


JULY 1, 2026 - JUNE 30, 2027







JULY 1, 2026 - JUNE 30, 2027



PLAN YEAR & EFFECTIVE DATES: ANNUAL ENROLLMENT DATES:
July 1, 2026 - June 30, 2027 May 1, 2026 - May 15, 2026
• Full-time employees working an average of 30 hours or more per week are eligible for benefits.
Congratulations on your new employment! Your employment means more than just a paycheck. Your employer also provides eligible employees with a valuable benefits package. Above you will find eligibility requirements and below you will find information about how to enroll in these benefits as a new employee.
New employees working 30+ hours per week are eligible for benefits. Please contact the Amherst County Human Resources department for more information and benefit effective dates. Please refer to the Enrollment Instructions page and the New Hire Onboarding Guide on your client microsite or pages 16 through 21 of your Benefits Guide for more information on how to enroll.
Be sure to also review your group’s custom benefits website, that allows for easy, year-round access to benefit information, live chat support, benefit explainer videos, plan certificates and documents, and carrier contacts and forms.
www.PierceGroupBenefits.com/AmherstCountyGovernment


- Individual Maximum: $4,400/year Max
-Family Maximum: $8,750/year Max
HSA plans can only be established in conjunction with a qualified High-Deductible Health Plan (HDHP)
Amherst County Government contributes $1,500 per year, paid out in monthly installments, to eligible employees accounts.

- Medical Reimbursement: $3,400/year Max | $300/year Min
- Dependent Care Reimbursement: $7,500/year Max
*You will need to re-enroll in the Flexible Spending Accounts if you want them to continue next year.
If you do not re-enroll, your contribution will stop effective June 30, 2026.









When do my benefits start? The plan year for Colonial Life Insurance Products, The Local Choice Benefits (Anthem Health, Delta Dental of VA, and Anthem Blue View Vision), Flex Facts Health Savings Accounts, Flex Facts Flexible Spending Accounts, Ameritas Dental (Stand-Alone Policy), Anthem Blue View Vision (Stand-Alone Policy) and CHUBB Long Term Care runs from July 1, 2026, through June 30, 2027.
When do my deductions start? Deductions for Colonial Life Insurance Products, The Local Choice Benefits (Anthem Health, Delta Dental of VA, and Anthem Blue View Vision), Flex Facts Health Savings Accounts, Flex Facts Flexible Spending Accounts, Ameritas Dental (Stand-Alone Policy), Anthem Blue View Vision (Stand-Alone Policy) and CHUBB Long Term Care start June 2026 for all enrolled employees.
Why have my Medical Bridge benefits not started yet? The Health Screening Rider on the Colonial Medical Bridge plan has a 30-day waiting period for new enrollees. Coverage, therefore, will not begin until July 31, 2026.
How do Flexible Spending Account (FSA) funds work, and do my FSA funds have to be used by a specific deadline?
Flexible Spending Account expenses must be incurred during the plan year to be eligible for reimbursement. After the plan year ends, an employee has 45 days to submit claims for incurred qualified spending account expenses (or 90 days after employment termination date). If employment is terminated before the plan year ends, the spending account also ends. Failure to use all allotted funds in the FSA account will result in a “Use It or Lose It” scenario. Your plan also includes a rollover provision! This means that if you have money left in your FSA at the end of the plan year, you can carryover up to $680 into the next plan year. Any remaining funds beyond $680 is forfeited under the “Use It or Lose It” rule.
My spouse is enrolled in an Health Savings Account (HSA), am I eligible for an FSA? As a married couple, one spouse cannot be enrolled in a Medical Reimbursement FSA at the same time the other opens or contributes to an HSA.
How do Dependent Care Account (DCA) funds work and when do they need to be used? Dependent Care Accounts are like FSA accounts and allow you to request reimbursement up to your current balance. However, you cannot receive more reimbursement than what has been deducted from your pay. After the plan year ends, an employee has 45 days to submit claims for incurred qualified dependent care expenses (or 90 days after employment termination date). Any remaining funds in your DCA account must be utilized before the deadline. Failure to use all allotted funds in the DCA account will result in a “Use It or Lose It” scenario. Your plan includes a grace period which is an additional 2.5 months (running July 1, 2027, through September 15, 2027), during which you can incur eligible expenses that can be reimbursed. Therefore, you have from July 1, 2026, through September 15, 2027, to incur qualified expenses eligible for reimbursement. If you do not incur qualified expenses by September 15, 2027, and/or file by September 30, 2027, any contributions are forfeited under the “Use It or Lose It” rule.
When will I get my card? If you will be receiving a new debit card, whether you are a new participant or to replace your expired card, please be aware that it may take up to 30 days following your plan effective date for your card to arrive. Your card will be delivered by mail in a plain white envelope. During this time you may use manual claim forms for eligible expenses. Please note that your debit card is good through the expiration date printed on the card.
I want to sign my family up for benefits as well, what information will I need? If signing up for any coverage on your spouse and/or children, please have their dates of birth and social security numbers available when speaking with the Benefits Representative.
What does Pre-Tax vs. Post-Tax Change? Pre-Tax benefits take funds directly from your paycheck to cover benefits before going through State and Federal taxing process. Post-Tax collects funds for benefits after taxes have been taken out. Please be aware there are certain coverages that may be subject to federal and state tax when premium is paid by pretax deduction or employee contribution.
Can I change my benefit elections outside of the enrollment period? Elections made during this enrollment period CANNOT BE CHANGED AFTER THE ENROLLMENT PERIOD unless there is a family status change, otherwise known as a qualifying life event (Mid-Year Events), as defined by the Internal Revenue Code. Examples of Mid-Year Events can be found in the chart on the next page. Once a Mid-Year Event has occurred, an employee has 30 days to notify PGB’s VA Employee Services at 1-800387-5955 to request a change in elections.
I have a pre-existing condition. Will I still be covered? Some policies may include a pre-existing condition clause. Please read your policy carefully for full details.
The benefit elections you make during Annual Enrollment or as a New Hire will remain in effect for the entire plan year. You will not be able to change or revoke your elections once they have been made unless a Mid-Year Event (status change) occurs. The summary of events that allow an employee to make benefit changes and instructions for processing those life event changes can be reviewed in the chart below.
Make elections within 30 days of hire date. Documentation is required.
Add your new spouse to your elections within 30 days of the marriage date. A copy of the marriage certificate must be presented.
Birth or Adoption of a Child
Remove the former spouse within 30 days of the divorce. Proof of the divorce will be required. A copy of the divorce decree must be presented.
You and your dependents are not eligible until the next Annual Enrollment period.
Dependent Aging Out
Enroll the new dependent in your elections within 30 days of the birth or adoption date, even if you already have family coverage. A copy of the birth certificate, mother’s copy of birth certificate, or hospital discharge papers must be presented. Once you receive the child’s Social Security Number, don’t forget to update your child’s insurance information record.
Your spouse is not eligible until the next Annual Enrollment period.
Remove or update dependent elections within 30 days of the dependent aging out. For more information and assistance, please call PGB Employee Services at 800-387-5955.
Benefits are not available for the divorced spouse and will be recouped if paid erroneously.
Death of a Spouse or Dependent
Remove the dependent from your elections within 30 days from the date of death. Death certificate must be presented.
The new dependent will not be covered until the next Annual Enrollment period.
Change in Spouse’s Employment or Coverage
Add or drop benefits from your elections within 30 days of the event date. A letter from the employer or insurance company must be presented.
Coverage for the dependent will end at the time of the dependent aging out and the policyholder must remove/update the dependent elections in order for the change to be reflected in the employee’s deductions.
You could pay a higher premium than required and you may be overpaying for coverage required.
You will not be able to make changes until the next Annual Enrollment period.
The examples included in this chart are not all-inclusive. Please speak to a Benefits Representative to learn more.
Mid-Year Event
Part-Time to Full-Time or Vice Versa
Transferring Employers
Change your elections within 30 days from the employment status change to receive COBRA information or to enroll in benefits as a full-time employee. Documentation from the employer must be provided.
If you are transferring from one PGB client to another, some benefits may be eligible for transfer. Please call PGB Employee Services at 800-387-5955 for more information and assistance.
Benefits may not be available to you or your dependents if you wait to enroll in COBRA. Full-time employees will have to wait until the next Annual Enrollment period.
Loss of Government or Education Sponsored Health Coverage
Entitlement to Medicare or Medicaid
If you, your spouse, or a dependent loses coverage under any group health coverage sponsored by a governmental or educational institution, you may be eligible to add additional coverage for eligible benefits.
You may lose the opportunity to transfer benefits.
Non-FMLA Leave
If you, your spouse, or dependent becomes entitled to or loses coverage under Medicare or Medicaid, you may be able to change coverage under the accident or health plan.
You and your dependents are not eligible until the next Annual Enrollment period.
You and your dependents are not eligible until the next Annual Enrollment period.
An employee taking a leave of absence, other than under the Family & Medical Leave Act, may not be eligible to re-enter the Flexible Benefits program until next plan year. Please contact your Benefit Administrator for more information.
Your individual supplemental/voluntary policies through Colonial Life are portable! To move them from payroll deduction to direct billing, please complete and submit the Payment Method Change Form to Colonial Life within 30 days of retiring. You are also eligible for post-employment Dental, Vision, and Telemedicine benefits through PGB. Please visit: www.piercegroupbenefits.com/ individualcoverage or call our Employee Services at 800-387-5955 for more information and assistance.
You and your dependents are not eligible until the next Annual Enrollment period.
If you do not transfer your policies from payroll deduction to direct billing, Colonial Life will terminate your policies resulting in a loss of coverage.
The examples included in this chart are not all-inclusive. Please speak to a Benefits Representative to learn more.
During your annual enrollment period, a PGB Benefits Representative will be available by appointment to meet with you one-on-one to help you evaluate your benefits based on your individual and family needs, answer any questions you may have, and assist you in the enrollment process. If you prefer, you may also self-enroll online following the instructions on the next page of this guide.
YOU CAN MAKE THE FOLLOWING BENEFIT ELECTIONS DURING THE ANNUAL ENROLLMENT PERIOD:
• Enroll in, change, or cancel The Local Choice benefits (Anthem Health, Delta Dental of VA, and Anthem Blue View Vision).
• Enroll in, change, or cancel Health Savings Accounts.+
• Enroll/Re-Enroll in Flexible Spending Accounts.+
• Enroll in, change, or cancel Dental Insurance (Stand-Alone Policy).*
• Enroll in, change, or cancel Vision Insurance (Stand-Alone Policy).*
• Enroll in, change, or cancel Long Term Care Benefits.
• Enroll in, change, or cancel Colonial coverage.
+You will need to re-enroll in the Health Savings Accounts and Flexible Spending Accounts if you want them to continue each year.
*The Dental and Vision Stand-Alone Policies are for employees who have waived coverage under the Local Choice (Health, Dental, & Vision) plan. Employees enrolled in the Local Choice plan may not enroll in the Dental or Vision Stand-Alone Policies.
You can view details about what benefits your employer offers, view educational videos about all of your benefits, download forms, chat with one of our knowledgeable Benefits Representatives, and more on your personalized benefits website. To view your custom benefits website, visit:
www.PierceGroupBenefits.com/AmherstCountyGovernment
1.
Amherst Count y offers an excellent benefits package which includes the following employer paid and voluntar y benefits for full-time employees:
• Employer subsidized medical, dental and vision insurance
• Voluntary supplemental health insurance policies through Colonial Life
• Required participation in the Virginia Retirement System plans and a voluntary deferred Compensation Plan
• Employer paid life insurance and optional voluntary life insurance through Securian/Minnesota Life
• Paid Leave Benefits
• Employee Assistance Plan (EAP) through HealthWorks.
More information is provided about these benefits below and in Employee Navigator.
Please call HR at 434-946-9420 if you have any additional questions about employee benefits.
Summaries of the Amherst County’s medical, dental and vision plans offered are provided in Employee Navigator. For dependents to be covered, the employee must be on the same plan as the dependents.
Amherst County offers two different medical plans through Anthem TLC (The Local Choice). Your TLC benefits are all inclusive and include medical, dental and vision coverage. Dental is provided through Delta Dental of Virginia and Vision is through Anthem Blue View Vision. If you enroll in The Local Choice, you will receive your member card(s) in the mail.
Amherst County offers a standalone dental plan for employees who do not enroll in one of The Local Choice plans. This plan is offered through Delta Dental of VA.
Amherst County offers a standalone dental plan for employees who do not enroll in one of The Local Choice plans. This plan is offered through Anthem Blue View Vision.
Amherst County offers voluntary supplemental health benefits through Flex Facts, Colonial Life, and CHUBB. Employees may put aside funds on a pre-tax basis in a Flexible Spending Account (FSA) or Health Savings Account (HSA) and/or purchase supplemental health insurance plans for Medical Bridge, Cancer, Accident, Short Term Disability, Term Life, Whole Life, Critical Illness, and Long Term Care.
Flex Facts is our Flexible Spending Account (FSA) and Health Savings Account (HSA) administrator. An FSA allows you to put away money from your payroll on a pre-tax basis to pay for qualified health expenses such as co-pays, deductibles, prosthetics, etc., and/or child care. An HSA is a type of personal savings account that can be used to pay for qualified medical expenses. You can put money into an HSA and withdraw it tax-free, as long as you use it for expenses like deductibles, co-payments, and coinsurance. HSAs can only be used when paired with a High Deductible Health Plan (HDHP). Please note, you can not be enrolled in an FSA at the same time you open or contribute to an HSA.
LIFE
Colonial Life offers supplemental benefits that can be customized to employees’ needs.
CHUBB provides professional and general coverage for long term care facilities.
Amherst County employees are eligible to participate in the state’s Virginia Retirement System (VRS). The state mandated required employee contribution is 5% of your monthly gross pay which is withheld on a pre-tax basis. There are three plans – eligibility is based on your hire date and prior VRS service credit – and HR assigns you to the appropriate plan when we set you up in the Employee Navigator system. You are enrolled with VRS automatically when Finance completes your first full month’s payroll. You should receive a letter from VRS when that occurs.
This plan is the original VRS pension plan. If you were hired prior to July 1, 2010 and were vested in the plan as of January 1, 2013, then you will be enrolled in Plan 1.
This plan is also a traditional pension plan with a lower multiplier than Plan 1. If you were hired between July 1, 2010 and December 31, 2013 and were not vested in Plan 1 on January 1, 2013, then you will be enrolled in Plan 2. If you are employed in a hazardous duty position, you will be either a Plan 1 or Plan 2 participant.
The Hybrid plan is a combination of a traditional pension plan and deferred compensation. If you are not in a hazardous duty position and you were hired on January 1, 2014 or later, or you were rehired on January 1, 2014 with no prior service credits in VRS, you will be enrolled in the Hybrid plan. For Hybrid employees, your 5% payroll contribution is split with 4% going to your pension plan and 1% going to deferred compensation. The deferred compensation portion is administered by VOYA and includes an employer match. You may voluntarily choose to contribute up to an additional 4% of your pay to the deferred compensation portion of your retirement. Contribution increase requests are completed online at varetire.org.
After one calendar year of employment, Hybrid employees receive paid short and long term disability. If you are in the Hybrid plan and you choose to purchase short and/or long term disability through one of the supplemental health vendors, you will want to cancel it at that point. State law greatly limits the benefit that the vendor is allowed to pay if you have employer paid short and/or long term disability.
Amherst County also offers a deferred compensation plan through Nationwide Retirement Solutions. Employees assigned to Plan 1 or Plan 2 or those Hybrid employees who have exceeded the allowable voluntary contribution in the Hybrid plan may participate. A 1:1 employer match of up to $100 per month is available. You may contact Senior Retirement Specialist Charlie Brennan at 804-314-9521 or stop by HR for a Retirement Planning 101 guide.
Amherst County provides employer paid group term life insurance at no cost to you through Securian/Minnesota Life. Coverage starts on your first day of employment. The benefit is twice your annual salary (rounded up to the next one thousand) at the time of death. You may purchase additional optional group term life insurance through Securian/Minnesota Life for yourself, your spouse or your children. If you do not purchase optional life insurance in your first 30 days of employment, a Certificate of Insurability form for the person(s) you are trying to insure must be completed and the Securian/Minnesota Life underwriters will determine whether you are eligible to purchase additional life insurance at that time.
Amherst County provides paid vacation leave, sick leave, personal leave and personal business leave for employees. New employees are granted and may begin to use personal leave and personal business leave upon hire. Except in emergency situations, all employee absences must be pre-approved by the employee’s direct supervisor. Annual leave and sick leave accrues at the end of each full calendar month of employment during the six month probationary period but may not be used until the new employee is released from probation. Other types of available leave include paid holidays, civic leave, military leave, FMLA, and administrative leave. Leave benefits and accrual rates are outlined in Section 6 of the Amherst County HR Regulation. The most current version of the HR Regulation may be found on the Human Resources page of the county website at www.countyofamherst.com.
EMPLOYEE ASSISTANCE PROGRAM 7.
Amherst County offers an Employee Assistance Program (EAP) through HealthWorks. Confidential professional counseling at no cost may be accessed by calling 434-200-6000. HealthWorks also offers a Work-Life Balance portal which can provide additional information and valuable resources for full time employees. If you are interested, please inquire at HR how to access the portals.
Below is a series of instructions outlining the enrollment process. Please have the following information available before you begin:
• Username and password. If you have forgotten your password, please visit the enrollment website and select “Reset a forgotten password”.
• Social security numbers of the spouse or any dependents you wish to enroll
• Dates of birth for the spouse and any dependents you wish to enroll
• Beneficiary names and social security numbers
• If you are a new employee, please refer to the New Hire information on the Eligibility Requirements page of this guide or contact PGB Employee Services at 800-387-5955 between 8:30am and 5:00pm for assistance.
• If you are an existing employee and unable to log into the online system, please contact the PGB Employee Services at 800-387-5955, or speak with the Benefits Representative assigned to your location.
First time users: Click on your Registration Link in the email sent to you by your admin or Register as a new user. Create an account, and create your own username and password.
Returning users: Visit the enrollment website below and click Login. Log in with the username and password you previously selected.
To login, visit: www.employeenavigator.com/benefits/account/login
After you login click Let’s Begin to complete your required tasks.
Complete any assigned onboarding tasks before enrolling in your benefits.
Once you’ve completed your tasks click Start Enrollment to begin your enrollments.
TIP: If you hit “Dismiss, complete later” you’ll be taken to your Home Page. You’ll still be able to start enrollments again by clicking “Start Enrollments”
After clicking Start Enrollment, you’ll need to complete some personal & dependent information before moving to your benefit elections.
To enroll dependents in a benefit, click the checkbox next to the dependent’s name under: Who am I enrolling?
Below your dependents you can view your available plans and the cost per pay. To elect a benefit, click Select Plan underneath the plan cost.
Click Save & Continue at the bottom of each screen to save your elections.
If you do not want a benefit, click Don’t want this benefit? at the bottom of the screen and select a reason from the drop-down menu.
If you have elected benefits that require a beneficiary designation, Primary Care Physician, or completion of an Evidence of Insurability form, you will be prompted to add in those details.
Review the benefits you selected on the enrollment summary page to make sure they are correct then click Sign & Agree to complete your enrollment.
You can either print a summary of your elections for your records or login at any point during the year to view your summary online.
To complete any required HR tasks, click Start Tasks. If your HR department has not assigned any tasks, you’re finished!
TIP: If you miss a step, you’ll see Enrollment Not Complete in the progress bar with the incomplete steps highlighted. Click on any incomplete steps to complete them.

