











Plan Year March 1, 2026 – February 28, 2027
A comprehensive guide to your DeSoto County Board of Supervisors employee benefits program

see page 14 for more
www.medben.com
www.bhsgonline.org/search_provider/search_provider.asp www.hstconnect.com
https://hcpdirectory.cigna.com/web/public/consumer/ directory/search?consumerCode=HDC054


We value your contributions as a County employee and are proud to be able to reward your hard work and dedication with another year of affordable and generous healthcare. When choosing a prospective employer, considering the overall benefits package is wise. Many other organizations pass on the entire premium cost to their employees, resulting in lower net wages. We continue to offer reduced premiums to our employees, as the Board of Supervisors absorbs the majority of cost.
Preventive care still remains at the top of our plan, with 100% coverage for annual wellness visits, two mammograms and one colonoscopy per member each year.
Additionally, we will continue to provide every full time employee with a Basic Life Policy, an AD&D policy (Accidental Death & Dismemberment) and household access to our EAP (Employee Assistance Program). These benefits are a nice addition to our Medical, Dental & Vision offerings. Those wishing to amplify their insurance coverage may also choose from our variety of supplemental policies, depending on their individual needs.

PERS is adding a new tier for members hired after March 1. The Board of Supervisors is currently contributing at a rate of 18.4%. We can look ahead to a contribution rate of 18.9% effective July 1, 2026.
Our hope is that our employees are able to see their cost savings when they do have to use their Medical benefits. Remember that you also have the freedom to choose who you see, as we do not have a required network. Although, if you use Baptist affiliated providers, there are savings for out of pocket costs.
We wish each of you a successful and prosperous year as we move the County forward, together. If you ever have questions or need assistance, please reach out to HR; Our door is always open.




You are eligible for benefits if you are a regular, fulltime employee working an average of 30 hours per week. Your coverage is effective on the first of the month following 30 days of employment. You may also enroll eligible dependents for benefits coverage. The cost for coverage depends on the number of dependents you enroll and the benefits you choose. When covering dependents, you must select and be on the same plans.
Your legal spouse
Children under the age of 26, regardless of student, dependency, or marital status
Children over the age of 26 who are fully dependent on you for support due to a mental or physical disability, and who are indicated as such on your federal tax return
Open Enrollment is your opportunity to choose benefits for the upcoming plan year, March 1, 2026 through February 28, 2027.
You must complete the enrollment process within 30 days of your date of hire. If you do not enroll by your effective date, you will need to wait until the next Open Enrollment to enroll unless you experience a Qualifying Life Event (QLE) (details below).
Enrollment is presently managed by Human Resources. Please visit them at:
Human Resources
365 Losher Street, Suite 205A Hernando, MS 38632

Once you elect your benefit options, they remain in effect for the entire plan year until the following Open Enrollment. You may only change coverage during the plan year if you have a QLE, which includes:
Marriage, divorce, legal separation, or annulment
Birth, adoption, or placement for adoption of an eligible child
Death of your spouse or child
Change in your spouse’s employment status that affects benefits eligibility
Change in your child’s eligibility for benefits
Significant change in benefit plan coverage for you, your spouse, or child
FMLA leave, COBRA event, court judgment, or decree
Becoming eligible for Medicare, Medicaid, or TRICARE
Receiving a Qualified Medical Child Support Order
If you have a QLE and want to change your elections, you must notify Human Resources and complete your changes within 31 days of the event. You may be asked to provide documentation to support the change. Contact Human Resources for specific details.

As the DeSoto County Board of Supervisors continues to offer affordable, comprehensive medical plan coverage, we continue to partner with MedBen for the 2026-2027 plan year.
A reference-based pricing (RBP) medical plan does not use a provider network; rather, the plan pays providers a fair and reasonable fee for services based on price averages in your region. You may visit any provider (physician, hospital, or health care facility) you wish.
Our RBP plan offers a Preferred Hospital System that includes St. Elizabeth Physicians/St. Elizabeth Healthcare and Tri-Health (Baptist Hospital, St. Francis Hospital, and LeBonheur). All facilities in the Preferred Hospital System are guaranteed to not balance bill for services.
If you visit a provider outside the Preferred Hospital System and are billed, MedBen partners with Payor Compass , a patient advocacy company, who will contact the provider to resolve and write off the amount over the designated benefit.
Our employee benefits program offers medical plan coverage. To see a summary of the plan, contact Human Resources at 662-469-8020
To find an in-network provider, visit www.bhsgonline.org/ search_provider/search_provider.asp or call 800-522-2474 .
DeSoto County Board of Supervisors also offers you the option to enroll for telemedicine services. TelaMed PLUS gives you 24/7/365 access to U.S. boardcertified physicians and pediatricians through the convenience of email, phone, or smart device. This is a great alternative to urgent care and can also be a convenient option in lieu of a doctor’s visit. DeSoto County employees pay the cost of this benefit at $12 per month.
Contact TelaMed PLUS
Visit www.telamedplus.com
Call 855-847-3627

If you are taking a long-term generic medication,* you may be able to receive your 90-day supply at no cost ($0 copay, $0 shipping) through the RxnGo prescription drug program.
To see if your prescription is covered, visit www.rxngo.com , call 888-697-9646 , or contact HR.
*A long-term medication is taken for chronic conditions or long-term therapy. Examples include medication to manage high blood pressure, asthma, diabetes, birth control, and high cholesterol.


Refer to page 6 for a detailed explanation of RBP.
waived if admitted. Deductible waived if result of an accident.

