SIGHT TO LIFE BRINGING
2025 Annual Report





2025 Annual Report




As I reflect on the past year, I’m filled with pride and gratitude for the extraordinary accomplishments at the University of Colorado Anschutz Department of Ophthalmology.
It has been a year of remarkable growth, groundbreaking research, and continued dedication to our mission of bringing sight to life.
We’ve reached new heights in both scale and impact at the Sue Anschutz-Rodgers Eye Center. With more than 90 faculty members, we are now among the largest ophthalmology departments in the country — an achievement that speaks to the strength of our community and the breadth of our expertise. Our growth is not just in numbers, but in the depth of innovation and care we provide.
This year, we received a transformative $40 million gift to accelerate the translation of vision research into clinical care. We were also named as part of a cross-campus initiative awarded up to $46 million from Advanced Research Projects Agency for Health to pursue whole human eye transplantation, a bold step toward curing total blindness.
Our research continues to shape the future of ophthalmology. In the lab, Dr. Valeria Canto-Soler’s retinal organoid, winner of two NIH 3D Retina Challenge prizes, has been licensed by a major stem cell company and will soon be available to researchers worldwide. On the clinical side, our age-related macular degeneration team published a seminal study based on 12 years of data, offering new insights into disease progression and treatment.
In artificial intelligence (AI), we are leveraging a decade’s worth of clinical data to build algorithms that address the growing demands of vision care amid a shrinking workforce. These tools are poised to revolutionize how we diagnose and manage eye diseases, and they are already attracting top talent to our department.
Despite challenges in research funding and healthcare delivery, I remain more optimistic than ever. Our science is not only competitive; it’s relevant, translational, and making a real difference in patients’ lives. We’re also laying the groundwork for future growth, including exciting partnerships that position us at the forefront of academic-industry collaboration.

“Our growth is not just in numbers, but in the depth of innovation and care we provide.”
What inspires me most is the unwavering commitment of our faculty, trainees, and staff to advancing vision science and care. Their work, along with your support, make everything we do possible.
Thank you for being part of our journey. I invite you to explore the pages ahead and celebrate the remarkable progress we’ve made together.
Warmly,
Naresh Mandava, MD
Sue Anschutz-Rodgers Endowed Chair in Retinal Diseases
Professor and Chair, Department of Ophthalmology
Senior Associate Dean for Strategic Advancement, University of Colorado Anschutz School of Medicine
TOTAL FUNDING FOR SPONSORED RESEARCH GRANTS
TOTAL PUBLICATIONS ACTIVE CLINICAL TRIALS
$15.9M 144 34
NUMBER OF TECHNOLOGIES LICENSED IN TOTAL FUNDING RAISED FOR CU ANSCHUTZ DEPT. OF OPHTHALMOLOGY SPINOUT COMPANIES
13 $267M
SURGERIES BY CU ANSCHUTZ FACULTY
10,428
UNIQUE PATIENT VISITS BY CU ANSCHUTZ FACULTY
189,766
ADMINISTRATIVE STAFF RESEARCH STAFF
RESIDENTS
92 12 18 24 15 38 FACULTY FELLOWS
SECONDARY FACULTY
The anonymous gift will boost research into treating and curing eye diseases while investing in new technology and recruiting top talent.

The CU Anschutz Department of Ophthalmology received a historic $40 million gift in 2025 to treat and potentially cure eye diseases, increase focus on basic science, and harness artificial intelligence to revolutionize vision care in the years ahead. The generous investment has established the CU Department of Ophthalmology Research Endowment. Part of the gift is available for immediate use, including funding for critical basic science research in vision preservation and restoration, while the rest will provide ongoing support well into the future.
The donor, who has chosen to remain anonymous, and their family have been longtime patients at the Sue AnschutzRodgers Eye Center. Their gift reflects their deep appreciation for the exceptional care they’ve received and their desire for others to benefit from the same high-quality eye care at CU Anschutz for generations to come.
The investment will accelerate the innovative department’s endeavor in the quest to treat and cure eye disease.
“We have a tremendous opportunity to fuel our research enterprise which is fundamental to clinical care,” said Naresh Mandava, MD, professor and chair of the CU Anschutz Department of Ophthalmology and the Sue Anschutz-Rodgers
Endowed Chair in Retinal Diseases. “This gift will allow us to translate technology from the lab to the patient faster than before.”
The timing couldn’t be better.
Some 10,000 Americans turn 65 each day and that comes with an increase in diseases like glaucoma and macular degeneration.
“We have the chance to change the fate of those with these diseases with funding like this,” Mandava said.
The Sue Anschutz-Rodgers Eye Center is the sole academic eye center in Colorado and serves more than 115,000 patients a year. It has already launched a range of initiatives aimed at eradicating persistent eye diseases. They include:
• The CellSight program involves teams of investigators from across disciplines working to develop novel stem cell-based therapies to save and restore eyesight in blinding diseases.
• The CU Anschutz Age-Related Macular Degeneration (AMD) Registry allows researchers to investigate AMD, which is projected to affect almost 300 million people worldwide by 2040. Nearly 2,000 patients from the Sue Anschutz-Rodgers Eye Center are enrolled.
• Artificial intelligence is being used to build algorithms to help diagnose macular degeneration and glaucoma and screen for blinding diseases in infants.
115,000+
PATIENTS SERVED PER YEAR
“We are taking big datasets and seeing if we can identify the mechanisms that cause disease,” Mandava said. “We can also identify which patients will benefit from new drug therapies. So that opens the door for pharmaceutical companies to study their drugs on new patient populations earlier in the course of disease.”
The CU Anschutz Department of Ophthalmology is a national leader in innovation. It has won 60 patents since 2020. At least 13 technologies have been invented at CU Anschutz and licensed to industry, like the world-renowned Kahook Dual Blade, designed for minimally invasive glaucoma surgery. It was invented by Malik Kahook, MD, the Slater Family Endowed Chair in Ophthalmology and professor at the CU Anschutz School of Medicine
These innovations have spurred millions in investments, with several companies spun out of the department.
Mandava said he and his colleagues are honored that someone had enough confidence in the eye center to bestow such a large gift. It confirms just how precious sight is to people and the importance of vision science research programs.
“There is a tremendous responsibility that comes with this,” he said. “We have to deliver on every level to meet the full potential of this gift. And more importantly, we have to honor the intent of this investment which is to bring sight to patients.”
WON SINCE 2020

Learn more about our transformational vision science research.

The
Anschutz-
Eye Center is the only academic eye center in a 500 mile radius.
CU Anschutz ophthalmologists and rheumatologists work together to enhance the patient’s experience.
Since 2016, the CU Ocular Inflammation Multidisciplinary Clinic at the Sue Anschutz-Rodgers Eye Center has been a place where patients and trainees alike get a chance to see the complexities of medicine and the benefits of collaborating across specialties to provide individualized treatment.
“We started this clinic because rheumatologists deal with inflammation in the body and ophthalmologists deal with inflammation in the eye, but you can’t always deal with the eye alone or the body alone,” explains Alan Palestine, MD, CU Anschutz professor of ophthalmology and chief of the uveitis and ocular immunology service.
Normally, that would mean a patient spends a lot of time visiting different doctors, but the multidisciplinary clinic puts ophthalmology and rheumatology specialists and the patient all together in one room. This allows for a more holistic approach to assess the patient’s conditions and symptoms and discuss treatment options, which can be complex.
“When both doctors are in the same place at the same time seeing the patient simultaneously, we can make decisions right then and there instead of going back and forth over the course of several days or weeks,” Palestine says. “It’s better for the patient and it’s better for the doctors. We can initiate a change, and the patients only have to make one trip to CU Anschutz.”
The patients that Palestine and rheumatologist Jason Kolfenbach, MD, professor of medicine, see in the clinic typically have a systemic autoimmune disease with concurrent eye inflammation, but not always.
“We see patients with an established systemic autoimmune disease and secondary eye inflammation, but we also see patients with primary ocular inflammatory syndromes where management of medications to suppress their immune system may be challenging,” Kolfenbach says.
Medications used to treat these conditions often require expertise in ophthalmology and rheumatology because they can have an array of side effects, symptoms, or affect other organ systems.
A recent study authored by physicians in the clinic found that most patients seen in the multidisciplinary clinic had both ocular and systemic inflammatory disease, and they were treated with immunomodulatory therapies such as methotrexate, adalimumab, or rituximab.
More than 40% of clinic patients underwent a change in medication management as a result of their first evaluation with the physicians. Kolfenbach believes this is because of the specific expertise that rheumatologists and ophthalmologists bring to the multidisciplinary clinic, and the close working relationships formed between himself and the uveitis specialists.
“Based upon our joint evaluation, we commonly arrived at a new diagnosis and changed medical management for a substantial number of patients,” he says. “A new systemic diagnosis often provides new avenues for drug therapy, given the more limited treatment options for idiopathic uveitis. Our evaluation also allows us to identify concurrent health conditions that may increase the risk of certain therapies, so medication can be tailored to the specific patient.”

