Otolaryngology –Head and Neck Surgery
Chair’s Letter
In this edition of our newsletter, I’m delighted to share several exciting updates that reflect the continued growth and momentum of our Department of Otolaryngology – Head and Neck Surgery.
We’re especially pleased to welcome Dr. Nicole Ruszkay back to our pediatric otolaryngology team. A fellowship-trained pediatric otolaryngologist and former Hershey Medical Center resident, Dr. Ruszkay returns as an attending physician with exceptional expertise and a passion for caring for children. It’s rewarding to see one of our own come home to advance our mission and mentor the next generation.
This year also marks the launch of a unique collaboration with Sight & Sound Theatres to provide proactive vocal care for their professional performers – a partnership that beautifully blends clinical insight with the demands of the performing arts. You’ll learn more about the team leading this initiative in the pages ahead.
It was a pleasure reconnecting with so many alumni at the recent academy meeting in Indianapolis. Your ongoing engagement and support remain central to our collective success. We also encourage you to register for the upcoming Seaside Symposium in Otolaryngology – Head and Neck Surgery, taking place in Clearwater Beach from February 6-8, 2026.
Thank you for your partnership and for being an essential part of our community. Enjoy this edition, and warmest wishes for a joyful, healthy winter season.
Sincerely,

IN THIS EDITION
• Meet Dr. Ruszkay
• Thyroid Cancer Symptoms You Shouldn’t Ignore
• Seaside Symposium in Clearwater Beach
• Why Are My Ears Ringing? Tinnitus and Other Hearing Problems
• New Partnership with Sight & Sound Theatres
• Pediatric Inspire Implant
• Alumni and Friends Reception
• Recent Publications, Presentations, and Awards

David Goldenberg, MD, FACS Professor and Chair



Physician Spotlight
Meet Dr. Nicole Ruszkay
Dr. Nicole Ruszkay joined the Division of Pediatric Otolaryngology at Penn State Health in October 2025. She recently completed her fellowship training at the University of North Carolina Hospitals, bringing advanced expertise in pediatric otolaryngology – head and neck surgery.
Dr. Ruszkay provides comprehensive care for children with a wide range of conditions – from common issues such as ear infections to complex disorders like airway anomalies and head and neck tumors. She chose this specialty because of her passion for improving children’s health.

“The most rewarding part of being a pediatric otolaryngologist is helping to restore a child’s health and ability to connect with the world around them.”
A Chester County native, Dr. Ruszkay earned her medical degree from Drexel University College of Medicine and completed her residency in otolaryngology – head and neck surgery at Penn State Health Milton S. Hershey Medical Center, where she developed a strong foundation in caring for pediatric patients with complex needs. Upon graduation, she was honored with the Outstanding Otolaryngology Resident Award, as voted on by the otolaryngology faculty.
She has presented research at national, regional, and local conferences. Her interests include clinical outcomes, quality improvement, tracheostomy care, and medical education. During residency, Dr. Ruszkay was awarded a faculty research grant for her project focused on adenoid tissue microarchitecture in recurrent tonsillitis versus obstructive sleep apnea.
Dr. Ruszkay is also a member of the Alpha Omega Alpha Medical Honor Society, reflecting her commitment to excellence in medicine.
After completing residency training at Hershey Medical Center, we are proud to welcome Dr. Nicole Ruszkay back as an attending pediatric otolaryngologist and assistant professor at Penn State College of Medicine. She joins our pediatric otolaryngology team alongside Drs. Allison Keane, Gil Zoizner-Agar, and Victor Da Costa.
Dr. Ruszkay sees patients at the Otolaryngology – Head and Neck Surgery Clinic in Suite 400 of the University Physician Center in Hershey.
Outside of work, she enjoys boating, crabbing, cheering on the Philadelphia Eagles, and spending time with family and friends.



