CUTTING THE RED TAPE
Improving access to medicines
ANCHORING HEALTH FUNDING IN EVIDENCE
Inside AMA’s pre-Budget push

THE CALL OF THE COUNTRY






CUTTING THE RED TAPE
Improving access to medicines
ANCHORING HEALTH FUNDING IN EVIDENCE
Inside AMA’s pre-Budget push







It’s our first edition for 2026 and we have plenty of good summer reading.
Those of us with country roots know all too well the spell rural Australia can cast over you, always calling for your return to the fold after city studies or careers.
In this edition of NSW Doctor, we talk to Dr Sarah Woodford, a rural generalist now caring for the very people who featured heavily in her childhood in Gunnedah in the state’s north-west.
For Dr Woodford, life as a rural generalist provides job security, flexibility and professional development – while also allowing her to reconnect with the community that raised her. It’s a program that is helping boost medical practitioner numbers in regional hospitals, but it must also ensure GPs remain in the community where they are most needed. In this edition, we also talk to intensivist Dr Nhi
Ngyuen, once the calming face of COVID-19 in NSW, and now leading Nepean Hospital’s redevelopment, one of her many hats.
Over the years, she’s learnt that taking time for “deep listening to learn and understand perspectives achieves the best outcomes” - and she tells us why she isn’t finished just yet.
We hear from Dr John Sinn on the support he has received from AMA (NSW) in setting up and running his successful paediatric allergy practice. Dr Sinn has utilised our masterclasses, education sessions and workplace relations support and says “you know you have a team behind you”.
And lastly, 1145 new medical interns joined NSW hospitals recently. After many years of study, it is now time to navigate the complexities of our health system, build relationships and care for patients. To help shine a light, Dr Alan Pham shares tips on his first few days and week as a doctor-in-training.
I hope you enjoy this edition and thanks for being a part of AMA (NSW).
Australian Medical Association (NSW) Limited ACN 000 001 614
STREET ADDRESS
69 Christie Street
ST LEONARDS NSW 2065
MAILING ADDRESS
PO Box 121, ST LEONARDS NSW 1590 Telephone (02) 9439 8822
Outside Sydney Telephone 1800 813 423
Email magazine@amansw.com.au members@amansw.com.au www.amansw.com.au
The NSW Doctor is the quarterly publication of the Australian Medical Association (NSW) Limited.
Views expressed by contributors to The NSW Doctor and advertisements appearing in The NSW Doctor are not necessarily endorsed by the Australian Medical Association (NSW) Limited. No responsibility is accepted by the Australian Medical Association (NSW) Limited, the editors or the printers for the accuracy of the information contained in the text and advertisements in The NSW Doctor. The acceptance of advertising in AMA (NSW) publications, digital, or social channels or sponsorship of AMA (NSW) events does not in any way indicate or imply endorsement by the AMA.
AMA (NSW) BOARD
Dr Kathryn Austin, president
Dr Fred Betros, vice president
Dr Michael Bonning
Dr Costa Boyages
Dr Brian Fernandes
Dr Amandeep Hansra
Dr Jacqueline Ho
Dr Theresa Ly
Dr David Malouf
SECRETARIAT
Chief Executive Officer, Fiona Davies Director, Workplace Relations, Dominique Egan
Editor
Kate Benson kate.benson@amansw.com.au
Cover Photography
Tori Etheridge
Design
Cally Browning cally@barecreative..com.au
Advertising enquiries
Jacob Gormley Jacob.gormley@amansw.com.au
Welcome to the first edition of NSW Doctor for 2026. The year ahead is already shaping up to be one of great transition, renewed advocacy and strengthened support for the medical profession.
As many of you are already aware, AMA (NSW) long serving CEO Fiona Davies is stepping down from her role on July 1 after nearly three decades of service. Fiona has been an astute political operator and an extraordinary advocate for the medical profession, guiding the organisation through many troubled times. She’s also guided us through 13 presidents – with a 14th due before she departs.
We will ensure there are opportunities to farewell Fiona as we get closer to July.
We are now only 13 months from the next state election, and it is promising to be a tight contest. Last month, opposition leader Kellie Sloane named former education minister Sarah Mitchell as her health spokesperson. A strong opposition is essential in keeping a government accountable and we will continue our focus this year on greater hospital funding; supporting healthcare options and access for an ageing population; making preventative health care a priority to mitigate the burden on the health system and bolstering the health workforce via the expansion of consultant positions.
We have submitted our comprehensive pre-budget

submission, available on our website, to ensure these issues are front and centre for politicians this year.
This month, we’ve welcomed 1145 medical interns to our NSW hospitals, all embarking on incredible careers caring for others. We have already launched our 2026 Interns Program, offering free membership until April 15, alongside comprehensive career services, workplace guidance, and wellbeing support. This reflects AMA (NSW)’s commitment to fostering the next generation of clinicians.
We also embarking on our arbitration case for visiting medical officers in the NSW
Industrial Court, with the case starting in April. This has been a huge body of work over several years and I look forward to AMA (NSW) making real change in this space.
I look forward to working with members on our exciting and forward looking agenda, focusing on supporting doctors to do what they do best at every stage of their careers.
President@amansw.com.au
linkedin.com/in/kathrynaustin-a2929973/
www.facebook.com/amansw





Integrate with your PMS for a seamless payment & claims experience.
Process claims & quotes inperson or online.1
Add unlimited practitioners to a Tyro Health EFTPOS device, and settle funds separately



AMA (NSW) members get 3-months free EFTPOS rental. Scan to claim. T&Cs apply
Instant Medicare claims & rebates with Medicare Easyclaim & integrated PMS partners. 2
Secure payment links, deposits and payment holds, card on file and flexible instalment options.
Medicare, ECLIPSE, DVA, icare NSW, WorkSafe Victoria and other major workers’ compensation schemes

his year marks my last year as Chief Executive Officer of the Australian Medical Association (NSW).
While I have another edition (or two) of NSW Doctor to go, I am mindful of starting the difficult process of saying goodbye to the association and the profession I love. For this reason, I will indulge myself with my CEO columns to give some behind the scenes perspective on my time with AMA (NSW).
As I indicated in my email to members, I started with AMA (NSW) in June 1998. It was a time of Nokia phones and fax machines. The AMA (NSW) offices (in a different part of St Leonards) housed giant photocopiers and an endless amount of work and time was devoted to preparing large paper agendas which were mailed out to councillors prior to each meeting.
Council meetings were impressive, formal affairs. The mostly male council met in person - with limited crackly teleconference facilities. Dinner was by tradition served at the end of the meeting which must have made for some fractious discussions. Our regional councillors would fly in for the meeting, giving a rare night off for hard working regional doctors. They tended to celebrate accordingly.
Councillors stood to address the chair in meetings and there was a great sense of formality, but also an incredible sense of commitment to the business of the profession and the health system. In my first week, I was told that I would be in charge of Medical Practice Committee, then chaired by Dr