World-renowned melanoma oncologist Sapna Patel, MD, joins the Sue Anschutz-Rodgers Eye Center as a secondary faculty member to study eye cancer.
A specific strain of eye cancer, known as uveal melanoma, is a relatively rare but dangerous disease that can be deadly when it spreads to organs like the liver. “In uveal melanoma, about a third of patients die of their disease, and you can’t know just by looking at it,” says Scott Oliver, MD, associate professor in the CU Anschutz Department of Ophthalmology and director of the eye cancer program.
Melanoma oncologist Sapna Patel, MD, leader of the CU Cutaneous Oncology Program at the CU Anschutz Cancer Center, recently joined forces with Oliver, who is also a member of the CU Anschutz Cancer Center, to jointly treat uveal melanoma patients at the Sue AnschutzRodgers Eye Center.
“It’s great for patients to see the ophthalmologist and the cancer doctor together,” she says. “He dilates them, and then it takes about an hour for that dilation to take full effect, and since they’re not doing anything at that time, I slide in and do my visit with them rather than them having to navigate multiple clinics and different buildings.”
Patel’s mission at the CU Anschutz Cancer Center includes growing the rare-melanoma program, dealing mainly with non-sun-related melanomas. Patel, who has a secondary appointment in the Department of Ophthalmology, focuses much of her own research on uveal melanoma, which most commonly affects the eye’s middle layer, specifically the choroid layer, ciliary body, and the iris.
Through the joint clinic, Patel and Oliver, a vitreoretinal surgeon, have begun banking and sequencing donated patient uveal tumors.
“We hope in a few years we will have several hundred tumors where we know the sequence, we know the outcomes of these patients, and we can start to connect those dots,” she says. “Are certain mutations connected with a more aggressive form of this melanoma? And what are the mutations telling us about causative risk factors or opportunities to monitor for cancer recurrence?”
Oliver believes that the partnership with Patel and the CU Anschutz Cancer Center showcases the potential for expanding the eye cancer clinic at the Sue Anschutz-Rodgers Eye Center. “With future benefactor and grant support, we can fuel research advancements in uveal melanoma and other eye cancers, including retinoblastoma,” he says. “I am hopeful that this is just the beginning.”

“We hope in a few years we will have several hundred tumors where we know the sequence, we know the outcomes of these patients, and we can start to connect those dots.”
Christian Helfrich was diagnosed with bilateral retinoblastoma as a baby. Now, the 4-year-old boy is celebrating his road to recovery.
When Christian Helfrich, 4, rang the bell to signify he beat his cancer diagnosis, he was surrounded by his family, his community, his doctor, and all the major Colorado sports mascots.
“When we’re going to a sporting event, he’s going to a mascot event,” his mom, Melissa Helfrich, joked at the Make-A-Wish event in September 2024.
Mascots from professional Denver sports teams were in attendance, including Dinger, Miles, Bernie, Edson, Wooly, and Rocky. Various Denver-area high school mascots and community supporters showed their support for the Helfrich family’s monumental moment, too.
“He loves mascots. His face just lit up to see them all there,” says Scott Oliver, MD, associate professor of ophthalmology and Christian’s doctor throughout his treatment journey.
At 4 months old, during the first weeks of the COVID-19 pandemic, Christian was diagnosed with bilateral retinoblastoma, a rare eye cancer that forms in the retina of both eyes and most often occurs in young children.
Melissa and Justin Helfrich first noticed Christian had a white pupil in a photo taken with a flash when he was about 3 months old. The white pupil, called leukocoria, can serve as a warning sign that there is an ocular problem. Pediatricians screen for the disease with a red reflex test, but the cancer is so rare that it can be hard to spot.
To treat his cancer, Christian underwent five rounds of traditional chemotherapy and three rounds of intra-arterial chemotherapy (IAC), which is accomplished by doctors threading a catheter through the femoral artery, past the heart up through the carotid artery, and then into the artery that feeds the eye. Chemotherapy drugs are pumped through the vessel to directly target the tumor.
Oliver was able to save both of Christian’s eyes and preserve most of his vision. Now that Christian is in remission, his family says they want to bring awareness to the disease so that other families know what to look for to catch the cancer early and give doctors the best chance at beating it.

“The key thing to know is that in the U.S., retinoblastoma is one of the most survivable pediatric cancers,” Oliver says. “We want parents to be aware and watch for anything funny with their kids’ eyes. We want pediatricians to know that checking the red reflex really matters, and they have a chance to make a difference with that one very quick, very simple test.”

Watch an interview with Dr. Oliver and Christian’s family to learn more about retinoblastoma.
New Children’s Hospital Colorado eye clinic offers expert care, state-of-the-art equipment, and a whole lot of fun to young patients.
Helping pediatric patients feel comfortable in a doctor’s office can be a challenge, but that was exactly the goal in designing the new Eye Clinic at Children’s Colorado Outpatient Care at Fitzsimons Village Pavilion in Aurora.
Brightly painted walls and animal-coded hallways make the clinic a place that isn’t so daunting for young patients and their families. Village Pavilion Eye Clinic is an expansion from the main pediatric eye clinic across the street in the main Children’s Hospital Colorado building.
“The Village Pavilion is a playful space. It should be fun to come and see our staff,” says Chief of Pediatric Ophthalmology Emily McCourt, MD, a CU Anschutz associate professor of ophthalmology.
NEW PEDIATRIC PAVILION
9,500
SQUARE FEET
12 EXAM ROOMS
65%
INCREASED PATIENT ACCESS BY %
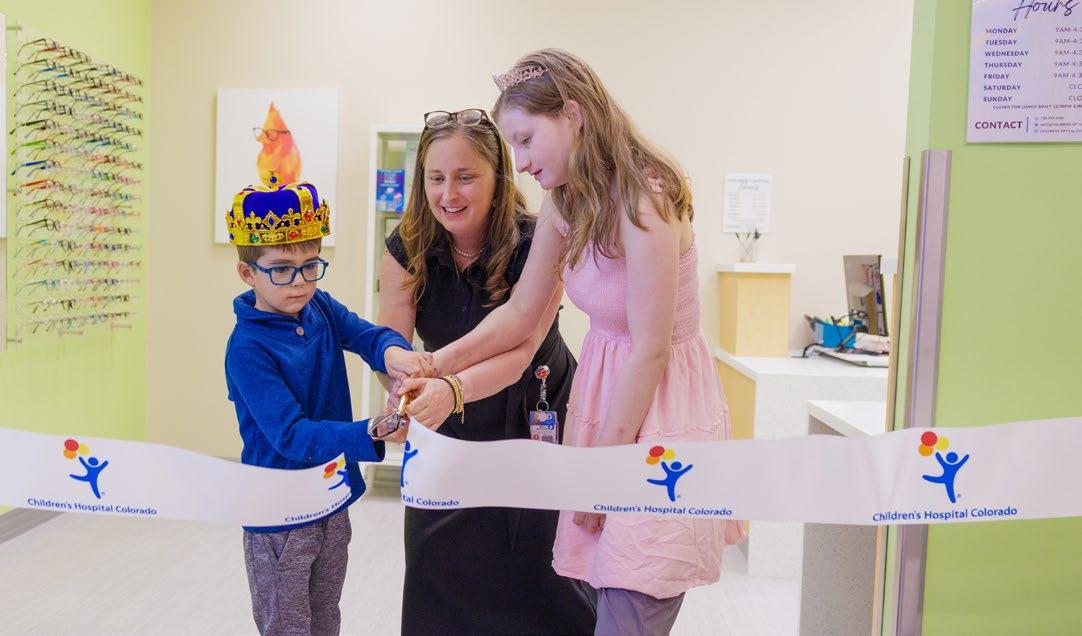
Today, more than a dozen CU Anschutz ophthalmologists and optometrists provide critical care and specialty expertise to patients at Children’s Hospital Colorado, which is located on the CU Anschutz medical campus.
The expansion has been on the minds of CU Anschutz eye doctors for years, especially as the need for pediatric ophthalmology services have grown in the region. As one of the largest pediatric eye centers in the country, the department has recently added several pediatric specialty-focused clinics, including glaucoma and uveitis, to cater to young patients who have different needs than adults.
At the main eye clinic at Children’s Hospital Colorado, clinicians will still see patients for some appointments, however, they will more often use the hospital space for hosting specialty clinics, tending to high-risk cases, and performing surgeries.
The Village Pavilion Eye Clinic, on the other hand, will be used mostly for traditional appointments. The 12 new exam rooms will allow dozens more patients to be seen each day.
Like the main Children’s Hospital Colorado eye clinic, the exam chairs at the Village Pavilion Eye Clinic are smaller, making them a better fit for kids, and there are kid-friendly touches throughout the space.
The space, being away from the main hospital, can also be more comforting for young patients who have had to undergo surgery and may find returning to that office overwhelming.
“Providing pediatric eye care in a pediatric setting is important for the comfort of the patient, and it really allows us to get a better exam,” McCourt, the Ponzio Family Chair for Pediatric Ophthalmology, says. “If the patient is comfortable, they like the space, and they’re having fun, then we’re able to get more information, and we’re better at giving accurate diagnoses and treatment plans.”

Pediatric patients share what excites them about the new eye clinic.

