community-based partners (e.g., nonprofit agencies) should be primarily responsible for submitting paperwork to enroll a child about to age out of foster care into Medicaid—and that they are documented as being a former foster child.
• OHA should offer briefings to child welfare agencies about work requirements and the FFY exemption, and share a clear process of what the child welfare agency should do to support its aging-out youths.
• OHA should pursue a proactive communications and relationship-building strategy, rather than encouraging new legislation that mandates child welfare agencies to share information.
• Engage social service providers to ask about the FFY exemption at the point of service. Upon intake, service providers, e.g., houseless shelters, food shelters, medical clinics, should ask every client if they have health insurance. For people within ages 19-26, they should also ask if they are a former foster youth and share information about the FFY exemption if so. OHA should work with service providers to encourage them to follow these steps.
• OHA should create one-pagers and flyers specifically about the FFY exemption to share with social service providers.
Recommendations
High-priority recommendations:
• Communicate to child welfare agencies that it is their responsibility to enroll aging-out foster youth. These agencies already support youth through the transition to adulthood and are best positioned to ensure eligible young people maintain Medicaid coverage.
Medium-priority recommendations:
• Engage social service providers to ask about the FFY exemption at the point of service. Social service providers can help identify eligible former foster youth in real time, though this approach is more diffuse and requires broader coordination.
Table 6. Recommendations and prioritizations for population-specific communications strategies
Population Strategy
Rural residents
Partner with rural CBOs
Engage healthcare providers, particularly FQHCs
Distribute communications through CCOs
Supplement mail communications with text messages and radio broadcasts
Prepare local and regional government offices
Houseless residents
Self-employed/ gig workers
Provide messaging through healthcare providers
Partner with CBOs and social service providers
Engage local health departments (city and county)
Run social media and text campaigns with action-oriented messaging
Work with orgs that support self-employed / gig workers to share information
Distribute information via tax preparation services and VITA sites
People with medical frailty
People with Limited English Proficiency (LEP)
Make accessible communications materials
Educate CCOs and healthcare providers on the medical frailty exemptions
Involve disability justice organizations
Make official documents in multiple languages
Share immigrant-relevant information
Broadcast on non-English-language radio stations
Engage CBOs that serve LEP populations
Caregivers Distribute caregiver-focused messaging in relevant healthcare settings
Partner with organizations that naturally interact with informal caregivers
Use school communication channels to reach adult relatives providing child care
Tribal residents Co-create an engagement timeline
Partner with indigenous healthcare providers
Engage directly with indigenous residents, according to best practices
Engage CBOs in urban areas
Note: Priority, scale, and cost scores are relative within each population, but should not be compared across population
People of Color Host briefings with trusted community leaders
Coach providers on culturally competent communications
Large Med. High
Med. Low Med. Former foster youth
Communicate to child welfare agencies about enrolling aging-out foster youth
Engage social service providers to ask about exemptions at the point of service
Large Med. High
Med. Med. Med.
Note: Priority, scale, and cost scores are relative within each population, but should not be compared across population
Conclusion
Ultimately, the long-term impacts of H.R. 1 on Oregon’s health care system will depend in large part on the state’s ability to successfully keep its population enrolled in the Oregon Health Plan. For the benefit of the health and the future of OHP and its members, it is imperative for OHA to prepare for work requirement implementation. By being strategic about the implementation of exemptions and definitions under the law; leveraging data for automatic, manual, and ex parte verification; and creating a population- and channel-specific communications strategy in collaboration with partners, OHA can design a system that maintains coverage under the OHP and minimizes burdens for its members.
First, OHA can minimize ambiguities in implementation by establishing clear definitions of who must comply with work requirements, who may be categorically exempt, and where administrative flexibility may mitigate coverage losses. This report identifies provisions related to caregiving and medical exemptions as key areas where the state should clarify ambiguities in the law. In cases of ambiguity, we recommend that OHA interpret these terms in ways that reflect the lived experience of people in Oregon and maintain access to coverage for those eligible. We also recommend that OHA take advantage of all of the optional exemptions provided in the law to exempt additional eligible applicants and members from work requirements.
Second, OHA can minimize burdens on applicants and members by relying on data to support automatic, manual, and ex parte verification of compliance and exemptions with work requirements. We recommend that OHA make updates to its OHP application and the ONE Eligibility system to assist with verification. We also recommend the use of additional data sources for ex parte verification, including data on medical claims, education, and incarceration. Finally, we recommend the state explore consent-based verification and set up data systems to prompt collaboration.
Finally, OHA can adopt a strategic communications strategy to ensure that all potential OHP applicants and members know of the upcoming changes to their
coverage and how to comply with the new changes. This will require using best practices for communications, such as plain language, message framing, and strategic timing of messages across channels. It will also require channel-specific communications campaigns across mail, text messaging, in-person activities (including flyering), alongside collaboration with community partners, agencies, and healthcare providers to share information in-person with Oregonians. Finally, an effective communications campaign will also recognize that certain groups will need targeted communications, such as Oregon residents that live in rural areas, are unhoused, or who speak a language other than English.
To assist with these goals, OHA should collaborate early with partners, including other government agencies, community-based organizations, hospitals, healthcare providers, FQHCs, CCOs, and community organizations. These partners will be essential for effectively reaching Oregon residents, testing communications strategies, collaborating on sharing data, and proactively identifying any issues as they arise.
Over the last several decades, OHA has been a leader in creating effective implementation strategies to promote access to care and minimize burdens for OHP applicants and members. The results of OHA’s efforts were demonstrated during the recent Medicaid redetermination process, when OHA significantly outperformed the nationwide average by keeping almost 95 percent of its members enrolled in Medicaid. While the fiscal realities are different from what they were during redetermination, we have no doubt that OHA can achieve similar levels of maintained coverage by effectively implementing the strategies outlined in this report. OHA has led the way nationally in setting a standard to provide a high level of coverage to everyone, regardless of their race, ethnicity, gender, or geographic location. We share this goal with OHA and look forward to its implementation of our recommendations.
About the Team


Isabella Belleza is from Fulton, Maryland, and graduated from Brown University with a B.A. in Public Policy. Her experiences in Southeast Asian American student organizing at Brown fostered her interest in higher education policy and led her to Asian and Pacific Islander American (APIA) Scholars. At APIA Scholars, she led advocacy campaigns focused on Minority-Serving Institutions and conducted research on the educational experiences of Asian American, Native Hawaiian, and Pacific Islander students. After Princeton, she hopes to work in government with a focus on promoting college affordability and student success at public colleges and universities. In her free time, Isabelle is an amateur adult figure skater, a competitive jump roper, and an enthusiastic foodie.
Shamik Bhat's experiences with healthcare across the United States led him to explore both medicine and health policy. At the University of Colorado, Denver, he studied biology and political science while working with Children's Hospital Colorado to build hands-on, unique educational experiences for patients. Having completed his third year of medical school at Yale, he’s exploring the many policy determinants of health at Princeton SPIA, ranging from housing policy to pharmaceutical price transparency. Shamik joined the Urban Institute's Health Policy team for the summer, where he helped the team actively fight against H.R.1's (The Big Beautiful Bill) cuts to healthcare programs, helped prepare state officials on how to respond to the cuts once passed, and led a paper on a novel health insurer fee states could levy to generate much-needed revenue. He ultimately hopes to use these experiences and lessons to better advocate for patients both in the hospital and on Capitol Hill.

Elena Conde is a lifelong New Yorker who works at the intersection of policy, strategy, and community engagement. Since completing this report, she has taken a leave of absence from her MPA to work full-time for NYC Mayor Zohran Mamdani. She is the Deputy Chief of Staff within the Mayor’s Office of Mass Engagement, a new office designed to elevate the perspectives of working-class New Yorkers across government. Previously, she served as a Policy Manager on the Mayor’s transition team, covering public safety, education, childcare, healthcare, and workers’ justice. Prior to Princeton, she served as a Deputy Chief of Staff with the NYC Council Progressive Caucus. She also worked as a community organizer with Make the Road New York. In her strategy consulting work, she advised clients such as the Bill and Melinda Gates Foundation and USAID on how to build effective philanthropic and nonprofit programs. Elena holds a Bachelor’s in Economics from Yale University. She is currently on leave with one semester left to finish her MPA from Princeton University. In all her work, she is motivated to build a better world where all can thrive.

Mera Cronbaugh is a Master in Public Affairs student at Princeton University focused on urban and social policy, graduating in May 2026. Mera serves on the editorial board of Princeton's Journal of Public and International Affairs and interned with Showing Up for Racial Justice. Prior to Princeton, Mera was a Senior Policy Associate at J-PAL North America, where she worked closely with local governments seeking to evaluate their social programs She holds a BS in Economics and Russian from the Ohio State University.

Faith Gay was born and raised in Los Angeles, CA, and in 2020, she graduated with a B.A. in international studies from American University in Washington, D.C. After graduating, she worked in anti-war organizing as a congressional lobbyist, primarily focusing on advocacy in favor of nuclear nonproliferation, U.S. military spending cuts, and global climate action. From 2024 to 2026, she served on the field-building committee of the Ploughshares Fund, a nuclear nonproliferation fund working to expand and organize the nonproliferation movement. While in graduate school, Faith’s engaged in strategic corporate research on the green manufacturing industry for labor rights organizations, in addition to assisting Southern, frontline, environmental justice groups in campaigns against corporate pollution.

Julia Heinzel was born and raised in Pennington, New Jersey, and is excited to be returning to her beloved home state. In 2019, she graduated from the University of Virginia with a degree in economics. Since then, she has worked at the Congressional Budget Office (CBO) in the Labor, Income Security, and Long-Term Analysis Division. At CBO, she has worked on estimating the labor market effects of a proposed policy to raise the minimum wage and modeling the economic effects of immigration. After Princeton, she hopes to use her quantitative background to craft policy to reduce income inequality and criminal justice reform. In her spare time, she loves to do crossword puzzles, go on hikes, and read.

Teddy Knox is a Master in Public Affairs candidate at SPIA focusing on economics, urban issues, and health policy. He previously worked at the public sector practice of Boston Consulting Group where he supported state and local government clients across topics including public health, public transit, higher education, and inclusive economic development. His work included supporting several states’ COVID response efforts and working to improve care access in rural areas.

Maya Pontón Aronoff grew up in Michigan and completed her bachelors at Princeton University before starting the Princeton MPA as a SINSI fellow in 2019. As a part of her fellowship she worked in the El Paso Federal Public Defender's Office and the Department of Energy Office of Equity & Economic Impact in Denver, before taking a year to work in Detroit for the Michigan Environmental Justice Coalition supporting grassroots environmental organizing against fossil fuel corporations. Maya has focused outside her 9-5 on local movement building for racial, environmental, and economic justice, from tenant to labor organizing, learning so much in all the beautiful places she's had the privilege to call home. She now lives in Weehawken, NJ, with her husband, great aunt, and reactive dog named Pacha. When she's not making public comment somewhere you can find her salsa dancing or drawing.

Matteo Treviño began his graduate education after seven years working for members of San Antonio’s City Council, primarily as a policy director and press liaison. He is proud to have been involved in establishing a $10M Climate Fund, expanding the Healthy Neighborhoods program, and developing a heat safety ordinance for construction workers. Prior to that, Matteo graduated from the University of Texas at San Antonio with a degree in philosophy.

Joshua Varcie was born and raised in Commerce Township, Michigan, a suburb of Detroit. Before attending Princeton, he worked as an Assistant Analyst in the Health Analysis Division of the Congressional Budget Office (CBO), where he contributed to analyses on prescription drugs, the Affordable Care Act (ACA), and long-term care. Prior to the CBO, Josh traveled the country campaigning for Joe Biden in five states during the 2020 presidential election. Josh is equally passionate about politics as he is about Detroit Lions football and can be found many Sundays rooting for his (suddenly good!) hometown team. He also plays the French horn and looks forward to exploring the biking trails near Princeton's campus. After Princeton SPIA, Josh hopes to serve in a role where he can use data and programming tools to solve pressing healthcare policy challenges, particularly at the federal level.
Policy Appendix 1. Definition of Serious Health Condition
“Serious Health Condition” is defined in Oregon Administrative Rule 471-070-1000:
(23) “Serious health condition” means an illness, injury, impairment, or physical or mental condition of a claimant or their family member that:
(a) Requires inpatient care in a medical care facility such as, but not limited to, a hospital, hospice, or residential facility such as, but not limited to, a nursing home or inpatient substance abuse treatment center;
(b) In the medical judgment of the treating health care provider poses an imminent danger of death, or that is terminal in prognosis with a reasonable possibility of death in the near future;
(c) Requires constant or continuing care, including home care administered by a health care professional;
(d) Involves a period of incapacity. “Incapacity” is the inability to perform at least one essential job function, or to attend school or perform regular daily activities for more than three consecutive calendar days. A period of incapacity includes any subsequent required treatment or recovery period relating to the same condition. The incapacity must involve one of the following:
(A) Two or more treatments by a health care provider; or
(B) One treatment plus a regimen of continuing care.
(e) Results in a period of incapacity or treatment for a chronic serious health condition that requires periodic visits for treatment by a health care provider, continues over an extended period of time, and may cause episodic rather than a continuing period of incapacity, such as, but not limited to, asthma, diabetes, or epilepsy;
(f) Involves permanent or long-term incapacity due to a condition for which treatment may not be effective, such as, but not limited to, Alzheimer’s Disease, a severe stroke, or terminal stages of a disease. The employee or family member must be under the continuing care of a health care provider, but need not be receiving active treatment;
(g) Involves multiple treatments for restorative surgery or for a condition such as, but not limited to, chemotherapy for cancer, physical therapy for arthritis, or dialysis for kidney disease that if not treated would likely result in incapacity of more than three calendar days;
(h) Involves any period of disability due to pregnancy, childbirth, miscarriage or stillbirth, or period of absence for prenatal care; or
(i) Involves any period of absence from work for the donation of a body part, organ, or tissue, including preoperative or diagnostic services, surgery, post-operative treatment, and recovery.
