








2 A message from Penny Fowler, HWT chairman and News Corp community ambassador
3 A message from Sarah Murdoch, MCRI co-chair and global ambassador
4 40 years of discovery and impact
8 Next-generation vaccine protection 10 Mini lungs fight respiratory diseases
Stem cells powering new therapies 16 Redefining concussion care for kids
Life-saving allergy breakthroughs
20 Obesity crisis warning 21 Shining a light on mental health
22 Genomic screening for newborns
24 AI detective helps cure epilepsy
26 Pill hope for children with dwarfism
28 The brilliant minds behind MCRI
32 The next chapter
At News in the Community, we are passionate about helping to build a better Australia.
And for the past 40 years, Murdoch Children’s Research Institute has helped build not only a better Australia, but a better world, discovering life-changing treatments and cures for conditions that a ect our sickest children.
This remarkable institution began its life thanks to Dame Elisabeth Murdoch, Rupert’s mother and our grandmother, who wanted an answer to a simple question.
She asked: “Why can’t we get down to the root cause of why these awful things happen to children?”
With the support of genetics pioneer and pediatrician Professor David Danks, they found the answer by establishing the original Murdoch Institute for Research in Birth Defects.
Since then, MCRI has grown from a genetics research institute into a global leader in child health, with 1800 researchers pioneering new discoveries into more than 150 childhood diseases.
MCRI is perhaps the most enduring legacy of Dame Elisabeth’s lifelong involvement with The Royal Children’s Hospital, which spanned more than 85 of her 103 years.
In her 20s, after winning a knitting competition at school, she joined the hospital’s management committee and later, as president, led the campaign to build a new children’s hospital.
It brought together two of her great loves — compassion and community.
This laid the foundations for the world-class precinct we know today,
incorporating MCRI within The Royal Children’s Hospital.
The largest research institute in Australia for child health, MCRI’s aim is to ensure all children are given the opportunity to live healthy and fulfilling lives.
Congratulations on your 40th anniversary and thank you to everyone who does so much to support MCRI’s life-saving work — from the thousands of researchers, sta , volunteers and donors to our News colleagues who help tell MCRI’s stories to the world.
Together you bring to life Granny’s vision to “always be committed to improving the lives of those less fortunate, less able and less equipped than yourself”.
PENNY FOWLER
HWT chairman and News Corp community ambassador


“Always be committed to improving the lives of those less fortunate, less able and less equipped than yourself.”
DAME ELISABETH MURDOCH

For more than 25 years, it has been one of the great privileges of my life to serve and support Murdoch Children’s Research Institute.
I still remember my first board meeting, feeling completely overwhelmed by the brilliance in the room and by the responsibility entrusted to us. That sense of honour has never left me.
Over these decades, I have watched the institute grow from a national leader into a global powerhouse in child health research. Today, the work of our researchers consistently places MCRI among the world’s top three pediatric research institutes for quality and impact.
For a country of our size, that is simply extraordinary. We truly do punch above our weight.
What makes me most proud is not simply our size or our reputation, but our impact.
From pioneering stem cell breakthroughs and heart regeneration research to transforming genomic medicine and diagnosing critically ill children in record time, our teams are changing what is possible for families.
MCRI is home to one of the world’s most ambitious child and parent health cohorts, called GenV. This nationally significant cohort of international importance ensures that discoveries today will shape healthier futures for decades to come.
None of this happens in isolation. It is powered by extraordinary scientific leadership, deep global partnerships and, critically, the unwavering belief of our philanthropic community.
As Dame Elisabeth so wisely said, philanthropy is not simply about giving, it is about being
truly involved in the causes you are passionate about.
When I reflect on MCRI now — its 1800 researchers, its collaborations across continents, its bold embrace of genomics, stem cell technology and AI — I often think how proud Dame Elisabeth would be.
Research transforms children’s lives. I know, because I have seen it first hand. And I remain as inspired today as I was 25 years ago by the promise of what comes next.
SARAH MURDOCH
MCRI co-chair and global ambassador
Ensuring the health of children from the day they are born has inspired four decades of groundbreaking discoveries
The biggest health challenges facing our kids today were barely on the radar 40 years ago.
From an initial focus on rare diseases and birth defects, MCRI has grown into a global force in research, tackling the most urgent and complex childhood diseases in Australia and around the world.
Today, 1800 world-leading researchers work across more than 150 diseases a ecting children, from allergies and genetic disorders to cancers and neurological conditions. They lead groundbreaking studies that deepen the

understanding of modern epidemics such as obesity and mental health conditions.
They drive scientific advances such as developing life-saving vaccines and creating human lung models in the lab using stem cells.
They can sequence all 20,000 human genes in days and apply genomic medicine directly in clinical settings for rapid diagnosis, prevention and early intervention.
And they harness cuttingedge technologies such as AI to pinpoint and remove tiny brain lesions responsible for seizures in children with epilepsy.
“For 40 years, we have scanned the horizon for what’s next and adopted new technologies,” MCRI director
Professor Kathryn North says.
“When genomic sequencing became fast and a ordable, we were ready, investing early in stem cell science and other transformative technologies.
“We will continue to harness new technologies to make the biggest impact on children’s health and take calculated risks to remain a global leader.”
Prof North says MCRI’s location within The Royal Children’s Hospital allows discoveries to be rapidly translated into better care.

“Clinicians in the hospital work side by side with our researchers, so questions arising in the hospital or community can be quickly answered by our researchers and translated into therapies
and interventions that best help children live healthy, fulfilled lives,” she says.
Prof North, who has been at the helm of MCRI since 2013, trained as a pediatrician.
“I really wanted to make a di erence to children’s health but then I found that by doing research you can influence the health of not just one child at a time, but many children all around the world,” she says.
“So, to me, that combination of being a children’s doctor but also doing research that helps children now and into future generations is the best possible job I could do.”
This magazine celebrates some of MCRI’s biggest breakthroughs of the past 40 years.
“I really wanted to make a difference to children’s health but then I found that by doing research you can influence the health of not just one child at a time, but many children all around the world.”
PROF KATHRYN NORTH MCRI director
Dame Elisabeth Murdoch and Professor David Danks shared a determination to improve the lives of children born with complex medical conditions. Their legacy lives on at MCRI
Murdoch Children’s Research Institute is one of the top three children’s research institutes globally, renowned for its pioneering work in the science of stem cell and genomic medicine, public health and infectious diseases.
Despite the many accolades, MCRI director Professor Kathryn North says the mission is far from complete.
“We have made profound advances in diagnosis, treatment and technologies that have helped children live healthier, longer lives,” Prof North says.
Professor David Danks and Dame Elisabeth Murdoch co-found the Murdoch Institute for Research In Birth Defects.
“But we still don’t have the cure for many (conditions) and children born today are anticipated to have shorter lifespans than their parents.
“The answer to these big issues is research, providing the evidence to underpin new approaches, new therapies and meaningful policy change.”
Prof North says that for the first time, evidence shows children are on a poorer health trajectory than their parents, with obesity, mental health issues, allergies and rare genetic diseases among the modern challenges MCRI is focused on tackling.
Discovery of the SRY gene solves the mystery of sex determination.

It has come a long way since the co-founders, philanthropist and child health advocate Dame Elisabeth Murdoch and pediatrician and genetics pioneer Professor David Danks, opened its doors 40 years ago.
A formidable pair, they were driven to “do something” about complex medical conditions a ecting children, with a determination to help them lead healthier, fuller lives.
Seeing children with terrible birth defects when she visited them in hospital had a profound impact on Dame Elisabeth, inspiring a lifelong commitment.
Then the Murdoch Institute for Research In Birth Defects, it merged with The Royal Children’s Hospital Research Institute in 2000 to become MCRI.
RV3 rotavirus vaccine shows strong immune response, paving the way for lifesaving birth-dose vaccines. Research shows introducing cooked egg to babies at four to six months lowers allergy risk, changing national guidance.
Australia’s first liver cell transplant introduces cell therapy for pediatric liver disease.
Mitochondrial “blueprint” advances diagnosis and treatment of rare metabolic disorders worldwide.
1986 2011 1988 2005 1990 2008 1994 2009 1999 2010 2000 2004
Victorian Clinical Genetics Services launches at MCRI.
Botox is proven safe and e ective for treating children with cerebral palsy.
The Murdoch Institute merges with The RCH Research Institute to form MCRI.
MCRI is recognised as a global leader in neonatal health research.
MCRI leads studies to optimise pneumococcal vaccines, helping reduce child mortality globally.
New MCRI campus opens within The Royal Children’s Hospital. Landmark HealthNuts study finds more than 10 per cent of infants have food allergy.
Dame Elisabeth’s commitment to improving child health has become her family’s legacy.
Along with generous financial contributions, family members have played active roles in championing MCRI’s work and helping elevate its global profile.
Dame Elisabeth is the mother of News Corp founder Rupert Murdoch. His daughter-in-law, Sarah Murdoch, the wife of Lachlan Murdoch, is co-chair and global ambassador of MCRI and founding chair of its Global Advisory Board.
Dame Elisabeth’s granddaughter, Penny Fowler, is chair of The Royal Children’s Hospital Good Friday Appeal.
Her mother, Janet Calvert-Jones (Dame Elisabeth’s daughter), was on MCRI’s board for 28 years and heavily involved in the annual Good Friday Appeal.

