OVERVIEW OF KINESIOLOGY TAPING
INTRODUCTION
Any physical therapist involved with assessing, treating, and rehabilitating sports-related injuries, or even patients who present with back and neck pain, will need to have the skill of taping.
Kinesiology taping is definitely the current buzzword in the field of sports medicine. This brightly colored tape is now a very common sight at all major sporting events throughout the world and is even seen at some recreational activities. Therefore, therapists need to master the techniques. They are relatively simple to learn and once applied in a specific way can improve the performance of an athlete as well as reducing any pain and swelling.
This book guides the reader toward having a better understanding of both why and when to apply kinesiology taping. It outlines how to effectively treat over 50 of the most common sports-related injuries, with the application of scientifically proven kinesiology taping methods (KTMs), and includes treatment guidelines for specific areas of the body that a patient/athlete might present with at a physical therapy clinic, e.g., lower back, sacroiliac joint (SIJ), and cervical spine (neck).
KTM techniques will be explained and illustrated for all the following areas of the body.
Plantar surface of the foot pain:
• Plantar fasciitis: proximal and distal pain
• Heel pain
• Fat pad syndrome
Ankle inversion sprain:
• Lateral ligaments
• Peroneal muscles
• Peroneal stabilization
• Self-taping
Achilles tendinopathy
• Self-taping
Calf strain/musculotendinous junction (MTJ) strain:
• Gastrocnemius
• Soleus
Medial shin pain:
• Medial tibial stress syndrome (shin splints)
• Periostitis
• Posterior compartment syndrome
Anterior shin pain:
• Anterior tibialis tendinopathy
• Anterior compartment syndrome
General knee pain:
Full knee taping for:
• Patellofemoral pain syndrome
• Patellar tendinopathy
• Osgood-Schlatter ’s disease
• Knee malalignment taping
Lateral knee pain:
• Iliotibial band friction syndrome
• Lateral collateral ligament (LCL) sprain
• Lateral meniscus pain
Medial knee pain:
• Medial collateral ligament (MCL) sprain
• Medial meniscus pain
Hamstring: generalized pain/fatigue
Hamstring strain:
• Medial strain: semitendinosus and semimembranosus
• Lateral strain: biceps femoris
Rectus femoris and quadriceps strain
Adductor strain
Gluteal and piriformis pain
Lower back pain:
• Lumbar spine pathology
• Facet joint syndrome
• Disc pathology
• Iliolumbar ligament sprain
• Multifidus strain
Sacroiliac joint (SIJ) dysfunction
• Big Daddy taping
• Quadratus lumborum (QL) strain
Rib/intercostal pain
Mid-thoracic pain:
• Rhomboid
• Lower trapezius
Posterior cervical pain:
• Facet joint
• Cervical muscles
• Cervical disc pain
Lateral cervical spine:
• Levator scapulae
• Upper trapezius strain
Postural taping
Pectoral strain
Shoulder pain:
• Rotator cuff tendinopathy of supraspinatus
• Subacromial bursitis
• Infraspinatus
Acromioclavicular joint (ACJ) sprain
Biceps tendinopathy: long and short head
Lateral elbow pain:
• Lateral epicondylitis (tennis elbow)
Medial elbow pain:
• Medial epicondylitis (golfer ’s elbow)
• Ulnar nerve
Forearm and wrist pain:
• Carpal tunnel syndrome
• Median nerve
• Tenosynovitis
Wrist pain:
• De Quervain’s tendinosis
• Intersection syndrome
Osteoarthritis (OA) of the first carpometacarpal (CMC) joint
Kinesiology taping to control edema:
• Ankle edema
• Knee edema
• Quadriceps/hematoma/edema
• Forearm/compartment syndrome/ edema
• Shoulder edema
HISTORY OF KINESIOLOGY TAPING
In the 1970s a Japanese chiropractor, Dr. Kenzo Kase, started using a unique type of taping method, which led to the
development of a new form of sports tape. He was keen to develop a new style of taping compared to the standard form of athletic strapping and taping, such as the zinc oxide (Z/O) technique. He felt this conventional method provided support to the muscles and joints but would sometimes restrict the range of motion (ROM), and in certain applications this technique could limit, and potentially inhibit, the natural healing process. After extensive research, Dr. Kase developed the Kinesio Taping® technique and Kinesio Tex® tape: a taping system that naturally assists in the healing of damaged tissue by encouraging lymphatic drainage and provides support to the joints and muscles without causing restriction to the ROM. This form of kinesiology taping then went on to be widely seen at the 1988 Seoul Olympics as 50,000 rolls of kinesiology tape were donated to 58 countries, which gave the taping product great exposure throughout the athletic world.
KINESIOLOGY TAPING METHOD
The KTM is another “tool” for the toolbox that can be used effectively in any sports- or non-sports-related setting. It can be applied in the comfort of a clinic or while treating an athlete at the side of the field or in the dressing room. It can even be applied to a hill walker on top of a mountain.
