

Beyond The Pitt:
A Moment of Visibility and Unity for Emergency Medicine
SCIENTIFIC ASSEMBLY HIGHLIGHTS


EDITORIAL STAFF
Victoria Selley, MS, DO, FACOEP, Editor
Regina Hart, DO, Assistant Editor
Ariana Cranston, OMS-IV
ACOEP-RSO Student Social Chair
Amanda Mahan, MA, ACOEP Executive Director
Megan Heller, ACOEP Association Manager
Claire Krzyzewski, Graphic Designer
The Pulse is a copyrighted quarterly publication distributed at no cost by ACOEP to its Members, Colleges of Osteopathic Medicine, sponsors, exhibitors, and liaison associations recognized by the national offices of ACOEP.
The Pulse and ACOEP accept no responsibility for the statements made by authors, contributors, and/ or advertisers in this publication; nor do they accept responsibility for consequences or response to an advertisement. All articles and artwork remain the property of The Pulse and will not be returned.
Display advertisements are accepted by the publication. Please contact ACOEP at info@acoep.org for the specific rates, due dates, and print specifications.
Deadlines for the submission of articles are as follows: January issue due date is November 15; April issue due date is February 15; July issue due date is May 15; October issue due date is August 15. The Editorial Board of The Pulse reserve the right to decline advertising and articles for any issue.
©ACOEP 2026 – All rights reserved. Articles may not be reproduced without the expressed, written approval of ACOEP and the author.
ACOEP is a registered trademark of the American College of Osteopathic Emergency Physicians.
5
16
18
PRESIDENT’S REPORT
Benjamin Godfrey, DO, FACOEP-D
A MESSAGE FROM THE PRESIDENT-ELECT
John Dery, DO, FACOEP-Dist, FACEP, FAWM
EXECUTIVE DIRECTOR’S DESK
Amanda Mahan, MA
WOMEN’S COMMITTEE UPDATE
Jacqueline M. Dziedzic, DO, FACEP, FACOEP
WELLNESS COMMITTEE UPDATE
AAO’s Osteopathic Education Service at SA25 20
ACOEP PRACTICE ADVOCACY COMMITTEE UPDATE
Jeremy Selley, DO, FACOEP

This is my first President’s Message, and to be transparent, I am having difficulty deciding what to write to you all about. First, I want to thank all of you for your continued support. Thank you for re-electing me to my final term on the Board and allowing me to serve as your President this year. The past six years have been a valuable learning experience, and I have had the pleasure of meeting and working with some stellar members.
Our specialty prides itself on improvising, adapting, and overcoming the challenges before us. As a night shift doc, working in the trenches, I definitely see a lot of challenges… workplace violence, the rise of AI, CMGs and their increasing reliance on APPs over physicians in the name of profit, the continued loss of reimbursement and revenue over time due to government cuts which are then compounded by inflation, to name a few. On the other hand, what a time to be alive and working in healthcare!
As a matter of keeping you informed, I was privileged to participate in the All EM AI Summit in fall of last year. Most of the stakeholders were present (ACEP, ACOEP, AAEM, ABEM, AOBEM, CORD, EMRA, SEMPA, to name a few). Together, we started creating the framework and guardrails for AI use in the EM space to increase our capabilities, protect our patients and protect our role and jobs in the future. AI has the
PRESIDENT’S REPORT
Benjamin Godfrey, DO, FACOEP-D
PRESIDENT’S REPORT
promise of making our jobs easier from an information gathering and documentation standpoint, a potential to improve our decisionmaking skills in real time and effect innovative and personalized care for our patients. However, like any tool, it’s all in how it’s used. We do not want our physician decision making and prescribing data to be collected, aggregated by third party corporations and then used to create a virtual physician, displacing the physical physician from the bedside.
The technology and science at our fingertips are impressive, but it is nothing without us… the end user, operator and interface between the patient and The System. This is where we can shine! The more we can focus back on the patient, listen to their stories, fill in the missing pieces, and guide them towards health, the better it will be for everyone.
I was recently working an overnight moonlighting shift at a facility about one hundred miles from my home. I had a 17-year-old female, brought it by her parents for intractable vomiting for months. The parents were adamant that the patient be admitted, as they were at their wits end. The patient had a history of multiple psychiatric problems and reported that she had chronic epigastric pain and vomited up to one hundred times per day. However, she wasn’t losing weight. Her dental exam and didn’t support bulimia, and her parents denied ever seeing self-induced vomiting behavior.
If anything, it was spontaneous. After ruling out gallbladder, pancreatic, gastrointestinal pathologies with labs, ultrasound, and CT, I reluctantly called the on-call physician for the patient’s pediatrician. They refused to admit, as everything was normal. The parents, as expected, were not happy with that result. I then decided to dive a little deeper into the vomiting history.
The patient described that she didn’t typically experience nausea prior to vomiting. Also, she said that what came up tasted the same as when she swallowed it. That clinched it for me. The patient had rumination syndrome. With a working diagnosis in hand, a treatment plan with diaphragmatic breathing, re-swallowing, Baclofen, Pepcid, Reglan, and a referral to a pediatric gastroenterologist in Houston, the parents were relieved. A frustrating and tense situation was de-escalated because I took the extra time to listen, address their concerns and was able to figure out the puzzle at 2am on a weekend.
As we move forward into the future, with all the challenges and technological marvels that surround us, I encourage you all to maintain and foster human connection with your family, friends, and your patients. Their care, your career, longevity, and happiness depend on it. –•–
Benjamin Godfrey, DO, FACOEP-D President, ACOEP

Awinter challenges into the promise of a much needed spring, I am honored to invite you to our upcoming Spring Seminar in Orlando, Florida. In listening to our membership and your feedback, our leadership team has arranged an amazing opportunity to gather at the beautiful Loews Portofino Bay Hotel at Universal Orlando - a venue that combines worldclass educational opportunities with exceptional family-friendly amenities. While Orlando is synonymous with Disney and Universal Studios, I encourage you to explore the some other outstanding alternative attractions that won’t break the family budget; ICON park with its observation wheel and attractions, Gatorland for authentic Florida Wildlife experience, and my personal favorite, the Orlando Science Center offering engaging experiences at a fraction of the theme park prices. The spring weather in Central Florida is simply

