THE ROLE OF COMMUNITY HEALTH IMPACT
ASSESSMENTS IN RETROFIT









This workbook has been developed through a collaboration between the National Retrofit Hub and Centric Lab, supported by Impact on Urban Health, as part of the Measuring Outcomes and Impact Evaluation project. The work explored how broader outcome measurement could accelerate retrofit delivery and support better policy, funding, and delivery decisions, particularly in a fiscally constrained environment.
A key finding was the importance of place-based data that reflects lived experience and provides a nuanced understanding of local needs, opportunities, and challenges. This workbook aims to offer one way to generate such data. It also draws on extensive research developed by Centric Lab, which approaches health ecologically, recognising how place, systems, and lived experience interact to shape wellbeing over time. That research underpins the approach taken throughout.

Centric Lab is a Community Interest Company dedicated to advancing health justice by co-creating knowledge, tools, and narratives that support grassroots movements and organisations addressing structural inequities.
Their interdisciplinary team of neuroscientists, health researchers, and urban geographers investigates how biological inequity affects racialised and marginalised communities, and they build healing strategies that centre lived experience and community expertise.
Since 2016, Centric Lab has developed open-access programmes and research collaborations across the UK to strengthen advocacy work, improve material conditions, and surface non-western epistemologies, all while fostering autonomy and equitable access to evidence and infrastructure for health justice.
The National Retrofit Hub (NRH) is a Community Interest Company focused on improving how housing retrofit is delivered at scale.
We do this by convening the retrofit community, building and sharing evidence on what works, and supporting action that leads to better outcomes for homes, buildings, and places.
Title image, and images on pages 7, 20, 35 + 39 are credited to Angela Grabowska & Paul Stringer
CHIA Scenario
Retrofit, Health & CHIAs
Retrofit & CHIA - The Potential Retrofit & CHIA - Examples
Wider Context of Health & Homes Policy Recommendations Part 2
The Who
Roles at a Glance
Group Archetype 1
Group Archetype 2
Group Archetype 3
The How - CL-HIA
The How - CHIA Provocations When Thinking About Place Case Study


About this document:
This document is structured in two main parts.
Part 1 explores the theoretical background and context to health, health justice, and the relationship to retrofit.
Three different health impact assessment approaches are explained.
Part 2 takes a more practical form. Here you will find out about who can and should use these assessments. There is guidance about how to use them, with further resources signposted to at the end.

Retrofit sits at the centre of a growing challenge facing homes across the UK. Poor housing quality, rising living costs, insecure tenure, and environmental stressors are placing increasing pressure on people, families, and communities. These pressures are closely linked to health outcomes, from exposure to damp and mould through to anxiety, stress, and reduced wellbeing.
At the same time, retrofit is often delivered in environments shaped by urgency, limited capacity, and competing priorities. Under pressure, it can become fragmented, focused on individual homes, measures, or compliance requirements rather than wider outcomes. This is not a failure of intent or effort. It reflects the systems within which retrofit is planned and delivered, including policy design, funding constraints, data availability, and organisational capacity.
What remains less well embedded is a consistent way of connecting retrofit and health that is grounded in place, informed by lived experience, and capable of supporting better decisions across policy, funding, and delivery. Creating space to step back, reflect, and reconnect these elements is not a luxury. It is essential to delivering retrofit that improves longterm outcomes for people and communities.


The National Retrofit Hub (NRH) exists to support this kind of progress. The NRH works across housing, health, local government, industry, and community action to strengthen the conditions needed for effective retrofit delivery. Its focus is on alignment, coordination, evidence, and practical tools that help connect national ambition with local, place-based delivery. This workbook sits within that role.



Retrofit is the upgrading of our existing homes, buildings and places to make them healthier to live in, better able to cope with climate change and longer lasting, while using less energy and producing less carbon (both operational and embodied).



Community Health Impact Assessments, or CHIAs, provide a structured, community-led way to understand how health and wellbeing are shaped by place and by the systems people interact with every day.
A CHIA enables communities to define what health means in their own context and to assess how a proposed or existing intervention, such as a retrofit strategy or project, may affect health outcomes. It brings together lived experience, local knowledge, and evidence to surface the social, commercial, and political determinants of health that are often missed by standard datasets or top-down approaches.
Facilitating a CHIA reflects a justice-led approach aligned with the values of the World Health Organization, including participation and voice, equity, long-term sustainability, and the ethical use of evidence.
Treating retrofit solely as an exercise in improving individual homes risks severing the relationships that shape how people live, in community, in kinship, and with one another. CHIAs offer a way to reconnect retrofit with these wider systems, supporting more informed decisions, stronger collaboration, and outcomes that extend beyond energy performance alone.
A Community Health Impact Assessment (CHIA) is a way for a community to ask: “How will this decision affect our health?”
It is a structured community-led process that brings residents into the conversation early, to define what health and wellbeing mean to them and assess how a proposed policy, plan or project, such as a retrofit programme, may impact their lives.


This playbook is not only for end users that will design and implement a CHIA in their own community, but also those that can advocate for localised and nuanced understandings of people and place. This includes but is not limited to community groups, combined and local authorities, and advocacy organisations.
Whether or not you are working in health or retrofit, a CHIA could be a meaningful tool that furthers your advocacy journey. It provides an essential evidence base, offering a granular understanding of the context of place and people in which national or local policy is being delivered.
The CHIA is:
• a tool to baseline your community’s health
• a tool to assess the impact of an anticipated or present change
• a process to connect your community to deepen your mutual and collective understanding of your health in place
• an opportunity to identify and build upon health giving and life affirming infrastructures and activities in your community
• an opportunity to surface and spotlight what needs changing
More detail about user archetypes is provided in Part 2.



In this first part of the workbook we set out the context for understanding why health and health equity matters when talking about retrofit, and retrofit strategy design.
We explain what a Health Impact Assessment is, and how a Community Health Impact Assessment differs, giving some example scenarios.
Finally we set out the potential for adopting tools such as CHIA in retrofit and situate our work within the current discourse across the industry on the matter.
Homes should be a sanctuary. They are where we rest, recover and feel safe. When the conditions inside our homes make that difficult, they stop feeling safe and start becoming a source of stress.
Stress is disease. Whilst our bodies have a natural stressresponse-system, and can handle short bursts of stress, the over-engagement of that system can have negative impacts on our health.
Decades of research1 have shown that stress is not just personal. It is shaped by the environments we live in, including our housing, our neighbourhoods, and the wider social and economic systems around us. These environments can create both physical and psychological stress.
An example of an environmental stressor could be poor air quality in the home. Tiny particles in polluted air can be breathed in, enter the bloodstream, and cause inflammation.
An example of a psychological (or psychosocial) stressor could be the ongoing experience of marginalisation and fear. When this continues over many years, or across generations, it keeps the body in a constant state of alert.
When stress like this does not stop, it builds up in the body. This is known as allostatic load. Over time, the body’s key systems, including the immune and hormonal systems, begin to
struggle. This increases the risk of illness.


