

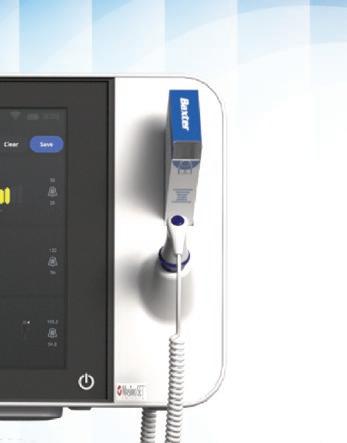
Robotic Process Automation in Supply Chain Work
Healthcare systems are using robotic process automation to streamline repetitive tasks, boost efficiency, and free staff for higher-value work.










2 A Preventable Cancer is Taking More Young Lives
Colorectal cancer has become the top cause of cancer death for Americans under 50, even as deaths from lung, breast and other cancers decline, raising the stakes for screening, advocacy and health equity.
10 From Contract to P&L
How baseline choice shapes reported value. 14 Robotic Process Automation in Supply Chain Work
Healthcare systems are using robotic process automation to streamline repetitive tasks, boost efficiency, and free staff for higher-value work.
The Journal of Healthcare Contracting is published bi-monthly by Share Moving Media
350 Town Center Ave, Ste. 201 Suwanee, GA 30024
Phone: 770/263-5262 FAX: 770/236-8023 e-mail: info@jhconline.com www.jhconline.com
PUBLISHER John Pritchard jpritchard@sharemovingmedia.com
22 Using AI Will Generate Supply Chain Savings for Health Systems
24 Poking a Round Peg Through a Square Deal?
Decisions on legality of mergers-andacquisitions frequently a head-scratcher.
26 Healthcare Distributors Offer Lessons on Leadership
DIRECTOR OF BUSINESS DEVELOPMENT Anna McCormick amccormick@sharemovingmedia.com EDITOR Graham Garrison ggarrison@sharemovingmedia.com
Laura Gantert lgantert@sharemovingmedia.com
ART DIRECTOR Brent Cashman bcashman@sharemovingmedia.com
The Journal of Healthcare Contracting (ISSN 1548-4165) is published bi-monthly by Share Moving Media, 350 Town Center Ave, Ste 201, Suwanee, GA 30024.
Copyright 2026 by Share Moving Media All rights reserved.
Please note: The acceptance of advertising or products mentioned by contributing authors does not constitute endorsement by the publisher. Publisher cannot accept responsibility for the correctness of an opinion expressed by contributing authors.
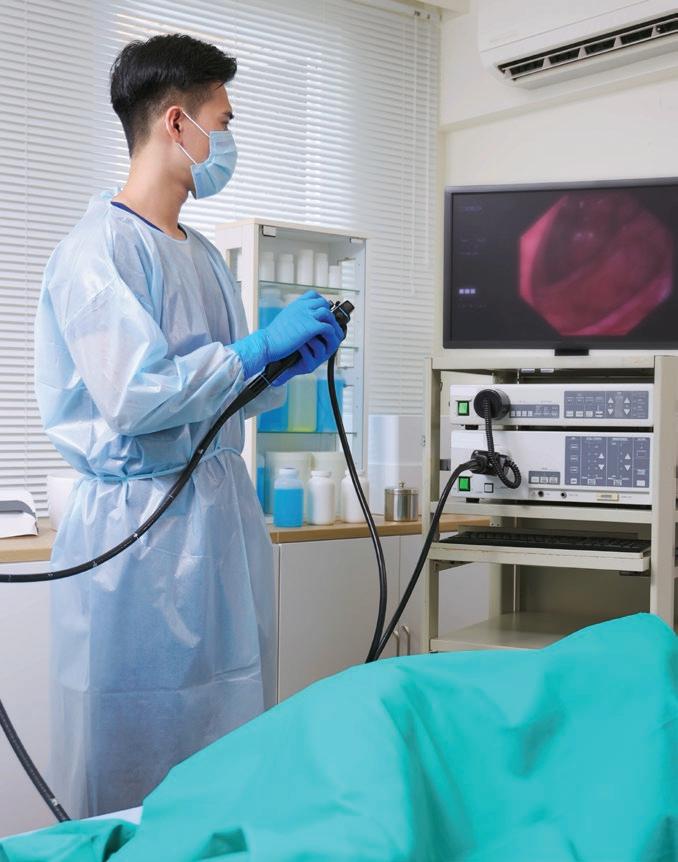
A Preventable Cancer is Taking More Young Lives
Colorectal cancer has become the top cause of cancer death for Americans under 50, even as deaths from lung, breast and other cancers decline, raising the stakes for screening, advocacy and health equity.
A new study from the American Cancer Society (ACS) reveals that cancer mortality among Americans under age 50 has dropped sharply overall, but one disease bucks the trend.
According to research published Jan. 22 in the Journal of the American Medical Association, the U.S. cancer death rate for people younger than 50 fell by 44% from 25.5 per 100,000 in 1990 to 14.2 per 100,000 in 2023 – largely due to significant decreases in deaths from lung, breast, brain cancers, and leukemia.
However, colorectal cancer was the lone exception, rising steadily and becoming the leading cause of cancer death in this age group in 2023 after increasing 1.1% per year since 2005.
Rebecca Siegel, MPH, senior scientific director of surveillance research at the ACS and lead author of the report, said: “The steady rise in colorectal deaths under 50 is even more alarming compared to the dramatic declines for lung and breast, even as breast cancer incidence is climbing.”
Siegel added that while the reasons for the rising numbers remain unclear, “lives can be saved now through symptom awareness and destigmatization, and more screening uptake, as three in four people under 50 are diagnosed with advanced disease.”
For the study, scientists analyzed trends in the annual numbers of cancer
deaths and age-standardized rates per 100,000 men and women aged 0-49 years for the top 5 cancer-related deaths during 1990-2023 in the U.S. They used data from the National Center for Health Statistics as provided by the Surveillance, Epidemiology, and End Results (SEER) program at the National Cancer Institute.
The ACS said results showed that 1,267,520 people died from cancer in the U.S. before age 50 from 1990 through 2023, and the overall death rate decreased by 44%. Four of the five leading causes of cancer death decreased, with the average annual decline during 2014-2023 ranging from 0.3% for brain cancer and 1.4% for breast cancer to 2.3% for leukemia and 5.7% for lung cancer.
Only CRC mortality increased annually for people under 50. Lung cancer and leukemia dropped from ranking first to fourth and third to fifth, respectively, whereas breast cancer remained the second leading cancer death overall and first in women. Cervical cancer ranked third in women in 1990 and 2023, despite a continuous decline throughout the study period. The cancer distribution in men mirrored the overall pattern, with breast cancer replaced by non-Hodgkin lymphoma (4th) in 1990 and pancreatic cancer (5th) in 2023.
“We weren’t expecting colorectal cancer to rise to this level so quickly, but now it is clear that this can no longer be called an old person’s disease. We must double down on research to pinpoint what is driving this tsunami of cancer in generations born since 1950,” said Dr. Ahmedin Jemal, senior vice president, surveillance, prevention, and health services research at the ACS and senior author of the study. “In the meantime, people 45-49 years make up 50% of di -
agnoses under 50, so increased screening uptake will prevent disease as well as death.”
Catching it early
CRC is one of the most preventable and treatable cancers when found early, according to the Centers for Disease Control and Prevention (CDC). That’s in part because CRC grows slowly, often starting as a small, noncancerous polyp. Over time, some polyps can turn into cancer.
Stool-based tests are noninvasive and can be completed at home. These include the fecal immunochemical test (FIT) and guaiac-based fecal occult blood test (gFOBT), which look for hidden blood in the stool, as well as FIT-DNA tests, which detect both blood and abnormal DNA linked to cancer or polyps. These tests are typically repeated every one to three years, depending on the method used. A positive result requires follow-up with a diagnostic colonoscopy.
“Fight CRC advances health equity by targeting resources and culturally appropriate education to clinics and communities that need them most and by pushing state and federal policy to close coverage and access gaps.”
Another reason why early screening is so essential: Colorectal cancer often produces no early warning signs, especially for adults age 45 and older, the CDC says. When symptoms do occur, they may include persistent changes in bowel habits, such as diarrhea or constipation; blood in or on the stool; a feeling that the bowel does not empty completely; ongoing abdominal pain, cramps or aches; and unexplained weight loss. Because these signs can also stem from non-cancer causes, health officials urge individuals experiencing any of them to consult a clinician promptly. Health experts stress that multiple colorectal cancer screening options are available, allowing patients and providers to choose an approach that fits individual risk, preferences, and access to care. Screening tests generally fall into two categories: stool-based tests and visual exams of the colon and rectum.
Visual exams allow clinicians to directly examine the colon. Colonoscopy, considered the most comprehensive option, enables providers to detect and remove precancerous polyps during the same procedure and is usually performed every 10 years for average-risk adults. Other options include flexible sigmoidoscopy and CT colonography, also known as virtual colonoscopy, which are performed at shorter intervals.
Advocacy efforts
The increase in colorectal cancer among younger adults is shifting public health toward earlier screening, better symptom recognition and risk-based approaches, said Anjee Davis, CEO of Fight Colorectal Cancer, an organization that works to empower individuals, influence policy, and accelerate breakthroughs that improve
prevention, care and outcomes. Fight CRC’s efforts include educating providers and the public, expanding digital navigation tools, and advocating for coverage reforms so people ages 45 to 49 and symptomatic younger patients are identified and tested promptly.
Fight CRC’s advocacy program mobilizes patients, caregivers and supporters to influence public policy at both the federal and state levels. Through initiatives such as Call-on Congress and the State Catalyst Program, advocates receive training and tools to engage lawmakers on issues including access to screening, affordability of care and research funding. These efforts ensure that colorectal cancer remains a visible priority in health policy discussions.
Fight CRC also plays a significant role in advancing research and innovation. The organization supports research focused on prevention, early detection and treatment, while emphasizing patient involvement in the scientific process. Its Research Advocacy Training and Support (RATS ) program equips advocates to participate in clinical trial design, advisory panels and funding decisions, helping ensure that research reflects real-world patient needs.
In addition, Fight CRC offers a range of education and support resources for patients and caregivers navigating a colorectal cancer diagnosis. These include medically reviewed educational materials, community connections, and digital tools such as ChatCRC, an AI-powered chatbot designed to provide personalized guidance on screening, treatment options, and survivorship.
Community engagement and awareness are further strengthened through national campaigns and events, including United in Blue during Colorectal Cancer
An AI-enabled patient chat for colorectal cancer patients and caregivers
Davis said technology will make screening and diagnosis more accurate, less invasive, and more personalized. Even initial outreach efforts can be boosted by the latest advances in communication tools.
Fight Colorectal Cancer’s AI-enabled patient chat, ChatCRC, is an artificial intelligence–powered chatbot created to support people affected by colorectal cancer – including patients, caregivers and clinicians – by providing accurate, accessible information and personalized responses related to colorectal cancer prevention, screening, diagnosis, treatment and care management.
ChatCRC delivers 24/7 interactive support, helping users ask questions and receive immediate answers about topics like risk factors, screening options, treatment side effects, wellness strategies and available resources. It’s designed to remove complex medical jargon so information is easier to understand, and it can even be accessed by SMS text message for users without internet access.
While the tool provides tailored information and connects users with educational resources, clinical trial info and support groups, it does not offer medical advice or replace consultation with a healthcare provider.
