A guide to
Multiple System Atrophy Trust
Our Vision
A World Free of MSA
Our Mission
To find the cause, and ultimately cure, for MSA. Until that day we will do all we can to support people affected by MSA and work to ensure that they are not alone on their individual journeys.
Six things to take away…
1. Create a network of support around you
2. Educate yourself about MSA
3. Plan ahead – it helps avoid a crisis
4. Arrange regular reviews with the professionals
involved in your care
5. Get advice on financial affairs and care support
6. Plan enjoyable activities with family and friends.
The aim of this guide is to explain what MSA is. It includes information about the symptoms that may occur, how these symptoms can be managed and tries to answer some frequently asked questions. We hope it will help support you and your family but if you have questions or want further guidance, please contact us at the Multiple System Atrophy Trust (‘the Trust’).
Most people have never heard of multiple system atrophy (MSA). Many healthcare professionals are often unfamiliar with the condition. It is rare, sometimes not recognised and, as you will probably know by now, often difficult to diagnose.
We offer information, support and education and fund research into MSA. Our services are free to people living with MSA and their families and friends, and we are entirely funded by voluntary donations. If you have not done so already we encourage you to register with us.
We have a range of information materials on living with MSA which you can view or download from our website www.msatrust.org.uk.
This Guide is not intended to replace advice from your Specialist. Any issues raised through reading this information should be discussed with your doctors and healthcare professionals.
We are happy for you to reproduce the information in this guide but please acknowledge the Multiple System Atrophy Trust as the source.
What is multiple system atrophy?
Multiple system atrophy (MSA) is a progressive neurological disorder that affects adult men and women. It is caused by degeneration or atrophy (shrinking) of nerve cells in several (or multiple) areas of the brain. This can result in problems with movement, balance and autonomic functions of the body such as bladder and blood pressure control.
There is a list of common terms on page 27 with helpful explanations of words and references used throughout this Guide.
How common is MSA?
MSA is a rare disease and diagnosis is difficult. It can take several visits to a Neurologist to get a diagnosis. Research suggests it affects about 4.5 people per 100,000. This means at any one time there are about 3,300 people living with MSA in the UK and Ireland.
Who gets MSA?
MSA usually starts between the ages of 40-60 years. It can affect people younger and older but isn’t known to occur in people under the age of 30. MSA does not appear to be hereditary although current research is examining if individuals may have a genetic predisposition to develop the disease. The importance of environmental factors is not clear and there is still much to understand about the condition. We do know it is not infectious or contagious and has no connection with the much more common neurological disease, multiple sclerosis (MS).
What does MSA mean?
The condition was previously called ‘Shy-Drager Syndrome’. The term ‘multiple system atrophy’ was first introduced in 1969. It took some years for the term ‘MSA’ to be widely adopted until an international consensus of medical experts recommended in 1996 the name multiple system atrophy (MSA) be used. They also recommended the terms ‘MSA-C’ and ‘MSA-P’ be specified to indicate whether a person’s early symptoms are predominantly cerebellar (see common terms, page 27) or Parkinsonian respectively.
MSA stands for:
Multiple - more than one
System - brain structures that control different functions
Atrophy - cell shrinkage and loss
This means that cells are damaged in areas of the brain which control different body functions. The three areas most often affected are the basal ganglia, cerebellum and brain stem.
How are the nerve cells in the brain damaged by MSA?
Nerve cells in the affected areas of the brain atrophy or shrink, this shrinkage can sometimes be seen on MRI scans. The shrinkage is caused by abnormal alphasynuclein protein building up in the nerve cells which then causes them to die. Loss of these nerve cells shows up as shrinkage in the affected area of the brain.
We all have alpha-synuclein in our brains. Abnormal protein deposits in the cells of the control centres of the brain involved in movement, balance and autonomic function, damages these areas and causes symptoms of MSA.
Why do nerve cells become damaged?
It is still unclear why alpha-synuclein gathers together and the cells become damaged in people with MSA. Further research is being conducted into why and how this happens, some funded by the MSA Trust. The progression of damage is also unclear and is different for each individual. Studies of the brains of people who have been affected by MSA compared to unaffected brains are aiding research.
How is MSA diagnosed?
The diagnosis of MSA is a clinical one and depends on a specialist recognising a combination of symptoms and signs using a specific set of criteria. There is not a test that can give a clear positive or negative indication of MSA. Many neurological conditions look similar in the early stages so it’s important that a more common or treatable condition is ruled out before a diagnosis of MSA is made. Improved brain scanning techniques may show abnormalities in some people with MSA but it is not unusual for a standard MRI brain scan to be normal.