As you continue forward, you will be asked to review, acknowledge, download, and complete required forms requested by your employer. There are instructions listed for each form and this guide is built to be used in conjunction with them.
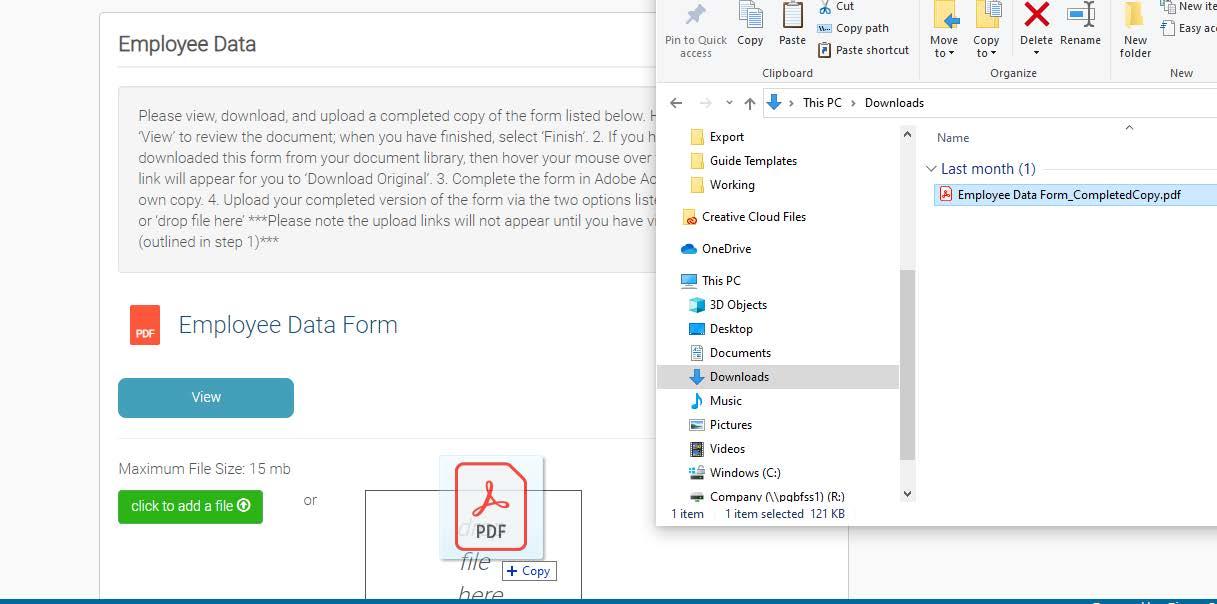
1. For most of the forms, you will see a set of instructions that reads as: “ Please view, download, and upload a completed copy of the form listed below…”.
a. Read through the Helpful Steps listed in the instructions: i. Click ‘View’ to review the document; when you have finished, select ‘Finish’.
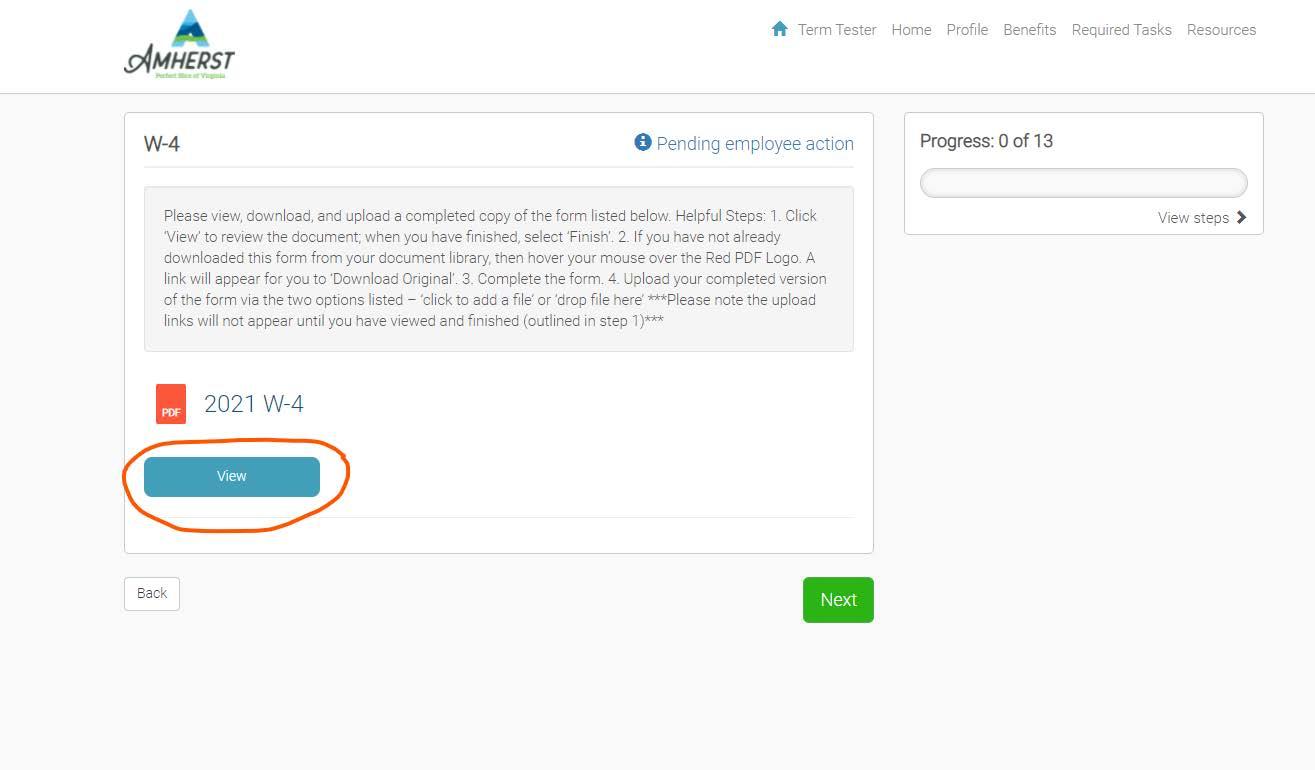
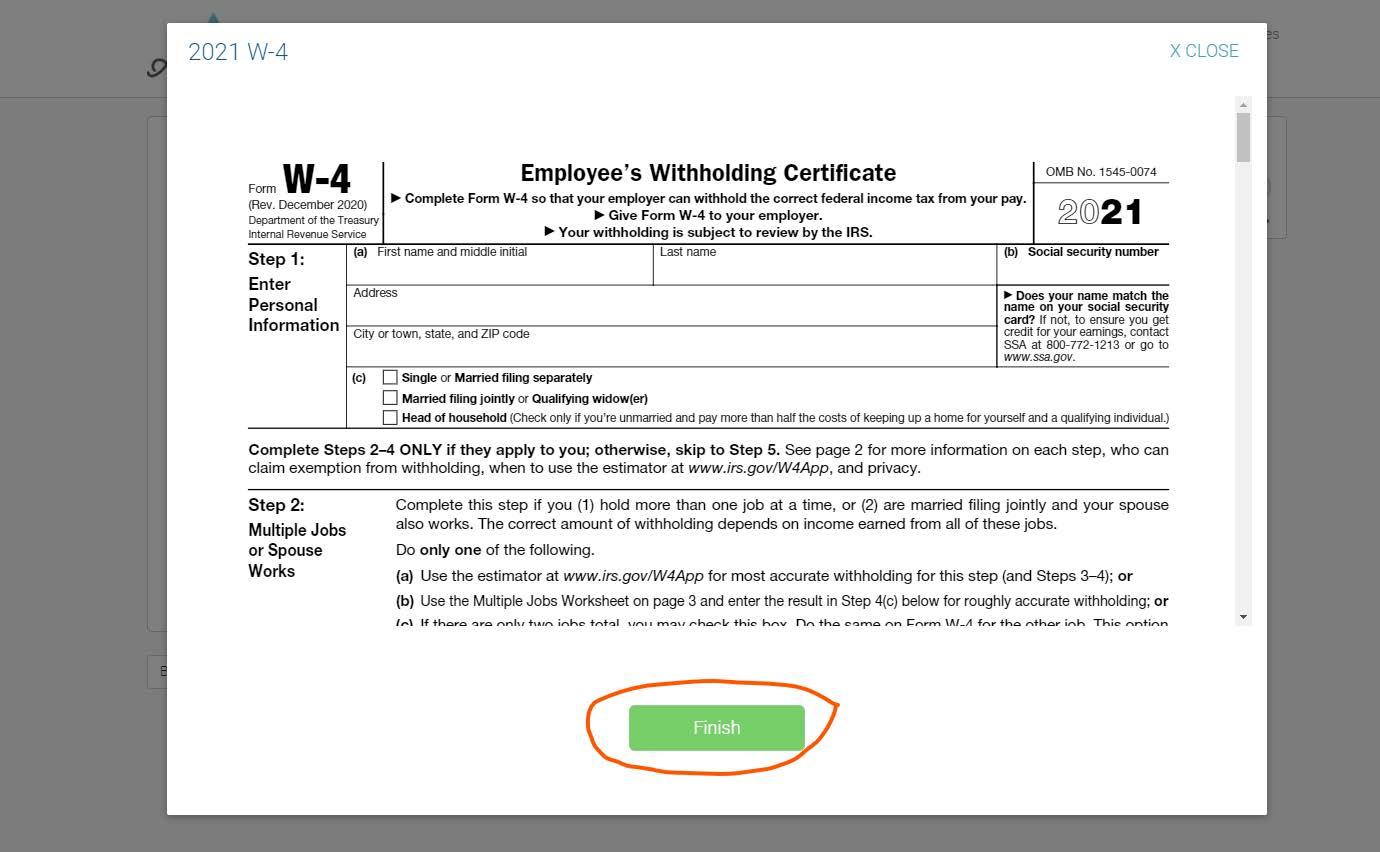
ii. If you have not already downloaded this form from your document library, then hover your mouse over the Red PDF Logo. A link will appear for you to ‘Download Original’.

iii. Complete the form in Adobe Acrobat and save your own copy.
1. Please keep in mind that no matter which web browser (Google Chrome, Microsoft Edge/Internet Explorer, Mozilla Firefox), you will want to open the form in Adobe. If you open it elsewhere, the electronic signature field may not appear. Also, if you are havi ng trouble locating the form you downloaded, then search your file directory for your ‘Downloads’ folder (example pictured below).

iv. Upload your completed version of the form via the two options listed –1. Click to add a file
a. Click the link for ‘Click to add a file’. This should open up your file directory. Navigate to where your signed and completed version of the form is saved. Select the file, click Open.
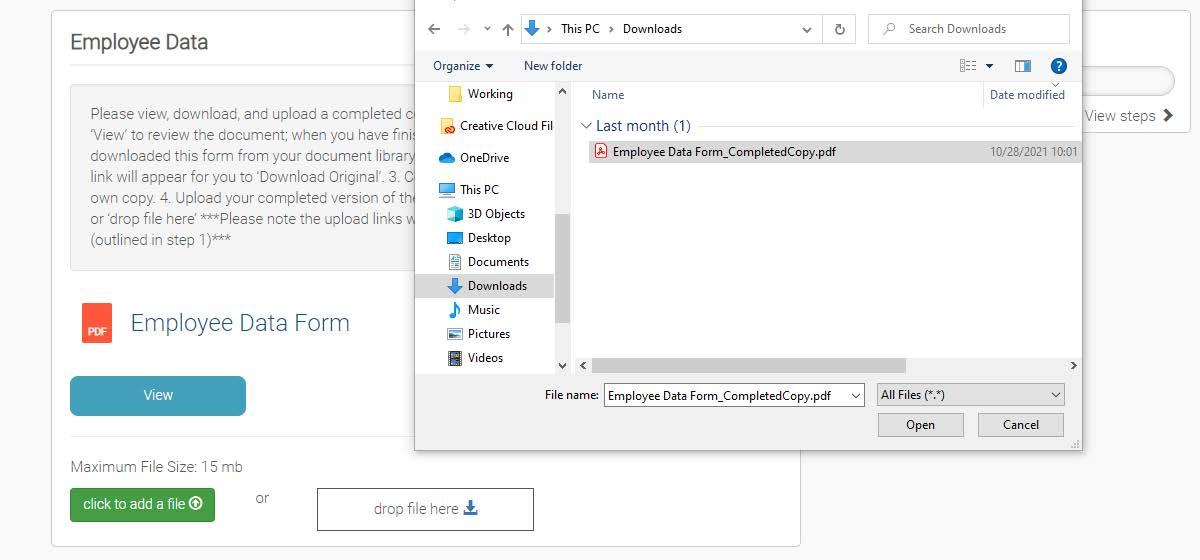
b. You should see a status bar appear below the link reflecting if the upload was successful.
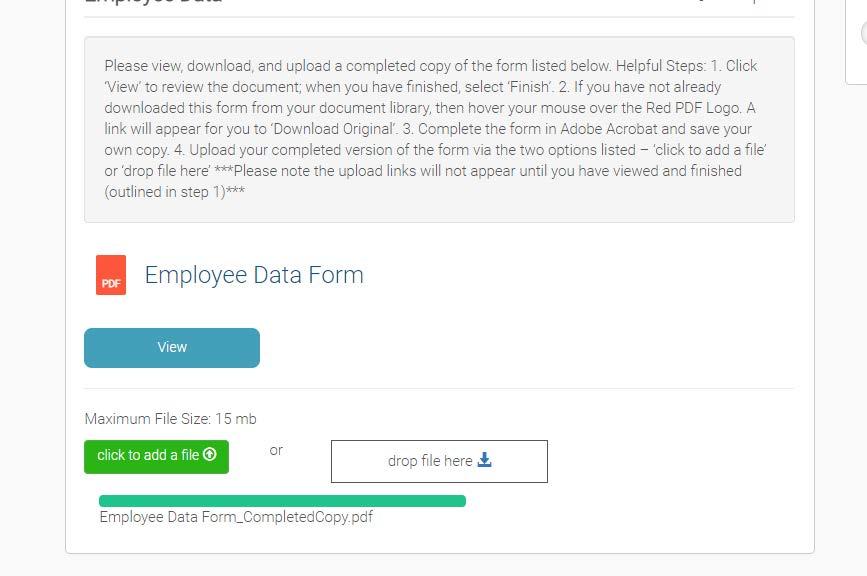
2. Drop file here
a. If you choose this method, you will open your file directory to where your signed and completed version of the for m is saved. Then simply select and drag the file over the ‘Drop file here link.
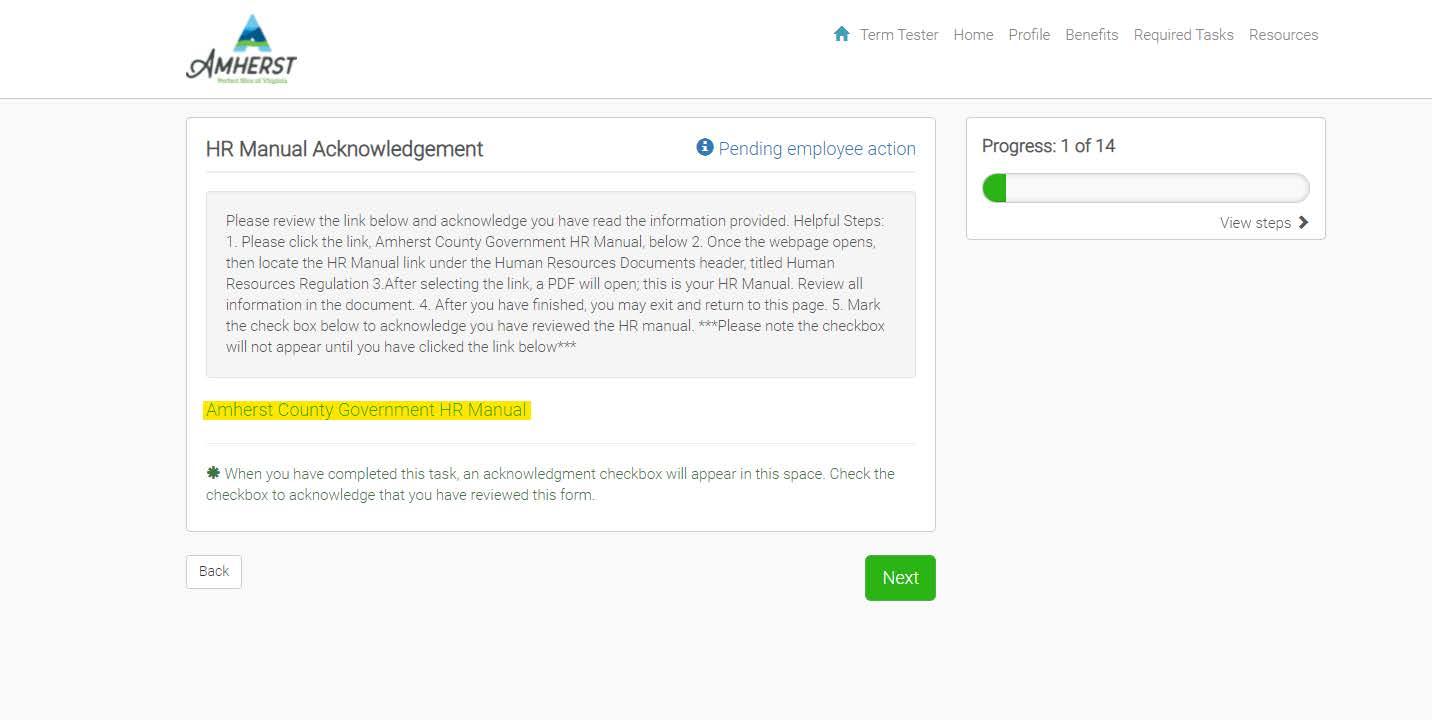
2. The other task you may be asked to complete is to review and acknowledge a webpage.
a. For this task, the instructions will start with, “Please review the link below and acknowledge you have read the information provided …” . Follow the Helpful Steps:
i. Please click the link, Amherst County Government HR Manual, below
ii. Once the new webpage opens, then locate the HR Manual link under the Human Resources Documents header, titled Human Resources Regulation
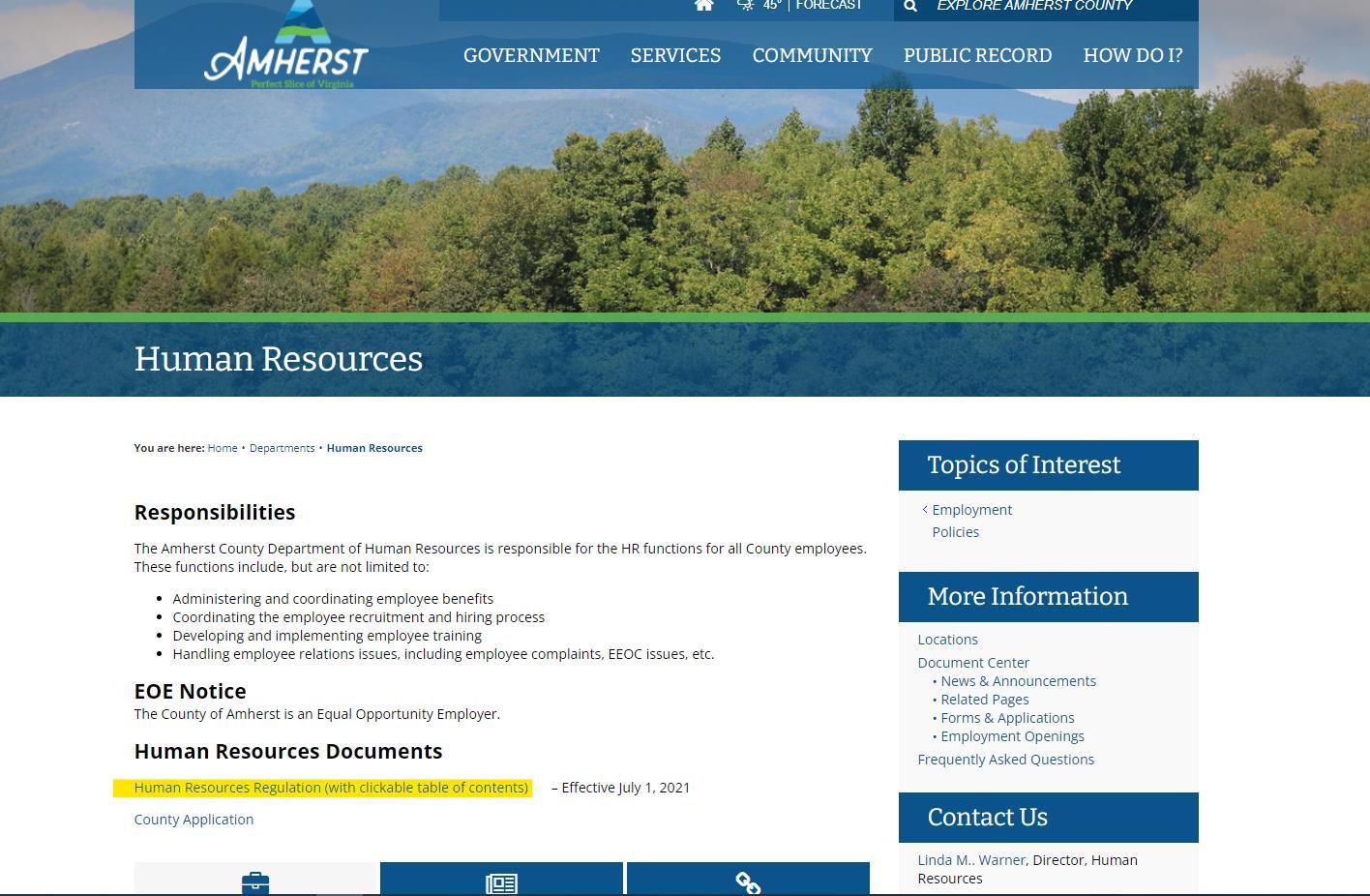
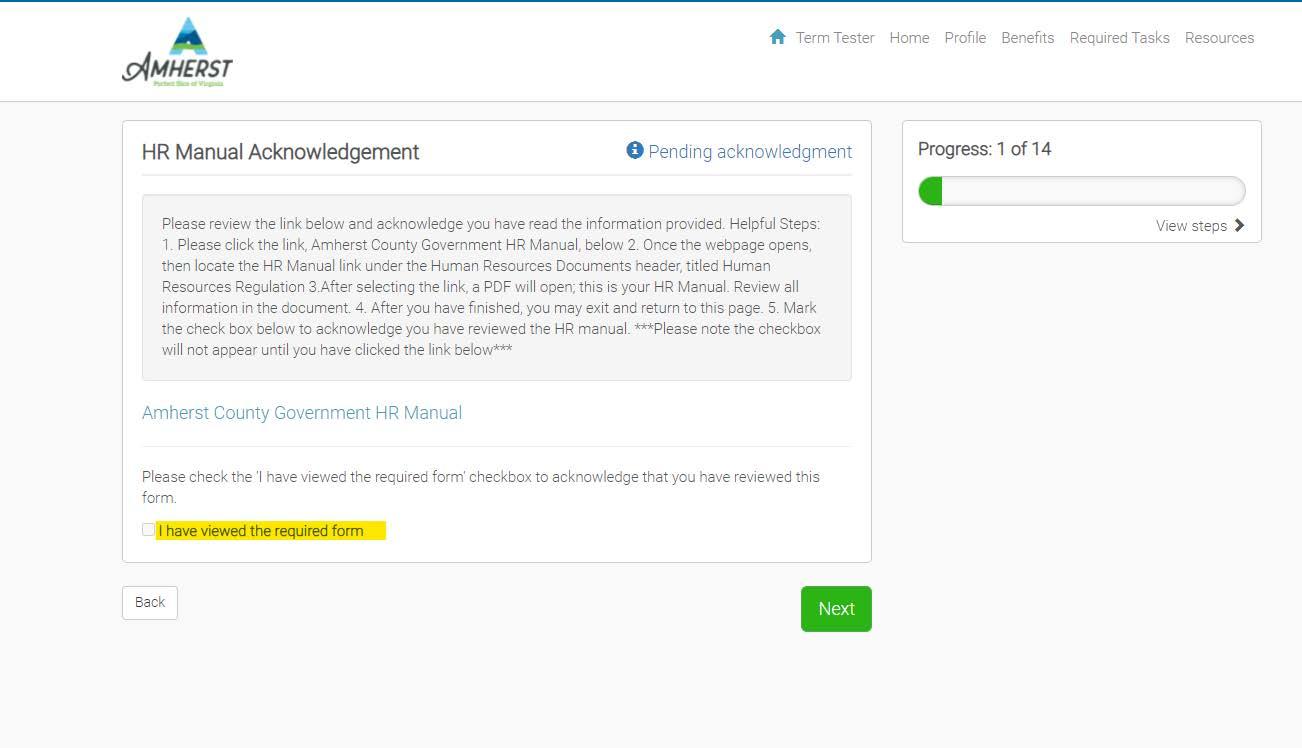
iii. After selecting the link, a PDF will open; this is your HR Manual. Review all information in the document.

iv. After you have finished, you may exit and return to the original Employee Navigator page. Mark the check box below to acknowledge you have reviewed the HR manual.






