
















TEAM IRELAND AT THE WORLD RESCUE CHALLENGE














IRELAND







First Responders and the Problem of Bringing the Job Home PROTECTING MENTAL HEALTH
TAKING ON THE WORLD VETERAN & CAMINO WALKER

































TEAM IRELAND AT THE WORLD RESCUE CHALLENGE














IRELAND







First Responders and the Problem of Bringing the Job Home PROTECTING MENTAL HEALTH
TAKING ON THE WORLD VETERAN & CAMINO WALKER





























HARBOUR OF MARY
Cuan Mhuire is Ireland’s largest multi-site provider of Detoxification & Treatment for Alcohol, Drug & Gambling Addiction.
Cuan Mhuire has CHKS Accreditation & ISO 9001:2015 Certification
It has Residential Treatment Centres at:
Athy, Co. Kildare T: 059 8631493
E: athy@cuanmhuire.ie
Bruree, Co. Limerick T: 063 90555
E: bruree@cuanmhuire.ie
Coolarne, Co. Galway T: 091 797102 E: coolarne@cuanmhuire.ie
Farnanes, Co.Cork T: 021 7335994
E: farnanes@cuanmhuire.ie
Newry, Co Down, BT35 8RL, United Kingdom
T: 0044 2830849010
E: newry@cuanmhuire.ie





Dear readers,
Editor: Adam Hyland
Contributors: Adam Hyland
Creative Director: Jane Matthews
Cover Credit: Adam Hyland
Photography:
HSE, NAS, Adobe, Adam Hyland, Óglaigh na hÉireann/Irish Defence Forces, An Garda Síochána, Road Safety Authority, Dublin Fire Brigade, Coast Guard, Jimmy Fullam, Mercier Press, Bloomsbury, Irish Academic Press, Transworld, Dubai Ambulance Service, Durite, University of Miami.
Production Executive: Claire Kiernan
Publisher: Ashville Media Group, Unit 55, Park West Road, Park West Industrial Estate, Dublin 12, D12 X9F9.
Tel: (01) 432 2200
Fax: (01) 676 6043
Managing Director: Gerry Tynan
Chairman: Diarmaid Lennon
Publisher’s Statement:
The information in Ambulance Ireland is carefully researched and believed to be accurate and authoritative, but the Publisher cannot accept responsibility for any errors or omissions. Statements and opinions expressed herein are not necessarily those of the Editor or the Publisher.
Copyright © Ashville Media Group Ltd. No part of this publication may be reproduced, stored in a retrieval system or transmitted in any form or by any means without written permission from the Publisher.
Welcome to the 2026 edition of Ambulance Ireland. As always, we bring you the latest news and features covering Ireland’s medical and emergency services sectors, as well as interesting and inspiring stories from our frontline personnel and from around the globe.
The dedication and commitment of all emergency service and frontline personnel is a constant that we must all be grateful for, and we must remember that a huge amount of thanks must go to those people who help keep us safe. Thanks must also go to all who gave their time to make the features in this issue possible.
Jimmy Fullam’s personal motto of “Always think of others” has seen him walk more than 8,000km across six full Camino Walks, two Ignatian Ways, and two Famine Trails, with each step dedicated to raising funds for charities close to his heart. Last year, he took on a Camino trek with his son that exemplified the message of hope he carries with him, showing the path to recovery is both a physical and spiritual journey. It was my pleasure to talk to him about his journey, what he has learned along the way, and what it can teach others.
A very important aspect of mental health for emergency service personnel is the problem of bringing the job home with you. It is not always easy, but there are steps you can take to ensure the stress experienced as a first responder doesn’t carry over into your home life. With invaluable input from Michelle O’Toole, Project Lead on Hugs@Home at the RCSI, and Dublin Fire Brigade’s Critical Incident Stress Management Coordinator Joe Dromgoole, we take a look at how to recognise the signs that you may be taking the stress home, and what you and others can do to help.
We also take a look at how “Team Ireland” consisting of members of Dublin Fire Brigade, Carlow Fire and Rescue and Dublin Civil Defence got on when they travelled to Croatia for the World Rescue Challenge extrication event.
Also included are a review of the Defence Forces and Coast Guard’s year to see just what is involved in protecting us and keeping us safe on land and at sea.
Elsewhere, we look at the latest road safety stats and campaigns, the HSE’s investment in mental health, the debate around drone defibrillator delivery, and see what’s new in the world of emergency services technology.
Best wishes,
PATH TO HOPE
The Camino and the Remarkable Journey of Jimmy Fullam
22 PROTECTING MENTAL HEALTH How First Responders Can Prevent Bringing the Job Home 32 TAKING ON THE WORLD Team Ireland at the World Rescue Challenge
The Latest in Nationwide Health, Medical and Emergency Services News
HSE Ambulance sta have reported widespread abuse of the system whereby people are calling an ambulance to be used as a “taxi service”. As reported by Tralee Councillor Angie Baily, they allege people often ring ambulances at night if they can’t get a taxi, are transported to hospital, only to immediately leave and walk the rest of the way home. These claims have been echoed by sta nationwide, according to Cllr Baily. Paramedics have also raised concerns about families calling ambulances for elderly relatives to e ectively leave older family members in hospital care so they can go on holiday. Emergency service workers have warned that unless misuse is tackled, ambulance availability will be compromised, increasing the risk that those in genuine medical distress may not receive help in time. Because ambulance call-outs are free and paramedics are legally required to respond to every emergency call, crews must attend even when it becomes apparent that there is no genuine medical emergency. It is currently a criminal o ence to knowingly call an ambulance without good reason, with the potential of fines or even jail time, but prosecutions are rare.
A total of 202 organ transplants from 97 people took place in Ireland in 2025, according to the HSE’s Organ Donation Transplant Ireland O ice. Across the country’s three national transplant centres, 140 kidney, nine heart, 15 lung, 33 liver and five pancreas transplants were completed. This includes kidney transplants from 29 living donors. The number of deceased donors was 68. Dr Colm Henry, HSE Chief Clinical O icer, said: “I want to express my deepest gratitude to organ donors and their families who, through their extraordinary generosity, gave the precious gift of life this year. Your selfless decision to donate has saved lives and o ered hope to others at a di icult time for you.
The Defence Forces have retired their fleet of 27 light armoured vehicles purchased in 2010 at a cost of €20million. The South-African made light armoured tactical vehicles (LTAVs) had mostly been deployed on overseas missions in the Middle East and Africa, as well as being used as part of Ireland’s contribution to the EU Battlegroup, but had seen infrequent actual operational use. Government spend on the Defence Forces has stepped up in the last year, with the planned purchase of a new fleet of vehicles to replace the LTAVs and complement the 80-strong fleet of Mowag armoured personnel carriers on the cards. These new vehicles will have “level four” armour capable of stopping high-calibre rounds and the ability to be fitted with mortar systems. As well as the purchase of the new fleet, the acquisition of 24 Armoured Utility Vehicles (AUVs) in 2017 has further reduced the need for the LTAVs, which as of January had yet to be o icially withdrawn from service but had been consigned to storage. The Mowag vehicles, first purchased in 1999, are expected to remain in service beyond 2030 thanks to a recent mid-life refit. Defence and Security Analyst Declan Power, has suggested Ireland should look to countries closer to home when buying military vehicles and equipment, prioritising countries with similar operational environments and close political and logistical ties. “This country should be looking at purchasing from France, the UK, and the Nordic states,” he said. “These are our neighbours. They’re our partners. They understand the kind of military environments we operate in.”
World-first clinical trials focused on bringing long-term relief to people su ering from chronic musculoskeletal pain are to begin in Ireland. A consortium involving medtech and digital healthcare companies and researchers from the RCSI and University of Galway, will use €6.6million in funding to carry out the RECAP project: Resorbable Embolization for Chronic musculoskeletal Pain. Patients will have access to breakthrough pain treatment developed by CrannMed and a recovery programme developed by Salaso Health Solutions with the support of clinical specialists. In the first trial, a patient will receive an injection to selectively block blood flow to the site of pain, reducing inflammation and stray nerve endings. The second trial will assess the recovery process of patients, supported by an AI-enabled self-management platform in real-time, with the impact monitored closely. The trials will allow scientists and researchers to develop new imaging techniques, smart trial designs and pain measurement methodologies needed to make the solution standard within healthcare systems.
The HSE’s Health App now has more than 125,000 users, with more than 210,000 downloads made since its launch in early 2025. The latest update released last November includes significant enhancements including showing patents hospital waiting lists they are on, access to information on GP referrals, and expanded health data for patients on the Structured Chronic Disease Management Programme, including diagnosis and vital measurements. “This app is transforming how patients manage their health from viewing hospital appointments to checking GP referrals and their own vaccination records,” said Health Minister Jennifer Carroll MacNeill. “These features give people more control and convenience and there’s even more coming later this year, ensuring the app continues to evolve to meet patient needs.”
Ireland has retained its position as the EU country with the highest self-reported rate of good health. The latest State of Health in the EU Country Health Profiles shows that four in five Irish adults rate their health as good or very good. Highlights in Ireland’s Country Health Profile include that life expectancy was 82.9 (1.5 years above EU average), smoking prevalence fell to 14% (EU average is 19%), health spend per capita is 17% above the EU average, our mortality rate is 21% lower than the EU average. However, in-patient care accounted for 35% of health expenditure, above the EU average of 28%, while 5% of adults reported unmet needs for primary care (above the EU average of 3%). This year’s Country Health Profile also notes a rise in the number of young people using e-cigarettes, and the number of people classified as having obesity 19% is also above the EU average of 15%.

For the first time, a sum of €2million has been invested specifically in women’s health research by the Minister for Health. Funding of €1million each year in 2026 and 2027 has been ringfenced by the Health Department’s Women’s Health Fund, which will be allocated to Applied Partnership Awards scheme recipients to address historic gaps in knowledge and understanding of women’s health issues and the impact of gender on health outcomes and experiences. A formal call for research proposals was launched in January, with up to ten awards to be granted. Specific themes looked for included postpartum mental health, endometriosis, menstruation, and culturally sensitive healthcare. “Our recent evidence and gap review across 38 OECD countries, including Ireland, identified clear gaps in women’s health research,” said Chief Executive of the Health Research Board Dr Gráinne Gorman. “By delivering this funding we aim to address those gaps, inform better care and improve outcomes for women.”
MEDICAL AND EMERGENCY SERVICES NEWS FROM AROUND THE WORLD

Following the introduction of bodycams last year, parliament has strengthened legislation to increase penalties for violence and threats against the country’s medical personnel, including doctors, paramedics and ambulance drivers while on duty. e legislation introduces a new article establishing speci c criminal liability for actions that endanger the life, health, and safety of medical workers. Penalties will now amount to around €3,000 in nes, 300 hours of community service, or a two-year jail term. More serious o ences such as violence that endangers life or health will carry prison sentences of ten years. According to the Ministry of Health, more than 280 assaults on healthcare personnel have been recorded in Kazakhstan since 2019. In tandem with the legal changes, the government is expanding protective measures with round-the-clock police posts established at 152 hospitals nationwide.

