Empathy Effect

BU Receives Major NIH Grant for Women’s Research BU-AMP Collaborates on Stroke Treatment, Primary Care Programs By The Numbers
The How sharing personal narratives is transforming medical training DONOR FY 2025 REPORT


BU Receives Major NIH Grant for Women’s Research BU-AMP Collaborates on Stroke Treatment, Primary Care Programs By The Numbers
The How sharing personal narratives is transforming medical training DONOR FY 2025 REPORT

Dear Alumni, Friends, and Colleagues, Greetings! Our cold New England winter is beginning to thaw, finding us more than halfway through the 2025–26 academic year. Before we know it, graduation will be here!
This edition of BU Medicine celebrates the many contributions of our students, faculty, staff, and alumni. Our cover story highlights the Students Perspective Initiative, which pairs talks by students who have endured diseases or medical conditions with medical school lectures investigating those topics—underscoring how sharing personal narratives is transforming medical education.
We also showcase our MA in Mental Health Counseling & Behavioral Medicine program, now in its 25th year, which until recently averaged 90-100 applicants annually for approximately 30-40 spots. Since 2017, the number of applicants has increased significantly, reaching 626 for 48 spots in the 2025 entering class.
We celebrate a five-year, $4.5M grant from the National Institutes of Health (NIH) Building Interdisciplinary Research Careers in Women’s Health program to further women’s health research and spur career growth for young investigators. The prestigious award will connect junior and senior faculty interested in women’s health research, largely focusing on addiction science, maternal-child health, and sex influences on health outcomes.
We mark the first time Boston University has received a multi-PI Medical Scientist Training Program grant from the NIH. The five-year, $1.6M award will help recruit, train, and inspire four or more students a year to become clinician-scientists by providing research and clinical training leading to an MD/PhD.
We feature a group of medical students who traveled to Malawi as part of BU’s Global Health Summer Scholarship to work on improving water chlorination practices in rural communities, and also give an interesting update on the BU-Armenia Partnership, which has been reinvigorated by some additional funding from the late Edward Avedisian (CFA’59,’61, Hon.’22) and his wife Pamela (Hon.’23), part of their $100M gift to the school.
Closer to home, we highlight a peer-led high school student program on overdose prevention created by the students and BU/Boston Medical Center addiction and harmreduction researchers.
Boston University Medicine
Boston University Medicine is published by the Chobanian & Avedisian School of Medicine Communications Office.
Maria Ober
Associate Dean, Communications
design & production
Boston University Creative Services
contributing writers
Alene Bouranova, Jessica Colarossi, Gina DiGravio, Doug Fraser, Molly Glass, Sarah Rowan
photography
Jake Mackey, Cydney Scott
Please direct any questions or comments to:
Maria Ober
Communications Office
Boston University Medical Campus
85 East Newton Street, M810H Boston, MA 02118
P 617-358-7869 | E mpober@bu.edu 0326
Our Giving section and Donor Report pay tribute to your impactful gifts. We gratefully acknowledge the long-standing generosity of the Karin Grunebaum Cancer Research Foundation, which has given the school more than $2.4 million since 1984 to fund a professorship, an annual faculty fellowship focused on cancer research, and medical student research. We also recognize a generous gift from Monita Lam establishing the Kum Fung Lau Fund, which supports key research initiatives at the BU Alzheimer’s Disease Research Center in the fight against Alzheimer’s disease. The fund is named after Lam’s mother, who died of the disease in 2002.
Our Alumni section celebrates the 2025 Alumni Awards recipients: Humanitarian awardee Larry Nichter, MD’78; Distinguished Alumni awardee Ziv Haskal, MD’86; Emerging Leaders awardee Stephanie Feldman, MD’14; and Medical Sciences Distinguished Alumni awardee Vladimir Kefalov, PhD’99.
Thank you for your ongoing commitment to our school and your generous support for our outstanding students, faculty, and staff on the front lines of science and medicine.
Please enjoy this issue of BU Medicine. Best Regards,

Hee-Young Park, PhD Dean Ad Interim, Chobanian & Avedisian School of Medicine
Associate Dean of Faculty Affairs
Carolann S. Najarian Professor and Chair, Medical Sciences & Education Professor of Dermatology


Speaking to 138 first-year medical students taking the initial step of their medical training, White Coat Ceremony keynote speaker and CEO emeritus of Providence Health & Services Rod Hochman, MD’79, CAS’79, reflected on donning his own white coat for the first time 50 years ago. “If you’d asked me back then what my career would look like, I would have been mostly wrong. There are easier career paths—business, finance, consulting—but none will offer the kind of fulfillment that comes from a life spent healing, listening, and making a difference,” he said.
Hochman and his wife Nancy, Sargent ’77,’83, recently donated $10 million to build
the new Rod Hochman Family Clinical Skills & Simulation Center.
Organized by the Student Affairs office, the traditional ceremony held last August 4 on Talbot Green featured faculty members helping new students put on, for the first time, the iconic physician’s white coat symbolizing the transfer of knowledge from one generation to the next.
“Donning the white coat symbolizes your entry and commitment to the professional expectations, responsibilities, and obligations of becoming a doctor,” said Interim Medical School Dean Hee-Young Park, PhD.
Associate Dean of Student Affairs Angela Jackson, MD, told students the ceremony was “visible evidence you are joining this
Jake Mackey
Organized by the Student Affairs office, the traditional ceremony on Talbot Green featured faculty members helping new students put on, for the first time, the iconic physician’s white coat symbolizing the transfer of knowledge from one generation to the next.
profession, taking your first steps along the path to a demanding but rewarding and meaningful career in medicine.”
Selected from a pool of 11,484 applicants, the 177th entering class includes students from 32 states and 17 countries, speakers of 28 different languages, and an age range of 20 to 30s, said Kristen Hanssen, MD, associate dean of admissions.
Their personal stories vary as well.
Medical school wasn’t always a certainty for William Wang, whose parents immigrated from China and worked long days at their restaurant; Wang helped out after school and on weekends and holidays. Limited finances meant the family had to travel long distances to get affordable healthcare,
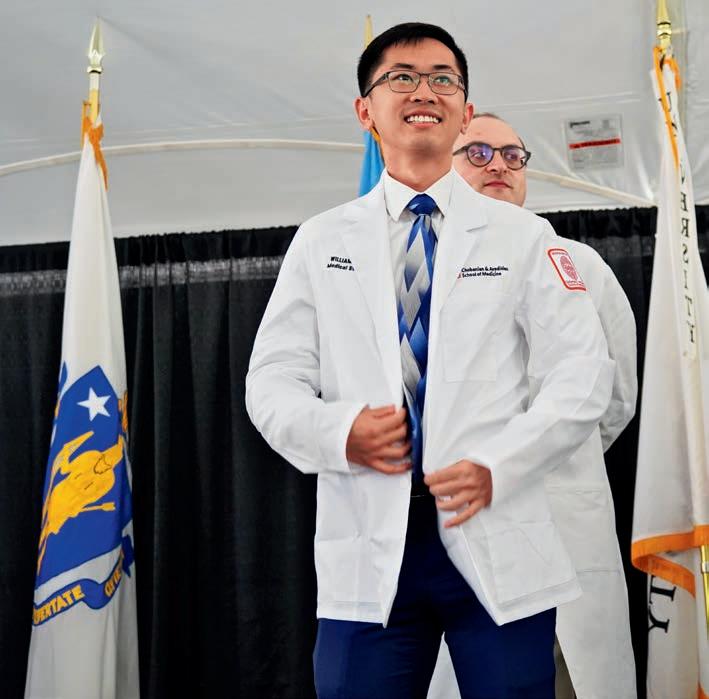
which fueled Wang’s desire to become a physician.
The restaurant faltered soon after Wang graduated from BU with a degree in biomedical engineering. “At the time, I thought if I went to medical school, I wouldn’t be able to help the family and I’d just accumulate more debt,” he said.
After four years working at a private equity firm, family finances had improved, and Wang continued his medical school journey.
Hellen Edwards always wanted a medical career, but for financial and personal reasons, the Hawaii native joined the Reserve Officers’ Training Corps as a BU freshman chemistry major. Now 34 and an Air Force
major, Edwards is returning to the University with 10 years of active duty behind her, including postings in Montana; Okinawa, Japan, and Washington, D.C., where she led monitoring efforts related to biological threats and weapons of mass destruction.
“That desire to practice medicine never really left me,” said Edwards. “After all these other experiences, I came back to medicine and serving people. That’s where my heart is.”
Lifelong gymnast Alma Kuc’s resilience was tested in January 2025, when her family home burned to the ground in the Los Angeles Palisades fire. A member of the Polish national gymnastics team and an All-American at UC Berkley who competed
The unexpected illness and death of two mentors in Eric Yang’s formative years propelled him into a medical career. A gifted clarinetist, Yang was devastated by the death from cancer of a teacher who had guided him into a prestigious precollege music program at Juilliard. When dementia forced a second mentor into early retirement, Yang’s career focus shifted from music to biomedical science.
in two world championships, Kuc had seen her share of success as well as failure as an athlete.
Coping with injuries that required four major surgeries and involved extensive rehabs convinced her to enter medical school and become a physician. “I’ve become resilient, and gymnastics has helped with that because you fall a lot and you just have to keep on going,” she said.
Amarachi “Amy” Opara knows firsthand what a debilitating disease can do to a child and family. Starting at a young age and continuing through high school and college, Opara helped care for her younger sister, who has cerebral palsy and other developmental issues, while her mother, a pharmacist originally from Nigeria, worked long hours to support the family.
“It’s what brought me to medicine,” said Opara. “It all stems from growing up with a sister with special needs.”
The unexpected illness and death of two mentors in Eric Yang’s formative years propelled him into a medical career. A gifted clarinetist, Yang was devastated by the death from cancer of a teacher who had guided him into a prestigious precollege music program at Juilliard. When dementia forced a second mentor into early retirement, Yang’s career focus shifted from music to biomedical science. “I wanted answers to questions like, ‘Why were they taken away from me?’” he recalled.
Yang majored in neuroscience at the University of Pennsylvania, followed by two years as a clinical research coordinator at Children’s Hospital of Philadelphia, where he developed an interest in gene therapies for leukodystrophies. He intends to continue research in medical school.
“The best way to understand the newest developments in rare diseases is to be directly involved,” said Yang ●


On August 1, physician assistant students officially marked their entry into the professional study and practice of medicine during their White Coat Ceremony.
The cohort’s 20 students comprise the tenth class of the Chobanian & Avedisian School of Medicine Physician Assistant (PA) program, which graduated its first students in 2016. Since then, the program has graduated more than 200 students.
PA Program Director Susan White, MD, and Graduate Medical Sciences Assistant Dean of Master’s Programs Theresa Davies, PhD, spoke during the ceremony. Robert Lowe, MD, associate professor of medicine/ gastroenterology, delivered the keynote address.
“Congratulations as you receive your white coats,” Davies told the assembled students. “It’s amazing, and you should be very proud. Congratulations as well to your
parents who have supported you to this point. You should be so proud as well. You have incredible faculty serving you, and you have bright futures. We will be celebrating you and your program all year.”
Davies encouraged the cohort to “explore Boston; be a student, grow and learn.”
In his keynote address, Lowe described the White Coat Ceremony as the start of a great journey and an invitation to work hard throughout what will be a challenging, but worthwhile, curriculum and career.
“Nothing that’s worthwhile is easy,” he said. “The program is tough. When you’re done, it’s still tough. But you’re going to step up and do it.”
Ultimately, Lowe reminded them, the white coat is a symbol. “You will be the person to help when needed. On the days you’re not wearing [the white coat], you’ll still be the person to step forward.”
He also told the class they will gain a unique perspective on life.
“The things we do are incredible, but also an incredible privilege.”
Each student joined the PA faculty individually to receive their white coats as Associate Director of Clinical Education Michael Smith, MS, PA-C, announced names. Students were coated by Dan Tzizik, MPAA, MPH, PA-C, and Robert O’Brien, MHS, PA-C, both associate directors of didactic education for the program.
After being coated, students were led by Class of 2024 President Elise McIntosh, PA-S, in reciting the Physician Assistant Professional Oath invoking the professional and ethical responsibilities they will honor throughout their careers as physician assistants.
“Congratulations on taking your first step to joining the PA profession,” White concluded. “You are our tenth class, and this is a wonderful milestone for us. We are very happy to have you here and look forward to getting to know you.” ●
Applications for the master’s in Mental Health Counseling & Behavioral Medicine program have skyrocketed. Now in its 25th year, the program until fairly recently averaged 90–100 applicants annually for approximately 30–40 spots. Since 2017, the number of applicants has significantly increased, reaching 626 for 48 spots in the 2025 entering class.
“It’s become wildly competitive,” said Laurie Craigen, PhD, associate professor of psychiatry and assistant director of the program. She fully expects applications will top 700 during the next admissions cycle.
The increase is partly due to a demand/ supply issue. A 2022 Kaiser Family Foundation/CNN survey found that 90% of the public believes there is a mental health crisis in the United States, and one-third of respondents reported that they couldn’t get the mental health services they needed. The US Bureau of Labor Statistics projects a 17% jump in the number of jobs in substance abuse, behavioral disorders, and mental health counselors between 2024 and 2034, nearly six times the average 3% job increase, for all jobs.
“I can’t tell you how much busier I’ve been post-COVID,” said Stephen Brady, PhD, MA, associate professor of psychiatry and a program founder.
Brady, who served as program director for 20 years, said the reasons for the jump in applicants at BU are complex, but unique features of the program make it especially popular.
“We had an initial large jump in appli-

cants in 2013 after we were accredited by the Council for Accreditation of Counseling and Related Educational Programs (CACREP),” said Brady, who also cited contributing factors including more faculty and staff time devoted to recruitment, a growing recognition of the importance of integrated care models, and coursework focused on behavioral medicine. In addition, the program’s medical campus location, affiliation with Boston Medical Center (BMC), and BU’s reputation for research and medical education impress prospective students.
Graduates of the Mental Health Coun-
seling & Behavioral Medicine program find employment as mental health counselors in integrated healthcare, trauma counseling, substance abuse recovery, and private practice.
“I was really attracted to the program because it offered integrated training between medicine and behavioral health. I knew I wanted to work in a healthcare setting, and you need to have that type of training,” said Tasha Ferguson, MA’08, LMHC, senior director of the Behavioral Health Crisis Continuum and executive director of the BEST Center of Excellence, located at BMC.
“Having at least a basic understanding of medication is important because a multidisciplinary team is often going to be master’s level staff and prescribers, nurse practitioners, or psychiatrists. Speaking a similar language, having a similar frame of reference, just puts you so much further ahead, in terms of being able to work together.”
While the stereotype is generally that of a mental health counselor meeting clients one-on-one in an office, mental health, like other health disciplines, is increasingly being integrated into medical settings with teams of physicians and nurses. According to Brady, the program was designed to prepare students to work in clinical settings and incorporates required courses in neuroscience, behavioral medicine, and psychopharmacology. “That’s what differentiates us from the [mental health counseling] programs affiliated with schools of education and social work,” says Brady.
Craigen believes that recent applicants were seeking a more fulfilling work experience.
“I think that we have very impressive people who are drawn to wanting to make a difference . . . and there is nothing more beautiful than being a part of somebody’s healing story,” she said. Students also realize that the path to a mental health counseling career is much shorter than that of a physician. “With a master’s degree, you literally can start your own mental health or behavioral medicine business, and I think that’s a draw for a lot of students.”
Increasing awareness by the public and by the healthcare community of the benefits of mental health counseling, along with its validation through accreditation, has helped open up employment opportunities.
“BU’s program has certainly benefitted from having a solid reputation,” said Jonathan Waldo, MA’14, LMHC, associate director of clinical training for the master’s program. Similar to medical students, master’s candidates in mental health counseling spend half their time in clinical settings. The requirement of 1,000 supervised hours counseling patients is critical to getting licensed. That time is split between a one-semester practicum in the first year and a two-semester internship in the second. Postgraduates are still considered trainees and need two years of supervised work to qualify as a Licensed Mental Health Counselor (LMHC).
While the stereotype is generally of a mental health counselor meeting clients one-on-one in an office, mental health, like other health disciplines, is increasingly being integrated into medical settings with teams of physicians and nurses.
Waldo is responsible for placing students in clinical settings for their practicums and internships, and the program’s success in achieving those placements is also a significant draw for students.
Graduation from a CACREP-accredited program is a requirement for licensing in Ohio, Kentucky, North Carolina, and Florida, and to be hired by the Veteran’s Administration. Graduates from CACREP-accredited programs also meet the educational requirements for licensing in most states
and receive an expedited review for the educational component of LMHC licensing.
“Our program was one of the first to get that accreditation,” said Waldo. “That has been a big draw for informed applicants. Prospective students appreciate that an independent organization has ensured that the education provided to them is aligned with high quality of care, being prepared to succeed, and getting licensure.”
Naomi Szanto, MA’21, LHMC, was looking for just that in a mental health counseling program and said the CACREP accreditation impresses employers.
Szanto works as a behavioral health clinician focused mainly on children’s eating disorders at Lexington Pediatrics, which is affiliated with Boston Children’s Hospital, and like Ferguson, found the science component in the BU program to be an asset.
“Part of the program emphasizes working on a multidisciplinary team,” said Szanto. “At Lexington Pediatrics, I work closely with pediatricians, a dietitian, and a psychiatric nurse practitioner. This collaboration allows us to take a holistic approach to each patient’s care, and I love being able to learn from and understand their perspectives. I’m really not surprised that this program is so popular. I think it offers really great training for clinicians who want to enter the mental health field—and we need them.” ●
Tasha Ferguson, MA’08, LMHC

