













Balfour Beatty plead not guilty in nuclear site fatality prosecution
CJC consults on new rules governing the use of AI in preparing court documents
says Law Society
13 Another expert has a bad day
ACCOUNTANCY
15 Avoiding potential problems caused by share plans
16 Periodical payment orders vs lump sum settlements – is one better than the other?
17 Government to crack down on gambling operator sport sponsorship
17 More than £1.1m seized in currency exchange raid
DIGITAL FORENSICS
19 Authenticity in internal investigations: a digital forensics perspective
POLICE CUSTODY
21 Behind the cell door: expert eyes uncover healthcare claims in custody
LIPREADING
22 When the camera speaks: the forensic lipreader in modern litigation
FORENSIC DOCUMENT EXAMINATION
23 Forensic document examiners – the gatekeepers of authenticity
PROPERTY, CONSTRUCTION & ENGINEERING
25 When metal fails before the law: the science of metal failure extends to the courtroom
27 Boundary, rights of way & easement disputes: expert evidence can decide the outcome
29 Engineering insight is crucial in structural defect litigation
FIRE INVESTIGATION
30 Industry flags lift fire safety as critical risk in major retrofit programmes
31 Nearly half of all fire safety inspections unsatisfactory
MARITIME DISPUTES
32 Cargo at risk in times of geopolitical conflict
EQUESTRIAN ACCIDENTS
33 When equestrian sport turns to forensic scrutiny
ENVIRONMENTAL ISSUES
34 The fiduciary duty disconnect: who has responsibility on climate?
35 Pollutions cost farm over £18,000
TREES AND THE LAW
36 Branching out: the growing role of arboricultural experts in legal cases
37 Why health & safety is too important to be left to chance
TRANSLATING & INTERPRETING
39 Mistranslation is not a minor error: it is an evidential risk



NEWS
49 Costs judge caps medical agency mark-ups at 25% in expert fee ruling
51 MDU responds to PAC report on reducing the costs of clinical negligence
53 Law on AI must be changed to protect injured people
53 BAPRAS marks anniversary with travelling exhibition
55 Expert witness in Lucy Letby trial did not disclose hospital investigation
57 Clinical negligence victims ‘need closure’ as case delays hit record highs
59 Mother dies after being given wrong antibiotics
61 Addenbrooke’s Hospital agrees £1m settlement in stroke misdiagnosis case
63 RCP responds to the publication of the National Cancer Plan for England
64 Surgical drain was left in woman’s body for 11 years after hysterectomy
URGENT CARE
65 Urgent care claims require experts in front-line clinical practice
CARDIOLOGY
67 BCS signs joint statement of support for the ‘BRITISH’ trial
VASCULAR SURGERY
68 Chronic limb-threatening ischaemia
SEPSIS IN A&E
71 Sepsis in the emergency department: recognising the ‘red flags’ is crucial
DELAYED DIAGNOSIS
72 Seconds count – the consequences of diagnostic delay in time-critical claims
ORTHOPAEDICS
73 Clarifying care standards is central in shoulder and elbow surgery claims
75 Orthopaedic surgery comes under scrutiny in complex injury disputes
77 Orthopaedic expertise in an evolving legal landscape
79 ARMA launches new strategy to make musculoskeletal health a national priority
81 The medicolegal implications of complications following spinal surgery
83 Foot and ankle surgery: functional impact is key in assessing claims
85 The 1% problem: how known surgical risk becomes misinterpreted as negligence
87 Hand surgery: recent UK claims and the role of expert evidence
HARLEY STREET
91 The Harley Street advantage: prestige and professionalism can strengthen a case
UROLOGY
93 Litigation claims in urology contribute to significant NHS payouts
DENTISTRY & MAXILLOFACIAL SURGERY
95 Implant failure and how it affects the cost of a claim
OBSTETRICS & GYNAECOLOGY
99 Royal colleges respond to interim investigation report
99 Report shows rise in endometriosis diagnosis times
OCCUPATIONAL THERAPY
100 Functional impact, not just diagnosis: the occupational therapist’s medico-legal contribution
PSYCHIATRIC & PSYCHOLOGICAL ISSUES
101 Assessing neurodiversity in the family court
103 UK’s top psychiatrist raises alarm over threat posed by ‘silent mental health pandemic’
103 BPS welcomes guidance that unregulated psychologists should not give evidence
105 Behind the scenes of psychological assessments in legal cases
PAEDIATRIC CARE
106 Small patients, big consequences: the growing complexity of paediatric litigation
ENT SURGERY
107 Sound judgement: ENT cases demand careful expert evidence
BURNS LITIGATION
109 Burns litigation in the spotlight
HERNIA SURGERY
111 Hernia surgery under the microscope as claims rise
OPHTHALMOLOGY & OPTOMETRY
113 ‘Utilise primary care’ to



[EXPERT EVIDENCE has never been more visible, or vital, across the legal landscape. High-profile cases show how lapses in health and safety can have devastating consequences – and how expert testimony is central to both establishing accountability and guiding regulatory compliance. On a construction site or in court, specialist insight can be the difference between clarity and confusion, justice served and lessons not learned.
• As courts handle increasing volumes of complex evidence, new rules governing AI in court documents are shaping expert engagement. From automated summaries to predictive analytics, AI promises efficiency –but raises questions about accuracy, bias and the integrity of expert opinion. Traditional skills, from forensic document examination to lipreading analysis, remain essential, with human oversight ensuring nuanced interpretation is never lost.
• Financial expertise continues to play a pivotal role. Debates over Periodical Payment Orders versus lump sum settlements highlight the importance of long-term planning, risk assessment and clear modelling. Experts help the courts understand projected care needs, inflation and award sustainability, proving that meticulous analysis is as crucial in finance as it is in forensics.
• Safety and risk extend beyond boardrooms. Behind the cell door, health and safety in police custody demands expert scrutiny to ensure welfare, interpret incidents and evaluate compliance. In the built environment, fire safety in residential and commercial properties is under intense focus – including evacuation plans and firefighting access.
• The physical world also presents complex challenges. Metallurgical and welding disputes rely on forensic insight, while boundary and rights-of-way cases demand precise historical, legal and technical knowledge. Even in conflict zones, experts assessing cargo must consider logistics, contractual obligations and risk exposure.
• Environmental and animal-related disputes are similarly intricate. Whether investigating injuries, land management or liability, these specialists operate at the intersection of natural behaviour, human activity and statutory frameworks, showing that expertise is not just knowledge – it’s context.
• Across all disciplines, one principle remains constant: precision matters. Every report, opinion and calculation contributes to a chain of evidence courts rely on. From forensic lipreading and document authentication to financial projections or structural assessments, expert credibility underpins both justice and safety. In an age of AI, global conflict and complex regulations, the expert witness is not a luxury – they are essential guarantors of accuracy and fairness.
• Today’s cases are diverse, yet share a common thread: the need for clear, defensible and authoritative expertise. Whether in court, a factory or a police cell, expert witnesses turn knowledge into actionable understanding and ensure that when the facts matter most, they are understood – and acted upon. q
Ian Wild, Director of Business Development Your Expert Witness





[BALFOUR BEATTY GROUP LIMITED have pleaded not guilty to health and safety offences following a worker fatality at AWE plc's Aldermaston nuclear site. The infrastructure company appeared at High Wycombe Magistrates Court for a prosecution instigated by the Office for Nuclear Regulation (ONR), the UK’s independent nuclear regulator.
The company is facing two health and safety charges following alleged breaches of the Health and Safety at Work etc. Act 1974 Section 2(1), and 3(1).
[ THE CIVIL JUSTICE COUNCIL (CJC) has launched an eightweek consultation to address whether procedural rules are needed to govern the use of AI by legal representatives for the preparation of court documents, such as:
• Statements of case
• Skeleton arguments and other advocacy documents
• Witness statements
• Expert reports
Part 8 of the consultation also examines this question in relation to experts in the preparation of their reports.
It cites the Bond Solon Expert Witness Survey 2025, which reported that 20% of respondents had used AI in their role as an expert witness and suggested that ‘perhaps this is the time for strong guidance from the judiciary in terms of court rules, protocols and case law dealing with AI’.
It also cites the American case of Kohls v Elison No 24-cv-3754 (D Minn 10 January 2025) in which an expert witness used AI to draft his report and accidentally submitted misinformation.
The CJC proposes extending the statement of truth in PD35 3.3 to allow a further requirement that ‘the expert explains what use of AI has been made other than for transcription (or other administrative uses) and that the expert identifies the AI tools used’.
The consultation remains open for responses until 14 April 2026.
The many issues arising from the use of AI are of vital importance for all expert witnesses and the subject will be covered in depth at the Bond Solon Expert Witness Conference on 6 November. You can attend the conference venue in Westminster and benefit from the networking opportunities that this brings. Alternatively, if your preference is for virtual attendance, then Bond Solon are live-streaming the event and you will be able to view and interact with the live sessions, engage and connect with other delegates and sponsors via the conference app.
All of the speakers’ talks are being recorded and will be available to virtual and in-person delegates to watch on the conference app after the event.
A corporate booking discount is available for group bookings. Visit www.bondsolon.com/courses/bond-solon-expert-witness-conference/, email expertwitness@bondsolon.com or call 020 7549 2549 for more information. q
They relate to an incident which occurred at the Aldermaston site in West Berkshire on 6 July 2023 when a 58-year-old male construction worker from East London died after sustaining fatal injuries.
The trial date has not yet been scheduled. ONR will announce details of the date and location of the trial when available.
ONR regulates the work at AWE's Aldermaston and Burghfield sites, which covers the entire life cycle of nuclear warheads – from initial concept, assessment and design, through to component manufacture and assembly, in-service support, and finally decommissioning and disposal.
The incident was a conventional health and safety matter and there was no radiological risk to the public. q




[
PIECEMEAL REFORM of the criminal justice system – a vital public service – will not tackle the court backlogs, the Law Society of England and Wales warned ahead of the second reading of the Courts and Tribunals Bill in March.
“A fair, coordinated, whole-system approach, including sustained investment in the workforce, infrastructure and technology, is needed to restore confidence in this vital public service,” said immediate past president of the Law Society Richard Atkinson.
“The UK government must also reduce the overall volume of cases entering the system and take action to resolve persistent failures of prisoners being brought to court on time."
Ahead of the second reading the Law Society said:
• Removing a defendant’s right to elect jury trial and moving to judge-only hearings are significant departures from Sir Brian Leveson’s recommendations and we oppose them
• The government’s modelling does not provide good enough evidence that judge only trials would reduce the backlogs

• If the government insists on implementing the Crown Court Bench division, this radical change proposed by Sir Brian of a judge sitting with two magistrates should be tested by a pilot against the twin objectives of ensuring trials are fair and reducing the backlogs
• Retrospectively removing the right to jury trial to defendants already in the system
will lead to legal challenges causing further delay and uncertainty for victims and defendants
• The bill will result in more unrepresented defendants in the magistrates’ courts unless the legal aid means test there is levelled up with that for the Crown Court
• Retaining large volumes of cases in the magistrates’ courts will result in lower remuneration for criminal legal aid solicitors, putting further pressure on already fragile legal aid firms. This is despite the claim in the impact assessment that there will be no impact on small firms.
“There are no quick fixes,” Richard Atkinson added, “the government must avoid implementing standalone measures that risk diminishing fairness and trust in the system, such as changing from jury trials to judgealone, particularly without convincing evidence they will bring the backlog down significantly.
“Piecemeal reforms accompanied by isolated injections of funding will not be enough to restore this vital public service back to health.” q


By Chris Makin chartered accountant, accredited civil mediator and accredited expert determiner
[ RECENTLY I wrote about Jeff Davidson, a friendly chap I had known for many years and, like me, one of the early practitioners of forensic accounting. He came a cropper in a case concerning the ‘diversion’ of £1,900,000,000 (yes, really!) from a Ukrainian bank. This was a huge case which was heard over 43 days, with one claimant (the bank), eight defendants and a huge crowd of KCs and junior counsel in what must have been a very crowded courtroom.
The crux of the expert’s behaviour was that he was disciplined for an unconnected matter and was excluded from membership of ICAEW, but he didn’t tell anybody. The fact that Jeff had been criticised in other cases, and the fact that the Charity Commission are investigating the whereabouts of £500,000 from a charity of which he and his wife were sole trustees (now removed) didn’t help him. And when it came out that he was no longer a chartered accountant and shouldn’t be acting as an expert witness, one of his responses was a refusal to be examined on these other cases from a fear of selfincrimination. That says it all.
They say that you wait ages for a bus, and then three come all at once. Well, I am determined to act properly as an expert so that I don’t become the third bus – but we do have a second bus, and again he is an expert with a high profile, who I have known for many years. He is a chartered accountant called Vivian Cohen.
The case was Peter Marples & Ors v Secretary of State for Education [2025] EWHC 2794 (Ch). The facts of the case are simple. Marples had been a partner at KPMG and the lead partner in their education service. After he left KPMG, he and his family set up a company to provide apprenticeship training services. He had a valuable contract for that with the Skills Funding Agency, part of the DfE.
The company was to be sold, so Marples told the SFA of the change in ownership. Their chief executive replied, disapproving of the purchaser. The deal collapsed, the Marples family lost £27m plus a possible £10m in loan notes, and the company lost its contract over allegations of data manipulation, causing its shares to be worthless.
The Marples family brought a claim against the DfE for negligence and misfeasance in public office. The outcome is not relevant to us, though I believe the claim failed. But what does interest us is the behaviour of the Marples’s expert, one Vivian Cohen. Interestingly, the expert for the opposing party was the same Jeff Davidson, though this time he did not come under criticism. I merely question how he could practise as an expert now with no professional qualification.
Now, any litigation lawyer will know off by heart the words of Lord Wilberforce in Whitehouse v Jordan [1981] 1 All ER 267, as I do: “The report of the expert shall be the independent product of the expert, uninfluenced as to form and content by the exigencies of litigation.”
These words resound through Cresswell J’s seminal case of the Ikarian Reefer [1993] and the Civil Procedure Rules. In short, the expert’s opinions are their own, and neither instructing lawyer nor client can interfere with them. And it’s not only the expert’s report: Questions of the Expert and the Joint Statement of Experts are part of the report, and they become the expert’s evidence in chief at trial. They are his/her opinions alone.
So what happens if the client insists on playing a part in writing the expert’s report and the joint statement? Knowing Vivian as I do, he is a really gentle gentleman, and I can see that he would find it hard to resist if Mr Marples, who I do not know, approached him at all forcefully. But such an approach led to dire consequences for Vivian and for Mr Marples.

It emerged (the judgment does not say how) that Mr Marples, himself a qualified accountant, had worked closely with Mr Cohen both in writing the expert report and in compiling Mr Cohen’s part of the Joint Statement. An application was made to the court for permission of this expert’s evidence to be revoked, or for this evidence to be given no weight. This was serious; it would have left the claimant family with no expert evidence.
But after repeating much of what I say above about experts and the CPR, the trial judge said: “The expert’s role is to provide independent assistance to the Court by way of objective unbiased opinion on matters within their expertise.” This is fundamental to all the expert work I do, and it should apply to all experts – indeed, it must.
The judgment sets out the degree of involvement which Mr Marples had in Mr Cohen’s work, the number of times drafts were passed between the two of them. Mr Cohen even warned Mr Marples not to tell the solicitors the two of them were working together, so he knew full well that this was improper.
The judge, Rajah J, even said that he did not know the extent of the joint working: “I do not accept that I have been given the full story of the involvement of Peter Marples in the preparation of Mr Cohen’s expert report and the joint statement. It seems to me that both have approached the work on expert evidence as a joint exercise, with Mr Cohen happy to defer to Mr Marples as the client.”
The conclusion was unavoidable: “I have no confidence in Mr Cohen’s ability to act in accordance with his obligations as an expert witness. I accordingly refuse the claimants permission to rely upon the evidence and reports of Mr Cohen.”
There was a further embarrassment for Vivian. The judge pointed out that he had been criticised as an expert at least twice before.
In Pepe’s Piri Piri Ltd v Aljunaid [2019] EWHC 2097 (Ch) the judge said he had ‘approached the exercise more as an advocate than as an expert complying with the requirements of CPR Part 35’ and for having expressed an ‘understanding of his role as being to present the case of the party instructing him in the most favourable light’. That’s so wrong!
When he was reminded of that case by the judge, Vivian said he couldn’t remember it. Again, that says it all. q
[ CHRIS MAKIN was one of the first 30 or so chartered accountants to become an Accredited Forensic Accountant and Expert Witness – see www. icaew.com/about-icaew/find-achartered-accountant/find-anaccredited-forensic-expert

He is also an accredited civil and commercial mediator and an accredited expert determiner. Over the last 30 years he has given expert evidence at least 100 times and worked on a vast range of cases. For CV, war stories and much more go to the website at www.chrismakin.co.uk – now with videos! q


By Sarah Anderson, director of RM2 Employee Ownership Ltd
[WHEN REVOLUT’S SHARE PLAN controversy left former employees facing unexpected and significant tax bills, many company directors probably assumed it was a problem faced only by big companies. But the issues it highlighted – confusion over tax treatment, poor communication with leavers and incorrect assumptions about plan rules – can arise in businesses of every size.
For any business where share plans form part of the reward package, getting this wrong carries consequences far beyond a tax bill. If the plan behind it is poorly structured or badly managed, you are not just creating a legal and tax headache, but breaking faith with the people who backed you.
Share plans sit at the intersection of employment law, tax law and corporate governance. It is this complexity that catches companies out in predictable ways.
The most common failure is not considering what happens when someone leaves. Many businesses allow former employees to retain options or shares without fully understanding the tax consequences. What looked like a valuable benefit can become a liability for the employee, whilst the reputational and legal exposure for the company can be severe.
Tax-advantaged schemes such as the Enterprise Management Incentive (EMI) or Company Share Option Plan (CSOP) can be enormously effective, but their advantages are conditional. The right paperwork, processes and professional advice must be in place not just at the point of setup, but at every key moment: annual HMRC filings, grant, exercise and any corporate events such as funding rounds, restructurings or exits.
Leaver provisions are also rarely considered with sufficient care. Should departing employees keep their shares, potentially expanding your share register over time, or should the company retain the right to compel a sale, and if so, at what price?
If a corporate transaction arises and the business has lost contact with some of its shareholders, the consequences can range from the inconvenient to the deal-threatening. Is your share register accessible to the team responsible for employee offboarding, so that appropriate actions can be taken promptly?
Communication is another common failure point. Vague promises about what shares will be worth or how they will be taxed, without the detail to support them, store up trouble. Tax treatment can change and corporate structures evolve, so what was true at grant may not be true at exercise. When employees discover the gap between expectation and reality, the fallout is rarely quiet.
Five steps to keeping your scheme safe
A well-structured, properly managed scheme remains one of the most effective ways to align your team with the long-term success of the business, but the plan should be a living document, not a box to tick at the outset.
Consider leavers: decide upfront whether options should lapse on departure and under what circumstances. Good and bad leaver provisions need to be clearly defined in the plan rules, aligned with the Articles of Association and understood by participants. Internal procedures must ensure that leaver treatment is dealt with promptly and consistently.
Plan rules: tax-advantaged schemes carry real benefits that can be lost if the rules are not followed correctly. Take advice at the point of grant, at the point of exercise and whenever anything significant changes in the business, ideally beforehand.
Communicate clearly: you do not need to explain every possible tax scenario to every participant, but you do need to flag the moments that matter: when tax positions might change, when decisions need to be made and when individuals should seek independent advice.

Don’t overpromise: avoid making definitive statements about tax outcomes or financial returns, which depend on factors outside the company’s control, such as legislative changes or the individual’s personal tax position.
Review regularly: a plan that works well for a business at one stage of its development may be wholly unsuitable as the company grows, restructures or changes ownership. Regular reviews are a valuable investment in the integrity of the promise made to your team, and a clear signal to option holders that the company takes its obligations seriously.
The Revolut story will fade from the headlines, but the lesson it offers is permanent: equity is only as valuable as the trust that surrounds it. Get the structure right and your share plan becomes one of the most powerful tools available to your business. Get it wrong and it could undermine the trust you have worked hard to build. q

By Elen Davies-Kay, client director at Frenkel Topping
[
FRENKEL TOPPING exists to enhance life after life-changing events, combining unmatched knowledge, experience and understanding with a complete commitment to every individual the company works with.
I’ve been part of Frenkel Topping for over ten years, and I’m very proud to be a member of this team that works solely with vulnerable clients in the financial advice space – it enables us to become immersed in the communities we serve and to gain a unique perspective on our clients’ needs.
For me, as well as my team, this helps us to keep the focus on getting the best outcomes to create brighter tomorrows for our clients.
My colleagues and I all bring a distinctive skillset to this mission. I am so lucky to work with clients that inspire me every day, and I’m privileged to support, guide, and help clients and their families. A key part of this role for me is to ensure that my clients all receive the best advice that is tailored for them.
One of the questions I’m often asked by lawyers is whether a Periodical Payment Order (PPO) is better than a lump sum settlement. What is crucially important to remember is that there is no such thing as a ‘one size fits all’ approach. Every client is
different and therefore every approach needs to be different. As financial advisers, we are often asked the question ‘do you think a PPO or lump sum settlement is best?’ Although I may have an instinct of what could be better for the client thanks to the experience I’ve gained over the years, it would be remiss of me to suggest either option without undertaking a full analysis.
That analysis involves using complex cashflow modelling tools together with detailed mathematics to see what levels of risk are involved for the client and what both options are able to provide for the client longer term.
As someone who deals with vulnerable individuals every day, I’m passionate about ensuring that every settlement is right for each of my clients because I’ve spent my career understanding what vulnerable clients need. Our clients often come to us from a place of trauma, recovering from a life-changing injury. It’s my job both to support their solicitor achieve an appropriate settlement, and to give them as much support and reassurance whilst they navigate their post settlement chapter in life, helping them understand how the settlement


can work for them and what life could look like for them and their family.
A PPO can provide certainty and help clients feel secure that these costs are futureproofed at the conclusion of their claim. In many cases, claimants might need to factor in care and case management costs, a change or even an end to their career and potentially deputyship costs. The security, tax and low risk nature of a PPO could offer huge reassurance, particularly if these costs are running at a high level or when considering uncertainty surrounding life expectancy.
On the other hand, there are clients that feel strongly about wanting a clean break from the defendant – a PPO can’t provide that, but a lump sum can, and it’s vital that we take client preference into consideration when making recommendations.
I’m always happy to have discussions with the client at the right stage in their case and support a solicitor when talking to their clients in order to explain what either position could look like after settlement. My support can also take the form of an analysis report of the settlement for solicitors ahead of Joint Settlement Meetings (JSMs) so they can walk in with a strong argument to help secure the best outcome for their client.
I am often found attending JSMs in person together with my laptop and analysis tools, to offer my guidance and expertise, as offers are coming in from the other side, in order to help support the instructing solicitor and counsel determine whether those offers are right for the client, ahead of agreeing and finalising settlement. q
• If you have a case that you’d like to discuss with one of our experts, contact the team via email; enquiries@frenkeltopping.co.uk
[UNLICENSED GAMBLING OPERATORS
face being blocked from sponsoring British sports teams, including Premier League clubs, as the Government sets out plans to consult on a ban as part of its crackdown on illegal gambling.
Ministers are deeply concerned about the dangers posed by the unlicensed gambling market, which has been linked to organised crime. Unlicensed operators do not adhere to laws and guidelines designed to protect customers, including mandatory financial vulnerability checks, responsible advertising and fair terms. They often lack data protections, leaving customers vulnerable to fraud and identity theft.