There are a number of symptoms that healthcare professionals might note and highlight when referring to a specialist for a possible MSA diagnosis. These are:
• Erectile dysfunction in men and sexual dysfunction in women
• Bladder issues including urgency, frequency, nocturia (passing urine at night) and retention (inability to empty the bladder)
• Postural hypotension (also called Orthostatic hypotension) which is a sudden drop in blood pressure when changing position – particularly from lying or sitting to standing
• Poor response to Levodopa (a commonly used Parkinson’s Disease drug)
• Cold extremities
• Difficulty speaking and swallowing
• Inspiratory sighs/ stridor (a high-pitched breath sound)
• Faster progression than Parkinson’s Disease and Cerebellar ataxia.
Symptoms
Although there is currently no specific treatment to modify disease progression there are ways of managing many of the symptoms of MSA. Trials of possible medicines to treat symptoms are continually being explored.
What are the first signs of MSA?
For men, the first symptom is often erectile dysfunction (inability to achieve or sustain an erection). Other causes may be explored by a doctor before connecting it to a neurological cause. Both men and women may have early bladder problems including urgency, frequency, nocturia (night time passing of urine) and retention (not emptying the bladder fully). Often these bladder issues are linked to other causes such as ageing.
Other early problems can be feeling stiff and slow as well as changes in handwriting. Some people become clumsy or unsteady when walking. If blood pressure control has been affected, people may feel dizzy when standing up or experience episodes of fainting.
What happens next?
MSA is a progressive disease, which means that unfortunately symptoms will worsen over time. As things progress, people will need help to manage day to day living. The speed of these changes is difficult to predict as people with MSA experience the condition differently and the rate of progression varies.
Some people feel they cope better if they know what lies ahead. However, others may prefer to receive information in smaller amounts or at different times. Even within the same family, people may choose to access information at different times. Whilst MSA progression is very individual and unpredictable, you can discuss how your journey may look with your specialist or one of our MSA Health Care Specialists.
The symptoms that may be experienced include:
Parkinsonism
• Feeling slow and stiff when moving
• Difficulty in starting to move
• Writing becoming small and spidery
• Difficulty turning in bed
Cerebellar
• Feeling clumsy, dropping things
• Finding it difficult to fasten buttons
• Feeling unsteady in crowds
• Unable to balance without support
• Difficulty writing
• Slurred speech
Autonomic
• Difficulties with sexual function
• Bladder problems
• Feeling dizzy or fainting (blood pressure problems)
• Pain around neck and shoulders (known as ‘coat-hanger pain’)
• Altered bowel function
• Cold hands and feet
• Problems with sweating control
Other problems
• Weakness in arms and legs
• Uncontrollable laughing or crying (called emotional lability)
• Restless sleep
• Nightmares
• Noisy breathing during the day, excessive snoring at night
• Unintentional sighing
• Weak, quiet voice
• Difficulty with chewing, swallowing and coughing at mealtimes
• Blurred vision.
There are ways of managing and alleviating symptoms. These include lifestyle adaptations, medications for specific symptoms and ensuring you get the support and advice of professionals involved in your care.
Remember we are here to help.
Treatment and management
Treatment for people with MSA involves a combination of medication, specialised equipment and the involvement of therapists to manage specific symptoms. This diagram shows how members of a multidisciplinary team may be involved in your care in conjunction with you and your GP.
ou and your GP
•Neurologist/Specialis t
• Parkinson'sDiseaseNurseSpecialist/ NeurologicalNurseSpecialist
•MSATrustandMSAHealthCareSpecialists
•Physiotherapist
•SpeechandLanguageTherapist
• Occupational Therapist
• Carer Support
• Palliative Care Specialists
• Bladder and Bowel Specialist
•CommunityNursesandMatrons
• FallsClinic
•Dietician
•SocialWorkerandCareServices
• Counsellor
•Neuropsychologist
Treatment
The complex nature of MSA means that the best treatment is gained from a team approach, involving a group of health and social care professionals.
Ideally, you will be supported by your GP who will act as a care coordinator and refer you to other members of the team. It is quite possible your GP has not previously seen a patient with MSA but we can provide specific medical information for them. Likewise, members of the team may not have treated anyone with MSA but don’t be discouraged by this. Please ask them to contact us for information, or get them to look at our website section for health and care professionals.
What medication can I take?
The medicines you are prescribed will vary depending on your symptoms. Medications are very individual and what works for one person may not be effective for another. Your specialist will prescribe the best combination to meet your needs. Below are some of the medications and treatments commonly used in MSA.
Movement problems
Drugs to help stiffness and slowness are the same drugs used in Parkinson’s Disease. They are often not as effective in MSA and can make blood pressure problems worse. It may take time to find what suits you and if a medication is not useful it may be reduced or discontinued on the advice of your specialist.
