








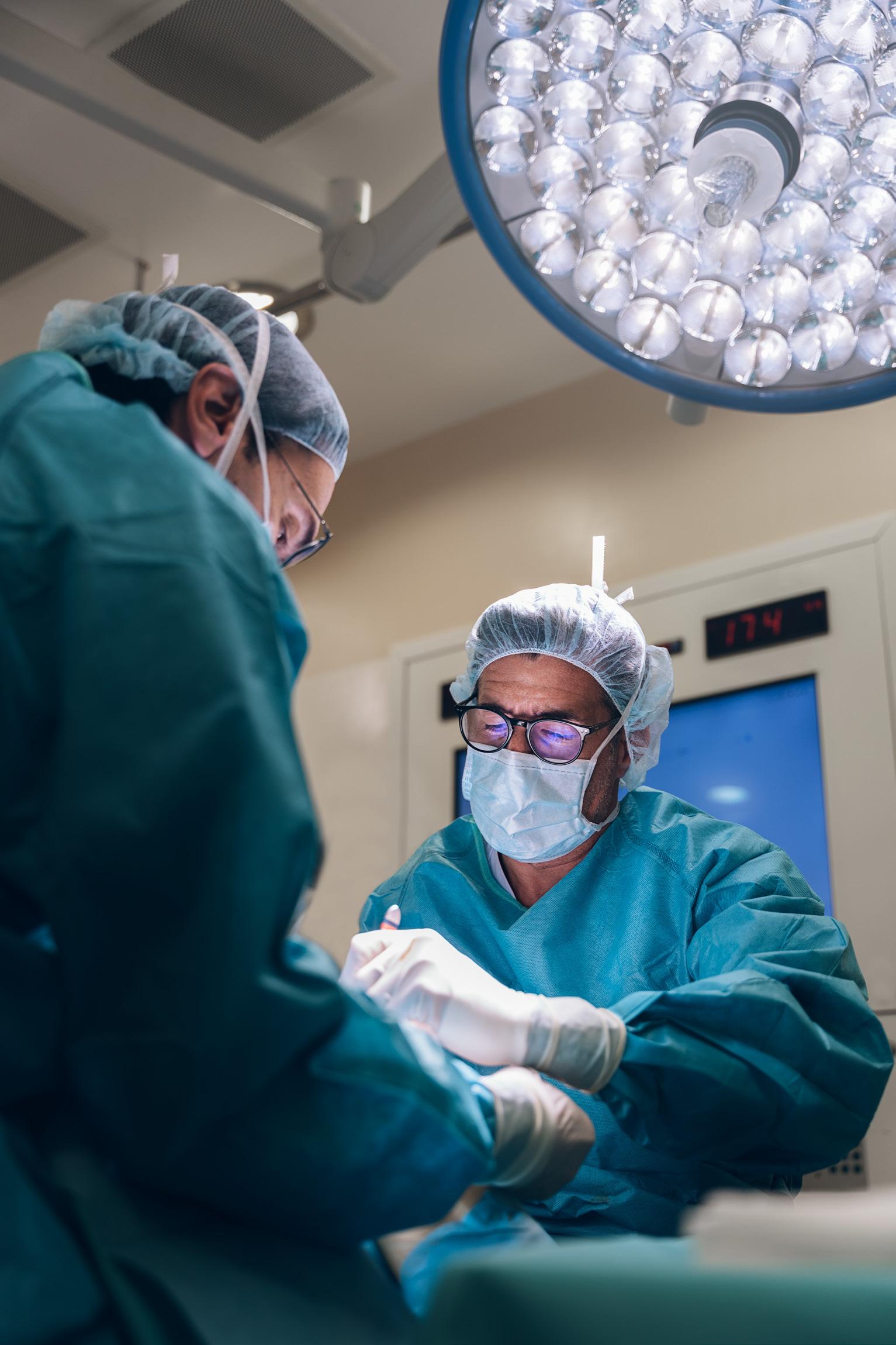
In the turbulent world of medicine, support you can trust means a lot.
We can give you that, because it’s our world too. Our discretionary indemnity gives us the flexibility to help even in the most unusual circumstances, while our legally trained doctors, specialist solicitors and case managers are ready to support you through the most daunting of legal challenges. We’re here for you 24/7 in a medicolegal emergency – and to help you cope with the everyday challenges, we build counselling and wellbeing support into every membership.


Welcome to Issue 32 of the Medico-Legal Magazine, produced by SpecialistInfo and publishing partner Iconic Media Solutions Ltd.
In this first issue of 2026, we have several articles including:
Mr Jonathan Dunne, Consultant Plastic Surgeon, discussing the standard of care in skin cancer cases; and
Tonia Goman , Certified Expert Witness, Skin Camouflage Consultant, covers the effects of scarring on victims of personal injury and clinical negligence; and
Altaf Patel , Director, Cromptons Solicitors, explains Complex Regional Pain Syndrome in a medico-legal context; and
Muiris Lyons, CEDR, reviews Alternative Dispute Resolution use in clinical negligence cases.
In our Expert Witness Directory we showcase more featured experts, who are available for instruction now.
Once again , the magazine will be circulated to up to 40,000 people in the industry, including doctors, insurance companies, law firms and medico-legal agencies. It has a dedicated website www.medicolegalmagazine.co.uk and a page on the Medico-Legal Section of the Specialistinfo. com website, where all the back issues can be viewed. Printed copies can be ordered from Iconic Media.
Specialistinfo maintains a database of contact details for up to 90,000 UK consultants and GPs, including approximately 11,000 consultants and GPs who undertake medico-legal work. We also provide Medico-Legal courses for expert witnesses and promote the members of the Faculty of Expert Witnesses (the FEW).
We welcome feedback from our readers, so please contact us with any suggestions for areas you would like to see covered in future issues or share your news and experiences with us.
Lisa
Cheyne
Specialistinfo
Medico-Legal Magazine
Beyond Office Hours: Ensuring Expert Reports Reach Solicitors in Time By Mark Nicol
Expert Witness Directory 06 09 12 16 19 22 23 29
Management of Skin Cancer - How Does a Plastic Surgeon help to Deliver the Standard of Care? By Mr Jonathan Dunne
A New Era for ADR in Clinical Negligence? By Muiris Lyons
When Visible Scarring Matters: The Role of Skin Camouflage in Clinical Negligence and Personal Injury Claims By Tonia Goman
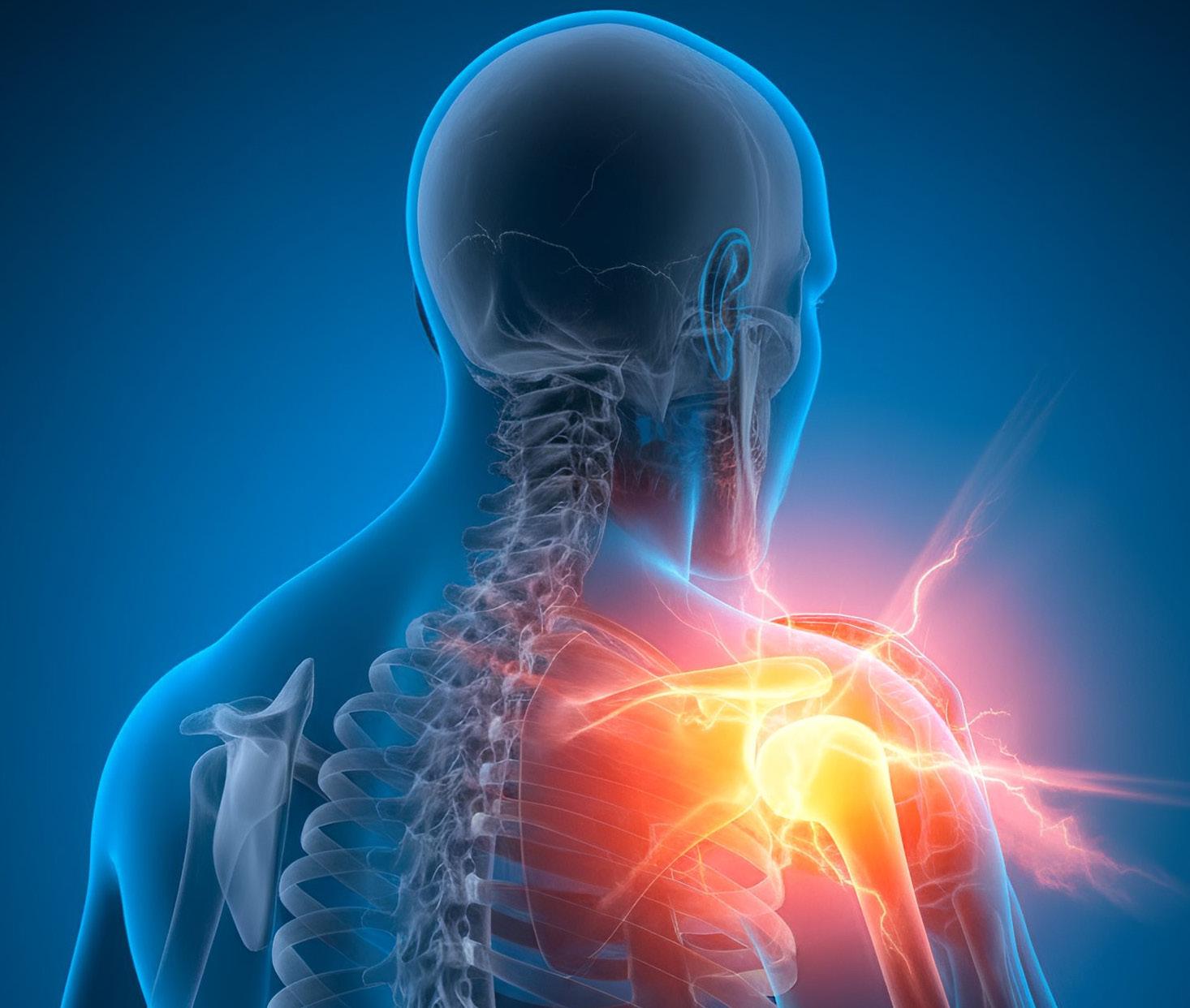
Understanding Complex Regional Pain Syndrome in a Medico-Legal Context By Altaf Patel
SpecialistInfo Medico-Legal Courses 2026 By Lisa Cheyne
Medico-Legal News By Lisa Cheyne
Presented by:

SpecialistInfo t: +44 (0) 14 2356 2003 e: magazine@specialistinfo.com www.specialistinfo.com
Published by:

Iconic Media Solutions t: +44 (0) 20 3693 1940 e: info@iconicmediasolutions.co.uk www.iconicmediasolutions.co.uk
Medico-Legal Magazine is published by Iconic Media Solutions Ltd. Whilst every care has been taken in compiling this publication, and the statements contained herein are believed to be correct, the publishers do not accept any liability or responsibility for inaccuracies or omissions. Reproduction of any part of this publication is strictly forbidden. We do not endorse, nor is Iconic Media Solutions Ltd, nor SpecialistInfo affiliated with any company or organisation listed within.


ExamWorks UK is a leading provider of integrated health, injury and rehabilitation solutions. Operating as a group of specialist companies, we cover every stage of the rehabilitation journey. Under the ExamWorks UK umbrella, our portfolio includes case management and rehabilitation providers such as Enable Therapy Services, Rehab Direct and 3d Rehabilitation. Together, we deliver a wide spectrum of services, from Immediate Needs Assessments (INA) and diagnostic procedures (including MRI scans and medical consultations) to a comprehensive range of therapies, like physiotherapy and psychotherapy.
We are recognised for our expertise in managing longterm conditions (LTC) such as chronic pain and functional neurological disorders, areas in which we’ve built expert capability over more than three decades. Our interventions are designed to enhance individual resilience and promote overall wellbeing and recovery. Collectively, we offer an end-to-end solution for every stage of the case lifecycle.
Our tailored, efficient treatment pathways help individuals recover their health and restore their lifestyle following injury or trauma, supporting them in regaining their full potential.
Functional Neurological Disorder (FND) refers to neurological symptoms that are not caused by structural neurological disease. The symptoms can include seizures, weakness, tremors, sensory issues, or difficulties with movement or speech. These symptoms are real, often debilitating, and typically result from a complex interplay between psychological and neurological factors.
Studies from the British Psychological Society estimate that between 50,000 - 100,000 individuals are affected by FND in the UK1. The symptoms of FND can present in many forms but the main areas are; sensory, memory, fatigue, movement disorders and seizures. FND is not treated with traditional rehabilitation methods and often requires a multidisciplinary approach.
Functional Neurological Disorder is often misunderstood and can be frightening for those experiencing symptoms. Across the ExamWorks UK businesses, claimant care is at the heart of our approach and our teams of expert clinical case managers provide informed support, reassurance and their clinical insight to liaise with all litigation parties.
1. FND is poorly understood and can be frightening for those with a diagnosis.
2. FND is difficult to manage with many challenges, but not impossible!
3. Key prognostic indicator is acceptance of the diagnosis.
4. Consistent messaging and long-term reinforcement is crucial for a good outcome.
Functional Neurological Disorder (FND) can present some of the most complex challenges for insurers. Although trauma and psychological stress are not the sole cause of FND, these are the conditions that can cause FND to be triggered. FND can present in many different ways and can be difficult to diagnose. Without a direct and informed approach, this can cause prolonged and costly litigation.
At ExamWorks UK we offer a comprehensive service that focuses on the complex individual needs of a claimant and utilises a multidisciplinary team to focus on both physical and mental rehabilitation. This approach has been devised to enhance claimant engagement, management of symptoms and litigation outcomes.
Please contact Thom Soutter
Email: thom.soutter@examworks.co.uk
www.examworks.co.uk
1.[Bennett, K., Diamond, C., Hoeritzauer, I., et al. (2021) A practical review of functional neurological disorder (FND) for the general physician. Clinical Medicine 21(1), 28-36.]