The government’s new consultation on sports sponsorship, to be launched this spring, will mitigate the risks associated with the illegal market and help eliminate unfair competition for properly regulated firms.
Culture Secretary Lisa Nandy said: “When placing a bet on the big match, fans deserve to know the sites they’re using are properly regulated, with the right protections in place. It’s not right that unlicensed gambling operators can sponsor some of our biggest football clubs, raising their profile and potentially drawing fans towards sites that don’t meet our regulatory standards.”
The new measures would mean gambling companies without a UK licence would be restricted from entering into any sponsorship arrangements with sports clubs, including in the Premier League, where a number of clubs currently carry sponsorship from operators not licensed in Great Britain.
Last year the Premier League voluntarily committed to removing all gambling sponsorship from the front of shirts by the end of the 2025-26 season.
However gambling operators, including those that are unlicensed, are currently able to strike deals, including logos on shirt sleeves, that give them a major presence in the country’s most-watched sports league.
Clubs are currently not acting unlawfully in maintaining these sponsorship arrangements as long as the gambling operators are not accessible to UK consumers. However, ministers believe there is a
[OVER 100 HMRC OFFICERS were involved in a raid on a currency exchange office in London in October, seizing more than £1.1m in cash together with gold, electronic devices and paper records.
Investigators arrested seven men and searched nine business and residential properties along with four vehicles, as part of a criminal investigation into alleged money laundering.
The cash was seized under the Proceeds of Crime Act, along with gold, electronic devices and paper records. A further £120,000 was discovered during a search of one of the vehicles.
Margaret Mousley, Deputy Director at HMRC’s Fraud Investigation Service, commented: “We will always be on the side of the lawabiding majority and will investigate any business suspected of laundering the proceeds of crime. This is a significant amount of money, and the courts have agreed we can hold it for six months while our investigations continue.” q
strong case for stopping unlicensed sponsorship altogether given the brand visibility could drive consumers towards unlicensed sites operating outside the Gambling Commission’s regulatory protections.
Gambling Minister Baroness Twycross said: “We know the real harm that unregulated gambling can cause, exploiting vulnerable people and leaving consumers without the protections they deserve. This consultation, alongside the work of our Illegal Gambling Taskforce, shows how seriously this government is taking the issue. We will not hesitate to act where we see people being put at risk.”
This consultation forms part of the government’s separate, wider work to address concerns around gambling. In January, the government launched an Illegal Gambling Taskforce, bringing together major companies including Google, Mastercard, TikTok and Visa alongside law enforcement and gambling bodies to tackle illegal gambling.
The taskforce, led by Baroness Twycross, will focus on three areas: stopping illegal operators from advertising on social media platforms, preventing payments to unlicensed sites and improving cross-agency collaboration.
This work is distinct from the consultation, though both reflect the government’s broader commitment to protecting consumers and tackling illegal gambling. q


By Ryan Shields, digital forensics expert witness at S-RM
[ IN MY PREVIOUS ARTICLES , I explored the growing challenges of authenticity in the context of deepfakes and document disputes in litigation. Many of the same issues arise long before matters reach the courtroom – during internal investigations conducted by organisations in response to allegations of misconduct, regulatory concerns or whistleblowing reports.
In fact, internal investigations often present an even more complex evidential landscape, where decisions may be made on the basis of incomplete information, tight timelines and evolving factual narratives.
Internal investigations are increasingly data driven. Emails, instant messages, documents, system logs, call recordings and other digital data frequently sit at the centre of an investigation. As with litigation, the authenticity of this material is critical. If the evidence relied upon is incomplete, altered or misunderstood, the conclusions of an investigation – and the decisions that follow –may be fundamentally flawed.
The authenticity challenge when collecting evidence
Unlike litigation, internal investigations often begin informally. Data may be collected by IT teams, HR or external advisors before forensic specialists are engaged. In many cases, material is provided to investigators in the form of screenshots, PDFs, exported message threads or forwarded emails. While these may capture the apparent content of a communication, they rarely preserve the underlying metadata or contextual artefacts that allow authenticity to be properly assessed at a later date.
For example, a screenshot of an instant message may appear to evidence inappropriate conduct. However, without access to the underlying message database, it may be impossible to confirm whether the message was sent, received, deleted, edited or even fabricated. Similarly, an email forwarded as an attachment may lack routing information, server headers or timestamps that would allow an investigator to validate when and how it was sent.
Internal investigations frequently rely on employee cooperation and self-disclosure, which can further complicate matters. Devices may have been used for both personal and corporate activity, accounts may span multiple platforms, and records may be selectively produced. Without forensic discipline, investigators risk accepting evidence at face value when its authenticity has not been tested.
Source evidence and context are key
From a digital forensics perspective, the most reliable way to address authenticity concerns is through access to source evidence. This may include corporate laptops, mobile devices, servers, backups, cloud-based accounts such as Microsoft 365 and Google Workspace, or collaboration platforms like Teams and Slack. Source evidence allows investigators to move beyond isolated documents and reconstruct context. For example, forensic analysis may reveal draft versions of a document, evidence of copying or backdating, or contemporaneous communications discussing its creation. Message databases can show whether content was deleted, edited or forwarded, and whether screenshots align with actual records held on a device or server.
This contextual analysis is particularly important where employee accounts are disputed. In internal investigations, it is becoming

increasingly common for individuals to deny authorship of documents or messages, or to allege that evidence has been manipulated. Forensic artefacts –such as user account activity, device usage patterns and application logs – can corroborate or challenge these assertions in a way that standalone documents cannot.
importance of early evidence handling
One of the most significant risks to authenticity in internal investigations arises at the earliest stages. Well-intentioned actions – such as asking an employee to ‘send over’ relevant messages, copying files to a USB drive or taking screenshots for convenience –can irreversibly damage the evidential value of data.
Actions taken without forensic consideration may overwrite metadata, alter timestamps or destroy artefacts that indicate how evidence was created or modified. In some cases, investigative steps themselves can introduce doubt about authenticity, particularly if the matter later becomes subject to regulatory scrutiny or litigation. Once questions are raised about how evidence was collected, the focus can quickly shift from the alleged misconduct to the integrity of the investigation itself.
From a digital forensics perspective, the manner in which evidence is obtained is often as important as the content of the evidence.
The absence of a clear audit trail documenting who collected the data, when it was collected and how it was handled can significantly weaken the evidential weight of otherwise probative material. Where evidence has been selectively copied, manually curated or reformatted, it may no longer be possible to demonstrate that it represents a complete and accurate record.
Early engagement of digital forensics specialists can help ensure that evidence is preserved in a defensible manner. This does not necessarily mean full forensic imaging in every case, but it does require a clear strategy for evidence collection, preservation and review that anticipates potential authenticity challenges.
Proportionate steps – such as targeted forensic captures, preservation of cloud-based accounts or the secure acquisition of mobile device data – can safeguard key artefacts while minimising disruption to the business.
Authenticity is a foundational issue in internal investigations. As digital evidence plays an ever-greater role in shaping investigative findings, organisations must be confident that the material they rely upon is genuine, complete and properly understood.
From a digital forensics standpoint, authenticity is rarely established by reviewing documents in isolation. It is built through context, corroboration and careful analysis of source evidence. By recognising authenticity as a proactive consideration – and by involving forensic expertise early – organisations can conduct internal investigations with greater confidence, defensibility and integrity. q
• If you require support in relation to authenticity issues arising during an internal investigation, please don’t hesitate to contact me by emailing r.shields@s-rminform.com


[HEALTHCARE DELIVERED within police custody suites and places of detention is no longer hidden from scrutiny. In recent years, deaths in custody, allegations of neglect and concerns about safeguarding have attracted sustained public attention and rigorous legal examination.
For litigation solicitors, the instruction of experienced medical and nursing experts in this specialist field has become central to the effective investigation and presentation of both civil and criminal proceedings.

Custody healthcare sits at the intersection of medicine, law and public protection. Across the United Kingdom, clinical services in police stations are typically delivered by forensic nurses, advanced clinical practitioners, paramedics and, in some areas, forensic physicians. In prisons, primary care teams work alongside mental health in-reach and substance misuse services. These environments are governed by a distinct statutory and regulatory framework, including the Police and Criminal Evidence Act 1984 and its accompanying Codes of Practice, as well as oversight from bodies such as the Care Quality Commission.
For solicitors, the value of an independent expert lies not simply in clinical knowledge, but in contextual understanding. Detention settings present unique pressures: time-sensitive decision-making, incomplete histories, intoxication, behavioural disturbance and variable access to secondary care. The expert must be able to assess care against recognised standards, while appreciating the operational realities faced by custody staff and clinicians.
A significant proportion of claims and inquests concern suicide and selfharm. Detainees frequently present with complex mental health histories, substance misuse and acute distress. Experts are commonly asked to consider whether appropriate reception screening took place, whether known risk factors were identified, and whether observation levels and safeguarding measures were proportionate. Documentation is often pivotal: custody records, healthcare notes and risk assessment tools must be analysed to determine whether warning signs were missed or escalation pathways inadequately followed.
Substance misuse represents another high-risk area. Acute alcohol withdrawal, opioid toxicity and mixed drug intoxication demand careful monitoring and evidence-based intervention. Allegations frequently centre on failure to recognise deterioration, inadequate vital sign monitoring, or delay in transfer to hospital. A forensic healthcare expert will address whether assessment was sufficiently thorough, whether clinical scoring systems were applied correctly, and whether pharmacological management was appropriate. In fatal cases, the issue of causation may require detailed examination of timing, symptom progression and the foreseeability of collapse.
The use of force in custody introduces a further complexity. Where restraint precedes serious injury or death, expert opinion may be required on positional asphyxia, head injury, excited delirium and the interaction between restraint techniques and underlying pathology. Crucially, the expert will consider the medical oversight of the incident: was there adequate post-restraint monitoring, were red flags recognised and was timely medical escalation undertaken? Such analysis may be central in civil claims, criminal prosecutions or disciplinary proceedings.
Deaths in custody invariably engage the coronial jurisdiction. Inquests often explore not only individual clinical decisions but systemic failings. Independent experts assist the court by clarifying standards of care, identifying breaches where present, and addressing causation. They may also contribute to consideration of future risk and lessons to be learned. Given the public interest dimension of such cases, clarity, independence and methodological rigour are essential.
For instructing solicitors, careful expert selection is critical. This is a niche field requiring recent frontline experience in custody or prison healthcare, familiarity with multi-agency working, and a sound grasp of medico-legal duties under the Civil Procedure Rules.
Experts must be comfortable navigating large volumes of material, including CCTV logs, use-offorce records and incident reports, and distilling these into a coherent and balanced opinion.
As with all clinical negligence matters, the application of established legal principles remains central. The court will look to the expert to address whether the standard of care fell below that of a reasonably competent practitioner in that field, and whether any breach caused or materially contributed to the harm alleged. In custody cases, the added dimension of safeguarding vulnerable adults and the state’s duty of care heightens the scrutiny applied.
Healthcare in detention settings is, by its nature, delivered to a vulnerable and often marginalised population. The legal system has recognised that transparency and accountability are essential. For solicitors acting for families, detainees, public authorities or healthcare providers, early and strategic instruction of an experienced forensic medical or nursing expert can be decisive.
In an area where clinical judgement, custodial practice and human rights considerations converge, robust and independent expert evidence remains the cornerstone of fair and defensible outcomes. q


[WITH CCTV, body-worn video and mobile telephone recordings being routinely deployed in litigation, it is increasingly common for crucial footage to exist without usable sound.
Whether due to technical limitations, environmental interference or the absence of an audio function, the lack of recorded speech can leave a significant evidential gap. In such circumstances, the instruction of a forensic lipreader may prove highly significant.
A forensic lipreader is a specialist trained to interpret speech by analysing lip movements, facial expression and contextual features captured on video. They can provide a reasoned opinion as to what is likely to have been said, together with a clear explanation of the limitations inherent in the material examined. This can represent a valuable addition to the evidential landscape in both criminal and civil proceedings. In criminal matters, silent footage can assume particular importance. Exchanges between suspects prior to an alleged assault or dialogue captured within a custody environment may all carry probative weight. A forensic lipreader may be asked to consider whether threats were made, instructions issued or admissions expressed.
Such analysis can corroborate or undermine witness accounts, assist in establishing intent and clarify the sequence of events. In cases involving allegations of conspiracy or joint participation, even a brief exchange may be of considerable relevance.
The relevance of lipreading evidence extends beyond the criminal courts. In civil claims and personal injury litigation, disputes frequently arise as to what was said at a critical moment.
On construction sites, in industrial premises or during workplace operations, CCTV may record conversations where verbal instructions are central to liability. A claimant may contend that no warning was provided; a defendant may assert that clear directions were given. Where audio is absent, a forensic lipreader can assist the court by assessing whether the visible speech patterns are consistent with one version of events or another.
Conversations at the scene of a road traffic collision, exchanges between employees during a suspected staged incident, or discussions within commercial premises can be scrutinised. While lipreading evidence is seldom determinative in isolation, it may expose inconsistencies between

contemporaneous footage and subsequent accounts,.
For instructing solicitors, it is essential to recognise both the strengths and limitations of lipreading evidence. The reliability of any interpretation depends significantly upon video quality, frame rate, lighting, camera angle and the visibility of the speaker’s mouth. Obstructions, facial hair, rapid speech and regional variations in articulation may all affect clarity. A responsible expert will identify such constraints expressly and may provide a graded assessment of certainty rather than an absolute conclusion.
A compliant report should detail the expert’s qualifications, methodology, assumptions and any alternative interpretations considered. Courts are alert to the potential for overstatement, and lipreading evidence is ordinarily evaluated alongside other strands of evidence rather than in isolation.
Where silent footage lies at the centre of a factual dispute, early consideration of forensic lipreading expertise can assist in clarifying issues and informing case strategy. It has the capacity to convert silent images into meaningful, admissible evidence capable of assisting the court in determining what was, in all probability, said. q

[ IN AN ERA DEFINED by digital transformation and hybrid working practices, the written word remains at the heart of legal disputes. Contracts, wills, corporate agreements and other formal documents underpin countless civil and criminal cases.
Yet with the proliferation of electronic signatures, scanned documents and digital communication, courts are increasingly confronted with contested documents and questioned authenticity. In this landscape, forensic document examiners have emerged as indispensable expert witnesses, providing clarity and certainty where doubt could otherwise prevail.
Forensic document examiners are specialists trained to analyse the authenticity, origin and integrity of documents. Their work encompasses both traditional handwritten materials and digital records, spanning everything from contracts and letters to wills, deeds, and internal corporate communications.
In practice, these experts assess whether a document is genuine, has been altered or contains inconsistencies that might indicate forgery or fraud. By applying scientific techniques and established methodologies, they help courts distinguish between legitimate documents and material that has been manipulated.
The rise in electronic signatures and digital correspondence has added new layers of complexity to this work. Modern examiners are not limited to pen-and-ink analysis; they must also interrogate metadata, examine file histories and verify electronic signature protocols. In contested contracts, for example, the timing and provenance of an electronic signature can be crucial in determining enforceability. Similarly, in disputed wills, digital records and scanned copies may require careful scrutiny to ensure they faithfully represent the testator’s intentions. The hybrid nature of today’s working environment, with a mix of hard-copy and digital workflows, makes the expertise of document examiners increasingly relevant.
Traditional techniques remain equally vital. Handwriting comparison, ink differentiation, page sequencing and detection of physical alterations are all tools in the examiner’s arsenal. Advanced methods, such as ink dating or spectral analysis, can reveal subtle changes, while page substitution or layering may expose attempts to introduce fraudulent material. In civil and criminal proceedings alike, such findings can be pivotal, whether establishing the validity of a commercial agreement, confirming the authorship of a contested note or identifying falsified evidence in fraud investigations.
Crucially, forensic document examiners do more than provide technical assessments. Their role as expert witnesses extends to translating complex scientific findings into language the court can

readily understand. Reports must be impartial, clearly articulated and robustly reasoned, allowing courts to evaluate evidence without requiring specialist knowledge themselves. This ability to bridge technical detail and legal standards ensures that their conclusions carry weight and can withstand scrutiny during cross-examination.
The presence of a qualified document examiner can influence case strategy from the outset. Early instruction allows solicitors to identify potential weaknesses, corroborate witness accounts or challenge the authenticity of opposing evidence. In contested wills, for example, an examiner may clarify whether a signature is genuine or produced under duress. In criminal cases, their expertise can be critical in identifying forged identification documents or falsified records.
As disputes over written evidence continue to rise, the contribution of forensic document examiners is increasingly indispensable. By combining scientific rigour with clear, impartial explanation, these experts safeguard the reliability of documents that underpin legal claims. For solicitors, understanding when and how to instruct a document examiner is now central to managing risk, supporting client positions and ensuring that courts are presented with evidence they can trust.
In a world where a signature can be scanned, copied or digitally manipulated, forensic document examiners remain the gatekeepers of authenticity, providing courts with certainty amidst growing complexity. q


[MODERN INFRASTRUCTURE depends on complex engineered components and welded structures operating under demanding conditions – when those systems fail, the consequences often extend beyond engineering and into the courtroom.
Increasingly, courts face technical questions that only specialised metallurgical and welding experts can answer. Did poor fabrication lead to failure? Was inspection adequate? Did corrosion or a hidden metallurgical defect trigger the breakdown of a structure?
Once largely confined to sectors such as oil and gas or conventional power generation, these disputes are now emerging across a wider industrial landscape. Hydrogen infrastructure, energy-from-waste facilities and major civil engineering projects are pushing materials and fabrication processes into new territory.
As projects become larger and more complex, failures can involve significant financial losses, operational disruption and reputational damage. In such circumstances, expert evidence from metallurgists and welding specialists plays a vital role in helping courts determine where liability lies.
The forensic examination of welds and materials
One of the most common tasks for expert witnesses is assessing whether fabrication and welding were carried out correctly. Many structural failures can be traced to small deviations from approved welding procedures or inadequate control of heat input during fabrication. Problems such as incomplete fusion, porosity, residual stresses or incorrect weld profiling can significantly reduce the fatigue strength of a structure.
Metallurgical experts examine the physical evidence left behind by the failure. Techniques such as fractography, metallography and mechanical testing allow specialists to identify how cracks initiated and propagated through the material. These analyses can reveal whether defects originated during manufacture, developed through operational stresses or arose from material weaknesses present from the outset. By comparing findings with relevant engineering codes and specifications, experts help courts understand whether construction standards were properly followed.
Inspection and quality assurance frequently come under scrutiny –even well-fabricated components can fail if defects are not detected before entering service. Expert witnesses therefore analyse inspection regimes, including non-destructive testing methods such as ultrasonic testing or radiography. Their role is to determine whether inspection procedures were appropriate and competently carried out, and whether warning signs were missed that might have prevented a failure.
The importance of expert metallurgical analysis was illustrated in a case some years ago in the Court of Appeal: Promet Engineering (Singapore) PTE Ltd v Sturge. The dispute concerned fatigue cracking discovered in an offshore accommodation platform. Investigations showed that the cracking originated in welds containing latent defects caused by incorrect profiling during fabrication.
Expert metallurgical evidence demonstrated that these defective welds acted as the starting point for fatigue cracks that later spread into structural elements of the platform. The court ultimately accepted that the weld defects constituted physical damage under the relevant insurance policy.
Although the case centred on insurance coverage rather than negligence, it demonstrated how detailed technical analysis of weld defects can play a decisive role in legal outcomes.
Beyond fabrication issues, experts are often asked to investigate corrosion and environmental degradation. Components operating in harsh industrial environments may be exposed to extreme temperatures, chemical attack or cyclic pressure loading. These
conditions can accelerate corrosion processes or promote crack growth within welded joints.
Metallurgical specialists analyse the type and progression of corrosion to determine whether protective measures – such as coatings or appropriate material selection – were adequate. Their findings help establish whether deterioration was foreseeable and whether preventative maintenance or design choices might have mitigated the problem.
Underlying metallurgical defects can present an additional challenge. Variations in alloy composition, improper heat treatment or microstructural inconsistencies may reduce a material’s mechanical performance. Using laboratory techniques such as microscopy and chemical analysis, experts can identify these hidden issues and explain their significance in clear terms for the court.
For legal teams, credible expert testimony is often critical in technical disputes. Courts increasingly expect expert witnesses to present objective, scientifically robust opinions capable of withstanding detailed scrutiny. Well-supported analysis can clarify the chain of events leading to failure and sometimes facilitate settlement before trial.
As infrastructure and energy technologies continue to evolve, the demand for metallurgical and welding expertise in litigation is likely to grow. When structures fail, determining the true cause requires careful scientific investigation – an area where expert witnesses play an essential role in helping courts reach informed and balanced decisions. q




[ DISPUTES INVOLVING LAND BOUNDARIES , rights of way and easements remain among the most common – and often the most contentious – forms of property litigation in the UK.
What may begin as a disagreement between neighbours about the position of a fence, access across land or the right to use a pathway can quickly escalate into a complex legal matter requiring detailed technical analysis. In many of these cases, the outcome ultimately depends on the independent evidence of specialist expert witnesses capable of interpreting historical documents, mapping evidence and physical site conditions.
As land becomes increasingly valuable and intensively developed, the likelihood of such disputes has grown. Subdivision of land, redevelopment of older sites and changes in property ownership can bring previously dormant issues to the surface. When historic rights or boundaries are unclear – or when longstanding arrangements are challenged – solicitors frequently turn to expert surveyors or land specialists to provide impartial analysis.
Boundary disputes are perhaps the most familiar of these conflicts. Although title plans registered with the Land Registry provide an indication of property boundaries, they are generally drawn to a general boundary rule and rarely determine the precise legal line. As a result, disagreements often arise about whether a fence, wall, hedge or structure sits on one property or another.
An expert specialising in boundary determination will typically examine a wide range of evidence. This may include historical conveyances, title deeds, transfer plans, historic mapping, aerial photography and physical site features. In many cases, older documents must be carefully interpreted in the context of modern mapping systems. Even small discrepancies in scale, measurement or interpretation can have significant implications.
Physical features on the ground can also provide important clues. Walls, hedgerows, ditches, fences and long-standing occupation patterns may reflect historic boundary arrangements. However, these features change over time, meaning that expert analysis must consider whether a physical marker represents the original boundary or a later alteration. The expert’s role is to reconcile documentary evidence with the current physical landscape to form an objective opinion on where the legal boundary is most likely to lie.
Closely related to boundary disputes are conflicts involving rights of way and easements. These cases often arise where one landowner claims the right to pass over another’s property, either through express legal grant or through long-standing use. Such access rights may involve driveways, footpaths, farm tracks or service routes used by neighbouring properties.
Where a right of way is expressly granted in a deed, disputes may centre on the interpretation of the document itself. Questions may arise about the width of the route, the type of use permitted or whether changes in land use have exceeded the original intention of the easement. Experts are frequently asked to analyse historical conveyancing documents, mapping evidence and site conditions to determine how the right was intended to operate.
Under English property law, a right may arise where use has continued openly and without permission for at least twenty years – prescriptive easement. Establishing such a claim requires careful examination of witness evidence, historical mapping and patterns of land occupation.
Expert witnesses may be instructed to review aerial photographs, historic Ordnance Survey mapping and documentary records to determine whether the claimed route existed and was used consistently over the relevant period. They may also assess whether the physical layout of the land supports or contradicts the alleged long-standing access.

Such disputes are often highly emotive because they arise between neighbours or adjoining landowners whose relationships may already be strained. For this reason, the expert’s independence is particularly important. Courts rely on impartial technical evidence to move beyond conflicting personal accounts and establish a factual understanding of the land in question.
An essential part of the expert’s role is presenting complex historical and technical material in a clear and accessible way. Boundary and easement disputes frequently involve documents that may be decades or even centuries old. Plans may be handdrawn, written descriptions ambiguous and historical references difficult to interpret without specialist knowledge.
A well-prepared expert report will therefore carefully explain how each piece of evidence has been analysed. Plans, diagrams and annotated mapping are often used to illustrate the relationship between historical documents and present-day site conditions. This structured approach allows the courts to understand not only the conclusion but also the reasoning behind it.
In many boundary and easement disputes, a robust CPR35compliant report can prove decisive. Clear, well-supported expert evidence often helps narrow the issues in dispute and may even lead to settlement before trial. Where cases do proceed to court, the expert’s ability to explain complex land evidence under cross-examination can play a crucial role in determining the final outcome. q





[STRUCTURAL DISPUTES involving buildings and infrastructure are an increasingly common feature of construction litigation. As property values rise and development intensifies, disagreements over structural integrity, land movement and building performance frequently escalate into formal legal claims.
In many of these cases, solicitors, insurers and courts rely heavily on the independent analysis of chartered engineers to establish the technical facts behind the dispute.
Chartered engineers acting as expert witnesses play a critical role in helping legal teams understand complex structural issues. Their task is to provide impartial, technically sound opinions based on engineering principles, site inspections, documentary evidence and industry standards. When structural defects or failures are alleged, their expertise often becomes central to determining whether a problem arose from design deficiencies, construction errors, inadequate maintenance, environmental conditions or neighbouring activities.
One of the most common issues is subsidence.
elements such as beams, columns, foundations or floor systems were capable of safely carrying the loads imposed upon them. In some cases, engineers will need to evaluate whether remedial works have been appropriately designed and whether a building can safely remain in service.

Movement in the ground beneath a property can cause cracking, distortion of walls, sloping floors and damage to structural elements. While the symptoms may be visible, the underlying cause is often far more complex. Chartered engineers are frequently instructed to investigate whether subsidence has resulted from soil shrinkage, leaking drains, nearby excavation, defective foundations or tree root activity.
A thorough subsidence investigation typically involves detailed site inspections, structural crack monitoring, soil analysis, foundation exposure and a review of historical construction records. Engineers may also examine drainage systems and consider the geological conditions present at the site. Their findings can determine whether the damage is progressive, historic or related to a specific event. In many cases, expert evidence can distinguish between genuine structural subsidence and minor cosmetic cracking caused by normal building movement.
Another area where chartered engineering expertise is regularly required is the design and stability of retaining walls. Retaining structures are commonly used to support soil at different ground levels. When such structures fail or show signs of distress – such as bulging, cracking or leaning – the consequences can be serious, potentially leading to property damage, land slippage or personal injury.
Such disputes often centre on questions of design adequacy, construction quality and drainage provision. Chartered engineers will typically assess whether the wall was correctly designed to withstand lateral earth pressures, surcharge loads and water build-up behind the structure. They may also investigate as to whether appropriate reinforcement, foundations and drainage systems were installed in accordance with accepted practice. By analysing construction drawings, material specifications and site conditions, the expert can determine whether the wall’s failure resulted from poor design, substandard construction or external factors such as increased loading or ground movement.
Load-bearing assessments represent a third major category of structural disputes. Alterations to buildings – particularly the removal of internal walls or the installation of new structural openings – can significantly affect the distribution of loads within a structure. In domestic properties, issues frequently arise where renovations have been undertaken without adequate structural design or compliance with building regulations. In commercial or industrial buildings, disputes may involve heavier structural loads, equipment installations or changes in occupancy use.
Chartered engineers are often instructed to establish whether structural
Expert reports are particularly valuable in structural disputes because they translate complex engineering analysis into language that the courts can understand. By presenting clear reasoning and objective conclusions, the expert helps the court identify the true cause of the structural issue and determine whether there has been a breach of professional duty or contractual obligation.
Credible engineering evidence can often lead to disputes being resolved before they reach trial. Early expert involvement can clarify liability, highlight weaknesses in competing arguments and provide a technical foundation for settlement negotiations. Joint expert meetings can further narrow the issues in dispute, saving both time and legal costs.
As property development becomes more complex and structural claims continue to increase, the contribution of chartered engineers in the litigation process is likely to remain indispensable. Their ability to combine rigorous technical investigation with clear, independent reporting ensures that courts and legal professionals are equipped with the expert insight needed to resolve structural disputes fairly and effectively. q

[AS THE INDUSTRY WORKS to align ageing building stock with Building Safety Act (BSA) requirements and evolving evacuation standards, fire safety in lifts is emerging as a growing concern for construction and building management professionals.
With thousands of high-rise and complex residential buildings now undergoing remediation and safety reviews, attention is increasingly turning to vertical transportation systems and their role in evacuation and firefighter access, particularly in older buildings where upgrading lift infrastructure is technically complex.
Against this backdrop, new research commissioned by PEW Electrical reveals that 63% of professionals say that lifts are a major concern when it comes to fire safety in buildings, while 48% say they expect less than half of operational lifts are compliant with fire safety standards.
It found that while understanding of regulatory requirements is improving, delivery on site remains challenging. In fact, over a third (35%) of professionals say that the main difficulty with meeting standards is technical complications in the lift shaft itself, reflecting the reality of retrofitting systems that were never designed to meet modern evacuation or
firefighting lift requirements.
Concern doesn’t end there: fire risk assessments continue to attract criticism. 39% say that fire risk assessments are inconsistent, varying between contractor and assessors, and nearly one in five (18%) say that ‘no one’ complies with the processes, raising concerns about how reliably lift-specific risks are being captured in building safety strategies.
However, there are signs that capability is improving. 66% say that the industry is prepared to meet modern evacuation and firefighting lift standards such as BS EN 81-72, while 57% say they are confident that lift design standards align with current building safety expectations, suggesting that while confidence in frameworks is growing, practical implementation remains the bigger hurdle.
Jason Clark, registered engineer and chairman at PEW Electrical, said: “What we’re seeing is a sector that understands the importance of lift fire safety, but the reality is that many existing buildings simply weren’t built with modern evacuation or firefighting lift requirements in mind. Fire safety performance has to be designed and delivered, not assumed.”
“Lifts sit at the intersection of fire strategy, accessibility and emergency response. If they’re

treated as a standalone package rather than as a critical part of the whole building safety system, gaps in technical understanding or assessment can create real risk for residents and first responders.”
With remediation programmes continuing across the UK and scrutiny from the Building Safety Regulator increasing, lift industry leaders warn that fire safety will remain a pressure point unless technical guidance, assessment practices and supply chain coordination improve in parallel with regulatory reform.
PEW Electrical is urging main contractors, developers, designers and specifiers to engage specialists early to avoid gaps in technical knowledge that could undermine wider building safety strategies. q

[THE LATEST FIGURES from GOV.UK show that fire safety concerns are at an all-time high, with the number of unsatisfactory audits and formal notices served soaring. Of the 51,026 fire safety audits carried out in 2024/25, 42% (21,312) were found to be unsatisfactory, with almost 3,000 premises served formal notices.
Unsatisfactory fire safety audits have increased steadily over the last eight years, while formal notices served to premises owners have also risen alarmingly.
The statistics also raise concerns about the lack of fire safety audits carried out on a yearly basis, with just 2% of the 2.5 million premises that require regular audits having them carried out in each of the last six years. These premises should ideally be audited by a competent person every three years.
Analysis of the statistics from the UK’s leading smoke ventilation manufacturer, Sertus, suggest that while there has been an alarming number of unsatisfactory audits and formal notices served, the industry has been forced to take building fire safety more seriously since the Grenfell disaster.
Richard White, commercial director at Sertus, believes that there has been a change in how audits are being approached, with those in charge benefiting from the new legislation and processes put in place in recent years.
He said: “While the statistics may be alarming on the face of it, I’d argue that the increase is likely happening because of the implementation of the Building Safety Regulator and new legislation. There is a proper process in place now, and there wasn’t before. More people are beginning to understand what good looks like when it comes to fire safety.”
There’s positivity that the industry is now placing additional emphasis on protecting the life of citizens, which is a direct reflection of the changes driven by Dame Judith Hackitt with the backing of HSE and Ministry of Housing, Communities and Local Government.