• Levodopa (Madopar or Sinemet)
• Amantadine (Symmetrel)
• Dopamine Agonists (may be used in conjunction with Levodopa)
Physiotherapy can prove helpful and also provide you with tips to get you moving. Your physiotherapist can give you
specific exercises to do which may help to prevent falls.
Balance difficulties
Feeling unsafe on stairs and elsewhere may be due to problems with balance and people often feel they need to hold on to things for support. Physiotherapists, Occupational Therapists and the Falls Team can provide advice and equipment to help you move safely. For example, they can suggest where handrails can help or where raised seating can aid people when rising to stand.
Difficulties with bladder control
Urology and continence specialists can assess your symptoms and recommend treatment to help manage bladder issues.
People may also find that they are not fully emptying their bladder when urinating. If you are leaving behind some urine it can make you more likely to experience urine infections (see section on ‘Antibiotics’ on page 17). If this becomes a major problem, there is currently no effective medication for this and bladder surgery is very unlikely to lead to improvement. Intermittent catheterisation, either by you or a carer, is the best management. Catheterisation is the process of putting a tube into the bladder to allow urine to drain. This may be done intermittently and then removed. Or it may be placed permanently, either through the urethra or through the abdominal wall. A continence advisor can help you learn the technique. People with MSA who have postural hypotension produce less urine during the day and more at night. There are medications such as DDAVP/ Desmopressin that can help with nocturia. These do have side effects so will be discussed between you and your specialist, if it is thought they may be helpful.
Also, you may want to think about having a commode or urinal at your bedside to reduce the effort of getting to the
bathroom. This is especially important if you have low blood pressure (postural hypotension) or are prone to falls. We have a factsheet on ‘Continence in MSA’.
Constipation
Constipation is common in people living with MSA. It is to be avoided where possible as straining could affect your blood pressure and make other symptoms worse. It is important to drink plenty of fluids and eat a well-balanced diet. Dietary fibre, especially cereal-derived fibre, may not help with bowel emptying. Daily medication to prevent constipation is often needed to maintain a regular bowel habit. Suppositories can be helpful to avoid straining. For some people with MSA loose bowel movements or diarrhoea can be troublesome. There is a specific factsheet on ‘Bowel Management in MSA’ available from the Trust, and a Dietitian can also provide more advice.
Sexual Function
For men, erectile dysfunction (inability to achieve or sustain an erection) is often the first symptom of MSA. Men often take medication for this problem such as sildenafil (Viagra), tadalafil (Cialis) or vardenafil (Levitra). However, these medications can worsen blood pressure control, so other measures may be an option. Woman may also experience impaired libido and sexual function. Seeking help on this issue is therefore important so you should not be embarrassed to talk with your doctor, who can support you and refer you to a specialist if neccessary. We have a ‘Relationships and Sex’ factsheet available to support you.
Dizziness
Dizziness may be due to your blood pressure falling when you stand up or change position. This drop in blood pressure is called postural hypotension or orthostatic hypotension. There
are several ways to relieve this. These include increasing your fluid and salt intake as well as leg exercises to help blood flow in your calves. It is important that you avoid sudden changes in position like quickly rising to your feet and plan your periods of activity accordingly. Abdominal binders and compression hosiery can also be helpful. If the drop in blood pressure is significant, and cannot be managed by practical methods, medications may be suggested by your specialist:
• Fludrocortisone - A steroid, taken in very small doses
• Ephedrine - Works quickly to raise blood pressure; usually taken three times a day
• Midodrine - Works quickly to raise blood pressure within 30-60 minutes; usually taken three times a day. Only prescribed by specialists.
We have a ‘Living with Postural Hypotension’ factsheet available in print or to download on our website (including an ‘easier to read’ leaflet version with a checklist).
Antibiotics
An infection in someone with MSA can suddenly worsen all symptoms of MSA and should be promptly treated with antibiotics. Urinary and respiratory infections are the most common.
People with MSA may not have a raised temperature with an infection. If there is a sudden worsening of MSA symptoms, health and care professionals should always consider if an infection is present.
Swallowing
Coughing whilst eating and drinking may be an indication of swallowing difficulties. Coughing is a normal reaction to help prevent food going into your lungs and causing infection. A Speech and Language Therapist can assess the safety of your swallow and, together with a Dietitian, can advise on the best type of food for you.
Sleep disorders
You may experience irregular breathing at night. Missing a breath or not taking deep enough breaths (sleep apnoea) can sometimes happen and may be associated with increased snoring. If you feel tired and lethargic during the day, it may mean that you have a sleep disturbance.