Policy Appendix 2. Maps
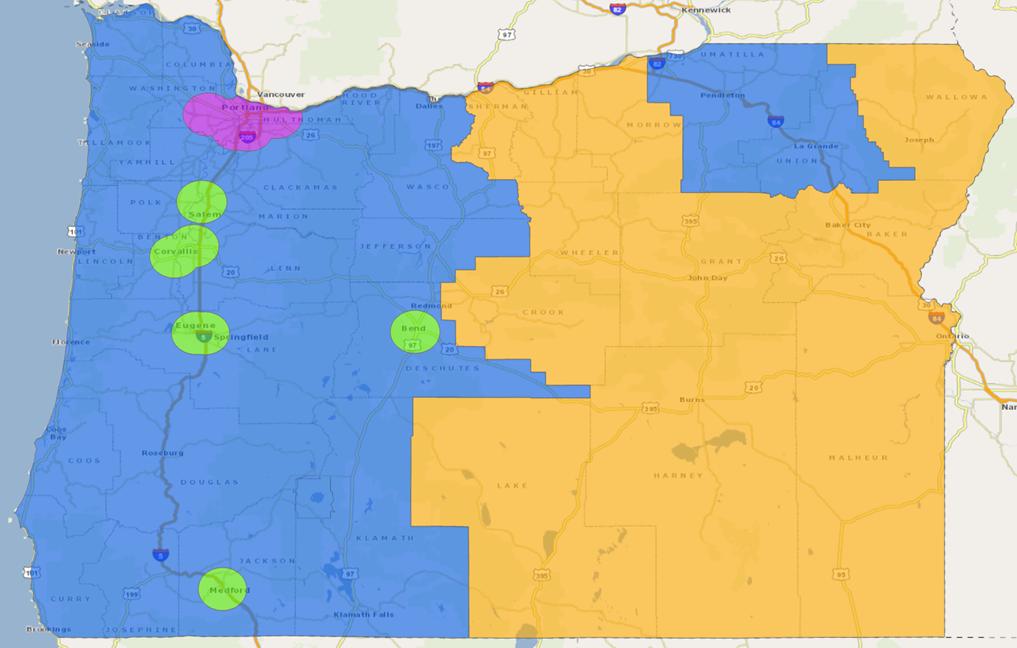
Policy Appendix Figure 1. Map of Oregon by area type
Area Types: Large Urban (Purple), Urban (green), Rural (blue), Remote Access (Orange)
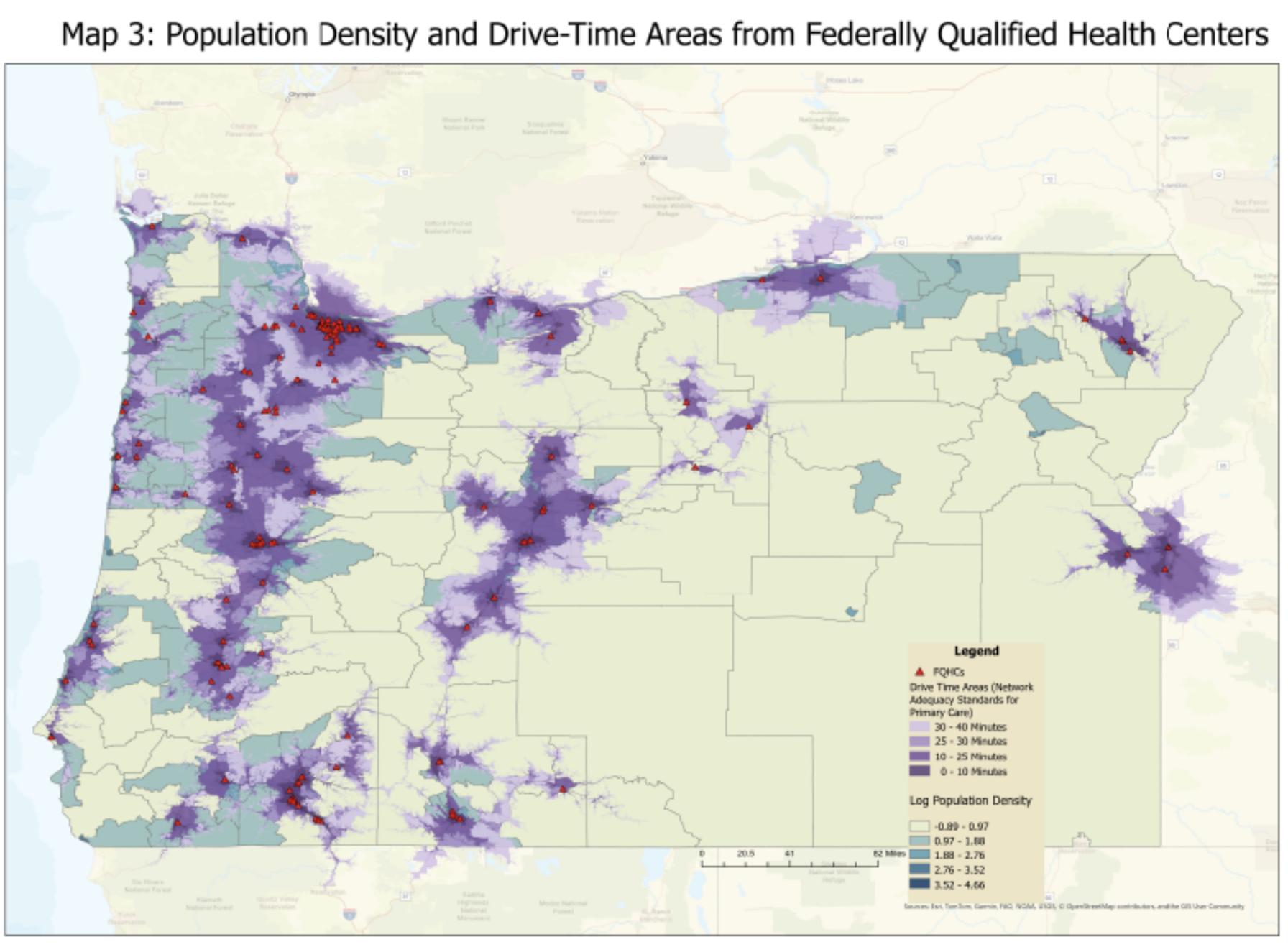
Policy Appendix Figure 2. Map of Oregon by population density and drive time from an FQHC
Data
Data Appendix 1. Methodology for determining the size of the potential population subject to work requirements
This report uses 1-year estimates from the 2023 American Community Survey to estimate the universe of potential Medicaid enrollees subject to work requirements. The American Community Survey is a survey conducted annually by the Census Bureau that contains a nationally representative sample of households and individuals living in institutions.234 The survey provides detailed information about a household and individual’s characteristics, including demographics, geographic location, income, health insurance status, and disability.
To generate estimates, this report utilizes an enhanced version of the ACS dataset from IPUMS.235 The IPUMS data includes a variable that assigns each individual to a health insurance unit using a process designed by the State Health Access Data Assistance Center (SHADAC).236 A health insurance unit (HIU) is a grouping of individuals that would likely share eligibility for family health insurance benefits. While the members of an HIU are sometimes the same as the members of a household, important differences arise that make the HIU a more accurate variable for analysis. The IPUMS data also includes an HIU-level calculation of income relative to Federal Poverty Level (FPL) from SHADAC, which is useful for calculating eligibility for Medicaid.
To create these estimates, we first define the Medicaid-eligible population subject to work requirements. Medicaid work requirements apply to adults in the Medicaid expansion population who are eligible for benefits based on their Modified Adjusted Gross Income (MAGI). Therefore, this report defines the work requirement population as anyone in the ACS data between the ages of 19 and 64 and lives in a health insurance unit with MAGI between 0 percent and 138 percent of the Federal Poverty Line (FPL). This definition will include some individuals who are not eligible for Medicaid. We choose this expansion definition because it represents the most expansive definition of the population of interest.
The next step is to determine which individuals fall into which statutory groups for the purposes of exemption or compliance among the work requirement population. In many cases, the data contains a variable that can be used to directly determine whether an individual falls into a statutory group. Other cases require outside data sources. In cases of uncertainty, a broader definition of a statutory group is favored over a limited definition. Appendix Table 1 presents the operationalized definitions, data source(s), and estimates of the population size for each statutory group.
This analysis is subject to limitations. For one thing, ACS data is self-reported. A wide body of literature suggests that self-reported data may lead to systematic errors in estimates.237 The potential for such errors should be taken into account, but are likely not sufficient to drastically alter the size of the estimates. Second, the operationalized definitions of certain statutory groups are limited to definitions in the law, some of which are expected to change after the release of guidance from the Centers for Medicare and Medicaid Services (CMS). This guidance could significantly impact the report’s estimates, especially if the guidance is more restrictive than the report’s definitions. Finally, the operationalized definitions are subject to data limitations, and therefore do not always match exactly to the population of interest. For this reason, estimates should be considered preliminary and subject to uncertainty.
Data Appendix Table 1. Operationalization of estimates of the work requirement population in each statutory group
Statutory Group Definition Source(s) IPUMS Variable(s)
Exemptions
Member of a household receiving SNAP and is not exempt from SNAP work requirements
Parent, guardian, caretaker relative, or family caregiver of a dependent child age 13 and under
Medically frail – have a significant physical, intellectual, or developmental disability that interferes with one or more activities of daily living
Medically frail– have substance-use disorder
The lower bound estimate includes individuals in the ACS who self-report receiving SNAP and have usual hours per work greater than 20 hours per week. The upper bound estimate includes any individual who self-reports having SNAP.
An individual who self-reports they have a child in the home that is 13 years of age or younger
ACS (IPUMS)
Medically frail – have disabling mental disorder
Individual who self-reports they have one or more self-reported limitations to activities of daily living (physical, mobility, self-care, hearing, or vision) in the ACS
ACS (IPUMS) YNGCH
Parent, guardian, caretaker relative, or family caregiver of a disabled individual
The lower bound represents the share of the Medicaid population ages 19-64 that KFF classifies as having severe substance use disorder only. The upper bound represents the share of that population that KFF classifies as having any substance use disorder.
The lower bound represents the share of the Medicaid population ages 19-64 that KFF classifies as having serious mental illness only. The upper bound represents the share of that population that KFF classifies as having serious or moderate mental illness.
An individual who lives in a household where at least one member of the household besides themselves self-reports they have a disability that affects at least 1 activity of daily living. The estimate likely undercounts the share of people eligible for an exemption because it does not take into account individuals who provide care for those who live outside the home.
ACS (IPUMS) DIFFPHYS, DIFFMOB, DIFFCARE, DIFFEYE, DIFFHEAR
American Indian or Alaska Native (AI/AN)
Meeting TANF work requirements
An individual who self-reports they are of American Indian or Alaska Native descent.
ACS (IPUMS) DIFFPHYS, DIFFMOB, DIFFCARE, DIFFEYE, DIFFHEAR
ACS (IPUMS) RACAMIND
Note: This table calculates the share of the work requirement population that will qualify for an exemption for a given statutory group or be determined to be compliant under a compliance pathway. Individuals may qualify for multiple exemptions or may comply with; therefore, the totals in the table will be greater than 100%.
Statutory Group Definition
Former foster youth under age 26
Living in a county with high unemployment rate
Postpartum
Pregnant
Participating in a drug or alcohol addiction treatment program
The number of people in the former foster youth under age 26 expansion category per OHA administrative data
An individual who self-reports living in a county that has an unemployment rate greater than 8% or greater than 1.5 times the national average unemployment rate
An individual who self-reports having a child in the last 12 months
The total number of women ages 19-44 multipled by the share of women who self-reported having a child in the last 12 months multiplied by 0.75
The number of clients in Oregon age 18+ enrolled in a program times 0.21, which is the estimated share of the population with substance abuse disorders on Medicaid.
OHA
Veteran with disability rated as total
Inmate of a public institution
Recently released from incarceration within the past 90 days
Medically frail– blind or disabled
Living in a county impacted by a federally declared emergency or disaster
Receiving inpatient hospital care, nursing facility services in an intermediate care facility for individuals with intellectual disabilities, inpatient psychiatric hospital services, or such other services of similar acuity
The number of veterans who have a self-reported disability rating greater than or equal to 70 percent.
The number of people released from jail in a year in Oregon according to the Oregon Health Authority times 90/365.
The number of people released from jail in a year in Oregon according to the Oregon Health Authority times 90/365.
The number of people in the medically frail pathway (??)
No federally declared disasters under the Stafford Act are active in Oregon.
Not estimable with current data sources.
ACS (IPUMS); BLS Local Area Unemployment Statistics COUNTYFIP
ACS (IPUMS) FERTYR
ACS (IPUMS) FERTYR
SAMHSA, KFF
ACS (IPUMS)
OHA
OHA
Note: This table calculates the share of the work requirement population that will qualify for an exemption for a given statutory group or be determined to be compliant under a compliance pathway. Individuals may qualify for multiple exemptions or may comply with; therefore, the totals in the table will be greater than 100%.
Statutory Group Definition
Traveling for an extended period to access medically necessary care for a serious or complex medical condition that is not available in the individual’s community for either themselves or their dependent(s)
Medically frail – have a serious or complex medical condition
Compliance
Income of at least $580/ month (as of 2025), equivalent to working at least 41 hours per month in Oregon
Average monthly income of at least $580/month for seasonal worker over six month period
80 hours of work program
80 hours of community service
At least half-time enrollment in educational program
80 hours combination of work, work program or school
Not estimable with current data sources.
Not estimable with current data sources.
The number of people who report a monthly income (annual income / 12) > $580 or report working greater than 40 hours per month (usual hours worked per week * 4)
Not estimable with current data sources.
ACS (IPUMS) INCTOT, UHRSWORK
The number of people who report spending more than 79 hours per month under a work training time code (daily minutes / 60 * 30 days/month)
The number of people who report spending more than 79 hours per month under a volunteering time code (daily minutes / 60 * 30 days/month)
The number of people who report being enrolled in school
The number of people who report being enrolled in school, working at least 40 hours per month, or a monthly income > $580
ATUS (IPUMS) tutier2code, tuactdur
ATUS (IPUMS) tutier1code, tuactdur
ACS (IPUMS) SCHOOL
ACS (IPUMS) SCHOOL, INCTOT, UHRSWORK
Note: This table calculates the share of the work requirement population that will qualify for an exemption for a given statutory group or be determined to be compliant under a compliance pathway. Individuals may qualify for multiple exemptions or may comply with; therefore, the totals in the table will be greater than 100%.
Statutory Group Share of Work Requirement Population Source(s) IPUMS Variable(s)
W-2 recipients The number of people who report being in the following classes of workers: wage/salary, private, wage/salary at a non-profit, wage/salary, government, federal government employee, Armed forces, state government employee, and local government employee
Self-employed The number of people who report being in the following classes of workers: self-employed employer, self-employed working on own account, self-employed not incorporated, self-employed incorporated
Likely gig workers The number of people who report being in the following 4 industries: couriers and messengers, taxi and limousine service, independent artists, writers, and performers, and child care services; and are in the self-employed category (not likely to have a W-2)
UI recipients The number of people who report being unemployed
ACS (IPUMS) CLASSWKRD
ACS (IPUMS) CLASSWKRD
ACS (IPUMS) CLASSWKRD, IND
ACS (IPUMS) EMPSTAT
Data Appendix 2. Example list of medical conditions
Medical condition Description
Sickle cell disorder SICKLE-CELL DISEASE WITHOUT CRISIS ICD-10
Sickle cell disorder SICKLE-CELL/HB-C DISEASE WITHOUT CRISIS ICD-10 D5720
Sickle cell disorder SICKLE-CELL/HB-C DISEASE WITH ACUTE CHEST SYNDROME
Sickle cell disorder SICKLE-CELL/HB-C DISEASE WITH SPLENIC SEQUESTRATION
Sickle cell disorder SICKLE-CELL/HB-C DISEASE WITH CRISIS, UNSPECIFIED ICD-10
Sickle cell disorder SICKLE-CELL THALASSEMIA WITHOUT CRISIS
Sickle cell disorder SICKLE-CELL THALASSEMIA WITH ACUTE CHEST SYNDROME
Sickle cell disorder SICKLE-CELL THALASSEMIA WITH SPLENIC SEQUESTRATION
Sickle cell disorder SICKLE-CELL THALASSEMIA WITH CRISIS, UNSPECIFIED
Sickle cell disorder OTHER SICKLE-CELL DISORDERS WITHOUT CRISIS ICD-10
Sickle cell disorder OTHER SICKLE-CELL DISORDERS WITH ACUTE CHEST SYNDROME
Sickle cell disorder OTHER SICKLE-CELL DISORDERS WITH SPLENIC SEQUESTRATION
Sickle cell disorder OTHER SICKLE-CELL DISORDERS WITH CRISIS, UNSPECIFIED
Sickle cell disorder Lyfgenia NDC-5-4-1
73554-1111-1
Sickle cell disorder Casgevy NDC-5-3-2 51167-290-09
Sources:
https://www.michigan.gov/-/media/Project/Websites/mdhhs/Folder3/Folder65/Folder2/Folder165/Folder1/Folder265/ Attachment_D_-_Medically_Frail_Process.pdf
https://www.cbo.gov/system/files/2024-12/60775-sickle-cell-disease_final.pdf
https://www.fda.gov/media/174610/download?attachment
https://www.cms.gov/icd10m/version372-fullcode-cms/fullcode_cms/P0306.html
Data Appendix Table 2. Identifying sickle cell disorder for the purposes of medical exemptions
Data Appendix 3. Example report from state data agencies to ONE Eligibility System
SAMPLE SAMPLE SAMPLE Y
SAMPLE SAMPLE SAMPLE N
SAMPLE SAMPLE SAMPLE N
SAMPLE SAMPLE SAMPLE Y
SAMPLE SAMPLE SAMPLE N
Mental Disorder Permanent
SAMPLE SAMPLE SAMPLE Y Pregnancy Temporary
Data Appendix Table 3. Example report from state data agencies to ONE Eligibility System
Communications
Communications Appendix 1. Sample flyers
Communications Appendix Figure 1 shows three examples of flyers from unwinding: (A) from CMS, (B) from the City of Philadelphia, and (C) from Partners for Kids. Table 1 summarizes some of the strengths and weaknesses of each flyer, according to design best practices.