A new Cabinet-backed bill aimed at closing gaps in pre-hospital medical services has been announced by the Government of Cyprus. New legislation will allow for the creation of a National Ambulance Authority to establish a uni ed system for emergency medical response. e National Ambulance Authority will be designated as essential national infrastructure operating under the Ministry of Health, with responsibilities including dispatching and transporting patients to A&E departments, responding to urgent mass-casualty incidents, and managing both national emergency call coordination centre and poison control centre. Transitional measures ensure that the State Health Services Organization (OKYPY) will continue providing emergency pre-hospital services until it becomes nancially and administratively autonomous.


e Katsina State Government has unveiled 15 new ambulances aimed speci cally at strengthening response and reducing fatalities arising from road accidents on major highways. e ambulances are to be deployed along major highways to ensure victims of road accidents and other medical emergencies receive timely attention. Governo Dikko Umaru Radda said the initiative would improve medical care, especially for accident victims on busy inter-state routes. Chief of Sta , Abdulkadir Mamman Nasir, said the ambulances are equipped with modern life-support facilities and will be manned by trained paramedics. He added that the initiative complements ongoing investments by the state government in healthcare services across the state.
Two thirds of people who showed hesitancy regarding receiving COVID-19 shots went on to receive the vaccine, according to a new study of more than 1million people by Imperial College London. e research studied people in England between January 2021 and March 2022, and found that there was a general decline in vaccine hesitancy during those 15 months. Some 64% of those who were reluctant to receive the vaccine went on to do so. Participants were asked whether they had been or intended to get vaccinated. ose who refused the vaccine, or were sceptical about vaccination, were asked about their reasons for hesitancy from a checklist of 23 options. Overall, 3.3% of participants reported some degree of COVID-19 vaccine hesitancy and subsequent vaccination data was available through NHS records linkage for 24,229 (64%) of them. e researchers identi ed eight categories of vaccine hesitancy including concerns about e ectiveness and side e ects, perception of low risk from COVID-19 and mistrust of vaccine developers, and fear of vaccines and reactions. Among the hesitant who provided a reason for hesitancy, 41% reported concerns around long-term health e ects, 39% that they wanted to wait to see whether the vaccine worked, and 37% that they had concerns about side e ects.


Last year was an exceptionally busy and demanding period for the Irish Coast Guard, with almost 2,800 incidents responded to, according to the organisation’s annual end of year summary of statistics.
In total, there were 2,793 incidents recorded, ranging from search and rescue operations to maritime casualty responses, as well as pollution control and preparedness activities.
e Coast Guard also assisted An Garda Síochána in open country missing person searches and mountain rescue, the National Ambulance Service in providing an Air Ambulance and Helicopter Medical Emergency Service (HEMS) both inland and to island communities, as well as provision of other supports to the Emergency Services.
e 44 Coast Guard Units mobilised on 1,187 separate occasions, continuing to play a vital role in safeguarding communities nationwide. Collaboration remained central to e orts, with the three Rescue Coordination Centres in Dublin, Malin, and Valentia tasking RNLI lifeboats on 798 occasions and activating the community inshore rescue service 121 times.
e Coast Guard helicopters conducted 933 missions, including 190 air ambulance ights in support of o shore island communities.
In terms of lives saved, which the Coast Guard de ne as “assistance provided that prevented loss of life, severe risk to life, and/or delivery to appropriate medical care”, critical assistance was provided to

1,941 persons over the course of the year.
e Irish Coast Guard also reached a major milestone in its aviation capability in 2025, with the AW189 helicopters operated by Bristow Ireland commencing operations from bases in Shannon, Dublin and Sligo, and Fixed Wing operations going live from Shannon in September. is strategic expansion ensured that the IRCG has responded more e ectively to emergencies, ensuring rapid deployment and improved coverage across Ireland’s coastline and inland areas throughout 2025.
e additional aviation capacity proved critical in 2025, a year marked by extreme and unpredictable weather conditions. ese conditions placed unprecedented demands on emergency

services, requiring rapid and coordinated responses across multiple regions. With increased resources and operational exibility, the Coast Guard also delivered enhanced support for Principal Response Agencies (PRAs) nationwide, ensuring that communities a ected by ooding, coastal emergencies, and other weatherrelated incidents received assistance and life-saving interventions.
Another major development was the beginning of construction of a new Coast Guard station in Greystones, Co Wicklow, in November 2025, with Minister with special responsibility for the Irish Cost Guard Seán Canney, o cially turning the sod for the new site.
e Greystones/Wicklow Coast Guard Unit (CGU), which has a proud history dating back to the 1920s, delivers land, cli , and maritime search and rescue services across a catchment area from Shanganagh and Bray as far south as Brittas. Sta ed entirely by volunteers, the unit includes 32 personnel and responded to more than 50 incidents last year. eir work regularly involves collaboration with other emergency services, including Dun Laoghaire CGU, the Dublin-based R116 IRCG helicopter, An Garda Síochána, Greystones Fire Service, and the RNLI. e new station will provide t-forpurpose welfare and operational facilities, including an operations room, a training room, kitchenette, drying room, stores, boathouse, changing facilities, and boat launch facilities.
Speaking at the event, Minister Canney said: “Our Coast Guard volunteers are the backbone of maritime search and rescue in Ireland. e Greystones/Wicklow
Unit has saved countless lives over its long history, and this new station will ensure they have the facilities they need to continue their vital work for generations to come. Today’s sod-turning is a tangible demonstration of our commitment to supporting these dedicated volunteers and the communities they serve.”
With the ongoing public safety message of having the capacity to Raise the Alarm and Stay A oat central to the prevention of drownings at sea, along the coast and on inland waterways, the Coast Guard’s core message of Stay A oat – Stay in Touch continues to be shared on www.safetyonthewater.gov.ie and across multiple media, and highlights the importance of never engaging in any commercial or recreational boating activity without wearing a life jacket or Personal Flotation Device, coupled with the capacity to raise the alarm via VHF radio, Personal Locator Beacon (PLB) or EPIRB.
e message also makes clear that any maritime or coastal activity should be supported by informing shore-based colleagues of intended activity and anticipated return time. Mobile phones, it stresses, should not be considered a suitable substitute or be relied upon as the only means of emergency communication at sea.
A series of awareness campaigns across the major Bank Holidays were launched to underline this safety message, outlining that practical and simple steps can save lives, such as checking the weather forecast and times of tides for your local area; swimming at lifeguarded beaches and within your depth; and ensuring
2025 WAS A YEAR THAT TRULY TESTED THE RESILIENCE AND CAPABILITY OF THE IRISH COAST GUARD”

that you have the right equipment for the water-based activity you are about to undertake, will help ensure you return home safely.
“2025 was a year that truly tested the resilience and capability of the Irish Coast Guard,” said Ms Joanna Cullen, Assistant Secretary at the Department of Transport with responsibility for the Irish Coast Guard. “ e extreme weather conditions we faced demanded rapid, coordinated responses, and I am proud of how our teams rose to the challenge. e successful transition of three bases and the introduction of Fixed Wing operations from Shannon have been game-changers, enabling us to respond faster and more e ectively than ever before. ese advancements, combined with the dedication of our volunteers and partners, ensured that communities across Ireland received the life-saving support they needed when it mattered most.”

















Specialise in:
Regular dentistry • Cosmetic dentistry • Bleaching
Crowns • Bridge crossing • Gum shields
Also:
• PRSI holders:
- 1 free examination per year


• Medical Card holders very welcome:
- Two free fillings per year
- All extractions free
- 1 Free dental examination per year
TEL:


Unfortunately, 2025 was a grim year when it came to road fatalities in Ireland, with the number of deaths recorded increasing from 175 in 2024 to 190 in 2025, resulting from a total of 179 fatal collisions.
ese devastating gures show that despite the work of An Garda Síochána and the Road Safety Authority, there are still far too many people not heeding the simple messages of driving safely, at a sensible speed, and without distraction. Alarmingly, there was an increase in the number of deaths of more vulnerable road users, with 45 pedestrians killed
on our roads in 2025, 14 cyclists, 30 motorcyclists, and three e-scooter drivers or passengers. e number of cyclists killed was the highest since 2017 while the number of motorcycle fatalities was the highest since 2007. Overall, these gures show that there was an average of 15 road fatalities every month last year.
Minister of State with responsibility for Road Safety, Seán Canney TD, said: “Last year was an incredibly di cult year on Irish roads. Too many families have faced heartbreak. Too many
communities have been le grieving. It is a stark reminder that road safety is not just a policy area or a set of statistics – this is about people’s lives, about loved ones, about futures changed in an instant.
“My absolute priority as Minister for Road Safety is to make Irish roads safer for everyone, and I will continue to work closely with all road safety stakeholders in the New Year to achieve this.”
Sam Waide, Chief Executive of the RSA, added: “It is with great sadness that we acknowledge the tragic loss of life on Ireland’s roads in 2025. We are deeply concerned by the increase in fatalities, particularly among our most vulnerable
We are asking everyone to play their part. A safe journey is the responsibility of every driver”
road users – cyclists, pedestrians and motorcyclists.
“With sustained political commitment, a whole-of-government response, and adequate resourcing and funding, I rmly believe we can reverse this tragic increase in road deaths.”
Assistant Commissioner Catharina Gunne, An Garda Síochána, Roads Policing and Community Engagement, also said: “2025 has been a devastating year for the families of the 190 persons who died on our roads. Each of these deaths has had a profound impact on their loved ones, families, friends, colleagues and communities.
“An Garda Síochána remains committed to improving road safety and minimising the number of deaths and serious injuries on our roads, and will continue to do so in 2026, targeting
those drivers with the most risky and dangerous driving behaviours.
“As a society we all need to work together to bring real impact to ‘Vision Zero’, Ireland’s Road Safety Strategy 2030. We once again need to adjust attitudes to driver behaviour and make driving while under the in uence of any intoxicant, inappropriate speed and driving while distracted unacceptable behaviours. As a society we all need to call them out! By working together as communities, we can all make our roads safer in 2026.”
However, the trend towards dangerous driving and the high rate of road fatalities seems to be continuing into 2026. At the time of writing, there have already been 17 road fatalities in the rst six weeks of the year (nine drivers, two passengers, and six pedestrians).
In e orts to stop dangerous driving, gardaí carried out two major road tra c enforcement campaigns at the end of 2025 and start of 2026. e rst, over the Christmas period from 1 December to 5 January, saw almost 10,000 checkpoints (both statutory Mandatory Intoxicant Testing (MIT) and highvisibility policing) carried out, with 765 people arrested for driving under the in uence (56% alcohol and 44% drugs). Almost 26,500 drivers were detected for speeding o ences, while almost 3,000 vehicles were seized for a range of o ences. Nearly 1,700 Fixed Charge Notices were issued for the o ence of using a mobile phone while driving and more than 450 Fixed Charge Notices were issued to vehicle users for nonwearing of seatbelts.
Shockingly, 59% of these other o ences were for having no insurance, which recent gures show has become a growing problem.