Peter Arnold who had been the long standing chair of Federal Council. Peter (who would hate my referring to him as chair instead of chairman) was an accomplished GP and medical leader. He kindly but firmly corrected my minutes, noting my issues with apostrophes. Peter Arnold was followed by Professor Kerryn Phelps in the early stages of her rapid rise through medical politics.
The business of the AMA was conducted by email in part but much more by meetings and letters. I started at the AMA not long after the major VMO dispute of the early 1990s. It was also soon after the provider number dispute which had been a formative issue for so many doctors in training and medical students. Indemnity and hospital funding were the other major issues of the day.
The AMA was also starting work on a novel new concept - the idea of safe working hours for doctors in training. The AMA’s first report into safe hours, launched in 2000, was
groundbreaking for its time. In the first few years of the survey working hours of 100 to 150 hours per week were standard. Clearly, while there is a long way to go, it is remarkable to have seen the complete change to the conversation around the issue.
The benefit of being with the AMA (NSW) during all of these years is that I have seen the commitment and determination of doctors over many years.
In my experience, doctors have always been effective and listened to because they worked hard and they were smart. They put their patients first and were willing to step up. As long as those attributes remain at the foundation of the medical profession and the AMA, the profession will continue to be effective.
Fiona.davies@amansw.com.au
www.facebook.com/amansw
https://au.linkedin.com/company/ ama-nsw
Dr Sarah Woodford has returned to the town that raised her, helping rebuild rural healthcare from the inside out. She tells Jacob Gormley why coming home was the best decision she ever made.
When Dr Sarah Woodford walks down the main street of Gunnedah, the faces are familiar. She waves to a teacher who once helped her through high school maths, checks in on an elderly neighbour, and later that afternoon, treats a child she has known since birth.
For Dr Woodford, medicine in Gunnedah is more than a career. It is a homecoming. “I grew up here, so I knew how incredible our local doctors were,” she says. “But I also saw how few there were. Rural healthcare professionals have always been thin on the ground.”
Today, as a rural generalist trainee based in her hometown, Dr Woodford has come full circle, helping to strengthen the very system that once inspired her. But her path to rural medicine was not straightforward. Like many young people from regional towns, she thought she would have to build her future elsewhere.
“I moved to Sydney for university and pretty quickly discovered the city was not for me,” she recalls. “I became involved with the Australian Medical Students’ Association’s Rural Health Committee and learned a lot about the challenges facing rural healthcare, but that was still quite theoretical at the time.”
The turning point came during residency, when she completed a general practice rotation in Scone.
“That was when it really clicked. I realised rural generalism was the best way to serve the breadth of a community. You can provide comprehensive, high quality general practice care, use your emergency skills when needed, and pursue additional training in an area your community genuinely needs.”
For Dr Woodford, that specialty area is child and adolescent health, a field that allows her to combine clinical skill with a lifelong passion for supporting young people and families.
Her journey back to Gunnedah was supported by the Rural Generalist Single Employer Pathway, or RGSEP, an innovative program that gives doctors in training one continuous contract across both hospital and community settings. The pathway was developed to make rural generalist training more sustainable, predictable and attractive.
Instead of juggling multiple shortterm contracts, trainees have the security of a single employer, NSW Health, while they rotate through hospital and general practice placements.
“The pathway has allowed me to stay connected to the hospital system while doing my general practice training,” Dr Woodford explains. “That is a huge benefit. Working between the public health system and the community
under one contract has made the constant transition between the two really smooth.”
She says the stability has also strengthened her relationships with patients and colleagues. “It has allowed me to maintain professional contacts and friendships that would otherwise be disrupted by contract changes. I have also had financial stability, since my income does not rely solely on billings, and I have kept my NSW Health leave entitlements, which gives me peace of mind.”
That blend of job security, flexibility and professional development sets the RGSEP apart.
For many young doctors, the uncertainty of short-term contracts or income fluctuations can be a major deterrent to rural work. The single employer model helps address those concerns by providing parity in pay with hospital-based colleagues, access to leave and superannuation, and a smoother training experience overall. For NSW Health and for rural communities, it is a mutually beneficial system, ensuring both continuity of care and retention of medical talent.
Returning to her hometown was not just a professional decision for Dr Woodford. “It means so much to come back and work in the community that raised me,” she says. “I am supervised by the same

doctors who treated me when I was a child. I get to look after people I know and care about. That is really special.”
The Gunnedah practice is collegial and supportive, offering both autonomy and mentorship. “I get a lot of autonomy in managing patients, but I also know there is always back up when I need it. The team culture is fantastic, and I get to see such a wide variety of medicine. No two days are ever the same.”
Alongside her general practice work, Dr Woodford contributes to the paediatrics department at Tamworth Hospital and takes part
in college training initiatives, giving her a diverse professional life while keeping her roots firmly planted in Gunnedah.
While the professional rewards are clear, Dr Woodford says the human side of rural practice keeps her grounded. “In rural medicine, you see the impact of your work immediately. You might help stabilise someone in the emergency department one night and then follow up with their family in clinic the next week. You become part of their story.”
That continuity of care, from birth through to aged care, is something

rural generalists experience more deeply than most, and it is what makes their role so vital to the health of regional and remote communities.
“People underestimate how deeply fulfilling it can be,” Dr Woodford says. “You are not just treating illnesses. You are building relationships that last decades. You are part of the community’s rhythm.”
The rural generalist model is increasingly recognised as one of the most effective ways to deliver equitable healthcare outside metropolitan centres. In September 2025, the Medical Board of Australia formally recognised Rural Generalist Medicine as a distinct field of specialty practice, a major milestone in strengthening and professionalising the rural workforce. According to the Federal Department of Health and Aged Care, more than 1,500 doctors nationwide are now training as rural generalists, with NSW and Queensland leading the uptake.
The NSW Rural Generalist Single Employer Program is currently in its pilot and evaluation phase, with future expansion expected to depend on the outcomes of ongoing reviews and funding cycles.
Since joining the program, Dr Woodford has seen the difference it makes not only for doctors but for the community. “Having a consistent presence in town really builds trust. Patients do not feel like their doctor is changing every few months. That stability matters, especially for chronic care and mental health.”
It is also changing perceptions among young doctors who might not have previously considered

a rural path. “People sometimes think working rurally means limiting your options,” she says. “It is the opposite. You get to practise a broader scope of medicine, develop unique procedural skills and contribute to something bigger, your community’s wellbeing.”
For junior doctors or medical students considering a rural career, Dr Woodford’s message is simple: say yes. “It is the most rewarding career you could ask for. You serve a population that is both medically fascinating and deeply appreciative. You get to manage everything from preventative health to palliative care, and you genuinely make a difference.”
As for those curious about the RGSEP specifically, she is unequivocal in her support. “If
having one contract between a GP practice and a hospital appeals to you, if you value stability, fair pay and access to your NSW Health leave. Every new program has challenges, but I have felt really supported by the RGSEP team. We are all working towards the same goal, better rural healthcare.”
AMA (NSW) regional specialist Dr Tom Gleeson said “AMA (NSW) had long advocated for the Rural Generalist Single Employer Program and we are pleased to see young doctors and their communities benefiting from this model”.
“I commend Dr Woodford’s commitment to rural generalist medicine. I think she has cracked the code to fulfilment by choosing a specialty that deeply connects with her local community and
It is the most rewarding career you could ask for. You serve a population that is both medically fascinating and deeply appreciative.”
provides her with constant interest and variability in the day, whether that be in general practice or at the local hospital. This is exactly what rural communities need.”
At the end of the day, it all comes back to Gunnedah.
“This community shaped me,” Dr Woodford says. “To come home and give something back, that is incredibly fulfilling. I feel like I am part of something that matters.”
Members are owners of Avant and serve on the Board. They ensure all profits are reinvested to benefit members.
We advocate for doctors’ interests, and offer a wealth of education, advisory services and grants.
Members have preferential access to, and savings on, a suite of Avant products and services.