Communications Appendix Figure 1. Three sample flyers
Flyer
A
Strengths
• Key message is highly visible
• Clear, simple action steps
B
C
• Strong, urgent key message (“You must act to keep your coverage”)
• Specific relevant information including timeline
• Clear, simple action steps
• Specific relevant information including timeline
• Clear, simple action steps
Weaknesses
• Key message is vague
• Action steps could include more detail (e.g., phone numbers, websites)
• Key message should be more visible
• No photo
• Dense, less-relevant information in bottom half of flyer
• Key messages conveying legitimacy
Communications Appendix Table 1. Strengths and weaknesses of sample flyer designs
Communications Appendix 2. Examples of web design
A well-designed webpage will more closely resemble the SBA’s Covid-19 relief page and less the DOD’s FOIA page, as highlighted by the Center for Plain Language’s 2021 Report Card. Source: Center for Plain Language, 2021.

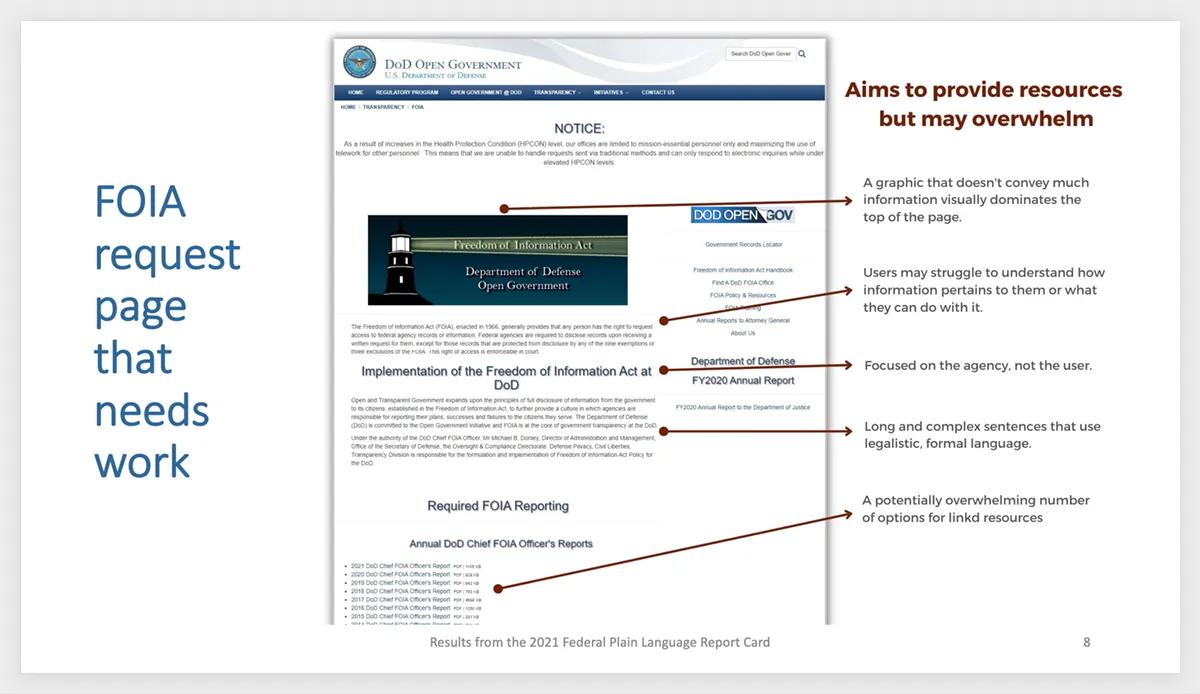
Communications Appendix Figure 3. U.S. Department of Defense FOIA page
Communications Appendix 3. Ladder of engagement framework
In this appendix, we share additional notes on the ladder of engagement framework..
Strategy 1: Sharing Physical Information
• Flyers and fact sheets are most important to share, but OHA can also include branding guidelines, postcards, and social media graphics and sample captions. OHA can follow similar protocols to what it did with ‘OHP Covers Me!’
• In addition to providing physical materials, we recommend that OHA offer a web-version of these materials as well. Having a single comprehensive PDF is useful, but PDFs are generally less accessible than a standard webpage. Having a standard webpage also allows partners to send it to one another, rather than OHA needing to be a central node sharing information.
OHA’s Office of External Affairs should ensure community partners have information about work requirements and how their members can comply. Share flyers and fact sheets on a webpage and ensure these partners post them in public places. Community partners may include: public state and municipal buildings, including public schools, grocery stores, food pantries, community centers, houseless shelters, libraries, public housing authorities, universities and community colleges, small businesses, civil rights organizations.
Strategy 2: Sharing In-Depth Information
People with close relationships with patients can more actively engage with supporting clients to maintain their health insurance than someone simply passing by in a grocery store. Therefore, OHA should invest in sharing in-depth information with these groups.
These groups include:
• Healthcare providers, who can be an excellent resource to help clients keep their health insurance and be aware of upcoming changes to their health insurance.
• Healthcare organizations such as CCOs, hospitals, FQHCs, and clinics
• Social service agencies within Oregon, whose clientele will likely have reliance on Medicaid
• Community organizations with deep ties to their community who regularly see community members in person, such as churches, mosques, synagogues.
To share information with these groups, OHA should still share the physical information they shared in strategy #1. However, OHA can also share additional physical information, given this group may have closer communication with clients. For instance, OHA should also build and disseminate cards that providers and intake at healthcare institutions can pass out to clients. These should have information that clearly says: “Make sure you can keep your health insurance. Check here to see if work requirements apply to you.” It should have a link to OHA’s website to learn about work requirements, OHA’s seal, and a phone number.
With these groups, OHA should also host briefings to ensure people clearly understand how they can be advocates to their community members for maintaining insurance coverage.A sample agenda for one of these briefings could include:
• What is at stake with work requirements: How many people could lose health insurance and go without needed care.
• Why it is essential for healthcare providers to get involved: Healthcare providers have access to communities in ways that OHA does not.
• Briefing on the 101 of work requirements: What work requirements are, how people can comply, and who is exempt.
• How healthcare leadership and providers can support: What their role is — e.g., sharing information verbally, posting information, verifying if their patient has a condition that can qualify them for an exemption – especially medical frailty, caregiving, or if they traveled a great distance to receive care.
• Open Q&A session.
OHA should lead briefings with healthcare organizations and providers about what work requirements are and how healthcare providers and organizations can support with compliance. Also share physical information – flyers, fact sheets, and cards with information about compliance – with healthcare organizations and providers. If possible, also lead briefings with social welfare agencies and well-trusted community groups.
Strategy 3: Co-Creation Of Strategy
Additional detail: Working with the Beneficiary Advisory Council (BAC):
OHA should raise the following questions in a series of its monthly BAC meetings to scope out member suggestions on work requirements implementation, before then sharing meeting outcomes in its BAC distribution list:
• “What are the best ways to inform people about whom the work requirement policies will and will not apply to?”
• “What organizations are trusted sources to deliver this type of information?”
• “How would you like OHA to communicate with you to share relevant information about this policy?”
• “How would you like to communicate challenges or issues to OHA?”
OHA should seek feedback from hospitals, FQHCs, CCOs, and Beneficiary Advisory Council around how well work requirements are being implemented and how effective OHA communications are. Also seek feedback from groups that represent groups with low insurance rates that often have lower levels of trust in medical systems – e.g., people of color, tribal communities, immigrants.
Communications Appendix 4. People of Color in Oregon
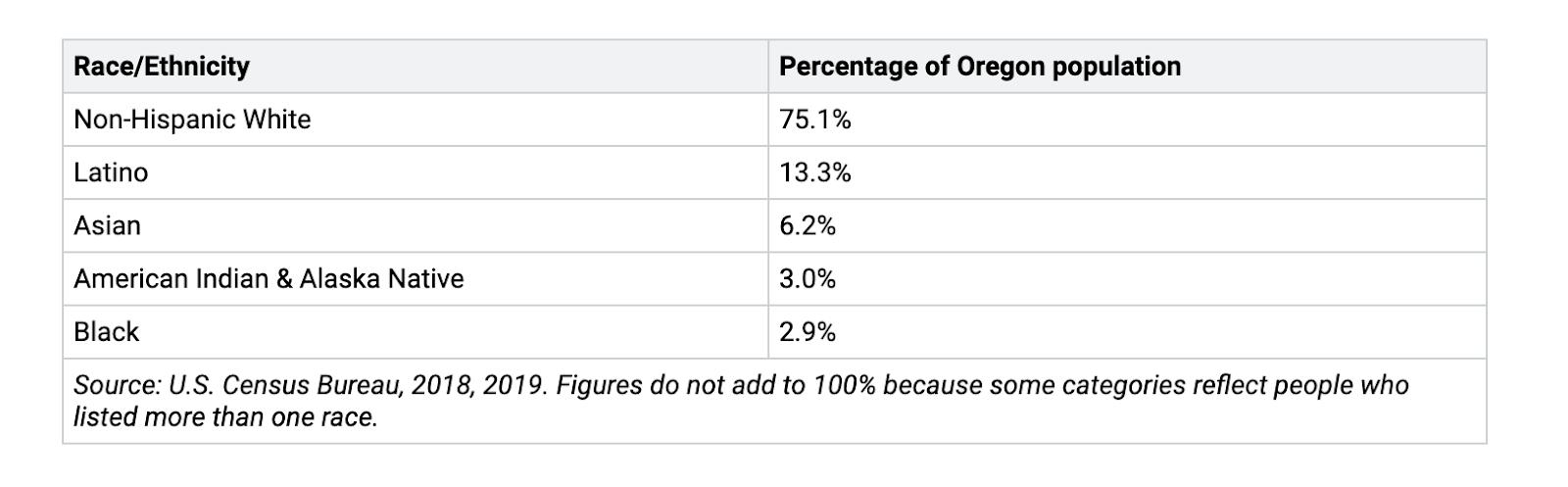
Communications Appendix Figure 4. Racial demographics of Oregon
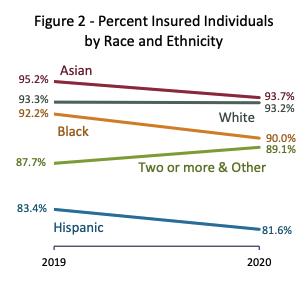
Communications Appendix Figure 5. Insurance rates in Oregon, 2019-2020
Endnotes
1. Oregon Department of Administrative Services, “Estimated Impacts of H.R. 1,” August 11, 2025, https://www. oregon.gov/das/Financial/Documents/Federal-Impact-HR1-Initial-Analysis.pdf.
2. Commonwealth Fund, “How Medicaid and SNAP Cutbacks in the ‘One Big Beautiful Bill’ Would Trigger Big and Bigger Job Losses Across States,” June 23, 2025, https://doi.org/10.26099/tryd-ht51.
3. Dan Meuse, “Medicaid Work Reporting Requirements: Implementation Basics and State Decision Points,” State Health & Value Strategies, August 15, 2025, https://shvs.org/medicaid-work-reporting-requirements-implementationbasics-and-state-decision-points/.
4. Amina Khalique et al., The Trump Administration’s One Big Beautiful Bill Act Will Drive Up Costs in Oregon (Center for American Progress, 2025).
5. Mia Maldonado, “Republican Tax Bill Could Slash Billions for Oregon Health Plan, State Officials Say,” Health, Oregon Capital Chronicle, June 4, 2025, https://oregoncapitalchronicle.com/2025/06/04/republican-tax-bill-could-slashbillions-for-oregon-health-plan-state-officials-say/.
6. Margaret Coker, “Georgia’s Medicaid Work Requirement Program Spent Twice as Much on Administrative Costs as on Health Care, GAO Says,” North Carolina Health News (North Carolina), September 27, 2025, https://www. northcarolinahealthnews.org/2025/09/27/georgias-medicaid-work-requirement-program-spent-twice-as-much-onadministrative-costs-as-on-health-care-gao-says/.
7. An Act to Provide for Reconciliation Pursuant to Title II of H. Con. Res. 14, Pub. L. Nos. 119–21 (2025), https:// www.congress.gov/bill/119th-congress/house-bill/1/text.
8. “OHP Enrollment Report,” Oregon Health Authority, https://www.oregon.gov/oha/hpa/analytics/pages/medicaidenrollment.aspx.
9. Office of Health Analytics, “Health Insurance Coverage,” Oregon Health Authority, September 2024, https://www. oregon.gov/oha/HPA/ANALYTICS/Documents/OHIS-coverage-summary.pdf.
10. Office of Health Analytics, “Health Insurance Coverage.”
11. State Plans for Medical Assistance, 42 U.S.C. 139a, accessed December 9, 2025, https://www.ssa.gov/OP_Home/ ssact/title19/1902.htm.
12. Oregon Health Authority, “Oregon’s Health System Transformation: CCO Metrics 2015 Final Report,” June 23, 2016, https://www.oregon.gov/oha/HPA/ANALYTICS/CCOMetrics/2015-CCO-Performance-Report.pdf.
13. Oregon Health Authority, “OHP Enrollment Report.”
14. Oregon Health Authority, “OHP Enrollment Report.”
15. “Healthier Oregon,” Oregon Health Authority, accessed December 9, 2025, https://www.oregon.gov/oha/hsd/ohp/ pages/healthier-oregon.aspx.
16. “Medicaid Management Information System: HPA Data Profile,” Oregon Health Authority, May 2025, https://www. oregon.gov/oha/HPA/ANALYTICS/Documents/Dataprofile_MMIS.pdf.
17. LaVonne Griffin-Valade and Kip Memmott, The Oregon Eligibility System Appropriately Determines Eligibility, but Input Errors Continue to Occur, Audit nos. 2024–27 (Oregon Secretary of State, 2024), https://sos.oregon.gov/audits/ Documents/2024-27.pdf.
18. Jennifer Tolbert and Bradley Corallo, “An Examination of Medicaid Renewal Outcomes and Enrollment Changes at the End of the Unwinding,” KFF, September 18, 2024, https://www.kff.org/medicaid/an-examination-of-medicaidrenewal-outcomes-and-enrollment-changes-at-the-end-of-the-unwinding/.
19. “Coordinated Care Organizations (CCOs) in Oregon: How They Work and Future Opportunities,” United States of Care, n.d., accessed November 29, 2025, https://unitedstatesofcare.org/wp-content/uploads/2022/04/CCO-OregonOverview.pdf.
20. “Estimated Impacts of H.R. 1,” Department of Administrative Services Chief Financial Office, August 11, 2025, https://www.oregon.gov/das/Financial/Documents/Federal-Impact-HR1-Initial-Analysis.pdf.
21. “About Redetermination,” CareOregon, accessed December 9, 2025, https://www.careoregon.org/providers/aboutredetermination.
22. “Impact of Federal Requirements & Funding Cuts to Oregon Health Plan (OHP/Medicaid),” Oregon Health Authority, June 4, 2025, https://www.oregon.gov/oha/Documents/Federal-Budget-Impacts-Medicaid.pdf.
23. Oregon Health Authority, “OHP Enrollment Report.”
24. Pamela Herd et al., “Introduction: Administrative Burden as a Mechanism of Inequality in Policy Implementation,” RSF: The Russell Sage Foundation Journal of the Social Sciences 9, no. 5 (2023): 1–30, https://doi.org/10.7758/ RSF.2023.9.5.01.
25. Pamela Herd and Donald Moynihan, “Administrative Burdens in the Social Safety Net,” Journal of Economic Perspectives 39, no. 1 (2025): 129–50, https://doi.org/10.1257/jep.20231394.
26. Herd and Moynihan, “Administrative Burdens in the Social Safety Net.”
27. Adrianna McIntyre et al., “New Medicaid Enrollment Barriers and Lessons From Unwinding,” JAMA Health Forum 6, no. 9 (2025): e254849, https://doi.org/10.1001/jamahealthforum.2025.4849.
28. Laura Wheaton et al., The Impact of SNAP Able-Bodied Adults Without Dependents (ABAWD) Time Limit Reinstatement in Nine States (Urban Institute, 2021), https://www.urban.org/research/publication/impact-snap-ablebodied-adults-without-dependents-abawd-time-limit-reinstatement-nine-states.
29. Wheaton et al., The Impact of SNAP Able-Bodied Adults Without Dependents (ABAWD) Time Limit Reinstatement in Nine States.