A professor of ophthalmology and the vice chair for quality and clinical affairs, Dr. Davidson leads comprehensive ophthalmologists and optometrists while advancing clinical quality initiatives across the department. As the Endowed Chair in Eye Care Innovation, his work focuses on improving patient outcomes through strategic oversight and peer collaboration. A cataract, cornea, and refractive surgeon, he is also the team ophthalmologist for the Colorado Avalanche and the Denver Nuggets.
In fiscal year 2025, he was especially proud of his role on the board of directors of the CEDARS/ ASPENS Society, contributing to the advancement of ophthalmic surgical education and excellence in patient care.
Outside of work, Dr. Davidson enjoys traveling, hiking, biking, skiing, and cherishes time spent with close friends and family.
With no cure and limited treatment options, AMD robs millions of people of their central vision, but CU Anschutz researchers have gained vital insights about the disease from a patient registry.
Anne Lynch, MD, distinctly remembers the day the Sue AnschutzRodgers Eye Center’s age-related macular degeneration (AMD) registry enrolled its first patient on July 9, 2014.
“We were just so delighted,” says Lynch, a professor of ophthalmology and epidemiology, and director of the Division of Ophthalmic Epidemiology in the CU Anschutz Department of Ophthalmology. “Since that day, we’ve had so many motivated patients enroll who realize how important this registry is and how it enables research that helps us understand the condition.”
By 2040, it’s projected that AMD will impact an estimated 288 million people worldwide. Damage to the macula progressively diminishes central vision. In dry AMD, which accounts for about 80% of cases, parts of the macula thin as small clumps of protein called drusen form. In wet AMD, which is rarer, new blood vessels grow under the retina and leak blood and fluid. Wet AMD leads to faster vision loss.
The registry holds repositories of electronic data, imaging data, and blood samples for biomarker studies that allow researchers to further investigate the disease. Now in its 11th year of operation, the registry includes close to 2,000 patients. It’s also been the foundation for more than 30 published manuscripts, including a recent seminal publication in JAMA Ophthalmology, as well as nearly 50 presentations at various meetings and conferences around the world.
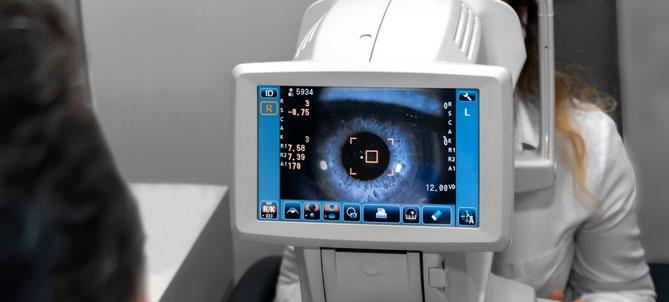
2,000
“We are proud of how our retinal specialists and the registry team have worked together to create this rich, highly curated registry of patients over the last decade,” says AMD specialist Naresh Mandava, MD, professor and chair of the Department of Ophthalmology.
When a patient is first recruited into the registry, they give enrollment samples of their blood and complete multimodal imaging. Physicians analyze these images and classify the case into early AMD, intermediate AMD, and advanced types of AMD, which include geographic atrophy and neovascular AMD. Then, each year after that, the registry team collects another blood sample from each patient on the registry and connects it to their imaging. This allows the researchers to study changes over time.
“Longitudinal studies are difficult because they require deep commitment and large investments to retain the confidentiality, quality, and integrity of the data collected,” Mandava says. “They also require teams that stay together for many years with a deep commitment to discovery, and I am proud that we have that here.”
AMD researchers in the department have used the registry for several investigations on the epidemiology of AMD, the complement system, proteomics, inflammation, and imaging. Lynch, Mandava, and the team of registry researchers and staff say the first decade is just the beginning for the registry.
“Our team is grateful for the dedication and commitment these patients have to the registry,” Lynch says. “We have to keep working for them toward new interventions and slowing the progression of this terrible disease.”
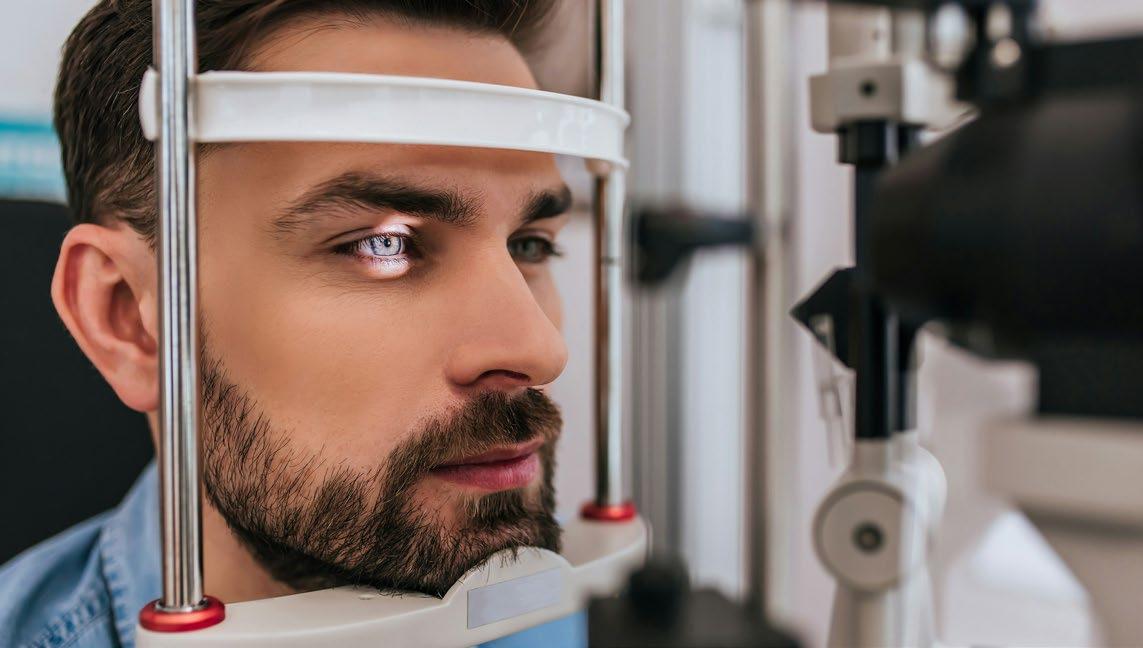
Ocular surface irritation and allergy visits more than doubled alongside higher concentrations of some pollutants.
Daily visit counts at the Sue Anschutz-Rodgers Eye Center significantly increase when certain ambient particulate matter (PM) levels in the Denver metro region are higher, according to a new study by CU Anschutz ophthalmology researchers.
In analyzing more than 144,000 ocular surface irritation and allergy patient visits to the eye center between 2015 and 2023, the researchers discovered that visits more than doubled when the particulate matter from air pollution was prevalent.
This research, published in the journal Clinical Ophthalmology, points to a possible association between climate conditions and the eyes.
“There are a lot of ways climate factors impact our health, but the eye is the organ that is the least studied,” says the study’s lead author, Jennifer Patnaik, PhD, MHS, assistant professor of ophthalmology and epidemiology.
25
ACTIVE RESEARCH GRANTS
16
ACTIVE PRINCIPAL INVESTIGATORS
224 PATENT APPLICATIONS
Despite being understudied, ophthalmologists know that the eyes can be affected by the environment. The ocular surface is directly exposed to environmental factors, making it highly susceptible to airborne pollutants like particulate matter.
“These pollutants can destabilize the tear film, cause inflammation, and exacerbate existing conditions such as dry eye and allergies, particularly in urban and industrialized regions,” explains study senior author Malik Kahook, MD, professor, vice chair of translational research, and Slater Family Endowed Chair in Ophthalmology.
The study specifically looked at concentrations of small PM in the range of 10 micrometers or less (PM10) and PM in the range of 2.5 micrometers or less (PM2.5) in diameter because of their known health effects.
“Pollutants like PM10 and PM2.5 are small enough to penetrate and adhere to the ocular surface, disrupting the tear film and triggering inflammation,” says Kahook. “Additionally, many contain toxic chemicals that activate oxidative stress pathways, further damaging the sensitive tissues of the eye.”
As the concentration level of particulate matter increased, so did the number of visits. Patnaik says this type of gradient effect can be difficult to establish with smaller datasets but gives important credibility to the findings because it shows that there’s likely a strong association between the two.
Patnaik says the researchers see value in studying the Denver metro region and would like to extend the research nationally or even globally, as pollution can differ greatly from one location to another. More data increases confidence in the link and can play an important foundational role in policies and regulation that directly benefit ocular and overall health.

The Doni Solich Family Chair in Ocular Stem Cell Research, Dr. Canto-Soler is a professor of ophthalmology and the director of CellSight. She leads cutting-edge research in regenerative medicine, focusing on developing therapies for retinal degenerative diseases. Her team pioneered the use of human induced pluripotent stem cells (hiPSCs) to generate miniature light-sensitive human retinas in laboratory dishes — providing a powerful platform for disease modeling and therapeutic development.
RESEARCHERS HARD AT WORK
$1.8M
DIRECT DEPARTMENT
SUPPORT FOR RESEARCH
$6.1M BLUE RIDGE FUNDING
In fiscal year 2025, she was especially proud of receiving a $9.2M Anschutz Acceleration Initiative grant to advance stem cell-based retinal transplants for geographic atrophy, a severe form of dry age-related macular degeneration.
Outside of work, Dr. Canto-Soler enjoys hiking, biking, fishing, skiing, and spending time with friends and family.
CU Anschutz-led team receives up to $46 million ARPA-H award. Funds will allow researchers to work toward restoring vision to patients with total blindness.
An award from the Advanced Research Projects Agency for Health (ARPA-H) Transplantation of Human Eye Allografts (THEA) program totaling up to $46 million is set to aid CU Anschutz researchers working to cure total blindness through human eye transplantation.
The award will support the work of the Total Human Eyeallotransplantation Innovation Advancement (THEIA) project team led by CU Anschutz.
Principal investigator and surgeon-scientist Kia Washington, MD, professor of surgery and secondary faculty member in the CU Anschutz Department of Ophthalmology, and co-principal investigator Christene A. Huang, PhD, transplant immunologist, will guide the effort.
Currently, there has never been a successful whole human eye transplant for the restoration of vision.
“We believe the great advancements over the last two decades in technology, transplantation surgery, and regenerative medicine now make restoration of vision possible,” Washington said.
ARPA-H is a federal agency established to advance high-potential, high-impact biomedical and health research that cannot be readily accomplished through traditional research or commercial activity.
The CU Anschutz team, which includes primary ophthalmology faculty members Valeria Canto-Soler, PhD, Mi-Hyun Nam, PhD, Alan Palestine, MD, Sudharshan Srivatsan, MD, and Natalia Vergara, PhD, will start by working with animal models to forward optic nerve regenerative strategies, immunosuppression, and postoperative care, with the goal of advancing to human trial studies.
Canto-Soler — professor of ophthalmology and director of CellSight, the ocular stem cell and regeneration research program based at the Sue Anschutz-Rodgers Eye Center — has been working with her team to make strides toward restoring vision to patients experiencing irreversible blindness due to diseases such as age-related macular degeneration (AMD).

