
Hacking the matrix TO BREACH CANCER’S TOUGHEST BARRIERS
Welcome

Dear Garvan family,
Sometimes the most important discoveries come from looking at old problems in entirely new ways – through fresh perspectives, cutting-edge technology or often both, working in tandem.
In this issue, you’ll learn why some childhood cancers stop responding to chemotherapy and how we found a drug that works differently. You’ll discover an innovative approach to pancreatic cancer where immune cells become smart drug delivery systems. And finally, you’ll find out about our new clinical trial for liver cancer.
These advances happen when we have the right people asking the right questions. This year, we’ve welcomed two exceptional scientists from leading institutions – Dr Clare Puttick and Dr Carlson Tsui – while celebrating Dr Etienne Masle-Farquhar and Dr Seyhan Yazar establishing their own labs. I’m also delighted to share that we have appointed Garvan’s first Chief Translation Officer, Dr Rachel Galimidi, who will help accelerate our discoveries from lab to clinic.
From a clinical trial for liver cancer to understanding the earliest changes in multiple sclerosis, the research in this issue represents our commitment to transforming how diseases are diagnosed and treated.
Your partnership brings this extraordinary science into the world. Thank you for your continued support.
Yours sincerely,
Cover image: A killer immune cell probes the dense collagen matrix surrounding a tumour. By mapping these physical barriers, researchers are learning how to engineer therapies that can bypass them.
Credit: Biro Lab
Mapping MS

What if the earliest signs of multiple sclerosis (MS) could be detected before irreversible damage occurs? MS is a complex autoimmune disease shaped by both genetics and the environment, yet its earliest biological triggers remain hidden.
Following her recent appointment to Garvan’s Faculty, Dr Seyhan Yazar has established a lab to investigate how genetic risk and environmental exposures interact to drive autoimmune disease, with an initial focus on uncovering the biological changes that occur long before MS is diagnosed.
“In the future, I hope our work shifts the paradigm of MS care from a ‘one-size-fitsall’ approach to true precision medicine,” says Dr Yazar. “By understanding the unique interplay between a person’s genetics and their environment, we aim to enable earlier diagnosis and develop tailored management strategies.”
Professor Benjamin Kile Executive Director and CEO
Her lab is looking for the specific biological ‘fingerprints’ of MS that differentiate how the disease manifests in different people – helping clinicians better predict the treatments most likely to work for each person.
Dr Seyhan Yazar
Discoveries in Focus

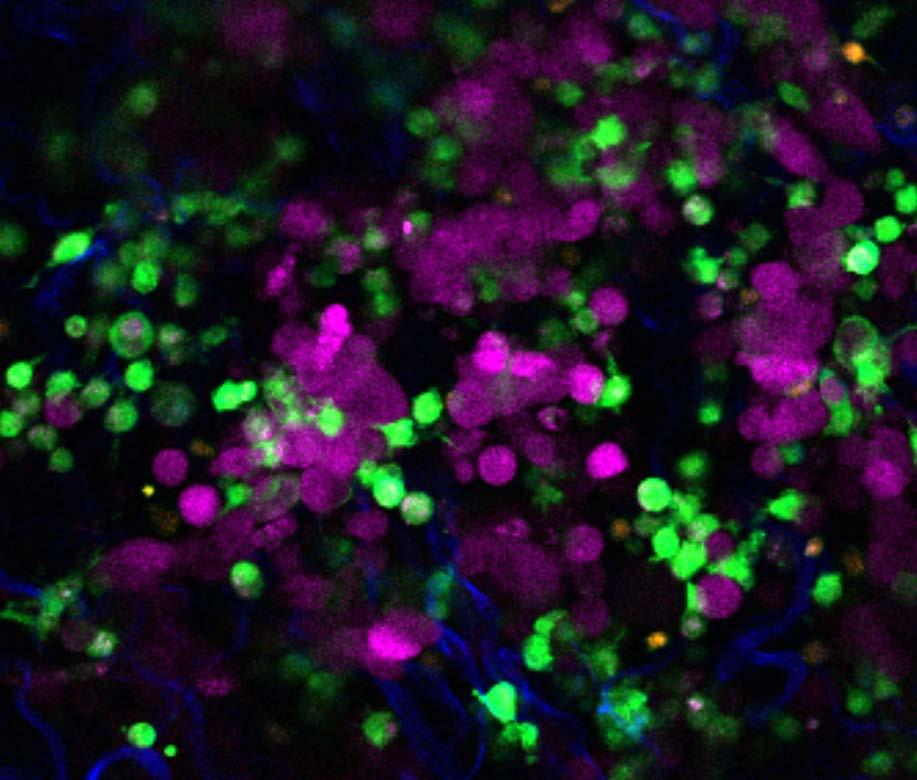
The skin’s battlefield
In this striking snapshot of the skin’s microscopic battlefield, Dr Yuki Keith captures the immune system going on the offensive. Using real-time imaging at Garvan’s ACRF INCITe Centre, Dr Keith – a dermatologist-turned-researcher in Garvan’s Phan Lab – reveals immune cells called macrophages (green) surrounding and ‘nibbling’ on melanoma cells (magenta).
While other immune cells (orange) stand guard, collagen fibres (blue) are the structural backdrop of the skin. For Australia, which has the world’s highest melanoma rates, this work is vital. By witnessing how these macrophages ingest tumour cells, Dr Keith aims to unlock new ways to prime the body’s own defences against aggressive skin cancers.
Dr Yuki Keith
Charles’s story
Medical research gave Charles an ‘extra life’ – now he’s ensuring others get the same chance.