An out-of-pocket maximum is the most you could pay for covered services. If you have other family members in this plan, they need to meet their own individual out-of-pocket maximum until the overall family out-of-pocket maximum has been met. Out-of-pocket expenses include deductibles, copays (medical and pharmacy), and coinsurance.



Our dental plan helps you maintain good oral health through affordable options for preventive care, including regular dental checkups and orthodontics. Coverage is provided through Cigna
You may choose to see an in-network or out-of-network provider. When you use in-network providers, you receive benefits at a discounted network cost. You must meet a calendar year deductible (except for preventive care services), then the plan pays a percentage of covered care costs.
To find an in-network provider, visit www.cigna.com or call 800-997-1654 .

Class 1 – Preventive & Diagnostic Care
Oral exam, bitewing X-rays (one set per calendar year), cleanings, sealants, space maintainers, emergency care for pain relief, topical fluoride treatment (two applications per year for children up to age 19)
Class II – Basic Restorative Care
Oral surgery, fillings, routine extractions, denture repair and adjustments, periodontics, endodontics
Class III – Major Restorative Care
Crowns, inlays and onlays, bridgework, dentures
Class IV – Orthodontia
Child(ren) to age 19
*Out-of-network services are paid at the 90th percentile.
**Deductible applies to Basic and Major services only.


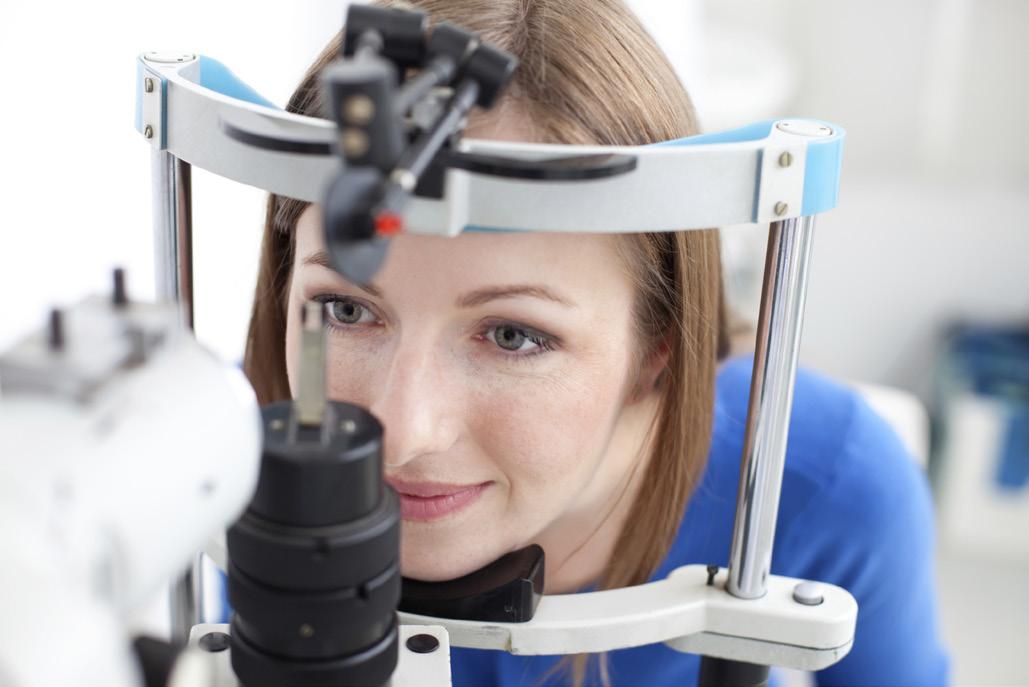
Our vision plan provides quality care to help preserve your health and eyesight. In addition to identifying vision and eye problems, regular exams can detect certain medical issues such as diabetes and high cholesterol.
You may seek care from any licensed optometrist, ophthalmologist, or optician, but plan benefits are better if you use an in-network provider. Coverage is provided through Cigna .
To find an in-network provider, visit www.cigna.com or call 800-997-1654 .
Standard Lenses
Single Vision
Lined Bifocal
Lined Trifocal
Lenticular
Lenses (in lieu of eyeglasses)
Elective
Medically Necessary
Exam
Lenses
Frames
Contacts


Life and Accidental Death and Dismemberment (AD&D) insurance through Symetra are important parts of your financial security, especially if others depend on you for support. With Life insurance, your beneficiary(ies) can use the coverage to pay off your debts such as credit cards, mortgages, and other final expenses. AD&D coverage provides specified benefits for a covered accidental bodily injury that causes dismemberment (e.g., the loss of a hand, foot, or eye). In the event that death occurs from an accident, 100% of the AD&D benefit would be payable to your beneficiary(ies). As you grow older, your Life and AD&D coverage amount reduces to 65% at age 70, and 50% at age 75.
Basic Life and AD&D insurance are provided at no cost to you. If you become terminally ill with a life expectancy of 12 months or less, you may request up to 50% of your coverage to be paid in advance. Upon termination of employment, coverage may be converted/ported to an individual policy. See the plan summary for details.
You may purchase additional Life and AD&D insurance for you and your eligible dependents. If you decline Voluntary Life and AD&D insurance when first eligible or if you elect coverage and wish to increase your benefit amount at a later date, Evidence of Insurability (EOI) — proof of good health — may be required before coverage is approved. You must elect Voluntary Life and AD&D coverage for yourself in order to elect coverage for your spouse or children.
If you become terminally ill with a life expectancy of 12 months or less, you may request up to 50% of your coverage to be paid in advance (maximum $250,000). Upon termination of employment, coverage may be converted/ported to an individual policy. See the plan summary for details.
$10,000 increments up to $500,000 (not to exceed 5x your annual salary)
Life Guaranteed Issue*: $180,000
AD&D Guaranteed Issue*: $500,000
$5,000 increments up to $250,000 (not to exceed 100% of the employee amount)
Spouse
Life Guaranteed Issue*: $25,000
AD&D Guaranteed Issue*: up to 100% of employee amount
$10,000
Child