Checkpoints have shown a huge number of people under the influence or driving without insurance

More than 19,600 uninsured vehicles were seized by gardaí in 2025”
According to the Motor Insurers’ Bureau of Ireland (MIBI), more than 19,600 uninsured vehicles were seized by gardaí in 2025. is brings to 38,546 the number of uninsured vehicles seized in the rst 24 months since the introduction of the Irish motor insurance database system in 2024.
is is a horrifying statistic that shows there is a huge number of people driving on Irish roads who feel they do not have to comply with the very basics of car ownership, and who are content to risk injury or loss of life to other road users with no recourse for compensation.
e second major Road Safety and Tra c Enforcement campaign was carried out over the new St Brigid’s Day bank holiday from 29 January to 3 February, and the stats show the same worrying gures. During this time, almost 3,500 motorists were detected speeding, 193 were arrested on suspicion of driving under the in uence, more than 660 vehicles were detained (50% for no insurance), and almost 400 drivers were detected driving while using a mobile phone.
is last gure emphasises the huge problem of getting the message across that driving while distracted by a mobile phone or other device can be extremely dangerous. Over the last ve years, An Garda Síochána has issued almost 110,000 Fixed Charge Notices for holding a mobile phone while driving, and gures show there has been a 30% increase in such incidents since 2022.
An Observational Survey on Mobile Device Usage carried out by the Road Safety Authority during September and October 2025, found that 8% of motorists were using a mobile phone while driving, up 2% from 2024. e percentage of drivers seen using a handheld mobile device increased on motorways (+10%) and urban roads (+2%) in the 2025 study, with a slight improvement seen on rural 80km/h and 100km/h roads.
Speaking about these gures, Minister Canney, said: “One of the most dangerous behaviours on our roads is driving while distracted. Driving while using a mobile device is utterly unacceptable but unfortunately, this behaviour has
become far too common on our roads. Driving any vehicle requires your full attention, and it is unacceptable to put lives at risk by picking up the phone –whatever the reason. Too many families and communities have lost loved ones to road tra c collisions, and I appeal to all road users to put your devices away and to drive in a manner that protects the safety of other road users.”
Assistant Commissioner Gunne added: “Driving requires your full attention. When you pick up a mobile phone, read a message, or interact with any device behind the wheel, you are placing yourself, your passengers, and every other road user at risk. No call, message or noti cation is worth a life. Put the phone away, remove distractions, and stay focused on the road.
“We are asking everyone to play their part. A safe journey is the responsibility of every driver. By eliminating distractions and making safe decisions, you can help ensure that all road users arrive home safely.”
With the Garda message of safe driving not getting through to some, the organisation did turn to the public for help with a new tip-o line set up in 2024 to ag dangerous driving on Irish roads, but this has seen mixed results. Although there were almost 8,000 submissions, these led to a conviction rate of just 1.8%, with the inability to upload images or recordings to the platform cited as a reason for the low gure.
While encouraging the public to call out dangerous driving is a positive move, the number of road fatalities occurring in Ireland despite the ongoing e orts of An Garda Síochána and the Road Safety Authority shows that the onus is really on us, not just to call out others, but to receive the message loud and clear that it is not ok to drive dangerously, or while distracted, or at excessive speed, and that such behaviour can lead to tragedy. Only when we all agree on this, and act accordingly, will we see the number of tragedies on our roads decrease.
When a child loses their home, they lose their entire world.

There are almost 4,000 children homeless in Ireland. Donate now.

focusireland.ie 1850 204 205





































The Defence Forces Saw Developments at Home and Abroad in 2025
BELOW: The Air Corps conducts a wide variety of missions in the air domain and continues to support Defence Forces operations across the maritime and land environments


Following the publication at the end of 2024 of a “highlights reel” of its main events, at the end of 2025 the Irish Defence Forces once more shared with the public the events of the year in a more traditional statement, recapping the main activities of the Army, Air Corps and Naval Service.
In 2025, the Irish Defence Forces saw recruitment reach a 20-year high, with 788 people joining the force, up from 708 in 2024 and 415 in 2023. Applications for General Service Recruitment were 34% above 2024 and 83% more than 2023, while Cadet applications increased by 21% in 2025 compared to the previous year.
e Naval Service also saw an increase in numbers, with 784 personnel now in service, up from 719 in 2024. In the last few months of the year, 156 recruits had been inducted, re ecting an increase of 59, more than the total number of inductions in 2024.
is increase in numbers is set to improve further on the back of a record €1.5billion ve-year Defence Sectoral National Development Plan budget set out by Government in October 2025, with training capacity to be expanded this year as the force aims to reach its recruitment target of 850 people at what is an increasingly contentious time for security in European countries.
At home, the Army carried out 124 operations to support the civil powers in 2025. Most of these were in support of An Garda Síochána and included bomb squad call outs, prisoner escorts, explosives escorts, cash escort and special search operations.
Troops also continued to carry out 365day armed guard operations at the Central Bank, a Military Police Detachment at Government Buildings, and supported the provision of security for visiting foreign aircra landings at various airports within the State.
Abroad, the Army continues to have the longest unbroken record of overseas service since rst deploying a United Nations mission in 1958. e largest such
deployment remained as the UN Interim Force in Lebanon (UNIFIL), where approximately 360 Irish soldiers currently serve alongside the Polish Army. is includes an Infantry Battalion who patrol along the Blue Line frontier between Israel and Lebanon. e UNIFIL mandate has been extended to 31 December 2026 with a full withdrawal of all UNIFIL assets to occur in 2027.
While the majority of Irish troops serving abroad are based at Camp Shamrock in South Lebanon, personnel also served in Bosnia and Herzegovina, Kosovo, Hungary and Strasbourg. ere are currently 430 Irish soldiers serving overseas, deployed across 12 missions in 13 countries.
Up to 30 personnel currently serve with EUMAM-UA (EU Military Assistance Mission - Ukraine) delivering specialised training in areas such as tactical combat casualty care, drill instructor training, and junior leadership training to the Ukrainian Armed Forces.
e Defence Forces also took part in the large-scale MILEX 2025 military exercise in Hungary to develop the EU Rapid Deployment Capacity, with 139 Irish troops playing roles in mission planning, logistics and eld operations within the German-led EU Battlegroup.
Within this Battlegroup, Irish forces were on high-readiness standby for the entirety of 2025 as part of a 2,000-personnel EU commitment.
In March, a major change to the Defence Forces’ stance on deployment overseas was introduced, with Cabinet approval given to dra legislation that changes Ireland’s “triple lock” approach whereby troop deployments of more than 12 personnel require the approval of the UN, Government and the Dáil.
e proposed change, which some in opposition fear removes Ireland’s position of neutrality, would mean removing the need for UN approval and raising to 50 the number of troops that can be deployed without sign o from the Dáil.
Tánaiste and Foreign A airs Minister Simon Harris said the removal of the triple lock system is about “sovereignty”. “We have a very proud track record in the

ABOVE: In 2025, the Air Corps helped with six international resupply flights








Ireland has partnered with Poland on the UNIFIL mission, enhancing and developing our interoperability with Partner Nations


Brig Gen Rossa
was appointed as Chief of Sta of the Irish Defence Forces





country of peacekeeping,” he said. “But the idea that any permanent member of the security council can have a veto, including Vladimir Putin, on where our defence forces go is not democratic.”
He added that it was “important” for decisions on peacekeeping to be taken in Ireland.
In June, Brig Gen Rossa Mulcahy was appointed as Chief of Sta of the Irish Defence Forces. Announcing the appointment, the Defence Forces said that Brig Gen Mulcahy has more than 35 years of experience across a variety of roles, both at home and overseas. He has served in deployments to Lebanon, Syria and Afghanistan with the United Nations and NATO. He had held the role of Assistant Chief of Sta since 2021.
He holds bachelor’s degrees from the National University of Ireland Galway and University College Dublin, and a master’s degree in Leadership Management and Defence Studies, is a graduate of the Defence Forces’ Senior Command and Sta Course and the US Army Command and General Sta College.
e Air Corps of the Defence Forces also had a busy year, responding to
254 emergency missions, helping the National Ambulance Service with the transportation of critically ill patients across the country. It also completed 36 inter-hospital transfer missions, delivering vital air ambulance support both nationally and internationally.
e Air Corps also helped with six international re-supply ights, ensuring critical logistical support to deployed Defence Forces personnel, and supported the defence contribution to the European Union Battlegroup completing three missions transporting personnel and equipment.
ere was expansion too, with the arrival of a third Airbus C295 and the introduction of the Dassault Falcon 6X, signi cantly strengthening operational and strategic airli capacity.
e Naval Service continued to patrol Ireland’s seas, with Joint Task Force Operations carried out with An Garda Síochána and Revenue’s Customs Service to suppress illegal drug tra cking by sea. It was deployed on 18 occasions for Harbour Protection and Port Security taskings, search and recovery of missing persons and routine mechanical
engineering work on the Naval Service eet. Maritime resource protection missions saw 196 sheries boardings conducted, resulting in one detention. e number of patrols also increased dramatically in 2025 following successive years of declining activity.
As part of the new Defence Sectoral National Development Plan, it was announced in October that the Irish Navy will see signi cant investment in advanced sub-surface detection systems that include towed array sonar upgrades that provide enhanced underwater acoustic awareness to better detect and track objects and activities beneath the waves, a sonobuoy project that supports anti-submarine and sub-surface monitoring missions, and an expansion of the P60 eet.
Additionally, to underpin operational improvements, €400million was allocated for naval infrastructure. is includes the development and modernisation of naval berthage facilities, which will support extended deployments, improved maintenance throughput, and enhanced logistics for surface and sub-surface assets.
e country saw some high-pro le visitors in 2025, as well as a presidential election. For the Presidential Inauguration Ceremony of Catherine Connolly on November 11 at Dublin Castle, 350 members took part. is included a Captain’s Tri-Service Guard of Honour, a Captain’s Escort of Honour, a 21 Gun Artillery Salute, two Army Bands, Air Corps Fly Past, Flag O cers and Military Police.
State ceremonial honours were a orded to South African President Cyril Ramaphosa in October and Ukrainian President Volodymyr Zelensky in December at Áras an Uachtaráin and Government Buildings.
e Defence Forces also participated in other annual State commemoration ceremonies, including the commemoration of the 109th anniversary of the Easter Rising at the GPO, the 1916 Leaders Commemoration at Arbour Hill and the National Day of Commemoration in Royal Hospital Kilmainham.

