










The use of platelet-rich fibrin in dental implantology represent a cutting-edge advancement in oral health care, enhancing healing and integration for patients undergoing dental implant treatment This comprehensive guide explores how PRF technology harnesses the body's innate regenerative abilities to enhance bone and soft-tissue healing, thereby increasing long-term success rates for implant procedures Learn practical insights from expert leader Dr Richard J Miron about the science, clinical application, and future trends transforming implant dentistry
Definition of platelet-rich fibrin �PRF�
Overview of dental implants and their healing process
Importance of regenerative medicine in implant dentistry
Platelet-rich fibrin in dental implantology utilizes a patient's own blood-derived platelet concentrates to support and accelerate the natural healing around dental implants PRF is a biomaterial composed of a fibrin mesh enriched with platelets and growth factors, essential for tissue regeneration
Dental implants require successful integration with the surrounding bone and soft tissues for long-term stability. The healing process can be complex, especially when bone volume is insufficient or softtissue quality is compromised. Regenerative medicine
techniques, such as PRF application, play a critical role in enhancing these biological processes by providing concentrated autologous growth factors that promote faster, more effective healing
As implant dentistry advances, combining traditional surgical protocols with regenerative technologies like PRF offers patients improved comfort, quicker recovery times, and better overall implant outcomes. These innovations exemplify how modern dentistry is moving beyond mechanical replacements to biologically driven solutions.
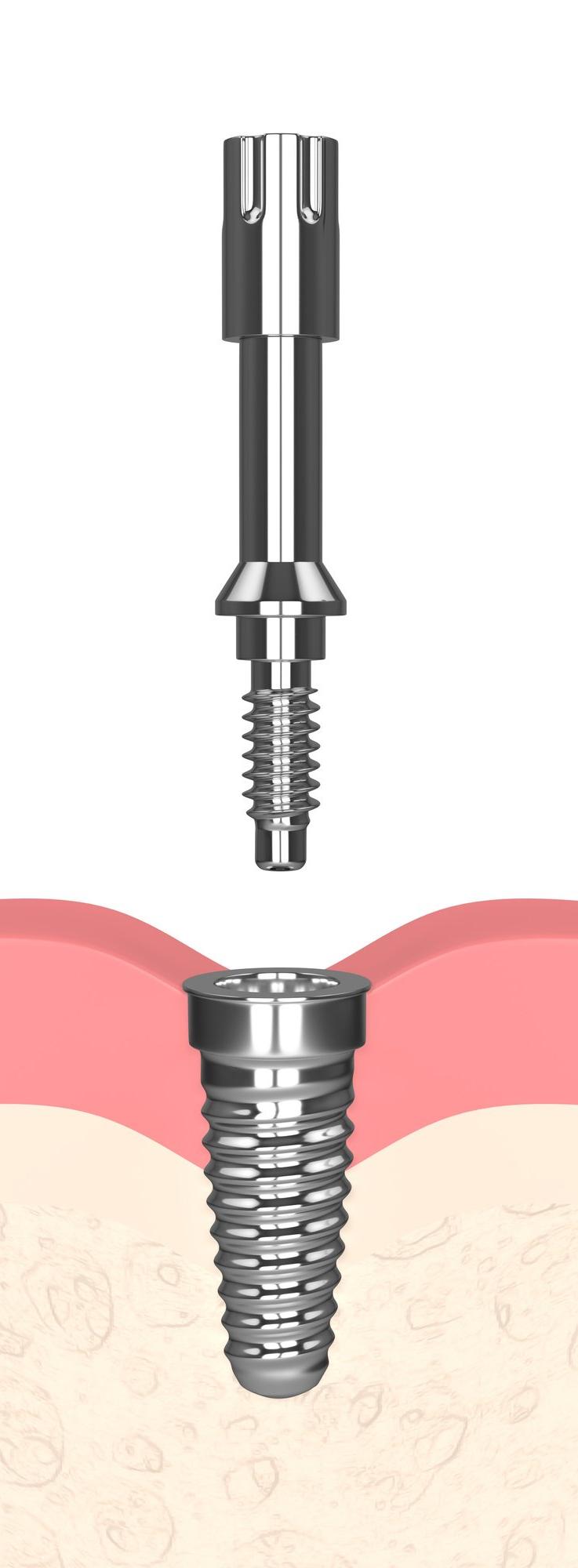
The science behind platelet-rich fibrin and its application How PRF enhances healing in dental implant procedures Key factors influencing implant success Advances in implant dentistry and future trends
“
Platelet concentrates like PRF harness your body's intrinsic ability to heal by concentrating growth factors from your own blood, significantly enhancing tissue regeneration around dental implants.