Building interdisciplinary research careers in women’s health program support will also spur investment in earlycareer faculty
The National Institutes of Health (NIH) has awarded Boston University a $4.5 million grant to further women’s health research and spur career growth for young investigators.
The prestigious five-year award from the Building Interdisciplinary Research Careers in Women’s Health (BIRCWH) program, a NIH-funded research and career development initiative, will connect senior and junior faculty interested in women’s health research.
“The BIRCWH award reflects Boston University’s dual mission: to educate and empower future leaders from all sectors of society and to conduct research that advances knowledge and delivers meaningful societal impact,” says Kenneth Lutchen, BU’s vice president and associate provost for research. “By investing in cross-disciplinary mentorship and discovery, BU is helping to drive a convergent approach necessary to address the challenges in women’s health.”
BU’s BIRCWH grant provides funding for three early-career faculty members per year to participate in a two-year program. They will perform research under the mentorship of senior BU faculty, receive individualized career development support, and participate in regular research meetings and annual conferences. The program will largely focus on the themes of addiction science, maternal and child health, and sex influences on health outcomes. It will be led by Emelia Benjamin, MD, ScM, the Chobanian & Avedisian School of Medicine’s Jay and Louise Coffman Professor in Vascular Medicine and
associate dean of faculty development ad interim, Elisha Wachman, MD’06, a professor of pediatrics at the medical school, and Joyce Wong, PhD, a College of Engineering Distinguished Professor of Engineering. Wachman and Benjamin also hold positions at Boston Medical Center, BU’s primary teaching hospital; Wachman is a neonatologist and vice chair of pediatric academic research, and Benjamin is a cardiologist.
The three lead the Women’s Health Affinity Research Collaborative (ARC) at the BU Evans Center for Interdisciplinary Biomedical Research and say the BU BIRCWH program will boost the number of highly trained scientists tackling issues like maternal and reproductive health, as well as help disseminate more research in women’s health areas.
“Women’s health, including addressing sex-based differences in healthcare, represents one of our most critical challenges,” says Wong, a professor of biomedical engineering and of materials science and engineering whose research focuses on using bioengineering to support maternal and child health. “We are thrilled by this opportunity, because the BU BIRCWH program uniquely integrates engineering, basic science, and clinical translational medicine— perfectly aligning with BU’s mission to tackle major societal challenges. This program, together with ARC, will unite our women’s health research community to accelerate progress in this essential field.”
The grant links multiple BU schools across the Charles River and Medical Campuses, as well as affiliated sites, such as the Veterans Affairs Healthcare System. Almost 30 faculty members have signed on to be BU BIRCWH senior mentors; in addition to ENG and the medical school, mentors from BU’s School of Public Health, College of Arts & Sciences, the Henry M. Goldman School of Dental Medicine, and Sargent College of Health &

“Women’s health, including addressing sex-based differences in healthcare, represents one of our most critical challenges.”
JOYCE WONG, PROFESSOR OF BIOMEDICAL ENGINEERING AND MATERIALS SCIENCE AND ENGINEERING
Rehabilitation Sciences volunteered.
“The BU BIRCWH grant represents an important partnership across multiple BU schools and Boston Medical Center, with the participation of accomplished faculty mentors from across disciplines,” says Wachman, a leader in the field of substance use disorders in pregnancy.
The award represents BU’s second BIRCWH grant; the first ran from 2002 to 2014.
“[These] awards can launch an earlycareer investigator’s research career,” says Benjamin, a widely recognized expert on the epidemiology of atrial fibrillation and other cardiovascular conditions. “In these challenging fiscal times, we are grateful to be able to support the early-career scientists from across BU seeking to improve women’s health across the country.” ●

The group traveled to Malawi as part of BU’s Global Health Summer Scholarship program
In the summer of 2025, four Boston University medical students, Michalina Jadick, CAS’22, MD’28, Jazmine Johnson, MD’28, Brent Leung, MD’24,’28, and Diego López, MD’28, spent a month in Malawi, a landlocked country in southeastern Africa, working to improve water chlorination practices in rural communities
But that’s not the work they had originally planned to do.
The Global Health Summer Scholarship program provides funding for Chobanian & Avedisian School of Medicine students to travel abroad and undertake a research, language immersion, or a community health project in the summer between their first and second years of study. Through the program, these students were set to partner with the nonprofits Bridges to Malawi
and K2 TASO to help distribute Artemisia annua, more commonly known as mugwort or wormwood, in low-resource communities. When it’s ingested as tea, the plant serves as a natural antimalarial treatment.
A few weeks before the students were set to depart, the nonprofits decided to redirect their focus to water treatment rather than antimalarial efforts. That meant the students had to come up with a new project proposal—and fast.
The students received word of the change in May. Their flights were booked for early June.
“In the span of maybe two weeks, all four of us banded together to iron out the details of a new project to resubmit to BU and the National Health Science Research Committee in Kasungu, Malawi, so we would have per-
mission to [do our work there],” Jadick says.
The decision to focus their efforts on drinking water made sense.
Drinking water in Kasungu’s villages often comes from wells, rivers, or ponds, and can contain waterborne illnesses, especially during the country’s rainy season. Adding just a teaspoon of chlorine solution to 20 liters of water renders the water drinkable for 24 hours.
Bridges to Malawi, a US-based organization, and K2 TASO, its Malawian counterpart, work with the local government to distribute buckets of chlorine stock solution to 24 designated health centers across Kasungu. From there, either a representative from a village will pick up the solution and bring it back to the community, or a local health official will pick it up and deliver it to the villages in their district.
The distributions occur roughly twice a month—primarily during rainy season—and are usually accompanied by education sessions on how to use the solution. But because water treatment happens at the household level, results vary widely.
That’s where the students came in.
They interviewed government officials and nonprofit staff to figure out how the chlorine solution was prepared, distributed, and explained, went along on distribution trips, and helped lead education sessions.
From there, the students created a qualitative survey about chlorination practices for Kasungu residents, then used the survey to conduct interviews with 100 residents, with the help of an interpreter from K2 TASO. (The students credit the nonprofit and its director, Peter Minjale, as integral to their
efforts.) The survey’s aim was to establish where breakdowns in the process occurred.
“The goal of our project was to help ensure that folks are able to get chlorine throughout the year, and not just during the rainy season, when [incidents of waterborne] diarrheal illnesses are higher,” Johnson says. “Seeing some of these seemingly small challenges to keeping water clean was really enlightening for both us and the organizations we worked with.”
As the students learned, almost everyone believed in the efficacy of chlorine; the issues were in administration. When treating water with chlorine, you have to stir vigorously, then wait 30 minutes for the chemical to take effect, but not everyone waited the whole 30 minutes—or even knew it was necessary. Some also added too much chlorine, which can be dangerous over time, or didn’t follow anticontamina-

tion practices, like keeping water covered after it was treated. The biggest issue by far, however, was that not everyone knew when and where to find the chlorine.
The students presented the survey they created, plus their initial findings, to K2 TASO, community health officials, the District Health Research Committee of Kasungu, and Rudolf Zinkanda Banda, the District Environmental Health Officer. They also presented it to the National Health Sciences Research Committee of Malawi, a national body that oversees all research operations across Malawi.
Going forward, K2 TASO can use the survey to conduct regular interviews and identify pain points; the data also adds legitimacy to the nonprofit’s efforts. “One of the things we talked about in various meetings was the utility of having formal research done,” Jadick says. “Now, when these organizations go to the government and say, ‘We need more chlorine to give to people,’ they actually have evidence to support why they need it.”
When not busy working on the project, all four students spent time in clinical spaces; K2 TASO conducts regular mobile health clinics in rural communities and director Minjale also works as a physician. As rising second-year medical students, the four couldn’t act as full providers, López says. But they could administer malaria tests, listen to patients’ hearts and lungs, take down medical history, and guide patients through physical exam maneuvers.
“Seeing how medicine is practiced in a low-resource setting was incredibly eye-opening,” Diego López, MD’28, says. “Providers can’t just order a gazillion laboratory tests, or imaging, like we do here. Observing the ways they’ve learned to manage complicated chronic conditions, for example, was incredibly impactful.”
He and his fellow students plan to return to Malawi to continue the work they started this summer. And all say they see themselves going into global health in the future.
“Seeing the beauty and resilience of people who’ve adapted to make the best out of difficult circumstances illuminated something in a way that I can’t really put into words,” López says. “I just know that it’s something I want to keep participating in and learning from.” ●
Vickery Trinkaus-Randall, PhD, professor of biochemistry & cell biology, and ophthalmology, and Steven Borkan, MD, associate professor of medicine, have received the prestigious multi-PI Medical Scientist Training Program (MSTP) grant from the National Institutes of Health (NIH). The five-year, $1.6M award will help recruit, train, and inspire four or more MD/ PhD students a year to become clinician-scientists by providing research and clinical training leading to an MD/PhD. It is the first time BU has received an MSTP grant for its MD/PhD program.
The MD/PhD program’s mission is to educate talented students to become clinician-scientists who solve healthcare challenges and improve human health and prevent disease. Trinkaus-Randall and Borkan codirect the program.
“The BU Medical Scientist Training Program, now partially funded by the new NIH grant, will support our trainees with an extensive mentoring network, supporting infrastructure and innovative programs and the pursuit of long-term careers that dually conduct rigorous research and clinical practice to improve human health,” said Trinkaus-Randall.
“Our courses, mentoring system, and exposure to a unique healthcare setting have enhanced student commitment to clinician-scientist careers, as evidenced by the increased number of recent graduates who have applied and been accepted into physician-scientist training programs and other research-oriented residencies,” added Borkan.
To aid current and future students and enhance the skills of trainees, the researchers have developed a new course, Enterprising, Mentoring, Balance, Resilience & Adeptness in Clinician-Scientist Education (EMBRACE), which will be facilitated by faculty from the mental health counseling program and other BU educators. This new funding allows the Medical Science Training Program to expand and include additional students


The
five-year, $1.6M award will help recruit, train, and inspire four or more MD/PhD students a year to become clinician-scientists by providing research and clinical training leading to an MD/ PhD. It is the first time BU has received an MSTP grant for its MD/PhD program.
Trinkaus-Randall and Borkan believe that EMBRACE will promote the resilience and self-confidence needed to sustain a healthy work-life balance, allowing students to thrive through the stress of long years of training with multiple transitions and avoid burnout.
“Our
courses, mentoring system, and exposure to a unique healthcare setting have enhanced student commitment to clinician-scientist careers, as evidenced by the increased number of recent graduates who have applied and been accepted into physician-scientist training programs and other researchoriented residencies.”
STEVEN BORKAN, MD, ASSOCIATE PROFESSOR OF MEDICINE
Trinkaus-Randall has been funded by the NIH since 1985 for her research on developing a synthetic cornea and corneal wound healing and served on many study sections. Before assuming the position of codirector of the MD/PhD program, she served as director of the Cell & Molecular Biology graduate program and chaired PhD student advising under the Program in Biomedical Sciences.
In addition to his interest in educating medical students and staff, Borkan studies the cellular mechanisms of acute kidney injury and supervises the care of underserved patients. Borkan has received several teaching awards and is the senior author of numerous publications in the pathobiology of acute kidney injury. He has been an active, NIH-funded principal investigator for 25 years. ●
Creating a curriculum for teens, by teens: students from a Roxbury school met with researchers all summer to learn about opioid overdose prevention
All summer of 2025, in a classroom normally occupied by aspiring doctors and healthcare professionals at the medical school, Boston high school students met to build something important. The students, most of them rising seniors at the John D. O’Bryant School of Math & Science in Boston’s Roxbury neighborhood, gathered once a week to cocreate (alongside BU medical professionals) a curriculum meant to teach their peers about drug overdoses: what they are, how to prevent them, how to recognize someone in distress, and what to do about it.
The program they devised—largely built by teenagers, for teenagers—could help fill a critical educational gap, says Sarah Bagley, an associate professor of medicine and pediatrics in the school’s Clinical Addiction Research & Education (CARE) Unit. For adults, Bagley says, treating and preventing opioid overdoses generally means treating drug addiction, too. But this isn’t usually the case when it comes to young people and teenagers, who more often overdose accidentally and aren’t necessarily addicted to opioids.
“We think that some of the risk factors for youth are a little bit different,” says Bagley, who is also a primary care physician at Boston Medical Center (BMC), Boston’s safety-net hospital. “Not as many of them may have opioid use disorder, and therefore may not need treatment to prevent overdose.”
For adults, she says, preventing overdose likely means using methadone and suboxone—medical interventions that help reduce a patient’s withdrawal symptoms and cravings for opioids. But this sort of protracted medical care may not be necessary to treat a young person experiencing an opioid overdose.
“A lot of teenagers are using drugs maybe for the first time or intermittently, and are accidentally or unknowingly exposed to fentanyl. This potent opioid can then lead to an overdose,” she says. “The opportunity to prevent that introduction from happening isn’t necessarily engaging them in treatment—it’s making sure they understand that the drug supply has a lot of fentanyl in it. It’s a different approach.”
The question then becomes how to build an educational model that will reach busy teenagers and also be understandable and approachable. It’s a question Bagley and her colleagues at BMC and the schools of medicine and public health put to the experts: teenagers themselves. They launched an equity-centered, peer-led overdose prevention program at the O’Bryant School, cocreated directly with students, to address this critical public health challenge.

“Our group has been thinking a lot about how to provide more community-based education, so that youth can learn about those risks for themselves, but also so they can talk to their friends and family and other people in their community about overdose,” Bagley says. More than 40 high school students applied to join the program. The researchers narrowed it down to about half that, 17 students.
Throughout the summer, a team of BU and BMC addiction and harm-reduction researchers met with the O’Bryant students to teach them about public health, social determinants of opioid abuse, overdose risk, and more. The students then broke into groups to design an overdose prevention curriculum. One group built a website filled with useful information about the risk factors for overdose; another produced short, catchy videos about how to compassionately confront a friend who may be using drugs; and another designed a presentation on recognizing signs of an overdose and what to do about it.
The students and researchers continue to explore ways to get these robust, peer-designed resources into the hands of Boston students.
“The final products that these students created are amazing,” Bagley says. “They’re educational while still being accessible. They’re just wonderful resources.” ●

Both offer a novel approach that uses art to improve clinical diagnoses, become comfortable with ambiguity
One evening last fall, medical residents from Boston Medical Center (BMC) found themselves on the Charles River Campus in the College of Fine Arts’ quiet, spacious Faye G., Jo, and James Stone Gallery, viewing art ranging from sculpture to contemporary and abstract paintings done by BU art students. The residents were there as part of the VITAL (Visual Thinking & Art in Learning
Medicine) program, a new educational initiative designed to immerse BMC residents and fellows in the language and skills of the arts that translate to the medical field. By using art as the vehicle, early-career physicians can delve into the gray areas of medicine—like observation, interpretation, empathy, and ambiguity.
Using humanities and the arts to educate the next generation of doctors has gained in popularity, and BU is no exception. VITAL
is one of two recently launched programs at BMC—the other is the MANET Project (Museum Art in Neurology Education Training). Both programs create learning experiences that cannot be gained from medical textbooks and hospital shifts.
VITAL began in 2025 and is overseen by Deepthi Gunasekaran, MD, a nephrologist and assistant professor of medicine and Gopala Krishna Yadavalli, MD, an infectious disease expert and clinical associate professor of medicine in collaboration with Lissa Cramer, director of BU Art Galleries. Together, they create interactive, hands-on learning experiences that help foster visual thinking strategies that get young doctors to explore questions like, “What do you see? What do you see that makes you say that?” Yadavalli says. “There’s no right or wrong here. But it is important to understand why we’re thinking the way we’re thinking.”
Led by Pria Anand, MD, an assistant professor of neurology at the medical school and director of the Adult Neurology Residency program at BMC, the MANET Project is a unique collaboration between BMC
and curators at the Harvard Art Museums. Started in 2024 by Tatiana Greige, MD, then BMC chief resident, now a neurohospitalist at MaineHealth Maine Medical Center, the collaboration is the first of its kind, art-based neurology program in the country. After just one semester, the 17 residents in the initial cohort were shown to have dramatically improved their observational skills. The findings, led by Anand, Greige, and other BU colleagues, were published in Neurology Education. The program is now a regular part of neurology training, of which Anand is particularly proud.
“To be a good neurologist, you have to be interested in someone else’s subjective experience to understand the depth of someone’s symptoms, and how those symptoms are affecting their life,” Anand says. “Neurology forces you to contend with how you perceive the world, and there’s a long tradition of using art as a way to understand someone
else’s experience of neurologic illness.” For example, art or drawing can be a way to understand a person’s visual distortion from a migraine or to communicate with someone who has lost their speech from a stroke, or other symptoms that can be difficult or impossible to articulate.
During a recent trip to the Harvard Art Museums, a group of 30 residents was brought to three different works, guided by Jen Thum, Harvard Art Museums’ associate director of academic engagement and campus partnerships and research curator. They stopped in front of a large painting titled Four Stops, by Nina Chanel Abney, an American artist known for works that combine aspects of representation and abstraction. They had 15 minutes to absorb the scene and discuss what they were seeing—people sitting in a subway car, colors dripping and blending, a floating blue face in the shape of a balloon. They then moved on to a gallery filled
with art from ancient Egypt. There, Thum explained the story of a 4,000-year-old tomb relief on display—how it tells the story of the person and family it is memorializing, yet was sawed into pieces when it was taken from the tomb and is now missing information. The group discussed how in the hospital, doctors are often given only pieces of a person’s story and must do their best to understand the full picture. Last, they viewed some of the museum’s photography collection, including Dorothea Lange’s iconic Depression-era black and white photo, Migrant Mother, Nipomo, California.
“This is an incredible program for Boston Medical Center, especially as a safety-net hospital,” Anand says. “We care for a diverse group of patients, and I think to serve that community in a way that provides the best possible care, being empathetic, and being able to see perspectives different than your own is really important.” ●
BMC medical residents view an ancient tomb relief during a recent visit to the Harvard Art Museums. They discussed the importance of interpreting history and understanding individual stories like the one depicted in the damaged relief.


