Dragon Products Group: Tanks & Trailers/Rigs/Pump & Power/PES
Tiger Rental Group: Offshore/Industrial/Safety/PMI
Modern AgILE Group: Modern Ag/Rancher Supply/ National Chassis/Modern Polymer Products/Pipe & Extrusions


Dragon Products Group: Tanks & Trailers/Rigs/Pump & Power/PES
Tiger Rental Group: Offshore/Industrial/Safety/PMI
Modern AgILE Group: Modern Ag/Rancher Supply/ National Chassis/Modern Polymer Products/Pipe & Extrusions

Medical
Medical/Dental
UnitedHealthcare
www.myuhc.com
877-277-6091
877-816-3596 Dental
800-638-3120 Vision
Health Savings Account
HSA Bank
www.hsabank.com
855-731-5220
Employee Assistance Program
UnitedHealthcare
www.liveandworkwell.com
877-660-3806
Human Resources
The Modern Group health.insurance@modernusa.com 409-951-4001



Your benefits program offers three medical plan options. To help you make an informed choice and compare your options, a Summary of Benefits and Coverage for each plan is available on the ADP enrollment website.
There are special notifications relating to your medical plans contained on the ADP enrollment website. These include the Women’s Health and Cancer Rights Act of 1998, Special Enrollment Rights, Medicare Drug Coverage, HIPAA Privacy Practices, and Premium Assistance Under Medicaid and CHIP programs.
The Modern Group pharmacy benefit options qualify as creditable coverage, because they are at least as generous as the plan provided under Medicare Part D. This means employees eligible for Medicare can participate in the pharmacy plans offered by The Modern Group and do not have to pay a penalty once they leave The Modern Group plan to enroll for Medicare Part D.
If you have any questions about this process, call our claim service team at 888-299-2070 between 8:00 a.m. and 8:00 p.m. ET.
1. Member claims portal – Log in to myuhcfp.com and click the “Start a Claim” icon
2. Hard copy claim form – Request the claim form from your HR representative. Complete, sign, date, and send the form via fax or mail to the contact details listed on the claim form. You may also email the completed form to fpcustomersupport@uhc.com. Please note, this is an unsecured email address.
3. Phone – Confirm telephonic access with your HR representative. Then, call us toll-free at 866-556-8298. Monday through Friday, 8:00 a.m. to 8:00 p.m. ET.
We are pleased to confirm that we will remain with UnitedHealthcare (UHC) for the policy year June 1, 2026 through May 31, 2027. There will be no change in benefits and no increase in employee contributions for the new policy year. We are pleased to confirm that there has been no change in employee premiums for any plan since we went with UHC five years ago.
This guide is your opportunity to learn more about the benefits that are available to you and your eligible dependents beginning June 1, 2026. Take time to evaluate your coverage options and determine which plans best meet your health care and financial needs. Being a wise consumer can support your health and maximize your health care dollars.
Each year during Open Enrollment (OE), you have the opportunity to make changes to your benefit plans. The enrollment decisions you make this year will remain in effect through May 31, 2027. After OE you may make changes to your benefit elections only when you have a Qualifying Life Event (QLE).
You will have 30 days to make your benefit elections and submit supporting documentation to Human Resources. Changes will be effective on the day of the event and must be consistent with your QLE. If you do not make your changes during the 30-day period, your changes cannot be made until the next OE period.

