










• CATARACT SURGERY
• GLAUCOMA
• CORNEAL DISORDERS
• OCULOPLASTICS
• DIABETIC EYE CARE
• MACULAR DEGENERATION
• LASIK SURGERY
• DRY EYE
CHESTER COUNTY
• EYE EMERGENCIES
• ROUTINE EYE CARE
• CONTACT LENSES























• CATARACT SURGERY
• GLAUCOMA
• CORNEAL DISORDERS
• OCULOPLASTICS
• DIABETIC EYE CARE
• MACULAR DEGENERATION
• LASIK SURGERY
• DRY EYE
• EYE EMERGENCIES
• ROUTINE EYE CARE
• CONTACT LENSES











Being healthy starts well before you ever get sick and need a doctor. Preventative health care can go a long way toward keeping your immune system strong and helping you physically and mentally cope better with stress.
Everyone knows to eat a balanced diet, but it’s still one of the most important factors in good health. Eating lots of fruits, vegetables and whole grains, while avoiding too many rich and heavy foods, can help you have more energy and feel better. A healthy diet can also help stave off conditions like diabetes, heart disease and obesity or help you in controlling those conditions.
Regular exercise can also help you feel better overall, in addition to managing longterm health conditions such as diabetes. Your joints last longer and hurt less if you’re exercising regularly, plus getting outside and working up a sweat is good for your mental health. Find physical activity that you enjoy and can do regularly. This can be high-intensity exercises like running, hiking, kickboxing or weightlifting, or low-intensity exercises like walking, yoga and pilates.
The CDC suggests seven to nine hours of sleep a night for adults. Simply being in bed for that long isn’t sufficient, though; you need good quality sleep at night. If you’re waking

up after eight hours of sleep and still feeling tired, waking up multiple times a night or if you snore or gasp for air while you sleep, you’re probably not getting enough deep sleep. Try to go to bed and get up at the same time every day and cultivate other good sleep habits, including reducing screen time
right before bed; having a quiet, dark room; keeping screens out of the bedroom; and not eating large meals or drinking caffeine right before you go to bed.
See your doctor for an annual physical to get your blood pressure and cholesterol checked
and get any tests you may need (such as mammograms and pap smears for women and prostate exams for men). Make sure you’re up to date on vaccines, and take this chance to talk over any concerns or ask questions. You should see a dentist twice a year and see an eye doctor regularly as well.























New location in nearby Exton
WhenLawrence M. Grello, MS, PT, was undergoing his training to become a licensed physical therapist two decades ago, he noticed that there were three prominent schools of thought in the science of healing the body. The first prescribed an exercise-based form of therapy, the other a modality-based therapy and the third took a manualbased approach. Rarely did Larry see therapists pull the best from each of these applications.
When he became the owner of Integrated Physical Therapy 15 years ago, Larry sought to change that paradigm, and integrated all modalities into the company’s practice. Today, at the company’s three locations in Bryn Mawr, King of Prussia and now Exton, patients at Integrated Physical Therapy receive
does just that – heal.
“We don’t fix people here,” Larry said from the 2,800-square-foot Exton location, which opened in October 2018. “We facilitate a person’s healing and well-being, and we treat everyone as an individual. We’re getting rid of the road blocks and the hurdles that prevent you from attaining that decreased pain, that peak performance, or that comfort level and the functional levels of movement.”
Integrated Physical Therapy is a fully licensed, direct access clinic that provides the highest quality, one-on-one therapy for neck and back injuries; degenerative spinal conditions; chronic shoulder, back, knee, jaw and neck pain; sports-related injuries; migraines and headaches; and concussions. Larry and his fully-trained and licensed team of therapists also treat arthritis, stenosis, jaw pain, Fibromyalgia, Post-Concussion Syndrome, and rotator cuff injuries.
Customized programs at Integrated Physical Therapy involve a threestep program of healing that often brings positive results in as little as 72 hours following an injury:
• A physical examination to identify the problem areas
• A complete evaluation to determine therapy needs and

• The creation of a personalized treatment plan that allows
At Integrated Physical Therapy, patients will never be subject to a “cookie cutter” approach to healing. Every therapist works with a customized treatment plan that’s been tailored to each individual’s needs, a prescription for health that leads to faster recovery times and more

“Everybody’s different, and that plays into how the body heals,” he said. “Healing starts with evaluation and listening, and it’s where we find out what’s important to that person. Being compassionate to those emotions and guiding that person through that experience toward healing is all part of what we do. It’s about finding out what is important to them, and then facilitating their health and well-being.”
“The body is a self-correcting mechanism. We just have to figure out what components that need to get out of the way, in order for that process can begin again.”
The unique approach to healing at Integrated Physical Therapy doesn’t just attract patients in Chester County and the Philadelphia area; it’s very normal for therapists to welcome patients from northern New Jersey, Northern and Western Pennsylvania and Delaware.
Very often, the first step to an individual’s method of healing can be found in the place where his or her body’s history resides: the body’s fascial area, a connective tissue that attaches, stabilizes, encloses, and separates muscles and other internal organs. “The fascial component of a body tells us everything about a person – the change in relationships between muscles, and the person’s posture, mobility and flexibility, and how it’s driving stress and strains into an area that’s dysfunctional,” Larry said. “By changing that paradigm, an individual’s posture, strength and core strength improves, and allows them to become more comfortable in their movement patterns.”
At Integrated Physical Therapy, healing doesn’t end when the pain ends. It’s the integration of a sound, responsive and healthy body that improves an individual’s overall vitality, mind and spirit, that begins with welcoming an individual to “own” their way back to health.
“Healthcare is trying to create these algorithms on how we standardize care, but the wild card in all of this is the person’s experiences and perceptions, and what they believe in their own mind,” Larry said.“Every patient has his or her own perspectives on their
individual health, but people will excel more often then not if they’re vested in what they’re doing – if they see that it is important and personal to them. Once that’s established, a person’s outcome will always be better.”
Physical Therapy
www.Integrated-PT.com
855 Springdale Drive, Suite 110, Exton, Pa. 19341 • (484) 874-2130
Monday-Thursday, 8 a.m. - 8 p.m. Friday, 8 a.m. - 4 p.m.
Offices also at 211 S Gulph RD, King of Prussia, PA (610) 265-2230
940 Haverford Rd Bryn Mawr, PA (610) 527-0178
Call today for a free consultation
Integrated Physical Therapy accepts most insurance plans



