

Artificial intelligence in audiology, and


Artificial intelligence in audiology, and
LATEST STATS ON ENT SURGERY
Data shows waiting times have dropped but ENT still has the longest waits
TINNITUS INNOVATION AND MANAGEMENT
A world first diagnostic tool and tailored treatment plus management insights 40
CONFERENCE PREVIEWS What to expect at The Sound Exchange '26 and the ASOHNS conference
The only RESOLUTION you need. Don’t look back and say “should’ve...”
Start the year with confidence. Choose the business that’s making a real difference - to its customers and its people. Make the resolution that matters. Join Specsavers. Scan to find out more.


Public patients waiting for ear, nose and throat (ENT) elective surgery in 2024-25 faced the longest delays of any surgical specialty in Australia, according to new data.
The information also revealed that more than one in four public patients waiting for surgery to repair a hole in their eardrum were waiting more than a year for the procedure.
ENT surgery waiting times have dropped but are still long. Image: Herjua/stock.adobe.com.
the AIHW National Elective Surgery Waiting Times Data Collection.
It revealed how long patients waited for admission from public elective surgery waiting lists based on the area of clinical expertise of the doctor performing the planned elective surgery.
The Australian Institute of Health and Welfare (AIHW) data showed patients needing ENT surgery were waiting longer on average than other surgical patients, and waiting longer at the extreme end of waits.
“In 2024–25, the area of surgical speciality with the highest median (50th percentile) and highest 90th percentile waiting times was otolaryngology, head and neck surgery (99 days and 397 days,
respectively),” the AIHW said.
“The surgical specialities that had the highest proportions of patients who waited more than 365 days to be admitted were otolaryngology, head and neck surgery (14.4%) and orthopaedics (10.8%) respectively.”
The institute released updated data on its AIHW Hospitals platform on 10 December 2025. The source of information was
It included waiting times for otolaryngology, head and neck surgery (ear, nose and throat or ENT surgery).
The analysis also found that waiting times had dropped in recent years for ENT surgery.
While half of patients needing ENT surgery were admitted for surgery within 99 days in 2024-25, this was down from half being admitted within 111 days in 2023-24 and 104 days in 2022-23.
Additionally, in 2024-25, 90% requiring ENT surgery
The Australian Government is helping to fund a local invention pioneered by ENT surgeons and scientists that aims to be the first product to safeguard cochlear health.
The technology – Hear Alert – measures electrical impedances of cochlear implant electrodes to signal drops in hearing. The technology is being designed to integrate into cochlear implants to alert wearers when adjustments with an audiologist are required for optimal hearing performance, enabling on-demand rather than scheduled review.
team had received a $1.38 million NHMRC development grant to “ensure high value clinical review after cochlear implantation”.
Chief investigator, ENT surgeon Professor Stephen O'Leary from The Royal Victorian Eye and Ear Hospital, said the project would “deliver the first product to safeguard cochlear health by monitoring implant performance and alerting patients when a clinic visit is truly needed”.
“As patient numbers grow, the demand for clinic visits rises, outstripping resources.
To overcome this problem, low value visits – those that do not improve the patient’s hearing –must be eliminated.
“The solution is Hear Alert. Our novel cochlear health monitoring product continuously measures the electrical impedances of the implant’s electrodes.
were admitted within 397 days compared with 90% being admitted within 432 days in 2023-24, and 507 days in 2022-23.
The proportion of patients waiting more than one year for ENT surgery was 14.4% in 2024-25 down from 16.6% in 2023-24 and 17.4% in 2021-22.
The analysis showed there were 60,031 elective ENT surgery admissions in Australia in 2024-25 in public hospitals.
The data also revealed that more than one in four Australians on public hospital elective surgery waiting lists for repair of a perforated eardrum wait more than a year.
The AIHW said that in 2024-25,
continued page 8

“Disturbances in cochlear health that adversely affect hearing are identified by impedance changes, triggering a high-value clinic visit that improves the patient’s hearing.”
Hear Alert is founded on impedance-related IP from
On 23 January 2026, Mr Mark Butler, Minister for Health, announced the Hear Alert/University of Melbourne continued page 8
“Cochlear implants transform lives by restoring hearing, but less than 10% of those eligible receive an implant. A significant barrier to patient access and market growth is the cost of running cochlear implant clinics,” he told HPA
more than ever, says Ms Dawn Rollings, managing director of Starkey Hearing Technologies ANZ. Rollings discusses balancing business success and compassionate care in modern healthcare leadership.

GN Hearing’s Accelerate Partnership Program is designed around the needs of every Independent Customer. By working together, we can achieve more and help your business grow.
At GN Hearing, we’re committed to supporting all our Independent Customers - not just the top performers. Our Accelerate Partnership Program is designed to help those who trust our brand in various areas, including:
Unlike other Australia and New Zealand hearing aid manufacturers, GN Hearing ANZ will not compete with you by owning retail stores. As a customer-obsessed organisation, we uphold ‘solely a manufacturer’ status as a trusted innovative partner, where our objective is, ‘if you win, we win’.
As part of this commitment, we offer Beltone as a dedicated brand for the Independent channel – giving you a distinct identity, tailored support and a premium portfolio your clients cannot find in retail chains, helping you differentiate and grow.

Beltone is an Independent premium product range, giving you the opportunity to build a unique value proposition for your clients.
As your trusted partner, Beltone offers a comprehensive portfolio of premium tailored hearing solutions.
Contact your GN Hearing Account Manager today to learn more about how to become a member of Accelerate Partnership Program!

The industry’s

Founder Damien Fechner explains his Australian first AI audiology scribe.

18
Audiologists and AI experts discuss what's happening and predict what's to come.

26

This edition, coinciding with Tinnitus Awareness Week, features Melbourne researcher Associate Professor Mehrnaz Shoushtarian, whose work sits at the cutting edge of objective tinnitus diagnosis. HPA also investigates tinnitus care at the coalface, hearing from audiologists whose every day work helps those with bothersome tinnitus –

Ms Sarah Swann from the University of Melbourne, Ms Pia Nairn from Lions Hearing Clinic, and also Dr Celene McNeill from Sydney who discusses an innovative multidisciplinary model.
Our other theme is artificial intelligence in audiology. Audiologist and AI expert, Ms Dianne Rafter, explains what’s happening and predicts what’s coming, while University of Technology Sydney lecturer Dr Julia Dray provides insight into a national initiative focused on testing and guiding AI adoption in healthcare.

Business help for independent clinics
What's GN Hearing ANZ's Accelerate Partnership Program all about?
28 OPSM welcomes audiology
EssilorLuxottica has launched a new hearing care option in ANZ.


There's a summary from experts who spoke at GN Hearing ANZ’s AI in audiology symposium. And an indepth look at Australia’s first audiology AI scribe, AudZone. Its founder, Sydney audiometrist Mr Daniel Fechner has left no stone unturned in developing an operating system that caters for everything an audiology clinic needs, including Hearing Services Program compliance.
Starkey’s research and development team has celebrated 300 years of collective experience in artificial intelligence. Dr Dave Fabry and Mr Amit Shar expand on the company’s industry-leading AI and DNN.
A new chapter in hearing care in Australia and New Zealand has begun with EssilorLuxottica’s OPSM stores now offering audiology services, including Nuance Audio Glasses, alongside optometry care. We hear about the model and client feedback from audiologists Ms Marisa Varrica and Ms Naomi Nicolinas. GN’s Accelerate Partnership Program which provides business solutions to loyal independent audiology clinics is in the spotlight along with Specsavers’ audiology partners explaining why it's a great place to work. Finally, there’s a surgeon’s view of Oticon Medical’s Sentio System and previews of The Sound Exchange '26 and the 76th ASOHNS’ scientific meeting.
HELEN CARTER Editor



Just as HPA went to print, one of the largest health infrastructure projects built in Victoria, the $1.1 billion redevelopment of Frankston Hospital, opened with a new name – PENINSULA UNIVERSITY HOSPITAL. Ms Mary-Anne Thomas, Victorian Minister for Health, said it had capacity to treat up to 35,000 more patients every year. It includes a new and expanded emergency department, 15 new operating theatres and
Weird
Japanese researchers have developed a device that uses sound waves to detect helium leaks. Excess helium can displace oxygen in a confined space, leaving less oxygen for people to breathe. Writing in Applied Physics Letters, they said they hope to expand the device to locate leakage points in 3D space and develop the system into a portable device. It includes cylinders and triangles that share apexes. Microphones record the sound signal in corner cylinders and speakers under these cylinders generate sound waves.
Wonderful
An Oregon cafe that takes orders in sign language has become a cherished space for the Deaf community, providing a unique gathering place and employment for those who are deaf or hard of hearing. US newspaper the Daily Record says American Sign Language, or ASL, is the main language at Woodstock Cafe in Portland. Non-ASL speakers use a microphone that transcribes their order onto a screen. People have moved from across the country to work at the cafe which also hosts weekly ASL meetups and game nights.
Wacky
more beds. The hospital offers a children’s audiology service, ENT surgery and ENT research led by ENT surgeon Mr Andrew Martin. IN OTHER NEWS, the National Acoustic Laboratories (NAL) has announced its NAL-NL3 is now integrated into MedRx Studio Software version 1.3.2, providing hearing care professionals with access to NAL’s next-generation, evidence-based hearing aid fitting system. Dr Brent Edwards, NAL director, said it marked one of the first global implementations of NAL-NL3 within a verification and test ecosystem. “The
integration reflects a longstanding collaboration between NAL, MedRx, and the broader Demant Group, demonstrating how translational research and industry partnership accelerate access to advanced clinical tools that support people with hearing difficulties,” he said. FINALLY, the Bionics Institute has partnered with Swinburne University of Technology in Melbourne in a first-of-its-kind collaboration to accelerate the development of life-changing medical devices. The partnership aims to progress medical device innovation to the clinic.
Image: gpointstudio/stock.adobe.com.
hearingpractitionernews.com.au
Published by: 379 Docklands Drive, Docklands VIC 3008 T: 03 9690 8766 www.primecreative.com.au
Chief Executive Officer Christine Clancy christine.clancy@primecreative.com.au
Intracochlear electrocochleography during cochlear implant surgery may enable hearing preservation in most recipients, says Dr Christo Bester from Ear Science Institute Australia. Page 45
University of Auckland researchers have used spoons to reveal auditory illusions, helping them better understand how our brains process and interpret what we’re hearing. Associate Professor Sam Schwarzkopf told the NZ Herald, that his team blindfolded people and discovered people mishear the sound of two spoons being hit in front of them as coming from behind them. They said in Perception that this revealed a gap in understanding of how we hear sounds and where sounds are.
CI DAY 25 February
Cochlear is hosting a live online Q&A on International Cochlear Implant Day for people considering an implant. cochlear.com Complete calendar page 51
The World Health Organization theme is, "From communities to classrooms: hearing care for all children". who.int/campaigns/worldhearing-day/2026
Publisher Sarah Baker sarah.baker@primecreative.com.au
Managing Editor Myles Hume myles.hume@primecreative.com.au
Editor Helen Carter helen.carter@primecreative.com.au
B usiness Development Manager Luke Ronca luke.ronca@primecreative.com.au
Client Success Manager
Karyssa Arendt karyssa.arendt@primecreative.com.au
Head of Design Blake Storey
Ar t Director Bea Barthelson
Subscriptions T: 03 9690 8766 subscriptions@primecreative.com.au
Cover – Image: Bionics Institute. Trialling the fNIRS tinnitus cap.

The Publisher reserves the right to alter or omit any article or advertisement submitted and requires indemnity from the advertisers and contributors against damages or liabilities that arise from material published. © Copyright – No part of this publication can be reproduced, stored in a retrieval system or transmitted in any means electronic, mechanical, photocopying, recording or otherwise without the permission of the publisher.
continued from page 3
28.3% of public patients requiring myringoplasty or tympanoplasty waited more than 365 days.
The situation had improved though, as 32.7% of those on the list in 2023-24 waited longer than a year for the procedures, and nearly 40% (39.2%) waited more than 365 days in 2022-23.
In 2024-25, half waiting for myringoplasty/tympanoplasty were admitted within 264 days – down from 292 days in 2020-21. And 90% were admitted within 559 days, lower than 694 days in 2023-24.
Myringoplasty repairs a perforation (hole) in the tympanic membrane while tympanoplasty is a broader term including surgery to repair a hole in the eardrum with or without reconstruction of the hearing bones (ossicles).
Infection or injury can cause a ruptured eardrum, and it may affect hearing or balance. While most cases heal without treatment, some need surgery.
Indigenous patients had reduced waits for myringoplasty/ tympanoplasty, with the median wait for non-Indigenous patients being 273 days, compared with 233 days for Indigenous patients. The median wait is the mid-point in waiting times with half of patients waiting less than or equal to the median number of days, while half were on the list for longer than the median waiting time.

“5.6% WAIT MORE THAN A YEAR FOR GROMMET SURGERY.” AIHW
Figures were also released for myringotomy, surgery which makes a small incision in the eardrum often accompanied by insertion of grommets. This drains fluid and relieves pressure to treat chronic ear infections such as otitis media (glue ear.)
Overall, half of patients needing myringotomy were admitted within 80 days for the procedure, down from 88 in 2023-24. And 90% of patients were admitted within 329 days for myringotomy, down from 352 days in 2020-21, with 5.6% waiting more than a year.
Grommet surgery reduces the risk of long-term hearing loss by draining fluid from the middle ear and preventing recurrent infections that can damage the eardrum or ear bones. It provides immediate improvement in hearing and reduces the need for antibiotics.
This surgery is particularly important for children as ear infections and hearing loss impacts learning at school and socialisation.
The analysis revealed details for septoplasty, an ENT procedure to straighten a deviated nasal septum which can cause a long-term blocked nose and breathing difficulties. In 2024-25, half were admitted within 320 days, and 90% within 563 days. But 30.8% waited longer than a year. Additionally, 1.3% of emergency department presentations in public hospitals were for ear/ mastoid process diseases. These presentations were higher in younger patients, accounting for 1.9% of presentations in children aged 0-4, and 2.2% in children aged five to 14 years.
continued from page 3
the University of Melbourne. The research optimises this IP to best predict an impending drop in hearing so that the impedance measures are optimised for commercial development, Prof O'Leary said.
“Our idea is that Hear Alert will continuously monitor the implant’s electrodes for changes that signal a drop in hearing,” he said. “When intervention is needed, the system will trigger a clinic visit. Instead of routine appointments, care will be on demand, saving time, reducing unnecessary visits, and freeing up clinic capacity for more people to access implants.”
He said the researchers vision was that Hear Alert would help patients and cochlear implant clinics. “For patients, they will have optimal hearing at all times and will only need to go to the clinic when cochlear implant adjustments are required.
“Clinics will run more efficiently, improving their viability and increasing their capacity,” he said. Prof O’Leary, the William Gibson Chair of Otolaryngology at the University of Melbourne, said
that with the technology, cochlear implant clinics should have the resources to help more people with hearing impairment.
“With Hear Alert, cochlear implant recipients will have the assurance of knowing that their hearing is optimal, and when it’s not, they’ll be alerted to attend clinic,” he said. “We expect it will save health system resources, save patients’ time, and reduce disruption by avoiding unnecessary clinic visits. Patients will be at the centre of their own care.”

idea of using the implant to make electrical measurements probing how the ear is doing after surgery, to make sure we catch any changes as they happen to improve the recipient’s clinical journey.”
Fellow investigator, scientist Dr Christo Bester from the University of Melbourne’s Department of Otolaryngology told HPA: “We completed an NHMRC funded project called “Hear Assure” that revolved around the first stages of this –alerting the client and clinician that a change in hearing was likely.
“We have a fair amount of research data that has been tested and found to have good results but we don’t have the product-integrated version that we will develop as part of the funding. The idea is to take our research results and turn them into something Cochlear can integrate into all its devices. The new NHMRC development grant is based on the
Dr Bester said they trialled Hear Alert impedance monitoring in 40 human cochlear implant recipients. They tied changes they saw in the implants with what happened in clinical appointments and found most patients come back for appointments to check how they are doing but in most cases, nothing was changed in the programming so there was no clinical need for the appointment.
“In patients where there was a big change in their programming, we could see the change in their implant prior to that appointment – hence our belief that monitoring the implant will tell us whether patients need to come in for urgent appointments, or if they can skip follow up appointments if they don’t feel the need to visit their clinician,” he said. Other team members are Dr Tayla Razmovski, Prof Robert Briggs, Mr Joerg Pesch, Prof James Bailey, Prof Richard Dowell and Dr Zachary Smith.


Your Patients Deserve Better than Generic - So do You!
You did not choose independence to deliver cookie-cutter care. You chose it because every patient deserves your full attention, your clinical expertise, and your time.
So, why trust your documentation to generic AI that was not built for Audiology?
AudZone:







HSP-ready Notes and:
Compliance Checker (!!)
50+ Audiology Templates
Document Automation (Cosi, Reports, DVA Docs)
Clinically Aware Workflows Made for Long Consults
Double your time: 4 weeks FREE TRIAL
No Credit Card Required
Generic AI: Not HSP Aware Note Compliance?
Limited Templates What’s COSI?? Who is DVA??
More Manual editing Made for Short Appts.

AudZone was created to support clinicians who refuse to compromise on patient care
New research has revealed alarming rates of hearing loss among adolescents, with 6.2% experiencing sensorineural hearing loss and 12.9% showing signs of probable noise-induced hearing damage by age 18. The authors of the landmark longitudinal study said it highlighted the important need for hearing protection among teens. They suggested regular hearing screenings during adolescence could catch problems before they worsen. The study was part of one of the world’s largest birth cohorts, the Generation R Study which studies children from infancy to adulthood.
Digital health and allied health bodies have released a national plan to empower allied health professionals and enable more connected care for Australians. The plan aims to improve the way health information is shared and accessed digitally. The Australian Digital Health Agency and the Department of Health, Disability and Ageing, with support from Allied Health Professions Australia, released the plan in December 2025. The National Allied Health Digital Uplift Plan sets out a coordinated pathway to uplift digital capability across the nation’s allied health workforce so Australians can benefit from their broad care teams sharing key health information between them.
Specsavers has been ranked in the World’s Best Workplaces list for the second year in a row, placing 12th. Moving up four places from last year, the optical and audiology business is the top retailer in the list. Great Place to Work, a global authority on workplace culture, chose Specsavers from organisations that took part in Great Place to Work’s employee survey process. The survey represents 25 million employees worldwide and had more than nine million responses. Mr John Perkins, Specsavers CEO, said all staff should be really proud of the recognition.
A Western Australian audiology team has won a WA Department of Health excellence award for its innovative project which reduced ear, nose and throat (ENT) waiting list times across three hospitals.
The Audiology Advanced Scope Practitioner Project received the 2025 WA Health Excellence Awards Excellence in Sustainability award which recognised projects that delivered high-value health care.
The project introduced a model that empowered senior audiologists to independently manage suitable ENT patients such as those with otitis media under approved protocols at three public hospitals – Fiona Stanley Hospital, Royal Perth Hospital and Sir Charles Gairdner Hospital.
This reduced ENT waitlists, improved access to care, and used health resources sustainably by allowing audiologists to perform initial assessments, triage, and even some management tasks previously done only by ENT specialists.
The project aligned with global trends in advanced allied health roles to tackle healthcare backlogs, proving successful in improving efficiency and patient outcomes.
Below: (L-R) Dr Sara Pearson, A/Prof Dayse Távora–Vieira and audiologist Dr Roberta Marino with the award.
The WA Health Department awarded 10 team or project awards that celebrated excellence and innovation in service delivery statewide. It said the individuals and teams “made remarkable contributions to the system and embodied a commitment to
willingness to improve health outcomes for the community”.
Audiologist, and hearing implant and balance specialist Associate Professor Dayse Távora–Vieira said she was incredibly proud that the award recognised the audiology team.
A/Prof Távora–Vieira is from Fiona Stanley Hospital and is head of State-Wide Audiology, Fiona Stanley Fremantle Hospitals Group, Royal Perth Hospital and Sir Charles Gairdner Hospital.
“This achievement goes far beyond an award,” she said.
“It represents meaningful, sometimes life-changing outcomes for our patients.
“Through this project, we’ve been able to provide care to patients who had been on the waitlist for many years. Seeing these individuals finally receive the assessment and support they have been waiting for has been one of the most rewarding aspects of this journey.”
She said what made the achievement even more special was who had earned it.
“We are one of the smallest teams across three large tertiary hospitals, but every single day, this team shows that size has nothing to do with impact,” she said. “Their dedication, professionalism, compassion, and relentless commitment to excellence in patient care are second to none.”