Awareness Month and signature fundraising initiatives like Climb for a Cure.
Together, these programs reflect Fight CRC’s comprehensive approach: driving policy change, accelerating research, and supporting patients at every stage of their journey. As colorectal cancer rates continue to rise, particularly among younger adults, the organization’s multifaceted strategy aims to ensure that progress keeps pace with the growing need.
Addressing disparities and gaps
Disparities in colorectal cancer risk and outcomes across different populations or
regions are both large and avoidable, said Fight CRC’s Davis. Black, Hispanic, rural, low income and uninsured communities shoulder a disproportionate burden.
“Fight CRC advances health equity by targeting resources and culturally appropriate education to clinics and communities that need them most and by pushing state and federal policy to close coverage and access gaps,” she said. “This is evident in places with constrained or limited access to endoscopy.”
Davis said barriers to care for younger patients are practical and solvable: cost, access, awareness, provider recommendation and follow up after
abnormal tests. “Fight CRC pushes systemic solutions such as mailed outreach, patient navigation, no cost follow up for diagnostic colonoscopy and state level quality measures so that noninvasive testing translates into timely diagnosis and care,” she said. “These barriers are most acute where Medicaid expansion and coverage policies vary.”
At the national level, the Centers for Disease Control and Prevention’s (CDC) Colorectal Cancer Control Program (CRCCP) is driving measurable increases in colorectal cancer screening by partnering with clinics, hospitals and other health care organizations to implement proven strategies that help detect cancer early and save lives.
The CRCCP targets adults aged 45 to 75, particularly in clinics where fewer than 60% of patients are up to date on screening – often in lower-income or medically underserved communities.
At the heart of the program are evidence-based interventions recommended by the Guide to Community Preventive Services. These include regular assessment and feedback to healthcare providers on their screening recommendations, electronic or written provider reminders for due or overdue tests, and targeted patient reminders via mail, email or phone.
The CRCCP also works to remove structural barriers that can hinder screening access. Efforts range from extending clinic hours and offering stool tests in nonclinical settings like vaccination sites to providing patient navigation services, transportation, childcare and simplified paperwork, all aimed at making screening more accessible and less burdensome.
By collecting and analyzing clinic data, the CDC says it can identify where screening gaps remain and adjust
strategies to maximize impact. Public health evaluations indicate that these interventions have increased screening rates, particularly in clinics serving underserved populations, though challenges remain in closing gaps across all regions.
Health officials emphasize that increasing colorectal cancer screening not only saves lives by detecting precancerous conditions early but also reduces long-term health care costs, lost wages and the burden on patients, employers and insurers.
In a compelling example of the CRCCP’s real-world impact, a free clinic in West Virginia dramatically increased its screening rate through tailored interventions supported by CDC funding. At Wheeling Health Right, only 9% of eligible patients were screened initially,
In another example of the CRCCP’s influence, a public health clinic in St. Petersburg, Florida, more than doubled its colorectal cancer screening rate by adopting a series of targeted outreach and follow-up strategies. Before partnering with the Florida Department of Health’s Colorectal Cancer Control Program, only about one-third of eligible patients were being screened. With CDC support, the clinic hired a full-time patient navigator, developed daily electronic reports of screening needs, and implemented a robust reminder system that combines pre-visit and follow-up calls and letters.
One especially effective innovation allowed clinic staff to collect stool samples while patients were already visiting for
Success stories from participating organizations show that reaching 80% is achievable with coordinated effort, tailored outreach and systematic follow-up.
largely because the clinic relied on an older fecal occult blood test that many patients found inconvenient. By switching to the easier fecal immunochemical test (FIT), training staff on screening guidelines, updating electronic records, and implementing follow-up phone reminders, the clinic saw its screening rate jump first to 53% in 2017 and then to more than 67% in 2018 – a 58% overall increase over two years. Staff calls alone boosted FIT return rates by nearly 40%, underscoring the power of patient engagement and simple systemic changes in improving health outcomes. Despite progress, about one-third of patients still need screening, and clinic leaders plan to continue adapting strategies to raise rates even further.
other services, escorting them to the restroom and providing results the same day. These combined efforts helped boost screening from 34% to over 75%.
80% in Every Community
Another major health equity campaign is gaining momentum across the United States with a shared aim: get at least 80% of eligible adults screened for colorectal cancer in every community nationwide. The initiative, 80% in Every Community, is led by the American Cancer Society National Colorectal Cancer Roundtable (ACS NCCRT) – a coalition of health systems, community organizations, employers, health plans and other partners
committed to reducing colorectal cancer deaths through increased early detection.
The 80% in Every Community campaign builds on earlier national efforts – including the original 80% by 2018 pledge – by focusing not just on overall national targets but on ensuring that every community, regardless of location, income or racial and ethnic makeup, reaches screening rates of at least 80%. This expanded focus on health equity aims to close persistent gaps in access to lifesaving colorectal cancer tests.
What counts as a “community” under the initiative is intentionally flexible: it can be a city, county, state, a patient
population served by a particular health system, a workforce group, or a racial or ethnic community striving together toward higher screening rates.
ACS NCCRT encourages organizations to commit to the goal, adopt screening improvement strategies, share best practices and use a suite of available tools and resources to support their outreach work. There is also a social engagement aspect: partners and supporters share progress and stories using #80inEveryCommunity to help raise awareness and inspire action.
Success stories from participating organizations show that reaching 80% is
Polyps in the colon or rectum
Most colorectal cancers start as a growth on the inner lining of the colon or rectum. These growths are called polyps. Polyps are quite common, especially as you get older. Most polyps are benign, or noncancerous. Some types of polyps can change into cancer over time (usually over many years). The chance of a polyp turning into cancer depends on the type of polyp it is. There are different types of polyps.
` Adenomatous polyps (adenomas): These polyps sometimes change into cancer. Because of this, adenomas are called a precancerous condition. The 3 types of adenomas are tubular, villous, and tubulovillous. Tubular adenomas are the most common type of adenomatous polyps. Villous adenomas are the least common type of adenomatous polyps, but are more likely to change into cancer.
` Hyperplastic polyps and inflammatory polyps: These polyps are more common, but in general they are not precancerous. Some people with large (more than 1cm) hyperplastic polyps might need colorectal cancer screening with colonoscopy more often.
` Sessile serrated polyps (SSP) and traditional serrated adenomas (TSA): These polyps are often treated like adenomas because they have a higher risk of changing into cancer.
Source: American Cancer Society
achievable with coordinated effort, tailored outreach and systematic follow-up. A core part of the initiative’s strategy includes addressing barriers to care, particularly in underserved populations, and investing in data tracking to monitor progress.
As the campaign moves forward, its leaders emphasize collaboration and shared responsibility in eliminating colorectal cancer disparities and ensuring that everyone – regardless of where they live – can benefit from timely, lifesaving screening.
Reversing the trend
Taken together, the data point to a clear and urgent message: while cancer outcomes for younger Americans have improved dramatically overall, colorectal cancer is moving in the opposite direction–and it does not have to. With effective screening tools, proven public health strategies and growing advocacy to expand access and awareness, experts say the means to reverse this trend already exist.
The challenge now is turning knowledge into action, ensuring that age, income, geography or insurance status no longer stand between patients and early detection. As researchers, clinicians, advocates and communities align around that goal, the hope is that colorectal cancer will soon follow the same downward trajectory as other cancers – and that fewer lives will be lost to a largely preventable disease.
Whether at the national or local level, Fight CRC’s Davis said simplicity is key to effective screening strategies. “Simple, well-designed systems work: mailed noninvasive tests, patient navigation, and programs that remove cost and logistical barriers,” she said.
The Supply Chain Reset
Healthcare doesnʼt have a savings problem. It has a proof problem.
The next era of supply chain is built on verified savings, executive governance and artificial intelligence (AI)-powered execution — not assumptions.
At University Hospitals Health System (UH), supply chain was redesigned to operate like a financial control center.
Partnering with Premier, UH embedded governance, aligned clinicians with analytics, and hardwired zero-waste execution.
Delivered measurable cost improvement across supplies, pharmacy and clinical utilization.
Case in Point
By embedding cost intelligence directly into clinical workflow, a $100-plus item review threshold was introduced, ensuring higher-cost supplies were opened only when clinically necessary, resulting in $8 million in sustained annual savings.