The Building Safety Act 2022 was brought in off the back of the Grenfell tragedy to implement stricter regulatory frameworks for the design, construction and management of higher risk buildings. Alongside this, Fire Safety Act 2021 was also introduced and clarifies that the Responsible Person for a building must manage and reduce the risk of fire.
The two pieces of legislation have driven increasing scrutiny from auditors, as they are now more likely to capture any areas of non-compliance due to the liability and risk if a fire was to break out. The Building Safety Act in particular places particular emphasis on early-stage design, ensuring compliant application of fire safety equipment, such as smoke ventilation, is in place. q

[ESCALATING GEOPOLITICAL CONFLICT in key global shipping corridors presents significant challenges for the cargo and maritime sector. Reports of vessels being struck by projectiles and notices from carriers terminating voyages highlight the operational and financial risks confronting the industry. As uncertainty increases, so too does the potential for disputes requiring detailed technical analysis from expert witnesses.
Large volumes of cargo remain in transit through affected regions, representing substantial value and exposure for owners and insurers. Commercial shipping is being advised to avoid high-risk areas where possible and to seek alternative routes. Where diversion is not feasible, carriers may terminate voyages, requiring cargo owners either to accept higher charges or arrange alternative transport.
The immediate impact is likely to be higher costs. Carriers face rising fuel prices, which are generally passed on to cargo owners via surcharges and increased freight rates. Additional war-risk insurance, where obtainable, adds further cost. Combined with rerouting, port congestion and the logistics of discharging and re-forwarding cargo, these factors may substantially disrupt the delivery of goods.
These developments raise complex insurance and legal questions, precisely the types of issues for which independent expert witnesses are instructed. Cargo owners may seek to recover onforwarding or re-forwarding costs under their insurance policies. Under Institute Cargo Clauses (A), Clause 12 provides cover for forwarding charges where these arise ‘as a result of the operation of a risk covered by this insurance’. Where war risks are excluded under Clause 6, however, whether such costs are recoverable is far from clear, raising difficult questions of causation.
Voyage termination and rerouting are also likely to cause substantial delays. Delay itself is typically an excluded peril under Clause 4.5. Where cargo becomes commercially unusable or significantly devalued during


transit, disputes may arise as to whether the loss constitutes mere delay or a constructive total loss. Determining this distinction often requires expert evidence relating to cargo condition, timelines and valuation.
Further complexity arises as owners seek additional war-risk or strikes and terrorism cover. Where conflicts involve multiple actors – including groups designated as terrorist organisations by some states – it may be increasingly difficult to distinguish whether a loss arises from war, terrorism or other causes. Cargo discharged at ports for extended periods may also face heightened risks of theft, deterioration or accidental damage. Independent marine surveyors, logistics specialists and insurance experts may be required to assess loss causation and cargo condition in such circumstances.
The potential for disputes increases where cargo owners obtain ‘buy-back’ cover or multiple policies from different insurers. Where events are poorly documented or occur across several stages of transit, disagreements could arise over which policy responds. Expert witnesses are often critical in reconstructing events and providing technical analysis to support or challenge competing claims.
Freight forwarders also face challenges. Notices of voyage cancellation, rerouting and emergency surcharges from shipping lines can be difficult to pass on to customers, particularly under long-term service agreements. While most bills of lading include force majeure provisions and liberty clauses allowing deviation in the event of hindrances, courts interpret such clauses narrowly. Carriers remain under a continuing duty of care for cargo while in their custody. Disputes over the reasonableness of carrier decisions, the handling of cargo during diversion, and the validity of notices are all areas where expert evidence can prove decisive.
In such circumstances, operational disruption and financial exposure go hand in hand with complex contractual and insurance challenges. Expert witnesses – ranging from marine surveyors and logistics specialists to insurance and maritime law experts – play an essential role in helping courts, arbitrators and insurers understand the technical realities behind claims. Their input can be decisive in clarifying liability, causation and valuation issues in an increasingly uncertain environment. q

[ IN AUGUST 2025, the equestrian community in Aston-le-Walls, Northamptonshire, was shaken by the tragic death of 37-year-old rider Sarah Yorke, who suffered fatal injuries during a cross-country phase at the horse trials.
Ms Yorke fell when negotiating a solid obstacle on the course and, despite receiving immediate medical attention, she could not be saved. The event was subsequently abandoned and organisers held a full review of the incident in accordance with established safety protocols.
Such incidents, while thankfully rare, underscore the inherent risks in equestrian sport and the critical importance of thorough investigation when accidents result in death or serious injury. For solicitors involved in claims, understanding how equestrian accidents are investigated – and how evidence is assembled – is essential when advising clients.
The framework of inquiry
Accident investigations in equestrian events typically involve multiple strands. Initially, event organisers and governing bodies such as British Eventing launch internal reviews to examine course design, obstacle construction, ground conditions, supervision and compliance with sport-specific safety standards. The objective at this stage is not to assign blame, but to identify contributing factors and whether any procedural safeguards were breached.
Parallel to this, statutory agencies such as the Health and Safety Executive may become involved if the circumstances suggest a breach of the Health and Safety at Work etc. Act 1974 or equivalent jurisdictional obligations. Their remit includes assessing whether reasonable steps were taken to protect participants, whether risk assessments were adequate and how emergency response arrangements were deployed on the day. In complex cases, these investigations can stretch into months as evidence is gathered and analysed.
The role of forensic evidence
Forensic evidence plays a central part in establishing an accurate narrative of events. Photographs and video footage from course cameras, judges’ vantage points and competitors can illuminate the dynamics of a fall. Veterinary reports provide insight into a horse’s condition and behaviour at the time of the accident, potentially identifying factors such as preexisting lameness, fatigue or an environmental trigger that may have caused a spook or misstride. Medical records for the rider are also meticulously reviewed to determine the severity of injuries sustained.
Expert witnesses are often instructed to interpret this material. Equine and human biomechanics specialists, veterinary pathologists and accident reconstruction experts can analyse footage and physical evidence to offer neutral opinions on key questions: Could the obstacle have contributed to a rotational fall? Was there any indication that surface conditions increased risk? Were welfare and safety protocols properly implemented?
Legal implications and liability
In cases where negligence or breach of duty is alleged, expert evidence is vital. A solicitor advising an injured rider, or the estate of a deceased participant, must consider whether there was a failure in duty of care by event organisers, course designers or other responsible parties. Proof of negligence often hinges on demonstrating a departure from established practice that materially contributed to the accident. Conversely, defendants may call experts to show adherence to recognised standards and that the accident was an unfortunate but unforeseeable occurrence inherent to the sport.
Accident investigations can also have regulatory and sport governance consequences. Findings may lead to revisions in eventing rules, course design and protective equipment standards. They are intended to inform practice across future competitions to help prevent recurrence.

For solicitors, translating the technical findings of accident investigation into clear, client-friendly advice is crucial. Clients often arrive with deeply personal concerns – the physical and psychological impact of injury, the loss of a loved one or uncertainty over whether justice will be served. Expert reports must be explained in terms that are legally relevant, highlighting points of strength and vulnerability in a claim.
Accidents such as the fatal fall at Aston-le-Walls remind us that equestrian sport, like many high-risk activities, straddles the line between accepted risk and potential liability. Comprehensive investigation, supported by robust expert evidence, ensures that the courts receive an accurate and impartial account of what occurred. In a field where every detail can influence a case, early and strategic engagement with forensic and technical expertise can make all the difference. q

By Dr Mark Hinnells, director of Susenco Consulting Ltd


[ FIDUCIARY DUTY is when one person has an obligation in law to act in the best interests of another. It has usually been seen as financial and relatively short term.
Currently the fiduciary duties of various actors – including cabinet ministers, fund or investment managers and company directors –are defined in different places in different ways, in a combination of
law, policy and guidance, some of which is litigable and some is not. Increasingly, a longer time frame is being applied to fiduciary duty. As the impacts and costs of climate change are better understood, the risk to assets, investments, companies, financial systems and ultimately GDP becomes ever more obvious.
The Paris Agreement 2015 committed to returning global

greenhouse gas emissions to net zero by mid-century to mitigate the worst effects of climate change. Such a target requires co-ordinated action across the global economy. Surely then, a joined-up approach to fiduciary responsibility is now necessary, connecting the legal and ethical obligations of, for example, cabinet ministers, fund managers and corporate directors. Is this for government to work out, or for courts to point out?
Cabinet ministers don’t have fiduciary duties in the same way that company directors or pension trustees do, but courts and constitutional practice in Westminster-style systems treat their responsibilities as fiduciary in nature. Ministers also obviously have political constraints and a duty to follow the law.
The testing of whether ministers have complied with law has become more common in the UK. For example, Friends of the Earth v Secretary of State for BEIS (2022) successfully challenged the UK’s net zero strategy for failing to meet obligations laid out in the UK Climate Change Act 2008 (as amended). Judgements challenging ministers may become more common in other jurisdictions, following the ICJ Advisory Opinion on ‘Obligations of States in Respect of Climate Change’ July 2025 and the Inter-American Court of Human Rights (Advisory Opinion 32) July 2025.
Those who invest on other people’s behalf – fund managers for pensions, life insurance and other investment products – have a fiduciary duty to beneficiaries. In the UK climate change is now on the face of pensions legislation (Pensions Schemes Act 2021, s124). The climate and ESG component of fiduciary duty continues to be tested in court – Butler-Sloss v Charity Commission (2022), McGaughey & Davies v Universities Superannuation Scheme Ltd (2023) and in the US Wong v New York City Employees Retirement System
In Canada currently, four young people whose pensions mature after 2050 have taken the Canada Pension Plan Investment Board (CPP Investments) to court, claiming CPP is breaching its duty to invest in their best interests by failing to protect their pensions from climate risk. This case raises a further layer of conflict in that fiduciary duty to younger people may be different from those about to retire, since the longer a pension has to run, the more exposed to climate risk it is.
At the corporate level, company directors’ duties vary by jurisdiction, but alongside a fiduciary duty some jurisdictions, such as Hong Kong, include a range of duties onto which climate risk can be mapped. For example, a duty of care, including a reasonable degree of skill, care and attention to major issues like climate risk; a duty to invest prudently, implying risk management and foresight; a duty to keep accounts and records including, where required, reporting and evidence of consideration of ESG and climate issues; a duty to inform and consult on major risks and opportunities like climate; and a duty to take professional advice as climate is unlikely to be a specialism of trustees. All this said, the commercial courts are currently reluctant to interfere with how directors discharge their duties as in ClientEarth v Shell plc 2023
Siloed fiduciary duties are thus insufficient, where international agreements like the Paris Agreement on achieving net zero carbon by mid-century is clear, as is the ICJ Advisory Opinion on ‘Obligations of States in Respect of Climate Change’. There is a clear need for a cascading fiduciary duty, from states to cabinet ministers, to fund managers and company directors. Alignment needs transparency, long-termism, climate literacy and accountability.
In the meantime, there is a need for advice, arbitration and, if necessary, litigation to test the obligations of those with a fiduciary duty in respect of climate and ESG. Susenco would be happy to assist. q
• For more on climate change, ESG and fiduciary duty, see the other blogs by Dr Mark Hinnells in this journal and the seminar given by Dr Mark Hinnells for Hong Kong Trustees Association. More information is at www.susenco.com
[A CHIPPENHAM-BASED FARMING PARTNERSHIP has been hit with £18,744 in penalties after two slurry spills polluted the Bristol Avon river in Chippenham.
In a prosecution brought by the Environment Agency, JD Spencer Farm Partnership of Manor Farm, Langley Burrell, Chippenham, pleaded guilty at Swindon Magistrates’ Court to four offences on 6 March 2026. The partnership was fined £7,000, a victim surcharge of £2,800 and costs of £8,944.
The farm was charged on two counts of illegal water discharge activities and two charges of failing to plan the spreading of slurry.
The first incident, which occurred in November 2023, led to slurry entering a tributary of the Bristol Avon. Downstream water samples showed very low dissolved oxygen levels and the presence of significant quantities of ammonia in the water.
During a formal interview, co-owner of the farm, Winston Spencer, denied that he had been recently spreading slurry or that he had pumped from the farm’s slurry lagoon onto the fields. He did, however, admit that his slurry and parlour washings stores were full and that slurry run-off had occurred. He suggested this had been due to heavy rainfall washing off slurry which he had spread the previous month.
The second incident, in March 2024, resulted in slurry pollution to a watercourse at Langley Burrell, Chippenham.
David Womack, senior environment officer, said: “This incident was avoidable and should never have happened. Farmers have a responsibility to ensure their organic manures are properly stored and spread. If farmers have concerns about not having sufficient slurry storage capacity, we recommend they contact us.
“We can give advice on current legislation, help ensure slurry calculations are accurate and reduce the pollution risk by identifying non-compliant structures.” q

[AS URBAN DEVELOPMENT, climate change and public safety concerns converge, the role of arboricultural experts in legal proceedings has expanded significantly. Solicitors increasingly rely on specialist opinion when disputes arise over tree safety, root-related subsidence, planning matters and personal injury claims. From local authority obligations to private property disputes, expert input is now central to establishing facts and assessing liability.
Arboricultural experts are routinely instructed to assess the condition and management of trees, whether in public parks, residential gardens or commercial sites. In civil disputes, they provide guidance on issues such as alleged breaches of Tree Preservation Orders, encroachment onto neighbouring properties or damage caused by invasive roots to buildings. Their evaluations help determine whether proper maintenance and risk mitigation measures were in place and whether any harm could have been reasonably foreseen.
Root-related subsidence and structural damage represent a common source of litigation. An arboricultural report may examine soil type, tree species, moisture content and historical growth patterns to establish causation and contributory factors. Similarly, in planning disputes, experts advise on potential ecological impacts of tree removal or development near protected specimens, ensuring compliance with statutory obligations and environmental considerations.
Personal injury claims are another area where arboricultural evidence is invaluable. Falling branches, obstructed pathways and inadequate pruning can lead to significant harm. Expert reports clarify the standard of care expected of landowners or authorities, assess whether inspections and maintenance were appropriate and provide a balanced, impartial opinion on liability. These insights assist
defendants and claimants alike in understanding the strengths and weaknesses of a case.
In an increasingly litigious environment, arboricultural expertise ensures that legal decisions are informed by objective, technically grounded analysis. In civil, insurance or planning-related matters, early engagement with an expert can provide clarity, manage risk and support a robust evidential foundation.
As awareness of tree safety and ecological obligations grows, the demand for specialist arboricultural opinion continues to rise, highlighting the critical role these experts play in modern legal practice. q


By Mark Chester
[ AS SOMEONE who has worked in the land-based sectors all their life, I am very familiar with both the role of health and safety in day to day activities, and also the reaction many give to its mention. Eyes roll and there are shrugged shoulders with mutterings of paperwork and process that are out of control. The reality, and the consequences of not taking it seriously, are very different.
Many of the precautions we take in managing health and safety are born from the experience of others, and responding to accidents, whether near-goes or those with life-changing outcomes.
Being from a farming background, I am familiar with the risks that many face on a daily basis and the reliance on personal judgement. I also appreciate how dangerous some of the equipment used and situations faced can be – and how ready they are to catch out the unwary or ill-experienced.
Some risks may be more obvious. Others can apply widely and several are ones I am learning to adapt to. In my work as an expert witness operating in the world of trees, I have been asked to investigate a number of cases where there have been life-changing accidents. There is usually a claim for compensation to cover costs of on-going medical support and adapting to a new way of life.
A common theme is emerging for me. It is noticeable how often people underestimate the risks involved with tasks that seem familiar but, if not undertaken with training on a regular basis, can easily catch the operator unaware and cause problems which may be severe.
Many a farmer, faced with needing to prune or fell trees on their land, will have a chainsaw. They may have also completed the basic training in using this kit. However, felling trees and logging timber is often not as straight forward as may be perceived. Different species respond in different ways. The timber of a fallen tree responds in a different way to that of an upright and then freshly felled specimen. And when an operator isn’t working with a chainsaw on a regular basis, refresher training becomes important.
Themes are emerging for me. These include individuals being unaware that they are not adequately trained, a lack of awareness of the correct training, both among operators and their clients or employers. Correct training and procedures can be regarded as luxuries, and it is sadly only when dealing with the consequences that the limitation of this attitude becomes apparent.
Chainsaws need to be treated with respect. An advertising campaign was recently launched by Lantra to emphasise this; injuries can happen all too easily.
Practical issues such as lone working, the need for reliable mobile phone reception and the location of the nearest A & E hospital may seem obvious but, in my experience, are often not.
I survey trees, including on development sites, on a regular basis. Usually, visits are undertaken without incident. Indeed, during COVID, one client, running a housing association, was discussing any specific risks that needed to be considered. I explained that I was going to be walking around the grounds looking at the trees, as any resident would do. We agreed that this should be reasonably safe.
However, occasionally, the unexpected can catch me out. Visiting one site with development potential, the client brief was that there was a single tree on some scrubland on a gently sloping site. As I explored the site, finding the plot to be a steeply sloping hillside, I realised that it was uneven terrain with the main road at the bottom and few obstacles in the way if I slipped. I then found there was no phone reception or internet for WhatsApp calls in the event of an accident. I proceeded with my descent with considerable care.
For another case, I was surveying trees within the grounds of a university campus. On day one, I found the area for surveying and proceeded with the task – I was told that I didn’t need to sign in. On day two, which happened to be a Friday, I visited reception, signed in and received a visitor pass. I found later in the day that the fenced
area I was working in had been locked. Friday was early closing for the weekend, and the security team was unaware I was on site. My visitor pass proved very valuable, as it contained the phone number of the reception team and someone soon came to unlock the main gate.

My recent health and safety experience as an expert witness has focused on personal injuries, some of them life changing, as a result of work place accidents. However, those relating to tree safety, and to a tree falling on to a person, have been a feature for claims over the past two decades.
The limitations of surveys and lack of credentials of surveyors are recurring themes for such claims. When a surveyor is not adequately trained for the role, they are more likely to overlook features such as structural weaknesses or the presence of decay, which the trained surveyor is experienced to identify.
The process of identifying health and safety issues, and how to manage them, especially in land-based settings, is a specialist skill. It is one requiring a trained assessor, whether in-house or employing consultants. When this doesn’t happen, problems can emerge. In one case, I was instructed to assess liability following an accident allegedly caused by the failure of an unsafe tree. The tree was within the communal grounds of a site managed by a management company. The company emphasised how they had arranged for a specialist to survey the tree which had been in a good condition when last surveyed. A storm was blamed for the damage.
It was when I began to investigate that the account began to unravel. There was no storm in the area, nor were there any records of the survey and the surveyor was unable to cite any specific training in surveying trees. The presence of dead wood on other trees within the grounds indicated the absence of an active management programme. The defendants soon settled the claim.
This case highlighted one of the key aspects of health and safety which is easily overlooked and misunderstood: who is responsible for the management of this within an operation. This is not something that can be out-sourced. The owner of an organisation is responsible for ensuring it is properly managed and, where it is delegated to members of staff, that they are adequately trained for their roles. The caveat is where someone is self-employed and works for several clients. In such a situation, they take responsibility for their own health and safety.
Health and safety is a specialist area. Fortunately, there are organisations, including HSE and Lantra, which can help advise on where to get advice. Lantra leads on training in skills in the landbased sector, which includes the use and operation of chainsaws, felling trees and tree surveying.
Whilst the explanation of lack of knowledge may be understandable, it is not a defendable position. Information is readily available. In exploring cases this year, I have been able to guide clients to the National Farmers’ Union, Health & Safety Executive and Lantra.
There is also a network of advisors who can guide on what you are doing right and where you need to make changes. I am called in when something has gone wrong and, usually, correct process has not been followed. I prefer the cases I am instructed on to be acts of nature rather than human failure.
Much of my work involves claims for compensation. When the claim relates to the loss of a tree or damage to property, the settlement is usually sufficient to compensate for what has been lost. When the claim is based on a personal injury, which may have been lifechanging and could have been avoidable, the cost is greater.
It is for those situations where I would wish to take parties back in time and suggest they review their approach to health and safety. It is too important to be left to change or whatever reason might be cited. It matters, as life matters. q

By Rebecca Guthrie, Translate Hive
In an increasingly international legal landscape, language is no longer a background consideration. It is a frontline risk. For expert witnesses, solicitors and insurers alike, the quality of translation and interpretation can directly affect credibility, admissibility and outcomes.

[EXPERT EVIDENCE is built on precision. Whether it is a medicolegal report, an engineering opinion, a forensic schedule or a witness statement, every word carries weight. When that evidence crosses linguistic borders, accuracy is no longer just desirable. It is essential.
Yet too often, translation is treated as an administrative afterthought. A box to tick. A cost to minimise. That approach is no longer sustainable.
Courts are seeing an increase in cases involving non-English speakers, foreign documentation and international evidence chains. Road traffic accidents involving overseas drivers, cross-border employment disputes, asylum and immigration matters, international commercial litigation and multi-jurisdictional insurance claims are now routine rather than exceptional. With this comes a heightened scrutiny of how language is handled.
A poorly translated report does not simply read badly. It can alter meaning, introduce ambiguity and undermine expert independence. In the worst cases, it can render evidence unreliable or inadmissible.
From an expert witness perspective, this presents a real professional risk. Experts are instructed for their clarity, authority and objectivity. If their opinion is filtered through an inaccurate translation, their reputation can be affected despite having done nothing wrong. Subtle errors in technical terminology, measurement units, causation language or professional qualifiers can materially change how evidence is interpreted by the court. This is particularly acute in technical disciplines.
Engineering reports rely on precise descriptions of force, mechanism and probability. Medical reports depend on correct anatomical, diagnostic and prognostic terminology. Accident reconstruction, fire investigation and financial forensics all involve specialist language that generic translators are not trained to handle.
Legal translation is not the same as general translation. Expert evidence translation is a specialist discipline in its own right.
The challenge is compounded by procedural obligations. Under the Civil Procedure Rules, experts have a duty to the court. That duty includes ensuring that their evidence is clear, accurate and capable of being properly understood. If an expert knows their report will be translated, there is an implied responsibility to ensure that the translation process itself does not distort their opinion.
This is where a structured, expert-led approach to language services
becomes critical. High-quality legal translation should mirror the standards expected of expert evidence itself. That means subjectmatter specialists, documented quality assurance, transparent workflows and a clear audit trail. It also means understanding how expert reports are used in practice, from disclosure and joint statements to cross-examination.
For example, a translated report may later be challenged line by line in court. If the translator cannot justify their word choices or lacks familiarity with the underlying discipline, the expert may be placed in an uncomfortable position, forced to explain or defend wording they did not write.
Equally, interpretation during conferences, hearings or joint expert meetings carries its own risks. An interpreter who does not understand technical nuance can inadvertently lead discussions, soften conclusions or misrepresent levels of certainty. That can influence settlement decisions and judicial impressions in ways that are difficult to correct after the fact.
What is needed is a shift in mindset. Language should be treated as part of the evidence chain, not an external bolt-on. Just as experts expect proper instructions, clear scope and appropriate fees for their work, translation and interpretation should be commissioned with the same level of professional care.
That includes early identification of language needs, matching linguists to subject matter, ensuring confidentiality and data security, and maintaining consistency across multiple documents and stages of litigation.
Technology has a role to play, but it must be used responsibly. AI-assisted tools can support efficiency and consistency, but expert evidence still demands human oversight. Context, intent and professional judgement cannot be automated away. A human-in-theloop approach is not a luxury. It is a safeguard.
For expert witnesses, solicitors and insurers, the message is clear. Language accuracy is no longer a peripheral concern. It is a strategic and professional one.
As cases become more complex and more international, those who treat translation as a core evidential discipline will protect their credibility, reduce risk and ultimately serve the court better. In expert evidence, every word matters. Ensuring those words survive translation intact is not optional. It is part of doing the job properly. q


















COLLISION INVESTIGATION & RECONSTRUCTION

COMPLIANCE CONSULTANTS


COMPUTER & MOBILE FORENSICS



DIGITAL TECHNOLOGY

ENERGY CONSULTANTS




EQUESTRIANS

ERGONOMICS

FINANCIAL SERVICES



















Andrew F Acquier BA FRICS
Chartered Art & Antiques Surveyor
Expert witness reports and representation at court for matters involving:
• Divorce settlements • Insurance valuation disputes • Arts litigation
• Contentious Probate • Associate member of Resolution for many years
www.andrewacquier.co.uk
Clarke Gammon
Chartered Surveyors with experience in All Aspects of Property • Residential property values
• Asset valuations • Land values and more www.clarkegammon.co.uk
Crowe Expert Witness Services
Forensic and Tax Resolutions Specialists Audit / Tax / Advisory / Consulting Smart decisions. Lasting value. www.crowe.co.uk
DRC Forensics Limited




DRC Forensics Limited offers the complete range of forensic accounting & litigation support: • Fraud • Money laundering
• Partnership disputes • Loss of profit • Professional negligence www.drcforensics.co.uk
FHDI - Kathryn Thorndycraft-Pope

Dr Dan Jones PhD, MSc, BSc, MA, MEWI Cert
Foremost international Japanese Knotweed, Himalayan Balsam and Giant Hogweed expert.
• Residential, commercial, government • Independent audit
• Engineering & construction • Industrial & infrastructure
www.advancedinvasives.com
Mr Chris Makin
• Chartered Accountant • Accredited Civil Mediator
• Accredited Expert Determiner
www.chrismakin.co.uk
Andrew Smith FPC III CeMAP
Financial Conduct Authority Compliance & Risk Consultant
Cases relating to FCA compliance in consumer credit and mortgage lending.
• Mediation • Arbitration • Adjudication • Expert Determination
www.paxen.co.uk
Simon Quinton Smith BSc FRICS MI Hort
Expert Witness to the Garden Centre & Horticultural Industry • Rent Reviews • Lease Renewals
Valuation
Planning



Compensation
Tax Issues
www.quintonedwards.co.uk
Colin Todd – Fire Safety Expert • Fire safety management • Fire risk assessment

Mr Roger Flaxman ACII MAE
Chartered Insurance Practitioner with more than two decade’s experience serving as an expert witness in matters of insurance practice, broker’s duty of care, insurance market procedure and as an advocate in the resolution of disputed insurance claims.
Examining documents & handwriting • to determine authenticity • to expose forgery • to reveal aspects of origin. Electro Static Detection Apparatus and Mi-Scope used. www.forensichandwriting.co.uk www.flaxmanpartners.co.uk