The HSE published its National Service Plan 2026 at the start of the year, setting out the delivery of a range of health and social care services to be provided within its €29billion budget.
e major highlight is the completion of the National Children’s Hospital in Dublin that has seen many delays and rising costs, but the plan also includes the delivery of 428 community beds and 177 acute beds, plus ve new surgical hubs.
e HSE also promises to deliver a single point of access to disability, mental health and primary care services for children to improve timely access to the right care, and to provide greater access to services in the evenings and on weekends.
ere will be an expansion of core disability services including residential supports with the delivery of 199 residential placements, 58 de-congregation transitions, and 45 transitions from nursing homes for people under 65.
e Maternity and Newborn Electronic Health Record system will be deployed in four of the remaining 13 maternity units across the country, while the Shared Care Record will be implemented in the Dublin South East region and two other regions.
Speaking about the HSE’s priorities for 2026, Mr Ciarán Devane, HSE Chairperson, said: “ e 2026 plan represents a continuation of our reform journey towards a health and social care system that is accessible, supportive, sustainable, and responsive to the needs of all. Our priority for 2026 is to improve access to care by making signi cant improvements to waiting times for both emergency and scheduled care. Part of this will be expanding and strengthening health and social care capacity to meet the increasingly complex needs of a growing, ageing, and diverse population. More, however, will be using our existing resources to best e ect, innovating our processes to ensure our colleagues are supported to have the time and resources to continue to deliver great care.”
Minister for Health Jennifer Carroll MacNeill said: “ e Government’s priority for 2026 is to improve healthcare access and quality across all health regions. is will be achieved through targeted investment that supports the shi to community-based care, reduces hospital overcrowding, and delivers services closer to home. Investment will be directed where it delivers the greatest impact for patients and return for taxpayers on the State’s sustained healthcare funding over the past decade.”
HSE CEO Mr Bernard Gloster added: “ is transition to population-focused funding aligns resources with need and empowers health regions to deliver integrated, responsive care, with the ultimate goal of achieving better health outcomes. 2026 is the rst year and rst major step towards the type of resource allocation and the pathway set by the Minister is clear – we must look at all resources existing and new together to achieve the priorities for the people.”


THE INSIGHTS GENERATED FROM THESE PROJECTS WILL HELP US BUILD A MORE RESPONSIVE, INCLUSIVE, AND EFFECTIVE MENTAL HEALTH SERVICE FOR EVERYONE”
Funding Aims to Enhance Understanding and Create Insights
Mental Health research in Ireland received a welcome boost in January when Minister for Mental Health
Mary Butler TD announced a €3million investment to advance understanding in areas such as youth mental health, ADHD in adults, women’s mental health and loneliness in older people.
A grant of €1million over a ve-year period will establish a new all-island Collaborative Research Network in mental health led by Maynooth University
in partnership with the University of Galway and the National Suicide Research Foundation at University College Cork. is new research network will embed lived experience in mental health research through co-production of studies between academics and public involvement, whilst also building capacity and career opportunities for researchers in the area of mental health. It will also coordinate mental health research by identifying research gaps and fostering partnerships between academic institutions in Ireland and internationally.
“ e new all-island Collaborative Research Network will transform how research is coordinated, build research capacity, embed lived experience within research projects, and ensure research ndings are translated into real-world impact,” Minister Butler said.
“I am delighted to see Maynooth University leading out on this critical initiative and continuing to develop their health faculty and expertise,” added Minister for Further and Higher Education, Research, Innovation and
Science, James Lawless. “Research and informed analysis brings multiple bene ts to solving societal challenges such as in the mental health arena. Breakthroughs o en emerge from unexpected inquiries and leading-edge research recognises and supports that. is funding demonstrates the whole of government response around mental health and our continued spearheading of scienti c excellence to inform policy interventions across government.”

A further €2million will fund ten separate mental health research projects through the Applied Partnership Awards scheme, which brings together knowledge users and researchers to co-develop projects that address real-world needs in health and social care, directly delivering on commitments in the National Mental Health Research Strategy and Sharing the Vison: A Mental Health Policy for Everyone.
e investments are supported by the Health Research Board’s dedicated mental health research budget which has tripled since 2022, with the funded projects re ecting Sharing the Vision’s emphasis on the need for whole-of-government and whole-of-population approaches to mental health.
e ten research projects are:
• Improving the Mental Health and Wellbeing of Priority Population Groups: An Evaluation of the Act Belong Commit Mental Health Promotion Initiative in Community Settings – Prof Margaret Barry (University of Galway) & Dr Aisling Sheehan (Health Service Executive)
• Project ACCESS (Advancing Care


through Single-Session erapy): Examining the Implementation of Timely Youth Mental Health Interventions in Jigsaw Ireland – Dr Amanda Fitzgerald (University College Dublin) & Dr Je Moore (Jigsaw – e National Centre for Youth Mental Health)
• Exploring Experiences and Coproducing Supports to Promote Mental Wellbeing and Improve Access to Mental Health Services for Children with Physical Disabilities in Ireland – Dr Jennifer Ryan (RCSI University of Medicine and Health Sciences) & Mr Michael Walsh (Central Remedial Clinic)
• Improving Outcomes for Children in Care – Prof David Hevey (Trinity College Dublin) & Mr Robert O’Connor (Tusla Child and Family Agency)
• Designing an Integrated Women’s Mental Health Service: Enhancing Quality and Integration of Women’s Mental Healthcare – Dr Anne Doherty (University College Dublin) & Dr Richard Du y ( e Rotunda Hospital)
• Enabling General Practitioners to Develop an Extended Role in Adult ADHD Diagnosis and Management in Primary Care – Prof Emma Wallace (University College Cork) & Dr Aoife O’Sullivan (Irish College of General Practitioners)
• SMILE MS: Supporting Mental Health by Improving the Lives and Emotional Wellbeing of People with Multiple Sclerosis – Dr Rebecca Maguire (Maynooth University) & Ms Mary McCusker (Multiple Sclerosis Society of Ireland)
• Understanding and Addressing Mental Health, Loneliness and Quality of Life
in Older People Living with HIV in Ireland: A Pathway to Social Prescribing – Dr Louise Brennan (Trinity College Dublin) & Professor David Robinson (St James’s Hospital Dublin)
• Shi ing the Paradigm- Empowering Paramedic Educators to Better Support Practitioner Mental Health, through an Evidence-Based, Sca olded Teaching Faculty Curriculum – Dr Michelle O’Toole (RCSI University of Medicine and Health Sciences) & Mr Brendan Cawley (Pre-Hospital Emergency Care Council)
• Integrating Smoking Cessation Interventions into Mental Health Services: National Survey, Guideline Development and Pilot Service Evaluation – Prof Brian O’Donoghue (University College Dublin) & Professor John Lyne (Newcastle Hospital Greystones)
Speaking about these projects, Minister Butler said: “ e ten funded research projects will make a tangible di erence whether it’s reducing waiting times for young people through single-session intervention approaches or exploring how GPs can play a greater role in supporting adults with ADHD. e insights generated from these projects will help us build a more responsive, inclusive, and e ective mental health service for everyone.”
Health Research Board CEO Gráinne Gorman added: “ is recent investment demonstrates the power of co-production and collaboration in driving research that improves mental health and wellbeing, especially among priority and underserved populations, across the island of Ireland.”
First Responders Often Face the Challenge of Bringing the Job Home With Them, So How Can You Recognise the Signs in Yourself and Others, and What Can Help?
The work of rst responders and the impact it can have on their mental health is something not ordinarily understood by those who don’t work on the frontlines, and this includes family and friends. It is of the utmost importance that if you are a ected by what happens at work, you know there are ways to cope, and people to reach out to, and that it is ok to do so. e tendency is to believe it is best not to bring the job home with you, but that is easier said than done. So how do you deal with it? How do you ag up with your partner, family, friends or colleagues that you may need to talk? What should you do if these people recognise something is impacting your relationships? How should you structure these discussions? Whether you feel the job is impacting your home life, or you are concerned about a colleague, get that conversation started.
Teacher Practitioner in the School of Medicine and Principal Investigator of the HUGS@Home programme at the RCSI SIM Centre for Simulation Education and Research at the Royal College of Surgeons

Through our experience, we’ve come to realise that the job always comes home with you, whether you realise it or not. Signs can be physical, emotional, behavioural, cognitive or spiritual. Some are easily recognisable by yourself or others, and some will only be picked up by those who know you well. These are:
1Physical body cues: Tight jaw/ shoulders, headaches, shallow breathing, jumpiness, poor sleep or vivid recall dreams.

First responders switch between two very di erent worlds. On duty they make fast, highstakes decisions with clear roles and expectations and an adrenaline-ready nervous system. At home, the tempo is so er but messier – children can’t nd their shoes, dinner’s late, the dog’s barking - and there’s no protocol to follow. at change of gears can be jarring and the nervous system doesn’t always regulate. e same protective habits that keep us safe (focus, emotional armour, scanning for risks) can sometimes look like distance, impatience, or over-protection in family life. From the family perspective, the challenges are missed celebrations, accommodating irregular moods and sleep schedules, and o en, the lack of communication. None of this means we’re broken: it means our brain and body are doing exactly what they were trained to do at work. With self-awareness, checkins with family/friends, and the teamwork already used on the job, rst responders can adapt smoothly between work and home mode.
2Emotional: Mood shifts, irritability, flatness, withdrawing from the people who usually refill your cup.
3Behavioural: Over-monitoring children, needing perfection, more alcohol/sugar/ca eine, doom-scrolling on your phone, skipping exercise/hobbies.
4Relationship signals: more arguments, distance, less a ection.

The main thing is to acknowledge that stress will come home at some point and shows up in di erent forms. These are a few simple techniques to avoid it impacting family life:
1Think about how you switch o work mode, sometimes called a transition ritual. For some, that’s showering before leaving work, changing clothes, literally leaving the uniform at work. For others it might be a podcast/music in the car on the way home, box breathing techniques or exercise.
2Protect the basics: sleep, hydration, nutrition, movement, connection with others. These are sometimes considered psychological PPE.
3Limit unhealthy coping mechanisms such as alcohol/drugs, media overload, and swap for a walk/ stretch, conversation with a friend.
4Talk about what’s lingering. You don’t need to share any graphic details: “I need to decompress/walk the dog … and then I can …”
So how do you start the conversation with loved ones or a trained professional? Choose carefully who you need the listener to be. Family, friends, spouse, are good for connection and social support, whereas work colleagues or professionals might be better suited for more technical or clinical unpacking of the event. Simple conversation starters could be: “I think I’m bringing stu home lately, can we chat about this after dinner? I don’t need suggestions or fixing, just listening - is now a good time?” Importantly, always protect children from these conversations. And what if a loved one recognises that your relationships are being impacted by work and suggests you seek help? Don’t get defensive: remember they are bringing it up because they care. Acknowledge their support and ask what they have noticed. Share what support looks like for you, and realise they also may need support. Try involve them in the next steps: peer support, professional support (GP, Counsellor), family support.
H.U.G.S is a simple structure for healthy conversations
One speaks, one listens. No fixing. “What’s happening? How are you feeling right now?”
Reflect back. “So you’re wired and tired after a tough call; did I get that right?”
Guide towards healthy coping mechanisms. Slow breaths, short walk, tea, shoulder-toshoulder activity.
“What helps tonight?” Agree a small action (early night, arrange peer support) and a quick check-in tomorrow.
Do we need further help?
For more information on resources, visit www.hugsathome.eu or the new social enterprise website www.hugscommunity.ie or see us on LinkedIn www.linkedin.com/company/ hugs-community/
One organisation that takes the issue of mental health very seriously is Dublin Fire Brigade, who have their own dedicated Critical Incident Stress Management (CISM) team and approach to mental health awareness. They endeavour to educate all DFB members - who are all both firefighters and paramedics - and their families on the importance of talking about mental health, and recognising when somebody might need to have that conversation.

