












Whether or not you want to live forever, I think it’s fair to say that most of us want to live as healthily as we can, for as long as possible.
In the cover story for this Hole Health special section, we call that longevity. More broadly, I think there’s another word that describes the sentiment: sustainability.
Sustainability is a core value in Jackson Hole. Most people know it from conversations we have about preserving our lands, our environment and the living beings within it. To me, health care deserves a spot in the conversation.
And health care, just like the climate, is changing.
Costs are piling up for hospitals and insurers alike, influencing negotiations between the two. Populations are getting older — including in Teton County — and more dependent on medical care. All of that is taking place as federal decisions likely lead to more people not getting health insurance at all.
In this special section, we take a peek at how the fallout
is influencing local patients and providers alike. The impact includes beloved doctors who are starting new ventures, whether that be concierge medicine in Jackson Hole or orthopedic surgery in Teton Valley. We explore what people can do if they are uninsured. And we dive into what health expertise looks like in the halls of our state government.
The News&Guide also tried to explore what sets the Hole’s health apart from that of other communities. It’s undeniable that the Teton region is known for its intense physical activity, whether that be from pumping iron or Strava stats.
Sustaining the self, I learned from our reporters’ inquiries, is part of the path to ascending new heights.
Just like I don’t know how long I’ll live, I don’t know what the future looks like for health care in Jackson Hole. All we can focus on, today, is keeping an eye on how to keep it going — healthily, sustainably — as long as possible.
— Alex Viveros Health Reporter
Published by
PUBLISHER
Adam Meyer
EDITOR IN CHIEF
Johanna Love
MANAGING EDITOR
Billy Arnold
SECTION EDITOR
Alex Viveros
PHOTOGRAPHERS
Bradly J. Boner, Kathryn Ziesig, Charlie Nick
EDITORIAL DESIGN
Andy Edwards
CONTRIBUTORS
Jeannette Boner, Jasmine Hall, Charley Sutherland, Christina MacIntosh
COPY EDITING: Sarah Sellergren
CREATIVE DIRECTOR
Sarah Wilson
ADVERTISING DESIGN ARTISTS
Lydia Redzich, Luis Ortiz, Chelsea Robinson
DIRECTOR OF ADVERTISING
Karen Brennan
MULTIMEDIA SALES MANAGERS
Tim Walker, Chad Repinski
DIGITAL CAMPAIGN MANAGER: Tatum Mentzer
DIRECTOR OF OPERATIONS AND SALES: Tom Hall
PRODUCTION MANAGER: Dale Fjeldsted
PRESS SUPERVISOR: Stephen Livingston
PREPRESS SUPERVISOR: Lewis Haddock
PRESSMEN: Gunner Heller, Angel Aguilar
CIRCULATION MANAGER: Jayann Carlisle
CIRCULATION: RuLinda Roice, Gunner Heller, Angel Aguilar, Anthony Sosa Sedeno
CEO: Kevin B. Olson
©2026 Teton Media Works
Jackson Hole News&Guide
P.O. Box 7445, 1225 Maple Way, Jackson, WY 83002
Phone: 307-733-2047; Web: JHNewsAndGuide.com
Maintaining physical and cognitive functionality as long as possible is focus of new Wilson clinic.

By Alex Viveros
Donna Marts has shown off her strength over 65 years. Literally.
In her 40’s, Marts started lifting free weights at the gym. She blossomed, progressing into heavier, heavier and heavier things. Twentyodd years later, the 10-time world champion powerlifter has racked up her accolades, including one for a record-setting near-400 pound deadlift.
Like many exercise buffs that call Jackson Hole home, Marts is looking to what’s next. Breaking existing powerlifting records and hiking the Sleeping Indian are on her bucket list. Still, there’s one obstacle that even the most fit struggle to outrun.
”You lose strength as you age,” Marts said. “There’s no magic trick for that.”
When it comes to powerlifting, Marts is focusing on improving her squat and deadlift form to compensate for Father Time. More broadly, she’s joined other Teton County residents who have recently looked to so-called longevity care.
To some people, the word “longevity” might suggest the premise of wanting to live forever, or at least longer than what might be biologically predicated. But for Marts and others, that’s not necessarily the case. Instead, the hope is that certain lifestyle changes may lead to a quality life for longer.
In Jackson Hole, that ideal could mean keeping up until the clock runs out.
“Ideally, I would be 105, just gotten through my tram lap, and drop dead,” Marts said. “I don’t want to be sitting on the couch, watching other people enjoy things. I want to be able to do things until I drop.”
For Marts and over a dozen other residents, optimizing one’s lifespan involves care at Grand Health, a new longevity clinic in Wilson. Beyond the specific advice she gets there, her goals may help paint a picture of what sets aging in the Tetons apart.
”We live in the most gorgeous place in the universe,” Marts said. “Why would you not want to be able to hike everything possible?”
ER to Wilson
For over a decade, Tobin Dennis has treated people through some of the worst days of their lives. An emergency medicine physician at St. John’s Health, he is responsible for helping people who roll

for a
Jan. 30 at Grand Health Clinic. As Jackson Hole’s first longevity healthcare clinic, Grand Health uses modern medicine to promote long-term well-being through implementing personalized health monitoring and focusing on physical and mental wellness to help combat health issues and build a stronger foundation.
through the emergency department. Responding to accidents, strokes and heart attacks comes with the territory.
Dennis, who grew up in Jackson, initially did his residency at Virginia Tech, where he noticed that admitted patients were generally sicker than Teton County residents. More young people, for example, came in with cardiovascular crises. When he started working at St. John’s Health in 2019, he observed a difference in people’s health.
”I saw the transition from seeing populations in Virginia compared to the population in Teton County, and just the differences in outcomes that we had, which I thought was most likely due to the physical fitness levels of everybody,” Dennis said. He thought “there’s probably something significant to what we
can do to change outcomes by orders of magnitude.”
The idea of longevity, which can mean different things to different people, caught his eye. For Dennis, longevity meant improving the quality — though not necessarily the length — of someone’s life for longer. Others agreed.
“You could be 90 years old, hit the slopes … so you have the physical functionality to get out and actually do activities that you want to do,” said Thomas M. Holland, a physician-scientist at the Rush Institute for Healthy Aging in Chicago. “The idea of longevity, or being a super-ager, is maintaining your cognitive and physical functionality for as long as possible.”
Last year, Dennis’ interest materialized into
The model allows providers more time with (fewer) patients, and comes with hefty price tag.

