

HOSPIT AL MEDICINE
WINTER NEW SLETTER 2026

IN THIS IS SUE
Accomplishments
Check out our top Division of Hospital Medicine (DHM) accomplishments from the last quarter!
Stay up to date with the latest
Discover our recently published research and articles featuring team members from our division!
Explore the daily happenings in hospital medicine that build into our efforts to improve lives through excellence in patient care, education, and cutting-edge innovation.
Winter Spotlight
This spotlight highlights our Visiting Scholar, Dr. Taiju Miyagami and our Global Health Scholar, Dr. Philip Angelides. Check out their incredible impact on the team so far!
Stay Connected
Stay


As we close out another productive quarter, I find myself reflecting on the many wins and new opportunities across our division. I am deeply grateful to work alongside such thoughtful, dedicated, and compassionate clinicians who continue to show up for our patients, learners, and each other every day. This period has also marked meaningful growth in our research efforts. Over the past year, our division contributed nearly 200 peer-reviewed publications, a remarkable achievement that reflects both the depth of expertise and the collaborative spirit of our team. In addition to these publications, our faculty and staff have shared their work through articles and invited speaking opportunities, helping advance hospital medicine well beyond our institution. These accomplishments represent countless hours of inquiry, mentorship, and teamwork.
Thank you for taking the time to read this newsletter and celebrate these achievements with us. I am excited to continue building on this momentum together in the months ahead."
#CUDHM ACCOMPLISHMENT
DHM Top Quarterly Accomplishments
These are just a few highlights of the many accomplishments for our incredible team.
Advancing Patient Safety Through Thoughtful Systems Improvement
1
Behind the scenes, meaningful progress was made to continually work to improve patient safety and quality,and optimize our clinical operations. This quarter focused on identifying opportunities to strengthen post-discharge result follow-up by reviewing cases, partnering with patient safety colleagues, and beginning development of a clear electronic health record process map. This work reflects the divisionʼs commitment to proactive problem-solving and continuous improvement. Read more about this incredible work on page 10 of this newsletter.
Second Cohort of the Clinical Excellence Society (CES)
Help us congratulate the most recent inductees to the Department of Medicine CES. This society recognizes exceptional faculty members in the CU Anschutz Department of Medicine for their commitment to patient care. These inductees will also serve as advisors to the Department of Medicine leadership team on identifying future inductees, on ways to build clinical excellence, and on addressing such issues as burnout, wellness, and equity. Congratulations Susan Calcaterra, MD, MPH, MS and Cason Pierce, MD!
3
2
Building Community Through Engagement and Professional Growth
This quarter, the Division of Hospital Medicine continued to invest in the well-being of our people by creating intentional spaces for connection, creativity, and restoration. Weekly writing opportunities provided colleagues with a consistent space to connect, share ideas, and engage in creative practice—building community while encouraging reflection and expression. In parallel, wellness small grants invited team members to propose ideas to support their own health and well-being, reinforcing a culture where wellness is shaped by the voices of our community. Team bonding activities further supported connection and balance beyond daily clinical work.
We also kicked off the year with our annual writing challenge, which saw strong participation from more than 50 individuals representing multiple states, universities, and institutions—making it one of the most broadly engaged challenges to date. Together, these consistent opportunities help foster a supportive, creative, and encouraging environment for our team.

NEWEST TEAM MEMBER S
Welcome the Newest #CUDHM Team Additions


Past DHM Fellowship Graduates

The individuals below are recent graduates from our Advanced Practice Fellowship program, who have decided to join our team full-time. Welcome!



Staff Highlight - Research Services Project Manager

Nick Kendell, MS
Please join us in welcoming one of the newest members of our CUDHM admin team, Nick, who joined in November! As our Research Services Project Manager, Nick is already making an impact, supporting healthcare and community initiatives with Dr. Lily Cervantes—including advocacy and research focused on the Latino/x community.
Nick brings a wealth of experience from his prior roles at the University of Iowa Hospitals and Clinics, Department of Otolaryngology, and the Fred Hutch Vaccine Trials Unit, where he focused on research and data coordination. His expertise has already proven invaluable in his current work, and weʼre excited to see his continued contributions to the team.
Outside of work, Nick is a passionate Broncos fan, enjoys watching football, works as an Analyst for Sports Illustrated, and hosts his own podcast covering all things Broncos.
Julie Delgado, PA-C
Jessica Gerlach, PA-C
Morgan Orand, PA-C
Nick Kendell, MS
Ariel Redell, BS
C UDHM WINS
Wins & Awards

