

CLINICAL LEADERSHIP IN A CHANGING
CLIMATE
Paul Manning, chief executive of Circle Health, discusses transitioning from the operating theatre to the boardroom
THE SURGICAL CAPACITY CHALLENGE
RCS president Tim Mitchell on why an increase in consultants isn’t matched by an increase in the number of operating theatres
THE SERIOUS SIDE OF ROBOTIC
COMPANIONS
Ageless Innovation CEO Ted Fischer talks about tech-enabled solutions for healthy ageing

WELCOME MARCH 2025
“For the patient who has come to hospital expecting surgery, having prepared psychologically and made the necessary arrangements in their personal life, a last-minute cancellation is absolutely devastating,” says Tim Mitchell. “Sadly, this is not an uncommon story. It reflects a combination of pressures coming together across the system.”
While the elective recovery backlog remains a top priority for the government, here the president of the Royal College of Surgeons of England talks to Healthcare Today about the urgent need for capital investment, the shift toward preparation lists to keep patients fit for surgery, and the expanding role of robot-assisted technology in the modern operating theatre.
Also in this issue, Circle Health chief executive Paul Manning discusses the group’s evolving relationship with the NHS; Ted Fischer of Ageless Innovation explains the benefits of robotic pets for the elderly; and much more...
We hope you enjoy!


30-33

36-39

REVISED STANDARDS FOR MEDICAL DEVICES
THE British Standards Institution (BSI) has published a revised standard to provide a framework to assess the biological safety of medical devices, ensuring materials that come into contact with the human body are safe, effective, and meet global regulatory expectations.
First developed to bring scientific rigor and consistency to biocompatibility testing, the standard has evolved to reflect advances in material science, toxicology, and risk management. The sixth edition introduces significant updates, including alignment with the standard enhanced guidance on exposure duration, device characterisation, and biological hazard identification, and a new annexe explaining the rationale behind the revised biological effects tables.
“This revised standard reflects a new era in biological evaluation, one that is evidence-led, globally harmonised, and designed to support both patient safety and innovation,” said Michelly Kelly, chair of the National Committee for the Biological Evaluation of Medical Devices.
“This revision strengthens the way manufacturers assess biological safety by encouraging data-driven evaluations that enhance patient and user protection, reduce unnecessary animal testing, and streamline global regulatory approval. It also supports innovation across emerging technologies such as combination products and wearables, helping organisations bring safe, effective, and compliant medical devices to market more efficiently,” she continued.
The new BS EN ISO 10993-1 provides the general principles for biological evaluation of medical devices within a risk management process. It guides manufacturers in determining which tests are necessary based on the device’s nature, contact type, and duration, ensuring appropriate safety assessment while avoiding unnecessary testing.
This latest revision emphasises risk-based decisionmaking, harmonisation with regulatory frameworks, and the integration of toxicological and material science data to improve patient outcomes and streamline global compliance.

PAC SAYS THE FAILED TO ACT
AREPORT from the Public Accounts Committee (PAC) has found that not only has the government’s liability for clinical negligence quadrupled over the past two decades to £60 billion last year, the Department of Health and Social Care (DHSC) is unable to show any meaningful action taken to address this, and the NHS has not done enough to tackle the underlying causes of patient harm.
The report paints a picture of a system overwhelmed by safety recommendations that it cannot action, with evidence that, despite the NHS in England keeping a plethora of data on patient harm, its fragmented nature does not amount to good information which could identify and address clinical negligence’s underlying causes. This builds on the broader report published by the committee at the end of November that found that, despite spending £3.24 billion on transforming diagnostic and surgical services, NHS England has missed its recovery targets. It also confirms the repeated failings of maternity services highlighted by Healthcare Today
The PAC has highlighted the problem of disproportionate legal costs in clinical negligence claims again. Claimant legal fees more than tripled to £538 million last year, while claims with damages of £25,000 or less cost far more in fees than victims receive, with a cost-to-damages ratio of 3.7 to 1. The government’s previous plans to limit the amount paid to lawyers in lower-value cases were not implemented as planned two years
ago, it says, and alternative mechanism and reduce costs
Recent increases to £3.6 billion last significantly to the end of the decade. the PAC dating DHSC has not committed improvements clinical negligence review announced not have an expected
The report calls to learn lessons maternity care plans to reduce costs of claims
The report shows infants and children reaching £325 failings last year.
130 brain injury settled every year, of 11-12 years to cost both for the financially. Evidence from the Royal Gynaecologists workforce is struggling delivering increasingly College pointed woman currently list stood shoulder would stretch over
THE GOVERNMENT HAS ACT ON PATIENT SAFETY

and the DHSC should develop an mechanism to speed up decisions costs for these cases.
increases in settlement costs (tripling last year) are likely to rise more than £4 billion a year by decade. Despite warnings from back to 2002, it says that the committed to acting to make to the fundamental issues of negligence until the completion of a announced last year, for which it did expected date.
calls in particular for the DHSC lessons from its failure to improve in England, and set out how it reduce the incidence of harm and the in this area.
shows settled claims involving children increasing significantly, million in claims for paediatric year. The inquiry heard that 120injury cases involving children are year, but it can take an average to resolve each claim, at a high the victim’s experience and Evidence to the PAC’s inquiry College of Obstetricians and Gynaecologists suggested that the maternity struggling under the pressure of increasingly complex care. As the pointed out earlier this year, if every currently on a gynaecological waiting shoulder to shoulder, the queue over 191 miles.
Finally, the report notes that claims being settled on the basis of how much a victim’s care would cost in the private sector, rather than in the NHS, stem from a law from 1948. The inquiry heard that this is a major contributory factor to the increasing cost of very high-value cases of more than £1 million.
“Clinical negligence is the second-largest financial liability across government, but represents to our committee a different matter entirely from other large items like nuclear decommissioning or pensions. This is a swelling accounting of profound suffering,” said Geoffrey Clifton-Brown, chair of the Public Accounts Committee. “The rising costs of such claims are diverting resources away from frontline care, badly in need of them. That is why it feels impossible to accept that, despite two decades’ worth of warnings, we still appear to be worlds away from government or NHS engaging with the underlying causes of this issue.”
Many suggestions have been made about how to cut negligence costs, but the PAC has made six specific recommendations. It has asked the DHSC both to explain its operational plan to tackle clinical negligence, including key milestones for achieving reductions in claim costs and volumes, and to publish David Lock’s review of clinical negligence within six months of it being completed.
It has also recommended that a national framework for improving patient safety with clear targets for annual improvement be set up. “We are concerned there is far too little data on the factors behind clinical negligence,
given its huge impact on people’s lives and NHS finances,” the report says.
The DHSC should establish a national system for sharing data between trusts and analysing trends. “If there are barriers to sharing protected data, it should develop analysis on an anonymised basis to pull out lessons and provide early warning alerts to trusts,” it suggests.
It is echoing the emphasis on a failure of maternity care and has recommended that the DHSC publish the review by Valerie Amos, Baroness Amos, into maternity services within two months, alongside its response and set out how it plans to reduce the incidence of harm and the costs of claims in maternity care.
Next, an alternative dispute mechanism should be set up to speed up decisions and reduce costs for less complex cases. As part of this, it recommends that the DHSC look at international examples, such as in New Zealand and Sweden, of non-adversarial and ombudsman models and assess how our ombudsman system could be improved.
Finally, the DHSC should develop, within six months, proper estimates of the impact of assuming health and social care for clinical negligence victims by the private sector. It should set out, by the same deadline, additional measures which it judges would effectively guard against the risk of paying twice for the care of those it has harmed and an indicative timeline for their potential implementation.

A BROAD WELCOME FOR
UNDER the government’s national cancer plan, every patient will be given a tailored plan that looks beyond just treatment and diagnosis to cover the full impact of cancer on their life, from anxiety and fatigue to diet and returning to work.
They will also receive an end-oftreatment summary to end the cliff edge many face when chemotherapy or surgery finishes – giving them clear guidance on warning signs, who to call with concerns, and where to find ongoing support like physiotherapy, counselling or local cancer groups.
Even after successful treatment, some patients find themselves unable to return to the lives they had before diagnosis. The psychological toll of cancer can be devastating and longlasting with anxiety, depression and trauma persisting long after physical recovery. The personalised cancer plan ensures patients receive the mental health support they need to rebuild their lives.
“If you’ve ever sat in a waiting room dreading what comes next or laid awake at 3am wondering how you’ll pay the bills while you’re off work for
treatment, you’ll know that cancer doesn’t just attack your body - it takes over your whole life. I was fortunate. I had a supportive employer, a family who could rally around me, and the financial security to focus on getting better. But I know that’s not everyone’s reality – and it shouldn’t be based on luck,” said secretary of state for health and social care Wes Streeting, who is now cancer-free following a kidney cancer diagnosis in 2021.
Through the NHS app, patients in England will be able to book screening appointments, access prehabilitation programmes, view their patient record, check their personalised cancer plan, and provide feedback on their care. They will also be connected to cancer charities for specialist support as soon as they are diagnosed.
By 2035, the government hopes that every cancer patient will have a named neighbourhood care lead responsible for joining up their care after treatment meaning no more being passed from pillar to post.
New standards will be introduced by 2028 to help patients get fit for treatment and recover quickly
afterwards, including prehabilitation, rehabilitation and physical activity programmes.
“Being diagnosed with cancer affects every part of your life and the lives of the people around you, which is why the NHS is committed to supporting people with cancer in every possible way,” said Peter Johnson, NHS England’s national clinical director for cancer.
“A personalised cancer plan will bring all this together, helping people face cancer with the right care, at the right time, in the right way,” he added.
The news about the new personalised approach to cancer treatment was widely welcomed.
“The plan’s promise of a tailored support plan for everyone, alongside a named neighbourhood cancer lead and connecting people to cancer charities for support, will make a real difference,” said Gemma Peters, chief executive of the charity Macmillan Cancer Support.
“This is a truly landmark moment. For the first time, children and young people have a dedicated chapter in the National Cancer Plan, a clear
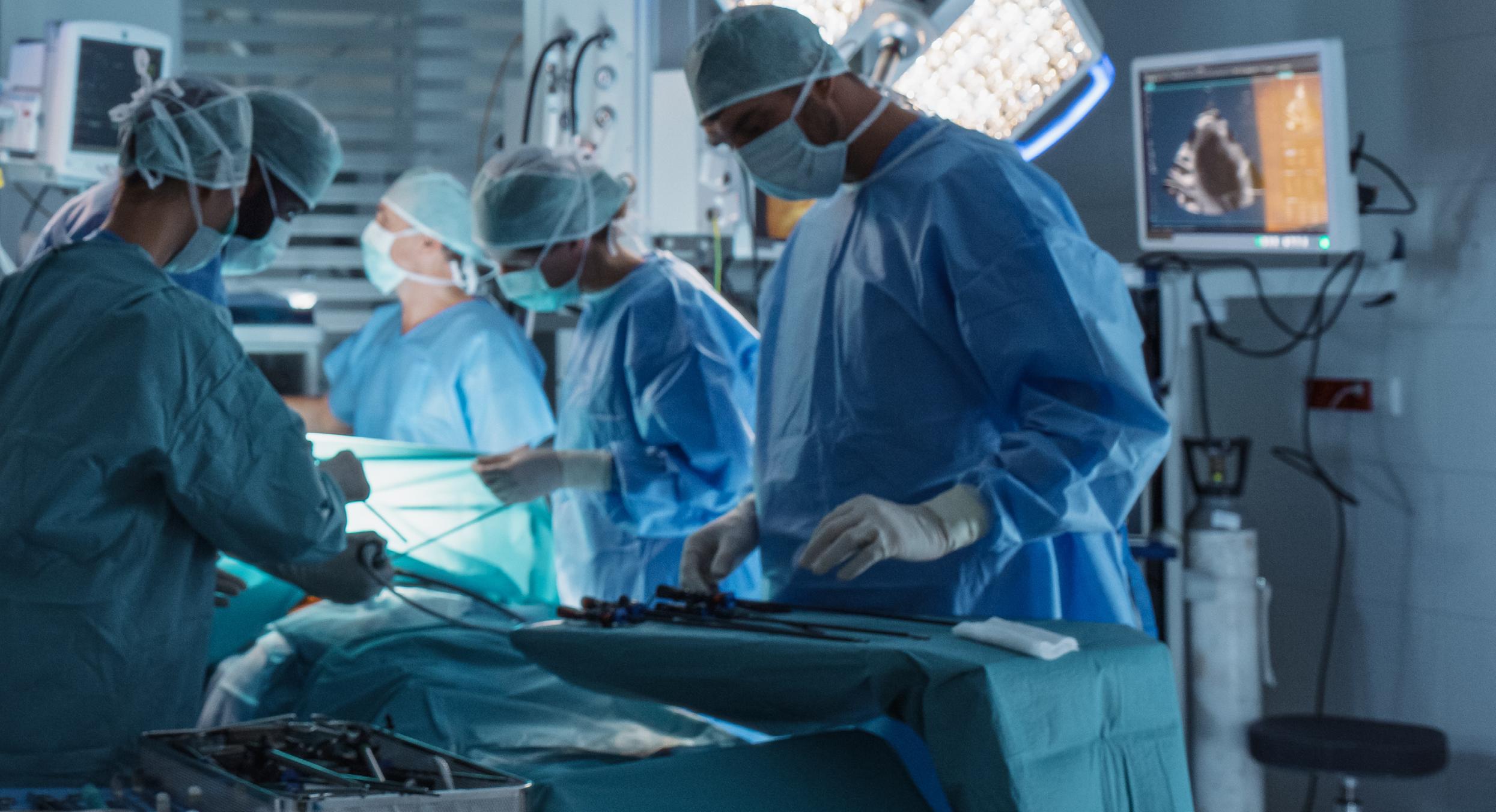
NATIONAL CANCER PLAN
recognition that their needs are distinct, complex and deserve focused attention,” agreed Rachel Kirby-Rider, chief executive of the charity Young Lives vs Cancer.
“This is a landmark moment for the 260,000 people living with or in remission from blood cancer in England and one we’ve been calling for over many years,” said Helen Rowntree, chief executive of Blood Cancer UK. “Survival for blood cancer patients has fallen behind other nations of similar wealth and health, and people with blood cancer face some of the toughest odds. This plan could change that, but only if it’s delivered properly.”
The private sector is also on board. David Hare, chief executive of the Independent Healthcare Providers Network (IHPN), said that private sector would make a significant contribution to meeting the NHS’ cancer targets. He pointed out that the plan committed to significant new investment to deliver 9.5 million additional tests and scans by 2029, of which NHS England has made clear that more than one third will need to come from the independent sector.
“This will help create significant
new additional diagnostics capacity without the need for additional public capital spending, and will help to drive up the overall productivity of services – key in improving patients’ access to care,” he said.
Kidney Cancer UK chief executive Malcolm Packer emphasised that early diagnosis was key and welcomed the massive investment in additional diagnostic tests.
He pointed to research that Britain’s leading kidney cancer charity had published earlier this month which showed that one-in-five (20%) kidney cancer patients are being diagnosed at Stage 4, which results in harsher treatments, reduced quality of life, and significantly higher mortality rates.
Mortality rates have grown over recent decades, increasing by 73% since the 1970s.
Research also shows that threequarters (74-75%) of people diagnosed with Stage 3 kidney cancer survive for at least five years – though for those diagnosed at Stage 4, when the cancer has spread to distant organs, five-year survival falls significantly to around 10-15%.
The five-year survival rates in the UK are among the lowest in Europe.
Kidney cancer now ranks as the UK’s sixth most common cancer with around 13,800 new cases each year –that’s roughly 38 new diagnoses every day. Around 4,700 people die from the disease annually, amounting to about 13 deaths per day.
“The finding that just over 20% of patients are now being diagnosed with Stage 4 kidney cancer represents a concerning year-on-year increase,” said Grant Stewart, professor of surgical oncology at Cambridge and consultant urologist at Addenbrooke’s Hospital.
“Kidney cancer often presents with non-specific or subtle symptoms, which can be overlooked or misattributed, leading to delays in diagnosis. These delays can significantly limit treatment options and adversely affect patient outcomes.”
As Streeting himself said in a speech at Royal Free Hospital in North London in early February early diagnosis is literally life changing. “I was lucky, my cancer was caught early,” he said.