I chair the Board of Avant and it’s really important that we have doctors representing members and our profession on that board. Our job is to put the member view on the table whenever decisions are being made.
Dr Steven Hambleton AM
General Practitioner, Chair Avant Mutual


Making sure you have the correct processes in place to collect, use and disclose patient information is essential to ensure you are compliant with your privacy law obligations writes Senior Workplace Relations Advisor Anastasia Livanova
Consent is a fundamental principle of privacy law, giving patients control over how their personal and health information is handled. In New South Wales, private practices operate within robust privacy frameworks that outline clear requirements for handling patient information. Understanding these requirements is essential for not only complying with privacy laws but also for maintaining the trust that sits at the heart of the doctor/ patient relationship.
This article explores what consent means in the context of handling patient information, the processes that can undermine its validity and the practical steps practices can take to implement compliant and patient-centred consent systems.
In New South Wales, the collection and handling of personal and health information in healthcare settings is governed by the Health Records and Information Privacy Act 2002 (HRIP Act) and the Privacy Act 1988 (Cth), which incorporates the Australian Privacy Principles (APPs). These laws set out how personal and health information must be handled. Central to these requirements is the concept of consent.
Consent is more than a check box. It is a two-way communication process ensuring patients can make informed decisions.
For consent to be valid, it must be freely given without pressure or coercion, based on clear information, specific to the stated purpose, current and up to date and provided by a patient who has the capacity to make decisions.
Consent may be implied or express given in writing, orally, or in any form where the intention is clearly communicated. While signed consent is preferred, a record setting out the details of a discussion will carry significant evidentiary weight if a dispute later arises.
As noted above. consent can take different forms. Express consent is clearly and unmistakably communicated and can be documented in various ways, such as a signed hardcopy form, a digitally signed document or a verbal agreement recorded in the patient’s file.
On the other hand, implied consent is inferred from a patient’s actions. When a patient attends a
consultation and provides health information to their treating doctor for the provision of a medical service, consent to the collection and use of the information to the provision of the health service may be implied in most circumstances.
Every practice must maintain a clear and accessible privacy policy describing how it manages patients’ personal and health information. This should include information on collection, use and disclosure, data storage and security and complaint processes.
The policy should be easily accessible to patients and reflect current practice operations. If you don’t already have one in place, AMA (NSW) has a privacy policy template that members can tailor to ensure it accurately reflects the processes and procedures in place at their practice.
Consent, express or implied is required to collect, use and disclose health information. The primary purpose for which health information is collected is usually the provision of a health service. This may be conveyed to patients in the privacy policy and / or consent and patient registration forms and during consultations.
Information may be used and disclosed for the purpose of providing a health service. This may include disclosure to other health service providers involved in the provision of the patient’s care.
. Using information for a secondary purpose, for example, disclosure to the patient’s insurer, typically requires express consent from the patient.. Information may be disclosed without express consent for a secondary purpose if:
• the patient would reasonably expect the secondary use;
• the use is directly related to providing healthcare;
• the use is required or authorised by law; or
• the use is necessary to prevent a serious threat to life, health, or safety.
A warning about bundled consent and opt-out mechanisms
When obtaining patient consent, practices must take care with their approaches to avoid the questioning of the validity of consent, particularly bundled consent and opt-out mechanisms.
Bundled consent occurs when consent for different purposes are combined into one broad agreement. This approach can make it difficult for patients to understand each purpose for which their information will be used. As a result, bundled consent increases the risk that patients feel pressured into an all or nothing decision and can undermine the core elements of valid consent. For example, a consent form that records the patient’s consent for the collection of their health information and that also permits
the practice to use images for promotional or educational purposes.
Opt-out mechanisms pose similar challenges. Opt-out mechanisms treat a patient’s inaction as agreement, assuming the patient has read, understood, and considered the information provided. In reality, a missed checkbox or unreturned form does not guarantee valid consent. If the opt-out option is unclear, buried, or bundled with other information, it is unlikely to be considered informed.
To ensure valid consent, practices should:
• Avoid broad, bundled consent forms.
• Provide clear, separate explanations for each purpose requiring consent.
• Allow patients to agree to or decline each purpose individually.
• Use opt-out mechanisms only where the purpose is low risk, clearly explained and easy for patients to understand. These purposes will be very limited in a health context,
• Prioritise express consent, obtained through a clear conversation or written agreement.
By designing consent processes that emphasise clarity, choice, and transparency, practices reinforce that consent is a two-way communication process.
A word about artificial intelligence
As artificial intelligence (AI) scribes become more common, new

considerations arise for patient consent and transparency. These technologies introduce additional layers of data handling, making it essential for practices to clearly communicate how patient information will be collected, handled and stored.
Practices using AI scribe tools should:
• Verify that AI providers comply with Australian privacy laws.
• Inform patients upfront about the use of AI scribe tools and explain their purpose in the clinical documentation processes.
• Obtain consent each time an AI scribe is used. This step is critical, as failing to do so may amount to a criminal offence in New South Wales and some other jurisdictions.
• Update privacy notices and policies to reflect the use of AI scribe tools within the practice.
As technology evolves, clear communication helps patients understand how their information is managed and reduces concerns. By treating consent as an ongoing conversation rather than a box to tick, practices can stay compliant with privacy laws while building stronger relationships with their patients.
If you need assistance with implementing these processes or understanding your obligations, contact the Workplace Relations team on (02) 9439 8822 or via email at workplace@amansw.com.au

A recent federal court ruling against Woolworths and Coles has clarified how annual salaries must be managed. The message for medical practices is clear, entitlements must be met each pay period and accurate records are essential, writes workplace relations advisor, Kain Hourn.
Ensuring staff are paid correctly is a fundamental obligation of employers, and, more than that, a cornerstone of good workplace practice. While employers may aim to simplify payroll by offering annual salaries under the assumption the above-award rate will cover all their bases, a recent Federal Court decision involving Woolworths and Coles shows that this approach can carry significant risk if not properly managed.
This article explores how an aboveaward payment is commonly made, summarises key findings from the case, and provides practical considerations for medical practices to ensure they are compliant in the future.
The two main approaches to payment of staff
Employers generally take one of two approaches when paying award-covered employees:
1. Award-Based Hourly Rate
The first is to be paid an hourly rate according to their classification under the relevant Modern Award (or higher where competitively necessary). The employee will receive payment for overtime, penalty rates, and
other entitlements as they are incurred.
2. Above-Award Hourly Rate or Annual Salary to Set-Off Entitlements
Employers may pay an employee an above-award rate, either as an hourly rate or through an annual salary, and then “set-off” award entitlements against that higher rate of pay. Practically, this means that the above-award pay must be high enough to sufficiently cover all relevant minimum pay obligations the employer is required to meet, and their contract will outline this in a “set-off” clause.
While the second method may offer administrative convenience, it carries inherent risk if the practice owners “set and forget” the above-award figure. An employer must consistently review their pay and entitlements to ensure the above-award rate is sufficient.
For example, if an employee works a significant amount of overtime, their minimum entitlements may exceed the salary they’re normally paid. At this point, a top up payment must be made to prevent underpayment.
It’s for this reason AMA NSW typically advises against this arrangement, particularly when the salary that is to be offered is not sufficiently greater than the employee’s minimum entitlements.
The recent Federal Court of Australia decision
On 5 September 2025, the Federal Court of Australia handed down its decision in FWO v Woolworths Group Limited; FWO v Coles Supermarkets Australia Pty Ltd, following claims by the Fair Work Ombudsman and claims made in multiple class actions. These claims centred on the alleged underpayment of salaried store managers and supervisors; approximately 19,000 at Woolworths and 8,750 at Coles.
Although relevant employees were covered by the General Retail Industry Award 2020, the case has attracted widespread attention due to its implications for employers using similar salary arrangements under other Modern Awards including those in private medical practice where staff are employed under the Health Professional and Support Services Award 2020 or the Nurses Award 2020


