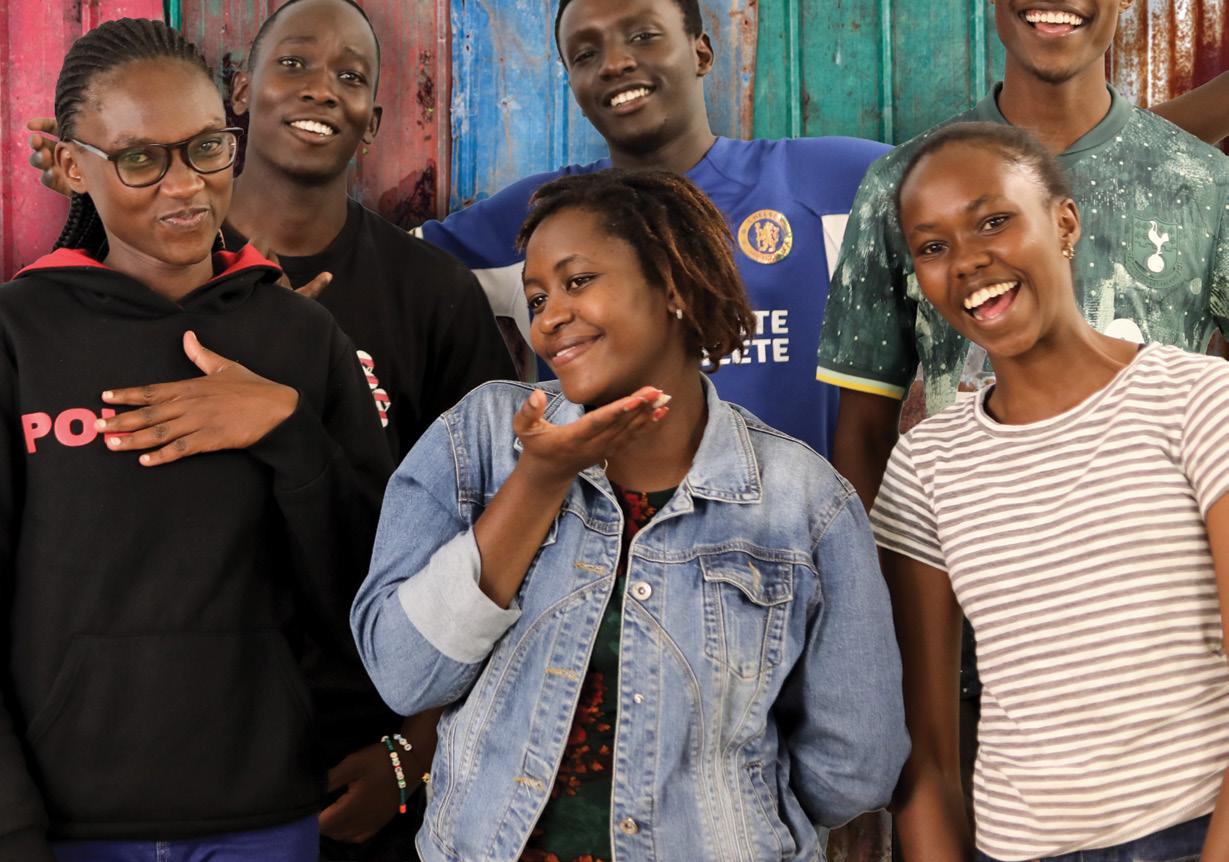NEW YORK CITY PARTNERSHIP PILOT GRANTS
Project Title
They Don’t Believe Us: Changing the Narrative for Patients with Sickle Cell Disease with an Acute Painful Episode Presenting to the Emergency Department Through the Implementation and Evaluation of a Standardized Pain Protocol
Hope Bodega: An Equity-Centered Resiliency Research Project and Intervention
Postpartum Transitions in Healthcare (PATH)
Harnessing Optimism and Perseverance in the Face of Long COVID~Español (HOPE-LC~Español)
Principal Investigators
Dave A. Holson, MD, MPH
NYC Health + Hospitals/Queens and Icahn School of Medicine at Mount Sinai
Impact on Healthcare Utilization and Care Experience after Medicaid Expansion Among Older Immigrant Adults in New York State
Devin Madden, PhD, MPH Icahn School of Medicine at Mount Sinai
Sarah Nowlin, PhD, MSN, RN Icahn School of Medicine at Mount Sinai
Eric Watson, PhD Icahn School of Medicine at Mount Sinai
Amelia Hicks, PhD (co-principal investigator) Icahn School of Medicine at Mount Sinai
Ellerie Weber, PhD, MBA Icahn School of Medicine at Mount Sinai
Mehak Paul, MBBS, MPH (co-principal investigator)
NYC Health + Hospitals/Elmhurst
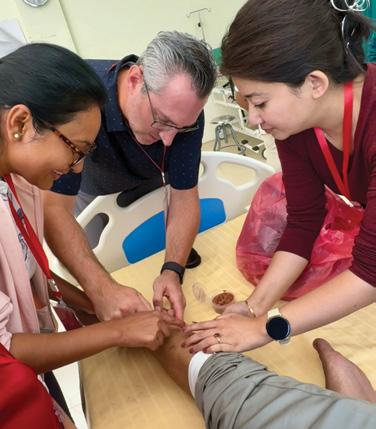
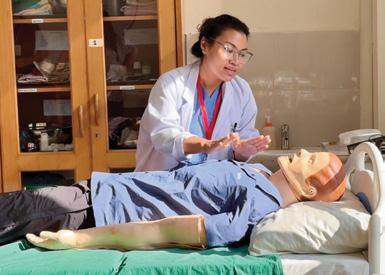
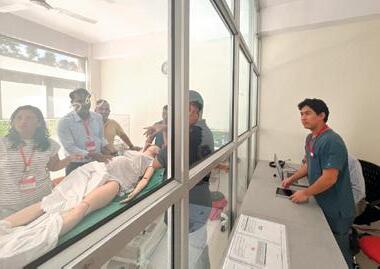
AMPATH KENYA PILOT GRANTS AND YOUTH LEADER GRANTS
Due to a changing funding landscape for ongoing, lifesaving AMPATH Kenya programs, funding for pilot grants was redirected into the Mount Sinai Youth Fund , which has been used to provide essential medicines to existing clients of AMPATH Kenya programs, fund peer support initiatives, invest in startup costs for a new adolescent health clinic in Kitale, Kenya, and fund other critical needs across the partnership.
