

2025 Annual Report

A Letter from the Chief Innovation Officer
As we close out another transformative year at Boston Children’s Hospital, I am proud to reflect on the remarkable progress our Innovation Team has made in advancing our mission to improve the health and well-being of children and families everywhere. Innovation at Boston Children’s has always been more than a function; it is a fundamental mindset that empowers us to anticipate the future of pediatric care, translate ideas into impact, and ensure that our patients benefit from the very best that science, technology, and human creativity can offer.
This year, our team continued to serve as a catalyst across the institution: identifying unmet clinical needs, supporting our clinicians and researchers as they bring new solutions to life, and accelerating the development and deployment of technologies that enhance care delivery Whether through digital health tools that increase access, data-driven insights that improve clinical decision-making, or new care models that personalize and elevate the patient experience, our work is rooted in a commitment to meaningful, measurable value for our patients and providers.
Importantly, innovation at Boston Children’s is never pursued in isolation. Our team operates at the intersection of clinical excellence, research leadership, and operational expertise. We collaborate deeply with our colleagues across departments, as well as with industry partners, startups, policymakers, and community organizations These partnerships enable us to translate bold ideas into scalable solutions, ensuring that
innovations born here have the potential to improve pediatric care globally
This year’s achievements are a testament to the dedication, creativity, and perseverance of our innovation ecosystem. But even more inspiring are the ideas still emerging, the problems we have yet to solve, and the future we are actively shaping together.
I am immensely grateful to our clinicians, researchers, staff, collaborators, and supporters who make this work possible. The Innovation Team is here to serve as a bridge connecting ideas to resources, challenges to solutions, and imagination to real-world impact. Together, we are building a more responsive, equitable, and visionary future for pediatric care.
Thank you for your continued partnership and for the trust you place in us. I look forward to another year of discovery, creativity, and progress driven by our shared commitment to the children and families who inspire everything we do.

John Brownstein SVP & Chief Innovation Officer
IDHA Over the Years
2016–2018: Foundations of Innovation
• Formally launched the Accelerator Program under the Innovation and Digital Health Accelerator (IDHA).
• Primary focus was on supporting BCH innovators through the successful commercialization of novel digital health solutions.
• Formed the IDHA Advisory Board and solidified industry partnerships to support our mission.
2019-2022: Scaling Innovation
• Expanded focus to include strategic partnerships and capital investments with enterprise-aligned startups.
• Accelerator program launched 'Advisory Services' offering to support a greater number of innovators.
• During the pandemic, the team led the hospital’s COVID-19 Innovation Task Force to support staff solutions to pandemic-related challenges.
2023-Present: Focused Innovation
• Team begins to support AI & emerging technology efforts for the hospital, including sourcing & prioritization, governance, capacity building, and development.
• With fewer resources, the Accelerator Program sharpens its focus on select incubations, where unmet healthcare needs and Boston Children's competitive advantage are highly aligned.
Across the Innovation Team



The Accelerator Program leverages the expertise of Boston Children’s Hospital to build new digital health solutions that will be impactful beyond the walls of the hospital.
The Accelerator Program unlocks access to Boston Children’s expertise through digital innovations that can improve healthcare delivery and outcomes for pediatric patients everywhere. The Program’s goal is to develop new software-based solutions – either internally with the Program’s full-stack development team or in partnership with external entities – that can find sustainability and achieve long-lasting impact without ongoing hospital support.
The team conducts market research, considers novel hospital insights, and collaborates with Boston Children’s staff to uncover innovation opportunities. The Accelerator Program takes a problem-first approach to innovation, focusing on identifying pain points and understanding the needs of those experiencing the pain points before scoping, designing, and developing a solution. The approach incorporates a range of different activities including interviews, market research, workflow mapping, and validation testing to ensure that solutions effectively address unmet needs. Solutions have emerged from the program as new standalone ventures or as new products with codevelopment partners that can include digital health startups, technology companies, or nonprofits.