RISE IN DATA BREACHES ACROSS UK AMBULANCE SERVICES
THE scale of data security incidents affecting ambulance services across the UK is rising as emergency responders face growing digital and cyber-related threats.
Research from Data Breach Claims UK shows that more than 4,000 data breaches have been recorded by UK ambulance services over the past three years. Official figures show that ambulance services recorded 1,212 data breaches in 2022/23, rising sharply to 1,460 in 2023/24. Over the past year, reports continued to climb, with 1,521 breaches logged, indicating a sustained upward trend.
The findings come amid wider concerns about cybersecurity in emergency services. Earlier this year, cybersecurity firm NCC Group published research warning of escalating digital threats to blue light services, including a 15% increase in ransomware attacks during 2024,
which can disrupt critical systems and delay emergency responses.
“Ambulance services handle some of the most sensitive personal data that exists, including medical records, emergency care notes and contact details for patients and their families,” said Tekena Bobmanuel, data breach solicitor for JF Law in Liverpool.
“When that information is mishandled, lost, or accessed without authorisation, the consequences for those affected can be extremely distressing,” he added.
London Ambulance Service NHS Trust recorded the largest volume, with 904 data breaches, followed by East of England Ambulance Service NHS Trust, which logged 716 incidents.
The Welsh Ambulance Service logged 675 cases, and the South Central Ambulance Service NHS Trust and the North West Ambulance Service NHS Trust logged 459 and 390 cases respectively.
Data breaches within ambulance services can impact patients, staff and third parties such as relatives or carers. While cyberattacks often attract the most attention, many incidents arise from more routine causes, including human error, IT system failures and the loss of devices containing personal data.
As digital patient records continue to expand across the NHS, maintaining robust data protection practices remains essential to preserving public trust and preventing further financial and operational strain on ambulance services nationwide.
“Many people wrongly assume that a data breach is something they simply have to accept, particularly when it involves a public service,” said Bobmanuel. “In reality, UK data protection law gives individuals the right to seek compensation if a failure to protect their personal data has caused emotional harm, anxiety or financial loss.”

ACCORDING to the latest Global State of Patient Safety report, Britain is struggling in a number of metrics, including mortality rates, surgical complications and waiting times.
While Norway is ranked first out of 38 Organisation for Economic Cooperation and Development (OECD) countries for patient safety, the UK languishes in 21st place.
The Global State of Patient Safety 2025 report from the Institute of Global Health Innovation at Imperial College London and Patient Safety Watch highlights some global difficulties with patient safety.
It highlights excess mortality across 38 countries for people with severe mental illness as a major concern.
For people with bipolar disorder, excess mortality has risen by 41% since 2015, and by 21% in the same period for people with schizophrenia. But there are some areas for optimism too.
Average waiting times for selected planned procedures, which increased during the pandemic, are largely returning to pre-pandemic levels. Average rates of maternal deaths, stillbirths and neonatal deaths continue to fall, and neonatal mortality rates (deaths of babies under 28 days old) have fallen 46% since 2000.
The report, however, paints a damning picture of healthcare safety in the UK, which has not improved in the rankings at all since the previous report in 2023.
“Tens of thousands of lives could be saved every year if the UK matched the patient safety performance of the world’s best health systems, according to this report,” said Jeremy Hunt, former health secretary and chair of Patient Safety Watch.
The UK is struggling on a number of metrics.
THE UK PATIENT
If the UK had matched the rate of treatable mortality in Switzerland, which leads in this measure, it could have had 22,789 fewer deaths in 2021.
Although the neonatal mortality rate in the UK fell between 2000 and 2017, it has plateaued since then. If the UK matched the neonatal mortality rate Japan, for example, it could have had 1,123 fewer neonatal deaths in 2023.
OECD rates for four out of five indicators for surgical complications have fallen since 2009, but the UK recorded the highest complication rates for three of the indicators using the latest available data. And perhaps most brutally, the UK has higherthan-average waits for more complex procedures.
“Behind every statistic in this report is a person who should still be alive,
UK LANGUISHES IN PATIENT SAFETY REPORT
“Improving patient safety in the NHS is not optional – it is fundamental to saving lives, supporting staff, and restoring confidence in the health service,” he added.
The report builds on the recommendations made in the 2023 report with three core areas of patient safety.
First, to create a more comprehensive set of global patient safety indicators,
could 2021. rate 2017, UK rate of had 2023. complications complication using perhaps complex report alive, and a family whose lives have been permanently changed. The gap between where the UK is on patient safety and where we could be – if we matched the best performing health system – represents around 22,000 lives every year. That’s 60 lives every day,” said James Titcombe, chief executive of Patient Safety Watch, and one of the report’s authors.
the report is encouraging international organisations focused on safety and quality to develop a roadmap to improve data coverage in lowerand middle-income countries. The improvements of maternal and neonatal safety data show how collective action can lead to global coverage, further supporting safety improvement efforts.
Second, to support improved adoption of best practice in patient safety, it is advising countries to learn from best practice in core aspects of patient safety.
These complement emerging resources, including the WHO Global Knowledge Sharing Platform for Patient Safety.
Third, to help ensure patients, families and carers become active
partners in the delivery of safe care, it is advocating national and international action to address the inequities in safe care identified in this report.
“It is imperative that we tackle care deficiencies now to prevent patient safety risks later. Patient safety is everyone’s responsibility, and our report suggests how healthcare teams in one part of the system can support safety in another,” said Bryony Dean Franklin, director of the NIHR North West London Patient Safety Research Collaboration at the Institute of Global Health Innovation, and one of the report’s authors.
“As healthcare professionals, there is much more we can – and must – do to foster multi-disciplinary teamworking and cross-sector collaboration to improve patient safety,” she added.



HEALTHCARE IN THE POLITICAL CROSSFIRE
How US policy shifts are shaping clinical decision-making in the UK
FREE WEBINAR with Emergency Physician turned Healthcare Strategist Dr. Adam Brown Wednesday, March 11th at 1pm GMT
DEBATE OVER USE OF PHYSICIAN ASSOCIATES REOPENS
THE United Medical Associate Professionals (UMAPs) trade union has reopened the debate about the use of physician associates (PAs), anaesthesia associates (AAs) and surgical care practitioners (SCPs).
The long-running debate about their use appeared over after the government accepted all the recommendations of an independent review – the Leng Review – at the end of July last year, on how they are and can be used.
Launched in November 2024, a review chaired by Gillian Leng looked into the safety of the roles of PAs and AAs and how they support wider health teams. She made 18 recommendations aimed at providing clarity to patients and improving patient safety, all of which were accepted by health and social care secretary Wes Streeting.
“The terrible impact of the Leng Review recommendations should have been entirely obvious to both the government and NHS England,” said UMAP general secretary Stephen Nash.
“Effectively sidelining some 3,500 highly qualified medical professionals was clearly going to be disastrous for patients, associates, and doctors alike. Yet at no point did the health secretary make any assessment of how this would harm medical associates or restrict patients’ access to care.”
The survey found that PAs’ scope of practice has been drastically reduced, resulting in lengthening patient waiting times in both secondary care and general practice.
More than three-quarters (76%) of PAs say their scope of practice has been restricted since the publication of the Leng Review.
The number of PAs averaging more than 11 patient interactions (including consultations, follow-ups, results and referrals) per shift has dropped since the Leng Review, while the number of those averaging only one to five interactions has more than quadrupled.
Two in five PAs report worsening patient waiting times in their departments since the publication of the Leng Review, and according to PAs in general practice, there has
been an increase in longer patient waiting times of one to four weeks and four to eight weeks, and a drop in patients being seen in a matter of days.
“Far from protecting patients, it is increasingly looking like these changes were cooked up to mollify the increasingly radical BMA, which at the time of the review was threatening major strike action. That is why we are challenging the irrational recommendations in our judicial review, ensuring that PAs and AAs can go back to caring for patients and helping our doctor colleagues to shoulder the burden,” said Nash.
UMAPs surveyed 459 PAs currently working clinically across NHS England between mid-December and midJanuary, representing a 13% response rate from an estimated population of approximately 3,500 clinical PAs.
The sample includes a spread across NHS England regions and departments, with 47% of respondents working in general practice and 27% in urgent and emergency care. Over half have been working as a PA for more than five years.
RADIOLOGY NEGLIGENCE COSTS NHS
£230 MILLION
THE financial impact of diagnostic imaging failures within the NHS is growing as mounting demand and staffing pressures continue to strain radiology services nationwide.
Data obtained by Medical Negligence Assist shows that NHS trusts in England have collectively paid out more than £230 million in compensation since 2020 to patients who brought claims linked to radiology-related mistakes.
Each year, millions of scans are carried out across the NHS, and the vast majority are completed accurately. When errors occur, however, such as missed findings, delayed reporting, or scans not being performed at all, the consequences for patients can be serious and long-lasting.
Over the past ten years, the number of settled radiology negligence claims has risen by around 30%, marking one of the sharpest increases among all clinical negligence specialities. This trend reflects growing pressure on diagnostic services as demand for imaging continues to climb.
“Radiology is a key part of modern
healthcare and includes diagnostic tests such as X-rays, MRI scans, CT scans and ultrasounds. These tools are a vital step in identifying a patient’s condition and ensuring they receive the appropriate treatment,” said Sophie Cope, medical negligence solicitor for JF Law.
“When something goes wrong at this stage, whether a scan is carried out to a poor standard, misinterpreted, delayed, or never carried out in the first place, the impact on a patient’s health can be profound.”
Between 2020 and 2025, a total of 2,163 radiology-related claims were brought against NHS trusts in England. Of these, 1,520 claims were settled, with the highest annual total recorded last year, when 504 claims were made.
As Healthcare Today pointed out last year, the early retirement of radiologists means that workforce shortages are affecting patient safety.
Radiology mistakes can arise from a range of causes, including human error, inadequate supervision, outdated equipment, or high
workloads. These incidents are commonly categorised as diagnostic errors, which are regarded as among the most serious patient safety failures due to their direct impact on treatment outcomes and prognosis.
NHS trusts paid a total of £231 million in compensation for radiology-related claims over the past five years. The highest annual payout occurred in 2022/23, when settlements reached £58.5 million.
While some claims involved severe outcomes, including delayed cancer diagnoses and fatalities, the most frequently recorded injury was unnecessary pain and suffering, accounting for 261 claims during the five-year period.
Among individual trusts, University Hospitals Sussex NHS Foundation Trust recorded the highest overall compensation total, paying out £13.4 million in radiology-related settlements since 2020.
“Many of these errors are avoidable. When a patient is harmed because standards have fallen short, they have every right to question what went wrong,” said Cope.
BREAST CANCER BLOOD TEST CAN PREDICT TREATMENT RESPONSE
ANEW blood test can predict how well patients with advanced breast cancer will respond to targeted therapies even before treatment begins.
A team from the Institute of Cancer Research, London, used a liquid biopsy to detect the presence of tiny amounts of cancer DNA in the blood at the start of treatment and four weeks into the treatment. They compared the levels of this DNA with patients’ outcomes, including how long it took for a cancer to grow, and how well the cancer was responding to treatment.
The researchers, based at the Breast Cancer Now Toby Robins Research Centre at The Institute of Cancer Research, saw a strong association between low levels of circulating tumour DNA (ctDNA) at the start of treatment and treatment response. A similar association was seen after four weeks, one treatment cycle.
The results show that it is possible to monitor how well treatment is working through a non-invasive blood test, meaning patients who are not responding well could be identified and moved to alternative treatments sooner.
“Our study shows that a simple blood test could give us an early and reliable indication of whether treatment is working for people with metastatic breast cancer,” said study lead Nicholas Turner, professor of molecular oncology at the Institute of Cancer Research, London, and consultant medical oncologist at The Royal Marsden NHS Foundation Trust.
“By tracking changes in tumour DNA in the blood just a few weeks into treatment, we can begin to identify who is likely to benefit and who may need a different approach sooner. This
has the potential to make treatment decisions faster, more personalised and ultimately more effective for people living with metastatic breast cancer,” he added.
In the study, funded by Breast Cancer Now, Cancer Research UK, and the NIHR Biomedical Research Centre at The Royal Marsden NHS Foundation Trust and the Institute of Cancer Research, the team analysed blood samples from 167 people with advanced breast cancer.
The patients were enrolled in the plasmaMATCH trial – a study run by the ICR’s Clinical Trials and Statistics Unit (ICR-CTSU), and funded by Stand Up To Cancer, a joint fundraising campaign from Cancer Research UK and Channel 4.
The team grouped the patients based on their type of breast cancer and the specific mutations in their genes.
The first group consisted of patients whose cancers had an ESR1, HER2, AKT1, AKT or PTEN mutation, and who received targeted treatments matched to those mutations. The second group consisted of people with triple-negative breast cancer and no targetable mutation. These people received a combination of the
PARP inhibitor olarparib and the ATR inhibitor ceralasertib.
For patients in the second group, low ctDNA levels before treatment began were associated with longer progression-free survival – 10.2 months, compared with 4.4 months. In this group, the percentage of patients who responded to treatment – either seeing their tumours shrink or disappear – was 40% for those with low ctDNA levels, compared with 9.7% for those with higher levels.
A similar, but weaker, association was also observed between pre-treatment ctDNA levels and clinical outcomes in the first group.
In the second group, the blood test after four weeks of treatment also showed a strong link between ctDNA levels and patient outcomes. Patients whose ctDNA was no longer detectable had their cancer kept at bay for 12 months, compared with 4.3 months in patients who still had detectable ctDNA. Treatment response was also significantly higher for those with undetectable ctDNA, with 85.7% responding to therapy, versus 11.4% among those with detectable ctDNA.
The researchers now hope to validate their findings in larger studies.

PHARMACY2U ACQUIRES CARE QUALITY PHARMACY
PHARMACY2U, Britain’s largest digital pharmacy, has acquired Care Quality Pharmacy. It is the company’s first move into the care home pharmacy sector.
Financial terms have not been disclosed.
Founded in 2013, Coventry-based Care Quality Pharmacy is one of the largest care home pharmacies in England. It provides prescription and NHS services to a wide range of independent and national care home groups, extra care services, and domiciliary care agencies.
Additional services include paper-based and electronic MAR charts (eMAR), care planning integrations, eLearning, as well as face-to-face training and support through compliance visits and audits.
“Care homes are responsible for an important portion of all prescription medications dispensed in the UK, predicated on service quality and reliability, making the market a natural extension for Pharmacy2U,” said Pharmacy2U chief executive Kevin Heath.
“This acquisition is an important step in delivering [our] growth strategy and is fully aligned with our approach of partnering with high-quality businesses that leverage our scale and core competencies,” he added.
In May last year, the digital pharmacy partnered with IT developer Healthcode to deliver prescriptions more efficiently by integrating secure electronic prescriptions and a next-day delivery service.
NHS BACKS AI NOTE-TAKING
WHILE some scepticism remains from doctors about the use of AI within a healthcare setting, the government, business and consumers have embraced the technology wholeheartedly. The latest Barclays Business Prosperity Index showed that healthcare companies plan to increase investment in AI over the next 12 months, and the recent EY Consumer Health Study indicated a strong appetite from consumers for smart homes and digital health solutions to help them age independently.
The government is now backing the use of AI note-taking rules in surgeries.
It is encouraging NHS organisations across England to take advantage of a new national registry of 19 suppliers for the technology, which captures clinician-patient conversations and uses AI to generate real-time transcriptions and clinical summaries.
It believes that embracing the cuttingedge tools, known as ambient voice technologies, could save clinicians up to two or three minutes for each patient consultation, which would free up more time for them to see other patients.
“AI notetaking tools will help free up more time for clinicians to focus on their patients, rather than typing up notes or looking at a screen –enhancing the quality of consultations and improving overall patient satisfaction,” said NHS England national chief clinical information officer Alec Price-Forbes. “We are working with NHS organisations to help them implement the technology
safely and effectively – helping to make the NHS the most AI-enabled healthcare system in the world, as we shift from analogue to digital.”
NHS England has published a selfcertified registry for the technology, which requires suppliers to comply with standards on clinical safety, technology and data protection.
The registry of suppliers is being launched following NHS guidance published last year advising NHS organisations to use AI notetaking tools which are safe, evidence-based and deliver benefits for patients.
AI notetaking technology tested across nine NHS sites has been proven to free up clinicians to spend nearly a quarter more time with patients. An NHS England-sponsored study published last year found that AIscribing technology can reduce clinician workload while improving patient care, with the potential to unlock millions of pounds worth of activity if rolled out nationally. Led by Great Ormond Street Hospital for Children NHS Foundation Trust’s Innovation Unit (GOSH DRIVE), it was conducted across nine NHS sites in London to assess the impact of an AIscribing tool.
More than 17,000 patient encounters were evaluated across a diverse range of sites, including hospitals, GP practices, mental health services and ambulance teams.
Results showed a 23.5% increase in direct patient interaction time during appointments, alongside an 8.2% reduction in overall appointment length when AI-scribes were used. A&E saw particularly strong results, with a 13.4% increase in patients seen per shift.