When retired hotel manager Charles visited his GP in 2015 for a routine skin check, he expected to be in and out in 15 minutes. Instead, the discovery of a swollen lymph gland triggered a whirlwind 72-hour diagnosis of Merkel cell carcinoma (MCC), a rare and aggressive skin cancer.
What followed was a swift but extensive healthcare journey: surgery to remove 46 lymph nodes from his neck and 25 sessions of precision radiotherapy. Though he was initially given the all-clear, the news came with a stark warning; his radiologist told him that if the cancer returned, the outlook would be terminal. Three years later, that possibility became a reality when scans revealed a four-centimetre tumour had spread to his lungs.

Facing this devastating development in his 80s, Charles’s resilience was put to the ultimate test. Under the care of Dr Venessa Chin, an oncologist at St Vincent’s Hospital and Research Officer at Garvan, Charles tolerated his treatment remarkably well. Against all odds, he was cancer-free less than a year later, attributing his ‘extra life’ to the clinical expertise and medical research that guided his care.
While he focused on his physical recovery – even asking his doctors at one point when he’d waterski again – he also began to reflect on the science that was making his recovery possible. This profound sense of gratitude shifted Charles’s focus from his own recovery to the legacy he wanted to leave behind.
His journey with cancer became the inspiration to support the Garvan Institute, ensuring that future discoveries continue to turn the tide for patients facing aggressive diseases.
I firmly believe that medical research has kept me alive, there’s
no question about it.
Charles, Partner for the Future
With that in mind, Charles became a Garvan Partner for the Future, pledging a gift in his Will to support medical research.
“I’ve now had 10 years of extra life,” he says. “You can’t pay somebody to save your life. But you can leave money towards something that might help somebody else. There are millions of charities one could give to,” he says. “But Garvan achieves so much.”
“In terms of my Will, I believe I’m leaving them a legacy; that supporting medical research will enable somebody to benefit from it – the same way I have.”
Charles, Partner for the Future
Family runs strong

Sydney construction company Belmadar helped Team Garvan achieve its best-ever City2Surf result last year, raising a record $68,110 for medical research – more than double their previous effort.
Led by managing director Alfredo Marrocco, son of founder Domenico Marrocco, Belmadar’s enduring commitment to Garvan’s blood cancer research began after their beloved Domenico’s death from acute myeloid leukaemia (AML) in 2015. Their decade-long commitment has now raised over $210,000.
The funds support research led by Dr Jim Blackburn, developing genetic tests to detect mutations that cause AML and other blood cancers. These tests could help clinicians identify the specific genetic changes driving each patient’s cancer, potentially leading to more targeted treatment approaches. The Marrocco family is proud that through their legacy, this support has enabled discoveries not only in blood cancer research, but in other diseases too.