From navigating complex clinical demands to innovating new ways to support patients and the community, the team continuously strived to do better, elevate care, and support one
“Their work is thoughtful and grounded in genuine patient-centred values,” she said.
“And we could not have achieved this alone. Many ENT doctors, nurses, and allied health colleagues have been essential partners throughout this work.
“Their support, collaboration, and belief in the value of this pathway were critical in helping us deliver better, sustainable care
She said the award reflected the collective spirit behind the project: "teamwork, resilience, and a shared commitment to doing what’s right for our patients.”
Australians have rated Starkey as the top pick in Canstar Blue’s latest hearing aid ratings, receiving five-star reviews for overall satisfaction, performance, design and durability.
Survey respondents rated Starkey as the best-rated hearing aid brand.
Apart from five-star ratings in four categories, Starkey’s hearing aids also received four stars for being user friendly, offering value for money, and battery and charging performance.
Starkey previously won the hearing aids rating award in 2021 and was equal winner in 2022.
The Canstar Blue comparison website surveyed 437 Australians on the brands they had bought and used in the past five years. Research was completed and published in December 2025.
Only brands with a minimum of 30 responses were included. Six major brands/companies were represented. Details of the sub-categories are:

• O verall satisfaction measures consumer satisfaction with a hearing aid brand as an individual score –respondents were asked about overall satisfaction with the brand. It was not a combined total of all ratings.
• Value for money represents quality and longevity of the product for the price paid.
• B eing user friendly represents the hearing aids being simple to manage and control, with clear guidelines for everyday use.
• D urability includes how the hearing aids maintain
Above: The Canstar logo, and Starkey's Edge AI hearing aids. Images: Canstar Blue/ Starkey.
performance over time despite frequent use.
• B attery and charging performance include battery performance over the device's lifetime, and if it offers multiple charging options and fast charging.
• D esign means it allows for comfortable use without compromising functionality.
• Performance covers how well the hearing aid supports hearing needs in different environments.
“Starkey sells a variety of hearing aids to suit different degrees of hearing loss,” Canstar Blue said on its website. “The brand’s hearing aids are assisted by artificial intelligence and come in several styles including in-ear, invisible and in-canal to suit individual preferences and needs.”
Canstar Blue said the winner received the highest overall satisfaction rating once all scores from the overall satisfaction criteria were combined and averaged.
GN Hearing ANZ has announced key leadership appointments and organisational changes for 2026 which it said were designed to strengthen its commercial focus and position the business for continued success.
Audiologist Mr Christopher Brew, formerly training manager and senior product specialist ANZ, was promoted to head of sales for Australia and New Zealand. He assumes full responsibility for all sales channels across ANZ and reports to Mr Paul Jones, general manager ANZ.
GN said Brew had been leading key parts of the sales function, and with his experience in driving growth and operational excellence across the hearing industry, combined with clinical expertise and commercial leadership, he was positioned to accelerate GN’s sales performance and reinforce its presence in the market.
In sales, audiologist and speech pathologist, Ms Laura White will continue to report to Brew as product specialist field manager, with an expanded scope across Australia and New Zealand.
Mr John Bullion will continue to
lead the account manager team as sales manager – independent channel and oversee the independent sales strategy with an extended remit covering Australia and New Zealand, reporting to Brew.
GN said it was also reshaping its product management and audiology leadership to meet demands of a more complex product landscape and expanding global portfolio.
Audiologist Ms Lisa McBride, formerly product and audiology manager ANZ, has moved into a global role as senior audiological product marketing manager and is now a member of GN Hearing’s global product marketing and brand strategy team.
GN said the appointment recognised her impact and contribution in ANZ and the wider business.
In her new role she will help elevate product launches and sell strategies globally while remaining closely connected to the ANZ market.
Audiologist and speech language pathologist Ms Kristy Kroutz was promoted to product manager

Above: (L-R, clockwise) Christopher Brew, Lisa McBride, John Bullion, Kristy Kroutz and Laura White. Images: GN Hearing ANZ, GN.
for Australia and New Zealand from associate product manager.
GN said she owned the full product strategy and roadmap, providing comprehensive lifecycle management across the portfolio.
Kroutz reports to Jones.
GN said the changes demonstrated its commitment to building stronger leadership to better serve customers.
“This is about building the future of our company,” Jones said.
“By empowering our people and aligning around customers and partners, we are setting ourselves up to succeed in 2026 and beyond.
"I’m excited for what we will achieve together.”
The new president for Audiology Australia (AudA), Ms Lia Traves, is looking forward to working with the organisation to prepare members for regulation during unprecedented change for the profession.
The board appointed Traves, a Brisbane audiologist with more than 30 years’ experience, on 20 November 2025 after its annual general meeting. She has served on the board for two years including one as co vice-president.
There is also a new vice-president, Dr Emma Laird, La Trobe University senior audiology lecturer and NHMRC research project lead investigator. Co-opted board director Mr David Frost, former CFO, Australian Institute for Teaching and School Leadership, was appointed treasurer.
Dr Paola Incerti, senior research audiologist, National Acoustic Laboratories, Ms Janice Pollard, chief audiologist, Sonic Equipment, and Ms Emma Rushbrooke, consultant and former director of clinical governance, research, and training, Hear and Say Brisbane, were confirmed as new board members from nine candidates.
Traves said she looked forward to working closely with the board
and team led by CEO Ms Leanne Emerson as they prepared members for regulation. “This is a time of unprecedented change for the audiology profession in Australia,” Traves said. “We are united, with one clear goal: to advocate for the best possible outcomes for audiologists and clients.”
AudA said Traves brought valuable insights to the presidency including from her role as director audiology at Children’s Health Queensland. She also sits on state-wide audiology and allied health committees and national audiology working groups.
Emerson congratulated the new appointees. “Lia’s experience will help Audiology Australia continue to navigate sector challenges, strengthen the organisation for the future, and drive strong leadership in clinical guidance that will enhance the quality, visibility and authority of audiologists,” she said.
Traves succeeds outgoing president Dr Barbra Timmer, who chose to step down from the position after six years but will remain on the board and support the incoming president as immediate past president.
“I’d like to thank Barbra,” Traves said.

“Since her appointment in 2019, she has helped lead Audiology Australia through a pandemic, lockdowns, the evolution of our complaints body, return of in-person events, and the Decision RIS consultation process.” Terms ended for former co-vice president Ms Yetta Abrahams, who advised of her intention to retire from the board, and board members Dr Jessica Vitkovic, former AudA president (2018–2019), and Ms Emma Ramsay, former treasurer, who retired from the board after serving their maximum nine-year terms.
The Australian College of Audiology incorporating HAASA (ACAud inc. HAASA) has announced a leadership transition as it “continues to strengthen its readiness for an evolving regulatory environment".
"Following a period of organisational development and growth, Dr Sonj Hall has concluded her role as CEO effective 12 January 2026," the organisation said in a media release.
"The Board thanks Dr Hall for her contribution during this phase of the organisation’s evolution." To ensure continuity and momentum, continuing vice-chair Ms Marguerite Rushworth had assumed interim executive responsibility for operational matters, under delegated authority. Ms Kylie Dicieri, who was reappointed chair, would continue to lead its advocacy agenda and stakeholder engagement, providing senior-level continuity as
regulatory reform progressed.
"ACAud inc. HAASA remains focused on strong governance, effective advocacy, and delivery of key initiatives, including its upcoming National Congress," the organisation said. "All programs and services will continue as planned."
Dicieri, an Adelaide audiologist, was re-appointed chair for the
development. She has lived experience of unilateral hearing loss.
Grigor, an independent clinic owner with 34 plus years of experience with a career spanning clinical practice, management, and business ownership. Priya is Signia Hearing's business unit manager for NSW/ACT/ SA. With degrees in audiology, speech language pathology and an MBA, she has more than two decades in clinical and corporate roles across Australia








Also continuing on the board are secretary Dr Vijay Marimuthu, treasurer Mr Joe Bayer, and board directors Mr Mark Paton, Ms Helen King, Mr Andrew Sharrock and Mr Leo Tutt AM. The board thanked Ms Janette Brazel and Mr Stephen Dimitri who stepped down, saying their dedication, contributions, time and expertise made a lasting impact.

Nuance Audio Glasses deliver “consistent benefits for users in everyday communication” according to clinical findings from two studies evaluating their performance.
EssilorLuxottica markets its revolutionary glasses as an open-ear hearing solution built into smart eyewear for adults with mild to moderate hearing loss.
“One insight stands out across both studies: users prefer to wear Nuance Audio Glasses in the real, noisy conversations that matter most to them,” said Dr Tami Harel, chief of audiology of Nuance Audio, EssilorLuxottica. “These results mark an important achievement in terms of the post-market clinical validation of the product for early-stage hearing support.”
Dr Harel presented findings from studies conducted at the National Acoustic Laboratories (NAL) and Western University Canada, at the 69th EUHA (European Union of Hearing Aid Acousticians) Congress in Germany. They evaluated controlled laboratory performance and real-world listening experiences.
The NAL study assessed laboratory performance and short supervised real-world use. It found a 3.48 dB improvement in signal-to-noise ratio (SNR), a clinically meaningful gain in speech-in-noise performance, and 70% of participants reported improved communication ability after three hours of real-world use.
Participants’ top communication goals were met in 84%–95% of cases, and they preferred using the glasses more as the acoustic environment became more challenging. The Canadian study evaluated the glasses in controlled yet realistic noise conditions. Results demonstrated up to 29% improvement in speech understanding in challenging acoustic conditions, and significant reduction in listening effort measured through standardised rating scales.
Below: The glasses are available

Australia’s Hearing Care Industry Association (HCIA) has appointed its first independent chair, audiologist Ms Nina Quinn, and announced several other appointments.
Ms Donna Edman is HCIA’s newly appointed CEO and Mr Grant Ewer, managing director for retail ANZ at WSA and a board member of the New Zealand Hearing Industry Association, has joined HCIA board as a director.
Quinn and Ewer are filling vacancies after Mr James Benston stepped away as chair and director following his promotion to president of WSA’s Asia-Pacific region.
Quinn and Ewer were appointed at the organisation’s 2025 annual general meeting in November, where Mr Adam Redman, company secretary, was reappointed deputy chair. Redman is a member of Amplifon Australia’s leadership team and head of regulatory and public affairs.
Quinn has served as an HCIA member since 2008 and was appointed to the board as an independent director from 1 July 2021. She has worked for government providers, industry manufacturers, Neuromonics tinnitus solution, and was CEO and managing director of Neurosensory.
She was the audiologist representative on the OHNS Clinical


Committee as part of the Medicare Taskforce (2018-2023), has been an Audiology Australia federal councillor, and worked on taskforces and committees to improve access to, and quality of, hearing care for Australians. Edman has a longstanding interest in hearing health having consulted to and advised Deafness Forum Australia, First Voice which she is an independent director of, The Shepherd Centre, Cochlear, and many other health care organisations. She was appointed by the then Health Minister to the committee that established the first Roadmap for Hearing Health and Wellbeing.
Ewer’s expertise in the industry spans retail strategy, governance, and innovation, and he has overseen WSA’s ANZ clinical network, delivering hearing services across more than 100 locations.
nib is the first major health fund to partner with Specsavers Audiology, offering eligible customers access to hearing aids at no, or lower out-of-pocket costs. Specsavers said the initiative aimed to help break down financial barriers to better hearing and improve access to hearing care for Australians.
It said that, through this national partnership, eligible nib customers with extras cover that includes hearing aids, and those who qualify for the Hearing Services Program, could access hearing devices at Specsavers Audiology at no or reduced cost.
Mr James Barr, nib Group’s Australian private health insurance chief executive, said: “Cost is one of the biggest barriers to hearing health in Australia, with many people delaying treatment.
“At nib, we are lowering costs to
help make hearing aids accessible to more Australians. Our customers can combine government support with their nib extras cover to access high-quality hearing devices at no or lower out-of-pocket costs, aiming to improve health outcomes.”
Mr Nick Taylor, Specsavers chief audiologist, said: “This partnership with nib will help more Australians access high-quality hearing care at Specsavers. We encourage everyone to book a hearing check when they turn 50 – not just to catch early signs of hearing loss, but to support long-term cognitive health.
“Hearing aids have proven benefits for improving communication which can help users stay cognitively and socially active.”
He said nib customers could access exclusive hearing aid offers through Specsavers Audiology.
Ear Science Institute Australia’s research manager, Dr Rob Eikelboom, has been named Australia’s leading researcher in audiology, speech and language pathology for the second consecutive year by The Australian’s Research magazine.
Others in the sector also honoured for the second year in a row were The University of Queensland (UQ), Professor Richard Harvey and Macquarie University.
The magazine used publicly available data on Google Scholar to assess Australia’s top research performers and institutions across 250 fields of research.
Ranking is based on the quality and impact of their work measured by the number of citations for papers published (by the individual or the institution) in the top 20 journals of each field in the past five years, ensuring only recent
quality work is assessed.
UQ was named the leading research institution in Australia for audiology, speech and language pathology.
In the otolaryngology field, Macquarie University was named Australia’s leading institution while Professor Richard Harvey from Macquarie University was the nation’s leading researcher in otolaryngology.

Dr Eikelboom, Corporate and Adjunct/Associate Professor at the University of Western Australia, has expertise in clinical research, epidemiology and telehealth.
His collaborative approach in integrating research with clinical practice has made him an integral part of the Ear Science team since he joined in 2001. He works closely with its team of researchers and clinicians and national and international institutions.
“Rob is a treasured senior
Dr Rob Eikelboom was recognised for his contribution to the hearing health of humanity. Image: Ear Science Institute Australia.
research leader at Ear Science who exemplifies our values and is devoted to conducting impactful research that is relevant and changes lives for the better,” said Ear Science Institute Australia CEO, Adjunct/Associate Professor UWA Sandra Bellekom.
“He leads quietly and sets an extraordinary example for the many early career researchers that he mentors – being both highly productive and efficient. With collaborations spanning the planet, Rob is a highly sought after research partner in many areas of ear and hearing science.”
His research in 2025 has included a report on cochlear implantation procedures in Australia over the past 23 years, a paper on the impact of cochlear implants on partner relationships, and a review of ear and hearing services to remote communities in the East Pilbara over the last 10 years.
Winners of the 2026 Endeavour Awards, Australia’s premier celebration of excellence and innovation in manufacturing, will be announced at a ceremony in Brisbane in May.
Award recipients will be revealed at a gala dinner on 13 May 2026 at The Westin during Australian Manufacturing Week.
For the first time, innovators in Australia’s healthcare and hearing care sectors were invited to nominate for the new Innovation in Healthcare Technology Award which recognises technologies that improve healthcare and medical manufacturing.
The category is for companies developing innovative health solutions, including medical devices, digital health platforms, biotechnologies, and pharmaceuticals.
Eligible technologies must have undergone advancements within two years before nominations closed on 13 February 2026. Products and technologies must be manufactured and/or commercially available in Australia. Nominees may also be eligible for the Manufacturer of the Year

The awards honour the achievements of individuals and organisations who are driving Australian manufacturing forward. T hey are presented annually by Manufacturers’ Monthly magazine and website published by Melbourne-based company Prime Creative Media, a trade media and events company that also publishes Hearing Practitioner Australia. The event is recognised as the
Above: The event is recognised as the manufacturing industry’s night of nights.
manufacturing industry’s night of nights, bringing together leaders, innovators, and rising stars to celebrate success, share stories, and connect with peers shaping the future of Australian manufacturing.
Companies and individuals from the hearing care sector were invited to submit their nominations and showcase the projects, technologies, and people making an impact on the industry’s growth and resilience. For more information including tickets to attend see endeavourawards.com.au

AudZone is being heralded as the first audiology AI scribe and operating system purpose-built for Australian hearing care. HPA delves into its unique benefits and advantages.
As the founder of the first smart artificial intelligence (AI) platform developed specifically for audiology clinics in Australia, Sydney audiometrist
Mr Daniel Fechner is excited about how his product can solve multiple industry pain points and generate more revenue for clinics.
“AudZone is the first AI scribe designed specifically for Australian hearing care, with built-in HSP compliance and an audiology-specific clinical depth that generic AI scribes can’t match,” he says.
The note-taker, compliance control and operating system is tuned for Australian hearing care standards and clinical best practices to improve audiology clinic workflows, he adds
Fechner says the biggest advantage over generic tools is that it includes Hearing Services Program (HSP) compliance checks along with HSP compliant templates.
“Many audiology clinics today rely on AI scribes that were originally built for GPs and hospital notes – not HSP audits and audiogram analysis,” he says. “In our tests on 90-minute audiology consultations, these generic health scribes captured only about 70% of HSP requirements, often missing critical documentation.
“Using the same transcript, AudZone’s AI generated note achieved 100% compliance using our compliance checker.”
HSP is a clinic-level responsibility, not just a clinician’s responsibility, with the risk
of paying back funds to the government for non-compliance large and real, Fechner says. “Current generic scribes are not specifically tuned for audiology, so often omit important details required for compliance over longer appointments.”
The system builds better and more efficient businesses, he says, by saving practitioners time and clinics money, including through this improved compliance.
The platform includes more than 50 audiology-specific templates automatically matched to appointment type. Apart from hearing assessments and hearing aid fitting, templates include tinnitus, wax removal, auditory processing disorder (APD), cochlear implants, hearing implants, and vestibular diagnosis and rehabilitation.
Templates for HSP compliance cover current contracts.
When an appointment starts, the platform automatically loads requirements to be completed in each consultation. If it’s for a HSP patient, a HSP real-time checklist appears to keep the consult on track.
“The AI listens and generates a note structured to HSP requirements,” Fechner says. “It compares this information with the HSP contract requirements and gives the clinician a compliance score.”
The score highlights areas for improvement which managers or supervisors can use for KPIs. Clinics can
also set minimum compliance scores.
“Owners might want clinicians to be minimum 90% compliant and say anyone over 95% gets a bonus, because with the next HSP audit, they won’t need to pay back anything to the government for that clinician,” Fechner says.
Templates can also be customised so companies or clinics can audit their own requirements for any appointment type.
“It’s super helpful for small clinics that don't have the funds to pay someone to check HSP compliance, and for big clinics that don't have the overview of all clinicians,” Fechner says. It’s also ideal for graduates or new staff not familiar with clinic protocols.
Fechner says AudZone is an AI tool that helps clinicians write better notes and patient reports but “the major advantage is built-in HSP compliance – no other AI scribe has that.”
The Australian Department of Health, Disability and Ageing manages and funds the HSP which provides vouchers towards hearing aids and care for eligible patients.
“There's quite a load on an audiology business as HSP regulation deems the clinic/business responsible for its clinicians being compliant with the program,” Fechner says. “If a clinic is audited and not all notes are compliant, it must pay back HSP funding which can be significant annual revenue.”
This frequently happens, he adds.
“If a practice has several practitioners with eight appointments each a day, how is the clinic owner ensuring they’re compliant?" he asks. "Some employ people to read notes and others allocate this role to clinical staff.”
But under AudZone, this tedious, time-consuming task is automated.
It’s also the first AI scribe that can analyse hearing tests, Fechner says.
“When uploading hearing tests, the system automatically analyses if the client fits the minimum hearing loss threshold to qualify for the HSP,” he says.
“It helps practitioners write better clinical reports because the AI understands the patient better. It imports audiograms and integrates objective test data with conversation context. It also integrates with CounselEar CRM (customer relationship management) software or can be used as standalone software for any other CRM system.”
Unlike generic scribes, AudZone can drop in a PDF or image of an audiogram or use a photo of a coffee-stained hand-written audiogram and convert it to a clean clinical audiogram. Audiogram data is available for notes, reports, compliance checks, and counselling tools.
Practitioners upload scanned/hand-written forms in AudZone. These include the Hearing Handicap Inventory Assessment (HHIA), Tinnitus Functional Index (TFI), Tinnitus Handicap Inventory (THI), Client Oriented Scale of Improvement (COSI), and International Outcome Inventory for Hearing Aids (IOI-HA)
AI scores them automatically, stores them in outcome tracking, and pulls them into notes/reports.
“If done digitally, like with the HHIA, the client answers questions on the screen and gets an immediate score so the clinician doesn’t have to calculate it,” Fechner explains.
Any dropped images, PDFs,
tympanograms, otoscopy photos, and so on become part of the patient context. These assets can be embedded directly in the report builder and exported as PDFs or word documents.
“Most generic AI scribes only ‘hear’ the transcript. They don’t see your audiogram, your outcome questionnaires, or your otoscopy images – and they can’t relate them to each other,” he adds. “AudZone doesn’t just transcribe; it actually understands audiology data.”
HHIA tracking also includes visual progress charts, and evidence-based tools demonstrate treatment effectiveness.
Another unique feature is patient history inclusion across appointments.
“While most notes in other AI scribes may be based on one session, because AudZone is patient-based rather than session-based, it knows when the client last visited, what happened in that appointment and includes this information. Our AI can summarise all visits in one report,” Fechner says.
A clinician can ask it how the patient’s tinnitus handicap changed over the past three visits and the system knows because it has audiograms, questionnaires and notes all in one place. It also works perfectly with long-term cases or complex clients.
“AudZone offers clinical memory and reasoning, not just documentation,” he adds.
It’s also a document operating system for hearing care. It can create notes including