Lifetime Maximum Covered Services
Doctor's Visits (Outpatient or In-Office)
Primary Care Physician Visits -
Chiropractic, Spinal Manipulations (30 visit limit)
Specialist Visits -
Chiropractic, Spinal Manipulations (30 visit limit)
Shots - Allergy or Therapeutic InjectionsDoctor's Office, ER, or Outpatient Setting
Diagnostic Tests, Labs, and X-Rays
Specific conditions/diseases at doctor's office, ER, or Outpatient Setting
Preventive Care Visits
Emergency Room Visits
Hospital & Other Services (Pre-certification may be required)
Ambulance Services
Inpatient Hospital Services
Outpatient Hospital Services
Outpatient Diagnostic Test, Labs, and X-Rays
Outpatient Therapy Services - Occupational, Speech, Physical, Cardiac, Chemotherapy, Radiation, Infusion, & Respiratory
Diabetic Equipment
Maternity
Prenatal & Provider Services- PCP
Prenatal & Provider Services - Specialist
Hospital Services for Delivery
Diagnostic Tests, Labs, and X-Rays
Behavioral Health
Inpatient Treatment/Residential Treatment
Partial Hospitalization (Day) Program
Outpatient Professional Provider Services
Prescription Drug Benefit*
Retail Pharmacy (up to a 34-day supply) Rx
- Individual/Family

Anthem can help you make the most of your benefts so you can be your healthiest. Take advantage of these wellness programs and services included in your health plan.
The SydneySM Health mobile app gives you a quick connection to beneft information, tools, and helpful resources. Download the app today and log in using your anthem.com username and password to:
• View your ID card.
• See all your medical and pharmacy benefts and claims.
• Easily chat with customer service.
• Connect quickly to virtual care and wellness resources.
• Track your health goals and ftness.


Simplify your healthcare by downloading Sydney Health today
Anthem Health Guides are specially trained to answer your health plan questions and steer you to the right programs and support for your unique needs. Your guide will also remind you of any screenings or routine exams that are due, help you save money on your prescription drugs, compare costs for care, and fnd in-network doctors in your area. Call 800-552-2682, Monday to Friday 8:00 a.m. to 6:00 p.m.
Life can be challenging, and Anthem EAP is here to help. Your EAP includes up to 4 free, confdential counseling sessions per issue per plan year for you, your covered dependents, and members of your household. It’s also a valuable source for information about emotional well-being, childcare and elder care resources, fnancial and legal issues, and smoking cessation. Go to anthemeap.com, and log in using Commonwealth of Virginia as your company, and then select The Local Choice, or call 855-223-9277.
Using the Sydney Health app, you can have a private, secure, video visit wherever you are with a doctor.
Urgent care virtual visits are available on demand 24/7. Virtual appointments can also be scheduled to meet with a therapist, psychologist, psychiatrist, or a sleep specialist, Monday to Friday 9 a.m. to 9 p.m. Eastern time.
No cost for Key Advantage Plans. Twenty percent coinsurance, after deductible for HDHP plans.
24/7 NurseLine has registered nurses ready and willing to help you at any time of the day. They are excellent resources for:
• Minor health issues that can be handled at home.
• Directing you to the correct doctor, health professional, or specialist.
• Determining which facility type is the best choice for your issue.
Call 800-337-4770 anytime day or night. Your call is always free and completely confdential.


Enroll in Future Moms by calling 800-828-5891 within the frst 16 weeks of pregnancy for free pre- and post-natal support that can help ensure a healthy pregnancy. Once your baby is born, use LiveHealth Online for virtual visits with a certifed lactation consultant, counselor, or registered dietitian at no extra cost through the Future Moms with Breastfeeding Support program. Key Advantage Expanded or Key Advantage 250 members: Enroll within the frst 16 weeks and your plan will waive the hospital copayment for delivery.
Extra support for members with:
• Asthma
• Diabetes
• Coronary artery disease
• Heart failure
• Chronic obstructive pulmonary disease (COPD)
• Hypertension
ConditionCare provides Nurse Care Managers who work with you or a covered
family member to help you better understand and manage a condition and meet personalized health goals. Call 844-507-8472 to enroll or we may call you to see if you would like to participate.



During those moments when you feel overwhelmed, your Employee Assistance Program (EAP) is here for you with real-life tips, tools, articles, webinars, and links to helpful resources. As always, your EAP is private, confidential, and included as part of your benefits.1 EAP is available to all employees and household members or dependents, even if you are not enrolled in an Anthem medical plan.
Connect with a mental health professional for a variety of matters, including in moments of crisis. In-person and virtual options are available. Virtual options are offered through Headway, Talkspace or LiveHealth Online.
Find resources for career, parenting, healthy communication, and balancing work and family.
Talk with a professional and find resources that can help you take charge of your finances.
For questions or issues, you have access to your EAP 24/7. Contact your EAP by calling 855-223-9277 or visit anthemeap.com/the-local-choice
Access on-line resources and legal help in-person or by phone for each issue, each year, at no added cost.2 You or eligible family members can call EAP and request a consultation for each separate issue, with a network attorney at no cost.
Emotional Well-being resources connect you to one-on-one coaching, self-help digital tools and access to articles, podcasts, and webinars for help with depression, anxiety, relationships, and alcohol use.
Take self-assessments to get personalized recommendations on the best resources for your needs.
View all your benefits and access wellness tools to improve your overall health with the Sydney HealthSM app
The Sydney Health mobile app works with you by guiding you to better overall health — and for you by bringing your benefits and health information together in one convenient place. Sydney Health has everything you need to know about your benefits, so you can make the most of them while taking care of your health.
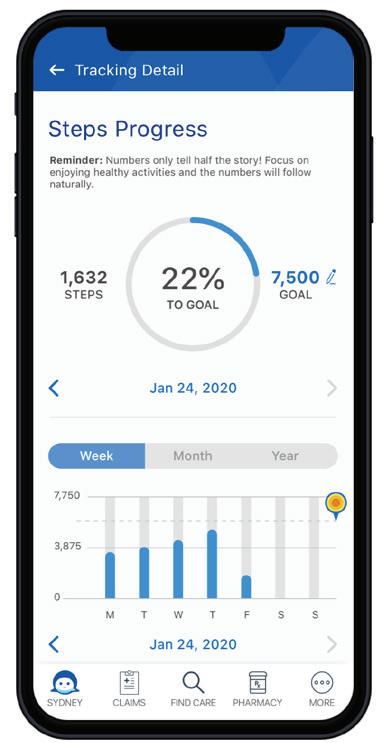
} Reminding you about important
} Planning and tracking your health goals, fitness, and rewards
} Giving you instant access to your preventive care needs* medical, dental and vision benefits and claims*
} Storing your member ID card so you can show, email, or fax it right
} Guiding you with insights based on from your phone your history and changing health needs
Simplify your healthcare by downloading Sydney Health today
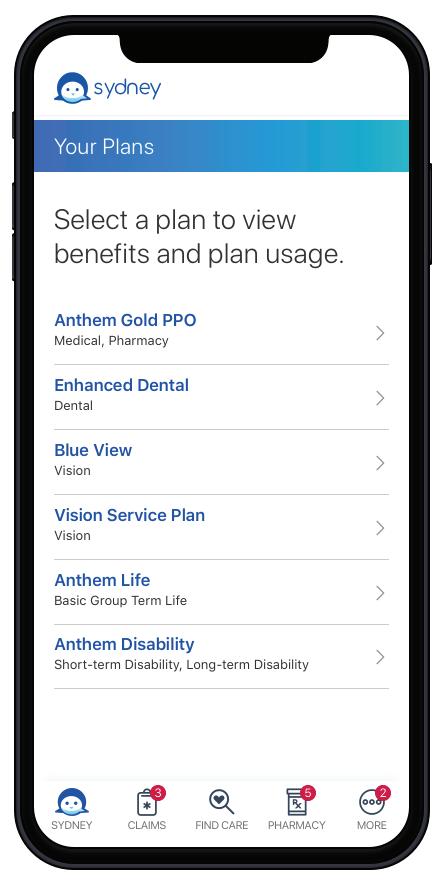
} Providing answers quickly through
} Empowering you with personalized real-time live chat with an Anthem tools to find doctors, hospitals, labs, and representative other health care providers in your plan and compare costs.*
} Connecting you to virtual care options for primary, urgent or
} Helping you manage prescriptions and specialty care save money by comparing pharmacy costs and locating coupons


You have an allowance for eyeglass lenses or contact lenses every plan year. You pay the remaining cost for frames and lenses after Your Health Plan’s Reimbursement.
Covered Services
Routine eye exam
Standard eyeglass lenses (in lieu of contact lenses)
Polycarbonate lenses included at no additional cost for children under 19 years old
Eyeglass frames
Contact lenses1 (in lieu of eyeglass lenses)
Elective Conventional2
Elective Disposable2
Non-Elective2
Retinal Imaging
At member’s option can be performed at time of eye exam
Lens options
UV coating, tints, standard scratch-resistant
Blue View Vision Network (once per plan year)
You pay $15 copayment
You pay $20 copayment
Plan pays up to $100* retail allowance
Plan pays up to $100 allowance then 15% discount off remaining balance
Plan pays up to to $50
Plan pays up to: $50 single lenses; $75 bifocal; $100 trifocal
Plan pays up to $80
Plan pays up to $80
Plan pays up to $100 allowance (no additional discount)Plan pays up to $80
Covered in full
Not more than $39
You pay $15
Standard polycarbonate (Adult) You pay $40
Standard progressive (in addition to bifocal copayment)
Standard anti-reflective
Other add-ons
(i.e. high index lenses, anti-fog coating)
You pay $65
You pay $45
You pay 20% off retail
*You may select a frame greater than the covered allowance and receive a 20% discount for any additional cost over the allowance.
Plan pays up to $210
Not available
Not available
Not available
Not available
Not available
1 Declining Balance. Your plan has a declining balance allowance. This means if you do not use your allowance all at once, the remainder will be available for you to use at a later time. However, any remaining balance will not carry over to the next benefit year. All services or supplies using the declining balance for a benefit period must be received In-Network based on where the first paid claim is incurred..
2 Elective contact lenses are typically elected in lieu of eyeglass lenses. Non-Elective contact lenses are medically necessary contacts when glasses are not an option for vision.
Enrollment in a HDHP allows you to set up a personal Health Savings Account (HSA) through a bank or other financial institution to help you manage healthcare expenses or save for retirement. HSAs were created as part of Medicare reform legislation in 2003. An HSA is a tax-favored account that allows those covered by a HDHP to pay for certain qualified medical expenses. It can help you save on the cost of your health insurance and healthcare expenses, and also help pay for covered services before you satisfy the health plan deductible. If you decide to set up an HSA to work with your HDHP, confer with your tax advisor, bank or other financial institution.
The following web sites are a good place to start learning more about HSAs.
• www.treasury.gov – Provides an overview of HSAs, answers to frequently asked questions and important IRS forms and applications. Search using keyword HSA.
• www.irs.gov – Provides information about how HSAs impact your Federal taxes and qualified medical expenses (Publications 969 and 502). Search using keyword HSA.
• www.hhs.gov – Provides general information about HSAs and other tax-favored health plans. Search using keyword HSA.
Note: If you have an HSA, you cannot also have a Flexible Spending Account unless it is limited in scope. More information is available from tax consultants or financial institutions.
You have an allowance for eyeglass lenses or contact lenses every plan year. You pay the remaining cost for frames and lenses after Your Health Plan’s Reimbursement.
Routine eye exam
Standard eyeglass lenses (in lieu of contact lenses)
Polycarbonate lenses included at no additional cost for children under 19 years old
Eyeglass frames
Contact lenses1 (in lieu of eyeglass lenses)
Elective Conventional2
Elective Disposable2
Non-Elective2
Retinal Imaging
At member’s option can be performed at time of eye exam
Lens options
UV coating, tints, standard scratch-resistant
Blue View Vision Network (once per plan year)
You pay $40 copayment
You pay $20 copayment
Plan pays up to $100* retail allowance
Plan pays up to $100 allowance then 15% discount off remaining balance
Plan pays up to $100 allowance (no additional discount)
Plan pays up to $250 allowance
Not more than $39
You pay $15
Standard polycarbonate (Adult) You pay $40
Standard progressive (in addition to bifocal copayment)
Standard anti-reflective
Other add-ons (i.e. high index lenses, anti-fog coating)
You pay $65
You pay $45
You pay 20% off retail
*You may select a frame greater than the covered allowance and receive a 20% discount for any additional cost over the allowance.
Plan pays up to to $50
Plan pays up to:
$50 single lenses;
$75 bifocal;
$100 trifocal
Plan pays up to $80
Plan pays up to $80
Plan pays up to $80
Plan pays up to $210
Not available
Not available
Not available
Not available
Not available
1 Declining Balance. Your plan has a declining balance allowance. This means if you do not use your allowance all at once, the remainder will be available for you to use at a later time. However, any remaining balance will not carry over to the next benefit year. All services or supplies using the declining balance for a benefit period must be received In-Network based on where the first paid claim is incurred..
2 Elective contact lenses are typically elected in lieu of eyeglass lenses. Non-Elective contact lenses are medically necessary contacts when glasses are not an option for vision.
You have an allowance for eyeglass lenses or contact lenses every plan year. You pay the remaining cost for frames and lenses after Your Health Plan’s Reimbursement.
Routine eye exam
Standard eyeglass lenses (in lieu of contact lenses)
Polycarbonate lenses included at no additional cost for children under 19 years old
Eyeglass frames
Contact lenses1 (in lieu of eyeglass lenses)
Elective Conventional2
Elective Disposable2
Non-Elective2
Retinal Imaging
At member’s option can be performed at time of eye exam
Lens options
UV coating, tints, standard scratch-resistant
Blue View Vision Network (once per plan year)
You pay $35 copayment
You pay $20 copayment
Plan pays up to $100* retail allowance
Plan pays up to $100 allowance then 15% discount off remaining balance
Plan pays up to $100 allowance (no additional discount)
Covered in full
Not more than $39
View
Plan pays up to to $50
Plan pays up to:
$50 single lenses;
$75 bifocal; $100 trifocal
Plan pays up to $80
Plan pays up to $80
Plan pays up to $80
Plan pays up to $210
You pay $15
Standard polycarbonate (Adult) You pay $40
Standard progressive (in addition to bifocal copayment)
Standard anti-reflective
Other add-ons (i.e. high index lenses, anti-fog coating)
You pay $65
You pay $45
You pay 20% off retail
*You may select a frame greater than the covered allowance and receive a 20% discount for any additional cost over the allowance.
Not available
Not available
Not available
Not available
Not available
1 Declining Balance. Your plan has a declining balance allowance. This means if you do not use your allowance all at once, the remainder will be available for you to use at a later time. However, any remaining balance will not carry over to the next benefit year. All services or supplies using the declining balance for a benefit period must be received In-Network based on where the first paid claim is incurred..
2 Elective contact lenses are typically elected in lieu of eyeglass lenses. Non-Elective contact lenses are medically necessary contacts when glasses are not an option for vision.






Effective Date: 7/1/2026
Deductible $25/Calendar Year Type 2 & 3
1
(per person) $1,500 per calendar year
Enrollment
Orthodontia Summary - Adult and Child Coverage
Sample Procedure Listing (Current Dental Terminology © American Dental Association.) Type 1 Type 2 Type 3
⚫ Routine Exam
(2 per benefit period)
⚫ Bitewing X-rays (1 per benefit period)
⚫ Full Mouth/Panoramic X-rays (1 in 3 years)
⚫ Periapical X-rays
⚫ Cleaning
(2 per benefit period)
⚫ Fluoride for Children 18 and under (1 per benefit period)
⚫ Sealants (age 15 and under)
⚫ Space Maintainers
Ameritas Information
We're Here to Help
⚫ Fillings for Cavities
⚫ Restorative Composites (anterior and posterior teeth)
⚫ Endodontics (nonsurgical)
⚫ Endodontics (surgical)
⚫ Periodontics (nonsurgical)
⚫ Periodontics (surgical)
⚫ Simple Extractions
⚫ Complex Extractions
⚫ Anesthesia
⚫ Onlays
⚫ Crowns (1 in 5 years per tooth)
⚫ Crown Repair
⚫ Denture Repair
⚫ Implants
⚫ Prosthodontics (fixed bridge; removable complete/partial dentures) (1 in 5 years)
This plan was designed specifically for the associates of AMHERST COUNTY BOARD OF SUPERVISORS, VA. At Ameritas Group, we do more than provide coverage - we make sure there's always a friendly voice to explain your benefits, listen to your concerns, and answer your questions. Our customer relations associates will be pleased to assist you 7 a.m. to midnight (Central Time) Monda y through Thursday, and 7 a.m. to 6:30 p.m. on Friday. You can speak to them by calling toll -free: 800-487-5553. For plan information any time, access our automated voice response system or go online to ameritas.com.
Dental Network Information
To find a provider, visit ameritas.com and select FIND A PROVIDER, then DENTAL. Enter your criteria to search by location or for a specific dentist or practice. California Residents: When prompted to select your network, choose the Ameritas Network found on your ID Card or contact Customer Connections at 800 -487-5553.
Your provider network is Ameritas Classic and Plus Network.

While we don't require a pretreatment authorization form for any procedure, we recommend them for any dental work you conside r expensive. As a smart consumer, it's best for you to know your share of the cost up front. Simply ask your dentist to submi t the information for a pretreatment estimate to our customer relations department. We'll inform both you and your dentist of the e xact amount your insurance will cover and the amount that you will be responsible for. That way, there won't be any surprises on ce the work has been completed.
If a member does not elect to participate when initially eligible, the member may elect to participate at the policyholder's next enrollment period. This enrollment period will be held each year and those who elect to participate in this policy at that ti me will have their insurance become effective on July 1. If you do not enroll during your company's open enrollment period, then you will be su bject to the Late Entrant Provision.
We strongly encourage you to sign up for coverage when you are initially eligible. If you choose not to sign up during this initial enrollment period, you will become a late entrant. Late entrants will be eligible for only exams, cleanings, and fluoride a pplications for the first 12 months they are covered.
This document is a highlight of plan benefits provided by Ameritas Life Insurance Corp. as selected by your employer. It is not a certificate of insurance and does not include exclusions and limitations. For exclusions and limitations, or a complete list of covered procedures, contact your benefits administrator.






Welcome to your Blue View Vision plan!
You have many choices when it comes to using your benefits. As a Blue View Vision plan member, you have access to one of the nation’s largest vision networks. You may choose from many private practice doctors, local optical stores, and national retail stores including LensCrafters®, Target Optical®, and most Pearle Vision® locations. You may also use your in-network benefits to order eyewear online at Glasses.com and ContactsDirect.com. To locate a participating network eye care doctor or location, log in at anthem.com, or from the home page menu under Care, select Find a Doctor. You may also call member services for assistance at 1-866-723-0515
Out-of-Network – If you choose to, you may instead receive covered benefits outside of the Blue View Vision network. Just pay in full at the time of service, obtain an itemized receipt, and file a claim for reimbursement up to your maximum out-of-network allowance.
Routine Eye Exam
A comprehensive eye examination
Eyeglass Frames
One pair of eyeglass frames
Eyeglass Lenses (instead of contact lenses)
One pair of standard plastic prescription lenses
Single vision lenses
Bifocal lenses
Trifocal lenses
Eyeglass Lens Enhancements
$20 Copay
$130 Allowance, then 20% off any remaining balance
$20 Copay
$20 Copay
$20 Copay
Reimbursed Up To $42
Reimbursed Up To $45
Reimbursed Up To $40
Reimbursed Up To $60
Reimbursed Up To $80
Once every calendar year
Once every calendar year
Once every calendar year
When obtaining covered eyewear from a Blue View Vision provider, you may choose to add any of the following lens enhancements at no extra cost
Lenses (for a child under age 19)
Standard polycarbonate (for a child under age 19)
Factory Scratch Coating
Contact Lenses (instead of eyeglass lenses)
$0 Copay
$0 Copay
$0 Copay
No allowance when obtained out-of-network
Same as covered eyeglass lenses
Contact lens allowance will only be applied toward the first purchase of contacts made during a benefit period. Any unused amount remaining cannot be used for subsequent purchases in the same benefit period, nor can any unused amount be carried over to the following benefit period.
Elective conventional (non-disposable) OR
Elective disposable OR
Non-elective (medically necessary)
Contact lens fit and follow-up
$130 Allowance, then 15% off any remaining balance
$130 Allowance (no additional discount)
Covered in full
Reimbursed Up To $105
Reimbursed Up To $105
Reimbursed Up To $210
Once every calendar year
A contact lens fitting and up to two follow-up visits are available to you once a comprehensive eye exam has been completed
Standard contact lens fitting
Premium contact lens fitting
$0 Copay 10% off retail price, then apply $55 allowance
Reimbursed Up To $35
Reimbursed Up To $35
Once every calendar year
Retinal Imaging – at member’s option, can be performed a time of eye exam
Eyeglass lens upgrades
When obtaining eyewear from a Blue View Vision provider, you may choose to upgrade your new eyeglass lenses at a discounted cost. Eyeglass lens copayment applies.
Conventional Contact Lenses (non-disposable type)
1 Please ask your provider for his/her recommendation as well as the available progressive brands by tier.
2 Please ask your provider for his/her recommendation as well as the available anti-reflective brands by tier.
Cannot be combined with any other offer. Discounts are subject to change without notice. Discounts are not covered benefits under your vision plan and will not be listed in your certificate of coverage. Discounts will be offered from in-network providers except where State law prevents discounting of products and services that are not covered benefits under this plan. Discounts on frames will not apply if the manufacturer has imposed a no discount on sales at retail and independent provider locations.
Some of our in-network providers include:

Savings on items like additional eyewear after your benefits have been used, non-prescription sunglasses, hearing aids and even LASIK laser vision correction surgery are available through a variety of vendors. Just log in at anthem.com, select discounts, then Vision, Hearing & Dental.
* Discounts cannot be used in conjunction with your covered benefits.
OUT-OF-NETWORK
If you choose to receive covered services or purchase covered eyewear from an out-of-network provider, network discounts will not apply and you will be responsible for payment of services and/or eyewear materials at the time of service. Please complete an out-of-network claim form and submit it along with your itemized receipt to the fax number, email address, or mailing address below. To download a claim form, log in at anthem.com, or from the home page menu under Support select Forms, click Change State to choose your state, and then scroll down to Claims and select the Blue View Vision Out-of-Network Claim Form. You may instead call member services at 1-866-723-0515 to request a claim form.
TO FAX: 866-293-7373
TO EMAIL: oonclaims@eyewearspecialoffers.com
TO MAIL: Blue View Vision Attn: OON Claims P.O. Box 8504 Mason, OH 45040-7111
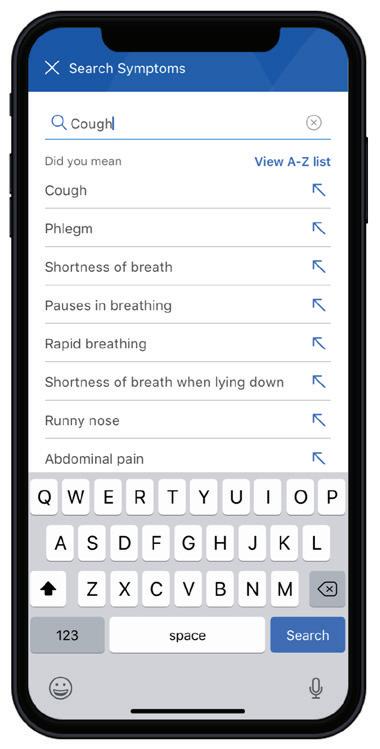
Here’s how to find one fast on our mobile app, Sydney, or anthem.com.
To search on the app, you’ll need a username and password.
Select Find a Doctor
Search for a provider
Click on the name of an eye care provider to learn more
On anthem.com, log in as a member with your username and password, or your member ID card number.
You can also search as a guest. Just select a plan or network, or search by all plans and networks.*
You can search based on type of provider or facility, locations near you or a provider’s name.
Find out about their training, specialties, languages spoken, location and phone number.
Keep in mind, you’ll get the most from your benefits — and save money — when you use a provider in your plan.
Download our Sydney mobile app today to easily access your plan.