Voluntary Life and AD&D for your child – $500 (birth to 6 months)/$10,000 (6 months to 19 years or age 26 if fulltime student)
*During your initial eligibility, you can receive coverage up to the Guaranteed Issue amount without needing to provide EOI — proof of good health. Coverage amounts that require EOI will not be effective until approved by the insurance carrier.
A beneficiary is the person or entity you designate to receive the death benefits of your Life and AD&D insurance policies. You can name more than one beneficiary and you can change beneficiaries at any time. If you name more than one beneficiary, you must identify the share for each.


Disability insurance provides partial income protection if you are unable to work due to a covered accident or illness. We provide Short Term Disability (STD) to all eligible full-time employees working at least 30 hours per week at no cost. We offer Long Term Disability (LTD) insurance for you to purchase. Coverage is provided through Symetra
STD coverage pays a percentage of your weekly salary for up to 25 weeks if you are temporarily disabled and unable to work due to an illness, non-work-related injury, or pregnancy. STD benefits are not payable if the disability is due to a job-related injury or illness.
LTD insurance pays a percentage of your monthly salary for a covered disability or injury that prevents you from working for more than 90 days. Benefits begin at the end of an elimination period and continue while you are disabled up to Social Security Normal Retirement Age (SSNRA).
Pre-existing Condition Exclusion 6/12**
*This is your waiting period before you qualify for this benefit. You do not have to be completely disabled to qualify and days do not have to be consecutive.
**Benefits may not be paid for any condition treated within six months prior to your effective date until you have been covered under this plan for 12 months.


Additional benefits are available on a voluntary basis.
You may be able to defer a portion of your compensation. Reach out to Empower Retirement at 855-756-4738 with questions.
Aflac benefits are paid directly to you. Use the cash benefit to offset out-of-pocket medical expenses or meet financial obligations that continue regardless of your ability to work.
Accident insurance
Cancer insurance
Critical Illness insurance
Hospitalization insurance
Short Term Disability
Whole Life insurance
Contact Aflac
Contact Joanie Mills at 662-934-5707 or joanie_mills@us.aflac.com for more information.

Personal issues, planning for life events, or managing daily life can affect your work, health, and family. Our Employee Assistance Program (EAP), offered through CONCERN, provides short-term counseling for you and any member of your household at no cost to you. The services are confidential and available 24 hours a day, seven days a week. Online resources are also available. Visit www.concernhealth.com and identify your employer as DeSoto County Board of Supervisors or the Sheriff’s Department.
If you need to talk about a problem, simply call for an appointment.
During your first visit or two, the CONCERN counselor will listen to gain a clear understanding of your problem. They will help you sort through your options and develop a problem resolution plan. Help can usually be found through continued short-term counseling.
If additional or specialized help is needed, your counselor will put you in touch with a qualified professional or a support group best suited to assist. Your counselor will remain available to you until you feel the difficulties are under control.
CONCERN maintains strict confidentiality. No one will know of your participation unless you tell them or give your counselor permission to speak with someone. CONCERN complies with all state and federal laws regarding patient confidentiality.
Contact CONCERN EAP
Visit www.concernhealth.com
Call 901-458-4000


The Public Employees’ Retirement System of Mississippi (PERS) serves those who serve others by providing guaranteed lifetime retirement benefits, as well as disability and survivor protection.
Established by the Mississippi Legislature in 1952, PERS provides more than $3.3 billion to more than 118,000 retirees. Active members total more than 146,000 employees working in state government, public schools, universities, community colleges, municipalities, counties, legislature, highway patrol, and other such public entities from the Gulf of Mexico to the Tennessee border, and from the Alabama line to the Mississippi River.
The PERS of Mississippi is a government-defined benefit pension plan qualified under Section 401(a) of the IRS. This is a retirement system for nearly all nonfederal public employees in the state.
Visit www.pers.ms.gov
Call 601-359-3589 or 800-444-PERS
Presently, employees are required to contribute 9% of their gross income. Our Board of Supervisors generously contributes 18.4% of the employee’s gross income. In July 2026, the Board’s contribution will increase to 18.9%.
If you were hired on or after March 1, 2026 , your 9% contribution will be divided into two retirement accounts:
4% – Defined Benefit Pension – provides regular monthly income for life.
5% – Defined Contribution account – works like a personal retirement savings account.
For everyone else hired before March 1, 2026, you will continue to contribute your entire 9% into your Defined Benefit Pension.
Scan the QR code to visit PERS online or go to www.pers.ms.gov