Prof Kathryn North recruited as MCRI director, starting her tenure in 2013.
Children’s Bioresource Centre launches, enabling largescale population health research and biobanking.
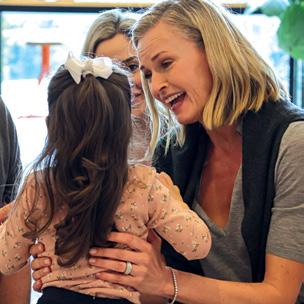
Sarah Murdoch says MCRI has not historically enjoyed the level of funding that, for example, US institutes receive.
Ahighlight of Prof Danks’s career before he retired in 1995 was helping discover the genetic cause of Menkes syndrome, a rare disorder that a ects copper levels in the body, leading to brain damage, growth issues and death.
He was succeeded in 1995 by geneticist Professor Bob Williamson, a central figure in gene cloning.
In almost 10 years as director, Prof Williamson helped move the institute from being an excellent but (in world terms) tiny medical genetics group to an integrated, internationally respected child health institute.
He passed the baton to leading population health expert Professor Terry Dwyer.
“Despite this, MCRI is still in the global top three for research impact — showing what a great investment MCRI is,” she says. “Philanthropy is critical — I have seen first hand the di erence it makes, particularly in seeding research.
“We want to continue to attract the brightest minds in research to create lasting, multigenerational impact and we also hope to inspire others who have the capacity to donate to ensure MCRI can thrive in the long term.”
Sarah says Dame Elisabeth would be incredibly proud. “It is truly breathtaking to contemplate the breadth and depth of the work of the institute, its impact on medical advances globally, and the potential it has to change the lives of children for generations to come,” she says.
RV3 rotavirus birth-dose vaccine achieves greater than 90 per cent immune response.
Mackenzie’s Mission carrier screening program launches, helping families prevent severe genetic conditions.
Achondroplasia growth therapy improves height and reduces complications for children with dwarfism.
reNEW Stem Cell Medicine
consortium launches across three continents to accelerate stem-cell therapies.
National Allergy Centre of Excellence is established.
World-first Strep A human challenge model fast-tracks vaccine development.
AI tool detects tiny brain lesions in epilepsy patients.
GenV recruits 116,000 participants.
Pharmacogenomics personalises child cancer treatments.
Concussion Essentials Clinic launches.
Global childhood obesity study warns one-third of children may be overweight by 2050.
Lab-grown blood stem cells o er hope for children with leukaemia and bone marrow failure.
Vaccine research with the potential to prevent thousands of childhood deaths worldwide is a key focus at MCRI.
A next-generation oral rotavirus vaccine, called RV3-BB, is one of the latest advancements from MCRI researchers and the culmination of decades of work that started with the late Professor Ruth Bishop’s discovery of rotavirus in 1973.
Rotavirus is the most common cause of severe diarrhoea in children aged under five years, causing more than 230,000 deaths every year, mainly in low-income countries.
Unlike existing rotavirus vaccines, RV3-BB can be administered soon after birth, closing the gap in protection for vulnerable newborns.
A world-first clinical trial in Indonesia found 94 per cent of infants were protected against severe rotavirus gastroenteritis in their first year of life and 75 per cent were protected for up to 18 months after three

A next-generation rotavirus vaccine builds on a decades-old, life-saving legacy
single doses of the new RV3-BB vaccine, the first administered within five days of birth.
Additional MCRI research suggests the timing of the first dose within a baby’s first five days helps shape early gut microbiome in a way that improves the body’s response to the new vaccine.
The RV3-BB vaccine is based on a rotavirus strain that was isolated by Prof Bishop, Professor Graeme Barnes and colleagues in the nurseries of Melbourne’s Royal Women's Hospital. This strain was found not to cause symptoms in the babies who were infected and instead provided them with protection against severe gastroenteritis.
Prof Bishop’s original rotavirus discovery at The Royal Children’s Hospital in 1973 led to the development of the first oral vaccines for babies older than six weeks.
These vaccines have had a significant impact in Australia. Since being added to the routine immunisation schedule
in 2007, the number of rotavirus cases has decreased across all ages, including an 85 per cent drop in severe gastroenteritis hospitalisations in children aged under five.
While the World Health Organization recommends all children receive a rotavirus vaccine, an estimated 94 million infants globally still do not have access to the vaccine.
The new RV3-BB vaccine provides a window of opportunity to protect millions more children.
“In low-resource settings, birth o ers the best opportunity for contact between mother, baby and health services. RV3BB provides an ideal vaccination opportunity,” lead researcher Professor Julie Bines says.

MORE INFORMATION: How the new rotavirus vaccine could save millions of babies
94% of infants were protected against severe rotavirus gastroenteritis in their first year of life.

A new trial aims to accelerate a breakthrough Strep A vaccine
Avaccine for a common cause of sore throats is a step closer thanks to a new human challenge trial at MCRI.
The trial is a collaboration between MCRI and Doherty Clinical Trials Limited and will see healthy adult volunteers infected with a particular strain of Strep A in a safe, clinical setting to better understand and prevent diseases caused by the common bacteria.
Human challenge trials allow researchers to study the course of infection in real time and develop a model of infection that allows drug and vaccine candidates to be tested far more rapidly and e ciently than traditional trials.
Strep A infections a ect about 750 million people and kill more than 500,000 globally every year, more than influenza, typhoid or whooping cough.
They typically cause a sore throat, which usually resolves. But they can also lead to scarlet fever, skin sores and life–threatening conditions such as toxic shock syndrome and flesh-eating disease.
There’s also the possibility of serious postinfectious illnesses such as acute rheumatic fever, rheumatic heart disease and kidney disease.
Tropical diseases group team leader Dr Josh Osowicki says developing a Strep A vaccine would be a global game changer and the only plausible way to prevent these potentially serious infections.
“A Strep A vaccine would not only prevent Strep A infections but also prevent invasive Strep A disease, which can be devastating for adults and children,” Dr Osowicki says.
Doherty Clinical Trials chief executive Dr Andrew Brockway says launching the study is a major step forward for Australian medical research.
“Human challenge trials are an essential part of the global infectious disease toolkit, and the ability to conduct a study such as this positions Australia among a select group of countries capable of conducting these complex, high-impact studies,” Dr Brockway says.
Doherty Clinical Trials chief scientific o cer
Professor James McCarthy says the study will “accelerate the development of new vaccines and treatments that could save lives globally”.
Lisa and Lucy

MCRI is part of an international e ort to develop a vaccine combating more pneumococcal strains
Anew pneumococcal vaccine that aims to shield children from up to seven extra strains of the nasty bug is being tested by MCRI scientists in an international trial.
Pneumococcal is a common but potentially dangerous infection caused by bacteria that live in the nose and throat. The infection can cause fever, headaches, sinus pain and ear and lung infections, with serious complications including meningitis, septicaemia, bone infections, joint infections, hearing loss, kidney failure, loss of limbs and intellectual disability.
The Australian Centre for Disease Control recorded 371 serious pneumococcal cases in children aged four and under last year.
While the National Immunisation Program o ers a vaccine covering 13 of the more than 90 pneumococcal types, the trial vaccine could protect children against an additional eight strains.
Pediatric nurse and mum Lisa Blackbourn enrolled her youngest daughter, Lucy McCarthy, in the important trial when she was born in 2025.
“It is an absolute honour for Lucy to be part of this,” Lisa says. “I have seen babies a ected by a lot of illnesses that are preventable. This study can help increase the coverage of the vaccine to stop more preventable illnesses.”
MCRI vaccine uptake group leader Professor Margie Danchin says having a vaccine that can o er broader protection is crucial.
“There are more than 90 di erent strains of the pneumococcal bacteria and no vaccine is able to protect against every strain,” Prof Danchin says.
“But our trial of this new pneumococcal vaccine, which has shown good results in earlier studies and will protect against 21 strains, has the potential to save more lives.”
Groundbreaking mini-lung models are giving scientists new insight into respiratory infections and hope for life-changing treatments
Mini lungs created in the MCRI lab using stem cells could unlock cures for respiratory illnesses including the common cold.
Researchers have developed highly sophisticated miniature lung models, incorporating many of the di erent cells that make up human lungs.
The models help scientists better understand respiratory diseases and why some patients become sicker than others.
The research also has the potential to drive new treatments — and even cures — for infections such as rhinovirus, which causes the common cold, and respiratory syncytial virus (RSV), the leading cause of respiratory infections in children and responsible for 12,000 infant hospitalisations in Australia each year.