How you handle stress is a huge factor in the rest of your health as well as your overall quality of life; poor stress management can make you feel under the weather, exacerbate conditions you already have, interrupt your sleep, and cause you to have a shorter fuse in dealing with people or issues and feeling overwhelmed when dealing with problems.
If it goes on long enough, your brain is exposed to cortisol, which can weaken your immune system as well. The National Association of Mental Illness talked about stress, what to watch out for and how you can handle this normal part of life in a healthy way.
Like other conditions, stress can cause physical symptoms, including headaches, difficulty sleeping, jaw pain, appetite changes, frequent mood swings,
having difficulty concentrating and feeling overwhelmed and unable to deal with difficulties that come your way.
Stress is a part of everyday life, so it’s important to know where it is likely to come from in your life. Your job, family relationships, financial worries, school, health concerns, not getting enough sleep and not eating well can all lead to stress, which, while it may not be overwhelming at first, can
become that way if not handled well. On top of this stress, other life events can make you even more vulnerable, such as experiencing a major life change (moving, the death of a loved one, starting a new job, having a child, getting married), feeling alone or without a social network for support.
Everyone handles stress a little differently, so don’t feel bad if your friend’s way of coping doesn’t work for you.
NAMI suggested starting with accepting your needs — know what your triggers are, avoid them if possible or allow time and energy to handle them. Schedule your days so you have time to take breaks as needed, you’re getting enough sleep, you have time for hobbies or reading or other self-care; exercise; and eat well. Lean on your support network and consider talking to a therapist or support group. Be careful not to self-medicate with alcohol and drugs.

Weight is no one’s favorite topic, but it is an important factor in your health. Being overweight or obese puts people at greater risk of being diagnosed with chronic conditions like diabetes, arthritis and heart disease, it puts greater stress on your joints and can make exercise harder and have an overall greater sense of dissatisfaction with your health.

That means maintaining or reaching a healthy weight. According to the Centers for Disease Control and Prevention, what that number looks like is different for everyone; talk to your doctor to find out what range you should be in, and, as you’re making lifestyle changes, think more about how much energy you have, how your clothes are fitting and how you’re feeling than just the number on the scale.
Healthy weight management will not happen through fad diets or even short-term
changes. For most people, it doesn’t mean cutting out certain foods either. If you love cookies, any long-term diet that doesn’t include cookies isn’t likely to be successful for you. Instead, find a lifestyle that includes a mix of healthy eating and regular exercise.
The first step is to determine the number of calories you need in a day. The standard 2,000 recommended daily allowance is more than many American adults need.
Once you know your calorie count, start planning meals that
fit into your intake, provide the nutrients you need and taste good. A healthy diet is full of fruits, vegetables, whole grains and low-fat dairy products; lean meat like poultry and fish, as well as other lean proteins like beans, eggs and nuts; and is low in saturated and trans fats, cholesterol, salt and added sugars.
This necessitates avoiding processed foods, which means more cooking and meal preparation on your part, but there are shortcuts or different methods that will still taste good
and be healthy — use frozen, already sliced or canned fruits and vegetables (just make sure canned fruit is packed in juice, not syrup); substitute brown rice for white rice; and find healthier substitutions for ingredients in your favorite dishes or different ways of cooking, such as sautéing instead of deep frying food.
For high-calorie foods like desserts, chips, French fries, cheese and anything with butter, keep them as part of your diet, but cut back how much you eat and how frequently.

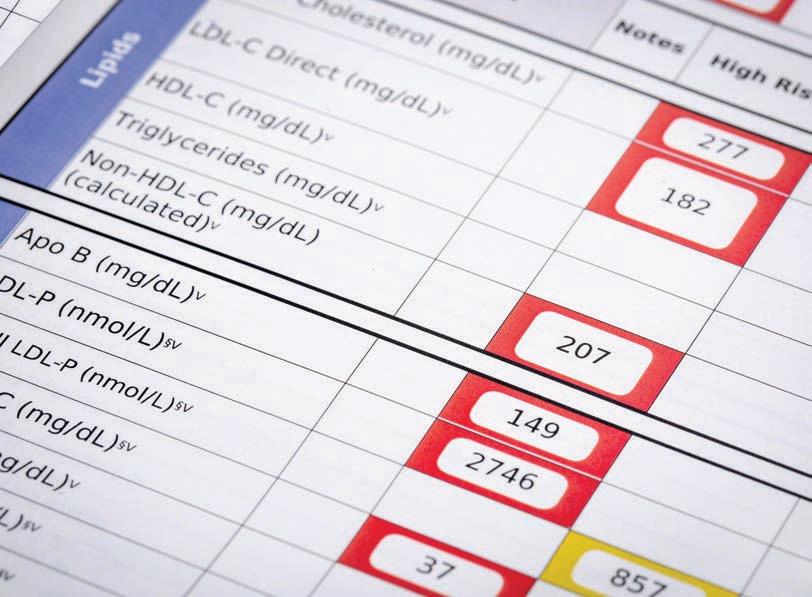
Every time you go to the doctor, she’s going to take a couple of numbers that can tell you a lot about your health. High cholesterol and high blood pressure can both lead to or be symptomatic of serious chronic diseases like heart disease, diabetes and stroke.
The CDC talks about both of these conditions, what to know and how you can make lifestyle changes to keep these numbers in a healthy range.
Blood cholesterol is a waxy, fat-like substance that your body produces naturally and uses to make hormones and digest fatty foods. Animal products like eggs, meat and cheese contain dietary cholesterol.
High cholesterol, which about one in six Americans has, could be caused by a number of factors, including family history, health conditions like obesity and lifestyle habits such as a diet high in saturated and trans fats, not getting enough exercise, smoking or drinking too much alcohol.
While there is medication to treat high cholesterol, you can make several lifestyle changes to manage your cholesterol more naturally. Eat foods that are low in saturated fats, like fruits, vegetables and whole grains; high in fiber, like beans; lean meats like fish and chicken; and foods with unsaturated fats like nuts and olive oil. Regular exercise, quitting smoking and keeping your weight under control also can help you manage your cholesterol.
High blood pressure, also known as hypertension, has two measurements: systolic blood pressure, the top number, measures the pressure in the blood vessels when the heart beats, and the bottom number, the diastolic pressure, measures the pressure in the vessels when the heart is resting between beats. A normal blood
pressure is 120/80; anything over 140/90 is high.
Hypertension can make your arteries hard, which means less oxygen is moving through your body, which can lead to heart attack, heart failure or a stroke. Left untreated, it can lead to chronic kidney disease.
Although about a third of Americans have high blood pressure, it doesn’t have any
symptoms, so without getting checked by a doctor, you may not know if you have it. There isn’t any one identifiable cause, in most cases, although genetics, age, obesity and a poor diet are contributors. To manage it naturally, it’s a similar diet if you’re watching your cholesterol, with the added measure of watching out for your sodium intake.