FF/P and CISM Coordinator with DFB, Joe Dromgoole, outlines how they can help:
Studies have shown that there are two reasons why re ghters cope with trauma:
• Having the support of their front-line colleagues
• Having the caring support of loved one
erefore, rst responders are unique in having the support of two families – one at home and one at work. Every recruit re ghter has ve contact days with the CISM team during training to highlight the potential critical incidents they will be exposed to, and the stress response they may experience. ey are also shown the support network the CISM team o ers. e CISM team acknowledge the importance of the support structure that families o er. It is important that families are made aware of the potential impact these Critical Incidents can have on rst responders. To this end, we organise a family night during recruit training, where we highlight all these potential impacts, enabling families to understand the stresses of the job. is support is paramount to reducing the impact of highly stressful work, helps create a positive work/life balance, and allows for self-care to take place. Families are best positioned to recognise irregular behaviours, such as irritability and sleeplessness. If family members witness unusual behaviour, we encourage them to talk to the rst responder about what is going on. ese members hopefully will be willing to talk. With family and DFB support we can e ectively manage that situation, allowing us to build resilience through experience.
Under the ICISF CISM Model, one-to-one individual support (Assisting Individuals in Crisis) is called the SAFER-R model, which includes steps like stabilisation, acknowledgment of the crisis, facilitation of coping, and referral for further care if needed. It serves as a specialised, short-term intervention designed to help firefighters cope with the immediate psychological and emotional impact of a critical incident. The purpose of this intervention is to:
“Emotional First Aid”: Individual crisis intervention is not psychotherapy, it is an acute, emergency mental health approach like physical first aid. It aims to stabilise the firefighter emotionally and cognitively so they can function and make decisions safely.
2Normalise Stress Reactions: The intervention helps the firefighter understand that their reactions, such as anxiety, confusion, or being emotionally overwhelmed, are normal responses to abnormal events. This reduces feelings of isolation or fear of “losing control”.
3Restore Coping Strategies: Critical incidents often disrupt natural coping mechanisms. One-to-one support assists in re-establishing their own, normal coping skills and fosters resilience, enabling the person to regain a sense of control.
4Reduce Risk of Long-Term Psychological Harm: By addressing acute stress early, the intervention lowers the likelihood of developing more severe conditions such as PTSD, depression, or maladaptive coping behaviours.
The CISM team will have no more than three points of contact with the firefighter. Often, these are done by meeting for a co ee in person, but can be done over the phone. If after three points of contact the firefighter is still struggling, we would refer them onto either DCC Sta Support or a Mental Health Professional. We don’t have to wait until after the three points of contact, we can recommend referral after our first contact.
If you need to contact us, the CISM team is made up of a Coordinator, three senior mentoring peer support workers and 23 active peer support workers. There are four CISM phones manned 24/7. I would encourage any firefighter who needs support to contact any of these numbers so we can arrange confidential advice and support for you:
CISM 1: 086 815 0181
CISM 2: 087 210 5276
CISM 3: 086 815 0183
CISM Coordinator: 087 950 7225
DFB
























































































































































“THE MAIN THING IS TO ACKNOWLEDGE THAT STRESS WILL COME HOME AT SOME POINT AND IT SHOWS UP IN DIFFERENT FORMS”
First responders have a unique bond with their colleagues. This enables them to identify areas of concern. Because of the nature of the job, we work in very close proximity to each other and spend a lot of time together. This creates an environment where we get to know each other’s idiosyncrasies, character traits, etc. As a result, we are also in a unique position to know when something “is o ” with a colleague. We can have good days and bad days. The problem is when bad days become more frequent. The natural response is to ask how they are doing? Based on the interaction, the first responder can identify that there is an issue and seek assistance themselves. Or they may ask for help or assistance in getting support. When the answers to these questions don’t sit right, or the first responder is displaying signs and symptoms of distress, their colleagues or o icers can contact us. This has happened numerous times in the past, and we then get as much information as possible and contact the person involved. One of the important aspects of the CISM team is surveillance, knowing the signs and symptoms of distress and spotting it in each other. To this end, we have trained up more than 50 of our Station O icers to the level of peer support worker so we can identify first responders who are struggling much earlier. The plan is to train up every Station O icer to this level.
As first responders we can be exposed to Stress Crossover. We work in a highintensity work environment. We can face life-threatening situations, traumatic incidents, and unpredictable schedules. This creates chronic stress that doesn’t simply “switch o ” after a shift. Long shifts often lead to poor sleep quality, which a ects mood, patience, and family interactions. Exposure to trauma (injuries, fatalities, disasters) can lead to emotional exhaustion or PTS symptoms, which spill into personal life. At home, first responders are expected to be present and emotionally available, but the mental load from work can make that di icult. Much like a free taker in Gaelic or rugby goes through the same ritual prior to taking every free kick or penalty to get their mind in focus, a first responder should do the same. As Michelle O’Toole says above, this might involve using the gym in the station after work, showering to symbolically wash the working day o , changing out of uniform, listening to music or a podcast going home rather than the news. Breathing exercises or meditation can also work. Structured downtime is important. While this can be di icult with busy family lives, have a scheduled recovery time after intense shifts before engaging in family responsibilities. Try to avoid or limit unhealthy coping mechanisms such as alcohol/drugs, ca eine, and the “what if” mind game (replaying the events). Studies have shown that a 30-minute walk can have the same e ects on the mind as a mild antidepressant. It is always good to talk, so talk with colleagues prior to leaving work about anything bothering you. Talk to loved ones in a general way about the event (nothing specific or graphic). Let them know how you are feeling, what space you need.
When a first responder is struggling and bringing job-related stress home, it’s important to approach the situation with care and awareness, and recognise signs and symptoms:
• Irritability, withdrawal, or emotional numbness
• Trouble sleeping or constant fatigue
• Increased alcohol use or unhealthy coping habits
• Di iculty engaging with family or friends
1LISTEN, DON’T FIX: Sometimes they need to vent, they are not looking for solutions. Use active listening and don’t interrupt: “That sounds really tough. How are you coping?”
2If the situation warrants, encourage them to get professional help. First, contact the CISM team and speak to one of the peer support workers. This can then be followed by using the sta support counselling services or Mental Health Professional used by Dublin Fire Brigade. It’s important to realise that seeking help is a normal response, seen as a strength, not a weakness. It’s important to maintain
confidentiality and trust. O er support without judgment.
3Involve family education to help family understand the nature of the job and its emotional toll. It’s important that spouses/partners know how to contact the CISM team if needed.
4Watching out for Red Flags is extremely important: Expressions of hopelessness or suicidal thoughts, severe withdrawal and/or substance abuse. If these appear, escalate immediately to Mental Health Professionals or Crisis Support.




The Camino and the Remarkable Journey of Jimmy Fullam
“You don’t do Camino Walks with your body, you do them with your mind,” says Defence Forces veteran Jimmy Fullam. “It will always get you where you need to be, stage by stage, just like life. You don’t need to be a super t, just some tness and inspiration.” He should know, having undertaken a huge number of Walks for charities including Focus Ireland, the Organisation of National Ex-Service Personnel (ONE), his own ex-unit the 5th Infantry Battalion Veteran’s Association, LauraLynn, Simon Community, and most recently in 2025, Coolmine erapeutic Community.
His personal motto of “Always think of others” has seen him cover more than 8,000km across six full Caminos, two Ignatian Ways, two Famine Trails and Dolomite Trails. For him, it’s not just a physical journey, but a spiritual one that has sent him on his own road to recovery, spreading a message of hope for people who feel they have none le . He speaks from experience, having undertaken a long and demanding road towards his own recovery from alcohol addiction.
Jimmy always had an itch to join the Army, and on his 17th birthday, walked to Cathal Brugha Barracks to sign up. Sworn in the next day and posted to Limerick, he soon became Southern Command Boxing Champion, then All-Army Featherweight Champion. In 1979, having moved to the 5th Infantry Battalion Collins Barracks, he was also selected for the Battalion soccer team, winning league and cup medals and an All-Army Cunningham Cup.
Halfway through his second term, things started to fall apart. “I got married to my wife Violet in 1980 and I knew it was time to leave the Army a er six years,” he says. “I wanted a di erent life. I became a taxi driver in 1984 and have been doing it ever since!
“I’d already started drinking heavily, and when I le the Army, I started drinking more. Before I knew it, I couldn’t live without a drink, ended up sick drunk and in all sorts of trouble, made a lot of promises to my wife that I would stop, and I completely abused the word ‘sorry’ to the point where I never use it now. I always say ‘I regret’. ‘Sorry’ lost all meaning.”

In his mid-40s, Jimmy realised his problem was something that required help, but it took a moment of clarity and unexpected spirituality to force that change.
“My wife was ready to leave me, but I didn’t know,” he says. “I got out of bed to nd her cleaning the house, she was looking beautiful. I knew there was something strange going on. She smiled at me in a way I had never seen before, and my heart sank. I walked into the bathroom and dropped to my knees, saying ‘Please somebody help me’. It was the rst time I ever asked for help, and it was an awakening. I made a conscious decision to stop.
“I got up o my knees and looked in the mirror, and I saw a vision in my mind’s eye of the Sacred Heart. at moment shook me. I went downstairs and asked my wife to give me a li to an AA meeting. She said I could go myself, so I
went to a meeting that night and haven’t stopped since. at was 13 years ago.
“Six months later when things had turned a corner, I was sober, my wife handed me a letter to read. It said she was leaving me, but as I broke down, she pointed to the date she had written it. It was from that day six months earlier, when she was about to walk out the door, but I had asked for help, so she stayed.”
Back on the right track, Jimmy still felt there was something missing in his life that would help him start on a new path, and it was then that serendipity seemed to intervene with a series of chance meetings.
“I was sober four years, had done the 12 Step programme, had spent time in a monastery emptying myself spiritually, but there was something missing I couldn’t put my nger on,” Jimmy says. “I was trying to nd that spirituality that would make me believe my mother, who had



died in my arms and had always wanted to see me sober, was looking down on me, but I didn’t know where to turn.
“I picked up a passenger in my taxi to bring him to the airport, and when I asked him where he was going, he said the Camino de Santiago. I had never heard of it, but he told me about this pilgrimage walk in Spain and I was intrigued. He told me to watch the lm e Way, and from there everything started to fall into place. Six months later, I went on my rst Camino.”
A fellow taxi driver and professional climber Lee Gallagher brought Jimmy to the Dublin/Wicklow Mountains to get a taste of hiking and being in nature before he set o .
Embarking on the 800km Camino Francés, he had a second chance encounter that opened his eyes to the opportunity to heal and nd meaning.
“I was sitting in a place called Logroño when a man in his 70s asked to sit with me,” Jimmy says. “He said he was a eologian and was on a di erent Camino Walk to me, from Loyola towards Barcelona. Intrigued, I asked him about it, and he detailed the life of St Ignatius of Loyola for me. e story resonated with
me. He had been a soldier, had faced many challenges before founding the Jesuits. Before he le , this man said ‘You will walk many more Caminos, and you will walk the Ignatian Way’. I still had 450km le on this walk, but all I could think about was this man. I don’t know if he was a real man or just sent to give me a message.
“I still think a higher power sent me that passenger in my taxi who rst told me about the Camino, and that messenger I met on my rst Camino who told me I would do many more. ey sent me on my way.”