Chelsey Skeete, PhD’25, had a passion for science long before she matriculated into Boston University
Chobanian & Avedisian School of Medicine in 2020
Born and raised in Boston, Skeete remembers participating in science fairs throughout the city and gravitating toward science books, even as a young child. As she progressed through school, teachers and mentors encouraged her to pursue extracurricular outreach opportunities that would bolster her interest in scientific research.
“To be able to research, to ask questions, to be comfortable not knowing things, to explore in the lab—and to have an impact on the community through your findings—was very important to me,” Skeete said.
That drive propelled Skeete’s professional path to STEM, first taking her to Boston College for her bachelor’s degree in biology and then to BU Graduate Medical Sciences for her PhD, where Skeete successfully defended her dissertation in June 2025.
As an undergraduate student in 2019, Skeete joined the summer cohort of BU’s Summer Training as Research Scholars (StaRS), an on-site summer research program that offers academically talented undergraduates an opportunity to work with a faculty mentor on an independent biomedical research project.
After a summer working under Lee Quinton, PhD, in the Pulmonary Center, she knew that the BU Medical Campus was where she wanted to be for the next chapter of her education.
“Everything was just very collaborative,” Skeete said. “All the graduate students had very complex projects, but the campus was set up with all these different cores and labs who were willing to share information and willing to have multilab meetings on a weekly basis.”
Skeete applied to the Program in Biomedical Sciences (PiBS), which offers students the opportunity to rotate through three laboratories during their first year before specializing in their second year, and matriculated in fall 2020.
Her rotations helped Skeete solidify her interest in host-pathogen interactions and she chose to specialize in the department of virology, immunology & microbiology (VIM), joining the lab of Rahm Gummuluru, PhD, professor and vice chair of VIM.
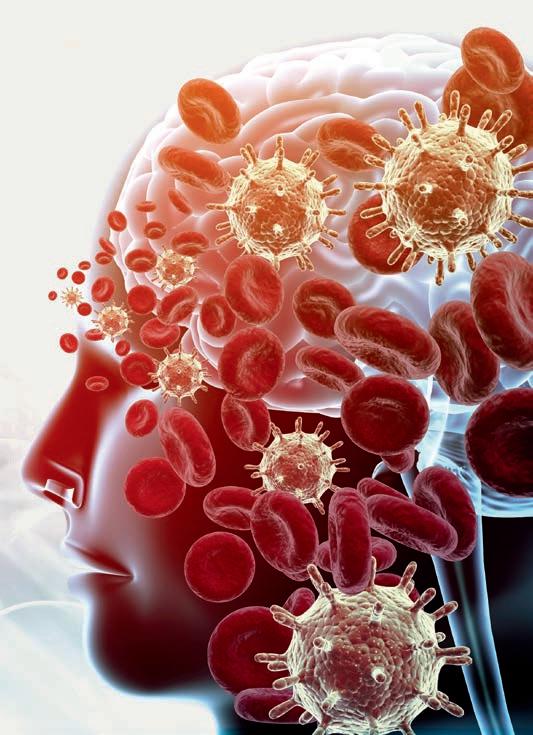
Skeete’s dissertation research focused on the effects of opioids on individuals infected with HIV in the brain.
A new project at the time, Skeete’s research examined how this intersection can impact a person from an immunology lens, and how opioid use with an HIV diagnosis affects inflammation and leads to different neurocognitive disorders.
“People with HIV who are also using drugs or opioids are often overlooked in our healthcare system,” Skeete said. “They often have limited resources, and it’s important that we continue to research the best practices and ways to help them.”
Skeete’s project gave her the opportunity to collaborate with
“People with HIV who are also using drugs or opioids are often overlooked in our healthcare system. They often have limited resources, and it’s important that we continue to research the best practices and ways to help them.”
CHELSEY SKEETE
different labs and cores at the Medical Campus. She worked closely with the lab of Gustavo Mostoslavsky, MD, PhD, in the Center for Regenerative Medicine to cultivate a specific type of brain cell called microglia. Her research findings highlight how opioid treatment enhances multiple stages of HIV-1 replication and virus-induced inflammation in microglia.
“In science, there is always going to be trial and error,” Skeete said, “I’m just very grateful for a team that was willing to stick through the process and be able to look and see how, together, we could improve the overall model until it became a well-established model.”
Skeete presented her research at the Society for Neuroscience Conference in 2023. Her work, “Mu opioid receptor activation in microglia enhances HIV-1 infection and HIV-infection-induced inflammatory responses,” was published in Frontiers in Immunology in October 2025.
“While it’s important to gain those wet lab skills and those analytical and critical thinking skills, it’s also important to learn how to communicate your research to broad ranges of audiences,” Skeete said.
Skeete is also involved in the community, both on and off campus, and volunteers with the National Association for the Advancement of Colored People (NAACP), working with high school students to inspire their passion for STEM through outreach programs.
During her time at GMS, Skeete served as a student liaison to leadership to advocate for student concerns and brainstorm ideas to improve campus culture and build community and a sense of belonging for all student populations. She also returned to the STaRS program as a mentor in 2023 and 2024, where she guided undergraduate students on their research projects and presentations.
Skeete said she values the different mentors and support systems she built throughout her academic journey: “They were key in encouraging me along the way, especially when challenges came and it seemed like the whole world was against what I was trying to do.”
Skeete is ready to move into the next step of her professional career and has accepted a program manager position with Novartis, where she will lead an outreach program in STEM education.
“It’s so important to me that we continue to equip the next generation of scientists, to really teach them how to think as scientists and encourage them in their calling within STEM,” she said. ●

Ann McKee, MD, a William Fairfield Warren Distinguished Professor of Neurology and Pathology, has been selected as the recipient of a three-year, $450,000 Zenith Fellows Award from the Alzheimer’s Association for her project, “Contribution of Microvascular Alterations to Tau Progression in AD and CTE.” Zenith Fellows Awards are among the most prestigious worldwide in Alzheimer’s disease (AD) research
Through her work with the BU Alzheimer’s Disease Research Center and the Framingham Heart Study, McKee helped define microvascular injury and the neuropathology of aging and AD. She is a board-certified neurologist and neuropathologist whose research has significantly advanced scientific understanding of posttraumatic neurodegeneration and CTE.
“Through our prestigious Zenith Fellows Awards, the Alzheimer’s Association is proud to fund researchers making major strides in dementia research,” said Heather Snyder, PhD, Alzheimer’s Association senior vice president of medical and scientific relations. “Dr. McKee’s work reflects the bold, innovative science that moves us closer to breakthrough treatments and, ultimately, a future free of Alzheimer’s and other dementias.”
With funding from Zenith Society members, the program has provided more than $48 million in awards to 152 leading Alzheimer’s researchers in nine countries since 1991. The awards continue to be supported by members of the Alzheimer’s Association Zenith Society, who have an exceptional commitment to the advancement of Alzheimer’s and other dementia research.
Kirsten Austad, MD, MPH, Named National Academy of Medicine Fellow

Kirsten Austad, MD, MPH, assistant professor of family medicine, has been named the National Academy of Medicine’s 2025–2027
James C. Puffer, MD/American Board of Family Medicine (ABFM) Fellow
Chosen for her professional qualifications, reputation and accomplishments, and the relevance of her current field of expertise to the work of the National Academies of Sciences, Engineering, and Medicine, Austad will collaborate with eminent researchers, policy experts, and clinicians from across the country during the two-year fellowship.
Austad joins Alyssa Tilhou, MD, PhD, assistant professor of family medicine, a 2024 recipient. Of the 18 Puffer Fellowships awarded BU over the years, two have gone to the department of family medicine, the only department to have multiple faculty members recognized.

Emelia Benjamin, MD, ScM, FAHA, has received the 2025 Eugene Braunwald Academic Mentorship Award at the American Heart Association’s Scientific Sessions 2025.
Named for legendary cardiologist Eugene Braunwald, the award honors an individual with a sustained record of excellence in teaching and mentoring the next generation of
faculty researchers, educators, and healthcare professionals. Recipients of the award are recognized for their lasting impact on cardiovascular care and research through their extensive mentoring of residents and fellows.
Benjamin is the Jay and Louise Coffman Professor in Vascular Medicine at the School of Medicine and professor of epidemiology at the School of Public Health. She has developed and led ongoing faculty development programs that support early- and mid-career clinicians and researchers from diverse backgrounds. She has also directed multiinstitutional research fellowships supported by the American Heart Association (AHA) and the National Institutes of Health (NIH), including an ongoing international atrial fibrillation genetics fellowship and an NIH K12 program, Boston University Building Interdisciplinary Research Careers in Women’s Health. Her NIH-funded research has focused on atrial fibrillation, mobile health, inflammation, and chronic pain. She has served as principal investigator or coinvestigator for NIH-funded trials continuously since 1998.
Benjamin’s career legacy is reflected in the success of her trainees, many of whom received NIH Career Development Awards reflecting the strength of their mentorship and training and went on to launch numerous careers in cardiovascular research. In her numerous roles at the AHA, Benjamin has advocated for early-career scientists, including serving as former chair of the Council on Functional Genomics and Translational Biology to develop a strong Early Career Committee, participating on many early career panels, and mentoring individual members.
“I am deeply honored to be recognized with this award,” said Benjamin. “Mentoring has been one of the most meaningful parts of my career. There is nothing more fulfilling than seeing my mentees thrive, whether in research, clinical care, or academic leadership. I owe the successes of my career to my mentees. It is especially humbling to receive an award named for Dr. Eugene Braunwald, whose legacy as a mentor and scientist has informed my career and generations of cardiovascular health scientists and clinicians.” ●

BY DOUGLAS FRASER
his first year of
a
it was hard to understand, and commiserating with one of my classmates who told me, ‘Well, you’re in luck because I was born with a congenital heart disease,’” recalls Bergenholtz, now in his third year in the Mount Sinai Internal Medicine Residency Program in New York City.
“She started explaining things to me in a very nuanced way, and I thought, people who have their own experience with illness have this great opportunity to be able to teach it,” he says.
He decided to propose the idea of pairing talks by students who have endured diseases or medical conditions with medical school lectures investigating those topics. With the approval of curriculum course directors, he sent out a request for volunteers to tell their stories and volunteered to share his own medical experience with Crohn’s disease.
“When you’re learning it from somebody who’s lived it you can empathize, and I think you internalize that information a lot better,” Bergenholtz explains. “It’s like learning from real life versus a textbook.”
His idea caught on with students and educators and, five years later, the Students Perspective Initiative (SPI) is a firmly established feature of a BU medical education, with each student
talk drawing 25 to 160 classmates. In July 2025, Bergenholtz, Elyse Olesinski, MD’25, and third-year medical student Sarah Horn published a paper on the program in Medical Science Educator. In November, Horn presented the paper and the program as one of three medical education innovation projects selected by the Association of American Medical Colleges for their annual meeting in San Antonio, Texas.
According to Associate Dean of Medical Education Priya Garg, MD, SPI is both innovative and unique—BU and other medical schools have long brought patients into classrooms to discuss their medical histories, but BU’s program may be the first to have students discuss their own medical conditions.
“It’s definitely different when students see a classmate describing their condition and they get a chance to hear how it impacts the life of someone they can relate to,” says Garg. “There’s something special about hearing your peers talk about what they have experienced in healthcare.”
“These are the kinds of activities that give color and vibrance to a medical education experience,” says Jonathan Wisco, PhD, codirector of Principles Integrating Science, Clinical Medicine and Equity (PISCEs), the academic science curriculum for medical and physician assistant students. “Students
come to BU because that they know these extracurricular activities are going to inform all of the things that they are required to know and do.”
Typically, a call for volunteers goes out in the first few weeks of first- and second-year classes in advance of the shift to more clinical studies, when firstperson experiences are most effective. Once volunteers are selected, instructors are contacted to arrange a time slot immediately following course content, or as close to that as possible. Students are advised on presenting, but ultimately, their talk’s style and content is up to them; some incorporate research and use PowerPoint slides, while others give more personal talks.
“People who want to share their story know what they need or want to say,” says Bergenholtz, who launched a similar program in New York City at the Icahn School of Medicine at Mount Sinai.
Before leaving BU, Bergenholtz passed the torch to Olesinski, then a second-year MD student and now a first-year internal medicine resident at Massachusetts General Hospital.
Olesinski has found that the presentations benefit both the presenters and the students in the audience, and is gratified at how many medical students want to share their medical stories—a process she initially thought would be hindered by privacy concerns.
“I told my own story, and what it came down to was this desire to share what had happened to me,” she says.
As a teenager, Olesinski was diagnosed with atypical hemolytic uremic syndrome triggered by a bacterial infection. The condition causes small blood vessel damage and red blood cell breakdown and can result in kidney injury—with the potential for renal failure and even death. As part of her treatment, Olesinski had a port surgically implanted in her chest to allow medication to be infused directly
“It’s definitely different when students see a classmate describing their condition and they get a chance to hear how it impacts the life of someone they can relate to.”
- Priya Garg, MD, associate dean of medical education

into her bloodstream every two weeks. As someone with the blended identities of both patient and physician, she felt this gave her an enhanced perspective for her interactions with patients.
“I’m interested in specializing in oncology, and in the cancer world people have ports for chemotherapy. We access those ports all the time, and people say that it’s uncomfortable,” says Olesinski. “We might say it’s not that big of a deal, that this person just doesn’t have good pain tolerance. But, unless you’ve personally had a needle stuck in there, you don’t know that it’s actually quite painful.
“I think this program helps us see the bigger picture, to see that our therapies and procedures are not completely without harm or consequences, even if the side effects seem small. It makes doctors more careful, more mindful. It certainly makes
me more patient when I have people bring up their concerns.”
The SPI program fits in nicely with the new curriculum, says Horn, who was in the second class that fully integrated the new approach to learning. “One of the major changes in the new curriculum was the transition from lectures, where you’re sitting and passively listening, to teambased learning, where you learn from your peers.”
Caitlin Neri, MD, MPH, a clinical associate professor and PISCEs codirector, recalls two students, both survivors of childhood cancer, who approached her with the idea of sharing their stories. One had Hodgkin’s lymphoma at age ten; the other had leukemia as a toddler.
“They did it together and it was really special,” says Neri, a pediatric hematologist who teaches first- and second-year medical students.
Neri notes another aspect of the presentations that resonated with students: “The class really liked it because here were these two young people who had these serious diseases as children and had survived and thrived. Obviously, the students who are coming forward to speak are doing pretty well. They’ve come out the other side, and that can be uplifting and positive.”
Presenting is an affirmative experience for the student speakers, too, and often becomes part of their journey to healing.
“People generally said that it was a cathartic experience,” says Bergenholtz. “I think it’s good to be able to share with your peers something that you know deeply about yourself, and to feel that you are helping people like yourself, that next generation of doctors who will be better equipped to help people who have the same illness you have.” ●

“Obviously, the students who are coming forward to speak are doing pretty well. They’ve come out the other side, and that can be uplifting and positive.”
- Caitlin M. Neri, MD, MPH
For patients with major strokes, the time to meaningful intervention is critical; care must be administered within an hour or two. Stroke centers typically have trained personnel, advanced equipment, and a dedicated intensive care unit. But, as recently as a decade ago, Armenia had no stroke centers.
“Today, Armenia has five stroke centers that did not exist 10 years ago,” said BU neurology professor Viken Babikian, MD, a member of the Armenian Stroke Council who has worked with his Armenian neurological colleagues for more than two decades as part of the BU-Armenia Partnership (BU-AMP).

Dr. Aram Kaligian (Boston University), Dr. Kristina Mnatsakanyan (HENAR Foundation), Dr. Ara Arshamyan (associate physician, family medicine department, National Institutes of Health), Dr. Samvel Hayrumyan (RA Ministry of Health Family Medicine Consultant), Dr. Gohar Yerimyan (dean, National Institutes of Health), Dr. Samvel Hovhannisyan (head of the family medicine department, National Institutes of Health), Dr. Alexander Bazarchyan (director, National Institutes of Health), Dr. Jeffrey Markuns (Boston University), Mrs. Yelena Abovyan (director, HENAR Foundation), Dr. Arman Voskerchyan (cofounder, HENAR Foundation).
Initiated by Aram Chobanian, MD, in 1991 when he was dean of the medical school, the BU-AMP has been reinvigorated by some additional funding from Pamela and Edward Avedisian, part of Edward Avedisian’s $100 million gift to the medical school.
Recently, BU-AMP Director Aram Kaligian, MD, MPH, an assistant professor of family medicine, teamed up with Jeff Markuns, MD, EdM, director of BU’s Global Health Collaborative, to shore up primary care in Armenia by deploying a capacity-building template that the collaborative has employed successfully in other countries.
Primary care is widely considered the gatekeeper for a healthcare system. Studies have shown that a robust primary care system improves healthcare access and reduces child mortality and incomebased mortality disparities at a relatively low cost.
BU-AMP recently launched two new programs, the Rural Family Medicine Fellowship in 2024 that provides additional training to new doctors
working in rural areas of Armenia, and the Master’s Degree in Health Professions Education program, focused on training healthcare leaders and medical school faculty on effective medical education pedagogy.
Armenia is a landlocked country of approximately three million people, nearly two million of whom live in cities and the rest in rural mountainous areas.
The country has a relatively high level of life expectancy of 75–76 years.
“But if you look deeper, the level of noncommunicable diseases— cardiovascular disease (CVD), pulmonary diseases, diabetes, and cancer is depressing,” said Arman Voskerchyan, MD, cofounder of key BU local partner Health Network for Armenia (HENAR).
Cardiovascular disease, cancer, and diabetes account for 75% of all deaths.
“Significantly higher than in other countries,” said Voskerchyan, who attributed this to behavioral risk factors like smoking and diet that could be addressed with patient education and early diagnosis in primary care settings.
But Armenian medical schools produce too few primary care doctors to meet the need, and graduates are generally inexperienced with patient interactions and care, said HENAR CEO Yelena Abovyan. These schools train physicians using a curriculum that emphasizes academics but largely lacks hands-on experience with patients.
“Armenia’s healthcare system is highly focused on hospital care, with less attention paid to prevention and primary care,” added Voskerchyan.
“Physicians and nurses are unevenly distributed across the regions, especially in remote regions, and medical education is inadequate to address the current challenges in healthcare.”
Working with the ministry of health and HENAR, BU-AMP built a hybrid version of the Master’s Degree in Health Professions Education program Markun developed at BU to introduce curriculum development skills to Armenian medical residency program leaders, with the goal of expanding curriculum development training into a competency-based
medical education system similar to that of the US.
Alvard Hovhannisyan, MD, has been a practicing physician in the capital city of Yerevan for 18 years. An associate professor of infectious diseases at Yerevan State Medical University, she is enrolled in the new master’s program that held its first sessions in September 2025. She will take BU’s online courses for a year, participate in three workshops, and then spend six weeks at Boston University in the summer of 2026.
“I really gained a lot of basic and very deep knowledge as a medical student, but practical work was lacking,” said Hovhannisyan. “We went to departments, we saw how doctors manage patients, how they performed some procedures, but we never did it ourselves.”
Armenian medical residents are not paid a salary and tend to gravitate towards more lucrative specialties.
According to Abovyan, while 30–40% of US students go into primary care, just 10–15% do so in Armenia, meaning there are fewer family and primary care physicians to staff rural clinics and an overcrowding of specialists in cities. Moreover, those that do choose to work in rural areas tend to be so inexperienced
with patient diagnosis that clients travel long distances to see veteran doctors in city hospitals.
Partnering with the Armenian Ministry of Health, HENAR, and other institutions, in the spring of 2024 BU-AMP launched the Rural Family Medicine Fellowship (RFMF) program, recruiting faculty from experienced physicians working in rural clinics who were then trained in competency-based medical education.
The fellows—nine newly graduated family medicine physicians assigned to rural clinics—were instructed in a six-week intensive healthcare academy followed by weekly lectures and workshops.
In the fall of 2024, the RFMF fellows participated in rotations at faculty member clinics to improve their diagnostic interactions with patients.
“The classroom-style learning that had been taught in previous decades often answered the question, ‘What do you know?’” explained Henry Louis, MD, director of the Armenian Rural Health Family Medicine Fellowship initiative and master’s in Health Professions Education (MPHE) program. “We’re trying to introduce, and Armenian universities are trying to adopt, ‘What can you do? What is your competency?’” to translate something read in a book to real-life patients.”

