






In our recent webinar we were introduced to the ‘Evidence Pie’ which is a practical tool used to support building the evidence base to inform local decision making and offers a common language for discussing research and evidence across sectors, that can be adapted to meet local needs.
This e-bulletin includes articles from projects and initiatives that use practical methods, resources and examples that others could benefit from.
Getting to know our members: Adam Jones
Shared Lives: Building a bridge from hospital back to home
Tess Seymour,Communications and Engagement Officer, Ategi
Addressing inequalities in bowel cancer screening - Cancer Research UK’s tool for assessing interventions
Hope Walters,Strategic Evidence Manager, Cancer Research UK
Emma Fox,Strategic Evidence Engagement Manager, Cancer Research UK
The Evidence Pie: Putting Evidence at the Heart of Better Decisions
Amy Lloyd, Research and Evidence Lead, Rhondda Cynon Taf Health Determinants Research Collaboration On
Dr Michaela James,Research Officer, Swansea University

We are getting to know our members and would like to help our members to get to know each other. This month we’re meeting Adam Jones, Senior Policy Officer.
Please tell us a bit about yourself and your current work
I’ve recently returned to Public Health Wales after four years working with Welsh Government on the design, delivery and implementation of the Basic Income for Care Leavers in Wales pilot. In my Public Health Wales role, I have worked on policy analysis and research and contributed to policy design on a range of topics, most notably sexual health, the potential implications of Brexit on public health in Wales and some of the economic factors affecting public health.
What motivated you to join this network?
Once upon a time I was one of the Network Coordinators, from 2009-2016, as the All Wales Sexual Health Network
Coordinator, and was involved in the development of Public Health Network Cymru from its launch. I’ve always believed that the Network is a fantastic vehicle for encouraging collaboration and sharing knowledge and experience, as it’s always been my belief that no one person or service can address the challenges that public health in Wales or beyond faces. We need to work together, and the Network helps to facilitate that.
What are the benefits for you in being a member of this network?
It’s vital to be kept up-todate with developments in Wales, and to learn from the experiences of others. The webinars and events held by the Network certainly help with this. The Network has always shone a light on the work of the whole public health system.
What is one thing you would like to share with other members of the network?
Keep going! This is never an easy line of work, there are often new or emerging challenges, and it often takes a long time to see improving outcomes, but we need to be patient, persistent and continually listen, learn and improve.
Are you happy for your email address to be shared on the e-bulletin?
Yes – adam.jones2@wales.nhs. uk
If you would like to feature in a future edition, please email us at publichealth.network@ wales.nhs.uk

The challenge: leaving hospital safely
Across the UK, many people are medically ready to leave hospital but remain there longer than needed because the right support is not in place at home. These delays can affect people’s wellbeing and independence and place additional pressure on hospital beds and staff. Social care-related delays now account for a significant proportion of delayed hospital discharges (1). For adults with additional needs, leaving hospital can feel daunting. Returning straight home is not always safe or possible,
yet prolonged hospital stays carry risks of deconditioning and declining mental wellbeing. Shared Lives offers a community-based, personcentred alternative that helps bridge the gap between hospital care and life back in the community.
Shared Lives: a community-based approach
Shared Lives is a model of support where adults with additional needs are supported by approved carers in real home environments. Support is based on everyday life, relationships, and
belonging rather than clinical care, helping people build confidence, routines, and independence.
For people leaving hospital, Shared Lives can offer shortterm support in a safe, home-like setting when returning directly home is not suitable. This approach aligns with national guidance on hospital discharge, which highlights the importance of addressing people’s social needs alongside medical care to support recovery and reduce readmissions (2).
In Wales, the NHS Wales Home First principle