Washington will lead the overall scientific team and partner with Srivatsan on the oculofacial plastic and orbital surgery team, while Huang’s team will study how the immune system reacts to the new eye.
“Our goal is to make it easier for the body to accept the new eye without rejecting it. To do that, we will create practical methods to manage inflammation and prevent transplant rejection,” Huang said.
The team said the work could also be translated to other parts of the body as well.
“The techniques and advancements we develop could be used to treat blindness while offering new solutions for other neurodegenerative disorders that impact the central nervous system,” Washington said. “For example, treating conditions like spinal cord injuries or brain damage. This could also be used in progressive brain disorders like Alzheimer’s and Parkinson’s disease.”
The transformative project will be in collaboration with several partners from across the country.
The Foundation Fighting Blindness will manage reporting for the effort while various institutions will aid in research that ranges from genetics to creating protocols for donation surgery.
This includes investigators at Johns Hopkins University, the University of Wisconsin, Indiana University, the University of Southern California, the National Eye Institute, and Cedars Sinai Medical Center.

Learn more about this pioneering research aimed at curing total blindness.
During SpaceX’s Polaris Dawn’s multi-day, high-altitude mission in September 2024, the crew conducted health impact research to better understand spaceflight-associated neuro-ocular syndrome (SANS). Prem Subramanian, MD, PhD, professor and chief of neuro-ophthalmology at CU Anschutz, in collaboration with CU Boulder aerospace engineering assistant professor Allie Hayman, PhD, sent specialized optical equipment to gather data from the astronauts’ eyes.
“This project is an amazing collaboration with astronauts who are forging the way for deep space exploration,” Subramanian says. “It’s the first time we can get dynamic information on how the body reacts to the transition to spaceflight.”
For some time, astronauts have noticed vision changes during long-duration space missions. Since NASA began post-mission MRI brain scans on astronauts in 2011, more than half have been diagnosed with potential increased intercranial pressure and optic disc swelling.
“We’re trying to figure out what’s causing these eye changes,” Subramanian says. “One theory is that it may be a balance between intraocular pressure and intracranial pressure, or pressure in the blood vessels that alters fluid dynamics in the eye socket. All those things are probably interacting to cause this problem.”
Subramanian sent up SENSIMED Triggerfish lenses, which are “smart” contact lenses to track eye pressure fluctuation and changes in cornea dimensions in glaucoma patients. Adjoint CU Anschutz ophthalmology professor Kaweh Mansouri, MD, contributed to the development of these lenses, which contain sensors that monitored astronauts’ eyes during launch and as they transitioned to microgravity.
The team also used a device called the QuickSee, which measured astronauts’ refractive error, when the shape of the eye changes and keeps light from focusing correctly on the retina.
“We’re looking for changes in the axial length of the eye, because we know that the eye gets a little shorter when you go into space,” Subramanian explains. “We’re trying to get more

concrete data on which layers of the eye are changing because that helps us understand what could be driving the optic nerve swelling.”
“Solving this problem can help advance deep space exploration,” Subramanian says. “SANS is considered by NASA to be the number two hazard behind radiation exposure that need countermeasures in order for humans to pursue long-duration spaceflight.”
“It’s gratifying to be able to participate in research like this,” he continues. “It is an acknowledgment of the longstanding expertise we have at the University of Colorado, in ophthalmology as well as aerospace medicine.” Subramanian and Hayman plan to publish their findings in the near future.

Listen to Dr. Subramanian discuss how space travel affects the eyes.
Graduating residents will use their expertise to care for patients across the country.
In June, CU Anschutz Department of Ophthalmology PGY-4 residents celebrated their graduation after four years of long clinic days, honing surgical techniques, and gaining invaluable knowledge. All six residents have placed for the upcoming year as ophthalmologists across the US.
Anne Strong Caldwell, MD, and Dallin Milner, MD, both started vitreoretinal diseases and surgery fellowships in the fall; Caldwell at Tufts University and Milner at Emory University. Garrett “Conner” Nix, MD, will remain affiliated with CU Anschutz, serving patients at Denver Health.
Three of the residents are moving into positions at private practices: Matthew Tukel, MD, in Michigan, where he is completing an oculoplastic, orbital, and reconstructive surgery fellowship; Jonathan Volkin, MD, in Colorado; and Stephanie Wangyu, MD, in California.
“It is exciting to honor the Sue Anschutz-Rodgers Eye Center graduating ophthalmology residency class of 2025,” says Naresh Mandava, MD, professor and chair of ophthalmology. “This group of remarkable ophthalmologists will serve patients in Atlanta, Boston, Denver, Detroit, and San Francisco.
The CU Anschutz faculty are so proud of the hard work and dedication of this class, and we look forward to the wonderful things they are going to accomplish in the future.”
Throughout his time at the Sue AnschutzRodgers Eye Center, graduating resident Jonathan Volkin, MD, appreciated the support and encouragement of faculty members and the technological advancement of the facilities. The ambulatory operating rooms allow for a much higher volume of surgeries than other academic eye centers. He credits the team, technology, and hands-on experience with expanding his breadth of knowledge.
“One of the greatest things about the Eye Center is the volume and range of pathology you see. It’s invaluable and makes you comfortable managing anything from the easy to the complex,” Volkin says. The University of Colorado Anschutz is an amazing place to have these opportunities.”
24

This year’s six graduating ophthalmology residents completed 5,877 surgical procedures during their training. The average number of cases completed by each graduating resident was 978. Below is the breakdown of the average surgical experience.
Collaboration with ophthalmic hospitalists accelerates ophthalmology residency training and enhances patient experiences.
It is a busy morning in the emergency department at the UCHealth University of Colorado Hospital, and a second-year ophthalmology resident has been paged to the emergency room for consultation on an eye trauma case. Daniel J. Ozzello, MD, an assistant professor of ophthalmology, joins to help evaluate the patient.
A fellowship-trained oculofacial plastic and orbital surgeon, Ozzello is an ophthalmic hospitalist, which is an ophthalmologist who specializes in coordinating the care of complex eye patients admitted to the hospital. In his role, he also trains residents at the Sue Anschutz-Rodgers Eye Center on providing this care.
The CU Anschutz Department of Ophthalmology is one of only a few academic eye centers in the United States with an ophthalmic hospitalist who support residents.
According to Naresh Mandava, MD, professor and chair of ophthalmology, in many other programs, ophthalmology attending physicians are available to consult via phone, but they are not often in the hospital room with the on-call second-year residents.
Throughout their training, CU Anschutz ophthalmology residents are exposed to a high volume of eye cases as they rotate at four different Denver metro area hospitals, including UCHealth, Denver Health, Children’s Hospital of Colorado, and the Rocky Mountain Regional Veterans Affairs Medical Center, each with a wide range of patient populations with distinct clinical challenges.
When the second-year residents begin their inpatient training at UCHealth, they receive significant one-on-one coaching about every aspect of patient care.
“More autonomy comes as they gain experience, and I become more of a consultant for them instead of a coach,” says Ozzello, who also serves as director of the residency program.

The Sue Anschutz-Rodgers Eye Center serves the largest geographic segment of the nation among academic eye centers.
“Our residents are some of the busiest in the country because they have patients who are transferred in from all over the United States,” Mandava says. “Working in collaboration with Ozzello and other faculty attendings offers them the opportunity to grow as clinicians and practice safely in high-pressure environments.”
The large patient population equates to diverse pathology, allowing the residents to experience an array of cases, from routine conditions to rare vision-threatening and lifethreatening cases.
“They aren’t just seeing these cases once,” Ozzello says. “They’re seeing them over and over and becoming some of the best trained ophthalmologists because of that. My goal is that by the time a resident finishes their training with me, they feel like they can handle anything that comes in the door.”
4
Julia Xia, MD, CU Anschutz’s first uveitis fellow, reflects on unique training.
Julia Xia, MD, the first-ever uveitis fellow at the CU Anschutz Department of Ophthalmology, was originally drawn to neuroscience before finding her path to medicine. Now, after completing her residency training and a “life-changing fellowship” at the Sue AnschutzRodgers Eye Center, she is the first ophthalmologist at EyeHealth Northwest, a private practice in Oregon, who is specially trained in treating uveitis — a broad term for a type of eye inflammation that can lead to vision problems and permanent blindness.
“My residency and fellowship training gave me a strong clinical and surgical foundation,” she says. “Thanks to CU Anschutz, I feel well prepared for a lot of the urgent issues that arise in my clinic.”
During her residency, Xia was exposed to different subspecialties in ophthalmology, and uveitis caught her attention.
“I noticed that uveitis patients were the ones who I kept thinking about after treating them. The complexity of their problems stood out to me,” Xia says. “My residency uveitis mentors, Dr. Alan Palestine and Dr. Amit Reddy, showed me that treating uveitis can be fascinating and rewarding, and they were a huge reason why I chose to pursue a uveitis fellowship.”
At the same time, Xia was interested in working as a comprehensive ophthalmologist and performing eye surgeries.
“Cataract surgeries are such a joyous part of ophthalmology because it’s a procedure that can improve someone’s vision overnight. It’s rewarding and instantly gratifying, and it really makes me love my job,” she says.
Xia was initially torn on which route to take, but when she expressed her interests to her mentors, they helped carve a new path for her, creating a uveitis fellowship at the Sue Anschutz-Rodgers Eye Center that has both clinical uveitis training as well as cataract and minimally invasive glaucoma surgical training. “It was the best fellowship year I could have asked for,” she says.