“For family doctors in rural regions, the main goal is to keep them there, and to give them more physician and leadership skills,” said Marina Melkumova, MD, a pediatrician and core faculty member in the RFMF program.
“It’s been about one year for the Rural Family Medicine Fellowship program, and you can see these changes,” she said. “The physicians have become more confident, more skilled.”
A second group of rural family medicine fellows began in October 2025. When the initial class graduates in 2026, they will teach new cohorts of primary care physicians, staffing clinics in some of the most remote and underserved areas of Armenia.
“We brought them together to learn leadership skills; to learn quality improvement, medical skills, and understanding. We walk them through clinical cases, show them how to run their clinic, how to be leaders,” said Louis, “It’s a holistic approach towards supporting doctors who otherwise wouldn’t have much support.”
Abovyan believes that Armenia’s relatively small population works in its favor when it comes to retraining the 800–1,000 medical faculty in a medical competency curriculum; instead of a thesis, the healthcare master’s degree candidates are required to train 20–30 faculty members each in 20 “train-thetrainer” workshops. As the program progresses, the number of those who have been retrained goes up logarithmically.
“You don’t need to do many years of producing multiple cohorts of graduates. We consider three to five cohorts, and you’ll have reached this critical mass,” she said.
“What we’re trying to do is invest in those people who are going to be the movers down the road,” said Markuns of the master’s students. “Medical educators and primary care physicians are rarely sitting in positions of power. If we can train these champions who really have that experience of seeing what’s happened in the US, they become the people that the technocrats and the ministry of health turn to for help.” ●

In what is believed to be the first review to summarize evidence on the effect of unconditional cash transfers (UCTs) on postpartum health outcomes in the US, researchers have found strong evidence that UCTs increase breastfeeding rates and result in little to no difference in postpartum mood.
“UCTs provide low-income parents with the ability to cover expensive costs following childbirth, which can ease financial strain and allow more time to rest and bond with their baby. Healthier parents and children mean fewer hospital visits, better child development, and stronger families, all of which can save the public money in the long run and build healthier, thriving communities,” explained corresponding author Mara Murray Horwitz, MD, MPH, assistant professor of medicine.
The researchers reviewed research articles to see how different types of UCT programs—including social programs such as tax credits, disability benefits
Based on their review in the Annals of Internal Medicine, the researchers concluded that UCTs increased breastfeeding across a variety of different settings and populations.
from Social Security, and direct cash transfers—affect postpartum (0–2 years after delivery) health outcomes in the US. After finding all eligible articles, they conducted a dual-data extraction, followed by a study quality and strength-of-evidence assessment for each eligible article. Ultimately, they found 11 reports from six studies. Four of these studies analyzed three social programs, and two were experiments that gave cash directly to low-income people after giving birth.
Based on their review in the Annals of Internal Medicine, the researchers concluded that UCTs increased breastfeeding across a variety of different settings and populations. Breastfeeding can improve maternal health in many ways, such as lowering the risks of future high blood pressure, diabetes, breast cancer, and ovarian cancer. “Future studies should examine more closely the mechanisms by which UCTs increase breastfeeding, and any other factors that play into it such as work or childcare, so that interventions can be designed for maximum impact,” said Murray Horwitz. ●
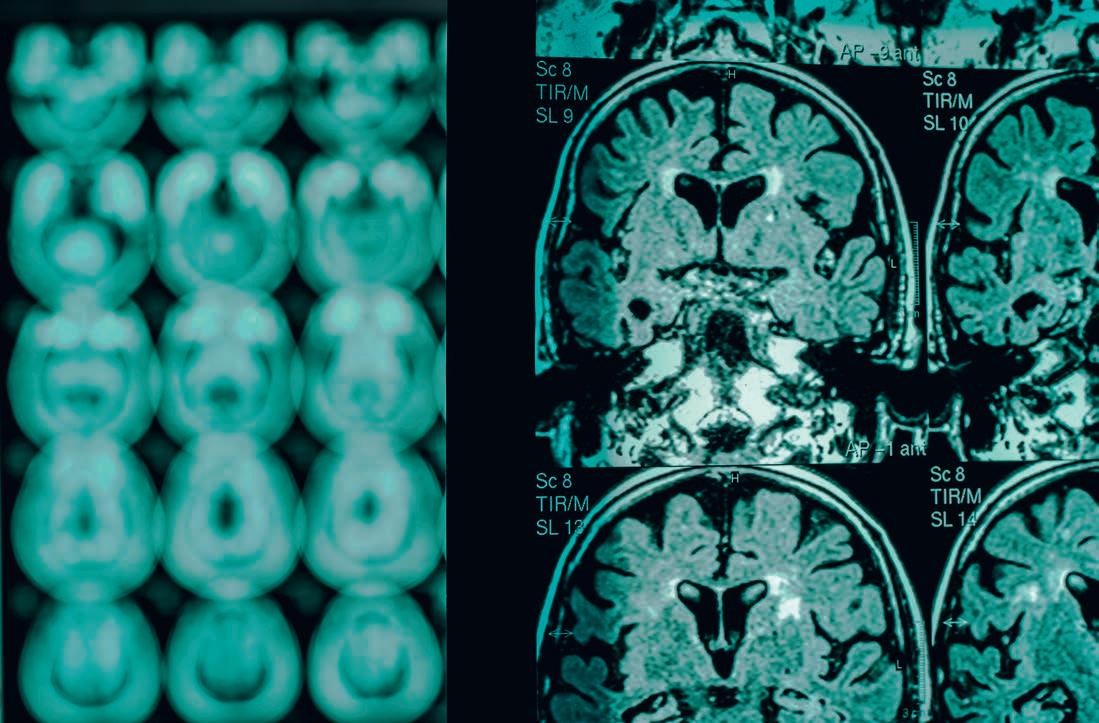
Researchers have built an artificial intelligence (AI) tool that can accurately predict key signs of Alzheimer’s disease (AD)—such as the presence of sticky proteins called amyloid beta and tau—using common and less expensive tests like brain scans, memory checks, and health records.
“We used data from multiple international research cohorts, allowing us to predict the presence of these sticky proteins, even checking specific brain areas,” explained corresponding author Vijaya B. Kolachalama, PhD, FAHA, associate professor of medicine and computer science. “While popular new blood tests can somewhat detect signs of Alzheimer’s, they can’t reveal exactly where in the brain the issues are occurring—unlike our AI tool, which provides important, location-specific detail.”
Kolachalama and his team gathered information from seven different cohorts totaling 12,185
Kolachalama believes this breakthrough could make checking for AD easier and less costly for everyone.
participants including age, health history, memory test scores, genetic information, and brain scans. They trained an AI model on this data to learn patterns that match the presence of sticky proteins seen in expensive scans and even designed the model to work if some of the information was missing. They then tested it on a separate group of people not used in training and found that the AI correctly predicted who had high amyloid or tau levels. These findings appeared in the journal Nature Communications
Kolachalama believes this breakthrough could make checking for AD easier and less costly for everyone. “The tool can help doctors quickly pick people for treatment with new drugs or to participate in research studies, thus saving time and money while reaching more patients who might not have access to costly and complicated tests. For the public, this means faster diagnoses, fewer unnecessary exams, and hope for treatments that slow the disease, improving daily life for those affected and their loved ones,” he said. ●

A study published in Nature has revealed a cascade of repetitive head impact (RHI)-related brain injuries resulting in brain cell loss, inflammation, and vascular damage in young former contact sport athletes. Notably, many of the changes were seen in athletes before the onset of Chronic Traumatic Encephalopathy (CTE).
“These results have the potential to significantly change how we view contact sports. They suggest that exposure to RHI can kill brain cells and cause long-term brain damage, independent of CTE,” said corresponding author Jonathan Cherry, PhD, assistant professor of pathology & laboratory medicine and director of the digital pathology core at the BU CTE Center.
To identify the earliest changes from RHI, researchers performed single nucleus RNA sequencing on the frozen human brain tissue from 28 men between the ages of 25 and 51. They were divided into three groups: a control group of eight men who didn’t play contact sports; an RHI group comprising eight American football players and a soccer player, none of whom were diagnosed with CTE; and a CTE group of 11 contact-sport athletes with low-stage (defined as Stage 1 or 2) CTE. All results were further validated and confirmed in larger sample sets and through comparison to other published studies.
The study showed similar levels of vascular injury and inflammation in athletes without CTE, suggesting that RHI-related brain injury is not solely dependent on CTE.
“This groundbreaking study shows that repetitive hits to the head, including concussions and the more frequent nonconcussive impacts, cause brain damage in young people even before CTE. These findings should serve as a call to reduce head hits in contact sports at all levels, including youth, high school, and college,” said coauthor Ann McKee, MD, director of the BU CTE Center and William Fairfield Warren Distinguished Professor of Neurology and Pathology. ●

Despite progress in recent decades to reduce the burden of cardiovascular disease (CVD), it remains the leading cause of death in the US and worldwide. Data within the past 10 years indicates deceleration and reversal of declines in CVD morbidity and mortality, trends that may be further accelerated by the prevalence of low heart health, particularly among young adults.
A study in JAMA Network
Open has found that among young adults, unfavorable patterns of heart health through young adulthood were associated with increased risk for CVD later in life.
A study in JAMA Network Open has found that among young adults, unfavorable patterns of heart health through young adulthood were associated with increased risk for CVD later in life.
“While research has begun to characterize cardiovascular health in young adults and its long-term association with premature cardiovascular disease, few studies have examined longitudinal patterns of heart health in young adulthood,” explained corresponding author Donald Lloyd-Jones, MD, ScM, professor of medicine and director of the Framingham Heart Study.
In 2022, the American Heart Association introduced the concept of Life’s Essential 8 (LE8) as a way for people to assess their current heart health and to find ways to measurably improve it by making simple lifestyle changes. The researchers looked at the LE8 scores of several thousand young adults starting at age 18 who were part of the Coronary Artery Risk Development in Young Adults/ CARDIA study, observing how the scores changed over 20 years, and then, how those patterns related to poor outcomes such as heart attacks and strokes in the subsequent 20 years. They found that those whose LE8 scores were always high were at very low risk for later heart attacks and strokes, those who started with only moderate heart health and maintained it over time were at twice the risk, and those who went from moderate to low heart health over time were at 10 times higher risk for heart attacks and strokes. ●