By Mark Nicol, Director, Expert Witness Gateway
In urgent litigation, delay is rarely caused by the expert’s clinical work. More often, it is created by the mechanics around it: emails missed, attachments blocked, admin teams restricted to office hours, and multiple handoffs between solicitor, agency and expert. The Expert Witness Gateway exists to remove that friction — not by changing the expert’s duties, but by giving both parties a secure, structured and always-available workflow that matches the reality of modern court timetables.
This case study from February 2026 illustrates why that matters.
The problem: short timeframes and late-arriving evidence
In many medico-legal matters, the expert’s report cannot be finalised until late-stage evidence is available. Haematology is a good example: results may be required to confirm a diagnosis, exclude differential causes, interpret bruising or bleeding presentations, or provide an evidential foundation for causation and timing opinions. Those results are produced by laboratories operating on their own processing windows, and they do not adapt to the court’s timetable simply because a hearing is imminent.
In this case, the hearing was listed for Monday 2 February 2026. The haematology testing was essential to the
expert’s analysis and needed to be considered before the report could be completed. Despite appropriate pursuit of the outstanding results, the laboratory did not issue them until Sunday 1 February 2026 — less than 24 hours before the hearing.
That is not unusual. It is, however, the precise scenario in which traditional instruction models often fail: where the expert is ready to work, the evidence arrives late, and the remaining risk sits entirely in how quickly the completed report can be transmitted, acknowledged, and made usable for court the next morning.
Under a typical agency-led process, the final step is often the slowest. Even if the expert works on a weekend, the report may still be routed through agency administration for formatting, logging, and onward transmission. If the report is finished on a Sunday, the agency may not even see it until staff return on Monday morning. At that point, the report must still be checked, processed, and forwarded to the solicitor — with the very real prospect that the legal team receives it too late to prepare, comply with directions, or deploy it effectively at the hearing.


This is not a criticism of agency staff; it is a structural limitation. If access, processing and onward delivery rely on office-hours workflows, then the system cannot cope with late-breaking evidence in a case listed for Monday morning. The effect is predictable: the report arrives at the point of maximum urgency, leaving the solicitor with little time to review, consider instructions, address questions, or integrate it into the hearing bundle and submissions.
The Gateway model: direct, secure, 24/7 collaboration
The Expert Witness Gateway is built around a different principle: the expert and the instructing solicitor should be able to collaborate and exchange key documents securely at the pace demanded by the case — including outside conventional business hours — while maintaining clear structure, auditability, and professional boundaries.
In this case, once the laboratory results were received on Sunday 1 February 2026 , the expert was able to complete the report that same day. Crucially, the report did not need to “wait for Monday” to reach the solicitor. The expert uploaded it straight to the Gateway immediately upon completion.
Because the Gateway provides 24/7 access for authorised users, the solicitor was able to log in and access the report on the Sunday evening. That single feature — round-the-clock access to the authoritative final document — converted what could have been a Monday-morning crisis into a controlled, manageable situation. The solicitor had the report in hand ahead of the hearing, with sufficient time to read it, identify any practical points, and ensure everything required for Monday 2 February 2026 was ready.
Efficiency matters, but the more important point is effectiveness: the ability for an expert opinion to be delivered in a way that is actually usable for court.
A report received after a hearing begins may be academically excellent, but functionally irrelevant. The Gateway’s workflow prevents that failure mode by removing unnecessary intermediaries in the final mile, without removing the safeguards that solicitors
and experts need. The expert remains responsible for the content and independence of their opinion; the solicitor remains responsible for case management and compliance. What changes is the reliability of delivery and access at critical times.
In practical terms, the Gateway improves effectiveness in four ways:
1. Continuity under time pressure
The report can be delivered immediately when it is ready, even if that happens on a weekend or late evening.
2. Reduced risk of missed communications
The report is uploaded to a central case space, reducing dependence on email chains, file size limits, and inbox oversight.
3. Immediate solicitor access and readiness
The instructing team can retrieve the report as soon as it is uploaded, enabling preparation for hearings and conferences without delay.
4. Clearer collaboration
A shared platform supports structured case handling, helping both parties keep pace with tight timetables and late evidence.
This February 2026 case demonstrates a simple truth: when the evidence arrives late, the only way to meet the court’s timetable is to remove avoidable delay everywhere else. The Expert Witness Gateway did not change when the lab released results; it changed what happened next.
The expert completed the report on Sunday 1 February 2026, uploaded it immediately, and the solicitor accessed it the same evening — fully prepared for the Monday 2 February 2026 hearing. Under a traditional agency model, the report would likely have been trapped behind office hours, with the solicitor receiving it too late.
In urgent cases, that difference is decisive. The Gateway’s 24/7, secure, direct access model turns fragile workflows into resilient ones — ensuring that when an expert works at pace, the process around them can keep up.







By Mr Jonathan Dunne, Consultant Plastic Surgeon, Imperial College NHS Trust
What does your role as Lead for Skin Cancer at Imperial involve?
As a Consultant Plastic Surgeon and Clinical Lead for S kin Cancer at Imperial College Healthcare NHS Trust, I am responsible for the strategic direction, clinical delivery and governance of one of the UK’s largest tertiary skin cancer services. My role includes chairing multidisciplinary team meetings, developing and refining clinical pathways, ensuring adherence to national standards, and leading quality improvement initiatives across the full patient journey — from suspected cancer referrals through to complex oncological care for advanced disease.
Imperial serves as a major referral centre for complex and high-risk cases, and my clinical practice focuses on advanced melanoma, aggressive non-melanoma skin cancers, recurrent tumours, and patients requiring complex reconstruction, particularly within the head and neck.
Alongside my clinical work, I hold significant research leadership roles and am currently Principal
Investigator for the MelMart study at Imperial as well as Chief Investigator of the international DEPLOY trial in desmoplastic melanoma.
Through this combination of clinical leadership, tertiary referral work and research governance, I have developed a comprehensive understanding of the entire skin cancer pathway — from diagnosis and surgical management to long-term follow-up and surveillance. When in the skin cancer clinical pathway are patients referred to you as a plastic surgeon?
Patients are typically referred for excision biopsy — particularly for facial lesions — as well as for management of larger tumours, sentinel lymph node biopsy, lymph node clearance, and regional or metastatic disease. I also receive tertiary referrals from across the south of England for complex head and neck reconstruction, including microvascular free tissue transfer and management of facial palsy related to skin cancer.
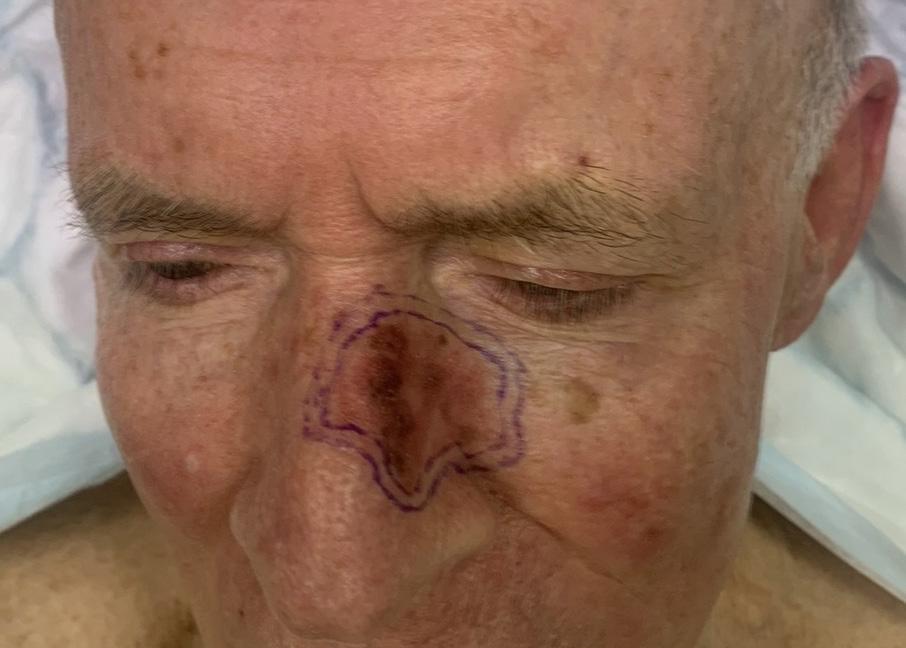
Typical cases include melanoma requiring wide local excision and sentinel node biopsy; high-risk or


recurrent basal and squamous cell carcinomas; lesions in cosmetically or functionally critical facial areas; reconstruction following Mohs surgery; complex head and neck reconstruction after oncological clearance; and lymph node surgery for metastatic disease.
What treatment options do you offer?
I provide comprehensive surgical management for skin cancer, including:
• Wide local excision for melanoma
• Sentinel lymph node biopsy
• Reconstruction after Mohs micrographic surgery
• Complex reconstruction using local, regional and free tissue transfer techniques
• Management of advanced and recurrent disease
• Functional reconstruction, particularly in the head and neck
All care is delivered through evidence-based, multidisciplinary practice. I have a keen research interest with over 60 peer-reviewed publications in skin cancer, and combine academic expertise with clinical decisionmaking. My background in craniofacial and facial palsy surgery also allows me to prioritise long-term functional and aesthetic outcomes alongside effective tumour clearance - often central issues in medicolegal cases.
What type of skin cancer cases are you seeing in your medico-legal workload?
My medicolegal work focuses on delayed diagnosis of skin cancers; failure to biopsy or inappropriate initial management; inadequate excision margins; errors in histopathology interpretation or staging; delays in referral; inadequate follow-up or surveillance; and suboptimal reconstruction resulting in avoidable functional or aesthetic deficit.
Cases commonly involve melanoma, squamous cell carcinoma and basal cell carcinoma, as well as rarer
aggressive tumours such as Merkel cell carcinoma and pleomorphic dermal sarcoma.
I am frequently instructed to assess staging, prognostic implications and the impact of delay on outcome, and to provide opinion on standard of care, guideline adherence and causation in complex cases.
Are any key themes emerging?
Recurring themes in my medico-legal work include diagnostic delay and failure to refer appropriately to specialist multidisciplinary services, underestimation of aggressive histological subtypes, inadequate documentation and safety-netting, and reconstructive decisions that compromise long-term functional outcomes.
A growing focus is the interface between primary, secondary and tertiary care, particularly whether escalation occurred appropriately within the pathway. Working within a high-volume tertiary centre and leading international research allows me to assess not only what occurred, but what would reasonably have been expected in contemporary UK practice.
What kind of cases can you help with?
I can prepare medicolegal reports on breach of duty, causation and condition and prognosis in skin cancer cases, and accept direct instructions from solicitors as well as specialist medicolegal agencies.
My experience across high-volume tertiary care, academic research, and complex reconstruction allows me to analyse cases with both oncological precision and surgical nuance.