In 2020, Chester County Hospital will complete a 250,000 square foot expansion and 26,000 square foot renovation plan that will make world-class health care accessible to all of Chester County.
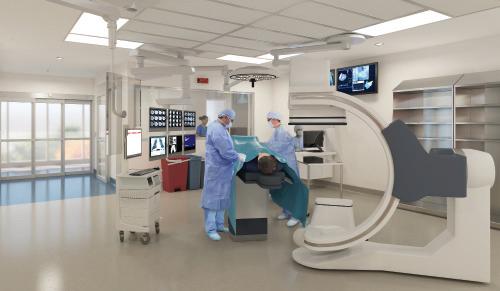
The project will include 15 state-of-the-art operating rooms, three high-tech labs for cardiac catheterization and electrophysiology, and new areas for interventional cardiology and pre-admission testing. These additions will aid the hospital’s nationally recognized medical staff, nurses and care teams in providing the highest quality care possible to patients.
The expansion will also include a 99-bed tower featuring private patient rooms for peaceful healing, an expanded Emergency Department with thirteen additional rooms for expedited care, a new community pharmacy, calming public spaces and interior courtyard, and additional dining and shopping options in the new café bistro and Gift Shop.
Planning an expansion of this size and complexity requires consensus building among multiple stakeholders. To get a true idea of the time and effort that has been invested, imagine the undertaking as an iceberg and the construction as the tip that sits above the water’s surface. We physically only see a small part of the larger picture.
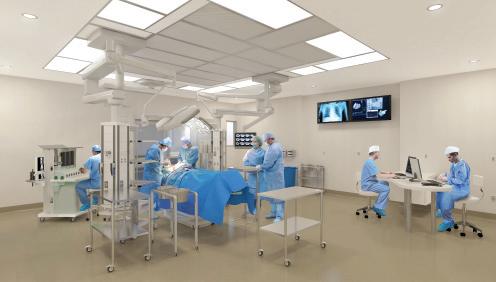
For over two years, beginning in 2015, the hospital engaged architects, clinicians and other stakeholders to seek their input on areas throughout the hospital, including the operating rooms, Post-Anesthesia Care Unit, Intensive Care Unit, patient rooms and Emergency Department. Both 3D models and full-scale mock-ups were utilized to test and ensure that the design was optimized for the experience of both the medical provider and the patient.
The planning committee also incorporated concepts from evidence-based design to plan for the ultimate healing environment. For example, operational ow mapping from the patient experience perspective revealed opportunities to eliminate unnecessary steps, allowing caregivers to provide more effective direct patient care.
The design meetings concluded before the start of construction. Similar planning sessions are expected to begin in the coming months, but this time they will address how to best incorporate new and updated spaces into the rest of the hospital so they function seamlessly.
The expansion will promote an environment that fosters healing by giving patients and their families choice and control, and offers care providers a compelling place to work.

This new space will resonate with the needs of patients, families and medical providers and will support the values of a community-based hospital. Chester County will bene t from having urban innovation right here in the suburbs. The expansion will allow more space for the most sophisticated medical procedures, provide more personalized care for inpatients, increase the patient care space in the Emergency Department and allow local residents and the surrounding communities to stay close to home to receive the highest quality of care.
“The community we serve relies on our mission-based approach to care, our reputation for quality, and our history of providing advanced clinical services,” said Michael J. Duncan, President and CEO of Chester County Hospital.
“This expansion project, which is a tes-

tament to Chester County Hospital’s partnership with Penn Medicine, highlights the hospital’s and the health system’s commitments to expand lifesaving treatments and programs in the community. The venture also accommodates anticipated growth and will continue the hospital’s movement towards world-class health care for all of Chester County,” Duncan added.

It is an elegant, forward-looking design rooted in the hospital’s architectural tradition as well as its lasting mission: To be the leading provider of care in the region and a national model for quality, service excellence and scal stewardship.
For more information, visit ChesterCountyHospital.org/ Expansion
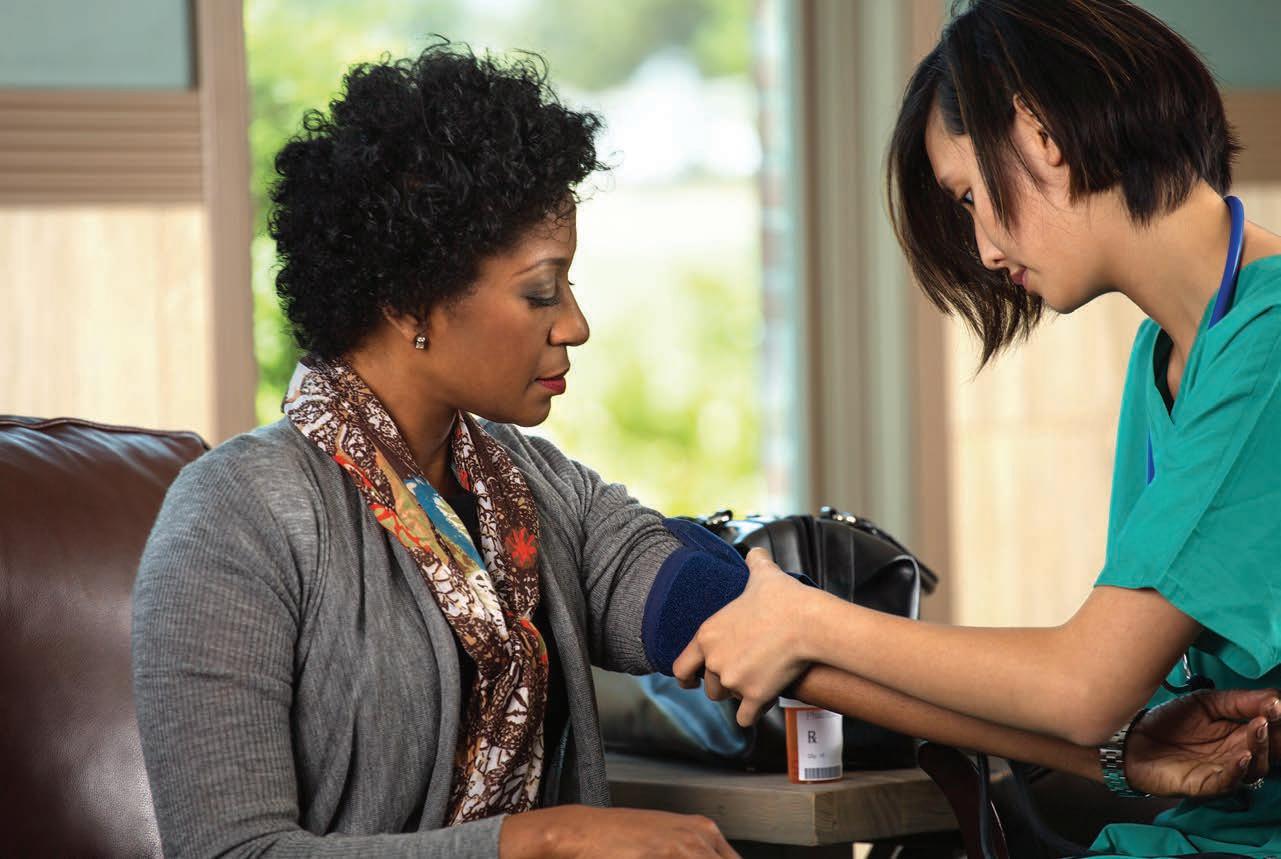
Taking your blood pressure is one of the first tasks your doctor does when you arrive for any appointment.
It can be a cause for concern for many people; high blood pressure, or hypertension, can increase a person’s risk for heart disease and stroke, two of the leading causes of death for Americans. The Centers for Disease Control and Prevention talks about what you need to know about blood pressure. Blood pressure is measured by two numbers. The systolic blood pressure, the number that comes first, measures the pressure in the blood vessels when the heart beats. The second number, diastolic blood pressure, measures the pressure in the vessels when the heart is resting between beats. A normal
blood pressure is 120/80. When it reaches 140/90, that is considered high blood pressure.
The risks of high blood pressure
About a third of American adults have high blood pressure. There are no symptoms, so getting it checked regularly (if not at the doctor’s office, many pharmacies have blood pressure machines) is likely the only way to know if you’re at risk. Hypertension can harden your arteries, which means less oxygen-carrying blood is getting to your heart and brain. This can lead to chest pain, heart failure or heart attack, or burst arteries to the brain, causing