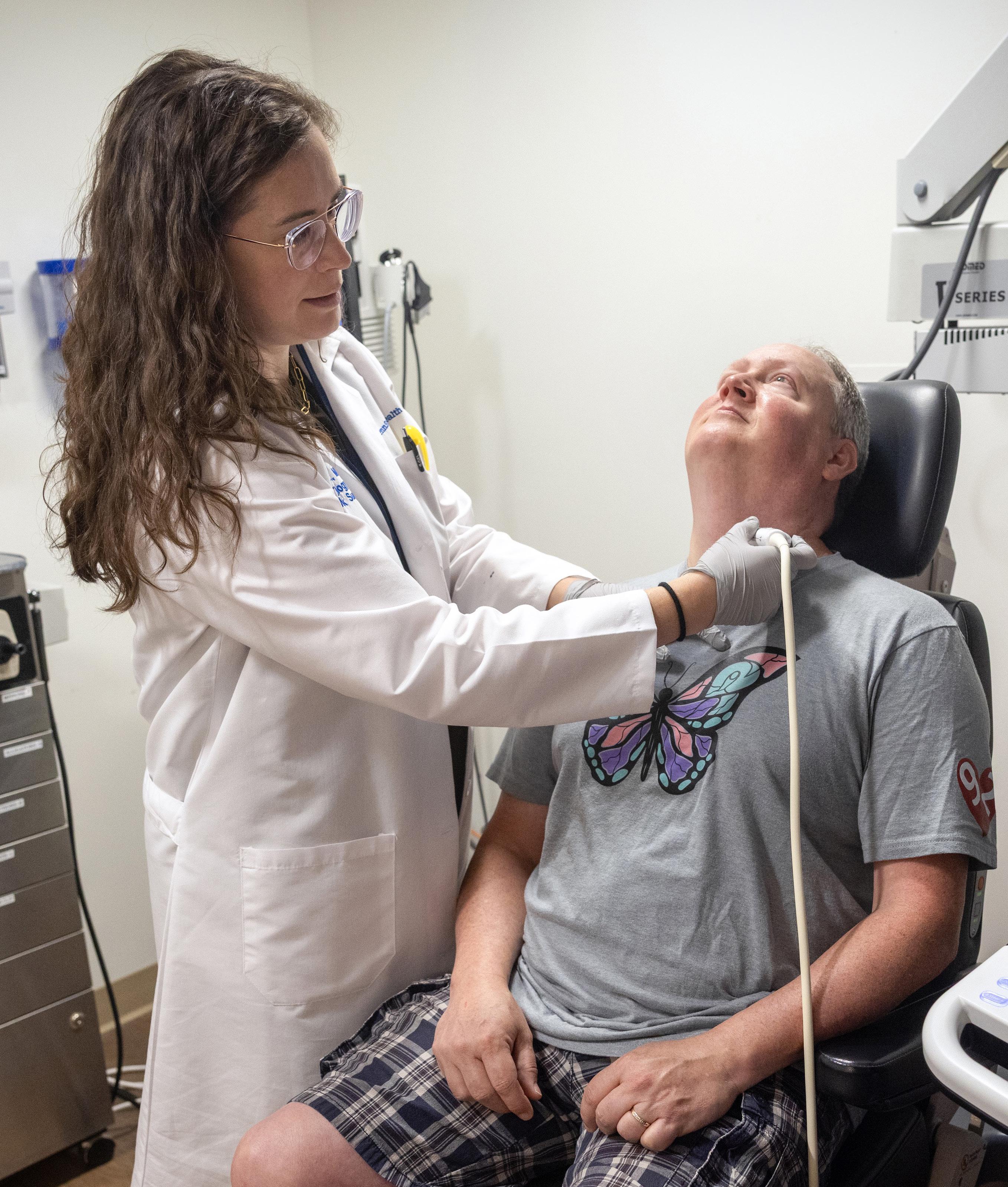
Thyroid Cancer Symptoms
You Shouldn’t Ignore
Tom Murphy, a 54-year-old from East Petersburg, was driving home from Myrtle Beach, South Carolina, late last summer when his friend urged him to see a doctor about his persistent cough.
Murphy went to his primary care physician. As she checked his neck, she paused. Suddenly, Murphy recalled something.
“There were times before when I felt like there might be a bump on the left side of my neck, but nothing that really jumped out,” he says. “I thought maybe it was just a muscle.”
His doctor felt a lump there, too. It signaled a bigger problem unrelated to his cough. Imaging tests and a biopsy confirmed it – the lump was thyroid cancer.
“Sometimes people overlook thyroid cancer symptoms because they assume it’s nothing or they’re too young for cancer,” says Dr. Emily Funk, head and neck surgical oncologist and microvascular reconstructive surgeon at Penn State Health Otolaryngology – Head and Neck Surgery. “It’s always worth getting evaluated because the earlier you identify thyroid cancer, the easier it is to treat.”
The American Cancer Society estimates that about 44,020 Americans have been or will be diagnosed with thyroid cancer by
the end of 2025. About 2,290 will die from it.
What is thyroid cancer?
Your thyroid is a butterfly-shaped gland toward the front of your neck, just under your Adam’s apple. What does the thyroid do? A lot. It secretes hormones that regulate body temperature and metabolism.
“It acts like the body’s thermometer,” Funk says.
Thyroid cancer develops when thyroid cells mutate and multiply. Some risk factors include high radiation exposure or some inherited genetic mutations. However, the cause of most cases is unknown.
Thyroid cancer is classified into four types:
• Papillary thyroid cancer: Makes up 8 in 10 thyroid cancers and is the most treatable. This is the type that Murphy had.
• Follicular thyroid cancer: Makes up 1 in 10 thyroid cancers. It’s more likely to spread, making treatment more difficult.
• Medullary thyroid cancer: Less than 5% of thyroid cancers, affecting the thyroid’s C cells, which regulate calcium.
• Anaplastic thyroid cancer: Makes up 2% of thyroid cancers. It can grow and spread quickly.
Who’s at risk?
Thyroid cancer is an uncommon cancer overall, but one of the most common among young adults. The average age at diagnosis is 51.
“I see many patients with thyroid cancers in their 30s, 40s and 50s,” Funk says. “While not common, we sometimes see it in teenagers, too.”
Thyroid cancer is three times more common in women than in men. It’s 40% to 50% less common in Black people than in any other racial or ethnic group.
How is thyroid cancer detected?
A painless lump or neck swelling is the most common symptom. Some people also notice hoarseness or trouble swallowing.
Murphy’s experience, where a doctor notices a
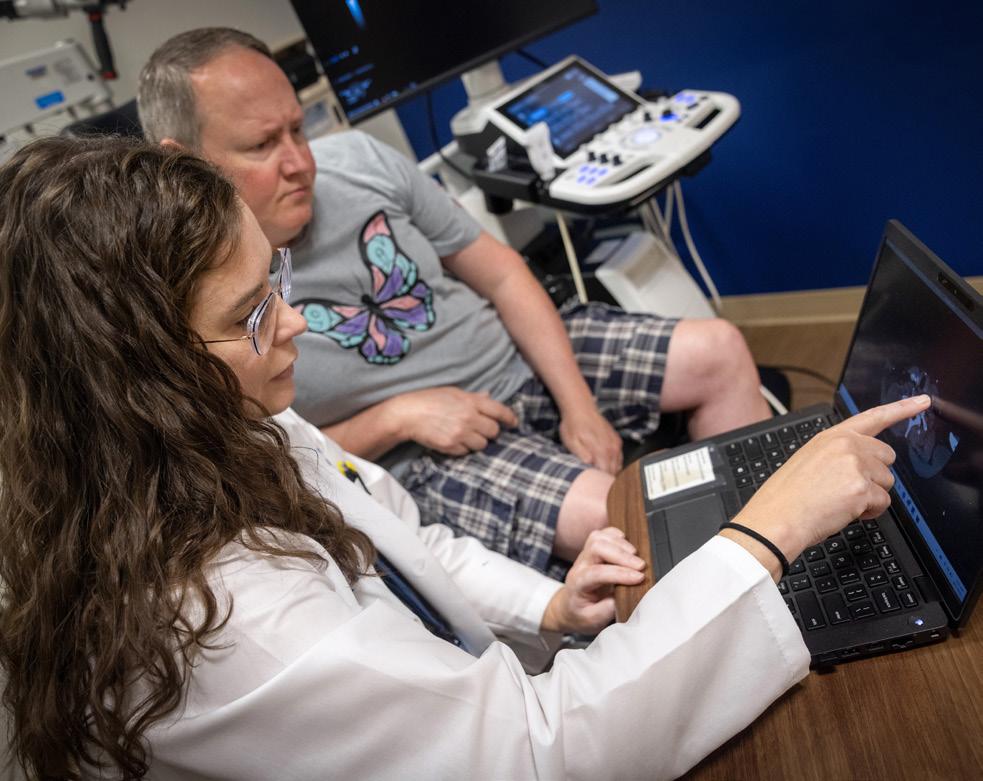

