Cancer Care



As cancer treatment shifts to take-home therapies, Extend Cancer Pharmacist Network empowers community pharmacists to deliver expert, local oncology support across Ontario.
Jason Wentzell, Oncology Pharmacist & Founder Extend Cancer Pharmacist Network
Cancer care in Canada is changing. More people are being treated with take‑home cancer medicines, which means care is no longer limited to hospitals and cancer centres. The Extend Cancer Pharmacist Network (ECPN) was created to support the existing cancer care system and make sure patients receive accessible and timely support wherever they live — especially in their local community pharmacy.
ECPN’s vision is simple and powerful: to collaborate with, support, and enable com munity pharmacists to provide exceptional cancer care to their patients. Community phar macists are among the most accessible and trusted health
professionals in Canada. ECPN helps them build the confi dence and knowledge needed to support people living with cancer, close to home and close to family.
expertise
Today, many cancer treatments are taken by mouth at home. While this offers convenience, it can also create gaps in care if patients do not have easy access to oncology expertise. ECPN bridges this cancer care gap by connecting community pharmacists with specialized oncology pharmacists, edu cation, and real‑time clinical support. This ensures patients receive safe medication use,
side‑effect monitoring, and clear guidance throughout their treatment.
For patients, the benefit is meaningful. They can ask questions, manage symp toms, and receive ongoing support from their community pharmacy team who are also familiar with their other medi cations and health conditions. This team‑based approach helps patients feel supported, informed, and confident during an often overwhelming time.
By strengthening com munity pharmacies, ECPN is helping to bring high‑quality cancer care closer to home — improving access, safety, and peace of mind for patients across Ontario.


Thanks to The Princess Margaret, cancer care in Canada continues to evolve and improve.
Tania Amardeil
Cancer care in Canada is among the best in the world. Princess Margaret Cancer Centre is ranked Canada’s top oncology hospi tal and among the top 10 worldwide.
Mediaplanet spoke with two leaders at The Princess Margaret to learn more about recent developments in radia tion medicine. First, we spoke with Dr. David Kirsch, Head of the Radiation Medicine Program, about adaptive radiation therapy and theranostics.
What is adaptive radiation therapy, and why is it a breakthrough for patients?
With adaptive radiation therapy, we get a new scan, either MRI or CT, right before the radiation is delivered, allowing us to modify the radiation plan accordingly. This can limit the radiation dose going to healthy organs while ensuring the tumour is fully targeted.
Which patients are seeing the greatest benefit from adaptive radiation therapy today?
We’re seeing the clearest benefits in cancers where the tumour or nearby organs change position from day to day, such as cancers in the pelvis. Daily imaging allows us to adjust for things