“I’m hopeful that the unique fellowship at CU Anschutz will continue to interest candidates in the future. Uveitis is a small specialty, but there’s a lot of need for it across the country.” Fellowship
1 Cornea, External Diseases, & Refractive Surgery
2 Glaucoma
1 Neuro-Ophthalmology
1 Oculofacial Plastic & Orbital Surgery
1 Pediatric Ophthalmology & Adult Strabismus
1 Uveitis
4 Vitreoretinal Diseases & Surgery
Jennifer Lopez, MD, joined the Sue Anschutz-Rodgers Eye Center after completing the department’s vitreoretinal diseases and surgery fellowship.
Ophthalmologist Jennifer Lopez, MD, may have never discovered her passion for treating patients’ eyes if not for a two-week elective she took on a whim during medical school. Now, after years of training and honing her skills, she is joining the CU Anschutz Department of Ophthalmology as a new faculty member after completing the CU Vitreoretinal Diseases and Surgery Fellowship this past summer.
As a retina specialist and surgeon, Lopez will help care for the thousands of patients in Colorado with retinal diseases, detachment or tears, and other retina-related issues. In her new role, she looks forward to teaching trainees while simultaneously improving clinical care for patients from diverse backgrounds — particularly Spanish-speaking patients who she can communicate with directly.
“It’s exciting because it feels like I’ve worked my whole life toward getting to this point,” Lopez says. “There are some fears with becoming an attending, but because I trained here, I’m very close with all the other attendings and know I’ll have their support if needed. We have an amazing program here with phenomenal clinicians, surgeons, and educators.”
Faculty at the Sue Anschutz-Rodgers Eye Center are thrilled about Lopez joining the team, says Scott Oliver, MD, chief of the retina service, director of the retina fellowship program, and an associate professor of ophthalmology.
“She is a gifted ophthalmic surgeon who showed early talent for managing very difficult cases, a talented investigator with interest in social determinants of health, and a caring, compassionate physician,” Oliver says. “She fits the culture of our group and was a unanimous choice.”
As an attending, Lopez now works as a retina specialist at the Sue Anschutz-Rodgers Eye Center and Denver Health, where she is eager to help improve care for patients.
“There are so many patients, especially at Denver Health, who come in with end-stage diabetic retinopathy. A lot of them speak Spanish as their primary language, and I speak Spanish. For many of them, it’s their first time even seeing a provider who speaks the same language as them,” she says. “I feel really fulfilled because I’m able to help in a different way by helping them understand their condition better.”

“Developing and improving access to care for our underserved populations is really important to me,” she adds. “During my fellowship, I grew as a clinician and as a surgeon. I’m now ready to be an independent surgeon, to make decisions on my own, and to teach future generations.”

Discover more about the CU Anschutz ophthalmology education programs.
Saif Aldeen Alryalat, MD
Michael Gilhooley, MD
Zafar Gill, MD
Cecillia Hernandez, MD
Jennifer Lopez, MD
Melissa Suggs, MD
Anthony Tang, MD
Julia Xia, MD
Lama Assi, MD
Samantha Butterfield, MD
Hannah Chen, MD
Abraham Hang, MD
Amy Huang, MD
Sanjana Jaiswal, MBBS
Jessica Kraker, MD
Anne Strong Caldwell, MD
Dallin Milner, MD
Garrett Conner Nix, MD
PGY-4
Hosanna Evie, MD
Joana Karanxha, MD
Ian McClain, MD
Air Stoner, MD
Conner Style, DO
Tiffany Wu, MD
PGY-3
Soufiane Azargui, MD
Emmeline Kim, MD
Kenten Kingsbury, MD
Randy Lu, MD
Max Mayeda, MD
Nick Tan, MD
Matthew Tukel, MD
Jonathan Volkin, MD
Stephanie Wangyu, MD
Brittany Perzia, MD
Yaqoob Qaseem, MD
Sean Rodriguez, MD
Meredith Spitz, MD
PGY-2
Lauren Arguinchona, MD
Sofia De Arrigunaga, MD
Matthew Lam, MD
Nikhil Mandava, MD
Ellie Rhodes, MD
Olivia Ritter, MD
Intern*
Kelly Acuña, MD
Spencer Burt, MD
Emely Carmona, MD
Kathleen Ho, MD
Reilley Knott, MD
Jennifer Lai, MD
*Intern year is completed in partnership with the CU Anschutz Department of Internal Medicine.

An associate professor of ophthalmology, Dr. Chen serves as the Division Chief of Ophthalmology at Denver Health Medical Center. A cornea and external disease expert, he cares for patients with a wide range of eye conditions. Dr. Chen is actively involved in resident education. His academic and clinical efforts are centered on improving access to eye care and advancing health equity, particularly for marginalized and underserved populations. Outside of work, he enjoys spending time with his family and participating in his church community.
Clinicians say matching visually impaired students with the right tools can have a lifelong impact.
In the fall of 2024, faculty in the CU Anschutz Department of Ophthalmology began bringing their expertise to schools throughout the state for low vision evaluations that help students with vision impairments reach their full potential in the classroom and beyond.
“Our work is different from what you typically think of with school screenings. For the most part, we’re working with students who have already been identified as having a visual impairment,” says David Simpson, OD, FAAO, assistant professor of ophthalmology.
“The clinics are a good opportunity to collaborate with students, their family members, and teachers of students with visual impairments (TSVIs) to make sure they’ve all got the right tools and can optimize them for the student’s learning abilities,” he continues.
Simpson and Kara Hanson, OD, FAAO, associate professor of ophthalmology and director of the Low Vision Rehabilitation Service, partnered with the Colorado Department of Education to complete clinics in four Colorado communities over several months, serving dozens of students.

The clinics started in 1998 after a group of teachers from Colorado’s Western Slope requested more solutions from the Colorado Department of Education to assist students with low vision. Then, there were no optometrists specializing in low vision in that region and only a handful in the state’s more urban communities.
The agency assembled the Low Vision Task Force, offered training to TSVIs to become certified low vision therapists, and funded regional low vision clinics across the state at no cost to families or school districts.
Colorado Springs optometrist Thomas Theune, OD, became the task force’s first low vision specialist. When Theune retired in 2023, clinicians at the Low Vision Rehabilitation Service at the Sue AnschutzRodgers Eye Center continued the effort, providing opportunities available to students and their families.
At each visit, a clinician performs an assessment of visual function and then works closely with a certified low vision therapist who is also a TSVI to find the best mechanisms that can help that individual student. Different tools often vary from student to student, so getting the right formula of resources is significant.
“Having the TSVI included in these visits means that the student and their family get two different perspectives,” Hanson says. “Families get the educator’s perspective and the optometric perspective. As a team, we can determine the level of functional vision that a student has and what they need to meet their goals.”
Jim and Anita Reichert have committed to donating a portion of their estate to CU Anschutz ophthalmology researchers who investigate inherited retinal disease.
When Jim Reichert gets an early start hiking a Colorado fourteener, he sometimes notices that the morning light peeking through the leaves appears a bit pixelated. It’s the only symptom he can currently tie to retinitis pigmentosa (RP), an inherited retinal disease that slowly leads to irreversible vision loss.
Eventually, Reichert, who is in his mid-60s, may lose his sight completely, just as his father did. But he hopes future research will make a different outcome possible for others. He and his wife, Anita Reichert, have committed to donating a portion of their estate to ophthalmology investigators who focus on inherited retinal disease, including RP, at the Sue AnschutzRodgers Eye Center, where he is a patient.
“This gift comes full circle for me,” he says. “Inherited retinal diseases don’t get as much attention as some other areas in health research, and there are so many variations, so it’s needed, and we have the means. Maybe we can have an impact.”
The bulk of the donation will likely happen decades from now, after the Reicherts die, but they’ve already started making monthly gifts to a fund that benefits the researchers now, hoping to kickstart discoveries that will help patients who share Jim Reichert’s diagnosis and others like it. The fund is also open to anybody else who wishes to donate.
Inherited retinal diseases encompass a broad spectrum of degenerative conditions, explains retinal specialist Marc Mathias, MD, associate professor of ophthalmology. In RP, there’s typically a genetic basis to the condition, although some patients may not have a family history. RP leads to the gradual degeneration of photoreceptors. Rods — specialized cells in the eye — that control night and peripheral vision typically degenerate first, followed by cones, which control central, color, and daytime vision.
In RP specifically, there are at least 100 genes that have been found to cause the disease. This presents a significant challenge to finding individual cures. There are overall no cures for RP and only one FDA-approved gene therapy treatment for a rare form of RP that affects 1-2% of patients.