PROGRAM ACTIVITIES
Educate staff on digital health innovation to encourage and support entrepreneurship
Identify promising innovation opportunities
Endocrine Survivorship Tracking and Risk Tool (EndoSTAR)
A clinician-designed tool enabling endocrinologists to more easily surface relevant survivorship guidelines improving efficiency and consistency in care for young cancer survivors without adding burden
Conceptualize and design sustainable digital health solutions in partnership with internal subject matter experts
MyFriendBen Massachusetts
Develop and validate effective solutions for long-term impact beyond the hospital
Launch incubated solutions through sustainable pathways and encourage ongoing success outside of the enterprise
Positive Fitness Hub for Congenital Heart Disease
A co-development partnership bringing MyFriendBen’s public benefits eligibility screener to Massachusetts, helping families and the staff who support them to access a single, trusted front door to the social safety net
A web-based educational hub that scales the positive fitness framework, giving providers access to the knowledge and tools needed to help children with heart disease thrive
EndoSTAR Endocrine Survivorship Tracking and Risk Tool
Cardiac Fitness Incubation Concept
Partnership with Boston Children’s Cardiac Fitness Program
EndoSTAR is a Boston Children’s Hospital–built clinical workflow tool designed to simplify how clinicians access and act on guideline-based survivorship screening recommendations for childhood and young adult cancer survivors. Developed in close partnership with experts from the Neuroendocrinology and Cancer Survivorship Program at Boston Children’s, EndoSTAR supports more consistent, guideline-concordant care without replacing clinical judgment or altering established clinical content.
The Challenge
Childhood and young adult cancer survivors often require longterm, risk-based endocrine surveillance informed by complex and evolving guidelines. The knowledge of how to appropriately screen patients for downstream endocrine effects from cancer treatment is specialized, even among endocrinologists.
To ensure clinical alignment with the most up-to-date guidelines, clinicians consult the academic literature and, in many cases, lean on their expert peers to confirm approach. This process can be burdensome, both for the treating provider and for the expert clinician.
At institutions like Boston Children’s, clinicians can consult their colleagues with extensive experience treating this patient population, but many institutions and providers don’t have access to this specialized expertise.
The Solution: EndoSTAR
EndoSTAR was built to make survivorship guidance easier to access and apply during routine care. Rather than introducing new clinical rules or automated decision-making, the EndoSTAR tool:
Utilizes expert-created logic rules to surface guidelines aligned with standard practice of care
Centralizes guideline-based endocrine survivorship recommendations and source references in a clear, clinician-friendly format
Fits naturally into existing clinical workflows
Preserves clinician autonomy and judgment
Why This Matters
EndoSTAR highlights how thoughtfully designed, clinician-centered tools can reduce provider burden and extend the impact of Boston Children’s clinical expertise.

Our Approach
The idea for this initiative was surfaced by clinician innovators who partnered with the Accelerator Program to create an impactful solution.
Key elements of the approach included:
Co-design with clinicians: Input from frontline endocrinologists informed solution purpose and tool design to ensure usability
Expert collaboration: Expert endocrinologists acted as development partners alongside nnovation team to ensure clinical relevance and validity
Rapid-cycle learning: A brief, anonymous clinician survey was launched to evaluate ease of use, trust, confidence, perceived time savings, and overall satisfaction
Early Impact Validation
To evaluate EndoSTAR’s impact, the team launched an IRB-exempt study focused on clinician experience. Approximately 40–60 pediatric endocrinology clinicians are eligible to participate, including attending physicians, fellows, and advanced practice providers caring for cancer survivors.
What’s Next
Upcoming clinical survey to understand:
• Ease of accessing survivorship screening guidelines through EndoSTAR
• Clinician confidence in delivering guidelineconcordant care
• Perceived time savings during clinical encounters
• Trust in the tool as a supportive, non-intrusive resource
The goal of the study is to validate the tool’s impact on the clinician experience at Boston Children’s. If internal impact is validated, the team’s efforts will shift to finding a sustainable pathway for the tool that will allow it to be accessible to clinical teams beyond the hospital.
As part of our broader innovation portfolio, EndoSTAR represents a successful partnership with clinicians and an ongoing collaboration to extend their expertise to support gold-standard care beyond the Boston Children’s community.
MyFriendBen Massachusetts Unlocking the Social Safety Net for Families
Cardiac Fitness Incubation Concept
Partnership with Boston Children’s Cardiac Fitness Program
Boston Children’s Hospital partnered with MyFriendBen to bring their state-based social benefits eligibility screener to Massachusetts. By adapting their open-source benefits eligibility screener for Massachusetts–specific programs and rules, the partnership aims to help families more easily understand and access public benefits, tax credits, and nonprofit resources.