“We hope our fundraising leads to earlier detection, more effective treatments, and ultimately, a future where other families don’t have to face the heartbreak of losing a loved one too soon,” says Alfredo.

(Left to right) Dr Jim Blackburn, Michelle Uhlhorn, Luke Civitarese, Kirsten Griffiths, Josh Levitt, Lidia Marrocco, Alessia Marrocco, Alfredo Marrocco, Nick Gaglianocelebrating their record City2Surf donation
The Belmadar team. (Left to right) Nick Gagliano, Domenico Marrocco, Alfredo Marrocco, Millie Mayn, Kerri Eagle
Unlocking hope
Neuroblastoma is notorious for resisting chemotherapy, often with tragic results for the children it affects. Our new study shows how an existing drug could overcome this deadly resistance.


For Stacey and Andy, watching their two-year-old son Asher endure nearly two years of intensive cancer treatment was devastating. Despite chemotherapy, surgery to remove a 10cm tumour, bone marrow transplant, radiation and immunotherapy, Asher’s neuroblastoma eventually stopped responding to treatment. He passed away in May 2023, aged four and a half.
Neuroblastoma, a cancer that develops from immature nerve cells, is the most common solid tumour in young children after brain cancer. Asher’s story reflects a harsh reality: when this aggressive cancer returns, current treatments save fewer than one in ten children. Now, Garvan researchers have discovered why these cancers become resistant – and identified a drug combination that could bypass this deadly defence mechanism.
Neuroblastoma cancer cells
Asher and his parents

The team, led by Associate Professor David Croucher, studied tumour samples from children at diagnosis and after relapse. They found that many chemotherapy drugs depend on a cellular ‘switch’ called the JNK pathway to trigger cancer cell death. In resistant tumours, this switch stops working.
“We discovered that relapsed neuroblastomas have essentially learned to ignore the signals that should tell them to die,” says Associate Professor Croucher. “It’s like having a fire alarm that no longer triggers the sprinkler system – the warning is there, but nothing happens.”
Rather than trying to fix the broken switch, the researchers looked for drugs that could trigger cell death through alternative routes. Screening FDA-approved medicines with paediatric safety data, they identified romidepsin, currently used for certain lymphomas, as particularly effective against neuroblastoma cells regardless of whether the JNK pathway works.
In collaboration with the Children’s Cancer Institute, the team tested the combination in preclinical models of relapsed neuroblastoma. Adding romidepsin to standard chemotherapy reduced tumour growth and extended survival compared to chemotherapy alone. Importantly, lower doses of chemotherapy achieved the same cancer-killing effect when combined with romidepsin – potentially reducing side effects for young patients.
Behind every statistic is someone’s loved one, understanding these molecular mechanisms gives us hope we can develop more effective treatments for patients and their families who currently face limited options.
Associate Professor David Croucher
The findings, published in Science Advances, represent an important step in understanding treatment resistance. Because romidepsin is already approved and has been tested for safety in children, development could be faster than for entirely new drugs. However, further study and clinical trials are still needed to establish safety and effectiveness in neuroblastoma patients.
For families like Asher’s, who witness their children’s remarkable courage through gruelling treatments that may ultimately fail, this research honours their experience by working towards answers. The goal is simple: fewer children lost to this devastating disease.
Neuroblastoma: The facts
• Most common solid tumour in children outside the brain
• Typically diagnosed before age 2
• Develops from nerve cells in adrenal glands or along spine, chest, abdomen or pelvis
• Half of patients have high-risk disease with tumours already spread

Associate Professor David Croucher
Resistance isn’t futile
Garvan researchers are engineering immune cells that sense cancer’s defensive barriers and respond with targeted drug release, while virtual reality helps them understand how killer cells navigate tissue.
On level 9 of The Kinghorn Cancer Centre, researcher Jakson Playford grips two controllers while wearing a virtual reality (VR) headset. On the screen, we see what he sees: one of the immune system’s killer cells caught at the centre of a glowing web of collagen fibres, probing for a way to squeeze through any gaps.
This VR system, built from vast amounts of microscopy data – equivalent to eight months of continuous highdefinition Netflix streaming – is helping Associate Professor Maté Biro’s lab understand how immune cells interact with the barriers that protect tumours.
Cells are not just bags of chemicals – they can push, pull, feel their surroundings – and we need to understand those abilities to equip them with new ways to kill cancer.