THE ON-DECK CIRCLE
By John Dery DO FACOEP-Dist, FACEP, FAWM President-Elect
A MESSAGE FROM THE PRESIDENT-ELECT
magnificent, making this an ideal time to combine professional development with family recreation. As we plan for this gathering, I want to address three critical challenges confronting our specialty - issues that demand our immediate attention and collective action. These challenges not only impact our daily practice, but also shape the future of Emergency Medicine, and the care we provide to our communities.
The Unmonitored Prescription Crisis: Direct-to-Consumer Medications
We are witnessing an alarming proliferation of direct-to-consumer (DTC) prescriptions services that bypass traditional medical oversight. Most concerning is the rapid expansion of GLP-1 receptor agonist medications for weight loss and others, such as testosterone and other hormone replacement therapy delivered directly to patients through online platforms with minimal medical supervision.
The FDA reported 520 adverse events related to compounded Semaglutide and 480 events for compounded Tirzepatide as of April 2025, though these numbers likely represent significant underreporting. Many of these adverse events resulted from dosing errors, with patients inadvertently administering 5 to 20 times their intended dose due to unclear instructions or unfamiliarity with insulin syringes.1 Emergency departments are increasingly
encountering patients with severe gastrointestinal complications, electrolyte arrangements, and acute pancreatitis linked to unsupervised GLP-1 use.
The problem extends beyond GLP-1 medications. Direct to consumer platforms, marketing testosterone replacement, compounded weight loss, formulations, and “GLP-1– like” supplements, create safety concerns. These products often lack FDA approval, proper quality control, and adequate patient screening. Healthcare providers report increasing cases of hepatic toxicity from oral “GLP1-like” supplements marketed as cheaper alternatives to injectable medications. 2
As emergency physicians, we must remain vigilant in obtaining comprehensive medication histories, specifically asking about online prescriptions, compounded medications, and over-thecounter weightloss supplements. When FDA resolved medication shortages ended for Semaglutide and tirzepatide in early 2025, compounding pharmacies were required to cease production, yet many DTC platforms continue offering “customized” versions by adding ingredients or altering formulations. 3 This regulatory gray area creates confusion for patients and complications for emergency providers attempting to coordinate care.
continued on page 6
The Boarding Crisis: Emergency Medicine at Breaking Point Emergency department boarding has evolved from an operational challenge to a full-blown public health crisis. Recent data reveals that by 2024, even during months would typically lower boarding rates, the percentage of patients waiting four or more hours for inpatient beds exceeded the peak rates observed before the COVID19 pandemic.4 In January 2022, 40% of patients boarded for more than four hours, and 6% waited 24 hours or longer – levels that have remained persistently elevated.
The Agency for Healthcare Research and Quality convened a landmark summit in October 2024; bringing together stakeholders to address this crisis.5 The summit emphasized that boarding is not an emergency department problem, but rather a symptom of systemic healthcare delivery failures driven by misaligned economic incentives that pressure hospitals to maintain high inpatient census levels. When hospital occupancy exceeds 85%, boarding times routinely suppressed the recommended four hour threshold, with median boarding times reaching 6.58 hours.6
This crisis, disproportionately affects vulnerable populations. Data demonstrates that boarding during peak periods increased most rapidly for patients age 65 and older, whose primary language is neither English or Spanish,