“The
HSP assessment notes, referral letters, GP reports, medical reports, internal summaries and can add images, graphs, logos and branding.
Documents can be auto-generated using conditional logic and follow instructions such as, “Only generate this report if a full assessment is completed” .
The system can also create fillable PDFs such as DVA forms, COSI forms or any other form practitioners wish to fill using the session data. These fillable PDFs are automatically created with fields correctly labelled, unlike with some generic AI scribes, Fechner adds.
“People just drop in their PDF and Audzone’s AI does the hard work for them,” he says.
Additionally, a hearing simulator provides visual and audio simulation of a patient’s hearing loss, building understanding and treatment acceptance.
“We are planning features that can use data it's gathering to run reports on clinics and analyse how much time was spent on activities in each appointment including things that increase conversion,” Fechner says. “This can show how clinicians are performing; if a clinician does certain things and they’re doing much better than others, the company can ask all practitioners to include this factor in appointments to increase conversions.”
AudZone will also be able to assist
major advantage is built-in HSP compliance – no other AI scribe has that. And AudZone doesn’t just transcribe; it actually understands audiology data.”
Daniel Fechner AudZone

supervision if clinics have students or graduates by highlighting fields requiring more attention. And it can give feedback on how warm and empathetic practitioners are and even how well the patient understood.
The system is built for long hearing appointments, not 10-minute GP consults, including multi-hour recording stability. Its clinically aware recorder doesn’t get hijacked by audiometer microphones or USB interfaces and it features automatic recovery if a PC crashes or the audiometer is unplugged, Fechner says.
“It’s programmed to seamlessly work with equipment in an audiology clinic without interfering with the many microphones or other equipment such as audiometers,” he says.
It can also be used for meetings with staff, vendors and clinical training and will draft notes, reports and even compliance checks for these.
Fechner believes it’s unfair to charge practitioners who work part time, a full-time subscription. His model is based around the industry being predominantly female including many young mothers working part-time.
“We’re an on-demand platform so after signing on for a base cost, we don’t charge
for days you don’t work, are on holiday or sick. It only charges for the time the tool helps you and it's not a lock-in contract but a monthly subscription,” he says.
Base cost is $45 per clinician per month (including eight recording days) plus $5 per day that the practitioner works beyond the included allowance. Monthly fees are capped at $105, and the maximum annual price is $540 (for a casual worker), $780 (part-time) and $1260 (full-time.)
“We suggest the clinic pays for an account and adds its practitioners,” Fechner says. “It’s a clinical tool and a clinic investment; the clinic reaps the reward of more appointments and money, better compliance and patient records, and less HSP payback.”
The tool helps practices generate more revenue by freeing practitioners to perform more consultations.
From a wellbeing perspective, clinicians can leave work on time instead of staying back to write notes. “It saves one to two hours a day per clinician which would normally be spent taking notes, summarising and adding them to medical records,” Fechner says.
“It transforms hours of paperwork into minutes with intelligent note taking that captures every clinical detail. Practitioners can add at least two more appointments
per day, a conservative annual equivalent of saving $15,000 per practitioner a year,” he adds. “For a clinic with four clinicians, that’s roughly $60,000/year in extra revenue.”
Fechner funds AudZone from his clinic, Ear Studio, in Sydney. It’s been a major undertaking and he believes it has accounted for every critical element Australian hearing care practitioners and their patients need in an audiology appointment.
He says AudZone takes user feedback and requests seriously and is constantly improving the software and adding innovative features.
“It’s an Australian owned and designed platform – the data stays in Australia and does not go offshore,” he says. “The platform meets Australian standards of HSP requirements and Australian Privacy Principles.”
Since its soft launch in May 2025, 80 practitioners have signed on. “Feedback has been brilliant,” Fechner says. “They love it.”
Hearing Business Alliance members qualify for a 10% discount, and all plans include all current features.
“Now’s the time to stop trusting a generic AI scribe with your HSP contract and hearing-specific documentation and try AudZone, a full audiology operating system,” Fechner says.
For more information see audzone.com. au.



Artificial intelligence has transformed hearing aids, fitting software, clinic note-taking and administration, and patient apps. HPA explores current and future uses of the technology.
After more than 20 years working in hearing care and seeing the huge influence of technology on the sector, audiologist Ms Dianne Rafter decided to go a step further to research the impact of artificial intelligence (AI) on audiology.
Rafter enrolled in a Masters of Technological Futures and is now a future tech and change readiness advisor, along with being sales and marketing manager for Sonova in New Zealand.
“The master's degree is a great future lens of how technology will change the way we work,” she says. “AI was a big topic, but at that point, it was more theoretical than practical. Now we know AI can change the way we work in everything we do from a clinical perspective, an admin perspective, in research, how we teach; in every aspect of audiology, AI is going to impact how we do things today and in the future.”
Rafter says a key finding from her research was that “the more people empowered and talking about AI, the more we as an industry can decide the industry's future, instead of just waiting for disruption to happen to us”.
“Awareness and basic understanding are important because this technology is so powerful and it will impact on so many different layers; the more you have a basic understanding of how it works and the potential changes, the more you can be part of and a voice in the change,” she adds.
Initially audiology colleagues didn’t know much about the technology, she says. She wanted to find out how audiology would react and adapt and what the future would look like so she interviewed hearing practitioners and other professionals.
Rafter began and continues raising
awareness about AI through workshops, training sessions, conference talks and articles. More people saw the potential and started to come on the journey.
“At first they believed nothing would change and no technology could do their job,” Rafter says. “Now conversations are more advanced. People have a better understanding; there's more excitement around how it can help and aid the work we're doing.”
AI in hearing care has evolved from theoretical to practical applications, she adds, including automating tasks, enhancing patient care and predicting hearing loss. Real-time troubleshooting exists and could expand in future along with personalised coaching and hearing screening.
Already some AI can track a person’s voice and notice if they start raising their voice routinely or are missing certain words. In future this could become early hearing loss screening, Rafter suggests.
The technology is so powerful, it could potentially change everything in the future, she adds. Healthcare and systems globally are struggling due to the ageing population, burnt out workforces, access and equity issues, she says. “There’s a landscape of healthcare being a bit of a broken system and technology is often seen as the solution to many of these problems; it’s a way of democratising access and inequality."
Patients are changing and becoming more empowered and knowledgeable with various types and ages having different access to information. “They’re looking for more of a partnership than a traditional model

where the professional tells you what to do,” Rafter says.
Personalised and precision medicine is another theme focusing on preventive measures and treatment plans tailored to the individual’s genetics and environmental factors. “The advancement of medical and scientific discoveries with AI will be big for all parts of medicine and there's definitely a place for hearing,” Rafter says. “Prevention and treatment of sensorineural hearing loss is one area we could see medical changes.”
Already there’s been advances and successful trials in gene therapy for inherited forms of deafness. AI is heavily involved in gene therapy, accelerating research, improving precision, personalising treatments and transforming everything from target identification to manufacturing.
AI’s ability for pattern prediction and big data sets also opens research opportunities at a faster pace, Rafter adds. And service delivery is another field the technology can
assist with including telecare and devices for measurement at home. In some hearing aids with AI, data enables continual monitoring of environments, automatically or allowing patient adjustments to improve hearing clarity and reduce noise. Data can also be fed back remotely to practitioners and hearing aid manufacturers to enable real time or future troubleshooting.
Rafter says the audiologists’ role will look different in the future as will every job with more empowered technology.
“For audiology and many other professionals, we need to look at the human potential of the industry – what we are doing from a human-to-human perspective that is unique and can't be replaced by technology, or that humans would prefer to have people do – the sharing connection,” she says.
“I think there's still going to be a place for humans to be there for the whole journey, seeing patients, supporting them and giving them personal support from an expert.”

if it’s noticed they aren’t wearing their hearing aids and remind them, along with the benefits, Rafter says.
Clients may read about hearing devices on large language model chatbots such as ChatGPT which have good information, she says, so practitioners should at least be at the same level.
“If you're talking about AI and hearing technology, you must know how to pitch with credibility because if someone comes in knowing a lot about the tech and wants to understand how a deep neural network works in a hearing aid and you can't talk about that credibly, they're potentially not going to pay more for the tech,” Rafter says.
Others may have heard conspiracy theories about “AI listening and recording conversations” and might not want this tech in hearing aids. Having enough knowledge to talk about that and allay concerns is also important, she adds.
Other applications include software that leverages advanced AI algorithms based on more than 10,000 ear images taken from over 4,000 children to assess and triage patients with ear conditions. DrumBeat. ai enables uploading of eardrum photos captured with an otoscope to diagnose acute and chronic otitis media in outback areas.
Coaching and motivation are other areas where AI can assist including texting people
Administration is a big area that AI can help with – booking appointments, appointment reminders, automating filing, writing first drafts of patient reports and to do lists.
“Basically, anything you're doing in audiology, there's a use case where AI can help, augment and uplift you and your business,” she says. “But where do you start? I'd suggest AI scribes as there's big uptake from audiologists and it’s an easy win.
“Our human potential is not writing notes and doing reports but patient contact so the more we can optimise that by letting scribes write patient notes and reports, the better.”
She suggests thinking of an AI scribe as being like an intern or graduate – you must still check output for accuracy as it's a medical record.
Checking journal references provided by AI is also advised, says Dr Julia Dray, an interdisciplinary researcher and lecturer at the University of Technology Sydney (UTS). Her work spans speech pathology, psychology, genetic counselling, digital health, and the responsible integration of GenAI in education and mental health care.
This caution matters, she says, because AI can hallucinate details, including fabricated or inaccurate references, with recent studies having found chatbots generate inaccurate
health references about 20% of the time, particularly in health and mental health related content.
To help address this risk, Dr Dray contributes to a national initiative focused on rigorously testing and guiding AI adoption in healthcare. As part of her work at UTS, she leads a project in the Graduate School of Health AI Research Node, where 38 academics are researching AI’s real-world impacts, and testing, evaluating and shaping how Australia can adopt AI safely, ethically and with patients at the centre.
The evidence-based interrogation includes how AI is influencing patient behaviour, clinical conversations and frontline decision-making – critical insights for determining when and how AI can genuinely support human-led health care.
“We’re studying how to provide protection to patients and health professionals and integrate AI to lighten the load, reduce staff burnout, shortages and long wait lists – what can AI feasibly and sensibly help with without taking over what humans are doing,” she says. “We want to know what questions community members and health professionals think we could help answer or investigate and are open to collaborating and to receive funding.”
This is needed as Dr Dray says new research shows Australians are turning to AI tools for health advice, with almost half having


recently used generative AI, and one in 10 adults consulting platforms like ChatGPT for health information. This means that they’re arriving at appointments with AI-generated ‘first opinions’. Health literacy is important for patients including understanding and preparing questions to help them advocate for and have self-determination in their own care, she says.
“They might come with goals for therapy or thoughts about solving problems hearing in noisy environments,” Dr Dray says. “It can be problematic if patients use AI advice as an objective, hard source of truth which is different from using it to prepare and approach an appointment with curiosity and still understand and respect that health professionals have training and will respectfully challenge them with their own knowledge.”
Human oversight is needed on AI generated information from chatbots such as ChatGPT, Gemini and Copilot which draw from a mix of huge amounts of information they were trained on, and in some cases, on information from the entire web, allowing them to answer from a broad net, she adds.
“It might not just be academic-based papers or tested theories but any source such as opinion pieces, social media, marketing information or advertisements,” Dr Dray says. “Algorithms the chatbots learn may be biased and miss important elements including health settings and diverse populations because they've found predominant populations and trends and base answers on this.
“They might miss patients using different languages or living in rural areas.”
Some information shared online may include personal experience, rather than formal evidence. “This is not to speak poorly of community members and lived experience because I'm incredibly dedicated to lived experience in research and healthcare; people should feel validated and respected as the expert in their health journey,” Dr Dray says.
“In supporting patients who come to
us prepared for their appointment we can acknowledge they've researched and validate it by saying it’s great they’ve brought concerns, we want to complement what they’ve brought with our expertise, ideas and integrate them.”
Practitioners should work with AI, ensuring to uphold professional standards and have human knowledge in the room, she adds.
If using AI assisted scribes, Dr Dray says to ask for patient consent to record the appointment, reassuring them professional and ethical standards will be upheld, (and ensuring this is firmly in place) and be familiar with where the data is held.
Australian Privacy Principles and Australian Government cyber security standards and data security recommendations urge information about Australians be retained here rather than offshore.
“I don’t think AI will ever replace hearing professionals, but it will assist and lighten the load in administration and other areas,” she says. “AI could provide care between human care appointments – in between sessions there may be things AI supports.”
While an initial appointment to receive hearing aids is needed, the tech is enabling more appointments via telehealth and some troubleshooting including fitting. “We still need human experts in the room to guide us though,” she adds. And while AI can’t yet read eye contact, facial expression or body language, she says it’s coming.
Other current and predicted advances

were explored at an in-person and online symposium on the future of AI in hearing aid technology, organised in Sydney by GN.
Dr Andrew Dittberner, GN Hearing’s chief scientific officer and part of GN’s advanced science group, told participants current deep neural network (DNN) technology in hearing aids is first generation DNN noise reduction.
DNN speech enhancement denoises or reduces noise while trying to preserve speech. “The DNN basically emulates single channel noise reduction – there’s a speech signal and noise in between,” he says. “The actual speech signal still has noise embedded in it. It sounds less noisy, but voice intelligibility doesn’t significantly improve. As better AI algorithms come along, they could theoretically rebuild the speech signals if they have enough data to reconstruct them without any noise.”
He says this could potentially give unlimited SNR (single number rating which measures noise reduction) if the size and number of processors needed could be overcome since hearing aids are known for miniaturisation.
“Ten years from now, or even earlier, I believe hearing in noise will no longer be the number one problem if we can get some of this stuff to work together – that’s the potential of DNN denoising and that’s what exciting,” he says.
Dr Dittberner, who has worked in hearing research for 20 years, has a Master of Science in neuropsychology and a PhD in hearing science, is an Adjunct Professor at Vanderbilt University, and has served on government and industry research working groups in the US.
Dr Megan Quilter, GN Hearing’s lead audiologist, says everyone in the industry can contribute to the evolution of the next generation of hearing aid technology. “This industry is moving forward and it’s moving quickly,” she adds.
Dr Quilter says GN’s DNN is currently being validated in real world settings using ecological momentary assessment (EMA) to capture real time speech understanding, listening effort, sound quality, and social engagement. Information from clients on the street using DNN in hearing aids feeds into their smartphones via GN’s LifeData dashboard which turns the data into insights for researchers and clinicians, minimising recall bias.
“EMA can tell when patients are struggling to hear such as at a party and asks them
“Basically, anything you're doing in audiology, there's a use case where AI can help, augment and uplift you and your business.”
Dianne Rafter Audiologist and future tech advisor
to answer a few questions. When the client returns to their audiologist, they can see the noise level and settings from that event and tailor a solution. It provides real world outcomes and better validity,” she says.
“It’s improved patient outcomes, they and their audiologists have a better understanding of what’s going on with their auditory lifestyle, it leads to better counselling and engagement and more trust.” The feedback has also helped manufacturers understand where patients are struggling and what features resonate with people. “We’ve made changes in fitting software and products based on what people have told us,” Dr Quilter says.
“It fosters different conversations with patients on what adjustments to do, enables better engagement with patients and they find it empowering.”
Dr Quilter and GN Hearing’s senior audiological product marketing manager, audiologist Ms Lisa McBride, are working on an EMA project across four countries including Australia to validate DNNs in everyday life and are seeking audiologist and patient input. It will study speech understanding including in noise, listening effort, social engagement and sound quality to shed light on whether DNN helps users follow conversations in noisy places.

Dr Padraig Kitterick, head of audiological science at NAL, says the system has incorporated AI, specifically neural networks and machine learning, in its development.
“Unlike its predecessors which were based on data from hundreds or thousands of participants, NAL-NL3 was developed by analysing millions of historical hearing aid fittings and data points from real-world user feedback to create more precise and personalised amplification targets,” he says.
“We’ve been challenged with DNN in the real world,” Dr Quilter says. “People need more education and a better handle on it, when to use it and why because people (some clients and audiologists) are confused.
“One audiologist thought DNN could help with tinnitus, which we do not believe it does, some patients use DNN in quiet which is not what we expected, others don’t see a difference, so we want to know why. We want to know what triggers a person to want DNN on and why they choose it. Much of the time clients say they want a hearing aid with AI or DNN but don’t know what that means.”
Dr Quilter says explaining AI and DNN to patients was a challenge. “Some ask me, ‘Is it like Alexa on my ears?’; I say it isn’t and try not to get into the specific AI,” she says. “What I’ve found useful is to say that hearing aids with AI can recognise patterns, just like you recognise your child’s voice, they look for speech and cut out the rest of the noise.”
McBride says it's important to ensure hearing aid AI technologies use an intelligence augmented approach to empower users, rather than devices.
Meanwhile, a global optimisation algorithm and DNN mapping of audiograms to target are at the heart of the National Acoustic Laboratories new NAL-NL3 hearing aid fitting prescription software.
Dr Jessica Monaghan, senior research scientist leading AI research at NAL, told the symposium it was the first update of the fitting formula in 15 years.
“This data-driven approach, enhanced by AI analysis, allows the system to provide a more accurate and individualised fitting solution for a wider range of patient needs.”
Dr Monaghan says machine learning has evolved a great deal and hearing aids have changed a lot since NAL-NL2. “NAL-NL3 is a modular fitting system rather than one fitting prescription, with modules for unique patient types or listening environments including music and novel hearing technologies,” she says. NAL will release new modules over time based on audiologists’ needs, and priorities of hearing aid companies such as specialised models and extended high frequencies. Many hearing aids can amplify at higher frequencies now which NAL-NL2 can’t provide targets for.

researcher. The module, based on the NL3 script and audiograms, gives people control over tone and volume. “In noisy environments there’s no big difference in NAL-NL3 and the Comfort In Noise Module in speech intelligibility, but people prefer it. Anyone who is curious to try it should be offered it including people who have difficulty hearing in noise or discomfort in noise,” he says. “You can compare their speech in noise ability with Comfort In Noise and let them try both at home.”
A major benefit is the software can fit hearing aids to people with normal audiograms or minimal hearing loss who struggle to hear. In 2025, 31 clinicians nationwide in 33 clinics validated the module in 251 general appointments with clients.
“They found NAL-NL3 easier to fit in 60% of new and experienced hearing aid users, easier to fit to target and for trickier audiograms, while 40% found it similar to NAL-NL2,” Dr Monaghan says.
NAL director, Dr Brent Edwards, says there's much excitement around this application as thousands of audiologists worldwide – who previously lacked confidence in fitting these patients or the benefits – could now fit this underserved group instead of turning them away.
A Comfort In Noise Supplemental Module is available for people who struggle in noisy environments, says Mr Matt Croteau, NAL audiologist, acoustic engineer and
Croteau says the Minimal Hearing Loss Module was an unmet need and NAL researchers are seeking opinions from practitioners on what future modules they could develop. Dr Kitterick says NAL wants to measure the benefits of AI in hearing aids. “There are many different applications of AI in hearing aids and the capabilities of the AI processors in hearing aids will become more varied,” he says. “Every producer of devices uses different ways to measure the benefits of such new technology. We'd love collaboration and are considering ways to measure these new technologies with input from hearing aid companies, clinicians and NAL so we all have information, and can test and understand results. As an industry and sector we could then address this challenge and receive information about what benefits AI brings and in what listening situations or challenges. We’re at early stages of how we address this as an industry and sector.”
Starkey’s research and development team has celebrated more than 300 years of collective experience in artificial intelligence. DAVE FABRY and AMIT SHAHAR expand on development of the company’s industry-leading AI and deep neural networks.
As one of the leading experts who has helped write the roadmap for advances in hearing technology, Mr Amit Shahar is a huge advocate for artificial intelligence (AI) and what it has done for people with hearing loss.
He believes that, in the future, hearing aids that incorporate AI and deep neural networks (DNNs) will become the gateway to other devices for people to monitor and improve their health.
“In future, DNNs will be everywhere, and hearing aids will become more personalised,” he says. “They will understand the environment better and be much smarter. I strongly believe hearing aids will become the gateway to other devices – personal assistants that seamlessly connect to other devices, and health will be part of it.”
Shahar, Starkey’s senior vice president of advanced development, revealed his predictions in a Starkey Sound Bites podcast with audiologist Dr Dave Fabry, Starkey’s chief hearing health officer. They also discussed the company’s journey to become an industry-leader in AI and DNN, including the strategic decision to establish a global research and development (R&D) presence.