a stroke. Untreated high blood pressure can also contribute to chronic kidney disease.
Causes of high blood pressure
Most adults with hypertension don’t have an identifiable cause, according to the Mayo Clinic. This type, called primary hypertension, tends to develop gradually over time, with risk factors like age, genetics, being overweight, not eating a healthy diet or using tobacco. Secondary hypertension is caused by an underlying condition like kidney problems, genetic defects, certain medications or thyroid problems, and it tends to appear suddenly and cause higher
blood pressure than primary hypertension.
Preventing or treating high blood pressure
There are a number of nonmedical options to control hypertension. A healthy diet that is low in salt, fat and cholesterol, and full of fresh fruits and vegetables can help to keep your blood pressure low. Physical activity can help as well. If you’re not exercising at all right now, ease into it with short, brisk walks a few times a day five days a week. There also are medications that treat high blood pressure. Talk to your doctor about what treatment regimen is best for you.

It’s not just feeling sad, anxious, worried or stressed. Depression and anxiety are serious mental illnesses that require the same level of treatment and care that a physical illness does. A quarter of the U.S. population suffers from either anxiety or depression, according to the National Association on Mental Illness.
About 18 percent of adults and 8 percent of children and teens suffer from an anxiety disorder, making it the most common mental health concern in the country. There is not one disease; the spectrum of anxiety disorders share a persistent, excessive fear or worry in situations that should not be threatening. Other symptoms could include:
• Feeling tense or jumpy.
• Restlessness or irritability.
• Feelings of dread or apprehension.
• Anticipating the worst and signs of dangers.
• Pounding or racing heart, shortness of breath.
• Sweating, twitches, shaking.
• Headaches, fatigue, insomnia.
• Upset stomach or frequent urination.
Anxiety disorders can be caused by genetics or stressful or traumatic life events. It can be hard to diagnose because the physical symptoms of anxiety often look like heart disease or other conditions. Treatment can include therapy, prescription medication and treatments like relaxation or stress-management techniques.
Almost 7 percent of the U.S. population has depression, according to NAMI. Depression looks different depending on the person, which can make it hard to diagnose. Common symptoms are:
• Changes in sleep patterns and appetite.
• Difficulty concentrating.
• Loss of energy or interest in activities.
• Hopelessness.
• Physical aches and pains.
• Thoughts of suicide or suicidal ideation.
• Fatigue.
• Feelings of guilt or low self-worth.
Science also hasn’t found a determinant cause for depression. It can be brought on by a life event, such as a crisis or a physical illness, but often it’s not triggered by anything. Early life trauma, genetics and drug and alcohol abuse can cause actual changes in the brain, which can lead to depression.

While treatment for depression often is as unique as the symptoms, most people do find relief either on their own or by
combining different strategies.
Cognitive behavioral therapy and interpersonal therapy and medications like antidepressants and mood stabilizers are often prescribed. Exercise can help with prevention and mild symptoms.



Not your ears.
orient recognize focus separate


For more than a century Friends Home in Kennett has opened its doors to senior members of the community. Located at 147 West State Street in the heart of Kennett Square, last year it has marked its 120th anniversary. Though of Quaker origins, persons from all religions are welcomed. Christine Mc Donald, Executive Director noted that: “everyone – staff, volunteers, and the Board of Directors – associated with Friends Home are dedicated to fulfilling the Home’s mission of providing quality, affordable care for seniors.”
As the needs of residents changed and increased, so have the programs and services offered by Friends Home. Independent Living one bedroom apartments offer residents the opportunity to be a part of the Friends family while continuing to be independent. The invitation to join in trips and activities, head into town for a meal – or join others in the dining room, give the feeling of belonging. Also, as a fully licensed Personal Care facility, residents with basic physical and/or minor cognitive care needs choose studio or one bedroom apartments in the main building of Friends Home. All residents are individually assessed before acceptance to be certain their needs fall within the scope of our service. In addition to amenities such as housekeeping, laundry, Personal Care residents receive assistance with basic personal care. According to McDonald, “it is not about filling rooms – never was – it is important to us to know that we can and do have residents
that can safely benefit from our programs and services.”
A third facet of Friends Home is its licensed skilled nursing unit, Linden Hall which features private and semi-private rooms with a capacity of 20 residents. Though consideration is given to current residents in need of skilled care, when there is availability, we welcome all who wish to apply to be a member of the family.
Most recently, Friends Home recognized that a piece was missing. Soon to open is the Supportive Independent Living wing in the Garden Court section of the building. Persons who choose and are accepted into the SIL will have the best of both worlds. The independence of apartment living, without the need to walk between buildings for meals. They also can have limited medical or care needs and, as in the case of Independent Living, small pets are permitted on a case-by-case basis. Should more care be needed, they simply relocate to the Personal Care floor.

