













































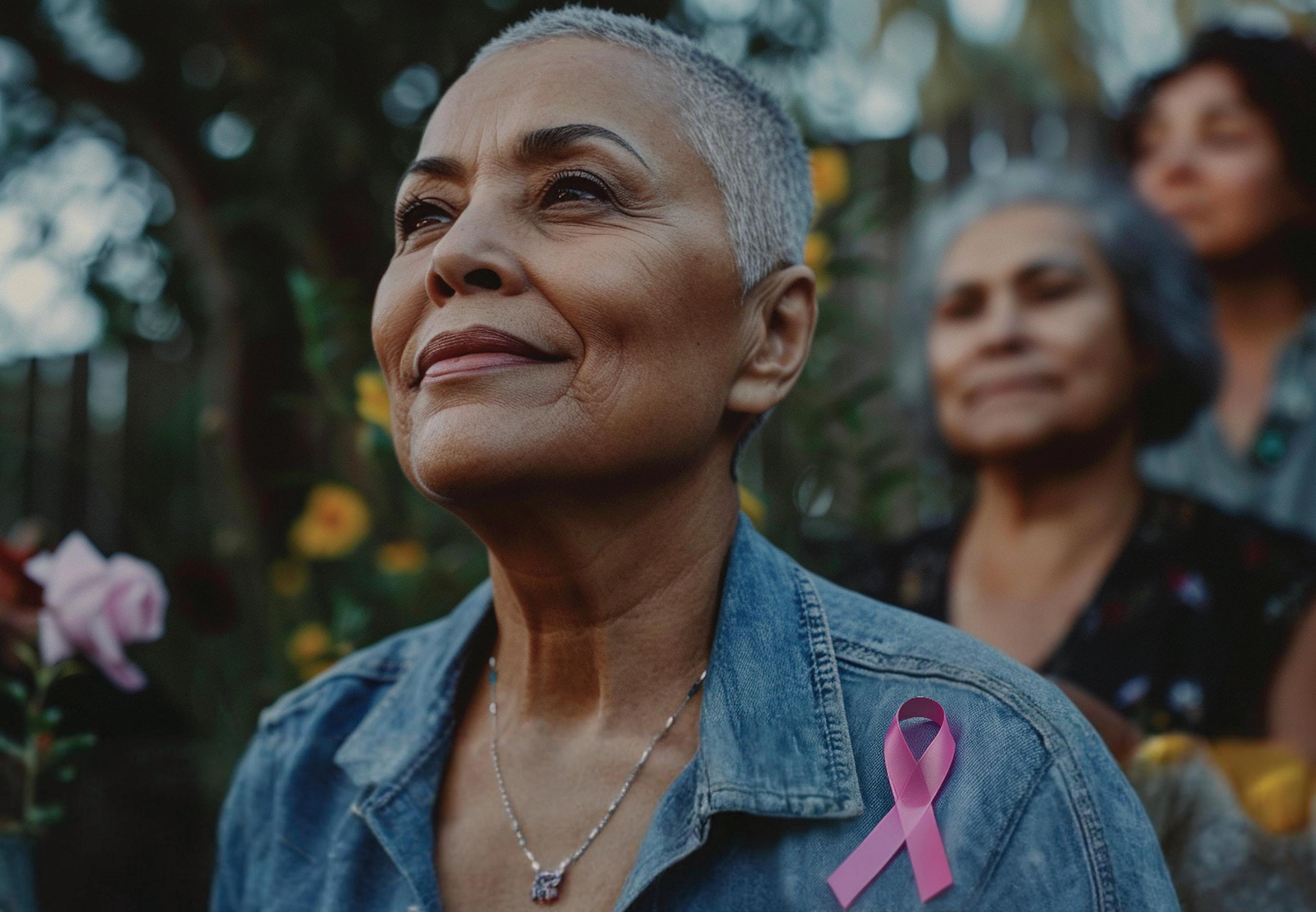
































































































































































































































































































































































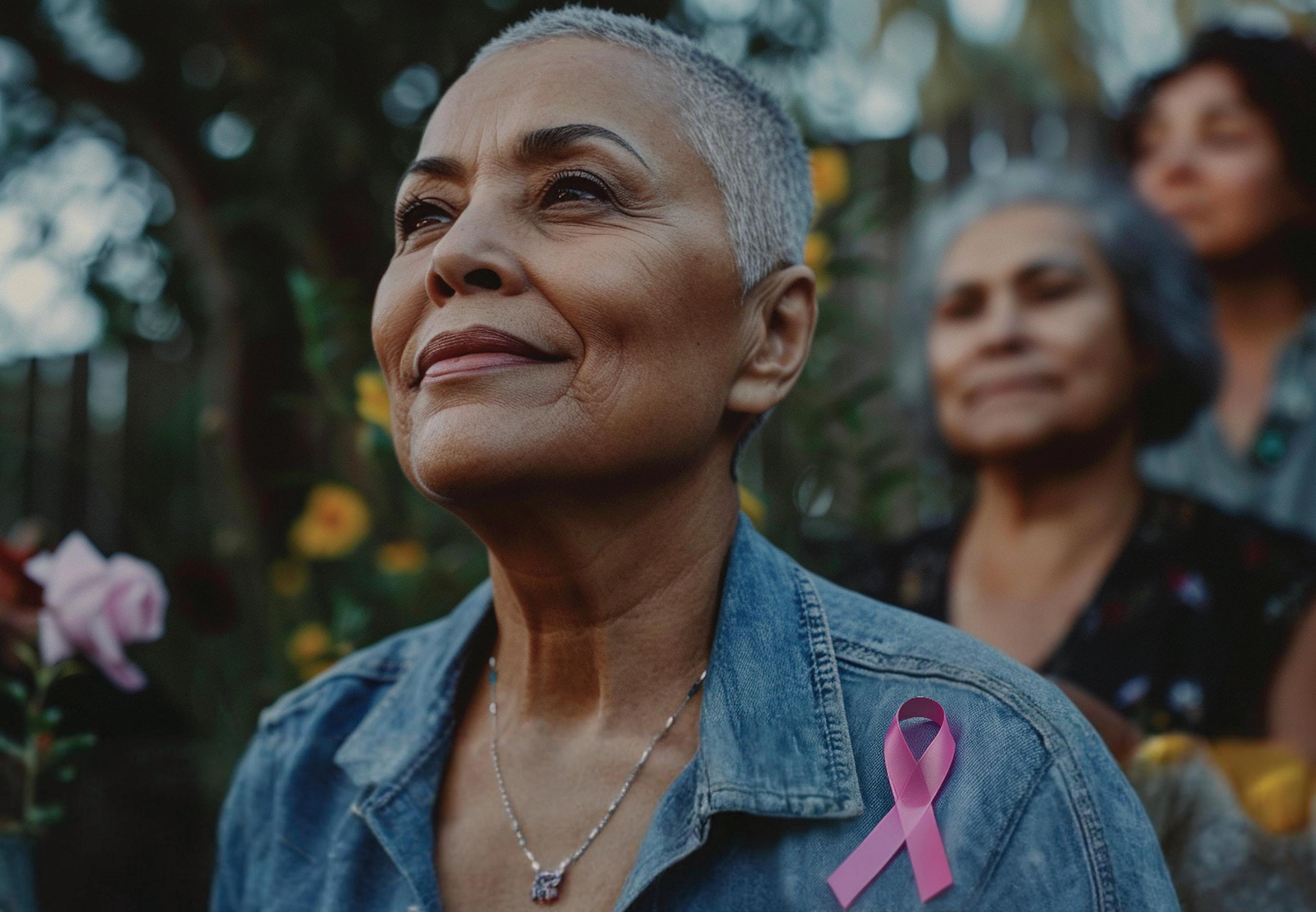





























































































































































































































































































































by: Dorothy Leone Glasser & Harsha Vyas, MD, FACP
Georgia patients are struggling to balance high healthcare costs with other daily living essentials.

These aren't just statistics. They represent real Georgians making impossible choices between medications, groceries, rent, and other living expenses. Over 50% of Georgia adults living below the federal poverty line have two or more chronic conditions and rely on consistent access to affordable medications to manage their health. For patients already stretched to their breaking point, relief from burdensome costs should come from programs designed to make healthcare access more affordable. Unfortunately, one such federal program has lost sight of its original intent.
In 1992, Congress created the 340B program with a clear, honorable mission: improving medication access for vulnerable patients. Under the program, eligible hospitals and clinics serving low-income and uninsured patients can purchase outpatient drugs directly from pharmaceutical manufacturers at deeply discounted prices – typically 20–50% below market rates, and sometimes for as little as a penny. The intended execution was straightforward. Hospitals are expected to use the savings accrued to reduce out-of-pocket costs for patients in need or invest in expanded charity care and community health services. Today, however, a lack of federal transparency and accountability policies have allowed the program to go off track.
Over the last two decades, 340B has grown exponentially and is now the second largest federal prescription drug program behind Medicare Part D, yet so many Americans are unaware of the program’s existence. The numbers alone show just how broken the 340B program is. Across the country, 340B hospitals are marking up drugs purchased through the program, billing patients and their insurers full price for discounted treatments and pocketing the difference. Medicine price markups are over six times higher at 340B hospitals than at independent clinics.