and African-American patients.4 The impact extends far beyond wait times – boarding correlates with increased patient, morbidity, mortality, workplace violence against healthcare workers, and accelerated clinician turnover.7
As emergency positions, we must continue advocating for systemic solutions. Multiple professional organizations have successfully lobbied for the formation of national boarding task force, and is currently working with CMS to maintain quality measures that incentivize reducing boarding times. At our Spring Seminar, we will dedicate programming to sharing evidence based strategies for mitigating boarding’s impact on patient care and provider wellness.
Physician Wellness: Addressing Burnout in Emergency Medicine
For the second consecutive year, emergency medicine leads all specialties in physician burnout, with 52-63% of emergency physicians reporting symptoms. 8, 9 Well overall Physician burnout has decreased from pandemic peaks from 53% in 2022 down to 43.2% in 2024 across all specialties10 -Emergency Medicine continues to experience disproportionately high rates.
A groundbreaking 2025 study examining the workforce impact of boarding found alarming connections between operational dysfunction and clinician wellness. Survey respondents reported that boarding contributes to moral injury – the psychological distress experience when bureaucratic
policies prevent physicians from providing to care they know patients require.⁷ This moral injury, combined with increased workplace violence, nursing shortages requiring emergency positions to assume additional tasks, an extreme shift work demands, creates a perfect storm, threatening the sustainability of our specialty.⁹
Female emergency physicians in particular experience, burnout rate rates at 27% higher than their male counterparts, even after adjusting for age, specialty, and other factors10 the consequences extend beyond individual wellness – burned out physicians are more likely to reduce clinical hours or leave practice entirely, exacerbating workforce shortages at a time when an emergency department volumes continue rising. Approximately 15% of emergency medicine workforce has worked at locum tenens positions, reflecting the specialty’s staffing challenges.11
Despite the sobering statistics, there are reasons for optimism. Healthcare systems are increasingly recognizing physician wellness as essential to quality care. Organizations implementing evidence-based wellness initiatives - including adequate staffing, streamlined documentation systems, and supportive work environments - demonstrate measurable improvements in burnout rates and job satisfaction 10 ACOEP remains committed to supporting our members through wellness Programming, advocacy for systemic change, and fostering
La community where emergency physicians support one another.
Looking Forward: Join Us in Orlando
These challenges – unmonitored prescription services, the boarding crisis, and Physician burnout – are interconnected manifestations of systemic pressures on emergency medicine. Yet they also represent opportunities for innovation, advocacy, and collective action. Our Spring Seminar will address each of these issues through cutting-edge educational sessions, collaborative, problemsolving workshops, and networking opportunities with colleagues facing similar challenges.
I encourage you to register today for our spring convention at the Loews Portofino Bay Hotel. Beyond the exceptional CME Programming, you’ll find a supportive community of osteopathic emergency physicians committed to clinical excellence and professional advocacy. Whether you’re seeking to expand your knowledge base, reconnect with colleagues, or simply recharge in the Florida sunshine with your
family, this gathering offers something for everyone.
Emergency medicine as a specialty stands at a critical juncture. The decisions we make today – as individual clinicians, as a specialty organization, and advocates for our patients, and ourselves will determine the future of emergency care for
REFERENCES
years to come. I am confident that together, we will rise to meet these challenges and emerge, stronger, more resilient, and better equipped to serve our communities.
I look forward to seeing you in Orlando this April. –•–
John Dery DO FACOEP-Dist, FACEP, FAWM
President-Elect, ACOEP
1. Drug Information GRoup, University of Illinois Chicago. What are the safety concerns reguardingcompounded GLP-1 receptor agonists? August 2025.
2. University of Kansas Health System. Don’t be fooled by GLP1-like claims. October 2025
3. Milligan. Six things for healthcare stakeholders to know about GLP-1s and compounding. 2025
4. Janke A, et al. Hospital boarding of patients in the emergency department increasingly common,2017-24. Health Affairs. 2025; 44(2). Doi:10.1377/hlthaff.2024.01513
5. Michael SS, Bruno S, Sessums, LL. Building a public-private partnership to confront theemergency department boarding crisis. Health Affairs Scholar. 2025;3(4):qxaf014.
6. Yale School of Medicine. Emergency department crowding hits crisis levels, risking patient safety.Yale News, October 6, 2024
7. Workforce impact of emergency department boarding. Health Affairs. 2025; Collection August.
8. Becker’s Hospital Review. The most burnt-out physicians specialties, January 25, 2024.
9. Medscape. Seeking solutions to burnout among emergency physicians, December 18, 2024.
10. American Medical Association. Which physician specialities are seeing a drop in burnout? May 13,2025.
11. Medics Healthcare Solutions. A system under strain:rising demands in emergency medicine.November 5, 2025
oews Portofino Bay Hotel is located on the grounds of Universal Orlando Resort, putting you steps from Universal Studios Florida, Universal’s Islands of Adventure, and Universal CityWalk. Beyond the parks, Orlando offers a vibrant mix of shopping, dining, and entertainment options:
• Universal CityWalk – A lively waterfront district with restaurants, live music, shops, and nightlife, easily accessible by water taxi or a short walk.
• International Drive – Orlando’s main entertainment corridor with attractions, outlet shopping, and dining just a short drive away.
• Icon Park – Home to The Wheel, Madame Tussauds, SEA LIFE Aquarium, and numerous restaurants and bars.
• Downtown Orlando – About 20–25 minutes away, featuring cultural venues, sports arenas, and local restaurants.
• Family Attractions – SeaWorld, Discovery Cove, and Walt Disney World are within a 20–30 minute drive.
Registered attendees will also have access to exclusive discounts on Universal Orlando theme-park tickets and perks associated with staying at an official Universal Orlando Resort hotel.

Purchase Theme Park Tickets


THANK YOU EXHIBITORS + SPONSORS









EXECUTIVE DIRECTOR’S DESK
Amanda Mahan, MA Executive Director
IN THE PITT -- A MOMENT OF CHALLENGE, A MOMENT OF OPPORTUNITY
Greetings ACOEP Family,
As we step into Spring 2026, I know many of you are feeling the weight of what seems like nonstop turbulence—rapid federal policy shifts, unstable funding, inconsistent guidance, rising administrative burdens, and the constant expectation to adapt faster than ever before. And this isn’t only an emergency medicine story.
Earlier this year, in my role as President of AOSED (the Association of Osteopathic State Executive Directors), I spoke at the AOA Midyear Meeting about the long arc of disruption our broader osteopathic community has been navigating. On behalf of my fellow state and specialty affiliate executive directors nationwide, I highlighted the lingering downstream effects of single accreditation, the decoupling of AOA membership from board certification, increasing competition across the ecosystem, and the fragmentation of what was once a more unified osteopathic identity in a video report.
These forces have challenged the clarity, cohesion, and connection that once came more naturally to our profession—and they inevitably affect the College. Layer that with the pressures of 2026—fast-moving federal changes, public health uncertainty, and members who understandably prioritize what is immediate, clear, and reliable— and we find ourselves at a pivotal moment. Loyalty and tradition alone no longer sustain engagement; responsiveness and relevance do.
That’s why this is such an important time for ACOEP. We are actively examining how to collaborate and partner more intentionally across the osteopathic and emergency medicine landscape while staying firmly grounded in what makes our College strong and uniquely ours. Striking that balance—deepening connection without diluting
identity—is central to our leadership conversations right now.
But this cannot be a one-sided process. We exist to serve you, and your voice is essential as we shape the path ahead. What does meaningful partnership look like to you? What should we protect fiercely, and where should we evolve boldly? I genuinely welcome your thoughts and feedback as we navigate this moment together.
Now More Than Ever, Engagement Matters
In the midst of disruption, I believe wholeheartedly that there has never been a more important time to engage in your professional community. Whether through our educational offerings, leadership development, advocacy efforts, or mentorship pathways, ACOEP is here to support you.
One of the most direct and meaningful ways to make an impact is to get involved with ACOEP’s committees. These groups drive our mission every day and give members a powerful voice in where we go next.
You can explore opportunities here
A National Spotlight on Emergency Medicine
On a brighter note, many of you have shared your reactions to the hit series The Pitt—and I’ll admit, I’ve been tuning in too. The show has shined a rare, authentic spotlight on emergency medicine, offering the public a glimpse into the pace, complexity, emotional intensity, and teamwork that characterize your daily work. It has certainly deepened my own appreciation for the realities you face shift after shift.
At a time when your work is under unprecedented strain, seeing the nation appreciate your expertise and humanity feels especially meaningful. Let’s use this moment

of visibility to continue raising the profile of osteopathic emergency physicians everywhere.
Help Us Tell Your Story
This year, we launched a new, streamlined form to lift up the incredible work happening within our community. Share your news— or highlight a colleague doing something extraordinary.
Submit your updates here
Your stories help us celebrate our shared strengths and remind one another what makes this profession exceptional.
See You in Orlando
I can’t wait to connect with many of you at our Spring Seminar in Orlando this April. Event details
Please come find me, say hello, and share your thoughts—about identity, collaboration, disruption, or simply how things are going in your corner of the world. My door is always open, and your voices will continue to shape where we go next.
Thank you for your resilience, your leadership, and the extraordinary work you do every day. –•–
Warmly,
Amanda Mahan
Executive Director, ACOEP President, AOSED amandam@affinity-strategies.com