Adrienne Mann, MD
Awarded American Medical
Association Women
Physicianʼs Section (WSP)
Inspiration Award

Henry Kramer, MD
Selected as an SHM Senior Fellow of Hospital Medicine


Molly McCullough, PA-C, MPAS
Received Office of Advanced Practice (OAP) Rising Star Award
Sarah Stella, MD
Grant from Caring for Denver Foundation supporting ongoing care coordination for the Social Impact Partnership to Pay for Results Act (SIPPRA) Program
Grant Highlight: Expanding Virtual Addiction Medicine Consult Services Across A Few Colorado Hospitals
We (CU Division of Hospital Medicine), Dr. Susan Calcaterra and Dr. Hemali Patel, representing the UCHealth Virtual Health Center) received a grant from UPL-CU Medicine to develop and implement a virtual addiction consultation service. Our DHM Addiction Medicine team will provide dedicated addiction care to patients hospitalized at Greeley Hospital, Medical Center of the Rockies, and Memorial Central Hospital, starting March 2, 2026.

Susan Calcaterra, MD, MPH, MS

Hemali Patel, MD
We are grateful to UPL and CU Medicine for supporting this work across the system.
C UDHM WINS





Sansrita Nepal, MD
Mentor for American College of Physician Advisors “Cultivating Physician Advisor Leaders 25–26” Program
Adam Meyer, MD
Associate Chief Medical
Officer (ACMO) for Patient Flow & Capacity Management
Erin Szemak, NP
Co-Director for the Division of Hospital Medicine Advanced Practice Fellowship
Rebecca Allyn, MD
Director of Faculty
Advancement for the CU Division of Hospital Medicine




Bobbie Jo Dodson, DO
Program Director for new Integrated Medical and Psychiatric Care Unit
Rob Broadhurst, MD
Associate Director of Evidence-Based Medicine for CU School of Medicine
Caitlin Dietsche, MD
Medical Director for the Division of Hospital Medicine Advanced Practice Fellowship
Anna Maw, MD
Selected for Competency Standards in AI Team for Association of American Medical Colleges




PUBLICATIONS & AR TICLES
Recent Articles
MEDICAL
EDUCATION & OPPORTUNITIES
MEDICAL WORK DESIGN
CU Anschutz Educator Helps Students Get Published in Medical Journals
CU Anschutz Department of Medicine Article Written by Tayler Shaw, Featuring Ben Vipler, MD
Bridging Decision-Making and Bedside Realities: Understanding the Context of Administrative Harm Society of Hospital Medicine Webinar (1 of 2), Featuring Marisha Burden, MD, MBA, FACP, SFHM; Kris Gaw, MBA; Alan Hathcock, MD, MPH; Luci Leykum, MD, MBA, MSC
ADDICTION MEDICINE
POINT OF CARE
ULTRASOUND (POCUS)
Study Finds Take-Home Methadone at Hospital Discharge Can Be a Critical Turning Point in Opioid Recovery
CU Anschutz Article Written by Laura Kelly, Featuring Susan Calcaterra, MD, MPH
Teaching the Magic of POCUS: Research Aims to Improve Physician Training on Portable Ultrasounds
CU Anschutz Department of Medicine Article Written by Tayler Shaw, Featuring Amiran Baduashvili, MD
CU Anschutz Hospital Medicine Program Helps Institutions Develop Successful Advanced Practice Providers
CU Anschutz Department of Medicine Article Written by Tayler Shaw, Featuring Amiran Baduashvili, MD APP CONSULTING PROGRAM
Many More Denver Teens Have Experienced Homelessness Than Official Counts Show
HOMELESSNESS
CU Anschutz Article Featuring by Joshua Barocas, MD, and Matthew Westfall, MD
CUDHM DAILY
Recent Speaking Opportunities
Susan Calcaterra, MD, MPH, MS - Presented two talks at AMERSA (Association for Medical Education and Research in Substance Use and Addiction) in Portland, Oregon:
◦ 11.13.25: “Assessment of an Electronic Health Record
Intervention to Increase In-Hospital Opioid Use Disorder
Treatment: An Interrupted Time Series Analysis”
◦ 11.14.25: “Implementing Take-Home Methadone: Results from Three Geographically Diverse Healthcare Systems”