In more ‘built environment’ terms, it’s like unchecked wear-and-tear in a home. If small problems such as damp, cracks or leaks are ignored, the damage builds up over time. Eventually, the structure itself is affected. Sometimes with catastrophic effects.
The body works in a similar way. When stress is constant and nothing changes, the strain builds up and begins to affect core systems. Unlike a house, we can’t replace neurobiological systems. That is why reducing stress in people’s homes and communities is essential, alongside creating conditions that increase healing pathways and support recovery.
READ MORE ABOUT DATA FOR HEALTH JUSTICE HERE https://www.thecentriclab.com/data-for-health-justice
Allostatic load is the cumulative damage that chronic stress does to the body over time
Health inequities are avoidable differences in health outcomes. They are not random. They result from structural inequities built into the systems that shape daily life.
Structural inequities include poor housing, limited access to green space, high levels of pollution, inadequate transport, and poor access to healthcare and nutritious food. These conditions create ongoing disadvantage for marginalised and discriminated groups.
These disadvantages shape unequal access to the social and environmental conditions that determine health, leading to unequal health outcomes2.
In turn, health inequities reinforce structural inequities. Poor health can limit people’s ability to work, learn, and participate fully in society, which deepens poverty, exclusion, and disadvantage.
This creates a reinforcing feedback loop, a vicious cycle in which structural inequities produce poor health, and poor health further entrenches those same inequities. Breaking this cycle requires policy designers and practitioners to prioritise health at the individual, community, and population levels.
The participatory role of the CHIA helps identify through people’s lived experiences how different policy-led systems interact and can either risk acting as a pathway to poor health or as a potentially health affirming intervention.


Language is important as it has the power to either build consensus or cause confusion around crucial topics. The following terms are important to define if health justice is the goal.
Injustice can be defined as a situation or condition that is unfair and is lacking justice3.
Social injustice can be defined as ‘the denial or violation of economic, sociocultural, political, civil, or human rights of specific populations or groups in the society based on the perception of their inferiority by those with more power or influence’4 .
Environmental injustice, a form of social injustice, can be defined as the disproportionate exposure of certain populations, including ethnic minority populations and people living in poverty, to environmental hazards5.
Health Justice can be defined as the equity created by community leaders to support the abolition of systems that lead to contamination, pollution, discrimination, and prejudice.
The CHIA is a practical approach to build that equity with partners where identification of community-led solutions is a key facet.


Centric Lab has 3 working definitions to cover the term ‘community’:
• Local: meaning a group of people within a specific geographical area;
• Organised: meaning a group of people within a relative geographical area representing collective interests for the betterment of the geographical area;
• Identity Oriented: meaning a group, or groups, of people who have defined, and protected, characteristics such as gender identities, racial(ised) identities, and class identities.
Taking these definitions allows practitioners and programme designers to be more accurate with their terminology, methods, and goals and lean into existing networks.
For example, evidence shows that some groups choose not to participate in broad, ‘catch-all’ public meetings. As a result, the insights gathered in these settings can overlook those who are most marginalised. Taking a CHIA-focused approach with groups such as neurodivergent communities or women’s groups can not only generate richer, more nuanced understanding, but also create opportunities for new partners and stakeholders to join the conversation and support delivery.
The World Health Organization defines the health impact assessment (HIA) as “an approach used to systematically judge the potential health effects of a policy, strategy, plan, programme or project on a population, particularly on vulnerable or disadvantaged groups. HIAs can help to identify the distribution of those effects within the population, generate evidence for proper action to avoid and mitigate sometimes unintended health risks, and promote health opportunities.”
HIAs are predominantly conducted within technocratic or policy spaces, without the input of broad stakeholder groups, such as the community that is most impacted. As processes they can also rely heavily on secondary quantitative data that draws assertions and conclusions that can be at times unethical and inaccurate.



A traditional HIA is generated by the assessing organisation selecting a number of determinants of health and defining criteria within them to judge whether the plan/policy/intervention will address that determinant.
In spatial planning, an HIA typically considers the following as determinants of health:
• Housing design and affordability
• Access to health and social care services and other social
• infrastructure
• Access to open space and nature
• Air quality, noise and neighbourhood amenity
• Accessibility and active travel
• Crime reduction and community safety
• Access to healthy food
• Access to work and training
• Social cohesion and inclusive design
• Minimising the use of resources
• Climate change
Many of these are useful, however a community may see others that build on these and are more pertinent to their lived experience.


Community led HIAs bring data from the community into HIA templates, typically from community leaders who represent their groups and bring key issues or concern into the mix. They are a first, incomplete, step towards complete Community Health Impact Assessments. To conduct one with community based data with community leaders ensures a certain degree of accuracy and generates a level of accountability for those involved. It is important to note that whilst qualitative data from the community is being collected this way, it still falls under a format that the community have not designed as relevant to them.
A Community Health Impact Assessment (CHIA), is the traditional process flipped on its head, where the assessment is created by a community who is likely to be impacted by future changes. Through facilitation and conversation they uncover which determinants of health are relevant to them and how these are at play in their lives. They consider how these may be measured and impacted, in ways that are accurate and meaningful for them, and through this process provide a level of analysis and insight into the relationship of place on their health.
In doing so, a process is created through which the community can deepen their understandings of the conditions and systems that shape and determine their collective health. The process
covers broader discussions of how life plays out within our lived and built environments. Invariably, gathering to talk about our health in community will capture how we live, the safety and comfort of our homes, and the ways in which our homes and environments enable or inhibit our wellness physically, mentally and socially.

• A method where community leaders work to bring major issues to surface.
• An imperfect bridge that allows for capturing key insights from key stakeholders.
• Ideally used when time scales are limited.
• Typically led by a person with authority who convenes a number of close contacts in respected and trusted positions within the community to consult on the process.
• Ideal for when resources and scope are limited.
Let’s imagine that an authority is gearing up for a big project or policy shift. Numerous actors and agendas are at play and time is limited as proposals and plans need to be sorted within a relatively short time frame. Here, a community-leaders HIA is an approach that can bring key voices to the conversation - such as how extreme heat is experienced by different demographics or how care needs differ and influence the use of energy and utilities the home. In practice, an organiser from an authority who has built existing and trusted relationships is able to convene a number of community leaders who can share insights by following a structured template. In theory, this can take place over an afternoon workshop at a friendly, safe, and accessible location to all participants. The insights are gathered and discussed in the same workshop - or in another workshop if time and resources permitwhere all can give consent to and approval that their contributions have been recorded accurately. These insights are then able to be summarised and provided to project leads to incorporate into plans in order to reduce externalities.



In 2024, community liaison officers joined a programme run by Centric Lab. After a learning course, a grant was allocated to Support Staffordshire to facilitate workshops with 2 demographic groups on their experiences of the health impacts of extreme weather and how existing built environment assets can adapt to improve wellbeing and quality of life. Through intimate and controlled workshops participants shared insights with each other and gave consent for their anonymised reflections to support a policy initiative that Support Staffordshire created. The policy briefing was shared throughout the local authority and further internal-training was implemented to ensure the authority’s uptake of lived experience knowledge.