Kinesiology taping is not a “stand-alone” treatment as it is normally combined with other physical therapies, e.g., softtissue treatments such as muscle energy techniques (METs), myofascial techniques, and joint mobilizations. Once this taping system has been thoroughly understood and practically applied, then and only then, it will provide an adjunct to any treatment protocol to assist the overall well-being of patients and sporting athletes.
COMPARISON OF KINESIOLOGY TAPE VS. CONVENTIONAL ATHLETIC TAPE
Most types of athletic tape have very little or no stretch; however, kinesiology tape is very elastic and can be stretched longitudinally up to 120–180% of its original size. In addition, the thickness of kinesiology tape and its elasticity are similar to those of human skin.
When non-elastic athletic tape is applied to an injury, the rigidity of the tape can cause a restriction, or it can even prevent movement of the taped area. This is desirable for severe injuries where immobilization is necessary to prevent further damage. Most injuries, however, do not require full immobilization, and this is where the flexibility of kinesiology tape comes into its own. KTM can therefore provide support to injured muscles and joints while still allowing a safe and painfree ROM, unlike conventional taping. This enables patients and athletes to continue training or competing while they recover from lower-back and neck pain, as well as minor to moderate sports-related injuries.
When conventional athletic tape is applied there is the possibility that circulation can be compromised, plus the issue of removing the tape after every sporting event. Kinesiology tape, on the other hand, can be worn for many days, providing support and therapeutic benefits “24/7.” In addition, this tape does not cause problems to the underlying tissues or restriction to the associated joint(s). Another benefit is that once kinesiology tape is removed it does not tend to leave any glue-like residue, unlike conventional athletic strapping and taping products.
Kinesiology tape also tends to be thinner and more elastic than conventional tape, and most of the kinesiology taping products have been designed to provide “uni-directional” elasticity, i.e., stretch in length but not in width. Each company that produces a kinesiology taping product claims that the stretching capability is critical because it provides the same elasticity as human skin (even though each company claims slight variations in the amount of this perceived stretching capability: Rocktape® claims that its tape has approximately 180% stretch, and KT Tape® claims 140% stretch for its product).
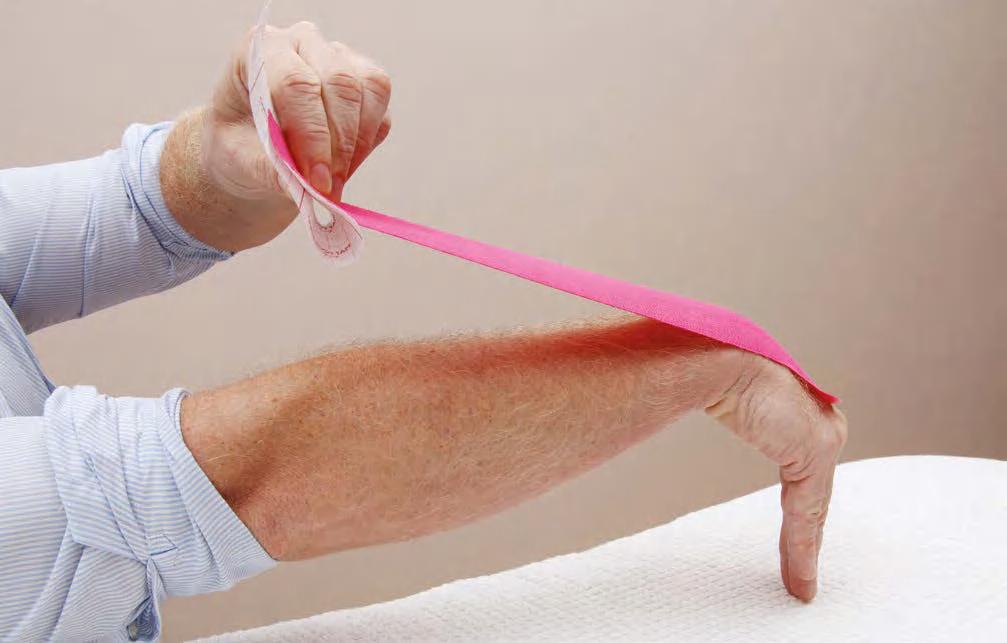
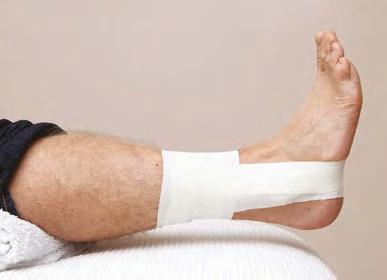
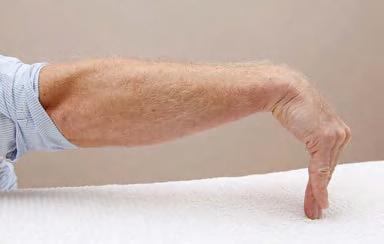
Perhaps the main difference between kinesiology tape and other athletic tapes can be seen in the specific method of application (Fig. 1.1). Conventional athletic
Figure 1.1 Comparison of conventional taping vs. kinesiology taping.
tape is typically wrapped tightly around an injured area to promote stability, and in some cases athletic tape can be applied to provide immobility. However, kinesiology tape is applied over and around the contours of the muscles and the associated joints, and the amount of stretch applied to the tape can vary depending on the purpose of the application.