The case centred on two key questions:
1. Can “set-off” clauses offset entitlements across multiple pay periods?
Coles and Woolworths argued that clauses in the staff contracts allowed them to set-off these entitlements across a 26-week period. Over that period, staff were not underpaid.
However, the Federal Court disagreed. It found that above-award payments paid
on one pay period can set-off entitlements within that pay period (usually a fortnight or a month), they could not be used to set-off entitlements in another pay period. The obligation on employer’s is to ensure there no underpayment in each pay period.
2. Do employers need to keep records of overtime for salaried staff?
Record keeping obligations under the Fair Work Act and Regulations require employers to record the amount of overtime worked,
The Woolworths and Coles decision is a timely reminder for private practices that wage compliance cannot be a “set and forget” exercise.”


start/finish times, and any agreements for time off in lieu of overtime, and must keep these records for seven years.
It was argued by Coles and Woolworths that because their employee contracts stated that any additional overtime payments were included in their aboveaward salaries, they did not need to keep separate overtime records as there were no additional payments to make.
Significantly, this argument was rejected by the Court. Under the Act and Regulations, employers must keep time and wages records regardless of how the employee is paid as, and be able to provide them in support of the payments made to employees, if required.
So, what does this mean for medical practices? The Court’s decision has two major considerations:
• All employee award entitlements must be paid each pay period regardless of whether the employee is remunerated on the basis of an hourly rate or annualised salary.
• Record keeping is essential. Employers must maintain accurate records of hours worked, including overtime, for all staff, including salaried staff. Beyond legal compliance, it provides critical evidence in the event an underpayment claim is made against them.
Following the Federal Court’s Decision, medical practices should take the following steps:
• Review your employment contracts for salaried staff: Ensure there is no contractual wording that stipulates minimum pay entitlements are averaged over multiple pay periods, or offset by payments in other periods. Seek professional advice about changes that you may be contemplating regarding contractual arrangements.
• Audit pay processes: If you conduct an annual audit to confirm a salaried employee’s annual remuneration is sufficient, change this to a review at the end of every pay cycle. This helps identify shortfalls early.
• Ensure compliance with record keeping obligations: For staff on annual salaries, record actual hours worked, including overtime, and calculate the minimum entitlements they should receive. This ensures compliance and helps confirm that salaries meet requirements under the Award.
The Woolworths and Coles decision is a timely reminder for private practices that wage compliance cannot be a “set and forget” exercise. While annual salaries and aboveaward arrangements may offer convenience, they come with additional obligations. These
Employers may pay an employee an above-award rate, either as an hourly rate or through an annual salary, and then “set-off” award entitlements against that higher rate of pay.”
include ensuring employee entitlements are met in every pay period and maintaining accurate records of hours worked, including overtime.
By reviewing contracts, auditing pay processes regularly, and implementing robust recordkeeping systems, practices can significantly reduce the risk of underpayment claims in the future.
If you’re unsure whether your current arrangements comply with the Fair Work Act 2009 and Awards, or if you’d like assistance reviewing contracts and payroll processes, please contact the AMA (NSW) Workplace Relations team via email at workplace@amansw.com.au or call (02) 9439 8822
MA (NSW) has lodged its 2026–27 pre-budget submission calling for health funding to be anchored in evidence and population need. Policy Manager Marita O’Toole outlines the key priorities needed to support an ageing population, strengthen the workforce and deliver sustainable healthcare across NSW.
AMA (NSW) has provided a pre-budget submission to the NSW Government to outline our suggested health budget priorities for the 2026-2027 financial year. The next budget will be delivered in June this year.
We have emphasised that the challenge of delivering healthcare for an ageing and increasingly complex population requires a greater investment in preventative healthcare, the consultant workforce and stable, multi-year funding certainty across all local health districts.
The Special Commission of Inquiry into Healthcare Funding was unequivocal that past NSW Health budgets were not grounded in evidence, and population need. We call for the NSW Government to implement its own report and prioritise health in the 2026-27 budget.
Our key priorities are for the NSW government to:
1. Reformulate the funding model to develop a new ‘base’ that is grounded in evidence and population need.

2. Prioritise multi-year funding across all local health districts to support predictable service and workforce planning across the health system.
3. Invest in prevention as a wholeof-government priority and to quarantine a minimum 5 per cent of the health budget towards prevention related activities.
4. Allocate a greater number of
consultant positions across NSW public hospitals to support efficient, quality care and bolster workforce attraction and retention
5. Maintain and build facilities that support world class diagnosis and treatment that enable residents of NSW to access timely, quality healthcare irrespective of where they live.


Welcome to the latest edition of Financial Paracetamol.
As always, if you have any questions relating to anything in this edition, please don’t hesitate to get in touch with our award-winning team.
The First Home Guarantee now allows all Australians to buy with just a 5% deposit and no LMI. It’s a major shift, but it doesn’t take away the longstanding benefits available to medical professionals.
Lenders factor in your future earning trajectory which can increase how much you can borrow.
Many banks still offer up to 95% LVR with no LMI for eligible medical professionals, helping you buy sooner with less red tape.
Specialist medical finance teams understand rotations, contract roles and variable income, making the process smoother.

Stuart Chan, Partner 1800 988 522
medical@cutcher.com.au

cutcher.com.au
These policies also apply to scenarios the government scheme can’t cover, including investment properties and refinancing.
While the public is gaining access to a lower-deposit pathway, doctors still hold a meaningful advantage. If you’re weighing up your next step contact us on 1800 988 522 or visit cutcher.com.au.


Early Career (Locum/ Hospital Employee) >
• Medical Indemnity
• Income Protection
• Life and TPD
As your medical career grows, so does your exposure. The insurance that protected you as a locum or hospital employee won’t always be enough once you’re running your own rooms, employing staff or purchasing valuable equipment.
Insurance breakdown: which insurances you need and when. For tailored advice,
Transition to Private Practice >
• Business Insurance
• Practice Indemnity
• Property and Equipment Cover
Retirement is something many doctors look forward to, but the real challenge is knowing how much super you’ll need to maintain your lifestyle. The Association of Superannuation Funds of Australia estimates a comfortable retirement at around $690,000 for couples and $595,000 for singles. But for most medical professionals with higher living costs, those benchmarks fall short.
If your household spends about $150,000 a year, maintaining that level in retirement could mean needing up to $3 million in super. With Division 296 on the horizon, doctors nearing the $3 million mark should review their strategies because once your balance tips over that threshold, the new tax rules can significantly impact your long-term outcomes.
Our advisors can help you build comfort and clarity in your retirement planning.
Established or Growing Practice >
• Management Liability
• Cyber Insurance
• Expanded Business Interruption Cover
What is Division 296?
Extra 15% tax on earnings above $3m
25% above $10m
Applies per individual
Unrealised gains no longer taxed
Thresholds indexed (reduces bracket creep)
From locum shifts to running your own practice: When your cover needs an upgrade. The tailored financial service for doctors in training.