Trusted by Clinicians, Chosen by Patients
Located in the Harley Street Health District, Pharmacierge supports over 4,500 GPs and Consultants with seamless, secure e-Prescribing apps tailored for private practitioners.
With our state-of-the-art robotically enabled dispensary and nationwide delivery, we ensure your patients receive their medications promptly, while you prescribe with confidence - anytime, anywhere.
mPrescribe®
Revolutionises private prescribing by allowing you to prescribe flexibly without a laptop, for delivery to your patients nationwide.
Medication range
Due to the range of specialists we support, we stock and source medication not typically found outside of a hospital setting, including refrigerated, controlled, injectable and biologic medication.
Courier delivery
We include same weekday delivery to London postcodes, or next weekday nationally as standard. International deliveries are also available.

"Your mobile app changed my life!"
— Dr Dominic Paviour, Consultant Neurologist "Intuitive and secure."
— Dr Tim Wigmore, Consultant Intensivist & Anaesthetist
Join thousands of clinicians today. Download the app and register online www.pharmacierge.com/register




NEW GUIDANCE FOR IONISING RADIATION USE
THE Health Research Authority has published new guidance for the set-up of NHS studies involving ionising radiation and the interpretation of the Ionising Radiation (Medical Exposures) Regulations.
The guidance is for all those involved in the set-up and delivery of research studies involving ionising radiation as part of medical (diagnostic or therapeutic) exposures delivered in the NHS in England, Wales and Northern Ireland.
It has been developed in response to inconsistencies in the interpretation of Ionising Radiation (Medical Exposures) Regulations in NHS organisations’ standard operating procedures. This has resulted in unnecessary steps in the set-up of research studies involving ionising radiation exposures, which causes delays.
“Protecting research participants always comes first, and IR(ME)R is a critical part of that, where studies involve ionising radiation,” said Health Research Authority chief executive Matt Westmore.
“But there isn’t always enough capacity to carry out all the radiation reviews that are needed when they are needed. The HRA supports study-wide radiation reviews that reduce the need for duplicate reviews at site, and provides consistent technical information to help set up and start early. This guidance will help local reviewers make the best use of those national assessments,” he continued.
The inconsistencies were identified by the UK Clinical Research Delivery (UKCRD) programme, a cross-sector programme of work of which the Health Research Authority is part.
HOW TO COUNTER THE USE OF AI IN INTERVIEWS
THE use of artificial intelligence by students in interviews has become such an issue that there are growing calls to ban virtual interviews altogether to stop cheating. In September last year, the Four Nation Postgraduate National Recruitment Programme Board published a position statement on the issue.
Although it recognised that some applicants may use assistive technologies to support communication or processing needs, it was very clear.
“To ensure a fair and equitable interview experience for all applicants, the use of AI technologies, including but not limited to AIgenerated responses, virtual assistants, real-time transcription tools, and automated scripts, will not be permitted during online interviews,” it said.
Some Trusts have even refined the guidance further about how AI can and cannot be used. Leeds and York Partnership NHS Foundation Trust, for example, has published its own guide to using AI in recruitment.
Now the Confederation of British Surgery (CBS) has echoed the concerns of the wider sector around the reports of ambient AI being used in interviews to decide who is accepted into surgical training vacancies.
“CBS wholeheartedly supports this call for a return to face-to-face interviews in light of a situation that seriously compromises fairness and integrity,” said CBS president Mark Henley.
“Our profession is built on trust and accountability, and by allowing

applicants who have not upheld those values at the very first stage of their careers, we risk undermining the credibility of the surgical training system as a whole,” he added.
Ambient AI is a type of artificial intelligence system that can run in the background, constantly active and responsive. In the context of interviews, it can listen, analyse and respond without prompting, meaning that the interviewee will get real-time suggested answers displayed on their device screen.
As the interview will also be on a screen, and the AI response appears as an overlay, the candidate will exhibit few telltale eye movements, and there will be no need for them to type the questions into the software. For this reason, it is very difficult to detect if a candidate is using it. The real-world issue with this is that a candidate could appear to be prepared, well-structured, and knowledgeable about a certain
subject, thus falsely enhancing their potential, whilst potentially knowing very little about what they are speaking about.
Virtual interviews and virtual technical assessments have recently been in the news due to big tech companies having concerns around candidate integrity.
Google has reintroduced in-person interviews for this very reason, amid reports that more than 50% of candidates are using AI tools to solve coding challenges during virtual interviews.
Other corporations reimplementing face-to-face interviews, or rejecting remote hiring, include such companies as McKinsey, Cisco and Deloitte.
The virtual interviews in question are overseen by Medical and Dental Recruitment and Selection (MDRS), the national body responsible for running and coordinating recruitment for all postgraduate medical and dental training across the UK.
MDRS brought in virtual interviewing during and after the COVID-19 pandemic, allowing applicants to log in remotely and take their interviews online.
“The best way to definitively eliminate AI use in interviews is to conduct them face-to-face. We therefore strongly urge MDRS to immediately revert to face-to-face interviews for the upcoming recruitment rounds for both core surgical training and for higher speciality training, to protect the validity and integrity of the selection process, and the safety of our patients,” said Oliver Townsend, president of the British Orthopaedic Trainees Association.
AI-ENABLED STETHOSCOPES HELP DIAGNOSE HEART CONDITIONS
ANEW AI-enabled stethoscope designed to detect serious heart conditions spots them faster and more frequently in primary care.
The clinical trial, called TRICORDER, led by researchers at Imperial’s National Heart and Lung Institute and Imperial College Healthcare NHS Trust, and supported by the Imperial Biomedical Research Centre (BRC), examined if the technology could detect heart conditions such as heart failure, arrhythmias and valve disease.
The study found that although the technology worked well, it didn’t significantly increase the overall number of heart failure diagnoses. This was primarily because too many GPs did not use the device consistently in routine clinical practice.
When doctors used the AI stethoscope as intended, the technology detected

these cardiovascular conditions faster and more frequently. This suggests the device performed well, but it will only have a significant impact on patient care when doctors use it frequently and receive the training to do so correctly.
“Our trial suggests AI tools like smart stethoscopes help us detect heart conditions earlier, but only if they are used and properly integrated into everyday clinical practice,” said Patrik Bachtiger, one of the researchers who led the study.
“Although the technology performed well, the impact it could have in the real world depends on doctors being able to use the technology easily during busy clinics.”
The TRICORDER trial involved 205 NHS GP practices and more than 1.5 million registered patients in the UK.
Over the year-long study, doctors performed nearly 13,000 AIassisted heart examinations. Patients examined with the AI stethoscope had significantly higher detection rates – nearly twice as many new heart failure cases and three times as many detections of irregular heart rhythms – compared to patients who were not examined with the AI device.
GMC PLACES CONDITIONS ON BASILDON UNIVERSITY HOSPITAL
THE General Medical Council (GMC) has placed conditions on the anaesthetics training programme at Basildon University Hospital, part of Mid and South Essex NHS Foundation Trust, following issues relating to patient safety and the quality of postgraduate medical education.
The GMC said that it had taken this action to address a range of issues, including “failures to protect doctors in training from sexual misconduct, misogyny and undermining behaviours, as well as inappropriate staffing levels within the department”.
As a result of these concerns,
doctors in training in anaesthetics are currently not working in the department, and the GMC has said that it will require evidence of change before conditions can be removed and before they can return.
“We work to make sure that education and training prepare doctors to deliver good, safe patient care by setting high standards and expected outcomes,” said the GMC’s director for education and standards Pushpinder Mangat.
“We need assurance that the required standards and the conditions imposed are being met, including the creation of a working culture where doctors can
raise issues openly, without fear of repercussions.”
The conditions for reinstatement include processes put in place that ensure the department is staffed with qualified educators; processes put in place to foster a culture where doctors in training can openly and safely raise concerns about patient safety, wellbeing, education, and training without the fear of adverse consequences; appropriate mechanisms in place that ensures doctors in training are not subjected to sexual misconduct; and governance systems which monitor and demonstrate quality in patient safety, education and training with accountability held at board level.
MHRA ISSUES GUIDANCE FOR MENTAL HEALTH APPS

THE Medicines and Healthcare products Regulatory Agency (MHRA) has published new advice on using apps and other digital tools to support mental health.
More people in the UK, particularly young people, are turning to digital tools for mental health support.
From symptom-tracking apps to virtual reality therapies, these products are now widely available and often used alongside NHS and community care, but it is not always clear which are reliable, safe or right for an individual.
“As a GP, I’ve seen how patients can benefit from accessing digital tools alongside traditional forms of care. This guidance supports better conversations between clinicians and patients and helps everyone ask the right questions about whether a tool is right for them,” said MHRA chair and Oxford University’s professor of primary care, Anthony Harnden.
The new online resources use short animations and real-world examples to show what safe, well-evidenced digital mental health technologies look like in practice, and explain how to report concerns through the MHRA Yellow Card scheme so action can be taken to protect others.
The guidance is aimed at anyone using these technologies, as well as parents and carers, and includes professionals who often recommend them, including teachers, nurses, GPs and mental health practitioners.
The advice is a five-point checklist for patients to use before they jump into a digital mental health tool.
First, does the product offer general wellbeing support, or does it claim to diagnose, treat or manage a mental health condition? Claims about medical benefits should be clearly explained and supported by evidence.
Second, who is it for? A tool built for adults may not be suitable for teenagers or children. Age and
intended users should be clearly stated.
Next, trustworthy products will explain how they have been tested or evaluated, for example, in a clinical study. People should be cautious of products that make big promises without clear supporting information.
Then, patients need to ask how the data is used and stored. These tools often collect very sensitive personal information. Patients should be able to easily find out how your data is stored and used.
And finally, patients should ask whether the tool is regulated as a medical device.
“As more people turn to digital mental health technologies for support, we need practical ways for regulators, developers, and healthcare providers to work together so that safe, effective interventions reach those who need them,” said head of digital technology, discovery research and mental health at Wellcome, Matthew Brown.

NHS WALES’ NEW APP CONTINUES TO EVOLVE
THE NHS Wales App is indeed the digital front door to the NHS. More than 650,000 people have registered to use the bilingual NHS Wales App since it launched in April 2023, equivalent to one in five adults in Wales.
In a written statement to the Senned at the end of January, Sarah Murphy, minister for mental health and wellbeing, said that more than 657,700 people have registered to use the app. Almost 5,000 people have been able to register using the new Welsh Identity Verification Service, which allows people’s identification to be verified at GP surgeries for those unable to use the standard NHS Login service. More than three million repeat prescriptions have now been ordered. People are able to view their health and prescription history, and access trusted health advice and information, including screening and wellbeing services via the app. It also allows people to use secure messaging and provide feedback.
Murphy also outlined new services that had been introduced over the last few months. People can also view their referral to a hospital waiting list and get details of their hospital appointments, including directions and supporting information.
“Future developments will include summary health records and test results being available for people on the app,” she said.
In a plenary statement to the Senned, Murphy explained that this isn’t just an app that allows us to check basic facts and figures about health services.
“This is a useful and powerful platform with a huge potential to change the way we all use and interact with our health service. It represents a fundamental shift in how we empower people to engage with their healthcare and health services,” she said, adding that it is “perfectly placed to evolve into the digital front door of the NHS”.
This stands in stark contrast to
Scotland, where the Scotland NHS app is rapidly turning into a disaster. In an interview at the end of last year, Neil Gray, Scotland’s secretary for health and social care, said he “can’t pretend to know” why Scotland’s NHS app is lagging behind England’s in development.
NHS Wales was happy to adapt NHS England’s app, while Scotland’s app is being developed independently by NHS Education for Scotland, in partnership with the Scottish government and local government group COSLA.
As Healthcare Today reported in December, the refusal of the SNPdominated parliament to reuse the NHS app was due to the “political optics of adopting an English solution”. Instead, it has already spent £17 million on its own app.
MyCare.scot, Scotland’s new health and social care online app, will be made available to everyone across Scotland from April, but it will not be completed until 2030.


THE PRIVATE SECTOR CAN HELP CUT COMMUNITY WAITING TIMES
THE Independent Healthcare Providers Network, the representative body for independent sector healthcare providers, has called for the private sector have a greater role in cutting NHS community waiting times.
NHS waiting lists have increased by 23% since 2022, and the establishment of a new target for 80% of community patients to receive treatment within 18 weeks appears a challenge.
“Independent health care providers working at scale are perfectly placed to apply their national-level understanding of what works when delivering services to local needs, supporting consistency of provision and improving patient outcomes and experiences,” a new report from the body says.
The report comes a year after prime minister Keir Starmer struck an agreement with the independent sector as part of plans to end the hospital waiting list backlog.
“When the waiting lists have ballooned to 7.5 million, we will not let ideology or old ways of doing things stand in the way of getting people’s lives back on track,” he said last January.
The IHPN’s new report argues that independent providers who deliver community care “at scale” have a vital contribution to make in bringing much-needed capacity and capability to local communities and achieve the NHS’s vision for “neighbourhood health”.
The industry body points out its members have a national footprint, with some providers delivering care covering around 10% of the population nationally. This means that they can use data and insight to understand and apply “what works” in pathway design across multiple contracts and areas.
They have the financial backing to invest in new and improved services, with access to private capital that public providers simply don’t have in the current fiscal climate.
IHPN members generally have centralised back-office functions, systems, processes, and skills which provide greater resilience and efficiency, which would be impossible for smaller local providers to achieve.
“We cannot fix the NHS by focusing solely on elective care while community services remain in a blind spot.
That approach is counter-productive and not in patients’ interests,” said IHPN’s director of policy Danielle Henry.
With NHS community services under huge strain and patients waiting far too long for much-needed care and support, significant capacity and resources will need to be brought in.
“Independent healthcare providers are already using their size and reach to deliver precisely the kind of accessible high-quality care to NHS patients that new Neighbourhood Health Services are seeking to achieve,” she added.