The prevalence of Alzheimer’s disease (AD) is approximately two times higher in African Americans (AA) compared to White/European-ancestry (EA) individuals living in the US. Some of this is due to social determinants of health such as disparities in healthcare access and quality of education, biases in testing, and higher rates of AD risk factors such as cardiovascular disease and diabetes in those who identify as African American.
In the largest AD study conducted in brain tissue from AA donors, researchers have identified many genes, a large portion of which had not previously been implicated in AD by other genetic studies, to be significantly more or less active in tissue from AD cases compared to controls. The most notable finding was a 1.5-fold higher level of expression of the ADAMTS2 gene in brain tissue from those with autopsy-confirmed AD. These findings appeared online in the journal Alzheimer’s & Dementia
According to the researchers, this study is an important step in deciphering the genetic architecture and underlying mechanisms of AD risk in African Americans.
Using solicited specimens from 14 NIH-funded AD research centers across the country, the researchers generated and evaluated gene expression data derived from postmortem prefrontal cortex tissue from 207 AA brain donors (125 pathologically confirmed AD cases and 82 controls). They found the most significantly differentially expressed gene, ADAMTS2, was also the top-ranked gene in an independent study conducted by the same research team in brain tissue from a much larger sample of EA individuals.
“To our knowledge, this is the first time in similarly designed AD genetics studies that the most significant finding was the same in both white and African Americans,” said corresponding author Lindsay A. Farrer, PhD, chief of biomedical genetics at the school.
According to the researchers, this study is an important step in deciphering the genetic architecture and underlying mechanisms of AD risk in African Americans, considering evidence that nearly all the established AD risk variants are population-specific or have divergent frequencies across populations.●
With great appreciation, the Boston University Chobanian & Avedisian School of Medicine recognizes our donors for their contributions this past year. Their generosity supports the vital study and practice of medicine and research, and we deeply value the impact they have made on the school, on our students, and on our research.
GIVING LEVELS:
$100,000–$249,999 Bronze members
$250,000–$499,999 Silver members
$500,000–$999,999 Gold members
$1,000,000+
Platinum members
Keefer Society Recognition
• Invitation to the annual Chester S. Keefer, MD Society Dinner
• Honorary prism
■ 2025 Donor
■ Deceased
■ New Keefer Member
KEEFER SOCIETY CLASS OF 2025 INDUCTEES:
Platinum Level: Monita Lam
Bronze Level:
Mary C. Buletza, CPA, and Reverend Gary J. Breton
Larisa E. Connors, MD’98, and John M. Connors III
Dr. Helmuth Josef Resch
Ronda A. Rockett, MD’98, and Sean E. Rockett, MD
This year, the FY25 (July 1, 2024, to June 30, 2025) Chobanian & Avedisian School of Medicine donor rosters are available online. In this issue, only the Dean’s Advisory Board and the Chester S. Keefer, MD Society are listed. For a complete list of FY25 donors, including all individual and foundation giving, please scan the QR code above or visit our website at bumc.bu.edu/camed/giving/who-gives
The Chester S. Keefer, MD Society • The society is named in honor of Dr. Chester S. Keefer, a distinguished physician scientist who served as chairman of the Department of Medicine, dean of Boston University Chobanian & Avedisian School of Medicine, and director of Boston Medical Center. Keefer was responsible for laying the foundation for the medical center and as the dean of the school, he established a tradition of cutting-edge research that continues to this day.
The Chester S. Keefer, MD Society recognizes individuals whose personal philanthropy has helped advance the school by supporting the research and educational mission of Chobanian & Avedisian School of Medicine. In memory of Keefer, we honor the outstanding generosity of donors whose lifetime contributions to the school have reached $100,000 or more.
PLATINUM
Joel J. Alpert ■ and Barbara W. Alpert (SPH’79) ■
Edward Avedisian (CFA’59,’61, HON’22) ■ and Pamela A. Avedisian (HON’23)
Merwyn Bagan (CAMED’62, SPH’95) and Carol J. Bagan
Jag Bhawan and Pratibha G. Bhawan
Nancy L. Bucher ■
Howard D. Buzzee ■
Richard J. Catrambone (CAMED’92) and Sophia Catrambone ■
Shamim A. Dahod (CAMED’87, CGS’76, CAS’78) and Ashraf M. Dahod ■
Richard H. Egdahl, MD ■ and Cynthia Taft (GRS’77) ■
Ralph G. Ganick (CAMED’67, CAS’67) and Lois B. Ganick ■
Alan Gerry and Sandra Gerry
Jonathan P. Gertler (Questrom’99) and Jane R. Clark ■
Albert M. Ghassemian ■
Audrey & Martin Gruss Foundation
Lewis Heafitz and Ina B. Heafitz
Rod F. Hochman (CAMED’79, CAS’79) and Nancy J. Hochman (SAR’77,’83) ■
Stephen R. Karp (CAS’63) and Jill E. Karp ■
Sarkis J. Kechejian (CAMED’63) ■
Stanley H. Konefal (CAMED’47) ■ and Catherine M. Konefal ■
Monita Lam ■ ■
Sherry M. Leventhal and Alan M. Leventhal (HON’09)
Inez Lopez ■ Frank J. Miselis (CAMED’45) ■ and Theodora T. Miselis ■
Carl A. Olsson (CAMED’63) ■ and Mary D. Olsson
Peter T. Paul (Questrom’71)
Jerome S. Serchuck ■ and Joan S. Serchuck
Richard C. Shipley (Questrom’68,’72, HON’22) ■
Wesley R. Skinner ■ and Charlotte A. Skinner ■
Jack N. Spivack ■
Christine E. Stiefel ■
Helen L. Tarlow ■ and Sherwood J. Tarlow ■
Diane Tauber and Laszlo N. Tauber ■ GOLD
Norman W. Alpert and Jane D. Alpert
Karen H. Antman and Elliott Antman ■
Nancy Baler for G. Robert Baler (CAMED’50, CAS’47) ■
Anita B. Barkan (CAS’46) ■ and Donald B. Barkan (CAMED’45) ■
Paul C. Burke and Gloria J. Burke ■
Elizabeth C. Dooling (CAMED’65) ■
George A. Finley III and Phyllis A. Finley
Harold M. Ginzburg (CAMED’68, CAS’68) and Jenny Boyer ■
John L. Hall II (CAS’65) and Ann T. Hall
Joseph J. Konefal (CAMED’77) and Karen G. Konefal ■
Joseph B. Mizgerd and Ann F. Mizgerd ■ ■
Paul F. Nace, Jr.
Tania J. Phillips and Jeffrey S. Dover ■
Joelyn L. Rohman and Michael Rohman (CAMED’50) ■ ■
Albert Rosenthaler and Debbie Rosenthaler ■
Paul Rothbaum and Jean Rothbaum ■ Elayne Russek ■
Thomas J. Ryan ■ and Nancy T. Ryan Robert E. Schiesske (MET’78, Questrom’82) ■
Lee B. Silver (CAMED’82, CAS’82) and Rachelle L. Silver ■ Sumner Stone (CAMED’58) and Martha Skinner ■ Deborah W. Wilson (GRS’72) and John Wilson ■ Andrew Yee and Mirta Yee ■
SILVER
Erika Ebbel Angle (CAMED’12) and Colin Angle
William Y. Au (CAMED’55, CAS’51) ■ and Beverly N. Au ■
Donna R. Barnard (CAMED’65) and Douglas E. Barnard (CAMED’65) ■ Gerald Besson (CAMED’50) ■ and Eleanore S. Besson ■
Mary Ann Blount and James A. Blount, Jr. Helen L. Burr ■ and George Burr ■
David J. Caron and Susan M. Caron ■
Lin Castre and Abraham D. Gosman ■ Richard J. Cavell (CAMED’61) and Bonnie Cavell ■
Ann C. Cea (CAMED’67) and Anthony Tedeschi ■ Aram V. Chobanian (HON’06) ■ and Jasmine Chobanian ■
Andrew B. Crummy, Jr. (CAMED’55) ■ and Elsa E. Crummy ■
Jodi Dome Linger and Nicholas T. Linger ■ Idea S. Fiering ■
Frederick L. Fox (CAMED’68) and Gail P. Fox ■ ■
Laurie Girand and Scott McGregor
Burton P. Golub (CAMED’65) and Lee H. Golub ■
Robert C. Green and Sally E. McNagny
David T. Greenleaf (CAMED’65) and Katherine O. Greenleaf
Marvin J. Hoffman (CAMED’47) ■
Hideo H. Itabashi (CAMED’54, CAS’49) ■ and Yoko O. Itabashi ■
Donald M. Kaplan (CAMED’73) and Edna E. Kaplan (COM’88) ■ Denise S. Katsaros (Wheelock’69) and Arthur T. Katsaros ■ Reshma Kewalramani (CAMED’98, CAS’98) and Abhijit R. Kulkarni (ENG’93,’97) ■ Lenore Larkin and Harold S. Larkin ■
Patricia M. Leavitt (CAS’54, CAMED’58)
Susan E. Leeman
Henry T. Lew (CAMED’62) and Winifred Lew ■ ■
Douglas N. MacInnis (CAMED’46) ■
Barry M. Manuel (CAMED’58, CAS’54) and Patricia D. Manuel (SON’78, Wheelock’86) ■
Rita Z. Mehos
Steven A. Miller (CAMED’70, CAS’70) and Jacqueline H. Miller (CAS’70) ■ John H. Nichols, Jr. ■ Simon C. Parisier (CAMED’61) and Elaine S. Parisier ■ Peter E. Pochi (CAMED’55) ■
Jeffrey D. Tripp and M. Douglass Poirier (CAMED’76, CAS’73) ■ Allen Questrom (Questrom’64, HON’15) and Kelli Questrom (HON’15) ■ Ronald L. Ragland (CAMED’82) ■ Martin S. Rifkin (Questrom’82) and Judy A. Rifkin ■ Alexander M. Rodger ■ Paulette Samowitz ■
Richard D. Scott and Mary Scott ■ Ethan M. Shevach (CAMED’67, CAS’67) and Ruth S. Shevach ■ Louis W. Sullivan (CAMED’58, HON’90) and E. Ginger Sullivan ■ Mary U. Taylor ■ A. Raymond Tye (Questrom’47) ■ Martin L. Vogel (CAMED’53) and Phyllis M. Vogel
Arthur B. Wein (CAMED’39) ■ Madeline WIkler and Joseph M. Wikler ■ Amber Wong
Arnold Wong, Jr.
Jeremiah O. Young (CAMED’62) ■ and Beverly A. Young
Lily M. Young (CAMED’65) and John G. Johansson ■ The Family of Alan Ziskind ■ BRONZE Anonymous (4)
Carmela R. Abraham and Menachem E. Abraham
Winston D. Alt (CAMED’80) and Deborah A. Gribbon ■ Rahul S. Anand (CAMED’01, CAS’97) and Meredith Anand ■
Gerhard R. Andlinger ■ and Jeanne D. Andlinger
Michael L. Apuzzo (CAMED’65) ■
John T. Avellino and R. Ellen Avellino ■
Ruth M. Batson (Wheelock’76) ■
Robert M. Beazley ■
Melvin R. Berlin ■ and Randy L. Berlin
Deb Boedicker and Mackenzie Boedicker ■
David G. Bradley and Katherine B. Bradley
Yvonne K. Brockman and Stanley K. Brockman (CAMED’55) ■ ■
Alan J. Brody
Elizabeth R. Brown ■
Mary C. Buletza, CPA and Reverend Gary J. Breton ■ ■
Lisa B. Caruso (SPH’99) ■
Robert D. Champion and Marjorie Champion
Harold N. Chefitz (COM’55, CGS’53) and Charlotte M. Chefitz ■ Hsi-Pin Chen (CAMED’96,’96, CAS’89, SPH’91) and Kenneth E. Hancock (ENG’92,’01)
Yi-Chuan Ching (CAMED’58) and Helen Yu-Ching ■ ■
David J. Chronley (CAMED’74) and Marianne K. Chronley ■
Patricia A. Connolly (CAMED’84) ■
Larisa E. Connors (CAMED’98) and John M. Connors III ■ ■
Michael J. Critelli and Joyce M. Critelli
Suzanne Cutler (Questrom’61)
Clare L. Dana (CAMED’69)
R. Gordon Darby ■
Paul R. Dooling ■ and Sandra A. Danussi
David R. Edelstein (CAMED’80) and Eve L. Edelstein ■
E. Elaine Erbey (Wheelock’72)
Joseph S. Fastow (CAMED’70) and Ellen K. Fastow
Maurice R. Ferré (CAMED’92, CGS’81, SPH’92) and Maria D. Ferré
Joseph T. Ferrucci and Brenda Ferrucci
Samuel Finkielsztein and Gala Finkielsztein
Charles N. Freed ■ and Marlene Freed
Patricia L. Freysinger (SON’82)
Ronald S. Gabriel (CAMED’63) and Pamela Hobbs ■
Shahram S. Gholami (CAMED’96) and Neda Gholami ■
The Ginwala Family ■
Godley Family Foundation
Malcolm Gordon (CAMED’48) ■ and Nan Miller
Donald J. Grande (CAMED’73) and Elena M. Grande ■
Jack C. Guden ■
Haynes Family Foundation ■
Lea Highet and Ian Highet
Michael F. Holick and Sally A. Holick ■ Betsy E. Horen ■
Thomas R. Insel (CAMED’74, CAS’72, HON’20) and Deborah J. Insel (Wheelock’71)
Jeffrey R. Jay (CAMED’83, CAS’83) and Mary Ellen A. Jay ■
Earl G. Kendrick, Jr. and Randy Kendrick
The Kessler Family
Nasir A. Khan ■
Elaine B. Kirshenbaum (CAS’71, Wheelock’72, SPH’79) ■ and Howard D. Kirshenbaum ■
Shirley P. Klein (CAMED’68, CAS’68) ■
Rose Ann Kornfeld and Lewis F. Kornfeld, Jr. ■
Lawrence E. Langsam (Questrom’57) and Hannah S. Langsam
Estella I. Leach ■
Richard S. Leghorn ■
Ruth R. Levine ■ and Martin J. Levine ■
Rita E. Loos ■
Philip H. Lovett and Beatrice Liu ■
James H. Lowell II and Susan W. Lowell
The Estate of Lillian A. Luksis
Jules N. Manger (CGS’66) ■ and Janis G. Manger ■
Rocco S. Marino (CAMED’42) ■
Allan P. Markin and Patricia Markin
Hubert W. McDonald and Ann S. McDonald ■
JoAnn McGrath ■
Robert B. Melikian (CGS’60, CAS’62) ■
Robert Miselis and Cynthia Miselis
Ruth A. Moorman (CAS’88, Wheelock’89,’09) and Sheldon N. Simon
Charles Mosesian ■
Peter J. Mozden (CAMED’53) ■
Carolann S. Najarian (CAMED’80) and K. George Najarian
John Noble ■ and Ewa Kuligowska
Wilson Nolen and Eliot Nolen
Zein E. Obagi and Samar A. Obagi
Paul I. Ossen (CAMED’43) ■
William Patty and Eliot Patty
Louise E. Penta and P. A. Penta (CAMED’51) ■
Carol C. Pohl (CAMED’67) and Alan L. Pohl
Theodore Polos (CAMED’47) ■ and Jean Polos
Dr. Helmuth Josef Resch ■ ■
Ronda A. Rockett (CAMED’98) and Sean E. Rockett, MD ■ ■
Elihu Rose and Susan W. Rose
Doris M. Russell and Robert F. Russell (CAMED’46) ■ ■
Ralph L. Sacco (CAMED’83) ■ and Scott Dutcher
David J. Salant and Anne Salant
The Schulze Family
Charles L. Schwager (Questrom’66) and Evelyn C. Schwager (Questrom’66)
Richard Seeborg
Florence Seldin ■ and Ira L. Seldin ■ Leslie K. Serchuck (CAMED’90) ■
Muriel Shapiro and Arnold Shapiro ■
William F. Shields (CAMED’94, GRS’90) ■
The Shooshan Family ■
Stuart E. Siegel (CAMED’67, CAS’67) ■
Barry E. Sieger (CAMED’68) and Margarete Sieger ■
John Silber (HON’95) ■ and Kathryn U. Silber (HON’01) ■
Charles W. Smith and Hazel Smith ■
Gordon L. Snider ■
Edward Spindell (CAMED’53) ■ and Judith K. Spindell
Eliot B. Stewart and John M. Stewart ■
Elliott H. Sweetser (CAMED’43) ■ and Aileen B. Sweetser ■ Nevart Talanian ■
Gloria P. Talis ■ and George J. Talis (CAMED’50) ■
Alfred I. Tauber and Paula Fredriksen
Gerald Treece and Patricia Treece
Yolande Tsampalieros and Gabriel Tsampalieros ■ Marian A. Vita ■
David L. Walton (CAMED’83) and Machiko Nakatani ■ Burton White (CAMED’61) ■ and June S. White
Marcelle M. Willock (Questrom’89) ■
Henry R. Wolfe (CAMED’45) ■ and Grace A. Wolfe ■ Herbert H. Wotiz ■
Sam S. Wu (CAMED’92, CAS’87, GRS’90, SPH’92) and Patricia C. Tsang (CAMED’92, CAS’92, GRS’92)
Lawrence A. Yannuzzi (CAMED’64) and Julie Yannuzzi ■
Larry C. Young and Sue Young ■
MERCURY Anonymous (3)
Lawrence D. Ackman ■ and Ronnie Ackman
Noubar B. Afeyan and Anna Afeyan
Gerald Ajemian and Lucille Ajemian
Dwight M. Akers (CAMED’53) ■ and Beverly R. Akers ■
Max M. April (CAMED’85, CAS’81) and Pamela T. April (Questrom’83)
Carola A. Arndt (CAMED’78, CAS’78) ■
Amin Ashrafzadeh (CAMED’97, CAS’93) and Christine Ashrafzadeh (Questrom’96, CAS’92)
Sonya Nersessian (LAW’85) and Richard K. Babayan ■ Steven Baker ■ and Shirley Baker ■
Gary J. Balady and Rosemary Mehl ■
Elizabeth D. Barnett (CAMED’85) and Suleiman N. Mustafa-Kutana
Paul C. Barsam (STH’52) and Joyce L. Barsam
Howard C. Bauchner (CAMED’79) and Christine M. McElroy (GRS’81,’84) ■ Howard C. Beane (CAMED’57) ■ and Shirley T. Beane
John H. Bechtel (CAMED’50) ■ and Shirley F. Bechtel
Franklyn D. Berry (CAMED’41) ■ David W. Bishop (CAMED’46) ■ Elsa C. Bodon (CAMED’41) ■
James F. Bopp, Jr.
S. Arthur Boruchoff (CAMED’51) ■ and Anna Silverman-Boruchoff (CAMED’49) ■
Robert A. Cameron ■
Robert J. Carey (CAMED’54) ■ and Mary E. Carey (Wheelock’55)
Russell K. Carney and Geraldine Carney ■ David M. Center (CAMED’72, CAS’72) and Patricia Rabbett ■ Edmond E. Charrette (CAMED’62) and Maria T. Charrette ■ Jeremy Chess (CAMED’70, CAS’70)
Frank Citrone, Jr. and Carol Citrone
John P. Cloherty (CAMED’62) ■ John F. Cogan, Jr. ■ and Mary L. Cornille (GRS’87)
Alan S. Cohen (CAMED’52) ■ and Joan P. Cohen
DEAN’S ADVISORY BOARD
John T. Avellino ■
Gabriella J. Avellino, MD (CAMED’09,’13)
Deb Boedicker ■
Elizabeth R. Brown, MD ■ Richard J. Catrambone, MD, DMD (CAMED’92) ■
Jane R. Clark, MD ■
Larisa E. Connors, MD (CAMED’98) ■
Suzanne Cutler, PhD (QUESTROM’61)
Shamim A. Dahod, MD (CAMED’87, CGS’76, CAS’78) ■
David R. Edelstein, MD (CAMED’80) ■
Mary Jane R. England, MD (CAMED’64, Hon.’98) ■
Joseph S. Fastow, MD (CAMED’70)
Maurice R. Ferré, MD (CAMED’92, CGS’81, SPH’92) ■
Jonathan P. Gertler, MD (QUESTROM’99) ■
Shahram S. Gholami, MD (CAMED’96) ■
Burton P. Golub, MD (CAMED’65) ■
Rod F. Hochman, MD (CAMED’79, CAS‘79) ■
Christine S. Hunter, MD (CAMED’80, CAS’80) ■
Donald M. Kaplan, MD (CAMED’73) ■
Sarkis J. Kechejian, MD (CAMED’63) ■
Reshma Kewalramani, MD (CAMED’98, CAS’98) ■
Sherry M. Leventhal ■
Douglas M. Macdonald, PhD (CAMED’98, GRS’92) ■
Sarita A. Mohanty, MD, MPH (CAMED’98) ■
James A. Nassiri, MD (CAMED’97,’01) ■
Peter T. Paul (QUESTROM’71)
Tania J. Phillips, MD ■ Albert Rosenthaler ■ Pedram Salimpour, MD (CAMED’96,’00) ■
Leslie K. Serchuck, MD (CAMED’90) ■ Emily Wise Shanahan, MD (CAMED’09) ■ Richard C. Shipley (QUESTROM’68,’72, Hon.’22) ■
Louis Wade Sullivan, MD (CAMED’58, Hon.’90) ■
John K. Terzian, MD (CAMED’82, CAS’78) ■ Patricia Janine Williams, MD (CAMED’89, CAS’84) ■ Deborah Whittaker Wilson, PhD (GRS’72) ■
■ FY25 Donor
New DAB Members in Italics
Marian M. Cook
Ronald B. Corley and Janice Corley ■
Sidney Covich ■
Brit D’Arbeloff and Alexander V. D’Arbeloff ■
David P. DiChiara (CAMED’84, CAS’80) and Maria J. DiChiara ■
Paul E. Dixon, Jr. and Rebecca K. Dixon ■
Thomas J. Dowling, Jr. (CAMED’81, CAS’81) and Rosemary Dowling
Hilda R. Dressler (CAMED’34) ■
Carol A. Dyer and Gene Gordon (CAMED’46) ■
Alan M. Edelstein (Questrom’47, LAW’49) ■ and Sybil Edelstein ■
Alvin N. Eden (CAMED’52) ■ and Elaine R. Eden ■
Mary Jane R. England (CAMED’64, HON’98) ■
Michael J. Esposito (CAMED’49) ■
Geraldine L. Feldman (CAMED’69, CAS’69) ■
Judith N. Feldman ■ I. Howard Fine (CAMED’66) ■ and Victoria Fine
Bertha Offenbach Fineberg (CAMED’36) ■ and Nathan L. Fineberg (CAMED’30) ■
Nicholas J. Fiumara (CAMED’39) ■
Daphne H. Foster (CAS’79, Questrom’82) and Lawrence Foster
Beverly R. Franklin (CAS’44) ■ and William E. Franklin (CAMED’46) ■
Myrna Franzblau (Wheelock’73) ■ and Carl Franzblau
Monte Friedkin and Skeets Friedkin
Ray A. Garver ■ and Donna L. Garver ■
Marion L. Gendron (PAL’26) ■
George E. Ghareeb (CAMED’62) ■ and Nancy B. Ghareeb
Arnold Goldenberg (CAMED’54) and Gloria Goldenberg ■
Dorothy A. Gottlieb (CAS’76) and Leonard S. Gottlieb ■
Doris Grabosky ■ and Jack Grabosky ■
Ellen R. Grass ■
Robert E. Griffin and Cathleen Griffin
Morton S. Grossman (MET’42) ■ and Sylvia Grossman ■
Kenneth M. Grundfast and Ruthanne Grundfast
Fritz Grunebaum (HON’79) ■
Robert W. Healy (CAMED’67) and Bonnie M. Healy ■
Juan D. Hernandez Batista ■ and Maria A. Tavarez-De Hernandez
Arnold S. Hiatt
George L. Hines (CAMED’69, CAS’69) and Helene A. Hines (SAR’69)
Ann S. Hintlian ■ and Deran Hintlian
Michael G. Hirsh (CAMED’63) ■ and Carol N. Hirsh
Arline Housman ■ and Herbert E. Houseman ■ Charles Housman
Edward L. Housman (Questrom’42) ■ and Charolotte Houseman ■
John P. Howe III (CAMED’69, HON’19) and Tyrrell E. Flawn ■
James B. Howell (CAMED’65) ■ and Marlene A. Howell
Bernard L. Huang (CAMED’62, CAS’57)
■ and Ann M. Huang
Richard E. Hunter (CAMED’44) ■ and Minta L. Hunter ■
David Ingall (CAMED’57, CAS’52, GRS’53) ■ and Carol Ingall
Patricia K. Issarescu (CAMED’61) ■
Joseph A. Izzi, Sr. and Barbara A. Izzi
Peter F. Jeffries (CAMED’60) ■ and Jeanne F. Arnold (CAMED’61) ■
Clinton W. Josey, Jr. ■ and Betty Josey
Lori A. Jurado and Xavier Jurado
Esther B. Kahn (Wheelock’55, HON’86) ■
Charlotte A. Kaitz ■ and Louis L. Kaitz ■
Kenneth P. Kato (CAMED’89) and Nancy A. Nagy ■ Isabelle A. Katzer (Wheelock’68) ■
Damon J. Keith ■ The Kibrick Family
Burton I. Korelitz (CAMED’51) ■ and Ann Z. Korelitz
Conan Kornetsky ■
Bernard E. Kreger ■
Edward E. Krukonis (CAMED’63) ■ and Priscilla J. Krukonis
Saul Kurlat ■
Cecelia Lance
Charna C. Larkin and Alan B. Larkin ■
Robert E. Leach and Laurine Leach
Paul M. Leiman (CAMED’74, CAS’72) and Carol R. Leiman ■
Brian Levine and Beth Levine
Brigette Lonner and Joseph J. Lonner ■
Thomas A. MacLean (CAMED’64) and Colleen K. MacLean
William I. Malamud (CAMED’54) ■ and Camille C. Malamud ■
William M. Manger and Lynn S. Manger
Richard C. Marcus
Stella C. Martin and Clive R. Martin
Ronald P. McCaffrey and Maureen McCaffrey
John F. McCahan and Kathleen B. McCahan ■ ■
Edward J. McDonald, Jr. and Catherine A. McDonald
Jean E. McPhail ■
Robert F. Meenan (CAMED’72, Questrom’89)
Mark S. Michelman (CAMED’67) ■ and Susan F. Michelman ■
Daniel E. Moalli (CAMED’61) and Glenna M. Moalli
Jordan Monocandilos
Rodney A. Montag and Sally A. Montag
Sanford R. Montag and Nancy L. Montag
Thomas J. Moore and Mary C. Moore ■ Sunit Mukherjee (CAMED’89, CAS’89) and Sumeeta Mukherjee
Michael F. Mullarkey (CAMED’70) and Dawn Mullarkey (CAS’68)
Alan S. Multz (CAMED’85, CAS’81) and Michelle A. Multz ■ Praveen V. Mummaneni (CAMED’95, CAS’95) and Valli P. Mummaneni ■ G. Vijaya Naidu
Newton Family Fund
Merel G. Nissenberg
Dawn B. Norcia and David J. Norcia
N. Stephen Ober (CAMED’86, CAS’82)
John F. O’Brien (CAMED’59) ■ ■
Anne W. O’Connor and John F. O’Connor (CAMED’57) ■
Tim R. Palmer and Lynne L. Palmer
Hytho H. Pantazelos (CAMED’63) and Peter G. Pantazelos ■ ■
Dianne M. Parrotte (CAMED’79, CAS’79)
Edward F. Parsons (CAMED’65) ■
Jordan C. Paul and Valerie J. Paul ■ Lita Perkins ■ and John S. Perkins ■
Jona A. Perlmutter and Donna Perlmutter
Astrid O. Peterson (CAMED’77, CAS’74) ■
N. Neal Pike (LAW’37) ■
John I. Polk (CAMED’74, Wheelock’13) and Mary C. Nugent Polk (SON’76,’77)
Helen S. Ratner ■ and Frank Ratner (CAMED’47) ■ Iver S. Ravin (CAMED’40) ■
Nancy E. Rice (CAMED’65) and Millard J. Hyland
Joel A. Roffman (CAMED’75, CAS’72) and Nancy C. Roffman Bessie Rosenfield ■ and Louis I. Rosenfield ■ Gerald L. Ross ■
Melanie Rothbaum and David Rothbaum (CAMED’82) ■ Richard A. Rudders ■
Stephen W. Russell (CAMED’55) and Gail D. Russell
Pedram Salimpour (CAMED’96,’00) and Stacy Weiss ■
Hannah E. Sandson and John I. Sandson ■ Francis P. Saunders (CAMED’58) ■ and Lydia M. Saunders
Frank J. Schaberg, Jr. (CAMED’68, CAS’68) and Monica J. Schaberg (CAMED’68, CAS’68) ■ Alan L. Schechter (CAMED’78) and Genevieve Schechter
Harold S. Schell (CAMED’70) and Antoinette M. Schell ■ Rocco Schelzi ■
John Schieltz and Katie Schieltz ■ Herman Selinsky (CAMED’24) ■
Richard J. Shemin (CAMED’74, CAS’72) and Susan H. Shemin
Norton L. Sherman ■ and Claire M. Sherman
Richard L. Simmons (CAMED’59)
Kenneth B. Simons (CAMED’80) and Wendy A. Simons
Simon L. Strong (ENG’79, Questrom’91) and Sarah A. Strong
Lois N. Talis (PAL’49) ■
Tony Y. Tannoury and Viviane Tannoury
Stephen M. Tringale (CAMED’90, CAS’80, GRS’86) ■ Sanford W. Udis (CAMED’44) ■ Franz Waldeck ■ Carl W. Walter ■ and Margaret H. Walter ■ Murray Weinstock (CAMED’65) ■ and Gloria Weinstock
Sue Rosenwasser Weiss and Seymour Rosenwasser ■ Anthony Weldon
Judith F. Wellington and Peter S. Wellington ■ Jerrold Wexler and Joan Wexler
Robert H. Wexler ■ and Joanna B. Wexler ■ Alan Winters and Hope Winters
Robert A. Witzburg (CAMED’77) and Lorraine G. Witzburg (Wheelock’06) ■
Peak Woo (CAMED’78, CAS’78)
Earle G. Woodman (CAMED’58) ■ Moshe Yanai and Rachel Yanai
Charles R. Young ■ and Marion L. Young ■ Frances W. Young ■ Barry S. Zuckerman and Pamela A. Zuckerman
HONORARY
Dorothy C. Keefer (PAL’46,’48) ■ Ishebel K. Lyle ■ and Carl Lyle ■