By Alex Viveros
After nearly two decades of delivering babies in Teton County, Dr. Giovannina Anthony was burned out.
Newborns often pop up unpredictably, meaning Anthony would find herself awake at odd hours to welcome them into the world. A next day’s rest often wasn’t feasible either, as the obstetrician-gynecologist would have patients scheduled for checkups.
Though Anthony liked being busy, missing weekends, holidays and time spent with her daughter took a toll. Eventually, she felt sucked dry.
“The energy in medicine is a very giving, taking care of people type of energy,” Anthony said. “It’s hard to continue doing that when you don’t feel like you can take care of yourself.”
Still, Anthony was not ready to hang up her hat. Instead, she decided to join doctors across the country who are increasingly turning to concierge medicine, a health care model where patients pay an annual fee for all-access care from their preferred providers.
In Teton County, where small-town doctors are historically known for their engagement with patients and neighbors, she’s not alone.
“Quite honestly, I’ve been providing what amounts to concierge care for a long time,” said Dr. Brent Blue, a family medicine physician who opened a concierge medicine practice in Wilson late last year. “I just never charged for it.”
What does and doesn’t count as concierge medicine can be up to debate. But generally, patients pay thousands of dollars to access select
doctors around-the-clock. Given that concierge medicine doctors see fewer patients — at least in part because many don’t accept insurance — providers likely have more time to sit down with the people they’re treating.
“She has the time to talk you through things. She wants to get to know you as a human, not just what you’re there for,” said Lona Williams, one of Anthony’s patients. “I think that focuses her recommendations to a level that’s really handy.”
For Blue, who has practiced medicine in Jackson Hole for over four decades, concierge medicine reminded him of how private practices operated when he first came to the valley. That included increased access to physicians, he said — he remembered answering the telephone “basically 24/7.”
“I think it’s getting paid for what I’ve been doing all along,” Blue said. “But it’s also a return to taking care of the whole patient, and really being much more of a patient advocate.
“I think that unfortunately, medicine has gotten impersonal,” he added.
The concierge medicine model comes at a steep cost, making it out of reach for many Teton County residents.
Anthony charges $12,000 a year for an individual, which she said was “middle of the road” compared to other tiers. Elsewhere in the country, fees can range from $2,000 to well into the tens of thousands every year. Blue, for his part, charges $12,000 for an individual and $20,000 for a couple.
Based out of an office in Wilson called GMA Health, Anthony now treats about 35 patients year-round through the concierge model. That’s a
fraction of her previous patient numbers. She remembered seeing 15 to 20 patients a day, not including deliveries.
“I just don’t want a big practice. Because [in] concierge medicine, you still are accountable to your patients off hours,” Anthony said. “I’d rather have 50 patients than 5,000.”
All of Anthony’s patients have health insurance, which they use for care outside of the concierge clinic. That could include mammograms, specialist visits, and other services that Anthony refers them out to.
Anthony said she makes “a lot less money” from taking fewer patients. The tradeoff is more time to focus on individual patients, more time to spend with her family and more time to focus on abortion rights advocacy. Anthony was involved in three major abortion cases since 2022, efforts which ultimately led to the Wyoming Supreme Court ruling that two abortion bans in the state were unconstitutional.
“I am very passionate about reproductive justice and abortion rights, and that takes an incredible amount of time, too,” Anthony said. She made the transition to concierge medicine after her previous private practice had to close for financial reasons. “It was a perfect storm, in a way, where the practice had to close ... it forced me to rethink my career.”
A part of Anthony felt guilty for turning people away who wanted to use their health insurance, saying it was hard to say goodbye to patients she had seen for decades.
“That’s hard, because for decades, I never turned anybody away, ever,” Anthony said. “But that’s about making
my own boundaries, and ultimately, paying out of pocket is going to keep the practice small.”
Not accepting health insurance made running a practice simpler, Anthony said. She did not have to hire a billing company to help collect claims, and she did not have to negotiate with health insurers on reimbursement rates. The insurance model, she said, encouraged providers to move quickly and see as many patients as possible.
“Aside from having to deal with insurance companies for billing, on a day-to-day basis it’s really hard to not spend time with people when they need more time,” Anthony said.
That providers had to worry about seeing high patient volumes to pay the bills indicated that the health care system was “broken,” Anthony said.
“The system sucks you dry as a provider, and it doesn’t always provide the best service to the patient,” Anthony said.
“In order to provide the best service, I felt I had to go outside the system.”
Blue operates out of his concierge medicine practice in Wilson once a week, adding that his concierge patients have 24/7 access to him and are treated on a more personalized basis.
“A patient in the concierge practice will text me and I will text them back, no matter where they are or where I am,” said Blue, who also sits on the St. John’s Health Board of Trustees and is the Teton County Coroner. “I’ve texted people back or called them back or answered the phone when I’ve been overseas, thousands of miles away.”
The physician still operates a private practice with a traditional model, where he accepts patients
Move comes as health care pressures and recreation-driven growth reshape demand for specialty care.

By Jeannette Boner
For orthopedic surgeon Dr. Stefan Turkula, the move to private practice wasn’t about leaving Teton Valley Health. Instead, it was about finding a way to stay in Teton Valley and practice what he preaches.
“If I’m going to live here and be a surgeon here long term, I needed to have some control over my future,” he said from his new space along Ski Hill Road in Driggs, Idaho.
The shift comes at a moment of change in Teton Valley. Health care system pressures and rapid growth tied to the region’s recreation-driven economy are reshaping the traditional medical landscape.
Over the past two decades, Teton Valley has transformed from a primarily agricultural community into a year-round recreation hub. Fueled by demand for access to the Tetons’ peaks and open spaces, remote workers have relocated to the region, all as
outdoor recreation infrastructure continues to expand.
Growth at Grand Targhee Resort — including terrain expansion, lift upgrades and long-term base area development planning — has increased visitation and year-round activity, bringing more seasonal workers, visitors and part-time residents into the valley, according to an economic impact study.
That growth has driven demand across nearly every sector, including
housing, schools and roads. Increasingly, health care has been added to the mix. Orthopedic care has seen its own rise as more skiing, mountain biking, backcountry recreation and construction lead to musculoskeletal injuries, according to the National Library of Medicine.
Whether intended or not, Turkula’s exit came before a major change at his previous employer. As Teton Valley Health announced layoffs and hinted


For more than 13 years, Teton Behavior Therapy has been providing trusted, community-centered mental health care in the region. Growing each year to meet increasing demand, TBT has expanded its 501(c)(3) nonprofit initiatives to serve individuals and families across:
Jackson • Alpine • Pinedale • Driggs
(Nearly 50% of Teton County’s workforce commutes from these neighboring communities)
1,000+ individuals served annually
13,000+ mental health therapy sessions yearly
15+ free community workshops offered
Men’s Mental Health Initiative
School-based mental health support
Spanish-language services expanded Evening & weekend access increasing

As our region grows, so do the mental health needs of families, children, educators, hospitality workers, and caregivers. With community support, we will:
• Expand free and reduced mental health care
• Offer more free and accessible workshops
• Invest in prevention and early intervention
• Make sure help is available before a crisis