like bladder filling or tumour move ment, helping protect normal tissues while maintaining full tumour cover age. Adaptive therapy is also being used in other cancers, including head and neck cancers and sarcomas, as we continue to gather data to better under stand which patients benefit most.
Theranostics is described as a precision medicine approach. What is it, and how does it expand options for patients?
Theranostics is a way of delivering radiation therapy systemically, usually by intravenous injection, targeting the radiation medicine directly to tumour cells. It can travel throughout the body to treat microscopic disease.
We also spoke with Dr. Jan Seuntjens, medical radiation physicist and Head of Medical Physics at The Princess Margaret, about particle therapy and how AI enabled workflows are reshap ing radiation treatment delivery.
What is particle therapy, and what makes it different from conventional radiation?
With traditional radiotherapy, photon beams deliver the radiation dose to the tumour but also to surrounding tissues as the beam passes through
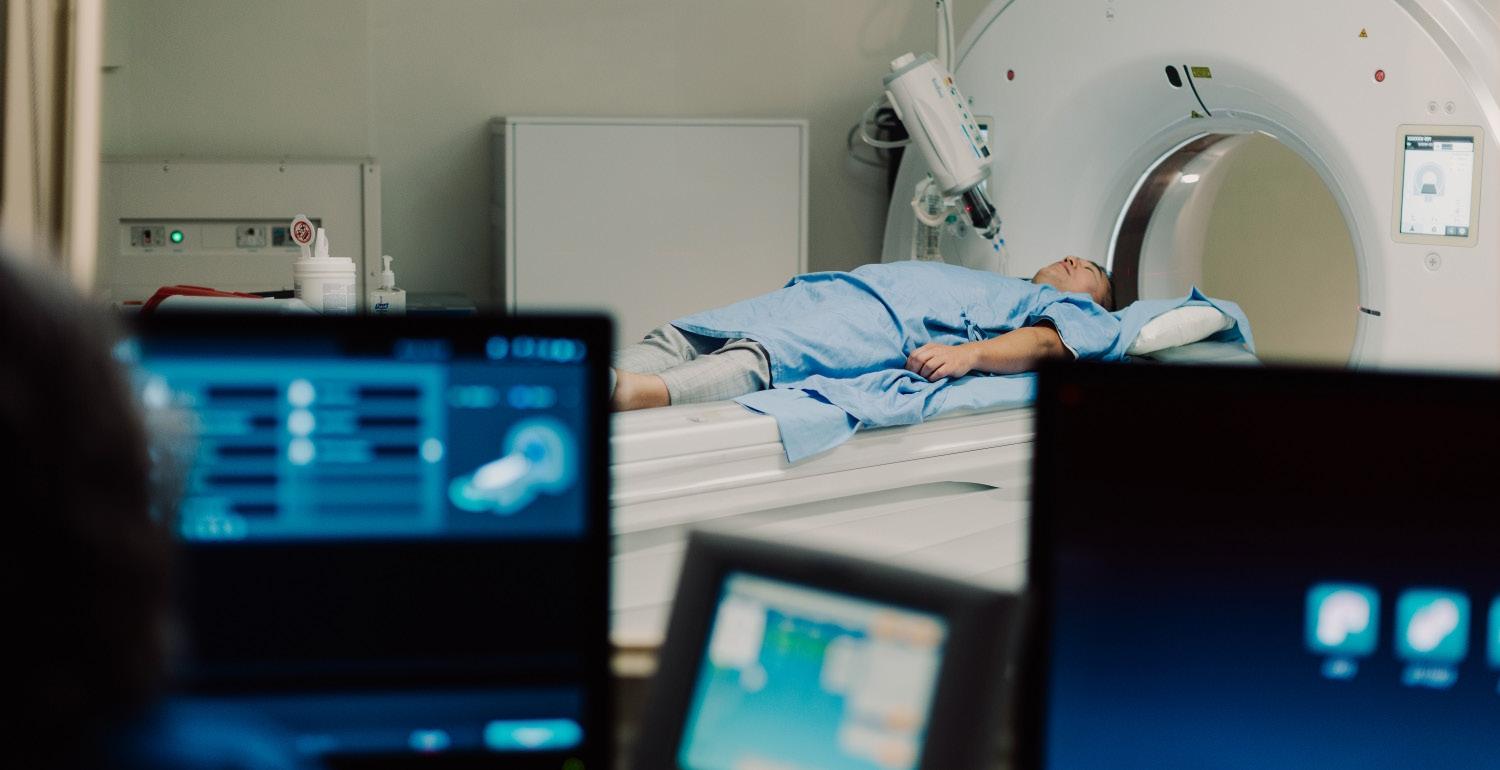
the target. With particle therapy, we can make the particles stop exactly in the tumour target, depositing all of their remaining energy, so there’s no radiation dose beyond the target.
How are AI and automation changing treatment planning and day-of delivery?
AI speeds up the segmentation process — outlining the tumour target and the normal tissues we need to spare. AI also automates the radiation planning process, with the plan reviewed and approved by the clinical team before delivery, so treatment can be adapted and adjusted minutes before it’s deliv ered. What used to take two weeks can now be done within an hour.
With faster AI-enabled workflows, what safeguards and teamwork are needed to deliver treatment safely?
We have three professions who col laborate: the radiation oncologist, the medical physicist, and the radiation therapist. Previously, our workflow followed a strictly sequential model, with tasks passed between professions and quality assurance embedded at specific checkpoints. In the AI enabled workflow, these quality assurance measures remain fully intact, but the process now emphasizes closer cross professional collaboration, with shared responsibility for deci sion making and verification.
This leadership in cancer care is supported by The Princess Margaret Cancer Foundation, which raises funds to advance research, acquire the most advanced technology, and support patient care, including innov ations in radiation medicine such as particle therapy, theranostics, and adaptive therapy.