Providing first class medical consulting and therapy rooms at prime locations in Central London and Liverpool
London
tenharleystreet.co.uk 020 7467 8300
Liverpool eightyeightrodneystreet.co.uk 0151 709 7066
Harley-quarter-ad-60x100.indd 1

MOMENTUM IN BRITAIN’S BIOTECH MARKET
Against a challenging market backdrop, the UK biotech sector ended last year with signs of renewed momentum and increased investor confidence.
According to the BioIndustry Association’s latest report, the UK retained its position as Europe’s leading national biotech market throughout the year, representing 30% of all European venture financing, despite a 13.2% year-on-year drop in venture capital investment, totalling £1.79 billion across 58 deals.
While much of last year was characterised by investor caution, the final quarter delivered an unmistakable shift. A record 22 completed deals –the highest quarterly deal count of the year. This renewed deal flow, the association said, signals the beginning of a healthier distribution of capital across the biotech ecosystem.
There is no getting away from the fact that almost half of total capital raised last year (47%) came from just two transactions in the first quarter. The investments in Isomorphic Labs and Verdiva Bio transactions contributed to a sharp rise in the average deal size to £30.8 million – up from £18.7 million in 2024.
13/10/2016 11:08
Beyond private capital markets, strategic transactions provided a strong indicator of sector confidence. MSD’s £7.5 billion acquisition of Verona Pharma was one of the largest global biotech exits in recent years and underscored sustained international appetite for high-quality UK biotech despite the absence of IPO activity. Major acquisitions by Sanofi and other global pharmaceutical leaders further reinforced this trend.
The macro-environment going into 2026 should also bolster UK biotech. The Nasdaq ended last year at an all-time high, investor sentiment is strengthening, and the association says the UK-US pharmaceutical trade deal has reinforced confidence in the UK market.
Crucially, it adds, last year saw the policy foundations laid for a new era of domestic capital deployment – most notably the Life Sciences Sector Plan, the Mansion House reforms, and the first evidence of pension-backed investment into the sector through the Draig Therapeutics financing and Aviva investing in Cambridge Innovation Capital.

BUSINESSES PLAN TO EXPAND FUNDED PMI SCHEMES
ALMOST a third of employers who don’t already offer private medical insurance (PMI) to employees are considering doing so within the next three years.
The findings from Broadstone’s second Employee Benefits Landscape Report found that the percentage of organisations without PMI but with definite plans to introduce it rose from 9% in 2023 to 11% last year, with those considering it increasing from 15% to 20%. Those with no PMI plans on the horizon fell from 74% to 68%.
The growth in healthcare benefits is seen across other areas. The proportion of employers offering clinic-based screenings rose from 20% in 2023 to 25% with the proportion of businesses providing onsite day screenings increased from 7% to 10%. Likewise, the health cash plan market expanded in 2024, which is reflected in the proportion of businesses offering this service to employees, moving from 24% in 2023 to 26% last year.
More than a quarter (26%) of employers are considering
introducing a health cash plan in the next three years.
“Healthcare benefits, such as private medical insurance (PMI) and health cash plans, are becoming an essential part of benefits packages, especially in competitive industry sectors,” said Broadstone’s head of health and protection Brett Hill.
“What’s particularly striking is the growing pipeline of employers actively planning to introduce or expand healthcare benefits over the next few years. Organisations are also taking a more preventative approach, with greater uptake of screenings and health cash plans, reflecting a broader shift towards early intervention and long-term workforce resilience,” he continued.
The growing corporate enthusiasm for PMI in the Broadstone report is echoed in the latest figures from the Association of British Insurers (ABI), which show that private medical insurance claims in 2024 jumped 13%, while Healthcode shows that this continued into 2025.
As Healthcare Today reported at the end of January, health insurers
processed a record £4 billion in individual and workplace private medical insurance claims in 2024 – up 13% compared to 2023 (£3.57 billion).
The ABI also said that the total number of people covered by health insurance increased 4% from 2023 to reach 6.5 million in 2024. Figures show 4.8 million of these people were covered by workplace policies – a second consecutive record in more than 30 years of data collection.
Fourth quarter data from Healthcode also showed that insured healthcare activity reached a peak in the final three months of 2025. The UK’s official clearing organisation for medical invoices processed three million invoices for private healthcare providers in the final three months of the year, up 5% both on the previous quarter and up 5% on the same period in 2024.
“The NHS remains under significant pressure, which means that businesses increasingly view access to timely diagnosis and treatment as a critical factor in supporting employee wellbeing, productivity and retention,” said Hill.





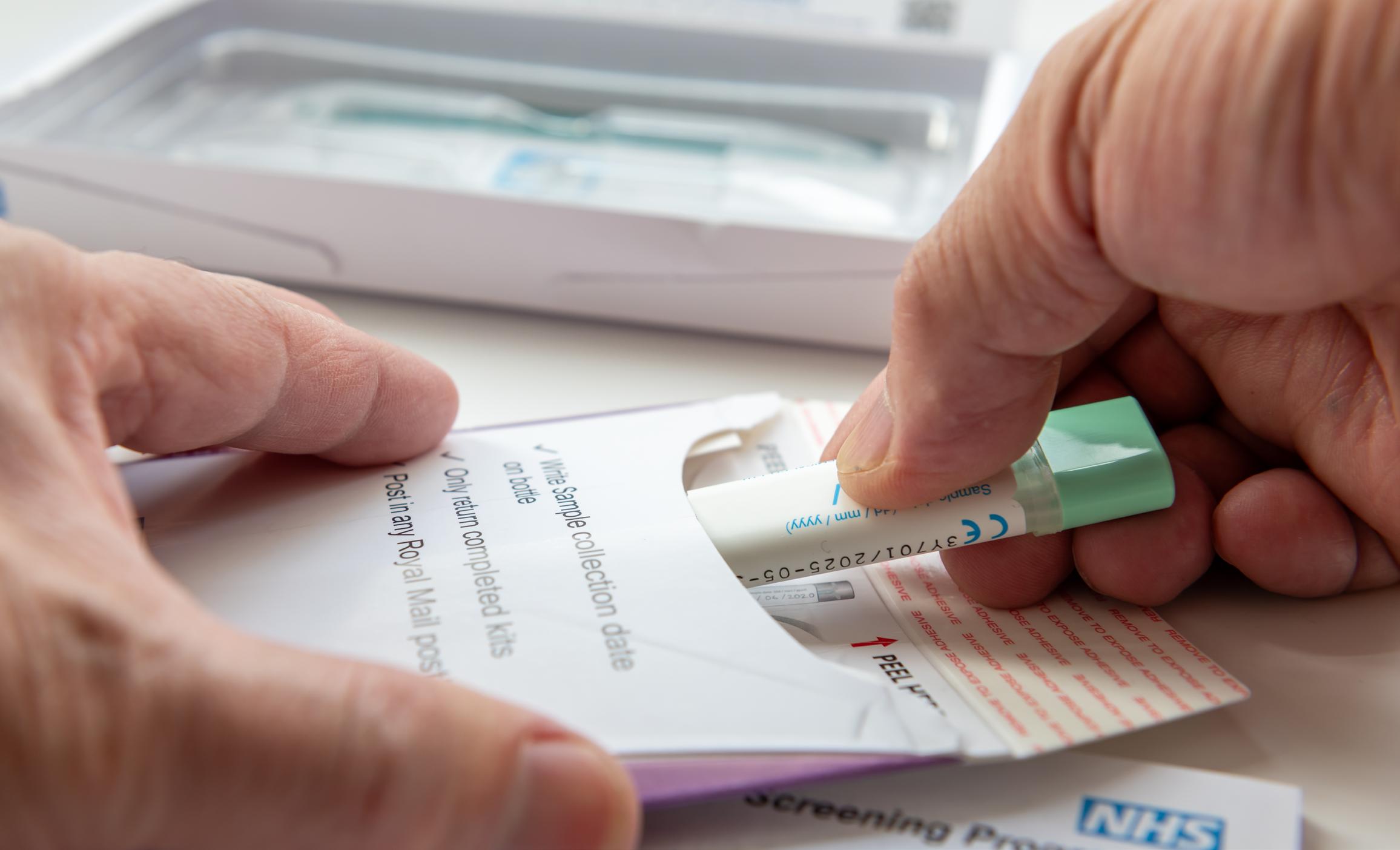
NHS ENGLAND TO INCREASE BOWEL CANCER SCREENING
NHS England has said that it is to lower the threshold for a homescreening kit to trigger urgent cancer testing in a move that could save thousands of lives.
The NHS estimates the change could help detect around 600 more bowel cancers early each year in England – around an 11% increase – and find 2,000 more people with high-risk polyps in their bowel, allowing patients to have preventative surgery before any cancers develop.
At the moment, the home-testing kit, known as the faecal immunochemical test (FIT), is offered to all people over 50 years old and checks for blood in a small stool sample, which can be a sign of bowel cancer. By reducing the level at which traces of blood in a FIT test trigger further investigation – from 120 micrograms of blood per gram of faeces down to 80 – the NHS will offer 35% more
screening colonoscopies each year to help diagnose or rule out bowel cancer.
“This is a major step forward in bowel cancer detection and will help save hundreds more lives from this devastating disease,” said Peter Johnson, national clinical director for cancer at NHS England.
“Testing at a lower threshold will now provide a better early-warning system for bowel cancer, helping us to spot and treat cancers earlier, often picking up problems before symptoms appear,” he continued.
Bowel cancer is the third most common cancer in the UK for both men and women, and the fourth overall, but screening can catch it early. It is estimated that, currently, around two in 100 people who take part in bowel screening will require further testing – this is expected to increase to three in 100 following the lowering of the threshold.
Once fully implemented, testing at the lower threshold is expected to reduce late-stage diagnoses and deaths from bowel cancer by around 6%, while it is estimated that preventing and detecting more cancers earlier will also save the NHS £32 million each year.
The roll-out follows a pilot at eight early-adopting services, where closer working between NHS screening and diagnostic teams has helped more people get checked sooner, with more than 60 additional cancers and nearly 500 high-risk polyps being found and treated.
“This vital step from NHS England to lower the threshold for further tests after bowel screening will save lives. It means more cancers will be detected at an earlier stage, when treatment is more likely to be successful, while also preventing some from developing in the first place,” said Michelle Mitchell, chief executive at Cancer Research UK.
TIM MITCHELL:
THE SURGICAL CAPACITY
IN THE current landscape of the NHS, the headlines are dominated by a recurring theme: a system under immense strain. While the elective recovery backlog remains a top priority for the government, the reality on the ground for surgical teams is one of many hurdles. From a crumbling estate and aging IT infrastructure to the critical shortage of intensive care beds, the path to the operating theatre has never felt more congested.
Tim Mitchell, president of the Royal College of Surgeons of England, speaks with Healthcare Today about the urgent need for capital investment, the shift toward preparation lists to keep patients fit for surgery, and the expanding role of robot-assisted technology in the modern operating theatre.
You can’t open a newspaper without being hit by issues of ward space, bed availability, theatre access and maintenance challenges of hospital theatres. How are they affecting surgical throughput at the moment?
It is a significant problem. We have recently conducted our second census of the surgical workforce, and it shows broadly similar findings to those from two years ago. Little has changed over that period. More than half of consultants and other staff report that one of their main frustrations is not being able to access operating theatres for a variety of reasons, some of which you have already mentioned.
One issue is simply the number of theatres available. The vast majority of consultant surgeons have two half-day operating lists or fewer in their weekly timetable. That is partly because, over the past 20 years, there has been a significant increase in the number of consultants without a matching increase in the number of operating theatres.
Even where facilities exist, there are staffing constraints. A fully functioning theatre requires a complete team – nurses, an anaesthetist and other theatre staff – as well as a hospital bed for
The president of the Royal College of talks about why an increase in consultants an increase in the number of operating
Written by Adrian Murdoch.
the patient afterwards. Critical care and intensive care beds are a particular pressure point. Many colleagues experience the frustration of arriving at work expecting to operate on a patient they have assessed and prepared, only for the case to be cancelled if, for example, a required intensive care bed is unavailable. Those beds cannot always be ring-fenced for surgical cases because of emergency demand.
For the patient, who has come to hospital expecting surgery, having prepared psychologically and made the necessary arrangements in their personal life, a last-minute cancellation is absolutely devastating. Sadly, this is not an uncommon story. It reflects a combination of pressures coming together across the system.
Surgical hubs – I think there are 123 in England at the moment – are seen as part of the solution to backlog challenges. Are they a sticking plaster or are they useful?
Surgical hubs are very useful and are part of the solution to this problem. The college has been advocating for them, particularly the concept of ringfenced facilities for elective, planned surgery, which is considered very important.
One of the difficulties is that hospitals are often full of emergency cases. Ring-fenced facilities allow surgical activity to continue even when the wider system is very busy. Surgical hubs are particularly suited to high-volume, low-complexity cases because they enable a large throughput, but they are not limited to these.
Surgical hubs must They need to add for it, with appropriate efficient use. It include training The surgical census concerned about access the operating training the next not be a future must be embedded expansion.
The Royal College that waiting lists as “preparation this mean?
The concept is someone on a then effectively about them until an operation arrives. times can be quite creates an opportunity patients are as the time they come That can include them to stop smoking, exercise, and to cardiovascular
The college contributes for Perioperative alongside the Royal Physicians and
MITCHELL:
CHALLENGE
Surgeons of England
consultants isn’t matched by operating theatres.
must not undermine existing capacity. add capacity rather than substitute appropriate staffing, rostering and is also important that surgical hubs training for the next generation of surgeons. census found that trainees are about their opportunities to operating theatre. Without next generation, there will service, so training embedded within service
College has suggested lists be thought of “preparation lists”. What does
to avoid placing waiting list and effectively forgetting until their turn for arrives. Waiting quite long, and this opportunity to ensure fit as possible by come in for surgery. include encouraging smoking, to to improve their fitness.
contributes to the Centre Perioperative Care (CPOC), Royal College of a number of other

organisations, with a focus on how to improve care in the perioperative period. A key element of that work is ensuring patients are in the best possible condition when they come in for surgery.
Experience after the COVID-19 pandemic illustrated the reverse situation, where the general health of patients deteriorated between being placed on a waiting list and eventually coming in for surgery. By the time they were called, their overall health was sometimes worse than when they were first listed.
This raises several considerations. An operation may no longer be appropriate, further tests may be needed to prepare for surgery, or treatment may be required for conditions such as high blood pressure or diabetes, which can delay surgery. The aim is to avoid putting people on a waiting list, calling them later, and finding that an opportunity has been lost either to improve their fitness for surgery or, if they are not in the right condition, to ensure surgery is safe at that point.
The Royal College has described the government’s waiting list pledge as “near impossible” to meet without urgent investment. What needs to happen now to make progress on waiting times? Is it just hard cash?
A huge amount of public money is spent on the health service, and it needs to be used as efficiently as possible. At the same time, there is a major problem with NHS estates. Some buildings are literally falling apart, including issues such as reinforced autoclaved aerated concrete, and there is a substantial maintenance backlog across NHS facilities, which has a significant impact.
IT systems are also not where they should be. Many clinicians find it frustrating that systems do not interact well with each other. There is
a strong view that capital investment is needed in estates and IT to help address these problems.
Alongside that, services need to be used as efficiently as possible to maintain throughput, including through measures such as surgical hubs. Returning to the 92% 18-week target by the end of this parliament is seen as very ambitious, and there is a view among a number of organisations that it may be extremely difficult to achieve.
It is difficult to identify a single solution. The reasons for the current situation are multifactorial, and any
solution therefore also has to be multifactorial. Investment in estates and IT is particularly important, especially when looking to the future.
Healthcare Today has written extensively about robotic-assisted surgery. Is it the Holy Grail that people think it is?
It is important to talk about robotassisted surgery rather than robotic surgery, because there can be a public perception of an autonomous robot carrying out an operation on its own. That is not where things stand. In robot-assisted surgery, the surgeon remains in control.
In certain fields, it has been a major advance. It is well established in prostate and kidney surgery and is becoming increasingly established in bowel surgery. From a clinical perspective, establishing evidence of effectiveness is paramount. Patients need to receive treatments that are proven to be safe and effective. That evidence base exists for prostate and kidney surgery and is developing in bowel surgery. There also needs to be suitable regulation and governance around how it is introduced. Systems should be introduced in a structured way, with each hospital having arrangements for oversight.
A key priority is equity of access –equal access for patients across the country and equal access to training for both current and future surgeons.
We have tried to highlight the issue of burnout in the medical profession, and it is an issue that the recent workforce census highlights. How can surgical careers be made more sustainable?
Indeed, this is borne out by our surgical census report, and it is a point we continue to highlight. We must recognise that our workforce is one of our strongest assets; we have a duty to protect and nurture them.
In my meetings with ministers, they have explicitly stated their intent to make the NHS the best employer in the country. That is the standard we should be aiming for, and there is now a genuine recognition of its importance.
The responsibility also lies with individual trusts in England and health boards across the devolved nations to acknowledge this and implement the necessary support.
We have seen examples of exemplary practice; Northumbria, for instance, is often held up as a beacon because of the immense support it offers its staff. We witnessed this first-hand during a visit to their hospital, which was, of course, the trust formerly led by Jim Mackey [now chief executive of NHS England].
We must be honest: across the board, workforce morale is currently poor. The NHS has functioned on goodwill for a very long time. Doctors, nurses, and all members of staff arrive at work with the sole intention of providing the best possible care; it is only right that we look after them in return.
What are your expectations for the next census report? What will you be turning to when the results come in that you won’t see change the most?
By the time of the next report, we hope to see a marked improvement in our core metrics. We want to see fewer colleagues reporting high levels of stress and burnout. We also want to see clinicians spending more time in the operating theatre, and for our trainees to report better access to high-quality training opportunities. Ultimately, we expect these improvements to translate into the broader metrics by which the health service is measured: increased productivity and a sustained reduction in the elective recovery backlog.
THE SILENT THE
THE primary care workforce crisis is usually framed as a numbers problem. Too few GPs and nurses are cited as the root cause of not enough capacity to meet demand.
But while these pressures are real, they mask a deeper and more uncomfortable truth: the system is losing clinicians not because they don’t want to care, but because the way we ask them to care has become psychologically unsustainable.
As a practising NHS GP, I see this daily. Primary care clinicians are carrying limitless patient demand within appointment structures that are no longer fit for purpose. Tenminute consultations are expected to absorb increasingly complex clinical presentations, safeguarding concerns,