Register Today for the 2026 Spring Seminar!
Click or scan QR code
Pre-Conference Sunday, April 19, 2026
10:00-11:00am ExComm Meeting 11:00am-12:00pm Finance Meeting
11:00-11:30am
North American Snake Envenomation: Practical Management for the Emergency Physician
11:30am-12:00pm Varices Gone Wild: Managing GI Bleeds When Help Isn’t Coming
12:00-12:30pm
Heat Illness in the ED: Recognition and Resuscitation
12:30-1:00pm Break
1:00-3:30pm Board Meeting
1:00-1:30pm Cardiothoracic Procedures: Chest Tubes, Pericardiocentesis, and Throacotomy
1:30-2:00pm Updates to the Knee Exam
2:30-4:30pm Thoracic Workshop
Day 2 Monday, April 20, 2026
7:00-7:30am Med Mal
7:30-8:30am Initiating MAT Treatment
8:00-8:30am Breakfast in Exhibit Hall
8:30-9:00am Substance use Ethics Panel
8:30am-12:30pm FOEM Case Poster Competition
9:00-9:30am Wound Management
9:30-10:30am EM Over Easy Live Show
10:30-11:00am Break in Exhibit Hall
11:00-11:30am Things to Stop Doing 11:30am-12:00pm Eye Emergencies
12:00-12:30pm Eye Trauma
1:30-5:00pm FOEM New Innovtions Competition
2:00-4:00pm Eye Workshop
2:30-3:00pm Break in Exhibit Hall
6:00-8:00pm Welcome Party
PRE RECORDED CONTENT (12 CME CREDITS)
• The 5 Papers You Need to Read This Year to Change Your Practice
• Advanced Hand Injuries - Radiographic Interpretation
• The Limping Child
• What the Hives?!
• Common Drug to Drug Interactions
• Child Abuse Recognition and Evaluation
• Mesenteric Ischemia
• Pre-Eclampsia and Eclampsia in the ED
• Modifying Standards of Care for the Unhoused
• Toxic Mushrooms
• Pediatric Congenital Heart Disease
• Bleeding Control
• Street Scanning: POCUS in Street Medicine
• Headaches with a Normal Neurological Exam You Can’t Miss
• Prevention in Medical Errors
• Florida Laws & Rules and Professional Medical Ethics
• Controlled Substance - 2 Hours
• Acute Pain Management for Chronic Opioids
• Opioid Use and Misuse
• MAT Pharmacology
• Controlled Substance TBD
Day 3 Tuesday, April 21, 2026
7:00-7:30am Human Trafficking
7:30-8:00am Pain Management / Opiod Alternatives
8:00-8:30am Breakfast in Exhibit Hall
8:30-9:30am Keynote Speaker
9:30-10:30am EM Over Easy Live Show
10:30-11:00am Break in Exhibit Hall
11:00-11:30am
The Department Dishcharge is the Treatment: Why the Last 5 Minutes Matter Most
11:00am-1:30pm FOEM Board Meeting
11:30am-12:00pm Post-Partum Hemorrhage
12:00-12:30pm The Procedure No One Wants to Do: Perimortum C-Sections
12:00-2:00pm FOEM Board Meeting
12:30-1:30pm Women in EM LuncheonWork Life Balance
2:00-4:00pm OB Emergencies Workshop
2:00-4:00pm Aesthetics Workshop
Day 4 Wednesday, April 22, 2026
7:00-7:30am Chained to Lactate, Freed by Light
7:30-8:00am
Cognitive Offloading in the ED: When AI Improves Clinical Judgement annnd When It Makes It Worse
8:00-8:30am Breakfast in Exhibit Hall
8:30-9:00am Pediatric Non-Invasive Ventilation
9:00-9:30am Sepsis After the Sepsis Bundles What Are We Actually Treating?
9:30-10:00am The Pediatric Airway
10:00-10:30am Risk Management Through Wrist Management
10:30-11:00am Break in Exhibit Hall
11:00-11:30am Pediatrics: Vascular Access Options
11:30am-12:30pm ACOEP Membership Meeting
2:00-4:00pm Pediatrics Workshop
5:00-9:00pm COLA / CORE Review
Day 5 Thursday, April 23, 2026
7:00-7:30am All the Diseases You Forgot About Because of Vaccines
7:30-8:00am Status Epilepticus
8:00-8:30am Breakfast in Exhibit Hall
8:30-9:00am A Sweet New Way to Treat Diabetes
9:00-9:30am Massive Transfusion
9:30-10:00am Aortic Catastrophes
10:00-10:30am Physicians as Athletes
10:30-11:00am Break in Exhibit Hall
11:00-11:30am Heme / Onc Emergencies
11:30am-12:00pm Food and Water Bourne Illnesses
12:00-12:30pm Peptides
CME Language: Attendees can earn at least 32.5 CME credits through general sessions and prerecorded content. Additional 12.5 CME credits are available through paid add-on workshops, bringing the current total to 45.0 credits. Access additional CME credits through pre-recorded content. We anticipate offering both AMA and AOA credits, pending final program approval.
The American College of Emergency Physicians (ACOEP) is accredited by the American Osteopathic Association (AOA) to provide osteopathic continuing medical education for physicians. The ACOEP designates this program for a maximum of 45.0 AOA Category 1-A credits and will report CME and specialty credits commensurate with the extent of the physician’s participation in this activity.
This activity has been submitted for AMA PRA Category 1 Credit™. Credit designation is pending and will be announced once approved.
RSO UPDATE
ACOEP RSO BOARD Nicole Gentile, DO, PGY-1 ACOEP-RSO President HELLO FROM THE RSO!
As the Resident Student Organization continues to grow, we’re proud to share an update on this past semester and what lies ahead for our EM community. This past semester, the ACOEP-RSO Swag Store went live with a wide range of merchandise including hats, sweatshirts, sweats, mugs, and bags available for purchase. The store gave students a fun way to represent emergency medicine and take pride in their involvement with ACOEP, at both conferences and beyond.
The fall conference in Nashville marked a significant milestone with the celebration of ACOEP’s 50th anniversary. We aimed to emphasize student engagement by thinking outside the box with conference activities while continuing to provide meaningful mentorship opportunities. The weekend featured a wellrounded mix of educational sessions, hands-on activities, and networking opportunities that brought students together from across the country. Our favorite guest speakers delivered high-
Spring Seminar 2026 RSO Schedule
PreConf Sunday, April 19, 2026
5:00-6:30pm RSO Happy Hour
Day 1 Monday, April 20, 2026
8:30-9:00am ACOEP RSO Welcome Address
8:30am-12:30pm FOEM Case Poster Competition
9:00am-12:00pm RSO Skills Labs
10:30-11:00am Break in Exhibit Hall
1:00-1:30pm How to Crush Your EM Audition
1:00-1:30pm Drowning
1:30-2:00pm Hyperthermia
1:30-2:00pm It’s Hot in Hurr: ER Approaches to Hyperthermia
1:30-5:0pm FOEM New Innovations Competition
2:00-2:30pm TBD
2:00-2:30pm Session Title TBD 1
2:30-3:00pm Break in Exhibit Hall
3:00-3:30pm Wellness That Actually Works
yield lectures on a range of topics, including quick tips on ventilation strategies, point-of-care ultrasound, habits of a successful medical student, global health in emergency medicine, and introductory trauma concepts.
One of the most memorable events of the conference was our Amazing Races competition, which took place throughout