lump during a checkup for something else, isn’t unusual, Funk says. Many thyroid tumors are found during X-rays or CT scans for unrelated issues.
Once a nodule is detected, an ultrasound test is used to see it more clearly. Next is a biopsy. A small sample of tumor cells is collected and analyzed in a lab to confirm whether the growth is benign or cancerous.
How is thyroid cancer treated?
• Surgery. Thyroid cancer treatment usually starts with surgery. “For a small thyroid cancer, sometimes we can just remove one side of the thyroid,” Funk explains. “If it is larger or has more aggressive features, we might remove the entire thyroid gland.” Murphy had his whole thyroid gland taken out. His cancer had spread to his lymph nodes, requiring the removal of 44 nodes, too.
• Radioactive iodine. If the cancer has spread beyond the thyroid, as Murphy’s did, radioactive iodine treatment may follow surgery. “This treatment destroys tiny cancer cells that could be left behind or circulating in the bloodstream,” Funk says.
• Targeted chemotherapy or immunotherapy. Cancer-targeting medications are sometimes used for particularly aggressive thyroid cancers, anaplastic thyroid cancer or cancer that has spread.
Murphy says he is grateful he got help before his cancer grew. “If you think you feel a lump somewhere, get it checked.”

JOIN US! CLEARWATER FLORIDA BEACH


Registration now open for participants and vendors!
February 6-8, 2026
Hyatt Regency Clearwater Beach Resort and Spa
Scan QR code for full details on the event website:


Registration is open for the Seaside Symposium in Otolaryngology – Head and Neck Surgery, taking place February 6-8, 2026, in Clearwater Beach, Florida.
Co-hosted by the University of Tennessee Health Science Center and Penn State College of Medicine, this conference is designed for otolaryngologists, physician assistants, nurse practitioners, nurses, and other healthcare professionals.
• Evidence-based updates across a wide range of otolaryngology topics
• Networking with healthcare professionals
• 12.75 CME/CEU credits provided
A block of rooms has been reserved at Hyatt Regency Clearwater Beach Resort and Spa. Full details on hotel booking and course registration can be found on the event website.


Why are my ears ringing? Tinnitus and other hearing problems
Susan Bianco, an 87-year-old from Lancaster, realized she was losing her hearing when she found herself constantly asking her husband to repeat himself. She was also struggling during phone calls and social events.
“It is very hard to hear in a crowd,” she says. “I can’t understand what one person is saying if other people are talking.”
Then, Bianco started to hear something new: an annoying buzzing in her ears that gets louder when she is tired.
Bianco is among the 13% of U.S. adults – and 27% of adults 65 and older – who have trouble hearing, reports the Centers for Disease Control and Prevention. She is also among the
10% with tinnitus – a ringing in the ears often linked with hearing loss. The risk of hearing loss and tinnitus increases with age and noise exposure.
“You can’t stop aging, but you can take steps to conserve your hearing and reduce your risk of developing hearing loss and tinnitus,” says Dr. Jackie Price, audiologist at Penn State Health.
What is tinnitus?
Tinnitus is a ringing, buzzing, hissing or whooshing sound in one or both ears. Some people say it sounds like cicadas or a freight train, Price says.
“For some people, the noise is constant
and bothersome, interfering with their productivity and quality of life,” Price says.
The noise does not come from an external source. It stems from a miscommunication between your brain and ears.
Other common sound-related disorders include hyperacusis, which makes everyday sounds feel too intense, and misophonia, where certain sounds trigger strong emotional reactions.
What
causes
tinnitus and hearing loss?
Tinnitus and other sound-related disorders are often early signs of hearing loss, Price says.
Hearing loss starts with damage to tiny hair cells inside your cochlea, a snail-shaped organ in your inner ear. These hair cells convert sound waves into signals your brain can understand. When they are damaged, they can no longer communicate with your brain properly. The result is that you cannot hear as well. The messages between your brain and ears can also become distorted, creating the sounds of tinnitus.
Hearing loss and sound disorders can affect more than just your ears. They often affect sleep, concentration and relationships. They can also speed up cognitive decline, raise depression risk and increase the risk of falls.
How can hearing loss and tinnitus be prevented?