Upon returning home, Jimmy got in touch with the Jesuits to nd out more about Ignatius and the Ignatian Way. It was then that he was put in touch with arguably the most in uential person to come into his life: Fr Brendan McManus SJ, who has accompanied Jimmy on not just several Walks, but on a path through life that continues to this day.
“He intrigued me, and was intrigued by me,” says Jimmy. “I told him about my plans and based on his own experience, he advised me not to travel alone because



there are ve peaks in the rst eight days of the Ignatian Way, with dangerous terrain, and if you get injured you are in trouble.”
A plan was put in place, with Fr Brendan agreeing to meet Jimmy in Logroño a er the rst eight stages. Jimmy’s nephew David accompanied him over the mountains, and along the way, they discovered they were both on a path to recovery.
ey met Fr Brendan before David went home, but on their rst day together with 400km in front of them, Fr Brendan was called away to a funeral, leaving Jimmy to walk through wilderness, su ering dehydration and exhaustion, not meeting another pilgrim along the route, following the Pyrenees and the Ebro River on his le until he could reunite with Fr Brendan again.
Before then though, Jimmy faced a crossroads that could have changed his life for the worse again, but he found solace in the teachings of Ignatius that Fr Brendan had passed on, and which forms a major
Grants Trust and Foundations Executive with Coolmine Therapeutic Community MacDara O’Shea on Jimmy’s Fundraising
“Endeavours like Jimmy and Ciaran Fullam’s Camino Walk for Coolmine are incredibly important to us because community led fundraising directly supports people on their recovery journey. Their e orts help us raise the vital funds needed to provide treatment, family support, and programmes. Their Camino became a powerful advertisement for what Coolmine o ers in terms of rebuilding lives and reconnecting families.
“When our graduates share their stories publicly, it helps break down stigma and barriers for others who may be afraid to seek help. These success stories matter deeply to us: they open doors for others to follow the same path, inspiring future participants, families, and supporters to believe that recovery is possible.
“Jimmy and Ciaran are the embodiment of Coolmine’s ethos of giving back, lifting others, and showing that recovery is a transformative journey. They have actively chosen to help the next group of clients succeed on their own recovery paths, just as they were once supported themselves. This spirit of giving back is not only vital for those entering recovery, but deeply valuable for participants like Jimmy and Ciaran too. Their act of selflessness allows them to see how far they’ve come, and to appreciate the strength, compassion, and resilience they now carry.
“This transformation moves them away from the isolation and self focus of addiction and into a place of connection, empathy, and purpose. They also become role models, showing their peers, especially those just beginning their journey, what recovery can look like. Role modelling is a core part of Coolmine’s ethos, inspiring others to act in a way that transforms the individual in their mindset and behaviour. Jimmy and Ciaran’s journey captures all of this.”
part of the book they later co-wrote about this trip, Brothers In Arms (so-called because of Jimmy’s army past and because they are both Dire Straits fans).
“ e route I was supposed to take in Zaragoza had been turned into a junction,” Jimmy says. “So, I went to the bus station but there wasn’t a bus for hours. Sitting in 44C heat, I thought my credit card had been hacked and I had lost my glasses. Looking around exhausted, wondering if this was all worth it, I saw every second premises was a bar. Temptation was right there, but Brendan had taught me the Ignatian
Way of just sitting and observing, the principles of going from a di cult situation, from desolation, and turning it into consolation. Within half an hour I had my credit card back, found my glasses, and was back on track.”
Jimmy also received a lot of help and support on daily calls from ex-soldier and Dublin Fire Brigade member Ken Cleary who gave great advice on health and safety, and retired soldier Peter Downes.
He also received a lot of support from his ex-5th Battalion colleagues: Tipp Ryan, Kevin Corcoran, Mick O’Brien, Marlo, Christy Mahon, Joe McDonagh, Tomo

McCann, Noel Corr, Eamonn Doyle, Eddie Costigan, Tony Murray, and retired Air Corp Piper Pat Cleary, who gave great advice. One particular person who got him involved in the Veterans Association, Larry Jones, was a huge help along the way. “His o ers of kindness were typical of a Veteran,” Jimmy says. “To name them all, I’d probably have to write a book!”
Reunited with Fr Brendan, Jimmy completed the Ignatian Way and was soon planning his next pilgrimage walk. One he is eager to discuss is the Famine Trail from Strokestown to Dublin that he completed twice with Army veterans. Having joined the Battalion Veterans Association in 2020, he has been very active with the 5th Infantry Battalion Veteran’s Association, the Organisation of National Ex-Service Personnel (ONE), and Brú na bhFiann (Home of the Brave), the homeless veteran facility.
Jimmy enjoys working with Veterans Support O cer Tony Sta ord, Brú na bhFiann House Manager Richard Dillon, ONE CEO Cormac Kirwan and Marketing and Fundraising O cer Paul Clarke who he says “do a lot of great work for this cause” and adds that walking with ten veterans for seven days brought him back to his earlier days when he was in the Army.
“ anks to the support group on this Walk led by the Chairman Pat Mulcahy
McKee Barracks, Michael Kinehan, Noel Kelly, Jim Kearns, Kevin Martin, Sammy Dermot McIlwaine, Eoin Feeney, support driver Dave Buckley of Civil Defence, Paul Clarke for organising it,” he says, “and huge thanks to the Army for accommodating us on that Walk and for supporting us two years in a row.
“Marching down North Wall Quay on the last leg with my comrades, with pipes and colours to a ceremony t for royalty laid on by Paul Clarke, and with the Lord Mayor of Dublin present, to see my whole family there to greet me was for me recovery at its highest, and this brought tears to my eyes,” he adds.
Honoured by Dublin Lord Mayor Caroline Conroy for his endeavours on the rst Famine Trail, Jimmy’s drive to help raise money for charities has seen him take on further Caminos, with last year’s from Ferrol to Santiago in aid of Coolmine particularly special to him. “ ere was a catharsis in doing each walk, and to help Coolmine erapeutic Community was important to me,” he says. “My son Ciarán came out of Coolmine four years ago, they were a big help to him and his partner, and this had a ripple e ect on me wanting to help people on the path to recovery.”
With his nephew David also on board, Jimmy found no shortage of company. “It ended up that people my son knew, who helped each other through recovery, all came on board too,” he says. “Each day we walked we shared our experiences of how it was and how it is today. I hope to bring more people in the same boat back for another Camino!
“We ended up calling it the ‘Camino of Hope’ because we were sending that message to those still nding their way out of the darkness of addiction, acting as beacons of recovery, resilience and gratitude.
“If I can put a roof over someone’s head for the night, or give them a meal they wouldn’t have gotten otherwise, then I am glad to do these walks and raise money for charities. It is about awareness too. Maybe people will look at what I do and it might
resonate with them.
“I never knew the meaning of the word ‘Gratitude’ when I was younger, but it is a big part of my recovery. I have come a long way, literally. Life is precious to me and I try to live it in a good way, helping others.”
Jimmy heads to Tampa, Florida, in March to walk in their St Patrick’s Day Parade with the Pat Mulcahy Group of Veterans, having become a minor celebrity when Brothers In Arms was launched there. He is keen to thank his American friends who have supported him or accompanied him on his many Walks.
“My friends in America always get behind me, they are very good to me,” he says. “Steve Krist, who I met in 2021 on the Camino Francés in the middle of nowhere, was another messenger sent to me. Also ex-marine Lt Colonel John Tempone, a great friend and comrade, who sadly passed away shortly a er I took ten marines along with Fr Brendan on an 11-stage trek of the Ignatian Way, was another. Also Fr Zach and Pete Kelly, Bruce McDonald, Tim, Dan and Tony.
“If someone had told me years ago that I was going to walk thousands of kilometres, raise a lot of money, go to America and meet famous people, and write a book, I would have said you were mad.”
Jimmy is already planning his next Walk for 2026, and looks forward to helping raise funds and awareness for charity, but he is also relishing the sense of achievement in his own recovery.
“You couldn’t write this script,” he says, “it is a journey and a path that continues, it never stops. While there are people who need help, you can take them on the journey too, and that is what I plan to do.”
Jimmy would like to thank his wife Violet, his children and grandchildren, who have been a special part of his recovery and without whom he might not have been successful. He would also like to thank the ONE, 5th Infantry Battalion Association, Michael Kinahan and all the lads from the Pat Mulcahy Group McKee Barracks, ex-Air Corps John Maguire for all his help and support in this story, all his American friends, and all who donated to him in his journey.

The Waiting Time Action Plan 2026 was launched at the end of January by Minister for Health Jennifer Carroll MacNeill, setting out how Government plans to improve access to hospital care.
It follows on from previous Plans rst started in 2021 against the backdrop of increased demand for planned care services and the subsequent lengthening of time patients are le waiting for an appointment or procedure.
Overseen by the Waiting List Task Force, which is co-chaired by the Secretary General of the Department of Health and the CEO of the HSE, the Plan sets out six overarching and interconnected targets to be achieved through the delivery of 36 actions under the themes of “Reforming Planned Care”, Enabling Planned Care”, and “Capacity Optimisation”. ese are:
• Sláintecare Wait Time Targets: 50% of patients to be waiting less than the Sláintecare wait time targets of 10 weeks for Outpatient Department
(OPD) appointments and 12 weeks for In-patient (IPDC) procedures; and 65% of patients to be waiting less than the Sláíntecare wait time target of 12 weeks for Gastrointestinal (GI) Scopes.
• Weighted Average Wait Time: Reducing the weighted average time to <5.5 months for OPD and IPDC and to <3.5 months for GI Scopes.
• Patients waiting less than 12 months: 90% of patients to be waiting less than 12 months for rst access to OPD services.
• OPD New to Return Ratio: To achieve an OPD new to return ratio of 1:2:0.
• Chronological Scheduling: To have 85% of routine elective appointments/ procedures chronologically scheduled.
• Elective surgery same day of admission: 83% of in-patients to have their principal elective procedure conducted on day of admission.
“ e Waiting Time Action Plan is a multifaceted approach with one overarching aim, to ensure people get access to faster care and achieve better health outcomes,” said Minister Carroll MacNeill. “It will ensure that we build on the progress we
The Latest Action Plan Aims to Improve Access to Hospital Appointments
have already made in reforming our health service and continue to boost productivity and e ciency, while developing alternative care pathways and shi ing towards care in community settings.”
Between 2016 and 2021, the weighted average waiting time for each of OPD, IPDC and GI Scopes increased, but since then, metrics have improved. As of December 2025, the weighted average waiting time for patients on the total hospital waiting list improved by 46% from 12.2 months to 6.6 months.
OPD waiting times have been reduced from 12.8 months in 2021 to 6.8 months, IPDC waiting times were reduced from 9.1 months to 6.4 months, and GI Scope waiting times have been reduced from 6.9 months to 3.5 months.
However, meeting the new targets will not be easy. ere is an ever-increasing number of people on waiting lists, with approximately 754,000 patients on active hospital waiting lists by the end of 2025, representing an increase of 11.8% since 2024.