30. Herd and Moynihan, “Administrative Burdens in the Social Safety Net.”
31. Herd and Moynihan, “Administrative Burdens in the Social Safety Net.”
32. “Application for Oregon Health Plan Benefits,” Oregon Health Authority, May 1, 2020, https://sharedsystems. dhsoha.state.or.us/DHSForms/Served/he7210.pdf.
33. Leah Chan, Georgia’s Pathways to Coverage Program: The First Year in Review (Georgia Budget & Policy Institute, n.d.), https://gbpi.org/wp-content/uploads/2024/10/PathwaystoCoverage_PolicyBrief_2024103.pdf.
34. The law differentiates between populations that are excluded and excepted. Throughout this report, we use the term “exempted” to refer to this population more broadly.
35. Sueann Ramella, “The Invisible Work of Caregiving: A Radio Special on the Caregiving World Part 1,” Northwest Public Broadcasting, May 22, 2025, https://www.nwpb.org/uncategorized/2025-05-22/caregiving-radio-special-hour-one.
36. Justice in Aging et al., “Recommendations for Mitigating Harms to People with Disabilities, Older Adults, and Caregivers from Medicaid Work Requirements,” Justice in Aging, December 2025, https://justiceinaging.org/wp-content/ uploads/2025/12/NHeLP_JIA_Bazelon_RecsforMitigatingHarmstoPWD_OlderAdults_WorkReq_122025.pdf.
37. Chairman Mike Crapo, “Finance Committee Title,” US Senate Committee on Finance, August 2025, https://www. finance.senate.gov/imo/media/doc/finance_committee_summary3.pdf.
38. “Person with a Disability” Defined, 174.107 Oregon Revised Statutes § State Government, Government Procedures, Land Use, accessed December 9, 2025, https://oregon.public.law/statutes/ors_174.107.
39. Interviews with partners
40. Food and Nutrition Service, “A Short History of SNAP,” U.S. Department of Agriculture, accessed December 9, 2025, https://www.fns.usda.gov/snap/history.
41. Food and Nutrition Service, “A Short History of SNAP.”
42. Food and Nutrition Service, “SNAP Work Requirements,” U.S. Department of Agriculture, accessed December 9, 2025, https://www.fns.usda.gov/snap/work-requirements.
43. David Inbody, “12-Month Eligibility for Oregon Health Plan Post-Partum Benefits,” Memo to Coordinated care organizations, April 1, 2022, https://www.oregon.gov/oha/HSD/OHP/Announcements/12-month%20eligibility%20for%20 Oregon%20Health%20Plan%20post-partum%20benefits.pdf.
44. Food and Nutrition Act of 2008, Pub. L. Nos. 88–525 (2025), https://www.govinfo.gov/content/pkg/COMPS-10331/ pdf/COMPS-10331.pdf.
45. Definitions Relating to Institutional Status, 435.1010 Code of Federal Regulations, accessed December 9, 2025, https://www.ecfr.gov/current/title-42/part-435/section-435.1010.
46. Evelyne P. Baumrucker, Medicaid and Incarcerated Individuals, In Focus no. IF11830 (Congressional Research Service, 2024), https://www.congress.gov/crs-product/IF11830.
47. Baumrucker, Medicaid and Incarcerated Individuals.
48. Vikki Wachino, “To Facilitate Successful Re-Entry for Individuals Transitioning from Incarceration to Their Communities,” Letter, n.d., accessed December 9, 2025, https://www.medicaid.gov/sites/default/files/Federal-PolicyGuidance/Downloads/sho16007.pdf.
49. Elizabeth Hinton et al., “A Closer Look at the Work Requirement Provisions in the 2025 Federal Budget Reconciliation Law,” KFF, July 30, 2025, https://www.kff.org/medicaid/a-closer-look-at-the-work-requirementprovisions-in-the-2025-federal-budget-reconciliation-law/.
50. “State Alternative Benefit Plans and 1115 Waivers Medical Frailty Definitions,” Harvard Law School Center for Health Law and Policy Innovation, n.d., accessed December 9, 2025, https://chlpi.org/wp-content/uploads/2025/11/StateABP-and-1115-Medical-Frailty-Definitions_uploaded-11.17.25.pdf.
51. Arkansas, “Arkansas Alternative Benefit Plan,” Application to Centers for Medicare & Medicaid Services, June 26, 2023, https://humanservices.arkansas.gov/wp-content/uploads/3.1-AttachL-AltBenefitPlan.pdf.
52. Exempt Individuals, 440.315 Code of Federal Regulations (2013), https://www.ecfr.gov/current/title-42/part-440/ section-440.315.
53. Kentucky Department for Medicaid Services, 1115 Demonstration Extension Request (Team Kentucky Cabinet for Health and Family Services, 2022), https://www.chfs.ky.gov/agencies/dms/Documents/1115ExtensionNoLetter.pdf.
54. Robert Gordon, “More Than 100,000 Michigan Residents Nearly Lost Medicaid Coverage Under Work Requirements,” The Commonwealth Fund, May 12, 2025, https://doi.org/10.26099/8XP5-7397.
55. “Attachment D: Medically Frail Identification Process,” Michigan Department of Health and Human Services, n.d.
56. “Attachment D: Medically Frail Identification Process.”
57. Meaning of Blindness as Defined in the Law, 404.1581 Code of Federal Regulations (1983), https://www.ssa.gov/ OP_Home/cfr20/404/404-1581.htm.
58. Health Systems Division: Addiction Services, 415-050–0105 Oregon Administrative Rules, accessed December 10, 2025, https://secure.sos.state.or.us/oard/viewSingleRule.action?ruleVrsnRsn=300322.
59. Mental Illness, 436-035–0400 Oregon Administrative Rules § Department of Consumer and Business Services, Workers’ Compensation Division (2025), https://oregon.public.law/rules/oar_436-035-0400.
60. Brian J. Miller et al., “Mortality and Medical Comorbidity among Patients with Serious Mental Illness,” Psychiatric Services (Washington, D.C.) 57, no. 10 (2006): 1482–87, https://doi.org/10.1176/ps.2006.57.10.1482.
61. Aging and People with Disabilities and Development Disabilities, 411-320–0020 Oregon Administrative Rules, accessed December 9, 2025, https://secure.sos.state.or.us/oard/viewSingleRule.action?ruleVrsnRsn=315547.
62. Definitions, 471-070–1000 Oregon Administrative Rules, accessed December 9, 2025, https://www.law.cornell.edu/ regulations/oregon/Or-Admin-Code-SS-471-070-1000.
63. Brian W. Ward, “Multiple Chronic Conditions and Labor Force Outcomes: A Population Study of U.S. Adults,” American Journal of Industrial Medicine 58, no. 9 (2015): 943–54, https://doi.org/10.1002/ajim.22439.
64. “Network Adequacy - Time and Distance Rules for Providers,” Oregon Health Authority, accessed November 15, 2025, https://www.oregon.gov/oha/hsd/ohp/pages/network.aspx.
65. The GIS analysis measured travel times around FQHCs, given the importance of these clinics in providing primary care to rural and frontier populations. Other providers such as private practices are not included in the analysis.
66. Centers for Medicare & Medicaid Services, “Long-Term Care Hospital PPS,” CMS.Gov, accessed November 15, 2025, https://www.cms.gov/medicare/payment/prospective-payment-systems/long-term-care-hospital.
67. Governor Tina Kotek, “Section 1115 Demonstration Waiver Extension Request,” Letter to Drew Snyder et al., March 20, 2025.
68. “Oregon Minimum Wage,” Bureau of Labor and Industries, accessed December 9, 2025, https://www.oregon.gov/ boli/workers/pages/minimum-wage.aspx.
69. Bureau of Labor and Industries, “Oregon Minimum Wage.”
70. Higher Education Act of 1965, Pub. L. Nos. 119–21 (2025), https://www.govinfo.gov/content/pkg/COMPS-765/pdf/ COMPS-765.pdf.
71. Higher Education Act of 1965.
72. Carl D. Perkins Career and Technical Education Improvement Act of 2006, Pub. L. Nos. 109–270 (2006), https:// www.congress.gov/bill/109th-congress/senate-bill/250.
73. U.S. Department of Education, “Half-Time Enrollment,” StudentAid.Gov, accessed December 9, 2025, https:// studentaid.gov/help-center/answers/article/half-time-enrollment.
74. See, e.g., census date information for Oregon State University: https://financialaid.oregonstate.edu/census-date, and census date information for Portland State University: https://www.pdx.edu/student-finance/disbursement.
75. “Enrollment,” University of Oregon, accessed December 9, 2025, https://financialaid.uoregon.edu/enrollment.
76. Lauren Bauer et al., “Which Nontraditional Students Are Also in the Labor Force?,” Brookings Institution, December 7, 2023, https://www.brookings.edu/articles/which-nontraditional-students-are-also-in-the-labor-force/.
77. Alyssa Stefanese Yates, Student-Parent Data: What We Know, What We Don’t, and How to Find Out, Carnegie Classifications (American Council on Education, Carnegie Foundation for the Advancement of Teaching, Imaginable Futures, n.d.).
78. Alice Burns et al., “How Will the 2025 Reconciliation Law Affect the Uninsured Rate in Each State?,” KFF, August 20, 2025, https://www.kff.org/uninsured/how-will-the-2025-reconciliation-law-affect-the-uninsured-rate-in-each-state/.
79. Jennifer Wagner et al., A Guide to Reducing Coverage Losses Through Effective Implementation of Medicaid’s New Work Requirement (Center on Budget and Policy Priorities, 2025), https://www.cbpp.org/research/health/a-guide-toreducing-coverage-losses-through-effective-implementation-of-medicaids.
80. Griffin-Valade and Memmott, The Oregon Eligibility System Appropriately Determines Eligibility, but Input Errors Continue to Occur.
81. Bradley Corallo and Jennifer Tolbert, “Understanding Medicaid Ex Parte Renewals During the Unwinding,” KFF, October 2, 2023, https://www.kff.org/medicaid/understanding-medicaid-ex-parte-renewals-during-the-unwinding/.
82. Tolbert and Corallo, “An Examination of Medicaid Renewal Outcomes and Enrollment Changes at the End of the Unwinding.”
83. Griffin-Valade and Memmott, The Oregon Eligibility System Appropriately Determines Eligibility, but Input Errors Continue to Occur.
84. “MAGI-Based Eligibility Verification Plan,” Oregon Health Authority, July 5, 2016, https://www.medicaid.gov/ medicaid/eligibility/downloads/oregon-verification-plan-template-final.pdf.
85. Daniel Tsai, Financial Eligibility Verification Requirements and Flexibilities, Informational Bulletin (Centers for Medicare & Medicaid Services, 2024).
86. Sarah Kliff et al., “‘A Big Positive’: How One Company Plans to Profit From Medicaid Cuts,” The New York Times, November 3, 2025, https://www.nytimes.com/2025/11/03/health/medicaid-cuts-equifax-data.html.
87. “Minimum and Maximum Weekly Benefit Amounts to Increase for New Unemployment Insurance and Paid Leave Oregon Claims,” Oregon Employment Department, June 3, 2025, https://www.oregon.gov/employ/NewsAndMedia/ Documents/2025-06-03-Minimum-Maximum-Weekly-Benefit-Amounts.pdf.
88. Mark A. Crabtree, “Oregon Family, Paid Leave Changes Effective July 1, 2024,” Jackson Lewis, April 3, 2024, https://www.jacksonlewis.com/insights/oregon-family-paid-leave-changes-effective-july-1-2024.
89. Christopher L. Rowe et al., “Using ICD-10-CM Codes to Detect Illicit Substance Use: A Comparison with Retrospective Self-Report,” Drug and Alcohol Dependence 221 (April 2021): 108537, https://doi.org/10.1016/j. drugalcdep.2021.108537.
90. Centers for Medicare & Medicaid Services, “Transitioning to ICD-10,” CMS.Gov, February 25, 2015, https://www. cms.gov/newsroom/fact-sheets/transitioning-icd-10.
91. Centers for Medicare & Medicaid Services, “Data Disclosures and Data Use Agreements (DUAs),” CMS.Gov, accessed December 10, 2025, https://www.cms.gov/data-research/cms-data/data-disclosures-and-data-use-agreementsduas.
92. “All Payer All Claims Reporting Program,” Oregon Health Authority, https://www.oregon.gov/oha/hpa/analytics/ pages/all-payer-all-claims.aspx.
93. “Prescription Drug Monitoring Program,” Oregon Health Authority, accessed December 10, 2025, https://www. oregon.gov/oha/ph/preventionwellness/safeliving/pdmp/pages/index.aspx.
94. “Oregon State Cancer Registry (OSCaR),” Oregon Health Authority, accessed December 10, 2025, https://www. oregon.gov/oha/ph/diseasesconditions/chronicdisease/cancer/oscar/pages/index.aspx.
95. “Cancer Reporting,” Oregon Health Authority, accessed December 10, 2025, https://www.oregon.gov/oha/ ph/diseasesconditions/chronicdisease/cancer/oscar/pages/reporting.aspx; Public Health Division, 333-010–0000 Oregon Administrative Rules, accessed December 10, 2025, https://secure.sos.state.or.us/oard/displayDivisionRules. action;JSESSIONID_OARD=AajA3Un2PKiX-yZmqD_bhzPpjasK5vESisCyOUhkVrBWmi_yEdlz!-1969788327?selecte dDivision=1225.
96. Oregon Health Authority: Cancer Reporting Standards and Forms”, accessed December 11, 2025, https://www. oregon.gov/oha/PH/DISEASESCONDITIONS/CHRONICDISEASE/CANCER/OSCAR/Pages/reporting.aspx
97. “Sharing Oregon State Hospital Encounter Information in the PointClickCare Platform: Information Sheet,” HIT Commons, n.d., accessed December 10, 2025, https://ohlc.org/wp-content/uploads/2024/09/OSH-ADT-Brief-9-19-24.pdf.
98. David Inbody and Oregon Health Plan hospital providers, “Reporting Inpatient Hospital Admissions and Discharges,” Memo, January 9, 2024.
99. “Suspension of Medicaid Coverage for Incarcerated Adults,” KFF, January 2025, https://www.kff.org/medicaid/ state-indicator/suspension-of-medicaid-coverage-for-incarcerated-adults/.
100. “Community Population Profile,” Oregon Department of Corrections, August 1, 2025, https://www.oregon.gov/ doc/Documents/community-profile.pdf.
101. “AIC Population Profile,” Oregon Department of Corrections, December 1, 2025, https://www.oregon.gov/doc/ Documents/inmate-profile.pdf.
102. Additional Processing Instructions for Suspension and Reinstatement Actions on 3BOP, GN 02607.794 Program Operations Manual System (POMS) (2023), https://secure.ssa.gov/poms.nsf/lnx/0202607794.
103. PUPS Skeleton Records, GN 02607.520 Program Operations Manual Systems (POMS) (2023), https://secure.ssa. gov/poms.nsf/lnx/0202607520.
104. Conrad Wilson, “Oregon Governor Signs Bill To Track Info About Jail Inmates,” Oregon Public Broadcasting, May 23, 2019, https://www.opb.org/news/article/oregon-governor-kate-brown-signs-bill-to-track-information-jailinmates/.
105. Michael Reese and Heidi Steward, “Oregon Department of Corrections Healthcare Delivery System Assessment,” Memo to Elizabeth Falcon, July 25, 2025, https://www.oregon.gov/doc/Documents/ODOC_Falcon_Report.pdf.
106. If OHA is able to use HECC data to verify enrolled students ex parte, then a large portion of students will not need data-supported verification. However, non-exparte data-supported verification of students will still be impactful, given that HECC data from some institutions will not be able to verify students.
107. Hinton et al., “Work Requirement Provisions.”
108. Food and Nutrition Service, “SNAP Work Requirements.”
109. See: Steady IQ, Truv, truework, and Plaid
110. Sam Whitehead and Rae Ellen Bichell, “Officials Show Little Proof That New Tech Will Help Medicaid Enrollees Meet Work Rules,” KFF Health News, October 23, 2025, https://kffhealthnews.org/news/article/medicaid-eligibility-toolpilot-test-work-requirements-ai-louisiana-arizona-georgia/.