In October 1998, Congress enacted the Women’s Health and Cancer Rights Act of 1998. This notice explains some important provisions of the Act. Please review this information carefully.
As specified in the Women’s Health and Cancer Rights Act, a plan participant or beneficiary who elects breast reconstruction in connection with a mastectomy is also entitled to the following benefits:
All stages of reconstruction of the breast on which the mastectomy was performed;
Surgery and reconstruction of the other breast to produce a symmetrical appearance; and
Prostheses and treatment of physical complications of the mastectomy, including lymphedema.
Health plans must determine the manner of coverage in consultation with the attending physician and the patient. Coverage for breast reconstruction and related services may be subject to deductibles and coinsurance amounts that are consistent with those that apply to other benefits under the plan.
This notice is being provided to ensure that you understand your right to apply for group health insurance coverage. You should read this notice even if you plan to waive coverage at this time.
Loss of Other Coverage or Becoming Eligible for Medicaid or a state Children’s Health Insurance Program (CHIP)
If you are declining coverage for yourself or your dependents because of other health insurance or group health plan coverage, you may be able to later enroll yourself and your dependents in this plan if you or your dependents lose eligibility for that other coverage (or if the employer stops contributing toward your or your dependents’ other coverage). However, you must enroll within 31 days after your or your dependents’ other coverage ends (or after the employer that sponsors that coverage stops contributing toward the other coverage).
If you or your dependents lose eligibility under a Medicaid plan or CHIP, or if you or your dependents become eligible for a subsidy under Medicaid or CHIP, you may be able to enroll yourself and your dependents in this plan. You
must provide notification within 60 days after you or your dependent is terminated from, or determined to be eligible for, such assistance.
If you have a new dependent as a result of a marriage, birth, adoption, or placement for adoption, you may be able to enroll yourself and your dependents. However, you must enroll within 31 days after the marriage, birth, or placement for adoption.
To request special enrollment or obtain more information, contact:
DeSoto County Human Resources 365 Losher Street, Suite #205A Hernando, MS 38632 hr@desotocountyms.gov 662-469-8020
Please read this notice carefully and keep it where you can find it. This notice has information about your current prescription drug coverage with DeSoto County Board of Supervisors and about your options under Medicare’s prescription drug coverage. This information can help you decide whether or not you want to enroll in a Medicare drug plan. Information about where you can get help to make decisions about your prescription drug coverage is at the end of this notice.
If neither you nor any of your covered dependents are eligible for or have Medicare, this notice does not apply to you or the dependents, as the case may be. However, you should still keep a copy of this notice in the event you or a dependent should qualify for coverage under Medicare in the future. Please note, however, that later notices might supersede this notice.
1. Medicare prescription drug coverage became available in 2006 to everyone with Medicare. You can get this coverage through a Medicare Prescription Drug Plan or a Medicare Advantage Plan that offers prescription drug coverage. All Medicare prescription drug plans provide at least a standard level of coverage set by Medicare. Some plans may also offer more coverage for a higher monthly premium.


2. DeSoto County Board of Supervisors has determined that the prescription drug coverage offered by the DeSoto County Board of Supervisors medical plan is, on average for all plan participants, expected to pay out as much as the standard Medicare prescription drug coverage pays and is considered Creditable Coverage
Because your existing coverage is, on average, at least as good as standard Medicare prescription drug coverage, you can keep this coverage and not pay a higher premium (a penalty) if you later decide to enroll in a Medicare prescription drug plan, as long as you later enroll within specific time periods.
You can enroll in a Medicare prescription drug plan when you first become eligible for Medicare. If you decide to wait to enroll in a Medicare prescription drug plan, you may enroll later, during Medicare Part D’s annual enrollment period, which runs each year from October 15 through December 7 but as a general rule, if you delay your enrollment in Medicare Part D after first becoming eligible to enroll, you may have to pay a higher premium (a penalty).
You should compare your current coverage, including which drugs are covered at what cost, with the coverage and cost of the plans offering Medicare prescription drug coverage in your area. See the Plan’s summary plan description for a summary of the Plan’s prescription drug coverage. If you don’t have a copy, you can get one by contacting DeSoto County Board of Supervisors at the phone number or address listed at the end of this section.
If you choose to enroll in a Medicare prescription drug plan and cancel your current DeSoto County Board of Supervisors prescription drug coverage, be aware that you and your dependents may not be able to get this coverage back. To regain coverage, you would have to re-enroll in the Plan, pursuant to the Plan’s eligibility and enrollment rules. You should review the Plan’s summary plan description to determine if and when you are allowed to add coverage.
If you cancel or lose your current coverage and do not have prescription drug coverage for 63 days or longer prior to enrolling in the Medicare prescription drug coverage, your monthly premium will be at least 1% per month greater for every month that you did not have coverage for as long as you have Medicare prescription drug coverage. For example, if nineteen months lapse without coverage, your premium will always be at least 19% higher than it would have been without the lapse in coverage.
For more information about this notice or your current prescription drug coverage:
Contact the Human Resources Department at 662-4698020.
NOTE: You will receive this notice annually and at other times in the future, such as before the next period you can enroll in Medicare prescription drug coverage and if this coverage changes. You may also request a copy.
For more information about your options under Medicare prescription drug coverage:
More detailed information about Medicare plans that offer prescription drug coverage is in the “Medicare & You” handbook. You will get a copy of the handbook in the mail every year from Medicare. You may also be contacted directly by Medicare prescription drug plans. For more information about Medicare prescription drug coverage:
Visit www.medicare.gov.
Call your State Health Insurance Assistance Program (see the inside back cover of your copy of the “Medicare & You” handbook for their telephone number) for personalized help.
Call 1-800-MEDICARE (1-800-633-4227). TTY users should call 877-486-2048 .
If you have limited income and resources, extra help paying for Medicare prescription drug coverage is available. Information about this extra help is available from the Social Security Administration (SSA) online at www.socialsecurity.gov, or you can call them at 800-7721213 . TTY users should call 800-325-0778 .
Remember: Keep this Creditable Coverage notice. If you enroll in one of the new plans approved by Medicare which offer prescription drug coverage, you may be required to provide a copy of this notice when you join to show whether or not you have maintained creditable coverage and whether or not you are required to pay a higher premium (a penalty).
March 1, 2026
DeSoto County Human Resources 365 Losher Street, Suite #205A Hernando, MS 38632 hr@desotocountyms.gov 662-469-8020