Shahar oversees Starkey’s advanced development teams across the globe, who work in concert to integrate AI and DNN into the company’s hearing aid technology.
He is a technology executive with extensive experience in systems and software engineering plus product development focusing on human-computer interaction, advanced sensing and AI. Shahar reports to Starkey’s chief technology officer and executive vice president of engineering Dr Achin Bhowmik.
“The hearing aid industry wasn’t on my bucket list,” Shahar says in the podcast. “I started in the defence industry then consumer electronics and the health industry before moving to Intel. I went from augmented reality to virtual reality, robot drones and mobile phones.”
Eight years ago, Dr Bhowmik contacted him. “I wasn’t looking to move but he called and explained about his vision to change the industry. He said he needed me to execute it. I saw the spark in his eye and that’s how I found my way to the hearing aid

industry,” Shahar says.
Shahar has spent his entire career working on sensors, AI, and human interfaces – similar to the work he now does at Starkey, creating and developing new technology for Starkey products.
“What we see in today’s products, we started to develop five, six, seven years ago,” he says. “What we’re working on now, we’ll see in products in six years.”
Dr Fabry, on the other hand, spent decades immersed in hearing healthcare, initially from a practitioner’s perspective and is now also immersed in AI. While he saw incremental improvements over time, he says he's witnessed vast tech improvements since Dr Bhowmik and Shahar joined the company.
“Since they joined, they really have differentiated us from the rest of the industry by focusing on hearing and bringing in AI,” Dr Fabry says. “We put the AI in hearing aids by starting to focus on hearing aids that could help people hear better but also live better through health and wellness features such as falls alert and prevention, and virtual assistants.”
Shahar says every company needs to balance releasing products, fixing issues, incremental improvements and support, against developing tech and future products.
“The most successful tech companies in the world create a separate group for
advanced development that focus on development for the future,” he says.
“When Starkey decided to strategically become a tech leader, we created an advanced development group chartered with developing new tech and bringing it to market. We’re not a research group and we don’t just create papers and go to conferences; our job is to bring this tech into products in collaboration with engineering groups and everyone.”
Starkey invested substantially in the group, bringing in resources and recruiting the best talent it could find.
“It was very important if we wanted to become a tech leader in this industry, and we now have more than 300 years of collective work experience in AI,” he says.
Today its biggest investments are in better hearing, improving sound quality, developing more tools for clinicians, more tech and intelligent assistants.
“But we put the most effort into hearing,” Shahar says. “AI will eventually run every aspect of algorithms and that’s where we are putting in a lot of our effort.”
Traditional algorithm development gives computers and hearing aids specific rules and instructions – telling devices how to perform in various situations. But when they come across something they haven't seen, these devices may not know what to do, creating limitations.
Machine learning learns from data. When a device such as a hearing aid encounters an unknown situation, machine learning

helps it decide how to respond, based on patterns it has learned over time.
Giving a computer information and letting it figure it out provides enormous flexibility, the same way the human brain works, and this is how DNNs work, Shahar adds.
“One big advantage of DNN is that it’s better in real life environments,” he says. “Two hearing aids on paper look the same and test the same in a laboratory but you should always prefer the one with DNN because it does a better job in uncertainty, in dynamic environments, when things change.”
DNN is better in non-stationary environments and in speech in noise, he adds. “In any acoustic scenario, it is much better at classifying what the environment is, it allows better end-to-end optimisation, is more personalised, and better at taking new data and fusing it.”
Hearing aids can automatically classify an acoustic environment as quiet, noisy, windy, musical and there is 85% agreement between human and AI-driven classification, he says. For those who want this improved, the Starkey team developed Edge Mode+ to improve environment classification by a further 15% to 20%.
Edge Mode+ captures listeners’ intent combined with AI-driven classification.
Hearing aid wearers can say they’re in a challenging, noisy environment and AI helps determine if it is noisy music which is of interest and the person wants to hear, versus noise.
“It’s a very successful feature and is getting better over time,” Shahar says. “It constantly adjusts looking for the best scenario for the patient.”

Below: (L-R) Starkey’s Edge AI CIC (completely in canal), and mRIC (micro receiver-in-canal) hearing aids.
Dr Fabry agrees it’s one of the most widely used features and is increasingly being used by wearers in lieu of manual programs in restaurants, crowds and music.
DNNs require a lot of computing power, and the only way to incorporate them is to “bake it into the hardware”, Shahar says.
He says Starkey took the neural network and put it in its hearing aids, inside the
silicon on the chip as part of the hearing aid. “That’s what allowed us to open the door to all sorts of new capabilities that weren’t possible before,” he says.
In 2023, Starkey introduced a version of hearing aids featuring a neural accelerator capable of running sophisticated DNN-driven processing for better hearing.
With this came a rapid transition to rechargeable batteries, Dr Fabry says. This version with a DNN accelerator on the chip gave up to 51 hours’ with the RIC-RT model using Edge Mode+ which used DNN application situationally or automatically throughout the day, he says. “If you turn it on in the morning it just goes all day.”

The Edge AI mRIC is small and discrete.

Dr Fabry says what was done with this hearing aid was nothing short of remarkable. It took anxiety for hearing aid users off the table by making them confident that when they bought these devices, and even years later when putting them on, regardless of how much they engage with Edge Mode+, they’ll still automatically get all day battery life, he says.
Shahar says the team took time to develop the technology from the ground up. It considered that a separate chip would not be as efficient and would be a power drag compared with an optimised neural network incorporated into the one chip.
He says AI in hearing aids means better personalised solutions and a faster first fit. DNN improves speech enhancement and suppresses noise and machine learning in various forms helps clinicians in fitting and improving fittings.
Other Starkey innovations his team has helped spearhead include incorporating automatic REMs (real ear measurements) for every patient to NAL-NL2 software targets and using machine learning ability to optimise to prescription target faster than human capability.
The team also developed world first fall detection, alert and prevention features in
Starkey’s latest hearing aids. “We strongly believe in the importance of that for our patients,” Shahar says.
Hearing care is healthcare as even mild hearing loss places people at three times the risk of falling, Dr Fabry adds.
He says the team was also instrumental in improvements in self-checking features including evaluation within seconds of how often wax guards should be replaced in hearing aids.
“All patients should learn how to use this as they’ll have a better experience and could avoid issues,” Shahar adds.
“We want the technology running in the background to become more sophisticated and see how things are going all the time, allowing clinicians to get more information about what’s going on. When patients come in, practitioners would already know what happened and have a record of what should be done.
“We’re trying to get the best product and best solution to the patient.”
Starkey’s Edge AI hearing aids, which launched in Australia and New Zealand in February 2025, have all the AI and DNN features and benefits profiled in this article. Starkey says these translate to 30% better speech identification than its previous hearing aids, and DNN processing which is 100 times more powerful, enhancing sound clarity and streaming range.
See starkeypro.com.au.











GN Hearing ANZ’s Accelerate Partnership Program supports independent audiology clinics by providing comprehensive business solutions beyond product sales. H PA gains an insight into the program.
Running an independent audiology clinic is no small feat, particularly when hearing practitioners’ primary focus is patient care. Amid busy schedules and growing clinical demands, the business side of practice can easily slip down the priority list, leaving little time to plan marketing or manage growth.
That’s where GN Hearing Australia and New Zealand’s Accelerate Partnership Program comes in. Designed for loyal customers, the program offers independent audiology clinic owners access to practical business and marketing support at no cost, helping practices thrive without taking focus away from patients.
The program, which has evolved over seven years, covers everything from advice on establishing an independent clinic to business planning, marketing support and materials, and access to marketing, business and human resources consultants. Its four pillars are business consulting and development, business support and services, lead generation support and design services, and training and knowledge development. Support can include awareness campaigns, print advertisements and business promotion flyers with the clinic’s branding, events and open days, and assistance with website development.
GN consultants can also visit clinics to assess business health, while marketing specialists can develop tailored plans and coach practitioners on how to run campaigns effectively. The program also provides access to premium products and discounts on equipment.
Ms Eva Gajos, marketing manager for
GN Hearing ANZ, says the service is designed to support often-time poor independent practitioners.
“We recognise the unique challenges they face as an independent clinic owner, particularly in managing time and resources,” she says.
Independent audiology businesses are the backbone of a strong, diverse hearing care sector, adds Mr Paul Jones, GN Hearing's ANZ general manager.
“In an increasingly complex and competitive market, clinics require more than just great products – they need practical business solutions that support efficient operations, sustainable growth, and genuine independence,” he says.


about how we can support them.”
“GN Hearing’s Accelerate Partnership Program is designed as a true partnership, giving clinics access to the tools, insights and support they need to strengthen their businesses, enhance the patient experience and stay focused on what matters most: delivering outstanding hearing care.”
The program’s theme is ‘going beyond a transaction’ and beyond simply supplying great products. Its success is measured by long-term business growth rather than short-term sales outcomes, Gajos says.
“We want to be perceived as a genuine partner for independent clinics,” she says. “While some competitors may offer loyalty points and programs, our program focuses on business solutions.
“There’s no cost associated with it. To become a partner, a clinic must be independent and have Beltone business with us. From there, we start a conversation
Gajos says GN understands that independent clinics typically work with multiple manufacturers. Clinics can sell other brands and still participate in the Accelerate program, provided they sell Beltone hearing aids.
GN offers Beltone’s latest hearing innovations exclusively to independent clinics in Australia and New Zealand.
“Our Beltone range is the only hearing aid brand in this market available exclusively to independent clinics,” she says. “But modern business isn’t just about products, transactions or discounts. It’s about supporting independent businesses to grow and remain viable.
“As a manufacturer, we feel a responsibility to support our independent clients in a competitive landscape.”
Gajos says audiologists and audiometrists have invested their hearts and lives into hearing care.
“The business side is something they must do on top of that, and we want to make that easier for them, be their

sounding board, experts they can come to and bounce ideas off, ask for direction and help improve their business acumen,” she says.
Mr John Bullion, sales manager –independent channel at GN Hearing ANZ, says the program began modestly more than seven years ago but has since expanded significantly.
He oversees the independent sales strategy across Australia and New Zealand and leads four account managers who provide commercial guidance through the program.
“Account managers are separate from our product specialists, who are audiologists focused on technical and product support,” he says.

“Our account managers work with independent clinic owners on proactive strategies, bringing ideas on how to differentiate themselves, improve efficiencies and boost profitability. That is their sole role.”
In South Australia, GN has a joint product and account manager. There are two similar hybrid roles in New Zealand, and another hybrid role is planned for Western Australia.
“The account manager roles are complemented by the broader suite of solutions available through the program,” Bullion says.
The partner network has grown steadily, with many independents taking up GN’s offer of business support, he adds.
Gajos says some practitioners may not initially know what their business challenges are, but account managers can help identify underlying issues and suggest solutions or referrals to consultants.
Bullion says assistance is highly tailored.
“A practitioner might say they want to run an open day, for example,” he says. “We’ll explore whether that’s because it’s worked before, or because they’re unsure what else to do. By asking the right questions, we can clarify what they want to achieve, what message they want to communicate, and how they want to be perceived in their community.”
Account managers may suggest alternative approaches if another solution is better suited to the clinic’s goals.

Gajos adds that the strength of the program lies in the relationship between account managers and clinics.
“It’s not about throwing ideas at people to see what sticks,” she says. “If the clinic doesn’t have clarity around its goals, those ideas may not deliver value.”
She stresses the program is not designed as a short-term fix for underperformance but as a pathway to sustainable, long term success.
Account managers act as business partners, reviewing clinics from multiple angles including lead generation, margins and service mix. For more complex issues, practitioners can be referred to external consultants.
Bullion says GN works with consultancies that understand the independent audiology sector, enabling faster and more meaningful impact.
“We have tools that help clinics understand efficiency, profitability and the financial impact of business decisions,” he says.
“It's not always about, ‘I need more people through the door’. Through our market improvement tools, we can show many ways of improving the profitability of their business.”
Bullion says there are numerous success stories where clinics can directly link GN’s recommendations to measurable returns on investment.
“We evaluate each intervention, looking at costs, outcomes and impact on sales,” he says. “That helps determine whether to repeat, refine or change an approach.”
“It's not always about, ‘I need more people through the door’. Through our market improvement tools, we can show many ways of improving the profitability of their business.”
John Bullion
GN Hearing ANZ
account managers and consultants can provide business advice to independent clinics with a Beltone account.
Recent initiatives include a webinar with a HR consultancy on recruitment, which was well received by partners.
Many marketing assets focus on hearing awareness rather than brand promotion.
“Posters highlighting hearing loss prevalence or tinnitus awareness prompt people to book a hearing test,” Gajos says.
Account managers can also help facilitate connections between clinics and local healthcare providers to build referral pathways and awareness of services and support that hearing practitioners provide.
“Sometimes audiologists don't feel confident or are too time poor to initiate these conversations about how they can work together,” Bullion says. “We can do the leg work where appropriate – establish a line of communication and identify the right people to speak to and potentially organise for the audiologist to present. We arrange it but they’re always the face of the audiology clinic.”
Accelerate partners qualify for discounts on services and equipment, including impression scanners, with finance options also available.
GN’s Emerge program supports clinicians looking to establish independent practices from the ground up. The platform officially launched in October 2025, though GN has supported start-ups for some time.
“Emerge covers everything from mission statements and finance to rental agreements, demographics and location selection,” Bullion says.
“It helps with the things clinicians may not initially consider when setting up a business. Where needed, we can also refer them to independent advisers.”
Gajos says Accelerate is designed to deliver lasting benefits.
“We want independent clinics to feel supported, confident and not overwhelmed,” she says.
Independent clinics with Beltone accounts wanting to discuss joining the Accelerate program can contact John Bullion on jbullion@GNhearing.com or 0414 784 443.

EssilorLuxottica has launched a new hearing care option for Australia and New Zealand through its first direct-to-consumer audiology service in OPSM stores.
As the inaugural audiologist to work in an OPSM store in NSW, Ms Marisa Varrica is excited to be on the frontline of a new chapter in hearing care for Australia.
“It’s a great opportunity to build audiology from the ground up within an already trusted and established brand,” she says. “I started in October 2025 in our biggest store in Castle Hill. I'm really enjoying it and am surprised at how quickly it's grown in a short amount of time.”
Varrica works across three stores in the Sydney suburbs of Castle Hill, Rouse Hill and Bankstown. She’s found that when people in store for optometry services are offered a hearing test, most take it positively.
“They’re surprised we now offer hearing services, but it’s been positive,” she adds. “A lot of patients say they'd been meaning to get their hearing checked but hadn’t got around to it.
“They appreciate the convenience of having eye and ear care under the same roof. It’s a familiar environment where they've received trusted optometry care so it makes an easier transition into audiology.”
Some in the team have been with OPSM for 20 years and patients have seen the same practitioner, making it a family feel.
OPSM’s parent company, EssilorLuxottica, launched the service last year. Ms Naomi Nicolinas, EssilorLuxottica director of audiology services ANZ, says the company is a global leader in vision care, bringing together world class innovation, iconic eyewear brands, and a trusted retail network across more than 150 countries.
“Its ongoing investment in med-tech, smart eyewear and emerging sensory solutions including Nuance Audio Glasses are shaping a future where vision and
hearing care are more integrated, accessible, and preventative,” she says.
“OPSM has an extensive store footprint with more than 419 stores across Australia and New Zealand. With the introduction of audiology services, we are now able to offer truly integrated sensory care under one roof by bringing together hearing screenings, diagnostic assessments, and hearing solutions alongside comprehensive optical care.”
Nicolinas says audiology is being progressively rolled out across its OPSM network, with seven stores currently offering audiology services and additional locations planned throughout the year across Australia and New Zealand.
“The model is distinct in its ability to normalise hearing care within a familiar, trusted retail health setting, providing customers with convenient access to both hearing and eyecare support in one location,” she adds.
Vision and hearing loss affect similar demographics, particularly older adults, and integrating eye and hearing care in the same location provides a more holistic and efficient approach for patients by addressing multiple sensory issues at a single point of service.
Varrica agrees eye and ear care are a natural fit, and says retail and optometry staff also initiate conversations around hearing.
OPSM audiologists deliver hearing care for adults including diagnostics, treatment such as hearing aids and rehabilitation. Additionally, OPSM is a contracted Hearing Services Program (HSP) provider and is able to provide hearing care for eligible patients through the HSP and the Department of
Veterans Affairs. Children and those under 26 are referred to Hearing Australia for free or government subsidised hearing care.
Varrica says hearing screenings are offered to all existing and new customers. “Hearing screenings have been built in to the in-store experience with customers made aware that audiology is now part of the services available," she says. "The aim is to make hearing health more accessible, creating opportunities for people to engage with their hearing alongside their eye care."
The baseline screening gives an indication of hearing, and if a loss is detected, the person is referred for a complimentary full hearing assessment.
“It’s also about making hearing care more available close to where people live, creating awareness and accessibility across locations,” Varrica says. “It’s incredibly rewarding and I love the variety the role brings. I’m proud of the progress we've made, especially being able to see a wide range of patients and see the positive impacts on people's lives through a more collaborative approach to patient-centred care, which is what motivates me the most.”
Many found to have hearing loss through the screening go on to have an assessment. “The full hearing assessment allows for a better understanding of their hearing health” she says. “We determine the type and severity of hearing loss through a comprehensive test battery, so we can find the best solution for the individual.”
Patients receive an in-store hearing aid demonstration and wear the devices in the shopping centre to experience enhanced hearing in a real-world environment.
“My job is to educate so our patients are making an informed decision," Varrica says.
"We have a selection of devices in store so patients have the ability to go home with hearing devices on the same day.”
OPSM offer a 30-day satisfaction period on hearing devices to ensure customers have time to experience the benefits, make adjustments and are comfortable with their hearing solution.
While at high school, Varrica did work experience with a speech pathologist and loved it so completed her Bachelor of Speech and Hearing Sciences at Macquarie University intending to become a speech pathologist. “When I started learning about audiology, it sparked my passion for hearing care and desire to make a positive difference in peoples’ lives," she says. "I love that through standardised tests we determine the type and degree of hearing loss and can provide a solution to help people hear better through technology.”
She graduated with a Master of Clinical Audiology from Macquarie University and completed Certificate II in Auslan. While studying she worked at a shoe store, progressing to manager; a great foundational experience in leadership and providing customer service. “I love interacting and talking to people. Hearing connects us with people and the world around us which is so important for our social interactions and cognitive health,” she says.

Post graduation, Varrica worked at Bay Audio as a provisional audiologist then a clinical audiologist for 18 months, across different clinics – a job she also enjoyed.
“Previously I worked in an established clinical setting, but working at OPSM allows me to have more independence and responsibility managing and shaping patient care to achieve best outcomes,” she says.
“At OPSM, I’ve taken on more of a leadership role, helping to shape the way we deliver audiology services. EssilorLuxottica delivers excellent customer care which integrates with my values.” Varrica supports and collaborates with multiple teams, integrating audiology alongside optometry.

“I work closely with optometry and retail teams to create a more holistic approach,” she says. “Each store has its own team, rhythm and community which keeps the role dynamic. We've been streamlining processes to ensure the customer journey is consistent across all our OPSM stores to deliver a high quality and standardised level of care.”
EssilorLuxottica provides foundation understanding of hearing care by training eye care and retail staff in hearing screening, how to service hearing aids and devices, and conversations around hearing. Varrica has helped with this training and education including raising awareness around the importance of early detection and addressing hearing loss. “I also did training at head office learning the systems and how audiology would be integrated,” she adds.
All stores with audiology have been fitted with sound treated rooms, doors and insulation. Audiologists are contracted as employees, as are optometry and retail workers. “I love working with the OPSM team. Everyone’s been so supportive – the retail team, optometrists, executives and particularly director of audiology Naomi Nicolinas who has been incredible. I'm grateful to be part of the team and excited for the future of audiology at OPSM.”
EssilorLuxottica’s revolutionary hearing aid glasses – Nuance Audio Glasses – are also on sale in OPSM stores. They have directional microphones and open-ear speakers embedded in their frame arms and are designed for people with a mild to moderate hearing loss.
“There are demos in all stores and there's been strong interest, especially from people who are not quite ready for traditional hearing aids, or who are having a bit of trouble but not a significant loss,” Varrica says. “There’s great feedback around the discretion of the glasses and combining vision and the hearing component. People are seeing ads and coming in.”
The glasses don’t require an audiology prescription, and their sale is generally handled by retail and optometry teams if prescription lenses are needed. Varrica often gives patients an introduction and explanation though.
“You can have plano lenses if you don’t need prescription lenses,” she adds. “It’s a good segue and conversation starter about hearing and can help people take the first step in doing something about their hearing.