Sarguni Singh, MD - Gave a talk titled “Post-Hospital Transitions in Older Adults with Cancer: Insurance, Outcomes, and Opportunities for Palliative Care” at the University of Colorado 2025 Palliative Care Days Conference
Ben Vipler, MD - Presented 2 workshops at the international conference on residency education in Quebec City on October 31:
◦ Itʼs a two-way street: Fostering healthy dialogue between trainees and faculty to promote program and individual growth


◦ Elevate your career: Mastering personal branding in academic medicine
Kim Indovina, MD - Virtual presentation at Nexus Summit 2025 on Interprofessional Education
◦ Indovina K, Yates L, Estes K, Akerman A, Waterhouse J, Trujillo J, Nordon-Craft A. Leveraging geri-educators to enhance interprofessional collaborative practice education. Oral presentation. Nexus Summit, Sept 2025.

Rebecca Allyn, MD - Oral presentation at the American Conference on Physician Health in Boston, MA on “Clinician and Patient Impact of an Ambient AI Intervention in an FQHC Network”.
Michelle Knees, DO; Claire Brickson, MD - External invited grand rounds: Brickson C, Knees M. Triage, Test, Treat, and… Text? Secure Messaging in Hospital Medicine. Virginia Commonwealth University Division of Hospital Medicine Ground Rounds; Oct 2025; Virtual

Quality Improvement Initiatives DHM DAILY
The CUDHM Quality and Patient Safety Program is dedicated to ensuring quality care to patients through the promotion of a culture of iterative improvement and by developing hospitalist leaders in quality and patient safety.
We focus on six major priorities in Quality in the following domains:
Patient Experience Highlight
Opportunities in Provider Listening
Small, intentional moments can improve how heard patients feel. Recent feedback highlighted opportunities such as more consistent afternoon check-ins and clearer explanations of how technology is used during visits. Focusing on these practices supports transparency, builds trust, and enhances the overall patient experience.

Patient Safety Highlight

Some of our ongoing project include modifying order panels with smart language to guide and reduce dosing errors. We are also implementing a new 72 hour fast pathway and orderset. Other recent cases have highlighted opportunities to improve how pending test results are tracked and followed up after hospital discharge. We are actively working to clarify and standardize workflows within the electronic health record to support timely, reliable post-discharge follow-up. This work is made possible through the ongoing efforts of our patient safety team, whose expertise and partnership help drive continuous improvement in patient care.
Tip of the month: Consider including a separate section in discharge summaries for any incidental findings during hospitalization and recommended plan for work-up
Diagnostic Cross Check Campaign DHM DAILY
What is the ADEPT Program?

Members of the CU Anschutz Division of Hospital Medicine are partnering with the University of California San Francisco team and are participating in and leading key aspects of the AHRQ-funded Achieving Diagnostic Excellence through Prevention and Teamwork (ADEPT) study. ADEPT builds on the earlier AHRQ-funded study, Utility of Predictive Systems in Diagnostic Errors (UPSIDE).
UPSIDE is defining risk factors, underlying causes, and the prevalence of diagnostic errors among patients admitted to hospitals in our 55-hospital research collaborative, the Hospital Medicine
Reengineering Network (HOMERuN). UPSIDE has developed reference standard approaches to adjudicating diagnostic errors, identified factors associated with errors, and built strong collaborations with participating sites and national organizations. Together, this work creates a powerful opportunity to transform how diagnostic process evaluation programs improve patient safety.
ADEPT will build on UPSIDE to create a learning health system that integrates diagnostic error and process assessments into existing quality and safety programs. It will also support data sharing, infrastructure, and expertise to accelerate improvement in diagnostic performance and lay the groundwork for efforts that continue beyond the duration of the grant.
Why does Cross-check Matter?