The Challenge
Families across Massachusetts face significant barriers to accessing public benefits and assistance programs even when they are eligible. Complex and inconsistent eligibility rules, fragmented information spread across dozens of agencies, and timeintensive application processes create confusion and frustration.
For clinicians, social workers, and patient navigators, the lack of a centralized, easy-touse eligibility tool limits their ability to efficiently support families experiencing food insecurity, housing instability, and other social needs.
The Solution: MyFriendBen Massachusetts
MyFriendBen is a nonprofit developing technology to improve the process for securing public benefits. They have developed a state-specific, open-source, comprehensive benefits eligibility screener. The screener brings together more than 50 federal, state, and local programs including public benefits, tax credits, and nonprofit resources into a single, user-friendly experience.
Through this co-development effort, Boston Children’s acted as an anchor partner in Massachusetts, collaborating with MyFriendBen to:
• Provide expertise from clinical staff and our program partners to customize the screener for Massachusetts–specific eligibility rules and programs
• Ensure the tool reflects the real-world needs of families and frontline staff
• Facilitate local and statewide connections to help build a network of partners in Massachusetts
The Massachusetts version of MyFriendBen enables users to enter basic household information and receive a personalized list of programs they may qualify for, along with links to next steps, without requiring identifiable personal data.
Why This Matters
Access to public benefits is a powerful lever for improving child and family health. By increasing household economic stability, benefits such as SNAP, housing assistance, and tax credits can reduce food insecurity, housing instability, and other social stressors that drive poor health outcomes and higher health care costs.
Early Impact and Promise
Nationally, MyFriendBen is live in five states: Colorado, Illinois, North Carolina, Massachusetts, and Texas. To date, the platform has served more than 75,000 families with over $47MM in secured benefits and tax credits out of over $1.35B in benefits identified. The Massachusetts launch builds on this momentum, positioning the state to unlock millions of additional public dollars for residents.
Importantly, the tool supports both direct use by families and potential integration into navigator, social work, and care coordination workflows, extending its reach well beyond a single setting.
Our Approach
This initiative was built through a multi-sector collaboration that combined clinical insight, legal expertise, and product infrastructure.
Key elements of the approach included:
Health system leadership: Boston Children’s Department of Accountable Care and Clinical Integration, the Social Work Program, and the Accelerator Program served as implementation and learning partners, grounding the tool in real clinical and patient-facing workflows.
Expert partnership: MyFriendBen provided the national open-source platform, policy engine, and technical infrastructure, while partners such as the Safety Net Project at Harvard Law School contributed deep expertise in benefits eligibility.
Human-centered design: Tool customization prioritized clarity, accessibility, and equity particularly for households below 200% of the federal poverty level.
Statewide launch: Boston Children’s in-kind resource investment, along with financial and in-kind support from other state and national partners, will enable the Massachusetts screening tool to be launched statewide. Once launched, the tool will be accessible to families at no cost.
What’s Next
Following launch, the partnership will focus on real-world use, feedback collection, and external evaluation to assess impact and inform continuous improvement. There are also opportunities to expand the range of programs, languages, and integrations supported by the tool.
Innovation Focus: Social drivers of health, benefits access, open-source infrastructure, equity
Positive Fitness Hub Scaling Positive Fitness Principles to Providers Everywhere
Cardiac Fitness Incubation Concept
Partnership with Boston Children’s Cardiac Fitness Program
Boston Children’s Hospital’s Cardiac Fitness Program is a national leader in supporting children and adolescents with congenital or pediatric-acquired heart disease through safe participation in physical activity. By integrating supervised exercise, education, and mindset support into cardiac care, the program improves confidence, wellbeing, and long-term quality of life for patients and families. The Accelerator Program and the Cardiac Fitness Program are collaborating on the creation of a Positive Fitness educational platform to expand access to the principles of Positive Fitness through clinician-facing training and support.
The Challenge
Positive Fitness is a powerful way to improve outcomes for children with CHD, but it has not yet been broadly incorporated into standard care practices. Physical activity is an essential component of healthy childhood and has proven benefits across a range of outcomes, but children with CHD are less fit than their peers and their fitness levels decline more rapidly.