In 2025, Arnhold Institute faculty published more than 70 scholarly peer-reviewed journal articles. This essential literature informs policy and practice, contributing to better care, health, and well-being for underserved people around the world.
Choudhury N, Wu WJ, Khatri R, Tiwari A, Thapa A, Adhikari S, Basnett I, Bhandari V, Bhatta A, Bogati B, Bhatt LD, Citrin D, Halliday S, Khadka S, Ksetri YKB, Kunwar LB, Magar KR, Marasini N, Maru D, Nirola I, Paudel R, Rai B, Schwarz R, Saud S, Sharma D, Niraula GD, Shrestha R, Thapa P, Rayamazi HJ, Maru S, Sapkota S. “Now that they come to our doorsteps to teach us these things…” - Postpartum contraception outcomes from a pre-post effectiveness-implementation study of an integrated community health worker intervention in rural Nepal. Reprod Health. 2025 Dec 22;22(1):258.
Poor HD, Eisenberg E, Saini S, HannahClark S, Zhang J, Lee AG, Serrao G, Powell C, Ventetuolo CE, Padilla M. Sotatercept Is Associated with Improved Lung Function in Sarcoidosis-Associated Pulmonary Hypertension. Chest. 2025 Dec 16:S0012-3692(25)05844-1. Epub ahead of print.
O’Donovan J, Baskin C, Katzen LS, Jiménez A, Iberico M, Kok M, Cook J, Ballard M, Ishimwe AB, Martin L, Kawooya P, Aranda Z, Mantus M, Kumar MB, Finnegan KE, Mudhune SA, Dennis M, Palazuelos D, Mbewe D, Nshimayesu M, Vaughan K. Costs and cost-effectiveness of community health worker programmes focussed on noncommunicable diseases in low- and middle-income countries (2015-2024): A scoping literature review. BMJ Glob Health. 2025 Dec 10;10(12):e018035.