• A method in which the community redesigns the assessment itself, using lived experience of how systems affect their lives.
• Communities are equipped with resources to facilitate the process over a sustained period.
• Best suited to long-term planning and structural change.
• Led by trusted people within the community, independent of direct control by authorities.
• Can be delivered by social enterprises or change-making charities as part of wider systems change work.
• Power is shifted from authorities to community organisations, giving communities sovereignty and real decision-making control.
Imagine a community, whether defined by place, identity or shared experience, where health outcomes are poor and wellbeing is declining. Addressing this requires more than small adjustments. It calls for systems change. A CHIA creates space for that shift. It helps surface how current policies, assumptions and decision-making processes are contributing to health inequalities. For example, a community may feel that its culture and history are not understood or reflected in local policy. Even where intentions are good, decisions can miss the mark. Over time, this disconnect can reinforce poor health outcomes and erode trust.
The CHIA centres imagination, cultural competency, and experience to navigate these challenges.
It begins by shaping working practices around people’s real needs; creating space for those most affected to share their stories without constraint; opening room to imagine a healthier future; and asking how processes can work better. These insights are then brought together to redefine what good community health looks like from the community’s perspective. The final output is still an assessment with indicators and metrics, but one that reveals how wider determinants of health drive poor outcomes.



In 2018, residents in Southall began to notice that a putrid gasoline-like smell in the air was coinciding with increased rates of sore chests, eyes, increased asthma related problems and headaches. Existing regulations and policies meant halting the redevelopment of a contaminated land site, the source of the community’s experiences, was difficult. Over the years, Clean Air for Southall & Hayes (CASH) wanted to demonstrate that the oversights from planning, policy, and regulatory systems were letting people like them down. In 2022 Centric Lab partnered with CASH to reimagine the HIA with the question “what if the HIA was designed by people like us, would the approaches have been different; would we have fallen so ill?” Together, they developed a new template, a CHIA. It became both a practical toolkit for other communities and the foundation of a learning programme to support wider adoption. The process and its outcomes have since been documented in peer-reviewed journals.
Retrofit provides a catalyst to understand how we live and experience our homes and neighbourhoods, the ways in which our lived experience of these places can shape us and be shaped, and how these experiences run deep into impacting our bodies and how they function. Retrofit is not only a technical field, but also a relational one, and is deeply embedded in systems of governance and ways of living. It therefore has the opportunity to contribute to human health both materially, structurally, and relationally.
Embedding community health impact approaches from the start of retrofit programmes and initiatives can lead to processes that remain intact for future impact measurement and evaluation because the foundation of investment and observation of the reality of the place has been established. When patterns of living are collectively observed and noted, the relationality of what goes on in our homes and streets becomes clearer.
A CHIA necessitates systemic thinking because it ultimately identifies the structural determinants of health by which we understand how our health is at risk.
For example, a community that may be experiencing widespread black mould in their homes and respiratory concerns will have established the links between housing and health. The use of a CHIA reveals not only the conditions of the homes, but why they are like that, and the other factors impacting their health.


This might include the experiences of dealing with building management, concerns around overcrowding, or the costs and decision making powers around property maintenance. These factors touch on social, political and commercial determinants of health through the recounting of lived experience, highlighting also the compounding inequities and nuances that could be lost without involving the community.
Doing this in the context of retrofit further brings to light how retrofit is not simply about technical changes to a home, but challenging the relational assumptions around how decisions are made, and how both have implications on community health.
Conducting a CHIA also brings data into context, it speaks directly to the structures at play in place, with people, not as an abstract but as a real, lived and shared experience.
It creates and uses place-based data, creating the potential for area health profiles, taking into consideration not only the building profiles and energy use of space, but how people’s health is determined by the organisation, design, use, quality and decisions made of their homes.
Through a bottom-up approach to an HIA, the CHIA exposes lived experience of systems, moving from broad generalisations to tangible and measurable impacts on community, as well as providing pathways for changes to be made to mitigate the risks and harms of them. A bottomup approach also gives nuance to flattened assumptions that certain interventions are invariably good for health on paper, and shows areas of intervention that are most likely to be effective.
A CHIA is not only a technical and tangible output that can be used to baseline a community’s health against any anticipated changes in their lived environments. It also creates a shared evidence base for a community that may have experienced long term individual and collective gaslighting from structural sources6. For many this evidence base is a key component of their healing, and the activation of their agency.
A CHIA enables the building of social capital by deepening mutual understanding of ecological health, the idea that we are only as healthy as the environments we live in. The process often strengthens social bonds as people connect through shared experiences and recognise how their lives overlap and affect one another. When the links between place and collective health are clearly understood and validated, solidarity can grow. This can increase agency, as the group not only names the ways their health is negatively affected, but also identifies the assets, relationships and opportunities available to them and how these might be organised.
This type of process also brings forward the behavioural realities of a place that someone outside those homes may struggle to see. For example, it can surface how often and in what ways kitchens and bathrooms are used. These insights can highlight patterns that contribute to what makes a home inefficient, and whether the home is equipped for the way people actually live. As a result, CHIA recommendations can extend beyond emission reduction to address health, comfort and everyday usability.


A CHIA can take multiple forms, there are as many approaches to it as there are communities, existing examples of CHIAs conducted by community can be found on Centric Lab’s website7 .

A community first approach to retrofit that considers the neighbourhood, people’s lived experiences, and how they live, produces different insights into where and how retrofit can lead to wider health benefits.
A community-level approach to retrofit can reveal shared challenges that are best solved collectively. A neighbourhood might identify excessive solar gain on south-facing walls as a major driver of heat stress. By agreeing on a nature-based solution such as sustained and long term tree planting combined with sustainable urban drainage system, residents can address thermal regulation, comfort, flood resilience and energy consumption in a way that could also benefit from economies of scale. This kind of coordinated action also creates wider social value and may unlock complementary funding streams from departments focused on health, environment, or community wellbeing.


A community relate their high energy usage to a lack of safe, welcoming communal spaces where resources can be shared. By improving public spaces, making them greener, safer, and more inclusive, the community can reduce isolation, shift activity solely out of individual homes, and lower overall energy demand. A solution can be seen laterally in understanding how to make public spaces safer, greener, and more inclusive.
A community discusses how noise pollution in their local area is a factor of their poor health. Schemes that deliver wall insulation and window repair can have a social impact as well as addressing thermal comfort. Equally, a cost effective solution to noise pollution may also be the introduction of green walls that absorb sound, lower urban heat island effect, and improve air quality in the local area, giving retrofit organisations the abilities to partner with other urban wellbeing and built environment stakeholders and funders.
A community discusses the lack of skills training and employment opportunities for local residents as a key factor in their health outcomes. Therefore, instituting a skills based programme designed around maintenance can ensure that installations and asset based interventions are managed by the people who live in their areas, rather than often costly outsourced firms.
The community health impact assessment is a pathway that illuminates the barriers to health people experience whilst offering key co-design opportunities for solution making. Through the solution making process scheme designers and authorities can look laterally to tackle the wider determinants of health and achieve wider policy and legislative goals.
At the end of the day, that “what” is still happening; the re-engineering of our built environment to be more adaptive to climate, health, and energy requirements, but “how” it is being delivered - and sometimes with who - is different. The more we see retrofit as an extension of our social fabric, the closer we’ll see its rewards.
There are various existing Health Impact Assessments, and Resident Impact Assessments of housing and retrofit schemes, conducted by a range of institutions8, 9, 10, 11 including the NHS, Public Health Departments, housing providers and waste authorities. In most of these cases, a broad understanding of health and its determinants are already at play and being measured. Through these processes there are shared understandings of the ways in which our housing and living conditions are impacting health outcomes, and powerful communications on just how important our living environments are, not just on our individual health but our collective and social health too.
“Homes should be warm, safe, ventilated, not overcrowded, affordable, accessible, and provide a sense of security and community.”15
“Our home is not just a dwelling place. It should be a place of comfort, shelter, safety & warmth. . . it is the main setting for our health throughout our lives.”16
The 2022 publication of the Warm Homes Prescription12 further illustrates the details of how our housing impacts health, that it is not just about the affordability or security that the housing provides, but also the quality, comfort and possibility that housing enables.