Studies of your sleeping behaviour can be carried out at a sleep centre to see how this may be affecting you. It could be necessary to have some breathing assistance at night from a piece of equipment called a Continuous Positive Airway Pressure Machine (CPAP) (see Common Terms on page 28). This equipment can help improve your quality of sleep and can travel with you wherever there is electrical power.
Emotional reactions
Emotional reactions may be appropriate in the situation, but the behaviour or expression may be stronger, louder, or last longer than would be usual for you. This is called emotional lability. For example, a person may be genuinely happy but once the laughter has started they may be unable to stop or regulate the behaviour. This could include laughing (or crying) too loudly, too much, or for too long. Please see out factsheet for further information about uncontrollable laughing and crying.
An individual living with MSA may also show extreme but genuine emotional responses, including sadness and grief, despair, frustration and irritability, anger, anxiety and depression, joy, happiness and pleasure. Please see the Emotional Support resource on our website or request our booklet for further support.
Aids and equipment
There are many items, aids and pieces of equipment that
may prove useful to help overcome some of the difficulties connected with MSA. However, some of these can be expensive so you should discuss with the relevant therapist in your support team before buying anything. It may be possible to get some items of equipment via your local authority or the NHS. If you would like further information about aids and equipment, please contact the Trust or refer to our website.
We also fund voice banking at the MSA Trust so get in touch with us for more information on this service.
What about complementary therapies?
Some people with MSA find complementary therapies helpful, particularly to aid relaxation and improve comfort and general well-being. Some therapies can help specifically with muscle spasm and pain management. Please discuss with your specialist or GP before trying any complementary therapies.
It is important that you tell any complementary therapist that you have MSA. Some treatments may lower your blood pressure further so you should let your therapist know if you have low blood pressure, particularly postural hypotension. Use a therapist who is a member of the appropriate governing body and is able to demonstrate their current competence and experience. Bear in mind that very few therapies are funded on the NHS. For further advice, contact the Institute for Complementary and Natural Medicine (see page 35) or download our factsheet on Complementary Therapies.
Would counselling be helpful?
Many people find counselling helpful in coming to terms with a diagnosis of MSA and the changes it brings. Please see the emotional impact pages on our website for more information or ask us to send you a copy of our Emotional Support booklet.
Communication
Over time MSA causes challenges with speech and communication. It is important that people are referred to a Speech and Language Therapist. The Speech and Language Therapist will make an assessment and then recommendations to help with communication. They may recommend simple aids such as using a communication chart or the use of technology, and this may include voice banking. Many people find their voice varies at different times of day or when they are fatigued. Peoples voices may become quiet, so a voice amplifier may be helpful.
Frequently Asked Questions
Try not to be worried if professionals that you meet have not heard of MSA. They are experts in their professional role with much to offer you, and can become experts in MSA through caring for you.
Be prepared to cope with questions about MSA by:
• Having a standard answer ready such as “it’s like Parkinson’s Disease but I have extra problems such as low blood pressure”
• Having this guide and the Trust’s information materials handy to show your family and friends
• Giving your GP and therapists the Trust’s contact details so they can get further information themselves
• Giving your care professionals and family carers contact details for the MSA Health Care Specialists so that they can seek guidance on how best to support you (see page 34).
How is MSA different from Parkinson’s Disease?
Many people with MSA may have received an initial diagnosis of Parkinson’s Disease (PD) or cerebellar ataxia because they both cause similar symptoms initially. Additional problems that develop in MSA which are unusual in early PD may have made your neurologist suspect that you do not have typical Parkinson’s but a “parkinsonism”- one of which is MSA. The changes in the brain in MSA are different from that of PD.
Will my children or family get MSA?
There is no evidence that MSA is a hereditary condition and it is not contagious or infectious. You may read or hear about genetic factors; this does not mean that there is a known faulty gene. As a greater understanding of genetic makeup is achieved, there is increasing interest as to whether an individual’s specific unique combination of genes can cause them to be more susceptible to developing conditions like MSA.
Will I experience cognitive difficulties?
People with MSA might experience cognitive difficulties, including cognitive slowing and cognitive dysfunction as the illness progresses. People may find they struggle with planning, organising, memory, attention, problem-solving and flexible thinking. Emotional control can be affected. Giving people more time to think and answer, and also concentrating on one task at a time are strategies that can help. Fatigue and tiredness can also affect cognitive abilities. This will likely come on gradually. Confusion or hallucinations are not usual in MSA, unless there is an acute infection which can sometimes cause a sudden onset of these symptoms. The symptoms should subside after treatment.
Can I travel abroad on holidays?