SILENT EMERGENCY BEHIND WORKFORCE CRISIS
Anshumen Bhagat, NHS GP principal and chief medical officer at private healthcare provider GPDQ, argues that mental health is central to successful health systems.
administrative burdens and emotional labour – all within fragmented systems that rarely speak to one another. The expectation is not just clinical competence, but infinite resilience.
This erosion of well-being is no longer anecdotal.
The 2024 NHS Staff Survey revealed that 41% of staff reported being unwell due to work-related stress in the past year. That figure should concern us not only as clinicians but as leaders and system designers. Burnout is not a personal failure; it is a predictable outcome of poorly designed operating models.
Mental health is infrastructure, not a soft
issue
In healthcare, we are comfortable talking about infrastructure in terms of estates, digital systems or workforce numbers. We are far less comfortable recognising that clinician mental health is core infrastructure too. When clinicians feel they can never finish their day because work is endlessly unfinished and emotionally unresolved, the system accumulates hidden risk. This often surfaces as reduced decision quality, presenteeism, attrition and ultimately, compromised patient care.

From a business and governance perspective, this is not just a well-being issue. It is an operational and financial one. High turnover, sickness absence and reliance on short-term fixes cost organisations far more than investing in sustainable workforce design upfront.
If we want resilient healthcare systems, whether public, private or hybrid, we need models that align three fundamentals.
These are clinical autonomy, strong governance – with consistent standards, clear accountability and patient safety at scale – and flexible work design with careers that are sustainable over decades, not just tolerable for a few years.
There are solutions out there. Independent platforms that provide and support nationwide healthcare services are often built around these principles from the start.
The goal is not to pull clinicians away from the NHS, but to support them across portfolio careers that span NHS, private and hybrid settings. Variety of work as well as peer support and psychological safety are not indulgences - they are protective factors against burnout for healthcare professionals across the breadth of primary care.
Crucially, this approach does not mean lowering standards. In fact, strong clinical governance becomes even more important. Clinician-led decisionmaking and robust quality oversight
are what allow flexibility and scale to coexist. When clinicians are trusted and supported to work within well-governed systems, both quality and satisfaction improve.
Private and hybrid models as innovation testbeds
The reality is that the NHS, by its nature, is risk-averse and structurally constrained. That makes large-scale experimentation difficult. Private and hybrid models can act as testbeds for innovation to pilot new workforce structures, governance frameworks and uses of technology that prioritise both quality and clinician wellbeing. They allow faster iteration and the ability to design services around both patient outcomes and clinician experience.
The opportunity is not to pit sectors against one another, but to learn across them. What works in a well-governed private setting can inform NHS reform; what defines excellence in NHS care should set the benchmark everywhere else.
The workforce crisis will not be solved by recruiting more clinicians into systems that exhaust them. It will be solved by designing environments where clinicians can do their best work and feel professionally fulfilled, increasing the likelihood that they remain in practice for the long term. Portfolio careers, flexible models and psychologically safe working environments should be seen as sustainability tools, not exits from the system.
Mental health and well-being are not side conversations. They are signals telling us whether our systems are fit for the future. If we listen and design accordingly, primary care can move from survival mode to sustainability.
PAUL CLINICAL CHANGING
SINCE taking the helm of Circle Health in July last year, Paul Manning has moved quickly to implement a vision centred on clinical leadership. A career physician who transitioned from chief medical officer to chief executive, Manning brings a practitioner’s perspective to a massive organisation that includes 54 clinical sites and a network of 6,500 doctors. Here, he talks to Healthcare Today about drivers behind the surge in private medical insurance usage among younger demographics, the group’s evolving relationship with the NHS, and his plans to integrate high-acuity surgical care with new, digitally enabled preventative health platforms.

PAUL MANNING:
CLINICAL LEADERSHIP IN A CHANGING CLIMATE
The chief executive of Circle Health discusses transitioning from the operating theatre to the boardroom and why the future of the sector must be medically led.
Written by Adrian Murdoch.
Circle saw an 18% jump in private medical insurance-funder treatment last year. What is behind this growth?
There has been significant growth in the total market size, which really kicked off during the COVID-19 pandemic because access to healthcare became so difficult.
With corporately funded health insurance, there is often an initial period where new entrants lack cover or eligibility – sometimes for as long as 12 months – until the next rollover cycle. Since then, the number of lives covered has progressively increased. There is no doubt, however, that within that insured group, certain demographics are now using their insurance much more frequently than before. We have seen unprecedented growth in the 30-to-44-year-old age group using private medical insurance for primary care access; historically, we saw tiny volumes in that area, but it has now
become a substantial part of the business. Naturally, this leads to further healthcare encounters, as a reasonable proportion of those initial consultations develop into referrals and onward treatment. That is a key driver of the growth. Furthermore, there has been a notable rise in employee benefit trusts, with employers opting for these over traditional underwritten products to provide care for their staff. We are also seeing an increase in the use of the occupational health route, as companies strive to get people back to work more quickly, bypassing the inevitable delays currently found in some NHS facilities.
The government appears very open to working with the private sector in a way that previous governments haven’t. How does Circle view its role in complementing NHS capacity?
It is important to recognise that we are a very long-established, key supplier of services to the NHS and
I don’t see that changing. Naturally, the nature of that interaction shifts slightly with different administrations or – dare I say – various reorganisations of the NHS, and we have had to remain adaptable. It is also a regionally engaged customer rather than a centrally engaged one, and there are vast variations between the regions. Our strength lies in flexing to work with the NHS where appropriate.
While the NHS represents a relatively small part of our overall business – probably two-thirds, of our work comes through the privately funded route – it remains an important component, and we are proud of the contribution we make to the NHS in its various forms.
We have moved through the initial surprise of working with the private sector. How do you see it evolving from now on?
We are living in interesting times. Because we are in a financially constrained climate, certain parts of the NHS are facing material difficulties in deciding how best to deliver elective recovery targets.
Clearly, there is a focus on highpriority clinical conditions. I believe these will always be treated in the most accessible and appropriate location – primarily within mainstream NHS hospitals or, where
the independent sector can deliver to that standard, we will certainly do so, and we will do it quickly.
The difficulty regarding funding availability arises, perhaps, with routine elective care. Amidst financial constraints, there is an inevitable need to secure the best possible value for every pound spent, both within the NHS and the private sector. We are very much up for delivering that in the most cost-effective way possible. As an industry, and certainly as a company, we are absolutely committed to working within the tariff – or better, if we can – across all forms of care.
Circle absorbed BMI Healthcare in 2020 and was itself acquired by Abu Dhabi’s PureHealth in 2023. With rapid growth and ongoing integration how do you uphold clinical governance and consistent care standards?
Ultimately, that transformation is what I was put in place to deliver during my tenure as chief medical officer. We are a very large organisation, operating across 54 different clinical sites and a variety of back-office locations. We have assimilated not only BMI and Circle, but several new acquisitions as well – most recently, the Fairfield Independent Hospital near St Helens.
To manage this, we maintain a single clinical policy across the entire organisation. We have one Board Assurance Framework, one underlying Governance Assurance Framework, and a unified modus operandi regarding governance at every site. This is supported by a consistent cadence of governance and assurance meetings, strongly driven by a well-funded central clinical team as well as a medical team.
We have 6,500 doctors engaged with us across the organisation. They primarily operate under practising privileges, which are controlled locally by site registered

managers and the medical team. Regarding our clinical staff, we have an industry-leading programme of continuous improvement. We have an in-house learning and development department and an association with Liverpool John Moores University for professional development and continuous review.
At the board level, governance and the assurance of quality are our top priorities; it is the first matter we consider at every single operating board meeting to ensure it receives the time it deserves. We also participate in a large number of voluntary external accreditations. The vast majority of our sites are JAG accredited, and we are the only private provider to hold AfPP accreditation at each and every site.
We don’t shy away from external or mandated benchmarks. We now have a great relationship with the CQC. In fact, all but three of our facilities across the entire organisation – including our equivalents in Scotland and Wales – are now rated ‘good’ or
‘outstanding’. The only three that aren’t, I should add, simply haven’t been inspected for a very long time.
The recent report from the Public Accounts Committee on the costs of clinical negligence was an unpleasant wake-up call. How is Circle geared up to deal with these liabilities?
We take a rigorous in-house approach to malpractice and medical negligence. Each and every initial instruction, potential notification and subsequent letter of claim is reviewed by a full panel that includes the clinical and medical teams, alongside our in-house legal experts.
This allows us to identify litigation trends as they emerge, whether they relate to a specific facility or to broader clinical and medical practices. If we spot a pattern, we react to it immediately. While there is undeniably a growing climate of litigation, it is also vital to use this data as part of our consultant insights programme.
The digital enablement of healthcare isn’t just about the patient pathway or consumer interaction; it is about the provision of care itself.

This is a unique initiative which uses various digitally interactive data sources to monitor the performance and behaviour of all our medical practitioners. We take a similar approach with our nursing and clinical staff to drive continuous improvement and mitigate risk.
As a company, we are, of course, fully indemnified against these risks. Generally speaking, we maintain a relatively consistent rate of claims across the organisation; however, should we spot a specific concern or trend, we are all over it. Because the key clinical leaders are in the room working directly with the legal team, they are involved in every step of the pathway – right through to the decision to settle.
Circle has invested significantly in technology, digital pathways and robotic surgery. Is technology investment now essential?
If you had asked me ten years ago, I would have said the appetite for change was far lower, but we are seeing a real shift now.
This is particularly evident regarding robotics – not just hard-tissue robots in orthopaedics, but soft-tissue robots in intra-abdominal and visceral surgery.
Increasingly, doctors on postgraduate training programmes are using robotics in NHS hospitals. Since we only have these doctors for perhaps 5% or 10% of their working week – the vast majority of their time being spent in the NHS – what they do there fundamentally drives what they do in the private sector.
We are committed to facilitating the best technology for our doctors. As a company, we are already the largest centre for orthopaedic robotics for one of our key suppliers across Europe, the Middle East, and North Africa.
The digital enablement of healthcare isn’t just about the patient pathway or consumer interaction; it is about the provision of care itself. We want to be active in the low-acuity space, increasing our reach as people take more accountability for their health,
but also at the high-acuity end. We are seeing significant investment in cardiology and oncology, particularly at sites with intensive care facilities.
The nature of private healthcare is changing. It is no longer just about standard hip and knee replacements in provincial private hospitals; it is now about acute cardiac, intraabdominal, and thoracic care. We are seeing high demand for these services, not only from insurers but, interestingly, from self-pay customers as well.
Where do you see your priorities?
Is it the acute care that you’ve just outlined or preventative car? What will drive the next phase of Circle’s growth?
It is essentially a twofold strategy.
On the one hand, we are deeply committed to extending the duration of our relationship with customers who wish to take accountability for their own health.
You will see Circle Health roll out a digitally enabled interactive platform: a digital companion that allows patients to engage with a broad range of products, from primary care access and medical screening to sports-related care and chronic disease management. Ultimately, it will act as a friend to the patient as they transition into acute care, providing access to their diagnostics, their full medical record, and all clinical correspondence.
At the other end of the spectrum – the high-acuity end – there is significant frustration and, we believe, clear market demand. Wait times in the NHS for high-acuity surgery, such as a TAVI [transcatheter aortic valve implantation] in certain parts of the country, are now quite substantial. Consequently, we are seeing an ever-increasing drive toward high-acuity provision within our own facilities, particularly in the fields of cardiology and oncology.