“I had a couple who came in wanting Nuance glasses as the wife said her husband wasn’t answering her. After tests, I found he had a significant hearing loss and because the glasses are for mild to moderate hearing loss, he tried hearing aids and loved them.”
Varrica’s advice for audiologists considering a role with OPSM is to be open minded and embrace the collaboration with optometry.
“It’s an amazing opportunity for audiologists who enjoy teamwork, innovation and building something new," she says.
"You get to practise high quality clinical care while being part of a broader health environment. Don't be afraid to shape the way audiology is delivered; it's a chance to grow professionally and make a real difference in our patients’ lives.”
For more information, see opsm.com.au/ audiology.
FLEXIBLE




Australian surgeons are reporting success after implanting Oticon Medical’s first active transcutaneous bone anchored hearing solution, the Sentio System. HPA asks a leading ENT surgeon for insight into benefits and advantages.
Brisbane ENT surgeon Dr Andrew Chang has only implanted the Sentio System once, but he’s already concluded that it’s his preferred bone anchored hearing solution (BAHS).
As director of Mater Health Services ENT Department in Brisbane, and an otologist and cochlear/hearing implant surgeon at Queensland Children's Hospital, Dr Chang has been performing bone conduction implant surgery for about 10 years. He does 25 to 30 of the procedures annually.
A former senior otology and hearing implant Fellow at Cambridge University Hospitals NHS Foundation Trust, UK, he carried out his first Sentio implant in Brisbane in October 2025, two months after the product launched in Australia.
“The patient is very happy, and I have several more who are planning to have the procedure,” Dr Chang says. “She was an ideal candidate for bone conduction – she had conductive hearing loss from previous ear surgery and recurring otitis externa (inflammation of the passage of the outer ear) preventing her from wearing conventional hearing aids.”
The Sentio Ti implant is fully implanted under the skin with the only external part being the Sentio 1 Mini sound processor held over the implant by a magnet.
Oticon Medical says the Sentio delivers the proven benefits of the Ponto percutaneous system but in a transcutaneous option. Different from the Ponto, there is no connecting abutment visible on the skin's surface which is fixed to the implant in the skull bone. The Ponto’s sound processor clicks onto the abutment to deliver sound vibrations directly to the bone.
“I have personally gone away from
offering the abutment solution because where I am in Queensland, it gets very hot and humid in summer, and even recipients who take really good care of their abutment, often complain about redness, pain and discomfort throughout summer,” Dr Chang says.
“The heat and humidity make maintenance of their hair difficult; particularly for female patients, it's hard for them to do their hair with the abutment.
“I didn’t realise this until my first patient said the Sentio System was much better as she didn’t have to worry about anything getting caught on the abutment. With Sentio, patients do their normal hair care routine but must remember to take the processor off in the shower or when swimming.”
Dr Chang says the patient relayed that the external processor is so light that most of the time, she doesn’t even know it’s there.
“The better outcome is due to recipients wearing the sound processor for longer during the day because it’s more comfortable, which helps with their daily function,” he says. “They don't have to wear it for five hours then take it off and think

what they’re going to do (for hearing) for the next few hours.”
The processor is bigger with other devices, he adds. This means the magnet must be stronger which can tend to cause pressure over time.
“Many people say devices (that aren’t Sentio) are a bit uncomfortable to wear for 10 hours at once and they look forward to taking it off at the end of the day,” he says.
The clear advantage of the Sentio is that it has a better profile to the shape of the skull than other BAHS, Dr Chang says.
“The incision is much smaller than other implants because the implant is 28% smaller,” he says. “Also, it's not restricted in terms of previous surgery compared to other bone conduction implants.
“For example, if the patient has had extensive middle ear surgery or mastoidectomy, it is very hard to place those implants. You must push them back more and it becomes difficult to find an ideal location for a new implant.”
Additionally, the surgeon does not have to create a big bone well. “You can create a nice (up to) 3mm bone well in the cortex (outer layer) of the skull. You aren’t limited,
“The Sentio is innovative because it doesn’t require an anchoring screw to be implanted in the patient’s skull for the transmission of sound to occur.”
it’s like a little recess you can put in,” he says.
The procedure usually takes less than 60 minutes and going forward it should take about 30 minutes, he estimates. His first one took about 40 minutes due to becoming familiar with placement. Less anaesthesia time is also an advantage for the elderly and children.
Setup is simpler compared to other devices even from the starting point, he adds. Instead of three layers of draping, only two are needed.
The incision – about five centimetres long or less – can be directly behind the ear in the crease which gives enough room to access the skull. Surgeons make a standard pocket under the soft tissue of the scalp.
“The important part is that the implant is making good contact with the bone,” Dr Chang says. “The point where the Sentio is recessed into the bone – the size of that bony well, even though only (up to) 3mm deep – must allow good contact.
“You have to be precise as the implant must fit nicely into the circular recess and not have too much room around it.”
INNOVATIVE AND COMFORTABLE
The recess becomes a natural holder for the implant which sits inside. A small band is placed overtop and two screws hold it in place.
“The Sentio is innovative because it doesn’t require an anchoring screw to be implanted in the patient’s skull for the transmission of sound to occur,” Dr Chang says.
“It’s the smallest in terms of profile and length. The maximum skin thickness (behind the ear) it tolerates is about nine millimetres.
“If skin is thicker, it must be thinned down (shaved) so the external processor can make contact through the skin and magnet to the implant in the bone. This delivers sound vibrations directly to the bone, bypassing the outer and middle ear, enabling sound to be heard.”
Being thin, it is light and more comfortable than other transcutaneous implants, he reinforces.
Dr Chang says surgeons choose appropriate candidates to ensure they receive a good outcome. “It's usually for conductive hearing loss down to approximately 45 to 55 decibels,” he adds.
Oticon Medical says Sentio is also suitable for single sided deafness but the candidate must have essentially normal hearing thresholds on the other side.
For preoperative planning, he works with audiology colleagues to make sure a good bone conduction trial using a soft band occurs first to ensure there will be benefit from the implant.
Medically, Dr Chang makes sure patients don’t have a progressive loss that could impact on the long-term performance of the implant.
Dimensions of the implant.
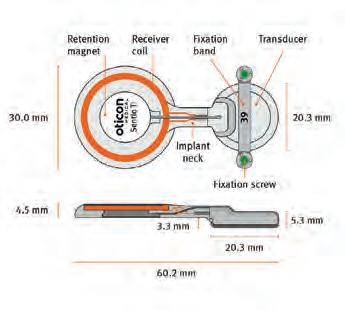
“Hearing loss has to be fairly stable,” he says. “Also knowing their previous ear surgery history is vital as is ensuring they're not going to have more ear surgery which may affect their hearing threshold, or the implant itself.” He also sends patients for a CT scan for pre-operative planning.
“I would suggest ENT surgeons think about and offer this option to patients because many times, my non-otological colleagues tell these patients, there's not much else that can be done for their hearing loss and just wear hearing aids,” Dr Chang says.
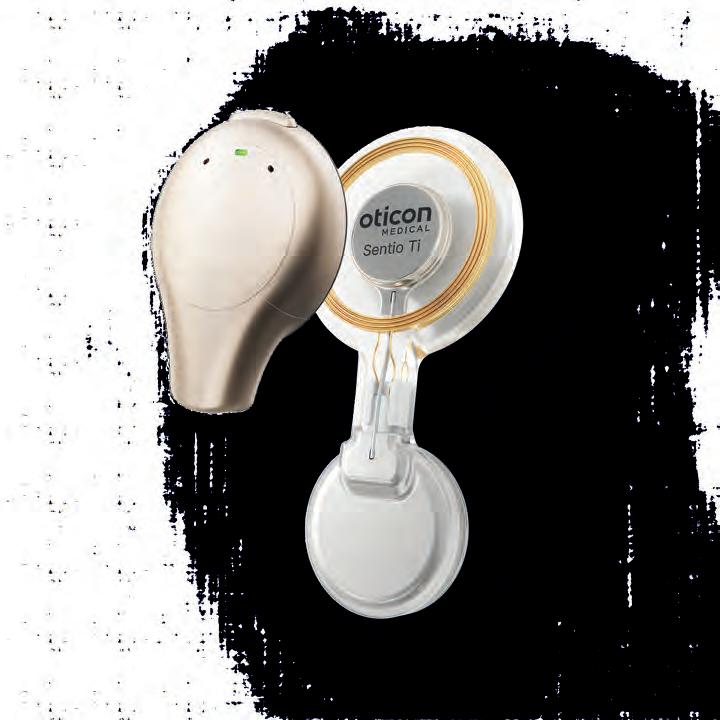
“This is fine and some people are happy with hearing aids but you always need to discuss other options, including hearing implants and refer appropriately if the patient wants to know more about it.
“I’ve had quite a few patients who’ve been told implants won’t work for them, without even seeing an audiologist with an interest in hearing implants or having any assessments done.”
Oticon Medical says the Sentio Ti implant is a ‘SuperPowerful’ implant developed to support patients whose hearing loss may deteriorate over time, without the need for additional surgeries. It says the aesthetics of the system are another big advantage, with sleek, stylish design.
“The external processor doesn’t look bulky, there’s a good selection of colour choices to blend in well with hair and it’s profiled better – aesthetically it looks good, which is important for patients’ acceptance and use,” Dr Chang says.
He doesn’t just see the Sentio as another option in the toolkit. “It's a superior option for people who have had extensive ear surgery as they will still benefit from having this bone conduction implant,” he says. “It’s also a better option for children because it’s smaller, slimmer and internal.
TGA-approved for children, it will be available earlier from around five years of age when they’re starting school.
“Although it’s indicated for children aged 12 and over, it hasn’t gone through the regulatory process yet for kids but it will happen soon. Most of my work in bone conduction implants is in children.
“It will be a definite advantage in children, particularly young children. Now they wear soft bands which are great, and are provided by Hearing Australia, but when
Dr Chang is already a convert but he has a final reminder for his surgical colleagues. “The advantages of the Sentio include the fact it’s surgically easier to implant, you don't have to do substantive drilling, you can use an incision behind the ear which is what most of us are comfortable with, and it has a slimmer profile compared to competitors.”
For information see oticonmedical.com.au.

Why is Specsavers such a popular place to work? Some of the network’s audiology partners and senior staff explain the reasons they chose a career in green.
Hearing care changes lives. A single conversation, a fitting, or a moment of clarity can open doors for patients to live fully and confidently. Audiology professionals carry this responsibility every day – but it’s impossible for practitioners to ‘pour from an empty cup’. For teams to give their best, businesses and leaders must create workplaces where clinicians feel valued, supported, and inspired.
Specsavers says this purpose of changing lives through better hearing is central to its philosophy – and this extends to its own people, too, with the business recently named the fourth Best Place to Work in Australia. In what’s the largest evaluation of workplace culture in Australia’s history, the program captured insights from 158,000 Australian employees across all sectors.
In this feature, some of Specsavers’ leadership team and audiology partners help us understand more about why hundreds of audiology professionals are joining the brand and if “life in green” is as good as it seems.
When you speak to people who work at Specsavers, the first thing that comes
through loud and clear is that everything starts with the patient.
Ms Kathryn Launchbury, senior professional services manager – audiology, explains: “When you authentically put patients first in every decision, you find that the rest flows through.
“Team members are happy because they’re making a difference and working toward a shared goal that aligns with their values; patients get what they need to live a full life without compromising due to factors like affordability; and products are designed and selected to meet the real-life needs of the patient.
“Our entire business is built with a focus on improving hearing outcomes for patients and making care and products accessible for everyone who needs them.”
Launchbury says clarity of purpose doesn’t just shape the patient experience, it shapes the workplace culture at Specsavers.
“It sounds so simple, but when you build a business around the reason why we all became audiology professionals – to help people hear better – you create an environment where people feel proud of what they do. That pride translates into
collaboration, growth, and a culture that is genuine.”
Mr Kieren Cullinan, audiology partner at Specsavers Belconnen ACT, agrees. He started working at Specsavers because it aligned with his values. What keeps him going is the impact he can make daily.
“Specsavers as a business is very genuine – what you see and hear, is what you actually get,” he says. “The culture is collaborative and the model is built around doing the right thing by patients, which is evident in every level of the business.
Having that encouraging and positive culture naturally brings out the best in people and subsequently fosters some amazing business opportunities.”
For many audiology professionals, career progression can feel limited, Specsavers says. But it says its joint venture partnership model allows clinicians to become business owners without compromising their values.
For Cullinan, becoming an audiology partner eventuated after realising he wanted to move upward in the industry, and owning a private practice wasn’t an option.
“The joint venture partnership model
lets you become your own boss, giving you the flexibility to invest as much time and effort as you’d like into the business, earning strong financial returns without compromising on clinical ethics from traditional sales pressures within the industry,” he says.
“And the best part is that your time spent growing and building the business won’t just disappear if you decide to leave – you are investing in your future.”
Similarly, Ms Gabrielle Brook, audiology partner at Specsavers Broadmeadows and Specsavers Craigieburn in Melbourne’s northern suburbs, shares that as a younger audiologist, she never thought owning her own practice would be possible until she learnt about Specsavers.
“The opportunity to become a partner and own my own business while still in my 20s was something I would never have been able to do on my own, financially or practically,” Brook says. “Working here has helped me reach my career goals so much faster, transitioning from an audiologist into an audiology partner.”
For audiology professionals not wanting to own a business, Launchbury says many other options are available.
“Specsavers is dedicated to continually upskilling our people to empower them to make great care even more accessible,” she says. “We understand partnership isn’t for everyone and for our many audiology professionals who aren’t partners, we provide an array of development, training and networking opportunities on top of those arranged by each local store.
“No matter where someone is in their professional journey, each opportunity helps to build a strong clinical framework, ensuring quality care is never compromised and audiology professionals have the autonomy they need to provide the best care for their patients.”
Specsavers’ integrated care model appears to be another reason why audiology professionals choose the network. By combining audiology and optometry under one roof, the organisation creates a seamless experience for patients and opens doors for clinicians to make a bigger impact, Specsavers says.
Mr Ben Scales, Specsaver’s director of growth – audiology ANZ, says: “One of the most unique and successful aspects of our


business model is the partnership between audiology and optics.
“Our screening process is a big team effort that incorporates everyone in store and in the support office. It’s been so successful that over the past five years, we’ve screened the hearing of more than four million Australians and New Zealanders.

“We have a single view of the patient and put the patient first. If we screen hearing while they have an eye test, it’s not only convenient but it grants access to assistance for people who haven’t even considered it.”
Most hearing loss is progressive and it can take people a long time to discover they can’t hear as well as they used to, he says, so being able to step in and make changes earlier can make a huge impact in people’s lives.
“It can be the difference between a grandparent feeling connected with their grandchildren; an employee being able to provide for their family longer; and people being able to continue with their hobbies and social groups,” Scales says.
‘’This is changing lives through better sight and hearing in action. It’s who we are, and that purpose is what everyone collaboratively works toward.”
This isn’t just operational efficiency – it’s a philosophy in action, Specsavers says. As Specsavers sees it, every screening is an opportunity to change a life, and every team member plays a role in that transformation.
This culture of teamwork is appreciated by clinicians and patients.
“For me, the best perk of working at Specsavers is the clinical independence you get while having a big, stable brand behind you.”
Gabrielle Brook Specsavers Broadmeadows and Craigieburn
Brook says: “I love our hearing screening program and that we offer free 15-minute hearing checks to anyone; it means we can educate clients early about their hearing health, even if they’re nowhere near thinking about hearing aids yet.”
She says providing a hearing service alongside optometry only has benefits.
“For me, the best perk of working at Specsavers is the clinical independence you get while having a big, stable brand behind you,” she adds.
“Clients also walk in already trusting the brand and are often already optics patients, which makes the whole journey easier and more positive from the start.
"Overall, the support and structure here really let you focus on meaningful clinical care.”
These answers make it clear that Specsavers is more than a workplace; it’s a platform for purpose, it says.
It’s where audiology professionals can deliver care that feels meaningful, backed by a structure that removes barriers and amplifies impact, Specsavers says.
It’s where independence meets security, and where ambition meets opportunity, it adds.
From Launchbury’s emphasis on patient-first principles to Scales’ vision of integrated care, and from Cullinan’s entrepreneurial leap to Brook’s passion for clinical autonomy, one thing is clear: Specsavers says it is working to create a new standard for what it means to work in hearing care.
Specsavers says that for those wondering if it’s as good as it sounds – the answer lies in the voices of those living it: clinicians who feel supported, valued, and empowered to do what they do best.
Australian researchers are trialling a world first tinnitus diagnostic tool which also aims to tailor treatment. For Tinnitus Awareness Week in February, HPA provides an update on the innovation and asks audiologists about trends and insights.
Biomedical engineer Associate Professor Mehrnaz Shoushtarian has spent more than seven years at the Bionics Institute in Melbourne immersed in the world of brain imaging using functional near-infrared spectroscopy (fNIRS).
Her goal, now within reach, is the development of an fNIRS device that hearing practitioners and ENT surgeons can routinely use in their clinics to diagnose tinnitus, and identify subtypes, enabling tailored treatment and monitoring of treatment effectiveness.
For A/Prof Shoushtarian, the Bionics Institute’s head of tinnitus research, it’s a major undertaking. She says there is currently no clinically available diagnostic test for tinnitus.
“Clinicians rely on patient reports –whatever the patient says they can hear,” she says. “Again, when trialling treatments, it's subjective – whatever the patient tells them. While it’s important to have patient input, it's not enough to give clinicians information on underlying brain activity and whether it changes with a particular treatment.”

“The light reflected back provides detailed information on brain activity which is recorded on a computer and analysed. This aims to set a baseline for tracking changes in the brain triggered by tinnitus.”
A/Prof Shoushtarian’s research interest has always been using non-invasive techniques to record brain activity and study how brain signals are affected by health conditions. When she joined the institute, Professor Colette McKay was investigating fNIRS for hearing conditions and suggested exploring use in tinnitus.
The safe, non-invasive fNRIS technique uses near-infrared light to record brain activity from different regions. “The technique involves placing a cap on the head like a swimming cap which shines gentle light onto the head, measuring changes in blood oxygen levels,” Dr Shoushtarian says.

A/Prof Shoushtarian’s pilot study with 25 tinnitus patients and 18 controls found the tool was 78% accurate at diagnosing tinnitus and achieved 87% accuracy in determining severity.
“We have done a larger study with 80 controls and 150 tinnitus patients and are currently writing up findings from the total dataset,” she says.
Published studies on smaller samples from the dataset confirmed the device could identify subtypes and monitor treatment. The studies could identify tinnitus laterality (sound heard on one side or both.)
A cochlear implant study where data was recorded with the implant turned on and off showed the device could detect severity changes within an individual, showing the potential to detect treatment effectiveness.
Plans include developing an accessible and affordable fNIRS device for audiology clinics.
“If it's developed and clinically available, it would be the world’s first diagnostic tool for tinnitus,” she says. “A tool like this could
provide information on underlying brain activity and tell us whether a treatment is effective and generating changes in brain activity.
“Some trials use brain stimulation for tinnitus and study how long to apply the stimulation over what period of time for it to have an effect so a tool like this could monitor those brain changes, rather than just asking if stimulation is helping.”
Her team includes research engineer, Ms Michelle Bravo, whose role includes data analysis, and institute chief technology officer, Professor James Fallon whose knowledge of auditory neuroscience is essential to the project. They’re comparing the fNIRS tool’s measurements with subjective ratings from patients using validated questionnaires such as the Tinnitus Handicap Inventory (THI).
The THI asks how tinnitus affects different aspects of a person's life and gives a score, providing a subjective measure of severity.
“We’re seeing if what we're measuring is agreeing with the person's score,” A/Prof Shoushtarian says.
“We study different aspects of these signals – resting state signals recorded while the person is at rest, and evoked recordings which are signals recorded in response to sound or visual stimuli.”
The test records six minutes of resting activity and 20 minutes of evoked responses. If treatments are being monitored, severity is tested before and after treatment, with severity based on brain signals.
“We’ve found there are differences in connectivity measures between people who have tinnitus and those who don't, which
agrees with previous fMRI research. But the benefit of fNIRS, if we can develop it further, is that it's more accessible than an MRI machine,” she adds.
This research found connectivity between signals in temporal and frontal regions was stronger in tinnitus patients at rest than controls. Similarly, brain responses to auditory or visual stimuli in evoked signals showed how the brain responded to stimuli, and this was not always the same in tinnitus and controls. “This helps us quantify tinnitus presence and severity,” she says.
A bigger dataset is helping develop refined measures of severity useful for monitoring treatments. “You don't want to just see if a person has gone from severe to mild tinnitus – you want to track mid ranges too to see if the tool provides more refined levels of accuracy.”
One vital use of the tool is to identify different types of tinnitus based on underlying brain activity patterns, which may help tailor treatment, she says.
“At the moment, anyone who hears a sound that's not present externally is known to have tinnitus, but there may be subgroups with different patterns of brain activity who would respond to different treatments,” A/Prof Shoushtarian says.
“Identifying subtypes could guide patients to different treatments. This is important because currently someone with tinnitus might try one thing, then another, year after year and eventually give up.”
Many of the Bionics Institute study participants had tried numerous things to manage their tinnitus and had virtually given up, she adds.
The institute’s team is undertaking another trial of 50 tinnitus patients being treated at The Melbourne Hearing Care Clinic in The University of Melbourne Department of Audiology and Speech Pathology and 20 controls who have tinnitus but are not receiving treatment.
“Once we have a bigger dataset, we hope this will determine which treatments help which subgroups,” A/Prof Shoushtarian says.
“For example, some use hearing aids for their tinnitus and find them useful, but others don’t; we can go back to the baseline brain activity and see which patients with certain patterns responded to hearing aids, and those with other patterns who didn’t.
“Our aim is to make the prototype device we’re using into a tool for use in audiology clinics. Our vision is that eventually anyone could have it and it would be user friendly enough for audiologists, audiometrists and ENT surgeons.”
If more funding can be attracted, she hopes it will be in clinics once regulatory approvals are completed. “The need is there and feedback from surgeons and audiologists at conferences is that they think a tool like this could help,” she says.
Senior audiologist and lecturer Ms Sarah
Swann, who has worked in The University of Melbourne’s tinnitus management clinic since it formed in 2017 and lectures on tinnitus to students, agrees that an objective measure of tinnitus is important “because of how complex the neural processes are in tinnitus”.
“It’s tricky because of how multifaceted tinnitus can be,” she says. “There's a difference between the trigger or the initial cause of the tinnitus, and how the brain processes and represents it. And how the limbic system becomes involved and creates an emotional connection to the tinnitus which can exacerbate the perception of it.”
The tinnitus clinic is the intervention arm for the Bionics Institute trial. “Our patients are having fNRIS measurements at baseline at the creation of their management plan then three and six months later,” Swann says.

we've recently refined protocols to include sound intolerance,” she adds.
“We will look at whether we can see differences in blood oxygenation patterns, exhibiting activity in different areas of the brain between controls who are not undergoing intervention for tinnitus and tinnitus patients who are undergoing interventional management.”
She believes the other aim – looking for patterns in tinnitus patients which dictate what level of success they might have with different types of management – will be the most beneficial for patients.
“If a person has a certain pattern of results or symptoms, and we see from these investigations if they're more likely to benefit from one type of management versus another, and we can objectively see a reduction in tinnitus that would be ideal,” she adds.
Swann has seen many severe tinnitus cases and uses personalised, multi-disciplinary approaches, including sound enrichment and habituation through apps.
Success rates are generally positive, with reductions in tinnitus severity observed at the three-month mark, she says. “The clinic has gone through a few evolutions, and
Swann was initially a musician who played the flute, and her husband is a professional tuba player who has tinnitus. She specialises in musicians’ hearing care with her PhD research aiming to develop a clinical protocol for musicians' hearing care.
“Tinnitus is a common comorbidity for musicians that occurs before hearing loss,” she says. “Our clinic tends to see patients on the more severe end, with referrals from GPs, ENTs, sometimes other audiology practices and self-referral.
“Patients complete the Tinnitus Functional Index (TFI) questionnaire to score severity. Sometimes they come in proactively because they're anxious it might worsen or become more bothersome and they don't want to reach that point.
“We see anyone with tinnitus that's bothersome enough to impact their health-related quality of life and aim to proactively manage it.”
Swann, and audiologist colleague Dr Philippa James who also works in the clinic, don’t discuss treating tinnitus. “We talk about managing tinnitus because we want to delineate the fact that we're not naming tinnitus on its own as a disease.
“It's a symptom of something, usually hearing related damage, so our management
strategy is always personalised, multi-factorial and often multi-disciplinary as we often refer for physiotherapy, dental treatment or psychology.
“If there's hearing loss, hearing aids might be discussed, and sound enrichment and habituation are almost always discussed.”