Protect your ears from loud noise: Use hearing protection when noise exceeds 85 decibels. That means wearing earplugs or earmuffs at concerts, sporting events, fireworks and when using power tools.
“I counsel people to wear hearing protection when they are mowing grass instead of listening to music through earbuds,” Price says. “It is like a double whammy because people have the noise from the mower, and then they crank up the music so they can hear it, and then they listen to excess noise for 45 minutes or more, sometimes twice a week.”
Choose the right earplugs or earmuffs: Buy earplugs or earmuffs with a Noise Reduction
Rating of at least 22 decibels. This number, listed on the product package, tells you how much sound the product will eliminate. Insert earplugs correctly for full protection.
“Take a foam earplug between your two fingers
and smoosh it down and roll it,” Price explains. “Then, when you go to put it in your ear, pull on your ear lobe with the opposite hand to open up the ear canal, insert the earplug and let it fully expand.”
Most foam earplugs are meant for one-time use to maintain a complete seal that keeps noise out.
How are hearing loss and tinnitus treated?
Hearing loss and tinnitus have no cure, but treatment can improve hearing and quality of life.
Hearing loss: Treatment depends on the cause and extent of the hearing loss. Often, hearing aids and other assistive devices are recommended.
Tinnitus: Tinnitus Retraining Therapy can help lessen the impact of tinnitus on daily life. This treatment combines counseling, which helps people cope with the sounds in their ears, with
sound therapy, which uses gentle white noise to shift focus away from tinnitus.
Bianco now wears hearing aids and recently started Tinnitus Retraining Therapy. Price programmed a soft, pleasant, constant noise into Bianco’s hearing aid as part of her sound therapy. Bianco hopes the new noise can help her feel less distracted by her tinnitus.
“It sounds like it’s raining, which is a sound I don’t mind too much,” Bianco says.
When to get a hearing test?
If you notice ringing in your ears, seek out a hearing evaluation, Price advises.
“Sometimes people think they hear fine, but there are signs of change inside the ear, such as hair cell damage or hearing loss at the highest frequencies,” Price says. “Testing can help you become better educated about what is going on so you can manage those changes.”
Dean’s List for Patient Experience
Jill McClelland, AuD, and Meghan Schmidt, PA-C, have been named to this year’s Dean’s List for Patient Experience. This recognition honors clinicians who achieved a 98% or higher patient satisfaction score for the fiscal year, reflecting their commitment to compassionate care and meaningful patient connections. Jill and Meghan’s dedication sets a high standard and exemplifies the very best of Penn State Health – way to go!


NEW STAFF
Welcome!







Dariann Angstadt
Speech-Language Pathologist
Pediatric Inpatient/Outpatient
Lauren Barnathan
Speech-Language Pathologist
Pediatric Inpatient
Colette Fisher
Speech-Language Pathologist
Catherine Hershey Schools for Early Learning
Ashley Hill
Medical Office Assistant
University Physicians Center
Nicole Kelley
Nurse Practitioner
Esteem Cosmetic Center
Facial Nerve Clinic
Christa Long
Medical Office Supervisor
University Physicians Center
Hannah Wood
Medical Office Assistant
University Physicians Center
ShENT faculty and resident team gathered for their annual fall team-building event – filled with festive fun, laughter, and camaraderie.

Dr. Rahul Shah, EVP and CEO of the American Academy of Otolaryngology – Head and Neck Surgery, delivered a visiting professor lecture on the future of healthcare leadership.

First annual ENT Faculty and Resident Basketball Tournament at the American Academy of Otolaryngology – Head and Neck Surgery Annual Meeting.

Dr. J.P. Gniady among the graduates of the 11th Annual Academic Healthcare Leadership Academy, a program to foster collaboration and strategic thinking across our academic health system.
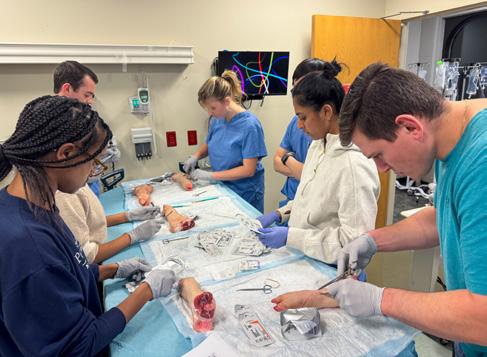
Dr. Emily Funk and resident team led medical students through suture techniques using pigs’ feet for a realistic soft tissue experience at the annual Suturing and Skills Night.
Elevating Care from Reactive to Proactive
Partnership with Sight & Sound Theatres
Sight & Sound Theatres is an entertainment company that produces Bible stories live on stage. Based in Lancaster County and known for its Broadway-style productions with panoramic stages, towering sets, live animals, special effects, music, and large casts. The shows are a major tourist attraction and draw millions of visitors annually.
Proactive Preventive Vocal Care
The Division of Communication Sciences and Disorders at Penn State Health is pioneering clinical partnership with Sight & Sound Theatres to establish a collaborative Vocal Strengthening Team
This initiative represents a strategic shift from traditional reactive treatment to proactive, preventative care – a cornerstone of modern
clinical practice. Led by laryngologist, Dr. J.P. Gniady and speech-language pathologists Aaron Ayala and Carrie Ruggiero, the program launches fully in 2026. This team will be providing crucial support through several key areas: delivering in-depth educational sessions on vocal health and hygiene; conducting vocal health screenings, including videostroboscopy, to establish baseline data; and offering consultative services by observing vocal rehearsals to identify potential stressors.
Crucially, the speech-language pathologists will be onsite at Sight & Sound weekly to provide dependable, preventative care. This consistent presence ensures early detection of vocal fatigue or inefficiency, helping to prevent minor concerns from escalating into career-interrupting injuries.