Navigate the obstacle course as a family; teams of 2-4. Course designed for families with children ages 5-12. Proceeds fund scholarships for children and family therapy. Register or sponsor at: www.tetonbehaviortherapy.com
Current, former lawmakers say more expertise is needed in Cheyenne.
By Jasmine Hall
This year, the Wyoming Legislature is likely wading into stem cell therapy, hospital bankruptcy, epinephrine delivery — and controversial issues like abortion.
But the Legislature is not made up of medical professionals. Far from it.
In 2017, the Wyoming Medical Society urged more health care providers to serve in the Wyoming Legislature. At the time, only 4% of lawmakers ever elected in the Legislature’s history had worked in the health care industry, according to the advocacy group representing more than 1,000 Wyoming physicians, medical students and residents. The Medical Society’s request had little impact.
In today’s 93-person citizen legislature, only four members are health care providers. However, there is also a veterinarian, the development director of a hospital, and a first responder.
“There’s very little medical knowledge in the Legislature, period,” said former Sen. Fred Baldwin, R-Kemmer, a physician’s assistant who was a medical resource during his 9 years in the Legislature. He chaired the Senate Labor, Health and Social Services Committee for four years.
The lack of medical professionals in office means that legislators have to rely on outside experts as they navigate a complicated and shifting medical landscape. Wyoming’s rural hospitals, including St. John’s Health, are facing narrower margins, labor shortages and increasing admin

issues tactfully, outside providers and advocates urge lawmakers to listen to medical professionals who give testimony. But the Covid-19 pandemic exacerbated a problem. Legislators, increasingly influenced by the far-right Wyoming Freedom Caucus, are more distrustful of medical institutions, some onlookers say.
Wyoming lawmakers, Baldwin said, don’t want to hear “outside facts.”
“It’s very difficult to educate the Legislature,” he added.
Sen. Evie Brennan, R-Cheyenne, is trying to balance her career in health care and politics.
She has been a nurse for 21 years and works at Cheyenne Regional Medical Center. Brennan takes a leave of absence during the session. Otherwise, she couldn’t work 12 hours, five days a week for a few months each year at the Capitol, then put in two 12 hour shifts at the hospital on the weekend.
Brennan is set to serve as the next Senate chair of the Labor, Health and Social Services Committee.
Brennan has seen legislators struggle to write and work through bills about controversial issues like abortion. She tries to protect unborn babies, while ensuring other people have access to care.
“I’m a very pro-life legislator,” she said. “But we need to make sure that we get there in a way that doesn’t hurt our health care system.”
Brennan joined the Senate in 2023, a year before Baldwin retired. She misses having him as a “second set of health care eyes in the Senate.”
“I have seen a lot of well intended but poorly written legislation,” she said.

In 2026, lawmakers have sponsored bills that would make Ivermectin an over-the-counter drug; authorize physicians to recommend and refer for stem cell therapy; require transparency about hospital service prices; increase certain Medicaid rates and more. They’re also involved in political battles about issues like abortion, which the Wyoming Supreme Court recently affirmed as a
To make sure the Legislature is handling those



Legislators, she said, often don’t understand the implications of their policy.
Rep. Lloyd Larsen, R-Lander, wants lawmakers without hands-on medical experience to do their homework.
When Larsen joined the Legislature in 2013, he was asked to serve on the Labor, Health and Social Services Committee. The committee was dealing with serious policy changes regarding Medicaid








By Jeannette Boner
There have been places and journeys that have surprised and delighted me, all at once.
None more so than this current medical journey — one that has whiplashed our family from one doctor to another, forced us to learn big, unpronounceable medical terms and navigate a new landscape in what is typically a pretty normal, humdrum cadence of life in the Tetons: work, play, rest, repeat.
Now, we are on a different schedule. It includes a lot more rest, a few more IVs and a deepening well of patience for the unknown. It includes the unsaid and the stunted conversations, rarely looking farther than the next day.
The future, for now, is measured in appointments, lab draws and the quiet choreography of waiting rooms.
But around each corner is sometimes something a little new, a little unexpected. Small joys that move the spirit forward in laugh-out-loud ways.
Today, I’m talking about the refrigerator inside the St. John’s Health oncology department.
It is, objectively, just a fridge. Black, plastic, like the one found in your first apartment or your parents’ old home. The low, steady hum of a machine doing exactly what it was designed to do.
But open it, and it feels a little like a community hug.
Inside, shelves are neatly stacked with juices, puddings, applesauce cups and varieties of cheese. Maybe a yogurt or two, if you time it right. Sometimes, there’s a rogue chocolate milk. Sometimes, there’s something someone clearly brought in because they thought, “Someone is going to need this today.”
Sometimes a well-stocked fridge can feed the soul.
This reporter’s husband, Brad, the News&Guide’s director of visuals, was diagnosed with cancer last fall. He is receiving care at St. John’s Health.
No one guards it. No one monitors it. It simply exists — quietly — for people who are navigating days that are heavier than most.
And on a morning when your brain is trying to hold new vocabulary, new risks, new possibilities and new fears all at once, opening that fridge can feel like opening a small promise:
You are allowed to need things right now.
You are allowed to be tired.
You are allowed to take something simple and good and just sit with it.
There is something deeply human about a shared fridge in a place built around serious medicine and serious conversations.
It feels like proof that even here — especially here — people understand that healing is not just procedures and protocols.
Sometimes it’s cold apple juice.
Sometimes it’s string cheese.
Sometimes it’s knowing someone stocked that shelf without needing to know who would take from it.
In a season of life where so much feels uncertain, I am unexpectedly grateful for a fridge that asks nothing and gives freely.
And for today, that feels like enough.
Contact Jeannette Boner at 307-7325901 or courts@jhnewsandguide.com.












Residents choose their indoor workout space based on location, price, equipment, culture.
By Charley Sutherland
Even though it may not be outfitted for certain gym rats, the Jackson/Teton County Community Recreation Center remains exceptionally popular, nearly two years after expanding.
“This is pretty sweet,” said wildland firefighter Jackson Ameden, 25, between tricep pulldown reps at the Rec Center on a Friday in January. Joggers behind him ran their laps along an indoor track, while climbers downstairs physically and mentally worked through problems on multicolored rock walls.
For Amedan, it was back day, meaning he was looking to get a “pretty gnarly pump.” But he also often likes to shoot hoops or play pickleball, both of which the Rec Center offers.
If he had to list a complaint about the Rec Center, he only has one.
“It’s missing the squat racks, but I do understand it could potentially create that ‘meathead vibe’ that they don’t want here,” Ameden said. “I think the meathead community in Jackson is pretty low, so I just don’t think that’s going to be as much of an issue as it could be in some other places.”
Since the Rec Center expanded in the spring of 2024, offering a wide array of activities for around $50 a month for residents, it has become a place where the athletic diversity of Jackson Hole’s community is on display. And despite the Rec Center’s popularity, a handful of private gyms have their own niches for residents to get their lift on.
“The Rec Center has not had a negative impact on us,” said Brooks Woodfin, owner of Gym22, a gym focused on personal training, classes and open gym to prep people for mountain sports. “We’re the only gym in the in the area that specializes in strongman training.”
To get a better sense of why Teton County residents choose certain gyms over others, the News&Guide spent a day scouting out the Rec Center and three private gyms. On top of revealing how the Rec Center has changed the exercise scene, their answers offer a peek into how Jackson Hole’s gym rats are finding places for their personalized goals.
To barbell or not to barbell Barbells came up time and time again at the Rec Center.
Sam Bergstrom, 26, a Park Service worker, has appreciated the Rec Center’s prices. She uses the pool, the sauna and steam room and fitness area.
The Rec Center could be improved with more room for mat workouts and a barbell bench press, Bergstrom said. More heavy equipment would not likely lead to a meathead takeover, she argued.
“I don’t know if there’s that many meatheads in Jackson,” Bergstrom said. “I feel like it would just add to what you’re able to do here.”
Limiting certain equipment was intentional. The Rec Center made the decision to leave out squat racks and bench press for safety and accessibility, Parks and Recreation director Tyler Florence said. Instead, he said machines and dumbbells offered a “low-barrier experience” for patrons.
Safety and space were also considered. It is easier to safely use a weight lifting machine than to safely lift with free weights, Florence said, reasoning that squat racks take up a lot of space and that it takes exercisers a lot of time to get their workout in.
“A person using a squat rack may