It could also be life-changing for children with genetic or chronic lung conditions such as cystic fibrosis and asthma, who are particularly vulnerable to serious complications from infections.
Historically, progress in developing new drugs for respiratory diseases has been very slow, according to Dr Rhiannon Werder, group leader of the MCRI lung disease lab.
“Part of the problem is that we haven’t always had the right models,” Dr Werder says.
“Human lungs are incredibly unique and complex, so they can’t be accurately studied in small animal models. And many of these viruses only infect humans, so we can’t use anything except a human model to fully understand them, which presents ethical challenges.”
Another factor is the historically low investment in respiratory research.
“That’s partly because society has just accepted respiratory illnesses as something we all have to live with, but that shouldn’t be the case,” Dr Werder says.
Dr Werder and her team have created multiple cell types for the mini-lung models, including the airway lining cells that form the first line of defence against infection, immune cells that reside in the lungs, and blood vessel cells that help oxygenate the blood.
“All of these pieces of the lung have been made previously, but nobody’s ever put them all together into one miniature lung model,” she says.
Dr Werder says the models can be customised according to
the disease the researchers are studying and, in some cases, even to the patient.
“We’ve built a strong foundational model and now we have the flexibility to mix and match or introduce new cells as di erent research questions arise,” she says.
The mini-lung models give scientists crucial insight into the early behaviour of lung infections and their impact on cells.
“To me, the real advantage is that patients usually don’t come to hospital until they’re already very sick, but in the lab we can study the chain of events that happens much earlier — what occurs in the initial stages of infection and how that might progress to severe illness requiring hospitalisation, or resolve before it ever gets to that point,” Dr Werder says.
“Those early events are almost impossible to capture in people because by the time they seek care, the infection is already well established.”
Dr Werder says this could be particularly life-changing for kids with cystic fibrosis or any chronic or even rare genetic lung disease.
“For these children, a respiratory infection is just so detrimental to their health in that moment, and every single infection makes their lung disease worse long term,” she explains.
“If we could prevent even a single respiratory infection in a year — let alone several — we could improve their lung function to levels we previously wouldn’t have thought possible.”
Dr Werder notes the research is still evolving, with the team having worked on building and refining the mini-lung models for about 3½ years.
“The ultimate goal is to translate what we’re learning in the lab into therapeutic candidates,” she says.
“We have promising leads, but further work with drug developers and clinical trials will be needed before treatments can reach patients.”
A blood sample is collected from a donor — either a healthy person or someone with a pre-existing lung disease such as cystic fibrosis.
The blood cells are then “reprogrammed” to become induced pluripotent stem cells (iPSCs).
This process resets an adult cell back to a flexible stem-cell state, similar to cells in early embryo development in the womb. Scientists do this by briefly introducing a small number of key biological signals. The cell stops acting like a blood cell and becomes an iPSC. At this stage, it has the potential to develop into almost any cell type in the body.
To turn an iPSC into a lung cell, a process called directed di erentiation is used. Cells are exposed to a carefully timed sequence of biological signals that mimic what happens during normal development in the womb.
The cells gradually change identity over days or weeks until they become specialised lung cells.

MORE INFORMATION: Using stem cells to create mini-lung models

“We’ve built a strong foundational model and now we have the flexibility
to mix and match or introduce new cells as different research questions arise.”
In many ways, Lewis Milne is your typical country kid.
He loves the outdoors, plays football and cricket, enjoys fishing and mountain biking, and last year received the Grey Wolf Award, the highest honour from Scouts Victoria for his age group.
It’s an impressive feat for any 12-year-old, let alone someone living with a genetic condition such as cystic fibrosis (CF).
Cystic fibrosis is a chronic illness that damages the lungs, digestive system and other organs. It has no cure and gets worse over time.
However, thanks to ongoing research — including trials at MCRI that Lewis has been part of — advances in treatments have significantly improved the lives of people with CF.
Lewis, pictured on the front cover in MCRI’s lung stem cell lab, has never let his condition become a roadblock.

“Having CF really doesn’t get in my way,” Lewis says.
It’s a perspective his family shares — and one they don’t take for granted after his challenging start to life.
Within 24 hours of being born, Lewis was airlifted to The Royal Children’s Hospital in Melbourne with a bowel obstruction called meconium ileus, which usually happens as a result of cystic fibrosis.
His cystic fibrosis diagnosis came as a shock to his mum, Justine, and dad, Nick. Despite being an inherited condition, no one else in his family has the condition.
“Nothing could have prepared us for what happened,” Justine says.
Cystic fibrosis is the most common life-limiting genetic condition a ecting Australians, with more than 3700 people living with CF in this country, according to Cystic Fibrosis Australia.
It a ects the cells that produce mucus, sweat and digestive fluids. A faulty gene makes the body’s internal tubes and ducts thick and sticky, clogging narrow passageways — particularly in the lungs and pancreas.
“Before Lewis was born, I knew nothing about CF besides the misconception that people with it had a very short lifespan. So I had a pretty bleak picture of what the future held for my son,” Justine says.
The Milne family, which also includes daughter Mia and son Owen, have had to educate themselves about CF.
They learnt early on about ivacaftor, a medication that targets specific genetic mutations, including the one Lewis has.
“Unfortunately, it wasn’t on the Pharmaceutical Benefits Scheme

(PBS) and would set back families $300,000 a year,” Justine recalls.
Ivacaftor was added to the PBS by the time Lewis was three. “It was a complete game changer. It has allowed him to participate in sport, go to camp, all the activities you take for granted in childhood. Even his asthma symptoms have subsided by proxy,” Justine says.
Justine says Lewis’s involvement with MCRI — especially its CF research team — has been life-changing.
“Just to be given the opportunity to be involved in treatment that could possibly help Lewis has been transformative to his quality of life,” she says. “I can’t even think of all the studies we’ve done, but we’ve learnt so much about Lewis’s condition in the process, and what the future holds for CF research and advancements.”
Now in secondary school, Lewis follows a multilayered approach to treatment — medication, physiotherapy and a special diet — giving him the freedom to live life fully.
However, he’s not without obstacles.
“Every person with CF has their own unique set of challenges, so a lot of Lewis’s health journey has involved trial and error,” Justine says.
“For instance, getting sick can quickly turn into a lung infection.”
Finding a balance between wanting to protect their son and wanting to give him the freedom to be an active, sporty kid has been a challenge for his parents.
“I think the real turning point came when we started to gain confidence in understanding his condition, along with the trust instilled by his medical team, and the support o ered,” Justine says.


The world-first development of lab-engineered blood stem cells could be a game changer for bone marrow transplants
Laboratory-grown blood stem cells that closely resemble those in the human body could pave the way for personalised treatments for children with leukaemia and bone marrow failure disorders.
The world-first lab-grown cells are being used in blood stem cell and bone marrow transplants.
“The ability to take any cell from a patient, reprogram it into a stem cell and then turn these into specifically matched blood cells for transplantation will have a massive impact on these vulnerable patients’ lives,” blood development lab group leader Associate Professor Elizabeth Ng says.
As part of the research, immune deficient mice were injected with the labengineered human blood stem cells. The blood stem cells became functional bone marrow at similar levels to that seen in umbilical cord blood cell transplants, a proven benchmark of success.
The research also found the lab-grown stem cells could be frozen before being successfully transplanted into the mice. This mimicked the preservation process of donor blood stem cells before being transplanted into patients.
Immune development group leader Professor Ed Stanley says being able to mimic human blood stem cells — which can create red blood cells, white blood cells and platelets — could lead to new treatment options for a range of blood disorders.
“Red blood cells are vital for oxygen transport and white

blood cells are our immune defence, while platelets cause clotting to stop us bleeding,” Prof Stanley says.
“By perfecting stem cell methods that mimic the development of the normal blood stem cells found in our bodies, we can understand and develop personalised treatments for a range of blood diseases, including leukaemias and bone marrow failure.”
Blood diseases lab group leader Professor Andrew Elefanty says a blood stem cell transplant is often a key part of life-saving treatment for childhood blood disorders but not all children can find an ideally matched donor.
“Mismatched donor immune cells from the transplant can attack the recipient’s own tissues, leading to severe illness or death,” Prof Elefanty says.
“Developing personalised, patient-specific blood stem cells will prevent these complications, address donor shortages and, alongside genome editing, help correct underlying causes of blood diseases.”
The breakthrough could help children such as Riya Mahajan, who was diagnosed at age 11 with aplastic anaemia, a rare and serious disorder where the body stops producing enough new blood cells.
Riya, now 16, and her family were in India when she started to feel fatigued, rapidly lost weight and developed bruises on her thighs.
Her mother, Sonali, says a blood test showed Riya had extremely low levels of platelets and red blood cells.
“The doctors told us she had bone marrow failure and she started needing regular platelet and blood transfusions to get her blood cell count up,” Sonali recalls.
The family fast-tracked their return to Australia and went straight to The Royal Children’s Hospital.
With Riya not responding to medication, a bone marrow transplant was recommended.
They tried for six months to find a perfectly matched donor and were losing hope.
“It caused us a huge amount of anxiety and was traumatic to see Riya struggle so much,” Sonali says.