It is important for us all to take holidays and have a change of scene if that is something we enjoy. If you like holidays in hot countries try to keep in the shade and drink plenty of fluids. Getting too warm can cause you to feel faint, especially if you have postural hypotension. You may become dehydrated more quickly and will need to drink extra fluids in hot weather.
Travel abroad is possible with the correct arrangements and good planning in place. Travel companies will need to be made aware of your special requirements and you will need to ensure the accommodation is suitable. There is a factsheet available from the Trust on holidays, with information about facilities in the UK and abroad, and details of companies that offer travel insurance to people with preexisting medical conditions.
What sort of a diet should I be on?
There is no special diet recommended for MSA, although
eating a balanced diet with fibre, protein, fresh fruit and vegetables is important. If you have postural hypotension there are some dietary suggestions to prevent a drop in blood pressure in our ‘Postural Hypotension’ factsheet. If you have swallowing difficulties, ask your Speech and Language Therapist for advice on the best type of food and drink for you.
I am worried about my family having to look after me
At some point you will need someone to help look after your everyday needs. Professionals within the health and social care systems can help you, and your family. You should ask your local Social Services Adult Disability Team to undertake a care needs assessment for you and a carer’s assessment for the person helping you with your everyday care needs.
Who can help me get things sorted out at home?
The assessments provided by Social Services Adult Disability Team (see above) should help identify the things you need help with. Other professionals, such as your GP, Occupational Therapist, Physiotherapist, Parkinson’s Nurse Specialist, MSA Health Care Specialist and our Social Welfare Specialists, will also be able to help you find the appropriate support. Citizens’ Advice, Carers UK and the Carers Trust are three organisations that can advise on help and support locally (see page 35).
I’m worried about my finances
Having MSA may mean that you have to stop working sooner than you anticipated - maybe before you can claim your pension. You may also face other additional costs.
There is a range of benefits and tax allowances available which the Trust’s Social Welfare Specialists can provide
support with claiming. Any entitlements will be assessed on your individual circumstances and the level of your disability, and this can be regularly reviewed if things change. Carers may also be entitled to benefits.
As well as our Social Welfare Specialists, the Trust also has factsheets summarising the benefits available. For a comprehensive assessment of entitlements, contact your local Social Services department or use the website www. turn2us.org.uk. Most people living with MSA will be eligible for some form of benefit so do claim if you can.
What about the future?
Many of the ideas and plans you had for your future will change once you have been diagnosed with MSA. People adjust to this change in different ways. There is no one plan to help you cope but there are many people out there who can offer help and support, not least of these is us at the MSA Trust. We have a ‘Planning for the Future’ resource on our website to support you in this area and a ‘I Wish I’d Known That A Year Ago’ factsheet. Thinking ahead and talking things through with your family can help.
Why has palliative care been mentioned?
Palliative care is about maintaining and maximising quality of life. It is the medical specialty focused on relief of pain, stress and other debilitating symptoms of serious illness. Hospice care and hospice services are one group of services providing palliative care which may be provided at any time during a person’s illness from the time of diagnosis onwards. Palliative care teams include specialist nurses, doctors and therapists. There is a factsheet on ‘Palliative Care’ available from the Trust and you may also find our Emotional Support resource (available on our website and as a booklet) helpful.
Research
Voluntary donations given to the Trust means we can fund research grants into MSA. We have a Scientific Advisory Panel which is made up of scientific and clinical experts in MSA. They look at the applications for research grants and judge which projects may be most worthwhile. We adhere to strict research and financial guidelines to ensure donations made to the Trust are managed properly. Our ‘Research Strategy’ can be viewed on our website.
Research
The MSA Trust fund and support research into MSA in the UK and Ireland, and work collaboratively with MSA Researchers worldwide. We are supported by an independent Scientific Advisory Panel (SAP), whose membership includes experts in clinical, scientific and research aspects of MSA, and people whose lives have been affected by MSA.