There is little comparison to the other communities in Chester County, Mc Donald offered. Some are large enough that they are pretty much self-sufficient. But those often require a large upfront pay-in and can also lack a neighborhood feel.
“Another thing is a lot of people want that walkability,” she said, pointing out the community’s prime location on State Street in Kennett Square. “They don’t want to necessarily be isolated. We’re never going to have a pool, but we have memberships to the YMCA. We’re not going to have a huge

library – we have a little library – but we go to the [Kennett] Library twice a month right up the street.”
A food court/market, bank and barber shop are all within walking distance, and some Friends Home residents take advantage of that. “We utilize the town, and as long as it’s deemed safe, our residents are free to go. One woman walks to church every Sunday,” McDonald said.
Residents also want to contribute to the community. “We have a lot of people who want to help out, so we try to do volunteer things. They want to be part of something larger than themselves,” McDonald said.
Friends Home is also making improvements and additions. There has been work on a four-season porch at Linden Hall as well as a covered connection between buildings. We are one community regardless of care level. The new connection will assist residents and visitors to walk comfortably from one building to the other. A bus was purchased to take residents on trips, and they’ve increased staff in the Community Life department, offering activities daily. “We have a lot of people here interested in gardening, so we’re looking to get a greenhouse,” she said.
McDonald said because of the Home’s longevity in the community, it’s offered many area residents peace of mind.
“There’s never been a concern that you would be cared for here at Friends Home,” she said, “and that’s what we want. A lot of people have lived [in the Kennett area] their whole lives and they said they always knew when the time came, they were going to move here. Or sometimes the children live in Kennett, and they say, ‘when Mom or Dad need help, I want to bring them back here.’
“It’s always had a reputation for excellent care. It’s not the fanciest, but the care and caring is there. A lot of staff are local Kennett people. Several of us walk to work. Several people have family members here. Some of the names have, for 50, 60, 70 years, been associated with the Friends Home.
“You know, when I first started, somebody who was in marketing


at a [larger] place told me, ‘You’ve got to change the name,’ because nobody calls them homes anymore.
“But I don’t think it’s a bad word,” McDonald said. “Because people come and go, their families come and go. People stop by and say ‘Hi.’ It’s very comfortable. This is their home.”

Maybe you’re in the thick of summer vacations, travel, kids being out of school and routines upended — or maybe it’s a normal day of work, school, family obligations, community service and more.
Taking care of yourself is critical. The National Association on Mental Illness compares it to putting on your own oxygen mask in an airplane before you can help anyone else. This is especially true for caregivers, doctors, counselors and others in a caring profession, but it’s a good skill for everyone to have.
Get enough sleep
The CDC recommends seven hours or more a night for adults. It’s not just about the hours logged, though; the quality of sleep is important as well. Signs of poor sleep quality are not feeling rested even after getting seven hours, waking up multiple times during the night, snoring or gasping for air. Ways to ensure good sleep habits are going to bed and getting up at the same time each day; having a quiet, dark bedroom; getting TVs out of the bedroom; and avoiding large meals, caffeine and alcohol before bedtime.
Stress management
Eliminating stress entirely is impossible, but using effective stress management techniques can help you alleviate negative health effects. The Mayo Clinic recommends identifying stress triggers (both positive and negative), then identifying what

you can control, even if it’s simply your reaction to that trigger. Cultivate a support group; practice deep breathing, yoga or other relaxation techniques; exercise regularly; and spend less time in front of a screen.
Eating well and exercising regularly
Eating a healthy, balanced diet can have positive effects
on any number of conditions like diabetes and heart disease and obesity, but it can also just make you feel better generally and give you more energy. Regular exercise offers the same benefits. This could be mountain climbing, running marathons or triathlons or other high-intensity exercises, but don’t discount the benefits of walking, yoga and other low-intensity exercises. All of it will help you feel better.
Pay attention to your body
Going to the doctor or needing a sick day rarely happens at a convenient time, and it’s easy for us to put those off. Depending on the ailment, though, not taking care of yourself can make it worse. Listen to what your body is telling you, take a rest day, see a doctor or otherwise do what you need to do so you can be healthy.


Heart disease is the No. 1 cause of death for Americans, for both men and women and most ethnicities; for American Indians and Asians/Pacific Islanders, heart disease is second to cancer in causes of death. More than 600,000 people die of heart disease every year; that represents 25 percent of all deaths in this country.
The good news is that while some aspects of heart disease are hereditary and all risk factors can’t be fully controlled, there are a number of lifestyle changes that can reduce the risk of a serious heart condition, like a heart attack, or help protect yourself from acquiring a heart condition. And, while heart disease looks different in everybody, there are symptoms to watch for. Since early action is critical in treating heart disease, that knowledge can save a life.
Most people recognize that chest pain is symptomatic of a heart attack, but there are other signs to look for as well. Pain or discomfort in the arms, back, neck, jaw or upper stomach; shortness of breath and nausea, lightheadedness or cold sweats all could indicate a heart attack. Women with heart disease are more likely to report chest pain that is sharp or burning. When in doubt, it’s better to seek treatment immediately. Almost half of sudden cardiac deaths occur before a person

can get to a hospital, which likely means early warning signs were ignored.
High cholesterol, hypertension and smoking are the major risk factors for heart disease; the CDC said about half of people with heart disease have at least one of these risk factors. Other chronic conditions or lifestyle choices that are risk factors are diabetes, being overweight or obese, having a poor diet, not getting sufficient exercise and excessive alcohol use.
Healthy habits like a balanced diet (whole foods with lots of color on your plate that comes from fruits and vegetables, not colored candy), getting plenty of exercise, quitting smoking and reducing your alcohol intake all reduce your risk of heart disease or a heart attack. You also want to keep your cholesterol, blood pressure and diabetes under control; take any medication you should be and see your doctor regularly.
Diabetes mellitus is a condition in which the body isn’t able to pull glucose out of the blood, which is how the body gets energy into the cells.
There are two types of diabetes. Type 1 diabetes, previously known as juvenile diabetes, is usually diagnosed in children and young adults. The body doesn’t produce insulin, which is needed to get glucose out of the bloodstream. It can be treated with insulin therapy. Only about 5 percent of diabetics have Type 1 diabetes. In Type 2 diabetes, the far more common form of the condition, the body produces insulin but doesn’t use it properly, so glucose builds up in the blood. This means your cells don’t get enough energy, and in the long term, high blood glucose levels can damage the eyes, kidneys, heart or nerves. While doctors can’t point to a single factor that leads to Type 2 diabetes, they have identified a number of risk factors, including being overweight or obese, not being physically active, high blood pressure or high cholesterol. There also are non-lifestyle factors. As people age, there is an increased risk for diabetes. African-Americans, MexicanAmericans, American Indians, Native Hawaiians, Pacific Islanders and Asian-Americans have a higher risk for Type 2 diabetes, as well as heart disease and stroke. People with immediate family members who have Type 2 diabetes are