take 15–20 minutes to complete their sets, including plate loading and unloading,” Florence wrote in an email.
“For that same square footage, a community center can often fit two or three machines that serve six different muscle groups and move three times as many people per hour.”
But although barbells aren’t available on the gym’s main floor, it may surprise residents to know that they could get their compound lifting on elsewhere in the facility. Rec Center leadership heard the feedback about equipment and does offer squat racks and bench presses in supervised fitness studios, Florence said. The Rec Center will continue to try to offer equipment that meets community needs, he added.
Still, the Rec Center’s restraint may lead to other gym’s gains.
Getting gains at smaller gyms
Vince Wisniewski, 37, chooses to exercise at Gym22, a gym focused on personal training for real-world Jackson activities like snowmobiling, biking, paddling, climbing and running. He likes the facility’s free weights and heavy kettlebells. As a chef, Wisniewski is used to spending a lot of time on his feet.
Gym22’s training has helped him develop a baseline level of fitness that allows him to feel good after a long shift. When he’s not in the

gym, he splitboards, rides at Jackson Hole Mountain Resort and runs. To him, the gym is worth it.
“I’m still making good enough money that I can afford to pay for this,” Wisniewski said. “I really appreciate supporting local businesses.”
Gym22 used to have a Kilter Board, a type of interactive climbing wall that lights up. But when the Rec Center opened its climbing gym, owner Woodfin sold it to a gym in Lander.
Elsewhere in town, lifters are making use of their preferred facilities.
Hannah Otto, a 26-year-old competitive Olympic weightlifter, needed a place where she could practice her snatch and clean and jerk. Those are not lifts she can practice at the Rec Center. Otto lifts at Athletic Club at Jackson Hole.
She does use the Rec Center for its indoor track.
“Mostly what I need is a platform and then some type of barbell and where I can drop the weights,” Otto said.
Hockey player Jack Conroy, 18, exercises at the gym at Jackson Hole Indoor, an indoor soccer and fitness facility south of town. He drives all the way from Wilson to get there.
As an athlete, Conroy has focused on explosiveness. Jackson Hole Indoor has a turf strip where Conroy
Mo Ellingson, Sandy Ostdiek and Vickie Bates were walking the track on a recent wintry day. Even with its immense popularity, workers keep the facility clean, the women said.
Bedirhan Yildirin, 24, also a server, said he likes to exercise at the Rec Center because it is close to his home. The people are super nice, Yildirin said, and no one has a big ego.
“Our community works a lot,” Yildirin said. “This is actually important so we can clear our minds.”
Griffin King, 47, has worked out at Gym22 for seven years. He has experienced a variety of injuries and said trainers at the gym help him work through those injuries.
Katie Cooper, 49, managing partner of the Snake River Grill, exercises at Jackson Hole Indoor. Cooper, who lives south of town, said the facility is a convenient option.
“The location for me was key because it holds me accountable,” Cooper said.
can push and pull sleds with weights for training.
“I love this place,” Conroy said of Jackson Hole Indoor.
Contact Charley Sutherland at 307-7327066 or county@jhnewsandguide.com.
JBy Christina MacIntosh
ackson could be America’s capital of Type 2 fun, or enjoyment that hurts in the moment but leaves a lasting reward.
In the shadow of the Tetons, it’s easy to find not-entirely-fun fun to be had, from a climb up the Grand to lapping Mount Glory at sunrise. Picnicking — biking to Jenny Lake, swimming across it, climbing the Grand Teton and then doing it all over again in reverse — is another feat on its way to becoming mainstream.
And that’s without even mentioning all the quotidian training required to be able to perform when the moment arises.
But passion can be a not-so-distant cousin of obsession. In Jackson Hole, therapists recommend keeping an eye on the gray area.
“The line between healthy and unhealthy is blurry,” therapist and mountain athlete Ryan Burke said.
Jackson therapists believe that there is more exercise addiction in Teton County than in other places. The line can be particularly difficult to discern in a community where the norm is, by many other communities’ standards, decidedly abnormal.
“It’s hard to see it in the lens of our community, because we do have such an intense, extreme, active community,” Charlotte Alexander, a therapist and executive director of The Mental Wellness Collaborative, said. “That’s kind of the biggest blinder — what is considered normal and healthy in our community.”
Exercise anywhere can be laden with unhealthy fixations on body image and health. In Jackson, social status and fitting in get added to the mix of pushing oneself to the limit.
“It really seems like when we are seeing all the hardest, most bada--things, or people trying to get fastest times, we get this perspective of ‘That’s what I should be doing,’” said Josie McKee, a Landerbased climbing coach, former climbing guide and former member of Yosemite Search and Rescue.
To be more anthropological, Burke refers to it as “monkey hierarchy stuff.”
Fitness trackers and apps like Strava — or even run of the mill social media platforms where athletic people share feats and objectives — can supercharge the impulse to view one’s achievements through the lens of other people’s.
“Comparing yourself to somebody else can push you to do more than you are capable of or should be doing,” said Deidre Ashley, executive director of Mental Health and Recovery Services of Jackson Hole.
Comparison could be a particular thief of joy to those who dedicate themselves to pushing their physical limits. Athletes already have a tendency to be obsessive in general, said Eden Morris, a dietitian in Teton Valley, Idaho. And young people, especially, are “vulnerable and impressionable,” Ashley said.
Maintaining joy, purpose and boundaries in athletic pursuits amid a high-performing, high-sending community takes practice.
“It’s a skill like training any muscle in your body, training those mental skills of self-awareness,” McKee said.
Red flags
Whether activity is healthy or unhealthy may have more to do with motive than miles.
“Externally, something can look healthy or unhealthy,” Burke said. “That doesn’t matter as much as what’s happening internally.”
When activity comes from a place of body image, social status, self worth or identity, that’s a bad sign.
“There’s a difference between a test and a challenge,” Burke said. “A challenge is good. A test of your self-worth is a problem.”
Alexander is wary of “shoulding” — someone feeling like they should be doing a certain activity. That can be for health, body image, validation or to keep up with others.
The phrasing of should “initiates a shame response,” Alexander said.
Another red flag would be giving up on other responsibilities to exercise. Maintaining work obligations and relationships with family and friends is crucial, Alexander said.
“Life is really about finding that balance,” Alexander said. “If any of those categories start taking over more time, energy and focus, then we want to ask if this is really healthy for us. Anything to the extreme, we want to look at and question.”
Putting off responsibilities and relationships could fall under an “inability to abstain,” Burke
said, which he likened to the way someone might feel about drugs or alcohol. Someone who has to work out every day or risk emotional dysregulation might have an inability to abstain, he said.
At that point “it’s not a coping skill anymore,” Burke said. “You need it to function normally.”
Balance in life can help people broaden their sense of identity to include things outside of athletic achievement. McKee, the climbing coach and guide, often works on helping clients rediscover other things they enjoy and that make them feel a sense of purpose.
“When people go hard all the time, their identity narrows into this one thing,” McKee said. “This activity is all of who I am and being successful in it is what everything is tied up in.”
Hinging so much self-worth on a singular physical activity can be risky, because injury and aging (see page 3) can take those things away.
“It can have really detrimental impacts on your mental health over time,” McKee said. “It can lead to depression and feeling like your life doesn’t have meaning.”
About a decade ago, Alexander drove by a woman running along the road. Though spotting runners isn’t unique in Jackson, the woman stood out be-