TAPE ADHESION
Generally speaking, athletic tapes tend to have an adhesive applied to them that is commonly called Z/O, and this sometimes leaves a residue on the skin after removal. In addition, some patients have been known to have an adverse reaction to this type of taping system. Most kinesiology taping products that are currently available to purchase from the marketplace have a unique acrylic-based adhesive, which is normally latex-free and hypoallergenic. The acrylic adhesive is much gentler on the skin than conventional athletic tape adhesive and seldom causes skin irritation or breakdown. It does not require the use of a protective under-wrap or pre-wrap to prevent skin damage, and can be applied directly to the skin on any area of the body.
The acrylic adhesive is generally applied to the back of the kinesiology tape in a wave-like pattern that creates alternating areas of adhesive and non-adhesive so that moisture can escape easily from the taped area. In addition, the cotton fabric dries quickly so that kinesiology tape can be worn comfortably throughout showering and even swimming. A quick pat with a dry towel and it’s back to its original state with no residual moisture to irritate the skin and lead to potential bacterial growth.
Even more importantly, it is felt that the alternating ridges of adhesive create a pressure differential in the tissues under the tape. In theory this will allow the tape to interact with pain receptors (nociceptors), blood vessels, and the lymphatic system to assist in relieving pain and reducing the inflammation.
TYPES OF KINESIOLOGY TAPE
There are many varieties of kinesiology taping products available on the market, and when I wrote the second edition of book in 2019, there were 70 different types of kinesiology tape.
How to Choose the Right Type of Kinesiology Tape
I have tried and tested many varieties of kinesiology tape and the top brands tested better than the easily available, cheaper options. My team and I are based at the sports injury clinic for the University of Oxford and, therefore, have been able to try most of the top brands on both elite athletes and non-athletic patients alike. All the betterquality kinesiology taping products tested well, with some variations among stretch, tape feel, adhesive quality, etc. Maybe try a few and find your own preference.
I like the phrase used by the kinesiology taping product company Rocktape (who I consider to be one of the leaders in the field). The company mentions in its literature that there are essentially two types of tape: “cheap and good tape.” Rocktape highly recommends avoiding cheap tape on patients as it often peels and frays much faster than high-quality tape. Reports of
skin reactions are also more frequent with cheap tape. As Rocktape suggests, I would personally avoid the cheaper and less known or tested products.
Personal Recommendations
Patients, and especially athletes, say to me on a regular basis that the main problem with wearing any type of tape whether athletic or kinesiology tape is the ability of the product to stay on the body during exercising. Some tapes, they complain, just fall off and refuse to stay on.
Rocktape is a company that I recommend highly and I have used its products many times on athletes and other patients (Fig. 1.2). They have various kinesiology taping products on the market and I am a huge fan of their alternative designs and funky colors, and all without compromising the effectiveness of the tape.
Rocktape also offers other versions of its standard product. There is a more waterproof form, and this is called the Rocktape H2O. This has been designed for athletes in more water-based sports, such as surfers and swimmers. They also produce a more sensitive version, called Rocktape RX, designed for the more sensitive population such as the elderly and children, because it contains less acrylic than the standard taping product. If you have larger athletes or want to cover a wider area of the body, then a 4 in (10 cm) (wide) version is available; this is also known as the Big Daddy (Fig. 1.3)!
Rocktape is currently my sponsor and the main kinesiology taping product I have used consistently over many years, both in my practice as a clinician at the University of Oxford and for training purposes on my
Bodymaster Method® “Kinesiology Taping for the Athlete Masterclass.”
Rocktape is used for each of the demonstrations in this book, as well as the individual videos that are shown on YouTube. You can access these for FREE by using the accompanying QR codes.
Some features of Rocktape®:
• 100% cotton
• Designed in California
• Latex-free
• 170–180% stretch
• Hypoallergenic
• Water resistant
• Allows the skin to breathe
Figure 1.3 16.4 ft × 4 in (5 m × 10 cm) (Big Daddy) Rocktape®.
Figure 1.2 16.4 ft. × 2 in. (5 m × 5 cm) Rocktape®.
• Ultra flexible and moldable to the body ’ s contours
• Thickness and weight of the tape are similar to those of human skin
• Easily tolerated with very few contraindications
• Allows the natural joint and muscle ROM and does not restrict motion (often a problem with conventional athletic tape)
• Elastic properties to help support and reduce muscle fatigue
• Helps assist the flow of lymphatic drainage
• Can be worn for 3–5 days without re-application
• Cost-effective patient management, i.e., 10–12 applications per roll.
