






With over 25 years of specialist expertise, Regal Fire & Protection is the UK’s trusted partner for fire door installation, maintenance and inspection — certified by BMTRADA and holding CHAS Elite accreditation.


Complete compliance assessment of all fire doors.
BMTRADA certification provided — ensuring your building meets every regulatory requirement.
Fully certified fire door sets installed by qualified specialists. Every component is compatible, tested and documented for full traceability.
Legal compliance under the Regulatory Reform (Fire Safety) Order. Ongoing maintenance contracts with digital reporting and client portal access.
Chief Editor
Tani Johnson
tj@carehomemagazine.co.uk
Publication Manager
James Davies james@carehomemagazine.co.uk
Tel: 01795 509 112
Credit Facilities
Manager
Gwen Lee
creditcontrol@cimltd.co.uk
Tel: 01795 509 103
Design and Production
James Taylor james@cimltd.co.uk
Grant Waters grant@cimltd.co.uk
Administration Manager
Natalie Woollin admin@cimltd.co.uk
Head of Digital
Xhulio Bishtaja press@carehomemagazine.co.uk
Marketing Manager
Lucas Payne lucas@cimltd.co.uk
Social Media Manager
Lily Lawson press@carehomemagazine.co.uk
Director
Tom Woollin tom@cimltd.co.uk
Managing Director
John Denning
As the sector evolves, our understanding of care environments also changes. This month’s issue highlights two key areas shaping the future: interior design and innovation. These are no longer just about aesthetics or expansion; they focus on creating spaces that promote wellbeing, dignity, and operational efficiency.

Throughout our features, industry experts share insights into how care settings can and should evolve. From early development stages to detailed design, there’s increasing awareness that the built environment significantly impacts residents, staff, and operators.
In Dishing Up, we explore how a braai can provide a great summer dining experience, adaptable, social, and flavourful. This concept suits care settings by offering flexibility for various dietary needs.
Meanwhile, Editor’s Day Out features Advinia’s Chef of the Year finals, showcasing the sector’s passion and the role of food in enriching residents’ lives. We also revisit the past with this month’s Activity of the Month, highlighting May Day and traditional May Fair celebrations, which foster reminiscence and joy through music, movement, flowers, and shared traditions.
As always, this issue aims to inform, inspire, and support you in creating the best possible care environments, offering practical ideas and new perspectives as we approach summer.

Nitesh Somani discusses his new role as Chair of Championing Social Care and how he plans to elevate social care’s profile across the UK.
Discover the increasing significance of interior design in care environments, with expert insights on how well-designed spaces can improve wellbeing, aid dementia support, and foster a genuine sense of home for residents.
Take a closer look at the importance of offering residents a diverse and inclusive drinks menu, and how choice can encourage social interaction and improve quality of life.
Sector experts share their perspectives on the latest care home developments across the UK, highlighting key challenges, emerging trends, and what operators need to consider for future-ready environments.
Discover why a braai is the ideal summer dining option for care homes, offering flexibility, nutritional balance, and a sociable experience that can be easily adapted for all residents.
Join Care Home Magazine at Advinia’s Chef of the Year finals, where culinary talent, creativity, and resident-focused dining take centre stage in a celebration of care home hospitality.



KYN, London’s leading collection of residential and nursing care homes, has announced the commencement of construction on a new care home in Hammersmith, located on the River Thames. The development, named KYN Riverside, is scheduled to open in 2029.
Designed in collaboration with PRP Architects, KYN will transform a former office building on Chancellor’s Road, situated between Fulham Reach Boat Club and Riverside Studios. The redevelopment will upgrade the existing structure and create an elegant 45-bedroom care home reflecting KYN’s trademark design approach.
The design will prioritise river views, with bedrooms and communal areas on each floor orientated towards the Thames. A generous Walled Garden will provide seating and dining areas for residents and their families, with direct access to the Thames Path.
The site extends to approximately half an acre and is located close to Hammersmith Bridge and around

500 metres from the River Café. KYN will continue to partner with esteemed interior designer Nina Campbell, with artwork curated by Adam Ellis and landscape design by Randle Siddeley. The variety of spaces will include large, vibrant areas for socialising

and entertaining, as well as smaller semi-private spaces that complement the individual rooms.
Consistent with the existing residences in the collection, KYN Riverside will feature exceptional facilities, including The Great Room with garden access, the KYTH Spa and Rehab Studio, Home Cinema and Library. This considered design creates a sense of community while providing residents with peaceful retreats, enhancing overall comfort and wellbeing.
The development follows KYN’s ongoing expansion in London, including planned homes in Kensington and Highgate, due for completion in 2028, alongside its existing homes in Hurlingham and Bickley.
Caroline Naidoo, CEO at KYN, said: “At KYN, we are focused on redefining what later-life care can look and feel like. We design homes that combine high-quality nursing and residential care with thoughtful, residential environments that feel calm, private and familiar, while still enabling connection and community.”


and
• Cited in CQC reporting as supporting outstanding care
• Simple to install and use
• Watch via TVs, laptops, tablets and mobiles, 24/7
To subscribe, please visit tv.mylifefilms.org or for more information, email the team at info@mylifefilms.org

Vishal Shah talks about his and Championing Social Care’s mission to elevate the care sector’s profile.
Vishal Shah’s appointment as Chair of Championing Social Care (CSC) comes with both professional weight and personal meaning; something that becomes immediately clear in conversation. With a background in global finance and frontline healthcare, Shah offers a unique dual perspective, but it is his personal experience that most profoundly influences his outlook.
Reflecting on his upbringing in Birmingham, he was influenced by his family’s values that focused on community through their pharmacy business. He observed how vital human connection is in care, highlighting trust and reassurance over mere medication. Assisting his grandparents, particularly a grandmother with dementia, enhanced his appreciation for the skill and compassion of caregivers.
Although he began in the corporate sector at Goldman Sachs, PwC, and healthcare equity research, Vishal says his shift into healthcare was ultimately transformative. “It completely shifted my frame of reference,” he notes. “You quickly see the sector’s impact on lives.” This inspired a 20-year dedication to social care, leading to Banyan Care, a platform for integrated, values-led services in residential, home, and community settings.
Now, as Chair of CSC, Vishal is focused on something broader: changing how the sector is perceived. Championing Social Care, he explains, exists to “elevate the profile, perception and

recognition of social care.” It is a volunteer-led movement, driven by the belief that the sector’s story has not been told strongly enough. “Social care is vast, diverse and deeply skilled,” he says. “But social care is mostly not well understood, and too often it’s defined by its challenges rather than its strengths. That has to change.”
A key part of CSC’s work lies in its national programmes, which aim to both celebrate the sector and open it up to wider audiences. Initiatives such as Care Home Open Week, which last year saw over 5,500 services take part, are designed to bring communities into care settings and challenge outdated perceptions. Meanwhile, campaigns like Who Cares Wins target younger audiences, highlighting the breadth of career opportunities available.
At the heart of the organisation is its ambassadors community: a growing network of individuals committed to advocating for social
care. For Vishal, this collective approach is essential. “Real change doesn’t come just from one voice,” he says. “It comes from many, united by purpose.”
Looking ahead, Vishal is clear about his priorities. He wants to see social care recognised as an equal partner within the wider health system and as a fundamental pillar of society.
“This is a sector built on people,” he adds. “Its greatest asset is its workforce: their professional skill, their resilience, their compassion, their commitment.”
His message is both pragmatic and optimistic. While challenges remain, he believes the sector is entering a period of opportunity, particularly as innovation and technology begin to play a greater role. Under his leadership, CSC will continue to focus on telling that story, one that, as he puts it, “the sector itself already knows, but the world needs to hear.”



Level 2
Adult Care Worker
Level 3 Lead Adult Care Worker
Level 4 Lead Practitioner in Adult Care
Level 5 Leader in Adult Care

As Kara Healthcare continues its rapid expansion, CEO Nitesh Somani explains why a relentless focus on culture has been the true driver of growth, shaping teams, transforming homes and redefining what success looks like in care.
Many care providers measure growth by beds, buildings, and financials. However, at Kara Healthcare, the focus is different. CEO Nitesh Somani, it becomes clear that the organisation’s rapid expansion from a symbolic £1 acquisition to a broader portfolio of homes is driven not by financial tricks but by a more intangible and powerful factor: culture.
Nitesh states, “Great things in business are never done by one person. They’re done by a team.” This belief is central to Kara’s operating approach, where collective strength always surpasses individual effort. The core values: knowledge, ambition, resilience, and achievement, shape the way teams work, think, and feel.
This focus on culture is especially evident when Kara acquires new homes. Rather than imposing systems or processes from day one, the approach is deliberately human. “The biggest mistake people make is trying to fix operations before they fix belief,” Nitesh says. “Often, the teams we inherit aren’t lacking capability, they’re lacking confidence.”
The priority, therefore, is to restore pride and create psychological safety. By making staff feel valued and trusted, Kara unlocks discretionary effort, the kind that cannot be mandated. “People don’t perform their best when they’re pushed. They perform when they’re uplifted.”
Sustaining that culture at scale is often where organisations falter. Yet Kara’s leadership is clear: growth does not break culture; inconsistency does. The solution lies in maintaining a uniform experience across every home, supported by visible leadership and internal progression. The Kara Training Academy plays a central role here, equipping staff with skills, confidence and a sense of purpose. Importantly, the academy goes beyond traditional compliance training. From immersive team-building exercises to unconventional challenges designed to push past fears, the focus is on developing people, not just competencies. “When you

People don’t perform their best when they’re pushed. They perform when they’re uplifted.
invest in knowledge, you create leadership. When you invest in people, you create success,” Nitesh notes.
This people-first strategy is also Kara’s answer to the sector’s workforce challenges. Rather than relying on external recruitment or agency staff, the organisation has built a pipeline of internal talent. Career progression is tangible, with team members moving from frontline roles into leadership positions. The result is
strong retention and a workforce that is deeply aligned with the organisation’s values.
Ultimately, Kara Healthcare’s growth story defies traditional expectations. While financial performance, occupancy, and ratings have all improved, Nitesh emphasises that these are results, not the initial goals. He states, “When people feel valued, they stay longer, perform better, and deliver better care.”
In a sector under constant pressure, Kara’s model offers a clear message: if you get the culture right, everything else follows.




At Greetwell Purchasing Solutions, we provide expert purchasing support and comprehensive auditing across all commodity purchases to help you save money without compromising care. Get a free, no obligation review of how we can help you today: Call: 01522 244680 Email: support@greetwell.co.uk Visit: www.greetwell.co.uk
Juan Varela Area Manager, Birchgrove


Nightingale House, located in Clapham, is a care home for older Jewish people and is part of the Nightingale Hammerson charity, which has supported the older Jewish community for over 185 years.
They provide a full range of care, including residential, nursing, dementia, respite, rehabilitation and palliative care, all delivered in a way that reflects Jewish values and community.
Their commitment to exceptional care has been recognised with an Outstanding rating from the Care Quality Commission, placing Nightingale House among the top 3% of care homes in the UK.
Nightingale House is proud to have a multidisciplinary team to help meet Residents’ needs, including carers, nurses, NHS GPs 5 days a week, advanced nurse practitioners, occupational therapists, physiotherapists, a moving & handling advisor, a dietitian, a speech and language therapist, a psychologist, engagement leads, a relationship-centred care
Sponsored By

coordinator and spiritual care leads. These resources enable Residents to get prompt assessments, diagnoses, and medication, ensuring their care remains truly person-centred.
To uphold its mission of delivering excellent care, the home embarked on a major renovation and refurbishment to rejuvenate parts of the building, aligning with Nightingale Hammerson’s reputation for modern and innovative care. With the aim of creating a beautiful space that the Residents feel proud to live in

and that reflects the welcoming community.
Nightingale House recently opened its new Café and Lounge, providing a gorgeous space open to Residents, their friends and family, the community and the children and families from the home’s onsite nursery. During engagement activities, Residents often find themselves in the newly renovated Activity Hub. Dedicated, compassionate volunteers and engagement teams staff this space. To match their enthusiasm, Nightingale Hammerson has designed a spacious area for gathering, engaging, and interacting, regardless of the activity. On sunny days, the Activity Hub’s doors open to reveal the beautifully maintained gardens of Nightingale House.
Resident’s comfort, dignity and independence are at the heart of every decision made during the renovation process. Every detail has been designed with them in mind, from furniture that allows wheelchairs to fit easily underneath, to widened doorways for greater accessibility. Higher planter boxes mean Residents can continue gardening without bending over, while new beds and mattresses have been rolled out across all
rooms to ensure restful, supportive sleep. Nightingale House is also incorporating cutting-edge technology, including Teton, the AI-powered ambient monitoring platform, to enhance daily living and care. Every improvement reflects their commitment to creating a home where independence and wellbeing come first.
An on-site nursery, Apples and Honey Nightingale, is based in the grounds of Nightingale House. As pioneers of the first Intergenerational Programme in the UK, Nightingale Hammerson is hugely proud of its success and the impact it has on both older Residents and young nursery school attendees.
Apples and Honey Nightingale has had a significant impact on the Residents’ wellbeing and mood. It enhances joy and positivity, and the ambience in Nightingale House is all the more special because of the regular presence of noisy, happy toddlers.
Residents and children share common physical challenges, such as tool manipulation and hand-eye coordination. They support each other with tasks such as cutting, pottery and gardening. Other intergenerational activities include singing, a breakfast club, painting, buddied reading and harvesting honey.
The Residents benefit enormously from interaction with young people. Increased social engagement helps reduce isolation; they feel more integrated into the wider community and experience a sense of purpose as they share their life stories with the children.
One child told a Resident, “We love coming here as you are like our grandparents, but they live in a different country, so we can’t see them.”
Jenny Pattinson, the CEO at