THIS NOTICE OF PRIVACY PRACTICES DESCRIBES HOW MEDICAL INFORMATION ABOUT YOU MAY BE USED AND DISCLOSED AND HOW YOU CAN GET ACCESS TO THIS INFORMATION. PLEASE REVIEW IT CAREFULLY.
This Notice of Privacy Practices (the “Notice”) describes the legal obligations of DeSoto County Board of Supervisors’ Group Health Plan (the “Plan”) and your legal rights regarding your protected health information held by the Plan under the Health Insurance Portability and Accountability Act of 1996 (HIPAA) and the Health Information Technology for Economic and Clinical Health Act (HITECH Act). Among other things, this Notice describes how your protected health information may be used or disclosed to carry out treatment, payment, or health care operations, or for any other purposes that are permitted or required by law.
We are required to provide this Notice of Privacy Practices to you pursuant to HIPAA.
The HIPAA Privacy Rule protects only certain medical information known as “protected health information.” Generally, protected health information (PHI) is health information, including demographic information, collected from you or created or received by a health care provider, a health care clearinghouse, a health plan, or your employer on behalf of a group health plan, from which it is possible to individually identify you and that relates to:
1. Your past, present, or future physical or mental health or condition;
2. The provision of health care to you; or
3. The past, present, or future payment for the provision of health care to you.
If you have any questions about this Notice or about our privacy practices, and for any correspondence or requests related to the contents of this Notice, please contact:
DeSoto County Human Resources 365 Losher Street, Suite #205A Hernando, MS 38632 hr@desotocountyms.gov
662-469-8020
II. Effective Date
This Notice is effective February 15, 2026.
We are required by law to:
1. maintain the privacy of your PHI;
2. provide you with certain rights with respect to your PHI;
3. provide you with a copy of this Notice of our legal duties and privacy practices with respect to your PHI; and
4. follow the terms of the Notice that is currently in effect.
We reserve the right to change the terms of this Notice and to make new provisions regarding your PHI that we maintain, as allowed or required by law. If we make any material change to this Notice, we will provide you with a copy of our revised Notice of Privacy Practices.
Under the law, we may use or disclose your PHI under certain circumstances without your permission. The following categories describe the different ways that we may use and disclose your PHI. For each category of uses or disclosures we will explain what we mean and present some examples. Not every use or disclosure in a category will be listed. However, all of the ways we are permitted to use and disclose information will fall within one of the categories. Note that we will use and disclose PHI as described below unless otherwise prohibited or restricted by applicable state or other law, and that information can lose its protected status as PHI once re-disclosed by a recipient.
For Treatment. When and as appropriate, we may use or disclose medical information about you to facilitate medical treatment or services by health care providers. We may disclose medical information about you to providers, including doctors, nurses, technicians, medical students, or other hospital personnel who are involved in taking care of you. For example, we might disclose information about you with physicians who are treating you.
For Payment. We may use or disclose your protected health information to determine your eligibility for Plan benefits, to facilitate payment for the treatment and services you receive from health care providers, to determine benefit responsibility under the Plan, or to coordinate Plan coverage. For example, we may tell your health care provider about your medical history to determine whether a particular treatment is experimental,


investigational, or medically necessary, or to determine whether the Plan will cover the treatment. We may also share your protected health information with a utilization review or pre-certification service provider. Likewise, we may share your protected health information with another entity to assist with the adjudication or subrogation of health claims or to another health plan to coordinate benefit payments.
For Health Care Operations. We may use and disclose your protected health information for other Plan operations. These uses and disclosures are necessary to run the Plan. For example, we may use medical information in connection with conducting quality assessment and improvement activities; underwriting, premium rating, and other activities relating to Plan coverage; submitting claims for stop-loss (or excess-loss) coverage; conducting or arranging for medical review, legal services, audit services, and fraud and abuse detection programs; business planning and development such as cost management; and business management and general Plan administrative activities. However, we will not use your genetic information for underwriting purposes.
Substance Use Disorder (SUD) Treatment Information. Some of your health information may be part of a SUD patient record and subject to additional protections under federal law (42 CFR Part 2) governing confidentiality of SUD patient records.
If we receive or maintain any information about you from a SUD treatment program that is covered by 42 CFR Part 2 (a “Part 2 Program”) through a general consent you provide to the Part 2 Program to use and disclose the SUD patient record for purposes of treatment, payment or health care operations, we may use and disclose your SUD patient record for treatment, payment and health care operations purposes as described in this Notice. If we receive or maintain your SUD patient record through specific consent you provide to us or another third party, we will use and disclose your SUD patient record only as expressly permitted by you in your consent as provided to us. In no event will we use or disclose your SUD patient record, or testimony that describes the information contained in your SUD patient record, in any civil, criminal, administrative, or legislative proceedings by any Federal, State, or local authority, against you, unless authorized by your consent or the order of a court after it provides you notice of the court order.
To Business Associates. We may contract with individuals or entities known as Business Associates to perform various functions on our behalf or to provide certain types of services. In order to perform these functions or to provide these services, Business Associates will receive, create, maintain, transmit, use, and/or disclose your PHI, but only after they agree in writing with us to implement appropriate safeguards regarding your PHI. For example, we may disclose your PHI to a Business Associate to process your claims for Plan benefits or to provide support services, such as utilization management, pharmacy benefit management, or subrogation, but only after the Business Associate enters into a Business Associate contract with us.
Treatment Alternatives or
Services. We may use and disclose your protected health information to send you information about treatment alternatives or other health-related benefits and services that might be of interest to you.
As Required by Law. We will disclose your PHI when required to do so by federal, state, or local law. For example, we may disclose your PHI when required by national security laws or public health disclosure laws.
To Avert a Serious Threat to Health or Safety. We may use and disclose your PHI when necessary to prevent a serious threat to your health and safety, or the health and safety of the public or another person. Any disclosure, however, would only be to someone able to help prevent the threat. For example, we may disclose your PHI in a proceeding regarding the licensure of a physician.
To Plan Sponsors. For the purpose of administering the plan, we may disclose PHI to certain employees of the Employer. However, those employees will only use or disclose that information as necessary to perform plan administration functions or as otherwise required by HIPAA, unless you have authorized further disclosures. Your PHI cannot be used for employment purposes without your specific authorization.
In addition to the above, the following categories describe other possible ways that we may use and disclose your PHI without your specific authorization. For each category of uses or disclosures, we will explain what we mean and present some examples. Not every use or disclosure in a category will be listed. However, all of the ways we are permitted to use and disclose information will fall within one of the categories.