3:00-3:30pm Session Title TBD 2
3:30-4:00pm Wait...We Can Do That? - Preparing for Low-Occurrence ED Procedures
3:30-4:00pm Session Title TBD 4
4:00-4:30pm A Better Way to Pass Gas: How the PREOXI Trial Should Change the Way You Intubate
4:00-4:30pm GI Bleed
4:30-5:00pm Photosynthesis With a Body Count: Toxic Plants in the Sunshine State
4:30-5:00pm From Rambling to Ready: Confident Patient Presentations in the Emergency Department
6:00-8:00pm Welcome Party
Day 2 Tuesday, April 21, 2026
8:30-9:30am Keynote Speaker
9:30-11:00am So You Think You Can Teach
10:30-11:00am Break in Exhibit Hall
11:00-11:30am Learning from Fun: The Impact of Gamification in Medical Education
2:00-5:00pm Residency Fair
the streets of Nashville. Our RSO teams navigated the city while completing challenges that incorporated skills labs and clinical problem-solving, turning the city into an interactive and competitive learning experience. Another standout moment was the live recording of the EM Over Easy podcast, where hosts answered audience questions while sampling some of Nashville’s best hot wings, keeping the conversation as spicy as the food!
The conference concluded with a residency fair that hosted more than 30 programs. Using a speeddating format, students were able to interact directly with program representatives, ask questions, and gain insight into all of the different training environments. In addition to conference planning, we continued our
Mentorship Lecture Series via Zoom, ensuring that students nationwide could access educational content regardless of geographic location. These sessions focused on key aspects of the residency application process, including understanding SLOEs and navigating VSLO, learning how emergency medicine organizations can support students throughout their training, and strategies for succeeding during residency interviews. The series has served as a consistent and accessible resource for students at all stages of their medical education, with recorded sessions allowing students to revisit content on their own time.
Looking forward, we are excited to host the 2026 Spring Seminar in Orlando.One event
You Can Teach?”, where each student will present a ten-minute lecture on an EM topic of their choosing. The previous conference crowned three winners and we are eager to see the creativity, teaching skills, and innovation students will bring to the stage this spring!
Residency fair registration is currently open for participating programs, and additional lecturers, activities, and interactive events are actively being planned. ACOEP-RSO is looking forward to continuing to build opportunities that foster education, leadership development, and meaningful connections within our emergency medicine community. –•–
Nicole Gentile, DO, PGY-1 ACOEP-RSO President
Please direct questions to Thomas Creech, OMS-III at creecht5837@acom.edu


RSO AT THE 2025 SCIENTIFIC ASSEMBLY




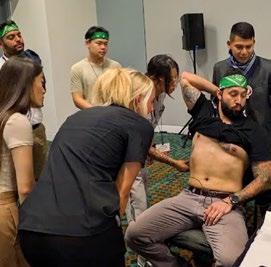




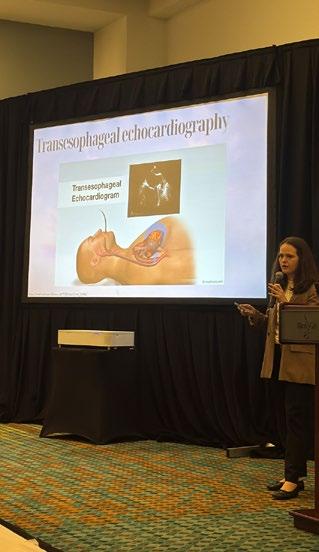



Registration is



Spring Seminar 2026 – Orlando, FL
Tuesday, April 21, 2026 | 2:00-5:00 PM
Loews Portofino Bay Hotel at Universal
• Recruit Top Talent: Meet driven and passionate students eager to join Emergency Medicine.
• Promote Your Program: Share what makes your residency unique in both structured and casual settings.
• Build Connections: Residency Speed Dating focused interactions, followed by open networking during the tabling hour.