NSW hospitals are lagging behind on discharge medications, putting patients at risk, writes, policy assistant Sophia Murphy.
NSW and ACT remain the only jurisdictions in Australia where patients discharged from hospital cannot access a safe supply of Pharmaceutical Benefits Scheme (PBS) medication.
All other state and territories have agreements in place, which allows hospitals to dispense up to 30 days’ worth of PBS medications. Instead, patients in NSW and ACT receive only a few days’ supply which can be as little as three days’ worth. This leaves individuals with no choice but to secure an urgent general practitioner appointment to continue their necessary treatment. This is not just inefficient. It’s unsafe.
This policy discrepancy may appear minor but, in the current healthcare landscape where GP appointments are becoming increasingly harder to secure, it has serious consequences. According to the Australian Bureau of Statistics, almost 30 per cent of Australians felt they waited longer than acceptable to get an appointment with a GP.
For many Australians, such as those with chronic conditions, mobility challenges and limited transport options, accessing a GP can be even more challenging. Any interruption to medication can be
dangerous. For example, a pause in blood thinners or heart medication can lead to readmission, strokes or another heart attack.
Introducing a Pharmacy Reform Agreement (PRA) between the Commonwealth and NSW and ACT would bring parity across all jurisdictions and in turn support a safer transition from hospital to home for all Australians.
When patients are discharged with a full month’s supply of medication, they are given the time to rest, recover and stabilise. Hospitalisation can be physically and emotionally draining so the ability to recuperate at home without pressures to obtain medication can be

critical. Furthermore, the need for immediate GP follow-up appointments places strain on an already stretched primary care system.
Moreover, the absence of a PRA threatens treatment continuity. PBS medications are not universally available in all community pharmacies. Hospital prescribed medication may differ from those stocked locally. Without a PRA, patients may have to switch medications after only a few days, increasing the risk of adverse effects. Continuity of care is a key principle of NSW health, but the current PBS discharge system actively undermines this.
The lack of a PRA also means that Indigenous patients in NSW and the ACT are excluded from the Department of Health, Disability and Ageing Closing the Gap PBS Co-payment Program, which was extended to all public hospitals with a PRA in January 2025. This program is designed to reduce financial barriers to essential medications for Aboriginal and Torres Strait Islander peoples. Without a PRA, Indigenous patients in NSW and ACT are being denied access to a nationally endorsed initiative that directly supports health equity and improves outcomes.
The Federal Government has already recommended the establishment of a PRA in NSW and ACT. The Pharmaceutical Reform Agreement Review Report (March 2024) and the Mid-Term Review of the National Health Reform Agreement (NHRA) Addendum 2020–2025 (October 2023) both explicitly call for NSW and ACT to implement a PRA.

While a prospective, nationally consistent, multilateral PRA is being considered to replace existing bilateral agreements in all states and territories, there is currently no clear timeline for its implementation. Historically, these negotiations take considerable time. Time that patients in NSW and ACT who are facing unnecessary risks, costs, and barriers to care, don’t have.
AMA (NSW) therefore continues to advocate for the Australian Government to urgently establish a bilateral interim PRA. This would provide an immediate and practical solution, ensuring patients can access safe, affordable, and uninterrupted medication upon discharge from hospital. It would align NSW with other states standards, reduce pressure on primary care, and uphold the principles of continuity, equity, and safety.
The absence threatens treatment continuity. PBS medications are not universally available in all community pharmacies. Hospital prescribed medication may differ from those stocked locally.”
The Mandatory Disease Testing Act is not supported by clinical evidence, writes Sophia Murphy.
In 2025, AMA (NSW) was invited by the NSW Department of Communities and Justice and NSW Police Force to make a submission to inform the legislative review of the Mandatory Disease Testing Act (MDT Act) (2021).
AMA (NSW) maintains its strong stance against this legislation, consistent with what we voiced in 2018 when it was proposed, and during the initial review conducted by the Ombudsman in 2023.
The MDT Act
The MDT Act (2021) mandates blood testing of individuals in
circumstances where their bodily fluid - blood, saliva, semen or faeces - comes into contact with a health, emergency or public sector worker due to deliberate action.
The Act’s objectives are to “provide mandatory testing when a worker is at risk of contracting a bloodborne disease, to protect and promote the health and wellbeing of health, emergency and public sector workers” (Mandatory Disease Testing Act 2021 no 13).
There is no doubt that blood borne viruses (BBV) are a serious health concern with public health significance, and we appreciate the fear of contracting these
viruses as a public sector worker. However, AMA (NSW) strongly believes that the objects of this Act are not supported by clinical evidence or best practice. This not only drains already scarce resources but contributes to the spread of misinformation. AMA (NSW) stands strongly against this, advocating for informed, expert driven health policy.
Clinical evidence contradicts perceived risk
Whilst the Act aims to reduce risk of BBV transmission, clinical evidence and data undermines this. Workers have next to no risk
of contracting a bloodborne disease in these instances. The Police and Blood-Borne Viruses 2023 report, confirms “there have been no recorded incidences of occupational transmission of HIV to a police officer in Australia” (Australasian Society for HIV, Viral Hepatitis and Sexual Health Medicine 2023.) It further states that you cannot contract hepatitis B, hepatitis C or HIV by saliva, sweat, faeces or blood exposure to unbroken skin.
Despite this, the 2025 Ombudsman report, Mandatory Disease Testing in NSW, highlights that all MDT applications involved either saliva (62.3 per cent), blood (14.2 per cent) or both (23.5 per cent). The inclusion of low-risk bodily fluids within the scope of this legislation not only misrepresents clinical evidence and contributes to misinformation but is a waste of public health resources. This diverts attention away from proven prevention strategies and care, reinforcing stigma and undermining rational, clinical based, expert driven health messaging.
Additionally, the reliability of testing is compromised by window periods for BBV detection. A negative result from a third party does not guarantee the absence of infection because it can take up to three months until transmission can be detectable. On the other hand, a positive test of a third party does not mean transmission has occurred. The reality is that testing cannot provide relief to workers or be indicative of appropriate management processes.
Contrary to its objectives, this Act does not encourage workers to seek timely medical advice. Best practice protocols already dictate that any exposure to bodily fluids should be treated as potentially dangerous, with immediate assessment by a health professional and initiation of postexposure prophylaxis (PEP) within 72 hours where required. These protocols are independent of third-party test results and should remain so.
A 2025 survey led by the NSW Ombudsman found that no workers altered their treatment plans based on MDT outcomes. Further, many reported that the process increased their stress and negatively impacted their wellbeing. The Act is purporting ill-advised assurance to those requesting a test, so what is the real agenda?
AMA (NSW) strongly advocates for health policy grounded in ethics, evidence, and respect for individual rights. Mandatory testing undermines patient autonomy and violates core bioethical principles, including informed and voluntary consent. The Act also compromises privacy by disclosing sensitive health information against an individual’s desire and permission to share that information.
The inclusion of minors in the MDT process is also particularly troubling. HIV prevalence among
AMA (NSW) strongly believes that the objects of this Act are not supported by clinical evidence or best practice. This not only drains already scarce resources but contributes to the spread of misinformation.”
individuals under 19 years is extremely low with only three new cases reported in 2024 in NSW. Subjecting minors to invasive procedures like venipuncture without direct health benefit is ethically problematic. The NSW Ombudsman’s 2025 report further raises serious concerns about the disproportionate targeting of Aboriginal and Torres Strait Islander communities, who represent 3.4 per cent of the population but were the subject of 28 per cent of MDT applications. This both perpetuates stigma toward those with BBV and discrimination against vulnerable populations.
Overall, AMA (NSW) urges the government to repeal this Act. Further, we advocate for its allocated resources to be shifted to genuine, clinical based policies that provide reliable health information, medical and pastoral support, and holistic post-incident care for all parties involved.









m a t t e r s . S h a r e y o u r s a n d h e l p

Dr Nhi Nguyen helped guide us through the COVID-19 pandemic and shaped the future of intensive care in NSW.
She talks to Jacob Gormley on why she isn’t done just yet.