MCRI’s stem cell breakthroughs are providing hope for young heart patients and their families
James Thornton was born with half a heart. His rare condition, known as hypoplastic left heart syndrome, is caused when the structures on the left side of the heart don’t develop properly in utero.
“Despite being a half match, the specialist decided I would be her donor.”
Riya remained in hospital for three months following her transplant in June 2023.
Without a perfect donor match, Riya’s platelet count took more time to return to normal, she required longer immunosuppressive therapy and was more susceptible to infections.
Sonali says MCRI’s laboratorygenerated blood stem cells are a “blessing to so many families”.
“The fact that one day there could be targeted treatments for children with leukaemia and bone marrow failure disorders is life-changing,” she says.

His mum, Nikki Burgess, and dad, David Thornton, were given the options to terminate the pregnancy, go full term and do palliative care or have three risky heart surgeries after James was born. They opted for the surgeries.
Now 16, sports-mad James can’t play footy but dreams of being a commentator.
He is “truly confident” the team at MCRI will find a cure for conditions such as his.
Stem cell medicine theme director Professor Enzo Porrello heads a lab developing cellular treatments for congenital heart disease in children. His pioneering work includes the creation in 2017 of the world’s most complex 3D miniature models of human heart tissue.
He and his team now create thousands of these beating heart tissues every week, enabling experiments at a scale not previously imagined.
“By creating bioengineered heart tissues from stem cells, we hope to support heart function in children like James with congenital heart defects, prevent their hearts from failing and ultimately for them not to need a heart transplant,” he says.

From a world-class treatment clinic to innovative diagnostic tools to groundbreaking research, MCRI is leading the way in detecting and managing concussion in the four million children worldwide who are a ected each year.
The MCRI concussion team helped design and build the Concussion Essentials (HeadCheck) app, now regarded as the gold standard for identifying and managing concussion in junior sports. Launched in 2018 in partnership with the AFL and The Royal Children’s Hospital, the app has been downloaded more than 50,000 times.
Last year, MCRI also opened the Concussion Essentials Clinic
As concern grows about concussion, MCRI is reshaping care for children
for children aged eight to 18 with persisting symptoms. The service is also being expanded via telehealth to families in regional areas and non-Englishspeaking communities.
Pediatric neuropsychologist Professor Vicki Anderson says the clinic, launched as part of a clinical trial to evaluate evidence-based treatments and assess clinical outcomes, is a game changer for children, who can take twice as long as adults to recover from a concussion.
“Concussions are common during childhood and while most children will recover fully, there remain inconsistencies in clinical management across Australia,” Prof Anderson says.
“Timely recognition and
treatment for concussion is key to preventing long-term symptoms such as poor mental health, memory loss and sensitivity to light.
“Unlike in adults, the developing brain responds di erently to concussion, so preventing the long-term e ects requires child-specific diagnosis, acute management and recovery protocols.”
Netballer Emma Henry developed anxiety, headaches and a sense of hopelessness and had trouble concentrating after her second concussion in a year.
“I found it very hard to be motivated for school and everyday life,” she says. “Doing the simplest of tasks such as a walk was di cult. Not being
able to complete these tasks got me quite disheartened, which impacted my mental health.”
The Concussion Essentials Clinic will also provide online and in-person training to educate health care workers in bestpractice concussion care.
Prof Anderson says while there is growing community concern around head injuries, it is important for children and young people to continue being active.
She says providing the latest resources and targeted care is crucial. “Parents, coaches and teachers are becoming more aware of the potential long-term impacts of repeat, untreated head knocks and concussions,” she says. “Children shouldn’t return to sport too soon after a concussion because their reaction times can be slower.
“However, we don't want the fear of concussion to discourage participation. It’s important that children spend time playing, exploring outside and continuing to participate in sport, all of which have enormous benefits for physical and mental health and wellbeing.”
The clinic was announced as a new MCRI-led study found no brain tissue damage di erences in children with persistent concussion symptoms.
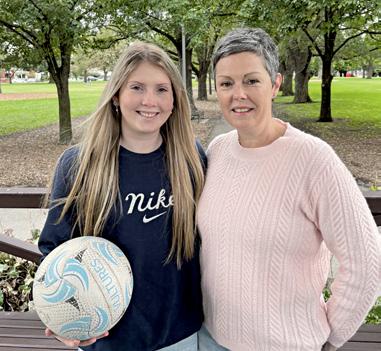
“Unlike in adults, the developing brain responds differently to concussion, so preventing the long-term effects requires child-specific diagnosis, acute management and recovery protocols.”
It reported those who took longer to recover from a concussion weren’t more likely to have white matter damage in their brain than a child who bounced back quickly.
Other cutting-edge MCRI research has paved the way for a simple blood test to detect children with lingering concussion symptoms.
Researcher Ella Swaney says there is a growing need for a tool that can help identify those at risk of delayed recovery.
About 25 to 30 per cent of children who are a ected by concussion have long-term symptoms and about half never seek medical care. Symptoms, including headaches, di culty remembering and sensitivity to light, can last for months, while mental health conditions can persist for several years.
“Delayed recovery from concussion spans emotional, behavioural, physical and cognitive symptoms, which can a ect the wellbeing of the child, delaying their return to school and sport,” Ella says.
“Early detection of children at risk of delayed recovery is crucial to ensure e ective treatment and targeted follow-up.”
In the world-first study, published in the Journal of Neurotrauma in 2024, blood samples were collected from 80 children, aged five to 18 years, who presented to The Royal Children’s Hospital emergency department less than 48 hours after a concussion.
A protein called alpha-1-ACT was found to be “significantly lower” in children who went on to have a delayed recovery.
“If it does hold up in further studies, clinicians could really use this to identify children who are in need of treatment,” Ella says.
Melbourne mum Karen Payne, whose daughter, Mackenzie, 18, was knocked out playing netball and su ered ongoing nausea, confusion, memory loss and poor mental health, had no idea the symptoms of a single concussion could linger for so long.
Karen says MCRI’s chronic concussion program — involving weekly physiotherapy and psychology — was an “absolute lifesaver” for her daughter, who missed weeks of school and didn’t return to netball for five months.
“Anything that can help speed up the process would make a world of di erence,” she says.
Football player Alannah Green, 15, experienced a bad head knock while playing in 2024.
Her symptoms, including blood noses and sensitivity to light and noise, surfaced that night and persisted for months.
Alannah’s mum, Danielle, says it wasn’t until her daughter joined a Concussion Essentials Clinic recovery program that she began to improve. “The clinic not only helped Alannah to get back physically, but also allowed her the safe space to talk about her feelings while she dealt with these tough, ongoing symptoms,” Danielle says.
by


MCRI researchers are setting the benchmark in pioneering food allergy therapies that could change the lives of millions of children
Australia has the highest reported rates of childhood food allergy in the world.
Peanut allergies — one of the most common causes of lifethreatening anaphylaxis — have increased by more than 350 per cent in Australia since 1995.
To help change the trajectory of allergic disease, MCRI hosts various clinical trials and studies as well as two national allergy research collaborations — the National Allergy Centre of Excellence and the Centre for Food Allergy Research.
Current trials are testing di erent ways to build tolerance to allergens and retrain the immune system, including through food allergen patches, oral immunotherapy and monthly injections.
In one immunotherapy trial, 46 per cent of children no longer

had allergic reactions by the end of the study, which saw them given a combination of a good bacteria probiotic and peanut protein in increasing amounts over 18 months. The benefits were sustained for most of these children four years after stopping daily therapy.
The immunotherapy stimulated the immune system to become less sensitive to peanuts, while the probiotic was thought to improve safety and tolerability.
MCRI is now working to develop the therapy into a globally available product and also trialling similar therapies for other food allergies, including to egg.
While not a cure, the therapy could lead to the first treatment options that provide meaningful and long-lasting benefits,
allowing kids to eat food safely and reducing the risk of an allergic reaction from an accidental exposure.
The research could change the lives of millions of people with food allergies around the world.
In food allergy, the immune system incorrectly identifies the specific food as a threat when it enters the body.
Mild symptoms can include skin rash or hives, face swelling, vomiting and tummy pain.
Anaphylaxis is a severe and potentially fatal allergic reaction, marked by noisy or di cult breathing, persistent coughing, voice change, going pale and floppy, or collapsing.
Eggs, milk, peanuts, tree nuts, wheat, soy, fish and shellfish account for more than 90 per cent of childhood food allergies in this country.
30% or 8.2 million Australians reported living with allergic disease in 2024, up from 19.6 per cent (4.1 million) in 2007.