Nightingale Hammerson, said “[they] are reminded every day that care isn’t something you do to someone, it’s something you build with them. It begins with noticing: noticing that someone now prefers their tea a little weaker, that a familiar song from years gone by brings a smile to their face. Sometimes, a quiet moment is more comforting than questions.
That is why everything we do at Nightingale House is based on relationship-centred care. Relationship-centred care goes beyond outstanding clinical standards or beautifully designed buildings. It recognises that wellbeing is shaped by the connections between Residents and teams, families and carers and the wider community that surrounds each person.
We take time to understand each Resident’s history, preferences, routines and values to form the foundation of their care plan. When carers know Residents well, they can anticipate needs, notice subtle changes and provide support that feels personal rather than processdriven. Families often tell us that what reassures them most is not only the professionalism of our teams but the genuine warmth and affection they see in everyday moments.
Relationship-centred care is something we believe should always be at the heart of life in our care homes. It’s a practical, evidenceinformed approach that enhances Residents’ quality of life, and it’s why we place such importance on building and nurturing meaningful relationships in our homes.”
Nightingale Hammerson’s staff turnover stands at just 8.1%; across social care, workforce retention remains one of the greatest challenges of our time. Nationally, turnover in care homes averages around 24%. The low staff turnover reflects not luck, but a deliberate culture built on care, purpose and professional growth.
The team are excited to start welcoming the wider community into Nightingale House following recent renovations; the home has been transformed into a central hub for gathering, celebrating and connecting. From community events and cultural celebrations to learning opportunities and social activities, the home’s doors are open for everyone to come together, share experiences, and enjoy the home’s vibrant life.
Nightingale Hammerson stands out for its strong commitment to Research & Innovation. Through Reach by Nightingale Hammerson, a free digital platform, the organisation shares expert advice from its teams with professionals, carers and families, extending its impact far beyond its homes.
In the past year alone, it has supported more than 30 research projects and produced over 100 practical advice films. Building on this momentum, plans are underway for its sixth annual Care Home Research Forum, taking place on 5th November at Hammerson House, Wohl Campus.







Interior design is playing an increasingly strategic role in the success of care homes. In 2026, the focus goes beyond aesthetics, shaping environments that support wellbeing, operational efficiency, and regulatory compliance. Here are five essential design features every new care home should prioritise.
Dementia-informed design is now a baseline expectation rather than a specialist add-on. Clear wayfinding, colour contrast, memory cues, and unobtrusive safety features help residents maintain independence and reduce anxiety. Thoughtful layouts minimise confusion and support routine, while familiar, domestic-style environments promote comfort, dignity, and a stronger sense of identity for residents living with cognitive decline.
Care homes in 2026 must accommodate a wide range of activities within adaptable environments. Multiuse lounges, dining areas, and activity rooms allow operators to respond to changing resident needs throughout the day. Flexible design maximises space efficiency, supports varied programming, and enables homes to create vibrant, engaging environments without increasing overall footprint or compromising operational flow.
Integrating nature into interior spaces has proven benefits for mental and physical wellbeing. Large windows, indoor planting, natural materials, and direct access to gardens or courtyards help reduce stress and improve mood. Biophilic design also enhances air quality and light levels, creating calmer, more restorative environments that positively impact the experiences of both residents and staff.
Technology in care homes is becoming increasingly discreet yet powerful. From silent nurse call systems to circadian lighting and acoustic management, the goal is seamless integration. Residents benefit from enhanced safety and comfort without feeling surrounded by clinical equipment, while staff gain access to efficient, responsive systems that support high-quality care delivery behind the scenes.
5 4 3 2 1
Design expectations continue to rise, with care homes drawing inspiration from boutique hospitality settings. High-quality furnishings, layered lighting, and tactile materials create warmth and familiarity. Attention to detail in finishes, such as soft textiles, artwork, and personalised spaces, helps move away from institutional aesthetics, supporting resident dignity while also appealing to prospective families and stakeholders.









An exploration of how thoughtful design can balance clinical performance with comfort and dignity in modern care homes, from kitchens and communal spaces to artwork, with insight from Signature.
Balancing clinical performance with comfort and dignity is one of the defining challenges in modern care home design. From kitchens and communal spaces to artwork and marketing suites, today’s homes prove that operational efficiency and regulatory compliance can sit seamlessly alongside warmth, familiarity and a genuine sense of home.
In contemporary care home developments, the tension between clinical necessity and residential comfort is no longer viewed as a compromise to be managed, but as a design challenge to be solved. Operators and designers are increasingly aligned in the belief that environments supporting higher acuity care must still feel instinctively domestic: places where residents live, not simply receive care.
At Signature at Weybridge, this philosophy is evident from the moment of arrival. The design approach begins with a deliberate rejection of institutional cues: no clinical corridors, no dominant nurses’ stations, and no overtly medicalised finishes. Instead, the emphasis is on creating the impression of a well-appointed private residence. Lighting, flooring, furniture, and artwork are all specified with this in mind, while essential clinical infrastructure is carefully integrated to support care delivery without defining the aesthetic.
This “design discipline” is

increasingly critical across all areas of the home, including those traditionally considered purely functional, such as the catering kitchen.
While rarely seen by residents or visitors, the catering kitchen is one of the most operationally intensive spaces within a care home. Its design must support efficiency, hygiene compliance and staff workflow, while enabling the delivery of high-quality, appetising meals that contribute directly to resident wellbeing.
A well-designed kitchen begins with zoning: clear separation between preparation, cooking, plating and cleaning areas ensures compliance with infection control
standards while streamlining movement. Equipment selection is equally important; appliances must be robust and efficient, but also flexible enough to accommodate varied dietary requirements, from texture-modified meals to culturally specific dishes.
Adjacency planning is key. Direct, discreet connections between the kitchen and dining spaces allow food to be served promptly and at the correct temperature, preserving both nutritional value and presentation. At Weybridge, the emphasis on restaurant-style dining reinforces this connection; what happens in the kitchen is intrinsically linked to the social experience of mealtimes.
Critically, the kitchen must also support staff. Logical layouts, ergonomic workstations, and intuitive storage reduce physical
strain and improve productivity, ultimately leading to better service delivery. In this sense, operational efficiency becomes a foundation for resident experience rather than a competing priority.
The transition from kitchen to dining space is where clinical function meets hospitality design. At Weybridge, restaurant-style dining areas are carefully planned to encourage conversation and choice, avoiding institutional layouts in favour of smaller, more intimate table arrangements.
Equally important is the inclusion of flexible, informal spaces such as bistro-style cafés. Designed to operate beyond fixed mealtimes, these areas act as social anchors within the home: places where residents can gather for coffee, read the newspaper or engage in spontaneous interaction.
Achieving this requires careful specification: acoustic treatments to prevent noise from becoming overwhelming, lighting schemes that transition from day to evening, and furniture that accommodates both wheelchair users and ambulant residents. The result is a space that feels intuitive and inviting rather than programmed or prescriptive.
Beyond individual rooms, the overall layout of a care home plays a crucial role in shaping the experience it offers. Large-scale developments, particularly those accommodating over 100 residents, risk feeling impersonal if not carefully structured.
At Weybridge, the solution lies in breaking down scale into recognisable “neighbourhoods.” Rather than long, anonymous corridors, the floorplate is organised into smaller clusters of apartments centred around shared spaces. This approach is particularly important in dementia care, where familiarity and legibility of space directly impact confidence and independence.
Wayfinding strategies are embedded into the design from the

outset. Colour differentiation, tactile cues, clear sightlines, and access to natural light all support orientation, while the ability of residents to personalise their apartments reinforces a sense of identity and belonging.
The goal is not simply ease of navigation, but the creation of environments that feel comprehensible and reassuring, spaces that residents can understand and make their own.
Artwork is often underestimated in care environments, yet it plays a significant role in shaping atmosphere and emotional response. At Weybridge, artwork is curated as part of a broader strategy of sensory layering, contributing to a cohesive, residential aesthetic.
Rather than generic or overly clinical pieces, artwork selections aim to evoke familiarity, warmth and interest. This might include landscapes, local references or pieces that resonate with residents’ lived experiences. Placement is equally important—artworks act as visual landmarks, supporting wayfinding while adding character to communal areas.
Combined with soft furnishings, textures, and carefully considered lighting, artwork helps to soften the environment, ensuring that
even highly functional spaces feel comfortable and lived-in.
Ultimately, the success of any care home design lies in its ability to support residents not just clinically, but emotionally and socially.
At Weybridge, one of the most consistent pieces of feedback from families is the reassurance of seeing their relative settled, content and engaged.
Spaces such as the bistro have had a particularly strong impact, creating informal environments for interaction and fostering a sense of community. Meanwhile, the careful integration of clinical requirements ensures that care delivery remains efficient and effective without dominating the lived experience.
This is the essence of designing to feel like home. It is not about disguising care, but about embedding it within environments that respect individuality, support independence and promote wellbeing.
As care needs become more complex, this approach will only grow in importance. The challenge for designers and operators is clear: to continue evolving environments that meet the highest standards of care while never losing sight of what matters most—the simple, fundamental feeling of being at home.
Fire doors are a critical yet often overlooked element of care home safety. Regal Fire & Protection explores the legal responsibilities, technical complexities and maintenance demands that make effective fire door management essential to protecting residents, staff and buildings alike.
Care homes present a fire safety challenge unlike almost any other building type. Residents may have limited or no ability to selfevacuate, corridors are in constant use around the clock, and staffing ratios, particularly overnight, place greater reliance on the building itself to contain and control fire. In this context, passive fire protection is not a background consideration; it is central to life safety strategy. At the heart of that strategy sits one critical component: the fire door.
Too often treated as a compliance formality, fire doors are in reality complex, engineered systems designed to hold back fire and smoke long enough to protect escape routes and enable phased evacuation. When specified, installed and maintained correctly, they save lives.
Fire door compliance remains a commonly misunderstood aspect of building management in the care sector. Although operators often uphold strict clinical governance standards, from medication management to safeguarding, the physical structure of the building does not always benefit from the same disciplined oversight.
This oversight gap presents considerable risk. According to the Regulatory Reform (Fire Safety) Order 2005, the Responsible Person has a legal duty to ensure proper maintenance and suitability of fire safety measures, including fire doors.

One of the key reasons fire door compliance is often mishandled is a fundamental misunderstanding of what a fire door actually is. It is not a single product, but a complete assembly.
A compliant fire door set includes the door leaf, frame, hinges, intumescent and smoke seals, glazing (where applicable), ironmongery, and closing device; all of which must be compatible and tested together to achieve a certified fire resistance rating. The integrity of the system depends on every component performing as intended.
A single point of failure, an incorrectly specified hinge, a poorly fitted seal, or a non-compliant closer can compromise the entire assembly. Even seemingly minor deviations, such as excessive gaps between the door and frame, can prevent intumescent materials from expanding effectively under heat,
allowing fire and smoke to pass through.
For care home operators, this makes the choice of contractor particularly important. Competence, certification and traceability are not optional extras; they are essential safeguards.
In an increasingly scrutinised regulatory and insurance environment, third-party certification provides a critical layer of assurance. Certified contractors operate under independently audited schemes that verify both competence and consistency of delivery.
This is particularly relevant in care settings, where operators must be able to demonstrate not only that fire safety measures are in place, but that they have been installed and maintained by appropriately qualified professionals. Insurers are
also placing growing emphasis on certificated products and installers, often making them a condition of cover.
Working with accredited specialists helps create a clear audit trail: something that can prove invaluable during inspections by regulators or in the aftermath of an incident.
Installation is just the beginning. In busy environments like care homes, fire doors experience constant wear and tear. Frequent use by staff, residents, and visitors, often with mobility aids or wheelchairs, can quickly cause damage, misalignment, or component failure. Doors may be propped open, closers disconnected, or seals degraded over time. In dementia care settings, behavioural patterns can further increase the risk of damage or interference.
Therefore, regular inspection and maintenance are crucial. Industry guidelines advise checking fire doors at least twice a year, with more frequent inspections every three months or even monthly in high-traffic areas or newly occupied buildings.
A thorough inspection should assess:
• The condition of the door leaf and frame
• The integrity and compression of seals
• The functionality of hinges and closers
• The presence and condition of glazing
• The accuracy of gaps between door and frame
• Correct signage and overall operation
Failure in any one of these areas can render the door non-compliant, regardless of how well it was originally installed.
A common pitfall in fire door management is reliance on reactive maintenance; addressing issues only when they become visible

or problematic. This approach is inherently risky, particularly in care environments where undetected faults can persist unnoticed.
A more robust model is planned, with preventative maintenance supported by structured inspection regimes and digital reporting. Modern systems now allow operators to maintain a live record of each fire door, including its specification, inspection history, identified defects and remedial actions.
This shift from reactive to proactive management not only reduces risk but also strengthens an operator’s ability to demonstrate compliance in a clear, evidencebased way.
Central to effective fire door management is the fire door register: a comprehensive record of all fire doors within a building. This should include each door’s location, fire rating, certification details, installation date, contractor information and full maintenance history.
Increasingly, enforcement authorities view the absence of such a register as a red flag, indicating a lack of systematic oversight. Conversely, a wellmaintained register provides tangible proof that fire safety responsibilities are being actively managed.
For care home operators, this is not simply an administrative exercise. It is a critical component of risk management and regulatory compliance, providing clarity and accountability across the entire estate.
Fire door compliance should be approached with the same discipline as any other high-risk operational area within a care home. That means engaging competent, certified contractors; implementing structured maintenance programmes; maintaining accurate, accessible records; and embedding fire safety into day-to-day operational culture.
In a sector where resident vulnerability is high and evacuation is complex, there is little margin for error. Fire doors are not passive features; they are active life safety systems that must perform under the most extreme conditions.
Getting them right is not just about meeting regulatory requirements. It is about protecting lives, safeguarding staff, and ensuring that care environments remain safe, resilient and fit for purpose at all times.