Cross-check Accomplishments (so far)
The Diagnostic Cross-check is an opportunity to huddle with our critical care colleagues at RRT and synthesize diagnostic information and plan in a structured way. The cross-check has been implemented at 10+ hospitals with our outcomes below!


Strengthening Global Connections & Educational Opportunities WINTER SPO TLIGHT

Taiju Miyagami, MD, PhD is our very first Visiting Scholar and is visiting from Juntendo University of Tokyo. He originally planned to stay for nine months but decided to extend his stay for a full year. Read what he has to say about his experience in this program so far.

Q: Tell us about your experience in the Visiting Scholar Program. What have you been focusing on?

A: The Clinical Scholars Program, primarily led by Amiran Baduashvilli, MD, has offered many highly educational sessions. I have been focusing on understanding and improving diagnosis in the hospital. Iʼm particularly interested in interprofessional collaboration and plan to start a study this January investigating how RNs communicate diagnostic concerns to physicians and barriers they encounter to collaboration. I also plan to investigate improvement opportunities in prevention and diagnosis of hospital-onset sepsis, in particular aspiration pneumonia.
I also participated in the Foundations in Healthcare Leadership program led by the Institute of Healthcare Quality Safety and Efficiency (IHQSE), including CUDHM faculty Jeff Glasheen, MD and Katie Raffel, MD. During my time in Japan, there hasn't been a lot opportunity to properly consider leadership before, so this was a valuable chance to think about how to become a better leader in my department and hospital.
Q: You recently attended a diagnostic excellence conference, DEX25, in Michigan. What did you present on?
A: At DEX25, I delivered a research proposal in a Shark Tank session-- where I presented a one slide proposal on personality traits and association with cognitive bias, followed by a Q&A! It was engaging, and I received very valuable feedback. I also had the opportunity to design and lead a workshop on cognitive load and diagnosis impact with David Kimpl, MD and David Scudder, MD. This is a truly wonderful memory.
"I am deeply grateful to everyone, starting with Katie, for being so kind to me since I arrived. I'm also impressed by how everyone possesses a strong professional mindset in their areas of expertise and specialization."
Strengthening Global Connections & Educational Opportunities WINTER SPO TLIGHT