recognises that for most people, home, or a homelike environment, is the best place to recover. Longer hospital stays can contribute to loss of strength, reduced independence, and poorer mental well-being (3).
Evidence and local context
Evidence from an NDTi evaluation of a Shared Lives intermediate care pilot found that short-term, family-based support can help people regain confidence, rebuild routines and reconnect with their communities following hospital discharge (4). Local initiatives such as Safe at Home in Cardiff and Vale also demonstrate the value of community-based alternatives, reducing pressure on hospitals while improving outcomes for individuals (5).
A real example: Dennis’ story
Dennis, a man in his 70s from Cardiff, spent four months in hospital following a serious health episode. Although medically ready for discharge, he did not feel safe returning home. Through Shared Lives, Dennis moved into a carer’s home for a short period, receiving non-clinical, everyday support such as shared meals, companionship and gentle encouragement.
This stable environment helped Dennis rebuild confidence and feel secure while longer-term housing was arranged. After a few weeks, he was able to move
into a new flat with improved mental well-being, increased independence, and stronger community connections. Shared Lives provided continuity, reassurance, and practical support at a critical transition point.
Shared Lives shows how relationship-based, community care can play a vital role in supporting people to leave hospital safely and avoid unnecessary extended stays. Home-like environments, time, and human connection are often as important as formal care services in recovery.
Health and social care partners are encouraged to consider Shared Lives as part of local discharge pathways and community support options. By working together across systems, we can reduce pressure on hospitals, support independence, and help people rebuild their lives in ways that feel stable, meaningful, and their own
. Further information and references
Learn more about Shared Lives with Ategi: https://www.ategi.org.uk/ becoming-a-shared-livescarer/
Shared Lives: Building a bridge from hospital back to home (Ategi): https://www.ategi.org.uk/ news/shared-lives-building-abridge-from-hospital-back-tohome/
References Care Quality Commission, The state of health care and adult social care in England 2023–24 — https:// assets.publishing.service.gov.uk/media/671b5ce3044f28e776c609dc/ care-quality-commissionthe-state-of-health-care-andadult-social-care-in-england2023-to-2024.pdf
GOV.WALES, Home First: your hospital discharge — https://www.gov.wales/homefirst
National Development Team for Inclusion (NDTi), Shared Lives Intermediate Care — https://www.ndti.org. uk/resource/shared-livesintermediate-care/ Home First: Reducing hospital stays and improving patient wellbeing, Cardiff and Vale University Health Board — https://www.gvs.wales/ news/home-first-reducinghospital-stays-and-improvingpatient-wellbeing/
Safe at Home supports patients to receive urgent care at home, Cardiff and Vale UHB — https://cavuhb.nhs. wales/news/latest-news/safeat-home-supports-patients-toreceive-urgent-care-at-home/
Research | Practice | Commentary
Hope Walters,
Strategic Evidence Manager, Cancer Research UK
Bowel cancer is the fourth most common cancer in the UK, and survival is significantly higher when it is diagnosed early. Screening plays a vital role, with most cancers detected through screening identified at an early stage (stage I or II). In Wales, around a third (34.5%) of people invited to take part in bowel screening do not participate, and uptake is considerably lower in some demographic groups. Investigating barriers and facilitators to taking part in bowel cancer screening and designing interventions to support informed participation and reduce inequalities is
Emma Fox, Strategic Evidence Engagement Manager, Cancer Research UK
an active area of research. However, it can be a difficult research space to navigate with little consensus on which interventions are most effective.
Cancer Research UK’s Strategic Evidence team carried out a research mapping exercise to better understand who is less likely to take part in screening and why. This brought together evidence on demographic groups with lower uptake and the barriers or facilitators they report. Then Behaviour change frameworks - including the Capability, Opportunity, Motivation Behaviour model
(COM B) and the Integrated Screening Action Model (I SAM) - were applied to identify potential interventions that could address these barriers. Each intervention was assessed for strength of evidence, likely impact on participation, and potential to reduce inequalities.
The findings were brought together in an interactive resource known as the Bowel Grid. This tool presents evidence in an accessible, userfriendly format to support those working to increase informed participation in bowel screening. By combining insights from the tool with