This autologous approach minimizes risk and maximizes healing potential, providing dental implants with a stronger biological foundation and shorter recovery times. By aligning surgical technique with the bodyʼs own capacity to regenerate, clinicians can unlock more predictable outcomes across a wide range of case complexities.
Composition and preparation of PRF from the patientʼs blood, the role of platelets and growth factors in tissue regeneration, and differences between PRF and other platelet concentrates like PRP form the scientific backbone of this therapy. Platelet-rich fibrin in dental implantology relies on a simple yet powerful biological concept: concentrating a patientʼs own platelets to harness their natural healing capabilities. Blood is drawn and placed in a centrifuge, where it is spun to separate its components by density. The PRF layer includes a fibrin scaffold loaded with platelets, growth factors, and white blood cells, all of which play essential roles in tissue repair and regeneration.
The growth factors released by the platelets stimulate cell migration, proliferation, and differentiation the processes required to build new bone and soft tissue around implants. Compared to platelet-rich plasma �PRP�, PRF contains a fibrin matrix that serves as a scaffold to support cells and prolong the release of growth factors, thereby providing sustained healing benefits. This distinction makes PRF advantageous for dental implant cases that require robust and long-lasting tissue support.
Through this approach, dental practitioners can improve the biological foundation for implants, reduce recovery times, and promote better integration of the implant with the patientʼs jawbone and gums, leading to more predictable treatment outcomes. Dr. Miron highlights, "The body's an amazing thing. PRF leverages your own healing potential by giving concentrated growth factors in the exact ratios that they're needed, significantly speeding up tissue regeneration and improving the integration of tissues around dental implants. " This biologically active scaffold also creates a favorable environment for regenerative cells and other reparative cells to thrive.

The preparation of plateletrich fibrin is straightforward yet precise. A small vial of the patient's own blood is drawn, typically around 10 ml, and placed into a centrifuge. This process separates the blood into distinct layers based on density, isolating a fibrin matrix rich in platelets and growth factors. Dr. Miron states, "We take a small vial of blood, spin it in a centrifuge to concentrate platelets, and apply this 10x growth factor-rich fibrin scaffold around the implant site, accelerating healing and improving outcomes. " The PRF clot is then carefully applied around the dental implant site to promote accelerated softtissue healing and bone regeneration, reducing complications and improving long-term implant stability.
• • • Acceleration of soft tissue and bone regeneration
Improved integration of implants with surrounding tissues
Reduction in healing time and patient discomfort
• • • Use in bone grafting and soft tissue grafting procedures Support in complex fullmouth dental implant cases
Successful patient outcomes increasingly rely on these regenerative techniques, as PRF not only expedites healing but also promotes highquality tissue formation, ensuring long-lasting implant stability and function. The combined impact of biologically active scaffolds and controlled growth factor release translates to improved osseointegration, better soft-tissue seals around abutments, and more predictable esthetic results.