cause Alexander had seen her while skiing earlier that day.
Alexander, who was knackered after a full day on the mountain, felt the impulse to compare herself.
“That was a rare occurrence because I just happened to be driving past her,” Alexander said. “Things like Strava make it even more in your face.”
According to “social facilitation theory,” a psychological concept, humans perform better on tasks in the presence of others.
“We do better when someone is watching,” Burke said, adding that competition is an important part of athletics.
Comparing oneself to others is not inherently bad, the therapist and mountain athlete said.
“It could be healthy, or very much could be maladaptive,” Burke said.
He added that people are interested in Strava and other social media platforms because humans are a social species and want to know what other people are up to.
And, potentially, how they compare.
“They really want to know how they stack up, and that’s okay,” Burke said.
Without self-reflection and perspective, exposure to the activities of others can become unconscious and unhealthy, Burke said.
“You’re in a town full of abnormalities as far as exercise goes,” Burke said. “If you compare yourself with those people — on apps, in particular — your tribe is getting pretty big and pretty elite pretty quickly.”
Fitness trackers, in general, have pros and cons, therapists said. They allow people to compete against themselves and stay accountable to their personal goals. But they also can provide fodder for obsessive tendencies.
“As soon as you become obsessed with the numbers, whatever it is is no longer healthy for you,” Morris said.
Numbers can also take athletes out of the mindfulness of exercise, Ashley said.
McKee helps her clients get in touch with the meaning they tie to their athletic activities. It’s an ongoing practice, amid mental noise and external input from other people and social media.
“It’s not just something that you can sit down and answer once,” McKee said. “Like training any other skill or muscle in the body. You don’t go to the gym once and do one bench press, and then you’re strong.”
The mindfulness training involves returning to the idea of who someone wants to be, how an activity adds meaning to their life and the mental skills they still need to develop to do it in a healthy fashion.
Self-reflection is an important part of uncovering unhealthy tendencies. But talking to friends, family or a therapist can help, too, Burke said.
“I don’t think anyone on their own is a great judge of that,” Burke said.
Contact Christina MacIntosh at 307-732-5911 or environmental@jhnewsandguide.com.
By Charley Sutherland
Amy Gardiner isn’t sure what’s next.
Gardiner runs the 23-yearold Teton Free Clinic, a free primary medical care resource for low-income and uninsured Teton County residents. But because of recent indecision in the nation’s capital, the clinic’s groove may look different this year.
As health insurance premiums soar for many Teton County residents, likely leading some to go uninsured, Gardiner is expecting to see more patients at the clinic.
“I do anticipate that we’ll see an increase,” Gardiner said. “We haven’t yet.”
The nonprofit clinic on Broadway just west of St. John’s Health is mostly staffed by a team of volunteer nurses and doctors and is funded through grants and donations. The clinic is open on Tuesday evening and Wednesdays by appointment.
In October, politicians in Washington D.C. shut down the federal government for the longest stretch in U.S. history. Subsidies that made Obamacare Marketplace health insurance cheaper for thousands of Wyomingites were at the heart of the shutdown debate. Senate Democrats wanted to extend the subsidies, while Republicans were satisfied with letting them expire.
Seven Senate Democrats and one independent voted to end the shutdown without securing the subsidies. The subsidies expired at the beginning of the year.
In Jackson Hole, where many residents don’t get health insurance through employers, residents are feeling the heat. That left many with a difficult choice: spend drastically more on health insurance, or risk it

and live uninsured or underinsured.
The policy shift affected Gardiner herself, who purchases health insurance through the Marketplace. For her family of four, Gardiner’s premium went from $39,000 a year to $52,000 a year.
Now-uninsured people faced with similar premium spikes could turn to resources like the free clinic to treat several health issues, including high blood pressure, heart disease and diabetes. The clinic also offers health education options and preventative measures.
The Centers for Medicare and Medicaid Services released data in January showing that around 5,000 fewer Wyomingites have enrolled in Obamacare plans so far, compared to last year. As people get their first bills, more could choose to drop their insur-
ance, experts have warned.
To qualify for health care at the clinic, residents must earn less than 250% of the federal poverty level. For a single person that’s $40,000 a year. Patients need to bring some form of identification and proof of residency or employment in Teton County.
The subsidy expiration is set to deal the biggest blow to people making over 400% of the federal poverty level. Those people would not currently have access to the free clinic. Leaders at the free clinic have not discussed whether to expand income qualifications, Gardiner said.
Wyoming is one of 10 states that have not expanded Medicaid, meaning the federal health insurance program is limited almost exclusively to children and disabled adults. The free clinic helps
bridge the gap for its clientele — which, in Teton County, includes workers.
“They’re the fabric of our community,” Gardiner said. “They’re people who work in the trades, people who work for the ski resorts, people who work for the Grand Teton Lodge Company, people who work in hotels, restaurants, construction and landscaping.”
If more patients do come, the clinic can handle it — to a point.
“We can accommodate an increase of patients, at least for now,” Gardiner said. “Certainly, with the more patients that we see, the harder I have to work at fundraising.”
At the end of December, the Centers for Medicare and Medicaid Services announced Wyoming will receive $205 million in federal funding through a so-called “Rural Health Transformation Program.” That program was established through the Trump-backed “One Big Beautiful Bill Act.”
State officials have proposed putting much of that money into a “perpetuity fund,” said Jenn Lowe, the executive director of Healthy Wyoming, a coalition that advocates for Medicaid expansion in the state. The fund would be like a savings account. Within a few years, it would generate revenue for other health programs, like funding for “critical access hospitals” and regionalization of Emergency Medical Services.
The Wyoming Department of Heath also proposed “BearCare,” a state-run health care plan for catastrophic emergencies, which might help protect otherwise uninsured people from financial ruin. But it’s unlikely lawmakers will approve BearCare, Lowe said.
“You know what’s missing from that proposal is any support for healthcare