111. Kliff et al., “‘A Big Positive’: How One Company Plans to Profit From Medicaid Cuts.”
112. For more detailed consideration of data-sharing partnerships with educational institutions, see the “Education” section above.
113. Wagner et al., A Guide to Reducing Coverage Losses Through Effective Implementation of Medicaid’s New Work Requirement.
114. “Developing Effective Data Use Agreements (DUAs),” Comprehensive Opioid, Stimulant, and Substance Use Program (COSSUP), n.d., https://www.abtglobal.com/sites/default/files/files/Projects/PDFs/2025/developing-effectiveduas_0.pdf.
115. HB3361 2017 Regular Session - Oregon Legislative Information System, 3361, Oregon State Legislature 2017, accessed December 12, 2025, https://olis.oregonlegislature.gov/liz/2017R1/Measures/Overview/HB3361.hb
116. “Data Policies / Agreements,” Results for America, accessed December 12, 2025, https://2020state. results4america.org/state-standard-of-excellence/data-policies--agreements.html.
117. Results for America, “Data Policies / Agreements.”
118. “CBO’s Agreements to Access Data Since September 30, 2024,” Congressional Budget Office, September 25, 2025, https://www.cbo.gov/publication/61548.
119. “State Data Use Agreement Example (Louisiana),” Centers for Medicare & Medicaid Services Medicaid Innovation Accelerator Program, n.d., https://www.medicaid.gov/state-resource-center/innovation-accelerator-program/ iap-downloads/program-areas/la-dua-example.pdf.
120. “Health Equity Plan Definitions,” Oregon Health Authority, accessed December 12, 2025, https://www.oregon. gov/oha/ei/pages/hec%20plan%20definitions.aspx.
121. Griffin-Valade and Memmott, The Oregon Eligibility System Appropriately Determines Eligibility, but Input Errors Continue to Occur.
122. Benjamin D. Sommers et al., “Medicaid Work Requirements — Results from the First Year in Arkansas,” New England Journal of Medicine 381, no. 11 (2019): 1073–82, https://doi.org/10.1056/NEJMsr1901772.
123. “Plain Language Guide Series,” Digital.Gov, September 23, 2025, https://digital.gov/guides/plain-language.
124. Whitney Quesenbery and Sean Johnson, “Center for Civic Design,” October 15, 2025, Zoom.
125. Arkansas Medicaid Work and Community Engagement Requirement: Community Response (Arkansas Center for Health Improvement, 2019), https://achi.net/wp-content/uploads/2019/10/190917A_AR-Works-Interviews-Report.pdf.
126. “Five Steps to Plain Language,” Center for Plain Language, December 6, 2016, https://centerforplainlanguage.org/ learning-training/five-steps-plain-language/.
127. Ken Alltucker, “Medicaid Name Changes Confuse the Public: What It Means for Your Health Insurance Coverage,” USA TODAY, July 30, 2025, https://www.usatoday.com/story/money/2025/07/30/medicaid-name-changeconfuse-public-private-insurance/85403874007/.
128. A Field Guide to Fix Government Forms (The Lab @ DC, 2025), https://static1. squarespace.com/static/5d2361aa11fed60001f7ab3a/t/68d19c78f652e37bff2f1080/1758567544111/ A+Field+Guide+to+Fix+Government+Forms_The+Lab.pdf.
129. https://digital.gov/guides/plain-language
130. Massachusetts Digital Service, “How to Conduct a Plain Language Review,” Mass.Gov, accessed December 1, 2025, https://www.mass.gov/info-details/how-to-conduct-a-plain-language-review.
131. Melissa Morales and Kevin Caudill, “Rapid Message Test Insights to Inform 2024 Medicaid Renewal Messaging,” State Health & Value Strategies, January 8, 2024, https://shvs.org/rapid-message-test-insights-to-inform-2024-medicaidrenewal-messaging/.
132. “Usability Testing Toolkit,” Center for Civic Design, October 30, 2025, https://civicdesign.org/tools/usabilitytesting/. Note: For administrative simplicity, the Center for Civic Design collects minimal information about their interviewees. Aside from their feedback on the prototype, they collect their age, race, and, in the case of Medicaid prototypes, whether they are a Medicaid beneficiary. Such minimal data collection exempts them for typical research standards.
133. Patricia Boozang et al., “Federal Ruling Provides Text Messaging Flexibility to Support State’s Unwinding Efforts,” State Health & Value Strategies, January 27, 2023, https://shvs.org/federal-ruling-provides-text-messagingflexibility-to-support-states-unwinding-efforts/.
134. Maren N. Robinson et al., “Mass Media Health Communication Campaigns Combined with Health-Related Product Distribution: A Community Guide Systematic Review,” American Journal of Preventive Medicine 47, no. 3 (2014): 360–71, https://doi.org/10.1016/j.amepre.2014.05.034.
135. Julie Bataille and Kevin Caudill, “State Strategies for Sequencing Enrollee Communications When Medicaid Continuous Coverage Ends,” State Health & Value Strategies, August 3, 2022, https://shvs.org/state-strategies-forsequencing-enrollee-communications-when-medicaid-continuous-coverage-ends/.
136. Matt Darling, “What Can Be Learned from States That Made Good Faith Efforts with Work Requirements?,” Substack newsletter, Can We Still Govern?, August 25, 2025, https://donmoynihan.substack.com/p/what-can-be-learnedfrom-states-that.
137. Arkansas Medicaid Work and Community Engagement Requirement: Community Response.
138. Center for Civic Design, Form Letters That Actually Inform, September 2, 2025, https://civicdesign.org/formletters-that-actually-inform/.
139. Medicaid and CHIP Eligibility Renewals: A Communications Toolkit (Centers for Medicare & Medicaid Services, 2023).
140. Medicaid & CHIP Renewals: Reaching Children and Families in School-Based and Early Education and Care Settings (Centers for Medicare & Medicaid Services, 2024); Medicaid and CHIP Renewals: A Faith-Based
Communications Toolkit (Centers for Medicare & Medicaid Services, 2024); Medicaid and CHIP Renewals: PatientCentered Messaging for Clinical Offices and Health Care Settings (Centers for Medicare & Medicaid Services, n.d.).
141. Medicaid and CHIP Eligibility Renewals: A Communications Toolkit.
142. Boozang et al., “Federal Ruling Provides Text Messaging Flexibility to Support State’s Unwinding Efforts.”
143. Melissa Morales et al., “Optimizing SMS Strategies for Outreach to Medicaid and Marketplace Enrollees,” State Health & Value Strategies, May 16, 2024, https://shvs.org/optimizing-sms-strategies-for-outreach-to-medicaid-andmarketplace-enrollees/.
144. Morales et al., “Optimizing SMS Strategies for Outreach to Medicaid and Marketplace Enrollees.”
145. GSA Blog Team, “Making Government Text Messaging More Effective with Notify.Gov,” U.S. General Services Administration, December 17, 2024, https://www.gsa.gov/blog/2024/12/17/making-government-text-messaging-moreeffective-with-notifygov.
146. Boozang et al., “Federal Ruling Provides Text Messaging Flexibility to Support State’s Unwinding Efforts.”
147. Morales et al., “Optimizing SMS Strategies for Outreach to Medicaid and Marketplace Enrollees.”
148. GSA Blog Team, “Making Government Text Messaging More Effective with Notify.Gov.”
149. Matthew Lee Smith et al., “Effectiveness of the Radio as a Health Information Source,” Journal of Radio & Audio Media 18, no. 2 (2011): 196–211, https://doi.org/10.1080/19376529.2011.615776.
150. “FM Broadcast Station Classes and Service Contours,” Federal Communications Commission, accessed December 10, 2025, https://www.fcc.gov/media/radio/fm-station-classes.
151. “Rural Project Summary: Coast to Forest: Mental Health Promotion in Rural Oregon and Beyond,” Rural Health Information Hub, accessed December 12, 2025, https://www.ruralhealthinfo.org/project-examples/1096.
152. B. Milton et al., “The Impact of Community Engagement on Health and Social Outcomes: A Systematic Review,” Community Development Journal 47, no. 3 (2012): 316–34, https://doi.org/10.1093/cdj/bsr043.
153. Susan K. Riesch et al., “Community Outreach and Engagement Strategies from the Wisconsin Study Center of the National Children’s Study,” Public Health Nursing (Boston, Mass.) 30, no. 3 (2013): 254–65, https://doi.org/10.1111/ phn.12018.
154. Rhiannon Euhus et al., “5 Key Facts About Medicaid Coverage for People Living in Rural Areas,” KFF, June 26, 2025, https://www.kff.org/medicaid/5-key-facts-about-medicaid-coverage-for-people-living-in-rural-areas/.
155. Oregon Health Authority, “OHP Enrollment Report.”
156. Oregon Areas of Unmet Health Care Need Report (Oregon Office of Rural Health, 2025), https://www.ohsu.edu/ sites/default/files/2025-09/AUHCN%20Report_2025%20-%20FINAL.pdf.
157. Franklin Holcomb Spurbeck et al., 2024 Oregon Statewide Homelessness Estimates (Portland State University Homeless Research & Action Collaborative, 2025).
158. U.S. Centers for Disease Control & Prevention, “About Homelessness and Health,” Homelessness and Health, October 15, 2024, https://www.cdc.gov/homelessness-and-health/about/index.html.
159. D. Keith McInnes et al., “Opportunities for Engaging Low-Income, Vulnerable Populations in Health Care: A Systematic Review of Homeless Persons’ Access to and Use of Information Technologies,” American Journal of Public Health 103, no. Suppl 2 (2013): e11–24, https://doi.org/10.2105/AJPH.2013.301623.
160. Harmony Rhoades et al., “No Digital Divide? Technology Use among Homeless Adults,” Journal of Social Distress and the Homeless 26, no. 1 (2017): 73–77, https://doi.org/10.1080/10530789.2017.1305140.
161. Elizabeth M Allen et al., “Communicating Effectively With People Experiencing Homelessness to Prevent Infectious Diseases,” The Journal of Infectious Diseases 226, no. Suppl 3 (2022): S340–45, https://doi.org/10.1093/infdis/ jiac336.
162. The Re-Employment of Oregon (Oregon Employment Department, 2022), https://www.dol.gov/sites/dolgov/files/ eta/Performance/pdfs/annual_economic_reports/PY2021/OR%20PY21%20Economic%20Analysis%20Report.pdf.
163. The Re-Employment of Oregon; “The State of Gig Economy in Oregon,” Neilsberg Research, December 12, 2022, https://www.neilsberg.com/insights/the-state-of-gig-economy-in-oregon/.
164. 2022 Annual Report (Common Sense Institute, n.d.), accessed December 12, 2025, https://www. commonsenseinstituteus.org/about/annual-reports/2022-annual-report.
165. KATU Staff, “Number of Oregonians Working Multiple Jobs Rises Again in 2024, Ahead of National Average,” KATU (Portland, Oregon), April 28, 2025, https://katu.com/news/local/number-of-oregonians-working-multiple-jobsrises-again-ahead-of-national-average-employment-workers-portland-job-oregon-department-bureau-labor-april-20242025.
166. “Gig Economy Data Hub,” GigEconomyData.Org, accessed December 12, 2025, https:///gigeconomydata.org/ home.
167. Suzanne Wikle et al., States Can Reduce Medicaid’s Administrative Burdens to Advance Health and Racial Equity (Center on Budget and Policy Priorities, 2022), https://www.cbpp.org/research/health/states-can-reduce-medicaidsadministrative-burdens-to-advance-health-and-racial.
168. GigEconomyData.Org, “Gig Economy Data Hub.”
169. Noah Lang, “How Medicaid Redetermination Impacts Gig Economy Workers,” Stride Blog, n.d., accessed December 12, 2025, https://blog.stridehealth.com/post/how-medicaid-redetermination-impacts-gig-economy-workers.
170. See Data section for sources and methods used to obtain these estimates.
171. Alice Burns and Sammy Cervantes, “5 Key Facts About Medicaid Coverage for People with Disabilities,” KFF, February 7, 2025, https://www.kff.org/medicaid/5-key-facts-about-medicaid-coverage-for-people-with-disabilities/.
172. Burns and Cervantes, “5 Key Facts About Medicaid Coverage for People with Disabilities.”
173. Rashmi Goyat et al., “Racial/Ethnic Disparities in Disability Prevalence,” Journal of Racial and Ethnic Health Disparities 3, no. 4 (2016): 635–45, https://doi.org/10.1007/s40615-015-0182-z.
174. One Department Serving Rural America: HHS Rural Task Force Report to the Secretary (U.S. Department of Health & Human Services, 2002), https://www.govinfo.gov/content/pkg/GOVPUB-HE-PURL-LPS21888/pdf/GOVPUBHE-PURL-LPS21888.pdf.
175. Julia Métraux, “Trump’s War on Medicaid Will Institutionalize Millions of People,” Mother Jones, January 31, 2025, https://www.motherjones.com/politics/2025/01/trump-medicaid-institutionalization-hcbs-cuts-gop/.
176. Burns and Cervantes, “5 Key Facts About Medicaid Coverage for People with Disabilities.”
177. “Effective Communications,” Northwest ADA Center, accessed December 12, 2025, https://nwadacenter.org/ toolkit/effective-communications.
178. “Best Practices for Accessible Communications,” National Center on Health, Physical Activity and Disability (NCHPAD), September 5, 2024, https://www.nchpad.org/resources/best-practices-for-accessible-and-inclusivecommunications/.
179. Department of Justice, Civil Rights Division, “ADA Best Practices Tool Kit for State and Local Governments,” National Association of County & City Health Officials (NACCHO), accessed December 12, 2025, https://www.naccho. org/resource-hub-articles/ada-best-practices-tool-kit-for-state-and-local-governments.
180. “State Immigration Data Profiles: Oregon,” Migration Policy Institute, accessed December 12, 2025, https://www. migrationpolicy.org/data/state-profiles/state/language/OR.
181. Authors’ analysis of data from Migration Policy Institute.
182. “How Many Immigrants Are in Oregon?,” USAFacts, accessed December 12, 2025, https://usafacts.org/answers/ how-many-immigrants-are-in-the-us/state/oregon/.
183. Enrollment and Access Barriers for People with Limited English Proficiency, Brief (MACPAC, 2024).
184. Michael Wong et al., “Addressing Language Barriers in U.S. Healthcare: The Role of CLAS Standards, Telehealth, and Policy in Supporting Limited English Proficiency Populations,” Health Sciences Review 17 (December 2025): 100249, https://doi.org/10.1016/j.hsr.2025.100249.
185. Ana Gonzalez-Barrera et al., “Language Barriers in Health Care: Findings from the KFF Survey on Racism, Discrimination, and Health,” KFF, May 16, 2024, https://www.kff.org/racial-equity-and-health-policy/language-barriersin-health-care-findings-from-the-kff-survey-on-racism-discrimination-and-health/.
186. Hamutal Bernstein et al., Immigrant Families Express Worry as They Prepare for Policy Changes (Urban Institute, 2025), https://www.urban.org/sites/default/files/2025-03/Immigrant-Families-Express-Worry-as-They-Prepare-for-PolicyChanges.pdf.
187. “Caregiver Statistics: Demographics,” Family Caregiver Alliance, accessed November 29, 2025, https://www. caregiver.org/resource/caregiver-statistics-demographics/.
188. Women and Caregiving: Facts and Figures (Family Caregiver Alliance, n.d.), accessed December 12, 2025, https:// www.caregiver.org/resource/women-and-caregiving-facts-and-figures/.
189. Family Caregiver Alliance, “Caregiver Statistics.”
190. Ramella, “The Invisible Work of Caregiving.”
191. Ramella, “The Invisible Work of Caregiving.”
192. “Resources for Area Agencies on Aging,” Oregon Department of Human Services, accessed December 12, 2025, https://www.oregon.gov/odhs/providers-partners/community-services-supports/pages/area-agencies-aging.aspx.
193. “Learn About Oregon’s ADRC,” Oregon Department of Human Services, accessed December 12, 2025, https:// www.oregon.gov/odhs/providers-partners/community-services-supports/pages/adrc.aspx.
194. Members of state-recognized tribes are not exempt; Oregon does not have any state-recognized tribes, but it may have some indigenous residents who are members of state-recognized tribes elsewhere.