Singing Voice Specialist
A key strength of this collaboration lies in the unique expertise of our singing voice specialist, Aaron Ayala, who holds a Master of Voice Pedagogy and has over 25 years of performance experience. This role is vital because it bridges the clinical world of voice science with the artistry and technical demands of vocal performance.
A singing voice specialist understands the specific acoustic and aesthetic requirements of different performance styles, allowing the team to offer interventions that are not only physiologically sound but also technically relevant to the performers. They can communicate corrective strategies using the precise language and concepts that the performers and their vocal coaches already understand.
This expertise ensures our preventative strategies are seamlessly integrated into rehearsals, directly enhancing vocal technique, reducing the risk of injury from misuse, and guaranteeing the highest standard of specialized care for the entire company.
This groundbreaking partnership not only protects the health and careers of professional voice users in our community, but also proudly expands the scope and visibility of Penn State Health’s expertise in specialized laryngeal care.
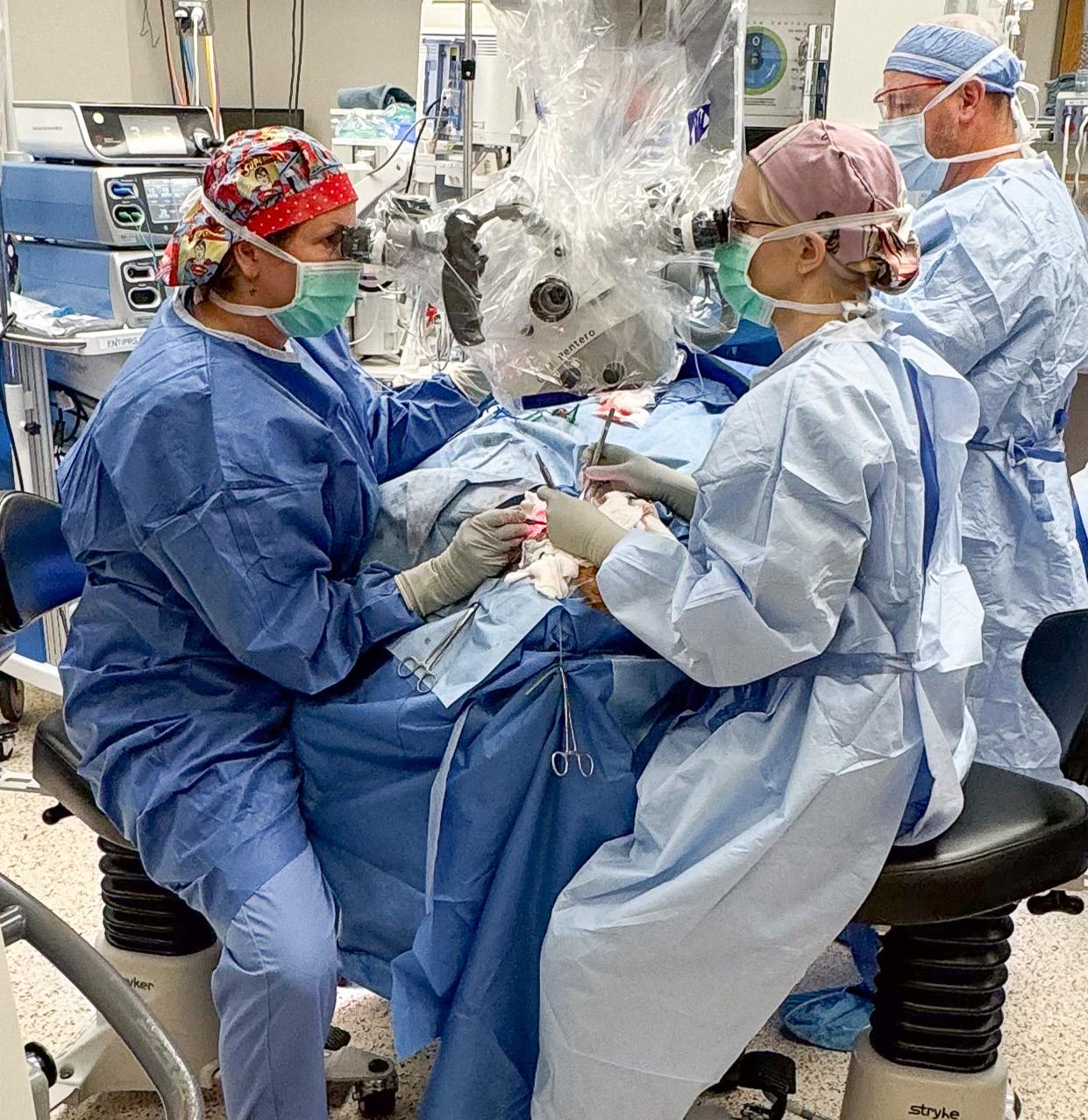
PENN STATE HEALTH IS HIRING a fulltime, BC/BE otolaryngologist fellowshiptrained in facial plastic and reconstructive surgery to join our team at the assistant professor level. This academic position offers a diverse scope of practice, including reconstructive and aesthetic care, clinical responsibilities, teaching, and research opportunities. The role also includes work at our off-site cosmetic center.