WOMEN’S COMMITTEE UPDATE
BUILDING COMMUNITY
Sofia Ferrezza OMS-II Touro College of Osteopathic Medicine
What does it look like to prioritize wellness in a profession defined by high expectations, long hours, and constant demands? In collaboration with the ACOEP’s Wellness Committee, the Women & Wellness Happy Hour—held this past fall during the Scientific Assembly in Nashville—was held to offer a space for connection, conversation, and community support.
Hosted alongside a busy national conference, the informal setting encouraged authentic dialogue and meaningful connections among physicians at various stages of training and practice. The event reinforced the idea that wellness should be an ongoing priority rather than an afterthought. By creating dedicated spaces for connection, participants


ACOEP WOMEN IN EM COMMITTEE
Jacqueline M. Dziedzic, DO, FACEP, FACOEP
Chairwoman

were able to share experiences, learn from one another, and feel supported. The Women & Wellness Happy Hour served as a powerful reminder that community itself is a vital tool in promoting well-being.
During the event, guest speaker Dr. Brie Howerton highlighted how the integration of osteopathic manipulative treatment (OMT) within emergency medicine reflects a commitment to wholeperson care. She emphasized that osteopathic treatments reinforce physician-patient connections, aligning philosophy with practice in ways that benefit both patient care and physician well-being. Having effective, non-pharmacologic tools to address pain and discomfort can enhance clinical confidence, improve patient satisfaction, and reduce reliance on medications when appropriate. For many practitioners, the ability to incorporate OMT fosters a deeper sense of purpose and alignment with osteopathic principles, which can be grounding in the fast-paced ED environment.
One of the most impactful aspects of the Women & Wellness Happy Hour was how approachable the space felt across all levels of training. Medical students, residents, and attending physicians connected easily in an atmosphere
that encouraged relaxed, genuine conversation. Attendees expressed how meaningful it was to hear directly from practicing DOs who actively incorporate osteopathic principles into emergency medicine, particularly when discussions addressed practical realities of documentation and billing. Equally notable was the enthusiasm from attending physicians at seeing such strong trainee engagement, reinforcing a shared commitment to the future of osteopathic emergency medicine.
Looking ahead, the Women’s Committee remains dedicated to creating opportunities that promote connection, inclusivity, and professional growth. Events like the Women & Wellness Happy Hour provide a foundation for continued engagement and dialogue within the osteopathic emergency medicine community.
This spring, we look forward to continuing these conversations at the Women in EM Luncheon on Tuesday, April 21st, from 12:30 to 1:30 PM, featuring guest speaker Dr. Jamie Hope. We encourage readers to stay connected, participate in upcoming events, and explore ways to integrate wellness—both personal and professional—into daily practice.




WELLNESS COMMITTEE UPDATE
FIGHTING THE STIGMA: A REVIEW OF THE PREVALENCE OF SUBSTANCE USE DISORDERS AMONG PHYSICIANS AND THE RESOURCES AVAILABLE TO THEM
It finally happened. I was coerced into watching “The Pitt” via a constant onslaught of text messages filled with intrigue from loved ones back home. The show did not disappoint, capturing much of the heartbreak mixed with the weird moments that inevitably occur in the Emergency Department. One character was particularly fascinating as it highlighted a theme somewhat taboo in the medical space, the physician with a substance use disorder (SUD). This article seeks to explore the prevalence of physicians with SUDs in the United States, populations most at risk, current resources available, and avenues to improve access to treatment in the future.
The prevalence of SUD among physicians is similar to the general population, with 10-15% of US physicians identified as having a SUD 1,2 . This is likely an underestimation due to fear of loss of employment opportunity and social stigma. The specialties noted to have the highest rates of SUDs are anesthesia, emergency medicine (EM), and psychiatry, with EM physicians comprising 7-18% of this population2 . It is no surprise that the specialties most affected by substance misuse have the easiest access to controlled substances and work in high acuity, high-stress environments. Some sources have cited the personality type this career attracts as a reason why EM physicians are more prone to SUDs1. The instant gratification of emergency medical care is something many of us consider a perk of the job, a dopamine rush to the same reward centers involved in addiction disorders.
Most clinicians who struggle with SUDs are referred to a physician health program (PHP). PHPs are nonprofit organizations often funded by state licensing agencies to provide comprehensive, confidential treatment for substance use and mental health disorders 3. These programs offer counseling, pharmacologic treatment, and a network of professionals familiar with the complexities of seeking treatment while employed as a clinician 3 . PHPs are particularly useful as they implement longterm accountability through a five-year substance monitoring program and can assist with medical license reinstatement if necessary 3,4. EM physicians do particularly well with PHPs when it comes to long-term recovery, with 84% of EM physicians achieving sobriety and successful return to clinical practice at 5 years1. Early intervention can be sought using primary care physicians, who can readily connect their clinician patients to cognitive behavioral specialists, treat underlying mental health disorders, and assist with early referral to PHPs5. Additionally, more physicians from multiple specialties are becoming certified to manage opioid
SOURCES
By Morgan Irvin,
use disorder and alcohol use disorder pharmacologically with medications like Suboxone and Naltrexone 5
There are several projects advocating for better protection for clinicians with SUDs and increasing the availability of treatment resources. The “ALL IN: Caring for Caregivers coalition”, an advocacy group of the Lorna Breen Foundation, encourages local credentialing bodies to remove stigmatizing language from their applications 6 . Specifically, a Minnesota bill set to be submitted in the 2026 general election is proposing a change in language to questions regarding mental health disorders on credentialing applications as an attempt to remove barriers for physicians seeking treatment through a PHP 7
As these topics make their way into popular culture with shows like “The Pitt”, it is important to highlight the mental health problems clinicians face, especially those with stigmatized health conditions. This can be accomplished through continued advocacy, awareness about current rights and resources for clinicians, and early referral for intervention in cases of suspected SUD. –•–
1. Rose JS, Campbell M, Skipper G. Prognosis for Emergency Physician with substance abuse recovery: 5-year outcome study. West J Emerg Med. 2014 Feb;15(1):20-5. doi: 10.5811/westjem.2013.7.17871. PMID: 24696748; PMCID: PMC3952884.
2. Srivastava AB. Impaired Physicians: Obliterating the Stigma. American Journal of Psychiatry Residents’ Journal. 2018;13(3):4-6. doi:https://doi.org/10.1176/appi.ajp-rj.2018.130303
3. Virtual Mentor. 2003;5(12):568-571. doi: 10.1001/virtualmentor.2003.5.12.cprl1-0312.
4. Savage S. Mission, Vision And Values. Memberclicks.net. Published 2026. Accessed February 2, 2026. https://fsphp.memberclicks.net/mission-vision-and-values
5. Fitzgerald RM. Caring for the Physician Affected by Substance Use Disorder. Am Fam Physician. 2021 Mar 1;103(5):302-304. PMID: 33630553.
6. About Us - All In for Mental Health. All In for Mental Health. Published October 31, 2025. Accessed February 5, 2026. https://drlornabreen.org/allinformentalhealth/about-us
7. SF3531- 119th Congress 119 (2025-2027) Minnesota Equal Rights Ammendment.; 2025. https://www.revisor.mn.gov/bills/93/2024/0/SF/3531/versions/0/pdf/


Are You Following EM Over Easy?