Rebecca Ruscoe, Senior Project Coordinator at Boutique Care Homes, shares how Catalyst Interiors delivered exceptional dementia-informed design at Keymer Hall.
What initially led you to partner with Catalyst Interiors?
We were drawn to Catalyst Interiors because of their extensive expertise in dementiainformed design and their clear understanding of how it should shape the built environment. It was important for us to work with a designer who could deliver not only a visually appealing home but, more importantly, a space that truly supports our residents and enhances their quality of life.
How would you describe the collaborative process?
In one word, exceptional. Every interaction, from start to finish, has been highly collaborative and delivered to an impressive standard. They took the time to understand our vision and brought it to life with great care and expertise. Nothing is ever too much trouble; they are always willing to listen and thoughtfully consider every idea, even the more unconventional ones.
In what ways did their design approach align with your vision?
By working closely with our design team and project manager, Catalyst fully understood our vision for a Boutique Care Home and successfully translated those ideas into reality. They brought a wealth of knowledge and experience, delivering homes that are both functional and thoughtfully designed. Our vision has always been to create inviting, welcoming homes with a genuine sense of comfort and familiarity, while ensuring residents feel safe

and secure; something Catalyst has consistently achieved.
What tangible impact have the interiorscompleted had on resident wellbeing, staff experience, and overall occupancy or market positioning?
Every care home designed by Catalyst results in a beautiful, calm environment with a natural and intuitive flow. Fabrics and furnishings are carefully selected to avoid anything heavy or oppressive, creating light, airy, and welcoming interiors. Importantly, back-of-house areas have not been overlooked; staff benefit from the same high-quality finishes, reflecting a consistent and thoughtful design approach throughout.
Were there any standout elements that exceeded your expectations?
Every time I walk into a completed care home, I am struck by the
attention to detail and the lengths Catalyst goes to in creating interiors genuinely rooted in the local area. It is very important to Boutique Care Homes that each home becomes an integral part of its wider community, and Catalyst has consistently supported this. Whether through locally inspired artwork, bespoke spaces that reflect local character, or showcases of regional craftsmanship, they ensure every home feels both distinctive and connected to its surroundings.
was experienceyour of working with
The Catalyst team is always readily available and highly responsive to enquiries, not only from us but also from main and sub-contractors. They are an integral part of the project team. Any issues during the build are addressed promptly and efficiently, with minimal disruption, ensuring a smooth, well-managed delivery.
catalystinteriors.co.uk

Catalyst Interiors is revolutionising the world of interior design with our ground-breaking experiential approach to dementia care environments!
• Residential Care • Nursing Care • Dementia/Memory Care
• Retirement Living • Care Villages • Assisted Living
• Medium Secure • Mental Health Services • Addiction • Autism

Scan here to see our award-winning care home interiors


Interior design plays a far greater role in care homes than many realise. Care UK’s Sophia Wolsey Hurst explains how it shapes daily life, comfort and connection for residents.
When asked about the most rewarding part of her job, Sophia is clear: “Design is a long process, but when a home is completed, you finally get to see your vision come to life. The best part of that is seeing a resident move in and see them enjoy and interact with what you’ve created. To have designed a space that they and their loved ones feel at home and safe in, and a place where they can find joy, is really special. It’s what drives the design team to create the best environment possible.”
Care UK’s small but mighty team of interior designers are responsible for supporting not only new build homes, but also refurbishments of existing homes across England, Scotland and Wales, some of which have been with the provider since the 1980s.
The team recognise that each care home is individual and needs to be treated as such. Every new-

build care home is inspired by the local area, helping residents feel a sense of familiarity from the minute they move into their new home. For example, a newly-opened care home in Southampton, The Wickets, is inspired by the county’s cricket scene. This theme is present throughout, particularly in the artwork, where specifically sourced

images and 3D elements, including an old Hampshire cricket ball, bat, and wickets, are on display. These encourage conversations between residents, their loved ones and carers on a daily basis.
The designers work closely with the construction and development teams, but just as importantly, they engage operational colleagues by sharing plans from the outset. This collaborative approach helps them understand the practical needs of residents and colleagues, enabling them to shape thoughtfully designed spaces that support everyday living.
A welcoming impression is key in all Care UK homes, which is why the team take inspiration from the
hospitality sector for key parts of their design. “You want someone to greet you straight away at a friendly but official front desk”, Sophia explains, “and then you want everything else to feel homely, not sterile and neutral, as has sometimes been the case with care homes.”
The team loves using texture and colour in their designs and is always looking for new inspiration, from their natural surroundings and, often, from bars, restaurants and hotels, which can inspire the cinema rooms, in-house pubs and bars, dining rooms or lounges at Care UK homes. The team always want to try different things: “this can range from designing a new piece of furniture, to simply re-colouring a pattern on a curtain fabric!” Sophia says.
Interior design is also moving on, the team notes. The postwar themes that have regularly been present in care homes are being updated for today’s residents, ensuring that artwork and accessories feel dynamic and engaging: shifting the dynamic towards familiar references from the 1970s and 1980s.
Functionality is a key consideration in any care home design and, as a result, bespoke joinery has become a significant part of the design process. From TV units, to the bar and its surroundings, and even built-in bookcases – the team must ensure the items are suitable and accessible for residents and colleagues to use, all whilst remaining aesthetically pleasing.
The team is also moving towards a more functional approach to dementia suites, experimenting with how to keep residents safe whilst they engage with familiar hobbies. Where non-operational sewing machines and typewriters have previously been on display to evoke residents’ memories, there are ongoing discussions about replacing such items with usable, tactile objects. Artwork is changing too, a cluster of vintage holiday posters asks the question “where

have you visited on holiday?”, all of which benefit conversation and reminiscence.
Common challenges, particularly in older care homes, are a lack of day space. The three interior designers at Care UK, Sophia, Sarah Mossman and Katharine Shea, prioritise the creation and design of these new spaces wherever they can. Within dementia suites, they recognise that the need for additional spaces, such as a ‘quiet lounge’ or a space for care sessions, is crucial. In a recent refurbishment at Blossomfield Grange in Solihull, the team added an extra dining room to the dementia suite, helping residents enjoy calmer mealtimes.
There’s a lot to consider on dementia floors. Within the décor, strong patterns are avoided, and items must be carefully selected to ensure sufficient contrast between furniture, flooring, and walls, enabling residents to easily identify seating. Throughout the corridors, handrails will contrast with the wall colours, aiding with residents’ orientation, mobility and independence.
As well as innovative, personalised design, the team
know that it is important for their work to speak to customers. Recently, they’ve worked with Care UK’s digital marketing team and Imagineer to create virtual marketing suite tours that walk you through all upcoming newbuild homes in 3D. This will not only help relatives explore the intricacies of the design prior to the home’s completion, but will, most importantly, allow potential residents to familiarise themselves with their new home.
In keeping with Care UK’s commitment to responsible corporate citizenship, the design team champions sustainable suppliers. During refurbishments, they will work with Shackletons to recycle furniture that the home no longer needs. Repurposed materials play a central role across our new builds and refurbishments; curtain and upholstery fabrics are made from recycled plastic bottles, and carpets are woven with reused fibres.
“Our job isn’t complete until residents feel at home. It’s a privilege to work on something as important as this.”
Modal AV explores how integrated audio-visual systems are reshaping care home environments, using discreet technology to enhance comfort, dignity and atmosphere, proving that the best-designed spaces are the ones where the technology is felt, not seen.
Modal AV has developed integrated systems for care homes throughout the Home Counties and beyond. The consistent theme? Technology that you experience: music, lighting, and ambiance that create a homely feel.
Walk into a well-designed care home today, and you shouldn’t notice the technology. You should notice the warmth of the lighting, the music drifting gently through the lounge, the way a resident can settle into an armchair without a single cable, remote, or flashing indicator pulling them out of the moment. That is the brief we work on at Modal AV, and it is as much an interior design brief as a technical one.
Care environments have historically leaned towards feeling clinical, partly by necessity, partly by default. Bright overhead lighting, visible cabling, bulky televisions and obtrusive speakers all contribute to a hospital feel that sits uncomfortably with the growing expectation that care homes should look and feel like premium residential spaces. Having designed integrated AV systems for many care homes, we have learned that the hardware itself has to recede before the atmosphere can come forward.
Our approach is to specify equipment that disappears into the architecture. In-ceiling speakers flush-fit into plaster and can be painted to match; projection is hidden behind motorised screens; televisions sit within joinery or art frame housings. Lighting, controlled through Crestron, shifts in colour temperature throughout the day,

Our approach is to specify equipment that disappears into the architecture.
cool and energising in the morning, warm and restful by evening, giving rooms the same circadian quality a well-designed home would have. Nothing blinks. Nothing hums. Nothing announces itself.
Where a human interface is needed, we favour small, discreet touchscreens installed in commonuse rooms and communal spaces. These tidy up what would otherwise be a clutter of remote controls, light switches and thermostats into a single, elegant panel. A resident, or a member of staff working on their behalf, can adjust music, lighting, heating and window shading from one place, using clear, simple controls. For residents with cognitive difficulties, the reduction in visual and operational clutter matters enormously. For interior designers, the reduction in wall hardware means a cleaner elevation and more freedom with finishes.
Good AV in a care setting should feel like good hospitality. It should make a space more welcoming, more comfortable, more dignified, and it should do so without ever drawing attention to itself. When a family member visits and comments on how lovely the lounge feels, without noticing why, we have done our job properly. The technology is there, working hard in the background, but the experience is entirely human.
modalav.co.uk

The British Institute of Cleaning Science’s CPSS brings structured, professional training to the sector, helping teams deliver consistent, accountable standards across every environment.
We all appreciate cleanliness, whether at work, home, or while caring for loved ones. In residential care homes, cleanliness goes beyond appearances; it directly affects health outcomes, residents’ dignity, infection prevention, and overall quality of life. In these settings, cleaning professionals play a crucial, skilled role vital to the safety and wellbeing of residents, staff, and visitors.
At BICSc, we have consistently supported cleaning operatives. Our mission is based on the conviction that structured training and recognised standards are crucial for achieving consistent, measurable hygiene improvements. Therefore, we created the Cleaning Professional’s Skills Suite (CPSS), which provides cleaning staff with practical, evidence-based skills that have a tangible impact in care environments.
Traditionally, cleaning in care settings has been viewed simply as a checklist task. CPSS redefines this approach by emphasising the importance of understanding why cleaning matters and how to do it effectively and efficiently. It incorporates key principles such as using colour-coded systems to control cross-contamination and following correct cleaning sequences. The program also covers chemical selection, proper dilution, usage, and compliance with local and national policies. Through hands-on training and assessments, staff learn about proper disinfectant contact times, identify high-touch areas, and determine appropriate cleaning frequencies. This ensures that

cleaning is not only visibly thorough but also effectively minimises infection risks.
One of the biggest challenges in care settings is maintaining consistency across teams, shifts, and multiple sites. Without standardised training, quality can vary, creating dangerous hygiene gaps. CPSS provides a unified framework ensuring every operative is trained and assessed to the same high standard. Facilities often report improved audit scores, fewer corrective actions, and greater confidence during inspections.
Standardisation breaks the cycle of ‘cleaning how you were shown’, where poor practices are passed down informally. Instead, staff follow proven, compliant methodologies that deliver predictable, repeatable results, essential for infection prevention and control (IPC). Trained professionals become a cornerstone of IPC, working alongside clinical teams to protect vulnerable residents, particularly those with compromised immunity. Beyond clinical results, professional cleaning upholds resident dignity and comfort. Staff are trained to clean occupied spaces with respect and minimal
disruption, adhering to policy. Families and residents often cite cleanliness as a key factor in satisfaction surveys and quality ratings. Additional benefits include increased efficiency; proper techniques and chemical dilution help reduce waste, lower costs, extend equipment lifespan, and boost productivity.
CPSS users frequently report lower supply expenses, improved time management, and more sustainable operations. Crucially, CPSS enhances the reputation of cleaning professionals. Recognised training improves recruitment, retention, and team morale, especially in sectors with workforce shortages. Valued, skilled staff work better with care teams, promoting improved collaboration and outcomes.
In care environments, the difference between routine cleaning and professional standards is critical. It is the difference between appearance and genuine assurance, between increased risk and real protection. For residents who rely on these spaces daily, professional cleaning delivers safety, dignity, and true reassurance always.


The BICSc Cleaning Professional’s Skills Suite translates training into real, measurable improvements in hygiene in care environments. Choose from our wide range of courses to enhance skill sets.