Premier is more than a GPO. Weʼre the strategic partner helping health systems prove performance — and sustain it. Register for the Webinar
The Supply Chain Reset: How Health Systems Deliver Savings with AI, Governance and Zero Waste
2025 Cardinal Health™ Lab Briefings A year
in review
Total attendees
10,688
In 2025, Cardinal Health’s PACE-accredited Lab Briefings webinar series continued to lead the way in providing trusted monthly education designed for laboratory professionals. Each session connected the lab community with leading experts to address critical challenges and deliver actionable knowledge to help lab professionals thrive in a rapidly evolving healthcare landscape.
Total credit hours earned
117,568
The art of urine culture stewardship Hottest topics
CAP accreditation checklist updates Chemical safety in the workplace
January
Topic:
Lab payment and policy outlook for 2025
Speaker: Dennis Weissman, M.S.
Febuary
Topic:
2024 CAP accreditation checklist updates
Speaker: Stephen Sarewitz, MD, FCAP Gregory Gagnon, MD, FCAP
Top attendees Laboratory Manager Laboratory Director
Medical Laboratory Scientist
March
Topic: Chemical safety in the workplace
Speaker: Margaret Blaetz, CLC, MLT(AMT), Mcm, MLT(ASCP), CCCP(AAPOL)
April
Topic: The clinical lab’s role in promoting better patient outcomes
Speaker: James Crawford, MD, Ph.D.
May
Topic: Beyond the label: novel applications of cardiac biomarkers
Speaker: Christopher W. Farnsworth, Ph.D., DABCC
June
Topic: From hidden to found: Giving a voice to medical lab science
Speaker: Austin Korczak, MLS (ASCP)CM
“Very informational webinar! I learned a lot and the speaker was incredibly knowledgeable on the subject.” – Webinar series attendee