Dr. David Kirsch Head of the Radiation Medicine Program, The Princess Margaret

Dr. Jan Seuntjens, Medical Radiation Physicist and Head of Medical Physics, The Princess Margaret
To learn more, visit thepmcf.ca
This article was sponsored by The Princess Margaret Cancer Foundation


An evolution in cancer care; this Canadian research network increased collaboration to advance individualized treatment for cancer patients.
Sonya
Friesen
Today we know cancer is many diseases, occur ring when healthy cells develop mutations that allow them to grow unchecked. Being a disease of the genomes, cancers show unique char acteristics at a molecular and cellular (DNA) level which can dictate how an individual case will progress and how it might respond to treatment.
Precision oncology aims to evalu ate specific genomic abnormalities in cancerous tumours and use that infor mation to deliver more personalized treatment to patients based on these individual characteristics. While some cancer patients in Canada are already benefitting from this approach, there’s still a lot of work to be done to better understand the genomic alterations that lead to cancer in each individual and how best to target them. Unlocking these discoveries relies heavily on the ability for researchers to have access to high quality, well annotated data— more than any one cancer centre in Canada generates.
In a Canadian first, researchers from across the country have part nered with the Terry Fox Research Institute and the Terry Fox Founda tion to establish the Marathon of Hope
Cancer Centres Network (MOHCCN), a national collaboration that brings together patients, researchers, oncol ogists, administrators, and donors to support a unified cancer strategy and expand access to precision oncology for more Canadians.
Now comprising 54 cancer centres across all 10 provinces, the Network has created a national data resource called the Gold Cohort. This resource includes clinical and genomic data from 15,000 sequenced genomes from Canadian cancer patients, one of the world’s largest and most complete cancer care resources.
“This solution is a tremendous accomplishment for Canadians: it is the first time for us to work together at this scale to build a resource and national strategy to accelerate pre cision oncology for the benefit of all cancer patients," said Dr. André Veillette, the Network’s Executive Dir ector. "The Gold Cohort demonstrates the power of this collaboration to shape cancer research and care today and into the future.”
Building a national cancer resource
A comprehensive resource that includes genomic and clinical data from diverse
cancer patients across Canada, the Gold Cohort has successfully captured genomic data from 15,000 patients in February 2026, a key milestone for the project, funded by Health Canada and other partners. It will be instrumental in the future of cancer care in Canada and is also one of the richest resources of its kind globally.
Husband and father of two daugh ters, Dan Murphy is a member of the Network’s Patient Working Group. The Stage IV pancreatic cancer patient, who lives in Toronto, has contributed his data to the cohort. "I am living proof of the benefit of precision oncol ogy. The Gold Cohort is helping to give more patients being diagnosed with cancer reason to have hope."
Through the MOHCCN Gold Cohort, Canadian cancer leaders are working to ensure that patient care is not only more personalized, but that each case has a higher chance of success. Understanding genomic differences will play a pivotal role in this evolution. The MOHCCN doesn’t plan to stop at 15,000 patients, and the hope is that the database can continue to grow, deepening clinical knowledge of cancer genomes and building a brighter future for cancer patients worldwide.

Dr. André Veillette Executive Director, Marathon of Hope Cancer Centres Network

Dan Murphy Member of Patient Working Group, Marathon of Hope Cancer Centres Network
To learn more about the Network, our Gold Cohort and how we are transforming cancer research and care for patients, visit marathonofhope cancercentres.ca
This article was sponsored by Terry Fox


An innovative oral therapy represents the first major brain cancer advancement in nearly 25 years for a group of brain tumours known as lowgrade gliomas. Sustained research is needed to drive future breakthroughs. Anne Papmehl
Each year, about 3,300 Can adians are diagnosed with a form of brain or other nervous system cancer, while about 2,600 will die from the disease.1
One of those types is known as glioma. Gliomas are diffuse tumours of the brain that start in the glial cells in the central nervous system.2 Unlike discrete tumours, gliomas have no clear boundaries and spread into sur rounding healthy brain. High grade gliomas are fast moving, with poor prognosis for long term survival. Low grade gliomas may grow more gradually but can still have a pro found impact on daily life, often causing debilitating symptoms such as headaches, seizures, vision changes, speech difficulties, and balance issues.
“Unfortunately, these low grade