local data and community knowledge, teams can identify evidence-based interventions that are likely to help more people take part in screening. Examples of interventions included in the tool include telephone reminders/ advice, annual re-invitation, and providing information opportunistically during healthcare appointments.
Since its launch in October 2025, the Bowel Grid has supported Bowel Screening Wales in shaping their strategy to reduce inequalities in screening participation. Peyton Jones, Quality and Service Improvement Manager, said: “The Cancer Research UK Bowel Grid is a valuable resource for Bowel Screening Wales, enabling us to prioritise our equality work plans in areas supported by robust evidence. At the same time, it highlights gaps in the current evidence base, allowing us to explore these areas further and develop projects that enhance the bowel grid’s usefulness for future research.”
Feedback from users across the UK has been positive, with many reporting that the tool helps guide and prioritise local action.
The Bowel Grid offers a clear, accessible way to explore evidence on interventions that support informed participation in bowel screening and
address inequalities. We encourage health professionals, commissioners and programme leads to use the tool to identify approaches that best fit their local populations and to explore opportunities to implement and evaluate interventions. Strengthening the evidence base will help ensure more people benefit from early diagnosis.
Download the tool to explore the data and evidence, as well as practical tools and guidance for implementation and evaluation of interventions to reduce inequalities.
For questions or feedback, email seinbox@cancer.org.uk
Research
Rhondda Cynon Taf Health Determinants Research
Collaboration (RCT HDRC) has placed the Evidence Pie at the heart of its mission to embed evidence-informed decision making across Rhondda Cynon Taf Council. Developed to respond to varied understandings of what “evidence” means in practice, the Evidence Pie provides a shared language that is accessible to Council staff, elected members, voluntary sector organisations,
and the public. Its purpose is to establish a common framework that supports consistent conversations about the value of combining different forms of evidence.
The Evidence Pie has been used to raise awareness of the value of using different types of evidence. It became clear early on that staff, elected members, partner organisations and the public all interpreted ‘evidence’ differently, sometimes leading
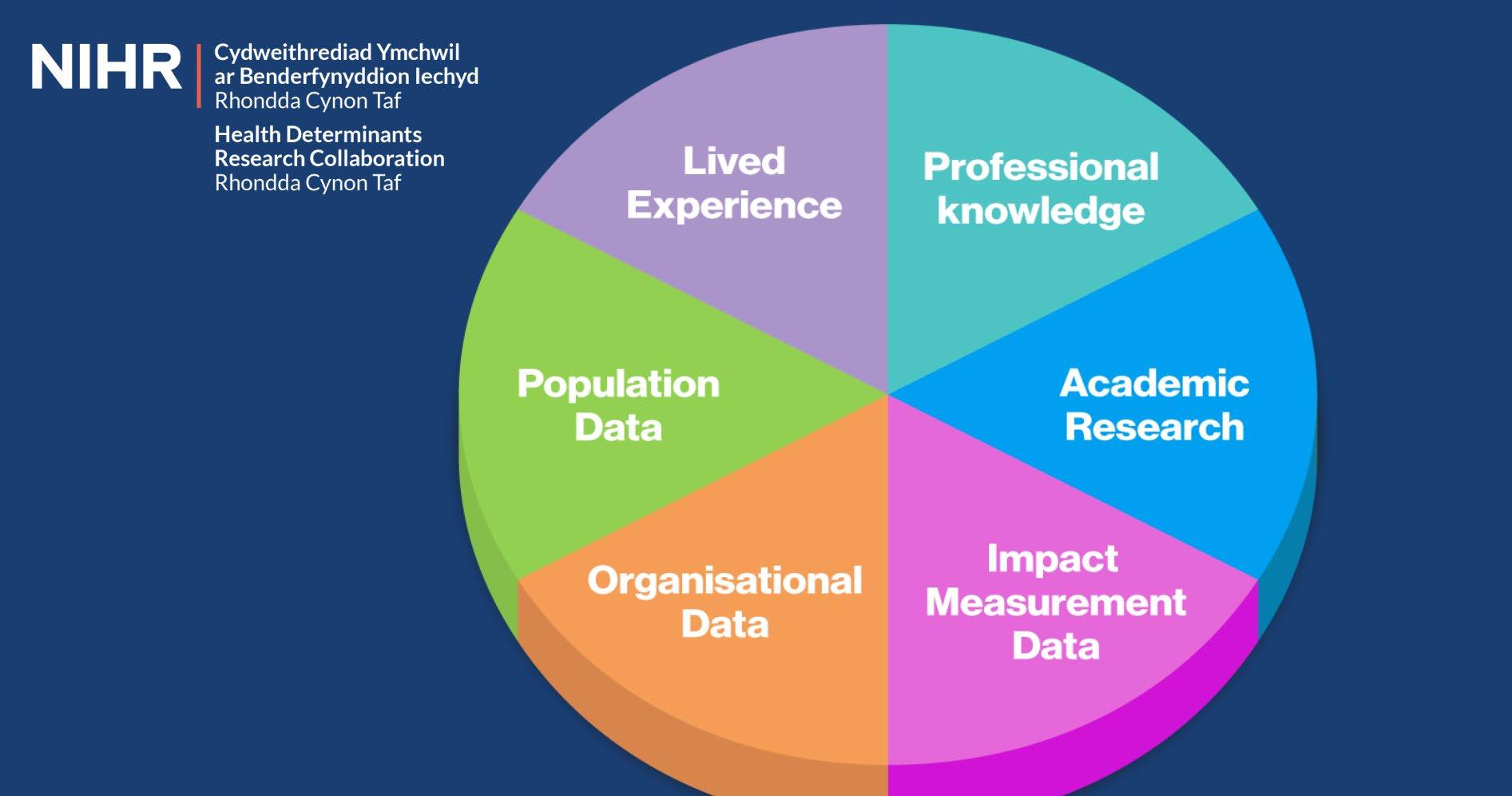
to narrow or inconsistent approaches to gathering and using information. The Evidence Pie addresses this by setting out six equally important types of evidence: lived experience, professional knowledge, organisational data, population-level data, impact measurement, and academic research. These categories broaden understanding of what counts as evidence and legitimise the insight that staff and communities already hold,
reinforcing that evidence is more than numbers, and that qualitative experience holds equal weight.
The Evidence Pie has been integrated into formal training and tailored support to help staff develop the skills and confidence to use different forms of evidence. Training workshops have been delivered across the Council, and integrated into senior and middle management courses, emphasising that evidence-informed decision making is everyone’s responsibility and that all staff, regardless of role, contribute expertise in at least one type of evidence. The approach has enabled teams to reflect on their current strengths and gaps, identify opportunities for improvement, and build confidence in using evidence to inform their practice. The Evidence Pie has enabled open discussion about the realities of evidence use and is helping to cultivate a supportive culture where evidence is routinely considered, and where staff feel more able to discuss challenges honestly.
The Evidence Pie is also shaping the systems that support evidence-informed decision making. Council structures, policies, and processes have been adapted to encourage use of different forms of evidence. Service areas now report on the different types of evidence they use to assess impact. Six
members of the public have been recruited to a Community Voice Team to help integrate lived experience into Council decisions. Rhondda Cynon Taf Health Determinants Research Collaboration is also strengthening infrastructure between partner organisations to address knowledge gaps and create opportunities to share expertise, including through collaborative research proposals that meet the needs of staff and residents.
Overall, the Evidence Pie is enabling Rhondda Cynon Taf Health Determinants Research Collaboration to build a shared language, increase organisational confidence in using varied evidence, and establish a clear, inclusive framework for improving decision making across Council services. We are proud that many other local authorities across the UK are drawing on the learning from the Evidence Pie in their own work.
For more information, please visit https://makeachange. rctcbc.gov.uk/
or click here to watch a recent webinar explaining more about The Evidence Pie