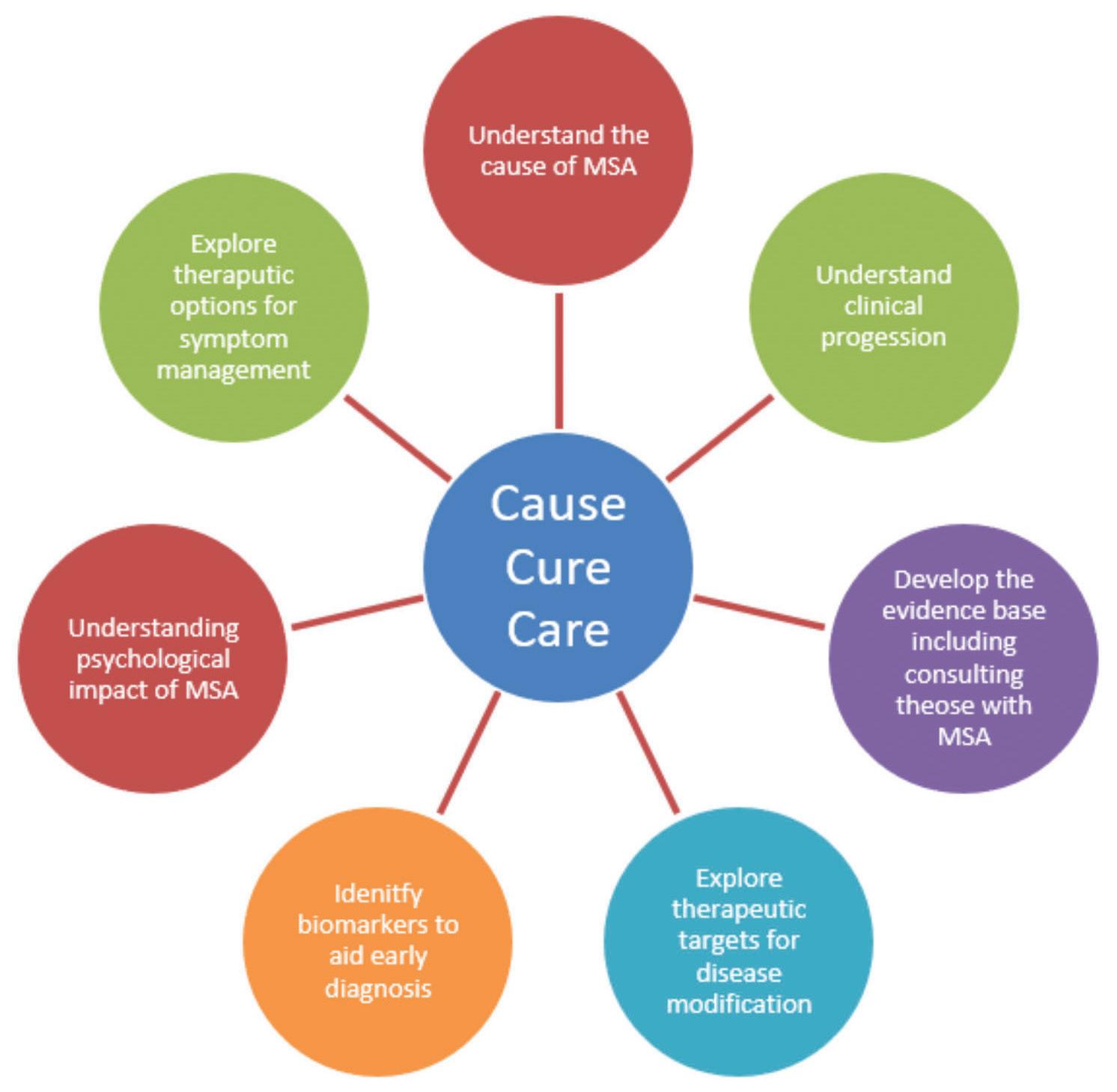
These are our research priorities:
Our research strategy, research results and current research opportunities are available on our website www.msatrust. org.uk/causeand-cure/.
What is a brain bank?
There are several brain banks in the UK and Ireland that register people who would like to donate their brain or tissue for research purposes. If this is something you feel you might be prepared to do, please talk to your local specialist. Brains unaffected by neurological conditions are also needed, so family members may also consider donating their brains for research purposes. There is a factsheet on ‘Brain and Tissue Donation’ available from the Trust.
Common terms
The following is an explanation of words and references used throughout this Guide. If you would like a more detailed explanation of anything mentioned in this publication, please contact us on 0333 323 4591 or email support@msatrust.org.uk.