For more information, please visit pennstatehealth.org/careers.
Pediatric Inspire Implant
Down Syndrome & Obstructive Sleep Apnea
Penn State Health Golisano Children’s Hospital is now offering an advanced treatment option for children with Down syndrome who suffer from obstructive sleep apnea and are unable to tolerate CPAP therapy.
Multidisciplinary Care Team
Led by a team of pediatric otolaryngologists and sleep medicine specialists, Penn State Health is the first in central Pennsylvania to offer the pediatric Inspire implant. Inspire therapy is the first FDA-approved treatment for obstructive sleep apnea that works inside the body to address its root cause.
A small device, implanted during a minimally invasive procedure, delivers gentle stimulation to keep the airway open throughout sleep.
Pediatric Patients with Down Syndrome
Each year, approximately 6,000 babies are born with Down syndrome in the United States. About 60% of these children develop obstructive sleep apnea due to anatomical and physiological factors such as smaller airways, lower muscle tone, and larger tongue size.
Children with Down syndrome who meet certain eligibility requirements may be candidates for Inspire therapy.
This exciting advancement in treatment options positions Penn State Health at the forefront of innovative pediatric care, reinforcing our commitment to improving outcomes and enhancing the well-being of patients.
Milestone Inspire V Device Implant
The Inspire V device is the newest generation of Inspire’s implantable system for treating moderate to severe obstructive sleep apnea. This advanced implant features an integrated respiratory sensor, eliminating the need for a separate sensing lead and enabling seamless respiratory sensing within the device itself. Dr. Guy Slonimsky and Dr. Neerav Goyal provide adult Inspire implants at Penn State Health locations, including Hershey Medical Center, Holy Spirit Medical Center, and Lancaster Medical Center.


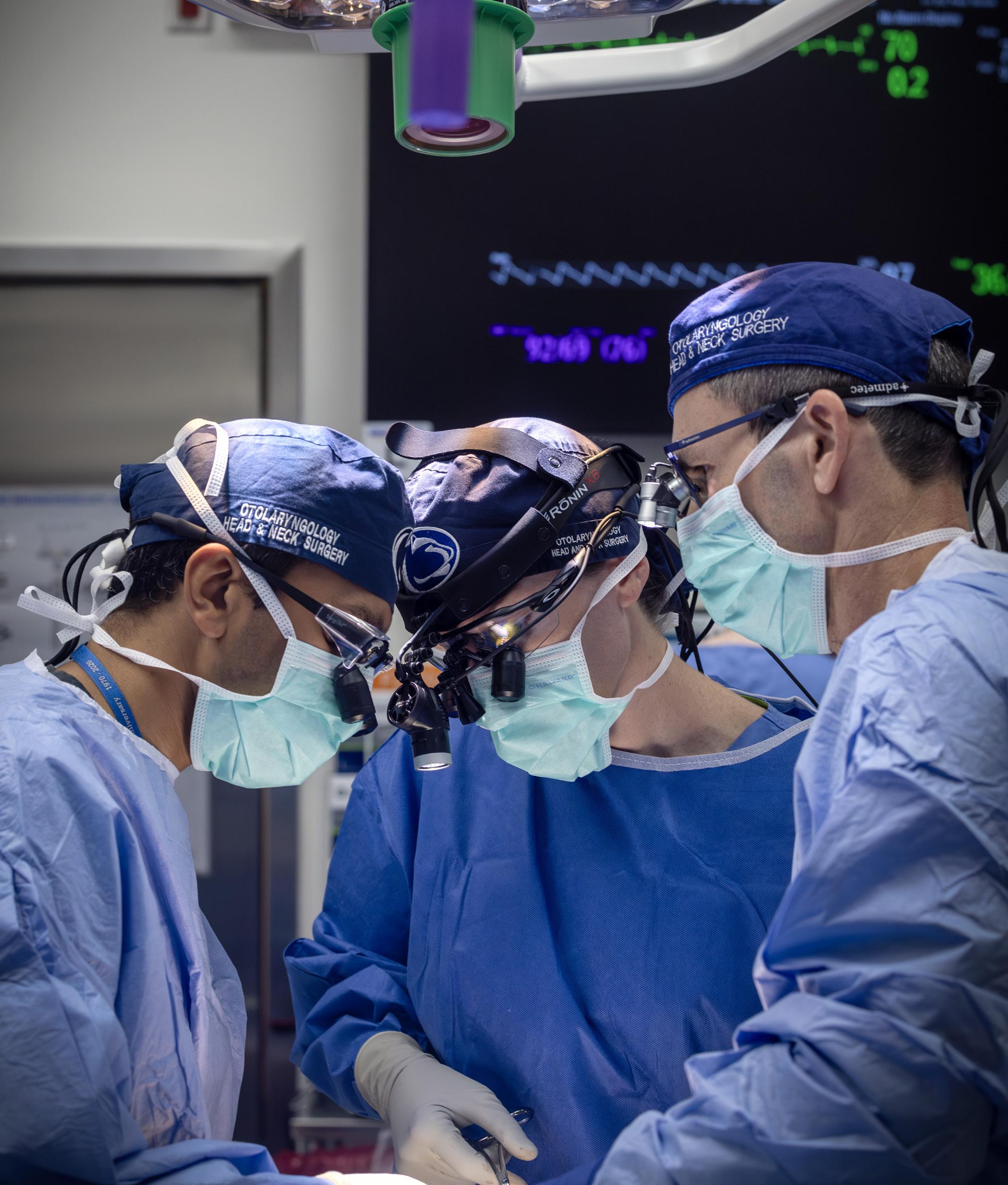
Alumni & Friends Reception Academy Meeting in Indianapolis




The Penn State Alumni & Friends Reception at the American Academy of Otolaryngology – Head and Neck Surgery Annual Meeting in Indianapolis, Indiana, brought together attendees from near and far, including alumni, colleagues, and department members, for an evening of connection and celebration. Thank you to everyone who joined us to mark another fantastic year!
Baby Announcements
JUNE 2025

AUGUST 2025


Julio de Leon, MD (PGY-1 resident) and Natalie de Leon welcomed a baby girl, June Olivia de Leon.
Christopher Tseng, MD (PGY-3 resident) and Deborah Tseng welcomed a baby girl, Katherine Amelia Tseng.