The work addresses one of oncology’s most pressing challenges: pancreatic cancer, where tumours surround themselves with tissue up to ten times stiffer than normal. This dense barrier of collagen mesh blocks immune cells and drugs alike, contributing to a five-year survival rate of just 13 per cent.
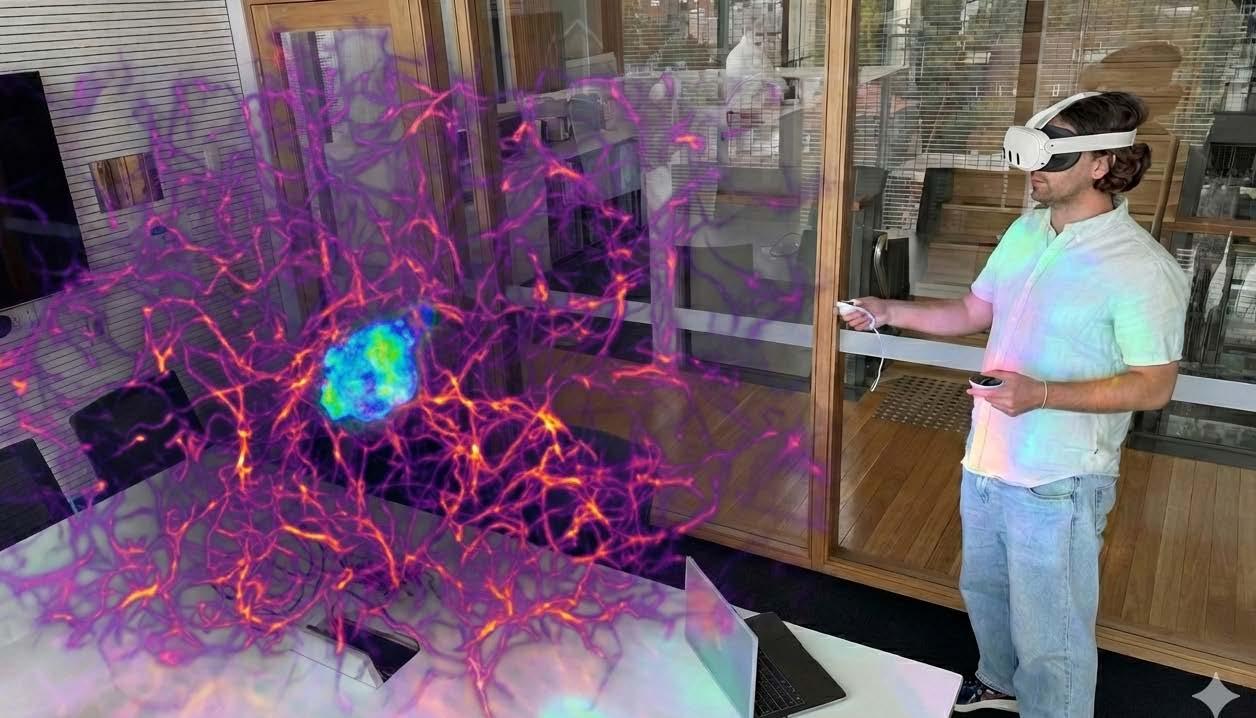
Inside the matrix: tracking a killer immune cell (green blue) trapped in a dense mesh of cancer’s protective barrier (pink purple). The image was generated using Gemini.
Associate Professor Maté Biro
Associate Professor Maté Biro
Rather than trying to bulldoze through these barriers, Associate Professor Biro’s team is taking a different approach. They’re engineering immune cells to become smart drug delivery systems. When these modified cells encounter the abnormally rigid tissue around tumours, they’ll release therapeutic proteins a thousand times smaller than them, that can slip through where the cells themselves cannot. “It’s like having soldiers who can advance right to the castle walls and then fire arrows through the loopholes,” Associate Professor Biro explains.
The trick involves giving the cells molecular sensors that detect mechanical force. Like a pressure-sensitive switch, these sensors activate when they feel the stiffness surrounding cancerous tissue – triggering the cell to produce cancer-fighting drugs on the spot. The forces involved are incredibly subtle, ten thousand times smaller than the weight of a grain of salt on your hand.