CONVENIENCE A CLINICAL
PRESCRIPTION weight-loss injections, such as GLP-1 treatments, have changed the conversation around weight management. For the right patient, used for the right reason, they can be clinically significant when prescribed and supported appropriately. Some patients describe feeling better supported and more confident in managing their health when treatment is prescribed carefully and followed up appropriately.
That is precisely why safeguards matter. These are powerful prescription-only medicines, not cosmetic quick fixes. If we treat them like a shortcut, we turn something that should be a clinical intervention into an avoidable source of harm.
The uncomfortable truth is that demand is moving faster than good practice. Many people seeking weight-loss support are not chasing a fad; they are exhausted after countless attempts to change and have learned to brace themselves for judgment. Others arrive with expectations shaped by what they have seen online, like fast results and little to no mention of side effects or follow-up care. In that environment, a prescriber’s role is not simply to approve or decline, but to assess risk, support patients through difficult decisions and keep the focus on outcomes that last.
Pharmacies should only prescribe when they have enough confidence that it is right for the person in front of them. In a clinic, that confidence is built through conversation, observation, and the
face-to-face. be optimism. From worry dramatic On prepared much that’s history, aside goals, what avoid from difficulties being entire usual automatically inappropriate, prescriber more This falls, professional people is built put before it is permission are rather means decision assessment,
Hira
CONVENIENCE CANNOT BE CLINICAL STANDARD
Hira Malik, superintendent pharmacist and co-founder at Oushk Pharmacy, wants to raise the bar for prescribing weight-loss injections online.
kind of context that comes from being face-to-face. Online, the context must earned and not replaced by speed or optimism.
From the front line, the cases that worry clinicians most are rarely the dramatic ones, but the plausible ones. On paper, the patient who is well prepared and keen can often have too much uncertainty underneath. Whether that’s an incomplete or dishonest health history, symptoms that are brushed aside or unrealistic and unhealthy goals, sometimes the red flag is not what someone says, but what they avoid saying. This can be everything, from a reluctance to talk about past difficulties with food, discomfort with being weighed, or a desire to keep the entire journey private without involving usual healthcare support. None of this automatically means the medicine is inappropriate, but it does mean the prescriber needs to slow down and ask more difficult questions.
This is where online prescribing rises or falls, with the service either supporting professional judgment or nudging people towards a quick yes. If a model built around speed, the prescriber is put under pressure to deliver a decision before they can form a defensible view. If is built around care, the prescriber has permission to be cautious, and patients are supported through that caution rather than bounced out the door. This means treating prescribing as a clinical decision first, supported by structured assessment, appropriate follow-up and
the freedom for prescribers to pause or decline when information is incomplete.
Weight-loss injections are not a oneand-done prescription, but a treatment journey. People may experience side effects, struggle to stay on track, or find the pace of change difficult to manage without appropriate support, while others may need reassurance and guidance or a clear prompt to seek medical advice. But most of all, they need honesty upfront. The best outcomes tend to come when people understand what they are starting, what will be expected of them, and what support they will receive if things do not go smoothly.
This is not about making online care harder for the sake of it. Done well, prescribing online can widen access and reduce barriers, especially for people who find in-person appointments difficult to fit around work, caring responsibilities or mobility issues. The danger is inconsistency. In a fragmented market, the easiest route often becomes the most popular one, and that creates a race to the bottom. Where prescribing thresholds vary widely across providers, risk is raised for the whole sector. They raise the risk for the whole sector. The impact shows up later, in complaints, health scares, damaged trust and tighter scrutiny for everyone.
For healthcare leaders, the business implications are as clear as the clinical ones. A lax approach may deliver quick growth, but it also stores up
liability. Unsafe prescribing does not remain a private matter. It becomes an operational disruption, a reputational risk, and an erosion of confidence in digital healthcare more broadly. The organisations that will still be standing in five years are not the ones that moved fastest in a gold rush. They are the ones who built trust early and protected it consistently.
The sector doesn’t need broad statements of intent, but a shared baseline that protects patients wherever they go. In practice, that means clear expectations around assessment quality, the ability for prescribers to pause or decline when information is incomplete and a defined commitment to followup rather than transactional supply. Online prescribing can be a legitimate part of modern healthcare, but only if it behaves like healthcare in the moments that matter most. If we get this right, the upside is significant and longlasting. Patients who meet the criteria can receive treatment that is both safe and respectful, rather than rushed or transactional. Prescribers can practice with confidence instead of secondguessing every decision, providers can build reputations that actually hold up under scrutiny, and digital healthcare can earn trust on its own merits, not by leaning on the credibility of traditional systems.
This is the moment for health providers, industry leaders, and regulators to stop pretending the only options are over-restriction or reckless access. A clearly defined minimum standard that prioritises patient welfare overgrowth metrics or conversion rates is essential. If online prescribing is to remain sustainable, raising standards now is not optional. It is the cost of long-term credibility.
THE SERIOUS SIDE ROBOTIC COMPANION
WHEN Ted Fischer first began to explore robotic companion pets, he was sceptical himself. But as health systems grapple with ageing populations, staff shortages and rising demand, attention is beginning to look beyond drugs to non-pharmacological ways of supporting wellbeing.
Here, the chief executive of Ageless Innovation speaks to Healthcare Today about loneliness, dementia and connection, and why technology designed to bring joy may have a more serious role in modern care than many assume.
What problem does Ageless Innovation solve that medicine and traditional care don’t?
I used to lead a team at Hasbro focused on new innovation. As we began our research, two things became very clear. First, we were seeing huge numbers of unintended users of our products. And second, there was this incredible unmet need among older adults for interactive companionship that no one was talking about.
We found that we have the greatest impact in a couple of key areas. The first is loneliness and isolation, often alongside depression. The second is Alzheimer’s, dementia and related conditions, including cognitive decline. We now have more than a dozen published research papers that speak to the efficacy and impact of these highly non-traditional interventions.
Ultimately, it’s about joy and happiness. I say it all the time – I’m not medically trained – but when people are happy, they feel better. And we’ve seen that play out millions of times over the course of our journey.
Loneliness, cognitive decline and loss of purpose are often treated as soft problems. How do you convince doctors that addressing them should be central rather than an optional extra?
It was actually clinicians themselves who began to notice the effect. They were seeing the anecdotal evidence on the ground and did the work needed to prove and validate it.
Ted Fischer, the chief executive of Ageless talks about non-pharmacological, tech-enabled for healthy ageing, including Joy for All
Written by Adrian Murdoch.
We launched the brand in 2015, and in 2018, my team and I spun the business out of Hasbro so that we could focus entirely on this population.
By 2020, in the US at least, that evidence had translated into formal recognition. We were approved by the Centers for Medicare and Medicaid Services, meaning our products could be covered for specific need states. At the same time, we were working with the NHS in the UK. Once that approval came through, adoption accelerated. Across care homes, assisted living, memory care and other settings, clinicians and practitioners could identify individuals who would genuinely benefit from interaction with a companion pet.
Critics often dismiss robotic pets as gimmicks or infantilising. What evidence do you have that this works?
There have been critics from the very beginning. One of the reasons I think we’ve succeeded is that we never assumed we knew what older adults wanted. We asked them, and we involved them directly in the design and development process.
When we designed our cats, for example, the details really mattered. People told us the paw pads were important – they wanted them to feel realistic. So that’s what we built.
All of this was driven by a simple principle: we’re not trying to fool anyone. It’s not our reality that matters, it’s theirs. We follow a person-centred design philosophy, which means recognising that every individual is different. If someone can have a real cat or dog and gets love and fulfilment from that, that’s fantastic. But there is a significant group of people who can’t and who deeply miss that companionship and interaction.
This solution isn’t But we’ve now and what we forming.
People immediately happens, something the magic begins.
Is the approach different in the
Not really – it’s similar. We won a couple of years date, well over pets have been need state is we see through in the US. These care homes or lonely or isolated by someone within – often a professional likely to benefit. distributed through
We now operate 20 countries, the systems may the underlying remarkably consistent. that sense, this the human condition. Across the developed world, populations ageing rapidly, challenges that with that demographic shift are broadly
SIDE OF COMPANION PETS
Ageless Innovation, tech-enabled solutions
All
Companion Pets.
isn’t right for everyone. Nothing is. now seen more than 750,000 adoptions, see again and again is a relationship
immediately name their pets, and once that something changes. That’s where some of begins.
approach to the programme the UK?
it’s actually very won an NHS contract years ago now, and to over 1,000 companion been distributed. The much the same as what through Medicare and Medicaid These are people living in or independently, who are isolated and are identified within the care system professional caregiver – as benefit. The pets are then through those channels.
operate in more than and while may differ, underlying need looks consistent. In this is about condition. developed populations are rapidly, and the that come demographic broadly similar.

Are there differences in impact across settings – care homes, hospitals, community care, people living alone?
There can be differences, but when a pet belongs to you, there’s a sense of ownership and attachment that seems to deepen the outcome and the impact. That personal relationship matters.
That said, many organisations use the pets in different ways. Care homes, for example, might purchase a number of pets and use them in group settings, bringing them out for shared activities and then putting them away again. Some memory care units keep a few pets available to use at specific moments. When someone becomes agitated or is struggling with a transition, staff may bring a pet out to help calm and soothe them. What’s important is that this can sometimes replace what would previously have been a psychotropic medication, which was often the default response to agitation or distress. Instead, a cat is placed on someone’s lap, they begin to settle, and the situation de-escalates more gently.
Do you see these tools as preventative or primarily as supportive?
Yes, I think it’s both. These interventions are being used in reactive and proactive ways. We’ve run studies with people who are gifted the companion pets, measuring outcomes at three, six, nine and 12 months across a range of recognised scales. In the US, we also run formal programmes that produce monthly and quarterly reports, with a clear performance threshold: we’re expected to deliver at least a 20% improvement in quality of life.
The proactive benefit shows up over the longer term. One study in New York illustrates this particularly well. Researchers used a pain scale in which a score of ten indicates a very high likelihood of an emergency department admission. Over a year, measured at regular intervals, they saw the average pain score among people gifted the companion cats fall
from around seven to just two.
That has significant implications, both for individual health and wellbeing and for pressure on the system. If fewer people are presenting to emergency departments, and a simple, non-traditional intervention like a companion pet is helping people feel less pain, that’s a meaningful outcome – not just clinically, but economically as well.
What role do families play in adoption and acceptance?
Families already know more than they think they do. On the direct-toconsumer side, where the product is typically bought as a gift for an older loved one, around 70% of purchasers are daughters or sons buying for a parent or grandparent. It’s closer to 80% when you include wider family carers. These are people who have actively gone looking for something –whether through online searches, word of mouth or evidence around dementia and other need states – because they’re trying to help someone they care about. We do offer guidance on how to introduce a companion pet, but ultimately, it comes down to knowing your loved one. There’s no single right way.
Let’s talk ethics. Is emotional attachment to robots a deception? Where do you draw the ethical line?
We have never set out to replace human interaction. Our aim has always been to create products that bring happiness and joy. What we’ve discovered is that they actually enhance human interaction rather than detract from it.
Let me give you an example that is typical. I have numerous letters from children whose parents are living in nursing homes. They often describe a similar situation: a mother or father who has been there for years, has no friends, doesn’t socially engage, and is effectively alone despite being surrounded by other people. Families gift a companion cat, hoping it might
offer some comfort. What they find instead is that the cat becomes a focal point. Other residents want to come over, ask about it, touch it, and interact with it.
Suddenly, someone who was withdrawn becomes the centre of attention. They start going to bingo. They won’t go anywhere without the cat. People gather around, conversations start, and the entire dynamic shifts.
The same is true in dementia and Alzheimer’s care, where interaction can become especially difficult. What we hear from caregivers as loneliness deepens or cognitive decline progresses, conversations can become harder and harder. But when the cat is in the room, the focus shifts. The pet becomes a bridge.
Almost without exception, what we’ve seen is that these companions don’t reduce human interaction in any way. They make it easier, particularly in situations that are otherwise very difficult to navigate.
Looking ahead, do you expect companion technologies to remain niche or to become as normal as mobility aids or telecare?
I spent the week before last at [the consumer electronics trade show] CES in Las Vegas, and it’s clear that the idea of the companion robot has already taken shape. You can already see it in professional care settings. Where it gets more nuanced is around form. Interaction with animals is a normal part of life across the entire lifespan. What we’ve consistently heard from caregivers is that companion pets remove a difficult emotional and visual barrier.
It’s been a fascinating journey, and we’re continuing to innovate in what our pets can do. But the most important principle will never change: anything we create has to enhance the relationship between the person and the product. If it doesn’t do that, it doesn’t belong.

When a pet belongs to you, there’s a sense of ownership and attachment that seems to deepen the outcome and the impact.

BLOOD CANCERS EXCLUDED FROM
AS WORLD Cancer Day approaches, the publication of the government’s long-awaited National Cancer Plan for England represents a defining moment for cancer care. The plan has the potential to transform outcomes for patients for years to come, but only if it reflects the realities of all cancers.
Blood cancers are the fifth most common cancer type in the UK, impacting hundreds of thousands of people, and are the third biggest cause of cancer deaths. There are 60,000 people in the UK who are currently living with a leukaemia diagnosis alone.
However, they have been consistently overlooked in a system designed around stageable, solid tumours. Unlike tumours, blood cancers cannot be staged, and as a result, they are excluded from current early diagnosis targets and performance measures. No national cancer policy to date has focused on monitoring progress in early diagnosis for leukaemia and other blood cancers.
At Leukaemia UK, we have been campaigning for the government to recognise the unique challenges faced by people with leukaemia and other blood cancers in the National Cancer Plan, and to take urgent action to stop them devastating lives.
CANCERS MUST NOT BE FROM NATIONAL TARGETS
Fiona Hazell, chief executive of Leukaemia UK, says that the National Cancer Plan must commit to earlier diagnosis targets for leukaemia.
As leukaemia and other blood cancers cannot be treated surgically, they often require immediate and aggressive treatment, meaning early diagnosis of the disease is vital to give people the best chance of survival.
However, a recent study commissioned by Leukaemia UK found that one-in-four leukaemia patients in England currently experience an avoidable delay in their diagnosis – resulting in worse outcomes for patients and avoidable costs for the NHS.
Many people who present with the signs and symptoms of leukaemia experience a delay in escalation at the GP level.
We speak to patients every day whose leukaemia symptoms were initially missed, often on multiple occasions.
Those who do have their symptoms escalated often face delays in being referred for a full blood count test, which can rule leukaemia in or out, due to capacity issues in phlebotomy services.
Currently, 37% of leukaemia cases are diagnosed in emergency settings such as A&E, far higher than the cancer average of 21%. This significantly impacts the effectiveness of treatment, prognosis and survival rates for patients.
For those diagnosed with Acute Myeloid Leukaemia (AML), a particularly aggressive form of the disease where symptoms escalate rapidly, this impact is stark.
One-year mortality for AML patients diagnosed in an emergency setting is 67%, compared to 48% for those diagnosed in a non-emergency setting. Reduction of leukaemia emergency diagnosis will both save lives and ease some of the pressures on the NHS.
Half of the people currently diagnosed with leukaemia in the UK won’t survive for more than five years. Even more alarmingly, if no action is taken, nearly 80% of those diagnosed with AML today will not survive until the end of this parliament.
This is simply unacceptable, particularly when we know five-year survival rates are higher in several European countries, and when progress has been made for other common cancers.
At Leukaemia UK, we hear stories every day from patients and their families highlighting the devastating consequences of a delay in diagnosis.
As the National Cancer Plan is finalised, the government has a once-in-ageneration chance to change this and commit to increasing survival and improving the lives of those with leukaemia. This can only be done with a focused commitment to earlier diagnosis, faster pathways, and policies that truly reflect the realities of blood cancer.
A recent response from the Department of Health and Social Care confirmed that it shares these concerns about
existing early diagnosis targets and recognises there is more to be done to improve outcomes for non-stageable cancers such as leukaemia.
They are also considering the feasibility of adopting new metrics to track progress for non-stageable cancers as part of the upcoming plan.
This is encouraging, but for the thousands of people living with leukaemia and those yet to be diagnosed, it is now vital that this recognition translates into meaningful policy change.
The National Cancer Plan must introduce a new early diagnosis metric for non-stageable cancers so that blood cancers are no longer excluded from national targets.
It must also commit to practical, evidence-based solutions that we know can make a difference, including a commitment to faster referral for a full blood count test, clearer guidelines for escalation and better follow-ups to help diagnose leukaemia earlier and reduce emergency diagnosis.
A best-practice timed pathway for leukaemia would ensure that anyone with an abnormal full blood count is seen by a specialist within one week.
With a focused commitment to better diagnosis, treatment and care, it is possible to increase survival and improve the lives of those with leukaemia.
We are ready to work with the government and all those with the power to drive change, to move towards a future where leukaemia and other blood cancers no longer devastate lives.
CANCER CARE: SEEING THE WHOLE PICTURE
CANCER care is one of Scotland’s most urgent health system challenges, and alarmingly, one in two patients will have a cancer diagnosis in their lifetime. Thousands of people each year experience the fear and uncertainty while waiting for a cancer diagnosis.
For me, the importance of timely diagnosis is personal. In my early 30s, I was recalled following a routine cervical screening. Even though I worked in the NHS at the time, the experience was frightening.
My diagnostic journey was completed in days, but these were some of the longest days of my life. I still remember the medical director (my gynaecologist) phoning me with the good news. Speed really mattered to me as it meant the uncertainty didn’t drag on.
Two decades later, I was recalled from the breast screening programme. Once again, the service moved quickly, with a same-day diagnostic visit within 48 hours.
The fear returned and was all consuming. Once again there was compassion, dignity and speed. This should be the rule, not the exception, but for many, pathways diagnosis is taking too long.
The national framework
Scotland already has a planned, coordinated approach with its National Framework for Effective Cancer Management, published in March last year. The report sets out the right objectives and highlights how
Donna Smith, director of strategic solutions at Insource, explains how cancer data can be used to improve performance and reduce delays.
a joined-up approach should follow ten recommended steps to streamline pathways and enhance data reporting collectively across the country –something it aimed to put into action within three years.
Scottish health boards are working hard to implement the framework in their areas, yet the pace of improvement still feels too slow for those waiting for a diagnosis and treatment today.
Understanding diagnostic bottlenecks, systemic pressures, and socioeconomic impacts is all possible with real-time data and the right analytical focus.
Cancer waiting times are on the agenda for every Scottish NHS board and the latest Public Health for Scotland figures show incremental improvements, with 31-day targets being met.
However, only 69.9% of patients referred with an urgent suspicion of cancer begin treatment within the 62-day target window. This falls far short of the 95% standard that has not been met since 2012.
These headline figures don’t reveal the full picture: they do not show how the NHS across Scotland is missing out on the opportunity to carry out a systematic review of how cancer pathway delivery is failing and where delivery could be significantly improved.
The Danish example
A question I often hear is where to invest first: workforce, equipment or data? In reality, these are not competing choices. They are interdependent.
Without high-quality, real-time data, the workforce cannot be deployed effectively, equipment cannot be used efficiently, and bottlenecks aren’t identified early enough.
Data acquisition and visibility are not luxuries. They are key enablers to maximise the impact of every pound spent and every professional’s effort to improve patient outcomes.
Real-time insights enable the targeted deployment of capacity and optimised use of equipment to make the greatest difference. With consistent definitions and interoperable datasets, boards can rapidly test and spread improvements, reduce unwarranted variation, manage inequalities, support recruitment to clinical trials, and so much more.
This data-driven approach has been proven elsewhere and was fundamental to transforming cancer care in Denmark, identifying two key blockages of understanding and optimising the pathway, and then using the data to improve the system infrastructure and progress patients through the system.