As a six-year-old, Dr Nhi Nguyen escaped Vietnam by boat. That early experience of uncertainty and survival shaped her deep empathy and unwavering commitment to care, qualities that have defined her career in medicine.
Today, she is the Clinical Director, Intensive Care NSW, providing
state-wide leadership across the intensive care network. Her role involves guiding critical care strategy, supporting clinicians, and ensuring patients receive timely, coordinated care. But her impact goes far beyond the ICU.
During the COVID-19 pandemic, Nhi served as the state’s ICU clinical advisor. It was a time of disruption, but also of innovation.
“It was a privilege to be part of the state’s COVID-19 pandemic response,” she says.
“It was a period of personal and professional growth for me, a time where careful communication was so important to balance the stress which comes with uncertainty with the reassurance that all our efforts were to prepare our staff and community for the challenges ahead.”
She reflects that the most important lesson from that time was “how well we can all work together when needed.” Collaboration between clinicians, management and the Ministry of Health became the foundation for rapid, adaptive care.
“Taking time for deep listening to learn and understand perspectives achieves the best outcomes,” she says. “I’ve learned to be more comfortable asking for clarity about what problem we are trying to solve and how we might stop doing things which do not work.”
Nhi is also a key figure in the Single Digital Patient Record program the largest digital health transformation in NSW history. Her advocacy ensures clinicians are engaged in shaping technology that supports, rather than complicates, care delivery.
Locally, she leads the Nepean Hospital Redevelopment, a multistage infrastructure project that’s reshaping healthcare in western Sydney. “Infrastructure provides an opportunity to explore new models of care which may improve efficiencies,” she says. “Importantly, new modern buildings hopefully will improve the staff and patient experience during care delivery.”
Her governance contributions are equally significant. Since 2019, Nhi has served on the Nepean Blue Mountains Local Health District Board, including roles as Deputy Chair and Chair of the Safe Care Board Sub-Committee. She’s also a former Chair of the Nepean Medical Staff Council.
She’s passionate about prevention and community partnerships. “If we can be a role model for our children showing the benefits of healthy

eating, physical activity and care for ourselves and each other, as a community we will reap the rewards in the future.”
After 25 years as an AMA (NSW) member, Nhi sees the organisation as a vital voice in shaping healthcare. “Over the years, I have continued my membership because it is important to be a member of a professional group from whom opinions and perspective are respected and sought by health system managers,” she says.
Whether she’s leading state-wide ICU strategy, shaping hospital infrastructure, or advocating for digital transformation, Nhi’s work is driven by a clear purpose: to create a health system that listens, adapts, and delivers care that truly matters.
“We need to understand the systems and problems that damage our health,” she says, “so we can build healthier spaces for our communities and for the generations to come.”
Taking time for deep listening to learn and understand perspectives achieves the best outcomes, I’ve learned to be more comfortable asking for clarity about what problem we are trying to solve.”
AMA (NSW) is committed to supporting members at every stage of their professional journey. Jacob Gormley speaks with paediatric allergist Dr John Sinn about building a specialised private practice and the practical support that helps keep it running.
Dr John Sinn runs The Paediatric Allergy Centre in Chatswood, a highly specialised practice supporting children with complex and lifethreatening allergies. Alongside private practice, he is a senior staff specialist neonatologist at Royal North Shore Hospital and a professor at Macquarie University.
Dr Sinn’s path to private practice
was driven by a desire to do things differently. After training in paediatric allergy at Royal Prince Alfred Hospital in the late 1990s, he began questioning whether standardised food challenges were always delivering safe and reliable outcomes for families.
“Through discussions with food scientists, I became aware that allergen proteins can vary
significantly between food sources,” Dr Sinn says. “That helped explain why some children could pass a hospital food challenge, then have a severe reaction at home. It raised concerns about giving families a false sense of security.”
To address this, Dr Sinn established The Paediatric Allergy Centre and developed the Personalised Allergy Management (PAM)
program, which supports children to gradually build tolerance to allergens including nuts, egg, cow’s milk, seafood and fruit.
“It’s incredibly rewarding to see children who were previously anaphylactic regain confidence and quality of life,” he says. “Watching skin prick tests turn negative after PAM never gets old.”
Running a highly specialised practice comes with its own challenges, particularly when it comes to staffing, compliance and workplace relations.
“In private practice, AMA support becomes essential,” Dr Sinn says. “They are the backbone of our practice.”
He says AMA (NSW) has been particularly valuable in navigating workplace relations, staff entitlements and dismissals, as well as reviewing policies and patient consent forms.
“It’s a legal minefield if you’re new to private practice,” he says. “Having access to clear, reliable advice means we can deal with issues properly and confidently, without immediately needing to engage expensive lawyers.”
Dr Sinn also credits AMA education and masterclasses with helping his practice stay informed and compliant.
“The practice manager masterclasses were extremely helpful,” he says. “They provide a broad understanding of the issues you face in private practice, from staffing to regulatory changes. With AMA support, you know you have a team behind you.”

At The Paediatric Allergy Centre, empathy and accessibility are central to how care is delivered. Families are supported not only through consultations, but between appointments, with clear communication and education designed to reduce anxiety and empower parents.
“Our patients are dealing with fear every day,” Dr Sinn says. “Managing allergy isn’t just about avoidance. It’s about confidence, understanding and support.”
That approach has built strong trust, with families travelling from interstate and overseas to access the PAM program, often through word-of-mouth referrals.
For Dr Sinn, AMA membership provides reassurance behind the scenes, allowing him to focus on patient care and innovation.
“When you’re running a practice, you need to know help is there when issues arise,” he says. “AMA gives us that confidence.”

Secure, seamless & made for Australian healthcare.
Experience seamless, secure, and reliable virtual care with Medihost Telehealth - your trusted partner in modern healthcare delivery.
Whether you’re a solo GP or a multi-site practice, Medihost Telehealth helps you connect with your patients - anytime, anywhere. Book your free demo today. Our solution brings you:
Effortless video consultations with no downloads or logins required. End-to-end encryption for patient privacy and peace of mind.
Custom branding to reflect your practice’s identity.