“One
of the most valuable CE presentations I have attended. Clear, concise and easy to understand.”
– Webinar series attendee
August
Topic:
Evaluating urine fentanyl tests for clinical implementation
Speaker: Rongrong Huang, Ph.D.
November
Topic:
The intricacies and complexities of pharyngitis diagnostics
Speaker: Susan Butler-Wu, Ph.D., D(ABMM), FIDSA
September
Topic:
Data-driven optimization of diagnostic thresholds
Speaker: Jieli Shirley Li, MD, Ph.D., DABCC, FCACB
October
Topic: Lab compliance and test utilization: Prepare for 2026 and beyond
Speaker: Andrew Fletcher, MD, MBA, CPE, CHCQM, FCAP Danielle Tangorre, JD, MS
Explore our full archive of webinars. Earn CE credits for up to six months after the live event.
From Contract to P&L
How
baseline choice shapes reported value.
BY BRETT WEBSTER
In healthcare contracting, value is rarely disputed in principle. The friction emerges later, when sourcing reports one number, finance validates another, and both are technically correct within their own logic. More often than not, the root cause is not execution or compliance, but the baseline chosen to measure impact.
Two baselines dominate contracting analytics: Last Price Paid (LPP) and Weighted Average (WA). Each has legitimate use cases. Each can also obscure reality when applied indiscriminately. Understanding their behavior across price enhancement and conversion projects is essential if reconciliation is the goal rather than simply reporting value.
Last Price Paid: Powerful, intuitive and dangerous
Last Price Paid is attractive because it feels concrete and is simple. It reflects the most recent transaction before a
new contract takes effect and therefore resonates with operational stakeholders. For conversion projects in particular, LPP often captures the full economic delta between the old product and the new one.
However, LPP carries a structural weakness that becomes apparent over time: it is path dependent.
If prices fluctuate during the year, LPP implicitly embeds all prior volatility into the baseline. A late-year price spike, distributor adjustment, or short-term surcharge can dramatically inflate the apparent value of a subsequent contract, even if that contract merely restores pricing to historical norms.

In this scenario, LPP-based savings include two fundamentally different effects:
` True price reduction relative to a stable historical rate
` Cost avoidance from preventing a temporary or unsustainable price from persisting
Both are real. But when they are reported as a single figure, reconciliation becomes difficult. Finance may see a reduction that never existed in the run-rate, while sourcing sees total value that was legitimately negotiated.
This issue is amplified when the contract cycle does not align with the fiscal year. A price spike late in Q4 followed by a new contract on January 1 can produce dramatic “savings” on paper, even though the organization never intended to budget at the inflated rate.
Weighted Average: Stable,
defensible and incomplete
Weighted Average addresses many of LPP’s weaknesses by smoothing volatility across a defined historical period. By anchoring the baseline to actual utilization patterns, WA better reflects the economic reality that finance recognizes in budgets and forecasts.
For price enhancement projects, WA often produces numbers that reconcile more cleanly to the P&L. It avoids overstating value tied to anomalous transactions and reduces the risk of reporting savings that exceed prior-year spend.
The tradeoff is that WA can understate total value in certain conversion scenarios. When a project eliminates exposure to future price increases or shifts volume away from an unfavorable mix, WA captures only what changed relative to history, not what was prevented from happening.
From a sourcing perspective, this can feel punitive. From a finance perspective, it feels credible. The tension is not about correctness, but about intent.
Where baselines collide
Conversion projects expose the philosophical divide between LPP and WA most clearly.
Using LPP, a conversion may show substantial value by comparing the new item to the most expensive legacy product still in use. Using WA, the same project may appear modest because the baseline reflects blended historical behavior rather than worst-case exposure.
Neither view is wrong. But they answer different questions:
` LPP answers: What is the total value relative to what we were most recently paying?
` WA answers: What is the sustainable reduction relative to how we actually operated?
Problems arise when organizations expect one baseline to serve both purposes simultaneously.
Even in straightforward renegotiations without a conversion, baseline choice matters. If LPP reflects a latecycle increase, reported savings may include avoided escalation rather than true reduction. If WA spans periods of atypical utilization, it may dampen legitimate improvements.
In both cases, reconciliation fails not because value is absent, but because its components are blended beyond recognition.
Why reconciliation fails without a clear baseline
Reconciliation is not about matching a sourcing report to a ledger line item exactly. It is about ensuring that the directional logic aligns. When baselines are inconsistent, finance sees variance where sourcing sees success.
The most common failure modes include:
` Savings reported against a baseline that was never budgeted
` Avoided costs reported as reductions
` Annualized projections compared to partial-year actuals
` Conversion value conflated with utilization growth or decline
None of these are analytical errors. They are framing errors.
A better path forward: Separating total value from reconcilable value
The tension between sourcing and finance does not come from disagreement about whether value exists. It comes from trying to force a single number to serve two different purposes:
demonstrating total economic impact and reconciling cleanly to the P&L. A more durable approach accepts that these are related but distinct objectives and designs the methodology accordingly.
The path forward is twofold:
` Total Value should answer the question sourcing leaders care about: What is the full economic impact of this decision relative to what we would otherwise have paid?
` Reconcilable Value should answer the question finance cares about: What portion of that impact can reasonably be expected to show up in budget and actuals?
Both can be derived from the same data, but they require different reference points. The bridge between them is not guesswork. It is the explicit identification of cost avoidance.
A concrete example
Consider a conversion from two clinically equivalent, dual-sourced implants to a single sole-source product.
` Product A
` Early-year price: $1,000
` Midyear contract increase to $1,050
` Equal usage at both prices in prior year (average price $1,025)
` Product B
` Stable price throughout the year
` Price: $950
` New Product C
` Sole-source conversion price: $850
Immediately, the limitations of a single baseline become apparent.
Why LPP alone breaks down
Last Price Paid is not a stable concept in this scenario.
` For Product A, LPP is $1,050.
` For Product B, LPP is $950.
` At the system level, LPP depends entirely on which SKU happened to be purchased most recently.
If Product A was purchased last, the conversion appears dramatically more valuable than if Product B was purchased last, even though nothing operationally changed.
Weighted Average as the reconcilable anchor
Weighted Average avoids this instability. Using WA, the baseline reflects how the organization actually behaved over the year, smoothing timing effects and eliminating dependence on transactional order.
If historical utilization was, for example, 75% Product A and 25% Product B, the blended weighted average baseline is: (0.75 × $1,025) + (0.25 × $950) = $1,006.25
Against the new price of $850, the reconcilable cost reduction is: $1,006.25 − $850 = $156.25 per unit. This is the portion of value finance can reasonably expect to see reflected in run-rate expense reduction, assuming comparable utilization.
Recovering total value without sacrificing credibility
Where sourcing often feels shortchanged is that this approach understates exposure avoided. That exposure is real, and it should be measured, but not conflated with reduction.
To calculate total value, LPP is still useful but must be applied correctly.
Instead of a single LPP, use product-level LPPs and preserve the historical mix:
` Product A LPP: $1,050
` Product B LPP: $950
Assuming the same 75/25 mix, the LPP-based blended baseline becomes: (0.75 × $1,050) + (0.25 × $950) = $1,025
Total value relative to LPP is therefore: $1,025 − $850 = $175 per unit
The missing link:
Cost avoidance made explicit
The difference between these two figures is not an error, but insight.
` Total Value (LPP-based): $175 per unit
` Reconcilable Cost Reduction (WA-based): $156.25 per unit
` Cost Avoidance: $18.75 per unit
That $18.75 represents avoided exposure tied to timing and price escalation, not a reduction in historical run-rate cost. By isolating it explicitly, sourcing retains credit for full economic impact while finance maintains confidence in what should reconcile.
Why this framework scales
This approach works cleanly when there is a single incumbent product, where the distinction between LPP and WA is straightforward. It also scales to more
complex, multi-SKU conversions without introducing arbitrariness.
The key principles remain consistent:
` Use Weighted Average to anchor reconcilable cost reduction.
` Use product-level Last Price Paid, preserved by historical mix, to calculate total value.
` Treat the difference as cost avoidance, not as a rounding error or modeling artifact.
By design, this framework produces two numbers that answer two different questions, while remaining mathematically and conceptually linked.
Why this matters
When total value and reconcilable value are forced into a single figure, credibility suffers. When they are presented side by side, with cost avoidance clearly defined, the conversation changes. Finance no longer has to challenge sourcing’s math, and sourcing no longer has to defend value that is real but misunderstood.
This is not about adding complexity for its own sake. It is about acknowledging that healthcare contracting decisions shape both what we spend and what we avoid spending. Measuring both, transparently and intentionally, is how organizations move from debating savings numbers to reconciling value with confidence.
Next in this series: why midyear contract implementations create the illusion of “missing savings,” and how annualization, timing, and partial-year realization distort both sourcing reports and financial forecasts.
Healthcare needs distributors that are more than just box movers
When you choose Cardinal Health, you’re joining a community committed to diagnostic quality and supply chain resiliency. With a dedicated, clinical lab pointof-contact, on-hand capital equipment experts and supportive suppliers (including exclusive relationships), our teams of professionals are all invested in championing your success.
Your priorities are our priorities. That's why we offer competitively priced, quality products that are locally stocked for your convenience. And we’re constantly expanding our portfolio, with over 1,000 product launches across 29 suppliers this year.
We support all testing disciplines, including:
• Anatomic pathology/ histology
• Blood bank
• Capital equipment
• Clinical chemistry
• Coagulation
• Hematology
• Laboratory equipment
• Laboratory essentials
• Microbiology
• Molecular diagnostics
• Point of care & infectious disease
• Research essentials
• Specimen collection
• Specimen collection kits
• Urinalysis
• Virology