Niu L, Liu S, Chen R, Wang Y, Zhang J, Lin S, Li Y, Pagán JA, Moran AE, Diaz A. Association of childhood maltreatment with hypertension outcomes in adulthood: A systematic review and meta-analysis. Child Abuse Negl. 2025 Dec 10;172:107840. Epub ahead of print.
Stansert Katzen L, Miyares M, Vaughan K, Baskin C, Ballard M, Kok M, Jimenez A, Iberico M, Cook J, Bienvenue Ishimwe A, Martin L, Kawooya P, Aranda Z, Mantus M, Bruce Kumar M, Finnegan KE, Mudhune S, Dennis M, Palazuelos D, Mbewe D, Nshimayesu M, Revill P, O’Donovan J. Economic evaluations of community health worker programs focussed on neglected tropical diseases in low- and middle-income countries (2015-2024): A scoping literature review. PLOS Glob Public Health. 2025 Dec 5;5(12):e0005551.
Nowlin SY, Boychuk N, Essein N, Glazer K, Howell FM, Burdick M, Oshewa O, Monterroso M, Rodriguez A, Cabrera C, Maru S, Lewey J, Howell EA, Levine L, Janevic T. Engagement with a Text-Based, Bilingual Blood Pressure Monitoring Program during Postpartum among a Multiethnic Population. MCN Am J Matern Child Nurs. 2026 Jan-Feb 01;51(1):20-28. doi: 10.1097/ NMC.0000000000001156. Epub 2025 Dec 3. PMID: 40960287; PMCID: PMC12672030.
Brewer NT, Tomar A, Perkins R, DarvilleSanders G, Fisher-Borne M, Footman A, Naavaal S, Oliver K, Saslow D, Brandt HM. Identifying HPV vaccination research priorities for the US. Hum Vaccin Immunother. 2025 Dec;21(1):2590263. Epub 2025 Dec 2.
Hauschildt KE, Thornton JD, Brown C, Hope AA, Jain S, Valley TS, Aslakson RA, Carlton EF, Iwashyna TJ, Mikkelsen M, Boen C, Dzeng E, Falvey J, George N, Hotchkin D, Khandelwal N, Khatri UG, McPeake J, Nadig NR, Oyesanya TO, Amiri I, Ashana DC. A Research Agenda to Mitigate Racial and Ethnic Disparities in U.S. Critical Care Medicine: An Official American Thoracic Society Research Statement. Am J Respir Crit Care Med. 2025 Dec;211(12):2268-2288.
Davis KP, Rudd T, Wilkinson TA, Ott MA, Meredith AH. Assessing Healthcare Utilization Postpharmacist Contraception Prescribing Among College-Aged Students. J Pediatr Adolesc Gynecol. 2025 Dec;38(6):735738. Epub 2025 May 15.
Schödel MM, Zimet GD, Cheng ER, Ott MA. Philadelphia’s Adolescent Vaccine Self-Consent Regulation: Provider Perspectives, Implementation Barriers, and Implications for Practice. J Adolesc Health. 2025 Nov 20. Epub ahead of print.
Reuveni I, Katz CL, Tene O, DeLisi LE. From 9/11/2001 to October 7, 2023The PreAct conference, NYC, June 2025: Preparing for mental health response to mass trauma. Psychiatry Res. 2025 Nov 20:116855. Epub ahead of print.
Wahl B, Menon GI, Nyhan K, Ren Y, Coria AL, Mukherjee B. Global health data precarity: Safeguarding the Demographic and Health Survey program as a global public good. Sci Data. 2025 Nov 19;12(1):1827.
Chory A, Kiptui R, Kirwa S, Genberg B, Embleton L. Perceptions about the use of direct cash-transfers to increase housing stability and HIV services utilization among street-connected young women in Western Kenya. Discover Public Health. 2025 Nov 18;22(1):705.
McCuskee S, Kowalski R, Mei C, Zebrowski A, Patel A, Zajac L, Zikry H, Ayyash A, DeFelice N. Concurrent Viral Transmission and Wildfire Smoke Events Following COVID-19 Pandemic School Closures in New York City: Associations of a Large Natural Experiment With Acute Care for Pediatric Asthma, 20182023. J Am Coll Emerg Physicians Open. 2025 Nov 17;7(1):100273.