A Q&A with Stuart Hulbert, Joint Managing Director at Brents Insurance, on the shifting risk landscape in the care sector and why a tailored, value-led approach to insurance is now essential for operators.
Can you introduce Brents Insurance and your role in the care sector?
Brents Insurance is an independent, Chartered insurance broker with extensive experience supporting care home operators throughout the UK. We serve providers from single-site residential homes to large multi-location groups, offering customised insurance and risk management solutions that address the complexities of modern care. Our role goes beyond policy arrangements; we act as a strategic partner, helping operators identify, understand, and reduce risks, while ensuring their insurance coverage is effective when it is needed most.
How is the risk landscape changing for care home operators?
The risk landscape has changed considerably. Traditional risks like property damage and employer’s liability still exist, but new complexities have emerged, especially in litigation related to safeguarding and clinical care. Increased regulatory oversight and accountability further add to these challenges. Workforce issues, such as staffing shortages and dependence on agency staff, are also creating additional risks. Moreover, digital transformation exposes organisations to cyber threats and data protection concerns.
Cost pressures are unavoidable, but concentrating solely on premium can pose significant risks. Typical problems involve outdated valuations of buildings

and contents, insufficient business interruption periods, and liability limits that no longer align with current claims environments. Restrictive policy language or exclusions often go unnoticed until a claim occurs. Insurance should be evaluated based on value rather than cost, especially in a sector where a single uninsured loss could cause severe operational and financial impacts.
As expectations from regulators like the Care Quality Commission grow, insurance can proactively aid compliance efforts. An effective program should bolster robust risk management, offer access to specialist services like legal and HR support, and align with governance standards. In this situation, insurance evolves beyond mere safety coverage, enhancing an operator’s overall compliance strategy.
Each care home is unique, and
a “one-size-fits-all” approach seldom offers sufficient protection. Elements like the type of care, resident acuity, property features, and staffing structures all impact risk. A customised program ensures coverage aligns with the actual risk profile of the facility, minimising gaps that occur with standard policies.
Several risks remain underestimated, including cyber threats from increased digital reliance, vulnerabilities in the workforce, and rising clinical complexity as residents present with more advanced conditions. Supply chain disruptions also impact repairs and medical supplies. Acknowledging these risks is key to building resilience. In this dynamic and changing sector, insurance should offer clarity, confidence, and support. We aim to foster long-term partnerships, ensuring coverage adapts to the challenges and opportunities that care providers face.
brentsinsurance.co.uk



You deserve insurance that works as hard as you do.
Established in Brentwood in 1963, an essential part of the Brents service is our philosophy of teamwork. Our friendly staff make it their business to understand our customers’ requirements, plus they have a detailed knowledge of the UK care sector insurance market to secure competitive terms and cover.
• Residential care
• Nursing care
• Elderly care
• Domiciliary care
• Mental Health
• Children’s care
We can arrange your Care Home Insurance with independent, impartial advice so that the cover arranged meets your requirements and that of the regulator and Local Authority.
Contact us today to find out how we can support you with your care business insurance.
01277 223344
https://brents-care.co.uk/




Laura Willoughby MBE, Co-founder of Club Soda, discusses how changing drinking habits are reshaping social moments in care, with a focus on choice and alcohol-free options.
Reading the headlines, you’d be forgiven for thinking its only younger people changing how they drink. But that’s not quite true.
Older drinkers (55+) are among the most likely to drink regularly, and sometimes above recommended guidelines, but they are also increasingly cutting down. Health is the big driver: medication, sleep, long-term conditions, just feeling the impact more.
So, when people arrive in a care setting, you’re not dealing with one type of drinker at all; it’s a real mix. There will be residents who have never drunk for religious or personal reasons, others who may be drinking at harmful levels, and plenty who’ve already spent years moderating their intake for health or lifestyle reasons.
That makes creating social moments around drinks both more complex, making what you choose to serve more important.
Already, over half of those aged 55+ only consume one drink per occasion, and more than a third are choosing alcohol-free drinks. But what hasn’t changed is the reason people drink in the first place: to socialise.
For many older adults, their social life has historically centred around the pub. Research from CAMRA suggests 74% of people say pubs are important for reducing loneliness. That tells you something important. It’s not the strength of the drink that matters; it’s the

shared experience. So, we should not automatically default to alcohol as a shorthand for being social. And that’s the bit care settings can hold onto.
I know care environments deal with a huge range of needs, so none of this is one-size-fits-all. But there
are some simple ways drinks can support wellbeing.
Done well, drinks can play a much bigger role than just refreshment. They can help mark celebrations and milestones, bring visiting family and friends into the moment, create a natural shift from day to evening, and add a sense of occasion to everyday life.
Because drinks are rarely just about what’s in the glass. They’re about identity, routine and connection. And today’s residents didn’t grow up on sherry. They grew up in the 60s to 80’s, where we shifted to cross-gender socialising, wine with dinner, maybe the odd cocktail if they were feeling fancy.
So, when the choice becomes “tea, coffee or a sherry”, it does not replicate the social experience they remember - and tea is what you have been drinking all day. It does not feel special.
There’s also a very practical side to this. You may have residents who are psychologically dependent on drinking, or who should not drink due to health conditions, such as dementia and Alzheimer’s.
Guidance from Alzheimer’s Society highlights that alcohol can increase confusion, dehydration and risk, and may interact with medication. For some residents, it simply won’t be appropriate. But that doesn’t mean removing the moment altogether.
In practice, many care teams already manage this by pouring drinks themselves, keeping bottles out of sight and offering smaller measures, or even running an alcohol-free environment.
But alcohol-free options take this a step further. They allow residents to keep the ritual, a drink with dinner, something in hand in the evening, without the same risks.
We had a customer in our shop buying alcoholfree wine in bulk for her
mum with dementia. She was a heavy drinker but could not tell that the wine was alcohol-free. This helped her daughter manage her moods and expectations without the side effects of alcohol. Majestic Wine tells me that care homes are among the largest purchasers of its alcohol-free selection.
One of the most useful insights is that requests for alcohol are often about something else: boredom, habit, a cue for social interaction (this applies to everyone, not just older people!).
So the answer isn’t just swapping the drink, it’s creating better moments.
Some homes are already moving toward relaxed social gatherings, music or themed evenings, and shared food-and-drink moments. Because what people are often looking for is the atmosphere the pub once provided, not necessarily the alcohol itself. We’re starting to see glimpses of this done well (and I’m always keen to hear more).
In the Netherlands, De Hogeweyk Dementia Village recreates everyday environments, including cafés and bars, where residents can socialise as they always have. In the UK, providers like Care UK and Barchester Healthcare are investing more in experienceled care, from themed events to hospitality-style dining. The direction is clear: care is becoming more social, more personalised, and more like real life. Drinks should follow.

This doesn’t need a big overhaul; a few practical shifts can make a real difference. Offering more than one alcoholfree option, a beer and something sparkling, helps normalise choice and promotes inclusion. Keeping familiar rituals, like a pre-dinner drink or

something in the evening, maintains a routine. And using alcohol-free options can help manage risk without removing choice.
It also comes down to confidence: training staff to offer alternatives, rather than waiting to be asked, and focusing on the overall atmosphere, not just the drink itself.
There’s also a big opportunity around celebration milestones. A birthday or family visit shouldn’t mean defaulting to sugary soft drinks. There are now alcohol-free sparkling wines and grown-up alternatives that feel just as special. And as family members may have driven to the care home, this means they are fully included too.
We know from hospitality that better alcohol-free options help people stay engaged, socialise for longer, and feel more included. The same applies in a care setting. It can be directly linked to wellbeing. Because people don’t stop being social when they move into care. And sometimes, what they really want isn’t alcohol, it’s the socialising around it.
Club Soda is a social impact business and advocates for the availability, visibility and celebration of low and no alcohol drinks to help society change drinking for good.

ONLY £24 per month, per property

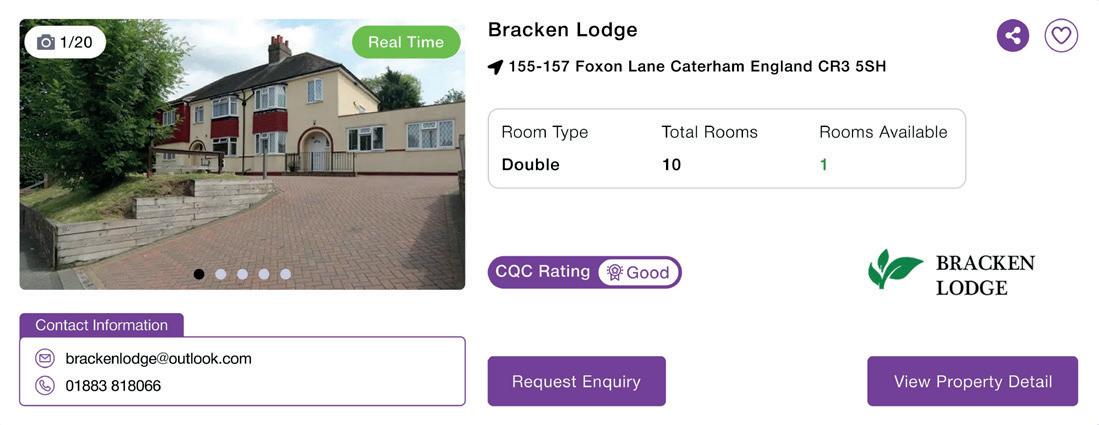
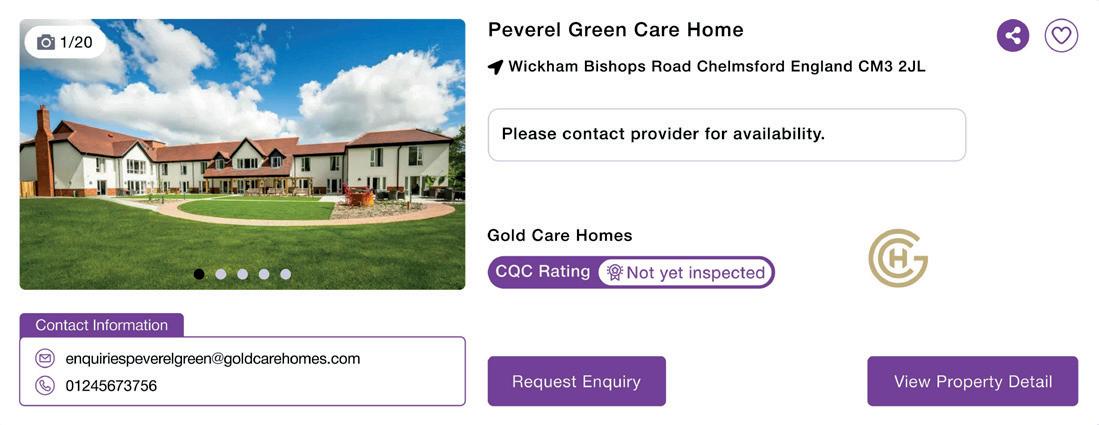




Launching a new care home development is a complex process, shaped by regulatory pressures, financial constraints, and operational realities. This article explores five key challenges developers must navigate to deliver successful, sustainable, and residentfocused care environments.
Securing planning permission and aligning with local authorities are among the initial challenges for new care home projects. Navigating zoning laws, community concerns, and changing regulations can cause significant delays. Developers need to balance financial viability with social value by clearly showing community benefits, workforce impacts, and sustainability to gain approval and build stakeholder trust.
Construction cost inflation and supply chain volatility continue to pressure budgets for new care home schemes. Fluctuating material prices, contractor availability, and extended lead times create uncertainty at every stage. Effective procurement strategies, early contractor engagement, and contingency planning are essential to maintain programme timelines, protect margins, and avoid compromising on build quality or regulatory compliance standards through delivery phases.
Workforce planning is a critical but often underestimated challenge in new care home developments. Recruiting, training, and retaining skilled staff in a competitive labour market requires early strategic focus. Location, transport links, and local demographics all influence staffing viability. Without a robust workforce model, even the most well-designed facility can struggle to operate effectively and deliver consistent, high-quality care outcomes.
Designing for compliance while delivering a homely, resident-centred environment presents a complex balancing act. Regulations around fire safety, accessibility, infection control, and dementia-friendly design must be fully integrated without creating an institutional feel. Successful schemes prioritise thoughtful layouts, natural light, and intuitive wayfinding, ensuring environments support both operational efficiency and resident wellbeing without compromising on statutory requirements at any stage.
5 4 3 2 1
Securing funding and demonstrating long-term financial viability remain persistent challenges for developers entering the care sector. Lenders and investors require detailed evidence of occupancy projections, fee structures, and operating costs. Market saturation in certain regions adds complexity. A clear business case, supported by demographic data and realistic assumptions, is essential for attracting investment and ensuring sustainable returns over time.