A positive mindset (e.g., sense of meaning, optimism, confidence) is also related to improved health outcomes. Both physical fitness and a positive mindset are modifiable through training. However, many providers supporting patients with CHD lack the awareness, education, and understanding of exercise and positive fitness principles to effectively incorporate it into clinical care.
As survival improves and CHD becomes a lifelong condition for many patients, the absence of integrated physical fitness and positive mindset training for pediatric patients with CHD represents a growing gap in care.
Why This Matters
The Solution
The Positive Fitness Hub is designed to scale the knowledge and tools needed to incorporate the principles of Positive Fitness into cardiac care. The platform’s content will be built on clinical expertise gained from over two decades of work in this space. The initial iteration of the web-based platform will focus on provider-facing resources including:
• A central hub with educational content, certification programs, and training for providers to understand the methodology and framework behind positive fitness
• Actionable tools for providers to deliver positive fitness to their patients
• A connected community of professionals to establish a network of providers committed to delivering positive fitness to pediatric CHD patients
Through a technology-enabled approach, the platform aims to rapidly expand the reach of our clinical expertise and leadership, creating a pathway for increased access to positive fitness principles through provider education and training.
Children with CHD are living longer, fuller lives and the approach to care and systems supporting that care must evolve accordingly. The Positive Fitness Hub aims to begin a shift in the care model from one that focuses on limitations to one that prioritizes potential. This work reflects Boston Children’s role as a national leader in pediatric innovation: translating deep, transformational subspecialty expertise into scalable solutions that support lifelong health.
Impact and Potential
The Positive Fitness Hub has strong potential to improve outcomes across multiple dimensions. For providers, it expands their ability to support pediatric patients with CHD. For patients and families, it improves access to elements of positive fitness through the care team’s incorporation of positive fitness principles into the care plan. Over time, broader participation in positive fitness could contribute to increased participation in physical activity, improved confidence and self-efficacy, and improved clinical outcomes, including functional capacity, muscle strength, and reduced hospital utilization while also generating long-term health economic value.
Our Approach
The Accelerator Program is partnering with the Cardiac Fitness Program to develop an initial iteration of the Positive Fitness Hub. Through a structured discovery and design process, the team will scope a solution, create new educational content informed by clinical expertise, and create a website for broad dissemination.
Key elements of the approach include:
Human-centered discovery, including analysis of provider survey data from past training and network building events held by the team and interviews with providers in the space
Thoughtful product design leveraging both the Accelerator team’s digital experience and insights gained from the discovery
Iterative scoping and validation to ensure the platform delivers meaningful value immediately while also planning for additional content and components
What’s Next
Boston Children’s Hospital has received a philanthropic gift to support efforts to expand access to Positive Fitness. With dedicated funding, the team will complete discovery, design and develop a web-based educational hub, launch the website for early users, and create a pathway through which the solution can find sustainability. This groundwork will inform additional content creation, website expansion to additional audiences (like patient families), long-term sustainability opportunities, and even additional product incubation in the positive fitness space.
Expert-crafted content created by Boston Children’s national thought leaders in this space
Emerging Tech Innovation focuses on enabling development of novel technology, driving adoption of new deployments, and measuring the impact of emerging technology applications at Boston Children’s Hospital.
PROGRAM ACTIVITIES
Emerging Tech Innovation focuses on translating emerging technologies into meaningful pediatric healthcare solutions, ensuring that innovation is both mission-aligned and built for long-term sustainability. Through a combination of innovation builds, business development, institutional capacity building, and thought leadership, the team helps position Boston Children’s at the forefront of responsible technology adoption while remaining closely attuned to evolving market trends.
This work builds on Boston Children’s deep experience adapting cutting-edge technologies for pediatric use, including prior efforts across social media research, voice technologies, and immersive platforms such as AR/VR and spatial computing.
Current Focus: Harnessing AI to Drive Progress
Today, the portfolio is primarily focused on artificial intelligence and generative AI, reflecting their growing relevance across clinical care, research, and operational domains. By supporting staff, strengthening institutional readiness, and advancing sustainable products, platforms, and ventures, Emerging Tech Innovation fosters a culture of innovation that empowers employees and maximizes the potential for lasting impact on patients, families, and the broader healthcare ecosystem.