CARE: PICTURE
Much has been written about Denmark’s success in recent years. Comparable to the UK, and a valid benchmark, in the 1990s, both countries had similarly poor cancer survival rates, according to International Cancer Benchmarking Partnership (ICBP) data. Today, Denmark has achieved some of the biggest improvements among ICBP members. Sadly, the same progress has not been mirrored across the UK.
A key driver of Denmark’s turnaround has been its use of real-time, comprehensive data, including stageat-diagnosis reporting. Data has helped inform the national strategy and plan, enabling targeted action, continuous learning, and observable improvements.
Population-level data continues to guide Denmark’s efforts, revealing that diagnosis rates remain higher than the EU average (partly due to increased screening), prevention and public health initiatives still need strengthening, and longer waits for first treatment correlate with poorer outcomes.
Applying the approach in Scotland
Closer to home, some of Scotland’s cancer programmes and board-level initiatives are demonstrating what is possible when data and improvement go hand in hand.
Within just 100 days, NHS Greater Glasgow and Clyde reduced their longest


diagnosed cancer waits by 42%. That’s been made possible with access to complete, accurate data that identified and removed key bottlenecks in selected pathway cohorts to speed up the process between referral and diagnosis, supporting the longest waiting patients to get their treatment faster.
Data can, and should, be used to replicate similar successes across the whole of Scotland to identify constraints, redesign flows, and allow quicker diagnosis and faster access to treatment for all.
Cancer does not observe board boundaries, yet accountability structures do.
Each Scottish health board, rightly, has the responsibility for meeting waiting time standards.
However, this fragments the ownership of the end-to-end pathway. Patients travel for diagnostics and treatment, capacity varies by site and specialty, information often sits in local systems and patients can get lost in the system.
Without a single, coherent national view of demand, capacity, activity and waits, unintentional variation is created, effort is duplicated, and opportunities are missed to treat patients sooner.
The solution is a shared, near-realtime, visible pathway management that follows the patient rather than the organisation. When boards see the same data, in the same way, mutual aid becomes practical, escalation becomes timely, and patients experience a more seamless journey.

A targeted model
The targeted operating model for oncology can be delivered at pace, with this cross-boundary visibility, delivered through complete and consistent datasets, with a single operational view linking demand, staffing, chair time, pharmacy preparation and transport.
With that visibility, Scotland can deliver timely starts, minimise cancellations and deliver safe and equitable access across sites.
It’s about uncovering where the real issues lie and tackling them. It isn’t about blame. It’s about focusing effort and resources where they will count most.
Scotland has many of the right components and the right ambition set out in the National Framework to solve the cancer challenge. By treating data as an enabler, not a competitor for resource, improvement can be accelerated across Scotland in a way that is practical for operational teams and tangible for patients.
The correct solutions, to the real problems, will reduce waiting times.
We can make that happen now and give every cancer patient in Scotland an equal chance.
Accurate, real-time cancer data doesn’t just inform, it empowers. And that power, used now, not later, is what will finally break the cycle of delay.
Scotland’s cancer patients deserve nothing less, and they deserve it now.
IMMERSIVE virtual reality (VR) therapy is entering care pathways faster than the governance around it. I do not say that to slow innovation down. I say it because immersion changes the risk profile of digital health in a way many teams still underestimate.
A standard app delivers content. Immersion delivers an environment. The nervous system does not treat that difference as cosmetic. It responds as if it is inside a space, not looking at a screen. That is why immersive interventions can feel so effective. It is also why the usual shortcuts in digital health stop being safe once you scale.
When a patient reports discomfort after an app, it often gets framed as user experience. When a patient reports overload after immersion, the questions become clinical immediately. Who screened suitability? Who defined exposure limits? Who supervised? Who documented adverse effects? Who decided the session should continue?
Immersion turns digital delivery into accountability.
A paper last year on neuropsychological safety in virtual therapeutic environments makes a point that private providers, outpatient settings, and any service building VR into a pathway should take seriously. Early wins in pilots are common, but real-world variability arrives fast. panic activation, nausea that does not resolve quickly, dissociation, symptom rebound, or simple intolerance to sensory load are not rare edge cases. They are predictable when exposure rules are undefined.
This is the part that gets missed in the rush to deploy. Undefined exposure rules do not stay neutral. they become incidents, complaints, and reputational damage. They also become legal vulnerability, not
THE ETHICS OF IMMERSION VR THERAPY

because providers are careless, but because they cannot demonstrate that they operated within a defensible standard of care.
The governance gap shows up clearly in private settings because adoption can be fast, and supervision models vary. Another paper on VR in private psychological practice maps the same issue from a professional risk angle. When a headset becomes part of routine delivery, the soft parts of practice become hard requirements. Screening, dosing logic, supervision, and adverse event capture are no longer nice to have. They become the difference between an intervention that can be defended and an experience that can only be explained after something goes wrong.
Responsible governance
So what does responsible governance look like when a provider wants to use immersive
Nargiz Noimann, founder about the patient safety virtual reality
therapy in a way that is credible, safe and sustainable?
It starts with a mindset shift. session length is dose, not scheduling. In immersive formats, dose is not only time. It is intensity, sensory load, interactivity, and the degree of presence the environment creates. If a provider cannot define dose ranges and clear stop criteria, they cannot honestly claim they are delivering a controlled intervention.
Screening also has to be concrete. Providers need explicit exclusion criteria and escalation rules for seizure risk, significant vestibular sensitivity, acute psychosis, and high dissociation vulnerability.
This is not about treating patients as fragile. It is about matching exposure to physiology. In immersion, the

founder of X-Technology, writes safety and liability gap in reality therapy.
same stimulus can regulate one person and destabilise another.
Supervision must be defined just as clearly. Immersion can look calm on the outside while the patient is shutting down internally. A trained observer is not there to police. They are there to recognise overload early and to end the session before the nervous system crosses a threshold that is harder to reverse. That training should include what to look for, what to do, and how to document it.
Then there is adverse event capture. Too many programmes treat discomfort as noise. In a regulated care culture, it is a signal. If you cannot record and categorise nausea, panic activation, dissociative responses, symptom rebound, or delayed agitation, you cannot
improve protocols and you cannot demonstrate duty of care. This is also where complaints become sharper, because patients often describe not only the experience but the feeling that nobody expected a negative response.
Informed consent has to reflect reality. A signature is not enough. Patients need a clear explanation of what immersion can trigger, what sensations can occur, what signs indicate overload, and what support exists if an effect lingers beyond the session. If an incident is reviewed later, the question will not be whether the technology is innovative. It will be whether the provider communicated risk responsibly and operated within defined boundaries.
Frameworks in place
The good news is that the UK already has frameworks that help teams think in the right way, even when immersive therapy sits between wellness and clinical service.
The National Institute for Health and Care Excellence (NICE) created an Evidence Standards Framework that links evidence expectations to function and risk.
That logic matters for immersive interventions because it pushes providers and developers to align claims with the level of proof required, instead of jumping from early pilots to broad conclusions.
Regulatory clarity matters too. Medicines and Healthcare products Regulatory Agency (MHRA) guidance on software and AI as a medical device makes a point that many teams try to avoid until late. intended purpose and claims influence whether a product falls into regulated territory. Even when a specific immersive experience is not regulated as a medical device, provider governance still carries weight because it defines how the intervention is used, monitored, and documented.
I see 2026 as a turning point. Immersive therapy is moving from novelty to routine exposure. When something becomes routine, its failures stop being surprising. They become systemic. That is why governance cannot be treated as an afterthought or a later phase.
The field does not need to slow down. It needs to be professionalised. That means treating neuropsychological safety as a standard that is designed, documented, and audited, not a hope that patients will tolerate the experience.
If those rules are defined early, immersive therapy can earn trust, attract serious clinical partners, and integrate into pathways without the predictable cycle of early excitement followed by backlash after preventable incidents. If they are not defined, the standard will be written after the fact by complaints, lawyers, and reputational damage.
THE FUTURE OF PERSONALISED CARE
THE global healthcare landscape is undergoing a seismic shift as ageing populations and rising demand for long-term care increasingly outstrip the supply of traditional clinical resources. The industry faces the critical dual challenge of maintaining high standards of patient safety while delivering personalised care at scale, and the answer lies at the intersection of Artificial Intelligence and remote monitoring technology. Deploying these tools effectively requires a robust ethical framework to ensure that the most vulnerable members of society, particularly the elderly community, truly benefit from these advancements.
Leading this technological revolution are initiatives that are reshaping doorstep primary health and social care through patented digital safeguarding technology and innovative smartwatches for remote medical monitoring.
These advancements demonstrate how AI can serve as a compassionate and vigilant partner in patient safety. Traditionally, patient safety has been reactive, responding to falls or managing sudden illnesses after they occur, but this model is no longer sustainable in stretched healthcare systems.
A proactive approach is essential to anticipate risks before they become emergencies, and AI excels at this. By analysing vast datasets, from vital signs to movement patterns, AI algorithms can detect subtle deviations that the human eye might miss, transforming the home into a safe, medically monitored environment that allows the elderly to age in place with dignity.
Samit Biswas, founder and chief executive of CareSafe, explains how AI and ethical technology are redefining patient safety.
Tracking health metrics
Central to this new ecosystem are medical-grade smartwatches designed for the nuances of elderly care. Unlike standard consumer wearables, these devices serve as a lifeline, continuously tracking critical health metrics such as heart rate variability, oxygen saturation, and sleep quality.
Their true power lies in integration with digital safeguarding technology, creating a constant safety net. Instead of merely recording data, the system interprets it to identify anomalies, such as a subtle change in gait that might precede a fall or an unexpected spike in heart rate at rest. These insights are transmitted in real time to monitoring centres and care teams, enabling preventative intervention and shifting the paradigm from reacting to emergencies to preventing them entirely.
The integration of AI into healthcare raises valid concerns about privacy, data security, and the potential dehumanisation of care. These challenges are addressed through a commitment to ethical AI. This approach prioritises transparency, ensuring that algorithms assist rather than replace human decision-making by providing actionable insights to trained clinicians. Security is also paramount, with sensitive health data protected by military-grade encryption and rigorous certification standards that safeguard user privacy. Furthermore, ethical AI is human-centric, designed to respect the individual by learning each user’s specific baseline
health metrics. This personalisation ensures that alerts are accurate and relevant, reducing alarm fatigue for carers and anxiety for families.
Support of intelligent technology
The ambition of these technologies is global, aiming to deliver tailored, AI-driven primary health and social care solutions to elderly communities worldwide. Whether in rural areas or urban centres, the need for safe, monitored independence is universal. By combining the physical presence of vetted carers and mobile clinical units with the digital vigilance of smart monitoring devices, a hybrid care model emerges. This holistic approach allows technology to handle continuous monitoring, freeing human carers to focus on companionship, empathy, and hands-on support.
As the future of healthcare unfolds, it is clear that patient safety cannot rely solely on human vigilance but requires the unwavering support of intelligent technology. However, technology without ethics is hollow. This new era fuses digital safeguarding with ethical AI and robust remote monitoring to protect and empower patients, demonstrating that with the right tools, the elderly community can live safer, healthier, and more independent lives.
In this context, AI becomes more than a cold calculation; it transforms into a protective embrace that extends the reach of compassionate care.

CARE

“ESSENTIALLY LIKE-FOR-LIKE” THE MOST DANGEROUS PHRASE
THERE is a phrase I am hearing with increasing frequency from clinicians reviewing their indemnity arrangements:
“I’ve been told the policies are essentially like for like.” On the surface, it sounds reassuring. Efficient. Convenient. In reality, it is often an oversimplification, and in some cases, a dangerously misleading one.
Medical indemnity is not a commodity. It is not broadband. It is not car insurance. And reducing complex contractual protections to “like for like” does a disservice to clinicians making decisions that could define their professional future. This is not about criticising competition. A healthy market is important. But clarity matters. And language matters.
Indemnity is structural — Not cosmetic
Two policies can appear similar at a headline level:
• The same indemnity limit
• A comparable premium
• The same specialty declared
But the real protection lies beneath the surface.
When comparing indemnity arrangements, meaningful differences can exist in:
• Claims conditions
• Notification requirements
• Consent provisions
• Retroactive dates
• Run-off structures
• Aggregation wording
• Exclusions relating to cosmetic or evolving procedures

George Maughan, THEMIS’ director of insurance services, reveals why medical indemnity cover is not one size fits all.
• The contractual versus discretionary nature of the promise to indemnify
• Additional protections outside of normal cover
• The credibility of the legal team that will support you
These are not minor technicalities. They form the framework that determines how a claim is handled, and whether a clinician is protected in the way they expect. To suggest these nuances are “essentially the same” without careful analysis is, at best, incomplete and at worst, wilfully lazy.
Beyond the core policy: The additional protections that matter
Another area often overlooked in “like for like” comparisons is the additional protections wrapped around the core indemnity. Many products provide extensions or ancillary protections that sit above and beyond standard civil negligence cover.
These may include, for example:
• Regulatory and disciplinary defence
• Criminal defence costs arising from clinical practice
• Coroner’s inquests
• Media or reputational support
• Good Samaritan acts
• Public liability or entity extensions
• Breach of confidentiality or data-related liabilities
• Employment support
The breadth, limits, triggers, and conditions attached to these protections can vary significantly between providers. Two policies might both offer £10 million indemnity but differ materially in how they respond to a GMC investigation or a coroner’s inquest. These differences are rarely visible in a simple premium comparison. Yet they can be pivotal in moments of professional stress.
Claims-made is not claims-made is not claims-made
Take claims-made policies as an example. Two providers may both offer a claims-made structure. That does not mean they operate identically.
Key questions include:
• What triggers notification?
• How is prior knowledge defined?
• What happens if practice changes?
• What are the conditions attached to run-off?
• How are defence costs treated within the limit?
• Similarly, an occurrencebased policy may appear straightforward - until exclusions, territorial restrictions, or sub-limits are examined.
Structure matters. Wording matters. Conditions matter.
LIKE-FOR-LIKE”
PHRASE IN MEDICAL INDEMNITY?
The myth of interchangeability
One of the underlying problems is the assumption that medical malpractice policies are interchangeable. They are not.
Indemnity providers operate with different risk appetites, different pool compositions, different capital structures, and different longterm strategies. These factors influence not only pricing, but claims philosophy and sustainability. When a clinician is told a policy is “like for like,” an important question follows:
On what basis?
• Was the comparison limited to limit and price?
• Was the wording reviewed lineby-line?
• Were exclusions mapped?
• Were additional protections compared?
• Was the claims handling philosophy considered?
• Was the long-term resilience of the indemnity pool assessed?
Without that depth, “like for like” becomes shorthand for “superficially similar.”
Risk has become more complex
The claims environment is evolving. Severity is increasing. Legal costs are rising. Cosmetic and elective work carry distinct litigation patterns. Patient expectations continue to shift.
At the same time, clinicians’ practices are more diverse than ever:
• Mixed NHS and private work
• Entity and individual exposure
• Cosmetic alongside reconstructive
• Advisory, medico-legal, or digital health activity
In such an environment, the idea that policies can be casually categorised as interchangeable should give us pause.
Brokers and responsibility
Most brokers work hard for their clients. Many provide thoughtful guidance. But simplification can creep in, particularly when market competition intensifies.
Reducing indemnity to a price comparison risks turning a professional safeguard into a procurement exercise. As clinicians, you would not accept a colleague describing two surgical approaches as “essentially like for like” without understanding anatomy, technique, and outcome data. Indemnity deserves the same intellectual discipline.
The real question to ask
If you are reviewing your cover and hear the phrase “like for like,” consider asking:
• Can you walk me through the key structural differences?
• How do notification and prior knowledge provisions compare?
• Are there differences in retroactive protection?
• What are the run-off conditions?
• What additional protections are included; and how do their limits differ?
• How does each provider construct and protect its indemnity pool?
If those questions cannot be answered clearly, the comparison may not be complete.
This is not about fear - It is about understanding
This is not an argument that one model is universally better than another. It is not an attempt to create alarm. It is a call for precision.
Medical indemnity is there for the worst day of your career. It is activated in moments of stress, scrutiny, and uncertainty. At that point, nuance becomes everything.
The time to understand difference is before a claim arises; not after.
A consultative approach
At THEMIS, we believe indemnity conversations should be consultative, not transactional.
That means:
• Understanding the detail of a clinician’s work
• Discussing how practice evolves over time
• Explaining policy structure clearly
• Being transparent about what is and is not covered
• Ensuring clinicians understand their obligations under the policy
Comparison is entirely appropriate. Switching providers can be appropriate. Markets should compete. But comparison should be rigorous, not reductive. Because when it comes to professional protection, “essentially like for like” may be the most expensive assumption a clinician ever makes.