The annual report of the director of Public Health in East Sussex in 2019/2020 was titled “Health & Housing - You Cannot Maintain Good Health Without Good Housing”13. Recognising that the quality of housing impacts significantly on the health of its occupants, the public health team in East Sussex went on to develop an Housing Retrofit Strategy for the borough and in doing so articulated the connection between health and housing and the opportunity of retrofit to have a positive impact on public health in the region.
The question is not whether or not there are established links between retrofit and people’s health, this is already well documented. Rather, what data are we using to understand this relationship? Are we using accurate and inclusive methods to measure and capture people’s direct lived experience.
The opportunity that we see for the CHIA is not simply to conduct impact assessments for health in retrofit for the purposes of enhanced evaluation, we see this as an opportunity to build the processes and conditions for us all to organise our retrofit journeys with the nuances of the ways in which communities are organised and live, for the greatest possible health outcome for all, and there is no way to do this without including the experiences and imaginations of those living in the homes and streets that will be retrofitted.
Furthermore, the opportunity for a CHIA in retrofit is also to be a catalyst14 for embedding and integrating ecological understandings of health in programmes, and for a community to be better equipped and ready to respond to change. All this because a nuanced baseline of their collective health and the determinants of it now exists. It means that communities are working with greater clarity of which parts of the puzzle impact their health, what to feed into, and what to organise for and around.
1. Adopt an Ecological Approach to Health in Retrofit Policy
Treat Retrofit as a Neighbourhood-Scale Opportunity
Design funding and regulatory mechanisms that support retrofit at community or neighbourhood scale, not only individual homes.
Embed Health, Place and Ecological Thinking in Retrofit Strategy
Require all national retrofit programmes to use an ecological health model, so that interventions consider environmental and psychological stressors alongside material conditions.
Mandate Community-First Approaches in Retrofit Design
Require CHIAs (Community Health Impact Assessments) as a standard early-stage requirement for publicly funded retrofit schemes.
2. Centre Communities, Lived Experience and Equity
Engage Specialist and Marginalised Communities as Core Contributors
Ensure retrofit programmes include structured engagement with demographic groups (e.g., neurodivergent communities, older adults, culturally specific groups).
Prioritise CHIAs for specialist demographic groups
Direct early CHIA investment toward groups where impact is highest, and partner with aligned organisations (e.g., Autism UK, Centre for Aging Better, Shelter, Age UK).
Uphold equitable and inclusive practice standards
Require all community related work to follow “nothing about us without us” principles and include safeguards against harm from poorly prepared engagement.


3. Build Strong Delivery Ecosystems and Accountability
Leverage Community Leaders and Civil Society Networks
Formally recognise and resource community leaders, support networks, and civil society organisations as delivery partners.
Partner with Social Impact and Community Organisations
Enable and fund social impact organisations (e.g., Civic Square, East Marsh United, Julie’s Bicycle) to deliver CHIAs as part of national retrofit programmes.
Strengthen the Role of Public Health Departments
Position public health teams as required co-producers or reviewers of CHIAs within retrofit programmes.
Integrate CHIA Findings into Policy and Scheme Design
Mandate that CHIA outputs directly inform scheme rules, funding criteria, delivery expectations, and accountability frameworks.



In this second part of the workbook we set out the practical elements of going about conducting a Community Health Impact Assessment.
Having explained the differences between the types of Health Impact Assessments in Part One, we set out three group archetypes and which assessment type would be of most benefit in each given situation.
We set out the principles of engagement, and an overview of the steps involved. Finally we direct users to the printable workbook resources.


As set out in the Introduction, this workbook supports both community practitioners and advocates who want to use a Community Health Impact Assessment (CHIA) to understand local people and places more deeply.
A CHIA provides a baseline of community health, helps assess the effects of current or future changes, strengthens community connection, highlights existing health-promoting assets, and brings needed changes into focus.
In the following pages we highlight three archetypal users of this workbook. The following groups may identify themselves in one or more of these archetypes.
• Community groups in the retrofit, material and built environment space
• Community groups in the health and social justice space
• Tenants or residents that are not yet organised but on the brink of change in their neighbourhoods, or those that are recognising community health concerns in their area as a result of living environments
• Those that are able to further the use of this tool on the ground - cheerleaders that can influence the take up the tool
• Those that can incorporate this tool into design specifications, strategic or policy documents, or directly into retrofit scheme requirements
This tool also enables different communities and groups to work together and collaborate on overlapping concerns and experiences through a shared entry point.
The three archetypes are:
Group Archetype 1 - Local Resident Groups
Group Archetype 2 - Retrofit Ready Groups
Group Archetype 3 - Professional Class Groups
And to recap, the assessment types are:
HIA = Health Impact Assessment
CL-HIA = Community Leader Health Impact Assessment
CHIA = Community Health Impact Assessment
The following table sets out the most appropriate impact assessment method for each of the groups identified. This is a guideline rather than a rigid rule.


This visualisation is intended to ensure that the right people are in the right place. Each actor can move across, however they retain control and domain over responsibilities.
Group Archetype 1

Community and resident groups self-organise to explore how retrofit can impact their health.
Group Archetype 2

Community organisations and leaders leverage their positions in power to bring forward community imaginations and visions for long term stewardship.
Group Archetype 3

Public health professionals work in tandem to co-create a Community HIA that can be used by authorities going forward.
Community groups can use the CHIA resources to investigate how the systems around them influence their health and then create plans to articulate how retrofit can impact them.
Community leaders build on the grassroots work by residents and use the CL-HIA to bring forward critical issues on retrofit to authorities when timescales are short.
Public health professionals work alongside community leaders and residents to produce a new HIA. As a longer term process this is about creating new infrastructure going forward and building the necessary political capital for new introducing the new CHIA to policies.


The first archetype is a group of residents that are about to experience a change in their locality, this could be a major infrastructure development, demolition to their homes, major refurbishment to their homes or a land use change in the area surrounding their homes.