* If you don’t know the name of your plan or network, check with your human resources department or benefits administrator.
online, retailand independent providers
Between work and their personal lives, your employees are busy. So we want to make things a little easier for them. With Blue View VisionSM, they have benefts that are easy to use and make it convenient for them to get care from independent, retail and i online vision care specialists. Choose from over 38,000 eye doctors at over 27,000 locations nationwide.
Check out this list of other Blue View Vision retailers and vision care specialists in your plan. Choose from over 4,240+ regional eye care locations close to work and home.
Abba Eye Care
All About Eyes
America’s Best
Bard Optical
Boscov’s Optical
C&B Optical One
Clarkson Eyecare
Cohen’s Fashion Optical
Crown Optical
Devlyn Optical
Doctor’s Vision Center
Dr. Tavel Family Eye Care
Drs. May & Hettler
Eye Assoc. of New Mexico
Eye Boutique
Eyeglass World
Eye-Mart Optical Outlet
FirstSight Vision Services
For Eyes Optical
Gulf Coast Optometry
Heartland Vision
Henry Ford OptimEyes
Herslof Opticians
ILORI
Marion Eye Centers & Optical
Meijer Optical
Midwest Eye Consultants
Midwest Vision Centers
MyEyeDr.
MyEyeLab
National Vision
Nationwide Vision Center
Northeastern Eye Institute
Oakley Store
We defne retail providers as practices that have 20 or more i locations. The retail providers listed here can be found in or nearby major shopping centers and offer night and weekend hours. Many also have on-site labs, which makes it easier for your employees to get their glasses in about an hour or even the same day.
If your employees need help fnding a vision care provider, i let them know they can use the provider search at anthem.com.
Optical Shop of Aspen
Optical Shoppe in Fred Meyer
OPTYX
Ossip Optometry
Rx Optical
Schaeffer Eye Center
SEE, Inc.
Shopko Eye Care Center
Site for Sore Eyes
Southwestern Eye Center
Sterling Vision Care
SVS Vision
Texas State Optical Today’s Vision
Union Eye Care
US Vision
Vision World
Vogue Vision Centers
Wing Eyecare
Wisconsin Vision
For more information Call your Anthem representative or broker.
FY2027 Dental Rates - Ameritas
FY2027 Vision Rates - Blue View Vision







y An HSA is a personal savings account that allows you to set aside pre-tax dollars for current and future healthcare expenses for you and your dependents.
y You are eligible to open an HSA if you are enrolled in an HSAeligible high-deductible health plan.
y Your HSA is funded by payroll deduction, online banking transfer or a direct contribution.
y Use your funds to pay for current healthcare expenses, preserve your funds for tax-free growth, or invest your funds for long-term savings.
y HSA-eligible health plans typically have lower monthly premiums, giving you an opportunity to contribute those savings into an HSA.
y Your HSA stays with you, even if you leave your employer.
y Unlike an FSA, unused funds stay in your account from year to year and earn interest tax-free.
y Money goes in tax-free, grows tax-free and withdrawals are taxfree if used on eligible items.
y Once your account balance reaches $1,000, savings can be invested for growth, just like a 401k.
A powerful tool for retirement savings
y Maintain a $1,000 balance in your cash account to start investing.
y Withdrawals for qualified medical expenses are tax-free.
y Move your investment funds to your cash account at any time.
y You must have funds in your HSA before you can spend them.
y You can change your contribution amount at any time.
y Save your receipts because the IRS may audit your HSA transactions.
Swipe your Flex Facts debit card to pay for eligible expenses or pay with your personal funds and reimburse yourself.
y C Copays, deductibles, coinsurance
y P Prescriptions
y D Dental exams, x-rays, orthodontia
y V Vision exams, frames, contact lenses
y Physical therapy and chiropractic care
y F First aid kits
y O Over-the-counter medications
y A And much more
y You can claim a tax deduction for any direct contributions you make to your account with post-tax dollars.
• The largest selection of guaranteed HSAeligible products
• Phone and live chat support available 24 hours a day / 7 days a week
• Fast and free shipping on orders over $50
• Use your HSA card or any other major credit card for purchases

Eligibility List
Search comprehensive list of eligible products and services.

FSA Calculator
Estimate how much you can save with an HSA.

Learning Center
Easy tips and resources for living with an HSA.

Savings Center
Your funds go further with the HSA Store rewards program.
Take control of your health and wellness with guaranteed HSA-eligible essentials. Pierce Group Benefits partners with the HSA store to provide one convenient location for Heath Savings Account holders.
Click or Scan to Shop Now


Click on the video below to learn more about Flexible Spending Accounts!




Participating in an FSA is like receiving a 30% discount from your medical providers.
A medical FSA is a flexible spending account that allows you to set aside pre-tax dollars for eligible medical, dental, and vision expenses for you and your dependents.
Choose an annual election amount, up to $3,400*. This amount will be deducted from your paychecks in equal installments throughout the year. Your full election will be available for spending on the first day of the plan year!
Almost everyone has some level of out of pocket medical costs. If you expect to incur medical expenses, you’ll want to take advantage of the savings this plan offers.
Money contributed to a healthcare FSA is free from federal and most state taxes. On average, participants enjoy a 30% tax savings on their annual contribution, saving up to $1,020 per year!
Your election can only be changed during the plan year if you experience a qualifying event. Save your receipts. You may need itemized invoices to verify card swipes or for claim reimbursements. If your employment terminates, your account will be terminated.
Up to $680 of unused funds will rollover into the next plan year. Unused funds over this amount will be forfeited at the end of the plan year.
Reminder: You can't contribute to an FSA and HSA within the same plan year.
Swipe your Flex Facts debit card to pay for eligible expenses or pay with your personal funds and submit a claim for reimbursement.
• Copays, deductible, coinsurance
• Doctor office visits, lab work, x-rays
• Hospital charges
• Dental and orthodontia
• Vision exams, glasses, contact lenses, laser vision correction
• Physical therapy
• Chiropractic care
• Medical supplies and first aid kits
• Rx and over-the-counter meds
• And much more...
Visit http://fsastore.com/ FlexfactsEL for full list.
• The largest selection of guaranteed FSAeligible products
• Phone and live chat support available 24 hours a day / 7 days a week

Eligibility List
Search comprehensive list of eligible products and services.

FSA Calculator
Estimate how much you can save with an FSA.
• Fast and free shipping on orders over $50
• Use your FSA card or any other major credit card for purchases

Learning Center
Easy tips and resources for living with an FSA.

Savings Center
Your funds go further with the FSA Store rewards program.
Take control of your health and wellness with guaranteed FSA-eligible essentials. Pierce Group Benefits partners with the FSA store to provide one convenient location for Flexible Spending Account holders.
Click or Scan to Shop Now


Click on the video below to learn more about Dependent Care Accounts!




Participating in a dependent care FSA is like receiving a 30% discount from your care providers.
A dependent care FSA (DCA) is a flexible spending account that allows you to set aside pre-tax dollars for dependent care expenses that allow you to work or look for work This includes daycares, babysitters and before/after school care.
Choose an annual election amount, up to $7,500/ family. This amount will be deducted from your paychecks in equal installments throughout the year.
Child and dependent care is a large expense for many families. If you pay for care of dependents in order to work, you’ll want to take advantage of the savings this plan offers.
Money contributed to a dependent care FSA (DCA) is free from federal and most state taxes. On average, participants enjoy a 30% tax savings on their annual contribution, saving up to $2,250 per year!
Funds will be made available in your DCA account, as deductions are taken each payroll.
Your election can only be changed during the plan year if you experience a qualifying event.
Save your receipts. You may need itemized invoices to verify card swipes or for claim reimbursements. If your employment terminates, your account will be terminated. You will have an additional 2.5 month grace period to spend your DCA funds after the plan ends. Be sure to spend your funds by then, as unspent funds will be forfeited
Swipe your Flex Facts debit card to pay for eligible expenses or pay with your personal funds and submit a claim for reimbursement.
• Your qualifying child under age 13
• Your spouse or qualifying adult child or relative who is physically or mentally incapable of self-care
• Before school or after school care for children 12 and younger
• Custodial care for adult dependents
• Licensed day care centers
• Nanny / Au Pair
• Nursery Schools or preschools
• Late Pick-up fees
• Summer or Holiday day camps
A full list of eligible expenses can be found at www.flexfacts.com.
our app


Click on the video below to learn more about Long Term Care Benefits!




Learn more about our 7702(b) Qualified Long Term Care offering, with favorable interest rates and benefits to ensure your clients are better protected.
LBT provides a tax-qualified LTC Benefit that complies with this provision of the tax code and may satisfy future state mandates as Qualified Long Term Care.
After 10 years, paid-up benefits begin to accrue. At any point thereafter, if you stop paying the premium, a reduced paid-up benefit is issued and can never lapse.
Based on a 3% interest rate and mortality assumptions, the full death benefit is designed to last through age 99 for non-tobacco users and age 95 for tobacco users.

Our Life Insurance premiums never change and are only due until age 100. And as long as premiums are paid, coverage won’t lapse, lasting until employees reach their 121st birthday.
Pays benefits for Long Term Care services
and
Employees can take these benefits with them, even if they change jobs.

Chubb’s Workplace Benefits product series is designed to empower you with innovative and flexible benefits solutions to better meet your customer’s needs.
For about the same premium, LifeTime Benefit Term (LBT) provides higher death benefits than permanent life insurance and lasts to age 121. Plus offers additional benefits.
LBT’s innovative design provides life time guarantees at a fraction of the cost of permanent life insurance. And flexibility allows you to customize benefits for Long Term Care (LTC) and double or triple the policy value.
Death Benefit is guaranteed 100% when it is needed most—during the working years when a family is relying on income. While the policy is in force, the death benefit is 100% guaranteed
The full death benefit is designed to last through age 99 for nontobacco users and age 95 for tobacco users based on the current interest rate and mortality assumptions.
Chubb is the marketing name used to refer to subsidiaries of Chubb Limited providing insurance and related services. This insurance product is underwritten by Combined Insurance Company of America, Chicago, IL, a Chubb company. www.chubbworkplacebenefits.com

When employees need LTC, death benefits can be paid early for home health care, assisted living, adult day care and nursing home care. Early payments equal 4% of the death benefit per month for up to 25 months. Premiums are waived while this benefit is being paid.
Once the full death benefit has been paid in advance for LTC, payments can be extended. Choose between 25 and 50 months of LTC Benefit Extension to double or triple the value.
Accelerating the life coverage for LTC benefits can reduce the death benefit to $0. This rider restores the life coverage to either 25% or 50% of the death benefit on which the LTC benefits were based, therefore assuring a death benefit available up to the insured’s age 121.
Lifelong protection with premiums beginning as low as $3 per week.
Dependable
Guaranteed life insurance premium and death benefits last a lifetime.
Fully Portable and Guaranteed Renewable for Life
Employee coverage cannot be cancelled as long as premiums are paid as due.
LifeTime Benefit Term protects families with money that can be used any way they need. Often it is used to pay for mortgage or rent, education for children and grandchildren, family debt and final expenses.
Long Term Care is expensive, and LifeTime Benefit Term can help. It pays death benefits in advance for home health care, assisted living, adult day care and nursing home and waives life insurance premiums. And with Extension of Long Term Care, benefits can last for more than 6 years, in essence, tripling the policy value
Life insurance premiums will never increase and are guaranteed through age 100.
After 10 years, paid-up benefits begin to accrue. At any point thereafter, if premiums stop, a reduced paid up benefit is guaranteed. Flexibility is perfect for retirement.
After coverage has been in force for two years, employees can receive 50% of their death benefit immediately, up to $100,000, if they are diagnosed as terminally ill.
Waiver of Premium Benefit
Waives premium if employee becomes totally disabled.
For the same premium, LifeTime Benefit Term provides higher benefits than permanent life Insurance and lasts to age 121.
* LTC and Extension of Benefits premiums may be adjusted based upon the experience of the group or other group characteristics that may affect results. Premiums will not be increased solely because of an independent claim.
This document is only a brief description of Group Policy Form No. P34544. See the policy for complete details about features, benefits, exclusions and limitations that may vary by state. The availability of this product, riders or optional benefits are subject to underwriting approval.


Click on the video below to learn more about Cancer Benefits!






Hopefully, you and your family will never face cancer. If you do, a financial safety net can help you and your loved ones focus on what matters most — recovery.
If you were diagnosed with cancer, you could have expenses that medical insurance doesn’t cover. In addition to your regular, ongoing bills, you could have indirect treatment and recovery costs, such as child care and home health care services.
Cancer coverage from Colonial Life & Accident Insurance Company can help protect the lifestyle you’ve worked so hard to build. It provides benefits you can use to help cover:
■ Loss of income
■ Out-of-network treatment
■ Lodging and meals
■ Deductibles and co-pays
Travel expenses
When the couple traveled several hundred miles from their home to a top cancer hospital, they used the policy’s lodging and transportation benefits to help with expenses.
Paul and Kim were preparing for their second child when they learned Paul had cancer. They quickly realized their medical insurance wouldn’t cover everything. Thankfully, Kim’s job enabled her to have a cancer insurance policy on Paul to help them with expenses.
Out-of-pocket costs
The policy’s benefits helped with deductibles and co-pays related to Paul’s surgery and hospital stay.

■ Coverage options are available for you and your eligible dependents.
■ Benefits are paid directly to you, unless you specify otherwise.
■ You’re paid regardless of any insurance you may have with other companies.
■ You can take coverage with you, even if you change jobs or retire.
Experimental care Follow-up evaluations
Paul used his plan’s benefits to help pay for experimental treatments not covered by his medical insurance.
Paul has been cancer-free for more than four years. His cancer policy provides a benefit for periodic scans to help ensure the cancer stays in check.
Our cancer insurance offers more than 30 benefits that can help you with costs that may not be covered by your medical insurance.
Treatment benefits (inpatient or outpatient)
■ Radiation/chemotherapy
■ Anti-nausea medication
■ Medical imaging studies
■ Supportive or protective care drugs and colony stimulating factors
■ Second medical opinion
■ Blood/plasma/platelets/ immunoglobulins
■ Bone marrow or peripheral stem cell donation
■ Bone marrow or peripheral stem cell transplant
■ Egg(s) extraction or harvesting/ sperm collection and storage
■ Experimental treatment
■ Hair/external breast/voice box prosthesis
■ Home health care services
■ Hospice (initial or daily care)
■ Surgical procedures
■ Anesthesia
■ Reconstructive surgery
■ Outpatient surgical center
■ Prosthetic device/artificial limb
■ Transportation
■ Companion transportation
■ Lodging
■ Hospital confinement
■ Private full-time nursing services
■ Skilled nursing care facility
■ Ambulance
■ Air ambulance
Additional benefits
■ Family care
■ Cancer vaccine
■ Bone marrow donor screening
■ Skin cancer initial diagnosis
■ Waiver of premium

For an additional cost, you may have the option of purchasing additional riders for even more financial protection against cancer. Talk with your benefits counselor to find out which of these riders are available for you to purchase.
■ Diagnosis of cancer rider — Pays a one-time, lump-sum benefit for the initial diagnosis of cancer. You may choose a benefit amount in $1,000 increments between $1,000 and $10,000. If your dependent child is diagnosed with cancer, we will pay two and a half times ($2,500 - $25,000) the chosen benefit amount.
■ Diagnosis of cancer progressive payment rider — Provides a lump-sum payment of $50 for each month the rider has been in force and before cancer is first diagnosed.
■ Specified disease hospital confinement rider — Pays $300 per day if you or a covered family member is confined to a hospital for treatment for one of the 34 specified diseases covered under the rider.
If cancer impacts your life, you should be able to focus on getting better — not on how you’ll pay your bills. Talk with your Colonial Life benefits counselor about how cancer insurance can help provide financial security for you and your family.
We will not pay benefits for the diagnosis of internal cancer or skin cancer that is a pre-existing condition, nor will we pay benefits for the treatment of internal cancer or skin cancer that is a pre-existing condition unless the covered person has satisfied the six-month pre-existing condition limitation period shown on the Policy Schedule. Pre-existing condition means a condition for which a covered person was diagnosed prior to the effective date of this policy, and for which medical advice or treatment was recommended by or received from a doctor within six months immediately preceding the effective date of this policy.
We will not pay benefits for cancer or skin cancer:
■ If the diagnosis or treatment of cancer is received outside of the territorial limits of the United States and its possessions; or
■ For other conditions or diseases, except losses due directly from cancer.
The policy and its riders may have additional exclusions and limitations. For cost and complete details of the coverage, see your Colonial Life benefits counselor. Coverage may vary by state and may not be available in all states. Applicable to policy form CanAssist-VA and rider forms R-CanAssistIndx-VA, R-CanAssistProg-VA and R-CanAssistSpDis-VA.
Cancer insurance helps provide financial protection through a variety of benefits. These benefits are not only for you but also for your covered family members.