An ambitious new development from Dunham Care and Back to the Garden Childcare will bring together luxury residential care and a nature-led nursery, creating a connected, community-focused environment that supports wellbeing, purpose and meaningful intergenerational interaction.
Dunham Care and Back to the Garden Childcare have announced plans for a £13 million intergenerational development in the heart of Bowdon, Cheshire, with completion scheduled for October 2026. The scheme, Bowdon Manor, will bring together a 51-bedroom luxury care home and a purpose-built, nature-inspired children’s nursery, creating a shared environment designed to foster meaningful connections across generations.
Situated on the historic site of the former Bowdon Hotel, the development has been carefully conceived to respect the character of its surroundings while delivering a sustainable, future-focused care setting. The design prioritises both functionality and wellbeing, incorporating landscaped outdoor areas and flexible communal spaces that encourage interaction between residents and children in a safe and structured way.
The concept builds on the proven intergenerational model already established in Lymm, where a Dunham Care home operates alongside a Back to the Garden nursery. At Bowdon Manor, this approach will again underpin the day-to-day experience, with opportunities for shared activities such as storytelling, music sessions, gardening, and arts-based programmes. These interactions are intended to deliver measurable benefits: residents can experience reduced social
isolation and improved emotional wellbeing, while children are supported in developing empathy, communication skills, and social confidence.
Internally, the care home will offer 51 en-suite bedrooms alongside a range of high-quality amenities, including lounges, dining areas, and dedicated wellbeing spaces. The interiors have been designed to balance comfort with a sense of dignity, avoiding institutional aesthetics in favour of a more residential, hospitality-led environment.
Adjacent to the care home, the Back to the Garden Bowdon nursery will accommodate approximately 90 children. The setting will follow the provider’s established nature-led, childcentred ethos, featuring open-plan learning environments, outdoor play areas, and creative studios that encourage exploration and independence through natural materials and sensory experiences.
A key aspect of the scheme is the integration between the two settings. Shared gardens and carefully planned communal zones will enable regular, organic interaction while maintaining appropriate safeguarding and operational boundaries. As intergenerational care models continue to gain traction across the sector, Bowdon Manor represents a significant investment in a model that prioritises connection, community, and holistic wellbeing.
“Seeing the smiles, laughter,

and warmth shared between generations in Lymm has been incredibly powerful,” said Emma James, Operations Director at Back to the Garden Childcare & Dunham Care. ” We’re reducing isolation, strengthening community, and creating happiness in the everyday moments that matter most.”
Chris McGoff, CEO of Dunham Care and Back to the Garden Childcare, added: “This development represents the future of intergenerational, connected care. The success at Lymm inspired us to bring this model to Bowdon, where the benefits for children and older residents will continue to flourish.”

Subsidium explains how fully managed devices, from encryption to real-time tracking, remove the burden of IT management and ensure care providers remain secure, compliant, and focused on delivering quality care.
In care settings, staff are increasingly becoming accidental IT technicians: resetting passwords, troubleshooting Wi-Fi, and dealing with faulty devices. Every minute spent resolving technical issues is time taken away from residents.
At Subsidium, devices arrive ready to use and fully managed from day one. There’s no setup, no stress, and no disruption. Supporting over 50,000 devices across more than 250 care providers, we ensure your technology stays in the background so care remains front and centre.
Focus on care. We’ll handle the rest.
Many providers purchase off-theshelf devices, only to spend days manually configuring each one.
This often creates an immediate bottleneck in digital adoption.
Subsidium eliminates this challenge through Zero-Touch Deployment.
Provisioning goes far beyond simple delivery; it’s about total preparation. Before a device even reaches your home, it is fully enrolled, encrypted, and pre-loaded with your required clinical software. This means your digital systems are ready to go from the moment the device is powered on.
By removing the logistical burden of setup, we enable instant digital transformation. Your infrastructure is clinical-grade from day one, without adding further pressure to already stretched frontline teams.

The Passcode Trap: When staff leave, devices can become locked and unusable. We resolve access issues remotely in seconds.
Update Fatigue: Security patches and app updates are handled automatically, running quietly overnight, never during critical care moments like medication rounds.
Hardware Health: Devices are monitored in real time, allowing us to detect and address potential failures before they impact your team.
For the Care Quality Commission (CQC), unmanaged devices present a clear risk. Under Regulations 12 (Safe Care and Treatment) and 17 (Good Governance), providers must demonstrate strong control over both data and equipment.
Since these safeguards are
integrated into our provisioning process, each Subsidium device is compliant right after unboxing.
With Subsidium, data encryption is enabled; settings can be restricted and applications protected through kiosk mode; updates occur automatically to keep software secure and current; and every device features GPS tracking so you can determine its location.
Choosing Subsidium means more than simply purchasing software - it’s an investment in a complete, clinical-grade ecosystem. We remove the technical complexity, ensuring your infrastructure is secure, compliant, and future-proof.
By managing the technology behind the scenes, we free your teams from the role of “accidental IT technicians” and allow them to focus on what matters most: delivering high-quality care.
Don’t let your hardware become a barrier to care.
subsidium-ms.com
Don’t let unmanaged devices steal valuable time from your residents.
Subsidium currently manages over 50,000 devices across the care sector. We turn chaotic, vulnerable tablets into secure, clinical tools instantly. From Kiosk Mode to overnight updates, we handle the entire lifecycle behind the scenes.

No distractions. No data risks. Just technology that works, so your team can too.
Book a demo today

Signature, Boutique, Greetwell and Business Support Experts share how new care homes are being designed to meet rising acuity: combining flexibility, efficiency and a more future-proof approach from the outset.

Across the UK, the profile of care home residents is evolving rapidly. Individuals are entering care later in life, often with more advanced conditions, increased clinical complexity, and elevated expectations for both the environment and the care experience. As a result, new care home projects are being redesigned from the ground up, not only to meet higher-acuity needs but also to proactively address them. For operators, developers, and suppliers, the focus has shifted from merely modifying existing buildings to creating environments that inherently accommodate future needs without requiring adaptation.
A prominent and consistent theme emerging from recent innovations is the shift towards embedded flexibility in care design. Instead of creating environments for a fixed care model, providers are embedding adaptability in response to residents’ changing needs.
At Signature Care Homes, this principle is fundamental. Their newest developments focus on supporting an “elasticity of care,” allowing residents to age in place across a full continuum: from independent living to nursing, dementia, and palliative care. This impacts the building’s design, with integrated clinical infrastructure, assisted bathroom features, and nurse call systems from the start, ensuring the environment can seamlessly scale to higher dependency levels. Similarly,
Boutique Care Homes employs a subtle yet structured strategy. While offering a hospitality-focused setting, they include dedicated spaces, such as their “nostalgia community,” to cater to residents with higher care needs. Importantly, this does not create a visual break from the rest of the home. Design consistency is preserved, with only specific modifications such as dementia-friendly signage and themed navigation added where necessary. Overall, this results in a transition in care levels that doesn’t feel clinical or disruptive. This approach mirrors a wider industry trend: future-proofing is now about integrating capacity invisibly from the start, rather than adding it later.
As resident needs grow more

complex, the clash between clinical practicality and hospitalityinspired design becomes more evident. Instead of choosing one over the other, leading providers are addressing this challenge by collaborating early.
Signature refers to this as a “productive tension” between disciplines. By involving clinical and design teams early in the concept phase, they ensure that neither aspect is an afterthought. The hospitality vision establishes the goals, high-quality interiors, lifestyle amenities, and a homely atmosphere, while clinical needs set the operational boundaries. Good design results from balancing these elements.
Similarly, Boutique adopts this approach by discreetly hiding clinical infrastructure in backof-house areas. Residents enjoy themed interiors, local motifs, and welcoming communal spaces, rather than overtly medical settings. This approach is especially crucial as expectations evolve; residents now anticipate well-designed homes and demand the same quality in care environments. Ultimately, this leads to a new design language in care, where clinical functions are present but subtly integrated.
While new developments often focus on resident experience,
operational efficiency remains essential, especially as cost pressures grow. Floorplate design plays a strategic role; at Boutique, layouts are precisely arranged to match staffing ratios with bed counts, ensuring effective care and financial viability. Poor spatial planning can increase staffing needs, making it crucial to get this right during design.
Procurement strategies are also moving earlier in the process.
Steve Gibson from Greetwell Purchasing Solutions notes that many operators still see procurement as a post-build step. In reality, decisions about kitchens, storage, and service flows impact long-term operational success. Data insights are increasingly important: analysing purchasing trends, such as demand for special diets or allergen-free products, can guide kitchen design, storage, and workflow before construction starts. This is especially vital in highdependency settings with complex, less predictable nutritional needs.
Flexibility remains vital; kitchens and service systems must adapt to evolving resident profiles rather than being optimised for a single operating model.
Alongside design and operations, financial structuring is increasingly shaping new developments.
Business Support Experts
emphasize a significant, often overlooked opportunity through Capital Allowances.
These tax reliefs can considerably lower the net cost of a project but are often underused because they aren’t considered early enough. Incorporating tax planning into the design stage can influence key decisions, such as opting for demountable partitions instead of fixed ones, which can unlock higher tax relief. In high-demand settings where specialized equipment and flexible spaces are common, opportunities for optimization grow even more.
These changes have substantial effects: better cash flow and lower capital costs can be the difference between a project proceeding or not, especially in high-cost areas with strong demand for beds but tight margins. As development costs rise, financial efficiency becomes a crucial part of the overall strategy, not just an administrative concern.
Geography continues to significantly influence new care provision, but the situation is complex. In Greater London and the South East, providers highlight a clear shortage of purpose-built, high-quality homes.
Despite considerable development activity, demand surpasses supply due to dense,

ageing populations and inadequate modern facilities. Signature’s focus on London reflects this, aiming at areas where families struggle to find appropriate care options. Similarly, Boutique recognises ongoing demand throughout the South East, noting that much of the current care home stock no longer meets modern standards. Features now standard, such as ensuite wetrooms, are often missing in older homes, indicating a need for both new capacity and upgrades to outdated facilities.
Nationally, the issue isn’t about pinpointing a single hotspot but about understanding localised pressure points. As Greetwell’s data indicates, relying solely on national averages can be misleading. The demand for higher-acuity care varies across regions, and new developments need to be tailored to local needs.
Sustainability is becoming a more integral part of new care home developments, with the scope broadening from just energy efficiency. From a building performance standpoint, providers are adopting a fabric-first strategy, emphasising insulation and construction quality to reduce
energy demand before adding mechanical solutions. Technologies like photovoltaic panels, battery storage, and heat pumps are increasingly common, along with LED lighting and smart controls. Yet, sustainability also encompasses operational and experiential aspects. Efficient layouts can lessen staffing demands; streamlined supply chains reduce waste; and environments that promote wellbeing, through natural light and outdoor access, enhance long-term resident outcomes. Procurement also contributes, prioritising sustainable purchasing not for premium costs but for better visibility, less waste, and stronger supplier accountability. When integrated early, such practices support both environmental aims and cost efficiency.
An often-overlooked element of new developments is how they connect with the local community. For Boutique, community engagement serves both wellbeing and business goals. By welcoming local groups and activities into their spaces, they foster environments that feel connected rather than isolated.
This approach benefits residents by keeping them engaged with the outside world and also enhances local reputation and referral opportunities. In competitive markets, such visibility can be as important as traditional marketing, as trust built through community involvement becomes a unique and hard-to-copy advantage.
As the sector develops, so do expectations. Features that once set premium care homes apart, such as private apartments, high-quality dining, and wellness amenities, are now becoming commonplace.
Meanwhile, residents’ clinical needs are growing more complex, placing greater demands on buildings, systems, and staff. The sector’s clear response is: build once, and build it right. This involves integrating clinical capabilities, operational efficiency, financial strategies, and sustainability from the beginning, all while creating environments that truly feel like home.
The next generation of care homes will be judged not just by their ability to adapt to change, but by how effectively they can anticipate it.
Supporting social care to use tech and data safely
FREE Independent guidance, advice and elearning
Choose and use the right technology
Strengthen digital and data governance
Build digital and data skills
Access and share data safely Manage suppliers and contracts
Keep up to date with new tech

Find out how Yorkare Homes partnered with Syndora Alto to deliver a flexible, integrated approach to nurse call and digital care recording; modernising services while maintaining continuity and enhancing day-to-day care delivery.
Yorkare Homes is advancing its approach to care delivery through a strategic partnership with Syndora Alto, implementing a flexible, integrated model for nurse call and digital care recording across its portfolio.
Recognising the need to balance innovation with operational continuity, Yorkare has adopted a dual-approach rollout. In newly developed homes, the group has implemented CHARIS, a fully digital nurse call system designed to deliver real-time alerts, intelligent room displays and robust wireless connectivity. In parallel, established homes have been upgraded with AltoEnhance, enabling seamless integration with existing nurse call infrastructure without requiring a full system replacement.
This hybrid model allows Yorkare to modernise at pace while maintaining service continuity: an essential consideration in live care environments. Across both settings, the technology is designed to support responsive, person-centred care, ensuring staff can act quickly and confidently when residents require assistance.
A defining feature of the implementation is the integration between nurse call systems and handheld digital care record devices. Alerts are automatically logged within individual care plans, strengthening accountability, improving visibility and creating a more comprehensive, real-time picture of each resident’s care journey. For frontline teams, this

reduces administrative burden and frees up more time for direct care, while providing management with actionable insights into call volumes, response times and emerging trends.
Jonathan Garton, Operations Director at Yorkare Homes, highlights the impact of the rollout: “We began our partnership with Syndora by installing the system in a new-build site, and the process was seamless. The engineers were professional and methodical, ensuring not only that the system was fully operational, but that staff were confident using it before leaving.”
He continues: “We later implemented the hybrid model across several established homes, integrating it with existing equipment. The transition was completed in under 48 hours, with no disruption to residents’ access to call bells at any stage. Continuity of care was clearly prioritised.”
Ongoing support has also been a key differentiator. Kieran Stanley, System Coordinator, notes: “The level of customer service has been exceptional. With 24-hour remote support and responsive on-site engineering when required, the aftercare matches the quality of the technology itself.”
For Yorkare Homes, the result is a more connected, data-driven care environment that enhances responsiveness, strengthens oversight and supports more efficient workflows. The partnership with Syndora Alto demonstrates how a considered, flexible approach to digital transformation can deliver tangible benefits across both new and existing care settings.
syndoraalto.com