Market Intelligence & Regulatory Monitoring
Capacity
Building
A clinician-led AI tool that helps care teams learn from prior similar patients, with the potential to dramatically reduce time to insight for complex pediatric cases
Governance & Prioritization
MedTutor
A precision education platform that uses AI to ensure every medical learner regardless of site or background achieves core clinical and equity competencies
Design & Implementation
Change
Management & Impact
Measurement
NEST NEST is an application that supports clinicians by combining patient data, note templates, and large language models (LLMs) to generate higher quality clinical notes
Cardiac Fitness Incubation Concept
Clinical Doppelganger Accelerating pediatric insights
Partnership with Boston Children’s Cardiac Fitness Program
Clinical Doppelganger is a clinician-led innovation at Boston Children’s Hospital designed to help clinicians learn from prior patients with similar clinical characteristics when caring for complex cases. By combining large language models (LLMs) with cloud-scale infrastructure, the project enables clinicians and researchers to identify and review comparable patients based on clinical context, supporting faster, more informed decision-making.
The Challenge
Treating medically complex pediatric patients often requires clinicians to reason through nuanced combinations of anatomy, interventions, physiology, and outcomes. While electronic health records contain rich historical data, that information is largely locked in unstructured clinical narratives, making it difficult to learn from prior similar cases in a timely way.
Traditional search tools fall short for these scenarios. For example, identifying patients with a specific congenital heart defect who developed a particular complication after a specific surgery and responded well to a nonstandard intervention would be challenging and time-intensive to research. As a result, clinicians spend significant time manually reviewing charts, limiting their ability to quickly apply prior experience at scale.
Why This Matters
The Solution: Clinical Doppelganger
Clinical Doppelganger enables clinicians to ask natural language questions and rapidly surface prior patients with similar clinical characteristics their “doppelgangers.” The system reasons over context, connecting diagnoses, procedures, lab values, and outcomes to generate clinically meaningful cohorts.
The following elements enable this:
An agentic LLM that transforms unstructured clinical narratives into searchable signals.
These signals are joined with structured data, allowing clinicians to move from a question to a relevant cohort in minutes.
Results are source-attributed and interpretable, allowing clinicians to review underlying patient data and apply judgment.
As pediatric care becomes increasingly specialized, the ability to learn from prior patients at scale is critical. Clinical Doppelganger demonstrates how AI can augment clinical expertise by making institutional knowledge accessible when and where it is needed.

Our Approach
Boston Children’s has built a complete, endto-end pipeline to operationalize Clinical Doppelganger, combining clinical expertise with scalable cloud services.
Key elements of the approach included:
Clinician-led design ensuring the system supports real diagnostic and treatment reasoning
Transformation of unstructured data into semantic embeddings and sparse lexical representations
Integration of structured and unstructured signals to capture both clinical meaning and numeric measurements
Early Impact
Clinicians demoing Clinical Doppelganger report strong enthusiasm for its ability to reduce time to insight and surface relevant prior experience that would otherwise be difficult to find. Early impact includes:
• Substantially reduced manual chart review for complex cases
• Faster cohort development for clinical decision support and research
• Increased confidence in exploring alternative approaches informed by prior outcomes
The team is targeting up to an 80% reduction in chart review time for complex cases, freeing clinicians to focus more on care decisions and less on data retrieval. To date, the pipeline has processed more than 6,000 complex pediatric cardiac ICU cases, generating a knowledge base with hundreds of structured measurements and thousands of semantic representations.
What’s Next
The Clinical Doppelganger roadmap includes expanding beyond the cardiac ICU to additional ICUs and clinical specialties, integrating into electronic health record workflows, and supporting quality improvement and research through faster cohort identification. We will share learnings with other pediatric and adult health systems, extending the impact of this work beyond Boston Children’s.
Innovation Focus Areas: Workflow enablement, guideline-based care, clinician experience
Cardiac Fitness Incubation Concept
Partnership with Boston Children’s Cardiac Fitness Program
MedTutor Precision education for equitable medical training
MedTutor is a precision-education platform developed at Boston Children’s Hospital that uses large language models (LLMs) to create immersive, multi-stage clinical encounters with virtual patients, families, and care teams. By pairing these encounters with automated, competency-based assessment and personalized feedback, MedTutor transforms medical education from episodic exposure into a systematic, equitable pathway to mastery.