ACROSS the UK, urgent and emergency care teams are facing unprecedented pressure with rising demand, workforce strain and fragmented digital pathways creating bottlenecks that delay care and increase riskfor both patients and clinicians.
While services like NHS 111, Clinical Assessment Units (CAS), Out of Hours, Urgent Treatment Centres (UTCs), ED and Same Day Emergency Care (SDEC) have made strides in digital triage, one challenge continues: the patient journey between first contact and clinician consultation.
CLEO Systems believes that transforming this ‘in-between’ stage is the key to unlocking safer, faster, more efficient care. And that’s exactly what its Virtual Waiting Room (VWR) technology is designed to do.
A smarter way to manage patient flow
Built to ease the burden on clinicians and healthcare services by intelligently automating and

CLEO Systems explains why intelligent automation can help to ease the burden on clinicians and healthcare services.
streamlining patient flow, the CLEO Virtual Waiting Room addresses that critical first stage in the patient / clinician journey.
It’s not just a digital queue. It’s an intelligent, real-time queue management solution built to streamline patient flow, reduce missed contacts and free clinicians from unnecessary administrative tasks.
But the real innovation lies in how intelligently the queue works.
When a case enters the VWR system, intelligent mapping priorities cases based on urgency, availability and clinician expertise.
Clinicians have a clear view of the patient record before they speak to the patient.
Patients are invited to join the virtual queue with a friendly automated message and when a clinician is ready to speak to a patient - instead of staff manually calling each patient before a consultation - a process that can consume minutes per contact and slow down servicesclinicians simply log in and take the next assigned call where the patient is ready to speak to them.
The VWR can be optimised to include the organisations, business rules, DX Code, expected consultation length and safe waiting thresholds.
The result? The right patient is connected to the right clinician at exactly the right time. What could be simpler?
An immediate impact on efficiency and patient safety
For overstretched healthcare environments, the benefits are clear.
HOW
HOW CLEO’S VIRTUAL WAITING ROOM IS TRANSFORMING EMERGENCY CARE

VWR connects patients and clinicians creating a 50% increase in clinician productivity, services using CLEO’s Virtual Waiting Room report increasing capacity to five or six consultations per hour, simply by removing the friction from manual contact and scheduling processes.
Other key advantages include enhanced patient satisfaction and reduced no shows and failed contact.
Patients receive real-time updates, greater transparency and reassurance that their consultation is on track, while automated communication means fewer missed or repeated calls, saving both time and frustration.
The platform ensures that clinically dependent patients are seen promptly based on safe criteria, not manual decision-making.
CLEO Virtual Waiting Room also provides seamless digital integration and works alongside existing patient management systems,
including CLEO Urgent Care, with no disruption to existing infrastructure.
There are also real-time analytics which help service leads monitor performance, understand pressure points and drive continuous improvement, while full DCB0129 clinical safety compliance gives providers confidence in safe, robust deployment.
Designed with the NHS, for the NHS
CLEO Systems isn’t a newcomer to urgent and emergency care technology. With more than 20 years of collaboration with the NHS, CLEO’s mission has remained the same: to empower clinicians with intuitive digital tools that improve efficiency and elevate the patient experience.
As part of a UK social enterprise, CLEO is aligned with the NHS Long Term Plan to make digitally enabled care mainstream and to place technology at the heart of every outof-hospital service. Being patientfirst, not paper-first, CLEO’s in-house
clinicians and developers work directly with NHS partners to design solutions that meet the real-world needs of call handlers, clinicians and patients across the Integrated Urgent and Emergency Care (IUEC) landscape.
Simplifying connected care
With demand on urgent care services continuing to rise, the need for smarter, more connected digital systems has never been greater.
CLEO Virtual Waiting Room is proving that technology can do more than digitise a process, it can redefine an entire workflow.
By removing administrative burdens, reducing missed contacts, and enabling safer prioritisation, CLEO Systems is helping urgent care teams deliver faster, more efficient and more reassuring experiences for patients.
This is the future of patient flow. And it’s available today. Click here for more information.
THE 10-POINT PLAN MODERN MEDICAL
THIS article outlines a practical ten-point plan to help healthcare leaders build resilient, highperforming practices in an increasingly complex environment.
Healthcare has evolved. Regulation is tighter. Patient expectations are higher. Administrative demands are heavier. In this landscape, sustainable success doesn’t happen by accident, it is engineered through disciplined practice management. At Medserv, we work with practices across the country and consistently see that high-performing clinics share ten defining characteristics.
Here is our ten-point plan to building a future-ready medical practice.
1.
Put the patient at the centre
Patient-centred care is not a slogan; it is a strategy.
Every operational decision, from scheduling systems to communication protocols, should enhance the patient experience rather than complicate it. When teams are trained in empathy, communication, and clarity, consultations run more smoothly, expectations are managed better, and loyalty strengthens. Operational efficiency and patient-centred care are not opposing forces. Done correctly, they reinforce each other.
2. Digitise core operations
Paper-based systems and fragmented processes are no longer viable.
Success in medical practice today requires more than clinical excellence. It demands operational clarity, financial discipline, digital confidence, and an unwavering commitment to patient experience, says Medserv’s Derek Kelly.
Modern practice management software integrates scheduling, billing, reporting, and patient records into one ecosystem. Automation reduces administrative burden, minimises human error, and frees clinical teams to focus on care delivery. Technology should not add complexity; it should remove friction.
3. Engineer your appointment system
Time is a clinical asset. An optimised scheduling model reduces idle gaps, manages demand, and improves provider productivity. Smart reminder systems decrease no-shows and late cancellations, protecting both revenue and access.
When appointment systems are strategically designed rather than reactively managed, capacity increases without increasing stress.
4. Clarify roles and empower your team
High-performing practices operate with precision.

Clear responsibilities, defined workflows, and consistent communication eliminate duplication and confusion. Ongoing training and structured performance reviews ensure standards remain high and bottlenecks are addressed early.
A coordinated team not only works faster, it works smarter.
5. Strengthen revenue cycle discipline
Revenue leakage is one of the most common hidden threats to practice sustainability.
Automated billing processes, systematic claim reviews, and proactive denial management protect cash flow. Efficient revenue cycle management ensures that services delivered translate into revenue received, promptly and accurately. Financial health enables clinical excellence.
PLAN TO SUCCESS IN MEDICAL PRACTICE

6. Build a strong digital presence
Today’s patients research before they book. A visible, professional online presence, supported by search optimisation, targeted communication, and reputation management, strengthens credibility and attracts new patients. Digital marketing is no longer optional; it is a core growth lever. Practices that control their digital narrative control their growth trajectory.
7. Treat data protection as a leadership responsibility
Regulatory compliance is not simply an administrative requirement; it is a trust commitment.
Robust GDPR compliance, secure data systems, and staff education around cybersecurity safeguard both patients and reputation. In an era of increasing digital risk, governance must be proactive, not reactive.
8. Measure what matters
You cannot improve what you do not measure. Successful practices monitor key performance indicators such as patient satisfaction, waiting times, claim rejection rates, and revenue trends. Regular review of performance data enables informed decision-making and early intervention.
Data transforms management from guesswork into strategy.
9. Embed a culture of continuous improvement
Operational excellence is not a one-time project. The most resilient practices actively seek feedback from patients and staff, review processes regularly, and remain open to change. Small, incremental improvements compound over time, creating meaningful long-term gains. Adaptability is a competitive advantage.
10. Focus on what you do best and outsource the rest
Clinical expertise is your core competency. Outsourcing specialised administrative functions such as billing or practice management can reduce internal strain while improving accuracy and performance. Strategic partnerships provide access to advanced systems and expertise that may not be sustainable in-house.
Delegation, when done wisely, strengthens control rather than weakens it.
A final word
Success in modern medical practice requires balance: efficiency without sacrificing compassion, growth without losing control, and innovation without compromising compliance.
At Medserv, we believe operational excellence is not about cost-cutting alone, it is about creating an environment where clinicians can focus on care, patients feel valued, and the business remains financially secure.
The practices that thrive in today’s healthcare landscape are those that view management not as an administrative necessity, but as a strategic discipline. With clarity, structure, and the right support, success is not just possible... It is sustainable.
Discover more about Medserv here.
CLINICAL NEGLIGENCE REFORM
ON 30 January 2026, the House of Commons Public Accounts Committee (PAC) published its long-awaited report Costs of Clinical Negligence. While few in healthcare or medico-legal practice will be surprised by its conclusions, the report is notable for the strength of its criticism of government inaction, the breadth of its recommendations, and the urgency with which it calls for reform.
This article explains what the report is, why it was prepared, what it says - particularly its recommendationsand what key stakeholders should be doing now.
What is the PAC and why this report matters
The Public Accounts Committee is Parliament’s principal body for scrutinising public expenditure and value for money. It does not make policy, but its reports carry significant political and practical weight, particularly where there has been repeated failure to act.
The PAC has examined clinical negligence before, most notably in reports in 2002 and 2017, and again in its recent reviews of the Department of Health and Social Care’s (DHSC) annual accounts.
The 2026 report follows a National Audit Office (NAO) investigation last year and evidence sessions with DHSC, NHS England and NHS Resolution. The well-known backdrop is stark. Clinical negligence is now the second-largest liability on the government’s balance sheet, exceeded only by nuclear decommissioning.
At a time when the NHS is being asked to make savings of at least £1 billion over the next three years,
Neil Rowe, head of practice at Maulin Law, delves into the PAC’s latest call to action.

the PAC’s central message is that rising negligence costs are diverting money away from frontline careand that this has been allowed to continue for far too long.
The scale of the problem
The figures set out in the report are sobering:
• The total provision for clinical negligence in England has risen to £60 billion.
• Annual settlement costs have tripled since 2006-07, reaching £3.6 billion in 2024-25, and are forecast to exceed £4 billion p.a. by the end of the decade.
• A very small number of highvalue claims - predominantly obstetric brain injury casesaccount for a disproportionate share of costs, with an average value of £11.2 million per claim.
• Legal costs remain a major concern, particularly in lowervalue cases where costs can be almost four times the damages paid.
Behind these numbers, the PAC repeatedly emphasises, lie serious and often devastating incidents of patient harm.
Key themes and findings
Although the report ranges widely, several themes recur.
1. Failure of leadership and coordination
The PAC is highly critical of DHSC in successive governments, concluding that it has failed to take “any meaningful action” to tackle rising negligence costs despite years of warnings.
Of particular concern is the Department’s reluctance to commit to reform while awaiting the outcome of an ongoing review by David Lock KC - without even being able to provide a completion date.
By contrast, NHS Resolution is praised for its more proactive approach, including increased use of early settlement, mediation and alternative dispute resolution.
2. Patient safety and the complaints system
The report unsurprisingly makes clear that preventing harm is the most effective way to reduce negligence costs. Yet the PAC finds the current patient safety landscape fragmented and overwhelmed by recommendations that are not translated into action.
The NHS complaints system is described as confusing and ineffective, with poor communication and delays often driving patients towards litigation simply to obtain answers or accountability.
The PAC highlights evidence that early, compassionate responses - including explanations and apologies - can reduce both claim volumes and costs.
3. Data: “a plethora of data and no information”
Despite the NHS holding vast amounts of data on patient safety incidents and claims, the PAC
REFORM BACK IN THE SPOTLIGHT
concludes that this information is not being used effectively to identify trends or prevent recurrence. There is no coherent national system for learning from claims, and limited investment in analytics risks the NHS falling behind Claimant law firms increasingly using artificial intelligence.
4. Maternity care as a systemic failure
Maternity services inevitably receive scrutiny. The PAC links high-value claims to longstanding workforce, training and patient safety problems in maternity and neonatal care.
While initiatives such as NHS Resolution’s Early Notification Scheme are welcomed, the Committee is clear that incremental measures are not enough without addressing systemic causes.
5. Legal costs and structural drivers of claims inflation
Two legal drivers receive sustained attention. First, disproportionate legal costs in low-value claims, and the failure to implement fixed recoverable costs reforms previously proposed. Secondly, the continued requirement - dating back to the Law Reform (Personal Injuries) Act 1948 - to calculate damages on the assumption that future care will be privately funded, even where Claimants may later rely on NHS or publicly funded social care.
The PAC’s recommendations
The report contains a detailed and demanding set of recommendations, including that:
• DHSC must publish a clear operational plan to reduce claim volumes and costs, with measurable milestones.
• The David Lock KC review should be published in full within six months of completion.
• A national patient safety framework should be established, with clear targets and accountability.
• The NHS complaints system should be reformed to increase resolution without litigation.
• The NHS should estimate and track the cost of treating avoidable harm.
• A national system for sharing and analysing claims and safety data should be created, including exploration of AI tools.
• The Amos Review into maternity and neonatal services should be published promptly, alongside a clear action plan.
• Alternative, non-adversarial mechanisms for resolving lower-value claims should be developed, drawing on international models.
• The government should urgently clarify its position on fixed recoverable costs.
• DHSC should assess the financial impact of assuming private care in damages and consider legislative change to prevent double payment.
What should stakeholders do now?
For healthcare leaders, whether in the private sector as well as in the NHS, the report reinforces the need to treat patient safety, complaints handling and learning from harm as strategic priorities, not compliance exercises. Investment in staff
training, culture, and early resolution mechanisms is no longer optional.
For clinicians, the report underlines the importance of candour, documentation and engagement with patients after adverse events. Many claims arise not solely from harm, but from how that harm is handled.
For NHS or med mal lawyers, and indemnifiers, the direction of travel is clear: greater emphasis on early resolution, alternative dispute mechanisms, data-driven risk identification and - potentially - significant reform to costs and damages frameworks. Stakeholders should engage constructively with consultations that are likely to follow, particularly on fixed recoverable costs and care models.
Finally, for policymakers, the PAC’s message is unequivocal. Further delay risks not only financial unsustainability, but continued harm to patients and yet further erosion of trust in the system. There may not be a single “silver bullet” solution, but the status quo is no longer defensible.
Conclusion
Last year I wrote extensively on the pressures faced by the health sector and the need for clinical negligence reform in many aspects. That there appears to have been little practical progress in a time of crisis is a disappointment that everyone will share.
Whether the PAC’s report will mean this time will be different remains to be seen. However, for all involved in healthcare and clinical negligence, this report should be treated as the loudest call to action yet, rather than another warning filed and forgotten.

Published by Healthcare Today Media Ltd. Healthcare Today is editorially independent. Material is governed by copyright.
No part of this publication may be reproduced, stored in a retrieval system or transmitted in any form without permission, unless for the purposes of reference and comment.
© Healthcare Today Media Ltd 2025 Registered office: Connect 38, 1 Dover Place, Ashford, Kent, TN23 1FB

Tell us your news: Contact: Adrian Murdoch adrian.murdoch@healthcaretoday.com +44 (0)7983 407607
Advertise with us: Advertise with us: Contact: Jake Sackman jake.sackman@healthcaretoday.com +44 (0)7785 803226
To download a copy of our media pack, click here.