Forensic Collision Investigation & Reconstruction Ltd
Specialists in the analysis of road traffic collisions
• Collision Reconstruction • Expert Witness
• Vehicle Examinations
www.FCIR.co.uk
Formedecon Ltd
Forensic & Investigative Services to the Legal Profession
• All Aspects of Forensic Work Undertaken
• LAA and Privately Funded • Free Estimates www.Formedecon.com


Means of escape • Fire protection of buildings


Specialist Timber Consultancy and Training since 1991 • Site visits & investigations
Structural surveys
Desktop analysis & review of documents
Species identification
Fire engineering • Application of fire safety legislation • Fire detection and alarm systems www.cstodd.co.uk www.woodexperts.com



[THE MEDICO-LEGAL LANDSCAPE continues to evolve at a rapid pace, driven by the twin pressures of increasingly complex clinical practice and rising expectations for accountability. In this issue, we explore how expert evidence informs decisions across a spectrum of disciplines – from orthopaedics and cardiology to psychiatry and paediatric care – and how courts, regulators and professional bodies are responding to new challenges.
• The Medical Defence Union has recently responded to the Public Accounts Committee’s report on reducing the costs of clinical negligence, highlighting the importance of patient safety as well as managing long-term costs. While the report offers practical recommendations for managing claims, experts across specialities remind us that victims of clinical negligence continue to face prolonged delays, with case backlogs hitting record highs and the need for closure becoming ever more pressing.
In a striking illustration of both the human and financial stakes, Addenbrooke’s Hospital has agreed a £1m settlement in a stroke misdiagnosis case, while another report reveals that a surgical drain was left in a patient’s body for eleven years after a hysterectomy.
• Emerging technologies also demand attention. The current law on artificial intelligence has been criticised for failing to protect injured patients, underscoring the urgent need for legislative reform as AI becomes increasingly integrated into diagnostics, imaging and treatment planning. Expert witnesses are uniquely positioned to guide the court on both the potential and the limitations of these tools, providing evidence-based assessment of clinical outcomes in cases where technology intersects with human error.
• Specialist societies are marking milestones while contributing to public engagement. The British Association of Plastic, Reconstructive and Aesthetic Surgeons (BAPRAS) has commemorated its 80th anniversary with a travelling exhibition exploring the remarkable history of the speciality. Meanwhile, the Royal College of Physicians (RCP) has issued a response to the newly published National Cancer Plan for England, focusing on both prevention and improving survival rates.
• Across clinical domains, expert testimony remains pivotal. Orthopaedic surgeons continue to clarify standards of care in complex shoulder, elbow and spinal cases, while musculoskeletal health advocates, including ARMA, push for national prioritisation of prevention and timely intervention. In urgent care, minor injury and emergency settings, the interface between front-line clinical practice and medico-legal scrutiny has never been more critical, particularly in time-sensitive conditions such as sepsis and chronic limb-threatening ischaemia. Meanwhile, specialist insights in dentistry, urology, ophthalmology and paediatric care highlight how even seemingly routine interventions carry medicolegal implications that require precise evaluation.
• Beyond the operating theatre, occupational therapists, psychologists and psychiatrists provide vital perspectives on functional impact, mental capacity and neurodiversity, shaping outcomes in family, civil and criminal proceedings.
Their contributions underscore a central theme: expert evidence is not merely descriptive but interpretive, bridging clinical knowledge and judicial decision making. q




[ A LANDMARK RULING by a senior costs judge has imposed a 25% cap on the mark-up that medical agencies can take on their expert’s fees – a decision likely to have significant implications for the personal injury litigation market.
In JXX v Archibald , Senior Costs Judge Rowley addressed a long-running dispute about how fees charged by medical reporting organisations (MROs) should be treated during costs assessments. The case concerned the level of mark-up agencies apply to the fees charged by medical experts who provide reports in personal injury claims.
Judge Rowley ruled that MRO fees should be treated as disbursements, rather than as outsourced work carried out by solicitors. As a result, agencies will not be required to provide the detailed itemised breakdowns that law firms must produce when presenting their own bills of costs. For many agencies and claimant firms, this clarification resolves uncertainty over the level of transparency required when such costs are challenged.
However, the judgment also introduced a significant new limitation. The court concluded that the recoverable mark-up applied by medical agencies to experts’ fees should not exceed 25%.
The ruling arose in two joined cases in which Judge Rowley examined the charges applied by different MROs. Evidence before the court showed that the agency Premex had applied uplifts of 35% or 45% on expert fees. Meanwhile Medical and Professional Services Limited (MAPS) was found to have applied mark-ups ranging from 20% to as high as 104%.
Judge Rowley said these figures demonstrated that agency charges were largely influenced by ongoing commercial arrangements rather than the needs of individual cases. He noted that the fees charged by agencies ‘plainly reflect variations resulting from ongoing commercial relationships between the solicitors and MROs rather than any case-specific factors’. While he emphasised that such relationships were not inherently problematic, he said they could not justify any particular percentage between the parties.
Given the range of figures presented to the court, Judge Rowley said it was necessary to adopt a cautious approach: “I am not persuaded that even the range of 30% to 53% generally charged can be considered reasonable, let alone the outlier percentages, some of which result from fixed sums having been claimed.”
Although the ruling confirmed that agency fees themselves remain recoverable, the 25% limit represents a substantial reduction for some providers operating in the personal injury sector.
Premex, one of the agencies involved in the litigation, described the judgment as a mixed outcome. Wayne Brannan, the company’s commercial director, said it was welcome that the court had confirmed that MRO fees are legitimate disbursements and do not require ‘breakdowns of breakdowns’ or identification of specific unrecoverable elements.
However, he warned that the cap on mark-ups could create significant commercial challenges. Brannan said: “Whilst it is undoubtedly good news to have confirmation that MRO fees are disbursements, the assessment of a recoverable fee of 25% of the expert’s fee is both disappointing and concerning.”
He added that agencies incur real costs when arranging medical evidence, particularly when operating at scale or offering deferred payment terms that allow claimants to obtain expert reports without paying upfront.
“The logical conclusion of a decision like this,” he said, “is that injured claimants – who in the main cannot afford to pay up front for medical evidence – will again suffer either by having to cover these costs from damages or simply be unable to access medical evidence at all.”
Slater and Gordon, which represented JXX, one of the claimants, said the ruling recognised the important role played by medical reporting organisations in the personal injury system. However, the firm noted that the 25% ceiling had not been proposed by either side in the case, raising questions about its practical impact.
Madelene Holdsworth, managing director at Slater and Gordon, said the firm relied on established relationships with agencies such as Premex to provide claimants with access to a nationwide network of medical experts. She added that the firm was reviewing the judgment carefully with clients and other parties involved in the case.
She also highlighted the need to maintain ‘equality of arms’ between claimants and defendants, warning that restrictions on recoverable costs could undermine claimants’ ability to secure high-quality expert evidence.
Similar concerns were raised by Thompsons Solicitors, which acted for claimant JXX. Partner Henrietta Phillips said: “We welcome the court’s finding that, in principle, all elements of the MRO fees are recoverable from the defendants.
“This is an important result for injured people, as it helps ensure they can access the independent medical evidence needed in personal injury claims, and underlines the crucial role MROs play in supporting access to justice.
“However, we are concerned that the maximum recoverable mark-up decided by the judge will mean that, in many cases, the shortfall will be yet another deduction from claimants’ compensation.
“We are firmly of the belief that the system should be structured so that all reasonable costs of bringing a successful personal injury claim are fully recoverable, and that injured claimants should not be forced to fund legal costs out of the compensation intended to restore them, so far as money can, to the position they would have been in if the injury had not happened.”
Judge Rowley acknowledged in his judgment that the ruling may not be the final word on the issue, noting that one or both sides may seek permission to appeal. q



[ RESPONDING TO THE Public Accounts Committee (PAC) report on reducing the costs of clinical negligence, Thomas Reynolds, Director of Policy and Communications at the Medical Defence Union (MDU), said: “It’s clear that Parliament has run out of patience with the failure of successive governments to take control of soaring clinical negligence costs.
“The MDU’s patience is equally, if not more, exhausted. MPs have now set a six-month deadline for action and we’ll be holding the Government to account to make sure they meet it. We need concrete action to end this huge financial drain on the NHS and the public purse.”
The report, published in January, examined the cost of clinical negligence in England, including why liabilities and settlement costs have risen significantly over time, the impact on NHS resources and the systemic factors that drive claims. It also highlighted the importance of patient safety, early resolution and coordinated action to reduce avoidable harm and manage long-term costs more effectively.
It heavily criticised the Department of Health and Social Care (DHSC) for failing to control rising clinical negligence costs, which reached £3.6bn in 2024-25 and are projected to exceed £4bn annually by the decade's end. Total liabilities have reached £60bn, with the committee demanding urgent action, including a national patient safety framework and publication of the delayed David Lock KC review.
The PAC report, along with a recent National Audit Office (NAO) report, highlighted the need for a less adversarial system and faster, more efficient dispute resolution to prevent further depletion of frontline NHS resources.
Thomas Reynolds continued: “The MDU has been sounding the alarm bell for years about two issues the report highlights. We strongly support the recommendation to repeal outdated legislation which risks the NHS paying twice for claimants’ care. We are particularly pleased that the Committee is supporting our call for data from government on the cost to the taxpayer of the current approach. Currently, there’s none – and that’s not good enough.
“Secondly, capping legal fees for lower value clinical negligence cases can’t come soon enough to control spiralling claimant legal fees. We urge the Government to get on with it and finally introduce fixed recoverable costs for lower value claims, which has been continuously delayed since the change of Government in 2024.
“We join the Public Accounts Committee in calling for publication of the long-awaited Lock Review into the current clinical negligence regime. This review was commissioned as part of the NHS 10 Year Plan and is intended to outline to ministers how to fix the broken system. Given the public interest in this issue, that review’s findings and recommendations must see the light of day as quickly as possible. This is all about transparency.
“Decades of inaction on clinical negligence has allowed costs to balloon, so we are pleased to see that MPs are putting pressure on Government to act. This is a chance to put an end to the millions of pounds being unnecessarily diverted from frontline patient care. We’ll be following next steps closely to ensure the Government sticks to the timetable that’s been set out and finally shifts the dial on this issue.” q




[LAWS IN THE UK need an urgent update so patients who suffer injuries where faulty artificial intelligence (AI) is used in their treatment can pursue compensation, personal injury lawyers say.
An independent national commission is working with experts, including from Google and top clinicians, to draw up new regulations for the use of AI in NHS care.
“The law is lagging behind when people are injured and AI technology is involved. AI use in healthcare is set to be transformative in providing rapid, accurate diagnosis and personalised treatment, so it’s key that if patients are hurt due to negligence where AI plays a part that they have a clear and accessible route to redress through the courts in the UK,” said Pauline Roberts, from the Association of Personal Injury Lawyers (APIL).
“People injured by medical products that utilise AI are forced to take on well-resourced manufacturers, sometimes based abroad, by pursuing product liability claims, which are notoriously complex, costly and lengthy,” she went on.
AI-powered radiology has already been used to help diagnose cancer or covid from chest imaging, for example. Technology is being trialled to speed up patient discharges from hospital with AI enhanced robots assisting in minimally invasive procedures, thus reducing recovery time.
“The law must keep pace with the latest use of technology, including AI use in healthcare so injured people can avoid a ‘David and Goliath’ battle to secure the compensation they need to get their lives back on track,” said Pauline.
“The legal framework around injuries caused by products involving AI generally, not just their use in healthcare, needs to be reviewed to ensure that if someone is needlessly injured, they receive the timely help and compensation that they need,” she added.
APIL has responded to the Medicines and Healthcare products Regulatory Agency’s call for evidence to inform the recommendations of the National Commission as it develops the new regulation framework for AI use in healthcare. q
[AS PART of its 80th anniversary celebrations the British Association of Plastic, Reconstructive and Aesthetic Surgeons (BAPRAS) is proud to present a travelling exhibition exploring the remarkable history of reconstructive plastic surgery.
The exhibition, The Evolution of Tissue Transfer Techniques, will be on display at the Museum of the Royal College of Surgeons of Edinburgh, on 25-26 March 2026.
The exhibition offers a fascinating journey through the key developments that have shaped modern reconstructive plastic surgery. From the earliest skin grafting methods to the microvascular revolution of the 1960s and 70s, the exhibit traces the ingenuity and innovation that has defined this specialty.
Visitors will have the opportunity to explore a curated display of historic surgical instruments and equipment, each telling its own story about how reconstructive techniques developed over time. The exhibition describes the surgical milestones that made it possible to transfer tissue from one part of the body to another – restoring function, form and feeling for patients recovering from trauma, tumour, burns and congenital conditions.
The travelling exhibition is one of several events marking the association’s 80th anniversary in 2026, a year that will culminate in the BAPRAS Congress 2026, taking place in Liverpool on 2-4 December. q




[CHESHIRE POLICE and the Crown Prosecution Service (CPS) have confirmed they were not informed by a key expert witness before he gave evidence at the trial of former nurse Lucy Letby that he was under investigation over serious concerns about his medical work.
Professor Peter Hindmarsh provided crucial testimony in the case, supporting the prosecution’s claim that Letby had attempted to murder two babies by injecting insulin into their fluid bags. However, prior to his first appearance as a witness on 25 November 2022, Hindmarsh was subject to a formal investigation by University College London Hospitals NHS Trust (UCLH), with input from Great Ormond Street Hospital, into multiple serious concerns, including allegations that he had harmed patients.
Criminal procedure rules require expert witnesses to disclose to the party instructing them any information ‘that might reasonably be thought capable of undermining the expert’s opinion or detract from the credibility or impartiality of the expert’. Senior legal figures have confirmed that this includes investigations conducted by an expert’s employer, particularly if they raise questions about competence or professional conduct.
Glyn Maddocks KC, joint secretary of the all-party parliamentary group on miscarriages of justice, said: “As I understand the rules, in order to be open and transparent with the court, this expert should have disclosed this investigation, so that its relevance and importance could be assessed. It’s vitally important that the integrity of experts is retained at all times.”
Tim Green KC, a barrister with expertise in disclosure rules, added that a physician with experience giving expert evidence would generally be expected to reveal an internal investigation, especially if it had reached an adverse conclusion, so that the instructing lawyers could ensure the expert complies with the disclosure rules before giving evidence.
Letby was convicted of murdering seven babies and attempting to murder seven others at the Countess of Chester Hospital across two trials in 2023 and 2024. The two insulin-related cases were pivotal, forming part of only three convictions that were unanimous.
Letby has consistently maintained her innocence, and her lawyer, Mark McDonald, submitted an application to the Criminal Cases Review Commission (CCRC) last year, arguing that the convictions were unsafe.
The CCRC is reviewing the application, which is supported by reports from 27 experts, including a panel led by Canadian neonatologist Dr Shoo Lee. These reports challenge the prosecution’s medical evidence, asserting that the babies’ deaths resulted from natural causes and lapses in care, with no evidence of deliberate harm or insulin poisoning.
Hindmarsh was one of eight expert witnesses called by the prosecution. He was a consultant paediatric endocrinologist and clinical director for paediatrics at UCLH and also held an honorary consultant position at Great Ormond Street. However, his contract with Great Ormond Street was terminated in July 2022, four months before he gave evidence. Cheshire police confirmed that Hindmarsh did not disclose this to them at the time.
When questioned by the lead CPS barrister about his honorary consultant role in November 2022, Hindmarsh did not make it clear that his contract had been terminated. Great Ormond Street subsequently referred its concerns to the General Medical Council (GMC), which opened an investigation on the same day Hindmarsh first appeared in court. UCLH followed with a similar referral.
Hindmarsh disclosed his GMC investigation to Cheshire police on 14 December 2022, almost three weeks after his first witness appearance. Neither the police nor the CPS had been informed prior to

his testimony, and the jury was not made aware of the investigations.
The allegations against Hindmarsh were never formally adjudicated, as he voluntarily removed himself from the GMC register of doctors in November 2024. A spokesperson for Cheshire police confirmed that the disclosure occurred in December 2022 and was subsequently communicated to the CPS.
Mark McDonald has indicated he will submit Hindmarsh’s nondisclosure as further evidence in support of Letby’s CCRC application, noting that it raises questions over the expert’s credibility and integrity. q


[
MOUNTING DEFENCE TIMES and rising liabilities are delaying access to justice for claimants in clinical negligence cases, with new figures showing record costs and unresolved claims.
Law firm Veritas Solicitors, which specialises in clinical negligence, says it is now routine for defendants to take up to nine months filing defences – described as a ‘record high’ by the firm’s lawyers.
Delays are mounting, they say, despite procedural rules allowing around six weeks, leaving claimants waiting months for cases to progress.
Claimant legal costs in clinical negligence cases have also reached their highest level on record, with NHS Resolution figures showing costs surpassed £600m last year for the first time, while the average time from notification to settlement remained at around 1.7 years – raising concerns about ongoing delays within the system.
Clinical negligence liabilities have now surpassed £60bn, highlighting how delays at the defence stage are prolonging justice and driving up costs for both claimants and the NHS.
Amina Ali, Partner and Head of Clinical Negligence at Veritas Solicitors, said: “Increasing delays in cases being resolved have significant consequences for claimants, and are mainly due to the lack of proactivity on the part of defendants.
“People face delayed access to justice, postponed compensation and increased stress, at a time when many are seeking muchneeded closure after going through terrible ordeals. For some clients who are unable to work due to negligence or have been left out of pocket, it delays recovery of their compensation.”
Most claims are resolved before reaching court, but more complex cases are increasingly held up at the defence stage, with NHS Resolution data showing 1,099 more clinical negligence claims were notified than settled last year, adding to the growing backlog.
“Defence extensions cannot be the norm, as it undermines access to justice,” Amina added. “Without stricter oversight from the courts in cracking down on defendants seeking endless extensions, these delays are likely to continue into 2026, increasing the need for experienced legal representation.
“Improving early engagement from the defendant and a more disciplined approach in allowing defence extensions would make a significant difference in ensuring people can access justice without avoidable delay.”
The Manchester-based firm says defence delays are particularly frustrating for clients, as delays in litigation are already long due to a lack of court resources.
Currently, the Civil Procedure Rules 1998 allow defendants

around six weeks to file a defence, with an extension beyond this requiring permission from the court.
The objective of the rules is to ensure cases are dealt with fairly and at proportionate cost, but as NHS legal costs increased by 7% to £181.3m, prolonged defence delays risk undermining that objective.
As clinical negligence litigation becomes more complex and time-consuming, delays in filing defences are a defining factor in whether the system can deliver timely justice. q




[ A CORONER HAS RULED that the death of a young mother from sepsis following a routine medical procedure was contributed to by neglect after she was given inappropriate antibiotics for a serious infection. An inquest in December heard that the failure to prescribe the correct medication in time significantly reduced her chances of survival.
Aleisha Rochester, a 33-year-old bank cashier from Croydon in south London, died in August 2023 after complications developed following surgery to remove abscesses from her left armpit and groin. The inquest heard that her condition deteriorated rapidly after the infection was not treated with antibiotics capable of targeting the bacteria responsible.
Rochester had undergone what was described as a routine day procedure on 5 August 2023 at St Thomas’ Hospital to remove the abscesses. She had a history of hidradenitis suppurativa, a chronic skin condition that causes painful abscesses and inflammation. Initially discharged following the surgery, she began to feel increasingly unwell within days.
Assistant coroner Sian Reeves said that Rochester’s surgical wound in her left armpit became infected after 10 August. As her symptoms worsened, she sought medical help on multiple occasions from both her GP and hospital services. Despite these consultations, the infection continued to progress.
On 15 August she was prescribed antibiotics, but the coroner found that the medication given did not comply with the antimicrobial prescribing guidelines used at St Helier Hospital. Crucially, the drugs did not provide effective coverage against a Gram-positive organism, which the coroner said was the most likely pathogen responsible for the infection.
The inquest also heard that before prescribing this combination of antibiotics, the surgical team had not consulted the hospital’s microbiology department for specialist advice. Such consultation is typically recommended where complex infections or unusual cases are involved.
A further drug was prescribed the following day, on 16 August, and this treatment was consistent with the hospital’s guidelines. However, by that point Rochester’s condition had already deteriorated significantly. She was admitted to intensive care on 17 August suffering from septic shock and multiple organ failure. Medical staff also identified signs of infection in her lungs. Despite aggressive treatment in intensive care, including a full antibiotic regime, mechanical ventilation and intensive medical support, her condition continued to worsen. In the early hours of 19 August Rochester suffered a cardiac arrest. Attempts to resuscitate her were unsuccessful.
Delivering her conclusion, Reeves ruled that Rochester should have been prescribed the appropriate antibiotics on 15 August. Had that happened, she would most likely have survived. As a result, the death was recorded as having been contributed to by neglect.
Rochester’s death has had a profound impact on her family, particularly her young son Xavier, who was only five at the time and is now eight. Her mother, Lorna, described her daughter as a loving and devoted parent whose life was cut tragically short.
She said Aleisha had been a compassionate and ambitious woman who had hoped to start her own business. She also spoke about the close relationship between Rochester and her son, describing the bond between them as evident to everyone who knew them.
According to her family, the loss has left a lasting void. They say the most painful aspect of the tragedy is knowing Rochester will never see her son grow up or share in the milestones of his life.
The family has now launched legal action against the NHS trust involved in her care.
Rochester’s mother has said the family hopes speaking publicly about what happened will help raise awareness of sepsis and the importance of prompt and appropriate treatment. She also expressed concern that similar mistakes could occur again if lessons are not fully learned.
In response to the coroner’s findings, Dr Richard Jennings, group chief medical officer for St George’s, Epsom and St Helier University Hospitals, acknowledged the failings identified at the inquest. He said the trust deeply regretted that Rochester had not been given the correct antibiotics and offered condolences to her family.
Jennings stated that the trust had taken steps to reduce the risk of similar incidents in future. These include providing additional training to staff to improve the early recognition of sepsis and introducing measures to ensure antibiotic prescribing is done correctly.
Although such changes may help prevent similar tragedies, Rochester’s family say the loss of a daughter and mother remains something they will never fully come to terms with. q



[A HOSPITAL TRUST at the centre of two high-profile investigations has agreed to pay a £1m legal settlement after it admitted doctors failed to diagnose that a patient had suffered a stroke.
Lisa, from Bishop’s Stortford, was 31 at the time and says she was told she had likely been suffering from stress and was sent home. She went on to have a second stroke that left her confined to a wheelchair for a year and with ongoing mobility issues.
Lisa was first taken by ambulance to Addenbrooke’s Hospital –governed by the Cambridge University Hospitals NHS Foundation Trust – after she suffered paralysis down her left side. The mother-of-two, who was on maternity leave with her youngest daughter at the time, was not referred to a stroke specialist.
She was discharged after medical staff told her an eight-hourdelayed CT scan had been inconclusive. Her condition worsened the following day and she returned to Addenbrooke’s. It was then discovered she had suffered a second stroke and she remained in hospital for five weeks.
Lisa said: “I had my first stroke at 5pm but only had a brain scan at midnight. That was inconclusive and I wasn’t given any medication, not even aspirin.
“I was then advised to go home and that the reason I was like how I was might have been a cause of stress, and that if my situation remained the same to speak to a GP on Monday.
“I left the hospital in a wheelchair and had to be carried up to bed at home by my husband. My parents were in Spain at the time and got the first flight home when they realised how serious it was.
“I was lying in bed on Sunday morning and I wanted to go downstairs. My dad carried me down and put me on the sofa, but that’s when my family saw that my face had dropped and my speech was slurred. It was quite clear I was having a stroke.”
Lisa was discharged from hospital earlier than anticipated as specialists expressed concerns about her mental health as she was unable to spend time with her family. She had to sleep downstairs for six weeks and was in a wheelchair for 12 months.
Lisa has since returned to part-time work in her role as a bookkeeper but is unable to hold a manual driver’s licence. She now suffers with significant issues to her left arm and hand. A further operation on her left foot and ankle has so far had a negative effect.
She said: “I remain in chronic pain on a daily basis. I’ve just now resigned myself to this being my new normal. I used to be fit and active and I was really positive of making a 100 per cent recovery. But when I realised that was never going to happen it was really mentally upsetting.
“I still try to enjoy my life as best as I can but it’s easier said than done – in the summer my mood goes up, but in the winter, it goes down. I’m no longer the same person – it’s changed my life completely.”
Cambridge University Hospitals NHS Foundation Trust, currently under patient safety investigations relating to suspended orthopaedic surgeon Kuldeep Stohr and its neuroscience unit, admitted a breach of duty of care.
It admitted that had Lisa ‘received prompt and appropriate’ initial treatment she would have had a ‘substantially better outcome’ from her stroke and would ‘likely have made a much better overall recovery’.
Medical negligence compensation specialists Hudgell Solicitors, who represented Lisa, alleged that administration of thrombolysis –an emergency procedure that breaks down blood clots – as soon as Lisa arrived at Addenbrooke’s would have avoided progression of a second stroke.
Although the trust also initially indicated an admission that its errors caused Lisa’s second stroke, it then changed its position and denied this had been the case.
This meant lawyers had to prepare for the matter to be heard in court
by a judge, but just five weeks before the case was due to be heard, the trust made a £1m offer to cover damages for Lisa and for legal costs.
Clinical negligence solicitor Hayley Collinson, of Hudgell Solicitors, said: “This has been a heartbreaking case. Lisa’s life has changed forever. She is unlikely to have the levels of independence she once cherished and will never get back those lost months of watching her children develop and thrive. This was an utterly preventable situation in which basic mistakes at Addenbrooke’s have been exposed.
“Cambridge University Hospitals NHS Foundation Trust firstly admitted a breach of duty, and that its error had caused the second stroke, but it then changed its position on causation which held up the process and prolonged the litigation.
“Thankfully, we were able to secure Lisa an interim payment of £50,000 before the claim was settled to help fund various therapies. With two huge investigations still ongoing, the governance of this trust and the conduct of staff at Addenbrooke’s is rightly under the spotlight.”
Lisa added: “I’m still angry that I was not believed from the off – not least because it was obvious I was half-paralysed. I’m also angry that they left me untreated for so long, that I didn’t get referred (to a stroke unit) and wasn’t given thrombolysis at the time.
“My anger has lessened over the years, but I think, looking back, we probably should have insisted on staying in hospital when we were first advised to go home and demanded a second opinion. You trust the experts, though, and that’s where the real anger comes from. I do feel I’ve been badly let down.
“Hudgells have been amazing from the start in what was a messy litigation, and now it’s over we can move on.” q