By Alex Viveros
Many Jacksonites, like Americans across the country, are grappling with increasing health insurance costs.
“Lack of affordability and access to health care is a really big problem in this country,” said Travis Riddell, director of the Teton County Health Department. “It’s a failure in the health care market, where it cannot serve the people that it is designed to serve, or at least not in their entirety.”
For people who obtained insurance on the Obamacare Marketplace, where premiums recently skyrocketed for many, the cost hikes might mean going uninsured entirely. Those people are likely asking the question, “What now?”
“This is a tough situation,” Riddell said. “I think we have a few resources in this community that can help those people.”
The Affordable Care Act, more commonly known as Obamacare, created the Health Insurance Marketplace, which intended to provide affordable health plans to people unable or unwilling to get coverage elsewhere. But key federal subsidies that made those plans cheaper expired earlier this year, leading to sticker shock for many en-
Continued from 12
clinics, free rural healthcare clinics,” Lowe said.
Lowe is not certain officials could fund free clinics through the rural health transformation program.
Franz Fuchs, deputy director of the Department of Health, said free clin-
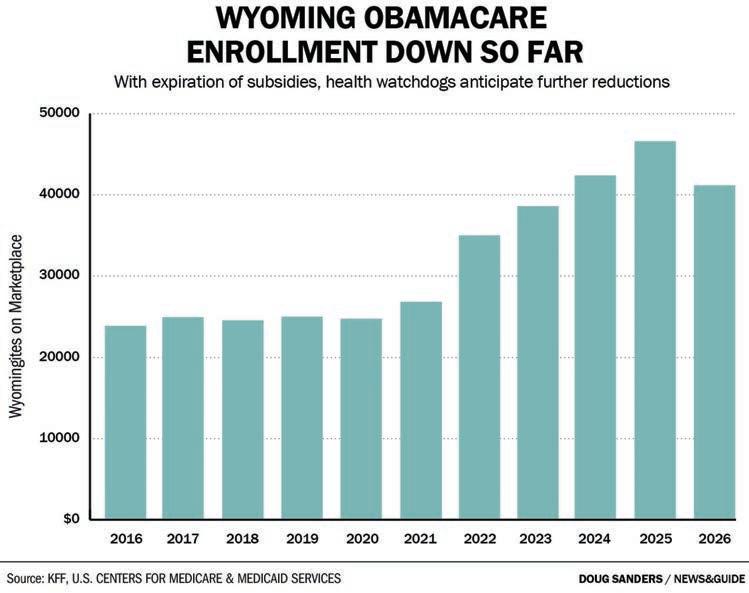
rollees who saw their new rates. In Wyoming, Obamacare Marketplace enrollment has dropped 10.9%, so far.
People without health insurance still have access to rights and resources they might not be aware of, according to Riddell and health insurance
ics could apply for funds through the program.
Because of Jackson Hole’s wealth and robust philanthropic community, the free clinic may be able to meet the rising need, Lowe said. Other parts of the state might not be so lucky.
“I fully expect that there will be more people that need free health care clinics because they can’t afford


experts. Beyond that, cautiously looking into alternate options and lobbying lawmakers for change may be worth a shot, they said.
Health insurance, under the United States’ system, can help protect people against risk and financial ruin, Riddell
to go to the hospital and they don’t have insurance,” Lowe said. “I expect that these free health care clinics will continue to be challenged in securing funding.”
said. Though people can take proactive steps to try to protect their health, managing health risk is tricky, he said. Sudden health issues can be unpredictable.
“You never know when some bad actor on the Pass is going to cause an insurance claim for your auto insurance. Health is similar,” Riddell said. “We can do many things to improve the odds of having good health, but it’s an area where unfortunately, it’s not entirely within our control, and calamity can strike.”
In Jackson Hole, where many residents enjoy extreme outdoor recreation, the risk of injury may prompt uninsured people to think twice before skiing a challenging line, or climbing a more tenuous route. But advising people how to manage their comfort with personal risk in a changing heath insurance landscape is challenging.
“It’s hard to tell people who like to do these activities that you shouldn’t do these because of the risk of being uninsured,” said Kevin Callison, an associate professor in the Department of Health Policy and Management at Tulane University. “If you can minimize your risk for needing to show up in the emergency department with a broken
See UNINSURED on 15
The free clinic has seen a number of calls from folks asking about qualifications to receive care at the clinic, Gardiner said. Those people about whether to go uninsured.
“Living here in Teton County, people are forced to make hard decisions every day, whether that’s to pay their rent or buy groceries,” Gardiner said. “Or do I pay for my health insurance.”
Contact Charley Sutherland at 307-732-

the opening of a longevity practice, dubbed Grand Health. Upon signing up for an out-of-pocket quarterly fee — ranging from $1,250 to $6,250 — clients could access providers who would keep tabs on their diet, physical fitness and progression toward personalized goals.
Grand Health’s focuses include evaluating muscle mass, body composition, trying to prevent heart attacks, and improving a biomarker called VO2 max — the maximum rate of oxygen a person can consume while exercising. Higher VO2 maxes mean that a person’s heart and lungs are more effectively bringing oxygen to muscles, which has been linked with increased longevity.
Holland backed up the science behind Grand Health’s biomarker tracking, saying certain markers could help monitor risk for heart attack, stroke or diabetes.
“Having objective data that tells you either that you’re stable, that you’re improving, or that you need a bit more work, is important,” Holland said. “Having all of these metrics, being a bit more thoughtful and having a bit more precision and approach is an ideal scenario.”
After measuring a client’s base, Grand Health then works with people over time to get them closer to their given long-term health goals. That setup was ideal to Holland, who said more oversight and accountability could help people stay on task.
“Having a hands-on, very personalized, precise intervention, it’s good,” said Holland, who runs a clinical trial evaluating the impact of lifestyle changes on cognitive decline. “Certainly, clinics that are directed toward it are going to have a bit more of a plan of action in how they’re approaching these components.“
As a powerlifter, Marts was initially drawn to Grand Health for its DEXA

scan, an X-ray machine that analyzes bone health and muscle mass. She decided to give the facility’s other offerings a try.
“I thought ‘Well yeah, maybe you can turn this old powerlifter into a more healthy person,’” Marts said.
“Instead of just a strong old lady.”
The clinic is intended to be preventative, Dennis said. People who have colds or other acute illness should see their primary care doctors, he said.
“I’m not a specialist in primary care,” Dennis said. “I’m quick to admit when I’m out of my element.”
More time
Longevity is appealing for Marts as she starts to think of her life after lifting. Though she doesn’t plan to
throw in the towel on exercise, she’s prepping to eventually transition from brute-strength lifting to more endurance-focused activities like hiking, biking and kayaking.
“I’m starting to realize that I would rather spend more time in the outdoors, because we live in the most gorgeous place in the universe,” Marts said. “I’ve had a good run. Couple more world records maybe, or bump the ones I have, then maybe I can hang it up.”
Challenging oneself with new things is an important part of maintaining both physical and cognitive longevity, Holland said.
“That’s such a lovely mentality to have,” Holland said of Marts’ goals. “That’s some really great forward
thinking, as well — what’s the next step in my evolution?”
Goals vary from person to person. One person might want to walk the Great Wall of China, while another might want to be able to get down on the ground and play with their grandkids.
“It’s always great fun talking to people and understanding what those motivations are,” Holland said. “But it also helps guide how you’re doing things.”
Mercedes Huff, a real estate agent who moved to the valley 54 years ago, doesn’t go jumping into Corbet’s Couloir. Instead, the 76-year-old’s longevity goals involve hitting the groomers with her two grandchildren.
“It’s not just a question of adding years,” Huff, who is a Grand Health client, said. “You want to add them in a healthy way that you feel good, and you feel like doing things and participating and being part of the community.”
Those who might not have the money for a specialized clinic could still find ways to improve their longevity. Being thoughtful about physical activity — including avoiding things that would lead to injury — strengthening diet, and keeping oneself socially engaged were all good starting points, Holland said.
“It’s never too early or too late to start making positive lifestyle changes,” Holland said. “There’s always an opportunity to improve health, and especially improve health for enhancing health and lifespan, and in that vein, longevity.
“For everybody, today is day zero,” he added.
As Marts thought about her goals, she said she intends to climb Sleeping Indian this year. It won’t be easy, she said. But that didn’t seem to matter.
”We have a finite time on this earth,” she said. “You might as well maximize what you can.”
Contact Alex Viveros at 307-732-5909 or alexv@jhnewsandguide.com.