There are no changes in the benefit programs for the new plan year. Please keep in mind the following free programs that are available to all members:
The Price Edge program ensures you pay the lowest cost for medications remains in effect. This program guarantees the lowest possible cost for generic and some non-covered medications by searching for coupons from vendors like GoodRx, which can lower your out-of-pocket cost for certain medications. This happens automatically at the pharmacy; no action is needed by the plan participant. This program applies to all plans, including the Health Savings Account (HSA) plan, where employees pay the discounted actual cost until they meet their deductible. Refer to page 11 for more details.
The Accident and Hospital indemnity plans continue to include the Benefit Assist feature. This provision automatically files claims for these coverages based on data from the medical plan. See more details about the coverage on pages 18-19. These coverages pay claims in addition to the medical coverage, effectively reducing your out-of-pocket cost for covered accident and hospitalizations.
We continue to offer Teladoc benefit support programs for diabetes, prediabetes, and hypertension management. If you have any of these conditions, you can enroll in this program at no cost. It offers valuable monitoring tools, support, and resources to help you effectively manage your condition and improve your well-being. If you are not already enrolled, consider joining as the program is continuous.
You will continue to have access to the UHC Tier 1 Provider network of physicians and facilities. Tier 1 providers are screened and approved by UHC for cost-effective, quality care using the best and latest technology. This results in better outcomes and lower costs for you. We strongly encourage you to take advantage of this benefit feature, because it provides higher benefits and access to top-quality care at affordable prices. See page 6 for more information on the UHC Tier 1 Provider program.
Log on to ADP to access the Open Enrollment Wizard, which will automatically appear on your screen when you log in. Click Start This Enrollment or click Remind Me Later to enroll later.
Add anyone who will be covered as a dependent or a beneficiary.
You have two options:
Click Walk Me Through My Benefit Options to review your benefit options.
Click I Know What I Want To Change to begin making your enrollment elections.
Consider your level of coverage. This is the only time you will be able to change coverage this year unless you have a QLE.
Review current dependents and enroll or unenroll as necessary.
Edit your plan to review your elections and make any necessary changes.
Choose a beneficiary(ies) for Life insurance and indicate the share percentages.
You have two options:
Click Finish Later to save your changes and continue at a later time. You can select this option anytime during the process.
Click Review and Complete to finalize your elections and submit for approval.
Step 5: Print the Review Your Benefit Elections Page for Your Records.

After you click Complete Enrollment, your elections will be forwarded to Human Resources, who will send you an approval email.
You are eligible for benefits if you are a regular, full-time employee working 30+ hours per week. Your coverage is effective the first of the month after you have completed 60 days of full-time employment. You may also enroll eligible dependents for benefits coverage. The cost for coverage depends on the number of dependents you enroll and the plans you choose. When covering dependents, you must select and be on the same plans.
Your legal spouse if your spouse does not have coverage available from an employer-provided medical plan
Children under age 26 regardless of student, dependency, or marital status
Children over age 26 who are fully dependent on you for support due to a mental or physical disability and who are indicated as such on your federal tax return
Your benefit elections remain in effect for the entire plan year until the following OE. You may only change coverage during the plan year if you have a QLE such as marriage, divorce, birth or adoption, loss of other coverage, etc. You must notify Human Resources within 30 days if any of these events occur. Contact Human Resources for a full list of QLEs.


The medical plan options through UHC are designed to protect you and your family from major financial hardship in the event of illness or injury. Each time you seek medical care, you decide whether to use in-network or out-of-network providers. Both you and the company benefit from significant discounts through negotiated rates when you use UHC Tier 1 providers. To access a list of Tier 1 and non-Tier 1 PPO providers, visit www.myuhc.com or call 877-277-6091 for assistance.
The High Deductible Health Plan (HDHP) offers the freedom to see the provider of your choice, and preventive care is fully covered in-network. When you use in-network providers, you receive benefits at a discounted network cost. You pay more for out-of-network providers. However, in exchange for a lower per-paycheck cost, the HDHP requires that you satisfy a higher deductible for almost all health care expenses, including prescriptions. Once your in-network combined deductible for medical and pharmacy is met, the plan pays 100%. Out-of-network providers will be reimbursed at the out-of-network benefit amount. If you enroll in the HDHP, you may be eligible to open an HSA. See page 11 for more information about the HSA.

Premium Plus Plan
Ultimate Plan
The Preferred Provider Organization (PPO) plan options offer the freedom to see any provider when you need care. When you use Tier 1 providers, you receive benefits at a discounted network cost. You pay more for services if you use non-Tier 1 PPO or out-of-network providers. There is no deductible for preventive care, which is covered at 100% in-network. While not required, it is recommended you select a Tier 1 primary care physician (PCP) to manage your care.
If you enroll in the Premium Plus or Ultimate medical plan, you will pay less using Tier 1 providers.
Copays for Tier 1 providers are less than non-Tier 1 PPO providers
Primary Care – $0 Tier 1 versus $30 or $40 nonTier 1 PPO (depending on plan)
Specialist Care – $40 Tier 1 versus $100 non-Tier 1 PPO
Coinsurance is 10% for Tier 1 providers and 30% for non-Tier 1 PPO providers