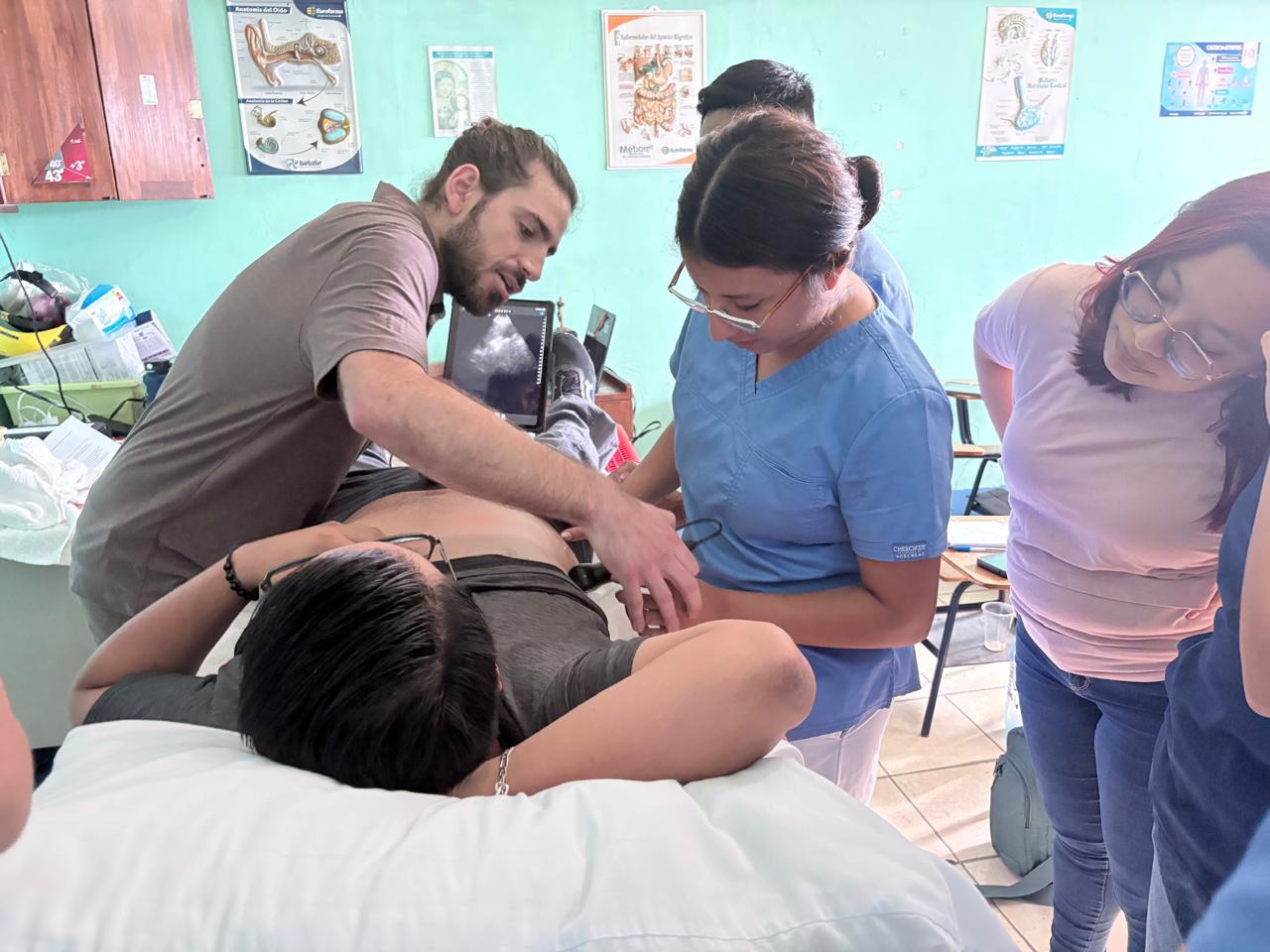

Dr. Philip Angelides is our Global Health Scholar this year, a program that prepares future hospitalist leaders for work in resource-limited settings through combined international and academic training. As part of this scholarship, Dr. Angelides is leading a Point of Care Ultrasound (POCUS) curriculum for students and internal medicine faculty in Coatepeque, Guatemala. Following a successful pilot, the program is transitioning to focus on training the hospitalists in a
ward-based, train-the-trainer model designed to develop local POCUS champions and ensure sustainability.


In Guatemala, the project partnered closely with Dr. Leon, Dr. Juarez (Director of Hospital Nacional de Coatepeque), Dr. Bolaños, and an engaged group of medical students whose enthusiasm and commitment were central to the curriculumʼs success. The work was built on foundational efforts initiated by Dr. Angeline Sawaya, whose early vision helped launch the curriculum and support its ongoing evaluation, and Dr. Jake Gamboa, whose interdisciplinary anesthesiology partnership contributed meaningfully to the programʼs success.
“Learning from Dr. Leon and collaborating with my anesthesia colleagues Vikas and Kimberly—who have made this experience both deeply educational and genuinely enjoyable—has been a highlight of my time at Hospital Nacional de Coatepeque. I see a strong opportunity for a bidirectional CU–Coatepeque partnership to expand diagnostic capacity and point-of-care ultrasound in ways that advance health equity locally while also informing and improving care back home.”
This work was further supported by sustained mentorship and institutional guidance from Drs. Reem Hanna, Carolina Ortiz, Dan Olson, Michelle Fleshner, Lisa Umphrey, Elizabeth Brickley and Marisha Burden. Their advocacy, support, and guidance were critical to the curriculumʼs development and success, and this collaborative effort contributed to an invitation to present the project in an open plenary at the Society of Hospital Medicine Converge 2026, with Dr. Leon as first author alongside Himmer Hip, a Guatemalan medical student, as co author.
Outside of global health, Dr. Angelides mentors several residents and medical students. In the past month, this mentorship has already led to notable scholarly successes, with Dr. Angelides serving as senior author or supporter, including:
• Second place at the Society of Hospital Medicine Abstract Competition (Houston Chapter)
• Accepted abstracts at the Consortium of Universities for Global Health and the Texas Chapter of the American College of Physicians, with additional submissions accepted to SGIM and underway for peer-reviewed Infectious Disease journals
• Longitudinal scholarly mentorship of a CU third year medical student through the Guatemala POCUS project
We are proud of the meaningful impact Dr. Angelides has made in a short amount of time and look forward to seeing his work continue to grow.
Photo's courtesy of Travis Mendoza
STAY CONNEC TED
Recent & Upcoming Dates
National Hospitalist Day MAR 5 SHM Regional POCUS Course MAR 12-13 MAR 24