Integrated workflows that fit your clinics needs.
AI scribe to automatically generate clinical notes, saving time & improving accuracy.
Medihost Solutions is a valued sponsor of AMA (NSW)
Doctors’ Health NSW encourages clinicians to pause, reconnect and seek genuine support. As Dr Katherine Hutt writes, real wellbeing comes from community and conversation, not constant productivity or carrying the weight of medicine alone.
As we reflect on the last year, I always promise myself I will be more organised. Yet somehow the same patterns return: juggling deadlines, squeezing in too many patients, doing late-night online shopping (because now we can all stay busy 24/7), and overfilling the caravan for the holiday that kept me hanging on by a thread. It is a chaotic and messy time, and in all the rush it can be hard to pause and truly look back at the year that has passed.
So as we begin this new year, I want to take a moment to breathe and reflect on a year in doctors’ health in NSW. What have we done, and what have we learned?
Our 2025 Impact Report is full of people. 345 doctors and medical students called our 24/7 phone line last year and shared their stories with the doctors on our team. These were important conversations. Our doctors listened with care while callers struggled with overwhelm, loneliness, exam failure, or the growing feeling that they were in the wrong job. What helped was the chance to talk to a colleague who genuinely understood. They found a connection, and together they worked through the next steps.
We also watched rooms come alive with talking and deep listening during the workshops and

education sessions we ran with 1,670 doctors and medical students across NSW. These moments reminded people that we are part of a professional village, and that connection with colleagues can be one of our greatest supports. We created time and space for real conversations, for vulnerability, for sharing difficult experiences. We saw the impact on both the speaker and the listener. Both walked away feeling a little lighter.
The holiday period can feel overwhelming. Even when it is joyful, there is always so much to be done. For some of us it also brings grief or loneliness that feels even more isolating when everyone else seems festive. At the exact time when connection matters most, doctors are very good at convincing ourselves that friends
and colleagues are too busy and that we should not bother them.
So here is my suggestion as we move into the new year. Be the one to make the first move. Tell your friends and colleagues you are never too busy to take their call. Remind your registrar that you are around if they need a chat. Let a colleague know you can always make time for a coffee.
Be part of a profession that looks after its own.
Our doctors are here 24/7 and ready for a chat. Our Impact Report is available for summer reading, and I hope the stories inspire you to nurture your own peer support network with the people around you. Luckily kindness is one gift that never goes out of fashion.
Doctors’ Health Advisory Service (DHAS) is a confidential, 24-hour support service for medical professionals across Australia, including doctors and medical students.
Support is available via the national helpline on (02) 9437 6552.
Each November, Rural Health Month brings together rural health professionals to share knowledge and build connection. In this feature, Theo Clark reflects on how the initiative continues to strengthen the rural health workforce.
They say tradition is not the worship of ashes, but the preservation of fire. By this measure, the annual series of events known as Rural Health Month launched by RDN’s Rural Health Pro in 2020, are now ‘tradition’, in the most meaningful sense of the term.
Each year in November, through training and networking events, the flame of passion for rural health is passed between colleagues and between generations. The National Rural and Remote Health Awards kicked off celebrations in Canberra in early November, while the Rural Allied Health Conference took place in Tamworth and online mid-month.
Late November, the action shifted to Sydney for the Practice Managers Conference, Rural GPs Conference, and Medical Student Rural Inspiration Conference, along with other co-located training events.
In an interview with ABC Canberra, RDN Chair Professor Peter O’Mara was asked why it was important to celebrate rural health annually in this way. “There’s stories that are shared that can be taken to other communities and applied to allow good things to happen,” he answered.
National Rural Health Commissioner Professor Jenny May summed up the spirit of Rural Health Month on the sidelines of the Sydney

conferences: “It’s the collegiality, it’s the networking and it’s the continuing professional development, where people who’ve got really important roles in our rural communities can get together and share stories.”
In short, the events break down barriers of isolation. “You get to meet like-minded people and discuss cases - and feel you’re not the only one alone in the world out in the rural community,” said veteran Warialda GP Dr Di Coote.
“We feel refreshed, we share ideas, we network, and as junior, we learn from our forebearers about how to manage these challenges but also to have that sense of ‘I see you, I hear you’,” said Orange Junior Medical Officer Dr Pippa Kensit.
Enthusiasm like this has proven infectious, as more and more young doctors embrace a passion for rural health through programs like the NSW Rural Resident Medical Cadetships, to which Dr Kensitt belongs.
Long live the new tradition of Rural Health Month – may it keep this flame of passion alive!

Doctors
In our work at the Medical Benevolent Association NSWACT (MBA NSW-ACT), we often speak with doctors at points of deep uncertainty. Some are still working and caring for patients but quietly know they have been struggling. Others reach out after a sudden shift such as illness, relationship breakdown or unplanned leave. No matter how it begins, the experience is rarely simple and life can become tangled quickly.
When a doctor calls, we often say, “There is always an answer, we just don’t know what it is yet.” By taking that moment to pause, doctors usually start to see things differently. From there, we work together to untangle what’s happening- sometimes through a single conversation, sometimes


over time as circumstances evolve and new information becomes clearer.
Dr Michael Ungar, a leading resilience researcher from Canada, describes resilience as something built through relationships and context- the presence of support, structure, and shared problem-solving (Ungar, 2018). This aligns closely with what we observe every day.
In our conversations, those elements become visible: a clearer plan, restored confidence, and a sense that life is no longer unfolding alone but with guidance and practical support. In our experience, certain patterns make a difference:
• Early contact: reaching out before things unravel reveals more options.
• Identifying the real issue: the
presenting problem isn’t always the most important one, and careful reflection can reveal what truly needs attention.
• Perspective: seeing life through a calmer lens rather than through exhaustion or self-criticism can shift the way forward.
• Mobilising supports: bringing the right people or systems into the picture helps stabilise complex situations.
• Taking manageable steps: progress builds through small, workable actions rather than trying to fix everything at once.
For close to 130 years, MBA NSWACT has walked alongside doctors as they navigate challenging experiences. For confidential, free support from our social work team, please call 02 9987 0504.





As more than 1,145 interns begin their medical careers across NSW hospitals, Dr Alan Pham reflects on his early years as a junior medical officer. Drawing on experience across the Blacktown, Mount Druitt and Bathurst network, he shares practical lessons on workload, imposter syndrome and the value of peer support.

My first day
My initial two years as a JMO in the Blacktown, Mount Druitt, and Bathurst network were a hectic whirlwind of activity. I found it challenging to juggle daily ward duties, overtime shifts, research activities, figuring out my career path, and planning the way forward. Additionally, I had personal commitments, AMA (NSW) Doctors-in-Training Committee responsibilities, caring for a newborn baby boy, and making time for the gym and my well-being. Honestly, it was a lot.
During my struggles to balance different parts of my life, I depended greatly on the incredible colleagues around me. I’ll never forget the words of support, encouragement, and camaraderie from particular surgeons, ID regs, a few particular bosses, and especially my fellow interns and residents, who I eventually realised were all in the same boat as me and similarly looking for support.
I wish I knew:
• It’s not always my responsibility to gauge the urgency of each task. However, it is my duty to monitor all jobs, inform my team about updates, and convey what still needs to be done.
• Imposter syndrome is not something you grow out of. You just get better at managing it, and balance it out with experience, insight, and feedback.
• There is always time for a short break. No matter how

I’ll never forget the words of support, encouragement, and camaraderie from particular surgeons, ID regs, a few particular bosses, and especially my fellow interns and residents”
crazy things got. Luckily, I had amazing nurses and allied health working alongside me on the ward.
Advice for future interns:
• Every rotation has something new to offer, no matter what speciality you end up in. Absorb and learn everything you can because you never know what might be useful later.
• Your registrars and consultants are not infallible. They can make mistakes, too, and at times, you may be the one to notice them. Never feel embarrassed about double-checking things for your patients. Just make sure you ask respectfully.
Everyone values your input, engagement, and feedback. Whether it’s your unit Quality Assurance initiatives, facility General Clinical Training Committee, network Resident Medical Officers’ Association, Health Education and Training Institute committee, the Australian Health Practitioner Regulation Agency Medical Training Survey, or the AMA (NSW) Doctors-inTraining Committee. Your time and opinions are valued. Reflect on your experiences, document, and share them. Together, our efforts make the system better for everyone, patients and doctors alike.