Scientific investigators are looking at gene therapies as well as gene agnostic therapies, which don’t require knowing the genetic basis of the disease. These requires preserving or restoring rod and cone function and could have a broader application.
“We’re working hard on research to try and find more treatments that may be able to preserve vision and even regenerate vision that patients have lost,” Mathias says. “I’m grateful for the Reicherts and what they’re doing. These funds can help our mission.”
“It takes a team to help our patients, many of whom want to maintain independence and navigate the world,” he adds. “The Reicherts are making a difference for our researchers, clinicians, and for fellow and future patients.”
To contribute to the Reichert Inherited Retina Disease Fund, please contact Michael Tortoro by phone: 303-724-7618.

Watch a mini documentary about retinitis pigmentosa, featuring Dr. Mathias.
Naresh Mandava named as CU Anschutz School of Medicine senior associate dean for strategic advancement.
This spring, the CU Anschutz School of Medicine Dean, John Sampson, MD, PhD, MBA, announced new key leadership positions to ensure the school maintains programs of excellence in clinical care, research, and education.

Five senior leaders were appointed, effective May 1, 2025, to roles within the school, including Naresh Mandava, MD, chair of the Department of Ophthalmology, who was named senior associate dean for strategic advancement to build on his successful fundraising efforts for the school. He will continue serving as chair of ophthalmology in addition to his dean role.
“I am honored to be able to serve the CU Anschutz and the overall campus in this expanded capacity. I am excited to partner with our faculty, staff, and hospital partners to expand our philanthropic efforts and showcase why CU Anschutz is a top-tier academic medical center destination,” Mandava says.
Building on his success in securing transformative gifts for the Sue Anschutz-Rodgers Eye Center, in his role as senior associate dean for strategic advancement, Mandava will champion benefactor support as a member of the Dean’s leadership team. He will also help advance key strategic priorities for the School of Medicine, including strengthening translational research and expanding AI partnerships.

Watch Dr. Mandava and Dean Sampson discuss philanthropic priorities for the CU Anschutz School of Medicine.

A professor of ophthalmology and translational AI scientist, Dr. Kalphathy-Cramer is the ophthalmology division chief of artificial medical intelligence, where she leads cross-disciplinary teams focused on advancing ocular imaging and AI-driven diagnostics to improve patient outcomes.
In fiscal year 2025, she was especially proud of developing computational models to study geographic atrophy and launching the “oculomics” initiative, which explores ocular imaging as a window into systemic disease.
Philanthropic support has been instrumental in enabling her team’s bold, exploratory ophthalmic AI research and accelerating innovations that would not be possible through traditional grant mechanisms.
Outside of work, she enjoys travel, tennis, cooking, reading, and exploring Colorado’s natural beauty.
The Slingsby family, with three generations of CU-trained doctors, supports the Sue AnschutzRodgers Eye Center’s mission.
When J. Geoffrey “Geoff” Slingsby, MD, decided to pursue his residency training at the University of Colorado Department of Ophthalmology in 1977, he didn’t know how special the university would become to his future family.
Growing up in Rapid City, South Dakota, as the son of an OB-GYN, he was drawn to the world of medicine at a young age. After completing medical school in Atlanta, he “jumped at the chance” to join the ophthalmology residency program at CU — the same university where his father had received residency training.
“The CU residency program was very well led,” he says, explaining he found influential mentors at CU who taught him how to become an excellent clinician who works hard and with integrity.
While at CU, he also reconnected with Jacalyn “Jackie” Slingsby, a CU medical technology student who would later become his wife and the mother of their two children. After completing his vitreoretinal surgery fellowship in California, Geoff and Jackie Slingsby returned to Rapid City in 1982 and he took over a private practice from another ophthalmologist.
“It was very busy from day one. In the beginning, I was the only retina specialist in town, but shortly after, another specialist began working at a different practice in the same region,” he says. “Together, we were able to provide essentially a full spectrum of retinal care to patients in the area.”
He retired in 2022, but the Slingsby name lives on at the South Dakota ophthalmology practice — now, through his son Taylor Slingsby, MD, who followed in his father’s footsteps by completing his ophthalmology residency training at the Sue AnschutzRodgers Eye Center in 2020.
“He was very happy with his residency training at CU,” Geoff Slingsby says. “He went on to do his retina fellowship at the Cincinnati Eye Institute and then decided to come home to Rapid City and bring his advanced skills in vitreoretinal surgery to the practice.”
Their other son, Jason Slingsby, is also a CU alum, graduating from the Boulder campus with his bachelor’s degree in chemical engineering.
Geoff and Jackie Slingsby now continue their family’s CU tradition by donating funds to the Department of Ophthalmology, supporting future generations of ophthalmologists and the department’s pursuit of improving care at the Sue Anschutz-Rodgers Eye Center
“With my father, me, and my son going to the CU Anschutz and getting excellent training there, supporting CU is a legacy for us,” Geoff Slingsby says. “Whatever way we can help, that’s what we want to do.”

Jeffrey Bennett, MD, PhD
Michael Chen, MD
Richard Davidson, MD
Michael Erlanger, MD
Darren Gregory, MD
Eric Hink, MD
Malik Kahook, MD
Todd Kingdom, MD
Naresh Mandava, MD
Fiscal Year 2026
(Effective July 1, 2025)
Mariam Ahmad, MD
Associate Clinical Professor
Valeria Canto-Soler, PhD Professor
Niranjan Manoharan, MD
Associate Professor
Jennifer Patnaik, PhD, MHS
Associate Professor
Michael Puente Jr., MD Associate Professor
Emily McCourt, MD
Scott Oliver, MD
Jeffrey Olson, MD
Sapna Patel, MD
Victoria Pelak, MD
Michael Puente, MD
Leo Seibold, MD
Michael Taravella, MD
Fiscal Year 2025
(Effective July 1, 2024)
Cara Capitena Young, MD
Associate Professor
Karen Christopher, MD Associate Professor
Tianjing Li, MD, PhD, MHS Professor


Garrett “Conner” Nix, MD, earned his medical degree from the University of Tennessee after spending two Fulbright years in Madrid. Dr. Nix completed his ophthalmology residency at the University of Colorado Anschutz in 2025. He brings strong clinical and surgical expertise in comprehensive ophthalmology and will train residents at Denver Health.

Travis Redd, MD, MPH, joins the Sue Anschutz-Rodgers Eye Center as the new section chief of cornea and external diseases. Dr. Redd earned his medical and public health degrees from Oregon Health & Science University (OHSU), where he also completed his ophthalmology residency. He then completed a cornea and external disease fellowship at the Francis I. Proctor Foundation at the University of California, San Francisco, before joining the faculty at the OHSU Casey Eye Institute.
Dr. Redd leads an internationally recognized research program at the intersection of artificial intelligence and global health, contributing to the development and implementation of AI tools that expand equitable access to care. He serves as co-chair of the AAO Artificial Intelligence Committee and directs multiple National Institute of Health and Department of Defense funded studies. His clinical expertise includes complex infectious and pediatric corneal disorders.


Rachel Scott, MD, earned her medical degree from Baylor College of Medicine after double majoring in Molecular, Cellular, and Developmental Biology and Religious Studies at Yale University. She completed her ophthalmology residency at the University of Colorado, followed by a global ophthalmology fellowship at Stanford University, where she trained in complex cataract surgery and residency development abroad. Dr. Scott is passionate about medical education and improving access to care.

Katherine Lucarelli, MD, earned her medical degree from the University of Wisconsin School of Medicine and Public Health after completing a Bachelor of Science in Biology and Spanish at the University of Wisconsin–Madison. She completed her ophthalmology residency at the University of Illinois at Chicago, serving as Chief Resident, and an ASOPRS oculoplastics fellowship at UCLA. Dr. Lucarelli’s research addresses eyelid disease and healthcare disparities.

Sudarshan Srivatsan, MD, earned his medical degree from the University of Michigan and a holds a BS in biomedical engineering from Northwestern University. He completed his ophthalmology residency at the University of Illinois at Chicago followed by an ASOPRS oculoplastics fellowship at the University of Utah. Dr. Srivatsan’s research spans orbital, lacrimal, and eyelid disease, surgical education, and artificial intelligence in diagnosis.

Jennifer Lopez, MD, earned her medical degree from the New York University Grossman School of Medicine and completed her ophthalmology residency at the University of Southern California/LAC+USC Medical Center, where she served as Chief Resident. From there, she completed a vitreoretinal fellowship at the Sue Anschutz-Rodgers Eye Center at the University of Colorado Anschutz. Dr. Lopez’s research focuses on diabetic retinopathy screening and the application of artificial intelligence in ophthalmology.

Jared Sokol, MD, earned his medical degree from the University of Chicago Pritzker School of Medicine and an MBA from the Booth School of Business. He completed his ophthalmology residency at Massachusetts Eye and Ear/Harvard Medical School and a vitreoretinal fellowship at Stanford University’s Byers Eye Institute. Dr. Sokol’s research focuses on artificial intelligence applications in ophthalmology and surgical innovation.
Cue the applause: congratulations to our faculty for their well-deserved recognitions.

Michael Puente, MD, was awarded the 2025 Crystal Cornea Award from the Eye Bank Association of America. Dr. Puente’s groundbreaking research and advocacy have helped raise awareness around corneal donation policies and expanded access for more donors.

Ram Nagaraj, PhD, was named a Gates Institute 2024 Grubstake Fund Awardee! Dr. Nagaraj, along with Mi-Hyun Nam, PhD, and Jesse Smith, MD, have identified a gene capable of preserving retinal endothelial cell function. Their intravitreal single-dose gene therapy aims to prevent vision loss by directly targeting capillary cell death.