CU Thrive: Wellbeing Innovation Day
Announcements
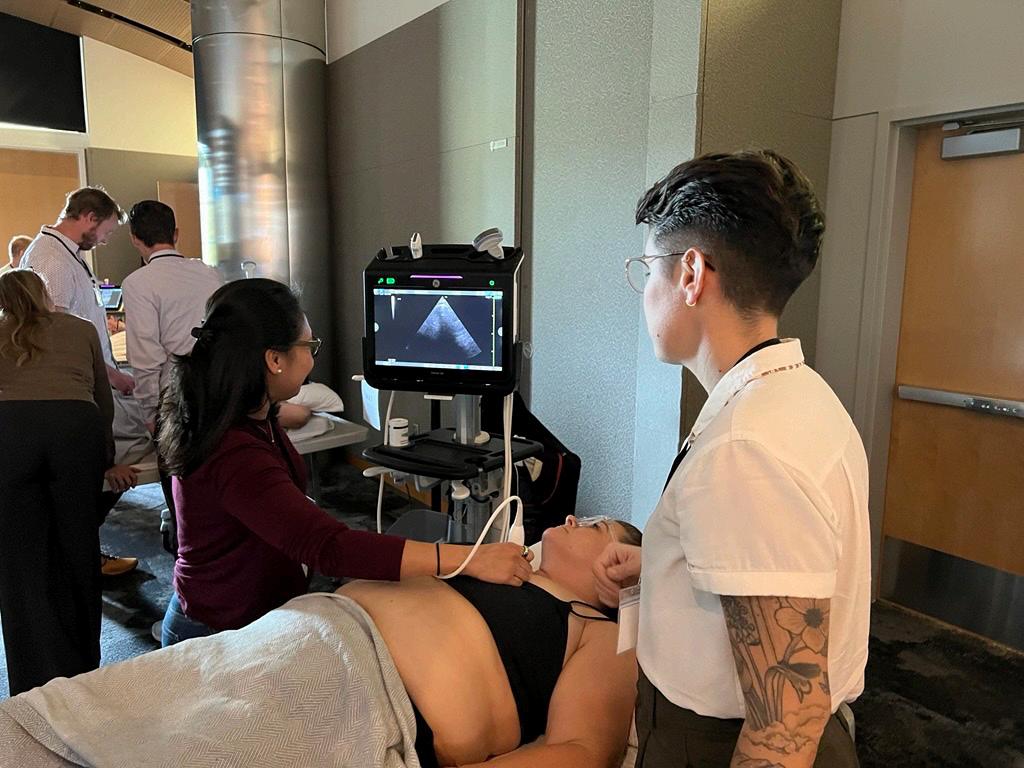
Applications are open for our March 2026 POCUS Course
Start of SHM Annual Conference MAR 30

Expand your ultrasound skills by joining our Society of Hospital Medicine (SHM) Point of Care Ultrasound (POCUS) Regional Course March 12-13, 2026. The course curriculum focuses on the most relevant POCUS applications for generalist providers caring for hospitalized patients. Participants will learn best practices of ultrasound-guided techniques for bedside procedures such as thoracentesis, central venous access, lumbar puncture, and paracentesis. Youʼll gain practical skills in image acquisition, interpretation, and clinical integration.
This immersive two-day workshop includes:
◦ 3:1 participant-to-instructor ratio
◦ Live model scanning and procedure-based practice
◦ Up to 16 AMA PRA Category 1 Credit(s)™
Learn more on our website and secure your spot today!




A Chance to be Featured
For marketing content, please send your submission to Kelsey Hussey, MS at kelsey.hussey@cuanschutz.edu. Please our hashtag #CUDHM or tag us in your post!