Since 2022, we have supported over 60 innovative projects, with grants ranging from £2,500 to £199,000, funding vital areas of research often overlooked by traditional research councils and funders.
Submit your Expression of Interest today at thempsfoundation.org Closing date – 1 May 2026 at 17.00 BST




By Muiris Lyons, CEDR
The clinical negligence litigation landscape is changing rapidly, and alternative dispute resolution (ADR) is now central to how claims are managed and resolved.
The National Audit Office in its report on the Costs of Clinical Negligence published on 17 October 2025 confirmed that in 2024/25 NHS Resolution (NHSR) resolved 83% of clinical negligence cases without litigation (pre-issue). The figure was 66% in 2006/07. 1 One of the reasons for this significant improvement is the increased prevalence of mediation within clinical negligence.
NHSR explains that its mediation service supports patients, families, and NHS staff in working together towards resolution of incidents, complaints, legal claims, and costs disputes—avoiding unnecessary expense, time, stress, and potential emotional distress. The service provides access to an independent, accredited mediator, selected from a panel drawn from a wide range of backgrounds.
CEDR has been at the forefront of this development partnering with NHSR since the introduction of
the mediation scheme in 2016. CEDR’s specialist clinical negligence panel brings together decades of experience, legal and medical expertise, and a commitment to achieving the best outcomes for all parties.
This year, NHS Resolution (NHSR) renewed its fouryear contracts with a select panel of ADR providers, including CEDR, to deliver mediation services in clinical negligence and personal injury claims. The new contract does more than extend the current mediation scheme—it introduces Early Neutral Evaluation (ENE) as an additional tool to help parties resolve disputes earlier and more efficiently.
Mediation is now a well-established part of the clinical negligence process. Since NHSR adopted mediation in 2016, more than 2,000 claims have been referred2, with consistently high settlement rates—79% of mediations in 2023/24 resulted in resolution on the day or within 28 days3. The innovation in this new contract is the integration of ENE. Piloted successfully in 2023/24,


ENE provides the parties with a confidential, non-binding and without prejudice opinion from an independent evaluator with specialist knowledge of the subject matter to give an assessment of the merits of their respective claims. For claimant and defendant lawyers alike, ENE can be a valuable reality check: clarifying the strengths and weaknesses of a case, narrowing the issues in dispute, and often paving the way to earlier settlement.
The NHSR mediation service has developed significantly since its inception:
• 2016 – Scheme launched as a pilot focused solely on clinical negligence claims.
• 2018 – Scheme made permanent and scope expanded to include personal injury claims against NHS organisations (such as employer’s liability and public liability cases).
• 2024 – New four-year contracts awarded to CEDR and other providers, confirming mediation as a core part of NHSR’s dispute resolution approach and adding Early Neutral Evaluation (ENE) as a further option.
This evolution reflects NHSR’s growing confidence in mediation and its willingness to broaden ADR opportunities for both clinical negligence and personal injury claims.
Neutrality has always been the cornerstone of mediation. Yet, as the practice of mediation continues to evolve, there is increasing debate about whether mediators should remain strictly facilitative or, at times, adopt a more evaluative approach. Many mediators now agree that there is a place for constructive honesty, provided it is offered at the right moment and in the right way.
In my own mediation experience, the evaluative element often arises as a natural extension of the process. When discussions stall or the parties reach an impasse — and where they have chosen a mediator precisely because of that mediator’s depth of expertise — it is not uncommon to be asked for a view. For those mediators who also hold judicial or part-time judicial appointments, the question is sometimes put directly: “How would you approach this issue if you were hearing it as a judge?”
This is where the value of experience comes to the fore. With more than 30 years in clinical negligence practice, including as head of one of the UK’s leading claimant firms and a former President of the Association of Personal Injury Lawyers, I have occasionally been asked to offer a neutral perspective grounded in lived expertise. Until now, that evaluative role has been ad hoc. Under the new NHSR scheme, however, Early Neutral Evaluation (ENE) is formally recognised as an official tool in the mediator’s toolbox. A deep understanding of the clinical negligence landscape, combined with formal ENE accreditation, enables us to provide parties with a structured, credible reality check that can unlock settlement, or at the very least narrow the issues for trial.
CEDR ran its first ENE accreditation course in October, and I was delighted to be among the first clinical negligence mediators to become formally accredited under the scheme. This combination of professional training and practical experience means parties will be able to access ENE through the NHSR process with clear parameters and the reassurance of a formally recognised framework.
Taken together, mediation and ENE offer a flexible ADR toolkit — one that can be tailored to the nature of the dispute and the stage of proceedings, helping parties find resolution earlier, more efficiently, and with greater confidence.
It's helpful to review the NHSR’s renewed commitment to mediation under the new 4-year scheme in the context of the data available from the latest NHSR Annual Report. This was published in July 2025 and shows a 4.7% increase in claims last year from 13,784 to 14,428 4 and claims for the last four years present a significant upward trend. However, most of this reflects the inclusion of GP and other claims previously dealt with by medical protection societies from 2020/21 onwards, rather than an underlying rise in claims against the NHS. If you strip out the impact of including GP claims, hospital (CNST) claims have remained relatively constant over the last four years post-Covid.


Based on the NHSR Report, the financial cost of clinical negligence continues to rise. In 2024/25 NHS Resolution paid out £3.088 billion in clinical negligence payments, up from £2.821bn the previous year (+6.8%). 5 Of this:
• £2.286bn represented damages (+6%),
• £620m was claimant legal costs (+11%), and
• £181m was NHS defence costs (+6%).
At the balance sheet level, NHSR’s provision for accumulated clinical negligence liabilities as at 31 March 2025 was £60bn, with high-value obstetric claims accounting for the majority of that exposure. 6
There were only 24 clinical negligence claims which went to trial in 2024/25, and in those the claimant was successful in only 9 (37.5%). 7
According to analysis published by Legal Futures (29 September 2025) 8, the financial and market
pressures in clinical negligence are continuing to grow. In particular, they point to the 5% increase in claims reported and the 3.5% increase in claims registered with the Compensation Recovery Unit (CRU). They highlight that the market is expanding: law firm revenues from clinical negligence work rose to £1.7bn (+8.1%), 9 while total NHS expenditure on claims hit £3.1bn.
Traditionally, mediation was often a settlement option prior to trial, alongside or instead of a Round Table Meeting (RTM) or Joint Settlement Meeting (JSM). However, with NHSR’s commitment to resolving more cases pre-issue to reduce costs, there is now a far more significant role for early, pre-issue mediations. These early interventions can help parties narrow the issues, clarify positions, and even if the case does not settle, set the stage for more efficient litigation. The growth in pre-issue mediations is a testament to the effectiveness of ADR in delivering better outcomes for all stakeholders.


The message from NHSR’s latest figures, the new contract, and wider market trends is clear: ADR is no longer an optional extra in clinical negligence. It is central to how claims are being managed and resolved. Mediation has already proven its worth, and the introduction of ENE offers an additional pathway to early, constructive resolution. For claimant and defendant lawyers alike, engaging with ADR is not just about saving costs—it’s about achieving better outcomes for clients, patients, and the NHS.
CEDR’s dedicated panel of clinical negligence specialists—including highly experienced former litigators now working as neutrals—is well placed to help parties navigate this new era of ADR.
If you would like to discuss a clinical negligence claim or explore how mediation or ENE could help resolve your dispute, please contact the CEDR clinical negligence panel.
Muiris Lyons is a CMC registered and CEDR-accredited mediator and is one of the first to achieve formal accreditation by CEDR for Early Neutral Evaluation (ENE).

CURRENT ROLE
Consultant Plastic and Reconstructive
Surgeon, Clinical Lead for Skin Cancer
Imperial College Healthcare NHS Trust
2020 – present
FELLOWSHIPS
Skin Cancer & Mohs Surgery
Craniofacial Surgery
Head & Neck Surgery / Trauma
EDUCATION
University of Bristol
BSc (Hons) Medical Microbiology
MBChB
University of Leeds
MSs Health Research
Royal College of Surgeons of England
FRCS (Plastic Surgery)
With more than 30 years’ experience as a leading clinical negligence litigator — including over 15 years as Head of Department at one of the UK’s top claimant firms and a former President of the Association of Personal Injury Lawyers — he brings unparalleled insight into the complexities of high-value and sensitive claims. Muiris is passionate about the use of ADR to achieve better outcomes for clients, practitioners, and the NHS alike.
References:
[1] Para 17 NAO ReportCosts of Clinical Negligence 17.10.25
[2] CEDR figures
[3] The NHSR report states: "In 2024/25 a total of 138 claims proceeded to mediation with 73% of the claims settling on the mediation day or within 28 days of the mediation.”
[4] NHSR. Annual Report and Accounts 2024/25 17.07.25 p23
[5] Supra p43
[6] NAO Report p4
[7] NHSR Report p45
[8] Legal Futures (29 Sept 2025): ‘Strong growth predicted for clinical negligence market’ – summarising 2024/25 totals and CRU registrations.
[9] In its UK clinical negligence 2025 market trends report, IRN combined these figures (allowing for 20% to go towards after-the-event insurance premiums) with estimated success fees, payments from other sources like legal expenses insurance, and cases involving non-NHS providers.
Mr Jonathan Dunne is a Consultant Plastic Surgeon at Imperial College Healthcare NHS Trust and holds the role of Clinical Lead for Skin Cancer. Here, he is also the Chief Investigator and Principal Investigator for a number of international skin cancer research trials. He works in the independent sector at Montrose London and King Edward VII Hospital.
In addition to his skin cancer practice, Mr Dunne has extensive experience in facial and head & neck surgery, burns, wound care and aesthetics He undertakes emergency plastic surgery in support of the Trust’s major trauma team.
In addition to his clinical commitments, Mr Dunne has published more than 60 scientific articles and several book chapters primarily in the field of skin cancer and co-authored the Oxford Handbook of Head and Neck anatomy. He is a trustee of the Malawi Burns Trust and is a member of the national committee for BFIRST (British Foundation for International Reconstructive Surgery and Training).
Mr Dunne has undertaken Bond Salon expert witness training and provides expert advice on breach of duty, causation, condition and prognosis. He currently undertakes 50 reports per year with a 60:40 split for defendants and claimants
He takes direct instructions from solicitors and also works through a number of specialist medicolegal agencies.