They often recommend sound enrichment apps which can be personalised. “Most of the time if the person has hearing aids, I have them stream through an app into their hearing aids for sound enrichment,” Swann says.
“It's always helpful to discuss tinnitus models, how it emerges, how it's processed in the brain and the different neurophysiological pathways to create an understanding of their tinnitus. Understanding triggers and exacerbating factors is also helpful along with understanding vigilance, hypervigilance and redirection strategies.”
A review occurs at three months, the plan may be tweaked, and another review happens 12 months later, with the aim to have patients self-manage through a personalised plan. The TFI verifies the plan.
“We almost always see a reduction in tinnitus at three months,” Swann says, but success rates also depend on the person, their self-efficacy, self-advocacy and adherence to the plan, with mental health playing a vital part.
“Sometimes we see great success, especially if there's hearing loss causing tinnitus, and they're wearing hearing aids for tinnitus,” she adds.
While there’s greater hope nowadays thanks to more awareness and management options – including the condition being discussed more openly among patients and clinicians – Swann says patients often say they mentioned it years ago to doctors who advised nothing could be done.
“Advice about just trying to ignore it and forget it is unhelpful, and people are relieved when they see us and find that – just because there's no cure – doesn't mean
there's not successful and accessible ways of managing the severity and impact,” she says.
“People often ask if it will go away, get better, become less loud and it’s hard to answer those questions, but when there’s less of an impact which equates to them noticing it less, this means it feels to them as if it's quieter, is getting better and is not as impactful.”
Language used is important because practitioners want to give hope and empathy but also realistic expectations, she adds.
Swann believes there may be increased prevalence because of recreational sound exposure. “There definitely seems to be more links between hidden hearing loss and tinnitus prevalence because we often see normal audiograms and tinnitus. A normal audiogram doesn't mean there's not underlying damage to the hearing system.
“That's often the case with excessive noise (workplace) exposure or sound exposure including for recreation or pleasure or for professional musicians.”
She cites the use of earbuds and headphones in young people for music and gaming as one possible cause. But the rise of sound cancelling and good quality headphones translating to improvements in sound quality and noise cancellation mean the volume can be turned down for the same amount of enjoyment, which is more protective.
She has had teenage patients with tinnitus, and even a boy aged 10 who was getting tinnitus spikes after drumming. A discussion about sound exposure, noise dosages, the importance of safe listening, safe practice methods, hearing protection, earplugs and reassurance led to a great outcome.
“Education is important and people appreciate it – they leave feeling better in themselves, hopeful and having a greater understanding of what tinnitus is and that it’s not necessarily a sign that they have a disorder or hearing loss,” Swann adds.
She says more than three hours a day of listening using headphones is not advisable including for gaming. “I'm sure there has
been an increase in tinnitus in young people but there's also a push for education, and commercialisation and trending of earplugs such as at music festivals,” she says.
“They're more stylish and accepted than they used to be which is fantastic.”
Education in health lessons at school is taking off. Swann presented on sound exposure, hearing protection and tinnitus at a meeting of music teachers in Melbourne in January. Her discussion of the topics in an ABC segment is also widely circulated among secondary school music students.
Additionally, a collaboration between The University of Melbourne Department of Audiology and the Conservatorium of Music provides hearing screenings for music students, hearing protection funded by the conservatorium and education on hearing protection and sound exposure.
Other trends the clinic is noting include more tinnitus cases among perimenopausal or menopausal women, due possibly to hormonal links.
Swann says audiologists graduating nowadays are more knowledgeable about tinnitus, sound intolerance, misophonia, hyperacusis and acoustic shock.
Her PhD aims to create a set of hearing aid fitting protocols for musicians and protocols to help manage sound exposure. It’s involved interviewing musicians with hearing loss who wear hearing aids, including one publication, and an upcoming literature review.
She’s now recruiting musicians with hearing loss for a ‘hearing aid for live music’ listening project. “They can be retired, amateur, professional or still practising, preferably who wear hearing aids, and we’ll fit them with hearing aids programmed specifically and modified with different parameters to improve music sound quality,” she adds.
Swann leads the Audiology Australia Musicians Hearing Group, which has 53 members who are clinicians, audiologists,

and hearing or music psychology researchers. Its meetings cover themes including hearing rehabilitation, protective practices for musicians, sound disorders and tinnitus.
One of her bugbears is that tinnitus investigations and management are not claimable on Medicare. “Tinnitus can be debilitating and is economically costly so it would be great to see more public funding pathways for management – outside of DVA and HSP programs – including private health insurance,” Swann says.
Perth audiologist Ms Pia Nairn from Lions Hearing Clinic also specialises in tinnitus management, having trained in Tinnitus Retraining Therapy and cognitive behavioural therapy. Nairn, who also works as a clinical trainer, notes greater acceptance and openness to mental health support among tinnitus patients.
“Help seeking and acceptance of the impact of mental health conditions now mean people are more open to discussing contributing factors; my conversations have changed a bit as people are more forthcoming and willing to see a psychologist or try mindfulness-based strategies,” Nairn says.

“That’s been the biggest shift – that we can do more things in parallel. When you recommend something that may be beneficial, they're not so resistant. More people are researching tinnitus and the detail of information we're giving now is more specific as they may be more informed or misinformed in some cases from Dr Google.”
She emphasises the importance of personalised treatment including sound-based strategies, counselling, customising education, discussing effectiveness of apps, and the potential of bimodal devices.
“Apps are great because they often follow the audiological approach combined with CBT, and they're good for remote patients who can't come into a clinic to continue treatment,’ Nairn adds.
“Good ones include MindEar and OTO, and others designed by audiologists and psychologists. There's been evidence that Lenire bimodal somatosensory tongue stimulation also helps some people.
“I don’t think there's anything out there that's a step above anything else. Some audiological management strategies and counselling tend to, in the long term, be proven to be the most effective or equally effective.”
Free apps for sound enrichment and mindfulness can also be coupled with counselling, Nairn says, but sometimes there are more complex factors involved and seeing a psychologist can be of infinite value.
“The one thing I always try and instil in my tinnitus clients, is that everyone with
tinnitus can be helped,” she adds. “The most devastating thing is when someone says they previously saw somebody who told them nothing could be done. With tinnitus, and particularly tinnitus with hearing loss, we have pretty good success rates.”
Nairn says tinnitus can be severe, chronic, intermittent or constant. Patients seek treatment when it becomes bothersome, as validated by the TFI or THI. People with mild to moderate tinnitus probably need counselling and support to help prevent it from progressing in severity, she adds.
“The earlier you intervene and educate, you can stop it getting worse or skyrocketing later,” she says. “It’s a normal function of the auditory system to get tinnitus in quiet, it's just what the brain's doing with the signal, and whether you have it penetrating everyday life as well when there's sound around. It’s all about tinnitus impact, what the brain is doing with that signal and how it's prioritising it over other stuff in the environment.”
In normal to mild hearing loss, hearing aids can be an effective tool for tinnitus management, Nairn says, although the level of benefit varies significantly between individuals. “For this reason, Lions Hearing Clinics sometimes offer a two-week hearing aid trial focused specifically on tinnitus relief rather than hearing improvement, allowing us to determine potential benefit for each person,” she says.
“It's not just sticking them in and expecting miracles. It's realistic expectations. I had one patient who had the mildest hearing loss and even in the clinic, the demo ones neutralised his tinnitus.”
It also depends on the origin of the tinnitus signal; if it’s just the cochlea, or further up, she says. The tinnitus signal is spontaneous activity but if you give it a true sound, it may
suppress the tinnitus signal, she explains.
“In some people, sound will inhibit the tinnitus signal and many people with tinnitus say when they're in the shower, it sort of washes out their tinnitus a bit –that’s masking and is why sound can be so effective.” For others, adding sound worsens tinnitus, Nairn says. For some with hearing loss and tinnitus, the devices don't eliminate tinnitus but push it to the background.
“The downside of a trial is that if you give someone a treatment or management strategy, they want to know if it's working so pay more attention to their tinnitus – has it increased or decreased during treatment?” she says. “This searching behaviour is a challenge, but you've just got to work with the person and work it out.”
Swann and Nairn believe more audiologists should train in tinnitus management.
“We're not psychologists and many people with tinnitus who really struggle have mental health issues they're worried about. Audiologists might think, 'What if my client has suicidal ideations?; how will I manage that effectively?” Nairn says.
“Some hearing practitioners might not have the emotional capacity, time or personality for tinnitus treatment as it’s a lot of counselling. Not everyone's wired that way, but I think everyone should have a knowledge of some basic strategies, how to reassure clients and referral pathways.”
Lions Hearing Clinic has trained its clinicians in basic counselling, how to identify if more help’s needed and when to refer. Celebrities opening up also help create awareness. When Australian cricket great Mr Justin Langer revealed his tinnitus struggles and how Lions Hearing Clinic had helped, it drove many to seek help. “One client heard him on the radio and said, 'Justin Langer told me to come see you!” Nairn says.
A compelling, evidence-based blueprint for high quality tinnitus care was offered at Tinnitus Talk Day 2025, says Brazilian-born Sydney audiologist Dr CELENE MCNEILL PhD. She reports on lessons learnt from the event that focused on multidisciplinary management models.
By Dr Celene McNeill PhD, audiologist Healthy Hearing & Balance Care
Tinnitus Talk Day 2025, chaired by ENT specialist Dr Clarice Saba in Salvador, Brazil, presented a robust and coordinated model of tinnitus care. The event challenged the prevailing belief that tinnitus is largely untreatable and emphasised its nature as a symptom with diverse potential causes.
The Brazilian approach integrates medical and allied health specialists from the outset, offering a comprehensive protocol that may be relevant for Australian practitioners.
MULTIDISCIPLINARY INVESTIGATION
In Brazil, the ENT specialist serves as the case manager for tinnitus patients. A detailed hour-long case history is considered essential, providing the foundation for exploring possible auditory, metabolic, vascular, somatosensory, psychological and iatrogenic contributors.
This depth of inquiry reflects the understanding that tinnitus is rarely caused by a single system and is instead frequently multifactorial.

After the initial consultation, patients undergo an extensive audiological assessment. Standard auditory testing includes air and bone conduction audiometry, speech perception testing, loudness discomfort levels, tympanometry, acoustic reflexes, otoacoustic emissions and auditory evoked potentials.
Vestibular function tests which often include VEMPs (vestibular evoked myogenic potentials), nystagmography, calorics and vHIT (video head impulse test), help identify peripheral and/or central involvement of the audio-vestibular pathway.
Tinnitus-specific measures such as pitch and loudness matching, minimum masking levels and residual inhibition provide further insight into tinnitus characteristics and their relationship with auditory function.
A defining feature of the Brazilian diagnostic model is its thorough investigation of metabolic factors. Clinicians routinely assess fasting glucose and insulin, HbA1c, lipid profiles, thyroid function, sex hormones when indicated, and micronutrient levels including vitamin B12, vitamin D, iron studies and magnesium.
Abnormalities in these areas are recognised as potential contributors to cochlear and
A physiotherapist palpating trigger points which can refer symptoms to the ear.
neural instability. Several cases presented demonstrated full tinnitus resolution once metabolic dysfunctions, particularly insulin resistance and dyslipidaemia, were appropriately managed.
Vascular causes are also explored in depth in cases of pulsatile tinnitus.
Vascular tinnitus typically presents as a pulsatile, heartbeat-synchronous sound and may indicate disturbed blood flow near the auditory system.
Diagnostic considerations include arterial disorders such as carotid atherosclerosis, dissection or aberrant carotid anatomy; venous contributors such as idiopathic intracranial hypertension, venous sinus stenosis, high-riding jugular bulbs or sigmoid sinus anomalies.
Systemic influences including anaemia, hyperthyroidism and uncontrolled hypertension are also investigated as well as imaging pathways commonly involving brain MRI (magnetic resonance investigation), MRA (magnetic resonance angiography), CTA (computed tomography angiography) and temporal bone CT and MRI scans, depending on the suspected mechanism.
Somatosensory factors receive the same level of attention as auditory and metabolic contributors. This reflects the growing body of evidence that cranial-cervical structures can significantly influence tinnitus perception.
Dentists undertake a comprehensive evaluation of temporomandibular joint (TMJ) dysfunction, assessing joint mechanics, loading patterns, and disc behaviour. This occurs alongside screening for bruxism (teeth grinding), both sleep-related and awake, given its strong association with muscular hyperactivity and referred ear symptoms.
Occlusion relationships and the presence of joint inflammation are also reviewed, as these can contribute to altered sensory input along the trigeminal pathway.
Physiotherapists complement this by performing a detailed cervical assessment, examining posture, segmental mobility, cervical-cranial alignment, and myofascial integrity. Palpation of trigger points in the sternocleidomastoid, upper trapezius, masseter, and sub-occipital muscles is routine, as these structures frequently refer symptoms into the ear.
Clinicians also evaluate for neural irritation, including involvement of the greater occipital, auriculotemporal, and trigeminal branches, which can interplay with auditory circuits at the level of the dorsal cochlear nucleus.
A key part of this assessment involves exploring whether the tinnitus can be modulated through somatic manoeuvres such as jaw protrusion, clenching, lateral deviation, neck rotation, or
resistance-based movements which are interpreted as a meaningful clinical sign that implicates musculoskeletal or neural pathways in the tinnitus experience. When modulation is present, it helps clinicians triage patients more effectively toward targeted interventions, such as TMJ stabilisation, bite-splint therapy, cervical physiotherapy, myofascial release, dry needling, posture correction, or trigeminal-focused neural-modulation strategies. This structured and deliberate approach not only improves diagnostic clarity but also expands the therapeutic avenues available, reinforcing the message that many tinnitus presentations are both interpretable and treatable when somatosensory mechanisms are properly investigated.
Iatrogenic contributors are also carefully evaluated. Medications such as aminoglycosides, platinum-based chemotherapeutics, loop diuretics, high-dose s alicylates, certain antidepressants, anti-epileptics and anti-malarials are well recognised for their ototoxic potential. Withdrawal from benzodiazepines or antidepressants may also provoke tinnitus due to acute neurochemical shifts. Non-pharmaceutical factors, including acoustic trauma from MRI scanners or surgical drilling, traumatic ear wax removal, ototoxic ear drops in the presence of tympanic membrane perforation and dental procedures involving prolonged mouth opening or high-frequency drilling, are also considered.

Image: Celene McNeill.
“Meaningful improvement, often resolution, is achievable when tinnitus is approached as a multisystem symptom and addressed within a coordinated, patient-centred, multidisciplinary framework.”
sound generators, notch therapy, auditory training, tinnitus retraining therapy (TRT) and, when required, hearing implants. These are supported by structured audiological counselling, regular follow-up and monitored by questionnaires such as Tinnitus Reaction Questionnaire (TRQ) and Tinnitus Handicap Inventory (THI).
Although complete resolution is less common in tinnitus caused purely by sensorineural hearing loss, a significant reduction in tinnitus perception, improvements in function and quality of life are routinely achieved when audiological treatment is integrated with broader care. When metabolic abnormalities are identified, treatment may involve dietary modification, medical management of glucose or lipid disorders, correction of micronutrient deficiencies and hormonal treatment when appropriate.
Seminar outcomes showed that addressing metabolic dysfunction can lead not only to symptom reduction but, in many cases, total elimination of tinnitus perception.
Preventative education plays a critical role in reducing recurrence. Psychological support is incorporated early. Cognitive behavioural therapy, acceptance and commitment therapy, mindfulness-based approaches and sleep-focused interventions help patients reduce tinnitus-related distress, enhance emotional regulation and improve habituation.
When psychiatric intervention is required, appropriate medication management further supports recovery.
An innovative feature of the seminar was a mind–body workshop for tinnitus patients and professionals with participants using dance and music as tools for teaching auditory anatomy, sensory integration and autonomic regulation.
This approach promoted relaxation, acceptance and social connection, and participants reported immediate benefit. While not a substitute for clinical treatment, such interventions may offer meaningful adjunctive support.
Psychological contributors are assessed in parallel rather than as an afterthought. Psychiatric and psychological evaluation focuses on anxiety, depression, panic symptoms, insomnia, hyper-vigilance and catastrophic thinking patterns. These factors may not cause tinnitus but strongly influence the degree of distress and the ability to habituate.
Audiological rehabilitation forms the therapeutic backbone in most cases. Interventions may involve hearing aids,

Vascular causes are addressed according to their underlying mechanism. Treatment may include medical management of hypertension, thyroid disease or anaemia; weight management and cerebrospinal fluid regulation for idiopathic intracranial hypertension; endovascular interventions such as venous sinus stenting; or surgical management of vascular tumours or fistulas. Many patients experience substantial improvement once blood-flow turbulence is corrected.
Somatosensory tinnitus is managed through dental and physiotherapy interventions, often with excellent outcomes. TMJ rehabilitation, splint therapy, cervical physiotherapy, manual therapy, dry needling, myofascial release, postural correction and treatment for bruxism or malocclusion are commonly employed.
Numerous cases presented demonstrated complete resolution once musculoskeletal contributors were treated.
Iatrogenic tinnitus is managed through careful medication review, supervised tapering of medication when appropriate, counselling on ototoxic risks, protection against high-level clinical noise and rehabilitation for TMJ or cervical strain after dental or surgical procedures.
The Brazilian model demonstrates that thorough assessment and interdisciplinary collaboration significantly improve diagnostic accuracy and treatment outcomes. It also highlights variability in international systems. Brazilian ENTs generally have more clinical availability and fewer surgical obligations than Australian ENTs, who manage higher surgical loads and serve a population with a substantially lower ENT-per-capita ratio.
Brazilians may consult ENTs directly but Australians must obtain a GP referral for Medicare coverage. This barrier can delay care, particularly when GPs lack specialised training in tinnitus assessment.
In Australia, audiologists are well placed to be the first port of call due to in-depth hearing health expertise. But many cases involve systemic, vascular or musculoskeletal factors that need medical oversight. Developing clearer referral pathways, stronger inter-professional relationships and broader diagnostic frameworks may enhance outcomes for Australian patients. The Brazilian model demonstrates meaningful improvement, and in many cases, complete resolution, are achievable when tinnitus is approached as a multisystem symptom and addressed within a coordinated, patient-centred, multidisciplinary framework.


