Staying Safe with Opioids at Home: The Role of Naloxone in the Care of Older Adults
By Elana Kieffer, MBA Director of Strategic Alliances, Gerontological Society of America
Many of us, especially as we age, are prescribed opioids for pain relief, due to health conditions or when recovering from surgery. While opioids used for pain relief as prescribed by a health care provider, especially taken short-term, are generally safe, there is always a risk of an overdose. It is important to note that not all opioids a person may have in their home were prescribed for them by a health care provider. If you or a loved one has opioids in the home, there are many ways to store opioids safely and steps to take if you think someone has had an overdose.
Opioids are powerful and potentially addictive drugs that are sometimes needed for treating severe pain. When you or someone you live with or care for is interacting with opioids, you, family members, caregivers, friends, and other acquaintances must know about the adverse effects of these drugs and how to recognize and respond in cases of apparent overdoses.

Narcan) is a medication that can be used to restore breathing in people who have overdosed on opioids. You can also purchase naloxone without a prescription by paying for it out-of-pocket.
There are questions you should ask the prescribing provider when considering opioids for your treatment plan or for someone who you provide care for. There are also important questions to ask your pharmacist about methods for safely and securely storing and disposing of opioids.
Physicians, dentists, and other health professionals grew accustomed over the years to prescribing opioids for a variety of relatively simple surgeries and minor conditions. Many of these situations are now recognized as responding well to nonopioid therapies such as over-the-counter analgesics. Ask your health care provider if nonprescription drugs or other non-opioid prescription medications could be strong enough to relieve pain when considering using opioids.
Questions to Ask Your Health Care Provider
• Do I really need opioids?
• Would something with fewer side effects be enough to stop my pain?
• Will you prescribe naloxone in addition to the opioid so that my insurance covers it?
• What is the best way to dispose of leftover medication when I no longer need it?
If you or someone you care for is prescribed an opioid medication, be sure to ask for and fill a prescription for naloxone. Naloxone (also commonly known as the brand name
People often do not take all the opioid medication they are given at the pharmacy, and these leftover medications lie forgotten in drawers and medication cabinets for long periods of time. Pets and children may discover and eat them. Teenagers or adults who are experimenting with drugs or addicted to opioids may find and take these drugs. You never know when naloxone may be needed.
When opioids are present in the home, they must be stored properly—safely away from pets, children, and drug-seeking adolescents and adults. Recommended practices for the storage of opioids include the following:
• Use a locked cabinet or a medication lock box or drawer.
• Avoid storage in easily accessible areas such as bathrooms or kitchens.
• Keep opioids and other medications in their original containers with information on proper use and side effects.
• Keep track of the number of tablets or capsules remaining in the home.
• Educate all family members and caregivers on the risks associated with opioid use.
• Avoid storage in purses or bags to prevent theft or pilfering.
• Keep medications in locked containers when traveling and maintain a list of all transported medications.
Just as safe storage is important, opioids should be disposed of properly. The best way to dispose of opioids safely
is by taking them to a collection site registered by the U.S. Drug Enforcement Administration (DEA). You can find one close to you by going to https://www. deadiversion.usdoj.gov/drug_disposal/ drug-disposal.html and selecting “Search for Year Round Pharmaceutical Disposal Locations.”
These drop-off locations are usually pharmacies or law enforcement agencies. Consumers can also ask pharmacists for pre-addressed envelopes to mail unneeded opioids back to the pharmacy.
When those options are not available, the next best choice is making the drug products unpalatable or impossible to use before disposing of them in household trash. One method is mixing crushed-up drug products with coffee grounds, cat litter, or dirt. Another is to dissolve the products in water mixed with vinegar or dish soap and then soak up the solution using paper towels.
High-risk products such as hydrocodone and fentanyl can be flushed down the toilet when other options are not feasible. Check the U.S. Food and Drug Administration (FDA) Remove the Risk medication flush list at https://www.fda.gov/drugs/disposalunused-medicines-what-you-shouldknow/drug-disposal-fdas-flush-listcertain-medicines to determine whether a product can be safely flushed.