info@lexmed.co.uk
linkedin.com/in/jonathandunne-1a098a59/


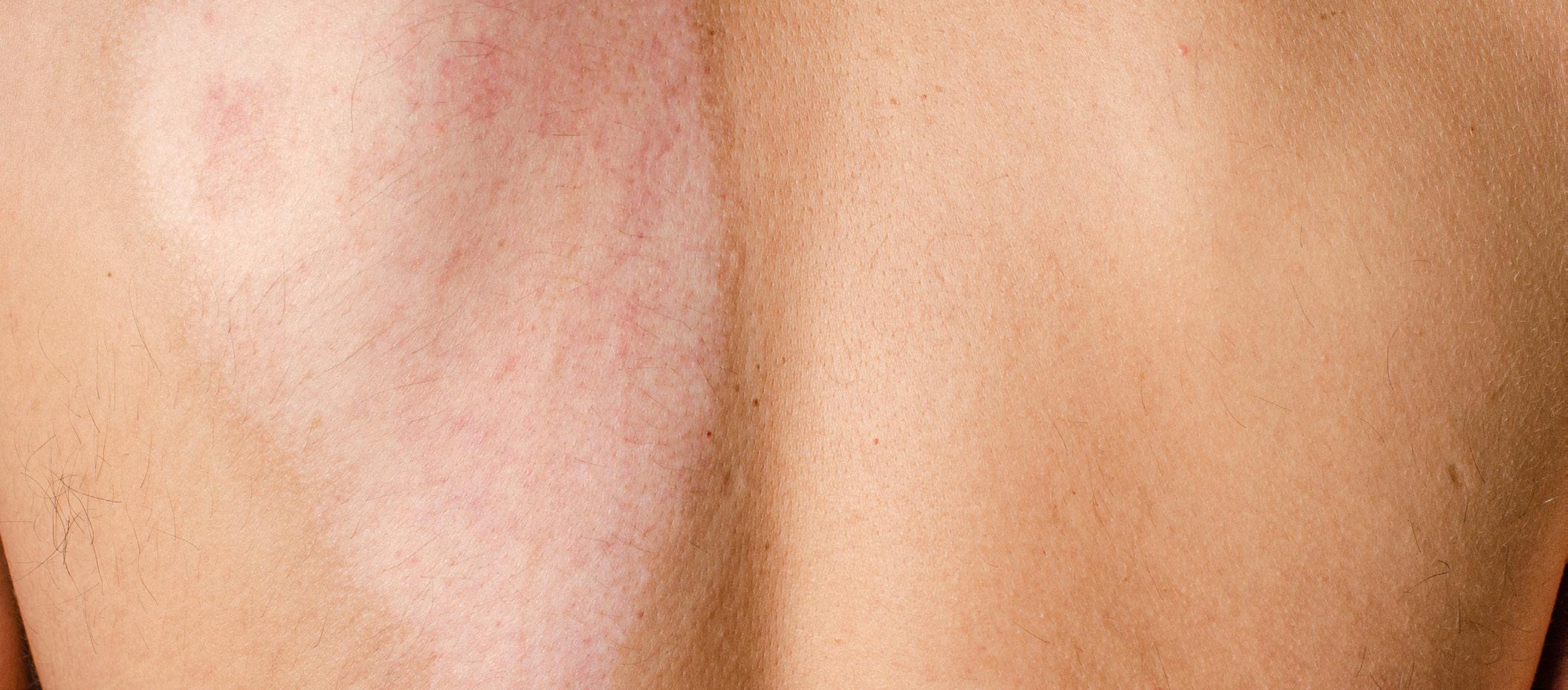
By Tonia Goman, Certified Expert Witness, Skin Camouflage Consultant
When physical injuries heal, the medical treatment may conclude. However, for many individuals, the adjustment to visible scarring continues long after the wound itself has resolved.
Scarring can be immediately visible, particularly when affecting the face, neck, or hands. In other cases, scars may be concealed by clothing but still influence behaviour, for example avoiding short sleeves, shorts, swimming, gym activities, or holidays in warmer climates. The impact is not always constant, but it can be situational and emotionally significant.
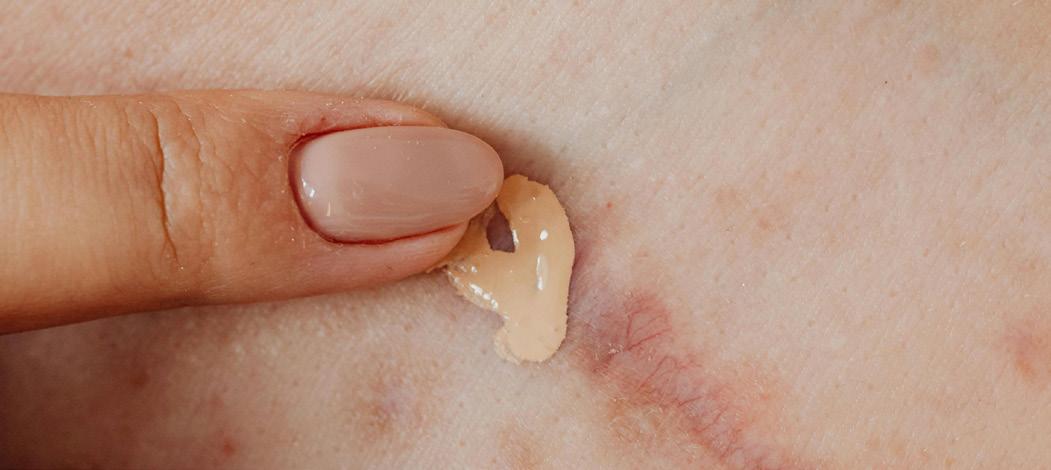
In cases where a scar differs in tone from the surrounding skin and creates visible contrast, skin camouflage can offer a temporary and proportionate option to reduce that difference.
Traditional skin camouflage involves the use of specialist, highly pigmented creams and setting products designed to blend areas of altered pigmentation with surrounding skin. It does not alter
scar texture or remove the scar itself, but it can reduce colour contrast and therefore visual prominence. The products are temporary, water-resistant, and removable.
Alternative options such as medical tattooing or micropigmentation may be considered in some circumstances, though these are semi-permanent procedures and fall outside the scope of traditional camouflage practice. For certain small, indented scars, silicone fillers such as Dermaflage may also be appropriate as an adjunct.
Within the medicolegal context, the role of the skin camouflage expert is to provide independent assessment of suitability and realistic future need. The focus is not about improving appearance for its own sake, but about managing visible colour difference where it may influence clothing choices, social situations, or confidence.


A CPR35-compliant report will typically address whether camouflage is appropriate for the specific scar or scars, the type of products likely to be required, and any practical considerations relating to access or application. In most cases, assessment is undertaken face-to-face, which allows accurate colour matching and more precise costing.
Where circumstances require a remote consultation, suitability can usually be determined and product requirements estimated from good-quality photographic evidence. However, remote assessment does not permit exact colour matching, and quantum calculations are therefore necessarily based on reasoned estimation rather than direct in-person testing.
In litigation, the issue extends beyond clinical suitability to proportionality of cost. Many individuals choose to use camouflage only occasionally, for example during holidays, social events or in warmer weather when clothing changes, rather than as a daily measure. In these circumstances, projections are based on the individual’s stated intention regarding frequency of use, together with product shelf life and realistic replacement cycles.
When approached in this way, skin camouflage evidence provides the court with a structured and proportionate assessment of both practical management and financial impact. It allows rehabilitation options to be considered realistically, without overstating need or reducing the significance of visible scarring in everyday life.
In the medicolegal context, a comprehensive consultation extends beyond colour matching. It usually includes practical instruction, discussion of application challenges, and consideration of how the individual is realistically likely to use camouflage. This ensures that recommendations are workable in everyday life and defensible within litigation.
Many scars arising from trauma or medical treatment are physically asymptomatic. Others may be raised, hypersensitive, or intermittently itchy, particularly where hypertrophic or keloid features are

present. However, even in the absence of physical symptoms, visible difference can influence behaviour, clothing choices, social interaction, intimacy, and professional confidence.
Some scarring is routinely concealed by clothing but still shapes decision-making, such as avoiding shorts, swimwear, or gym environments. In other cases, individuals report reluctance to attend social events or answer the door without first applying camouflage. The impact is therefore not necessarily physical, but behavioural.
Skin camouflage does not remove injury, nor does it alter identity. Its value lies in restoring choice. The ability to decide when and whether to conceal visible pigmentary change can support confidence and autonomy without committing to permanent alteration.
Use is often intermittent and situation specific. This pattern of discretionary application is relevant when considering both suitability and proportionality within medicolegal reporting.
While skin camouflage is a practical intervention rather than a therapeutic one, enabling individuals to manage visible difference can support confidence and longer-term adjustment.
The financial implications of skin camouflage vary according to the size, location and visibility of the scarring involved. Some individuals may choose to use camouflage only occasionally, while others, particularly where larger body areas or the face are affected, may require a more long-term approach.


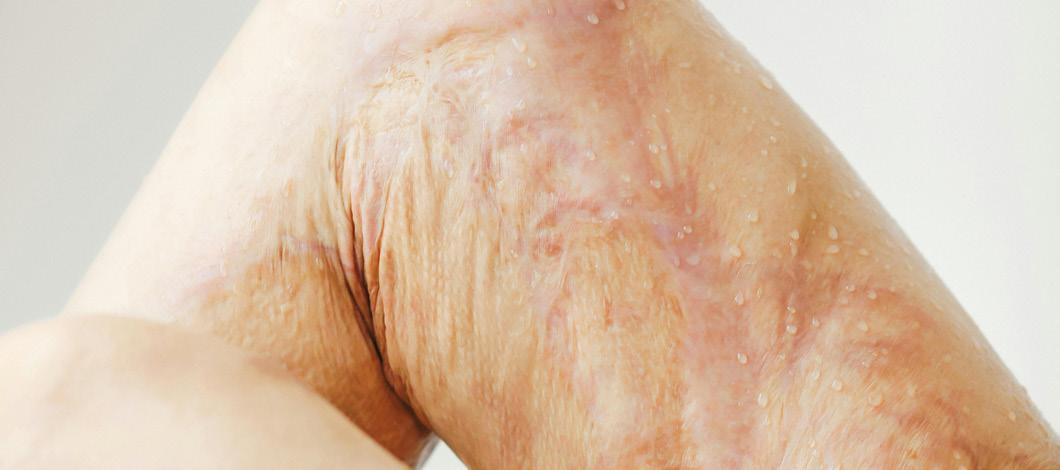
Camouflage creams are highly pigmented and typically used sparingly. When correctly applied and set, they can remain effective for several days and are generally water-resistant, allowing use to be planned around specific occasions rather than requiring daily application.
However, manufacturer-recommended shelf life, commonly around 24 months once opened, usually determines replacement cycles rather than frequency of use alone. Even where application is infrequent, products cannot reasonably be relied upon beyond this period due to potential changes in texture and performance.
In cases involving larger surface areas or deeper pigmentary change, greater product volume and a neutralising base layer may be required. Accessories such as sponges and fixing tools should also be considered, with replacement cycles reflecting realistic anticipated use.
The key consideration is proportionality. Cost projections are based on how the individual is likely to use camouflage in practice, rather than assuming either maximum or minimal usage without explanation. There are occasions where camouflage may not be appropriate or proportionate at all and recognising this forms part of the overall assessment. What Courts and Solicitors Should Expect
Skin camouflage is a specialist but increasingly relevant consideration within clinical negligence and personal injury claims, particularly in cases involving burns, visible trauma, or surgical intervention resulting in lasting pigmentary change.
Where instructed, solicitors can expect a clear explanation of suitability, proportionate and transparent costing grounded in realistic anticipated
use, acknowledgement of any limitations of assessment, and confirmation of independence with no commercial affiliation to product suppliers.
When visible scarring remains permanent, skin camouflage offers a reversible and proportionate option for managing its appearance. Properly assessed and transparently costed, it can sit appropriately within the medicolegal framework alongside surgical and dermatological opinion.
“Delivering the truth: Why NHS maternity care is broken and how we can fix it together”
BY LORIN LAKASING
‘Tells
the truth to power on maternity services with solutions that need to be heard.’ Iain Dale, political journalist and broadcaster
Pre-order now or available from 21st October in all good bookshops, and on Amazon.





By Altaf Patel, Director, Cromptons Solicitors – altaf.patel@cromptonssolicitors.co.uk
Altaf Patel is an APIL accredited senior litigator specialising in Serious, catastrophic injury and medical negligence. He has a special interest in Complex Regional Pain Syndrome and is also a founding trustee of the charity Burning Nights CRPS support.
Complex Regional Pain Syndrome, commonly known by the acronym, ‘CRPS’, is a rare and chronic condition that affects the nervous system, causing intense and often debilitating pain. It is a poorly understood disorder that can develop after an injury or surgery but can also occur without any obvious trigger.
CRPS remains one of the most problematic diagnoses encountered in medicolegal work. Although recognised within mainstream pain medicine, it continues to generate significant controversy in litigation due to its protean presentation, uncertain mechanisms and reliance on clinical assessment rather than confirmatory
testing. These features place CRPS at the centre of disputes concerning diagnosis, causation, credibility and long-term loss.
CRPS is mostly seen in adults, with research showing a higher prevalence in females than males by a ratio of 3-4:1. It has however also been found to affect children and teenagers.
CRPS is thought to be the most painful pain condition known to modern medicine falling at no. 42 on the McGill Pain Index.
CRPS is conventionally subdivided into the following categories:
• Type I, where no specific nerve injury is demonstrated.
• Type II, where a definable nerve injury is present.
• CRPS with some remitting features, and
• CRPS – NOS – Not otherwise Specified, where patients may not fully meet diagnostic criteria

The clinical picture often includes severe and persistent pain disproportionate to the precipitating event, sensory disturbance, temperature or colour asymmetry, sweating abnormalities, movement restriction, weakness, and trophic changes. Importantly, these features are neither static nor universally present, and prominence may fluctuate over time.
Despite ongoing research, CRPS lacks a definitive biomarker. Diagnosis therefore rests on clinical evaluation, guided by the Budapest Criteria, which requires a combination of reported symptoms and observed signs across multiple categories.
The Budapest Criteria, first proposed in 2004, provides the accepted clinical framework for diagnosing CRPS. The criteria emphasise a combination of disproportionate pain, reported symptoms and objectively observed signs, whilst excluding alternative explanations.
First, the individual must experience continuing pain that is disproportionate in duration and/or severity to the original injury or precipitating event. This assessment is necessarily contextual and depends on the expected recovery trajectory for the relevant trauma or injury. A deviation from the usual course of healing should prompt consideration of CRPS, rather than being regarded as diagnostic in isolation.
Second, the patient must report symptoms from at least three or more recognised categories:
• Sensory , which includes features such as hyperaesthesia or hypersensitivity in the affected limb;
• Vasomotor , which encompasses temperature asymmetry and/or changes in skin colour compared with the contralateral limb;
• Sudomotor/oedema , such as swelling, altered sweating, or sweating asymmetry;
• Motor/trophic , which includes reduced range of movement, motor dysfunction (for example weakness, tremor, or dystonia), and/or trophic changes affecting skin, hair, or nails.