At the annual Keefer Society Scholarship Dinner, the conversations between donors and the students they have supported hum steadily in the background through the speeches, the awards, and the meal. Nearly 100 donors and students attended the dinner.
“They are wonderful, wonderful people,” said Ann Cea, MD’67, a radiologist and the medical coordinator for the New York State Department of Health Office of Professional Medical Conduct.
Third-year medical student Molly Geraghty, a beneficiary of the Cea Scholarship Fund, stood alongside Cea in the Fenway Room of the Hotel Commonwealth in Boston at the September 25 event.
“Molly is the perfect example of someone pursuing something that they love, and I’m very proud of what she’s doing,” said Cea.
“I come from a long line of public school teachers; no one in medicine for generations, if ever,” said Geraghty. “Having someone who is there to support me and show that they believe in my potential really means a lot.”
Established to recognize donors whose
lifetime contributions have reached $100,000 or more, the Keefer Society honors Chester S. Keefer, MD, medical school dean from 1955 to 1960. The school’s scholarship endowment has grown from $15 million 26 years ago to more than $164 million today.
After his parents passed away, cardiologist Daniel Kirshenbaum, MD’11, decided to continue supporting the Elaine B. and Howard D. Kirshenbaum Scholarship Fund in their memory.
“I’m very grateful that I’ve been given the opportunity to help people,” Kirshenbaum said. “I think when you are working so hard to study, to be a doctor, to try to help other people, to have to worry about your finances, debt, and lifelong obligations is just very difficult. Anything I can do to make that easier is something I want to do.”
Los Angeles native and second-year medical student Ruby Nguyen said his father fled the Cambodian genocide, his mother the Vietnam War. Today, Nguyen’s father repairs jewelry and his mother works in a nail salon.
His older brother’s death from brain cancer propelled Nguyen into medicine. He worked for five years before he entered medical
school; first as a research coordinator at the University of California Irvine and then as a contract teacher for the US Department of Education. Nguyen received a scholarship from the Sumner Stone, MD’58, and Martha Skinner, MD, Endowed Scholarship Fund.
“Without the scholarship, I honestly don’t even know if I could have attended medical school,” he said. “I probably would have stayed in California if not for the scholarship. It was pretty much the deciding factor in coming to BU.”
The funding helps attract the best students and diversifies the student body.
As invited student speakers, second-year medical students Grace Johnson and Brianna Chambers shared their stories with the dinner guests.
“I am the proud daughter of two hardworking parents. My father worked at the post office, and my mother was the first in her family to graduate from college,” Chambers, a Kenneth C. Edelin Scholarship Fund recipient, told the audience. “From her, I learned that education was not just about earning a degree, but also about breaking barriers and opening doors.”
Her mother currently teaches in a public school.
Copresident of the BU Chapter of the Student National Medical Association, a national organization that designs and develops mentorship and service programs for underrepresented students, Chambers is also a member of the student group Creating Leadership and Education to Address Racism, which helps medical students understand racism in medicine.
Her medical school research is focused on gestational weight gain and its impact on metabolism and cardiovascular risk later in life.
“None of this would be possible without the support I’ve received,” Chambers said. “Scholarships give us the ability to concentrate on our education, our research, and our community service.”
Johnson, who is supported by the Dr. Trevor J.G. Phillips and Dr. Mark R. Dover Endowed Scholarship Fund, told the audience that her path to medicine was shaped by the experience of her grandmother, a stroke survivor.
“Witnessing the end of her life introduced
my desire to become a physician who honors patients’ priorities and dignity at every stage,” she said.
Before entering medical school, Johnson spent two years as a research assistant at Boston Children’s Hospital, working with the Medical Critical Care team in the Medical Intensive Care Unit helping parents navigate the difficult questions of treatment and healthcare.
“Bearing witness to these conversations— painful, human, and profoundly compassionate—affirmed the kind of physician I want to be, one who brings empathy, candor, and humility to the discussion of how patients want to live and die.”
Advocacy has been central to Johnson’s medical school experience. In the summer of 2025, she participated in the Medical Student Summer Research Program, developing an educational tool on Extreme Risk Protection Orders that allow providers to remove firearms from individuals who might harm

themselves or others. She also leads the Disability and Identity Vertical Integration Group, which advocates for curriculum changes.
“Scholarships relieve the financial burden and allow students like me to pursue what inspires us most,” Johnson said.
The Keefer Society inducted new members, including Larisa Connors, MD’98, and John
Connors, who established the Larisa E. and John Connors III Endowed Scholarship Fund; Monita Lam, who established the Kum Fung Lau Fund, named for her mother, to benefit BU’s Alzheimer’s Disease Research Center; and Ronda Rockett, MD’98, and Sean Rockett, MD, who support the Applebaum-Rockett Scholarship Fund ●
The American Lung Association of Massachusetts has made a significant investment in Boston-based lung health research by awarding 12 researchers, including four from BU, grants to study lung health. Boston received more of the 130 total grants awarded across the US than any other city. The organization awarded Boston researchers a total of $800,000 in grants for up to two years.
“We are proud to welcome these researchers to the American Lung Association’s elite team to help advance our mission to save lives by improving lung health and preventing lung disease. More than 35 million Americans live with lung disease, and as we face new challenges with cuts to federal funding and changes in research priorities, lung health research is more important than ever,” said Ashley Carrier, executive director of the Lung Association in Massachusetts. “We are proud
to fund these incredible local researchers to help us realize our vision of a world free of lung disease.”
The BU researchers:
• Ahmed A. Raslan, PhD, research assistant professor of medicine, received the Dalsemer Interstitial Lung Disease Award for the project, “Targeting Endothelial Cells in Small Lung Capillaries to Halt Progression of Lung Fibrosis.”
• Shawn Lyons, PhD, assistant professor of biochemistry, received the Emerging Respiratory Pathogen Award for the project, “Exploiting Weak Spot in How Viruses Operate to Combat Severe Respiratory Infections.”
• Liangliang Hao, PhD, assistant professor of biomedical engineering at the College of Engineering, received the Innovation Award
for the project, “Developing Innovative Early Detection Test for IPF.”
• Ignaty Leshchiner, PhD, assistant professor of computational biomedicine, received the Innovation Award for the project, “Predicting When Lung Cancer Will Return.”



Each funded project undergoes a rigorous scientific peer-review process, ensuring that only the most promising, innovative, and impactful research receives support. In addition to funding individual researchers, the American Lung Association Research Institute also supports the Airways Clinical Research Centers Network, the nation’s largest nonprofit network of clinical research centers dedicated to asthma and Chronic Obstructive Pulmonary Disease (COPD) treatment research. ●
The donation comes at a key time for the center and its research
When her mother began to show signs of memory loss and cognitive decline, Monita Lam turned to Boston University’s medical community for support. “The doctors at BU helped me understand the complexities of Alzheimer’s,” she says. “They taught me how to care for my mother with
compassion and knowledge, and they helped me feel less alone.”
Recently, Lam has made a personally meaningful and generous gift to the University’s Alzheimer’s Disease Research Center (BU ADRC) to honor her beloved mother and to support groundbreaking research in the fight against the disease.
By establishing the Kum Fung Lau

Fund—named for her mother, who died in 2002—Lam seeks to recognize the immense responsibility caregivers and doctors face in managing diseases like Alzheimer’s and to inspire others to give back. Her gift will support key research initiatives at the BU ADRC.
“We have made huge strides in diagnosing Alzheimer’s disease within a person’s lifetime,” says Ann McKee, BU William Fairfield Warren Distinguished Professor of Neurology and Pathology and director of the BU ADRC. “The Kum Fung Lau endowment will go primarily toward early detection, early intervention, and treatment, as well as leadership training that will help researchers keep on track with the progress we’ve made.”
McKee also emphasizes the importance of private gifts, particularly in a time of uncertain federal funding, when some grants have been halted. “Philanthropy allows us to continue without staff reductions, lab shutdowns, or stopping the ongoing experiments,” she says.
The BU ADRC is focused on detecting Alzheimer’s as early as possible—ideally before symptoms or pathology appear—and intervening through clinical trials. With a recent shift toward precision medicine over one-size-fits-all approaches, researchers are developing new strategies to that end. These include identifying how specific physical characteristics, such as how a person’s genes interact with environmental factors, and data from wearable devices like watches can inform targeted therapies that move from the lab bench to patient care.
“We’re extremely grateful to Monita for her very generous gift in her mother’s name,” says McKee. “It will allow us to accelerate all our cutting-edge research.”
Lam says she hopes her story is a powerful reminder that philanthropy is not only a tribute to those we love, but also a lifeline to those still waiting for answers.
“We can’t afford to wait for a cure,” she says. ●

Advancing cancer research is a deeply personal issue to the trustees of the Karin Grunebaum Cancer Research Foundation, which was founded in 1958 following the death of 39-year-old Karin Grunebaum three months after she gave birth to her fourth child. Today, three of those children lead the foundation, in addition to three grandchildren and eight faculty members from the schools of medicine at Boston University and Harvard University.
Within months of her death, Grunebaum’s husband Fritz endowed the foundation in her honor. Its mission: to advance cancer research with the hope that other families could avoid a similar loss.
Since 1984, the Grunebaum Foundation has given more than $2.4 million to the School of Medicine, where it funds medical student research, a professorship, and an annual fel-
lowship, all focused on cancer research.
Julie Palmer, ScD, MPH, director of the BU Slone Epidemiology Center and codirector of the Boston University-Boston Medical Center Cancer Center, is the current Karen Grunebaum Professor in Cancer Research. “This endowed professorship has allowed me to recruit outstanding early-career cancer researchers, conduct high-risk innovative pilot studies, and enhance cross-disciplinary interactions among researchers at the BU-BMC Cancer Center,” she said.
“We’re honored to be able to support both research and the scientists who are advancing the understanding, diagnosis, and treatment of cancer,” added Steven Wallach, foundation chair and the oldest of Karin Grunebaum’s children.
A recent point of pride was the 2023 Nobel Prize awarded to Drew Weissman, MD’87, GRS’87, Hon.’23, for discoveries on
mRNA technology with corecipient Katalin Karikó, PhD, which laid critical groundwork for COVID-19 vaccines. Weissman was supported by the foundation when he was a PhD student at the medical school in the 1980s.
“It was thrilling to witness the achievements of Dr. Weissman and to think that our family played a small role early in his career,” said Wallach.
The foundation has funded fellowships for assistant professors who have been instrumental to dozens of faculty just starting out.
“I’m honored to have been selected as a Karin Grunebaum Faculty Research Fellow,” says Mollie Barnard, ScD, assistant professor of medicine. “The fellowship has been an important catalyst for my work evaluating how metabolic health influences the immune response to breast cancer.”
The commitment to early-career scientists extends to medical students participating in cancer research projects. “The Grunebaum Foundation has funded stipends for many students in our summer research program,” says Matthew Layne, PhD, associate professor of biochemistry & cell biology and assistant dean of research. “These stipends enable students to live in Boston over the summer and engage in full-time cancer research with our faculty mentors.”
Tom Clarke, PhD, assistant professor of pathology & laboratory medicine and a former Grunebaum fellow, mentored a medical student in his lab who received a summer research stipend from the foundation. “After completing her research, she went on to win a Best Poster Award, an exciting milestone that reflects the impact of student-driven research,” Clarke said.
Whether supporting future physicians, early-career or established scientists, members of this multigenerational family have devoted decades and millions of dollars to generations of researchers who share their commitment to saving lives. “We have always thought of the foundation members as part of our family,” said Steven Wallach, “not just because our family established the foundation, but because since its inception, we have personally met with each sponsored fellow, 114 and counting, and have directly listened to, supported, and followed their individual ideas for eradicating cancer. Thanks to the efforts of our ‘extended family,’ we are making significant progress towards that critical goal.” ●
Speaking at the fourth annual Alan and Sybil Edelstein Professionalism and Ethics in Medicine Lecture, Alan Carver, MD’95, chair of the pain and palliative medicine section of the American Academy of Neurology, noted that interest has noticeably increased in endof-life studies and care.
Twenty-five years ago, a handful of people might populate the audience at an end-oflife care talk, but today, many more attend.
“There has been a greater focus than ever before on these issues,” Carver said.
Nearly 100 people participated in the November 12 Edelstein virtual lecture on “The Ethics of End-of-Life Care,” which considered various impacts on patients, families, and medical staff.
“Most people don’t want to talk about it,” said moderator David Edelstein, MD’80. Edelstein, former chief of otolaryngology at Manhattan Eye, Ear & Throat Hospital and a clinical professor at Weill Cornell Medical College, and his sister Marcia Edelstein Herrman, MD’78, founded the lecture series in honor of their parents, Alan and Sybil.
The lecture focuses on a different topic each year.
Edelstein touched on his own end-oflife experiences involving his parents, family members, and friends.
“If there’s no advance directive, what do doctors do?” Edelstein asked. “They advocate for the best care available. But that’s not so easy to do sometimes when things are happening quickly with your patient.”
Carver described what he called an ethical imperative: “The right to excellence at the end of life.” Patients, family, and physicians often misinterpret a fatal diagnosis and “Do Not Resuscitate” orders as signaling the end of care.
“Palliative care is never about stopping or withdrawing care. It’s all about living with incurable illness as well as possible,” he said. “It’s really about life.”
Fourth-year medical student Brandon Oddo said medical students often don’t get

a lot of advice on how to process that fatal diagnosis for patients—or for themselves.
“This gap may be in part due to a hidden curriculum that implies that death is medical failure, but I find that the growing respect for hospice and palliative medicine is challeng-
“Palliative care is never about stopping or withdrawing care. It’s all about living with incurable illness as well as possible. It’s really about life.”
ALAN CARVER, MD’95
ing that,” said Oddo, cofounder of Grieving, Reflecting, and Cultivating Empathy (GRACE), a student-led organization that helps students discuss loss and understand grief.
“I think a humbled, even reverent recognition of the messiness of the end of life is, in its totality, crucial to developing moral character and informing proper responses in this setting.”
Shelly Rambo, PhD, a professor at BU’s School of Theology and former interim dean, teaches chaplains how to help families navigate end-of-life ethics.
“Research describes how hospitals and hospital staff respond to death by avoiding
it, distancing themselves from it, focusing on its technical aspects and managing it,” said Rambo, quoting from the book Paging God by Wendy Cadge, PhD, president and professor of sociology at Bryn Mawr College.
“Most people have not sat down to think about their own wishes for end-of-life care,” said Beth Rooney Suereth, CAS’85, who served as a family caregiving consultant for AARP Public Policy Institute in Washington, D.C., and founded Caregiving Pathways, a family caregiver support organization.
Instead, patients and families are typically surprised when hospitals shift from curative to comfort care. Most are unaware of the benefits of a physician order for life-sustaining treatment (POLST). Signed by a physician, physician assistant, or nurse practitioner, this document specifies the treatment the patient desires for medical procedures like resuscitation and other medical interventions, along with medically assisted nutrition and hydration. “It is more specific than any other advance directives,” noted Suereth.
There are also financial considerations. “I see families who have medical bills from end-of-life care, and they’ve seen the suffering that somebody endured for care that wasn’t effective and certainly didn’t provide any additional quality of life. The ultimate goal is quality of life at the end of life,” Suereth said, urging families to discuss everything ahead of time, including who has a say in making decisions.
“You can plan and prepare, or react and regret.” ●