leg, that’s probably a good thing to do. But at the same time, you want people to exercise and be outside.”
Negotiate
Instead, people could look to ways to either get free care or lower-cost care in their communities. For non-emergency visits, like urgent care or treating chronic conditions, Riddell pointed Teton County residents toward the Teton Free Clinic, a nonprofit that provides primary medical care for people who make under 250% of the federal poverty level (see page 14).
In a crisis, people should not think twice about going to the emergency room, Riddell said. Federal law requires hospitals to treat people presenting with emergency conditions, regardless of their ability to pay.
“If we’re talking about something that is truly emergent, life-threatening, please don’t let your lack of insurance put your life in any further jeopardy,” Riddell said. “I’d rather be alive and bankrupt, I suppose, than not alive.”
The list price for hospital services may shock anybody who gets a bill. But those prices are high for a reason. Health insurance companies negotiate down lower rates. Experts said that everyday people, too, can negotiate down their initial hospital bill.
“If you negotiate with the hospital or provider, they may offer a discount — in some cases a very steep discount — on care for people who don’t have insurance,” Callison said. “I think that is one thing that people don’t always realize.”
St. John’s Health has financial assistance programs, including discounts and its charity care program. The hospital suggested that people call in advance of care to see what they may be eligible for.
“It happens that people sometimes
have medical bills that they can’t afford,” said Karen Connelly, the hospital’s chief communications officer. “We regularly have conversations with people about ways they can pay their bills, and how they might be eligible for some of the programs we have.”
Local health insurance brokers could help individuals get a better sense of other health plans that might be available to them, Riddell said.
Some consumers who were previously on the Obamacare Marketplace may also look to a “Wild West” of health coverage options. But those plans aren’t bound to protections passed under the Affordable Care Act, like requiring insurance companies to cover people with pre-existing medical conditions. People who consider those plans should be careful to read the fine print to ensure that their ailment is covered.
Even the least generous Marketplace plans “are still going to provide some protection in case you really get sick,” said Benjamin Sommers, a health economist and primary care doctor at the Harvard T.H. Chan School of Public Health. “That’s not always the case for some of these other unregulated plans.”
Advocate
Though Congress did not extend the Marketplace subsidies earlier this year, federal lawmakers still could. Asking state legislators to expand Medicaid — Wyoming is one of 10 states that has not done so — may also give more Wyomingites coverage, Sommers said.
“We’ve seen coverage rates rise in this country. We’ve seen them fall depending on who’s running the White House, who’s running Congress, who the governors are,” he added. “Elections matter.”
Contact Alex Viveros at 307-732-5909 or alexv@jhnewsandguide.com







may not understand the administrative and governmental sides of it.
and other health insurance. At the time, Larsen said he “couldn’t even spell Medicaid.”
He studied concepts and definitions that would come “naturally to a health care professional,” and eventually became vice-chair of the House Labor Committee. Studying the subject, he said, is “the most important thing you can do as a legislator.” But lawmakers can also lean on health care associations, like the Wyoming Hospital Association or the Wyoming Medical Society, to help them learn. Those groups aren’t the “enemy,” Larsen said.
Turning away
Even doctors and other medical professionals have their limitations, according to Larsen. While doctors may be experts on health care and its challenges in a frontier state, they
That means it’s “critical that all lawmakers have reliable access to credible, nonpartisan clinical expertise when making policy decisions that impact health care,” Bush said.
A lack of expertise in the room can create “unintended consequences,” she added.
“Without a strong foundational understanding, there is a tendency to underestimate implementation hurdles, inflate projected savings, or create administrative burdens that ultimately divert clinicians away from patient care,” she said.
But having experience or doing the research doesn’t always mean lawmakers will listen.
Baldwin said his experience was beginning to fall on deaf ears before he left the Legislature. He remembers a day when he stood up to speak on the floor of the Senate. He explained


a medical concept and why Senators should change a bill.
“One of the other senators got up and said, ‘You know, we all love our medical provider and we go to him a lot. He cares for us and he does things for us, but we’ve been lied to before.’”
Baldwin wasn’t directly being called a liar. The charge was directed at his profession as a whole.
“That carried more weight than what I said,” he said.
Aversion to many medical institutions was exacerbated by the Covid-19 pandemic, Baldwin said. The Legislature held a special session to push back against federal mask and vaccine mandates. But reservations existed well before then, Baldwin said, with pushes for alternative medicine or the anti-vaccine movement.
“It just gets a little bit worse each year,” Baldwin said.
Bush, from the Medical Society, also sees lawmakers turning away from expertise. Associations like the Wyoming Medical Society, are “sometimes marginalized and unfairly characterized as nefarious.”
Baldwin and Brennan, the nurse now chairing the Senate Health committee, agree about some things, like the Legislature’s cultural shift. But they disagree about what that means.
Brennan, for her part, understands why some people are skeptical of medical professionals.
During Covid-19, the medical establishment’s reaction to the spreading virus was immediate and fearbased, she said. Health professionals didn’t have a lot of information.
“We continued with the same things that we had put in place when we had no information, instead of quickly changing what we were doing as a society,” she said. “We were slow

Lloyd Larsen, R-Lander, listens to a speaker during the morning session of the 68th Wyoming Legislature Jan. 17, 2025 in the House Chambers.
to respond.”
The thousands of medical professionals in an association also might not always share the same opinions, Brennan said, particularly on moral and ethical issues like abortion or gender-affirming care for transgender patients.
“When it comes to these things that are very personal beliefs, even the medical community is split over what they think should be done in those situations,” she said.
Baldwin is less understanding of the shift.
Many mistrustful lawmakers are Wyoming Freedom Caucus members or allies. The caucus won’t budge in general and won’t listen to “logical reasons to change policy,” Baldwin said.
“All these people, including the Freedom Caucus, need to be more open,” he said.
Baldwin and Brennan agree: Health policy is nuanced, and impacts everyone in Wyoming.
“We all need health care,” Brennan said. “So it’s important for somebody who understands the system and the language and what’s going on to be in the Legislature in order to help create better policy.”
Contact Jasmine Hall at 307-732-7063 or state@jhnewsandguide.com.