Discover how easyResidences is approaching new care home development at Manor Farm in Kessingland, balancing live construction with resident wellbeing to create a future-focused home.
Since its launch in Autumn 2025, easyResidences has signalled a new approach in the care sector, offering homes designed for real people with genuine ageing experiences. These homes are high-quality properties with modern interiors, accessible layouts, fully furnished ensuite bedrooms, and shared indoor and outdoor spaces for communal enjoyment.
The groundbreaking ceremony took place in December 2025, initiating the project for Morrison Care Group, KRG Healthcare’s management, and staff. They faced the challenge of building a new facility while residents stayed in the existing care home on the same site. This situation, though not unprecedented, demands meticulous planning, ongoing review, and clear communication among all parties.
Before laying a single foundation at Manor Farm, comprehensive risk assessments addressed the complex task of building a future care home alongside an operational one. With residents living nearby, the risk of disruption had to be minimised, including access route segregation, noise and vibration during sleep hours, dust and air quality management given existing residents’ respiratory vulnerabilities, and safeguarding utilities such as power, water, and emergency systems throughout construction.
Infection prevention was critical; construction protocols were integrated with the home’s existing IPC framework to ensure safety. A

Principal Designer and Principal Contractor were appointed in accordance with CDM 2015 standards, with a live risk register reviewed continuously throughout each construction phase.
Throughout the project, the operational home’s registered manager played a key role in site governance. At Manor Farm, resident welfare is the overriding priority that guides all construction decisions. This dedication to care and communication defined every stage of the subsequent project.
Before digging began, archaeologists surveyed the site designated for the new development. Their work concluded in October 2025, when a team member visited the residents to share their discoveries. These included the remains of a 13th-14th Century farmstead located beneath the car park, and an 11th/12th Century jug handle.
This meeting with residents marked a crucial step in the
development process, enabling them to participate actively and safely in shaping their new community. As construction got underway, one resident even took a supervised tour of the site to discuss the project with the construction team.
A rainy start to 2026, combined with the large trenches on site, prevented residents from attending external visits to inspect the work. Nonetheless, the home’s activities coordinator took a supervised tour around the site to take photographs, which were later shared with the residents. The dining room at the current Manor Farm offers a safe spot to watch the evolving new development, with residents enjoying observing the construction team at work, sparking conversations and photo opportunities.
By the end of March, with much of the severe winter weather behind them, the foundations and substructure work were almost finished. This included building two lift shaft bases and installing external and internal drainage systems, and preparing for the ground-floor concrete slab. Once this was done, work on the superstructure began, with external block and brickwork rising to 1500mm, and scaffold installation was scheduled.
Whenever possible and practical, the building team visited residents to update them on the development’s progress. This helped residents feel involved and understand the visible changes happening outside.
Managing the care home alongside ongoing building work has required careful planning among the developer, operator, and construction team in a true partnership spirit.
Early considerations related to parking, safe access to the existing care home, external storage space,

and the safety of residents near the construction site were prioritised to ensure a smooth start as everyone adjusted to their ‘new normal’. The construction team quickly established safety walkways and accessible routes with disability access, enabling residents to continue reaching the community, friends, family, and staff. The main entrance of the care home was relocated to another part of the building to allow safe access.
The Manor Farm team has been flexible and maintained strong, clear communication about planned changes, which has been crucial to the project’s success so far. Their top priority has remained providing a calm, safe, and reassuring environment for residents, especially those with dementia. Despite these ongoing efforts, Manor Farm also received an unannounced routine inspection from the EHO, which resulted in it retaining its 5-star rating. This highlights the team’s dedication to delivering outstanding service even amid significant transformation. To date, noise disruptions have
been minimal, and residents have shown curiosity about the project, watching it take shape.
As the weather improves and the garden at the far end of the property undergoes a Spring transformation, residents can enjoy the sunshine peacefully, listening to birds and watching squirrels visit along the fence.
Everyone at the home is eager for the opportunities the development will offer, including upgraded facilities, improved living spaces, and beautiful grounds that will enhance residents’ quality of life.
Registered Manager Kylie Child, with many years at the home, is optimistic about Manor Farm’s future, stating, “We are sure to face more challenges as the build progresses, but everyone so far has shown resilience and excitement. We look forward to the benefits the new build will bring.”
With summer approaching and a strong team in place, the first easyResidences care home appears to have a bright future.
Bringing on new technological developments which help make care homes run more smoothly and efficiently is an important aspect of improving care. In the case of fire detection, it is a fundamental consideration in protecting both residents and staff from the threat of fire, but also, in doing so, ensuring that it has minimum impact on the day-to-day running of a home.
Siemens has introduced the new Cerberus Nova fire detectors, which are aiming to transform traditional fire detection into proactive, smart, connected safety solutions through cloud connectivity.
Central to the new detectors is automated Disturbance-Free Testing (DFT) technology, which runs self-checks around the clock, reducing potential downtime for systems. Digital fire service solutions are replacing costly and time-consuming on-site visits. In a care home, such visits can be particularly disruptive to residents, who may be confused or upset by unfamiliar visitors, and can also affect the day-to-day running of the home. With the advent of remote services enabled by digitalisation, monitoring and intervention can be conducted offsite, allowing service providers to interrogate and even alter systems remotely. This not only reduces costs but also enhances flexibility through remote access 24/7.

This not only reduces costs but also enhances flexibility through remote access
24/7.
With the support of the Smoke Entry Supervision (SES) technology, which monitors smoke entry points in real time, safety teams can intervene immediately before risks escalate. Additionally, the ASAplus technology of Cerberus Nova, incorporating multi-wavelength optical and dual-thermal detection, minimises false alarms, reducing unnecessary evacuations. Given the nature of the elderly occupants of a care
home and their mobility issues, potential cognitive impairment, hearing loss, or other medical conditions, this needs to be a particular focus when selecting an appropriate method to protect the occupants and the care home itself from the threat of fire.
With many care home providers operating multiple, widely distributed buildings, centralised fire safety management can be essential. Siemens Cerberus Nova detectors help facility teams maintain consistent protection standards across all sites by
providing continuous monitoring, reducing the risk of unnecessary disruptions, and supporting proactive maintenance. This holistic approach provides oversight of widely dispersed facilities and ensures reliable, resilient operations across the entire building portfolio. Multi-site dashboards can provide the locations of all sites in one place, with a status bar indicating the status of each in real time, using a simple colour-coded approach to identify sites where problems may be occurring.
siemens.com/en-gb/

Symphony Sound discusses the growing importance of integrated hearing technology in the design of care homes.
Hearing accessibility is rapidly emerging as a defining feature of high-quality care environments, yet it is still too often treated as an afterthought. For forward-thinking operators and developers, this approach is no longer sustainable.
Symphony Sound, a specialist provider of assistive listening and acoustic technology, is addressing this gap by embedding inclusive sound design directly into newbuild care homes.
Rather than retrofitting solutions post-completion, Symphony Sound collaborates with architects, developers and operators from the earliest design stages. The aim is to ensure hearing accessibility is considered as fundamental as lighting, heating or connectivity. This approach not only creates a more seamless solution but also eliminates the cost and disruption associated with later adaptations.
At the planning stage, several key elements must be prioritised. Acoustic performance is critical, requiring careful management of background noise, echo and reverberation through both material selection and spatial layout. Built-in infrastructure is equally important, ensuring spaces are equipped with the necessary wiring and connectivity to support integrated systems.
Communal areas such as lounges, dining rooms and activity spaces should be designed for flexibility, supporting both group interaction and one-to-one communication. Inclusive technology must cater to

hearing aid users and non-users alike, while remaining intuitive for staff to operate consistently. Addressing these considerations early ensures a discreet, effective solution that integrates naturally into the environment.
The benefits for residents are immediate and meaningful. Symphony Sound’s room-based systems are designed to improve clarity in everyday interactions, particularly for those living with hearing loss, dementia or cognitive decline. Residents are better able to follow conversations, engage in activities and respond to staff, leading to increased participation and confidence.
Reduced cognitive strain is another key outcome. When listening becomes easier, residents experience less fatigue and confusion, supporting greater independence. Just as importantly, improved inclusion in daily life contributes to stronger emotional wellbeing and reduced feelings of isolation.
For operators, the advantages
extend beyond resident wellbeing. Families are increasingly seeking care environments that actively support sensory needs, making integrated hearing technology a powerful differentiator. Developments that prioritise accessibility are better positioned to drive occupancy and strengthen their market position. There are also clear operational efficiencies. Improved communication reduces repetition and misunderstanding, easing the burden on staff and enabling more effective care delivery. At the same time, providers benefit from enhanced reputation, demonstrating a commitment to innovation and quality.
Hearing technology in care settings is set to advance rapidly, with smart, connected systems, personalised listening experiences and data-led insights shaping the next generation of care environments. For providers aiming to stay ahead, the message is clear: embed hearing accessibility at the design stage, invest in scalable solutions, and treat sound as a core component of wellbeing; not an optional extra.

Why backing your ‘go-to’ staff as trainers strengthens confidence, consistency and care; by Ashlyn Cartwright, Training Manager at Abuka.
Over the years I’ve learned that the important elements of learning in care homes don’t happen in front of a projector. It’s the stuff you can’t get really from a manual, for example an experienced carer showing a new starter the knack for using a standing hoist with a resident who gets anxious during transfers. It’s not just about the safe use of equipment but also about the eye contact and the reassurance. Staff may have completed a course, but it’s these day-to-day learning that help them turn knowledge into confident practice.
In almost every care home I visit, there are one or two people the team naturally turn to for guidance and advice. They’re the ones who get tapped on the shoulder with quick questions, who are asked to show a newer colleague how something should be done, who step in when someone looks unsure. In practice, they’re already