THIS ISSUE OF BU MEDICINE FEATURES
A COVER STORY ON THE Student Perspectives Initiative, a student-led effort that utilizes the pedagogy of narrative medicine to further clinical learning, empathy, and humanism in medicine. The preclinical initiative pairs talks by student peers who have experienced disease and other medical conditions with clinically relevant curriculum lectures investigating those topics, emphasizing personal storytelling and narrative as educational tools in humanizing physicians and building the relationship between practitioner and patient.
We welcomed the Class of 2029 to our campus in August with a White Coat address from Rod Hochman, MD’79, CAS’79. Dr. Hochman addressed our new class with candor and encouragement, urging our students to embrace both the challenges and the joys that lie ahead as they begin
their medical careers. This year we also included words of encouragement from our alumni in each incoming student’s folder to remind them that no matter how challenging things become, they have a supportive community behind them. Thank you to our alumni for sharing your experience and wisdom with the entering Class of 2029.
Each year as first-year students receive their new stethoscopes during our annual Lorraine Stanfield Lecture, I am honored to commemorate the legacy of my former teacher and colleague, the late Lorraine Stanfield, MD. Made possible by the generosity of more than 80 alumni, the distribution of 138 stethoscopes is an important milestone for students as they embark on their unique medical education journeys. Since 2007, our alumni have donated more than 2,500 stethoscopes, and we remain deeply grateful for their steadfast commitment to supporting the next generation of physicians.
Ricardo Cruz, MD’11, MA’07, MPH’03, assistant professor of medicine and assistant dean of student affairs, was keynote speaker. He shared with students that their stethoscope is more than a tool to examine a patient: “it represents a physician’s role as a healer and caregiver.”
During our annual Alumni Weekend in September we welcomed home hundreds of alumni for memorable events including a Red Sox game, tours of the School of Medicine and Boston Medical Center, and class dinners. We honored Stephanie Feldman, MS’10, MD’14; Larry Nichter, MD’78, CGS’71, CAS’73; Ziv Haskal, MD’86, CAS’86; and Vladimir Kefalov, PhD, GMS’99 during our Alumni Awards Luncheon, a meaningful occasion for us to celebrate their remarkable careers as
they were joined by family, friends, and former classmates. We also welcomed new Alumni Association President Aleksander Chudnovsky, MD’01, at the luncheon with the ceremonial passing of the gavel. We greatly look forward to benefiting from Dr. Chudnovsky’s invaluable expertise as the new president of our Alumni Board.
Sadly, Elizabeth Dooling, MD’65, passed away on December 16 (see In Memoriam, page 48). A gifted pediatric neurologist and teacher and an invaluable board member, Dr. Dooling was dedicated to nurturing new students and committed to our mission and community. She will be greatly missed. Our office remains committed to fostering meaningful connections between alumni and the school of medicine. We are proud of our alumni and here to provide opportunities for you to reconnect with classmates, share your life updates and experience, and inspire the next generation of health professionals. We hope you will join us at future alumni events and invite you to visit our alumni web pages, where you can find opportunities to mentor students or host gatherings with your former classmates.
Thank you for your support and engagement. It is your involvement that keeps our community vibrant and thriving.
Sincerely,

Heather Miselis, MAMS’00, MPH’00, MD’04 Associate Dean for Alumni Affairs
Through alumni generosity, stethoscopes and other instruments are distributed to first-year students

In keeping with the event’s focus on the physical examination, speakers at the 8th Annual Lorraine Stanfield, MD, Memorial Doctoring Lecture held on August 25 in Hiebert Lounge emphasized the importance of listening. Key points included being able to hear what the body—and person—were communicating about their health, whether through the new stethoscopes first-year students received from alumni or by listening to patients telling their stories.
“These stethoscopes are more than just a tool to help you examine a patient. They represent a physician’s role as a healer and caregiver,” said keynote speaker Ricardo Cruz, MD’11, MA’07, MPH’03, assistant professor of medicine and assistant dean of student affairs.
“We listen to the body to understand, diagnose, and treat illness, {but the stethoscope} also represents presence. When we
utilize the stethoscope, we should be attentive and present, not only listening to the patient’s body but listening to their stories.”
Stanfield, who died of breast cancer in 2017 at 56, worked for two decades as a primary care physician caring for underserved patients at Dorchester House Health Center (DotHouse). A much-beloved teacher, advisor, mentor, and clinician who won the highest teaching awards from the school and University as well as the prestigious Leonard Tow Humanism in Medicine Award for clinical excellence, Stanfield was remembered with great affection and admiration by those who knew her.
“She was someone who loved students deeply. She listened to everyone in a way that you would want to be listened to, whether you were a patient or a friend,” recalled Priya Garg, MD, associate dean of medical education.
Heather Miselis, MAMS’00, MPH’00, MD’04, associate dean for alumni affairs,
worked with Stanfield at DotHouse and remembered her as a talented educator and compassionate human being.
Miselis noted that 80+ alumni paid for the 138 instrument kits that included a stethoscope, patella hammer, tuning forks, ophthalmoscope, and an otoscope. Since 2007, more than 2,500 instrument kits for first-year students have been funded through the Alumni Association.
“I think the stethoscope specifically is something we’ve been thinking about, some of us, since childhood,” said first-year medical student Anya Sanchorawala. The daughter of two physicians, as a child Sanchorawala dressed up as a doctor for Halloween, wearing her parents’ scrubs and draping her father’s stethoscope over her shoulders.
“It’s been a big symbol of what it means to be a physician, and I’m grateful to now have one,” said Sanchorawala. “I feel like I’m finally there, in the medical community, with my parents.”
“It means a lot that I received my stethoscope from someone who was educated here at BU. Hopefully, I’m in a position to do the same someday,” said first-year student Ishasn Oza. “As a physician, you not only have to take care of your patients but also make sure the next generation of physicians is being properly educated and has the tools they will need to save lives.”
Alison Chilcott credited family support for helping her down the path to medical school and embraced her new “family” in the medical community: “It’s like transferring the support of family to people who will take me even further.”
A month into his first year and with his first exam looming, Denis Pegosyan cited the lecture as a refreshing break from academics, noting, “It’s nice to take a step back, zoom out, and see what this is really all about: helping other human beings.”
Stanfield’s memory continues to inspire students. “Seeing how many people were moved by her, were influenced by her, gives me a lot of hope that I will be trained by people who want to continue her legacy,” Chilcott said. ●
Aleksander Chudnovsky, MD’01, Named New Alumni Association President

The 2025 Alumni Award winners, from left, Humanitarian awardee Larry Nichter, MD’78, CGS ‘71, CAS’73, Distinguished Alumni awardee Ziv Haskal, MD’86, CAS’86, Emerging Leaders awardee Stephanie Feldman, MS’10, MD’14, and Medical Sciences Distinguished Alumni awardee Vladimir Kefalov, PhD, GMS’99.
Accepting the Humanitarian Award at the annual Alumni Awards Ceremony and Luncheon on September 26 of Alumni Weekend, Larry Nichter, MD’78, CGS’71, CAS’73, cited the motto of the national medical honor society Alpha Omega Alpha: “To be worthy to serve the suffering.”
A globally recognized plastic surgeon and founder of a nonprofit dedicated to training surgeons in underserved regions worldwide, Nichter described health as a fundamental human right and stressed that no life is more important than another.
“Most medical students start with these humanistic beliefs and values but financial, family, and lifestyle pressures can sometimes turn medicine into a job and not a calling,” he said. “Striving to make the world better and equipping others to do the same, I believe, is a very powerful antidote to all that.”
“Our school truly values and treasures all the contributions that our alumni make through the incredible work that they do in the local and global communities,” said Dean Ad Interim Hee-Young Park, PhD, in opening remarks.
Other alumni honored at the event included Stephanie Feldman, MS’10, MD’14 (cardiooncology); Ziv J. Haskal, MD’86, CAS’86
(interventional radiology); and Vladimir Kefalov, PhD, GMS’99 (photoreceptor physiology).
The ceremony also marked the passing of the gavel from Alumni Association President Daniel Oates, MD’00, to his successor, Aleksander Chudnovsky, MD’01.
Associate Dean of Graduate Medical Sciences Jamie McKnight, PhD, MA, introduced Kefalov, the recipient of the Graduate Medical Sciences Distinguished Alumni Award, as one of the world’s top electrophysiologists working in vision research.
Born in Bulgaria, Kefalov earned his PhD in cellular biophysics from BU, studying photoreceptor physiology under M. Carter Cornwall, PhD, professor emeritus of pharmacology, physiology & biophysics. Kefalov is currently a professor and vice chair for research at University of California Irvine Department of Ophthalmology.
“Boston was just an amazing place to be a student and to live, and Boston University has made a great impact on my career,” said Kefalov, who returned to BU in January to address the pharmacology, physiology & biophysics department at their annual retreat.
“It was just wonderful to see how vibrant and strong and diverse the department is, with many researchers, and many, many students doing amazing work,” he said.
Feldman, who received the Emerging Leaders Award, is a national leader in cardiooncology and serves as the director of the New York-Presbyterian/Weill Cornell Medical College Cardio-Oncology program. Her clinical research focuses on cardiovascular risk assessment in patients being treated with potentially cardiotoxic cancer therapies.
“I feel incredibly lucky to have found a field that I am passionate about and where I have the opportunity to make a meaningful difference,” she said, adding that exam scores or hours spent studying were not what set her up for success. “It was the people. What [mentors] say and do truly matters.”
Introducing Distinguished Alumni Award recipient Ziv Haskal, MD’86, Associate Dean of Alumni Affairs Heather Miselis, MAMS’00, MPH’00, MD’04, noted that he is known worldwide as an interventional radiologist “whose groundbreaking research and innovations have transformed our daily medical practice.”
“Our school truly values and treasures all the contributions that our alumni make through the incredible work that they do in the local and global communities.”
DEAN AD INTERIM HEE-YOUNG PARK, PHD
A professor of radiology and medical imaging at the University of Virginia School of Medicine, Haskal has delivered more than 700 lectures, received numerous honors, and served as editor of three prestigious medical journals.
He spoke of his BU medical school education being set back a year after he was hit by a car. When he returned, still suffering from a damaged knee, the late John “Jack” O’Connor, MD’57, then dean of admissions and chair of pediatric radiology, took Haskal under his wing. Under O’Connor’s mentorship, Haskal pivoted from medicine to radiology.
“He nudged me into a residency that was beyond my reach,” said Haskal.
“I never took an English class in college, I never wanted to write, I never wanted to do research, and somehow, I’ve had guidance and curiosity. What it means is that, if there are any students here today, you can look at what I did. It was just a series of steps and opportunities, and [advice from] the people who guide you.”
Outgoing Alumni Association President Oates introduced incoming President Chudnovsky, a urologist and the global clinical program lead in late development oncology at the biopharmaceutical company AstraZeneca.
“Congratulations to all our alumni award recipients today. It is an honor to be a graduate of the Chobanian & Avedisian School of Medicine with such distinguished contemporary alumni,” Chudnovsky said. “I look forward to an exciting year as I continue to collaborate with our alumni board and roll out the expanded alumni awards, which more broadly recognize the outstanding and innovative work of our alumni.” ●
Following a national search, Quinnipiac University has appointed Lisa Coplit, MD’97, as dean of the Frank H. Netter MD School of Medicine. Coplit had served as interim dean at the North Haven, Connecticut, school since July 2025.
“Dr. Coplit has distinguished herself as a national leader who translates vision into measurable impact,” said Quinnipiac Provost Debra Liebowitz. “She brings a clear sense of institutional priorities and mission, the boldness to innovate that this moment demands, and a dedication to excellence in education and patient care that makes our graduates the medical leaders of tomorrow.”
A founding leader of the Frank H. Netter MD School of Medicine, Coplit has held several senior positions since the school’s inception, including associate dean for faculty development, interim senior associate dean for education, and senior associate dean for faculty affairs.
Before joining Quinnipiac, Coplit served as director of the Institute for Medical Education at the Icahn School of Medicine at Mount Sinai in New York, where she advanced institutional faculty development programs and recognition systems for physician and scientist educators.
Board certified in internal medicine, Coplit has held clinical appointments at St. Vincent’s Medical Center in Bridgeport, Connecticut; Mount Sinai Medical Center in New York; the East Harlem Health Outreach Project Clinic at Mount Sinai; and the Boston Veterans Administration Medical Center. She has been recognized with multiple awards for teaching excellence.
Coplit earned her MD from the Chobanian & Avedisian School of Medicine in 1997 and completed her residency and chief resident training in internal medicine at Boston Medical Center. She is also an

alumna of the Harvard Macy Program for Physician Educators and the Stanford Faculty Development Program in Clinical Teaching Skills.
“I am profoundly honored to be named the next dean of the Frank H. Netter MD School of Medicine. Serving as interim dean has been the most meaningful chapter of my professional life, and I am inspired every day by our extraordinary students and our deeply committed faculty, staff, clinical partners, and colleagues across the university. Together, we will ensure that QU Netter continues to grow as a leader in pioneering, community-engaged, and humanistic medical education, improving the health of the communities we serve while shaping the future of medicine.” ●
Eliot Slater of Marblehead, Massachusetts, writes, “Although I failed to both publish anything scientific or add new members to my family, I did manage to celebrate my 95th birthday this year, and if my wife Miriam and I make it to November 23, we will have been married 70 years. Both Mim and I are in good health and are currently living in an excellent assisted living facility. My email address is eliots3131@gmail.com, and I would love to hear from any ‘55 classmates who happen to read the above. With best wishes to all, Chuck Slater.”

Artemis Simopoulos of Washington, D.C., writes, “It has been a very busy year with travel to Greece and China. In China I gave four presentations in various cities (Nanchang, Shanghai, Zhengzhou, and Guangzhou) on my book,The Healthiest Diet for You: Scientific Aspects, which has been translated into Chinese and is in the process of being published. In the meantime, I am negotiating translations in Italian and Spanish and am very pleased with the success of the book. Another major international publication is my paper on ’Omega-3, Omega-6, Omega-9 Fatty Acids: Sources, Metabolism and Supplements’ in the UNESCO (United Nations Educational, Scientific and Cultural Organization) encyclopedia, the official encyclopedia for the United Nations. In November 2025, I gave the keynote presentation on ’A Balanced Omega-6/Omega-3 Ratio is Essential for Health and Healthy Longevity’ at the newly established Hellenic Healthy Longevity Institute in Athens, Greece. With the hope that similar Institutes will be developed worldwide.”
Ethan Shevach of Rockville, Maryland, writes, “After 55 years as a senior scientist at the National Institute of Allergy and Infectious Diseases, NIH, I have decided to retire and close my laboratory. After two years of internal medicine training as a resident at the Bronx Municipal Hospital (Albert Einstein Medical School), I was fortunate to get an appointment as a commissioned officer in the US Public Health Service (the so-called “Yellow Berets”). I entered the Clinical Center of the NIH on July 1, 1969, as a clinical associate in what was then called the Laboratory of Clinical Investigation; I spent a year taking care of patients with a wide variety of immunologic and infectious diseases and then began my lab training. I never believed at that time that I would spend my entire career at the NIH doing basic research in immunology. It has been a privilege to watch the field of immunology develop over the past fifty years and to have been able to make what I hope were significant contributions. After writing more than 450 papers, I still have about five or six more to finish as I begin my retirement. I met my wife, Ruth, when she was a med tech across the street at what was then University Hospital. We just celebrated our 58th anniversary. We have two sons and five grandchildren.”

Carol O’Neil of Walpole, Massachusetts, writes, “As I approach 80, I marvel at all the improvements and options in disease treatments. I enjoy retirement, using my experience and judgment to help friends and family navigate this complex and increasingly bureaucratic medical world. I do wish that I had kept my license! I miss being a PCP.”
James Brasic of Baltimore, Maryland, writes, “Johns Hopkins student Neeraj Kadubandi and I presented his project, funded by his Provost Undergraduate Research Award from Johns Hopkins University, at the International Congress of Parkinson’s Disease and Movement Disorders in Honolulu, Hawaii, on October 5, 2025.”