Most resolve during primary school but allergies to peanuts, tree nuts, fish and shellfish are more likely to be lifelong.
Ju Lee Ng’s daughter, Stella, 13, was diagnosed with a peanut allergy at 18 months old after breaking out in hives from a meal containing traces of the nut. But Ju Lee says Stella has been in clinical remission for almost four years since taking part in a MCRI allergy trial and now eats peanuts regularly.
“Stella’s quality of life has improved considerably since the trial,” Ju Lee says. “Her level of anxiety has reduced dramatically and she has the freedom to enjoy di erent types of food. We previously had to avoid travel to countries that use lots of peanuts in the food, including Malaysia, where my husband and I are from.
Mealtimes can be stressful for families a ected by food allergies. With no current cure, allergy management relies on strict avoidance of allergens and knowing how to respond to accidental exposures and allergic reactions. The Allergy Friendly Family Cookbook is developed by world-leading allergy researchers and specialists from MCRI, in partnership with taste.com.au, and features more than 100 allergy friendly recipes and evidence-based advice for families.

Food allergies are just one piece of Australia’s increasing allergic disease burden — and one focus of MCRI allergic disease research.
Published by HarperCollins, it is $28 at shop.rch.org.au/products/the-allergyfriendly-family-cookbook
“Shortly after Stella achieved remission, we were so excited to travel on a family holiday to Thailand. We tried local dishes and enjoyed an amazing holiday without the stress that Stella could have an allergic reaction.”
In another study, MCRI researchers discovered a link between exposure to higher levels of air pollution as a baby and childhood peanut allergies.
“The rise in allergy prevalence has occurred at a similar time to increased urbanisation, leading to the belief that environmental factors may be contributing to high allergy rates,” Associate Professor Rachel Peters says.
Assoc Prof Peters, from MCRI’s population allergy research group, says policies aimed at tackling air pollution could potentially reduce the development and persistence of peanut allergy. “Improving city design to support greater air quality regulation, better promoting public transport and switching to non-combustion fuels may help turn the tide on peanut allergy,” she says.
The 2025 Costly Reactions: The economic and social cost of allergic disease in Australia report, which involved MCRI, revealed 30 per cent or 8.2 million Australians reported living with allergic disease in 2024, up from 19.6 per cent (4.1 million) in 2007.
MCRI population allergy research group leader and National Allergy Centre of Excellence director Professor Kirsten Perrett says environmental changes such as urbanisation and air pollution, modern lifestyle factors including sanitisation, and increased awareness are possible drivers of the growth.
“Australia has some of the highest allergy rates globally, including the world’s highest reported rate of infant food allergy, a ecting one in 10 babies,” Prof Perrett says.
“The burden isn’t just physical; for many families, allergic disease disrupts daily life and brings financial and emotional strain.
“Through national research collaboration, we’re now better placed than ever to understand these complex conditions and deliver more targeted, e ective responses.”

The number of overweight and obese children will skyrocket in Australia in the next five years without urgent intervention.
A global study, led by MCRI, also reports one in three children and adolescents in Australia will be obese by 2050 without changes supported by strong investment in health programs.
Young women aged 15 to 24 years are most at risk of living with obesity in Australia.
Globally, a third of children and adolescents is forecast to be overweight (385 million) or obese (360 million) by 2050.
This equates to 356 million children aged five to 14 years and 390 million aged 15 to 24 years, with one in six facing obesity.
The global obesity rate among five- to 24-year-olds tripled from 1990 to 2021, rising by 244 per cent to 174 million, suggesting current approaches to combat obesity are failing.
Lead researcher Dr Jessica Kerr says a five-year action plan is needed to target the drivers of obesity: nutrition, activity, lifestyle and environments where families live.
“The systems and the environment and the policies are what really need to change rather than blaming parents,” Dr Kerr says.
The researchers studied more than 200 countries, finding the drivers of obesity are complex, shaped by interacting
MCRI is leading the push for urgent action to combat the obesity epidemic in children

social, genetic, biological and environmental influences.
“In Australia we live in an environment surrounded by abundant, a ordable ultraprocessed foods, with junk foods marketed as health foods to our babies and toddlers,” Dr Kerr says.
“Some people are more negatively a ected by these environments, such as those with genetic predispositions, and it’s really hard to be healthy surrounded by an obesitypromoting environment.”
Dr Kerr says it is also important not to write o the results as a lost cause.
“Too often the issue is ignored as too big or too complex,” she says. “And we do actually show (in the study) several regions of the world in a position to avoid obesity epidemics.
Unfortunately, Australia isn’t one of those.”
Dr Kerr says the observational
study found prevention is key as obesity rarely resolves after adolescence.
Dr Kerr says the study is an urgent call to action, with possible changes including:
• Reducing sugar-sweetened beverages and unhealthy foods;
• Adding subsidies to healthy foods to make them more a ordable;
• Improving marketing regulations and food labelling.
“This giant burden will not only cost the health system and the economy billions, but complications including diabetes, cancer, heart problems, breathing issues, fertility problems and mental health challenges will negatively impact our children and adolescents now and into the future,” Dr Kerr warns.
“Despite these findings … our results provide optimism that this trajectory can be avoided if action comes before 2030.”


Landmark MCRI research is helping Australia tackle unprecedented rates of youth anxiety and depression
Almost three quarters of Australian teenagers have experienced clinically significant levels of anxiety or depression symptoms by the age of 18, alarming MCRI research has revealed.
And most of these teens have struggled for lengthy periods, with two-thirds of su erers reporting issues during three di erent times in their adolescence.
Adolescent health group leader Professor Susan Sawyer says that despite growing concerns about adolescent mental health, few previous
studies have comprehensively charted the course of common mental disorders across the key life stage of adolescence.
“To our knowledge, this longitudinal study shows the highest cumulative incidence of clinically significant symptoms of common mental disorders that has ever been reported across adolescence from any country,” Prof Sawyer says.
Prof Sawyer says the data “suggests that even the most well-resourced country would struggle to provide adequate treatment if every young person sought help”.
“Beyond clinical care, we urgently need to fund, develop and evaluate preventive strategies that aim to reduce the onset and chronicity of depression and anxiety,” Prof Sawyer says.
Child to Adult Transition Study (CATS) researchers surveyed more than 1200 Melburnians about their recent anxiety and depression symptoms every year from the ages of 10 to 18.
They found 74 per cent had “clinically significant” levels at least once, which means their symptoms had reached the same level patients with a formal anxiety or depression diagnosis would typically record on those questionnaires.
The study found 84 per cent of surveyed girls had such symptoms, compared to 61 per cent of boys.
Girls with symptoms were also more likely to have them for longer, with 70 per cent reporting issues over three or more annual surveys, compared to 49 per cent in the male group.
Child to Adult Transition Study researcher Dr Ellie Robson
says while there have been “longstanding concerns of a youth mental health crisis”, the team did not expect rates to be so high or long-lasting.
“For those who did reach high symptoms, the majority reached these symptoms at three waves or more, which is pretty significant and it’s quite concerning,” Dr Robson says.
She says increases tended to align with “stressful” times including the transition to high school, exams, the onset of puberty and the Covid-19 pandemic.
“We were also surprised that in those who experienced mental health concerns during the pandemic years, that the overwhelming majority had onset of mental health concerns prior to the pandemic,” she says.
Dr Robson says today’s youth face unique challenges, including social media and increasing rates of family separation. But greater awareness about mental health could also be contributing to reporting rates.
“Adolescents today are growing up in a distinctly di erent psychosocial landscape than earlier generations, one that is characterised by greater mental health literacy, reduced stigma and, at times, the glamorisation of mental health problems,” Dr Robson says.
“Given this context, our next step will be to explore what impact these reported symptoms have on the functioning and health outcomes of contemporary adolescents.” MORE INFORMATION: Why mental health research is important