gliomas affect mostly younger patients between the ages of 30 and 40 who are in the prime of life,” says Dr. Farshad Nassiri, a neurosurgeon and scientist at the University Health Network in Toronto, Ont.
But there’s hope. Recent research advancements have identified a specific gene mutation called isocitrate dehydrogenase (IDH) in low grade gli omas, which has led to a new targeted oral therapy for grade 2 IDH mutant glioma. “The drug inhibits the specific protein that allows the cells to divide uncontrollably, essentially putting the brakes on the engine that drives the tumour cells,” says Dr. Nassiri.
Fighting for a better future for patients
Angela
Scalisi, Chair of Brain Cancer
Canada (BCC), wishes this treatment had been available when her brother Bernardo was diagnosed in 2013 at age 26. “At the time, the ability to identify genetic markers was not at the fore front, and treatment options were limited. Had he been diagnosed today and able to access this new treatment, I believe the outcome may have been different,” she says. Bernardo passed away in January 2025.
Scalisi’s personal experience drove her to found BCC in 2015, which is now a national leader in funding and advo cating for brain cancer research.
RESOURCES:
1. Brain and other nervous system cancer statistics | Canadian Cancer Society
2. https://cancer.ca/en/cancewr-information/resources/ glossary/g/glioma
Learn more about how you can help support innovations in brain cancer research by visiting braincancer canada.ca
This article was made possible by the support of Servier Canada.
Detecting ovarian cancer earlier is complex, but new research is showing promise in diagnosing it sooner.
Meaghan Ince
Ovarian cancer is caused by abnormal cell growth in or near the ovaries, but many don’t know that the most common form of the disease begins in the fal lopian tubes. At this stage, women may not experience symptoms, making ovarian cancer difficult to detect early.
Dr. Andrea Neilson, a Vancouver based gynecologic oncologist and Ovarian Cancer Canada funded researcher is working to change this. She is developing a new tool that would detect abnormal cells in the fallopian tubes before they become cancerous. “This is a very ambitious project. Things like this have been studied before, but not with today’s biomedical technology,” says Dr. Neilson.
Closing the gap in ovarian cancer care
An estimated 3,100 Canadians are diagnosed with ovarian cancer each year — 56 per cent of
them will die within 5 years. Carol Lee McInnis was one of them, leaving behind her husband, Ron, and their daughter Lindsay.
“She was full of life,” says Ron. “She golfed, she curled, she biked, she was an artist, but it all changed so quickly.” High school sweethearts, the two looked forward to seeing their grand children grow up and spending time in Prince Edward Island. But after a 15 month journey with advanced ovarian cancer, she passed away in January 2021.
Determined to change this story for other families, McInnis organized a fundraiser in Carol Lee’s memory to support ovarian cancer research. Funding innovative research like Dr. Neilson’s helps close gaps in care, improving early detection and leading to higher survival rates, “If we can increase the number of stage one patients we find even a little bit, we’re going to cure so many more people.”

Learn more and donate at ovariancanada.org
This article was sponsored by Ovarian Cancer Canada