Just north of us in North Carolina, an investigation led by the State Treasurer found that 340B hospitals overcharged state employees and teachers living with cancer for treatments purchased through 340B, marking up drugs over five times their acquisition cost and collecting over $6,000 in average profits per claim. For every $10 the most profitable 340B hospitals collect in profit, just $1 is invested in charity care. A recent poll found that Americans across the country are tired of unfair and unaffordable hospital practices, especially aggressive markups. Nine in 10 Americans are concerned about hospital medicine markups.
To dispense outpatient medications purchased through the program, 340B hospitals are able to set up contract arrangements with any number of pharmacies in any location, many of which are owned by the nation’s largest pharmacy benefit managers (PBMs). As of October 2025, about two-thirds of the entire U.S. pharmacy industry were operating as 340B contract pharmacies. Both PBMs and 340B contract pharmacies can profit significantly from dispensing marked up 340B medicines.
Discounted 340B medication purchases reached over $81 billion in 2024 – a 23% increase from just the year prior. If 340B operated as intended, growth of this magnitude should be driving better patient outcomes or increased levels of charity care at 340B entities. Instead, we’ve seen large hospital systems and for-profit companies take advantage of loopholes in the program to maximize their own profits while patients are left behind.
More than 12% carry medical debt.



Georgia residents continue to report that they have delayed or skipped care due to costs, yet almost a third of Georgia's 340B hospitals provide charity care levels below the national average. Over 50% of Georgia 340B disproportionate share hospitals collect more in 340B profits than is spent on charity care. Of the many 340B contract pharmacies supposedly serving low-income Georgians, 40% are actually located in affluent neighborhoods and another 30% aren't located in Georgia at all.
The impact of hospitals trying to maximize 340B profits ripples throughout our local healthcare system, leading to higher costs for businesses and workers, taking resources away from the government, and incentivizing healthcare consolidation that shifts patients to 340B-owned and more expensive facilities. 340B abuse imposes substantial costs on local businesses and workers, costing Georgia employers and workers approximately $187 million annually through lost drug rebates. It also diverts billions of dollars in federal and state tax revenue that could go toward local schools, infrastructure, and public services into the pockets of hospitals and profiteering middlemen.
The ability to profit deeply from 340B also grants large hospital systems the upper hand in the market, giving them leverage over smaller, independent clinics and driving increased consolidation. Because 340B hospitals can purchase discounted 340B medications that independent practices cannot access, they’re incentivized to acquire independent providers — especially oncologists and other specialists who prescribe high-cost therapies — and exploit those margins to their advantage. Meanwhile, independent practices struggle to compete on equal footing and often face pressure to sell or merge.
340B profits have evolved into a powerful financial lever for large hospital systems. Drug margins are routinely used to subsidize specialist compensation packages that independent community
practices cannot realistically match. This creates a market distortion: physicians are not migrating because care is better coordinated or more efficient, but because the reimbursement architecture rewards hospital ownership.
In oncology, the effect is particularly pronounced. High-cost infused therapies generate significant 340B spreads, making cancer specialists attractive acquisition targets. Hospitals can offer lucrative employment models funded in part by drug margins, effectively locking oncologists into large systems and accelerating the absorption of independent practices.
The downstream consequence is geographic imbalance. Urban hospital systems accumulate oncology capacity, while rural and underserved communities lose it. The financial incentives embedded in 340B do not encourage distribution of specialists to areas of greatest need — they concentrate them where margins are highest.
As a community oncologist practicing in rural Georgia, I have watched this dynamic unfold in real time in just the last 15 years.
When independent practices disappear, patients do not just lose a business. They lose proximity, continuity, and often affordability. For a rural patient with cancer, consolidation can mean hours of additional travel, longer wait times, higher facility fees, and delayed treatment.
That is not an unintended side effect, it is the predictable outcome of a program that rewards consolidation over community-based care.
