HOW DOES KINESIOLOGY TAPING WORK?
Any type of injury or trauma to the body will set off the body’s natural protective mechanism known as the inflammatory response (Fig. 1.4). The main identifiable signs of this response are: pain, swelling, heat, and redness, as well as restriction to the ROM.
Kinesiology taping has been clinically shown to help with the natural response to inflammation as it targets different receptors within the somatosensory system. Correct application of KTMs helps alleviate pain and encourages the facilitation of lymphatic drainage by microscopically lifting the skin. This lifting effect helps create distortions in the skin, thus increasing interstitial space and allowing a decrease in the inflammatory process for affected areas (Fig. 1.5(a, b)).
As shown with Figure 1.5a, the underlying nerve endings, lymphatic vessels, and blood vessels are in a state of “compression” due to an injury. Any type of injury will cause inflammation, as explained earlier, and this natural process will produce some form of swelling one common type of swelling is a hematoma and subsequently pressure will build up within the tissue. This naturally occurring process, with the increased pressure that is building up within the soft tissues, will start to irritate the nociceptors (pain receptors) and pain will be perceived. As I often quote during my kinesiology taping courses, “swelling causes pressure
Figure 1.4 The inflammatory process.
Skin
Pain receptors compressed
Blood and lymph vessels compressed
Buildup of lymphatic fluid
Inflamed muscle
Dermis compressed
Skin
Pain receptors decompressed
Blood and lymph vessels dilated
Lymphatic fluid drained
Uninflamed muscle
and pressure causes pain; to reduce the pain we have to reduce the pressure, and this is where specific kinesiology taping procedures can be utilized to assist in the reduction of the pressure that has built up within the soft tissues.” Other treatment methods can also be used at the same time as kinesiology taping, e.g., ice packs and non-steroidal antiinflammatory drugs (NSAIDs).
As mentioned earlier, when kinesiology tape is applied to the skin it causes a “lifting ” or
Dermis decompressed
“convolution” of the epidermis. This process is discussed by Capobianco and van den Dries (2009) in their book Power Taping, where the “lifting ” of the skin is referred to as the biomechanical lifting mechanism (BLM). They state that “ The BLM lifts the skin microscopically, which allows fluid to move more freely. This allows more blood to flow into the injured area, thereby accelerating recovery and repair and also allows lymph fluid to more easily drain from the area, thus decreasing inflammation.”
Figure 1.5b Cross-section of skin with tape applied.
K tape
Figure 1.5a Cross-section of skin without tape applied.
(See Fig. 1.5b for an example of this process.)
Kinesiology taping methods have been used in the clinical setting for many years and can be specifically applied to the athlete/ patient based upon their therapeutic needs. In turn, these therapeutic needs are based on the outcome of the initial physical examination and dictate the specific requirements for the kinesiology taping application, as well as other alternative treatments or modalities.
HOW TO USE AND APPLY KINESIOLOGY TAPE
Kinesiology taping products tend to come in a standard size and length, normally 2 in × 6 ft 6 in (5 cm × 5 m). The therapist then decides on how and when to use this standard taping product, as they will need to pre-cut the tape for the individual patient or athlete who visits the clinic. However, some kinesiology taping products come in an already pre-cut form, which in theory makes “life” a little bit easier. My preference is to pre-cut the size and shape of the tape myself at the time of the application. This is mainly because I assess and treat a lot of elite athletes who participate in rowing as a sport, and these women and men tend to be very tall: some of the men reaching a height of 6 ft 5 in (1 m 95 cm) plus. A standard pre-cut piece of tape might be appropriate for someone who is 5 ft 3 in (1 m 60 cm) in height, but not for someone who is taller.
There are a few unique taping designs that can be created from a single piece of tape, as shown by Figure 1.6. It is very common, in all methods of kinesiology taping, to start with a single “I” strip, where the therapist will have decided on the specific length to use
Figure 1.6 Different shapes of kinesiology taping applications.
depending on the height, size, and area of the athlete/patient. The standard-sized “I” strip can then be modified into a smaller version of the same strip or made into the shape of an “X” by crossing over two smaller “I” strips. The standard “I” strip can also be made into a “Y” shape or another specialized shape like a “fan.” The “fan” technique is generally used to help control lymphatic drainage, as demonstrated in Chapter 9. The direction and the amount of stretch applied to the kinesiology tape can also be changed at the time of application as these will be determined by the individual needs of the athlete/patient.
Why the Different Colors and Patterns?
• Black “I” strip
• Beige “ Y” strip
• Blue “fan” strip
• Pink smaller “I” strip.