For more information, talk with your benefits counselor.
Air ambulance
Transportation to or from a hospital or medical facility [max. of two trips per confinement]
Ambulance
Transportation to or from a hospital or medical facility [max. of two trips per confinement]
Anesthesia
Administered during a surgical procedure for cancer treatment
■ General anesthesia
■ Local anesthesia
Anti-nausea medication
$2,000 per trip
$250 per trip
25% of surgical procedures benefit
$50 per procedure
$60 per day administered or Doctor-prescribed medication for radiation or chemotherapy [$240 monthly max.] per prescription filled
Blood/plasma/platelets/immunoglobulins
A transfusion required during cancer treatment [$10,000 calendar year max.]
Bone marrow donor screening
Testing in connection with being a potential donor [once per lifetime]
Bone marrow or peripheral stem cell donation
Receiving another person’s bone marrow or stem cells for a transplant [once per lifetime]
Bone marrow or peripheral stem cell transplant
Transplant you receive in connection with cancer treatment [max. of two bone marrow transplant benefits per lifetime]
Cancer vaccine
An FDA-approved vaccine for the prevention of cancer [once per lifetime]
Companion transportation
Companion travels by plane, train or bus to accompany a covered cancer patient more than 50 miles one way for treatment [up to $1,500 per round trip]
Egg(s) extraction or harvesting/sperm collection and storage
Extracted/harvested or collected before chemotherapy or radiation [once per lifetime]
■ Egg(s) extraction or harvesting/sperm collection
■ Egg(s) or sperm storage (cryopreservation)
Experimental treatment
Hospital, medical or surgical care for cancer [$15,000 lifetime max.]
Family care
Inpatient or outpatient treatment for a covered dependent child [$3,000 calendar year max.]
Hair/external breast/voice box prosthesis
Prosthesis needed as a direct result of cancer
Home health care services
Examples include physical therapy, occupational therapy, speech therapy and audiology; prosthesis and orthopedic appliances; rental or purchase of durable medical equipment [up to 100 days per covered person per lifetime]
Hospice (initial or daily care)
An initial, one-time benefit and a daily benefit for treatment [$15,000 lifetime max. for both]
■ Initial hospice care [once per lifetime]
■ Daily hospice care
$250 per day
$50
$1,000
$10,000 per transplant
$50
$0.50 per mile
$1,500
$500
$300 per day
$60 per day
$500 per calendar year
$175 per day
$1,000
$50 per day
Hospital confinement
Hospital stay (including intensive care) required for cancer treatment
■ 30 days or less
■ 31 days or more
$350 per day
$700 per day
Lodging $80 per day
Hotel/motel expenses when being treated for cancer more than 50 miles from home [70-day calendar year max.]
Medical imaging studies
Specific studies for cancer treatment [$450 calendar year max.]
Outpatient surgical center
Surgery at an outpatient center for cancer treatment [$1,200 calendar year max.]
Private full-time nursing services
Services while hospital confined other than those regularly furnished by the hospital
Prosthetic device/artificial limb
A surgical implant needed because of cancer surgery [payable one per site, $6,000 lifetime max.]
Radiation/chemotherapy
[per day with a max. of one per calendar week]
■ Injected chemotherapy by medical personnel
■ Radiation delivered by medical personnel
[per day with a max. of one per calendar month]
■ Self-injected
■ Pump
■ Topical
■ Oral hormonal [1-24 months]
■ Oral hormonal [25+ months]
■ Oral non-hormonal
Reconstructive surgery
A surgery to reconstruct anatomic defects that result from cancer treatment [min. $350 per procedure, up to $3,000, including 25% for general anesthesia]
$225 per study
$400 per day
$150 per day
$3,000 per device or limb
$60 per surgical unit
Second medical opinion $300
A second physician’s opinion on cancer surgery or treatment [once per lifetime]
Skilled nursing care facility
Confinement to a covered facility after hospital release [up to 100 days per covered person per lifetime]
Skin cancer diagnosis
A skin cancer diagnosis while the policy is in force [once per lifetime]
Supportive or protective care drugs and colony stimulating factors
Doctor-prescribed drugs to enhance or modify radiation/chemotherapy treatments [$1,600 calendar year max.]
Surgical procedures
Inpatient or outpatient surgery for cancer treatment [min. $350 per procedure, up to $6,000]
$175 per day
per day
$70 per surgical unit
Transportation $0.50 per mile
Travel expenses when being treated for cancer more than 50 miles from home [up to $1,500 per round trip]
Waiver of premium Is available
No premiums due if the named insured is disabled longer than 90 consecutive days
The policy has limitations and exclusions that may affect benefits payable. Most benefits require that a charge be incurred. Coverage may vary by state and may not be available in all states. For cost and complete details, see your benefits counselor.
This chart highlights the benefits of policy forms CanAssist-NJ and CanAssist-VA. This chart is not complete without form 101505-NJ or 101481-VA.
THE POLICY PROVIDES LIMITED BENEFITS. For cost and complete details of the coverage, see your Colonial Life benefits counselor. Coverage may vary by state and may not be available in all states. Coverage is dependent on answers to health questions. Applicable to policy forms CanAssist-VA and rider forms R-CanAssistIndx-VA, R-CanAssistProg-VA and R-CanAssistSpDis-VA.
Cancer Insurance Benefits
Level 1Level 2Level 3Level 4
$2,000$2,000$2,000$2,000
Maximum trips per confinement 2222
Ambulance, per trip
Anesthesia, General Air Ambulance, per trip
$250$250$250$250
Maximum trips per confinement 2222
Anesthesia, Local, per procedure Anti-Nausea Medication, per day
Maximum per month
Blood/Plasma/Platelets/Immunoglobulins, per day
Maximum per year
Bone Marrow or Peripheral Stem Cell Donation, per lifetime
Bone Marrow or Peripheral Stem Cell Transplant, per transplant
25% of Surgical Procedures Benefit
$25$30$40$50
$25$40$50$60
$100$160$200$240
$150$150$175$250
$10,000$10,000$10,000$10,000
$500$500$750$1,000
$3,500$4,000$7,000$10,000
Maximum transplants per lifetime 2222
Companion Transportation, per mile
Maximum per round trip
Egg(s) Extraction or Harvesting or Sperm Collection, per lifetime
Egg(s) or Sperm Storage, per lifetime
Experimental Treatment, per day
Maximum per lifetime
Family Care, per day
Maximum per year
Hair/External Breast/Voice Box Prosthesis, per year
Home Health Care Services, per day
$0.50$0.50$0.50$0.50
$1,000$1,000$1,200$1,500
$500$700$1,000$1,500
$175$200$350$500
$200$250$300$300
$10,000$12,500$15,000$15,000
$30$40$50$60
$1,500$2,000$2,500$3,000
$200$200$350$500
$50$75$125$175
Benefit payable for at least and not more than 100 days per covered person per lifetime
Hospice, Initial, per lifetime
Hospice, Daily
Maximum combined Initial and Daily per lifetime
Hospital Confinement, 30 days or less, per day
Hospital Confinement, 31 days or more, per day
$1,000$1,000$1,000$1,000
$50$50$50$50
$15,000$15,000$15,000$15,000
$100$150$250$350
$200$300$500$700
Benefit payable for up to 365 days per covered person per calendar year.
Lodging, per day
$50$50$75$80
Maximum days per year 70707070
Medical Imaging Studies, per study
Maximum per year
Outpatient Surgical Center, per day
Maximum per year
Private Full-time Nursing Services, per day
Prosthetic Device/Artificial Limb, per device or limb
Maximum per lifetime
$75$125$175$225
$150$250$350$450
$100$200$300$400
$300$600$900$1,200
$50$75$125$150
$1,000$1,500$2,000$3,000
$2,000$3,000$4,000$6,000
Radiation/Chemotherapy
Benefit payable period can exceed but will not be less than 365 days per covered person per lifetime
Injected chemotherapy by medical personnel, per day with a maximum of one per calendar week
Radiation delivered by medical personnel, per day with a maximum of one per calendar week
Self-Injected Chemotherapy, per day with a maximum of one per calendar month
Pump Chemotherapy, per day with a maximum of one per calendar month
Topical Chemotherapy, per day with a maximum of one per calendar month
Oral Hormonal Chemotherapy (1-24 months), per day with a maximum of one per calendar month
Oral Hormonal Chemotherapy (25+ months), per day with a maximum of one per calendar month
Oral Non-Hormonal Chemotherapy, per day with a maximum of one per calendar month
Reconstructive Surgery, per surgical unit
Minimum per procedure
Maximum per procedure, including 25% for general anesthesia
Second Medical Opinion, per lifetime
Skilled Nursing Care Facility, per day, up to days confined
$250$500$750 $1,000
$250$500$750 $1,000
$150$200$300 $400
$150$200$300 $400
$150$200$300 $400
$150$200$300 $400
$100$150$250 $350
$150$200$300 $400
$40$40$60 $60
$100$150$250$350
$2,500$2,500$3,000$3,000 $150$200$300 $300
$50$75$125 $175
Benefit payable for at least and not more than 100 days per covered person per lifetime
Skin Cancer Initial Diagnosis
Supportive/Protective Care Drugs/Colony Stimulating Factors, per day
Surgical Procedures
Transportation
Waiver of Premium
Additional Riders may be available at an additional cost
What is not covered by the policy
Pre-Existing Condition Limitation
$300$300$400 $600
$50$100$150
We will not pay benefits for the diagnosis of internal cancer or skin cancer that is a pre-existing condition nor will we pay benefits for the treatment of internal cancer or skin cancer that is a preexisting condition, unless the covered person has satisfied the six-month pre-existing condition limitation period.
Pre-existing condition means a condition for which a covered person was diagnosed prior to the effective date of the policy and for which medical advice or treatment was recommended by or received from a doctor within six months immediately preceding the effective date of the policy.
We will not pay benefits for cancer or skin cancer:
■ If the diagnosis or treatment of cancer is received outside of the territorial limits of the United States and its possessions; or
■ For other conditions or diseases, except losses due directly from cancer.


Click on the video below to learn more about Critical Illness Benefits!





Chris was mowing the lawn when he suffered a stroke. His recovery will be challenging and he's worried, since his family relies on his income. HOW
The lump-sum payment from his critical illness insurance helped pay for:

When life takes an unexpected turn due to a critical illness diagnosis, your focus should be on recovery — not finances. Colonial Life’s group critical illness insurance helps provide financial support by providing a lump-sum benefit payable directly to you for your greatest needs. Coverage amount:
For illustrative purposes only.
Available coverage for spouse and eligible dependent children at 50% of your coverage amount
Cover your eligible dependent children at no additional cost
Receive coverage regardless of medical histor y, within specified limits
Works alongside your health savings account (HSA)
Benefits payable regardless of other insurance
Subsequent diagnosis of a different critical illness2
If you receive a benefit for a critical illness, and are later diagnosed with a different critical illness, 100% of the coverage amount may be payable for that particular critical illness.
Subsequent diagnosis of the same critical illness2
If you receive a benefit for a critical illness, and are later diagnosed with the same critical illness,3 25% of the coverage amount may be payable for that critical illness.
For more information, talk with your benefits counselor.
Preparing for the unexpected is simpler than you think. With Colonial Life, youʼll have the support you need to face lifeʼs toughest challenges.
1. Refer to the certificate for complete definitions of covered conditions.
2. Dates of diagnoses of a covered critical illness must be separated by more than 180 days.
3. Critical illnesses that do not qualify include: coronary artery disease, loss of hearing, loss of sight, loss of speech, and occupational infectious HIV or occupational infectious hepatitis B,C,or D.
THIS INSURANCE PROVIDES LIMITED BENEFITS
Insureds in MA must be covered by comprehensive health insurance before applying for this coverage.
EXCLUSIONS AND LIMITATIONS FOR CRITICAL ILLNESS
We will not pay the Critical Illness Benefit, Benefits Payable Upon Subsequent Diagnosis of a Critical Illness or Additional Critical Illness Benefit for Dependent Children that occurs as a result of a covered person’s: alcoholism or drug addiction; felonies or illegal occupations; intoxicants and narcotics; suicide or injuring oneself intentionally, whether sane or not; war or armed conflict; or pre-existing condition, unless the covered person has satisfied the pre-existing condition limitation period shown on the Certificate Schedule on the date the covered person is diagnosed with a critical illness.
PRE-EXISTING CONDITION LIMITATION
We will not pay a benefit for a pre-existing condition that occurs during the 12-month period after the coverage effective date. Pre-existing condition means a sickness or physical condition for which a covered person was treated, had medical testing, received medical advice or had taken medication within 12 months before the coverage effective date.
This information is not intended to be a complete description of the insurance coverage available. The insurance or its provisions may vary or be unavailable in some states. The insurance has exclusions and limitations which may affect any benefits payable. Applicable to policy form GCI6000-P and certificate form GCI6000-C (including state abbreviations where used, for example: GCI6000-C-TX). For cost and complete details of coverage, call or write your Colonial Life benefits counselor or the company.

Rebecca

When life takes an unexpected turn, your focus should be on recovery — not finances. Colonial Life’s group critical illness insurance helps relieve financial worries by providing a lump-sum benefit payable directly to you to use as needed. Coverage amount: ____________________________
Available coverage for spouse and eligible dependent children at 50% of your coverage amount
Cover your eligible dependent children at no additional cost
Receive coverage regardless of medical histor y, within specified limits
Works alongside your health savings account (HSA)
Benefits payable regardless of other insurance
For more information, talk with your benefits counselor.
Subsequent diagnosis of a different critical illness2
If you receive a benefit for a critical illness, and are later diagnosed with a different critical illness, 100% of the coverage amount may be payable for that particular critical illness.
Subsequent diagnosis of the same critical illness2
If you receive a benefit for a critical illness, and are later diagnosed with the same critical illness,3 25% of the coverage amount is payable for that critical illness.
Reoccurrence of invasive cancer (including all breast cancer)
If you receive a benefit for invasive cancer and are later diagnosed with a reoccurrence of invasive cancer, 25% of the coverage amount is payable if treatment-free for at least 12 months and in complete remission prior to the date of reoccurrence; excludes non-invasive or skin cancer.
Preparing for the unexpected is simpler than you think. With Colonial Life, youʼll have the support you need to face lifeʼs toughest challenges.
1. Refer to the certificate for complete definitions of covered conditions.
2. Dates of diagnoses of a covered critical illness must be separated by more than 180 days.
3. Critical illnesses that do not qualify include: coronary artery disease, loss of hearing, loss of sight, loss of speech, and occupational infectious HIV or occupational infectious hepatitis B,C,or D.
THIS INSURANCE PROVIDES LIMITED BENEFITS
Insureds in MA must be covered by comprehensive health insurance before applying for this coverage.
EXCLUSIONS AND LIMITATIONS FOR CRITICAL ILLNESS
We will not pay the Critical Illness Benefit, Benefits Payable Upon Subsequent Diagnosis of a Critical Illness or Additional Critical Illness Benefit for Dependent Children that occurs as a result of a covered person’s: alcoholism or drug addiction; felonies or illegal occupations; intoxicants and narcotics; suicide or injuring oneself intentionally, whether sane or not; war or armed conflict; or pre-existing condition, unless the covered person has satisfied the pre-existing condition limitation period shown on the Certificate Schedule on the date the covered person is diagnosed with a critical illness.
EXCLUSIONS AND LIMITATIONS FOR CANCER
We will not pay the Invasive Cancer (including all Breast Cancer) Benefit, Non-Invasive Cancer Benefit, Benefit Payable Upon Reoccurrence of Invasive Cancer (including all Breast Cancer) or Skin Cancer Initial Diagnosis Benefit for a covered person’s invasive cancer or non-invasive cancer that: is diagnosed or treated outside the territorial limits of the United States, its possessions, or the countries of Canada and Mexico; is a pre-existing condition, unless the covered person has satisfied the pre-existing condition limitation period shown on the Certificate Schedule on the date the covered person is initially diagnosed as having invasive or non-invasive cancer. No pre-existing condition limitation will be applied for dependent children who are born or adopted while the named insured is covered under the certificate, and who are continuously covered from the date of birth or adoption.
PRE-EXISTING CONDITION LIMITATION
We will not pay a benefit for a pre-existing condition that occurs during the 12-month period after the coverage effective date. Pre-existing condition means a sickness or physical condition for which a covered person was treated, had medical testing, received medical advice or had taken medication within 12 months before the coverage effective date. This information is not intended to be a complete description of the insurance coverage available. The insurance or its provisions may vary or be unavailable in some states. The insurance has exclusions and limitations which may affect any benefits payable. Applicable to policy form GCI6000-P and certificate form GCI6000-C (including state abbreviations where used, for example: GCI6000-C-TX). For cost and complete details of coverage, call or write your Colonial Life benefits counselor or the company.
SC

For more information, talk with your benefits counselor.
The first diagnosis building benefit rider provides a lump-sum payment in addition to the coverage amount when you are diagnosed with a covered critical illness or invasive cancer (including all breast cancer). This benefit is for you and all your covered family members.
First diagnosis building benefit
Payable once per covered person per lifetime
¾ Named insured
¾ Covered spouse/dependent children
Accumulates $1,000 each year
Accumulates $500 each year
The benefit amount accumulates each rider year the rider is in force before a diagnosis is made, up to a maximum of 10 years.
If diagnosed with a covered critical illness or invasive cancer (including all breast cancer) before the end of the first rider year, the rider will provide one-half of the annual building benefit amount. Coronary artery disease is not a covered critical illness. Non-invasive and skin cancer are not covered cancer conditions.
This information is not intended to be a complete description of the insurance coverage available. The insurance or its provisions may vary or be unavailable in some states. The insurance has exclusions and limitations which may affect any benefits payable. Applicable to policy form GCI6000-P and certificate form GCI6000-C (including state abbreviations where used, for example: GCI6000-C-TX) and rider form R-GCI6000-BB. For cost and complete details of coverage, call or write your Colonial Life benefits counselor or the company.

The sudden onset of an infectious or contagious disease can create unexpected circumstances for you or your family. The infectious diseases rider provides a lump sum which can be used toward health care expenses or meeting day-today needs. These benefits are for you as well as your covered family members.
1. Refer to the certificate for complete definitions of covered diseases.
THIS INSURANCE PROVIDES LIMITED BENEFITS.
EXCLUSIONS AND LIMITATIONS FOR INFECTIOUS DISEASES RIDER
We will not pay benefits for a covered infectious disease that occurs as a result of a covered person’s: alcoholism or drug addiction; felonies or illegal occupations; intoxicants and narcotics; suicide or injuring oneself intentionally, whether sane or not; war or armed conflict; or pre-existing condition, unless the covered person has satisfied the pre-existing condition limitation period shown on the Certificate Schedule on the date the covered person is diagnosed with a covered infectious disease.
PRE-EXISTING CONDITION LIMITATION
We will not pay a benefit for a pre-existing condition that occurs during the 12-month period after the coverage effective date. Pre-existing condition means a sickness or physical condition for which a covered person was treated, had medical testing, received medical advice or had taken medication within 12 months before the coverage effective date. This information is not intended to be a complete description of the insurance coverage available. The insurance or its provisions may vary or be unavailable in some states. The insurance has exclusions and limitations which may affect any benefits payable. Applicable to policy form GCI6000-P and certificate form GCI6000-C (including state abbreviations where used, for example: GCI6000-C-TX) and rider form R-GCI6000-INF. For cost and complete details of coverage, call or write your Colonial Life benefits counselor or the company.

For more information, talk with your benefits counselor.
The debilitating effects of a progressive disease not only impact you physically, but financially as well. Changes in lifestyle may require home modification, additional medical treatment and other expenses. These benefits are for you as well as your covered family members.
Payable for each covered progressive disease once per covered person per lifetime
This benefit is payable if the covered person is unable to perform two or more activities of daily living2 and the 90-day elimination period has been met.
1. Refer to the certificate for complete definitions of covered diseases.
2. Activities of daily living include bathing, continence, dressing, eating, toileting and transferring.
THIS INSURANCE PROVIDES LIMITED BENEFITS.
EXCLUSIONS AND LIMITATIONS FOR PROGRESSIVE DISEASES RIDER
We will not pay benefits for a covered progressive disease that occurs as a result of a covered person’s: alcoholism or drug addiction; felonies or illegal occupations; intoxicants and narcotics; suicide or injuring oneself intentionally, whether sane or not; war or armed conflict; or pre-existing condition, unless the covered person has satisfied the preexisting condition limitation period shown on the Certificate Schedule on the date the covered person is diagnosed with a covered progressive disease.
PRE-EXISTING CONDITION LIMITATION
We will not pay a benefit for a pre-existing condition that occurs during the 12-month period after the coverage effective date. Pre-existing condition means a sickness or physical condition for which a covered person was treated, had medical testing, received medical advice or had taken medication within 12 months before the coverage effective date. This information is not intended to be a complete description of the insurance coverage available. The insurance or its provisions may vary or be unavailable in some states. The insurance has exclusions and limitations which may affect any benefits payable. Applicable to policy form GCI6000-P and certificate form GCI6000-C (including state abbreviations where used, for example: GCI6000-C-TX) and rider form R-GCI6000-PD. For cost and complete details of coverage, call or write your Colonial Life benefits counselor or the company.







You never know when a disability could impact your way of life. Fortunately, there’s a way to help protect your income. If an accident or sickness prevents you from earning a paycheck, disability insurance can provide a monthly benefit to help you cover your ongoing expenses.
Can you afford to not protect your paycheck?
You don’t have the same lifestyle expenses as the next person. That’s why you need disability coverage that can be customized to fit your specific needs.
After calculating your monthly expenses, your benefits counselor can help you complete the benefits worksheet.
How much coverage do I need?
Monthly benefit amount for off-job accident and off-job sickness: ______________
Choose a monthly benefit amount between $400 and $6,500.*
If your plan includes on-job accident/sickness benefits, the benefit is 50% of the off-job amount.
How long will I receive benefits?
Benefit period: _______ months
The partial disability benefit period is three months.
When will my total disability benefits start?
After an accident: _______ days After a sickness: _______ days
Total disability definition
Totally disabled or total disability means you are: unable to perform the material and substantial duties of your job, not working at any job, and under the regular and appropriate care of a physician.
If you are able to return to work part-time after at least 14 days of being paid for a total disability, you may be able to still receive 50% of your total disability benefit.
We will waive your premium payments after 90 consecutive days of a covered disability.
Geographical limitations
If you are disabled while outside of the United States, Canada or Mexico, you may receive benefits for up to 60 days before you have to return to the U.S. in order to continue receiving benefits.
Issue age
Coverage is available from ages 17 to 74.
Keep your coverage
You can keep your coverage to age 75 at no additional cost, even if you change jobs, as long as you pay your premiums when they are due.
Your premium is based on your age when you purchase coverage and the amount of coverage you are eligible to buy. Your premium will not change as you age.*
For more information, talk with your benefits counselor.
We will not pay benefits for losses that are caused by, contributed to by or occur as the result of: alcoholism or drug addiction, aviation, cosmetic surgery, felonies or illegal occupations, intoxicants and narcotics, psychiatric or psychological conditions, suicide or injuries which you intentionally do to yourself, war or armed conflict. We will not pay for losses due to you giving birth within the first nine months after the coverage effective date of the policy. We will not pay for loss when the disability is a pre-existing condition as described in the policy.
For cost and complete details, see your Colonial Life benefits counselor. Applicable to policy form ISTD3000-VA and rider form ISTD3000-ADIB-VA. This is not an insurance contract and only the actual policy and rider provisions will control.

For more information, talk with your benefits counselor.
Although illnesses and accidents are often associated with disabilities, mental disorders can also leave you unable to earn an income.
If you’re disabled with a covered psychiatric or covered psychological condition, disability insurance from Colonial Life & Accident Insurance Company pays a monthly benefit that can help provide financial support while you focus on recovery.
There is a maximum six-month benefit period limitation for any one occurrence of a psychiatric or psychological condition. There is a three-month benefit period limitation if you have a three-month benefit period.
There is a 24-month cumulative lifetime maximum benefit period for all psychiatric or psychological conditions. This maximum includes a combination of total disability and partial disability occurrences.