A Team of Dublin Firefighters, Carlow Fire and Rescue and Dublin Civil Defence Competed Very Well at the World Rescue Challenge, writes DFB Firefighter/Paramedic Stephen Wade
Agroup of Fire ghter/ Paramedics from Dublin Fire Brigade, members of Dublin Civil Defence and Carlow Fire and Rescue Service took to the international stage as ‘Team Ireland’ to take part in the World Rescue Challenge in September.
Before that event, there was the small matter of competing in the National Extrication and Trauma Challenge that took place on 26 May, when teams from across the country, as well as from Luxembourg and Manchester, descended on the Dublin Fire Brigade Training Centre.
An award ceremony was held on-site, and when the nishing positions were announced, it was revealed that DFB had secured the winning place for the second year in a row, therefore qualifying to compete at the World Rescue Challenge in Karlovac, Croatia.
For the rst time in the team’s history, a week-long training programme was put together by District O cer Declan Rice, which allowed the team to spend a week in the Training Centre ne-tuning extrication and trauma scenarios. is time was also used to produce LearnPro
material and assess new RTC equipment. Assessors from around the country were also invited to appraise the team’s performance and make some tweaks; (we thank you for your time and guidance).
In between training scenarios, D/O Rice encouraged open and frank discussion. Everyone was to speak up, opinions mattered, and ideas on what went well and what needed improvement were discussed, regardless of rank or experience in the team. By the end of the week, a lot of improvements had been made and both teams were feeling good about the challenge ahead. e Trauma Team had also been given an opportunity to train for




the new Mass Casualty Incident scenario under the tuition of Fire ghter/Advanced Paramedic Eithne Scully.
is year we adopted the “Team Ireland” approach of Stronger Together, and so it was that DFB was joined by our colleagues from Dublin Civil Defence and Carlow Fire and Rescue Service. Team Ireland le Dublin Airport bound for Zagreb, where we were met with an incredible level of hospitality from the Zagreb Fire Service who collected us from the airport and provided us with two minibuses for as long as we needed them.
Day 1 of the competition saw our rst Team take to the extrication pit for a challenging scenario which presented a patient with a catastrophic haemorrhage to the arm trapped in an overturned car, with access obstructed by another car and various immovable objects of road furniture. David Lorenzo and Liam Ca ery had to work hard, creating space by reforming the roof while Eithne Scully stabilised the patient before he could be extricated. Meanwhile, Paul Stanley quickly assessed a patient in the second car before stepping him out and handing him over with minor injuries. is is an example of the multiple jobs being undertaken at once, and Stephen Bon l and Keith Russell ensured we had multiple pieces of equipment being used in tandem to ensure the goal of a 25-minute extrication and handover was achieved. e team were praised for their communication, patient handling, and incident command.
Day 2 saw the new trauma team consisting of Andy Dowling and Aaron Cullen take to the pit. ey were faced


with a complex scenario which comprised of two patients, one critical and one with non-life-threatening injuries. Aaron Cullen took to treating the critical patient while Andy Dowling assessed and treated the second patient. roughout the scenario, both team members had to continuously communicate with each other, ensuring neither patient deteriorated while preparing them for transport. All of this had to be done within 14 minutes, with one minute allowed for a full handover of both patients. e assessors in this case were emergency medicine consultants from Romania and Spain, so no chance of winging it!
On Day 3, Aaron Cullen and Stephen Wade were joined by two re ghters from France for the newly introduced Mass Casualty Incident. It soon transpired that the French re ghters were trained to Emergency First Response level, so it would take a huge amount of team work to recognise each team’s abilities and limitations when it came to triaging and stabilising casualties, particularly with the language barrier. e scenario presented an RTC involving a minibus and pedestrians amounting to eight patients with injuries ranging from cuts
and bruises to catastrophic haemorrhages and traumatic brain injuries. Despite the challenges of working with French colleagues with di erent skillsets, the team managed to treat all casualties and nished in 4th place, just four points behind the winning team. e margins are so tight at this level!
Outside of the competition pits, there were several workshops from subject matter experts on new technologies including Virtual Reality, Lithium-Ion battery res and new vehicle construction. ere was something for everyone on the social calendar; also swaps night, live bands, and museums.
Between scenarios over the four days, the team also got to take in the local area and amenities, including the 10metre diving board on the Korana River. One particular team member, Liam Ca ery, made the climb of no returns when he went to the 10metre board only to nd a crowd of local re ghters had gathered on the nearby bridge to watch him make the long step from the top board. A er a few short minutes of gentle encouragement from the team and a growing crowd of spectators, Liam made the jump, the ripple of which is still making its way down river. Not wanting to be upstaged,

he was soon followed by D/O Rice and Lorenzo.
It was a very successful week in which the team continued to show its progression at World level. ey performed to the highest standards and the I.C. Stephen Bon l came in 4th position overall, while the other teams had a top ten nish out of 72 teams. When a date is set for training to recommence in the new year, it will be advertised on the ‘Request to Speak’ bulletin and any potential new members, regardless of watch, service, sex, size, or experience, all are eagerly welcomed to attend, to watch, or get involved!
THE MARGINS ARE SO TIGHT AT THIS LEVEL!”


While the delivery of food and other goods by drone is becoming more commonplace, this technology’s potential to quickly bring vital medical assistance to people in any location is, as yet, untapped in our country.
e ability to get a de brillator to a
patient experiencing cardiac arrest is central to survival rates, so it would seem to be a no-brainer that drones could play a vital part in delivering these emergency care devices, but their introduction seems to have hit a crossroads, leaving their proposed introduction somewhat up in the air, so to speak.
e idea has been discussed at council level. In November of last year, drone delivery company Manna were in contact with local councillors in Blanchardstown, with CEO Bobby Healy, who said he had already been in discussions with the National Ambulance Service (NAS), asking for backing to progress an
THE SURVIVAL RATE FOR SOMEBODY WHO GOES INTO CARDIAC ARREST OUT OF HOSPITAL IS CURRENTLY AROUND 8%”
emergency de brillator initiative.
He said the company needed the HSE, NAS and Dublin Fire Brigade to nish up a memorandum of understanding setting out the emergency response pathway to move the project forward.
e collaboration with the HSE came at the end of 2024, with a simulation test of drone delivery of a de brillator spearheaded by the Digital Hub’s designer in residence, Dr Glenn Curtin, with cooperation from the NAS, the Community First Responder programme and the HSE. It saw a Manna drone y from their hub in Blanchardstown to an address in a nearby housing estate in just two minutes.
“ e successful roll-out of a community de brillator delivery initiative in Dublin 15 has the potential to materially improve emergency response outcomes for all residents, and Manna is proud to be a part of this vitally important community service,” Healy said when discussing his initiative with local councillors.
He had raised the idea of drone delivery of de brillators at the Oireachtas Joint Committee on Transport last July, and discussed how his company was moving beyond takeaway deliveries.
“We’ve worked with Dublin Fire Brigade and the National Ambulance Service to launch a de brillator drone delivery pilot in Dublin 15 – potentially saving lives where every second counts,” Mr Healy’s written statement said. “Per the HSE, rolling this out nationally could help save up to 900 liver per year in Ireland.”
However, it was le unclear whether the initiative had ever even gotten o the ground.
In November, a spokesperson for the NAS said that while it had informal discussions regarding the service as
a trial community rst responder scheme, it didn’t progress and discussions had closed out. is, they said, was because the NAS isn’t the primary pre-hospital emergency care provider for emergency calls in the area and “as such, engagements with other State bodies would rst have to conclude”. e primary care provider in this case is Dublin Fire Brigade.
A spokesperson for Dublin City Council, which oversees DFB, said there has been discussions between Manna and a doctor in relation to trialling de brillator delivery, but Dublin Fire Brigade “did not receive any further details and have no further insight into this project”. Since then, a spokesperson has con rmed that this was still the case and DFB had no plans to further its involvement.
e proposal to help deliver de brillators to emergencies in the area – and the call for local councillor support – meanwhile, has refocused debate on public opinion as to what drones should, and shouldn’t, be used for.
Fianna Fáil Councillor JohnKingsley Onwumereh said the idea of Manna moving into de brillator delivery has always been on the cards, saying it did seem to get the support of councillors when it was rst raised. He added that it would impact wider public attitudes towards drones, saying: “Personally, I think it’s going to be a game-changer in terms of perceptions.”
Labour Councillor John Walsh also commented at the time, saying he thinks there is a place for drone technology, particularly its appropriate use in the urgent delivery of medical products, but that “de brillators shouldn’t be an a erthought to promote a large-scale drone delivery service”.
Co-lead for the HSE’s National Heart Programme, Joe Galvin, weighed in on the subject, saying: “ e survival rate for somebody who goes into cardiac arrest out of hospital is currently around 8%. At the moment, the average emergency medical services response time in urban areas is 11 minutes and in rural areas is 18 minutes. e likelihood that somebody will survive drops by 10% each minute from onset of the cardiac arrest to de brillation or the arrival of an ambulance. Anything that can reduce the times to de brillation, is going to save lives.
“At the moment, community rst responder teams – local volunteers with paramedic training – are alerted when a call comes to the dispatch centre, and they can grab the nearest de brillator and run there. Drones could potentially help de brillators get there faster. ey can y at 60km an hour, so in ve minutes they can get 5km. Will it work? I truly don’t know. But I think there is untapped potential.”
Government agencies have worked on a pilot drone de b delivery project as part of the Drone Innovation Partnership made up of academics from Maynooth university working with Dublin City Council and the Irish Aviation Authority, with the issue of drone dock stations a key challenge, but as yet any results have been kept internal.
Attitudes towards drone use, it appears, depends very much on what they are being used for, and the potential to bring de brillators to those in critical need in a short space of time does seem to meet with approval from the general public. While surveys conducted by Dublin City Council suggest the number of people who feel positive about drone technology overall has fallen from 84% to 54% in four years, those who feel positive about its use for emergency services stood at 94%.
So, public backing is there, and it may simply be a matter of emergency services organisations guring out how best to e ciently, and legally, use them in rst response scenarios, but for now, we needn’t look to the Irish skies for help from above just yet.
Durite, a UK supplier of vehicle safety and electrical components, has launched a new LED warning light that combines standard amber LED strobing with a new highintensity non-visible intelligent illumination (HINVII) system to improve visibility in low-light conditions and enhance safety for on-site personnel. The device produces a distinctive purple flash to activate high-visibility materials such as PPE clothing, signs, cones and machinery and make them appear brighter without creating a distracting glare. The new warning lamp includes multi-programmable flash patterns and operates on 12/24V systems. It can withstand vibration, water and dirt, making it ideal for road-side incidents in low light. “This patented technology enables emergency fleets to access precision warning lighting which quite literally cuts through the dark,” says John Nobbs, UK Sales Director for Durite. “By enhancing visibility without increasing visual noise, it empowers fleet and emergency service operators to improve crew safety without compromising performance or compliance. Truly, a leap forward in lighting safety.”