Organ and Tissue Donation. If you are an organ donor, we may release your PHI after your death to organizations that handle organ procurement or organ, eye, or tissue transplantation or to an organ donation bank, as necessary to facilitate organ or tissue donation and transplantation.
Military. If you are a member of the armed forces, we may release your PHI as required by military command authorities. We may also release PHI about foreign military personnel to the appropriate foreign military authority.
Workers’ Compensation. We may release your PHI for workers’ compensation or similar programs, but only as authorized by, and to the extent necessary to comply with, laws relating to workers’ compensation and similar programs that provide benefits for work-related injuries or illness.
Public Health Risks. We may disclose your PHI for public health activities. These activities generally include the following:
1. to prevent or control disease, injury, or disability;
2. to report births and deaths;
3. to report child abuse or neglect;
4. to report reactions to medications or problems with products;
5. to notify people of recalls of products they may be using;
6. to notify a person who may have been exposed to a disease or may be at risk for contracting or spreading a disease or condition;
7. to notify the appropriate government authority if we believe that a patient has been the victim of abuse, neglect, or domestic violence. We will only make this disclosure if you agree, or when required or authorized by law.
Health Oversight Activities. We may disclose your PHI to a health oversight agency for activities authorized by law. These oversight activities include, for example, audits, investigations, inspections, and licensure. These activities are necessary for the government to monitor the health care system, government programs, and compliance with civil rights laws.
Lawsuits and Disputes. If you are involved in a lawsuit or a dispute, we may disclose your PHI in response to a court or administrative order. We may also disclose your PHI in response to a subpoena, discovery request, or other lawful process by someone involved in a legal dispute, but only if efforts have been made to tell you about the request or to obtain a court or administrative order protecting the information requested.
Law Enforcement. We may disclose your PHI if asked to do so by a law-enforcement official.
1. in response to a court order, subpoena, warrant, summons, or similar process;
2. to identify or locate a suspect, fugitive, material witness, or missing person;
3. about the victim of a crime if, under certain limited circumstances, we are unable to obtain the victim’s agreement;
4. about a death that we believe may be the result of criminal conduct; and
5. about criminal conduct.
Coroners, Medical Examiners, and Funeral Directors. We may release PHI to a coroner or medical examiner. This may be necessary, for example, to identify a deceased person or determine the cause of death. We may also release medical information about patients to funeral directors, as necessary to carry out their duties.
National Security and Intelligence Activities. We may release your PHI to authorized federal officials for intelligence, counterintelligence, and other national security activities authorized by law.
Inmates. If you are an inmate of a correctional institution or are in the custody of a law-enforcement official, we may disclose your PHI to the correctional institution or law-enforcement official if necessary (1) for the institution to provide you with health care; (2) to protect your health and safety or the health and safety of others; or (3) for the safety and security of the correctional institution.
Research. We may disclose your PHI to researchers when:
1. The individual identifiers have been removed; or
2. When an institutional review board or privacy board has reviewed the research proposal and established protocols to ensure the privacy of the requested information and approves the research.