The $250 per confinement copay is waived, and coinsurance is less if admitted to a Tier 1 hospital
The $100 copay for outpatient surgery is waived, and coinsurance is less when using a Tier 1 provider
Telemedicine visits are $0
There are no requirements to use a Tier 1 provider. If your current provider is not designated as Tier 1, you do not have to change providers, but you may pay more for care. You may select a Tier 1 provider at anytime for primary or specialty care.
Locate a Tier 1 Provider
To locate a Tier 1 provider or facility, log in at www.myuhc.com and access the Provider Directory. Look for providers designated with the Tier 1 blue dot symbol. The list of Tier 1 providers is updated annually. Employees living outside the Tier 1 geographic area will receive Tier 1-level benefits using their current providers.
This is how it looks on www.myuhc.com
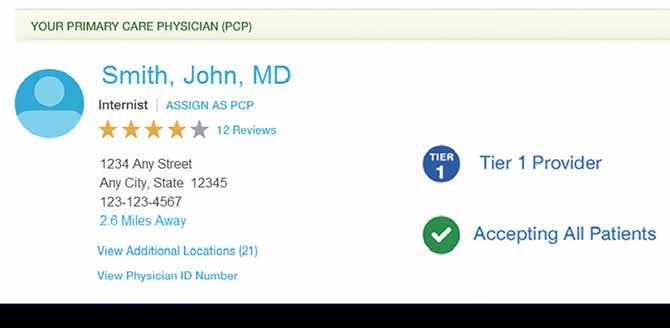




1 Applies toward deductible.
2 Your cost after the deductible is met.
3 After deductible.
If there are not at least two Tier 1 PCPs within 30 miles of your home, you may be classified as an out-of-area member and will receive Tier 1 benefits with your current PPO providers. This applies only to employees living in Wyoming and a few additional rural locations.
To find a provider or to look up your current provider prior to your effective date:
Visit www.whyuhc.com/nexus2
Click on Health Plans.
Select Nexus ACO OAP “Plan Details.”
Then search the provider network.
Note: Pharmacy information is not available until after your effective date.
Call the number on the back of your ID card or log in at www.myuhc.com
Click on Doctor Search and search by ZIP code, name, provider type, or facility.
Tier 1 – If you are enrolled in the Premium Plus or Ultimate medical plan, search for providers with the Tier 1 symbol and pay $0 for primary care or $40 for specialist care.

PPO Network – Providers in the PPO network but without the Tier 1 symbol are considered in-network, but you pay more than for Tier 1 providers.
Out-of-Network – Providers not included in the PPO network, or without a Tier 1 symbol, are considered out-of-network.
Remember, you can select a Tier 1 provider at anytime. If your provider is not a Tier 1 provider, be sure your provider is a member of the PPO network to receive in-network benefits.

Your UHC pharmacy benefit now includes Price Edge, a discount solution for covered generics and select non-covered drugs.
Use your current network pharmacy—no setup needed.
Get automatic savings on some covered medications.
Receive discounts on non-covered and OTC drugs with a doctor’s prescription.
Download the Price Edge app or visit www.myuhc.com

Call the number on the back of your ID card or log in at www.myuhc.com.
Click on the Pharmacies & Prescriptions tab.
Select one of the following options:
Find price and medication
Find alternatives
Locate pharmacy
Manage home delivery
www.myuhc.com is a personalized website that helps you access and manage your health plan and information. Use it to:
Find network doctors and facilities.
Check your coverage and claims status.
Review preventive care services.
Print a temporary ID card.
Access the Virtual Visits telemedicine services.
Compare costs for treatment and care.
Set Up Your Account
Go to www.myuhc.com.
Click on Register Now. You will need your ID card or your Social Security number and date of birth.
Follow the step-by-step instructions.
UHC Mobile App
For quick and easy access to your www.myuhc.com account, download the UnitedHealthcare app and use it to:
Access resources such as Virtual Visits.
View your copay and coinsurance information for common medical visits.
View and share your medical ID card.
View claims information and updated deductible and coinsurance amounts.
And more!