[THE ROYAL COLLEGE OF PHYSICIANS (RCP) has welcomed the ambition set out in the National Cancer Plan and its clear focus on prevention, earlier diagnosis, improving survival and supporting people to live well with and beyond cancer.
The National Cancer Plan sets out how we will improve cancer care so that three out of four people diagnosed with cancer survive for five years or more by 2035.
The plan was shaped by an extensive call for evidence exercise held from 29 April 2025. The more than 11,000 responses received played an essential role in developing the plan.
Physicians across the NHS will recognise the scale of the challenge and the urgency of action, particularly after years of missed cancer waiting time standards and widening inequalities in outcomes.
RCP clinical vice president and consultant medical oncologist, Dr Hilary Williams, said: “The ambition in this plan is right. Earlier diagnosis, faster access to treatment and better support for people living with cancer must be nonnegotiable, and it’s good to see commitments on lung cancer screening and tightening up rules around sunbed use. But the delivery of this plan will depend on sustained investment in the physician workforce. This is particularly important in areas of deprivation, where the lack of NHS staff delays both diagnostics and treatment.
“We also welcome the recognition that cancer care does not end when treatment does. Supporting people to live well with cancer, addressing inequalities in access and outcomes, and ensuring joinedup care across hospital and community services are all areas where physicians are ready to play a central role.
“We are extremely pleased that recommendations from our position statement on acute and supportive oncology are reflected in the plan and we look forward to working with the government and other Royal Colleges to review and modernise multidisciplinary team working and develop clear and consistent standards for acute and supportive oncology. Too many cancers are currently diagnosed in hospital emergency departments – a more proactive, system-wide, preventative approach is needed.
“We particularly welcome the emphasis on preventative healthcare, expanding community diagnostics and reducing variation between regions. However, these reforms will only succeed if matched with longterm workforce planning and investment in services that means we can effectively manage the toxicity of new cancer drugs and recognise unmet needs at an earlier stage. At their best, acute and supportive oncology services can reduce pressure on acute care, alleviate

The RCP looks forward to working with government and the NHS to turn this ambition into meaningful, measurable improvements in cancer outcomes and patient experience. q

[A WOMAN has received a five-figure settlement after a surgical drain from a hysterectomy was left in her body for more than a decade.
Sophie Bainbridge, medical negligence solicitor at law firm Leigh Day, said: “A woman, who we have called Lauren, attended Queen’s Hospital Burton for a hysterectomy in 2012. During the surgery, a surgical drain was inserted. The drain was noted to have been removed at 8pm the next day, and Lauren was discharged from the hospital three days later.
“Nearly four years later, Lauren was suffering from loose stools and swelling on the right side of her back and went to her GP. As she had a family history of bowel cancer, she had a blood test, colonoscopy and an abdominal examination, but the results suggested everything was normal.”
Lauren suffered episodes of pain, nausea and urgency to go to the toilet for the next seven years. In 2023, 11 years after the initial surgery, Lauren suffered excruciating pain on her lower left side. She vomited and struggled to breathe. After going to the toilet, she noticed that she had lost a lot of blood.
Lauren attended A&E at Queen’s Hospital the following afternoon. Following a scan, Lauren overheard a junior doctor say on the phone, 'what about the tube?', before mentioning the need to admit her and to start intravenous antibiotics.
Lauren was told that she still had a drain in her body, that her colon was inflamed, and that she needed to be admitted to hospital. She was then asked if she had had surgery recently and, as she had not, was instead told that she could be discharged with a prescription for antibiotics. 10 days later, Lauren returned to the hospital for a CT scan, which

confirmed the presence of the drain in her abdomen and inflammation around her colon. An urgent colonoscopy was arranged, and Lauren had to have a further surgery for the drain to be removed.
Lauren was told that the drain was longer than initially thought, and she could see from the imaging that it was bent, jagged and could move around. She could see that pieces had broken off the drain and asked whether these were still in her body. Whilst a full body scan showed no other pieces of drain, Lauren was still concerned.
Following the surgery to remove the drain, Lauren was sore, tired and shocked at what had happened. The events were distressing for her whole family, due to their history of colon cancer. Lauren’s bowel and abdominal symptoms resolved following the drain’s removal.
Lauren instructed Leigh Day to investigate the care she was provided with. University Hospitals of Derby and Burton NHS Foundation Trust admitted that Lauren received inadequate care during the surgery in 2012 and this caused her pain and suffering and the need for further surgery 11 years later when the drain was discovered.
Lauren said: “The experience was shocking, more so after the event, with the lack of genuine regret or regard to the potential risks to health or even life expressed by Queen’s Hospital. I would like to add that my consultant, however, was amazing and without whom, I could have had a very different outcome”
Sophie Bainbridge commented: “This is a truly shocking case. My client suffered over a decade of medical trauma due to a drain that should have been removed the day after her surgery. I hope that the trust’s admission of liability and the settlement bring her some closure following this awful ordeal.” q

[ THE ROLE OF urgent care and minor injuries clinicians in personal injury litigation has grown markedly in recent years. As front-line practitioners, they are often the first point of contact for patients presenting with injuries ranging from simple lacerations to complex musculoskeletal trauma.
In claims where initial assessment, triage decisions, wound management, safeguarding or failure to recognise red-flag symptoms are questioned, expert evidence from experienced urgent care clinicians has become increasingly valuable.
Urgent care centres and minor injury units operate at the intersection of primary and secondary care, requiring clinicians to make rapid, high-stakes decisions. In medico-legal disputes, the court must determine whether these decisions met the expected standard of care. An expert witness in urgent care provides clarity, assessing whether clinical actions – or omissions – were reasonable in the context of available resources, presenting symptoms and prevailing professional guidance.

of serious injury or systemic illness can carry serious consequences. Experts can help the courts understand the subtleties of risk assessment in a fast-paced environment. By examining records, triage notes and follow-up plans, they determine whether any oversight constituted a departure from accepted standards or reflected the inherent uncertainty of front-line practice.
Beyond establishing breach, expert opinion supports the assessment of causation and prognosis. By clarifying the likely progression of an injury under reasonable care, experts inform both liability and the quantification of damages. Their reports are structured to meet court expectations, providing independent, balanced and evidencebased commentary that solicitors can rely on when presenting or defending claims.
One common area of scrutiny involves triage and initial assessment. Experts evaluate whether the patient’s history and presenting signs were appropriately interpreted, whether vital signs and risk factors were considered and whether referral or escalation pathways were correctly followed. Failure to identify potentially serious conditions – such as compartment syndrome, head injuries or vascular compromise – can lead to significant complications. The expert’s role is to explain, in clear and impartial terms, whether any delay or misjudgement contributed materially to the outcome.
Wound management and musculoskeletal injury care are also frequent subjects of claims. Clinicians must assess severity, select appropriate interventions and provide clear discharge advice. Experts review documentation, consider whether management adhered to accepted standards and evaluate the implications of any deviation. For instance, inadequate wound care may result in infection or delayed healing, while incorrect splinting or fracture immobilisation can contribute to malunion or chronic pain.
Safeguarding concerns are another critical area. Urgent care clinicians are often the first professionals to encounter potential abuse or neglect. Evidence may be sought to assess whether concerns were appropriately recognised, documented and escalated. The expert’s analysis can clarify whether the clinician acted within the bounds of professional duty and current statutory guidance.
Red-flag recognition is central to urgent care practice. Missed signs

Experts provide objective insight into complex clinical decisions, reduce ambiguity in disputed facts and assist in establishing whether outcomes arose from accepted risk or substandard practice. Their input ensures that courts receive a comprehensive, clinically grounded perspective on front-line care, bridging the gap between medical complexity and legal analysis.
In an era of increasing scrutiny on initial assessment and triage, urgent care and minor injuries clinicians offer crucial expertise. Their input allows courts to evaluate claims fairly, ensuring that both patients and healthcare professionals are treated justly. q




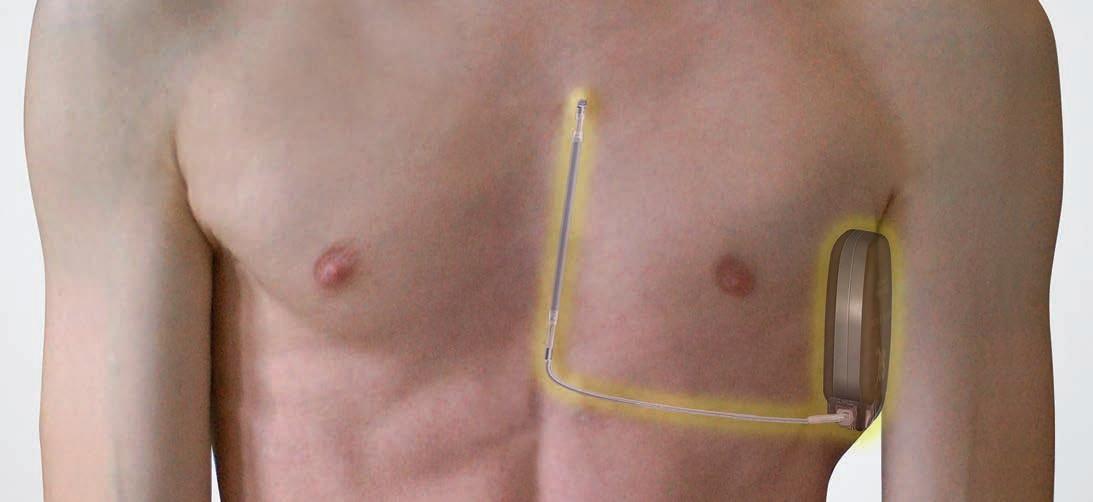
[THE BRITISH CARDIOVASCULAR SOCIETY (BCS) has joined three other organisations in signing a joint statement supporting the BRITISH Trial: a National Priority for Improving Care in NICM – a major UK-led clinical trial funded by the British Heart Foundation (BHF).
Together with the British Heart Rhythm Society, the British Society for Heart Failure and the British Society of Cardiovascular Magnetic Resonance, BCS recognises the importance of the trial and its potential to shape future recommendations for implantable cardioverter defibrillator (ICD) implementation in non-ischaemic cardiomyopathy (NICM).
Non-ischaemic cardiomyopathy is a heart muscle disease leading to dysfunction that is not caused by coronary artery disease, blockages or heart attacks. It stems from diverse causes such as genetics, viral infections, toxins or autoimmune conditions. Symptoms include fatigue, shortness of breath and leg swelling, with treatments ranging from medication (beta-blockers) to device implantation.
The statement of support also highlights the value of national collaboration and encourages all centres involved in caring for patients with NICM to support recruitment processes within their local pathways.
In the letter the four societies jointly recognise the importance of the BRITISH Trial and strongly support its successful completion.
The letter states: “BRITISH is a major British Heart Foundationfunded, UK-led clinical trial designed to determine whether cardiovascular magnetic resonance can guide decisions regarding implantable cardioverter defibrillator therapy in patients with nonischaemic cardiomyopathy. This is a longstanding and clinically

significant question that directly impacts treatment decisions, resource use, patient experience and future guideline development.
“Current international guidelines acknowledge the uncertainty regarding ICD benefit in NICM, and the absence of definitive evidence supporting imaging-based risk stratification. BRITISH is uniquely positioned to address this gap and to generate high-quality, UK-derived evidence that may influence practice nationally and internationally.
“Over 500 patients have now been randomised across participating centres, reflecting substantial effort from clinical and research teams. The study aims to recruit 1,252 patients and is behind schedule - as such, continued and enhanced recruitment is essential to ensure the study reaches the required sample size and delivers conclusive results.”
The four societies jointly:
• Affirm the scientific importance of the BRITISH Trial and its potential to shape future recommendations for ICD implantation in NICM.
• Encourage all centres involved in the care of patients with NICM to actively identify eligible patients and support recruitment processes within their local pathways.
• Highlight the value of national collaboration, noting that the UK has an opportunity to demonstrate international leadership in device therapy and advanced cardiac imaging research.
The letter concludes: “The societies are fully supportive of BRITISH and encourage all centres to work with local research teams and the study investigators to help complete this important trial.” q

By Philip Coleridge Smith DM MA BCh FRCS, Consultant Vascular Surgeon, Medical Director of
[CHRONIC LIMB-THREATENING ISCHAEMIA (CLTI) is a condition affecting the lower limbs in which blocked arteries no longer provide sufficient blood flow to maintain the leg in good health. The consequence of this is that the leg gradually deteriorates with pain, skin ulcers and infection. The need for major limb amputation is a common consequence of CLTI. About 12,000 patients per year present to the NHS with this condition.
The causes of CLTI are smoking, diabetes and old age. These cause the development of atheroma in the arteries leading to narrowing and eventual closure of the arteries. This is the same mechanism that may lead to heart attacks and strokes that also affect this group of patients.
Smoking used to be the most common cause of narrowed arteries. However, in the last half-century the prevalence of smoking has fallen from 40% of the population to about 11%. This has been associated with a substantial reduction in smokingrelated diseases.
However, over this period type 2 diabetes has become much more frequent with as many as 7% of the population affected. A substantial proportion of patients with CLTI are now affected by type 2 diabetes which is present in 50-70% of this patient group.
The onset of CLTI is usually insidious since arteries often occlude gradually giving the opportunity for a collateral (alternative) route of blood supply to evolve over a period of time. Where a larger artery occludes suddenly the patient may notice an abrupt deterioration in their symptoms.
Surgery
be mistaken for an adequately perfused limb.
Diagnosis depends on asking the patient, and potential claimant, the correct questions. Delay in diagnosis and treatment may lead to a major limb amputation. In patients presenting with foot pain the presence of a smoking history and diabetes should be obtained. If the pain occurs at night and is relieved by hanging the leg down, limb ischaemia may be present. A history of pain in the calf on walking, leading up to the current presentation, suggests that limb ischaemia may be present.
Clinical examination should assess the colour and temperature of the limb. CLTI usually results in coldness of the peripheries. Assessment of the pulses should reveal the state of circulation in the limb. Sometimes all the pulses are absent, sometimes only those at and below the knee. However, palpation of ankle pulses may lead to confusion; these may be difficult to feel and the clinician may mistakenly feel his own pulse. ‘Capillary refilling time’ – after compression with the finger of the examiner – is often assessed in place of palpation of the pulses. However, this is a very unreliable clinical sign, especially in ‘sunset foot’.
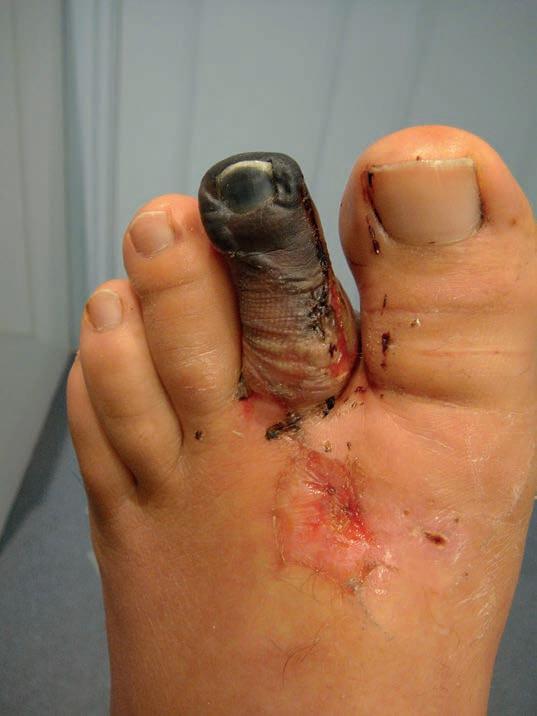
A patient with CLTI presents with gangrene affecting only one toe
Common symptoms include ‘rest pain’ and ischaemic ulceration of the foot or ankle. Rest pain occurring in the foot is very severe and is attributable to lack of adequate blood flow. This is especially likely to occur at night when the blood pressure falls during sleep. Patients find that sitting with the leg dependent relieves the pain since this increases the arterial pressure in the foot. Patients frequently sleep in a chair to minimise pain at night.
Patients with CLTI commonly present to their general practitioner with pain in the foot or foot ulceration. Sometimes the blood supply to one or more toes fails abruptly leading to presentation with gangrene of the toes (pictured). When the foot becomes generally short of blood flow, all blood vessels in the skin dilate leading to a red foot which is cold to the touch, contrasting with paleness of the rest of the limb. This is sometimes known as ‘sunset foot’ and can
Where doubts about the adequacy of circulation arise, these should be checked by Doppler ultrasound insonation of the foot and ankle pulses. Measurement of ankle blood pressure is also very useful to indicate the quality of the circulation of the foot and can readily be done in general practice. Absent ankle pulses or reduced ankle pressures are indicative of limb ischaemia.
Mistaken diagnosis of patients presenting to GPs, A&E departments and urgent care centres is common in this condition. Symptoms may be attributed to gout (acute inflammation of the one of the joints of the foot), plantar fasciitis or sciatica. This may lead to incorrect treatment being provided over a period of weeks or months. The resulting delays permit deterioration of the limb with gradual destruction of the foot by CLTI.
A number of publications show that delayed treatment of CLTI leads to adverse outcomes, including loss of the limb and loss of the patient. The Vascular Society of Great Britain and Ireland advises that patients with suspected CLTI should be referred to the vascular ‘hot’ clinic (or A&E department if the need is urgent) for review within one week with completion of investigations and treatment within one further week. For diabetic patients with a new foot ulcer, referral to the diabetic foot multidisciplinary team within one day is recommended by NICE Guidelines with review by the MDT within one further day. Failure to consider and comply with these guidelines may be considered to fall below an acceptable standard of care.
The main aim is to restore blood flow to the ischaemic limb as soon as feasible, sometimes as an emergency. This can be done using either open surgical bypass techniques or endovascular techniques such as balloon angioplasty and stenting of narrowed or blocked arteries. Available evidence is that both are equally effective. However, this group of patients commonly have arterial disease affecting all arteries in the body.
The risks of heart attack and stroke during or after interventions are common. Guidelines recommend use of ‘best medical therapy’ to treat this risk including prescription of aspirin, statins, blood pressure controlling medicine, anticoagulant drugs and treatment of diabetes to ensure good control of blood sugars.
The results of treatment for CLTI reflect the extent of generalised arterial disease in this patient group. Known adverse events arising from treatment include heart attack, stroke and death. The Society for Vascular Surgery, European Society for Vascular Surgery and World Federation of Vascular Societies have published global guidelines which make many recommendations concerning the management of this condition.
These guidelines assert: “CLTI is an end-stage manifestation of systemic atherosclerosis. It is frequently accompanied by clinically significant CVD, resulting in exceedingly high mortality from stroke and myocardial infarction. In the absence of aggressive identification and treatment of risk factors and associated comorbid conditions, the prognosis of CLTI is usually poor, with a mortality rate of 20% to 26% within one year of diagnosis. In a study of 574 patients with CLTI who did not undergo revascularisation after two years, 31.6% had died, primarily of CVD, and 23% required major amputation.”
Detailed outcome studies of CLTI show that in patients who

undergo vascular surgical treatment, life expectancy is about four years and less in diabetic patients. This will lead to limitation of the quantum in such cases and is a consideration when litigation relates to patients with CLTI.
Patients presenting with chronic limb-threatening ischaemia face a number of hurdles when seeking medical treatment for severe pain in the lower limb. Although CLTI is a common condition, the diagnosis is often not recognised by GPs and emergency care physicians. This may lead to delayed diagnosis which prejudices successful treatment by vascular surgeons to restore blood flow. Even if treatment is completed successfully, life expectancy of affected patients is limited and this should be considered when embarking on litigation. q




[SEPSIS IS ONE of modern medicine’s most urgent clinical emergencies. In the United Kingdom it affects hundreds of thousands of people each year, and when not recognised or treated promptly it can rapidly progress to organ failure, longterm disability or death.
Despite decades of national guidance and improvement programmes, delay and misdiagnosis remain persistent safety concerns, leading not only to tragic health outcomes but a growing volume of clinical negligence claims. In this challenging landscape, independent expert evidence from experienced emergency medicine clinicians is crucial in helping courts determine whether care met the standards reasonably expected.
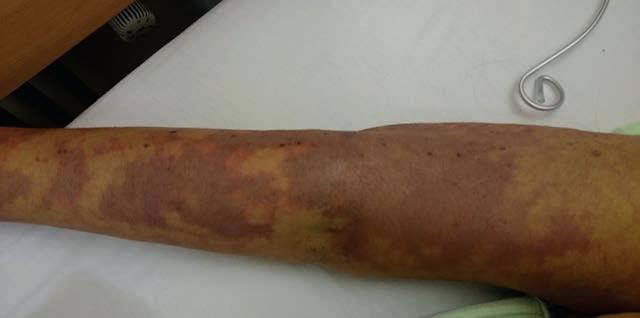
Emergency departments (EDs) are unique high-pressure environments. Clinicians must triage patients with undifferentiated symptoms, often relying on rapid clinical judgement, vital sign observations and decision-making tools such as the National Early Warning Score (NEWS) to identify those at risk of deterioration.
In sepsis cases, early identification and immediate treatment –including administration of antibiotics – are vital. National guidance stresses that patients with suspected sepsis should be screened and treated within an hour to optimise outcomes; however, less than half of high-risk cases currently receive antibiotics within this time frame.
The focus in claims invariably turns to whether sepsis ‘red flags’ were recognised and acted on appropriately. Experts in emergency medicine are often instructed to analyse triage decisions, escalation pathways, documentation of observations and the timing of interventions. They assist the court in understanding not only the clinical picture but the context in which decisions were made – including crowded waiting rooms and resource constraints.
A central task for the ED expert is to assess whether clinicians identified and responded to sepsis red flags – altered mental state, tachycardia, hypotension, elevated respiratory rate, fever or signs of organ dysfunction. The expert reviews whether vital signs were measured and documented systematically, whether the NEWS scoring was applied correctly and whether results were acted upon in line with accepted practice. Failure to do so can significantly worsen the outcome and forms a common basis for litigation.
Experts also scrutinise the escalation of care. In busy EDs, junior staff may make early assessments but it is expected that concerns are escalated promptly to senior clinicians when sepsis is suspected. A failure to escalate is often central to delayed diagnosis claims. In many cases, gaps in documentation or ambiguous notes complicate the picture. Legal teams frequently instruct experts to interpret records where red flags were present but not clearly recorded or where follow-up plans were inadequate. The court may be asked to consider whether, on the balance of probabilities, a reasonable clinician would have taken different actions had key signs been recognised.
Safety netting – advising a patient when to return to care if symptoms worsen – is another area where expert evidence can be decisive. Effective safety netting can mitigate risk by ensuring patients know when deterioration warrants urgent reassessment. Experts examine whether such advice was appropriate, clear and reasonable.
Arguably the most crucial component of expert evidence in sepsis claims is the assessment of causation. It is not sufficient to demonstrate a delay in diagnosis or treatment; the expert must explain how that delay materially contributed to harm and what the likely outcome would have been with timely recognition and intervention. For example,
earlier senior review and a faster start of antibiotic therapy may have prevented organ failure or prolonged hospitalisation.
Emergency medicine experts are also able to contextualise human factors that influence performance in the ED. They explain to the court how high patient volumes, cognitive overload and competing clinical priorities can affect decision making. While such factors do not excuse substandard care, they can help to explain why errors occur and whether those errors fall within the scope of reasonable practice.
Sepsis litigation presents complex challenges where clinical urgency, variable presentation and imperfect documentation intersect. Independent, court-compliant expert evidence plays a pivotal role in navigating these disputes, helping courts understand whether clinical actions were reasonable and how timing affected outcome. q

[ THE TIMING of diagnosis and intervention in modern clinical negligence litigation can be just as critical as the technical skill with which treatment is delivered. Delays in recognising or responding to a medical condition and failure to interpret diagnostic findings accurately can transform a potentially straightforward recovery into long-term disability or even fatality.
For solicitors handling time-critical claims, high quality evidence from clinicians experienced in acute and emergency care is essential to determine whether care standards met those reasonably expected and, crucially, whether any delay contributed materially to harm.
Delayed diagnosis and diagnostic error claims span a wide range of clinical scenarios – from missed fractures and overlooked symptoms of internal disease to failure to appreciate the red flags of sepsis, stroke or cancer. A timely and accurate diagnosis frequently dictates the window for effective treatment. An expert witness helps the court understand not only what did happen but what should reasonably have happened, given the available evidence.
A well-known example in the UK is that of Hotson v East Berkshire Area Health Authority [1988] UKHL 1. In that case, a teenage boy who had fallen from a tree was examined in hospital, but an incorrect initial diagnosis was made. Avascular necrosis of the hip – a serious condition – was not identified until five days later. By that time, the blood supply to the hip had deteriorated, leading to deformity, limited mobility and permanent disability.