Ages: 17-49
Ages: 50-64
Ages: 65-74
Ages: 17-49
Ages: 50-64
Ages: 65-74







If you are in an accident, your focus should be on recovery, not how you’re going to pay your bills. Colonial Life Accident Insurance can pay benefits directly to you to use however you like — from medical costs to everyday expenses — offering financial support when you need it.
coverage includes:
• Benefits payable directly to you
• No medical questions to qualify for coverage
• Coverage for simple and complex injuries
• Benefits payable regardless of other insurance
• Worldwide coverage
• Works alongside your Health Savings Account (HSA)
Olivia was driving to the store when she got into a car accident. Olivia’s accident benefits helped cover her annual deductible and co-payments.
Olivia arrived by ambulance at the nearest emergency room and received immediate care.
The doctor ordered an X-ray and discovered Olivia had fractured her thigh (femur). He also ordered a CT scan of her head to check for a brain injury.
Olivia was admitted to the hospital for surgery on her leg. She was confined for three days.
Olivia had eight sessions of physical therapy to help regain the strength in her leg.
Over the next several weeks, she had six follow-up appointments with her doctor.
For illustrative purposes only for covered accidents. Benefit amounts may vary and may not cover all expenses.
• Ambulance
•
• X-ray
• Medical imaging (CT) • Thigh fracture — femur (surgical)
• Hospital admission
• Surgery (exploratory/arthroscopic)
• Hospital confinement (3 days)
• Physical therapy (8 days)
• Medical equipment (crutches)
follow-up treatment (6 visits)
Benefits are per covered person per covered accident unless stated otherwise.
Accident emergency treatment......................... $125
Hospital emergency room, urgent care facility or physician’s office
Accidental injury due to an automobile accident1 ........ $250
Air ambulance ..................................... $2,400
Ambulance — ground or water ......................... $250
Observation room .............................. $175 per day
(up to two days per calendar year)
X-ray................................................. $40
Burn ....................................... $1,000–$15,000 (based on size and degree)
Burn — skin graft .............. 50% of applicable burn benefit
Coma ............................................. $15,000
(lasting for seven or more consecutive days)
Concussion $200
Dislocation — separated joint
• Non-surgical — repair .......................
$125–$2,750
Examples: elbow: $600 | ankle: $1,250 | hip: $2,750
• Incomplete dislocation — or dislocation without anesthesia 25% (payable as a % of the applicable dislocation benefit)
• Surgical — repair ............................ $250–$5,500 Examples: elbow: $1,200 | ankle: $2,500 | hip: $5,500
Emergency dental work .......................... $125–$350
Dental extraction or dental crown, denture or implant
Eye injury — with surgical repair or removal of a foreign object ............................ $350
Fracture — complete
• Non-surgical — repair $300–$3,750 Examples: hand/foot: $475 | collarbone: $775 | leg: $1,250
• Chip fracture ....................................... 25% (payable as a

Hearing-loss injuries2 .................................. $140
Knee cartilage — torn — with surgical repair ............. $800
Laceration ...................................... $30–$750 (based on repair and length)
Ruptured disc — with surgical repair $950
Tendon/ligament/rotator cuff — with surgical repair
• One ............................................... $800
• Two or more ...................................... $1,600
Hospital admission
$1,250
Hospital confinement $300 per day (up to 365 days)
Hospital sub-acute intensive care unit confinement ............................. $400 per day (up to 30 days)
Intensive care unit admission
$2,500
Intensive care unit confinement $550 per day (up to 15 days)
Blood/plasma/platelets — transfusion
$400 Surgery $250–$1,900 (based on type of repair and surgery)
Transportation for hospital confinement .. $700 per round trip (up to three round trips, 50+ miles from home)
Lodging–companion .......................... $150 per day (up to 30 days)
Accident follow-up treatment, including transportation/telemedicine
$55 (up to six benefits per covered person per covered accident and up to 12 benefits per covered person per calendar year)
Medical equipment
• Tier 1...............................................
$40
Arm sling, cane, medical ring cushion, neck brace or wrist/ankle splint
• Tier 2 $125
Bedside commode, cold therapy system (cryotherapy), crutches, leg brace, shower chair, walker or walking boot
• Tier 3 ............................................. $250
Back brace, body jacket, continuous passive movement (CPM), halo, electric scooter, hospital bed (including rental), knee scooter, stair lift chair or wheelchair
Medical imaging study — CT, CAT scan, EEG, EMG, MR or MRI. .
(one per calendar year)
$250
Pain management for epidural anesthesia — non-surgical $125
Post-traumatic stress disorder (PTSD) ................. $250
Prosthetic device/artificial limb
• One ............................................... $950
• More than one .................................... $1,900
• Repair/replacement3 .......................... $475/$950
Rehabilitation unit confinement $175 per day (up to 15 days, not to exceed 30 days per calendar year)
Therapy — occupational, physical or speech ...... $45 per day (up to 10 days)
Accidental dismemberment ................. $1,050–$40,000
• Loss, loss of use or paralysis – hand, arm, foot, leg, sight of eye
• Loss, loss of use – finger, toe, partial dismemberment of finger or toe
Accidental death
• Named insured, spouse .......................... $40,000
• Child $10,000
Accidental death common carrier
Examples of common carriers are mass transit trains, buses and planes
• Named insured, spouse .......................... $160,000
• Child ........................................... $30,000
For more information, contact your Colonial Life benefits counselor.
1 Requires transportation by a licensed professional air ambulance or ambulance (ground or water).
2 One benefit for each injured ear per covered person per lifetime.
3 One repair or replacement per prosthetic device/artificial limb per covered person per lifetime.
HEALTH SAVINGS ACCOUNT (HSA) COMPATIBLE
This plan is compatible with HSA guidelines and any other HSA plan in which a covered family member may participate. It may also be offered to employees who do not have HSAs.
THIS POLICY PROVIDES LIMITED BENEFITS.
This coverage is a supplement to health insurance. It is not a substitute for essential health benefits or minimum essential coverage as defined in federal law. Insureds in some states must be covered by comprehensive health insurance before applying for this coverage.
EXCLUSIONS
We will not pay benefits for losses that are caused by, contributed to by or occur as the result of a covered personʼs felonies or illegal occupations, sickness, suicide or injuries which any covered person intentionally does to himself, war or armed conflict.
This information is not intended to be a complete description of the insurance coverage available. The policy or its provisions may vary or be unavailable in some states. The policy has exclusions and limitations which may affect any benefits payable. Applicable to policy form IAC4000-VA. For cost and complete details of the coverage, call or write your Colonial Life benefits counselor or the company.
Underwritten by Colonial Life & Accident Insurance Company, Columbia, SC. © 2024 Colonial Life & Accident Insurance Company. All rights reserved. Colonial Life is a registered trademark and marketing brand of Colonial Life & Accident Insurance Company.

This benefit increases the amount you receive by 20% for your covered eligible benefits, giving you more financial protection for the unexpected.
The active lifestyles benefit is available to you with accident coverage, as well as all your covered family members.
Eligible benefits1
• Concussion
• Dislocation
• Emergency dental work
• Eye injuries
• Fractures
• Knee cartilage (torn)
• Laceration
• Medical imaging study
• Ruptured disc with surgical repair
• Surgery
‐ cranial, open abdominal, thoracic/hernia
‐ exploratory and arthroscopic
• Tendon/ligament/rotator cuff with surgical repair
• X-ray
Example of a benefits calculation
$2,500 Eligible benefits
$2,500 x 20% $500 Eligible benefit amount Active lifestyles benefit Active lifestyles benefit calculation
$2,500 + $500
$3,000 Eligible benefit amount Active lifestyles benefit
Total
For illustrative purposes only
To learn more, talk with your Colonial Life benefits counselor.
1 Active lifestyles benefit applies to any combination of these injuries or services due to a covered accident.
HEALTH SAVINGS ACCOUNT (HSA) COMPATIBLE
This plan is compatible with HSA guidelines and any other HSA plan in which a covered family member may participate. It may also be offered to employees who do not have HSAs.
THIS POLICY PROVIDES LIMITED BENEFITS.
This coverage is a supplement to health insurance. It is not a substitute for essential health benefits or minimum essential coverage as defined in federal law. Insureds in some states must be covered by comprehensive health insurance before applying for this coverage.
ADDITIONAL DISCLOSURES FOR KENTUCKY
Eligibility for benefits: We will pay benefits for a covered accident if any covered person sustains an injury as a result of a covered accident if:
• the covered accident occurs while the policy is in force;
• the covered accident occurs on or after the policy coverage effective date;
• the covered accident is an accident type listed on the policy schedule; and
• the covered accident is not excluded by name or specific description in the policy.
Noncancellable: This policy is noncancellable. We have no right to change the premiums we charge on this policy. Any riders attached to this policy may be subject to a change in premium. The premium can be changed following the approval of the Commissioner of Insurance only if we change it on all riders of the same kind in force in the state where the policy was issued.
What is not covered by this policy: We will not pay benefits for losses that are caused by, contributed to by or occur as a result of the covered person’s felonies or illegal occupations, hazardous avocations, racing, semi-professional or professional sports, sickness or injuries which any covered person intentionally does to himself, war or armed conflict. In addition, we also will not pay the Accidental Dismemberment due to Catastrophic Accident benefit for injuries that are caused by or are the result of birth or intoxicants, narcotics and hallucinogencis.
This information is not intended to be a complete description of the insurance coverage available. The policy or its provisions may vary or be unavailable in some states. The policy has exclusions and limitations which may affect any benefits payable. Applicable to policy form IAC4000 (including state abbreviations where used, for example: IAC4000-TX). For cost and complete details of coverage, call or write your Colonial Life benefits counselor or the company. An insurance producer may contact you.
Underwritten by Colonial Life & Accident Insurance Company, Columbia, SC. © 2024 Colonial Life & Accident Insurance Company. All rights reserved. Colonial Life is a registered trademark and

These benefits can help with medical costs related to a hospital stay for a covered sickness, including costs that your health insurance may not cover, such as co-pays and deductibles.
The sickness hospital confinement rider is optional coverage available to you and all your covered family members.
Daily sickness hospital confinement
To learn more, talk with your Colonial Life benefits counselor.
$100 per day
Up to 30 days per covered person per confinement for a covered sickness
Re-confinement for the same or related condition within 90 days of discharge is considered a continuation of a previous confinement.
HEALTH SAVINGS ACCOUNT (HSA) COMPATIBLE
This plan is compatible with HSA guidelines and any other HSA plan in which a covered family member may participate. It may also be offered to employees who do not have HSAs.
THIS POLICY PROVIDES LIMITED BENEFITS.
This coverage is a supplement to health insurance. It is not a substitute for essential health benefits or minimum essential coverage as defined in federal law. Insureds in some states must be covered by comprehensive health insurance before applying for this coverage.
EXCLUSIONS AND LIMITATIONS
We will not pay benefits for losses that are caused by, contributed to by or occur as the result of accidental injuries, alcoholism or drug addiction, dental procedures, elective procedures and cosmetic surgery, felonies or illegal occupations, psychiatric or psychological conditions, intoxicants and narcotics, psychiatric or psychological conditions, suicide or injuries which you intentionally do to yourself, war or armed conflict and well baby care.
PRE-EXISTING CONDITION LIMITATION
Pre-existing condition means a sickness or physical condition, whether diagnosed or not, for which a covered person was treated, had medical testing, received medical advice, or had taken medication within 12 months before the rider coverage effective date shown on the rider schedule. After this rider has been in force for 12 months from the rider coverage effective date shown on the rider schedule, we will pay benefits as stated in the rider for any loss as the result of a pre-existing condition not excluded by name or specific description if the covered loss began at least 12 months after the rider coverage effective date.
STATE VARIATIONS FOR EXCLUSIONS AND LIMITATIONS
AK: Replace “alcoholism or drug addiction” with “intoxicants or narcotics.”
DE: Replace “alcoholism or drug addiction” with “substance abuse.”
FL: Replace “psychiatric or psychological conditions” with “mental or nervous disorders.”
IL: Pre-existing Condition Limitation definition also includes “produced symptoms.”
LA: Replace “alcoholism or drug addiction” with “intoxicants and narcotics.”
ME: Pre-existing Condition Limitation definition does not include “had taken medication.”
MO: Replace “alcoholism or drug addiction” with “substance abuse.”
MT: Pre-existing Condition Limitation definition does not include “whether diagnosed or not” or “had medical testing.”
NC: Pre-existing Conditions Limitation definition also includes “If a covered person is 65 or older when this policy is issued, pre-existing conditions for that covered person will include only conditions specifically eliminated by rider.”
OK: Replace “psychiatric or psychological conditions” with “mental or emotional conditions.”
SC: Replace “psychiatric or psychological conditions” with “mental or emotional disorders.”
SD: Not applicable to “alcoholism or drug addiction.”
UT: Replace “psychiatric or psychological conditions” with “mental or nervous disorders.”
VT: Not applicable to “alcoholism or drug abuse, psychiatric or psychological conditions, well baby care,” or the limitation for giving birth within the first nine months after the rider coverage effective date.
ADDITIONAL DISCLOSURES FOR THE STATE OF KENTUCKY
Eligibility for Benefits: We will pay the benefits for a covered accident if any covered person sustains an injury as a result of a covered accident if:
• The covered accident occurs while the policy is in force;
• The covered accident occurs on or after the policy coverage effective date;
• The covered accident is on an accident type listed on the policy schedule; and
• The covered accident is not excluded by name or specific description in the policy.
What is not covered by this policy: We will not pay benefits for losses that are caused by, contributed to by or occurs as a result of the covered person’s felonies or illegal occupations, hazardous avocations, racing, semi-professional or professional sports, sickness or injuries which any covered person intentionally does to himself, war or armed conflict. In addition, we also will not pay the Accidental Dismemberment due to Catastrophic Accident benefit for injuries that are caused by or are the result of birth or intoxicants, narcotics, and hallucinogenics.
Termination of this Rider: This rider will terminate on the earliest of: the date the policy to which this rider is attached terminates; the date premium for this rider is not paid by the end of the grace period; or the date we receive your written request to terminate this rider.
Noncancellable: This policy is noncancellable. We have no right to change the premiums we charge on this policy. Any riders attached to this policy may be subject to a change in premium. The premium can be changed following the approval of the Commissioner of Insurance only if we change it on all riders of the same kind in force in the state where the policy was issued. This information is not intended to be a complete description of the insurance coverage available. The policy or its provisions may vary or be unavailable in some states. The policy has exclusions and limitations which may affect any benefits payable. Applicable to policy form IAC4000 and rider form R-SHC4000 (including state abbreviations where used, for example: IAC4000-AL). For cost and complete details of coverage, call or write your Colonial Life benefits counselor or the company.
Underwritten by Colonial Life & Accident Insurance Company, Columbia, SC.
© 2024 Colonial Life & Accident Insurance Company. All rights reserved. Colonial Life is a registered trademark and marketing brand of Colonial Life & Accident Insurance Company.

This benefit can help pay your medical expenses if you receive a non-fatal gunshot wound. It offers you a lump sum benefit for a covered injury that you can use where you need it the most.
Gunshot wound $_____________________
Guaranteed issue
You can get this coverage without answering any health questions.
On/off-job coverage
You may receive benefits regardless of whether the injury occurs on or off the job.
Direct payment
Benefits are payable directly to you regardless of any other insurance coverage you may have.
This policy covers a non-fatal gunshot wound from a conventional firearm that requires treatment by a doctor and overnight hospitalization within 24 hours of the injury. If you’re shot more than once in a 24-hour period, we can pay benefits only for the first wound.
For more information, talk with your Colonial Life benefits counselor.
HEALTH SAVINGS ACCOUNT (HSA) COMPATIBLE
This plan is compatible with HSA guidelines and any other HSA plan in which a covered family member may participate. It may also be offered to employees who do not have HSAs.
THIS POLICY PROVIDES LIMITED BENEFITS .
This coverage is a supplement to health insurance. It is not a substitute for essential health benefits or minimum essential coverage as defined in federal law. Insureds in some states must be covered by comprehensive health insurance before applying for this coverage.
EXCLUSIONS
We will not pay benefits for losses that are caused by, contributed to by or occur as the result of your felonies or illegal occupations, suicide or injuries which you do to yourself, war or armed conflict.
STATE VARIATIONS FOR EXCLUSIONS AND LIMITATIONS
CT: Not applicable to “or illegal occupations”.
ID: This is a rider R-GSW4000-ID.
MD: Not applicable to “or illegal occupations”. This is a rider R-GSW4000-MD.
MI: Not applicable to “suicide or injuries which you do to yourself”.
MT: Not applicable to “suicide or injuries which you do to yourself”.
OH: This is a rider R-GSW4000.
OR: Not applicable to “or illegal occupations”.
ADDITIONAL DISCLOSURES FOR KENTUCKY:
Eligibility for Benefits: We will pay the benefits for a covered accident if any covered person sustains an injury as a result of a covered accident if:
• The covered accident occurs while the policy is in force;
• The covered accident occurs on or after the policy coverage effective date;
• The covered accident is on an accident type listed on the policy schedule; and
• The covered accident is not excluded by name or specific description in the policy.
What is not covered by this policy: We will not pay benefits for losses that are caused by, contributed to by or occurs as a result of the covered person’s felonies or illegal occupations, hazardous avocations, racing, semi-professional or professional sports, sickness or injuries which any covered person intentionally does to himself, war or armed conflict. In addition, we also will not pay the Accidental Dismemberment due to Catastrophic Accident benefit for injuries that are caused by or are the result of birth or intoxicants, narcotics, and hallucinogencis.
Noncancellable: This policy is noncancellable. We have no right to change the premiums we charge on this policy. Any riders attached to this policy may be subject to a change in premium. The premium can be changed following the approval of the Commissioner of Insurance only if we change it on all riders of the same kind in force in the state where the policy was issued.
This information is not intended to be a complete description of the insurance coverage available. The policy or its provisions may vary or be unavailable in some states. The policy has exclusions and limitations which may affect any benefits payable. Applicable to policy form IAC4000 (including state abbreviations where used, for example: IAC4000-TX). For cost and complete details of coverage, call or write your Colonial Life benefits counselor or the company. An insurance producer may contact you.
Underwritten by Colonial Life & Accident Insurance Company, Columbia, SC.
© 2024 Colonial Life & Accident Insurance Company. All rights reserved. Colonial Life is a registered trademark and marketing brand of Colonial Life & Accident Insurance Company.


Click on the video below to learn more about Medical Bridge Benefits!





For more information, talk with your benefits counselor.
Our Individual Medical BridgeSM insurance can help with medical costs that your health insurance may not cover. These benefits are available for you, your spouse and eligible dependent children.
Hospital confinement $
Maximum of one benefit per covered person per calendar year
Observation room..................................................................................
Maximum of two visits per covered person per calendar year
Rehabilitation unit confinement
$100 per visit
$100 per day
Maximum of 15 days per confinement with a 30-day maximum per covered person per calendar year
Waiver of premium
Available after 30 continuous days of a covered hospital confinement of the named insured
Health savings account (HSA) compatible
This plan is compatible with HSA guidelines. This plan may also be offered to employees who do not have HSAs.
Colonial Life & Accident Insurance Company’s Individual Medical Bridge offers an HSA compatible plan in most states.
THIS POLICY PROVIDES LIMITED BENEFITS.
EXCLUSIONS
We will not pay benefits for losses which are caused by: alcoholism or drug addiction, dental procedures, elective procedures and cosmetic surgery, felonies or illegal occupations, pregnancy of a dependent child, psychiatric or psychological conditions, suicide or injuries which any covered person intentionally does to himself or herself, war, or giving birth within the first nine months after the effective date of the policy. We will not pay benefits for hospital confinement of a newborn who is neither injured nor sick. We will not pay benefits for loss during the first 12 months after the effective date due to a pre-existing condition. A pre-existing condition is a sickness or physical condition for which a covered person was treated, had medical testing, received medical advice or had taken medication within the 12 months before the effective date of the policy. For cost and complete details, see your Colonial Life benefits counselor. Applicable to policy number IMB7000 (including state abbreviations where used, for example: IMB7000-TX). Coverage may vary by state and may not be available in all states. This is not an insurance contract and only the actual policy provisions will control.