When you have questions about your health care, get answers quickly and reliably from UHC’s Advocate4Me
The Advocate4Me program connects you with a personal advocate who helps you navigate the health care system to get the information and support you need. Your advocate consults with experts who specialize in clinical medicine, behavioral health, wellness, pharmaceuticals, and cost management. Your advocate can also help you understand your overall health benefits plan so you can make informed health care decisions.
Your advocate is a single point of contact to help you resolve issues and guide you to the right resources. Health resources and tools are accessible online 24/7, and advocates are available by phone Monday through Friday from 7:00 a.m. to 10:00 p.m. CT.
Nurse Advocate
A clinically licensed expert (LPN or RN) who can provide health education
Health Advocate
A claims and wellness expert
Benefit Advocate
A customer service expert
Complex or recurring conditions
Treatment options/decision support
Long-term care
Pharmaceutical information
Program enrollment
Benefits and claims support
Preventive care and basic health education
High-cost system use (e.g., out-of-network or denied claims)
Member tools
Questions and answers
Procedure costs
Understanding your benefits
Physician verification and appointment scheduling
Call the phone number listed on your health plan ID card to contact an advocate.
The Teladoc Health suite of programs includes multi-condition support to comprehensively address diabetic needs. Diabetes and prediabetes management programs support members regardless of where they are on their journey to improved health. These solutions care for the whole person by integrating mental health and leveraging personalized and dedicated expert coaches for a unified experience with sustainable results.
Cellular-enabled proprietary blood glucose monitor with unlimited test strips and personalized real-time feedback and messaging
Data-driven personalized insights lead to best-in-class engagement
Robust goal setting, nutrition tracking, and activity recommendations
Connected scale and syncing with activity trackers enable effortless data collection
Evidence-based curriculum, health challenges, and coach-facilitated group sessions
CDC-certified diabetes prevention program with nutrition tracking and activity recommendations
Smart blood pressure monitor
Personalized action plan and oneon-one expert coaching
Robust goal setting, nutrition tracking, and activity recommendations
UHC will approach eligible members to enroll in this voluntary program.
If you enroll in the HDHP HSA plan, you may be eligible to open an HSA through HSA Bank. An HSA is a personal savings account you can use to pay qualified out-of-pocket medical expenses with pretax dollars. You own and control the money in your HSA. The money in your account (including interest and investment earnings) grows tax-free, and if the funds are used to pay for qualified medical expenses, it is spent tax-free. There is no “use it or lose it” rule — you do not lose your money if it is not spent during the calendar year — and there are no vesting requirements or forfeiture provisions. The account automatically rolls over year after year and, since it is an individual account, the balance is yours to keep even if you change health plans or jobs.
You are eligible to open and contribute to an HSA if you:
Are enrolled in an HSA-eligible HDHP (the HDHP HSA plan)
Are not covered by another non-HDHP, such as your spouse’s health plan or Health Care Flexible Spending Account
Are not eligible to be claimed as a dependent on someone else’s tax return
Are not enrolled in Medicare, Medicaid, or TRICARE
Have not received Veterans Administration benefits
You can use the money in your HSA to pay for qualified medical expenses now or in the future. Your HSA can be used for your expenses and those of your spouse and dependents, even if they are not covered by the HDHP.
Your contributions to your HSA may not exceed the 2026 maximum amounts established by the IRS. The annual contribution maximums are based on the coverage option you elect:
Individual – $4,400
Family – $8,750
Employees age 55 or older may make an additional catchup contribution of up to $1,000 each year.

Once you enroll in the HDHP medical plan, you may be eligible to open an HSA administered by HSA Bank. You will then receive a debit card to manage your HSA account reimbursements. Keep in mind, available funds are limited to the balance in your HSA. To open and manage your account, go to www.hsabank.com
Always ask your health care provider to file your claims with your care provider so network discounts can be applied. Then you can pay the provider with your HSA debit card based on the balance due after discount.
You, NOT your employer, are responsible for maintaining ALL records and receipts for HSA reimbursements in the event of an IRS audit.
Note: You may open an HSA at any financial institution of your choice. However, payroll deductions are available only when you open your HSA through HSA Bank.
As a UHC member, you have access to quality national telemedicine services as part of your medical plan. Virtual Visits can be a cost-effective alternative to visiting a convenient care clinic, urgent care center, or emergency room. You have access to the following telemedicine providers: Amwell, Doctor on Demand, Optum Virtual Care, Teladoc, and Walmart Virtual Health
You can connect with a board-certified doctor via phone without leaving your home or office. Your cost is often the same or less than a visit to your PCP. Care is available day or night, weekdays, weekends, and holidays. Telemedicine services should only be used for minor, nonlife-threatening conditions such as:
Sore throat
Headache
Stomachache
Cold and flu
Allergies
Fever
Urinary tract infections
Register for Virtual Visits so you are ready to use this valuable service when and where you need it. Once your account is set up, a doctor is just a call or click away.
Visit www.myuhc.com/virtualvisits
Call 877-277-6091
Download the UnitedHealthcare app
Becoming familiar with your medical care options can save time and money.
Telemedicine – Access to care via phone, online video, or mobile app whether you are home, at work, or traveling; medications can be prescribed
Allergies
Cough/cold/flu
Rash
Stomachache
Doctor’s Office – Generally, the best place for routine preventive care; established relationship; able to treat based on medical history
Infections
Sore and strep throat
Vaccinations
Minor injuries, sprains, and strains
Retail Clinic – Usually lower out-of-pocket cost than urgent care; when you can’t see your doctor; located in stores and pharmacies
Common infections
Minor injuries
Pregnancy tests
Vaccinations
Urgent Care – When you need immediate attention; walk-in basis is usually accepted
Sprains and strains
Minor broken bones
Small cuts that may require stitches
Minor burns and infections
Hospital ER – Life-threatening or critical conditions; trauma treatment; multiple bills for doctor and facility
Chest pain
Difficulty breathing
Severe bleeding
Blurred or sudden loss of vision
Major broken bones
Freestanding ER – Services do not include trauma care; can look similar to an urgent care center, but medical bills may be 10 times higher
Most major injuries except trauma
Severe pain