More lives could be saved by a change to the heel-prick test that has provided routine screening for more than half a century
Hundreds of additional rare but serious childhood conditions stand to be detected by expanding the routine newborn heel-prick test to include genomic screening.
The heel-prick test has been one of Australia’s most successful public health programs for more than 50 years. It involves collecting a few drops of blood from newborns — usually within 72 hours of birth — to screen for a range of disorders.
Today, the program screens for 34 conditions.
But a study led by MCRI and Victorian Clinical Genetics Services has found genomic
screening — a test that reveals a person’s entire genetic makeup — could easily be included as part of the newborn heel-prick test and deliver results for hundreds of treatable conditions within 14 days.
Clinical geneticist Professor Zornitza Stark says the BabyScreen+ pilot study highlights how genomic newborn screening could save lives by enabling earlier diagnosis and treatment.
“Newborn screening for rare conditions is one of the most e ective public health interventions,” Prof Stark says. “But the increased capacity of genomic medicine to diagnose
and treat rare diseases has challenged the ability of newborn screening programs to keep pace.
“Our study found incorporating genomic sequencing provides the opportunity to substantially expand the range of conditions screened for, including those that predispose people to childhood cancers, as well as cardiac and neurological disorders, not detectable with current standard technologies.”
One in 1000 newborns receives an abnormal result from the existing heel-prick test. This makes a huge di erence to their future, allowing treatments to start early, to
newborns receives an abnormal result from the existing heel-prick test.

prevent permanent damage that would have occurred had the early diagnosis not been made. The screening also helps researchers better understand the incidence and progression of disorders to fine-tune treatments and the advice given to parents.
The BabyScreen+ study screened 1000 newborns in Victoria for changes in 605 genes associated with early-onset, severe, treatable conditions using genome sequencing.
It found 16 babies had an increased likelihood of a genetic condition. Of these, only one was detected by the standard newborn screening.
One baby was diagnosed with a rare and severe immunodeficiency disorder, with the early diagnosis enabling rapid treatment, including a successful bone marrow transplant.
Parents of the newborns enrolled in the study were glad to have taken part, with 99.5 per cent believing the genomic testing should be available to all babies, and 93 per cent willing to recommend it to family and friends.
“Genomic sequencing at birth

would enable many newborns to be diagnosed and treated earlier, improving patient and family health outcomes,”
Dr Sebastian Lunke says. “It could also potentially be vital to lifelong health, with the data stored and available to screen at any time.”
However, he says practical and ethical concerns need to be addressed.
“Generating genomic data introduces complexities spanning privacy, data usage and, potentially, insurance implications,” he says.
“We need to carefully think about how and when this information is best presented to parents to enable considered and informed choices.
“We need to progress this research to make sure our health care system makes decisions on robust evidence and builds the capacity to harness this technology responsibly on a mass scale.”

MORE INFORMATION: Adding genomic screening to the
Genomic testing meant early diagnosis and vital treatment for this happy child
The BabyScreen+ study was a game changer for little Giselle Ghattas.
It’s hard to imagine the bubbly bub has a rare and serious immunodeficiency condition that can lead to tissue damage, organ failure and even death.
Because of its rarity, hemophagocytic lymphohistiocytosis (HLH) can also be di cult to detect, which can worsen its impact.
Giselle, now 19 months, was diagnosed almost by chance after her dad, Justin Ghattas, and mum, Scarlett Morwood, signed up to participate in the BabyScreen+ trial.
When doctors called to say the screening had detected the serious condition requiring immediate intervention, it was devastating but also quite possibly life-saving.
“We got that call sitting at our dining table having lunch and I just wept,” Scarlett says.
“We went from having a normal, healthy kid to thinking our baby could die, in one phone call. So it was really terrifying.”
Trial head Professor Zornitza Stark says: “It was absolutely heartbreaking to give that diagnosis to them because I knew that she was going to become unwell very quickly.”
Giselle’s condition deteriorated within weeks. She was admitted to hospital and underwent intensive treatment, including a long list of medications, chemotherapy and then a stem cell transplant.
Although a strain on her little body, the early intervention boosted her chances of survival.
Giselle was one of 16 babies identified through the genomic screening trial as having an increased likelihood of a genetic condition. She and another baby were in the most severe category, while the others required more minor interventions.
The traditional heel-prick test detected only one of those cases.

Kids like Royal and John are seizure-free thanks to a detector that can pinpoint tiny brain lesions other scans miss
Researchers have discovered a cure for drug-resistant epilepsy in children after creating an “AI detective” that locates brain lesions smaller than a blueberry.
Spotting these tiny seizurecausing lesions with medical imaging alone has been di cult and often delayed life-changing surgery for young children.
Now, using it with an advanced AI tool, 11 Australian children with uncontrolled seizures have been cured after taking part in a landmark study.
again
Royal Naneer successfully underwent surgery after scans aided by the AI detector identified a blueberry-sized lesion on his brain.
Royal, 6, had been having increasingly frequent seizures, the worst episode involving 19 seizures in two hours.
Transferred to The Royal Children’s Hospital after antiseizure medication failed to help and a traditional MRI did not provide answers, Royal was given a scan using the AI detector. The tiny brain lesion, or cortical dysplasia, was found, paving the way for his life-changing surgery in 2024.
His mum, Gurjinder, says the youngster has not had a seizure since.
“The whole ordeal took a huge toll on our family and we were struggling mentally,” she says. “We were so lucky that we quickly picked up that something was wrong because young children can’t always explain what they are going through. Royal is back to his calm, friendly, patient self.”
Neuorolgist Dr Emma Macdonald-Laurs says AI and big data will be increasingly integrated into medical care.
“I think what AI can do for medicine is get from A to B much faster. Rather than waiting years for a diagnosis, it can happen much quicker,” Dr Macdonald-Laurs says.
The researchers say the new epilepsy detector tool, developed by a team at MCRI and The Royal Children’s Hospital, will help deliver a more accurate diagnosis that will lead to faster referrals for epilepsy surgery, fewer seizures in children and improved longterm outcomes.
Before using the AI detector’s keen eye, 80 per cent of trial participants had their diagnosis missed by humans studying their MRI results.
“Identifying the cause early lets us tailor treatment options and helps neurosurgeons plan and navigate surgery,” neurologist Dr Emma Macdonald-Laurs says.
“With more accurate imaging, neurosurgeons can develop a safer surgical road map to avoid important blood vessels and brain regions that control speech, thinking and movement and without removing healthy brain tissue.”
Dr Macdonald-Laurs says being able to find the lesions is key.
“That’s what the AI detective does; it helps us find the really tiny ones,” she says.
“One of the most common lesions we see in children is called dysplasia, but these are di cult to see on MRI, so they are frequently missed and many children are not considered as surgical candidates.
“Our aim was to make a tool that helps us find them faster so that children can be referred earlier for potentially curative epilepsy surgery.”

The AI detective helped find a tiny lesion in the brain of trial participant John Kounadis, 11, which had triggered uncontrolled seizures for three years.
Dr Macdonald-Laurs says John’s MRI did not detect a lesion, but he continued to have seizures multiple times a night.
“We were able to run the detector on John’s scan and found that it highlighted this very small area in his right frontal lobe,” she says.
“After careful review of this area and our neuroscientists doing some reformatting of his brain into a 3D model … we felt confident this was the reason for his seizures and he was able to undergo surgery and has not had a seizure since.”
Epilepsy is the most common neurological condition in childhood, a ecting one in 200 Australian children.
With additional funding, the researchers next want to do more tests in pediatric hospitals across Australia.
“We want to test the tool in clinical settings where we haven’t diagnosed a lesion and also look to understand what clinicians, parents and children think about using AI in this way,”
Dr Macdonald-Laurs says.
“We are not just looking at the AI solution, we’re looking at it in conjunction with all the patient’s data, and still getting the human expert to confirm that the abnormality is present.
“That is key. I wouldn’t want to put anyone forward for brain
surgery unless I was convinced that we definitely can see an abnormality there.”
Before using the AI detector’s keen eye, 80% of trial participants had their diagnosis missed by humans studying their MRI results.
Dr Macdonald-Laurs says the impact of frequent, uncontrolled seizures can include learning di culties, intellectual disability and loss of friendships and “the opportunity to be a kid”.
There can also be parental stress, relationship breakdowns, mental illness, medication side e ects, loss of independence and, in some children, even injury from seizures or sudden, unexplained death.
John’s parents, Spiros and Irine Kounadis, were desperate for answers when their previously healthy only son suddenly started having seizures at night.
“It completely rocked our world,” Spiros says.
“We asked family here and in Greece if anyone else had similar symptoms, but no one did.”
They agreed to join the trial and John had brain surgery in May 2025. “I’m just back to normal,” John says.
Asked if he was worried about undergoing brain surgery, the articulate and confident youngster says: “I just wanted to get it out of me.”
To his family, John is a hero.
“The morning of the surgery John woke up early after a good night’s sleep and said, ‘Let’s go do this’. I am very proud of him,” Spiros says.