JEWISH DOCTORS CARRY ‘PSYCHOLOGICAL WEIGHT’ OF BONDI ATTACK WHILE TREATING VICTIMS
Dr Kathryn Austin
The Australian December 19

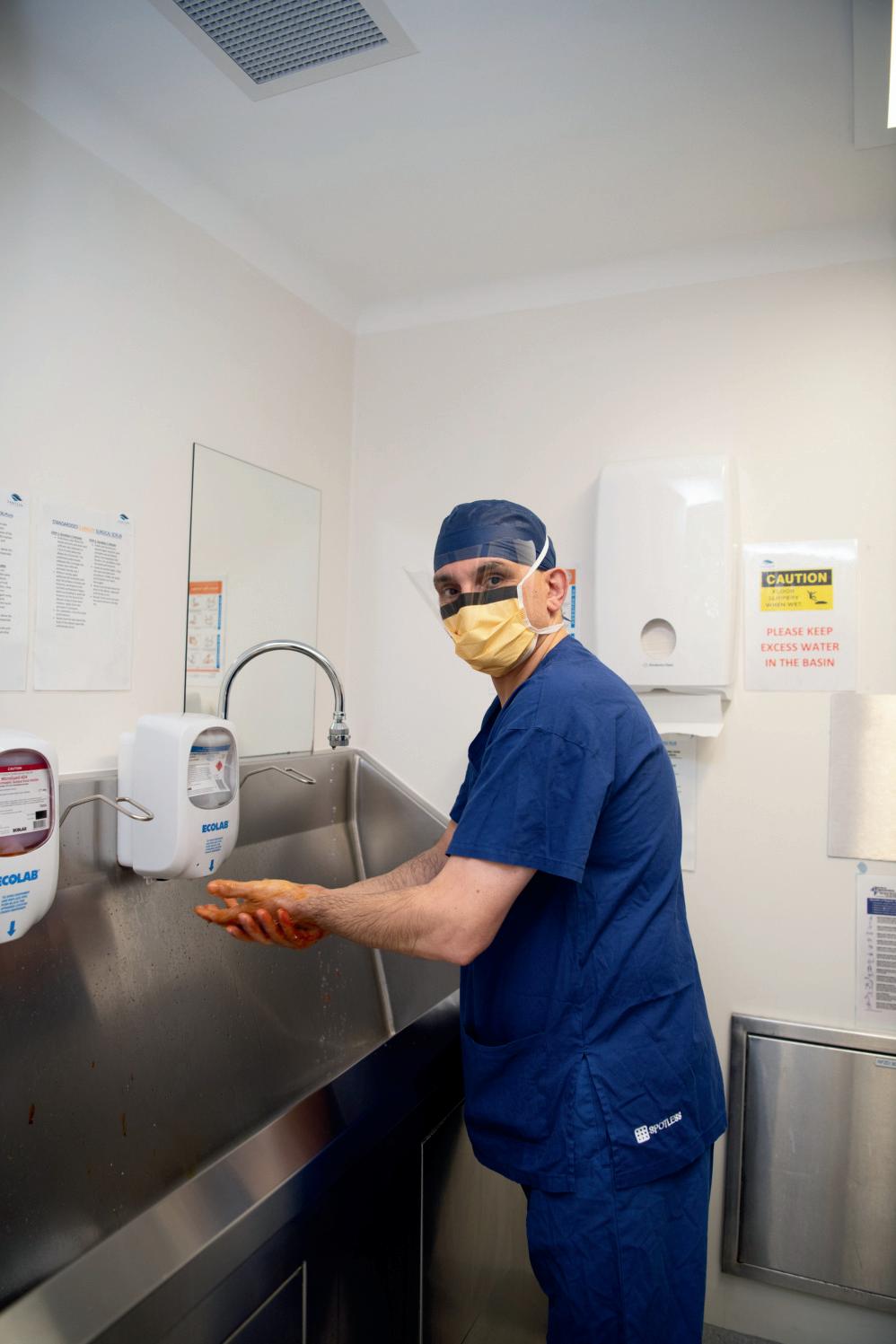

WAITS OF UP TO EIGHT YEARS TO SEE GUT AND COLON SPECIALISTS AT JOHN HUNTER
Dr Fred Betros
The Newcastle Herald
December 1


BED BLOCK, WAIT TIMES, BOTTLENECKS: SYDNEY’S BEST AND WORST HOSPITALS REVEALED
Dr Fred Betros
Sydney Morning Herald
December 10


HOSPITAL PATIENTS DESERVE BETTER THAN A FIGHT OVER FUNDS
Dr Kathryn Austin
The Australian November 19

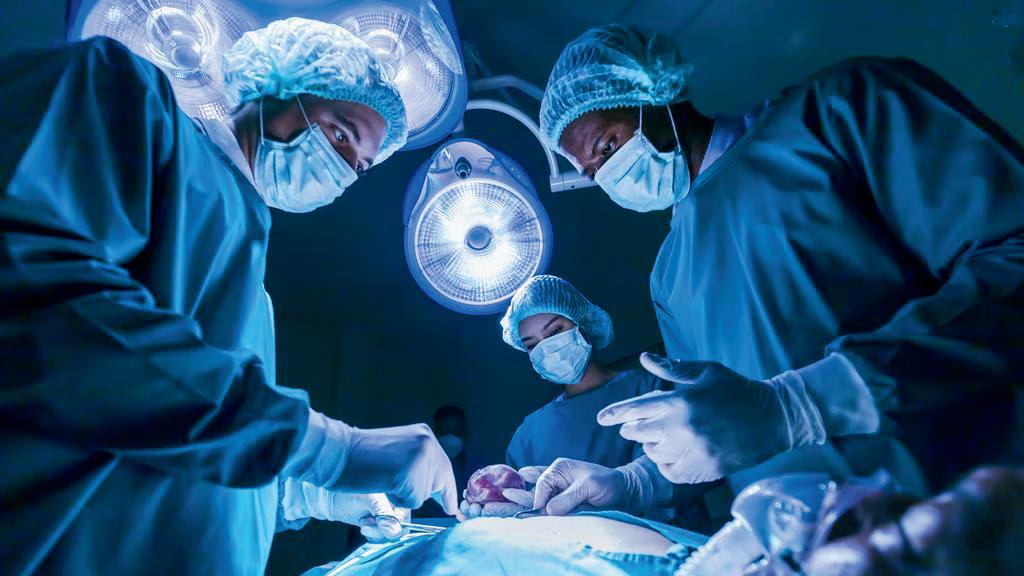
ELECTIVE SURGERIES SLUMP AS NSW HEALTH CATCHES UP ON OVERDUE WAITLIST
Dr Kathryn Austin
The Daily Telegraph

NEW NASAL SPRAY INFLUENZA VACCINE
Dr Ken McCroary Seven News
September 16

September 10

MELATONIN OVERUSE
Dr Michael Bonning Ten News
November 14


NORTHERN BEACHES HOSPITAL PUBLIC BUY BACK WARNING
Dr David Dickison and Dr Karen Shaw
ABC tv
September 16


NEW RURAL HEALTH GAME PLAN SHOWS PROMISE
Dr Kathryn Austin The Medical Republic
October 18

AMA (NSW) members came together at the Museum of Sydney to mark the end of the year, providing an opportunity to thank members for their ongoing support and reflect on the collective work and achievements of the medical community over the past year.

















can find a comprehensive list of benefits and more information at www.amansw.com.au or email members@amansw.com.au

















































Refer a colleague to join AMA (NSW) and receive an e-Gift Card for every successful sign-up.

What you’ll receive:
$100 for each Doctor in Training (DiT) referral
$200 for each non-DiT referral