Natalia Vergara, PhD, received the CU Anschutz Graduate School’s Dean’s Master’s Mentoring Award in recognition of her exemplary master’s mentoring in modern human anatomy.
A recent bibliometric study of over 1,500 publications found CU Anschutz ophthalmology faculty members Malik Kahook, MD, and Leonard Seibold, MD, in the top 10 most productive authors globally about minimally invasive glaucoma surgery (MIGS).
Tianjing Li, MD, PhD, MHS, was recognized as one of the most “Highly Cited Researchers of 2024 and 2025” by Clarivate!
Lynn Hassman, MD, PhD, received a grant from Birdshot Uveitis Society of North America (BUSNA).
A peek inside the department.
PGY-3 resident, Soufiane Azargui, MD, presented his poster “Long-Term Change in Astigmatic Axis and Power after Cataract Surgery in the Pediatric Population: The Case for Selection of Toric IOLs” at the AAPOS 2025 conference.

This spring, our research faculty gave Congressman Jason Crow (CO-06) a guided tour of our CellSight lab and discussed our efforts to save and restore sight in patients with blinding eye diseases.

In the moving short documentary “All Eyes on Hope,” ultra runner and Paralympian Jason Romero shares his journey of vision loss and resilience. The film, which premiered this year, features Marc Mathias, MD, as he examines Jason and discusses his retinitis pigmentosa diagnosis.

Sue Anschutz-Rodgers Eye Center clinicians ran the Colfax Marathon this summer. Their relay team, Retina JedEYES, completed the race in 4 hours 2 minutes, and 21 seconds!

In August, Natalia Vergara, PhD, Christopher Gelston, MD, and Joseph Brzezinski, PhD, were inducted into the Academy of Medical Educators.

After more than two decades of dedicated service to the department, we celebrated the retirement of Gaylian Howard, executive assistant to the chair. Prior to serving as Dr. Mandava’s EA, Gaylian held numerous other CU ophthalmology administrative roles, including residency coordinator.

Each spring, residents enjoy a fun-filled day at a department sponsored resident retreat. This year, they completed a ropes course in the mountains alongside a handful of faculty members.

Outside of work, two of our musically gifted faculty perform in local orchestras. Melanie Akau, OD, (pictured) is a first violinist in the Denver Philharmonic Orchestra, while French horn player, Prem Subramanian, MD, PhD, is a member of the Colorado Wind Ensemble.
Thank you to those who have made our endowed chair appointments possible, and to the faculty members who carry out our department’s mission. Endowed chairs allow our faculty to engage in specialized research and dedicate their time to elevated academic pursuits.






M. Valeria Canto-Soler, PhD
Doni Solich Family Endowed Chair in Ocular Stem Cell Research

Richard Davidson, MD
Endowed Chair in Eye Care Innovation

Malik Kahook, MD
Slater Family Endowed Chair in Ophthalmology

Emily McCourt, MD
Ponzio Family Endowed Chair for Pediatric Ophthalmology at Children’s Hospital Colorado
Scott Oliver, MD
Vitale-Schlessman Endowed Chair in Retinal Diseases
Alan Palestine, MD
Endowed Chair in Ocular Inflammation
Jayashree Kalpathy-Cramer, PhD
Endowed Chair in Ophthalmic Data Sciences