The Challenge
Despite advances in medical education, training still relies heavily on unpredictable clinical encounters, static case vignettes, and assessments that do not fully capture real-world clinical reasoning or equity-focused care. Learners may graduate without ever encountering critical scenarios, receive feedback too late to influence learning, or advance with hidden competency gaps that surface only under pressure. These limitations create variability in preparation across training sites and learner backgrounds, unintentionally reinforcing inequities in confidence and readiness. Meanwhile faculty lack timely, granular insight into where learners are struggling, making it difficult to target coaching or adapt curricula in real time.
Why This Matters
The Solution: MedTutor
MedTutor addresses these challenges through a precision-education platform that enables learners to practice and be assessed on complex clinical and equity-related competencies in a consistent, scalable way.
Through LLM-powered virtual encounters, learners engage in realistic clinical scenarios that adapt to their level and learning needs. An agentic assessment framework evaluates each interaction against validated competency standards including ACGME core competencies and milestones, AAMC diversity, equity, and inclusion competencies, and emerging structural competency frameworks.
Rather than providing answers, MedTutor uses Socratic dialogue to promote active clinical reasoning. The system identifies individual learning gaps in real time and generates targeted micro-vignettes designed to strengthen specific skills, while grounding all content in verified sources and applying regular bias audits to ensure equitable assessment.
Medical education shapes the quality, safety, and equity of care for decades to come. When training depends on chance encounters and uneven feedback, gaps in preparation can persist and compound particularly for learners training in resource-constrained settings or serving diverse patient populations.

Our Approach
This initiative was investigator-designed and clinician-led, with close collaboration between the cardiac ICU team and the innovation team.
Key elements of the approach included:
Competency-first design, mapping learner performance to approx. 40 measurable clinical & equity competencies
Continuous feedback loops that combine immediate guidance with longitudinal performance tracking
Faculty-centered analytics, providing actionable insight to guide coaching, rounds, and curriculum refinement
Early Impact
Early pilot users report high engagement and increased confidence in clinical reasoning. Faculty note improved visibility into learner strengths and gaps, enabling more focused coaching and support.
As MedTutor scales, the expected impact includes:
• Faster time-to-competency comparable to one-on-one tutoring
• Reduced variability in competency attainment across learner demographics
• Improved integration of health equity considerations into clinical reasoning
• More agile, data-informed curriculum improvement
What’s Next
The MedTutor roadmap includes expanding across training levels and institutions, integrating additional competency frameworks, and validating impact on both educational equity and clinical practice.
Longer term, the team plans to publish open implementation resources to enable adoption by resource-limited programs, extending the benefits of precision education beyond Boston Children’s and helping ensure that every learner has a clear, supported path to clinical and professional excellence.
Innovation Focus Areas: Continuing medical education, responsible AI deployment, addressing bias
Cardiac Fitness Incubation Concept
Partnership with Boston Children’s Cardiac Fitness Program
NEST Clinical Intelligence Transform clinical documentation & workflows
This project aims to reduce documentation burden for clinicians at Boston Children's Hospital by using patient data, structured note templates, and HIPAA-compliant large language models (LLMs) to generate complete first drafts of clinical notes, starting with anesthesia pre-op notes and CICU progress notes. NUSC combines data from EPIC and other clinical systems with BCH standard templates to produce notes that are complete, consistent, and reliable.
The Challenge
Clinicians creating progress notes struggle because critical patient information is dispersed across many parts of the chart, requiring them to search through vitals, device data, telemetry, labs, imaging, consults, medications, and overnight events just to understand the patient’s current state. This makes it time-consuming and cognitively taxing to assemble an accurate, up-to-date picture of a critically ill patient.
As a result, important details can be missed, clinical reasoning becomes harder to document and note quality can vary depending on how efficiently each clinician can find and synthesize fragmented data. Furthermore, this impacts accuracy of ICD-10 coding because relevant clinical details are often buried in lengthy, unstructured notes, requiring manual review and interpretation.