Solan MJ, Calcano GA, Fernandez XMM, de Anderson XRFS, de Alonso MCP, Fallar R, Aloysi AS, Katz CL, Gupta DR. Assessing the Utility of Mental Health Training of Primary Care Professionals and Psychologists in the Dominican Republic. Psychiatr Q. 2025 Nov 15. Epub ahead of print.
Curtis SA, Jhawar R, Bellis J, McCuskee S, Devine L, Roberts JD. A pilot study of dronabinol for the treatment of pain in sickle cell disease. Pilot Feasibility Stud. 2025 Nov 12;11(1):139.
McHenry MS, Masese ER, Kinyanjui D, Were E, Carlucci JG, Humphrey JM, Wahome E, Munyoro D, White G, Nafiseh A, Cunningham K, Cory M, Nyalumbe M, Ombitsa RA, Ott MA, Halverson C. Ethical considerations for research involving pregnant women with HIV and their children. AIDS. 2025 Nov 1;39(13):18661877. Epub 2025 Sep 25.
Poor HD, Zhang J, Hannah-Clark S, Saini S, Eisenberg E, Wang J, Lee AG, Serrao G, Schotland H, Rogers L, Smith BM, Beasley MB, Li M, Powell CA, Ventetuolo CE, Padilla M. Sotatercept Improves Small Airway Disease and Hyperinflation in Patients with Pulmonary Hypertension. medRxiv [Preprint]. 2025 Oct 9:2025.
Titus AR, Kanchi R, Adhikari S, Thorpe LE, Lee DC, Baum A, Schwartz MD. Timevarying associations between diabetes and mortality following COVID-19: Evidence from a U.S. Veteran population. PLoS One. 2025 Oct 8;20(10):e0333052.
Vreeman RC, Yiannoutsos CT, Edmonds A, Leroy V, Fatti G, Kosalaraksa P, Pinto J, Musick B, Nyandiko W, Twizere C, Amorissani-Folquet M, Mbewe S, Mejia F, Scanlon ML, Martin R, Wools-Kaloustian K; IeDEA. Rates of adherence, adherence measurement, and support services for children and adolescents living with HIV followed in global sites of the International Epidemiology Databases to Evaluate AIDS (IeDEA). BMC Pediatr. 2025 Oct 2;25(1):706.
Jacobs-McFarlane C, Liu A, McCrary B, McCuskee S, Wexler MG, Stidham E, Zhang B, Glassberg J, Curtis S. Buprenorphine Is Associated With Lower Home Opioid Use and Acute Care Utilization in Sickle Cell Disease. Pain Manag Nurs. 2025 Oct;26(5):585-591. Epub 2025 May 29.
Kaali S, Michelle L, Mujtaba MN, Tsotetsi K, Yussif T, Colicino E, Osei M, Awuni S, Probst-Hensch N, Chillrud S, Jack D, Asante KP, Röösli M, Lee AG. Early Life Cookstove Interventions and Children’s Blood Pressure: Evidence from the Ghana Randomized Air Pollution and Health Study. Environ Res. 2025 Sep 30:122994. Epub ahead of print.
Boyce D, Katz CL. A keynote in two parts: The intersection of emergency management and disaster mental health, and a vision of disaster mental health that emerges from its challenges. Psychiatry Res. 2025 Sep 28;353:116750. Epub ahead of print.
Ciemins EL, Rooney A, Yaun JA, Saxena K, Schmier JK, Dempsey AF, Oliver K. Initiating Human Papillomavirus Vaccination at Age 9: Strategies for Success From 5 US Health Systems. Acad Pediatr. 2025 Sep-Oct;25(7):102869. Epub 2025 Jun 7.
Dangal RK, Barun K, Thapa D, Anderson K MA, Shrestha R, House DR. Enhancing Emergency Medicine Services at Rural Outreach Centers: A Comprehensive Needs Assessment for Project ECHO Education Program. Kathmandu Univ Med J (KUMJ). 2025 Sep;23(91):55-60.
Sampath V, Payne-Sturges D, Slopen N, Harnett N, Lee AG, Nadeau K, Taylor NK, Burghardt L. Call to action: recognize and prevent the effects of extreme heat on early childhood development and health. Front Public Health. 2025 Aug 25;13:1654097.