doing a lot of the training – it just isn’t called that.
There is a risk in leaving all of this completely informal as valuable knowledge can sit with a small number of individuals and, if they move on, a great deal of experience moves with them.
This is where a more deliberate
approach to developing internal trainers can make a difference. Rather than assuming informal support will just happen, it means pausing to ask: who do people turn to already, and what would it look like to support them properly in that role? A Train-the-Trainer approach is one way of doing this; not necessarily to replace all external training, but to give those trusted colleagues the time, skills and framework to share their expertise in a clear and consistent way.
When organisations begin to do this, a few things tend to change. First, learning starts to feel closer to the reality of the service. An internal trainer understands the people being supported, the rhythm of the day and where the pressure points are. They know the shortcuts people are tempted to take and the situations that staff find most difficult, often because they’ve been there themselves.
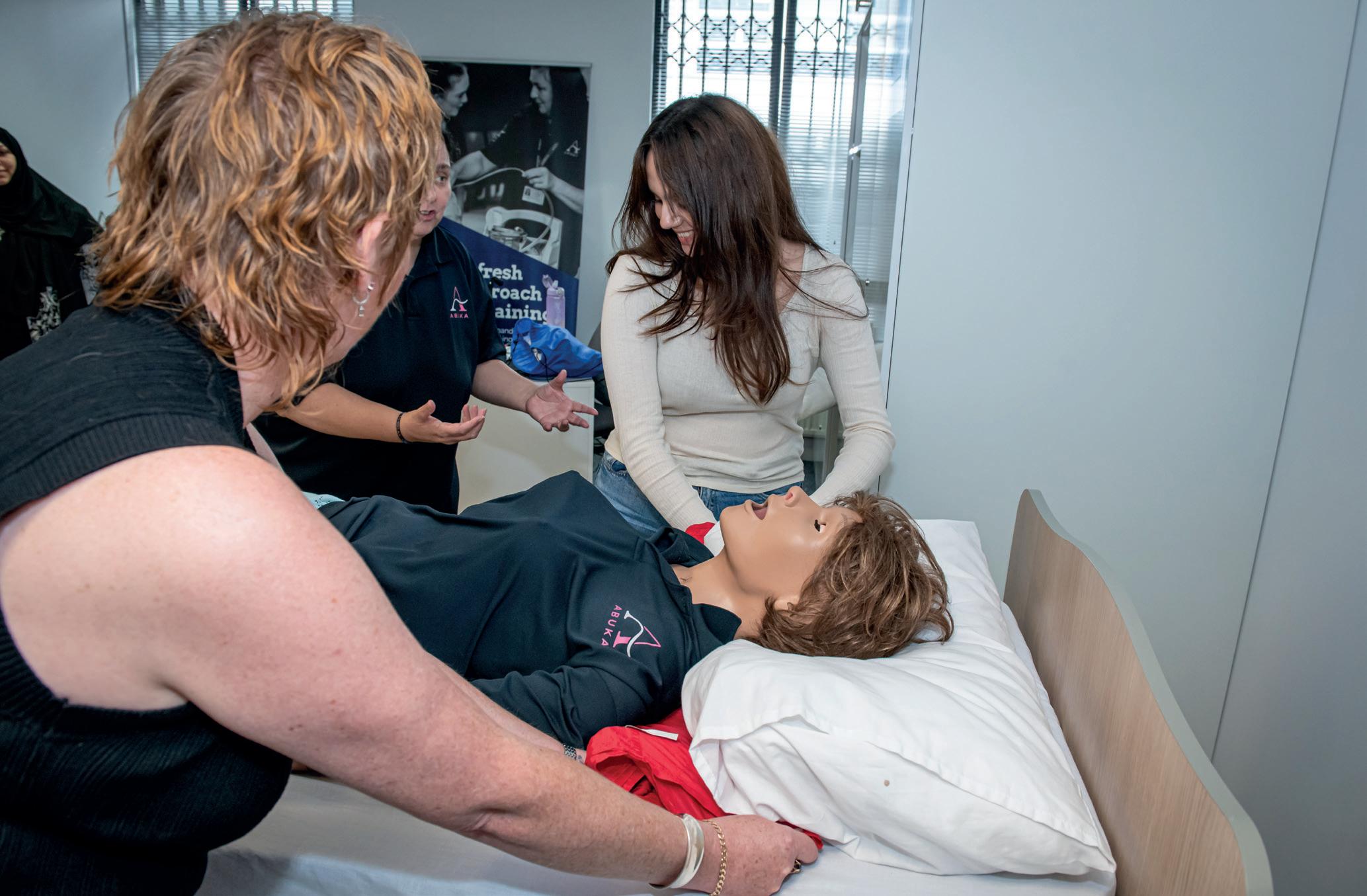
Learning can become more continuous including sessions delivered on the “shop floor” in real care homes to help new starters, address skills gaps, upskill staff or introduce new practices.
Training can be customised to a care home’s unique policies and specific service user needs to aid personalisation. Formal sessions can be scheduled around daily routines and staff shifts, reducing the need for travel and minimising
operational disruption.
It can reduce reliance on external training providers, especially for statutory and mandatory subjects and perhaps those less common topics required by your specific care home.
For many providers, the first motivation to explore internal trainers is practical. Having more inhouse capacity can make training more flexible and help new starters get up to speed more quickly when
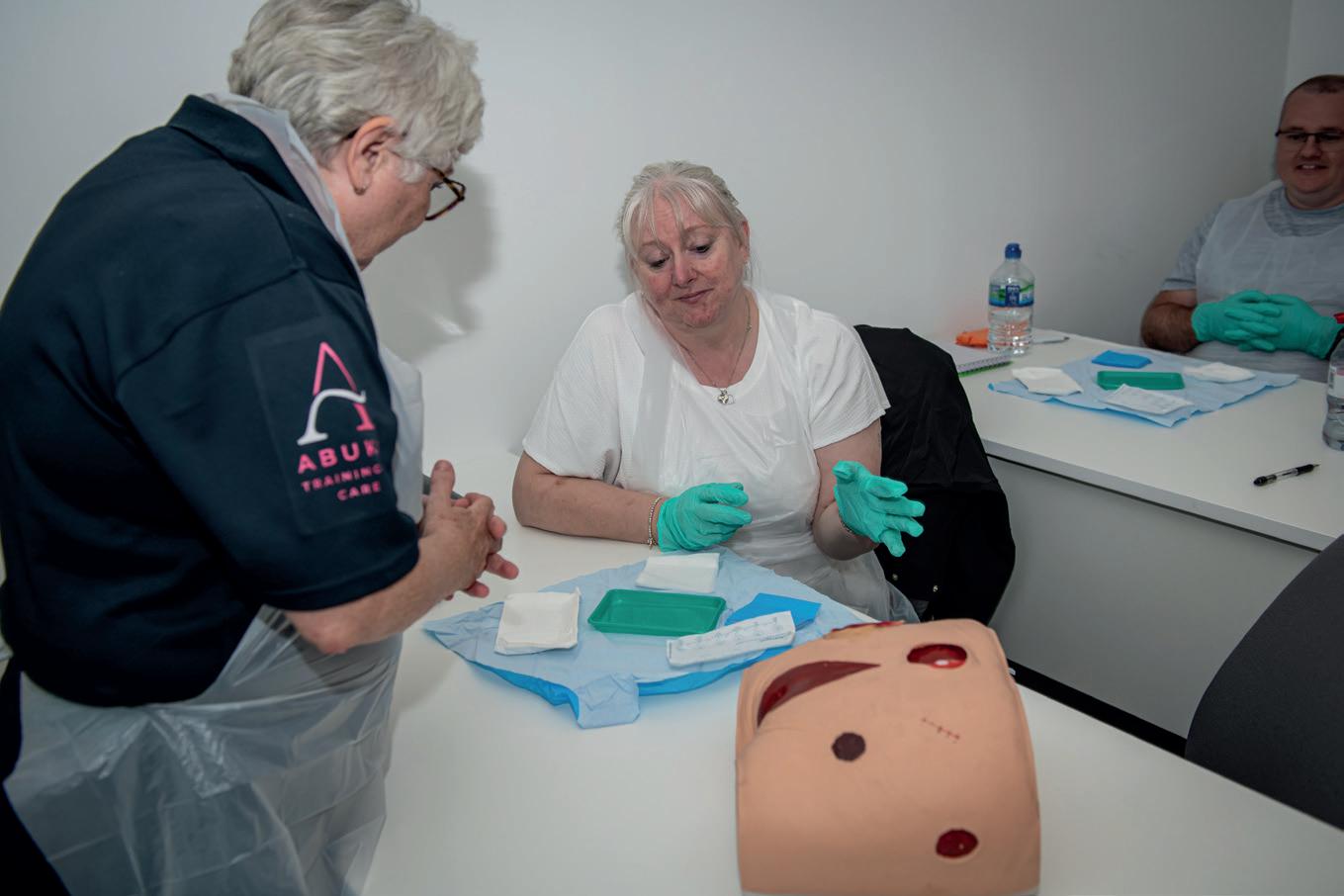
teams are changing or growing. Those are important benefits in a sector where time and resources are under constant pressure.
None of this is a magic fix, and developing internal trainers won’t look the same in every organisation. But I have consistently seen that when learning becomes part of the day-to-day life of a service – and when there are people on the team who feel equipped and supported to lead that learning –staff feel more confident and better supported in their work. In turn, the impact is felt by the people in those services and by their families.
If you’re starting to picture the “go-to” people in your own service as you read this, it might be the right moment to think about how you could support them more intentionally in that role.
At Abuka, we work with care providers to develop internal trainers through practical, experience-led programmes designed around the realities of care. We build their knowledge, skills and confidence, ultimately helping turn the “go-to” people into a training asset.
In this Q&A, Michael D’souza, Commercial Development Manager at Business Support Experts (BSE), shares how smarter tax planning and capital allowances can drive financial efficiency and support growth in the care sector.
Business Support Experts specialises in commercial tax relief, helping UK businesses maximise their tax savings and enhance financial efficiency. While we serve various sectors, our primary expertise is in assisting care home operators, who often face distinct financial and regulatory challenges.
Our goal is to help care providers identify and claim reliefs they might not realise they qualify for, such as Capital Allowances. These incentives can provide significant cash flow benefits that can then be reinvested in facilities, staff, and resident care.
We adopt a comprehensive, hands-on approach, managing the entire process to ensure claims are accurate, compliant, and fully optimised.
In a sector with slim margins and increasing demand, our mission is to give care home operators the financial flexibility and confidence to focus on delivering excellent care.
Capital Allowances are often overlooked in the care sector. Many operators are unaware that parts of their property, such as fixtures, fittings, and integral features, can qualify for relief, leading to missed opportunities for significant tax savings that could be reinvested in their business.
We encourage operators to engage with a specialist as early as possible, ideally at the point of acquisition, development, or refurbishment. Taking a proactive, consultative approach allows us to identify opportunities from the outset, streamline the process, and typically secure a quicker and often greater financial benefit.
Our approach remains consistent whether we handle a new development or an existing care home. We aim to deliver strong, fully compliant claims while maximising all available reliefs.
The main difference lies in the opportunity type: new builds or recent projects often enable more immediate and optimised claims, whereas existing care homes may require a review of past expenditures. Nonetheless, our methodology is unchanged; thorough, consultative, and dedicated to securing the best possible results for the client.
Tax efficiency and solid financial planning are becoming increasingly vital as providers develop the next generation of care homes. Facilities serving residents with higher dependency levels usually

require greater initial investments in construction and specialised equipment. Effective tax strategies help operators improve cash flow and retain more capital within the business, supporting expansion through new locations, extensions, or refurbishments of existing facilities.
As demand in the sector continues to grow, the ability to reinvest wisely and scale operations will be crucial. Therefore, proactive tax planning should be considered a key component of long-term strategic success.
businesssupportexperts.co.uk/ contactchm/

Discover how much your business could reclaim through Capital Allowances.
• 15-minute initial call at your convenience
• Any UK income or corporation tax-paying entity may qualify
• No fees unless you receive a claim
Claim relief on longterm business assets that aren’t in your P&L—let us help you get back what’s rightfully yours.


Celebrate the season with a care home-friendly take on the traditional May Fair, offering adaptable, dementia-friendly activities that encourage reminiscence, creativity and meaningful social interaction.
The arrival of May has long been associated with renewal, colour and community spirit. Rooted in centuries-old traditions, the British May Fair offers a rich and highly adaptable theme for care home activities; one that naturally lends itself to reminiscence, creativity and social engagement. For operators, it provides a structured yet flexible framework to deliver meaningful experiences that can be scaled to suit a wide range of abilities and interests.
At its core, a May Fair is about celebration. Historically marking the transition into warmer months, it combines visual spectacle with simple, joyful rituals, many of which will resonate strongly with older generations. This makes it an ideal focal point for activity programming, particularly when the emphasis is placed on participation, choice and accessibility.
When translating a May Fair into a care home setting, the key is to balance authenticity with practicality. Not every element needs to be recreated in full; instead, focus on capturing the atmosphere through a series of smaller, manageable activities that can run throughout the day or week.
Start with the environment. Bunting is an easy, low-cost way to transform communal spaces, corridors or dining areas. Residents can be actively involved in creating decorations using simple materials: paper, glue, string and scissors. This activity can be adapted for varying

dexterity levels, with pre-cut shapes or templates available for those who may struggle with fine motor tasks. For more independent residents, designing and assembling bunting offers a sense of ownership over the celebration. Layer in seasonal touches using traditional spring flowers such as primrose, gorse and lesser celandine. Even where fresh flowers are not practical, artificial alternatives can still deliver visual impact. Arranging flowers, whether individually or in small groups, provides both sensory stimulation and a familiar, calming activity, particularly for those living with dementia.
Maypole dancing is one of the most recognisable elements of a May Fair, but it doesn’t need to be physically demanding to be effective. A simplified version can be created using a lightweight pole or even a seated adaptation with ribbons attached to a central point. Residents can participate by holding ribbons and moving them rhythmically, either standing or seated. Music plays an important role here: traditional folk tunes or songs from residents’ younger years can enhance the sense of occasion and encourage engagement. For those who prefer
not to take part directly, watching the activity still contributes to the communal atmosphere and offers a valuable social touchpoint.
The tradition of the May Queen provides an opportunity to celebrate individuals within the home while reinforcing a sense of occasion. This can be approached in a way that prioritises inclusivity; rather than a competitive selection, consider inviting residents to volunteer or rotate the role across different units or groups.
The crowning itself can be a simple but meaningful ceremony, perhaps accompanied by music or readings. It creates a focal moment within the day and encourages wider participation from residents, staff, and even visiting family members.
Flower crown making is a particularly effective activity within this theme, combining creativity with tactile engagement. It also supports reminiscence, as many residents may recall similar crafts from earlier life experiences.
The process can be broken down into manageable steps using measuring tape, florist wire, florist tape, scissors, ribbon and flowers. Staff or more able residents can assist with the initial shaping of the crown, while others contribute by selecting and attaching flowers. This division of tasks ensures inclusivity while maintaining a sense of shared achievement.
For residents with limited dexterity, consider pre-assembling the base and offering larger, easierto-handle floral elements. The finished crowns can then be worn during the celebration, reinforcing a sense of participation and pride.
While the visual and creative aspects of a May Fair are important, the underlying value lies in how activities are delivered. A

successful programme will take into account individual interests and preferences.
For residents living with dementia, familiarity and repetition are key. Using recognisable materials, seasonal cues, and gentle prompts can help anchor the activity in something meaningful. Avoid overly complex instructions and instead focus on sensory engagement: textures, colours and simple actions.
Equally, providing a balance between group and individual activities ensures that all residents can participate in ways that suit them. Some may thrive in the energy of a communal celebration, while others will benefit more from quieter, one-to-one interactions.
From an operational perspective, simplicity is essential. Activities should be easy to set up, require minimal specialist equipment and be deliverable within existing staffing levels. Preparing materials in advance, such as pre-cut bunting shapes or partially assembled flower crowns, can significantly reduce the workload on the day. Risk assessments should also
be conducted, particularly when using tools such as scissors or wire. Opt for safety scissors where appropriate and ensure staff are available to support residents who may need assistance.
Finally, consider how the activity fits into the wider daily routine. Integrating elements of the May Fair into mealtimes, music sessions or outdoor activities can help extend the experience without placing additional strain on resources.
The strength of a May Fair theme lies in its versatility. It can be scaled up into a full-day event or broken down into a series of smaller activities delivered over time. More importantly, it offers a platform for meaningful engagement; combining reminiscence, creativity and social connection in a way that feels both natural and enjoyable.
For care home operators, this is exactly the kind of activity that delivers value beyond the immediate moment. It supports wellbeing, fosters community and reinforces a sense of identity and belonging, outcomes that sit at the heart of high-quality care.
Aneil Manmohan, Head Chef at Nesbit House Care Home in Orpington, Kent, shares his delicious BBQ lamb chops recipe, a firm favourite with residents at the home.