Thirdly clinicians must identify at least one objectively demonstrable sign in two or more of these categories at the time of examination. These may include evidence of hyperalgesia or allodynia on sensory testing, measurable temperature or colour asymmetry, oedema or sweating asymmetry or disturbance in observable limbs, or demonstrable motor limitation, dysfunction, or trophic change.
Finally, diagnosis requires that no other condition more adequately accounts for clinical findings.
In medicolegal contexts, CRPS is often challenged because diagnosis depends substantially on subjective experience and examiner interpretation. Absence of a diagnostic test means that opinions must be justified by reference to methodology rather than conclusion.
Common evidential weaknesses can include:
• failure to document contemporaneous objective signs,
• retrospective labelling of symptoms as CRPS,
• inadequate consideration of differential diagnoses such as peripheral neuropathy, infection, inflammatory arthropathy, or functional neurological disorder.
A defensible medicolegal opinion should demonstrate not merely that CRPS is possible, but that diagnostic criteria were met at the relevant time and applied correctly.
Causation represents a frequent point of contention. CRPS is unusual in that it may follow relatively trivial trauma or injury and yet not all such trauma or injury results in CRPS. This disconnect complicates legal analysis somewhat.
From a medicolegal standpoint, the expert must address the nature and timing of the alleged trauma or injury, the chronology of symptom development and progression, absence or presence of competing explanations and whether the proposed causal mechanism is medically coherent.


It is insufficient to rely on temporal association alone. Courts require a reasoned explanation linking the index incident to the onset of the symptoms based on the “balance of probabilities”.
CRPS cases frequently invite scrutiny of symptom validity due to the subjective nature of pain and what sometimes presents as a dramatic level of reported disability. However, medicolegal experts must take care not to equate diagnostic uncertainty with fabrication.
Inconsistencies, surveillance material, or functional variation should be analysed within a biopsychosocial framework. Fluctuating ability is not uncommon in chronic pain cases and does not, of itself, negate diagnosis.
A balanced report must acknowledge both supportive and unsupportive features, allowing the Court to weigh the evidence rather than being directed toward a predetermined conclusion.
Outcomes in CRPS can vary widely with some patients showing substantial improvement, particularly with early diagnosis and active rehabilitation, while others develop persistent pain and functional limitation. Unfortunately, CRPS often remains undiagnosed and/or misdiagnosed leading to chronicity of the condition.
When advising the Court, prognosis should be evidence-based and avoid deterministic assumptions. Relevant considerations should include symptom duration, consistency of clinical findings, treatment response, psychological comorbidity, and observed function in daily life. Where psychological comorbidity is concerned, it is essential to distinguish between psychosomatic illness, functional mechanism and biopsychosocial disease models particularly when future care, employment capacity, or dependency are in issue.
Symptoms of CRPS are underpinned by identifiable physiological processes affecting the peripheral and central nervous system. Although many of these processes are not readily demonstrable on routine
imaging or laboratory testing, their presence is inferred from reproducible clinical signs observed on examination and from established neurobiological models. While psychological factors may influence pain perception, coping strategies, and functional outcomes, as they do in many chronic medical conditions, they cannot provide an adequate or complete explanation for the objective autonomic, sensory, and motor abnormalities observed in CRPS and therefore to characterise the condition as psychologically generated risks conflating modulation of symptoms with causation.
In a medicolegal assessment context, failure to maintain this distinction may lead to erroneous conclusions regarding diagnosis, causation, and credibility.
Medicolegal reporting therefore requires not only explicit reference to recognised diagnostic criteria but also careful consideration and documentation of observed behaviour and signs, transparent discussion of potentially alternative diagnosis with acknowledgment of uncertainty where it exists. Such discipline is key in cases where polarised views between experts are common and where expert credibility is frequently tested in Court.
CRPS presents not only significant biopsychosocial and psychosomatic challenges but also a convergence of medical complexity and legal difficulty. Its significance in litigation arises less from its rarity than from the challenges it poses to presentation of symptoms and traditional evidential frameworks. For courts to assess CRPS claims fairly, expert evidence must be methodical, analytical, and firmly anchored in established clinical principles.







S p e c i a l i s t I n f o h a s b e e n p r o v i d i n g h i g h l y
S p e c i a l i s t I n f o h a s b e e n p r o v i d i n g h i g h l y
a c c l a i m e d C P D a c c r e d i t e d M e d i c o - L e g a l C o u r s e s
a c c l a i m e d C P D a c c r e d i t e d M e d i c o - L e g a l C o u r s e s
S p e c i a l i s t I n f o h a s b e e n p r o v i d i n g h i g h l y
f o r d o c t o r s s i n c e 2 0 0 7 . I n 1 8 y e a r s w e h a v e
f o r d o c t o r s s i n c e 2 0 0 7 . I n 1 8 y e a r s w e h a v e
a c c l a i m e d C P D a c c r e d i t e d M e d i c o - L e g a l C o u r s e s
t r a i n e d o v e r 2 , 5 0 0 m e d i c a l p r o f e s s i o n a l s .
t r a i n e d o v e r 2 , 5 0 0 m e d i c a l p r o f e s s i o n a l s .
f o r d o c t o r s s i n c e 2 0 0 7 . I n 1 8 y e a r s w e h a v e
t r a i n e d o v e r 2 , 5 0 0 m e d i c a l p r o f e s s i o n a l s .
O u r t u t o r s a r e l e a d i n g p r a c t i s i n g B a r r i s t e r s ,
O u r t u t o r s a r e l e a d i n g p r a c t i s i n g B a r r i s t e r s ,
M e d i a t o r s & P e r s o n a l I n j u r y S o l i c i t o r s . W e
M e d i a t o r s & P e r s o n a l I n j u r y S o l i c i t o r s . W e
O u r t u t o r s a r e l e a d i n g p r a c t i s i n g B a r r i s t e r s ,
w o r k c l o s e l y w i t h t h e m t o d e v e l o p o u r c o u r s e
w o r k c l o s e l y w i t h t h e m t o d e v e l o p o u r c o u r s e
M e d i a t o r s & P e r s o n a l I n j u r y S o l i c i t o r s . W e
p r o g r a m m e a n d t o b u i l d o u r p a n e l o f e x p e r t s
p r o g r a m m e a n d t o b u i l d o u r p a n e l o f e x p e r t s
w o r k c l o s e l y w i t h t h e m t o d e v e l o p o u r c o u r s e
( T h e F a c u l t y o f E x p e r t W i t n e s s e s – T h e F E W )
( T h e F a c u l t y o f E x p e r t W i t n e s s e s – T h e F E W )
p r o g r a m m e a n d t o b u i l d o u r p a n e l o f e x p e r t s
( T h e F a c u l t y o f E x p e r t W i t n e s s e s – T h e F E W )
A n d r e a B a r n e s - S p e c i a l i s t P e r s o n a l I n j u r y &
A n d r e a B a r n e s - S p e c i a l i s t P e r s o n a l I n j u r y &
C l i n i c a l N e g l i g e n c e B a r r i s t e r a n d M e d i a t o r
C l i n i c a l N e g l i g e n c e B a r r i s t e r a n d M e d i a t o r
A n d r e a B a r n e s - S p e c i a l i s t P e r s o n a l I n j u r y &
( N o r m a n t o n C h a m b e r s )
( N o r m a n t o n C h a m b e r s )
C l i n i c a l N e g l i g e n c e B a r r i s t e r a n d M e d i a t o r
J o n a t h a n D i n g l e – M e d i a t o r , E d u c a t o r ;
J o n a t h a n D i n g l e – M e d i a t o r , E d u c a t o r ;
( N o r m a n t o n C h a m b e r s )
C o u r s e a n d F a c u l t y D i r e c t o r a t T h e S o c i e t y
C o u r s e a n d F a c u l t y D i r e c t o r a t T h e S o c i e t y
J o n a t h a n D i n g l e – M e d i a t o r , E d u c a t o r ;
o f M e d i a t o r s
o f M e d i a t o r s
C o u r s e a n d F a c u l t y D i r e c t o r a t T h e S o c i e t y
o f M e d i a t o r s
P l e a s e b e a w a r e : R u l e s f o r e x p e r t e v i d e n c e h a v e c h a n g e d s i n c e
P l e a s e b e a w a r e : R u l e s f o r e x p e r t e v i d e n c e h a v e c h a n g e d s i n c e
2 0 2 0 a n d i t i s r e c o m m e n d e d t h a t a l l e x p e r t s b o o k a n u p d a t i n g
2 0 2 0 a n d i t i s r e c o m m e n d e d t h a t a l l e x p e r t s b o o k a n u p d a t i n g
U P C O M I N G
C O
U P C O M I N G
C O U R S E S
C O U R S E S
P E R S O N A L I N J U R Y
P E R S O N A L I N J U R Y
W e d n e s d a y 1 1 M a r c h t h
W e d n e s d a y 1 1 M a r c h t h
E R S O N A
£ 3 9 5 + v a t M i d d l e T e m p l e , L o n d o n
£ 3 9 5 + v a t M i d d l e T e m p l e , L o n d o n
W e d n e s d a y 1 1 M a r c h t h
£ 3 6 0 + v a t v i r t u a l c l a s s r o o m
£ 3 6 0 + v a t v i r t u a l c l a s s r o o m
£ 3 9 5 + v a t M i d d l e T e m p l e , L o n d o n
£ 3 6 0 + v a t v i r t u a l c l a s s r o o m
C L I N I C A L N E G L I G E N C E
C L I N I C A L N E G L I G E N C E
T h u r s d a y 1 2 M a r c h t h
T h u r s d a y 1 2 M a r c h t h
C L I N I C A L N E G L I G E N C E
£ 3 9 5 + v a t M i d d l e T e m p l e , L o n d o n
£ 3 9 5 + v a t M i d d l e T e m p l e , L o n d o n
s e s s i o n t o e n s u r e t h e y a r e c o m p l i a n t .
P l e a s e b e a w a r e : R u l e s f o r e x p e r t e v i d e n c e h a v e c h a n g e d s i n c e
s e s s i o n t o e n s u r e t h e y a r e c o m p l i a n t .
2 0 2 0 a n d i t i s r e c o m m e n d e d t h a t a l l e x p e r t s b o o k a n u p d a t i n g
s e s s i o n t o e n s u r e t h e y a r e c o m p l i a n t
T h u r s d a y 1 2 M a r c h t h
£ 3 6 0 + v a t v i r t u a l c l a s s r o o m
£ 3 6 0 + v a t v i r t u a l c l a s s r o o m
£ 3 9 5 + v a t M i d d l e T e m p l e , L o n d o n
£ 3 6 0 + v a t v i r t u a l c l a s s r o o m
S
YOUR PLACE TODAY
BOOK YOUR PLACE TODAY
T o b o o k y o u r p l a c e , u s e t h e Q R c o d e o r v i s i t
T o b o o k y o u r p l a c e , u s e t h e Q R c o d e o r v i s i t
w w w . s p e c i a l i s t i n f o . c o m / c o u r s e - c a l e n d a r
w w w . s p e c i a l i s t i n f o . c o m / c o u r s e - c a l e n d a r
T o b o o k y o u r p l a c e , u s e t h e Q R c o d e o r v i s i t
o r y o u c a n e m a i l l i s a @ s p e c i a l i s t i n f o . c o m
o r y o u c a n e m a i l l i s a @ s p e c i a l i s t i n f o . c o m
w w w . s p e c i a l i s t i n f o . c o m / c o u r s e - c a l e n d a r
o r c a l l u s o n 0 1 4 2 3 7 8 7 9 8 4
o r c a l l u s o n 0 1 4 2 3 7 8 7 9 8 4
o r y o u c a n e m a i l l i s a @ s p e c i a l i s t i n f o . c o m
o r c a l l u s o n 0 1 4 2 3 7 8 7 9 8 4 BOOK YOUR PLACE TODAY
Scan the QR code to see our 2026 Course Calendar
Scan the QR code to see our 2026 Course Calendar

£ 1 9 5 + v a t v i r t u a l c l a s s r o o m M E D I C O - L
C R E T A R Y O N L I N E C O U R S E
M E D I C O - L E G A L S E C R E T A R Y O N L I N E C O U R S E
£ 1 9 5 + v a t v i r t u a l c l a s s r o o m M E D I C O - L E G A L S E C R E T A R Y O N L I N E C O U R S E
W e d n e s d a y 1 5 A p r i l t h
W e d n e s d a y 1 5 A p r i l t h
£ 1 9 5 + v a t v i r t u a l c l a s s r o o m
W e d n e s d a y 1 5 A p r i l t h
E X P E R T R E A C C R E D I T A T I O N
E X P E R T R E A C C R E D I T A T I O N
W e d n e s d a y 1 0 J u n e t h
W e d n e s d a y 1 0 J u n e t h
E X P E R T R E A C C R E D I T A T I O N
£ 3 9 5 + v a t M i d d l e T e m p l e , L o n d o n
£ 3 9 5 + v a t M i d d l e T e m p l e , L o n d o n
W e d n e s d a y 1 0 J u n e t h
£ 3 6 0 + v a t v i r t u a l c l a s s r o o m
£ 3 6 0 + v a t v i r t u a l c l a s s r o o m
£ 3 9 5 + v a t M i d d l e T e m p l e , L o n d o n
£ 3 6 0 + v a t v i r t u a l c l a s s r o o m
C O U R T R O O M S K I L L S
C O U R T R O O M S K I L L S
T h u r s d a y 1 1 J u n e t h
T h u
£ 4 4 0 + v a t M i d d l e T e m p l e , L o n d o n
£ 3 9 5 + v a t v i r t u a l c l a s s r o o m
, L
£ 3 9 5 + v a t v i r t u a l c l a s s r o o m
n d
£ 3 9 5 + v a t v i r t u a l c l a s s r o o m C O U R T R O O M S K I L L S