Dr Michaela James, Research Officer, Swansea University
Schools are a key part of children’s daily lives, yet their voices are often missing from the data used to shape education and public health policy. HAPPEN (Health and Attainment of Pupils in a Primary Education Network) was created to change that. Co-produced with schools, HAPPEN is a child-centred research and feedback tool that helps schools better
understand pupils’ health and wellbeing while contributing to a unique national dataset. HAPPEN supports schools to make evidence-informed decisions and provides policymakers with timely, relevant insight into what really matters to children.
HAPPEN is a Wales-wide school-based survey and research network that captures
children’s self-reported experiences of wellbeing, play, relationships, screen use, physical activity and mental health. The survey is designed to be accessible and engaging for children, ensuring their perspectives are central rather than filtered through adult assumptions. We have currently had over 50,000 responses to the HAPPEN Survey with 650 schools
registered to take part.
Schools receive annual tailored reports that support reflection, school improvement planning and conversations with pupils, staff, parents and local partners. In HAPPEN, schools are not just data providers; they help shape the questions, interpretation and outputs.
The subsequent enriched dataset has been used to explore key public health priorities [1–4]. It allows researchers and policymakers to respond quickly to emerging issues while also tracking longer-term trends. This combination of rapid response and longitudinal insight is novel, and vital.
HAPPEN has empowered schools with data they can understand and use. Schools report greater confidence in identifying priorities, advocating for resources, and embedding wellbeing into everyday practice. Particularly in line with the Curriculum for Wales Health and Wellbeing Area of Learning Experience. HAPPEN provides robust, child-centred evidence that reflects lived experience rather than proxy measures. Findings from HAPPEN have informed local and national discussions on wellbeing, ensuring that children’s voices are present in decision-making. Current work
includes an evaluation of the national roll-out of free school meals, wellbeing in additional learning needs, screen time use and engagement, healthy relationships, play (and play sufficiency).
HAPPEN shows that it is possible to generate highquality, policy-relevant data while directly benefiting schools and pupils. Our call to action is simple: invest in approaches that value children’s perspectives, empower schools, and connect research to real-world decisions. If we want effective public health and education policy, we must start by listening to children.
Further information and resources: HAPPEN Wales HAPPEN Factsheets
1. James M, Marchant E, Defeyter MA, Woodside J, Brophy S. Impact of school closures on the health and well-being of primary school children in Wales (UK): a routine data linkage study using the HAPPEN Survey (20182020). BMJ Open. 2021;11. https://doi.org/10.1136/ bmjopen-2021-051574.
2. Marchant E, Todd C, James M, Crick T, Dwyer R, Brophy S. Primary school staff perspectives of school closures due to COVID-19, experiences
of schools reopening and recommendations for the future: a qualitative survey in Wales. PLoS One. 2020. https://doi.org/10.1101/2020. 11.06.20227108.
3. James M, Rasheed M, Bandyopadhyay A, Mannello M, Marchant E, Brophy S. The Effect COVID Has Had on the Wants and Needs of Children in Terms of Play: Text Mining the Qualitative Response of the Happen Primary School Survey with 20,000 Children in Wales, (UK) between 2016 and 2021. Int J Environ Res Public Health. 2022;19:12687. https://doi.org/10.3390/ ijerph191912687.
4. James M, Adebayo M, Bianchim MS, Hughes L, Mannello M, Marchant E, et al. To what extent does selfreported physical activity impact children’s wellbeing and mental health? Insights from school-aged children in Wales. PLoS One. 2025;20 5 May. https://doi.org/10.1371/ journal.pone.0313970.