At Nesbit House Care Home, I’m always looking for ways to bring a bit of excitement and comfort to our residents at mealtimes. Whenever I can, I take the opportunity to get the two big BBQs at the home going. This style of cooking is something close to me; what I’d call a braai, from my South African heritage, and it brings a real sense of warmth and familiarity. While BBQ is often seen as a bit indulgent, I like to show that it can be both nutritious and accessible, without losing those bold, comforting flavours people enjoy.
Everything I cook is centred around the residents. With BBQstyle cooking, you can build deep flavour naturally, which means we can keep dishes balanced without relying on heavy ingredients. I tend

to use lean proteins like chicken or fish, paired with grilled vegetables, so meals still deliver what residents need nutritionally: good protein for maintaining strength, fibre for digestion, and plenty of vitamins to support overall health.
Of course, in a care home, texture and dietary needs are just as important as flavour. It’s really important to me that everyone can enjoy the same meal, regardless of their individual requirements. Our BBQ dishes are always adapted where needed; whether that’s soft and bite-sized or minced and moist options, pureed versions, or adjustments for low-salt, diabeticfriendly, or allergen-aware diets.
A lot of that comes down to how we cook. Slow-cooking meats makes them naturally tender and easier to eat, and vegetables are prepared so they stay soft while still retaining their goodness. When someone needs a modified texture, we don’t just serve something completely different: we adapt the same dish. That way, the flavour, the look, and the overall experience are still there. It’s important to us that dignity and enjoyment are never
Ingredients
Lamb chops - Rib or loin chops, approximately 2–3 cm thick
Marinade
1/4 cup olive oil
2 tbsp Worcestershire sauce
2 tbsp red wine vinegar or lemon juice
2 cloves garlic, crushed
1 tbsp fresh rosemary (or 1 tsp dried)
1 tsp dried thyme
1 tsp smoked paprika
1 tsp ground coriander
1 tsp salt
1/2 tsp black pepper
1 tsp brown sugar
Method
1. Prepare and marinate
Combine all marinade ingredients in a bowl and mix well. Coat the

lost. I always say, a modified diet shouldn’t mean a lesser experience.
Another benefit of BBQ-style cooking is that it’s a healthier approach overall. Grilling means we don’t need to rely on excess fats, and we can control exactly how much salt or sugar goes into each dish. You still get that satisfying taste, just in a more balanced way.
Beyond the nutrition, there’s something about BBQ that really brings people together. The smell alone can get people interested in food again, especially for residents who may have lost their appetite.
lamb chops evenly, cover, and refrigerate for at least 2 hours (or overnight if time allows). Remove from the fridge 30 minutes before cooking to bring to room temperature.
2. Preheat the grill
Preheat a gas grill to high heat for 10–15 minutes, then reduce to medium-high. If possible, create two heat zones — one side hotter for searing and the other slightly cooler for finishing.
3. Cook the lamb chops
Remove excess marinade and place the chops onto the hotter side of the grill. Cook for 2–3 minutes on each side to develop colour. Transfer to the cooler side and continue cooking for a further 2–3 minutes, depending on thickness. Ensure the meat is cooked through but remains tender and juicy.
4. Rest before serving
More than that, it often brings back memories - family gatherings, summer days, being outdoors. Creating that feeling again, even in a care home setting, adds something really, really special to the dining experience.
For me, it’s never just about the food on the plate. It’s about creating meals that support health while also bringing enjoyment and a sense of occasion. If I can take something as familiar as a BBQ and adapt it so every resident can be part of it, then I know I’m doing my job right.
Allow the chops to rest for 5 minutes before serving. This helps retain moisture and improves tenderness.
Serving Suggestions
I serve with familiar, comforting sides such as:
• Soft tomato and onion salad
• Mild yellow rice or mashed potatoes
• A small spoon of chutney for added flavour
• Warm, soft bread or flatbreads
Chef’s Note
For residents who may require softer textures, chops can be finished in a covered tray with a small amount of stock to gently tenderise further. Always ensure seasoning is balanced and not too strong, keeping dishes enjoyable and accessible for all.
A new report from Lakeland Dairies, supported by Consultant Dietitian Rachael Masters (MSc, BSc), finds the care sector at a tipping point, with 74% of operators concerned about their ability to meet residents’ nutrition and hydration needs amid rising complexity and cost pressures.
Care catering is evolving beyond just meal delivery to focus on providing measurable nutritional value, even in more complex settings. The report ‘The Care Kitchen Reset: The Future of Care Catering’ highlights ongoing sector challenges, with 43% of operators noting increased resident nutritional needs over the past five years. Meanwhile, 71% cite rising ingredient costs as a barrier to maintaining food quality, despite 90% still committed to high standards. These combined pressures are prompting operators to reconsider how they deliver care and value through their food offerings.
Catering is crucial in care settings. For 90% of residents, food influences their choice of a care home, and 87% consider mealtimes the most important part of their day. This makes catering teams vital for both resident wellbeing and the care home’s success. As expectations grow, there is an increasing need for reliable, highquality dining experiences that also address complex nutritional needs.
Rather than introducing additional processes or increasing workload, the report identifies a more effective solution: strengthening the foundations of everyday cooking. By enriching base ingredients, kitchens can increase calorie and protein density without increasing portion sizes, labour or waste.

This approach enables care homes to deliver enhanced nutrition in a way that is both practical and scalable; an important consideration in a resourceconstrained environment.
Dairy-based ingredients play a key role in this strategy due to their versatility, enabling kitchens to enhance meals for residents with smaller appetites or special diets. The report indicates that 90% of operators find ingredients like cream and milk powder improve the food and drink experience, while 88% see them as effective for supporting nutritional goals. When used strategically, these ingredients can boost both the nutritional value and the general appeal of common dishes.
Rachael Masters, Consultant Dietitian, emphasises that catering teams are now being asked to deliver “meaningful nutritional
support” in increasingly complex care environments. She notes that the solution lies not in adding more processes, but in making smarter use of core ingredients to enhance energy, protein and key nutrients. Paul Jennings, Head of Food UK & International at Lakeland Dairies, echoes this view, highlighting ingredient strategy as a practical way for operators to build quality, consistency and resilience into their menus without adding complexity.
As the sector continues to navigate financial pressures and rising expectations, the message is clear: the future of care catering will depend on how effectively kitchens can optimise their foundations. By focusing on enriched ingredients and smarter menu design, operators can protect both nutritional standards and operational efficiency, delivering better outcomes for residents without increasing strain on already stretched teams.


Discover how Advinia’s Chef of the Year competition in Manchester set a new benchmark for how care providers can place lived experience at the heart of dining.
Some moments in the care sector quietly challenge long-held assumptions.
Advinia’s Chef of the Year competition, held at Food Sorcery in Manchester, was one such example; it appeared to be a standard culinary contest with six chefs, experienced judges, and a kitchen full of effort and pride.
Johnny Hazell, Joe Oliver, Rob Henry, and Donnie Munro brought expertise spanning compliance, systems, product development and large-scale catering. However, what distinguished this event was more significant: six residents sat alongside industry professionals, playing a key role in selecting the winner, with residents sharing equal status with professional judges, reflecting a genuine shift where lived experience is valued as expertise rather than an afterthought.
From the moment the day began, there was a palpable sense of energy in the room. Chefs moved with purpose, plating dishes that needed to meet a very specific brief: restaurant-quality food that could realistically be delivered in a care home environment. It is a balance that is often underestimated: flavour, nutrition, presentation, and scalability all need to coexist. Here, that challenge was embraced.
Rob, the Head of Culinary Solutions and Compliance at EFgroup, who supported the event, emphasised its importance. With over 10 years at the company, he has witnessed firsthand the talent within care kitchens.
“Care homes aren’t graveyards for retired chefs,” he remarked. “It’s heartening to see the camaraderie among the chefs and the lively

energy in the kitchen.”
This camaraderie was visible throughout the day. Despite the competitive nature of the event, there was mutual respect among the chefs and an understanding that everyone was united by a common goal: enhancing residents’ dining experiences.
And that purpose ran deeper than just the food.
Sarah, Advinia’s Head of Dementia Care, brought new depth to the day. Having joined just seven months ago, she has begun transforming the understanding and support of dementia throughout the organisation.
Her efforts include creating training programs that reach all levels of the company, not only direct care staff, so that even chefs and housekeeping personnel are prepared to better assist residents. Her drive is rooted in personal experience; after caring for her grandmother with dementia for seven years, she sums up her work as: “My passion is my purpose.”
That ethos was reflected in the food itself. Every dish presented had to consider not only taste and
presentation, but also accessibility, nutrition, and the specific needs of residents, particularly those living with dementia. Texture, fortification, and ease of eating were all part of the judging criteria: a reminder that in care settings, food is never just food.
Throughout the competition, the judges provided detailed, practical feedback. Dishes were assessed not only on flavour and presentation but also on their feasibility in a care home kitchen. One dish, a jerk chicken, was praised for its visual appeal. Another impressed with its technical ambition, recreating a Tunnock’s-style teacake that demonstrated both skill and a clear understanding of how to fortify desserts effectively.
There was also a strong operational lens applied. Considerations around scalability, consistency, and the realities of catering for large numbers were central to the discussion, reinforcing the idea that excellence in this sector is as much about delivery as it is about creativity.
What made the judging process especially impactful was its
alignment with the residents’ perspectives. While professionals focused on evaluating technique and feasibility, the residents assessed a similarly vital aspect: how the food made them feel.
Residents arrived dressed for the occasion, clearly aware that this was not an ordinary day out. There was pride in their role, excitement in their voices, and genuine engagement with the process. They asked questions, shared opinions, and, most importantly, were listened to.
Helena, one of the resident judges, who also got to present an award, perfectly expressed the mood: “I enjoyed our day out so much… so much delicious food.”
Dennis commented on the special occasion: “I really liked dressing up nicely for the event, which made it feel even more memorable… I felt so happy and proud to be asked to serve as a judge.” For Enid and Fred, the experience extended beyond that day. Their daughter later shared how meaningful it was to see photos capturing them smiling, engaged, and visibly enjoying themselves. In a sector where families often worry about connection and quality of life, moments like these are truly significant. Even residents with specific needs felt the impact. John, who follows an easy-to-chew diet, still participated in the experience, showing that, with proper inclusion,

everyone can be involved.
The dishes themselves reflected a wide range of influences and approaches. From Balmoral Chicken Wellington to smoked haddock fishcakes, from Polish-inspired pork rolls to comforting chicken and leek pie, there was a clear effort to balance familiarity with creativity. Some chefs leaned into nostalgia, others into cultural exploration, but all remained grounded in the realities of care catering.
Ultimately, it was Jake WalkerMacey who took the title, his chicken and leek pie resonating strongly with both judges and residents alike. It was a fitting winner: a dish rooted in comfort, executed with care, and perfectly suited to its environment.

However, the true aim of the competition went beyond identifying a single winner. It was about transforming expectations. In care settings, food is often seen solely as a functional necessity to fulfil nutritional needs with little regard for other aspects.
Events like this challenge that view, showing that food can be a source of joy, identity, and connection. They also emphasise an equally vital point: residents are not just passive recipients of care but active participants in shaping their experience. By centring residents in its Chef of the Year competition, Advinia has not only created a memorable event but also established a new standard: one where voices are valued, preferences respected, and experiences enriched.
If the lively atmosphere in that Manchester kitchen was any indication, this standard could soon become the norm across the sector.
Mark Dale, Head of Hospitality at Advinia, said: “The B Happie Star Chef of the Year reimagines how we recognise culinary talent, with residents at the heart of the process. The winner was chosen by resident judges and supported by our valued supply partners. Every chef who entered was deserving; while there could only be one winner, each should feel proud. The passion and dedication shown throughout made this a success for everyone involved.”
Tajá, Director of Operations, Quality & Compliance at Meadowbanks Care Home, discusses how to strengthen systems, invest in staff development, and build a culture of consistency to drive high-quality, person-centred care.
With over ten years in the care sector, I possess a clinical nursing background complemented by formal leadership and management qualifications. My responsibilities include operational delivery, governance, compliance, recruitment, safeguarding, and service development. I prioritise working closely with care teams, residents, families, local authorities, and healthcare partners to ensure care remains safe, compassionate, and truly person-centred.
Additionally, I focus on fostering a positive workforce culture where colleagues feel valued, supported, and encouraged to grow. When staff are confident and engaged, resident outcomes improve, and the entire home benefits.
On joining Meadowbanks, I saw significant potential. The setting is a clear strength, with spacious accommodation, attractive grounds, and a tranquil lakeside aspect that enhances residents’ wellbeing. There was already a warm, caring ethos, underpinned by a committed team and positive community links. Alongside this, there were opportunities to drive greater consistency, strengthen systems, and introduce innovation, particularly through the effective use of digital tools.
Early assessment highlighted challenges around organisation, communication, and consistency of practice. Processes required a clearer structure, with defined accountability and more robust frameworks to support decisionmaking. Workforce development was also a priority. Investing in high-quality training, coaching,

and leadership support is essential to ensure every team member understands expectations and feels equipped to deliver excellent care.
We have since implemented a series of targeted improvements. Investment in digital care planning and recording has enhanced accuracy, accessibility, and oversight. We have expanded training provision through structured programmes and eLearning, and reinforced risk management through stronger assessments and documentation. Operationally, workflows have been streamlined to improve coordination across departments. At the same time, we have enriched the resident experience by broadening activities, strengthening community engagement, improving communication with families, and making thoughtful environmental enhancements to create a more homely, high-quality setting.
Culture underpins all of this work. Systems provide the framework,
but people deliver the difference. I prioritise a culture defined by kindness, professionalism, accountability, and teamwork. Open communication is encouraged, with staff supported to share ideas, raise concerns, and take ownership of their roles.
Looking ahead, the ambition is to position Meadowbanks among the leading residential homes in the region. This will be driven by continuous quality improvement, sustained investment in people, ongoing upgrades to the environment, and a more strategic use of technology. We also intend to further develop our premium offering, ensuring residents benefit from a truly outstanding standard of living.
Ultimately, the goal is clear: to be recognised for excellence, innovation, and authentic personcentred care, where residents feel respected and fulfilled, families feel confident, and staff take pride in their work.