All the tapes in Figure 1.6 have the same therapeutic value, regardless of color and pattern. However, depending on the sport and patient/athlete gender, the red/pink kinesiology tape is popular and is thought to be more stimulating. This color, as well as
appearing to be more vibrant, is considered to stimulate certain senses within the brain and may produce a placebo effect. The blue, on the other hand, is generally considered to be a soothing color that can calm the mind and aid concentration.
How Much Stretch to Apply to the Tape?
How much stretch should be applied to the kinesiology tape? This is a commonly asked question and there are some simple rules to follow:
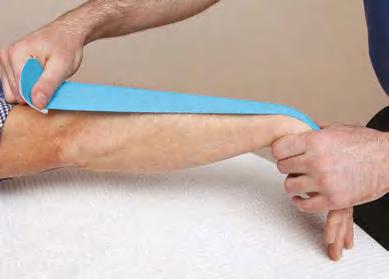
• Method 1: when applying the kinesiology tape to the patient, there is usually little to no stretch on the tape as the tissue of the patient has already been guided into a pre-stretched position prior to the application. Demonstrated in this chapter by a pre-stretch to the forearm extensors as shown in Figure 1.8.
• Method 2: think of this as the “decompression” strip or, in more simplistic terms, the “pain-relieving” strip. This tape can be applied with a range of 25–100% stretch, as this will help offload the specific area of pain, as demonstrated in this chapter by Figures 1.13 and 1.14.
However, there are some exceptions to the first rule of “pre-stretch” the tissue before you apply the first taping application with “little to no stretch.” Some KTMs require stretching the tape as well as pre-stretching the muscle, e.g., if you want to stabilize and offload an area of pain, such as the plantar surface of the foot with a common condition such as plantar fasciitis. With this type of kinesiology taping method, as shown in the demonstration (see page 34), I place the plantar surface of the foot into a
pre-stretched position and apply between 75 and 100% stretch to the kinesiology tape. This is a typical exception to the standard first rule of kinesiology taping. This method, in my experience of kinesiology taping, works very well to help reduce the pain, even though there is no current research for this theory.
Another exception to the first kinesiology taping rule is where there is “no stretch” applied to the patient’s tissue and maximum stretch is applied to the kinesiology tape. Let’s take an area of the body that is very commonly injured: a sprain of the lateral ligaments of the ankle joint. The first tape should be applied at 100% stretch as the ankle has not been put into an inverted position to initiate the stretch of soft tissues. This is because the position of inversion would place the ankle in a potentially vulnerable state. Instead, apply the kinesiology tape at 100% stretch with the ankle in a dorsiflexed and slightly everted position. Then apply the tape from the medial malleolus to the lateral malleolus, as shown in Chapter 2, Figure 2.5. This technique is similar to a “stirrup” method of taping and is used to provide joint stability. To recap this technique: if applying 100% stretch to the kinesiology tape then this will assist in stabilizing the joint and, in theory, is similar to conventional athletic taping principles.
The taping techniques described in this book show the variations in the amount of stretch that can be applied to the tape, i.e., ranging from 10 to 100%. However, I personally feel that there are a multitude of ways to apply kinesiology tape and I have had the good fortune of being able to modify some of the methods I was taught. In this book I will be demonstrating the techniques that currently work for me, based on my athletes and patients.
Rocktape has another saying: “ We believe there is no ‘right way ’ to tape for any given problem.” I truly believe in what Rocktape says; for an example of this you can watch, on YouTube, 15 different ways to apply kinesiology tape to the hamstrings, and you will naturally think to yourself, which technique of the 15 demonstrated is the correct one? Well, in theory, they all are correct, as the physical therapist who is applying the technique to the patient on the video is hopefully showing the technique that works for them in their clinic.
When I teach the Bodymaster Method
“Kinesiology Taping for the Athlete Masterclass” I try to emphasize the following fact: it is the patient who will decide if the taping technique applied is working or not. As the physical therapist you will apply the kinesiology tape to patients in the way you were taught by your tutor. However, you will need the necessary experience and underlying knowledge of functional anatomy to have the ability to change the technique to meet the individual demands of your athlete/patient.
BENEFITS OF KINESIOLOGY TAPING
Kase et al. (1996, 2003) claimed four main benefits for the application of kinesio tape:
1. Normalization of muscular function
2. Increased vascular and lymphatic flow by eliminatination of tissue fluid or bleeding beneath the skin
3. Reduction of pain through neurological suppression
4. Correction of possible joint misalignment by relieving abnormal muscle tension and helping to influence the function of fascia and muscle.
Murray and Husk (2001) suggested a fifth mechanism:
5. Increased proprioception through increased stimulation to cutaneous mechanoreceptors.
In addition, Kase described Kinesio Taping applications for both “muscle facilitation” and “muscle inhibition” techniques. If kinesio tape is applied from the muscle origin to the insertion with stronger tension, i.e., 50–75% of its original length, this may enhance muscle contraction. However, applying kinesio tape may reduce muscle contraction from the muscle insertion to the origin with weaker tension, i.e., 15–25% of its original length (Kase et al. 2003).