Claire Llewellyn, Student in NPTC Group of Colleges, Trinity St Davids University South Wales
A Silent Killer: My Story is a short awareness film about hypertension and the devastating consequences of not taking prescribed medication. The film shares my personal experience of being diagnosed with high blood pressure, feeling well, and not realising the serious risks involved.
Hypertension is often symptom-free, which can lead people to underestimate its danger. In my case, this resulted in a brain haemorrhage, permanent brain damage and epilepsy. This project is important because it puts a real face to an invisible condition and highlights how a simple daily tablet can prevent lifechanging outcomes. My film is a personal, first-hand account of living with untreated hypertension and its longterm impact. In 2015, I was diagnosed with high blood pressure but felt healthy and experienced no warning signs. Like many people, I did not understand why hypertension is often described as a “silent killer”. The film explains how damage can occur long before symptoms appear and why medication adherence is critical.
Several years later, I suffered a brain haemorrhage while alone at home, caused by uncontrolled blood pressure. My family were told that the next 24 hours were critical and that my condition could change minute by minute. I survived, but I now live with permanent brain damage and epilepsy, requiring around 30 tablets a day to manage my health.
Hypertension is a major risk factor for stroke and brain haemorrhage and is widely recognised as a leading cause of preventable illness. However, many people still do not take their medication as prescribed because they feel well. This film uses lived experience rather than medical language to communicate risk in a way that is relatable, emotional and memorable, supporting public health messages around prevention and early intervention. The film has helped start honest conversations about hypertension, medication and risk, particularly among people who previously believed high blood pressure was not serious. Viewers have reported that the film made them reflect on their own health and medication habits and encouraged them to take
their condition more seriously. By showing the real, long-term consequences of untreated hypertension, the project has increased awareness that missing medication can have irreversible outcomes.
Public Health Wales have requested to share the film within their meetings, recognising its value as a powerful education and engagement tool. The key message is simple: take your medication, even when you feel fine. Hypertension does not always cause symptoms, but the damage it causes can be permanent and life changing. A few seconds a day to swallow a tablet can prevent strokes, brain injury and lifelong disability.
My call to action is for individuals to take responsibility for their prescribed treatment, for families to encourage loved ones to do the same, and for health organisations to use real stories alongside clinical information. Lived experience can save lives.
For further information about the film and this story please contact Claire Llewellyn: 338927@nptcgroup.ac.uk