• They may be new to organising
• They may have already gathered as a group without the appropriate tools for documenting their experiences
• They may have been organising but not gaining traction for lack of evidence
• They are motivated to halt or pause the drivers of change through evidencing the harm or disruption
• They sense that there are financial and political drivers behind the change that are detrimental to the community and as a result their health
• They are looking for tools to collectively witness and affirm the moment, and the impact of the change being introduced
For example, a housing estate is being earmarked for demolition for future regeneration, residents are to be ‘decanted’ into temporary accommodation far away from their community. The assumption for demolition and regeneration has overpowered the possibilities of refurbishment and retrofit, the demolition and displacement will have huge impacts on residents’ individual and collective health.
In this case, using a CHIA would bring in different levels and layers of decision makers that may have previously been outside of the conversation, such as Public Health teams.
The second audience is organised community groups that are preparing for, or already progressing, retrofit works in their homes.
This includes the NRH Retrofit Connect Cohort*, as well as other Retrofit Ready Groups who are on the cusp of delivery or already have works in the pipeline.
* See appendix for definition of Retrofit Connect Cohort



For these groups, retrofit is already an established part of their journey, and it is broadly understood that retrofit will make their homes more energy efficient, comfortable, saving on bills in the long term, and is likely beneficial for their health.
• They may share a belief that retrofit is good for health without the data and shared understanding as to why
• They may be working across multiple projects, intuiting the connections and throughlines but looking to consolidate and illuminate these understandings
• They may be invested in conducting processes differently, in a way that is more inclusive of their community
• They may have reservations or concerns about decision making processes, delivery schedules, the short to long term impacts that retrofit works could have on their stress, their mental and social health
• They may be seeing retrofitting their built environments as an opportunity to reshape the relations in their communities, making the spaces more fit for purpose
For example, a community are preparing to embark on a large scale retrofit of their street or neighbourhood, there are many standards and guidelines available for how to go about this process, however there are particular experiences and a unique context that are not being considered in these standards.
The CHIA would be an opportunity to take stock of everyone’s contexts and experiences and how this process could have impacts on their health and that of the community at large.


Another audience group for this playbook are those that work on public health and macro social determinants of health, those that design and implement policies related to retrofit, housing, social participation and democratic processes.

In many instances, local authorities lack localised data and nuanced, granular understandings of people and place, making monitoring and evaluation difficult, as well as efforts to meaningfully analyse policies in action. Sometimes social participation projects, such as one off workshops or short series of workshops, roundtables and stakeholder engagement interviews, are short term, under resourced and overly output oriented.
This can make community engagement extractive and surface level, reducing communities’ willingness to go in depth, both in sharing what is currently happening for them and in imagining what could be possible.
A CHIA is a more time and energy intensive process that requires a longer term level of resourcing, commitment and vulnerability. It is a foundation for building community social capital. When communities can collectively determine and define baseline criteria of their health, communities are able to draw their observation to patterns, conditions and dependencies. This in itself is an important process for creating the environment in which trust can be built, and effective monitoring and evaluation to take place.
This archetype group includes:
• An organisation that is able to influence policy
• An organisation that is able to resource and fund this type of work
• A Public Health Department
• A Housing or Planning Department
• A Patient Participation Group
• A charity that represents and advocates for specific groups and demographics
A CHIA can be championed by institutional or professional partners who see the value in accurate, place-based data that takes into consideration the nuances of place, and the particular experiences of people in their homes. It furthers health equity by providing space for lived experience to reflect how the determinants of health impact and compound certain experiences. The process also furthers more democratic engagement with people in their lived environments, and may mitigate future preventable health risks. The CHIA as a whole can be championed as a tool to integrate health and community participation in retrofit or housing schemes.
Note, the steps set out below are as a guide, more detailed guidance is within the workbooks on Centric Lab’s website.
Once you have identified that the CL-HIA approach is the most appropriate for you or your group, read the “Community Leaders Health Impact Assessment (CL-HIA) Workbook”. This is available here on the Centric Lab website.
A person with good ties to the community uses the CL-HIA workbook to hold a number of workshop sessions.
Consideration is given to the principles for equitable engagement in establishing the workshop environment.
Prepare to host a session with Community Leaders. These leaders should be people who hold trusted leadership from the community they represent who have consent to communicate key insights on their behalf.



Identify and create baseline data with community leaders that helps external stakeholders understand those communities. This will likely include both publicly available data (in the context of housing this could include English Housing Survey, EPC database, Index of Multiple Deprivation) and more crucially, the sort of lived experience data that is missed by external data observatories.
Discuss how key determinants of health (housing, transport, employment, etc.) show up for the communities represented by session leaders.
This can be done generally or in relation to a specific proposal. For example, housing might be explored in terms of overall condition and care within the community, or in relation to a proposed local-authority retrofit programme.
Capture insights collaboratively and with consent with Community Leaders
New technologies are all well and good, but we need gutters repaired, roof tiles replaced, and general repair first.
It just feels that every decision about our local environment is being made for new people and not those of us who have been here for decades.
For us, being near green space isn’t enough, it’s not safe. What would help us is community-led security.
A problem we routinely face with housing and our health is when landlords are slow to act to address noise.
There are often promises of employment with regeneration but the conditions offered are so bad
Use the macro-environmental lens from the workbook - natural, built, social, economic, and political systems - to understand how these determinants shape local health conditions.
For example, Consider how something like housing and the natural environment interact to impact health. Could our housing have more biodiversity around it or be made from more natural sustainable materials.

Access to Green Space
What else?




Identify the criteria with the Community Leaders to judge the intervention proposed (retrofit programme for example).
Setting the health determinant in the context of the environmental context, questions about the proposal can be identified.
These questions can set out indicators that can then be used to assess the proposal in question.
These insights are turned into questions for decision making stakeholders to address:
Assessment Criteria Details/evidence Potential Stakeholders
Does the proposal ensure that immediate condition needs are met?
Does the proposal provide a level of community oversight for influence?
Does the proposal bring forward enforcement standards to ensure quality and robust delivery?
Does the proposal offer employment opportunities with secured rights?
Does the proposal address the culturally appropriate safety needs of local residents in creating new outdoor spaces?


The main difference to the CL-HIA process is the preparation steps.
Then follow the same steps as in the CL-HIA process:
Step 1 – Baseline
Step 2 – Insights on Health Determinants
Step 3 – Assessment of Intervention
Once it has been identified that a CHIA process is the most appropriate approach for you or your group, the first step is to create the conditions for a healthy working environment.
As a group of people who don’t normally work together it’s important to set boundaries and expectations together. Recommendations for how to go about this are set out in the “Facilitating a Community Health Impact Assessment (CHIA)” workbook.
Invest the time in learning to use good facilitation skills and methods to ensure a safe and welcoming space is created. Again, more details are in the workbook linked above.
Prepare the programme of activity and co-learning sessions with your community.
It is recommended that setting out a Theory of Change is a useful beginning point to build a collective understanding of what the ultimate goal is.
A Theory of Change is “a description of why a particular way of working will be effective, showing how change happens in the short, medium and long term to achieve the intended impact.”
I’m always battling to be heard about the mould in my apartment. No-one seems to take responsibility and I’m just sitting here depressed about what’s going in my
Does the proposal increase accountability and lines of communication between members of the public/ residents and those operating spaces?
They say that local jobs are important to their decisions in who gets the big contracts but we don’t see local people getting decent jobs.
Does the proposal ensure that employment offered provides secure employment conditions and a fair living wage?
It is important to note that the very idea of a CHIA is that it is co-created by the community, and driven by the community, so once the process is underway, it may change shape and direction to meet the needs of the community. What is set out above is one example.