For more information, talk with your benefits counselor.
Our Individual Medical BridgeSM insurance can help with medical costs that your health insurance may not cover. These benefits are available for you, your spouse and eligible dependent children.
Hospital confinement $
Maximum of one benefit per covered person per calendar year
Observation room
Maximum of two visits per covered person per calendar year
Rehabilitation unit confinement
$100 per visit
$100 per day
Maximum of 15 days per confinement with a 30-day maximum per covered person per calendar year
Waiver of premium
Available after 30 continuous days of a covered hospital confinement of the named insured
Diagnostic procedure
Tier 1 $250
Tier 2
Maximum of $500 per covered person per calendar year for all covered diagnostic procedures combined
Outpatient surgical procedure
Tier 1 $
Tier 2 $
Maximum of $___________ per covered person per calendar year for all covered outpatient surgical procedures combined
The following is a list of common diagnostic procedures that may be covered.
Tier 1 diagnostic procedures
Breast
– Biopsy (incisional, needle, stereotactic)
Diagnostic radiology
– Nuclear medicine test
Digestive
– Barium enema/lower GI series
– Barium swallow/upper GI series
– Esophagogastroduodenoscopy (EGD)
Ear, nose, throat, mouth
– Laryngoscopy
Gynecological
– Amniocentesis
– Cervical biopsy
– Cone biopsy
– Endometrial biopsy
– Hysteroscopy
– Loop electrosurgical excisional procedure (LEEP)
Tier 2 diagnostic procedures
Cardiac
– Angiogram
– Arteriogram
– Thallium stress test
– Transesophageal echocardiogram (TEE)
Liver – biopsy
Lymphatic – biopsy
Miscellaneous
– Bone marrow aspiration/biopsy
Renal – biopsy
Respiratory
– Biopsy
– Bronchoscopy
– Pulmonary function test (PFT)
Skin
– Biopsy
– Excision of lesion
Thyroid – biopsy
Urologic
– Cystoscopy
Diagnostic radiology
– Computerized tomography scan (CT scan)
– Electroencephalogram (EEG)
– Magnetic resonance imaging (MRI)
– Myelogram
– Positron emission tomography scan (PET scan)
The surgeries listed below are only a sampling of the surgeries that may be covered. Surgeries must be performed by a doctor in a hospital or ambulatory surgical center. For complete details and definitions, please refer to your policy.
Tier 1 outpatient surgical procedures
Breast
– Axillary node dissection
– Breast capsulotomy
– Lumpectomy
Cardiac
– Pacemaker insertion
Digestive
– Colonoscopy
– Fistulotomy
– Hemorrhoidectomy
– Lysis of adhesions
Skin
– Laparoscopic hernia repair
– Skin grafting
Ear, nose, throat, mouth
– Adenoidectomy
– Removal of oral lesions
– Myringotomy
– Tonsillectomy
– Tracheostomy
– Tympanotomy
Tier 2 outpatient surgical procedures
Breast
– Breast reconstruction
– Breast reduction
Cardiac
– Angioplasty
– Cardiac catheterization
Digestive
– Exploratory laparoscopy
– Laparoscopic appendectomy
– Laparoscopic cholecystectomy
Ear, nose, throat, mouth
– Ethmoidectomy
– Mastoidectomy
– Septoplasty
– Stapedectomy
– Tympanoplasty
Eye
– Cataract surgery
– Corneal surgery (penetrating keratoplasty)
– Glaucoma surgery (trabeculectomy)
– Vitrectomy
EXCLUSIONS
Gynecological
– Dilation and curettage (D&C)
– Endometrial ablation
– Lysis of adhesions
Liver
– Paracentesis
Musculoskeletal system
– Carpal/cubital repair or release
– Foot surgery (bunionectomy, exostectomy, arthroplasty, hammertoe repair)
– Removal of orthopedic hardware
– Removal of tendon lesion
Gynecological
– Hysterectomy
– Myomectomy
Musculoskeletal system
– Arthroscopic knee surgery with meniscectomy (knee cartilage repair)
– Arthroscopic shoulder surgery
– Clavicle resection
– Dislocations (open reduction with internal fixation)
– Fracture (open reduction with internal fixation)
– Removal or implantation of cartilage
– Tendon/ligament repair
Thyroid
– Excision of a mass
Urologic
– Lithotripsy
We will not pay benefits for losses which are caused by: alcoholism or drug addiction, dental procedures, elective procedures and cosmetic surgery, felonies or illegal occupations, pregnancy of a dependent child, psychiatric or psychological conditions, suicide or injuries which any covered person intentionally does to himself or herself, war, or giving birth within the first nine months after the effective date of the policy. We will not pay benefits for hospital confinement of a newborn who is neither injured nor sick. We will not pay benefits for loss during the first 12 months after the effective date due to a pre-existing condition. A pre-existing condition is a sickness or physical condition for which a covered person was treated, had medical testing, received medical advice or had taken medication within the 12 months before the effective date of the policy. For cost and complete details, see your Colonial Life benefits counselor. Applicable to policy number IMB7000 (including state abbreviations where used, for example: IMB7000-TX). Coverage may vary by state and may not be available in all states. This is not an insurance contract and only the actual policy provisions will control.

Individual Medical BridgeSM insurance’s health screening benefit can help pay for health and wellness tests you have each year.
screening $_____________
Maximum of one health screening test per covered person per calendar year; subject to a 30-day waiting period
Blood test for triglycerides
Bone marrow testing
Breast ultrasound
CA 15-3 (blood test for breast cancer)
CA 125 (blood test for ovarian cancer)
CEA (blood test for colon cancer)
Carotid Doppler
Chest X-ray
Colonoscopy
Echocardiogram (ECHO)
Electrocardiogram (EKG, ECG)
Fasting blood glucose test
Flexible sigmoidoscopy
Hemoccult stool analysis
Mammography
Pap smear
PSA (blood test for prostate cancer)
Serum cholesterol test for HDL and LDL levels
Serum protein electrophoresis (blood test for myeloma)
Skin cancer biopsy
Stress test on a bicycle or treadmill
Thermography
ThinPrep pap test
Virtual colonoscopy


For more information, talk with your benefits counselor.
Individual Medical BridgeSM offers two optional benefit riders – the daily hospital confinement rider and the enhanced intensive care unit confinement rider. For an additional cost, these riders can help provide extra financial protection to help with out-of-pocket medical expenses.
Daily hospital confinement rider
Per covered person per day of hospital confinement
Maximum of 365 days per covered person per confinement
Enhanced intensive care unit confinement rider
Per covered person per day of intensive care unit confinement
Maximum of 30 days per covered person per confinement
Re-confinement for the same or related condition within 90 days of discharge is considered a continuation of a previous confinement.
$100 per day
$500 per day
EXCLUSIONS
We will not pay benefits for losses which are caused by: alcoholism or drug addiction, dental procedures, elective procedures and cosmetic surgery, felonies or illegal occupations, pregnancy of a dependent child, psychiatric or psychological conditions, suicide or injuries which any covered person intentionally does to himself or herself, war, or giving birth within the first nine months after the effective date of the rider. We will not pay benefits for hospital confinement of a newborn who is neither injured nor sick. We will not pay benefits for loss during the first 12 months after the effective date due to a pre-existing condition. A pre-existing condition is a sickness or physical condition for which a covered person was treated, had medical testing, received medical advice or had taken medication within the 12 months before the effective date of the rider. For cost and complete details, see your Colonial Life benefits counselor. Applicable to rider numbers R-DHC7000 and R-EIC7000 (including state abbreviations where used, for example: R-DHC7000-TX and R-EIC7000-TX). Coverage may vary by state and may not be available in all states. This is not an insurance contract and only the actual policy or rider provisions will control.
|
which Colonial Life is the marketing brand.







Life insurance needs change as life circumstances change. You may need different coverage if you’re getting married, buying a home or having a child.
Term life insurance from Colonial Life provides protection for a specified period of time, typically offering the greatest amount of coverage for the lowest initial premium. This fact makes term life insurance a good choice for supplementing cash value coverage during life stages when obligations are higher, such as while children are younger. It’s also a good option for families on a tight budget — especially since you can convert it to a permanent cash value plan later.
n A beneficiary can receive a benefit that is typically free from income tax.
n The policy’s accelerated death benefit can pay a percentage of the death benefit if the covered person is diagnosed with a terminal illness.
n You can convert it to a Colonial Life cash value insurance plan, with no proof of good health, to age 75.
n Coverage is guaranteed renewable up to age 95 as long as premiums are paid when due.
n Portability allows you to take it with you if you change jobs or retire.
Two options are available for spouse coverage at an additional cost: You may add a Children’s Term Life Rider to cover all of your eligible dependent children with up to $20,000 in coverage each for one premium.
1. Spouse Term Life Policy: Offers guaranteed premiums and level death benefits equivalent to those available to you –whether or not you buy a policy for yourself.
2. Spouse Term Life Rider: Add a term rider for your spouse to your policy, up to a maximum death benefit of $50,000; 10-year and 20-year are available (20-year rider only available with a 20- or 30-year term policy).
The Children’s Term Life Rider may be added to either the primary or spouse policy, not both.
How much coverage do you need?
£ YOU $ ___________________
Select the term period:
£ 10-year
£ 15-year
£ 20-year
£ 30-year
£ SPOUSE $ ___________________
Select the term period:
£ 10-year
£ 15-year
£ 20-year
£ 30-year
Select any optional riders:
£ Spouse term life rider
$ _____________ face amount for ________-year term period
£ Children’s term life rider
$ _____________ face amount
£ Accidental death benefit rider
£ Critical illness accelerated death benefit rider
£ Waiver of premium benefit rider
At an additional cost, you can purchase the following riders for even more financial protection.
Your spouse may receive a maximum death benefit of $50,000; 10-year and 20-year spouse term riders are available.
You can purchase up to $20,000 in term life coverage for all of your eligible dependent children and pay one premium. The children’s term life rider may be added to either your policy or your spouse’s policy – not both.
The beneficiary may receive an additional benefit if the covered person dies as a result of an accident before age 70. The benefit doubles if the accidental bodily injury occurs while riding as a fare-paying passenger using public transportation, such as ridesharing services. An additional 25% will be payable if the injury is sustained while driving or riding in a private passenger vehicle and wearing a seatbelt
If you suffer a heart attack (myocardial infarction), stroke or end-stage renal (kidney) failure, a $5,000 benefit is payable.1 A subsequent diagnosis benefit is included
Premiums are waived (for the policy and riders) if you become totally disabled before the policy anniversary following your 65th birthday and you satisfy the six-month elimination period.3
1 Any payout would reduce the death benefit. Benefits may be taxable as income. Individuals should consult with their l egal or tax counsel when deciding to apply for accelerated benefits.
3 You must resume premium payments once you are no longer disabled.
If the insured dies by suicide, whether sane or insane, within two years (one year in ND) from the coverage effective date or the date of reinstatement, we will not pay the death benefit. We will terminate this policy and return the premiums paid without interest, minus any loans and loan interest to you.
This information is not intended to be a complete description of the insurance coverage available. The policy or its provisions may vary or be unavailable in some states. The policy has exclusions and limitations which may affect any benefits payable. Applicable to policy forms ICC18-ITL5000/ITL5000 and rider forms ICC18-R-ITL5000-STR/RITL5000- STR, ICC18-R-ITL5000-CTR/R-ITL5000-CTR, ICC18-R-ITL5000-WP/R-ITL5000-WP, ICC18-R-ITL5000-ACCD/RITL5000- ACCD, ICC18-R-ITL5000-CI/R-ITL5000-CI, ICC18-R-ITL5000-CC/R-ITL5000-CC. For cost and complete details of the coverage, call or write your Colonial Life benefits counselor or the company.