Gennings C, Midya V, Renzetti S, DeFelice N. Weighted quantile sum (WQS) mixedeffects model. MethodsX. 2025 Aug 22;15:103580.
Olasehinde O, Wuraola F, Di Bernardo M, Knapp G, Aderounmu A, Omisore A, Oladele A, Awe MO, Mohammed T, Romanoff A, Kingham TP, Mango V, Adisa A, Alatise O. Breast Cancer-Related Lymphedema: A Common Challenge among Nigerian Breast Cancer Survivors. Breast Care (Basel). 2025 Aug 21. Epub ahead of print.
Juarez R, Phankitnirundorn K, Ozorio Dutra SV, Bond-Smith D, Lee AG, Maunakea AK. Health and Social Support in the Aftermath of the Maui Wildfires. JAMA Netw Open. 2025 Aug 1;8(8):e2525430.
Lopez-Perez PE, Portillo EN, Silver M, Coria A. Inequities in Length of Stay for Pediatric Patient Families Using Languages Other Than English for Care. Hosp Pediatr. 2025 Aug 1;15(8):645-651.
Baldwin MK, Bell AJ, Hoopes AJ, Narasimhan S, Ott MA. Society of Family Planning Research Practice Support: Researcher and institutional review board considerations for sexual and reproductive health research with minor adolescents. Contraception. 2025 Aug;148:110935.
Squeri B, Huang J, Chavez S, Nowlin S. Getting the Full Picture: Nurses Use Video Visits to Enhance Telephone Triage for Homebound Patients. Home Healthc Now. 2025 Jul-Aug 01;43(4):206-212.
O’Donovan J, Kumar MB, Ballard M, Mchenga M, Martin L, Dennis M, Mantus M, Jiménez A, Sirmareza T, Cook J, Kawooya P, Aranda Z, Ishimwe AB, Praha RD, Finnegan KE, Ruffing K, Kok M, Iberico M, Palazuelos D, Witter S, Rao M, Dhillon RS, Napier HG, Nkenfack M, Katzen LS, Makhupula L, Odera M, Nshimayesu M, Vaughan K. Costs and cost-effectiveness of integrated horizontal community health worker programmes in low- and middleincome countries (2015-2024): A scoping literature review. BMJ Glob Health. 2025 Jul 22;10(7):e017852.
Baskin C, Westgate CC, Shellaby L, Ballard M, Rogers A, Hofmann R, Raghavan M, Palazuelos D, Lindsay S, Keronyai PP, French M, Ganjian N, Rapp S, Tiedt S, López Castañeda C, Nsubuga DN, Aidam J, Razafinjato B, O’Donovan J. Essential aid made fully visible: understanding the proCHW financing landscape analysing accessible donor data sources. BMJ Glob Health. 2025 Jul 15;10(7):e017453.
Bowling M, Langer S, Saracino C, Shrestha R, Joshi A, Kutzin J, Strother C, House DR. Developing a pediatric emergency medicine simulation-based learning curriculum in Nepal. Int J Emerg Med. 2025 Jul 1;18(1):116.
Grubner A, Fisher P, Suozzo D, Bowling M. Bilious Emesis and Back Pain in an 11-Year-Old Girl. Pediatr Rev. 2025 Jul 1;46(7):391-394.
Ott MA, Hoopes AJ, Sucato GS, LeroyMelamed M; Committee on Adolescence. Contraception for Adolescents: Policy Statement. Pediatrics. 2025 Jul 1;156(1):e2025072217.
Ott MA, Sucato GS, Leroy-Melamed M, Hoopes AJ; Committee on Adolescence. Contraceptive Counseling and Methods for Adolescents: Clinical Report. Pediatrics. 2025 Jul 1;156(1):e2025072218.
Opel DJ, Diekema DS; Committee on Bioethics. New and Evolving Dimensions in the Pediatrician-Family-Patient Relationship: Maintaining and Managing Boundaries: Clinical Report. Pediatrics. 2025 Jul 1;156(1):e2025072215.
Singh M, Nyandiko W, Delong A, Ashimosi C, Munyoro D, Lidweye J, Nyagaya J, Biegon W, Aluoch J, Chory A, Sang E, Jepkemboi E, Orido M, Novitsky V, Hogan JW, Vreeman R, Kantor R. Challenges Faced by Perinatally-Infected Kenyan Adolescents and Youth Living with HIV During the COVID-19 Pandemic. AIDS Behav. 2025 Jul;29(7):2249-2257. Epub 2025 Mar 20.