When thinking about place, we need to see it as a living entity, made up of people’s experiences. It’s not just physical allocations of assets, it’s the experiences of them that define place.
To support good facilitation it’s a good idea to do some baseline research and ask questions with people. From their lived experiences, you start to see what matters and how retrofit becomes a broader place, social, and community based issue, rather than purely a matter of homes and heating.
Each initial investigation can open up rich conversations and insights from people who love, know, and care about where they live.

How multi-generational is the neighbourhood?
What’s the social capital of the neighbourhood?
How has politics been a part of the neighbourhood’s history?
What’s the history of the place, what has once been there?
What’s the spatial history of the place?
What are the community assets to be leveraged?
What novel geospatial datasets can you use to understand more about the place?


The Portland Inn Project CIC is a creative arts project for a community in Stoke On Trent with an aim to achieve community cohesion, economic, social and cultural development by involving the community in development of a pioneering community space, cultural hub and social enterprise.
On a December evening, members of the community gathered with people from the National Retrofit Hub and Centric Lab to explore how a CHIA may further their work in the neighbourhood. Over a number of hours (and snacks) we all shared stories and ideas of how retrofit could make an impact to the community and improve their health and quality of life. Here are some examples:


The area has high levels of noise and air pollution so wall and window insulation is key.
Absent landlords mean that it’s important for any agenda to have strong enforcement. There is a real fear of displacement from retrofit costs resulting in higher rents.
Wants Stoke to move away from the “Sick City” nickname it was given in the past - can retrofit build new pride?
Can retrofit be delivered in such a way that there’s accountable lines of communication between residents and authorities?
What’s the role that children have in this? How can their views, experiences, and lives be considered in project planning?
Any strategy should lean into the strong bonds the community have with each other.
Everyone reported that gutters and water overflow was ruining outdoor spaces and leading to mould development.
Collectively imagined taking over an abandoned shop and turning it into a community kitchen.
There is a strong steer here that policy designers and public health officials need to approach the health impacts of retrofit through a systemic lens. The insight also points towards the importance of building social capital and drawing on asset-based community development, while embedding robust governance throughout. And when it comes to insulation for thermal comfort, the message is that these measures should also be understood and communicated as ways to shield homes from unwanted noise and air pollution, not just to keep heat in.
When preparing to embark on your chosen method of assessment, it’s important to create the conditions for equitable engagement. The following is a list of such conditions to accommodate in your preparations.
The Principles for Equitable Engagement allow facilitators to abide by the Gunning Principles17, which form a strong legal foundation from which the legitimacy of public consultations is assessed.
The Gunning Principles are four guidelines ensuring fair and transparent public consultations in the UK, established in 1985, which mandate clear communication, stakeholder engagement, and consideration of responses.
The Principles for Equitable Engagement that follow have been developed through a combination of the Gunning Principles and practice based experience.



Collectivity can be defined as ‘the experience or feeling of sharing responsibilities, experiences, [or] activities’. In the context of equitable engagement, it means working collectively (i.e., as a group) towards a goal. Endeavour to include as many diverse voices possible and identify traumainformed methods for including those who may shy away from large spaces. Be sure to recognise who is not present as well.
In the context of equitable engagement with community expertise, selfawareness means being aware of yourself and your role in the collective; it means being aware of what you know, what you don’t know, and what you can’t know. For successful, equitable engagement with community expertise, the ‘outsider’ must be aware of the limits of their expertise.
It is important to establish honest and transparent working relationships between those working as a collective through open lines of communication. This can be facilitated through open group conversations, in a safe and equitable space, where members can talk honestly and open about: Reasons for being a part of the project; Intentions; Aims of the project; Expertise/skills and their limitations; Compensation/pay.
You have to be flexible; you have to be open to modifications of your original idea and willing to make compromises. The willingness to listen, learn, be proven wrong, and adapt is key to equitable engagement with community expertise. Being self-aware and honest is only valuable when
translated into action, i.e., into changes that serve the overall purpose of gaining a true understanding of a phenomenon and, ultimately, benefiting the community.
Each group or collection of people from a community should have the opportunity to practice their work in dignifying spaces. This means that organisers and authorities should consider spaces that are inspiring, well ventilated, catered, and accessible to all. This often means additional resourcing but it is essential. Equally, all engagement opportunities should provide a form of remuneration to participants. If “professionals” are paid for their time, then why shouldn’t the experts of place be too?
The community should benefit equally, if not more, from the relationship than ‘outsiders’. It’s important that ‘outsiders’ recognise that communities are always imparting and sharing their expertise, and, thus, are always benefiting the ‘outsider’ and providing a valuable contribution to the aims and success of the collective work. Therefore, open discussions from the outset of any collaboration should carefully consider in what way the project/’outsider’ can positively contribute to both individual community members and the community as a whole during any engagement sessions.


Any project or work that involves members of the community is carefully considered and guaranteed from the very start of the project. Examples can be: Developing a long-term partnership; Building a community panel for the future; Training the community to do their own research; Securing funding for future community-led research; Providing employment opportunities
Community sovereignty can be defined as the power of the community to control their own governance over their community. It means empowering communities to develop their own research agenda and to access funding for research. This includes access, control, and ownership over information and data
Informed consent is usually used within the context of healthcare with its formal definition being “Informed the process in which a health care provider educates a patient about the risks, benefits, and alternatives of a given procedure or intervention”. We want to extend this definition outside healthcare and into equitable engagement. Many words that we use could be alien or have very different meanings depending on cultural context. It is also important to note the consent is procedural rather than a stand alone moment. It might be a good idea for the objectives and progress of the study to be laid out in a communal knowledge portal like a Google doc or a website.
Note: These practice recommendations follow the headings and format of the policy recommendations in Part 1 for ease of reference


1. Adopt an Ecological Approach to Health in Retrofit Policy
Treat Retrofit as a Neighbourhood-Scale Opportunity
Delivery teams should analyse local lived experience, patterns of use, and neighbourhood dynamics to identify where retrofit can generate wider health benefits.
Embed Health, Place and Ecological Thinking in Retrofit Strategy
Practitioners should assess environmental and psychosocial stressors alongside physical housing conditions when designing retrofit interventions.
Mandate Community-First Approaches in Retrofit Design
Begin engagement by mapping community priorities and lived realities before selecting technical measures or housing archetypes.
2. Centre Communities, Lived Experience and Equity
Engage Specialist and Marginalised Communities as Core Contributors
Work with these communities to understand lived realities, such as preferences for baths over showers, and integrate these insights into design decisions that improve health and quality of life.
Prioritise CHIAs for specialist demographic groups
Use existing operational networks to support smoother adoption, richer insight gathering, and clearer pathways to policy implementation.
Uphold equitable and inclusive practice standards
Practitioners should use equitable engagement methods, centre lived experience, and ensure communities have agency throughout the process.
3. Build Strong Delivery Ecosystems and Accountability
Leverage Community Leaders and Civil Society Networks
Invite insight from trusted relationships to gather insight, build legitimacy, and support residents to shape local places.
Partner with Social Impact and Community Organisations
Embed retrofit within broader community missions for a just and regenerative transition, centering these organisations’ long-standing relationships and convening power.
Strengthen the Role of Public Health Departments
Public health practitioners should apply health-systems expertise to ensure CHIAs are robust, actionable, and aligned with health equity goals.
Integrate CHIA Findings into Policy and Scheme Design
Delivery teams should treat CHIA findings as actionable evidence, using them to refine design choices, mitigate risks, and maximise health and wellbeing outcomes.