The House of Lords ultimately found that the evidence did not satisfy the legal test of causation on the balance of probabilities, but the case highlights how expert medical evidence on timing, diagnosis and natural disease progression is central to the issue of responsibility for deterioration following delayed care.
Solicitors instructing experts in delay cases are advised to consider several core areas of focus. Firstly, what was the presentation to healthcare services, and were clearly abnormal signs or symptoms appropriately investigated? This may involve interpreting notes from general practice, emergency departments and diagnostic imaging. The expert will assess whether investigations such as scans, blood tests or referrals to specialists should reasonably have been undertaken earlier.
Secondly, once an abnormality was identified, did clinicians act promptly? Examples abound in clinical negligence practice where delayed follow up of abnormal test results, failure to admit for urgent review or misinterpretation of radiology have allowed conditions to worsen. Delays in diagnosing and treating liver or lung cancer, for example, commonly result in reduced treatment options and poorer prognosis; similar patterns are seen with unrecognised sepsis or strokes where every hour can significantly affect the outcome.
Thirdly, and perhaps most challenging, is the task of causation analysis. It is not enough to show that care was delayed. The expert must explain, with reference to accepted clinical evidence, how and to what extent that delay caused or materially contributed to the claimant’s deterioration. Did the delay reduce the likelihood of successful intervention? Would earlier surgery, treatment or referral have altered the trajectory of disease?
Prognosis opinions are another vital component in these claims. Where pre-existing pathology or comorbidities are present, experts must distinguish the natural progression of disease from harm attributable to delayed care. Careful, independent analysis will allow the court to weigh the counterfactual scenario – what would likely have occurred with timely, competent treatment – against the reality of the claimant’s current condition.
In summary, delay, deterioration and diagnostic error claims demand expert witnesses who can articulate not only clinical detail but also the interplay of timing, decision making and outcome. Their specialist opinion helps bridge the gap between complex medicine and legal standards, enabling the courts to arrive at fair, evidence-based conclusions in some of the most challenging clinical negligence cases. q

[SHOULDER AND ELBOW CONDITIONS are a frequent source of both personal injury and clinical negligence litigation. From traumatic rotator cuff tears and complex fractures to nerve injuries and failed joint replacements, these cases often involve significant pain and long-term functional impairment.
The central issue is rarely the diagnosis itself, but whether the standard of care met the level expected of a reasonably competent orthopaedic surgeon.
Shoulder surgery commonly addresses rotator cuff pathology, instability, impingement and degenerative joint disease. Elbow procedures may involve fracture fixation, ligament reconstruction, ulnar nerve decompression or total elbow arthroplasty.
While many operations are routine in experienced hands, both joints are anatomically intricate and technically demanding. Complications can include stiffness, persistent pain, infection, nerve damage and failure of repair.
In the medico-legal context, expert orthopaedic opinion is essential in distinguishing recognised complications from negligent treatment. An expert will
review the entirety of the clinical pathway: initial presentation, imaging, conservative management, timing of surgery, operative technique and post-operative rehabilitation. Particular scrutiny is often applied to decision-making. Was surgery indicated at the material time? Were non-operative options appropriately explored? Was there an unreasonable delay that materially affected the outcome?
Consent is another consideration. Patients undergoing shoulder or elbow procedures must be informed of material risks such as re-tear of a repaired tendon, ongoing stiffness, neurovascular injury or the possibility of limited functional improvement. An expert assesses whether the consent discussion, as documented in the records, reflects a meaningful exchange tailored to the patient’s circumstances rather than a generic recital of risks.
Technical performance is evaluated against accepted orthopaedic practice. In shoulder arthroscopy, for example, careful portal placement and recognition of anatomical structures are critical to avoid iatrogenic injury. In elbow fracture fixation, restoration of alignment and joint congruity is essential to minimise long-term dysfunction. An
experienced expert will analyse operative notes, imaging and follow-up records to determine whether the approach and execution were reasonable.
Causation analysis can often be complex. A poor outcome does not, in itself, establish breach of duty. Degenerative conditions may progress despite appropriate management and traumatic injuries may carry an inherently guarded prognosis. The expert must therefore separate the natural history of the condition from any additional harm attributable to substandard care.
Quantum often turns on functional limitation. Reduced shoulder elevation or compromised elbow extension can significantly impair employment, particularly in manual occupations. Expert opinion on prognosis, need for revision surgery and long-term restriction informs both liability negotiations and valuation of damages.
For solicitors handling orthopaedic claims, early instruction of a specialist in shoulder and elbow surgery ensures clarity on breach, causation and prognosis. For experts in this subspecialty, the medico-legal arena demands balanced, independent analysis and the ability to explain complex anatomy and surgical decision-making in clear, measured terms. q




[ORTHOPAEDIC SURGERY is increasingly under the medico-legal microscope. With advances in surgical techniques and heightened expectations for functional recovery, solicitors are seeing a rise in claims where post-operative complications, disputed decision-making and longterm outcomes are contested.
From traumatic fractures to elective joint replacements, courts rely heavily on independent orthopaedic experts to clarify whether care met the accepted standard at the time, particularly where consent, operative technique, fixation choices and rehabilitation planning are in question.
The role of the orthopaedic expert begins with a meticulous review of medical records, operative notes and imaging. In trauma cases, this often involves assessing whether fractures were identified and managed promptly, whether fixation was appropriate and whether post-operative protocols were adhered to.
In elective procedures, including joint replacement or spinal surgery, experts evaluate surgical indications, choice of prosthesis and intra-operative technique. Disputes frequently arise over whether the surgeon’s decisions reflected a responsible body of opinion or fell below the standard reasonably expected of a competent specialist.
Consent is a recurrent focus in litigation. Courts require evidence that patients were informed of material risks, alternatives and potential complications. Experts scrutinise documentation to determine whether the discussion was adequate and whether it aligns with recognised standards. Failure to properly inform a patient of the likelihood of persistent pain, restricted mobility or the need for revision surgery can form the basis of a claim, even when the surgery itself was technically competent.
delays or omissions contributed to ongoing disability.
Assessing causation and prognosis is frequently challenging. Preexisting conditions, co-morbidities and degenerative changes can obscure the relationship between treatment and outcome. Experts must separate the natural history of disease from any additional harm caused by surgical intervention or delay. Their opinion guides the court in understanding how injury and treatment interact with pre-existing pathology, enabling a balanced assessment of liability and the valuation of damages.
Technical execution is another area of close examination. Orthopaedic surgery is inherently precise, and even minor deviations can lead to significant functional impairment. Experts assess whether alignment, fixation and soft tissue handling were appropriate and whether operative notes support the conclusion that accepted standards were followed. In complex trauma or revision surgery, this analysis is vital in distinguishing unavoidable complications from substandard care.
Rehabilitation and post-operative care form a further dimension of expert assessment. Appropriate physiotherapy, monitoring for complications and timely intervention in response to adverse signs can markedly influence outcome. Courts often rely on orthopaedic experts to determine whether post-operative management was sufficient or whether

Orthopaedic experts are particularly valuable in cases involving spinal surgery, complex joint procedures, fracture management, missed injuries and revision operations. They provide independent, court-compliant reports that translate clinical complexity into reasoned opinion on breach, causation and functional outcome. By interpreting operative records and imaging in the context of accepted practice, they clarify whether care met the standard expected and the likely trajectory of recovery.
For solicitors instructing orthopaedic experts, early engagement can sharpen case strategy and strengthen negotiations. In contested claims, the expert’s impartial and authoritative opinion is pivotal in assisting courts to understand intricate surgical issues, evaluate long-term consequences and reach fair and proportionate outcomes. q


By Mr Simon Wimsey FRCS (Tr & Orth), Consultant Orthopaedic Surgeon
[THE ROLE of the orthopaedic expert witness continues to evolve in response to judicial expectation, procedural reform and increasingly complex medical claims.
In disputes involving the hand, wrist and elbow – whether arising from personal injury, industrial disease or clinical negligence –the court relies on experts not merely for clinical knowledge, but for clear, disciplined reasoning on causation, breach, prognosis and functional impact.
Since 2013, I have worked as an APIL Tier 1 expert with Bond Solon CertMR and clinical negligence training, preparing over 1,100 orthopaedic reports. This experience has consistently reinforced that credibility before the court depends as much on methodology and independence as on surgical experience.
Upper limb pathology frequently presents with diagnostic and causal uncertainty. Conditions such as hand-arm vibration syndrome (HAVS), nerve injury, missed fractures and evolving compartment syndrome often lack a single defining event. The expert’s task is therefore not simply to state an opinion, but to explain how that opinion has been reached, addressing competing explanations and evidential gaps in a structured and transparent manner.
HAVS litigation offers a useful illustration of the court’s approach to expert evidence. These cases commonly involve prolonged exposure histories, delayed symptom reporting and confounding risk factors such as smoking or non-occupational cold exposure.
Courts have consistently favoured expert opinions that demonstrate careful
reconstruction of exposure, application of recognised diagnostic criteria and reasoned differentiation between occupational and nonoccupational causes. Conversely, opinions that rely on assumption, or fail to engage with alternative explanations, have been given little weight. For the expert witness, HAVS claims highlight the importance of analytical discipline and an evidence-led approach.
Similar issues arise in clinical negligence cases involving fluid extravasation injuries. Although such cases may initially appear to concern acute care or nursing practice, the downstream orthopaedic consequences – soft tissue necrosis, nerve damage and longterm loss of hand function – often fall within orthopaedic expertise.
Courts have scrutinised whether early signs of extravasation were recognised, whether escalation was appropriate, and whether evolving compartment syndrome should reasonably have been anticipated.
Expert evidence has been most persuasive where it clearly explains the clinical decisionmaking process at each stage, rather than applying retrospective hindsight.
The broader legal context reinforces these expectations. The Supreme Court decision in Jones v Kaney [2011] removed expert witness immunity from suit, underlining that experts are accountable for the quality and integrity of their work. While now well established, its implications remain highly relevant: inadequately reasoned opinions or failures of professional care in medico-legal work carry real risk.
Judicial criticism has increasingly focused

on expert reports containing unsupported assertions, unexplained conclusions or opinions that stray beyond the expert’s true area of expertise. This is particularly pertinent in orthopaedics, where overlapping subspecialties and multidisciplinary care can blur professional boundaries. Experts must be vigilant in defining the limits of their competence and resisting the temptation to fill evidential gaps with speculation.
Further guidance can be found in Wye Valley NHS Trust v Murphy [2024], where the court examined inconsistencies in the factual accounts provided to multiple experts. The case serves as a reminder that expert opinion is only as reliable as the factual assumptions on which it is based, and that experts must remain alert to discrepancies that may undermine the integrity of their conclusions.
Taken together, these developments emphasise core principles for the modern orthopaedic expert witness: independence from the instructing party; adherence to one’s genuine area of expertise; reasoned, evidence-based analysis; procedural fluency with the Civil Procedure Rules; and clear communication for a non-clinical audience. Guidance from professional bodies, including the British Orthopaedic Association, remains a valuable reference point in maintaining these standards.
As the interface between medicine and law continues to sharpen, the expert witness plays a pivotal role in assisting the court. Only by combining clinical insight with intellectual rigour, transparency and independence can orthopaedic expert evidence continue to command judicial confidence and fulfil its proper function. q


[THE Arthritis and Musculoskeletal Alliance (ARMA) has launched a bold new five-year strategy to transform how musculoskeletal (MSK) health is recognised, prevented and treated across the UK.
MSK conditions are the leading cause of pain and disability, affecting more than 20 million people. They limit independence, reduce healthy life expectancy, drive economic inactivity and place major pressure on health and care services. Yet MSK health remains consistently overlooked in national policy and investment.
ARMA’s 2026-2031 strategy 20 Million Reasons sets out how the UK-wide alliance of patient organisations, professional bodies and research groups will change that. It commits ARMA to securing stronger political and senior NHS leadership, shifting the system towards prevention and neighbourhood-based support, tackling inequalities and improving access to timely, effective MSK care.
The strategy positions MSK health as fundamental to the nation’s wellbeing and prosperity and calls for collective action to make it impossible to ignore. Adrian Bradley, chief executive of ARMA, said: “MSK health must not be overlooked. It’s central to our nation’s health and prosperity. If we invest in prevention, whole system change and better treatment and care in every community, we can improve millions of lives and secure a decade of better health and wellbeing.”
Justine Clarke, chief operating officer of the British Orthopaedic Association, said: “We strongly support ARMA’s strategy and its ambition to make musculoskeletal health a national priority. Relieving pain and restoring function is fundamental to improving quality of life, reducing inequality and enabling people to remain active and independent. ARMA’s collective voice is critical in ensuring MSK health


receives the political focus and investment it warrants. By working together across the MSK community, we can turn evidence and lived experience into meaningful policy change and make MSK health impossible to ignore.” q





By Mr Alexander Montgomery MBchB MRCS (Eng) Dipl Orth Eng FRCS (Eng), Consultant Spinal Surgeon
[SPINAL SURGERY may be contemplated for several conditions, including congenital abnormalities, degenerative conditions, traumatic injury and tumours. Often, these procedures are complex. Therefore, the frequency of complications is relatively high, occurring in up to 20% of patients. While some of these unwanted effects are mild, others can be devastating for the patient and even lead to death.
Spinal surgery complications can be divided into those that arise during surgery itself, and issues that become apparent after the procedure, including those with delayed onset.
Of the intraoperative complications, neurological injuries are probably the most feared. They arise when either the spinal cord or one or more nerve roots are damaged and take the form of a worsening of current neurological status or a new neurological deficit. Several measures can be taken to avoid neurological injury during surgery, including careful planning, positioning of the patient before and during the procedure, and intraoperative electrophysiologic monitoring which allows issues to be identified quickly.
The use of high-dose steroids can also help to reduce traumatic oedema and the potential for spinal compression. If compression does occur, it should be relieved immediately, even to the extent of reversing deformity correction if necessary.

for adequate wound closure. Signs of infection or dehiscence should be treated promptly with antibiotics.
As the causal organisms can differ from those commonly seen in orthopaedic surgery, infections may present in an unusual way, and often there is insidious infection without widespread systemic involvement. Therefore, clinicians should maintain a high index of suspicion for signs of infection.
Although cerebral spinal fluid (CSF) leaks can occur intraoperatively, they can also cause issues postoperatively, as they can impair wound healing and promote infection. In patients with cancer, leaks can also lead to intradural tumour seeding. In the event of a leak, repair should be undertaken immediately, as ongoing leaks can lead to cerebrospinal fluid hypotension and intracranial subdural haematomas.
Temporary lumbar drainage may be needed to decrease the level of hydrostatic pressure on the repaired area. CSF leaks rarely cause longer term effects, but can slow down recovery and wound healing, and can lead to the need for further surgery.
Injuries to adjacent structures can occur during spinal surgery. In the posterior approach to the facet joints, and in the anterior approach to the organs and blood vessels. Major vascular damage can be lifethreatening and immediate attempts should be made to control the bleeding. Vascular surgeons are often present, and may be required to repair the damage. Oesophageal and bowel injuries may also require specialist interventions. Damage to the gastrointestinal tract can significantly increase the risk of infection and consideration should be given to appropriate management postoperatively.
The risk of misplaced screws causing damage to adjacent structures can be reduced by the use image intensifier, or navigated operating techniques, which have a higher level of screw placement accuracy.
Issues with wound healing are the most frequently encountered of the postoperative complications. Management of wound breakdown can be challenging and lead to considerable morbidity. Additionally, surgery involving removal of a tumour or other resected tissue can create a large dead space within the spine that must also be addressed. These cases often benefit from intervention by a plastic surgeon to ensure adequate closure of the dead space and coverage of the surgical site. Plastic surgery may also be required in cases of repeated wound infection or breakdown. Wounds in the sacral area are particularly prone to breakdown, as there is limited soft tissue available
Failure of spinal reconstruction can also be a major issue. This may be due to poor surgical technique, poor bone quality which impedes healing, and instrumentation failure. The latter can be particularly difficult to manage, as scarring and broken bone or instrumentation can present the surgeon with even fewer options for repair than for the original procedure. Further surgery is warranted if the failure increases the risk of further injury to the patient or causes mobility-limiting pain.
As well as the risk of complications themselves, several additional issues must be considered during surgery for spinal tumours. This type of surgery requires the suspension of adjuvant therapies such as chemotherapy to allow the healing of the surgical site. Surgical complications, especially if they involve wound healing, may prolong the time that a patient goes without these life-prolonging therapies and could ultimately shorten the patient’s life.
This is compounded by the fact that patients with cancer are more likely to develop a surgical site infection, due to immunosuppressive therapies, previous radiation of the site, and comorbidities such as anaemia and poor nutritional status. In patients with a relatively long life expectancy, the long-term durability of the procedure must also be considered. Therefore, emphasis on maintaining or restoring biomechanical function of the spine with bony fusion is important. Several other factors increase the risk of complications following spinal surgery. These include blood loss during surgery, duration of surgery, procedures involving more than one site, and comorbid conditions, including atrial fibrillation, metastatic tumours and obesity. Patient age may also be a factor. Therefore, assessment of the patient’s current disease status, comorbidities and neurological status must be fully investigated before surgery takes place, as these will determine the expected surgical benefits and anticipated complications.
The patient should be given reasonable expectations regarding useful neurological function and pain reduction after surgery, which will reduce the likelihood of subsequent litigation for negligence. q
• Mr Alexander Montgomery is a Consultant Spinal Surgeon and regional Chair of Spinal Surgery for North East London and Essex. Twelve years ago, he established the spinal trauma unit at The Royal London Hospital (Barts Health NHS Trust) which is now the largest in the country.
Mr Montgomery performs spinal surgery using microscopes and minimally invasive techniques. He performs anterior, posterior and lateral minimal access approaches for lumbar surgery, anterior and posterior cervical surgery, and complex deformity cases.
He accepts adult instructions for claimant or defendant in medical negligence and personal injury cases.
For further information contact Medicolegal Partners by emailing info@medicolegal-partners.com


[FOOT AND ANKLE CONDITIONS present unique challenges in both clinical and medicolegal contexts. Injuries range from simple fractures and sprains to complex midfoot and hindfoot reconstructions, while degenerative conditions such as osteoarthritis and tendon dysfunction, and deformities like hallux valgus, often require surgical intervention.
For instructing solicitors, understanding the nuances of foot and ankle surgery is essential to establishing breach of duty and evaluating claims.
Foot and ankle surgery encompasses a broad spectrum of procedures – from minimally invasive arthroscopy to open reconstruction, osteotomies, tendon repairs, ligament reconstruction and joint replacement. While many are highly successful in restoring mobility and reducing pain, complications can arise. These include infection, non-union or malunion of fractures, nerve injury, persistent pain, stiffness and recurrence of deformity. Differentiating between recognised surgical risk and substandard care is critical in assessing claims.
understand whether any adverse outcome reflects unavoidable risk or substandard practice.
Post-operative care and rehabilitation are equally important. Successful recovery often depends on adherence to physiotherapy, gradual weightbearing protocols and monitoring for complications. Failure to provide adequate follow-up, or delay in recognising complications, can exacerbate injury and form the basis of litigation. Expert analysis in this area clarifies whether post-operative management met the standards expected of a competent specialist.
Functional impact is a key consideration in quantifying damages. Reduced ankle dorsiflexion, limited subtalar motion or chronic forefoot pain can affect walking, standing, employment and daily living activities. Experts can provide an objective assessment of functional limitation, prognosis and the potential need for further interventions. That opinion informs both liability assessment and valuation of losses, assisting solicitors in presenting coherent, evidence-based arguments to the court.
An expert orthopaedic surgeon specialising in foot and ankle surgery plays a vital role in interpreting clinical records and operative notes. Their assessment begins with reviewing diagnostic imaging, pre-operative evaluation, surgical planning and post-operative management. For traumatic injuries, they can evaluate whether timely intervention was undertaken, whether fixation and alignment were achieved according to accepted standards, and whether appropriate post-operative rehabilitation was prescribed.
In elective procedures, such as bunion correction or ankle arthroplasty, the focus often shifts to surgical technique, appropriateness of the chosen procedure and informed consent.
Consent is frequently a focus in claims involving elective surgery. Courts expect evidence that patients were made aware of any material risks. An expert will assess whether consent discussions were documented, clear and personalised, rather than generic or incomplete. This analysis can determine whether a breach of duty arose from the consent process or from technical execution of the surgery.
Surgical technique is central to the expert’s evaluation. Foot and ankle surgery demands precision, given the intricate anatomy and weight-bearing function of the region. Errors in alignment, fixation or soft tissue handling can have long-term functional consequences. Experts assess whether recognised techniques were followed, whether any deviations were justified and whether operative records demonstrate careful planning and execution. This helps the court

Instructing a foot and ankle specialist expert witness ensures that claims are evaluated by practitioners with both technical expertise and experience in medico-legal reporting. Such specialists enable solicitors to navigate claims with confidence, ensuring that both the technical and practical consequences of an injury are accurately represented and fairly evaluated. q


By Professor Paul Y F Lee, consultant orthopaedic surgeon, Honorary Professor of Sports Medicine and expert witness
[IN ORTHOPAEDIC MEDICO-LEGAL PRACTICE few concepts are as persistently misunderstood as low-probability surgical risk. A complication may be rare, recognised and widely documented, yet once it occurs it is often reinterpreted as evidence of fault.
This phenomenon – which may be termed the 1% problem – arises when probability is retrospectively collapsed into certainty, and risk is mistaken for negligence.
The difficulty is not confined to one side of litigation. It affects claimant and defence cases alike and is driven by a failure to distinguish clearly between risk, mechanism and responsibility.
Risk is not negligence
Negligence requires a departure from reasonable practice. It also requires logic and common sense. Surgery involves intervening in complex biological systems, and even when care is reasonable, adverse outcomes may occur. The fact that a complication is uncommon does not make it illegitimate, nor does its occurrence alone establish breach. A poor outcome is not, in itself, proof of negligent care.
The 1% problem emerges when expert reasoning begins with outcome rather than with the decision making, execution and systems in place at the time. Courts are then presented with conclusions that rely on hindsight rather than disciplined analysis.
Consent and the myth of numerical thresholds
Modern consent law has decisively moved away from percentagebased disclosure. There is no legal rule that fixes material risk at 0.5%, 1% or any other figure. Materiality is contextual. A low-probability risk may be material because of its consequences, the patient’s occupation, lifestyle or stated priorities.
Equally, however, consent recognises residual risk. It does not guarantee outcome. The occurrence of a disclosed risk does not retrospectively convert appropriate care into negligence. The 1% problem arises when risk is accepted in theory but treated as unacceptable once it materialises.
The critical corrective to the 1% problem is mechanism-based analysis. Complications should not be assessed by name alone, but by how, when and under whose control they occurred.
Hip dislocation provides a useful illustration. It is a recognised complication of hip arthroplasty, yet its medico-legal significance varies entirely with context.
A dislocation occurring weeks after surgery, during independent mobilisation, in a patient with recognised instability risk factors, may remain within the spectrum of accepted risk, provided reconstruction was reasonable and precautions appropriate.
By contrast, a dislocation occurring immediately post-operatively – during transfer or recovery, before the patient has mobilised or exercised meaningful control – requires a different analysis. In such circumstances, attributing causation to patient behaviour is rarely logical. Responsibility narrows to two domains: the inherent stability of the reconstruction, and the healthcare system responsible for handling and positioning. What is ordinarily a recognised risk may cease to be

one, not because dislocation occurred, but because its timing and mechanism are inconsistent with reasonable care.
versus negligence
Importantly, not every early dislocation represents negligence. Surgery can involve mishap without fault. The decisive factor is often what happens next.
An early dislocation that is promptly recognised, safely reduced, properly investigated, clearly documented and honestly explained to the patient may represent a complication or operative mishap rather than negligent care.
However, if the event is missed, dismissed, inappropriately attributed to the patient, poorly documented or followed by delayed or incomplete explanation, the focus shifts. What may have begun as a complication can evolve into a breach – not necessarily because the dislocation occurred, but because of a failure to recognise, respond or communicate reasonably once it did.
This distinction is critical. Negligence often lies not in the initial event, but in the unreasonable failure to respond appropriately to it.
The 1% problem is exacerbated when responsibility is forced into a single category. In reality, adverse outcomes often arise from an interaction between surgical execution, implant behaviour, patient physiology and post-operative systems of care.
A mechanically unstable reconstruction may predispose to dislocation. Equally, unsafe handling during transfer can convert a stable construct into an unstable event. Medico-legal analysis must allow for both possibilities and resist the temptation to default either to outcome-based blame or blanket acceptance of risk.
The role of the expert is not to excuse complications nor to assume fault, but to explain why an event occurred, whether it was preventable, and where control lay at the relevant moment. This requires moving beyond labels and percentages and towards structured, logical analysis grounded in mechanism and context.
When that approach is taken, the 1% problem largely dissolves. Some cases will properly support claims; others will not. What matters is that responsibility is attributed on the basis of evidence, reasonableness and common sense – not assumption.
Low-probability risk is an inherent feature of surgery. Treating its occurrence as automatic proof of negligence serves neither patients nor the courts. Understanding when risk remains risk – and when it becomes failure – is where modern medico-legal analysis must now focus. q
• Professor Paul Y F Lee is a consultant orthopaedic surgeon, Honorary Professor of Sports Medicine and expert witness specialising in biomechanics, imaging and causation analysis. He and his team at MSK Doctors operate across London and Lincolnshire, with offices in London, Marylebone and near Liverpool Street Station.
Urgent expert opinion can be provided by prior agreement



[HAND AND WRIST INJURIES are among the most common presentations in trauma and orthopaedic practice. From sports injuries and falls to workplace accidents and missed fractures, these cases frequently lead to prolonged pain, functional impairment and, increasingly, medicolegal claims.
In the United Kingdom, recent legal developments highlight both the human cost of substandard hand care and the vital role that independent expert witnesses play in unraveling complex clinical evidence.
A recent case involved a delayed diagnosis of a scaphoid fracture – a classic hand injury in which early recognition is crucial to prevent long-term disability. A man in his 30s presented with wrist pain after a fall and was discharged with a diagnosis of soft tissue injury, but no specialist scaphoid imaging was obtained.
Over the next 18 months he suffered persistent pain and loss of grip strength, which ultimately led to invasive bone grafting surgery and significant scarring because the fracture had gone unrecognised for too long. The claim was settled with an admission of failure to consider a scaphoid fracture and arrange appropriate imaging.
The case highlights the medicolegal importance of specialist interpretation of early imaging and clinical signs. A hand and wrist surgery expert witness assesses whether the initial assessment met the standard expected of a competent clinician, whether critical investigations were omitted and whether any delay materially worsened the outcome. In claims involving subtle musculoskeletal injuries, such as those of the scaphoid or triangular fibrocartilage complex, early diagnosis can dictate whether conservative management or surgery will be sufficient.
Another example from past reporting illustrates the long-term impact of missed hand fractures. A 43-year-old woman from Essex received compensation after a fracture at the base of the thumb was not identified at the time of injury, leaving her with ongoing pain and functional limitations that affected even basic tasks, such as lifting small objects, more than six years later.
Such cases emphasise how expert evidence must address not only the merits of the clinical decisions made at the time but also the lifelong consequences for daily living and work, forming a critical input to quantifying damages.
Beyond fractures, hand surgery claims often involve disputes over surgical technique, fixation choice or post-operative management. In scenarios where internal fixation devices have been poorly positioned, tendon repairs have failed or nerve damage has occurred, experts in hand and wrist surgery are tasked with determining whether the surgeon’s approach conformed to accepted practice at the time and whether any departure from that standard caused or materially contributed to the claimant’s disability.
National trends in orthopaedic litigation reinforce the relevance of these specific claims. Musculoskeletal injuries – including upper limb and hand injuries – continue to feature heavily in clinical negligence statistics, with surgical errors, delays in treatment and decision-making errors among the most costly categories.
Expert witnesses also play a vital role in interpreting gaps in documentation and the wider context of care. Emergency department and outpatient records may lack detail on the rationale for clinical decisions, or fail to record specific hand tests and comparison imaging. An expert scrutinises such records alongside accepted clinical protocols, offering the court reasoned conclusions on whether, on the balance of probabilities, a different course of action would have been preferred by a responsibly competent clinician.
For claimants who have experienced prolonged pain, dysfunction or loss of employment due to hand injury, expert evidence is central
to establishing the degree of functional impairment and ongoing care needs. Hand surgery experts provide structured evaluation of grip strength, dexterity, sensory deficits and muscle wasting, linking these findings to realistic projections of recovery, rehabilitation and future therapeutic interventions.
As hand and wrist claims continue to be brought before the courts or settled in the shadow of litigation, the role of independent expert witnesses remains indispensable. Their expert opinion helps bridge complex clinical evidence and legal standards, ensuring that both breach of duty and the true impact on quality of life are clearly understood and fairly represented in every case. q


David Berry PhD FRC Path MFSSoc MRSC
Independent Toxicology Consultant
Specialist in Clinical and Forensic Toxicology with particular emphasis on drugs (both illicit and therapeutic) and alcohol. www.toxicologyservices.co.uk
Mr Timothy Burge MBChB FRCS FRCS(Plast) DMCC MSc
Consultant Burns & Plastic Surgeon
• Cosmetic and aesthetic surgery of the breast and trunk
• Burns • Trauma • Scars
Clinics in Birmingham, Bristol, Cardiff, London and Salisbury. www.clifton-plastic-surgery.co.uk


Professor Paul J Ciclitira MB PhD FRCP MRCS FRCP AGAF
Professor of Gastroenterology with particular interest in food allergy, including Coeliac disease, peptic ulcer, inflammatory bowel disorder and hepatology. www.profpaulciclitira.co.uk
Mr Philip Coleridge Smith DM MA BCh FRCS
Consultant Vascular Surgeon 20 years of:
• Defendant instructions • Claimant instructions
• Single joint expert • Court experience