195. Lyric Aquino, “Medicaid Cuts Could Strip Critical Funding from Tribal Health Clinics, Including in Rural Oregon,” Health Care, Underscore Native News, August 27, 2025, https://www.underscore.news/justice/health-care/ medicaid-cuts-could-strip-critical-funding-from-tribal-health-clinics-including-in-rural-oregon/.
196. Melanie Henshaw, “Northwest Tribes Sound Alarm about Cuts to Health Care, Education and Other Key Services,” Politics, Oregon Capital Chronicle, March 22, 2025, https://oregoncapitalchronicle.com/2025/03/22/northwesttribes-sound-alarm-about-cuts-to-health-care-education-and-other-key-services/.
197. “Tribal Engagement Toolkit,” Oregon Department of Human Services, accessed December 12, 2025, https://www. oregon.gov/odhs/providers-partners/seniors-disabilities/Documents/tribal-toolkit.pdf.
198. Coalition of Communities of Color and Portland State University, The Native American Community in Multnomah County: An Unsettling Report (Coalition of Communities of Color, n.d.), accessed December 12, 2025, https://www. coalitioncommunitiescolor.org/research-and-publications/the-native-american-community-in-multnomah-county-anunsettling-report.
199. “Tribal Consultation and Urban Indian Health Program Confer Policy,” Oregon Department of Human Services, October 6, 2023, https://sharedsystems.dhsoha.state.or.us/DHSForms/Served/me010-028.pdf.
200. “Portland Area,” Indian Health Service (IHS), accessed December 12, 2025, https://www.ihs.gov/portland/.
201. “Rural Tribal Clinics,” Oregon Health & Science University, accessed December 12, 2025, https://www.ohsu.edu/ oregon-office-of-rural-health/rural-tribal-clinics.
202. Amanda D Boyd et al., “Communication about COVID-19 with Urban American Indian and Alaska Native Peoples: The Role of Health Literacy, Trust, and Information Source,” Journal of Public Health 47, no. 3 (2025): 460–68, https://doi.org/10.1093/pubmed/fdaf050.
203. Coalition of Communities of Color and Portland State University, The Native American Community in Multnomah County.
204. Oregon Department of Human Services, “Tribal Engagement Toolkit.”
205. Jeff Mapes, “How Oregon’s Statistics on Race Often Get Misinterpreted,” Oregon Public Broadcasting, August 10, 2020, https://www.opb.org/article/2020/08/10/how-oregons-statistics-on-race-often-get-misinterpreted/. See Appendix.
206. We’re All Connected: OHA’s Strategic Plan to Eliminate Health Inequities (Oregon Health Authority, 2024), https://sharedsystems.dhsoha.state.or.us/DHSForms/Served/le-683051.pdf.
207. “Health Insurance Coverage Type by Race / Ethnicity,” State Health Access Data Assistance Center (SHADAC), accessed December 12, 2025, https://statehealthcompare.shadac.org/table/29/health-insurance-coverage-type-by-race-ethn icity#39/5,4,1,10,86,9,8,6,39,40,41,42,238,43,239/76/57,58. See Appendix.
208. Data Brief: COVID-19 and the Changes to Oregon Residents’ Health Insurance Coverage, Brief (Oregon Health Authority, 2021), https://www.oregon.gov/oha/HPA/ANALYTICS/Documents/Coverage-stats-Jan2021-1-26-21-final.pdf.
209. We’re All Connected: OHA’s Strategic Plan to Eliminate Health Inequities.
210. OHSU.Edu. “Racism in Oregon’s Health Care System.” 2020. https://www.ohsu.edu/sites/default/files/2021-01/ NA%20Brief_Experiences%20of%20Racism_FINAL%2011.18.20.pdf.
211. Matthew A. Kaczynski et al., “Perceived Discrimination in the Healthcare Setting and Medical Mistrust: Findings from the Health Information National Trends Survey, 2022,” Journal of General Internal Medicine 40, no. 11 (2025): 2491–98, https://doi.org/10.1007/s11606-025-09369-x.
212. Maryam Jafari Bidgoli et al., “Perceived Discrimination in Health Care Settings and Care Delays in Patients With Diabetes and Hypertension,” JAMA Network Open 8, no. 3 (2025): e250046, https://doi.org/10.1001/ jamanetworkopen.2025.0046.
213. Wikle et al., States Can Reduce Medicaid’s Administrative Burdens to Advance Health and Racial Equity.
214. Renuka Rayasam and Sam Whitehead, “The First Year of Georgia’s Medicaid Work Requirement Is Mired in Red Tape,” KFF Health News, September 13, 2024, https://kffhealthnews.org/news/article/georgia-medicaid-workrequirement-red-tape/.
215. Natasha P. Malmin et al., “Health Disparities and the Influence of Culturally Competent Care in Overall Health and Healthcare Utilization among Hispanics in a Southeastern US Community,” Hispanic Health Care International: The Official Journal of the National Association of Hispanic Nurses 23, no. 4 (2025): 196–205, https://doi. org/10.1177/15404153241289550; Cindy Brach and Irene Fraserirector, “Can Cultural Competency Reduce Racial And Ethnic Health Disparities? A Review And Conceptual Model,” Medical Care Research and Review: MCRR 57, no. Suppl 1 (2000): 181–217, https://doi.org/10.1177/1077558700057001S09.
216. Jafari Bidgoli et al., “Perceived Discrimination in Health Care Settings and Care Delays in Patients With Diabetes and Hypertension.”
217. Medicaid and CHIP Learning Collaboratives, “Ensuring Continuity of Coverage for Foster Youth Aging Out of Foster Care and Young Adults Eligible for the Former Foster Care Group,” The Coverage Learning Collaborative, September 9, 2019.
218. Medicaid and CHIP Learning Collaboratives, “Continuity of Coverage for Foster Youth.”
219. Medicaid and CHIP Learning Collaboratives, “Continuity of Coverage for Foster Youth.”
220. Amelia Coffey et al., Young People and Medical Assistance: Medicaid and the Children’s Health Insurance Program (Urban Institute, 2021), https://www.urban.org/sites/default/files/publication/103584/young-people-and-medicalassistance_1.pdf.
221. Arizona Section 115 Waiver: Draft Amendment Request: Former Foster Youth Annual Automatic Renewal (Arizona Health Care Cost Containment System, 2023), https://azahcccs.gov/Resources/Downloads/Federal/ FormerFosterYouthWaiverAmendmentProposal.pdf.
222. Arizona Section 115 Waiver: Draft Amendment Request: Former Foster Youth Annual Automatic Renewal.
223. Zachary Scherer, “Older Adults Who Are Foreign Born Less Likely to Live Alone Than Native Born,” Government, America Counts, August 31, 2020, https://www.census.gov/library/stories/2020/08/young-adults-mostlikely-to-change-living-arrangements.html.
224. Medicaid and CHIP Learning Collaboratives, “Continuity of Coverage for Foster Youth.”
225. Morales et al., “Optimizing SMS Strategies for Outreach to Medicaid and Marketplace Enrollees.”
226. Amelia Templeton, “Oregon’s Governor Convened a Group to Advise on Medicaid Funding Crisis. It’s Meeting behind Closed Doors,” Health, Oregon Public Broadcasting, November 17, 2025, https://www.opb.org/article/2025/11/17/ oregon-kotek-group-advise-medicaid-funding-crisis/.
227. Dana Hittle et al., “Addressing H.R.1 Impacts on SNAP and Medicaid in Oregon,” Presentation, Senate Committee on Health Care, September 30, 2025.
228. Tolbert and Corallo, “An Examination of Medicaid Renewal Outcomes and Enrollment Changes at the End of the Unwinding.”
229. McIntyre et al., “New Medicaid Enrollment Barriers and Lessons From Unwinding.”
230. Strengthening Cross-Agency Collaboration Across Medicaid and Other State Partners to Support Work Requirements Implementation (Center for Health Care Strategies, 2025), https://www.chcs.org/resource/strengtheningcross-agency-collaboration-across-medicaid-and-other-state-partners-to-support-work-requirements-implementation/.
231. Oregon Health Authority Strategic Plan (Oregon Health Authority, 2024), https://sharedsystems.dhsoha.state.or.us/ DHSForms/Served/le-609702.pdf#page=20.
232. Mia Ives-Rublee and Kennedy Andara, “House Republican Budget Bill Proposes Weakening Support for Homeless Individuals,” Center for American Progress, May 21, 2025, https://www.americanprogress.org/article/houserepublican-budget-bill-proposes-weakening-support-for-homeless-individuals/.
233. Wilson Criscione, “Why Unhoused People in the US Are Choosing to Go to Jail: ‘I Kept Reoffending,’” Society, The Guardian, November 2, 2022, https://www.theguardian.com/society/2022/nov/02/unhoused-people-sheltershomelessness-to-jail-cycle.
234. https://www.census.gov/programs-surveys/acs.html
235. Steven Ruggles, Sarah Flood, Matthew Sobek, Daniel Backman, Grace Cooper, Julia A. Rivera Drew, Stephanie Richards, Renae Rodgers, Jonathan Schroeder, and Kari C.W. Williams. IPUMS USA: Version 16.0 2023 1-year ACS estimates. Minneapolis, MN: IPUMS, 2025. https://doi.org/10.18128/D010.V16.0
236. https://shadac-pdf-files.s3.us-east-2.amazonaws.com/s3fs-public/publications/2021%20HIU%20Defining%20 families%20brief.pdf
237. https://www.nber.org/system/files/working_papers/w25143/w25143.pdf
Bibliography
2022 Annual Report. Common Sense Institute, n.d. Accessed December 12, 2025. https://www.commonsenseinstituteus. org/about/annual-reports/2022-annual-report.
A Field Guide to Fix Government Forms. The Lab @ DC, 2025. https://static1.squarespace. com/static/5d2361aa11fed60001f7ab3a/t/68d19c78f652e37bff2f1080/1758567544111/ A+Field+Guide+to+Fix+Government+Forms_The+Lab.pdf.
Additional Processing Instructions for Suspension and Reinstatement Actions on 3BOP, GN 02607.794 Program Operations Manual System (POMS) (2023). https://secure.ssa.gov/poms.nsf/lnx/0202607794.
Aging and People with Disabilities and Development Disabilities, 411-320–0020 Oregon Administrative Rules. Accessed December 9, 2025. https://secure.sos.state.or.us/oard/viewSingleRule.action?ruleVrsnRsn=315547.
“AIC Population Profile.” Oregon Department of Corrections, December 1, 2025. https://www.oregon.gov/doc/Documents/ inmate-profile.pdf.
Allen, Elizabeth M, Betsy Smither, Lindsey Barranco, et al. “Communicating Effectively With People Experiencing Homelessness to Prevent Infectious Diseases.” The Journal of Infectious Diseases 226, no. Suppl 3 (2022): S340–45. https://doi.org/10.1093/infdis/jiac336.
Alltucker, Ken. “Medicaid Name Changes Confuse the Public: What It Means for Your Health Insurance Coverage.” USA TODAY, July 30, 2025. https://www.usatoday.com/story/money/2025/07/30/medicaid-name-change-confusepublic-private-insurance/85403874007/.
An Act to Provide for Reconciliation Pursuant to Title II of H. Con. Res. 14, Pub. L. Nos. 119–21 (2025). https://www. congress.gov/bill/119th-congress/house-bill/1/text.
“Application for Oregon Health Plan Benefits.” Oregon Health Authority, May 1, 2020. https://sharedsystems.dhsoha.state. or.us/DHSForms/Served/he7210.pdf.
Aquino, Lyric. “Medicaid Cuts Could Strip Critical Funding from Tribal Health Clinics, Including in Rural Oregon.” Health Care. Underscore Native News, August 27, 2025. https://www.underscore.news/justice/health-care/medicaid-cutscould-strip-critical-funding-from-tribal-health-clinics-including-in-rural-oregon/.
Arizona Section 115 Waiver: Draft Amendment Request: Former Foster Youth Annual Automatic Renewal. Arizona Health Care Cost Containment System, 2023. https://azahcccs.gov/Resources/Downloads/Federal/ FormerFosterYouthWaiverAmendmentProposal.pdf.
Arkansas. “Arkansas Alternative Benefit Plan.” Application to Centers for Medicare & Medicaid Services. June 26, 2023. https://humanservices.arkansas.gov/wp-content/uploads/3.1-AttachL-AltBenefitPlan.pdf.
Arkansas Medicaid Work and Community Engagement Requirement: Community Response. Arkansas Center for Health Improvement, 2019. https://achi.net/wp-content/uploads/2019/10/190917A_AR-Works-Interviews-Report.pdf.
“Attachment D: Medically Frail Identification Process.” Michigan Department of Health and Human Services, n.d.
Bataille, Julie, and Kevin Caudill. “State Strategies for Sequencing Enrollee Communications When Medicaid Continuous Coverage Ends.” State Health & Value Strategies, August 3, 2022. https://shvs.org/state-strategies-for-sequencingenrollee-communications-when-medicaid-continuous-coverage-ends/.
Bauer, Lauren, Eloise Burtis, Olivia Howard, and Sarah Yu Wang. “Which Nontraditional Students Are Also in the Labor Force?” Brookings Institution, December 7, 2023. https://www.brookings.edu/articles/which-nontraditionalstudents-are-also-in-the-labor-force/.
Baumrucker, Evelyne P. Medicaid and Incarcerated Individuals. In Focus No. IF11830. Congressional Research Service, 2024. https://www.congress.gov/crs-product/IF11830.
Bernstein, Hamutal, Dulce Gonzalez, and Diana Guelsepe. Immigrant Families Express Worry as They Prepare for Policy Changes. Urban Institute, 2025. https://www.urban.org/sites/default/files/2025-03/Immigrant-Families-ExpressWorry-as-They-Prepare-for-Policy-Changes.pdf.
“Best Practices for Accessible Communications.” National Center on Health, Physical Activity and Disability (NCHPAD), September 5, 2024. https://www.nchpad.org/resources/best-practices-for-accessible-and-inclusivecommunications/.
Boozang, Patricia, Kinda Serafi, and Alex Dworkowitz. “Federal Ruling Provides Text Messaging Flexibility to Support State’s Unwinding Efforts.” State Health & Value Strategies, January 27, 2023. https://shvs.org/federal-rulingprovides-text-messaging-flexibility-to-support-states-unwinding-efforts/.
Boyd, Amanda D, Austin Henderson, Azhar Uddin, et al. “Communication about COVID-19 with Urban American Indian and Alaska Native Peoples: The Role of Health Literacy, Trust, and Information Source.” Journal of Public Health 47, no. 3 (2025): 460–68. https://doi.org/10.1093/pubmed/fdaf050.
Brach, Cindy, and Irene Fraserirector. “Can Cultural Competency Reduce Racial And Ethnic Health Disparities? A Review And Conceptual Model.” Medical Care Research and Review: MCRR 57, no. Suppl 1 (2000): 181–217. https://doi. org/10.1177/1077558700057001S09.
Bureau of Labor and Industries. “Oregon Minimum Wage.” Accessed December 9, 2025. https://www.oregon.gov/boli/ workers/pages/minimum-wage.aspx.
Burns, Alice, and Sammy Cervantes. “5 Key Facts About Medicaid Coverage for People with Disabilities.” KFF, February 7, 2025. https://www.kff.org/medicaid/5-key-facts-about-medicaid-coverage-for-people-with-disabilities/.
Burns, Alice, Jared Ortaliza, Justin Lo, Matthew Rae, and Cynthia Cox. “How Will the 2025 Reconciliation Law Affect the Uninsured Rate in Each State?” KFF, August 20, 2025. https://www.kff.org/uninsured/how-will-the-2025reconciliation-law-affect-the-uninsured-rate-in-each-state/.
CareOregon. “About Redetermination.” Accessed December 9, 2025. https://www.careoregon.org/providers/aboutredetermination.
Carl D. Perkins Career and Technical Education Improvement Act of 2006, Pub. L. Nos. 109–270 (2006). https://www. congress.gov/bill/109th-congress/senate-bill/250.
Center for Civic Design. Form Letters That Actually Inform. September 2, 2025. https://civicdesign.org/form-letters-thatactually-inform/.