Michael Kushlan of Mountain View, California, writes, “I was very happy to see Class of 2025 graduates accepted for their internships at the Harvard hospitals. After graduating, I went to the Beth Israel for internship. Yes, I was an intern at the The House of God, written by one of my fellow interns! Almost all of it was true. But equally important, we were treated as colleagues by the attending staff from day one. I suspect attendings were rooting around for interesting cases in the hospital; I would occasionally get a call from an attending I didn’t know and I could call on anybody in the system to discuss a case. I get a Beth Israel alumni magazine, and they mentioned that they had a good number of interns from BU. One thing I am proud of—we can handle ourselves with the best of them!”
Louis Scheinman of Toronto, Ontario, Canada, writes, “I retired in 2022 after thoroughly enjoying a wonderful surgical career for more than four decades. I’m now thoroughly enjoying a second wonderful career as an equity options trader, even more fun than taking out gallbladders. I recently wrote a mathematics paper which I hope to have published, but it’s not the same quality of groundbreaking work as was my paper published 20 years ago. My family, with four grandkids including a set of boy/girl twins, is doing well. I’d so much love to hear from old friends and classmates. I can be reached at louscheinman@gmail.com. All the best from Toronto, Canada to all of you!”
Suzanne (Stelmach) Tuluri of Salisbury, North Carolina, writes, “I am happily (if not healthily!) retired from the US Navy after 24.5 years of service. I spent the next 18 years in a volunteer position as a child abuse pediatrician and have been fully retired since then. I am married to Sam Tuluri, another retired Navy peditrician, in a smallish city 30 miles north of Charlotte that we chose to be near our girls (my stepdaughters) and their families. Three grandsons are growing up too quickly!”
John Adams of Wrentham, Massachusetts, writes, “Retiring after 40-plus years of practice in primary care. Life is good, MS has slowed me down a bit, but I will be able to get more rest, exercise, and time to spend with two-and-a-half-year-old Zach. Wishing everyone well.”
Stephen Saris of Sharon, Massachusetts, writes, “Hello to all. Similar to my classmates, I am in my early 70s. Still practicing neurosurgery, though transitioning progressively to retirement. I am also recently a grandfather, the proud father of two wonderful daughters who have brought into the world two equally wonderful grandsons. I practice at Brigham and Women’s Hospital, our crosstown rival.”
Gail Schonfeld of East Hampton, New York, writes, “I received the American Academy of Pediatrics (AAP) Awards Pediatrician for

Outstanding Contributions ‘Buzzy Award,’ sponsored by the AAP Section on Administration and Practice Management (SOAPM), in September 2025. The AAP is an organization of 67,000 primary care pediatricians, pediatric medical subspecialists, and pediatric surgical specialists dedicated to the health, safety, and wellbeing of infants, children, adolescents, and young adults. The prestigious Charles ‘Buzzy’ Vanchiere Award is given to those who have made outstanding contributions toward the education and advocacy of pediatricians in administration, practice management, and payment. Dr. Vanchiere’s legacy lives on through this honor, which reflects his spirit of advocacy, mentorship, and service. As a long-standing member of SOAPM, I have consistently shared timely, accurate, and practical insights into the complexities of practice management—especially from the lens of the small independent practice.”
Jacob Asher of Menlo Park, California, writes, “On a recent east coast trip in October from my California home, I was fortunate to have a wonderful reunion with dear friends and classmates Jeff Wilson, MD’82, and Dan Steigman, MD’82, at Jeff’s house in Newton, Massachusetts. All three of us are enjoying retirement. In addition to an improved tennis game and returning to skiing, I enjoy sharing my insights into commercial health insurance gained from my second career as a health plan medical officer with residents and physicians.”
Ram Kalus of Charleston, South Carolina, writes, “Having lived in Tel Aviv from 2017–2023, I’ve had probably the most impactful years of my life, including caring for patients and identifying victims of the October 7

Hamas attack and performing surgery in Lviv, Ukraine, on war victims. I am back at my plastic surgery practice in Charleston/ Mt. Pleasant, South Carolina (Plastic Surgery of the Carolinas) which I founded in 1997, with an emphasis on breast reconstruction. I am thankful every day for my family, my health, and for the privilege of doing what I love every day, while impacting however I can on my patients’ quality of life.”
Alan Ettinger of Dix Hills, New York, writes, “Based in part upon our grant-supported research on music and health, I am part of a musical group, the Synaptic Groove Band. We perform concert/lectures for the lay public on the health benefits of music. We have also performed for the Long Island Music & Entertainment Hall of Fame, medical staff societies, and assorted disease-related organizations.”
Ronald Lindsay of Saint Johns, Florida, writes, “I recently published a series of essays reflecting on my decades of work in pediatric systems reform, rural innovation, and interdisciplinary care. The pieces trace a journey that began in Hartford, Conneticut and extended through military medicine, academic leadership, and national research networks. My work has been referenced by Yale Medicine and BU’s CAS and MD journals, highlighting the enduring impact of regional roots and ethical witness. Now retired from clinical practice, I continue to write, consult, and speak on healthcare systems, legacy, and public testimony.”
Peter Mulhern of Ocala, Florida, writes, “I completed my career in orthopedic surgery as of January 31, 2025. After my residency at Georgetown in 1988, I practiced in Lynn
and then Worcester until 2002. I divorced in 1998, with three children from my first marriage. I moved to north Georgia outside of Chattanooga, Tennessee, until 2011 and then Ocala, Florida, until 2016. I remarried in 2003 with one more child and most recently worked in Galesburg and Mt. Vernon, Illinios, until January 2025. I am presently working part time around Tampa, Florida, with Medical Marijuana certification and considering a career in wound care management with recent certification in that field as well. I have one grandchild back in Worcester and my youngest daughter is about to finish USF and is heading for medical school after a year off. Happy to be back in Florida for another 30 years!”

Stephen Corn of Norton, Massachusetts, writes, “Greetings. We are all doing well, and our wonderful son has become a firstyear law student at his first-choice school. I am confident that he will help make the world a better place! Having served over 25 years on the faculty of Harvard Medical School clinically and as director of clinical innovation at two Harvard-affiliated teaching hospitals, I continue to oversee several companies based on my inventions and lead TheAnswerPage.com, a website I founded in 1998 through which my incredible wife and I provide multiaccredited, continuing medical education focused on the endocannabinoid system and medical cannabis. Our work now spans New York to Hawaii—where we deliver the state-required courses for healthcare professionals—and beyond, an exciting and deeply meaningful endeavor. Related to this work, we were honored to receive the Special Award for Medical Cannabis Education from the International Association of Cannabinoid Medicine. Outside of work, I stay active through sports, travel, and, of course, by driving my nitrous oxide–fuel-injected track cars on international speedways, which somehow seems fitting for an anesthesiologist! Best wishes to my professors and classmates.”
Arnold Pallay of Montville, New Jersey, writes, “I am currently a practicing physician and executive medical director, and recently, was named a “2025 Healthcare Hero” by NJBIZ Magazine, a leading business journal covering New Jersey. The Healthcare Heroes Awards program was created to recognize excellence, promote innovation, and honor the efforts of individuals and organizations making a significant impact on the quality of healthcare throughout New Jersey. I’m also proud “GePa” of four—soon to be five—wonderful grandkids with Robin, two in South Carolina and two in North Jersey. Three of our four children are engineers; my eldest is a political editor-in-chief. I’ll probably continue practicing medical genetics with population health for a few more years as I slow down my primary care office workload.”
Mubin Syed of Springfield, Ohio, writes, “I began researching the link between the devastating Colonial-Era famines and today’s epidemic of diabetes and heart disease in South Asian communities, an exploration that revealed how intergenerational trauma and forced nutritional deprivation have shaped our collective health. This work led to an invitation to deliver a TEDx talk in India, where I shared how historical hunger and survival adaptations may still influence our metabolism today. The research gained international attention and was featured in a UK Guardian video that has been viewed over one million times. Building on that momentum, I recently published a book titled Healing from Our History: How Colonial-Era Famines Led to a Modern South Asian Health Crisis. Most recently, I appeared as a guest in a “Council on Foreign Relations” video discussing how food is being weaponized in

Gaza, Sudan, and Ukraine—drawing parallels between historical famines and the politics of hunger today. While my research centers on South Asian communities, my broader mission is to educate and empower everyone to achieve their best health, particularly those of South Asian origin, who carry a unique historical and genetic legacy of resilience and risk.”
Kathleen Kelly of Franconia, New Hampshire, writes, “It was lovely to catch up with classmates who were able to attend the 35th reunion. It still boggles my mind that it feels like only a minute ago I attended my father’s (MD’59) 35th reunion. This year marked my transition to retirement rather ahead of schedule to accommodate family care needs. We are now living over our garage in Franconia, in a room smaller than our camper, with four dogs while the house gets renovated. Anyone visiting the Mt. Washington Valley with a sense of adventure and humor (and no white pants) is welcome to drop in. Call to confirm we’ll be here, as we are still commuting to the seacoast periodically.”
Keira Mason of Wellesley Hills, Massachusetts, writes, “Having been a pediatric anesthesiologist at Boston Children’s Hospital for over 20 years, I am proud of my fifth book titled Mason‘s Pediatric, Sedation Outside of the Operating Room. I am also excited to announce that I have started a travel agency, Seek And Savor Travel. After 35 years of travel, almost five years independently, I am finally following my dream. This travel agency is unique in that it offers fixed group departures for two to 16 persons to destinations during times of special celebrations, festivals, and special natural events. The
Mongolian Eagle Hunting festival, the Naam festivals in Mongolia, the sacred and special festivals in Bhutan, trekking to see the rare mountain gorilla in Uganda, and the sacred and rarely-seen yogurt, horse, and new year’s festivals in Tibet are just a sampling. I would be so honored if my classmates and fellow alumni could support my dream. Please follow us on Instagram. I will offer special discounts for all BU alums.”
Elliott Leitman of West Chester, Pennsylvannia, writes, “My wife Silvia and I completed our first medical mission to Trinidad in July, where our multispecialty team saw over 7,000 patients. From an orthopedic standpoint, I saw more than 300 patients during our four-day clinic.”
Frank MacMillan of Stratham, New Hamphshire, writes, “Many updates—we got a dog, Luna, who marches to her own drumbeat. I took a new job in Dartmouth, New Hampshire, this year after dipping a toe in retirement for three months over the winter. I like working. I like taking call much less. The new job is hospital call once every 12 weeks, so I think I will last in practice a bit longer. My eldest, Erica (31), is getting married next December; she was on stage with me during our graduation and is now a labor and delivery nurse in Sarasota, Florida. The ‘littles’ are 24; my daughter Brenna is a 4th-grade teacher in McLean, Virginia, and my son Dan is starting PA school at Albany Med in December. We are finally empty-nesters. I’m losing my resident snowblower just in time for winter. Very happy to have seen many classmates this past month for our 30th reunion in Boston, Massachusetts, at the Westin Copley!”
Scott Goldstein of Dresher, Pennsylvannia, writes, “It’s hard to believe it has been almost 30 years since graduation. I continue to work in both a multispecialty ophthalmology practice in Philadelphia and serve on the adjunct faculty at the University of Pennsylvania. I am equally proud to note that I just completed a two-year term as the president of the Pennsylvania Academy of Ophthal-
mology and six-year term as treasurer of the American Society of Ophthalmic Plastic and Reconstructive Surgery. I owe so much to our education at BU!”
Michael Phelan of Millersville, Maryland, writes, “I was honored and privileged to be the Robert Krane Visiting Professor for BU Chobanian & Avedisian School of Medicine Department of Urology in June 2025. This event was hosted by Dr. Toby Chai, chair of the department of urology, and his faculty. Great to see my former medical school urology mentors Drs. Richard Babayan, former Chair of Urology, and Robert Oates, MD’82.”

Lisa Coplit of Hamden, Connecticut, writes, “Quinnipiac University has appointed Dr. Lisa Coplit as dean of the Frank H. Netter MD School of Medicine, following a national search. Dr. Coplit, who has served as interim dean since July 2025, assumes the role effective immediately. I am profoundly honored to be named the next dean of the Frank H. Netter MD School of Medicine. Serving as interim dean has been the most meaningful chapter of my professional life, and I am inspired every day by our extraordinary students and our deeply committed faculty, staff, clinical partners, and colleagues across the university. Together, we will ensure that QU Netter continues to grow as a leader in pioneering, community-engaged, and humanistic medical education, improving the health of the communities we serve while shaping the future of medicine.”
Adam Kanter of Laguna Beach, California, writes, “After 15 years as the chief of spinal neurosurgery at University of Pittsburgh Medical Center, I moved to southern California and became the chief of neurosurgery
and EMD at Hoag Neurosciences Institute. Got an executive MBA from UCLA as well last year. Can’t practice medicine anymore without understanding the business! Five kiddos—two through college, one halfway, and the last two applying now! Emptynesting in ten months and counting! Life is good.”
Johanna Fifi of New York, New York, writes, “I am just finishing up my term as president of the Society of NeuroInterventional Surgery (SNIS). It’s been quite a busy, hectic year of meetings and travel with SNIS, as well as with my work at Mount Sinai, where I see kids and adults, and with the family. My kids are now 12 and nine and we enjoy spending time together traveling in and outside the city.”
Daniel Oates of Quincy, Massachusetts, writes, “It was great to see so many who came from far and wide to celebrate our 25th medical school reunion, watching the Red Sox make their playoff-clinching walkoff win, visiting old favorites, and seeing everything that is new at the medical school and BMC. Hope that everyone can return for our 30th in 2030!!”

Kerryane Monahan of Vero Beach, Florida, writes, “After many years in secondary education, I returned to my BU anatomy roots as an assistant professor of biology, teaching anatomy at Indian River State College. It was apparently a good career change, as I was just awarded a three-year endowed chair to rethink our curriculum and write a new laboratory manual for our introductory anatomy
and physiology course. I’m really excited to put my anatomical education and research experience to good use again. I even hear the voices of my former professors come right out of my mouth during lectures and labs some days!”
Karl Kwok of Baldwin Park, California, writes, “Recently featured in two Kaiser Permanente commercials, ‘I Need an MRI’ and ‘Meat Sweats’.”
Luisa Feng of Amherst, Massachusetts, writes, “I graduated from the Mental Health Counseling and Behavioral Medicine program and after living in California and Hawaii, came back to obtain my LMHC (Licensed Mental Health Counselor) for Massachusetts a few years ago. My husband and I live in Western Massachusetts with our two little ones, missing the ocean but couldn’t imagine raising our kids anywhere else.”

Oscar Gonzalez of Ayer, Massachusetts, writes, “Sigma Lab Consulting, my consulting business addressing workflow friction in biopharma teams and organizations through workflow design, execution, and adoption, has hit its third year, a venture that began with fellow Questrom alumnus Lawrence Wong (Questrom’20). As we continue supporting organizations, I have recently finished my self-published manuscript, Predictably Broken: Straight Talk on the Failures in Biopharma and How to Fix Them, expected to
be available in early 2026. Our flagship product based on the teachings of Predictably Broken will also become available in early 2026. Throughout all of this, I continue to raise my two young boys with my wife Michelle, and prepare our home for the next addition to our family expected in March 2026.”

Laura Klein of Dallas, Georgia, writes, “As a proud 2017 graduate of the Healthcare Emergency Management program in Graduate Medical Sciences, I’m excited to share where my path has led since graduation. I currently serve as the managing director for the Douglas County Fire/EMS Department in Georgia, overseeing a wide range of projects including development of Key Performance Indicator reports and performance metrics, department accreditation, public communications and digital outreach, and management of a $10M federal grant. The skills I gained at BU, particularly in strategic thinking, crisis management, and interagency coordination, laid the foundation for everything I do today. Since graduating, I’ve worked across several sectors, including government policy, air transportation, healthcare (both public and private), higher education, and international business collaborations. I’ve also developed a strong background in continuity of operations planning and data analytics, with a specialty in predictive modeling. Now, I’m exploring new openings in the private sector and would welcome opportunities to connect with fellow alumni who may be hiring, collaborating, or simply open to networking. Feel free to
reach out. I’d love to reconnect and hear where your journey has taken you.”
Andrew Chu of Fullerton, California, writes, “I’m faculty at Stanford, where I do work in AI and informatics. I’m also an indie filmmaker and my short film, Life Support, is screening at dozens of film festivals around the world! My wife and I named the main character after our cute little one-year-old, Sara.”
Anne Wells of San Antonio, Texas, writes, “It’s been an exciting year! I’m thrilled to share that I am an MD/PhD student at UT San Antonio and successfully defended my PhD in Neuroscience with work focused on the genetic basis of cognition. I also just got married to my beautiful wife, Annie, who also is an MD/PhD student, now finishing her PhD! The best is yet to come!”

Roya Edalatpour of Baltimore, Maryland, writes, “I married Mohammed Toure last June in Philadelphia. We met in Boston in 2021, while I was attending medical school at Boston University and Mohammed was completing his PhD at MIT. The celebration was made even more special by the presence of many former classmates who joined us for the occasion. I am now a first-year neurocritical care fellow at Johns Hopkins University and Mohammed serves as associate director of business development at Flagship Pioneering. We are thrilled to begin this new chapter of our lives together in Baltimore, Maryland.” ●


Diane Crocker of Chevy Chase, Maryland, passed away on July 22, 2025.

Robert Kenerson of Winchester, Massachusetts, passed away on September 6, 2025. 19 68

Allan Garfield of Santa Rosa, California, passed away on July 17, 2025. ●
Continued from page 47
Pediatric Neurologist Elizabeth C. Dooling, MD’65, Passionate Supporter

“We will miss her wisdom, enthusiasm for medicine as a career, and her personal support for our students.”
DEAN EMERITA KAREN ANTMAN, MD
Elizabeth C. Dooling, MD’65, passed away on December 16, 2025, at her Boston home. A pediatric neurologist who specialized in the diagnosis and treatment of neurological disorders among children, she dedicated most of her professional years to Massachusetts General Hospital, where she served as director of the Pediatric Rehabilitation Unit and director of the training program in Pediatric Neurology.
Born in Boston on October 6, 1937, Dooling earned a BA from Vassar College in 1959 before matriculating to Boston University School of Medicine. At MGH, she received numerous awards, including 1992 Teacher of the Year in pediatric neurology and the 2013 Brian McGovern Award for Clinical Excellence. She received an honorary doctor of humanities from New England School of Law in 1985.
“Liz was a special person. Despite her own busy career in pediatric neurology at MGH, she continued to support our students with her advice for the school on both curriculum and student life,” said Dean Emerita Karen Antman, MD. “We will miss her wisdom, enthusiasm for medicine as a
career, and her personal support for our students.”
Dooling was known for her compassion and her unflagging devotion to patients.
“If you (are) the parent of a neurologically challenged or compromised child and you feel lost…and don’t know where to turn, then (open the door to) Elizabeth Dooling’s office, where the most considerate, conscientious, and compassionate caretaker that has ever graced this earth will await you with open arms,” a colleague and fellow neurologist wrote in his McGovern Award nomination remarks.
Dooling gave back to the medical school in many ways. An alumni board member, she was recognized by the Alumni Office for leading their annual phonathon from the 1970s until 2014.
Over a lifetime of philanthropy, she generously supported medical education, contributing more than $700,000 to student scholarships as a member of the Keefer Society and the Annual Fund Leadership Giving Society. She also volunteered at the Black Alumni Symposia and established the Christmas-Eastman-Fuller Endowed Scholarship fund to honor three pioneering BU medical school graduates: Black psychiatrist June Jackson Christmas, MD’49; Charles Eastman, MD’1890, one of the first Native American physicians; and Solomon Carter Fuller, MD’1887, the nation’s first Black psychiatrist.
Well-known and admired by Chobanian & Avedisian School of Medicine students, Dooling purchased more than 1,800 copies of Atul Gawande’s book, Being Mortal: Medicine and What Matters in the End, personally handing a copy to each first-year student for twelve years; for the last eight, she did so at the annual Lorraine Stanfield, MD, Memorial Doctoring Lecture.
“Aunt Libby” to her family, Dooling leaves behind 10 nieces and nephews, more than two dozen grand nieces and nephews, and many Boston-area cousins and their families. She will be dearly missed. ●