2-5 minutes average wait 24 hours a day, 7
minutes average wait Office hours vary
minutes average wait Generally includes evening, weekend, and holiday hours
Minimal wait
Note: Examples of symptoms are not inclusive of all health issues. Wait times described are only estimates. This information is not intended as medical advice. If you have questions, please call the phone number on the back of your medical ID card.
Becoming familiar with your options for medical care can save you time and money.
NON-EMERGENCY CARE
Access to care via phone, online video, or mobile app whether you are home, work, or traveling; medications can be prescribed
VIRTUAL VISITS/ TELEMEDICINE
Allergies
Cough/cold/flu
Rash
Stomachache
Behavioral health
24 hours a day, 7 days a week
Generally, the best place for routine preventive care; established relationship; able to treat based on medical history
Office hours vary
DOCTOR’S OFFICE
Usually lower out-of-pocket cost than urgent care; when you can’t see your doctor; located in stores and pharmacies
Hours vary based on store hours
Infections
Sore and strep throat
Vaccinations
Minor injuries, sprains and strains
Common infections
Minor injuries
Pregnancy tests
Vaccinations
RETAIL CLINIC
When you need immediate attention; walk-in basis is usually accepted
Generally includes evening, weekend, and holiday hours
URGENT CARE
Life-threatening or critical conditions; trauma treatment; multiple bills for doctor and facility
24 hours a day, 7 days a week
Sprains and strains
Minor broken bones
Small cuts that may require stitches
Minor burns and infections
Chest pain
Difficulty breathing
Severe bleeding
Blurred or sudden loss of vision
HOSPITAL ER
Services do not include trauma care; can look similar to an urgent care center, but medical bills may be 10 times higher
24 hours a day, 7 days a week
Major broken bones
Most major injuries except trauma
Severe pain
Minimal
Note: Examples of symptoms are not inclusive of all health issues. Wait times described are only estimates. This information is not intended as medical advice. If you have questions, please call the phone number on the back of your medical ID card.
Our dental plan helps you maintain good oral health through affordable options for preventive care, including regular checkups and other dental work. Premium contributions for dental will be deducted from your paycheck on a pretax basis. Coverage is provided through UHC.
The dental plan is available on a stand-alone basis for all tiers of coverage, independent of the medical plan. It is not necessary to enroll in the medical plan to enroll in the dental plan.
Two levels of benefits are available with the DPPO plan depending on whether your dentist is in-network or out-of-network. You have the flexibility to select the provider of your choice, but your level of coverage may vary based on the provider you see for services. Staying in-network and going to a contracted DPPO provider will provide you with the highest level of benefits and the deepest discounts the plan offers.

1 When you use out-of-network providers, your benefits will be paid based on a contracted fee schedule (a set amount for each type of service that is determined by UHC). If your dentist’s fee is lower than the scheduled fee, the plan will pay benefits based on the actual fee. If the fee is higher, the plan will pay benefits based only on the scheduled fee, and you are responsible for the difference. Pretreatment review is highly recommended when the dental treatment proposed is more than $200.
2 Calendar year is January 1 to December 31. Your calendar year deductible and maximum benefit will reset every January 1.