MORE INFORMATION: Epilepsy and seizures
John’s many trips to hospital in an ambulance after a seizure have left an impression on him. He now wants to be a paramedic.
Dr Macdonald-Laurs says he will be a great asset.
“That’s why I love doing this work, because there are stories like this in epilepsy surgery where you can really change the course of someone’s life,” she says.
MAIN Casper, 6, has been in the vosoritide trial since he was five months old.
INSET Daisy and Justin Broadway with Casper.


A daily oral medication could o er a new alternative to injections for Australian children with achondroplasia

Adaily tablet has been e ective at increasing height and improving proportional limb growth in children with achondroplasia, the most common form of dwarfism, in a promising study led by MCRI researchers.
The phase II study found experimental drug infigratinib is safe and e ective in treating children with achondroplasia aged three to 11 years.
Sponsored by BridgeBio Pharma Inc, the study involved 72 children with achondroplasia from Australia, the UK, the US, Spain, France and Canada.
It reported the medication was e ective at increasing the rate of growth by 2.5cm a year for up to 18 months during treatment, increasing overall height and improving the upper-to-lowerbody segment ratio. Participants experienced minor side e ects from the treatment but none had serious adverse reactions.
Achondroplasia is the most common form of skeletal dysplasia or dwarfism, a ecting around one in 20,000 babies in Australia. The genetic condition can cause serious medical complications such as spinal cord compression, sleep apnoea, bowed legs, narrowing of the spinal canal and recurrent ear infections. Children with achondroplasia are 50 times more likely to die before the age of five than their peers.
Currently, the only approved therapy for children with achondroplasia in Australia is
vosoritide, a daily injection, which was added to the Pharmaceutical Benefits Scheme last year.
MCRI, the largest vosoritide clinical trial site in the world, has previously found vosoritide not only improves bone growth development in patients from as young as four months up to 18 years, but can also reduce their chances of sudden infant death syndrome (SIDS), sleep apnoea and needing surgery.
Daisy and Justin Broadway’s son, Casper, 6, was diagnosed with achondroplasia as a newborn.
“During my pregnancy, it was suspected that Casper had the condition, which we had confirmed through genetic testing when he was 10 days old,” Daisy says.
“I was filled with worry and anxiety when we received the diagnosis. As a first-time mum you are going through all the emotions of learning how to care for a baby and then having this unfamiliar condition to get your head around as well was a lot to digest. It was a huge learning curve for us trying to understand what his future would look like.”
To try to give Casper the best start to life, Daisy enrolled him in the vosoritide trial at MCRI when he was five months old. She says it has been remarkable to see the positive changes in her son.
“Casper has no spinal compression, his limbs are more
1 in 20,000 babies in Australia is affected by achondroplasia or dwarfism.
proportionate and his legs are less bowed,” she says. “He is healthy and happy and a lot of that we contribute to the vosoritide treatment.
“We did a lot of research into the condition when Casper was born and there were some very sobering statistics. But it’s reassuring to learn that vosoritide can help improve the quality of life of young children with achondroplasia and ultimately avoid some of the long-term health complications.”
Clinical geneticist Professor Ravi Savarirayan says the new study finding that a daily infigratinib tablet is e ective and safe for children with achondroplasia could lead to another treatment option and improve their quality of life.
“This is especially important for those children who can’t tolerate daily injections and in parts of the world where oral medications are more practicable than injections,”
Prof Savarirayan says.


“Genomics is a rapidly advancing field and it is exciting to be part of work that is making a tangible difference to the lives of many people.”
PROF JOHN CHRISTODOULOU Theme director — genomic medicine
Your work and impact: My work sits at the intersection of clinical genetics and research: I am helping uncover the genetic causes of rare childhood diseases, translating those discoveries into clinical practice and pushing for equitable access to genomic diagnostics and therapies. This enables more children with rare diseases to receive a diagnosis, informs improved care and treatment development and expands reproductive options for families.
Proudest achievement: The system I have helped build that has changed how rare disease is diagnosed and managed in Australia. I have had the privilege of working with incredibly talented people across the country to help move genomic medicine in Australia from an academic idea to a routine clinical reality for children with rare diseases. Genomics is a rapidly advancing field and it is exciting to be part of work that is making a tangible di erence to the lives of many people.
Hope for the future: We are at a point where the tools to diagnose and understand rare genetic diseases are maturing at the same time inside a health system and research culture that is finally ready to use them. The hope is this confluence of skills and knowledge will lead to the development of precision therapies that can transform the lives of a ected individuals and their families.
Birthday wish: My wish is that MCRI remains at the forefront of building a future where Australia becomes a place where a child’s rare genetic condition is met with immediate understanding, coordinated expertise and genuine hope for intervention.
“We are grateful to be able to support new low-middle income country leaders who will spearhead equitable research advances into the future.”
PROF ANDREW STEER Theme director — infection, immunity and global health
Your work and impact: Infectious diseases are the leading cause of childhood morbidity, mortality and hospitalisation globally. The burden falls disproportionately on low-middle income countries, where 83 per cent of the global population lives and where 10 per cent of children in the poorest countries die before age five — necessitating a global, equity-focused approach.
Proudest achievement: Our team has delivered major advances in the prevention and treatment of childhood infectious diseases globally, including discovery of rotavirus through to vaccine development that has prevented countless infant deaths from diarrhoeal disease. We’ve also optimised pneumococcal vaccine dosing schedules to save a greater

number of lives at lower cost and we’re helping improve access to life-saving oxygen therapy. Together, these achievements have shaped global guidelines, strengthened health systems and saved children’s lives at scale worldwide. Hope for the future: New vaccines and reenergised e orts to more widely deploy existing vaccines to combat infection diseases and reduce inequity. Most importantly, we are grateful to be able to support new low-middle income country leaders who will spearhead equitable research advances into the future.
Birthday wish: The gift of time — to reflect on the advances made in child health over the past 40 years and to think about how MCRI will help improve the health and wellbeing of all children in the next 40 years.
“We are in such an incredible time in scientific history where our technology has advanced to the point where what was science fiction in my childhood is becoming mainstream.”
PROF MELISSA LITTLE Chief scientist
Your work and impact: My team is using stem cells to create models of the human kidney. We use these to model kidney disease to better understand the problem and find new treatments. We are also using these stem cells to try to build kidney tissue to treat kidney failure. Proudest achievement: I am most proud that our research is focused on what comes next and the outcomes for patients are always front of mind. I am also proud of the team at MCRI and how we work together locally and globally to make a di erence.

Hope for the future: We are in such an incredible time in scientific history where our technology has advanced to the point where what was science fiction in my childhood is becoming mainstream. My hope is that we can work together to harness this opportunity to improve the future for our own children and grandchildren.
Birthday wish: That the future for my own grandchildren is even better than today.
“My team uses patientderived stem cells to grow beating human heart tissue that helps us uncover how heart disease develops, and we are exploring new ways to protect and repair damaged heart muscle.”
PROF ENZO PORRELLO Theme director — stem cell medicine

Your work and impact: My work focuses on developing new treatments for heart disease, one of the most common health issues in children, a ecting up to one in 100 births. My team uses patient-derived stem cells to grow beating human heart tissue that helps us uncover how heart disease develops, and we are exploring new ways to protect and repair damaged heart muscle.
Proudest achievement: When I was recruited to MCRI in 2017, we sat down with cardiac surgeons and cardiologists from The Royal Children’s Hospital to discuss the possibility of growing human heart tissue from stem cells to repair damaged heart tissue and restore function to the failing heart. Almost a decade later we have demonstrated that this approach is safe and e ective in animal models and we have now spun out this technology into a biotechnology company called
Ibnova Therapeutics. We aim to initiate first-in-human clinical trials in the next few years. Hope for the future: We are living in one of the greatest eras of scientific and medical advancement in human history. What seemed like science fiction only a decade ago is now a reality. The convergence of genomics, stem cell technologies and artificial intelligence holds tremendous promise for ushering in a new generation of advanced therapies for currently incurable conditions.
Birthday wish: My birthday wish for MCRI is that our worldleading research contributes to the development of a new generation of transformative therapies for currently incurable conditions, reaching every child who needs them.
“We have led the world in the design and implementation of innovative treatments to support optimal development, quality of life and community participation of these young people.
PROF VICKI ANDERSON Theme director — clinical sciences