Center for Civic Design. “Usability Testing Toolkit.” October 30, 2025. https://civicdesign.org/tools/usability-testing/.
Center for Plain Language. “Five Steps to Plain Language.” December 6, 2016. https://centerforplainlanguage.org/learningtraining/five-steps-plain-language/.
Centers for Medicare & Medicaid Services. “Data Disclosures and Data Use Agreements (DUAs).” CMS.Gov. Accessed December 10, 2025. https://www.cms.gov/data-research/cms-data/data-disclosures-and-data-use-agreementsduas.
Centers for Medicare & Medicaid Services. “Long-Term Care Hospital PPS.” CMS.Gov. Accessed November 15, 2025. https://www.cms.gov/medicare/payment/prospective-payment-systems/long-term-care-hospital.
Centers for Medicare & Medicaid Services. “Transitioning to ICD-10.” CMS.Gov, February 25, 2015. https://www.cms.gov/ newsroom/fact-sheets/transitioning-icd-10.
Chairman Mike Crapo. “Finance Committee Title.” US Senate Committee on Finance, August 2025. https://www.finance. senate.gov/imo/media/doc/finance_committee_summary3.pdf.
Chan, Leah. Georgia’s Pathways to Coverage Program: The First Year in Review. Georgia Budget & Policy Institute, n.d. https://gbpi.org/wp-content/uploads/2024/10/PathwaystoCoverage_PolicyBrief_2024103.pdf.
Coalition of Communities of Color and Portland State University. The Native American Community in Multnomah County: An Unsettling Report. Coalition of Communities of Color, n.d. Accessed December 12, 2025. https://
www.coalitioncommunitiescolor.org/research-and-publications/the-native-american-community-in-multnomahcounty-an-unsettling-report.
Coffey, Amelia, Gina Adams, and Heather Hahn. Young People and Medical Assistance: Medicaid and the Children’s Health Insurance Program. Urban Institute, 2021. https://www.urban.org/sites/default/files/publication/103584/ young-people-and-medical-assistance_1.pdf.
Coker, Margaret. “Georgia’s Medicaid Work Requirement Program Spent Twice as Much on Administrative Costs as on Health Care, GAO Says.” North Carolina Health News (North Carolina), September 27, 2025. https://www. northcarolinahealthnews.org/2025/09/27/georgias-medicaid-work-requirement-program-spent-twice-as-muchon-administrative-costs-as-on-health-care-gao-says/.
“Community Population Profile.” Oregon Department of Corrections, August 1, 2025. https://www.oregon.gov/doc/ Documents/community-profile.pdf.
Congressional Budget Office. “CBO’s Agreements to Access Data Since September 30, 2024.” September 25, 2025. https:// www.cbo.gov/publication/61548.
“Coordinated Care Organizations (CCOs) in Oregon: How They Work and Future Opportunities.” United States of Care, n.d. Accessed November 29, 2025. https://unitedstatesofcare.org/wp-content/uploads/2022/04/CCO-OregonOverview.pdf.
Corallo, Bradley, and Jennifer Tolbert. “Understanding Medicaid Ex Parte Renewals During the Unwinding.” KFF, October 2, 2023. https://www.kff.org/medicaid/understanding-medicaid-ex-parte-renewals-during-the-unwinding/.
Criscione, Wilson. “Why Unhoused People in the US Are Choosing to Go to Jail: ‘I Kept Reoffending.’” Society. The Guardian, November 2, 2022. https://www.theguardian.com/society/2022/nov/02/unhoused-people-sheltershomelessness-to-jail-cycle.
Darling, Matt. “What Can Be Learned from States That Made Good Faith Efforts with Work Requirements?” Substack newsletter. Can We Still Govern?, August 25, 2025. https://donmoynihan.substack.com/p/what-can-be-learnedfrom-states-that.
Data Brief: COVID-19 and the Changes to Oregon Residents’ Health Insurance Coverage. Brief. Oregon Health Authority, 2021. https://www.oregon.gov/oha/HPA/ANALYTICS/Documents/Coverage-stats-Jan2021-1-26-21-final.pdf.
Definitions, 471-070–1000 Oregon Administrative Rules. Accessed December 9, 2025. https://www.law.cornell.edu/ regulations/oregon/Or-Admin-Code-SS-471-070-1000.
Definitions, 877-001–0006 Oregon Administrative Rules § Board of Licensed Social Workers. Accessed December 9, 2025. https://oregon.public.law/rules/oar_877-001-0006.
Definitions Relating to Institutional Status, 435.1010 Code of Federal Regulations. Accessed December 9, 2025. https:// www.ecfr.gov/current/title-42/part-435/section-435.1010.
Department of Justice, Civil Rights Division. “ADA Best Practices Tool Kit for State and Local Governments.” National Association of County & City Health Officials (NACCHO). Accessed December 12, 2025. https://www.naccho.org/ resource-hub-articles/ada-best-practices-tool-kit-for-state-and-local-governments.
“Developing Effective Data Use Agreements (DUAs).” Comprehensive Opioid, Stimulant, and Substance Use Program (COSSUP), n.d. https://www.abtglobal.com/sites/default/files/files/Projects/PDFs/2025/developing-effectiveduas_0.pdf.
Digital.Gov. “Plain Language Guide Series.” September 23, 2025. https://digital.gov/guides/plain-language.
Enrollment and Access Barriers for People with Limited English Proficiency. Brief. MACPAC, 2024.
“Estimated Impacts of H.R. 1.” Department of Administrative Services Chief Financial Office, August 11, 2025. https:// www.oregon.gov/das/Financial/Documents/Federal-Impact-HR1-Initial-Analysis.pdf.
Euhus, Rhiannon, Robin Rudowitz, Alice Burns, and Sammy Cervantes. “5 Key Facts About Medicaid Coverage for People Living in Rural Areas.” KFF, June 26, 2025. https://www.kff.org/medicaid/5-key-facts-about-medicaid-coveragefor-people-living-in-rural-areas/.
Exempt Individuals, 440.315 Code of Federal Regulations (2013). https://www.ecfr.gov/current/title-42/part-440/ section-440.315.
Family Caregiver Alliance. “Caregiver Statistics: Demographics.” Accessed November 29, 2025. https://www.caregiver.org/ resource/caregiver-statistics-demographics/.
Federal Communications Commission. “FM Broadcast Station Classes and Service Contours.” Accessed December 10, 2025. https://www.fcc.gov/media/radio/fm-station-classes.
Food and Nutrition Act of 2008, Pub. L. Nos. 88–525 (2025). https://www.govinfo.gov/content/pkg/COMPS-10331/pdf/ COMPS-10331.pdf.
Food and Nutrition Service. “A Short History of SNAP.” U.S. Department of Agriculture. Accessed December 9, 2025. https://www.fns.usda.gov/snap/history.
Food and Nutrition Service. “SNAP Work Requirements.” U.S. Department of Agriculture. Accessed December 9, 2025. https://www.fns.usda.gov/snap/work-requirements.
GigEconomyData.Org. “Gig Economy Data Hub.” Accessed December 12, 2025. https:///gigeconomydata.org/home.
Gonzalez-Barrera, Ana, Liz Hamel, Samantha Artiga, and Marley Presiado. “Language Barriers in Health Care: Findings from the KFF Survey on Racism, Discrimination, and Health.” KFF, May 16, 2024. https://www.kff.org/ racial-equity-and-health-policy/language-barriers-in-health-care-findings-from-the-kff-survey-on-racismdiscrimination-and-health/.
Gordon, Robert. “More Than 100,000 Michigan Residents Nearly Lost Medicaid Coverage Under Work Requirements.” The Commonwealth Fund, May 12, 2025. https://doi.org/10.26099/8XP5-7397.
Goyat, Rashmi, Ami Vyas, and Usha Sambamoorthi. “Racial/Ethnic Disparities in Disability Prevalence.” Journal of Racial and Ethnic Health Disparities 3, no. 4 (2016): 635–45. https://doi.org/10.1007/s40615-015-0182-z.
Griffin-Valade, LaVonne, and Kip Memmott. The Oregon Eligibility System Appropriately Determines Eligibility, but Input Errors Continue to Occur. Audit Nos. 2024–27. Oregon Secretary of State, 2024. https://sos.oregon.gov/audits/ Documents/2024-27.pdf.
GSA Blog Team. “Making Government Text Messaging More Effective with Notify.Gov.” U.S. General Services Administration, December 17, 2024. https://www.gsa.gov/blog/2024/12/17/making-government-text-messagingmore-effective-with-notifygov.
HB3361 2017 Regular Session - Oregon Legislative Information System, 3361, Oregon State Legislature 2017. Accessed December 12, 2025. https://olis.oregonlegislature.gov/liz/2017R1/Measures/Overview/HB3361.
Health Systems Division: Addiction Services, 415-050–0105 Oregon Administrative Rules. Accessed December 10, 2025. https://secure.sos.state.or.us/oard/viewSingleRule.action?ruleVrsnRsn=300322.
Henshaw, Melanie. “Northwest Tribes Sound Alarm about Cuts to Health Care, Education and Other Key Services.” Politics. Oregon Capital Chronicle, March 22, 2025. https://oregoncapitalchronicle.com/2025/03/22/northwesttribes-sound-alarm-about-cuts-to-health-care-education-and-other-key-services/.
Herd, Pamela, Hilary Hoynes, Jamila Michener, and Donald Moynihan. “Introduction: Administrative Burden as a Mechanism of Inequality in Policy Implementation.” RSF: The Russell Sage Foundation Journal of the Social Sciences 9, no. 5 (2023): 1–30. https://doi.org/10.7758/RSF.2023.9.5.01.
Herd, Pamela, and Donald Moynihan. “Administrative Burdens in the Social Safety Net.” Journal of Economic Perspectives 39, no. 1 (2025): 129–50. https://doi.org/10.1257/jep.20231394.
Higher Education Act of 1965, Pub. L. Nos. 119–21 (2025). https://www.govinfo.gov/content/pkg/COMPS-765/pdf/ COMPS-765.pdf.
Hinton, Elizabeth, Amaya Diana, and Robin Rudowitz. “A Closer Look at the Work Requirement Provisions in the 2025 Federal Budget Reconciliation Law.” KFF, July 30, 2025. https://www.kff.org/medicaid/a-closer-look-at-the-workrequirement-provisions-in-the-2025-federal-budget-reconciliation-law/.
“Impact of Federal Requirements & Funding Cuts to Oregon Health Plan (OHP/Medicaid).” Oregon Health Authority, June 4, 2025. https://www.oregon.gov/oha/Documents/Federal-Budget-Impacts-Medicaid.pdf.
Inbody, David. “12-Month Eligibility for Oregon Health Plan Post-Partum Benefits.” Memo to Coordinated care organizations. April 1, 2022. https://www.oregon.gov/oha/HSD/OHP/Announcements/12-month%20 eligibility%20for%20Oregon%20Health%20Plan%20post-partum%20benefits.pdf.
Indian Health Service (IHS). “Portland Area.” Accessed December 12, 2025. https://www.ihs.gov/portland/.
Ives-Rublee, Mia, and Kennedy Andara. “House Republican Budget Bill Proposes Weakening Support for Homeless Individuals.” Center for American Progress, May 21, 2025. https://www.americanprogress.org/article/houserepublican-budget-bill-proposes-weakening-support-for-homeless-individuals/.
Jafari Bidgoli, Maryam, Hui Wang, Casey Macander, and Abbey Gregg. “Perceived Discrimination in Health Care Settings and Care Delays in Patients With Diabetes and Hypertension.” JAMA Network Open 8, no. 3 (2025): e250046. https://doi.org/10.1001/jamanetworkopen.2025.0046.
Justice in Aging, National Health Law Program, and Judge David L. Bazelon Center for Mental Health Law. “Recommendations for Mitigating Harms to People with Disabilities, Older Adults, and Caregivers from Medicaid Work Requirements.” Justice in Aging, December 2025. https://justiceinaging.org/wp-content/uploads/2025/12/ NHeLP_JIA_Bazelon_RecsforMitigatingHarmstoPWD_OlderAdults_WorkReq_122025.pdf.
Kaczynski, Matthew A., Gregorio Benitez, Fadi Shehadeh, Eleftherios Mylonakis, and Mark A. Fiala. “Perceived Discrimination in the Healthcare Setting and Medical Mistrust: Findings from the Health Information National Trends Survey, 2022.” Journal of General Internal Medicine 40, no. 11 (2025): 2491–98. https://doi.org/10.1007/ s11606-025-09369-x.
KATU Staff. “Number of Oregonians Working Multiple Jobs Rises Again in 2024, Ahead of National Average.” KATU (Portland, Oregon), April 28, 2025. https://katu.com/news/local/number-of-oregonians-working-multiple-jobsrises-again-ahead-of-national-average-employment-workers-portland-job-oregon-department-bureau-labor-april2024-2025.
Kentucky Department for Medicaid Services. 1115 Demonstration Extension Request. Team Kentucky Cabinet for Health and Family Services, 2022. https://www.chfs.ky.gov/agencies/dms/Documents/1115ExtensionNoLetter.pdf.
KFF. “Suspension of Medicaid Coverage for Incarcerated Adults.” January 2025. https://www.kff.org/medicaid/stateindicator/suspension-of-medicaid-coverage-for-incarcerated-adults/.
Khalique, Amina, Kennedy Andara, Natalie Baker, Sara Partridge, and Kyle Ross. The Trump Administration’s One Big Beautiful Bill Act Will Drive Up Costs in Oregon. Center for American Progress, 2025.
Kliff, Sarah, Margot Sanger-Katz, and Asmaa Elkeurti. “‘A Big Positive’: How One Company Plans to Profit From Medicaid Cuts.” The New York Times, November 3, 2025. https://www.nytimes.com/2025/11/03/health/medicaid-cutsequifax-data.html.
Lang, Noah. “How Medicaid Redetermination Impacts Gig Economy Workers.” Stride Blog, n.d. Accessed December 12, 2025. https://blog.stridehealth.com/post/how-medicaid-redetermination-impacts-gig-economy-workers.
“MAGI-Based Eligibility Verification Plan.” Oregon Health Authority, July 5, 2016. https://www.medicaid.gov/medicaid/ eligibility/downloads/oregon-verification-plan-template-final.pdf.
Maldonado, Mia. “Republican Tax Bill Could Slash Billions for Oregon Health Plan, State Officials Say.” Health. Oregon Capital Chronicle, June 4, 2025. https://oregoncapitalchronicle.com/2025/06/04/republican-tax-bill-could-slashbillions-for-oregon-health-plan-state-officials-say/.
Malmin, Natasha P., Shannon Owen, Diana Hoyos Lopez, Rebecca McKinney, and Vanessa Rodríguez. “Health Disparities and the Influence of Culturally Competent Care in Overall Health and Healthcare Utilization among Hispanics
in a Southeastern US Community.” Hispanic Health Care International: The Official Journal of the National Association of Hispanic Nurses 23, no. 4 (2025): 196–205. https://doi.org/10.1177/15404153241289550.
Mapes, Jeff. “How Oregon’s Statistics on Race Often Get Misinterpreted.” Oregon Public Broadcasting, August 10, 2020. https://www.opb.org/article/2020/08/10/how-oregons-statistics-on-race-often-get-misinterpreted/.
Mark A. Crabtree. “Oregon Family, Paid Leave Changes Effective July 1, 2024.” Jackson Lewis, April 3, 2024. https://www. jacksonlewis.com/insights/oregon-family-paid-leave-changes-effective-july-1-2024.
Massachusetts Digital Service. “How to Conduct a Plain Language Review.” Mass.Gov. Accessed December 1, 2025. https:// www.mass.gov/info-details/how-to-conduct-a-plain-language-review.
McInnes, D. Keith, Alice E. Li, and Timothy P. Hogan. “Opportunities for Engaging Low-Income, Vulnerable Populations in Health Care: A Systematic Review of Homeless Persons’ Access to and Use of Information Technologies.” American Journal of Public Health 103, no. Suppl 2 (2013): e11–24. https://doi.org/10.2105/AJPH.2013.301623.
McIntyre, Adrianna, Jinwoo Kim, and Benjamin D. Sommers. “New Medicaid Enrollment Barriers and Lessons From Unwinding.” JAMA Health Forum 6, no. 9 (2025): e254849. https://doi.org/10.1001/jamahealthforum.2025.4849.