Platelet-rich fibrin dental implants have revolutionized implant dentistry by providing enhanced regenerative support during critical phases of healing. PRF accelerates both soft tissue and bone regeneration, which is vital in patients requiring bone grafting or soft tissue augmentation before or during implant placement. Dr. Richard J. Miron explains, “With tissue engineering advancements like PRF, we can regrow bone and soft tissues more predictably, decreasing healing times and improving patient comfort throughout. ” In clinical practice, PRF is used to support graft material handling, improve wound healing, and reduce complications such as infection or implant failure. Complex cases, including fullmouth dental implants where extensive reconstruction is necessary, particularly benefit from PRFʼs enhanced healing properties. Patients often report reduced swelling and pain, and faster recovery when PRF protocols are integrated into their treatment plans
• •
• Medical conditions affecting implant success (e.g., diabetes, osteoporosis)
Importance of bone volume and quality
Patient lifestyle factors and expectations
Evaluating medical history, systemic health, and bone quality is essential to determine if a patient is a good candidate for implants and PRF� enhanced healing.
Successful dental implant outcomes with PRF also depend heavily on patient candidacy. A thorough evaluation of medical history is critical, including factors like diabetes, osteoporosis, medication use, and age. These variables affect healing and the success of implant integration. Dr. Miron emphasizes, "The day you place the implant is the most important day of that implants life. Proper planning, diagnosis, and use of technologies like PRF are critical to long-term success. " A customized treatment plan based on evidence-based medicine ensures that PRF is optimally integrated into the surgical protocol, resulting in superior outcomes.
Every implant case is unique; therefore, treatment timing, bone and soft-tissue grafting requirements, and the use of biologic agents such as PRF must be personalized. Evidencebased protocols guide specialists to determine when bone regeneration is needed, how long healing phases should last, and how to manage systemic health to optimize results. Not all patients are equally suited for platelet-rich fibrin dental implants. Careful evaluation is critical to achieve optimal results. Dr. Miron highlights the importance of reviewing a patientʼs medical history, including chronic diseases such as diabetes or osteoporosis, which
can affect bone metabolism and the healing response. Bone volume and quality determine whether regenerative procedures like PRF will be effective in supporting the implant. Patients with inadequate bone may require additional grafting, aided by PRF, to improve their chances of successful integration. Moreover, patient lifestyle factors such as smoking, medication usage, and oral hygiene habits must be considered to set realistic treatment expectations. Educated clinicians also emphasize transparency with patients about timelines and possible challenges. Some patients prefer quicker options like dentures, while others are willing
to undergo regenerative protocols, knowing the benefits of improved long-term implant success. Informed decision-making tailored to each individual's health profile leads to better overall satisfaction and clinical outcomes.
Growth factors and biomaterials improving bone grafting
Emerging biological agents like exosomes and Periosomes
Integration of systemic health management in implant success
The future of implant dentistry lies in regenerative medicine and understanding systemic healthʼs impact on oral healing. Recent advances in platelet-rich fibrin therapy in dental implantology and regenerative medicine continue to push the boundaries of what is possible in implant dentistry. New biomaterials enhanced with growth factors improve bone graft stability and accelerate healing. Emerging biological agents, such as exosomes and specialized vesicles
called Periosomes, are poised to enable targeted tissue regeneration, potentially revolutionizing periodontal and bone repair. Moreover, understanding a patientʼs systemic health such as vitamin D levels or inflammatory status—has become increasingly important in predicting and improving implant success. Dr. Miron emphasizes, “We now know that systemic health profoundly affects how implants integrate. Managing these factors alongside regenerative techniques offers a holistic path to better outcomes. ” The integration of these
next-generation therapies represents the future where personalized regenerative dentistry will optimize healing, reduce complications, and enhance patient quality of life.