Your work and impact: We work with children and families experiencing challenges to optimise outcomes and help them live healthy, happy lives. Our researchers target and solve major pain points in child health. It’s inspiring to see my team tackle some of the most severe medical problems and solve or reduce them through innovative thinking, hard work and passion for kids’ health. In my role, I get to contribute to MCRI’s strategic direction, mentor talented researchers and collaborate with colleagues across many areas of clinical research to support our institute’s superstars.
Proudest achievement: The opening of the Concussion Essentials Clinic in 2025, which allows us to deliver our research findings directly to children with concussion to accelerate recovery. It has a real-life impact for many Victorian children and their families, treating 20 kids each week, with 90 per cent full recovery rate. The future is exciting, with new funding to be rolled out across Australia this year. Our work in mental health has also highlighted the unique vulnerability of children with chronic illness (head injury epilepsy, cancer, neurodisability), the impact on brain development and cognitive and social growth, and the importance of supporting their mental health and wellbeing. We have led the world in the design and implementation of innovative treatments to support optimal development, quality of life and community participation of these young people. Hope for the future: The amazing talent, drive and innovation of emerging researchers mean our children and children's children are in good hands! Advances in research methods and capacity dramatically increase the quality and impact of our work and our capacity to change lives: advanced therapies, opportunities for national and international networks, AI, a focus on including the child’s voice in our research, and emphasis on ensuring our work is not just well published but also changes clinical practice and kids’ lives. Birthday wish: Honouring the early visionaries who laid the foundations for four decades of growth, discovery and impact for children, and hoping the current and upcoming researchers sustain the talent and drive for the institute to continue to accelerate its impact.

“My wish is that every Australian child has the same chance at a healthy, happy life, no matter who they are, where they live or their circumstance — I know it is possible and I know we can do it now.”
PROF SHARON GOLDFELD Theme director — population health
Your work and impact: Population health research focuses on the factors that influence the health of children and young people across entire populations. We use this evidence to develop e ective prevention, early interventions and treatment strategies. We can also inform policy change so all children and young people — regardless of background or location — can experience the best possible and most equitable health outcomes. Proudest achievement: The 2009 national rollout of the Australian Early Development Census, measuring the development of all children starting school every three years. It proved population-level data collections can be delivered at scale and meaningfully inform policy and practice. It also paved the way for transformative initiatives such as MCRI’s GenV study, embedding data as a key part
of the national policymaking machinery. I'm proud of the legacy this work will leave through the continued translation of research into better outcomes for children and young people globally. Hope for the future: The convergence of the growing ability to harness rich population-level data to help us both understand and intervene, together with the growing policy interest in making a di erence to the outcomes for Australia’s children. It feels that we are at a moment when we can e ectively and e ciently design solutions that deliver greater, faster and more equitable impact for children and young people. Birthday wish: My wish is that every Australian child has the same chance at a healthy, happy life, no matter who they are, where they live or their circumstance — I know it is possible and I know we can do it now.
MCRI’s 40th anniversary is a moment to celebrate four decades of discovery and impact — and to look to the future.
The brightest minds in medical research will keep MCRI at the cutting edge of e orts to tackle the most pressing health challenges facing children in the decades to come.
An unprecedented population data project helping shape the health of the nation, safer childhood cancer treatments and a study monitoring the impact of Australia’s worldfirst teen social media ban are among exciting emerging priorities.


MCRI’s Generation Australia project will be a “treasure trove” of population health data, made freely available to researchers worldwide.
It brings together two landmark projects: GenV, which is tracking the health of 50,000 Victorian children, and ORIGINS, which is following 10,000 WA children and their families.
Together, as Generation Australia, they will transform the health and wellbeing of children — now and for generations to come.
GenV data is already being used to identify and solve complex health problems, including whether blood pressure checks should begin in childhood, who is likely to have a heart attack by age 50, predicting neurodevelopmental disorders to enable earlier intervention, and
examining links between urban heat and mental health.
Mental health, climate, obesity and heart health will be in the spotlight for Generation Australia.
Generation Australia director Professor Melissa Wake says it will be one of the great studies of its time.
She says the project can be thought of as a living laboratory that will not only save time and money, but also help solve the “big and connected health and social problems” facing families today.
“Generation Australia is designed not just to watch but to fix. We will discover new strategies to help all children and adults to thrive, prevent illness and manage today’s complex, interconnected and emerging challenges,” Prof Wake says.

Reducing the brutal side e ects of cancer treatments in kids is the focus of a pioneering genetics project.
Led by MCRI, with $1.76 million in funding from the Children’s Cancer CoLab, the project will explore how a child’s genes are impacted by cancer therapies, with the aim of boosting safety and e ectiveness of the treatments.
Despite childhood cancer cure rates having reached 85 per cent, most children are treated with drugs developed for adults, causing uncertainty about how each child’s body will respond to toxicities of treatment.
Project lead Professor Rachel Conyers says pharmacogenomics, which uses genetic information to predict drug responses, could help reduce side e ects caused by cancer treatments.
85% of childhood cancers are cured but most are treated with drugs developed for adults.
“Pharmacogenomics is like having a personalised instruction manual for each child’s body, telling doctors which medications will work best and which doses will be safest,” she says.
“This information is crucial because children process medications di erently from adults, yet most treatment guidelines are based on adult research.”
Prof Conyers’ team interviewed 30 people with a lived experience of childhood cancer to help guide the direction of the project, which is a collaboration with the Peter MacCallum Cancer Centre, Monash Children’s Hospital, Princess Máxima Center for Pediatric Oncology and The Royal Melbourne Hospital.


The world will be watching MCRI’s Connected Minds Study, which will measure the impact of Australia’s landmark teen social media ban.
The study will examine whether blocking under 16s from social media platforms including Instagram, Facebook, TikTok, Snapchat and YouTube has been e ective at changing their phone use patterns and improving their mental wellbeing.
“Some evidence links social media use to adolescent mental and physical health, but a clear cause-and-e ect relationship hasn’t been proven,” Professor Susan Sawyer says.
“Crucially, we need to hear from young people and their families about what they think about the restrictions and, ultimately, what changes it makes to their lives, to better inform debates around the potential harms or benefits of social media.”
Researchers from MCRI and Deakin University are studying the experiences of teens aged 13 to 16, along with those of their parents, using surveys conducted before and after the age restrictions came into e ect on December 10, 2025.
De-identified information is collected on the amount of time spent on social media, sleep, physical activity and young people’s feelings about social connectedness.
“With Australia leading the world on delaying social media for young people, we have a major social experiment ahead of us,” Prof Sawyer says.
“The restrictions have generated a lot of interest globally, with many countries seeking to adopt similar restrictions.
“Our findings will help us to advocate for young people, better inform policy decisions and determine whether further regulations on social media companies are warranted.”





News Corp Australia is helping MCRI change the lives of sick children through our News in the Community program
Giving back is at the heart of News in the Community. It’s why News in the Community supports a variety of organisations committed to improving the lives of Australians and the communities in which we all live and work.
Murdoch Children’s Research Institute is one such organisation.
For 40 years, MCRI has been working to understand, treat and cure childhood illnesses, becoming a global leader in the field.
There’s a natural alignment: MCRI was co-founded by Dame Elisabeth Murdoch in 1986 and its life-saving work is embodied in News in the Community’s key Healthy Nation pillar.
As a company of storytellers, editorial coverage has anchored News Corp Australia’s support of MCRI. From page-one splashes on world-first discoveries and heartwarming features on children
whose lives are changed by the latest medical breakthroughs to breaking news on a visit by Queen Mary and King Frederik of Denmark, these important stories have been told across our mastheads and websites.
Fundraising has also been a focus. The Good Friday Appeal, an important part of News in the Community, raised more than $25 million for The Royal Children’s Hospital this year, with a portion supporting MCRI, based at the hospital’s Parkville campus in Melbourne.
The wider News Corp Australia family has also pitched in.
A collaboration between MCRI, HarperCollins and taste.com.au saw the publication of The Allergy Friendly Family Cookbook in 2023. Along with recipes, it contains advice to help families navigate the challenges of living with food allergies.

And former stablemate Foxtel established a national treadmill challenge, the Foxtel Lap, before getting behind the MCRI Step-a-thon, to raise more than $6 million over 10 years.
“We’re proud to support MCRI’s life-changing work — and to help share the stories that inspire understanding, action and hope for families across Australia,” News Corp Australasia executive chairman Michael Miller says.



in the Community supports a variety of organisations and projects that make a di erence to communities around the




MCRI: Celebrating 40 Years of Impact is produced for News Australia by

GENERAL MANAGER
Marie Joyce
CONTENT DIRECTOR
Michelle Rose
EDITOR
Kamahl Cogdon
LEAD ART DIRECTOR
Meisha Reynolds
DESIGNER
Michael Owen
WRITER
Charlotte Brundrett
SUB-EDITORS
Cathy Laird
Joanne Trzcinski
Monique Gill
PHOTOGRAPHY MCRI
News Australia
Getty Images