The following are some sample slides from the toolkits that are designed to help facilitators develop health impact assessment methods.
Resources from the online Ecological Health course from Centric Lab and partners may also prove to be useful grounding for those investigating the topics of health and place18.





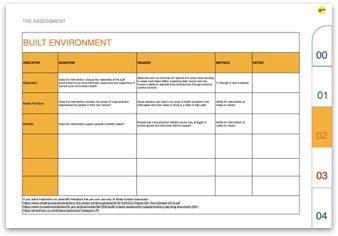
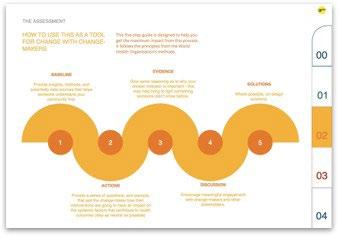

This light-touch approach is designed to support community leaders work with speed to capture key insights about community health and the impacts that a policy, plan, or project may have.
These sample pages show how the toolkits guide facilitators through a series of stages in order to quickly yet robustly produce a communityleader’s HIA.
Click HERE to access the toolkit

Or scan here to download
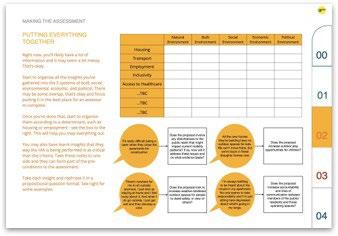


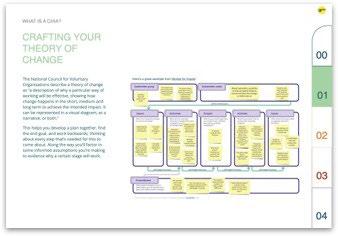



This toolkit is designed for collaborations between civil society organisations and public health teams to create a community health impact assessment from the ground up.
It is a more time intensive but rewarding process.
These sample pages show how the toolkits guide facilitators through a series of stages in order to quickly yet robustly produce the assessment..
Click HERE to access the toolkit

Or scan here to download
When facilitated appropriately, conducting a CHIA with communities brings out incredible insights into how communities and residents perceive their environments, and how their imaginations lead to solutions.
Research can never replace people’s histories and experiences with the places they live. They can reveal key opportunities to drastically change their environments and create conditions for better health outcomes.
It’s the facilitator’s role to create the space for this and to acknowledge this knowledge and expertise.


Retrofitting our nation’s homes has the potential to change the lives and the economy on an unprecedented scale. How that is done is the art within the science. Aligning the missions of retrofit with the wider public health (and social wellbeing agenda) is a winning tactic. Health is a unifier, we are all just lumps of cells with beating hearts.
Healthcare and feeling healthy are key pathways to happiness and social wellbeing. As such, understanding how the practice and process of retrofit aligns with this notion will be crucial to a public and systemic uptake. This workbook has focused on demonstrating how a community health impact assessment is a mechanism to achieving that goal.
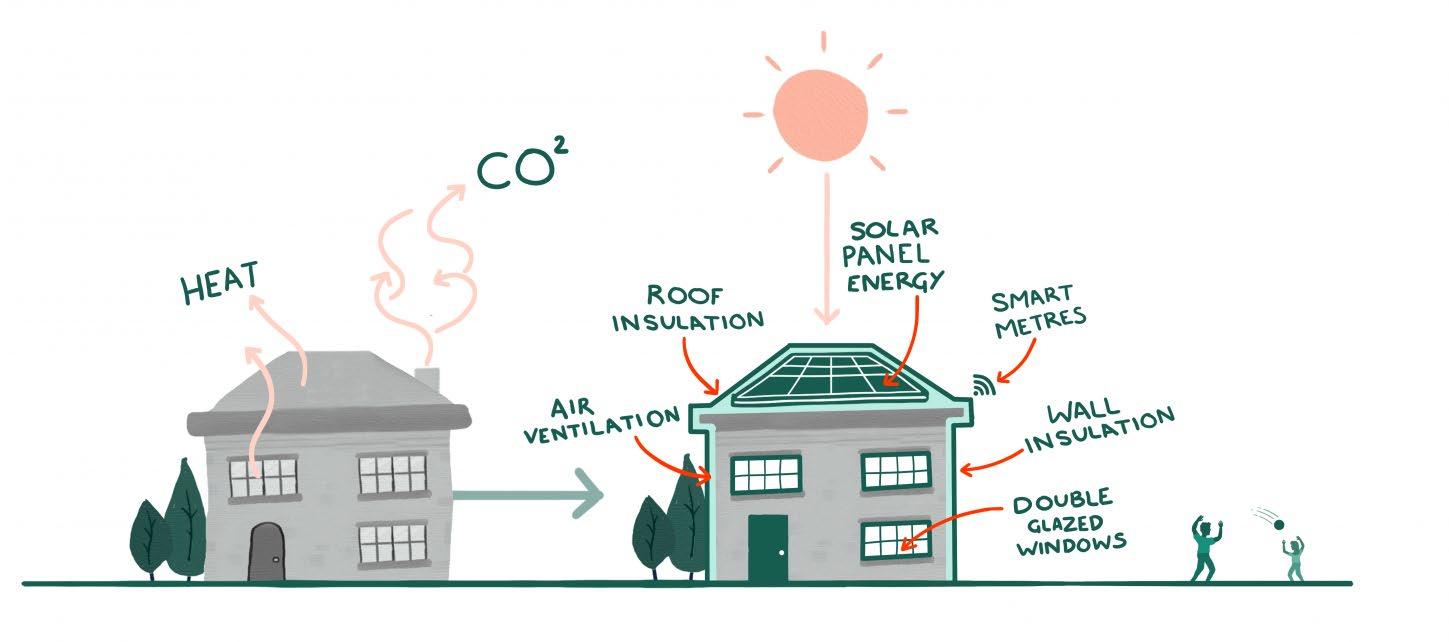

This section is intended to provide some baseline understandings of health to support learning and action.
Split into four sections of Place, Community, Health, and Data these insights build capacity for understanding health ecologically and why new approaches are needed.
Each section has three categories: Introductory, Technical, Political. Within each category is a learning developed from Centric Lab’s research library.