By Lisa Cheyne, Medico-Legal Manager, SpecialistInfo
A round-up of news in the industry of the first quarter of 2026
The Civil Procedure (Amendment) Rules SI2026/97 were laid before Parliament on the 5th February 2026 and come into force (generally) on the 6th April 2026.
Changes include:
Ordering a party to request another person to disclose a document
31.12A. "The court may order a party to request any person to produce for disclosure and inspection any document which may support the case or adversely affect the case of any party to the proceedings.”
Online Procedure Rules (OPR)
When Schedule 4 of the Judicial Review and Courts Act 2022 comes into force it will amend the Civil Procedure Act 1997 to ensure that CPR’s
are written in a way so that they do not impact practice and procedure governed by the OPR’s.
The Practice Direction Update has also been approved, which contains a suite of amendments in support of the Civil Procedure (Amendment) Rules 2026 (above) including:
Statutory appeals and appeals subject to special provision – Amendments to update PD52D to clarify the process for appeals by professionals regulated under the Anaesthesia Associates and Physician Associates Order 2024
Extending the Mediation Pilot PD51ZE until April 2027.
Read more: https://www.justice.gov.uk/courts/ procedure-rules/civil



The NHS has initiated a pilot program utilizing artificial intelligence (AI) and robotic technology to detect lung cancer at early stages. This program employs AI to analyse scans for small nodules, smaller than a grain of rice, and uses robotic bronchoscopy for precise biopsies in hard-to-reach areas, aiming to streamline diagnosis and tackle health inequalities.
The pilot comes alongside plans for the NHS to expand lung cancer screening, ensuring every eligible person is invited for checks in less than five years, no matter where they live, to tackle inequalities in cancer outcomes as part of the National Cancer Plan. Lung cancer contributes to a whole year of the nine-year life expectancy gap between richer and poorer parts of England.
The expansion is set to see the NHS invite 1.4 million people for a lung cancer check next year alone. The programme is expected to diagnose up to 50,000 cancers by 2035 and at least 23,000 at an earlier stage, potentially saving thousands of lives.
The pilot is funded through the NHS Cancer Programme Innovation Open Call (SBRI Healthcare) and is the first NHS pilot to integrate Optellum’s AI risk stratification with Intuitive’s Ion robotic bronchoscopy in a single end-to-end lung cancer diagnostic pathway.
Read more: https://www.england.nhs.uk/2026/01/ nhs-launches-trailblazing-ai-and-robot-pilot-tospot-lung-cancer-sooner/
A sad case from the end of 2025 highlighting the difficulty for any doctor with personal caring responsibilities to balance providing safe care for patients with care of dependents.
GP, Dr Helen Eisenhauer, needed to leave work on time, at 4:45pm as her childcare ended at 6pm, over an hour later. To ensure she would not be late, she added two in-person appointments into her diary at the end of the shift, which had actually taken place by phone earlier in the day. When a colleague noticed that there were no notes to accompany those appointments, she retrospectively added notes including saying she had examined a patient. When later challenged about this “examination”, she did not initially admit to the wrongdoing.
The MPTS hearing concluded that, as well as being dishonest, she put her own interests above those of her patients’ and had taken on additional locum session work without making appropriate fallback provision for childcare.
Her “own interests” in this case were needing to collect her children 1 hour and 15 minutes after her shift should have finished, a time allowance in most work settings that would be considered appropriate, especially taking into account that most standard childcare provision ends at 6pm.
Dishonesty is not acceptable from a doctor, but Dr Eisenhauer had an unblemished career up to this point. This case highlights that the current NHS workforce is often a hostile and inflexible environment for those juggling a medical career with a family.
Read more: https://www.mpts-uk.org/-/media/ mpts-rod-files/dr-helen-eisenhauer--09-dec-25.pdf


The Royal College of Midwives called on Government to take urgent action with its Safe Staffing = Safe Care campaign this January.
The campaign highlights that 87% of midwives believe their units are not safely staffed, with maternal deaths in the UK rising by 20% over the last decade.
The Five Key Demands from the RCM are:
1. Deliver safe staffing through dedicated, multi-year funding via a national maternity and neonatal action plan to end chronic understaffing in hospital and community settings.
2. Protect a learning profession by providing midwives and maternity support workers with 52 hours of protected, salaried time to supervise students and complete essential continuing professional development.
3. Amplify midwives’ voices by mandating a Director of Midwifery in every Trust and ensuring sufficient consultant midwives are in post as a non-negotiable standard.
4. Improve health and prevention by funding protected time for midwives and MSWs to develop cultural competence and deliver safe, equitable care for every mother and birthing person.
5. Invest in workplaces and birthplaces by prioritising poor maternity estates for urgent improvement through ring-fenced capital funding.
In response, the Department for Health and Social Care stated it is "on a mission" to improve services, citing a £131 million investment in infrastructure and ongoing work with NHS England to enhance training.
Read more: https://rcm.org.uk/mediareleases/2026/01/enough-is-enough-royalcollege-of-midwives-calls-on-government-to-takeurgent-action-with-safe-staffing-campaign/
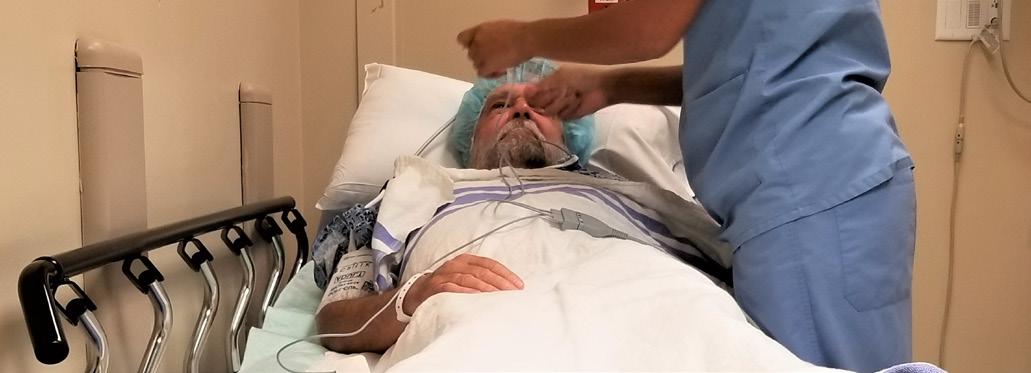
Corridor care in the NHS refers to the practice of treating patients in non-designated clinical areas, such as hospital corridors, waiting rooms, or cupboards, due to severe overcrowding, bed shortages, and system-wide pressures. Once considered a rare emergency measure, it has become increasingly routine, with reports indicating a significant rise in 12-hour waits in these environments, particularly affecting older and vulnerable patients.
New analysis by the Royal College of Emergency Medicine (RCEM) reveals that there were nearly 5,000 deaths associated with long A&E waits before admission in England last summer (1 June to 30 September 2025).The President of the RCEM, Dr Ian Higginson, described the findings as “appalling”.
“There is absolutely rock-solid evidence that long waits in the emergency departments are associated with an increased risk of dying - and that's what really worries us,” Dr Higginson said.
Reports from the Royal College of Nursing (RCN) and Royal College of Physicians (RCP) highlight that this is still a nationwide crisis, with nearly 70% of nursing staff reporting daily use of such spaces. Patients often face a lack of privacy, dignity, and access to essential equipment like oxygen or call bells, leading to increased risk of harm and, in some cases, death.
The crisis is driven by a lack of available beds and delays in discharging patients, often caused by bottlenecks in social care.
The Health Secretary, Wes Streeting, has expressed a commitment to ending this practice over the course of the current Parliament, acknowledging that the situation is "unsafe and undignified".
Read more: https://www.rcn.org.uk/employmentand-pay/Safe-staffing/Corridor-care






Jess’s Rule requires GP teams to critically re-evaluate a diagnosis if a patient presents three times with the same or escalating symptoms or concerns. It is led by the Department of Health and Social Care (DHSC) and NHS England and is supported by the Royal College of General Practitioners (RCGP).
Jessica Brady passed away due to cancer in December 2020 at the age of 27. In the 5 months leading up to her death, Jess had 20 consultations with her GP practice, and her cancer had not been diagnosed. Jess was then admitted to hospital with stage 4 adenocarcinoma and passed shortly afterwards. Since then, Jess’s family have campaigned for primary care staff to elevate a patient’s case for review after their third appointment with their practice about a condition or symptom.
Posters reminding GP teams of Jess’s Rule and the importance of critically re-evaluating a diagnosis if a patient presents three times with the same or escalating symptoms or concerns are being sent to every practice in England.
This rule follows the successful establishment of Martha’s Rule, after the tragic death of a 13-yearold girl from sepsis despite the attempts of her parents to raise the alarm. This allows a second opinion to be sought within a legal and procedural framework to ensure that patients, their families/ carers, and staff have unimpeded access 24/7 to a rapid review by a critical care outreach team when there are concerns that a patient is deteriorating and those concerns are not being addressed.

Read more: https://www.england.nhs.uk/longread/jesss-rule-three-strikes-and-we-rethink/ https://pedmore-medical.com/marthas-law-andthe-medico-legal-imperative-of-second-opinions/
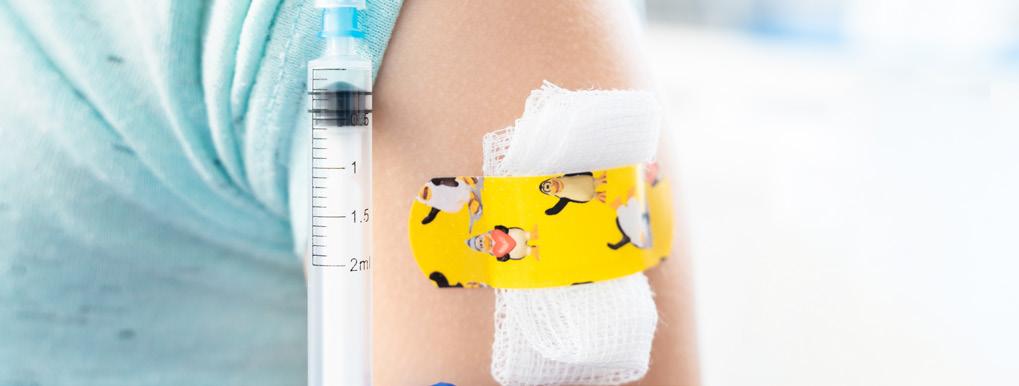
MPs from the Health and Social Care Committee warned in their recent report, First 1000 Days: a renewed focus, that falling vaccination rates are part of a range of problems that have left England with some of the worst health outcomes in Europe among young children.
The report, published in January, warns, “The continuing decline in childhood vaccination levels since 2012 is a national disgrace,” adding that “children should not be dying of entirely


preventable diseases.” Speaking on behalf of the cross-party committee, the Labour MP Paulette Hamilton said, “Children growing up in our country today stand too great a chance of becoming overweight, developing asthma or tooth decay, or catching life threatening yet preventable diseases due to missed vaccines.”
A recent BMJ article reports that in 2024 the UK recorded the highest number of measles cases since 2012, with 2911 confirmed cases and one death. Eleven infants died from whooping cough in 2024.
The report states, “vaccination is one of the most effective public health interventions, yet uptake has declined steadily since 2012, with stark regional and ethnic disparities. We recommend reinstating the 95% coverage target in NHS planning guidance and committing to achieve it
by the end of this Parliament. The Government should accelerate pilots for health visitor-led vaccination delivery and ensure Integrated Care Boards have named leads for coordinating local vaccination strategies.”
A government spokesperson said it is introducing a new £2m pilot scheme for health visitors to try to reach families who are facing barriers to vaccination and, “Parents are now also able to protect their children from chickenpox through the MMRV [measles, mumps, rubella, and varicella] vaccine, which is free for the first time ever. We’re also backing our Best Start Family Hubs with an extra £500m, giving families access to joined-up health and children’s services right in their own community.”
Read more: https://publications.parliament.uk/pa/ cm5901/cmselect/cmhealth/802/report.html
MA(Oxon) BM BCh FRCSEd (Gen. Surg)
Consultant Hepatopancreaticobiliary (HPB) & General Surgeon
Mr Mark Duxbury is a Consultant Surgeon with an active NHS and private clinical practice in Glasgow, specialising in diseases of the liver, pancreas, biliary tree and gallbladder. He also has expertise in laparoscopic and complex hernia surgery.
Mr Duxbury has over 15 years’ medicolegal experience and accepts expert witness instructions for cases including:
• General, emergency and trauma surgery
• Gallstones and gallbladder disease
• Complex hernia surgery
• Gastrointestinal surgery
• Laparoscopic surgery