Make sure to listen to the official podcast of ACOEP wherever you listen to podcasts. Listen Now!

PRACTICE ADVOCACY COMMITTEE UPDATE
ACOEP PRACTICE ADVOCACY COMMITTEE
Jeremy Selley, DO, FACOEP
Joseph Leary, DO, MPH
Practice Advocacy Committee, ACOEP
ADVOCACY IN ACTION: NATIONAL LEGISLATIVE UPDATES IMPACTING EMERGENCY MEDICINE
Over the past year, the national health policy landscape has increasingly centered on issues that directly affect emergency physicians—most notably reimbursement and insurance industry behavior. While comprehensive reform remains elusive, recent legislative and regulatory activity reflects growing recognition that the sustainability of emergency medicine is a national concern.
Progress on Physician Reimbursement
Physician reimbursement remains a top federal advocacy priority. After years of inflationadjusted Medicare payment erosion, Congress has begun to acknowledge the unsustainable path facing frontline physicians and the practices that support them.
Recent federal action includes targeted, though limited, relief:
• A temporary 2.5% payment increase, passed as part of the One Big Beautiful Bill Act (H.R. 1), mitigating scheduled Medicare Physician Fee Schedule cuts.
• Small but permanent baseline updates under MACRA (Medicare Access and CHIP Reauthorization Act of 2015), including a 0.75% annual increase for qualifying participants in advanced alternative payment models (APMs) and a 0.25% increase for other physicians.
• A positive 0.49% budgetneutrality adjustment,
offering modest stabilization within the existing framework. These measures represent real advocacy wins. However, they do not reverse more than a decade of cumulative payment decline relative to inflation.
Emergency physicians continue to practice within a system that has not kept pace with rising labor costs, regulatory burden, or uncompensated care.
Temporary fixes help—but they are not structural reform.
Confronting Harmful Insurance Practices
Reimbursement pressures are compounded by increasingly complex and often burdensome insurance practices. Administrative delays, prior authorization barriers, retroactive denials, and aggressive payment reductions continue to strain emergency practices nationwide.
Federal policymakers have responded with several initiatives:
• Prior authorization reform, particularly in Medicare Advantage plans, aimed at improving transparency and reducing inappropriate delays in care.
• Continued refinement of the No Surprises Act (NSA) and the independent dispute resolution (IDR) process.
• The proposed No Surprises Act Enforcement Act (H.R. 4710/S. 2420), bipartisan legislation intended to strengthen accountability for insurers who fail to comply with statutory payment timelines or arbitration determinations.
Congressional oversight has also intensified. The House Energy and Commerce Committee’s Subcommittee on Health has recently held hearings examining insurer consolidation and vertical integration—specifically the growing trend of major insurers owning physician groups,
ADVOCACY & INVOLVEMENT LINKS
ACOEP ADVOCACY UPDATES
acoep.org/advocacy-update
JOIN THE PRACTICE ADVOCACY COMMITTEE
acoep.org/about-acoep/committees
DONATE TO A PAC
NEMPAC (ACEP) | OPAC (AOA)
KNOW YOUR LEGISLATORS
Find Your Rep/Senator
ATTEND NATIONAL ADVOCACY EVENTS
D.O. Day on the Hill (AOA)
ACEP Leadership & Advocacy Conference
TAKE ACTION NOW
ACEP 911 Grassroots Network
AOA Grassroots Action Center
pharmacies, and pharmacy benefit managers (PBMs). During these hearings, members of both parties, including Rep. Alexandria OcasioCortez (D-NY) and Rep. Greg Murphy, MD (R-NC), pressed insurance executives on market concentration, reimbursement practices, and the potential conflicts of interest that arise when insurers both finance and deliver care. Lawmakers raised concerns about reduced competition, downward pressure on physician reimbursement, and diminished patient access to independent practices. Several members indicated that additional legislative action may be necessary to address anticompetitive consolidation and restore balance within the health care marketplace.
Despite these efforts, emergency physicians continue to face delayed payments, systematic underpayment, and administrative interference that directly threaten the financial stability of emergency departments— particularly those serving vulnerable communities.
RAND Report: A National Call to Sustain Emergency Care
Adding weight to these concerns is the recent RAND report outlining strategies for sustaining emergency care in the United States. The analysis confirms what many emergency physicians experience daily: the emergency care system is under significant financial and operational strain.
Among its findings:
• Chronic underfunding driven by declining reimbursement and uncompensated care burdens.
• The indispensable role of emergency departments as the nation’s health care safety net.
• The need for payment stabilization mechanisms and reforms addressing insurer behavior.
The RAND report provides objective validation of our concerns and strengthens the case for targeted policy solutions. It gives lawmakers credible, data-driven evidence that emergency medicine requires deliberate support to remain viable.
Ongoing Challenges
Even with recent progress, structural challenges persist:
• Emergency departments continue to absorb unsustainable levels of uncompensated and undercompensated care.
• Insurance payment delays and post-payment denials remain common.
• Long-term physician payment reform remains unresolved.
Advocacy, therefore, is not optional—it is essential.
How Emergency Physicians Can Make a Difference
Emergency physicians have more influence than we sometimes realize.
Begin by contacting your state and U.S. representatives. Let them know you are an emergency physician practicing in their district and offer to serve as a resource when healthrelated bills are being considered. Legislators often lack real-time clinical insight. When we step forward early, we help shape conversations before key votes occur.
Participate in advocacy events such as ACEP’s Leadership and Advocacy Conference (LAC) or DO Day on the Hill. If your schedule does not allow in-person participation, consider supporting medical political advocacy committees (PACs) such as USACS PAC, NEMPAC, FOMA PAC, EMRA PAC, or state-level PACs like FCEP PAC. Engagement—whether through time or financial support— helps secure access and build relationships.
As the saying goes, “If you are not at the table, you are on the menu.” Contributions and involvement help open doors to meaningful dialogue. Legislators may not always vote as we hope, but engagement ensures emergency medicine remains part of the discussion.
Finally, share real-world experiences. Policy changes when the human impact becomes clear.
When appropriate and compliant with patient privacy protections, describe examples of delayed care due to prior authorization, coverage denials that limited access to
specialty services, or reimbursement instability that jeopardized services in your community. If patients and families are willing to share their stories—through written testimony or direct conversation—the impact can be profound.
Data informs policy. Stories move people. When lawmakers understand how payment cuts or insurer practices translate into real harm for patients in their own districts, the conversation shifts. Those are often the moments when meaningful change becomes possible.
Conclusion
Recent legislative activity offers cautious optimism, but it also reinforces an enduring truth: reform occurs only when physicians remain engaged.
The RAND report confirms that sustaining emergency care requires deliberate policy action. Increased congressional scrutiny of insurer practices underscores that accountability remains unfinished work.
Everyone wants higher reimbursement. Everyone wants stability. Yet over the past decade, emergency physicians have faced repeated cuts, expanding administrative burden, and mounting financial pressure. If that trend continues, we should not be surprised.
Advocacy does not happen passively. If we are unwilling to show up, build relationships, or financially support those advocating on behalf of our specialty, we should anticipate continued erosion of both reimbursement and influence.
The question is not only what policymakers will do for emergency medicine.
The real question is: What are we willing to do for our profession today?
Make the commitment.
Engage. Support.
Speak up.
Our patients, our practices, and the future of emergency medicine depend on it.

