Audiology Australia’s main professional development event for the 2026-27 CPD cycle will be in Sydney in May 2026.
Delegates at Audiology Australia’s immersive, hands-on event The Sound Exchange ’26 will dive deep into one of four specialised audiology streams, each delivered through two days of expert-led masterclasses.
Attendees can register in one stream during the main program on days two and three, 12-13 May 2026, at Accor Stadium, Sydney Olympic Park.
They can also register for one of three optional pre-conference workshops on the afternoon of day one, 11 May 2026.
Ms Leanne Emerson, CEO of Audiology Australia (AudA), says The Sound Exchange ’26 is the organisation’s number one practical and immersive event for the 2026-27 CPD cycle.
She says it supports practitioners to gain practical skills and knowledge in a subject matter of their choosing.
“By grouping you with other attendees of your chosen stream throughout the duration of the event, you’ll be encouraged to remain focused as you deep dive into a specialised area of audiology,” she says.
“Each session flows on from the next, supporting you to gradually build your competencies through hands-on practice, guided application and real-world learning. By the end of the event, you’ll be able to
take what you learn from the conference to the clinic.”
Emerson says AudA wanted to bring back at least one of the leads from its sold-out streams at the 2024 conference.
“This led to us resecuring the compelling Mr Dominic Power, who will once again lead the popular Management of Chronic Conductive Hearing Loss in Adults,” she says.
“We have Professor Harvey Dillon, Ms Lucy Shiels, and Dr Grace Nixon, who will co-lead the Assessment and Management of Children with Listening Difficulties stream. Harvey needs no introduction given his tremendous impact and presence in the sector, while Lucy’s and Grace’s research focusing on various areas of auditory processing disorder make them the perfect co-leads.”
Dr Philippa James will lead the stream on Identification and Support of Tinnitus and Hyperacusis.
“Philippa trained under Ms Myriam

Westcott and her approach integrating cognitive behavioural therapy, acceptance and commitment therapy, and mindfulness psychosocial strategies into her clinical practice makes her an ideal fit for bringing together the stream’s various learning goals,” Emerson says.
Mr Keith Chittleborough, an independent Melbourne audiologist, will lead the Extending Your Diagnostic Test Battery stream.
“Keith has made waves in the audiology community these last few years thanks to his increasing social media presence, and we are excited for his stream’s take on sharing underused clinical tools and why they matter, to help give audiologists the confidence to use them back in the clinic,” Emerson says.
The optional workshops allow audiologists to upskill in an additional subject matter to their stream. They are also compelling options to choose on their own if delegates can’t make the rest of the conference, she adds.
“The Sound Exchange ’26 is Audiology Australia’s number one practical and immersive event for the 2026-27 CPD cycle.”
Leanne Emerson Audiology Australia





Professor Harvey Dillon, Macquarie University, and Ms Lucy Shiels and Dr Grace Nixon, both from The University of Melbourne and Melbourne Hearing Care Clinic
This stream focuses on diagnosing and addressing listening difficulties, including auditory processing disorders, in children. It introduces a relatively new, cohesive test battery assessing abilities that may affect speech identification in noise. Participants will have hands-on experience administering and receiving the tests. Explanations of the tested abilities and an overview of typical result patterns will be complemented by clinical case studies. It covers management options including an overview of auditory training programs, wireless remote microphone technology and low-gain hearing aids. Evidence supporting options will be reviewed, along with clinical considerations such as device options, validation and funding considerations. Approaches and options discussed are also applicable to adults.
Mr Keith Chittleborough, Earman Audiology
Audiology is more than selling hearing aids. It is excellent diagnostics and smart clinical decision-making and then selling hearing aids. Many powerful diagnostic tools are left ignored. Most aren't complicated and some are already installed on computers. They have the potential not just to change patients’ lives, but to make our work more rewarding and more profitable. We’ll take a handful of underused clinical tools, show you when they matter, and give you the confidence to use them in the clinic. Some include: Otoscopy –we’ll compare your otoscope to digital camera otoscopy, head-loupes and a medical microscope; Extended high-frequency audiometry, because the cochlea doesn’t magically stop at 8kHz; Speech testing in noise: Are you ANL, ACT or QuickSin curious? Let’s play those lists together; DPOAES: Great diagnostic audiologists do them. Want to follow their example?

Mr Dominic Power, Melbourne Hearing Care Clinic
The diagnosis and management of conductive and mixed hearing loss is fundamental in audiology. This stream will review pathologies associated with conductive hearing loss and new trends in medical and surgical treatment for adults and children. It will focus on the audiologist’s role in rehabilitation and options available for clients where there has been a fundamental change in their ear geometry. There will be practical guidance on the fundamentals of taking an ear impression and more complex procedures for ears requiring mastoid packing. It will review device options including ear mould and hearing device selection, software settings and hands-on training with contemporary bone conduction devices. *Note, this contains the same learning goals as The Sound Exchange ’24 so if you attended that, we recommend taking another stream.

Dr Philippa James, Melbourne Hearing Care Clinic and DWM Audiology
Tinnitus is common and debilitating among help-seeking patients presenting to audiology clinics. So is hyperacusis which develops in half of patients with bothersome tinnitus but is under identified and rarely supported in clinical practice. How can we as audiologists best support our patients with bothersome tinnitus and associated reduced sound tolerance? This clinically focused stream will explore tinnitus history-taking, education, counselling, support avenues and referral pathways. It will review and provide hands-on opportunity to explore tinnitus assessment and support tools including questionnaires, tinnitus apps, and tinnitus features in current hearing aid technology. A review of hyperacusis identification and support will be included, including an overview of device options that can support desensitisation.
Each workshop lasts for three hours and is taught by several speakers.
“In the Towards Managing Sub-Clinical Hearing Difficulties: From Identification to Intervention workshop, Dr Bec Bennett, Dr Sriram Boothalingam, Dr Jess Monaghan and Mr Matt Croteau from the National Acoustic Laboratories will share tools and strategies that clinicians can use to work more effectively with adults with sub-clinical hearing difficulties,” Emerson explains.
“This is a population group that has traditionally been underserved, and we are excited for these strategies to be shared at the conference.”
Sharing the News, a workshop chiefly led by people with lived experience of hearing loss – a topic highly requested by AudA members – highlights the importance of hearing directly from consumers, ensuring the content is grounded in real-world experiences and reflects what truly matters to those living with hearing loss.
“Sydney Children's Hospital Network head of audiology Ms Fiona Duncan, clinical psychologist Ms Alice Brennan
and Deaf Children Australia’s Ms Renee Fayad and Ms Tamara Trinder Scacco will be running the workshop, sharing how audiologists can further support families of children when they first receive the news that their child is deaf or hard of hearing,” Emerson says.
“Finally, Ms Celia Gomes Chapman and Mr Trong Nguyen from Interacoustics will run a workshop titled The Right Balance: Enhancing your vHIT and VEMP Technique, which is a hands-on, practical session designed to help audiologists with a demonstrated interest in performing vestibular assessments.”
More than 20 exhibitors comprising a variety of retailers, educational organisations, industry suppliers and manufacturers will participate in a trade expo.
Delegates can network during morning tea, lunch and afternoon tea breaks, and there will be a dedicated chance for networking at a welcome reception at Accor Stadium on the Tuesday night,
12 May which will feature drinks, canapes and entertainment.
Fifteen CPD points are on offer for the live event – 12 points (category 1.1 and 1.4) for the masterclass stream and three points (category 1.4) for a workshop. Five additional points (category 1.2) will be made available for those who watch the online learning package which is included in all full registrations.
“As always, attendees will be able to save by registering by our early bird deadline –11 March 2026,” Emerson says. “Audiology Australia members also enjoy additional savings over non-members, and, to support the next generation, we provide a considerable reduction in registration fees for student members who are looking to upskill while studying.
“If you want a PD opportunity where you can take what you learn from the conference to the clinic the next day, and where you’ll be left with a series of actions to further build your clinical competencies, The Sound Exchange is the event for you.”
Register at soundexchange.com.au.


ENT surgeons and nurses will converge on Hobart in March for the 76th ASOHNS annual scientific meeting and otorhinolaryngology nurses conference.
The latest advancements in surgical techniques, emerging technologies, and evidence-based practices that are shaping the future of ENT care will be explored at the 76th ASOHNS annual scientific meeting.
The Australian Society of Otorhinolaryngology, Head and Neck Surgery (ASOHNS) annual scientific meeting is the largest gathering of OHNS surgeons, surgical trainees, registrars and medical students in Australia and New Zealand.
The meeting, at the Hotel Grand Chancellor Hobart, will be from Friday 20 to Sunday 22 March 2026. It will be in conjunction with the Otorhinolaryngology Head & Neck Nurses Group (OHNNG’s) 29th annual scientific conference on 20 and 21 March 2026.
Workforce, innovation, sustainability and excellence are the themes of the ASOHNS meeting. Hobart ENT surgeon Dr Dan McCormick is convenor of the meeting, with the scientific program led by Melbourne ENT surgeon Dr Sor Way Chan.
They say the program will feature a diverse range of keynote speakers, interactive workshops, and cutting-edge research presentations.
“The ASOHNS meeting has always been a cornerstone event for our community, fostering collaboration, innovation, and knowledge-sharing among specialists from across the country and beyond,” the convenors say.
Dr Julie Agnew, ASOHNS president, adds:
“We are excited by the opportunity to host the 76th ASOHNS ASM in the exciting and beautiful city of Hobart for the first time since 1991.
"A beautiful and welcoming state like Tasmania is an excellent conference location. The subspecialty team has been working hard to assemble a panel of local and international speakers that will inspire all of us.
“We hope to discuss some of the challenges of regional Australia including workforce, sustainability and remoteness through an exciting program.”
Mr Marin Duvnjak, OHNNG president, says the nurses conference continues its tradition of bringing together nursing professionals from across Australia to share insights, latest clinical practices, and innovations in ENT and head and neck care.
“The program will feature expert-led presentations, case studies, and interactive discussions focused on advancing patient outcomes and professional development,” he says.



to paediatric mastoiditis, osteomyelitis, melioidosis and computer vision models to identify anatomical structures in endoscopic ear surgery.
Pre-conference workshops for ASOHNS delegates on Thursday 19 March include a paediatric ENT workshop, Indigenous health workshop, head and neck ultrasound workshop, and a complex airway symposium.
Other ASOHNS events include a trade exhibition, welcome reception, gala dinner, women in ENT breakfast and Lark guided whisky tasting tour.
A welcome reception at the Hotel Grand Chancellor on the Friday evening and a gala dinner at Wrest Point Casino on the Saturday night are open to delegates from both surgeons’ and nurses’ conferences.
Otology sub–committee member Dr Claire Iseli has co-ordinated a strong otology program that highlights the positive collaboration and multi-disciplinary teams within the specialty. Sydney ENT surgeon Professor Catherine Birman and ENT surgeon Dr Peter Monksfield from Birmingham, UK will be keynote speakers for this program.
Audiologist Dr Jaime Leigh from The Royal Victorian Eye and Ear Hospital, who is clinical lead, Victorian Cochlear Implant Program, will also present.
In the general otology concurrent session, topics range from the ergonomics of endoscopic surgery and the 3D exoscope in otologic and lateral skull base surgery,
Artificial intelligence is another popular topic in general otology, with presenters to discuss how AI is revolutionising hearing loss diagnosis, an AI tool for post grommet follow up to support ENT surgery delivery, cholesteatoma mapping using AI, and AI classification of middle ear disease.
The implantable hearing technology concurrent session covers topics ranging from cochlear implant revisions to implant outcomes using local anaesthesia in the very elderly, expanding implant candidacy and device use in single sided deafness.
The impacts of cochlear implants on functional balance will also be discussed along with long term safety and performance of a new active transcutaneous bone anchored hearing implant system.
Topics explored in a concurrent session covering vestibular and lateral skull base will include Medicare funded deafness genetic testing, implications for health services of registration of audiologists, head injury and hearing loss, pulsatile tinnitus, vestibular schwannoma and stapedial synkinesis.
For more information and to register for the ASOHNS conference visit asm.asohns.org. au/au.
For more information and to register for the nurses’ conference, see ohnng.com.au/ registration/.
A consultant laryngologist at the National Centre for Airway Reconstruction, Imperial College Healthcare, London, Dr Al Yaghchi manages the full spectrum of laryngeal disorders with specialist interest in airway stenosis and complex dysphagia. He has a PhD in molecular oncology studying oncolytic viruses in head and neck cancers and an active clinical research program in voice, airway and swallowing disorders. An internationally renowned specialist in gender-affirming voice surgery, he introduced several voice feminisation procedures to the UK including his own modification to the Wendler Glottoplasty technique and vocal fold muscle reduction. He is a founding member of the International Association of TransVoice Surgeons.
Prof Birman is an ENT surgeon at the Children’s Hospital at Westmead, Royal Prince Alfred Hospital, Macquarie University Hospital, and Hornsby Ku-ring-gai Hospital in Sydney. She specialises in paediatric and adult cochlear implants, otology and paediatric ENT. Prof Birman has extensive experience in hearing loss and cochlear implants having performed more than 2,000 cochlear implant procedures. She has published and presented extensively on cochlear implant outcomes, innovative cochlear implant devices, bone conduction implantable hearing devices, and paediatric conditions. Prof Birman has participated in several clinical trials and grants, including the gene therapy trials involving BDNF and NT3 DNA using electroporation; and adenovirus vector gene therapy for congenital OTOF genetic auditory neuropathy.


The Representative Director of Withsim Clinic, Bundang, South Korea, Dr Cho graduated from Korea University in Seoul, South Korea, and trained in otolaryngology-head and neck surgery at Korea University Anam Hospital. He maintains an active busy practice using ultrasound, focused exclusively on patients with a lump on the neck including thyroid nodules, salivary disease, lymphadenopathy and soft tissue diseases. Dr Cho is active in research on office-based head and neck ultrasound performed by surgeons and ultrasonography-guided procedures (radiofrequency ablation, sclerotherapy and core needle biopsy). He has overseen more than 20 international and domestic head and neck ultrasound courses for surgeons.
Prof Gross completed a head and neck surgery and oncology fellowship at Memorial Sloan Kettering Cancer Centre and has since developed an international reputation as a thought-leader in head and neck cancer. He is currently professor in the Department of Head and Neck Surgery and medical director of perioperative surgical services at MD Anderson Cancer Center. Prof Gross’s clinical and research interests focus on improving functional outcomes using transoral robotic surgery (TORS) for HPV-associated oropharynx cancer and neoadjuvant approaches to head and neck cancers including aggressive cutaneous squamous cell carcinoma (CSCC). He is an expert in surgeon-led clinical trials, including a registrational-intent randomised phase three trial using neoadjuvant immunotherapy for advanced, resectable CSCC.


A professor of otolaryngology – head and neck surgery at the University of South Florida College of Medicine, Dr Magnuson is a pioneer in the field of robotic surgery for the head and neck. He is also the founding partner of AdventHealth Medical Group Otolaryngology and Head & Neck Surgery at Celebration, medical director of head and neck surgery, AdventHealth Florida and chief medical officer of the AdventHealth Nicholson Center. A specialist in treating patients with tumours or cancer of the head and neck with expertise in head and neck reconstruction after cancer surgery, Dr Magnuson is dedicated to ongoing research, clinical trials and training on trans oral robotic surgery (TORS).
Director of endoscopic skull base surgery and a professor of otolaryngology and, by courtesy, of neurosurgery at Stanford, Prof Patel is an expert in advanced endoscopic sinus and skull base surgery, treating patients with a wide variety of rhinologic complaints, including chronic sinus infection or inflammation, sinus disease that has failed medical therapy, and olfactory disorders. Prof Patel continues to perform research in the areas of endoscopic sinus surgery and chronic rhinosinusitis in the immunosuppressed patient population and is collaborating with neuroscientists and engineers to develop technology that she hopes will eventually help cure patients with olfactory loss.
Dr Thevasagayam is a consultant ENT/airway surgeon at the Sheffield Children’s Hospital and the clinical director for surgery,. He is also an examiner and member of the European Board of ORL-HNS and DO-HNS. Dr Thevasagayam is the honorary secretary for the British Association for Paediatric Otolaryngology. His interests include airway surgery, sleep surgery, drooling, sialendoscopy and inducible laryngeal obstruction. Dr Thevasagayam is interested in non-technical factors and cognitive bias and has lectured on the Hillsborough Disaster and learning from error.



Hearing Practitioner Australia is the only dedicated business-to-business publication for the nation’s hearing industry. Established out of a desire for premium, local and independent content for audiologists, audiometrists, otolaryngologists/ENTs and other Australian hearing professionals, HPA brings industry-specific reporting and analysis, in addition to the latest in news, business, products, policy, and research, plus more.