The following is a description of disclosures of your PHI we are required to make.
Government Audits. We are required to disclose your PHI to the Secretary of the United States Department of Health and Human Services when the Secretary is investigating or determining our compliance with the HIPAA privacy rule.
Disclosures to You. When you request, we are required to disclose to you the portion of your PHI that contains medical records, billing records, and any other records used to make decisions regarding your health care benefits. We are also required, when requested, to provide you with an accounting of most disclosures of your PHI if the disclosure was for reasons other than for payment, treatment, or health care operations, and if the PHI was not disclosed pursuant to your individual authorization.
Personal Representatives. We will disclose your PHI to individuals authorized by you, or to an individual designated as your personal representative, attorney-infact, etc., so long as you provide us with a written notice/ authorization and any supporting documents (i.e., power of attorney). Note: Under the HIPAA privacy rule, we do not have to disclose information to a personal representative if we have a reasonable belief that:
1. You have been, or may be, subject to domestic violence, abuse, or neglect by such person; or
2. Treating such person as your personal representative could endanger you; and
3. In the exercise of professional judgment, it is not in your best interest to treat the person as your personal representative.
Spouses and Other Family Members. With only limited exceptions, we will send all mail to the employee. This includes mail relating to the employee’s spouse and other family members who are covered under the Plan and includes mail with information on the use of Plan benefits by the employee’s spouse and other family members and information on the denial of any Plan benefits to the employee’s spouse and other family members. If a person covered under the Plan has requested Restrictions or Confidential Communications (see below under “Your Rights”), and if we have agreed to the request, we will send mail as provided by the request for Restrictions or Confidential Communications.
Authorizations. Other uses or disclosures of your PHI not described above will only be made with your written authorization. For example, in general and subject to specific conditions, we will not use or disclose your psychiatric notes; we will not use or disclose your PHI for marketing; and we will not sell your PHI, unless you give us a written authorization. You may revoke written authorizations at any time, so long as the revocation is in writing. Once we receive your written revocation, it will only be effective for future uses and disclosures. It will not be effective for any information that may have been used or disclosed in reliance upon the written authorization and prior to receiving your written revocation.
You have the following rights with respect to your PHI: Right to Inspect and Copy. You have the right to inspect and copy certain PHI that may be used to make decisions about your Plan benefits. If the information you request is maintained electronically, and you request an electronic copy, we will provide a copy in the electronic form and format you request, if the information can be readily produced in that form and format; if the information cannot be readily produced in that form and format, we will work with you to come to an agreement on form and format. If we cannot agree on an electronic form and format, we will provide you with a paper copy.
To inspect and copy your PHI, you must submit your request in writing. If you request a copy of the information, we may charge a reasonable fee for the costs of copying, mailing, or other supplies associated with your request.
We may deny your request to inspect and copy in certain very limited circumstances. If you are denied access to your medical information, you may request that the denial be reviewed by submitting a written request.
Right to Amend. If you feel that the PHI we have about you is incorrect or incomplete, you may ask us to amend the information. You have the right to request an amendment for as long as the information is kept by or for the Plan.
To request an amendment, your request must be made in writing. In addition, you must provide a reason that supports your request.

We may deny your request for an amendment if it is not in writing or does not include a reason to support the request. In addition, we may deny your request if you ask us to amend information that:
1. is not part of the medical information kept by or for the Plan;
2. was not created by us, unless the person or entity that created the information is no longer available to make the amendment;
3. is not part of the information that you would be permitted to inspect and copy; or
4. is already accurate and complete.
If we deny your request, you have the right to file a statement of disagreement with us and any future disclosures of the disputed information will include your statement.
Right to an Accounting of Disclosures. You have the right to request an “accounting” of certain disclosures of your PHI. The accounting will not include (1) disclosures for purposes of treatment, payment, or health care operations; (2) disclosures made to you; (3) disclosures made pursuant to your authorization; (4) disclosures made to friends or family in your presence or because of an emergency; (5) disclosures for national security purposes; and (6) disclosures incidental to otherwise permissible disclosures.
To request this list or accounting of disclosures, you must submit your request in writing. Your request must state the time period you want the accounting to cover, which may not be longer than six years before the date of the request. Your request should indicate in what form you want the list (for example, paper or electronic). The first list you request within a 12-month period will be provided free of charge. For additional lists, we may charge you for the costs of providing the list. We will notify you of the cost involved and you may choose to withdraw or modify your request at that time before any costs are incurred.
Right to Request Restrictions. You have the right to request a restriction or limitation on your PHI that we use or disclose for treatment, payment, or health care operations. You also have the right to request a limit on your PHI that we disclose to someone who is involved in your care or the payment for your care, such as a family member or friend. For example, you could ask that we not use or disclose information about a surgery that you had.
Except as provided in the next paragraph, we are not required to agree to your request. However, if we do agree to the request, we will honor the restriction until you revoke it or we notify you.
We will comply with any restriction request if (1) except as otherwise required by law, the disclosure is to a health plan for purposes of carrying out payment or health care operations (and is not for purposes of carrying out treatment); and (2) the PHI pertains solely to a health care item or service for which the health care provider involved has been paid in full by you or another person.
To request restrictions, you must make your request in writing. In your request, you must tell us (1) what information you want to limit; (2) whether you want to limit our use, disclosure, or both; and (3) to whom you want the limits to apply-for example, disclosures to your spouse.
Right to Request Confidential Communications. You have the right to request that we communicate with you about medical matters in a certain way or at a certain location. For example, you can ask that we only contact you at work or by mail.
To request confidential communications, you must make your request in writing. We will not ask you the reason for your request. Your request must specify how or where you wish to be contacted. We will accommodate all reasonable requests.
Right to Be Notified of a Breach. You have the right to be notified in the event that we (or a Business Associate) discover a breach of unsecured PHI.
Right to a Paper Copy of This Notice. You have the right to a paper copy of this notice. You may ask us to give you a copy of this notice at any time. Even if you have agreed to receive this notice electronically, you are still entitled to a paper copy of this notice.
If you believe that your privacy rights have been violated, you may file a complaint with the Plan or with the Office for Civil Rights of the United States Department of Health and Human Services. To file a complaint with the Plan, contact the person listed in the Contact Information section of this Notice. All complaints must be submitted in writing.
You will not be penalized, or in any other way retaliated against, for filing a complaint with the Office for Civil Rights or with us.