• Bile duct injury
• Complex biliary surgery
• Liver and pancreatic surgery for benign disease and cancer
He understands his duties to the court and can serve as a witness on behalf of claimants/pursuers, defendants/defenders, as a single joint expert and has mediation experience.
Mr Duxbury serves as an expert witness across the UK and Republic of Ireland. He understands the requirements of instructing solicitors, the restricted timescales for civil litigation, and the limitations of expertise. All reports represent an independent opinion on the standard of care and will contain a clear summary of the key background medical information and conclusions, as required.
On request, Mr Duxbury will provide a fee estimate and timescale for report preparation Legal Aid cases, agency instructions, and fixed fee work are accepted.
Deferred payment can be arranged (by prior agreement only). Secure electronic systems are used. Where appropriate, reports are produced in accordance with current UK Civil Procedure Rules Data are managed in accordance with GDPR.
www MarkDuxbury info/medicolegal Mark Duxbury@iCloud com 0141 2016665

7TH MAY 2026, DE VERE GRAND CONNAUGHT ROOMS, LONDON, UK
The Medico-Legal Conference has now firmly established itself as the UK’s leading event bringing together medico-legal professionals, industry experts, and suppliers. Attend to experience our high level programme of speakers, interactive exhibition zone, and networking.
The conference is being held at De Vere Grand Connaught Rooms on Thursday 7th May 2026.
Benefits of Attending:
• Be updated on the latest medico-legal developments, reforms and issues
• Hear from lawyers involved in some of the most complex medico-legal cases
• Learn more from medics about the challenges facing the NHS from an expert witness point of view
• Gain insight into writing medico-legal reports and where experts go wrong
• Enjoy excellent networking opportunities, including a Champagne reception





























The Medico-Legal Conference has now firmly established itself as the UK's leading event bringing together medico-legal professionals, industry experts, and suppliers. Attend to experience our high-level programme of speakers, interactive exhibition zone, and networking.


For more information and to book your place please visit:





The conference is being held at De Vere Grand Connaught Rooms on Thursday 7th May 2026.







•






•
•
•
•
•
•
Be nefits of Atte nding:
Book now and benefit from our 30% off offer
• Enjoy excellent networking opport unities, including a Champagne reception
Be nefits of Atte nding:
• Learn about the increasing role of mediation in settling medico-legal claims
some of the most recent high profile cases
• Be updated on the latest medico-le gal developments, reforms and i ssues
• Learn about the increasing role of mediation in settling medico-legal claims
• Be updated on the latest medico-le gal developments, reforms and i ssues
• ficulties
• Be updated on the latest medico-le gal developments, reforms and i ssues
Be nefits of Atte nding: 6 Hou r s C PD
• in some of the most recent high profile cases
Be nefits of Atte nding:
of speakers, interactive exhibition zone, and networking. The conference is being held at De Vere Grand Connaught Rooms on Thursday 7th May 2026.
• in some of the most recent high profile cases
• Enjoy excellent networking opport unities, including a Champagne reception
• in some of the most recent high profile cases
• Learn about the increasing role of mediation in settling medico-legal claims
E ss entia l fo r Do ct ors, L aw yer s and a ll t hos e in v ol ved i n the M ed ic o-L ega l Pr of
• Be updated on the latest medico-le gal developments, reforms and i ssues
• ficulties Enjoy excellent networking opport unities, including a Champagne reception
• Learn about the increasing role of mediation in settling medico-legal claims
• Be updated on the latest medico-le gal developments, reforms and i ssues
• ficulties
6 Hou r s C PD
• fic
• in some of the most recent high profile cases
• Learn about the increasing role of mediation in settling medico-legal claims
• ficulties
and benefit from our
6 Hou r s C PD
• Enjoy excellent networking opport unities, including a Champagne reception
• in some of the most recent high profile cases

• ficulties


• Enjoy excellent networking opport unities, including a Champagne reception
• Learn about the increasing role of mediation in settling medico-legal claims
E ss entia l fo r Do ct ors, L aw yer s and a ll t hos e in v ol ved i n the M ed ic o-L ega
• Enjoy excellent networking opport unities, including a Champagne reception




• Learn about the increasing role of mediation in settling medico-legal claims
• Enjoy excellent networking opport unities, including a Champagne reception
• ficulties
• ficulties
E ss entia l fo r Do ct ors, L aw yer s
• Enjoy excellent networking opport unities, including a Champagne reception
• Be updated on the latest medico-le gal developments,
• Enjoy excellent networking opport unities, including a Champagne reception
6 Hou r s C PD































Over 5,000 Experts across over 125 disciplines
Expertise on all case types
Dedicated Clinical Negligence and Serious Injury case handlers
A complete range of rehabilitation services, surgical procedures
When you instruct with Speed Medical, your efficient, supported, and



Work opportunities across a breadth of case types

Dedicated support from our Expert Liaison team
Professional development opportunities & exclusive training discounts
Access to our online portal to enable efficient case management
a



MB ChB BSc LMCC MD FRCPC FRCSCplas FRCSEd(Plast) MRCEM
Consultant Plastic & Reconstructive Surgeon | Senior Emergency Physician | Expert Witness
t: +44 7852 136 413
e: paul@paulbaguley.co.uk w: www.paulbaguley.co.uk

Mr Paul Baguley is a triple-qualified Consultant in Paediatric Medicine, Emergency Medicine, and Plastic & Reconstructive Surgery, with additional expertise in Paediatric Plastic Surgery. Over a forty-year career, he has combined frontline emergency practice with complex reconstructive and aesthetic surgery. As a Senior Physician in both adult and paediatric emergency medicine, he brings unique crossspecialty insight to medico-legal work. Mr Baguley provides
balanced, evidence-based expert reports on breach of duty, causation, and prognosis for claimant and defendant solicitors across the UK and Ireland.
Consulting at A Vita, 22 High Street, Yarm, TS15 9AE

Consultant
Respiratory Physician
t: +44 07961 231 45
e: mazhar.chaudri@nhs.net

Dr Mazhar Chaudri has been a Consultant Respiratory Physician at Russells Hall Hospital in Dudley, West Midlands since April 2004. He is the Trust lung cancer lead and Clinical Director of the Dudley Lung Cancer Screening programme. He is interested in interventional procedures such as bronchoscopy, endobronchial ultrasound, medical thoracoscopy and indwelling pleural catheter insertion and management. Dr Chaudri achieved the Cardiff University Bond Solon Expert Witness Certificate (CUBS) in 2018 and undertakes instructions as an expert witness, preparing medico-legal reports on various respiratory cases,
including clinical negligence, personal injury and occupational lung disease. He used to sit on the British Thoracic Society Specialist Advisory Group on Interventional Procedures and undertake lung cancer peer review for NHS England and NHS Improvement.
Consultant Plastic Surgeon (GMC: 2702249)
t: +44 07515 094 348
e: info@clifton-plastic-surgery.co.uk
w: clifton-plastic-surgery.co.uk
• Consultant Plastic Surgeon since 1996 and has a broad experience having worked in the Army, the NHS and the
Private Sector.


Over 20 years of experience writing reports and receives about 300 instructions per year.
• Instructed by Claimants, Defendants, and as a Joint Expert.
• Aware of the Part 35 requirements of an Expert Witness and has obtained Part 1 of the Certificate of Medical Reporting (Bond Solon).
• Has experience appearing in court as an expert witness.
• Appointments are available in Bristol, London, Cardiff, Birmingham and Salisbury.
• All reports are produced within agreed timescales, usually 6 weeks, which can be expedited.

t: +44 0208 383 2026
e: andrew.chukwuemeka@nhs.net

Acting for Claimants, Defendants and as a single joint expert, a Consultant Cardiothoracic Surgeon with Imperial College Healthcare NHS Trust, he is Medical Director at Hammersmith Hospital and was previously Clinical Director for Cardiac Sciences (Cardiology, Cardiothoracic and Vascular Surgery). His clinical interests include Chest Trauma, Aortic Surgery including Transcatheter Aortic Valve Implantation (TAVI), Heart Valve and Coronary Artery Bypass Surgery. Mr Chukwuemeka was the Royal College of Surgeons’ Regional Specialty Advisor and served on the Medical Technologies Committee at NICE. He serves on the NHSE - Clinical Reference Group for Cardiac Services, NHSE - London Clinical Senate Council and the Medicines and Healthcare products Regulatory Agency (MHRA).


Podiatric Consultant and Gait Specialist
t: +44 0207 636 4465
e: clinic@gaitandposture.com w: www.gaitandposture.com

David Simon Costain is a Podiatric Consultant and Gait Specialist, based in Harley Street, London. He has over 45 years of experience in Podiatry and is the CEO of the Gait & Posture Centre.
He specialises in the analysis of gait related musculo-skeletal problems relating to foot and leg malfunction, dividing his time between his private practice and expert witness work. He focuses on Personal Injury cases where approximately 75% of his work is for the claimant, and 25% for the defendant.

BSc MBBS MD FRCR
Expert Radiology Witness
t: +44 07733 156 406
e: suprio.ganguly@nhs.net

Dr Suprio Ganguly has over 37 years' experience of radiology practice earned in five countries spanning three continents, traversing both military and civilian sectors. Dr Ganguly is on the GMC's Expert Witness and Associate Medical Performance Assessor panels. Dr Ganguly undertakes expert witness instructions, including the preparation of medico-legal reports and giving evidence in court in clinical negligence cases relating to Neuro, Chest, abdomen and pelvis, Gynaecology
EMAIL ME and obstetrics, Paediatric, Cancers, Trauma, and Emergency radiology. Dr Ganguly can act on behalf of either claimant or defendant or as a Single Joint Expert. He has provided expert witness evidence in the coroner's, judicial, and military courts.

T: +44 (0)20 8852 8522
E: eyes@dbcg.co.uk
Office: Docklands Business Centre, 10-16 Tiller Road, London E14 8PX
EYE-LAW CHAMBERS® was founded in 2017 through the consolidation of leading medicolegal practices. Specialising exclusively in eye and vision-related medicolegal matters, the team offers high-quality CPR35-compliant expert opinion across issues involving causation, liability, condition, and prognosis. A corporate membership in The Academy of Experts since 2019, EYE-LAW CHAMBERS® acts as trusted expert medicolegal providers through its unwavering commitment to expertise, timeliness, and service. Based in London and
CONTACT US operating internationally, for civil and criminal courts and tribunals across the UK, Republic of Ireland, mainland Europe, Africa, and Asia, EYE-LAW CHAMBERS® delivers comprehensive Expert reports within four weeks of instruction.
Certified Expert Witness – Skin Camouflage

t: +44 7817 297286
e: tonia@skincamouflage-bristol.co.uk
w: www.skincamouflage-bristol.co.uk

Tonia Goman is a Certified Expert Witness and specialist Skin Camouflage Practitioner with over twenty years’ clinical experience in dermatology and scar management. She provides independent CPR-compliant medicolegal reports for claimant and defendant solicitors nationwide, including remote assessments, treatment planning and detailed quantum costings. Tonia advises on the suitability, application and long-term requirements of medical-grade skin camouflage for scars, burns and
disfigurement. Originally trained with the British Association of Skin Camouflage, she works independently from her Bristol clinic and offers consultations and expert assessments across the UK, both remotely and face-to-face. Tonia provides balanced, practical and evidence-based expert opinion to the courts.