Dr Sam Creavin MPhil MBChB MRCP(UK) MRCGP PhD CUBS
General Medical Practitioner

• Delayed diagnosis: cancer, sepsis, spinal disorders, ectopic pregnancy, diabetes, heart disease • Instructed by GMC and NHS resolutions 60/40 split • Quick turnaround. Authoritative, logical and reasoned reports. www.gpexpertwitness.com
Chris Dawson MS FRCS LLDip
Consultant Urologist with 22 years experience of medico legal report writing and expert witness work and has completed over 2,100 reports. He also regularly completes Fitness to Practice reports for the General Medical Council.
www.chrisdawson.org.uk
Mr Mark Duxbury MA (Oxon) DM FRCSEd (Gen Surg)
Consultant Hepatobiliary, Pancreatic & General Surgeon
• General & emergency surgery • Hernia surgery
• Liver & pancreatic surgery • Gallbladder & biliary surgery
Equip2Speak
Medico-legal Consultancy for Assistive Technology (AT) & Speech and Language Therapy (SLT)
• Specialists in Brain and Spinal Injury
• Justified Evidence & Expertise in Immediate & Lifetime Needs
• Experienced in Complex & High-Value Claims


Mr Kim Hakin FRCS FRCOphth
Consultant Ophthalmic Surgeon and Expert Witness on ophthalmological matters
www.kimhakin.com

Mr Vijay Joshi MBChB, LL.B (Hons), FRCSEd (C-Th), PGCert (Medical Law)
Consultant Thoracic Surgeon
Personal injury and clinical negligence cases relating to diseases and injuries of the chest. Preparation of medicolegal reports and giving evidence in court.
www.thoracicexpertwitness.co.uk
Atul Khanna FRCS (Plast)
Consultant Plastic, Reconstructive and Hand Surgeon
• Hand surgery • Soft tissue injury • Burns management
• Medical negligence in cosmetic surgery www.atulkhanna.co.uk/expert-witness/
Dr Raj Kumar – Dental Expert
Causation and Liability and Condition and Prognosis Reports
• General dentistry • Cosmetic dentistry • Patient consent
• Dental implantology • Orthodontics • Facial aesthetics
07802 456 804 | info@dentalexpert.me | www.dentalexpert.me
Kulvinder Lall Consultant Cardiothoracic Surgeon
Instructions taken in cases relating to cardiac and thoracic surgery, including aspects relating to surgical care and those following trauma to the structures of the chest.
www.kulvinderlall.com




Mr Brian Leatherbarrow BSc MBChB DO FRCS FRCOphth
Consultant Ophthalmic, Oculoplastic & Orbital Surgeon
• Complications of cosmetic eyelid surgery • Eyelid reconstructive surgery • Eyelid and orbital tumours and trauma • Loss of an eye / socket reconstructive surgery • Thyroid eye disease • Ptosis surgery
www.medicolegalophthalmology.co.uk
Mr Richard Matthews MB BS FRCS FRCSE MAE
PLASTIC & HAND SURGEON

• Claimant/Defendant/Joint Instruction
• Laparoscopic surgery • Hepatobiliary surgery www.markduxbury.info/medicolegal www.equip2speak.co.uk
Dr Lance N. Forbat BSc (Hons) MD FRCP FRCP (Glasgow)
Consultant Cardiologist
Experienced in writing medico-legal reports on all aspects of adult cardiology – specialising in angina, heart failure, arrhythmias and pacing.
www.heartattacksymptoms.co.uk

Mr Matthews is well versed in the provision of Medical Reports relating to Personal Injury ranging from scarring through trauma, including burns and scalds, to non-bony hand injuries.
www.richardmatthewsmedicolegal.uk
Mr Lindsay Muir MB MCh(Orth) FRCS(Orth)
Consultant Hand Surgeon
• Amputation • Nerve injury • Dupuytren’s disease
• Scaphoid fracture
• Finger fracture
• Tendon injury
Consultant Orthopaedic Surgeon – Upper Limb Specialist. Expertise in all upper limb conditions and treatment. Shoulder, elbow, wristand hand injuries. www.yorkshire-upperlimb.co.uk www.adsummedicolegal.com & www.britishveininstitute.com
• Hand surgery
• Wrist fracture www.tmhc.co.uk
Mr Abraham Odumala
MBBS M.MedSci FWACS FRCS FRCS(Tr & Orth)




Dr Shanthi Paramothayan
BSc PhD MBBS LLM MScMedEd FHEA FCCP FRCP
Consultant Respiratory Physician specialising in negligence cases relating to all aspects of respiratory medicine. www.paramothayan.com
Jonathan Park Consultant Ophthalmologist
MB ChB (Hons) BSc (Hons) FRCOphth
Clinical negligence (ophthalmology) and personal injury (non-surgical ocular trauma) cases. Can act on behalf of either claimant or defendant or as a Single Joint Expert. www.jonathan-park.co.uk
Dr Nick Plowman MA MD FRCP FRCR
Consultant in Clinical Oncology
Specialist areas of expertise include radiation therapy, chemotherapy, immunotherapy and genomics as well as delay in diagnosis. This applies to adults and children. drnickplowman.com
Dr Stuart Porter Chartered Physiotherapist
PhD MCSP HCPC BSc Hons Grad Dip Phys MLACP PgCAP Cert.MHS SFHEA
Specialist areas of expertise include: • Clinical negligence
• Breach of duty • Allegations of inappropriate contact
• Assessment of adults and children • HCPC investigations. stuartbporter@aol.com
Dr Samy Sadek MBBS BSc MCEM FCEM
Consultant in Emergency Medicine & Pre-Hospital Care
• Minor injuries • Major trauma
• Medical emergencies
• Criminal and forensic cases




Prof. Elizabeth J. Soilleux MA MB BChir PhD FRCPath PGDipMedEd Expert Witness Pathologist with a particular interest in haematopathology. Short reports on specimens, full court compliant reports and expert biopsy reporting. www.expertwitnesspathologist.co.uk

Mr Bernard Speculand MDS FDS FFD FRACDS (OMS) Consultant Oral and Maxillofacial Surgeon. Personal injury and clinical negligence cases for claimant, defendant and as Single Joint Expert. Special interest is TMJ Surgery.
Yvette Young (Secretary) T: 0121 605 1884 E: info@medsecadmin.co.uk www.birminghamtmj.co.uk
Dr Ian Starke MSc MD FRCP
Stroke Medicine and Medicine for the Elderly Reports and examinations for clinical negligence and personal injury cases in stroke medicine and geriatric medicine www.expertwitnessinstrokes.co.uk
Mr. William E G Thomas Bsc, MBBS, FRCS, MS
Consultant Surgeon specialising in general surgery, hernia surgery, gastrointestinal surgery, hepatobiliary-pancreatic surgery, laparoscopic surgery and endocrine surgery T: 0114 262 0852 E: wegthomas@btinternet.com W: www.wegthomas.com



Lymm Eye Clinic
Mr Sameer Singh MBBS BSc FRCS Orth
Consultant Orthopaedic Surgeon • All aspects of trauma – soft tissue and bone injuries • Upper and lower limb disorders and injuries
• Whiplash injuries • Expert Witness for defence and claimant Clinic locations – London, Milton Keynes and Bedford
• Reports on survivability and cause of death. www.drsamysadek.com www.orthopaedicexpertwitness.net


Lymm Eye Clinic are a team of leading, independent ophthalmology experts covering all aspects of ophthalmology. www.lymmeyeclinic.co.uk
DR S V MEDICALS (Mr Sen Venkat)

MSc Ortho (London) FRCS Consultant Orthopaedic Surgeon • Whiplash injuries • General trauma • Sports injuries
• Clinical negligence work • Joint replacement surgery of hip and knee • Hand, shoulder, elbow and wrist injury www.drsvmedicals.co.uk
Ms Leyla Ziyal MPhil AFBPsS CPsychol
HCPC Registered clinical Neuropsychologist
• Neuropsychological assessment and rehabilitation
• Depression • Occupational stress • PTSD • Anxiety www.accentpsychology.co.uk






[ IN LITIGATION , perception and presentation matter. While the strength of any medico-legal case rests ultimately on evidence, the standing and credibility of the instructed expert can significantly influence how that evidence is received.
Few addresses in the world carry the professional weight and recognition of Harley Street. For generations, it has been synonymous with clinical excellence, discretion and specialist expertise. Instructing an expert witness with a Harley Street address sends a clear and immediate message: this is a practitioner operating at the highest level of their profession.
Situated in the heart of London’s medical district, Harley Street has long been regarded as a centre of private medical practice and specialist consultancy. Its name is recognised not only across the United Kingdom but internationally, associated with leading consultants in surgery, psychiatry, orthopaedics, neurology, dentistry and a wide range of allied health disciplines. That reputation has not arisen by chance. It reflects a concentration of experienced clinicians who have built distinguished careers, often combining senior NHS appointments with respected private practice. For solicitors seeking authoritative expert opinion, this concentration of expertise is highly relevant. Experts based in Harley Street practices are frequently at the forefront of their fields. Many contribute to national guidelines, publish in peer-reviewed journals and maintain active clinical workloads. This ongoing engagement with contemporary practice strengthens the quality of their medico-legal opinions. Courts and counsel alike place considerable weight on experts who demonstrate not only historical experience but current, hands-on clinical involvement.
Credibility in the courtroom extends beyond qualifications alone. An expert’s ability to present clear, balanced and independent opinion is paramount. Harley Street practitioners are often well versed in the demands of litigation. Regularly instructed in complex personal injury and clinical negligence cases, they understand the procedural framework, the importance of court-compliant reporting and the necessity of maintaining impartiality. Their reports tend to reflect careful reasoning, transparent methodology and a structured approach to breach, causation and prognosis.
Facilities and infrastructure also play a part. Harley Street consulting rooms are typically well equipped, providing an appropriate and professional environment for medico-legal assessments. For claimants, attendance at a recognised medical address can reinforce confidence in the process. For solicitors, it offers reassurance that assessments will be conducted in a setting conducive to thorough examination and accurate reporting. In higher value or sensitive cases, this level of presentation can carry subtle but meaningful influence.
There is, of course, no legal presumption that a Harley Street expert’s evidence is inherently superior to that of a consultant practising elsewhere. The court’s focus remains firmly on expertise, independence and reasoning. However, reputation and perception cannot be ignored. The Harley Street name is embedded in public and professional consciousness as a benchmark of quality. Instructing an expert from this district reflects a deliberate commitment to instructing at a premium level.
In complex or high-profile litigation, that commitment may be particularly important. Where issues of surgical technique, psychiatric diagnosis, capacity assessment or long-term prognosis are vigorously contested, the standing of the expert can affect how confidently the opinion withstands scrutiny. A well-established Harley Street consultant, accustomed to joint meetings and crossexamination, is likely to approach such scrutiny with measured assurance.

From a client-care perspective, instructing a Harley Street expert may also provide reassurance. Claimants often feel anxious about medico-legal examinations. Attendance at a respected and discreet practice can enhance their sense of being taken seriously. Defendants, too, may view such instruction as evidence that the matter is being addressed with appropriate gravity and professionalism.
Importantly, the value of a Harley Street expert lies not merely in the address itself but in what it represents. It signifies seniority, specialisation and a track record of clinical excellence. It suggests familiarity with complex cases and an understanding of the standards expected by the courts. It communicates that the instructing solicitor has prioritised quality and authority.
For experts practising in this distinguished district, the medicolegal arena provides an opportunity to apply their clinical expertise within a structured legal framework. For solicitors, instruction of a suitably qualified Harley Street specialist can clarify issues, strengthen negotiation position and, where necessary, present compelling evidence at trial.
Ultimately, litigation demands independent, reasoned and proportionate opinion. When that opinion is delivered by a practitioner whose professional base is synonymous with excellence, it reinforces the seriousness and credibility of the case. Instructing a Harley Street expert is therefore more than a logistical choice. It is a statement of intent: that the matter will be supported by authoritative expertise and conducted to the highest professional standards. q



[ONE OF THE MOST WIDELY REPORTED recent cases involved the death of a 73-year-old man following elective urological surgery at a private hospital commissioned by the NHS. After an optical urethrotomy procedure, the patient developed sepsis and multi-organ failure and died three days later.
In a Prevention of Future Deaths report, the assistant coroner found ‘gross failures’ in clinical governance of the Community Urology Service. The service, staffed by non-consultant grade doctors working without effective oversight from a consultant-led team, failed to recognise or escalate signs of deterioration, a deficiency the coroner concluded had materially contributed to the patient’s death.
The case highlights how systemic issues and failures in escalation pathways within urology services can precipitate catastrophic outcomes.
For legal teams, it serves as a stark reminder of how expert witnesses in urological practice may be required not only to analyse clinical action but also to address governance, staffing, escalation and care pathways. In particular, expert evidence can assist the court in understanding whether a reasonably competent urologist, operating under the pressures and constraints at the time, would have recognised the signs of sepsis and ensured appropriate review and escalation.
Complications arising from delays in urological procedures often become the foundation of negligence claims. A notable case concerned the delayed removal of a ureteric stent. After undergoing a cystoscopy and stent placement for a ureteric stone, a patient experienced prolonged pain, haematuria and bladder discomfort because the elective follow-up surgery to remove the stent was not booked properly.
By the time the stent was eventually removed under general anaesthetic – after becoming malpositioned and encrusted – the patient had suffered significant morbidity and additional operative risks. A formal complaint and investigation revealed failings in the care pathway and the NHS trust ultimately admitted liability, settling the claim.
This example demonstrates how tracking systems, procedural booking, follow-up care and patient communication are critical issues in litigation. Urology experts are often instructed to determine whether such delays constitute departures from accepted practice, whether complications were predictable and how earlier intervention might have altered the clinical course.
Misdiagnosis or delayed diagnosis of urological conditions, particularly renal or bladder cancer, continues to be a significant area of concern. Whilst no specific recent news case focuses solely on cancer misdiagnosis in urology, solicitors regularly report claims arising where abnormal imaging or symptoms were not investigated or escalated in line with accepted diagnostic pathways.
Independent urological experts are central in these claims, analysing whether imaging interpretation, referral patterns and clinical thresholds met the standard reasonably expected of a competent clinician, and whether earlier diagnosis would likely have improved treatment options and outcomes.
Data from NHS Resolution’s Freedom of Information (FOI) disclosures illustrate that urology has historically been a consistent contributor to NHS clinical negligence payouts. Earlier FOI data shows claims for failures in treatment, delays in diagnosis, informed consent failures and failure to recognise complications have accounted for significant payouts within the specialty over many years.
Further supporting this, recent academic analysis of malpractice litigation
and formal complaints to the General Medical Council reveals that urology sits within the broader pattern of surgical specialties prone to disputes.
The common denominator across these cases is the indispensable role of expert witnesses. Whether the issue is delay or error in diagnosis, failure of follow-up, procedural harm or governance shortfalls, solicitors rely on specialists with active clinical practice and deep subspecialty insight to help the court determine:
• What was the standard of care at the time of treatment?
• Did the clinician’s actions align with accepted practice?
• Could earlier or different intervention have materially changed the outcome?
• What is the prognosis and expected long-term functional impact on the claimant?
Expert evidence in urology cases must be detailed, impartial and rooted in contemporaneous guidance. It often involves nuanced interpretation of imaging, surgical planning, follow-up systems and multidisciplinary input.
Whilst not always headline-dominating, urology claims encompass a wide clinical and legal scope – from procedural complications and governance failures to diagnostic delays with long-term consequences. As these cases continue to feature in clinical negligence practice, the demand for authoritative, independent expert evidence in urology remains strong. q



By Dr Raj Kumar BDS LDS RCS MAGDS RCSED MSC ImpDent, Dental Surgeon
[DENTAL IMPLANTS have been used for over 60 years to replace missing teeth, either as single units or as part of dental bridges. The most common material used is titanium alloy, which has been scientifically studied since implants were first introduced into clinical practice.
When preparing reports on causation and prognosis, I am frequently asked: How long is this implant likely to last?; Can the claimant reasonably claim the cost of future replacement implant crowns?; If so, how many replacements should be allowed for over a lifetime?
It is well recognised that a natural tooth can last a patient’s lifetime if they have a clear medical history, good oral hygiene and good dietary control. Conversely, patients who do not look after their teeth may suffer premature tooth loss due to decay or periodontal disease.
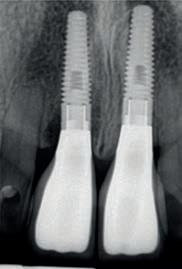
These factors must be taken into account when preparing cost reports for claimants. It is the responsibility of the dental expert to review the claimant’s dental history prior to the accident and assess whether the lost tooth would reasonably have been expected to last for the claimant’s lifetime.
Although implants have been used for many decades, there are relatively few long-term studies with sufficiently large patient numbers to provide consistent evidence regarding longevity. Most published studies last between five and 15 years and typically involve smaller patient cohorts, which limits the strength of the conclusions that can be drawn.
Many scientific studies are retrospective and are often carried out by the clinician who placed the implants, usually within specialist practices where standards of placement and aftercare are higher than in general practice. This may not reflect everyday clinical reality.

Ideally, a robust scientific study assessing implant longevity would include a large number of patients, a large number of implants placed by multiple operators and long-term follow-up of at least 10-15 years. Unfortunately, most available studies fall short of this ideal, meaning that we cannot state with certainty how long all implants will last, even when well maintained.
One of the largest published studies (D. French et al) reports over 22 years of follow-up and includes nearly 11,000 dental implants. It was a retrospective longitudinal cohort study of implants placed by a single specialist periodontist between 1995 and 2019.
The study reported higher implant failure rates in the following groups: patients with multiple implants compared to single implants; heavy smokers; patients with diabetes; implants placed in grafted bone; short implants (6mm or less).
At first reading, this study may give the impression that implants can reliably last up to 22 years or more. However, there are important limitations: all implants were placed by a single specialist operator, which is unusual in routine implant dentistry and may overestimate success rates; the average implant follow-up period was relatively short (mean 4.5 years), meaning that relatively few implants were actually observed for 15-20 years.
The reported cumulative implant survival rates were: 3 years – 98.9%; 5 years – 98.5%; 10 years – 96.8%; 15 years – 94%.
Cumulative survival represents a statistical estimate of the probability that an implant survives to a given time point, based on all available data.
Although the maximum follow-up extended to over 22 years, the study does not clearly report how many implants were actually observed beyond 15 years. Many implants may only have been followed for a short period.
The study used Kaplan-Meier survival analysis, which counts every failure event when it occurs, treats patients who have not yet failed (or who are lost to follow-up) as ‘censored’ rather than failures, and continuously updates survival probability over time.
As long as some implants remain under observation at later time points, the model can calculate long-term survival estimates, even if most implants were followed for much shorter periods. This can result in optimistic projections of long-term survival.
Other studies have reported that:
• Dental implants are not 100% successful and there is a risk of failure within 10-15 years, commonly due to peri-implantitis. Removal of a failed implant can be traumatic and may result in significant bone loss.
Subsequent replacement implants may need to be placed under more difficult clinical conditions (Setzer and Kim).
• All restorations require replacement cycles over a patient’s lifetime (Holm Pedersen).
Conclusion
Based on the available evidence and my own clinical experience of over 30 years:
• A single implant can reasonably be expected to last between 10 and 20 years, depending on patient risk factors and maintenance.
• Implant-supported bridges are more difficult to keep clean and are subjected to increased loading due to additional pontic teeth. Their expected lifespan is therefore typically 10 to 15 years.
My experience is that some implant failures can occur early. Once an implant has successfully integrated however, many remain functional for 20 years or more, although gradual bone loss and implant exposure can occur over time.
For the purpose of costing future treatment I generally allow for replacement every 20 years in patients without significant risk factors. In patients with increased risk, I apply a more cautious 15-year replacement cycle.
This approach reflects both the published evidence and real-world clinical experience. q



[THE Royal College of Obstetricians and Gynaecologists (RCOG) has responded to the interim report from the National Maternity and Neonatal Investigation, chaired by Baroness Amos.
The report highlighted many themes that have appeared in previous reports such as racism and discrimination, workforce pressure, crumbling and underfunded estates and infrastructures, lack of multidisciplinary teamwork, cultural and leadership failures, and an overall lack of empathetic listening to women and their families.
RCOG president Dr Alison Wright commented: “Last summer, Wes Streeting stood before our members and said that he would take personal responsibility for turning things around after years of under-investment and stalled progress. We were very encouraged by this commitment and remain ready and willing to work with the Secretary of State to support rapid progress.
“Today’s interim report is a compassionate and comprehensive whole system review. However, we are hearing that women are losing faith in the system and staff are struggling under rising workloads and increasingly complex care. We need action and investment to deliver the improvements so desperately needed by women, families and staff.
“Once the final report is published, we look forward to seeing tangible improvements in staffing shortages, training time, modernising equipment, and improved estates and processes for
reviews when families experience harm or loss.
“The RCOG remains absolutely committed to supporting progress and we look forward to being invited to formally provide evidence to the ongoing Review and being part of the taskforce. We are concerned to hear from our members that many have not yet received the survey to be able to contribute their individual perspectives directly.
“Pregnant women and families who have experienced harm, or the tragedy of losing a much-loved baby, and staff that go to work every day under unacceptable pressures, need and deserve better.”
The Royal College of Midwives (RCM) has described the report as harrowing. “For years, the RCM has argued that staffing and funding are not keeping pace with the growing complexity of maternity care and these findings reinforce that.
“Even Trusts meeting recognised staffing targets may not have safe staffing in practice. Without ring-fenced investment in the workforce and infrastructure, midwives will not be able to deliver the safe care women and babies deserve,” said RCM chief executive Gill Walton.
“We are also deeply troubled by the findings on racism and discrimination, experienced both by women using services and by the staff working in them. This is not a secondary issue – tackling racism and discrimination is fundamental to improving outcomes for all women,” she added. q
[ A NEW REPORT by Endometriosis UK has found that the average time to receive a diagnosis of endometriosis in the UK has now reached nine years and four months – an increase from an average of eight years reported in 2020.
“This rise in the time taken to get a diagnosis is deeply concerning. Endometriosis is a serious, often debilitating, long-term condition that can devastate women’s daily lives, yet too many are still waiting far too long for the care they need and deserve,” said RCOG’s president Dr Alison Wright.
“With hundreds of thousands of women already on gynaecology waiting lists, we know this delay will contribute to existing delays in accessing care.
“The Royal College of Obstetricians and Gynaecologists is calling on the Government to go further and faster in tackling elective gynaecology waiting lists, by promoting Women’s Health Hubs and addressing the underlying capacity issues in gynaecological staffing and theatre capacity, which contribute to these delays.
“We urgently need sustained investment in research, to better understand endometriosis, to develop faster diagnostic tools like ultrasound and biomarkers, and more effective treatments, and to address inequalities in women’s experiences and outcomes.” q



[ IN PERSONAL INJURY and clinical negligence litigation, diagnosis alone rarely tells the whole story. A fracture, brain injury or chronic pain condition may be clearly documented, yet the real question for the court is this: how does it affect day-to-day life? This is where the occupational therapist (OT) becomes indispensable.
An experienced medico-legal OT moves beyond clinical labels to examine functional reality. Through objective assessment, they evaluate how an injury influences activities of daily living such as washing, dressing, cooking, mobility and managing domestic responsibilities. They consider not only what a claimant can do in a clinical setting, but what they can sustain safely, reliably and repeatedly in their home and community.
For solicitors, this evidence is central to quantifying loss. An OT identifies whether assistance is reasonably required, distinguishing between gratuitous care provided by family members and professional support that may be necessary in the future. They analyse the level, frequency and type of care needed, through observation and recognised assessment tools. This provides a defensible framework for valuing past and future care claims.
Accommodation and equipment needs are another core component of OT evidence. Where mobility is compromised, the therapist evaluates the suitability of the current home environment and outlines proportionate recommendations, whether minor adaptations or significant structural alterations. Their expertise ensures that recommendations are clinically justified and cost-effective, reducing the risk of speculative or inflated claims.
Return-to-work capacity is often a contentious issue. An OT assesses

transferable skills, cognitive and physical tolerances, fatigue patterns and environmental barriers. Rather than offering a simplistic ‘fit’ or ‘unfit’ opinion, they provide nuanced analysis of phased return, workplace adjustments and alternative vocational pathways.
This balanced approach assists both claimant and defendant representatives in evaluating residual earning capacity and future disadvantage on the labour market.
Crucially, the occupational therapist’s report must be court-compliant. Experienced experts understand the requirements of independence, transparency and reasoned opinion. They set out the factual basis of their conclusions, identify any limitations in the evidence, and clearly distinguish between observed fact and professional opinion. This clarity enhances credibility and withstands scrutiny in court.
Prognosis and rehabilitation planning also fall squarely within the OT’s remit. By identifying realistic therapeutic goals and timeframes, the therapist informs not only damages but also case management decisions. Early expert input can support interim rehabilitation, aligning with the wider objectives of restoration and recovery.
Instructing a specialist OT provides a bridge between medical evidence and financial quantification. Their analysis transforms abstract impairment into measurable functional consequence. For experts practising in this field, the opportunity to contribute meaningfully to the justice process – through robust, impartial and practically grounded opinion – continues to grow.
In an environment where courts demand clarity and proportionality, the occupational therapist offers precisely what is required: structured, evidence-based insight into how injury shapes everyday life. q

By Lisa Crowther of Carter Brown
[ IN FAMILY COURT PROCEEDINGS, decisions about children’s welfare, parenting capacity and contact arrangements often hinge on the careful assessment of individual functioning and needs.
Historically, neurodiversity – the natural variation in cognitive processing associated with conditions such as autism spectrum disorder (ASD), attention-deficit/hyperactivity disorder (ADHD), dyslexia and related profiles – has been largely overlooked within assessment frameworks, often being dealt with as a discrete concept via different, and notably separate, channels.
As defined by the National Autistic Society: “Neurodiversity is a way of saying that human brains are different to each other. This is a biological fact. No two brains (or nervous systems) are the same.” The family court, practitioners therein, and allied professionals have had to pivot to ensure that the needs of neurodivergent individuals are fully considered and necessary adaptations made, ensuring optimal participation in proceedings.

among women and minority ethnic groups, can further obscure identification. When cognitive or processing differences are identified, an important aspect of assessment in family proceedings is the use of specialist intermediaries or communication assessments. Under Part 3A and Practice Direction 3AA of the Family Procedure Rules 2010, adjustments such as intermediaries can be appointed to facilitate understanding and communication – particularly in evidencegiving or cross-examination. It is important to note that this is still a developing area and guidance for professionals, for example the Advocates Gateway Toolkits, is somewhat splintered with autism, ADHD, dyslexia, dyspraxia and learning disabilities, which can all co-exist, straddling three different toolkits – 3, 4 and 5. There remain tensions between legal and medical perspectives, alongside differing views across professional disciplines, which need to be overcome as understanding and practice develops.
The publication of Guidance on Neurodiversity in the Family Justice System for Practitioners by the Family Justice Council in 2025 was key. The guidance recognises that failure to account for neurodivergence can affect two core dimensions of family proceedings: the substantive assessments undertaken by experts and the capacity of the neurodivergent person to participate fully and fairly in proceedings. Where a party is unable to participate in this manner, their access to justice is obstructed.
Since 2024, Carter Brown has been working closely with its experts to develop its offering for neurodivergent individuals and those representing them. Our focus has been on offering robust assessments, completed in line with NICE and UKAAN guidance, using multidisciplinary teams of experts, experienced in providing reports within family proceedings, thereby combining the requisite clinical experience with Practice Direction 25 compliance.
In practice, for clients coming to our service, every assessment begins with identification through screening. Where there is an existing clinical diagnosis, practitioners will record this and consider its implications for engagement, decision-making, stress tolerance and communication. Where no previous diagnosis exists, our experts will use a variety of structured screening tools to sensitively identify possible neurodivergent traits that may be affecting an individual’s interactions in the world at large and more specifically within the legal process.
If potential neurodivergence is identified, the court and professionals may wish to seek further information. This can include input from health, education or social care records, reports from family or carers, or formal full psychological assessment (incorporating neurodivergence). Such assessments seek to establish whether a person’s presentation meets diagnostic criteria but also to map out an individual’s unique profile of strengths, challenges and reasonable adjustments required within the court context.
A neuro-affirming approach is taken to all assessments, stepping away from traditional diagnostic models, which may view autistic behaviours, for example, as inherently problematic and deficit-based.
Critical to the fairness of assessment is the avoidance of misinterpretation. Behaviours associated with neurodivergence –such as differences in eye contact, speech patterns or processing speed – can be mistakenly attributed to resistance, evasiveness or poor parenting if context is ignored. Underdiagnosis, particularly
With roughly one in seven in the UK being neurodivergent, embedding neurodiversity-aware assessment practices at every stage is essential not only for procedural fairness but also for achieving outcomes that genuinely serve the best interests and participation rights of neurodivergent individuals in family proceedings. q