New Parent Health Information Resources published by Public Health Wales –Supporting Families Across Wales
This webinar highlighted how embedding these resources into your programmes and services and offering them to our families, help to create a consistent, trusted parenting offer across Wales.
Explore our video library on our website
Introducing the ‘Evidence Pie’ with Health Determinants Research Collaboration (HDRC) Rhondda Cynon Taf
Join us for this webinar with Zoe Lancelott and Rhianydd Davies from the National Institute for Health and Care Research (NIHR) Health Determinants Research Collaboration (HDRC), Rhondda Cynon Taf.
Launch of Teg I Bawb / Fair for All: A Strategic Action Plan to address health inequalities through Primary Care
This webinar launches a Fairer Primary Care – Fair for All, Teg I Bawb, action plan that has been developed by reviewing the evidence, data and iterative rounds of face to face and online workshops, and extensive engagement and collaboration with patients, health professionals, senior leaders, community groups, and experts by experience across the Primary Care system in Wales.
View all our videos


Tooth decay in young children in Wales continues to fall, but inequalities remain
24-02-2026

Wales leads globally in recognising social connections as a public health priority
18-02-2026

Welsh public backs stronger support for women’s health and wellbeing after pregnancy
11-02-2026
Loneliness, social isolation and social connection in Wales: A public health perspective
Public Health Wales
Trade, Trade Agreements and Tariffs and the Impact on Health, Wellbeing and Equity in Wales
Public Health Wales

Every child in Wales deserves the best start in life. To help families feel confident and supported, Public Health Wales, on behalf of Welsh Government, created a complete, evidence-based set of four resources for parents covering the early years.
At our recent webinar we heard how using these resources within programmes and services and offering them to families, helps to create a consistent, trusted parenting offer across Wales. This helps to reduce misinformation, strengthen key messages, and improve outcomes, while aligning with national strategies.
For our upcoming ebulletin, we would like to hear how you are using these (or similar) resources, when working with parents. We welcome examples of work from national, regional, or local programmes. We are particularly interested in
• Short case studies
• Practical tips and examples
• Lessons learned
• Ideas that others across Wales could adopt or
adapt.
Our article submission form will provide you with further information on word count, layout of your article and guidance for images.
Please send articles to publichealth.network@wales. nhs.uk by 19 March 2026