at greater risk as well.
Type 2 diabetes isn’t always noticeable. The symptoms make come on slowly and often don’t offer a perfect match. The ADA estimates more than 7 million people who have diabetes are undiagnosed. Symptoms of Type 2 diabetes include frequent urination and feeling hungry and thirsty, blurred vision, cuts and bruises that are slow to heal, weight loss and tingling, pain or
numbness in hands and feet.
Often people with Type 2 diabetes can control their blood glucose levels through non-medical means like balanced, healthy eating and physical exercise. However, Type 2 diabetes often gets worse over time, so many people need medication; your doctor may prescribe oral medications or insulin.
Pregnant women with high blood glucose levels during
their pregnancy have a condition known as gestational diabetes, which the CDC estimates affects almost 10 percent of pregnant women. Doctors believe hormones from the placenta block the action of the mother’s insulin. It may also occur when the mother’s body can’t make all the insulin it needs. Pregnant women should be tested and gestational diabetes can be treated fairly easily.


Influenza isn’t just a cold on steroids. This disease, which resurfaces every fall and can be a health risk well into the next spring, can knock even the healthiest people out of commission for a week to 10 days.
While flu can be dangerous to infants, elderly adults, pregnant women and people with weakened immune systems or chronic illness, for most people it’s not deadly, just extremely unpleasant. It’s good to be aware of the symptoms and know how to treat them.
According to the Mayo Clinic, early symptoms of the flu appear like a common cold, though they are likely to come on quickly and then get much worse than a cold. Common symptoms of the flu include a fever higher than 100 degrees; aching muscles;
chills and sweats; headache; a dry, persistent cough; fatigue; weakness; nasal congestion; and a sore throat.
Most people with the flu don’t need to see a doctor; stay home for at least a full day after your fever subsides (your coworkers and fellow students will thank you), rest, drink lots of fluids and treat the symptoms as necessary to remain comfortable. If you or a family member are at risk of complications, see a doctor immediately. Taking antiviral drugs within the first two days may shorten the length of your
illness and help prevent other problems.
Those who are at risk and should seek medical care include the elderly and very young; people who live or work in facilities like hospitals or nursing homes; people with weakened immune systems, like those who have cancer or are going through chemotherapy; people with chronic illnesses like asthma, diabetes or heart disease; pregnant women; and people with obesity.
Getting a vaccine is your first and best option for prevention; it makes you less likely to get
sick and likely will reduce the severity of the illness if you do get sick. Other ways to prevent the spread of disease is regularly washing your hands, using alcohol-based hand sanitizer if soap and water aren’t available; cover your mouth and nose when you cough or sneeze; and avoid crowds. Flu spreads more easily when people are close to each other, such as in child care centers, schools, auditoriums, public transportation, and perhaps most importantly, doctor’s offices and emergency rooms during flu season.

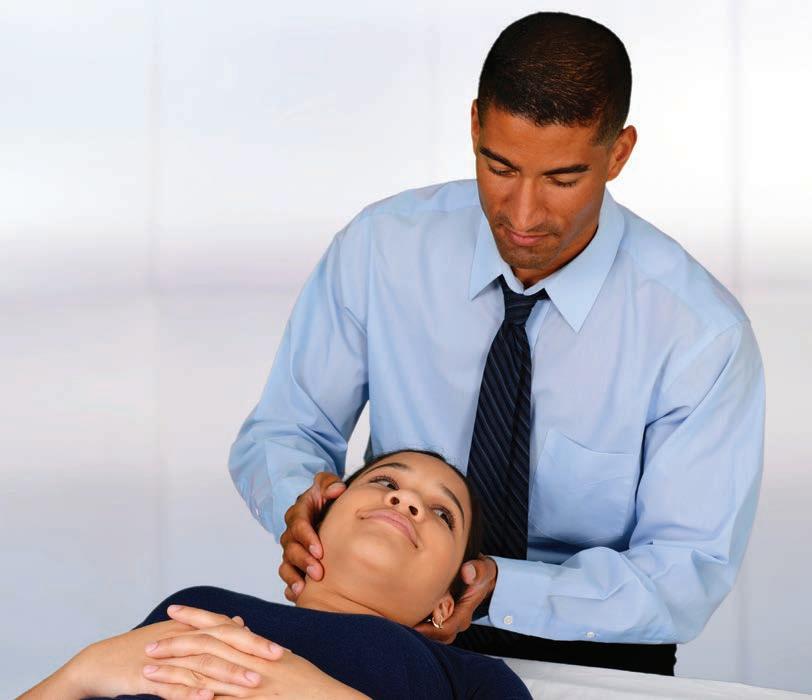
Trained to carefully examine and treat muscles, joints, connective tissue and bones, chiropractors can identify and relieve the underlying causes of pain.
Trained to carefully examine and treat muscles, joints, connective tissue and bones, chiropractors can identify and relieve the underlying causes of pain.
Chiropractic specialties can vary across practices, but most professionals are focused on alternatives to drugs or surgery, restoration of nervous system functions, pain relief, pediatric care solutions, massage therapy and relief of headaches, digestive issues, insomnia and asthma.
How do you know if a visit to the chiropractor is right for you?
Chiropractors can offer treatment to alleviate pain, whether you were hurt in a vehicle accident or have recently been experiencing painful symptoms caused by some other source.
What Does a Visit Cost?
Visits vary by practice but can actually save you money in the long run, depending on your medical conditions. That’s because chiropractors don’t prescribe medications or perform expensive surgeries.
Chiropractic care also can help you minimize or avoid the need for lengthy or costly physical therapy. By making adjustments or offering alternative solutions, a chiropractor may be able to keep you out of the operating room.
Call around to different chiro-
practors in your area to ask about rates and find out if your issue can be treated in their offices.
More than Pain Relief
Many chiropractors offer health and wellness programs that focus on not only your physical health but your men-
tal and psychological health, as well.
Most chiropractors encourage you to make lifestyle changes that will improve your health, which in turn can decrease your susceptibility to injury and pain. Everyone knows that people who are more physically active generally have less stress and anxiety in their lives. Because chiropractors encourage exercise and increased physical activity to help alleviate pain, visiting one can lead to positive changes that contribute to an overall better quality of life.