Our vision plan offers quality care to help preserve your health and eyesight. Regular exams can detect certain medical issues such as diabetes and high cholesterol, in addition to vision and eye problems. You may seek care from any vision provider, but the plan will pay the highest level of benefits when you see innetwork providers. Coverage is provided through UHC


Life and Accidental Death and Dismemberment (AD&D) insurance through UHC are important parts of your financial security, especially if others depend on you for support. With Life insurance, your beneficiary(ies) can use the coverage to pay off your debts such as credit cards, mortgages, and other final expenses. AD&D coverage provides specified benefits for a covered accidental bodily injury that causes dismemberment (e.g., the loss of a hand, foot, or eye). In the event that death occurs from an accident, 100% of the AD&D benefit would be payable to your beneficiary(ies). To elect dependent coverage, you must first enroll in employee coverage.
You may buy more Life and AD&D insurance for you and your eligible dependents. You may increase your amount by $10,000 and your spouse's by $5,000 without submission of Evidence of Insurability (EOI). Your election amount cannot exceed the Guaranteed Issue amount outlined below. All other amounts require EOI and approval from UHC before your coverage goes into effect. If you did not elect voluntary Life and AD&D coverage for yourself, your spouse, or your dependent when first eligible, UHC requires EOI for any amount of coverage you select.
Rates for these coverages are available through the online enrollment system. You must elect voluntary coverage for yourself in order to elect coverage for your spouse or children. If you leave The Modern Group, you may be able to take the insurance with you.
Increments of $10,000 up to $200,000

Disability insurance provides partial income protection if you are unable to work due to a covered accident or illness while insured. The Modern Group offers Short Term Disability (STD) insurance for you to purchase through UHC
Employee
Spouse
Child(ren)
Birth to age 26
Guaranteed Issue $200,000
Increments of $5,000 up to $50,000
Guaranteed Issue $50,000
$5,000 or $10,000
You may purchase up to $200,000 without providing EOI. If you enroll your spouse when first eligible, you may buy up to $50,000 without providing EOI. If you do not enroll during this OE period, you will be required to provide EOI to enroll.
Your Life and AD&D coverages are convertible if you terminate employment or become disabled. Coverage also terminates after 90 days if you are unable to work due to accident or sickness. You may convert the coverages at that time.
If you are temporarily disabled and unable to work due to a pregnancy, illness, or non-work-related injury, STD coverage will pay 60% of your weekly salary (up to a maximum of $1,000 per week) for up to 13 weeks. Rates are available through the ADP enrollment website.
If you did not elect voluntary STD when first eligible, UHC requires EOI and approval for coverage.
Accident insurance through UHC pays a fixed benefit directly to you in the event of an off-the-job accident, regardless of any other coverage you may have. Benefits are paid according to a fixed schedule for hospitalizations, fractures and dislocations, emergency room visits, major diagnostic exams, physical therapy, and more. Please refer to the benefit summary for details. Rates are available through the ADP enrollment website.

Confinement $175 per day per confinement
Intensive Care Unit
Specific Sum Injuries
Dislocations, ruptured discs, eye injuries, fractures, lacerations, concussions, etc.
Wellness Benefit
Employee
Spouse
Accidental Death & Dismemberment*
Employee
Spouse
$2,000 plus $500 per day
$75-$5,500
$50 $50
Child $25,000
*Percentage of benefit paid is dependent on type of loss.
Hospital Indemnity insurance through UHC provides financial assistance to enhance your current coverage. It helps you avoid utilizing your savings or borrowing money to cover out-of-pocket costs that health insurance was never intended to cover. Hospital Indemnity insurance can help with expenses such as transportation and meals for family members, childcare, or time away from work. Rates are available through the ADP enrollment website.
Hospital/ICU Admission*
Hospital/ICU Confinement*
Health Screening/Wellness
$1,000 per admission plus $100 per day up to 364 days limited to one admission per insured per benefit year
$1,000 per admission plus $100 per day limited to 30 days per insured per benefit year
$50
*Pre-existing Conditions Limitation: Benefits may not be paid for a condition for which you have consulted with a physician, received treatment, or taken prescribed medications within three months prior to your effective date until you have been covered under this plan for 12 months and been treatment-free for six months.
New employees who enroll in Hospital Indemnity insurance will not need to provide EOI when electing coverage. If you did not select Hospital Indemnity insurance when first eligible, you may elect coverage during OE. EOI and approval are required before your coverage begins.