“We were interested in seeing exactly how collagen fibres are displaced from their resting positions when a cell pushes through,” says Dr Peter Newman, who leads the VR integration.
We can identify which fibres are under tension, which are compressed, and map out that mechanical landscape the cell is navigating.
Dr Peter Newman
This three-dimensional understanding of cellular mechanics underpins the team’s broader research strategy. Creating the visualisation needed artificial intelligence to computationally track the fibres. By understanding these mechanical interactions, the researchers can better calibrate their engineered cells – determining precisely what level of stiffness should trigger drug release.
If successful, this approach could transform treatment for pancreatic cancer and potentially other solid tumours that create similar barriers. Instead of accepting these defences as insurmountable obstacles, the team is turning them into the very trigger for treatment – a conceptual shift that could offer hope where little exists today.
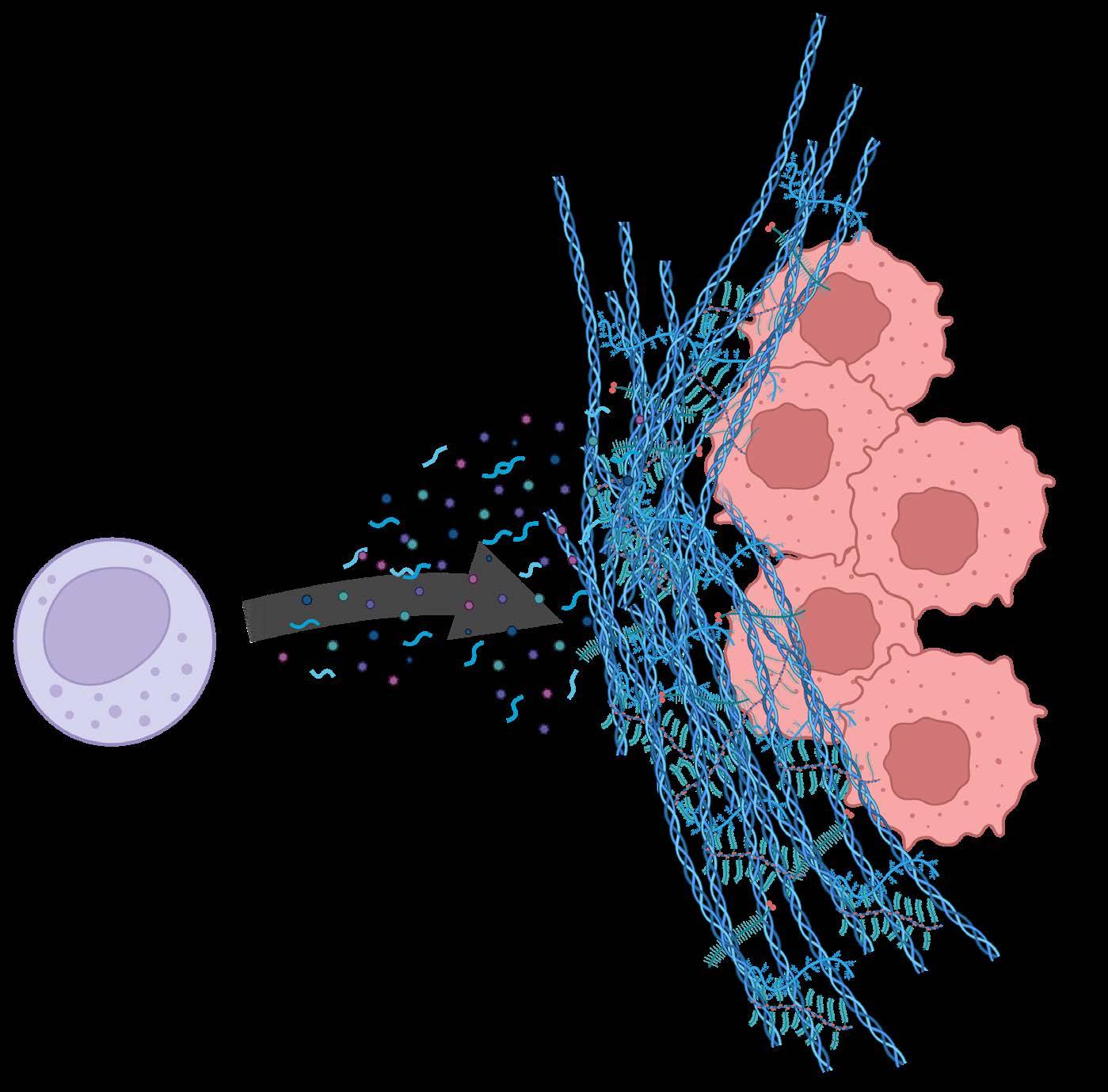
Therapeutic proteins released
Special delivery
The immune system’s cells are too large to squeeze through pancreatic cancer’s dense barriers. But the therapeutic proteins they will release upon sensing the stiffness of the barrier are a thousand times smaller –small enough to slip through where the cells cannot.
Immune cell
Collagen mesh
Cancer cells
New liver cancer clinical trial
A Garvan trial is testing a combination of two already approved drugs to deplete the environment around liver cancers and to prevent recurrence.