Ballard M. Q&A with Madeleine Ballard. Med. 2025 Jun 13;6(6):100745.
Gigase FAJ, Suleri A, Isaevska E, Rommel AS, Boekhorst MGBM, Dmitrichenko O, El Marroun H, Steegers EAP, Hillegers MHJ, Muetzel RL, Lieb W, Cecil CAM, Pop VJM, Breen M, Bergink V, de Witte LD. Inflammatory markers in pregnancy - identifying drivers in four large cohorts. Front Immunol. 2025 Jun 9;16:1561798.
Saxena K, Ai L, Martino A, Mohamed AFS, Wang D, Zheng Y, Oliver K. Human papillomavirus vaccine administration opportunities at well visits in adolescents. BMC Public Health. 2025 Jun 4;25(1):2084.
Khatri UG, Lopez C, Yen YT, Ling EJ, Richardson LD, Ngai KM. Receipt of Buprenorphine and Naltrexone for Opioid Use Disorder by Race and Ethnicity and Insurance Type. JAMA Netw Open. 2025 Jun 2;8(6):e2518493.
Khatri UG, Hakes JK, Buckler D, Zebrowski A, Winkelman T. Individualand Area-Level Incarceration and Mortality. JAMA Netw Open. 2025 Jun 2;8(6):e2513537.
Mezzich JE, Rodriguez-Bores L, Camarena-Robles E. Patterns and innovations in the unfolding of Latin American psychiatry and mental health. World Psychiatry. 2025 Jun;24(2):285286.
Baron S, Cuervo I, Wilets I, Cruz J, Gonzalez A, Flores D, Harari H. A Qualitative Study of the Ethics of Community Scientists’ Role in Environmental Health Research from the Perspective of Community Scientists and Institutional Review Board Staff. Environ Health Perspect. 2025 May;133(5):57019. Epub 2025 May 23.
Walker A, Bowling M, Thamburaj R, Akhtar R. Persistent Sore Throat and Dysphagia in a Teenager. Pediatr Rev. 2025 Jun 1;46(6):341-344.
Coritsidis A, Arniella G, Berhane T, Madden D, Ruiz J, Vangeepuram N, Oliver K. Sustaining Communities and Community Health Workers: Lessons Learned From Community Health Workers’ Experience During the COVID-19 Pandemic. J Ambul Care Manage. 2025 Jul-Sep 01;48(3):159-168.
O’Donovan J, Baskin C, Stansert Katzen L, Ballard M, Kok M, Jimenez A, Iberico M, Cook J, Bienvenue Ishimwe A, Martin L, Kawooya P, Aranda Z, Mantus M, Bruce Kumar M, Finnegan KE, Mudhune S, Dennis M, Palazuelos D, Mbewe D, Nshimayesu M, Vaughan K. Costs and cost-effectiveness of community health worker programs focussed on HIV, TB and malaria infectious diseases in lowand middle-income countries (20152024): A scoping literature review. PLOS Glob Public Health. 2025 May 9;5(5):e0004596.
Zhou S, Kagoya EK, Coria A, Beck A, Evert J, Haque M, Lamb MM, Rule AR, Umphrey L. Income-Based Disparities in Perceived Benefits and Challenges of Virtual Global Health Activities
During the COVID-19 Pandemic: Mixed Methods Analysis. J Med Internet Res. 2025 May 7.
MacMurdo MG, Bayram H, Brigham E, Croft D, Goobie G, Lee AG, Myers LC, Nassikas N, Radbel J. Letting Cooler Heads Prevail: The Necessity of Occupational Regulation of Heat and Smoke Exposure. Am J Respir Crit Care Med. 2025 May 2. Epub ahead of print.
Gillette E, Nyandiko W, Chory A, Scanlon M, Aluoch J, Koros H, Ashimosi C, Biegon W, Munyoro D, Lidweye J, Nyagaya J, DeLong A, Kantor R, Vreeman R, Naanyu V. Risks and benefits of engaging youth living with HIV in research: Perspectives from Kenyan youth, caregivers, and subject matter experts. BMC Med Ethics. 2025 May 16;26(1):63.