[ THE President of the Royal College of Psychiatrists (RCPsych), Dr Lade Smith CBE, is calling on the UK Government to address the ‘silent mental health pandemic’ affecting people across England.
She said: “People are unable to get the help they need when they need it, leaving them to suffer from depression, post-traumatic stress disorder, schizophrenia and other severe mental illnesses with insufficient support and treatment and this affects their life chances.
“It is atrocious that they are increasingly only able to access care when they reach a crisis point because services are overwhelmed and under resourced. This crisis is of pandemic proportion and yet the needs of those with severe mental illness are rarely acknowledged.
“As a forensic psychiatrist, I see this on the frontline every day – patients who don’t have timely access to appropriate treatments are at greater risk of relapsing, becoming more unwell and, on rare occasions, posing a danger to themselves or others. This is simply unacceptable. Mental health patients, clinicians and services are blamed when people become so unwell they go into crisis –

but they often wouldn’t reach this point if they could get care and treatment earlier.
“No one should have their life defined by their illness, and there are effective treatments available for even the most severe mental health conditions, but services are struggling to manage millions of additional patients. The longer we ignore the scale of this challenge the harder it will be to overcome.”
[ PRESIDENT OF THE FAMILY DIVISION, Sir Andrew McFarlane, has recommended that expert witness psychologists should only be used as experts in family court cases if they are registered with a relevant statutory body.
Welcoming the news, Chair of the British Psychological Society’s (BPS) Expert Witness Advisory Group, Dr Andy Siddaway said: “We welcome this guidance as there have been growing concerns about the instruction of expert witnesses who are not suitably qualified for the role. The current system allows courts to instruct individuals who are not subject to professional regulation, which means there is no clear route for parties to raise concerns about an expert's conduct or competence.
“At present, it is possible for individuals with no recognised qualifications to offer services under self-described titles such as ‘forensic assessor’, with little assurance of competence or accountability. While all experts are required to assist the court by clearly setting out their expertise in each case (typically via a CV), anyone who claims to offer psychological services can currently do so.”
Judge McFarlane also indicated that chartered status with the BPS could be used as an alternative to registration with the HCPC. The BPS is not the statutory regulator of psychologists. It is the society's position that all chartered psychologists acting as expert witnesses should also be registered with the HCPC q
RCPsych is calling on the Government to ensure that community mental health services have the resources they need to consistently deliver early intervention, continuity of care and assertive outreach, which all help patients engage with their treatment for as long as necessary and reduce the likelihood of relapse and mental health crisis. q


By Dr Laura Pipon-Young, Clinical Psychologist and Chartered Psychologist
[IN MY WORK as a clinical psychologist, I am frequently instructed in legal cases where psychological assessments play a central role. These instructions arise across a wide range of settings, including family and criminal proceedings, civil litigation, immigration matters, employment disputes and questions of mental capacity.
Despite their regular use, I often find that the process behind psychological assessments is not always fully understood. So, let me give you a brief insight into what sits behind the report, and why careful assessment and formulation are essential to providing meaningful psychological evidence to the court.
The secrets behind…
There is no single type of ‘legal psychological assessment’. Each assessment must be shaped by the specific legal question being asked and the context in which it sits. Psychologists may be instructed to assess cognitive functioning, capacity, psychological injury, risk or neurodevelopmental conditions such as autism or ADHD. The approach taken should always be proportionate, evidence-based and tailored to the referral question.
Psychologists and psychiatrists: complementary expertise
One area that commonly causes confusion is the distinction between psychologists and psychiatrists. Psychiatrists are medically trained doctors who can prescribe medication, diagnose psychiatric disorders and, where appropriate, detain individuals under the Mental Health Act. Their expertise is particularly relevant where there is a clear psychiatric presentation, such as psychosis, bipolar disorder, perinatal mental illness or drug-induced conditions.
Psychologists, by contrast, are not medical doctors and do not prescribe medication. Our training focuses on psychological theory, assessment and formulation. We undertake cognitive, intellectual and personality assessments, assess mental capacity where cognitive factors are central, and conduct structured risk assessments. In practice, psychologists and psychiatrists often work collaboratively, bringing different but complementary perspectives to complex cases.
What does a psychological assessment actually involve?
Psychological assessments are multi-method and should never rely on a single source of information. A core component is a detailed clinical interview, which explores an individual’s developmental history, mental health, current functioning and relevant life experiences. This is often combined with psychometric testing, such as measures of intellectual ability, memory or executive functioning, alongside validated questionnaires and semi-structured interviews.
Where risk is a concern, structured risk assessment tools may be used. However, it is important to emphasise that no test or tool can be interpreted in isolation. Psychological evidence relies on the integration of test results with clinical judgement, observation and contextual understanding.
Collateral information gathering is a vital part of any robust assessment. Medical records, educational reports and previous

assessments often provide rich contemporaneous information, including chronology, prior interventions and diagnostic history. Where appropriate, consultation with other professionals or third parties further strengthens the reliability of conclusions.
One of the most important aspects of a psychological assessment is formulation. Applied psychologists are trained to synthesise information using psychological theory and evidence. I often use the ‘5 Ps’ model, which considers presenting problems, predisposing factors, precipitating factors, perpetuating factors and protective factors.
Formulation allows the psychologist to move beyond description and towards explanation. It helps to clarify why an individual is experiencing difficulties at a particular point in time, what maintains those difficulties, and what may help reduce risk or support improvement. In legal contexts, this narrative understanding is often more useful than diagnosis alone.
Cognitive assessments are frequently requested in legal settings, particularly where intellectual functioning, learning disability or capacity is in question. While IQ testing can provide valuable information, scores should always be reported as ranges and interpreted alongside background history and observed effort. A score of 70 or below forms part of the cognitive criterion for a learning disability, but it is only one element of a broader diagnostic framework.
Similarly, assessments for autism and ADHD require specialist expertise. Diagnosis should never be based solely on self-report, online questionnaires or internet searches. Best practice involves a detailed developmental history, third-party information, collateral records and, where appropriate, the use of gold-standard tools such as the ADOS2 or DIVA. Issues such as masking or exaggeration are carefully considered within a structured and evidence-based assessment process.
Risk assessments may address concerns relating to violence, self-harm, suicide, sexual risk, child neglect or domestic abuse. Contemporary practice recognises the limitations of relying on any single method. Actuarial tools offer statistical grounding, while structured professional judgement approaches allow for individualised analysis. Clear reasoning, transparency and an acknowledgment of uncertainty are essential when presenting opinions on risk.
From the court’s perspective, the most helpful psychological reports are those that are clear, balanced and focused on the questions being asked. They explain how conclusions have been reached, acknowledge limitations and avoid unnecessary jargon. Above all, psychological evidence should support informed decision-making by offering a coherent, evidence-based understanding of the individual and the issues before the court. q
[PAEDIATRIC CARE OCCUPIES a uniquely sensitive position within the healthcare and legal landscape. When things go wrong in the treatment of children, the consequences can be profound and long-lasting. As a result, paediatric care features prominently in clinical negligence litigation.
One of the most litigated areas involves failures in neonatal and perinatal care. Allegations frequently concern delayed recognition of sepsis, hypoxia or metabolic disorders in the hours and days following birth. Where injury occurs, the financial value of claims can be significant due to lifelong care needs. Courts will examine fetal monitoring records and neonatal observations in detail.
Delayed diagnosis is a recurring theme. Conditions such as meningitis, appendicitis or diabetic ketoacidosis can initially present with nonspecific symptoms in children. Claims often focus on whether clinicians appropriately recognised ‘red flag’ signs and provided adequate safetynetting advice.
The challenge for the court is to distinguish between the inherent diagnostic uncertainty of early presentation and a breach of duty. Contemporary practice guidance from bodies such as the Royal College of Paediatrics and Child Health is frequently scrutinised when assessing standards of care.
Safeguarding failures also generate litigation. Paediatricians and emergency clinicians are expected to identify and escalate concerns regarding non-accidental injury. Allegations may arise either from missed signs of abuse or, conversely, from inappropriate referrals causing family distress. These cases demand careful, balanced expert analysis and an appreciation of multi-agency safeguarding frameworks.
Chronic disease management presents a further area of risk. Children with epilepsy, asthma or diabetes require coordinated, long-term care. Litigation may arise where there has been inadequate monitoring, poor communication between primary and secondary care, or failure to adjust treatment appropriately. In such cases, causation can be particularly complex, especially where the child had pre-existing vulnerabilities.
Consent and capacity issues in paediatrics add another legal dimension. Although parents or guardians usually provide consent, older children may have sufficient maturity to make decisions themselves. The principles established in Gillick v West Norfolk and Wisbech Area Health Authority remain central in determining when a child can consent to treatment. Disputes may arise where treatment was undertaken without appropriate parental involvement, or where disagreements between clinicians and families escalated into legal proceedings.
From a litigation perspective, paediatric cases frequently require input from multiple experts, including paediatricians, neurologists, educational psychologists and care experts to assess long-term needs. Detailed analysis of growth charts, developmental milestones and school records may be required to establish causation and prognosis.
Ultimately, paediatric care litigation underscores the importance of meticulous documentation, effective communication with families and robust escalation systems. For solicitors, early instruction of experienced paediatric experts is essential.
Balanced, authoritative expert opinion assists the court in navigating the fine line between unavoidable clinical complexity and negligent care, ensuring that outcomes are both legally sound and clinically informed. q

[
EAR, NOSE AND THROAT (ENT) litigation remains a steady and often complex strand of clinical negligence work in the UK. Claims frequently raise intricate questions of anatomy, consent, surgical technique and timely diagnosis.
For claimant and defendant solicitors alike, these cases demand careful expert analysis and a clear understanding of both primary and secondary care pathways.
One of the most common areas of dispute concerns delayed or missed diagnosis of head and neck cancers. Malignancies of the larynx, pharynx and oral cavity may initially present with relatively non-specific symptoms such as persistent hoarseness, dysphagia or unilateral ear pain. Litigation often centres on whether a GP or hospital clinician ought reasonably to have referred the patient under the urgent suspected cancer pathway at an earlier stage.
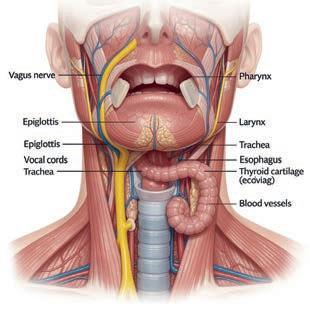
In cases involving laryngeal cancer, for example, the distinction between an early lesion treatable with radiotherapy and advanced disease requiring laryngectomy can have life-changing consequences. Courts will closely examine compliance with national guidance and the adequacy of safetynetting advice.
Surgical claims form another substantial category. Procedures such as septoplasty, functional endoscopic sinus surgery and tonsillectomy are routinely performed across the NHS and private sector. Although generally safe, complications including haemorrhage, septal perforation, cerebrospinal fluid leak or dental injury can give rise to allegations of negligent technique.
In tonsillectomy claims, post-operative bleeding remains a recognised risk; the legal question is rarely the occurrence of bleeding itself, but

whether the patient was appropriately consented and whether any delay in responding to deterioration fell below a reasonable standard of care.
Otology cases frequently involve hearing loss following surgery or infection. Claims may arise from alleged failure to diagnose cholesteatoma, leading to progressive conductive hearing loss or intracranial complications. Where surgery is undertaken, such as mastoidectomy, disputes can focus on facial nerve injury or balance disturbance.
The evidential burden often includes detailed review of operative notes, audiograms and imaging, alongside expert opinion on causation and long-term prognosis.
Paediatric ENT litigation presents its own challenges. Delayed recognition of airway obstruction, epiglottitis or peritonsillar abscess can result in catastrophic outcomes. In children with recurrent infections, arguments sometimes arise about whether earlier intervention would have prevented complications such as hearing impairment affecting educational development. These cases frequently require multidisciplinary expert input, including paediatrics, audiology and speech and language therapy.
Across all categories, informed consent remains central. Claimants increasingly allege that material risks – such as altered sense of smell after sinus surgery or changes in voice following thyroid or laryngeal procedures – were not adequately explained. Detailed documentation of consent discussions is therefore critical.
Cases often turn on fine clinical judgments rather than obvious errors. Clear, balanced expert evidence can assist the court in distinguishing between an unfortunate complication and a breach of duty, ensuring that outcomes are fair to both patients and clinicians. q




[RECENT MONTHS have seen injuries caused by burns emerge more prominently in UK personal injury reporting, with cases settling outside court and specialist medico-legal evidence playing a pivotal role in securing fair outcomes for claimants.
One of the more notable examples involves a Windsor hotel agreeing compensation with a guest who sustained serious burns from a red-hot towel rail that was not fitted with a thermostat. The case illustrates how ordinary environments can harbour hidden dangers that give rise to injury claims.
Burn injuries are among the most complex and life-changing forms of trauma encountered in personal injury practice. They can result from exposure to thermal heat, scalding liquids, electrical sources or chemical agents, and their impact extends far beyond the acute wound phase. Unlike many other injuries, burns often require long-term multidisciplinary care, complex reconstruction and ongoing rehabilitation. They may leave survivors with significant scarring, contractures and psychological distress that endures for years.
Expert witnesses are crucial to establishing the chain of causation and the full extent of ramifications. In the UK there is a well-established pool of burns and reconstructive surgery specialists available to provide independent medico-legal evidence, from acute management and debridement to scar reconstruction and functional prognosis.
An expert in burns medicine – often a consultant plastic and reconstructive surgeon with burn care subspecialty expertise – is typically instructed at an early stage to evaluate whether the handling of the incident and subsequent treatment met the relevant standards. Their assessment will cover:
• How and why the burns occurred and whether the environment or product posed an unreasonable risk of harm.
• Initial clinical management, including fluid resuscitation, wound debridement, infection control and the timing of surgical intervention.
• Progression and complications, such as hypertrophic scarring, contracture formation or functional limitation affecting hands, feet or joint regions.
• Reconstructive options and rehabilitation planning, including the potential for further surgery, grafting procedures or specialist therapy.
• Long-term prognosis and quality of life impact, addressing both physical function and psychological effects such as anxiety, depression or post traumatic stress.
Experts not only review medical records and imaging, but often juxtapose clinical notes against accepted standards of care to determine whether an earlier or different intervention might have materially affected outcomes. Their insight is indispensable when a defence argues that complications were unavoidable and not the result of substandard practice.
Burn injuries can be deceptively complex – something as simple as a towel rail or hot surface in a leisure setting may lead to severe damage with lifelong consequences. In the Windsor hotel case, the availability of expert opinion helped resolve a claim without the need for protracted litigation.
Experts also help in quantifying loss, including assessments of ongoing healthcare needs, assistive devices, adaptations to home and workplace environments and future care costs. These projections are essential to ensuring that settlements reflect the full social and economic effect of the burns injury, rather than just the immediate clinical episode.
Instructing the right expert helps legal teams navigate not just clinical complexity, but also ancillary issues such as product safety standards, mechanical faults in consumer devices or failure in workplace health and safety protocols. For example, electrical burns or chemical exposures might implicate a manufacturer’s duty of care, requiring experts to comment not only on medical management but on causal links to defective equipment or inadequate warnings.
Burns litigation sits at the intersection of acute trauma care, long-term rehabilitation and personal injury law. With claim volumes rising and
injuries often severe in consequence, expert witnesses in burns medicine are playing an increasingly central role in guiding courts towards informed, proportionate outcomes. Their clinical insight helps ensure that compensation awards reflect both the physical and lasting human cost of an injury. q




[HERNIA REPAIR remains one of the most frequently performed general surgical procedures. Inguinal, incisional and ventral hernias account for tens of thousands of operations each year, undertaken in both NHS and independent settings.
While the majority of patients experience good outcomes, the sheer volume of procedures inevitably generates a proportion of complications. In recent years, an increase in medico-legal claims –particularly those involving mesh implantation, delayed diagnosis, nerve injury and chronic post-operative pain – has placed hernia surgery firmly under closer scrutiny.
For claimant and defendant solicitors alike, the distinction between a recognised complication and a breach of duty is rarely straightforward. It is here that the role of the expert witness becomes pivotal.
Recognised risk or substandard care?
Hernia repair, whether open or laparoscopic, carries welldocumented risks. These include recurrence, infection, seroma formation, chronic groin pain and, in rare cases, visceral or vascular injury. The use of synthetic mesh, now standard in most adult repairs, has reduced recurrence rates but introduced its own profile of potential complications – including mesh migration, erosion, chronic inflammatory response and neuropathic pain.
The question is not whether a complication occurred, but whether the care fell below the standard expected of a reasonably competent surgeon. An experienced surgical expert will consider relevant guidance from organisations such as the National Institute for Health and Care Excellence and the Royal College of Surgeons of England, alongside peer-reviewed literature and accepted practice at the time.
Expert analysis begins with a careful review of records: pre-operative assessment, imaging, clinic correspondence, consent documentation, operative notes and post-operative follow-up. The expert must then determine whether the management was consistent with a responsible body of surgical opinion.
Patient selection and pre-operative assessment
A common area of dispute in hernia litigation concerns patient selection. Was surgery necessary at all? In some minimally symptomatic inguinal hernias, watchful waiting may be appropriate. Conversely, failure to operate on a symptomatic or enlarging hernia may result in incarceration or strangulation, leading to emergency surgery and significantly higher risk.
Experts are often asked to assess whether appropriate risk evaluation took place. Did the surgeon properly take into account comorbidities such as obesity, diabetes or smoking status, all of which may increase wound complications and recurrence rates? In incisional and complex ventral hernias, was adequate imaging obtained and, where necessary, multidisciplinary input sought?
Consent is another key issue in hernia-related claims, particularly where mesh is used. Clinicians must take reasonable care to ensure patients are aware of material risks and reasonable alternatives.
An expert witness will examine whether risks such as chronic postoperative pain, testicular complications or mesh-related problems were discussed clearly and in terms meaningful to the patient. Generic consent forms are rarely decisive. Instead, experts assess whether the clinical records demonstrate a genuine, patient-centred discussion.
Technical performance is frequently examined in cases involving nerve damage or chronic groin pain. During open inguinal repair,
careful identification and protection of the ilioinguinal, iliohypogastric and genitofemoral nerves is expected. Laparoscopic procedures require equally careful attention to mesh placement and fixation.
An expert’s task is not to judge with hindsight but to determine whether the operative note demonstrates a methodical and competent approach. Inadequate documentation can itself become an important issue, as the court may draw inferences where the operative record is sparse or unclear.
The duty of care extends beyond the operating theatre. Experts frequently examine whether post-operative complaints were managed appropriately. Persistent pain, infection or suspected recurrence require timely investigation and follow-up. Failure to respond to repeated GP consultations or hospital attendances may allow complications to progress unnecessarily.
Mesh-related claims present particular challenges. Public scrutiny has heightened patient awareness, yet not every adverse outcome indicates negligence. Courts therefore depend on balanced expert opinion to explain the evidence base for mesh use and the realistic incidence of complications.
For solicitors handling hernia claims, early instruction of a specialist expert can clarify breach, causation and prognosis. In a field where high procedural numbers inevitably generate disputes, authoritative and independent expert evidence remains essential to achieving fair and proportionate outcomes. q



[AT A TIME when public confidence in accessing GP services is fragile, it is vital that the Government acts to ensure that all patients can visit an optician in the community if they think they have an eye problem, in the same way the public can go to a community pharmacy for a range of health issues, according to Adam Sampson, chief executive of the Association of Optometrists (AOP).
Commenting on new polling from the Health Foundation and Ipsos, which found that nearly half of the public (48%) delayed or avoided contact with their GP practice about a health concern, he said: “It’s clear that the public are reluctant to contact their GP because they have concluded the service is overstretched and inaccessible.
“This represents a risk not only to individual health outcomes, but will add greater strain on the Government’s commitment to improve the NHS by shifting health care out of hospitals into the community and from sickness to prevention.
“Primary care is the front door to the NHS. General practice is a cornerstone of the service, but to ensure GPs are able to offer the support the public expect, it is essential that all of primary care –community pharmacies, dental practices and opticians – are fully able to each play their part to improve access to healthcare.
“Currently, primary eye care services are an under-utilised clinical resource. Every day, optometrists manage common eye conditions and eye problems on the High Street, reduce avoidable pressure on GPs and hospital eye departments, playing a crucial role in identifying wider health issues – from diabetes to hypertension – through routine sight tests.

“But while such services exist in most parts of the UK, there are parts of England where they are not yet in place. At a time when confidence in accessing GP services is fragile, it is vital that the Government acts to close the gaps so that all patients can visit an optician in the community if they think they have an eye problem, in the same way the public can go to a community pharmacy for a range of health issues.
“With the right commitment from Government, community optometry – just like community pharmacy – can do so much more to provide timely, local, NHS-funded care and ensure the public are not delaying treatment that could prevent avoidable sight loss.”
As part of its One million appointments campaign the AOP calls on the Government and NHS in England to support a nationwide eye care service delivered in High Street opticians for all common eye conditions and problems, to improve access for patients. q

ACCIDENT & EMERGENCY MEDICINE


CARDIOLOGISTS & CARDIOTHORACIC SURGEONS



DENTAL & ORTHODONTIC EXPERTS









GASTROINTESTINAL & COLORECTAL SURGEONS

GENERAL SURGEONS




HAEMATOLOGY


MEDICAL NEGLIGENCE


NEONATAL MEDICINE

NEUROLOGY


NEUROSURGEONS





NURSING, CARE & REHABILITATION CONSULTANTS













































PSYCHIATRISTS & PSYCHOLOGISTS







SPEECH & LANGUAGE THERAPY

THORACIC SURGEONS










EXPERTS FOR MEDIA is a regular section in Your Expert Witness for experts who wish to offer their views and the benefit of their experience to the vast range of print and broadcast media.
Ever wondered how news teams find the experts they consult to explain the ramifications of breaking news stories, seemingly at the drop of a hat? Or how the producers of TV drama series ensure their stories are accurate and reflect the realities of the professions they portray?
The fact is that researchers consult registers of experts and expert periodicals just as lawyers do. In fact, Your Expert Witness is receiving an increasing number of enquiries from media researchers and public relations agencies looking to locate appropriate experts to inform their clients.
Experts for Media is therefore an ideal space to attract their attention. For prices and to book your space, contact Ian on 0161 710 3880 or via ian@dmmonline.co.uk .
Joanne Caffrey Expert Witness & Trainer
Ms Joanne Caffrey undertakes expert witness instructions in cases relating to the following police topics:
• Use of force
• Custody procedures
• Drink/drug driving
• Ligature deaths
T: 07528 800 720 E: joanne_caffrey@sky.com
Professor Stephen Clark

Professor Clark has extensive experience in medicolegal and coronial expert witness work. He can be instructed nationwide in personal injury and clinical negligence cases relating to all aspects of cardiothoracic surgery and transplantation.
T: 0191 213 7445 M: 07779 273388 E: stephen.clark18@nhs.net and clarkmedicolegal@icloud.com

T: 01865 307433 or 07508 617949 E: jeremycrew@urologyoxford.com W: www.oxfordurology.co.uk Mr Jeremy Crew

Mr Jeremy Crew has offered a medicolegal service for over sixteen years. He provides expert medical opinion, medico-legal reports and court attendance on all aspects of urology including clinical negligence, personal injury and criminal matters.


Dr Dan Jones PhD MSc BSc MA MEWI Cert Ecological Consultant

Dan is the UK’s foremost authority on the ecology and management of Japanese Knotweed, Himalayan Balsam, and Giant Hogweed. Dan is the lead author of the world’s largest field trial on Japanese Knotweed control, a study that has fundamentally changed how government and industry manages infestations. As a Full Member of The Academy (MA) and a Certified Expert Witness (MEWI Cert), he provides ‘commercially independent’ testimony that is indispensable for both claimants and defendants in civil claims. T: 07967 408844 E: daniel@advancedinvasives.com W: www.advancedinvasives.com
Laird Assessors Automotive Expert
Laird Assessors are the UK’s leading independent automotive expert witness firm supporting claimant, defendant and criminal solicitors – from instruction to court. Laird provide intelligence to the automotive world predominantly relating to crashed vehicles.

T: 0151 342 9961 E: enquiries@laird-assessors.com W: www.laird-assessors.com
Mr Jonathan Luck FRCS FRCOphth Consultant Ophthalmologist
Mr Jonathan Luck has over 20 years of experience in medicolegal work. Experience of giving evidence in court including cross examination. Rapid turnaround of reports. Full consulting and diagnostic facility for Condition and Prognosis reports. Holder of the Bond Solon Cardiff University Civil Expert Witness Certificate.

E: jon.luck@nhs.net W: www.jonathanluckmedicolegal.org.uk
Chris Makin FCA FCMI FAE QDR MCIArb Chartered Accountant • Accredited Civil Mediator • Accredited Expert Determiner
Chris Makin was one of the first chartered accountants to become an Accredited Forensic Accountant and Expert Witness. He is also an accredited civil and commercial mediator and an accredited expert determiner. Over the last 30 years he has given expert evidence at least 100 times and worked on a vast range of cases.
T: 01924 495888 or 07887 660072 E: chris@chrismakin.co.uk W: www.chrismakin.co.uk

Mr Luke Meleagros BSc MBBS MD FRCS Consultant Surgeon
Mr Meleagros Completes 3-4 expert reports per month on medical negligence cases and abdominal injury/major abdominal trauma cases. He has reported extensively on cases involving abdominal laparoscopy surgery and hernia surgery.
T: 0208 527 0977 E: L.Meleagros@btinternet.com
Sec: jawdobson@gmail.com

Kathryn Thorndycraft-Pope Examination of Documents and Handwriting

FHDI provides an independent document examination service, giving unbiased professional advice for criminal or civil litigation.
• Handwriting • Alterations • Indentations • Authenticity
T: 01569 764508 M: 07710 655838 E: fhdi@icloud.com W: www.forensichandwriting.co.uk