KT Tape also outlines the benefits of kinesiology taping in the following product information from its website: “KT Tape is applied along muscles, ligaments, and tendons (soft tissue) to provide a lightweight, strong, external support that helps to prevent injury and speed recovery. KT Tape works differently for different injuries. KT Tape can lift and support the kneecap, holding it in place for runner ’s knee. KT Tape can support sagging muscles along the arch of the foot, relieving the connective tissues for plantar fasciitis. Depending on how it is applied, KT Tape supports, enables, or restricts soft tissue and its movement. By stretching and recoiling like a rubber band, KT Tape augments tissue function and distributes loads away from inflamed or damaged muscles and tendons, thereby protecting tissues from further injury. KT Tape also reduces inflammation and increases circulation which prevents muscle cramping and lactic acid buildup.”
Kinesiology taping can be a valuable addition to the treatment protocol as it has been shown to have positive physiological effects on the skin, lymphatic vessels, and subsequently circulatory system, as well as having a physiological effect on the fascia, muscles, ligaments, tendons, and joints. Kinesiology taping can also be used in conjunction with a multitude of other treatments and modalities within the clinical setting and is very effective during the rehabilitative process. It can also be applied to an acute or chronic injury that has been sustained, as well as being used for preventative measures.
Kinesiology tape can be applied to the body in many ways and has the ability to assist the re-education of the neuromuscular system, reduce pain, control inflammation, enhance performance, stabilize joints, prevent injury, and promote good circulation and healing. It also assists in returning the body to its natural homeostasis.
However, it is important to conduct a physical therapy assessment of the athlete/ patient as this is the key to deciding the best treatment protocol, and whether kinesiology taping is recommended. Information gained from this assessment/consultation is essential for obtaining the desired results from a kinesiology taping application, as well as any other treatment modalities.
SUMMARY OF THE USES FOR KINESIOLOGY TAPING
• Provides support for weak or injured muscles without affecting the normal ROM. This allows full participation in therapeutic exercises and/or sports training and minimizes the risk of
developing compensatory imbalances or injuries.
• Activates muscles that have been weakened after injury or surgery, improving the quality of contractions and speeding up the recovery process.
• Stabilizes the area without restricting the movement like conventional athletic tape.
• The athlete and patient can remain active during the sport/activity.
• Relaxes, and can offload, overused and overstrained muscles.
• Assists the re-education of the neuromuscular system.
• Accelerates blood flow to the injured area to speed up the healing process.
• Helps to reduce pain.
• Reduces edema by removal of lymphatic fluid.
• Can enhance athletic performance and endurance.
• Corrects postural imbalance and improves the ROM.
• Inhibits muscles that are tight, fatigued, or overused and allows them to relax.
• Helps prevent injury.
• Psychological benefits as well as a placebo effect.
PRECAUTIONS/ CONTRAINDICATIONS FOR KINESIOLOGY TAPING
Kinesiology taping is generally safe for everyone, ranging from the very young to the very old and from the very fit to the not so fit. It is a therapeutic taping technique not only offering athletes and patients the support they are looking for but also enabling rehabilitation from their condition. Hence the athlete/patient can remain active throughout their sport or even their day-to-day activities.
With all types of taping methods, there are some precautions and potential contraindications you need to check before the application of the tape. Listed below are some examples (although there is no current evidence in support of this information).
Precautions
• Allergic reactions to tape
• Deep vein thrombosis and phlebitis
• Axillary and popliteal areas as these body regions are sensitive
• Local or distant sites of cancer
• Fragile skin, e.g., in the elderly or with specific medical conditions
• Skin healing in early phase.
Contraindications
• Infected areas of the skin
• Dermatological skin conditions like eczema and dermatitis
• Cellulitis
• Broken skin and wounds
• Skin reactions to kinesiology tape.
While teaching a course on kinesiology taping, I mentioned that there are very few contraindications to the use of kinesiology tape. However, there was an emergencyroom nurse on the course who, while at work, witnessed a gentleman with kinesiology tape adhered to his shoulder skin, who was subsequently referred to the plastic surgery department to remove the tape. The reason behind this admission was that after his morning shower he decided to use a hair dryer on the kinesiology tape, which subsequently overheated the acrylic glue causing it to
adhere directly to his skin. This gentleman should have simply patted the kinesiology tape dry with a towel. Please be careful if using an external source to dry the kinesiology tape as it is not needed and may be detrimental.
KINESIOLOGY TAPING APPLICATIONS
There are many different ways of applying kinesiology tape and the preferred style can vary among tutors. I think it is best to stick to some simple rules, and once one process has been learnt it can then be adapted according to the needs of the athlete/patient.
General rules before application
• Always check for a history of allergies to tape adhesives.