SEPTEMBER
2025

Kasra Ziai, MD (resident alumni) and Assal Ziai welcomed a baby boy, Rumi Pasha Ziai.
Recent Publications
LaBarge B, Lorenz FJ, Gniady JP. Association of Laryngeal Dystonia With Common Neurologic Disorders. Laryngoscope. Jul 2025.
Meci A, Goyal N, Goldenberg D. Branchial Cleft Cyst Carcinoma Remains Grossly Over Diagnosed: A Large Database Analysis. Laryngoscope. Aug 2024.
Meci A, Goyal N, Goldenberg D. The Malignant Transformation Rate of Oral Carcinoma In Situ. Laryngoscope. Aug 2025.
Chan K, Goyal N, et al. Practice Patterns in Management of Low- to Intermediate-Grade Salivary Gland Carcinoma: A Multi-Institutional Study. Laryngoscope Investig Otolaryngol. Sept 2025.
Lorenz FJ, Schopper HK, Walen SG. The Role of Toxins and Fillers in Optimizing Perioral Rejuvenation. Facial Plast Surg. Oct 2025.
Ma C, Parikh A, Lighthall JG. Evaluation and Treatment Planning to Maximize Perioral, Submental, and Neck Aesthetics. Facial Plast Surg. Oct 2025.
Lighthall JG, Bloom JD. Guest Editor Issue Titled, “Aesthetic Management of the Lips, Chin and Submentum”. Facial Plast Surg. Oct 2025.
Choi KY, Chan K, Van Dyke E, Van Scoy LJ. Exploratory Qualitative Analysis of Needs Assessment and Obstacles Faced by Head and Neck Cancer Patients in Central Pennsylvania. Laryngoscope Investig Otolaryngol. Jul 2025.
Recent Presentations
Goldenberg D. Radiofrequency Ablation for Thyroid Nodules. Thyroid RFA Workshop at Thammasat University. Bangkok, Thailand. Nov 2025. Oral Presentation.
Goldenberg D. Clinical Correlates in the Head and Neck. Thammasat University and Chulabhorn International College of Medicine. Bangkok, Thailand. Nov 2025. Oral Presentation.
Chi JJ, Moneta LB, Schopper HK, Newsome H. Common facial injuries for the otolaryngologist:
From initial repair to scar management. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Poster Presentation.
Durfee QC, Stancliff H, Eberly HW, Meci AV, Goyal N. Quality and Reliability of YouTube Videos for Patient Education in Surgical Drains. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Poster Presentation.
Eberly HW, Aziz M, Lorenz FJ, Schopper HK, Lighthall JG. Does Electrical Stimulation Therapy Influence Synkinesis in Facial Paralysis? A Systematic Review. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Oral Presentation.
Eberly HW, Yeakel HA, Meci AV, Lighthall JG. Evaluating Quality and Reliability of YouTube Videos for Patient Education in Facial Paralysis. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Poster Presentation.
Goldenberg D. Leading with Purpose: Advancing Collaborative Tracheostomy Care from Hospital to Home. 9th International Tracheostomy Symposium. Chicago, IL. Oct 2025. Oral Presentation.
He M, Pandian V, Brenner M. Tracheostomy Across Contexts: A Cluster Analysis of Global Care Trends (2015–2025). 9th International Tracheostomy Symposium. Chicago, IL. Oct 2025. Poster Presentation.
Hughes S, Ji Q, Brenner M, Pandian V. Intrahospital Transport of Adults with Surgical Airways: A Scoping Review of Risks and Outcomes. 9th International Tracheostomy Symposium. Chicago, IL. Oct 2025. Poster Presentation.
Hughes S, Ji Q, Brenner M, Pandian V. Laryngotracheal Sequelae Following Endotracheal Intubation in the ICU: A TriNetX Database Analysis. 9th International Tracheostomy Symposium. Chicago, IL. Oct 2025. Poster Presentation.
Kulkarni P, Chan K, Tseng C, Milarachi E, Goldrich D, LaBarge B, Walter V, Goyal N, Broach J, Goldenberg D. PTPR Family Deletions Are Associated with More Structural Instability in Tongue Cancer in the Young. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Oral Presentation.
Kulkarni P, Hollenbeak C, Goldenberg D, Goyal N. Cost-effectiveness of near Infrared Autofluorescence for Parathyroid Gland Identification During Total Thyroidectomy. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Oral Presentation.
Li S (Moderator), Puram SV, Pipkorn P, Ziegler AM. Reconstruction Showdown Panel Discussion. AAOHNS Annual Meeting. Indianapolis, IN. Oct 2025. Panel Presentation.
Lorenz FJ, Ma C, Parikh A, Walen S. Respiratory Complications Following Septoplasty in Patients with OSA: Is it Necessary to Admit After Surgery?. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Oral Presentation.
Ma C, Givens A, McGinn J, Goyal N, Slonimsky G, Damah M, Owoo C, Goldenberg D. Experience of a Head and Neck Otolaryngology Surgical Skills and Cadaveric Dissection Bootcamp in Ghana. AAOHNS Annual Meeting. Indianapolis, IN. Oct 2025. Poster Presentation.
McClelland J. Incorporating Hearing Instrument Specialists and Audiology Assistants into the Audiology Practice. Pennsylvania Academy of Audiology. King of Prussia, PA. Sep 2025. Oral Presentation.
Meci A, Ji Q, Goldenberg D, Goyal N, Pandian V. Impact of Planned Tracheostomy Timing on Survival and Complications in Critically Ill Patients. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Oral Presentation.
Meci A, Kulkarni P, Givens A, Stancliff H, Milarachi E, Chan E, Goldenberg D. Performance of the ThyroSeq multigene genomic classifier: A ten-year institutional experience. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Oral Presentation.
Meci A, Milarachi EN, Gniady JP. Mental Health and Sleep Outcomes Among Patients Diagnosed with Chronic Cough. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Oral Presentation.
Meci A, Kulkarni P, Milarachi E, Funk E, Goyal N. Palliative Care Usage and Outcomes Among Patients with Advanced Head and Neck Cancer. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Oral Presentation.
Meci A, Slonimsky G, Funk E, Goyal N. Comparing AI Chatbots for Patient Education on Topics in Head and Neck Surgery. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Oral Presentation.
Milarachi E, Sciscent B, Lorenz J, Gniady J, Goyal N. Adherence to Clinical Practice Guidelines: Hoarseness. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Oral Presentation.
Mohammadi MA, Pandian V, Azimi AV. Enhancing Critical Care Nurses’ Suctioning Skills Using Structured Education: A Quasi-Experimental Study. 9th International Tracheostomy Symposium. Chicago, IL. Oct 2025. Poster Presentation.
Murphy P, Goshert A, Mowatt T, McClelland J, Hanbidge L. State Board and Legislative Updates in Audiology. Pennsylvania Academy of Audiology. King of Prussia, PA. Sep 2025. Panel Presentation.
Nikander M, McClelland J, Parsons A, Lucas L. Audiology Assistants and Hearing Instrument Specialists in the Audiology Office. Pennsylvania Academy of Audiology. King of Prussia, PA. Sep 2025. Oral Presentation.
Pandian V. Automated Suctioning in Action: Experimental Evaluation of Device Efficiency and Reliability. 9th International Tracheostomy Symposium. Chicago, IL. Oct 2025. Oral Presentation.
Pandian V, Brenner M. Beyond the ICU: Longitudinal Healthcare Costs of Tracheostomy in a Nationally Insured Cohort. 9th International Tracheostomy Symposium. Chicago, IL. Oct 2025. Poster Presentation.
Rothka AJ, Aziz M, Nguyen K, Lorenz FJ, Schopper HK, Lighthall JG. Evaluating Dog BiteInduced Facial Trauma: A Study from a Single Tertiary Care Center. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Oral Presentation.
Stancliff H, Durfee QC, Eberly HW, Meci AV, Goyal N. Assessing the Quality of Tracheotomy Education on YouTube: Insights and Implications. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Poster Presentation.
Nairns L. The Speech-Language Pathologist’s Contribution to a Multidisciplinary Tracheostomy Team: Barriers, Benefits, Implementation, and Outcomes . ASHA Convention. Washington, DC. Nov 2025. Poster Presentation.
Evitts P, Blackburn E, Reichwein, et al. Using Translational Science to Increase Care to Rural Populations. ASHA Convention. Washington, DC. Nov 2025. Poster Presentation.
Nairns L, Hartman O, Bazhan S, Schwanger J. Does Liquid Food Coloring Change the Consistency of Thickened Liquids?. ASHA Convention. Washington, DC. Nov 2025. Poster Presentation.
Bren J. Pediatric Cardiac Lusoria: What are we missing?. ASHA Convention. Washington, DC. Nov 2025. Poster Presentation.
Welch S, Edwards E. Joining Forces: The Importance of SLP and BCBA Collaboration in Autism and Neurodivergent Care. ASHA Convention. Washington, DC. Nov 2025. Oral Presentation.
Stancliff H, Durfee QC, Eberly HW, Meci AV, Goyal N. A Comprehensive Analysis of Gastrostomy Tube Education Across YouTube. AAO-HNS Annual Meeting. Indianapolis, IN. Oct 2025. Poster Presentation.