MBChB, LL.B (Hons), FRCSEd (C-Th), PgCert (Medical Law)
e: vijayjoshi@doctors.net.uk
w: www.thoracicexpertwitness.co.uk
Mr Joshi is an award winning, US and UK trained Consultant Thoracic Surgeon (in practice since 2018). He takes instructions on cases related to lung / thoracic cancers, pleural and airway diseases, sarcoma and many other lung / chest related conditions. He has a
regular, ongoing trauma practice and can opine on both rib and sternal injury. Mr Joshi has been preparing reports since 2019 and has given evidence in Court. He is formally trained through Bond Solon and has CUBS certification. He takes instruction for both claimant and defense as well as a joint expert.
Consultant Plastic, Reconstructive and Hand Surgeon
t: +44 07360 750 011
e: mrkplastics2021@gmail.com
w: www.atulkhanna.co.uk/expert-witness

Mr Khanna is a substantive NHS Consultant in Plastic, Reconstructive and Hand Surgery at The Sandwell and West Birmingham NHS Trust and has been involved in medical legal work since 1998. In this period he has provided over 4000 medical reports. He has prepared a chapter for the Encyclopedia of Forensic & Legal Medicine entitled "Medical malpractice in Cosmetic and Plastic Surgery".
Areas of expertise:
• Hand surgery: Sequelae of hand injuries and surgery
• Soft tissue injury:
• Burns management: Sequelae of disability following burns injury, scarring and surgery
• Medical negligence in Cosmetic Surgery
MB ChB PhD MRCP MRCPath

Consultant Paediatric Haematologist

t: +44 07802 456 804
w: www.dentalexpert.me
w: www.forma.co.uk
e: info@dentalexpert.me

Dr Raj Kumar has written over 500 reports in matters arising from patient and regulatory complaints, dental negligence and accidental injuries. Dr Kumar currently completes about 150 reports annually; 70:30 claimant defendant ratio. Clinical negligence, Condition and Prognosis, Road traffic accidents and Clinical Fraud are all covered. Dr Kumar has appeared in court hearings at least 5 times on behalf of claimants and defendants, including Regulatory matters. Dr Kumar qualified from Guys Hospital in 1989 with a
BDS. In 1990 he obtained his LDS RCS from the Royal College of Surgeons London. Dr Kumar holds a Masters degree in Advanced General Dentistry from the Royal College of Surgeons and a Masters in Implantology from the University of Madrid.
EMAIL ME


t: +44 07596 852 737
Mr. Damian Lake MB,Ch.B,FRCOphth,LLM.
w: www.medicolegalorthopaedics.com
w: www.upperlimbsurgery.net

e: appointments.shyamkumar@gmail.com
Mr Kumar is a Consultant Orthopaedic Surgeon, specialising in trauma and upper limb conditions, with a focus on medicolegal practice since 2011. He serves on the Orthopaedic trauma rota at the Royal Lancaster Infirmary. He holds an LLM in Medical Law & Ethics and is on the Medicolegal Committee of the British Orthopaedic Association. He is on the panel of performance assessors
Consultant Orthopaedic Surgeon for the General Medical Council and is an examiner for the FRCS (Tr& Orth) and Royal College of Surgeons. He provides concise medical reports for clinical negligence and personal injury cases, with clinics in Manchester, Lytham, Bolton and Lancaster.
Consultant Cardiothoracic Surgeon
w: www.damianlake.com
e: info@damianlake.com

Mr. Lake is a Consultant Ophthalmologist currently practising in Kent, Sussex and London. In 2008 Mr. Lake became a Consultant at the Queen Victoria NHS hospital, East Grinstead. He became Clinical Director of the service for five years, and responsible for the UK’s first Eye Bank. Mr. Lake has represented the hospital at National level at OTAG (Ocular Tissue Advisory Group to NHSBT) and as Chair of the OTTSG (Ocular Tissue and transplant Standards Group of the Royal College of Ophthalmology.) In 2022, Mr. Lake obtained a Masters degree (with merit) in Law from The University of Cardiff. In 2023, Mr. Lake founded The Sight Centre Group and opened clinics and hospitals in Tunbridge Wells, Kent, dedicated to excellence in eye care. He continues as the Medical Director and a practising Consultant. Mr. Lake has produced medico legal reports since 2008, with an approximate 50:50 split, Defendant: Claimant ratio.

Consultant Orthopaedic and Trauma Surgeon

e: cardiothoraciclegal@icloud.com w: www.cardiothoracic-surgeon.co.uk
Kulvinder Lall is one of the top cardiothoracic surgeon’s in the UK, with particular expertise in aortic valve replacement, mitral valve repair, coronary artery bypass graft, and thoracic aortic aneurysm. Mr Lall is listed on the General Medical Council Specialist Register as a specialist in cardiothoracic surgery. Qualifying in 1989 from the University of London, he has trained in cardiothoracic surgery in London, Glasgow & Sydney. He was appointed to St Bartholomew’s Hospital as one of the youngest cardiac surgeons in the UK aged 36. As an NHS Surgeon he has performed in excess of 5,000 heart operations with outstanding results as measured by The Care Quality Commission & Department of Health.
As a leading cardiothoracic surgeon, he has published in over 15 peer reviewed worldwide journals and is actively involved in NHS research. He teaches extensively in China, Europe, Hong Kong and Israel, and was the first implanter of a stentless heart valve in Asia (Beijing 2010).

Consultant Ophthalmologist
t: +44 1225 821741
e: jon.luck@nhs.net
w: www.jonathanluckmedicolegal.org.uk

A practicing NHS Consultant Ophthalmologist, Mr Luck has over 25 years’ experience in providing medicolegal opinion and reports. He will accept instructions as an Expert Witness in most aspects of general ophthalmology, but has a special interest in Cataract Surgery, Trauma, Laser Eye Surgery and Paediatric Ophthalmology (including alleged non-accidental injury). He aims to provide timely,
reasoned, logical, and thorough medical reports, which can be fully CPR Part 35 Compliant, or short ‘screening’ reports, according to his instructions. Mr Luck regularly undertakes CPD in medicolegal matters and was awarded the Cardiff University Bond Solon Expert Witness Certificate in 2019.


Dr Neil Mo
BSc (Hons), MSc, MBBCh, FRCP
Consultant Rheumatologist
t: +44 0800 433 2380
e: enquiries@drneilmo.com
w: www.drneilmo.com

Dr Neil Mo is a consultant rheumatologist and clinical lead in Swansea Bay University Health Board. He was previously a consultant in Charing Cross and Hammersmith Hospitals. He has received training in report writing and courtroom skills, and has produced over 300 medicolegal reports. He provides comprehensive, authoritative and well balanced
reports with a quick turnaround time. He has expertise in all areas of adult rheumatology, and maintains his clinical and medicolegal knowledge to deliver an up to date expert opinion. He is experienced with risk management within the NHS and has undergone training with NHS resolution.
MA MD FRCP FRCR
Senior Clinical Oncologist
t: +44 020 7631 1632
e: nplowman@doctorplowman.com
w: www.drnickplowman.com
ME

Dr P N Plowman is senior clinical oncologist to St Bartholomew's Hospital, London and has a paediatric interest and on the staff of Great Ormond Street Hospital. He has a long history of medicolegal work with around 50 new instructions each year. He has been an expert
in the Tobacco Litigation and the class action of 22,000 USA women claiming breast cancer caused by HRT. Most of his instructions are to do with delay to diagnosis of cancer or causation aspects of cancer treatments' complications.
EMAIL ME
Dr David Newby
BSc MBChB
FRCA LLM

Consultant Paediatric and Adult Anaesthetist
t: +44 07428 467 803
e: ddp.medicolegal@gmail.com

w: www.anaesthesiamedicalexpert.co.uk
Dr David Newby is a substantive anaesthetic consultant at Ipswich Hospital. He is the lead anaesthestist for paediatric services and established and runs the consultant-led paediatric preoperative assessment clinic. His adult work
includes orthopaedic trauma and vascular surgery.
Areas of particular expertise: anaesthesia for children in the district general hospital
• paediatric preoperative assessment
• TIVA in children
In addition to:
• all aspects of adult perioperative care, including preoperative assessment
• high-risk surgery
• awareness under anaesthesia
• anaphylaxis
• shared-decision making
Dr Ana Phelps MD, PhD, FRCP, RCPathME
Substantive Consultant Geriatrician
t: +44 07970 627 996
e: ana.phelps@nhs.net

Dr Phelps is a substantive Consultant Geriatrician at Buckinghamshire Healthcare NHS Trust. She is an experienced Medical Examiner, regularly reviewing hospital mortality cases and advising doctors on medical certification of cause of death and when to refer to a Coroner. Her expertise includes Orthogeriatrics, Frailty, Dementia, Peri-operative Medicine and complex cases in patients >65y. Her medico-legal practice includes medical negligence, second opinions, decisions on escalation
and resuscitation, coroner reports, ethical situations, inappropriate/ harmful testing and treatments, and breeches in communication. She can provide comprehensive case reviews and expert opinion on the quality of the care provided at the different stages of care.
EMAIL ME
Lecturer in Physiotherapy | Expert Witness | Author
t: +44 7530 479177
e: stuartbporter@aol.com

Dr Stuart Porter is a Chartered Physiotherapist and an Expert Witness with extensive experience. He is also an international textbook author. His medico-legal practice encompasses breach of duty, causation, and condition-andprognosis matters within physiotherapy, rehabilitation, and wider neuro musculoskeletal healthcare in adults and children. He accepts instructions on behalf of both Claimants and Defendants, including legal aid rates, providing independent expert opinion in accordance with the Civil Procedure Rules (CPR Part 35) and associated Practice Directions. His reports address standards of physiotherapy practice, assault, negligence and criminal claims, the appropriateness
of interventions in relation to accepted professional and evidential standards. Dr Porter routinely analyses the adequacy of physical assessment, documentation, treatment protocols, patient consent, and continuity of care.
EMAIL ME


FRCS(Tr & Orth) FRCS MCh(Orth) MS(Orth) DNB(Orth) MBBS
Consultant Trauma & Orthopaedic Surgeon
t: +44 0161 393 3059 e: nikhil.shah@consultantcare.com

Mr Nikhil Shah can act as an expert witness in personal injury and clinical negligence cases, taking instructions from either claimant or defendant or as a Single Joint Expert. He can provide medico legal reports for personal injury claims involving:
• Trips and slips
• Pelvic and acetabular fractures
• Low velocity impact cases
• Whiplash
• Long bone and articular fractures
• Ankle, knee and hip fractures, lower limb injuries Soft tissue injuries
Mr Shah can provide clinical negligence related reports in his specialist areas of expertise concerning:
• Primary and revision hip and knee replacements
• Pelvic and acetabular fractures
• Long bone and periarticular trauma
Lead Consultant in Emergency Medicine, Princess Elizabeth Hospital, Guernsey
t: +44 07839 755 001 e: thesens@msn.com

Medico Legal Expert since 1996 Experience as independent expert for claimant, defence & SJE.
Areas of interest:
• Clinical Negligence
• Personal Injury
• Hand Injury
• Resuscitation
• Trauma, Burns, Sedation & Acute Pain
• Musculoskeletal injuries CPR Part35 trained
• MEDCO accredited
• Up to date medico-legal CPD portfolio
• Reports vetted by solicitors
• Consultation Venues at: Chester (Cheshire, Northwest & North Wales), Guernsey & Jersey
• Happy to provide pro-bono opinion Member of EWI, APIL, Law Society.
(Trauma and Orthopaedics)
t: +44 07506 504 351
e: Sophie.medicolegal@outlook.com w: www.paulwj.com

Mr Whittingham-Jones is a consultant Hip and Knee surgeon with an NHS and private practice. He has
produced over 1000 reports since 2013. Reports are accurate, concise and well reasoned. He is always happy to talk through any issues with reports. Having a particular interest in breach of duty cases, he will provide full reports or desktop screening reports as required.





t: +44 7915 423 924 e: medicalreport@btinternet.com

Mrs Webber has been a consultant urological surgeon for over 25 years, working in both the NHS and the private sector. She is based at the Victoria Hospital in Kirkcaldy, part of NHS Fife University Health Board. She has been in medicolegal practice since 2007 and currently writes 75 reports per year. She undertakes cases from all parts of the United Kingdom and the Irish Republic.
Areas of expertise:
• Injuries to the genitourinary tract, including renal and pelvic trauma
• Clinical negligence, including
• Delayed diagnosis of urological conditions
• Complications following the implantation of TVT/TOT mesh devices
• Urinary sepsis
• Management of stone disease Informed consent






For 25 years, we’ve helped law firms to build stronger cases by providing access to specialist medical experts for comprehensive medico-legal reports.

Why choose Premex+?
With over 7,000 experienced medical specialists, each hand-selected for their subject matter knowledge and medico-legal experience, we deliver professional medical reports for your complex cases.
What sets us apart:
Specialist team, with on average 5+ years of experience working on complex cases
Tailored solutions for each case
Secure data handling –ISO27001 certified
Extensive industry experience www.premexplus.co.uk