Janevic T, Birnie L, Belfon K, Glenn L, Maru S, Reynolds S, Eniola F, Kim H, Howell FM, Fox A, Weber E. Immigrant Inequities in Uninsurance and Postpartum Medicaid Extension: A Quasi-Experimental Study in New York City, 2016-2021. Am J Public Health. 2025 May;115(5):732-735. Epub 2025 Feb 27.
Coria AL, Wahl B, Thacker N, Vreeman R, Zühlke L. USAID’s Role in Saving Children’s Lives: Past Legacy and Future Directions. Pediatrics. 2025 Apr 24. Epub ahead of print.
Harp RD, Holcomb KM, Retkute R, Prusokiene A, Prusokas A, Ertem Z, Ajelli M, Kummer AG, Litvinova M, Merler S, Piontti APY, Poletti P, Vespignani A, Wilke ABB, Zardini A, Smith KH, Armstrong P, DeFelice N, Keyel A, Shepard J, Smith R, Tyre A, Humphreys J, Cohnstaedt LW, Hosseini S, Scoglio C, Gorris ME, Barnard M, Moser SK, Spencer JA, McCarter MSJ, Lee C, Nolan MS, Barker CM, Staples JE, Nett RJ, Johansson MA. Evaluation of the 2022 West Nile virus forecasting challenge, USA. Parasit Vectors. 2025 Apr 23;18(1):152.
Embleton L, Sudjaritruk T, Machado DM, Chihota B, Musabyimana F, Jesson J, Apondi E, Puthanakit T, Luque MT, van Dongen NE, Murenzi G, Amorissani-Folquet M, Kwena Z, Perreras N, Rouzier V, Lyamuya R, Anderson K, Elul B, Leroy V, Enane LA, Martin R, Lancaster K, Parcesepe AM, Vreeman R; IeDEA. Characterizing adolescent and youth-friendly HIV services: A cross-sectional assessment across 16 global sites. J Int AIDS Soc. 2025 Apr;28(4):e26437.
House DR, Amatya Y, Nti BK, Russell FM. Clinical Prediction Models for Pneumonia in Children Presenting to an Emergency Department in a Resource-Limited Setting Using Lung Ultrasound Diagnosis as the Gold Standard. Cureus. 2025 Mar 28;17(3): 1.
Tosi M, Winkler M, Zubizaretta N, Nisenholtz M, Spangenberg M, Tappenden KA, Iyer K. Chronic intestinal failure knowledge among a cohort of ASPEN registered dietitians: Response to a membership survey. Nutr Clin Pract. 2025 Mar 11. Epub ahead of print.
Cid ME, Yang Z, Glassberg J, McCuskee S, Hua M. Epidemiology of Intensive Care Use for Patients With Sickle Cell Disease in New York State. Chest. 2025 Mar 10. Epub ahead of print.
Khatri UG, Sondheim SE. Unmasking Racial and Ethnic Disparities in Prehospital Sedation and Restraint Practices-Beyond the Straps. JAMA Netw Open. 2025 Mar 3.
Mills AN, Dubois B, Lesseur C, Rommel AS, Tubassum R, Kaplowitz E, Boychuk N, Stern T, Chen J, Lieb W, Janevic T, Jessel RH. Impact of antenatal SARS-CoV-2 infection on development of hypertensive disorders of pregnancy in a large, diverse cohort. Pregnancy Hypertens. 2025 Feb 25;39. Epub ahead of print.
Liu A, Jacobs-McFarlane C, Sebastiani P, Glassberg J, McCuskee S, Curtis S. Plasma-free hemoglobin is associated with LDH, AST, total bilirubin, reticulocyte count, and the hemolysis score in patients with sickle cell anemia. Ann Hematol. 2025 Feb 19. Epub ahead of print.
Maru S, Porchia-Albert C, Lockworth K, Hall C, Boychuk N, Calliste N, Cooke C, Gebara S, Haq K, Harishankar K, James R, Janevic T, Mathurin K, Nowlin S, Rivera A, Rodriguez A, Schwartz R, St Clair V, Whaley S, Whitney A. Building HOPE: Integrating communitybased doula care in public hospitals in New York City. Health Aff Sch. 2025 Feb 14;3.