We're a preferred laboratory distributor and product advisor to top healthcare providers, and we have been for decades.1 Count on us for financial savings, operational efficiencies and supply continuity through our rich history of distribution excellence, industry-leading lab expertise delivered by a strategic, responsive team of 200 lab professionals and clinically equivalent Cardinal Health™ Brand products.
Transparency without the hidden costs or fees. One point of contact. Deep supplier relationships. Always-on service. That’s the Cardinal Health way.
We are your lab advisor. Expertise. Choice. Efficiency. Savings.
Robotic Process Automation in Supply Chain Work
Healthcare systems are using robotic process automation to streamline repetitive tasks, boost efficiency, and free staff for higher-value work.
BY R. DANA BARLOW
Editor’s note: The following is third in a multipart series.
When people talk of robots in supply chain, they likely envision myriad mobile vehicles roaming around, or a chorus of articulating arms moving packages with some degree of synchronicity, or even drones buzzing around overhead.
However, robotics extends beyond physical machines or vehicles in consistent, if not constant, motion. The category also includes high-tech software to handle a different kind of mundane, repetitive work that leans toward mental than physical fatigue: Robotic Process Automation (RPA).
In determining the need to invest in RPA for relevant supply chain areas and functions, such as procure-to-pay (P2P) processes, healthcare supply chain executives and leaders acknowledge they approach their assessment and decision in much the same way they investigate automated guided vehicles (AGV) and automatic mobile robots (AMRs).
Mapping tasks
Livonia, Michigan-based Trinity Health began their own evaluation by starting from scratch, listing, mapping and recording the steps team members take to learn how, when and where RPA could simplify workflow, according to Kristyl Tucker, director, Continuous Improvement and Customer Service Operations.
“Our investment decisions begin with disciplined process assessment,” Tucker told The Journal of Healthcare Contracting. “In 2019, we cataloged dozens of manual, repetitive tasks across Procurement and Accounts Payable and applied an intelligent Automation Assessment framework to evaluate them for automation