Continued from 4
with insurance, in Driggs. That office, which he converted from part of his airplane hanger, had “no overhead,” he said. To afford overhead and staffing in Wilson under a traditional model, Blue would have to see 10 or 15 patients a day, he said.
“I don’t want to sit there and work my a-- off just so I could be in Wilson,” Blue said. “I’d rather do a concierge type practice, have time to spend with the patients, take good care of the patients. So that’s why it’s limited to 30 new patients.”
So far, Blue has nine patients at his concierge practice in Wilson. Though 30 is the limit, he would be “fine” if he ended up with 10 or 15.
Anthony has transitioned from OB/ GYN to only doing gynecology and women’s health. She no longer does major surgical procedures.
“I really liked it, but you can’t have everything,” Anthony said. “You can’t expect patients to pay out of pocket for surgery. It’s too expensive. They want to use their insurance.”
Dr. Travis Riddell, a pediatrician and the director of the Teton County Health Department, said concierge medicine can provide a good model for doctors and patients alike. Health care has become more consolidated into a smaller number of traditional outlets, he said, adding that care can feel more impersonal.
“For people seeking a bygone and perhaps simpler time when it was easier to get ahold of your doctor, easier to get that direct relationship, I think the ... concierge model can be attractive,” Riddell said.
Even St. John’s Health, which operates under a traditional health care model, has fielded interest in concierge medicine from patients who have been treated under the model elsewhere. Though the hospital was more focused on increasing efficiency and how many more patients they could see, Chief Com -



munications Officer Karen Connelly said concierge medicine helped keep “valued providers” like Anthony and Blue in Jackson Hole.
“This is the way they can make it work and continue to practice medicine in the community,” Connelly said. “It’s not surprising that they would choose this model.”
St. John’s had been told by some patients that the hospital’s providers had given them the same level of attention as concierge providers they had seen elsewhere in the country, Connelly said.
Riddell worries about how concierge medicine’s increase might affect patients at a public health and community level. The model wasn’t “really scalable” to cover the entirety of Teton County, he said.
“It would take a whole lot of concierge doctors in this town to be able to cover every resident,” Riddell said. “That’s without even thinking about the cost to folks, which is just going to be out of reach for portions of our population.”
Anthony wouldn’t have entered concierge medicine right out of training. For young doctors, concierge medicine patient numbers aren’t high enough to get “great” experience, she said. Philosophically, she went into medicine to help people — she saw her transition to concierge medicine as a ramp to her eventual retirement, a move that allowed her to develop other aspects of her career.
The rise of concierge medicine, to her, pointed to fractures in the health care system.
“As providers, we don’t want to be forced to worry about the money we’re bringing in, and to see high volumes in order to pay the bills,” Anthony said. “It tells us that the system is broken, because it’s forcing patients and doctors to go outside the system to find a rewarding career and a rewarding experience.”
Contact Alex Viveros at 307-732-5909 or alexv@jhnewsandguide.com.






at potential merger options at the end of January, Turkula was moving into a new practice space along Ski Hill Road, looking west toward the Tetons.
The quiet, bright orthopedic office serves as a temporary location while he searches for a larger, permanent space. For now, waiting rooms fill with teens and adults, skiers and farmers, all seeking treatment and recovery.
“As the valley grows, you’re going to see more independent practitioners,” Turkula said. “That’s just market economics.”
Turkula will still perform surgeries at Teton Valley Health as part of an agreement with the hospital. But private practice gives him something he said modern rural medicine doesn’t always guarantee: control over when, and where, he can operate.
“I still do surgery at the hospital,” he said. “I love the staff there.”
“People deserve choice,” he said.
Clinically, Turkula’s approach centers on what he calls the “patient experience” — focusing as much on communication, access and coordination as on the surgical procedure itself.
“My number one goal is that patients have a good experience,” he said.
“The surgery is only a small part of what patients go through,” he added. “The rest is communication, scheduling, follow-up, and feeling like someone is guiding you through it.”
“The most exciting innovation in orthopedics is happening in joint preservation and biologics.”
— Stefan Turkula ORTHOPEDIC SURGEON
He spoke positively about hospital leadership, emphasizing his decision to leave was about professional sustainability, not dissatisfaction.
Private practice, he said, allows him to pursue credentialing at other regional hospitals, creating redundancy if operating rooms close or if capacity tightens.
As the population expands and outdoor participation increases, Turkula predicts that demand for orthopedic care will rise. That leaves room for independent specialists to work alongside hospital-employed physicians.
His clinical specialty focuses largely on knee and shoulder care, particularly joint preservation The procedures are designed to repair or maintain a patient’s natural joint and delay or avoid replacement when possible.
“We want to preserve joints whenever we can,” he said.
“The most exciting innovation in orthopedics is happening in joint preservation and biologics,” he said.
Turkula treats patients across most age groups and measures success not just by surgical outcomes, but by whether patients can return to the activities that define their daily lives. No matter what those daily lives might entail.
“Anyone is an athlete,” he said. “Whether that’s skiing, gardening or helping take care of someone at home.”
He is also affiliated with the national Joint Preservation Center, made up of fellowship-trained surgeons who share research, case consultation and

emerging technologies.
In orthopedic medicine, a growing number of surgeons are shifting toward joint preservation, according to the Joint Preservation Center.
Historically, many of these programs were concentrated in large metropolitan medical centers. But as research, training and surgical technology become more widely available, similar models are appearing in smaller regional communities.
For recreation-based regions like Teton Valley — where orthopedic injuries are common and the population continues to grow — that shift could mean more options for patients seeking specialized care closer to home.
Turkula said he is also thinking long term about the valley’s medical landscape.
“In a perfect world,” he said, “you build a place where everything is in one spot — clinic, surgery center, physical therapy, performance.”
In an ideal scenario, he said, he would like to help develop a comprehensive orthopedic campus that could include fellowship-trained surgeons, an outpatient surgery center, physical therapy and sports performance services — a one-stop model he believes could lower costs, increase access and potentially make the region a destination for orthopedic care.
For now, he said, that vision remains aspirational, though he has begun early conversations about what such a model could look like.
“We’re here,” he said. “We’re seeing patients.”
For him the goal is simple, if ambitious: build a practice model that allows him to remain rooted in Teton Valley while offering high-level orthopedic care typically associated with larger regional or academic centers. And do it in a way that keeps patients close to home.
Contact Jeannette Boner at 307-7325901 or courts@jhnewsandguide.com.




And we’re lucky! Because having you as our audience pushes us—in typical mountain style—to deliver content that supports the true meaning living fully. With up-close profiles of artisans who make jobs out of a passion, cutting-edge ways to deal with modern health issues, and farm-fresh recipes you’ll dog ear and return to for seasons to come, we’ve got the local culture on lockdown.


Heart Disease is the leading cause of death in the U.S., yet 80% of heart disease and strokes are preventable through healthy lifestyle choices.*
What you eat matters. A diet rich in fruits, vegetables, whole grains, and lean proteins can significantly lower your risk.
You can move your way to a healthier heart. Regular physical activity, just 30 minutes a day, can make a big difference.*
High blood pressure is often called the "silent killer" because it shows no symptoms. Make sure to know your numbers! †
Smoking increases the risk of heart disease by 2–4 times, but quitting can improve your heart health almost immediately.*
* Source: American Heart Association † Source: CDC
February is American Heart Month! Learn more about our cardiology services here: www.stjohns.health/cardiology