Smartwatches from brands including Apple, Google and Samsung with built-in ECG sensors could be better at detecting life-threatening heart rhythm disorders than a conventional check-up, according to a study by Amsterdam University Medical Centre. The research focused on atrial fibrillation, which often occurs irregularly and causes no noticeable symptoms in many people and found smartwatches help spot disorders earlier and more reliably than a GP visit. In the study, half of 437 patients over 65 with an elevated stroke risk wore smartwatches for at least 12 hours a day over six months while the other half received standard care without digital monitoring. Atrial fibrillation was found four times more often in the smartwatch group than in the control group, with 21 users diagnosed and treated compared to five in the control group. All five patients in the non-watch group had symptoms and visited a doctor because they felt unwell. In the smartwatch group 57% were asymptomatic, and would likely not have learned their heart was out of rhythm without the watch.
Dubai’s ambulance service has unveiled an AI-powered “Smart First Aid Kit” in the form of a digital platform and mobile app aimed at improving public awareness of rst aid and emergency response. e tool aims to provide fast, accurate medical guidance and educational content focused on preventative healthcare through interactive digital channels, helping people handle emergency situations before ambulance crews arrive. Similar to the audio instructions on a de brillator, it will use technology akin to conversational AI tools, whereby users can describe a situation or ask a question to receive clear, step by step guidance on how to respond. e service will also include explainer videos and digital simulations to demonstrate procedures in a simple and accessible manner.


US-based chemical analysis specialists 908 Devices Inc have produced their new VipIR, a 3-in-1 handheld analyser o ering rapid chemical identi cation through a single sample analysis. ey say it sets a new benchmark for quick and reliable eld-based chemical identi cation of unknown bulk solids and liquids, including dangerous compounds that will help HazMat teams make decisions on the spot. eir patented Smart Spectral Processing (SSP) algorithm dynamically combines data from Fourier Transform Infrared and Raman spectroscopy to analyse complicated or mixed chemicals from a single sample. e VipIR includes a vast collection of more than 39,000 chemical spectra encompassing ordinary compounds, chemical warfare agents, dangerous industrial products, pharmaceuticals, illegal drugs and explosives, as well as fast data uploads, simpli ed reporting, integrated Wi-Fi, and a light yet robust construction. “VipIR is rede ning chemical analysis at the point of need with its combination of lab-grade analytical technologies, sophisticated algorithms and a simple, smart work ow that provides one con dent result,” said Kevin J. Knopp, CEO and Co-founder of 908 Devices. “ is new chemical analyser reinforces our commitment to providing frontline teams with next-generation tools that deliver con dent, reliable answers.”
Researchers at the University of Miami School of Medicine have developed a simple wipe test that reveals per- and poly uoroalkyl substances (PFAS) on protective gear without damaging it, ultimately aiming to create tools to help re ghters reduce exposure to chemicals linked with cancer. Researchers swabbed high-contact areas of turnout gear and SCBA masks with damp polypropylene wipes and analysed the extracts using advanced mass spectrometry. ey also used physiologically-based toxicokinetic modelling to estimate how surface contamination could translate into internal exposure. e aim now is to develop a PFAS dashboard powered by AI-driven analytics that can be installed at every re station to map contamination hotspots and predict risk trends, and alert re ghters to high levels of contamination risk.
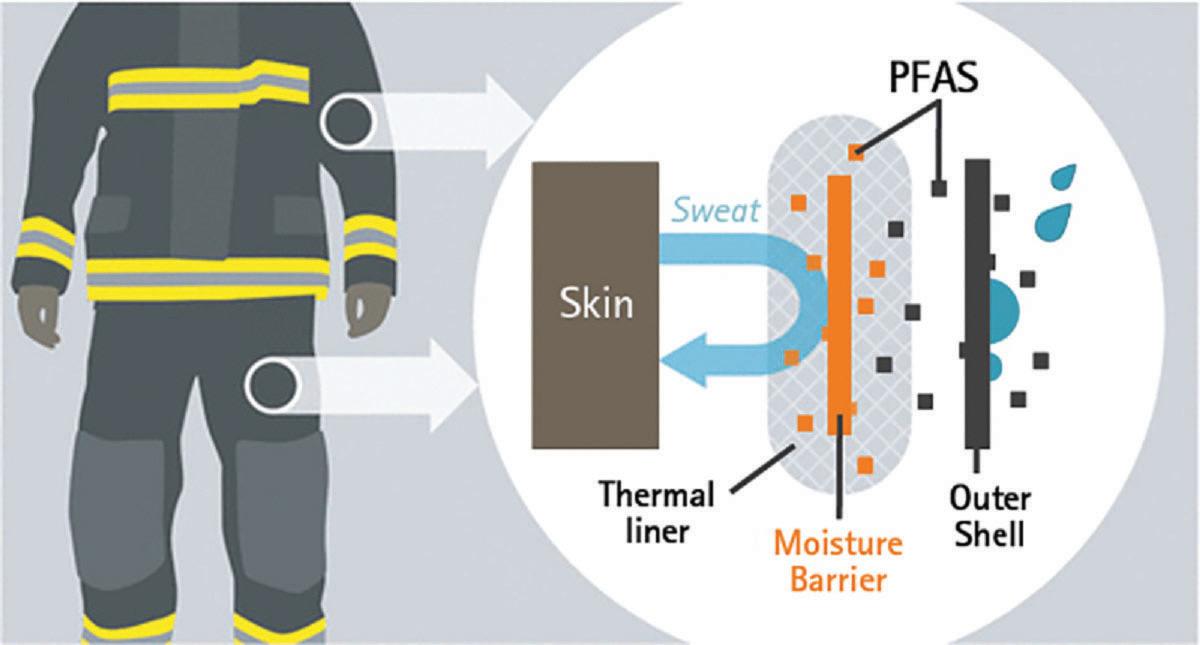

SOMEWHERE COLD: A YEAR LIVING IN THE HIGH ARCTIC
Author: Dr Geraldine Osborne
Publisher: Mercier Press
Available: Easons, Hodges & Figgis, Dubray Books
Price: €19.99
In 1989, Dr Geraldine Osborne decided on a remarkable lifestyle change. Leaving their home in Beara, Co Cork, she took her husband Danny and three young children aged ve, two and one, to one of the most isolated parts of the world, the Inuit settlement of Grise Fjord, 1,000km above the Arctic Circle in Canada. Although she had never been further north than Scotland, artist Danny had been part of the rst Irish Arctic Expedition in 1981 and ever since then had fought an urge to return. When he persuaded his wife to pack up their belongings to live in temperatures of -40C over the course of a year, they both knew their family was in for an unforgettable experience, they just didn’t know if it was going to be for good or bad.
Immersing themselves in the local Inuit community, they learned to dogsled in preparation for a perilous journey across the frozen sea to retrace the route of the last Inuit migration to Greenland the following spring (ultimately cancelled due to rising temperatures), donned caribou skins and got used to eating raw sh to survive in the harshest of climates. Osborne writes with warmth, humour and compelling honesty about trying to balance her maternal instincts to protect her children from very real hazards – crippling cold, dangerous animals –with the desire to embrace a once-in-a-lifetime adventure.
What may seem mundane is made very interesting as she describes in fascinating detail the nuts and bolts of living in dark and sub-zero conditions, and although anchored in lived experience, these insights reach far beyond the speci cs of her own story to speak of the universal human need for connection with the land. Along the way, she describes how her family forged deep connections with the local Inuit community, who shared their traditional knowledge, country food, and exceptional resilience, a bond that is still going strong today as the Osbornes returned in 2001 to live another 12 years in the frozen North. Looking back at her time there in 1989, Osborne now re ects on the bonds her family formed: “I’m amazed at how we managed to do so well, especially having so little money. But we were committed to making it work, and many people were incredibly generous towards us. For Inuit, sharing is part of their culture, it’s integral to who they are. As a hunting society, private property is of little interest to them because living and working cooperatively is vital for survival in that harsh environment.”
In her own words, the author returned to Ireland and her work, and only found the time to piece her story together a er retiring 30 years later, and with a compelling blend of travel narrative, family memoir and cultural observation, richly illustrated with photographs, this book details an extraordinary decision to embrace the unknown and is well worth the read.

AUTHOR: TANYA SWEENEY
PUBLISHER: TRANSWORLD AVAILABLE: EASONS, HODGES & FIGGIS, DUBRAY BOOKS
PRICE: €14.99
Hailed by the Irish Times as “a future classic” that renews faith in the art of novel writing, this work by Pakistani-American author Mueenuddin is the long-awaited follow-up to his critically acclaimed collection of short stories, Other Rooms, Other Wonders, written all the way back in 2009. The years in between were spent crafting this excellent story, and it has been worth the wait. It reads a little like a short story collection in itself, interweaving as it does several characters living in modern Pakistan that gradually tie together into the larger narrative. It is, in a way, a state of the nation overview, leading us through the castes and classes of the country, from the cocaine-fuelled parties and American-education of the wealthy, to the arranged marriages, feudal law and days spent simply farming of the lower echelons of society. Throughout, the author shows great skill in displaying the folly of human behaviour with a dry wit, making for a thoroughly enjoyable, if lengthy, read.
Described as a cross between Baby Reindeer and Fleabag, this debut novel from newspaper columnist Tanya Sweeney has already gathered a lot of fans. Its popularity lies partly in the fact that it dives head first into the growing problem of ‘parasocial’ lives, but also because it is, despite having the disturbing premiss of a woman obsessed with a male celebrity to the point of believing they have a relationship, quite funny. Thirty-something Esther is walking in a park in London when she locks eyes with actor Ted and feels a spark she hasn’t felt before. Journeying down a rabbit hole, she researches his career, reads every interview he ever did, and joins his online fan club to watch his every move. When Ted gets a new celebrity girlfriend, Esther’s life begins to spiral as she leaves her husband, takes all their savings and buys a plane ticket to Canada where he lives, determined to make him realise they are supposed to be together. It would be scary if it wasn’t so funny, but in this day and age when social media and the internet can dictate our every decision, there is still menace behind the laughs.

AUTHOR: DANIYAL MUEENUDDIN
PUBLISHER: BLOOMSBURY
AVAILABLE: EASONS, HODGES & FIGGIS, DUBRAY BOOKS
PRICE: €22

A winner of the Eason’s Favourite Book of the Year 2025 and an entry on numerous sports book of the year lists last year, this shocking depiction of the rise and fall of one of hurling’s most iconic stars is a riveting but tragic read. The story has been covered extensively across the media and in a two-part RTÉ documentary, but it is well worth diving into this very well-researched book to find out just how baffling the actions of Carey became, as the author interviews many people taken in by his lies who were not called upon in court. Whereas the documentary leans towards having sympathy for a fallen hero, here the facts are laid bare: The five-time All-Ireland winner conned friends, business partners and an adoring public in a truly awful fashion by claiming to have cancer requiring multiple trips to the US, defrauding them of their money to fund his own failing business and lifestyle, ultimately ending in a jail term. Although a failing business is the reason Carey gives, there is a sense here that there is much more to it, but what really went through his head is still anybody’s guess.
AUTHOR: EIMEAR NÍ BHRAONÁIN
PUBLISHER: IRISH ACADEMIC PRESS
AVAILABLE: EASONS, HODGES & FIGGIS, DUBRAY BOOKS PRICE: €19.99


•Full range available 400VA to 6.4MVA
•400VA to 10KVA in stock
•Next day delivery
• Free site surveys
• Full software & network adapters
• 24/7 maintenance cover