ROBOTIC PROCESS AUTOMATION
based on process, data, technology and people characteristics.
“We piloted our first automation using HP’s UFT as a proof of concept, and the success was clear,” she continued. “Depending on the solution and adoption, we could fully recoup our investment within one to two years. That proof point gave us the confidence to expand and establish RPA as a standard capability. Since then, we’ve scaled to more than 20 bots in production, automating 2.7 million transactions and delivering nearly $4 million in value.”
If anything, RPA could be viewed as supply chain’s version of the decision support systems that assist clinicians to make more accurate and informed diagnoses on patients, whether that involves interpreting diagnostic images, laboratory test results or surgical direction.
‘’That’s a great analogy,” Tucker acknowledged. “Just as clinical decision support systems help providers make faster, more informed decisions, RPA in Supply Chain acts as a digital assistant that streamlines operational decisionmaking. Bots surface exceptions, route tasks intelligently and ensure data integrity, allowing our teams to focus on strategic work, supplier relationships and valuebased decisions. It’s not about replacing judgment, but enhancing it with timely, accurate information and automation.”
Trinity prioritized high-volume, error-prone activities and used a scoring framework to assess automation potential, according to Tucker. “While our proof of concept was on HP’s UFT, we intentionally kept our process documentation and automation logic platform-agnostic,” she indicated. “Our team drove the strategy, governance and pipeline development, while the bots themselves enabled scale
by handling increasing volumes without additional headcount. Once a bot is built and stable, it can process thousands of transactions with minimal oversight.”
Tucker adds that the scale expansion may have started with staff direction but could be routinely managed by the RPA software, but only within the framework they design and maintain.
RPA could serve as a baseline technology for provider organizations of any size, scope and scale to test the robotic waters, particularly covering administrative tasks, according to Jeffrey Stephens, senior vice president, Supply Chain Management, Memorial Hermann Health System, Houston.
your decision. It’s just a simple cost and benefit analysis. Whoever tries to sell us a product like this needs to understand how we operate and what applications we need, followed by the costs to invest in the technology to see if it’s worth it.”
Cleveland Clinic embarked on its own RPA investigation as it strives to ramp up automation within its facilities.
“When looking at RPA opportunities, we focus on processes that create the greatest impact across the overall operation, not just within a single team or function,” said Steve Downey, vice president, Chief Supply Chain and Support Services Officer. “We evaluate both cost savings and quality improvements.
As with any automation, labor, manpower and workflow can feel some pressure, resulting potentially in reallocation or reduction.
“With RPA we have moved 15 to 20 different manual tasks to the system, so I would say to the smaller facility to focus on RPA for sure,” Stephens recommended.
While it may be easy for supply chain executives to lump robotic technology in with artificial intelligence (AI) capabilities, any administrative, financial and operational assessment would be the same, Stephens insists.
“We would be interested if we could understand the applications and benefits of the software as it applies to supply chain,” he noted. “Just as with the AMRs, you really have to ask a lot of good questions to truly understand what are the benefits to your team and operation. Once you understand those benefits, then you attach a cost to it, just like we did with the AMRs. Then you can make
RPA can reduce manual effort, but it also enhances consistency and accuracy in repetitive processes. The goal is to free up our teams for higher-value work while improving speed and reliability across the supply chain. We also consider scalability – whether the automation can be expanded to other areas once proven successful. Ultimately, the decision is based on where automation will make the most meaningful difference in performance, accuracy, and caregiver or customer experience.”
Picking products
Once supply chain identifies and establishes the need for digital assistance in the form of RPA, then the vendor selection commences.
“Our technology choice was guided by pragmatism and scalability,” Trinity’s Tucker explained. “We initially tested UFT but quickly realized that to expand across the enterprise, we needed a platform that was more flexible, cloud-capable and supportive of citizen developers. After vendor evaluations, we selected UiPath as our standard.”
Three fundamental questions anchored Trinity’s decision, according to Tucker. ` Will this solve our problems efficiently and integrate easily with our critical systems such as PeopleSoft, Outlook, and ServiceNow?
` Can we implement it with the resources we have?
` Does it deliver measurable value?
Trinity didn’t let the enduring hype around this technology influence their perspective, choosing to pursue potential solutions pragmatically and thinking longterm rather than investing in the shiny new tool dominating buzzworthy conversations.
“We stayed grounded by focusing on business outcomes rather than technology trends,” she said. “Our guiding principle was, ‘Does this solve a real problem?’ That mindset helped us avoid chasing hype and instead build a sustainable automation program that delivers measurable value.”
Memorial Hermann’s Stephens reiterates applying the same philosophy for evaluating robots to RPA.
“This is basic stuff that all supply chain people will know,” he said. “Questions include how easy is it to use? And then how will it integrate into operations, including your current system and your normal workflows. Do you have to change your workflows to be able to use RPA? We know we’ll be doing some of that when we implement Oracle. We’ll
change certain processes to mirror what Oracle says we should do. We’re not going to go the other way around and make Oracle customize what they’re doing to our processes. You have to look at the costs to change some existing workflows versus the costs the vendor will apply to you to customize their system for you.”
Don’t be so quick to outsource everything, Cleveland Clinic’s Downey cautions.
“In most cases, we build our own RPA solutions, leveraging tools already available across the enterprise,” he noted. “If the automation need is more complex, we explore external solutions, evaluating both the ROI and the potential for a strong partnership with the vendor.”
Three questions Downey poses when choosing a vendor’s solution:
` Does it deliver measurable value?
“Will it save costs, improve quality, or increase operational efficiency?”
` Is it scalable? “Can the solution grow and adapt as our processes evolve?”
` Is the partnership sustainable?
“Do we have confidence in the vendor’s ability to support, update and collaborate long-term?”
Process appeal for RPA in P2P
Healthcare supply chain teams may look for RPA to satisfy various needs, including accuracy, speed, workflow efficiency.
“Efficiency comes from turning daily pain points into automated workflows that scale,” Tucker indicated. “Our ‘RoboRoute’ process alone has processed over 769,000 invoices, saving $1.5 million and 64,000 hours. Across the portfolio, we’ve automated 2.7 million transactions, saved 130,000 hours and delivered nearly $4 million in value.
“For us, efficiency is not just about speed. It is about resilience, accuracy and the ability to redeploy people to meaningful work that requires judgment,” she added.
From an accuracy standpoint, one question revolves around timing. Do you need to start with clean data before you can reap RPA benefits fully or can you get by with using RPA to help scrub data along the way?
“Clean data is ideal, but not always a prerequisite,” Tucker said. “In fact, one of RPA’s strengths is its ability to help clean and standardize data as part of the automation process. For example, bots can identify and correct formatting issues, flag missing fields and apply business rules consistently. So, while we aim for clean data upfront, we also use RPA to improve data quality over time as the process runs.”
Stephens references accuracy and big picture views as potential gains from RPA use.
“It’s understanding everything that’s going on from a global supply chain standpoint so that we can do a better job of managing backorders because ever since COVID it’s become whack-a-mole in terms of things that show up,” he observed. “As far as backorder management goes, we’ve had to add several FTEs just to be able to help us manage all these backorders. Using RPA to be able to understand how a strike in Malaysia or a fire at a refinery or a cyclone in southeast Asia would affect global production of masks, gloves and gowns and other PPE would be huge. Piecing all of that together to create a picture of what could happen or will happen is something that could be very valuable.”
RPA offers considerable opportunities in navigating around and through crises and disasters, according to Stephens.
ROBOTIC PROCESS AUTOMATION
“Right now, we’re doing it manually by partnering with our key suppliers to share with us as much information and notice as they possibly can on everything from raw materials to being able to get product to us,” he said. “When we look at things like reducing our dependency on offshore and nearshore companies toward onshore companies – all those things that supply chain’s been talking about for the last five years – this is where RPA could really help us.”
RPA creates efficiencies by automating repetitive, transactional tasks, like copying and pasting data or updating multiple systems and it removes the manual, human element from these processes, reducing errors and freeing up staff to focus on higher-value work, Downey emphasizes.
“Beyond individual automations, we’re on a broader journey to centralize, standardize, and automate,” he noted. “We’re looking for areas where similar work is being done in multiple ways or across different locations. By consolidating and standardizing those processes, we create the foundation for automation to be most effective — scalable, consistent and impactful across the organization.”
Some might question how RPA interfaces or integrates with supply chain and other internal information technology systems.
For Trinity, it’s not an issue.
“Our bots are embedded directly into system workflows,” Tucker said. “They run queries against PeopleSoft, resolve exceptions and feed updates back automatically. This includes correcting tax codes, closing PO lines, emailing suppliers with payment information, or obtaining PO confirmations. The design principle is simple. RPA should feel invisible to the end user. Processes move faster with
fewer interruptions. This seamless integration has driven strong adoption across Procure-to-Pay.”
Cleveland Clinic has it under control, too.
“All RPA requests go through our centralized supply chain technology team, which provides governance and oversight,” Downey explained. “The team evaluates how to best integrate information between systems and ensures the solution leverages the tools already available to us. This approach helps us standardize processes, maintain data integrity and optimize efficiency across our SCM and related systems.”
Labor, manpower equation
As with any automation, labor, manpower and workflow can feel some pressure, resulting potentially in reallocation or reduction. While this can be overtly noticed when AGVs, AMRs and articulating cobot arms are operating, the connection can be a bit more covert with software embedded within the guts of an organization.
Tucker dismisses any employment contention and stress.
“Our RPA journey has been intentionally people-centered,” she insisted. “RPA has served as a retention tool rather than a replacement strategy. By eliminating repetitive tasks such as invoice exceptions, duplicate check, and supplier outreach, we have freed staff to focus on more meaningful and value-added work.
“This shift has had a positive impact on retention and engagement,” Tucker continued. “Colleagues see that automation is not replacing them. It is enhancing their work. Bots have become digital team members who handle the mundane, while our people focus on the meaningful. This shift improves efficiency and boosts
morale. Staff feel their expertise is valued, and their roles are evolving rather than being replaced.”
The terms “meaningful” and “valueadded” work can be defined in different ways among various organizations, if the nebulous terms can be specified at all.
That’s not an issue at Trinity, which emphasizes the value of human ingenuity.
“By automating repetitive tasks, our teams have shifted focus to activities like supplier compliance, contract compliance reviews, root cause analysis of payment delays and process redesign,” Tucker said. “These are tasks that require human judgment, collaboration and strategic thinking, areas where our colleagues thrive and where their contributions drive real impact.”
Theoretically, Stephens acknowledges the specter of software-motivated labor reductions and reallocations but quickly redirects the technology toward the positive.
“The desire is to use the technological improvements as an enabler to upskill your folks so that they can be placed in the best positions possible to help your area drive key improvements,” he noted. “Right now, we’ve got analysts that help facilitate gathering all this information, running those reports, looking at all of this as part of their research. At some point, these same folks could lead efforts using RPA, implementing effective solutions so that SCM could improve and become more efficient operationally.”
Downey contends that the elimination, if not minimization, of repetitive, manual tasks to spend more time on “meaningful” work “makes roles more rewarding, which naturally helps with retention. It also lets us reallocate people to higher-value activities, supporting both their growth and the organization’s goals.”