Courtney Eisenhart, AuD confirmed by the PA State Senate for appointment to the State Board of Examiners in Speech-Language Pathology and Audiology.

DiGiovanni A, Lorenz FJ, Lighthall JG. Pediatric Microtia and Mental Health: Insights from a Large Database Analysis. 13th Pediatric Research Day. Hershey, PA. Nov 2025. Poster Presentation.
Kollipara V, Mukhtar H, Koka K, Lorenz FJ, Keane AM, Goldenberg D, Goyal N. Risk of Persistent Opioid Use After Oxycodone/Hydrocodone Prescribing in Pediatric Tonsillectomy: A TriNetX Database Study. 13th Pediatric Research Day. Hershey, PA. Nov 2025. Poster Presentation.
Whitaker M. Radiographic Imaging in Hearing and Balance: Clinical Correlates. Pennsylvania Academy of Audiology. King of Prussia, PA. Sep 2025. Oral Presentation.
Yeakel H, Meci A, Lighthall JG. A Cross-Sectional Analysis Helmets Use on Pediatric Facial Fracture Patterns while Bicycling. AAFPRS Annual Meeting. Los Angeles, CA. Sep 2025. Poster Presentation.

Glory Rodriguez, MA received the Growing the Future of Nursing Award from the Penn State Health Nursing Executive Council.
Jill McClelland, AuD elected Vice President of Government Affairs for the 2026 Pennsylvania Academy of Audiology Board of Directors.









UPCOMING EVENTS
FEBRUARY 6-8, 2026
Seaside Symposium in Otolaryngology – Head and Neck Surgery (Clearwater Beach, FL)
APRIL 2026
Let’s Get Ahead Campaign for Head and Neck Cancer Awareness Month
MAY 2, 2026
Annual Sporting Clay Shoot Fundraising Event (Annville, PA)
SPRING 2026
George H. Conner Visiting Professor Lecture (Hershey, PA)
MAY 30-31, 2026
Thyroid Radiofrequency Ablation Hands-On Training Course (Hershey, PA)
JUNE 2, 2026
Ferraro Resident Symposium in Otolaryngology (Hershey, PA)