Alpha-synuclein
A protein found in glial inclusion bodies
Ataxia
Unsteadiness and clumsiness
Autonomic
Part of the nervous system that controls essential body functions. These occur without our conscious awareness such as heart rate, blood pressure, bladder and sexual responses
Basal ganglia
The area of the brain that controls movement
Brain stem
The area of the brain that controls autonomic functions
Cerebellum
The area of the brain that controls balance and co-ordination
CISC
Clean Intermittent SelfCatheterisation is a technique to help empty your bladder completely
Bladder and Bowel Specialist
Someone, usually a nurse, who gives advice on managing bladder and bowel problems
CPAP machine
A machine that provides Continuous Positive Airway Pressure to help breathing whilst asleep
Degeneration
Gradual damage and deterioration
DNA
Deoxyribonucleic acid is the basic structure of all living things
Erectile dysfunction
Inability to achieve or maintain an erection
Glial inclusion bodies
Cell structures found in the damaged areas of the brain
Holistic care
Comprehensive patient care that considers the physical, emotional, social, economic and spiritual needs of the person
MRI scan
Magnetic Resonance
Imaging provides clear pictures of the brain and spinal cord
Multidisciplinary
A team composed of professionals from many disciplines (e.g. doctors, nurses, social workers, therapists)
Palliative care
Holistic care aimed at alleviating symptoms and maintaining well-being when a cure is not possible
Parkinsonism
Used to describe the characteristic symptoms associated with Parkinson’s disease
Postural or orthostatic hypotension
A fall in blood pressure on standing or sitting up that can cause dizziness or fainting (also called orthostatic hypotension)
Respite
A period of organised care, usually residential in a hospital or hospice, that enables your carer to have a break
Sleep apnoea
Periods during sleep when breathing is impaired or momentarily stops
Voice banking
Voice banking allows people to create a personalised synthetic voice for use in communication aids
References
The following are references to articles in medical journals that include technical terms but are valuable papers about MSA.
Wenning, G.K., Stankovic, I., Vignatelli, L., Fanciulli, A., CalandraBuonaura, G., Seppi, K., Palma, J.-A., Meissner, W.G., Krismer, F., Berg, D., Cortelli, P., Freeman, R., Halliday, G., Höglinger, G., Lang, A., Ling, H., Litvan, I., Low, P., Miki, Y., Panicker, J., Pellecchia, M.T., Quinn, N., Sakakibara, R., Stamelou, M., Tolosa, E., Tsuji, S., Warner, T., Poewe, W. and Kaufmann, H. (2022), The Movement Disorder Society Criteria for the Diagnosis of Multiple System Atrophy. Mov Disord, 37: 1131-1148. https://doi.org/10.1002/ mds.29005
Goh, Y. Y., Saunders, E., Pavey, S., Rushton, E., Quinn, N., Houlden, H., & Chelban, V. (2023). Multiple system atrophy. Practical neurology, 23(3), 208–221. https://doi.org/10.1136/pn-2020002797
Diedrich, A et al. Multiple System Atrophy (2018)
Meissner, W.G., Fernagut, P. O., Dehay, B., Péran, P., Traon, A.P. L., Foubert Samier, A., Lopez Cuina, M., Bezard, E., Tison, F. and Rascol, O. (2019), Multiple System Atrophy: Recent Developments and Future Perspectives. Mov Disord, 34: 1629-1642.
Mészáros L, Hoffmann A, Wihan J, Winkler J. Current Symptomatic and Disease-Modifying Treatments in Multiple System Atrophy. Int J Mol Sci. 2020;21(8):2775.
Wenning GK, Colosimo C. Geser F, Poewe W. Multiple system atrophy. Lancet Neurology 2004;3:93-103.
Wenning, Gregor K;Fanciulli, Alessandra (Eds). Multiple System Atrophy. Springer, 2014.
Multiple System Atrophy Trust
The Multiple System Atrophy Trust is the UK and Ireland’s leading charity supporting people affected by MSA. We support people living with MSA, their families, friends, carers and health and care professionals. We also fund vital research to find the cause, and one day, cure for MSA.
Multiple System Atrophy Trust
The Trust currently employs a small team of staff and MSA Health Care Specialists who provide the following services across the UK and Ireland:
• Telephone and email service offering support and information for people with MSA, carers, relatives, friends and health and social care professionals
• Guides and factsheets on a variety of aspects about living with MSA
• A regular magazine: MSA News
• Regional in-person and and digital Support Groups
• Comprehensive website: www.msatrust.org.uk
• Education sessions for health and care professionals
• Latest MSA research updates
• Supporting with access to further support services, welfare benefits and equipment
• Campaigning and advocating on behalf of people affected by MSA
• Facebook, X/Twitter, Instagram and HealthUnlocked Platforms
• Advice on organising or becoming involved in a fundraising event.
To ensure our services are accessible to everyone, the Trust is committed to providing its services to people with MSA and their families and friends, free of charge. People are free to access any or all of the services offered.
The Multiple System Atrophy Trust is a charity funded entirely by voluntary donations. In order for us to continue supporting people affected by MSA, please consider becoming a regular donor or organising a fundraising event.
Join us
If you have not already registered you can join us at the Trust by going to our website www.msatrust.org. uk. Alternatively, you can contact us on 0333 323 4591. Joining our MSA Trust community is free and gives you access to our MSA Health Care Specialist phone and email service, MSA News magazine three times a year, Support Group invitations and updates from us.