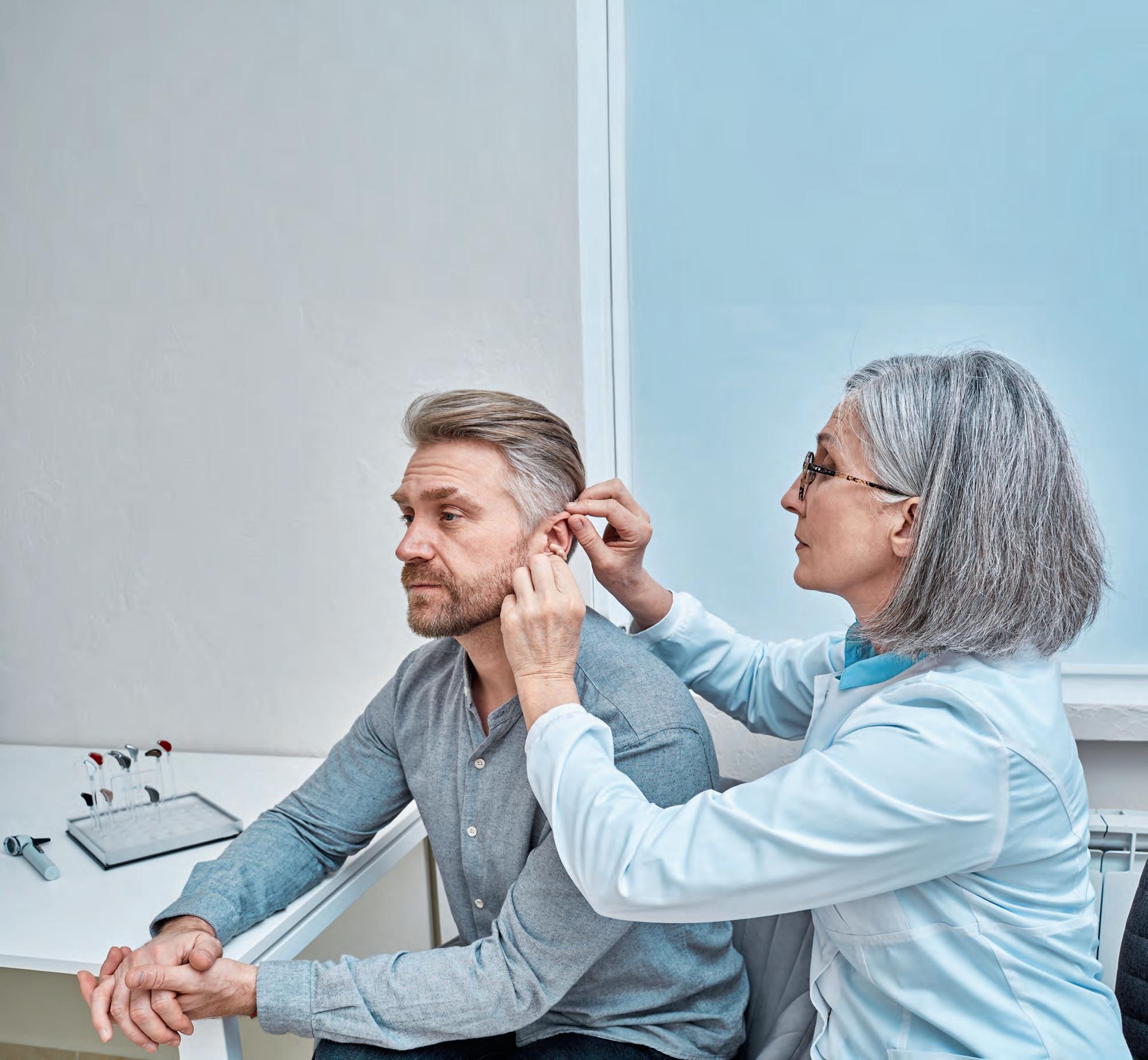


DR CHRISTO BESTER reviews two decades of electrocochleography-guided cochlear implantation, revealing recent success of real time hearing monitoring during surgery is helping preserve residual hearing.
ochlear implants are remarkably effective devices for restoring hearing in severe-toprofoundly deaf patients; except he modern candidate increasingly presents with serviceable residual low-frequency hearing, with some implanted with mild or even normal hearing thresholds below 1 kHz. When preserved, this ‘residual’ hearing significantly improves speech perception and quality-of-life outcomes. However, even with enhanced soft-surgery approaches and improved electrode design, about half of all recipients lose functional hearing during or after surgery. With real-time hearing monitoring, we have an opportunity to change this.
In the early 2010s, The University of Melbourne's Department of Otolaryngology, led by Professor Stephen O'Leary, began exploring a novel approach: using the cochlear implant electrode array itself to record acoustically evoked potentials during
This intracochlear electrocochleography (ECochG) captured the cochlear icrophonic (CM), a response primarily generated by the outer hair cells, directly from the implanted array. Using the implant's electrodes substantially enhanced recording quality, with successful recordings in individuals with up to 100 dB HL at the stimulation frequency.
Campbell and colleagues (2016) demonstrated feasibility, while O'Leary et al. (2020) showed that observational real-time CM recordings could predict hearing outcomes at three and 12 months post-operatively. A 30% CM drop predicted double the hearing loss compared with those showing preserved CM.
But this was feasibility, not clinical
utility. Signal interpretation required expert review in theatre, adding another trained observer. Real-time analysis was limited and confounded by unclear signals in moderate-to-severe hearing loss. Signal variability made interpretation controversial: fluctuations occurred even when hearing was preserved, possibly from interference between hair cell and neural potentials. Implementation barriers remained substantial.
We needed to demonstrate that surgeons could use ECochG feedback to improve outcomes. In 2022, we conducted the world's first randomised controlled trial of ECochG-triggered intervention. When surgeons were informed of CM drops during insertion, they could pause and slightly withdraw the electrode, allowing recovery before proceeding.
The intervention group showed significantly better hearing preservation (69% preserved versus 34% in controls).
The recently published Andonie et al. (2025) study in JAMA Otolaryngology represents a major advance. Analysing 112 patients across three international centres (Melbourne, Bern, and Zurich), the team implemented fully automated, objective ECochG analysis – no expert interpretation required.
The Australian investigators included myself and Dr Sudanthi Wijewickrema from The University of Melbourne Department of Surgery and Otolaryngology, and the department’s Prof Stephen O’Leary from The Royal Victorian Eye and Ear Hospital in Melbourne.
Not all CM events are equal. Persistent events (those from which CM amplitude never recovered) carried an adjusted odds ratio (OR) of 31.58 for hearing loss. Events happening near insertion end, representing most major CM decreases, occurred in the vulnerable region beyond 270° where the basilar membrane appears to be most susceptible to mechanical trauma, showing an even stronger association with hearing loss (OR 52.96).
Compared with our original, naïve 30% CM drop threshold, these automated approaches are substantially superior, as considering all CM events regardless of context showed much weaker association (OR 5.05).
These automated algorithms work independent of patient age, preoperative hearing levels, or implantation centre. With 77% of patients showing measurable CM responses, the approach is broadly applicable.
If automated analysis integrates into surgical tools in all operating theatres, insertion trauma may become limited to a small proportion of recipients. The addition of upcoming dexamethasone-eluting arrays could be another step-change toward hearing preservation. Complete hearing preservation (to within 10 dB of pre-operative thresholds) could become the norm. Instead of 23-30% (hearing) preservation rates, we may achieve preservation in most of our implant recipients.
Cochlear implantation already has substantially lower penetration in adults – only 10% of those who would benefit are implanted. If hearing preservation becomes reliable, how might we expand criteria? How do we counsel patients when expectations shift from "you'll likely lose residual hearing" to "we expect to preserve it"?
Technical challenges remain; 23% of our recipients lacked adequate CM signals to support interventional approaches. But the trajectory is clear: cochlear health monitoring has moved from experimental technique to evidence-based, automated clinical tool nearing routine delivery. The question for Australian clinicians: How do we optimise outcomes when preservation, not loss, becomes our baseline expectation?
ABOUT THE AUTHOR: Dr Christo Bester, a scientist who specialises in cochlear electrophysiology and cochlear mechanics, is research lead in clinical neurophysiology at Ear Science Institute Australia. He works jointly with Ear Science and the University of Melbourne Department of Surgery and Otolaryngology.








Extra support from support staff is a win for everyone, says CHEDY KALACH and HEATHER JOSEPH from the Australasian College of Audiometry.


CONTRARY TO THE BELIEF THAT TRAINING STAFF CONSUMES TIME THAT YOU DO NOT HAVE, WHEN DONE WELL, IT MULTIPLIES SKILLS AND EFFICIENCY.
hat if there was a better way to work smarter, not harder – increasing productivity while reducing workload and improving patient satisfaction?
You may be thinking this sounds familiar or unrealistic. It might work for others, but not for your clinic. If so, please hear us out.
You are experienced clinicians who stay current with technology, research, and professional standards. Through continuing education and engagement with professional bodies, you ensure the best possible outcomes for your patients. This is foundational – a non-negotiable – but perhaps there is a way of structuring your clinic that could better support how your time is used.
Assuming you have front-of-house staff or client service officers handling administrative tasks, what is their retention rate, and do they have genuine job satisfaction?
You have support staff because you need to be in clinic and do not have time to manage claims, organise appointments, and handle everything else. We hear you. However, are they always fully utilised while you are seeing patients?
Do you run late because a patient needs extra time, find you cannot proceed due to a wax build-up and are left with an unexpected gap, or discover that fittings or technical issues take time away from patients with more complex needs?
Individually, these moments feel minor. Collectively, they reduce appointment utilisation and quietly erode valuable clinical time.
If this resonates, we understand. And if your view is that a great front-of-house team is just as important as the clinician – first impressions matter and last – we completely agree. If a client is not welcomed well from the outset, it can quickly become an uphill battle.
Having worked in business and vocational training for many years, what we have seen repeatedly is that some of the strongest students are those already working in the industry or actively seeking a clear pathway forward. They are familiar with, or eager to learn, industry protocols, integrate well into clinical practice, and are receptive to training.
Have you asked your support staff whether they would be interested in progressing their career and becoming a clinical audiometrist? Could this be an opportunity lost if it is never explored?
It is often said that investing time and money into training staff is wasted because they will leave. The familiar response is: but what if they stay? Perhaps the more important question is what you are offering them in terms of job satisfaction and career progression.
PATHWAYS FOR TRAINEE AUDIOMETRISTS
If you already have front-of-house staff – or are recruiting – why not consider offering a pathway to become a trainee audiometrist?
While there is no formal traineeship in audiometry, employment contracts can still be structured in a traineeship-style arrangement.
Hiring or upskilling the right person – someone who fits your clinic culture – is often more important than the skills they currently possess. Skills can be taught; attitude and cultural fit are far harder to instil.

This model already works across many professions: dentists with hygienists, doctors with nurses, radiologists with radiographers, ophthalmologists with orthoptists, and beyond.
The Diploma of Audiometry offered through the Australasian College of Audiometry (AuCA) is a flexible, industry-designed course created by audiologists to address workforce training and retention
challenges. It equips students with essential clinical skills alongside the professional competencies required in modern practice.
In practice, this can involve an agreement with an existing employee, or a traineeship-style condition within a new employment contract, supported by a post-qualification clause. This attracts candidates seeking a career rather than just a job. A typical structure may involve a four-to-five-year commitment: qualification, internship, and post qualification employment.
During training, staff become increasingly valuable to the clinic –not only after qualification.
Because the program is vocational, staff can continue administrative work while gradually transitioning into clinical tasks as their competence grows. This frees clinicians to focus on complex care. For trainees, the benefits include job security, professional progression, improved satisfaction, and a nationally accredited qualification. If staff do leave, it is usually due to life circumstances. Agreements can include repayment clauses, but regardless, you have contributed meaningfully to someone’s long-term career and to the care of future patients.
Once qualified, staff progress through their ACAud inc. HAASA internship and become true clinical assets. With trained team members sharing the load, clinics can see more patients, focus on complex cases, or create space to work on the business — not just in it. Contrary to the belief that training staff consumes time that you do not have, when done well, it multiplies skills and efficiency.
One final thought: would you rather have trained staff leave after five years, or untrained staff stay for five years? Sustainable practices are built on culture, opportunity, and mutual respect – not just financia incentive.
Workers’ compensation lawyer STRATOS SAVVAS explains a noise-induced hearing loss case and implications.

THE MERE PRESENCE OF NOISE IN AN INDUSTRY IS NOT ENOUGH TO ESTABLISH LIABILITY; THE ACTUAL LEVEL AND DURATION OF EXPOSURE MUST BE CAPABLE OF CAUSING THE INJURY.
STRATOS SAVVAS
In a judgment handed down in 2025, the South Australian Employment Tribunal dismissed a worker's claim for compensation against a former employer for noise-induced hearing loss (NIHL). The case involved a detailed exploration of the ‘last noisy employer’ rule, with the central issue being which employer (if any) was responsible for the claimant’s hearing loss.
The claimant was diagnosed with NIHL and sought compensation for hearing loss. He had a history of working in noisy environments, including at an engineering company where he was employed for four years from 2012 to 2016. He subsequently worked for another engineering company (2017-2018) and then became the sole director of a business from 2018 onwards. The claimant brought his claim in November 2020 against a company that owned the first engineering company and was seeking to hold them liable. He claimed they were the last employer capable of causing his hearing loss. This was despite the fact that he had worked for two further employers after the first company.
Section 188(2) of South Australia’s Return to Work Act 2014 (RTW Act) states that unless there is proof to the contrary, a worker’s hearing loss is presumed to have arisen from the employment where they were last exposed to noise capable of causing such injury.
This ‘last noisy employer’ or ‘last in time’ rule is replicated in several
states, excluding Queensland. The rule simplifies the issue of liability for progressive conditions such as industrial deafness, where it is difficult to pinpoint exactly which employer caused the injury, and to what extent.
The ‘last noisy employer’ presumption still operates in Queensland, however the employer has an additional statutory right to seek contribution from previous employers who also exposed the worker to hazardous noise.
The tribunal heard evidence from the claimant, a former colleague, and two ear, nose and throat surgeons – one for the worker and one for the employer. They accepted the claimants' evidence that he spent limited time on-site (one to two hours a week) during his time with the second company and his business.
When on-site, he primarily communicated with workers, who would stop noisy work such as jackhammering while he was nearby. Both experts agreed this exposure was unlikely to have caused hearing loss. The tribunal was therefore satisfied that employment at the second company and his own business did not involve exposure to noise capable of causing the claimed hearing loss.
The tribunal then examined the claimant’s employment with the first engineering company. He alleged spending one to two hours daily on the workshop floor, where there was constant noise from welding, grinding, and cutting, though he admitted to wearing hearing protection at the time.

The tribunal then heard from the expert witnesses. The ENT surgeon for the claimant initially opined that the exposure with the first company was sufficient to cause NIHL, but in cross-examination he conceded that one to two hours of exposure at 91dB daily, while wearing hearing protection, might be within safe levels.
The consistent view of the ENT surgeon who gave evidence on behalf of the first company was that the noise levels at that company were unlikely to cause NIHL.
The tribunal ultimately preferred this evidence.
The tribunal found that the claimant successfully rebutted the presumption that employment at his last two workplaces caused his hearing loss. The onus then shifted to the company that owned the first workplace to prove that his duties there could not have caused the injury.
It was also held to have successfully rebutted the ‘last noisy employer’ presumption, as the evidence demonstrated the noise exposure during the claimant's employment there was not at a level capable of causing NIHL. Therefore, the tribunal confirmed the original decision to reject the claim for compensation.
This decision has several important implications for workers' compensation claims in South Australia and potentially other states, as well as for employers generally. Most notably, the ruling confirms that the legal presumption placing liability on the last employer can be defended, via robust, fact-specific evidence.
It also underscores the need for employers to maintain detailed records of workplace noise levels, the duration of exposure, and the use of hearing protection.
Lastly, the decision highlights that the mere presence of noise in an industry is not enough to establish liability; the actual level and duration of exposure must be capable of causing the injury.
For employers generally, the decision may encourage those in noisy workplaces to invest in noise surveys, ongoing audiometric testing, and noise control measures to proactively manage risk and gather data for potential future claims.
It also validates the importance of mandating and ensuring the correct and consistent use of hearing protection in the workplace.
Leadership matters now more than ever, says healthcare tech leader and audiologist DAWN ROLLINGS, as she discusses balancing business success and compassionate care in modern healthcare leadership.

that the intersection of business acumen and compassionate care is not just possible – it’s essential. My journey in healthcare leadership has been shaped by experiences where the needs of patients and staff could not be separated from the realities of running an efficient organisation.
I’ve seen firsthand how focusing solely on one side – whether financial performance or human connection – creates gaps that ultimately affect everyone. True leadership is about striking a dynamic balance, ensuring operational goals never overshadow the fundamental mission to care for people.
Leadership matters now more than ever. Modern healthcare leaders must navigate competing priorities, rapid change and the diverse needs of individuals and organisations. It’s a complex role requiring continual adaptation, strategic thinking and genuine compassion.
For decades, there has been a belief that strong leadership and genuine patient care are mutually exclusive, particularly in healthcare, where business priorities are sometimes seen as detracting from care. After more than 20 years in the field, I can confidently say this view is outdated. The best leaders seamlessly integrate compassionate care with effective business operations.
Running a healthcare organisation is not simply about turning a profit or keeping the doors open. Financial sustainability is essential to continue serving patients, employing staff and investing in innovation. But achieving this while delivering outstanding care is what
defines great leadership. It takes skill to manage resources, drive innovation and meet business targets without losing sight of the humans at the centre of it all – patients, families and staff. The most effective leaders inspire excellence while fostering empathy, trust and support.
One of the most pressing challenges for leaders today is workforce diversity. Healthcare teams often span four generations – Baby Boomers, Generation X, Millennials and Generation Z – each bringing different values, communication styles and expectations.
As a result, leaders must be flexible and adaptive. A one-sizefits-all approach is no longer effective. Flexibility means recognising that what motivates one person may not resonate with another, embracing new technologies while respecting the experience of seasoned professionals.
Listening actively, communicating transparently and being open to learning from others are essential leadership skills. Trust and open dialogue ensure team members feel valued and understood, strengthening both engagement and performance.
Resilience is another critical leadership quality. Healthcare and health technology are defined by constant change – from policy shifts and technological advances to global challenges such as the COVID-19 pandemic. Leaders must withstand pressure, recover from setbacks, and guide their teams through uncertainty.
Resilience isn’t about toughness alone. It’s about modelling calm decision-making, providing clarity and helping others find stability during turbulent times. Leadership sets the tone for organisational culture, shaping how staff engage with their work and how care is delivered.
I’ve seen how compassionate leadership can transform teams during difficult periods. When my
own team faced increased patient demand and staff shortages, prioritising open communication, regular debriefs and genuine support improved morale, strengthened unity and led to better patient outcomes. It reinforced my belief that caring leadership is not just compatible with operational success – it is essential to it.
Learning and innovation
Great leaders are committed to lifelong learning and open to innovation, including artificial intelligence. Used thoughtfully and ethically, AI can enhance decision-making, streamline administrative tasks and improve patient outcomes. By staying curious and collaborating with technology rather than resisting it, leaders ensure their teams are prepared for the future of care.
My studies toward a Doctor of Business Administration in International Business Communication have further shaped my leadership approach. They’ve strengthened my understanding of cross-cultural communication, strategic thinking and global trends – skills increasingly vital in diverse, multi-generational teams. These insights support clearer communication, stronger connection and more informed decision-making.
The ripple effect of leadership Leadership has a far-reaching impact. A leader’s actions influence morale, motivation and performance, shaping workplace culture and patient experience alike. When leaders act with integrity, empathy and vision, they inspire collaboration, growth and excellence.
Being a leader is a privilege that carries responsibility. It offers the opportunity to support others, shape careers and create a positive ripple effect across organisations and communities.
Name: Dawn Rollings
Qualifications: Audiology (BAAT I & II, Nat Dip MPPM UK) MBA
Affiliation: Starkey Hearing Technologies
ANZ managing director
Location: Sydney, Australia
Years in industry: 20+
"LEADERS
MUST WITHSTAND PRESSURE, RECOVER FROM SETBACKS, AND GUIDE THEIR TEAMS THROUGH UNCERTAINTY.”

Dr Amy Szarkowski has started a new role at NextSense Institute with a conjoint appointment at Macquarie University and the Australian Hearing Hub. A highly experienced psychologist with expertise in supporting young deaf or hard of hearing children and their families, she brings a wealth of knowledge from clinical work at Boston Children’s Hospital, leadership as ex-director of The Institute at the Children’s Center for Communication/Beverly School for the Deaf and pivotal contributions to the International Consensus Guidance on Family-Centred Early Intervention for DHH children. Her teaching and research spans Gallaudet University, Harvard Medical School, UMass Boston and Miyazaki International College.

Ms Emma Russell has been promoted to key account manager at Cochlear. She is excited to bring the learnings and experience from her previous account manager role to this new position, with a renewed focus on strengthening referral pathways and supporting the development of Cochlear implant programs across NSW. Russell graduated with a Bachelor of Science in Clinical Audiology, achieving first class honours in the UK in 2007. Since then, she has worked across the NHS, alongside ENT specialists, within hearing-aid manufacturers, and in a range of clinical roles. Across every role, her passion has remained the same: ensuring that everyone who needs it has access to the gift of hearing.

Mr Adam Mennella is GN Hearing’s new product specialist for northeast Queensland. He completed a Master of Audiology Studies at the University of Queensland, then for the next five years worked at many Bay Audio (later renamed Amplifon) locations in Brisbane. He gained experience in adult rehabilitation in private and government settings including understanding Hearing Services Program operations, training and mentoring graduates and new interns, solidifying his expertise in communication and hearing aid fittings, and expanding his passion for the Australian audiological community. In his new role, Mennella continues to increase and amplify client outcomes by supporting clinicians.
Hearing Implants Australia has two new audiologists, Ms Yashaswini Shivegowda (right) and Ms Mona Zabeti (left). Shivegowda completed her Bachelor of Audiology and Speech-Language Pathology at India's JSS Institute of Speech and Hearing and recently her Masters of Audiology at Macquarie University. She specialises in adult rehabilitation with sub-interests in vestibular, hearing aid and implantable solutions care. Zabeti, a highly qualified audiologist, specialises in adult vestibular assessment and rehabilitation. She completed audiology studies in Iran and has practised as an audiologist for more than 10 years. She's ACAud inc. HAASA certified and is doing the Macquarie University Masters of Audiology.


Ms Lisa Singer has been promoted to Cochlear key account manager, partnering with hearing health professionals nationwide to enhance patient access and strengthen clinical collaboration. After completing her Masters of Clinical Audiology at the University of Melbourne in 2009, she worked in hospitals and clinics across Australia and the UK, including The Royal Children’s Hospital, Barwon Health and Great Ormond Street Hospital. Her passion for equitable hearing care has taken her to remote communities in the NT, Pacific Islands and Zambia. Singer joined Cochlear ANZ in 2018. In her new role she hopes to expand access to cochlear implant services and foster stronger partnerships across the hearing industry.


Cochlear has promoted Ms Ashleigh Cowan to key account manager. She has a Masters of Audiology from UQ and degrees in psychology and business from QUT. She began her career with Attune, working across Queensland. She later became regional audiology and sales manager at Oticon, supporting Queensland, the NT and northern NSW, where she fostered relationships with hearing partners, coordinated national training, presented at events, and contributed to global product launches. As an audiologist interested in technology, it was a goal to work for Cochlear. Since joining Cochlear in 2023, she's focused on advocating for hearing health and innovation, and strengthening support for implant candidates, recipients, and providers.
To list an event in our calendar please email helen.carter@primecreative.com.au

WORLD HEARING DAY
Worldwide 6 March who.int/campaigns
76TH ASOHNS ASM Hobart, Australia 20-22 March asm.asohns.org.au
ACAUD INC.HAASA NATIONAL CONGRESS 2026 Gold Coast, Australia 22-24 April acaud.com.au
AMERICAN ACADEMY OF AUDIOLOGY AAA 2026 San Antonio, Texas 22-25 April audiology.org/aaa-annual-convention
QLD TEMPORAL BONE COURSE
Brisbane, Australia 8-9 May asohns.org.au
AUDIOLOGY AUSTRALIA’S THE SOUND EXCHANGE ‘26 Sydney, Australia 11-13 May soundexchange.com.au
IAA MEANS BUSINESS: BOOKKEEPING LIKE A BOSS Online recording 19 May independentaudiologists.net.au
WCA 2026 WORLD CONGRESS OF AUDIOLOGY Seoul, Korea 24-27 May wca2026seoul.com

inc. HAASA’s National Congress
will
ST VINCENT’S 41ST TEMPORAL BONE COURSE Sydney, Australia 19-21 June asohns.org.au
VCAA 2026 7TH VIRTUAL CONFERENCE ON COMPUTATIONAL AUDIOLOGY Online 25-26 June computationalaudiology.com
2026 AUSTRALIAN DEAF GAMES Sunshine Coast, Australia 4-11 July austdeafgames.org.au

Quality you can count on
Your patients depend on the technology you fit. Your reputation does too. That’s why, at Starkey, we put our hearing aids through the industry’s most comprehensive quality control process – so that every pair you fit performs as reliably on Day 1,000 as it does on Day One.
We push endurance and durability to the max – so our technology can be fit and worn with confidence.
• 500+ hours of high-stress testing
• Pro8 HydraShield® waterproof system is rated beyond IP68
• Significant investments made in quality innovations
Our custom products have an all-new shell resin that is up to 20x tougher.
Stronger material without sacrificing the ability for making modifications in the field.