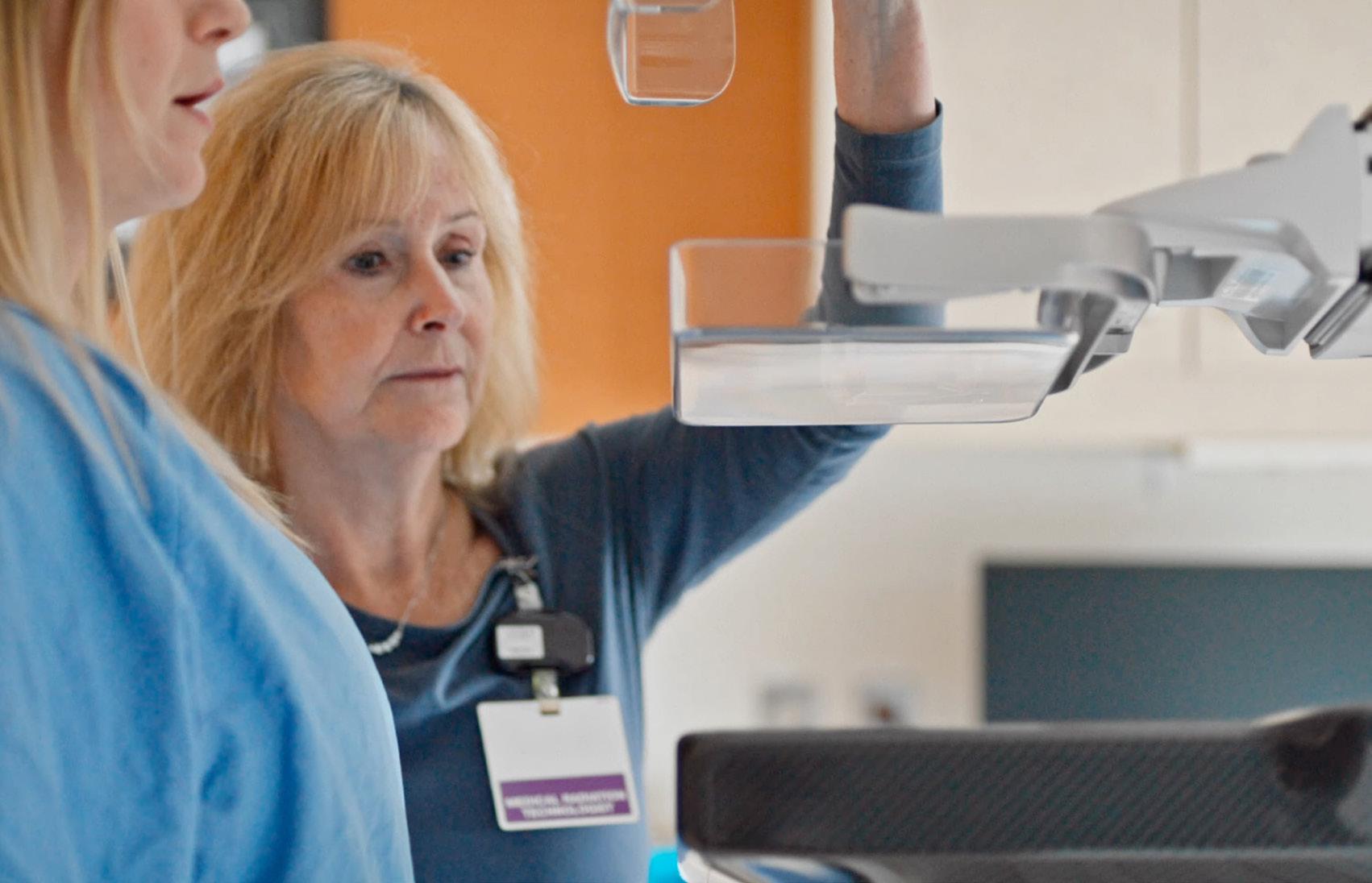
Regular screenings play a crucial role in detecting cancer early, improving health outcomes, and in many cases — saving lives.
Southlake Health
When people need healthcare, knowing that leading edge care is close to home makes a difference. From routine screening to innovative treatment, accessing care in a patient’s own community reduces travel time and stress, allowing healing to happen near loved ones.
This is especially true when it comes to Southlake Health’s approach to cancer care. Regular screenings play a crucial role in detecting cancer early, improving health outcomes, and in many cases, saving lives. When patients have to travel long distances, they may delay screening, which can lead to serious consequences.
Monique Rodrigue was almost one of those patients. During one of the busiest times of her life, Monique considered postponing a routine mammogram. Instead, she made an appointment at Southlake Health, a large community hospital just 10 minutes away from her home in New market, Ontario. Her mammogram detected stage one, triple positive breast cancer — an aggressive form of breast cancer.
Southlake is a designated hub for cancer care in Ontario and serves some of the fasted growing and aging communities in Canada. It provides publicly funded mammograms through the Ontario Breast Screening Program, as well as by referral from primary care provid ers. All women ages 40 and older can self refer for a mammogram.
After Monique’s mammogram, things moved quickly. She was called back for a biopsy, followed by a lump ectomy, chemotherapy and radiation treatment within weeks. Today, she is cancer free.
“I could not imagine going into Toronto for treatment, fighting traffic,” said Rodrigue. “Every day, I felt more and more confident in my decision to get care close to home.”
Timely cancer screening close to home is lifesaving. The need for accessible cancer screening and care is growing. The World Health Organization anticipates a 77 per cent increase in cancer diagnoses by 2050. In Canada, breast cancer is the second most diagnosed cancer, with an esti mated one in eight women expected to develop it in their lifetime.
By increasing our capacity and making mammograms more accessible, we’re helping more patients access the specialized care they need, close to home.

In recent years, Southlake has expanded its diagnostic and treatment capabilities with innovative technol ogies, supported by philanthropic investments from community donors and organizations. Three state of the art mammography machines were added to expand screening to an additional 1,500 patients annu ally. Two of the machines have biopsy capabilities that reduce appoint ment times and improve diagnostics capabilities. Southlake performs approximately 16,000 mammograms each year.
“The new mammography machines help Southlake meet the growing demand for breast cancer screenings and diagnostics, with the best technology available,” said Dr. Alisha Kassam, Physician Leader, Regional Cancer Program at South lake. “By increasing our capacity and making mammograms more access ible, we’re helping more patients access the specialized care they need, close to home.”
The message is clear: leading edge cancer care is not somewhere else. It’s available close to home.

Learn more at southlake.ca or by speaking with your health care provider about cancer screening.
This article was sponsored by Southlake Health