See what’s possible

Distributors and self-distributing health systems now have complete transparency of their Dukal products’ from purchase order to delivery.
Product Assigned at the Factory Level
Product Tracking at the Item Level
Compatible Excel Reporting
Automated Communication
Worldwide Tracking

Scan

> Learn more at dukal.info/insight
The effects of chronic disease in America
Currently, 6 in 10 Americans live with at least one chronic condition and 4 in 10 manage two or more. These diseases account for 8 in 10 of the leading causes of death nationwide. Contributing risk factors include physical inactivity, poor nutrition, tobacco use and excessive alcohol consumption.1,2
If a patient receives a chronic disease diagnosis, ongoing monitoring and treatment require continued lab testing throughout the rest of the patient’s life. These conditions present a growing strain on our health system and providers are looking for efficiencies in every area of their process.
Chronic disease costs the American medical system over $1 trillion annually — and is estimated to cost $47 trillion globally by 2030. 2






Every diagnosis begins with a lab test
Cardinal Health provides our distribution customers with robust capital equipment support to help increase lab capacity and diminish the strain of chronic disease. With Cardinal Health, you receive end-to-end support with single-source access to top manufacturers, expert consultation in equipment choice and assay menu expansion, extensive leasing options and access to a team of specialists that helps optimize your quality assurance program (QAP).





Cardinal Health™ Lab Capital Equipment Portfolio
bank
chemistry Quality control
No matter which equipment you choose, you’ll be connected to a community of over 200 Cardinal Health Lab experts who are here to serve you.
To connect with an expert and discuss available instruments and financing options, scan the QR code or visit cardinalhealth.com/labcapitalequipment
References: 1. CDC. About chronic diseases. Centers for Disease Control and Prevention. Published October 4, 2024. Accessed March 13, 2025. https://www.cdc.gov/chronic-disease/about/index.html 2. Hacker K. The burden of chronic disease. Mayo Clin Proc Innov Qual Outcomes. 2024;8(1):112-119. doi: https://doi.org/10.1016/j.mayocpiqo.2023.08.005
2025 Cardinal Health. All Rights Reserved. CARDINAL HEALTH and the Cardinal Health LOGO are trademarks of Cardinal Health and may be registered in the US and/or in other countries. All other trademarks are the property of their respective owners. Patent cardinalhealth.com/patents. Lit. No. 2LAB25-3607981-01 (09/2025)
Using AI Will Generate Supply Chain Savings for Health Systems

At the HITLAB symposium in New York City earlier this year, entrepreneurs shared how AI and novel data are being used to improve patient care and reduce health system costs. As a health system CFO for 30 years, I was struck by the number of elite students in attendance who are focused on healthcare careers, many with a specific interest in supply chain management.
When I began my CFO career, the supply chain was tucked away in a backroom, largely overlooked. But since the pandemic disruptions and the rise of international tariffs, supply chain management has moved to the forefront of health system leadership priorities. One key takeaway from the symposium was the growing visibility of data that CFOs previously lacked, data that is critical for forecasting and risk analysis.
Mark Van Sumeren, Chair of Healthcare and Life Sciences at LogicSource and a former EY partner who led the national healthcare supply chain consulting practice, emphasized the evolution of supply chain strategy. It is no longer about order-taking; it is now a C-suite-level decision about what to purchase and from whom.
During his remarks, Van Sumeren focused on the “front end” of the supply chain: sourcing and contracting. These are the foundations of effective procurement and executing them

BY DAVID KIRSHNER, MBA, CPA
professionally is where value creation begins. If the data is curated and the right questions are asked, the next generation of supply chain professionals can use AI to identify strategic partners and make more informed sourcing decisions.
Non-clinical spend often involves thousands of suppliers, each with unique service levels, terms, and pricing structures. This complexity challenges category managers to maintain competitive and consistently valuable vendor relationships. AI can help by improving visibility, accelerating sourcing, and, most importantly, enabling supply chain leaders to focus on strategy rather than day-to-day execution. Given the historical volume and fragmentation of non-clinical procurement, this shift is not just a productivity improvement; it is a strategic necessity.
Vendors have long capitalized on healthcare’s complexity, often applying a “wedding premium” to their pricing strategy by charging more simply because they can. Unit prices are not the only concern, as many contracts lack controls on utilization or performance measures. According to LogicSource’s experience, only one in four non-clinical contracts are well-negotiated.
“For a typical health system with annual net revenue of $1B,” Van Sumeren noted, “they will spend 20% of their annual revenue on non-clinical supply chain, or $200 million. Multiply that by a 10% savings, and that is $20 million back to the bottom line.”
Van Sumeren and others emphasized that AI alone does not drive value. Human judgment remains essential. With curated data and decision-making support from AI, future health system executive teams will be better equipped, with supply chain leaders contributing real-time expertise at the strategic level.



Poking a Round Peg Through a Square Deal?
Decisions on legality of mergers-and-acquisitions frequently a head-scratcher.
BY R. DANA BARLOW
Determining which companies “deserve” to merge or acquire a competitor seemed a bit more cut and dry during President Theodore Roosevelt’s trust-busting term roughly a century and a quarter ago.
Back then, corporate monopolies were brash, brazen and helmed by charismatic and influential business titans and tycoons who viewed the Sherman Act as impeding progress rather than epitomizing the Progressive Era.
Regulating railroad giant Northern Securities Co. and Standard Oil, among others, demonstrated the clear battlelines between management and worker, citizen consumer and profit-seeking producer.
Here in the second quarter of the 21st century, the image of corporate monopolies seems way more curious, nuanced, smoggy and subjective, leading some observers and pundits to parry and posit about playing games – economic and/or political – than protecting consumers and keeping supply chains fluid and open.
For example, back then railroads had reached the peak of their popularity as the root of national supply chain success. In fact, the healthcare group purchasing industry saw its birth from the railroad industry one year after Roosevelt left office and future Supreme Court Chief Justice William Taft occupied the White House. It would be several decades before the railway heat cooled to the point that supply chain’s predominantly channeling of