Meaning of Blindness as Defined in the Law, 404.1581 Code of Federal Regulations (1983). https://www.ssa.gov/OP_ Home/cfr20/404/404-1581.htm.
Medicaid & CHIP Renewals: Reaching Children and Families in School-Based and Early Education and Care Settings. Centers for Medicare & Medicaid Services, 2024.
Medicaid and CHIP Eligibility Renewals: A Communications Toolkit. Centers for Medicare & Medicaid Services, 2023.
Medicaid and CHIP Renewals: A Faith-Based Communications Toolkit. Centers for Medicare & Medicaid Services, 2024.
Medicaid and CHIP Renewals: Patient-Centered Messaging for Clinical Offices and Health Care Settings. Centers for Medicare & Medicaid Services, n.d.
“Medicaid Management Information System: HPA Data Profile.” Oregon Health Authority, May 2025. https://www.oregon. gov/oha/HPA/ANALYTICS/Documents/Dataprofile_MMIS.pdf.
Mental Illness, 436-035–0400 Oregon Administrative Rules § Department of Consumer and Business Services, Workers’ Compensation Division (2025). https://oregon.public.law/rules/oar_436-035-0400.
Métraux, Julia. “Trump’s War on Medicaid Will Institutionalize Millions of People.” Mother Jones, January 31, 2025. https:// www.motherjones.com/politics/2025/01/trump-medicaid-institutionalization-hcbs-cuts-gop/.
Meuse, Dan. “Medicaid Work Reporting Requirements: Implementation Basics and State Decision Points.” State Health & Value Strategies, August 15, 2025. https://shvs.org/medicaid-work-reporting-requirements-implementation-basicsand-state-decision-points/.
Migration Policy Institute. “State Immigration Data Profiles: Oregon.” Accessed December 12, 2025. https://www. migrationpolicy.org/data/state-profiles/state/language/OR.
Miller, Brian J., C. Bayard Paschall, and Dale P. Svendsen. “Mortality and Medical Comorbidity among Patients with Serious Mental Illness.” Psychiatric Services (Washington, D.C.) 57, no. 10 (2006): 1482–87. https://doi. org/10.1176/ps.2006.57.10.1482.
Milton, B., P. Attree, B. French, S. Povall, M. Whitehead, and J. Popay. “The Impact of Community Engagement on Health and Social Outcomes: A Systematic Review.” Community Development Journal 47, no. 3 (2012): 316–34. https:// doi.org/10.1093/cdj/bsr043.
“Minimum and Maximum Weekly Benefit Amounts to Increase for New Unemployment Insurance and Paid Leave Oregon Claims.” Oregon Employment Department, June 3, 2025. https://www.oregon.gov/employ/NewsAndMedia/ Documents/2025-06-03-Minimum-Maximum-Weekly-Benefit-Amounts.pdf.
Morales, Melissa, and Kevin Caudill. “Rapid Message Test Insights to Inform 2024 Medicaid Renewal Messaging.” State Health & Value Strategies, January 8, 2024. https://shvs.org/rapid-message-test-insights-to-inform-2024-medicaidrenewal-messaging/.
Morales, Melissa, Kenzie Perrow, and Kaylee O’Connor. “Optimizing SMS Strategies for Outreach to Medicaid and Marketplace Enrollees.” State Health & Value Strategies, May 16, 2024. https://shvs.org/optimizing-sms-strategiesfor-outreach-to-medicaid-and-marketplace-enrollees/.
Northwest ADA Center. “Effective Communications.” Accessed December 12, 2025. https://nwadacenter.org/toolkit/ effective-communications.
Office of Health Analytics. “Health Insurance Coverage.” Oregon Health Authority, September 2024. https://www.oregon. gov/oha/HPA/ANALYTICS/Documents/OHIS-coverage-summary.pdf.
OHSU.Edu. “Racism in Oregon’s Health Care System.” 2020. https://www.ohsu.edu/sites/default/files/2021-01/NA%20 Brief_Experiences%20of%20Racism_FINAL%2011.18.20.pdf.
One Department Serving Rural America: HHS Rural Task Force Report to the Secretary. U.S. Department of Health & Human Services, 2002. https://www.govinfo.gov/content/pkg/GOVPUB-HE-PURL-LPS21888/pdf/GOVPUB-HEPURL-LPS21888.pdf.
Oregon Areas of Unmet Health Care Need Report. Oregon Office of Rural Health, 2025. https://www.ohsu.edu/sites/ default/files/2025-09/AUHCN%20Report_2025%20-%20FINAL.pdf.
Oregon Department of Human Services. “Learn About Oregon’s ADRC.” Accessed December 12, 2025. https://www. oregon.gov/odhs/providers-partners/community-services-supports/pages/adrc.aspx.
Oregon Department of Human Services. “Resources for Area Agencies on Aging.” Accessed December 12, 2025. https:// www.oregon.gov/odhs/providers-partners/community-services-supports/pages/area-agencies-aging.aspx.
Oregon Department of Human Services. “Tribal Engagement Toolkit.” Accessed December 12, 2025. https://www.oregon. gov/odhs/providers-partners/seniors-disabilities/Documents/tribal-toolkit.pdf.
Oregon Health & Science University. “Rural Tribal Clinics.” Accessed December 12, 2025. https://www.ohsu.edu/oregonoffice-of-rural-health/rural-tribal-clinics.
Oregon Health Authority. “All Payer All Claims Reporting Program.” https://www.oregon.gov/oha/hpa/analytics/pages/allpayer-all-claims.aspx.
Oregon Health Authority. “Cancer Reporting.” Accessed December 10, 2025. https://www.oregon.gov/oha/ph/ diseasesconditions/chronicdisease/cancer/oscar/pages/reporting.aspx.
Oregon Health Authority. “Health Equity Plan Definitions.” Accessed December 12, 2025. https://www.oregon.gov/oha/ei/ pages/hec%20plan%20definitions.aspx.
Oregon Health Authority. “Healthier Oregon.” Accessed December 9, 2025. https://www.oregon.gov/oha/hsd/ohp/pages/ healthier-oregon.aspx.
Oregon Health Authority. “Network Adequacy - Time and Distance Rules for Providers.” Accessed November 15, 2025. https://www.oregon.gov/oha/hsd/ohp/pages/network.aspx.
Oregon Health Authority. “OHP Enrollment Report.” https://www.oregon.gov/oha/hpa/analytics/pages/medicaidenrollment.aspx.
Oregon Health Authority. “Oregon State Cancer Registry (OSCaR).” Accessed December 10, 2025. https://www.oregon. gov/oha/ph/diseasesconditions/chronicdisease/cancer/oscar/pages/index.aspx.
Oregon Health Authority. “Oregon’s Health System Transformation: CCO Metrics 2015 Final Report.” June 23, 2016. https://www.oregon.gov/oha/HPA/ANALYTICS/CCOMetrics/2015-CCO-Performance-Report.pdf.
Oregon Health Authority. “Prescription Drug Monitoring Program.” Accessed December 10, 2025. https://www.oregon. gov/oha/ph/preventionwellness/safeliving/pdmp/pages/index.aspx.
Oregon Health Authority Strategic Plan. Oregon Health Authority, 2024. https://sharedsystems.dhsoha.state.or.us/ DHSForms/Served/le-609702.pdf#page=20.
“Person with a Disability” Defined, 174.107 Oregon Revised Statutes § State Government, Government Procedures, Land Use. Accessed December 9, 2025. https://oregon.public.law/statutes/ors_174.107.
Public Health Division, 333-010–0000 Oregon Administrative Rules. Accessed December 10, 2025. https:// secure.sos.state.or.us/oard/displayDivisionRules.action;JSESSIONID_OARD=AajA3Un2PKiX-yZmqD_ bhzPpjasK5vESisCyOUhkVrBWmi_yEdlz!-1969788327?selectedDivision=1225.
PUPS Skeleton Records, GN 02607.520 Program Operations Manual Systems (POMS) (2023). https://secure.ssa.gov/poms. nsf/lnx/0202607520.
Ramella, Sueann. “The Invisible Work of Caregiving: A Radio Special on the Caregiving World Part 1.” Northwest Public Broadcasting, May 22, 2025. https://www.nwpb.org/uncategorized/2025-05-22/caregiving-radio-special-hour-one.
Rayasam, Renuka, and Sam Whitehead. “The First Year of Georgia’s Medicaid Work Requirement Is Mired in Red Tape.” KFF Health News, September 13, 2024. https://kffhealthnews.org/news/article/georgia-medicaid-workrequirement-red-tape/.
Reese, Michael, and Heidi Steward. “Oregon Department of Corrections Healthcare Delivery System Assessment.” Memo to Elizabeth Falcon. July 25, 2025. https://www.oregon.gov/doc/Documents/ODOC_Falcon_Report.pdf.
Results for America. “Data Policies / Agreements.” Accessed December 12, 2025. https://2020state.results4america.org/ state-standard-of-excellence/data-policies--agreements.html.
Rhoades, Harmony, Suzanne Wenzel, Eric Rice, Hailey Winetrobe, and Benjamin Henwood. “No Digital Divide? Technology Use among Homeless Adults.” Journal of Social Distress and the Homeless 26, no. 1 (2017): 73–77. https://doi.org/10.1080/10530789.2017.1305140.
Riesch, Susan K., Emmanuel Ngui, Carey Ehlert, et al. “Community Outreach and Engagement Strategies from the Wisconsin Study Center of the National Children’s Study.” Public Health Nursing (Boston, Mass.) 30, no. 3 (2013): 254–65. https://doi.org/10.1111/phn.12018.
Robinson, Maren N., Kristin A. Tansil, Randy W. Elder, et al. “Mass Media Health Communication Campaigns Combined with Health-Related Product Distribution: A Community Guide Systematic Review.” American Journal of Preventive Medicine 47, no. 3 (2014): 360–71. https://doi.org/10.1016/j.amepre.2014.05.034.
Rowe, Christopher L., Glenn-Milo Santos, Wiley Kornbluh, Sumeet Bhardwaj, Mark Faul, and Phillip O. Coffin. “Using ICD-10-CM Codes to Detect Illicit Substance Use: A Comparison with Retrospective Self-Report.” Drug and Alcohol Dependence 221 (April 2021): 108537. https://doi.org/10.1016/j.drugalcdep.2021.108537.
Rural Health Information Hub. “Rural Project Summary: Coast to Forest: Mental Health Promotion in Rural Oregon and Beyond.” Accessed December 12, 2025. https://www.ruralhealthinfo.org/project-examples/1096.
Scherer, Zachary. “Older Adults Who Are Foreign Born Less Likely to Live Alone Than Native Born.” Government. America Counts, August 31, 2020. https://www.census.gov/library/stories/2020/08/young-adults-most-likely-tochange-living-arrangements.html.
“Sharing Oregon State Hospital Encounter Information in the PointClickCare Platform: Information Sheet.” HIT Commons, n.d. Accessed December 10, 2025. https://ohlc.org/wp-content/uploads/2024/09/OSH-ADTBrief-9-19-24.pdf.
Smith, Matthew Lee, Mindy Menn, and E. Lisako J. McKyer. “Effectiveness of the Radio as a Health Information Source.” Journal of Radio & Audio Media 18, no. 2 (2011): 196–211. https://doi.org/10.1080/19376529.2011.615776.
Sommers, Benjamin D., Anna L. Goldman, Robert J. Blendon, E. John Orav, and Arnold M. Epstein. “Medicaid Work Requirements — Results from the First Year in Arkansas.” New England Journal of Medicine 381, no. 11 (2019): 1073–82. https://doi.org/10.1056/NEJMsr1901772.
Spurbeck, Franklin Holcomb, Jacen Greene, and Marisa Zapata. 2024 Oregon Statewide Homelessness Estimates. Portland State University Homeless Research & Action Collaborative, 2025.
“State Alternative Benefit Plans and 1115 Waivers Medical Frailty Definitions.” Harvard Law School Center for Health Law and Policy Innovation, n.d. Accessed December 9, 2025. https://chlpi.org/wp-content/uploads/2025/11/State-ABPand-1115-Medical-Frailty-Definitions_uploaded-11.17.25.pdf.
“State Data Use Agreement Example (Louisiana).” Centers for Medicare & Medicaid Services Medicaid Innovation Accelerator Program, n.d. https://www.medicaid.gov/state-resource-center/innovation-accelerator-program/iapdownloads/program-areas/la-dua-example.pdf.
State Health Access Data Assistance Center (SHADAC). “Health Insurance Coverage Type by Race / Ethnicity.” Accessed December 12, 2025. https://statehealthcompare.shadac.org/table/29/health-insurance-coverage-type-by-race-ethni city#39/5,4,1,10,86,9,8,6,39,40,41,42,238,43,239/76/57,58.
State Plans for Medical Assistance, 42 U.S.C. 139a. Accessed December 9, 2025. https://www.ssa.gov/OP_Home/ssact/ title19/1902.htm.
Strengthening Cross-Agency Collaboration Across Medicaid and Other State Partners to Support Work Requirements Implementation. Center for Health Care Strategies, 2025. https://www.chcs.org/resource/strengthening-crossagency-collaboration-across-medicaid-and-other-state-partners-to-support-work-requirements-implementation/.
Templeton, Amelia. “Oregon’s Governor Convened a Group to Advise on Medicaid Funding Crisis. It’s Meeting behind Closed Doors.” Health. Oregon Public Broadcasting, November 17, 2025. https://www.opb.org/article/2025/11/17/ oregon-kotek-group-advise-medicaid-funding-crisis/.
The Re-Employment of Oregon. Oregon Employment Department, 2022. https://www.dol.gov/sites/dolgov/files/eta/ Performance/pdfs/annual_economic_reports/PY2021/OR%20PY21%20Economic%20Analysis%20Report.pdf.
“The State of Gig Economy in Oregon.” Neilsberg Research, December 12, 2022. https://www.neilsberg.com/insights/thestate-of-gig-economy-in-oregon/.
Tolbert, Jennifer, and Bradley Corallo. “An Examination of Medicaid Renewal Outcomes and Enrollment Changes at the End of the Unwinding.” KFF, September 18, 2024. https://www.kff.org/medicaid/an-examination-of-medicaidrenewal-outcomes-and-enrollment-changes-at-the-end-of-the-unwinding/.
“Tribal Consultation and Urban Indian Health Program Confer Policy.” Oregon Department of Human Services, October 6, 2023. https://sharedsystems.dhsoha.state.or.us/DHSForms/Served/me010-028.pdf.
Tsai, Daniel. Financial Eligibility Verification Requirements and Flexibilities. Informational Bulletin. Centers for Medicare & Medicaid Services, 2024.
University of Oregon. “Enrollment.” Accessed December 9, 2025. https://financialaid.uoregon.edu/enrollment.
U.S. Centers for Disease Control & Prevention. “About Homelessness and Health.” Homelessness and Health, October 15, 2024. https://www.cdc.gov/homelessness-and-health/about/index.html.
U.S. Department of Education. “Half-Time Enrollment.” StudentAid.Gov. Accessed December 9, 2025. https://studentaid. gov/help-center/answers/article/half-time-enrollment.
USAFacts. “How Many Immigrants Are in Oregon?” Accessed December 12, 2025. https://usafacts.org/answers/howmany-immigrants-are-in-the-us/state/oregon/.
Wachino, Vikki. “To Facilitate Successful Re-Entry for Individuals Transitioning from Incarceration to Their Communities.” Letter. n.d. Accessed December 9, 2025. https://www.medicaid.gov/sites/default/files/FederalPolicy-Guidance/Downloads/sho16007.pdf.
Wagner, Jennifer, Symonne Singleton, and Maani Stewart. A Guide to Reducing Coverage Losses Through Effective Implementation of Medicaid’s New Work Requirement. Center on Budget and Policy Priorities, 2025. https://www. cbpp.org/research/health/a-guide-to-reducing-coverage-losses-through-effective-implementation-of-medicaids.
Ward, Brian W. “Multiple Chronic Conditions and Labor Force Outcomes: A Population Study of U.S. Adults.” American Journal of Industrial Medicine 58, no. 9 (2015): 943–54. https://doi.org/10.1002/ajim.22439.