Your Accident and Hospital Indemnity Coverages with Benefit Assist
With the UHC Benefit Assist program, enrolled employees can streamline the claims process for accident, and/or hospital indemnity protection plans.
By integrating medical and supplemental health benefits, Benefit Assist helps ensure that employees receive timely benefit payouts without the need for additional paperwork.
This program is available to eligible members enrolled in both UHC medical and supplemental health plans.

If supplemental health benefit is eligible for automatic payment — no paperwork is required from the employee.
Benefit Assist technology identifies a potential eligible claim.

If supplemental health benefit claim is not eligible for automatic payment, UHC reaches out directly to the employee via phone, email, letter, or text about their potential benefit.
Claim processed.
Final benefit determination and payment mailed.
The employee is connected with a claim specialist who will facilitate the filing on their behalf.
These additional benefits are included with your UHC voluntary Life, AD&D, and STD coverage.
UHC provides family wellness and security at the most difficult times and includes grief and financial counseling, legal support, and financial preparation.
Services for you and your family include:
Grief Support – Unlimited access to master's-level specialists 24/7 and up to two referrals for face-toface counseling.
Financial Support – One 30- to 60-minute financial consultation with a credentialed financial professional to assist with estate taxes and other financial matters.
Legal Assistance – One 30-minute consultation and discounts for continued services.

Wealth Management Account – An account with Optum Bank will automatically open for beneficiary payments of $5,000 or more and the option to open an account to manage your money (visit www.optumbank.com for more information).
For additional information, assistance, or to file a claim, visit www.myuhc.com or call 888-299-2070 Sunday through Saturday, 8:00 a.m. to 6:00 p.m. ET.
UHC provides guidance for your beneficiaries on closing your estate and protecting your identity. Services include:
Guidance Services – Assistance obtaining death certificate copies and notifying the Social Security Administration, credit reporting agencies, credit card companies, government agencies, and more.
Social Media Shutdown – Help closing social media accounts such as Facebook, Instagram, Twitter, LinkedIn, etc.
Fraud Resolution – Services include a credit report review, suppression of credit report or freezing/closing accounts, and full-service resolution if your identity is stolen or compromised. For more information or to request a complimentary guidebook, call 866-643-4241
UHC Global provides assistance for you and your dependents if you are traveling more than 100 miles from home. Representatives can help with trip planning or assist in an emergency while traveling. Additional services include:
Medical search, referral, and monitoring
Medical evacuation and return home
Replacement of medication and eyeglasses
Locating lost or stolen travel documents
Interpretation and translation
Create a UHC Global account for up-to-date travel alerts, travel tips, and more.
Visit www.uhcglobal.com
Select Member Log-in.
Select Visit Global Intelligence Center.
Select Create User.
Enter ID number 358231

Your voluntary Life and AD&D insurance also includes online will and trust services to help you:
Create and prepare a will
Locate nearby attorneys
Search legal forms
Find articles by legal experts
Access financial planning help and cost calculators
Visit www.liveandworkwell.com to register (use access code LIFEBENSVS).

UHC provides a confidential Employee Assistance Program (EAP) that helps you and your family members deal with personal concerns, work-related problems, and life’s toughest issues. Whether you are dealing with job pressures, substance abuse, or depression, our EAP services can help you 24/7.
Guidance and support are offered at no additional cost, including:
Unlimited telephone access to master's-level specialists
Up to three referrals for face-to-face counseling
One 30-minute legal consultation with an attorney by phone or in person
Discounted attorney’s fees for ongoing legal services
One 30- to 60-minute financial consultation to review estate taxes and other financial matters
Access to secure, online work/life resources at www.liveandworkwell.com
Call 877-660-3806 or visit www.liveandworkwell.com (log in using access code FP3EAP).



Dragon Products Group: Tanks & Trailers/Rigs/Pump & Power/PES
Tiger Rental Group: Offshore/Industrial/Safety/PMI
Modern AgILE Group: Modern Ag/Rancher Supply/ National Chassis/Modern Polymer Products/Pipe & Extrusions


This brochure highlights the main features of The Modern Group employee benefits program. It does not include all plan rules, details, limitations, and exclusions. The terms of your benefit plans are governed by legal documents, including insurance contracts. Should there be an inconsistency between this brochure and the legal plan documents, the plan documents are the final authority. The Modern Group reserves the right to change or discontinue its employee benefits plans anytime.