• Cleanse skin from any oil, cream, and massage wax and trim hair if needed.
• Measure and cut the tape into the size and shape required.
• Round off the corners at the end of each tape to prevent it from lifting/peeling (Fig. 1.7).
Figure 1.7 Rounding each corner of the kinesiology tape using a pair of scissors.
• Never stretch the ends of the tape, and leave around an inch of tape at each end that will remain un-stretched. Leaving no stretch at the ends of the kinesiology tape will avoid a “shearing ” type of tension to the skin and will limit any potential for irritation, as the tape is normally kept on for at least a few days.
During application pre-stretch
Before the kinesiology tape is applied to the area that is injured, guide and place the soft tissue of your athlete/patient, e.g., the muscle, into a position that will cause the tissue to be naturally stretched, as shown with Figure 1.8 for the forearm extensors.
Pre-stretch
Figure 1.8 Forearm extensors in a “pre-stretch.”
Please bear in mind that the patient is normally presenting with some type of pain or swelling, so only go as far as required until the patient is aware of the stretch and not to the point of discomfort.
Tape application/stabilizing technique
Before applying the kinesiology tape, expose the adhesive side of the tape so that it can be attached to the specific body area. It is
natural to want to “peel off ” the backing from the tape; however, this process is not needed as the tape can simply be “torn” across one of the squares as shown by Figure 1.9. This tearing will not damage the kinesiology tape as only the backing will be removed.
Figure 1.9 Tearing the backing from the kinesiology tape.
Apply a prepared “I” or “ Y” strip to the prestretched tissue of the body, with little to no stretch of the tape on first application. This technique will help stabilize the area, as shown with Figures 1.10 and 1.11. There are a few variations to this rule, as described throughout this book (e.g., plantar fasciitis, ankle, and knee).
Stabilize
No stretch
Figure 1.10 Self-application of kinesiology tape to the forearm, with little to no stretch of the tape. (The tissue of the forearm is in a pre-stretched position.)
Figure 1.11 Kinesiology tape applied by a physical therapist to the forearm, with little to no stretch of the tape.
Pain offload application/ decompression strip
The kinesiology tape (normally an “X,” “ Y,” or a smaller “I” strip) can be stretched between 25 and 100% of its original length. This type of application is commonly known as the pain relieving strip or decompression strip and is applied directly over the presenting area of pain.
If using a small “I” strip or a small “X” strip then it is easier to rip the backing off the tape by starting from the center of the tape, rather than starting from one end as would be the case for a longer “I” strip. Once the center has been split, peel back each end of the backing strips from the tape, and fold over the ends that have no stretch (similar to applying a plaster for a cut on the skin), as shown with Figure 1.12.
Once the ends have been folded over each other, the appropriate stretch is then applied to the center of the kinesiology tape, as shown by Figures 1.13 and 1.14.
The decompression strip of kinesiology tape, with the appropriate stretch added as
Figure 1.12 The ends of the small “I” strip are folded back like a plaster (and no stretch is applied to the kinesiology tape).
Figure 1.13 A stretch of 50% is applied to the center of the kinesiology tape by using the thumbs.
Figure 1.14 A stretch of 100% is applied to the center of the kinesiology tape by using the thumbs.
explained in each taping technique chapter, is then applied to the specific area of pain (as shown with Fig. 1.15).
Figure 1.15 The decompression strip is applied to the area of pain.
Once the kinesiology tape has been applied to the area, it then needs to be heat activated (not with artificial heat) to stimulate the acrylic adhesive on the back of the tape that adheres to the skin. Do this by rubbing the tape with either your hand or a piece of the backing tape that was removed from the kinesiology tape (Fig. 1.16).
Rub area to heat activate glue
Figure 1.16 Kinesiology tape applied by rubbing the area to generate heat and activate the glue.
How to prepare, cut, and apply kinesiology tape
After application
• The tape will need to be removed after a certain amount of time. It is normally left on the skin for between 3 and 5 days, even though it can be removed after the specific event or activity.
• If the kinesiology tape lifts or peels at the ends then it can be trimmed.
• On removal, do not rip the tape off as this can irritate the skin.
• It is easier to remove the kinesiology tape if it is moist or even wet.
• Apply a moisturizer to the skin after removal of the tape, as this will help reduce any potential irritation.
Things to remember
• Always check for a history of allergies to tape adhesives.
• Cleanse skin from any oil, cream, and massage wax and trim hair if needed prior to kinesiology taping application.
• Stretching the structure/tissue should always be comfortable and never painful for the patient/athlete.
• No stretch at either end of the tape.
• Heat activate the kinesiology tape after application.
• Remove after 3–5 days and it is easier to remove the kinesiology tape if it is wet.
• Moisturize the skin after tape removal.