Our health is influenced by our constant, dynamic, and biological interaction with the environments around us.
Some estimate that with each breath, we inhale more air molecules (25 sextillion or 25,000,000,000,000,000,000,000) than there are grains of sand on all the world’s beaches.
Biological Inequity refers to the “systematic, unfair, and avoidable stress-related biological differences which increase risk of disease, observed between social groups of a population”. Focused on articulating how particular social groups are disproportionately exposed.
We live in many environments; natural, built, social, economic, and political. Each of these environments can create both health pathways as well as stressors. For example, a good natural environment will be highly biodiverse, exposing us to a diversity of microbes that support gut health. Whereas, a bad economic environment will result in us working in unsafe, contaminated, and marginalising situations creating states of unjust stress. This means that assessing health ecologically allows us to look at the various place-based factors that influence health and account for externalities that may otherwise become determinants of health
We each inhale up to 15,000 litres of air every day, exposing our ‘walking ecosystems’ to an array of invisible biodiversity. We often speak of air in terms of its quality. Indeed, high levels of pollution and pathogens fill the air in many places and cause (preventable) diseases. This happens when we fail to respect air. It happens when we fail to foster kinship with the natural world; when we “bite the hand that feeds us”. It can be challenging to define ‘healthy air’. However, a good starting point is promoting air characterised by very low pollution and pathogen levels and the presence of beneficial microbiota and other biogenic compounds, such as phytoncides.
Given how much habitat plays a role in a person’s health, it is inaccurate to simply correlate poor health outcomes with a phenotype or “race”, additionally, it is more important to look at the interaction between a person in a specific place than just their “race”. Finally, it is a person who experiences the environment not their phenotype, race, or ethnicity. In other words if a Black person is living in a neighbourhood with clean air, water, access to healthcare, access to safety, access to nourishing food they will have very different health outcomes than a Black person living in an environment with high air pollution, no running water, no feelings of safety, etc.
Sources
https://www.thecentriclab.com/air-is-kin/who-are-air
https://www.thecentriclab.com/research-archive/obesity-classism-and-racism
https://en.wikipedia.org/wiki/Biological_inequity


A community is a group of people who have factors in common that socially, mentally, culturally, and spiritually bind them, such as living in the same area, or, among other things, their interests, work, gender, sexual identity, nationality, customs, language, activities, events, or ethnicity.
By neglecting people’s lived experience and relying on average effects from ‘large data’ only, we may miss important nuances of the association of a certain exposure with health.
Community health without community engagement leads to methods and programmes that happen to communities, not with, by, or for them.
We live in many environments; natural, built, social, economic, and political. Each of these environments can create both health pathways as well as stressors. For example, a good natural environment will be highly biodiverse, exposing us to a diversity of microbes that support gut health. Whereas, a bad economic environment will result in us working in unsafe, contaminated, and marginalising situations creating states of unjust stress. This means that assessing health ecologically allows us to look at the various place-based factors that influence health and account for externalities that may otherwise become determinants of health
It is not the job of practitioners to decide the cultural framing of health, it is a conversation to develop with communities. The terminology and framing used by practitioners are useful for developing a scholarly understanding of health and health phenomena, but every community will have its own cultural framing based on practises that may be internally developed or adapted from other environments. Lived experience is associated with knowledge, insights, and understanding of a phenomenon. In other words, lived experience is associated with expertise or ‘lived expertise’.
The UK COVID-19 response showed some data-based disparities, what the Ada Lovelace Institute refers to as the ‘the data divide,’ which include factors such as service accessibility, digital infrastructure, awareness of technologies, and familiarity or attitudes towards technology. Many of these outcomes are a result of using data as evidence in a situation where there is already a power inequity and distrust in structural stakeholders.
Sources
https://www.thecentriclab.com/research-archive/equitable-working-with-community-expertise
https://www.thecentriclab.com/research-archive/lived-experience-communities-and-health
Our health is influenced by our constant, dynamic, and biological interaction with the world around us. Epidemiologists have for many decades framed and understood health as an ecological phenomena.
Chronic stress resulting from our interactions with polluted, socially-unjust, and deprived environments can cause a biological wear-and tear on our hormonal, metabolic, and immune systems.


Viewing health, and designing policies and practices, around it solely as the function of behaviour and choices is scientifically inaccurate, opening up capacity for ignorance, bias and prejudice to create and entrench injustices.
Our body uses various systems, such as the hypothalamic-pituitary-adrenal axis (HPA-Axis) to observe changes in the environment in order to make adaptive changes within our bodies. For example, during a heatwave, our body will sense the change in temperature and through the communication between HPA-Axis, respiratory, and cardiovascular systems our body will go through a wide range of changes to adapt to the heat: we change our breathing rhythm, our heart starts to pump faster to move oxygen through all of our tissues, and, of course, we start to sweat to begin the cooling process.
When we are unable to restore against stressors and experience them chronically there are impacts to otherwise regularly occurring biological systems. Chronic stress increases the individuals ‘allostatic load’ level – which refers to the wear and tear of stress-related biological systems e.g., neuroendocrine, metabolic, immune systems. Neuroendocrinologist Robert Sapolsky’s work looks into factors such as non-life-threatening stressors, such as constantly worrying about heating or eating or losing your job, and how they trigger the release of adrenalin and other stress hormones, which, over time, can have devastating consequences to your health; “If you turn on the stress response chronically for purely psychological reasons, you increase your risk of adult onset diabetes and high blood pressure. If you’re chronically shutting down the digestive system, there’s a bunch of gastrointestinal disorders you’re more at risk for as well.”
The biomedical model of health failed to adequately account for wider causal psychological, and environmental factors and so there were calls to expand upon the biomedical model of health by acknowledging ‘top-down’ factors that also contribute to health and disease. This has come to be known as the biopsychosocial model of health, which emphasises an interplay between biological, psychological and socio-cultural factors in determining health and disease. Biological factors themselves are seen as necessary but not sufficient cause of disease, and so ‘top-down’ psychological, behavioural and socio-cultural factors must be be taken into account, where an individual’s health is a psychophysical phenomenon that is socially situated.
Sources
https://www.thecentriclab.com/research-archive/lived-experience-communities-and-health
https://www.thecentriclab.com/research-archive/the-history-of-disease
https://www.thecentriclab.com/research-archive/health-as-ecological


Data is factual information, such as measurements or statistics, used as a basis for reasoning, discussion, or calculation.
Data alone cannot provide us with the full phenomenological experience of health.
Data intentionally used for health justice considers the human, societal factors when creating ranges and values.
The purpose of data can be seen to:
1. Create an understanding of a phenomena
2. Document or measure a specific phenomena or experience.
3. Tangibly reflect what is usually intangible.
4. Creates opportunity to make informed decisions
5. Fill in gaps of knowledge that help individuals or groups make decisions at a variety of scales.
Sources
Most large-scale data studies are ‘multi-purpose’ studies. For example, large longitudinal studies collect data on a wide range of factors concerning people’s lives, so that many societal questions can be answered with the data collected. The richness of these data is a great advantage of large-scale studies. However, because the studies are multi-purpose, they do not provide specific data on a specific phenomenon. Thus, although there may be some data on some factors relevant for the phenomenon, many other important factors may not be captured. This means A) that an observed phenomenon cannot be explained fully and/or B) that the data provides a biased description of an unobserved phenomenon.
https://www.thecentriclab.com/research-archive/using-data-for-health-justice
https://www.thecentriclab.com/research-archive/data-culture-for-health-justice
https://www.thecentriclab.com/research-archive/macro-enviro-data-hj
Another damaging use of data-driven health is to directly conflict with, or erase, more localised or cultural knowledge that may not present as explicit data. To fully capture lived experience, we need to create an equitable data ecosystem where a community can gather their own data and have it be as important as the data gathered by practitioners.