You can’t predict your family’s future, but you can prepare for it.
Help give your family more peace of mind and coverage for final expenses with Colonial Life Individual Whole Life Plus insurance.
Benefits and features
Choose the age when your premium payments end — Paid-Up at Age 70 or Paid-Up at Age 100
Stand-alone spouse policy available even without buying a policy for yourself
Ability to keep the policy if you change jobs or retire
Built-in terminal illness accelerated death benefit that provides up to 75% of the policy’s death benefit (up to $150,000) if you’re diagnosed with a terminal illness1
Immediate $3,000 claim payment that can help your designated beneficiary pay for funeral costs or other expenses
Provides cash surrender value at age 100 (when the policy endows)
Spouse term rider
Cover your spouse with a death benefit up to $50,000, for 10 or 20 years.
Juvenile Whole Life Plus policy
Purchase a policy (Paid-Up at Age 70) while children are young and premiums are low — whether or not you buy a policy for yourself. You may also increase the coverage when the child is 18, 21 and 24 without proof of good health.
Children’s term rider
You may purchase up to $20,000 in term life insurance coverage for all of your eligible dependent children and pay one premium. The children’s term rider may be added to either your policy or your spouse’s policy — not both.
• Permanent life insurance coverage that stays the same through the life of the policy
• Premiums will not increase due to changes in health or age.
• Accumulates cash value based on a nonforfeiture interest rate of 3.75%2
• Policy loans available, which can be used for emergencies
• Benefit for the beneficiary that is typically tax-free
Your cost will vary based on the amount of coverage you select.
For use with your benefits counselor
How much coverage do you need?
YOU $
Select the option:
Paid-Up at Age 70
Paid-Up at Age 100
SPOUSE $
Select the option:
Paid-Up at Age 70
Paid-Up at Age 100
DEPENDENT STUDENT
$
Select the option:
Paid-Up at Age 70
Paid-Up at Age 100
Select any optional riders:
Spouse term rider
$ face amount for -year term period
Children’s term rider
$ face amount
Accidental death benefit rider
Critical illness accelerated death benefit rider
Guaranteed purchase option rider
An additional benefit may be payable if the covered person dies as a result of an accident before age 70, and doubles if the injury occurs while riding as a farepaying passenger using public transportation. An additional 25% is payable if the injury occurs while driving or riding in a private passenger vehicle and wearing a seatbelt.
If you suffer a heart attack, stroke or end-stage renal (kidney) failure, a $5,000 benefit is payable.1 A subsequent diagnosis benefit is included.
This rider allows you to purchase additional whole life coverage — without having to answer health questions — at three different points in the future. The rider may only be added if you are age 50 or younger when you purchase the policy. You may purchase up to your initial face amount, not to exceed a total combined maximum of $100,000 for all options.
Policy and rider premiums are waived if you become totally disabled before the policy anniversary following your 65th birthday and you satisfy the six-month elimination period. Once you are no longer disabled, premiums will resume.
* Whole Life Plus is a marketing name of the insurance policy filed as “Whole Life Insurance” in most
Waiver of premium benefit rider states.
1 Any payout would reduce the death benefit. Benefits may be taxable as income. Individuals should consult with their legal or tax counsel when deciding to apply for accelerated benefits.
2 Accessing the accumulated cash value reduces the death benefit by the amount accessed, unless the loan is repaid. Cash value will be reduced by any outstanding loans against the policy.
This life insurance does not specifically cover funeral goods or services and may not cover the entire cost of your funeral at the time of your death. The beneficiary of this life insurance may use the proceeds for any purpose, unless otherwise directed.
To learn more, talk with your benefits counselor.
EXCLUSIONS AND LIMITATIONS: If the insured dies by suicide, whether sane or insane, within two years (one year in ND) from the coverage effective date or the date of reinstatement, we will not pay the death benefit. We will terminate this policy and return the premiums paid without interest, minus any loans and loan interest to you.
This information is not intended to be a complete description of the insurance coverage available. The policy or its provisions may vary or be unavailable in some states. The policy has exclusions and limitations which may affect any benefits payable. Applicable to policy forms ICC19-IWL5000-70/ IWL5000-70, ICC19-IWL5000-100/IWL5000-100, ICC19-IWL5000J/IWL5000J and rider forms ICC23IWL5000-LTC/IWL5000-LTC, ICC19-R-IWL5000-STR/R-IWL5000-STR, ICC19-R-IWL5000-CTR/RIWL5000-CTR, ICC19-R-IWL5000-WP/R-IWL5000-WP, ICC19-R-IWL5000-ACCD/R-IWL5000-ACCD, ICC19-R-IWL5000-CI/R-IWL5000-CI, ICC19-R-IWL5000-CC/R-IWL5000-CC, ICC19-R-IWL5000GPO/R-IWL5000-GPO (including state abbreviations where applicable). For cost and complete details of the coverage, call or write your Colonial Life benefits counselor or the company.
Underwritten by Colonial Life & Accident Insurance Company, Columbia, SC. © 2023 Colonial Life & Accident Insurance Company. All rights reserved. Colonial Life is a registered trademark and marketing brand of Colonial Life & Accident Insurance Company.
Faster service than calling/emailing
Confirmation when a claim has been submitted
Simplified bill payment and management Answers to frequently asked questions and live chat assistance if you don’t see what you are looking for.
Find out how simple your claims and benefits experience can be by learning more about the Colonial Life for Policyholders portal. Just visit ColonialLife.com to see what this online account administration platform can do for you.
Colonial Life for Policyholders is an online portal created with you in mind. It’s the most convenient and efficient way to file a claim and manage your benefits.
File claims with a simple, guided form
Set up direct deposit for approved payments
BECOME A MEMBER TODAY:
View claim status or policy details anytime
Opt for instant alerts by email or text
Update your personal info & preferences
Go to ColonialLife .com/access to register. Click “create an account”, fill out the required information and click Submit Enjoy faster service and improved benefits awareness.
Filing online means never waiting for mail or dealing with fax machines and complex paper forms . Our guided question wizard walks you through the process and checks for missing information that could cause delays. Opting for direct deposit can also get approved payments to you up to a week faster than paper check.
Check your claim status by logging into your account at ColonialLife .com/access. You can also sign up for text or email alerts so you know instantly if status changes or more information is needed. For your convenience, you can login anytime with a mobile device to photograph and upload documents with your camera.
For the purpose of evaluating my application(s) for insurance submitted during the current enrollment and eligibility for benefits under an y insurance issued including checking for and resolving any issues that may arise regarding incomplete or incorrect information on my application(s), I hereby authorize the disclosure of the following information about me and, if applicable , my dependents, from the sources listed below to Colonial Life & Accident Insurance Company (Colonial) and its duly authorized representatives.
Health information may be disclosed by any health care provider or institution, health plan or health care clearinghouse that has any re cords or knowledge about me including prescription drug database or pharmacy benefit manager, or ambulanc e or other medical transport service. Health information may also be disclosed by any insuranc e company, Medicare or Medicaid agencies or the Medical Information Bureau (MIB). Health information includes my entire medical record, but does not include psychotherapy notes. Non-health information including earnings or empl oyment history deemed appropriate by Colonial to evaluate my application may be disclosed by any person or organization that has these records about me, including my employer, employer representative and compensation sources, insurance company, financial institution or governmental entities including departments of public safety and motor vehicle departments.
Any information Colonial obtains pursuant to this authorization will be used for the purpose of evaluating my application(s) for insu rance or eligibility for benefits. Some information obtained may not be protected by certain federal regulations governing the priva cy of health information, but the information is protected by state privacy laws and ot her applicable laws. Colonial will not re- disclose the information unless permitted or r equired by those laws. Re-disclosed information may no longer be protected by federal privacy laws.
This authorization is valid for two (2) years from its execution and a copy is as valid as the original. A copy will be included with my contract(s) and I or my authorized representative may request access to this information. This authorization may be revoked by me or my authorized representative at any time except to the extent Colonial has relied on the authorization prior to notice of revocation or has a legal right to contest coverage under the contract(s) or the contract itself. If revoked, Colonial may not be able to evaluate my application(s) for insurance or eligibility for benefits as necessary to issue my contract(s). I may revoke this authorization by sending written notice to: Colonial Life & Accident Insurance Company, Underwriting Department, P. O. Box 1365, Columbia, SC 29202.
You may refuse to sign this form; however, Colonial may not be able to issue your coverage. I am the individual to whom this authorization applies or that person's legal Guardian, Power of Attorney Designee, or Conservator.
(Printed name of individual (Social Security (Signature) (Date Signed) subject to this disclosure) Number)
If applicable, I signed on behalf of the proposed insured as ____________________(indicate relationship). If legal Guardian, Power of Attorney Designee, or Conservator.
(Printed name of legal representative) (Signature of legal representative) (Date Signed)
The Virginia Retirement System (VRS) Optional Group Life Insurance program gives you the opportunity to purchase additional insurance at favorable group rates on yourself and family. Optional group life is term insurance. Term insurance generally provides the largest immediate death protection for your premium dollar. The program is administered by the Virginia Retirement System, and is provided under a group policy issued by the Minnesota Life Insurance Company.
Questions about your employer paid and optional life insurance coverage can be submitted one of three ways:
By mail:
Securian Financial
PO Box 1193, Richmond, VA 23218-1193
By calling: 1-800-441-2258
Or by visiting their website: www.varetire.org/myvrs
Group Long Term Disability (LTD) insurance from The Standard helps provide financial protection for insured members by promising to pay a monthly benefit in the event of a covered disability.
This Group Short Term Disability (STD) program is provided for VRS Hybrid Plan Participants and administered by The Standard. This benefit helps provide financial protection for covered members by promising to pay a weekly benefit in the event of a covered disability.
Questions about your VACORP Short and Long Term Disability can be submitted one of two ways: Please refer to the plan summary document and your employee handbook for specific plan details, eligibility definitions, limitations, and exclusions.
By calling: 1-844-404-2111
Or by visiting their website: www.vacorp.org/coverage/hybrid-disability
Group health plans and health insurance issuers generally may not, under federal law restrict benefits for any hospital length of stay in connection with childbirth for the mother or newborn child to less than 48 hours following vaginal delivery, or less than 96 hours following a cesarean section. However, federal law generally does not prohibit the mother’s or newborn’s attending provider, after consulting with the mother, from discharging the mother or newborn earlier than 48 hours (or 96 hours as applicable). In any case, plans and issuers may not, under federal law, require that a provider obtain authorization from the plan or the issuer for prescribing a length of stay not in excess of 48 hours (or 96 hours).
In October 1998, Congress enacted the Women’s Health and Cancer Rights Act of 1998. This notice explains some important provisions of the Act. Please review this information carefully. As specified in the Women’s Health and Cancer Rights Act, a plan participant or beneficiary who elects breast reconstruction in connection with a covered mastectomy is also entitled to the following benefits: 1. All stages of reconstruction of the breast on which the mastectomy has been performed: 2. Surgery and reconstruction of the other breast to produce a symmetrical appearance; and 3. Prostheses and treatment of physical complications of the mastectomy , including lymphedemas. Health plans must provide coverage of mastectomy related benefits in a manner to determine in consultation with the attending physician and the patient. Coverage for breast reconstruction and related services may be subject to deductibles and insurance amounts that are consistent with those that apply to other benefits under the plan.
Premium Assistance Under Medicaid and the Children’s Health Insurance Program (CHIP)
If you or your children are eligible for Medicaid or CHIP and you’re eligible for health coverage from your employer, your state may have a premium assistance program that can help pay for coverage, using funds from their Medicaid or CHIP programs. If you or your children aren’t eligible for Medicaid or CHIP, you won’t be eligible for these premium assistance programs but you may be able to buy individual insurance coverage through the Health Insurance Marketplace. For more information, visit www.healthcare.gov.
If you or your dependents are already enrolled in Medicaid or CHIP and you live in a State listed below, contact your State Medicaid or CHIP office to find out if premium assistance is available.
If you or your dependents are NOT currently enrolled in Medicaid or CHIP, and you think you or any of your dependents might be eligible for either of these programs, contact your State Medicaid or CHIP office or dial 1-877-KIDS
NOW or www.insurekidsnow.gov to find out how to apply. If you qualify, ask your state if it has a program that might help you pay the premiums for an employer sponsored plan.
If you or your dependents are eligible for premium assistance under Medicaid or CHIP, as well as eligible under your employer plan, your employer must allow you to enroll in your employer plan if you aren’t already enrolled. This is called a “special enrollment” opportunity, and you must request coverage within 60 days of being determined eligible for premium assistance. If you have questions about enrolling in your employer plan, contact the Department of Labor at www.askebsa.dol.gov or call 1-866-444-EBSA (3272).
ALABAMA - MEDICAID
Website: myalhipp.com
Phone: 1-855-692-5447
ALASKA - MEDICAID
The AK Health Insurance Premium Payment Program
Website: myakhipp.com
Phone: 1-866-251-4861
Email: CustomerService@MyAKHIPP.com
Medicaid Eligibility: dhss.alaska.gov/dpa/Pages/ medicaid/default.aspx
ARKANSAS - MEDICAID
Website: myarhipp.com
Phone: 1-855-MyARHIPP (855-692-7447)
CALIFORNIA - MEDICAID
Website: www.dhcs.ca.gov/services/Pages/ TPLRD_CAU_cont.aspx
Phone: 916-440-5676
COLORADO - HEALTH FIRST COLORADO (MEDICAID) & CHILD HEALTH PLAN PLUS (CHP+)
Health First Colorado Website: www.healthfirstcolorado.com
Health First Colorado Member Contact Center: 1-800-221-3943/State Relay 711
CHP+: www.colorado.gov/pacific/hcpf/childhealth-plan-plus
CHP+ Customer Service: 1-800-359-1991/State Relay 711
Health Insurance Buy-In Program (HIBI): www.colorado.gov/pacific/hcpf/health-insurancebuy-program
HIBI Customer Service: 1-855-692-6442
GEORGIA - MEDICAID
Website: medicaid.georgia.gov/health-insurance premium-payment-program-hipp
Phone: 678-564-1162, ext. 2131
INDIANA - MEDICAID
Healthy Indiana Plan for Low-Income
Adults 19-64
Website: www.in.gov/fssa/hip
Phone: 1-877-438-4479
All other Medicaid Website: www.in.gov/medicaid
Phone: 1-800-457-4584
Medicaid Website: dhs.iowa.gov/ime/members
Medicaid Phone: 1-800-338-8366
Hawki Website: dhs.iowa.gov/Hawki
Hawki Phone: 1-800-257-8563
KANSAS - MEDICAID
Website: www.kdheks.gov/hcf/default.htm
Phone: 1-800-792-4884
KENTUCKY - MEDICAID
Kentucky Integrated Health Insurance
Premium Payment
Program (KI-HIPP) Website: chfs.ky.gov/agencies/dms/member/Pages/kihipp.aspx
Phone: 1-855-459-6328
Email: KIHIPP.PROGRAM@ky.gov
KCHIP Website: kidshealth.ky.gov/Pages/index.aspx
Phone: 1-877-524-4718
Kentucky Medicaid Website: chfs.ky.gov
Website: www.medicaid.la.gov or www.ldh.la.gov/lahipp
Website: www.flmedicaidtplrecovery.com/flmedicaidtplrecovery.com/hipp/index.html
Phone: 1-877-357-3268 FLORIDA - MEDICAID
Phone: 1-888-342-6207 (Medicaid hotline) or 1-855-618-5488 (LaHIPP)
MAINE - MEDICAID
Website: www.maine.gov/dhhs/ofi/public assistance/index.html
Phone: 1-800-442-6003
TTY: Maine Relay 711
- MEDICAID AND CHIP
Website: www.mass.gov/eohhs/gov/departments/ masshealth
Phone: 1-800-862-4840
MINNESOTA - MEDICAID
Website: mn.gov/dhs/people-we-serve/children-and-families/health-care/health-care-programs/programs-and-services/medical-assistance.jsp [Under ELIGIBILITY tab, see “What if I have other health insurance?”]
Phone: 1-800-657-3739
KANSAS - MEDICAID
Website: www.kdheks.gov/hcf/default.htm
Phone: 1-800-792-4884
MISSOURI - MEDICAID
Website: www.dss.mo.gov/mhd/participants/ pages/hipp.htm
Phone: 573-751-2005
MONTANA - MEDICAID
Website: dphhs.mt.gov/MontanaHealthcarePrograms/HIPP
Phone: 1-800-694-3084
NEBRASKA - MEDICAID
Website: www.ACCESSNebraska.ne.gov
Phone: 1-855-632-7633
Lincoln: 402-473-7000
Omaha: 402-595-1178
NEVADA - MEDICAID
Medicaid Website: dhcfp.nv.gov
Medicaid Phone: 1-800-992-0900
NEW HAMPSHIRE - MEDICAID
Website: www.dhhs.nh.gov/oii/hipp.htm
Phone: 603-271-5218
Toll free number for the HIPP program: 1-800-852-3345, ext. 5218
NEW JERSEY - MEDICAID AND CHIP
Medicaid Website: www.state.nj.us/humanservices/dmahs/clients/medicaid
Medicaid Phone: 609-631-2392
CHIP Website: www.njfamilycare.org/index.html
CHIP Phone: 1-800-701-0710
NEW YORK - MEDICAID
Website: www.health.ny.gov/health_care/ medicaid
Phone: 1-800-541-2831
NORTH CAROLINA - MEDICAID
Website: medicaid.ncdhhs.gov
Phone: 919-855-4100
NORTH DAKOTA - MEDICAID
Website: www.nd.gov/dhs/services/medicalserv/medicaid
Phone: 1-844-854-4825
OKLAHOMA - MEDICAID & CHIP
Website: www.insureoklahoma.org
Phone: 1-888-365-3742
OREGON - MEDICAID & CHIP
Website: healthcare.oregon.gov/Pages/index.aspx
Phone: 1-800-699-9075
PENNSYLVANIA - MEDICAID
Website: www.dhs.pa.gov/providers/Providers/ Pages/Medical/HIPP-Program.aspx
Phone: 1-800-692-7462
RHODE ISLAND - MEDICAID AND CHIP
Website: www.eohhs.ri.gov
Phone: 1-855-697-4347 or 401-462-0311
(Direct RIte Share Line)
SOUTH CAROLINA - MEDICAID
Website: www.scdhhs.gov
Phone: 1-888-549-0820
SOUTH DAKOTA - MEDICAID
Website: dss.sd.gov
Phone: 1-888-828-0059
TEXAS - MEDICAID
Website: gethipptexas.com
Phone: 1-800-440-0493
UTAH - MEDICAID
Medicaid Website: medicaid.utah.gov
CHIP Website: health.utah.gov/chip Phone: 1-877-543-7669
VERMONT - MEDICAID
Website: www.greenmountaincare.org Phone: 1-800-250-8427
VIRGINIA - MEDICAID AND CHIP
Website: www.coverva.org/hipp
Medicaid Phone: 1-800-432-5924
CHIP Phone: 1-855-242-8282
WASHINGTON - MEDICAID
Website: www.hca.wa.gov Phone: 1-800-562-3022
WEST VIRGINIA - MEDICAID
Website: mywvhipp.com
Toll-free phone: 1-855-MyWVHIPP (1-855-699-8447)
WISCONSIN - MEDICAID AND CHIP
Website: www.dhs.wisconsin.gov/badgercareplus/p-10095.htm Phone: 1-800-362-3002
WYOMING - MEDICAID
Website: wyequalitycare.acs-inc.com Phone: 307-777-7531
To see if any other states have added a premium assistance program since July 31, 2020, or for more information on special enrollment rights, contact either:
U.S. Department of Labor
Employee Benefits Security Administration www.dol.gov/agencies/ebsa 1-866-444-EBSA (3272)
U.S. Department of Health and Human Services Centers for Medicare & Medicaid Services www.cms.hhs.gov 1-877-267-2323, Menu Option 4, Ext. 61565
According to the Paperwork Reduction Act of 1995 (Pub. L. 104-13) (PRA), no persons are required to respond to a collection of information unless such collection displays a valid Office of Management and Budget (OMB) control number. The Department notes that a Federal agency cannot conduct or sponsor a collection of information unless it is approved by OMB under the PRA, and displays a currently valid OMB control number, and the public is not required to respond to a collection of information unless it displays a currently valid OMB control number. See 44 U.S.C. 3507. Also, notwithstanding any other provisions of law, no person shall be subject to penalty for failing to comply with a collection of information if the collection of information does not display a currently valid OMB control number. See 44 U.S.C. 3512. The public reporting burden for this collection of information is estimated to average approximately seven minutes per respondent. Interested parties are encouraged to send comments regarding the burden estimate or any other aspect of this collection of information, including suggestions for reducing this burden, to the U.S. Department of Labor, Employee Benefits Security Administration, Office of Policy and Research, Attention: PRA Clearance Officer, 200 Constitution Avenue, N.W., Room N-5718, Washington, DC 20210 or email ebsa.opr@dol.gov and reference the OMB Control Number 1210-0137.
INTRODUCTION: You’re getting this notice because you recently gained coverage under a group plan. This notice has important information about your right to COBRA continuation coverage, which is a temporary extension of coverage under the Plan. This notice explains COBRA continuation coverage, when it may become available to you and your family, and what you need to do to protect your right to get it. When you become eligible for COBRA, you may also become eligible for other coverage options that may cost less than COBRA continuation coverage.
The right to COBRA continuation coverage was created by a federal law, the Consolidated Omnibus Budget Reconciliation Act of 1985 (COBRA). COBRA continuation coverage can become available to you and other members of your family when group health coverage would otherwise end. For more information about your rights and obligations under the Plan and under federal law, you should review the Plan’s Summary Plan Description or contact the Plan Administrator.
You may have other options available to you when you lose group health coverage. For example, you may be eligible to buy an individual plan through the Health Insurance Marketplace. By enrolling in coverage through the Marketplace, you may qualify for lower costs on your monthly premiums and lower out-of-pocket costs. Additionally, you may qualify for a 30-day special enrollment period for another group health plan for which you are eligible (such as a spouse’s plan), even if that plan generally doesn’t accept late enrollees.
What Is Cobra Continuation Coverage?: COBRA continuation coverage is a continuation of Plan coverage when it would otherwise end because of a life event. This is also called a “qualifying event.” Specific qualifying events are listed later in this notice. After a qualifying event, COBRA continuation coverage must be offered to each person who is a “qualified beneficiary.” You, your spouse, and your dependent children could become qualified beneficiaries if coverage under the Plan is lost because of the qualifying event. Under the Plan, qualified beneficiaries who elect COBRA continuation coverage [choose and enter appropriate information: must pay or aren’t required to pay] for COBRA continuation coverage.
If you’re an employee, you’ll become a qualified beneficiary if you lose your coverage under the Plan because of the following qualifying events:
• Your hours of employment are reduced, or
• Your employment ends for any reason other than your gross misconduct.
• If you’re the spouse of an employee, you’ll become a qualified beneficiary if you lose your coverage under the Plan because of the following qualifying events:
• Your spouse dies;
• Your spouse’s hours of employment are reduced;
• Your spouse’s employment ends for any reason other than his or her gross misconduct;
• Your spouse becomes entitled to Medicare benefits (under Part
A, Part B, or both); or
• You become divorced or legally separated from your spouse. Your dependent children will become qualified beneficiaries if they lose coverage under the Plan because of the following qualifying events:
• The parent-employee dies;
• The parent-employee’s hours of employment are reduced;
• The parent-employee’s employment ends for any reason other than his or her gross misconduct;
• The parent-employee becomes entitled to Medicare benefits (Part A, Part B, or both);
• The parents become divorced or legally separated; or
• The child stops being eligible for coverage under the Plan as a “dependent child.”
Sometimes, filing a proceeding in bankruptcy under title 11 of the United States Code can be a qualifying event. If a proceeding in bankruptcy is filed with respect to Amherst County Government and that bankruptcy results in the loss of coverage of any retired employee covered under the Plan, the retired employee will become a qualified beneficiary. The retired employee’s spouse, surviving spouse, and dependent children will also become qualified beneficiaries if bankruptcy results in the loss of their coverage under the Plan.
When is COBRA continuation coverage available?
The Plan will offer COBRA continuation coverage to qualified beneficiaries only after the Plan Administrator has been notified that a qualifying event has occurred. The employer must notify the Plan Administrator of the following qualifying events:
• The end of employment or reduction of hours of employment;
• Death of the employee;
• The employee’s becoming entitled to Medicare benefits (under Part A, Part B, or both).
For all other qualifying events (divorce or legal separation of the employee and spouse or a dependent child’s losing eligibility for coverage as a dependent child), you must notify the Plan Administrator within 60 days after the qualifying event occurs. You must provide this notice to: Caitlin Jack at ccjack@countyofamherst.com. Applicable documentation will be required i.e. court order, certificate of coverage etc.
How is COBRA continuation coverage provided?
Once the Plan Administrator receives notice that a qualifying event has occurred, COBRA continuation coverage will be offered to each of the qualified beneficiaries. Each qualified beneficiary will have an independent right to elect COBRA continuation coverage. Covered employees may elect COBRA continuation coverage on behalf of their spouses, and parents may elect COBRA continuation coverage on behalf of their children.
COBRA continuation coverage is a temporary continuation of coverage that generally lasts for 18 months due to employment termination or reduction of hours of work. Certain qualifying events,
or a second qualifying event during the initial period of coverage, may permit a beneficiary to receive a maximum of 36 months of coverage.
There are also ways in which this 18-month period of COBRA continuation coverage can be extended:
Disability extension of 18-month period of COBRA continuation coverage: If you or anyone in your family covered under the Plan is determined by Social Security to be disabled and you notify the Plan Administrator in a timely fashion, you and your entire family may be entitled to get up to an additional 11 months of COBRA continuation coverage, for a maximum of 29 months. The disability would have to have started at some time before the 60th day of COBRA continuation coverage and must last at least until the end of the 18-month period of COBRA continuation coverage.
Second qualifying event extension of 18-month period of continuation coverage: If your family experiences another qualifying event during the 18 months of COBRA continuation coverage, the spouse and dependent children in your family can get up to 18 additional months of COBRA continuation coverage, for a maximum of 36 months, if the Plan is properly notified about the second qualifying event. This extension may be available to the spouse and any dependent children getting COBRA continuation coverage if the employee or former employee dies; becomes entitled to Medicare benefits (under Part A, Part B, or both); gets divorced or legally separated; or if the dependent child stops being eligible under the Plan as a dependent child. This extension is only available if the second qualifying event would have caused the spouse or dependent child to lose coverage under the Plan had the first qualifying event not occurred.
Are there other coverage options besides COBRA Continuation Coverage?: Yes. Instead of enrolling in COBRA continuation coverage, there may be other coverage options for you and your family through the Health Insurance Marketplace, Medicare, Medicaid, Children’s Health Insurance Program (CHIP), or other group health plan coverage options (such as a spouse’s plan) through what is called a “special enrollment period.” Some of these options may cost less than COBRA continuation coverage. You can learn more about many of these options at www.healthcare.gov.
Can I enroll in Medicare instead of COBRA continuation coverage after my group health plan coverage ends?: In general, if you don’t enroll in Medicare Part A or B when you are first eligible because you are still employed, after the Medicare initial enrollment period, you have an 8-month special enrollment period to sign up for Medicare Part A or B, beginning on the earlier of
• The month after your employment ends; or
• The month after group health plan coverage based on current employment ends.
If you don’t enroll in Medicare and elect COBRA continuation coverage instead, you may have to pay a Part B late enrollment penalty and you may have a gap in coverage if you decide you want Part B later. If you elect COBRA continuation coverage and later enroll in Medicare Part A or B before the COBRA continuation coverage ends, the Plan may terminate your continuation coverage. However, if Medicare Part A or B is effective on or before the date of
the COBRA election, COBRA coverage may not be discontinued on account of Medicare entitlement, even if you enroll in the other part of Medicare after the date of the election of COBRA coverage.
If you are enrolled in both COBRA continuation coverage and Medicare, Medicare will generally pay first (primary payer) and COBRA continuation coverage will pay second. Certain plans may pay as if secondary to Medicare, even if you are not enrolled in Medicare.
For more information visit https://www.medicare.gov/medicare-and-you.
If you have questions: Questions concerning your Plan or your COBRA continuation coverage rights should be addressed to the contact or contacts identified below. For more information about your rights under the Employee Retirement Income Security Act (ERISA), including COBRA, the Patient Protection and Affordable Care Act, and other laws affecting group health plans, contact the nearest Regional or District Office of the U.S. Department of Labor’s Employee Benefits Security Administration (EBSA) in your area or visit www.dol.gov/ebsa. (Addresses and phone numbers of Regional and District EBSA Offices are available through EBSA’s website.) For more information about the Marketplace, visit www.HealthCare. gov.
Keep your Plan informed of address changes: To protect your family’s rights, let the Plan Administrator knowabout any changes in the addresses of family members. You should also keep a copy, for your records, of any notices you send to the Plan Administrator.
Plan Contact Information
County of Amherst
ATTN: Caitlin Jack, Director of Human Resources
P.O. Box 390 Amherst, VA 24521
Phone: 434-946-9420
Fax: 434-946-9305
COBRA Administrator for Dental, Vision, FSA Coverage: Flex Facts
1200 River Avenue, Ste. 10E Lakewood, NJ 08701
Phone: 877-943-2287
Fax: 877-747-8564
COBRA Administrator for The Local Choice Benefits: DHRM – Office of Health Benefits
101 N.th Street, 13th Floor Richmond, VA 23219
Phone: 888-642-4414
We collect Non Public Information (NPI) about our customers to provide them with insurance products and services. This may include telephone number, address, date of birth, occupation, income and health history. We may receive NPI from your applications and forms. medical providers, other insurers, employers, insurance support organizations, and service providers.
We share the types of NPI described above primarily with people who perform insurance, business, and professional services for us, such as helping us pay claims and detect fraud. We may share NPI with medical providers for insurance and treatment purposes. We may share NPI with an insurance support organization. The organization may retain the NPI and disclose it to others for whom it performs services. In certain cases, we may share NPI with group policy holders for reporting and auditing purposes. We may share NPI with parties to a proposed or final sale of insurance business or for study purposes. We may also share NPI when otherwise required or permitted by law, such as sharing with governmental or other legal authorities. When legal necessary, we ask your permission before sharing NPI about you our practices apply to our former, current and future customers.
Please be assured we do not share your health NPI to market any product or service. We also do not share any NPI to market non financial products and services. For example, we do not sell your name to catalog companies.
The law allows us to share NPI as described above (except health information) will affiliates to market financial products and services. The law does not allow you to restrict these disclosures. We may also share with companies that help us market our insurance products and services, such as vendors that provide mailing services to us. We may share with other financial institution to jointly market financial products and services. When required by law, we ask your permission before we share NPI for marketing purposes.
When other companies help us conduct business, we expect them to follow applicable privacy laws.
We do not authorize them to use or share NPI except when necessary to conduct the work they are performing for us or to meet regulatory or other governmental requirements.
Our affiliated companies, including insurers and insurance service providers, may share NPI about you with each other. The NPI might not be directly related to our transaction or experience with you. It may include financial or other personal information such as employment history. Consistent with the Fair Credit Reporting Act, we ask your permission before sharing NPI that is not directly related to our transaction or experience with you.
We have physical, electronic and procedural safeguards that protect the confidentiality and security of NPI. We give access only to employees who need to know the NPI to provide insurance products or services to you.
You may request access to certain NPI we collect to provide you with insurance products and services, You must make your request in writing and send it to the address, telephone number and policy number if we have issued a policy. If you request, we will send copies of the NPI to you. If the NPI includes health information, we may provide the health information to you through a health care provider you designate. We will also send you information related to disclosures. We may charge a reasonable fee to cover our copying costs. This section applies to NPI we collect tor provide you with coverage. It does not apply to NPI we collect in anticipation of a claim or civil or criminal proceeding.
If you believe NPI we have about you is incorrect, please write us. Your letter should include your full name, address, telephone number and policy number if we have issued a policy. Your letter should also explain why you believe the NPI is inaccurate. If we agree with you, we will correct the NPI and notify you of the correction. We will also notify any person who may have received the incorrect NPI from us in the past two years if you ask us to contact that person.
If we disagree with you, we will tell you we are not going to make the correction, We will give the reason(s) for our refusal. We will also tell you that you may submit a statement to us.
Your statement should include the NPI you believe is correct. It should also include the reasons(s) why you disagree with our decision not to correct the NPI
in our files. We will file your statement with the disputed NPI. We will include your statement any time we disclose the disputed NPI. We will also give the statement to any person designated by your if we may have disclosed the disputed NPI to that person int he past two years.
Information regarding your insurability will be treated as confidential. Colonial or its reinsure(s) may, however, make a brief report thereon to the Medical Information Bureau, a nonprofit membership organization of life insurance companies which operates an information exchange on behalf of its members. If you apply to another Bureau member company for life or health insurance coverage, or a claim for benefits is submitted to such company, the Bureau, upon request, will supply such company with the information in its file.
Upon receipt of a request from you, the Bureau will arrange disclosure of any information it may have in your file. If you question the accuracy of information in the Bureau’s file, you may contact the Bureau and seek a correction in accordance with the procedure set forth in the federal Fair Credit Reporting Act. The address of the Bureau’s information office is: 50 Braintree Hill Park, Suite 400, Braintree, MA 02184-8734, telephone (617) 4263660.
Colonial or its reinsure may also release information in its file to other life insurance companies to whom you may apply for life or health insurance or to whom a claim for benefits may be submitted.
We are committed to being there for you and your family at every stage of life. Pierce Group Benefits makes it easy to stay protected!
The following benefits can be self-enrolled online or by contacting PGB Employee Services, with Individual and Family coverage options available for most plans. You are eligible to sign-up the first day after the end date of your employer-sponsored plan.
Your individual supplemental/voluntary policies through Colonial Life are portable! To transfer your benefits from payroll deduction to direct billing or automatic bank draft, please call Employee Services at 800-387-5955 within 30 days of becoming unemployed, switching careers, or retiring.
If you are transferring from a current PGB client to another, some benefits may be eligible for transfer. Please call Employee Services at 800-387-5955 for assistance.
Please visit www.piercegroupbenefits.com/individualcoverage or call 800-387-5955 for more information on these policies, as well as to enroll/continue your benefits.

Pierce Group Benefits is a leading full-service employee benefits administration and consulting agency serving employer groups across the Southeast. By leveraging market strength, exclusive partnerships, and industry expertise, we deliver trusted advice, products, and solutions that benefit employers and employees alike; delivered by one team and driven by one purpose — together we can do more.