Sophie Liao, MD
Robert H. Bell Endowed Chair in Ophthalmology

Naresh Mandava, MD
Sue Anschutz-Rodgers Endowed Chair in Retinal Diseases
Travis Redd, MD
Frank and Ann Taravella Endowed Chair in Corneal Disease
Prem Subramanian, MD, PhD
Clifford R. and Janice N. Merrill Endowed Chair in Ophthalmology
Artificial Medical Intelligence
Jayashree Kalpathy-Cramer, PhD
Chief, Division of Artificial Medical Intelligence in Ophthalmology Professor, Ophthalmology Director, Translational Informatics, CCTSI
Steve McNamara, OD Research Instructor, Ophthalmology
Praveer Singh, PhD Assistant Professor, Ophthalmology
Basic Science Research
Joseph Brzezinski, PhD Director, Research Director, Laboratory of Developmental Genetics, CellSight Associate Professor, Ophthalmology
M. Valeria Canto-Soler, PhD
Doni Solich Family Chair in Ocular Stem Cell Research Director, CellSight Director, 3DRet Lab, CellSight Professor, Ophthalmology
Daniel Denman, PhD* Assistant Professor, Physiology & Biophysics
Steven Droho, PhD Research Associate, Ophthalmology
Miguel Flores-Bellver, PhD Director, ExoSight Lab, CellSight Assistant Professor, Ophthalmology
Carl Frick, PhD+
Adjoint Assistant Professor, CellSight
Uday Kompella, PhD, FARVO, FAAPS*
Co-Director and Co-Founder, Colorado Center for Nanomedicine and Nanosafety Professor of Pharmaceutical Sciences, Ophthalmology, and Bioengineering
Daniel LaBarbera, PhD* Director, CU Center for Drug Discovery Professor, School of Pharmacy
Tim Lei, PhD*
Assistant Professor, University of Colorado - Denver
Andres Lisker, MD +
Adjoint Assistant Professor, CellSight
Marc Mathias, MD Director, Laboratory of Advanced Ophthalmic Surgery, CellSight Associate Professor, Ophthalmology
Ram Nagaraj, PhD Professor, Ophthalmology and Pharmaceutical Sciences
Rooban Babyantony Nahomi, PhD Research Scientist, Ophthalmology
Mi-Hyun Nam, PhD
Assistant Professor, Ophthalmology
Sudipta Panja, PhD Research Associate, Ophthalmology
Daewon Park, PhD*
Associate Professor, University of Colorado - Denver
Alon Poleg-Polsky, MD, PhD*
Assistant Professor, Physiology and Biophysics
Natalia Vergara, PhD
Director, Ocular Development and Translational Technologies Laboratory, CellSight Assistant Professor, Ophthalmology
Chris Yakacki, PhD*
Assistant Professor, University of Colorado - Denver
Wenbo Zhou, PhD
Research Associate, Ophthalmology
Joel Zylberberg, PhD + Adjoint Assistant Professor, Physiology & Biophysics
Comprehensive Eye Care
Christopher Allen, MD Instructor, Ophthalmology
Marilyn Dougherty, MD
Senior Instructor, Ophthalmology
Joel Goldstein, MD Associate Professor, Ophthalmology
Robert Keyser, MD Clinical Professor, Ophthalmology
Andrew Martin, MD Instructor, Ophthalmology
Garrett “Conner” Nix, MD
Assistant Residency Program Director Assistant Professor, Ophthalmology
William Roberts, MD Senior Instructor, Ophthalmology
Cornea, External Diseases, and Refractive Surgery
Travis Redd, MD, MPH
Frank and Ann Taravella Endowed Chair in Corneal Disease
Chief, Cornea and External Diseases Associate Professor, Ophthalmology
Michael Taravella, MD
Chief, Refractive Surgery
Director, Cornea, External Diseases, and Refractive Surgery Fellowship Professor, Ophthalmology
Michael Chen, MD
Ophthalmology Division Chief, Denver Health Medical Center
Associate Professor, Ophthalmology
Karen Christopher, MD
Associate Professor, Ophthalmology
Richard Davidson, MD
Endowed Chair in Eye Care Innovation Co-Medical Director, Rocky Mountain Lions Eye Bank
Vice Chair of Clinical Affairs and Quality, UCHealth Eye Centers Professor, Ophthalmology
Michael Erlanger, MD
Associate Professor, Ophthalmology
Christopher Gelston, MD
Associate Professor, Ophthalmology
Darren Gregory, MD Professor, Ophthalmology
Michael Wildes, MD
Clinical Director, Sue Anschutz-Rodgers Eye Center Assistant Professor, Ophthalmology
Ronald Wise, MD
Medical Director, UCHealth Eye Center - LoDo
Associate Professor of Clinical Practice, Ophthalmology
Ophthalmic Epidemiology
Anne Lynch, MD, MSPH Director, Ophthalmic Epidemiology Professor, Ophthalmology and Epidemiology
Alison Abraham, PhD, MS, MHS*
Vice Chair for Education, Colorado School of Public Health
Associate Professor, Epidemiology
Nathan Grove, MPH
Research Instructor
Tianjing Li, MD, PhD, MHS Director, Cochrane Eyes and Vision US Project Professor, Ophthalmology and Epidemiology
Alison Suhsun Liu, MD, PhD, MPH
Assistant Research Professor, Ophthalmology and Epidemiology
Jennifer Patnaik, PhD, MHS
Associate Professor, Ophthalmology and Epidemiology
Riaz Qureshi, MD
Assistant Professor, Ophthalmology and Epidemiology
Brandie Wagner, PhD*
Associate Research Professor, Colorado School of Public Health - Department of Biostatistics and Informatics
Glaucoma
Leonard Seibold, MD
Chief, Glaucoma Service Director, Glaucoma Fellowship Professor, Ophthalmology
Cara Capitena Young, MD
Medical Director, Sue Anschutz-Rodgers Eye Center Operating Room Associate Professor, Ophthalmology
Galia Deitz, MD, MPH
Section Chief, Ophthalmology, Rocky Mountain Regional VA Medical Center Assistant Professor, Ophthalmology
Malik Kahook, MD
Slater Family Endowed Chair in Ophthalmology
Vice Chair, Translational Research Professor, Ophthalmology
Gabriel Lazcano-Gomez, MD, OD + Adjoint Assistant Professor, Ophthalmology
Kaweh Mansouri, MD + Adjoint Professor, Ophthalmology
Mina Pantcheva, MD Associate Professor, Ophthalmology
Jeffrey SooHoo, MD, MBA
Associate Dean of Admissions and Student Affairs, University of Colorado School of Medicine
Associate Professor, Ophthalmology
Deidre St. Peter, MD Director, Wet Laboratory Assistant Professor, Ophthalmology
Optometry
Kaleb Abbott, OD, MS, FAAO Assistant Professor, Ophthalmology
Melanie Akau, OD, FAAO
Medical Director, Staff Education Instructor, Ophthalmology
Brian Bucca, OD, FAAO*
Chief of Eye Care at Barbara Davis Center
Associate Professor of Clinical Practice, Pediatrics - Barbara Davis Center
Angela Demetrulias, OD Instructor, Ophthalmology
C. Rob Graef, OD Assistant Professor, Ophthalmology
Cecelia Koetting, OD, FAAO, DipABO Assistant Professor, Ophthalmology
Stephanie Martich, OD Assistant Professor, Ophthalmology
Erica Tebon, OD Instructor, Ophthalmology
Shawna Vanderhoof, OD Instructor, Ophthalmology
Erin Van Dok, OD Clinical Instructor, Ophthalmology
Brittany Wright, OD, MS Assistant Professor, Ophthalmology
Neuro-Ophthalmology, Orbital Disease, and Adult Strabismus
Prem Subramanian, MD, PhD
Clifford R. and Janice N. Merrill Endowed Chair in Ophthalmology
Chief, Neuro-Ophthalmology Service
Chair, Faculty Promotions Committee
Vice Chair, Academic Affairs Professor, Ophthalmology
Jeffrey Bennett, MD, PhD* Professor, Ophthalmology and Neurology
Maria Nagel, MD* Professor, Ophthalmology and Neurology
*
Victoria Pelak, MD*
Professor, Ophthalmology and Neurology Director, Neuro-Ophthalmology Fellowship
Oculofacial Plastic and Orbital Surgery
Eric Hink, MD
Chief, Oculofacial Plastic and Orbital Surgery
Director, Oculofacial Plastic and Orbital Surgery Fellowship
Associate Professor, Ophthalmology
Sophie Liao, MD
Robert H. Bell Endowed Chair in Ophthalmology
Associate Chief Medical Officer, UCHealth - Ambulatory Associate Professor, Ophthalmology
Katherine Lucarelli, MD
Assistant Professor, Ophthalmology
Daniel J. Ozzello, MD
Ophthalmic Hospitalist
Director, Residency Program Director, Medical Student Education Assistant Professor, Ophthalmology
Sudarshan Srivatsan, MD
Assistant Professor, Ophthalmology
Kia Washington, MD*
Professor, Surgery - Plastic/Reconstructive, and Ophthalmology
Trevor Williams, PhD* Professor, School of Dental Medicine
Caroline Vloka, MD
Assistant Residency Program Director Assistant Professor, Ophthalmology
Todd Kingdom, MD*
Professor, Otolaryngology - Head and Neck Surgery
Ophthalmic Oncology
Scott Oliver, MD
Vitale-Schlessman Endowed Chair in Retinal Diseases
Chief, Retina Service
Director, Eye Cancer Program
Director, Vitreoretinal Diseases and Surgery Fellowship
Associate Professor, Ophthalmology
Eric Hink, MD
Chief, Oculofacial Plastic and Orbital Surgery Director, ASOPRS Fellowship in Oculofacial Plastic and Orbital Surgery
Associate Professor, Ophthalmology
Sophie Liao, MD
Robert H. Bell Endowed Chair in Ophthalmology
Associate Chief Medical Officer, UCHealth - Ambulatory
Associate Professor, Ophthalmology
Sapna Patel, MD, PhD* Professor, Medicine - Cancer Center, and Ophthalmology
Prem Subramanian, MD, PhD
Clifford R. and Janice N. Merrill Endowed Chair in Ophthalmology
Chief, Neuro-Ophthalmology Service
Chair, Faculty Promotions Committee Vice Chair, Academic Affairs Professor, Ophthalmology
Michael Taravella, MD
Chief, Refractive Surgery Director, Cataract, Cornea, and Refractive Surgery Fellowship Professor, Ophthalmology
Michael Wildes, MD
Clinical Director, Sue Anschutz-Rodgers Eye Center
Assistant Professor, Ophthalmology
Pediatric Ophthalmology and Adult Strabismus
Emily McCourt, MD
Ponzio Family Endowed Chair for Pediatric Ophthalmology Chief, Pediatric Ophthalmology Service Director, Pediatric Ophthalmology and Strabismus Fellowship Associate Professor, Ophthalmology
Mariam Ahmad, MD
Associate Professor of Clinical Practice, Ophthalmology
Rebecca Edwards Mayhew, MD, PhD Assistant Professor, Ophthalmology
Melissa Engle, OD, FAAO
Director, Pediatric Optometry Specialty Care Residency Program Director, Clinical Informatics, CHCO Department of Pediatric Ophthalmology Instructor, Ophthalmology
Robert Enzenauer, MD, MPH/MSPH Professor, Ophthalmology
Celeste Gomez, OD Instructor, Ophthalmology
John P. Gorham, MD Assistant Professor, Ophthalmology
Jennifer Jung, MD Director, Retinopathy of Prematurity Service
Associate Professor, Ophthalmology
Erin Major, OD Instructor, Ophthalmology
Lauren Mehner, MD, MPH
Medical Director, CHCO Pediatric Ophthalmology Clinic
Assistant Professor, Ophthalmology
Michael Puente, Jr., MD Director, UCHealth Adult Special Care Eye Clinic
Associate Professor, Ophthalmology
Rebecca Sands Braverman, MD Associate Professor, Ophthalmology
Casey Smith, MD Assistant Professor, Ophthalmology
Emma Stahr, OD Instructor, Ophthalmology
Uveitis and Ocular Immunology
Alan Palestine, MD
Endowed Chair in Ocular Inflammation Chief, Uveitis and Ocular Immunology Service Vice Chair, Clinical Research Professor, Ophthalmology
Lynn Hassman, MD, PhD
Assistant Professor, Ophthalmology
Jennifer Jung, MD
Director, Retinopathy of Prematurity Service
Associate Professor, Ophthalmology
Jason Kolfenbach, MD*
Associate Professor, MedicineRheumatology
Ruth Napier, PhD*
Associate Professor, MedicineRheumatology
Mina Pantcheva, MD Associate Professor, Ophthalmology
Amit Reddy, MD Director, Clinical Research Director, Resident Research Director, Uveitis and Ocular Immunology Fellowship
Assistant Professor, Ophthalmology
Vision Rehabilitation
Kara Hanson, OD, FAAO Director, Vision Rehabilitation Service Associate Professor, Ophthalmology
Cade Oost, OD, MS, FAAO Assistant Professor, Ophthalmology
David Simpson, OD, FAAO Assistant Professor, Ophthalmology
Scott Oliver, MD
Vitale-Schlessman Endowed Chair in Retinal Diseases
Chief, Retina Service Director, Eye Cancer Program Director, Vitreoretinal Diseases and Surgery Fellowship Associate Professor, Ophthalmology
Emily Cole, MD, MPH Assistant Professor, Ophthalmology
Talisa Forest (de Carlo), MD Director, Medical Imaging Assistant Professor, Ophthalmology
Stuart Fine, MD Clinical Professor, Ophthalmology
Jennifer Lopez, MD Assistant Professor, Ophthalmology
Naresh Mandava, MD
Sue Anschutz-Rodgers Endowed Chair in Retinal Diseases Chair, Department of Ophthalmology Senior Associate Dean for Strategic Advancement, University of Colorado Anschutz School of Medicine Professor, Ophthalmology
Niranjan Manoharan, MD Director, Informatics Associate Professor, Ophthalmology
Marc Mathias, MD
Director, Laboratory of Advanced Ophthalmic Surgery, Cellsight Associate Professor, Ophthalmology
Jeffrey Olson, MD
Associate Professor, Ophthalmology
Jesse Smith, MD
Associate Professor, Ophthalmology
Jared Sokol, MD Assistant Professor, Ophthalmology
Professor Emeritus
Philip Ellis, MD Professor Emeritus
J. Mark Petrash, PhD Professor Emeritus
Cover photo: CU professors sent SENSIMED Triggerfish® “smart” contact lenses to monitor changes to astronauts’ eyes on SpaceX’s Polaris Dawn mission. © Polaris Program / John Kraus, used with permission.
EDITOR
Emily Gibson
COPY EDITORS
Tayler Shaw
Mara Kalinoski
WRITERS
Emily Gibson
Mara Kalinoski
David Kelly

Toni Lapp
Kara Mason
Tayler Shaw
CONTRIBUTORS
Eimi Rodriguez-Cruz
Greg Glasgow
Mark Harden
Erin Hegel
Kelvin Oteng
Jason Owens
Michael Tortoro
Jesica Whittaker
Ashley Woodhouse
Tracey Yancey
GRAPHIC DESIGN
Collectively Creative
PHOTOGRAPHY
Children’s Hospital Colorado staff, CU Anschutz faculty, trainees, and staff, Melissa Helfrich, Justin Levitt, Jim and Anita Reichert, and, Geoff and Jackie Slingsby, all used with permission.
PRINTING
CU Anschutz Print Services