A new clinical trial co-led by Garvan and The Westmead Institute for Medical Research is seeking to test a combination therapy in early-stage liver cancer, with the hopes of improving survival rates for this deadly disease.
The trial, called DEFINERx050 is being co-led by Garvan’s Dr Ankur Sharma.
Over the last decade researchers have made a remarkable discovery that is transforming how we understand cancer – that the environment surrounding tumours is just as important as the cancer cells themselves. And liver cancer is no exception.
“We now understand that liver cancers need both ‘seed’ and ‘soil’ to grow. The cancer cell – seed – needs the right microenvironment – soil – around it to both provide nutrients and suppress the immune system from attacking and removing the cancer cells. In this way, cancer cells subvert the body’s systems to continue to grow unchecked,” says Dr Sharma.
This occurs because both liver cancer cells and those in the surrounding microenvironment are able to rapidly change their behaviour through reprogramming, a phenomenon called cell plasticity.
In a significant breakthrough, Dr Sharma discovered that certain reprogramming ‘signatures’ in the microenvironment make liver cancers more aggressive. Focusing on this new approach, Dr Sharma previously showed that liver cancer patients with these reprogramming signatures don’t respond well to current standard-of-care treatments. However, these
Dr Ankur Sharma
patients do respond to a combination of drugs called bevacizumab and atezolizumab which together work to actively target the environment around tumours. Atezolizumab reverses the immune suppression that cancer cells exert on their surroundings, allowing the immune system to enter and destroy the cancer cells, while bevacizumab affects the growth of cells that line blood vessels. This means blood vessels surrounding the tumour shrink, starving the tumour of vital nutrients. In Australia, this combination is already approved and subsidised for late-stage liver cancer but hasn’t yet been tested in the early stages of the disease. That’s the gap that the DEFINERx050 trial will fill, evaluating the effect of the combination treatment on high-risk, early-stage liver cancer patients, with a particular focus on cancer recurrence.
The trial is currently recruiting 208 people with earlystage hepatocellular carcinoma, the most common form of liver cancer, across five states and in 12 hospitals around Australia.
The great thing about this trial is that it’s testing a combination of drugs which are already approved and subsidised in Australia. If the trial is successful in reducing the recurrence of liver cancer, adoption into the clinic should be swift, and that’s great news for people living with this disease.
Dr
Ankur Sharma
This study has been approved by the Western Sydney Local Health District Human Research Ethics Committee with reference number 2024/ETH02271.
Dr Sharma is supported by the The Kinghorn Foundation.

About liver cancer
• Over 3,000 Australians are diagnosed and 2,500 die from liver cancer each year
• Only 1 in 4 people survive five years after diagnosis
• Hepatocellular carcinoma is the most common form, accounting for 90% of primary liver cancer cases
• Cases are increasing as more people are diagnosed with type 2 diabetes and fatty liver disease, risk factors for liver cancer
Interested to hear more from Dr Sharma?
Listen to his episode of our podcast, Medical Minds garvan.info/podcast-s3e9