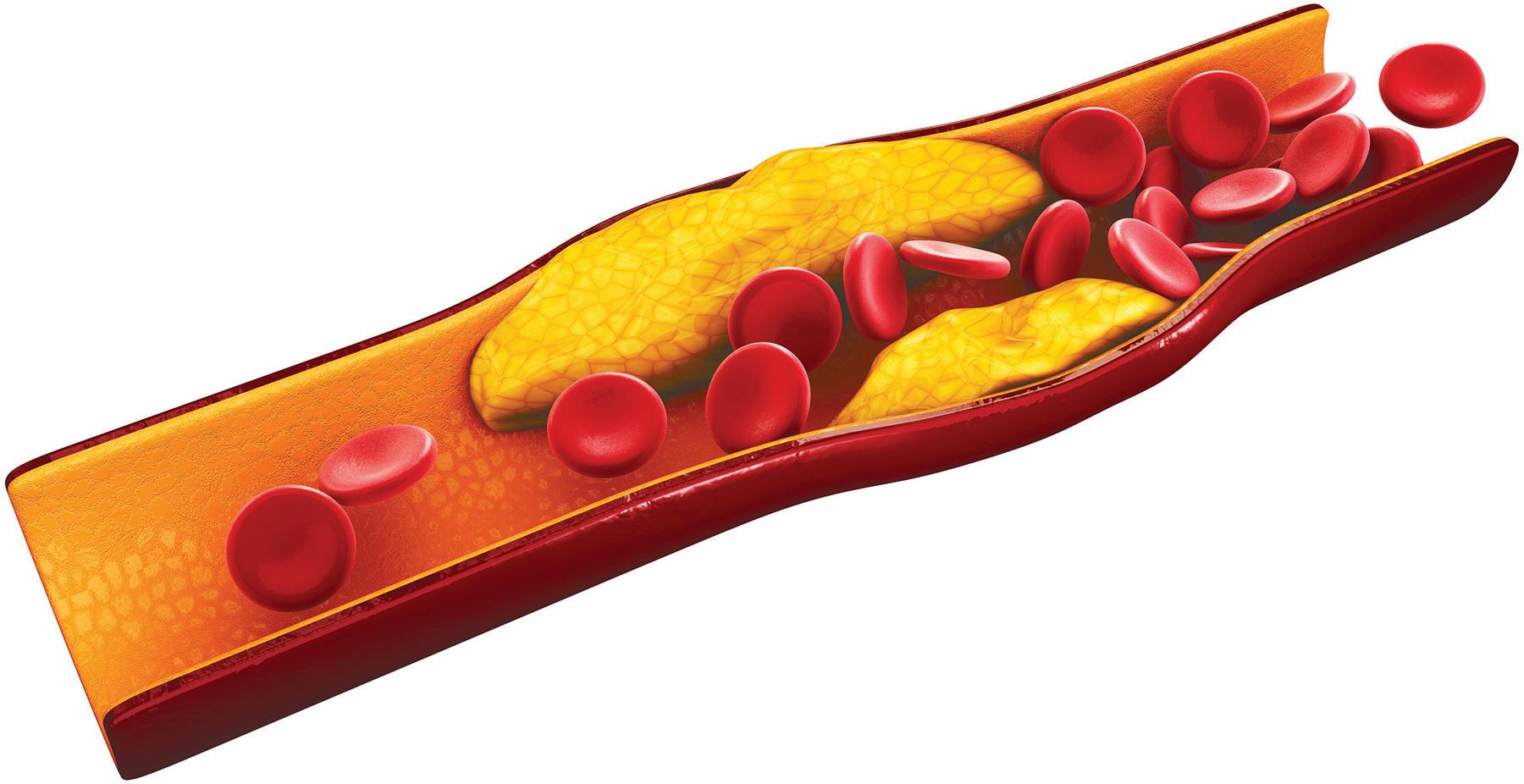
Too much of it can lead to a greater risk of heart disease and stroke.
Your body makes cholesterol in your liver and uses it. Dietary cholesterol is found in animal products like egg yolks, meat and cheese.
About one in six American adults has high cholesterol, which doesn’t manifest itself through any symptoms; your doctor will do a blood test to measure it.
Types of cholesterol
There are two types of cholesterol – low-density lipoprotein, known as LDL or
bad cholesterol, is most of the cholesterol in the body. High levels of LDL can increase the risk of heart disease and stroke. Too much LDL can build up on the walls of blood vessels; this buildup, called plaque, can cause blood vessels to narrow.
High-density lipoprotein, or good cholesterol, absorbs LDL and takes it back to the liver, which then flushes it from the body. High levels of HDL lower the risk of heart disease and stroke.
Risk factors for high cholesterol
High cholesterol could be
due to family history, lifestyle choices or certain health conditions like diabetes or obesity. Lifestyle factors that can contribute to high cholesterol include eating a diet high in saturated and trans fats, not getting enough exercise, using tobacco or drinking too much alcohol. Family history can also play a role, although that’s likely a combination of genetics and having a similar lifestyle.
cholesterol
Just as an unhealthy lifestyle can put you at greater risk of high cholesterol, a healthy
lifestyle can help you manage cholesterol. A diet that is low in trans and saturated fats — particularly from animal products — and added sugars, while eating lots of fruits, vegetables, high-fiber foods like beans, lean meats like fish and unsaturated fats like avocado, olive oil and nuts.
Regular exercise, limiting alcohol, giving up smoking and maintaining a healthy weight also can help control cholesterol. Talk with your doctor to determine if lifestyle changes will be sufficient or if you may need medication to control high cholesterol.
We’re outdoors more, enjoying nature and the sun and waterways and eating picnic food that may or may not have been cooked or stored properly. While it can be a lot of fun, it can also lead to various illness and conditions that can sideline your or your family for a weekend. Take steps to keep yourself healthy this summer.
More people outside means more infections from insect bites, which the CDC reported has increased at surprising rates in recent years. In 2016, almost 100,000 disease cases came from infected mosquitoes, ticks and fleas — triple the rates of a decade ago. Some of that could be attributed to new illnesses or diseases that have traveled from other countries.
To avoid infection while still enjoying the outdoors, always use insect repellent; wear long-sleeved shirts and pants when outdoors; treat boots, pants, socks and tents with permethrin; appropriately treat and frequently check pets for fleas and ticks; and take steps to keep your yard and surrounding areas free from pests.
Sun protection
It sounds simple, but protecting your skin from sun damage can drastically decrease your risk of skin cancer. According to the CDC, nearly 5 million Americans are treated for skin cancer annually. While most skin cancer is very treatable, it still costs upwards of $8 billion each year — and most of the damage could be prevented through proper care.
The CDC recommends
sunscreen of at least SPF 15 with frequent reapplication, covering all of their exposed skin (that includes the hairline, top of the head, ears, top of the feet and anywhere else the sun could hit). Wear a hat with a brim and take frequent breaks in the shade to stave off sunburn.
It’s the season of picnics, barbecues and potlucks — lots of opportunities to make or eat food in less than ideal conditions, which can lead to foodborne illnesses. One of the biggest culprits is mayonnaisebased foods like potato salad that
spent too long out of the fridge and spoiled. Make sure to keep foods at the proper temperatures and keep raw meat away from vegetables and fruit salads. Cook foods to the right temperatures and don’t let anything sit out too long. Wash your hands and cooking surfaces often.
Have you ever wondered what varicose veins actually are and how they come about? When once healthy vein walls become weakened over time, the vein grows in size leaving the valves unable to do their job properly. The vein becomes large and swollen, particularly in the legs, and can lead to symptoms such as itching, swelling, and/or a
tired and heavy feeling. In more severe cases, thrombophlebitis can occur. This happens when the blood sits in the large veins because it is not being returned up the leg properly and a clot forms in the superficial veins. Vein disease is progressive and if left untreated, it can lead to chronic swelling, discoloration and venous ulcers.
The first line of defense
in properly diagnosing varicose veins is with an ultrasound. The ultrasound will rule out any evidence of thrombus but also look at the superficial veins in detail. The varicose veins are often an issue that is secondary to venous reflux in one of the main superficial veins. Once the problematic vein is identified, a proper treatment plan can be devel-
oped. This often involves the closure of any refluxing veins, then focusing on the bulging varicosities that are the result of the severe venous insufficiency. Treatment of varicose veins may be different for each patient. Depending on the size and location of the individual's vein, the doctor will determine which option will be the best fit.