product shifted to semi-trailer trucks and other four-wheeled vehicles. Ironically, within the last few months, two railroad giants in the freight business – Union Pacific, which covers the U.S. west of the Mississippi and Norfolk Southern, which covers the U.S. east of the Mississippi –seek to create the nation’s first transcontinental freight railroad corporate that will dwarf its four more regional competitors.
Proponents of the deal crow about “eliminating time-consuming freight handoffs and moving trains more efficiently by consolidating loads.” Not surprisingly,
opponents cry about reduced competition and resulting price increases.
They’re far from alone in this. Take retail as another example – particularly office supplies.
Back in the late 1990s, Staples wanted to acquire/merge with Office Depot to consolidate “office-supply superstores” to two from three. Office Max was the third man out. The Federal Trade Commission blocked it on antitrust grounds, but roughly 15 years later allowed Office Depot and Office Max to merge. Why? Because the feds felt
enough competition existed with Amazon and Walmart that meant competition existed, consumers still had choices and prices likely wouldn’t increase. Note that 15 years earlier, Amazon was just an online bookstore created by Jeff Bezos and MacKenzie Scott, and Walmart’s office supply offerings kept pace with other department and grocery stores.
The difference now? Staples seeking to acquire/merge with Office Depot (including Office Max) now threatens to resurrect the old monopoly arguments from last century but without the essential background and context. To wit, Amazon Business, Costco Business and Walmart now dominate the office supplies market on convenience merits alone as well as their abilities to keep pricing in check. That’s part of the reason why government claims that refusing to let Staples hitch with Office Depot rings hollow because why would a bigger Staples raise prices to compete with Amazon, Costco and Walmart?
Back in the late 1990s, during the Clinton administration healthcare reform initiatives, healthcare providers and suppliers bristled at the federal government intrusion into clinical and financial management that directly impacted operations and supply chain.
As a result, mergers and acquisition efforts among the distribution and group purchasing organization industry segments bobbed and weaved through government intervention just as the online electronic commerce movement was blossoming and burgeoning. On the distribution side, we witnessed McKesson being allowed to merge with
and
HBO & Co. to bolster its information technology infrastructure and offering while being blocked to merge with Amerisource, which itself was allowed to merge with Bergen Brunswig. Meanwhile, Cardinal Health was blocked from acquiring Bergen Brunswig, but a year later allowed to acquire Baxter spinoff Allegiance Healthcare.
On the GPO side, VHA and University HealthSystem Consortium united to form Novation, while three regional
out for consumers. Red herrings or simple distractions?
The movie studios buried within media juggernauts represent the latest M&A wrinkle with Paramount Skydance wrangling with Netflix over Warner Bros. Discovery after Apple picked up MGM/UA in an industry seeing dramatic growth and interest in streaming content anywhere versus screening content in movie theaters. Most of the same competitive concerns remain with
What’s noteworthy is how federal regulators choose to block some companies from getting together while allowing others to continue gobbling up market share intermittently.
groups (American Healthcare Systems, Premier Health Alliance and SunHealth Alliance) fused into Premier.
Since then, the remaining companies expanded and grew even more through acquisitions and mergers as similar maneuvers engulfed the investor-owned hospital chains, payers and pharmacy benefit management companies that were scooped up by different retailers.
What’s noteworthy is how federal regulators choose to block some companies from getting together while allowing others to continue gobbling up market share intermittently. Further, as some companies grow larger and lower prices through higher volume sales and logistical process efficiencies you likely wonder whether government merely is manipulating commerce and playing games with corporate relationships or really looking
for The Journal of Healthcare Contracting.
affordable and convenient access to content being the twin tentpoles driving these business deals.
For every high-profile deal gone right or wrong, however, are myriad others cast away into historical footnotes – some of which crossed industry segments and raised competitive hackles in different ways, like a healthcare distributor and investor-owned hospital chain in the 1980s.
Regardless of brand name changes, contract renegotiations and management sifting, supply chain operations remain consistent, necessary and resolute. Everything (and everyone) runs on supply chain, which in this age of “influencers” should motivate The Journal of Healthcare Contracting readers to shake the dust off their boots and spurs and express their impact and power.
has nearly four decades of journalistic experience and has covered healthcare supply chain issues for more than 30 years. He can be reached at rickdanabarlow@wingfootmedia.biz
R. Dana Barlow serves as a senior writer
columnist
Barlow
Healthcare Distributors Offer Lessons on Leadership
Behind every contract negotiated and product delivered are healthcare distribution leaders who approach their work with a deep sense of responsibility and purpose. HIDA recently asked executives from key healthcare distributors for their perspective on leading teams, developing talent, and delivering patient care. Together, their perspectives illustrate how healthcare distribution leaders take their responsibilities seriously, making a daily commitment to serving the providers who depend on them.

If you could give your younger self one piece of advice, what would it be?
Kelley Moffett, Cardinal Health: Ask for the really hard, annoying assignments, the jobs that when they get handed out at the end of a meeting that no one wants to do. Raise your hand, ask for that job, take on that side hustle, that task. Because that is going to differentiate you, give you experiences that you wouldn’t normally get, and make you invaluable to the person who assigned it. It is an incredibly valuable way of learning; of becoming a trusted partner and somebody who people know can take on more.
What is one skill or mindset you think is critical for the next generation of leaders?
Patrick Jones, Thermo Fisher Scientific:
Stay curious about your industry. Stay curious about adjacent industries. Stay curious about your role, but also stay curious about where your colleagues are doing in different roles. I believe that the best leaders will have a certain understanding of many functions and many areas. They’re bringing different insights into their company, different insights to their team, and different insights to their customers.
How can leaders better serve their teams?
Brad Hilton, McKesson Medical-Surgical: I’ve been lucky enough to work with some great leaders that have been incredible role models on ways to lead teams and how to show up every single day. It’s about servant leadership and humility. If getting into leadership is about you and
your title and accomplishing things, I would strongly encourage you to consider whether leadership is the right career path for you. Because it is about serving the team. It’s about making the team better. When you have that mindset, great things can happen.
What skills should supply chain leaders develop for the future?
Charles Abbinanti, Dukal Corporation: Supply chain leaders need to be very agile and- and they need to be lifelong learners. They need to be people who feel very comfortable working in a cross-functional nature because of how supply chain has really now become ingrained into almost all aspects of our business.
Where does innovation open up opportunities in healthcare?
Emily Willburn Andrews, Willburn Medical Supply: Of course everyone’s talking about AI right now. But I really believe that the best way to make the biggest impact is to be as close as we can to our customer, and really hearing issues and solving their problems. Not just investing in technology for the sake of technology, but really to solve their needs and see true progress in healthcare.
KNOW THE DEALS
Now’s the time to act!
Midmark is offering limited-time promotions across featured product lines—each designed to help enhance your point of care ecosystem. From trade-in rewards to free maintenance kits and bonus rebates, these promotions deliver meaningful value on the equipment you trust.
Low Volume Examination Chair Trade-In to Trade-Up Promotion
Receive up to $400 when trading in any exam chair and purchasing an eligible Midmark model. Add delivery and trade-in removal services for $100 in bonus savings.
Scan for details.
High Volume Examination Chair Trade-In to Trade-Up Promotion
Rebates up to $500 + a bonus $150 with delivery and trade-in removal services.
Scan for details.
Procedure Chair Trade-In to Trade-Up Promotion
Get up to $850 back + an additional $150 with Midmark delivery and trade-in removal services.
Scan for details.
ECG Trade-In to Trade-Up Promotion
Save $200 when trading in an ECG for a new Midmark Digital ECG purchase—and save $50 more when you upgrade with a DICOM license.
Scan for details.
Sterilizer Trade-In to Trade-Up Promotion
Save up to $500 when trading in a sterilizer and purchasing an eligible Midmark model.
Scan for details.
Sterilizer Maintenance Kit Promotion
Get a free maintenance kit—a $225 value—when you register a new Midmark sterilizer.
Scan for details.










— Mark Welch, Senior Vice President, Novant Health