Treatment and Care
MSA Health Care
Specialists and Social
Welfare Specialists
Central access number
0333 323 4591
Chartered Society of Physiotherapy
0207 306 6666
www.csp.org.uk
Royal College of Speech and Language Therapists
0203 141 4600 www.rcot.co.uk
Housing Care www.housingcare.org
Bladder and Bowel
Community
0800 031 5406
www.bladderandbowel.org
Hypnotherapy Directory
0207 378 1200 www.rcslt.org College of Occupational Therapists
0333 325 2502 www.hypnotherapydirectory.org.uk
Hospice UK www.hospiceuk.org
Carers
Carers UK
0808 808 7777
www.carersuk.org
Carers Direct
0300 123 1053
www.nhs.uk/carersdirect
Carers Trust
0300 772 9600 www.carers.org
Age UK
0800 678 1602
www.ageuk.org.uk
Turn2Us
0808 802 2000 www.turn2us.org.uk Government
www.gov.uk
The Brain Charity 0800 008 6417 www.thebraincharity.org.uk
Rare Disease UKGenetic Alliance 0300 124 0441 www.raredisease.org.uk
The Patients Association 0800 345 7115 www.patients-association. org.uk
Communications, Mobility and Equipment
Communication equipment and support
0113 343 1533 www.communicationmatters. org.uk
Advice on wheelchair services
https://www.nhs.uk/ conditions/social-careand-support-guide/ care-services-equipmentand-care-homes/walkingaids-wheelchairs-andmobility-scooters/
or in Ireland
https://www.iwa.ie/
Forum of Mobility Centres
0800 559 3636 www.mobility-centres.org.uk
Disabled Living Foundation
0300 999 0004 www.livingmadeeasy.org.uk
Disability Rights UK www.disabilityrightsuk. org (includes UK National Key Scheme for over 9,000 accessible toilets)
0330 995 0400
Medic Alert
01908 951045 www.medicalert.org.uk
Other Organisations
Parkinson’s UK
0808 800 0303 www.parkinsons.org.uk
Citizens Advice Bureau
0808 223 1133
www.citizensadvice.org.uk
Brain Bank Enquiries
020 3456 7890
www.ucl.ac.uk/ion
Ways To Support the MSA Trust
We do not receive any Government or NHS funding and rely entirely on charitable donations to carry out our essential work. Please consider supporting the MSA Trust.
Regular Gifts
Regular donations are at the heart of every small charity – they allow us to plan our work with confidence, knowing that we will have the funds we need to kcontinue providing our services and support.
One-Off Donations
An individual gift, as and when you might have the means to offer one, could have an enormous impact on our work, for instance:
• £14 pays for an introductory call with one of our MSA Health Care Specialist Team for people newly diagnosed with MSA.
• £35 covers an hours MSA Healthcare Specialist attendance at NHS clinics.
• £100 can help us provide Voice Banking to aid communication for people with MSA.
Gift Aid
If you are a UK Taxpayer, any donation you make to the MSA Trust would be eligible for Gift Aid – meaning that we can claim an extra 25p on every £1 you give – so a gift of £100 could become £125!
Fundraising Events
We have supporters taking part in sponsored events like marathons, cycle rides and skydives. People also choose to raise awareness and funds for the Trust through community events like tea parties, raffles and charity balls.
Charity of the Year
If your workplace; a local business; or a high-street name are accepting nominations for a Charity of the Year, we would love you to suggest us.
Legacies
We are immensely grateful to anyone who wishes to remember the Trust and our essential work in their will.
If you would like more information about any of these options or other ways in which you can support our work, please contact us by calling 0333 323 4591, emailing fundraising@ msatrust.org.uk or visiting www.msatrust.org.uk.
Contribute to our magazine
Sharing your experiences and tips with other members helps keep it your magazine. Email support@msatrust.org.uk or call 0333 323 4591.
Volunteer at a local Support Group
We can offer guidance and encouragement to run, or help at, a local or digital MSA Support Group. Email or call us for more information.
Raise awareness about MSA
Share our information with family, friends and the health professionals you meet.
Follow us on Facebook, Instagram and X/Twitter
Multiple System Atrophy Trust
Thank you for your support
Disclaimer

Revision Date: 02/25
Review Date: 02/28
Version 5
We have taken every care to ensure the accuracy of the information contained in this publication. However, the information should not be used as a substitute for the advice from appropriately qualified professionals. Speak to your doctor, qualified health care professional or legal professional before taking any action. Please note that personal views and opinions expressed are not necessarily endorsed by the Trust. The resource is produced independently, is not influenced by sponsors and is free from endorsement.
References for this resource are available by contacting support@msatrust.org.uk. Your feedback helps us ensure we are delivering information to the highest standard. If you have any comments or suggestions, please contact us at support@msatrust.org.uk.