How to apply kinesiology tape
THE COLORED “STARS”
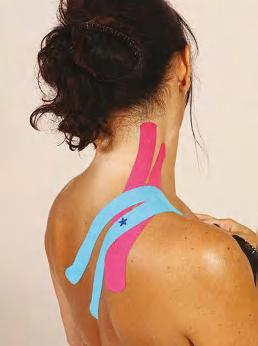
You might be wondering, especially if you have browsed through the book before reading this chapter, why there are colored stickers (or stars). For each of the individual kinesiology taping demonstrations I have placed some colored stickers (or stars) on specific areas of the body that relate directly to the pain or swelling that a patient might present with. I find this extremely beneficial, especially while lecturing to physical therapy students about the skills of kinesiology taping, as the application of a sticker enables accurate kinesiology taping.
Once the area of presenting pain has been located, then simply apply a sticker or mark the area as an exact guide as to where the kinesiology tape should be applied (Fig. 1.17). Once the area is
identified, preparation of the kinesiology tape can commence and the tape can be applied accordingly.
Reference to the individual videos using the QR code links is recommended as these explain when, where, and why I apply the colored stars as part of the kinesiology taping process.
TAPING AND FASCIAL TISSUE
Figure 1.17 The area of pain as indicated by the “stars.”
S = start; F = finish; and the directional arrow indicates the direction of the tape.
A quick look through the many pathologies covered by this text will confirm the fact that most soft-tissue injuries (plantar fasciitis, tendinopathies, ligament sprains, epicondylitis, tenosynovitis, to name a few) are not to the muscle fibers themselves, but directed more to their supportive elements, i.e., fascial tissues. Thankfully, the fascia has been the focus for a lot of research over the last two decades, a fact that has given us many new insights into, and appreciation of, its many functions.
Applying tape intelligently to address fascial pathologies necessitates some further understanding of the roles performed by this tissue type. Defined as the “soft tissue component of the connective tissue system that permeates the human body,” it includes all fibrous collagenous elements (Schleip et al. 2012). Its roles are to support and hold the organs and cells in place, giving them form and substance by holding them together, as well as providing both mechanical and chemical protection. The fascia provides boundaries, it contains and separates, and, perhaps most importantly for the purposes of this text, it allows movement. The fascial tissue transfers the force of muscle fiber contraction, as well as facilitating the necessary glide between structures, and is therefore especially
pertinent in our investigation into injury management.
We are all familiar with the muscle epi-, peri-, and endomysia: these are the fascial containers for the muscles, the bundles, and the individual fibers respectively. These muscle fiber “bags” come together to form the tendon, which blends into and becomes the periosteum, ligament, and joint capsule (Myers 2009). These dense tissues form the major force-transmission network through the body.
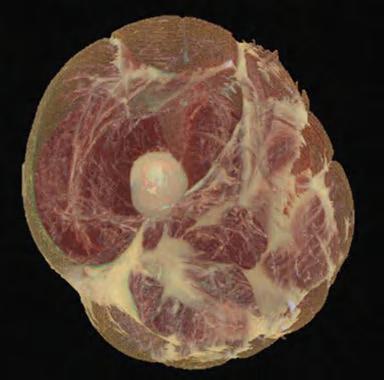
Figure 1.18 A modern rendition of the fascial net (from Jeff Linn using the Visible Human Data Project). Here we can see the thigh. This is a small section of what could be mapped in full, i.e., the fascial webbing of the body, which would include everything from the meninges to the organ bags and supports, the muscles’ epimysia, endomysia, and intermuscular septa, surrounded by the deep investing fascia and the superficial areolar and dermal layers.
Following Wolff ’s and Davis’s laws, the fascial tissues are adaptive and form themselves in response to the forces placed upon them. “Use it or lose it” is the
general advice given for many aspects of our biology. This is particularly true of the fascia, which will reinforce itself by laying down fibers in the direction of tension and varies its makeup according to the demands of the area (i.e., stronger or weaker pulls, which may be single- or multi-directional).
The linear pull of a muscle will be the primary defining dynamic of its associated fascia, but it will also transmit force horizontally beyond its connective tissue boundary. As we can see with Figure 1.18, the collagenous tissue forms a 3-dimensional web throughout the body and is capable of transmitting force to the surrounding tissue during contraction.
This not only disperses the force but also stimulates the many mechanoreceptors situated within the fascia and forms an important channel for exchange of proprioceptive information.
A fine balance must be made between using it enough and going too far too quickly. Unexpected or unusual loads will strain the tissue bonds, leading to injury and inflammation (Myers and Frederick in Schleip et al. 2012). By applying tape in certain directions, and with the appropriate load on the stretch, we can work to reduce the strain patterns and assist with the tissue healing by protecting the area.
By applying tape, and to influence local mechanics, the therapist will also alter the strain distribution and thereby the information that reaches the mechanoreceptors (Golgi’s organs, Ruffini’s endings, Pacini’s corpuscles, and free nerve endings) embedded within the collagenous tissues. This may increase the athlete’s ability to perform certain functions if the