If you or your children are eligible for Medicaid or CHIP and you’re eligible for health coverage from your employer, your state may have a premium assistance program that can help pay for coverage, using funds from their Medicaid or CHIP programs. If you or your children aren’t eligible for Medicaid or CHIP, you won’t be eligible for these premium assistance programs but you may be able to buy individual insurance coverage through the Health Insurance Marketplace. For more information, visit www. healthcare.gov
If you or your dependents are already enrolled in Medicaid or CHIP and you live in a State listed below, contact your State Medicaid or CHIP office to find out if premium assistance is available.
If you or your dependents are NOT currently enrolled in Medicaid or CHIP, and you think you or any of your dependents might be eligible for either of these programs, contact your State Medicaid or CHIP office or dial 1-877KIDS NOW or www.insurekidsnow.gov to find out how to apply. If you qualify, ask your state if it has a program that might help you pay the premiums for an employersponsored plan.
If you or your dependents are eligible for premium assistance under Medicaid or CHIP, as well as eligible under your employer plan, your employer must allow you to enroll in your employer plan if you aren’t already enrolled. This is called a “special enrollment” opportunity, and you must request coverage within 60 days of being determined eligible for premium assistance . If you have questions about enrolling in your employer plan, contact the Department of Labor at www.askebsa.dol.gov or call 1-866-444-EBSA (3272)
If you live in one of the following States, you may be eligible for assistance paying your employer health plan premiums. The following list of States is current as of January 31, 2026. Contact your State for more information on eligibility.
Website: http://myarhipp.com/
Phone: 1-855-MyARHIPP (855-692-7447)
To see if any other States have added a premium assistance program since January 31, 2026 , or for more information on special enrollment rights, can contact either:
U.S. Department of Labor Employee Benefits Security Administration www.dol.gov/agencies/ebsa 1-866-444-EBSA (3272)
U.S. Department of Health and Human Services Centers for Medicare & Medicaid Services www.cms.hhs.gov 1-877-267-2323, Menu Option 4, Ext. 61565
Under the Federal Consolidated Omnibus Budget Reconciliation Act of 1985 (COBRA), if you are covered under the DeSoto County Board of Supervisors group health plan you and your eligible dependents may be entitled to continue your group health benefits coverage under the DeSoto County Board of Supervisors plan after you have left employment with the company. If you wish to elect COBRA coverage, contact your Human Resources Department for the applicable deadlines to elect coverage and pay the initial premium.
Plan Contact Information
DeSoto County Human Resources 365 Losher Street, Suite #205A Hernando, MS 38632 hr@desotocountyms.gov 662-469-8020

When you get emergency care or get treated by an out-ofnetwork provider at an in-network hospital or ambulatory surgical center, you are protected from surprise billing or balance billing.
What is “balance billing” (sometimes called “surprise billing”)?
When you see a doctor or other health care provider, you may owe certain out-of-pocket costs, such as a copayment, coinsurance, and/or a deductible. You may have other costs or have to pay the entire bill if you see a provider or visit a health care facility that isn’t in your health plan’s network.
“Out-of-network” describes providers and facilities that have not signed a contract with your health plan. Out-ofnetwork providers may be permitted to bill you for the difference between what your plan agreed to pay and the full amount charged for a service. This is called “balance billing.” This amount is likely more than in-network costs for the same service and might not count toward your annual out-of-pocket limit.
“Surprise billing” is an unexpected balance bill. This can happen when you can’t control who is involved in your care—like when you have an emergency or when you schedule a visit at an in- network facility but are unexpectedly treated by an out-of-network provider.
You are protected from balance billing for:
Emergency services – If you have an emergency medical condition and get emergency services from an out-of- network provider or facility, the most the provider or facility may bill you is your plan’s innetwork cost-sharing amount (such as copayments and coinsurance). You cannot be balance billed for these emergency services. This includes services you may get after you are in stable condition, unless you give written consent and give up your protections not to be balanced billed for these post-stabilization services.
Certain services at an in-network hospital or ambulatory surgical center – When you get services from an in-network hospital or ambulatory surgical center, certain providers there may be out-of-network. In these cases, the most those providers may bill you is your plan’s in-network cost-sharing amount. This applies to emergency medicine, anesthesia, pathology, radiology, laboratory, neonatology, assistant surgeon, hospitalist, or intensivist services. These providers cannot balance bill you and may not ask you to give up your protections not to be balance billed.
If you get other services at these in-network facilities, outof-network providers cannot balance bill you, unless you give written consent and give up your protections.
You are never required to give up your protections from balance billing. You also are not required to get care outof-network. You can choose a provider or facility in your plan’s network.
When balance billing is not allowed, you also have the following protections:
You are only responsible for paying your share of the cost (like the copayments, coinsurance, and deductibles that you would pay if the provider or facility was in-network). Your health plan will pay outof-network providers and facilities directly.
Your health plan generally must:
• Cover emergency services without requiring you to get approval for services in advance (prior authorization).
• Cover emergency services by out-of-network providers.
• Base what you owe the provider or facility (costsharing) on what it would pay an in-network provider or facility and show that amount in your explanation of benefits.
• Count any amount you pay for emergency services or out-of-network services toward your deductible and out-of-pocket limit.
If you believe you have been wrongly billed, you may contact your insurance provider. Visit www.cms.gov/ nosurprises for more information about your rights under federal law.








This brochure highlights the main features of the DeSoto County Board of Supervisors employee benefits program. It does not include all plan rules, details, limitations, and exclusions. The terms of your benefit plans are governed by legal documents, including insurance contracts. Should there be an inconsistency between this brochure and the legal plan documents, the plan documents are the final authority. DeSoto County Board of Supervisors reserves the right to change or discontinue its employee benefits plans anytime.