Why This Matters
The Solution: NEST
The Note Enhancement & Support Tool (NEST) is an LLM-enabled clinical documentation + workflow layer that sits on top of a hospital’s EHR/warehouse data. It generates higher-quality clinical notes, powers workflows (e.g., coding, discharge readiness), and Q&A through naturallanguage interaction with the patient chart. NEST is the data layer on which many automations and workflows can be powered.
NEST will search across EPIC, Snowflake, and HL7 to identify relevant patient information. An LLM layer will take the key patient data points and information and create a readable and efficient, template-aligned anesthesiology pre-op note. This will support cardiologists with coalescing key patient information that lives across the patient medical record into a comprehensive and high quality pre-op note, saving the clinician time, increasing identification of key patient risk factors, and improving note quality.
Reduced documentation burden and with increased accuracy and fidelity, better data integration and synthesis, more consistent administrative outputs (coding/readiness/risk) grounded in chart data

Our Approach
We will prioritize development and validation of the Anesthesiology Pre-Op note use case before moving to the CICU progress note and subsequent use cases. The anesthesiology pre-op note use case presents our best opportunity to validate a single use case before extending functionality
Anesthesiology Pre-Op
An anesthesiology pre-operative note is a structured clinical document created by an anesthesiologist before a patient undergoes surgery. Its purpose is to ensure the patient is safe to proceed to the operating room and to guide the anesthesia plan.
What’s Next
CICU Progress Note communicates care team’s clinical reasoning, prioritizes active problems, and outlines plan for the next 24 hours to guide all providers involved in the patient’s care
We are still actively designing how NEST will support ICD-10 coding, but several options are under consideration. These include using retrieval-augmented generation (RAG) over ICD-10 guidelines, coding clinic examples, and similar past encounters to suggest more specific, appropriate codes; leveraging graph-based relationships between diagnoses, symptoms, labs, medications, and procedures to disambiguate and refine candidate codes; and applying consistency checks that flag missing or incompatible codes (for example, age- or pregnancy-inconsistent choices). Longer term, NEST could also generate short, clinician-friendly rationales for suggested codes and highlight related “phenotype bundles” (e.g., sepsis plus organ dysfunction) to reduce omissions and improve coding quality while keeping physicians in control.
Innovation Focus Areas: Supporting clinical workflows, reducing provider burnout, patient safety
Selected Enterprise AI Highlights
AI-Driven Translation: Lilt
Combining advanced machine learning with professional linguist review for highly accurate, cost-effective, and continuously-improving translations.
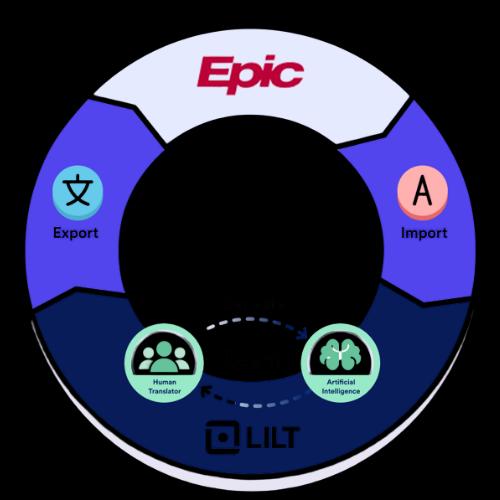
Early Results
Percent of inpatient discharge instructions translated (out of all eligible patients) increased from 8.4% in FY25 to 49% within pilot departments in first month
~40-70% improvement in average turnaround time (TAT) across top requested languages, meaning more patients leaving the hospital with translations in hand
What’s next?
• Epic integration & expansion to additional departments
• Exploration underway for additional use cases (e.g. medical records, consents)
Partnership with digital team, IT, clinicians, and language services.