Signs of Overdose and How to Help
The most common side effects of opioids are sedation, constipation, euphoria, and mood changes. It is important to know how to recognize, prevent, and manage these side effects. If they do occur, you must monitor the person who is taking opioids and be prepared to take prompt action.
Sleepiness and sedation are difficult to distinguish from opioid poisoning. As a family member or other caregiver, you can take the following actions to detect and manage sedation during opioid therapy:
• Watch diligently for signs of
excessive sedation, such as difficulty waking the person, dizziness, or confusion.
• Report to the person’s health care professionals all current medications, supplements, and nonprescription drugs as well as any recreational drug and alcohol use.
• Ensure that the person follows the prescribed dosing instructions and does not take extra doses.
• Encourage the person to avoid alcohol and other sedating drugs, including benzodiazepines such
as Valium and Xanax.
All these factors make it important for you to be alert to adverse effects or opioid poisoning. People with past histories of substance abuse may be on treatments such as methadone or buprenorphine, and these can increase the risk of opioid poisoning.
Safely using opioids requires attention to these instructions by everyone involved at all times:
• Never take more opioids than prescribed without first consulting the health care provider or pharmacist.
• Keep a record of any changes in signs and symptoms or reactions to the opioids during treatment.
• Ensure that you know the signs that indicate an emergency situation requiring immediate medical attention.
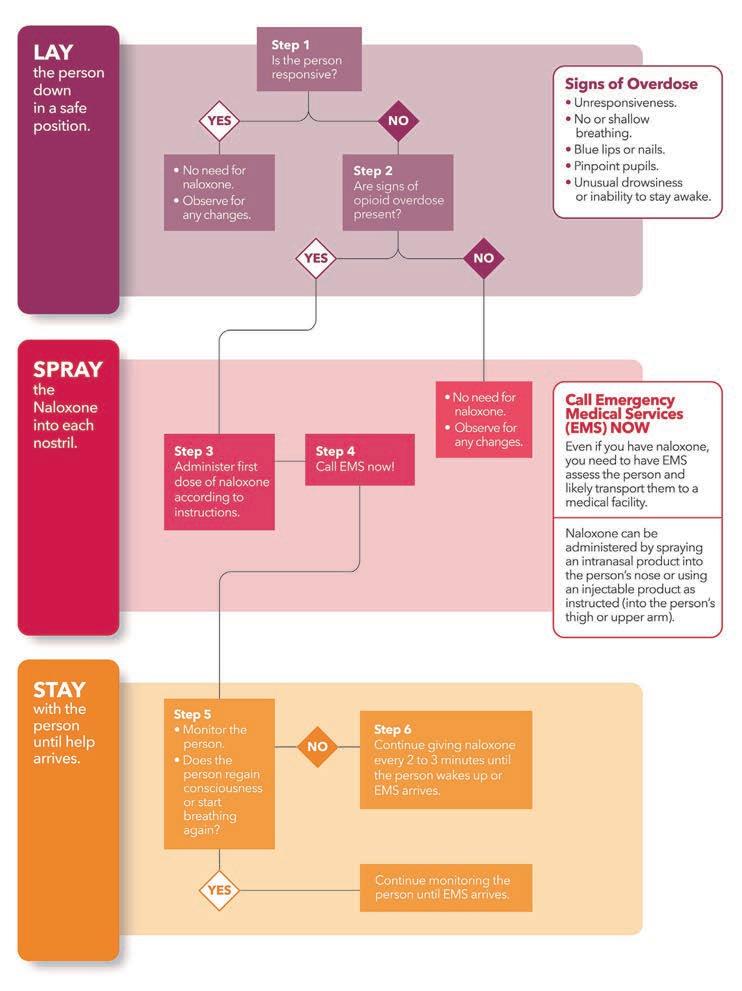
As shown in the decision tree on page 30, signs of potential opioid overdoses include excessive sleepiness or trouble staying awake, walking, or talking. Other signs of an overdose are slow or shallow breathing, snoring or gurgling sounds, pale or cold skin, blue lips or fingernails, or constricted (small) pupils. If these signs are present, call the person’s name loudly, shake them, and rub your knuckles on their sternum (center chest) to try and wake them up.
If the patient does not awaken, immediately administer naloxone. Lay the patient on their back and tilt their head up. Follow the instructions provided with the product you are using. For intranasal sprays, insert the nozzle into the nostril and press until the unit clicks to spray. For injectable naloxone, use the device as directed, injecting the medication into the outer thigh or upper arm (like an Epi-Pen).
Naloxone quickly reverses an overdose by blocking the effects of opioids. It can restore normal breathing within 2 to 3 minutes in a person whose breath has slowed, or even stopped, as a result of opioid overdose. After the naloxone dose is given, place the person on their side with the top leg bent to prevent choking if they vomit.
Call emergency medical services (911 in North America) immediately after administering the first dose of naloxone. Tell emergency services where you are and describe the patient’s condition. If you have experience monitoring someone’s vital signs, record their heart rate, breathing rate, and when possible, oxygenation and/or blood pressure. When help does arrive, give them the patient’s vital signs if you were able to take them.
Stay with the person until help arrives. The effects of

naloxone only last for up to 90 minutes, and the opioid still in the patient’s system could again suppress breathing.
Continue to observe the patient. If breathing is not restored after 3 minutes, give additional doses of naloxone every 2 to 3 minutes until help arrives. Emergency services can help you on the phone determine when you need to administer another dose.
Opioids are powerful drugs that can control severe pain. However, overdoses still can occur even in those who have been using opioids for a while. The body’s responses to opioids can change, doses can be increased, or therapy may be switched to a different opioid. Family members and caregivers play an essential role in opioid safety. By knowing what signs and symptoms to watch for and what to do for opioid poisoning, you can protect the health and lives of your family and friends.

About the Gerontological Society of America: GSA is the oldest and largest interdisciplinary organization devoted to research, education, and practice in the field of aging. GSA’s principal mission — and that of our 6,000 members — is to promote the study of aging and disseminate information to scientists, decision makers, and the general public.
Founded in 1945, GSA is the driving force behind advancing innovation in aging — both domestically and internationally. Our members come from more than 50 countries.
The Vision of GSA is Meaningful Lives as we Age.
Learn more at www.geron.org