50TH ANNIVERSARY PHOTO FLASHBACK!
Celebrating 50 Years at the Scientific Assembly
Our 50th Anniversary Scientific Assembly marked a milestone moment for emergency medicine. From dynamic Hippo Education sessions and a full day of EM podcast programming to hands-on workshops and two days of RSO activities, the meeting delivered education, connection, and inspiration.
Watch the Video!



The residency fair welcomed more than 30 programs, FOEM competitions highlighted emerging leaders, and the celebration concluded with a memorable awards and fellowship ceremony honoring excellence in our specialty.
Register for the 2026 Spring Seminar!








FOEM Fall Competition Award Winners
Scientific Assembly
Thank you for your participation! Best wishes in your future research endeavors.
Clinical Pathological Case Competition
1ST PLACE
Blake Chatham, DO
“First Time Seizure”

Faculty Discussants
1ST PLACE
Shawn Quinn, DO
“Teenage Fever Dream”

2ND PLACE
Katarina Werst, DO
“Your Favorite Chief Complaint: Weakness”

3RD PLACE
Dulari Patel, DO
“Splitting Up and Surviving –The Case of an Extensive Aortic Dissection”
2ND PLACE
Jennifer Jozefick, DO
“First Time Seizure”

Nancy Weber, DO, FACOEP, FACEP, MBA
“Your Favorite Chief Complaint: Weakness”

3RD PLACE
Natalie Siegfried, DO
“Severe Infectious Refractory Keratitis Requiring Escalated Antimicrobial Therapy and Surgical Intervention”

LAUNCH YOUR EMERGENCY MEDICINE RESEARCH CAREER:
The Foundation for Osteopathic Emergency Medicine (FOEM) offers a competitive Summer Research Internship that empowers osteopathic medical students to dive deeply into emergency medicine research. Participants will engage in a structured eight-week research experience that allows them to work closely with established investigators and clinical mentors in emergency medicine. Interns receive mentorship through literature review, study design,
data analysis, interpretation, and dissemination of results. In addition to skill development, the internship provides practical experience that can enhance future residency applications and professional opportunities within the osteopathic emergency medicine community.
their research at either ACOEP’s Scientific Assembly or Spring Seminar.
Beyond technical research skills, the FOEM Summer Research Internship reinforces the importance of evidence-based practice and academic engagement in osteopathic emergency medicine. By participating, students not only contribute to meaningful scientific work but also build networks within the ACOEP community that will position them as future leaders in emergency medicine research and patient care. –•–FOEM SUMMER INTERNSHIP APPLY TODAY
Helping to lessen financial barriers and support focus on scholarly activity, interns receive $4,000 in funding for the duration of the experience. Additionally, FOEM provides an extra stipend of $500 for interns who present
Oral Abstract Competition
1ST PLACE
Kiratpreet Sraa, OMS-II
“Retrospective Analysis of Central Line Complication Rates in a Rural Community Setting”

2ND PLACE
Madison Gackle, BS
“Assessing Treatment Compliance of Skin and Soft Tissue Infections to Published Guidelines”

The Board of Trustees of the Foundation for Osteopathic Emergency Medicine thanks you for participating in the competition and hope that you will participate in future events like this as a Resident or apply for research grants as a physician.

The Foundation is here to help serve the research needs of the specialty of emergency medicine and hopes that you have found the creation of a research paper a worthwhile experience worthy of repeating in the future.
3RD PLACE
Teddie Dombrowski, BS, OMS-II
“Race, Income, Insurance, and Transfers for Hospitalized Pediatric Emergency Department Patients”

Stay connected with the ACOEP family and enhance your networking opportunities by following us on social media! Whether you’re seeking to foster professional relationships, explore exciting events like our Scientific Assembly and Spring Seminar, or connect with fellow emergency medicine professionals, our social media channels offer a vibrant community and valuable updates. Join us as we build a supportive network that celebrates growth and collaboration in emergency medicine.
Follow us today and be part of our journey toward collective success!