InternalGPT
Initial Vision and Purpose: Built to unlock enterprise access to LLMs via a secure, cost-effective, HIPAA-compliant platform
Sustaining Value:
• Developed an assistant suite, enabling users to more easily derive value from the tool around specific use cases
• Multi-model access (currently all OpenAI models; bringing in Anthropic models next quarter)
• Built connections to additional data sources internally (e.g., Epic) and externally (e.g., PubMed) to continue expanding value and use case possibilities

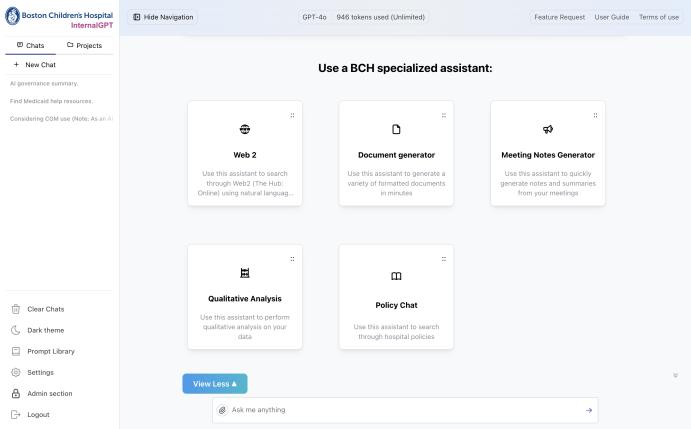
3.9K+ staff users

Intelligent Automation Program
Launched first automation in March 2024; deployments are now live across HR, Finance, Legal, Supply Chain, Patient Safety, and Clinical departments. Automations have become increasingly intelligent & agentic as the capabilities have advanced, broadening set of applicable use cases.
Impact areas
Reduction in time spent on manual & repetitive tasks


Amplification of workforce capacity without the need to back-fill roles
Improvement in staff productivity, with time spent on higher value activities
Support for BCH staff retention / increased job satisfaction
Reduction in operational friction and costs by automating high-volume workflows
Ambient Documentation: Abridge


43 deployed automations
45K+ hours saved $5.6M+ cost savings
After a bake-off between Nuance DAX Co-pilot and Abridge, Abridge was selected as the enterprise ambient clinical documentation partner. Broader enterprise roll-out took place in two parts in late 2025.
38.7K+
Reduce administrative burden
Improve time to completion of signed note 790
encounters in first quarter of fiscal year active providers in first quarter of fiscal year
Reduce time spent documenting in the EMR
Partnership with informatics, digital, IT, and clinicians.
Improve patient care delivery
Other projects and interest areas
Innovator's Assistant
The Accelerator Program's Innovation Assistant is a generative AI-powered chat bot that provides a la carte education and engagement meant to facilitate additional learning around topics including digital health innovation, software development, and entrepreneurship.
Asthma Environmental Risk Dashboard
Clinician-facing dashboard, conceptualized in partnership with the Pediatric Environmental Health Center, that utilizes publicly available location-based environmental data to help providers better understand climate and environmental vulnerability for their asthma patients and adjust or enhance care accordingly.
OpenAI Genetic Diagnostics
powerful AI models to help diagnose illnesses faster and create personalized treatment plans for patients with complex or rare diseases.
Apple Vision Pro Cyrano
This effort leverages cutting edge AR technology to expand the way we train clinicians, improving the quality of training and continuing education.
Trauma-Informed Care
Identifying opportunities alongside clinical psychologists in the Department of Anesthesia, Critical Care, and Pain Medicine to expand access to knowledge and improve the implementation of programs related to trauma-informed care.
Pediatric Point of Care Ultrasound
Exploring opportunities with the Emergency Medicine team to develop a digital solution in the point-of-care ultrasound space to support education, clinical, and quality assurance workflows, leveraging an extensive database of Boston Children's expert-reviewed studies.
Chronic Pain Management
Collaboration with the Comfort Ability Program to explore digital innovation opportunities supporting improved access to psychology-based interventions for pediatric chronic pain patients and families.
Letter of Medical Necessity
AI-supported drafting for letters of medical necessity, considering insurer requirements and ensuring clinical documentation to meet prior authorizations.
We are deeply grateful to the donors and advisors who make the work of the Innovation and Digital Health Accelerator possible. Your partnership, insight, and generosity enable us to explore and scale new technologies that meaningfully improve care for children, families, and clinicians. Beyond financial support, your guidance helps shape a thoughtful, responsible approach to innovation one grounded in clinical need, equity, and real-world impact. Together, we are accelerating progress at Boston Children’s Hospital and helping ensure that breakthrough ideas translate into better health outcomes for patients everywhere.
Thank you!
Innovation Team



Thank you to our wonderful team & supporters Thank you to our wonderful team & supporters