The two main treatment options that we offer differ in many aspects. Ultrasound Guided Sclerotherapy is a minimally invasive procedure that leaves a portion of the work for your body to take care of on it's own. Ambulatory Phlebectomy is a more involved procedure, however, the vein is permanently removed at the time of your visit.
Ultrasound Guided Sclerotherapy is one treat-
ment option which involves the injection of a medication directly into the varicose vein. This medicine will cause the blood within this vessel only to thrombose or clot off. The body's instinct is to then fight this clot, break it up and reabsorb it over time. The medication used is referred to as a sclerosant and different concentrations are used depending on the vein size.
Another treatment option
is Ambulatory Phlebectomy. This is a procedure that involves multiple small incisions through which the varicose vein is then removed in sections. This procedure is minimally invasive and can be performed in the comfort of our office. We use local anesthesia and offer the option of nitrous oxide (laughing gas) for ambulatory phlebectomies which help to relax the patient for a com-
fortable experience. We offer free verbal vein screenings each month to allow patients to express their concerns about their veins. This gives patients the opportunity to ask questions which helps us to better navigate you through the process of properly treating your venous insufficiency. Come to one of our FREE vein screenings or call (302) 731-0001 to schedule a free consult today.


Ditch the fad diets, the CDC recommends, and go for slow and sustainable weight loss — one to two pounds a week. Not only is this better for your body, but you’re more likely to keep the weight off. You’re not looking for a diet so much as a healthy, long-term lifestyle change.
This should include both different eating habits — more fruits and vegetables, fewer processed foods and fats — as well as regular exercise.
Even losing a small amount of your body weight can contribute to greater overall health, including lower blood pressure, cholesterol and blood sugars, all of which are risk factors for chronic conditions like diabetes and heart disease. People who lose weight also report better energy levels, physical mobility, mood and self-confidence.
Cutting back your calories is the biggest factor in weight loss, but doing it smartly means you won’t be hungry all the time. Eat lots of fruits, vegetables, whole grains, lowfat or fat-free dairy products, lean meats such as poultry and fish and other lean proteins, such as beans, eggs and nuts, while keeping your diet low in saturated and trans fats, cholesterol, salt and added sugars.
Healthy eating often requires more preparation, so look for shortcuts and plan ahead. You
can eat frozen and canned fruits and vegetables (though make sure canned fruit doesn’t have any added sugar) On your day off, make food that can be frozen and reheated. You can also substitute foods like whole wheat pasta and bread in your favorite recipes.
Tracking your calories can be very beneficial, as can measuring out your food so you’ll know exactly how much you’re eating. There are a number of mobile apps or websites that allow you to track your food and keep tabs on calories for you.
Most weight loss comes about from eating fewer calories, but exercise means burning more calories and quicker weight loss without having to cut out quite as many calories. To maintain weight, set a goal of 150 minutes of moderately intense aerobic activity per week. Moderate exercise means your breathing and heart rate are faster but you can still carry on a conversation. Build your way up to this if you don’t exercising regularly already.



Many people are familiar with the vaccination schedule for children, but did you know that adults need vaccines as well? According to the CDC, immunity from childhood vaccines can wear off, requiring boosters. Additionally, adults are at risk of different diseases than children are so require different vaccinations.
These shots are among the most convenient, effective and safest preventative care options available, particularly for people who are traveling to exotic places or working with at-risk groups.
Vaccinations are generally covered by health insurance.
What Vaccinations Do I Need?
Adults and children should get a flu vaccine every year. Protection doesn’t last from year to year because the flu virus mutates; scientists determine the strains of the virus that are most likely to infect people each year and prepare a vaccine for those strains. Although getting a vaccine doesn’t guarantee you won’t get sick, those who get the flu will likely be less sick if they got the flu shot.
The Tdap vaccine protects against whooping cough, tetanus and diphtheria and is safe for use in adults and children older than 7 years. Other routine vaccinations include the measles-mumpsrubella, chicken pox and polio vaccines. Most people get those as children.
Depending on where you’re traveling, certain vaccinations
are recommended or may even be required. The CDC recommends hepatitis A and typhoid vaccines when traveling to Mexico, for instance, as contaminated food or water could be a risk. Parts of Africa have an increased risk of cholera, and jungle areas are full of mosquitoes, so getting vaccinated for malaria is a good idea.
Talk to your doctor about activities that could put you at risk for other diseases. Travelers
who may come into contact with wild animals should consider a rabies vaccination. Depending on where you’re going and what you’re doing, meningitis, yellow fever and hepatitis B may be an issue. Check the CDC’s websites for recommended and required vaccines.
Getting a vaccine while pregnant also offers your baby
that protection, so the CDC recommends pregnant women get vaccinated for whooping cough and, if appropriate, the flu. Newborns do not get vaccinated for whooping cough right away, and this disease can be deadly for them. Other vaccines, like the MMR, should happen before pregnancy.
It also is safe to get vaccines while breastfeeding. Talk to your doctor about questions.






Introducing the Next Generation of Care.
We’re undergoing our largest expansion yet, implementing programmatic innovation to bring new possibilities for all who come to us for care. With 250,000 square feet of progressive design, we’re not only building a better space for healing, we’re defining the future of medicine in our community. Another reason your life is worth Penn Medicine.
See what’s coming.
ChesterCountyHospital.org/Expansion