Draucker CB, Carrión A, Ott MA, Hicks AI, Knopf A. A 4-Site Public Deliberation Project on the Acceptability of Youth SelfConsent in Biomedical HIV Prevention Trials: Assessment of Facilitator Fidelity to Key Principles. JMIR Form Res. 2025 Feb 13.
Jaguga F, Aalsma MC, Enane LA, Turissini M, Kwobah EK, Apondi E, Barasa J, Kosgei G, Olando Y, Ott MA. A qualitative pilot study exploring the acceptability of a peer provider delivered substance use brief intervention from the perspective of youth in Kenya. Subst Abuse Treat Prev Policy. 2025 Feb 11;20(1):6.
Hodgins S, Lehmann U, Perry H, Leydon N, Scott K, Agarwal S, Marcus H, Ved R, Olivas E, Ballard M, Mbewe D, Odera M, Petit Homme S, Otieno B, Wutete P, Chikumba A, Muyingo P, Kyakuha J, Harcourt E, Chowdhury M, Musoke D, Niyoyitungira T, Olaniran A, Williams JK, E Méllo LMBD, Dos Santos RC, Pinto ICM, Shrestha R, Sadruddin S, Morrow M, Sarriot E, Kok M, Pratap B. Comparing apples with apples: A proposed taxonomy for “Community Health Workers” and other front-line health workers for international comparisons. PLOS Glob Public Health. 2025 Feb 6;5(2):e0004156.
Romanoff A, Olasehinde O, Lynch K, Folorunso S, Omoyiola O, Omolade B, Omisore A, Okereke CE, Agodirin O, Muhammad AB, Ali N, Irowa O, Nweke NS, Nwokwu UE, Aderounmu A, Wuraola F, Kalvin HL, Kahn R, Fitzgerald G, Olcese C, Iasonos A, Mango VL, Ostroff JS, Vreeman R, Anderson BO, Kingham TP, Alatise OI. Health Care Professional Adherence to Breast Cancer Management Guidelines in Nigeria. JAMA Netw Open. 2025 Feb 3.
Wylie BJ, Kaali S, Duttweiler L, Ae-Ngibise KA, Mujtaba M, Tawiah C, Gibson E, Calafat AM, Ospina M, Jack DJ, Agyei O, Lee AG, Roberts DJ, Boamah-Kaali EA, FactorLitvak P, Modest AM, Hauser R, Coull BA, Asante KP. Evaluation of gestational nonpersistent pesticide exposure with newborn size and gestational length in rural Ghana using a novel time-varying extension of multiple informant models. Environ Int. 2025 Feb;196:109292. Epub 2025 Jan 28.
Janevic T, Howell FM, Burdick M, Nowlin S, Maru S, Boychuk N, Oshewa O, Monterroso M, McCarthy K, Gundersen DA, Rodriguez A, Katzenstein C, Longley R, Whilby KW, Lee A, Cabrera C, Lewey J, Howell EA, Levine LD. Racism and Postpartum Blood Pressure in a Multiethnic Prospective Cohort. Hypertension. 2025 Feb;82(2):206-215. Epub 2025 Jan 9.
Reuveni I, Tene O, Katz CL. The personal and the national: Lessons learned in the aftermath of the October 7 attacks in Israel. Psychiatry Res. 2025 Feb.
McCuskee S, Chiu YM, McCann M, Wright RJ, Glassberg JA. Exposure to public housing reverses the association between neighborhood disadvantage and eosinophilic inflammation in patients with sickle cell disease. medRxiv [Preprint]. 2025 Jan.
Huynh B, Ott MA, Tarvin SE. Experiences of sexual and reproductive health screening and counseling in the clinical setting among adolescents and young adults with rheumatic disease. Pediatr Rheumatol Online J. 2025 Jan 20;23(1):5.
Otero-Marquez O, Haq A, Muncharaz Duran L, Bellis J, McCuskee S, Ahsanuddin S, Rosen RB, Glassberg J, Chui TYP. Preferential Sites of Retinal Capillary Occlusion in Sickle Cell Disease. Invest Ophthalmol Vis Sci. 2025 Jan 2;66(1):57.
We invite you to join us in making a global impact.
Make a donation at https://bit.ly/aighdonate or scan the QR code below.