In the realm of platelet-rich fibrin in dental implantology, careful planning and diagnostics are crucial. Advanced imaging techniques, such as CBCT scans, allow clinicians to thoroughly assess bone anatomy, density, and proximity to vital structures. This information improves precise implant placement, which Dr. Miron calls “the most important day of the implantʼs life. ” Customized treatment plans incorporate both surgical and regenerative components tailored to the patientʼs unique anatomy and health profile. Proper diagnostics reduce the risk of complications, ensure optimal implant positioning, and maximize the regenerative potential of PRF and adjunct biomaterials. Emphasizing meticulous evidence-based planning underscores the clinicianʼs role as a skilled healthcare provider rather than merely a technician, fostering higher success rates and improved patient trust.

Despite its benefits, several misconceptions surround the use of platelet-rich fibrin in dental implantology Itʼs important to clarify that PRF does not regenerate teeth itself but enhances the healing of the tissues supporting both natural teeth and the implant site namely, bone, periodontal ligament, and soft tissues Immediate implant placement with PRF support is not suitable for every patient Complex cases often require staged regenerative procedures to rebuild adequate bone and soft tissue before implant placement Transparency about these timelines helps manage expectations and encourages patient compliance for follow-up care Understanding these realities empowers patients to make informed decisions and appreciate the biological basis of their treatments rather than expecting quick fixes or miracle cures
The necessity of realistic expectations regarding treatment duration

a qualified implant dentist with proper credentials
What is platelet-rich fibrin, and how does it work in dental implants? Platelet-rich fibrin is a blood-derived biomaterial that contains concentrated platelets and growth factors, enhancing tissue regeneration around implants, accelerating healing, and improving integration. How long does it take for dental implants to heal with PRF? Healing typically ranges from 4 to 7 months, including bone and soft-tissue regeneration, implant integration, and recovery, and PRF often reduces overall treatment time and discomfort. Are there any risks associated with using PRF in implant dentistry? PRF is autologous and safe, but proper technique is essential. Risks mainly relate to implant surgery itself, such as infection or failure, which PRF aims to minimize. Can PRF be used for all dental implant patients? While beneficial, candidacy depends on medical history, bone quality, and systemic health. A thorough evaluation by a qualified dentist determines suitability. What are the benefits of choosing a specialist for implant placement? Specialists have advanced training to manage complex cases, use evidence-based protocols, and integrate regenerative technologies such as PRF, resulting in better outcomes.

Platelet-rich fibrin �PRF) significantly enhances healing by concentrating growth factors from the patient's own blood.
Successful dental implant outcomes depend on thorough planning, patient health evaluation, and evidence-based treatment.
Advances in regenerative medicine, including PRF and emerging biological agents, are transforming implant dentistry.
Patients should seek qualified dentists and be wary of marketing claims promising instant results.
Ongoing research and education continue to improve implant success and patient comfort.


Dr. Richard Miron concludes, "Harnessing the body's natural healing through platelet-rich fibrin is a gamechanger in dental implantology, offering patients faster recovery and more predictable outcomes when applied with scientific rigor and transparency. " Dr. Richard Miron is currently lead educator and researcher at Advanced PRF Education and an Adjunct Visiting Faculty in the department of Periodontology in Bern, Switzerland where he completed his PhD studies since 2009. He has currently published over 400 peer-reviewed articles and lectures internationally on many topics relating to growth factors, bone biomaterials and guided bone regeneration. For the past 10 years, Dr. Miron has been recognized by Dentistry Today as being one of the top 100 CE providers in the country and the youngest to ever make the list. He is also the top ranked researcher on Platelet-Rich Fibrin therapy as per Expertscape independent review. He has recently been awarded many recent international prizes in dentistry and is widely considered as one of the top contributors to implant dentistry having won the ITI Andre Schroeder Prize, the IADR Young Investigator of the Year in the field of Implant Dentistry as well as the IADR Socransky Research award in the field of Periodontology �2020�. He has written 10 textbooks widely distributed in regenerative dentistry including his best-seller in 2019 titled: “Next Generation Biomaterials for Bone and Periodontal Regeneration” , in 2021 titled: “Understanding Platelet Rich Fibrin” and in 2023 titled: "Modern Implant Dentistry" .